Relapsing polychondritis and eye disease
|
|
|
- Caitlin Belinda Atkins
- 5 years ago
- Views:
Transcription
1 Brit. J. Ophthal. (I 974) 58, 6oo Relapsing polychondritis and eye disease D. A. R. McKAY, P. G. WATSON, AND A.J. LYNE Scleritis Clinic, Professorial Unit, Moorfields Eye Hospital, City Road, London, ECi V 2PD Relapsing polychondritis was first recognized as a clinical entity in I923 by Jaksch- Wartenhorst (I923) and reported by him under the title "polychondropathia". The term "relapsing polychondritis" was first used by Pearson, Kline, and Newcomer (I960). Up to I966, 49 cases had been described in the literature and these were reviewed by Dolan, Lemmon, and Teitelbaum (i 966). So far I 14 clinical cases have been described in the general medical literature. Migratory arthritis is frequently the earliest sign of the disease and is often accompanied by a febrile illness. Chrondritis, involving typically the external ear, follows at a variable interval after the onset of the disease. First one and then the other auricle becomes painful, swollen, and inflamed so that the pinna becomes distorted and floppy. The nasal, costal, tracheal, and laryngeal cartilage may also become involved, causing a characteristic saddlenosed deformity, tracheal collapse which may require urgent tracheostomy, or eventual death from acute bronchial collapse. Involvement of the inner ear may lead to auditory impairment, tinnitus, and vertigo. Myocardial and aortic involvement can result in valvular disease and aneurysm formation. Anaemia and a raised erythrocyte sedimentation rate (ESR) are common, and abnormal liver function tests have been recorded. Ocular signs were found in 6o per cent. of reported cases (Dolan and others, 1966). The first accurate description was that of Rucker and Ferguson (I965), and Anderson (I967) and Bergaust and Abrahamsen (I969) have since added further cases to the ophthalmic literature. In this Unit we have seen three cases of this condition, in one of whom the ocular manifestations were the primary presentation. The diagnosis ofrelapsing polychondritis should not be made until at least two or possibly three different sites are affected. Case reports Case I, a man aged 38, first attended the Scleritis Clinic of Moorfields Eye Hospital, City Road, in May, I965, with red eyes. A diagnosis of bilateral diffuse anterior necrotizing scleritis was made. He had been admitted to St. Andrew's Hospital, Bow, 8 months before with central chest pain and a swollen right ankle. He had a persistent fever and ulceration of the mouth and during admission he developed a mild jaundice which settled over a 2-week period. All investigations were normal including an electrocardiogram (ECG). i month later he developed a painful swollen left wrist and ankle. ACTH therapy was then started and led to a rapid improvement in his overall condition. 4 months before the eye signs appeared he again developed ulceration of his mouth and was given prednisolone 45 mg./day, which produced some improvement. Address for reprints: D. A. R. McKay, F.R.C.S., as above
2 Relapsing polychondritis and eye disease On his first admission to Moorfields (May, I965) with bilateral scleritis more severe in the right eye than the left, the visual acuity was 6/9 right, 6/6 left, unaided. Ocular examination was normal in all other respects. He had mild anaemia (Hb 8o per cent.) and an ESR of 29 mm. /Ist hr. An initial diagnosis of Behcet's disease was made; he was therefore given prednisolone 6o mg./day and his condition improved. He was discharged i month later on prednisolone 40 mg./day and Predsol eye drops. He required readmission 2 months later with severe pain in the right eye which improved with an increase in his steroid dosage to 8o mg. daily. About this time he developed an acutely inflamed right pinna, followed by severe tinnitus, vertigo, and deafness. In October, I965, he was admitted to the Metabolic Unit, St. Mary's Hospital, under Professor V. Wynn, for assessment of the steroid therapy, and his management has been shared since then. He was eventually stabilized on prednisolone I5 mg./day. In January, I966, the left pinna became swollen and the patient himself commented on the increasing deformity of the nasal cartilage. He again developed a severe left scleritis, and the steroid dose was temporarily increased to 8o mg./day with a good response. He was again extensively investigated but the only abnormal laboratory finding was an ESR of 39 mm./ist hr. Over the next 2 months he had further attacks of arthritis, mouth ulceration, and chest symptoms, all of which settled with boosting of the steroid intake. The various several attacks of scleritis have also responded well, and his present visual acuity is 6/6 right and left; the maintenance dose of prednisolone is 5 mg. three times a day. Case 2, a man aged 57 years, first presented to our Unit in October I968, with a painful red left eye. A diagnosis of simple episcleritis was made, and the condition responded well to Predsol eye drops 2-hourly; I2 months later the right eye became involved, and responded similarly. In June, 1970, he had a bilateral inguinal hernia repaired and about this time both ears became red and swollen, followed i month later by swelling of both knees and the left wrist. He was investigated by Dr. B. Gottlieb at St. Mary Abbotts Hospital, London. He was found to have a mild anaemia (Hb 85 per cent.), and the ESR was 55 mm./ist hr, negative Waaler-Rose test, negative urinary mucopolysaccharide, and a slight rise in the gamma globulin fraction of the serum proteins. Biopsy of the left ear showed necrotic cartilage and an inflammatory cell infiltrate, which consisted mainly of plasma cells. Anticartilage antibodies were demonstrated by an immunofluorescent technique (Godtfredsen, I 949). An audiogram showed hightone deafness. Once the diagnosis of relapsing polychondritis was made, he responded well to prednisolone by mouth and was maintained on 5 mg. three times a day. During the next I 2 months he was troubled by recurrent attacks of episcleritis, swelling of the left knee and both wrists, and further swelling and destruction of both external ears. He also had recurrent urinary tract infection and a sterile urethral discharge, and he passed a renal stone in July I97I. He has had one episode of right-sided laryngeal swelling. Recurrent skin rashes have also occurred, including a thoracic herpes zoster, necessitating a reduction in his steroid intake. At present his visual acuity is 6/9 right and left (corrected) and he is on maintenance therapy with prednisolone 15 mg./day and local steroid preparations to the eyes when necessary. Intraocular pressure has never been raised and there is as yet no sign of cataract formation. Case 3, a married woman aged 42 years, first attended the ophthalmic department in February, I970, when she was complaining of proptosis of the right eye for i week, and aching of the eye and orbit. She had also experienced double vision in all directions of gaze. The only significant past medical history was of thyrotoxicosis I0 years before, which had been treated with potassium perchlorate; the patient rapidly became euthyroid and there had since been no symptoms of thyroid dysfunction. Shortly after this episode she had noticed that the end of her nose had become depressed. She had been deaf since early childhood and there was a family history of perceptive deafness, her father and brother having similar symptoms. She had been helped by a hearing aid. 6oI
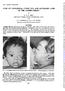
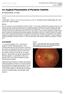
3 602 D. A. R. McKay, P. G. Watson, and A. Lyne Examination (February, 1970) Diplopia was present in all directions of gaze but most marked on elevation. There was definite proptosis and even more marked downward displacement of the right eye. The subconjunctival tissues in the region of the superior rectus were infiltrated. The corrected visual acuity was 6/6 in the right eye and 6/5 in the left. Central field testing showed no defect. There were no fundus abnormalities at this time. The intraocular pressure was 2I mm.hg in the right eye and I9 mm.hg in the left. Full investigations, which included x rays of the chest, skull, sinuses, orbits, small bones of the hands, feet, and wrists, and the neck, and full serological tests, were all negative. The erythrocyte sedimentation rate was 23 mm./ist hr (Westergren). Two biopsies of the infiltrated region of the superior rectus muscle revealed a lymphomatous type of deposit, and a non-specific chronic inflammatory reaction. It was therefore felt that this lesion was most likely to be an orbital lymphoma. Ear, nose and throat and neurosurgical opinions were sought, but no evidence of sinus or intracranial involvement was found. Progress After 3 months the proptosis had become more marked and an area of scleral thinning had appeared superiorly. The visual acuity remained unchanged but examination of the fundus showed retinal striae at the posterior pole. The vitreous remained clear and the disc margins were well defined. The scleral thinning suggested the presence of a posterior scleritis. The patient was therefore given systemic prednisolone 30 mg. daily. A dramatic improvement occurred within a few days, the proptosis resolved, and the pain disappeared. At this time the diagnosis of chronic relapsing polychondritis was made, and a maintenance dose of I0 to 15 mg. prednisolone daily was continued. The nose was operated upon in 1970; a plastic implant was inserted, but this unfortunately came out when the patient blew her nose. The Figure shows the facial appearance after the extrusion of the implant. FIGURE Destruction of nasal cartilage in a patient with relapsing polychondritis (Case 3), giving rise to a depression of the tip of the nose Biopsies of the nasal cartilage and of a section of the sixth costal cartilage were taken at the time of operation. The former showed aseptic necrosis and the latter was normal. Shortly after the birth of a normal female infant in May, I972, she suffered a relapse with recurrence of the proptosis and blurred vision. The corrected visual acuity was 6/i8, and the optic disc showed surrounding swelling with some small haemorrhages. Her condition returned to normal when the steroid dosage was increased. During April, 1974, she noticed a rapid loss of vision in the right eye; the visual acuity was reduced to counting fingers, the left remaining normal at 6/4. The pupillary reaction of the right eye was sluggish but the fundus showed no abnormality. The left eye was normal. The steroid dosage was increased to 20 mg. daily, and the visual acuity returned to normal within 5 days.
