Factors Associated with Dysfunctional Breathing in patients with Difficult to Treat Asthma
|
|
|
- Fay Phoebe Moody
- 5 years ago
- Views:
Transcription
1 Accepted Manuscript Factors Associated with Dysfunctional Breathing in patients with Difficult to Treat Asthma Eve Denton, MBBS Hons MPH FRACP, Janet Bondarenko, B Physio, TunnRen Tay, MBBS MRCP, Joy Lee, BHB MBChB FRACP, Naghmeh Radhakrishna, MBBS FRACP, Fiona Hore-Lacy, BNutSci Hons, Catherine Martin, PhD, Ryan Hoy, MBBS FRACP, Robyn O Hehir, FAHMS PhD FRACP, Eli Dabscheck, MBBS FRACP, Mark Hew, MBBS PhD FRACP PII: S (18) DOI: Reference: JAIP 1899 To appear in: The Journal of Allergy and Clinical Immunology: In Practice Received Date: 30 August 2018 Revised Date: 1 November 2018 Accepted Date: 19 November 2018 Please cite this article as: Denton E, Bondarenko J, Tay T, Lee J, Radhakrishna N, Hore-Lacy F, Martin C, Hoy R, O Hehir R, Dabscheck E, Hew M, Factors Associated with Dysfunctional Breathing in patients with Difficult to Treat Asthma, The Journal of Allergy and Clinical Immunology: In Practice (2019), doi: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
2 1 2 3 Factors Associated with Dysfunctional Breathing in patients with Difficult to Treat Asthma Authors: Eve Denton MBBS(Hons) MPH FRACP 1, 2, Janet Bondarenko B Physio 3 TunnRen Tay MBBS MRCP 1, Joy Lee BHB MBChB FRACP 1,Naghmeh Radhakrishna 1 MBBS FRACP 1, Fiona Hore-Lacy BNutSci(Hons) 1, Catherine Martin PhD 2, Ryan Hoy MBBS FRACP 1,2, Robyn O Hehir FAHMS PhD FRACP 1,4, Eli Dabscheck 1 MBBS FRACP 1, Mark Hew 1 MBBS PhD FRACP 1,2 1. Allergy, Asthma & Clinical Immunology, The Alfred Hospital, 55 Commercial Road, Melbourne 2. Public Health & Preventive Medicine, Monash University 3. Physiotherapy Department, The Alfred Hospital, Melbourne 4. Department of Medicine, Central Clinical School, Monash University Corresponding Author: Dr Eve Denton Respiratory Medicine, The Alfred Hospital 55 Commercial Road, Melbourne, Australia e.denton@alfred.org.au 24
3 Word count: Abstract: 197 Text: Conflicts of Interest: There are no conflicts of interest reported for any author in relation to this study. Funding: This research did not receive any specific grant from funding agencies in the public, commercial or not-for-profit sectors.
4 Abstract Background: Understanding of dysfunctional breathing in difficult asthma patients who remain symptomatic despite maximal inhaler therapy is limited Objective: We characterised the pattern of dysfunctional breathing in patients with difficult asthma and identified possible contributory factors. Methods: Dysfunctional breathing was identified in patients with difficult asthma using the Nijmegen questionnaire (score >23). Demographics, asthma variables, and comorbidities were assessed. Multivariate logistic regression was performed for dysfunctional breathing, adjusted for age, sex, body mass index and airflow obstruction. Results: Of 157 patients with difficult asthma, 73 (47%) had dysfunctional breathing. Compared to patients without dysfunctional breathing, those with dysfunctional breathing experienced poorer asthma status [symptom control, quality of life (QOL) and exacerbation rates] and greater unemployment. Additionally, more frequently they had elevated sino-nasal outcome test (SNOT- 22) scores, anxiety, depression, sleep apnoea and gastroesophageal reflux. On multivariate analysis, anxiety (OR=3.26, 95%CI , p=0.02), depression (OR= %CI , p=0.03) and SNOT-22 (OR % CI , 61 p=0.03) were independent risk factors for dysfunctional breathing Conclusion: Dysfunctional breathing is common in difficult asthma and associated with worse asthma status and unemployment. The independent association with
5 psychological disorders and nasal obstruction highlight an important interaction between comorbid treatable traits in difficult asthma
6 Highlights: 1. What is already known about this topic? Dysfunctional breathing is an important treatable trait in difficult asthma. Little is known about why it arises, whom it afflicts and who should be assessed. 2. What does the article add to our knowledge? This study found that dysfunctional breathing is present in almost 50% of difficult asthma patients, and associated with poorer asthma status and control. Anxiety, depression, and sino-nasal scores were independent risk factors for dysfunctional breathing. 3. How does the study impact current management guidelines? This study builds a profile of dysfunctional breathers in difficult asthma and highlights an important interaction between comorbid treatable traits. Key words: Asthma Difficult asthma Severe asthma Treatable trait Dysfunctional breathing Breathing pattern disorder Depression Anxiety Chronic rhinosinusitis
7 Abbreviations: ACQ6 Asthma Control Questionnaire 6 QOL quality of life AQLQ asthma-related quality of life HADS A and D Hospital Anxiety and Depression Scale RAST radioallergosorbent testing ENT Ear, Nose and Throat SNOT-22 sino-nasal outcome test OSA Obstructive sleep apnoea GORD Gastroesophageal reflux disease GERDQ Gastroesophageal reflux disease questionnaire VCD vocal cord dysfunction VCD Q vocal cord dysfunction questionnaire FEV1 Forced expiratory volume in one second FENO- Fractional exhaled nitric oxide ppb- parts per billion IgE immunoglobulin E BMI body mass index RCAT Rhinitis control assessment test SD standard deviation n number
8 Introduction A subgroup of asthma patients has difficult asthma, with uncontrolled disease despite maximal inhaled therapy. These patients experience significant morbidity, consume substantial healthcare resources, and present an ongoing clinical challenge.(1) Poor asthma control is manifested by residual symptom burden following treatment, but does not always correspond to the severity of airflow obstruction. One cause of disproportionate breathlessness in asthma is dysfunctional breathing, which is increasingly recognised but remains poorly understood.(2, 3) In dysfunctional breathing, a disruption to the normal biomechanical pattern of breathing results in respiratory and non-respiratory symptoms.(4) There are thought to be multiple different abnormal breathing patterns that fall under the umbrella of dysfunctional breathing including the most well described, hyperventilation, but other forms include deep sighing, thoracic-dominant breathing, mouth breathing, accessory muscle use at rest, and thoracoabdominal asynchrony. All are inefficient methods of breathing that can result in symptoms.(5) Furthermore, these patterns of dysfunctional breathing have been shown to commonly overlap within the same patient.(6) The presence of dysfunctional breathing can cause symptoms in asthma patients that are unresponsive to escalation of asthma therapies but responsive to breathing 145 retraining.(6) The Nijmegen questionnaire incorporates questions that cover four domains including symptoms related to the respiratory system, the peripheral and central
9 neurovascular systems and those related to anxiety.(7, 8) (9-11) The questionnaire is able to distinguish adults with hyperventilation from healthy controls,(7, 12) and also remains the only validated tool to detect hyperventilation in the presence of asthma.(13) We have previously reported the substantial presence of dysfunctional breathing in patients with difficult asthma.(14) Dysfunctional breathing occurring at this end of the asthma spectrum may well exert the greatest clinical impact, but also yield the maximum therapeutic potential. In this study, we therefore aimed to characterise the presence of dysfunctional breathing in a difficult asthma cohort and to identify risk factors which may contribute to its development. We assessed patient demographics, asthma variables and other comorbid treatable traits
10 Methods: Study design We included consecutive adult patients who underwent systematic assessment for difficult asthma at our institution between 1 st June 2014 and 31 st December 2017 as previously described.(15) Patients were referred to our difficult asthma program from specialist respiratory and allergy physicians with at least one of the following; severe or frequent asthma exacerbations despite treatment, inadequate control of asthma symptoms, unclear diagnosis, severe airflow obstruction and/or complex management issues. These patients underwent a structured evaluation process comprising a standardised history, examination, adherence monitoring (via electronic monitoring device where possible)(16) and a structured investigation process with the option for specific investigations and interventions based on clinical need. All patients evaluated via the program completed asthma and comorbidity questionnaires at baseline as well as lung function, skin prick testing and other investigations as clinically indicated. Asthma diagnosis was based on the demonstration of variable airflow obstruction via bronchodilator response, peak flow variability and/or bronchoprovocation testing in the presence of a consistent clinical history. Asthma control was assessed via the six-item Asthma Control Questionnaire (ACQ6), a validated questionnaire in asthma.(17-19). Quality of life (QOL) was assessed via the Asthma Quality of Life Questionnaire (AQLQ).(20-23) Ethics approval for this analysis was obtained from the Alfred Hospital Human Research Ethics Committee (Approval reference 285/15) and requirement for specific informed consent was waived.
