Comparison of the Efficacies of 0.94 mm and Double Silicone Tubes for Treatment of Canalicular Obstruction
|
|
|
- Heather Hubbard
- 5 years ago
- Views:
Transcription
1 pissn: eissn: Korean J Ophthalmol 2017;31(1):1-8 ht tps://doi.org/ /k jo Original Article Comparison of the Efficacies of 0.94 mm and Double Silicone Tubes for Treatment of Canalicular Obstruction Seong Chan Choi, Hye Sun Choi, Jae Woo Jang, Sung Joo Kim, Jung Hye Lee Department of Ophthalmology, Kim s Eye Hospital, Myung-Gok Eye Research Institute, Konyang University College of Medicine, Seoul, Korea Purpose: To compare the clinical effects of the single wide-diameter bicanalicular silicone tube and the double bicanalicular silicone tube in endonasal dacryocystorhinostomy (DCR) with canalicular trephinization for canalicular obstruction. Methods: We retrospectively reviewed the records of 121 patients with monocanalicular or common canalicular obstruction who had undergone endonasal DCR with random bicanalicular insertion of either double silicone tubes (insertion of two tubes into each canaliculus) or a single wide-diameter (0.94 mm) silicone tube. The tubes were removed at around 3 months after surgery. Results: This study included 79 eyes of 61 patients in the double-tube intubation group and 68 eyes of 60 patients in the single wide-diameter tube intubation group. Anatomical success, evaluated by syringing, was achieved in 72 of the 79 eyes (91.1%) in the double-tube intubation group and 60 of the 68 eyes (88.2%) in the single wide-diameter tube intubation group. Functional success was achieved in 65 of the 79 eyes (82.3%) in the double-tube intubation group and 61 of the 68 (89.7%) eyes in the single wide-diameter tube intubation group. There were no significant differences in the success rates of surgery between the two groups. One patient in the double-tube intubation group underwent conjunctivodacryocystorhinostomy (CDCR) and two in the wide-diameter tube intubation group underwent CDCR or reintubation to treat recurrence. Conclusions: Intubation using a single wide-diameter tube during endonasal DCR is as effective as double-tube intubation for the treatment of canalicular obstruction, with a lower rate of complications such as inflammation or patient discomfort. Key Words: Canaliculitis, Dacryocystorhinostomy, Intubation, Lacrimal duct obstruction The management of monocanalicular or common canalicular obstruction is challenging because of restenosis or Received: August 1, 2016 Accepted: October 5, 2016 Corresponding Author: Jung Hye Lee, MD. Department of Ophthalmology, Kim s Eye Hospital, #136 Yeongsin-ro, Yeongdeungpo-gu, Seoul 07301, Korea. Tel: , Fax: , katejung2000@gmail.com This study was presented at the 113th annual meeting of the Korea Ophthalmological Society at Gwangju, Korea in sticky adhesive changes often observed during follow-up. Management strategies for canalicular obstruction include external or endonasal dacryocystorhinostomy (DCR), balloon catheter dilation, conjunctivodacryocystorhinostomy (CDCR) using a Jones tube, and insertion of bicanalicular silicone tubes. Although CDCR with Jones tube intubation is a widely-used standard procedure performed for the treatment of canalicular obstruction, the procedure may be complicated by nasal bleeding, infection, dislocation of the tube, and the need for permanent retention of the tube [1] The Korean Ophthalmological Society This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( /by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. 1
2 Korean J Ophthalmol Vol.31, No.1, 2017 Many surgical techniques and instruments for stent placement have been described. The material of choice for stenting in the lacrimal system is silicone, which is generally inert within the system. Stents implanted within the nasolacrimal system prevent adherence of the mucosal lining of the ducts during healing and maintain long-term patency after removal. It has been shown that the greater is the diameter of the stent, the greater is the separation between the walls of the channel [2]. Silicone intubation methods such as the Crawford bicanalicular intubation method, Quickert-Dryden method, or silicone intubation using a Nunchaku-style tube have been introduced [3-5]. Bicanalicular silicone tube placement aims to maintain the anastomotic patency and stability of the epithelium of the canaliculus. However, many studies have reported that the long-term efficacy of silicone intubation for the treatment of stenotic or obstructed canaliculi