Fabian Speth 1, Johannes-Peter Haas 1 and Claas H. Hinze 2*
|
|
|
- George Adams
- 5 years ago
- Views:
Transcription
1 Speth et al. Pediatric Rheumatology (2016) 14:52 DOI /s CASE REPORT Open Access Treatment with high-dose recombinant human hyaluronidase-facilitated subcutaneous immune globulins in patients with juvenile dermatomyositis who are intolerant to intravenous immune globulins: a report of 5 cases Fabian Speth 1, Johannes-Peter Haas 1 and Claas H. Hinze 2* Abstract Background: High-dose intravenous immune globulins (IVIg) are frequently used in refractory juvenile dermatomyositis (JDM) but are often poorly tolerated. High-dose recombinant human hyaluronidase-facilitated subcutaneous immune globulins (fscig) allow the administration of much higher doses of immune globulins than conventional subcutaneous immune globulin therapy and may be an alternative to IVIg. The safety and efficacy of fscig therapy in JDM is unknown. Case Presentation: In this retrospective case series, five patients with steroid-refractory severe JDM were treated with high-dose fscig due to IVIg adverse effects (severe headaches, nausea, vomiting, difficult venous access). Peak serum IgG levels, muscle enzymes, the childhood myositis assessment scale and adverse effects were retrieved for at least 6 months following intiation of fscig. Data were analyzed by descriptive statistics. Patients initially received fscig 1 g/kg every 14 days, resulting in median IgG peak levels of 1901 mg/dl ( mg/dl), compared to median IgG peak and trough levels while previously receiving IVIg of 2741 mg/dl ( mg/dl) and 1351 mg/dl ( mg/dl). Additional antirheumatic therapies consisted of low-dose glucocorticoid therapy, methotrexate, mycophenolate mofetil and/or rituximab. Two patients maintained clinically inactive disease and three patients had only a partial treatment response. In the three patients with partial treatment response, fscig 1 g/kg was then given on days 1 and 6 of every 28-day cycle resulting in IgG peak levels of between mg/dl (previously mg/dl on the biweekly regimen), resulting in clinically inactive disease in two of the three patients. There were no relevant adverse effects that limited continuation of fscig treatment. Conclusions: High-dose fscig is well-tolerated in patients with JDM and high peak serum IgG levels can be achieved which may be important for treatment success. High-dose fscig may therefore be an alternative to high-dose IVIg and deserves further study. Trial registration: This is a case series and data were retrospectively registered. Keywords: Juvenile dermatomyositis, Intravenous immune globulins, Subcutaneous immune globulins, Recombinant human hyaluronidase * Correspondence: claas.hinze@ukmuenster.de 2 Klinik für Pädiatrische Rheumatologie und Immunologie, Universitätsklinikum Münster, Münster, Germany Full list of author information is available at the end of the article 2016 The Author(s). Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Speth et al. Pediatric Rheumatology (2016) 14:52 Page 2 of 5 Background Juvenile dermatomyositis (JDM) is a severe inflammatory myopathy characterized by vasculopathy affecting skin, muscle and sometimes internal organs [1]. While mortality is low with contemporary treatment, morbidities, such as dystrophic calcification, contractures and muscle weakness still cause a substantial long-term disease burden [2, 3]. However, little high-quality data from clinical trials exists to guide treatment decisions and treatment is mostly guided by expert opinion and consensus treatment protocols [1, 4 6]. There is evidence that the routine treatment of moderately-severe JDM should include high-dose steroids and methotrexate [7]. Additional steroid-sparing immunomodulatory therapies are often employed, especially including intravenous immune globulins (IVIg), hydroxychloroquine, cyclosporine, azathioprine, mycophenolate mofetil and rituximab. Even though randomized clinical trials for IVIg in JDM are lacking, it appears to be highly effective in severe or refractory JDM [8, 9]. Typically, the administration of up to 2 g per kg and month of IVIg are required to achieve treatment success, since antiinflammatory efficacy may depend on peak serum immune globulin (Ig)G levels [10, 11]. High-dose IVIg treatment causes adverse effects in 5-10 % of patients [11], including severe headaches, nausea, vomiting, aseptic meningitis, thrombosis and venous access may be difficult over time whereas subcutaneous Ig (SCIg) treatment is usually welltolerated [12]. However, since the extracellular matrix limits subcutaneous bulk fluid flow, the maximal volume infusible by standard SCIg in one site is 30 ml, effectively limiting the amount of Ig that can be applied in a single treatment and, thus, its utility as an anti-inflammatory therapy. By means of facilitating SCIg with recombinant human hyaluronidase (rhuph20) (fscig), a 20-fold higher volume of up to 600 ml fscig (equaling 60 g of Ig) can be administered at one site [13]. Cleaving hyaluronic acid increases permeability of the subcutaneous tissue markedly. Since rhuph20 is not available systemically, short-acting and non-immunogenic, and since tissue hyaluronic acid is rapidly resynthesized, there are typically no short-term or long-term adverse effects. Regarding the pharmacokinetics of fscig, the median time to reach peak serum IgG levels is five days [13]. fscig is currently approved for the use in patients with primary immunodeficiency disorders older than 18 years of age but has been tested in children older than two years of age. The safety and efficacy of high-dose fscig therapy in JDM is unknown. Case Presentation Patients Five patients with moderately severe or severe and refractory definitive JDM who had initially received IVIg were treated with fscig for at least six months were identified at the German Center for Pediatric and Adolescent Rheumatology in Garmisch-Partenkirchen between January 2012 and December 2015 [5]. Overall, 42 patients with JDM were treated at the center in that time frame, of whom 26 had received IVIg (62 %). Informed consent was obtained from all patients and guardians. Patient demographics, myositis-specific autoantibodies, clinical phenotype, disease severity [5], concurrent antirheumatic therapy and reasons for initiation of/switching to fscig treatment are shown in Table 1. Administration of subcutaneous immune globulins Patients 1 4 started fscig treatment 4 6 weeks after the last IVIg dose, and patient 5, who had not recently received IVIg, started fscig after a disease flare. All patients received high-dose fscig with recombinant human hyaluronidase (HyQvia, Baxalta, Unterschleißheim, Germany) between 1.7 to 2 g/kg per month (maximally 70 g per month) divided into two doses. Patients each received two inpatient training fscig treatments (first 0.3 g/kg, then 1 g/kg). Following hospital discharge, patients and parents received one or two fscig treatments at home guided by a nurse practitioner especially trained in the application of fscig. Eutectic mixture of local anesthetics was applied prior to the subcutaneous infusions and fscig was administered according to the manufacturer s instruction with maximal infusion rates of 160 ml/h (body weight <40 kg). Each individual fscig administration took on average three to four hours. For three patients, the regimen was later switched to two monthly fscig doses five days apart, i.e., the same monthly total dose was given divided into two doses at days 1 and 6 of each 28-day cycle. Data collection and analysis As part of the clinical routine at the center multiple clinical and laboratory parameters are collected prospectively for all patients with JDM. For this retrospective analysis, the following clinical and laboratory parameters were retrieved for analysis: serum IgG levels, muscle enzyme levels, childhood myositis assessment scale (CMAS) score, physician global assessment of disease activity, and potential treatment adverse effects. Data were analyzed using descriptive statistics. Serum IgG levels For the various time points of measuring serum IgG levels (before Ig therapy, peak/trough during IVIg, and peak during SCIg) up to nine different data point were available and mean IgG levels were calculated for each patient and time point. Overall, fscig treatment every 14 days resulted in median IgG peak levels, measured five days after administration, of 1901 mg/dl (range mg/dl), compared to median IgG peak (one day after dose) and trough levels (28 days after dose) while previously receiving IVIg 2 g per
