The efficacy of maggot debridement therapy a review of comparative clinical trials
|
|
|
- Dorcas Watkins
- 6 years ago
- Views:
Transcription
1 REVIEW ARTICLE The efficacy of maggot debridement therapy a review of comparative clinical trials Kian Zarchi, Gregor BE Jemec Zarchi K, Jemec GBE. The efficacy of maggot debridement therapy a review of comparative clinical trials. Int Wound J 2012; 9: ABSTRACT Over the last decade, maggot debridement therapy (MDT) has been recognized by many clinicians as a potential adjunct to conventional therapy, and many patients with non healing, chronic ulcers have been treated. Numerous case reports and case series have described the successful use of MDT in a variety of ulcers. However, comparative clinical trials and in particular randomized controlled trials investigating the efficacy of MDT are sparse. A systematic search in the literature showed three randomized clinical trials and five non randomized studies evaluating the efficacy of sterile Lucilia sericata applied on ulcers with various aetiologies. Of these, seven studies had debridement and/or healing as an outcome variable. When evaluating maggots as debriding agents, the studies report MDT as being significantly more effective than hydrogel or a mixture of conventional therapy modalities, including hydrocolloid, hydrogel and saline moistened gauze. However, the design of the studies was suboptimal, with important differences in the use of other therapies, such as compression, that may influence both debridement and healing between the compared groups, as well as inappropriately short follow-up times. The quality of the studies therefore makes it difficult to conclude that MDT shortens healing time. The poor quality of the data used for evaluating the efficacy of MDT highlights the need for more and better designed investigations. Key words: Biosurgery Chronic ulcer Debridement Larval therapy Maggot debridement therapy INTRODUCTION Debridement is an established procedure in wound management. It is thought to reduce the risk of infection and to promote wound healing through the removal of foreign debris and devitalized or contaminated tissue. However, there is a striking paucity of clinical evidence supporting its efficacy when dealing Authors: K Zarchi, MD, Department of Dermatology, Roskilde Hospital, Health Sciences Faculty, University of Copenhagen, Copenhagen, Denmark; GBE Jemec, MD, DMSc, Professor, Chairman, Department of Dermatology, Roskilde Hospital, Health Sciences Faculty, University of Copenhagen, Copenhagen, Denmark Address for correspondence: K Zarchi, MD, Department of Dermatology, Roskilde Hospital, Health Sciences Faculty, University of Copenhagen, 4000, Roskilde, Denmark kian_zarchi@yahoo.com with sloughy and necrotic wounds (1 4). There are a number of existing methods for debridement of chronic wounds, such as mechanical, surgical, autolytic and enzymatic. Each of these techniques has associated disadvantages, such as limited efficacy, need for anaesthesia, pain and mechanical damage to the underlying healthy tissue. Maggot debridement therapy (MDT) is a technique that has attracted some attention recently. Throughout history, MDT has been used in wound healing by various cultures, including Mayan, Burmese and Chinese and among Australian Aborigines (5). In 1557, Ambroise Paré, chief surgeon to Charles IX and Henri III, reported myiasis in the suppurative wounds of soldiers on the battlefield of St. Quentin (6,7). In 1829, Baron Dominique-Jean Larrey, surgeon maggot debridement therapy (MDT) is a technique that has attracted some attention recently throughout history, MDT has been used in wound healing by various cultures, including Mayan, Burmese and Chinese and among Australian Aborigines International Wound Journal 2012 Blackwell Publishing Ltd and Medicalhelplines.com Inc 469
2 the rising incidence of antibiotic resistance in the 1990s raised renewed interest in MDT the contrast with the number of published controlled clinical trials is striking; accordingly, we reviewed the available comparative clinical trials to assess the evidence base and efficacy of MDT a systematic electronic literature search of comparative clinical trials was carried out in Medline and Cochrane library trials had to include debridement and/or healing as an outcome variable in chief with the Napoleonic army, discovered the property of enhancement of granulation tissue and shortening of the healing process in wounds infected by maggots (8). However, the first clinical application of maggot therapy is credited to J.F. Zacharias and J. Jones, confederate medical officers during the American Civil War (9). Later, during World War I, William Baer, professor of orthopaedic surgery, who is considered to be the founder of the modern maggot therapy, noted that maggots assisted the healing process of two soldiers with compound femur fracture as well as abdominal and scrotal wounds (10). Baer refined the technique by using sterile maggots to prevent maggot-induced infections, a technique gradually popularized across North America and Europe during the 1930s. With the introduction of antibiotics in 1940s and the development of better surgical debridement and anaesthesia techniques, the popularity of maggot therapy gradually declined and became largely forgotten. However, the rising incidence of antibiotic resistance in the 1990s raised renewed interest in MDT. In the last decade, many patients with non healing, chronic ulcers have been treated with maggots, leading to MDT being recognized by many clinicians as an adjunct to conventional therapy. Numerous case series and case reports have described successful use of MDT among a variety of ulcers, including necrotizing fasciitis, perineal gangrene, post-surgical wound infections and burns (11 13). The contrast with the number of published controlled clinical trials is striking; accordingly, we reviewed the available comparative clinical trials to assess the evidence base and efficacy of MDT. METHODS A systematic electronic literature search of comparative clinical trials was carried out in Medline and Cochrane library, using a mixture of free text terms and medical subject headings including Maggo*, Larva*, Debridement, MDT and Biosurgery. We considered trials for inclusion if they compared MDT with other debridement therapy modalities. We included published papers and abstracts in English, Danish, Norwegian and Swedish, but placed no restrictions in terms of year of publication. Trials had to include debridement and/or healing as an outcome variable. We examined the reference lists of eligible trials for additional relevant evaluations. We found nine comparative clinical trials, of which eight met the inclusion criteria (Table 1). The larvae of the green bottle fly, Lucilia sericata, are the most commonly used and studied maggot species, but studies on the application of other species, such as Protophormia terraenovae, Lucilia cuprina, Lucilia illustris and Phormia regina, have also been published in the literature (14,15). Of the eight primary comparative trials included, seven used the maggot species L. sericata, while the other used L. cuprina. To maintain homogeneity of the evaluated data, the clinical trial using maggot species other than L. sericata was excluded. Of the remaining seven comparative clinical trials, three were randomized and four were non randomized. RESULTS Randomized controlled trials Between 2004 and 2007, a multicentre, randomized, controlled, single-blinded, open trial was conducted to investigate the efficacy of MDT compared with standard autolytic debridement technique, using hydrogel (Purilon; Coloplast Humlebaek, Denmark) (16). A total of 267 patients with at least one venous or mixed venous and arterial ulcers (ankle brachial pressure index (ABPI) > 0 60) with an area of 5 cm 2 or less with at least 25% coverage of slough or necrotic tissue were randomized to receive loose larvae, bagged larvae or hydrogel. Randomization was performed using permuted blocks with stratification by trial centre and ulcer area. Sterile L. sericata were applied loose or bagged on ulcers allocated to receive larvae therapy for 3 4 days, which could be repeated if additional larval therapy was assessed as necessary by the attending nurses. Patients in the control group received hydrogel covered with knitted viscose dressings as well as compression, depending on the ABPI and patient tolerance. The randomized treatment was applied in the debridement phase, which ended either when debridement was achieved according to the assessment of the attending nurses or when treatment was stopped before debridement because of, for example, patient request, which was classified as withdrawal. Debridement was defined as a cosmetically clean wound and was additionally assessed by masked independent 470 International Wound Journal 2012 Blackwell Publishing Ltd and Medicalhelplines.com Inc
