Airway stenting in excessive central airway collapse
|
|
|
- Berniece Garrett
- 5 years ago
- Views:
Transcription
1 Review Article on Aerodigestive Endoscopy Airway stenting in excessive central airway collapse Mihir Parikh, Jennifer Wilson, Adnan Majid, Sidhu Contributions: (I) Conception and design: All authors; (II) Administrative support: All authors; (III) Provision of study materials or patients: All authors; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Mihir Parikh. Center, 185 Pilgrim Road, Deac 201, Boston, MA 02215, USA. Abstract: In tracheobronchomalacia (TBM) and other disorders, weakened airway walls lead to expiratory central airway collapse (ECAC) and can cause symptoms of cough, dyspnea, retained secretions, and recurrent pulmonary infections. Diagnosis of severe ECAC is based on the presence of >90% expiratory airway collapse on dynamic computed tomography (CT) and/or bronchoscopy. We offer patients with severe ECAC a trial of airway stenting to determine whether splinting of the central airways leads to improvements in symptoms, quality of life, exercise capacity, or respiratory function. Patients who respond positively to airway stenting are considered for tracheobronchoplasty. Keywords: Tracheobronchomalacia (TBM); excessive dynamic airway collapse (EDAC); excessive central airway collapse (ECAC); tracheobronchoplasty; airway stenting Received: 11 February 2017; Accepted: 18 October 2017; Published: 22 November doi: /jovs View this article at: Introduction Excessive central airway collapse (ECAC) is an underrecognized syndrome characterized by excessive collapse and obstruction of the trachea and bronchi with expiration. ECAC includes tracheobronchomalacia (TBM) and excessive dynamic airway collapse (EDAC). TBM is defined by weakening of airway walls leading to collapse of lateral and anterior cartilaginous structures in the airways. In contrast, EDAC occurs when airway lumen is reduced due to excessive bowing of the posterior membrane on expiration. While the pathophysiology and morphology of TBM and EDAC are distinct, their clinical symptoms and management are similar. Patients with ECAC often present with symptoms of dyspnea, cough, wheezing, and frequent respiratory infections. Therapeutic options for ECAC are limited and include non-invasive therapies, such as continuous positive airway pressure (CPAP) or bi-level positive airway pressure (BiPAP), and more invasive options, including stent placement and tracheobronchoplasty (1). Here, we discuss the role of endobronchial stents in the management of ECAC. Patient selection and workup The exact prevalence of ECAC in adults remains unknown. This is partly due to persistent debate over diagnostic criteria for ECAC. The standard definition requires a greater than 50% reduction in airway cross-sectional area (CSA) with expiration for diagnosis of ECAC. This definition, however, is overly broad with as many as 78% of healthy, asymptomatic volunteers exceeding the threshold of 50% collapse of the airways (2). At our institution, we have increased the threshold to 70% reduction in CSA for diagnosis of ECAC based on evidence indicating that expiratory central airway collapse (ECAC) in normal individuals is 54% to 56%. A 70% reduction threshold is approximately one standard deviation higher than these normal controls (2). We limit treatment to those patients having severe ECAC, defined as a reduction of >90% in the CSA of the affected airways. ECAC can either be a congenital or an acquired condition. The acquired form can
2 Page 2 of 6 Journal of Visualized Surgery, 2017 be associated with traumatic injuries, prior tracheostomy or endotracheal intubation, or inflammatory conditions, such as relapsing polychondritis. In many patients, no clear cause is identified and their ECAC is classified as idiopathic. ECAC can also be classified based on the shape of the airways with dynamic respiratory maneuvers and based on whether airway collapse is due to weakness of the anterior cartilaginous rings or the posterior membrane (3). Patients with frown-shaped airways on expiration and lunate airways on inspiration are most amenable to surgical intervention with tracheobronchoplasty (4). Diagnosis of ECAC is based on identification of dynamic airway collapse with computed tomography (CT) scanning or direct visualization of airway collapse on bronchoscopy with forced expiratory maneuvers (5). Pulmonary function tests (PFTs) can show a range of patterns in patients with ECAC, including restrictive and obstructive ventilatory defects. Moreover, obstructive changes on PFTs can be due to concomitant obstructive lung disease, such as chronic obstructive pulmonary disease (COPD) or asthma, and not due to the ECAC itself (6). In many patients, the diagnosis and subsequent management of ECAC can be confounded by the presence of other pulmonary comorbidities, including COPD, asthma, laryngopharyngeal reflux (LPR), vocal cord dysfunction, and obstructive sleep apnea (7,8). Management options are limited. Medical treatments, including bronchodilators or inhaled corticosteroids, can provide some relief, particularly in patients with comorbid COPD or asthma. Mucociliary clearance techniques, including mucolytics and flutter valves, can assist patients with significant retained secretions. Pursed lip breathing and non-invasive positive pressure ventilation, including CPAP and BiPAP, can temporarily improve expiratory airflow to some degree. Invasive options to maintain or restore airway patency include tracheostomy or T-tube placement, stent placement and surgical intervention with tracheobronchoplasty (9). Airway stents predominantly have a role as trial therapy to determine the likelihood of successful symptom improvement with tracheobronchoplasty (10,11). Once a patient is diagnosed with severe ECAC and is being considered for definitive surgical intervention at our institution, we initiate a stent trial. We place tracheal and bronchial stents at sites of severe malacia (greater than 90% collapse of the airway with expiration). After a 2-week trial, patients are assessed for improvement in quality of life or in symptoms thought to be related to their ECAC. PFTs and 6-minute walk test (6MWT) are performed before and after stent placement to assess for objective improvements in respiratory function and exercise capacity, as measured by changes in forced vital capacity (FVC), expiratory volume during the first second of forced expiration (FEV1), and distance walked during 6MWT. The stents are removed within 2 weeks, and patients with subjective or objective improvement during the stent trial proceed to evaluation for tracheobronchoplasty (Figure 1). Based on our experience, approximately 60% to 75% of patients with ECAC will experience symptomatic improvement during the stent trial. Of those patients who responded positively to the stent trial, 80% will have improvements in quality of life after tracheobronchoplasty (12,13). Stent placement leads to improvements in respiratory symptoms, quality of life, and functional status in patients with ECAC (10). Despite limited data on longterm outcomes and complications after stent placement, our preference is to avoid definitive treatment of ECAC by stenting in patients who are able to undergo definitive surgical treatment because many