3 Table 1 Patient demographics, current antirheumatic therapy, reasons for initiation of subcutaneous immune globulins, and disease course following fscig therapy Patient Sex, age, age at disease onset, body weight 1 Male, 11 years, 9 years at disease 2 Female, 10 years, 8 years at disease 3 Female, 7 years, 5 years at disease onset, 20 kg 4 Male, 12 years, 8 years at disease 5 Female, 8 years, 5 years at disease onset, 20 kg Clinical phenotype and disease severity a, age at disease onset, MSA status prominent skin involvement, joint contractures, Anti-Mi-2 prominent vaculopathy, dysphagia, cutaneous ulcerations, myocarditis, joint contractures, calcinosis, Anti-TIF-1gamma prominent vasculopathy, cutaneous ulcerations, Anti-SRP and anti-mi-2 Classic, moderately severe JDM with nodular dystrophic calcification, anti-nxp-2 rhadomyolysis, failure to thrive and nephrolithiasis, MSA negative Disease activity at time of fscig initiation (however, recent recurrence after attempted IVIg discontiuation) Residual disease activity, vasculopathy (recent recurrence) (however, progressive calcinosis) Active skin and muscle disease (IVIg was discontinued 6 months earlier) Previous or concurrent antirheumatic treatments IVIg (60 g/month), fscig (70 g/month), PDN mg/kg/day, MTX 15 mg/ m 2 /week, HCQ IVIg (70 g/month), fscig (70 g/month), PDN 0.21 mg/kg/day, MMF 1200 mg/ m 2 /d, MTX 15 mg/m 2 /week, RTX (status post 375 mg/m 2 4), CYC (status post mg/m 2 ) IVIg (40 g/month), fscig (40 g/month), PDN mg/kg/day, MMF 1200 mg/ m 2 /d, MTX 15 mg/m 2 /week RTX (status post 375 mg/m 2 4 [first cycle], 750 mg/m 2 1 [second cycle]) IVIg (35 g/month), fscig (60 g/month) PDN 0.07 mg/kg/day, MMF 1200 mg/ m 2 /d, Colchicin IVIG (40 g/month), fscig (50 g/month) PDN 0.19 mg/kg/day, MMF 600 mg/ m 2 /d (diarrhea with higher doses), MTX 15 mg/m 2 /week Reason for initiation of fscig instead of IVIg, CMAS at time of fscig initiation CMAS 51 IVIg adverse effects (headaches), difficult peripheral venous access with port-a-cath CMAS not interpretable due to severity of contractures CMAS 52, residual disease activity with insufficient IVIg dose CMAS 52 CMAS 46 Disease course following initiation of fscig Within 3 months mild deterioration of CMAS (49 instead of 51); resolution after switching to fscig 5 days apart Stable mild residual disease activity even after switching to fscig 5 days apart Maintenance of clinically inactive disease; CMAS 52; fscig continued biweekly Maintenance of clinically inactive disease; CMAS 52; calcinosis decreasing; fscig continued biweekly Improvement but residual, mild proximal muscle weakness; normal muscle strength (inactive disease) after switching to fscig 5 days apart; CMAS 50; further PDN reduction Abbreviations: CYC cyclophosphamide, IVIg intravenous immune globulins, fscig subcutaneous immune globulins facilitated by recombinant human hyaluronidase, MMF mycophenolate mofetil, MSA myositis-specific antibodies, MTX methotrexate, PDN prednisolone, RTX rituximab a Definition of disease severity according to Huber et al. [5] Speth et al. Pediatric Rheumatology (2016) 14:52 Page 3 of 5
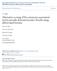
4 Speth et al. Pediatric Rheumatology (2016) 14:52 Page 4 of 5 kg and month of 2741 mg/dl (range mg/dl) and 1351 mg/dl ( mg/dl), respectively. In order to achieve higher peak serum levels and improved immunomodulatory efficacy, for three patients the fscig administration was switched to two monthly doses five days apart (i.e., days 1 and 6 of each 28-day cycle). Following fscig 1 g/kg on days 1 and 6, IgG serum levels on day 11 showed much increased IgG serum levels of 2846 mg/dl (up from 1901 mg/dl), 2300 mg/dl (up from 1774 mg/dl), and 2757 mg/dl (up from 1606 mg/dl). Individual levels and courses are also shown in Fig. 1. Disease activity Muscle enzymes remained stable and within normal limits. Patient 1 experienced mild worsening of the CMAS (from 51 to 49), which improved again when switched to fscig five days apart. Patient 2 had mild, stable residual disease despite switching to fscig five days apart. Patients 3 and 4 maintained clinically inactive disease and kept fscig 14 days apart. Patient 5 had resolution of skin disease but mild residual muscle weakness with fscig every 14 days which resolved after switching to fscig five days apart. Subcutaneous immune globulin administration and monitoring for adverse effects During and after fscig administration, the patients developed a localized subcutaneous pocket which resolved within 24 h. One patient (Patient 5) had transient mild headaches following administration of SCIg and a minor local site reaction. None of the patients required Fig. 1 IgG levels before initiation of Ig therapy, peak and trough serum IgG levels (during high-dose IVIg therapy) and peak levels during SCIg therapy. Values represent mean values and error bars standard deviation (if multiple measurements are available). The dashed lines represent the upper and lower limit of the normal range premedications (which all had required while receiving IVIg). There were no incidences of treatment abortion due to adverse effects. In three patients fscig five or 14 days apart was tolerated equally well. There was no evidence of dystrophic calcification at the site of fscig administration or elsewhere. All five patients reported that they strongly preferred treatment with fscig over IVIg, mostly due to the lack of adverse effects and the avoidance of hospitalization for i.v. therapy. Conclusions This is, to our knowledge, the first report on the treatment of severe refractory JDM with high-dose fscig. The application of standard preparations of SCIg (without recombinant human hyaluronidase) in moderately severe JDM (up to 1 g/kg and month) and refractory adult DM (up to 0.8 g/kg and month) resulting in improved quality of life has been reported previously [14 16]. While standard SCIg is typically applied between one and three times weekly (in clinical practice maximally 56 g per month), fscig may be applied less frequently, e.g., once monthly in case of primary immunodeficiency, since it shows a better bioavailability and in addition allows administration of up to 120 g of Ig per month [13]. We demonstrated that the administration of two doses of fscig separated by five days for a total dose of 2 g/kg and month results in peak serum IgG levels similar to those achieved by regular high-dose IVIg treatment but not by conventional SCIg treatment. It is suggested that high peak serum IgG levels may be necessary for immune modulatory efficacy of Ig therapy [10, 11]. We were able to avoid premedication before IgG application and used oral corticosteroids sparingly to avoid long-term steroid adverse effects. High-dose fscig therapy was well tolerated by our patients and even when given five days apart producing high IgG serum levels, we did not observe any relevant local or systemic adverse effects. Specifically, there was no evidence of increased local inflammation or dystrophic calcification at the administration sites and no evidence of aseptic meningitis or severe headaches. While high-dose IVIg treatment typically requires hospitalization and intravenous access, fscig can be administered without difficulty at home and may therefore be both time- and cost-saving [13, 17]. Our report is limited by the fact that this is a retrospective analysis of a small cohort of patients so that the assessment of treatment efficacy is very limited. In summary, high-dose fscig therapy may be an attractive treatment option for patients with moderately severe or severe refractory JDM as a remission maintenance treatment and potentially also as a remission induction therapy in case of IVIg intolerance, IgA deficiency or difficult venous access, in order to improve quality of life (avoiding hospital admissions) and to reduce cost of treatment.