4 Discussion Relapsing polychondritis and eye disease 603 The ocular manifestations of relapsing polychondritis are many and varied. The most common are episcleritis, scleritis, iritis, and keratoconjunctivitis sicca, but sclerokeratitis, conjunctivitis, exudative chorio-retinitis, exudative retinal detachment, optic neuritis, cataract, proptosis, and muscle paresis have been reported. In a case described by Rucker and Ferguson (I965) of a 41-year-old female patient, there was acute left proptosis with diplopia due either to lateral rectus involvement or to a sixth nerve paresis. This settled on treatment with steroids. Later the right eye became proptosed and also settled with treatment. Recently, Davies and Karseras (197 I) have described a further case of anterior and posterior scleritis with proptosis and a partial third nerve lesion. The seven cases reported by Anderson (I967) included signs of episcleritis, exudative retinopathy, which they describe as resembling Coats's disease, sclerokeratitis with progressive scleral thinning, and iritis. Bergaust and Abrahamsen (I969) described a case with multiple ocular complications including four attacks ofscierokeratitis, one attack ofsclero-iritis, one ofbilateral pan-uveitis, and an exudative chorio-retinopathy, also resembling Coats's disease. Eventual blindness has twice been described (Hilding, I952; Barth and Berson, I968). The first was due to a severe iritis with secondary glaucoma, leading to phthisis bulbi, and the second to bilateral corneal perforation. The most common manifestations seem to be episcleritis, iritis (Matas, 1970), and keratoconjunctivitis sicca. The first patient, who presented with a diffuse anterior necrotizing scleritis of the type commonly seen in patients with connective tissue disorders, had a severe generalized disease. The second patient never had any scleral involvement, the inflammation being confined to the episclera only. This presentation is unusual when other systemic connective tissue disease is present but does occur from time to time, particularly in patients with mild rheumatoid arthritis. The third patient presented with a posterior scleritis, proptosis, and reduced visual acuity due probably to the involvement of the sclera in the region of the optic nerve and posterior pole; in this respect the patient was similar to others we have seen with posterior scleritis both in presentation and in dramatic response to treatment. The usual exudative changes were absent in this patient. Because of the physiogenetic similarity between cartilage and sclera, the varied modes of presentation of these patients may be a manifestation of the inflammation of similar tissues at different sites. AETIOLOGY The aetiology of this condition is still obscure, although it is thought to belong to the family of "collagenoses" with an autoimmune complex background. Jaksch-Wartenhorst (1923), in his original article, attributed the cause, perhaps light-heartedly, to excessive consumption of alcohol! Dolan and others (I966) attempted to demonstrate immunofluorescent antibodies to cartilage with inconclusive results. These antibodies were found in Case 2; this patient also had raised gamma globulin fractions in the plasma proteins. Other laboratory investigations have also proved generally unhelpful. A high ESR is usually present, with a mild anaemia, but specific tests show no 'definite pattern. Antirheumatoid factor has been present in some cases, and an antithyroid antibody has been demonstrated in others. Kaye and Sones (I964) described a method of estimating urinary acid mucopolysaccharide, which was raised in patients with polychondritis, and Riggs and Wilson (I967) also found that such a test warranted inclusion in their investigation
5 604 D. A. R. McKay, P. G. Watson, and A. Lyne Hughes, Berry, Seifert, and Lessof (1972) discussed the use of tests for anticartilage antibodies, and also described the estimation of glycoaminoglycans in the cartilage matrix of affected individuals. Biopsy of affected cartilage and histological changes have been reported by Harwood (I958), who found replacement of cartilage by fibrous connective tissue, scattered calcification, and non-specific inflammatory signs. Verity, Larson, and Madden (I963) reported in detail the histological changes and, although there is no pathognomonic finding, the basophilic staining of the normal cartilage is usually lost while the diseased cartilage becomes acidophilic, dissolving and fragmenting from the edge towards the centre. The chondrocytes lose their cytoplasm, and eventually only nuclear remnants are found. The destroyed cartilage is replaced by fibrous connective tissue, often vascularized, growing in from the edges of the lesion. Similar changes were found in Case 3. DIFFERENTIAL DIAGNOSIS Before the diagnosis of relapsing polychondritis can be made, two or three sites including the ocular structures have to be involved. It is little wonder that diagnosis is difficult in the early stages as this has to be made on clinical grounds alone. This condition should be considered not only in patients presenting with scleral disease but also those who develop diffuse joint disease. It is interesting to note that two excellent reviews of ocular and joint disease (Godtfredsen, 1949; Stanworth, I95I) do not mention this condition. As demonstrated by Case I, both Reiter's disease and Behcet's disease can present a very similar picture and follow a similar course. Other conditions, including rheumatoid arthritis, Still's disease, Wegener's granulomatosis, Cogan's syndrome, and Sj6gren's syndrome, enter the differential diagnosis. Inflammation of the eye associated with inflammation and eventual destruction of the aural and nasal cartilage is diagnostic, and the condition should be suspected if there is associated chest pain (from involvement of the costal cartilages), tracheo-bronchial symptoms, migratory arthritis, or middle and inner ear disease. COURSE AND TREATMENT The cases so far described in the literature are equally spread between the sexes. The age at onset varied from 2 to 6i years (average 32). The duration of the disease varied from I to 24 years. The reported cause of death is usually acute respiratory collapse, and a number of survivors have required urgent tracheostomy. Other deaths have been caused by ruptured aortic and cerebral aneurysms and by myocardial valvular involvement. The disease may, in fact, run an acute fulminating course, but it more commonly follows a slow, low-grade, relapsing pattern. Treatment is essentially with anti-inflammatory agents. Steroids in an initial dosage of prednisolone 6o-8o mg./day or its equivalent bring about a marked and rapid improvement and this is the treatment of choice. A maintenance dose seems to be necessary to suppress the condition. If there is an exacerbation then the steroids must again be given in full dosage for a short period. Kaye and Sones (I964) reported good results with salicylates in a dosage of 2 to 5 g./day, but had no success with Plaquenil. The articular complications were successfully controlled with chloroquine on one occasion and our first patient responded well at one stage to systemic Tanderil. There is no doubt, however, that systemic steroids are the mainstay, and they can be supplemented by local steroids for recurrent ocular problems. Subconjunctival steroids should at all times be avoided - diseased sclera may often rupture at the site of such in jections (Watson, I972).
