Adoptive Immunotherapy for Posttransplantation Viral Infections
|
|
|
- Roger Ramsey
- 5 years ago
- Views:
Transcription
1 Biology of Blood and Marrow Transplantation 10: (2004) 2004 American Society for Blood and Marrow Transplantation /04/ $30.00/0 doi: /j.bbmt Adoptive Immunotherapy for Posttransplantation Viral Infections Catherine M. Bollard, Ingrid Kuehnle, Ann Leen, Cliona M. Rooney, Helen E. Heslop Center for Cell and Gene Therapy, Baylor College of Medicine, The Methodist Hospital, and Texas Children s Hospital, Houston, Texas Correspondence and reprint requests: Helen E. Heslop, Center for Cell and Gene Therapy, Baylor College of Medicine, 6621 Fannin St. MC , Houston, TX ( hheslop@bcm.tmc.edu). Received September 15, 2003; accepted September 30, 2003 ABSTRACT Viral diseases are a major cause of morbidity and mortality after hemopoietic stem cell transplantation. Because viral complications in these patients are clearly associated with the lack of recovery of virus-specific cellular immune responses, reconstitution of the host with in vitro expanded cytotoxic T lymphocytes is a potential approach to prevent and treat these diseases. Initial clinical studies of cytomegalovirus and Epstein-Barr virus in human stem cell transplant patients have shown that adoptively transferred donor-derived virus-specific T cells may restore protective immunity and control established infections. Preclinical studies are evaluating this approach for other viruses while strategies for generating T cells specific for multiple viruses to provide broader protection are being evaluated in clinical trials. The use of genetically modified T cells or the use of newer suicide genes may result in improved safety and efficacy American Society for Blood and Marrow Transplantation KEY WORDS Immunotherapy Viral infection Stem cell transplantation INTRODUCTION One of the major causes of morbidity and mortality in patients who receive allogeneic hematopoietic stem cell transplants (HSCT) is viral infection during the period of immune deficiency that follows the procedure. Recovery of antiviral immunity is dependent on engraftment and expansion of the donor immune system, which occurs by a combination of peripheral mature T-cell expansion and thymopoiesis [1]. The risk of viral infection relates to a number of factors, including the type of transplant, processing of the graft, and posttransplantation immunosuppression. In many cases, viral infection after bone marrow transplantation (BMT) results from reactivation of a latent virus, and herpes viruses such as cytomegalovirus (CMV), Epstein-Barr virus (EBV), and herpes simplex and herpes zoster are common viral pathogens that cause disease after transplantation. In addition, respiratory viruses such as adenovirus, influenza, and respiratory syncytial virus (RSV) also pose a serious problem in posttransplantation patients, who usually acquire the viruses from contact with infected individuals. Although pharmacologic agents are available for the prophylaxis and treatment of some of these viruses, they are expensive, have significant toxicities, and can delay viral-specific immune reconstitution. Because viral complications in these patients are clearly associated with the lack of recovery of virusspecific cellular immune responses, immunotherapeutic strategies to restore viral-specific immunity are an attractive alternative. The most important component of the cellular immune response that controls most viral infections is CD8 cytotoxic T lymphocytes (CTLs) that recognize peptides derived from viral proteins complexed to major histocompatibility complex (MHC) class I molecules. CD4 virus-specific T cells also play an essential role in providing help to CD8 cells and producing long-term immunity. Over the past decade, interest in immunotherapy approaches has been stimulated by studies showing that donor T cells have efficacy in treating viral infections [2,3]. Because unmanipulated T-cell populations also contain alloreactive T cells, a number of investigators have explored whether patients can be protected from such viruses by adoptive transfer of virus-specific 143
2 C. M. Bollard et al. Table 1. Different Sources of Antigens and Antigen-Presenting Cells in Preclinical and Clinical Studies Generating CMV-Specific CTLs Antigen Antigen-Presenting Cell Reference Virions Skin fibroblast Walter et al. [51] Retroviral vector encoding pp65 B lymphoblastoid cell line Sun et al. [36] Adenoviral vector encoding pp65 Dendritic cells Keever-Taylor et al. [56] Hamel et al. [72] Adenoviral vector encoding pp65 Dendritic cells and B lymphoblastoid cell line Sifi et al. [58] CMV antigen derived from CMV-infected lung fibroblasts Dendritic cells Peggs et al. [54] CMV lysate and antigen Peripheral blood mononuclear cells Einsele et al. [55] HLA-A*0201-restricted CMV peptide pp65( ) Dendritic cells and B lymphoblastoid cell line Szmania et al. [92] HLA-A*0201-restricted CMV peptide pp65( ) Dendritic cells Foster et al. [93] CTLs. Clinical trials have been undertaken that target CMV and EBV, and approaches that target other viruses are under development. There are several requirements for generating virus antigen specific CTLs ex vivo. First, virally infected cells must express unique proteins capable of providing epitopes for specific immune responses. It is crucial to know which antigens are expressed by virally infected cells and which antigens are most important for viral persistence and, thus, the best targets for immunotherapy strategies. The viral antigens expressed at different stages of viral infection have been well characterized for some viruses, such as CMV and EBV, but are less well defined for other viruses that cause morbidity, such as adenovirus. Over the past few years, antigen identification has been simplified by the availability of molecular techniques, and bioinformatics tools have enabled peptide mapping of specific epitopes recognized by CD4 and CD8 T cells. Another requirement is an effective antigen-presenting cell (APC) that must express MHC antigens, present relevant virus-derived peptides frequently enough and for sufficient duration to engage responder T cells, and express co-stimulatory molecules such as CD28 to induce T-cell activation. The choice of APC to study also depends on the type of antigen to be used and the proposed method of delivery. Table 1 shows, by using CMV as a model, that there is a wide range of possible choices for both APC and source of antigen. Some approaches use whole virions, whereas others use specific viral genes or peptides, and target cells include fibroblasts, dendritic cells (DCs), and B cells. One of the limitations of adoptive immunotherapy is the lack of a convenient source of APCs necessary to generate antigen-specific CTLs. Most current APCs used in clinical trials require prolonged in vivo culture or manipulation before the initiation of CTL generation. A number of approaches being explored in preclinical studies simplify this process. These include artificial APCs that express ligands for the T-cell receptor (TCR) and the CD28 and 4-1BB co-stimulatory surface molecules [4]; mouse fibroblasts retrovirally transduced with a single HLA/peptide complex along with the human accessory molecules B7.1, intercellular adhesion molecule-1, and leukocyte function-associated antigen [LFA]-3 [5]; and beads coupled to soluble HLA-immunoglobulin fusion protein and CD28-specific antibody [6]. It is also preferable when ex vivo CTL generation is undertaken that the donor be seropositive for the virus, because it is easier to reactivate a secondary immune response ex vivo than to generate a primary one. This is not a major limitation for approaches targeting EBV, because transfer of EBV-infected B cells in the infused product is the major cause of EBV lymphoproliferation. Recipients of seronegative donors are therefore at low risk of developing EBV lymphoma. However, CMV reactivation usually occurs from endogenous virus, and seropositive recipients with seronegative donors are a high-risk group. In preclinical studies, early selection of low-frequency virus-specific cells may enable CTL generation from seronegative donors [7]. IMMUNOTHERAPY TARGETING SPECIFIC VIRUSES Epstein-Barr Virus EBV is an enveloped herpesvirus with a 172-kilobase double-stranded DNA genome [8]. In the immunocompetent host, EBV infection results in a mild self-limiting illness [9]. Like other herpes viruses, EBV persists by a combination of latent infection in B cells and productive replication in B cells or mucosal epithelium. There are 3 types of EBV latency, which are defined by the number and type of latent proteins expressed on the host s B cells. In type 1 latency, only the EBNA1 gene is expressed, whereas in type 2latency, EBNA1, LMP1, and LMP2are expressed. B cells expressing type 3 latency express of all the 9 latency-associated EBV proteins, including the immunodominant EBNA3 viral antigens, and the presence of cell adhesion and co-stimulatory molecules that make these B cells highly immunogenic and, in the immunocompetent host, susceptible to immune-mediated killing by EBV-specific CTLs [10]. Type 3 latency is also demonstrated in vitro in immortalized EBV-transformed lymphoblastoid B-cell lines (LCL). 144
3 Adoptive Immunotherapy for Posttransplantation Viral Infections However, after transplantation, when CTL numbers or activity are suppressed, EBV-infected B cells expressing a type 3 latency may proliferate in an uncontrolled manner. This is also associated with an accumulation of EBV-infected B cells in the body, with increased levels of EBV DNA detected in the peripheral blood by polymerase chain reaction (PCR) [11-14], and, in many cases, with the development of lymphoma. Incidence. The reported incidence of lymphoproliferative disease (LPD) after HSCT ranges from 1% to 25% of transplant recipients [15]. The incidence is highest in the first 6 months after transplantation (120 cases per patients per year) [15]. In a multivariate analysis, the risk of LPD at 12months after HSCT was shown to be strongly associated with patients who received HSCT from HLA-mismatched family donors or unrelated donors [15]. Moreover, risk was increased depending on the posttransplantation immunosuppression regimen used or whether the marrow was depleted of T cells to prevent graftversus-host disease [16-20]. However, if both T and B cells were depleted simultaneously, the incidence was much lower [21]. Treatment with Pharmacologic Agents and Monoclonal Antibodies. A variety of therapeutic approaches to LPD after HSCT have been explored. Although withdrawal of immunosuppression is often effective in solid-organ recipients, this strategy is not usually effective in HSCT recipients because the developing donor-derived immune system cannot provide sufficient immune recovery to eradicate EBV-infected B cells. Chemotherapy regimens such as cyclophosphamide, hydroxydaunomycin, vincristine, and prednisone have been used to treat LPD after HSCT, but mortality is high secondary to significant toxicity [22]. Other drugs, including interferon- 2b and intravenous immune globulin, and antiviral agents such as acyclovir have also been used to treat LPD in this setting. However, a limitation with the use of antiviral agents is that EBV-transformed cells are latently infected, and these drugs block only active herpes virus replication and do not affect the growth of cells that are already transformed. The use of monoclonal anti B-cell antibodies such as anti-cd20 has also been investigated for the treatment of this disease. Although follow-up is relatively short and the number of patients in each series is relatively small, the overall response rates with anti-cd20 ranged from 69% to 100%, and this agent therefore represents a promising strategy for LPD after HSCT [23,24]. However, there are potential hazards of CD20 