Tracheal collapse diagnosed by multidetector computed tomography: evaluation of different image analysis methods
|
|
|
- Octavia Poole
- 5 years ago
- Views:
Transcription
1 Syddansk Universitet Tracheal collapse diagnosed by multidetector computed tomography: evaluation of different image analysis methods Nygaard, Mette; Bendstrup, Elisabeth; Dahl, Ronald; Hilberg, Ole; Rasmussen, Finn Published in: European Clinical Respiratory Journal DOI: / Publication date: 2017 Document version Publisher's PDF, also known as Version of record Document license CC BY Citation for pulished version (APA): Nygaard, M., Bendstrup, E., Dahl, R., Hilberg, O., & Rasmussen, F. (2017). Tracheal collapse diagnosed by multidetector computed tomography: evaluation of different image analysis methods. European Clinical Respiratory Journal, 4, [ ]. DOI: / General rights Copyright and moral rights for the publications made accessible in the public portal are retained by the authors and/or other copyright owners and it is a condition of accessing publications that users recognise and abide by the legal requirements associated with these rights. Users may download and print one copy of any publication from the public portal for the purpose of private study or research. You may not further distribute the material or use it for any profit-making activity or commercial gain You may freely distribute the URL identifying the publication in the public portal? Take down policy If you believe that this document breaches copyright please contact us providing details, and we will remove access to the work immediately and investigate your claim. Download date: 13. nov
2 European Clinical Respiratory Journal ISSN: (Print) (Online) Journal homepage: Tracheal collapse diagnosed by multidetector computed tomography: evaluation of different image analysis methods Mette Nygaard, Elisabeth Bendstrup, Ronald Dahl, Ole Hilberg & Finn Rasmussen To cite this article: Mette Nygaard, Elisabeth Bendstrup, Ronald Dahl, Ole Hilberg & Finn Rasmussen (2017) Tracheal collapse diagnosed by multidetector computed tomography: evaluation of different image analysis methods, European Clinical Respiratory Journal, 4:1, , DOI: / To link to this article: The Author(s). Published by Informa UK Limited, trading as Taylor & Francis Group. Published online: 08 Dec Submit your article to this journal Article views: 47 View related articles View Crossmark data Full Terms & Conditions of access and use can be found at
3 EUROPEAN CLINICAL RESPIRATORY JOURNAL, 2017 VOL. 4, RESEARCH ARTICLE Tracheal collapse diagnosed by multidetector computed tomography: evaluation of different image analysis methods Mette Nygaard a, Elisabeth Bendstrup a, Ronald Dahl c, Ole Hilberg a and Finn Rasmussen b a Department of Respiratory Diseases and Allergy, Aarhus University Hospital, Aarhus, Denmark; b Department of Radiology, Aarhus University Hospital, Aarhus, Denmark; c Department of Respiratory Medicine, Odense University Hospital, Odense C, Denmark ABSTRACT Background: The gold standard for diagnosing excessive tracheal collapse is still evaluation during bronchoscopy. Today, multidetector computed tomography (MDCT) is used to confirm a suspicion of abnormal tracheal collapse. There is no gold standard for computed tomography (CT) image analysis of tracheal collapse. Purpose: To evaluate four different methods for the diagnosis of tracheal collapse using the images obtained through MDCT to help clinicians evaluate the images in daily practice. Objectives: 374 consecutive high-resolution CT scans with full inspiratory and end-expiratory CT scans were retrospectively analyzed. Methods: The images were analyzed in four different ways. The degree of collapse was based on cross-sectional areas of individual locations or volumes of entire regions: (1) 1 cm above the carina, (2) the level of maximal collapse of the trachea, (3) the entire region from the carina to the thoracic inlet, and (4) the trachea and bronchial region as defined by the software. Results: We compared three existing and one new method for image analysis of tracheal collapse by MDCT. The prevalence of tracheal collapse varied from 10.7% to 19.5% in this cohort of patients suffering from mixed lung diseases when using an expiratory collapse of 50% as a threshold. The four methods were comparable with highly significant Pearsons correlation coefficients ( ). However, the four methods identified different patients with collapse of 50%. There was no correlation between symptoms and the degree of collapse. Conclusion: The different methods identify tracheal collapse in different patients. Hence, the diagnosis of excessive tracheal collapse can not rely solely on MDCT images. Generally, there is a poor correlation between symptoms and the degree of collapse in the different methods. However, when using the maximal collapse, there is some correlation with symptoms. When in doubt regarding the diagnosis, further investigations, such as bronchoscopy, should be carried out. ARTICLE HISTORY Received 10 January 2017 Accepted 22 October 2017 KEYWORDS excessive tracheal collapse; diagnosis; MDCT; prevalence; correlation; pulmonary function test Introduction Excessive tracheal collapse is characterized by flaccidity of the tracheal wall resulting in expiratory collapse of 50% of the central airways. The most frequent symptoms of tracheal collapse are cough, dyspnea, wheezing, and recurrent infections. This complicates diagnosis, as it mimics other and more common lung diseases [1]. The reported prevalence of tracheal collapse varies in different studies and depends both on the method used for diagnosing tracheomalacia and on the comorbidities of the patients [2 5]. The highest prevalence reported is 23% in patients with chronic bronchitis. In this single study, the diagnosis was solely based on bronchoscopy [2]. Another study reported a prevalence of 14.1% in patients with chronic cough [3]. The gold standard for diagnosing excessive tracheal collapse is still evaluation of the cross-sectional area of the trachea before and at forced expiration or cough during bronchoscopy. Until recently, this was the only available diagnostic option. With the introduction of multidetector computed tomography (MDCT), a noninvasive diagnostic tool is now available. This new tool poses new challenges such as standardization of a scanning protocol, standardization of image analysis, definition of the degree of airways collapse, and determination of the threshold for normal/abnormal airway collapse. Several methods for tracheal collapse evaluation of MDCT images have previously been used [6 8]. The most commonly used method is the determination of airway collapse at the localization of maximal collapse of the trachea [3,7,9]. In other methods, predetermined locations are used for establishing the CONTACT Mette Nygaard metnygch@rm.dk 2017 The Author(s). Published by Informa UK Limited, trading as Taylor & Francis Group. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
