IN 1988, Engstrom and Holland1 reported
|
|
|
- Barry Hutchinson
- 5 years ago
- Views:
Transcription
1 CLINICAL SCIENCES Chronic Varicella-zoster Virus Epithelial Keratitis in Patients With Acquired Immunodeficiency Syndrome Kenneth C. Chern, MD; Diana Conrad, MBBS, FRACO; Gary N. Holland, MD; Douglas S. Holsclaw, MD; Lee K. Schwartz, MD; Todd P. Margolis, MD, PhD Objective: To characterize further a chronic epithelial keratitis caused by varicella-zoster virus infection in patients with acquired immunodeficiency syndrome (AIDS). Methods: Patients with AIDS and chronic epithelial keratitis associated with varicella-zoster virus from 3 institutions were identified. Patient records were reviewed retrospectively for the following data: medical and demographic characteristics, techniques of diagnosis, physical findings, course, response to treatment, and outcome. Results: Sixteen patients were studied. CD4 + T- lymphocyte cell counts were available in 11 patients, with a median of /L (range, /L ). Two patients had no history of a zosteriform rash. In the remaining patients, the interval between rash and keratitis ranged from 0 days to 6 years. In all cases, the keratitis was chronic and characterized by gray, elevated, dendriform epithelial lesions that stained variably with fluorescein and rose bengal. The peripheral and midperipheral cornea was most commonly affected, and, in 13 of the 16 patients, the lesions crossed the limbus. Pain was a prominent feature, occurring in 12 of 16 patients. In 9 of 12 patients tested, varicella-zoster virus was identified by culture, direct fluorescent antibody testing, polymerase chain reaction testing, or a combination of these studies, with direct fluorescent antibody testing (6 of 8 positive results) and polymerase chain reaction testing (3 of 3 positive results) appearing to be the most sensitive. Response to antiviral medication was variable. Conclusions: In patients with AIDS, varicella-zoster virus may cause a chronic infection of the corneal epithelium. The keratitis is characterized by dendriform lesions, prolonged course, and frequently by extreme pain. It can occur without an associated dermatitis. Arch Ophthalmol. 1998;116: From The Francis I. Proctor Foundation and Department of Ophthalmology, University of California San Francisco Medical Center (Drs Chern, Holsclaw, and Margolis and Ms Conrad), the University of California Los Angeles Ocular Inflammatory Disease Center, the Jules Stein Eye Institute, Department of Ophthalmology, University of California Los Angeles School of Medicine (Dr Holland), and the Mount Zion Hospital, San Francisco (Dr Schwartz). IN 1988, Engstrom and Holland1 reported a case of chronic varicellazoster virus (VZV) keratitis that occurred in a patient with acquired immunodeficiency syndrome (AIDS). The keratitis was characterized by dendriform epithelial lesions and underlying anterior stromal haze. Varicella-zoster virus was cultured from corneal scraping, and the keratitis responded to topical acyclovir ointment therapy, thus distinguishing this form of VZV keratitis from the late pseudodendrites or mucus plaque keratopathy that has been described as a late complication of herpes zoster ophthalmicus. We have since examined 16 patients with AIDS who developed chronic epithelial dendriform keratitis in which VZV was the likely cause of the keratitis. In many of the patients, the clinical findings resemble those described by Engstrom and Holland and differ from previous descriptions of the acute and chronic corneal epithelial manifestations of VZV infection in immunecompetent patients. In this report, we further describe the chronic dendriform keratitis associated with VZV in patients with AIDS. RESULTS The clinical and laboratory features of 16 patients with AIDS and chronic epithelial keratitis associated with VZV are summarized in Table 1. All patients were men, ranging in age from 25 to 65 years (median, 36 years). CD4 + T-lymphocyte cell counts were available in 11 patients and ranged from 0 to /L (median, /L). There was a history of VZV infection in 15 of the 16 patients. Fourteen patients had cutaneous herpes zoster. Eight patients had herpes zoster ophthalmicus that began between 1 and 3 months before development of the keratitis. One patient had an episode of herpes zoster ophthalmicus 6 years before keratitis. In 1 additional patient, the onset of dendriform keratitis occurred concurrently with active herpes zoster ophthalmicus. Two patients had thoracic herpes zoster preceding the keratitis by 1 month and 18 months. One patient had primary VZV infection (chickenpox) 8 months before developing the keratitis. Two patients had no history of zosteriform rash. Two patients, 1 with and 1 without a his- 1011
2 PATIENTS AND METHODS We retrospectively reviewed the clinical records of 16 patients with AIDS and chronic VZV keratitis at 3 institutions. Patients were included if they had documented AIDS, chronic dendriform epithelial keratitis, and either dermatomal zoster within 6 months or laboratory evidence of VZV in corneal epithelial scrapings. Symptoms and signs at initial evaluation, treatment, diagnostic tests, course, and outcome were studied. REPRESENTATIVE CASE REPORTS Patient 2 A 35-year-old man with AIDS (CD4 + T-lymphocyte cell count, /L) developed progressive outer retinal necrosis syndrome of the right eye. He was treated with intravenous (IV) acyclovir and then received oral acyclovir. Two months later, he noted a foreign-body sensation in the left eye. Pseudodendrites present on the left cornea persisted for the next 5 months, despite therapy with topical trifluridine and IV acyclovir. He complained of chronic burning pain of the left eye that was unaffected by cycloplegia or oral amitriptyline hydrochloride, but completely relieved by topical proparacaine hydrochloride. He had no history of dermatomal herpes zoster. Examination of the left eye revealed multiple elevated, gray corneal pseudodendrites that crossed the limbus and stained well with rose bengal, but poorly with fluorescein dye (Figure 1, A). There was no inflammation in the anterior chamber or vitreous. Combined antiviral therapy (IV acyclovir and either topical trifluridine, topical vidarabine, or topical acyclovir) was ineffective in resolving the signs or symptoms. All antiviral drug therapy was stopped for 2 days, and the corneal lesions were scraped and cultured. Cytological examination revealed multinucleated giant cells and direct fluorescent antibody staining was positive for VZV antigen. Viral cultures were positive for VZV. Herpes simplex virus (HSV) was not detected with either direct fluorescent antibody staining or culture. Six months after the onset of the epithelial keratitis, therapy with oral sorivudine, 40 mg/d, was started. Within 10 days, the patient noted marked relief in symptoms and resolution of the epithelial lesions with a faint residual stromal haze contiguous with the limbus with no intervening clear zone. On day 17 of therapy with sorivudine, the epithelial pseudodendrites in the left eye recurred (Figure 1, B). By day 29 of sorivudine therapy, the pain had returned and multiple pseudodendrites were present on the left cornea. To control pain, Hess drops (0.5% cocaine and 3% epinephrine in a 2% boric acid solution) were administered every 4 to 6 hours with oral narcotics. Neither topical trifluridine, oral acyclovir, topical 10% acetylcysteine, nor an increase in the dose of oral sorivudine to 80 mg/d had any apparent therapeutic benefit. The patient died 6 weeks later. Patient 4 A 35-year-old man with AIDS (CD4 + T-lymphocyte cell count, /L) developed decreased vision, irritation, and redness of his right eye. One month before, he had a thoracic rash of unknown cause, but no recent facial dermatitis. On examination, the bulbar conjunctiva of the right eye was congested, most notably temporal to the limbus. Multiple, gray, raised dendriform lesions of the corneal epithelium stained poorly with fluorescein but well with rose bengal. There was a faint haze in the temporal corneal stroma, extending from the limbus with no intervening clear zone. Corneal sensation was normal except over the region of corneal stromal haze, where sensation was moderately decreased. The pseudodendrites were débrided, and tissue samples sent for laboratory analysis. Giemsa staining revealed multinucleated giant cells, direct immunofluorescence test result was negative for HSV antigen, but tory of dermatomal herpes zoster, had progressive outer retinal necrosis syndrome 3 and 8 weeks before developing the dendriform keratitis. The corneal epithelial lesions were usually multiple, elevated, gray dendriform in pattern and most commonly seen in the corneal periphery and midperiphery (Figure 3). The number and distribution of lesions changed with time. In 13 of the 16 patients, the corneal epithelial lesions were observed to cross the limbus on at least 1 examination. The lesions stained variably with fluorescein (Figure 4) and rose bengal, but, in most patients, staining with rose bengal was more prominent. There was variable loss of corneal sensation in 8 patients; 2 patients had normal corneal sensation. The keratitis was chronic in all 16 patients, persisting for 5 weeks to 14 months from initial examination to resolution or unavailability for follow-up. In 10 patients, there was an associated stromal keratitis. Eight of these patients had a faint stromal haze contiguous with the limbus without an intervening lucent area and best visualized with retroillumination. In all patients, the stromal haze was present in the quadrant corresponding to the epithelial lesions. One patient had mild stromal haze and corneal edema. An additional patient developed subepithelial infiltrates. In 12 of the 16 patients, pain was an important management issue. Corneal pain was variably described as a foreign-body sensation, reminiscent of a paper cut, or severe burning. For the 7 patients in whom the effect of topical anesthetics on the pain was documented, the anesthetic provided relief in all cases. The pain was difficult to control in 3 patients, who required systemic narcotics (2 patients), chronic topical anesthetic drops (3 patients), and retrobulbar alcohol (1 patient). Varicella-zoster virus was identified in the corneal epithelium of 9 patients by 1 or more of the following techniques: direct fluorescent antibody staining for VZV antigen (6 patients); viral culture of VZV (2 patients); and polymerase chain reaction amplification of VZV DNA (3 patients). A Giemsa stain of the epithelial scraping also demonstrated multinucleated giant cells in 3 of these 9 patients. All 6 clinical samples that had positive results for VZV antigen by direct fluorescent antibody staining had negative results by direct fluorescent antibody stain- 1012