therapy, because the profound B-cell depletion may further exacerbate immunodeficiency in transplant recipients and may result in selection of a CD20 population of proliferating B cells [25]. T-Cell Therapy for EBV. Immunotherapeutic strategies aimed at reconstituting T-cell responses to EBV have now been used for more than 10 years and have improved the outcome of EBV/LPD after transplantation. In addition, techniques to detect the disease early have been developed that allow preemptive therapy [11,26-28]. In the first reported study from Sloan- Kettering, unselected populations of donor lymphocytes were administered to HSCT recipients with established EBV/LPD [2]. The rationale for this strategy was that most EBV-seropositive individuals have a high frequency of EBV-specific precursors, so transfer of unmanipulated donor lymphocyte populations should be able to restore the immune response to EBV. In the Sloan-Kettering experience, the overall response rate was high: 20 of 22 patients attained complete remissions [17]. Other centers have seen lower response rates to donor leukocyte infusions [12]; this may reflect different patient populations or a better outcome with early diagnosis and treatment. Moreover, such therapy is limited by potentially fatal complications that arise from alloreactive T cells also present in the lymphocyte infusion [12,29]. One approach to overcome the problem of alloreactivity is to use antigen-specific T-cell lines, and results of clinical trials that have used this strategy to target EBV are summarized in Table 2. Although other treatment modalities such as rituximab are now available for the therapy of EBV lymphomas, this was an excellent model to evaluate antigen-specific CTLs because in most EBV-LPD cases that occur in hematopoietic stem cell recipients, the transformed cells are of donor origin and express all latent cycle virusassociated antigens, providing excellent targets for virus-specific T cells. EBV-transformed LCLs that express the same array of viral proteins can be readily prepared from any donor and provide a source of APCs that endogenously express the appropriate antigens for presentation of HLA class I restricted epitopes. Our group generated EBV-specific T-cell lines from donor lymphocytes and used them as prophylaxis and treatment for EBV-induced lymphoma in patients after HSCT [30-32]. APCs for CTL reactivation were generated by infecting donor peripheral blood mononuclear cells (PBMC) with a laboratory strain of EBV to generate a donor LCL line. These LCLs were irradiated and then used as APCs to stimulate and expand EBV-specific CTLs from the donor lymphocyte population. The resultant EBV-specific CTLs are polyclonal and contain both CD4 and CD8 EBV-specific T cells. This is considered advantageous because the presence of antigen-specific CD4-helper T cells is important for in vivo survival of cytotoxic CD8 T-cell populations. Since 1993, 58 patients who received a T cell depleted HSCT were given EBV CTLs prophylactically. The first 26 patients received CTLs that which were genetically modified with a retroviral vector that encoded the 145
4 C. M. Bollard et al. Table 2. Published Reports on Use of EBV-CytotoxicT Cells as Prophylaxis or Treatment for PTLD after BMT Study No. Patients (Patient Age Range) Type of Transplant Pathologic Evidence of PTLD Cytotoxic T-Cell (CTL) Lines and Dose Results Rooney et al. [32] Rooney et al. [32] and Gottschalk et al. [33] Gustafsson et al. [13] 39 (9 mo to 20 y) T cell depleted HSCT (mismatch related donor or matched unrelated donor) No prophylaxis study 3 (12-17 y) T cell depleted HSCT Yes lymphoblastic lymphoma 6 (1-39 y) T cell depleted HSCT or unmanipulated HSCT with ATG/OKT3 conditioning (mismatched or matched unrelated donor or matched related donor) No treatment based on increased EBV DNA levels Allogeneic (donorderived) EBV CTL: minimum dose of /m 2 and maximum dose of /m 2 Allogeneic (donorderived) EBV CTL /m 2 Allogeneic (donorderived) EBV CTL /m 2 No patients developed PTLD compared with 11.5% of controls: no toxicity 2 compete remissions, 1 died (no response to CTL secondary to tumor mutation resistant to CTL) 5 patients had decreased EBV DNA levels. 1 patient subsequently died of PTLD (CTL showed poor specificity for EBV targets on cytotoxicity assay) PTLD indicates posttransplantation lymphoproliferative disorder. neomycin-resistance gene. None of these patients who received EBV CTLs as prophylaxis developed LPD, compared with 11.5% in a comparable group that did not receive CTLs [16]. Nine patients had high EBV DNA levels in peripheral blood before CTL infusion, which was predictive of the imminent onset of EBV/ LPD, and had a rapid decrease in EBV DNA levels that correlated with an increase in EBV-specific CTL precursor frequency. By using conventional PCR and real-time PCR, the marker gene was identified in the peripheral blood up to 78 months after CTL (Table 2). Six patients have also been treated for established EBV lymphoma. The EBV-specific CTL therapy induced remissions in 5 patients, although in 1 case significant inflammation occurred at sites of disease after CTL administration [32]. The patient whose treatment failed was found to have an escape mutant in her tumor cells. Therefore, although the donor EBV CTL line recognized 2immunodominant HLA A11 restricted epitopes in EBNA3B, the patient s tumor cells had a mutation in the EBNA3B epitope, thereby rendering the tumor resistant to the donor CTL [33]. Although polyclonal CTL lines were used, such lines may have target antigen restriction after only 1 week of culture [34], and a restricted pattern of TCR use on spectratyping has been observed [35] that is likely due to the immunodominance of particular EBV-derived peptides presented in the context of different HLA types [10]. Therefore, the risk of tumor escape mutants remains a concern, as it does with the use of monoclonal antibody therapies. In addition, the infusion of CTL to patients with incipient or established disease warrants caution because of the risk of an inflammatory response at disease sites. However, adoptively transferred EBV CTLs do persist longterm and can prevent and effectively treat EBV-driven LPD. A study from Sweden has confirmed the efficacy of EBV-specific CTLs in reducing the viral load in patients with high EBV DNA levels after HSCT [13]. However, 1 of 6 patients who received EBV-specific CTLs subsequently developed overt EBV/LPD and died of progressive disease. In vitro testing of the donor CTL line of this patient showed that it lacked a strong EBV-specific component, which may explain this failure of CTL therapy. An additional limitation of CTL therapy is that because posttransplantation LPD requires immediate treatment, CTLs must be available at diagnosis. The generation of EBV-specific CTLs requires 2to 3 months, although use of EBV antigen loaded DCs as APCs can reduce this time. Another strategy recently described by Koehne et al. [34] is to select virusspecific cells early in culture by their susceptibility to transduction with a retroviral vector. Another concern is that if this strategy is used prophylactically, recipients are protected from only 1 of the many viruses that may cause morbidity and mortality during the period of immunosuppression after transplantation. Several groups have investigated approaches for modifying the LCLs used as APCs to generate multispecific CTLs. Transduction of LCLs with a retroviral vector encoding pp65 has allowed generation of CTLs specific for both CMV and EBV [36], whereas infection 146
5 Adoptive Immunotherapy for Posttransplantation Viral Infections of LCLs with adenovirus results in the generation of CTLs specific for both adenovirus and EBV [37]. Cytomegalovirus CMV is a member of the beta herpes viruses; its pathology is associated with its lytic cycle. CMV is latent in approximately 70% of individuals and replicates slowly in a wide range of cells, including epithelial cells and fibroblasts, and monocytes are thought to be the source of latent infection. Although rarely associated with significant illness in immunocompetent individuals, CMV causes significant morbidity and mortality in the immunocompromised host [38]. Incidence. In the absence of preventive measures, the incidence of CMV infection is 60% to 70% for seropositive allograft recipients in the first 100 days after transplantation. CMV causes interstitial pneumonitis, gastroenteritis, and a systemic wasting syndrome, and CMV seropositivity is an independent risk factor for adverse outcomes [39]. Further, with the increasing use of so-called submyeloablative or reduced-intensity, highly immunosuppressive conditioning regimens, higher rates of CMV infections and reactivation have been observed that are due to prolonged immune suppression [40,41]. In addition, the onset of CMV disease/reactivation is observed at later time points with these regimens (130 days versus 52 days after transplantation in recipients of fully ablative conditioning regimens), and late CMV disease has become a major problem [42]. Finally, CMV viremia in posttransplantation patients can result in prolongation of immunodeficiency and delay CMV-specific immune recovery and expansion even further. Prevention and Treatment with Pharmacologic Agents. The most frequently used drugs for prophylactic or preemptive antiviral therapy are ganciclovir and foscarnet. These drugs, in combination with intravenous immune globulin, have been successful in reducing the mortality associated with CMV disease and in preventing early CMV disease [43]. However, prophylaxis or preemptive treatment with ganciclovir or foscarnet has significant side effects (neutropenia and nephrotoxicity, respectively) and is expensive. Cidofovir has also been used as primary preemptive therapy after transplantation but is associated with renal toxicity, as well as a failure rate of up to 34% [44,45]. Patients receiving ganciclovir are more likely to develop myelosuppression that results in neutropenia and thrombocytopenia (frequency 41%-58%), which necessitates the administration of granulocyte colony-stimulating factor [46,47]. In addition, prophylactic or preemptive therapy delays recovery of CMV-specific CD4 and CD8 lymphocytes, and this results in an increased risk of developing persistent or late CMV disease ( 100 days after allogeneic BMT) [40]. T-Cell Therapy for CMV. Initially, studies performed in the murine CMV model showed that transfer of CD8 murine CMV specific CTLs protected the mice from fatal CMV infection. CMV-specific T-cell responses after HSCT have been studied by several groups. In a recent study with tetramers, Cwynarski et al. [48] studied 24 recipients of allogeneic stem cell transplants (SCT) and found that recovery of CMV-specific CTLs to levels /L was associated with protection from CMV disease. Further, although CMV-specific CTLs recovered approximately 50 days after transplantation in patients after matched related donor BMT, they were absent during the first 100 days in matched unrelated donor transplant recipients. Reconstitution of CD4 immunity showed similar kinetics [49]. Another group assessed not only the number, but also the function, of CMV-specific CTLs after HSCT by using tetramer and intracellular cytokine staining. They found that individuals who experienced CMV antigenemia had lower fractions of functional (tumor necrosis factor- secreting) CMV-specific CTLs present than subjects who did not (25% versus 65%; P.015). Furthermore, individuals at high risk for CMV reactivation, such as patients with acute graftversus-host disease, had significantly lower fractions of cytokine-producing CMV-specific T cells. These data suggest that the inability to control CMV reactivation after allogeneic SCT is due not only to low antigen-specific T-cell numbers, but also to impairment of the T-cell function in vivo [50]. Such studies help to confirm the rationale behind adoptively transferring donor-derived CMV-specific CTLs to at-risk patients after HSCT. The immune response to CMV is well understood, the CMV matrix protein pp65 has been identified as bearing immunodominant epitopes against a range of HLA backgrounds, and CD8 clones specific for pp65 protect against CMV disease in humans. In a proof-of-principle study, CMV prophylaxis with adoptively transferred, donor-derived CMV-specific CTLs was first explored by Walter et al. [51]. This group expanded and infused CMV-specific CD8 clones in a dose-escalation study in allogeneic matched sibling SCT recipients. There were no adverse events, and functional CMV-specific CD8 T- cell responses were detected in all patients after infusion [51]. However, the expansion of T-cell clones to achieve adequate dose levels is extremely time consuming. Also, the authors reported that the magnitude of their anti-cmv responses declined in those who lacked detectable CD4 CMV-specific T-cell responses, which is a concern when CD8 T-cell clones are used as opposed to polyclonal (CD4 and CD8 ) CTL lines. Further, studies have shown that CD4 T cells are required for long-term persistence of these adoptively transferred CD8 clones [52]. Nevertheless, 147