11 Patients were diagnosed with dysfunctional breathing if they had a positive Nijmegen Questionnaire defined by a score greater than 23 and accompanied by compatible clinical symptoms including excessive dyspnoea.(7, 12) As with any questionnaire the Nijmegen score has limitations including a variation in cut off scores used for detecting the presence of dysfunctional breathing in different studies, for this reason a sensitivity analysis was performed using the Nijmegen score as a continuous rather than dichotomous variable. With regard to other comorbidities, psychiatric history was assessed by a history of clinical diagnosis and the Hospital Anxiety and Depression Score (HADS A and HADS D), a questionnaire that has been validated to detect the presence of current anxiety and depression in an outpatient population. (24) A HADS A score of >11 signifies presence of anxiety and a HADS D score of >8 signifies the presence of depression.(24) Atopy was defined by the presence of allergen specific IgE by a positive skin prick test and/or positive serological testing (RAST) to common aeroallergens. Allergic rhinitis diagnosis was based on clinical allergist diagnosis in the presence of atopy and the level of symptom control was based on the Rhinitis Control Assessment Test (RCAT), a validated questionnaire that assesses rhinitis-specific symptoms.(25) Chronic rhinosinusitis diagnosis was based on clinical symptoms with a positive CT sinuses or compatible ear, nose and throat (ENT) specialist examination. Control of chronic rhinosinusitis symptoms was assessed using the validated Sinonasal outcome score (SNOT-22 score).(26) Obstructive sleep apnoea (OSA) was diagnosed on polysomnography. Gastro-oesophageal reflux (GORD) diagnosis
12 was based on compatible clinical symptoms plus an elevated GERD-Q score >2 or known history of GORD on acid suppression medication. Vocal cord dysfunction (VCD) was diagnosed clinically by a specialist in VCD (ENT surgeon, speech pathologist or respiratory physician) and supported by the Pittsburgh Index and the VCD-Q Questionnaires. A subgroup of patients had the diagnosis confirmed by visualisation of paroxysmal vocal fold motion on laryngoscopy. Statistical methods Nijmegen score was categorized, with a cut-off of >23 signifying the presence of dysfunctional breathing according to previously published data.(7, 27) Univariate and multivariate analysis were undertaken using logistic regression. Selected variables with p values <0.1 were included in the logistic regression model to determine factors independently associated with dysfunctional breathing. In addition, a decision was made a priori to include sex, age, FEV1 %predicted, and body mass index in the model regardless of p values on univariate analyses. Data were analysed with SPSS Version 24 (IBM, Armonk, NY)
13 Results: Patient Characteristics A total of 163 consecutive patients with difficult asthma underwent systematic assessment, of whom 157 completed Nijmegen questionnaires and were included for analysis. Among 157 included patients, the prevalence of dysfunctional breathing was 47% (73/157). The distribution of Nijmegen scores showed a biphasic elevation with peaks at 10 and 24 in what otherwise approximated a normal distribution. Baseline characteristics of the cohort are presented in Table 1, stratified by the presence or absence of dysfunctional breathing. 102 were female (65%). Female patients had significantly higher mean Nijmegen scores (24 versus 20, p=0.04). Mean age was 52 ±14 years (n=157) and significantly different between the sexes; females 49 ± 14 and males 56 ± 13 (p=0.005). There was no difference in mean age between those with and without dysfunctional breathing (p=0.7). Only 52% of the cohort were employed and those with dysfunctional breathing were significantly less likely to be employed (44% versus 61%, p=0.04). Lung function and phenotype There was no difference in FEV1% predicted, total serum IgE, blood eosinophils or FeNO in those with and without dysfunctional breathing (Table 1). Patients with the most severe degree of airflow obstruction (FEV1%predicted <40%) had similar Nijmegen scores to those with less severe airflow obstruction (mean 22.3 versus 22.5, p=0.95) Asthma control and quality of life
14 As expected, baseline asthma control overall was poor with mean number of severe exacerbations in the 6 months prior to review of 2.6 ± 2.1 and ACQ6 2.4 ± 1.3 (Table 1). Those with dysfunctional breathing had a significantly higher number of exacerbations in the 6 months prior to review (3 versus 2.5, p = 0.037) and a non-significant increase in reliever use in puffs per week (38 versus 27, p = 0.17). Those with dysfunctional breathing also had worse asthma control; ACQ 62.8 versus 2.1, p= Asthma-related quality of life, measured by the AQLQ, was worse in those with dysfunctional breathing (3.8 versus 4.6, p <0.001). Comorbidity diagnosis and control Body mass index (BMI) was elevated at baseline but did not differ significantly between those with and without elevated Nijmegen scores (p=0.5). Psychiatric comorbidity was frequent in the cohort with 25% of patients having anxiety and 29% depression. Those with positive Nijmegen scores had a significantly higher prevalence of comorbid anxiety (41% versus 11%, p<0.001) and depression (44% versus 18%, p=0.001). Similarly, there were higher HADS scores in those with positive Nijmegen scores, HADS A (10 versus 5.3, p <0.001) and HADS D (7.6 versus 3.6, p <0.001) scores. Allergic rhinitis and chronic rhinosinusitis were not more frequent in those with dysfunctional breathing (Table 1). However, symptom control scores were significantly worse with allergic rhinitis control, measured by RCAT, (19 versus 22, n = 151, p = 0.009) and sinonasal symptom scores, measured by SNOT-22, (47 versus 32, n = 155, p <0.001, MCID 9). OSA (41% versus 24%, n=157, p=0.02) and GORD (59% versus 35%, n=157, p=0.002) were significantly more frequent in those with dysfunctional breathing. Vocal
15 cord dysfunction was not found more frequently in dysfunctional breathing (Table 1) Multivariate analysis On multiple logistic regression, sinonasal symptoms (SNOT-22, OR % CI , p=0.03), anxiety (OR=3.26, 95%CI , p=0.02), and depression (OR= %CI , p=0.03) were all independent risk factors for dysfunctional breathing (Table 2). Results were similar when analysis was performed using Nijmegen score as a continuous rather than as a dichotomous variable (data not shown)
16 Discussion Given the extremely high prevalence of dysfunctional breathing in this difficult asthma cohort of almost 50% there is a profound need to enhance detection and treatment of dysfunctional breathing. In this study, patients with dysfunctional breathing had poorer asthma status and unemployment, which are key patient outcomes. Dysfunctional breathing was also independently predicted by anxiety, depression, and uncontrolled sino-nasal disease, suggesting an important interaction between multiple comorbid treatable traits (Figure 2). These findings offer potential mechanistic insights and novel treatment avenues for dysfunctional breathing. Breathlessness is common in difficult asthma patients and this breathlessness may sometimes be disproportionate to the degree of airway pathology.(4) Dysfunctional breathing is a common but under recognised cause of excessive breathlessness in this population, and is important to identify due to the potential for treatment.(28) Breathing re-training in mild-moderate asthmatics improves QOL and symptoms(29), and recent data from our group suggest similar benefits in more severe asthma.(6) It is possible that all difficult asthma patients may derive benefit from breathing retraining regardless of Nijmegen score. However in resource limited environments review of all patients by a specialist physiotherapist is not feasible and a method of identifying patients 345 who may benefit most is important The first key finding in this study was that psychiatric disease is independently associated with dysfunctional breathing among patients with difficult asthma.
17 This association has long been suspected even though previous evidence has been scarce. (30-33) After adjusting for multiple variables, difficult asthma patients with dysfunctional breathing were 3.3 times more likely to have anxiety and 2.8 times more likely to have depression than those without dysfunctional breathing. These are important findings, not least because these conditions are potentially treatable. Other data from our centre have revealed that breathing retraining improves Nijmegen scores but has no effect on HADS scores. This suggests that psychiatric disease should be specifically addressed alongside breathing retraining in those with both conditions.(6) The second key finding on multivariate analysis was that difficult asthma patients with dysfunctional breathing were more likely to have elevated sinonasal scores. This association is biologically plausible, as uncontrolled nasal congestion could leading to mouth breathing, itself a form of dysfunctional breathing.(30, 34) Therefore, assiduous attention to treating sino-nasal comorbidities may well be important to reduce dysfunctional breathing symptoms. Indeed, a previous longitudinal report from our centre found that improvements in both sino-nasal scores and Nijmegen scores could be achieved through active targeting of comorbidities in difficult asthma.(3) Comorbidities in difficult asthma are considered to be an important bundle of treatable traits, each of which may impact asthma control.(3, 35) The data from this study supports the hypothesis that interactions may also occur between these comorbid treatable traits.(3) It is possible that clusters of such
