Discontinuation of Secondary Prophylaxis against Disseminated Mycobacterium avium Complex Infection and Toxoplasmic Encephalitis
|
|
|
- Lauren Elliott
- 5 years ago
- Views:
Transcription
1 HIV/AIDS MAJOR ARTICLE Discontinuation of Secondary Prophylaxis against Disseminated Mycobacterium avium Complex Infection and Toxoplasmic Encephalitis Valérie Zeller, 1 Chantal Truffot, 2 Rachid Agher, 1 Philippe Bossi, 1 Roland Tubiana, 1 Eric Caumes, 1 Marc Jouan, 1 François Bricaire, 1 and Christine Katlama 1 Departments of 1 Infectious Diseases and 2 Bacteriology, Pitié-Salpêtrière Hospital, Paris, France We retrospectively studied outcomes for patients infected with human immunodeficiency virus who received highly active antiretroviral therapy (HAART) and had stopped receiving secondary prophylaxis against toxoplasmic encephalitis (TE) or disseminated Mycobacterium avium complex (MAC) infection. Nineteen patients had a history of TE, and 26 had a history of disseminated MAC infection. The median duration of secondary prophylaxis was 27 months, and the median duration of HAART before discontinuation of secondary prophylaxis was 22 months. Median CD4 + cell counts at the time of cessation of secondary prophylaxis against TE or disseminated MAC infection were 404 and 105 cells/mm 3, respectively. Plasma virus load was undetectable in 68% of the patients who had a history of TE and in 31% of patients who had a history of disseminated MAC infection. Patients were followed up for a median of 29 months after discontinuation of secondary prophylaxis; no relapses occurred in patients with a history of TE, and 3 relapses occurred in patients with a history of disseminated MAC infection (incidence, 4 relapses per 100 person-years). The use of highly active antiretroviral therapy (HAART) in recent years has markedly reduced the risk of opportunistic infections and death in HIV-infected patients [1, 2]. The clinical benefit is related to immune reconstitution, which is associated with a quantitative and qualitative improvement in CD4 cells [3, 4]. This raises the possibility that prophylaxis against opportunistic infections can be discontinued for patients with a good immunologic and virologic response to HAART. Indeed, simplification of therapy is a major factor in Received 15 June 2001; revised 1 October 2001; electronically published 24 January Reprints or correspondence: Dr. Valérie Zeller, Service des Maladies Infectieuses et Tropicales, CHU Pitié-Salpêtrière, Bd. de l Hôpital, Paris Cedex 013, France (valerie.zeller@psl.ap-hop-paris.fr). Clinical Infectious Diseases 2002; 34: by the Infectious Diseases Society of America. All rights reserved /2002/ $03.00 adherence to treatment and in the efficacy of antiretroviral drugs. Several prospective trials have shown that primary prophylaxis against opportunistic infections such as Pneumocystis carinii pneumonia, toxoplasmic encephalitis (TE), cytomegalovirus (CMV) retinitis, and disseminated Mycobacterium avium complex (MAC) infection can be safely discontinued for patients receiving HAART who have good immunologic and virologic response [5 12]. Discontinuation of secondary prophylaxis for opportunistic infections in patients successfully treated with HAART has been less widely investigated. Because of its high toxicity, CMV maintenance therapy was one of the first courses of prophylaxis to be evaluated in this respect. Several studies [13 16] have shown that CMV maintenance therapy can be discontinued in patients receiving HAART whose CD4 cell count remains 662 CID 2002:34 (1 March) HIV/AIDS
2 cells/mm 3 for 3 6 months [12]. More recently, 2 large studies (a cohort study and a randomized study) concluded that secondary prophylaxis against P. carinii pneumonia could be discontinued safely for patients receiving HAART in whom CD4 cell counts increase to 1200 cells/mm 3 [17, 18]. In contrast, few data are available on the safety of discontinuing secondary prophylaxis for other opportunistic infections, such as cerebral toxoplasmosis, disseminated MAC infection, and cryptococcal meningitis [19 22]. We undertook a retrospective study designed to evaluate outcomes for HIV-infected patients treated with HAART who discontinued secondary prophylaxis against TE and disseminated MAC infection. PATIENTS AND METHODS We reviewed the charts of all HIV-infected patients treated in the Department of Infectious Diseases at Pitié-Salpêtrière Hospital, Paris, who had a history of documented TE or disseminated MAC infection. Cerebral toxoplasmosis was diagnosed on the basis of a clinical and radiological response to specific treatment in patients who had clinical and neuroradiological evidence of a space-occupying cerebral lesion and who had IgG antibodies against Toxoplasma gondii (as determined by ELISA and an immunofluorescence assay). Disseminated MAC infection was diagnosed on the basis of 1 blood culture positive for MAC. Patients were included in the study if they were already receiving HAART when they stopped receiving secondary prophylaxis, and if they had at least 6 months of followup after discontinuing secondary prophylaxis. The following data were recorded for each patient: sex, age, risk factor for HIV infection, date of diagnosis and treatment of the opportunistic infection, date of initiation of HAART, date of cessation of secondary prophylaxis, and CD4 lymphocyte count and plasma virus load at diagnosis of the opportunistic infection, at initiation of HAART, and at discontinuation of secondary prophylaxis. All patients had their last follow-up visit during the period July December All clinical events that occurred after cessation of secondary prophylaxis were recorded. The following data were recorded for patients who died after June 1996: date of HAART initiation, date of cessation of secondary prophylaxis, and cause of death. Patients who died before June 1996 (i.e., before initiation of HAART) were excluded from the study. RESULTS One hundred thirteen patients with a history of TE and 49 patients with a history of disseminated MAC infection were seen in the Infectious Diseases Department of Pitié-Salpêtrière Hospital from June 1996 through December 2000 (figure 1). Twenty-six of these patients died. The causes of death are shown in figure 1. One patient died after a seizure at home, 1 month after starting treatment with sulfadiazine and pyrimethamine for cerebral toxoplasmosis. Another patient died of disseminated MAC infection; this patient had stopped taking both anti MAC and antiretroviral treatment. The other patients died of causes apparently unrelated to the opportunistic infection for which they were receiving prophylaxis. The cause of death was unknown for 7 patients, 6 of whom had not stopped taking secondary prophylaxis against the opportunistic infection. All 22 patients who were lost to follow-up for 11 year were still receiving secondary prophylaxis at the time of the last visit. Sixty-nine patients were still receiving secondary prophylaxis. Forty-five patients had stopped receiving secondary prophylaxis, for TE in 19 patients and for disseminated MAC infection in 26 patients (figure 1). The clinical characteristics of these 45 patients are shown in table 1. Forty-four patients (98%) were men, and the median age was 39 years (range, years). Risk factors for HIV infection were homosexual sexual activity for 27 patients (60%), heterosexual sexual activity for 10 patients (22%), injection drug use for 5 patients (11%), blood transfusion for 1 patient (2.2%), and undetermined factors for 2 patients (4.4%). Three of the 26 patients with a history of disseminated MAC infection experienced a relapse (incidence, 4 relapses per 100 person-years). The first patient developed disseminated MAC infection 2 months after starting primary prophylaxis with clarithromycin and 1 month after starting HAART. He was initially treated with a combination of ethambutol, clofazimin, ciprofloxacin, and azithromycin, but azithromycin was discontinued after 6 months because the infecting strain was resistant to clarithromycin (MIC, 128 mg/l) and the patient had poor compliance. The other drugs were maintained for an additional 6 months. The second patient was treated for disseminated MAC infection that developed 1 month after initiation of HAART with clarithromycin, ethambutol, and rifabutin for 12 months. Compliance with clarithromycin therapy was poor. Three months after they stopped receiving anti-mac treatment, both patients had clinical and radiological signs of joint and bone infection. Relapse of infection was diagnosed on the basis of a culture of a bone biopsy specimen (with use of Loewenstein-Jensen medium) that was positive for MAC. The infecting strains from both patients were susceptible to clarithromycin (MIC, 4 mg/l). At the time of relapse, the patients were afebrile, blood cultures for MAC remained negative, and the patients had a good immunologic and virologic response to HAART (CD4 cell count, 126 and 160 cells/mm 3, respectively; virus load,!200 copies/ml for both patients). Prolonged treatment (1 and 2 years, respectively) of the MAC infection relapse with HIV/AIDS CID 2002:34 (1 March) 663