6 C. M. Bollard et al. Table 3. Published Reports on the Use of CMV-CytotoxicT Cells as Prophylaxis or Treatment for CMV Infection after BMT Study No. Patients (Patient Age Range) Type of Transplant Clinical Evidence of CMV Disease Cytotoxic T-Cell (CTL) Lines and Dose Results Walter et al. [51] Einsele et al. [55] Peggs et al. [53], Peggs and Mackinan [94] Cobbold et al. [60] 14 (16-53 y) MRD BMT (unmanipulated graft); CSA or FK506 prophylaxis 8 (7 evaluable) (30-56 y) 13 (age not specified) 7 (age not specified) MRD, MMRD, and MUD (4 patients received CD34-selected stem cells); 6 had ATG; 7 had CSA Allogeneic MRD or MUD Allogeneic SCT (unmanipulated graft) No CMV colitis (n 1), CMV, interstitial pneumonitis (n 1) No administered when CMV DNA was detected No CD8 CMVspecific CTL clones /m 2 to /m 2 Polyclonal CD4 > CD8 CMVspecific CTL /m 2 Polyclonal CD8 and CD4 lines HLA peptideselected CD8 T cells to No toxicity; functional immunity detected in all; no patients developed CMV viremia or disease No toxicity; CMV DNA undetectable in 6/7 patients after CTL; Increased functional immunity in 5 patients; 2 non responders had increased immune suppression No toxicity, massive expansion, CMV-specific immune response Functional immunity detected in all; 1 patient with drug resistant CMV antigens became CMV negative MRD indicates matched related donor; CSA, cyclosporin A; MMRD, mismatched related donor; ATG, antithymocyte globulin; MUD, matched unrelated donor. no patient who received these infusions went on to develop CMV disease, which demonstrates the importance of functional CD8 T cells in the control of CMV reactivation after SCT [51]. One problem with the ex vivo generation of polyclonal CMV-specific CTLs is that unlike EBV-specific CTLs, which can be generated with autologous EBV-transformed LCLs as APCs, CTLs specific for CMV must be activated by exposure to CMV-infected fibroblasts or DCs transduced with 1 of the immunodominant CMV antigens, such as pp65 or pp150. Because of the requirement for donor fibroblasts as APCs in the study by Walter at al. [51], patients receiving transplants from unrelated donors, who are at increased risk of developing CMV reactivation, were excluded from this approach. Table 3 provides an outline of the published clinical trials that have used adoptively transferred CMVspecific CTLs. In one approach, Peggs et al. [53,54] generated CMV-specific CD4 and CD8 T cells by using 2or 3 stimulations with DCs pulsed with CMV antigen derived from a CMV-infected human lung fibroblast cell line. The use of the entire CMV antigen therefore enables a broad CTL response to be generated, as opposed to a solely pp65-specific response, for example. Patients were monitored for CMV reactivation, and T-cell lines were infused at the time of first PCR reactivity. There were no infusion-related toxicities, and none of the 13 patients treated with a single dose of 10 5 /kg CMV CTLs developed CMV disease, although 7 patients did develop CMV reactivation and were successfully treated with ganciclovir [53]. These results are encouraging, but potential problems remain, including the use of an allogeneic cell line to produce the CMV antigen, which could theoretically elicit an allospecific CTL response. In this study, grade I GVHD of the skin developed in only 3 patients, but these patients had early withdrawal of their GVHD prophylaxis, so it is unclear whether the cellular therapy precipitated the GVHD or not. Another problem with this approach and all other approaches that rely on DC stimulations is the logistic problem of generating adequate numbers of DCs to expand the CTLs. With the experience obtained with CMV-specific CTLs prophylactically, Einsele et al. [55] investigated the therapeutic application of adoptively transferring CMV-specific CTLs to patients with persisting or recurring CMV infection despite the prolonged use of antiviral medications. All the patients lacked measurable CMV-specific T-cell responses. Donor-derived PBMCs were pulsed with CMV lysate and expanded by using autologous irradiated feeder cells, CMV lysate, and interleukin-2. This group treated 8 patients who had received a CD34-selected SCT from a family donor. After transfer of T cells per square meter, there were no adverse events, and despite cessation of antiviral medications, the CMV load decreased significantly in 7 evaluable patients. In 5 patients, an increase in both CD4 and CD8 CMV- 148
7 Adoptive Immunotherapy for Posttransplantation Viral Infections specific T cells was seen, and the antiviral effect was sustained [55]. Two patients, however, had a reactivation of their CMV, but this was associated with an intensification of their immune suppression around the time of the T-cell infusion. The advantage with this approach is that it avoids the use of DCs and relies instead on the monocytes infected with the CMV lysate for antigen presentation. However, the CMV lysate contains infectious CMV, and this decreases the attractiveness of this approach in view of the risk of transferring live CMV to immunocompromised patients. Another strategy to generate donor-derived CMV-specific CTLs is the genetic modification of DCs that direct the CTL response to virally transduced genes [56,57]. This approach allows expression of whole proteins, which leads to the presentation of multiple undefined antigen epitopes. We found that although DCs expressing pp65 from an adenoviral vector effectively activated and expanded MHC class I and II restricted CMV-specific CTLs from PBMCs, the limiting monocyte-derived DC numbers hindered the expansion of the CTLs to the numbers necessary for adoptive transfer protocols [58]. We therefore assessed the feasibility of using 1 or 2stimulations with DCs transduced with the recombinant adenoviral vector expressing pp65 (Ad5f35pp65) followed by stimulations with LCLs transduced with the same Ad5f35pp65. Using this method, we were able to effectively expand pp65-specific CTL lines without competition from EBV-specific CTLs; this suggests that the critical point for expansion of these polyclonal, antigen-specific CTL lines was the unlimited source of APCs that could present antigens in the appropriate MHC context. On the basis of these results, a clinical trial has been initiated. Lucas et al. [59] have published a phase I/II clinical protocol for the generation and infusion of CMVspecific CTLs that also capitalizes on the LCLs as an effective and abundant source of APC. In their protocol, the CTL line is initiated by culturing donorderived PBMCs with irradiated donor-derived LCLs transduced with a retrovirus (murine stem cell virus) that expresses pp65. Two further stimulations with the transduced LCLs are performed before the CMVand EBV-specific cytolytic activity of the line are assessed. Clinical data are not yet available from this study. A final approach that avoids the use of an APC is to select donor-derived CMV-specific CD8 T cells after staining with HLA/peptide tetramers. In a study evaluating this approach, 4 patients received between and CMV tetramer-staining CTLs. CMV-specific CTLs were detectable at increasing levels in the peripheral blood after infusion, and all patients became CMV negative, including 1 patient with drug-resistant disease [60]. This approach is therefore promising but, again, is limited to a small number of donors who have a known HLA-restricted CMV peptide epitope. Other limitations are the risk of escape mutants because of the restricted virusspecific response transferred and the lack of a source of clinical-grade tetramer reagents. Adenovirus Adenoviruses are nonenveloped lytic DNA viruses capable of infecting most animal species. Pathogenicity varies according to group and type, and although acute infection is sometimes severe, it is rarely fatal in otherwise healthy adults. Initial infection ultimately results in cell destruction. However, adenoviruses do persist and can be detected months after primary exposure. Humans are susceptible to infection with 51 serotypes of adenovirus that form 6 distinct groups (A to F) [61]. Adenoviruses generally infect mucosal epithelium, but the serotypes differ in their tissue specificity and virulence [62]. After viral infection, transcription is temporally regulated, beginning with immediate early genes encoded in the E1A region, followed by the delayed early units E1B, E2, E3, E4, and L1. Approximately a third of the viral genome is devoted to counteracting the antiviral immune response. These viral immune-evasion strategies ensure prolonged survival of infected cells and facilitate virus transmission [63]. The early expression of immuneevasion genes is likely to inhibit immunity to most of the early and late antigens. For this reason, immunotherapeutic strategies need to target immunodominant virion proteins that access the endosomal/lysosomal pathway and cytosol by receptor-mediated endocytosis and endosomolysis and that are then presented to the immune response before immune-evasion functions are expressed. Incidence. The pathogenicity of adenoviruses varies according to group and type, and, although acute infection is sometimes severe, it is rarely fatal in otherwise healthy adults. Thus, in healthy individuals, the antiviral immune response of the host controls the extent of virus replication and spread. However, adenoviruses are one of a group of opportunistic pathogens of immunosuppressed patients, in whom severe, prolonged, and even fatal infections are common. The frequency of severe adenovirus disease is increasing in association with growing numbers of immunocompromised individuals, and fatality rates as high as 50% to 80% have been reported [64-66]. Lion et al. [65] prospectively studied the incidence of adenovirus infection and disease in 132consecutive pediatric SCT patients and found that 27% tested positive for adenovirus by PCR from multiple sites, including peripheral blood, stool, urine, and throat. It is important to note that 82% of patients who had detectable adenovirus in peripheral blood died from infectious compli- 149