18 comorbidities may exert a combined effects on asthma outcomes, and this area requires further study On univariate analysis, patients with dysfunctional breathing in our cohort experienced significantly more asthma exacerbations requiring oral corticosteroids. They also had worse asthma control and quality of life. The difference between AQLQ scores in those with positive Nijmegen compared to negative Nijmegen was statistically and clinically significant (0.93, minimal clinically important difference 0.5.) Thus the potential benefit of identifying and treating dysfunctional breathers amongst difficult asthma patients may be substantial. In this cohort, no association was found between lung function impairment and elevated Nijmegen scores. We specifically examined the subset of patients with the most severe airways obstruction, who might be postulated to have a higher likelihood of breathlessness due to organic disease. However, their Nijmegen scores were no different to those without severe airways obstruction. Similarly, inflammatory biomarker levels such as total serum IgE, atopic status, and serum eosinophils were unrelated to Nijmegen scores. These results highlight the need to investigate for dysfunctional breathing in all difficult asthma patients regardless of lung function impairment or inflammatory phenotype We found that those with dysfunctional breathing were significantly less likely on univariate analysis to be employed, an important finding given the relatively young population and the economic implications. Similar to previous data we
19 found an association between younger age and the presence of dysfunctional breathing. Unlike other studies we found no correlation between the presence of dysfunctional breathing and sex.(36) There was no statistically significant association found between the presence of dysfunctional breathing and VCD. It is possible that this association was underestimated due to our strict diagnostic criteria for VCD requiring patients to have either undergone laryngoscopy or been diagnosed by a specialist in this area. However, not all patients underwent laryngoscopy or were reviewed by VCD specialists. We used the presence of an elevated Nijmegen score to indicate the presence of dysfunctional breathing. Although the Nijmegen score has limited utility as a diagnostic tool, it remains the only validated method of diagnosing dysfunctional breathing in asthma patients. In the absence of a gold standard diagnosis this is the most widely used and practical diagnostic tool. Although data were collected prospectively the analysis was performed retrospectively and this could lead to information bias. This was an uncontrolled study and suffers from the lack of an appropriately matched control group. In conclusion, dysfunctional breathing affects almost half of patients with difficult asthma. It is independently associated with anxiety, depression and poorer upper airway scores, highlighting an interaction between comorbid treatable traits. These data highlight the importance of addressing dysfunctional
20 breathing in difficult asthma, and may offer enhanced diagnostic and treatment strategies. 424
21 References Israel E, Reddel HK. Severe and Difficult-to-Treat Asthma in Adults. New England Journal of Medicine. 2017;377(10): Radhakrishna N, Tay TR, Hore-Lacy F, Stirling R, Hoy R, Dabscheck E, et al. Validated questionnaires heighten detection of difficult asthma comorbidities. Journal of Asthma. 2017;54(3): Tay TR, Hew M. Comorbid treatable traits in difficult asthma: Current evidence and clinical evaluation. Allergy. 2017;73(7): Depiazzi J, Everard ML. Dysfunctional breathing and reaching one s physiological limit as causes of exercise-induced dyspnoea. Breathe. 2016;12: Boulding R, Stacey R, Niven R, Fowler SJ. Dysfunctional breathing: a review of the literature and proposal for classification. European Respiratory Review. 2016;25: Denton E, Bondarenko J, O'Hehir RE, Hew M. Breathing pattern disorderin difficult asthma: characteristics and improvement in asthma control and quality of life after breathing re-training. Allergy. 2018;0(ja). 7. van Dixhoorn J, Folgering H. The Nijmegen Questionnaire and dysfunctional breathing. ERJ Open Research. 2015;1(1): Courtney R, van Dixhoorn J, Greenwood KM, Anthonissen EL. Medically unexplained dyspnea: partly moderated by dysfunctional (thoracic dominant) breathing pattern. The Journal of asthma : official journal of the Association for the Care of Asthma. 2011;48(3): Han JN, Schepers R, Stegen K, Van den Bergh O, Van de Woestijne KP. Psychosomatic symptoms and breathing pattern. Journal of psychosomatic research. 2000;49(5): Hornsveld H, Garssen B. Hyperventilation syndrome: an elegant but scientifically untenable concept. The Netherlands journal of medicine. 1997;50(1): Prys-Picard CO, Kellett F, Niven RM. Disproportionate breathlessness associated with deep sighing breathing in a patient presenting with difficult-totreat asthma. Chest. 2006;130(6): van Dixhoorn J, Duivenvoorden HJ. Efficacy of Nijmegen Questionnaire in recognition of the hyperventilation syndrome. Journal of psychosomatic research. 1985;29(2): Grammatopoulou EP, Skordilis EK, Georgoudis G, Haniotou A, Evangelodimou A, Fildissis G, et al. Hyperventilation in asthma: a validation study of the Nijmegen Questionnaire--NQ. The Journal of asthma : official journal of the Association for the Care of Asthma. 2014;51(8): Radhakrishna N, Tay TR, Hore-Lacy F, Hoy R, Dabscheck E, Hew M. Profile of difficult to treat asthma patients referred for systematic assessment. Respiratory Medicine. 2016;117: Tay TR, Lee J, Radhakrishna N, Hore-Lacy F, Stirling R, Hoy R, et al. A Structured Approach to Specialist-referred Difficult Asthma Patients Improves Control of Comorbidities and Enhances Asthma Outcomes. Journal of Allergy and Clinical Immunology in Practice. 2017( (Electronic)).
22 Lee J, Ren Tay T, Radhakrishna N, Hore-Lacy F, Mackay A, Hoy R, et al. Non-adherence in the era of severe asthma biologics and thermoplasty. European Respiratory Journal Juniper EF, O byrne PM, Guyatt Gh, Ferrie Pj, King Dr. Development and validation of a questionnaire to measure asthma control. European Respiratory Journal. 1999;14(4): Jia CE, Zhang HP, Lv Y, Liang R, Jiang YQ, Powell H, et al. The Asthma Control Test and Asthma Control Questionnaire for assessing asthma control: Systematic review and meta-analysis. Journal of Allergy and Clinical Immunology. 2013;131(3): F Juniper E, Svensson K, Mörk A-C, Ståhl E. Measurement properties and interpretation of three shortened versions of the Asthma Control Questionnaire p. 20. Juniper EF, Guyatt GH, Epstein RS, Ferrie PJ, Jaeschke R, Hiller TK. Evaluation of impairment of health related quality of life in asthma: development of a questionnaire for use in clinical trials. Thorax. 1992;47(2): Juniper EF, Guyatt GH, Ferrie PJ, Griffith LE. Measuring Quality of Life in Asthma. American Review of Respiratory Disease. 1993;147(4): Mölken M, Custers F, Doorslaer E, Jansen CCM, Heurman L, Maesen FPV, et al. Comparison of performance of four instruments in evaluating the effects of salmeterol on asthma quality of life p. 23. Rowe BH, Oxman AD. Performance of an Asthma Quality of Life Questionnaire in an Outpatient Setting. American Review of Respiratory Disease. 1993;148(3): Law M, Naughton MT, Dhar A, Barton D, Dabscheck E. Validation of two depression screening instruments in a sleep disorders clinic. Journal of clinical sleep medicine : JCSM : official publication of the American Academy of Sleep Medicine. 2014;10(6): Schatz M, Meltzer Eo Fau - Nathan R, Nathan R Fau - Derebery MJ, Derebery Mj Fau - Mintz M, Mintz M Fau - Stanford RH, Stanford Rh Fau - Dalal AA, et al. Psychometric validation of the rhinitis control assessment test: a brief patient-completed instrument for evaluating rhinitis symptom control. Annals Allergy Asthma Immunology. 2010;104(2): Hopkins C, Gillett S, Slack R, Lund VJ, Browne JP. Psychometric validity of the 22-item Sinonasal Outcome Test. Clinical Otolaryngology. 2009;34(5): Vansteenkiste J, Rochette F, Demedts M. Diagnostic tests of hyperventilation syndrome. European Respiratory Journal. 1991;4(4): Holloway EA, West RJ. Integrated breathing and relaxation training (the Papworth method) for adults with asthma in primary care: a randomised controlled trial. Thorax. 2007;62(12): Bruton A, Lee A, Yardley L, Raftery J, Arden-Close E, Kirby S, et al. Physiotherapy breathing retraining for asthma: a randomised controlled trial. The Lancet Respiratory Medicine. 2018;6(1): Agache I, Ciobanu C, Paul G, Rogozea L. Dysfunctional breathing phenotype in adults with asthma - incidence and risk factors. Clinical and Translational Allergy. 2012;2:18-.
23 Mora JD, Grant L, Kenyon P, Patel MK, Jenner FA. Respiratory Ventilation and Carbon Dioxide Levels in Syndromes of Depression. British Journal of Psychiatry. 2018;129(5): Stevenson I, Ripley HS. Variations in respiration and in respiratory symptoms during changes in emotion. Psychosomatic Medicine. 1952;14: Gardner WN. The Pathophysiology of Hyperventilation Disorders. Chest. 1996;109(2): Bartley J. Nasal Congestion and Hyperventilation Syndrome. American Journal of Rhinology. 2005;19(6): Agusti A, Bel E, Thomas M, Vogelmeier C, Brusselle G, Holgate S, et al. Treatable traits: toward precision medicine of chronic airway diseases. European Respiratory Journal. 2016;47(2): Thomas M, McKinley RK, Freeman E, Foy C. Prevalence of dysfunctional breathing in patients treated for asthma in primary care: cross sectional survey. BMJ : British Medical Journal. 2001;322(7294): Figure Legends Figure 1 Distribution of Nijmegen scores amongst difficult asthma patients. The interrupted line indicates the cut-off score for dysfunctional breathing diagnosis Figure 2 A proposed paradigm of associations and consequences of dysfunctional breathing in difficult asthma
