SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison
|
|
|
- Iris Verity Franklin
- 6 years ago
- Views:
Transcription
1 SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about the risks and treatment in the event of an infectious agent exposure. In using this guidance, please consider that multiple routes of exposure may occur in a lab and that organism strains will sometimes be genetically modified to incorporate traits such as antimicrobial resistance. Research protocols and other available guidance such as Health Canada material safety data sheets will be provided as supporting information when available. It should be assumed that when exposures do occur, that the healthcare provider will be provided with information about the specific organism and strain involved, route of exposure, inoculum concentration, and victim vaccination and serological status, when available. This document was developed by UW Occupational Medicine in consultation with the UW Division of Infectious Disease. The information provided below is intended to provide guidance for treating physicians. Treatment and evaluation plans should be individualized to the patient based on the patient s symptoms, exposure risk, and underlying health status. If there are any questions about this document, please contact University Health Services, Occupational Medicine at Signs and Symptoms of Infection- Describe signs and symptoms associated with the agent. There are only three known cases of SIV seroconversion in the literature. In all three cases, patients remained entirely asymptomatic. CD4 counts demonstrated no laboratory evidence of decreased immunity. 3.0 Infectivity- Describe infective dose, relevant exposure routes (considering laboratory use), incubation period and potential severity of infection. The exact infective dose is unknown. The following is a list of potentially infectious material. Blood and blood products (serum/plasma) CSF Unfixed tissue and tissue cultures (viral stocks) Although there is no clear data, synovial fluid, pleural fluid, peritoneal fluid, pericardial fluid, saliva, semen/cervical secretions, breast milk, and amniotic fluid should also be considered infective Feces, nasal secretions, sputum, sweat, tears, and vomitus are not considered infectious. Routes of infection include the following Puncture wounds Exposure to non-intact skin (abrasions, cuts, dermatitis) Mucous membrane exposures (eyes, nose, mouth) It is unknown whether infection can occur via the respiratory tract. 12/2/13 Page 1 of 6
2 The incubation period for infection in humans after an identified exposure is unknown but estimated to be similar to HIV, with antibody conversion generally occurring within six months. Based on a blinded serosurvey in 1992, the CDC estimates 0.6% of laboratory workers handling SIV have antibodies to SIV. Of the three know cases of SIV seroconversion reported in the literature, two of the cases were associated with blood contaminated hollow bore needle stick injuries from an SIV positive monkey. The third case was in a laboratory worker with dermatitis who did not use gloves while handling SIV positive blood and tissue culture samples. The risk of SIV transmission is extrapolated from HIV transmission estimates. The average risk of transmission after a hollow bore needle puncture is 0.3%. Three factors increase this risk: a visibly blood needle, a needle that was previously in a blood vessel, and a deep puncture wound. The average risk of transmission after a mucous membrane exposure is 0.09%. 4.0 Description of First Aid - Provide an overview of first aid treatment of exposures considering that multiple routes of exposure could occur (needlestick, aerosol, eye, skin and ingestion). Cleanse the exposed area for a minimum of 15 minutes as soon as possible following exposure. 1. Eyes or mucous membranes: use sterile saline or water to irrigate for 15 minutes, preferably in an eye wash station. For all eye exposures, BOTH eyes should be irrigated. 2. Skin: wash with the disinfectant product approved for your laboratory for at least 15 minutes **ALL POTENTIAL EXPOSURES MUST BE REPORTED TO UW OCCUPATIONAL HEALTH ( ) **THE SIV STATUS OF THE ANIMAL SHOULD GENERALLY BE KNOWN. PLEASE NOTIFY THE VETERINARIAN and ask regarding the following: The viral load of the inoculum, whether it came from a recently infected animal and whether that animal was symptomatic or asymptomatic. 5.0 Urgency of Medical Care- Describe how soon medical attention should be sought, i.e. is an ER visit necessary, a visit to University Health Services, or simply schedule a visit with a personal physician. All exposures should be evaluated as soon as possible, preferably within 2 hours, to determine if post exposure prophylaxis (PEP) is warranted. If PEP is indicated, it needs to be administered promptly. UW UHS Occupational health should be contacted at or If they are closed (after hours, weekends and holidays), please proceed to the UWHC Emergency Department. 12/2/13 Page 2 of 6