8 C. M. Bollard et al. cations. This incidence increases in high-risk recipients who receive T cell depleted stem cells from unrelated or HLA-mismatched related donors. Approximately 70% of those with detectable adenovirus in the serum develop fatal adenoviral disease associated with hemorrhagic cystitis, pneumonia, nephritis, hepatitis, colitis, and pancreatitis [67,68]. SCT recipients succumb to a range of adenovirus serotypes; most commonly, types 7, 11, 34, and 35 from group B and types 2and 5 from group C have been detected. Pharmacologic Treatment. Treatment options for adenoviral disease are limited, with anecdotal reports of success with antiviral medications. The most frequently used drug for the treatment of adenoviral infections is cidofovir [69,70]. Although there are anecdotal reports of responses to cidofovir, there are no approved antiviral agents that have proven efficacy for the treatment of severe adenoviral disease, nor are there any prospective, randomized, controlled trials of potentially useful antiadenoviral therapies [67]. As seen with CMV infection, the increasing use of submyeloablative, highly T cell immunosuppressive conditioning regimens has resulted in higher rates of adenovirus infections/reactivations being observed. The onset of adenovirus disease/reactivation has recently been reported to occur at a median of 18 days after transplantation (range, day 7 today 100 or more) [65]. T-Cell Therapy for Adenovirus. Because viral complications in these patients are clearly associated with the lack of recovery of virus-specific cellular immune responses, reconstitution of the host with in vitro expanded CTLs is a potential approach to prevent and treat these diseases. However, no adenovirus-specific CD8 T epitopes have been described, so it is impossible to use a peptide-pulsed DC approach. In addition, as discussed previously, CMV-specific CTLs have been activated by DCs pulsed with CMV lysate, and a similar approach could be used for adenoviruses. However, this use of infectious adenovirus decreases the attractiveness of this approach (as it does for CMV) in view of the risk of transferring live adenoviruses to immunocompromised patients. A promising strategy for the generation of donorderived adenovirus-specific CTLs is to use an APC monocyte derived DC transduced with a replicationdefective adenoviral vector that directs the CTL response to viral capsid antigens [70]. This approach allows exposure to all proteins in the adenovirus protein coat, leading to the presentation of multiple undefined antigen epitopes [71]. To generate these adenovirus-specific T-cell lines, DCs were infected with either wild-type Ad5 or Ad5 strain dl312, an Ad5 mutant with the E1A and E3 regions deleted and consequently defective in early and late viral gene expression. It is important to note that the results showed that the adenovirus-specific CTLs generated in this way had extensive cross-reactivity in that CTLs generated with an Ad5 virus also lysed target cells infected with Ad11, Ad4, and Ad18 [71]. Such crossreactivity is important because it indicates that the adoptive transfer of adenovirus-specific CTLs generated in vitro against 1 adenovirus serotype may protect immunocompromised patients from infections by adenoviruses of many, if not all, serotypes. Regn et al. [37] confirmed the feasibility of the previously described approach and performed additional studies to simultaneously expand bispecific CTL populations by using LCLs that had been cocultured on a CD40 ligand expressing monolayer and infected with the Ad5 virus to prime autologous PBMCs. Using this methodology, they demonstrated that the resultant CTLs had specificity against both EBV and adenovirus and that this was mediated by both CD4 and CD8 T cells. Hamel et al. [72] have also generated bispecific CTLs for adenovirus and EBV and also for adenovirus and CMV [72]. They used DCs transduced with recombinant adenovirus encoding CMV pp65 or EBV EBNA 3C and used these cells to stimulate PBMCs. The resulting CTLs were able to kill target cells infected with laboratory strains of these viruses. To date there have been no clinical trials using adenovirus-specific CTLs. However, as a proof of principle for the use of T-cell therapy for adenoviral infection, 1 group reported a case of a 19-year-old man who underwent a T cell depleted 6/6 matched related donor BMT for T-cell lymphoblastic lymphoma [3]. His posttransplantation course was uncomplicated until day 42, when he presented with significant hemorrhagic cystitis secondary to adenovirus infection. The patient did not respond to foscarnet and was given donor leukocytes (10 6 CD3 cells per kilogram) on day 61. After 5 weeks, the patient s hematuria cleared, and urine adenovirus cultures were negative by day 94. This successful treatment of significant adenovirus infection with donor leukocyte infusion therefore supports the rationale for the adoptive transfer of adenovirus-specific CTLs. To assess the safety of donor-derived adenovirusspecific CTLs as prophylaxis and treatment after SCT, our group has developed a protocol that has been approved by our institutional review board and the Recombinant DNA Advisory Committee for the use of adenovirus-specific CTLs as prophylaxis or treatment of adenoviral infection after SCT. In this protocol, we aim to generate and expand adenovirusspecific CTLs by stimulating donor PBMCs with monocytes and LCLs transduced with an Ad5f35 vector. We have demonstrated that adenovirus-specific polyclonal T-cell lines with both cytotoxic and helper function can simply and reproducibly be expanded from healthy donors in vitro by using this method [73]. Further, these CTLs recognize and kill autolo- 150
9 Adoptive Immunotherapy for Posttransplantation Viral Infections gous cells infected with wild-type adenovirus isolates from multiple different serotypes and groups, implying that the virion proteins are responsible for generating at least some of our in vivo T-cell memory response to adenovirus and that T-cell epitopes that are recognized are conserved between different serotypes [73]. Thus, adenovirus immunotherapy is a practical objective that will determine whether virion proteins provide protective CTL epitopes. RESPIRATORY VIRUSES The respiratory viruses, particularly RSV, influenza, parainfluenza, and picornaviruses, are increasingly recognized as significant pathogens in posttransplantation populations. In a prospective surveillance study of 156 patients infected with RSV, influenza, or parainfluenza, 64% developed pneumonia and 30% died [74]. In a large prospective European Bone Marrow Transplantation Group study, over the course of 30 months, 40 patients developed respiratory viral infections, and the overall mortality rate was approximately 25% [75]. These studies further demonstrate the significant effect of human respiratory viruses in transplant-associated morbidity and mortality and particularly highlight the importance of focusing on strategies to prevent and treat such infections. One limitation of immunotherapy strategies for respiratory viruses is that, with the exception of influenza, knowledge of viral immunology is less complete than for CMV and EBV. Although there are some reports identifying epitopes for viruses such as RSV [76], there are no in vitro studies showing that it is possible to generate CTLs from BMT donors that recognize recipient infected cells. A second limitation is logistic in that these viruses cause the greatest morbidity in the early posttransplantation period, and it may not be feasible to generate CTLs in time to cover this period of high risk. There is one report suggesting that donor leukocytes may have activity in RSV: donor lymphocytes were administered to a patient with plasma cell leukemia who relapsed 1 year after transplantation and developed RSV-associated interstitial pneumonia [77]. One week after donor lymphocyte infusion (DLI) his respiratory status improved, with improved arterial oxygen pressures and a decrease in the pulmonary infiltrates detected on computed tomography. A repeat nasal swab was negative for RSV. However, his plasma cell leukemia rapidly progressed, and he died of septic shock approximately 3 weeks after DLI. RSV was not detected in the bronchoalveolar lavage fluid obtained after death [77]. This study therefore suggests a role for T-cell therapy in the management of RSV. It is of note that no inflammatory response was observed after DLI, as has been seen with EBV-specific CTL in the context of EBVassociated pulmonary disease [32]. The risk of a devastating inflammatory response with T-cell therapy is, however, a real possibility, and caution is warranted when immunotherapeutic approaches for respiratory diseases are considered. ALTERNATIVE STRATEGIES TO AUGMENT ANTIVIRAL IMMUNITY The strategies outlined previously to generate virus-specific CTLs target only 1 or 2viruses. The use of a broader range of donor T cells may provide more wide-ranging protection but carries the risk of alloreactivity. Two approaches are under evaluation to minimize alloreactivity. Donor T Cells Transduced with Suicide Genes One solution to the problem of alloreactivity when donor leukocyte infusions are administered is to transduce the T cells with a suicide gene. The suicide gene used most frequently is the herpes simplex virus 1 thymidine kinase gene, which renders transduced cells sensitive to ganciclovir so that they can be subsequently ablated should signs of GVHD develop. Several studies suggest that the use of such cells early or late after transplantation is associated with no acute toxicity; persistent circulation of the gene-modified cells and alloreactive T cells seem to be sensitive to ganciclovir [78,79]. However, 2concerns with this approach are that the transgene may be immunogenic [80] and that the ex vivo activation necessary for retroviral transduction may inhibit virus-reactive cells [81]. An alternative suicide gene that solves the immunogenicity problem is a chimeric human protein that expresses the Fas intracellular domain, with 2 copies of an FK506-binding protein. In vitro, transduced primary human T lymphocytes retrovirally transduced to express the Fas/FK506 chimeric protein functioned the same as untransduced cells. However, transduced cells rapidly underwent apoptosis with the addition of subnanomolar concentrations of AP1903, a bivalent dimerizer drug that binds FK506 binding protein and induces Fas cross-linking. T cells were eliminated regardless of their proliferation state, and this AP1903/Fas system contains only human components, suggesting that it may be a promising alternative to herpes simplex virus 1 thymidine kinase for the removal of alloreactive T cells and the prevention/ treatment of graft-versus-host disease [82]. Recent studies suggest that the problem of activation-induced cell death depleting tumor and virus-reactive cells from the final product can be overcome by using both CD3 and CD28 for T-cell activation [83]. Allodepleted T Cells An alternative strategy to reconstitute antigenspecific responses to multiple viruses, as well as tumor 151