3 Table 1 Comparative clinical trials evaluating the efficacy of MDT Authors Publ. date Design Cohort Number of participants Comparison Trial outcomes Follow-up Dumville et al. (16) 2007 RCT Venous or mixed arterial and venous ulcers (ABPI > 0 6) 248 MDT versus hydrogel Time to debridement, time to heal, HRQoL, overall bacterial load, adverse events, ulcer related pain. Markevich et al. (18) 2000 RCT Diabetic foot ulcers 140 MDT versus hydrogel Proportion of healed ulcers, 50% area reduction Wayman et al. (17) 2000 RCT Venous leg ulcers 12 MDT versus hydrogel Time to debridement, cost of treatment 1 month 6months Armstrong et al. (19) 2005 NCT Diabetic foot ulcers with vascular component 60 MDT versus conventional Sherman (20) 2002 NCT Diabetic foot and leg ulcers 18 MDT versus conventional Sherman (21) 2002 NCT Pressure ulcers 67 (in debridement and wound healing analysis), 103 (in adverse event analysis) Sherman et al. (22) 1995 NCT Pressure ulcer among spinal cord injured patients Sherman et al. (23) (this study did not meet the inclusion criteria, because of its outcome measures) Paul et al. (24) (this study did not meet the inclusion criteria, because of the use of L. cuprina) 2004 NCT Surgically closed, grafted or flapped ulcers of various aetiologies. MDT versus conventional 8 MDT versus conventional 25 MDT versus conventional 2009 NCT Diabetic foot ulcers 59 MDT (L. cuprina)versus conventional Time to heal, proportion of healed ulcers, infections, antibiotic-free days and amputations Time to debridement, changes in ulcer surface area, necrotic tissue and granulation tissue Time to debridement, changes in ulcer surface area, necrotic tissue and granulation, wound closure, adverse events Reduction in ulcer surface area and necrotic tissue Post-operative wound infections, adverse events 12 months 10 days Not specified Not specified: (at least 19 weeks?) 3 4 weeks during conventional therapy, not specified for MDT Not specified: ( the post-operative period ) Proportion of healed ulcers Not specified HRQoL, health-related quality of life; MDT, maggot debridement therapy; NCT, non randomized clinical trials; RCT, randomized clinical trials. International Wound Journal 2012 Blackwell Publishing Ltd and Medicalhelplines.com Inc 471
4 the authors found no evidence that debridement with loose or bagged larvae reduced the time of healing on venous leg ulcers however, time to debridement differed significantly between the groups assessors using digital photographs. Assessment of the efficacy of debridement was conducted blindly. In the post-debridement phase, patients received a standard knitted viscose dressing with or without compression. The follow-up period was 6 12 months. Of the 180 patients allocated to receive loose or bagged larvae, 10 did not receive the allocated treatment because of death, hospital admission, ulcer improvement or refusal to receive MDT. Of the remaining 170 patients, 75 (44%) withdrew from the treatment because of various reasons, such as increased slough (38 patients), patient request (10 patients) and adverse treatment reaction (14 patients). Of the 87 patients allocated to receive hydrogel, nine did not receive the allocated treatment, and of the remaining 78 patients, 34 (44%) withdrew because of various reasons, such as increased slough (16 patients), patient request (5 patients) and adverse treatment reaction (7 patients). The authors found no evidence that debridement with loose or bagged larvae reduced the time of healing of venous leg ulcers, compared with hydrogel. The median time to heal in the combined larvae and in the hydrogel group was 236 (95% CI: ) and 245 days (95% CI: 166 to upper limit not estimable), respectively. However, time to debridement differed significantly between the groups. The median time to debridement was shorter with loose larvae (14 days, 95% CI: 10 17) than with bagged larvae (28 days, 95% CI: 13 55) and hydrogel (72 days, 95% CI: ). The difference between loose and bagged larvae was not statistically significant. In total, 340 adverse events were reported in 131 patients. Of these 13 8% were classified as serious, corresponding to 14 6% events with loose larvae, 13 5% with bagged larvae and 13 5% with hydrogel. More patients in the combined larvae group experienced one or more adverse events than patients in the hydrogel group (51 7% versus 43 7%), but this difference was not statistically significant. Although significantly more pain was reported by patients in both larvae groups than the hydrogel group, the authors found no evidence of a difference in health-related quality of life between the groups. In 2000, Wayman et al. reported the results of a randomized, controlled trial evaluating the cost effectiveness of larval therapy (17). A total of 12 patients with sloughy venous leg ulcer, deemed to require debridement, were randomized to receive MDT or hydrogel (Intrasite gel; Smith & Nephew, London, UK). Patients were excluded if there was evidence of arterial insufficiency or if the patient had undergone previous failed therapy. The two groups were comparable in terms of age, sex, ulcer size and duration. The proportion of ulcer covered with slough in the MDT and hydrogel group was reported as 95% and 100%, respectively. Loose sterile L. sericata were applied to ulcers allocated to receive larvae therapy for a maximum of 72 hours. All patients were reviewed every 72 hours until debridement had occurred or for a maximum of 1 month. The outcome measures for effectiveness were whether debridement had occurred within the month and the time to debridement. Ulcers were considered debrided where the percentage surface area of slough was less than 5%. The authors reported that debridement occurred more rapidly in the MDT group, where patients required only one application of larvae. In the hydrogel group, debridement was achieved in only two patients within the month. The authors also reported that the median number of patient visits was 19 in the hydrogel group compared with 3 in the MDT group, but no references were made to the actual time to debridement. In 2000, Markevich et al. reported the results of a randomized, controlled trial evaluating the efficacy of MDT compared with hydrogel conducted among patients with diabetic foot ulcers (results available in abstract form only) (18). The authors identified diabetic neuropathy as the primary aetiology but did not make further references to inclusion and exclusion criteria. One hundred and forty patients were randomized to receive MDT (unknown whether loose or bagged) for 72 hours or hydrogel (unknown type). The authors reported the duration of the trial to be 30 months, while the follow-up was only 10 days. Despite the short follow-up, the proportion of completely healed ulcers was chosen as the primary outcome. In the MDT group, 7% (5/70) achieved complete healing, compared with 3% (2/70) in the hydrogel group. This difference was not statistically significant. However, reduction of more than 50% in wound area was achieved in 51% of patients (36/70) compared with 27% (19/70) 472 International Wound Journal 2012 Blackwell Publishing Ltd and Medicalhelplines.com Inc
