St Vincent s SportsMed
|
|
|
- Ilene Todd
- 5 years ago
- Views:
Transcription
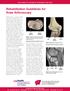
1 St Vincent s SportsMed Cartilage Transplantation In The Knee INTRODUCTION Normal articular cartilage is characterized by a smooth surface with very low friction and the ability to withstand repeated high loads. Loss of this smooth surface leads to pain, loss of motion, swelling and eventually deformity. This will ultimately result in degenerative osteoarthritis.(1,2) A variety of methods have been developed over the past 20 years and are now available to regenerate cartilage and effectively reproduce its natural characteristics. BACKGROUND Tissue engineering to treat cartilage injury has been in use for almost 20 years. Peterson and Brittberg first described their technique of autologous cartilage implantation (ACI) in They went on to publish their first clinical results in 1994.(3) The original technique delivered the grown cartilage cells as a suspension and was contained in a piece of the patients own periosteum (membranous sleeve from bone). This has been refined to its current state where the cells are imbedded on to a collagen scaffold, (see Fig 5) improving the surgical technique and potentially the results. ARTICULAR CARTILAGE AND INJURY Articular cartilage lesions are difficult to treat in part due to the distinctive structure and remarkable function of hyaline cartilage. Functional cartilage relies upon a homeostasis between water, chondrocytes (cartilage cells), macromolecules and type II collagen. The sparseness of cells, the unique architecture of cartilage and the fact that it is avascular, aneuric and alymphatic, give it superior loading characteristics but also the inability to spontaneously heal.(4,5) Injury to articular cartilage is common following sporting injuries, road accidents and even accidental falls in every day life. The injured cartilage produces a very poor healing response due to the lack of blood supply and limited inflammatory reaction, which is required for healing. The scarring that occurs in cartilage is inadequate and biomechanically inferior, making the surface more prone to accelerated wear and premature degenerative osteoarthritis. It would therefore seem logical to diagnose and subsequently treat articular cartilage defects early. The concepts that small lesions are insignificant is not supported and a recent study of elite soccer players demonstrated persistent knee pain due to chondral defects, even in lesions less than 10mm in diameter.(6) Pain probably occurs due to the irritation of nerve endings in subchondral bone. Significant advances have been made in the field of prosthetic joint replacement but articular cartilage defects in younger patients (under 50 years of age), remains a problem due to the limited lifespan of these prostheses. This has led to extensive research into the knee for a biological solution for cartilage defects. There are a number of techniques which attempt to produce regeneration of native articular cartilage. These include: 1. Microfracture 2. Osteochondral Autografts 3. Perichondral transfers 4. Allograft (cadaveric) donation 5. Autologous Chondrocyte Implantation (ACI). It is the latter technique which appears the most promising. 1
2 MAKING THE DIAGNOSIS OF A CARTILAGE LESION As is the case in all medical conditions, a thorough evaluation of the symptomatic patient including history, examination and assessment of investigations, is the key to diagnosing chondral lesions in the knee. Examination should document Body Mass Index (BMI), lower limb alignment, gait patterns, patellofemoral, meniscal and ligamentous evaluation, as well as signs attributable directly to cartilage lesions such as point tenderness, crepitus, catching and an effusion. Weight bearing radiographs can demonstrate arthritic changes, but isolated cartilage lesions are best seen on high resolution MRI or under direct vision using arthroscopy. MRI MRI is a non-invasive tool which is becoming increasingly useful in the diagnostic assessment of cartilage defects. Newer MRI sequences are being developed to assess the biomechanical and functional profile of articular cartilage. Some sequences will potentially have the ability to assess proteoglycan content,(7) a molecule crucial to adequate cartilage functioning. ARTHROSCOPY Inspection of the articular cartilage surfaces using arthroscopy may indeed be the gold standard for cartilage assessment. Despite being performed as an outpatient procedure and through key-holes it is still an invasive investigative tool. It does, however, allow critical assessment of cartilage surfaces as well as assessment of the rest of the knee including ligaments, menisci and global arthritic changes. The next stage in diagnostic arthroscopy is visualization of the joint through an arthroscope the size of an 18 guage needle so the procedure can be performed in the doctors office under local anaesthetic. This device is currently in use in selected units in the United States. ( Innervue Arthrotek) Once the diagnosis of a cartilage lesion is made (See Figure 1 and 2), clinical assessment and investigations are used to determine appropriateness for articular cartilage transplantation. THE IDEAL PATIENT Basic science research into the homeostasis of cartilage and increasing number of clinical reports has helped define a list of indications and contraindications for cartilage transplantation. Indications for ACI Age <55 years old Isolated, full thickness cartilage defect Femoral or Patellofemoral defect that is contained Compliant rehab patient Stable knee (Intact ligaments) Intact meniscal cartilage Normal alignment to lower extremities Contraindications to ACI Inflammatory or crystal arthritis Active infection Widespread advanced cartilage loss Age (relative) Some of these indications/contraindications can be controlled and patients can be made more appropriate for this surgery. For example, a malaligned knee can be corrected at the same time as the implantation of cartilage cells. Similarly, an unstable knee can have a ligament reconstruction and even a joint without a meniscus can have an artifical meniscus inserted. Age is relative, and a patient s physiological age is often a more reliable indicator of surgical candidacy.