is not high, especially in adults [6-9]. In order to improve the success rates of silicone intubation in adults with canalicular obstruction, Demirci and Elner [6], Hwang et al. [7], and Kim and Kim [9] performed double silicone intubation and reported high final rates of success in long-term follow-up. They concluded that double silicone intubation is an effective minimally invasive technique for the treatment of partial obstruction of the lacrimal apparatus. In addition, Hurwitz [2] introduced single wide-diameter (0.94 mm) silicone intubation to treat canalicular obstruction. The procedure is inexpensive and relatively nontraumatic, as verified by Yildiz et al. [10], who reported no complications associated with the larger tube size. In this study, we compared the clinical efficacies of double and single wide-diameter (0.94 mm) silicone tube intubations in the treatment of monocanalicular or common canalicular obstruction. Materials and Methods Clinical evaluation We retrospectively reviewed the medical records of 147 eyes of 121 patients (including 26 patients who had surgery on both eyes) who underwent either double or single wide-diameter (0.94 mm) silicone tube intubation for monocanalicular or common canalicular obstruction between January 2010 and December Approval from the institutional review board/ethics committee was obtained before starting the study. This study adhered to the tenets of the Declaration of Helsinki. Each of the intubations was performed using either two 0.64-mm (outer diameter) silicone tubes (You-Won Meditec, Seoul, Korea) or one 0.94-mm (outer diameter) silicone tube (You-Won Meditec). All of the patients were recruited from the outpatient clinic at Kim s Eye Hospital and were subjected to a thorough examination of the eyelid and lacrimal system, including examination of the puncta, conventional probing, syringing, and dacryocystography (DCG) with contrast. The diagnosis of canalicular obstruction and determination of the level of obstruction were based on the findings of lacrimal irrigation and probing. The patients included in this study exhibited complete canalicular obstruction, which was determined by the inability of the probe to pass beyond a soft stop as well as the inability to irrigate, which was confirmed by DCG. All of the patients were diagnosed as having monocanalicular or common canalicular obstruction. The level of canalicular obstruction was estimated in millimeters from the puncta to the end of the probe where the blockage was located. Distal canalicular obstruction was defined when the site of the obstruction was a distance 8 mm from the punctum. Common canalicular obstruction was confirmed by upper and lower canalicular syringing and probing. Patients with symptoms of dry eye caused by previous trauma or mass were excluded from this study. Patients who followed up for a period of less than 2 months were also excluded. Surgical technique Endonasal DCR was performed under general anesthesia. Vasoconstriction of the nasal mucosa was achieved by packing gauze soaked in lidocaine mixed with a 1 : 100,000 dilution of epinephrine. Conventional endonasal DCR with canalicular trephinization was performed once satisfactory anesthesia and nasal decongestion were achieved. Punctum dilatation was performed using a punctum dilator. A probe was inserted through the upper and lower puncta against the membrane obstructing the canaliculus. Then, a lubricated canalicular trephine with a stylet was inserted into the point of obstruction, where the stylet was removed, and the obstructed canaliculus was trephined by advancing the 2
3 SC Choi, et al. The Efficacy of 0.94 mm Silicone Tube in Canalicular Obstruction cutting part. Following this, the probe was reinserted to ensure that the obstruction was resolved. A 20-gauge endoilluminator probe, which allowed endonasal visualization of the location of the lacrimal sac by transillumination, was introduced through the canaliculus and advanced into the lacrimal sac. The nasal mucosa was dissected and cauterized by electrocautery, and a bony opening was created using a Kerrison punch, curette, or drill. The lacrimal sac was tented with a probe, incised using a sickle knife to create a posterior lacrimal sac, and removed using ethmoid forceps with or without diode laser. Two types of silicone tubes 0.64-mm-diameter and 0.94-mm-diameter silicone tubes (You-Won Meditec) were used. The patients were separated into two groups, one treated with double silicone intubation and