24 Tables: Table 1: Baseline characteristics of patients with difficult asthma (n = 157), comparing those with (Nijmegen score >23) and without dysfunctional breathing. Difficult asthma (n=157) No dysfunctional breathing (n=84) With dysfunctional breathing (n=73) p-value Demographics Age (mean ± SD) 52 ± ± ± Female sex n(%) 102 (65%) 51 (61%) 51 (70%) 0.23 Employed n(%) 82 (52%) 51/84 (61%) 31/70 (44%) 0.04 Smoker: never n(%) 88 (56%) 52/84 (62%) 36/73 (49%) ex 61 (39%) 27/84 (32%) 34/73 (47%) 0.25 current 7 (4.5%) 4/84 (5%) 3/73 (4%) Asthma variables Asthma duration (mean ± SD) 30.4 ± ± ± FEV1 (% predicted) 67 ± ± ± Blood eosinophils (10 9 /L) 0.34 ± ± ± FENO (ppb), n= ± ± ± Serum total IgE (ku/l) 515 ± ± ± Exacerbations in prior 6 months 2.6 ± ± ± Reliever use (puffs per week) 32 ± ± ± Six-item Asthma Control Questionnaire 2.4 ± ± ± Asthma Quality of Life Questionnaire 4.2 ± ± ± 1.2 <0.001 Comorbidities Obesity n(%) 82 (52%) 41/84 (49%) 41/73 (56%) BMI kg/m 2 (mean ± SD) 31.4 ± ± ± Chronic rhinosinusitis n(%) 63/157 (40%) 36/84 (43%) 27/73 (37%) SNOT-22 (mean ± SD) 39 ± ± ± 20 <0.001 Allergic rhinitis n (%) 82/157 (52%) 45/84 (54%) 37/73 (51%) RCAT (mean ± SD) 21 ± ± ± Anxiety- clinical diagnosis n(%) 39/130 (30%) 14/69 (20%) 25/61 (41%) Anxiety HADS A > 11 n(%) 38/154 (25%) 9/83 (11%) 29/71 (41%) <0.001 Depression- clinical diagnosis n(%) 44/130 (34%) 17/69 (25%) 27/61 (44%) Depression HADS D >8 n(%) 46/155 (30%) 15/84 (18%) 31/71 (44%) <0.001 VCD- clinical diagnosis n(%) 58/157 (37%) 27/84 (32%) 31/73 (43%) VCD on laryngoscopy n(%) 25/157 (16%) 13/84 (16%) 12/73 (16%) 0.87 Gastro-oesophageal reflux n(%) 72/157 (46%) 29/84 (35%) 43/73 (59%) Obstructive sleep apnoea n(%) 50/157 (32%) 20/84 (24%) 30/73 (41%) 0.02 SD standard deviation, n number, FEV 1 Forced expiratory volume in one second; FE NO - Fractional exhaled nitric oxide; ppb- parts per billion; IgE immunoglobulin E; BMI body mass index; SNOT-22 sino-nasal outcome test; RCAT Rhinitis control assessment test; HADS A and D Hospital Anxiety and Depression Scale; VCD Vocal cord dysfunction
25 Table 2: Multivariate analysis for dysfunctional breathing OR 95% CI p-value (*<0.05) Male sex Age FEV1 (% predicted) Body mass index Exacerbations in prior 6 months Asthma Control Questionnaire Asthma Quality of Life Questionnaire Anxiety on Hospital Anxiety and Depression Score Depression on Hospital Anxiety and Depression Score * * Sino Nasal Outcome Test * Obstructive Sleep Apnoea Gastroesophageal Reflux Disease OR; odds ratio, CI; confidence interval; FEV 1 ;Forced expiratory volume in one second
26
27
Difficult Asthma Assessment: A systematic approach
 Difficult Asthma Assessment: A systematic approach Dr Naghmeh Radhakrishna Respiratory, Sleep & Allergy Physician Allergy, Asthma & Clinical Immunology Service The Alfred Hospital Melbourne, Australia
Difficult Asthma Assessment: A systematic approach Dr Naghmeh Radhakrishna Respiratory, Sleep & Allergy Physician Allergy, Asthma & Clinical Immunology Service The Alfred Hospital Melbourne, Australia
Professor Richard Beasley
 Professor Richard Beasley University of Otago Director Medical Research Institute of New Zealand Wellington 14:00-14:55 WS #111: Towards Precision Medicine in Asthma -Treatable Traits 15:05-16:00 WS #121:
Professor Richard Beasley University of Otago Director Medical Research Institute of New Zealand Wellington 14:00-14:55 WS #111: Towards Precision Medicine in Asthma -Treatable Traits 15:05-16:00 WS #121:
Asthma COPD Overlap (ACO)
 Asthma COPD Overlap (ACO) Dr Thomas Brown Consultant Respiratory Physician Thomas.Brown@porthosp.nhs.uk Dr Hitasha Rupani Consultant Respiratory Physician Hitasha.rupani@porthosp.nhs.uk What is Asthma
Asthma COPD Overlap (ACO) Dr Thomas Brown Consultant Respiratory Physician Thomas.Brown@porthosp.nhs.uk Dr Hitasha Rupani Consultant Respiratory Physician Hitasha.rupani@porthosp.nhs.uk What is Asthma
compare patients preferences and costs for asthma treatment regimens targeting three
 APPENDIX I ADDITIONAL METHODS Trial design The Accurate trial lasted from September 2009 until January 2012 and was designed to compare patients preferences and costs for asthma treatment regimens targeting
APPENDIX I ADDITIONAL METHODS Trial design The Accurate trial lasted from September 2009 until January 2012 and was designed to compare patients preferences and costs for asthma treatment regimens targeting
F unctional breathing problems have been shown to result
 110 ASTHMA Breathing retraining for dysfunctional breathing in asthma: a randomised controlled trial M Thomas, R K McKinley, E Freeman, C Foy, P Prodger, D Price... See end of article for authors affiliations...
110 ASTHMA Breathing retraining for dysfunctional breathing in asthma: a randomised controlled trial M Thomas, R K McKinley, E Freeman, C Foy, P Prodger, D Price... See end of article for authors affiliations...
Prof Neil Barnes. Respiratory and General Medicine London Chest Hospital and The Royal London Hospital
 Prof Neil Barnes Respiratory and General Medicine London Chest Hospital and The Royal London Hospital ASTHMA: WHEN EVERYTHING FAILS WHAT DO YOU DO? South GP CME 2013, Dunedin Saturday 17 th August 2013
Prof Neil Barnes Respiratory and General Medicine London Chest Hospital and The Royal London Hospital ASTHMA: WHEN EVERYTHING FAILS WHAT DO YOU DO? South GP CME 2013, Dunedin Saturday 17 th August 2013
The impact of a dedicated physiotherapist clinic for children with dysfunctional breathing
 ORIGINAL ARTICLE PAEDIATRIC PULMONOLOGY The impact of a dedicated physiotherapist clinic for children with dysfunctional breathing Nicola J. Barker 1, Heather Elphick 1 and Mark L. Everard 2 Affiliations:
ORIGINAL ARTICLE PAEDIATRIC PULMONOLOGY The impact of a dedicated physiotherapist clinic for children with dysfunctional breathing Nicola J. Barker 1, Heather Elphick 1 and Mark L. Everard 2 Affiliations:
Clinical Implications of Asthma Phenotypes. Michael Schatz, MD, MS Department of Allergy
 Clinical Implications of Asthma Phenotypes Michael Schatz, MD, MS Department of Allergy Definition of Phenotype The observable properties of an organism that are produced by the interaction of the genotype
Clinical Implications of Asthma Phenotypes Michael Schatz, MD, MS Department of Allergy Definition of Phenotype The observable properties of an organism that are produced by the interaction of the genotype
NG80. Asthma: diagnosis, monitoring and chronic asthma management (NG80)
 Asthma: diagnosis, monitoring and chronic asthma management (NG80) NG80 NICE has checked the use of its content in this product and the sponsor has had no influence on the content of this booklet. NICE
Asthma: diagnosis, monitoring and chronic asthma management (NG80) NG80 NICE has checked the use of its content in this product and the sponsor has had no influence on the content of this booklet. NICE
Asthma: diagnosis and monitoring
 Asthma: diagnosis and monitoring NICE guideline: short version Draft for second consultation, July 01 This guideline covers assessing, diagnosing and monitoring suspected or confirmed asthma in adults,
Asthma: diagnosis and monitoring NICE guideline: short version Draft for second consultation, July 01 This guideline covers assessing, diagnosing and monitoring suspected or confirmed asthma in adults,
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss?
 ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
Clinical profile of patients with adult-onset eosinophilic asthma
 ORIGINAL ARTICLE ASTHMA Clinical profile of patients with adult-onset eosinophilic asthma Jantina C. de Groot 1, Huib Storm 2, Marijke Amelink 3, Selma B. de Nijs 3, Edwin Eichhorn 4, Bennie H. Reitsma
ORIGINAL ARTICLE ASTHMA Clinical profile of patients with adult-onset eosinophilic asthma Jantina C. de Groot 1, Huib Storm 2, Marijke Amelink 3, Selma B. de Nijs 3, Edwin Eichhorn 4, Bennie H. Reitsma
Somkiat Wongtim Professor of Medicine Division of Respiratory Disease and Critical Care Chulalongkorn University
 Somkiat Wongtim Professor of Medicine Division of Respiratory Disease and Critical Care Chulalongkorn University Asthma-related Comorbidities Comorbid conditions of the upper airways Rhinitis and Sinusitis
Somkiat Wongtim Professor of Medicine Division of Respiratory Disease and Critical Care Chulalongkorn University Asthma-related Comorbidities Comorbid conditions of the upper airways Rhinitis and Sinusitis
A comparison of global questions versus health status questionnaires as measures of the severity and impact of asthma
 Eur Respir J 1999; 1: 591±596 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 93-1936 A comparison of global questions versus health status questionnaires
Eur Respir J 1999; 1: 591±596 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 93-1936 A comparison of global questions versus health status questionnaires
Author s Accepted Manuscript
 Author s Accepted Manuscript Low levels of physical activity predict worse survival to lung transplantation and poor early postoperative outcomesphysical activity level in lung transplantation James R.
Author s Accepted Manuscript Low levels of physical activity predict worse survival to lung transplantation and poor early postoperative outcomesphysical activity level in lung transplantation James R.
