Skin Signs of Internal Disease: Case-based Challenges
|
|
|
- Frederica Thomas
- 5 years ago
- Views:
Transcription
1 Skin Signs of Internal Disease: Case-based Challenges Jeffrey P. Callen, MD Professor of Medicine (Dermatology) Chief, Division of Dermatology University of Louisville
2 Jeffrey P. Callen, MD Disclosure (previous 12 months) Consultant Biogen/IDEC, Lilly, Amgen Editorial Boards UpToDate (editor-in-chief, Dermatology), JAMA Dermatology (Associate Editor), Cutis, emedicine.com, Journal of Drugs in Dermatology, Medicine, Journal of Psoriasis and Psoriatic Arthritis Equity holdings (trust accounts) - Celgene; Pfizer; 3M; Johnson and Johnson; Merck; Abbott Laboratories; AbbVie; Procter and Gamble; CVS; Walgreens; Allergen; Amgen I will discuss off-label uses of some of the currently available agents and will identify which are labeled v. off-labeled uses. February 2018
3 Case 1
4 44-year-old man HPI: Presented in March 2017 with a 1-yr h/o skin ripping and genital edema affecting the penis and scrotum PMH: 3-year h/o Crohn s Disease with anorectal fistulas previously treated with adalimumab which was stopped due to MRSA abscesses. Vedolizumab was begun in January ROS: revealed h/o purulent drainage from the penis and inguinal lymphadenopathy, but was negative for abdominal pain, bleeding problems, cough, fevers/chills, joint aches, weight loss or gain Medications: Vedolizumab 300 mg IV q monthly, testosterone 0.75 mg q weekly, doxycycline, ibuprofen
5 What is your diagnosis? 1. Metastatic Crohn s disease 2. Hidradenitis suppurativa 3. Lymphedema 4. Sarcoidosis 5. Balanoposthitis
6 Course At the time of his visit, he informed us that he had seen urology and they had performed a biopsy of the penis and scrotum He was told that the findings were non-specific
7 What is the next step in evaluation of this patient? 1. Biopsy of the penis 2. Biopsy the perianal skin 3. Obtain the prior slide for review 4. Order Sacchyromyces Cerevisiae antibody 5. Order Antineutrophil cytoplasmic antibodies
8 Biopsy findings The slides from prior biopsies were obtained and revealed non-specific changes from the penis, but demonstrated focally granulomatous zones (non-caseating) as well as lymphocytic and plasmacytic inflammation which is compatible with Cutaneous Crohn s Disease (aka Metastatic Crohn s Disease)
9 What therapy should be recommended? 1. Oral metronidazole 2. SQ ustekinumab 3. Oral azathioprine 4. SQ methotrexate 5. SQ adalimumab 6. Oral mesalamine
10 Course His bowel disease was deemed to be reasonably well controlled, but his perianal fistula disease was active GI switched from vedolizumab to ustekinumab (GI dosing) We suggested the addition of metronidazole which he took for 3 months and reported little change
11
12 Which of the following statements is accurate? 1. Metastatic Crohn s disease is synonymous with cutaneous Crohn's disease 2. Presence or severity of metastatic Crohn s disease does not correlate with severity or activity of the GI disease 3. Treatment of underlying GI disease leads to resolution of skin lesions 4. Patients with metastatic Crohn s disease have less frequent involvement of the colon
13 Metastatic Crohn s Disease First described in 1965 by Parks, et al. A rare granulomatous inflammation of skin noncontiguous with the GIT May occur prior to, simultaneously with GI disease or following GI surgery The severity of skin involvement does not always parallel severity of GIT disease 56% genital involvement; 44% non-genital involvement (extremities, trunk, intertriginous/flexural skin, face/lips) Children tend to have more genital involvement than adults
14 From Thrash et al. JAAD (2) e1-e33.
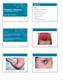
15 Crohn's disease of the vulva. From Barret M, et al: J Crohns Colitis Nov 16. pii: S (13)
16 Treatment options Topical, intralesional, systemic corticosteroids Antibiotics Dapsone Sulfasalazine Metronidazole Tetracycline Immunosuppressive agents: Azathioprine or 6-Mercaptopurine Mycophenolate mofetil Biologics: TNF-alpha inhibitors (infliximab, adalimumab, certolizumab, etc.) Ustekinumab Thalidomide Surgical debridement, hyperbaric oxygen, and fecal diversion useful in resistant cases
17
18
19 Conclusions Consider MCD in the clinical differential diagnosis of hidradentitis supprativa, dermatitis, intertrigo, chronic cellulitis, sarcoidosis, mycobacterial or fungal infections, erysipelas, etc. High degree of clinical suspicion is necessary Consider MCD particularly in children with genital and/or perianal fissures, ulcers, skin tags or unusual swelling
20 Case 2
21 63-year-old man 1-yr h/o waxing and waning eruption on the inner thighs and left inner arm. He denies any associated fever, chills, fatigue, night sweats, weight loss, abdominal pain, nausea, diarrhea. He said that the areas seems to flare after golfing or working outdoors. Outside biopsy in October 2016 interpreted as Sweet syndrome, in August 2017 as interstitial granulomatous dermatitis PMH: allergies, hypertension, GERD, prior hepatitis C Medications: baby aspirin, fexofenadine, atenolol, omeprazole, sertraline, tamsulosin
22 What is your diagnosis? 1. Granuloma annulare 2. Interstitial granulomatous dermatitis 3. Sweet syndrome 4. Palisaded neutrophilic and granulomatous dermatitis 5. Sarcoidosis
23 What is the most appropriate next step? 1. Obtain outside biopsies for review 2. Biopsy current eruption 3. Order a chest X-ray 4. Order an immunofixation electrophoresis 5. Order serologic testing for lupus and rheumatoid arthritis 6. All of the above
24 Evaluation The outside biopsies were reviewed and several new biopsies were performed which revealed changes c/w PNGD Laboratory testing revealed normal CBC, CMP, ANCA, IFE, RF, Hepatitis C viral load, ACE level, antiphospholipid antibodies, G-6PD, TMPT ANA 1:80, anti-ndna 58 IU/mL (nl <5), Ro/SS-A 48 AU/mL (nl < 40), Hepatitis C antibody, MTHFR polymorphism
25 What is the most appropriate diagnosis now? 1. Palisaded neutrophilic and granulomatous dermatitis 2. Sarcoidosis 3. Interstitial granulomatous dermatitis drug reaction 4. Interstitial granulomatous dermatitis 5. Reactive granulomatous dermatitis
26 What is the most appropriate therapy at this time? 1. Treat with prednisone 2. Treat with methotrexate 3. Treat with plaquenil 4. Treat with dapsone
