GUIDELINES FOR MANAGEMENT OF SUSPECTED RABIES EXPOSURES January, 2010
|
|
|
- Kristina Brittany Dalton
- 5 years ago
- Views:
Transcription
1 Ministry of Health and Long-Term Care Ministère de la Santé et des Soins de longue durée GUIDELINES FOR MANAGEMENT OF SUSPECTED RABIES EXPOSURES January, 2010 All suspected incidents must be reported to the local medical officer of health [Health Protection and Promotion Act, Reg. 557, s. 2 (1)] who can provide consultation and the necessary biologicals. The following is a condensed version of the Rabies Vaccine chapter in the Canadian Immunization Guide (Seventh Edition, Public Health Agency of Canada, 2006, pp ) and the National Advisory Committee on Immunization s Recommendations Regarding the management of Bat Exposures to Prevent Human Rabies (CCDR, November 2009). Text in italics has been added or substituted by the Ministry of Health and Long-Term Care based on the Rabies Prevention and Control Protocol, 2009). Please note that this document ONLY summarizes post-exposure prophylaxis guidelines. For information about pre-exposure management and vaccination of high-risk occupational categories, please see the relevant chapter in the Canadian Immunization Guide. Post-exposure management 1. Species of animal Squirrels, hamsters, guinea-pigs, gerbils, chipmunks, rats, mice or other rodents, rabbits and hares are only rarely found to be infected with rabies and are not known to have caused human rabies in North America; post-exposure prophylaxis should be considered only if the animal s behaviour was highly unusual. 2. Type of exposure Three broad categories of exposure are recognized as warranting post-exposure prophylaxis: bite, nonbite and bat exposures. Bite: This is defined as any penetration of the skin by teeth. Non-bite: This category includes contamination of scratches, abrasions or cuts of the skin or mucous membranes by saliva or other potentially infectious material, such as the brain tissue of a rabid animal. Petting a rabid animal or handling its blood, urine or feces is not considered to be an exposure, but such contact should be avoided. Being sprayed by a skunk is also not considered an exposure. Exposures incurred in the course of caring for humans with rabies could theoretically transmit the infection. No case of rabies acquired in this way has been documented, but post-exposure prophylaxis should be considered for exposed individuals. Bat exposures: With respect to human exposures to bats, post-exposure prophylaxis (PEP) is recommended only: when a bat bite or scratch has occurred, OR when there is direct contact with a bat (the bat should be observed to touch or land on the person) AND either of the following cannot be eliminated: a bat bite or scratch or saliva from a live bat entered an open wound or mucous membranes. 1
2 In an adult, a bat landing on clothing would be considered reason for PEP administration only if a bite, scratch, or saliva exposure into a wound or mucous membrane could not be ruled out. Therefore, if a bat lands on the clothing of a person who can be sure that a bite or scratch did not occur and that the bat s saliva did not contact an open wound or mucous membranes, then PEP is not required. In a child, any direct contact with a bat (i.e. the bat landing on or touching the child) should be considered a reason for PEP administration, including contact through clothes, as a history to rule out a bite, scratch or mucous membrane exposure may not be reliable. When a bat is found in the room with a child or adult who is unable to give a reliable history, assessment of direct contact can be difficult. Factors indicating that direct contact may have occurred in these situations include the individual waking up crying or upset while the bat was in the room, or observation of an obvious bite or scratch mark. Extreme care should be taken to ensure that there is no further exposure to the bat if it is captured or handled. In the event that the bat is captured, it should be submitted for rabies testing. Unless exposure to the bat is in the person s head or neck region, PEP can be delayed for up to 48 hours until the rabies test result on the bat is obtained. If PEP was initiated, it can be discontinued if the bat tests negative for rabies. Please note that spelunker exposure in caves will require special consideration. Rarely, transmission has been recorded when virus was inhaled, or infected grafts/organs were transplanted into patients. Post-exposure prophylaxis is warranted and recommended in rare instances of non-bite exposure, such as inhalation of aerosolized virus by spelunkers exploring caves inhabited by infected bats or by laboratory technicians homogenizing tissues infected with rabies virus. 3. Investigation of the incident Each incident of possible exposure requires a full investigation. This should include an assessment of the risk of rabies in the animal species involved and, in a low prevalence area such as Canada, the behaviour of the particular domestic animal implicated. An unprovoked attack is more likely to indicate that the animal is rabid. Nevertheless, rabid cats and dogs may become uncharacteristically quiet. Bites inflicted on a person attempting to feed or handle an apparently healthy animal should generally be regarded as provoked. Domestic pets with up-to-date rabies vaccination are unlikely to become infected with rabies. If vaccinated animals exhibit signs suggestive of rabies they must be carefully evaluated by a veterinarian. Any animal that has bitten a human and/or is suspected of being rabid should be reported to the local medical officer of health and to the nearest Canadian Food Inspection Agency (CFIA) veterinarian. These veterinarians are familiar with the regulations concerning rabies and, if necessary, will collect and ship appropriate specimens to a federal laboratory for diagnosis. Further information and advice is obtainable from the CFIA regional offices or local district office on the CFIA Web site ( or by consulting the blue pages of the local telephone directory. Signs of rabies cannot be reliably interpreted in wild animals. These animals should immediately be humanely killed in a way that does as little damage as possible to the head, which should be submitted for laboratory examination. Rabies virus is readily demonstrable in brains of animals that have neurologic symptoms. Stray or ownerless dogs or cats that seem healthy should be observed for evidence of rabies for 10 days if feasible, but if isolation and observation are not feasible, the animal should be euthanized and tested for rabies. Exotic pets (other than ferrets) should be treated as wild animals because the incubation period and period of rabies virus shedding in these animals are unknown. Recent information regarding the pathogenesis of rabies in domestic ferrets has prompted them to be considered in the same category as domestic dogs and cats rather than wild carnivores. 2