patients will develop a stent-related complication after approximately 2 weeks. Patients treated with airway stents for long term airway stabilization can develop significant granulation tissue at the proximal and distal ends of the stent leading to worsening airway stenosis and symptoms (10,13). Some patients will experience significant improvements during a stent trial but will be deemed poor surgical candidates for tracheobronchoplasty or will choose to defer surgical intervention. Surgical candidacy is based on a global assessment based on a patient s perceived fitness for surgery, individualized risk of surgery, and potential benefit gained from surgery. Patients may be unfit for surgery due to medical comorbidities or severely diminished FEV1/DLCO. Patients who are not surgical candidates must have optimal management of their medical comorbidities with maximal medical therapy for their ECAC. This can include noninvasive ventilation. If symptoms persist, then airway stents can be placed and maintained in these patients to restore airway patency for long-term definitive management but this can be a very arduous and often unsuccessful course. Equipment preferences We utilize both silicone and uncovered self-expanding metallic stents (SEMS) in our patients with ECAC. A Y-shaped silicone stent can be placed in patients with concomitant severe malacia in the distal trachea and bilateral main stem bronchi. These require rigid bronchoscopy for
3 Journal of Visualized Surgery, 2017 Page 3 of 6 Patient suspected of having TBM or EDAC based on consistent symptoms or dynamic CT findings Evaluation and optimization of medical comorbidities (e.g., COPD, asthma, GERD, laryngeal dysfunction) <90% dynamic airway collapse Medical management (e.g., Mucociliary clearance, mucolytics, positive pressure ventilation, pulmonary rehabilitation, etc.) Flexible bronchoscopy with dynamic expiratory maneuvers to assess for dynamic airway collapse >90% dynamic airway collapse Symptomatic or objective improvement Short-term trial of airway stenting Evaluation for surgical candidacy Surgical candidate No symptomatic or objective improvement Not a surgical candidate Tracheobronchoplasty Figure 1 Management pathway for patients with ECAC. ECAC, excessive central airway collapse. placement and can be prone to mucous plugging. In addition, a subset of patients will develop intractable coughing with these Y stents. However, they are easily removed and can be custom tailored to fit individual patient specifications. Utilization of SEMS for benign disease generally should be avoided despite the ease of placement. While the elastic properties of Nitinol-based SEMS allow them to conform to the shape of complex airways and to maintain their shape with cough and uncovered SEMS may preserve mucociliary clearance, there can be significant disadvantages to SEMS. These have been the subject of an FDA notification which warns about complications such as fracture, migration, granulation tissue, stenosis, and infection when SEMS are used to treat benign disease (14,15). With this caveat in mind, we have found that for short-term trial usage the complications rates for SEMS in ECAC are acceptably low. Therefore, as an initial intervention to assess a patient s candidacy for surgical tracheobronchoplasty we occasionally have utilized SEMS, especially in patients for whom cough may be their predominant complaint and may have the assessment of the benefit of airway stabilization confounded by a silicone Y stent-related cough (16,17). Procedure Prior to stent placement, patients with suspected ECAC are evaluated with dynamic flexible bronchoscopy under moderate sedation and sites of severe malacia (greater than 90% dynamic collapse) are identified with forced expiratory maneuvers (Figure 2). Stents are placed in the trachea, both main stem bronchi, and right bronchus intermedius at these sites of severe malacia. Stent placement in more distal segments increases the risk of mucous plugging and stent obstruction. The diameter of the stent is determined by measurements of airway diameter on CT scan and by direct measurement using an Aero Sizer tracheobronchial stent sizing device (Merit Medical) during flexible bronchoscopy. Stent length is based on the length of the malacic airway
4 Page 4 of 6 Journal of Visualized Surgery, 2017 Video 1. Dynamic airway maneuvers in a patient with ECAC Video 4. Balloon dilation of a tracheal stent Figure 2 Dynamic airway maneuvers in a patient with ECAC (18). ECAC, excessive central airway collapse. Available online: Figure 5 Balloon dilation of a tracheal stent (21). Available online: Video 2. Placement of an uncovered SEMS in the bronchus intermedius Figure 3 Placement of an uncovered SEMS in the bronchus intermedius (19). SEMS, self-expanding metallic stent. Available online: Video 3. Placement of an uncovered SEMS in the trachea Figure 4 Placement of an uncovered SEMS in the trachea (20). SEMS, self-expanding metallic stent. Available online: segment. We use the shortest stent length possible to minimize the impact on mucociliary clearance. We prefer to use uncovered SEMS as these tend to minimize the risk of mucous plugging, a common stent-related complication that can confound interpretation of the stent trial. We use silicone Y-stents if airway collapse is focused at the main carina or if the airway diameter is greater than 20 mm, which is the diameter of the largest uncovered selfexpanding airway metallic stent we carry. In most patients our practice is to place stents under rigid bronchoscopy. Y-silicone stents are placed into the malacic segments using the dedicated stent deployment device. Their position can then be adjusted using the rigid forceps. For SEMS, the rigid bronchoscope is positioned just proximal to the target airway segment and the stent is introduced through the rigid bronchoscope. The flexible bronchoscope or rigid camera is then introduced into the rigid bronchoscope and the SEMS is positioned and subsequently deployed into the target airway under direct visualization (Figures 3,4). Finally, we inflate a CRE Endovention Balloon (Boston Scientific) within the stent to achieve maximal deployment in the airway (Figure 5). Role of team members At our institution, the care of patients with ECAC is shared amongst a multi-disciplinary team of thoracic surgeons, interventional pulmonologists, laryngologists, gastroenterologists, chest radiologists, anesthesiologists, nurses, and physical therapists. Patients are initially evaluated by our thoracic surgeons and interventional pulmonologists to assess the presence and severity of symptoms attributable to ECAC as well as to optimize management of comorbid