6 Summary Relapsing polychondritis and eye disease 605 Three patients with relapsing polychondritis, who presented in the first instance to an eye department, are described. One patient had a diffuse anterior necrotizing scleritis, the second a simple episcleritis, and the third a posterior scleritis. All have made satisfactory progress with maintenance of good vision. Systemic steroid therapy appears to be the only satisfactory treatment; it must be given initially in high doses and reduced to a maintenance dose as soon as the ocular and systemic manifestations regress. All three patients still require maintenance dosage even after io, 7, and 4 years respectively. A brief review ofthe literature of this rare and interesting condition is included, and the aetiology discussed. References ANDERSON, B. (I967) Amer J. Ophthal., 64, 35 BARTH, W. F., and BERSON, E. L. (I968) Ibid., 66, 890 BERGAUST, B., and ABRAHAMSEN, A. M. (I969) Acta ophthal. (Kbh.), 47, I74 DAVIES, M. S., and KARSERAS, A. G. (I97I) Brit. J. Ophthal., 55, I96 DOLAN, D. L., LEMMON, G. B., and TEITELBAUM, S. L. (I966) Amer. J. Med., 41, 285 GODTFREDSEN, E. (I949) Brit. J. Ophthal., 33, 26I HARWOOD, T. R. (I 958) Arch. Path., 65, 8 I HILDING, A. C. (I952) Arch. intern. Med., 89, 445 HUGHES, R. A. C., BERRY, C. L., SEIFERT, M., and LESSOF, M. H. (I972) Quart. J. Med., 41, 363 JAKSCH-WARTENHORST, R. (I923) Wien. Z. inn. Med., 6, 93 KAYE, R. L., and SONES, D. A. (I964) Ann. intern. Med., 6o, 653 MATAS, B. R. (1970) Arch. Ophthal. (Chicago), 84, 474 PEARSON, C. M., KLINE, H. M., and NEWCOMER, V. D. (I960) New Engl. J. Med., 263, 51 RIGGS, R. H., and WILSON, j. w. (I967) Laryngoscope, 77, 534 RUCKER, C. W., and FERGUSON, R. H. (I965) Arch. Ophthal. (Chicago), 73, 46 STANWORTH, A. (I 95 I) Trans. ophthal. Soc. U.K., 7 1, I 89 VERITY, M. A., LARSON, W. M., and MADDEN, S. C. (I963) Amer. J. Path., 42, 251 WATSON, P. G. (1972) "Contemporary Ophthalmology Honouring Sir Stewart Duke-Elder", ed. J. G. Bellows, p. 77. Williams and Wilkins, Baltimore; Churchill Livingstone, Edinburgh. Br J Ophthalmol: first published as /bjo on 1 June Downloaded from on 2 September 2018 by guest. Protected by
Prednisolone-2 I -stearoylglycolate in scleritis
 Brit. j. Ophthal. (1970) 54, 394 Prednisolone- -stearoylglycolate in scleritis S. S. HAYREH* AND P. G. WATSON Scleritis Clinic, Moorfields Eye Hospital, City Road, London, E.C. i Scleritis is one of the
Brit. j. Ophthal. (1970) 54, 394 Prednisolone- -stearoylglycolate in scleritis S. S. HAYREH* AND P. G. WATSON Scleritis Clinic, Moorfields Eye Hospital, City Road, London, E.C. i Scleritis is one of the
arthritis "Contact lens" cornea in rheumatoid (opposite). Brit. J. Ophthal. (I970) 54, 410 Peterborough District Hospital
 Brit. J. Ophthal. (I970) 54, 410 "Contact lens" cornea in rheumatoid arthritis A. J. LYNE Peterborough District Hospital It has been noted that patients suffering from long-standing rheumatoid arthritis
Brit. J. Ophthal. (I970) 54, 410 "Contact lens" cornea in rheumatoid arthritis A. J. LYNE Peterborough District Hospital It has been noted that patients suffering from long-standing rheumatoid arthritis
Diffuse infiltrating retinoblastoma
 Brit. 1. Ophthal. (I 971) 55, 6oo Diffuse infiltrating retinoblastoma GWYN MORGAN Department of Pathology, Institute of Ophthalmology, University of London The term "diffuse infiltrating retinoblastoma"
Brit. 1. Ophthal. (I 971) 55, 6oo Diffuse infiltrating retinoblastoma GWYN MORGAN Department of Pathology, Institute of Ophthalmology, University of London The term "diffuse infiltrating retinoblastoma"
LEUKAEMIA*t INFILTRATION OF THE IRIS IN CHRONIC LYMPHATIC. pattemn * Received for pubiication November io, i967.
 Brit. J. Ophthal. (1968) 52, 781 INFILTRATION OF THE IRIS IN CHRONIC LYMPHATIC LEUKAEMIA*t BY BRIAN MARTIN The General Infirmary, Leeds OCULAR involvement is common in the leukaemias though the anterior
Brit. J. Ophthal. (1968) 52, 781 INFILTRATION OF THE IRIS IN CHRONIC LYMPHATIC LEUKAEMIA*t BY BRIAN MARTIN The General Infirmary, Leeds OCULAR involvement is common in the leukaemias though the anterior
Investigations. The blood count was normal with an erythrocyte. sedimentation rate of 5 mm. ist hr, and negative Waaler-
 Brit. J. Ophthal. (I975) 59, 149 Tolosa-Hunt syndrome The dangers of an eponym T. J. FOWLER, C. J. EARL, V. L. McALLISTER, AND W. I. McDONALD From the Institute of Neurology, National Hospitalfor Nervous
Brit. J. Ophthal. (I975) 59, 149 Tolosa-Hunt syndrome The dangers of an eponym T. J. FOWLER, C. J. EARL, V. L. McALLISTER, AND W. I. McDONALD From the Institute of Neurology, National Hospitalfor Nervous
SUPERVOLTAGE X-IURADIATION OF EPITHELIAL TUMOURS
 Brit. J. Ophthal. (1964) 48, 601. SUPERVOLTAGE X-IURADIATION OF EPITHELIAL TUMOURS OF THE LACRIMAL GLAND* BY ALY MORTADA Department of Ophthalmology, Faculty of Medicine, Cairo University, Egypt HOGAN
Brit. J. Ophthal. (1964) 48, 601. SUPERVOLTAGE X-IURADIATION OF EPITHELIAL TUMOURS OF THE LACRIMAL GLAND* BY ALY MORTADA Department of Ophthalmology, Faculty of Medicine, Cairo University, Egypt HOGAN
Optical coherence tomography findings in a child with posterior scleritis
 European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
European Journal of Ophthalmology / Vol. 18 no. 6, 2008 / pp. 1007-1010 SHORT OMMUNITIONS & SE REPORTS Optical coherence tomography findings in a child with posterior scleritis H. ERDÖL, M. KOL,. TÜRK
Trabeculectomy combined with cataract extraction: a follow-up study
 British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
UNIOCULAR APLASIA OF THE OPTIC NERVE*
 Brit. J. Ophthal. (1962) 46, 51. UNIOCULAR APLASIA OF THE OPTIC NERVE* BY FROMA SOMERVILLE London APLASIA of the optic nerve occurring as an isolated abnormality in an eye of normal external appearance
Brit. J. Ophthal. (1962) 46, 51. UNIOCULAR APLASIA OF THE OPTIC NERVE* BY FROMA SOMERVILLE London APLASIA of the optic nerve occurring as an isolated abnormality in an eye of normal external appearance
KERATO-CONJUNCTIVITIS SICCA TREATED WITH
 Brit. J. Ophthal. (1955), 39, 90. KERATO-CONJUNCTIVITIS SICCA TREATED WITH CORTISONE AND ACTH* BY STELLA EADIE AND MALCOLM THOMPSON Edinburgh THE effects of cortisone and ACTH in cases of kerato-conjunctivitis
Brit. J. Ophthal. (1955), 39, 90. KERATO-CONJUNCTIVITIS SICCA TREATED WITH CORTISONE AND ACTH* BY STELLA EADIE AND MALCOLM THOMPSON Edinburgh THE effects of cortisone and ACTH in cases of kerato-conjunctivitis
Temporal arteritis. Occurrence of ocular complications 7 years after diagnosis. University of Edinburgh, and Royal Infirmary of Edinburgh
 Brit. J. Ophthal. (I 972) 56, 584 Temporal arteritis Occurrence of ocular complications 7 years after diagnosis JAMES F. CULLEN Department of Ophthalmology, University of Edinburgh, and Royal Infirmary