5 Speth et al. Pediatric Rheumatology (2016) 14:52 Page 5 of 5 Generally, the use of IVIg or fscig in JDM may allow reduction of steroid use. Further formal testing of efficacy and safety by means of prospective clinical trials is desirable. Abbreviations CMAS: Childhood myositis assessment scale; fscig: Hyaluronidase-facilitated subcutaneous immune globulins; Ig: Immune globulin; IVIg: Intravenous immune globulins; JDM: Juvenile dermatomyositis; SCIg: Subcutaneous immune globulins Acknowledgements Not applicable. Funding Not applicable. Availability of data and materials The patient data were entered in the Excel spread sheets including their identification as only the investigator team had an access to them. Patients have not consented on presenting their full data to any third parties. Authors contributions FS was involved in the diagnosis, management of the patients, retrospective review of cases, data analysis and helped to draft the manuscript; JPH was involved in the diagnosis, management of the patients and retrospective review of cases; CH reviewed the cases, analyzed the data and drafted the manuscript. All authors read and approved the final manuscript. Competing interests The authors declare that they have no competing interests. methotrexate in new-onset juvenile dermatomyositis: a randomised trial. Lancet. 2016;387(10019): Lam CG, Manlhiot C, Pullenayegum EM, Feldman BM. Efficacy of intravenous Ig therapy in juvenile dermatomyositis. Ann Rheum Dis. 2011;70(12): Sansome A, Dubowitz V. Intravenous immunoglobulin in juvenile dermatomyositis four year review of nine cases. Arch Dis Child. 1995;72(1): Gelfand EW. Intravenous immune globulin in autoimmune and inflammatory diseases. N Engl J Med. 2012;367(21): Negi VS, Elluru S, Siberil S, Graff-Dubois S, Mouthon L, Kazatchkine MD, et al. Intravenous immunoglobulin: an update on the clinical use and mechanisms of action. J Clin Immunol. 2007;27(3): Stiehm ER. Adverse effects of human immunoglobulin therapy. Transfus Med Rev. 2013;27(3): Wasserman RL, Melamed I, Stein MR, Gupta S, Puck J, Engl W, et al. Recombinant human hyaluronidase-facilitated subcutaneous infusion of human immunoglobulins for primary immunodeficiency. J Allergy Clin Immunol. 2012;130(4): e Danieli MG, Moretti R, Gambini S, Paolini L, Gabrielli A. Open-label study on treatment with 20 % subcutaneous IgG administration in polymyositis and dermatomyositis. Clin Rheumatol. 2014;33(4): Danieli MG, Pettinari L, Moretti R, Logullo F, Gabrielli A. Subcutaneous immunoglobulin in polymyositis and dermatomyositis: a novel application. Autoimmun Rev. 2011;10(3): de Inocencio J, Enríquez-Merayo E, Casado R, et al. Subcutaneous Immunoglobulin in Refractory Juvenile Dermatomyositis. Pediatrics. 2016;137(4):e Ponsford M, Carne E, Kingdon C, Joyce C, Price C, Williams C, et al. Facilitated subcutaneous immunoglobulin (fscig) therapy practical considerations. Clin Exp Immunol. 2015;182(3): Consent for publication Individual patients and their parents consented to publication of their data. Ethics approval and consent to participate Individual patients and their parents consented to publication of their individual patient data. Author details 1 Deutsches Zentrum für Kinder- und Jugendrheumatologie, Garmisch-Partenkirchen, Germany. 2 Klinik für Pädiatrische Rheumatologie und Immunologie, Universitätsklinikum Münster, Münster, Germany. Received: 8 July 2016 Accepted: 8 September 2016 References 1. Feldman BM, Rider LG, Reed AM, Pachman LM. Juvenile dermatomyositis and other idiopathic inflammatory myopathies of childhood. Lancet. 2008;371(9631): Ravelli A, Trail L, Ferrari C, Ruperto N, Pistorio A, Pilkington C, et al. Long-term outcome and prognostic factors of juvenile dermatomyositis: a multinational, multicenter study of 490 patients. Arthritis Care Res. 2010;62(1): Robinson AB, Hoeltzel MF, Wahezi DM, Becker ML, Kessler EA, Schmeling H, et al. Clinical characteristics of children with juvenile dermatomyositis: the childhood arthritis and rheumatology research alliance registry. Arthritis Care Res. 2014;66(3): Dressler F, Huppertz HI. Juvenile dermatomyositis. Z Rheumatol. 2006;65(7): Huber AM, Robinson AB, Reed AM, Abramson L, Bout-Tabaku S, Carrasco R, et al. Consensus treatments for moderate juvenile dermatomyositis: beyond the first two months. results of the second childhood arthritis and rheumatology research alliance consensus conference. Arthritis Care Res. 2012;64(4): Robinson AB, Reed AM. Clinical features, pathogenesis and treatment of juvenile and adult dermatomyositis. Nat Rev Rheumatol. 2011;7(11): Ruperto N, Pistorio A, Oliveira S, Zulian F, Cuttica R, Ravelli A, et al. Prednisone versus prednisone plus ciclosporin versus prednisone plus Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
Understanding Myositis Medications
 Understanding Myositis Medications 2015 TMA Annual Patient Conference Orlando, Florida Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Disclosures Mallinckrodt: Research Grant Genentech:
Understanding Myositis Medications 2015 TMA Annual Patient Conference Orlando, Florida Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Disclosures Mallinckrodt: Research Grant Genentech:
Clinical Commissioning Policy Proposition:
 Clinical Commissioning Policy Proposition: Rituximab for the treatment of dermatomyositis and polymyositis (Adults) Reference: NHS England A13X05/01 Information Reader Box (IRB) to be inserted on inside
Clinical Commissioning Policy Proposition: Rituximab for the treatment of dermatomyositis and polymyositis (Adults) Reference: NHS England A13X05/01 Information Reader Box (IRB) to be inserted on inside
Arthritis Superspeciality Center, Hubli, Karnataka and 2 Department of Rheumatology, SDM Medical College, Dharwad, Karnataka, India.
 JOURNAL OF CASE REPORTS 2015;5(1):147-151 A Rare Case of Juvenile Dermatomyositis Vikram Haridas 1,2, Kiran Haridas 1 1,2 Arthritis Superspeciality Center, Hubli, Karnataka and 2 Department of Rheumatology,
JOURNAL OF CASE REPORTS 2015;5(1):147-151 A Rare Case of Juvenile Dermatomyositis Vikram Haridas 1,2, Kiran Haridas 1 1,2 Arthritis Superspeciality Center, Hubli, Karnataka and 2 Department of Rheumatology,
Takashi Yagisawa 1,2*, Makiko Mieno 1,3, Norio Yoshimura 1,4, Kenji Yuzawa 1,5 and Shiro Takahara 1,6
 Yagisawa et al. Renal Replacement Therapy (2016) 2:68 DOI 10.1186/s41100-016-0080-9 POSITION STATEMENT Current status of kidney transplantation in Japan in 2015: the data of the Kidney Transplant Registry
Yagisawa et al. Renal Replacement Therapy (2016) 2:68 DOI 10.1186/s41100-016-0080-9 POSITION STATEMENT Current status of kidney transplantation in Japan in 2015: the data of the Kidney Transplant Registry
Case Report Repository Corticotropin Injection for Treatment of Idiopathic Inflammatory Myopathies
 Case Reports in Rheumatology Volume 2016, Article ID 9068061, 4 pages http://dx.doi.org/10.1155/2016/9068061 Case Report Repository Corticotropin Injection for Treatment of Idiopathic Inflammatory Myopathies
Case Reports in Rheumatology Volume 2016, Article ID 9068061, 4 pages http://dx.doi.org/10.1155/2016/9068061 Case Report Repository Corticotropin Injection for Treatment of Idiopathic Inflammatory Myopathies
Autoantibodies in the Idiopathic Inflammatory Myopathies
 Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Patient characteristics associated with response to NSAID monotherapy in children with systemic juvenile idiopathic arthritis
 Sura et al. Pediatric Rheumatology (2018) 16:2 DOI 10.1186/s12969-017-0219-4 RESEARCH ARTICLE Open Access Patient characteristics associated with response to NSAID monotherapy in children with systemic
Sura et al. Pediatric Rheumatology (2018) 16:2 DOI 10.1186/s12969-017-0219-4 RESEARCH ARTICLE Open Access Patient characteristics associated with response to NSAID monotherapy in children with systemic
JUVENILE DERMATOMYOSITIS
 JUVENILE DERMATOMYOSITIS - how to diagnose, how to treat? Miloš Nikolić, MD, PhD Professor and Chairman Department of Dermatology, Division of Pediatric Dermatology University of Belgrade, School of Medicine,
JUVENILE DERMATOMYOSITIS - how to diagnose, how to treat? Miloš Nikolić, MD, PhD Professor and Chairman Department of Dermatology, Division of Pediatric Dermatology University of Belgrade, School of Medicine,
Recent advances in management of Pulmonary Vasculitis. Dr Nita MB
 Recent advances in management of Pulmonary Vasculitis Dr Nita MB 23-01-2015 Overview of the seminar Recent classification of Vasculitis What is new in present classification? Trials on remission induction
Recent advances in management of Pulmonary Vasculitis Dr Nita MB 23-01-2015 Overview of the seminar Recent classification of Vasculitis What is new in present classification? Trials on remission induction
4/16/2018. Demystifying weakness: how to approach refractory myositis. Objectives. Disclosures. Off-label uses for medications will be discussed
 Demystifying weakness: how to approach refractory myositis Jemima Albayda, MD Assistant Professor Johns Hopkins Myositis center Disclosures Off-label uses for medications will be discussed Objectives To
Demystifying weakness: how to approach refractory myositis Jemima Albayda, MD Assistant Professor Johns Hopkins Myositis center Disclosures Off-label uses for medications will be discussed Objectives To
Drug Class Prior Authorization Criteria Immune Globulins
 Drug Class Prior Authorization Criteria Immune Globulins Line of Business: Medicaid P & T Approval Date: August 16, 2017 Effective Date: August 16, 2017 This policy has been developed through review of
Drug Class Prior Authorization Criteria Immune Globulins Line of Business: Medicaid P & T Approval Date: August 16, 2017 Effective Date: August 16, 2017 This policy has been developed through review of
New Evidence reports on presentations given at EULAR Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis
 New Evidence reports on presentations given at EULAR 2011 Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis Report on EULAR 2011 presentations Anti-TNF failure and response to rituximab
New Evidence reports on presentations given at EULAR 2011 Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis Report on EULAR 2011 presentations Anti-TNF failure and response to rituximab
CT findings in patients with Cabazitaxel induced pelvic pain and haematuria: a case series
 Malalagama et al. Cancer Imaging (2017) 17:17 DOI 10.1186/s40644-017-0119-3 CASE SERIES CT findings in patients with Cabazitaxel induced pelvic pain and haematuria: a case series Geethal N. Malalagama
Malalagama et al. Cancer Imaging (2017) 17:17 DOI 10.1186/s40644-017-0119-3 CASE SERIES CT findings in patients with Cabazitaxel induced pelvic pain and haematuria: a case series Geethal N. Malalagama
Additional file 2: Details of cohort studies and randomised trials
 Reference Randomised trials Ye et al. 2001 Abstract 274 R=1 WD=0 Design, numbers, treatments, duration Randomised open comparison of: (45 patients) 1.5 g for 3, 1 g for 3, then 0.5 to 0.75 g IV cyclophosphamide
Reference Randomised trials Ye et al. 2001 Abstract 274 R=1 WD=0 Design, numbers, treatments, duration Randomised open comparison of: (45 patients) 1.5 g for 3, 1 g for 3, then 0.5 to 0.75 g IV cyclophosphamide
Subcutaneous Immune Globulin: Alternative Therapeutic Pathway for Patients With Primary Immunodeficiency
 Subcutaneous Immune Globulin: Alternative Therapeutic Pathway for Patients With Primary Immunodeficiency EDUCATIONAL OBJECTIVES Upon completion of this program, participants should be better able to: 1.