5 Journal of Visualized Surgery, 2017 Page 5 of 6 conditions, such as COPD, asthma, and obstructive sleep apnea. We also routinely refer patients to our colleagues in laryngology and gastroenterology to screen for gastroesophageal reflux, LPR and vocal cord dysfunction. Stenting and tracheobronchoplasty procedures are performed with the assistance of anesthesiologists and nurses with particular training in thoracic procedures, including the use of rigid bronchoscopy and jet ventilation. Post-operative management Complications of stent placement include those attendant to bronchoscopy and general anesthesia. These include airway obstruction, bleeding, pneumothorax, pneumomediastinum, and airway perforation (15). Post-procedure respiratory distress is of particular concern in patients with ECAC given their pre-existing central airway compromise and their tendency to develop intractable cough and bronchospasm. Stents, particularly non Y silicone stents, can also migrate in the airways. After stent placement, patients can also experience worsening cough, increased sputum production, mucous impaction, and ingrowth of granulation tissue with subsequent airway narrowing. These adverse sequelae can confound a stent trial and limit the ability to predict successful outcome after tracheobronchoplasty (4). Post-stent care is designed to minimize these adverse sequelae. Mucociliary clearance techniques are of vital importance to minimize the risk of mucous plugging and infection. Patients should be treated with daily mucolytics and are instructed to utilize a flutter valve or other oral oscillatory device. Airway humidification is achieved with daily treatment with nebulized saline. Nebulized acetylcysteine can be used in patients suffering from excessively thick or copious respiratory secretions. We remove silicone and SEMS under rigid bronchoscopy using rigid forceps. The most common complications after stent removal are respiratory distress secondary to laryngospasm, severe cough, or transient worsening of other ECAC-related symptoms. To minimize the risk of laryngospasm and cough we administer 15 ml of 1% lidocaine upon removal of the rigid bronchoscope at the vocal cords (5 ml) and the tracheobronchial tree (10 ml). In addition, we use NIV in the immediate post-operative period to mitigate the degree of central airway collapse. Conclusions ECAC, including the syndrome of TBM, is an underrecognized condition characterized by abnormal dynamic collapse of the central airways leading to cough, dyspnea, retained secretions, and recurrent infections. In patients with ECAC, restoration of airway patency with airway stenting can serve as a therapeutic trial to assess candidacy for tracheobronchoplasty or, in selected high-risk patients, as a long-term definitive management strategy. Airway stenting is a relatively safe procedure when performed by an experienced bronchoscopist, but appropriate patient selection and complex post-operative management require coordinated care by a dedicated team of thoracic surgeons, interventional pulmonologists, and others. Acknowledgements None. Footnote Conflicts of Interest: The authors have no conflicts of interest to declare. Informed Consent: Written informed consent was obtained for the recording and publication of patient videos in this manuscript. Identifying information, including names, initials, and hospital numbers, have been removed from all associated materials. References 1. Murgu S, Colt H. Tracheobronchomalacia and excessive dynamic airway collapse. Clin Chest Med 2013;34: Boiselle PM, O'Donnell CR, Bankier AA, et al. Tracheal collapsibility in healthy volunteers during forced expiration: assessment with multidetector CT. Radiology 2009;252: Ridge CA, O'donnell CR, Lee EY, et al. Tracheobronchomalacia: current concepts and controversies. J Thorac Imaging 2011;26: SP. Tracheobronchomalacia in adults. Semin Thorac Cardiovasc Surg 2010;22: Majid A, Gaurav K, Sanchez JM, et al. Evaluation of tracheobronchomalacia by dynamic flexible bronchoscopy. A pilot study. Ann Am Thorac Soc 2014;11: Majid A, Sosa AF, Ernst A, et al. Pulmonary function and flow-volume loop patterns in patients with tracheobronchomalacia. Respir Care 2013;58: Nataraj D, Majid A, Chuttani R, et al. Prevalence
6 Page 6 of 6 Journal of Visualized Surgery, 2017 of gastroesophageal rflux in patients with tracheobronchomalacia. Chest 2009;136:80S. 8. Ochs RA, Petkovska I, Kim HJ, et al. Prevalence of tracheal collapse in an emphysema cohort as measured with end-expiration CT. Acad Radiol 2009;16: Murgu SD, Colt HG. Treatment of adult tracheobronchomalacia and excessive dynamic airway collapse: an update. Treat Respir Med 2006;5: Ernst A, Majid A, Feller-Kopman D, et al. Airway stabilization with silicone stents for treating adult tracheobronchomalacia: a prospective observational study. Chest 2007;132: Ochoa S, Cheng GZ, Folch E, et al. Use of Self-expanding Metallic Airway Stents in Tracheobronchomalacia. J Bronchology Interv Pulmonol 2015;22:e9-e Majid A, Guerrero J, S, et al. Tracheobronchoplasty for severe tracheobronchomalacia: a prospective outcome analysis. Chest 2008;134: Ernst A, Odell DD, Michaud G, et al. Central airway stabilization for tracheobronchomalacia improves quality of life in patients with COPD. Chest 2011;140: Lund ME, Force S. Airway stenting for patients with benign airway disease and the Food and Drug Administration Advisory: A Call for Restraint. Chest 2007; 132: Casal RF. Update in airway stents. Curr Opin Pulm Med 2010;16: Majid A, Alape D, Kheir F, et al. Short-Term Use of Uncovered Self-Expanding Metallic Airway Stents for Severe Expiratory Central Airway Collapse. Respiration 2016;92: Murgu SD, Egressy K, Laxmanan B, et al. Central Airway Obstruction: Benign Strictures, Tracheobronchomalacia, and Malignancy-related Obstruction. Chest 2016;150: Parikh M, Wilson J, Majid A, S. Dynamic airway maneuvers in a patient with ECAC. Asvide 2017;4:509. Available online: articles/ Parikh M, Wilson J, Majid A, S. Placement of an uncovered SEMS in the bronchus intermedius. Asvide 2017;4:510. Available online: com/articles/ Parikh M, Wilson J, Majid A, S. Placement of an uncovered SEMS in the trachea. Asvide 2017;4:511. Available online: Parikh M, Wilson J, Majid A, S. Balloon dilation of a tracheal stent. Asvide 2017;4:512. Available online: doi: /jovs Cite this article as: Parikh M, Wilson J, Majid A, S. Airway stenting in excessive central airway collapse. J Vis Surg 2017;3:172.
Case Report Tracheomalacia Treatment Using a Large-Diameter, Custom-Made Airway Stent in a Case with Mounier-Kuhn Syndrome
 Case Reports in Pulmonology, Article ID 910135, 4 pages http://dx.doi.org/10.1155/2014/910135 Case Report Tracheomalacia Treatment Using a Large-Diameter, Custom-Made Airway Stent in a Case with Mounier-Kuhn
Case Reports in Pulmonology, Article ID 910135, 4 pages http://dx.doi.org/10.1155/2014/910135 Case Report Tracheomalacia Treatment Using a Large-Diameter, Custom-Made Airway Stent in a Case with Mounier-Kuhn
Accepted Manuscript. Robotic tracheobronchoplasty is feasible but which patients truly benefit? Steven Milman, MD, Thomas Ng, MD
 Accepted Manuscript Robotic tracheobronchoplasty is feasible but which patients truly benefit? Steven Milman, MD, Thomas Ng, MD PII: S0022-5223(18)32271-2 DOI: 10.1016/j.jtcvs.2018.08.028 Reference: YMTC
Accepted Manuscript Robotic tracheobronchoplasty is feasible but which patients truly benefit? Steven Milman, MD, Thomas Ng, MD PII: S0022-5223(18)32271-2 DOI: 10.1016/j.jtcvs.2018.08.028 Reference: YMTC
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction
 The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
Therapeutic Bronchoscopy Etiology - Benign Stenosis Post - intubation Trauma Post - operative Inflammatory Idiopathic
 Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Pulmonary Function and Flow Volume Loop Patterns in Patients with. *Adnan Majid, MD ¹, FCCP *Andres F.