3 The ideal surgical candidate is often difficult to find. The ideal candidate for Anterior Cruciate Ligament reconstruction is a young, continuingly active, well motivated patient with normal motion, full strength and normal biomechanics in the joint. One could argue that such a patient is too good to undergo the reconstruction. It is preferable to operate on patients without co-morbidities such as heart disease, hypertension, hypercholesterolaemia or diabetes, but this is often unavoidable and should not exclude patients with such conditions from at least consideration for operative procedures. The same is true for ACI. Even patients who are not the ideal patient or who have cartilage lesions that are not perfect for the procedure, should at least be assessed and ACI considered. Current recommendations suggest that patients who are perhaps borderline candidates for ACI should have as many variables adjusted (such as ligaments, alignment, and menisci) to make them more appropriate for the procedure and ultimately a better result.(8, 9, 10) THE PROCEDURE as per the Matrix enhanced Autologous Chondrocyte Implantation (MACI) see Figure 4 The completed process is a two stage procedure. Stage 1 Cell Harvest (Figure 1) The first surgery is arthroscopic and is often undertaken to diagnose and initiate treatment for suspected lesions. At arthroscopy, once a cartilage lesion is identified (see Fig 1and 2), good cartilage cells are harvested from the non-weightbearing area of the intercondylar notch. (This is the area that is commonly cleared during cruciate ligament reconstruction.) Approximately 200 mg of cartilage cells are desired. In practical terms, this is effectively, less cartilage than a tic-tac. The piece of cartilage is aseptically transferred to the cartilage laboratory and the chondrocytes are extracted. Under strict highly regulated conditions the cartilage cells are multiplied in vitro, seeded on to a porcine collagen bilayer membrane and then cryopreserved. The cells can then be stored until elective re-implantation. Stage 2 Re-implantation (Figures 6,7 and 8) The elective re-implantation can be performed as soon as the cells have multiplied adequately over the membrane (as soon as 4 weeks) or can be postponed until a more convenient time is available. An open arthrotomy is required for this part of the procedure. The cartilage defect is prepared to accept the graft and then the patient s chondrocyte-seeded membrane is fixed to the defect with fibrin glue. Concomitant procedures to improve biomechanics (cruciate ligament reconstruction, patellofemoral re-alignment, osteotomy) are usually performed with this surgery. The patients can be discharged home in 1-2 days usually dependant upon the concomitant procedures. Timing of surgery A time lag up to one year has traditionally been offered to patients between these two cartilage implantation stages. This wait and see how your knee goes now seems unwise due to irreversible changes seen in the ultrastructure and durability of articular cartilage when the conforming surfaces are altered.(11) It is becoming increasingly evident that significant defects in cartilage that are left unattended cause irreversible damage to adjacent surfaces. Intuitively this seems obvious as a pot-hole on one side of the joint must rub and wear the opposing surface. Translating this into clinical practice, however, is difficult but implies that once a full thickness cartilage lesion is identified, cartilage transplantation should be considered as soon as practicable. REHABILITATION Research focused specifically on rehabilitation after MACI is currently in a rapid growth phase with new basic science studies and clinical results reported every month. The lack of definitive research however, on the stress required to disrupt the cartilage graft has resulted in an over conservative approach to rehabilitation programmes. The past two years have seen rehab
4 recommendations shorten from originally 18 months to 12 months. This will shorten further as our understanding of this procedure improves. Orthopaedic surgeons have seen a similar evolution in Anterior Cruciate Ligament (ACL) accelerated rehab programmes. Low shear cyclical exercise is now commenced immediately following ACL surgery resulting in faster recovery and earlier return to sport. Braces are no longer recommended and crutches are discarded by 2 weeks. We know that the ACL graft matures beyond 12 months yet appropriate rehab allows a return to cutting sports at an average of 6 months. It is an accelerated approach such as this that we can expect to see with MACI. Current Recommendations MACI rehabilitation is driven by the fact that the procedure consists of 2 stages, the initial assessment and biopsy of cartilage and finally the implantation of cultured chondrocytes through an open arthrotomy. If the second stage procedure includes a re-alignment or ligament reconstruction, this will further slow the recovery time. The rehab also becomes specific depending on the site of the cartilage defect. A femoral condylar lesion needs to be protected from weight bearing but knee flexion is safe as long as it is undertaken in a manner to minimize shear forces. Comparatively, a patellofemoral lesion needs maximum protection from flexion/shear loads but will allow weight bearing. This means weight-bearing with the knee straight is allowed with patella lesions but stair climbing needs to be avoided in the early stage. The rehab for cartilage transplantation has been divided into 6 stages(12) PHASE I: Recovery and Protection Weeks 0-4 PHASE II: Inauguration Weeks 4-8 PHASE III: Maturation Weeks 8-12 PHASE IV: Integration Weeks PHASE V: Functional Adaptation Weeks PHASE VI: Return to Sports Weeks (Phases V and VI are dependant on specific sporting goals.) In brief, this means bracing and alteration in weight bearing for up to 3 months and restriction in sports from 6-12 months depending upon what the sport involves. RESULTS Fu et.al. reported over 80% of patients following ACI to femoral lesions had improvement in pain and function after 3 years follow-up.(14) Peterson et al found 82% patients were good to excellent 5-11 years after ACI.(15) 72% good to excellent results have recently been described in elite level soccer players.(13) This durability of ACI was found to be due to the hyaline-like cartilage repair tissue. Graft survivorship after 2 years is excellent.
5 COST ACI is a newer technique and more costly than traditional conservative therapies. However, there is more in evaluating the relative merits of a surgical procedure than its dollar value. Cartilage lesions cause pain, disability and time off work. The economic burden of a cartilage defect has recently been evaluated by Lindahl et al. Assessing 57 patients over 10 years they found the cost of absenteeism and disability due to a cartilage lesion to be USD $122,807 compared to USD $5,875 for the surgery.(16) CONCLUSION In summary, autologous cartilage transplantation to treat articular defects in the knee is now readily available. Good to excellent clinical results are approaching 15 years. Patients need to be appropriately selected and counseled on the limitations of this technique and advised of the comprehensive rehabilitation required to ensure the success of this procedure. REFERENCES 1. Buckwalter JA, Mankin HJ. Articualr cartilage. Part II: degeneration and osteoarthrosis, repair, regeneration, and transplantation. J Bone Joint Surg Am. 1997;79: Hunziker EB. Articular cartilage repair: basic science and clinical progress. A review of the current status and prospects. Osteoarthritis Cartilage. 2002; 10; Brittberg M, Lindahl A, Nilsson A, Ohlsson C, Isaksson O, Peterson L. Treatment of deep cartilage defects in the knee with autologous chondrocyte transplantation. N Engl J Med. 1994;331: Brower TD, Hsu WY. Normal articular cartilage. Clin Orthop 1969; 64: Cheung HS, Cottrey WH, Stephensen K, Nimmi ME. In vitro collagen biosynthesis in healing and normal articular cartilage. JBJS 1976; 60(8)A: Levy AS, Lohnes J, Sculley S, LeCroy M, Garrett W. Chondral delamination of the knee In soccer players. Am J sports Med 1996: 24(5) Sgaglione NA, Miniaci A, Gillogly SD, Carter TR. Update on advanced surgical techniques in the treatment of traumatic focal articular cartilage lesions in the knee. JARS 18. No2 2002; Mandelbaum BR, Browne JE, Fu F, et al. Articular cartilage lesions of the knee. Am J Sports Med. 1998;26: Minas T. The role of cartilage repair techniques, including chondrocyte transplantation, in focal chondral knee damage. Instr Course Lect. 1999;48: Peterson L, Brittberg M, Kiviranta I, Akerlund EL, Lindahl A. Autologous chondrocyte transplantation: biomechanics and long-term durability. Am J Sports Med. 2002;30: Rijk PC, Tigchelaar-Gutter W, Bernoski FP, Van Noorden CJF. Functional Changes in Articular Cartilage After Meniscal Allograft Transplantation: A Quantitative Histochemical Evaluation in Rabbits. AJARS Vol 22, No 2 Feb 2006; Hambly K, Bobic V, Wondrasch B, Van Assche D, Marlovits S. Autologous Chondrocyte Implantation Postoperative Care and Rehabilitation. Am J Sports Med Vol 34, No Mithöfer K, Peterson L, Mandelbaum B, Minas T. Articular Cartilage Repair in Soccer Players With Autologous Chondrocyte Transplantation: Functional Outcome and Return to Competition. Am. J. Sports Med., Nov 2005; 33: Fu F, Zurakowski D, Browne J, Mandelbaum B, Erggelet C, Moseley B, Anderson A, Micheli L. Autologous Chondrocyte Implantation Versus Debridement for Treatment of Full-Thickness Chondral Defects of the Knee. Am J Sports Med 33: (2005). 15. Peterson L, Brittberg M, Kiviranta I, Akerlund EL, Lindahl A. Autologous chondrocyte transplantation: biomechanics and long-term durability. Am J Sports Med. 2002;30: Lindahl A, Brittberg M, Peterson L. Health economic benefits following autologous chondrocyte transplantation for patients with focal chondral lesions of the knee. In Knee Surgery, Sports Traumatology, Arthroscopy. Vol 9, No.6. November 2001.