Case-Compare Impact Report
 Case-Compare Impact Report October 8, 20 For CME Activity: Developed through an independent educational grant from Genentech: Moderate to Severe Persistent Asthma: A Case-Based Panel Discussion (March
Case-Compare Impact Report October 8, 20 For CME Activity: Developed through an independent educational grant from Genentech: Moderate to Severe Persistent Asthma: A Case-Based Panel Discussion (March
Validation of the Asthma Quality of Life Questionnaire (AQLQ UK English Version) in Indian Asthmatic Subjects
 ORIGINAL ARTICLE Validation of the Asthma Quality of Life Questionnaire (AQLQ UK English Version) in Indian Asthmatic Subjects Sunil K. Chhabra and Shivu Kaushik Department of Cardiorespiratory Physiology,
ORIGINAL ARTICLE Validation of the Asthma Quality of Life Questionnaire (AQLQ UK English Version) in Indian Asthmatic Subjects Sunil K. Chhabra and Shivu Kaushik Department of Cardiorespiratory Physiology,
An Insight into Allergy and Allergen Immunotherapy Co-morbidities of allergic disease
 An Insight into Allergy and Allergen Immunotherapy Co-morbidities of allergic disease Carmen Vidal Athens, September 11, 2014 Pucci S & Incorvaia C, 2008; 153:1-2 1. The major player in driving the immune
An Insight into Allergy and Allergen Immunotherapy Co-morbidities of allergic disease Carmen Vidal Athens, September 11, 2014 Pucci S & Incorvaia C, 2008; 153:1-2 1. The major player in driving the immune
TARGET POPULATION Eligibility Inclusion Criterion Exclusion Criterion RECOMMENDATIONS
 TARGET POPULATION Eligibility Inclusion Criterion Exclusion Criterion RECOMMENDATIONS Recommendation PULMONARY FUNCTION TESTING (SPIROMETRY) Conditional: The Expert Panel that spirometry measurements FEV1,
TARGET POPULATION Eligibility Inclusion Criterion Exclusion Criterion RECOMMENDATIONS Recommendation PULMONARY FUNCTION TESTING (SPIROMETRY) Conditional: The Expert Panel that spirometry measurements FEV1,
Dysfunctional breathing phenotype in adults with asthma - incidence and risk factors
 Agache et al. Clinical and Translational Allergy 2012, 2:18 RESEARCH Open Access Dysfunctional breathing phenotype in adults with asthma - incidence and risk factors Ioana Agache 1*, Cristina Ciobanu 2,
Agache et al. Clinical and Translational Allergy 2012, 2:18 RESEARCH Open Access Dysfunctional breathing phenotype in adults with asthma - incidence and risk factors Ioana Agache 1*, Cristina Ciobanu 2,
Evaluation of Asthma Management in Middle EAst North Africa Adult population
 STUDY REPORT SUMMARY Evaluation of Asthma Management in Middle EAst North Africa Adult population Descriptive study on the management of asthma in an asthmatic Middle East Africa adult population Background/Rationale:
STUDY REPORT SUMMARY Evaluation of Asthma Management in Middle EAst North Africa Adult population Descriptive study on the management of asthma in an asthmatic Middle East Africa adult population Background/Rationale:
SGRQ Questionnaire assessing respiratory disease-specific quality of life. Questionnaire assessing general quality of life
 SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
I have no perceived conflicts of interest or commercial relationships to disclose.
 ASTHMA BASICS Michelle Dickens RN FNP-C AE-C Nurse Practitioner/Certified Asthma Educator Ferrell Duncan Allergy/Asthma/Immunology Coordinator, CoxHealth Asthma Center DISCLOSURES I have no perceived conflicts
ASTHMA BASICS Michelle Dickens RN FNP-C AE-C Nurse Practitioner/Certified Asthma Educator Ferrell Duncan Allergy/Asthma/Immunology Coordinator, CoxHealth Asthma Center DISCLOSURES I have no perceived conflicts
Outline FEF Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications?
 Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Life-long asthma and its relationship to COPD. Stephen T Holgate School of Medicine University of Southampton
 Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Outcome, classification and management of wheezing in preschool children Paul L.P. Brand
 Outcome, classification and management of wheezing in preschool children Paul L.P. Brand Princess Amalia Children s Clinic Isala klinieken, Zwolle the Netherlands p.l.p.brand@isala.nl Valle de la Luna,
Outcome, classification and management of wheezing in preschool children Paul L.P. Brand Princess Amalia Children s Clinic Isala klinieken, Zwolle the Netherlands p.l.p.brand@isala.nl Valle de la Luna,
2/4/2019. GOLD Objectives. GOLD 2019 Report: Chapters
 GOLD Objectives To provide a non biased review of the current evidence for the assessment, diagnosis and treatment of patients with COPD. To highlight short term and long term treatment objectives organized
GOLD Objectives To provide a non biased review of the current evidence for the assessment, diagnosis and treatment of patients with COPD. To highlight short term and long term treatment objectives organized
N ational and international guidelines on the treatment
 561 ASTHMA Predictors of therapy resistant asthma: outcome of a systematic evaluation protocol L G Heaney, E Conway, C Kelly, B T Johnston, C English, M Stevenson, J Gamble... See end of article for authors
561 ASTHMA Predictors of therapy resistant asthma: outcome of a systematic evaluation protocol L G Heaney, E Conway, C Kelly, B T Johnston, C English, M Stevenson, J Gamble... See end of article for authors
Global Initiative for Asthma (GINA) What s new in GINA 2017?
 Global Initiative for Asthma (GINA) GINA Global Strategy for Asthma Management and Prevention Asthma-COPD overlap The word syndrome has been removed from the previous term asthma-copd overlap syndrome
Global Initiative for Asthma (GINA) GINA Global Strategy for Asthma Management and Prevention Asthma-COPD overlap The word syndrome has been removed from the previous term asthma-copd overlap syndrome
Clinical Practice Guideline: Asthma
 Clinical Practice Guideline: Asthma INTRODUCTION A critical aspect of the diagnosis and management of asthma is the precise and periodic measurement of lung function both before and after bronchodilator
Clinical Practice Guideline: Asthma INTRODUCTION A critical aspect of the diagnosis and management of asthma is the precise and periodic measurement of lung function both before and after bronchodilator
Update on management of respiratory symptoms. Dr Farid Bazari Consultant Respiratory Physician Kingston Hospital NHS FT
 Update on management of respiratory symptoms Dr Farid Bazari Consultant Respiratory Physician Kingston Hospital NHS FT Topics The common respiratory symptoms Cough: causes, diagnosis and therapy Update
Update on management of respiratory symptoms Dr Farid Bazari Consultant Respiratory Physician Kingston Hospital NHS FT Topics The common respiratory symptoms Cough: causes, diagnosis and therapy Update
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: exhaled_nitric_oxide_measurement 2/2009 3/2018 3/2019 3/2018 Description of Procedure or Service Asthma is
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: exhaled_nitric_oxide_measurement 2/2009 3/2018 3/2019 3/2018 Description of Procedure or Service Asthma is
Is reslizumab effective in improving quality of life and asthma control in adolescent and adult patients with poorly controlled eosinophilic asthma?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is reslizumab effective in improving
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is reslizumab effective in improving
Nonadherence in the era of severe asthma biologics and thermoplasty
 ORIGINAL ARTICLE ASTHMA Nonadherence in the era of severe asthma biologics and thermoplasty Joy Lee 1,2, Tunn Ren Tay 1, Naghmeh Radhakrishna 1, Fiona Hore-Lacy 1, Anna Mackay 1,RyanHoy 1,2, Eli Dabscheck
ORIGINAL ARTICLE ASTHMA Nonadherence in the era of severe asthma biologics and thermoplasty Joy Lee 1,2, Tunn Ren Tay 1, Naghmeh Radhakrishna 1, Fiona Hore-Lacy 1, Anna Mackay 1,RyanHoy 1,2, Eli Dabscheck
Michael S. Blaiss, MD
 Michael S. Blaiss, MD Clinical Professor of Pediatrics and Medicine Division of Clinical Immunology and Allergy University of Tennessee Health Science Center Memphis, Tennessee Speaker s Bureau: AstraZeneca,
Michael S. Blaiss, MD Clinical Professor of Pediatrics and Medicine Division of Clinical Immunology and Allergy University of Tennessee Health Science Center Memphis, Tennessee Speaker s Bureau: AstraZeneca,
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma
 Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
The Asthma Guidelines: Diagnosis and Assessment of Asthma
 The Asthma Guidelines: Diagnosis and Assessment of Asthma Christopher H. Fanta, M.D. Partners Asthma Center Brigham and Women s Hospital Harvard Medical School Objectives Know how the diagnosis of asthma
The Asthma Guidelines: Diagnosis and Assessment of Asthma Christopher H. Fanta, M.D. Partners Asthma Center Brigham and Women s Hospital Harvard Medical School Objectives Know how the diagnosis of asthma
Common medically unexplained conditions (including PMS and fibromyalgia) and breathing pattern disorders 2008
 Common medically unexplained conditions (including PMS and fibromyalgia) and breathing pattern disorders 2008 Leon Chaitow ND DO www.leonchaitow.com Background Personal experience, and enquiry, suggests
Common medically unexplained conditions (including PMS and fibromyalgia) and breathing pattern disorders 2008 Leon Chaitow ND DO www.leonchaitow.com Background Personal experience, and enquiry, suggests
(Asthma) Diagnosis, monitoring and chronic asthma management
 Dubai Standards of Care 2018 (Asthma) Diagnosis, monitoring and chronic asthma management Preface Asthma is one of the most common problem dealt with in daily practice. In Dubai, the management of chronic
Dubai Standards of Care 2018 (Asthma) Diagnosis, monitoring and chronic asthma management Preface Asthma is one of the most common problem dealt with in daily practice. In Dubai, the management of chronic
KEY WORDS airflow limitation, airway hyperresponsiveness, airway inflammation, airway lability, peak expiratory flow rate
 Allergology International. 2013;62:343-349 DOI: 10.2332 allergolint.13-oa-0543 ORIGINAL ARTICLE Stratifying a Risk for an Increased Variation of Airway Caliber among the Clinically Stable Asthma Atsushi
Allergology International. 2013;62:343-349 DOI: 10.2332 allergolint.13-oa-0543 ORIGINAL ARTICLE Stratifying a Risk for an Increased Variation of Airway Caliber among the Clinically Stable Asthma Atsushi
2.6 MONITORING ASTHMA
 2.6 MONITORING ASTHMA 2.6.1 MONITORING ASTHMA IN ADULTS In the majority of patients with asthma symptom-based monitoring is adequate. Patients achieving control of symptoms with treatment have a low risk
2.6 MONITORING ASTHMA 2.6.1 MONITORING ASTHMA IN ADULTS In the majority of patients with asthma symptom-based monitoring is adequate. Patients achieving control of symptoms with treatment have a low risk
Phenotypes of asthma; implications for treatment. Medical Grand Rounds Feb 2018 Jim Martin MD DSc
 Phenotypes of asthma; implications for treatment Medical Grand Rounds Feb 2018 Jim Martin MD DSc No conflicts to declare Objectives To understand the varied clinical forms of asthma To understand the pathobiologic
Phenotypes of asthma; implications for treatment Medical Grand Rounds Feb 2018 Jim Martin MD DSc No conflicts to declare Objectives To understand the varied clinical forms of asthma To understand the pathobiologic
Guideline on the Management of Asthma in adults SHSCT
 CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Management of Asthma in adults Dr A John, Dr J Lindsay Respiratory Medicine/ MUSC Medicine Date Uploaded: 23/11/15 Review Date
CLINICAL GUIDELINES ID TAG Title: Author: Speciality / Division: Directorate: Management of Asthma in adults Dr A John, Dr J Lindsay Respiratory Medicine/ MUSC Medicine Date Uploaded: 23/11/15 Review Date
This is a cross-sectional analysis of the National Health and Nutrition Examination
 SUPPLEMENTAL METHODS Study Design and Setting This is a cross-sectional analysis of the National Health and Nutrition Examination Survey (NHANES) data 2007-2008, 2009-2010, and 2011-2012. The NHANES is
SUPPLEMENTAL METHODS Study Design and Setting This is a cross-sectional analysis of the National Health and Nutrition Examination Survey (NHANES) data 2007-2008, 2009-2010, and 2011-2012. The NHANES is
CHAPTER 5. Weekly self-monitoring and treatment adjustment benefit patients with partly controlled and uncontrolled asthma
 CHAPTER 5 Weekly self-monitoring and treatment adjustment benefit patients with partly controlled and uncontrolled asthma Victor van der Meer, Henk F. van Stel, Moira J. Bakker, Albert C. Roldaan, Willem
CHAPTER 5 Weekly self-monitoring and treatment adjustment benefit patients with partly controlled and uncontrolled asthma Victor van der Meer, Henk F. van Stel, Moira J. Bakker, Albert C. Roldaan, Willem
COPD and Asthma Update. April 29 th, 2017 Rachel M Taliercio, DO Staff, Respiratory Institute
 COPD and Asthma Update April 29 th, 2017 Rachel M Taliercio, DO Staff, Respiratory Institute What we ll be talking about COPD: diagnosis, management of stable COPD, COPD exacerbations Asthma: diagnosis,
COPD and Asthma Update April 29 th, 2017 Rachel M Taliercio, DO Staff, Respiratory Institute What we ll be talking about COPD: diagnosis, management of stable COPD, COPD exacerbations Asthma: diagnosis,
Public Dissemination
 1. THE ASTHMA CONDITION 9 18 3 30 A. Pathophysiology 4 6 0 10 1. Teach an individual with asthma and their family using simple language by illustrating the following with appropriate educational aids a.