 Pulmonary Function and Flow Volume Loop Patterns in Patients with Tracheobronchomalacia. *Adnan Majid, MD ¹, FCCP (amajid@bidmc.harvard.edu); *Andres F. Sosa, MD² (andres.sosa@umassmemorial.org); Armin
Pulmonary Function and Flow Volume Loop Patterns in Patients with Tracheobronchomalacia. *Adnan Majid, MD ¹, FCCP (amajid@bidmc.harvard.edu); *Andres F. Sosa, MD² (andres.sosa@umassmemorial.org); Armin
Interventional Pulmonology
 Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Double Y-stenting for tracheobronchial stenosis
 ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600
 Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
4/24/2017. Tracheal Stenosis. Tracheal Stenosis. Tracheal Stenosis. Tracheal Stenosis. Tracheal Stenosis Endoscopic & Surgical Management
 Endoscopic & Surgical Management Pressure ulceration Healing: granulation cicatrization contraction Ann Surg 1969;169:334-348 Gary Schwartz, MD Department of Thoracic Surgery and Lung Transplantation Baylor
Endoscopic & Surgical Management Pressure ulceration Healing: granulation cicatrization contraction Ann Surg 1969;169:334-348 Gary Schwartz, MD Department of Thoracic Surgery and Lung Transplantation Baylor
Endobronchial valve insertion to reduce lung volume in emphysema
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
Audra Fuller MD, Mark Sigler MD, Shrinivas Kambali MD, Raed Alalawi MD
 Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
Prevalence of tracheobronchomalacia and excessive dynamic airway collapse in bronchial asthma of different severity
 Dal Negro et al. Multidisciplinary Respiratory Medicine 2013, 8:32 ORIGINAL RESEARCH ARTICLE Prevalence of tracheobronchomalacia and excessive dynamic airway collapse in bronchial asthma of different severity
Dal Negro et al. Multidisciplinary Respiratory Medicine 2013, 8:32 ORIGINAL RESEARCH ARTICLE Prevalence of tracheobronchomalacia and excessive dynamic airway collapse in bronchial asthma of different severity
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Stents for airway strictures: selection and results
 Review Article Stents for airway strictures: selection and results Adil Ayub, Adnan M. Al-Ayoubi, Faiz Y. Bhora Department of Thoracic Surgery, Icahn School of Medicine, Mount Sinai Health System, New
Review Article Stents for airway strictures: selection and results Adil Ayub, Adnan M. Al-Ayoubi, Faiz Y. Bhora Department of Thoracic Surgery, Icahn School of Medicine, Mount Sinai Health System, New
Since central airway stenosis is often a lifethreatening. Double Y-stenting for tracheobronchial stenosis. Masahide Oki and Hideo Saka
 Eur Respir J 2012; 40: 1483 1488 DOI: 10.1183/09031936.00015012 CopyrightßERS 2012 Double Y-stenting for tracheobronchial stenosis Masahide Oki and Hideo Saka ABSTRACT: The purpose of the present study
Eur Respir J 2012; 40: 1483 1488 DOI: 10.1183/09031936.00015012 CopyrightßERS 2012 Double Y-stenting for tracheobronchial stenosis Masahide Oki and Hideo Saka ABSTRACT: The purpose of the present study
Wheeze. Dr Jo Harrison
 Wheeze Dr Jo Harrison 9.9.14 Wheeze - Physiology a continuous musical sound that lasts longer than 250 msec. can be high-pitched or low-pitched, consist of single or multiple notes, and occur during inspiration
Wheeze Dr Jo Harrison 9.9.14 Wheeze - Physiology a continuous musical sound that lasts longer than 250 msec. can be high-pitched or low-pitched, consist of single or multiple notes, and occur during inspiration
Tracheal Collapse: Medical Management Versus Implantable Stents
 What is Tracheal Collapse? The trachea (windpipe) is a large tube that is reinforced by cartilage rings. The trachea runs alongside of the esophagus (food pipe) and delivers air to the lungs. Tracheal
What is Tracheal Collapse? The trachea (windpipe) is a large tube that is reinforced by cartilage rings. The trachea runs alongside of the esophagus (food pipe) and delivers air to the lungs. Tracheal
Whistling in the Dark
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical problem-solving Whistling in the Dark Daniel A. Solomon, M.D., Christopher H. Fanta, M.D., Bruce D. Levy, M.D., and Joseph Loscalzo, M.D.,
T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical problem-solving Whistling in the Dark Daniel A. Solomon, M.D., Christopher H. Fanta, M.D., Bruce D. Levy, M.D., and Joseph Loscalzo, M.D.,
Temporary placement of metallic stent could lead to long-term benefits for benign tracheobronchial stenosis
 Original Article on Airway Obstruction Temporary placement of metallic stent could lead to long-term benefits for benign tracheobronchial stenosis Guo-Wu Zhou*, Hai-Dong Huang*, Qin-Ying Sun*, Ye Xiong*,
Original Article on Airway Obstruction Temporary placement of metallic stent could lead to long-term benefits for benign tracheobronchial stenosis Guo-Wu Zhou*, Hai-Dong Huang*, Qin-Ying Sun*, Ye Xiong*,
DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA
 Solunum 3, Özel Sayı 2: 260-264, 2001 DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA Jean F DUMON* M C DUMON* SUMMARY This article reports a 4-year
Solunum 3, Özel Sayı 2: 260-264, 2001 DUMON-NOVATECH Y-STENTS: A FOUR-YEAR EXPERIENCE WITH 50 TRACHEOBRONCHIAL TUMORS INVOLVING THE CARINA Jean F DUMON* M C DUMON* SUMMARY This article reports a 4-year
RESPIRATORY REHABILITATION
 RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
FOREIGN BODY ASPIRATION in children. Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital
 FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
Novatech Products for Interventional Pulmonology
 Novatech Products for Novatech and Boston Medical Products Bringing you the finest products for Novatech is a manufacturer of top-quality medical products used successfully worldwide in the growing specialty
Novatech Products for Novatech and Boston Medical Products Bringing you the finest products for Novatech is a manufacturer of top-quality medical products used successfully worldwide in the growing specialty
Subject Index. Bacterial infection, see Suppurative lung disease, Tuberculosis
 Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Airway stenosis: CT evaluation of endoscopic treatment
 Airway stenosis: CT evaluation of endoscopic treatment Poster No.: C-0334 Congress: ECR 2012 Type: Scientific Exhibit Authors: N. Maggialetti, M. Ficco, A. A. A. Stabile Ianora, M. Moschetta, A. Scardapane,
Airway stenosis: CT evaluation of endoscopic treatment Poster No.: C-0334 Congress: ECR 2012 Type: Scientific Exhibit Authors: N. Maggialetti, M. Ficco, A. A. A. Stabile Ianora, M. Moschetta, A. Scardapane,
MRSA pneumonia mucus plug burden and the difficult airway
 Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
ENDOBRONCHIAL ABLATIVE THERAPIES. Christopher Cortes, MD, FPCCP
 ENDOBRONCHIAL ABLATIVE THERAPIES Christopher Cortes, MD, FPCCP Choice of Ablative Therapy Size of the lesion Location of the lesion Characteristics of the lesion Availability of the different therapies
ENDOBRONCHIAL ABLATIVE THERAPIES Christopher Cortes, MD, FPCCP Choice of Ablative Therapy Size of the lesion Location of the lesion Characteristics of the lesion Availability of the different therapies
Therapeutic bronchoscopy for malignant airway stenoses: Choice of modality and survival
 Original Article Free full text available from www.cancerjournal.net Therapeutic bronchoscopy for malignant airway stenoses: Choice of modality and survival ABSTRACT Background: There are no data regarding
Original Article Free full text available from www.cancerjournal.net Therapeutic bronchoscopy for malignant airway stenoses: Choice of modality and survival ABSTRACT Background: There are no data regarding
Successful Endobronchial stenting for bronchial compression from a massive thoracic aortic aneurysm
 Successful Endobronchial stenting for bronchial compression from a massive thoracic aortic aneurysm Authors: David Comer (1), Amit Bedi (2), Peter Kennedy (2), Kieran McManus (2), and Werner McIlwaine
Successful Endobronchial stenting for bronchial compression from a massive thoracic aortic aneurysm Authors: David Comer (1), Amit Bedi (2), Peter Kennedy (2), Kieran McManus (2), and Werner McIlwaine
A 31-year-old female with a rare cause of recurrent lower lobar collapses
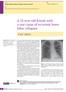 Radhika Banka, Dayle Terrington, Ajay V. Kamath radhika.banka@gmail.com Dept of Respiratory Medicine, Norfolk and Norwich University Hospital, Norwich, UK. A 31-year-old female with a rare cause of recurrent
Radhika Banka, Dayle Terrington, Ajay V. Kamath radhika.banka@gmail.com Dept of Respiratory Medicine, Norfolk and Norwich University Hospital, Norwich, UK. A 31-year-old female with a rare cause of recurrent
Bronchoscopy SICU Protocol
 Bronchoscopy SICU Protocol Updated January 2013 Outline Clinical indications Considerations Preparation Bronchoscopy technique Bronchoalveolar Lavage (BAL) Post-procedure Purpose Bronchoscopy is a procedure
Bronchoscopy SICU Protocol Updated January 2013 Outline Clinical indications Considerations Preparation Bronchoscopy technique Bronchoalveolar Lavage (BAL) Post-procedure Purpose Bronchoscopy is a procedure
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Varied Presentation and Management of Tracheal Polyps in Children Vinod M Raj 1, Varun Hathiramani 2, Swathi
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Varied Presentation and Management of Tracheal Polyps in Children Vinod M Raj 1, Varun Hathiramani 2, Swathi
Advanced Bronchoscopy
 Advanced Bronchoscopy Radial Jaw 4 Pulmonary Forceps Ultraflex Tracheobronchial Stent System CRE Pulmonary Balloon Alair Bronchial Thermoplasty Catheter CRE Pulmonary Balloon Radial Jaw 4 Pulmonary Forceps
Advanced Bronchoscopy Radial Jaw 4 Pulmonary Forceps Ultraflex Tracheobronchial Stent System CRE Pulmonary Balloon Alair Bronchial Thermoplasty Catheter CRE Pulmonary Balloon Radial Jaw 4 Pulmonary Forceps
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
External trauma (MVA, surf board, assault, etc.) Internal trauma (Endotracheal intubation, tracheostomy) Other
 Etiology External trauma (MVA, surf board, assault, etc.) Internal trauma (Endotracheal intubation, tracheostomy) Other Systemic diseases (vasculitis, etc.) Chemo/XRT Idiopathic Trans nasal Esophagoscope
Etiology External trauma (MVA, surf board, assault, etc.) Internal trauma (Endotracheal intubation, tracheostomy) Other Systemic diseases (vasculitis, etc.) Chemo/XRT Idiopathic Trans nasal Esophagoscope
Metallic stent and flexible bronchoscopy without fluoroscopy for acute respiratory failure
 Eur Respir J 2008; 31: 1019 1023 DOI: 10.1183/09031936.00099507 CopyrightßERS Journals Ltd 2008 Metallic stent and flexible bronchoscopy without fluoroscopy for acute respiratory failure S-M. Lin*,#, T-Y.
Eur Respir J 2008; 31: 1019 1023 DOI: 10.1183/09031936.00099507 CopyrightßERS Journals Ltd 2008 Metallic stent and flexible bronchoscopy without fluoroscopy for acute respiratory failure S-M. Lin*,#, T-Y.