3 Figure 1. Summary of outcomes for study patients with HIV infection who discontinued secondary prophylaxis (SP) against disseminated Mycobacterium avium complex (MAC) infection or toxoplasmic encephalitis. CMV, cytomegalovirus. specific multidrug regimens (which included clarithromycin, ethambutol, sparfloxacin, and amikacin) was successful in both patients. No additional relapses had occurred 16 and 19 months, respectively, after the end of treatment of the MAC infection relapse. Genotyping of the resistant and susceptible strains isolated from the first patient (by use of M. avium direct repetitive element PCR) revealed identical profiles. The third patient had disseminated MAC infection that was successfully treated with clarithromycin, ethambutol, and rifabutin for 12 months. His CD4 cell count was 107 cells/mm 3 when he stopped receiving anti-mac treatment. He experienced a late relapse 40 months after discontinuing maintenance treatment. At that time, he was severely immunodeficient (CD4 cell count,!50 cells/mm 3 ) and had had a high plasma virus load (1100,000 copies/ml) for 2.5 years. MAC was isolated from a subcutaneous abscess (2 colonies) and a blood culture (1 colony). Salvage antiretroviral therapy was started in October 2000, simultaneously with anti-mac treatment consisting of clarithromycin, rifabutin, and ethambutol. Six months later, at the time of this analysis, his condition was stable and a culture of a blood sample on Loewenstein-Jensen medium was sterile; however, antiretroviral therapy was virologically and immunologically ineffective (CD4 cell count, 1 cell/mm 3 ; plasma virus load, 400,000 copies/ml). Genotyping of the initial and relapse strains showed different profiles, which suggested reinfection, rather than relapse. An additional 25 clinical events occurred in 14 of the 45 patients after discontinuation of secondary prophylaxis: there were 11 viral infections (CMV in 5 patients, varicella-zoster virus in 4 patients, and herpes simplex virus in 2 patients), CID 2002:34 (1 March) HIV/AIDS
4 Table 1. Clinical characteristics of 45 patients with HIV infection who discontinued secondary prophylaxis against disseminated Mycobacterium avium complex (MAC) infection or toxoplasmic encephalitis. Characteristic Toxoplasmic encephalitis (n p 19) Disseminated MAC infection (n p 26) Duration of therapy, median months (range) Secondary prophylaxis 28 (9 69) 23 (6 48) HAART before discontinuation of secondary prophylaxis 29 (12 45) 13 (1 39) CD4 cell count by time point, median cells/mm 3 (range) At diagnosis of opportunistic infection 88 (1 220) 10 (1 171) At discontinuation of secondary prophylaxis 404 ( ) 105 (1 254) At last follow-up visit 497 (1 813) 309 (1 735) Patients per CD4 cell count category, no. (%) At discontinuation of secondary prophylaxis!50 cells/mm (27) cells/mm (19) cells/mm (31) 1200 cells/mm 3 19 (100) 6 (23) At last follow-up visit!50 cells/mm (11.5) cells/mm (4) cells/mm 3 1 (5) 3 (11.5) 1200 cells/mm 3 18 (95) 19 (73) Duration of elevated CD4 count a before discontinuation of secondary prophylaxis, no. (%) of patients 3 months 18 (95) 8 (31) 6 months 18 (95) 6 (23) Virus load, median copies/ml (% of patients with!200 copies/ml) At diagnosis of opportunistic infection 135,862 (0) 380,000 (4) At discontinuation of secondary prophylaxis 4478 (68) 83,864 (31) At last follow-up visit 1307 (52) 1851 (46) Duration of follow-up after discontinuation of secondary prophylaxis, median months (range) 20 (8 50) 35 (15 57) Relapse rate, % (95% CI) (0 24) NOTE. HAART, highly active antiretroviral therapy. a Greater than recommended threshold: for patients with toxoplasmic encephalitis, 1200 cells/mm 3 ; for patients with disseminated MAC infection, 1100 cells/mm 3 [23]. bacterial infections (pneumonia in 5 patients, sinusitis in 1 patient, colitis in 1 patient, cutaneous abscess in 1 patient, and catheter-related infection in 1 patient), 1 case of P. carinii pneumonia (in a patient with a history of MAC infection), 3 malignancies (progression of Kaposi s sarcoma in 1 patient, Castleman s disease in 1 patient, and rectal cancer in 1 patient), and 1 hip fracture. DISCUSSION The efficacy of HAART has raised the possibility that potentially toxic maintenance therapies against common opportunistic infections can be discontinued for patients whose CD4 cell count increases substantially during antiretroviral therapy. Good adherence to antiretroviral therapy is crucial to maintaining its efficacy and can be encouraged by use of simple, well-tolerated regimens. Therefore, clinicians managing HIV-infected patients should aim to minimize pill intake, drug toxicity, and potential drug interactions. To assess the feasibility of this objective in the post-haart era, we evaluated the safety of discontinuing secondary prophylaxis against 2 major opportunist infections: cerebral toxoplasmosis and disseminated MAC infection. In this retrospective series, there were no relapses in the 19 patients with a history of cerebral toxoplasmosis after a median HIV/AIDS CID 2002:34 (1 March) 665
5 follow-up of 20 months. All the patients had CD4 cell counts of 1200 cells/mm 3 when they discontinued secondary prophylaxis, and 95% of them maintained this level for 16 months. These results support the recommendations of recent draft of the US Public Health Service (USPHS) guidelines [23] and suggest that secondary prophylaxis for TE can be discontinued for patients receiving HAART whose CD4 cell counts remain 1200 cells/mm 3 for 3 6 months. Soriano et al. [20] described 9 patients treated with HAART who discontinued secondary prophylaxis for cerebral toxoplasmosis when their CD4 cell counts were 1100 cells/mm 3 and their plasma HIV RNA loads were!500 copies/ml. No relapses were noted during 18 months of follow-up. Data on discontinuation of secondary prophylaxis for disseminated MAC infection are more limited. Aberg et al. [19] described 4 patients with a history of disseminated MAC infection who were receiving HAART and discontinued their maintenance treatment when their CD4 cell counts were 1100 cells/mm 3 and their virus loads were!10,000 copies/ml. All had received a macrolide-based anti-mac regimen for at least 1 year. No relapses occurred during 8 13 months of followup. Soriano et al. [20] described 7 patients treated with HAART who discontinued maintenance treatment for MAC infection. No relapses occurred during 18 months of follow-up. More recently, Shafran et al. [22] conducted a retrospective study of 33 patients with a history of disseminated MAC infection who discontinued maintenance treatment while receiving HAART. At a median of 17 months of follow-up, only 1 patient experienced relapse (37 months after discontinuing MAC prophylaxis); it is noteworthy that this patient had uncontrolled HIV disease after having discontinued HAART. We retrospectively studied 26 patients who discontinued secondary prophylaxis for disseminated MAC infection while receiving HAART. When secondary prophylaxis was discontinued, the median CD4 lymphocyte count in these patients remained low (99 cells/mm 3 ); 7 patients (27%) had a CD4 count!50 cells/mm 3, and only 6 patients (23%) had CD4 count 1100 cells/mm 3 for at least 6 months. There were 3 relapses of MAC infection among these 26 patients during a median of 35 months of follow-up (range, months), corresponding to a relapse rate of 11.5% (95% CI, 0% 24%) and an incidence of 4 relapses per 100 person-years. This relapse rate is lower than was observed in the pre-haart era among patients receiving secondary prophylaxis. Two of these patients received suboptimal anti-mac therapy, possibly explaining the persistence and slow growth of mycobacteria in bone, despite immune restoration (CD4 cell counts, 1100 cells/mm 3 ). The third relapse occurred in a severely immunodeficient patient who had stopped receiving antiretroviral treatment. Genotyping of the 2 strains suggested reinfection rather than relapse. Our results suggest that specific immune responses to MAC are rapidly restored after initiation of HAART, even in patients with severe immunodeficiency and only partial viral suppression. Hadad et al. [24] described a patient who had 1 blood culture that grew a single colony of MAC and who was treated with HAART alone. Symptoms resolved completely, and subsequent blood cultures were negative for MAC. Havlir et al. [25] measured immune responses to M. avium before and during HAART in HIV-infected patients with a history of disseminated MAC infection. Proliferative responses to M. avium were present in 47% of patients before the initiation of HAART, in 61% of patients 3 months after the initiation of HAART, and in 77% of patients 6 months after the initiation of HAART. According to the 2001 USPHS guidelines [23], patients are thought to be at low risk for relapse of MAC infection once they have completed at least 12 months of anti-mac treatment and have had a sustained increase (at least 6 months) in their CD4 cell counts (to 1100 cells/mm 3 ) while receiving HAART. Our results, and those of Shafran et al. [22], support these guidelines and suggest that maintenance treatment for disseminated MAC infection can be stopped for patients receiving HAART whose CD4 cell counts remain 1100 cells/mm 3 for 3 6 months. Primary MAC infection should be treated with a combination of 3 drugs that includes clarithromycin. Optimal adherence to such regimens is crucial, but the minimum duration of anti-mac therapy in patients treated with HAART is unclear. Relapse and reinfection can occur in patients whose CD4 cell counts decrease to!100 cells/mm 3 while they are receiving HAART. Such patients should be monitored closely, and blood cultures (on Loewenstein-Jensen medium) should be performed regularly. Such patients may also qualify for a resumption of secondary prophylaxis. Furthermore, clinically atypical relapses can occur despite immune reconstitution in patients who have received suboptimal anti-mac treatment. We conclude that it is feasible and desirable to discontinue secondary prophylaxis for some common opportunistic infections in patients who have a satisfactory virologic and immunologic response to HAART. Acknowledgments We thank Jérome Briquet, Sophia Girard, Mélina LeBarbier, Jennifer LeGrand, and Fanny Pellegrin, for their help. References 1. Palella F, Delaney K, Moorman A, et al. Declining morbidity and mortality among patients with advanced human immunodeficiency virus infection. N Engl J Med 1998; 338: Miller V, Staszewski S, Nisius G, et al. Risk of new AIDS diseases in people on triple therapy. Lancet 1999; 353: Autran B, Carcelain G, Li TS, et al. Positive effects of combined anti- 666 CID 2002:34 (1 March) HIV/AIDS