1. THE ASTHMA CONDITION 9 18 3 30 A. Pathophysiology 4 6 0 10 1. Teach an individual with asthma and their family using simple language by illustrating the following with appropriate educational aids a.
Measure breath nitric oxide for airway inflammation with the NObreath FeNO monitor
 Measure breath nitric oxide for airway inflammation with the NObreath FeNO monitor British technology Improving asthma management, one breath at a time. www.bedfont.com w on 01622 851122 or email ask@bedfont.com
Measure breath nitric oxide for airway inflammation with the NObreath FeNO monitor British technology Improving asthma management, one breath at a time. www.bedfont.com w on 01622 851122 or email ask@bedfont.com
Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma Full Report 2007
 Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma Full Report 2007 TARGET POPULATION Eligibility Inclusion Criterion Exclusion Criterion RECOMMENDATIONS Selecting Initial Therapy
Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma Full Report 2007 TARGET POPULATION Eligibility Inclusion Criterion Exclusion Criterion RECOMMENDATIONS Selecting Initial Therapy
Changing Landscapes in COPD New Zealand Respiratory Conference
 Changing Landscapes in COPD New Zealand Respiratory Conference Dr Robert Young BMedSc MBChB DPhil (Oxon) FRACP FRCP Associate Professor Consultant Physician Changing Landscapes in COPD: Summary 1. Overview
Changing Landscapes in COPD New Zealand Respiratory Conference Dr Robert Young BMedSc MBChB DPhil (Oxon) FRACP FRCP Associate Professor Consultant Physician Changing Landscapes in COPD: Summary 1. Overview
WEBINAR. Difficult-to-treat and severe asthma: changing the paradigm
 WEBINAR Difficult-to-treat and severe asthma: changing the paradigm A multidisciplinary discussion on new therapies, and how to identify and manage difficult-to-treat and severe asthma DIFFICULT-TO-TREAT
WEBINAR Difficult-to-treat and severe asthma: changing the paradigm A multidisciplinary discussion on new therapies, and how to identify and manage difficult-to-treat and severe asthma DIFFICULT-TO-TREAT
Dysfunctional breathing: a review of the literature and proposal for classification
 REVIEW DYSFUNCTIONAL BREATHING Dysfunctional breathing: a review of the literature and proposal for classification Richard Boulding 1, Rebecca Stacey 1, Rob Niven and Stephen J. Fowler 1, Affiliations:
REVIEW DYSFUNCTIONAL BREATHING Dysfunctional breathing: a review of the literature and proposal for classification Richard Boulding 1, Rebecca Stacey 1, Rob Niven and Stephen J. Fowler 1, Affiliations:
TORCH: Salmeterol and Fluticasone Propionate and Survival in COPD
 TORCH: and Propionate and Survival in COPD April 19, 2007 Justin Lee Pharmacy Resident University Health Network Outline Overview of COPD Pathophysiology Pharmacological Treatment Overview of the TORCH
TORCH: and Propionate and Survival in COPD April 19, 2007 Justin Lee Pharmacy Resident University Health Network Outline Overview of COPD Pathophysiology Pharmacological Treatment Overview of the TORCH
Current Asthma Therapy: Little Need to Phenotype. Phenotypes of Severe Asthma. Cellular Phenotypes 12/7/2012
 Subbasement Membrane Thickness(µm) 12/7/212 Current Asthma Therapy: Little Need to Phenotype Phenotypes of Severe Asthma Most mild and to some degree moderate asthmatics respond well to currently available
Subbasement Membrane Thickness(µm) 12/7/212 Current Asthma Therapy: Little Need to Phenotype Phenotypes of Severe Asthma Most mild and to some degree moderate asthmatics respond well to currently available
What s new in COPD? Apichart Khanichap MD. Department of Medicine, Faculty of Medicine, Thammasat university
 What s new in COPD? Apichart Khanichap MD. Department of Medicine, Faculty of Medicine, Thammasat university Management stable COPD Relieve symptoms Improve exercise tolerance Improve health status Prevent
What s new in COPD? Apichart Khanichap MD. Department of Medicine, Faculty of Medicine, Thammasat university Management stable COPD Relieve symptoms Improve exercise tolerance Improve health status Prevent
The Asthma Quality of Life Questionnaire (AQLQ) Validation of a Standardized Version of the Asthma Quality of Life Questionnaire*
 Validation of a Standardized Version of the Asthma Quality of Life Questionnaire* Elizabeth F. Juniper, MSc; A. Sonia Buist, MD; Fred M. Cox, PhD; Penelope J. Ferrie, BA; and Derek R. King, BMath Background:
Validation of a Standardized Version of the Asthma Quality of Life Questionnaire* Elizabeth F. Juniper, MSc; A. Sonia Buist, MD; Fred M. Cox, PhD; Penelope J. Ferrie, BA; and Derek R. King, BMath Background:
How to distinguish between uncontrolled and severe asthma
 How to distinguish between uncontrolled and severe asthma Watch patient using their inhaler. Discuss adherence and barriers to use Compare inhaler technique with a devicespecific checklist, and correct
How to distinguish between uncontrolled and severe asthma Watch patient using their inhaler. Discuss adherence and barriers to use Compare inhaler technique with a devicespecific checklist, and correct
Diagnosis and Management of Asthma in Children based on the British Thoracic Society and Scottish Intercollegiate Guidelines Network September 2016
 Diagnosis and Management of Asthma in Children based on the British Thoracic Society and Scottish Intercollegiate Guidelines Network September 2016 Diagnosis: There is no lower limit to the age at which
Diagnosis and Management of Asthma in Children based on the British Thoracic Society and Scottish Intercollegiate Guidelines Network September 2016 Diagnosis: There is no lower limit to the age at which
Supplementary Online Content
 Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Online supplementary material
 Online supplementary material Add-on long-acting β2-agonist (LABA) in a separate inhaler as asthma step-up therapy versus increased dose of inhaled corticosteroid (ICS) or ICS/LABA combination inhaler
Online supplementary material Add-on long-acting β2-agonist (LABA) in a separate inhaler as asthma step-up therapy versus increased dose of inhaled corticosteroid (ICS) or ICS/LABA combination inhaler
Asthma and Vocal Cord Dysfunction
 Asthma and Vocal Cord Dysfunction Amy L. Marks DO, FACOP Pediatric Allergy and Immunology Assistant Professor of Pediatrics Oakland University William Beaumont School of Medicine Objectives: Understanding
Asthma and Vocal Cord Dysfunction Amy L. Marks DO, FACOP Pediatric Allergy and Immunology Assistant Professor of Pediatrics Oakland University William Beaumont School of Medicine Objectives: Understanding
7/7/2015. Somboon Chansakulporn, MD. History of variable respiratory symptoms. 1. Documented excessive variability in PFT ( 1 test)
 Definition of Asthma GINA 2010: Chronic inflammatory disorder of the airways Airway hyper-responsiveness Recurrent wheezing, breathlessness, chest tightness, coughing Variable, reversible airflow obstruction
Definition of Asthma GINA 2010: Chronic inflammatory disorder of the airways Airway hyper-responsiveness Recurrent wheezing, breathlessness, chest tightness, coughing Variable, reversible airflow obstruction
Do We Need Biologics in Pediatric Asthma Management?