3 6.0 Description of Medical Response- Provide an overview for clinical treatment of exposures to the agent considering that multiple routes of exposure could occur (needlestick, aerosol, eye, skin and ingestion) and that strains of agents will vary and sometimes include antimicrobial resistance. Initial Evaluation 1) Healthcare provider should re-wash the exposed area for 15 minutes as described above in First Aid section. 2) Healthcare provider should document date, time, and location of injury and the type of animal tissue or fluid involved in exposure. If available/relevant (see Indications for SIV Prophylaxis below), the viral load of the inoculum, whether the animal was symptomatic or asymptomatic, and whether the animal was recently infected should be recorded. The strain if SIV involved as well as any recombinants should be documented. 3) Evaluation of general health including potential pregnancy, medications and the date of the last tetanus booster. 4) If the exposure involved an animal, the healthcare provider will also evaluate for possible antibiotic prophylaxis and herpes B prophylaxis. 5) If an exposure has occurred, then blood work for SIV surveillance should be sent to the CDC. This includes HIV and SIV antibody tests as well as viral load testing. Please see the attached instructions Procedure for the collections and shipment of whole blood specimens to the CDC, IATA guidance document for shipping infectious substances, and IATA packing instructions for biologic specimens. These outline how the specimen should be collected, labeled and shipped. They also review who should be contacted and what information regarding the exposure should be provided. Indications for SIV Prophylaxis SIV postexposure prophylaxis for 4 weeks with a three drug regimen is recommended for exposure to any type of potentially infectious SIV material. Two drug regimens are no longer recommended for retrovirus postexposure prophylaxis. The current preferred three drug regimen is: Tenofovir-Emtricitabine (TDF/FTC 300/200 mg ; once daily ) plus Raltegravir (400 mg twice daily). Side effects: mild GI upset (nausea and vomiting 27%; diarrhea 21%; gas, pain or bloating 16%), headache (15%), fatigue (14%); Precautions / Interactions: hepatitis B, osteoporosis, renal disease This regimen avoids medications which should not be used during the first trimester of pregnancy, in women who are trying to conceive or are not using effective and consistent contraception, and avoids medications which can interact with omeprazole or similar acid lowering agents. 12/2/13 Page 3 of 6
4 The preferred three drug regimen for pregnant or breastfeeding (i.e. continues to breast feed though not recommended ) women is: Lopinavir/Ritonavir (LPV/r twice daily) and Zidovudine/Lamivudine (ZDV/3TC once daily) Side effects: GI upset, fatigue and headache Precautions / Interactions: hepatitis B, hemoglobin <9.5, neutrophil count < 1000; St John s wort should be avoided; co-administration with simvastatin or lovastatin increases the risk of myotoxicity; pravastatin does not interact and can be substituted. Other preferred regimens may be considered for specific medical histories or risk factors (renal disease, pregnancy or breastfeeding). SIV viruses with the M184V/I mutation or the K65R mutation also require an alternate regimen. These situations would require direct input from the UW Infectious Disease physician on-call. (Current approaches used by CDC include the following: Emtricitabine resistant viruses containing the M 184V/I mutation: tenofovir, raltegravir and darunavir boosted with ritonavir; Tenofovir resistant viruses containing the K65Rmutation, usually resistant to emtricitabine also: raltegravir, zidovudine, and darunavir boosted with ritonavir.) If it is decided to start PEP the following lab work should be obtained: CBC with differential Creatinine AST and ALT Urine pregnancy test in all women of childbearing age If PEP is prescribed, baseline lab work should be performed as outlined above. This should be repeated, with the exception of the urine pregnancy test, at 2 weeks and 4 weeks to assess for toxicity. At this 2 week mark, the worker should be seen by the clinician to ensure all wounds are healing properly and evaluate for medication side effects. Often, these can be handled symptomatically by prescribing anti-emetics and anti-motility agents. At the end of four weeks, the worker and clinician should follow-up. Any wounds should be inspected. Antivirals should be discontinued and the plan for follow up blood work (viral and antibody testing) reviewed. Follow-up All workers with an SIV exposure should be monitored for seroconversion and infection. Whole blood for SIV testing at the CDC should be drawn at the time of exposure, 3 weeks, 6 weeks, 3 months, 6 months and one year after. Procedure for the Collection and Shipment of Whole Blood Specimens to the CDC 1. Collect ml of EDTA-treated blood on Monday through Thursday using standard clinical venipuncture techniques. For samples collected outside this period please contact Bill Switzer at the CDC ( ; bis3@cdc.gov) to make other shipping arrangements. 2. All specimens and paperwork should be coded without any personal identifiers. 12/2/13 Page 4 of 6
5 3. Place the sample in a shipping container following the instructions found at the CDC or IATA websites ( and ship at room temperature to the CDC Serum Bank using an overnight, next morning delivery service. 4. Unless other arrangements are made, all shipments are to be sent to: CDC Serum Bank (STAT) Centers for Disease Control and Prevention 1600 Clifton Road NE Atlanta, GA Attention: Project Provide advance notice of the shipment by FAXing a copy of the shipment manifest to both Bill Switzer ( ) and the CDC Serum Bank ( ) the day the samples are collected. Alternatively, notification to Bill Switzer will suffice. bswitzer@cdc.gov 6. Please provide details of the specific exposure in an to Bill Switzer, including when, where, how the exposure occurred, the strain of SIV or SHIV involved, animal species, occupation, and antiretroviral treatment. (to be done by UHS) 7.0 Description of Medical Surveillance- Describe the advisability of medical surveillance strategies (in particular baseline and annual serology) for those working with the agent. If doing so would likely improve the identification, diagnosis or treatment of exposures, please indicate so. Surveillance, such as annual serology, for SIV is not indicated in the absence of exposure. 8.0 Considerations for Infection Control-Describe any special precautions required to prevent the further spread of infection. Include precautions for the healthcare, workplace, and home setting. The worker should be counseled to reduce risk for secondary transmission by avoiding unprotected sex, breast feeding, and blood or tissue donation during the incubation period. 9.0 Reporting-Describe any public health or federal regulatory reporting requirements. Include the timing and mechanism for reporting. Public Health: None Other: None 12/2/13 Page 5 of 6