3 positive for VZV antigen, and viral cultures were negative for both VZV and HSV. The patient was treated with oral acyclovir, 800 mg 5 times daily, and topical trifluridine every 3 hours. After 9 days of therapy, his symptoms had improved markedly and the corneal pseudodendrites had resolved; however, the corneal stromal haze had worsened, and there was now a mild anterior chamber inflammatory reaction. With the addition of topical 1% prednisolone acetate, the corneal haze promptly cleared. The trifluridine was discontinued, and the patient remained asymptomatic while receiving the oral acyclovir and topical corticosteroid drops for the next 7 weeks. He discontinued the acyclovir for financial reasons, and the pseudodendrites recurred 7 days later. Acyclovir and trifluridine drops were restarted, and, within 2 weeks, the pseudodendrites had disappeared. The patient remained free of active corneal lesions for the next month and was then unavailable for follow-up. Patient 6 A 38-year-old man with AIDS (CD4 + T-lymphocyte cell count, /L) came in with acute onset of right herpes zoster ophthalmicus and was admitted for IV acyclovir therapy. Ophthalmologic examination of the right eye revealed vesicular lesions around the eyelids, conjunctival injection and chemosis, punctate defects of the corneal epithelium, and small corneal pseudodendrites. Topical trifluridine was added to the therapy. Within 5 days, all the skin lesions had crusted over and the pseudodendrites had cleared. Antiviral therapy was discontinued shortly thereafter. During the next 2 months, the patient had 2 recurrences of corneal pseudodendrites. Each episode promptly resolved following therapy with oral acyclovir and topical trifluridine. He returned 4 months later with severe right eye pain and pseudodendrites over the superior third of the cornea. The pseudodendrites crossed the limbus and extended onto the bulbar conjunctiva. The pseudodendrites were gray, elevated, and stained poorly with fluorescein but extremely well with rose bengal (Figure 2, A). There was no loss of corneal sensation. The pseudodendrites were débrided, and tissue samples were sent for viral culture and immunofluorescence, both of which were negative for VZV and HSV. Despite treatment with acyclovir and trifluridine, the pain and pseudodendrites slowly worsened. Cycloplegia, topical 0.1% diclofenac sodium, systemic amitriptyline, topical 1% prednisolone acetate, and topical 3% acyclovir ointment failed to relieve the pain or have any apparent effect on the pseudodendrites. The pain became excruciating, and the patient began having suicidal ideation. The patient was admitted to the hospital for IV acyclovir therapy, 800 mg every 8 hours, with moderate, but incomplete resolution of his corneal disease after 2 weeks of therapy (Figure 2, B). Treatment was changed to IV foscarnet sodium, 3.7 g every 8 hours, with dramatic resolution of the pain and pseudodendrites (Figure 2, C). After 17 days of therapy, however, the foscarnet was discontinued because of unexplained fevers, elevated liver function test results, and granulocytopenia. Oral acyclovir, 800 mg 5 times daily, was resumed, but within 3 weeks the pseudodendrites had returned much more extensively than before (Figure 2, D). Recombinant human interferon alfa-2a was administered topically 4 times daily, but without improvement in signs or symptoms. All therapy was stopped for 24 hours, and the pseudodendrites were scraped for laboratory examination. Direct immunofluorescent antibody staining of the tissue was positive for VZV antigen and negative for HSV antigen. Giemsa staining of the tissue revealed multinucleated giant cells. The patient s pain became worse after debridement, and within 1 week the pseudodendrites had returned. Topical 10% acetylcysteine and oral sorivudine, 40 mg/d, had no obvious effect on signs or symptoms of the persistent keratitis. Pain control was achieved with systemic morphine sulfate and topical Hess drops until the patient died 14 months after the initial onset of the pseudodendrites. ing for HSV antigen. Both clinical samples that were positive for VZV by culture had negative results for HSV. All samples that had positive results for VZV DNA by polymerase chain reaction techniques had negative results for HSV and cytomegalovirus DNA. In 7 patients, the diagnosis was made clinically on the basis of a recent VZV dermatitis (within 3 months) and the findings of the characteristic keratitis, as described above. Herpes simplex virus was an unlikely cause of keratitis in these patients given the elevated and atypical appearance of the epithelial lesions, which lacked terminal bulbs and were not associated with ulceration. Furthermore, viral cultures of the corneal epithelium performed for 3 of the 7 eyes were negative for HSV. All 16 patients required prolonged courses of multiple antiviral medications for control of the keratitis. In 6 patients, the keratitis recurred when antiviral medications were discontinued. Seven patients had clinical features suggestive of drug resistance. Patient 2 failed to respond to IV acyclovir, topical acyclovir, vidarabine, and trifluridine. Furthermore, he had only a transient response to oral sorivudine. Patient 3 developed thoracic herpes zoster while receiving IV acyclovir. In vitro antiviral drug testing of this isolate revealed resistance to acyclovir. Patient 5 developed recurrent dendriform keratitis while taking oral acyclovir. Patient 6 developed recurrent pseudodendrites that failed to respond to oral acyclovir or sorivudine. This patient s keratitis responded partially to IV acyclovir and fully to foscarnet. Patient 10 had recurrence of dendriform lesions when famciclovir was discontinued. The lesions cleared completely with IV foscarnet. Patient 11 developed pseudodendrites while receiving maintenance IV foscarnet therapy for cytomegalovirus retinitis and had only a partial response to oral acyclovir. Patient 13 developed pseudodendrites that failed to respond to acyclovir or foscarnet. COMMENT We present a retrospective review of 16 patients with AIDS and low CD4 + T-lymphocyte cell counts who developed an unusual form of chronic epithelial keratitis, characterized by dendriform corneal lesions, pain, and variable clinical response to antiviral medications. 1013
4 A B Figure 1. Multiple elevated dendriform corneal epithelial lesions in patient 2 (A) highlighted by rose bengal staining. Both viral culture and direct fluorescent antibody staining were positive for varicella-zoster virus. Recurrent dendriform lesions (B) present while patient receiving oral sorivudine therapy. A B C Figure 2. Pseudodendrites on the right superior cornea and limbus in patient 6 (A) 4 months after an episode of herpes zoster ophthalmicus. Partial resolution of the lesions (B) was achieved with intravenous acyclovir sodium therapy. Complete disappearance (C) of the epithelial lesions achieved with treatment using intravenous foscarnet sodium. Fulminant recurrence of the pseudodendrites (D) 3 weeks following discontinuation of foscarnet treatment. D Laboratory evidence implicates VZV as the cause of this disorder. Direct fluorescent antibody staining and polymerase chain reaction testing confirmed the presence of VZV in 8 patients. In 2 of 9 patients in whom viral cultures of corneal epithelial scrapings were taken, VZV was isolated. Our inability to detect VZV in the remaining 7 patients by culture is not unusual, since VZV is highly cell associated and is difficult to culture, especially with the extremely small samples procured from corneal scrapings. A recent report 2 of keratitis caused by cytomegalovirus in a patient with AIDS showed that cytomegalovirus can also cause chronic dendriform keratitis. We did not consider cytomegalovirus to be a likely cause of the keratitis in our patients for several reasons. First, many of the patients had a recent history of VZV dermatitis. Second, in 9 of 12 patients, direct fluorescent antibody staining, polymerase chain reaction testing, or viral culture confirmed the presence of VZV in the corneal epithelium. Third, many of our patients responded to topical acyclovir, a drug with little activity against cytomegalovirus. Finally, although we did not specifically culture for cytomegalovirus in our epithelial 1014
5 Table 1. Clinical and Laboratory Characteristics of Patients With Chronic Varicella-zoster Virus (VZV) Epithelial Keratitis* Patient No./ Age, y CD4 + T- Lymphocyte Count, 10 9 /L Affected Eye Previous VZV Infection 1/53 0 OD Right V2 zoster 7 wk before, PORN syndrome OS 3 wk before 2/ OS PORN syndrome OS 8 wk before 3/ OD Thoracic VZV 1 mo before 4/ OD Primary zoster infection (chickenpox) 8 mo before 5/ OD V1, V2 zoster 4 wk before 6/ OD V1 zoster 6 wk before Cytologic Examination Findings Viral Identification Techniques DFA Staining for VZV Culture for VZV Results of PCR for VZV DNA Duration of Keratitis Treatment: Outcome ND ND ND ND 3 mo Oral acyclovir, trifluridine: resolved Multinucleated giant cells Positive Positive ND 6 mo Acyclovir: unresponsive Vidarabine: unresponsive Sorivudine: transient response ND Positive Negative ND 6 mo Oral acyclovir: resolved, Multinucleated Positive Negative ND 9 wk Oral acyclovir, trifluridine: resolved, giant cells ND ND ND ND 7 wk Oral and topical acyclovir: unresponsive Interferon alfa-2a: unresponsive IV acyclovir: partial response Multinucleated giant cells Positive Negative ND 14 mo Oral acyclovir, trifluridine: resolved, Sorivudine: unresponsive Interferon alfa-2a: unresponsive IV acyclovir: partial response Foscarnet: resolved 7/33 NA OU Thoracic zoster ND ND Positive ND 5 wk Oral acyclovir: resolved 18 mo before 8/41 NA OS V1 zoster ND Positive Negative ND 3 mo Oral acyclovir, trifluridine: resolved 9/ OD V1 zoster 5 mo before ND ND Negative ND 5 mo Vidarabine ointment, IV foscarnet: lost to follow-up 10/39 NA OD V1 zoster 4 mo before ND ND Negative ND 4 mo Acyclovir ointment: unresponsive Famciclovir: resolved, recurrence when discontinued IV foscarnet: resolved 11/43 0 OS V1 zoster 6 y before ND Positive ND Positive 3 mo Foscarnet: unresponsive Oral acyclovir: partial response 12/ OS None ND Negative ND Positive 12 mo Oral acyclovir, trifluridine: resolved, 13/29 NA OS V1 zoster ND Negative Negative ND 7 mo IV acyclovir, foscarnet, Trifluridine: partial response 14/38 NA OD V1 zoster ND ND ND ND 8 mo Oral acyclovir: resolved, 15/ OD V1 zoster ND ND ND Positive 3 mo Oral acyclovir: unresponsive Vidarabine: unresponsive Acyclovir ointment: resolved 16/ OD V1 zoster at initial examination ND ND ND ND 3 mo Oral and topical acyclovir: resolved *DFA indicates direct fluorescent antibody; PCR, polymerase chain reaction; V1, distribution of the first division of the fifth cranial nerve; V2, distribution of the second division of the fifth cranial nerve; NA, data not available; ND, test not done; PORN, progressive outer retinal necrosis; and IV, intravenous. This patient required narcotics for pain control. This patient developed acyclovir-resistant thoracic zoster. This patient required retrobulbar alcohol for pain. samples, we did not detect cytomegalovirus DNA by polymerase chain reaction in any of the 3 patients tested. The corneal epithelial lesions described in this study have features that distinguish them from both acute and chronic forms of VZV keratitis that have been described previously (Table 2). The acute epithelial dendriform lesions of VZV in immune-competent patients have been described 3-5 as small, fine, elevated intraepithelial lesions that occur several days following a rash and are accompanied by catarrhal conjunctivitis. These early dendriform lesions are self-limited with resolution within 6 days, found most frequently in the corneal periphery, and associated with loss of corneal sensation. Varicellazoster virus can be cultured from these lesions, but only within the first 48 to 72 hours after onset of cutaneous eruption. Superficial stromal infiltration can be seen with 1015