Subcutaneous Immune Globulin: Alternative Therapeutic Pathway for Patients With Primary Immunodeficiency EDUCATIONAL OBJECTIVES Upon completion of this program, participants should be better able to: 1.
Subcutaneous immunoglobulin therapy: a new option for patients with primary immunodeficiency diseases. Mai Thị Bích Ngọc
 Subcutaneous immunoglobulin therapy: a new option for patients with primary immunodeficiency diseases Mai Thị Bích Ngọc Background Primary immunodeficiency diseases (PIDD): group of over 150 disorders
Subcutaneous immunoglobulin therapy: a new option for patients with primary immunodeficiency diseases Mai Thị Bích Ngọc Background Primary immunodeficiency diseases (PIDD): group of over 150 disorders
The Hospital for Sick Children Technology Assessment at SickKids (TASK)
 The Hospital for Sick Children Technology Assessment at SickKids (TASK) THE USE OF BIOLOGIC RESPONSE MODIFIERS IN POLYARTICULAR-COURSE JUVENILE IDIOPATHIC ARTHRITIS Report No. 2010-01 Date: January 11,
The Hospital for Sick Children Technology Assessment at SickKids (TASK) THE USE OF BIOLOGIC RESPONSE MODIFIERS IN POLYARTICULAR-COURSE JUVENILE IDIOPATHIC ARTHRITIS Report No. 2010-01 Date: January 11,
Dosing schedules for IVIG: The use of an algorithm as a suggestion for personalized dosing
 Dosing schedules for IVIG: The use of an algorithm as a suggestion for personalized dosing 1 Disclosure The presentation contains information outside the labelled indication for intravenous immunoglobulin
Dosing schedules for IVIG: The use of an algorithm as a suggestion for personalized dosing 1 Disclosure The presentation contains information outside the labelled indication for intravenous immunoglobulin
Horizon Scanning Technology Summary. Abatacept (Orencia) for juvenile idiopathic arthritis. National Horizon Scanning Centre.
 Horizon Scanning Technology Summary National Horizon Scanning Centre Abatacept (Orencia) for juvenile idiopathic arthritis June 2007 This technology summary is based on information available at the time
Horizon Scanning Technology Summary National Horizon Scanning Centre Abatacept (Orencia) for juvenile idiopathic arthritis June 2007 This technology summary is based on information available at the time
Intravenous Immune Globulin in Amyopathic Dermatomyositis - Report of Two Cases and Review of the Literature
 Send Orders for Reprints to reprints@benthamscience.ae The Open Rheumatology Journal, 2015, 9, 77-81 77 Open Access Intravenous Immune Globulin in Amyopathic Dermatomyositis - Report of Two Cases and Review
Send Orders for Reprints to reprints@benthamscience.ae The Open Rheumatology Journal, 2015, 9, 77-81 77 Open Access Intravenous Immune Globulin in Amyopathic Dermatomyositis - Report of Two Cases and Review
Emerging Therapies for Lung Fibrosis. Helen Garthwaite Respiratory Registrar/ Clinical Research Fellow
 Emerging Therapies for Lung Fibrosis Helen Garthwaite Respiratory Registrar/ Clinical Research Fellow Lung Fibrosis/Interstitial Lung Disease Disease that affects the tissue that supports the lungs alveoli
Emerging Therapies for Lung Fibrosis Helen Garthwaite Respiratory Registrar/ Clinical Research Fellow Lung Fibrosis/Interstitial Lung Disease Disease that affects the tissue that supports the lungs alveoli
IMMUNOGLOBULIN REPLACEMENT THERAPY: ONE SIZE DOESN T FIT ALL
 PRIMARY IMMUNODEFICIENCIES IMMUNOGLOBULINS: ONE SIZE DOESN T FIT ALL IMMUNOGLOBULIN REPLACEMENT THERAPY: ONE SIZE DOESN T FIT ALL 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS IG IPOPI IV PID SC Immunoglobulins
PRIMARY IMMUNODEFICIENCIES IMMUNOGLOBULINS: ONE SIZE DOESN T FIT ALL IMMUNOGLOBULIN REPLACEMENT THERAPY: ONE SIZE DOESN T FIT ALL 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS IG IPOPI IV PID SC Immunoglobulins
Coverage Criteria: Express Scripts, Inc. monograph dated 12/15/ months or as otherwise noted by indication
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
Horizon Scanning Technology Summary. Adalimumab (Humira) for juvenile idiopathic arthritis. National Horizon Scanning Centre.
 Horizon Scanning Technology Summary National Horizon Scanning Centre Adalimumab (Humira) for juvenile idiopathic arthritis June 2007 This technology summary is based on information available at the time
Horizon Scanning Technology Summary National Horizon Scanning Centre Adalimumab (Humira) for juvenile idiopathic arthritis June 2007 This technology summary is based on information available at the time
IMMUNE GLOBULIN (IVIG AND SCIG) Brand Name Generic Name Length of Authorization Bivigam IVIG Per Medical Guidelines Carimune IVIG Per Medical
 Brand Name Generic Name Length of Authorization Bivigam IVIG Per Medical Guidelines Carimune IVIG Per Medical Guidelines Flebogamma IVIG Per Medical Guidelines Gammagard IVIG/SCIG Per Medical Guidelines
Brand Name Generic Name Length of Authorization Bivigam IVIG Per Medical Guidelines Carimune IVIG Per Medical Guidelines Flebogamma IVIG Per Medical Guidelines Gammagard IVIG/SCIG Per Medical Guidelines
Acute and chronic treatments
 21st Annual Meeting of the Swiss Stroke Society Lausanne, 11 January 2018 Vasculitis and stroke : Acute and chronic treatments Pr Mathieu ZUBER Service de Neurologie et NeuroVasculaire Groupe Hospitalier
21st Annual Meeting of the Swiss Stroke Society Lausanne, 11 January 2018 Vasculitis and stroke : Acute and chronic treatments Pr Mathieu ZUBER Service de Neurologie et NeuroVasculaire Groupe Hospitalier
ANCA+ VASCULITIDES CYCAZAREM,
 ANCA+ VASCULITIDES CYCAZAREM, q Comparison of 3 to 6 mo. oral CYC + CS then azathioprine or oral CYC for 12 mo.+ 10 mg/d CS. After 12 mo all the patients were treated with azathioprine q 150 patients followed
ANCA+ VASCULITIDES CYCAZAREM, q Comparison of 3 to 6 mo. oral CYC + CS then azathioprine or oral CYC for 12 mo.+ 10 mg/d CS. After 12 mo all the patients were treated with azathioprine q 150 patients followed
UNFOLDING NATURE S ORIGAMI: MEDICAL TREATMENT OF TAKAYASU ARTERITIS AND GIANT CELL ARTERITIS
 UNFOLDING NATURE S ORIGAMI: MEDICAL TREATMENT OF TAKAYASU ARTERITIS AND GIANT CELL ARTERITIS CanVasc meeting Montreal Nov 22 2012 Patrick Liang Service de rhumatologie Centre Hospitalier Universitaire
UNFOLDING NATURE S ORIGAMI: MEDICAL TREATMENT OF TAKAYASU ARTERITIS AND GIANT CELL ARTERITIS CanVasc meeting Montreal Nov 22 2012 Patrick Liang Service de rhumatologie Centre Hospitalier Universitaire
Treatment pathway for adult patients with immune (idiopathic) thrombocytopenic purpura (ITP)
 Prescribing Clinical Network Surrey (East Surrey CCG, Guildford & Waverley CCG, North West Surrey CCG, Surrey Downs CCG & Surrey Heath CCG) Crawley and Horsham & Mid-Sussex CCG Treatment pathway for adult
Prescribing Clinical Network Surrey (East Surrey CCG, Guildford & Waverley CCG, North West Surrey CCG, Surrey Downs CCG & Surrey Heath CCG) Crawley and Horsham & Mid-Sussex CCG Treatment pathway for adult
Favorable rituximab response in patients with refractory idiopathic inflammatory myopathies
 de Souza et al. Advances in Rheumatology (2018) 58:31 https://doi.org/10.1186/s42358-018-0030-z Advances in Rheumatology RESEARCH Favorable rituximab response in patients with refractory idiopathic inflammatory
de Souza et al. Advances in Rheumatology (2018) 58:31 https://doi.org/10.1186/s42358-018-0030-z Advances in Rheumatology RESEARCH Favorable rituximab response in patients with refractory idiopathic inflammatory
ENFERMEDADES AUTOINMUNES SISTÉMICAS. Dr. J. María Pego Reigosa
 ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. J. María Pego Reigosa ABSTRACT NUMBER: 888 PHASE 3 TRIAL RESULTS WITH BLISIBIMOD, A SELECTIVE INHIBITOR OF B-CELL ACTIVATING FACTOR, IN SUBJECTS WITH MODERATE-TO-SEVERE
ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. J. María Pego Reigosa ABSTRACT NUMBER: 888 PHASE 3 TRIAL RESULTS WITH BLISIBIMOD, A SELECTIVE INHIBITOR OF B-CELL ACTIVATING FACTOR, IN SUBJECTS WITH MODERATE-TO-SEVERE
TREATMENT OF ANCA-ASSOCIATED VASCULITIS
 TREATMENT OF ANCA-ASSOCIATED VASCULITIS Loïc Guillevin Hôpital Cochin, Université Paris Descartes Cours DU, 11 mars 2016 1 Disclosure of interest regarding this presentation Roche has provided, in part,
TREATMENT OF ANCA-ASSOCIATED VASCULITIS Loïc Guillevin Hôpital Cochin, Université Paris Descartes Cours DU, 11 mars 2016 1 Disclosure of interest regarding this presentation Roche has provided, in part,
Dermatomyositis Advice from Experts: Improving Your Medical Dermatology Diagnostic and Management Skills Jeffrey P. Callen, MD Professor of Medicine
 Dermatomyositis Advice from Experts: Improving Your Medical Dermatology Diagnostic and Management Skills Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville Learning Objectives
Dermatomyositis Advice from Experts: Improving Your Medical Dermatology Diagnostic and Management Skills Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville Learning Objectives
Dermatomyositis with Rapidly Progressive Interstitial Lung Disease Treated with Rituximab: A Report of 3 Cases in Japan
 CASE REPORT Dermatomyositis with Rapidly Progressive Interstitial Lung Disease Treated with Rituximab: A Report of 3 Cases in Japan Kenichiro Tokunaga 1 and Noboru Hagino 2 Abstract We performed a retrospective
CASE REPORT Dermatomyositis with Rapidly Progressive Interstitial Lung Disease Treated with Rituximab: A Report of 3 Cases in Japan Kenichiro Tokunaga 1 and Noboru Hagino 2 Abstract We performed a retrospective
Reviewer No. 2 checklist for: DMARDS Review for children. In the WHO Essential Medicines List
 Reviewer No. 2 checklist for: DMARDS Review for children In the WHO Essential Medicines List (1) Have all important studies that you are aware of been included? (2) Is there adequate evidence of efficacy
Reviewer No. 2 checklist for: DMARDS Review for children In the WHO Essential Medicines List (1) Have all important studies that you are aware of been included? (2) Is there adequate evidence of efficacy
The many faces of myositis. Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands
 The many faces of myositis Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands Outline of the presentation Classification Diagnosis Therapy Prognosis Diagnostic criteria
The many faces of myositis Marianne de Visser Academic Medical Centre Dept of Neurology Amsterdam The Netherlands Outline of the presentation Classification Diagnosis Therapy Prognosis Diagnostic criteria
MEDICATIONS: THE GOOD, THE BAD, THE UGLY
 MEDICATIONS: THE GOOD, THE BAD, THE UGLY July 13, 2013 Dr. Tanaz Kermani Assistant Clinical Professor of Medicine, Division of Rheumatology, David Geffen School of Medicine UCLA Dr. Robert Spiera Professor
MEDICATIONS: THE GOOD, THE BAD, THE UGLY July 13, 2013 Dr. Tanaz Kermani Assistant Clinical Professor of Medicine, Division of Rheumatology, David Geffen School of Medicine UCLA Dr. Robert Spiera Professor
Scottish Medicines Consortium
 Scottish Medicines Consortium romiplostim, 250 microgram vial of powder for solution for subcutaneous injection (Nplate ) No. (553/09) Amgen 08 May 2009 (Issued 4 September 2009) The Scottish Medicines
Scottish Medicines Consortium romiplostim, 250 microgram vial of powder for solution for subcutaneous injection (Nplate ) No. (553/09) Amgen 08 May 2009 (Issued 4 September 2009) The Scottish Medicines
thrombopoietin receptor agonists and University of Washington January 13, 2012
 Tickle me eltrombopag: thrombopoietin receptor agonists and the regulation of platelet production Manoj Menon University of Washington January 13, 2012 Outline Clinical case Pathophysiology of ITP Therapeutic
Tickle me eltrombopag: thrombopoietin receptor agonists and the regulation of platelet production Manoj Menon University of Washington January 13, 2012 Outline Clinical case Pathophysiology of ITP Therapeutic
Case Report High-Dose Subcutaneous Immunoglobulins for the Treatment of Severe Treatment-Resistant Polymyositis
 Case Reports in Rheumatology, Article ID 458231, 4 pages http://dx.doi.org/10.1155/2014/458231 Case Report High-Dose Subcutaneous Immunoglobulins for the Treatment of Severe Treatment-Resistant Polymyositis
Case Reports in Rheumatology, Article ID 458231, 4 pages http://dx.doi.org/10.1155/2014/458231 Case Report High-Dose Subcutaneous Immunoglobulins for the Treatment of Severe Treatment-Resistant Polymyositis
Subcutaneous ImmunoglobulinTherapy A New Way of Permanent Treatment in Primary Immunodeficiencies Gaby Strotmann
 Subcutaneous ImmunoglobulinTherapy A New Way of Permanent Treatment in Primary Immunodeficiencies Gaby Strotmann Immunodeficiency Department University Children s Hospital Dr. von Haunersches Kinderspital
Subcutaneous ImmunoglobulinTherapy A New Way of Permanent Treatment in Primary Immunodeficiencies Gaby Strotmann Immunodeficiency Department University Children s Hospital Dr. von Haunersches Kinderspital
budesonide, 3mg, gastro-resistant capsules (Budenofalk ) SMC No. (1043/15) Dr Falk Pharma UK Ltd
 budesonide, 3mg, gastro-resistant capsules (Budenofalk ) SMC No. (1043/15) Dr Falk Pharma UK Ltd 10 April 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
budesonide, 3mg, gastro-resistant capsules (Budenofalk ) SMC No. (1043/15) Dr Falk Pharma UK Ltd 10 April 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
Scottish Medicines Consortium
 Scottish Medicines Consortium eltrombopag, 25mg and 50mg film-coated tablets (Revolade ) No. (625/10) GlaxoSmithKline UK 09 July 2010 The Scottish Medicines Consortium (SMC) has completed its assessment
Scottish Medicines Consortium eltrombopag, 25mg and 50mg film-coated tablets (Revolade ) No. (625/10) GlaxoSmithKline UK 09 July 2010 The Scottish Medicines Consortium (SMC) has completed its assessment
TITLE: Rituximab for Granulomatosis with Polyangiitis or Microscopic Polyangiitis: A Review of the Clinical and Cost-effectiveness
 TITLE: Rituximab for Granulomatosis with Polyangiitis or Microscopic Polyangiitis: A Review of the Clinical and Cost-effectiveness DATE: 28 January 2015 CONTEXT AND POLICY ISSUES Granulomatosis with polyangiitis
TITLE: Rituximab for Granulomatosis with Polyangiitis or Microscopic Polyangiitis: A Review of the Clinical and Cost-effectiveness DATE: 28 January 2015 CONTEXT AND POLICY ISSUES Granulomatosis with polyangiitis
Subject: Remicade (Page 1 of 5)
 Subject: Remicade (Page 1 of 5) Objective: I. To ensure that Health Share/Tuality Health Alliance (THA) has a process by which the appropriate utilization of Remicade (Infliximab) for members whose diagnosis
Subject: Remicade (Page 1 of 5) Objective: I. To ensure that Health Share/Tuality Health Alliance (THA) has a process by which the appropriate utilization of Remicade (Infliximab) for members whose diagnosis
Childhood Primary Central Nervous System Vascultis Treatment Protocols
 Childhood Primary Central Nervous System Vascultis Treatment Protocols Last updated November 2015 Non-progressive large vessel primary CNS vasculitis* Adjunctive immunosuppression f 3 months IV Methylprednisolone
Childhood Primary Central Nervous System Vascultis Treatment Protocols Last updated November 2015 Non-progressive large vessel primary CNS vasculitis* Adjunctive immunosuppression f 3 months IV Methylprednisolone
EudraCT number: Page 8 of 42
 EudraCT number: 2012-001102-14 Page 8 of 42 5 Trial Synopsis Title Sponsor name North American Sponsor Disease Under Investigation An international, open label, randomised, controlled trial comparing rituximab
EudraCT number: 2012-001102-14 Page 8 of 42 5 Trial Synopsis Title Sponsor name North American Sponsor Disease Under Investigation An international, open label, randomised, controlled trial comparing rituximab
