Evaluation of Agent and Host Factors in Progression of Mycotic Keratitis
|
|
|
- Tyler Green
- 5 years ago
- Views:
Transcription
1 Evaluation of Agent and Host Factors in Progression of Mycotic Keratitis A Histologic and Microbiologic Study of 167 Corneal Buttons Geeta Kashyap Vemuganti, MD, 1 Prashant Garg, MS, 2 Usha Gopinathan, MSc, 3 Thomas J. Naduvilath, MSc, 3 Rajesh K. John, MSc, 4 Rajeev Buddi, MD, 4 Gullapalli N. Rao, MD 2 Purpose: To evaluate the host and agent factors in the progression of mycotic keratitis through the microbiologic evaluation and histologic study of human corneal buttons obtained at the time of therapeutic keratoplasty. Design: Retrospective noncomparative consecutive case series. Materials: One hundred sixty-seven corneal buttons from 148 patients of microbiologically diagnosed and treated cases of mycotic keratitis who underwent therapeutic keratoplasty between January 1995 and May Methods: Therapeutic penetrating keratoplasty, review of microbiologic results, histopathologic and microbiologic evaluation of the corneal buttons of mycotic keratitis Main Outcome Measures: Histologic evaluation of the buttons for morphologic changes, degree and distribution of inflammatory cells, presence or absence of fungal filaments, and their degree and distribution within the corneal buttons. Results: The diagnosis of fungal infection was made on corneal scrapings in 36 cases; whereas in 131 (78%), the fungus was grown in cultures and identified as Aspergillus in 55 (42%), Fusarium in 42 (32%), unidentified hyaline fungi in 22 (17%), dematiaceous (unidentified) in 4 (3%), and others in 8 (6%). The mean interval between diagnosis and keratoplasty was 19 ( 40) days. From the keratoplasty specimen, the fungus was identified at histologic examination in 127 of 167 (76%) buttons and grown by culture techniques in 76 of 115 (66%) buttons. The fungal species identified in the corneal button were Fusarium in 30 (39%); Aspergillus in 25 (33%); unidentified hyaline in 19 (25%), and others in 2 (3%). Fungus-positive corneal buttons had early surgery (mean, 15 days) compared with fungus-negative (39 days) corneal buttons (P ), with 93% fungus positivity in the buttons removed within 2 weeks and 42% after 2 months. In the fungus-positive buttons, there was an inverse correlation between the degree, distribution of inflammatory cells, and fungal filaments (r 0.255, P 0.024; r 0.199, P 0.027), respectively. The factors necessitating an early keratoplasty were heavy fungal load, deeper penetration of fungus, and possibly insufficient inflammation to combat infection. A granulomatous reaction was noted in the posterior stroma and around the fragmented Descemet s membrane in 23 buttons (13.8%), independent of fungal species. Inflammation was unaffected by elimination of fungus and increasing interval between diagnosis and treatment. Conclusions: Rapid progression of mycotic keratitis in the early phases is by agent factors such as heavy load and deeper penetration of the fungus, insufficient inflammatory response, and possibly relative ineffectiveness of antifungal agents. Progression in the later phase of mycotic keratitis need not necessarily be agent mediated; it could be either host-modulated, species-related, or drug resistance, thereby suggesting that ideal treatment regimens should include sensitivity-based antifungal therapy aided by in vivo monitoring of fungal filaments. Ophthalmology 2002;109: by the American Academy of Ophthalmology. Keratomycosis is a suppurative, ulcerative sight-threatening infection of the cornea that sometimes leads to loss of the Originally received: September 20, Accepted: February 6, Manuscript no Ophthalmic Pathology Centre, L. V. Prasad Eye Institute, Hyderabad, India. 2 Cornea Centre, L. V. Prasad Eye Institute, Hyderabad, India. 3 Jhaveri Microbiology Centre, L. V. Prasad Eye Institute, Hyderabad, India. 4 Public Health Ophthalmology Services, Milwaukee, Wisconsin. eye. Worldwide, the reported incidence of fungal keratitis is 17% to 36%, 1 3 whereas in India, it is 44% to 47%. 4 7 Despite advances in diagnosis and medical treatment of Presented in part at the annual meeting of the Association for Research in Vision and Ophthalmology, Fort Lauderdale, Florida, May Supported by the Hyderabad Eye Research Foundation, Hyderabad, India, and a grant from the US-India fund for scientific research (N ), New Delhi, India. Reprint requests to Geeta Kashyap Vemuganti, MD, Ophthalmic Pathology Service, Hyderabad Eye Research Foundation, L. V. Prasad Eye Institute, L. V. Prasad Marg, Banjara Hills, Hyderabad, AP, India by the American Academy of Ophthalmology ISSN /02/$ see front matter Published by Elsevier Science Inc. PII S (02)
2 Vemuganti et al Mycotic Keratitis A Histologic Study mycotic keratitis, 15% to 27% of patients require surgical intervention such as keratoplasty, enucleation, or evisceration because of either failed medical treatment or advanced disease at presentation There is no existing method, except confocal microscopy, 12 to assess whether the progression of the disease during treatment of mycotic keratitis is due to the persistence of the agent, an ongoing inflammatory response, or both. The outcome of mycotic keratitis depends ultimately on the interplay of the agent (virulence, resistance to drugs, and toxicity) and host factors (predisposing factors, inflammatory response, and hypersensitivity reactions) in addition to timely diagnosis and appropriate medical treatment. Insight into this complex pathogenic mechanism in keratomycosis could be obtained from animal experiments, impression debridement of corneal ulcers, diagnostic corneal biopsy, or from corneal buttons removed during penetrating keratoplasty for medically uncontrolled mycotic keratitis We have used a histologic evaluation of corneal buttons of mycotic keratitis to assess the role of agent factors, such as persistence of fungus, degree and distribution of filaments, and host factors, such as inflammatory response, tissue damage, and vascularization, to determine the progression of mycotic keratitis. Microbiologic evaluation of the mycotic ulcers at the time of diagnosis and at the time of therapeutic keratoplasty was also undertaken to assess the response to medical treatment. Material and Methods The medical, microbiologic, and histopathologic records of all culture-proven cases of fungal keratitis, which were managed surgically between January 1995 and May 1998 at the L. V. Prasad Eye Institute, a tertiary referral eye care center, were reviewed retrospectively. Patients with a clinical diagnosis of corneal ulcer were directed to the ulcer clinic and worked up extensively for the etiologic diagnosis. Once diagnosed microbiologically as having a fungal ulcer, the patients were preferably admitted as inpatients. The treatment was initiated with 5% natamycin instilled every half hour. Frequency of administration was reduced to 2 to 4 hours based on the clinical response as assessed by the reduction in the size of the epithelial defect and the size and depth of the stromal infiltrate. None of the patients received steroid treatment before or after diagnosis made at our institution. Oral ketoconazole, 200 mg twice daily, was added in severe ulcers. Surgical intervention with therapeutic keratoplasty was considered for failed medical treatment as assessed by an increase in the size of the epithelial defect, stromal infiltrates despite 5 to 7 days of treatment, limbal involvement, impending perforation, or advanced disease at presentation. Patients who underwent therapeutic penetrating keratoplasty were continued on antifungal medication until the possibility of recurrence was ruled out. Microbiology According to the institutional protocol, all ulcer patients were subjected to a complete microbiologic evaluation of the corneal scrapings according to the method described earlier. 18 The scraped material was smeared on glass slides and stained by Gram s and Giemsa stain for morphologic interpretation. The scraped material was inoculated on several media, including blood agar, chocolate agar, brain heart infusion broth, and Sabouraud s dextrose agar, to support the growth of bacteria, fungi, and Acanthamoeba. Microbiologic diagnosis of fungal keratitis was made if either fungal elements were identified in microscopic examination of the scraped material or if fungus grew from more than one medium in the absence of fungus in direct smears. The diseased corneal button removed during keratoplasty was divided into two halves. Routinely, the cornea was bisected by the operating surgeon through the lesional area, so as to provide representative tissues for both pathologic and microbiologic study. One half was subjected to microbiologic evaluation, and the other half was sent to the pathology laboratory for histologic evaluation. The former was divided into multiple pieces under laminar air flow and inoculated into several media as mentioned earlier. Complete microbiologic data of the half-corneal button obtained at the time of keratoplasty was, however, available in only 115 of 167 cases. Histopathology All the corneal button specimens were formalin-fixed, paraffinprocessed, and stained with routine hematoxylin eosin stain, periodic acid Schiff stain, and Gomori s methenamine silver stain. 19 A minimum of three glass slides with four sections each were studied by the same ophthalmic pathologist (GKV). Histologic changes in all layers of the cornea were noted. The presence or absence of inflammatory cells, type of cells, degree of inflammation, depth, and distribution of the cells was noted. The degree of inflammation was graded (in a semiquantitative way) as mild, moderate, or severe based on the density of inflammatory cells in the corneal tissues. Inflammation was considered mild if the background stroma and keratocyte nuclei were seen clearly; moderate if the keratocyte nuclei were obliterated, but the stroma was visible; and severe if there was complete obliteration of keratocyte nuclei and corneal stroma. Similarly, the presence or absence of fungal filaments, the number, distribution within the stroma, involvement beyond Descemet s membrane, and resected margins were noted. The fungal load was classified as mild, moderate, or severe based on the close packing of the fungal filaments as observed in more than two high-power fields. The person interpreting the histopathologic slides (GKV) was masked from microbiologic data (corneal scrapings and half-button data) of these cases. Correlation of Agent and Host Factors The patient details and the duration of treatment before keratoplasty were noted from the corneal database of our institution. We assessed the agent and host factors that are influenced by the duration of treatment (i.e., the interval between diagnosis and keratoplasty and also the influence of one on the other). The time interval was segregated into four phases for convenience: less than 2 weeks, 2 weeks to 1 month, 1 to 2 months, and more than 2 months. In 14 cases the data on time interval between diagnosis and keratoplasty was not available, hence these cases were excluded in the analysis when time frame was compared with other parameters. An attempt was made to evaluate the prognostic markers for perforation and regrafting. The statistical methods used in this study were chi-square test, Student s t test (risk factors for perforation and graft failure), Fisher s exact coefficient, Spearman s coefficient (inflammation vs. fungus degree and distribution), and analysis of variance (relationship of agent and host factors with duration of treatment). 1539