6 retroviral therapy on CD4 T cell homeostasis and function in advanced HIV disease. Science 1997; 277: Li TS, Tubiana R, Katlama C, Calvez V, Mohand HA, Autran B. Long lasting recovery in CD4 T cell function mirrors viral load reduction after highly active anti-retroviral therapy in patients with advanced HIV disease. Lancet 1998; 351: Furrer H, Egger M, Opravil M, et al. Discontinuation of primary prophylaxis against Pneumocystis carinii pneumonia in HIV-1 infected adults treated with combination antiretroviral therapy. N Engl J Med 1999; 340: Weverling G, Mocroft A, Lederberger B, Reiss P. Discontinuation of Pneumocystis carinii pneumonia prophylaxis after start of highly active antiretroviral therapy in HIV-1 infection. Lancet 1999; 353: Miro J, Lopez J, Podzamczer D, et al. Discontinuation of toxoplasmic encephalitis prophylaxis is safe in HIV-1 and T. gondii co-infected patients after immunological recovery with HAART: preliminary results of the GESIDA 04/98-B Study [abstract 230]. In: Program and abstracts of the 7th Conference on Retroviruses and Opportunistic Infections (San Francisco) Furrer H, Opravil M, Bernasconi, F, Telenti A, Egger M. Stopping primary prophylaxis in HIV-1 infected patients at high risk of toxoplasma encephalitis. Swiss HIV Cohort study. Lancet 2000; 355: Currier J, Williams P, Koletar S, et al. Discontinuation or Mycobacterium avium complex prophylaxis in patients with antiretroviral therapy-induced increases in CD4 cell count. Ann Intern Med 2000; 133: Furrer H, Telenti A, Rossi M, Lederberger B. Discontinuing of withholding primary prophylaxis against M. avium in patients on successful antiretroviral combination therapy: the Swiss HIV Cohort experience [abstract 246]. In: Program and abstracts of the 7th Conference on Retroviruses and Opportunistic Infections (San Francisco) El-Sadr W, Burman W, Grant L, et al. Discontinuation of prophylaxis against Mycobacterium avium complex disease in HIV-infected patients who have a response to antiretroviral therapy. N Engl J Med 2000; 342: Kovacs J, Masur H. Prophylaxis against opportunistic infections in patients with human immunodeficiency virus infection. N Engl J Med 2000; 342: Whitcup SM, Fortin E, Lindblad AS, et al. Discontinuation of anticytomegalovirus therapy in persons with HIV infection and cytomegalovirus retinitis. JAMA 1999; 282: Macdonald JC, Torriani FJ, Morse LS, Karavellas MP, Reed JB, Freeman WR. Lack of reactivation of cytomegalovirus retinitis after stopping CMV maintenance therapy in AIDS patients with sustained elevations in CD4 T cells in response to highly active antiretroviral therapy. J Infect Dis 1998; 177: Tural C, Romeu J, Sirera G, et al. Long-lasting remission of cytomegalovirus retinitis without maintenance therapy in human immunodeficiency virus infected patients. J Infect Dis 1998; 177: Jouan M, Savès M, Tubiana R, et al. Discontinuation of maintenance therapy for cytomegalovirus retinitis in HIV-infected patients receiving highly active antiretroviral therapy. AIDS 2001; 15: Lederberger B, Mocroft A, Reiss P, et al. Discontinuation of secondary prophylaxis against Pneumocystis carinii pneumonia in patients with HIV infection who have a response to antiretroviral therapy. N Engl J Med 2001; 344: Lopez Bernaldo de Quiros J, Miro J, Pena J, et al. A randomized trial of the discontinuation of primary and secondary prophylaxis against Pneumocystis pneumonia after highly active antiretroviral therapy in patients with HIV infection. N Engl J Med 2001; 344: Aberg J, Yajko D, Jacobson M. Eradication of AIDS-related disseminated Mycobacterium avium complex infection after 12 months of antimycobacterial therapy combined with highly active antiretroviral therapy. J Infect Dis 1998; 178: Soriano V, Dona C, Rodriguez-Rosado R, Barreiro P, Gonzalez-Lahoz J. Discontinuation of secondary prophylaxis for opportunistic infections in HIV-infected patients receiving highly active antiretroviral therapy. AIDS 2000; 14: Mussini C, Pini R, Borgi S, et al. Discontinuation of secondary prophylaxis for cryptococcal meningitis in AIDS patients receiving HAART [abstract 1912]. In: Program and abstracts of the 40th International Conference on Antimicrobial Agents and Chemotherapy (Toronto). Washington, DC: American Society for Microbiology, 2000: Shafran S, Gill M, Lalonde R, et al. Successful discontinuation of MAC therapy following effective HAART [abstratct 547]. In: Programs and abstracts of the 8th Conference on Retroviruses and Opportunistic Infections (Chicago) US Public Health Service (USPHS) and Infectious Diseases Society of America (IDSA). USPHS/IDSA Prevention of Opportunistic Infections Working Group USPHS/IDSA guidelines for the prevention of opportunistic infections in persons infected with human immunodeficiency virus. Available at: Accessed 23 January Hadad D, Lewi D, Pignatari A, Martins M, Vitti W, Arbeit R. Resolution of Mycobacterium avium complex following highly active antiretroviral therapy. Clin Infect Dis 1998; 26: Havlir D, Schrier R, Torriani F, Chervenak K, Hwang J, Boom WH. Effect of potent antiretroviral therapy on immune responses to Mycobacterium avium in human immunodeficiency virus infected subjects. J Infect Dis 2000; 182: HIV/AIDS CID 2002:34 (1 March) 667
ORIGINAL ARTICLE /j x
 ORIGINAL ARTICLE 10.1111/j.1469-0691.2006.01367.x Endemic fungal infections caused by Cryptococcus neoformans and Penicillium marneffei in patients infected with human immunodeficiency virus and treated
ORIGINAL ARTICLE 10.1111/j.1469-0691.2006.01367.x Endemic fungal infections caused by Cryptococcus neoformans and Penicillium marneffei in patients infected with human immunodeficiency virus and treated
Impact of highly active antiretroviral therapy on incidence and management of human immunodeficiency virus-related opportunistic infections
 Journal of Antimicrobial Chemotherapy (2004) 54, 849 853 DOI: 10.1093/jac/dkh438 Advance Access publication 29 September 2004 Impact of highly active antiretroviral therapy on incidence and management
Journal of Antimicrobial Chemotherapy (2004) 54, 849 853 DOI: 10.1093/jac/dkh438 Advance Access publication 29 September 2004 Impact of highly active antiretroviral therapy on incidence and management
Cryptococcosis of the Central Nervous System: Classical and Immune-Reconstitution Disease
 Cryptococcosis of the Central Nervous System: Classical and Immune-Reconstitution Disease Assist Prof. Somnuek Sungkanuparph Division of Infectious Diseases Faculty of Medicine Ramathibodi Hospital Mahidol
Cryptococcosis of the Central Nervous System: Classical and Immune-Reconstitution Disease Assist Prof. Somnuek Sungkanuparph Division of Infectious Diseases Faculty of Medicine Ramathibodi Hospital Mahidol
CONCISE COMMUNICATION
 611 CONCISE COMMUNICATION Risk for Preventable Opportunistic Infections in Persons with AIDS after Antiretroviral Therapy Increases CD4 + T Lymphocyte Counts above Prophylaxis Thresholds Mark S. Dworkin,
611 CONCISE COMMUNICATION Risk for Preventable Opportunistic Infections in Persons with AIDS after Antiretroviral Therapy Increases CD4 + T Lymphocyte Counts above Prophylaxis Thresholds Mark S. Dworkin,
AIDS at 25. Epidemiology and Clinical Management MID 37
 AIDS at 25 Epidemiology and Clinical Management Blood HIV Transmission transfusion injection drug use Sexual Intercourse heterosexual male to male Perinatal intrapartum breast feeding Regional HIV and
AIDS at 25 Epidemiology and Clinical Management Blood HIV Transmission transfusion injection drug use Sexual Intercourse heterosexual male to male Perinatal intrapartum breast feeding Regional HIV and
OI prophylaxis When to start, when to stop. Eva Raphael, MD MPH Family and community medicine, pgy-2 University of California, San Francisco
 OI prophylaxis When to start, when to stop Eva Raphael, MD MPH Family and community medicine, pgy-2 University of California, San Francisco Learning Objectives o Recognize when to start OI prophylaxis
OI prophylaxis When to start, when to stop Eva Raphael, MD MPH Family and community medicine, pgy-2 University of California, San Francisco Learning Objectives o Recognize when to start OI prophylaxis
To interrupt or not to interrupt Are we SMART enough?