6 Figure 3. Unstained, gray corneal epithelial lesions in patient 1. Figure 4. Corneal epithelial lesions in patient 12, which, unlike a dendrite caused by herpes simplex virus, are elevated without epithelial ulceration and lack terminal bulbs (fluorescein stain). Table 2. Comparison of Epithelial Dendritic Lesions Associated With Varicella-zoster Virus Feature Acute Dendrite Lesion* Late Pseudodendrite Lesion Chronic Infectious Lesion in Patients With AIDS Average age at keratitis onset y y 35 y Interval between zosteriform 2-3 d 2 wk-2 y 0-6 y rash and corneal lesions Appearance of dendritic lesion Small, fine, elevated stellate intraepithelial lesions Coarse, gray, elevated plaques with blunted ends Multiple, gray, elevated, epithelial lesions Location Peripheral Central or midperipheral Midperipheral and peripheral, crossing limbus Corneal sensation Decreased Decreased in 33% of patients Variable Epithelial staining Poorly with rose bengal and fluorescein Good with rose bengal Variable with rose bengal Stromal keratitis None Diffuse haze Sectoral haze Recoverable virus Yes No Yes Duration 1wk 1-8wk 5wkto14mo Responds to antiviral medications Yes No Yes *Data from Marsh et al. 3 Data from Marsh and Cooper. 6 AIDS indicates acquired immunodeficiency syndrome. In some cases of varicella-zoster virus, there is no history of rash. In acute dendrite lesions, virus is recoverable within the first 24 to 48 hours. resolution of the dendrites. Although our patients had replicating virus, their lesions differed from those of acute VZV in several ways. First, unlike the small, fine lesions that we have seen and have been described by Marsh et al 3 and others, 4,5 most of the lesions described herein were thick and discontinuous with blunt ends, bearing little resemblance to the Medusa-like lesions described by Pavan-Langston and McCulley. 4 Second, in 13 of the 16 affected eyes, the lesions crossed the corneal limbus. Third, the lesions in our patients were chronic, persisting for weeks to months, and, in many cases, first appeared months after a zosteriform rash. Chronic epithelial pseudodendrites, or mucus plaques, as described by Marsh and Cooper 6 and others 5,7 can occur from 7 days to 2 years following herpes zoster ophthalmicus. These transitory plaques are gray, elevated, linear or branching, and stain well with rose bengal and poorly with fluorescein. Abnormal accumulation of mucus, possibly a consequence of poor tear film quality, has been postulated to be the mechanism for the formation of these plaques, which frequently respond to topical mucolytics. Varicella-zoster virus has not been cultured from these lesions, and VZV antigen has not been detected. These lesions tend not to respond to antiviral medications. The clinical appearance of the dendriform lesions in our patients resembled in some ways that of mucus plaques; however, in contrast to the late lesions described by Marsh and Cooper 6 and others, 5,7 the epithelial lesions in our patients crossed the limbus, were associated with pain, and, in many cases, had either recoverable virus or VZV antigen. In addition, the epithelial lesions in many of our patients responded to antiviral medications, then worsened or recurred when the antiviral medications were discontinued. Mucolytics had no discernible effect on the epithelial lesions in our patients. The dendriform lesions described herein may therefore more closely resemble those described by Piebenga and Laibson 7 and more recently by Pavan-Langston et al. 8 In that study, 8 these lesions had a positive result for VZV DNA by polymerase chain reaction testing and responded variably to topical antiviral medications. To date, however, in patients without AIDS, we have been unable to amplify by polymerase chain reaction techniques VZV DNA from chronic mucus plaques that resemble lesions described by Marsh and Cooper. 6 A key feature of the epithelial lesions reported herein was their chronicity. Other VZV infections in patients with 1016
7 human immunodeficiency virus (HIV) have shown this propensity to chronicity. Chronic forms of herpes zoster dermatitis resulting in hyperkeratotic verrucous lesions have been recognized These lesions are thought to be caused by ongoing viral replication, possibly modified by drug resistance, 12 or be a limited form of lytic infection. 13 It is likely that the same mechanisms contribute to the chronic nature of the disease in our patients. Five of the 16 patients described herein developed keratitis without a preceding history of facial herpes zoster dermatitis, although 2 patients had prior thoracic herpes zoster and 1 patient had primary systemic herpes zoster. The development of VZV disease without skin eruption has been termed zoster sine herpete Varicellazoster virus ocular disease without skin manifestations has been described in both immunosuppressed and immunocompetent patients, including VZV iritis, 17 keratitis, 18 and VZV necrotizing retinitis. 19,20 The cases that presented sine herpete in this series suggest that it is important to consider VZV in the differential diagnosis of chronic dendriform keratitis in patients with HIV disease even in the absence of skin lesions. Pain was a prominent feature of the disease in 12 of the 16 patients. Since the pain was rapidly relieved by topical anesthesia, but not by tricyclic antidepressants, it was unlikely to be postherpetic neuralgia. The severity of the pain is exemplified by the 2 patients in whom systemic narcotics and chronic topical anesthetic drops were required for relief. An additional patient required a retrobulbar injection of alcohol to control the pain. All 4 patients without pain had preceding herpes zoster dermatitis in the distribution of the first division of the trigeminal nerve and loss of corneal sensation. Treatment of the keratitis was difficult. Based on our experience, we would recommend initial treatment with oral or topical acyclovir or trifluridine. In the event of treatment failure, alternative antiviral drugs, such as oral famciclovir, should be used. For thymidine kinase deficient strains of VZV, foscarnet or cidofovir, which do not depend on thymidine kinase for activation, should be considered. Although others 21 have reported that topical interferon alfa-2a may modify the severity of VZV in immunosuppressed patients, we found this treatment to have minimal effect in the 2 patients treated. As with other viral infections in patients with AIDS and low CD4 + T- lymphocyte cell counts, antiviral treatment is likely to be prolonged. In view of the recent success of Pavan- Langston et al 8 in using vidarabine for the treatment of 2 cases of late pseudodendrites, this drug should be considered. Varicella-zoster keratitis in HIV-infected patients should be differentiated from HSV keratitis, which has also been described in this population. 22,23 Perhaps more importantly, this disease must be differentiated from dry eye and exposure keratopathy, both of which are seen with high frequency in patients with AIDS who have low CD4 + T- lymphocyte cell counts. We have found the use of rose bengal to be valuable in helping to differentiate these entities. In summary, we believe that there may be forms of epithelial dendriform lesions associated with VZV that are distinct from the classic acute dendrites and late pseudodendrites described by Marsh and Cooper. 24 In our patients, we have found the chronic, dendriform epithelial lesions to have recoverable virus. Host immunosuppression and viral pathogenicity may play a role in the development and persistence of these lesions. Accepted for publication May 4, Supported, in part, by Research to Prevent Blindness Inc (New York, NY) Lew Wasserman Merit Award (Drs Holland and Margolis), the Ralph and Sophie Heintz Laboratory Fund, San Francisco, Calif (Dr Margolis), the Heed Ophthalmic Foundation, Chicago, Ill (Dr Chern), and by grant EY02162 from the National Eye Institute, National Institutes of Health, Bethesda, Md (Dr Margolis). Reprints: Todd P. Margolis, MD, PhD, Francis I. Proctor Foundation, Box 0944, University of California San Francisco Medical Center, San Francisco, CA ( tpms@itsa.ucsf.edu). REFERENCES 1. Engstrom RE, Holland GN. Chronic herpes zoster virus keratitis associated with the acquired immunodeficiency syndrome. Am J Ophthalmol. 1988;105: Wilhelmus KR, Font RL, Lehmann RP, Cernoch PL. Cytomegalovirus keratitis in acquired immunodeficiency syndrome. Arch Ophthalmol. 1996;114: Marsh RJ, Fraunfelder FT, McGill JI. Herpetic corneal epithelial disease. Arch Ophthalmol. 1976;94: Pavan-Langston D, McCulley JP. Herpes zoster dendritic keratitis. Arch Ophthalmol. 1973;89: Liesegang TJ. Corneal complications from herpes zoster ophthalmicus. Ophthalmology. 1985;92: Marsh RJ, Cooper M. Ophthalmic zoster: mucous plaque keratitis. Br J Ophthalmol. 1987;71: Piebenga LW, Laibson PR. Dendritic lesions in herpes zoster ophthalmicus. Arch Ophthalmol. 1973;90: Pavan-Langston D, Yamamoto S, Dunkel EC. Delayed herpes zoster pseudodendrites: polymerase chain reaction detection of viral DNA and a role for antiviral therapy. Arch Ophthalmol. 1995;113: Vaughan Jones SA, McGibbon DH, Bradbeer CS. Chronic verrucous varicellazoster infection in a patient with AIDS. Clin Exp Dermatol. 1994;19: Hoppenjans WB, Bibler MR, Orme RL, Solinger AM. Prolonged cutaneous herpes zoster in acquired immunodeficiency syndrome. Arch Dermatol. 1990;126: LeBoit PE, Limova M, Yen TS, et al. Chronic verrucous varicella-zoster virus infection in patients with the acquired immunodeficiency syndrome (AIDS): histologic and molecular biologic findings. Am J Dermatopathol. 1992;14: Jacobson MA, Berger TG, Fikrig S, et al. Acyclovir-resistant varicella zoster virus infection after chronic oral acyclovir therapy in patients with the acquired immunodeficiency syndrome (AIDS). Ann Intern Med. 1990;112: Nikkels AF, Rentier B, Pierard GE. Chronic varicella-zoster virus skin lesions in patients with human immunodeficiency virus are related to decreased expression of ge and gb. J Infect Dis. 1997;176: Lewis G. Zoster sine herpete. BMJ. 1958;2: Snoeck R, Gerard M, Sadzot-Delvaux C, et al. Meningoradiculoneuritis due to acyclovir-resistant varicella zoster virus in an acquired immune deficiency syndrome patient. J Med Virol. 1994;42: Gilden DH, Dueland AN, Devlin ME, Mahalingam R, Cohrs R. Varicella-zoster virus reactivation without rash. J Infect Dis. 1992;166(suppl 1):S30-S Schwab IR. Herpes zoster sine herpete. Ophthalmology. 1997;104: Silverstein BE, Chandler D, Neger R, Margolis TP. Disciform keratitis: a case of herpes zoster sine herpete. Am J Ophthalmol. 1997;123: Margolis TP, Lowder CY, Holland GN, et al. Varicella-zoster virus retinitis in patients with the acquired immunodeficiency syndrome. Am J Ophthalmol. 1991; 112: Stavrou P, Mitchell SM, Fox JD, Hope-Ross MW, Murray PI. Detection of varicellazoster virus DNA in ocular samples from patients with uveitis but no cutaneous eruption. Eye. 1994;8: Winston DJ, Eron LJ, Ho M, et al. Recombinant interferon alpha-2a for treatment of herpes zoster in immunosuppressed patients with cancer. Am J Med. 1988;85: Young TL, Robin JB, Holland GN, et al. Herpes simplex keratitis in patients with acquired immune deficiency syndrome. Ophthalmology. 1989;96: Hodge WG, Margolis TP. Herpes simplex virus keratitis among patients who are positive or negative for human immunodeficiency virus: an epidemiologic study. Ophthalmology. 1997;104: Marsh RJ, Cooper M. Ophthalmic herpes zoster. Eye. 1993;7:
Varicella-Zoster Virus Epithelial Keratitis in Herpes Zoster Ophthalmicus
 Varicella-Zoster Virus Epithelial Keratitis in Herpes Zoster Ophthalmicus Helena M. Tabery Varicella-Zoster Virus Epithelial Keratitis in Herpes Zoster Ophthalmicus In Vivo Morphology in the Human Cornea
Varicella-Zoster Virus Epithelial Keratitis in Herpes Zoster Ophthalmicus Helena M. Tabery Varicella-Zoster Virus Epithelial Keratitis in Herpes Zoster Ophthalmicus In Vivo Morphology in the Human Cornea
Condition: Herpes Simplex Keratitis
 Condition: Herpes Simplex Keratitis Description: Herpes simplex infection is very common but usually remains latent. When the virus is reactivated it travels along the trigeminal nerve to cause local infection
Condition: Herpes Simplex Keratitis Description: Herpes simplex infection is very common but usually remains latent. When the virus is reactivated it travels along the trigeminal nerve to cause local infection
Herpes Zoster Ophtalmicus in a HIV positive patient: A Case Report
 ISPUB.COM The Internet Journal of Neurology Volume 9 Number 2 Herpes Zoster Ophtalmicus in a HIV positive patient: A Case Report G Lopez Bejerano, Y Graza Fernandez Citation G Lopez Bejerano, Y Graza Fernandez..