5 in the hydrogel group, suggesting a significant difference in the two methods (Table 2). Non randomized controlled trials In 2005, Armstrong et al. reported the results of a non randomized, unblinded, open, retrospective review of patients with neuroischaemic diabetic foot ulcers who had been treated with either MDT or conventional therapy (19). Medical records were reviewed of non ambulatory diabetic wound patients who had a peripheral vascular disease, with at least 6 months of reliable follow-up data and who received MDT. Thirty patients met the inclusion criteria. Their data were compared with 30 age- and sex-matched control patients receiving contemporary standard wound care at the same institution. The authors reported that both groups were treated in a standardized manner according to the protocol and were followed in a high-risk diabetic foot clinic, but made no further references to the treatment modalities that they referred to as conventional therapy. In total, 27 patients (45%) healed during the 6-month review, where healing was defined as complete epithelialization. The proportion of patients healing in the MDT was 57% compared with 33% in the conventional therapy group. This difference was not statistically significant. Among the healed patients, time to heal in the maggot group was 18 5 ± 4 8 weeks versus 22 4 ± 4 4 weeks in the conventional group. The authors also reported significantly more antibiotic-free days during the 6 months of follow-up in patients who received MDT (127 ± 30 days versus 82 ± 42 days). In 2002, Sherman reported the results of a non randomized, unblinded, open, retrospective review of cases aimed at evaluating the efficacy of MDT in patients with pressure ulcers (20). Medical records were evaluated of 103 patients with 145 pressure ulcers who were referred to maggot therapy between 1990 and In total, 61 ulcers in 50 patients received MDT, while 84 ulcers in 70 patients did not receive maggot therapy. Fifty-one patients did not receive MDT on any wound. MDT was not administrated to these patients because of various reasons: the patient s doctor did not consent to maggot therapy (11 patients), the wound improved during baseline observation with conventional therapy alone (8 patients), the patients (2 cases) or their decision-making surrogates (2 cases), did not consent to therapy and patients were discharged, died or lost to follow-up (24 cases), before they could be treated. No reason was documented in four cases. Loose sterile L. sericata were applied for two 48-hour cycles per week. Conventional therapies included topical antimicrobial therapy (35%), acemannan hydrogel (10%), chemical debriding agents (8%), wet to dry dressings (8%), hydrocolloids and calcium alginates (6%), growth factors (4%) and multiple combinations of non surgical treatments (12%). Of the conventionally treated group, 17% received bedside or intra-operative surgical debridement. Evaluation of debridement and wound healing was carried out using digitalized images and tracings. Some wounds were excluded from the efficacy analysis, e.g. because of complex non planar topography, being photographed without the scale markers and follow-up shorter than 2 weeks. The efficacy analysis comprised 70% (43/61) of the wounds receiving MDT and 59% (43/84) of the wounds receiving conventional therapy. Ulcers in the MDT group were 60% larger, and maggot-treated patients were more often diabetic with spinal cord injuries and with higher average serum albumin. Otherwise there were no significant differences between the two treatment groups. The author reported that 80% (95% CI: 65 95) of maggot-treated wounds were completely debrided after 4 8 weeks, while complete debridement occurred in 48% (95% CI: 26 70) of wounds in the conventional therapy. Percentages of wounds that completely healed within 12 weeks for the MDT and conventional therapy group were 39% and 21%, respectively. This difference was not statistically significant. The average time until ulcers completely healed was 12 weeks (95% CI: 8 19) in the MDT group compared with 13 4 weeks (95% CI: 7 17) in the conventional therapy group. Pain complaints were reported in 4% of the maggot-treated patients. In 2002, Sherman reported the results of a non randomized, unblinded, open, case review attempting to evaluate the efficacy of MDT on diabetic foot and leg ulcers (21). Between 1990 and 1995, 26 patients with diabetic foot and leg ulcers were evaluated as candidates for MDT. Of these, eight were excluded because of the lack of sufficient baseline data. Of the 20 wounds on the remaining 18 patients, six wounds were treated only with conventional therapy, six wounds were treated with maggot International Wound Journal 2012 Blackwell Publishing Ltd and Medicalhelplines.com Inc 473
6 Table 2 Baseline characteristics of patients in the included studies Trials Groups Mean age (years) Ulcer size (cm 2 ) Proportion of ulcer covered with slough Ulcer duration (months) Dumville et al. (16) (venous or mixed arterial and venous ulcers) Markevich et al. (18) (diabetic foot ulcers) Wayman et al. (17) (venous leg ulcers) Armstrong et al. (19) (diabetic foot ulcers) Sherman (20) (diabetic foot ulcers) Sherman (21) (pressure ulcers) Sherman et al. (22) (pressure ulcers) MDT (loose) 74 1(SD:12 9) Median12 2 (range: ) At least 25% covered by slough or necrotic tissue MDT (bagged) 73 5(SD:12 2) Median17 3 (range: ) At least 25% covered by slough or necrotic tissue Control (hydrogel) 74 3(SD:12 8) Median 12 2 (range: ) At least 25% covered by slough or necrotic tissue 9 0 (Range: ) 6 9 (range: ) 8 0 (range: ) MDT 53 6(SD:15 4) for both groups 14 9 Not reported Not reported Control (hydrogel) 53 6(SD:15 4) for both groups 15 1 Not reported Not reported MDT 58 (48 72) 18 (13 25) 100% (80 100) 5 (2 8) Control (hydrogel) 54 (40 75) 16 (14 22) 95% (80 100) 4 (2 6) MDT 71 7(SD:6 8) 11 8(SD:4 5) Not reported Not reported Control (conventional therapy) 72 7(SD:6 8) 12 4(SD:6 7) Not reported Not reported MDT 63 (range: 53 74) 13 3(range: ) 38% (range: 0 90) 10 (44 weeks, range: 4 318) Control (conventional therapy) 68 (range: 53 82) 6 3(range: ) 44% (range: 0 100) 9 (40, weeks, range: 4 312) MDT 62 (range: 26 85) 22 1 (range: ) 31% (95% CI: 21 41) 8 3 (37 weeks, range: 5 207) Control (conventional therapy) 66 (range: 32 91) 14 0 (range: ) 34% (95% CI: 23 45) 7 6 (34 weeks, range: 4 208) MDT 58 (range: 44 68) 13 8 (range: ) 0 25%: five patients %: three patients Control (conventional therapy) The same patients as in the MDT group The same patients as in the MDT group 22% worsening during conventional therapy was reported, baseline data not specified Not reported Not reported MDT, maggot debridement therapy; SD, standard deviation. 474 International Wound Journal 2012 Blackwell Publishing Ltd and Medicalhelplines.com Inc
7 therapy, and eight wounds were treated with conventional therapy first followed by MDT. For the six wounds not treated with MDT, one patient underwent a below-knee amputation before maggot therapy was initiated, and in four patients consent to therapy was not given by the patient or the spouse. Conventional therapy included dry dressing or saline-moistened gauze (four wounds), topical antimicrobials (three wounds), acemannan hydrogel (one wound), hydrocolloid (one wound), unspecified multiple non surgical modalities (two wounds) and bedside surgical debridement (three wounds). MDT was administrated by applying loose sterile L. sericata to the wound for cycles of about 48 hours. One or two cycles were applied each week. The authors reported that a 50% reduction in necrotic surface area was reached after 9 days of MDT, whereas conventionally treated wounds did not reach that stage until Day 29. This difference was statistically significant. Within 4 weeks maggots-treated wounds were completely debrided, whereas wounds treated with conventional therapy for an average of 5 weeks were still covered with necrotic tissue over 33% of their surface. MDT was also associated with hastened growth of granulation tissue, resulting in 56% surface area coverage with granulation tissue within 4 weeks of treatment (19% at the baseline), whereas 15% of coverage with granulation tissue was reached in the conventional therapy group (18% at the baseline). The average time to wound closure in the maggot-treated group was 15 weeks (95% CI: 3 26) compared with 18 weeks (95% CI: 2 33) in the conventionally treated group. Two maggot-treated patients complained of pain during therapy, but the pain was not severe enough to cause cessation of treatment. The authors reported that the same two patients complained of pain during conventional dressing changes. In 1995, Sherman et al. reported the results of a case review aimed at evaluating the efficacy of MDT on pressure ulcers among spinal cord patients (22). Among 20 spinal injured patients with pressure ulcers treated with maggots, eight were followed for 3 4 weeks before MDT, thereby limiting the study group to eight patients. These patients were followed while receiving