 SMART To interrupt or not to interrupt Are we SMART enough? highly active antiretroviral therapy 5 1996 1997 10 25 43 45 35 metabolism 50 copies/ml lipodystrophy [fat redistribution syndrome] lactic acidosis
SMART To interrupt or not to interrupt Are we SMART enough? highly active antiretroviral therapy 5 1996 1997 10 25 43 45 35 metabolism 50 copies/ml lipodystrophy [fat redistribution syndrome] lactic acidosis
AIDS at 30 Epidemiology and Clinical Epidemiology and Management MID 37
 AIDS at 30 Epidemiology and Clinical Management Blood HIV Transmission transfusion injection drug use Sexual Intercourse heterosexual male to male Perinatal intrapartum breast feeding Adults and children
AIDS at 30 Epidemiology and Clinical Management Blood HIV Transmission transfusion injection drug use Sexual Intercourse heterosexual male to male Perinatal intrapartum breast feeding Adults and children
5/15/2017. What Does HIV/AIDS Look Like in DC in Potpourri of Challenges With Opportunistic Infections
 Potpourri of Challenges With Opportunistic Infections Henry Masur, MD Clinical Professor of Medicine George Washington University Washington, DC FORMATTED: 4/28/217 Learning Objectives After attending
Potpourri of Challenges With Opportunistic Infections Henry Masur, MD Clinical Professor of Medicine George Washington University Washington, DC FORMATTED: 4/28/217 Learning Objectives After attending
The importance of cohort collaborations for guiding clinical management of individuals with HIV infection
 The importance of cohort collaborations for guiding clinical management of individuals with HIV infection Caroline Sabin Professor of Medical Statistics and Epidemiology Royal Free and University College
The importance of cohort collaborations for guiding clinical management of individuals with HIV infection Caroline Sabin Professor of Medical Statistics and Epidemiology Royal Free and University College
Special populations. 11:30-11:40 Special populations (AIDS, etc...) Y. Van Laethem (Brussels)
 Special populations 11:30-11:40 Special populations (AIDS, etc...) Y. Van Laethem (Brussels) High persistant concentration in monocytes/polymorphonuclear leucocytes of : - azithromycin and clarithromycin
Special populations 11:30-11:40 Special populations (AIDS, etc...) Y. Van Laethem (Brussels) High persistant concentration in monocytes/polymorphonuclear leucocytes of : - azithromycin and clarithromycin
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 1999, by the Massachusetts Medical Society VOLUME 340 A PRIL 29, 1999 NUMBER 17 DISCONTINUATION OF PRIMARY PROPHYLAXIS AGAINST PNEUMOCYSTIS CARINII PNEUMONIA
The New England Journal of Medicine Copyright, 1999, by the Massachusetts Medical Society VOLUME 340 A PRIL 29, 1999 NUMBER 17 DISCONTINUATION OF PRIMARY PROPHYLAXIS AGAINST PNEUMOCYSTIS CARINII PNEUMONIA
When to start: guidelines comparison
 The editorial staff When to start: guidelines comparison The optimal time to begin antiretroviral therapy remains a critical question for the HIV field, and consensus about the appropriate CD4+ cell count
The editorial staff When to start: guidelines comparison The optimal time to begin antiretroviral therapy remains a critical question for the HIV field, and consensus about the appropriate CD4+ cell count
CMVR diagnoses and progression of CD4 cell counts and HIV viral load measurements in HIV patients on HAART
 Br J Ophthalmol 21;85:837 841 837 CMVR diagnoses and progression of CD4 cell counts and HIV viral load measurements in HIV patients on HAART Hadi J Zambarakji, Roger B Newson, Suzanne M Mitchell Department
Br J Ophthalmol 21;85:837 841 837 CMVR diagnoses and progression of CD4 cell counts and HIV viral load measurements in HIV patients on HAART Hadi J Zambarakji, Roger B Newson, Suzanne M Mitchell Department
Clinical Manifestations of HIV
 HIV Symptoms Diane Havlir, MD Professor of Medicine and Chief, HIV/AIDS Division University of California, San Francisco (UCSF) WorldMedSchool; July 2, 2013 1 Clinical Manifestations of HIV! Result from
HIV Symptoms Diane Havlir, MD Professor of Medicine and Chief, HIV/AIDS Division University of California, San Francisco (UCSF) WorldMedSchool; July 2, 2013 1 Clinical Manifestations of HIV! Result from
Immunodeficiencies HIV/AIDS
 Immunodeficiencies HIV/AIDS Immunodeficiencies Due to impaired function of one or more components of the immune or inflammatory responses. Problem may be with: B cells T cells phagocytes or complement
Immunodeficiencies HIV/AIDS Immunodeficiencies Due to impaired function of one or more components of the immune or inflammatory responses. Problem may be with: B cells T cells phagocytes or complement
Immune Reconstitution Inflammatory Syndrome - IRIS
 Immune Reconstitution Inflammatory Syndrome - IRIS Douglas G. Fish, MD Head, Division of HIV Medicine Albany Medical College Cali, Colombia March 25, 2010 I-Tech: Thank you International Training and
Immune Reconstitution Inflammatory Syndrome - IRIS Douglas G. Fish, MD Head, Division of HIV Medicine Albany Medical College Cali, Colombia March 25, 2010 I-Tech: Thank you International Training and
Management of Immune Reconstitution Inflammatory Syndrome (IRIS)
 Management of Immune Reconstitution Inflammatory Syndrome (IRIS) Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the IRIS Guideline
Management of Immune Reconstitution Inflammatory Syndrome (IRIS) Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the IRIS Guideline
HIV Update For the Internist
 HIV Update For the Internist Disclosures I declare that I have received no incentives, financial or otherwise, from pharmaceutical or biomedical companies relevant to the content of this talk. As an Infectious
HIV Update For the Internist Disclosures I declare that I have received no incentives, financial or otherwise, from pharmaceutical or biomedical companies relevant to the content of this talk. As an Infectious
Measure #161: HIV/AIDS: Adolescent and Adult Patients with HIV/AIDS Who Are Prescribed Potent Antiretroviral Therapy
 Measure #161: HIV/AIDS: Adolescent and Adult Patients with HIV/AIDS Who Are Prescribed Potent Antiretroviral Therapy 2012 PHYSICIAN QUALITY REPTING OPTIONS F INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION:
Measure #161: HIV/AIDS: Adolescent and Adult Patients with HIV/AIDS Who Are Prescribed Potent Antiretroviral Therapy 2012 PHYSICIAN QUALITY REPTING OPTIONS F INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION:
Risk Factors for Mortality in Patients with AIDS in the Era of Highly Active Antiretroviral Therapy
 Risk Factors for Mortality in Patients with AIDS in the Era of Highly Active Antiretroviral Therapy Douglas A. Jabs, MD, MBA, 1,2,3 Janet T. Holbrook, PhD, MPH, 3 Mark L. Van Natta, MHS, 3 Rebecca Clark,
Risk Factors for Mortality in Patients with AIDS in the Era of Highly Active Antiretroviral Therapy Douglas A. Jabs, MD, MBA, 1,2,3 Janet T. Holbrook, PhD, MPH, 3 Mark L. Van Natta, MHS, 3 Rebecca Clark,
HIV/AIDS MEASURES GROUP OVERVIEW
 2014 PQRS OPTIONS F MEASURES GROUPS: HIV/AIDS MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN HIV/AIDS MEASURES GROUP: #159. HIV/AIDS: CD4+ Cell Count or CD4+ Percentage Performed #160. HIV/AIDS: Pneumocystis
2014 PQRS OPTIONS F MEASURES GROUPS: HIV/AIDS MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN HIV/AIDS MEASURES GROUP: #159. HIV/AIDS: CD4+ Cell Count or CD4+ Percentage Performed #160. HIV/AIDS: Pneumocystis
Central Nervous System Immune Reconstitution Disease: Pathology
 Central Nervous System Immune Reconstitution Disease: Pathology F.Gray, H.Adle-Biassette, F.Héran, G. Pialoux, A.Moulignier, APHP Hôpital Lariboisière Université Paris VII Introduction of HAART, which
Central Nervous System Immune Reconstitution Disease: Pathology F.Gray, H.Adle-Biassette, F.Héran, G. Pialoux, A.Moulignier, APHP Hôpital Lariboisière Université Paris VII Introduction of HAART, which
The New England Journal of Medicine. Review Article
 Review Article Drug Therapy A LASTAIR J.J. WOOD, M.D., Editor PROPHYLAXIS AGAINST OPPORTUNISTIC INFECTIONS IN PATIENTS WITH HUMAN IMMUNODEFICIENCY VIRUS INFECTION JOSEPH A. KOVACS, M.D., AND HENRY MASUR,
Review Article Drug Therapy A LASTAIR J.J. WOOD, M.D., Editor PROPHYLAXIS AGAINST OPPORTUNISTIC INFECTIONS IN PATIENTS WITH HUMAN IMMUNODEFICIENCY VIRUS INFECTION JOSEPH A. KOVACS, M.D., AND HENRY MASUR,
Natural History of Untreated HIV-1 Infection
 Opportunistic infections Dr. Guido van den Berk December 2009 HIV [e] EDUCATION Natural History of Untreated HIV-1 Infection 1000 + CD4 Cells 800 600 400 Constitutional Symptoms Early Opportunistic Infections
Opportunistic infections Dr. Guido van den Berk December 2009 HIV [e] EDUCATION Natural History of Untreated HIV-1 Infection 1000 + CD4 Cells 800 600 400 Constitutional Symptoms Early Opportunistic Infections
CLINICIAN INTERVIEW PHARMACY MANAGEMENT OF HIV AND OPPORTUNISTIC INFECTIONS IN A HOSPITAL SETTING. Interview with Christopher Miller, PharmD, BCPS
 PHARMACY MANAGEMENT OF HIV AND OPPORTUNISTIC INFECTIONS IN A HOSPITAL SETTING Interview with Christopher Miller, PharmD, BCPS Dr Miller is currently employed in a joint position as an assistant professor
PHARMACY MANAGEMENT OF HIV AND OPPORTUNISTIC INFECTIONS IN A HOSPITAL SETTING Interview with Christopher Miller, PharmD, BCPS Dr Miller is currently employed in a joint position as an assistant professor
HIV: What Every Clinician Needs to Know ARIZONA STATE ASSOCIATION OF PHYSICIAN ASSISTANTS SPRING CONFERENCE BETTIE COPLAN MARCH 2018
 HIV: What Every Clinician Needs to Know ARIZONA STATE ASSOCIATION OF PHYSICIAN ASSISTANTS SPRING CONFERENCE BETTIE COPLAN MARCH 2018 Overview Overview recent trends in HIV incidence in the U.S. HIV screening
HIV: What Every Clinician Needs to Know ARIZONA STATE ASSOCIATION OF PHYSICIAN ASSISTANTS SPRING CONFERENCE BETTIE COPLAN MARCH 2018 Overview Overview recent trends in HIV incidence in the U.S. HIV screening
Other Diagnostic Tests
 Other Diagnostic Tests APTIMA HIV-1 RNA Qualitative Assay (approved in Oct 2006) Confirmation test (like Western Blot) Detects RNA of the HIV-1 virus (Nucleic Acid Amplification Test/ NAAT) First test
Other Diagnostic Tests APTIMA HIV-1 RNA Qualitative Assay (approved in Oct 2006) Confirmation test (like Western Blot) Detects RNA of the HIV-1 virus (Nucleic Acid Amplification Test/ NAAT) First test
(See the editorial commentary by Sasson et al. on pages 373 5)
 MAJOR ARTICLE HIV/AIDS Characteristics, Determinants, and Clinical Relevance of CD4 T Cell Recovery to!500 Cells/mL in HIV Type 1 Infected Individuals Receiving Potent Antiretroviral Therapy Gilbert R.