3 Ophthalmology Volume 109, Number 8, August 2002 Table 2. Histopathologic Features of Corneal Buttons Diagnosed as Fungal Keratitis Features No. of Cases (%) Epithelial ulceration 165 (98) Stromal thinning 109 (65) Stromal necrosis 138 (83) Perforation 40 (24) Vascularization 39 (23) the time of corneal scraping and from the corneal button obtained at the time of therapeutic keratoplasty are given in Table 1. Complete microbiologic study of the bisected corneal button obtained at the time of keratoplasty was available in 115 of 167 (68.9%) cases, of which 76 of 115 (66%) buttons revealed growth on cultures, as shown in Table 1. Histologic Data Figure 1. Age and gender distribution of the patients who underwent penetrating keratoplasty for fungal keratitis. Results Patients The number of patients with infectious keratitis attending our ulcer clinic between January 1995 and May 1998 was 1926, of which 644 (33.4%) were microbiologically diagnosed as having fungal keratitis; 148 patients (23%) required therapeutic penetrating keratoplasty. In addition, 19 patients required regrafting within the same period, resulting in 167 corneal buttons for this study. The age/gender distribution is given in Figure 1. The age of these patients ranged from 12 to 80 years, with a mean of years. There was a peak in the third decade, constituting 28.4% of all cases; 53.4% of cases were 40 years of age or younger. There were 104 (70%) males and 44 females (30%), with a male/female ratio of 2.3:1. The mean duration between the initial scraping and the time of penetrating keratoplasty was 19 days 40 days with a median of 8 days (1 331). One hundred five (62%) cases had undergone penetrating keratoplasty within 2 weeks, 28 (17%) between 2 weeks and 1 month, 13 (8%) between 1 and 2 months, and 7 (4%) more than 2 months after diagnosis was established. Microbiology The microbiologic diagnosis of mycotic keratitis was based on the identification of fungal filaments in the potassium hydroxide and calcofluor preparations in 36 cases, whereas growth on culture media was noted in 131 (78.4%) cases. The species identified at Table 1. Frequency and Spectrum of Fungal Agents Isolated from Cultures of Corneal Scrapings at Diagnosis and Corneal Buttons Removed during Therapeutic Penetrating Keratoplasty Species Scrapings Buttons No. of cases Aspergillus 55 (42%) 25 (33%) Fusarium 42 (32%) 30 (39%) Unidentified fungi 22 (17%) 19 (25%) Dematiaceous 4 (3%) Others 8 (6%) 2 (3%) The morphologic changes in the epithelium, Bowman s layer, and stroma are shown in Table 2. The absence of epithelium in two cases and intact Bowman s layer in 13 cases possibly represent a sampling error during bisection of the button, embedding, or cutting of the sections. Vascularization was noted in 39 cases (23%): localized to superficial stroma in 35 cases and deep stroma in 4 cases. Type, degree, and distribution of stromal inflammation is shown in Table 3. Inflammation was seen mostly involving all the layers (94, 60%), whereas in some cases it was restricted to either the anterior two thirds (23, 16%) or posterior one third (38, 24%) (Fig 2). Involvement beyond Descemet s membrane was noted in 55 (22%) cases, with or without demonstrable continuity thorough the posterior stroma. Perforation was evident on histologic examination in 40 (24%) buttons (Fig 3). The mean interval between diagnosis and keratoplasty in these cases was 21 days 54 days (median, 7 days). Giant cell reaction with or without granulomatous inflammation (Fig 4) was noted in 23 cases (13.8%). Granulomas were seen mostly in the deep stroma and along the fragmented Descemet s membrane, except in two cases, where they were seen in the superficial and midstroma. They were associated with identifiable perforation in 10 (43%) cases. The degree, orientation, and distribution of fungal filaments identified in 127 of 167 (76%) corneal buttons are shown in Table Table 3. Pattern of Inflammatory Response in Corneal Buttons with Fungal Keratitis Inflammation No. of Cases (%) Degree Mild 22 (14) Moderate 79 (50) Severe 66 (36) Location Anterior two thirds 25 (16) Posterior one third 38 (24) Diffuse* 94 (60) {Including anterior chamber involvement 55 (22)} Type of Infiltrate PMNs 112 (89) PMN LMNs 55 (11) Granulomatous reactions 23 (14) * Inflammation involving all layers of cornea and anterior chamber. LMNs lymphomononuclear cells; PMNs polymorphonuclear cells. 1540
4 Vemuganti et al Mycotic Keratitis A Histologic Study Figure 2. Light microscopic photographs of fungal keratitis showing epithelial ulceration with inflammatory infiltrates involving the full thickness of the corneal stroma. The inflammation was seen involving all layers (A) (stain, periodic acid Schiff; original magnification, 125), restricted to either the anterior two thirds (B) (stain, hematoxylin eosin; original magnification, 125), deeper one third of the stroma (C) (stain, hematoxylin eosin; original magnification, 125), and beyond the confines of the corneal stroma suggestive of extension into the anterior chamber (D) (stain, hematoxylin eosin; original magnification, 125). Figure 3. Section of the cornea showing perforation with a small fragment of uveal tissue seen adherent to the area of perforation. Figure 4. Granulomatous reaction (asterisks) in the posterior stroma and around the fragmented ends of Descemet s membrane in a microbiologically and histologically proven case of fungal keratitis (stain, hematoxylin eosin; original magnification, 250). 4. It is to be noted that fungal filaments were either seen in all layers (62, 49%) or restricted to the anterior two thirds (50, 39%) or to the posterior one third of the stroma (14, 11%) (Fig 5). Fungal filaments were noted in 32 of 40 (80%) corneal buttons with perforation. The fungal load in this group was mild/moderate in 13 buttons each and heavy in 6 cases. Regrafting was done in 19 cases during the study period. The mean interval between the initial graft and the regraft was 28 days 24.4 days (range, 5 98 days). Seventeen of these 19 cases (90%) had fungus in the primary (host) corneal button, with recurrence in 6 (32%) cases, proven by histology in 5 cases and by microbiologic techniques in 1 case. The fungus load in these cases was moderate (8) or heavy (7), accounting for 88% of funguspositive host corneas. The distribution was diffuse, involving all layers in nine cases, the anterior two thirds in eight cases; moderate in eight cases; and mild in two cases. Posterior and/or lateral resected margins were seen in 14 of 17 (82%) cases; anterior chamber involvement was seen in 8 (47%) cases. 1541
5 Ophthalmology Volume 109, Number 8, August 2002 Table 4. Density and Distribution of Fungal Filaments in Corneal Buttons with Fungal Keratitis Fungus No. of Cases (%) Degree Mild 31 (25) Moderate 50 (39) Severe 46 (36) Location Anterior two thirds 50 (39) Posterior one third 14 (12) Diffuse* 62 (49) Anterior Chamber 1 {Including anterior chamber involvement 52 (31)} Orientation Parallel 15 (12) Vertical 15 (12) Both 97 (76) Margins Involved 92 (72) Posterior 59 (64) Peripheral 4 (4) Both 29 (32) Not involved 35 (28) * Diffuse location of fungal filaments extending into anterior chamber. Correlation between Host Factors and Agent Factors In the fungus-positive group of corneal buttons, the degree and distribution of inflammatory cells was inversely proportional to the fungal load and distribution (Fig 6) (r 0.255, P 0.024; r 0.199, P 0.027, respectively). Moderate to heavy fungal load was associated with stromal thinning. However, there was no statistically significant difference in fungus distribution and the tissue reaction of both major species. Granulomatous inflammation did not correlate to presence of any one fungal species. Vascularization was noted in 39 corneal buttons, which were treated for a mean interval of 29 days, with persistence of fungal filaments in 28 of 39 (72%) cases. Risk Factors for Perforation and Graft Failure The histologic and microbiologically identified risk factors for perforation were fungal load (P ; relative risk, 0.72; ), depth of infiltration (P ; odds ratio, 1.57; 95% confidence interval, ), and Fusarium species (P ; odds ratio, 1.99; 95% confidence interval, ). Factors like duration of ulcer and inflammatory cell distribution in the perforated group and the nonperforated cases did not reveal any increased risk of perforation in the former group. There was no significant correlation between fungus load, depth of inflammation, and involvement of margins with graft failure compared with the rest of the cases. Regrafting had significant correlation with Aspergillus species (P 0.006; odds ratio, 2.1; 95% confidence interval, ). There was no increased risk of recurrence or regrafting with involvement of margins by the fungal filaments (P ). Factors Influenced by Interval between Diagnosis and Treatment After treatment, fungus was identified in the corneal buttons by histologic evaluation in 127 of 167 (76%) cases, whereas by microbiologic techniques it was grown from 76 of 115 (66%) buttons. The mean duration of medical treatment (i.e., interval between diagnosis and keratoplasty) in the fungus-positive cases was 15 days, whereas it was 39 days in the fungus-negative group, which was statistically significant (P ). The presence of fungus when plotted against duration of treatment revealed that fungus was present in 92% of corneal buttons that had a penetrating keratoplasty within 2 weeks compared with 43% of buttons that underwent penetrating keratoplasty after 2 months (Fig 7). The cases with heavy fungal load had a mean interval of 9 days between diagnosis and keratoplasty, whereas the moderate load had a mean interval of 12 days, and the mild load had a mean interval of 29 days. Corneal buttons with heavy fungal load were seen early compared with mild and moderate fungal load (P 0.048). Diffuse involvement of fungus had an interval of 11 days, whereas that in the anterior two thirds had 21 days, and the posterior one third had 6 days. The various species of fungus as seen at different time points revealed a slight increase in the presence of Aspergillus species after 2 months, which, however, was not significant (Fig 8). The presence or degree of inflammation did not vary with the interval between diagnosis and keratoplasty (Fig 7). The mean duration of treatment for buttons with mild inflammation was 21 days; for moderate inflammation, 20 days; and for severe inflammation, 16 days (P 0.536). However, diffuse inflammation involving all layers had a mean interval of 25 days, whereas that in the anterior two thirds had 31days, and the posterior one third had 6 days. The granulomatous reaction noted in 23 cases had a mean interval of 12 days between diagnosis and keratoplasty. It did not vary significantly with any particular species of fungus. There was no increase in the risk of perforation or graft failure with increasing time. Discussion Mycotic keratitis is an important ophthalmic problem in all parts of the world, because it leads to corneal blindness and sometimes loss of the eye. Despite advances in diagnostic methods and medical treatment, 20% to 25% of fungal keratitis cases required surgery in the form of therapeutic penetrating keratoplasty. 