I Need to Cough Ways to Keep Your Airways Clear
 I Need to Cough Ways to Keep Your Airways Clear 2018 Annual Cure SMA Conference Richard Kravitz, MD Duke University School of Medicine Duke University Medical Center Durham, North Carolina Presenters Jane
I Need to Cough Ways to Keep Your Airways Clear 2018 Annual Cure SMA Conference Richard Kravitz, MD Duke University School of Medicine Duke University Medical Center Durham, North Carolina Presenters Jane
Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012
 Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012 Recognize the importance of Pulmonary Function Testing in Cystic Fibrosis Be aware of different types
Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012 Recognize the importance of Pulmonary Function Testing in Cystic Fibrosis Be aware of different types
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery. By: Lillian Han
 Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Tracheobronchial stents are useful in the management
 Do Expandable Metallic Airway Stents Have a Role in the Management of Patients With Benign Tracheobronchial Disease? Brendan P. Madden, MD, FRCP, Tuck-Kay Loke, MRCP, and Abhijat C. Sheth, FRCS Department
Do Expandable Metallic Airway Stents Have a Role in the Management of Patients With Benign Tracheobronchial Disease? Brendan P. Madden, MD, FRCP, Tuck-Kay Loke, MRCP, and Abhijat C. Sheth, FRCS Department
Chapter 124: Congenital Disorders of the Trachea. Bruce Benjamin
 Chapter 124: Congenital Disorders of the Trachea Bruce Benjamin Investigation of the larynx and pharynx may be incomplete in infants and children with congenital abnormalities without investigation of
Chapter 124: Congenital Disorders of the Trachea Bruce Benjamin Investigation of the larynx and pharynx may be incomplete in infants and children with congenital abnormalities without investigation of
Expiratory central airway collapse in stable COPD and during exacerbations
 Leong et al. Respiratory Research (2017) 18:163 DOI 10.1186/s12931-017-0646-2 RESEARCH Expiratory central airway collapse in stable COPD and during exacerbations Paul Leong 1,2*, Anne Tran 1, Jhanavi Rangaswamy
Leong et al. Respiratory Research (2017) 18:163 DOI 10.1186/s12931-017-0646-2 RESEARCH Expiratory central airway collapse in stable COPD and during exacerbations Paul Leong 1,2*, Anne Tran 1, Jhanavi Rangaswamy
Respiratory distress in patients with central airway obstruction
 Indian J Thorac Cardiovasc Surg (2010) 26:151 156 DOI 10.1007/s12055-010-0021-0 ORIGINAL ARTICLE Respiratory distress in patients with central airway obstruction Mohamed Abdel Hamied Regal & Yasser Ahmed
Indian J Thorac Cardiovasc Surg (2010) 26:151 156 DOI 10.1007/s12055-010-0021-0 ORIGINAL ARTICLE Respiratory distress in patients with central airway obstruction Mohamed Abdel Hamied Regal & Yasser Ahmed
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Introduction to Interventional Pulmonology
 Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
What do pulmonary function tests tell you?
 Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
3. Identify the importance in the prehospital setting for the administration of nebulized bronchodilator.
 TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
Tracheal collapse diagnosed by multidetector computed tomography: evaluation of different image analysis methods
 Syddansk Universitet Tracheal collapse diagnosed by multidetector computed tomography: evaluation of different image analysis methods Nygaard, Mette; Bendstrup, Elisabeth; Dahl, Ronald; Hilberg, Ole; Rasmussen,
Syddansk Universitet Tracheal collapse diagnosed by multidetector computed tomography: evaluation of different image analysis methods Nygaard, Mette; Bendstrup, Elisabeth; Dahl, Ronald; Hilberg, Ole; Rasmussen,
Exercise-associated Excessive Dynamic Airway Collapse in Military Personnel
 Exercise-associated Excessive Dynamic Airway Collapse in Military Personnel Daniel J. Weinstein 1, James E. Hull 2, Brittany L. Ritchie 3, Jackie A. Hayes 2, and Michael J. Morris 2 1 Internal Medicine
Exercise-associated Excessive Dynamic Airway Collapse in Military Personnel Daniel J. Weinstein 1, James E. Hull 2, Brittany L. Ritchie 3, Jackie A. Hayes 2, and Michael J. Morris 2 1 Internal Medicine
Tracheal Stenosis Following Cuffed Tube Tracheostomy
 Tracheal Stenosis Following Cuffed Tube Tracheostomy Anatomical Variation and Selected Treatment Armand A. Lefemine, M.D., Kenneth MacDonnell, M.D., and Hyung S. Moon, M.D. ABSTRACT Tracheal stenosis resulting
Tracheal Stenosis Following Cuffed Tube Tracheostomy Anatomical Variation and Selected Treatment Armand A. Lefemine, M.D., Kenneth MacDonnell, M.D., and Hyung S. Moon, M.D. ABSTRACT Tracheal stenosis resulting
Anyone who smokes and/or has shortness of breath and sputum production could have COPD
 COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
Emphysema. Endoscopic lung volume reduction. PhD. Chief, department of chest diseases and thoracic oncology. JM VERGNON M.D, PhD.
 Emphysema Endoscopic lung volume reduction JM VERGNON M.D, PhD. PhD. Chief, department of chest diseases and thoracic oncology Genève 2010 INSERM IFR 143 Physiological concepts EMPHYSEMA Slide of Ch H
Emphysema Endoscopic lung volume reduction JM VERGNON M.D, PhD. PhD. Chief, department of chest diseases and thoracic oncology Genève 2010 INSERM IFR 143 Physiological concepts EMPHYSEMA Slide of Ch H
COPD. Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS
 IN THE NAME OF GOD COPD Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS Definition of COPD* COPD is a preventable and treatable chronic lung disease characterized by airflow limitation that is not fully
IN THE NAME OF GOD COPD Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS Definition of COPD* COPD is a preventable and treatable chronic lung disease characterized by airflow limitation that is not fully
Discussing feline tracheal disease
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Tracheobronchomalacia: morfologic evaluation in 64-MDTC.