Brit. J. Ophthal. (I 972) 56, 584 Temporal arteritis Occurrence of ocular complications 7 years after diagnosis JAMES F. CULLEN Department of Ophthalmology, University of Edinburgh, and Royal Infirmary
Hyalo-retinopathy in the clefting
 Brit. J. Ophthal. (I 974) 58, 96 Hyalo-retinopathy in the clefting syndrome R. DANIEL, J. J. KANSKI, AND M. G. GLASSPOOL Retinal Unit, Moorfields Eye Hospital, High Holborn, London, WCI V 7AN The hereditary
Brit. J. Ophthal. (I 974) 58, 96 Hyalo-retinopathy in the clefting syndrome R. DANIEL, J. J. KANSKI, AND M. G. GLASSPOOL Retinal Unit, Moorfields Eye Hospital, High Holborn, London, WCI V 7AN The hereditary
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Family studies in glaucoma
 Brit. j. Ophthal. (I 974) 58, 529 Family studies in glaucoma E. S. PERKINS Institute of Ophthalmology, University of London There is now strong evidence for a genetic basis to glaucoma. Numerous family
Brit. j. Ophthal. (I 974) 58, 529 Family studies in glaucoma E. S. PERKINS Institute of Ophthalmology, University of London There is now strong evidence for a genetic basis to glaucoma. Numerous family
OCULAR FINDINGS IN HAEMOCHROMATOSIS*
 Brit. J. Ophthal. (1953) 37, 242. OCULAR FINDINGS IN HAEMOCHROMATOSIS* BY J. R. HUDSON Institute of Ophthalmology, London HAEMOCHROMATOSIS is a rare condition, the chief clinical features of which are
Brit. J. Ophthal. (1953) 37, 242. OCULAR FINDINGS IN HAEMOCHROMATOSIS* BY J. R. HUDSON Institute of Ophthalmology, London HAEMOCHROMATOSIS is a rare condition, the chief clinical features of which are
AQUEOUS VEINS IN RABBITS*
 Brit. J. Ophthal., 35, 119. AQUEOUS VEINS IN RABBITS* BY D. P. GREAVES AND E. S. PERKINS Institute of Ophthalmology, London Director of Research, Sir Stewart Duke-Elder IN the course of investigations
Brit. J. Ophthal., 35, 119. AQUEOUS VEINS IN RABBITS* BY D. P. GREAVES AND E. S. PERKINS Institute of Ophthalmology, London Director of Research, Sir Stewart Duke-Elder IN the course of investigations
Scleritis LEN V KOH OD
 Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
CASE NOTES. nephritis, and diabetes. ACUTE RETINAL VASCULAR PROLIFERATION* Duke-Elder (1940), who states that it depends essentially on two factors;
 Brit. J. Ophthal. (1960) 44, 179. CASE NOTES ACUTE RETINAL VASCULAR PROLIFERATION* BY JOHN A. CHIVERS Dartford and Orpington Hospital Groups, Kent THs condition is described under its usual title retinitis
Brit. J. Ophthal. (1960) 44, 179. CASE NOTES ACUTE RETINAL VASCULAR PROLIFERATION* BY JOHN A. CHIVERS Dartford and Orpington Hospital Groups, Kent THs condition is described under its usual title retinitis
CHRONIC RETROBULBAR AND CHIASMAL NEURITIS*t
 Brit. J. Ophthal. (1967) 51, 698 CHRONIC RETROBULBAR AND CHIASMAL NEURITIS*t BY From the Department of Medicine, University of Bristol, and the United Bristol Hospitals AcuTE retrobulbar neuritis is a
Brit. J. Ophthal. (1967) 51, 698 CHRONIC RETROBULBAR AND CHIASMAL NEURITIS*t BY From the Department of Medicine, University of Bristol, and the United Bristol Hospitals AcuTE retrobulbar neuritis is a
Professor Helen Danesh-Meyer. Eye Institute Auckland
 Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Angle-closure glaucoma secondary to
 British Journal of Ophthalmology, 1978, 62, 330-335 Angle-closure glaucoma secondary to posterior scleritis M. P. QUINLAN AND R. A. HITCHINGS From the Department oj Clinical Ophthalmology, Institute of
British Journal of Ophthalmology, 1978, 62, 330-335 Angle-closure glaucoma secondary to posterior scleritis M. P. QUINLAN AND R. A. HITCHINGS From the Department oj Clinical Ophthalmology, Institute of
SEGMENTAL LESIONS OF THE RETINAL ARTERIES*
 Brit. J. Ophthal. (1960) 44, 562. SEGMENTAL LESIONS OF THE RETINAL ARTERIES* BY R. K. BLACH London FEW cases with segmental lesions of the retinal arteries have been described. Suganuma (1927) reported
Brit. J. Ophthal. (1960) 44, 562. SEGMENTAL LESIONS OF THE RETINAL ARTERIES* BY R. K. BLACH London FEW cases with segmental lesions of the retinal arteries have been described. Suganuma (1927) reported
RETINAL DETACHMENT AT THE POSTERIOR POLE*
 Brit. J. Ophthal. (1958) 42, 749. RETINAL DETACHMENT AT THE POSTERIOR POLE* BY CALBERT I. PHILLIPSt Institute of Ophthalmology, University oflondon THE common feature of the cases to be described in this
Brit. J. Ophthal. (1958) 42, 749. RETINAL DETACHMENT AT THE POSTERIOR POLE* BY CALBERT I. PHILLIPSt Institute of Ophthalmology, University oflondon THE common feature of the cases to be described in this
Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient
 CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
CM&R Rapid Release. Published online ahead of print September 20, 2012 as Aperture Acute Retinal Necrosis Secondary to Varicella Zoster Virus in an Immunosuppressed Post-Kidney Transplant Patient Elizabeth
Malawi. Ocular leprosy in. Clinical and therapeutic survey of 8,325 leprosy. patients
 Brit. 5. Ophthal. (I 970) 54, I 07 Ocular leprosy in Malawi Clinical and therapeutic survey of 8,325 leprosy patients U. TICHO AND I. BEN SIRA Eye Department, Hadassah Medical Centre, Jerusalem, Israel
Brit. 5. Ophthal. (I 970) 54, I 07 Ocular leprosy in Malawi Clinical and therapeutic survey of 8,325 leprosy patients U. TICHO AND I. BEN SIRA Eye Department, Hadassah Medical Centre, Jerusalem, Israel
Corneal blood staining after hyphaema
 Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Brit. J_. Ophthal. (I 972) 56, 589 after hyphaema J. D. BRODRICK Sheffield has been described as a rare complication of contusion injury in which a hyphaema of relatively long duration and a raised intraocular
Dr Jo-Anne Pon. Dr Sean Every. 8:30-9:25 WS #70: Eye Essentials for GPs 9:35-10:30 WS #80: Eye Essentials for GPs (Repeated)
 Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
CASE OF CONGENITAL CYSTIC EYE AND ACCESSORY LIMB OF THE LOWER EYELID*
 Brit. J. Ophthal. (1966) 50, 409 CASE OF CONGENITAL CYSTIC EYE AND ACCESSORY LIMB OF THE LOWER EYELID* BY N. S. C. RICE Department ofpathology, Institute of Ophthalmology, London, AND S. P. MINWALLA AND
Brit. J. Ophthal. (1966) 50, 409 CASE OF CONGENITAL CYSTIC EYE AND ACCESSORY LIMB OF THE LOWER EYELID* BY N. S. C. RICE Department ofpathology, Institute of Ophthalmology, London, AND S. P. MINWALLA AND
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS
 OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
OPHTHALMOLOGY REFERRAL GUIDE FOR GPS A guidebook to support general practitioners in the management and referral of a range of common eye problems. Contents 3 Introduction 4 Ophthalmic Workup 6 Acute Visual
UVEITIS A. D. RUEDEMANN, M.D.
