population in untreated coeliac disease
|
|
|
- Abraham Parks
- 6 years ago
- Views:
Transcription
1 Gut, 1983, 24, Human intestinal mucosal mast cells: expanded population in untreated coeliac disease S STROBEL,* A BUSUTTIL, AND ANNE FERGUSON From the University, of Edinburgh Gastro-lintestinial Uniit, and Department of Pathology, Western Genieral Hospital, Edinburgh SUMMARY Previous retrospective studies of intestinal mucosal mast cells in coeliac disease have given divergent results, and we have recently reported that inappropriate methodology could account for these discrepancies. In this prospective study, mucosal mast cell counts were performed in Carnoy fixed, peroral jejunal biopsy specimens from patients with coeliac disease, both untreated and treated with a gluten-free diet; and from controls (mainly irritable bowel syndrome). Mean mucosal mast cell count in 27 control subjects was 146/mm2, SD 29. Significantly higher values were obtained in untreated coeliac disease (mean 243, SD 41, p<o0ool) returning to the normal range in coeliacs treated with a gluten-free diet with normal jejunal biopsy morphology. In seven patients mucosal mast cell counts were performed in multiple jejunal biopsies, and these showed that mucosal mast cell distribution was not patchy. There was no evidence of degranulation of intestinal mucosal mast cells under the conditions of routine biopsy (overnight fast). An increase in mucosal mast cells in untreated coeliac disease may be one explanation for the high number of IgE positive stained cells in the intestinal mucosa that has been reported by some authors. Within the complex cellular infiltrate of jejunal mucosa, there is a population of mucosal mast cells. It has been suggested that degranulation of these intestinal mucosal mast cells may play a part in the pathogenesis of the clinical symptoms in food allergic diseases in the broadest sense such as coeliac disease' 2 and cow's milk protein intolerance.2 Evidence to support this postulate is scanty. There are three reports of mucosal mast cell counts in coeliac disease. Kumar and her colleagues3 reported values to be higher than normal in untreated coeliacs, remaining high after after treatment with a gluten-free diet; in another report counts were said to be low in untreated coeliac disease, returning to normal after gluten withdrawal,' and a third study (published in abstract) reported low mucosal mast cell counts in untreated coeliac disease, values remaining lower than normal after treatment.4 These discrepancies may be due to methodological errors in retrospective analysis of formalin-fixed jejunal biopsy specimens. We have recently ' Gcncr.ll Hospital. Edinburgh EH4 2XU. Received for publication 8 June 1982 reported the critical role of fixative on mucosal mast cell counts in normal human jejunal biopsies.5 We therefore performed a prospective study of mucosal mast cell counts in peroral jejunal biopsies and have studied coeliac patients, together with other patients having jejunal biopsy (usually for investigation of diarrhoea). Patients PATIENTS STUDIED Peroral jejunal biopsies from an unselected group of 57 patients were studied. Biopsy had been performed for diagnosis or follow-up of coeliac disease, or to exclude lactase deficiency as a factor in patients with irritable bowel syndrome or diarrhoea. In these patients, jejunal biopsy was taken with a Watson peroral biopsy capsule after an overnight fast. The biopsy was taken just distal to the ligament of Treitz, and divided into three parts; one was fixed in formalin for routine diagnostic pathology, one for disaccharidases estimation, and the third piece was Address for correspondence: Dr S Strobel. Gastro-Intestinal Unit. Western fixed in Carnoy's fixative for mast cell counts. Nineteen biopsies were from coeliac patients, showing subtotal or severe partial villous atrophy, 222
2 HIlUiflat itltestiltl mflucosai Itnast (ells: exptwtided p)opl(dtioti itl ulntreat(el (oeliac disease23 and had generalised disaccharidase deficiency; in 1 1 cases, biopsies were from coeliacs treated with a gluten-free diet and were histologically normal with normal disaccharidase activities; and there were 27 biopsies from patients with irritable bowel syndrome or in whom coeliac disease was ultimately excluded; all of these patients were taking normal diet, and in all cases both histopathology and disaccharidase content of the biopsies were normal. In seven patients multiple jejunal biopsies were taken with a Quinton hydraulic biopsy instrument. These were patients with malabsorption or diarrhoea in whom a patchy distribution of jejunal abnormality was suspected. Final diagnoses are given in the Table. Several biopsies were taken at each of three to five sites along the proximal jejunum, and one sample from each site was fixed in Carnoy's fixative. STAINING PROCEDURE After Carnoy fixation (minimum fixation time six hours) the tissue was paraffin embedded, 6,um sections cut, and mucosal mast cells were stained with Astra blue/safranin at ph 0-3 as previously described.5 6 METHOD FOR MAST CELL COUNTS5 Mast cells were counted in well-orientated sections cut perpendicular to the mucosa. The counts were performed on coded slides on a Leitz Dialux 20 EB microscope (eyepiece x 10, objective x40). A 100 mm2 eyepiece graticule, calibrated against a calibration slide, was used. The edge of the graticule was orientated along the muscularis mucosae at the base of the crypts. The area covered by the square of the graticule comprised % of the total depth of the mucosa (from the bottom of the crypt to the tip of the villus). For each biopsy, a minimum of 10 fields (290,um X 290,um; area mm2) were counted and the mucosal mast cell count per specimen was expressed as mucosal mast cells/mm2. No attempt was made to correct for the area covered Table by epithelium or lying between villi. This technique is similar to the mucosal unit counts, as applied to plasma cell counts.7 TATISTICS Results for the various groups were analysed by using Student's t test for unpaired observations. Results As in our previous work with operative biopsies of jejunum, the technique used gave excellent staining of mucosal mast cells in peroral jejunal biopsy specimens (Figs 1, 2). In those biopsies which contained muscularis mucosa with some submucosa, there was a difference in the staining patterns between the submucosal and mucosal (lamina propria) mast cells, the granules of the former being more intensely stained than those of lamina propria mucosal mast cells. This is further evidence supporting the existence of at least two different mast cell populations in the jejunum.t' " Intraepithelial granulated lymphocytes were not identified, even under oil immersion (x 100) in these jejunal biopsy specimens, although we had found such cells in operative jejunal biopsies.5 These findings highlight again the importance of optimal methodology and the problems of comparing features of surgical biopsies with biopsies taken perorally. Intraepithelial mast cells were occasionally seen (Fig. 3), their numbers being too small to allow any measurements of prevalence within a group of biopsies. A single mast cell in mitosis was found in a patient with untreated coeliac disease (Fig. 4) and in no patient was degranulation of mast cells observed. MUCOSAL MAST CELL COUNTS IN MULTIPLE BIOPSIES OF JEJUNUM Results for mucosal mast cell counts in the seven patients who had multiple biopsies are summarised in the Table. Diagnoses ranged from normal to MMC/mm2 at various sites in proximal jejunum* Diagnosis Histology Diarrhoea- lactase deficiency. previous radiotherapy Normal Severe diffuse enteritis Normal Coeliac. recently started on gluten-free diet 2( (1 173 Subtotal villus atrophy Delayed recovery from giardiasis () 230 Partial villus atrophy Functional diarrhoea Normal Relative of cocliac- lactase deficiency ) Normal Coeliac on normal diet Partial villus atrophv * Site 1 at ligament of Treitz; other biopsies at approximately 10 cm intervals beyond the ligament of Treitz. 223
3 224 Fig. 1 Jejunal biopsvhistologically normal mucosa. Several intensely stained mucosal mast cells can be identified, even at low magnification. Most mucosal mast cells are confined to the lamina propria around the crypts and in the lower part of the villi. The arrow indicates the cross-section ofmucosal mast cells. Carnov's, A BIS ph 03, x160. untreated coeliac disease, and, as indicated, similar mucosal mast cell counts were obtained at the various sites in each of the patients. MUCOSAL MAST CELL COUNTS IN COELIAC DISEASE AND CONTROLS Results of the mucosal mast cell counts in biopsies obtained with the Watson capsule are given in Fig. Fig. 2 Jejunal biopsy disease - with severe partial coeliac villus atrophv. Many mucosal mast cells can be seen as partly dark stained cells. even under low power. Carnov's, ABIS ph 03, x160. Strobel, Busuttil, and Ferguson 5. In the controls, mean mucosal mast cell count was 146 (SD 29/mm2). In untreated coeliac disease significantly higher values were obtained (243±41, p<o0oo1) and, with patients with normal jejunal morphology on a gluten-free diet, the value was similar to normal subjects (145±26) and significantly lower than in the untreated coeliac patients (p<o-ool).