6 PICTURES 1 Intraoperative arthroscopic photo of a cartilage defect being biopsied. 2 Intraoperative arthroscopic photo of full thickness cartilage defect. 3 Arthroscopic reassessment of a fully healed defect. 4 Schematic diagram representing the stages of MACI (Matrix enhanced Autologous Chondrocyte Implantation): 1.Debridement of the lesion. 2.Culturing of the cells on to the membrane. 3.Sizing the membrane to the defect. 4.Reimplantation of the chondrocyte rich membrane. 5 Scanning Electron Micrograph demonstrating viable cartilage cells amongst the collagen fibrils of the membrane. 6 The cartilage membrane is delivered to the operating room. 7 Stage II: Operative photograph of a full thickness femoral condyle lesion 8 Stage II: The same patient with a cartilage graft filling the defect. Diagrams and photos used with permission courtesy of Genzyme. Figure1 Figure 2 Figure 3 Figure 5 Figure 6 Figure 4 Figure 7 Figure 8 6
7 7
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT
 OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
OSTEOCHONDRAL ALLOGRAFT RECONSTRUCTION FOR MASSIVE BONE DEFECT Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati
TREATMENT OF CARTILAGE LESIONS
 TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
TREATMENT OF CARTILAGE LESIONS Angelo J. Colosimo, MD -Head Orthopaedic Surgeon University of Cincinnati Athletics -Director of Sports Medicine University of Cincinnati Medical Center -Associate Professor
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3
 AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR CHONDRAL KNEE DAMAGE B.A. Jalba 1, C.S. Jalba 2, F. Gherghina 3, M. Cruce 3 1-EMERGENCY CLINICAL HOSPITAL FLOREASCA BUCHAREST 2-EMERGENCY CLINICAL HOSPITAL SFANTUL
ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS
 ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS
ARTICULAR CARTILAGE RESTORATION: A REVIEW OF CURRENTLY AVAILABLE METHODS FOR REPAIR OF ARTICULAR CARTILAGE DEFECTS AMERICAN ACADEMY OF ORTHOPAEDIC SURGEONS 76TH ANNUAL MEETING FEBRUARY 25-28, 2009 LAS
Chondral Injuries in the Athlete
 Chondral Injuries in the Athlete Michael J. Stuart MD Professor of Orthopedic Surgery Chair, Division of Sports Medicine Mayo Clinic 2013 MFMER slide-1 Michael J. Stuart MD February 5, 2014 Financial Relationships
Chondral Injuries in the Athlete Michael J. Stuart MD Professor of Orthopedic Surgery Chair, Division of Sports Medicine Mayo Clinic 2013 MFMER slide-1 Michael J. Stuart MD February 5, 2014 Financial Relationships
Knee Preservation and Articular Cartilage Restoration
 Knee Preservation and Articular Cartilage Restoration With Special Thanks to Aaron Krych, MD and Riley Willims, MD Zak Knutson, MD Articular Cartilage Layer of tissue covering the bone which are part of
Knee Preservation and Articular Cartilage Restoration With Special Thanks to Aaron Krych, MD and Riley Willims, MD Zak Knutson, MD Articular Cartilage Layer of tissue covering the bone which are part of
Disclosures. How to approach cartilage repair. Articular Cartilage Problems: Surface Options
 Disclosures I have the following potential conflicts of interest: Consulting payments/royalties and research support directly related to products discussed: Vericel (ACI) [consultant] SLACK publishing
Disclosures I have the following potential conflicts of interest: Consulting payments/royalties and research support directly related to products discussed: Vericel (ACI) [consultant] SLACK publishing
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
OSTEOCHONDRAL ALLOGRAFTS AND AUTOGRAFTS IN THE TREATMENT OF FOCAL ARTICULAR CARTILAGE LESIONS
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-115 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
AUTOLOGOUS CHONDROCYTE IMPLANTATION FOR FOCAL ARTICULAR CARTILAGE LESIONS
 CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
CARTILAGE LESIONS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Articular Cartilage Surgical Restoration Options
 Articular Cartilage Surgical Restoration Options Randy Schwartzberg, M.D. Assistant Professor - UCF College of Medicine Rationale Our bodies do not make articular/hyaline cartilage. gics injections to
Articular Cartilage Surgical Restoration Options Randy Schwartzberg, M.D. Assistant Professor - UCF College of Medicine Rationale Our bodies do not make articular/hyaline cartilage. gics injections to
Autologous Chondrocyte Implantation. Gerard Hardisty FRACS
 Autologous Chondrocyte Implantation Gerard Hardisty FRACS Disclosure Orthopaedic Surgeons Strong as an OX and half as bright Orthopaedic Innovation Arthroscopy Joint replacement Trauma management MIS Early
Autologous Chondrocyte Implantation Gerard Hardisty FRACS Disclosure Orthopaedic Surgeons Strong as an OX and half as bright Orthopaedic Innovation Arthroscopy Joint replacement Trauma management MIS Early
PATIENT GUIDE TO CARTILAGE INJURIES
 Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Lucas Wymore, MD Sports Medicine 23000 Moakley Street Suite 102 Leonardtown MD 20650 Office Phone: 301-475-5555 Office Fax: 301-475- 5914 Email: lwymore@somdortho.com PATIENT GUIDE TO CARTILAGE INJURIES
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries. Cartilage Surgery. The Knee.