4 2 M. NYGAARD ET AL. degree of collapse in the trachea [4,5]. These locations differ, but most include levels 1 cm above the carina and the aortic arch [6 10]. There is no gold standard for computed tomography (CT) images analysis of tracheal collapse. To our knowledge, no studies have previously compared different image analysis methods with respect to identification of tracheal collapse. The aim of the present study was therefore to compare four different methods of high-resolution CT image analysis for tracheal collapse to help the clinician to appraise the CT images in the daily practice. Materials and methods Patients This study was approved by the Danish Data Protection Agency. During a 17-month period, 374 patients were referred to a high-resolution computed tomography (HRCT) scan performed in full inspiration and in end expiration. No participants were recruited exclusively for this study. The volume of tracheal collapse was measured retrospectively. The indication for HRCT is shown in Table 1. Patient files were scrutinized for data on age, respiratory symptoms (dyspnea, cough, and recurrent infection), smoking history, body mass index and pulmonary function data [forced expiratory volume in 1 s (FEV1), forced vital capacity (FVC), FEV1/FVC, forced expiratory flow (FEF25 75)]at3monthsbeforeand3monthsafterthe HRCT. Pulmonary function tests were analyzed in accordance with American Thoracic Society and European Respiratory Society guidelines [11] (Table 2) mm collimation, kv 120, mas/slice , rotation time 0.5 s, pitch 0.59, reconstruction thickness 0.9 mm, and increment 0.45 mm. A high-resolution kernel was used. Images were transferred to a picture-archiving communication system. During the scanning acquisition, an automatic voice recording instructed the patients to take a deep breath and hold it for end-inspiratory scanning. For endexpiratory scanning, the patients were instructed to take a deep breath, exhale, and hold it. Image interpretation Image assessment was performed on a dedicated CT workstation (Philips, Extended Brilliance workspace version 4.5.2) using standard lung window display settings (level: 500 hounsfield units (HU); width: 1500 HU). The images were retrospectively analyzed by a registrar in pulmonary medicine (M.N., with 5 years of experience in interpreting dynamic thoracic CT scans). Four different methods for calculation of tracheal collapse were performed: Method 1 The volume of a 10 mm CT slice located 1 cm above the carina as shown in Figure 1. Method 2 The volume of 10 mm CT slices from the level of the carina and every 1 cm until the thoracic inlet was examined. The location with maximal collapse was chosen as depicted in Figure 2. CT scan HRCT was performed on a multirow detector scanner (Philips Brilliance CT 64 or ICT 256, Philips Healthcare, Best, The Netherlands) and included a scan range of the whole chest in full inspiration and at end expiration. The CT acquisition parameters were mm or Table 1. Indication for performing the HRCT scans. Indication Number Percentage ILD a Emphysema (COPD) 14 4 Bronchiectasis Tracheomalacia Infiltrates LTX, BOS Dyspnea Other Combination of two of the above ILD = interstitial lung disease; COPD = chronic obstructive lung disease; LTX = lung transplant; BOS = bronchiolitis obliterans syndrome. a Known or referred on the suspicion of ILD. Method 3 Each 10 mm slice from the carina to the thoracic outlet was manually defined on both inspiratory and expiratory scans. The sum of these volumes was multiplied (Figure 3). Method 4 An automatic software segmentation technique of the lungs and the large airways was used to estimate the volume of the trachea (lung density, brilliance extended workspace) in the inspiratory and expiratory scan (Figure 4). The upper limit for the segmentation was the thoracic inlet. The lower limit was the carina. This method is fully automated and therefore without interobserver variability. The relative collapse in expiration was calculated as:
5 EUROPEAN CLINICAL RESPIRATORY JOURNAL 3 Table 2. Descriptive characteristics of the study population by the four different methods. Method 1 Method 2 Method 3 Method 4 Collapse 50 Collapse 50 Collapse 50 Collapse 50 Collapse 50 Collapse 50 Collapse 50 Collapse 50 Age, years 64* 56* 64* 56* 64* 56* 63* 56* Gender: Female, n (%) 29* (9) 150* (49) 43 (13) 144 (44) 41* (12) 146* (45) 23 (8) 145 (48) Male, n (%) 9* (3) 125* (39) 21 (6) 124 (37) 17* (5) 122* (37) 9 (3) 123 (41) BMI * 25.8* 27.6* 25.9* Lung function parameters: FEV1 (%predicted) FVC (%predicted) FEV1/FVC Flow-volume-loop with oscillation, n(%) 9* (67) 25* (16) 11 (30) 26 (16) 9 (26) 27 (17) 8*(38) 25*(16) Symptoms: Dyspnea, n (%) 26 (87) 164 (72) 44* (85) 158* (71) 39 (83) 159 (72) 23 (77) 159 (72) Cough, n (%) 21 (72) 138 (67) 34 (72) 134 (66) 31 (69) 131 (66) 17 (63) 135 (66) Rec.inf., n (5) 13 (45) 69 (35) 22 (46) 62 (32) 16 (37) 65 (34) 10 (38) 66 (34) Tobacco: Current, n (%) 3 (16) 30 (16) 6 (17) 34 (18) 2 (7) 36 (19) 3 (18) 37 (19) Former, n (%) 9 (47) 85 (45) 18 (51) 83 (44) 17 (55) 80 (42) 7 (42) 84 (44) Never, n (%) 7 (37) 74 (39) 11 (31) 73 (38) 12 (39) 71 (38) 7 (42) 72 (37) Method: 1: 1 cm above the carina; 2: max collapse; 3: sum of cross-sectional areas; 4: volume. FEV1 = forced expiratory volume in 1 s; FVC = forced vital capacity; FEF = forced expiratory flow. *p < Sample characteristics were examined, and continuous variables were compared by the unpaired t-test. The tests are considered one-sided, as an excessive tracheal collapse never would lead to an improvement in the pulmonary function tests. The categorical variables were analyzed using the chi-square analysis. The level of significance was set at p < 0.05 for all statistical analyses. All analyses were performed using statistical software (STATA, version 13). Results Study population Figure 1. Inspiratory sagittal reconstructed CT images of the air in the lungs and airways explaining Method 1: measurement of the cross-sectional area 1 cm above the carina. [(luminal area or volume at inspiration luminal area or volume at expiration)/luminal area or volume at inspiration] 100% Statistical analysis Normal distribution of all variables was confirmed by Q Q plots. The correlation between the different methods was primarily evaluated using Bland Altman plots. Afterwards, the Pearson correlation coefficient was used to evaluate the correlation between the different strategies for analyzing the images. A total of 353 HRCT scans met the inclusion criteria. The cohort consisted of 191 females (median age 55 years, range years) and 150 males (median age 60 years, range years). Patient demographics are listed in Table 2. Information on symptoms and spirometry was available in 225 subjects. Prevalence The prevalence of tracheal collapse varied from 10.7% to 19.5% when using an expiratory collapse of 50% as a threshold (Figure 5). The prevalences were significantly different from each other (p < 0.001). Using an expiratory collapse of 80% as threshold, only 1 3 patients were identified, and the prevalence decreased to <1% for all four methods. There was no significant difference between the prevalence of abnormal collapse in the three major lung disease groups: asthma ( ), chronic
6 4 M. NYGAARD ET AL. Figure 2. Method 2: paired end-inspiratory (a) and end-expiratory (b) sagittal reconstructed CT images showing maximal collapse of more than 50%. collapse (Method 2). The maximal collapse was located at the carina in 27% of patients (Figure 6). When evaluating the area at the carina and the lower 4 cm of the trachea, maximal collapse was identified in 78%. Thus, in our population, tracheal collapse was most pronounced in the distal part of the trachea. Correlations between the four different methods for measuring tracheal collapse were analyzed using Bland Altman plots. The plots were acceptable with a systematic difference between the methods (mean difference between 0.3 and 11 depending on compared methods). These results allowed us to use the pairwise linear regression analysis. The Pearson correlations were between r = and r = (p < 0.001). Figure 3. Inspiratory sagittal reconstructed CT images of the air in the lungs and airways explaining Method 3: measurement of the cross-sectional area every centimeter from the carina to the thoracic outlet. obstructive pulmonary disease (COPD) ( ), and interstitial lung diseases ( ) (p = , chi-square analysis) using three out of four methods. Measurement of the tracheal collapse The cross-sectional area was calculated every 1 cm from the carina to the thoracic inlet (Method 3) to determine the localization of maximal expiratory Correlation with age and gender Patients with expiratory tracheal collapse of 50% were significantly older than patients without collapse (63 years contra 56 years), and apparent for all four measuring methods (Table 2). For both genders, the highest prevalence of abnormal tracheal collapse was found in the age group between 70 and 79 years (females 38%, males 17%). The difference in average collapse between genders was statistically significant in method 1 and method 3 with significantly more women with collapse of 50% (p =0.014andp =0.028).Inmethod2and method 4, the difference was just insignificant (p = 0.056).