6 10.0 References: Wilson, D and L Chosewood. Biosafety in Microbiological and biomedical laboratories, 5 th edition. Revised December, Available at Guidelines for the Use of Antiretroviral Agents in HIV-1 Infected Adults and Adolescents; Update of March 27, 2012; Dept of Health and Human Services Document Revisions Revision History Revision Number Date Description of Revision Initial Approval 4/13/12 ASW original 1 4/2013 ASW edits 2 12/2/13 Changed to new format 12/2/13 Page 6 of 6
To provide the guidelines for the management of healthcare workers who have had an occupational exposure to blood and/or body fluids.
 TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
Clinical Education Initiative OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS. Antonio E. Urbina, MD
 Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison
 Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about
Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about
One of your office personnel
 Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison
 Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about the
Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about the
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Bloodbourne Pathogens (BBP) Occupational Post-Exposure Chemophrophylaxis
 Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Management of Workplace Exposure to Blood-borne Pathogens
 Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Blood/Body Fluid Exposure Option
 Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
INITIAL EVALUATION AND MANAGEMENT FOLLOWING EXPOSURE TO BLOOD OR BODY FLUIDS
 Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet. Instructions for Employees/Students:
 MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Needlestick and Splash Exposure Flow Chart Page 1 Clinical Practice Guidelines
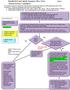 Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital
 HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
Exposures at Non-MUSC Clinical Sites
 BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
43. Guidelines on Needle stick Injury
 43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
Drew University Bloodborne Pathogens Exposure Control Plan and Procedures
 PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
PURPOSE To provide a written plan for preventing and/or minimizing exposure to bloodborne pathogens for those Drew University personnel who may be involved in the handling of human blood, blood products,
Blood-Borne Pathogens and Post-Exposure Prophylaxis
 Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
CONTINUING CARE ADMINISTRATIVE MANUAL POLICY
 CONTINUING CARE ADMINISTRATIVE MANUAL POLICY NUMBER III-10 DATE Draft June 8, 2010 PAGE 1 OF 3 APPROVED BY: SITE: CATEGORY TITLE: Vice President & Senior Operating Officer, Rehab & Continuing Care Edmonton
CONTINUING CARE ADMINISTRATIVE MANUAL POLICY NUMBER III-10 DATE Draft June 8, 2010 PAGE 1 OF 3 APPROVED BY: SITE: CATEGORY TITLE: Vice President & Senior Operating Officer, Rehab & Continuing Care Edmonton
Exposure. Blood. Department of Health & Human Services
 Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
HIV and PEP. LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED
 HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
Post-Sexual Exposure Prophylaxis (npep)
 Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS
 STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
STUDENT EXPOSURE TO BLOOD OR OTHER POTENTIALLY INFECTIOUS MATERIALS (See Bloodborne Pathogen Worksheet and Post Exposure Prophylaxis consent immediately following this policy ) 1. Student must report immediately
Bloodborne Pathogen Exposure STUDENT. Blood Borne Pathogen Exposure. Student. Rev:
 Blood Borne Pathogen Exposure Student INSTRUCTIONS 1. Student: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Blood Borne Pathogen Exposure Student INSTRUCTIONS 1. Student: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Bloodborne Pathogens Exposure Procedure
 Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Definitions. Appendix A
 Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
Definitions Appendix A 1. Blood means human blood, human blood components, and products made from human blood. 2. Bloodborne Pathogens means pathogenic microorganisms that are present in human blood and
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK)
 POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
Introduction to Blood Borne Pathogens
 Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Introduction to Blood Borne Pathogens What are blood pathogens? Any infectious microorganism in the human blood that can cause disease is a Blood borne pathogen. Three of these pathogens include hepatitis
Herpes B Virus Exposure Protocol
 Herpes B Virus Exposure Protocol ( This protocol has been revised based on new recommendations published in Clinical Infectious Diseases 2002; 35:1191-1203 which supercedes recommendations published in
Herpes B Virus Exposure Protocol ( This protocol has been revised based on new recommendations published in Clinical Infectious Diseases 2002; 35:1191-1203 which supercedes recommendations published in
Management of sharps injuries in the healthcare setting
 Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
Training for Employees of Taylor Special Care Services, Inc.
 Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
Bloodborne Pathogens Across the Continuum of Care Sue Sebazco, Arlington, Texas A Webber Training Teleclass
 Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Bloodborne Pathogens Training
 Bloodborne Pathogens Training OSHA S Bloodborne Pathogen Standard 29CFR 1910.1030 Employers must: Develop an Exposure Control Plan (ECP) that details their Bloodborne Pathogens (BBP) Program Provide employees
Bloodborne Pathogens Training OSHA S Bloodborne Pathogen Standard 29CFR 1910.1030 Employers must: Develop an Exposure Control Plan (ECP) that details their Bloodborne Pathogens (BBP) Program Provide employees
El Paso - Ambulatory Clinic Policy and Procedure
 Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
Infection Control Program (ICP) ICP Components 1. Exposure Determination 2. Control Methods A. Universal Precautions
 Compliance Assistance Guideline for the February 27, 1990, OSHA Instruction CPL 2 2.44B Enforcement Procedures for Occupational Exposure to Hepatitis B Virus and Human Immunodeficiency Virus from the U.S.
Compliance Assistance Guideline for the February 27, 1990, OSHA Instruction CPL 2 2.44B Enforcement Procedures for Occupational Exposure to Hepatitis B Virus and Human Immunodeficiency Virus from the U.S.
determine need but regimen does not change based on risk factor ED medicine attending meets
 HIV PEP Guidelines after Sexual Assault Harborview Medical Center January 2015 Initial risk assessment and discussion with patient about risk and PEP is by clinician who does exam (SANE, Ob-Gyn resident,
HIV PEP Guidelines after Sexual Assault Harborview Medical Center January 2015 Initial risk assessment and discussion with patient about risk and PEP is by clinician who does exam (SANE, Ob-Gyn resident,
3/23/2016. Managing Bloodborne Pathogen Exposures. Managing Bloodborne Pathogen Exposures
 This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
Contamination Incidents Frequently Asked Questions
 Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
You will now begin the Bloodborne Pathogen Refresher Training.
 You will now begin the Bloodborne Pathogen Refresher Training. The following program will review your occupational risks and the steps that you and your Client must take to reduce your risks of exposure.
You will now begin the Bloodborne Pathogen Refresher Training. The following program will review your occupational risks and the steps that you and your Client must take to reduce your risks of exposure.
PLEASE POST THIS PAGE IN AREAS WHERE HIV/SIV IS USED
 PLEASE POST THIS PAGE IN AREAS WHERE HIV/SIV IS USED Organism or Agent: UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY HUMAN IMMUNODEFICIENCY VIRUS (HIV) SIMIAN IMMUNODEFICIENCY
PLEASE POST THIS PAGE IN AREAS WHERE HIV/SIV IS USED Organism or Agent: UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY HUMAN IMMUNODEFICIENCY VIRUS (HIV) SIMIAN IMMUNODEFICIENCY
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
Revised April WGH ER #5 Hospital Rd. Whitehorse Phone: (867) Outside of Whitehorse: Local Community Health Centre/Clinic/ER
 Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV
 Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Kurdistan Board For Medical Specialties An exposure that might place health
Guidelines for Post- Exposure Prophylaxis for HAV, HBV, HCV & HIV By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Kurdistan Board For Medical Specialties An exposure that might place health
2014 OSHA Blood-borne Pathogens (BBP) Update JHS Annual Mandatory Education
 2014 OSHA Blood-borne Pathogens (BBP) Update 2014 JHS Annual Mandatory Education Objectives Discuss the epidemiology of Bloodborne Pathogens. List the statistics of HIV/AIDS cases Identify the correlation
2014 OSHA Blood-borne Pathogens (BBP) Update 2014 JHS Annual Mandatory Education Objectives Discuss the epidemiology of Bloodborne Pathogens. List the statistics of HIV/AIDS cases Identify the correlation
Universal Precautions
 Universal Precautions emphasizes the need for workers and students to consider all blood and body fluids as potentially infected with HIV, HBV, and / or other blood-borne pathogens, and to adhere rigorously
Universal Precautions emphasizes the need for workers and students to consider all blood and body fluids as potentially infected with HIV, HBV, and / or other blood-borne pathogens, and to adhere rigorously
B. Tasks and Procedures where employees, students or contractors can be exposed to bloodborne pathogens:
 Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Bloodborne Pathogens. Exposure Control Plan
 Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
Bloodborne Pathogens Exposure Control Plan Maryland Institute College of Art Revision Date(s): January 2007/January 2008 Maryland Institute College of Art (MICA) Subject: Occupational/Non-occupational
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Management
 01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Policy Definitions Establish protocol for management of occupational exposures to blood or potentially infectious materials.