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries Cartilage Surgery The Knee CARTILAGE INJURY Treatment of cartilage injury remains one of the most significant challenges
Does Autologous Chondrocyte Implantation Provide Better Outcomes Than Microfracture in the Repair of Articular Knee Defects?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2012 Does Autologous Chondrocyte Implantation
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2012 Does Autologous Chondrocyte Implantation
Why do they fail?? TOM MINAS MD MS. The Management of Failed Cartilage Repair Procedures PALM BEACH FL
 The Management of Failed Cartilage Repair Procedures Why do they fail?? TOM MINAS MD MS DIRECTOR, CARTILAGE REPAIR CENTER, PALEY ORTHOPEDIC INSTITUTE, PALM BEACH FL PROFESSOR EMERITUS, HARVARD MEDICAL
The Management of Failed Cartilage Repair Procedures Why do they fail?? TOM MINAS MD MS DIRECTOR, CARTILAGE REPAIR CENTER, PALEY ORTHOPEDIC INSTITUTE, PALM BEACH FL PROFESSOR EMERITUS, HARVARD MEDICAL
Introduction Knee Anatomy and Function Making the Diagnosis
 Introduction Knee injuries are a very common problem among active individuals. It is important for us to understand how your knee was injured. Most knee injuries are associated with non-contact mechanisms.
Introduction Knee injuries are a very common problem among active individuals. It is important for us to understand how your knee was injured. Most knee injuries are associated with non-contact mechanisms.
Joint Preservation Clinical Case
 Joint Preservation Clinical Case Jason M. Scopp, M.D. Director of Joint Preservation Peninsula Orthopaedic Associates, 1/19/19 Rational Rationale There are no absolutes. There is no dogma. Organize thoughts,
Joint Preservation Clinical Case Jason M. Scopp, M.D. Director of Joint Preservation Peninsula Orthopaedic Associates, 1/19/19 Rational Rationale There are no absolutes. There is no dogma. Organize thoughts,
Life. Uncompromised. The KineSpring Knee Implant System Surgeon Handout
 Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Life Uncompromised The KineSpring Knee Implant System Surgeon Handout 2 Patient Selection Criteria Patient Selection Criteria Medial compartment degeneration must be confirmed radiographically or arthroscopically
Treatment Options for Articular Cartilage Defects of the Knee
 Innovations Treatment Options for Articular Cartilage Defects of the Knee Alvin J. Detterline Steven Goldberg ernard R. ach, Jr. rian J. Cole The treatment of symptomatic articular cartilage defects of
Innovations Treatment Options for Articular Cartilage Defects of the Knee Alvin J. Detterline Steven Goldberg ernard R. ach, Jr. rian J. Cole The treatment of symptomatic articular cartilage defects of
Basics of Cartilage Restoration Introduction of TruFit
 Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
Basics of Cartilage Restoration Introduction of TruFit Philip A. Davidson, MD Heiden Orthopaedics Park City, Utah USA Smith & Nephew Seminar London, UK October 2008 Cartilage Restoration A wide realm between..
New Directions in Osteoarthritis Research
 New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
New Directions in Osteoarthritis Research Kananaskis October 22, 2015 Nick Mohtadi MD MSc FRCSC No conflicts of interest related to this presentation 1 Osteoarthritis: Disease? Fact of Life? Strong family
Cartilage Care in the Mature Female Athlete
 Cartilage Care in the Mature Female Athlete K. Linnea Welton, MD Hip Preservation Fellow Department of Orthopedic Surgery University of Colorado Women in Sports Medicine Conference February 24, 2018 Disclosures
Cartilage Care in the Mature Female Athlete K. Linnea Welton, MD Hip Preservation Fellow Department of Orthopedic Surgery University of Colorado Women in Sports Medicine Conference February 24, 2018 Disclosures
CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS
 CARTILAGE REPAIR TECHNIQUES CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS Written by Steffano Zaffagnini, Francesco Perdisa and Giuseppe Filardo, Italy Knee articular cartilage defects greater
CARTILAGE REPAIR TECHNIQUES CARTILAGE REPAIR PROCEDURES IN LARGE CARTILAGE DEFECTS Written by Steffano Zaffagnini, Francesco Perdisa and Giuseppe Filardo, Italy Knee articular cartilage defects greater
Increased Failure Rate of Autologous Chondrocyte Implantation After Previous Treatment With Marrow Stimulation Techniques
 Increased Failure Rate of Autologous Chondrocyte Implantation After Previous Treatment With Marrow Stimulation Techniques Tom Minas,* MD, MS, Andreas H. Gomoll, MD, Ralf Rosenberger, MD, Ronald O. Royce,
Increased Failure Rate of Autologous Chondrocyte Implantation After Previous Treatment With Marrow Stimulation Techniques Tom Minas,* MD, MS, Andreas H. Gomoll, MD, Ralf Rosenberger, MD, Ronald O. Royce,
Corporate Medical Policy
 Corporate Medical Policy Autologous Chondrocyte Implantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: autologous_chondrocyte_implantation 4/1996 6/2017 6/2018 6/2017 Description
Corporate Medical Policy Autologous Chondrocyte Implantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: autologous_chondrocyte_implantation 4/1996 6/2017 6/2018 6/2017 Description
Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee
 1 Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee Mitsuo Ochi, M.D. PhD Professor and chairman Department of Orthopaedic Surgery Graduate School
1 Histologic change of cartilage layer of osteochondritis dissecans before and after fixation in the knee Mitsuo Ochi, M.D. PhD Professor and chairman Department of Orthopaedic Surgery Graduate School
ARTICULAR CARTILAGE INJURY: EVALUATION AND WORK-UP ISMF Carlsbad Ca.
 ARTICULAR CARTILAGE INJURY: EVALUATION AND WORK-UP IMF 2018- Carlsbad Ca. Ken Zaslav MD Director: Cartilage Restoration Center ORTHO VIRGINIA: Richmond Virginia Clinical Prof. of Orthopedic urgery: V.C.U.
ARTICULAR CARTILAGE INJURY: EVALUATION AND WORK-UP IMF 2018- Carlsbad Ca. Ken Zaslav MD Director: Cartilage Restoration Center ORTHO VIRGINIA: Richmond Virginia Clinical Prof. of Orthopedic urgery: V.C.U.
CARTILAGE LESIONS IN THE PATELLOFEMORAL JOINT
 GENERAL OVERVIEW CARTILAGE LESIONS IN THE PATELLOFEMORAL JOINT Written by Mats Brittberg, Sweden The general low level of understanding of problems in the patellofemoral joint is reflected in the large
GENERAL OVERVIEW CARTILAGE LESIONS IN THE PATELLOFEMORAL JOINT Written by Mats Brittberg, Sweden The general low level of understanding of problems in the patellofemoral joint is reflected in the large
Medical Practice for Sports Injuries and Disorders of the Knee
 Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
Sports-Related Injuries and Disorders Medical Practice for Sports Injuries and Disorders of the Knee JMAJ 48(1): 20 24, 2005 Hirotsugu MURATSU*, Masahiro KUROSAKA**, Tetsuji YAMAMOTO***, and Shinichi YOSHIDA****
American Journal of Sports Medicine
 American Journal of Sports Medicine http://ajs.sagepub.com Prospective Evaluation of Concurrent Meniscus Transplantation and Articular Cartilage Repair: Minimum 2-Year Follow-Up LCDR John-Paul H. Rue,
American Journal of Sports Medicine http://ajs.sagepub.com Prospective Evaluation of Concurrent Meniscus Transplantation and Articular Cartilage Repair: Minimum 2-Year Follow-Up LCDR John-Paul H. Rue,
Evolution and Current Role of Autologous Chondrocyte Implantation for Treatment of Articular Cartilage Defects in the Football (Soccer) Player
 Evolution and Current Role of Autologous Chondrocyte Implantation for Treatment of Articular Cartilage Defects in the Football (Soccer) Player The Harvard community has made this article openly available.