10 C. M. Bollard et al. cells, would be to selectively deplete the graft of alloreactive cells that initiate graft-versus-host disease while preserving tumor- and virus-specific cells. Alloreactive cells express activation markers after exposure to alloantigens, including CD69, CD147, and the interleukin-2receptor CD25, which is expressed within the first 24 hours of T-cell activation. In a study using a CD25 immunotoxin to deplete alloreactive T cells ex vivo, the residual T cells were able to respond in a third-party mixed lymphocyte reaction or to viral or myeloid leukemia associated antigens [84]. In similar studies using CD69 and CD25 antibodies to deplete activated cells after culture of donor cells with recipient cells, the residual T-cell population retained helper and CTL responses against foreign antigens but was specifically devoid of responses to recipient HLA antigens [85-87]. Several groups are now initiating clinical trials with this strategy, and 1 study has been published [88]. Fifteen patients received 1 to allodepleted T cells per kilogram between days 15 and 47 after transplantation. No patient developed greater than grade II graft-versus-host disease, and evidence for early T-cell expansion was shown in 3 patients with continuing viral infections [88]. In comparison with similar patients who received CD34- selected haploidentical transplants alone, recipients of allodepleted cells seemed to have more rapid recovery of T-cell numbers and response to mitogen [88]. Grafting of Chimeric Receptors The generation of virus-specific T cells ex vivo is limited by the requirement for expression of an appropriate antigen by an effective APC and for a seropositive donor. One means of circumventing this problem is retroviral transduction of genes encoding a TCR from a T cell specific to a particular antigen presented on MHC, which should confer that specificity to the transduced cell, thereby bypassing the necessity to isolate and expand virus-specific CTLs from every donor. For example, transduction of a TCR specific for an LMP2peptide was able to transfer CTL activity from a LMP2peptide specific CTL clone to a stimulated PBMC population [89]. An alternate approach is to transduce T cells with chimeric receptors that are composed of an extracellular domain usually derived from immunoglobulin variable chains, which recognizes and binds target antigens attached to a segment of the TCR- chain, which transmits an activation signal to the T cell. In trials in solid tumors, T cells expressing transgenic antigenspecific receptors have had limited clinical success, in part because engagement of the chimeric receptor alone is insufficient to sustain T-cell growth and activation. One means of solving this problem is to transduce antigen-specific T cells rather than nonspecifically activated cells and take advantage of the costimulation provided to the native TCR by antigen; this approach has shown promise in preclinical studies with EBV-specific [90] or alloreactive T cells [91]. CONCLUSIONS AND FUTURE DIRECTIONS The association of viral infection with deficient viral immunity and the efficacy of donor leukocyte infusions for the treatment of various viral infections and virus-specific CTLs for the treatment of CMV and EBV demonstrates the potential of virus-specific immunotherapy. Current challenges are to define the immune response for some of the major pathogens, such as adenovirus, and to devise strategies to provide broad antiviral protection by either generating multivirus-specific CTLs or a T-cell product with a broad antiviral component but a low risk of alloreactivity. Finally, the availability of quantitative and functional assays of virus-specific immunity is critical for the detection and preemptive treatment of at-risk patients. ACKNOWLEDGMENTS This work was supported by NIH grants PO1 CA94237, CA61384, the GCRC at Baylor College of Medicine (RR00188), a Doris Duke Distinguished Clinical Scientist Award (H.E.H.), and the Amy Stelzer Manasevit Scholar Award (C.M.B.). REFERENCES 1. Weinberg K, Blazar BR, Wagner JE, et al. Factors affecting thymic function after allogeneic hematopoietic stem cell transplantation. Blood. 2001;97: Papadopoulos EB, Ladanyi M, Emanuel D, et al. Infusions of donor leukocytes to treat Epstein-Barr virus-associated lymphoproliferative disorders after allogeneic bone marrow transplantation. N Engl J Med. 1994;330: Hromas R, Cornetta K, Srour E, Blanke C, Broun ER. Donor leukocyte infusion as therapy of life-threatening adenoviral infections after T-cell-depleted bone marrow transplantation. Blood. 1994;84: Maus MV, Thomas AK, Leonard DG, et al. Ex vivo expansion of polyclonal and antigen-specific cytotoxic T lymphocytes by artificial APCs expressing ligands for the T-cell receptor, CD28 and 4-1BB. Nat Biotechnol. 2002;20: Latouche JB, Sadelain M. Induction of human cytotoxic T lymphocytes by artificial antigen-presenting cells. Nat Biotechnol. 2000;18: Oelke M, Maus MV, Didiano D, June CH, Mackensen A, Schneck JP. Ex vivo induction and expansion of antigen-specific cytotoxic T cells by HLA-Ig-coated artificial antigen-presenting cells. Nat Med. 2003;9: Savoldo B, Cubbage ML, Durett AG, et al. Generation of EBV-specific CD4( ) cytotoxic T cells from virus naive individuals. J Immunol. 2002;168: Rickinson AB, Kieff E. Epstein-Barr virus. In: Fields BN, Knipe 152
Multi-Virus-Specific T cell Therapy for Patients after HSC and CB Transplant
 Multi-Virus-Specific T cell Therapy for Patients after HSC and CB Transplant Hanley PJ, Krance BR, Brenner MK, Leen AM, Rooney CM, Heslop HE, Shpall EJ, Bollard CM Hematopoietic Stem Cell Transplantation
Multi-Virus-Specific T cell Therapy for Patients after HSC and CB Transplant Hanley PJ, Krance BR, Brenner MK, Leen AM, Rooney CM, Heslop HE, Shpall EJ, Bollard CM Hematopoietic Stem Cell Transplantation
Virological Surveillance in Paediatric HSCT Recipients
 Virological Surveillance in Paediatric HSCT Recipients Dr Pamela Lee Clinical Assistant Professor Department of Paediatrics & Adolescent Medicine Queen Mary Hospital LKS Faculty of Medicine, The University
Virological Surveillance in Paediatric HSCT Recipients Dr Pamela Lee Clinical Assistant Professor Department of Paediatrics & Adolescent Medicine Queen Mary Hospital LKS Faculty of Medicine, The University
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection. Masoud Mardani M.D,FIDSA
 Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
The future of HSCT. John Barrett, MD, NHBLI, NIH Bethesda MD
 The future of HSCT John Barrett, MD, NHBLI, NIH Bethesda MD Transplants today Current approaches to improve SCT outcome Optimize stem cell dose and source BMT? PBSCT? Adjusting post transplant I/S to minimize
The future of HSCT John Barrett, MD, NHBLI, NIH Bethesda MD Transplants today Current approaches to improve SCT outcome Optimize stem cell dose and source BMT? PBSCT? Adjusting post transplant I/S to minimize
Immunology Lecture 4. Clinical Relevance of the Immune System
 Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
PUO in the Immunocompromised Host: CMV and beyond
 PUO in the Immunocompromised Host: CMV and beyond PUO in the immunocompromised host: role of viral infections Nature of host defect T cell defects Underlying disease Treatment Nature of clinical presentation
PUO in the Immunocompromised Host: CMV and beyond PUO in the immunocompromised host: role of viral infections Nature of host defect T cell defects Underlying disease Treatment Nature of clinical presentation
Dr. Yi-chi M. Kong August 8, 2001 Benjamini. Ch. 19, Pgs Page 1 of 10 TRANSPLANTATION
 Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
One Day BMT Course by Thai Society of Hematology. Management of Graft Failure and Relapsed Diseases
 One Day BMT Course by Thai Society of Hematology Management of Graft Failure and Relapsed Diseases Piya Rujkijyanont, MD Division of Hematology-Oncology Department of Pediatrics Phramongkutklao Hospital
One Day BMT Course by Thai Society of Hematology Management of Graft Failure and Relapsed Diseases Piya Rujkijyanont, MD Division of Hematology-Oncology Department of Pediatrics Phramongkutklao Hospital
COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16
 COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16 Tumor Immunology M. Nagarkatti Teaching Objectives: Introduction to Cancer Immunology Know the antigens expressed by cancer cells Understand
COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16 Tumor Immunology M. Nagarkatti Teaching Objectives: Introduction to Cancer Immunology Know the antigens expressed by cancer cells Understand
TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer
 AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke, Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke, Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
T cell manipulation of the graft: Yes
 T cell manipulation of the graft: Yes J.H. Frederik Falkenburg Department of Hematology L M U C Allogeneic Hematopoietic Stem Cell Transplantation (SCT) for non-malignant disorders: no need for anti-tumor
T cell manipulation of the graft: Yes J.H. Frederik Falkenburg Department of Hematology L M U C Allogeneic Hematopoietic Stem Cell Transplantation (SCT) for non-malignant disorders: no need for anti-tumor
Administration of Tumor-Specific Cytotoxic T Lymphocytes Engineered to Resist TGF-ß to Patients with EBV-Associated Lymphomas
 Administration of Tumor-Specific Cytotoxic T Lymphocytes Engineered to Resist TGF-ß to Patients with EBV-Associated Lymphomas CM. Bollard, G Dotti, S Gottschalk, E Liu, A Sheehan, M Mims, H Liu, AP. Gee,
Administration of Tumor-Specific Cytotoxic T Lymphocytes Engineered to Resist TGF-ß to Patients with EBV-Associated Lymphomas CM. Bollard, G Dotti, S Gottschalk, E Liu, A Sheehan, M Mims, H Liu, AP. Gee,
EBV infection B cells and lymphomagenesis. Sridhar Chaganti
 EBV infection B cells and lymphomagenesis Sridhar Chaganti How EBV infects B-cells How viral genes influence the infected B cell Differences and similarities between in vitro and in vivo infection How
EBV infection B cells and lymphomagenesis Sridhar Chaganti How EBV infects B-cells How viral genes influence the infected B cell Differences and similarities between in vitro and in vivo infection How
CONTRACTING ORGANIZATION: Johns Hopkins University School of Medicine Baltimore, MD 21205
 AD Award Number: DAMD7---7 TITLE: Development of Artificial Antigen Presenting Cells for Prostate Cancer Immunotherapy PRINCIPAL INVESTIGATOR: Jonathan P. Schneck, M.D., Ph.D. Mathias Oelke, Ph.D. CONTRACTING
AD Award Number: DAMD7---7 TITLE: Development of Artificial Antigen Presenting Cells for Prostate Cancer Immunotherapy PRINCIPAL INVESTIGATOR: Jonathan P. Schneck, M.D., Ph.D. Mathias Oelke, Ph.D. CONTRACTING
Allo CTL Protocol Page 1 of 43 Version 0.8 dated August 15th, 2008
 Page 1 of 43 Version 0.8 dated August 15th, 2008 Most Closely HLA Matched Allogeneic Virus Specific Cytotoxic T- Lymphocytes (CTL) to Treat Persistent Reactivation or Infection with Adenovirus, CMV and
Page 1 of 43 Version 0.8 dated August 15th, 2008 Most Closely HLA Matched Allogeneic Virus Specific Cytotoxic T- Lymphocytes (CTL) to Treat Persistent Reactivation or Infection with Adenovirus, CMV and
Broad spectrum antiviral T cells for viral complications after hematopoietic stem cell transplantation
 Editorial Page 1 of 5 Broad spectrum antiviral T cells for viral complications after hematopoietic stem cell transplantation Britta Maecker-Kolhoff 1,2, Britta Eiz-Vesper 2,3 1 Department of Pediatric
Editorial Page 1 of 5 Broad spectrum antiviral T cells for viral complications after hematopoietic stem cell transplantation Britta Maecker-Kolhoff 1,2, Britta Eiz-Vesper 2,3 1 Department of Pediatric
CONTRACTING ORGANIZATION: Johns Hopkins University School of Medicine Baltimore, MD 21205
 AD Award Number: DAMD7---7 TITLE: Development of Artificial Antigen Presenting Cells for Prostate Cancer Immunotherapy PRINCIPAL INVESTIGATOR: Jonathan P. Schneck, M.D., Ph.D. Mathias Oelke, Ph.D. CONTRACTING
AD Award Number: DAMD7---7 TITLE: Development of Artificial Antigen Presenting Cells for Prostate Cancer Immunotherapy PRINCIPAL INVESTIGATOR: Jonathan P. Schneck, M.D., Ph.D. Mathias Oelke, Ph.D. CONTRACTING
TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer
 AD Award Number: W8XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
AD Award Number: W8XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
Haploidentical Transplantation Helen Heslop
 Haploidentical Transplantation Helen Heslop Outline Haplodentical transplantation Indications Regimens Outcomes KIR mismatching and NK cells Reconstituting T cell immunity Allodepleted T cells Cytotoxic
Haploidentical Transplantation Helen Heslop Outline Haplodentical transplantation Indications Regimens Outcomes KIR mismatching and NK cells Reconstituting T cell immunity Allodepleted T cells Cytotoxic
EBV in HSCT 2015 update of ECIL guidelines
 ECIL-6 EBV in HSCT 2015 update of ECIL guidelines Jan Styczynski (Poland, chair), Walter van der Velden (Netherlands), Christopher Fox (United Kingdom), Dan Engelhard (Israel), Rafael de la Camara (Spain),