the other with single 0.94-mm silicone intubation. In the double-tube intubation group, the original silicone tube was passed through both canaliculi and retrieved through the new opening. Subsequently, a second silicone tube of the same size was inserted in an identical way. During this procedure, additional dilatation of the puncta was performed using a trephine in cases of persistent stenosis. The ends of the silicone tubes were tied off using square knots, and, after the excess tube was cut, the remaining part was left behind for retraction. The knots were tied such that they would not be retracted up to the rhinostomy site or protrude from the nostril. In the single wide-diameter tube intubation group, one large silicone tube was passed through both canaliculi and retrieved through the new opening. The ends of this large tube were tied off with square knots, and, after the excess tube was cut, the remaining part was left behind for retraction. After intubation, the nasal cavity was packed with polyurethane foam soaked in antibiotics (Nasopore; Polyganics, Groningen, the Netherlands). Postoperatively, the patients were instructed to use antibiotics and steroid eye drops four times daily. They were also instructed to be careful when wiping or touching the corners of the affected eyes. Silicone tubes were removed during an outpatient visit approximately 3 months after surgery. However, if patients had persistent epiphora, tubes were left in place for a longer period. The silicone tubes were removed by cutting the interpunctal portions and retracting the ends from the nose. The patients were followed up for endoscopic removal of crusts as well as for monitoring the patency of the nasolacrimal duct system by syringing at 1 week and 1, 2, and 3 months after surgery as well as every 3 months thereafter. The anatomical, functional, and overall success rates of both groups were determined 3 months after surgery. Anatomical success was defined as either good fluid passage with no resistance or the absence of reflux during lacrimal irrigation. Functional success rate was determined by evaluating subjective ocular symptoms, and epiphora severity was assessed using the Munk score [11]. A Munk score of 0 to 1 defined the surgery as a functional success, while a score of 2 to 5 defined the surgery as a functional failure. Additionally, the data regarding patient age, sex, mean follow-up duration, number of reoperations, and laterality of involvement were reviewed. Complications related to the DCR or the tube itself were also investigated. Statistical analyses were performed using the commercially available software SPSS ver for Windows (SPSS Inc., Chicago, IL, USA). Differences in the parameters between the two groups were analyzed using the independent t-test, chisquare test, and Fisher s exact test. A p-value < 0.05 was considered to indicate significance. Results A total of 121 patients (average age, 57.0 ± 11.9 years; range, 16 to 86 years), including 21 male (17.4%) and 100 female (82.6%) patients, were evaluated in this study. There were no major intraoperative or immediate postoperative complications during endonasal DCR. Of the 121 patients, two silicone tubes were placed in 79 eyes of 61 patients, and a single wide-diameter silicone tube was placed in 68 eyes of 60 patients. There were no significant differences in the distribution of the clinical characteristics between the two groups. The mean follow-up period was 8.09 ± 5.91 months and 7.90 ± 4.59 months in the double-tube and single wide-diameter tube intubation groups, respectively. The patient demographics are summarized in Table 1. The success rates of both methods were evaluated at 3 months after surgery to compare the efficacies of the intubation materials. Upon lacrimal irrigation, 72 of the 79 eyes (91.1%) in the double-tube intubation group showed good fluid passage without resistance or reflux. In the single wide-diameter tube intubation group, 60 of the 68 eyes (88.2%) showed good fluid passage, and there was no statistically significant difference between the anatomical 3