 Do We Need Biologics in Pediatric Asthma Management? Ting Fan LEUNG, MBChB, MD, FRCPCH, FAAAAI Professor and Chairman Department of Paediatrics The Chinese University of Hong Kong Asthma and Allergy by
Do We Need Biologics in Pediatric Asthma Management? Ting Fan LEUNG, MBChB, MD, FRCPCH, FAAAAI Professor and Chairman Department of Paediatrics The Chinese University of Hong Kong Asthma and Allergy by
Development of a self-reported Chronic Respiratory Questionnaire (CRQ-SR)
 954 Department of Respiratory Medicine, University Hospitals of Leicester, Glenfield Hospital, Leicester LE3 9QP, UK J E A Williams S J Singh L Sewell M D L Morgan Department of Clinical Epidemiology and
954 Department of Respiratory Medicine, University Hospitals of Leicester, Glenfield Hospital, Leicester LE3 9QP, UK J E A Williams S J Singh L Sewell M D L Morgan Department of Clinical Epidemiology and
Primary Care Medicine: Concepts and Controversies Wed., February 17, 2010 Fiesta Americana Puerto Vallarta, Mexico Update on Asthma and COPD
 Primary Care Medicine: Concepts and Controversies Wed., February 17, 2010 Fiesta Americana Puerto Vallarta, Mexico Update on Asthma and COPD Talmadge E. King, Jr., M.D. Krevins Distinguished Professor
Primary Care Medicine: Concepts and Controversies Wed., February 17, 2010 Fiesta Americana Puerto Vallarta, Mexico Update on Asthma and COPD Talmadge E. King, Jr., M.D. Krevins Distinguished Professor
Interpreting thresholds for a clinically significant change in health status in asthma and COPD
 Eur Respir J 2002; 19: 398 404 DOI: 10.1183/09031936.02.00063702 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 Interpreting thresholds for
Eur Respir J 2002; 19: 398 404 DOI: 10.1183/09031936.02.00063702 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 Interpreting thresholds for
Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma
 Original Article Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma Feng-Jia Chen, Huai Liao, Xin-Yan Huang, Can-Mao Xie Department of Respiratory
Original Article Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma Feng-Jia Chen, Huai Liao, Xin-Yan Huang, Can-Mao Xie Department of Respiratory
National Asthma Educator Certification Board Detailed Content Outline
 I. THE ASTHMA CONDITION 9 20 1 30 A. Pathophysiology 4 6 0 10 1. Teach an individual with asthma and their family using simple language by illustrating the following with appropriate educational aids a.
I. THE ASTHMA CONDITION 9 20 1 30 A. Pathophysiology 4 6 0 10 1. Teach an individual with asthma and their family using simple language by illustrating the following with appropriate educational aids a.
COPD, Asthma, Or Something In Between? Sharon R. Rosenberg Assistant Professor of Medicine Northwestern University December 4, 2013
 COPD, Asthma, Or Something In Between? Sharon R. Rosenberg Assistant Professor of Medicine Northwestern University December 4, 2013 None Disclosures Definitions Asthma Asthma is a chronic inflammatory
COPD, Asthma, Or Something In Between? Sharon R. Rosenberg Assistant Professor of Medicine Northwestern University December 4, 2013 None Disclosures Definitions Asthma Asthma is a chronic inflammatory
Is CPAP helpful in severe Asthma?
 Is CPAP helpful in severe Asthma? P RAP UN KI TTIVORAVITKUL, M.D. PULMONARY AND CRITICAL CARE DIVISION DEPARTMENT OF MEDICINE, PHRAMONGKUTKLAO HOSPITAL Outlines o Obstructive sleep apnea syndrome (OSAS)
Is CPAP helpful in severe Asthma? P RAP UN KI TTIVORAVITKUL, M.D. PULMONARY AND CRITICAL CARE DIVISION DEPARTMENT OF MEDICINE, PHRAMONGKUTKLAO HOSPITAL Outlines o Obstructive sleep apnea syndrome (OSAS)
Measurement of Exhaled Nitric Oxide and Exhaled Breath Condensate in the Diagnosis and Management of Respiratory Disorders
 Measurement of Exhaled Nitric Oxide and Exhaled Breath Condensate in the Diagnosis and Management of Respiratory Disorders Policy Number: 2.01.61 Last Review: 9/2018 Origination: 2/2007 Next Review: 3/2019
Measurement of Exhaled Nitric Oxide and Exhaled Breath Condensate in the Diagnosis and Management of Respiratory Disorders Policy Number: 2.01.61 Last Review: 9/2018 Origination: 2/2007 Next Review: 3/2019
Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers?
 Disclosures: Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers? Stanley Fineman, MD Past-President, American College of Allergy, Asthma & Immunology Adjunct Associate
Disclosures: Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers? Stanley Fineman, MD Past-President, American College of Allergy, Asthma & Immunology Adjunct Associate
INDIVIDUAL DIFFERENCES INFLUENCE QUALITY OF LIFE IN ASTHMA PATIENTS: THE ROLE OF ANXIETY AND GENDER INTRODUCTION
 INDIVIDUAL DIFFERENCES INFLUENCE QUALITY OF LIFE IN ASTHMA PATIENTS: THE ROLE OF ANXIETY AND GENDER Maria Stavrinaki, M.Sc.¹ Maria Karekla, Ph.D.¹ Elena Hanna, M.A¹ Tonia Adamide, M.D.² Natalie Pilipenko,
INDIVIDUAL DIFFERENCES INFLUENCE QUALITY OF LIFE IN ASTHMA PATIENTS: THE ROLE OF ANXIETY AND GENDER Maria Stavrinaki, M.Sc.¹ Maria Karekla, Ph.D.¹ Elena Hanna, M.A¹ Tonia Adamide, M.D.² Natalie Pilipenko,
Dedicated Severe Asthma Services Improve Health-care Use and Quality of Life
 [ Original Research Asthma ] Dedicated Severe Asthma Services Improve Health-care Use and Quality of Life David Gibeon, MBChB ; Liam G. Heaney, MD ; Chris E. Brightling, PhD, FCCP ; Rob Niven, MD ; Adel
[ Original Research Asthma ] Dedicated Severe Asthma Services Improve Health-care Use and Quality of Life David Gibeon, MBChB ; Liam G. Heaney, MD ; Chris E. Brightling, PhD, FCCP ; Rob Niven, MD ; Adel
Function of the Respiratory System. Exchange CO2 (on expiration) for O2 (on inspiration)
 Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Asma e BPCO: le strategie terapeutiche
 Asma e BPCO: le strategie terapeutiche Dott. Marco Contoli ctm@unife.it Sezione di Medicina Interna e Cardio-Respiratoria Dipartimento di Scienze Mediche Università di Ferrara COPD Definition Chronic Obstructive
Asma e BPCO: le strategie terapeutiche Dott. Marco Contoli ctm@unife.it Sezione di Medicina Interna e Cardio-Respiratoria Dipartimento di Scienze Mediche Università di Ferrara COPD Definition Chronic Obstructive
Allergic Rhinitis: Effects on Quality of Life and Co-morbid Conditions
 Disclosures : Effects on Quality of Life and Co-morbid Conditions Nycomed Pharmaceutical Sepracor Pharmaceutical Michael S. Blaiss, MD Clinical Professor of Pediatrics and Medicine University of Tennessee
Disclosures : Effects on Quality of Life and Co-morbid Conditions Nycomed Pharmaceutical Sepracor Pharmaceutical Michael S. Blaiss, MD Clinical Professor of Pediatrics and Medicine University of Tennessee
LINEE GUIDA DELL ASMA: UP TO DATE
 LINEE GUIDA DELL ASMA: UP TO DATE Azienda Ospedaliera Pisana Università degli Studi di Pisa Pierluigi Paggiaro GINA International Executive Committee, Chairman GINA ITaly Cardio-Thoracic and Vascular Department,
LINEE GUIDA DELL ASMA: UP TO DATE Azienda Ospedaliera Pisana Università degli Studi di Pisa Pierluigi Paggiaro GINA International Executive Committee, Chairman GINA ITaly Cardio-Thoracic and Vascular Department,
FOR PUBLIC CONSULTATION ONLY. Evidence Review: Temperature-controlled laminar airflow device for persistent allergic asthma (children)
 Evidence Review: Temperature-controlled laminar airflow device for persistent allergic asthma (children) NHS England Evidence Review: Temperature-controlled laminar airflow device for persistent allergic
Evidence Review: Temperature-controlled laminar airflow device for persistent allergic asthma (children) NHS England Evidence Review: Temperature-controlled laminar airflow device for persistent allergic
Department of Pediatric Otolarygnology. ENT Specialty Programs
 Department of Pediatric Otolarygnology ENT Specialty Programs Staffed by fellowship-trained otolaryngologists, assisted by pediatric nurse practitioners, ENT (Otolaryngology) at Nationwide Children s Hospital
Department of Pediatric Otolarygnology ENT Specialty Programs Staffed by fellowship-trained otolaryngologists, assisted by pediatric nurse practitioners, ENT (Otolaryngology) at Nationwide Children s Hospital
Personalized medicine in childhood asthma. Dr Mariëlle Pijnenburg, Erasmus MC Sophia, Rotterdam, NL
 Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
UNDERSTANDING COPD MEDIA BACKGROUNDER
 UNDERSTANDING COPD MEDIA BACKGROUNDER What is COPD? Chronic Obstructive Pulmonary Disease (COPD) also called emphysema and/or chronic obstructive bronchitis* is a preventable lung disease caused by the
UNDERSTANDING COPD MEDIA BACKGROUNDER What is COPD? Chronic Obstructive Pulmonary Disease (COPD) also called emphysema and/or chronic obstructive bronchitis* is a preventable lung disease caused by the
Breathing training for dysfunctional breathing in asthma: taking a multidimensional approach
 REVIEW ASTHMA Breathing training for dysfunctional breathing in asthma: taking a multidimensional approach Rosalba Courtney Affiliation: School of Health Science, Southern Cross University, Lismore, Australia.