7 EUROPEAN CLINICAL RESPIRATORY JOURNAL 5 Figure 4. Automatic segmentation of the lungs and the airways at (a) full inspiration and at (b) end expiration. The red area shows the areas of the right lung with HU above 950 (inspiration) and 800 (expiration) respectively. The volume of the trachea and first generations of bronchi given by the software (Method 4) is shown in blue. 25% Prevalence 20% 19,5% (65/339) 17,8% (58/326) 15% 12,5% (39/314) 10,7% (34/311) 10% 5% 0% Method 1 Method 2 Method 3 Method 4 Figure 5. Prevalence of tracheomalacia using the four different methods and a threshold of 50% for maximal airway collapse. Correlation with symptoms, smoking, and BMI The relationship between three common respiratory symptoms, cough, dyspnea, and recurrent respiratory infections, and tracheal collapse, was evaluated. Significantly more patients in the group with collapse of 50% had dyspnea using method 2 (p < 0.05). They also showed a trend toward recurrent infections, albeit not insignificant (p = 0.07). The other methods revealed no significant relation between a tracheal collapse of 50% and dyspnea, recurrent infections, or cough (Table 2). The BMI was significantly higher in the group with collapse of 50% (BMI: ) when compared with the group without collapse (BMI: 25.9) when using methods 2 and 3 (p = and 0.039, t-test). When using method 1 (1 cm above the carina) and method 4 (volume given by the software), there was no difference. Correlation with physiological measurements There was no correlation between expiratory tracheal collapse and lung function tests using any of the four image-analysis methods (Table 3). However, we noticed a trend toward a correlation between the
8 6 M. NYGAARD ET AL Figure 6. Histogram of the number of patients with maximal collapse of the tracheal cross-sectional area at the carina (0) and every 1 cm until the thoracic inlet. Numbers are based on measurements from Method 3. tracheal collapse and the FEV1 and FVC when using method 2. The FEV1 and FVC were insignificantly (p = 0.06 and p = 0.09) lower in the group with tracheal collapse compared with the patients with normal tracheal function. The patients with tracheal collapse of 50% had a tendency toward oscillations on the flow-volume loops. In methods 1 and 4, the number of flow-volume loops with oscillations was significantly higher in the group with abnormal collapse ( 50%) than in the group with less collapsibility (p = 0.01 and p = 0.005). In method 2, there was a trend (p =0.06). Discussion In the present study, we compared three existing and one new method for image analysis of tracheal collapse by MDCT. The four methods were comparable with highly significant correlation coefficients ( ), but did not identify the same patients. Different groups of patients with airway collapse of 50% were identified depending on the method used for image analysis. Hence, in the clinical practice, it is important not to rely solely on the results of the MDCT but to investigate further, if there is a clinical suspicion of excessive tracheal collapse. There is no significant correlation between the degree of collapse seen on MDCT and clinical symptoms, making the diagnosis even harder. However, the correlation between the degree of collapse and symptoms has never been established in bronchoscopy either. In Figure 7, the overlap between the patients with tracheal collapse in the four methods is shown in a Venn diagram. It reveals no consistency between the patients diagnosed in the different methods. Thus, standardization of the MDCT method and correlation with other indices such as bronchoscopic detection of tracheal collapse and symptoms are needed. The prevalence of tracheal collapse in our cohort of patients with different lung diseases ranged from 10.7% to 19.5% depending on the method used for image analysis. Previously, other characteristics have been included in the diagnosis such as in the multidimensional classification system Functional status, Extent, Morfology, Origin and Severity of the abnormalities (FEMOS) that includes symptoms, etiology, morphology, extent, and severity of the collapse [12]. The method resulting in the highest prevalence of abnormal collapse is naturally the one using the maximal collapse at a certain level. In our study, the area with maximal collapse is based on measurements of the cross-sectional areas from the carina to the thoracic inlet. In a study by Lee et al., a radiologist determined the maximal collapse visually, while Ochs et al. used a technique similar to ours that minimizes the interobserver variation [13,14]. An important problem with this method is that patients with only minor localized collapse are also included, and the impact of this is unknown and questionable [15]. In our study, there were no patients with previous intubation trauma. Prolonged intubation may lead to a segmental collapse of the trachea, and such a localized collapse will also be diagnosed by the method using the maximal collapse. The method using the maximal collapse (Method 2) was the only method that revealed a significant correlation between symptoms and tracheal collapse. There was a higher percentage of patients suffering from dyspnea in the group of patients with tracheal collapse of 50% by the use of this method. Furthermore, there was a trend toward a higher risk of recurrent
9 EUROPEAN CLINICAL RESPIRATORY JOURNAL 7 Figure 7. Venn diagram showing the overlap between the patients with collapse of more than 50% in expiration using the four different methods. infections (p = 0.07), low FEV1 (p = 0.06), and FVC (p = 0.09) in the group with significant tracheal collapse. Methods 1 and 2 using only one location for evaluation of the collapsibility are rapid and easily performed. Previous studies have most often used the location 1 cm above the aortic arch for evaluation [7,9,10]. However, in our study, this was a rather rare location for the maximal collapse. When the method using only one level for evaluation of the collapse is applied, the most optimal location to measure is the distal levels of the trachea, as 78% of our patients had their maximal collapse there. As the clinical impact of expiratory tracheal collapse on imaging has not been determined, it is important to develop objective measurements for the diagnosis. In addition, it is important to relate bronchoscopic findings and MDCT to the symptoms presented by the patient. So far, no such studies have been published. The method using the cross-sectional areas from the carina to the thoracic inlet is more time-consuming with more interobserver variation, but the advantage is that the whole trachea is evaluated, thus providing information about both the severity and the disease extent. No readers of CT scans can rely only on software results. Some patients have extensive collapse making segmentation by the software impossible, and thus the radiologist has to evaluate pronounced collapse or consider other reasons for the inability for an automatic segmentation. However, when feasible, the fully automatic method is rapid without interobserver variation. Inherently, the inability of the software to generate the volume of the trachea in case of severe collapse poses major problems, as the most severely affected patients are not identified. Consequently, the correlation with symptoms and pulmonary function tests is low when using this method. All analysis methods found a significantly higher mean age in the group with tracheal collapse above 50% compared with the group with less collapse. It is tempting to impute the weakness of the tracheal wall to the general degenerative process of aging, but this needs to be proven. The patients with tracheal collapse had a higher mean BMI. It is questionable whether a difference in mean BMI of 1.5 is of clinical importance. However, this is in accordance with a recent study reporting a significantly higher degree of collapse in patients with COPD and a BMI 35 [6]. A higher intrathoracic pressure in this group of patients is thought to play a role. Such a relationship needs to be investigated in prospective studies in which a time volume curve of the trachea is compared with a time pressure curve during expiration. Previous studies have suggested 80% as the threshold for excessive tracheal collapse [10]. In our study, only a few patients were identified using an 80% threshold. The prevalence decreased to <1% independent of which of the four methods were used. The
10 8 M. NYGAARD ET AL. clinical significant threshold needs still to be defined, as we found no correlation between clinically relevant symptoms and the degree of collapse in the trachea. We acknowledge that there are several limitations in our study. The study is retrospective and observational in design. The indication for the MDCT scans was not to evaluate the collapsibility of the trachea. Our study is based on MDCT scans performed to diagnose a broad variety of lung diseases. The frequency of tracheal collapse was the same in obstructive airway diseases (asthma and COPD) and interstitial lung disease. The expiratory images were obtained at end expiration instead of during forced expiration, which was previously shown to lower the prevalence [16]. We believe that our results are transferable to patients suffering from chronic lung disease in general. The prevalence of tracheal collapse in healthy humans is not known, but we considered expiratory CT in healthy volunteers to be unethical and can therefore, however unlikely, not exclude tracheal collapse to be a common radiologic finding. Speculations on whether collapse of the trachea in expiration is a stationary condition or just one of many manifestations of severe lung diseases need to be explored in longitudinal studies. In conclusion, we have evaluated four different methods for the diagnosis of tracheal collapse using MDCT scanning. The different methods identify tracheal collapse in different patients depending on the method used. It is important to emphasize that there is a poor agreement between the four methods used for image analysis and a weak correlation between symptoms and degree of collapse. The software-generated results are easy and without interobserver variability, but do not identify severe collapse, thus making its use limited. The method using maximal collapse to identify patients reveals some correlations with both symptoms and pulmonary function tests, thus making this the method of choice for evaluating tracheal collapse on MDCT images. Research is warranted to determine which method correlates better with bronchoscopy, PFTs, or symptoms of tracheal collapse. A future study is planned to evaluate the tracheal collapse in expiration using both bronchoscopy and MDCT in different groups of patients suffering from known lung diseases. The correlation between the bronchoscopic results and the different image analysis will be examined and related to symptoms and pulmonary function tests. It is still uncertain if tracheal collapse is an independent concurrent disease, a