MAJOR ARTICLE HIV/AIDS Characteristics, Determinants, and Clinical Relevance of CD4 T Cell Recovery to!500 Cells/mL in HIV Type 1 Infected Individuals Receiving Potent Antiretroviral Therapy Gilbert R.
San Francisco AIDS Cases Reported Through December 31, 1998
 San Francisco AIDS Cases Reported Through December 31, 1998 San Francisco Department of Public Health HIV Seroepidemiology and Surveillance Section AIDS Surveillance Unit Contents Page Commentary: Trends
San Francisco AIDS Cases Reported Through December 31, 1998 San Francisco Department of Public Health HIV Seroepidemiology and Surveillance Section AIDS Surveillance Unit Contents Page Commentary: Trends
AIDS-Related Opportunistic Illnesses Occurring After Initiation of Potent Antiretroviral Therapy JAMA. 1999;282:
 ORIGINAL CONTRIBUTION AIDS-Related Opportunistic Illnesses Occurring After Initiation of Potent Antiretroviral Therapy The Swiss HIV Cohort Study Bruno Ledergerber, PhD Matthias Egger, MD Véronique Erard,
ORIGINAL CONTRIBUTION AIDS-Related Opportunistic Illnesses Occurring After Initiation of Potent Antiretroviral Therapy The Swiss HIV Cohort Study Bruno Ledergerber, PhD Matthias Egger, MD Véronique Erard,
ORIGINAL INVESTIGATION. CD4 T-Lymphocyte Recovery in Individuals With Advanced HIV-1 Infection Receiving Potent Antiretroviral Therapy for 4 Years
 CD4 T-Lymphocyte Recovery in Individuals With Advanced HIV-1 Infection Receiving Potent Antiretroviral Therapy for 4 Years The Swiss HIV Cohort Study ORIGINAL INVESTIGATION Gilbert R. Kaufmann, MD; Luc
CD4 T-Lymphocyte Recovery in Individuals With Advanced HIV-1 Infection Receiving Potent Antiretroviral Therapy for 4 Years The Swiss HIV Cohort Study ORIGINAL INVESTIGATION Gilbert R. Kaufmann, MD; Luc
Infections in immunocompromised host
 Infections in immunocompromised host Immunodeficiencies Primary immunodeficiencies Neutrophil defect Humoral: B cell defect Humoral: Complement Cellular: T cells Combined severe immunodeficiency Secondary
Infections in immunocompromised host Immunodeficiencies Primary immunodeficiencies Neutrophil defect Humoral: B cell defect Humoral: Complement Cellular: T cells Combined severe immunodeficiency Secondary
HAART. Graves HIV +/2. Highly active antiretroviral therapy : HAART human immunodeficiency virus : HIV-RNA acquired immunodeficiency syndrome : AIDS
 ,**- The Japanese Society for AIDS Research The Journal of AIDS Research HAART Graves HIV : HAART -+ CD. Graves HIV + : -, +333 1 CD.,/ml, HIV-RNA,..+* / copiesml HIV 2 EFV HAART CMV CMV GCV CAMEBRFBINHPZA,**+
,**- The Japanese Society for AIDS Research The Journal of AIDS Research HAART Graves HIV : HAART -+ CD. Graves HIV + : -, +333 1 CD.,/ml, HIV-RNA,..+* / copiesml HIV 2 EFV HAART CMV CMV GCV CAMEBRFBINHPZA,**+
HUMAN IMMUNODEFICIENCY VIRUS (HIV) NON-IMMEDIATE NOTIFICATION STD PROGRAM. Version
 1 HUMAN IMMUNODEFICIENCY VIRUS (HIV) NON-IMMEDIATE NOTIFICATION STD PROGRAM Event Name: Event Time Period: ADULT HIV 900 (AIDS.gov 12/31/2015) HIV Lifelong HIV (human immunodeficiency virus) is a retrovirus
1 HUMAN IMMUNODEFICIENCY VIRUS (HIV) NON-IMMEDIATE NOTIFICATION STD PROGRAM Event Name: Event Time Period: ADULT HIV 900 (AIDS.gov 12/31/2015) HIV Lifelong HIV (human immunodeficiency virus) is a retrovirus
Many highly active antiretroviral therapy PROCEEDINGS
 MAXIMIZING THE EFFECTIVENESS OF HIGHLY ACTIVE ANTIRETROVIRAL THERAPY: IS THERE A ROLE FOR QUADRUPLE REGIMENS? * François Raffi, MD, PhD ABSTRACT Although many highly active antiretroviral therapy (HAART)
MAXIMIZING THE EFFECTIVENESS OF HIGHLY ACTIVE ANTIRETROVIRAL THERAPY: IS THERE A ROLE FOR QUADRUPLE REGIMENS? * François Raffi, MD, PhD ABSTRACT Although many highly active antiretroviral therapy (HAART)
Supervised Treatment Interruption (STI) in an Urban HIV Clinical Practice: A Prospective Analysis.
 Supervised Treatment Interruption (STI) in an Urban HIV Clinical Practice: A Prospective Analysis. J.L. YOZVIAK 1, P. KOUVATSOS 2, R.E. DOERFLER 3, W.C. WOODWARD 3 1 Philadelphia College of Osteopathic
Supervised Treatment Interruption (STI) in an Urban HIV Clinical Practice: A Prospective Analysis. J.L. YOZVIAK 1, P. KOUVATSOS 2, R.E. DOERFLER 3, W.C. WOODWARD 3 1 Philadelphia College of Osteopathic
Lahey Clinic Internal Medicine Residency Program: Curriculum for Infectious Disease
 Lahey Clinic Internal Medicine Residency Program: Curriculum for Infectious Disease Faculty representative: Eva Piessens, MD, MPH Resident representative: Karen Ganz, MD Revision date: February 1, 2006
Lahey Clinic Internal Medicine Residency Program: Curriculum for Infectious Disease Faculty representative: Eva Piessens, MD, MPH Resident representative: Karen Ganz, MD Revision date: February 1, 2006
Department of Internal Medicine, Division of Infectious Disease, Washington University, St. Louis, Missouri
 MAJOR ARTICLE HIV/AIDS Discontinuation of Maintenance Therapy for Cryptococcal Meningitis in Patients with AIDS Treated with Highly Active Antiretroviral Therapy: An International Observational Study Cristina
MAJOR ARTICLE HIV/AIDS Discontinuation of Maintenance Therapy for Cryptococcal Meningitis in Patients with AIDS Treated with Highly Active Antiretroviral Therapy: An International Observational Study Cristina
Opportunistic infections in the era of cart, still a problem in resource-limited settings
 Opportunistic infections in the era of cart, still a problem in resource-limited settings Cristiana Oprea Victor Babes Clinical Hospital for Infectious and Tropical Diseases, Bucharest, Romania Assessment
Opportunistic infections in the era of cart, still a problem in resource-limited settings Cristiana Oprea Victor Babes Clinical Hospital for Infectious and Tropical Diseases, Bucharest, Romania Assessment
OCCURRENCE OF PNEUMOCYSTIS PNEUMONIA IN HIV-INFECTED PATIENTS AND THE INTERFERENCE OF THE HIGHLY ACTIVE ANTIRETROVIRAL THERAPY
 Received: August 24, 2007 Accepted: December 6, 2007 Abstract published online: December 17, 2007 Full paper published online: March 8, 2008 J. Venom. Anim. Toxins incl. Trop. Dis. V.14, n.1, p.152-160,
Received: August 24, 2007 Accepted: December 6, 2007 Abstract published online: December 17, 2007 Full paper published online: March 8, 2008 J. Venom. Anim. Toxins incl. Trop. Dis. V.14, n.1, p.152-160,
HIV 101: Overview of the Physiologic Impact of HIV and Its Diagnosis Part 2: Immunologic Impact of HIV and its Effects on the Body
 HIV 101: Overview of the Physiologic Impact of HIV and Its Diagnosis Part 2: Immunologic Impact of HIV and its Effects on the Body Melissa Badowski, PharmD, BCPS, AAHIVP Clinical Assistant Professor University
HIV 101: Overview of the Physiologic Impact of HIV and Its Diagnosis Part 2: Immunologic Impact of HIV and its Effects on the Body Melissa Badowski, PharmD, BCPS, AAHIVP Clinical Assistant Professor University
Low Incidence of Colonization and No Cases of Disseminated Mycobacterium avium Complex Infection (DMAC) in Brazilian AIDS Patients in the HAART Era
 252 BJID 2002; 6 (October) Low Incidence of Colonization and No Cases of Disseminated Mycobacterium avium Complex Infection (DMAC) in Brazilian AIDS Patients in the HAART Era Ângela Gadelha, Náurea Accácio,
252 BJID 2002; 6 (October) Low Incidence of Colonization and No Cases of Disseminated Mycobacterium avium Complex Infection (DMAC) in Brazilian AIDS Patients in the HAART Era Ângela Gadelha, Náurea Accácio,
Mortality Rates Among People With HIV, Long on the Wane, Continue to Drop HIV Medicine Feb 2013
 John F. White III, MD, MBA, FLMI VP and Medical Director American National Insurance Company 1 Mortality Rates Among People With HIV, Long on the Wane, Continue to Drop HIV Medicine Feb 2013 2 1 3 My Opinions
John F. White III, MD, MBA, FLMI VP and Medical Director American National Insurance Company 1 Mortality Rates Among People With HIV, Long on the Wane, Continue to Drop HIV Medicine Feb 2013 2 1 3 My Opinions
INTEGRATING HIV INTO PRIMARY CARE
 INTEGRATING HIV INTO PRIMARY CARE ADELERO ADEBAJO, MD, MPH, AAHIVS, FACP NO DISCLOSURE 1.2 million people in the United States are living with HIV infection and 1 in 5 are unaware of their infection.