 A. D. RUEDEMANN, M.D. The diagnosis of uveitis, especially of the low-grade recurring type, is one of the most exacting problems in medicine. Difficult to diagnose, difficult to treat, and offering a very
A. D. RUEDEMANN, M.D. The diagnosis of uveitis, especially of the low-grade recurring type, is one of the most exacting problems in medicine. Difficult to diagnose, difficult to treat, and offering a very
GLAUCOMA TREATED WITH DIAMOX*t PRELIMINARY REPORT OF 20 CASES
 Brit. J. Ophthal. (1955) 39, 659. GLAUCOA TREATED WITH DIAOX*t PRELIINARY REPORT O 20 CASES BY S.. DRANCE Oxford THE use of Diamox in logically follows riedenwald's concept that the bicarbonate ion is
Brit. J. Ophthal. (1955) 39, 659. GLAUCOA TREATED WITH DIAOX*t PRELIINARY REPORT O 20 CASES BY S.. DRANCE Oxford THE use of Diamox in logically follows riedenwald's concept that the bicarbonate ion is
HYPERPLASIA OF THE ANTERIOR LAYER OF THE IRIS STROMA*t
 Brit. J. Ophthal. (1965) 49, 516 HYPERPLASIA OF THE ANTERIOR LAYER OF THE IRIS STROMA*t BY MALCOLM N. LUXENBERG From the Bascom Palmer Eye Institute, Department of Ophthalmology, University of Miami School
Brit. J. Ophthal. (1965) 49, 516 HYPERPLASIA OF THE ANTERIOR LAYER OF THE IRIS STROMA*t BY MALCOLM N. LUXENBERG From the Bascom Palmer Eye Institute, Department of Ophthalmology, University of Miami School
Lymphangiectasia haemorrhagica
 Brit. 7. Ophthal. (i 969) 53, 274 Lymphangiectasia haemorrhagica conjunctivae PHILIP AWDRY Moorfields Eye Hospital, City Road, London, E.C. I Leber (i 88o) described a condition in which a connexion between
Brit. 7. Ophthal. (i 969) 53, 274 Lymphangiectasia haemorrhagica conjunctivae PHILIP AWDRY Moorfields Eye Hospital, City Road, London, E.C. I Leber (i 88o) described a condition in which a connexion between
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Herpes zoster ophthalmicus with trochlear
 Brit. J. Ophthal. (I 97I) 55, 76 I Herpes zoster ophthalmicus with trochlear nerve involvement after alcohol injection into the Gasserian ganglion ROBERT J.-NI. BOUCHERAT The Eye Hospital, 11'alton Street,
Brit. J. Ophthal. (I 97I) 55, 76 I Herpes zoster ophthalmicus with trochlear nerve involvement after alcohol injection into the Gasserian ganglion ROBERT J.-NI. BOUCHERAT The Eye Hospital, 11'alton Street,
RETINITIS PIGMENTOSA* A NEW THERAPEUTIC APPROACH
 Brit. J. Ophthal. (1963) 47, 144. RETINITIS PIGMENTOSA* A NEW THERAPEUTIC APPROACH BY LALIT P. AGARWAL, S. R. K. MALIK, MADAN MOHAN, AND P. R. KARWAL From the Department of Ophthalmology, All-India Institute
Brit. J. Ophthal. (1963) 47, 144. RETINITIS PIGMENTOSA* A NEW THERAPEUTIC APPROACH BY LALIT P. AGARWAL, S. R. K. MALIK, MADAN MOHAN, AND P. R. KARWAL From the Department of Ophthalmology, All-India Institute
Relapsing Polychondritis Presenting As Sub-Glottic Stenosis
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 12 Number 1 Relapsing Polychondritis Presenting As Sub-Glottic Stenosis M Ramdass, C Tilluckdharry, K Ali Citation M Ramdass, C Tilluckdharry,
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 12 Number 1 Relapsing Polychondritis Presenting As Sub-Glottic Stenosis M Ramdass, C Tilluckdharry, K Ali Citation M Ramdass, C Tilluckdharry,
Herpes Zoster Ophtalmicus in a HIV positive patient: A Case Report
 ISPUB.COM The Internet Journal of Neurology Volume 9 Number 2 Herpes Zoster Ophtalmicus in a HIV positive patient: A Case Report G Lopez Bejerano, Y Graza Fernandez Citation G Lopez Bejerano, Y Graza Fernandez..
ISPUB.COM The Internet Journal of Neurology Volume 9 Number 2 Herpes Zoster Ophtalmicus in a HIV positive patient: A Case Report G Lopez Bejerano, Y Graza Fernandez Citation G Lopez Bejerano, Y Graza Fernandez..
HLA-B27-related anterior Uveitis
 HLA-B27-related anterior Uveitis Nicholas Jones Manchester Uveitis Clinic The Royal Eye Hospital Manchester Anterior means anterior only IUSG classification: Anterior uveitis = Iris & pars plicata AU
HLA-B27-related anterior Uveitis Nicholas Jones Manchester Uveitis Clinic The Royal Eye Hospital Manchester Anterior means anterior only IUSG classification: Anterior uveitis = Iris & pars plicata AU
Rafik Girgis. Consultant Ophthalmic Surgeon ( Cataract & Primary Care)
 Rafik Girgis Consultant Ophthalmic Surgeon ( Cataract & Primary Care) Blepharitis Is a very common condition which usually bilateral & symmetrical. The main types are: Anterior, posterior or mixed Complications:
Rafik Girgis Consultant Ophthalmic Surgeon ( Cataract & Primary Care) Blepharitis Is a very common condition which usually bilateral & symmetrical. The main types are: Anterior, posterior or mixed Complications:
RETINITIS PIGMENTOSA*
 Brit. J. Ophthal. (1956) 40, 40. AUDIOMETRIC AND VESTIBULAR EXAMINATIONS IN RETINITIS PIGMENTOSA* BY Departments of Ophthalmology and Ear, Nose, and Throat of the Rothschild-Hadassah University Hospital,
Brit. J. Ophthal. (1956) 40, 40. AUDIOMETRIC AND VESTIBULAR EXAMINATIONS IN RETINITIS PIGMENTOSA* BY Departments of Ophthalmology and Ear, Nose, and Throat of the Rothschild-Hadassah University Hospital,
ADRENERGIC BLOCKING AGENTS*t A DOUBLE-BLIND TRIAL IN THE TREATMENT OF THE EYE SIGNS OF THYROID DISORDER
 Brit. J. Ophthal. (1968) 52, 616 ADRENERGIC BLOCKING AGENTS*t A DOUBLE-BLIND TRIAL IN THE TREATMENT OF THE EYE SIGNS OF THYROID DISORDER BY A. L. CROMBIE+ Professorial Unit, Eye Department, Royal Infirmary,
Brit. J. Ophthal. (1968) 52, 616 ADRENERGIC BLOCKING AGENTS*t A DOUBLE-BLIND TRIAL IN THE TREATMENT OF THE EYE SIGNS OF THYROID DISORDER BY A. L. CROMBIE+ Professorial Unit, Eye Department, Royal Infirmary,
THYROID EYE DISEASE ORBITAL DECOMPRESSION SURGERY
 THYROID EYE DISEASE ORBITAL DECOMPRESSION SURGERY What is thyroid eye disease (TED)? TED is an autoimmune condition where the body s own immune system attacks the tissues of the thyroid gland and the eye
THYROID EYE DISEASE ORBITAL DECOMPRESSION SURGERY What is thyroid eye disease (TED)? TED is an autoimmune condition where the body s own immune system attacks the tissues of the thyroid gland and the eye
cryotherapy Pigment fallout and uveitis after (Lincoff, Baras, and McLean, I965). Moorfields Eye Hospital, City Road, London, E.C.