ENFERMEDADES AUTOINMUNES SISTÉMICAS. Dr. José María Pego Reigosa
 ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. José María Pego Reigosa ABSTRACT NUMBER: 2754 Comparison of Individually Tailored vs Systematic Rituximab Regimens to Maintain ANCA-Associated Vasculitis Remissions:
ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. José María Pego Reigosa ABSTRACT NUMBER: 2754 Comparison of Individually Tailored vs Systematic Rituximab Regimens to Maintain ANCA-Associated Vasculitis Remissions:
Novel Therapies in Autoimmune Hepatitis
 Novel Therapies in Autoimmune Hepatitis Paul W. Rassam,MD Ass. Clinical Professor of Medicine Div. of Gastroenterology and Hepatology St George Hospital University Medical Center University of Balamand
Novel Therapies in Autoimmune Hepatitis Paul W. Rassam,MD Ass. Clinical Professor of Medicine Div. of Gastroenterology and Hepatology St George Hospital University Medical Center University of Balamand
Ig Therapy: One Size Does Not Fit All
 Ig Therapy: One Size Does Not Fit All Carla Duff, CPNP, MSN, IgCN Advanced Registered Nurse Practitioner University of South Florida Division of Allergy, Immunology, and Rheumatology 1 Objectives Understand
Ig Therapy: One Size Does Not Fit All Carla Duff, CPNP, MSN, IgCN Advanced Registered Nurse Practitioner University of South Florida Division of Allergy, Immunology, and Rheumatology 1 Objectives Understand
FOR PUBLIC CONSULTATION ONLY. Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD)
 Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD) NHS England FOR PUBLIC CONSULTATION ONLY Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4- RD) First published:
Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4-RD) NHS England FOR PUBLIC CONSULTATION ONLY Evidence Review: Rituximab for immunoglobulin G4-related disease (IgG4- RD) First published:
Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience
 Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience References Sanna G, Bertolaccini ML. Neuropsychiatric manifestations
Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience References Sanna G, Bertolaccini ML. Neuropsychiatric manifestations
The CARI Guidelines Caring for Australasians with Renal Impairment. Idiopathic membranous nephropathy: use of other therapies GUIDELINES
 Idiopathic membranous nephropathy: use of other therapies Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES No recommendations possible based on Level I or II evidence
Idiopathic membranous nephropathy: use of other therapies Date written: July 2005 Final submission: September 2005 Author: Merlin Thomas GUIDELINES No recommendations possible based on Level I or II evidence
Definitions. Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency)
 CROHN S DISEASE Definitions Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency) Recurrence: The reappearance of lesions after surgical resection Endoscopic remission:
CROHN S DISEASE Definitions Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency) Recurrence: The reappearance of lesions after surgical resection Endoscopic remission:
LONGITUDINAL TREATMENT PATTERNS AND ASSOCIATED OUTCOMES IN PATIENTS WITH NEWLY DIAGNOSED SYSTEMIC LUPUS ERYTHEMATOSUS. Hong Kan 7/12/2016
 LONGITUDINAL TREATMENT PATTERNS AND ASSOCIATED OUTCOMES IN PATIENTS WITH NEWLY DIAGNOSED SYSTEMIC LUPUS ERYTHEMATOSUS Hong Kan 7/12/2016 1 Acknowledgements Research conceptualization and design, programming
LONGITUDINAL TREATMENT PATTERNS AND ASSOCIATED OUTCOMES IN PATIENTS WITH NEWLY DIAGNOSED SYSTEMIC LUPUS ERYTHEMATOSUS Hong Kan 7/12/2016 1 Acknowledgements Research conceptualization and design, programming
Alternative scoring of the cutaneous assessment tool in juvenile dermatomyositis: Results using abbreviated formats
 Himmelfarb Health Sciences Library, The George Washington University Health Sciences Research Commons Rheumatology Faculty Publications Medicine 3-15-2008 Alternative scoring of the cutaneous assessment
Himmelfarb Health Sciences Library, The George Washington University Health Sciences Research Commons Rheumatology Faculty Publications Medicine 3-15-2008 Alternative scoring of the cutaneous assessment
Myositis and Your Lungs
 Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Abatacept (Orencia) for active rheumatoid arthritis. August 2009
 Abatacept (Orencia) for active rheumatoid arthritis August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
Abatacept (Orencia) for active rheumatoid arthritis August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
BIOLOGIC THERAPY : A NEW OPTION FOR TREATMENT JUVENILE IDIOPATHIC ARTHRITIS DR TON THAT HOANG
 BIOLOGIC THERAPY : A NEW OPTION FOR TREATMENT JUVENILE IDIOPATHIC ARTHRITIS DR TON THAT HOANG INTRODUCTION JIA is the most common chronic rheumatic inflammatory disease of childhood. If not successfully
BIOLOGIC THERAPY : A NEW OPTION FOR TREATMENT JUVENILE IDIOPATHIC ARTHRITIS DR TON THAT HOANG INTRODUCTION JIA is the most common chronic rheumatic inflammatory disease of childhood. If not successfully
Childhood Primary Central Nervous System Vascultis Treatment Protocols
 Childhood Primary Central Nervous System Vascultis Treatment Protocols Last updated December 2014 Non-progressive large vessel primary CNS vasculitis* Adjunctive immunosuppression f 3 months IV Methylprednisolone
Childhood Primary Central Nervous System Vascultis Treatment Protocols Last updated December 2014 Non-progressive large vessel primary CNS vasculitis* Adjunctive immunosuppression f 3 months IV Methylprednisolone
CENTENE PHARMACY AND THERAPEUTICS DRUG REVIEW 1Q18 January February
 BRAND NAME Soliris GENERIC NAME Eculizumab MANUFACTURER Alexion Pharmaceuticals, Inc. DATE OF APPROVAL October 23, 2017 PRODUCT LAUNCH DATE Currently commercially available REVIEW TYPE Review type 1 (RT1):
BRAND NAME Soliris GENERIC NAME Eculizumab MANUFACTURER Alexion Pharmaceuticals, Inc. DATE OF APPROVAL October 23, 2017 PRODUCT LAUNCH DATE Currently commercially available REVIEW TYPE Review type 1 (RT1):
Efficacy and Safety of Rituximab in the Treatment of Rheumatoid Arthritis and ANCA-associated Vasculitis
 New Evidence reports on presentations given at ACR/ARHP 2010 Efficacy and Safety of Rituximab in the Treatment of Rheumatoid Arthritis and ANCA-associated Vasculitis Report on ACR/ARHP 2010 presentations
New Evidence reports on presentations given at ACR/ARHP 2010 Efficacy and Safety of Rituximab in the Treatment of Rheumatoid Arthritis and ANCA-associated Vasculitis Report on ACR/ARHP 2010 presentations
Clinical Characteristics of Children With Juvenile Dermatomyositis: The Childhood Arthritis and Rheumatology Research Alliance Registry
 Arthritis Care & Research Vol. 66, No. 3, March 2014, pp 404 410 DOI 10.1002/acr.22142 2014, American College of Rheumatology ORIGINAL ARTICLE Clinical Characteristics of Children With Juvenile Dermatomyositis:
Arthritis Care & Research Vol. 66, No. 3, March 2014, pp 404 410 DOI 10.1002/acr.22142 2014, American College of Rheumatology ORIGINAL ARTICLE Clinical Characteristics of Children With Juvenile Dermatomyositis:
Cost-Motivated Treatment Changes in Medicare Part B:
 Cost-Motivated Treatment Changes in Medicare Part B: Implications for Non- Medical Switching September 2016 THE MORAN COMPANY 1 Cost-Motivated Treatment Changes in Medicare Part B: Implications for Non-Medical
Cost-Motivated Treatment Changes in Medicare Part B: Implications for Non- Medical Switching September 2016 THE MORAN COMPANY 1 Cost-Motivated Treatment Changes in Medicare Part B: Implications for Non-Medical
Treatment of Rheumatoid Arthritis: The Past, the Present and the Future