4 Human intestinal mucosal mast cells: expanded population in untreated coeliac disease Fig. 3 One intraepithelial and one lamina propria mast cell (arrowed) in a biopsy ofhistologically normaljejunum. Carnoy's, ABIS ph 0-3, x 750. Fig. 4 Mucosal mast cell in mitosis (arrowed) from a jejunal biopsy ofa coeliac patient. In the upper left corner of the preparation is a normal, non-dividing mucosal mast cells. Carnoy's, ABIS ph 03, x _ I 0 ±L COELIAC DISEASE COELIAC DISEASE 6.1. DISEASES PARTIAL OR NORMAL NORMAL SUBTOTAL VILLUS HISTOLOGY HISTOLOGY ATROPHY ( ON GF DIET ) Fig. 5 Mucosal mast cell counts (MMCImm2) in patients with coeliac disease, either with partial or subtotal villus atrophy, or with normal jejunal morphology on a glutenfree diet; in control patients with normal histology and disaccharidases.. al A A 0 225
5 226 Strobel, Butsluttil, and Fertliisoti Discussion In this prospective study of intestinal mucosal mast cells, we have demonstrated that the population of these cells is expanded in untreated coeliac disease. and that counts return to normal after successful treatment with a gluten-free diet. In order to perform this study, it was necessary to divide peroral jejunal biopsy specimens, and use different fixatives for diagnostic histopathology and for mucosal mast cell counts. It seems likely that the discrepant results in the literature for mucosal mast cell counts in coeliac disease' -3 4are attributable to inappropriate methodology in these earlier studies; these were retrospective reviews of tissues which had been processed for diagnostic purposes, and there is no indication that, in any of these studies, Carnoy's or a similar fixative, suitable for demonstration of mucosal mast cells, had been used. In two of the three previous reports, mast cell counts in formalinfixed specimens from coeliac patients were said to be lower than in controls. As we have now unequivocally shown that there are more mucosal mast cells in coeliacs, these earlier observations must have been due to differences between coeliacs and normal subjects in the susceptibility to the fixative-associated blocking which impairs histochemical staining of mast cell granules in formalinfixed mucosal biopsies. This may imply that, in coeliac disease, the mucosal mast cells are a younger, still dividing cell population,'2 13 cells which would have a lower glycosyl-aminoglycan content. We failed to find any evidence of degranulation of intestinal mucosal mast cells - another postulated explanation for a low mucosal mast cell count in tissue sections.1 4 It has been claimed that this phenomenon occurs in coeliac disease2 and in Crohn's disease. 14 The morphology of mucosal mast cells in untreated coeliac disease, however, appeared to be identical with that in treated coeliacs or in normal controls. Nevertheless, mast cell mediators could still contribute to mucosal damage even in coeliac disease, for intestinal mucosal mast cells are known to have the capacity to secrete mediators without visible evidence of degranulation.2"' Other workers'5'7 have approached the question of degranulation of mucosal mast cells by functional studies rather than by histopathology, and have estimated tissue contents of 5-hydroxytryptamine'5 or histamine16 in coeliac disease or Crohn's disease. 17 Increased levels of these constituents have been found in homogenised tissue preparations, findings in complete agreement with our demonstration of an expanded mucosal mast cell population in coeliac disease, although the sources of increased histamine or 5-hydroxytryptamine levels - mucosal mast cell or non-mast cell origin - are still unclear. lge-c(onitainlilng cells - the nature of whichi is unspecified - have been reported to be increased in number in coeliac disease, food allergic disease. and inflammatory bowel diseases. I2 There remains controversv as to whether these anti-lge positive cells are plasma cells. mast cells. eosinophils, or macrophages.2' Mucosal mast cells have been shown to contain IgE in rats.-2 Unfortunately, methods optimal for peroxidase staining of plasma cells are contraindicated for demonstration of mast cells in the same sections. and so it seems likelv that it will require immunoelectron microscopy of the IgEcontaining cells to reveal their exact nature. The complex immune response to gluten in coeliac disease produces an equally complex expansion of T and B cells in the intestinal mucosa. and also leads to an expanded intestinal mucosal mast cell population. Whether products of activated mast cells contribute to the tissue damage remains to be established. In this study, we have illustrated that with appropriate attention to methodology the morphology and numbers of mast cells in an intestinal mucosal biopsy can readily be documented. It remains now to establish whether mucosal mast cells play a part in conditions such as peptic ulcer, inflammatory bowel disease, infections, and gastrointestinal food allergies, and whether the number of intestinal mucosal mast cells relates in any way to the presence of IgE-mediated immune reactions in the gastrointestinal mucosae. We thank the nurses and the medical staff of the Gastrointestinal Unit for their help in carrying out this study, particularly Dr Philip Earnshaw who performed the multiple biopsies. We gratefully acknowledge the skilful technical assistance of Alexander Sutherland who processed the specimens, and of Dorothy Smith who performed the disaccharidase assays. We thank Mr J Paul, Medical Illustration Department, University of Edinburgh, for his help with the photography and Ms A Hardy for typing the manuscript. This work was supported in part by the Deutsche Forschungsgemeinschaft DFG(STR210/1), by the Coeliac Trust, and by the National Fund for Research into Crippling Diseases. References 1 Dollberg L, Gurevitz M, Freier S. Gastrointestinal mast cells in health, and in coeliac disease and other conditions. Arch Dis Childh 1980; 55:
6 Hultfl(utl ints(titia(l mulcosa tilist (cells: Xpa/)nld(l /)po)ulaiionl in unitreawd coliac disease Shiner M. Ultrastructural f'eatures of' allergic manifestations in the small intestine of children..sumd J Gasiroenierol 1981; 16: suppl Kumar P. O'Donoghue DP, Lancaster-Smith M. Cellular changes in the jejunal mucosa ffollowing thc reintroduction of gluten in treated coeliac disea.se. In: Edwards AM. Pepys J. eds. The mast cell. Tunbridge Wells: Pitman Medical. 1979: Kosnai 1. Kuitunen P. Savilahti E. Sipponen P. Mast cells in small intestine in cow's milk protein intoleratnce aind in celiac disease. Pediatr Res 1981; 15: Strobel S. Miller HRP. Ferguson A. Human intestinal mucosal mast cells: evaluation of fixation and staining techniques. J Clint Pathol 1981; 34: Bloom G, Kelly JW. The copper pthalocyanin dye 'Astrablau' and its staining properties. especially the staining of mast cells. Hi.stochemie 1960; 2: Brandtzaeg P, Baklien K, Fausa 0, Hoel PS. Immunohistochemical characteristics of local immunoglobulin formation in ulcerative colitis. Gastroenterology 1974; 66: Lloyd G, Green FHY, Fox H, Mani V, Turnberg LA. Mast cells and immunoglobulin E in inflammatory bowel disease. Gut 1975; 16: Takahashi T, Shimazu H, Yamagishi T, Masayohi T. G-cell populations in resected stomachs from gastric and duodenal ulcer patients. Gastroenterology 1980; 78: Miller HRP, Walshaw R. Immune reactions in mucous membranes. IV. Histochemistry of intestinal mast cells during helminth expulsion in the rat. Am J Pathol 1972; 69: Enerback L. Mast cells in rat gastrointestinal mucosa. II. Dye-binding and metachromatic properties. Acta Pathol Microbiol Scand 1966; 66: 3) Enerback L, Lowhagen GB. Long term increase of mucosal mast cells in the rat induced by administration of compound 48/80. (ell Tissue Res 1979; 198: Kaliner MA. Is a mast cell a mast cell a mast cel'l? J Allerg!' C/lin Immuniol 1980: 66: Dvorak AM, Monahan RA, Osage JE. Dickersin GR. Mast ccil degranulation in Crohn's disease. Lancet 1979; 1: (Challacombc DN. Dawkins PD, Baker D. Increascd tissue concentrations of 5-hydroxytryptamine in the duodenal mucosa of patients with cocalic disease. Giut 1977; 18: C halilcombe DN. Edwards JP, Baylis JM. Histamine relcase in post-challenge coeliac disease. Lancet 1980; 1: Bclus AD, Pearce FL, Gauldic J, Horsewood P. (ioodacre RL, Cole F Heaticy RV. Bienenstock J. Isolation and characteristics of mast cells from the lamina propria of the small bowel. In: Edwards AM, Pepys J. eds. The mast cell. Tunbridge Wells: Pitman Medical, 1979: Rosekrans PCM, Meijer CJLM, van der Waal AM, Lindeman J. Allergic proctitis. a clinical and an immunopathological entity. Gui 1980; 21: Heatley RV, Calcraft BJ, Fifield R. Rhodes J. Whitehead RH, Newcombe RG. Immunoglobulin E in rectal mucosa of patients with proctitis. Lancei 1975; 2: O'Donoghue DP, Kumar P. Rectal IgE cells in inflammatory bowel disease. Gut 1979; 20: Durkin HG, Bazin H, Waksman DH. Origin and fate of IgE-bearing lymphocytes. 1. Peyer's patches as differentiation site of cells simultaneously bearing IgA and IgE. J Exp Med 1981; 154: Mayrhofer G, Bazin, H, Gowans JL. Nature of cells binding anti-ige in rats immunized with Nippostrongylus brasiliensis: IgE synthesis in regional nodes and concentration in mucosal mast cells. Eur J Immunol 1976; 6: Gut: first published as /gut on 1 March Downloaded from on 27 June 2018 by guest. Protected by copyright.