5,20,21 Fungal keratitis is much more prevalent in tropical countries 2 4 and South India, 6 9 where fungi are present in the atmosphere and in the conjunctival sacs of asymptomatic individuals. 22,23 The most thought-provoking aspect of fungal keratitis is its pathogenesis, which involves the interplay of host and agent factors in the eye. 7 A few histologic studies on fungal keratitis published earlier 1,14,15,24 included cases with histologic evidence of fungus on sections, whereas in this study we included the cases that were clinically diagnosed and treated as fungal ulcer, irrespective of presence or absence of fungus in the histologic sections. These cases were microbiologically proven cases of fungal ulcers, adequately treated under supervision, and taken for penetrating keratoplasty only after ascertaining the disease progress at our institution. This study gives us the advantage of assessing the histologic and microbiologic factors involved in the progression of the disease (e.g., tissue inflammatory response, persistence of fungus after treatment), possible prognostic factors in evaluating the response to antifungal therapy, and thereby understanding the pathogenesis and progression of fungal keratitis. 1542
6 Vemuganti et al Mycotic Keratitis A Histologic Study Figure 5. The silver staining for fungus revealed fungal filaments involving the full thickness of the corneal stroma (A), restricted to the anterior two thirds (B), involving the posterior stroma and the anterior chamber (C), and extending into the anterior chamber (D) (stain, Gomori s silver methenamine; original magnification, 125). Figure 6. A and B, Section of the corneal button from a patient who underwent keratoplasty within 10 days of treatment shows minimal inflammation in the anterior stroma and mild inflammation in the posterior stroma. The same corneal section on silver staining shows dense fungal filaments anteriorly and few filaments extending into the posterior stroma, highlighting the inverse relationship of inflammation to fungal filaments (A: stain, hematoxylin eosin; original magnification 125; B: stain, Gomori s methenamine silver stain; original magnification, 125). The age group involved in this study ranged from 12 to 80 years, with a mean of 41 years. Although none of our cases were younger than 10 years old, as observed by Panda et al, 25 more than half of the patients were younger than 40 years of age; that could have a great impact on the economical burden. There was a preponderance of males as noted in other series from India and other countries, 1,6 which is possibly due to the relative frequency of outdoor activities of the males. Our hospital data revealed that 46.7% of patients with fungal keratitis are either agriculturists or manual laborers (unpublished data). The corneal morphology noted in this study is mostly similar to that described in other studies, except for the granulomatous reaction in the corneal stroma. 14,15 The granulomatous reaction was noted in 14% of cases, predominantly in the posterior stroma and around Descemet s membrane, similar to the 17.3% prevalence observed by Panda et al. 14 It did not show any specific association with the different species of fungus as identified from the corneal scraping or buttons. This type of inflammatory response in the cornea has been reported to be of nonspecific nature 26 because of herpetic keratitis 27 or Acanthamoeba keratitis
7 Ophthalmology Volume 109, Number 8, August 2002 Figure 7. Graph depicting the percentage of corneal buttons of various degrees of inflammation and fungus positivity in the corneal buttons removed at various intervals between diagnosis and treatment. In herpetic keratitis, the granulomatous reaction is suggested to be due to a viral antigen, altered cellular and/or basement membrane structures from the host, or both. In light of existing knowledge, the granulomatous inflammation in our series of microbiologically proven fungal keratitis, with evidence of fungus in 78% cases, could be either nonspecific, immune-mediated, or due to primary preexisting undetected viral infection in the patient. It is beyond the scope of this study to confirm or eliminate these causes; however, it does point toward the role of immunity and hypersensitivity in the progression of fungal keratitis. It is important to note that in the buttons positive for fungal filaments, the degree and distribution of inflammatory cells had a negative correlation with intensity and distribution of the fungal filaments. Although the correla- Figure 8. Graph representing the frequency of corneal buttons of varying fungal species as identified at the time of scraping compared with the time at which keratoplasty was undertaken for these cases. This is to assess the persistence of any particular species with increasing duration of medical treatment. 1544
8 Vemuganti et al Mycotic Keratitis A Histologic Study tion was weak (r ), it could be of clinical significance. This was our observation over the past few years, which could be confirmed by statistical evaluation in this large series of cases. It could be speculated that in the initial phase of mycotic keratitis, the polymorphonuclear cell infiltrates are beneficial in reducing the load of fungus by phagocytosis of the fungal filaments and destruction through the free radicals generated from the polymorphonuclear cells. 7 Another possible explanation for the inverse relationship of inflammatory infiltrates and fungus could be that the heavy fungal load and the toxins or enzymes inhibit the inflammatory response to perpetuate their growth. Interestingly, the corneal buttons obtained at the time of keratoplasty were negative for fungus in one fourth (24%) of the cases by histologic techniques and in one third (34%) by microbiologic techniques. Inflammation in this group was similar to that in the fungus-positive group, suggesting the persistence of inflammation after elimination of the agent (i.e., the fungus). It is evident that inflammation, once initiated, continues uninhibited even after the removal of the inciting agent. Further damage to the corneal tissues is possibly contributed to by the inflammatory mediators and not directly by agent factors. It is also evident from this study that the clinical parameters of the progression of the disease do not necessarily indicate the persistence of fungus, as has been generally assumed. It could be due to persisting inflammation, which may also be contributed to by the hypersensitivity reaction, as suggested by Thomas. 7 The hypothesis gains support in our study with a longer interval (39 days) between diagnosis and keratoplasty in the fungusnegative corneal buttons compared with the fungus-positive (15 days) group. We therefore speculate that the addition of an immunomodulating drug (possibly an antisteroidal drug) in addition to antifungal therapy would help in containing infection. In vivo monitoring of fungal filaments by confocal microscopy could aid the clinician in assessing the persistence or absence of fungus in the corneal tissues. The status of the fungus in the corneal buttons obtained at keratoplasty from patients who have been on continuous antifungal therapy could also reflect the in vivo effectiveness of the treatment protocols. Fungus was identified in 76% of our cases, similar to the 74% reported by Rosa et al, 1 whereas it was grown in 66% of our cases compared with 71% in their series. The presence of fungus and inflammation in the buttons after treatment suggests either overwhelming infection at presentation, inadequate medical treatment, lack of penetration of drugs, or in vivo resistance to the drugs. Although the treatment regimen in our series was not based on culture and sensitivity studies, a few interpretations are feasible. Our results suggest that the load of fungus and its penetration are important determinants of progression of the disease, necessitating early surgical intervention. The location of fungus in all layers or in the anterior two thirds in 88% of cases compared with 12% restricted to the posterior third contradicts previous observation of absence of fungus on the corneal surface. This would allow us to speculate that progression of the disease in the early stages with persistence of fungus anteriorly is possibly due to ineffectiveness of drugs rather than penetration of drugs. The presence of the fungus after 2 months, however, could be due to poor penetration of drug, resistance of fungus to drugs, or both. There is a relative increase in the number of cases with Aspergillus species, suggesting that the drug resistance could be species-specific. An in vitro susceptibility test for the fungal isolates could shed light on these findings. Another noteworthy observation was the presence of fungal filaments in 28 of 39 (78%) of the corneal buttons with vascularization. This is in contrast to the belief that vascularization represents the healing phase of the disease process. Other clinical factors such as history of trauma and systemic illness, which we did not include in this study, could shed light on the role of these factors in the progression of the disease. Although the need for surgical intervention by itself suggests a progressive disease, the addition of individual clinical parameters such as size of the infiltrate, stromal thinning at the time of diagnosis, and at the time of keratoplasty could have shed more light on the factors responsible for progression of this devastating disease. These factors that could not be addressed in this retrospective study should pave the way for another prospective study. By comparing the histologic parameters in the host and the donor corneal tissues, a few prognostic factors in the graft can be assessed. Regrafting was done in 19 cases, of which 90% had fungus in the host button and 5 (26%) had recurrence in the donor tissue. There was no statistical difference in the degree of inflammation, fungal load, and the duration of treatment in failed grafts and the other corneal tissues. However, graft failure with Aspergillus species was significant. There was no increased risk of recurrence or regrafting with involvement of the margins by the fungal filaments (P ). Earlier studies have shown that the results of surgical intervention are not adversely affected by the presence of fungus at the surgical margins. 20 It could be speculated that factors such as stromal necrosis, cytokines, associated local diseases, or systemic diseases may be more important than the presence of fungal filaments. Although not addressed in this study, our hospital ulcer data revealed predisposing ocular factors in 11.5% of cases, whereas systemic factors were noted in 9% of cases. Further prospective studies or animal experiments could help in assessing the prognostic factors in patients with fungal keratitis. In summary, both agent factors (heavy fungal load with deep penetration) and host factors (insufficient inflammatory response), possibly in addition to the relative ineffectiveness of antifungal agents, seem to influence the progression of mycotic keratitis in early stages, thereby justifying prompt surgical intervention. The late stages of mycotic keratitis could be attributed to the deleterious persistence of inflammation or possibly because of the resistant species of fungus. We therefore suggest that an ideal treatment protocol should include antifungal agents chosen by in vitro susceptibility of the fungus, the duration of which should be assessed by in vivo monitoring of fungal filaments, and, if required, the addition of antiinflammatory drugs should be considered in prolonged cases. 1545