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Policy Definitions Establish protocol for management of occupational exposures to blood or potentially infectious materials.
Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May Contains information for:
 APPENDIX A Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May 2018 BLOODBORNE PATHOGEN EXPOSURE INCIDENT PACKET Contains information for:
APPENDIX A Safety Regulations and Procedures Occupational Health Bloodborne Pathogens Exposure Control Plan S80.10, updated, May 2018 BLOODBORNE PATHOGEN EXPOSURE INCIDENT PACKET Contains information for:
SFAF CLINICAL PROTOCOLS
 SFAF CLINICAL PROTOCOLS Page 1 of Supersedes Date: December 31, 2016 Original Date: August 20, 2014 Version: 03 Policy Section: Patient Care Non-Occupational Post Exposure Prophylaxis Program Back ground:
SFAF CLINICAL PROTOCOLS Page 1 of Supersedes Date: December 31, 2016 Original Date: August 20, 2014 Version: 03 Policy Section: Patient Care Non-Occupational Post Exposure Prophylaxis Program Back ground:
Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis).
 LTHT Infection Control Policies Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis). This policy covers the immediate actions to
LTHT Infection Control Policies Needlestick Policy and Actions to be taken after Exposure to Blood and Body Fluids (including HIV Post- Exposure Prophylaxis). This policy covers the immediate actions to
Bloodborne Pathogens and Exposure Control
 Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
2017 BLOODBORNE PATHOGENS
 2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
Greenwood School District 50 OSHA UPDATE BLOODBORNE PATHOGENS
 Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
FOR INFECTION TO OCCUR: Bloodborne Pathogens are viral diseases that can infect a person if they are exposed Hepatitis B Hepatitis C HIV
 OCCUPATIONAL EXPOSURE TO BLOODBORNE PATHOGENS Bloodborne Pathogens are viral diseases that can infect a person if they are exposed Hepatitis B Hepatitis C HIV FOR INFECTION TO OCCUR: A germ Bloodborne
OCCUPATIONAL EXPOSURE TO BLOODBORNE PATHOGENS Bloodborne Pathogens are viral diseases that can infect a person if they are exposed Hepatitis B Hepatitis C HIV FOR INFECTION TO OCCUR: A germ Bloodborne
Post Exposure Prophylaxis (PEP)
 Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
PEDIATRIC EMERGENCY DEPARTMENT CLINICAL GUIDELINE: NON- OCCUPATIONAL EXPOSURE TO BLOOD-BORNE PATHOGENS (HIV, Hepatitis B, AND Hepatitis C)
 General Definition: Blood-borne pathogens are infectious agents that can be transmitted through contact with blood or certain other body fluids. The primary pathogens are HIV, Hepatitis B, and C. Before
General Definition: Blood-borne pathogens are infectious agents that can be transmitted through contact with blood or certain other body fluids. The primary pathogens are HIV, Hepatitis B, and C. Before
Infection Control Standard Precautions. CDC Recommendations: Application of Standard Precautions for All Patients
 Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Bloodborne Pathogens. Montclair Kimberley Academy 1
 Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
Colgate University. Bloodborne Pathogens Exposure Control Plan
 Colgate University Bloodborne Pathogens Exposure Control Plan COLGATE UNIVERSITY BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN I. STATEMENT OF POLICY It is the policy of Colgate University (CU) to limit or
Colgate University Bloodborne Pathogens Exposure Control Plan COLGATE UNIVERSITY BLOODBORNE PATHOGENS EXPOSURE CONTROL PLAN I. STATEMENT OF POLICY It is the policy of Colgate University (CU) to limit or
Blood-borne Pathogens Exposure Policy
 Blood-borne Pathogens Exposure Policy Contents Blood Borne Pathogen(s) Exposure (BBPE) -Post-Exposure Prophylaxis... 1 STUDENT CHECKLIST... 3 PROGRAM CHECKLIST... 4 PROVIDER CHECKLIST... 5 POST-EXPOSURE
Blood-borne Pathogens Exposure Policy Contents Blood Borne Pathogen(s) Exposure (BBPE) -Post-Exposure Prophylaxis... 1 STUDENT CHECKLIST... 3 PROGRAM CHECKLIST... 4 PROVIDER CHECKLIST... 5 POST-EXPOSURE