comorbidity, or a consequence of an underlying lung disease, and prospective studies are warranted. Disclosure statement No potential conflict of interest was reported by the authors. Funding This work was supported by the The Danish Lung Association. Notes on contributors Mette Nygaard is a Medical doctor from Aarhus University in Afterwards I have taken specialist training and now she is a specialist in pulmonary medicine. Together with her specialist training she have been doing a PhD in tracheomalacia which is due in Elisabeth Bendstrup, MD, PhD, is a consultant at Department of Respiratory Diseases and Allergy, Aarhus University Hospital, Denmark. She is a specialist in pulmonary diseases and her main research focus is interstitial lung diseases. Ronald Dahl, MD, DMSc is a specialist in respiratory medicine. His main research focus is pulmonology. Ole Hilberg, MD, DMSc, is a consultant at Department of Medicine, Vejle Hospital, Denmark. He is a specialist in respiratory medicine and his main research focus is pulmonology. Finn Rasmussen, MD, DMSc, is a consultant at Department of Radiology, Aarhus University Hospital, Denmark. He is a specialist in radiology and his main research focus is CT imaging of lung disorders. ORCID Elisabeth Bendstrup Ole Hilberg References [1] Carden KA, Boiselle PM, Waltz DA, et al. Tracheomalacia and tracheobronchomalacia in children and adults: an in-depth review. Chest. Division of Pulmonary and Critical Care Medicine, Beth Israel Deaconess Medical Center, 330 Brookline Ave, Boston, MA 02446, USA Mar;127(3): [2] Jokinen K, Palva T, Nuutinen J. Chronic bronchitis. A bronchologic evaluation. ORL J Otorhinolaryngol Relat Spec. SWITZERLAND. 1976;38(3): [3] Palombini BC, Villanova CA, Araujo E, et al. A pathogenic triad in chronic cough: asthma, postnasal drip syndrome, and gastroesophageal reflux disease Chest. United States Nov;136(5 Suppl):e30. [4] Wagnetz U, Roberts HC, Chung T, et al. Dynamic airway evaluation with volume CT: initial experience. Can Assoc Radiol J. Department of Medical Imaging, University Health Network, Toronto General Hospital,
11 EUROPEAN CLINICAL RESPIRATORY JOURNAL 9 Toronto, Ontario, Canada. Canadian Association of Radiologists. Published by Elsevier Inc Apr;61 (2): [5] Bhatt SP, Terry NLJ, Nath H, et al. association between expiratory central airway collapse and respiratory outcomes among smokers. JAMA. United States Feb;315(5): [6] Boiselle PM, O Donnell CR, Bankier AA, et al. Tracheal collapsibility in healthy volunteers during forced expiration: assessment with multidetector CT. Radiology. Center for Airway Imaging, Departments of Radiology, Beth Israel Deaconess Medical Center and Harvard Medical School, 330 Brookline Ave, Boston, MA 02215, USA Jul;252(1): [7] Boiselle PM, Litmanovich DE, Michaud G, et al. Dynamic expiratory tracheal collapse in morbidly obese COPD patients. COPD. 1From the Center for Airway Imaging and the Department of Radiology, Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA, USA. 2013;10(5): [8] Boiselle PM, Michaud G, Roberts DH, et al. Dynamic expiratory tracheal collapse in COPD: correlation with clinical and physiological parameters. Chest. From the Center for Airway Imaging and the Departments of Radiology ;142(6): doi: /chest Chest [9] O Donnell CR, Litmanovich D, Loring SH, et al. Age and sex dependence of forced expiratory central airway collapse in healthy volunteers. Chest. Division of Pulmonary, Critical Care and Sleep Medicine, Beth Israel Deaconess Medical Center, Boston, MA 02215, USA Jul;142 (1): [10] Boiselle PM, O Donnell CR, Loring SH, et al. Reproducibility of forced expiratory tracheal collapse: assessment with MDCT in healthy volunteers. Acad Radiol. Center for Airway Imaging and the Department of Radiology, Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA 02215, USA. AUR. Published by Elsevier Inc Sep;17(9): [11] Pellegrino R, Viegi G, Brusasco V, et al. Interpretative strategies for lung function tests. Eur Respir J. Internal Medicine, University of Genoa, V.le Benedetto XV, 6, Genova I-16132, Italy Nov;26 (5): [12] Murgu SD, Colt HG. Description of a multidimensional classification system for patients with expiratory central airway collapse. Respirology. Pulmonary and Critical Care Medicine, Department of Medicine, University of California School of Medicine, Irvine, California 92868, USA Jul;12(4): [13] Lee EY, Strauss KJ, Tracy DA, et al. Comparison of standard-dose and reduced-dose expiratory MDCT techniques for assessment of tracheomalacia in children. Acad Radiol. Department of Radiology, Children s Hospital Boston and Harvard Medical School, Boston, MA, USA. AUR. Published by Elsevier Inc Apr;17 (4): [14] Ochs RA, Petkovska I, Kim HJ, et al. Prevalence of tracheal collapse in an emphysema cohort as measured with end-expiration CT. Acad Radiol. Department of Radiological Sciences, David Geffen School of Medicine, University of California, Los Angeles, CA, USA Jan;16(1): [15] Ellingsen I, Holmedahl NH. Does excessive dynamic airway collapse have any impact on dynamic pulmonary function tests? J Bronchology Interv Pulmonol. Glittreklinikken AS, Hakadal, Norway Jan;21 (1): [16] Ferretti GR, Jankowski A, Perrin MA, et al. Multi-detector CT evaluation in patients suspected of tracheobronchomalacia: comparison of end-expiratory with dynamic expiratory volumetric acquisitions. Eur J Radiol. Department of Radiology, France Nov;68 (2):
Pulmonary Function and Flow Volume Loop Patterns in Patients with. *Adnan Majid, MD ¹, FCCP *Andres F.
 Pulmonary Function and Flow Volume Loop Patterns in Patients with Tracheobronchomalacia. *Adnan Majid, MD ¹, FCCP (amajid@bidmc.harvard.edu); *Andres F. Sosa, MD² (andres.sosa@umassmemorial.org); Armin
Pulmonary Function and Flow Volume Loop Patterns in Patients with Tracheobronchomalacia. *Adnan Majid, MD ¹, FCCP (amajid@bidmc.harvard.edu); *Andres F. Sosa, MD² (andres.sosa@umassmemorial.org); Armin
Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology
 Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
Supplementary Online Content
 Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
The Relationship among COPD Severity, Inhaled Corticosteroid Use, and the Risk of Pneumonia.
 The Relationship among COPD Severity, Inhaled Corticosteroid Use, and the Risk of Pneumonia. Rennard, Stephen I; Sin, Donald D; Tashkin, Donald P; Calverley, Peter M; Radner, Finn Published in: Annals
The Relationship among COPD Severity, Inhaled Corticosteroid Use, and the Risk of Pneumonia. Rennard, Stephen I; Sin, Donald D; Tashkin, Donald P; Calverley, Peter M; Radner, Finn Published in: Annals
Outline FEF Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications?
 Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
What do pulmonary function tests tell you?
 Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Prevalence of tracheobronchomalacia and excessive dynamic airway collapse in bronchial asthma of different severity
 Dal Negro et al. Multidisciplinary Respiratory Medicine 2013, 8:32 ORIGINAL RESEARCH ARTICLE Prevalence of tracheobronchomalacia and excessive dynamic airway collapse in bronchial asthma of different severity
Dal Negro et al. Multidisciplinary Respiratory Medicine 2013, 8:32 ORIGINAL RESEARCH ARTICLE Prevalence of tracheobronchomalacia and excessive dynamic airway collapse in bronchial asthma of different severity
collapse in patients with tracheobronchomalacia,
 J. Zhang 1,2 I. Hasegawa 1,3 H. Hatabu 1,3 D. Feller-Kopman 1,3 P. M. Boiselle 1,3 Received June 5, 2003; accepted after revision July 23, 2003. 1 Department of Radiology, Beth Israel Deaconess Medical
J. Zhang 1,2 I. Hasegawa 1,3 H. Hatabu 1,3 D. Feller-Kopman 1,3 P. M. Boiselle 1,3 Received June 5, 2003; accepted after revision July 23, 2003. 1 Department of Radiology, Beth Israel Deaconess Medical
HRCT Versus Volume Rendering (Three Colors, Three Densities Lung Images) in Diagnosis of Small Airway Disease: A Comparative Study
 Med. J. Cairo Univ., Vol. 84, No. 1, March: 359-364, 2016 www.medicaljournalofcairouniversity.net HRCT Versus Volume Rendering (Three Colors, Three Densities Lung Images) in Diagnosis of Small Airway Disease:
Med. J. Cairo Univ., Vol. 84, No. 1, March: 359-364, 2016 www.medicaljournalofcairouniversity.net HRCT Versus Volume Rendering (Three Colors, Three Densities Lung Images) in Diagnosis of Small Airway Disease:
Parametric response mapping
 Parametric response mapping Utility of a novel imaging biomarker in pulmonary disease Dharshan Vummidi MD, Lama VN MD, Yanik G MD, Kazerooni EA MD, Meilan Han MD, Galban C PhD Radiology, Pulmonary & Critical
Parametric response mapping Utility of a novel imaging biomarker in pulmonary disease Dharshan Vummidi MD, Lama VN MD, Yanik G MD, Kazerooni EA MD, Meilan Han MD, Galban C PhD Radiology, Pulmonary & Critical
Basic approach to PFT interpretation. Dr. Giulio Dominelli BSc, MD, FRCPC Kelowna Respiratory and Allergy Clinic
 Basic approach to PFT interpretation Dr. Giulio Dominelli BSc, MD, FRCPC Kelowna Respiratory and Allergy Clinic Disclosures Received honorarium from Astra Zeneca for education presentations Tasked Asked
Basic approach to PFT interpretation Dr. Giulio Dominelli BSc, MD, FRCPC Kelowna Respiratory and Allergy Clinic Disclosures Received honorarium from Astra Zeneca for education presentations Tasked Asked
Accepted Manuscript. Robotic tracheobronchoplasty is feasible but which patients truly benefit? Steven Milman, MD, Thomas Ng, MD
 Accepted Manuscript Robotic tracheobronchoplasty is feasible but which patients truly benefit? Steven Milman, MD, Thomas Ng, MD PII: S0022-5223(18)32271-2 DOI: 10.1016/j.jtcvs.2018.08.028 Reference: YMTC
Accepted Manuscript Robotic tracheobronchoplasty is feasible but which patients truly benefit? Steven Milman, MD, Thomas Ng, MD PII: S0022-5223(18)32271-2 DOI: 10.1016/j.jtcvs.2018.08.028 Reference: YMTC
Observer variation for radiography, computed tomography, and magnetic resonance imaging of occult hip fractures
 Observer variation for radiography, computed tomography, and magnetic resonance imaging of occult hip fractures Collin, David; Dunker, Dennis; Gothlin, Jan H.; Geijer, Mats Published in: Acta Radiologica
Observer variation for radiography, computed tomography, and magnetic resonance imaging of occult hip fractures Collin, David; Dunker, Dennis; Gothlin, Jan H.; Geijer, Mats Published in: Acta Radiologica
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Quantitative CT in Chronic Obstructive Pulmonary Disease: Inspiratory and Expiratory Assessment
 Cardiopulmonary Imaging Original Research kira et al. CT of Chronic Obstructive Pulmonary Disease Cardiopulmonary Imaging Original Research Masanori kira 1 Kazushige Toyokawa 1 Yoshikazu Inoue 2 Toru rai
Cardiopulmonary Imaging Original Research kira et al. CT of Chronic Obstructive Pulmonary Disease Cardiopulmonary Imaging Original Research Masanori kira 1 Kazushige Toyokawa 1 Yoshikazu Inoue 2 Toru rai
Pediatric chest HRCT using the idose 4 Hybrid Iterative Reconstruction Algorithm: Which idose level to choose?