3 Management of people after possible exposure to rabies Immediate washing and flushing of the wound with soap and water is imperative and is probably the most effective procedure in the prevention of rabies. Suturing the wound should be avoided if possible. Tetanus prophylaxis and antibacterial drugs should be given as required. The recommendations in the following table are intended as a guide and may need to be modified in accordance with the specific circumstances of the exposure. Table 12. Post-exposure Prophylaxis for Persons Not Previously Immunized Condition of animal of Animal species time of exposure Dog, cat or ferret Healthy and available for 10 days observation Rabid or suspected to be rabid*. Unknown or escaped Management of exposed person 2. At first sign of rabies in animal, give RabIg (local and intramuscular) and start HDCV or PCECV, unless bite wound to the head or neck (generally begin immediately see text below for other considerations) 2. RabIg (local and Intramuscular) and HDCV or PCECV Skunk, bat, fox, coyote, raccoon and other carnivores. Regard as rabid* unless geographic area is known to be rabies free 2. RabIg (local and intramuscular) and HDCV or PCECV** Livestock, rodents or lagomorphs (hares and rabbits) Consider individually. Consult appropriate public health and CFIA officials. Bites of squirrels, chipmunks, rats, mice, hamsters, gerbils, other rodents, rabbits and hares may warrant post-exposure rabies prophylaxis if the behaviour of the biting animal was highly unusual. Rablg = (human) rabies immune globulin, HDCV = human diploid cell vaccine (Imovax ), PCECV = purified chick embryo cell culture vaccine (RabAvert ) * If possible, the animal should be humanely killed and the brain tested for rabies as soon as possible; holding for observation is not recommended. Discontinue vaccine if fluorescent antibody test of animal brain is negative. ** See text for potential bat exposure. Schedule and dosage Post-exposure prophylaxis of previously unimmunized individuals Please refer to the ADVISORY: Changes to Rabies Post-Exposure Prophylaxis Rabies Vaccine Administration Schedule issued by the Peterborough County-City Health Unit on December 18, Post-exposure prophylaxis should be started as soon as possible after exposure and should be offered to exposed individuals regardless of the elapsed interval. When notification of an exposure is delayed, prophylaxis may be started as late as 6 or more months after exposure. Based on a risk assessment, and where the specimen is received at the lab within 48hrs of exposure, treatment may be withheld until the Fluorescent Antibody Test (FAT) result is available. The FAT report can be obtained within 6 to 24 hours from receipt of an animal specimen at the laboratory. If the suspect animal is 3
4 a cat, dog or ferret and is available for observation, then immunization may be withheld pending the animal s status after the 10-day observation period. However, if the bite wound is to the head and neck region, prophylaxis should generally begin immediately and not be delayed, unless a risk assessment would support a 10-day observation period instead. Considerations that may support delaying initiation of prophylaxis and instead observing the animal for a 10- day period include: if the animal is a domestic pet; if the animal is fully vaccinated; if the bite was provoked; and if there is very low prevalence of rabies in the area. If a rabies exposure is considered likely then post-exposure prophylaxis should never be delayed. The vaccine series may be discontinued after consultation with public health/infectious disease experts if the FAT of the brain of an animal killed at the time of attack is negative. However, if suspicion of rabies in the animal remains high, even in the presence of a negative test, the immunization series should be continued. The recommended dose of human RabIg is 20 IU/kg body weight. This formula is applicable to all age groups, including children. Preferably, the full dose of RabIg should be thoroughly infiltrated into the wound and surrounding area. If not anatomically feasible, any remaining volume of RabIg should be injected, using a separate needle and syringe, intramuscularly at a site distant from vaccine administration. When more than one wound exists, each should be locally infiltrated with a portion of the RabIg using a separate needle and syringe if possible. In such instances, the RabIg may be diluted 2- to 3-fold in a solution of 0.9% sodium chloride in order to provide the full amount of human RabIg required for good infiltration of sites at risk of rabies. If the site of the wound is unknown, the entire dose should be administered intramuscularly. Because of interference with active antibody production, the recommended dose should not be exceeded. Under no circumstances should vaccine be administered in the same syringe or at the same site as RabIg. Protective antibodies are present immediately after passive vaccination with RabIg, but they have a half-life of only approximately 21 days. Since vaccine-induced antibodies begin to appear within 1 week, there is no value in administering RabIg more than 8 days after initiating an approved vaccine course. RabIg is supplied in 2 ml vials containing 150 IU/ml. Use the following formulae to calculate the dose required and use the table to determine how many vials to order: 20 IU/kg x (client wt in kg) 150 IU/mL = dose in ml 9.09 IU/lb x (client wt in lb) 150 IU/mL = dose in ml TOTAL WEIGHT # OF VIALS TOTAL WEIGHT # OF VIALS To 33 lbs To 15 Kg lbs Kg lbs Kg lbs Kg lbs Kg lbs Kg lbs Kg lbs Kg lbs Kg lbs Kg 10 Post-exposure prophylaxis of previously immunized individuals Post-exposure prophylaxis for people who have previously received rabies vaccine differs according to which preparation of vaccine was received. 1. Two doses of HDCV or PCECV, one injected immediately and the other 3 days later, without RabIg, are recommended for exposed individuals with the following rabies immunization history: Completion of an approved course of pre-or post-exposure prophylaxis with HDCV or PCECV; Completion of immunization with other types of rabies vaccine or with HDCV or PCECV according to unapproved schedules as long as neutralizing rabies antibody has been demonstrated in serum (see serologic testing below). 4
5 2. A complete course of HDCV or PCECV plus RabIg is recommended for those who may have received rabies vaccines in the past but do not fulfill the criteria listed in point 1. A serum sample may be collected before vaccine is given, and if an acceptable antibody ( 0.5 IU/ml) is demonstrated, the course may be discontinued, provided that at least two doses of vaccine have been given. If in doubt, consultation with an infectious diseases or public health physician is recommended. Route of administration RabIg is always given intramuscularly. If possible, the full dose of RabIg should be thoroughly infiltrated into the wound and surrounding area. If this is not anatomically feasible, any remaining volume of RabIg should be injected, using a separate needle and syringe, intramuscularly at a site distant from vaccine administration. Rabies vaccine for post-exposure prophylaxis must be administered intramuscularly. Both HDCV and PCECV are approved in Canada for intramuscular (IM) use. Serologic testing Healthy people immunized with an appropriate regimen do not require routine post-immunization antibody determinations. Determination of post-immunization antibody titre may be advisable for those whose immune response may be reduced by illness, medication or advanced age. Corticosteroids, immunosuppressive agents and immunosuppressive illnesses may interfere with the antibody response. Where antibody levels are required, a sample of 5cc whole clotted blood, or serum therefrom, should be submitted to the nearest regional public health laboratory or directly to the Central Public Health Laboratory, 81 Resources Road, Toronto, Ontario M9P 3T1, telephone: (416) There is no charge for this test. To establish laboratory priority, please indicate the purpose of the sample. An acceptable antibody response is a titre of 0.5 IU/mL by the rapid fluorescent-focus inhibition test. Other considerations Vaccine interchangeability: wherever possible, an immunization series should be completed with the same product. However, if this is not feasible, RabAvert and Imovax Rabies are considered interchangeable in terms of indications for use, immunogenicity, efficacy and safety. FOR MORE INFORMATION: (Canadian Immunization Guide, 7th Edition) (HDCV/Imovax product monograph) (PCEC / RabAvert product monograph) (RabIg/Imogam product monograph) (Ministry of Natural Resources rabies in Ontario) (Canadian Food Inspection Agency rabies in Canada) (Centre for Disease Control and Prevention) (World Health Organization) 5
Guidance Document for the Management of Suspected Rabies Exposures
 Guidance Document for the Management of Suspected Rabies Exposures This document is in support of the Rabies Prevention and Control Protocol, 2008 (or as current) under the Ontario Public Health Standards.
Guidance Document for the Management of Suspected Rabies Exposures This document is in support of the Rabies Prevention and Control Protocol, 2008 (or as current) under the Ontario Public Health Standards.
