Pathology of Autoimmune Myelofibrosis A Report of Three Cases and a Review of the Literature
|
|
|
- Milo Berry
- 6 years ago
- Views:
Transcription
1 Hematopathology / AUTOIMMUNE MYELOFIBROSIS Pathology of Autoimmune Myelofibrosis A Report of Three Cases and a Review of the Literature Randall D. Bass, MD, 1 Vinod Pullarkat, MD, 2 Donald I. Feinstein, MD, 2 Anita Kaul, MD, 3 Carl D. Winberg, MD, 4 and Russell K. Brynes, MD 1 Key Words: Autoimmune myelofibrosis; Collagen vascular disease; Chronic idiopathic myelofibrosis Abstract We identified 3 patients with autoimmune myelofibrosis (AM) lacking American Rheumatism Association criteria for systemic lupus erythematosus (SLE). They had 1 or 2 cytopenias and lacked serologic evidence for SLE. Autoimmune features included psoriatic arthritis and positive direct Coombs test (DCT) result, DCT-positive autoimmune hemolytic anemia, and synovitis with polyclonal hypergammaglobulinemia. Bone marrow biopsy specimens from each patient were evaluated by routine morphologic and immunohistochemical examination. They demonstrated marked hypercellularity (2 cases) or hypocellularity (1 case), moderate erythroid hyperplasia (all cases) with left-shifted maturation (2 cases), intrasinusoidal hematopoiesis (all cases), slightly to moderately increased megakaryocytes (2 cases), and grade 3 to 4 reticulin fibrosis (all cases). All lacked basophilia, eosinophilia, bizarre megakaryocytes, clusters of megakaryocytes, and osteosclerosis. Mild to moderate bone marrow lymphocytosis was noted in all cases. In 2 cases, increased small T cells and B cells formed nonparatrabecular, loose aggregates. AM is a clinicopathologic entity that may lack features of SLE. Loose aggregates of bone marrow T and B lymphocytes and the absence of morphologic and clinical features of myeloproliferative disease or lowgrade lymphoproliferative disease are clues that distinguish AM from better known causes of bone marrow fibrosis. Bone marrow fibrosis is associated with numerous causes including myeloproliferative disease, other hematologic and nonhematologic malignant neoplasms, autoimmune disorders, and endocrine disorders. 1 Cases reported as autoimmune myelofibrosis (AM) have been associated with collagen vascular disease, in particular, systemic lupus erythematosus (SLE) This rare bone marrow failure syndrome may predate the diagnosis of SLE or SLE-like disease or develop during the course of documented disease. Rare cases of AM have been described in patients with Sjögren syndrome and progressive systemic sclerosis. 15,16 In addition, 1 case of AM has been described with a positive direct Coombs test result, splenomegaly, and bone marrow lymphoid infiltrate mimicking hairy cell leukemia. 17 AM typically occurs in females, with most cases developing before the age of 40 years Laboratory features of AM include anemia, thrombocytopenia, left-shifted granulocytes, rare circulating nucleated RBCs, serologic evidence of autoimmune disease, hypocomplementemia, and a positive direct Coombs test result. 2 Physical examination may demonstrate splenomegaly or hepatosplenomegaly and arthralgias or, less commonly, oral ulcers, gingival bleeding, petechiae, pleuritis, pericarditis, lymphadenopathy, and malar rash. 2 We describe 3 new cases of AM in order to further define the morphologic and immunohistochemical features characteristic of this entity and to review the clinical and pathologic features of cases reported in the literature. Case Reports Case 1 A 73-year-old white man with a 7-year history of psoriatic arthritis received a 5-week course of low-dose American Society of Clinical Pathologists Am J Clin Pathol 2001;116:
2 Bass et al / AUTOIMMUNE MYELOFIBROSIS methotrexate. Seven months later, he had fatigue, anemia, and thrombocytopenia. Skin lesions developed on the upper and lower extremities 1 month later. Physical examination demonstrated a fading erythematous rash on the knees and upper arms, hyperpigmented papular and raised lesions on upper and lower extremities (particularly feet and ankles), and no peripheral lymphadenopathy or splenomegaly. Skin biopsies of the raised lesions documented Kaposi sarcoma. Vitamin B 12 and folate levels, iron studies, prostate-specific antigen, and liver function tests were normal. Pertinent laboratory results are shown in Table 1. Computed tomography scans of the chest, abdomen, and pelvis were negative. Two bone marrow trephine biopsies performed 7 weeks apart showed myelofibrosis Table 2. Bone marrow aspiration attempts were unsuccessful on both occasions. The peripheral blood cytopenias improved after a course of corticosteroid therapy. Recent follow-up showed correction of the thrombocytopenia but persistent mild anemia requiring erythropoietin therapy. Kaposi sarcoma lesions responded to therapy with thalidomide. Case 2 A 48-year-old woman from El Salvador with a history of diabetes mellitus and Helicobacter pylori induced peptic ulcer disease was admitted with warm antibody (IgG) autoimmune hemolytic anemia and fever. Pertinent laboratory results are listed in Table 1. Two bone marrow trephine biopsies performed approximately 2 weeks apart showed myelofibrosis (Table 2). Both biopsies were associated with unsuccessful attempts at bone marrow aspiration. Cytogenetic evaluation of the bone marrow revealed a normal female karyotype (46,XX). Peripheral blood cytopenias improved during a 4-month course of prednisone. One year after diagnosis, a follow-up bone marrow trephine biopsy was performed with successful marrow aspiration. At the time of this biopsy, there was normalization of the peripheral blood counts. Case 3 A 40-year-old African American woman was examined because of left wrist synovitis, persistent night sweats, and a 30-pound weight loss. The synovitis resolved with nonsteroidal anti-inflammatory drug therapy. The pertinent laboratory results are listed in Table 1. She was transfusion dependent. Additional laboratory workup revealed a total protein of 7.6 g/dl (76 g/l; reference range, g/dl [62-79 g/l]) with serum IgG of 2,010 mg/dl (20.1 g/l; reference range, 768-1,632 mg/dl [ g/l]). An antinuclear antibody assay initially was positive with a titer of 1:160 and a speckled pattern, but was negative on repeated analysis. Serum iron studies and increased bone marrow storage iron were most consistent with anemia of chronic disease. Vitamin B 12 and folate levels were normal. Results of upper gastrointestinal endoscopy, colonoscopy, and barium studies of the small intestine for suspected chronic gastrointestinal bleeding were normal. A bone marrow trephine biopsy showed myelofibrosis (Table 2). The biopsy was associated with unsuccessful attempts at bone marrow aspiration. Recent follow-up indicates the CBC count normalized with prednisone therapy. Table 1 Clinical Features and Laboratory Data for 3 Cases Case 1 Case 2 Case 3 Age (y)/sex 73/M 48/F 40/F Associated conditions Psoriasis; Kaposi sarcoma Diabetes; peptic ulcer Synovitis Hepatosplenomegaly + WBCs/µL ( 10 9 /L) 4,600 (4.6) 3,200 (3.2) 6,800 (6.8) Hemoglobin, g/dl (g/l) 9.1 (91) 9.2 (92) 6.8 (68) Mean corpuscular volume, µm 3 (fl) 99 (99) 87 (87) 76 (76) Platelets, 10 3 /µl ( 10 9 /L) 77 (77) 192 (192) 358 (358) Reticulocyte count, % 0.9 (0.009) 3.0 (0.03) 2.8 (0.028) Antinuclear antibody + (1:160; speckled); (repeated) Antimitochondrial antibody ND ND Anti smooth muscle antibody ND ND Rheumatoid factor, IU/mL <20 ND ND Erythrocyte sedimentation rate (mm/h) 18 ND 85 Erythropoietin, miu/ml (IU/L) 31 (31) 148 (148) 36 (36) Direct Coombs test + + ND Autoimmune hemolytic anemia + Antibody specificity ND Anti-Fy a ND Warm autoantibody (IgG) + HIV ND ND SLE criteria* 1/11 1/11 1/11 ND, not done; +, positive or present;, negative or absent. * Four or more American Rheumatism Association criteria are required for the diagnosis of systemic lupus erythematosus (SLE) Am J Clin Pathol 2001;116: American Society of Clinical Pathologists