9 Ophthalmology Volume 109, Number 8, August 2002 References 1. Rosa RH Jr, Miller D, Alfonso EC. The changing spectrum of fungal keratitis in south Florida. Ophthalmology 1994;101: Upadhyay MP, Karmacharya PCD, Koirala S, et al. Epidemiologic characteristics, predisposing factors, and etiologic diagnosis of corneal ulceration in Nepal. Am J Ophthalmol 1991;111: Katz NN, Wadud SA, Ayazuddin M. Corneal ulcer disease in Bangladesh. Ann Ophthalmol 1983;15: Dunlop AA, Wright ED, Howlader SA, et al. Suppurative corneal ulceration in Bangladesh. A study of 142 cases examining the microbiological diagnosis, clinical diagnosis and epidemiological features of bacterial and fungal keratitis. Aust N Z J Ophthalmol 1994;22: Polack FM, Kaufman HE, Newmark E. Keratomycosis. Medical and surgical treatment. Arch Ophthalmol 1971;85: Srinivasan M, Gonzales CA, George C, et al. Epidemiology and aetiological diagnosis of corneal ulceration in Madurai, South India. Br J Ophthalmol 1997;81: Thomas PA. Mycotic keratitis an underestimated mycosis. J Med Vet Mycol 1994;32: Thomas PA, Geraldine P. Fungal keratitis due to Fusarium and other fungi. J Mycol Med 1992;2: Sharma S, Srinivasan M, George C. The current status of Fusarium species in mycotic keratitis in South India. Indian J Med Microbiol 1993;11: Reddy PS, Satyendran OM, Satapathy M, et al. Mycotic keratitis. Indian J Ophthalmol 1972;20: Mahajan VM. Ulcerative keratitis: an analysis of laboratory data in 674 cases. J Ocul Ther Surg 1985;4: Florakis GJ, Moazami G, Schubert H, et al. Scanning slit confocal microscopy of fungal keratitis. Arch Ophthalmol 1997;115: Hamilton HI, McLaughlin SA, Whitley EM, et al. Histopathological findings in corneal stromal abscesses of 11 horses: correlation with culture and cytology. Equine Vet J 1994;26: Panda A, Mohan M, Mukherjee G. Mycotic keratitis in Indian patients (a histopathological study of corneal buttons). Indian J Ophthalmol 1984;32: Naumann G, Green WR, Zimmerman LE. Mycotic keratitis: a histopathologic study of 73 cases. Am J Ophthalmol 1967;64: Ishibashi Y, Kaufman HE. Corneal biopsy in the diagnosis of keratomycosis. Am J Ophthalmol 1986;101: Ishibashi Y, Hommura S, Matsumoto Y. Direct examination vs culture of biopsy specimens for the diagnosis of keratomycosis. Am J Ophthalmol 1987;103: Kunimoto DY, Sharma S, Garg P, et al. Corneal ulceration in the elderly in Hyderabad, South India. Br J Ophthalmol 2000; 84: Prophet EB, Mills B, Arrington JB, Sobin LH. AFIP Laboratory Methods in Histotechnology. Washington, DC: Armed Forces Institute of Pathology, Killingsworth DW, Stern GA, Driebe WT, et al. Results of therapeutic penetrating keratoplasty. Ophthalmology 1993; 100: Wong TY, Ng TP, Fong KS, Tan DT. Risk factors and clinical outcomes between fungal and bacterial keratitis: a comparative study. CLAO J 1997;23: Ainley R, Smith B. Fungal flora of the conjunctival sac in healthy and diseased eyes. Br J Ophthalmol 1965;49: Sehgal SC, Dhawan S, Chibber S, et al. Frequency and significance of fungal isolations from conjunctival sac and their role in ocular infections. Mycopathologia 1981;73: Spencer WH, ed. Ophthalmic Pathology: An Atlas and Textbook, 4th ed. Philadelphia: W B Saunders, 1996;v.1, Panda A, Sharma M, Das G, et al. Mycotic keratitis in children: epidemiological and microbiologic evaluation. Cornea 1997;16: Green WR, Zimmerman LE. Granulomatous reaction to Descemet s membrane. Am J Ophthalmol 1967;64: Holbach LM, Font RL, Naumann GOH. Herpes simplex stromal and endothelial keratitis. Granulomatous cell reactions at the level of Descemet s membrane, the stroma, and Bowman s layer. Ophthalmology 1990;97: Mietz H, Font RL. Acanthamoeba keratitis with granulomatous reaction involving the stroma and anterior chamber. Arch Ophthalmol 1997;115:
Mycotic Keratitis in Patients Attending a Tertiary Care Hospital
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 10 (20) pp. 1665-1670 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.20.610.201
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 10 (20) pp. 1665-1670 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.20.610.201
Lamellar Keratoplasty for the Treatment of Fungal Keratitis
 Cornea 21(1): 33 37, 2002. 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Lamellar Keratoplasty for the Treatment of Fungal Keratitis Lixin Xie, M.D., Weiyun Shi, M.D., Zhaosheng Liu, M.D., and
Cornea 21(1): 33 37, 2002. 2002 Lippincott Williams & Wilkins, Inc., Philadelphia Lamellar Keratoplasty for the Treatment of Fungal Keratitis Lixin Xie, M.D., Weiyun Shi, M.D., Zhaosheng Liu, M.D., and
The Epidemiological Features and Laboratory Results of Fungal Keratitis
 Cornea 21(6): 555 559, 2002. 2002 Lippincott Williams & Wilkins, Inc., Philadelphia The Epidemiological Features and Laboratory Results of Fungal Keratitis A 10-Year Review at a Referral Eye Care Center
Cornea 21(6): 555 559, 2002. 2002 Lippincott Williams & Wilkins, Inc., Philadelphia The Epidemiological Features and Laboratory Results of Fungal Keratitis A 10-Year Review at a Referral Eye Care Center
Identification of Fungal Species in Proved Cases of Fungal Corneal Ulcer
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Identification of Fungal Species in Proved Cases of Fungal Corneal Ulcer Authors Madhusudhan C.N 1, Tanushree V 2, H.T.Venkategowda 3,
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x Identification of Fungal Species in Proved Cases of Fungal Corneal Ulcer Authors Madhusudhan C.N 1, Tanushree V 2, H.T.Venkategowda 3,
Fungal Infection of Sutureless Self-sealing Incision for Cataract Surgery
 Fungal Infection of Sutureless Self-sealing Incision for Cataract Surgery Prashant Garg, MS, 1 S. Mahesh, MD, 1 Aashish K. Bansal, MS, 1 Usha Gopinathan, PhD, 2 Gullapalli N. Rao, MD 1 Purpose: To report
Fungal Infection of Sutureless Self-sealing Incision for Cataract Surgery Prashant Garg, MS, 1 S. Mahesh, MD, 1 Aashish K. Bansal, MS, 1 Usha Gopinathan, PhD, 2 Gullapalli N. Rao, MD 1 Purpose: To report
Spectrum of Fungal Keratitis in North China
 Spectrum of Fungal Keratitis in North China Lixin Xie, MD, 1 Wenxian Zhong, MD, 1,2 Weiyun Shi, MD, 1 Shiying Sun, MD 1 Purpose: To report the epidemiological features, laboratory findings, and treatment
Spectrum of Fungal Keratitis in North China Lixin Xie, MD, 1 Wenxian Zhong, MD, 1,2 Weiyun Shi, MD, 1 Shiying Sun, MD 1 Purpose: To report the epidemiological features, laboratory findings, and treatment
Prevalence of Oculomycosis in a Tertiary Care Centre
 AJMS Al Ameen J Med Sci (2 011 )4 (4 ):3 3 4-3 3 8 (A US National Library of Medicine enlisted journal) I S S N 0 9 7 4-1 1 4 3 C O D E N : A A J M B G ORIGI NAL ARTICLE Prevalence of Oculomycosis in a
AJMS Al Ameen J Med Sci (2 011 )4 (4 ):3 3 4-3 3 8 (A US National Library of Medicine enlisted journal) I S S N 0 9 7 4-1 1 4 3 C O D E N : A A J M B G ORIGI NAL ARTICLE Prevalence of Oculomycosis in a
The Role of Ultrasonographic Biomicroscopy in the management of a patient with presumed Dematiaceous Mycotic Keratitis
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 6 Number 2 The Role of Ultrasonographic Biomicroscopy in the management of a patient with presumed Dematiaceous Mycotic Keratitis
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 6 Number 2 The Role of Ultrasonographic Biomicroscopy in the management of a patient with presumed Dematiaceous Mycotic Keratitis
INCIDENCE OF CURVULARIA ORGANISM IN MYCOTIC CORNEAL ULCER K. Anjaneyulu 1, Balla Vidya Sagar 2
 INCIDENCE OF CURVULARIA ORGANISM IN MYCOTIC CORNEAL ULCER K. Anjaneyulu 1, Balla Vidya Sagar 2 HOW TO CITE THIS ARTICLE: K. Anjaneyulu, Balla Vidya Sagar. Incidence of Curvularia Organism in Mycotic Corneal
INCIDENCE OF CURVULARIA ORGANISM IN MYCOTIC CORNEAL ULCER K. Anjaneyulu 1, Balla Vidya Sagar 2 HOW TO CITE THIS ARTICLE: K. Anjaneyulu, Balla Vidya Sagar. Incidence of Curvularia Organism in Mycotic Corneal
International Journal of Pharma and Bio Sciences
 Research Article Microbiology International Journal of Pharma and Bio Sciences ISSN 0975-6299 INFECTIVE KERATITIS - PREDISPOSING FACTORS, CLINICAL AND MICROBIOLOGICAL ANALYSIS WITH ANTIBIOTIC SUSCEPTIBILITY
Research Article Microbiology International Journal of Pharma and Bio Sciences ISSN 0975-6299 INFECTIVE KERATITIS - PREDISPOSING FACTORS, CLINICAL AND MICROBIOLOGICAL ANALYSIS WITH ANTIBIOTIC SUSCEPTIBILITY
Microbiological regional profile of infective keratitis
 Original Article Microbiological regional profile of infective keratitis Reena Gupta 1,*, Chekitaan Singh 2, Bella Mahajan 3, AK Khurana 4 1 Assistant Professor, 4 Senior Professor & HOD, PGIMS, Rohtak,
Original Article Microbiological regional profile of infective keratitis Reena Gupta 1,*, Chekitaan Singh 2, Bella Mahajan 3, AK Khurana 4 1 Assistant Professor, 4 Senior Professor & HOD, PGIMS, Rohtak,
Clinical Decision making in Infectious Keratitis
 Clinical Decision making in Infectious Stephen D. McLeod, MD Theresa M. and Wayne M. Caygill, MD Distinguished Professor and Chair Department of Ophthalmology Francis I. Proctor Foundation University of
Clinical Decision making in Infectious Stephen D. McLeod, MD Theresa M. and Wayne M. Caygill, MD Distinguished Professor and Chair Department of Ophthalmology Francis I. Proctor Foundation University of
A Clinical Microbiological Study of Corneal Ulcer Patients at Western Gujarat, India
 A Clinical Microbiological Study of Corneal Ulcer Patients at Western Gujarat, India Rajesh Somabhai Katara 1, Nilesh Dhanjibhai Patel 2, and Mala Sinha 3 1 Department of Microbiology, B. J. Medical College,
A Clinical Microbiological Study of Corneal Ulcer Patients at Western Gujarat, India Rajesh Somabhai Katara 1, Nilesh Dhanjibhai Patel 2, and Mala Sinha 3 1 Department of Microbiology, B. J. Medical College,
CORNEAL CONDITIONS CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
Treatment of fungal keratitis by penetrating keratoplasty
 1070 Shandong Eye Institute and Hospital, Qingdao 266071, PR China L Xie X Dong W Shi Correspondence to: Lixin Xie, MD, Shandong Eye Institute and Hospital, 5 Yanerdao Road, Qingdao 266071, PR China lixinxie@public.qd.sd.cn
1070 Shandong Eye Institute and Hospital, Qingdao 266071, PR China L Xie X Dong W Shi Correspondence to: Lixin Xie, MD, Shandong Eye Institute and Hospital, 5 Yanerdao Road, Qingdao 266071, PR China lixinxie@public.qd.sd.cn