 Journal of Physics: Conference Series PAPER OPEN ACCESS Pediatric chest HRCT using the idose 4 Hybrid Iterative Reconstruction Algorithm: Which idose level to choose? To cite this article: M Smarda et
Journal of Physics: Conference Series PAPER OPEN ACCESS Pediatric chest HRCT using the idose 4 Hybrid Iterative Reconstruction Algorithm: Which idose level to choose? To cite this article: M Smarda et
Tracheobronchomalacia: morfologic evaluation in 64-MDTC.
 Tracheobronchomalacia: morfologic evaluation in 64-MDTC. Poster No.: C-1779 Congress: ECR 2011 Type: Educational Exhibit Authors: C. A. P. Fontes, A. A. S. M. Santos, A. L. Ferreira Neto, E. Marchiori,
Tracheobronchomalacia: morfologic evaluation in 64-MDTC. Poster No.: C-1779 Congress: ECR 2011 Type: Educational Exhibit Authors: C. A. P. Fontes, A. A. S. M. Santos, A. L. Ferreira Neto, E. Marchiori,
APSR RESPIRATORY UPDATES
 APSR RESPIRATORY UPDATES Volume 4, Issue 7 Newsletter Date: July 2012 APSR EDUCATION PUBLICATION Inside this issue: Quantitative imaging of airways Small-Airway Obstruction and Emphysema in Chronic Obstructive
APSR RESPIRATORY UPDATES Volume 4, Issue 7 Newsletter Date: July 2012 APSR EDUCATION PUBLICATION Inside this issue: Quantitative imaging of airways Small-Airway Obstruction and Emphysema in Chronic Obstructive
Pulmonary Function Testing The Basics of Interpretation
 Pulmonary Function Testing The Basics of Interpretation Jennifer Hale, M.D. Valley Baptist Family Practice Residency Objectives Identify the components of PFTs Describe the indications Develop a stepwise
Pulmonary Function Testing The Basics of Interpretation Jennifer Hale, M.D. Valley Baptist Family Practice Residency Objectives Identify the components of PFTs Describe the indications Develop a stepwise
Airway stenting in excessive central airway collapse
 Review Article on Aerodigestive Endoscopy Airway stenting in excessive central airway collapse Mihir Parikh, Jennifer Wilson, Adnan Majid, Sidhu Contributions: (I) Conception and design: All authors; (II)
Review Article on Aerodigestive Endoscopy Airway stenting in excessive central airway collapse Mihir Parikh, Jennifer Wilson, Adnan Majid, Sidhu Contributions: (I) Conception and design: All authors; (II)
Outcomes in the NLST. Health system infrastructure needs to implement screening
 Outcomes in the NLST Health system infrastructure needs to implement screening Denise R. Aberle, MD Professor of Radiology and Bioengineering David Geffen School of Medicine at UCLA 1 Disclosures I have
Outcomes in the NLST Health system infrastructure needs to implement screening Denise R. Aberle, MD Professor of Radiology and Bioengineering David Geffen School of Medicine at UCLA 1 Disclosures I have
Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012
 Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012 Recognize the importance of Pulmonary Function Testing in Cystic Fibrosis Be aware of different types
Mai ElMallah,MD Updates in Pediatric Pulmonary Care XII: An Interdisciplinary Program April 13, 2012 Recognize the importance of Pulmonary Function Testing in Cystic Fibrosis Be aware of different types
Pulmonary Function Testing
 Pulmonary Function Testing Let s catch our breath Eddie Needham, MD, FAAFP Program Director Emory Family Medicine Residency Program Learning Objectives The Astute Learner will: Become familiar with indications
Pulmonary Function Testing Let s catch our breath Eddie Needham, MD, FAAFP Program Director Emory Family Medicine Residency Program Learning Objectives The Astute Learner will: Become familiar with indications
UNIT TWO: OVERVIEW OF SPIROMETRY. A. Definition of Spirometry
 UNIT TWO: OVERVIEW OF SPIROMETRY A. Definition of Spirometry Spirometry is a medical screening test that measures various aspects of breathing and lung function. It is performed by using a spirometer,
UNIT TWO: OVERVIEW OF SPIROMETRY A. Definition of Spirometry Spirometry is a medical screening test that measures various aspects of breathing and lung function. It is performed by using a spirometer,
Chapter 6. Hester Gietema Cornelia Schaefer-Prokop Willem Mali Gerard Groenewegen Mathias Prokop. Accepted for publication in Radiology
 Chapter 6 Interscan variability of semiautomated volume measurements in intraparenchymal pulmonary nodules using multidetector-row computed tomography: Influence of inspirational level, nodule size and
Chapter 6 Interscan variability of semiautomated volume measurements in intraparenchymal pulmonary nodules using multidetector-row computed tomography: Influence of inspirational level, nodule size and
How to treat COPD? What is the mechanism of dyspnea? Smoking cessation
 : The Increasing Role of the FP Alan Kaplan, MD, CCFP(EM) Presented at the Primary Care Today: Education Conference and Medical Exposition, Toronto, Ontario, May 2006. Chronic obstructive pulmonary disease
: The Increasing Role of the FP Alan Kaplan, MD, CCFP(EM) Presented at the Primary Care Today: Education Conference and Medical Exposition, Toronto, Ontario, May 2006. Chronic obstructive pulmonary disease
DOES SMOKING MARIJUANA INCREASE THE RISK OF CHRONIC OBSTRUCTIVE PULMONARY DISEASE?
 DOES SMOKING MARIJUANA INCREASE THE RISK OF CHRONIC OBSTRUCTIVE PULMONARY DISEASE Pubdate: Tue, 14 Apr 2009 Source: Canadian Medical Association Journal (Canada) Copyright: 2009 Canadian Medical Association
DOES SMOKING MARIJUANA INCREASE THE RISK OF CHRONIC OBSTRUCTIVE PULMONARY DISEASE Pubdate: Tue, 14 Apr 2009 Source: Canadian Medical Association Journal (Canada) Copyright: 2009 Canadian Medical Association
Small Airways Disease. Respiratory Function In Small Airways And Asthma. Pathophysiologic Changes in the Small Airways of Asthma Patients
 Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Differential diagnosis
 Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Anyone who smokes and/or has shortness of breath and sputum production could have COPD
 COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
PFT Interpretation and Reference Values
 PFT Interpretation and Reference Values September 21, 2018 Eric Wong Objectives Understand the components of PFT Interpretation of PFT Clinical Patterns How to choose Reference Values 3 Components Spirometry
PFT Interpretation and Reference Values September 21, 2018 Eric Wong Objectives Understand the components of PFT Interpretation of PFT Clinical Patterns How to choose Reference Values 3 Components Spirometry
PULMONARY FUNCTION. VOLUMES AND CAPACITIES
 PULMONARY FUNCTION. VOLUMES AND CAPACITIES The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer (spiro = breath, meter = to measure). A bell spirometer
PULMONARY FUNCTION. VOLUMES AND CAPACITIES The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer (spiro = breath, meter = to measure). A bell spirometer
Comparison of Virtual Bronchoscopy with Fiberoptic Bronchoscopy Findings in Patients Exposed to Sulfur Mustard Gas
 Comparison of Virtual Bronchoscopy with Fiberoptic Bronchoscopy Findings in Patients Exposed to Sulfur Mustard Gas Poster No.: C-487 Congress: ECR 212 Type: Scientific Exhibit Authors: S. Akhlaghpoor,
Comparison of Virtual Bronchoscopy with Fiberoptic Bronchoscopy Findings in Patients Exposed to Sulfur Mustard Gas Poster No.: C-487 Congress: ECR 212 Type: Scientific Exhibit Authors: S. Akhlaghpoor,
Coexistence of confirmed obstruction in spirometry and restriction in body plethysmography, e.g.: COPD + pulmonary fibrosis
 Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Pulmonary Function Testing
 In the Clinic Pulmonary Function Testing Hawa Edriss MD, Gilbert Berdine MD The term PFT encompasses three different measures of lung function: spirometry, lung volumes, and diffusion capacity. In this
In the Clinic Pulmonary Function Testing Hawa Edriss MD, Gilbert Berdine MD The term PFT encompasses three different measures of lung function: spirometry, lung volumes, and diffusion capacity. In this
Clinical and radiographic predictors of GOLD-Unclassified smokers in COPDGene
 Clinical and radiographic predictors of GOLD-Unclassified smokers in COPDGene Emily S. Wan, John E. Hokanson, James R. Murphy, Elizabeth A. Regan, Barry J. Make, David A. Lynch, James D. Crapo, Edwin K.