Management of Potential Rabies Exposures Guideline, 2018
 Ministry of Health and Long-Term Care Management of Potential Rabies Exposures Guideline, 2018 Population and Public Health Division, Ministry of Health and Long-Term Care Effective: January 1, 2018 or
Ministry of Health and Long-Term Care Management of Potential Rabies Exposures Guideline, 2018 Population and Public Health Division, Ministry of Health and Long-Term Care Effective: January 1, 2018 or
Rabies Epidemiology K require rabies post-exposure prophylaxis annually. Medical urgency, not medical emergency $300 million annually
 Rabies Rabies Epidemiology 16-39K require rabies post-exposure prophylaxis annually Medical urgency, not medical emergency $300 million annually About 1 or 2 cases of rabies annually in US Sources of Exposure
Rabies Rabies Epidemiology 16-39K require rabies post-exposure prophylaxis annually Medical urgency, not medical emergency $300 million annually About 1 or 2 cases of rabies annually in US Sources of Exposure
Protocol for Rabies Post-exposure Prophylaxis (RPEP) After Exposure to a Rabies Susceptible Animal 1,2
 Protocol for Rabies Post-exposure Prophylaxis (RPEP) After Exposure to a Rabies Susceptible Animal 1,2 Post-exposure Rabies Vaccine Schedule Update The March 19, 2010 issue of the Centers for Disease Control
Protocol for Rabies Post-exposure Prophylaxis (RPEP) After Exposure to a Rabies Susceptible Animal 1,2 Post-exposure Rabies Vaccine Schedule Update The March 19, 2010 issue of the Centers for Disease Control
Canadian Immunization Guide
 Home > Immunization & Vaccines > Canadian Immunization Guide > Rabies Vaccine Canadian Immunization Guide T [Previous page] [Table of Contents] [Next page] Part 4 Active Vaccines Rabies Vaccine Epidemiology
Home > Immunization & Vaccines > Canadian Immunization Guide > Rabies Vaccine Canadian Immunization Guide T [Previous page] [Table of Contents] [Next page] Part 4 Active Vaccines Rabies Vaccine Epidemiology
NEW YORK STATE DEPARTMENT OF HEALTH Updated February 1, 1999 Rabies Policies and Procedures (518) (518) (after hours)
 NEW YORK STATE DEPARTMENT OF HEALTH Updated February 1, 1999 Rabies Policies and Procedures (518) 474-3186 (518) 465-9720 (after hours) SUBJECT: Guidance Regarding Human Rabies Exposure and Treatment Decisions
NEW YORK STATE DEPARTMENT OF HEALTH Updated February 1, 1999 Rabies Policies and Procedures (518) 474-3186 (518) 465-9720 (after hours) SUBJECT: Guidance Regarding Human Rabies Exposure and Treatment Decisions
NEW JERSEY DEPARTMENT OF HEALTH & SENIOR SERVICES
 NEW JERSEY DEPARTMENT OF HEALTH & SENIOR SERVICES NEW JERSEY GUIDE TO POST-EXPOSURE RABIES PROPHYLAXIS FOR THE HEALTH CARE PROFESSIONAL July 2011 BACKGROUND Raccoon rabies entered New Jersey in the fall
NEW JERSEY DEPARTMENT OF HEALTH & SENIOR SERVICES NEW JERSEY GUIDE TO POST-EXPOSURE RABIES PROPHYLAXIS FOR THE HEALTH CARE PROFESSIONAL July 2011 BACKGROUND Raccoon rabies entered New Jersey in the fall
Rabies Prevention and Post- Deployment Assessments: Information for Providersand Public Health Personnel
 U.S. Army Public Health Command Public Health Notice Rabies Prevention and Post- Deployment Assessments: Information for Providersand Public Health Personnel December 2012 U.S. Army Public Health Command
U.S. Army Public Health Command Public Health Notice Rabies Prevention and Post- Deployment Assessments: Information for Providersand Public Health Personnel December 2012 U.S. Army Public Health Command
RABIES PROTECTION PROGRAM
 Page 1 of 5 STANDARD OPERATING PROCEDURES (SOP) SCOPE Rabies is a virus causing an acute central nervous system infection, which is typically transmitted by introducing the rabies virus into open cuts
Page 1 of 5 STANDARD OPERATING PROCEDURES (SOP) SCOPE Rabies is a virus causing an acute central nervous system infection, which is typically transmitted by introducing the rabies virus into open cuts
IMOGAM RABIES PASTEURIZED - HUMAN RABIES IMMUNOGLOBULIN. Active ingredient: Human proteins mg
 IMOGAM RABIES PASTEURIZED - HUMAN RABIES IMMUNOGLOBULIN COMPOSITION 1 ml of human rabies immunoglobulin contains: Active ingredient: Human proteins 100 180 mg containing (IgG class) human rabies immunoglobulins
IMOGAM RABIES PASTEURIZED - HUMAN RABIES IMMUNOGLOBULIN COMPOSITION 1 ml of human rabies immunoglobulin contains: Active ingredient: Human proteins 100 180 mg containing (IgG class) human rabies immunoglobulins
Policy Statement Rabies-Prevention Policy Update: New Reduced-Dose Schedule
 FROM THE AMERICAN ACADEMY OF PEDIATRICS Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children Policy Statement Rabies-Prevention Policy Update:
FROM THE AMERICAN ACADEMY OF PEDIATRICS Organizational Principles to Guide and Define the Child Health Care System and/or Improve the Health of all Children Policy Statement Rabies-Prevention Policy Update:
1.0 GOAL DEFINITIONS RISK ASSESSMENT...
 Chapter I - Management of Specific Diseases Table of Contents 1.0 GOAL... 2 2.0 DEFINITIONS... 2 3.0 RISK ASSESSMENT... 3 3.1 EXPOSURE HISTORY... 4 3.1.1 Bats... 6 3.1.2 Terrestrial Mammals... 7 3.1.3
Chapter I - Management of Specific Diseases Table of Contents 1.0 GOAL... 2 2.0 DEFINITIONS... 2 3.0 RISK ASSESSMENT... 3 3.1 EXPOSURE HISTORY... 4 3.1.1 Bats... 6 3.1.2 Terrestrial Mammals... 7 3.1.3
Twelve Common Questions About Human Rabies and Its Prevention
 Published in Infectious Diseases in Clinical Practice (2000) 9:202-207 Twelve Common Questions About Human Rabies and Its Prevention Robert V. Gibbons, MD, MPH Charles Rupprecht, DVM Viral and Rickettsial
Published in Infectious Diseases in Clinical Practice (2000) 9:202-207 Twelve Common Questions About Human Rabies and Its Prevention Robert V. Gibbons, MD, MPH Charles Rupprecht, DVM Viral and Rickettsial
OREGON PUBLIC HEALTH DIVISION IMMUNIZATION PROTOCOL FOR PHARMACISTS RABIES INACTIVATED VIRUS VACCINE FOR PRE-EXPOSURE PROPHYLAXIS ONLY
 OREGON PUBLIC HEALTH DIVISION IMMUNIZATION PROTOCOL FOR PHARMACISTS RABIES INACTIVATED VIRUS VACCINE FOR PRE-EXPOSURE PROPHYLAXIS ONLY Review 06-2010 No changes to the PRE-EXPOSURE protocol of 2008. See
OREGON PUBLIC HEALTH DIVISION IMMUNIZATION PROTOCOL FOR PHARMACISTS RABIES INACTIVATED VIRUS VACCINE FOR PRE-EXPOSURE PROPHYLAXIS ONLY Review 06-2010 No changes to the PRE-EXPOSURE protocol of 2008. See
PRODUCT MONOGRAPH. RabAvert. Rabies Vaccine. Freeze-dried vaccine for reconstitution with a diluent 2.5 IU of rabies antigen
 PRODUCT MONOGRAPH RabAvert Rabies Vaccine Freeze-dried vaccine for reconstitution with a diluent 2.5 IU of rabies antigen Therapeutic Classification: Active Immunising Agent GlaxoSmithKline Inc. 7333 Mississauga
PRODUCT MONOGRAPH RabAvert Rabies Vaccine Freeze-dried vaccine for reconstitution with a diluent 2.5 IU of rabies antigen Therapeutic Classification: Active Immunising Agent GlaxoSmithKline Inc. 7333 Mississauga
IMOGAM Rabies Pasteurized
 PRODUCT MONOGRAPH INCLUDING PATIENT MEDICATION INFORMATION IMOGAM Rabies Pasteurized Rabies Immune Globulin, Pasteurized (Human) Solution for Injection (150 IU/mL) 2.0 ml vials and 10.0 ml vials Passive
PRODUCT MONOGRAPH INCLUDING PATIENT MEDICATION INFORMATION IMOGAM Rabies Pasteurized Rabies Immune Globulin, Pasteurized (Human) Solution for Injection (150 IU/mL) 2.0 ml vials and 10.0 ml vials Passive
This is risky. Rabies. Are you at risk?