Evolution and Current Role of Autologous Chondrocyte Implantation for Treatment of Articular Cartilage Defects in the Football (Soccer) Player The Harvard community has made this article openly available.
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
OSCELL ARTICULAR CARTILAGE CELL IMPLANTATION (FEMORAL CONDYLE SITES) PATIENT ADVICE.
 OSCELL ARTICULAR CARTILAGE CELL IMPLANTATION ( SITES) PATIENT ADVICE. Anatomy of the Right Knee example of a femoral articular defect site Knee Straight Knee Bent KEY: Patella Kneecap Trochlea Groove on
OSCELL ARTICULAR CARTILAGE CELL IMPLANTATION ( SITES) PATIENT ADVICE. Anatomy of the Right Knee example of a femoral articular defect site Knee Straight Knee Bent KEY: Patella Kneecap Trochlea Groove on
Ideal Candidate for Cartilage Restoration. Large or Complex Lesions
 Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Complex Biological Knee Reconstruction: Bipolar, Multifocal Lesions and Osteoarthritis William Bugbee, MD Attending Physician, Scripps Clinic 18 th International Sports Medicine Fellow s Conference Ideal
Osteochondral allografting for all other joints is not covered as the evidence is insufficient to determine the
 Medical Coverage Policy Osteochondral Autologous Chrondrocyte Implantation for Focal Articular Cartilage Lesions EFFECTIVE DATE: 05 20 2008 POLICY LAST UPDATED: 10 16 2018 OVERVIEW A variety of procedures
Medical Coverage Policy Osteochondral Autologous Chrondrocyte Implantation for Focal Articular Cartilage Lesions EFFECTIVE DATE: 05 20 2008 POLICY LAST UPDATED: 10 16 2018 OVERVIEW A variety of procedures
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
Anterior Cruciate Ligament (ACL) Injuries Mark L. Wood, MD The anterior cruciate ligament (ACL) is one of the most commonly injured ligaments of the knee. The incidence of ACL injuries is currently estimated
ANTERIOR CRUCIATE LIGAMENT (ACL) INJURIES
 ANTERIOR CRUCIATE LIGAMENT (ACL) INJURIES WHAT IS THE ACL? The ACL is a very strong ligament on the inside of the knee. It runs from the femur (thigh bone) obliquely down to the Tibia (shin bone). The
ANTERIOR CRUCIATE LIGAMENT (ACL) INJURIES WHAT IS THE ACL? The ACL is a very strong ligament on the inside of the knee. It runs from the femur (thigh bone) obliquely down to the Tibia (shin bone). The
OSCELL ARTICULAR CARTILAGE CELL IMPLANTATION (PATELLOFEMORAL SITES) PATIENT ADVICE.
 OSCELL ARTICULAR CARTILAGE CELL IMPLANTATION ( SITES) PATIENT ADVICE. Anatomy of the Right Knee example of a trochlea articular defect site Knee Straight Knee Bent KEY: Patella Kneecap Trochlea Groove
OSCELL ARTICULAR CARTILAGE CELL IMPLANTATION ( SITES) PATIENT ADVICE. Anatomy of the Right Knee example of a trochlea articular defect site Knee Straight Knee Bent KEY: Patella Kneecap Trochlea Groove
Osteochondral Knee Injuries. Marc N Ialenti, MD PGY-4 8/19/14
 Osteochondral Knee Injuries Marc N Ialenti, MD PGY-4 8/19/14 Articular Cartilage Complex, layered structure Viscoelastic material Resist shear forces Variable loadbearing Range of motion Position Essential
Osteochondral Knee Injuries Marc N Ialenti, MD PGY-4 8/19/14 Articular Cartilage Complex, layered structure Viscoelastic material Resist shear forces Variable loadbearing Range of motion Position Essential
Osteochondritis Dissecans
 Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Osteochondritis Dissecans Introduction Osteochondritis dissecans (OCD) is a problem that affects the knee, mostly at the end of the big bone of the thigh (the femur). A joint surface damaged by OCD doesn't
Autologous Chondrocyte Implantation Improves Patellofemoral Cartilage Treatment Outcomes
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 000, pp. 000 000 2007 Lippincott Williams & Wilkins Autologous Chondrocyte Implantation Improves Patellofemoral Cartilage Treatment Outcomes Jack Farr,
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 000, pp. 000 000 2007 Lippincott Williams & Wilkins Autologous Chondrocyte Implantation Improves Patellofemoral Cartilage Treatment Outcomes Jack Farr,
A Patient s Guide to Osteochondritis Dissecans of the Knee
 A Patient s Guide to Osteochondritis Dissecans of the Knee 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Osteochondritis Dissecans of the Knee 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide. ACL Injury: Ø Frequently asked questions on injury, Ø Preoperative and postoperative. surgery and recovery.
 ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
Theoretical Background Cartilage
 Theoretical Background Cartilage NEW TECHNIQUES FOR CARTILAGE REPAIR AND REPLACEMENT Kevin R. Stone, M.D. Michael J. Mullin, ATC, PTA Injury to the cartilage of the knee joint is one of the most common
Theoretical Background Cartilage NEW TECHNIQUES FOR CARTILAGE REPAIR AND REPLACEMENT Kevin R. Stone, M.D. Michael J. Mullin, ATC, PTA Injury to the cartilage of the knee joint is one of the most common
Clinical Policy: Articular Cartilage Defect Repairs Reference Number: CP.MP.26
 Clinical Policy: Reference Number: CP.MP.26 Effective Date: 10/08 Last Review Date: 05/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.26 Effective Date: 10/08 Last Review Date: 05/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury
 Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
Mr Aslam Mohammed FRCS, FRCS (Orth) Consultant Orthopaedic Surgeon Specialising in Lower Limb Arthroplasty and Sports Injury I qualified from the Welsh National School of Medicine in Cardiff in 1984. I
Meniscal Tears/Deficiency in Athletes
 Meniscal Tears/Deficiency in Athletes A. Amendola MD Professor of Orthopaedic Surgery Director of Sports Medicine Duke University 1 2 Meniscal tears Introduction Meniscal tears are one of the most frequent
Meniscal Tears/Deficiency in Athletes A. Amendola MD Professor of Orthopaedic Surgery Director of Sports Medicine Duke University 1 2 Meniscal tears Introduction Meniscal tears are one of the most frequent
Treatment of Full-Thickness Chondral Defects in the Knee With Autologous Chondrocyte Implantation
 Treatment of Full-Thickness Chondral Defects in the Knee With Autologous Chondrocyte Implantation Scott D. Gillogly, MD 1 Thomas H. Myers, MD 2 Michael M. Reinold, PT, DPT, ATC, CSCS 3 Autologous chondrocyte
Treatment of Full-Thickness Chondral Defects in the Knee With Autologous Chondrocyte Implantation Scott D. Gillogly, MD 1 Thomas H. Myers, MD 2 Michael M. Reinold, PT, DPT, ATC, CSCS 3 Autologous chondrocyte
Anterior Cruciate Ligament Injuries
 Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
Anterior Cruciate Ligament Injuries One of the most common knee injuries is an anterior cruciate ligament sprain or tear.athletes who participate in high demand sports like soccer, football, and basketball
The American Journal of Sports Medicine
 The American Journal of Sports Medicine http://ajs.sagepub.com/ Recommendations and Treatment Outcomes for Patellofemoral Articular Cartilage Defects With Autologous Chondrocyte Implantation Cecilia Pascual-Garrido,
The American Journal of Sports Medicine http://ajs.sagepub.com/ Recommendations and Treatment Outcomes for Patellofemoral Articular Cartilage Defects With Autologous Chondrocyte Implantation Cecilia Pascual-Garrido,
Knee Articular Cartilage Restoration: From cells to the patient. Professor Lars Engebretsen, University of Oslo, Norway
 Knee Articular Cartilage Restoration: From cells to the patient Professor Lars Engebretsen, University of Oslo, Norway Much of this started in 1994: I 1989 Grande et al -cartilage cell transplantation
Knee Articular Cartilage Restoration: From cells to the patient Professor Lars Engebretsen, University of Oslo, Norway Much of this started in 1994: I 1989 Grande et al -cartilage cell transplantation
Disclosures 8/11/2017. ACI 2 Stage Technique Generation 1. Technical Improvements and Expansion of Indications based on evidence for ACI
 Technical Improvements and Expansion of Indications based on evidence for ACI Tom Minas MD MS Director, Cartilage Repair Center, Brigham and Women s, Hospital, Professor, Harvard Medical School, Boston
Technical Improvements and Expansion of Indications based on evidence for ACI Tom Minas MD MS Director, Cartilage Repair Center, Brigham and Women s, Hospital, Professor, Harvard Medical School, Boston
Knee Cartilage Transplants
 Knee Cartilage Transplants Date of Origin: 3/2005 Last Review Date: 8/23/2017 Effective Date: 8/23/2017 Dates Reviewed: Developed By: Medical Necessity Criteria Committee I. Description Allograft transplants
Knee Cartilage Transplants Date of Origin: 3/2005 Last Review Date: 8/23/2017 Effective Date: 8/23/2017 Dates Reviewed: Developed By: Medical Necessity Criteria Committee I. Description Allograft transplants
Failed Cartilage Repair
 Chapter 27 Failed Cartilage Repair Robert C. Grumet, Sarvottam Bajaj, and Brian J. Cole The management of traumatic and degenerative cartilage lesions is a known challenge given the limited vascularity
Chapter 27 Failed Cartilage Repair Robert C. Grumet, Sarvottam Bajaj, and Brian J. Cole The management of traumatic and degenerative cartilage lesions is a known challenge given the limited vascularity
Marrow (MSC) Stimulation Techniques: Microfracture/Microfracture Plus/Cartiform Kai Mithoefer, MD
 Marrow (MSC) Stimulation Techniques: Microfracture/Microfracture Plus/Cartiform Kai Mithoefer, MD Harvard Vanguard Medical Associates New England Baptist Hospital Boston, USA Cartilage Repair Marrow Stimulation
Marrow (MSC) Stimulation Techniques: Microfracture/Microfracture Plus/Cartiform Kai Mithoefer, MD Harvard Vanguard Medical Associates New England Baptist Hospital Boston, USA Cartilage Repair Marrow Stimulation
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Does Every Knee Need a Meniscus?
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/does-every-knee-need-a-meniscus/3799/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/does-every-knee-need-a-meniscus/3799/
AN OVERVIEW : Cartilage Treatment. Eric Thiel, MD. WVAM Conference 01/25/2019
 AN OVERVIEW : Cartilage Treatment Eric Thiel, MD WVAM Conference 01/25/2019 No Disclosure The Science of Hyaline Cartilage I. HYALINE CARTILAGE BASIC SCIENCE Normal Anatomy Cartilage is hypocellular, avascular,
AN OVERVIEW : Cartilage Treatment Eric Thiel, MD WVAM Conference 01/25/2019 No Disclosure The Science of Hyaline Cartilage I. HYALINE CARTILAGE BASIC SCIENCE Normal Anatomy Cartilage is hypocellular, avascular,
ACL Athletic Career. ACL Rupture - Warning Features Intensive pain Immediate swelling Locking Feel a Pop Dead leg Cannot continue to play
 FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
FIMS Ambassador Tour to Eastern Europe, 2004 Belgrade, Serbia Montenegro Acute Knee Injuries - Controversies and Challenges Professor KM Chan OBE, JP President of FIMS Belgrade ACL Athletic Career ACL
Anterior Cruciate Ligament (ACL)
 Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Anterior Cruciate Ligament (ACL) The anterior cruciate ligament (ACL) is one of the 4 major ligament stabilizers of the knee. ACL tears are among the most common major knee injuries in active people of
Rehabilitation Guidelines Following Microfracture Procedures to the Knee
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines Following Microfracture Procedures to the Knee There are two types of cartilage in the knee: meniscus and articular. One type of cartilage is the