INTEGRATING HIV INTO PRIMARY CARE ADELERO ADEBAJO, MD, MPH, AAHIVS, FACP NO DISCLOSURE 1.2 million people in the United States are living with HIV infection and 1 in 5 are unaware of their infection.
20 Years of Tears and Triumphs
 20 Years of Tears and Triumphs A Clinical Research Nurse s Perspective on HIV/AIDS Bobi Keenan, RN, ACRN Clinical Research Nurse UC Irvine Dept. of Medicine/Infectious Diseases Objectives 1. Understand
20 Years of Tears and Triumphs A Clinical Research Nurse s Perspective on HIV/AIDS Bobi Keenan, RN, ACRN Clinical Research Nurse UC Irvine Dept. of Medicine/Infectious Diseases Objectives 1. Understand
Antiviral Therapy 11:
 Antiviral Therapy 11:343 35 Change in T-lymphocyte count after initiation of highly active antiretroviral therapy in HIV-infected patients with history of Mycobacterium avium complex infection Estibaliz
Antiviral Therapy 11:343 35 Change in T-lymphocyte count after initiation of highly active antiretroviral therapy in HIV-infected patients with history of Mycobacterium avium complex infection Estibaliz
Clinical Case. Prof.ssa Cristina Mussini
 Clinical Case Prof.ssa Cristina Mussini Clinical history Male, born in Ivory Coast in 1968. HIV positive since dal 1998 Risk factor: heterosexual contacts He started antiretroviral therapy in 2001 with
Clinical Case Prof.ssa Cristina Mussini Clinical history Male, born in Ivory Coast in 1968. HIV positive since dal 1998 Risk factor: heterosexual contacts He started antiretroviral therapy in 2001 with
Antiviral Therapy 14:
 Antiviral Therapy 14:451 457 Short communication CD4 + T-cell percentage is an independent predictor of clinical progression in AIDS-free antiretroviral-naive patients with CD4 + T-cell counts >200 cells/mm
Antiviral Therapy 14:451 457 Short communication CD4 + T-cell percentage is an independent predictor of clinical progression in AIDS-free antiretroviral-naive patients with CD4 + T-cell counts >200 cells/mm
Tuberculosis among HIV-infected patients receiving HAART: long term incidence and risk factors in a South African cohort
 Tuberculosis among HIV-infected patients receiving HAART: long term incidence and risk factors in a South African cohort Stephen D. Lawn a,b, Motasim Badri a and Robin Wood a Objectives: To determine the
Tuberculosis among HIV-infected patients receiving HAART: long term incidence and risk factors in a South African cohort Stephen D. Lawn a,b, Motasim Badri a and Robin Wood a Objectives: To determine the
 http://www.savinglivesuk.com/ HIV Awareness Study Morning 24 th November 2017 Agenda HIV Basics & Stages of HIV HIV Testing, Health Advising & Sexual Health Saving Lives Antiretroviral Medication Antenatal/Postnatal
http://www.savinglivesuk.com/ HIV Awareness Study Morning 24 th November 2017 Agenda HIV Basics & Stages of HIV HIV Testing, Health Advising & Sexual Health Saving Lives Antiretroviral Medication Antenatal/Postnatal
Virologic and Immunologic Monitoring
 NEW YORK STATE DEPARTMENT OF HEALTH AIDS INSTITUTE HIV HCV SUBSTANCE USE LGBT HEALTH Virologic and Immunologic Monitoring Medical Care Criteria Committee, June 2016 TABLE OF CONTENTS Monitoring Intervals...1
NEW YORK STATE DEPARTMENT OF HEALTH AIDS INSTITUTE HIV HCV SUBSTANCE USE LGBT HEALTH Virologic and Immunologic Monitoring Medical Care Criteria Committee, June 2016 TABLE OF CONTENTS Monitoring Intervals...1
JMSCR Vol 3 Issue 10 Page October 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x DOI: http://dx.doi.org/10.18535/jmscr/v3i10.20 Drugs Related Changes of Haemoglobin and CD4 Counts in HIV-Infected Patients on Antiretroviral
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x DOI: http://dx.doi.org/10.18535/jmscr/v3i10.20 Drugs Related Changes of Haemoglobin and CD4 Counts in HIV-Infected Patients on Antiretroviral
Immunological recovery and antiretroviral therapy in HIV-1 infection
 Immunological recovery and antiretroviral therapy in HIV-1 infection Manuel Battegay, Reto Nüesch, Bernard Hirschel, Gilbert R Kaufmann Lancet Infect Dis 26; 6: 28 87 Division of Infectious Diseases and
Immunological recovery and antiretroviral therapy in HIV-1 infection Manuel Battegay, Reto Nüesch, Bernard Hirschel, Gilbert R Kaufmann Lancet Infect Dis 26; 6: 28 87 Division of Infectious Diseases and
Original Article. Noparat Oniem, M.D., Somnuek Sungkanuparph, M.D.
 Original Article Vol. 29 No. 1 Primary prophylaxis for cryptococcosis with fluconazole:- Oniem N & Sungkanuparph S. 5 Primary prophylaxis for cryptococcosis with fluconazole among HIV-infected patients
Original Article Vol. 29 No. 1 Primary prophylaxis for cryptococcosis with fluconazole:- Oniem N & Sungkanuparph S. 5 Primary prophylaxis for cryptococcosis with fluconazole among HIV-infected patients
Medical Overview March 7, Nina Lambert, NP Inova Juniper Program
 Medical Overview March 7, 2019 Nina Lambert, NP Inova Juniper Program Nina.lambert@inova.org Inova Juniper Program Sites Offering medical care, case management and mental health for youth and adults who
Medical Overview March 7, 2019 Nina Lambert, NP Inova Juniper Program Nina.lambert@inova.org Inova Juniper Program Sites Offering medical care, case management and mental health for youth and adults who
The New England Journal of Medicine THE COST EFFECTIVENESS OF COMBINATION ANTIRETROVIRAL THERAPY FOR HIV DISEASE. Study Design
 THE COST EFFECTIVENESS OF COMBINATION ANTIRETROVIRAL THERAPY FOR HIV DISEASE KENNETH A. FREEDBERG, M.D., ELENA LOSINA, PH.D., MILTON C. WEINSTEIN, PH.D., A. DAVID PALTIEL, PH.D., CALVIN J. COHEN, M.D.,
THE COST EFFECTIVENESS OF COMBINATION ANTIRETROVIRAL THERAPY FOR HIV DISEASE KENNETH A. FREEDBERG, M.D., ELENA LOSINA, PH.D., MILTON C. WEINSTEIN, PH.D., A. DAVID PALTIEL, PH.D., CALVIN J. COHEN, M.D.,
Prevention and Treatment of Selected Opportunistic Infections: A Guidelines Update
 Prevention and Treatment of Selected Opportunistic Infections: A Guidelines Update Constance A. Benson, MD Professor of Medicine Division of Infectious Diseases University of California, San Diego Disclosures
Prevention and Treatment of Selected Opportunistic Infections: A Guidelines Update Constance A. Benson, MD Professor of Medicine Division of Infectious Diseases University of California, San Diego Disclosures
Research Article Causes of Death in HIV Patients and the Evolution of an AIDS Hospice:
 Hindawi Publishing Corporation AIDS Research and Treatment Volume 2012, Article ID 390406, 7 pages doi:10.1155/2012/390406 Research Article Causes of Death in HIV Patients and the Evolution of an AIDS
Hindawi Publishing Corporation AIDS Research and Treatment Volume 2012, Article ID 390406, 7 pages doi:10.1155/2012/390406 Research Article Causes of Death in HIV Patients and the Evolution of an AIDS
Diagnosis and Initial Management of HIV/AIDS: What the Primary Care Provider Should Know
 Diagnosis and Initial Management of HIV/AIDS: What the Primary Care Provider Should Know Carolyn K. Burr, EdD, RN Co-Clinical Director Deputy Director François-Xavier Bagnoud Center December 17 th, 2013
Diagnosis and Initial Management of HIV/AIDS: What the Primary Care Provider Should Know Carolyn K. Burr, EdD, RN Co-Clinical Director Deputy Director François-Xavier Bagnoud Center December 17 th, 2013
Immune function in patients with HIV infection is
 Reconstitution of Immune Responses to Tuberculosis in Patients With HIV Infection Who Receive Antiretroviral Therapy* Neil W. Schluger, MD, FCCP; Daniel Perez, MD; and Yuk Ming Liu, MPH Study objectives:
Reconstitution of Immune Responses to Tuberculosis in Patients With HIV Infection Who Receive Antiretroviral Therapy* Neil W. Schluger, MD, FCCP; Daniel Perez, MD; and Yuk Ming Liu, MPH Study objectives:
HIV and Public Health: the Basics
 HIV and Public Health: the Basics Joy Zeh, RN, MS, Family Nurse Practitioner VCU HIV/AIDS Center HIV and Public Health: the Basics Epidemiology Related Infections and Co-Morbidities Spectrum of HIV Infection
HIV and Public Health: the Basics Joy Zeh, RN, MS, Family Nurse Practitioner VCU HIV/AIDS Center HIV and Public Health: the Basics Epidemiology Related Infections and Co-Morbidities Spectrum of HIV Infection
Antimycobacterial drugs. Dr.Naza M.Ali lec Dec 2018
 Antimycobacterial drugs Dr.Naza M.Ali lec 14-15 6 Dec 2018 About one-third of the world s population is infected with M. tuberculosis With 30 million people having active disease. Worldwide, 9 million
Antimycobacterial drugs Dr.Naza M.Ali lec 14-15 6 Dec 2018 About one-third of the world s population is infected with M. tuberculosis With 30 million people having active disease. Worldwide, 9 million
Review What s New in the 2009 US Guidelines for Prevention and Treatment of Opportunistic Infections Among Adults and Adolescents With HIV?