intestinal biopsies and a range of commonly used fixatives, to establish whether the method of fixation
 Human intestinal mucosal mast cells: fixation and staining techniques STEPHAN STROBEL, HUGH RP MILLER, ANNE FERGUSON J Clin Pathol 1981 ;34:851-858 evaluation of From the Gastro-Intestinal Unit, Western
Human intestinal mucosal mast cells: fixation and staining techniques STEPHAN STROBEL, HUGH RP MILLER, ANNE FERGUSON J Clin Pathol 1981 ;34:851-858 evaluation of From the Gastro-Intestinal Unit, Western
Prevalence of lactase deficiency in British adults
 Prevalence of lactase deficiency in British adults Gut, 1984, 25, 163-167 ANNE FERGUSON, DOROTHY M MACDONALD, AND W GORDON BRYDON From the Gastro-Intestinal Unit, University of Edinburgh, and Western General
Prevalence of lactase deficiency in British adults Gut, 1984, 25, 163-167 ANNE FERGUSON, DOROTHY M MACDONALD, AND W GORDON BRYDON From the Gastro-Intestinal Unit, University of Edinburgh, and Western General
Rectal mucosal plasma cells in inflammatory bowel
 Gut, 1983, 24, 519-524 Rectal mucosal plasma cells in inflammatory bowel disease B B SCOTT, ANNE GOODALL, P STEPHENSON, AND D JENKINS From the Departments of Medicine and Pathology, Lincoln County Hospital,
Gut, 1983, 24, 519-524 Rectal mucosal plasma cells in inflammatory bowel disease B B SCOTT, ANNE GOODALL, P STEPHENSON, AND D JENKINS From the Departments of Medicine and Pathology, Lincoln County Hospital,
embedded tissue-sections has the advantage of permanence of the sections and is more suitable for
 Gut, 1980, 21, 941-947 Immunoglobulin containing cells in inflammatory bowel disease of the colon: a morphometric and immunohistochemical study P C M ROSEKRANS,* C J L M MEIJER, A M VAN DER WAL, C J CORNELISSE,
Gut, 1980, 21, 941-947 Immunoglobulin containing cells in inflammatory bowel disease of the colon: a morphometric and immunohistochemical study P C M ROSEKRANS,* C J L M MEIJER, A M VAN DER WAL, C J CORNELISSE,
Lamina propria eosinophils and mast cells in ulcerative colitis: comparison between Asians and
 J Clin Pathol 199;43:27-31 ast Birmingham Hospital, Bordesley Green ast, Birmingham Department of Medicine G F A Benfield Department of Pathology R Bryan J Crocker Correspondence to: Dr J Crocker, Department
J Clin Pathol 199;43:27-31 ast Birmingham Hospital, Bordesley Green ast, Birmingham Department of Medicine G F A Benfield Department of Pathology R Bryan J Crocker Correspondence to: Dr J Crocker, Department
These studies were made at a time when it was not. yet fully established that mast cells could react with
 Gut, 1975, 16, 861-866 Mast cells and immunoglobulin E in inflammatory bowel disease G. LLOYD1, F. H. Y. GREEN, H. FOX, V. MANI2, AND L. A. TURNBERG2 From the Department ofpathology, University of Manchester,
Gut, 1975, 16, 861-866 Mast cells and immunoglobulin E in inflammatory bowel disease G. LLOYD1, F. H. Y. GREEN, H. FOX, V. MANI2, AND L. A. TURNBERG2 From the Department ofpathology, University of Manchester,
The cell population of the upper jejunal mucosa in tropical sprue and postinfective malabsorption
 Gut, 1974, 15, 387-391 The cell population of the upper jejunal mucosa in tropical sprue and postinfective malabsorption R. D. MONTGOMRY AND A. C. I. SHARR From the Metabolic Unit, ast Birmingham Hospital,
Gut, 1974, 15, 387-391 The cell population of the upper jejunal mucosa in tropical sprue and postinfective malabsorption R. D. MONTGOMRY AND A. C. I. SHARR From the Metabolic Unit, ast Birmingham Hospital,
Dissecting Microscope Appearance of
 Arch. Dis. Childh., 1967, 42, 626. Dissecting Microscope Appearance of Small Bowel Mucosa in Children JOHN WALKER-SMITH From Professorial Unit, Royal Alexandra Hospital for Children, Camperdown, Sydney,
Arch. Dis. Childh., 1967, 42, 626. Dissecting Microscope Appearance of Small Bowel Mucosa in Children JOHN WALKER-SMITH From Professorial Unit, Royal Alexandra Hospital for Children, Camperdown, Sydney,
Quantification of enterochromaffin cells with
 Archives of Disease in Childhood, 1984, 59, 523-527 Quantification of enterochromaffin cells with serotonin immunoreactivity in the duodenal mucosa in coeliac disease E E WHEELER AND D N CHALLACOMBE Somerset
Archives of Disease in Childhood, 1984, 59, 523-527 Quantification of enterochromaffin cells with serotonin immunoreactivity in the duodenal mucosa in coeliac disease E E WHEELER AND D N CHALLACOMBE Somerset
Increased numbers of IgE containing cells in gastric and duodenal biopsies. An expression of food allergy secondary to chronic inflammation?
 J Clin Pathol 1984;37:601-606 Increased numbers of IgE containing cells in gastric and duodenal biopsies. An expression of food allergy secondary to chronic inflammation? JP VAN SPREEUWEL,* J LINDEMAN,
J Clin Pathol 1984;37:601-606 Increased numbers of IgE containing cells in gastric and duodenal biopsies. An expression of food allergy secondary to chronic inflammation? JP VAN SPREEUWEL,* J LINDEMAN,
Quantitation of intraepithelial lymphocytes
 Gut, 1971, 12, 988-994 Quantitation of intraepithelial lymphocytes inhuman jejunum ANNE FERGUSON AND D. MURRAY From the University Departments ofbacteriology and Immunology (Western Infirmary) and Pathology
Gut, 1971, 12, 988-994 Quantitation of intraepithelial lymphocytes inhuman jejunum ANNE FERGUSON AND D. MURRAY From the University Departments ofbacteriology and Immunology (Western Infirmary) and Pathology
ranged from two months to 21 years (mean 5% years)
 Gut, 1978, 19, 754-758 Response of the skin in dermatitis herpetiformis to a gluten free diet, with reference to jejunal morphology B. T. COOPER, E. MALLAS, M. D. TROTTER, AND W. T. COOKE From the Nutritional
Gut, 1978, 19, 754-758 Response of the skin in dermatitis herpetiformis to a gluten free diet, with reference to jejunal morphology B. T. COOPER, E. MALLAS, M. D. TROTTER, AND W. T. COOKE From the Nutritional
Malignant histiocytosis of the intestine: the early histological lesion
 Gut, 1980, 21, 381-386 Malignant histiocytosis of the intestine: the early histological lesion P ISAACSON From the Department of Pathology, Faculty of Medicine, Southampton University Hospital, Southampton
Gut, 1980, 21, 381-386 Malignant histiocytosis of the intestine: the early histological lesion P ISAACSON From the Department of Pathology, Faculty of Medicine, Southampton University Hospital, Southampton
Cellobiose/mannitol sugar permeability test
 Cellobiose/mannitol sugar permeability test complements biopsy histopathology in clinical investigation of the jejunum S STROBEL, W G BRYDON, AND ANNE FERGUSON Gut, 1984, 25, 1241-1246 From the Gastro-Intestinal
Cellobiose/mannitol sugar permeability test complements biopsy histopathology in clinical investigation of the jejunum S STROBEL, W G BRYDON, AND ANNE FERGUSON Gut, 1984, 25, 1241-1246 From the Gastro-Intestinal
coeliac syndrome per day. Investigations showed a megaloblastic anaemia showed a flat mucosa. ileum were resected and he made an uninterrupted
 Gut, 1965, 6, 466 Post-mortem examination of a small intestine in the coeliac syndrome B. CREAMER AND P. LEPPARD From the Gastro-Intestinal Laboratory, St Thomas's Hospital, London EDITORIAL SYNOPSIS This
Gut, 1965, 6, 466 Post-mortem examination of a small intestine in the coeliac syndrome B. CREAMER AND P. LEPPARD From the Gastro-Intestinal Laboratory, St Thomas's Hospital, London EDITORIAL SYNOPSIS This
Three-dimensional structure of the human small intestinal mucosa in health and disease
 Gut, 1969, 10, 6-12 Three-dimensional structure of the human small intestinal mucosa in health and disease C. A. LOEHRY AND B. CREAMER From the Gastrointestinal Laboratory, St Thomas' Hospital, London
Gut, 1969, 10, 6-12 Three-dimensional structure of the human small intestinal mucosa in health and disease C. A. LOEHRY AND B. CREAMER From the Gastrointestinal Laboratory, St Thomas' Hospital, London
Gastric gland metaplasia in the small and
 Gut, 1977, 18, 214-218 Gastric gland metaplasia in the small and large intestine I. YOKOYAMA, S. KOZUKA, K. ITO, K. KUBOTA, Y. YOKOYAMA, AND T. KONDO From the Second Department of Surgery and the Second
Gut, 1977, 18, 214-218 Gastric gland metaplasia in the small and large intestine I. YOKOYAMA, S. KOZUKA, K. ITO, K. KUBOTA, Y. YOKOYAMA, AND T. KONDO From the Second Department of Surgery and the Second
Histopathology: gastritis and peptic ulceration
 Histopathology: gastritis and peptic ulceration These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual
Histopathology: gastritis and peptic ulceration These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus
 Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue
 A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue UCSF Liver and Gastrointestinal Pathology Update Sept. 4, 2009 How to Go Wrong When Evaluating Small Bowel Biopsies, Based on
A Practical Approach to Small Bowel Biopsies: All that flattens is not sprue UCSF Liver and Gastrointestinal Pathology Update Sept. 4, 2009 How to Go Wrong When Evaluating Small Bowel Biopsies, Based on
Rectal mucosa in cows' milk allergy
 Archives of Disease in Childhood, 1989, 64, 1256-1260 Rectal mucosa in cows' milk allergy N IYNGKARAN,* M YADAVt AND C G BOEYt Departments of *Paediatrics and tpathology, University Hospital, and tdepartment
Archives of Disease in Childhood, 1989, 64, 1256-1260 Rectal mucosa in cows' milk allergy N IYNGKARAN,* M YADAVt AND C G BOEYt Departments of *Paediatrics and tpathology, University Hospital, and tdepartment
HDF Case Whipple s disease
 HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
Is a raised intraepithelial lymphocyte count with normal duodenal villous architecture clinically relevant?