Clinical and radiographic predictors of GOLD-Unclassified smokers in COPDGene Emily S. Wan, John E. Hokanson, James R. Murphy, Elizabeth A. Regan, Barry J. Make, David A. Lynch, James D. Crapo, Edwin K.
6- Lung Volumes and Pulmonary Function Tests
 6- Lung Volumes and Pulmonary Function Tests s (PFTs) are noninvasive diagnostic tests that provide measurable feedback about the function of the lungs. By assessing lung volumes, capacities, rates of
6- Lung Volumes and Pulmonary Function Tests s (PFTs) are noninvasive diagnostic tests that provide measurable feedback about the function of the lungs. By assessing lung volumes, capacities, rates of
This is a cross-sectional analysis of the National Health and Nutrition Examination
 SUPPLEMENTAL METHODS Study Design and Setting This is a cross-sectional analysis of the National Health and Nutrition Examination Survey (NHANES) data 2007-2008, 2009-2010, and 2011-2012. The NHANES is
SUPPLEMENTAL METHODS Study Design and Setting This is a cross-sectional analysis of the National Health and Nutrition Examination Survey (NHANES) data 2007-2008, 2009-2010, and 2011-2012. The NHANES is
PULMONARY FUNCTION TESTS
 Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Wheeze. Dr Jo Harrison
 Wheeze Dr Jo Harrison 9.9.14 Wheeze - Physiology a continuous musical sound that lasts longer than 250 msec. can be high-pitched or low-pitched, consist of single or multiple notes, and occur during inspiration
Wheeze Dr Jo Harrison 9.9.14 Wheeze - Physiology a continuous musical sound that lasts longer than 250 msec. can be high-pitched or low-pitched, consist of single or multiple notes, and occur during inspiration
Increased difference between slow and forced vital capacity is associated with reduced exercise tolerance in COPD patients
 Yuan et al. BMC Pulmonary Medicine 2014, 14:16 RESEARCH ARTICLE Open Access Increased difference between slow and forced vital capacity is associated with reduced exercise tolerance in COPD patients Wei
Yuan et al. BMC Pulmonary Medicine 2014, 14:16 RESEARCH ARTICLE Open Access Increased difference between slow and forced vital capacity is associated with reduced exercise tolerance in COPD patients Wei
Case Report Tracheomalacia Treatment Using a Large-Diameter, Custom-Made Airway Stent in a Case with Mounier-Kuhn Syndrome
 Case Reports in Pulmonology, Article ID 910135, 4 pages http://dx.doi.org/10.1155/2014/910135 Case Report Tracheomalacia Treatment Using a Large-Diameter, Custom-Made Airway Stent in a Case with Mounier-Kuhn
Case Reports in Pulmonology, Article ID 910135, 4 pages http://dx.doi.org/10.1155/2014/910135 Case Report Tracheomalacia Treatment Using a Large-Diameter, Custom-Made Airway Stent in a Case with Mounier-Kuhn
CLINICAL SIGNIFICANCE OF PULMONARY FUNCTION TESTS
 CLINICAL SIGNIFICANCE OF PULMONARY FUNCTION TESTS Upper Airway Obstruction* John C. Acres, M.D., and Meir H. Kryger, M.D.t chronic upper airway obstruction is frequently unrecognized or misdiagnosed as
CLINICAL SIGNIFICANCE OF PULMONARY FUNCTION TESTS Upper Airway Obstruction* John C. Acres, M.D., and Meir H. Kryger, M.D.t chronic upper airway obstruction is frequently unrecognized or misdiagnosed as
Difference Between The Slow Vital Capacity And Forced Vital Capacity: Predictor Of Hyperinflation In Patients With Airflow Obstruction
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 4 Number 2 Difference Between The Slow Vital Capacity And Forced Vital Capacity: Predictor Of Hyperinflation In Patients With Airflow Obstruction
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 4 Number 2 Difference Between The Slow Vital Capacity And Forced Vital Capacity: Predictor Of Hyperinflation In Patients With Airflow Obstruction
DIAGNOSTIC NOTE TEMPLATE
 DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
Expiratory central airway collapse in stable COPD and during exacerbations
 Leong et al. Respiratory Research (2017) 18:163 DOI 10.1186/s12931-017-0646-2 RESEARCH Expiratory central airway collapse in stable COPD and during exacerbations Paul Leong 1,2*, Anne Tran 1, Jhanavi Rangaswamy
Leong et al. Respiratory Research (2017) 18:163 DOI 10.1186/s12931-017-0646-2 RESEARCH Expiratory central airway collapse in stable COPD and during exacerbations Paul Leong 1,2*, Anne Tran 1, Jhanavi Rangaswamy
9/22/2015 CONFLICT OF INTEREST OBJECTIVES. Understanding COPD - Recent Research and the Evolving Definition of COPD for MNACVPR
 Understanding COPD - Recent Research and the Evolving Definition of COPD for MNACVPR by Scott Cerreta, BS, RRT Director of Education www.copdfoundation.org scerreta@copdfoundation.org CONFLICT OF INTEREST
Understanding COPD - Recent Research and the Evolving Definition of COPD for MNACVPR by Scott Cerreta, BS, RRT Director of Education www.copdfoundation.org scerreta@copdfoundation.org CONFLICT OF INTEREST
Understanding COPD - Recent Research and the Evolving Definition of COPD for MNACVPR
 Understanding COPD - Recent Research and the Evolving Definition of COPD for MNACVPR by Scott Cerreta, BS, RRT Director of Education www.copdfoundation.org scerreta@copdfoundation.org CONFLICT OF INTEREST
Understanding COPD - Recent Research and the Evolving Definition of COPD for MNACVPR by Scott Cerreta, BS, RRT Director of Education www.copdfoundation.org scerreta@copdfoundation.org CONFLICT OF INTEREST
Citation for pulished version (APA): Kolmos, H. J. The future of infection control: Role of the clinical microbiology laboratory.
 Syddansk Universitet The future of infection control Role of the clinical microbiology laboratory Kolmos, Hans Jørn Publication date: 2011 Document version Early version, also known as pre-print Citation
Syddansk Universitet The future of infection control Role of the clinical microbiology laboratory Kolmos, Hans Jørn Publication date: 2011 Document version Early version, also known as pre-print Citation
S P I R O M E T R Y. Objectives. Objectives 2/5/2019
 S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
Improved image quality of low-dose thoracic CT examinations with a new postprocessing software*
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 11, NUMBER 3, Summer 2010 Improved image quality of low-dose thoracic CT examinations with a new postprocessing software* Anne Catrine Traegde Martinsen,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 11, NUMBER 3, Summer 2010 Improved image quality of low-dose thoracic CT examinations with a new postprocessing software* Anne Catrine Traegde Martinsen,
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Chronic Cough. Abhishek Kumar, MD, MPH Pulmonary and Critical Care Mercy Medical Center, Cedar Rapids, IA
 Chronic Cough Abhishek Kumar, MD, MPH Pulmonary and Critical Care Mercy Medical Center, Cedar Rapids, IA What we shall discuss? Cough anatomy and pathophysiology Common etiologies Work-up Role of spirometry/pulmonary
Chronic Cough Abhishek Kumar, MD, MPH Pulmonary and Critical Care Mercy Medical Center, Cedar Rapids, IA What we shall discuss? Cough anatomy and pathophysiology Common etiologies Work-up Role of spirometry/pulmonary
High resolution computed tomography (HRCT) assessment of β 2 -agonist induced bronchodilation in chronic obstructive pulmonary disease patients
 European Review for Medical and Pharmacological Sciences High resolution computed tomography (HRCT) assessment of β 2 -agonist induced bronchodilation in chronic obstructive pulmonary disease patients
European Review for Medical and Pharmacological Sciences High resolution computed tomography (HRCT) assessment of β 2 -agonist induced bronchodilation in chronic obstructive pulmonary disease patients
Triennial Pulmonary Workshop 2012
 Triennial Pulmonary Workshop 2012 Rod Richie, M.D., DBIM Medical Director Texas Life Insurance Company, Waco, TX EMSI, Waco, TX Lisa Papazian, M.D., DBIM Assistant Vice President and Medical Director Sun
Triennial Pulmonary Workshop 2012 Rod Richie, M.D., DBIM Medical Director Texas Life Insurance Company, Waco, TX EMSI, Waco, TX Lisa Papazian, M.D., DBIM Assistant Vice President and Medical Director Sun
SGRQ Questionnaire assessing respiratory disease-specific quality of life. Questionnaire assessing general quality of life
 SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
Pediatric High-Resolution Chest CT
 Pediatric High-Resolution Chest CT Alan S. Brody, MD Professor of Radiology and Pediatrics Chief, Thoracic Imaging Cincinnati Children s s Hospital Cincinnati, Ohio, USA Pediatric High-Resolution CT Short
Pediatric High-Resolution Chest CT Alan S. Brody, MD Professor of Radiology and Pediatrics Chief, Thoracic Imaging Cincinnati Children s s Hospital Cincinnati, Ohio, USA Pediatric High-Resolution CT Short
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss?
 ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
Combined pulmonary fibrosis and emphysema; prevalence and follow up among health-care personnel
 Combined pulmonary fibrosis and emphysema; prevalence and follow up among health-care personnel Poster No.: C-0698 Congress: ECR 2013 Type: Scientific Exhibit Authors: K. Chae, G. Jin, S. Chon, Y. Lee;
Combined pulmonary fibrosis and emphysema; prevalence and follow up among health-care personnel Poster No.: C-0698 Congress: ECR 2013 Type: Scientific Exhibit Authors: K. Chae, G. Jin, S. Chon, Y. Lee;
Change in health-related quality of life over 1 month in cancer patients with high initial levels of symptoms and problems
 Syddansk Universitet Change in health-related quality of life over 1 month in cancer patients with high initial levels of symptoms and problems Lund Rasmussen, Charlotte; Johnsen, Anna Thit; Petersen,
Syddansk Universitet Change in health-related quality of life over 1 month in cancer patients with high initial levels of symptoms and problems Lund Rasmussen, Charlotte; Johnsen, Anna Thit; Petersen,
Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma
 Original Article Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma Feng-Jia Chen, Huai Liao, Xin-Yan Huang, Can-Mao Xie Department of Respiratory
Original Article Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma Feng-Jia Chen, Huai Liao, Xin-Yan Huang, Can-Mao Xie Department of Respiratory
Analysis of Lung Function
 Computer 21 Spirometry is a valuable tool for analyzing the flow rate of air passing into and out of the lungs. Flow rates vary over the course of a respiratory cycle (a single inspiration followed by
Computer 21 Spirometry is a valuable tool for analyzing the flow rate of air passing into and out of the lungs. Flow rates vary over the course of a respiratory cycle (a single inspiration followed by
Airways Disease MDT - 6th May 2014
 Airways Disease MDT - 6th May 2014 The inaugural AD-MDT was held on 6/5/14. The AIM of the meeting is to develop the skills and knowledge to be able to run an AD-MDT - the time frame from the start to
Airways Disease MDT - 6th May 2014 The inaugural AD-MDT was held on 6/5/14. The AIM of the meeting is to develop the skills and knowledge to be able to run an AD-MDT - the time frame from the start to
Tests Your Pulmonologist Might Order. Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital
 Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
PULMONARY EMBOLISM ANGIOCT (CTA) ASSESSMENT OF VASCULAR OCCLUSION EXTENT AND LOCALIZATION OF EMBOLI 1. BACKGROUND
 JOURNAL OF MEDICAL INFORMATICS & TECHNOLOGIES Vol. 11/2007, ISSN 1642-6037 Damian PTAK * pulmonary embolism, AngioCT, postprocessing techniques, Mastora score PULMONARY EMBOLISM ANGIOCT (CTA) ASSESSMENT
JOURNAL OF MEDICAL INFORMATICS & TECHNOLOGIES Vol. 11/2007, ISSN 1642-6037 Damian PTAK * pulmonary embolism, AngioCT, postprocessing techniques, Mastora score PULMONARY EMBOLISM ANGIOCT (CTA) ASSESSMENT
Pulmonary Function Testing. Ramez Sunna MD, FCCP
 Pulmonary Function Testing Ramez Sunna MD, FCCP Lecture Overview General Introduction Indications and Uses Technical aspects Interpretation Patterns of Abnormalities When to perform a PFT 1. Evaluation
Pulmonary Function Testing Ramez Sunna MD, FCCP Lecture Overview General Introduction Indications and Uses Technical aspects Interpretation Patterns of Abnormalities When to perform a PFT 1. Evaluation
S P I R O M E T R Y. Objectives. Objectives 3/12/2018
 S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
Spirometry in primary care
 Spirometry in primary care Wednesday 13 th July 2016 Dr Rukhsana Hussain What is spirometry? A method of assessing lung function Measures volume of air a patient can expel after a full inspiration Recorded
Spirometry in primary care Wednesday 13 th July 2016 Dr Rukhsana Hussain What is spirometry? A method of assessing lung function Measures volume of air a patient can expel after a full inspiration Recorded
Ligation of lymph vessels for the treatment of recurrent inguinal lymphoceles following lymphadenectomy
 Syddansk Universitet Ligation of lymph vessels for the treatment of recurrent inguinal lymphoceles following lymphadenectomy Toyserkani, Navid Mohamadpour; Nielsen, Henrik Toft; Bakholdt, Vivi T.; Sørensen,
Syddansk Universitet Ligation of lymph vessels for the treatment of recurrent inguinal lymphoceles following lymphadenectomy Toyserkani, Navid Mohamadpour; Nielsen, Henrik Toft; Bakholdt, Vivi T.; Sørensen,
Syddansk Universitet. Stem cell divisions per se do not cause cancer. Wensink, Maarten Jan; Vaupel, James W. ; Christensen, Kaare
 Syddansk Universitet Stem cell divisions per se do not cause cancer Wensink, Maarten Jan; Vaupel, James W. ; Christensen, Kaare Published in: Epidemiology DOI: 10.1097/EDE.0000000000000612 Publication
Syddansk Universitet Stem cell divisions per se do not cause cancer Wensink, Maarten Jan; Vaupel, James W. ; Christensen, Kaare Published in: Epidemiology DOI: 10.1097/EDE.0000000000000612 Publication
Impact of the new ATS/ERS pulmonary function test interpretation guidelines
 Respiratory Medicine (2007) 101, 2336 2342 Impact of the new ATS/ERS pulmonary function test interpretation guidelines Mary Elizabeth Kreider a,, Michael A. Grippi a,b a Division of Pulmonary, Allergy,
Respiratory Medicine (2007) 101, 2336 2342 Impact of the new ATS/ERS pulmonary function test interpretation guidelines Mary Elizabeth Kreider a,, Michael A. Grippi a,b a Division of Pulmonary, Allergy,
Understanding the Basics of Spirometry It s not just about yelling blow
 Understanding the Basics of Spirometry It s not just about yelling blow Carl D. Mottram, RRT RPFT FAARC Technical Director - Pulmonary Function Labs and Rehabilitation Associate Professor of Medicine -
Understanding the Basics of Spirometry It s not just about yelling blow Carl D. Mottram, RRT RPFT FAARC Technical Director - Pulmonary Function Labs and Rehabilitation Associate Professor of Medicine -
Improvement of Image Quality with ß-Blocker Premedication on ECG-Gated 16-MDCT Coronary Angiography
 16-MDCT Coronary Angiography Shim et al. 16-MDCT Coronary Angiography Sung Shine Shim 1 Yookyung Kim Soo Mee Lim Received December 1, 2003; accepted after revision June 1, 2004. 1 All authors: Department
16-MDCT Coronary Angiography Shim et al. 16-MDCT Coronary Angiography Sung Shine Shim 1 Yookyung Kim Soo Mee Lim Received December 1, 2003; accepted after revision June 1, 2004. 1 All authors: Department
A time-honored but almost forgotten sign of COPD: sabersheath trachea as a marker of severe airflow obstruction
 A time-honored but almost forgotten sign of COPD: sabersheath trachea as a marker of severe airflow obstruction Poster No.: C-0958 Congress: ECR 2013 Type: Scientific Exhibit Authors: F. Ciccarese, A.
A time-honored but almost forgotten sign of COPD: sabersheath trachea as a marker of severe airflow obstruction Poster No.: C-0958 Congress: ECR 2013 Type: Scientific Exhibit Authors: F. Ciccarese, A.
PULMONARY FUNCTION TESTING. Purposes of Pulmonary Tests. General Categories of Lung Diseases. Types of PF Tests
 PULMONARY FUNCTION TESTING Wyka Chapter 13 Various AARC Clinical Practice Guidelines Purposes of Pulmonary Tests Is lung disease present? If so, is it reversible? If so, what type of lung disease is present?
PULMONARY FUNCTION TESTING Wyka Chapter 13 Various AARC Clinical Practice Guidelines Purposes of Pulmonary Tests Is lung disease present? If so, is it reversible? If so, what type of lung disease is present?