27 Course He was started on hydroxychloroquine 200 mg twice daily 2 weeks late an ophthalmologist called and reported that his eyes were crossing and he had double vision and advised that the hydroxychloroquine be stopped At that time, he reported that his rash had resolved and he was asymptomatic
28 What should be done at this time? 1. Observation 2. Start dapsone 3. Start methotrexate 4. Start azathioprine 5. Refer to rheumatology
29 Course He was not given any new therapy His eye symptoms resolved quickly He was seen 2 months later and remained asymptomatic and there was minimal erythema of the previously affected areas 1-month later he called to get treatment or further evaluation to get to the bottom of this
30
31
32
33
34
35 Case 3
36 35-year-old woman Developed purpuric lesions on the legs and arms in January 2015 Worsened in October 2015 at which time her internist sent her to a general surgeon for a skin biopsy which was interpreted as urticarial vasculitis Treated with intermittent prednisone tapers Noted to have elevated CRP, ESR and rheumatoid factor Referred to a rheumatologist in late 2015 whose evaluation excluded rheumatoid arthritis and treated with patient with colchicine 0.6 mg twice daily with little effect Rheumatologist referred the patient for management
37 HPI, PE and Labs: April 2016 Denied abdominal pain, blood in urine, headaches, muscle, joint, bone pain, shortness of air, alcohol consumption Labs sent from rheumatology ESR 39, Rheumatoid factor 950, ANA negative, ANCA negative, Antiglomerular basement membrane ab negative, elevated transaminases, negative hepatitis profile, and urinalysis which revealed hematuria but not proteinuria or casts. PMH: hypertension Medications: lisinopril PE: massively obese (BMI = 42 kg/m 2 ), purpuric lesions on legs, arms and buttocks
38 What should be done now? 1. Obtain slides from prior biopsy 2. Re-biopsy for routine processing 3. Biopsy for direct immunofluorescence microscopy 4. No additional biopsies are needed, go ahead and treat 5. 1,2 and 3
39 What laboratory testing should be performed? 1. ANA 2. Anti-Ro/SS-A 3. Repeat hepatitis profile 4. Cryoglobulin 5. ANCA
40 DIF result
41 DIF interpretation
42 Laboratory evaluation Abnormalities: AST 216 (nl < 46), ALT 439 (nl <69), Rheumatoid factor 426 IU (nl < 20), ANA 1:80 speckled, IFE polyclonal pattern, IgG 1910 (nl <1618), IgA 529 (nl <378), cryoglobulin IgM 2.0 mg/dl (nl = 0) Normal or negative CBC, urinalysis, total hemolytic complement, C2, ANCA, Ro/SS-A, La/SS-B, IgM level on IFE
43 What is this patient s diagnosis? 1. Henoch-Schönlein purpura 2. Hypersensitivity vasculitis 3. Vasculitis due to collagen vascular disease 4. Cryoglobulinemic purpura 5. Hyperglobulinemic purpura of Waldenstrom
44 What therapy should be administered now? 1. Dapsone 2. Leflunomide 3. Methotrexate 4. Azathioprine 5. Rituximab 6. Intravenous immune globulin 7. No therapy is needed
45 Course The patient was begun on dapsone and the dose escalated to 150 mg/day She was instructed to lose weight and a request was made for a liver biopsy to be performed and for her primary care physician to arrange for a dietitian to become involved The liver biopsy was performed, but the patient has not had meaningful weight reduction She continued over the next six months to have joint pain and showers of purpuric lesions, primarily on the legs
46 Subsequent Laboratory Evaluation 6-months AST 111 (nl < 46), ALT 146 (nl <56), urinalysis unremarkable, CBC normal Liver biopsy steatohepatitis with bridging fibrosis present 12-months AST 136, ALT 219, urinalysis nl, CBC normal, Rheumatoid factor months IFE IgG 1936 (nl < 1618), IgA 611 (nl< 378), Rheumatoid factor 241
47 What therapy should be administered now? 1. Add colchicine to the dapsone 2. Rituximab 3. Intravenous immune globulin 4. Azathioprine 5. Leflunomide
48 Course Colchicine was restarted and dapsone was continued No effect was noted Rituximab was initiated 18 months following initial presentation 1 gram initially, repeated at 2 weeks Follow-up at 21-months Clinically fewer lesions, but some continue Weight loss of only 10 pounds AST 37, ALT 43, IgG normal, IgA 386, Rheumatoid factor 183 Labs at 23 months AST and ALT normal, Rheumatoid factor 114
49 Cryoglobulinemic vasculitis v. Henoch-Schönlein purpura (aka IgA vasculitis) Arthritis Rheumatol Nov 14. [Epub ahead of print]
50 Inclusion criteria: purpura, histology of SVV, IgA predominant disease and at least one of the following: GI, renal or joint involvement Treatments compared corticosteroids alone, to corticosteroids plus cyclosphosphamide or colchicine Findings: CS alone was most effective Responses CS alone (64/80), CTX (23/30), colchicine (10/17) Arthritis & Rheumatology 2017; 69:
51 Comment Large cohort of patients Selected to include patients with evidence of systemic disease, particularly nephritis Limitations: Retrospective analysis Selection bias (referral bias) Underpowered to detect differences between CS and CS+CYT Small number of patients treated with colchicine No patients were treated with dapsone Arthritis & Rheumatology 2017; 69:
52 Study of 22 patients with IgA vasculitis At onset 21 had purpura (necrotic or bullous lesions 8), 18 had GI involvement (pain 18, hemorrhage 7), 20 had kidney involvement (15 had kidney biopsies), 17 had joint disease Indication for RTX refractory disease (8), relapse (8), contraindication to CS and/or immunosuppressive therapy (6) Rituximab either 375 mg/mm 2 x 4 wks or 1 gm infusions x 2 Arthritis & Rheumatology 2018; 70:
53 Arthritis & Rheumatology 2018; 70:
54 Remission was common, but relapse occurred in 35%, but retreatment was effective Adverse reactions: 2 patients had infusion reactions 1 with urticaria and one with dyspnea One patient with cirrhosis died due to pneumonia 60 months after infusions Limitations: Small sample size Use of concomitant therapies including immunosuppressives and ARBs or ACE inhibitors Inclusion of severe patients with nephritis Retrospective analysis Arthritis & Rheumatology 2018; 70:
55 Diagnosis cryoglobulinemic vasculitis v. HSP Dilemmas: in a patient with steatohepatitis Should patients with skin-only symptoms/signs be treated aggressively? What is the meaning of IgA deposition in the DIF result? What is the best therapy for this patient? When should the rituximab be re-administered?