 424 ORIGINAL ARTICLE Is a raised intraepithelial lymphocyte count with normal duodenal villous architecture clinically relevant? S Mahadeva, J I Wyatt, P D Howdle... See end of article for authors affiliations...
424 ORIGINAL ARTICLE Is a raised intraepithelial lymphocyte count with normal duodenal villous architecture clinically relevant? S Mahadeva, J I Wyatt, P D Howdle... See end of article for authors affiliations...
Timing of infiltration of T lymphocytes induced by gluten into the small intestine in coeliac disease
 J Clin Pathol 1987;40:741-745 Timing of infiltration of T lymphocytes induced by gluten into the small intestine in coeliac disease A R FREEDMAN,* J C MACARTNEY,t J M NELUFER,* P J CICLITIRA* From the
J Clin Pathol 1987;40:741-745 Timing of infiltration of T lymphocytes induced by gluten into the small intestine in coeliac disease A R FREEDMAN,* J C MACARTNEY,t J M NELUFER,* P J CICLITIRA* From the
Histologic Follow-up of People With Celiac Disease on a Gluten-Free Diet Slow and Incomplete Recovery
 Anatomic Pathology / HISTOLOGIC FOLLOW-UP OF PEOPLE WITH CELIAC DISEASE ON A GLUTEN-FREE DIET Histologic Follow-up of People With Celiac Disease on a Gluten-Free Diet Slow and Incomplete Recovery Peter
Anatomic Pathology / HISTOLOGIC FOLLOW-UP OF PEOPLE WITH CELIAC DISEASE ON A GLUTEN-FREE DIET Histologic Follow-up of People With Celiac Disease on a Gluten-Free Diet Slow and Incomplete Recovery Peter
Chronic immune colitis in rabbits
 Chronic immune colitis in rabbits A. S. MEE, J. E. McLAUGHLIN, H. J. F. HODGSON, AND D. P. JEWELL Gut, 1979, 20, 1-5 From the Academic Department of Medicine and Department of Histopathology, Royal Free
Chronic immune colitis in rabbits A. S. MEE, J. E. McLAUGHLIN, H. J. F. HODGSON, AND D. P. JEWELL Gut, 1979, 20, 1-5 From the Academic Department of Medicine and Department of Histopathology, Royal Free
Reintroduction of gluten in adults and children with treated coeliac disease
 Reintroduction of gluten in adults and children with treated coeliac disease PARVEEN J. KUMAR, D. P. O'DONOGHUE, KATHY STENSON, AND A. M. DAWSON From the Department of Gastroenterology, St. Bartholomew's
Reintroduction of gluten in adults and children with treated coeliac disease PARVEEN J. KUMAR, D. P. O'DONOGHUE, KATHY STENSON, AND A. M. DAWSON From the Department of Gastroenterology, St. Bartholomew's
Laboratory Methods for Diagnosing Celiac Disease. Vijay Kumar, PhD, FACB IMMCO Diagnostics, Inc. Buffalo, NY
 Laboratory Methods for Diagnosing Celiac Disease Vijay Kumar, PhD, FACB IMMCO Diagnostics, Inc. Buffalo, NY Prevalence of Celiac Disease Group With Symptoms Adults Children Associated Symptoms Chronic
Laboratory Methods for Diagnosing Celiac Disease Vijay Kumar, PhD, FACB IMMCO Diagnostics, Inc. Buffalo, NY Prevalence of Celiac Disease Group With Symptoms Adults Children Associated Symptoms Chronic
Collagenous colitis associated with small intestinal villous atrophy
 (Gut, 1986, 27, 1394-1398 Case report Collagenous colitis associated with small intestinal villous atrophy I HAMILTON, S SANDERS, D HOPWOOD, AND I A D BOUCHIER From the University Department of Medicine
(Gut, 1986, 27, 1394-1398 Case report Collagenous colitis associated with small intestinal villous atrophy I HAMILTON, S SANDERS, D HOPWOOD, AND I A D BOUCHIER From the University Department of Medicine
Confirming persistence of gluten intolerance in
 Archives of Disease in Childhood, 1975, 50, 259. Confirming persistence of gluten intolerance in children diagnosed as having coeliac disease in infancy Usefulness of onehour blood xylose test C. J. ROLLES,
Archives of Disease in Childhood, 1975, 50, 259. Confirming persistence of gluten intolerance in children diagnosed as having coeliac disease in infancy Usefulness of onehour blood xylose test C. J. ROLLES,
Lamina propria mast cells in biopsies from children with Crohn's disease
 J Clin Pathol 1986;39:279-283 Lamina propria mast cells in biopsies from children with Crohn's disease R ANDERON,* KBP LEUNG,t FL PEARCE,t JA WALKER-MTH* From the *Laboratory for Paediatric Gastroenterology,
J Clin Pathol 1986;39:279-283 Lamina propria mast cells in biopsies from children with Crohn's disease R ANDERON,* KBP LEUNG,t FL PEARCE,t JA WALKER-MTH* From the *Laboratory for Paediatric Gastroenterology,
Coeliac disease with histological features of peptic duodenitis: Value of assessment of intraepithelial lymphocytes
 420 4 Clin Pathol 1993;46:420-424 Department of Pathology, St James's Hospital and Trinity College, Dublin Ireland M D Jeffers D O'B Hourihane Correspondence to: Professor D O'B Hourihane Accepted for
420 4 Clin Pathol 1993;46:420-424 Department of Pathology, St James's Hospital and Trinity College, Dublin Ireland M D Jeffers D O'B Hourihane Correspondence to: Professor D O'B Hourihane Accepted for
Small intestine. Small intestine
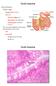 General features Tubular organ longest part; 5-6 m most of chemical digestion absorption of nutrients reabsorption of H2O occurs. Two structural features; maximize the lumenal surface area villi microvilli
General features Tubular organ longest part; 5-6 m most of chemical digestion absorption of nutrients reabsorption of H2O occurs. Two structural features; maximize the lumenal surface area villi microvilli
Increased mucosal damage during parasite infection
 Gut, 1980, 21, 37-43 Increased mucosal damage during parasite infection in mice fed an elemental diet ANNE FERGUSON, R F A LOGAN, AND T T MACDONALD' From the Gastro-Intestinal Unit, University oj Edinburgh,
Gut, 1980, 21, 37-43 Increased mucosal damage during parasite infection in mice fed an elemental diet ANNE FERGUSON, R F A LOGAN, AND T T MACDONALD' From the Gastro-Intestinal Unit, University oj Edinburgh,
DIGESTIVE TRACT ESOPHAGUS
 DIGESTIVE TRACT From the lower esophagus to the lower rectum four fundamental layers comprise the wall of the digestive tube: mucosa, submucosa, muscularis propria (externa), and adventitia or serosa (see
DIGESTIVE TRACT From the lower esophagus to the lower rectum four fundamental layers comprise the wall of the digestive tube: mucosa, submucosa, muscularis propria (externa), and adventitia or serosa (see
Primary mucinous adenocarcinoma developing in an ileostomy stoma
 Gut, 1988, 29, 1607-1612 Primary mucinous adenocarcinoma developing in an ileostomy stoma P J SMART, S SASTRY, AND S WELLS From the Departments of Histopathology and Surgery, Bolton General Hospital, Fan
Gut, 1988, 29, 1607-1612 Primary mucinous adenocarcinoma developing in an ileostomy stoma P J SMART, S SASTRY, AND S WELLS From the Departments of Histopathology and Surgery, Bolton General Hospital, Fan
Studies of intestinal fermentation in ulcerative
 Gut, 1968, 9, 51-56 Studies of intestinal fermentation in ulcerative colitis R. D. MONTGOMERY, A. C. FRAZER, CATHRYN HOOD, J. M. GOODHART, M. R. HOLLAND, AND R. SCHNEIDER From the Metabolic Unit, East
Gut, 1968, 9, 51-56 Studies of intestinal fermentation in ulcerative colitis R. D. MONTGOMERY, A. C. FRAZER, CATHRYN HOOD, J. M. GOODHART, M. R. HOLLAND, AND R. SCHNEIDER From the Metabolic Unit, East