 This is risky. Rabies Are you at risk? Are you at risk of rabies? You are at risk if you are in contact with potentially rabid animals: t Laboratory workers, veterinarians t Animal control workers, animal
This is risky. Rabies Are you at risk? Are you at risk of rabies? You are at risk if you are in contact with potentially rabid animals: t Laboratory workers, veterinarians t Animal control workers, animal
Rabies Vaccine IMOVAX RABIES
 046 90408-0 Rabies Vaccine IMOVAX RABIES WISTAR RABIES VIRUS STRAIN PM-1503-3M GROWN IN HUMAN DIPLOID CELL CULTURES Page 1 of 8 DESCRIPTION The Imovax Rabies Vaccine produced by Aventis Pasteur is a sterile,
046 90408-0 Rabies Vaccine IMOVAX RABIES WISTAR RABIES VIRUS STRAIN PM-1503-3M GROWN IN HUMAN DIPLOID CELL CULTURES Page 1 of 8 DESCRIPTION The Imovax Rabies Vaccine produced by Aventis Pasteur is a sterile,
RABIES. Zeliha Koçak Tufan, MD, Assoc. Prof. Yildirim Beyazit University Infectious Diseases & Clinical Microbiology Department
 RABIES Zeliha Koçak Tufan, MD, Assoc. Prof. Yildirim Beyazit University Infectious Diseases & Clinical Microbiology Department Please focus on the pathogenesis and prophylaxis plus wound care!! What is
RABIES Zeliha Koçak Tufan, MD, Assoc. Prof. Yildirim Beyazit University Infectious Diseases & Clinical Microbiology Department Please focus on the pathogenesis and prophylaxis plus wound care!! What is
Epidemiology of Rabies Post-exposure Prophylaxis in Ontario:
 Epidemiology of Rabies Post-exposure Prophylaxis in Ontario: 2007-2011 The CIPHI 2013 Ontario Branch Conference September 16-18, 2013 Karen Johnson, Senior Epidemiologist Communicable Diseases Prevention
Epidemiology of Rabies Post-exposure Prophylaxis in Ontario: 2007-2011 The CIPHI 2013 Ontario Branch Conference September 16-18, 2013 Karen Johnson, Senior Epidemiologist Communicable Diseases Prevention
SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1. Name of the product: 1.1 Product name: EQUIRAB Rabies Antiserum - Equine 1.2 Strength: 1000 I.U. / 5 ml 1.3 Pharmaceutical Dosage form: Injection 2. Qualitative and
SUMMARY OF PRODUCT CHARACTERISTICS 1. Name of the product: 1.1 Product name: EQUIRAB Rabies Antiserum - Equine 1.2 Strength: 1000 I.U. / 5 ml 1.3 Pharmaceutical Dosage form: Injection 2. Qualitative and
Clinical Pharmacology
 2 4 6 8 10 12 14 16 18 20 22 24 26 28 30 32 34 36 38 40 42 44 46 48 RabAvert Rabies Vaccine Rabies Vaccine for Human Use Description RabAvert, Rabies Vaccine, produced by Novartis Vaccines and Diagnostics
2 4 6 8 10 12 14 16 18 20 22 24 26 28 30 32 34 36 38 40 42 44 46 48 RabAvert Rabies Vaccine Rabies Vaccine for Human Use Description RabAvert, Rabies Vaccine, produced by Novartis Vaccines and Diagnostics
1.0 GOAL DEFINITIONS RISK ASSESSMENT...
 Chapter I - Management of Specific Diseases Table of Contents 1.0 GOAL... 2 2.0 DEFINITIONS... 2 3.0 RISK ASSESSMENT... 3 3.1 EXPOSURE HISTORY... 4 3.1.1 Bats... 5 3.1.2 Terrestrial Mammals... 6 3.1.3
Chapter I - Management of Specific Diseases Table of Contents 1.0 GOAL... 2 2.0 DEFINITIONS... 2 3.0 RISK ASSESSMENT... 3 3.1 EXPOSURE HISTORY... 4 3.1.1 Bats... 5 3.1.2 Terrestrial Mammals... 6 3.1.3
THERAPEUTIC CLASSIFICATION
 PRODUCT MONOGRAPH Rabies Immune Globulin [Human] HYPERRAB S/D Solvent / Detergent Treated 2 ml and 10 ml vials Injectable Solution Manufacturer s Standard THERAPEUTIC CLASSIFICATION Passive Immunizing
PRODUCT MONOGRAPH Rabies Immune Globulin [Human] HYPERRAB S/D Solvent / Detergent Treated 2 ml and 10 ml vials Injectable Solution Manufacturer s Standard THERAPEUTIC CLASSIFICATION Passive Immunizing
For the use only of registered medical practitioners or a hospital or a laboratory
 This package insert is continually updated: please read carefully before using a new pack! For the use only of registered medical practitioners or a hospital or a laboratory Package leaflet Rabipur PCEC
This package insert is continually updated: please read carefully before using a new pack! For the use only of registered medical practitioners or a hospital or a laboratory Package leaflet Rabipur PCEC
PRODUCT MONOGRAPH. RabAvert. Rabies Vaccine. Freeze-dried vaccine for reconstitution with a diluent 2.5 IU of rabies antigen
 PRODUCT MONOGRAPH RabAvert Rabies Vaccine Freeze-dried vaccine for reconstitution with a diluent 2.5 IU of rabies antigen Therapeutic Classification: Active Immunising Agent GlaxoSmithKline Inc. 7333 Mississauga
PRODUCT MONOGRAPH RabAvert Rabies Vaccine Freeze-dried vaccine for reconstitution with a diluent 2.5 IU of rabies antigen Therapeutic Classification: Active Immunising Agent GlaxoSmithKline Inc. 7333 Mississauga
Republic of the Philippines. Department of Health OFFICE OF THE SECRETARY. June 8, 2009 ADMINISTRATIVE ORDER. No:
 Republic of the Philippines Department of Health OFFICE OF THE SECRETARY June 8, 2009 ADMINISTRATIVE ORDER No: 2009-0027 1 / 22 SUBJECT: Amendment to AO 2007-0029 regarding the Revised Guidelines on. I.
Republic of the Philippines Department of Health OFFICE OF THE SECRETARY June 8, 2009 ADMINISTRATIVE ORDER No: 2009-0027 1 / 22 SUBJECT: Amendment to AO 2007-0029 regarding the Revised Guidelines on. I.
RabAvert Rabies Vaccine
 PRESCRIBING INFORMATION RabAvert Rabies Vaccine Rabies Vaccine for Human Use DESCRIPTION RabAvert Rabies Vaccine produced by GlaxoSmithKline GmbH is a sterile, freeze-dried vaccine obtained by growing
PRESCRIBING INFORMATION RabAvert Rabies Vaccine Rabies Vaccine for Human Use DESCRIPTION RabAvert Rabies Vaccine produced by GlaxoSmithKline GmbH is a sterile, freeze-dried vaccine obtained by growing
Updates in rabies vaccine protocols and diagnostic techniques used globally and nationally
 Updates in rabies vaccine protocols and diagnostic techniques used globally and nationally Susan Moore, Rabies Laboratory/KSVDL/College of Veterinary Medicine/Kansas State University, Manhattan, KS 66502,
Updates in rabies vaccine protocols and diagnostic techniques used globally and nationally Susan Moore, Rabies Laboratory/KSVDL/College of Veterinary Medicine/Kansas State University, Manhattan, KS 66502,
EASTERN ILLINOIS UNIVERSITY OCCUPATIONAL HEALTH FOR STUDENTS
 EASTERN ILLINOIS UNIVERSITY OCCUPATIONAL HEALTH FOR STUDENTS The Public Health Service of the U.S. Department of Health and Human Services has directed research/teaching institutions to develop programs
EASTERN ILLINOIS UNIVERSITY OCCUPATIONAL HEALTH FOR STUDENTS The Public Health Service of the U.S. Department of Health and Human Services has directed research/teaching institutions to develop programs
The Epidemiology of Human Rabies Postexposure Prophylaxis in Virginia, 2002 and 2003
 Virginia Commonwealth University VCU Scholars Compass Theses and Dissertations Graduate School 2011 The Epidemiology of Human Rabies Postexposure Prophylaxis in Virginia, 2002 and 2003 Marilyn Goss Haskell
Virginia Commonwealth University VCU Scholars Compass Theses and Dissertations Graduate School 2011 The Epidemiology of Human Rabies Postexposure Prophylaxis in Virginia, 2002 and 2003 Marilyn Goss Haskell
 Page 1 of 11 Medical Summary RABIES GENERAL INFORMATION Introduction Rabies is an acute, progressive infection of the central nervous system caused by neurotropic viruses in the family Rhabdoviridae, genus
Page 1 of 11 Medical Summary RABIES GENERAL INFORMATION Introduction Rabies is an acute, progressive infection of the central nervous system caused by neurotropic viruses in the family Rhabdoviridae, genus