3 Hematopathology / ORIGINAL ARTICLE Table 2 Peripheral Blood Smear Findings and the Initial Trephine Bone Marrow Biopsy Specimens: Morphologic Features and Reticulin Fibrosis Case 1 Case 2 Case 3 Peripheral blood smear morphologic features RBCs Moderate teardrop cells; Rare teardrop cells; Rare teardrop cells; rare nucleated RBCs rare nucleated RBCs rare nucleated RBCs WBCs Normal Mild left-shift Mild left-shift Platelets Normal Normal Rare giant forms Bone marrow biopsy Cellularity (%) Myeloid precursors Moderately Moderately Moderately Morphologic features Normal Mild hypersegmentation Normal Erythroid precursors Moderately ; left-shift Moderately ; left-shift Moderately ; left-shift Intrasinusoidal myeloid and erythroid precursors Megakaryocytes Moderately Slightly Moderately Size Normal Small Small Cluster formation Intrasinusoidal Lymphocytes Moderately Moderately Slightly Distribution Interstitial Interstitial Interstitial Aggregates Several, nonparatrabecular Many, nonparatrabecular Plasma cells Not increased Slightly Moderately Trabecular bone Normal Normal Thinned Reticulin fibrosis * Collagen fibrosis Large zones Large zones +, present (except for reticulin fibrosis);, absent;, decreased;, increased. * Scored on a 0-4+ scale. 19 Results Our patients ranged from 40 to 73 years in age and included 2 women and 1 man. All had signs and symptoms of autoimmune disease (psoriatic arthritis, autoimmune hemolytic anemia, and synovitis). None of our patients had conclusive serologic evidence of SLE, although one initially had a positive antinuclear antibody result. The American Rheumatism Association (ARA) has published criteria for the diagnosis of SLE. 18 These include cutaneous, renal, oral, rheumatologic, neurologic, hematologic, and serologic manifestations. Four or more features are required for this diagnosis. None of our patients demonstrated more than 1 criterion. They included thrombocytopenia (case 1), autoimmune hemolytic anemia (case 2), and synovitis (case 3). The morphologic features of the blood and bone marrow specimens are summarized in Table 2. At presentation, all patients had mild to moderate anemia, which was normochromic and normocytic (cases 1 and 2) or normochromic and microcytic (case 3). In all cases, rare to moderate teardrop cells and rare normoblasts were detected on the blood smears Image 1. The WBC count was mildly decreased in case 2 but normal in the other 2 cases. The WBCs were mildly left-shifted with rare myelocytes and occasional hypersegmented neutrophils (cases 2 and 3). Platelets were moderately decreased only in case 1. Rare circulating megakaryocytes were noted on the peripheral blood smear of case 2. Aspiration of the initial bone marrow was unsuccessful in all cases. The trephine biopsy cellularity was moderately hypocellular in case 1 and markedly hypercellular in the other 2 cases. Erythroid hyperplasia was present in all cases. In 2 cases, there was left-shifted erythroid maturation and increased pronormoblast islands. Intrasinusoidal hematopoiesis including megakaryocytes was identified in all cases Image 2. The number of megakaryocytes was moderately decreased in case 1 and slightly to moderately increased in the other 2 cases. Megakaryocytes were often small with hypolobated darkly staining nuclei (cases 2 and 3), but no megakaryocytes were found in clusters, nor were there bizarre shaped megakaryocytes. Marked, diffuse reticulin fibrosis was a consistent feature in all cases Image 3. In cases 1 and 3, large zones of collagen fibrosis also were seen. The initial trephine biopsy specimens demonstrated a moderate lymphocytosis with increased numbers of small lymphocytes. These cells had a delicate interstitial distribution in all cases and produced ill-defined, nonparatrabecular aggregates in cases 1 and 2 Image 4. Both components were composed of equal numbers of CD3+ T cells and CD20+ B cells. These lymphoid infiltrates failed to stain for kappa or lambda immunoglobulin light chain. Two patients had a mild to moderate increase in small, mature plasma American Society of Clinical Pathologists Am J Clin Pathol 2001;116:
4 Bass et al / AUTOIMMUNE MYELOFIBROSIS Image 1 (Case 1) Peripheral blood smear shows a rare normoblast and occasional teardrop erythrocytes (Wright- Giemsa, original magnification 200). Image 2 (Case 2) Markedly hypercellular bone marrow with intrasinusoidal hematopoiesis (H&E, original magnification 50). cells that expressed polytypic kappa and lambda immunoglobulin light chain staining. Follow-up bone marrow studies were performed only on case 2. The trephine and aspiration bone marrow biopsy specimens obtained following corticosteroid therapy showed marked hypercellularity with mild erythroid hyperplasia and moderately increased numbers of interstitial small lymphocytes and rare small, nonparatrabecular, poorly cohesive aggregates. Intrasinusoidal myeloid and erythroid hematopoiesis but no intrasinusoidal megakaryocytes were noted. A reticulin stain showed a marked delicate diffuse reticulin fibrosis, which was slightly less than that seen on the initial biopsy specimen. Immunohistochemical evaluation of the trephine biopsy specimen again demonstrated equal numbers of CD3+ T cells and CD20+ B cells within the interstitial infiltrate and lymphoid aggregates. Flow cytometric analysis of the bone marrow aspirate showed a normal distribution of T cells and B cells. Image 3 (Case 3) Bone marrow trephine biopsy specimen with marked, diffuse reticulin fibrosis and intrasinusoidal megakaryocytes (reticulin, original magnification 66). Image 4 (Case 2) Small, ill-defined, nonparatrabecular, lymphoid aggregate composed of small lymphocytes (H&E, original magnification 66). 214 Am J Clin Pathol 2001;116: American Society of Clinical Pathologists