Small intestinal mucosal patterns of coeliac disease and idiopathic steatorrhoea seen in other situations
 Gut, 1964, 5, 51 Small intestinal mucosal patterns of coeliac disease and idiopathic steatorrhoea seen in other situations R. R. W. TOWNLEY, M. H. CASS, AND CHARLOTTE M. ANDERSON From the Gastroenterological
Gut, 1964, 5, 51 Small intestinal mucosal patterns of coeliac disease and idiopathic steatorrhoea seen in other situations R. R. W. TOWNLEY, M. H. CASS, AND CHARLOTTE M. ANDERSON From the Gastroenterological
THE D-XYLOSE EXCRETION TEST IN COELIAC DISEASE IN CHILDHOOD
 Arch. Dis. Childh., 1963, 38, 476. THE D-XYLOE EXCRETON TET N COELAC DEAE N CHLDHOOD BY DOUGLA HUBBLE and HELA LTTLEJOHN From the Department of Paediatrics and Child Health, the University of Birmingham
Arch. Dis. Childh., 1963, 38, 476. THE D-XYLOE EXCRETON TET N COELAC DEAE N CHLDHOOD BY DOUGLA HUBBLE and HELA LTTLEJOHN From the Department of Paediatrics and Child Health, the University of Birmingham
Adult coeliac disease
 Postgrad. med. J. (August 1968) 44, 632-640. PATENTS with idiopathic steatorrhoea present in many different ways. The dominant feature of the clinical presentation in 100 patients is shown in Table 1.
Postgrad. med. J. (August 1968) 44, 632-640. PATENTS with idiopathic steatorrhoea present in many different ways. The dominant feature of the clinical presentation in 100 patients is shown in Table 1.
Lymphocytic Gastritis, Isolated Type Occurring in Family Members. A Case Report.
 Lymphocytic Gastritis, Isolated Type Occurring in Family Members. A Case Report. Alan Shienbaum, DO; AndriyPavlenko, MD; Jun Liu, MD, PhD; Janusz J Godyn, MD. Pathology Department, Kennedy University Hospitals,
Lymphocytic Gastritis, Isolated Type Occurring in Family Members. A Case Report. Alan Shienbaum, DO; AndriyPavlenko, MD; Jun Liu, MD, PhD; Janusz J Godyn, MD. Pathology Department, Kennedy University Hospitals,
Dermatitis herpetiformis: jejunal findings and skin response to gluten free diet
 Archives of Disease in Childhood, 1984, 59, 517-522 Dermatitis herpetiformis: jejunal findings and skin response to gluten free diet T REUNALA, I KOSNAI, S KARPATI, P KUITUNEN, E TOROK, AND E SAVILAHTI
Archives of Disease in Childhood, 1984, 59, 517-522 Dermatitis herpetiformis: jejunal findings and skin response to gluten free diet T REUNALA, I KOSNAI, S KARPATI, P KUITUNEN, E TOROK, AND E SAVILAHTI
EVIDENCE THAT ACTIVATED MUCOSAL T CELLS PLAY A ROLE IN THE PATHOGENESIS OF ENTEROPATHY IN HUMAN SMALL INTESTINE
 Published Online: 1 April, 1988 Supp Info: http://doi.org/10.1084/jem.167.4.1341 Downloaded from jem.rupress.org on September 23, 2018 EVIDENCE THAT ACTIVATED MUCOSAL T CELLS PLAY A ROLE IN THE PATHOGENESIS
Published Online: 1 April, 1988 Supp Info: http://doi.org/10.1084/jem.167.4.1341 Downloaded from jem.rupress.org on September 23, 2018 EVIDENCE THAT ACTIVATED MUCOSAL T CELLS PLAY A ROLE IN THE PATHOGENESIS
Spirochaetosis of the human rectum associated with an intraepithelial mast cell and IgE plasma cell response
 Gut, 1987, 28, 588-593 Spirochaetosis of the human rectum associated with an intraepithelial mast cell and IgE plasma cell response J-O GEBBERS, D J P FERGUSON, C MASON, P KELLY, AND D P JEWELL From the
Gut, 1987, 28, 588-593 Spirochaetosis of the human rectum associated with an intraepithelial mast cell and IgE plasma cell response J-O GEBBERS, D J P FERGUSON, C MASON, P KELLY, AND D P JEWELL From the
Expression of C-myc oncogene in coeliac disease
 J Clin Pathol 1987;40:307-311 Expression of C-myc oncogene in coeliac disease P J CICLITIRA,* J STEWART,J G EVAN,t D G D WIGHT, K SIKORAt From the *Division of Medicine, The Rayne Institute, The United
J Clin Pathol 1987;40:307-311 Expression of C-myc oncogene in coeliac disease P J CICLITIRA,* J STEWART,J G EVAN,t D G D WIGHT, K SIKORAt From the *Division of Medicine, The Rayne Institute, The United
children are shown in Table 1. Most children were under three years of age, and all were Caucasian,
 Gut, 1980, 21, 44-48 Microvillous surface area in secondary disaccharidase deficiency A D PHILLIPS', SARA AVIGAD, JOANNA SACKS, S J RICE, N E FRANCE, AND J A WALKER-SMITH From the Queen Elizabeth Hospital
Gut, 1980, 21, 44-48 Microvillous surface area in secondary disaccharidase deficiency A D PHILLIPS', SARA AVIGAD, JOANNA SACKS, S J RICE, N E FRANCE, AND J A WALKER-SMITH From the Queen Elizabeth Hospital
Coeliac Disease: Diagnosis and clinical features
 Coeliac Disease: Diagnosis and clinical features Australasian Gastrointestinal Pathology Society AGM 28 Oct 2016 Dr. Hooi Ee Gastroenterologist, Sir Charles Gairdner Hospital Coeliac disease Greek: koiliakos
Coeliac Disease: Diagnosis and clinical features Australasian Gastrointestinal Pathology Society AGM 28 Oct 2016 Dr. Hooi Ee Gastroenterologist, Sir Charles Gairdner Hospital Coeliac disease Greek: koiliakos
General Structure of Digestive Tract
 Dr. Nabil Khouri General Structure of Digestive Tract Common Characteristics: Hollow tube composed of a lumen whose diameter varies. Surrounded by a wall made up of 4 principal layers: Mucosa Epithelial
Dr. Nabil Khouri General Structure of Digestive Tract Common Characteristics: Hollow tube composed of a lumen whose diameter varies. Surrounded by a wall made up of 4 principal layers: Mucosa Epithelial
Low gluten diet in the treatment of adult coeliac disease: effect on jejunal morphology and serum anti-gluten antibodies
 Gut, 1988, 29, 1564-1568 Low gluten diet in the treatment of adult coeliac disease: effect on jejunal morphology and serum anti-gluten antibodies A M P MONTGOMERY, A K J GOKA, P J KUMAR, M J G FARTHING,
Gut, 1988, 29, 1564-1568 Low gluten diet in the treatment of adult coeliac disease: effect on jejunal morphology and serum anti-gluten antibodies A M P MONTGOMERY, A K J GOKA, P J KUMAR, M J G FARTHING,
MAST-CELLS are present in the digestive tract of all classes of vertebrates
 The Distribution of Mast-Cells in the Digestive Tract of Laboratory Animals: Its Bearings on the Problem of the Location of Histamine in Tissues By I. MOTA, A. G. FERRI, AND S. YONEDA 251 (From the Laboratory
The Distribution of Mast-Cells in the Digestive Tract of Laboratory Animals: Its Bearings on the Problem of the Location of Histamine in Tissues By I. MOTA, A. G. FERRI, AND S. YONEDA 251 (From the Laboratory
HISTOLOGY VIRTUAL LABORATORY GASTROINTESTINAL SYSTEM
 HISTOLOGY VIRTUAL LABORATORY GASTROINTESTINAL SYSTEM LIP (Slides GI 1, 2) Identify the outer portion lined by stratified squamous (keratinized) epithelium. Note the hair follicles and sebaceous glands
HISTOLOGY VIRTUAL LABORATORY GASTROINTESTINAL SYSTEM LIP (Slides GI 1, 2) Identify the outer portion lined by stratified squamous (keratinized) epithelium. Note the hair follicles and sebaceous glands
Rectal biopsy as an aid to cancer control in ulcerative colitis
 Rectal biopsy as an aid to cancer control in ulcerative colitis B. C. MORSON AND LILLIAN S. C. PANG From the Research Department, St. Mark's Hospital, London Gut, 1967, 8, 423 EDITORIAL COMMENT This is