Supplementary Appendix
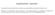 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Woodruff PG, Barr RG, Bleecker E, et al. Clinical significance
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Woodruff PG, Barr RG, Bleecker E, et al. Clinical significance
Respiratory Physiology In-Lab Guide
 Respiratory Physiology In-Lab Guide Read Me Study Guide Check Your Knowledge, before the Practical: 1. Understand the relationship between volume and pressure. Understand the three respiratory pressures
Respiratory Physiology In-Lab Guide Read Me Study Guide Check Your Knowledge, before the Practical: 1. Understand the relationship between volume and pressure. Understand the three respiratory pressures
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Spirometry. Obstruction. By Helen Grim M.S. RRT. loop will have concave appearance. Flows decreased consistent with degree of obstruction.
 1 2 Spirometry By Helen Grim M.S. RRT 3 4 Obstruction loop will have concave appearance. Flows decreased consistent with degree of obstruction. Volumes may be normal, but can decrease with severity of
1 2 Spirometry By Helen Grim M.S. RRT 3 4 Obstruction loop will have concave appearance. Flows decreased consistent with degree of obstruction. Volumes may be normal, but can decrease with severity of
Cigarette Smoking and Lung Obstruction Among Adults Aged 40 79: United States,
 NCHS Data Brief No. 8 January 25 Cigarette Smoking and Lung Obstruction Among Adults Aged 4 79: United States, 27 22 Ryne Paulose-Ram, Ph.D., M.A.; Timothy Tilert, B.S.; Charles F. Dillon, M.D., Ph.D.;
NCHS Data Brief No. 8 January 25 Cigarette Smoking and Lung Obstruction Among Adults Aged 4 79: United States, 27 22 Ryne Paulose-Ram, Ph.D., M.A.; Timothy Tilert, B.S.; Charles F. Dillon, M.D., Ph.D.;
Modifi ed CT perfusion contrast injection protocols for improved CBF quantifi cation with lower temporal sampling
 Investigations and research Modifi ed CT perfusion contrast injection protocols for improved CBF quantifi cation with lower temporal sampling J. Wang Z. Ying V. Yao L. Ciancibello S. Premraj S. Pohlman
Investigations and research Modifi ed CT perfusion contrast injection protocols for improved CBF quantifi cation with lower temporal sampling J. Wang Z. Ying V. Yao L. Ciancibello S. Premraj S. Pohlman
Research Protocol: Project summary
 Research Protocol: First clinical study with AiDA on patients as presented in the manuscript Can a single-breath nanoaerosol inhalation detect emphysema? A case-control study Project summary Nanoparticles
Research Protocol: First clinical study with AiDA on patients as presented in the manuscript Can a single-breath nanoaerosol inhalation detect emphysema? A case-control study Project summary Nanoparticles
COPD: early detection, screening and case-finding: what is the evidence? Prof. Jan-Willem Lammers, Md PhD Department of Respiratory Diseases
 COPD: early detection, screening and case-finding: what is the evidence? Prof. Jan-Willem Lammers, Md PhD Department of Respiratory Diseases «If you test one smoker with cough every day You will diagnose
COPD: early detection, screening and case-finding: what is the evidence? Prof. Jan-Willem Lammers, Md PhD Department of Respiratory Diseases «If you test one smoker with cough every day You will diagnose
Online Data Supplement. Prevalence of Chronic Obstructive Pulmonary Disease in Korea: Results of a Population-based Spirometry Survey
 Online Data Supplement Prevalence of Chronic Obstructive Pulmonary Disease in Korea: Results of a Population-based Spirometry Survey Dong Soon Kim, MD, Young Sam Kim MD, Kee Suk Chung MD, Jung Hyun Chang
Online Data Supplement Prevalence of Chronic Obstructive Pulmonary Disease in Korea: Results of a Population-based Spirometry Survey Dong Soon Kim, MD, Young Sam Kim MD, Kee Suk Chung MD, Jung Hyun Chang
ERS 2016 Congress Highlights Interstitial Lung Disease (ILD)
 ERS 216 Congress Highlights Interstitial Lung Disease (ILD) London, UK September 3 rd 7 th 216 The 26 th European Respiratory Society International Congress, (ERS) the largest respiratory meeting in the
ERS 216 Congress Highlights Interstitial Lung Disease (ILD) London, UK September 3 rd 7 th 216 The 26 th European Respiratory Society International Congress, (ERS) the largest respiratory meeting in the
Low-dose computed tomography (CT) protocol in the screening of patients with social exposure to asbestos
 Low-dose computed tomography (CT) protocol in the screening of patients with social exposure to asbestos Poster No.: C-3032 Congress: ECR 2010 Type: Scientific Exhibit Topic: Radiographers Authors: P.
Low-dose computed tomography (CT) protocol in the screening of patients with social exposure to asbestos Poster No.: C-3032 Congress: ECR 2010 Type: Scientific Exhibit Topic: Radiographers Authors: P.
COPD in Korea. Division of Pulmonary, Allergy and Critical Care Medicine of Hallym University Medical Center Park Yong Bum
 COPD in Korea Division of Pulmonary, Allergy and Critical Care Medicine of Hallym University Medical Center Park Yong Bum Mortality Rate 1970-2002, USA JAMA,2005 Global Burden of Disease: COPD WHO & World
COPD in Korea Division of Pulmonary, Allergy and Critical Care Medicine of Hallym University Medical Center Park Yong Bum Mortality Rate 1970-2002, USA JAMA,2005 Global Burden of Disease: COPD WHO & World
A method for the automatic quantification of the completeness of pulmonary fissures: evaluation in a database of subjects with severe emphysema
 Eur Radiol (2012) 22:302 309 DOI 10.1007/s00330-011-2278-0 CHEST A method for the automatic quantification of the completeness of pulmonary fissures: evaluation in a database of subjects with severe emphysema
Eur Radiol (2012) 22:302 309 DOI 10.1007/s00330-011-2278-0 CHEST A method for the automatic quantification of the completeness of pulmonary fissures: evaluation in a database of subjects with severe emphysema
behaviour are out of scope of the present review.
 explained about the test, a trial may be done before recording the results. The maneuver consists initially of normal tidal breathing. The subject then inhales to maximally fill the lungs. This is followed
explained about the test, a trial may be done before recording the results. The maneuver consists initially of normal tidal breathing. The subject then inhales to maximally fill the lungs. This is followed
National COPD Audit Programme
 National COPD Audit Programme Planning for every breath National Chronic Obstructive Pulmonary Disease (COPD) Audit Programme: Primary care audit (Wales) 2015 17 Data analysis and methodology Section 2:
National COPD Audit Programme Planning for every breath National Chronic Obstructive Pulmonary Disease (COPD) Audit Programme: Primary care audit (Wales) 2015 17 Data analysis and methodology Section 2:
Life-long asthma and its relationship to COPD. Stephen T Holgate School of Medicine University of Southampton
 Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Charles Darwin University
 Charles Darwin University Area-under-the-HbA1c-curve above the normal range and the prediction of microvascular outcomes an analysis of data from the Diabetes Control and Complications Trial Maple-Brown,
Charles Darwin University Area-under-the-HbA1c-curve above the normal range and the prediction of microvascular outcomes an analysis of data from the Diabetes Control and Complications Trial Maple-Brown,
11.3 RESPIRATORY SYSTEM DISORDERS
 11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
COUGH Dr. A m A it i e t sh A g A garwa w l Le L ctu t rer Departm t ent t o f f M e M dic i in i e
 COUGH Dr. Amitesh Aggarwal Lecturer Department of Medicine Cough is an explosive expiration that provides a normal protective mechanism for clearing the tracheobronchial tree of secretions and foreign
COUGH Dr. Amitesh Aggarwal Lecturer Department of Medicine Cough is an explosive expiration that provides a normal protective mechanism for clearing the tracheobronchial tree of secretions and foreign
To assess the pulmonary impairment in treated pulmonary tuberculosis patients using spirometry
 Original Research Article To assess the pulmonary impairment in treated pulmonary tuberculosis patients using spirometry Dhipu Mathew 1, Kirthana G 2, Krishnapriya R 1, Srinivasan R 3 1 Assistant Professor,
Original Research Article To assess the pulmonary impairment in treated pulmonary tuberculosis patients using spirometry Dhipu Mathew 1, Kirthana G 2, Krishnapriya R 1, Srinivasan R 3 1 Assistant Professor,
Dimensional quality control of Ti-Ni dental file by optical coordinate metrology and computed tomography
 Downloaded from orbit.dtu.dk on: Dec 20, 2017 Dimensional quality control of Ti-Ni dental file by optical coordinate metrology and computed tomography Yagüe-Fabra, J.A.; Tosello, Guido; Ontiveros, S.;
Downloaded from orbit.dtu.dk on: Dec 20, 2017 Dimensional quality control of Ti-Ni dental file by optical coordinate metrology and computed tomography Yagüe-Fabra, J.A.; Tosello, Guido; Ontiveros, S.;