CARTILAGE REPAIR INTRODUCTION. M. BERRUTO and G.M. PERETTI 1,2. Received January 6, Accepted January 8, 2013
 CARTILAGE REPAIR INTRODUCTION M. BERRUTO and G.M. PERETTI 1,2 Gaetano Pini Orthopedic Institute, Milan; 1 Department of Biomedical Sciences for Health, University of Milan, 2 IRCCS Galeazzi Orthopedic
CARTILAGE REPAIR INTRODUCTION M. BERRUTO and G.M. PERETTI 1,2 Gaetano Pini Orthopedic Institute, Milan; 1 Department of Biomedical Sciences for Health, University of Milan, 2 IRCCS Galeazzi Orthopedic
The Impact of Age on Knee Injury Treatment
 The Impact of Age on Knee Injury Treatment Focus on the Meniscus Dr. Alvin J. Detterline, MD Sports Medicine and Orthopaedic Surgery Towson Orthopaedic Associates University of Maryland St. Joseph Medical
The Impact of Age on Knee Injury Treatment Focus on the Meniscus Dr. Alvin J. Detterline, MD Sports Medicine and Orthopaedic Surgery Towson Orthopaedic Associates University of Maryland St. Joseph Medical
Knee chondral lesions treated with autologous chondrocyte transplantation in a tridimensional matrix: clinical evaluation at 1-year follow-up
 DOI 10.1007/s10195-009-0069-z ORIGINAL ARTICLE Knee chondral lesions treated with autologous chondrocyte transplantation in a tridimensional matrix: clinical evaluation at 1-year follow-up Félix Vilchez
DOI 10.1007/s10195-009-0069-z ORIGINAL ARTICLE Knee chondral lesions treated with autologous chondrocyte transplantation in a tridimensional matrix: clinical evaluation at 1-year follow-up Félix Vilchez
New Evidence Suggests that Work Related Knee Pain with Degenerative Complications May Not Require Surgery
 4 th Quarter 2017 New Evidence Suggests that Work Related Knee Pain with Degenerative Complications May Not Require Surgery By: Michael Erdil MD, FACOEM Introduction It is estimated there are approximately
4 th Quarter 2017 New Evidence Suggests that Work Related Knee Pain with Degenerative Complications May Not Require Surgery By: Michael Erdil MD, FACOEM Introduction It is estimated there are approximately
Cartilage Repair Center
 Cartilage Repair Center Tom Minas, MD, MS 901 45 th Street, Kimmel Building West Palm Beach, FL 33407 P: 561-844-5255 F: 561-844-5945 Gwen Watkins, Admin Ext 246 www.cartilagerepaircenter.org www.paleyinstitute.org
Cartilage Repair Center Tom Minas, MD, MS 901 45 th Street, Kimmel Building West Palm Beach, FL 33407 P: 561-844-5255 F: 561-844-5945 Gwen Watkins, Admin Ext 246 www.cartilagerepaircenter.org www.paleyinstitute.org
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells,
 What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
What is a Stem Cell? Most cells in the human body have an assigned purpose. They are liver cells, fat cells, bone cells, and so on. These cells can replicate more of their own kind of cell, but they cannot
ACL AND PCL INJURIES OF THE KNEE JOINT
 ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
ACL AND PCL INJURIES OF THE KNEE JOINT Dr.KN Subramanian M.Ch Orth., FRCS (Tr & Orth), CCT Orth(UK) Consultant Orthopaedic Surgeon, Special interest: Orthopaedic Sports Injury, Shoulder and Knee Surgery,
KNEE INJURIES IN SPORTS MEDICINE
 KNEE INJURIES IN SPORTS MEDICINE Irving Raphael, MD June 13, 2014 RSM Medical Associates Head Team Physician Syracuse University Outline Meniscal Injuries anatomy Exam Treatment ACL Injuries Etiology Physical
KNEE INJURIES IN SPORTS MEDICINE Irving Raphael, MD June 13, 2014 RSM Medical Associates Head Team Physician Syracuse University Outline Meniscal Injuries anatomy Exam Treatment ACL Injuries Etiology Physical
Osteo-chondral Transplantation (OATS) The Unhappy ACL. Dr Ivan Popoff Knee, Elbow & Shoulder Surgery
 Osteo-chondral Transplantation (OATS) The Unhappy ACL The Unhappy ACL ACL reconstruction highly successful surgery for restoring stability and return to pre-injury levels of sporting activity? Return to
Osteo-chondral Transplantation (OATS) The Unhappy ACL The Unhappy ACL ACL reconstruction highly successful surgery for restoring stability and return to pre-injury levels of sporting activity? Return to
Evaluation and Treatment of Knee Arthritis Classification of Knee Arthritis Osteoarthritis Osteoarthritis Osteoarthritis of Knee
 1 2 Evaluation and Treatment of Knee Arthritis John Zebrack, MD Reno Orthopaedic Clinic Classification of Knee Arthritis Non-inflammatory Osteoarthritis Primary Secondary Post-traumatic, dysplasia, neuropathic,
1 2 Evaluation and Treatment of Knee Arthritis John Zebrack, MD Reno Orthopaedic Clinic Classification of Knee Arthritis Non-inflammatory Osteoarthritis Primary Secondary Post-traumatic, dysplasia, neuropathic,
Rakesh Patel, MD 4/9/09
 Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Rakesh Patel, MD 4/9/09 Chondral Injuries Very common Present in 63-66% patients undergoing arthroscopy 11-19% full-thickness lesions Up to 79% patients with ACL deficient knee have some form of chondral
Osteochondral Problems of the Knee
 Arthroscopy: The Journal of Arthroscopic & Related Surgery Online October 1999, Supplement 1 Volume 15 Number 7
Arthroscopy: The Journal of Arthroscopic & Related Surgery Online October 1999, Supplement 1 Volume 15 Number 7
Horizon Scanning Centre November Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects
 Horizon Scanning Centre November 2014 Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects SUMMARY NIHR HSC ID: 8515 This briefing is based on information
Horizon Scanning Centre November 2014 Spheroids of human autologous matrix-associated chondrocytes (Chondrosphere) for articular cartilage defects SUMMARY NIHR HSC ID: 8515 This briefing is based on information
First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation
 First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation Bryan Van Dyke, DO Gregory C. Berlet, MD Justin L. Daigre, MD Christopher F. Hyer, DPM,
First Metatarsal Head Osteochondral Defect Treatment with Particulated Juvenile Cartilage Allograft Transplantation Bryan Van Dyke, DO Gregory C. Berlet, MD Justin L. Daigre, MD Christopher F. Hyer, DPM,
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
ANTERIOR CRUCIATE LIGAMENT INJURY
 ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
ANTERIOR CRUCIATE LIGAMENT INJURY WHAT IS THE ANTERIOR CRUCIATE LIGAMENT? The anterior cruciate ligament (ACL) is one of four major ligaments that stabilizes the knee joint. A ligament is a tough band
5:05 6:05 pm Live Surgery: office based Arthroscopy (Trice Medical) (1 hr) Surgeon: Sean McMillan, DO Moderator: Chris Uggen, MD
 AAOS Articular Cartilage Restoration: Current, Emerging, and Advanced Techniques Course # 3252 February 7-9, 2019 OLC Education and Conference Center, Rosemont, IL Course Directors: Kevin D. Plancher,
AAOS Articular Cartilage Restoration: Current, Emerging, and Advanced Techniques Course # 3252 February 7-9, 2019 OLC Education and Conference Center, Rosemont, IL Course Directors: Kevin D. Plancher,