Rectal biopsy as an aid to cancer control in ulcerative colitis B. C. MORSON AND LILLIAN S. C. PANG From the Research Department, St. Mark's Hospital, London Gut, 1967, 8, 423 EDITORIAL COMMENT This is
 SUMMARY Coeliac disease is a common food intolerance in Western populations, in which it has a prevalence of about 1%. In early infancy, when the transition is made to a gluten-containing diet (particularly
SUMMARY Coeliac disease is a common food intolerance in Western populations, in which it has a prevalence of about 1%. In early infancy, when the transition is made to a gluten-containing diet (particularly
without gut symptoms and in normal adults
 J Clin Pathol 1981;34:386-392 Jejunal mucosal morphometry in children with and without gut symptoms and in normal adults FJ PENNA,* ID HILL,t D KINGSTON,* K ROBERTSON,+ G SLAVIN,+ AND M SHINER* From the
J Clin Pathol 1981;34:386-392 Jejunal mucosal morphometry in children with and without gut symptoms and in normal adults FJ PENNA,* ID HILL,t D KINGSTON,* K ROBERTSON,+ G SLAVIN,+ AND M SHINER* From the
Protein synthesis by cultured jejunal mucosa from
 Gut, 1981, 22, 623-627 Protein synthesis by cultured jejunal mucosa from control subjects and patients with coeliac disease P E JONES,* C L L'HIRONDEL,t AND T J PETERS$ From the Department of Medicine,
Gut, 1981, 22, 623-627 Protein synthesis by cultured jejunal mucosa from control subjects and patients with coeliac disease P E JONES,* C L L'HIRONDEL,t AND T J PETERS$ From the Department of Medicine,
SAM PROVIDER TOOLKIT
 THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
Coeliac disease in Sudanese children
 Coeliac disease in Sudanese children G. I. SULIMAN1 Gut, 1978, 19, 121-125 From the Department ofpaediatrics and Child Health, Khartoum Civil Hospital, Khartoum, Sudan SUMMARY Coeliac disease has not hitherto
Coeliac disease in Sudanese children G. I. SULIMAN1 Gut, 1978, 19, 121-125 From the Department ofpaediatrics and Child Health, Khartoum Civil Hospital, Khartoum, Sudan SUMMARY Coeliac disease has not hitherto
Lactose Intolerance in Childhood Coeliac Disease
 Arch. Dis. Childh., 1968, 43, 433. Lactose Intolerance in Childhood Coeliac Disease Assessment of its Incidence and Importance ALEXANDER S. McNEISH and ELIZABETH M. SWEET From the Royal Hospital for Sick
Arch. Dis. Childh., 1968, 43, 433. Lactose Intolerance in Childhood Coeliac Disease Assessment of its Incidence and Importance ALEXANDER S. McNEISH and ELIZABETH M. SWEET From the Royal Hospital for Sick
TRICHURIASIS : LOCALIZED INFLAMMATORY RESPONSES IN THE COLON
 TRICHURIASIS : LOCALIZED INFLAMMATORY RESPONSES IN THE COLON Gurjeet Kaur 1, S Mahendra Raj 2 and Nyi Nyi Naing 3 Departments of 1 Pathology and 2 Medicine and the 3 Epidemiology and Medical Statistics
TRICHURIASIS : LOCALIZED INFLAMMATORY RESPONSES IN THE COLON Gurjeet Kaur 1, S Mahendra Raj 2 and Nyi Nyi Naing 3 Departments of 1 Pathology and 2 Medicine and the 3 Epidemiology and Medical Statistics
A HISTOLOGICAL STUDY OF THE EFFECTS OF NONSTEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs) ON THE GASTRIC AND DUODENAL MUCOSA
 A HISTOLOGICAL STUDY OF THE EFFECTS OF NONSTEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs) ON THE GASTRIC AND DUODENAL MUCOSA Abstract Pages with reference to book, From 287 To 290 Naheed Moghal, N.A. Jafarey
A HISTOLOGICAL STUDY OF THE EFFECTS OF NONSTEROIDAL ANTI-INFLAMMATORY DRUGS (NSAIDs) ON THE GASTRIC AND DUODENAL MUCOSA Abstract Pages with reference to book, From 287 To 290 Naheed Moghal, N.A. Jafarey
Rectal biopsy in patients presenting to an infectious disease unit with diarrhoeal disease
 Gut, 1979, 20, 141-148 Rectal biopsy in patients presenting to an infectious disease unit with diarrhoeal disease R. J. DICKINSON, H. M. GILMOUR, AND D. B. L. McCLELLAND' From the Department of Infectious
Gut, 1979, 20, 141-148 Rectal biopsy in patients presenting to an infectious disease unit with diarrhoeal disease R. J. DICKINSON, H. M. GILMOUR, AND D. B. L. McCLELLAND' From the Department of Infectious
Mucosal secretory IgA and secretory piece in adult
 Gut, 1973, 14, 778-783 Mucosal secretory IgA and secretory piece in adult coeliac disease R. J. SHINER AND JANET BALLARD' From the Medical Research Council Gastroenterology Unit, Central Middlesex Hospital,
Gut, 1973, 14, 778-783 Mucosal secretory IgA and secretory piece in adult coeliac disease R. J. SHINER AND JANET BALLARD' From the Medical Research Council Gastroenterology Unit, Central Middlesex Hospital,
Coeliac Disease Bible Class Questions and Answers
 Coeliac Disease Bible Class Questions and Answers Jan Hendrik Niess What is the definition of coeliac disease? Coeliac disease is an immune reaction to gluten (wheat, barely, rye) in an genetic predisposed
Coeliac Disease Bible Class Questions and Answers Jan Hendrik Niess What is the definition of coeliac disease? Coeliac disease is an immune reaction to gluten (wheat, barely, rye) in an genetic predisposed
Small intestinal structure and passive permeability in systemic sclerosis
 Gut, 198, 21, 293-298 Small intestinal structure and passive permeability in systemic sclerosis I COBDENM, J ROTHWELL, A T R AXON, M F DIXON, D J LINTOTT, AND N R ROWELL From the Gastroenterology Unit,
Gut, 198, 21, 293-298 Small intestinal structure and passive permeability in systemic sclerosis I COBDENM, J ROTHWELL, A T R AXON, M F DIXON, D J LINTOTT, AND N R ROWELL From the Gastroenterology Unit,
Transient paraproteinaemia in a patient with
 Transient paraproteinaemia in a patient with coeliac disease Gut, 1976,17, 735-739 A. S. PENA, JANNY v. NIEUWKOOP, H. R. E. SCHUIT, W. TH. J. M. HEKKENS, AND A. J. CH. HAEX From the Departments of Gastroenterology
Transient paraproteinaemia in a patient with coeliac disease Gut, 1976,17, 735-739 A. S. PENA, JANNY v. NIEUWKOOP, H. R. E. SCHUIT, W. TH. J. M. HEKKENS, AND A. J. CH. HAEX From the Departments of Gastroenterology
Collagenous gastritis and collagenous colitis: a report with sequential histological and ultrastructural findings
 Gut 1999;44:881 885 881 CASE REPORTS Wellcome Trust Research Laboratory, Christian Medical College and Hospital, Vellore 632004, India A B Pulimood B S Ramakrishna M M Mathan Correspondence to: Dr A B
Gut 1999;44:881 885 881 CASE REPORTS Wellcome Trust Research Laboratory, Christian Medical College and Hospital, Vellore 632004, India A B Pulimood B S Ramakrishna M M Mathan Correspondence to: Dr A B
Gastric epithelium in the duodenum
 Gastric epithelium in the duodenum A. H. JAMES From the Medical Unit, Cardiff Royal Infirmary, Cardiff, Wales Gut, 1964, 5, 285 EDITORIAL SYNOPSIS It has been found that a 'gastric' type of epithelium
Gastric epithelium in the duodenum A. H. JAMES From the Medical Unit, Cardiff Royal Infirmary, Cardiff, Wales Gut, 1964, 5, 285 EDITORIAL SYNOPSIS It has been found that a 'gastric' type of epithelium
Ultrastructural changes suggestive of immune. following gluten challenge. reactions in the jejunal mucosa of coeliac children