 Brit. J. Ophthal. (I 97) 57, 156 Pigment fallout and uveitis after cryotherapy A. H. CHIGNELL, R. S. CLEMETT, AND I. H. S. REVIE Moorfields Eye Hospital, City Road, London, E.C. i Cryotherapy, first advocated
Brit. J. Ophthal. (I 97) 57, 156 Pigment fallout and uveitis after cryotherapy A. H. CHIGNELL, R. S. CLEMETT, AND I. H. S. REVIE Moorfields Eye Hospital, City Road, London, E.C. i Cryotherapy, first advocated
Angle recession and secondary glaucoma
 Brit. j. Ophthal. (I973) 57, 6o8 Angle recession and secondary glaucoma D. MOONEY Kent County Ophthalmic and Aural Hospital, Maidstone In a previous article (Mooney, I972), the incidence and extent of
Brit. j. Ophthal. (I973) 57, 6o8 Angle recession and secondary glaucoma D. MOONEY Kent County Ophthalmic and Aural Hospital, Maidstone In a previous article (Mooney, I972), the incidence and extent of
Imaging in uveitis. Anthony Hall
 Imaging in uveitis Anthony Hall Causes of Vision Loss in Uveitis 1. Cystoid macular oedema 26% 2. Cataract 19% 3. Glaucoma 11% 4. Permanent macular damage 5% Rothova et al BJO 1996; 80: 332-336 Macular
Imaging in uveitis Anthony Hall Causes of Vision Loss in Uveitis 1. Cystoid macular oedema 26% 2. Cataract 19% 3. Glaucoma 11% 4. Permanent macular damage 5% Rothova et al BJO 1996; 80: 332-336 Macular
PENETRATING EYE INJUIRES
 PENETRATING EYE INJUIRES King Harold receives a mortal penetrating injury to the eye at the Battle of Hastings 1066, Detail Bayeux Tapestry, Eleventh century. Then Earl William came from Normandy into
PENETRATING EYE INJUIRES King Harold receives a mortal penetrating injury to the eye at the Battle of Hastings 1066, Detail Bayeux Tapestry, Eleventh century. Then Earl William came from Normandy into
Ocular Urgencies and Emergencies
 Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
BY N. N. SOODt AND V. J. MARMION- St. Paul's Eye Hospital, Liverpool
 Brit. J. Ophthal. (1964) 48, 609. SUPERFICIAL HERPETIC KERATITIS TREATED WITH 5-IODO-2'-DEOXYURIDINE* BY N. N. SOODt AND V. J. MARMION- St. Paul's Eye Hospital, Liverpool THE results of treating herpetic
Brit. J. Ophthal. (1964) 48, 609. SUPERFICIAL HERPETIC KERATITIS TREATED WITH 5-IODO-2'-DEOXYURIDINE* BY N. N. SOODt AND V. J. MARMION- St. Paul's Eye Hospital, Liverpool THE results of treating herpetic
Ocular warning signs in GP practice: Paediatric Eye Pointers
 Ocular warning signs in GP practice: Paediatric Eye Pointers Dr Benjamin Chang MB, BCh, BAO, MMedSci, FRCS(Irel), FRCS(Edin), FRCOphth(Lond) Senior Consultant Ophthalmology and Visual Sciences Khoo Teck
Ocular warning signs in GP practice: Paediatric Eye Pointers Dr Benjamin Chang MB, BCh, BAO, MMedSci, FRCS(Irel), FRCS(Edin), FRCOphth(Lond) Senior Consultant Ophthalmology and Visual Sciences Khoo Teck
JOB DESCRIPTION ENT/Ophthalmology with General Practice post GP+1
 JOB DESCRIPTION ENT/Ophthalmology with General Practice post GP+1 Job Title: Base: Responsible to: Working Hours: On-call: ST 1/2 ENT/Ophthalmology and GP Hospital Trust and GP practice Clinical Supervising
JOB DESCRIPTION ENT/Ophthalmology with General Practice post GP+1 Job Title: Base: Responsible to: Working Hours: On-call: ST 1/2 ENT/Ophthalmology and GP Hospital Trust and GP practice Clinical Supervising
_~~~~~~~~~~~~~~... I~~~~~~~~~~~~~~~~~~~~~~~~...x'..'.i ORBITAL BENIGN HAEMANGIO ENDOTHELIOMATA*
 '..,S''''. t ~~~~~~~~~~~~~~~~~~~~~~~. g.# lgl,~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~.%. : Brit. J. Ophthal. (1963) 47, 164. ORBITAL BENIGN HAEMANGIO ENDOTHELIOMATA* BY ALY MORTADA Faculty of Medicine, Cairo University,
'..,S''''. t ~~~~~~~~~~~~~~~~~~~~~~~. g.# lgl,~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~.%. : Brit. J. Ophthal. (1963) 47, 164. ORBITAL BENIGN HAEMANGIO ENDOTHELIOMATA* BY ALY MORTADA Faculty of Medicine, Cairo University,
PRECISION PROGRAM. Injection Technique Quick-Reference Guide. Companion booklet for the Video Guide to Injection Technique
 Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Injection Technique Quick-Reference Guide PRECISION PROGRAM Companion booklet for the Video Guide to Injection Technique Available at www.ozurdexprecisionprogram.com Provides step-by-step directions with
Retinal dialysis. procedures. The purpose of the present paper is to report the results of treatment of 62
 Brit. J. Ophthal. (I973) 57, 572 Retinal dialysis A. H. CHIGNELL Moorfields Eye Hospital, City Road, London, E.C. i Retinal dialysis is an important cause of retinal detachment and subsequent reduction
Brit. J. Ophthal. (I973) 57, 572 Retinal dialysis A. H. CHIGNELL Moorfields Eye Hospital, City Road, London, E.C. i Retinal dialysis is an important cause of retinal detachment and subsequent reduction
m ':~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~~N
 Brit. J. Ophthal. (1959) 43, 622. EPIPHORA A SYMPTOM OF EARLY HYPOTHYROIDISM* BY W. HAMILTON SMITH, K. G. HOWSAM, and J. J. BILLINGS Victorian Eye and Ear Hospital, Melbourne, Australia AMONG the many
Brit. J. Ophthal. (1959) 43, 622. EPIPHORA A SYMPTOM OF EARLY HYPOTHYROIDISM* BY W. HAMILTON SMITH, K. G. HOWSAM, and J. J. BILLINGS Victorian Eye and Ear Hospital, Melbourne, Australia AMONG the many
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
TREATMENT OF TRAUMATIC HYPHAEMA*t
 Brit. J. Ophthal. (1967) 51, 315 TREATMENT OF TRAUMATIC HYPHAEMA*t BY ARVO OKSALAt From the Ophthalmic Department, University Hospital, Turku, Finland THE treatment of traumatic hyphaema has attracted
Brit. J. Ophthal. (1967) 51, 315 TREATMENT OF TRAUMATIC HYPHAEMA*t BY ARVO OKSALAt From the Ophthalmic Department, University Hospital, Turku, Finland THE treatment of traumatic hyphaema has attracted
optic disc neovascularisation
 British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
Intracranial optic nerve angioblastoma
 Brit. J. Ophthal. (I974) 58, 823 Intracranial optic nerve angioblastoma F. H. STEFANI AND ELISABETH ROTHEMUND From the University Eye Clinic and the Max Planck Institute ofpsychiatry, Munich, Federal Republic
Brit. J. Ophthal. (I974) 58, 823 Intracranial optic nerve angioblastoma F. H. STEFANI AND ELISABETH ROTHEMUND From the University Eye Clinic and the Max Planck Institute ofpsychiatry, Munich, Federal Republic
VCRC-OMERACT ANCA-Vasculitis Outcome Measure Initiative Comparative Outcome Measure Exercise-Training Cases
 Introduction to Training Cases The purpose of this preliminary exercise is to familiarize you with the rules and logistics of the five instruments under study. Please do not read the Training Cases until
Introduction to Training Cases The purpose of this preliminary exercise is to familiarize you with the rules and logistics of the five instruments under study. Please do not read the Training Cases until
Case Report Atypical Presentation of Idiopathic Bilateral Optic Perineuritis in a Young Patient