56 Case 4
57 69-year-old woman 5-week h/o pruritic, blistering eruption on the neck, arms, legs and trunk PMH RA, COPD, former smoker Medications amlodipine, leflunomide, gabapentin, propranolol, adalimumab (previously treated with Golimumab and etanercept), three inhalers and OTC guaifenisen
58 What is your diagnosis? 1. Linear IgA bullous dermatosis 2. Dermatitis herpetiformis 3. Bullous pemphigoid 4. Epidermolysis bullosa acquisita 5. Bullous lupus erythematosus 6. Lichen planus pemphigoides
59
60 What is the best diagnosis now? 1. Linear IgA bullous dermatosis 2. Dermatitis herpetiformis 3. Bullous pemphigoid 4. Epidermolysis bullosa acquisita 5. Bullous lupus erythematosus 6. Lichen planus pemphigoides
61 Where should a biopsy be performed for immunoflouresence? 1. A fresh blister 2. An eroded area 3. Perilesional skin 4. Uninvolved skin on the buttocks 5. Previously involved skin that is clinically normal
62 IgA x 400
63 Which of the following diseases are associated with LABD? 1. Ulcerative colitis 2. Gluten sensitive enteropathy 3. Crohn s disease 4. Diabetes mellitus 5. Rheumatoid arthritis
64 Which of the following findings is more likely with Drug-induced LABD? 1. Mucosal involvement 2. Targetoid lesions 3. String of pearls distribution 4. Erosions
65
66
67 What is the best therapy for this patient? 1. Dapsone 2. Colchicine 3. Gluten free diet 4. Mycophenolate mofetil 5. Cyclosporin 6. Rituximab
68 Course Low-dose dapsone (75 mg three days per week, 50 mg on alternate days) resulted in control of her skin disease Mild anemia (hemoglobin 11 gm/dl) developed After 6-months of therapy she developed respiratory symptoms requiring oxygen
69 What testing should be performed now? 1. Methemoglobin levels 2. Reticulocyte count 3. High resolution CT scan 4. No additional testing is needed
70 How should dapsone be handled? 1. Stop it 2. Lower the daily dose 3. Administer vitamin E concomitantly 4. Add cimetidine therapy
71 Strategies for managing dapsone toxicity Co-administration of cimetidine might improve patient tolerance to dapsone by diminishing the formation of the methemoglobin-forming N-hydroxylated metabolites Brit. J. Clin Pharmac. 1992; Co-administration of vitamin E 800 U/d reduces hemolysis Arch Dermatol 1992; 128: 210-3
72 If you choose to stop the dapsone, what alternative therapy will you prescribe? 1. Colchicine 2. Prednisone 3. Nicotinamide and doxycycline 4. Mycophenolate 5. Rituximab
73 Br J Dermatol Jul;177(1):
74 Methods Retrospective case series; Autoimmune Inflammatory Bullous Disease referral centers Inclusion criteria: Adults (>15 yo) with idiopathic LABD; positive DIF linear pure IgA or predominant IgA+G/M deposits at the DEJ Exclusion critieria: <15 yo, drug-induced LABD, bullous lupus erythematous Drug-induced LABD any new drug within in 4 weeks before disease onset
75 Heterogeneous clinical presentation
76 Clinical presentation - II
77 Clinical Manifestations Skin lesions involved the head or neck of 29 patients (40%) and scalp of 16 patients (22%). String of pearls or herpetiform arrangement tended to be more frequent in patients with pure IgA deposits (P =.011) There were 43 patients (60%) who had mucosal involvement at diagnosis; 39 oral (91%), 18 nose and throat (42%), 15 eyes (35%), 10 genital (23%) and six anal (14%) Four of those with mucosal disease developed laryngeal stenoses or conjunctival synechiae
78 Co-morbidities IBD Crohn disease with sclerosing cholangitis (IgA anti-gp2 negative) Ulcerative colitis Malignancies Following diagnosis - Breast cancer, Hodgkin lymphoma (1 case each) Pre-diagnosis without recurrence one case each of liver, colon and prostate, colon and pancreas, or breast Paraproteinemia 1 with IgG monoclonal gammopathy of undetermined significance 1 with IgG myeloma
79 Treatments First-line therapy was potent (or highly potent) topical steroids alone for 29 patients (40%), combined with dapsone and/or sulfasalazine for 45 patients (63%). Overall, 16 patients (22%), all with mucosal involvement, required one or more adjunctive immunosuppressant Cyclophosphamide -15 Rituximab - 9 Mycophenolate mofetil - 4 Methotrexate - 2 Intravenous immunoglobulin (IVIg) - 3 TNF antagonists were used in combination with cyclosphosphamide - 2
80 Course 36% sustained CR Comment 29% CR w/ subsequent relapse 35% chronic lesions w/o CR Age >70 and lack of MM associated w/ CR Strengths/Weaknesses of this observational study (+) sample size, available data (-) Variability of therapies selected Analysis limited to complete responders Selection bias for severe cases
S003 CPC Self-Assessment
 S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
Case 1 History. William Tremaine, M.D. CP
 Extraintestinal Manifestations of IBD Case Studies William Tremaine, M.D. Case 1 History 18 year-old woman with Crohn s disease Onset at age 5: colonic & perianal Sulfasalazine, prednisone, mercaptopurine
Extraintestinal Manifestations of IBD Case Studies William Tremaine, M.D. Case 1 History 18 year-old woman with Crohn s disease Onset at age 5: colonic & perianal Sulfasalazine, prednisone, mercaptopurine
Cases I have Learned From. Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville
 Cases I have Learned From Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville Jeffrey P. Callen, MD Disclosure (previous 12 months) Consultant/Advisory board Auxilium Consultant
Cases I have Learned From Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville Jeffrey P. Callen, MD Disclosure (previous 12 months) Consultant/Advisory board Auxilium Consultant
More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa
 More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa Conflicts of Interest/Disclosure None Classification/Overview 1) Necrobiotic/Palisading
More Non-infectious Granulomatous Diseases! Karolyn Wanat, MD Assistant Professor, Dermatology & Pathology University of Iowa Conflicts of Interest/Disclosure None Classification/Overview 1) Necrobiotic/Palisading
COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS
 COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS Benjamin F. Chong, MD, MSCS February 17, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong, MD, MSCS F059 Complex
COMPLEX CUTANEOUS LUPUS CASES PEARLS AND PITFALLS Benjamin F. Chong, MD, MSCS February 17, 2018 CONFLICTS OF INTEREST D I S CLOSURE OF R E LATI ONSHIPS W I T H I NDUSTRY Benjamin Chong, MD, MSCS F059 Complex
First Name. Specialty: Fax. First Name DOB: Duration:
 Prescriber Information Last ame: First ame DEA/PI: Specialty: Phone - - Fax - - Member Information Last ame: First ame Member ID umber DOB: - - Medication Information: Drug ame and Strength: Diagnosis:
Prescriber Information Last ame: First ame DEA/PI: Specialty: Phone - - Fax - - Member Information Last ame: First ame Member ID umber DOB: - - Medication Information: Drug ame and Strength: Diagnosis:
Case 1. Debridement Cultures Keflex Silvadene
 The Red Breast Beth McLellan, M.D. Assistant Professor Division of Dermatology Albert Einstein College of Medicine Montefiore Medical Center Jacobi Medical Center Case 1 48 year old radiation oncologist
The Red Breast Beth McLellan, M.D. Assistant Professor Division of Dermatology Albert Einstein College of Medicine Montefiore Medical Center Jacobi Medical Center Case 1 48 year old radiation oncologist
Case Presentation. Rafid Asfar, MD
 Case Presentation Rafid Asfar, MD Introduction ANCA associated vasculitis may be localized or systemic, and can involve the eyes Ocular manifestations can occur in the absence of systemic disease in persons
Case Presentation Rafid Asfar, MD Introduction ANCA associated vasculitis may be localized or systemic, and can involve the eyes Ocular manifestations can occur in the absence of systemic disease in persons
A case of bullous pemphigoid following pemphigus foliaceus