conventional therapy, prescribed by their primary care teams. Conventional treatment modalities included thrice daily sterile normal saline (two patients), 0 5% sodium hypochloride (two patients), povidone iodine dressings (two patients), topical antimicrobial ointment (one patient) and knitted cellulose acetate impregnated with petrolatum emulsion (one patient). Patients were then treated with loose sterile L. sericata. Ulcers were evaluated visually and photographically every week, by an unblinded investigator. The authors reported that of ulcers with a 20% or larger necrotic base, none had debrided more than 50% during the 3 4 weeks before MDT. All such ulcers were reported completely debrided within 1 2 weeks after the initiation of MDT. The average change in ulcer surface area before MDT was an increase of 22% per week, whereas a decrease of 22% per week was reported after the initiation of MDT. No complications resulted from the MDT. DISCUSSION In recent years, it has been claimed that MDT should be recognized as an effective alternative to the conventional debridement methods. In this review, we undertook an investigation to determine whether the existing evidence in the literature supports such a claim. When evaluating therapy modalities in wound management, a variety of outcome measures, including infection rate, duration of hospital admission, post-operative complications, cost effectiveness and impact on the quality of life can provide valuable information. In this review, we aimed to evaluate the efficacy of maggots as debriding agents and solely focused on their impact on debridement and healing rate. Controlled trials, and in particular randomized controlled trials investigating the efficacy of MDT, are sparse. A systematic search in the literature showed three RCTs and five non randomized clinical trials (NCTs) evaluating the efficacy of sterile L. sericata applied to ulcers with various aetiologies. Of these, seven trials had debridement and/or healing as an outcome variable. Effectiveness of maggots as debriding agents was investigated in two RCTs and four NCTs, all suggesting MDT as being more effective than hydrogel and more efficient than a mixture of conventional therapy modalities including hydrocolloid, hydrogel and saline moistened gauze. However, the when evaluating therapy modalities in wound management, a variety of outcome measures, including infection rate, duration of hospital admission, post-operative complications, cost effectiveness and impact on the quality of life can provide valuable information in this review, we aimed to evaluate the efficacy of maggots as debriding agents and solely focused on their impact on debridement and healing rate International Wound Journal 2012 Blackwell Publishing Ltd and Medicalhelplines.com Inc 475
8 conclusions drawn by comparing MDT with conventional therapy among patients, who were referred to MDT because of inadequate therapeutic response to conventional methods, must be questioned accepting the premise that debridement is a prerequisite for healing, it is therefore difficult to draw the conclusion, that there is evidence suggesting that MDT shortens time to heal the studies highlight the need for more and better designed investigations in this area with standardized outcome variables that allow comparison across different studies similarly to studies of surgical techniques elsewhere quality of data in studies describing MDT is poor and the conclusions may therefore be questioned. The questionable quality of these trials is due to the following reasons: very short follow-up, limited number of patients, unclear inclusion and exclusion criteria, lack of clarity regarding whether treatment in the control group was administrated adequately, lack of blinding of outcome assessors and lack of randomization. The study of Dumville et al. is the only randomized clinical trial, following patients for longer than 1 month. Follow-up longer than 1 month must be considered as mandatory when outcome variables include time to heal. In the study of Wayman et al., the authors primarily focused on the cost effectiveness of the therapy and followed patients for a maximum of 1 month, while the follow-up was only 10 days in the study of Markevich et al.. Although, the study of Dumville et al. had an appropriate follow-up, the authors conducted the study on patients with venous or mixed venous and arterial ulcers (ABPI > 0 6) in whom compression must be regarded as the cornerstone of treatment. Reviewing the baseline data shows that 70% of patients treated with hydrogel received high compression compared with 53% in the MDT group. The dataset was therefore skewed, and their conclusion regarding MDT s impact on healing time must therefore be questioned. Unfortunately, the remaining studies have limited value if any definitive conclusion is to be drawn, although they can play an important role in showing some tendencies. The studies of Sherman et al. and Armstrong et al. aresubject to marked selection bias. Conclusions drawn by comparing MDT with conventional therapy among patients, who were referred to MDT because of inadequate therapeutic response to conventional methods, must be questioned. Accepting the premise that debridement is a prerequisite for healing, it is therefore difficult to draw the conclusion, that there is evidence suggesting that MDT shortens time to heal. The studies highlight the need for more and better designed investigations in this area with standardized outcome variables that allow comparison across different studies similarly to studies of surgical techniques elsewhere. REFERENCES 1 Gray M. Is larval (maggot) debridement effective for removal of necrotic tissue from chronic wounds? J Wound Ostomy Continence Nurs 2008;35: Kirshen C, Woo K, Ayella EA, SIbbald RG. Debridement: a vital component of wound bed preparation. Adv Skin Wound Care 2006;19: Schultz G, Mozingo D, Romanelli M, Claxton K. Wound healing and TIME; new concepts and scientific applications. Wound Repair Regen 2005;13(4 Suppl):S Saap LJ, Falanga V. Debridement performance index and its correlation with complete closure of diabetic foot ulcers. Wound Repair Regen 2002;10: Grossman J. Flies as medical allies. The world I 1994;9: Paré A. The battle of St. Quentin. In: Kenyes G, editor The Apologie and treatise of Ambriose Paré. Chicago: The University of Chicago Press,1952: Goldstein HI. Maggots in the treatment of wound and bone infections. J Bones Joint Surg Am 1931;13: Larrey D. Des vers ou larves de la mouche bleue. Clin Chir 1829;1:51. 9 Mumcuoglu KY. Clinical applications for maggots in wound care. Am J Clin Dermatol 2001;2: Baer WS. The treatment of chronic osteomyelitis with the maggots. J Bone Joint Surg 1931;13: Dunn C, Raghavan U, Pfleiderer AG. The use of maggots in head and neck necrotizing fasciitis. J Laryngol Otol 2002;116: Teich S, Myers RA. Maggot therapy for severe skin infections. South Med J 1986;79: Namias N, Varela JE, Varas RP, Quintana O, Ward CG. Biodebridement: a case report of maggot therapy for limb salvage after fourth-degree burns. J Burn Care Rehabil 2000;21: Nuesch R, Rahm G, Rudin W, Steffen I, Frei R, Rufli T, Zimmerli W. Clustering of bloodstream infections during maggot debridement therapy using contaminated larvae of Protophormia terraenovae. Infection 2002;30: Sherman RA, Pechter EA. Maggot therapy: a review of the therapeutic applications of fly larvae in human medicine, especially for treating osteomyelitis. Med Vet Entomol 1988;2: Dumville JC, Worthy G, Bland JM, Cullum N, Dowson C, Iglesias C, Mitchell JL, Nelson EA, Soares MO, Torgerson DJ, VenUS II. team. Larval therapy for leg ulcers (VenUS II): randomised controlled trial. BMJ 2009;338:b773. doi: /bmj.b Wayman J, Nirojogi V, Walker A, Sowinski A, Walker MA. The cost effectiveness of larval therapy in venous ulcers. J Tissue Viability 2000;10:91 4. Erratum in: J Tissue Viability 2001;11: Markevich YO, McLeod-Roberts J, Mousley M, Melloy E. Maggot therapy for diabetic neuropathic foot wounds. Diabetologia 2000;43 Suppl 1:A Armstrong DG, Salas P, Short B, Martin BR, Kimbriel HR, Nixon BP, Boulton AJ. Maggot therapy in lower-extremity hospice wound care: fewer 476 International Wound Journal 2012 Blackwell Publishing Ltd and Medicalhelplines.com Inc