5 Hematopathology / ORIGINAL ARTICLE Discussion AM has been identified in association with SLE, SLElike disease, rarely in Sjögren syndrome, and progressive systemic sclerosis The ARA requires a minimum of 4 criteria for the diagnosis of SLE. 18 A previous study of AM found 4 or more criteria in 5 of 8 cases. 2 Only 1 ARA feature was identified in each of our 3 cases: thrombocytopenia (case 1), autoimmune hemolytic anemia (case 2), and synovitis (case 3). Thus, none of our cases met standard criteria for the diagnosis of SLE. Rather, the abnormalities identified in these cases seem to be features of a heterogeneous group of autoimmune disorders associated with AM. Our 3 cases of AM had 1 or more cytopenias with rare to moderate teardrop cells, rare normoblasts, slightly leftshifted granulocytic maturation, and normal platelet morphologic features, with occasional giant platelets noted only in case 3. The lack of marked teardrop poikilocytosis and rarity of circulating immature myeloid precursor cells are useful features to differentiate AM from chronic idiopathic myelofibrosis. The bone marrow morphologic features of AM have been described inconsistently; hence, the main purpose for our study. We identified 25 cases of AM in the literature from 1966 to 2000 using the National Library of Medicine PubMed search service Morphologic assessment often was incomplete; however, the most commonly reported bone marrow biopsy features included the following: hypocellularity (10 of 21 evaluable cases); hypercellularity (8 of 21 evaluable cases, including 1 case of focal hypercellularity); normocellularity (3 of 21 evaluable cases); megakaryocytic hyperplasia (13 of 18 evaluable cases); and megakaryocyte clusters (4 of 4 evaluable cases). As expected, fibrosis was identified in all cases Bone marrow reticulin fibrosis or fibrosis was compared before and after corticosteroid therapy in a total of 15 cases. In 7 of these cases, there was no change in the degree of bone marrow reticulin fibrosis. However, peripheral blood parameters improved in 5 of these 7 cases after corticosteroid therapy. In the remaining 8 cases, bone marrow fibrosis following corticosteroid therapy was reportedly decreased in amount (4 cases), almost completely reversed (2 cases), and completely reversed (2 cases) with improvement or normalization of the peripheral blood parameters. The bone marrow trephine biopsy specimens in our cases differed from those described in the literature in that our cases were more often hypercellular and exhibited leftshifted erythroid hyperplasia and slightly to moderately increased numbers of megakaryocytes. Intrasinusoidal hematopoiesis including megakaryocytes, absence of megakaryocyte clusters, and marked reticulin fibrosis (case 2) with large zones of collagen fibrosis (cases 1 and 3) also were seen. A follow-up bone marrow biopsy specimen after corticosteroid therapy was available for only 1 case (case 2). Although counts normalized, there was no change in the morphologic features other than a slight decrease in reticulin fibrosis. Our remaining cases showed improvement in the CBC count after corticosteroid and erythropoietin therapy (case 1) and corticosteroid therapy alone (case 3). Bone marrow lymphoid infiltrates have been described in only 2 previously reported cases. 2,17 In both of these studies, the lymphoid infiltrate initially was thought to represent hairy cell leukemia. In 1 of these cases, the infiltrate was described as a lymphoid aggregate composed of mature lymphocytes. 2 In the other case, the bone marrow lymphoid infiltrate was described as a heavy spongy infiltration by large lymphocytic cells. 17 The lymphoid infiltrates in these cases were not further defined immunophenotypically. The bone marrow trephine biopsy specimens in our cases demonstrated slight to moderate lymphocytosis consisting of equal numbers of interstitial small T cells and B cells (all cases) and small, nonparatrabecular, loose lymphoid aggregates of similar composition (cases 1 and 2). In addition, 2 of our cases (cases 2 and 3) showed a mild to moderate increase in plasma cells with a polytypic immunoglobulin light chain staining pattern. This reactive lymphoid infiltration is consistent with an underlying autoimmune process. The differential diagnosis of AM includes myeloproliferative disorders (including the accelerated phase of chronic myelogenous leukemia, spent phase of polycythemia vera, and chronic idiopathic myelofibrosis), low-grade non- Hodgkin lymphoma, and hairy cell leukemia. Our cases lacked the characteristic features of myeloproliferative disorders in that there was no basophilia, eosinophilia, megakaryocyte clustering, or bizarre shaped megakaryocytes. Furthermore, morphologic and immunohistochemical features suggestive of malignant lymphoma or hairy cell leukemia were not identified. Although the cause of the bone marrow fibrosis is obscure, AM is a clinicopathologic manifestation of a diverse group of immune mediated disorders requiring a thorough clinical history and careful bone marrow morphologic assessment for accurate diagnosis. From the Departments of 1 Pathology and 2 Hematology, LAC+USC Medical Center and University of Southern California, Los Angeles; and Departments of 3 Hematology and 4 Pathology, Providence Saint Joseph Medical Center, Burbank, CA. Address reprint requests to Dr Brynes: USC Dept of Pathology, 2011 Zonal Ave, HMR 209, Los Angeles, CA References 1. McCarthy DM. Fibrosis of the bone marrow: content and causes. Br J Haematol. 1985;59:1-7. American Society of Clinical Pathologists Am J Clin Pathol 2001;116:
6 Bass et al / AUTOIMMUNE MYELOFIBROSIS 2. Paquette RL, Meshkinpour A, Rosen P. Autoimmune myelofibrosis: a steroid-responsive cause of bone marrow fibrosis associated with systemic lupus erythematosus. Medicine (Baltimore). 1994;73: Ramakrishna R, Kyle PW, Day PJ, et al. Evans syndrome, myelofibrosis and systemic lupus erythematosus: role of procollagens in myelofibrosis. Pathology. 1995;27: Borba EF, Pereira RM, Velloso ED, et al. Neutropenia associated with myelofibrosis in systemic lupus erythematosus. Acta Haematol. 1993;89: Hirose W, Fukuya H, Anzai T, et al. Myelofibrosis and systemic lupus erythematosus. J Rheumatol. 1993;20: Foley-Nolan D, Martin MF, Rowbotham D, et al. Systemic lupus erythematosus presenting with myelofibrosis. J Rheumatol. 1992;19: Matsouka C, Liouris J, Andrianakos A, et al. Systemic lupus erythematosus and myelofibrosis. Clin Rheumatol. 1989;8: Mouzan MI, Ahmad MA, Saleh MA, et al. Myelofibrosis and pancytopenia in systemic lupus erythematosus. Acta Haematol. 1988;80: Kaelin WG, Spivak JL. Systemic lupus erythematosus and myelofibrosis. Am J Med. 1986;81: Nanji AA, Jetha N. Myelofibrosis as a cause of pancytopenia in systemic lupus erythematosus [letter]. J Clin Pathol. 1984;37: Daly HM, Scott GL. Myelofibrosis as a cause of pancytopenia in systemic lupus erythematosus. J Clin Pathol. 1983;36: Lau KS, White JC. Myelosclerosis associated with systemic lupus erythematosus in patients in West Malaysia. J Clin Pathol. 1969;22: Inoue Y, Matsubara A, Okuya S, et al. Myelofibrosis and systemic lupus erythematosus: reversal of fibrosis with highdose corticosteroid therapy. Acta Haematol. 1992;88: Aharon A, Levy Y, Bar-Dayan Y, et al. Successful treatment of early secondary myelofibrosis in SLE with IVIG. Lupus. 1997;6: Marie I, Levesque H, Cailleux N, et al. An uncommon association: Sjögren s syndrome and autoimmune myelofibrosis [letter]. Rheumatology (Oxford). 1999;38: Gisser SD, Chung KB. Acute myelofibrosis in progressive systemic sclerosis: report of a case developing during longterm chlorambucil therapy and discussion of pathogenetic factors. Am J Med. 1979;67: Hasselbalch H, Jans H, Nielsen PL. A distinct subtype of idiopathic myelofibrosis with bone marrow features mimicking hairy cell leukemia: evidence of an autoimmune pathogenesis. Am J Hematol. 1987;25: Tan EM, Cohen AS, Fries JF, et al. The 1982 revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum. 1982;25: Bauermeister DE. Quantitation of bone marrow reticulin: a normal range. Am J Clin Pathol. 1971;56: Am J Clin Pathol 2001;116: American Society of Clinical Pathologists