 #2228 A case of bullous pemphigoid following pemphigus foliaceus Priyanka Vedak MD 1, Danielle Levine MD 1,3, Lyn Duncan MD 2,3, Hensin Tsao 1,3, Daniela Kroshinsky MD MPH 1,3 1. Department of Dermatology,
#2228 A case of bullous pemphigoid following pemphigus foliaceus Priyanka Vedak MD 1, Danielle Levine MD 1,3, Lyn Duncan MD 2,3, Hensin Tsao 1,3, Daniela Kroshinsky MD MPH 1,3 1. Department of Dermatology,
RHEUMATOLOGY OVERVIEW. Carmelita J. Colbert, MD Assistant Professor of Medicine Division of Rheumatology Loyola University Medical Center
 RHEUMATOLOGY OVERVIEW Carmelita J. Colbert, MD Assistant Professor of Medicine Division of Rheumatology Loyola University Medical Center What is Rheumatology? Medical science devoted to the rheumatic diseases
RHEUMATOLOGY OVERVIEW Carmelita J. Colbert, MD Assistant Professor of Medicine Division of Rheumatology Loyola University Medical Center What is Rheumatology? Medical science devoted to the rheumatic diseases
Pharmacy Prior Authorization
 Pharmacy Prior Authorization AETA BETTER HEALTH PESLVAIA & AETA BETTER HEALTH KIDS Humira (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information,
Pharmacy Prior Authorization AETA BETTER HEALTH PESLVAIA & AETA BETTER HEALTH KIDS Humira (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information,
BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123
 BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123 M55. 4/7 tender lesions on knee, legs and arms. Also iritis/ weight loss/headache, synovitis.?vasculitis. Sarcoidosis. Biopsy from left elbow
BSD Self Assessment Workshop 7 th July 2013 CASE 27 RAC6123 M55. 4/7 tender lesions on knee, legs and arms. Also iritis/ weight loss/headache, synovitis.?vasculitis. Sarcoidosis. Biopsy from left elbow
Incorporating Biologics Into Your Practice
 Incorporating Biologics Into Your Practice Jeffrey M. Sobell MD Tufts University School of Medicine SkinCare Physicians Ora Clinical Research Disclosure Of Relationships With Industry Amgen AbbVie Celgene
Incorporating Biologics Into Your Practice Jeffrey M. Sobell MD Tufts University School of Medicine SkinCare Physicians Ora Clinical Research Disclosure Of Relationships With Industry Amgen AbbVie Celgene
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT
 HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
Crohn s Disease. Resident Lecture 1/17/19
 Crohn s Disease Resident Lecture 1/17/19 Objectives Features/Classification of Crohn s Disease Medical Treatment Surgical Indications Surgical Considerations 2 Case 25 yo F presents to your office with
Crohn s Disease Resident Lecture 1/17/19 Objectives Features/Classification of Crohn s Disease Medical Treatment Surgical Indications Surgical Considerations 2 Case 25 yo F presents to your office with
Inflectra Frequently Asked Questions
 Inflectra Frequently Asked Questions 1. What is the funding status of Inflectra (infliximab)? Earlier in 2016, Inflectra (infliximab) was added to the Ontario Drug Benefit (ODB) Formulary as a Limited
Inflectra Frequently Asked Questions 1. What is the funding status of Inflectra (infliximab)? Earlier in 2016, Inflectra (infliximab) was added to the Ontario Drug Benefit (ODB) Formulary as a Limited
Stelara. Stelara (ustekinumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.90.04 Subject: Stelara Page: 1 of 9 Last Review Date: September 20, 2018 Stelara Description Stelara
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.90.04 Subject: Stelara Page: 1 of 9 Last Review Date: September 20, 2018 Stelara Description Stelara
Objectives. 3HP and Flu Syndrome What is the Underlying Mechanism? Case #1 3/23/2016. Christina T. Fiske, MD MPH March 30, 2016
 Objectives 3HP and Flu Syndrome What is the Underlying Mechanism? Christina T. Fiske, MD MPH March 30, 2016 Illustrate the side effect of 3HP flu like syndrome after its initiation to raise awareness in
Objectives 3HP and Flu Syndrome What is the Underlying Mechanism? Christina T. Fiske, MD MPH March 30, 2016 Illustrate the side effect of 3HP flu like syndrome after its initiation to raise awareness in
Pharmacy Prior Authorization
 Pharmacy Prior Authorization MERC CARE PLA (MEDICAID) Humira (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and date. Fax
Pharmacy Prior Authorization MERC CARE PLA (MEDICAID) Humira (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and date. Fax
2. Has the patient had a response to treatment? Y N. 3. Does the patient have a diagnosis of rheumatoid arthritis (RA)? Y N
 12/21/2016 Prior Authorization Aetna Better Health of West Virginia Humira (WV88) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and
12/21/2016 Prior Authorization Aetna Better Health of West Virginia Humira (WV88) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information, sign and
CHECK LIST FORM-MONTH 27 (Please note Month 27 is from enrolment not randomisation)
 CHECK LIST FORM-MONTH 27 (Please note Month 27 is from enrolment not randomisation) Participant Initials: Date of Birth: Were the following forms completed for this visit? Follow Up Form Done t Done BVASWG
CHECK LIST FORM-MONTH 27 (Please note Month 27 is from enrolment not randomisation) Participant Initials: Date of Birth: Were the following forms completed for this visit? Follow Up Form Done t Done BVASWG
THE TIP OF THE ICEBERG SAMER BOLIS, DO PGY-3 LEHIGH VALLEY HEALTH NETWORK, ALLENTOWN PA
 THE TIP OF THE ICEBERG SAMER BOLIS, DO PGY-3 LEHIGH VALLEY HEALTH NETWORK, ALLENTOWN PA Case The patient is a 48 year-old female, who recently returned from a trip to Puerto Rico. She presents to the ED
THE TIP OF THE ICEBERG SAMER BOLIS, DO PGY-3 LEHIGH VALLEY HEALTH NETWORK, ALLENTOWN PA Case The patient is a 48 year-old female, who recently returned from a trip to Puerto Rico. She presents to the ED
Pediatric Inflammatory Bowel Diseases
 Pediatric Inflammatory Bowel Diseases Michael Stephens, M.D. Denny Sanford Pediatric Symposium November 21 2014, Sioux Falls, SD 2014 slide-1 Disclosures I have nothing to disclose 2014 slide-2 Objectives
Pediatric Inflammatory Bowel Diseases Michael Stephens, M.D. Denny Sanford Pediatric Symposium November 21 2014, Sioux Falls, SD 2014 slide-1 Disclosures I have nothing to disclose 2014 slide-2 Objectives
Erythema gyratumrepens-like eruption in a patient with epidermolysisbullosaacquisita associated with ulcerative colitis
 Erythema gyratumrepens-like eruption in a patient with epidermolysisbullosaacquisita associated with ulcerative colitis A. España C. Sitaru* M. Pretel L. Aguado J. Jimenez# Department of Dermatology, University
Erythema gyratumrepens-like eruption in a patient with epidermolysisbullosaacquisita associated with ulcerative colitis A. España C. Sitaru* M. Pretel L. Aguado J. Jimenez# Department of Dermatology, University
Index. derm.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
Note: Page numbers of article titles are in boldface type. A Abatacept for DLE, 493 for SLE, 497 Ablative therapies, localized, for cutaneous T-cell lymphoma, 502 506. See also Cutaneous T-cell lymphoma,
Drugs and Applicable Coding: J-code: Enbrel-J1438; Humira-J0135; Remicade-J1745; Inflectra-Q5102; Cimzia-J0718; Simponi-J1602 Renflexis - pending
 Policy Subject: Anti-TNF Agents Policy Number: SHS PBD16 Category: Rheumatology & Autoimmune Policy Type: Medical Pharmacy Department: Pharmacy Product (check all that apply): Group HMO/POS Individual
Policy Subject: Anti-TNF Agents Policy Number: SHS PBD16 Category: Rheumatology & Autoimmune Policy Type: Medical Pharmacy Department: Pharmacy Product (check all that apply): Group HMO/POS Individual
ACP Rheumatology Pearls. Adam Q Carlson MD Assistant Professor UVA Rheumatology
 ACP Rheumatology Pearls Adam Q Carlson MD Assistant Professor UVA Rheumatology Disclosures I have no personal or professional disclosures Case #1 27 yo woman with a history of systemic lupus complicated
ACP Rheumatology Pearls Adam Q Carlson MD Assistant Professor UVA Rheumatology Disclosures I have no personal or professional disclosures Case #1 27 yo woman with a history of systemic lupus complicated