 Treatment of Rheumatoid Arthritis: The Past, the Present and the Future Lai-Ling Winchow FCP(SA) Cert Rheum(SA) Chris Hani Baragwanath Academic Hospital University of the Witwatersrand Outline of presentation
Treatment of Rheumatoid Arthritis: The Past, the Present and the Future Lai-Ling Winchow FCP(SA) Cert Rheum(SA) Chris Hani Baragwanath Academic Hospital University of the Witwatersrand Outline of presentation
Answers to Self Assessment Questions
 Answers to Self Assessment Questions 1. Which of the following findings is supportive of the diagnosis of multifocal motor neuropathy (MMN): A. Absence of conduction block (CB) on nerve conduction studies
Answers to Self Assessment Questions 1. Which of the following findings is supportive of the diagnosis of multifocal motor neuropathy (MMN): A. Absence of conduction block (CB) on nerve conduction studies
Juvenile idiopathic arthritis managed in the new millennium: one year outcomes of an inception cohort of Australian children
 Tiller et al. Pediatric Rheumatology (2018) 16:69 https://doi.org/10.1186/s12969-018-0288-z RESEARCH ARTICLE Open Access Juvenile idiopathic arthritis managed in the new millennium: one year outcomes of
Tiller et al. Pediatric Rheumatology (2018) 16:69 https://doi.org/10.1186/s12969-018-0288-z RESEARCH ARTICLE Open Access Juvenile idiopathic arthritis managed in the new millennium: one year outcomes of
SYNOPSIS (PROTOCOL WX17796)
 TITLE OF THE STUDY A prospective, randomized, double-blind, placebo-controlled, parallel group, multicenter, 52-week trial to assess the efficacy and safety of adjunct MMF to achieve remission with reduced
TITLE OF THE STUDY A prospective, randomized, double-blind, placebo-controlled, parallel group, multicenter, 52-week trial to assess the efficacy and safety of adjunct MMF to achieve remission with reduced
DocSpot what patients want to know
 DocSpot what patients want to know Professor Chris Denton Royal Free Hospital London, UK Madrid, February 2012 Copyright 2011 Raynaud's & Scleroderma Association. Charity Reg. No. 326306 DocSpot Live!
DocSpot what patients want to know Professor Chris Denton Royal Free Hospital London, UK Madrid, February 2012 Copyright 2011 Raynaud's & Scleroderma Association. Charity Reg. No. 326306 DocSpot Live!
Scottish Medicines Consortium
 Scottish Medicines Consortium abatacept, 250mg powder for concentrate for solution (Orencia ) No. (400/07) Bristol Myers Squibb Pharmaceuticals Ltd 10 August 2007 The Scottish Medicines Consortium has
Scottish Medicines Consortium abatacept, 250mg powder for concentrate for solution (Orencia ) No. (400/07) Bristol Myers Squibb Pharmaceuticals Ltd 10 August 2007 The Scottish Medicines Consortium has
New Drugs for Uveitis. Medical Eye Unit St Thomas Hospital
 New Drugs for Uveitis Miles Stanford Medical Eye Unit St Thomas Hospital x Epithelium x x Antigen Y Y Y Y IgG m cd4 IL-2 Y m + IL-12 Cytotoxic T B pmn Ig s PG s. LTB4 O - IL-6 TNFα IFNγγ IL-2 Th1 IL-10
New Drugs for Uveitis Miles Stanford Medical Eye Unit St Thomas Hospital x Epithelium x x Antigen Y Y Y Y IgG m cd4 IL-2 Y m + IL-12 Cytotoxic T B pmn Ig s PG s. LTB4 O - IL-6 TNFα IFNγγ IL-2 Th1 IL-10
Position Statement - Subcutaneous Immunoglobulin (SCIg)
 Position Statement - Subcutaneous Immunoglobulin (SCIg) Introduction Immunoglobulin replacement therapy (IRT) is used to treat adults and children with primary immune deficiencies (and other medical conditions).
Position Statement - Subcutaneous Immunoglobulin (SCIg) Introduction Immunoglobulin replacement therapy (IRT) is used to treat adults and children with primary immune deficiencies (and other medical conditions).
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 3 October 2012
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 3 October 2012 REMICADE 100 mg, powder for concentrate for solution for infusion B/1 vial (CIP code: 562 070-1) Applicant:
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 3 October 2012 REMICADE 100 mg, powder for concentrate for solution for infusion B/1 vial (CIP code: 562 070-1) Applicant:
Idiopathic inflammatory myopathies
 Myositis and cancer Idiopathic inflammatory myopathies Primary idiopathic polymyositis Primary idiopathic dermatomyositis Juvenile poly/dermatomyositis Myositis associated with another CTD Myositis associated
Myositis and cancer Idiopathic inflammatory myopathies Primary idiopathic polymyositis Primary idiopathic dermatomyositis Juvenile poly/dermatomyositis Myositis associated with another CTD Myositis associated
IVIG (intravenous immunoglobulin) Bivigam, Carimune NF, Flebogamma, Gammagard, Gammagard S/D, Gammaked, Gammaplex, Gamunex-C, Octagam, Privigen
 Pre - PA Allowance None Prior-Approval Requirements Diagnoses Patient must have ONE of the following documented indications: 1. Primary Immunodeficiency Disease (PID) with ONE of the a. Hypogammaglobulinemia,
Pre - PA Allowance None Prior-Approval Requirements Diagnoses Patient must have ONE of the following documented indications: 1. Primary Immunodeficiency Disease (PID) with ONE of the a. Hypogammaglobulinemia,
Sarcoidosis Case. Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA. WASOG: educational material
 Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Initial intravenous immunoglobulin doses should be based on adjusted body weight in obese patients with primary immunodeficiency disorders
 Ameratunga Allergy Asthma Clin Immunol (2017) 13:47 DOI 10.1186/s13223-017-0220-y Allergy, Asthma & Clinical Immunology CASE REPORT Open Access Initial intravenous immunoglobulin doses should be based
Ameratunga Allergy Asthma Clin Immunol (2017) 13:47 DOI 10.1186/s13223-017-0220-y Allergy, Asthma & Clinical Immunology CASE REPORT Open Access Initial intravenous immunoglobulin doses should be based
Pregabalin prescription for terminally ill cancer patients receiving specialist palliative care in an acute hospital
 Yajima et al. Journal of Pharmaceutical Health Care and Sciences (2016) 2:29 DOI 10.1186/s40780-016-0063-6 RESEARCH ARTICLE Open Access Pregabalin prescription for terminally ill cancer patients receiving
Yajima et al. Journal of Pharmaceutical Health Care and Sciences (2016) 2:29 DOI 10.1186/s40780-016-0063-6 RESEARCH ARTICLE Open Access Pregabalin prescription for terminally ill cancer patients receiving
EudraCT number: Page 9 of 46
 EudraCT number: 2012-001102-14 Page 9 of 46 5 Trial Synopsis Title Sponsor name North American Sponsor Japan Sponsor Ireland Sponsor Disease Under Investigation An international, open label, randomised,
EudraCT number: 2012-001102-14 Page 9 of 46 5 Trial Synopsis Title Sponsor name North American Sponsor Japan Sponsor Ireland Sponsor Disease Under Investigation An international, open label, randomised,
SYSTEMIC LUPUS ERYTHEMATOSUS: CURRENT CONCEPTS AND CLINICAL PEARLS. Dr Sheila Vasoo Consultant Division of Rheumatology NUHS
 SYSTEMIC LUPUS ERYTHEMATOSUS: CURRENT CONCEPTS AND CLINICAL PEARLS Dr Sheila Vasoo Consultant Division of Rheumatology NUHS Listen to the Patient Concepts Diagnosis Immunopathogenesis Clinical Pearls Disease
SYSTEMIC LUPUS ERYTHEMATOSUS: CURRENT CONCEPTS AND CLINICAL PEARLS Dr Sheila Vasoo Consultant Division of Rheumatology NUHS Listen to the Patient Concepts Diagnosis Immunopathogenesis Clinical Pearls Disease
Moderately to severely active ulcerative colitis
 Adalimumab in the Treatment of Moderate-to-Severe Ulcerative Colitis: ULTRA 2 Trial Results Sandborn WJ, van Assche G, Reinisch W, et al. Adalimumab induces and maintains clinical remission in patients
Adalimumab in the Treatment of Moderate-to-Severe Ulcerative Colitis: ULTRA 2 Trial Results Sandborn WJ, van Assche G, Reinisch W, et al. Adalimumab induces and maintains clinical remission in patients
A. B. Orandi 1*, K. W. Baszis 1, V. R. Dharnidharka 2, A. M. Huber 3, and M. F. Hoeltzel 4 for the CARRA Juvenile Myositis subgroup