2018 Infection Prevention and Control Update. Lisa Caffery, MS,BSN,RN- BC,CIC, FAPIC
 2018 Infection Prevention and Control Update Lisa Caffery, MS,BSN,RN- BC,CIC, FAPIC Influenza Influenza (1/19/18) Iowa activity IDPH has investigated 40 outbreaks in nursing homes 29 Deaths Activity will
2018 Infection Prevention and Control Update Lisa Caffery, MS,BSN,RN- BC,CIC, FAPIC Influenza Influenza (1/19/18) Iowa activity IDPH has investigated 40 outbreaks in nursing homes 29 Deaths Activity will
Rabies Immune Globulin (Human)
 14-7618-002 (Rev. April 1999) Rabies Immune Globulin (Human) BayRab Solvent/Detergent Treated DESCRIPTION Rabies Immune Globulin (Human) BayRab treated with solvent/detergent is a sterile solution of antirabies
14-7618-002 (Rev. April 1999) Rabies Immune Globulin (Human) BayRab Solvent/Detergent Treated DESCRIPTION Rabies Immune Globulin (Human) BayRab treated with solvent/detergent is a sterile solution of antirabies
Considerations for Tetanus While Treating an Exposure to Rabies
 Considerations for Tetanus While Treating an Exposure to Rabies Since rabies and tetanus are not as common in the United States (US) as they used to be, 1,2 people may not be fully aware of these diseases
Considerations for Tetanus While Treating an Exposure to Rabies Since rabies and tetanus are not as common in the United States (US) as they used to be, 1,2 people may not be fully aware of these diseases
Tetanus Immune Globulin (Human) Biological Page
 Tetanus Immune Globulin (Human) Biological Page Section 7: Biological Product Information Standard #: 07.322 Created by: Province-wide Immunization Program Standards and Quality Approved by: Province-wide
Tetanus Immune Globulin (Human) Biological Page Section 7: Biological Product Information Standard #: 07.322 Created by: Province-wide Immunization Program Standards and Quality Approved by: Province-wide
Produced by Agriculture and Extension Communications, Virginia Tech
 revised 2005 publication 420-036 Rabies: Its Ecology, Control, and Treatment Kari Signor, former student, Department of Fisheries and Wildlife Sciences, Virginia Tech James Parkhurst, associate professor,
revised 2005 publication 420-036 Rabies: Its Ecology, Control, and Treatment Kari Signor, former student, Department of Fisheries and Wildlife Sciences, Virginia Tech James Parkhurst, associate professor,
Rabies Immune Globulin (Human)
 08940054 (Rev. November 2010) Rabies Immune Globulin (Human) HyperRAB S/D Solvent/Detergent Treated DESCRIPTION Rabies Immune Globulin (Human) HyperRAB S/D treated with solvent/detergent is a colorless
08940054 (Rev. November 2010) Rabies Immune Globulin (Human) HyperRAB S/D Solvent/Detergent Treated DESCRIPTION Rabies Immune Globulin (Human) HyperRAB S/D treated with solvent/detergent is a colorless
Rabies. By Alexa Smith. Rabies Virus (Rabies); Etiological agent Family Rhabdoviridae. Genus- lyssavirus (1). Transmission:
 Rabies By Alexa Smith Rabies Virus (Rabies); Etiological agent Family Rhabdoviridae. Genus- lyssavirus (1). Transmission: The virus can enter a host via a parenteral route. The saliva of the infected host
Rabies By Alexa Smith Rabies Virus (Rabies); Etiological agent Family Rhabdoviridae. Genus- lyssavirus (1). Transmission: The virus can enter a host via a parenteral route. The saliva of the infected host
Animal Bites and Rabies. Patty W. Wright, M.D. 2018
 Animal Bites and Rabies Patty W. Wright, M.D. 2018 Objectives To inform participants about the treatment of common animal bites To discuss the indications for and administration of pre- and post-exposure
Animal Bites and Rabies Patty W. Wright, M.D. 2018 Objectives To inform participants about the treatment of common animal bites To discuss the indications for and administration of pre- and post-exposure
RABIPUR Product Information AUST R Page 1 of 14
 Page 1 of 14 DESCRIPTION RABIPUR Inactivated Rabies Virus Vaccine RABIPUR is an inactivated rabies virus vaccine, derived from the fixed-virus strain, Flury LEP. The virus is propagated in a Purified Chick
Page 1 of 14 DESCRIPTION RABIPUR Inactivated Rabies Virus Vaccine RABIPUR is an inactivated rabies virus vaccine, derived from the fixed-virus strain, Flury LEP. The virus is propagated in a Purified Chick
Rabipur is a white, freeze-dried vaccine for reconstitution with solvent prior to use. The solvent is clear and colourless.
 1. NAME OF THE MEDICINAL PRODUCT Rabipur Potency 2.5 IU/ml Powder and solvent for solution for injection Rabies, inactivated, whole virus vaccine 2. QUALITATIVE AND QUANTITATIVE COMPOSITION After reconstitution,
1. NAME OF THE MEDICINAL PRODUCT Rabipur Potency 2.5 IU/ml Powder and solvent for solution for injection Rabies, inactivated, whole virus vaccine 2. QUALITATIVE AND QUANTITATIVE COMPOSITION After reconstitution,
RABIES Pr P ese e n se t n er e : J. J. K a K m a bo b n o a n a (M.B. B Ch C. h B; B M.Med e ) d
 RABIES Presenter: J.J. Kambona (M.B.Ch.B; M.Med) OBJECTIVES At the end of this session each student will be able to: 1. Define rabies. 2. Describe the epidemiology of rabies. 3. Describe the cause of rabies.
RABIES Presenter: J.J. Kambona (M.B.Ch.B; M.Med) OBJECTIVES At the end of this session each student will be able to: 1. Define rabies. 2. Describe the epidemiology of rabies. 3. Describe the cause of rabies.
Research Animal Contact Program Handbook
 Research Animal Contact Program Handbook Florida Institute of Technology Office of Research Keuper 207 321-674-7274 fax: 321-674-8969 150 W. University Blvd.; Melbourne, Fl 32901 January 2019 Research
Research Animal Contact Program Handbook Florida Institute of Technology Office of Research Keuper 207 321-674-7274 fax: 321-674-8969 150 W. University Blvd.; Melbourne, Fl 32901 January 2019 Research
FACTORS AFFECTING COMPLIANCE TO RABIES POST-EXPOSURE PROPHYLAXIS AMONG PEDIATRIC PATIENTS SEEN AT THE RESEARCH INSTITUTE FOR TROPICAL MEDICINE
 56 ORIGINAL ARTICLE FACTORS AFFECTING COMPLIANCE TO RABIES POST-EXPOSURE PROPHYLAXIS AMONG PEDIATRIC PATIENTS SEEN AT THE RESEARCH INSTITUTE FOR TROPICAL MEDICINE AUTHORS: Ruth Faye Romero-Sengson *Philippine
56 ORIGINAL ARTICLE FACTORS AFFECTING COMPLIANCE TO RABIES POST-EXPOSURE PROPHYLAXIS AMONG PEDIATRIC PATIENTS SEEN AT THE RESEARCH INSTITUTE FOR TROPICAL MEDICINE AUTHORS: Ruth Faye Romero-Sengson *Philippine
THE ASSIST ANT SECRETARY OF DEFENSE
 THE ASSIST ANT SECRETARY OF DEFENSE 1200 DEFENSE PENTAGON WASHINGTON, DC 20301-1200 HEALTH AFFAIRS Nov 14, 2011 MEMORANDUM FOR ASSISTANT SECRETARY OF THE ARMY (MANPOWER AND RESERVE AFFAIRS) ASSISTANT SECRETARY
THE ASSIST ANT SECRETARY OF DEFENSE 1200 DEFENSE PENTAGON WASHINGTON, DC 20301-1200 HEALTH AFFAIRS Nov 14, 2011 MEMORANDUM FOR ASSISTANT SECRETARY OF THE ARMY (MANPOWER AND RESERVE AFFAIRS) ASSISTANT SECRETARY
DISEASE. Recommended Childhood Immunization Schedule, Minnesota, 1998
 MINNESOTA DEPAR ARTMENT OF HEALTH DISEASE CONTR ONTROL OL NEW EWSLETTER Volume 26, Number 4 (pages 29-36) May/June 1998 Recommended Childhood Immunization Schedule, Minnesota, 1998 The 1998 Recommended
MINNESOTA DEPAR ARTMENT OF HEALTH DISEASE CONTR ONTROL OL NEW EWSLETTER Volume 26, Number 4 (pages 29-36) May/June 1998 Recommended Childhood Immunization Schedule, Minnesota, 1998 The 1998 Recommended
Evidence to Recommendation Table 1
 Evidence to Recommendation Table 1 Questions: Can the duration of the entire course and/or the number of doses administered of current PEP regimens be reduced while maintaining immunogenicity and effectiveness?