Case Workshop of Society for Hematopathology and European Association for Haematopathology
 Case 148 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Robert P Hasserjian Department of Pathology Massachusetts General Hospital Boston, MA Clinical history
Case 148 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Robert P Hasserjian Department of Pathology Massachusetts General Hospital Boston, MA Clinical history
ADx Bone Marrow Report. Patient Information Referring Physician Specimen Information
 ADx Bone Marrow Report Patient Information Referring Physician Specimen Information Patient Name: Specimen: Bone Marrow Site: Left iliac Physician: Accession #: ID#: Reported: 08/19/2014 - CHRONIC MYELOGENOUS
ADx Bone Marrow Report Patient Information Referring Physician Specimen Information Patient Name: Specimen: Bone Marrow Site: Left iliac Physician: Accession #: ID#: Reported: 08/19/2014 - CHRONIC MYELOGENOUS
Bone Marrow Specimen (Aspirate and Trephine Biopsy) Proforma
 Bone Marrow Specimen (Aspirate and Trephine Biopsy) Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Sex Male Female Intersex/indeterminate Date
Bone Marrow Specimen (Aspirate and Trephine Biopsy) Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Sex Male Female Intersex/indeterminate Date
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Chronic Idiopathic Myelofibrosis (CIMF)
 Chronic Idiopathic Myelofibrosis (CIMF) CIMF Synonyms Agnogenic myeloid metaplasia Myelosclerosis with myeloid metaplasia Chronic granulocytic-megakaryocytic myelosis CIMF Megakaryocytic proliferation
Chronic Idiopathic Myelofibrosis (CIMF) CIMF Synonyms Agnogenic myeloid metaplasia Myelosclerosis with myeloid metaplasia Chronic granulocytic-megakaryocytic myelosis CIMF Megakaryocytic proliferation
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228
 2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
Ordering Physician CLIENT,CLIENT. Collected REVISED REPORT
 HPWET Hematopathology Consultation, MML Embed Client Hematopathology Consult REVISED INAL DIAGNOSIS Interpretation Peripheral blood, bone marrow aspirate and biopsies, bilateral iliac crests: 1. Normocellular
HPWET Hematopathology Consultation, MML Embed Client Hematopathology Consult REVISED INAL DIAGNOSIS Interpretation Peripheral blood, bone marrow aspirate and biopsies, bilateral iliac crests: 1. Normocellular
Pathology. #11 Acute Leukemias. Farah Banyhany. Dr. Sohaib Al- Khatib 23/2/16
 35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
Myelodysplastic Syndromes Myeloproliferative Disorders
 Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Case Presentation No. 075
 Case Presentation No. 075 Session 4. Myelodysplastic Syndrome Cristina Montalvo, MD Baylor College of Medicine Houston, Texas 2007 Workshop of Society for Hematopathology and European Association for Haematopathology
Case Presentation No. 075 Session 4. Myelodysplastic Syndrome Cristina Montalvo, MD Baylor College of Medicine Houston, Texas 2007 Workshop of Society for Hematopathology and European Association for Haematopathology
Polycthemia Vera (Rubra)
 Polycthemia Vera (Rubra) Polycthemia Vera (Rubra) Increased red cells Clonal Myeloid lineages also increased 2-13 cases per million Mean age: 60 years Sites of Involvement Bone marrow Peripheral blood
Polycthemia Vera (Rubra) Polycthemia Vera (Rubra) Increased red cells Clonal Myeloid lineages also increased 2-13 cases per million Mean age: 60 years Sites of Involvement Bone marrow Peripheral blood
Myeloid neoplasms. Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories:
 Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
2013 AAIM Pathology Workshop
 2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
Disclosures. Myeloproliferative Neoplasms: A Case-Based Approach. Objectives. Myeloproliferative Neoplasms. Myeloproliferative Neoplasms
 Myeloproliferative Neoplasms: A Case-Based Approach Disclosures No conflicts of interests regarding the topic being presented Adam M. Miller, MD PGY-4 Resident Physician Department of Pathology and Laboratory
Myeloproliferative Neoplasms: A Case-Based Approach Disclosures No conflicts of interests regarding the topic being presented Adam M. Miller, MD PGY-4 Resident Physician Department of Pathology and Laboratory
CASE 106. Pancytopenia in the setting of marrow hypoplasia, a PNH clone, and a DNMT3A mutation
 CASE 106 Pancytopenia in the setting of marrow hypoplasia, a PNH clone, and a DNMT3A mutation Gabriel C. Caponetti, MD University of Pennsylvania, US Clinical history 69, F peripheral neuropathy, refractory
CASE 106 Pancytopenia in the setting of marrow hypoplasia, a PNH clone, and a DNMT3A mutation Gabriel C. Caponetti, MD University of Pennsylvania, US Clinical history 69, F peripheral neuropathy, refractory
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD. Part 4 MYELOID NEOPLASMS
 HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA. April 16, 2008
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS LYMPHOMA April 16, 2008 FACULTY COPY GOAL: Learn the appearance of normal peripheral blood elements and lymph nodes. Recognize abnormal peripheral blood
Faculty of Medicine Dr. Tariq Aladily
 Iron deficiency anemia The most common anemia worldwide Only 10% of ingested iron is absorbed Most dietary iron occurs in meat products Absorbed in duodenum Hepcidin By inhibiting ferroportin, hepcidin
Iron deficiency anemia The most common anemia worldwide Only 10% of ingested iron is absorbed Most dietary iron occurs in meat products Absorbed in duodenum Hepcidin By inhibiting ferroportin, hepcidin
Hematopathology Case Study
 www.medfusionservices.com Hematopathology Case Study CV3515-14 JUNE Clinical Presentation: Clinical Information: A 42 year old male with history of chronic myelogenous leukemia (CML) presents with an elevated
www.medfusionservices.com Hematopathology Case Study CV3515-14 JUNE Clinical Presentation: Clinical Information: A 42 year old male with history of chronic myelogenous leukemia (CML) presents with an elevated
Pathology of Hematopoietic and Lymphoid tissue
 CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
CONTENTS Pathology of Hematopoietic and Lymphoid tissue White blood cells and lymph nodes Quantitative disorder of white blood cells Reactive lymphadenopathies Infectious lymphadenitis Tumor metastasis
ACCME/Disclosures 4/13/2016. Clinical History
 ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS which they or their spouse/partner
ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS which they or their spouse/partner
HEMATOPATHOLOGY (SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA): Rotation Director: Ying Li, M.D., Ph.D., Assistant Professor
 HEMATOPATHOLOGY (SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA): Rotation Director: Ying Li, M.D., Ph.D., Assistant Professor I. Description of the rotation: During this rotation, the resident will gain
HEMATOPATHOLOGY (SHANDS HOSPITAL AT THE UNIVERSITY OF FLORIDA): Rotation Director: Ying Li, M.D., Ph.D., Assistant Professor I. Description of the rotation: During this rotation, the resident will gain
MDS 101. What is bone marrow? Myelodysplastic Syndrome: Let s build a definition. Dysplastic? Syndrome? 5/22/2014. What does bone marrow do?