9 amputations and more antibiotic-free days. J Am Podiatr Med Assoc 2005;95: Sherman RA. Maggot versus conservative debridement therapy for the treatment of pressure ulcers. Wound Repair Regen 2002;10: Sherman RA. Maggot therapy for treating diabetic foot ulcers unresponsive to conventional therapy. Diabetes Care 2003;26: Sherman RA, Wyle F, Vulpe M. Maggot therapy for treating pressure ulcers in spinal cord injury patients. J Spinal Cord Med 1995;18: Sherman RA, Shimoda KJ. Presurgical maggot debridement of soft tissue wounds is associated with decreased rates of postoperative infection. Clin Infect Dis 2004;39: Epub 1 Sep Paul AG, Ahmad NW, Lee HL, Ariff AM, Saranum M, Naicker AS, Osman Z. Maggot debridement therapy with Lucilia cuprina:acomparison with conventional debridement in diabetic foot ulcers. Int Wound J 2009;6: International Wound Journal 2012 Blackwell Publishing Ltd and Medicalhelplines.com Inc 477
Safety, effectiveness and economic aspects of maggot debridement therapy for wound healing
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Safety, effectiveness and economic aspects of maggot debridement therapy for wound healing Jalal
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Safety, effectiveness and economic aspects of maggot debridement therapy for wound healing Jalal
Maggot Therapy. Bio 3323 Entomology. Teacher : Jon G. Houseman. Department of Biology. University of Ottawa
 Maggot Therapy ` By Bio 3323 Entomology Teacher : Jon G. Houseman February 9, 2004 Department of Biology University of Ottawa Maggot Therapy BBC journalist Georgina Kenyon describes the new fad in British
Maggot Therapy ` By Bio 3323 Entomology Teacher : Jon G. Houseman February 9, 2004 Department of Biology University of Ottawa Maggot Therapy BBC journalist Georgina Kenyon describes the new fad in British
Topical antimicrobials (antiseptics) Iodine, Silver, Honey
 Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
A Retrospective, Quality Improvement Review of Maggot Debridement Therapy Outcomes in a Foot and Leg Ulcer Clinic
 Feature A Retrospective, Quality Improvement Review of Maggot Debridement Therapy Outcomes in a Foot and Leg Ulcer Clinic Noreen Campbell, BScN, MA, LT, CWS; and Donna Campbell, RN Abstract Maggot debridement
Feature A Retrospective, Quality Improvement Review of Maggot Debridement Therapy Outcomes in a Foot and Leg Ulcer Clinic Noreen Campbell, BScN, MA, LT, CWS; and Donna Campbell, RN Abstract Maggot debridement
COMPARISON OF CURING COSTS BETWEEN MAGGOT AND CONVENTIONAL THERAPIES FOR CHRONIC WOUND CARE
 2 1 COMPARISON OF CURING COSTS BETWEEN MAGGOT AND CONVENTIONAL THERAPIES FOR CHRONIC WOUND CARE Suwannee Eamkong*, Sathirakorn Pongpanich and Chanapong Rojanaworarit College of Public Health Sciences,
2 1 COMPARISON OF CURING COSTS BETWEEN MAGGOT AND CONVENTIONAL THERAPIES FOR CHRONIC WOUND CARE Suwannee Eamkong*, Sathirakorn Pongpanich and Chanapong Rojanaworarit College of Public Health Sciences,
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
RESEARCH. Larval therapy for leg ulcers (VenUS II): randomised controlled trial
 Larval therapy for leg ulcers (VenUS II): randomised controlled trial Jo C Dumville, research fellow, 1 Gill Worthy, trial statistician, 1 J Martin Bland, professor of health statistics, 1 Nicky Cullum,
Larval therapy for leg ulcers (VenUS II): randomised controlled trial Jo C Dumville, research fellow, 1 Gill Worthy, trial statistician, 1 J Martin Bland, professor of health statistics, 1 Nicky Cullum,
Debridement: treatment, options and selection.
 This document is the Accepted Manuscript version of a Published Work that appeared in final form in Independent Nurse, copyright MA Healthcare, after peer review and technical editing by the publisher.
This document is the Accepted Manuscript version of a Published Work that appeared in final form in Independent Nurse, copyright MA Healthcare, after peer review and technical editing by the publisher.
This is a repository copy of Prescribing for the management of venous leg ulceration.
 This is a repository copy of Prescribing for the management of venous leg ulceration. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/95712/ Version: Accepted Version Article:
This is a repository copy of Prescribing for the management of venous leg ulceration. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/95712/ Version: Accepted Version Article:
o Venous edema o Stasis ulcers o Varicose veins (not including spider veins) o Lipodermatosclerosis
 Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
Wound Management. E. Foy White-Chu, MD, CWSP
 Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Maggot therapy in Pretoria, South Africa: an update
 Maggot therapy in Pretoria, South Africa: an update Herman J C du Plessis, MBChB, MMed(Sur)(Pret), FCS(SA), FACS Professor of Surgery, School of Medicine, Faculty of Health Sciences, University of Pretoria
Maggot therapy in Pretoria, South Africa: an update Herman J C du Plessis, MBChB, MMed(Sur)(Pret), FCS(SA), FACS Professor of Surgery, School of Medicine, Faculty of Health Sciences, University of Pretoria
The Georgetown Team Approach to Diabetic Limb Salvage: 2013
 The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
Cost and dressing evaluation of hydrofiber and alginate dressings in the management of community-based patients with chronic leg ulceration
 Cost and dressing evaluation of hydrofiber and alginate dressings in the management of community-based patients with chronic leg ulceration Harding K G, Price P, Robinson B, Thomas S, Hofman D Record Status
Cost and dressing evaluation of hydrofiber and alginate dressings in the management of community-based patients with chronic leg ulceration Harding K G, Price P, Robinson B, Thomas S, Hofman D Record Status
Pressure Ulcers: 3 Keys to Pressure Ulcer Management. Evidence Based Prevention & Management. I have no financial conflicts of interest
 Pressure Ulcers: Evidence Based Prevention & Management Madhuri Reddy, MD MSc I have no financial conflicts of interest I have nothing to disclose financially 3 Keys to Pressure Ulcer Management 1 3 Keys
Pressure Ulcers: Evidence Based Prevention & Management Madhuri Reddy, MD MSc I have no financial conflicts of interest I have nothing to disclose financially 3 Keys to Pressure Ulcer Management 1 3 Keys
A New Approach To Diabetic Foot Ulcers Using Keratin Gel Technology
 A New Approach To Diabetic Foot Ulcers Using Keratin Gel Technology Farheen Walid, BA, Shrunjay R. Patel, BSc, Stephanie Wu, DPM, MS Center for Lower Extremity Ambulatory Research (CLEAR), Scholl College
A New Approach To Diabetic Foot Ulcers Using Keratin Gel Technology Farheen Walid, BA, Shrunjay R. Patel, BSc, Stephanie Wu, DPM, MS Center for Lower Extremity Ambulatory Research (CLEAR), Scholl College
The Results Of Maggot Debridement Therapy In The Ischemic Leg: A Study On 89 Patients With 89 Wounds On The Lower Leg Treated With Maggots
 ISPUB.COM The Internet Journal of Surgery Volume 9 Number 1 The Results Of Maggot Debridement Therapy In The Ischemic Leg: A Study On 89 Patients With 89 Wounds On The Lower Leg Treated With Maggots P
ISPUB.COM The Internet Journal of Surgery Volume 9 Number 1 The Results Of Maggot Debridement Therapy In The Ischemic Leg: A Study On 89 Patients With 89 Wounds On The Lower Leg Treated With Maggots P
CLINICAL GUIDELINES FOR LARVAL THERAPY (MAGGOTS)
 CLINICAL GUIDELINES FOR LARVAL THERAPY (MAGGOTS) Introduction The use of maggots for wound debridement has a long history and the introduction of sterile maggots specifically bred for wound management
CLINICAL GUIDELINES FOR LARVAL THERAPY (MAGGOTS) Introduction The use of maggots for wound debridement has a long history and the introduction of sterile maggots specifically bred for wound management
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management
 An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
DEBRIDEMENT. Four Methods of Debridement
 Wound Definition Debridement is the removal of devitalized tissue and foreign matter from a wound. These materials support the growth of harmful organisms and may delay wound healing. Although debridement
Wound Definition Debridement is the removal of devitalized tissue and foreign matter from a wound. These materials support the growth of harmful organisms and may delay wound healing. Although debridement
Data extraction. Specific interventions included in the review Dressings and topical agents in relation to wound healing.