ISPUB.COM The Internet Journal of Neurology Volume 9 Number 2 Herpes Zoster Ophtalmicus in a HIV positive patient: A Case Report G Lopez Bejerano, Y Graza Fernandez Citation G Lopez Bejerano, Y Graza Fernandez..
Q: (picture of typical dendrite) What is the differential diagnosis and describe this entity? How would you treat and why?
 Q: (picture of typical dendrite) What is the differential diagnosis and describe this entity? How would you treat and why? Etiology/Risks: Critical symptoms: HSV is transmitted by direct contact of epidermis
Q: (picture of typical dendrite) What is the differential diagnosis and describe this entity? How would you treat and why? Etiology/Risks: Critical symptoms: HSV is transmitted by direct contact of epidermis
Condition: Herpes Zoster Ophthalmicus (HZO)
 Condition: Herpes Zoster Ophthalmicus (HZO) Description: Herpes zoster represents a reactivation of the varicella zoster virus (VZV) which leads to characteristic skin lesions and, in many cases, ocular
Condition: Herpes Zoster Ophthalmicus (HZO) Description: Herpes zoster represents a reactivation of the varicella zoster virus (VZV) which leads to characteristic skin lesions and, in many cases, ocular
Herpetic Eye Disease Jason Duncan, OD, FAAO Diplomate, American Board of Optometry Associate Professor, Southern College of Optometry
 Herpetic Eye Disease Jason Duncan, OD, FAAO Diplomate, American Board of Optometry Associate Professor, Southern College of Optometry I have what?! How to break the news Meet the Herpes Quick virology
Herpetic Eye Disease Jason Duncan, OD, FAAO Diplomate, American Board of Optometry Associate Professor, Southern College of Optometry I have what?! How to break the news Meet the Herpes Quick virology
Learning Objectives:
 Viral keratitis and antivirals Learning Objectives: Recognise and distinguish different types of viral keratitis HSV HZO Adenovirus Discuss the use of antiviral agents in the treatment of herpetic infections
Viral keratitis and antivirals Learning Objectives: Recognise and distinguish different types of viral keratitis HSV HZO Adenovirus Discuss the use of antiviral agents in the treatment of herpetic infections
Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient
 CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
D. 'endritic corneal lesions were considered
 Varicella dendritic keratitis* Anthony B. Nesburn, Adam Bonl,** John Pentelei-Molnar, and Richard Lazaro Atypical dendritic keratitis has been described following herpes zoster infection. This is the first
Varicella dendritic keratitis* Anthony B. Nesburn, Adam Bonl,** John Pentelei-Molnar, and Richard Lazaro Atypical dendritic keratitis has been described following herpes zoster infection. This is the first
H erpes simplex virus infection of the
 Herpes simplex keratitis An experimental study Samuel J. Kimura, Victor Diaz-Bonnet, and Masao Okumoto The incidence of complicated herpes simplex keratitis appears to have increased and the important
Herpes simplex keratitis An experimental study Samuel J. Kimura, Victor Diaz-Bonnet, and Masao Okumoto The incidence of complicated herpes simplex keratitis appears to have increased and the important
CORNEAL DENDRITE. What else do you want to know about this patient? What would be your initial treatment?
 Viral Keratitis CORNEAL DENDRITE What else do you want to know about this patient? What would be your initial treatment? Wilhelmus KR. Antiviral treatment and other therapeutic interventions for herpes
Viral Keratitis CORNEAL DENDRITE What else do you want to know about this patient? What would be your initial treatment? Wilhelmus KR. Antiviral treatment and other therapeutic interventions for herpes
Clinical Profile of Herpes Simplex Keratitis
 K V Raju MS, Jyothi PT MS, Shimna Iqbal MS Clinical Profile of Herpes Simplex Keratitis Original Article Abstract Aims To document the various clinical presentations and to assess the risk factors contributing
K V Raju MS, Jyothi PT MS, Shimna Iqbal MS Clinical Profile of Herpes Simplex Keratitis Original Article Abstract Aims To document the various clinical presentations and to assess the risk factors contributing
Dr Jo-Anne Pon. Dr Sean Every. 8:30-9:25 WS #70: Eye Essentials for GPs 9:35-10:30 WS #80: Eye Essentials for GPs (Repeated)
 Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
UCSF UC San Francisco Previously Published Works
 UCSF UC San Francisco Previously Published Works Title Unilateral Posterior Interstitial Keratitis as a Clinical Presentation of Herpes Simplex Virus Disease. Permalink https://escholarship.org/uc/item/8970f2fq
UCSF UC San Francisco Previously Published Works Title Unilateral Posterior Interstitial Keratitis as a Clinical Presentation of Herpes Simplex Virus Disease. Permalink https://escholarship.org/uc/item/8970f2fq
Herpes zoster. Diagnosis, Complications, Treatment, Prevention 서울대학교병원 FM R2 임하연
 Herpes zoster Diagnosis, Complications, Treatment, Prevention 2018.04.14 서울대학교병원 FM R2 임하연 1 2 Overview reactivation of lat ent VZV along sensory nerve VZV(varicella-zoster virus) Human herpes virus-3
Herpes zoster Diagnosis, Complications, Treatment, Prevention 2018.04.14 서울대학교병원 FM R2 임하연 1 2 Overview reactivation of lat ent VZV along sensory nerve VZV(varicella-zoster virus) Human herpes virus-3
1/3/17. ***Varicella-Zoster Virus*** Herpes DNA virus that causes 2 distinct syndromes
 Nathan Lighthizer, O.D., F.A.A.O. Assistant Dean, Clinical Care Services Director of Continuing Education Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Oklahoma College of Optometry
Nathan Lighthizer, O.D., F.A.A.O. Assistant Dean, Clinical Care Services Director of Continuing Education Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Oklahoma College of Optometry
5/24/17. ***Varicella-Zoster Virus*** Herpes DNA virus that causes 2 distinct syndromes
 Nathan Lighthizer, O.D., F.A.A.O. Assistant Dean, Clinical Care Services Director of Continuing Education Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Oklahoma College of Optometry
Nathan Lighthizer, O.D., F.A.A.O. Assistant Dean, Clinical Care Services Director of Continuing Education Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Oklahoma College of Optometry
Conjunctivitis in Cats
 Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Conjunctivitis in Cats (Inflammation of the Moist Tissues of the Eye) Basics OVERVIEW
Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Conjunctivitis in Cats (Inflammation of the Moist Tissues of the Eye) Basics OVERVIEW
Disease caused by herpes simplex virus
 Recurrence of herpes simplex virus in rabbit eyes: Results of a three-year study Peter R. Laibson and Sidney Kibrick Spontaneous reactivation of herpes simplex virus in rabbit ocular tissue was found on
Recurrence of herpes simplex virus in rabbit eyes: Results of a three-year study Peter R. Laibson and Sidney Kibrick Spontaneous reactivation of herpes simplex virus in rabbit ocular tissue was found on
CORNEAL CONDITIONS CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
Alphaherpesvirinae. Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV)
 Alphaherpesvirinae Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV) HERPES SIMPLEX VIRUS First human herpesvirus discovered (1922) Two serotypes recognised HSV-1 & HSV-2 (1962) HSV polymorphism
Alphaherpesvirinae Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV) HERPES SIMPLEX VIRUS First human herpesvirus discovered (1922) Two serotypes recognised HSV-1 & HSV-2 (1962) HSV polymorphism
a.superficial (adenoid layer).contain lymphoid tissue.
 Conjunctiva Dr. saifalshamarti Anatomy Microscopic: 1.Epithelium (non keratinized,includes goblet cell). 2.Epithelial basement membrane. 3.Stroma : a.superficial (adenoid layer).contain lymphoid tissue.