 Gut, 1973, 14, 1-12 Ultrastructural changes suggestive of immune reactions in the jejunal mucosa of coeliac children following gluten challenge MARGOT SHINER' From the Medical Research Council, Gastroenterology
Gut, 1973, 14, 1-12 Ultrastructural changes suggestive of immune reactions in the jejunal mucosa of coeliac children following gluten challenge MARGOT SHINER' From the Medical Research Council, Gastroenterology
What is your diagnosis? a. Lymphocytic colitis. b. Collagenous colitis. c. Common variable immunodeficiency (CVID) associated colitis
 Case History A 24 year old male presented with fatigue, fever, watery diarrhea, and a cough with sputum production for the past three weeks. His past medical history was significant for recurrent bouts
Case History A 24 year old male presented with fatigue, fever, watery diarrhea, and a cough with sputum production for the past three weeks. His past medical history was significant for recurrent bouts
possible in the present state of our knowledge. history of frequent, loose bowel actions for two relapse on its reintroduction is also necessary for
 Gut, 1970, 11, 743-747 A case of small-intestinal mucosal atrophy R. E. BARRY, JOHN S. MORRIS, AND A. E. A. READ From the Department of Medicine, Bristol Royal Infirmary SUMMARY A patient is described
Gut, 1970, 11, 743-747 A case of small-intestinal mucosal atrophy R. E. BARRY, JOHN S. MORRIS, AND A. E. A. READ From the Department of Medicine, Bristol Royal Infirmary SUMMARY A patient is described
Allergic disorders of the gastrointestinal tract
 Allergic disorders of the gastrointestinal tract Christopher Justinich, MD Introduction The patient with presumed food hypersensitivity continues to present a challenge for the clinician. In certain instances,
Allergic disorders of the gastrointestinal tract Christopher Justinich, MD Introduction The patient with presumed food hypersensitivity continues to present a challenge for the clinician. In certain instances,
A Chronic or Recurring Pattern of Esophagitis Resembling Allergic Contact Dermatitis
 Anatomic Pathology / Lymphocytic Esophagitis Lymphocytic Esophagitis A Chronic or Recurring Pattern of Esophagitis Resembling Allergic Contact Dermatitis Julianne K. Purdy, MD, Henry D. Appelman, MD, Christopher
Anatomic Pathology / Lymphocytic Esophagitis Lymphocytic Esophagitis A Chronic or Recurring Pattern of Esophagitis Resembling Allergic Contact Dermatitis Julianne K. Purdy, MD, Henry D. Appelman, MD, Christopher
of Nippostrongylus brasiliensis from the small
 Gut, 1977, 18, 182-186 Effect of iron and protein deficiency on the expulsion of Nippostrongylus brasiliensis from the small intestine of the rat T. D. BOLIN, A. E. DAVIS, A. G. CUMMINS, V. M. DUNCOMBE,
Gut, 1977, 18, 182-186 Effect of iron and protein deficiency on the expulsion of Nippostrongylus brasiliensis from the small intestine of the rat T. D. BOLIN, A. E. DAVIS, A. G. CUMMINS, V. M. DUNCOMBE,
Scalloped Valvulae Conniventes: An Endoscopic Marker of Celiac Sprue
 GASTROENTEROLOGY 1988;95:1518-22 Scalloped Valvulae Conniventes: An Endoscopic Marker of Celiac Sprue MANSOUR JABBARI, GARY WILD, CARL A. GORESKY, DONALD S. PAL Y, JOHN O. LOUGH, D. PAUL CLELAND, and DOUGLAS
GASTROENTEROLOGY 1988;95:1518-22 Scalloped Valvulae Conniventes: An Endoscopic Marker of Celiac Sprue MANSOUR JABBARI, GARY WILD, CARL A. GORESKY, DONALD S. PAL Y, JOHN O. LOUGH, D. PAUL CLELAND, and DOUGLAS
Case discussions. Case 1
 Case discussions Arzu Ensari 12 year old teen Case 1 Progressive cough and dysphagia following flu-like symptoms Family history of asthma Erythema in lower oesophagus 1 40 eos/hpf 2 What is Eosinophilic
Case discussions Arzu Ensari 12 year old teen Case 1 Progressive cough and dysphagia following flu-like symptoms Family history of asthma Erythema in lower oesophagus 1 40 eos/hpf 2 What is Eosinophilic
Why study T cell subsets in Crohn's
 Leading article Why study T cell subsets in Crohn's disease? Gut, 1983, 24, 687-691 Investigations of immunology in inflammatory bowel disease have always presented problems. The primary disease processes
Leading article Why study T cell subsets in Crohn's disease? Gut, 1983, 24, 687-691 Investigations of immunology in inflammatory bowel disease have always presented problems. The primary disease processes
Distribution of the Pores of Epithelial Basement Membrane in the Rat Small Intestine
 FULL PAPER Anatomy Distribution of the Pores of Epithelial Basement Membrane in the Rat Small Intestine Takashi TAKEUCHI 1) and Tatsuo GONDA 1) 1) Institute of Experimental Animals, Shimane Medical University,
FULL PAPER Anatomy Distribution of the Pores of Epithelial Basement Membrane in the Rat Small Intestine Takashi TAKEUCHI 1) and Tatsuo GONDA 1) 1) Institute of Experimental Animals, Shimane Medical University,
SMALL INTESTINAL EPITHELIAL CELL KINETICS AND PROTOZOAL INFECTION IN MICE
 00165085/78/7403-0496~02.00/0 GABTROENTEF.OLOGY 74:496-5@$1978 Copyright Q 1979 by the American Gastroenterological Association Vol. 74, No. 3 Printed in USA. SMALL INTESTINAL EPITHELIAL CELL KINETICS
00165085/78/7403-0496~02.00/0 GABTROENTEF.OLOGY 74:496-5@$1978 Copyright Q 1979 by the American Gastroenterological Association Vol. 74, No. 3 Printed in USA. SMALL INTESTINAL EPITHELIAL CELL KINETICS
Disaccharides and Cystic Fibrosis of the Pancreas*
 Arch. Dis. Childh., 1969, 44, 63. Disaccharides and Cystic Fibrosis of the Pancreas* I. S. E. GIBBONSt From The Hospital for Sick Children, Great Ormond Street, and Institute of Child Health, Guilford
Arch. Dis. Childh., 1969, 44, 63. Disaccharides and Cystic Fibrosis of the Pancreas* I. S. E. GIBBONSt From The Hospital for Sick Children, Great Ormond Street, and Institute of Child Health, Guilford
Kids Like to Break the Rules: Gastrointestinal Pathology in Children
 Kids Like to Break the Rules: Gastrointestinal Pathology in Children Jeffrey Goldsmith MD Director of Surgical Pathology, Beth Israel Deaconess Medical Center; Consultant in Gastrointestinal Pathology,
Kids Like to Break the Rules: Gastrointestinal Pathology in Children Jeffrey Goldsmith MD Director of Surgical Pathology, Beth Israel Deaconess Medical Center; Consultant in Gastrointestinal Pathology,
Refractory celiac disease (RCD) KASSEM BARADA LEBANESE SOCIETY OF GASTROENTEROLOGY NOVEMBER, 2014
 Refractory celiac disease (RCD) KASSEM BARADA LEBANESE SOCIETY OF GASTROENTEROLOGY NOVEMBER, 2014 Case scenario (1) A 49 year woman presents with intermittent watery diarrhea and bloating of two years
Refractory celiac disease (RCD) KASSEM BARADA LEBANESE SOCIETY OF GASTROENTEROLOGY NOVEMBER, 2014 Case scenario (1) A 49 year woman presents with intermittent watery diarrhea and bloating of two years
Subclass distribution of mucosal IgG-producing cells in gastritis
 Gut, 1989, 30, 322-326 Subclass distribution of mucosal IgG-producing cells in gastritis K VALNES AND P BRANDTZAEG From the Laboratory for Immunohistochemistry and Immunopathology (LIIPA T), Institute
Gut, 1989, 30, 322-326 Subclass distribution of mucosal IgG-producing cells in gastritis K VALNES AND P BRANDTZAEG From the Laboratory for Immunohistochemistry and Immunopathology (LIIPA T), Institute