 Tracheobronchomalacia: morfologic evaluation in 64-MDTC. Poster No.: C-1779 Congress: ECR 2011 Type: Educational Exhibit Authors: C. A. P. Fontes, A. A. S. M. Santos, A. L. Ferreira Neto, E. Marchiori,
Tracheobronchomalacia: morfologic evaluation in 64-MDTC. Poster No.: C-1779 Congress: ECR 2011 Type: Educational Exhibit Authors: C. A. P. Fontes, A. A. S. M. Santos, A. L. Ferreira Neto, E. Marchiori,
Intravascular Ultrasound (IVUS) and Optical Coherence Tomography (OCT)
 Intravascular Ultrasound (IVUS) and Optical Coherence Tomography (OCT) Clare McLaren Great Ormond Street Hospital London Introduction IVUS and OCT supplementary techniques to angiography provide information
Intravascular Ultrasound (IVUS) and Optical Coherence Tomography (OCT) Clare McLaren Great Ormond Street Hospital London Introduction IVUS and OCT supplementary techniques to angiography provide information
Disclosures. Learning Objectives. Coeditor/author. Associate Science Editor, American Heart Association
 Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule
 Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Flexible Bronchoscopy: More Than Just a Diagnostic Tool
 Flexible Bronchoscopy: More Than Just a Diagnostic Tool Kimberly M Baker-El Abiad, MD Division of Pulmonary, Critical Care, & Occupational Medicine 10/19/2018 Objectives Brief historical background on
Flexible Bronchoscopy: More Than Just a Diagnostic Tool Kimberly M Baker-El Abiad, MD Division of Pulmonary, Critical Care, & Occupational Medicine 10/19/2018 Objectives Brief historical background on
Airway Foreign Body in Children
 Joseph E. Dohar, M.D., M.S. Dr. Dohar Financial Disclosures Alcon consultant Incusmed consultant Otonomy consultant OrbiMed consultant Learning Objectives Identify clinical situations that may require
Joseph E. Dohar, M.D., M.S. Dr. Dohar Financial Disclosures Alcon consultant Incusmed consultant Otonomy consultant OrbiMed consultant Learning Objectives Identify clinical situations that may require
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
BiLevel Pressure Device
 PROCEDURE - Page 1 of 7 Purpose Scope Classes/ Goals Define indications and care settings for acute and chronic initiation of Noninvasive Positive Pressure Ventilation. Identify the role of Respiratory
PROCEDURE - Page 1 of 7 Purpose Scope Classes/ Goals Define indications and care settings for acute and chronic initiation of Noninvasive Positive Pressure Ventilation. Identify the role of Respiratory
Subglottic stenosis, with involvement of the lower larynx
 Laryngotracheal Resection and Reconstruction John D. Mitchell, MD n, Subglottic stenosis is being recognized with increasing frequency in adults, and may be the most frequent indication for airway intervention
Laryngotracheal Resection and Reconstruction John D. Mitchell, MD n, Subglottic stenosis is being recognized with increasing frequency in adults, and may be the most frequent indication for airway intervention
Anatomy and Physiology
 Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the
 Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
Tests Your Pulmonologist Might Order. Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital
 Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Airway Remodeling: Preliminary Experience with Bio-Absorbable Airway Stents in Adults Jaus MO, Gonfiotti A, Barale D, Macchiarini P
 Airway Remodeling: Preliminary Experience with Bio-Absorbable Airway Stents in Adults Jaus MO, Gonfiotti A, Barale D, Macchiarini P University Hospital Careggi Florence, Italy Disclosure Statement THE
Airway Remodeling: Preliminary Experience with Bio-Absorbable Airway Stents in Adults Jaus MO, Gonfiotti A, Barale D, Macchiarini P University Hospital Careggi Florence, Italy Disclosure Statement THE
Factors leading to tracheobronchial self-expandable metallic stent fracture
 GENERAL THORACIC SURGERY Factors leading to tracheobronchial self-expandable metallic stent fracture Fu-Tsai Chung, MD,* Shu-Min Lin, MD,* Hao-Cheng Chen, MD, Chun-Liang Chou, MD, Chih-Teng Yu, MD, Chien-
GENERAL THORACIC SURGERY Factors leading to tracheobronchial self-expandable metallic stent fracture Fu-Tsai Chung, MD,* Shu-Min Lin, MD,* Hao-Cheng Chen, MD, Chun-Liang Chou, MD, Chih-Teng Yu, MD, Chien-
Department of Thoracic Medicine, Chang Gung Memorial Hospital, Lin-Kuo Branch, Chang Gung Medical Foundation; Abstract
 DOI 10.6314/JIMT.2017.28(4).07 2017 28 243-251 Impacts of Airway Self-expandable Metallic Stent on Ventilator Weaning and Survival of Mechanically Ventilated Patients with Esophageal Cancer and Cental
DOI 10.6314/JIMT.2017.28(4).07 2017 28 243-251 Impacts of Airway Self-expandable Metallic Stent on Ventilator Weaning and Survival of Mechanically Ventilated Patients with Esophageal Cancer and Cental
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology
 Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
RESPIRATORY EMERGENCIES. Michael Waters MD April 2004
 RESPIRATORY EMERGENCIES Michael Waters MD April 2004 ASTHMA Asthma is a chronic inflammatory disease of the airways with variable or reversible airway obstruction Characterized by increased sensitivity
RESPIRATORY EMERGENCIES Michael Waters MD April 2004 ASTHMA Asthma is a chronic inflammatory disease of the airways with variable or reversible airway obstruction Characterized by increased sensitivity
Metallic Stent and Flexible Bronchoscopy without Fluoroscopy for
 ERJ Express. Published on January 9, 2008 as doi: 10.1183/09031936.00099507 Metallic Stent and Flexible Bronchoscopy without Fluoroscopy for Acute Respiratory Failure Shu-Min Lin, MD*,Ting-Yu Lin, MD*,
ERJ Express. Published on January 9, 2008 as doi: 10.1183/09031936.00099507 Metallic Stent and Flexible Bronchoscopy without Fluoroscopy for Acute Respiratory Failure Shu-Min Lin, MD*,Ting-Yu Lin, MD*,
Self-expanding metallic stents (SEMS) have gained widespread
 Bronchoscopic Extraction of Incorporated Self-Expanding Metallic Stents Sudish C. Murthy, MD, PhD, FACS, FCCP Self-expanding metallic stents (SEMS) have gained widespread acceptance as a treatment for
Bronchoscopic Extraction of Incorporated Self-Expanding Metallic Stents Sudish C. Murthy, MD, PhD, FACS, FCCP Self-expanding metallic stents (SEMS) have gained widespread acceptance as a treatment for
ISPUB.COM. Rare Cases: Tracheal/bronchial Obstruction. O Wenker, L Moehn, C Portera, G Walsh HISTORY ADMISSION
 ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
Section 4.1 Paediatric Tracheostomy Introduction
 Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation
 I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
Fariba Rezaeetalab Associate Professor,Pulmonologist
 Fariba Rezaeetalab Associate Professor,Pulmonologist rezaitalabf@mums.ac.ir Patient related risk factors Procedure related risk factors Preoperative risk assessment Risk reduction strategies Age Obesity
Fariba Rezaeetalab Associate Professor,Pulmonologist rezaitalabf@mums.ac.ir Patient related risk factors Procedure related risk factors Preoperative risk assessment Risk reduction strategies Age Obesity
Two Cases of Tracheal Disease Misdiagnosed as Difficult-to-Treat Asthma
 Two Cases of Tracheal Disease Misdiagnosed as Difficult-to-Treat Asthma Running-Head: Are you sure about the diagnosis of asthma? Ibrahim Onur Alici 1, Ozlem Kar Kurt 2, Adile Berna Dursun 3, Aydin Yilmaz
Two Cases of Tracheal Disease Misdiagnosed as Difficult-to-Treat Asthma Running-Head: Are you sure about the diagnosis of asthma? Ibrahim Onur Alici 1, Ozlem Kar Kurt 2, Adile Berna Dursun 3, Aydin Yilmaz
APSR RESPIRATORY UPDATES
 APSR RESPIRATORY UPDATES Volume 4, Issue 7 Newsletter Date: July 2012 APSR EDUCATION PUBLICATION Inside this issue: Quantitative imaging of airways Small-Airway Obstruction and Emphysema in Chronic Obstructive
APSR RESPIRATORY UPDATES Volume 4, Issue 7 Newsletter Date: July 2012 APSR EDUCATION PUBLICATION Inside this issue: Quantitative imaging of airways Small-Airway Obstruction and Emphysema in Chronic Obstructive
Endobronchial Management of Benign, Malignant, and Lung Transplantation Airway Stenoses
 Endobronchial Management of Benign, Malignant, and Lung Transplantation Airway Stenoses Joshua R. Sonett, MD, Robert J. Keenan, MD, Peter F. Ferson, MD, Bartley P. Griffith, MD, and Rodney J. Landreneau,
Endobronchial Management of Benign, Malignant, and Lung Transplantation Airway Stenoses Joshua R. Sonett, MD, Robert J. Keenan, MD, Peter F. Ferson, MD, Bartley P. Griffith, MD, and Rodney J. Landreneau,
Collaborating with interventional pulmonology in managing a massive tracheoesophageal fistula that extends from cricoid to carina: a case report
 DOI 10.1186/s40981-017-0133-2 CASE REPORT Collaborating with interventional pulmonology in managing a massive tracheoesophageal fistula that extends from cricoid to carina: a case report Luis E. Tollinche
DOI 10.1186/s40981-017-0133-2 CASE REPORT Collaborating with interventional pulmonology in managing a massive tracheoesophageal fistula that extends from cricoid to carina: a case report Luis E. Tollinche
AERO DV Tracheobronchial Direct Visualization Stent System
 AERO DV Tracheobronchial Direct Visualization Stent System Review Instructions For Use Before Using This System. Single Use Only Non-sterile MR Conditional CONTENTS Instructions for Use...............................