Conjunctiva Dr. saifalshamarti Anatomy Microscopic: 1.Epithelium (non keratinized,includes goblet cell). 2.Epithelial basement membrane. 3.Stroma : a.superficial (adenoid layer).contain lymphoid tissue.
Herpes simplex virus (HSV) stromal keratitis is the leading infectious cause of corneal blindness in
 Herpes Simplex Epithelial Keratitis and Proposed Treatments Andrea De Souza, OD I. Introduction Author s Bio Dr. Andrea De Souza received her Doctor of Optometry Degree in 2012 from the New England College
Herpes Simplex Epithelial Keratitis and Proposed Treatments Andrea De Souza, OD I. Introduction Author s Bio Dr. Andrea De Souza received her Doctor of Optometry Degree in 2012 from the New England College
Childhood corneal neovascularization
 Miltos Balidis PhD, FEBOphth, ICOphth Sotiria Palioura MD,PhD Childhood corneal neovascularization Opacities Cornea clarity is essential for optimal vision at any age. In childhood, loss of corneal transparency
Miltos Balidis PhD, FEBOphth, ICOphth Sotiria Palioura MD,PhD Childhood corneal neovascularization Opacities Cornea clarity is essential for optimal vision at any age. In childhood, loss of corneal transparency
founder of McDonald s Restaurants
 Press On Nothing in the world can take the place of persistence. Talent will not; nothing is more common than unsuccessful men with talent. Genius will not; unrewarded genius is almost a proverb. Education
Press On Nothing in the world can take the place of persistence. Talent will not; nothing is more common than unsuccessful men with talent. Genius will not; unrewarded genius is almost a proverb. Education
It has been estimated that 90% of individuals
 Famciclovir for Cutaneous Herpesvirus Infections: An Update and Review of New Single-Day Dosing Indications Manju Chacko, MD; Jeffrey M. Weinberg, MD Infections with herpes simplex virus (HSV) types 1
Famciclovir for Cutaneous Herpesvirus Infections: An Update and Review of New Single-Day Dosing Indications Manju Chacko, MD; Jeffrey M. Weinberg, MD Infections with herpes simplex virus (HSV) types 1
Prednisolone-2 I -stearoylglycolate in scleritis
 Brit. j. Ophthal. (1970) 54, 394 Prednisolone- -stearoylglycolate in scleritis S. S. HAYREH* AND P. G. WATSON Scleritis Clinic, Moorfields Eye Hospital, City Road, London, E.C. i Scleritis is one of the
Brit. j. Ophthal. (1970) 54, 394 Prednisolone- -stearoylglycolate in scleritis S. S. HAYREH* AND P. G. WATSON Scleritis Clinic, Moorfields Eye Hospital, City Road, London, E.C. i Scleritis is one of the
Strategies for Anterior Segment Disease Management Mile Brujic, OD, FAAO 1409 Kensington Blvd Bowling Green, OH
 Strategies for Anterior Segment Disease Management Mile Brujic, OD, FAAO 1409 Kensington Blvd Bowling Green, OH 43402 brujic@prodigy.net 419-261-9161 Summary As optometry s scope of practice continues
Strategies for Anterior Segment Disease Management Mile Brujic, OD, FAAO 1409 Kensington Blvd Bowling Green, OH 43402 brujic@prodigy.net 419-261-9161 Summary As optometry s scope of practice continues
8/7/12. Anterior Seg Grand Rounds Case III. New Advances in the Management of Viral Eye Disease. Slit lamp exam: Sign: 68 y.o.
 New Advances in the Management of Viral Eye Disease Anterior Seg Grand Rounds Case III 68 y.o. Caucasian female!! Dr.Paul Karpecki!! Corneal Services and Ocular Disease Research!! Koffler Vision Group
New Advances in the Management of Viral Eye Disease Anterior Seg Grand Rounds Case III 68 y.o. Caucasian female!! Dr.Paul Karpecki!! Corneal Services and Ocular Disease Research!! Koffler Vision Group
8/31/18. ***Varicella-Zoster Virus*** Herpes DNA virus that causes 2 distinct syndromes. Herpes DNA virus that causes 2 distinct syndromes.
 Nate Lighthizer, O.D., F.A.A.O. Assistant Dean, Clinical Care Services Director of Continuing Education Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Oklahoma College of Optometry
Nate Lighthizer, O.D., F.A.A.O. Assistant Dean, Clinical Care Services Director of Continuing Education Chief of Specialty Care Clinics Chief of Electrodiagnostics Clinic Oklahoma College of Optometry
OCULAR HERPES simplex virus
 CLINICAL SCIENCES Oral Acyclovir After Penetrating Keratoplasty for Herpes Simplex Keratitis Fabiana P. Tambasco, MD; Elisabeth J. Cohen, MD; Lien H. Nguyen, MD; Christopher J. Rapuano, MD; Peter R. Laibson,
CLINICAL SCIENCES Oral Acyclovir After Penetrating Keratoplasty for Herpes Simplex Keratitis Fabiana P. Tambasco, MD; Elisabeth J. Cohen, MD; Lien H. Nguyen, MD; Christopher J. Rapuano, MD; Peter R. Laibson,
Early and late stage ocular complications of herpes zoster ophthalmicus in rural South Africa
 Early and late stage ocular complications of herpes zoster ophthalmicus in rural South Africa Erik Schaftenaar, MD 1-3*, Christina Meenken, PhD 4, G. Seerp Baarsma, MD 2,5, James A. McIntyre, FRCOG 3,6,
Early and late stage ocular complications of herpes zoster ophthalmicus in rural South Africa Erik Schaftenaar, MD 1-3*, Christina Meenken, PhD 4, G. Seerp Baarsma, MD 2,5, James A. McIntyre, FRCOG 3,6,
Double-masked trial of topical acyclovir and steroids
 542 Department of Clinical Ophthalmology, Moorfields Eye Hospital, City Road, London EC1V 2PD R J Marsh M Cooper Correspondence to: R J Marsh, FRCS. Accepted for publication 28 February 1991 BritishlournalofOphthalmology,
542 Department of Clinical Ophthalmology, Moorfields Eye Hospital, City Road, London EC1V 2PD R J Marsh M Cooper Correspondence to: R J Marsh, FRCS. Accepted for publication 28 February 1991 BritishlournalofOphthalmology,
There is no direct financial or proprietary interest in any companies, products or services mentioned in this presentation.
 1 The content of this COPE Accredited CE Presentation was prepared independently by Michael Cooper, OD without input from members of the ophthalmic community. Dr. Cooper is affiliated with Allergan, Alcon
1 The content of this COPE Accredited CE Presentation was prepared independently by Michael Cooper, OD without input from members of the ophthalmic community. Dr. Cooper is affiliated with Allergan, Alcon
Subunit adjuvanted zoster vaccine: why the fuss?
 Subunit adjuvanted zoster vaccine: why the fuss? Soren Gantt, MD PhD MPH Pediatric Infectious Diseases Vaccine Evaluation Center BC Children s Hospital University of British Columbia Disclosures Research
Subunit adjuvanted zoster vaccine: why the fuss? Soren Gantt, MD PhD MPH Pediatric Infectious Diseases Vaccine Evaluation Center BC Children s Hospital University of British Columbia Disclosures Research
Early- and late-stage ocular complications of herpes zoster ophthalmicus in rural South Africa
 Tropical Medicine and International Health doi:10.1111/tmi.12654 volume 21 no 3 pp 334 339 march 2016 Early- and late-stage ocular complications of herpes zoster ophthalmicus in rural South Africa Erik
Tropical Medicine and International Health doi:10.1111/tmi.12654 volume 21 no 3 pp 334 339 march 2016 Early- and late-stage ocular complications of herpes zoster ophthalmicus in rural South Africa Erik
MedChem401 Herpesviridae. Herpesviridae
 MedChem401 Herpesviridae Members of the herpesvirus family have been identified in more than 80 different animal species Eight have been identified as human pathogens Herpes viruses are a leading cause
MedChem401 Herpesviridae Members of the herpesvirus family have been identified in more than 80 different animal species Eight have been identified as human pathogens Herpes viruses are a leading cause
Koppolu Sreedhar Reddy 1* and Venkata Prasanna DP 2
 e - ISSN - 2349-8005 INTERNATIONAL JOURNAL OF ADVANCES IN CASE REPORTS Journal homepage: www.mcmed.us/journal/ijacr EFFICACY OF TOPICAL ACYCLOVIR IN TREATMENT OF HERPETIC KERATITIS Koppolu Sreedhar Reddy
e - ISSN - 2349-8005 INTERNATIONAL JOURNAL OF ADVANCES IN CASE REPORTS Journal homepage: www.mcmed.us/journal/ijacr EFFICACY OF TOPICAL ACYCLOVIR IN TREATMENT OF HERPETIC KERATITIS Koppolu Sreedhar Reddy
HERPES SIMPLEX VIRUS (HSV)
 CLINICAL SCIENCES Modalities to Decrease Stromal Herpes Simplex Keratitis Reactivation Rates John D. Sheppard, MD; Michael L. Wertheimer, MD; Stephen V. Scoper, MD Objective: To evaluate the efficacy of
CLINICAL SCIENCES Modalities to Decrease Stromal Herpes Simplex Keratitis Reactivation Rates John D. Sheppard, MD; Michael L. Wertheimer, MD; Stephen V. Scoper, MD Objective: To evaluate the efficacy of
10 EYE EMERGENCIES. Who goes, who you better not send! Brant Slomovic, MD, FRCPC University Health Network
 10 EYE EMERGENCIES Who goes, who you better not send! Brant Slomovic, MD, FRCPC University Health Network DISCLOSURES I have none PVD CASE 1 WHAT IS A PVD? a process of aging (45-55) liquefaction of vitreous
10 EYE EMERGENCIES Who goes, who you better not send! Brant Slomovic, MD, FRCPC University Health Network DISCLOSURES I have none PVD CASE 1 WHAT IS A PVD? a process of aging (45-55) liquefaction of vitreous
PAINFUL PAINLESS Contact lens user BOV
 Common Causes Allergies Infections Ocular Cornea, uveitis, endophthalmitis Orbital Orbital cellulitis Inflammation Uveitis Scleritis / episcleritis Glaucomas Trauma Foreign bodies Chemical injuries History
Common Causes Allergies Infections Ocular Cornea, uveitis, endophthalmitis Orbital Orbital cellulitis Inflammation Uveitis Scleritis / episcleritis Glaucomas Trauma Foreign bodies Chemical injuries History
The Emergent Eye in the Acute Setting
 The Emergent Eye in the Acute Setting Todd P. Margolis MD, PhD Professor of Ophthalmology & Director of the F.I. Proctor Foundation UCSF Physical Exam-- Visual Acuity Essential Corrected visual acuity