Original Article Analysis of corneal injuries in King Mahendra Memorial Eye Hospital Bharatpur, Chitwan
 Kathmandu University Medical Journal (2006), Vol. 4, No. 1, Issue 13, 34-39 Original Article Analysis of corneal injuries in King Mahendra Memorial Eye Hospital Bharatpur, Chitwan Adhikari RK Senior Consultant
Kathmandu University Medical Journal (2006), Vol. 4, No. 1, Issue 13, 34-39 Original Article Analysis of corneal injuries in King Mahendra Memorial Eye Hospital Bharatpur, Chitwan Adhikari RK Senior Consultant
ACANTHAMOEBA KERATITIS A SIX YEAR EPIDEMIOLOGICAL REVIEW FROM A TERTIARY CARE EYE HOSPITAL IN SOUTH INDIA
 Indian Journal of Medical Microbiology, (2004) 22 (4):226-230 Original Article ACANTHAMOEBA KERATITIS A SIX YEAR EPIDEMIOLOGICAL REVIEW FROM A TERTIARY CARE EYE HOSPITAL IN SOUTH INDIA *P Manikandan, M
Indian Journal of Medical Microbiology, (2004) 22 (4):226-230 Original Article ACANTHAMOEBA KERATITIS A SIX YEAR EPIDEMIOLOGICAL REVIEW FROM A TERTIARY CARE EYE HOSPITAL IN SOUTH INDIA *P Manikandan, M
ETIOLOGY OF SUPPURATIVE CORNEAL ULCERS IN RURAL POPULATION OF NORTHERN INDIA
 RESEARCH ARTICLE ETIOLOGY OF SUPPURATIVE CORNEAL ULCERS IN RURAL POPULATION OF NORTHERN INDIA Sushil Ojha 1, *, Anupama Tandon 2, Dipendra Shukla 3, Neeraj Saraswat 4, Shweta Joshi 5 1 Senior Resident,
RESEARCH ARTICLE ETIOLOGY OF SUPPURATIVE CORNEAL ULCERS IN RURAL POPULATION OF NORTHERN INDIA Sushil Ojha 1, *, Anupama Tandon 2, Dipendra Shukla 3, Neeraj Saraswat 4, Shweta Joshi 5 1 Senior Resident,
Clinical study to identify causative organism in microbial keratitis, their sensitivity pattern and treatment outcome.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 10, Issue 3 (Sep.- Oct. 2013), PP 27-31 Clinical study to identify causative organism in microbial keratitis,
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 10, Issue 3 (Sep.- Oct. 2013), PP 27-31 Clinical study to identify causative organism in microbial keratitis,
GRANULOMATOUS INFLAMMATION IN ACANTHAMOEBA KERATITIS: AN IMMUNOHISTOCHEMICAL STUDY OF FIVE CASES AND REVIEW OF LITERATURE
 Indian Journal of Medical Microbiology, (2005) 23 (4):231-8 Original Article GRANULOMATOUS INFLAMMATION IN ACANTHAMOEBA KERATITIS: AN IMMUNOHISTOCHEMICAL STUDY OF FIVE CASES AND REVIEW OF LITERATURE *GK
Indian Journal of Medical Microbiology, (2005) 23 (4):231-8 Original Article GRANULOMATOUS INFLAMMATION IN ACANTHAMOEBA KERATITIS: AN IMMUNOHISTOCHEMICAL STUDY OF FIVE CASES AND REVIEW OF LITERATURE *GK
Direct microscopy in suppurative keratitis: a report from tertiary level hospital in Nepal
 Original article : a report from tertiary level hospital in Nepal Pooja Gautam Rai 1, Meenu Chaudhary 2, Ananda Kumar Sharma 2, Vijay Gautam 1 1 SagarmathaChoudhary Eye Hospital, Lahan, Siraha, Nepal 2
Original article : a report from tertiary level hospital in Nepal Pooja Gautam Rai 1, Meenu Chaudhary 2, Ananda Kumar Sharma 2, Vijay Gautam 1 1 SagarmathaChoudhary Eye Hospital, Lahan, Siraha, Nepal 2
Incidence of Corneal Ulcer in a Month of harvesting Season in a Tertiary Level Eye Hospital of Eastern Nepal
 Original Article Incidence of Corneal Ulcer in a Month of harvesting Season in a Tertiary Level Eye Hospital of Eastern Nepal Vijay Gautam, Abinash Chaudhary, Sanjay Kumar Singh, Pooja Gautam Rai Sagarmatha
Original Article Incidence of Corneal Ulcer in a Month of harvesting Season in a Tertiary Level Eye Hospital of Eastern Nepal Vijay Gautam, Abinash Chaudhary, Sanjay Kumar Singh, Pooja Gautam Rai Sagarmatha
H erpes simplex virus infection of the
 Herpes simplex keratitis An experimental study Samuel J. Kimura, Victor Diaz-Bonnet, and Masao Okumoto The incidence of complicated herpes simplex keratitis appears to have increased and the important
Herpes simplex keratitis An experimental study Samuel J. Kimura, Victor Diaz-Bonnet, and Masao Okumoto The incidence of complicated herpes simplex keratitis appears to have increased and the important
Original Research Article
 STUDY OF EPITHELIAL PHENOTYPE AFTER PTERYGIUM EXCISION BY USING CONJUNCTIVAL IMPRESSION CYTOLOGY. Dr. Sachin O. Agrawal*, Dr. Sudhir Pendke, Dr. Ravi Chauhan Department of Ophthalmology, Indira Gandhi
STUDY OF EPITHELIAL PHENOTYPE AFTER PTERYGIUM EXCISION BY USING CONJUNCTIVAL IMPRESSION CYTOLOGY. Dr. Sachin O. Agrawal*, Dr. Sudhir Pendke, Dr. Ravi Chauhan Department of Ophthalmology, Indira Gandhi
Corneal biopsy in keratitis performed with the microtrephine
 Graefe s Arch Clin Exp Ophthalmol (1999) 237:915 919 Springer-Verlag 1999 CLINICAL INVESTIGATION Sirpa Kompa Stéphanie Langefeld Bernd Kirchhof Norbert Schrage Corneal biopsy in keratitis performed with
Graefe s Arch Clin Exp Ophthalmol (1999) 237:915 919 Springer-Verlag 1999 CLINICAL INVESTIGATION Sirpa Kompa Stéphanie Langefeld Bernd Kirchhof Norbert Schrage Corneal biopsy in keratitis performed with
Post-LASIK infections
 Post-LASIK infections By Mohamed El-moddather Assiss. Prof. and head of department of ophthalmology AL-Azhar unizersity Assuit LASIK has become a common refractive procedure and is generally considered
Post-LASIK infections By Mohamed El-moddather Assiss. Prof. and head of department of ophthalmology AL-Azhar unizersity Assuit LASIK has become a common refractive procedure and is generally considered
A Study On Clinical And Microbiological Evaluation Of Corneal Ulcers In GGH, Kakinada During
 International Journal of scientific research and management (IJSRM) Volume 3 Issue 4 Pages 2564-2570 2015 \ Website: www.ijsrm.in ISSN (e): 2321-3418 A Study On Clinical And Microbiological Evaluation
International Journal of scientific research and management (IJSRM) Volume 3 Issue 4 Pages 2564-2570 2015 \ Website: www.ijsrm.in ISSN (e): 2321-3418 A Study On Clinical And Microbiological Evaluation
Clinical Profile of Herpes Simplex Keratitis
 K V Raju MS, Jyothi PT MS, Shimna Iqbal MS Clinical Profile of Herpes Simplex Keratitis Original Article Abstract Aims To document the various clinical presentations and to assess the risk factors contributing
K V Raju MS, Jyothi PT MS, Shimna Iqbal MS Clinical Profile of Herpes Simplex Keratitis Original Article Abstract Aims To document the various clinical presentations and to assess the risk factors contributing
Disease caused by herpes simplex virus
 Recurrence of herpes simplex virus in rabbit eyes: Results of a three-year study Peter R. Laibson and Sidney Kibrick Spontaneous reactivation of herpes simplex virus in rabbit ocular tissue was found on
Recurrence of herpes simplex virus in rabbit eyes: Results of a three-year study Peter R. Laibson and Sidney Kibrick Spontaneous reactivation of herpes simplex virus in rabbit ocular tissue was found on
EPIDEMIOLOGICAL AND MICROBIOLOGICAL PROFILE OF PATIENT S HAVING MICROBIAL KERATITIS
 Original Article EPIDEMIOLOGICAL AND MICROBIOLOGICAL PROFILE OF PATIENT S HAVING MICROBIAL KERATITIS Saurabh Patel 1, Akshay M Chaudhari 2, Trupti M Solu 3, Vaibhav Gharat 4 Financial Support: None declared
Original Article EPIDEMIOLOGICAL AND MICROBIOLOGICAL PROFILE OF PATIENT S HAVING MICROBIAL KERATITIS Saurabh Patel 1, Akshay M Chaudhari 2, Trupti M Solu 3, Vaibhav Gharat 4 Financial Support: None declared
Common Etiological Agents Causing Keratitis: A Study from a Tertiary Care Hospital in South India
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 7 (2017) pp. 1625-1633 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.607.196
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 7 (2017) pp. 1625-1633 Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2017.607.196
Microbial Keratitis in East Africa: why are the outcomes so poor?
 Europe PMC Funders Group Author Manuscript Published in final edited form as: Ophthalmic Epidemiol. 2011 August ; 18(4): 158 163. doi:10.3109/09286586.2011.595041. Microbial Keratitis in East Africa: why
Europe PMC Funders Group Author Manuscript Published in final edited form as: Ophthalmic Epidemiol. 2011 August ; 18(4): 158 163. doi:10.3109/09286586.2011.595041. Microbial Keratitis in East Africa: why
Eye Care for Animals Micki Armour VMD DACVO THE CORNEA
 Eye Care for Animals Micki Armour VMD DACVO THE CORNEA ANATOMY 0.5-0.6mm thick 4 primary layers Epithelium (5-7 cell layers) Stroma (90% total thickness) Descemet s membrane Endothelium (1 layer) ANATOMY-
Eye Care for Animals Micki Armour VMD DACVO THE CORNEA ANATOMY 0.5-0.6mm thick 4 primary layers Epithelium (5-7 cell layers) Stroma (90% total thickness) Descemet s membrane Endothelium (1 layer) ANATOMY-
ANNEX II: Atlas of histopathological lesions of Isolated Chicken Eyes
 ANNEX II: Atlas of histopathological lesions of Isolated Chicken Eyes (from Triskelion, Zeist, The Netherlands) 1. Introduction... 1 2. Semi-quantitative microscopic evaluation of the cornea... 1 3. Histopathology
ANNEX II: Atlas of histopathological lesions of Isolated Chicken Eyes (from Triskelion, Zeist, The Netherlands) 1. Introduction... 1 2. Semi-quantitative microscopic evaluation of the cornea... 1 3. Histopathology
INTRA-CORNEAL LAMELLAR KERATOPLASTY*
 Brit. J. Ophthal. (1960) 44, 629. INTRA-CORNEAL LAMELLAR KERATOPLASTY* BY TADEUSZ KRWAWICZ Ophthalmological Clinic, Medical Academy, Lublin, Poland THE operative technique of lamellar keratoplasty is still
Brit. J. Ophthal. (1960) 44, 629. INTRA-CORNEAL LAMELLAR KERATOPLASTY* BY TADEUSZ KRWAWICZ Ophthalmological Clinic, Medical Academy, Lublin, Poland THE operative technique of lamellar keratoplasty is still
M Rezanur Rahman, Gordon J Johnson, Rabiul Husain, Shahe A Howlader, Darwin C Minassian
 Br J Ophthalmol 1998;82:919 925 919 Institute of Ophthalmology, Department of Preventive Ophthalmology, University College London, Bath Street, London, EC1V 9EL M R Rahman G J Johnson D C Minassian Eye
Br J Ophthalmol 1998;82:919 925 919 Institute of Ophthalmology, Department of Preventive Ophthalmology, University College London, Bath Street, London, EC1V 9EL M R Rahman G J Johnson D C Minassian Eye
Topical 5% Natamycin With Oral Ketoconazole in Filamentous Fungal Keratitis: A Randomized Controlled Trial
 ORIGINAL CLINICAL STUDY With Oral in Filamentous Fungal Keratitis: A Randomized Controlled Trial Revathi Rajaraman, MS,* Parameshwar Bhat, MS,* Vikram Vaidee, DNB,* Sowmyalatha Maskibail, MS,* Anita Raghavan,
ORIGINAL CLINICAL STUDY With Oral in Filamentous Fungal Keratitis: A Randomized Controlled Trial Revathi Rajaraman, MS,* Parameshwar Bhat, MS,* Vikram Vaidee, DNB,* Sowmyalatha Maskibail, MS,* Anita Raghavan,
Corneal blood staining after hyphaema
 Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Acridine Orange Staining for Rapid Diagnosis of Acanthamoeba Keratitis
 Acridine Orange Staining for Rapid Diagnosis of Acanthamoeba Keratitis Tae-Won Hahn,* Terrence P. O Brien, Woo-Jin Sah* and Jae-Ho Kim* *Department of Ophthalmology, Catholic University Medical College,
Acridine Orange Staining for Rapid Diagnosis of Acanthamoeba Keratitis Tae-Won Hahn,* Terrence P. O Brien, Woo-Jin Sah* and Jae-Ho Kim* *Department of Ophthalmology, Catholic University Medical College,
Downloaded from:
 Burton, MJ; Pithuwa, J; Okello, E; Afwamba, I; Onyango, JJ; Oates, F; Chevallier, C; Hall, AB (2011) Microbial keratitis in East Africa: why are the outcomes so poor? Ophthalmic epidemiology, 18 (4). pp.