 101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
HEAMATOLOGICAL INDICES AND BONE MARROW BIOPSY
 HEAMATOLOGICAL INDICES AND BONE MARROW BIOPSY HEMATOCRIT Hematocrit is a measure of the percentage of the total blood volume that is made up by the red blood cells The hematocrit can be determined directly
HEAMATOLOGICAL INDICES AND BONE MARROW BIOPSY HEMATOCRIT Hematocrit is a measure of the percentage of the total blood volume that is made up by the red blood cells The hematocrit can be determined directly
Hematology Unit Lab 2 Review Material
 Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Myeloproliferative Disorders: Diagnostic Enigmas, Therapeutic Dilemmas. James J. Stark, MD, FACP
 Myeloproliferative Disorders: Diagnostic Enigmas, Therapeutic Dilemmas James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS
Myeloproliferative Disorders: Diagnostic Enigmas, Therapeutic Dilemmas James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS
Pathology of Hematopoietic and Lymphoid tissue
 Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Classification of Hematologic Malignancies. Patricia Aoun MD MPH
 Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Leukocytosis - Some Learning Points
 Leukocytosis - Some Learning Points Koh Liang Piu Department of Hematology-Oncology National University Cancer Institute National University Health System Objectives of this talk: 1. To provide some useful
Leukocytosis - Some Learning Points Koh Liang Piu Department of Hematology-Oncology National University Cancer Institute National University Health System Objectives of this talk: 1. To provide some useful
Warm Autoantibodies in a Patient with Hemophagocytic Lymphohistiocytosis: A Case Report
 Warm Autoantibodies in a Patient with Hemophagocytic Lymphohistiocytosis: A Case Report Emily Coberly, MD Department of Pathology and Anatomical Sciences University of Missouri Columbia April 30, 2013
Warm Autoantibodies in a Patient with Hemophagocytic Lymphohistiocytosis: A Case Report Emily Coberly, MD Department of Pathology and Anatomical Sciences University of Missouri Columbia April 30, 2013
APPROACHING TO PANCYTOPENIA
 APPROACHING TO PANCYTOPENIA P A T C H A R E E K O M V I L A I S A K, M. D. A S S I S T A N T P R O F E S S O R D I V I S I O N O F P E D I A T R I C H E M A T O L O G Y O N C O L O G Y, D E P A R T M E
APPROACHING TO PANCYTOPENIA P A T C H A R E E K O M V I L A I S A K, M. D. A S S I S T A N T P R O F E S S O R D I V I S I O N O F P E D I A T R I C H E M A T O L O G Y O N C O L O G Y, D E P A R T M E
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia. Abdallah Abbadi
 Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Anemia (3).ms4.25.Oct.15 Hemolytic Anemia Abdallah Abbadi Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k, retics 12%, LDH
Abstracting Hematopoietic Neoplasms
 CASE 1: LYMPHOMA PHYSICAL EXAMINATION 43yo male with a history of lower gastrointestinal bleeding and melena undergoing colonoscopy and biopsy to rule out neoplasm versus inflammation. Patient had no other
CASE 1: LYMPHOMA PHYSICAL EXAMINATION 43yo male with a history of lower gastrointestinal bleeding and melena undergoing colonoscopy and biopsy to rule out neoplasm versus inflammation. Patient had no other
Extramedullary precursor T-lymphoblastic transformation of CML at presentation
 Extramedullary precursor T-lymphoblastic transformation of CML at presentation Neerja Vajpayee, Constance Stein, Bernard Poeisz & Robert E. Hutchison Clinical History 30 year old man presented to the emergency
Extramedullary precursor T-lymphoblastic transformation of CML at presentation Neerja Vajpayee, Constance Stein, Bernard Poeisz & Robert E. Hutchison Clinical History 30 year old man presented to the emergency
The Complete Blood Count
 The Complete Blood Count (Cartesian Thinking at Its Best) A SEM Image of Normal Human Blood Laurie Larsson February 22, 2010 Anatomy and Philology II Dr. Danil Hammoudi Introduction A complete blood count
The Complete Blood Count (Cartesian Thinking at Its Best) A SEM Image of Normal Human Blood Laurie Larsson February 22, 2010 Anatomy and Philology II Dr. Danil Hammoudi Introduction A complete blood count
Year 2003 Paper two: Questions supplied by Tricia
 QUESTION 65 A 36-year-old man presents in a post-ictal state after an observed generalised seizure. Full blood investigation shows: haemoglobin 0 g/l [128-175] mean corpuscular volume (MCV) 106 fl [80-7]
QUESTION 65 A 36-year-old man presents in a post-ictal state after an observed generalised seizure. Full blood investigation shows: haemoglobin 0 g/l [128-175] mean corpuscular volume (MCV) 106 fl [80-7]
Disclosure BCR/ABL1-Negative Classical Myeloproliferative Neoplasms
 Disclosure BCR/ABL1-Negative Classical Myeloproliferative Neoplasms Sonam Prakash declares affiliation with Incyte Corporation: Advisor for Hematopathology Publications Steering Committee Sonam Prakash,
Disclosure BCR/ABL1-Negative Classical Myeloproliferative Neoplasms Sonam Prakash declares affiliation with Incyte Corporation: Advisor for Hematopathology Publications Steering Committee Sonam Prakash,
UNUSUAL PRESENTATIONS OF SYSTEMIC LUPUS ERYTHEMATOSUS
 UNUSUAL PRESENTATIONS OF SYSTEMIC LUPUS ERYTHEMATOSUS Presenter- Dr. Meghana B S Prof Dr. NAGARAJA B S Prof Dr. NIRMALA A C Dr. SIVARANJANI H Dr. B C PRAKASH Dr. MUMTAZ ALI KHAN A 60 year old lady, k/c/o
UNUSUAL PRESENTATIONS OF SYSTEMIC LUPUS ERYTHEMATOSUS Presenter- Dr. Meghana B S Prof Dr. NAGARAJA B S Prof Dr. NIRMALA A C Dr. SIVARANJANI H Dr. B C PRAKASH Dr. MUMTAZ ALI KHAN A 60 year old lady, k/c/o
MDS: Who gets it and how is it diagnosed?
 MDS: Who gets it and how is it diagnosed? October 16, 2010 Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine Weill Medical College of Cornell University The New York Presbyterian
MDS: Who gets it and how is it diagnosed? October 16, 2010 Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine Weill Medical College of Cornell University The New York Presbyterian
Hematopathology Lab. Third year medical students
 Hematopathology Lab Third year medical students Objectives Identify the lesion Know the specific name of the lesion Know associated disease Know relevant pathologic background Spherocytes: appear small,
Hematopathology Lab Third year medical students Objectives Identify the lesion Know the specific name of the lesion Know associated disease Know relevant pathologic background Spherocytes: appear small,
WBCs Disorders 1. Dr. Nabila Hamdi MD, PhD
 WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
Collected: , PM Sent: , PM Received: , PM Preliminary: , PM. Notification Status: COMPREHENSIVE DIAGNOSIS
 PATIENT Name:HIPAA, Compliant DOB: 03-25-1945 (60 yr) ID#: xxx-xx-0000 Sex: M Tel: xxx-xxx-xxxx SPECIMEN Your No:WS05-xxxx Case No:C05-00xxx Req. No:Txxxxx Collected: 06-08-05, PM Sent: 06-09-05, PM Received:
PATIENT Name:HIPAA, Compliant DOB: 03-25-1945 (60 yr) ID#: xxx-xx-0000 Sex: M Tel: xxx-xxx-xxxx SPECIMEN Your No:WS05-xxxx Case No:C05-00xxx Req. No:Txxxxx Collected: 06-08-05, PM Sent: 06-09-05, PM Received:
2013 Pathology Student
 About this guide If you re reading this introduction, it means you are probably either a) covering hematopathology in your pathology class right now, or b) studying for boards. Either way, you ve come
About this guide If you re reading this introduction, it means you are probably either a) covering hematopathology in your pathology class right now, or b) studying for boards. Either way, you ve come
MYELODYSPLASTIC SYNDROMES