Occupational Exposures to Bloodborne Pathogen (BBP) Training
 Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
Occupational Exposures to Bloodborne Pathogen (BBP) Training OSHA 29 CFR 1910.1030 Protects workers exposed to blood or other potentially infectious diseases Who are at Risk? Workers in many different
Emergency Department Blood/Body Fluid Exposure Instructions
 Emergency Department Blood/Body Fluid Exposure Instructions For employees sent to the Emergency Department after hours to be evaluated for needle stick / body fluid exposure 1. Floor or unit Charge RN
Emergency Department Blood/Body Fluid Exposure Instructions For employees sent to the Emergency Department after hours to be evaluated for needle stick / body fluid exposure 1. Floor or unit Charge RN
Information for Health Care Workers
 Information for Health Care Workers This Bulletin highlights precautions to be taken by health care workers who may be exposed to blood and body fluids. In general, workers should minimize direct contact
Information for Health Care Workers This Bulletin highlights precautions to be taken by health care workers who may be exposed to blood and body fluids. In general, workers should minimize direct contact
Bloodborne Pathogens Training (OHS_BIO500) Course Material
 Introduction (OHS_BIO500) Course Material Welcome to the Bloodborne Pathogens (BBP) Training Course (OHS_BIO500). UAB Campus Employees whose job duties put them at increased risk for exposure to bloodborne
Introduction (OHS_BIO500) Course Material Welcome to the Bloodborne Pathogens (BBP) Training Course (OHS_BIO500). UAB Campus Employees whose job duties put them at increased risk for exposure to bloodborne
Confronting Ebola. Keeping NY patients and healthcare workers safe and healthy
 Confronting Ebola Keeping NY patients and healthcare workers safe and healthy All materials provided by Centers for Disease Control and Prevention. October 16, 2014 What You Need to Know about Ebola The
Confronting Ebola Keeping NY patients and healthcare workers safe and healthy All materials provided by Centers for Disease Control and Prevention. October 16, 2014 What You Need to Know about Ebola The
Influenza-Associated Pediatric Mortality rev Jan 2018
 rev Jan 2018 Infectious Agent Influenza A, B or C virus BASIC EPIDEMIOLOGY Transmission Transmission occurs via droplet spread. After a person infected with influenza coughs, sneezes, or talks, influenza
rev Jan 2018 Infectious Agent Influenza A, B or C virus BASIC EPIDEMIOLOGY Transmission Transmission occurs via droplet spread. After a person infected with influenza coughs, sneezes, or talks, influenza
Management of Exposure to Needlestick Injuries & Body Fluids
 Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Universal Precautions
 Universal Precautions James Madison University Brought to you by Office of Health Promotion, JMU Health Center (2007) Purpose of this Training Teach the principles behind the prevention of disease transmission.
Universal Precautions James Madison University Brought to you by Office of Health Promotion, JMU Health Center (2007) Purpose of this Training Teach the principles behind the prevention of disease transmission.
Blood Borne Pathogen Exposure Employee
 Blood Borne Pathogen Exposure Employee INSTRUCTIONS 1. Employee: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
Blood Borne Pathogen Exposure Employee INSTRUCTIONS 1. Employee: Get name, DOB and, if available, health record number of source patient Obtain form and assist your supervisor with providing information
The OSHA Standard. The OSHA Standard. The OSHA Standard
 Bloodborne Pathogen Training 1 What are Bloodborne Pathogens? We already have learned that pathogens are infectious agents that can cause us to get sick like viruses or bacteria or germs or parasites.
Bloodborne Pathogen Training 1 What are Bloodborne Pathogens? We already have learned that pathogens are infectious agents that can cause us to get sick like viruses or bacteria or germs or parasites.