Burton, MJ; Pithuwa, J; Okello, E; Afwamba, I; Onyango, JJ; Oates, F; Chevallier, C; Hall, AB (2011) Microbial keratitis in East Africa: why are the outcomes so poor? Ophthalmic epidemiology, 18 (4). pp.
Department of Microbiology, MMC&RI, Mysore, Karnataka, India.1- Associate Professor, 2- Professor and HOD
 Original Article ISSN (o):2321 7251 Microbiological profile of Ulcerative Keratitis in a tertiary care hospital Amrutha Kumari B 1, D. Venkatesha 2 Department of Microbiology, MMC&RI, Mysore, Karnataka,
Original Article ISSN (o):2321 7251 Microbiological profile of Ulcerative Keratitis in a tertiary care hospital Amrutha Kumari B 1, D. Venkatesha 2 Department of Microbiology, MMC&RI, Mysore, Karnataka,
Sclerokeratoplasty David S. Chu, M.D. Cases
 Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Demographic profile of Suppurative keratitis
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. V (August. 2016), PP 01-05 www.iosrjournals.org Dr.Bapanapalli Sailaja 1, Dr.Bapanapalli
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. V (August. 2016), PP 01-05 www.iosrjournals.org Dr.Bapanapalli Sailaja 1, Dr.Bapanapalli
International Journal of Science and Research (IJSR)
 1 M.D. (Microbiology), Professor & HOD of Microbiology, Govt. Thoothukudi Medical College 2 M.S., D.O., FICO., Associate Prof., Department of Ophthalmology, Tirunelveli Medical College 3 M.S., Assistant
1 M.D. (Microbiology), Professor & HOD of Microbiology, Govt. Thoothukudi Medical College 2 M.S., D.O., FICO., Associate Prof., Department of Ophthalmology, Tirunelveli Medical College 3 M.S., Assistant
EPIDEMIOLOGY AND OUTCOME OF CORNEAL ULCER IN YAZD SHAHID SADOUGHI HOSPITAL
 EPIDEMIOLOGY AND OUTCOME OF CORNEAL ULCER IN YAZD SHAHID SADOUGHI HOSPITAL M. R. Shoja * and M. Manaviat Department of Ophthalmology, Shahid Sadoughi Hospital, School of Medicine, Yazd University of Medical
EPIDEMIOLOGY AND OUTCOME OF CORNEAL ULCER IN YAZD SHAHID SADOUGHI HOSPITAL M. R. Shoja * and M. Manaviat Department of Ophthalmology, Shahid Sadoughi Hospital, School of Medicine, Yazd University of Medical
GAFFI Fact Sheet. Keratitis refers to inflammation (usually an infection) of the normally transparent DARKER AREAS AND
 Fungal Keratitis GAFFI Fact Sheet GLOBAL ACTION FUND FOR FUNGAL INFECTIONS Keratitis refers to inflammation (usually an infection) of the normally transparent DARKER AREAS AND cornea of the eye, which
Fungal Keratitis GAFFI Fact Sheet GLOBAL ACTION FUND FOR FUNGAL INFECTIONS Keratitis refers to inflammation (usually an infection) of the normally transparent DARKER AREAS AND cornea of the eye, which
Patient characteristics, diagnosis, and treatment of non-contact lens related Acanthamoeba keratitis
 Br J Ophthalmol 2000;84:1103 1108 1103 Jhaveri Microbiology Centre, LV Prasad Eye Institute, LV Prasad Marg, Banjara Hills, Hyderabad-500 034, India S Sharma Cornea Service P Garg G N Rao Correspondence
Br J Ophthalmol 2000;84:1103 1108 1103 Jhaveri Microbiology Centre, LV Prasad Eye Institute, LV Prasad Marg, Banjara Hills, Hyderabad-500 034, India S Sharma Cornea Service P Garg G N Rao Correspondence
Mycotic keratitis is an important ophthalmologic problem
 CLINICAL SCIENCES Spectrum of Fungal Keratitis in North India Anuradha Chowdhary, MD,* and Kirti Singh, MD, DNB, FRCS Purpose: To report the epidemiologic features and laboratory results of 191 consecutive
CLINICAL SCIENCES Spectrum of Fungal Keratitis in North India Anuradha Chowdhary, MD,* and Kirti Singh, MD, DNB, FRCS Purpose: To report the epidemiologic features and laboratory results of 191 consecutive
Condition: Herpes Simplex Keratitis
 Condition: Herpes Simplex Keratitis Description: Herpes simplex infection is very common but usually remains latent. When the virus is reactivated it travels along the trigeminal nerve to cause local infection
Condition: Herpes Simplex Keratitis Description: Herpes simplex infection is very common but usually remains latent. When the virus is reactivated it travels along the trigeminal nerve to cause local infection
FUNGAL CORNEAL ULCER. Arundhati Dvivedi final year p.g Dept.of Ophthalmology 2018/7/31
 FUNGAL CORNEAL ULCER Arundhati Dvivedi final year p.g Dept.of Ophthalmology Introduction: Fungal Keratitis is one of the most difficult forms of microbial keratitis to diagnose & to treat successfully
FUNGAL CORNEAL ULCER Arundhati Dvivedi final year p.g Dept.of Ophthalmology Introduction: Fungal Keratitis is one of the most difficult forms of microbial keratitis to diagnose & to treat successfully
Subject Index. Atopic keratoconjunctivitis (AKC) management 16 overview 15
 Subject Index Acanthamoeba keratitis, see Infective keratitis Acute allergic conjunctivitis AKC, see Atopic keratoconjunctivitis Allergy acute allergic conjunctivitis 15 atopic keratoconjunctivitis 15
Subject Index Acanthamoeba keratitis, see Infective keratitis Acute allergic conjunctivitis AKC, see Atopic keratoconjunctivitis Allergy acute allergic conjunctivitis 15 atopic keratoconjunctivitis 15
EPIDEMIOLOGY OF BACTERIAL KERATITIS IN A REFERRAL CENTRE IN SOUTH INDIA
 Indian Journal of Medical Microbiology, (2003) 21 (4):239-245 Original Article EPIDEMIOLOGY OF BACTERIAL KERATITIS IN A REFERRAL CENTRE IN SOUTH INDIA *MJ Bharathi, R Ramakrishnan, S Vasu, R Meenakshi,
Indian Journal of Medical Microbiology, (2003) 21 (4):239-245 Original Article EPIDEMIOLOGY OF BACTERIAL KERATITIS IN A REFERRAL CENTRE IN SOUTH INDIA *MJ Bharathi, R Ramakrishnan, S Vasu, R Meenakshi,
A Comparative Study for the Diagnosis of Microbial Keratitis Using Different Techniques.
 A Comparative Study for the Diagnosis of Microbial Keratitis Using Different Techniques 1 Rania A. Khattab, 2 Mohamed Shafik, 1 Salwa A. Rasmy, 2 Dalia G. Said, 2 Maha M. Abdelfatah and 1 Yasser M. Ragab
A Comparative Study for the Diagnosis of Microbial Keratitis Using Different Techniques 1 Rania A. Khattab, 2 Mohamed Shafik, 1 Salwa A. Rasmy, 2 Dalia G. Said, 2 Maha M. Abdelfatah and 1 Yasser M. Ragab
Selected Diseases of the Cornea Dick Dubielzig July 20 th, 2009
 Selected Diseases of the Cornea Dick Dubielzig July 20 th, 2009 Canine Collagenolytic Keratitis Canine Collagenolytic Keratitis 270 cases (1.5%) Usually associated with suppurative keratitis Collagenolytic
Selected Diseases of the Cornea Dick Dubielzig July 20 th, 2009 Canine Collagenolytic Keratitis Canine Collagenolytic Keratitis 270 cases (1.5%) Usually associated with suppurative keratitis Collagenolytic
Prednisolone Sodium Phosphate Ophthalmic Solution USP, 1% (Sterile) Rx only
 Prednisolone Sodium Phosphate Ophthalmic Solution USP, 1% (Sterile) Rx only DESCRIPTION Prednisolone Sodium Phosphate Ophthalmic Solution, 1%, is a sterile solution for ophthalmic administration having
Prednisolone Sodium Phosphate Ophthalmic Solution USP, 1% (Sterile) Rx only DESCRIPTION Prednisolone Sodium Phosphate Ophthalmic Solution, 1%, is a sterile solution for ophthalmic administration having
ISHAM Symposium: S33: Ocular aspects of Fungal Infections Friday, 8 May 2015, ; MR101/102 Level 1
 ISHAM Symposium: S33: Ocular aspects of Fungal Infections Friday, 8 May 2015, 14.15 15.45; MR101/102 Level 1 Chairs: Ariya Chindamporn, TH and Phillip A Thomas, IN 14:15-14:35 AGENDA Clinical overview
ISHAM Symposium: S33: Ocular aspects of Fungal Infections Friday, 8 May 2015, 14.15 15.45; MR101/102 Level 1 Chairs: Ariya Chindamporn, TH and Phillip A Thomas, IN 14:15-14:35 AGENDA Clinical overview
Deep Anterior Lamellar Keratoplasty - Techniques
 Deep Anterior Lamellar Keratoplasty - Techniques SHERAZ DAYA MD FACP FACS FRCS(Ed) FRCOphth Financial Disclosure Company Code 1. Abbott Medical Optics Inc. S 2. Bausch + Lomb C,L 3. Carl Zeiss Meditec
Deep Anterior Lamellar Keratoplasty - Techniques SHERAZ DAYA MD FACP FACS FRCS(Ed) FRCOphth Financial Disclosure Company Code 1. Abbott Medical Optics Inc. S 2. Bausch + Lomb C,L 3. Carl Zeiss Meditec
Acanthamoeba Keratitis in a Non-contact Lens Wearer: A Challenge in Diagnosis and Management
 JOURNAL OF CASE REPORTS 2014;4(2):419-423 Acanthamoeba Keratitis in a Non-contact Lens Wearer: A Challenge in Diagnosis and Management Dian Eka Putri, Lukman Edwar, Made Susiyanti Department of Ophthalmology,
JOURNAL OF CASE REPORTS 2014;4(2):419-423 Acanthamoeba Keratitis in a Non-contact Lens Wearer: A Challenge in Diagnosis and Management Dian Eka Putri, Lukman Edwar, Made Susiyanti Department of Ophthalmology,
Factors Affecting Treatment Outcome of Graft Infection Following Penetrating Keratoplasty
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(5):301-308 http://dx.doi.org/10.3341/kjo.2015.29.5.301 Original Article Factors Affecting Treatment Outcome of Graft Infection Following Penetrating
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(5):301-308 http://dx.doi.org/10.3341/kjo.2015.29.5.301 Original Article Factors Affecting Treatment Outcome of Graft Infection Following Penetrating
Corneal Ulceration. Client Information Sheet Copyright Bilton Veterinary Centre All rights Reserved. What is the cornea?