 MYELODYSPLASTIC SYNDROMES Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra university hospital, Isfahan university of medical sciences Key Features ESSENTIALS OF DIAGNOSIS Cytopenias
MYELODYSPLASTIC SYNDROMES Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra university hospital, Isfahan university of medical sciences Key Features ESSENTIALS OF DIAGNOSIS Cytopenias
Hematology Unit Lab 1 Review Material
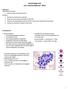 Hematology Unit Lab 1 Review Material - 2018 Objectives Laboratory instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Hematology Unit Lab 1 Review Material - 2018 Objectives Laboratory instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
BLASTIC CRISIS AND MYELOFIBROSIS SIMULTANEOUS COMPLICATIONS IN A CASE OF CHRONIC MYELOCYTIC LEUKEMIA
 BLASTIC CRISIS AND MYELOFIBROSIS SIMULTANEOUS COMPLICATIONS IN A CASE OF CHRONIC MYELOCYTIC LEUKEMIA Abstract Pages with reference to book, From 151 To 153 Khalid Hassan ( Department of Pathology (Haematology)
BLASTIC CRISIS AND MYELOFIBROSIS SIMULTANEOUS COMPLICATIONS IN A CASE OF CHRONIC MYELOCYTIC LEUKEMIA Abstract Pages with reference to book, From 151 To 153 Khalid Hassan ( Department of Pathology (Haematology)
Study of advantages and disadvantages of bone marrow trephine biopsy over bone marrow aspiration
 Original article: Study of advantages and disadvantages of bone marrow trephine biopsy over bone marrow aspiration 1 Dr. Smita Bhadekar *, 2 Dr.Sunita Patil 1Assistant Professor, Dept. of Pathology, BJGMC,
Original article: Study of advantages and disadvantages of bone marrow trephine biopsy over bone marrow aspiration 1 Dr. Smita Bhadekar *, 2 Dr.Sunita Patil 1Assistant Professor, Dept. of Pathology, BJGMC,
High Impact Rheumatology
 High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls
 Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure
 Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY
 V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY Kharkov Regional Centre of Cardiovascular surgery V.N. Karazin Kharkov National University Department of Internal Medicine Immune thrombocytopenic purpura Abduyeva
V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY Kharkov Regional Centre of Cardiovascular surgery V.N. Karazin Kharkov National University Department of Internal Medicine Immune thrombocytopenic purpura Abduyeva
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms. Daniel A. Arber, MD Stanford University
 Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
Myelodysplastic Syndrome: Let s build a definition
 1 MDS: Diagnosis and Treatment Update Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine Weill Medical College of Cornell University The New York Presbyterian Hospital Myelodysplastic
1 MDS: Diagnosis and Treatment Update Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine Weill Medical College of Cornell University The New York Presbyterian Hospital Myelodysplastic
Evaluation of Bone Marrow Biopsies and Aspirates ANNA PORWIT DEPARTMENT OF PATHOLOGY, LUND UNIVERSITY
 Evaluation of Bone Marrow Biopsies and Aspirates ANNA PORWIT DEPARTMENT OF PATHOLOGY, LUND UNIVERSITY DISCLOSURES NONE Learning objectives To review the rules of BMA evaluation To review the main issues
Evaluation of Bone Marrow Biopsies and Aspirates ANNA PORWIT DEPARTMENT OF PATHOLOGY, LUND UNIVERSITY DISCLOSURES NONE Learning objectives To review the rules of BMA evaluation To review the main issues
Anemia (3).ms Hemolytic Anemia. Abdallah Abbadi Feras Fararjeh
 Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
Anemia (3).ms4.26.2.18 Hemolytic Anemia Abdallah Abbadi Feras Fararjeh Case 3 24 yr old female presented with anemia syndrome and jaundice. She was found to have splenomegaly. Hb 8, wbc 12k, Plt 212k,
Disorders of Blood Cells & Blood Coagulation
 Disorders of Blood Cells & Blood Coagulation HIHIM 409 WBC count RBC count WBC differential Hemoglobin (HGB) Hematocrit (HCT) % of volume occupied by RBCs CBC Red cell indices Mean cell volume (MCV) average
Disorders of Blood Cells & Blood Coagulation HIHIM 409 WBC count RBC count WBC differential Hemoglobin (HGB) Hematocrit (HCT) % of volume occupied by RBCs CBC Red cell indices Mean cell volume (MCV) average
CLINICO-PATHOLOGICAL CONFERENCE CLASS OF 2007/2012 PHASE IIIB SESSION 2010/2012
 CLINICO-PATHOLOGICAL CONFERENCE CLASS OF 2007/2012 PHASE IIIB SESSION 2010/2012 PRESENTATION OF CASE A 62-year-old woman was seen in the outpatient cancer center of this hospital because of anemia and
CLINICO-PATHOLOGICAL CONFERENCE CLASS OF 2007/2012 PHASE IIIB SESSION 2010/2012 PRESENTATION OF CASE A 62-year-old woman was seen in the outpatient cancer center of this hospital because of anemia and
r). SUPPLEMENTARY/SECOND OPPORTUNITY EXAMINATION PAPER nnmlbih UNIVERSITY Sophia Blaauw INSTRUCTIONS FACULTY OF HEALTH AND APPLIED SCIENCES
 r). nnmlbih UNIVERSITY OF SCIEFICE nnd TECHNOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES QUALIFICATION: BACHELOR OF MEDICAL LABORATORY SCIENCES QUALIFICATION CODE: 08BMLS
r). nnmlbih UNIVERSITY OF SCIEFICE nnd TECHNOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES QUALIFICATION: BACHELOR OF MEDICAL LABORATORY SCIENCES QUALIFICATION CODE: 08BMLS
The Power of Peripheral Blood Smears: Apparent Diagnostic Clues (Part 1) (Wednesday, October 19, 2011)
 The Power of Peripheral Blood Smears: Apparent Diagnostic Clues (Part 1) (Wednesday, October 19, 2011) By Gene Gulati, Ph.D., SH(ASCP) Conflict of Interest None Plan for the Course Review blood smears,
The Power of Peripheral Blood Smears: Apparent Diagnostic Clues (Part 1) (Wednesday, October 19, 2011) By Gene Gulati, Ph.D., SH(ASCP) Conflict of Interest None Plan for the Course Review blood smears,
SB 6331 (scanned slide available) Keith Duncan; Mills-Peninsula Hospital 52-year-old male with painful right parotid mass.
 SB 6331 (scanned slide available) Keith Duncan; Mills-Peninsula Hospital 52-year-old male with painful right parotid mass. SB 6332 Shyam Raghavan/Don Born; Stanford 77-year-old male with right
SB 6331 (scanned slide available) Keith Duncan; Mills-Peninsula Hospital 52-year-old male with painful right parotid mass. SB 6332 Shyam Raghavan/Don Born; Stanford 77-year-old male with right
The Internists Approach to Polycythemia and Implications of Uncontrolled Disease
 The Internists Approach to Polycythemia and Implications of Uncontrolled Disease Mary Jo K. Voelpel, DO, FACOI, MA, CS Associate Clinical Professor MSU-COM Disclosures NONE Overview 1. Objectives 2. Case
The Internists Approach to Polycythemia and Implications of Uncontrolled Disease Mary Jo K. Voelpel, DO, FACOI, MA, CS Associate Clinical Professor MSU-COM Disclosures NONE Overview 1. Objectives 2. Case
FBC CASES Vernon Louw Clinical Haematology 2010
 FBC CASES Vernon Louw Clinical Haematology 2010 FOR EACH OF THE FOLLOWING PATIENTS, SELECT THE MOST LIKELY FINDING FROM THE ANALYSIS OF THE PERIPHERAL BLOOD. A patient with infectious mononucleosis. A
FBC CASES Vernon Louw Clinical Haematology 2010 FOR EACH OF THE FOLLOWING PATIENTS, SELECT THE MOST LIKELY FINDING FROM THE ANALYSIS OF THE PERIPHERAL BLOOD. A patient with infectious mononucleosis. A
Bone marrow histopathology in Ph - CMPDs. - the new WHO classification - Juergen Thiele Cologne, Germany
 Bone marrow histopathology in Ph - CMPDs - the new WHO classification - Juergen Thiele Cologne, Germany Current issues in MPNs concerning morphology 1.Prodromal stages of disease 2.Impact of histopathology