MMS Pharmacology Lecture 2. Antirheumatic drugs. Dr Sura Al Zoubi
 MMS Pharmacology Lecture 2 Antirheumatic drugs Dr Sura Al Zoubi Revision Rheumatoid Arthritis Definition (RA): is the most common systemic inflammatory disease characterized by symmetrical inflammation
MMS Pharmacology Lecture 2 Antirheumatic drugs Dr Sura Al Zoubi Revision Rheumatoid Arthritis Definition (RA): is the most common systemic inflammatory disease characterized by symmetrical inflammation
Vulval dermatoses. Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough
 Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Autoimmune Diseases with Oral Manifestations
 Autoimmune Diseases with Oral Manifestations Martin S. Greenberg DDS, FDS RCSEd Professor Emeritus Department of Oral Medicine University of Pennsylvania Disclosure Statement I have no actual or potential
Autoimmune Diseases with Oral Manifestations Martin S. Greenberg DDS, FDS RCSEd Professor Emeritus Department of Oral Medicine University of Pennsylvania Disclosure Statement I have no actual or potential
9/25/2013 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE)
 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
Interesting Case Series. Linear IgA Bullous Dermatosis
 Interesting Case Series Linear IgA Bullous Dermatosis Sean Chen, BA, a Peter Mattei, MD, a Max Fischer, MD, MPH, a Joshua D. Gay, PA-C, b Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS, b and Leigh Ann
Interesting Case Series Linear IgA Bullous Dermatosis Sean Chen, BA, a Peter Mattei, MD, a Max Fischer, MD, MPH, a Joshua D. Gay, PA-C, b Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS, b and Leigh Ann
Sarcoidosis Case. Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA. WASOG: educational material
 Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Rheumatology Primer: What Labs and When
 Rheumatology Primer: What Labs and When Irina Konon, MD Department of Internal Medicine Division of Rheumatology Medical College of Wisconsin Disclosures None 1 Objective Discuss principles of laboratory
Rheumatology Primer: What Labs and When Irina Konon, MD Department of Internal Medicine Division of Rheumatology Medical College of Wisconsin Disclosures None 1 Objective Discuss principles of laboratory
1. Background: Infliximab is administered parenterally; therefore, it is not covered under retail pharmacy benefits.
 Subject: Infliximab (Remicade ) Original Original Committee Approval: October 13, 2006 Revised Last Committee Approval: December 3, 2008 Last Review: October 19, 2007 1. Background: Infliximab is a genetically
Subject: Infliximab (Remicade ) Original Original Committee Approval: October 13, 2006 Revised Last Committee Approval: December 3, 2008 Last Review: October 19, 2007 1. Background: Infliximab is a genetically
CIMZIA (certolizumab pegol)
 Pre - PA Allowance None Prior-Approval Requirements Age Diagnoses 18 years of age or older Patient must have ONE of the following: 1. Moderate to severe Crohn s Disease (CD) a. Inadequate response, intolerance
Pre - PA Allowance None Prior-Approval Requirements Age Diagnoses 18 years of age or older Patient must have ONE of the following: 1. Moderate to severe Crohn s Disease (CD) a. Inadequate response, intolerance
Recalcitrant Warty Erythroderma With Severe Pruritus. Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University
 Recalcitrant Warty Erythroderma With Severe Pruritus Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Gil Yosipovitch,
Recalcitrant Warty Erythroderma With Severe Pruritus Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Gil Yosipovitch,
Coverage Criteria: Express Scripts, Inc. monograph dated 12/15/ months or as otherwise noted by indication
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
Beyond Anti TNFs: positioning of other biologics for Crohn s disease. Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center
 Beyond Anti TNFs: positioning of other biologics for Crohn s disease Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center Objectives: To define high and low risk patient and disease features
Beyond Anti TNFs: positioning of other biologics for Crohn s disease Christina Ha, MD Cedars Sinai Inflammatory Bowel Disease Center Objectives: To define high and low risk patient and disease features
Ulcerative Colitis Therapy. Faculty Disclosure. Acknowledgements 28/11/2013. Amy Morse November 30/13
 Ulcerative Colitis Therapy Amy Morse November 30/13 GI for GP s Jasper AB Faculty Disclosure Faculty: Amy Morse Relationships with commercial interests: Grants/Research Support: Therapeutic Fellowship
Ulcerative Colitis Therapy Amy Morse November 30/13 GI for GP s Jasper AB Faculty Disclosure Faculty: Amy Morse Relationships with commercial interests: Grants/Research Support: Therapeutic Fellowship
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES. R e g i S C A R PATIENT'S DATA. Age country of birth
 REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
Treatment of Inflammatory Bowel Disease. Michael Weiss MD, FACG
 Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
What prescribers need to know
 HUMIRA Citrate-free presentations in an Electronic Medical Record (EMR) What prescribers need to know 2 / This is your guide to identifying HUMIRA Citrate-free presentations in your Electronic Medical
HUMIRA Citrate-free presentations in an Electronic Medical Record (EMR) What prescribers need to know 2 / This is your guide to identifying HUMIRA Citrate-free presentations in your Electronic Medical
Crohn's disease CAUSES COURSE OF CROHN'S DISEASE TREATMENT. Sulfasalazine
 Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
Crohn's disease Crohn's disease is an inflammatory condition of the digestive tract that affects children and adults. Common features of Crohn's disease include mouth sores, diarrhea, abdominal pain, weight
Scleritis LEN V KOH OD
 Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
HELPING YOU AND YOUR PATIENTS TALK OPENLY ABOUT MODERATELY TO SEVERELY ACTIVE RA
 SIMPONI ARIA (golimumab) is indicated for the treatment of adults with moderately to severely active rheumatoid arthritis (RA) in combination with MTX, active psoriatic arthritis, and active ankylosing
SIMPONI ARIA (golimumab) is indicated for the treatment of adults with moderately to severely active rheumatoid arthritis (RA) in combination with MTX, active psoriatic arthritis, and active ankylosing
Significance. Outline and Objectives. S007 Systemic Therapies for Medical Oncology
 S007 Systemic Therapies for Medical Oncology Anisha B. Patel, M.D. Assistant Professor, Dermatology UT MD Anderson Cancer Center UT Health Science Center Houston Safety considerations Outline and Objectives
S007 Systemic Therapies for Medical Oncology Anisha B. Patel, M.D. Assistant Professor, Dermatology UT MD Anderson Cancer Center UT Health Science Center Houston Safety considerations Outline and Objectives
Systemic Medications for the Dermatology Toolbox: Azathioprine
 Systemic Medications for the Dermatology Toolbox: Azathioprine Wynnis Tom, M.D. Associate Clinical Professor University of California, San Diego and Rady Children s Hospital Faculty Disclosure Information
Systemic Medications for the Dermatology Toolbox: Azathioprine Wynnis Tom, M.D. Associate Clinical Professor University of California, San Diego and Rady Children s Hospital Faculty Disclosure Information
ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה
 ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה Presentation: S.A is 25 years old. Referred to a gastroentrologist because of abdominal pain and bloody diarrhea in the last few weeks.
ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה Presentation: S.A is 25 years old. Referred to a gastroentrologist because of abdominal pain and bloody diarrhea in the last few weeks.