 2009 Guidelines Volume 17 Issue 3 July/August 2009 Review What s New in the 2009 US Guidelines for Prevention and Treatment of Among Adults and Adolescents With HIV? John T. Brooks, MD, Jonathan E. Kaplan,
2009 Guidelines Volume 17 Issue 3 July/August 2009 Review What s New in the 2009 US Guidelines for Prevention and Treatment of Among Adults and Adolescents With HIV? John T. Brooks, MD, Jonathan E. Kaplan,
Journal of Antimicrobial Chemotherapy Advance Access published December 30, 2005
 Journal of Antimicrobial Chemotherapy Advance Access published December 30, 2005 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dki472 Safety and factors predicting the duration of first and second
Journal of Antimicrobial Chemotherapy Advance Access published December 30, 2005 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dki472 Safety and factors predicting the duration of first and second
Survival of HIV-infected patients in the intensive care unit in the era of highly active antiretroviral therapy
 Thorax Online First, published on May 2, 27 as.36/thx.26.72256 Survival of HIV-infected patients in the intensive care unit in the era of highly active antiretroviral therapy SJ Dickson, S Batson 2, AJ
Thorax Online First, published on May 2, 27 as.36/thx.26.72256 Survival of HIV-infected patients in the intensive care unit in the era of highly active antiretroviral therapy SJ Dickson, S Batson 2, AJ
QUARTERLY HIV/AIDS SURVEILLANCE REPORT
 QUARTERLY HIV/AIDS SURVEILLANCE REPORT San Francisco Department of Public Health HIV/AIDS Cases Reported Through September 2010 Contents Page Surveillance Summary..... 1 Table 1: Adult/Adolescent HIV/AIDS
QUARTERLY HIV/AIDS SURVEILLANCE REPORT San Francisco Department of Public Health HIV/AIDS Cases Reported Through September 2010 Contents Page Surveillance Summary..... 1 Table 1: Adult/Adolescent HIV/AIDS
Pneumococcal pneumonia in HIV-infected patients by antiretroviral therapy periods
 DOI: 10.1111/j.1468-1293.2008.00546.x r 2008 British HIV Association HIV Medicine (2008), 9, 203 207 ORIGINAL RESEARCH Pneumococcal pneumonia in HIV-infected patients by antiretroviral therapy periods
DOI: 10.1111/j.1468-1293.2008.00546.x r 2008 British HIV Association HIV Medicine (2008), 9, 203 207 ORIGINAL RESEARCH Pneumococcal pneumonia in HIV-infected patients by antiretroviral therapy periods
CHART ELEVEN (11) KENYAN FIGURES (KENYA DEMOGRAPHIC HEALTH SURVEY REVISED 2004)
 CHART ELEVEN (11) KENYAN FIGURES (KENYA DEMOGRAPHIC HEALTH SURVEY REVISED 2004) Adults living with HIV/AIDS - 1.1 million Children - 150,000 Number using ART - 24,000 Number needing ARVs - 200,000 National
CHART ELEVEN (11) KENYAN FIGURES (KENYA DEMOGRAPHIC HEALTH SURVEY REVISED 2004) Adults living with HIV/AIDS - 1.1 million Children - 150,000 Number using ART - 24,000 Number needing ARVs - 200,000 National
Preventing Mycobacterium avium complex in patients who are using protease inhibitors: a cost-effectiveness analysis Bayoumi A M, Redelmeier D A
 Preventing Mycobacterium avium complex in patients who are using protease inhibitors: a cost-effectiveness analysis Bayoumi A M, Redelmeier D A Record Status This is a critical abstract of an economic
Preventing Mycobacterium avium complex in patients who are using protease inhibitors: a cost-effectiveness analysis Bayoumi A M, Redelmeier D A Record Status This is a critical abstract of an economic
Cerebral Toxoplasmosis in HIV-Infected Patients. Ahmed Saad,MD,FACP
 Cerebral Toxoplasmosis in HIV-Infected Patients Ahmed Saad,MD,FACP Introduction Toxoplasmosis: Caused by the intracellular protozoan, Toxoplasma gondii. Immunocompetent persons with primary infection
Cerebral Toxoplasmosis in HIV-Infected Patients Ahmed Saad,MD,FACP Introduction Toxoplasmosis: Caused by the intracellular protozoan, Toxoplasma gondii. Immunocompetent persons with primary infection
Dr Jayanta K Panda Associate Professor, Medicine SCB Medical College, Cuttack
 Dr Jayanta K Panda Associate Professor, Medicine SCB Medical College, Cuttack Case reports Prevalence Persistently Low CD4 Counts in Patients with Suppressed HIV RNA Immunologic Recovery Based on Specific
Dr Jayanta K Panda Associate Professor, Medicine SCB Medical College, Cuttack Case reports Prevalence Persistently Low CD4 Counts in Patients with Suppressed HIV RNA Immunologic Recovery Based on Specific
Title: Revision of the Surveillance Case Definition for HIV Infection and AIDS Among children age > 18 months but < 13 years
 06-ID-02 Committee: Infectious Disease Title: Revision of the Surveillance Case Definition for HIV Infection and AIDS Among children age > 18 months but < 13 years Statement of problem: Advances in HIV
06-ID-02 Committee: Infectious Disease Title: Revision of the Surveillance Case Definition for HIV Infection and AIDS Among children age > 18 months but < 13 years Statement of problem: Advances in HIV
Immune Reconstitution Syndrome in HIV: Validating a Case Definition and Identifying Clinical Predictors in Persons Initiating Antiretroviral Therapy
 MAJOR ARTICLE HIV/AIDS Immune Reconstitution Syndrome in HIV: Validating a Case Definition and Identifying Clinical Predictors in Persons Initiating Antiretroviral Therapy Jaime Robertson, 1 Matthew Meier,
MAJOR ARTICLE HIV/AIDS Immune Reconstitution Syndrome in HIV: Validating a Case Definition and Identifying Clinical Predictors in Persons Initiating Antiretroviral Therapy Jaime Robertson, 1 Matthew Meier,
Department of Clinical Epidemiology, Institute of Infectious Disease and Epidemiology, Tan Tock Seng Hospital, Singapore 2
 Original Article 563 Causes of Death and Factors Associated with Early Death Among Human Immunodeficiency Virus (HIV)-Infected Persons in Singapore: Pre-Highly Active Antiretroviral Therapy (HAART) and
Original Article 563 Causes of Death and Factors Associated with Early Death Among Human Immunodeficiency Virus (HIV)-Infected Persons in Singapore: Pre-Highly Active Antiretroviral Therapy (HAART) and
Overview on Opportunistic Infections of the Central Nervous System
 Second HIV Infection and the Central Nervous System: Developed and Resource-Limited Settings Venice, Italy April 14 16, 2007 Overview on Opportunistic Infections of the Central Nervous System Adriana Ammassari
Second HIV Infection and the Central Nervous System: Developed and Resource-Limited Settings Venice, Italy April 14 16, 2007 Overview on Opportunistic Infections of the Central Nervous System Adriana Ammassari
OPPORTUNISTIC INFECTIONS. Institute of Infectious Diseases, Pune India
 OPPORTUNISTIC INFECTIONS Institute of Infectious Diseases, Pune India DISCLOSURES Nothing to declare Outline The problem Bacterial Fungal Protozoal Viral Decline in OI prevalence in HAART era: USA CROI
OPPORTUNISTIC INFECTIONS Institute of Infectious Diseases, Pune India DISCLOSURES Nothing to declare Outline The problem Bacterial Fungal Protozoal Viral Decline in OI prevalence in HAART era: USA CROI
Principles of Antiretroviral Therapy
 Principles of Antiretroviral Therapy Ten Principles of Antiretroviral Therapy Skills Building Workshop: Clinical Management of HIV Infection and Antiretroviral Therapy, 11 th ICAAP, November 21st, 2011,
Principles of Antiretroviral Therapy Ten Principles of Antiretroviral Therapy Skills Building Workshop: Clinical Management of HIV Infection and Antiretroviral Therapy, 11 th ICAAP, November 21st, 2011,
Immunodeficiency. (2 of 2)
 Immunodeficiency (2 of 2) Acquired (secondary) immunodeficiencies More common Many causes such as therapy, cancer, sarcoidosis, malnutrition, infection & renal disease The most common of which is therapy-related
Immunodeficiency (2 of 2) Acquired (secondary) immunodeficiencies More common Many causes such as therapy, cancer, sarcoidosis, malnutrition, infection & renal disease The most common of which is therapy-related
Quarterly Journal of Medicine, New Series 70, No. 262, pp , February 1989
 Quarterly Journal of Medicine, New Series 70, No. 6, pp. 6-74, February 989 The Efficacy and Toxicity of Azidothymidine (AZT) in the Treatment of Patients with AIDS and AIDS-related Complex (ARC): An Open
Quarterly Journal of Medicine, New Series 70, No. 6, pp. 6-74, February 989 The Efficacy and Toxicity of Azidothymidine (AZT) in the Treatment of Patients with AIDS and AIDS-related Complex (ARC): An Open
GOALS AND OBJECTIVES INFECTIOUS DISEASE
 GOALS AND OBJECTIVES INFECTIOUS DISEASE Infectious Disease and HIV Overview: The Infectious Diseases Program at the University of Southern California prepares trainees for the management of problems in
GOALS AND OBJECTIVES INFECTIOUS DISEASE Infectious Disease and HIV Overview: The Infectious Diseases Program at the University of Southern California prepares trainees for the management of problems in
European Guidelines. for the Clinical Management and Treatment of HIV Infected Adults
 European Guidelines for the Clinical Management and Treatment of HIV Infected Adults 2005 These Euroguidelines result from the comparison of guidelines from several European countries and from a discussion