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses
 Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Bloodborne Infectious Diseases
 Bloodborne Infectious Diseases Dr. Kaya Süer Near East University Faculty of Medicine Infectious Diseases and Clinical Microbiology Bloodborne Pathogens Bloodborne pathogens Pathogenic organisms present
Bloodborne Infectious Diseases Dr. Kaya Süer Near East University Faculty of Medicine Infectious Diseases and Clinical Microbiology Bloodborne Pathogens Bloodborne pathogens Pathogenic organisms present
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Prophylaxis
 01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Establish protocol for management of occupational exposures to blood or potentially infectious materials. All employees of
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Establish protocol for management of occupational exposures to blood or potentially infectious materials. All employees of
BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM
 Page 1 of 13 BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM INTRODUCTION The attached materials will assist in teaching the information about bloodborne pathogens for health care workers as required
Page 1 of 13 BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM INTRODUCTION The attached materials will assist in teaching the information about bloodborne pathogens for health care workers as required
May Safety Subject. Bloodborne Pathogens
 May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
May Safety Subject Bloodborne Pathogens Everyone is at risk to contact bloodborne pathogens. Some more than others. Universal precautions means treating all objects as potentially contaminated Personal
EQuIP 5 - This version June 2011 Revision Due June 2014
 Preamble Rockingham Peel Group Non-Occupational Post-Exposure Prophylaxis (NPEP) To Prevent HIV in Western Australia Protocol The purpose of this protocol is to clarify the appropriate use and methods
Preamble Rockingham Peel Group Non-Occupational Post-Exposure Prophylaxis (NPEP) To Prevent HIV in Western Australia Protocol The purpose of this protocol is to clarify the appropriate use and methods
HIV Management Update 2015
 9/30/15 HIV Management Update 2015 Larry Pineda, PharmD, PhC, BCPS Visiting Assistant Professor Pharmacy Practice and Administrative Science ljpineda@salud.unm.edu Pharmacist Learning Objectives Describe
9/30/15 HIV Management Update 2015 Larry Pineda, PharmD, PhC, BCPS Visiting Assistant Professor Pharmacy Practice and Administrative Science ljpineda@salud.unm.edu Pharmacist Learning Objectives Describe
BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees
 BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees Buncombe County Public Schools require employees to receive annual training for Bloodborne Pathogens. This online training
BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees Buncombe County Public Schools require employees to receive annual training for Bloodborne Pathogens. This online training
Blood Borne Pathogens. Becky Walch, R.N. Micheel Valdez, L.V.N.
 Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
Safety Committee Prototypical Safety Program Manual
 1 Bloodborne Pathogens Exposure Control Plan Policy The Department Bloodborne Pathogens Exposure Control Plan is designed to comply with the requirements of the OSHA Bloodborne Pathogens Standard, 29 CFR
1 Bloodborne Pathogens Exposure Control Plan Policy The Department Bloodborne Pathogens Exposure Control Plan is designed to comply with the requirements of the OSHA Bloodborne Pathogens Standard, 29 CFR
Postexposure prophylaxis (PEP)
 Postexposure Prophylaxis Against Human Immunodeficiency Virus MICHAEL A. TOLLE, MD, MPH, and HEIDI L. SCHWARZWALD, MD, MPH, Baylor College of Medicine, Houston, Texas Family physicians often encounter
Postexposure Prophylaxis Against Human Immunodeficiency Virus MICHAEL A. TOLLE, MD, MPH, and HEIDI L. SCHWARZWALD, MD, MPH, Baylor College of Medicine, Houston, Texas Family physicians often encounter
WVU Occupational Medicine Program for evaluation and treatment of persons exposed to Lentivirus Vectors
 Hazard Description: Lentivirus vector systems are derived from HIV and similar viruses because of being very effective at inserting genetic material into the genome of target cells. While most researchers
Hazard Description: Lentivirus vector systems are derived from HIV and similar viruses because of being very effective at inserting genetic material into the genome of target cells. While most researchers
Guidelines for Implementing Pre-Exposure Prophylaxis For The Prevention of HIV in Youth Peter Havens, MD MS Draft:
 Guidelines for Implementing Pre-Exposure Prophylaxis For The Prevention of HIV in Youth Peter Havens, MD MS Draft: 10-2-2015 Clinical studies demonstrate that when a person without HIV infection takes
Guidelines for Implementing Pre-Exposure Prophylaxis For The Prevention of HIV in Youth Peter Havens, MD MS Draft: 10-2-2015 Clinical studies demonstrate that when a person without HIV infection takes
Hepatitis B is a virus that attacks the liver. It is highly infectious. Hepatitis B is transmitted primarily