Lupus. Fast facts. What is lupus? What causes lupus? Who gets lupus?
 Lupus Systemic lupus erythematosus, referred to as SLE or lupus, is sometimes called the "great imitator." Why? Because of its wide range of symptoms, people often confuse lupus with other health problems.
Lupus Systemic lupus erythematosus, referred to as SLE or lupus, is sometimes called the "great imitator." Why? Because of its wide range of symptoms, people often confuse lupus with other health problems.
Доверяй, но проверяй {Doveryai, no proveryai} Trust, but Verify. Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville
 Доверяй, но проверяй {Doveryai, no proveryai} Trust, but Verify Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville Jeffrey P. Callen, MD Disclosure (previous 12 months)
Доверяй, но проверяй {Doveryai, no proveryai} Trust, but Verify Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville Jeffrey P. Callen, MD Disclosure (previous 12 months)
10/25/2018. Autoimmunity and how to treat it. Disclosure. Why do we get autoimmunity? James Verbsky MD/PhD Pediatric Rheumatology/Immunology
 Autoimmunity and how to treat it James Verbsky MD/PhD Pediatric Rheumatology/Immunology Disclosure None I will mention drug names and some brand names but I have no financial interest or any other ties
Autoimmunity and how to treat it James Verbsky MD/PhD Pediatric Rheumatology/Immunology Disclosure None I will mention drug names and some brand names but I have no financial interest or any other ties
Recognizing Pyoderma Gangrenosum in a Patient with History of Essential Thrombocytosis
 Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 17 ISSN 2379-1039 Recognizing Pyoderma Gangrenosum in a Patient with History of Essential Thrombocytosis * Amier Ahmad, Md ; Kevin
Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 17 ISSN 2379-1039 Recognizing Pyoderma Gangrenosum in a Patient with History of Essential Thrombocytosis * Amier Ahmad, Md ; Kevin
Efficacy and Safety of Treatment for Pediatric IBD
 Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Associate Professor of Clinical Pediatrics Division of Gastroenterology,
Efficacy and Safety of Treatment for Pediatric IBD Andrew B. Grossman MD Co-Director, Center for Pediatric Inflammatory Bowel Disease Associate Professor of Clinical Pediatrics Division of Gastroenterology,
Rayos Prior Authorization Program Summary
 Rayos Prior Authorization Program Summary FDA APPROVED INDICATIONS AND DOSAGE FDA-Approved Indications: 1 Agent Indication Dosage Rayos (prednisone delayedrelease tablet) as an anti-inflammatory or immunosuppressive
Rayos Prior Authorization Program Summary FDA APPROVED INDICATIONS AND DOSAGE FDA-Approved Indications: 1 Agent Indication Dosage Rayos (prednisone delayedrelease tablet) as an anti-inflammatory or immunosuppressive
Antirheumatic drugs. Rheumatic Arthritis (RA)
 Antirheumatic drugs Rheumatic Arthritis (RA) Disease Modifying Antirheumatic drugs (DMARDs) DMARDs are used in the treatment of rheumatic arthritis RA and have been shown to slow the course of the disease,
Antirheumatic drugs Rheumatic Arthritis (RA) Disease Modifying Antirheumatic drugs (DMARDs) DMARDs are used in the treatment of rheumatic arthritis RA and have been shown to slow the course of the disease,
Case Report Henoch-Schönlein Purpura with Adalimumab Therapy for Ulcerative Colitis: A Case Report and Review of the Literature
 Case Reports in Rheumatology Volume 2016, Article ID 2812980, 4 pages http://dx.doi.org/10.1155/2016/2812980 Case Report Henoch-Schönlein Purpura with Adalimumab Therapy for Ulcerative Colitis: A Case
Case Reports in Rheumatology Volume 2016, Article ID 2812980, 4 pages http://dx.doi.org/10.1155/2016/2812980 Case Report Henoch-Schönlein Purpura with Adalimumab Therapy for Ulcerative Colitis: A Case
Fever of unknown origin
 Fever of unknown origin Case B History of the present illness 75 years old women presented at our hospital with since months daily fevers between 38 to 39.5 Celsius (100.4-103.1 F) with night sweats. Her
Fever of unknown origin Case B History of the present illness 75 years old women presented at our hospital with since months daily fevers between 38 to 39.5 Celsius (100.4-103.1 F) with night sweats. Her
Guideline on the clinical management of Henoch Schonlein Purpura (HSP)
 Guideline on the clinical management of Henoch Schonlein Purpura (HSP) Purpose To ensure a standardised approach in the management of children with HSP in southern Derbyshire. Scope The scope of this guideline
Guideline on the clinical management of Henoch Schonlein Purpura (HSP) Purpose To ensure a standardised approach in the management of children with HSP in southern Derbyshire. Scope The scope of this guideline
Medical Therapy for Pediatric IBD: Efficacy and Safety
 Medical Therapy for Pediatric IBD: Efficacy and Safety Betsy Maxwell, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Pediatric IBD: Defining Remission
Medical Therapy for Pediatric IBD: Efficacy and Safety Betsy Maxwell, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Pediatric IBD: Defining Remission
Serologic Markers CONVENTIONAL ANTIBODIES ANTIBODIES UNCONVENTIONAL. AIH Type I
 Autoimmune Hepatitis By Thomas Frazier Objective What we need to know about AIH Diagnosis Treatment Difficulties in both Liver transplantation concerns AASLD Guidelines: Hepatology. 2010 Jun;51(6):2193-213.
Autoimmune Hepatitis By Thomas Frazier Objective What we need to know about AIH Diagnosis Treatment Difficulties in both Liver transplantation concerns AASLD Guidelines: Hepatology. 2010 Jun;51(6):2193-213.