ECIL-6 EBV in HSCT 2015 update of ECIL guidelines Jan Styczynski (Poland, chair), Walter van der Velden (Netherlands), Christopher Fox (United Kingdom), Dan Engelhard (Israel), Rafael de la Camara (Spain),
Diagnosis of CMV infection UPDATE ECIL
 UPDATE ECIL-4 2011 Recommendations for CMV and HHV-6 management in patients with hematological diseases Per Ljungman, Rafael de la Camara, Hermann Einsele, Dan Engelhard, Pierre Reusser, Jan Styczynski,
UPDATE ECIL-4 2011 Recommendations for CMV and HHV-6 management in patients with hematological diseases Per Ljungman, Rafael de la Camara, Hermann Einsele, Dan Engelhard, Pierre Reusser, Jan Styczynski,
Antiviral Drugs Lecture 5
 Antiviral Drugs Lecture 5 Antimicrobial Chemotherapy (MLAB 366) 1 Dr. Mohamed A. El-Sakhawy 2 Introduction Viruses are microscopic organisms that can infect all living cells. They are parasitic and multiply
Antiviral Drugs Lecture 5 Antimicrobial Chemotherapy (MLAB 366) 1 Dr. Mohamed A. El-Sakhawy 2 Introduction Viruses are microscopic organisms that can infect all living cells. They are parasitic and multiply
Manipulation of T Cells in the Thnsplant Inoculum
 International Journal of Cell Cloning 4: 122-126 Suppl 1 (1986) Manipulation of T Cells in the Thnsplant Inoculum J. Kersey Bone Marrow Transplantation Program, University of Minnesota, Minneapolis, MN,
International Journal of Cell Cloning 4: 122-126 Suppl 1 (1986) Manipulation of T Cells in the Thnsplant Inoculum J. Kersey Bone Marrow Transplantation Program, University of Minnesota, Minneapolis, MN,
Federica Galaverna, 1 Daria Pagliara, 1 Deepa Manwani, 2 Rajni Agarwal-Hashmi, 3 Melissa Aldinger, 4 Franco Locatelli 1
 Administration of Rivogenlecleucel (Rivo-cel, BPX-501) Following αβ T- and B-Cell Depleted Haplo-HSCT in Children With Transfusion-Dependent Thalassemia Federica Galaverna, 1 Daria Pagliara, 1 Deepa Manwani,
Administration of Rivogenlecleucel (Rivo-cel, BPX-501) Following αβ T- and B-Cell Depleted Haplo-HSCT in Children With Transfusion-Dependent Thalassemia Federica Galaverna, 1 Daria Pagliara, 1 Deepa Manwani,
EBV Infection and Immunity. Andrew Hislop Institute for Cancer Studies University of Birmingham
 EBV Infection and Immunity Andrew Hislop Institute for Cancer Studies University of Birmingham EBV Introduction Large ds DNA virus Spread by saliva contact Lifelong infection Predominantly B-lymphotropic
EBV Infection and Immunity Andrew Hislop Institute for Cancer Studies University of Birmingham EBV Introduction Large ds DNA virus Spread by saliva contact Lifelong infection Predominantly B-lymphotropic
Transplantation. Immunology Unit College of Medicine King Saud University
 Transplantation Immunology Unit College of Medicine King Saud University Objectives To understand the diversity among human leukocyte antigens (HLA) or major histocompatibility complex (MHC) To know the
Transplantation Immunology Unit College of Medicine King Saud University Objectives To understand the diversity among human leukocyte antigens (HLA) or major histocompatibility complex (MHC) To know the
Appendix E1. Epidemiology
 Appendix E1 Epidemiology Viruses are the most frequent cause of human infectious diseases and are responsible for a spectrum of illnesses ranging from trivial colds to fatal immunoimpairment caused by
Appendix E1 Epidemiology Viruses are the most frequent cause of human infectious diseases and are responsible for a spectrum of illnesses ranging from trivial colds to fatal immunoimpairment caused by
TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer
 AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke,. CONTRACTING ORGANIZATION: Johns Hopkins
AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke,. CONTRACTING ORGANIZATION: Johns Hopkins
Dr. Joseph McGuirk Professor of Medicine, BMT Medical Director, Interim Director, Division of Hematology/Oncology
 Advances in Autologous and Allogeneic Stem Cell Transplantation Dr. Joseph McGuirk Professor of Medicine, BMT Medical Director, Interim Director, Division of Hematology/Oncology April 12, 2014 Disclosures
Advances in Autologous and Allogeneic Stem Cell Transplantation Dr. Joseph McGuirk Professor of Medicine, BMT Medical Director, Interim Director, Division of Hematology/Oncology April 12, 2014 Disclosures
Tumors arise from accumulated genetic mutations. Tumor Immunology (Cancer)
 Tumor Immunology (Cancer) Tumors arise from accumulated genetic mutations Robert Beatty MCB150 Mutations Usually have >6 mutations in both activation/growth factors and tumor suppressor genes. Types of
Tumor Immunology (Cancer) Tumors arise from accumulated genetic mutations Robert Beatty MCB150 Mutations Usually have >6 mutations in both activation/growth factors and tumor suppressor genes. Types of
SEVENTH EDITION CHAPTER
 Judy Owen Jenni Punt Sharon Stranford Kuby Immunology SEVENTH EDITION CHAPTER 16 Tolerance, Autoimmunity, and Transplantation Copyright 2013 by W. H. Freeman and Company Immune tolerance: history * Some
Judy Owen Jenni Punt Sharon Stranford Kuby Immunology SEVENTH EDITION CHAPTER 16 Tolerance, Autoimmunity, and Transplantation Copyright 2013 by W. H. Freeman and Company Immune tolerance: history * Some
Michael Grimley 1, Vinod Prasad 2, Joanne Kurtzberg 2, Roy Chemaly 3, Thomas Brundage 4, Chad Wilson 4, Herve Mommeja-Marin 4
 Twice-weekly Brincidofovir (BCV, CMX1) Shows Promising Antiviral Activity in Immunocompromised Transplant Patients with Asymptomatic Adenovirus Viremia Michael Grimley 1, Vinod Prasad, Joanne Kurtzberg,
Twice-weekly Brincidofovir (BCV, CMX1) Shows Promising Antiviral Activity in Immunocompromised Transplant Patients with Asymptomatic Adenovirus Viremia Michael Grimley 1, Vinod Prasad, Joanne Kurtzberg,
M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology
 Code : AS-2246 M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology A. Select one correct option for each of the following questions:- 2X10=10 1. (b)
Code : AS-2246 M.Sc. III Semester Biotechnology End Semester Examination, 2013 Model Answer LBTM: 302 Advanced Immunology A. Select one correct option for each of the following questions:- 2X10=10 1. (b)
Transplant Booklet D Page 1
 Booklet D Pretest Correct Answers 4. (A) is correct. Technically, performing a hematopoietic stem cell transplant is one of the simplest transplantation procedures. The hematopoietic stem cells are infused
Booklet D Pretest Correct Answers 4. (A) is correct. Technically, performing a hematopoietic stem cell transplant is one of the simplest transplantation procedures. The hematopoietic stem cells are infused
What s a Transplant? What s not?
 What s a Transplant? What s not? How to report the difference? Daniel Weisdorf MD University of Minnesota Anti-cancer effects of BMT or PBSCT [HSCT] Kill the cancer Save the patient Restore immunocompetence
What s a Transplant? What s not? How to report the difference? Daniel Weisdorf MD University of Minnesota Anti-cancer effects of BMT or PBSCT [HSCT] Kill the cancer Save the patient Restore immunocompetence
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_ transplantation_for_primary_amyloidosis 2/2001 11/2018 11/2019 11/2018 Description
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_ transplantation_for_primary_amyloidosis 2/2001 11/2018 11/2019 11/2018 Description
NIH Public Access Author Manuscript Cytotherapy. Author manuscript; available in PMC 2012 May 1.
 NIH Public Access Author Manuscript Published in final edited form as: Cytotherapy. 2011 May ; 13(5): 518 522. doi:10.3109/14653249.2011.561983. Manufacture of GMP-grade Cytotoxic T Lymphocytes specific
NIH Public Access Author Manuscript Published in final edited form as: Cytotherapy. 2011 May ; 13(5): 518 522. doi:10.3109/14653249.2011.561983. Manufacture of GMP-grade Cytotoxic T Lymphocytes specific
08/02/59. Tumor Immunotherapy. Development of Tumor Vaccines. Types of Tumor Vaccines. Immunotherapy w/ Cytokine Gene-Transfected Tumor Cells
 Tumor Immunotherapy Autologous virus Inactivation Inactivated virus Lymphopheresis Culture? Monocyte s Dendritic cells Immunization Autologous vaccine Development of Tumor Vaccines Types of Tumor Vaccines
Tumor Immunotherapy Autologous virus Inactivation Inactivated virus Lymphopheresis Culture? Monocyte s Dendritic cells Immunization Autologous vaccine Development of Tumor Vaccines Types of Tumor Vaccines
Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach
 Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach Oncolytic immunotherapy Oncolytic immunotherapy the use of a genetically modified virus to attack tumors and induce a systemic immune response
Oncolytic Immunotherapy: A Local and Systemic Antitumor Approach Oncolytic immunotherapy Oncolytic immunotherapy the use of a genetically modified virus to attack tumors and induce a systemic immune response
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/20522 holds various files of this Leiden University dissertation. Author: Stevanović, Sanja Title: Exploiting HLA-class II disparity for anti-tumor immunity
Cover Page The handle http://hdl.handle.net/1887/20522 holds various files of this Leiden University dissertation. Author: Stevanović, Sanja Title: Exploiting HLA-class II disparity for anti-tumor immunity
T lymphocytes targeting native receptors
 Cliona M. Rooney Ann M. Leen Juan F. Vera Helen E. Heslop T lymphocytes targeting native receptors Authors address Cliona M. Rooney 1, Ann M. Leen 1, Juan F. Vera 1, Helen E. Heslop 1 1 Center for Cell
Cliona M. Rooney Ann M. Leen Juan F. Vera Helen E. Heslop T lymphocytes targeting native receptors Authors address Cliona M. Rooney 1, Ann M. Leen 1, Juan F. Vera 1, Helen E. Heslop 1 1 Center for Cell
Determinants of Immunogenicity and Tolerance. Abul K. Abbas, MD Department of Pathology University of California San Francisco
 Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
5/9/2018. Bone marrow failure diseases (aplastic anemia) can be cured by providing a source of new marrow
 5/9/2018 or Stem Cell Harvest Where we are now, and What s Coming AA MDS International Foundation Indianapolis IN Luke Akard MD May 19, 2018 Infusion Transplant Conditioning Treatment 2-7 days STEM CELL
5/9/2018 or Stem Cell Harvest Where we are now, and What s Coming AA MDS International Foundation Indianapolis IN Luke Akard MD May 19, 2018 Infusion Transplant Conditioning Treatment 2-7 days STEM CELL
RAISON D ETRE OF THE IMMUNE SYSTEM:
 RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Acquired Immunity Innate immunity: (Antigen nonspecific) defense
RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Acquired Immunity Innate immunity: (Antigen nonspecific) defense
Class I Ag processing. TAP= transporters associated with antigen processing Transport peptides into ER
 Antigen processing Class I Ag processing TAP= transporters associated with antigen processing Transport peptides into ER Proteosome degrades cytosolic proteins Large, multi-subunit complex Degrades foreign
Antigen processing Class I Ag processing TAP= transporters associated with antigen processing Transport peptides into ER Proteosome degrades cytosolic proteins Large, multi-subunit complex Degrades foreign
TRANSPLANT IMMUNOLOGY. Shiv Pillai Ragon Institute of MGH, MIT and Harvard
 TRANSPLANT IMMUNOLOGY Shiv Pillai Ragon Institute of MGH, MIT and Harvard Outline MHC / HLA Direct vs indirect allorecognition Alloreactive cells: where do they come from? Rejection and Immunosuppression
TRANSPLANT IMMUNOLOGY Shiv Pillai Ragon Institute of MGH, MIT and Harvard Outline MHC / HLA Direct vs indirect allorecognition Alloreactive cells: where do they come from? Rejection and Immunosuppression
Improving the Outcome of Stem Cell Transplants for Cancer Treatment Using Multivirus-Specific T Cells (Viralym-M)
 OFF-THE-SHELF T CELL THERAPY FOR CANCER PATIENTS FOLLOWING STEM CELL TRANSPLANT Improving the Outcome of Stem Cell Transplants for Cancer Treatment Using Multivirus-Specific T Cells (Viralym-M) Ann M.