Case Report. Byung Ill Lee, MD and Byoung Min Kim, MD Department of Orthopedic Surgery, Soonchunhyang University Hospital, Seoul, Korea
 Case Report Knee Surg Relat Res 2015;27(4):263-268 http://dx.doi.org/10.5792/ksrr.2015.27.4.263 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Concomitant Osteochondral utograft Transplantation
Case Report Knee Surg Relat Res 2015;27(4):263-268 http://dx.doi.org/10.5792/ksrr.2015.27.4.263 pissn 2234-0726 eissn 2234-2451 Knee Surgery & Related Research Concomitant Osteochondral utograft Transplantation
Novel Techniques in Articular Cartilage Restoration
 21 Novel Techniques in Articular Cartilage Restoration Adam B. Yanke, MD and Brian J. Cole, MD, MBA PART ONE: DENOVO NT Introduction DeNovo NT (Zimmer) is minced (1-mm cubes) juvenile allograft cartilage
21 Novel Techniques in Articular Cartilage Restoration Adam B. Yanke, MD and Brian J. Cole, MD, MBA PART ONE: DENOVO NT Introduction DeNovo NT (Zimmer) is minced (1-mm cubes) juvenile allograft cartilage
Evaluation and Treatment of Intra-articular Fractures. Benjamin Maxson, DO Florida Orthopaedic Institute Orthopaedic Trauma Service
 Evaluation and Treatment of Intra-articular Fractures Benjamin Maxson, DO Florida Orthopaedic Institute Orthopaedic Trauma Service Disclosures Nothing to disclose Articular Fractures: Overview Require
Evaluation and Treatment of Intra-articular Fractures Benjamin Maxson, DO Florida Orthopaedic Institute Orthopaedic Trauma Service Disclosures Nothing to disclose Articular Fractures: Overview Require
Cartilage repair update: Indications are being refined and the future is bright
 Cartilage repair update: Indications are being refined and the future is bright ORTHOPEDICS TODAY 2008; 28:46 September 2008 Cartilage is a highly structured tissue with low cellularity and virtually no
Cartilage repair update: Indications are being refined and the future is bright ORTHOPEDICS TODAY 2008; 28:46 September 2008 Cartilage is a highly structured tissue with low cellularity and virtually no
ACL Rehabilitation and Return To Play
 ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
ACL Rehabilitation and Return To Play Seth Gasser, MD Director of Sports Medicine Florida Orthopaedic Institute Introduction Return to Play: the point in recovery from an injury when a person is safely
Periarticular knee osteotomy
 Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Periarticular knee osteotomy Turnberg Building Orthopaedics 0161 206 4803 All Rights Reserved 2018. Document for issue as handout. Knee joint The knee consists of two joints which allow flexion (bending)
Osteoarthritis. Dr Anthony Feher. With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides
 Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
Osteoarthritis Dr Anthony Feher With special thanks to Dr. Tim Williams and Dr. Bhatia for allowing me to use some of their slides No Financial Disclosures Number one chronic disability in the United States
James C. Y. Chow, M.D., Michael E. Hantes, M.D., Jean Benoit Houle, M.D., and Charalampos G. Zalavras, M.D.
 Arthroscopic Autogenous Osteochondral Transplantation for Treating Knee Cartilage Defects: A 2- to 5-Year Follow-up Study James C. Y. Chow, M.D., Michael E. Hantes, M.D., Jean Benoit Houle, M.D., and Charalampos
Arthroscopic Autogenous Osteochondral Transplantation for Treating Knee Cartilage Defects: A 2- to 5-Year Follow-up Study James C. Y. Chow, M.D., Michael E. Hantes, M.D., Jean Benoit Houle, M.D., and Charalampos
Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation for the Repair of Chondral Defects of the Knee
 International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine Cancun, Mexico MAY 12 16, 2019 Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation
International Society of Arthroscopy, Knee Surgery and Orthopaedic Sports Medicine Cancun, Mexico MAY 12 16, 2019 Mid-Term Clinical Outcomes of Atelocollagenassociated Autologous Chondrocyte Implantation
Anterior Cruciate Ligament (ACL) Injuries
 Anterior Cruciate Ligament (ACL) Injuries This article is also available in Spanish: Lesiones del ligamento cruzado anterior (topic.cfm?topic=a00697) and Portuguese: Lesões do ligamento cruzado anterior
Anterior Cruciate Ligament (ACL) Injuries This article is also available in Spanish: Lesiones del ligamento cruzado anterior (topic.cfm?topic=a00697) and Portuguese: Lesões do ligamento cruzado anterior
Epidemiology. Meniscal Injury & Repair. Meniscus Anatomy. Meniscus Anatomy
 Epidemiology 60-70/100,000 per year Meniscal Injury & Repair Arthroscopic Mensiscectomy One of the most common orthopaedic procedures 20% of all surgeries at some centers Male:Female ratio - 2-4:1 Younger
Epidemiology 60-70/100,000 per year Meniscal Injury & Repair Arthroscopic Mensiscectomy One of the most common orthopaedic procedures 20% of all surgeries at some centers Male:Female ratio - 2-4:1 Younger
AMIC or ACI for arthroscopic repair of grade IV acetabular cartilage defects in femoroacetabular impingement.
 AMIC or ACI for arthroscopic repair of grade IV acetabular cartilage defects in femoroacetabular impingement. Dr. Andrea Fontana Istituto Auxologico Italiano Milan - Italy Introduction Chondropathies of
AMIC or ACI for arthroscopic repair of grade IV acetabular cartilage defects in femoroacetabular impingement. Dr. Andrea Fontana Istituto Auxologico Italiano Milan - Italy Introduction Chondropathies of
Anterior Cruciate Ligament Surgery
 Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Anatomy Anterior Cruciate Ligament Surgery Roger Ostrander, MD Andrews Institute Anatomy Anatomy Function Primary restraint to anterior tibial translation Secondary restraint to internal tibial rotation
Standard of Care: Autologous Chondrocyte Implantation (ACI)
 BRIGHAM & WOMEN S HOSPITAL Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: Autologous Chondrocyte Implantation (ACI) ICD-9 Code: 718.0 Articular cartilage disorder APTA Practice
BRIGHAM & WOMEN S HOSPITAL Department of Rehabilitation Services Physical Therapy Case Type / Diagnosis: Autologous Chondrocyte Implantation (ACI) ICD-9 Code: 718.0 Articular cartilage disorder APTA Practice
Rehabilitation Guidelines for Knee Arthroscopy
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
Medical Diagnosis for Michael s Knee
 Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
Medical Diagnosis for Michael s Knee Introduction The following report mainly concerns the diagnosis and treatment of the patient, Michael. Given that Michael s clinical problem surrounds an injury about
Patellofemoral Pathology
 Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
Patellofemoral Pathology Matthew Murray, MD UT Health Science Center/UT Medicine Sports Medicine and Arthroscopic Surgery I have disclosed that I am a consultant for Biomet Orthopaedics. Anterior Knee