 Systematic reviews of wound care management: (2) dressings and topical agents used in the healing of chronic wounds Bradley M, Cullum N, Nelson E A, Petticrew M, Sheldon T, Torgerson D Authors' objectives
Systematic reviews of wound care management: (2) dressings and topical agents used in the healing of chronic wounds Bradley M, Cullum N, Nelson E A, Petticrew M, Sheldon T, Torgerson D Authors' objectives
Advancing the science of wound bed preparation
 Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Larval therapy was first discovered to have the ability. Larval therapy applied to a large arterial ulcer: an effective outcome
 Larval therapy applied to a large arterial ulcer: an effective outcome Linda Rafter Abstract This article is a review of larval therapy and includes a case study that uses larval therapy in the treatment
Larval therapy applied to a large arterial ulcer: an effective outcome Linda Rafter Abstract This article is a review of larval therapy and includes a case study that uses larval therapy in the treatment
TITLE: Non-Surgical Debridement for Chronic Lower Extremity Wounds: Clinical Effectiveness and Guidelines
 TITLE: Non-Surgical Debridement for Chronic Lower Extremity Wounds: Clinical Effectiveness and Guidelines DATE: 05 December 2013 RESEARCH QUESTIONS 1. What is the clinical evidence regarding the effectiveness
TITLE: Non-Surgical Debridement for Chronic Lower Extremity Wounds: Clinical Effectiveness and Guidelines DATE: 05 December 2013 RESEARCH QUESTIONS 1. What is the clinical evidence regarding the effectiveness
Slough is a complex, generally fibrinous,
 Article Management of slough in diabetic foot wounds Steve Young A common presentation of diabetic foot wounds is a chronic ulcer with a yellowcoloured, viscous adherent layer of debris. This yellow wound
Article Management of slough in diabetic foot wounds Steve Young A common presentation of diabetic foot wounds is a chronic ulcer with a yellowcoloured, viscous adherent layer of debris. This yellow wound
JMSCR Vol 06 Issue 03 Page March 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i3.55 Thesis Paper A Prospective Comparative
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i3.55 Thesis Paper A Prospective Comparative
Consider the possibility of pressure ulcer development
 Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Accelerate wound healing of acute and chronic wounds in patients with Diabetes: Experience from Mexico using supplementary haemoglobin spray.
 Accelerate wound healing of acute and chronic wounds in patients with Diabetes: Experience from Mexico using supplementary haemoglobin spray. Obdulia Lopez Lopez 1, Fredrik Elg 2 Peter Engels 3, 1 Universidad
Accelerate wound healing of acute and chronic wounds in patients with Diabetes: Experience from Mexico using supplementary haemoglobin spray. Obdulia Lopez Lopez 1, Fredrik Elg 2 Peter Engels 3, 1 Universidad
Mean percent reduction in ulcer area from baseline at six weeks 62 % SANTYL Ointment + supportive care* + sharp debridement 1 (P<0.
 Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Honey has been used in wound care since the
 Honey as a dressing for chronic wounds in adults Carolyn Fox Carolyn Fox is Clinical Nurse Specialist - Tissue Viability, University Hospital Lewisham, London Series editor: Peter Griffiths Honey has been
Honey as a dressing for chronic wounds in adults Carolyn Fox Carolyn Fox is Clinical Nurse Specialist - Tissue Viability, University Hospital Lewisham, London Series editor: Peter Griffiths Honey has been
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Authors' objectives To assess the value of treatments for foot ulcers in patients with Type 2 diabetes mellitus.
 A systematic review of foot ulcer in patients with Type 2 diabetes mellitus - II: treatment Mason J, O'Keeffe C, Hutchinson A, McIntosh A, Young R, Booth A Authors' objectives To assess the value of treatments
A systematic review of foot ulcer in patients with Type 2 diabetes mellitus - II: treatment Mason J, O'Keeffe C, Hutchinson A, McIntosh A, Young R, Booth A Authors' objectives To assess the value of treatments
Venous. Arterial. Neuropathic (e.g. diabetic foot ulcer) Describe Wound Types & Stages of. Pressure Ulcers. Identify Phases of Healing & Wound Care
 A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
36 Urey Court, Irvine, CA ~ Fax: ~ ~
 B T E R BIO-THERAPEUTICS EDUCATION & RESEARCH FOUNDATION 36 Urey Court, Irvine, CA 92617 ~ Fax: 949-679-3001 ~ info@bterfoundation.org ~ www.bterfoundation.org Advancing Healthcare through Education &
B T E R BIO-THERAPEUTICS EDUCATION & RESEARCH FOUNDATION 36 Urey Court, Irvine, CA 92617 ~ Fax: 949-679-3001 ~ info@bterfoundation.org ~ www.bterfoundation.org Advancing Healthcare through Education &
Many patients with chronic wounds. Case reports. The use of Prontosan in combination with Askina Calgitrol : an independent case series
 Case reports The use of Prontosan in combination with Askina Calgitrol : an independent case series Author: Liezl Naude Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald
Case reports The use of Prontosan in combination with Askina Calgitrol : an independent case series Author: Liezl Naude Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald
Larval Debridement Therapy Making healing possible
 Larval Debridement Therapy Making healing possible What is Larval Debridement Therapy (LDT)? The term Larval Debridement Therapy describes the use of maggots, precisely the larvae of the green bottle blowfly
Larval Debridement Therapy Making healing possible What is Larval Debridement Therapy (LDT)? The term Larval Debridement Therapy describes the use of maggots, precisely the larvae of the green bottle blowfly
Making the Most of your Dressing Products Catherine Hammond CNS/CNE
 Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
The beneficial effects of maggots have been known for. The antimicrobial activity of maggots: in-vivo results RESEARCH PAPER
 97_101_JTV_Maggots 24/6/04 12:13pm Page 1 The antimicrobial activity of maggots: in-vivo results P Steenvoorde 1, GN Jukema 2 1 Section of Traumatology, Department of Surgery, Leiden University Medical
97_101_JTV_Maggots 24/6/04 12:13pm Page 1 The antimicrobial activity of maggots: in-vivo results P Steenvoorde 1, GN Jukema 2 1 Section of Traumatology, Department of Surgery, Leiden University Medical
Clinical Policy: EpiFix Wound Treatment
 Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
The word debridement derives from the
 Advertorial Is the scalpel the only way to debride? Duncan Stang Citation: Stang D (2013) Is the scalpel the only way to debride. The Diabetic Foot Journal 16: 74 8 Article points 1. A range of debridement
Advertorial Is the scalpel the only way to debride? Duncan Stang Citation: Stang D (2013) Is the scalpel the only way to debride. The Diabetic Foot Journal 16: 74 8 Article points 1. A range of debridement
Disclosures. Outpatient NPWT Options Free up Hospital Beds, but Do They Work? Objectives. Clinically Effective: Does it Work?