 Case Reports in Ophthalmological Medicine Volume 2016, Article ID 6741925, 4 pages http://dx.doi.org/10.1155/2016/6741925 Case Report Atypical Presentation of Idiopathic Bilateral Optic Perineuritis in
Case Reports in Ophthalmological Medicine Volume 2016, Article ID 6741925, 4 pages http://dx.doi.org/10.1155/2016/6741925 Case Report Atypical Presentation of Idiopathic Bilateral Optic Perineuritis in
Bilateral common carotid occlusion with hypoxic ocular sequelae
 Brit. J. Ophthal. (1971) 55, 383 Bilateral common carotid occlusion with hypoxic ocular sequelae C. T. HART AND S. HAWORTH Cheltenham A patient is described who was referred with anterior uveitis; following
Brit. J. Ophthal. (1971) 55, 383 Bilateral common carotid occlusion with hypoxic ocular sequelae C. T. HART AND S. HAWORTH Cheltenham A patient is described who was referred with anterior uveitis; following
Relapsing polychondritis in a patient with Takayasu disease; A rare association with fatal outcome
 Case Report Relapsing polychondritis in a patient with Takayasu disease; A rare association with fatal outcome Ausaylah Burqan Department of Medicine, Division of Rheumatology, King Hussain Medical Center,
Case Report Relapsing polychondritis in a patient with Takayasu disease; A rare association with fatal outcome Ausaylah Burqan Department of Medicine, Division of Rheumatology, King Hussain Medical Center,
MALIGNANT SALIVARY GLAND TUMOURS OF THE
 Brit. J. Ophthal. (1963) 47, 279. MALIGNANT SALIVARY GLAND TUMOURS OF THE NASAL SINUSES AND EXOPHTHALMOS* BY ALY MORTADA Department of Ophthalmology, Faculty of Medicine Cairo University, Egypt TUMOURS
Brit. J. Ophthal. (1963) 47, 279. MALIGNANT SALIVARY GLAND TUMOURS OF THE NASAL SINUSES AND EXOPHTHALMOS* BY ALY MORTADA Department of Ophthalmology, Faculty of Medicine Cairo University, Egypt TUMOURS
H erpes simplex virus infection of the
 Herpes simplex keratitis An experimental study Samuel J. Kimura, Victor Diaz-Bonnet, and Masao Okumoto The incidence of complicated herpes simplex keratitis appears to have increased and the important
Herpes simplex keratitis An experimental study Samuel J. Kimura, Victor Diaz-Bonnet, and Masao Okumoto The incidence of complicated herpes simplex keratitis appears to have increased and the important
non-perforating injury
 Brit. J. Ophthal. (I 972) 56, 418 Anterior chamber angle tears after non-perforating injury DAVID MOONEY Croydon Eye Unit, Croydon, Surrey Recession of the anterior chamber angle is a common finding after
Brit. J. Ophthal. (I 972) 56, 418 Anterior chamber angle tears after non-perforating injury DAVID MOONEY Croydon Eye Unit, Croydon, Surrey Recession of the anterior chamber angle is a common finding after
Work Sheet And Course Hand Out
 Work Sheet And Course Hand Out This course provides the primary care health professional with a basic understanding of the eye, its function and the assessment of common sight- and non-sight threatening
Work Sheet And Course Hand Out This course provides the primary care health professional with a basic understanding of the eye, its function and the assessment of common sight- and non-sight threatening
EXUDATIVE DIABETIC RETINOPATHY* SPONTANEOUS CHANGES AND EFFECTS OF A CORN OIL DIET
 Brit. J. Ophthal. (1963) 47, 666. EXUDATIVE DIABETIC RETINOPATHY* SPONTANEOUS CHANGES AND EFFECTS OF A CORN OIL DIET BY R. C. KING, J. H. DOBREE, D'A. KOK, W. S. FOULDS, AND W. G. DANGERFIELD St. Bartholomew's
Brit. J. Ophthal. (1963) 47, 666. EXUDATIVE DIABETIC RETINOPATHY* SPONTANEOUS CHANGES AND EFFECTS OF A CORN OIL DIET BY R. C. KING, J. H. DOBREE, D'A. KOK, W. S. FOULDS, AND W. G. DANGERFIELD St. Bartholomew's
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
ROLE OF ORAL GLYCEROL IN GLAUCOMA*
 Brit. J. Ophthal. (1965) 49, 660 ROLE OF ORAL GLYCEROL IN GLAUCOMA* BY P. AWASTHI AND S. N. SRIVASTAVA Department of Ophthalmology,_Sarojni Naidu Medical College, Agra, India IN cases of acute glaucoma
Brit. J. Ophthal. (1965) 49, 660 ROLE OF ORAL GLYCEROL IN GLAUCOMA* BY P. AWASTHI AND S. N. SRIVASTAVA Department of Ophthalmology,_Sarojni Naidu Medical College, Agra, India IN cases of acute glaucoma
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Fluorescein angiography in the differential diagnosis of sclerokeratitis
 British Journal of Ophthalmology, 1987, 71, 145-151 Fluorescein angiography in the differential diagnosis of sclerokeratitis PETER WATSON AND SARAH BOOTH-MASON From the Scleritis Clinic, Moorfields Eye
British Journal of Ophthalmology, 1987, 71, 145-151 Fluorescein angiography in the differential diagnosis of sclerokeratitis PETER WATSON AND SARAH BOOTH-MASON From the Scleritis Clinic, Moorfields Eye
VISUAL PROGNOSIS OF PROLIFERATING DIABETIC
 Brit. J. Ophthal. (1963) 47, 611. VISUAL PROGNOSIS OF PROLIFERATING DIABETIC RETINOPATHY* BY WILLIAM PARKES BEETHAM From the Harvard Medical School, the Massachusetts Eye and Ear Infirmary, and the New
Brit. J. Ophthal. (1963) 47, 611. VISUAL PROGNOSIS OF PROLIFERATING DIABETIC RETINOPATHY* BY WILLIAM PARKES BEETHAM From the Harvard Medical School, the Massachusetts Eye and Ear Infirmary, and the New
Rare Presentation of Ocular Toxoplasmosis
 Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Case Report Rare Presentation of Ocular Toxoplasmosis Rakhshandeh Alipanahi MD From Department of Ophthalmology, Nikookari Eye Hospital, Tabriz University of Medical Sciences, Tabriz, Iran. Correspondence:
Giant cell arteritis
 Postgraduate Medical Journal (May 1974) 50, 265-269. R. G. TURNER M.B., B.S. J. HENRY M.B., B.S. Giant cell arteritis A. I. FRIEDMANN F.R.C.S. D. GERAINT JAMES M.D., F.R.C.P. The Medical Ophthalmology
Postgraduate Medical Journal (May 1974) 50, 265-269. R. G. TURNER M.B., B.S. J. HENRY M.B., B.S. Giant cell arteritis A. I. FRIEDMANN F.R.C.S. D. GERAINT JAMES M.D., F.R.C.P. The Medical Ophthalmology
LECOM Health Ophthalmology
 Patient Name: Date of Birth: New Patient Questionnaire Your answers will be used by your healthcare provider get an accurate history of your medical conditions and ocular concerns. If you are uncomfortable
Patient Name: Date of Birth: New Patient Questionnaire Your answers will be used by your healthcare provider get an accurate history of your medical conditions and ocular concerns. If you are uncomfortable
Differential diagnosis of the red eye. Carol Slight Nurse Practitioner Ophthalmology
 Differential diagnosis of the red eye Carol Slight Nurse Practitioner Ophthalmology The red eye Conjunctivitis HSV Keratitis Acute angle closure glaucoma Anterior Uveitis Red eye Scleritis Subconjunctival
Differential diagnosis of the red eye Carol Slight Nurse Practitioner Ophthalmology The red eye Conjunctivitis HSV Keratitis Acute angle closure glaucoma Anterior Uveitis Red eye Scleritis Subconjunctival
COMMUNICATIONS PHOTOCOAGULATION OF THE RETINA* OPHTHALMOSCOPIC AND HISTOLOGICAL FINDINGS. photocoagulation of the rabbit's retina.