 BLOOD BORNE PATHOGENS TRAINING FOR SCHOOL STAFF Blood Borne Pathogen (BBP): A blood borne pathogen is defined as an organism found in human blood or other infected body fluids that may cause disease in
BLOOD BORNE PATHOGENS TRAINING FOR SCHOOL STAFF Blood Borne Pathogen (BBP): A blood borne pathogen is defined as an organism found in human blood or other infected body fluids that may cause disease in
Bloodborne Pathogens. Kathleen Stefek, RN, MSN
 Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
Effective Date: 6/10/2013 Review Date: 6/10/2016
 Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Clinical management of non-occupational and occupational exposure to blood borne pathogens. - A Pocket Reference -
 Pocket P.E.P. Clinical management of non-occupational and occupational eposure to blood borne pathogens Development Team: Deborah Yoong, PharmD 1 1, 2, 3 Kevin Gough, MD, MEd 1 Positive Care Clinic, Toronto,
Pocket P.E.P. Clinical management of non-occupational and occupational eposure to blood borne pathogens Development Team: Deborah Yoong, PharmD 1 1, 2, 3 Kevin Gough, MD, MEd 1 Positive Care Clinic, Toronto,
Self-Instructional Packet (SIP)
 Self-Instructional Packet (SIP) Advanced Infection Prevention and Control Training Module 1 Intro to Infection Prevention Control February 11, 2013 Page 1 Learning Objectives Module One Introduction to
Self-Instructional Packet (SIP) Advanced Infection Prevention and Control Training Module 1 Intro to Infection Prevention Control February 11, 2013 Page 1 Learning Objectives Module One Introduction to
SUBJECT: Management of Human Body Fluids/Waste (Bloodborne Pathogens)
 Page 1 of 6 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 PURPOSE To establish uniform procedures for the safe management of human body fluids
Page 1 of 6 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 PURPOSE To establish uniform procedures for the safe management of human body fluids
For. Correctional. Officers. Your. Health Risks. in Correctional Settings. Facts. About HIV
 For Correctional Officers Your Health Risks in Correctional Settings Facts About HIV Working in close quarters with inmates in a correctional facility puts correctional officers (COs) at increased risk
For Correctional Officers Your Health Risks in Correctional Settings Facts About HIV Working in close quarters with inmates in a correctional facility puts correctional officers (COs) at increased risk
Goldenrod Hills Community Action. Bloodborne Pathogen (BBP) Training according to OSHA Standard 29 CFR
 Goldenrod Hills Community Action Bloodborne Pathogen (BBP) Training according to OSHA Standard 29 CFR 1910.1030 Welcome to GHCA s Bloodborne Pathogen Training based upon the Occupational Safety and Health
Goldenrod Hills Community Action Bloodborne Pathogen (BBP) Training according to OSHA Standard 29 CFR 1910.1030 Welcome to GHCA s Bloodborne Pathogen Training based upon the Occupational Safety and Health
A. Background for Trainer: B. What OSHA Requires: Bloodborne Pathogens. Lesson Plan 6080a
 Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
Lesson Plan 6080a This training session outline is designed to follow the accompanying booklet, OSHA s Bloodborne Pathogens Standard. The booklet reviews what employees who are potentially exposed to the
Haemophilus influenzae, Invasive Disease rev Jan 2018
 Haemophilus influenzae, Invasive Disease rev Jan 2018 BASIC EPIDEMIOLOGY Infectious Agent Haemophilus influenzae (H. influenzae) is a small, Gram-negative bacillus, a bacterium capable of causing a range
Haemophilus influenzae, Invasive Disease rev Jan 2018 BASIC EPIDEMIOLOGY Infectious Agent Haemophilus influenzae (H. influenzae) is a small, Gram-negative bacillus, a bacterium capable of causing a range
BAY-ARENAC BEHAVIORAL HEALTH AUTHORITY POLICIES AND PROCEDURES MANUAL
 Page: 1 of 8 Policy Bay-Arenac Behavioral Health Authority (BABHA) is committed to high standards of employee and consumer safety practices. This standard will include the prevention, surveillance, identification
Page: 1 of 8 Policy Bay-Arenac Behavioral Health Authority (BABHA) is committed to high standards of employee and consumer safety practices. This standard will include the prevention, surveillance, identification
Safety Tips from the WorkSafe People
 Blood Borne Pathogens Training HIV/AIDS Hepatitis B Determining Exposure Protecting Yourself Preventing Exposure during an Emergency HIV/AIDS Definition: AIDS stands for Acquired Immune Deficiency Syndrome.
Blood Borne Pathogens Training HIV/AIDS Hepatitis B Determining Exposure Protecting Yourself Preventing Exposure during an Emergency HIV/AIDS Definition: AIDS stands for Acquired Immune Deficiency Syndrome.
Bloodborne Pathogens Training For School Personnel
 Bloodborne Pathogens Training For School Personnel OSHA Defined: Occupational Safety and Health Administration Published a standard to reduce or eliminate health risk, resulting in: Annual training of
Bloodborne Pathogens Training For School Personnel OSHA Defined: Occupational Safety and Health Administration Published a standard to reduce or eliminate health risk, resulting in: Annual training of