AERO DV Tracheobronchial Direct Visualization Stent System Review Instructions For Use Before Using This System. Single Use Only Non-sterile MR Conditional CONTENTS Instructions for Use...............................
COPD Management in LTC: Presented By: Jessica Denney RRT
 COPD Management in LTC: Presented By: Jessica Denney RRT Sponsored by Z & D Medical Services, Diamond Sponsor Seizing Opportunities to Provide Individualized Treatment and Device Selection for your COPD
COPD Management in LTC: Presented By: Jessica Denney RRT Sponsored by Z & D Medical Services, Diamond Sponsor Seizing Opportunities to Provide Individualized Treatment and Device Selection for your COPD
Comparison of Virtual Bronchoscopy with Fiberoptic Bronchoscopy Findings in Patients Exposed to Sulfur Mustard Gas
 Comparison of Virtual Bronchoscopy with Fiberoptic Bronchoscopy Findings in Patients Exposed to Sulfur Mustard Gas Poster No.: C-487 Congress: ECR 212 Type: Scientific Exhibit Authors: S. Akhlaghpoor,
Comparison of Virtual Bronchoscopy with Fiberoptic Bronchoscopy Findings in Patients Exposed to Sulfur Mustard Gas Poster No.: C-487 Congress: ECR 212 Type: Scientific Exhibit Authors: S. Akhlaghpoor,
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Endoscopic Removal of Metallic Airway Stents*
 bronchoscopy Endoscopic Removal of Metallic Airway Stents* William Lunn, MD, FCCP; David Feller-Kopman, MD, FCCP; Momen Wahidi, MD; Simon Ashiku, MD; Robert Thurer, MD, FCCP; and Armin Ernst, MD, FCCP
bronchoscopy Endoscopic Removal of Metallic Airway Stents* William Lunn, MD, FCCP; David Feller-Kopman, MD, FCCP; Momen Wahidi, MD; Simon Ashiku, MD; Robert Thurer, MD, FCCP; and Armin Ernst, MD, FCCP
Metallic Stent Placement for the Management of Tracheal Carina Strictures and Fistulas: Technical and Clinical Outcomes
 Vascular and Interventional Radiology Original Research Kim et al. Outcomes of Tracheal Stent Placement Vascular and Interventional Radiology Original Research Jinoo Kim 1 Ji Hoon Shin 2 Jin-Hyoung Kim
Vascular and Interventional Radiology Original Research Kim et al. Outcomes of Tracheal Stent Placement Vascular and Interventional Radiology Original Research Jinoo Kim 1 Ji Hoon Shin 2 Jin-Hyoung Kim
Proceedings of the 36th World Small Animal Veterinary Congress WSAVA
 www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
SPIRATION. VALVE SYSTEM For the Treatment of Emphysema or Air Leaks.
 SPIRATION VALVE SYSTEM For the Treatment of Emphysema or Air Leaks. 0000 ENGINEERED FOR AIRWAY MANAGEMENT Inspired by aerodynamics, the Spiration Valve redirects air away from diseased or damaged lung
SPIRATION VALVE SYSTEM For the Treatment of Emphysema or Air Leaks. 0000 ENGINEERED FOR AIRWAY MANAGEMENT Inspired by aerodynamics, the Spiration Valve redirects air away from diseased or damaged lung
Case Report. Management of recurrent distal tracheal stenosis using an endoprosthesis: a case report* Abstract. Introduction.
 121 Case Report Management of recurrent distal tracheal stenosis using an endoprosthesis: a case report* André Germano Leite 1, Douglas Kussler 2 Abstract The authors report the case of a patient with
121 Case Report Management of recurrent distal tracheal stenosis using an endoprosthesis: a case report* André Germano Leite 1, Douglas Kussler 2 Abstract The authors report the case of a patient with
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (1), Page
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (1), Page 3516-3520 Severe Tracheomalacia Secondary to Double Aortic Arch. Any Role in Posterior Aortopexy? A Case report Bayan Almehamadi
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (1), Page 3516-3520 Severe Tracheomalacia Secondary to Double Aortic Arch. Any Role in Posterior Aortopexy? A Case report Bayan Almehamadi
ORIGINAL ARTICLE. The Use of Balloon-Expandable Metallic Stents in the Treatment of Pediatric Tracheomalacia and Bronchomalacia
 ORIGINAL ARTICLE The Use of Balloon-Expandable Metallic Stents in the Treatment of Pediatric Tracheomalacia and Bronchomalacia Robert H. Furman, MD; Carl L. Backer, MD; Michael E. Dunham, MD; James Donaldson,
ORIGINAL ARTICLE The Use of Balloon-Expandable Metallic Stents in the Treatment of Pediatric Tracheomalacia and Bronchomalacia Robert H. Furman, MD; Carl L. Backer, MD; Michael E. Dunham, MD; James Donaldson,
NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP)
 Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