Etanercept for Treatment of Hidradenitis
 Home Search Browse Resources Help What's New About Purpose Etanercept for Treatment of Hidradenitis This study is currently recruiting patients. Sponsors and Collaborators: University of Pennsylvania Amgen
Home Search Browse Resources Help What's New About Purpose Etanercept for Treatment of Hidradenitis This study is currently recruiting patients. Sponsors and Collaborators: University of Pennsylvania Amgen
Elevated Serum Creatinine, a simplified approach
 Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Five things not to miss in Dermatology. Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine
 Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Five things not to miss in Dermatology Dr Judy Wismer Associate Clinical Professor Michael G DeGroote School of Medicine Key Descriptives Fever, skin pain Purpura, necrosis Bullae, Mucosal, Skin sloughing
Chronic Granulomatous Disease Managing GI Issues
 Chronic Granulomatous Disease Managing GI Issues N I C H O L A S H A R T O G, M D D i r e c t o r o f P e d i a t r i c / A d u l t P r i m a r y I m m u n o d e f i c i e n c y C l i n i c A s s i s t
Chronic Granulomatous Disease Managing GI Issues N I C H O L A S H A R T O G, M D D i r e c t o r o f P e d i a t r i c / A d u l t P r i m a r y I m m u n o d e f i c i e n c y C l i n i c A s s i s t
Michael P. Heffernan, M.D San Luis Dermatology & Laser Clinic Director, US Probity Medical Research
 Michael P. Heffernan, M.D San Luis Dermatology & Laser Clinic Director, US Probity Medical Research mpheffernanmd@gmail.com DISCLOSURES Consultant, Speaker, Investigator: Abbvie, Amgen, Brickell Biotech,
Michael P. Heffernan, M.D San Luis Dermatology & Laser Clinic Director, US Probity Medical Research mpheffernanmd@gmail.com DISCLOSURES Consultant, Speaker, Investigator: Abbvie, Amgen, Brickell Biotech,
Subject: Remicade (Page 1 of 5)
 Subject: Remicade (Page 1 of 5) Objective: I. To ensure that Health Share/Tuality Health Alliance (THA) has a process by which the appropriate utilization of Remicade (Infliximab) for members whose diagnosis
Subject: Remicade (Page 1 of 5) Objective: I. To ensure that Health Share/Tuality Health Alliance (THA) has a process by which the appropriate utilization of Remicade (Infliximab) for members whose diagnosis
INFLIXIMAB Remicade (infliximab), Inflectra (infliximab-dyyb), Ixifi* (infliximabqbtx), Renflexis (infliximab-abda)
 Pre - PA Allowance None Prior-Approval Requirements Diagnoses Patient must have ONE of the following: 6 years of age or older 1. Moderate to severe Crohn s disease (CD) a. Patient has fistulizing disease
Pre - PA Allowance None Prior-Approval Requirements Diagnoses Patient must have ONE of the following: 6 years of age or older 1. Moderate to severe Crohn s disease (CD) a. Patient has fistulizing disease
Definitions. Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency)
 CROHN S DISEASE Definitions Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency) Recurrence: The reappearance of lesions after surgical resection Endoscopic remission:
CROHN S DISEASE Definitions Clinical remission: Resolution of symptoms (stool frequency 3/day, no bleeding and no urgency) Recurrence: The reappearance of lesions after surgical resection Endoscopic remission:
Understanding Myositis Medications
 Understanding Myositis Medications 2015 TMA Annual Patient Conference Orlando, Florida Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Disclosures Mallinckrodt: Research Grant Genentech:
Understanding Myositis Medications 2015 TMA Annual Patient Conference Orlando, Florida Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Disclosures Mallinckrodt: Research Grant Genentech:
Management of Pyoderma Gangrenosum Mentoring in IBD XVII
 Management of Pyoderma Gangrenosum Mentoring in IBD XVII Scott Walsh MD PhD FRCPC Division of Dermatology Sunnybrook Health Sciences Centre University of Toronto Pyoderma Gangrenosum: A pathological
Management of Pyoderma Gangrenosum Mentoring in IBD XVII Scott Walsh MD PhD FRCPC Division of Dermatology Sunnybrook Health Sciences Centre University of Toronto Pyoderma Gangrenosum: A pathological
Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS
 Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS Introduction: There is perhaps no rheumatic disease that evokes so much fear and confusion among both patients
Arthritis & Rheumatology Clinics of Kansas PATIENT EDUCATION SYSTEMIC LUPUS ERYTHEMATOSUS Introduction: There is perhaps no rheumatic disease that evokes so much fear and confusion among both patients
Nursing Perspective on iraes: Patient Education, Monitoring and Management
 Nursing Perspective on iraes: Patient Education, Monitoring and Management Rebecca Lewis, CRNP Nurse Practitioner University of Pittsburgh-HCC Shadyside Disclosures No relevant financial relationships
Nursing Perspective on iraes: Patient Education, Monitoring and Management Rebecca Lewis, CRNP Nurse Practitioner University of Pittsburgh-HCC Shadyside Disclosures No relevant financial relationships
Lupus Related Kidney Diseases. Jason Cobb MD Assistant Professor Renal Division Emory University School of Medicine October 14, 2017
 Lupus Related Kidney Diseases Jason Cobb MD Assistant Professor Renal Division Emory University School of Medicine October 14, 2017 Financial Disclosures MedImmune Lupus Nephritis Kidney Biopsy Biomarkers
Lupus Related Kidney Diseases Jason Cobb MD Assistant Professor Renal Division Emory University School of Medicine October 14, 2017 Financial Disclosures MedImmune Lupus Nephritis Kidney Biopsy Biomarkers
GASTROENTEROLOGY ESSENTIALS
 GASTROENTEROLOGY ESSENTIALS Practical Gastroenterology 8/25/2018 Jahnavi Koppala, MBBS Abdullah Abdussalam, MD A 48-year-old male was evaluated for noncardiac chest pain. Treatment with PPI twice daily
GASTROENTEROLOGY ESSENTIALS Practical Gastroenterology 8/25/2018 Jahnavi Koppala, MBBS Abdullah Abdussalam, MD A 48-year-old male was evaluated for noncardiac chest pain. Treatment with PPI twice daily
Ali Keshavarzian MD Rush University Medical Center
 Treatment: Step Up or Top Down? Ali Keshavarzian MD Rush University Medical Center Questions What medication should IBD be treated with? Can we predict which patients with IBD are high risk? Is starting
Treatment: Step Up or Top Down? Ali Keshavarzian MD Rush University Medical Center Questions What medication should IBD be treated with? Can we predict which patients with IBD are high risk? Is starting
RAPIDLY FAILING KIDNEYS. Dr Paul Johny 2 nd yr DNB Medicine Resident
 RAPIDLY FAILING KIDNEYS Dr Paul Johny 2 nd yr DNB Medicine Resident Mr Z 67yrs old Occupation : Retired officer from electricity board Chief complaints : Fever : 5 days Right lower limb swelling and pain
RAPIDLY FAILING KIDNEYS Dr Paul Johny 2 nd yr DNB Medicine Resident Mr Z 67yrs old Occupation : Retired officer from electricity board Chief complaints : Fever : 5 days Right lower limb swelling and pain
Annual Rheumatology & Therapeutics Review for Organizations & Societies
 Annual Rheumatology & Therapeutics Review for Organizations & Societies Update on Granulomatosis with Polyangiitis (Wegener s) Philip Seo, MD, MHS Director, Johns Hopkins Vasculitis Center Director, Johns
Annual Rheumatology & Therapeutics Review for Organizations & Societies Update on Granulomatosis with Polyangiitis (Wegener s) Philip Seo, MD, MHS Director, Johns Hopkins Vasculitis Center Director, Johns
Drug Class Prior Authorization Criteria Therapeutic Agents in Rheumatic and Inflammatory Diseases
 Drug Class Prior Authorization Criteria Therapeutic Agents in Rheumatic and Inflammatory Diseases Line of Business: Medicaid P & T Approval Date: August 16, 2017 Effective Date: August 16, 2017 This policy
Drug Class Prior Authorization Criteria Therapeutic Agents in Rheumatic and Inflammatory Diseases Line of Business: Medicaid P & T Approval Date: August 16, 2017 Effective Date: August 16, 2017 This policy
Myositis and Your Lungs
 Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
Myositis and Your Lungs 2013 TMA Annual Patient Meeting Louisville, Kentucky Chester V. Oddis, MD University of Pittsburgh Director, Myositis Center Myositis Heterogeneous group of autoimmune syndromes
1 P a g e. Systemic Juvenile Idiopathic Arthritis (SJIA) (1.3) Patients 2 years of age and older with active systemic juvenile idiopathic arthritis.