Evidence to Recommendation Table 1 Questions: Can the duration of the entire course and/or the number of doses administered of current PEP regimens be reduced while maintaining immunogenicity and effectiveness?
LONG-TERM PROTECTIVE RABIES ANTIBODIES IN THAI CHILDREN AFTER PRE-EXPOSURE RABIES VACCINATION
 LONG-TERM PROTECTIVE RABIES ANTIBODIES IN THAI CHILDREN AFTER PRE-EXPOSURE RABIES VACCINATION Supawat Chatchen, Shakil Ibrahim, Pataporn Wisetsing and Kriengsak Limkittikul Department of Tropical Pediatrics,
LONG-TERM PROTECTIVE RABIES ANTIBODIES IN THAI CHILDREN AFTER PRE-EXPOSURE RABIES VACCINATION Supawat Chatchen, Shakil Ibrahim, Pataporn Wisetsing and Kriengsak Limkittikul Department of Tropical Pediatrics,
RABIES IMMUNOGLOBULIN. Kanishka Singh Choudhary* and Gunjan Jadon Shrinathji Institute of Pharmacy, Nathdwara. (Raj.)
 Available online on www.ijarpb.com Review Article Received on 17/12/2013; Revised on 20/12/2014; Accepted 28/12/2013; Abstract RABIES IMMUNOGLOBULIN Kanishka Singh Choudhary* and Gunjan Jadon Shrinathji
Available online on www.ijarpb.com Review Article Received on 17/12/2013; Revised on 20/12/2014; Accepted 28/12/2013; Abstract RABIES IMMUNOGLOBULIN Kanishka Singh Choudhary* and Gunjan Jadon Shrinathji
Economical intradermal rabies vaccine application By F.X Meslin and M.Warrell at the occasion of the international seminar on "intradermal
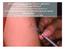 Economical intradermal rabies vaccine application By F.X Meslin and M.Warrell at the occasion of the international seminar on "intradermal immunization: an alternative route for vaccine administration"
Economical intradermal rabies vaccine application By F.X Meslin and M.Warrell at the occasion of the international seminar on "intradermal immunization: an alternative route for vaccine administration"
SUMMARY OF PRODUCT CHARACTRISTICS
 1. NAME OF THE MEDICINAL PRODUCT Purified, Inactivated, Lyophilized Rabies Vaccine, Prepared on Vero Cells INDIRAB 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Qualitative Formula per dose of 0.5 ml (Single
1. NAME OF THE MEDICINAL PRODUCT Purified, Inactivated, Lyophilized Rabies Vaccine, Prepared on Vero Cells INDIRAB 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Qualitative Formula per dose of 0.5 ml (Single
Philippe Lagacé Wiens M.D., DTM&H, FRCPC
 Philippe Lagacé Wiens M.D., DTM&H, FRCPC ay yah FYAH lah yer kuhl 1. Describe the pathogenesis (steps in causing disease) of the rabies virus starting from the bite of an infected animal death of the
Philippe Lagacé Wiens M.D., DTM&H, FRCPC ay yah FYAH lah yer kuhl 1. Describe the pathogenesis (steps in causing disease) of the rabies virus starting from the bite of an infected animal death of the
Rabies. By Rosa Reynoso. Rabies; Etiological Agent: Rhabdoviridae family Lyssavirus genus type (4)
 Rabies By Rosa Reynoso Rabies; Etiological Agent: Rhabdoviridae family Lyssavirus genus type (4) Transmision: It is a zoonotic disease transmitted from infected animals to humans (4). Infected animals
Rabies By Rosa Reynoso Rabies; Etiological Agent: Rhabdoviridae family Lyssavirus genus type (4) Transmision: It is a zoonotic disease transmitted from infected animals to humans (4). Infected animals
RABIES PREVENTION IN TEXAS
 RABIES PREVENTION IN TEXAS Texas Department of State Health Services Zoonosis Control Stock No 6-108 Revised January 2016 1 CONTENTS INTRODUCTION 3 RABIES BIOLOGICALS 4 RATIONALE OF TREATMENT 5 MANAGEMENT
RABIES PREVENTION IN TEXAS Texas Department of State Health Services Zoonosis Control Stock No 6-108 Revised January 2016 1 CONTENTS INTRODUCTION 3 RABIES BIOLOGICALS 4 RATIONALE OF TREATMENT 5 MANAGEMENT
GENUS LYSSAVIRUS IT IS ALMOST A 100% FATAL DISEASE OF HUMANS AND OTHER ANIMALS.
 GENUS LYSSAVIRUS RABIES VIRUS IT IS ALMOST A 100% FATAL DISEASE OF HUMANS AND OTHER ANIMALS. IT HAS BEEN KNOWN SINCE THE 23 CENTURY B.C. RABIES IS PRESENT IS THE SALIVA OF RABID ANIMALS AND IS TRANSMITTED
GENUS LYSSAVIRUS RABIES VIRUS IT IS ALMOST A 100% FATAL DISEASE OF HUMANS AND OTHER ANIMALS. IT HAS BEEN KNOWN SINCE THE 23 CENTURY B.C. RABIES IS PRESENT IS THE SALIVA OF RABID ANIMALS AND IS TRANSMITTED
Zoonosis = an infection or infestation which is shared in nature by man and lower vertebrate animals.
 Zoonosis = an infection or infestation which is shared in nature by man and lower vertebrate animals. For the purposes of this presentation, "zoonotic disease" will be defined as a disease that is caused
Zoonosis = an infection or infestation which is shared in nature by man and lower vertebrate animals. For the purposes of this presentation, "zoonotic disease" will be defined as a disease that is caused
Hepatitis B Immune Globulin Biological Page
 Hepatitis B Immune Globulin Biological Page Section 7: Biological Product Information Standard #: 07.233 Created by: Approved by: Province-wide Immunization Program Standards and Quality Province-wide
Hepatitis B Immune Globulin Biological Page Section 7: Biological Product Information Standard #: 07.233 Created by: Approved by: Province-wide Immunization Program Standards and Quality Province-wide
To provide the guidelines for the management of healthcare workers who have had an occupational exposure to blood and/or body fluids.
 TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
(cf / / Exposure Control Plan for Bloodborne Pathogens)
 All Personnel BP 4119.43 UNIVERSAL PRECAUTIONS 4319.43 In order to protect employees from contact with potentially infectious blood or other body fluids, the Governing Board requires that universal precautions
All Personnel BP 4119.43 UNIVERSAL PRECAUTIONS 4319.43 In order to protect employees from contact with potentially infectious blood or other body fluids, the Governing Board requires that universal precautions
Management of Exposure to Needlestick Injuries & Body Fluids
 Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Drew University Bloodborne Pathogens Exposure Control Plan and Procedures
 PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
ORV STRATEGY USING RABORAL V-RG FOR CONTROLLING RACOON RABIES
 ORV STRATEGY USING RABORAL V-RG FOR CONTROLLING RACOON RABIES Emily W. Lankau DVM, PhD Scientific Consultant Merial, A Sanofi Company RABORAL V-RG : Product Description Produced by Merial Limited - Athens,
ORV STRATEGY USING RABORAL V-RG FOR CONTROLLING RACOON RABIES Emily W. Lankau DVM, PhD Scientific Consultant Merial, A Sanofi Company RABORAL V-RG : Product Description Produced by Merial Limited - Athens,
Diane Lockman, Public Health Nurse. Marilyn Mitchell, Registered Nurse. Sue Mulhall, Public Health Nurse
 Diane Lockman, Public Health Nurse Marilyn Mitchell, Registered Nurse Sue Mulhall, Public Health Nurse Agenda Pre-evaluation Minimizing Your Risk Emergency Service Worker Exposures Scenarios Questions
Diane Lockman, Public Health Nurse Marilyn Mitchell, Registered Nurse Sue Mulhall, Public Health Nurse Agenda Pre-evaluation Minimizing Your Risk Emergency Service Worker Exposures Scenarios Questions
September 24, Dr. Amanda House: As far as I am aware, there are no definitive ante-mortem diagnostic tests for rabies in the horse.
 September 24, 2009 Equine Rabies: What Every Horse Owner Should Know Guest: Hello, I recently purchased a TB Broodmare and would like to vaccinate her against Rabies. She is in foal on a April 06 2009
September 24, 2009 Equine Rabies: What Every Horse Owner Should Know Guest: Hello, I recently purchased a TB Broodmare and would like to vaccinate her against Rabies. She is in foal on a April 06 2009
Continuing Dilemma in Endemic Infection: Rabies in Focus Nancy N. Bermal, MD Fellow: PPS, PIDSP
 Continuing Dilemma in Endemic Infection: Rabies in Focus Nancy N. Bermal, MD Fellow: PPS, PIDSP Conflict of Interest Disclosure Currently an employee of GSK Phils Objective To provide update to rabies
Continuing Dilemma in Endemic Infection: Rabies in Focus Nancy N. Bermal, MD Fellow: PPS, PIDSP Conflict of Interest Disclosure Currently an employee of GSK Phils Objective To provide update to rabies
Presented by. Professor Dr. Md. Zakir Hossain. Professor & Head Department of Medicine Rangpur Medical College & Hospital
 Rabies Presented by Professor Dr. Md. Zakir Hossain MBBS, FCPS, MD(Internal Medicine), FACP Professor & Head Department of Medicine Rangpur Medical College & Hospital Rangpur Medical College Rangpur Medical
Rabies Presented by Professor Dr. Md. Zakir Hossain MBBS, FCPS, MD(Internal Medicine), FACP Professor & Head Department of Medicine Rangpur Medical College & Hospital Rangpur Medical College Rangpur Medical
PATIENT INFORMATION LEAFLET
 PATIENT INFORMATION LEAFLET Read all of this leaflet carefully before you receive this vaccine. - Keep this leaflet. You may need to read it again. - If you have further questions, please ask your doctor
PATIENT INFORMATION LEAFLET Read all of this leaflet carefully before you receive this vaccine. - Keep this leaflet. You may need to read it again. - If you have further questions, please ask your doctor
Safety Committee Prototypical Safety Program Manual
 1 Bloodborne Pathogens Exposure Control Plan Policy The Department Bloodborne Pathogens Exposure Control Plan is designed to comply with the requirements of the OSHA Bloodborne Pathogens Standard, 29 CFR
1 Bloodborne Pathogens Exposure Control Plan Policy The Department Bloodborne Pathogens Exposure Control Plan is designed to comply with the requirements of the OSHA Bloodborne Pathogens Standard, 29 CFR
Rabies Prevention Outreach Program Information for Providers
 Rabies Prevention Outreach Program Information for Providers Contents Provider Message Evaluation & Treatment Algorithm Information on Rabies Animal Exposure Questionnaire/Interview Form Evaluating Rabies
Rabies Prevention Outreach Program Information for Providers Contents Provider Message Evaluation & Treatment Algorithm Information on Rabies Animal Exposure Questionnaire/Interview Form Evaluating Rabies
Rabies. By Sarah C. Rivera
 Rabies By Sarah C. Rivera Etiologic Agent: As a current veterinary technician, rabies is a word spoken all too often and without thinking twice. The clinic where I work is an approved rabies quarantine
Rabies By Sarah C. Rivera Etiologic Agent: As a current veterinary technician, rabies is a word spoken all too often and without thinking twice. The clinic where I work is an approved rabies quarantine
AUSTRALIAN PRODUCT INFORMATION RABIPUR (INACTIVATED RABIES VIRUS VACCINE) POWDER FOR INJECTION
 AUSTRALIAN PRODUCT INFORMATION RABIPUR (INACTIVATED RABIES VIRUS VACCINE) POWDER FOR INJECTION 1 NAME OF THE MEDICINE RABIPUR Inactivated Rabies Virus vaccine 2 QUALITATIVE AND QUANTITATIVE COMPOSITION
AUSTRALIAN PRODUCT INFORMATION RABIPUR (INACTIVATED RABIES VIRUS VACCINE) POWDER FOR INJECTION 1 NAME OF THE MEDICINE RABIPUR Inactivated Rabies Virus vaccine 2 QUALITATIVE AND QUANTITATIVE COMPOSITION
Blood/Body Fluid Exposure Option
 Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
The Bloodborne Pathogen Standard. An Overview
 The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
Rabies. By: Christopher Solomon. Disease: Rabies etiologic agent: Lyssavirus (1)
 Rabies By: Christopher Solomon Disease: Rabies etiologic agent: Lyssavirus (1) Transmission: Transmission of this disease is most often transmitted by the bite of an infected or rabid animal (2). Reservoirs:
Rabies By: Christopher Solomon Disease: Rabies etiologic agent: Lyssavirus (1) Transmission: Transmission of this disease is most often transmitted by the bite of an infected or rabid animal (2). Reservoirs:
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
ALAT - Chapter 4. Occupational Health and Safety. Dr. Carrie Freed, DACLAM, DVM, MLAS
 ALAT - Chapter 4 Occupational Health and Safety Dr. Carrie Freed, DACLAM, DVM, MLAS Freed.36@osu.edu, 292-7319 OSHA Every institution with an animal research program must have an occupational health and
ALAT - Chapter 4 Occupational Health and Safety Dr. Carrie Freed, DACLAM, DVM, MLAS Freed.36@osu.edu, 292-7319 OSHA Every institution with an animal research program must have an occupational health and
Laboratory confirmation requires at least one of the following: isolation of Y. pestis four-fold or greater rise in antibody to Y. pestis.
 Plague Epidemiology in New Zealand Twenty-one cases of plague were recorded in New Zealand between 1900 and 1911, but none has been recorded since then. However, both species of rodent flea necessary for
Plague Epidemiology in New Zealand Twenty-one cases of plague were recorded in New Zealand between 1900 and 1911, but none has been recorded since then. However, both species of rodent flea necessary for
CHEROKEE COUNTY SCHOOL DISTRICT
 For Protection against Infectious Diseases Universal Precautions refers to a set of basic procedures designed to protect against infectious diseases that are transferred by blood and body fluids. Using
For Protection against Infectious Diseases Universal Precautions refers to a set of basic procedures designed to protect against infectious diseases that are transferred by blood and body fluids. Using
1. Councillor W. Stewart s report dated 15 Nov 99 is immediately attached.
 8. OTTAWA-CARLETON WILDLIFE CENTRE COMMITTEE RECOMMENDATION That Council approve funding for the Ottawa-Carleton Wildlife Centre in the amount of $143,000, as a pre-commitment to the 2000 Regional Budget.
8. OTTAWA-CARLETON WILDLIFE CENTRE COMMITTEE RECOMMENDATION That Council approve funding for the Ottawa-Carleton Wildlife Centre in the amount of $143,000, as a pre-commitment to the 2000 Regional Budget.