ORIGINAL ARTICLE Histopathological features of coeliac disease in a sample of Sudanese patients
 Malaysian J Pathol 2016; 38(3) : 267 272 ORIGINAL ARTICLE Histopathological features of coeliac disease in a sample of Sudanese patients MA Noha MOKHTAR, SO MEKKI, HMY MUDAWI*, SH SULAIMAN**, MA TAHIR,
Malaysian J Pathol 2016; 38(3) : 267 272 ORIGINAL ARTICLE Histopathological features of coeliac disease in a sample of Sudanese patients MA Noha MOKHTAR, SO MEKKI, HMY MUDAWI*, SH SULAIMAN**, MA TAHIR,
Small Intestinal Biopsy in a Patient with Crohn's Disease of the Duodenum
 GASTROENTEROLOGY 76:1009-1014, 1979 Small Intestinal Biopsy in a Patient with Crohn's Disease of the Duodenum The Spectrum of Abnormal Findings in the Absence of Granulomas MICHAEL D. SCHUFFLER and ROBERT
GASTROENTEROLOGY 76:1009-1014, 1979 Small Intestinal Biopsy in a Patient with Crohn's Disease of the Duodenum The Spectrum of Abnormal Findings in the Absence of Granulomas MICHAEL D. SCHUFFLER and ROBERT
ulcer-associated duodenitis correlation between area
 J Clin Pathol 1981 ;34:1181-1186 Measurements of intestinal villi in non-specific and ulcer-associated duodenitis correlation between area of microdissected villus and villus epithelial cell count MAHMUD
J Clin Pathol 1981 ;34:1181-1186 Measurements of intestinal villi in non-specific and ulcer-associated duodenitis correlation between area of microdissected villus and villus epithelial cell count MAHMUD
Evaluation of Serosal Nerves in Hirschsprung Disease
 Evaluation of Serosal Nerves in Hirschsprung Disease Mudassira and Anwar ul Haque Department of Pathology, Pakistan Institute of Medical Sciences, Islamabad. Introduction: For the diagnosis of Hirschsprung
Evaluation of Serosal Nerves in Hirschsprung Disease Mudassira and Anwar ul Haque Department of Pathology, Pakistan Institute of Medical Sciences, Islamabad. Introduction: For the diagnosis of Hirschsprung
HISTOPATHOLOGICAL STUDY OF ENDOSCOPIC BIOPSIES OF STOMACH
 HISTOPATHOLOGICAL STUDY OF ENDOSCOPIC BIOPSIES OF STOMACH Pages with reference to book, From 177 To 179 Javed Iqbal Kazi, Syed Mahmood Alam ( Departments of Pathology, Jinnah Postgraduate Medical Centre,
HISTOPATHOLOGICAL STUDY OF ENDOSCOPIC BIOPSIES OF STOMACH Pages with reference to book, From 177 To 179 Javed Iqbal Kazi, Syed Mahmood Alam ( Departments of Pathology, Jinnah Postgraduate Medical Centre,
PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT.
 PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT. OESOPHAGEAL LESIONS OESOPHAGITIS AND OTHER NON NEOPLASTIC DISORDERS Corrosive Gastroesophageal reflux (GERD), Pills, Acid intake,
PATHOLOGY OF NON NEOPLASTIC LESIONS OF THE UPPER GASTROINTESTINAL TRACT. OESOPHAGEAL LESIONS OESOPHAGITIS AND OTHER NON NEOPLASTIC DISORDERS Corrosive Gastroesophageal reflux (GERD), Pills, Acid intake,
This is the second learning component (Learning Component 2) in our first learning module (Learning Module 1). In this component we review a very
 This is the second learning component (Learning Component 2) in our first learning module (Learning Module 1). In this component we review a very basic response to injury inflammation. We ll look at examples
This is the second learning component (Learning Component 2) in our first learning module (Learning Module 1). In this component we review a very basic response to injury inflammation. We ll look at examples
'Chronic duodenitis': A clinical pathological entity?
 Gut, 1965, 6, 376 'Chronic duodenitis': A clinical pathological entity? I. T. BECK, D. S. KAHN, M. LACERTE, J. SOLYMAR, U. CALLEGARINI, AND M. C. GEOKAS with the assistance of E. PHELPS From the Department
Gut, 1965, 6, 376 'Chronic duodenitis': A clinical pathological entity? I. T. BECK, D. S. KAHN, M. LACERTE, J. SOLYMAR, U. CALLEGARINI, AND M. C. GEOKAS with the assistance of E. PHELPS From the Department
Are Gastrointestinal Mucosal Mast Cells Increased in Patients With Systemic Mastocytosis?
 Anatomic Pathology / GASTRODUODENAL MAST CELLS IN MASTOCYTOSIS Are Gastrointestinal Mucosal Mast Cells Increased in Patients With Systemic Mastocytosis? Sabine I. Siegert, MD, 1 Joachim Diebold, MD, PhD,
Anatomic Pathology / GASTRODUODENAL MAST CELLS IN MASTOCYTOSIS Are Gastrointestinal Mucosal Mast Cells Increased in Patients With Systemic Mastocytosis? Sabine I. Siegert, MD, 1 Joachim Diebold, MD, PhD,
SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST QUESTIONS. Ver. #
 SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST Ver. #5-02.12.17 GUIDELINES FOR DEVELOPING SELF-ASSESSMENT MODULES TEST The USCAP is accredited by the American Board of Pathology (ABP) to offer
SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST Ver. #5-02.12.17 GUIDELINES FOR DEVELOPING SELF-ASSESSMENT MODULES TEST The USCAP is accredited by the American Board of Pathology (ABP) to offer
The permeation of gastric epithelial cells by leucocytes
 Gut, 1964, 5, 160 The permeation of gastric epithelial cells by leucocytes D. D. GIBBS From the Department of Medicine, The London Hospital EDITORIAL SYNOPSIS The cytological observations reported here
Gut, 1964, 5, 160 The permeation of gastric epithelial cells by leucocytes D. D. GIBBS From the Department of Medicine, The London Hospital EDITORIAL SYNOPSIS The cytological observations reported here
Mast cells are heavily granulated wandering
 ORIGINAL PAPER Distribution and density of mast cells in camel small intestine and influence of fixation techniques M.B. Al-Zghoul, 1 R.K. Al-Rukibat, 2 M. Alghadi, 1 T. Caceci, 3 Z. Bani Ismail 4 1 Department
ORIGINAL PAPER Distribution and density of mast cells in camel small intestine and influence of fixation techniques M.B. Al-Zghoul, 1 R.K. Al-Rukibat, 2 M. Alghadi, 1 T. Caceci, 3 Z. Bani Ismail 4 1 Department
Fibrin thrombi, a cause of clindamycin-associated
 Gut, 1976, 17, 483487 Fibrin thrombi, a cause of clindamycin-associated colitis? W. V. BOGOMOLETZ From the Department of Pathology, Queen Mary's Hospital, London summary Rectal biopsies from five patients
Gut, 1976, 17, 483487 Fibrin thrombi, a cause of clindamycin-associated colitis? W. V. BOGOMOLETZ From the Department of Pathology, Queen Mary's Hospital, London summary Rectal biopsies from five patients
Sheila E. Crowe, MD, FRCPC, FACP, FACG, AGAF Department of Medicine University of California, San Diego
 Severe and Emergency Presentations of Celiac Disease Sheila E. Crowe, MD, FRCPC, FACP, FACG, AGAF Department of Medicine University of California, San Diego Case Presentation (1) 63 year old male transferred
Severe and Emergency Presentations of Celiac Disease Sheila E. Crowe, MD, FRCPC, FACP, FACG, AGAF Department of Medicine University of California, San Diego Case Presentation (1) 63 year old male transferred
Anatomy & Histology of The Small intestine
 Anatomy & Histology of The Small intestine Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Jejunum Ileum Histology: Duodenum, jejunum, and ileum
Anatomy & Histology of The Small intestine Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Jejunum Ileum Histology: Duodenum, jejunum, and ileum