OFF-THE-SHELF T CELL THERAPY FOR CANCER PATIENTS FOLLOWING STEM CELL TRANSPLANT Improving the Outcome of Stem Cell Transplants for Cancer Treatment Using Multivirus-Specific T Cells (Viralym-M) Ann M.
RAISON D ETRE OF THE IMMUNE SYSTEM:
 RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Adaptive Immunity Innate immunity: (Antigen - nonspecific) defense
RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Adaptive Immunity Innate immunity: (Antigen - nonspecific) defense
Recommendations for VZV management in. Dan Engelhard, Pierre Reusser, Rafael de la Camara, Hermann Einsele, Jan Styczynski, Kate Ward, Per Ljungman
 Recommendations for VZV management in patients Cas cliniques with leukemia Dan Engelhard, Pierre Reusser, Rafael de la Camara, Hermann Einsele, Jan Styczynski, Kate Ward, Per Ljungman Introduction Acute
Recommendations for VZV management in patients Cas cliniques with leukemia Dan Engelhard, Pierre Reusser, Rafael de la Camara, Hermann Einsele, Jan Styczynski, Kate Ward, Per Ljungman Introduction Acute
MUD SCT. Pimjai Niparuck Division of Hematology, Department of Medicine Ramathibodi Hospital, Mahidol University
 MUD SCT Pimjai Niparuck Division of Hematology, Department of Medicine Ramathibodi Hospital, Mahidol University Outlines Optimal match criteria for unrelated adult donors Role of ATG in MUD-SCT Post-transplant
MUD SCT Pimjai Niparuck Division of Hematology, Department of Medicine Ramathibodi Hospital, Mahidol University Outlines Optimal match criteria for unrelated adult donors Role of ATG in MUD-SCT Post-transplant
KEY WORDS: Alternative donor stem cell transplantation, Acute lymphoblastic leukemia, GVHD, Leukemia relapse
 Comparable Outcome of Alternative Donor and Matched Sibling Donor Hematopoietic Stem Cell Transplant for Children with Acute Lymphoblastic Leukemia in First or Second Remission Using Alemtuzumab in a Myeloablative
Comparable Outcome of Alternative Donor and Matched Sibling Donor Hematopoietic Stem Cell Transplant for Children with Acute Lymphoblastic Leukemia in First or Second Remission Using Alemtuzumab in a Myeloablative
Management of Viral Infections in HCT
 Management of Viral Infections in HCT Alison Coats, APRN-BC Liza Rodriguez, APRN, AOCNP Objectives Recognize viral infections that affect patients after hematopoietic cell transplant (HCT) Describe the
Management of Viral Infections in HCT Alison Coats, APRN-BC Liza Rodriguez, APRN, AOCNP Objectives Recognize viral infections that affect patients after hematopoietic cell transplant (HCT) Describe the
Antiviral Adoptive Immunotherapy for Primary Immunodeficiency Disorders. Speaker Disclosures
 3/27/218 Antiviral Adoptive Immunotherapy for Primary Immunodeficiency Disorders Michael Keller, MD Program for Cell Enhancement & Technologies for Immunotherapy (CETI) Director: Dr. Catherine Bollard
3/27/218 Antiviral Adoptive Immunotherapy for Primary Immunodeficiency Disorders Michael Keller, MD Program for Cell Enhancement & Technologies for Immunotherapy (CETI) Director: Dr. Catherine Bollard
Transfusion Medicine: New Clinical Applications of Cellular Immunotherapy
 Transfusion Medicine: New Clinical Applications of Cellular Immunotherapy Malcolm Brenner (Chair), Claudia Rossig, Uluhan Sili, James W. Young, and Els Goulmy There is now clear clinical evidence that
Transfusion Medicine: New Clinical Applications of Cellular Immunotherapy Malcolm Brenner (Chair), Claudia Rossig, Uluhan Sili, James W. Young, and Els Goulmy There is now clear clinical evidence that
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_cell_transplantation_for_cll_and_sll 2/2001
Corporate Medical Policy Hematopoietic Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_cell_transplantation_for_cll_and_sll 2/2001
The Adaptive Immune Response: T lymphocytes and Their Functional Types *
 OpenStax-CNX module: m46560 1 The Adaptive Immune Response: T lymphocytes and Their Functional Types * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution
OpenStax-CNX module: m46560 1 The Adaptive Immune Response: T lymphocytes and Their Functional Types * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution
Herpesviruses. Virion. Genome. Genes and proteins. Viruses and hosts. Diseases. Distinctive characteristics
 Herpesviruses Virion Genome Genes and proteins Viruses and hosts Diseases Distinctive characteristics Virion Enveloped icosahedral capsid (T=16), diameter 125 nm Diameter of enveloped virion 200 nm Capsid
Herpesviruses Virion Genome Genes and proteins Viruses and hosts Diseases Distinctive characteristics Virion Enveloped icosahedral capsid (T=16), diameter 125 nm Diameter of enveloped virion 200 nm Capsid
Revista Cubana de Hematología, Inmunología y Hemoterapia. 2017; 36 (Suplemento).
 Depletion of TCR alpha/beta+ T-lymphocytes from grafts for haplo haematopoietic CELL transplantation (HCT) in children Heilmann C, Ifversen M, Haastrup E, Fischer-Nielsen A. Haematopoietic Cell Transplantation
Depletion of TCR alpha/beta+ T-lymphocytes from grafts for haplo haematopoietic CELL transplantation (HCT) in children Heilmann C, Ifversen M, Haastrup E, Fischer-Nielsen A. Haematopoietic Cell Transplantation
Third line of Defense
 Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
Complications after HSCT. ICU Fellowship Training Radboudumc
 Complications after HSCT ICU Fellowship Training Radboudumc Type of HSCT HSCT Improved outcome due to better HLA matching, conditioning regimens, post transplant supportive care Over one-third have pulmonary
Complications after HSCT ICU Fellowship Training Radboudumc Type of HSCT HSCT Improved outcome due to better HLA matching, conditioning regimens, post transplant supportive care Over one-third have pulmonary
Defensive mechanisms include :
 Acquired Immunity Defensive mechanisms include : 1) Innate immunity (Natural or Non specific) 2) Acquired immunity (Adaptive or Specific) Cell-mediated immunity Humoral immunity Two mechanisms 1) Humoral
Acquired Immunity Defensive mechanisms include : 1) Innate immunity (Natural or Non specific) 2) Acquired immunity (Adaptive or Specific) Cell-mediated immunity Humoral immunity Two mechanisms 1) Humoral
1. Overview of Adaptive Immunity
 Chapter 17A: Adaptive Immunity Part I 1. Overview of Adaptive Immunity 2. T and B Cell Production 3. Antigens & Antigen Presentation 4. Helper T cells 1. Overview of Adaptive Immunity The Nature of Adaptive
Chapter 17A: Adaptive Immunity Part I 1. Overview of Adaptive Immunity 2. T and B Cell Production 3. Antigens & Antigen Presentation 4. Helper T cells 1. Overview of Adaptive Immunity The Nature of Adaptive
Severe Viral Related Complications Following Allo-HCT for Severe Aplastic Anemia
 Severe Viral Related Complications Following Allo-HCT for Severe Aplastic Anemia Liat Shragian Alon, MD Rabin Medical Center, ISRAEL #EBMT15 www.ebmt.org Patient: 25-year-old male No prior medical history
Severe Viral Related Complications Following Allo-HCT for Severe Aplastic Anemia Liat Shragian Alon, MD Rabin Medical Center, ISRAEL #EBMT15 www.ebmt.org Patient: 25-year-old male No prior medical history
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases. Abul K. Abbas UCSF
 Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Shiv Pillai Ragon Institute, Massachusetts General Hospital Harvard Medical School
 CTLs, Natural Killers and NKTs 1 Shiv Pillai Ragon Institute, Massachusetts General Hospital Harvard Medical School CTL inducing tumor apoptosis 3 Lecture outline CD8 + Cytotoxic T lymphocytes (CTL) Activation/differentiation
CTLs, Natural Killers and NKTs 1 Shiv Pillai Ragon Institute, Massachusetts General Hospital Harvard Medical School CTL inducing tumor apoptosis 3 Lecture outline CD8 + Cytotoxic T lymphocytes (CTL) Activation/differentiation
Structure of viruses
 Antiviral Drugs o Viruses are obligate intracellular parasites. o lack both a cell wall and a cell membrane. o They do not carry out metabolic processes. o Viruses use much of the host s metabolic machinery.
Antiviral Drugs o Viruses are obligate intracellular parasites. o lack both a cell wall and a cell membrane. o They do not carry out metabolic processes. o Viruses use much of the host s metabolic machinery.