Bone marrow histopathology in Ph - CMPDs - the new WHO classification - Juergen Thiele Cologne, Germany Current issues in MPNs concerning morphology 1.Prodromal stages of disease 2.Impact of histopathology
Western Health Specialist Clinics Access & Referral Guidelines
 Haematology Specialist Clinics at Western Health: Western Health runs MBS funded Specialist Clinics on a Wednesday and Thursday afternoon at its Sunshine Hospital site for patients who require assessment
Haematology Specialist Clinics at Western Health: Western Health runs MBS funded Specialist Clinics on a Wednesday and Thursday afternoon at its Sunshine Hospital site for patients who require assessment
20/20 PATHOLOGY REPORTS
 20/20 PATHOLOGY REPORTS Improving the Physician Experience. Enhancing the Patient Experience. We are LabTest Diagnostics. LabTest Diagnostics has a full-service laboratory with state-of-the-art equipment
20/20 PATHOLOGY REPORTS Improving the Physician Experience. Enhancing the Patient Experience. We are LabTest Diagnostics. LabTest Diagnostics has a full-service laboratory with state-of-the-art equipment
Deconstructing the CBC
 Deconstructing the CBC Dr. Ann M. Wexler Solano Hematology Oncology September 10, 2017 What Are the Major Components of Blood? Red Blood Cells (also called erythrocytes) White Blood Cells (also called
Deconstructing the CBC Dr. Ann M. Wexler Solano Hematology Oncology September 10, 2017 What Are the Major Components of Blood? Red Blood Cells (also called erythrocytes) White Blood Cells (also called
Anemia in the elderly. Nattiya Teawtrakul MD., PhD
 Anemia in the elderly Nattiya Teawtrakul MD., PhD Contents Definition of anemia in the elderly The impact of anemia in the elderly Etiology of anemia in the elderly Management of anemia in the elderly
Anemia in the elderly Nattiya Teawtrakul MD., PhD Contents Definition of anemia in the elderly The impact of anemia in the elderly Etiology of anemia in the elderly Management of anemia in the elderly
MYELOPROLIFERATIVE DISEASE. Dr Mere Kende MBBS (UPNG), MMED (Path),MAACB, MACTM, MACRRM (Aus) Lecturer-SMHS UPNG
 MYELOPROLIFERATIVE DISEASE Dr Mere Kende MBBS (UPNG), MMED (Path),MAACB, MACTM, MACRRM (Aus) Lecturer-SMHS UPNG Myeloproliferative Diseases Essential to diagnosis Acquired clonal abnormalities of the hematopoietic
MYELOPROLIFERATIVE DISEASE Dr Mere Kende MBBS (UPNG), MMED (Path),MAACB, MACTM, MACRRM (Aus) Lecturer-SMHS UPNG Myeloproliferative Diseases Essential to diagnosis Acquired clonal abnormalities of the hematopoietic
Antinuclear antibodies positive patient with splenic infarct a diagnostic dilemma
 www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Antinuclear antibodies positive patient with splenic infarct a diagnostic dilemma Sabina Langer, Ravi Daswani, Rahul Arora, Nitin Gupta, Anil
www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Antinuclear antibodies positive patient with splenic infarct a diagnostic dilemma Sabina Langer, Ravi Daswani, Rahul Arora, Nitin Gupta, Anil
Bone marrow morphology in reactive conditions. Kaaren K. Reichard, MD Mayo Clinic Rochester
 Bone marrow morphology in reactive conditions Kaaren K. Reichard, MD Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Outline of Presentation Brief introduction General
Bone marrow morphology in reactive conditions Kaaren K. Reichard, MD Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Outline of Presentation Brief introduction General
Bone marrow fibrosis as a feature of systemic lupus erythematosus: a case report and literature review
 Chalayer et al. SpringerPlus 2014, 3:349 a SpringerOpen Journal REVIEW Open Access Bone marrow fibrosis as a feature of systemic lupus erythematosus: a case report and literature review Émilie Chalayer
Chalayer et al. SpringerPlus 2014, 3:349 a SpringerOpen Journal REVIEW Open Access Bone marrow fibrosis as a feature of systemic lupus erythematosus: a case report and literature review Émilie Chalayer
Does Morphology Matter in 2017
 Does Morphology Matter in 2017 ISLH May 2017 Kathryn Foucar Distinguished Professor Emerita kfoucar@salud.unm.edu Objectives Recognize unique RBC and WBC abnormalities in non-neoplastic disorders Learn
Does Morphology Matter in 2017 ISLH May 2017 Kathryn Foucar Distinguished Professor Emerita kfoucar@salud.unm.edu Objectives Recognize unique RBC and WBC abnormalities in non-neoplastic disorders Learn
Correspondence should be addressed to Anas Khanfar;
 Case Reports in Oncological Medicine, Article ID 949515, 4 pages http://dx.doi.org/10.1155/2014/949515 Case Report Durable Hematological and Major Cytogenetic Response in a Patient with Isolated 20q Deletion
Case Reports in Oncological Medicine, Article ID 949515, 4 pages http://dx.doi.org/10.1155/2014/949515 Case Report Durable Hematological and Major Cytogenetic Response in a Patient with Isolated 20q Deletion
74y old Female with chronic elevation of Platelet count. August 18, 2005 Faizi Ali, MD Hematopathology Fellow
 74y old Female with chronic elevation of Platelet count August 18, 2005 Faizi Ali, MD Hematopathology Fellow Clinical History Patient is a 74y old otherwise healthy Caucasian female with no major complaint
74y old Female with chronic elevation of Platelet count August 18, 2005 Faizi Ali, MD Hematopathology Fellow Clinical History Patient is a 74y old otherwise healthy Caucasian female with no major complaint
CHAPTER:4 LEUKEMIA. BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY 8/12/2009
 LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data
 Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
WHO Update to Myeloproliferative Neoplasms
 WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
The ABCs of Waldenström s Macroglobulinemia (WM)
 The ABCs of Waldenström s Macroglobulinemia (WM) Jeffrey V. Matous MD Colorado Blood Cancer Institute IWMF Ed Forum May 2017 Objectives Describe the roots underneath WM Review incidence, possible risk
The ABCs of Waldenström s Macroglobulinemia (WM) Jeffrey V. Matous MD Colorado Blood Cancer Institute IWMF Ed Forum May 2017 Objectives Describe the roots underneath WM Review incidence, possible risk
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Osteosclerotic Myeloma (POEMS Syndrome)
 Osteosclerotic Myeloma (POEMS Syndrome) Osteosclerotic Myeloma (POEMS Syndrome) Synonyms Crow-Fukase syndrome Multicentric Castleman disease Takatsuki syndrome Acronym coined by Bardwick POEMS Scheinker,
Osteosclerotic Myeloma (POEMS Syndrome) Osteosclerotic Myeloma (POEMS Syndrome) Synonyms Crow-Fukase syndrome Multicentric Castleman disease Takatsuki syndrome Acronym coined by Bardwick POEMS Scheinker,
Case Report Myeloid Neoplasms in the Guise of Nutritional Deficiency
 Hindawi Publishing Corporation Case Reports in Hematology Volume 2012, Article ID 826939, 5 pages doi:10.1155/2012/826939 Case Report Myeloid Neoplasms in the Guise of Nutritional Deficiency Veda Parthasarathy
Hindawi Publishing Corporation Case Reports in Hematology Volume 2012, Article ID 826939, 5 pages doi:10.1155/2012/826939 Case Report Myeloid Neoplasms in the Guise of Nutritional Deficiency Veda Parthasarathy
Acute Immune Thrombocytopenic Purpura (ITP) in Childhood
 Acute Immune Thrombocytopenic Purpura (ITP) in Childhood Guideline developed by Robert Saylors, MD, in collaboration with the ANGELS team. Last reviewed by Robert Saylors, MD September 22, 2016. Key Points
Acute Immune Thrombocytopenic Purpura (ITP) in Childhood Guideline developed by Robert Saylors, MD, in collaboration with the ANGELS team. Last reviewed by Robert Saylors, MD September 22, 2016. Key Points