 Orandi et al. Pediatric Rheumatology (2017) 15:71 DOI 10.1186/s12969-017-0199-4 RESEARCH ARTICLE Open Access Assessment, classification and treatment of calcinosis as a complication of juvenile dermatomyositis:
Orandi et al. Pediatric Rheumatology (2017) 15:71 DOI 10.1186/s12969-017-0199-4 RESEARCH ARTICLE Open Access Assessment, classification and treatment of calcinosis as a complication of juvenile dermatomyositis:
Evolving Uses of IVIG in myositis
 Evolving Uses of IVIG in myositis Rossitza I. Chichkova, MD, MS Associate Professor Depts of Neurology and Internal Medicine University of South Florida, Tampa, FL Immune Function In Normal State: Protects
Evolving Uses of IVIG in myositis Rossitza I. Chichkova, MD, MS Associate Professor Depts of Neurology and Internal Medicine University of South Florida, Tampa, FL Immune Function In Normal State: Protects
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU
 Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Canadian Society of Internal Medicine Annual Meeting 2016 Montreal, QC
 Canadian Society of Internal Medicine Annual Meeting 2016 Montreal, QC Update on the Treatment of Rheumatoid Arthritis Sabrina Fallavollita MDCM McGill University Canadian Society of Internal Medicine
Canadian Society of Internal Medicine Annual Meeting 2016 Montreal, QC Update on the Treatment of Rheumatoid Arthritis Sabrina Fallavollita MDCM McGill University Canadian Society of Internal Medicine
Treatment of Susac s Syndrome (SS)
 Treatment of Susac s Syndrome (SS) Ideal Treatment of SS Ideally, treatment of SS should be based on: An accurate understanding of the immunopathogenesis (cause) of the disease. An accurate understanding
Treatment of Susac s Syndrome (SS) Ideal Treatment of SS Ideally, treatment of SS should be based on: An accurate understanding of the immunopathogenesis (cause) of the disease. An accurate understanding
Research Article. Disease management in pediatric lupus: could it pose a burden?
 Disease management in pediatric lupus: could it pose a burden? Aims: To identify disease management-related activities that could pose a burden to patients with systemic lupus erythematosus (SLE) and their
Disease management in pediatric lupus: could it pose a burden? Aims: To identify disease management-related activities that could pose a burden to patients with systemic lupus erythematosus (SLE) and their
This month, we are very pleased to introduce some new tests for Scleroderma as well as some test changes to our existing scleroderma tests/panels.
 February 20, 2017 Client Letter Test Update February 2017 Dear Colleague: This month, we are very pleased to introduce some new tests for Scleroderma as well as some test changes to our existing scleroderma
February 20, 2017 Client Letter Test Update February 2017 Dear Colleague: This month, we are very pleased to introduce some new tests for Scleroderma as well as some test changes to our existing scleroderma
Long-term follow-up of sporadic inclusion body myositis treated with intravenous immunoglobulin: a retrospective study of 16 patients
 Long-term follow-up of sporadic inclusion body myositis treated with intravenous immunoglobulin: a retrospective study of 16 patients C. Dobloug, R. Walle-Hansen, J.T. Gran, Ø. Molberg Section of Rheumatology,
Long-term follow-up of sporadic inclusion body myositis treated with intravenous immunoglobulin: a retrospective study of 16 patients C. Dobloug, R. Walle-Hansen, J.T. Gran, Ø. Molberg Section of Rheumatology,
Uveitis unplugged: systemic therapy
 Uveitis unplugged: systemic therapy Hobart 2017 Peter McCluskey Save Sight Institute Sydney Eye Hospital Sydney Medical School University of Sydney Sydney Australia No financial or proprietary interest
Uveitis unplugged: systemic therapy Hobart 2017 Peter McCluskey Save Sight Institute Sydney Eye Hospital Sydney Medical School University of Sydney Sydney Australia No financial or proprietary interest
Evidence Review: Title. Month/ Year. Evidence Review:
 Evidence Review: Title Month/ Year Evidence Review: Rituximab for connective tissue disease associated interstitial lung disease October 2014 Standard Operating Procedure: NHS England Evidence Review:
Evidence Review: Title Month/ Year Evidence Review: Rituximab for connective tissue disease associated interstitial lung disease October 2014 Standard Operating Procedure: NHS England Evidence Review:
DRUG THERAPY
 www.pediatric-rheumathology.printo.it DRUG THERAPY NSAIDS NON-STEROIDAL ANTI-INFLAMMATORY DRUGS They are symptomatic anti-inflammatory, anti febrile (fever) and analgesic (pain reducing) medications. Symptomatic
www.pediatric-rheumathology.printo.it DRUG THERAPY NSAIDS NON-STEROIDAL ANTI-INFLAMMATORY DRUGS They are symptomatic anti-inflammatory, anti febrile (fever) and analgesic (pain reducing) medications. Symptomatic
Childhood Arthritis and Rheumatology Research Alliance consensus clinical treatment plans for juvenile dermatomyositis with skin predominant disease
 Kim et al. Pediatric Rheumatology (2017) 15:1 DOI 10.1186/s12969-016-0134-0 RESEARCH ARTICLE Open Access Childhood Arthritis and Rheumatology Research Alliance consensus clinical treatment plans for juvenile
Kim et al. Pediatric Rheumatology (2017) 15:1 DOI 10.1186/s12969-016-0134-0 RESEARCH ARTICLE Open Access Childhood Arthritis and Rheumatology Research Alliance consensus clinical treatment plans for juvenile
Regulatory Status FDA- approved indication: Simponi and Simponi ARIA are tumor necrosis factor (TNF) blockers indicated for the treatment of: (2-3)
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 9 Last Review Date: March 16, 2018 Simponi / Simponi
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.51 Subject: Simponi / Simponi ARIA Page: 1 of 9 Last Review Date: March 16, 2018 Simponi / Simponi
Scottish Medicines Consortium
 Scottish Medicines Consortium infliximab 100mg powder for intravenous infusion (Remicade ) No. (364/07) Schering-Plough UK Ltd 6 April 2007 The Scottish Medicines Consortium (SMC) has completed its assessment
Scottish Medicines Consortium infliximab 100mg powder for intravenous infusion (Remicade ) No. (364/07) Schering-Plough UK Ltd 6 April 2007 The Scottish Medicines Consortium (SMC) has completed its assessment
2013 National Treatment Survey. Immune Deficiency Foundation
 2013 National Treatment Survey Immune Deficiency Foundation IDF 2013 Treatment Survey Mail-based, pencil & paper survey Over 75 Main questions Survey in the field December 2013-March 2014 IDF mail invitation
2013 National Treatment Survey Immune Deficiency Foundation IDF 2013 Treatment Survey Mail-based, pencil & paper survey Over 75 Main questions Survey in the field December 2013-March 2014 IDF mail invitation
Significance of antibody testing in idiopathic inflammatory myopathies
 2/0/20 Significance of antibody testing in idiopathic inflammatory myopathies Jiří Vencovský Institute of Rheumatology, Prague Diagnosis Polymyositis Juvenile DM (JPM) Paraneoplastic Myositis in overlap
2/0/20 Significance of antibody testing in idiopathic inflammatory myopathies Jiří Vencovský Institute of Rheumatology, Prague Diagnosis Polymyositis Juvenile DM (JPM) Paraneoplastic Myositis in overlap
Case study 1: A Bayesian clinical trial in children with polyarteritis nodosa (PAN)
 Case study 1: A Bayesian clinical trial in children with polyarteritis nodosa (PAN) Catrin Tudur Smith Department of Biostatistics University of Liverpool cat1@liv.ac.uk CLINICAL TRIALS IN SMALL POPULATIONS
Case study 1: A Bayesian clinical trial in children with polyarteritis nodosa (PAN) Catrin Tudur Smith Department of Biostatistics University of Liverpool cat1@liv.ac.uk CLINICAL TRIALS IN SMALL POPULATIONS