The Emergent Eye in the Acute Setting Todd P. Margolis MD, PhD Professor of Ophthalmology & Director of the F.I. Proctor Foundation UCSF Physical Exam-- Visual Acuity Essential Corrected visual acuity
Disseminated shingles acyclovir
 Disseminated shingles acyclovir The Borg System is 100 % Disseminated shingles acyclovir Two developed disseminated herpes zoster, one developed cytomegalovirus. Reduced response to acyclovir,. Disseminated
Disseminated shingles acyclovir The Borg System is 100 % Disseminated shingles acyclovir Two developed disseminated herpes zoster, one developed cytomegalovirus. Reduced response to acyclovir,. Disseminated
Challenging Anterior Segment Cases. Benjamin P. Casella, OD, FAAO
 Challenging Anterior Segment Cases Benjamin P. Casella, OD, FAAO Bpc81@aol.com Disclosures Have lectured or been a consultant for: Allergan Carl Zeiss Hydrogel Vision 31yoWM My eye is irritated, and I
Challenging Anterior Segment Cases Benjamin P. Casella, OD, FAAO Bpc81@aol.com Disclosures Have lectured or been a consultant for: Allergan Carl Zeiss Hydrogel Vision 31yoWM My eye is irritated, and I
History. Examination. Diagnosis/Course
 History A 51 year-old female with a history of chronic dry eyes and photosensitivity was referred for evaluation. She reported a five year history of symptoms of frequent irritation and photophobia in
History A 51 year-old female with a history of chronic dry eyes and photosensitivity was referred for evaluation. She reported a five year history of symptoms of frequent irritation and photophobia in
Trifluridine Ophthalmic Solution, 1% Sterile
 Trifluridine Ophthalmic Solution, 1% Sterile DESCRIPTION Trifluridine (also known as trifluorothymidine, F 3 TdR,F 3 T), is an antiviral drug for topical treatment of epithelial keratitis caused by herpes
Trifluridine Ophthalmic Solution, 1% Sterile DESCRIPTION Trifluridine (also known as trifluorothymidine, F 3 TdR,F 3 T), is an antiviral drug for topical treatment of epithelial keratitis caused by herpes
Viral keratitis Mark Daniell Head of Cornea RVEEH
 Viral keratitis Mark Daniell Head of Cornea RVEEH Typical presentation 77year old man 4 weeks right eye red and painful. POH Nil PMHx: HTN, osteoporosis, obesity VAR HM, VAL 6/6-3 IOP R 15, L 8 Microbial
Viral keratitis Mark Daniell Head of Cornea RVEEH Typical presentation 77year old man 4 weeks right eye red and painful. POH Nil PMHx: HTN, osteoporosis, obesity VAR HM, VAL 6/6-3 IOP R 15, L 8 Microbial
Dry Eye Assessment and Management Study ELIGIBILITY OCULAR EVALUATION FORM
 Page 1 of 13 BEFORE COMPLETING THE OCULAR EXAMINATION, YOU MUST BE ABLE TO ANSWER YES TO THE FOLLOWING QUESTIONS: Have you done MMP9? (SVonly) The Following are done at Baseline: Have you done Tear Osmolarity?
Page 1 of 13 BEFORE COMPLETING THE OCULAR EXAMINATION, YOU MUST BE ABLE TO ANSWER YES TO THE FOLLOWING QUESTIONS: Have you done MMP9? (SVonly) The Following are done at Baseline: Have you done Tear Osmolarity?
Page 1 RED EYES. conjunctivitis keratitis episcleritis / scleritis. Frank Larkin Moorfields Eye Hospital. acute glaucoma anterior uveitis
 The RED EYE and ALLERGIC EYE DISEASE DIAGNOSIS & MANAGEMENT Frank Larkin Moorfields Eye Hospital RED EYES conjunctivitis keratitis episcleritis / scleritis acute glaucoma anterior uveitis post-op. / trauma
The RED EYE and ALLERGIC EYE DISEASE DIAGNOSIS & MANAGEMENT Frank Larkin Moorfields Eye Hospital RED EYES conjunctivitis keratitis episcleritis / scleritis acute glaucoma anterior uveitis post-op. / trauma
Darren J. Guffey, MD; Sarah B. Koch, MD, MBA; Leonora Bomar, MD; William W. Huang, MD, MPH
 PEDIATRIC DERMATOLOGY Herpes Zoster Following Varicella Vaccination in Children Darren J. Guffey, MD; Sarah B. Koch, MD, MBA; Leonora Bomar, MD; William W. Huang, MD, MPH PRACTICE POINTS Most children
PEDIATRIC DERMATOLOGY Herpes Zoster Following Varicella Vaccination in Children Darren J. Guffey, MD; Sarah B. Koch, MD, MBA; Leonora Bomar, MD; William W. Huang, MD, MPH PRACTICE POINTS Most children
What are some common conditions that affect the cornea?
 What are some common conditions that affect the cornea? Injuries After minor injuries or scratches, the cornea usually heals on its own. Deeper injuries can cause corneal scarring, resulting in a haze
What are some common conditions that affect the cornea? Injuries After minor injuries or scratches, the cornea usually heals on its own. Deeper injuries can cause corneal scarring, resulting in a haze
EPIDEMIOLOGY. Erik A. Severson, MD; Keith H. Baratz, MD; David O. Hodge, MS; James P. Burke, PhD
 EPIDEMIOLOGY Herpes Zoster Ophthalmicus in Olmsted County, Minnesota Have Systemic Antivirals Made a Difference? Erik A. Severson, MD; Keith H. Baratz, MD; David O. Hodge, MS; James P. Burke, PhD Objective:
EPIDEMIOLOGY Herpes Zoster Ophthalmicus in Olmsted County, Minnesota Have Systemic Antivirals Made a Difference? Erik A. Severson, MD; Keith H. Baratz, MD; David O. Hodge, MS; James P. Burke, PhD Objective:
VIROPTIC Ophthalmic Solution, 1% Sterile (trifluridine ophthalmic solution)
 VIROPTIC Ophthalmic Solution, 1% Sterile (trifluridine ophthalmic solution) PRODUCT OVERVIEW: VIROPTIC SOLUTION DESCRIPTION VIROPTIC is the brand name for trifluridine (also known as trifluorothymidine,
VIROPTIC Ophthalmic Solution, 1% Sterile (trifluridine ophthalmic solution) PRODUCT OVERVIEW: VIROPTIC SOLUTION DESCRIPTION VIROPTIC is the brand name for trifluridine (also known as trifluorothymidine,
Ulcerative Keratitis (Type of Inflammation of the Cornea) Basics
 Ulcerative Keratitis (Type of Inflammation of the Cornea) Basics OVERVIEW Keratitis is inflammation of the cornea; the cornea is the clear outer layer of the front of the eye The corneal epithelium is
Ulcerative Keratitis (Type of Inflammation of the Cornea) Basics OVERVIEW Keratitis is inflammation of the cornea; the cornea is the clear outer layer of the front of the eye The corneal epithelium is
APPENDIX II: Corneal Penetration and Median Effective Dose of Antiviral Agents
 APPENDIX II: Corneal Penetration and Median Effective Dose of Antiviral Agents Median Effective Dose (ED50) The median effective dose is a statistically derived dose of drug expected to produce a certain
APPENDIX II: Corneal Penetration and Median Effective Dose of Antiviral Agents Median Effective Dose (ED50) The median effective dose is a statistically derived dose of drug expected to produce a certain
Photodynamic therapy for IMMK in horses
 Photodynamic therapy for IMMK in horses Overview Immune mediated keratitis in horses Traditional treatment options Sustained release implant Photodynamic therapy Use in veterinary medicine Treatment for
Photodynamic therapy for IMMK in horses Overview Immune mediated keratitis in horses Traditional treatment options Sustained release implant Photodynamic therapy Use in veterinary medicine Treatment for
Herpes Simplex Keratitis in South India: Clinico-Virological Correlation
 Herpes Simplex Keratitis in South India: Clinico-Virological Correlation N.P. Pramod,* P. Rajendran,* K. Ananda Kannan and S.P. Thyagarajan* *Department of Microbiology, Dr. ALM Post Graduate Institute
Herpes Simplex Keratitis in South India: Clinico-Virological Correlation N.P. Pramod,* P. Rajendran,* K. Ananda Kannan and S.P. Thyagarajan* *Department of Microbiology, Dr. ALM Post Graduate Institute
Antiviral Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018
 Antiviral Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 Viruses Viruses are the smallest infective agents, consisting of nucleic acid (DNA or RNA) enclosed
Antiviral Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 Viruses Viruses are the smallest infective agents, consisting of nucleic acid (DNA or RNA) enclosed
Eye infections. Hossain Jabbari, MD, MPH, ID & TM Infectious Diseases Dept., Digestive Diseases Research Institute (DDRI) TUMS
 Eye infections Hossain Jabbari, MD, MPH, ID & TM Infectious Diseases Dept., Digestive Diseases Research Institute (DDRI) TUMS Eye: An overview Eye: An overview The eye is one of the most complex parts
Eye infections Hossain Jabbari, MD, MPH, ID & TM Infectious Diseases Dept., Digestive Diseases Research Institute (DDRI) TUMS Eye: An overview Eye: An overview The eye is one of the most complex parts
Key issues in varicella-zoster virus latency
 Journal of NeuroVirology, 8(suppl. 2): 80 84, 2002 c 2002 Taylor & Francis ISSN 1355 0284/02 $12.00+.00 DOI: 10.1080/13550280290101058 Key issues in varicella-zoster virus latency Peter GE Kennedy Department
Journal of NeuroVirology, 8(suppl. 2): 80 84, 2002 c 2002 Taylor & Francis ISSN 1355 0284/02 $12.00+.00 DOI: 10.1080/13550280290101058 Key issues in varicella-zoster virus latency Peter GE Kennedy Department
Various presentations of herpes simplex retinochoroiditis A case series
 Various presentations of herpes simplex retinochoroidits 47 Various presentations of herpes simplex retinochoroiditis A case series M. T. K. Perera 1, T. S. Keragala 1, M. Gamage 2 The Journal of the College
Various presentations of herpes simplex retinochoroidits 47 Various presentations of herpes simplex retinochoroiditis A case series M. T. K. Perera 1, T. S. Keragala 1, M. Gamage 2 The Journal of the College
Antiviral Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018
 Antiviral Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 Viruses Viruses are the smallest infective agents, consisting of nucleic acid (DNA or RNA) enclosed
Antiviral Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 Viruses Viruses are the smallest infective agents, consisting of nucleic acid (DNA or RNA) enclosed
OOGZIEKTEN VOOR DE HUISARTS F. GOES, JR.