 4/16/16 Disclosures Consultant, Volcano Corporation Outpatient Options Free up Hospital Beds, but Do They Work? UCSF Vascular Symposium 16 Jonathan Labovitz, DPM Medical Director, Foot & Ankle Center Associate
4/16/16 Disclosures Consultant, Volcano Corporation Outpatient Options Free up Hospital Beds, but Do They Work? UCSF Vascular Symposium 16 Jonathan Labovitz, DPM Medical Director, Foot & Ankle Center Associate
I n the twenty first century, when modern
 REVIEW Larval therapy from antiquity to the present day: mechanisms of action, clinical applications and future potential Iain S Whitaker, Christopher Twine, Michael J Whitaker, Mathew Welck, Charles S
REVIEW Larval therapy from antiquity to the present day: mechanisms of action, clinical applications and future potential Iain S Whitaker, Christopher Twine, Michael J Whitaker, Mathew Welck, Charles S
Hyperbaric Oxygen Utilization in Wound Care
 Hyperbaric Oxygen Utilization in Wound Care Robert Barnes, MD, CWS Hyperbaric Center Sacred Heart Medical Center Riverbend Springfield, Oregon No relevant disclosures Diabetes and lower extremity wounds
Hyperbaric Oxygen Utilization in Wound Care Robert Barnes, MD, CWS Hyperbaric Center Sacred Heart Medical Center Riverbend Springfield, Oregon No relevant disclosures Diabetes and lower extremity wounds
Exudate in the early stages of wound healing
 Products & technology Wound management with the Biatain Silicone foam dressing: A multicentre product evaluation Authors: Hugues Cartier, Simon Barrett, Karen Campbell, Jan Forster, Mike Schmalzbauer,
Products & technology Wound management with the Biatain Silicone foam dressing: A multicentre product evaluation Authors: Hugues Cartier, Simon Barrett, Karen Campbell, Jan Forster, Mike Schmalzbauer,
DRESSING SELECTION. Rebecca Aburn MN NP Candidate
 DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
How Wounds Heal: A Guide for the Wound-care Novice
 C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
Emil Schmidt Wound Care specialist SDHB - Otago
 Prospective randomised trial of low frequency ultrasound debridement (LFUD) in management of lower limb wounds Krysa J, Schmidt E, Thomson I, van Rij A Emil Schmidt Wound Care specialist SDHB - Otago Background
Prospective randomised trial of low frequency ultrasound debridement (LFUD) in management of lower limb wounds Krysa J, Schmidt E, Thomson I, van Rij A Emil Schmidt Wound Care specialist SDHB - Otago Background
Disclosures for Tarik Alam. Wound Bed Preparation. Wound Prognosis. Session Objectives. Debridement 4/26/2015
 Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
CASE 1: TYPE-II DIABETIC FOOT ULCER
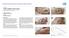 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
A comprehensive study on effect of collagen dressing in diabetic foot ulcer
 Original Research Article A comprehensive study on effect of collagen dressing in diabetic foot ulcer Sivakumar 1, S. Shanmugam 2* 1 Associate Professor, 2 Senior Assistant Professor Department of General
Original Research Article A comprehensive study on effect of collagen dressing in diabetic foot ulcer Sivakumar 1, S. Shanmugam 2* 1 Associate Professor, 2 Senior Assistant Professor Department of General
Chapter. Introduction
 Chapter 1 Introduction Introduction A long history of maggot therapy Maggot-therapy is a medical curiosity that has had little influence on the course of modern medicine. 2 This statement might have been
Chapter 1 Introduction Introduction A long history of maggot therapy Maggot-therapy is a medical curiosity that has had little influence on the course of modern medicine. 2 This statement might have been
Interesting Case Series. Skin Grafting in Pyoderma Gangrenosum
 Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
Interesting Case Series Skin Grafting in Pyoderma Gangrenosum Marco Romanelli, MD, PhD, Agata Janowska, MD, Teresa Oranges, MD, and Valentina Dini, MD, PhD Department of Dermatology, University of Pisa,
Precise excision. Preserve viable tissue and reduce time to closure (1,2)
 Precise excision Preserve viable tissue and reduce time to closure (1,2) Precision to preserve Conventional surgical excision Non-viable tissue VERSAJET II excision More precise tissue removal Non-viable
Precise excision Preserve viable tissue and reduce time to closure (1,2) Precision to preserve Conventional surgical excision Non-viable tissue VERSAJET II excision More precise tissue removal Non-viable
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
DEBRIDEMENT. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
Sterilisation of Lucilia cuprina Wiedemann maggots used in therapy of intractable wounds
 Tropical Biomedicine 22(2): 185 189 (2005) Sterilisation of Lucilia cuprina Wiedemann maggots used in therapy of intractable wounds Mohd Masri, S., Nazni, W.A., Lee, H.L., T. Rogayah, T.A.R. and Subramaniam,
Tropical Biomedicine 22(2): 185 189 (2005) Sterilisation of Lucilia cuprina Wiedemann maggots used in therapy of intractable wounds Mohd Masri, S., Nazni, W.A., Lee, H.L., T. Rogayah, T.A.R. and Subramaniam,
Larval debridement therapy: vascular wound management
 Larval debridement therapy: vascular wound management aling Wounds uk PUBLISHED BY: Wounds UK Enterprise House 1 2 Hatfields London SE1 9PG, UK Tel: + 44 (0)20 7627 1510 Fax: +44 (0)20 7627 1570 www.wounds-uk.com
Larval debridement therapy: vascular wound management aling Wounds uk PUBLISHED BY: Wounds UK Enterprise House 1 2 Hatfields London SE1 9PG, UK Tel: + 44 (0)20 7627 1510 Fax: +44 (0)20 7627 1570 www.wounds-uk.com
Use of Non-Contact Low Frequency Ultrasound in Wound Care
 Use of Non-Contact Low Frequency Ultrasound in Wound Care BLAIRE CHANDLER SEPTEMBER 29, 2015 VCU DPT CLASS OF 2016 Objectives Patient case overview Examine clinical evidence Review intervention of interest
Use of Non-Contact Low Frequency Ultrasound in Wound Care BLAIRE CHANDLER SEPTEMBER 29, 2015 VCU DPT CLASS OF 2016 Objectives Patient case overview Examine clinical evidence Review intervention of interest
Clinical Policy Title: Debridement of diabetic foot ulcers
 Clinical Policy Title: Debridement of diabetic foot ulcers Clinical Policy Number: CCP.1200 Effective Date: January 1, 2016 Initial Review Date: October 19, 2015 Most Recent Review Date: October 2, 2018
Clinical Policy Title: Debridement of diabetic foot ulcers Clinical Policy Number: CCP.1200 Effective Date: January 1, 2016 Initial Review Date: October 19, 2015 Most Recent Review Date: October 2, 2018
Negative Pressure Wound Therapy
 Ontario Health Technology Assessment Series 2010; Vol. 10, No. 22 Negative Pressure Wound Therapy An Evidence Update Presented to the Ontario Health Technology Advisory Committee in September 2010 December
Ontario Health Technology Assessment Series 2010; Vol. 10, No. 22 Negative Pressure Wound Therapy An Evidence Update Presented to the Ontario Health Technology Advisory Committee in September 2010 December
A new classification of the diabetic ischaemic foot promotes a modern approach to treatment. Michael Edmonds King s College Hospital London
 A new classification of the diabetic ischaemic foot promotes a modern approach to treatment Michael Edmonds King s College Hospital London Disclosure Speaker name: Michael Edmonds... I have the following
A new classification of the diabetic ischaemic foot promotes a modern approach to treatment Michael Edmonds King s College Hospital London Disclosure Speaker name: Michael Edmonds... I have the following
Ray Norris, Rachel Henchy
 Use of low frequency ultrasound therapy in the treatment of recalcitrant leg ulcers: case series This series of case reports looks at the efficacy of low frequency ultrasound using the MIST Therapy System
Use of low frequency ultrasound therapy in the treatment of recalcitrant leg ulcers: case series This series of case reports looks at the efficacy of low frequency ultrasound using the MIST Therapy System
2008 American Medical Association and National Committee for Quality Assurance. All Rights Reserved. CPT Copyright 2007 American Medical Association
 Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Larval debridement therapy (LDT)
 Meeting report Appropriate use of larval debridement therapy in diabetic foot management: consensus recommendations Paul Chadwick, Joanne McCardle, Elaine Ricci, Duncan Stang, Stella Vig Recent evidence
Meeting report Appropriate use of larval debridement therapy in diabetic foot management: consensus recommendations Paul Chadwick, Joanne McCardle, Elaine Ricci, Duncan Stang, Stella Vig Recent evidence