The Adaptive Immune Responses
 The Adaptive Immune Responses The two arms of the immune responses are; 1) the cell mediated, and 2) the humoral responses. In this chapter we will discuss the two responses in detail and we will start
The Adaptive Immune Responses The two arms of the immune responses are; 1) the cell mediated, and 2) the humoral responses. In this chapter we will discuss the two responses in detail and we will start
Principles of Adaptive Immunity
 Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Understanding the role of ex vivo T cell depletion
 Prevention of graftversus-host disease (GVHD) Understanding the role of ex vivo T cell depletion Information for patients undergoing allogeneic stem cell transplantation in AML and their families 2 This
Prevention of graftversus-host disease (GVHD) Understanding the role of ex vivo T cell depletion Information for patients undergoing allogeneic stem cell transplantation in AML and their families 2 This
HLA-DR-matched Parental Donors for Allogeneic Hematopoietic Stem Cell Transplantation in Patients with High-risk Acute Leukemia
 BRIEF COMMUNICATION HLA-DR-matched Parental Donors for Allogeneic Hematopoietic Stem Cell Transplantation in Patients with High-risk Acute Leukemia Shang-Ju Wu, Ming Yao,* Jih-Luh Tang, Bo-Sheng Ko, Hwei-Fang
BRIEF COMMUNICATION HLA-DR-matched Parental Donors for Allogeneic Hematopoietic Stem Cell Transplantation in Patients with High-risk Acute Leukemia Shang-Ju Wu, Ming Yao,* Jih-Luh Tang, Bo-Sheng Ko, Hwei-Fang
Stem Cell Sources 2/22/13. Cellular Therapy Today and Tomorrow. Cellular Therapy in HCT. Bone Marrow
 2/22/13 Cellular Therapy Today and Tomorrow Robert S. Negrin, MD Division Chief, Stanford Bone and Marrow Transplant Program Professor of Medicine Cellular Therapy in Clinical Medicine Established Hematopoietic
2/22/13 Cellular Therapy Today and Tomorrow Robert S. Negrin, MD Division Chief, Stanford Bone and Marrow Transplant Program Professor of Medicine Cellular Therapy in Clinical Medicine Established Hematopoietic
Barry Slobedman. University of Sydney. Viruses in May 11 th May, 2013
 Barry Slobedman University of Sydney Viruses in May 11 th May, 2013 Outline Human cytomegalovirus (CMV) impact on the community Three phases of infection Focus on the dormant (latent) phase of infection
Barry Slobedman University of Sydney Viruses in May 11 th May, 2013 Outline Human cytomegalovirus (CMV) impact on the community Three phases of infection Focus on the dormant (latent) phase of infection
Test Bank for Basic Immunology Functions and Disorders of the Immune System 4th Edition by Abbas
 Test Bank for Basic Immunology Functions and Disorders of the Immune System 4th Edition by Abbas Chapter 04: Antigen Recognition in the Adaptive Immune System Test Bank MULTIPLE CHOICE 1. Most T lymphocytes
Test Bank for Basic Immunology Functions and Disorders of the Immune System 4th Edition by Abbas Chapter 04: Antigen Recognition in the Adaptive Immune System Test Bank MULTIPLE CHOICE 1. Most T lymphocytes
Mucosal Immune System
 Exam Format 100 points - 60 pts mandatory; 40 points where 4, 10 point questions will be chosen Some open-ended questions, some short answer. Kuby question Cytokines Terminology How do cytokines achieve
Exam Format 100 points - 60 pts mandatory; 40 points where 4, 10 point questions will be chosen Some open-ended questions, some short answer. Kuby question Cytokines Terminology How do cytokines achieve
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for Waldenstrom Macroglobulinemia File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem_cell_transplantation_for_waldenstrom_macroglobulinemia
Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for Waldenstrom Macroglobulinemia File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem_cell_transplantation_for_waldenstrom_macroglobulinemia
General Terms: Appendix B. National Marrow Donor Program and The Medical College of Wisconsin
 Glossary of Terms This appendix is divided into two sections. The first section, General Terms, defines terms used throughout the CIBMTR data collection forms. The second section, FormsNet TM 2 Terms,
Glossary of Terms This appendix is divided into two sections. The first section, General Terms, defines terms used throughout the CIBMTR data collection forms. The second section, FormsNet TM 2 Terms,
Antigen Presentation and T Lymphocyte Activation. Abul K. Abbas UCSF. FOCiS
 1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
VIRUSES AND CANCER Michael Lea
 VIRUSES AND CANCER 2010 Michael Lea VIRAL ONCOLOGY - LECTURE OUTLINE 1. Historical Review 2. Viruses Associated with Cancer 3. RNA Tumor Viruses 4. DNA Tumor Viruses HISTORICAL REVIEW Historical Review
VIRUSES AND CANCER 2010 Michael Lea VIRAL ONCOLOGY - LECTURE OUTLINE 1. Historical Review 2. Viruses Associated with Cancer 3. RNA Tumor Viruses 4. DNA Tumor Viruses HISTORICAL REVIEW Historical Review
Immunology. Anas Abu-Humaidan M.D. Ph.D. Transplant immunology+ Secondary immune deficiency
 Immunology Anas Abu-Humaidan M.D. Ph.D. Transplant immunology+ Secondary immune deficiency Transplant Immunology Transplantation is the process of moving cells, tissues or organs from one site to another
Immunology Anas Abu-Humaidan M.D. Ph.D. Transplant immunology+ Secondary immune deficiency Transplant Immunology Transplantation is the process of moving cells, tissues or organs from one site to another
The Immune System. These are classified as the Innate and Adaptive Immune Responses. Innate Immunity
 The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
T Cell Development. Xuefang Cao, MD, PhD. November 3, 2015
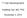 T Cell Development Xuefang Cao, MD, PhD November 3, 2015 Thymocytes in the cortex of the thymus Early thymocytes development Positive and negative selection Lineage commitment Exit from the thymus and
T Cell Development Xuefang Cao, MD, PhD November 3, 2015 Thymocytes in the cortex of the thymus Early thymocytes development Positive and negative selection Lineage commitment Exit from the thymus and
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Antiviral Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018
 Antiviral Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 Viruses Viruses are the smallest infective agents, consisting of nucleic acid (DNA or RNA) enclosed
Antiviral Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 Viruses Viruses are the smallest infective agents, consisting of nucleic acid (DNA or RNA) enclosed
Third line of Defense. Topic 8 Specific Immunity (adaptive) (18) 3 rd Line = Prophylaxis via Immunization!
 Topic 8 Specific Immunity (adaptive) (18) Topics - 3 rd Line of Defense - B cells - T cells - Specific Immunities 1 3 rd Line = Prophylaxis via Immunization! (a) A painting of Edward Jenner depicts a cow
Topic 8 Specific Immunity (adaptive) (18) Topics - 3 rd Line of Defense - B cells - T cells - Specific Immunities 1 3 rd Line = Prophylaxis via Immunization! (a) A painting of Edward Jenner depicts a cow
Persistent Infections
 Persistent Infections Lecture 17 Biology 3310/4310 Virology Spring 2017 Paralyze resistance with persistence WOODY HAYES Acute vs persistent infections Acute infection - rapid and self-limiting Persistent
Persistent Infections Lecture 17 Biology 3310/4310 Virology Spring 2017 Paralyze resistance with persistence WOODY HAYES Acute vs persistent infections Acute infection - rapid and self-limiting Persistent
3.1 Clinical safety of chimeric or humanized anti-cd25 (ch/anti-cd25)
 3 Results 3.1 Clinical safety of chimeric or humanized anti-cd25 (ch/anti-cd25) Five infusions of monoclonal IL-2 receptor antibody (anti-cd25) were planned according to protocol between day 0 and day
3 Results 3.1 Clinical safety of chimeric or humanized anti-cd25 (ch/anti-cd25) Five infusions of monoclonal IL-2 receptor antibody (anti-cd25) were planned according to protocol between day 0 and day
The Contribution of Homeostatically Expanded Donor CD8 T Cells to Host Reconstitution Following Syngeneic Hematopoietic Cell Transplantation
 University of Miami Scholarly Repository Open Access Dissertations Electronic Theses and Dissertations 2008-07-24 The Contribution of Homeostatically Expanded Donor CD8 T Cells to Host Reconstitution Following
University of Miami Scholarly Repository Open Access Dissertations Electronic Theses and Dissertations 2008-07-24 The Contribution of Homeostatically Expanded Donor CD8 T Cells to Host Reconstitution Following
Human Cytomegalovirus Latency-Associated Proteins Elicit Immune-Suppressive IL-10 Producing CD4 + T Cells
 Human Cytomegalovirus Latency-Associated Proteins Elicit Immune-Suppressive IL-10 Producing CD4 + T Cells Gavin M. Mason, Sarah Jackson, Georgina Okecha, Emma Poole, J. G. Patrick Sissons, John Sinclair,
Human Cytomegalovirus Latency-Associated Proteins Elicit Immune-Suppressive IL-10 Producing CD4 + T Cells Gavin M. Mason, Sarah Jackson, Georgina Okecha, Emma Poole, J. G. Patrick Sissons, John Sinclair,
Central tolerance. Mechanisms of Immune Tolerance. Regulation of the T cell response
 Immunoregulation: A balance between activation and suppression that achieves an efficient immune response without damaging the host. Mechanisms of Immune Tolerance ACTIVATION (immunity) SUPPRESSION (tolerance)
Immunoregulation: A balance between activation and suppression that achieves an efficient immune response without damaging the host. Mechanisms of Immune Tolerance ACTIVATION (immunity) SUPPRESSION (tolerance)
Mechanisms of Immune Tolerance
 Immunoregulation: A balance between activation and suppression that achieves an efficient immune response without damaging the host. ACTIVATION (immunity) SUPPRESSION (tolerance) Autoimmunity Immunodeficiency
Immunoregulation: A balance between activation and suppression that achieves an efficient immune response without damaging the host. ACTIVATION (immunity) SUPPRESSION (tolerance) Autoimmunity Immunodeficiency
CELL BIOLOGY - CLUTCH CH THE IMMUNE SYSTEM.
 !! www.clutchprep.com CONCEPT: OVERVIEW OF HOST DEFENSES The human body contains three lines of against infectious agents (pathogens) 1. Mechanical and chemical boundaries (part of the innate immune system)
!! www.clutchprep.com CONCEPT: OVERVIEW OF HOST DEFENSES The human body contains three lines of against infectious agents (pathogens) 1. Mechanical and chemical boundaries (part of the innate immune system)
Haploidentical Transplantation today: and the alternatives
 Haploidentical Transplantation today: and the alternatives Daniel Weisdorf MD University of Minnesota February, 2013 No matched sib: where to look? URD donor requires close HLA matching and 3-12 weeks
Haploidentical Transplantation today: and the alternatives Daniel Weisdorf MD University of Minnesota February, 2013 No matched sib: where to look? URD donor requires close HLA matching and 3-12 weeks
Scott Abrams, Ph.D. Professor of Oncology, x4375 Kuby Immunology SEVENTH EDITION
 Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 13 Effector Responses: Cell- and Antibody-Mediated Immunity Copyright 2013 by W. H.
Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 13 Effector Responses: Cell- and Antibody-Mediated Immunity Copyright 2013 by W. H.
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Chapter 22: The Lymphatic System and Immunity
 Bio40C schedule Lecture Immune system Lab Quiz 2 this week; bring a scantron! Study guide on my website (see lab assignments) Extra credit Critical thinking questions at end of chapters 5 pts/chapter Due
Bio40C schedule Lecture Immune system Lab Quiz 2 this week; bring a scantron! Study guide on my website (see lab assignments) Extra credit Critical thinking questions at end of chapters 5 pts/chapter Due
Trends in Hematopoietic Cell Transplantation. AAMAC Patient Education Day Oct 2014
 Trends in Hematopoietic Cell Transplantation AAMAC Patient Education Day Oct 2014 Objectives Review the principles behind allogeneic stem cell transplantation Outline the process of transplant, some of
Trends in Hematopoietic Cell Transplantation AAMAC Patient Education Day Oct 2014 Objectives Review the principles behind allogeneic stem cell transplantation Outline the process of transplant, some of
ATA129 for Epstein-Barr virusassociated. lymphoproliferative disorder
 March 2017 Horizon Scanning Research & Intelligence Centre ATA129 for Epstein-Barr virusassociated post-transplant lymphoproliferative disorder NIHR HSRIC ID: 10876 Lay summary ATA129 is a new treatment
March 2017 Horizon Scanning Research & Intelligence Centre ATA129 for Epstein-Barr virusassociated post-transplant lymphoproliferative disorder NIHR HSRIC ID: 10876 Lay summary ATA129 is a new treatment
Translating EBV Immunology from Bench to Bedside: Somnium Animadverto A Dream Realized
 Translating EBV Immunology from Bench to Bedside: Somnium Animadverto A Dream Realized Epstein-Barr Virus Human herpesvirus 90% population infected Associated with many other cancers latent infection.persists
Translating EBV Immunology from Bench to Bedside: Somnium Animadverto A Dream Realized Epstein-Barr Virus Human herpesvirus 90% population infected Associated with many other cancers latent infection.persists