Conditions that mimic neoplasia in the bone marrow. Kaaren K. Reichard Mayo Clinic Rochester
 Conditions that mimic neoplasia in the bone marrow Kaaren K. Reichard Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Learning Objectives Multiple conditions in
Conditions that mimic neoplasia in the bone marrow Kaaren K. Reichard Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Learning Objectives Multiple conditions in
CASE REPORTS. Jorida Kuçaj 1, Sotiraq Lako 1, Etleva Gjoshe 1, Teuta Dedej 2. Abstract
 CASE REPORTS ALBANIAN MEDICAL JOURNAL methotrexate therapy and hyperleukocytosis after filgrastim administration to a patient with subacute cutaneous Lupus Erythematosus Jorida Kuçaj 1, Sotiraq Lako 1,
CASE REPORTS ALBANIAN MEDICAL JOURNAL methotrexate therapy and hyperleukocytosis after filgrastim administration to a patient with subacute cutaneous Lupus Erythematosus Jorida Kuçaj 1, Sotiraq Lako 1,
Taking The Fear Out of Abnormal CBC s Problems of Production, Destruction or loss
 Taking The Fear Out of Abnormal CBC s Problems of Production, Destruction or loss Joanne Eddington, MN, FNP, AOCN Providence Oncology and Hematology Care Clinic - Eastside Blood Cell Abnormalities Abnormalities
Taking The Fear Out of Abnormal CBC s Problems of Production, Destruction or loss Joanne Eddington, MN, FNP, AOCN Providence Oncology and Hematology Care Clinic - Eastside Blood Cell Abnormalities Abnormalities
Severe anemia CASE DISCUSSION ANGELA SHIH, MD, RUBY E. KASSANOFF, MD, AND BASEL ALTRABULSI, MD
 CASE DISCUSSION Severe anemia ANGELA SHIH, MD, RUBY E. KASSANOFF, MD, AND BASEL ALTRABULSI, MD CASE PRESENTATION ANGELA SHIH, MD: A 35-year-old, previously healthy homosexual man was admitted because of
CASE DISCUSSION Severe anemia ANGELA SHIH, MD, RUBY E. KASSANOFF, MD, AND BASEL ALTRABULSI, MD CASE PRESENTATION ANGELA SHIH, MD: A 35-year-old, previously healthy homosexual man was admitted because of
Avoiding Early Cancer Claims. Presentation #4. Hank George, FALU
 Avoiding Early Cancer Claims Presentation #4 Hank George, FALU Hematology and High Risk of Early Cancer Claims Mild Anemia in elders is underpriced by insurers most likely because of its high prevalence
Avoiding Early Cancer Claims Presentation #4 Hank George, FALU Hematology and High Risk of Early Cancer Claims Mild Anemia in elders is underpriced by insurers most likely because of its high prevalence
Participants Identification No. % Evaluation. Mitotic figure Educational Erythrocyte precursor, abnormal 1 0.
 Cell Identification Mitotic figure 212 99.5 Educational Erythrocyte precursor, abnormal BMD-02 The arrowed cell is a mitotic figure. It was correctly identified by 99.5% of the participants. A cell containing
Cell Identification Mitotic figure 212 99.5 Educational Erythrocyte precursor, abnormal BMD-02 The arrowed cell is a mitotic figure. It was correctly identified by 99.5% of the participants. A cell containing
CD34 positive dysplastic giant platelets masquerading as blasts on flow cytometry
 CD34+ Giant Platelets Hematopathology - September 2016 Case Study CD34 positive dysplastic giant platelets masquerading as blasts on flow cytometry Anmaar Abdul-Nabi 1,*, Yvette Reese 2, Susan Treese 2,
CD34+ Giant Platelets Hematopathology - September 2016 Case Study CD34 positive dysplastic giant platelets masquerading as blasts on flow cytometry Anmaar Abdul-Nabi 1,*, Yvette Reese 2, Susan Treese 2,
Hematology 101. Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD
 Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
Collect and label sample according to standard protocols. Gently invert tube 8-10 times immediately after draw. DO NOT SHAKE. Do not centrifuge.
 Complete Blood Count CPT Code: CBC with Differential: 85025 CBC without Differential: 85027 Order Code: CBC with Differential: C915 Includes: White blood cell, Red blood cell, Hematocrit, Hemoglobin, MCV,
Complete Blood Count CPT Code: CBC with Differential: 85025 CBC without Differential: 85027 Order Code: CBC with Differential: C915 Includes: White blood cell, Red blood cell, Hematocrit, Hemoglobin, MCV,
Peripheral Blood Smear: Diagnostic Clues and Algorithms
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Hematology: Challenging Cases with Your Participation COPYRIGHT
 Hematology: Challenging Cases with Your Participation Reed E. Drews, MD Beth Israel Deaconess Medical Center Harvard Medical School Boston, MA Question 1 Question 1 64-year-old man is evaluated during
Hematology: Challenging Cases with Your Participation Reed E. Drews, MD Beth Israel Deaconess Medical Center Harvard Medical School Boston, MA Question 1 Question 1 64-year-old man is evaluated during
Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies
 Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies Directions: Each of the numbered items or incomplete statements in this section is followed by answers or by completions of the statement.
Medical Immunology Practice Questions-2016 Autoimmunity + Case Studies Directions: Each of the numbered items or incomplete statements in this section is followed by answers or by completions of the statement.
Approach to a pale child
 Approach to a pale child Dr. Dafalla Ahmed Babiker Jazan university objectives Definition of anemia Classification and causes Important points in history and physical examination Investigations. Definition
Approach to a pale child Dr. Dafalla Ahmed Babiker Jazan university objectives Definition of anemia Classification and causes Important points in history and physical examination Investigations. Definition
12 Dynamic Interactions between Hematopoietic Stem and Progenitor Cells and the Bone Marrow: Current Biology of Stem Cell Homing and Mobilization
 Table of Contents: PART I: Molecular and Cellular Basis of Hematology 1 Anatomy and Pathophysiology of the Gene 2 Genomic Approaches to Hematology 3 Regulation of Gene Expression, Transcription, Splicing,
Table of Contents: PART I: Molecular and Cellular Basis of Hematology 1 Anatomy and Pathophysiology of the Gene 2 Genomic Approaches to Hematology 3 Regulation of Gene Expression, Transcription, Splicing,
Case Report. Introduction. Mastocytosis associated with CML Hematopathology - March K. David Li 1,*, Xinjie Xu 1, and Anna P.
 Mastocytosis associated with CML Hematopathology - March 2016 Case Report Systemic mastocytosis with associated clonal hematologic non-mast cell lineage disease (SM-AHNMD) involving chronic myelogenous
Mastocytosis associated with CML Hematopathology - March 2016 Case Report Systemic mastocytosis with associated clonal hematologic non-mast cell lineage disease (SM-AHNMD) involving chronic myelogenous
Diagnostic challenge: Acute leukemia with biphenotypic blasts and BCR-ABL1 translocation
 Case Study Diagnostic challenge: Acute leukemia with biphenotypic blasts and BCR-ABL1 translocation Ling Wang 1 and Xiangdong Xu 1,2,* 1 Department of Pathology, University of California, San Diego; 2
Case Study Diagnostic challenge: Acute leukemia with biphenotypic blasts and BCR-ABL1 translocation Ling Wang 1 and Xiangdong Xu 1,2,* 1 Department of Pathology, University of California, San Diego; 2
Myelodysplastic Syndrome Case 158
 Myelodysplastic Syndrome Case 158 Dong Chen MD PhD Division of Hematopathology Mayo Clinic Clinical History 86 year old man Persistent borderline anemia and thrombocytopenia. His past medical history was
Myelodysplastic Syndrome Case 158 Dong Chen MD PhD Division of Hematopathology Mayo Clinic Clinical History 86 year old man Persistent borderline anemia and thrombocytopenia. His past medical history was