 Brit. J. Ophthal. (1963) 47, 577. COMMUNICATIONS PHOTOCOAGULATION OF THE RETINA* OPHTHALMOSCOPIC AND HISTOLOGICAL FINDINGS BY A. LAVYEL Haifa, Israel SINCE the introduction of the photocoagulator by Meyer-Schwickerath
Brit. J. Ophthal. (1963) 47, 577. COMMUNICATIONS PHOTOCOAGULATION OF THE RETINA* OPHTHALMOSCOPIC AND HISTOLOGICAL FINDINGS BY A. LAVYEL Haifa, Israel SINCE the introduction of the photocoagulator by Meyer-Schwickerath
Case Presentation. Rafid Asfar, MD
 Case Presentation Rafid Asfar, MD Introduction ANCA associated vasculitis may be localized or systemic, and can involve the eyes Ocular manifestations can occur in the absence of systemic disease in persons
Case Presentation Rafid Asfar, MD Introduction ANCA associated vasculitis may be localized or systemic, and can involve the eyes Ocular manifestations can occur in the absence of systemic disease in persons
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC
 CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
CONSENT FOR CATARACT SURGERY REQUEST FOR SURGICAL OPERATION / PROCEDURE AND ANAESTHETIC Your doctor has indicated that the condition of your eye appears stable and your cataract surgery and/or implantation
CASE REPORT A CASE SHOWING COMBINED FEATURES OF ACUTE RHEUMATISM AND RHEUMATOID ARTHRITIS
 CASE REPORT A CASE SHOWING COMBINED FEATURES OF ACUTE RHEUMATISM AND RHEUMATOID ARTHRITIS BY C. ELAINE FIELD, M.D., M.R.C.P. (From the Children's Unit, Hempstead House Emergency Hospital) 'There are not
CASE REPORT A CASE SHOWING COMBINED FEATURES OF ACUTE RHEUMATISM AND RHEUMATOID ARTHRITIS BY C. ELAINE FIELD, M.D., M.R.C.P. (From the Children's Unit, Hempstead House Emergency Hospital) 'There are not
Pit-like changes of the optic nerve head
 Pit-like changes of the optic nerve head in open-angle glaucoma British Journal of Ophthalmology, 1978, 62, 389-393 RONALD L. RADIUS, A. EDWARD MAUMENEE, AND WILLIAM R. GREEN From the Wilmer Ophthalmologic
Pit-like changes of the optic nerve head in open-angle glaucoma British Journal of Ophthalmology, 1978, 62, 389-393 RONALD L. RADIUS, A. EDWARD MAUMENEE, AND WILLIAM R. GREEN From the Wilmer Ophthalmologic
Note: This is an outcome measure and can be calculated solely using registry data.
 Measure #191 (NQF 0565): Cataracts: 20/40 or Better Visual Acuity within 90 Days Following Cataract Surgery -- National Quality Strategy Domain: Effective Clinical Care DESCRIPTION: Percentage of patients
Measure #191 (NQF 0565): Cataracts: 20/40 or Better Visual Acuity within 90 Days Following Cataract Surgery -- National Quality Strategy Domain: Effective Clinical Care DESCRIPTION: Percentage of patients
chamber pigment in the anterior L beration of iris phenylephrine hydrochloride solution. After instillation of io per cent.
 Brit.. Ophthal. (I 97 I) 55, 544 L beration of iris chamber After instillation of io per cent. hydrochloride solution J. L. AGGARWAL AND B. BEVERIDGE Wolverhampton and Midland Counties Eye Infirmary pigment
Brit.. Ophthal. (I 97 I) 55, 544 L beration of iris chamber After instillation of io per cent. hydrochloride solution J. L. AGGARWAL AND B. BEVERIDGE Wolverhampton and Midland Counties Eye Infirmary pigment
Combined Infliximab and Rituximab in Necrotising Scleritis
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Case History. Slit lamp exam: Clinical Pearls in the Management of Iritis. 2- injection: Irregular SPK and staining AC: grade 3 cell & flare
 Clinical Pearls in the Management of Iritis Paul Karpecki, OD, FAAO Corneal Services and Ocular Disease Research Koffler Vision Group-Lexington, KY 68 y.o. Caucasian female Complains of photophobia and
Clinical Pearls in the Management of Iritis Paul Karpecki, OD, FAAO Corneal Services and Ocular Disease Research Koffler Vision Group-Lexington, KY 68 y.o. Caucasian female Complains of photophobia and
J.P.S. Bakshi Manual of Ophthalmological Disorders
 J.P.S. Bakshi Leseprobe von J.P.S. Bakshi Herausgeber: Cosmic Healers India http://www.narayana-verlag.de/b5605 Im Narayana Webshop finden Sie alle deutschen und englischen Bücher zu Homöopathie, Alternativmedizin
J.P.S. Bakshi Leseprobe von J.P.S. Bakshi Herausgeber: Cosmic Healers India http://www.narayana-verlag.de/b5605 Im Narayana Webshop finden Sie alle deutschen und englischen Bücher zu Homöopathie, Alternativmedizin
ISPUB.COM. An Atypical Presentation of Posterior Scleritis. A Ramanathan, A Gaur CASE REPORT
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 2 A Ramanathan, A Gaur Citation A Ramanathan, A Gaur.. The Internet Journal of Ophthalmology and Visual Science. 2009
Retinal embolism after hysterosalpingography
 Brit. J. Ophthal. (I 973) 57, i 66 Retinal embolism after hysterosalpingography A. M. CHARAWANAMUTTU,* J. HUGHES-NURSE,t AND J. D. HAMLETTt From St. Paul's Eye Hospital*, Liverpool, The Gynaecology Department,
Brit. J. Ophthal. (I 973) 57, i 66 Retinal embolism after hysterosalpingography A. M. CHARAWANAMUTTU,* J. HUGHES-NURSE,t AND J. D. HAMLETTt From St. Paul's Eye Hospital*, Liverpool, The Gynaecology Department,
Masquerade Scleritis CASE REPORT INTRODUCTION
 Ocular Immunology and Inflammation, 13:479 482, 2005 Copyright c Taylor & Francis Inc. ISSN: 0927-3948 print; 1744-5078 online DOI: 10.1080/09273940591004133 CASE REPORT Masquerade Scleritis Chrysanthi
Ocular Immunology and Inflammation, 13:479 482, 2005 Copyright c Taylor & Francis Inc. ISSN: 0927-3948 print; 1744-5078 online DOI: 10.1080/09273940591004133 CASE REPORT Masquerade Scleritis Chrysanthi
Orbital facia. Periororbital facia Orbital septum Bulbar facia Muscular facia
 Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
She has a health visitor.
 Demonstration Site Title: Can ibuprofen, sulfasalazine or hormone replacement therapy cause posterior vitreous detachment? Enq. No:171 Due By: 16/05/2018 17:00:00 Comments: Answer by end of day. Date completed:
Demonstration Site Title: Can ibuprofen, sulfasalazine or hormone replacement therapy cause posterior vitreous detachment? Enq. No:171 Due By: 16/05/2018 17:00:00 Comments: Answer by end of day. Date completed:
UNDERSTAND MORE ABOUT UVEITIS UVEITIS
 UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
Ross. *March, 1927, an attempt was made to classify congenital defects
 608 'HE BRITISH JOURNAL OF OPHTHALMOLOGY A CASE OF ATYPICAL COLOBOMA ASSOCIATED WITH ABNORMAL RETINAL VESSELS BY IDA MANN AND JAMES A. LONDON CARLISLE Ross IN a paper on" Certain abnormal conditions of
608 'HE BRITISH JOURNAL OF OPHTHALMOLOGY A CASE OF ATYPICAL COLOBOMA ASSOCIATED WITH ABNORMAL RETINAL VESSELS BY IDA MANN AND JAMES A. LONDON CARLISLE Ross IN a paper on" Certain abnormal conditions of
New vessel formation in retinal branch vein occlusion
 Brit. 7. Ophthal. (I 976) 6o, 8io New vessel formation in retinal branch vein occlusion JOHN S. SHILLING AND EVA M. KOHNER From the Retinal Diagnostic Unit, Moorfields Eye Hospital, London Neovascularization
Brit. 7. Ophthal. (I 976) 6o, 8io New vessel formation in retinal branch vein occlusion JOHN S. SHILLING AND EVA M. KOHNER From the Retinal Diagnostic Unit, Moorfields Eye Hospital, London Neovascularization
Haemorrhagic glaucoma
 Brit. j. Ophthal. (I97I) 55, 444 Haemorrhagic glaucoma Comparative study in diabetic and nondiabetic patients P. H. MADSEN From the Departments of Ophthalmology and Internal Medicine, the University Hospital,
Brit. j. Ophthal. (I97I) 55, 444 Haemorrhagic glaucoma Comparative study in diabetic and nondiabetic patients P. H. MADSEN From the Departments of Ophthalmology and Internal Medicine, the University Hospital,
"A" AND "V" PHENOMENA*t
 Brit. J. Ophthal. (1966) 50, 718 "A" AND "V" PHENOMENA*t DHANWANT SINGH, GURBUX SINGH, L. P. AGGARWAL, AND PREM CHANDRA BY From the Department of Ophthalmology, Government Medical College, Patiala, and
Brit. J. Ophthal. (1966) 50, 718 "A" AND "V" PHENOMENA*t DHANWANT SINGH, GURBUX SINGH, L. P. AGGARWAL, AND PREM CHANDRA BY From the Department of Ophthalmology, Government Medical College, Patiala, and