 OOGZIEKTEN VOOR DE HUISARTS F. GOES, JR. HET RODE OOG F. GOES, JR. Condition Signs Symptoms Causes Conjunctivitis Viral Normal vision, normal pupil size Mild to no pain, diffuse Adenovirus (most common),
OOGZIEKTEN VOOR DE HUISARTS F. GOES, JR. HET RODE OOG F. GOES, JR. Condition Signs Symptoms Causes Conjunctivitis Viral Normal vision, normal pupil size Mild to no pain, diffuse Adenovirus (most common),
Focusing on A&E. By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel
 Focusing on A&E By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel 01752 439331 Email sandra.cooper5@nhs.net sandracooper041@btinternet.com THINGS TO WORRY ABOUT WITH ANY EYE PROBLEM CHANGES IN VISION
Focusing on A&E By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel 01752 439331 Email sandra.cooper5@nhs.net sandracooper041@btinternet.com THINGS TO WORRY ABOUT WITH ANY EYE PROBLEM CHANGES IN VISION
Eye Care for Animals Micki Armour VMD DACVO THE CORNEA
 Eye Care for Animals Micki Armour VMD DACVO THE CORNEA ANATOMY 0.5-0.6mm thick 4 primary layers Epithelium (5-7 cell layers) Stroma (90% total thickness) Descemet s membrane Endothelium (1 layer) ANATOMY-
Eye Care for Animals Micki Armour VMD DACVO THE CORNEA ANATOMY 0.5-0.6mm thick 4 primary layers Epithelium (5-7 cell layers) Stroma (90% total thickness) Descemet s membrane Endothelium (1 layer) ANATOMY-
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
Antiviral Agents I. Tutorial 6
 Antiviral Agents I Tutorial 6 Viruses, the smallest of pathogens, are unable to conduct metabolic processes on their own, they use the metabolic system of the infected cell to replicate ( intracellular
Antiviral Agents I Tutorial 6 Viruses, the smallest of pathogens, are unable to conduct metabolic processes on their own, they use the metabolic system of the infected cell to replicate ( intracellular
Conjunctivitis in Dogs
 Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Conjunctivitis in Dogs (Inflammation of the Moist Tissues of the Eye) Basics OVERVIEW
Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Conjunctivitis in Dogs (Inflammation of the Moist Tissues of the Eye) Basics OVERVIEW
Bilateral acute retinal necrosis in a patient with multiple sclerosis on natalizumab
 Bilateral acute retinal necrosis in a patient with multiple sclerosis on natalizumab Arjun B. Sood, Emory University Gokul Kumar, Emory University Joshua Robinson, Emory University Journal Title: Journal
Bilateral acute retinal necrosis in a patient with multiple sclerosis on natalizumab Arjun B. Sood, Emory University Gokul Kumar, Emory University Joshua Robinson, Emory University Journal Title: Journal
Dr.saifalshamarti. Objective. Where is cornea? Functions of the cornea
 Cornea Dr.saifalshamarti Objective Functions Anatomy: detailed description of the 5 layers: epithelium, Bowman s layer, stroma, Descement s membrane, endothelium. Diseases of the cornea: - infection: bacterial
Cornea Dr.saifalshamarti Objective Functions Anatomy: detailed description of the 5 layers: epithelium, Bowman s layer, stroma, Descement s membrane, endothelium. Diseases of the cornea: - infection: bacterial
Natural history of herpes zoster ophthalmicus: predictors of postherpetic neuralgia and ocular involvement
 British Journal of Ophthalmology, 1987, 71, 353-358 Natural history of herpes zoster ophthalmicus: predictors of postherpetic neuralgia and ocular involvement S P HARDNG,' J R LPTON,' AND J C D WELLS2
British Journal of Ophthalmology, 1987, 71, 353-358 Natural history of herpes zoster ophthalmicus: predictors of postherpetic neuralgia and ocular involvement S P HARDNG,' J R LPTON,' AND J C D WELLS2
NIH Public Access Author Manuscript J Neurol Sci. Author manuscript; available in PMC 2010 February 24.
 NIH Public Access Author Manuscript Published in final edited form as: J Neurol Sci. 2009 January 15; 276(1-2): 196 198. doi:10.1016/j.jns.2008.09.025. Recurrent varicella zoster virus myelopathy Don Gilden
NIH Public Access Author Manuscript Published in final edited form as: J Neurol Sci. 2009 January 15; 276(1-2): 196 198. doi:10.1016/j.jns.2008.09.025. Recurrent varicella zoster virus myelopathy Don Gilden
Herpes simplex virus infections of the eye and their management with acyclovir
 Journal of Antimicrobial Chemotherapy (1983) 12, Suppl. B, 39-43 Herpes simplex virus infections of the eye and their management with acyclovir M. G. Falcon Eye Department, St Thomas' Hospital, London
Journal of Antimicrobial Chemotherapy (1983) 12, Suppl. B, 39-43 Herpes simplex virus infections of the eye and their management with acyclovir M. G. Falcon Eye Department, St Thomas' Hospital, London
Lymphotropic Virus Type 1 Infection
 JOURNAL OF CLINICAL MICROBIOLOGY, Sept. 1992, p. 2487-2491 0095-1137/92/092487-05$02.00/0 Copyright 1992, American Society for Microbiology Vol. 30, No. 9 Immunoelectron Microscopy for Rapid Diagnosis
JOURNAL OF CLINICAL MICROBIOLOGY, Sept. 1992, p. 2487-2491 0095-1137/92/092487-05$02.00/0 Copyright 1992, American Society for Microbiology Vol. 30, No. 9 Immunoelectron Microscopy for Rapid Diagnosis
Isolation of herpes simplex virus from the cornea in
 British Journal of Ophthalmology, 1982, 66, 643-647 Isolation of herpes simplex virus from the cornea in chronic stromal keratitis C. SHIMELD, A. B. TULLO, D. L. EASTY, AND J. THOMSITT* From the Department
British Journal of Ophthalmology, 1982, 66, 643-647 Isolation of herpes simplex virus from the cornea in chronic stromal keratitis C. SHIMELD, A. B. TULLO, D. L. EASTY, AND J. THOMSITT* From the Department
Differential Diagnosis of Conjunctivitis and Keratoconjunctivitis
 Differential Diagnosis of Conjunctivitis and Keratoconjunctivitis Dr. Victor Malinovsky 2006 Mechanical-Physical Trauma Corneal Abrasions Abrasions (interpalpebral/variable): a focal loss of epithelium
Differential Diagnosis of Conjunctivitis and Keratoconjunctivitis Dr. Victor Malinovsky 2006 Mechanical-Physical Trauma Corneal Abrasions Abrasions (interpalpebral/variable): a focal loss of epithelium
Ganciclovir-resistant CMV retinitis in a patient with wild-type plasma CMV. North Carolina School of Medicine, Chapel Hill, NC
 JCM Accepts, published online ahead of print on 15 February 2012 J. Clin. Microbiol. doi:10.1128/jcm.00029-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 Ganciclovir-resistant
JCM Accepts, published online ahead of print on 15 February 2012 J. Clin. Microbiol. doi:10.1128/jcm.00029-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 Ganciclovir-resistant
ZEDS Coordinators Conference Call May 30, :00 AM EDT
 ZEDS Coordinators Conference Call May 30, 2018 11:00 AM EDT Participating Clinical Centers (PCC): Status Updates Centers Green Lighted for Screening and Randomization N=56 Study Participants Screened N=93
ZEDS Coordinators Conference Call May 30, 2018 11:00 AM EDT Participating Clinical Centers (PCC): Status Updates Centers Green Lighted for Screening and Randomization N=56 Study Participants Screened N=93
INTERNATIONAL JOURNAL OF PHARMACEUTICAL RESEARCH AND BIO-SCIENCE
 Amar PP,, 2014; Volume 3(3): 123-127 INTERNATIONAL JOURNAL OF PHARMACEUTICAL RESEARCH AND BIO-SCIENCE A REVIEW ON HERPES ZOSTER AMAR PP 1, AJINKYA C 2, TOHID NB 2, ROHIDAS P 2, AVINASH C 2 1. Assistant
Amar PP,, 2014; Volume 3(3): 123-127 INTERNATIONAL JOURNAL OF PHARMACEUTICAL RESEARCH AND BIO-SCIENCE A REVIEW ON HERPES ZOSTER AMAR PP 1, AJINKYA C 2, TOHID NB 2, ROHIDAS P 2, AVINASH C 2 1. Assistant
Differential diagnosis of the red eye. Carol Slight Nurse Practitioner Ophthalmology
 Differential diagnosis of the red eye Carol Slight Nurse Practitioner Ophthalmology The red eye Conjunctivitis HSV Keratitis Acute angle closure glaucoma Anterior Uveitis Red eye Scleritis Subconjunctival
Differential diagnosis of the red eye Carol Slight Nurse Practitioner Ophthalmology The red eye Conjunctivitis HSV Keratitis Acute angle closure glaucoma Anterior Uveitis Red eye Scleritis Subconjunctival
Rare Presentation of Ocular Toxoplasmosis
 Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Subject Index. Atopic keratoconjunctivitis (AKC) management 16 overview 15
 Subject Index Acanthamoeba keratitis, see Infective keratitis Acute allergic conjunctivitis AKC, see Atopic keratoconjunctivitis Allergy acute allergic conjunctivitis 15 atopic keratoconjunctivitis 15
Subject Index Acanthamoeba keratitis, see Infective keratitis Acute allergic conjunctivitis AKC, see Atopic keratoconjunctivitis Allergy acute allergic conjunctivitis 15 atopic keratoconjunctivitis 15
Prof Dr Najlaa Fawzi
 1 Prof Dr Najlaa Fawzi is an acute highly infectious disease, characterized by vesicular rash, mild fever and mild constitutional symptoms. is a local manifestation of reactivation of latent varicella
1 Prof Dr Najlaa Fawzi is an acute highly infectious disease, characterized by vesicular rash, mild fever and mild constitutional symptoms. is a local manifestation of reactivation of latent varicella
March 1, 2006 Table of Contents. What is the best treatment for patients with an outbreak of herpes zoster?