European Guidelines for the Clinical Management and Treatment of HIV Infected Adults 2005 These Euroguidelines result from the comparison of guidelines from several European countries and from a discussion
Advanced HIV Disease / AIDS
 Advanced HIV Disease / AIDS Technical Summary for Activists Gilles Van Cutsem, SAMU, MSF Objectives Why is increased investment in Advanced HIV Disease (AHD) / AIDS critical? What are the issues? What
Advanced HIV Disease / AIDS Technical Summary for Activists Gilles Van Cutsem, SAMU, MSF Objectives Why is increased investment in Advanced HIV Disease (AHD) / AIDS critical? What are the issues? What
10/17/2015. Chapter 55. Care of the Patient with HIV/AIDS. History of HIV. HIV Modes of Transmission
 Chapter 55 Care of the Patient with HIV/AIDS All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. History of HIV Remains somewhat obscure The earlier
Chapter 55 Care of the Patient with HIV/AIDS All items and derived items 2015, 2011, 2006 by Mosby, Inc., an imprint of Elsevier Inc. All rights reserved. History of HIV Remains somewhat obscure The earlier
Recurring and Emerging Questions Related to Management of HIV-Related Opportunistic Infections. Objectives. Henry Masur MD
 Recurring and Emerging Questions Related to Management of HIV-Related Opportunistic Infections Henry Masur MD Clinical Professor of Medicine George Washington University School of Medicine Objectives To
Recurring and Emerging Questions Related to Management of HIV-Related Opportunistic Infections Henry Masur MD Clinical Professor of Medicine George Washington University School of Medicine Objectives To
Herpes virus co-factors in HIV infection
 Herpes virus co-factors in HIV infection Dr Jane Deayton Barts and the London Queen Mary School of Medicine Introduction Herpes viruses very common and often coexist with HIV Establish life-long latent
Herpes virus co-factors in HIV infection Dr Jane Deayton Barts and the London Queen Mary School of Medicine Introduction Herpes viruses very common and often coexist with HIV Establish life-long latent
Hospitalization and Mortality among HIV-Infected Children after Receiving Highly Active Antiretroviral Therapy
 MAJOR ARTICLE HIV/AIDS Hospitalization and Mortality among HIV-Infected Children after Receiving Highly Active Antiretroviral Therapy Thanyawee Puthanakit, 1 Linda Aurpibul, 1 Peninnah Oberdorfer, 2 Noppadon
MAJOR ARTICLE HIV/AIDS Hospitalization and Mortality among HIV-Infected Children after Receiving Highly Active Antiretroviral Therapy Thanyawee Puthanakit, 1 Linda Aurpibul, 1 Peninnah Oberdorfer, 2 Noppadon
MYCOBACTERIUM AVIUM COMPLEX
 MYCOBACTERIUM AVIUM COMPLEX Mycobacterium avium complex (my-koe-back-teer-ee-um ay-vee-um complecks) disease is among the most common bacterial infections in people living with HIV. In one study, MAC bacteria
MYCOBACTERIUM AVIUM COMPLEX Mycobacterium avium complex (my-koe-back-teer-ee-um ay-vee-um complecks) disease is among the most common bacterial infections in people living with HIV. In one study, MAC bacteria
Neuroradiology of AIDS
 Neuroradiology of AIDS Frank Minja,, HMS IV Gillian Lieberman MD September 2002 AIDS 90% of HIV patients have CNS involvement 1 10% of AIDS patients present first with neurological symptoms 2 73-80% of
Neuroradiology of AIDS Frank Minja,, HMS IV Gillian Lieberman MD September 2002 AIDS 90% of HIV patients have CNS involvement 1 10% of AIDS patients present first with neurological symptoms 2 73-80% of
227 28, 2010 MIDTERM EXAMINATION KEY
 Epidemiology 227 April 28, 2010 MIDTERM EXAMINATION KEY Select the best answer for the multiple choice questions. There are 64 questions and 9 pages on the examination. Each question will count one point.
Epidemiology 227 April 28, 2010 MIDTERM EXAMINATION KEY Select the best answer for the multiple choice questions. There are 64 questions and 9 pages on the examination. Each question will count one point.
Individual Study Table Referring to the Dossier SYNOPSIS. Final Clinical Study Report for Study AI424136
 Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Reyataz Name of Active Ingredient: Individual Study Table Referring to the Dossier (For National Authority Use Only) SYNOPSIS for
Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Reyataz Name of Active Ingredient: Individual Study Table Referring to the Dossier (For National Authority Use Only) SYNOPSIS for
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 2001, by the Massachusetts Medical Society VOLUME 344 J ANUARY 18, 2001 NUMBER 3 A RANDOMIZED TRIAL OF THE DISCONTINUATION OF PRIMARY AND SECONDARY PROPHYLAXIS
The New England Journal of Medicine Copyright, 2001, by the Massachusetts Medical Society VOLUME 344 J ANUARY 18, 2001 NUMBER 3 A RANDOMIZED TRIAL OF THE DISCONTINUATION OF PRIMARY AND SECONDARY PROPHYLAXIS
Clarithromycin. Brand Name: Biaxin Drug Class: Opportunistic Infection and Other Drugs
 Brand Name: Biaxin Drug Class: Opportunistic Infection and Other Drugs Drug Description is a semisynthetic macrolide antibiotic. It differs structurally from erythromycin by methylation of a hydroxyl group
Brand Name: Biaxin Drug Class: Opportunistic Infection and Other Drugs Drug Description is a semisynthetic macrolide antibiotic. It differs structurally from erythromycin by methylation of a hydroxyl group
Reasons why we will never forget. Andrea Antinori INMI L. Spallanzani IRCCS, Roma
 Reasons why we will never forget Andrea Antinori INMI L. Spallanzani IRCCS, Roma SMRs according to time spent with CD4 count >500/mm3 after cart initiation in MSM 80,642 HIV-infected individuals eligible
Reasons why we will never forget Andrea Antinori INMI L. Spallanzani IRCCS, Roma SMRs according to time spent with CD4 count >500/mm3 after cart initiation in MSM 80,642 HIV-infected individuals eligible
The management of opportunistic infections and cancer in HIV disease
 The management of opportunistic infections and cancer in HIV disease Highlights Botes ME, MBChB Department of Internal Medicine, University of Pretoria and Private Practitioner, Muelmed Hospital, Pretoria
The management of opportunistic infections and cancer in HIV disease Highlights Botes ME, MBChB Department of Internal Medicine, University of Pretoria and Private Practitioner, Muelmed Hospital, Pretoria
Clinical response to Highly Active Antiretroviral Treatment (HAART) in a patient with Kaposi's sarcoma: A case presentation
 ISPUB.COM The Internet Journal of Infectious Diseases Volume 6 Number 2 Clinical response to Highly Active Antiretroviral Treatment (HAART) in a patient with Kaposi's sarcoma: A case presentation Y Graza,
ISPUB.COM The Internet Journal of Infectious Diseases Volume 6 Number 2 Clinical response to Highly Active Antiretroviral Treatment (HAART) in a patient with Kaposi's sarcoma: A case presentation Y Graza,
Avascular Necrosis of Bone in Patients with Human Immunodeficiency Virus Infection: Report of 6 Cases and Review of the Literature
 BRIEF REPORT HIV/AIDS Avascular Necrosis of Bone in Patients with Human Immunodeficiency Virus Infection: Report of 6 Cases and Review of the Literature Patricia Brown and Lawrence Crane Division of Infectious
BRIEF REPORT HIV/AIDS Avascular Necrosis of Bone in Patients with Human Immunodeficiency Virus Infection: Report of 6 Cases and Review of the Literature Patricia Brown and Lawrence Crane Division of Infectious
CMV. Inclusions predominantly in endothelial cells. Immunostaining greater sensitivity than H&E alone.
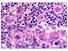 CMV Inclusions predominantly in endothelial cells. Immunostaining greater sensitivity than H&E alone. CMV inclusions are often present in a very patchy distribution Carefully examine all levels CMV CMV
CMV Inclusions predominantly in endothelial cells. Immunostaining greater sensitivity than H&E alone. CMV inclusions are often present in a very patchy distribution Carefully examine all levels CMV CMV
HIV AND LUNG HEALTH. Stephen Aston Infectious Diseases SpR Royal Liverpool University Hospital
 HIV AND LUNG HEALTH Stephen Aston Infectious Diseases SpR Royal Liverpool University Hospital Introduction HIV infection exerts multiple effects on pulmonary immune responses: Generalised state of immune
HIV AND LUNG HEALTH Stephen Aston Infectious Diseases SpR Royal Liverpool University Hospital Introduction HIV infection exerts multiple effects on pulmonary immune responses: Generalised state of immune
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 3/ Issue 14/Apr 07, 2014 Page 3633
 STUDY OF INCIDENCE & RISK FACTORS FOR IMMUNE RECONSTITUTION INFLAMMATORY SYNDROME (IRIS) IN ADULT HIV PATIENTS IN NAGPUR REGION Saurabh G. Agarwal 1, R. M. Powar 2, Supriya S. Tankhiwale 3 HOW TO CITE
STUDY OF INCIDENCE & RISK FACTORS FOR IMMUNE RECONSTITUTION INFLAMMATORY SYNDROME (IRIS) IN ADULT HIV PATIENTS IN NAGPUR REGION Saurabh G. Agarwal 1, R. M. Powar 2, Supriya S. Tankhiwale 3 HOW TO CITE