REVIEW ASTHMA Breathing training for dysfunctional breathing in asthma: taking a multidimensional approach Rosalba Courtney Affiliation: School of Health Science, Southern Cross University, Lismore, Australia.
Accepted Manuscript. Robotic tracheobronchoplasty is feasible but which patients truly benefit? Steven Milman, MD, Thomas Ng, MD
 Accepted Manuscript Robotic tracheobronchoplasty is feasible but which patients truly benefit? Steven Milman, MD, Thomas Ng, MD PII: S0022-5223(18)32271-2 DOI: 10.1016/j.jtcvs.2018.08.028 Reference: YMTC
Accepted Manuscript Robotic tracheobronchoplasty is feasible but which patients truly benefit? Steven Milman, MD, Thomas Ng, MD PII: S0022-5223(18)32271-2 DOI: 10.1016/j.jtcvs.2018.08.028 Reference: YMTC
COPD and Asthma: Similarities and differences Prof. Peter Barnes
 and Asthma: Similarities and Differences and Asthma: 1 Imperial College Peter Barnes FRS, FMedSci, National Heart & Lung Institute Imperial College, London, UK p.j.barnes@imperial.ac.uk Royal Brompton
and Asthma: Similarities and Differences and Asthma: 1 Imperial College Peter Barnes FRS, FMedSci, National Heart & Lung Institute Imperial College, London, UK p.j.barnes@imperial.ac.uk Royal Brompton
ASTHMA & RESPIRATORY FOUNDATION NZ ADULT ASTHMA GUIDELINES: A QUICK REFERENCE GUIDE 1
 ASTHMA & RESPIRATORY FOUNDATION NZ ADULT ASTHMA GUIDELINES: A QUICK REFERENCE GUIDE 1 1. Richard Beasley, Bob Hancox, Matire Harwood, Kyle Perrin, Betty Poot, Janine Pilcher, Jim Reid, Api Talemaitoga,
ASTHMA & RESPIRATORY FOUNDATION NZ ADULT ASTHMA GUIDELINES: A QUICK REFERENCE GUIDE 1 1. Richard Beasley, Bob Hancox, Matire Harwood, Kyle Perrin, Betty Poot, Janine Pilcher, Jim Reid, Api Talemaitoga,
DIFFICULT ASTHMA. Dr. Prathyusha Dr. S.Balasubramanian KKCTH
 DIFFICULT ASTHMA Dr. Prathyusha Dr. S.Balasubramanian KKCTH CASE SUMMARY 11 yr old girl, Neyveli Treated as moderate persistent asthma x 5 years On Seroflo [ LABA + steroid ] 250 2 puffs BD and intermittent
DIFFICULT ASTHMA Dr. Prathyusha Dr. S.Balasubramanian KKCTH CASE SUMMARY 11 yr old girl, Neyveli Treated as moderate persistent asthma x 5 years On Seroflo [ LABA + steroid ] 250 2 puffs BD and intermittent
Chronic rhinosinusitis (CRS) is an inflammatory disease
 Original Research Sinonasal Disorders Association between Asthma and Chronic Rhinosinusitis Severity in the Context of Asthma Control Otolaryngology Head and Neck Surgery 2018, Vol. 158(2) 386 390 Ó American
Original Research Sinonasal Disorders Association between Asthma and Chronic Rhinosinusitis Severity in the Context of Asthma Control Otolaryngology Head and Neck Surgery 2018, Vol. 158(2) 386 390 Ó American
Asthma Pathophysiology and Treatment. John R. Holcomb, M.D.
 Asthma Pathophysiology and Treatment John R. Holcomb, M.D. Objectives Definition of Asthma Epidemiology and risk factors of Asthma Pathophysiology of Asthma Diagnostics test of Asthma Management of Asthma
Asthma Pathophysiology and Treatment John R. Holcomb, M.D. Objectives Definition of Asthma Epidemiology and risk factors of Asthma Pathophysiology of Asthma Diagnostics test of Asthma Management of Asthma
Lecture 11: Clustering to discover disease subtypes and stages
 MACHINE LEARNING FOR HEALTHCARE 6.S897, HST.S53 Lecture 11: Clustering to discover disease subtypes and stages Prof. David Sontag MIT EECS, CSAIL, IMES Outline of today s class 1. Overview of clustering
MACHINE LEARNING FOR HEALTHCARE 6.S897, HST.S53 Lecture 11: Clustering to discover disease subtypes and stages Prof. David Sontag MIT EECS, CSAIL, IMES Outline of today s class 1. Overview of clustering
11/15/2017. Highgate Private Hospital (Royal Free London NHS Foundation Trust) Causes of chronic cough
 A whistle stop of Chronic Cough For 10min consultations.. Dr Dean Creer Consultant Chest Physician (MBChB, FRCP) Highgate Private Hospital (Royal Free London NHS Foundation Trust) E: drcreer.pa@gmail.com(secretary)
A whistle stop of Chronic Cough For 10min consultations.. Dr Dean Creer Consultant Chest Physician (MBChB, FRCP) Highgate Private Hospital (Royal Free London NHS Foundation Trust) E: drcreer.pa@gmail.com(secretary)
Patient Information Series
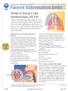 A M E R I C A N T H O R A C I C S O C I E T Y Patient Information Series What Is Vocal Cord Dysfunction (VCD)? Vocal Cord Dysfunction means that your vocal cords do not act normally. With VCD, instead
A M E R I C A N T H O R A C I C S O C I E T Y Patient Information Series What Is Vocal Cord Dysfunction (VCD)? Vocal Cord Dysfunction means that your vocal cords do not act normally. With VCD, instead
Research in Real Life
 Research in Real Life Study 1: Exploratory study - identifying the benefits of pmdi versus Diskus for delivering fluticasone/salmeterol combination therapy in patients with chronic obstructive pulmonary
Research in Real Life Study 1: Exploratory study - identifying the benefits of pmdi versus Diskus for delivering fluticasone/salmeterol combination therapy in patients with chronic obstructive pulmonary
DR REBECCA THOMAS CONSULTANT RESPIRATORY PHYSICIAN YORK DISTRICT HOSPITAL
 DR REBECCA THOMAS CONSULTANT RESPIRATORY PHYSICIAN YORK DISTRICT HOSPITAL Definition Guidelines contact complicated definitions Central to this is Presence of symptoms Variable airflow obstruction Diagnosis
DR REBECCA THOMAS CONSULTANT RESPIRATORY PHYSICIAN YORK DISTRICT HOSPITAL Definition Guidelines contact complicated definitions Central to this is Presence of symptoms Variable airflow obstruction Diagnosis
Which asthma patient has allergic airway inflammation?
 Which asthma patient has allergic airway inflammation? C o n t r o l l i n g A l l e r g i c A s t h m a Several underlying diseases can present symptoms similar to asthma. Therefore, a correct diagnos
Which asthma patient has allergic airway inflammation? C o n t r o l l i n g A l l e r g i c A s t h m a Several underlying diseases can present symptoms similar to asthma. Therefore, a correct diagnos
ASTHMA. Dr Liz Gamble BRI
 ASTHMA Dr Liz Gamble BRI Diagnosis Clinical: wheeze, breathlessness, chest tightness, cough Variable airflow obstruction: peak flow chart, spirometry with reversibility to bronchodilators Airways hyper-responsiveness
ASTHMA Dr Liz Gamble BRI Diagnosis Clinical: wheeze, breathlessness, chest tightness, cough Variable airflow obstruction: peak flow chart, spirometry with reversibility to bronchodilators Airways hyper-responsiveness
Asthma in Children with Sickle Cell Disease
 December 18, 2018 Asthma in Children with Sickle Cell Disease Robyn Cohen, MD, MPH Director, Division of Pediatric Pulmonology and Allergy Associate Professor of Pediatrics Boston University/Boston Medical
December 18, 2018 Asthma in Children with Sickle Cell Disease Robyn Cohen, MD, MPH Director, Division of Pediatric Pulmonology and Allergy Associate Professor of Pediatrics Boston University/Boston Medical
COPD or not COPD, that is the question.
 COPD or not COPD, that is the question. Asthma-COPD Overlap Syndrome: ACOS Do we really need this? Michelle Harkins Disclosure Slide Slide help - William Busse, MD Organizational Interests ATS, ACCP, ACP
COPD or not COPD, that is the question. Asthma-COPD Overlap Syndrome: ACOS Do we really need this? Michelle Harkins Disclosure Slide Slide help - William Busse, MD Organizational Interests ATS, ACCP, ACP
Manuscript type: Research letter
 TITLE PAGE Chronic breathlessness associated with poorer physical and mental health-related quality of life (SF-12) across all adult age groups. Authors Currow DC, 1,2,3 Dal Grande E, 4 Ferreira D, 1 Johnson
TITLE PAGE Chronic breathlessness associated with poorer physical and mental health-related quality of life (SF-12) across all adult age groups. Authors Currow DC, 1,2,3 Dal Grande E, 4 Ferreira D, 1 Johnson