 March 1, 2006 Table of Contents FPIN's Clinical Inquiries Treatment of Herpes Zoster Clinical Question What is the best treatment for patients with an outbreak of herpes zoster? Evidence-Based Answer Resolution
March 1, 2006 Table of Contents FPIN's Clinical Inquiries Treatment of Herpes Zoster Clinical Question What is the best treatment for patients with an outbreak of herpes zoster? Evidence-Based Answer Resolution
Laboratory diagnosis of congenital infections
 Laboratory diagnosis of congenital infections Laboratory diagnosis of HSV Direct staining Tzanck test Immunostaining HSV isolation Serology PCR Tzanck test Cell scrape from base of the lesion smear on
Laboratory diagnosis of congenital infections Laboratory diagnosis of HSV Direct staining Tzanck test Immunostaining HSV isolation Serology PCR Tzanck test Cell scrape from base of the lesion smear on
VZV, EBV, and HHV-6-8
 VZV, EBV, and HHV-6-8 Anne Gershon Common Features of Herpesviruses Morphology Basic mode of replication Primary infection followed by latency Ubiquitous Ability to cause recurrent infections (reactivation
VZV, EBV, and HHV-6-8 Anne Gershon Common Features of Herpesviruses Morphology Basic mode of replication Primary infection followed by latency Ubiquitous Ability to cause recurrent infections (reactivation
BY N. N. SOODt AND V. J. MARMION- St. Paul's Eye Hospital, Liverpool
 Brit. J. Ophthal. (1964) 48, 609. SUPERFICIAL HERPETIC KERATITIS TREATED WITH 5-IODO-2'-DEOXYURIDINE* BY N. N. SOODt AND V. J. MARMION- St. Paul's Eye Hospital, Liverpool THE results of treating herpetic
Brit. J. Ophthal. (1964) 48, 609. SUPERFICIAL HERPETIC KERATITIS TREATED WITH 5-IODO-2'-DEOXYURIDINE* BY N. N. SOODt AND V. J. MARMION- St. Paul's Eye Hospital, Liverpool THE results of treating herpetic
The chemical name of acyclovir, USP is 2-amino-1,9-dihydro-9-[(2-hydroxyethoxy)methyl]-6Hpurin-6-one; it has the following structural formula:
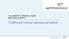
![The chemical name of acyclovir, USP is 2-amino-1,9-dihydro-9-[(2-hydroxyethoxy)methyl]-6Hpurin-6-one; it has the following structural formula: The chemical name of acyclovir, USP is 2-amino-1,9-dihydro-9-[(2-hydroxyethoxy)methyl]-6Hpurin-6-one; it has the following structural formula:](/thumbs/74/71271167.jpg) Acyclovir Ointment, USP 5% DESCRIPTION Acyclovir, USP, is a synthetic nucleoside analogue active against herpes viruses. Acyclovir ointment, USP 5% is a formulation for topical administration. Each gram
Acyclovir Ointment, USP 5% DESCRIPTION Acyclovir, USP, is a synthetic nucleoside analogue active against herpes viruses. Acyclovir ointment, USP 5% is a formulation for topical administration. Each gram
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
HSV DNA replication. Herpesvirus Latency. Latency and Chemotherapy. Human Herpesviruses - subtypes. Acyclovir (acycloguanosine) {Zovirax}
 Human Herpesviruses - subtypes Herpes Simplex I (HSVI) - herpes labialis (cold sores) herpes keratitis (eye infections) HSVII - herpes genitalis (genital herpes) Varicella Zoster virus (VZV) Chicken pox
Human Herpesviruses - subtypes Herpes Simplex I (HSVI) - herpes labialis (cold sores) herpes keratitis (eye infections) HSVII - herpes genitalis (genital herpes) Varicella Zoster virus (VZV) Chicken pox
Eye Examination Techniques in Horses
 Eye Examination Techniques in Horses Dennis E. Brooks DVM, PhD Dip ACVO University of Florida brooksd@mail.vetmed.ufl.edu Basic Instruments How to tell the potential of vision? PLRs (retina, CN 2, chiasm,
Eye Examination Techniques in Horses Dennis E. Brooks DVM, PhD Dip ACVO University of Florida brooksd@mail.vetmed.ufl.edu Basic Instruments How to tell the potential of vision? PLRs (retina, CN 2, chiasm,
Nonulcerative Keratitis (Type of Inflammation of the Cornea) Basics
 Nonulcerative Keratitis (Type of Inflammation of the Cornea) Basics OVERVIEW Keratitis is inflammation of the cornea; the cornea is the clear outer layer of the front of the eye The corneal epithelium
Nonulcerative Keratitis (Type of Inflammation of the Cornea) Basics OVERVIEW Keratitis is inflammation of the cornea; the cornea is the clear outer layer of the front of the eye The corneal epithelium
Recommendations for VZV management in. Dan Engelhard, Pierre Reusser, Rafael de la Camara, Hermann Einsele, Jan Styczynski, Kate Ward, Per Ljungman
 Recommendations for VZV management in patients Cas cliniques with leukemia Dan Engelhard, Pierre Reusser, Rafael de la Camara, Hermann Einsele, Jan Styczynski, Kate Ward, Per Ljungman Introduction Acute
Recommendations for VZV management in patients Cas cliniques with leukemia Dan Engelhard, Pierre Reusser, Rafael de la Camara, Hermann Einsele, Jan Styczynski, Kate Ward, Per Ljungman Introduction Acute
Effect of acyclovir on acute and latent herpes simplex virus infections in the rabbit. Melvin D. Trousdale, Edmund C. Dunkel, and Anthony B.
 Effect of acyclovir on acute and latent herpes simplex virus infections in the rabbit Melvin D. Trousdale, Edmund C. Dunkel, and Anthony B. Nesburn Acyclovir, a new potent antiviral drug, was used to treat
Effect of acyclovir on acute and latent herpes simplex virus infections in the rabbit Melvin D. Trousdale, Edmund C. Dunkel, and Anthony B. Nesburn Acyclovir, a new potent antiviral drug, was used to treat
Summary code for ocular herpes simplex
 Brit. Y. Ophthal. (I975) 59, 539 ummary code for ocular herpes simplex JOHN McKINNON*, JAME McGILLt, AND BARRIE R. JONE From the Department of Clinical Ophthalmology, Institute of Ophthalmology, Moorfields
Brit. Y. Ophthal. (I975) 59, 539 ummary code for ocular herpes simplex JOHN McKINNON*, JAME McGILLt, AND BARRIE R. JONE From the Department of Clinical Ophthalmology, Institute of Ophthalmology, Moorfields
Human Herpes Viruses (HHV) Mazin Barry, MD, FRCPC, FACP, DTM&H Assistant Professor and Consultant Infectious Diseases KSU
 Human Herpes Viruses (HHV) Mazin Barry, MD, FRCPC, FACP, DTM&H Assistant Professor and Consultant Infectious Diseases KSU HERPES VIRUS INFECTIONS objectives: ØTo know the clinically important HHVs. ØTo
Human Herpes Viruses (HHV) Mazin Barry, MD, FRCPC, FACP, DTM&H Assistant Professor and Consultant Infectious Diseases KSU HERPES VIRUS INFECTIONS objectives: ØTo know the clinically important HHVs. ØTo
Nonulcerative Keratitis (Type of Inflammation of the Cornea) Basics
 Nonulcerative Keratitis (Type of Inflammation of the Cornea) Basics OVERVIEW Keratitis is inflammation of the cornea; the cornea is the clear outer layer of the front of the eye The corneal epithelium
Nonulcerative Keratitis (Type of Inflammation of the Cornea) Basics OVERVIEW Keratitis is inflammation of the cornea; the cornea is the clear outer layer of the front of the eye The corneal epithelium
Viroptic (trifluridine) solution [Monarch Pharmaceuticals, Inc.]
![Viroptic (trifluridine) solution [Monarch Pharmaceuticals, Inc.] Viroptic (trifluridine) solution [Monarch Pharmaceuticals, Inc.]](/thumbs/94/118693790.jpg) Viroptic (trifluridine) solution [Monarch Pharmaceuticals, Inc.] Description VIROPTIC is the brand name for trifluridine (also known as trifluorothymidine, F3TdR,F3T), an antiviral drug for topical treatment
Viroptic (trifluridine) solution [Monarch Pharmaceuticals, Inc.] Description VIROPTIC is the brand name for trifluridine (also known as trifluorothymidine, F3TdR,F3T), an antiviral drug for topical treatment
EYE CARE PROTOCOL FOR PATIENTS IN ITU
 EYE CARE PROTOCOL FOR PATIENTS IN ITU Back to contents Developed by SUE LIGHTMAN PROFESSOR OF CLINICAL OPHTHALMOLOGY/CONSULTANT OPHTHALMOLOGIST MOORFIELDS EYE HOSPITAL Amended for UCLU ICU by Caroline
EYE CARE PROTOCOL FOR PATIENTS IN ITU Back to contents Developed by SUE LIGHTMAN PROFESSOR OF CLINICAL OPHTHALMOLOGY/CONSULTANT OPHTHALMOLOGIST MOORFIELDS EYE HOSPITAL Amended for UCLU ICU by Caroline
Breaking the Cycle. Yijie (Brittany) Lin, MD, MBA, Reena Garg, MD New York Eye and Ear Infirmary of Mount Sinai
 Lin, Garg Ophthalmology Times 1 Breaking the Cycle Yijie (Brittany) Lin, MD, MBA, Reena Garg, MD New York Eye and Ear Infirmary of Mount Sinai Abstract A 32 year-old female with a history of LASIK surgery
Lin, Garg Ophthalmology Times 1 Breaking the Cycle Yijie (Brittany) Lin, MD, MBA, Reena Garg, MD New York Eye and Ear Infirmary of Mount Sinai Abstract A 32 year-old female with a history of LASIK surgery