 What is the cornea? Corneal Ulceration The cornea is the central clear part of the eye that is surrounded by the white of the eye called the Sclera. Looking through the cornea, you can see the coloured
What is the cornea? Corneal Ulceration The cornea is the central clear part of the eye that is surrounded by the white of the eye called the Sclera. Looking through the cornea, you can see the coloured
Innovation In Ophthalmology
 Innovation In Ophthalmology INVELTYS TM Approval August 2018 Disclaimers and Notices This presentation contains forward-looking statements within the meaning of the Private Securities Litigation Reform
Innovation In Ophthalmology INVELTYS TM Approval August 2018 Disclaimers and Notices This presentation contains forward-looking statements within the meaning of the Private Securities Litigation Reform
The Bhaktapur eye study: ocular trauma and antibiotic prophylaxis for the prevention of corneal ulceration in Nepal
 388 Br J Ophthalmol 2001;85:388 392 ORIGINAL ARTICLES Clinical science The Bhaktapur eye study: ocular trauma and antibiotic prophylaxis for the prevention of corneal ulceration in Nepal M P Upadhyay,
388 Br J Ophthalmol 2001;85:388 392 ORIGINAL ARTICLES Clinical science The Bhaktapur eye study: ocular trauma and antibiotic prophylaxis for the prevention of corneal ulceration in Nepal M P Upadhyay,
NON TRADITIONAL MANAGEMENT OF FUNGAL KERATITIS
 NON TRADITIONAL MANAGEMENT OF FUNGAL KERATITIS MOHAMED SAAD,MD PROF. OF OPHTHALMOLOGY ASSIUT UNIVERSITY HOSPITAL FINANCIAL DISCLOSURE: No financial interest. 1 Fungal keratitis is a sight-threatening condition
NON TRADITIONAL MANAGEMENT OF FUNGAL KERATITIS MOHAMED SAAD,MD PROF. OF OPHTHALMOLOGY ASSIUT UNIVERSITY HOSPITAL FINANCIAL DISCLOSURE: No financial interest. 1 Fungal keratitis is a sight-threatening condition
Original Article. Fungal keratitis in Melbourne INTRODUCTION ABSTRACT METHODS
 Original Article Clinical and Experimental Ophthalmology 2007; 35: 124 130 doi:10.1111/j.1442-9071.2006.01405.x Fungal keratitis in Melbourne Prashant Bhartiya FRCS, 1,2 Mark Daniell FRANZCO, 1,2 Marios
Original Article Clinical and Experimental Ophthalmology 2007; 35: 124 130 doi:10.1111/j.1442-9071.2006.01405.x Fungal keratitis in Melbourne Prashant Bhartiya FRCS, 1,2 Mark Daniell FRANZCO, 1,2 Marios
DALK IN DANGEROUS INFECTIONS
 32 INTERNATIONAL CONGRESS of the HELLENIC SOCIETY OF INTRAOCULAR IMPLANT AND REFRACTIVE SURGERY CORNEA ROUND TABLE: STROMAL REPAIR DALK IN DANGEROUS INFECTIONS, MD Clinica Degli Occhi Sarnicola, Grosseto
32 INTERNATIONAL CONGRESS of the HELLENIC SOCIETY OF INTRAOCULAR IMPLANT AND REFRACTIVE SURGERY CORNEA ROUND TABLE: STROMAL REPAIR DALK IN DANGEROUS INFECTIONS, MD Clinica Degli Occhi Sarnicola, Grosseto
Causes of suppurative keratitis in Ghana
 1024 Korle Bu Teaching Hospital, University of Ghana, Accra, Ghana M Hagan M Newman Worthing Hospital, Park Avenue, Worthing, England E Wright Institute of Ophthalmology, Department of Preventive Ophthalmology,
1024 Korle Bu Teaching Hospital, University of Ghana, Accra, Ghana M Hagan M Newman Worthing Hospital, Park Avenue, Worthing, England E Wright Institute of Ophthalmology, Department of Preventive Ophthalmology,
Fungal Keratitis CURRENT CONCEPTS. Aetiology. Epidemiology. Fungi causing human keratitis. Predisposing factors. Local
 June 2008 N. Bindu - Fungal Keratitis 169 CURRENT CONCEPTS Fungal Keratitis Dr. N. Bindu MS Fungal infections of the cornea constitute an important eye problem in outdoor workers in tropical & subtropical
June 2008 N. Bindu - Fungal Keratitis 169 CURRENT CONCEPTS Fungal Keratitis Dr. N. Bindu MS Fungal infections of the cornea constitute an important eye problem in outdoor workers in tropical & subtropical
Subcutaneous Fungi 10/13/2009. General Characteristics. Pathogenesis. Epidemiology. Laboratory Diagnosis. Specimens. Growth rate: 1-4 weeks
 General Characteristics Growth rate: 1-4 weeks Subcutaneous Fungi Clinical Laboratory Science Program Carol Larson MSEd, MT(ASCP) Dematiaceous septate hyphae Hyaline septate hyphae Branching GPR Epidemiology
General Characteristics Growth rate: 1-4 weeks Subcutaneous Fungi Clinical Laboratory Science Program Carol Larson MSEd, MT(ASCP) Dematiaceous septate hyphae Hyaline septate hyphae Branching GPR Epidemiology
Spectrum of Mycotic corneal ulcers in Mid Western peripheral region of Terrain belt of Nepal and Indo-Nepal Border
 Nepal Journal of Medical Sciences Original Article Spectrum of Mycotic corneal ulcers in Mid Western peripheral region of Terrain belt of Nepal and Indo-Nepal Border Bastola P, 1* Mishra A, 2 Chaudhary
Nepal Journal of Medical Sciences Original Article Spectrum of Mycotic corneal ulcers in Mid Western peripheral region of Terrain belt of Nepal and Indo-Nepal Border Bastola P, 1* Mishra A, 2 Chaudhary
2016 Week 2. Corneal Ulcer Culture Collection & Foreign Body Removal
 2016 Week 2 Corneal Ulcer Culture Collection & Foreign Body Removal Collection of corneal ulcer specimen Entering acuities Thorough SLE; anesthetic likely necessary for SLE & definitely for corneal ulcer
2016 Week 2 Corneal Ulcer Culture Collection & Foreign Body Removal Collection of corneal ulcer specimen Entering acuities Thorough SLE; anesthetic likely necessary for SLE & definitely for corneal ulcer
AUSTRALIAN PRODUCT INFORMATION FLAREX (FLUOROMETHOLONE ACETATE) EYE DROPS SUSPENSION
 AUSTRALIAN PRODUCT INFORMATION FLAREX (FLUOROMETHOLONE ACETATE) EYE DROPS SUSPENSION 1 NAME OF THE MEDICINE Fluorometholone acetate. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION The active ingredient in
AUSTRALIAN PRODUCT INFORMATION FLAREX (FLUOROMETHOLONE ACETATE) EYE DROPS SUSPENSION 1 NAME OF THE MEDICINE Fluorometholone acetate. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION The active ingredient in
NEW ZEALAND DATA SHEET 1. PRODUCT NAME
 NEW ZEALAND DATA SHEET 1. PRODUCT NAME Flucon fluorometholone 0.1% Eye Drops Suspension 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each ml of Flucon contains 1.0 mg of fluorometholone (0.1% w/v). Excipient
NEW ZEALAND DATA SHEET 1. PRODUCT NAME Flucon fluorometholone 0.1% Eye Drops Suspension 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each ml of Flucon contains 1.0 mg of fluorometholone (0.1% w/v). Excipient
Introduction. Study of fungi called mycology.
 Fungi Introduction Study of fungi called mycology. Some fungi are beneficial: ex a) Important in production of some foods, ex: cheeses, bread. b) Important in production of some antibiotics, ex: penicillin
Fungi Introduction Study of fungi called mycology. Some fungi are beneficial: ex a) Important in production of some foods, ex: cheeses, bread. b) Important in production of some antibiotics, ex: penicillin
INVELTYS (loteprednol etabonate ophthalmic suspension) 1%, for topical ophthalmic use Initial U.S. Approval: 1998
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use INVELTYS safely and effectively. See full prescribing information for INVELTYS. INVELTYS (loteprednol
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use INVELTYS safely and effectively. See full prescribing information for INVELTYS. INVELTYS (loteprednol
Dr Jo-Anne Pon. Dr Sean Every. 8:30-9:25 WS #70: Eye Essentials for GPs 9:35-10:30 WS #80: Eye Essentials for GPs (Repeated)
 Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Dr.saifalshamarti. Objective. Where is cornea? Functions of the cornea
 Cornea Dr.saifalshamarti Objective Functions Anatomy: detailed description of the 5 layers: epithelium, Bowman s layer, stroma, Descement s membrane, endothelium. Diseases of the cornea: - infection: bacterial
Cornea Dr.saifalshamarti Objective Functions Anatomy: detailed description of the 5 layers: epithelium, Bowman s layer, stroma, Descement s membrane, endothelium. Diseases of the cornea: - infection: bacterial
JMSCR Vol 05 Issue 03 Page March 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i3.201 Etiological Profile of Proptosis A Prospective
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i3.201 Etiological Profile of Proptosis A Prospective
Epidemiology of Microbial Keratitis in a Tertiary Care Center in Karachi
 Original Article Epidemiology of Microbial Keratitis in a Tertiary Care Center in Karachi Qamar Riaz, Umar Fawwad, Nasir Bhatti, Aziz ur Rehman, Mazhar ul Hasan Pak J Ophthalmol 2013, Vol. 29 No. 2.....................................................................................................
Original Article Epidemiology of Microbial Keratitis in a Tertiary Care Center in Karachi Qamar Riaz, Umar Fawwad, Nasir Bhatti, Aziz ur Rehman, Mazhar ul Hasan Pak J Ophthalmol 2013, Vol. 29 No. 2.....................................................................................................