The Management of Lower Limb Oedema. Catherine Hammond CNS/CNE 2018
 The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
Diabetic Foot Ulcer Treatment and Prevention
 Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
Clinical Policy Title: Vacuum assisted closure in surgical wounds
 Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
Prontosan. Clean. Easy Wound Healing. Wound Cleansing
 Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
First Coast Service Options (FCSO) Medicare Policy Primer
 First Coast Service Options (FCSO) Medicare Policy Primer Medicare Jurisdiction (JN) Florida, Puerto Rico and U.S. Virgin Islands Application of Skin Substitute Grafts for the treatment of DFU and VLU
First Coast Service Options (FCSO) Medicare Policy Primer Medicare Jurisdiction (JN) Florida, Puerto Rico and U.S. Virgin Islands Application of Skin Substitute Grafts for the treatment of DFU and VLU
TITLE: Debridement Procedures for Managing Diabetic Foot Ulcers: A Review of Clinical Effectiveness, Cost-effectiveness, and Guidelines
 TITLE: Debridement Procedures for Managing Diabetic Foot Ulcers: A Review of Clinical Effectiveness, Cost-effectiveness, and Guidelines DATE: 15 September 2014 CONTEXT AND POLICY ISSUES The rising prevalence
TITLE: Debridement Procedures for Managing Diabetic Foot Ulcers: A Review of Clinical Effectiveness, Cost-effectiveness, and Guidelines DATE: 15 September 2014 CONTEXT AND POLICY ISSUES The rising prevalence
Independent evaluation of BEMER physical vascular regulation therapy
 of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Do all foam dressings have the same efficacy in the treatment of chronic wounds? Janice Bianchi, David Gray, John Timmons, Sylvie Meaume
 Do all foam dressings have the same efficacy in the treatment of chronic wounds? The challenge of chronic wounds remains significant both in terms of clinical management, impact on patients and cost to
Do all foam dressings have the same efficacy in the treatment of chronic wounds? The challenge of chronic wounds remains significant both in terms of clinical management, impact on patients and cost to
The VERSAJET II Hydrosurgery System
 Precise Excision The VERSAJET II Hydrosurgery System The VERSAJET II Hydrosurgery System The VERSAJET II system enables a surgeon to precisely select, excise and evacuate nonviable tissue, bacteria and
Precise Excision The VERSAJET II Hydrosurgery System The VERSAJET II Hydrosurgery System The VERSAJET II system enables a surgeon to precisely select, excise and evacuate nonviable tissue, bacteria and
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Managing Wounds. Esther White Tissue Viability Nurse
 Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
PRODIGY Quick Reference Guide
 PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
PRODIGY Quick Venous leg ulcer infected How do I assess a venous leg ulcer? Chronic venous insufficiency and venous hypertension result from damage to the valves in the veins of the leg and inadequate
Multidisciplinary approach to BTK Y. Gouëffic, MD, PhD
 Multidisciplinary approach to BTK Y. Gouëffic, MD, PhD Department of vascular surgery, University Hospital of Nantes, France Response to the increased demand of hospital care Population is aging Diabetes
Multidisciplinary approach to BTK Y. Gouëffic, MD, PhD Department of vascular surgery, University Hospital of Nantes, France Response to the increased demand of hospital care Population is aging Diabetes
Medical technology guidance
 NICE provided the content for this booklet which is independent of any company or product advertised Medical technology guidance The Debrisoft monofilament debridement pad for use in acute or chronic wounds
NICE provided the content for this booklet which is independent of any company or product advertised Medical technology guidance The Debrisoft monofilament debridement pad for use in acute or chronic wounds
Hyperbaric oxygen therapy Villanueva E, Johnston R, Clavisi O, Burrows E, Bernath V, Rajendran M, Wasiak J, Fennessy P, Anderson J, Harris A, Yong K
 Hyperbaric oxygen therapy Villanueva E, Johnston R, Clavisi O, Burrows E, Bernath V, Rajendran M, Wasiak J, Fennessy P, Anderson J, Harris A, Yong K Authors' objectives To assess the effectiveness of hyperbaric
Hyperbaric oxygen therapy Villanueva E, Johnston R, Clavisi O, Burrows E, Bernath V, Rajendran M, Wasiak J, Fennessy P, Anderson J, Harris A, Yong K Authors' objectives To assess the effectiveness of hyperbaric
DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR
 ORIGINAL ARTICLE DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR Ghulam Shabbier, Said Amin, Ishaq Khattak, Sadeeq-ur-Rehman Department of Medicine Khyber Teaching Hospital
ORIGINAL ARTICLE DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR Ghulam Shabbier, Said Amin, Ishaq Khattak, Sadeeq-ur-Rehman Department of Medicine Khyber Teaching Hospital
a,b and the annual cost of diabetic neuropathy is estimated to be $10.91 billion in the United States alone. 3
 eplasty: Vol. 11 A Prospective Study of Negative Pressure Wound Therapy With Integrated Charles M. Zelen, DPM,, FACFAS a,b Brian Stover, DPM, a Professional Education and b esearch Institute, oanoke, Department
eplasty: Vol. 11 A Prospective Study of Negative Pressure Wound Therapy With Integrated Charles M. Zelen, DPM,, FACFAS a,b Brian Stover, DPM, a Professional Education and b esearch Institute, oanoke, Department
PluroGel Burn and Wound Dressing Chicago. 23 May 2014
 PluroGel Burn and Wound Dressing Chicago 23 May 2014 A NEW, BREAKTHROUGH SURFACTANT BASED BIOMATERIAL WITH A SPECIAL MOLECULAR STRUCTURE PLUROGEL BIOMATERIAL SPECIAL MOLECULAR STRUCTURE PLUROGEL MICELLE
PluroGel Burn and Wound Dressing Chicago 23 May 2014 A NEW, BREAKTHROUGH SURFACTANT BASED BIOMATERIAL WITH A SPECIAL MOLECULAR STRUCTURE PLUROGEL BIOMATERIAL SPECIAL MOLECULAR STRUCTURE PLUROGEL MICELLE
Regenerative Tissue Matrix in Treatment of Wounds
 Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
I ve a drawer full of dressings i don t know how to use!
 I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
Diabetic Foot Ulcer. A Complete Solution. Therapy Approach with Adapted Products
 Diabetic Foot Ulcer A Complete Solution Therapy Approach with Adapted Products A Complete Solution for Diabetic Foot Ulcers This booklet focuses on the recommended treatment of diabetic foot ulcers. Diabetes
Diabetic Foot Ulcer A Complete Solution Therapy Approach with Adapted Products A Complete Solution for Diabetic Foot Ulcers This booklet focuses on the recommended treatment of diabetic foot ulcers. Diabetes
Nanogen Aktiv. Naz Wahab MD, FAAFP, FAPWCA Nexderma
 Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Understanding Debridement
 Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
Palmetto Medicare Policy Primer
 Palmetto Medicare Policy Primer Medicare Jurisdiction (JM) NC, SC, WV & VA Application of Skin Substitutes LCD #L36466 Indications Presence of neuropathic diabetic foot ulcer(s) having failed to respond
Palmetto Medicare Policy Primer Medicare Jurisdiction (JM) NC, SC, WV & VA Application of Skin Substitutes LCD #L36466 Indications Presence of neuropathic diabetic foot ulcer(s) having failed to respond
A Prospective Study of Negative Pressure Wound Therapy With Integrated Irrigation for the Treatment of Diabetic Foot Ulcers
 A Prospective Study of Negative Pressure Wound Therapy With Integrated Irrigation for the Treatment of Diabetic Foot Ulcers Charles M. Zelen, DPM, FACFAS, a,b Brian Stover, DPM, a David Nielson, DPM, a,b
A Prospective Study of Negative Pressure Wound Therapy With Integrated Irrigation for the Treatment of Diabetic Foot Ulcers Charles M. Zelen, DPM, FACFAS, a,b Brian Stover, DPM, a David Nielson, DPM, a,b
CPAG Summary Report for Clinical Panel URN 1779, Hyperbaric Oxygen Therapy for Diabetic Lower Limb Ulceration Refractory to Best Standard Care
 MANAGEMENT IN CONFIDENCE CPAG Summary Report for Clinical Panel URN 1779, Hyperbaric Oxygen Therapy for Diabetic Lower Limb Ulceration Refractory to Best Standard Care The Benefits of the Proposition No
MANAGEMENT IN CONFIDENCE CPAG Summary Report for Clinical Panel URN 1779, Hyperbaric Oxygen Therapy for Diabetic Lower Limb Ulceration Refractory to Best Standard Care The Benefits of the Proposition No
The Triangle of Wound Assessment
 The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