IMMUNOGENICITY AND FEASIBILITY OF PURIFIED CHICK EMBRYO CELL VACCINE
 IMMUNOGENICITY AND FEASIBILITY OF PURIFIED CHICK EMBRYO CELL VACCINE S. Sehgal M. Bhardwaj D. Bhattacharya ABSTRACT Two hundred seventy-one children reported at the WHO Collaborative Centre for Rabies
IMMUNOGENICITY AND FEASIBILITY OF PURIFIED CHICK EMBRYO CELL VACCINE S. Sehgal M. Bhardwaj D. Bhattacharya ABSTRACT Two hundred seventy-one children reported at the WHO Collaborative Centre for Rabies
Recommendations on pre-exposure rabies vaccine schedules
 Recommendations on pre-exposure rabies vaccine schedules 25 Jan 2018 PATRICK SOENTJENS Chief Medical Physician Travel Clinic ITM, Antwerp Med LtCol Leading Physician ID4C/Travel Clinic Mil Hospital, Brussels
Recommendations on pre-exposure rabies vaccine schedules 25 Jan 2018 PATRICK SOENTJENS Chief Medical Physician Travel Clinic ITM, Antwerp Med LtCol Leading Physician ID4C/Travel Clinic Mil Hospital, Brussels
Infectious Diseases Protocol, 2018
 Ministry of Health and Long-Term Care Infectious Diseases Protocol, 2018 Population and Public Health Division, Ministry of Health and Long-Term Care Effective: January 1, 2018 or upon date of release
Ministry of Health and Long-Term Care Infectious Diseases Protocol, 2018 Population and Public Health Division, Ministry of Health and Long-Term Care Effective: January 1, 2018 or upon date of release
SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison
 SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
Bloodborne Pathogens. Kathleen Stefek, RN, MSN
 Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
CNS MODULE. Dr Hamed Al-Zoubi Ass. Prof. of Microbiology
 CNS MODULE Dr Hamed Al-Zoubi Ass. Prof. of Microbiology Enteroviruses Picornaviridae family 1. Enteroviruses a) Polioviruses types 1, 2 and 3 b) Coxsackieviruses A1-A24 (no A23), B1-B6 c) Echoviruses 1
CNS MODULE Dr Hamed Al-Zoubi Ass. Prof. of Microbiology Enteroviruses Picornaviridae family 1. Enteroviruses a) Polioviruses types 1, 2 and 3 b) Coxsackieviruses A1-A24 (no A23), B1-B6 c) Echoviruses 1
Public Health Brief. A Newsletter on Current Public Health Topics
 Public Health Brief A Newsletter on Current Public Health Topics Serving Adams, Arapahoe and Douglas Counties Phone 303/220-9200 Fax 303/741-4173 Follow us on Twitter @TCHDHealth and @TCHDEmergency Time
Public Health Brief A Newsletter on Current Public Health Topics Serving Adams, Arapahoe and Douglas Counties Phone 303/220-9200 Fax 303/741-4173 Follow us on Twitter @TCHDHealth and @TCHDEmergency Time
Alberta s Response Plan (2005)
 W E S T N I L E V I R U S : Alberta s Response Plan (2005) Alberta s West Nile virus Response Plan (2005) An Interdepartmental Plan Under the leadership of the Provincial Health Office, five government
W E S T N I L E V I R U S : Alberta s Response Plan (2005) Alberta s West Nile virus Response Plan (2005) An Interdepartmental Plan Under the leadership of the Provincial Health Office, five government
Herpes B Virus Exposure Protocol
 Herpes B Virus Exposure Protocol ( This protocol has been revised based on new recommendations published in Clinical Infectious Diseases 2002; 35:1191-1203 which supercedes recommendations published in
Herpes B Virus Exposure Protocol ( This protocol has been revised based on new recommendations published in Clinical Infectious Diseases 2002; 35:1191-1203 which supercedes recommendations published in
Rabies Response. Briefing for the Defense Health Board
 Rabies Response Briefing for the Defense Health Board Steven B. Cersovsky, MD, MPH LTC(P), MC, USA Director, Epidemiology & Disease Surveillance 14 November 2011 UNCLASSIFIED Briefing Outline PURPOSE:
Rabies Response Briefing for the Defense Health Board Steven B. Cersovsky, MD, MPH LTC(P), MC, USA Director, Epidemiology & Disease Surveillance 14 November 2011 UNCLASSIFIED Briefing Outline PURPOSE:
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK)
 POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison
 Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about
Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about
Below you will find information about diseases, the risk of contagion, and preventive vaccinations.
 Vaccinations Below you will find information about diseases, the risk of contagion, and preventive vaccinations. DTP - Diphtheria Tetanus Polio Yellow fever Hepatitis A Typhoid fever Cerebrospinal meningitis
Vaccinations Below you will find information about diseases, the risk of contagion, and preventive vaccinations. DTP - Diphtheria Tetanus Polio Yellow fever Hepatitis A Typhoid fever Cerebrospinal meningitis
SCIENTIFIC STUDY GROUP ON TRAVEL MEDICINE NATIONAL CONSENSUS MEETING 2018
 SCIENTIFIC STUDY GROUP ON TRAVEL MEDICINE WETENSCHAPPELIJKE STUDIEGROEP REISGENEESKUNDE/GROUPE D'ETUDE SCIENTIFIQUE DE LA MEDECINE DES VOYAGES NATIONAL CONSENSUS MEETING 2018 Neder-over-Heembeek, October
SCIENTIFIC STUDY GROUP ON TRAVEL MEDICINE WETENSCHAPPELIJKE STUDIEGROEP REISGENEESKUNDE/GROUPE D'ETUDE SCIENTIFIQUE DE LA MEDECINE DES VOYAGES NATIONAL CONSENSUS MEETING 2018 Neder-over-Heembeek, October
Bloodborne Pathogens Exposure Procedure
 Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Immunization for Adult Hematopoietic Stem Cell Transplant (HSCT) Recipients
 Immunization for Adult Recipients January 4, 201 Immunization for Adult Hematopoietic Stem Cell Transplant () Recipients Revision Date: January 4, 201 Note: This guide is meant to supplement existing recommendations
Immunization for Adult Recipients January 4, 201 Immunization for Adult Hematopoietic Stem Cell Transplant () Recipients Revision Date: January 4, 201 Note: This guide is meant to supplement existing recommendations
Immunization for Child Hematopoietic Stem Cell Transplant (HSCT) Recipients
 Immunization for Child Recipients January 4, 201 Immunization for Child Hematopoietic Stem Cell Transplant () Recipients Revision Date: January 4, 201 Note: This guide is meant to supplement existing recommendations
Immunization for Child Recipients January 4, 201 Immunization for Child Hematopoietic Stem Cell Transplant () Recipients Revision Date: January 4, 201 Note: This guide is meant to supplement existing recommendations
Chapter 6 Occupational Health. Occupational health program Staff immunization Communicable disease management Disease specific recommendations
 Chapter 6 Occupational Health Occupational health program Staff immunization Communicable disease management Disease specific recommendations Region of Peel Public Health June 2011 Region of Peel Public
Chapter 6 Occupational Health Occupational health program Staff immunization Communicable disease management Disease specific recommendations Region of Peel Public Health June 2011 Region of Peel Public
FACT SHEET FOR ADDITIONAL INFORMATION CONTACT
 FACT SHEET FOR ADDITIONAL INFORMATION CONTACT Caroline Calderone Baisley, MPH, RS Michael S. Long, MS Director of Health Director of Environmental Services Tel. 203-622-7836 Tel: 203-622-7838 FREQUENTLY
FACT SHEET FOR ADDITIONAL INFORMATION CONTACT Caroline Calderone Baisley, MPH, RS Michael S. Long, MS Director of Health Director of Environmental Services Tel. 203-622-7836 Tel: 203-622-7838 FREQUENTLY