HISTOMORPHOLOGICAL SPECTRUM OF BREAST LESIONS
 HISTOMORPHOLOGICAL SPECTRUM OF BREAST LESIONS Kiran H. S, Jayaprakash Shetty, Chandrika Rao Assistant Professor, Department of Pathology, Yenepoya Medical College, Mangalore. Professor, Department of Pathology,
HISTOMORPHOLOGICAL SPECTRUM OF BREAST LESIONS Kiran H. S, Jayaprakash Shetty, Chandrika Rao Assistant Professor, Department of Pathology, Yenepoya Medical College, Mangalore. Professor, Department of Pathology,
Trifluridine Ophthalmic Solution, 1% Sterile
 Trifluridine Ophthalmic Solution, 1% Sterile DESCRIPTION Trifluridine (also known as trifluorothymidine, F 3 TdR,F 3 T), is an antiviral drug for topical treatment of epithelial keratitis caused by herpes
Trifluridine Ophthalmic Solution, 1% Sterile DESCRIPTION Trifluridine (also known as trifluorothymidine, F 3 TdR,F 3 T), is an antiviral drug for topical treatment of epithelial keratitis caused by herpes
2046: Fungal Infection Pre-Infusion Data
 2046: Fungal Infection Pre-Infusion Data Fungal infections are significant opportunistic infections affecting transplant patients. Because these infections are quite serious, it is important to collect
2046: Fungal Infection Pre-Infusion Data Fungal infections are significant opportunistic infections affecting transplant patients. Because these infections are quite serious, it is important to collect
Photodynamic therapy for IMMK in horses
 Photodynamic therapy for IMMK in horses Overview Immune mediated keratitis in horses Traditional treatment options Sustained release implant Photodynamic therapy Use in veterinary medicine Treatment for
Photodynamic therapy for IMMK in horses Overview Immune mediated keratitis in horses Traditional treatment options Sustained release implant Photodynamic therapy Use in veterinary medicine Treatment for
Koppolu Sreedhar Reddy 1* and Venkata Prasanna DP 2
 e - ISSN - 2349-8005 INTERNATIONAL JOURNAL OF ADVANCES IN CASE REPORTS Journal homepage: www.mcmed.us/journal/ijacr EFFICACY OF TOPICAL ACYCLOVIR IN TREATMENT OF HERPETIC KERATITIS Koppolu Sreedhar Reddy
e - ISSN - 2349-8005 INTERNATIONAL JOURNAL OF ADVANCES IN CASE REPORTS Journal homepage: www.mcmed.us/journal/ijacr EFFICACY OF TOPICAL ACYCLOVIR IN TREATMENT OF HERPETIC KERATITIS Koppolu Sreedhar Reddy
Histopathological Study of Lacrimal Gland Tumors
 ORIGINAL ARTICLE Pratikkumar B. Desai 1, Ami Shah 2 1 4 th Year Resident, Pathology Department, B.J.Medical College, Civil Hospital, Ahmedabad 2 Associate Professor, M. J. Institute of Ophthalmology, Civil
ORIGINAL ARTICLE Pratikkumar B. Desai 1, Ami Shah 2 1 4 th Year Resident, Pathology Department, B.J.Medical College, Civil Hospital, Ahmedabad 2 Associate Professor, M. J. Institute of Ophthalmology, Civil
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endothelial_keratoplasty 9/2009 6/2018 6/2019 6/2018 Description of Procedure or Service Endothelial keratoplasty
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endothelial_keratoplasty 9/2009 6/2018 6/2019 6/2018 Description of Procedure or Service Endothelial keratoplasty
Spectrum of causative agents of suppurative keratitis in sub- Himalayan region of North India a prospective study
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 8 Ver. IV (Aug. 2015), PP 79-84 www.iosrjournals.org Spectrum of causative agents of suppurative
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 8 Ver. IV (Aug. 2015), PP 79-84 www.iosrjournals.org Spectrum of causative agents of suppurative
Relationship between limbal incisions. angle. and the structures of the anterior chamber
 Brit. _7. Ophthal. (I 973) 57, 722 Relationship between limbal incisions and the structures of the anterior chamber angle MOHAMED I. AYOUB AND AHMED H. SAID Department of Ophthalmology, Faculty of Medicine,
Brit. _7. Ophthal. (I 973) 57, 722 Relationship between limbal incisions and the structures of the anterior chamber angle MOHAMED I. AYOUB AND AHMED H. SAID Department of Ophthalmology, Faculty of Medicine,
Actinomycosis and aspergillosis in the nose of a diabetic: A case report
 Volume 2 Issue 3 2012 ISSN 2250-0359 Actinomycosis and aspergillosis in the nose of a diabetic: A case report 1 Meenu Khurana Cherian 1*, Rajarajeswari 2 1 Department of ENT, Gulf Medical College Hospital
Volume 2 Issue 3 2012 ISSN 2250-0359 Actinomycosis and aspergillosis in the nose of a diabetic: A case report 1 Meenu Khurana Cherian 1*, Rajarajeswari 2 1 Department of ENT, Gulf Medical College Hospital
Comparison of prognostic value of Roper Hall and Dua classification systems in acute ocular burns
 1 Cornea and Refractive Surgery Services, Dr Rajendra Prasad Centre for Ophthalmic Sciences, All India Institute of Medical Sciences, New Delhi, India 2 Department of Biostatistics, All India Institute
1 Cornea and Refractive Surgery Services, Dr Rajendra Prasad Centre for Ophthalmic Sciences, All India Institute of Medical Sciences, New Delhi, India 2 Department of Biostatistics, All India Institute
PAINFUL PAINLESS Contact lens user BOV
 Common Causes Allergies Infections Ocular Cornea, uveitis, endophthalmitis Orbital Orbital cellulitis Inflammation Uveitis Scleritis / episcleritis Glaucomas Trauma Foreign bodies Chemical injuries History
Common Causes Allergies Infections Ocular Cornea, uveitis, endophthalmitis Orbital Orbital cellulitis Inflammation Uveitis Scleritis / episcleritis Glaucomas Trauma Foreign bodies Chemical injuries History
VIROPTIC Ophthalmic Solution, 1% Sterile (trifluridine ophthalmic solution)
 VIROPTIC Ophthalmic Solution, 1% Sterile (trifluridine ophthalmic solution) PRODUCT OVERVIEW: VIROPTIC SOLUTION DESCRIPTION VIROPTIC is the brand name for trifluridine (also known as trifluorothymidine,
VIROPTIC Ophthalmic Solution, 1% Sterile (trifluridine ophthalmic solution) PRODUCT OVERVIEW: VIROPTIC SOLUTION DESCRIPTION VIROPTIC is the brand name for trifluridine (also known as trifluorothymidine,
S carring of the cornea as a result of suppurative keratitis is
 1211 WORLD VIEW Aetiology of suppurative corneal ulcers in and south, and epidemiology of fungal keratitis A K Leck, P A Thomas, M Hagan, J Kaliamurthy, E Ackuaku, M John, M J Newman, F S Codjoe, J A Opintan,
1211 WORLD VIEW Aetiology of suppurative corneal ulcers in and south, and epidemiology of fungal keratitis A K Leck, P A Thomas, M Hagan, J Kaliamurthy, E Ackuaku, M John, M J Newman, F S Codjoe, J A Opintan,
INDICATIONS For steroid responsive inflammation of the palpebral and bulbar conjunctiva, cornea, and anterior segment of the eye globe.
 Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM PRED FORTE Sterile Eye Suspension COMPOSITION PRED FORTE Sterile Eye Suspension contains: Prednisolone acetate 10 mg/ml Preservative:
Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM PRED FORTE Sterile Eye Suspension COMPOSITION PRED FORTE Sterile Eye Suspension contains: Prednisolone acetate 10 mg/ml Preservative:
GENERAL INFORMATION CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL TRANSPLANTATION WHAT IS CORNEAL TRANSPLANTATION? A corneal transplant is an operation where a damaged or diseased cornea is replaced with donated, healthy tissue. Also called
GENERAL INFORMATION CORNEAL TRANSPLANTATION WHAT IS CORNEAL TRANSPLANTATION? A corneal transplant is an operation where a damaged or diseased cornea is replaced with donated, healthy tissue. Also called
ISPUB.COM. Management of Mycotic Keratitis. V Sharma, M Purohit, S Vaidya INTRODUCTION
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 6 Number 2 V Sharma, M Purohit, S Vaidya Citation V Sharma, M Purohit, S Vaidya.. The Internet Journal of Ophthalmology and Visual
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 6 Number 2 V Sharma, M Purohit, S Vaidya Citation V Sharma, M Purohit, S Vaidya.. The Internet Journal of Ophthalmology and Visual
Role of ASOCT in Intracorneal Foreign Body
 Diagnostics Ocular Trauma Role of ASOCT in Intracorneal Foreign Body Tarun Arora MD, DNB, FICO Tarun Arora MD, DNB, FICO, Vijay Kumar Sharma MS, Rajesh Sinha MD, DNB, FRCS Cornea, Lens and Refractive Surgery
Diagnostics Ocular Trauma Role of ASOCT in Intracorneal Foreign Body Tarun Arora MD, DNB, FICO Tarun Arora MD, DNB, FICO, Vijay Kumar Sharma MS, Rajesh Sinha MD, DNB, FRCS Cornea, Lens and Refractive Surgery
Distinction layer by layer. HRT II Rostock Cornea Module
 Distinction layer by layer HRT II Rostock Cornea Module Homogenously illuminated, undistorted images Movie capture Manual Pachymetry Epithelial and intra-corneal pachymetry Full corneal thickness Post-LASIK
Distinction layer by layer HRT II Rostock Cornea Module Homogenously illuminated, undistorted images Movie capture Manual Pachymetry Epithelial and intra-corneal pachymetry Full corneal thickness Post-LASIK
Corneal nerve alterations in acute Acanthamoeba and fungal keratitis: an in vivo confocal microscopy study
 (212) 26, 126 132 & 212 Macmillan Publishers Limited All rights reserved 95-222X/12 www.nature.com/eye CLINICAL STUDY Corneal nerve alterations in acute Acanthamoeba and fungal keratitis: an in vivo confocal
(212) 26, 126 132 & 212 Macmillan Publishers Limited All rights reserved 95-222X/12 www.nature.com/eye CLINICAL STUDY Corneal nerve alterations in acute Acanthamoeba and fungal keratitis: an in vivo confocal
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress MANAGEMENT OF CORNEAL ULCERS IN SMALL ANIMALS Robin G Stanley, BVSc(Hons), FACVSc-Ophthalmology Animal Eye Care
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress MANAGEMENT OF CORNEAL ULCERS IN SMALL ANIMALS Robin G Stanley, BVSc(Hons), FACVSc-Ophthalmology Animal Eye Care
PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia)
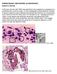 PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia) A 46-year-old man with AIDS was admitted to the hospital for complaints of a persisting fever and dry cough. A chest radiograph showed bilateral
PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia) A 46-year-old man with AIDS was admitted to the hospital for complaints of a persisting fever and dry cough. A chest radiograph showed bilateral