 LENGTH OF AUTHORIZATION: Initial: 3 months for Crohn s or Ulcerative Colitis; 1 year for all other indications. Renewal: 1 year dependent upon medical records supporting response to therapy and review
LENGTH OF AUTHORIZATION: Initial: 3 months for Crohn s or Ulcerative Colitis; 1 year for all other indications. Renewal: 1 year dependent upon medical records supporting response to therapy and review
Immune Modulating Drugs Prior Authorization Request Form
 Patient: HPHC member ID #: Requesting provider: Phone: Servicing provider: Diagnosis: Contact for questions (name and phone #): Projected start and end date for requested Requesting provider NPI: Fax:
Patient: HPHC member ID #: Requesting provider: Phone: Servicing provider: Diagnosis: Contact for questions (name and phone #): Projected start and end date for requested Requesting provider NPI: Fax:
Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis
 GLOMERULONEPHRITIDES Vivette D Agati Jai Radhakrishnan Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis Heavy Proteinuria Renal failure Low serum Albumin Hypertension
GLOMERULONEPHRITIDES Vivette D Agati Jai Radhakrishnan Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis Heavy Proteinuria Renal failure Low serum Albumin Hypertension
Fever in Lupus. 21 st April 2014
 Fever in Lupus 21 st April 2014 Fever in lupus Cause of fever N= 487 % SLE fever 206 42 Infection in SLE 265 54.5 Active SLE and infection 8 1.6 Tumor fever 4 0.8 Miscellaneous 4 0.8 Crucial Question Infection
Fever in Lupus 21 st April 2014 Fever in lupus Cause of fever N= 487 % SLE fever 206 42 Infection in SLE 265 54.5 Active SLE and infection 8 1.6 Tumor fever 4 0.8 Miscellaneous 4 0.8 Crucial Question Infection
THE KIDNEY AND SLE LUPUS NEPHRITIS
 THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
Disclaimer. This is a broad survey and cannot cover all differential diagnoses or each condition in thorough detail
 Objectives Pediatric Infections: Differentiating Benign from Serious Eileen Klein, MD, MPH Rashes Infectious vs non-infectious Viral vs bacterial Respiratory and GI illnesses When do you treat When do
Objectives Pediatric Infections: Differentiating Benign from Serious Eileen Klein, MD, MPH Rashes Infectious vs non-infectious Viral vs bacterial Respiratory and GI illnesses When do you treat When do
Medical Management of Rheumatoid Arthritis (RA)
 Medical Management of Rheumatoid Arthritis (RA) Dr Lee-Suan Teh Rheumatologist Royal Blackburn Hospital Educational objectives ABC Appreciate the epidemiology of RA Be able to diagnosis of RA Competent
Medical Management of Rheumatoid Arthritis (RA) Dr Lee-Suan Teh Rheumatologist Royal Blackburn Hospital Educational objectives ABC Appreciate the epidemiology of RA Be able to diagnosis of RA Competent
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 3 October 2012
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 3 October 2012 REMICADE 100 mg, powder for concentrate for solution for infusion B/1 vial (CIP code: 562 070-1) Applicant:
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 3 October 2012 REMICADE 100 mg, powder for concentrate for solution for infusion B/1 vial (CIP code: 562 070-1) Applicant:
Autoimmunity and autoinflammation
 Autoimmunity and autoinflammation Primary immunodeficiencies Autoimmunity and autoinflammation 1 Primary immunodeficiencies List of some common abbreviations APECED CAPS CGD CINCA CRMO CVID FCAS FMF HIDS
Autoimmunity and autoinflammation Primary immunodeficiencies Autoimmunity and autoinflammation 1 Primary immunodeficiencies List of some common abbreviations APECED CAPS CGD CINCA CRMO CVID FCAS FMF HIDS
Immunosuppressants. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
What is Crohn's disease?
 What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
Inflammatory Bowel Disease Medical Exam Questionnaire
 Patient Name: MR: Date: Name DOB / / Age Marital Status Race Gender M / F Height Present Weight Usual Weight Insurance Managed Care Self referral Yes No Yes No Yes No Primary Care Physician Referring Physician
Patient Name: MR: Date: Name DOB / / Age Marital Status Race Gender M / F Height Present Weight Usual Weight Insurance Managed Care Self referral Yes No Yes No Yes No Primary Care Physician Referring Physician
Anti-Tumor Necrosis Factor (Anti-TNF)
 Anti-Tumor Necrosis Factor (Anti-TNF) 110465 Anti-TNF.indd 1 9/20/16 9:01 AM s About your medicine Anti-tumor necrosis factor (anti-tnf) is a type of medicine called biologic agent that targets substance
Anti-Tumor Necrosis Factor (Anti-TNF) 110465 Anti-TNF.indd 1 9/20/16 9:01 AM s About your medicine Anti-tumor necrosis factor (anti-tnf) is a type of medicine called biologic agent that targets substance
Patient #1. Rheumatoid Arthritis. Rheumatoid Arthritis. 45 y/o female Morning stiffness in her joints >1 hour
 Patient #1 Rheumatoid Arthritis Essentials For The Family Medicine Physician 45 y/o female Morning stiffness in her joints >1 hour Hands, Wrists, Knees, Ankles, Feet Polyarticular, symmetrical swelling
Patient #1 Rheumatoid Arthritis Essentials For The Family Medicine Physician 45 y/o female Morning stiffness in her joints >1 hour Hands, Wrists, Knees, Ankles, Feet Polyarticular, symmetrical swelling
GRANULOMATOSIS WITH POLYANGIITIS
 What is granulomatosis with polyangiitis (GPA)? Granulomatosis with polyangiitis (GPA) is a form of vasculitis a family of rare disorders characterized by inflammation of the blood vessels, which can restrict
What is granulomatosis with polyangiitis (GPA)? Granulomatosis with polyangiitis (GPA) is a form of vasculitis a family of rare disorders characterized by inflammation of the blood vessels, which can restrict
Rheumatoid arthritis
 Rheumatoid arthritis 1 Definition Rheumatoid arthritis is one of the most common inflammatory disorders affecting the population worldwide. It is a systemic inflammatory disease which affects not only
Rheumatoid arthritis 1 Definition Rheumatoid arthritis is one of the most common inflammatory disorders affecting the population worldwide. It is a systemic inflammatory disease which affects not only
Is it Autoimmune or NOT! Presented to AONP! October 2015!
 Is it Autoimmune or NOT! Presented to AONP! October 2015! Four main jobs of immune system Detects Contains and eliminates Self regulates Protects Innate Immune System! Epithelial cells, phagocytic cells
Is it Autoimmune or NOT! Presented to AONP! October 2015! Four main jobs of immune system Detects Contains and eliminates Self regulates Protects Innate Immune System! Epithelial cells, phagocytic cells
MEDICATIONS: THE GOOD, THE BAD, THE UGLY
 MEDICATIONS: THE GOOD, THE BAD, THE UGLY July 13, 2013 Dr. Tanaz Kermani Assistant Clinical Professor of Medicine, Division of Rheumatology, David Geffen School of Medicine UCLA Dr. Robert Spiera Professor
MEDICATIONS: THE GOOD, THE BAD, THE UGLY July 13, 2013 Dr. Tanaz Kermani Assistant Clinical Professor of Medicine, Division of Rheumatology, David Geffen School of Medicine UCLA Dr. Robert Spiera Professor
Dermatomyositis Advice from Experts: Improving Your Medical Dermatology Diagnostic and Management Skills Jeffrey P. Callen, MD Professor of Medicine
 Dermatomyositis Advice from Experts: Improving Your Medical Dermatology Diagnostic and Management Skills Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville Learning Objectives
Dermatomyositis Advice from Experts: Improving Your Medical Dermatology Diagnostic and Management Skills Jeffrey P. Callen, MD Professor of Medicine (Dermatology) University of Louisville Learning Objectives