4 Korean J Ophthalmol Vol.31, No.1, 2017 success rates of the two groups. Functional success rate, as assessed by the Munk score [11], was 82.3% (65 of 79 eyes) in the double-tube group and 89.7% (61 of 68 eyes) in the single wide-diameter tube intubation group; the difference between the functional success rates of the two groups was not statistically significant (Table 2). Additionally, long-term success rates for both methods were evaluated. Six months after the surgery, 64 eyes of the double-tube intubation group and 39 eyes of the single wide-diameter intubation tube group were followed. The anatomical success rate was 89.1% in the double-tube intubation group and 87.2% in the single wide-diameter tube Table 1. Clinical characteristics of the patients Double-tube intubation group Single wide-diameter tube intubation group p-value No. of patients (eyes) 61 (79) 60 (68) - Mean age (yr) 56.8 ± ± * Sex (male : female) 14 : 47 7 : Operated side (right : left) 40 : : Values are presented as mean ± standard deviation unless otherwise indicated. * By independent t-test; By Pearson s chi-square test. Table 2. Comparison of the postoperative parameters of the two groups Double-tube intubation group (n = 79) Single wide-diameter tube intubation group (n = 68) p-value Mean follow-up period (mon) 8.09 ± ± * Anatomical success 72 (91.1) 60 (88.2) Functional success assessed by Munk score 65 (82.3) 61 (89.7) Overall success 65 (82.3) 55 (80.9) Reoperation 1 (1.6) 2 (3.3) Values are presented as mean ± standard deviation or number (%). * By independent t-test; By Pearson s chi-square test; Munk score criteria was defined as follows: grade 0, no epiphora; grade 1, occasional epiphora requiring dabbing less than twice a day; grade 2, epiphora requiring dabbing 2 to 4 times daily; grade 3, epiphora requiring dabbing 5 to 10 times daily; grade 4, epiphora requiring dabbing more than 10 times per day; grade 5, constant tearing. Munk score: 0 1, success; 2 5, failure; By Fisher s exact test. Table 3. Postoperative success rates in the two groups of patients treated for canalicular obstruction 3 mon Double-tube intubation group Single wide-diameter tube intubation group p-value No. of eyes Anatomical success 72 (91.1) 60 (88.2) * Functional success 65 (82.3) 61 (89.7) * 6 mon No. of eyes Anatomical success 57 (89.1) 34 (87.2) * Functional success 51 (79.7) 33 (84.6) * 12 mon No. of eyes Anatomical success 7 (63.6) 14 (82.4) * Functional success 4 (36.4) 14 (82.4) Values are presented as number (%). * By Pearson s chi-square test; By Fisher s exact test. 4
5 SC Choi, et al. The Efficacy of 0.94 mm Silicone Tube in Canalicular Obstruction intubation group, while the functional success rate was 79.7% in the former group and 84.6% in the latter. These slight differences in success rates were not statistically significant. Twelve months after the surgery, 11 eyes of the double-tube intubation group and 17 eyes of the single wide-diameter tube intubation group were followed. The anatomical success rate was 64.6% in the double-tube intubation group and 88.4% in the singe wide-diameter intubation group, while the functional success rate was 36.4% (4 of 11 eyes) in the former group and 82.4% (14 of 17 eyes) in the latter. This difference between groups was statistically significant (p = 0.020) (Table 3). The level of obstruction was assessed as described earlier. The most common site of obstruction was the common canaliculus, which was found to be obstructed in 54.4% of the cases in the double-tube intubation group and 69.1% of the cases in the single wide-diameter tube intubation group. Although the incidence of distal canaliculus obstruction was higher in the double-tube intubation group than in the single wide-diameter tube intubation group, there was no significant difference in incidence between the two groups (p = 0.068) (Table 4). While one patient in the double-tube intubation group underwent reoperation for epiphora by CDCR, two patients in the single wide-diameter tube intubation group underwent reoperation for recurrence, one by CDCR and the other by reintubation (Table 5). There were no significant differences in the final anatomical or functional success rates between the two groups. However, there were differences between the two groups in terms of the occurrence of minor postoperative complications such as the formation of lower punctal slit, minor inflammation near the canaliculi, reobstruction, and granulation near the bony opening in the nasal cavity. The rates of incidence of inflammation and reobstruction were similar between the two groups. However, the rates of incidence of granulation and postoperative complications were higher in the double-tube intubation group than in the single wide-diameter tube intubation group. Extrusion or malpositioning of the silicone tubes was easily corrected using a nasal endoscope and intranasal forceps. In cases of patients with granulated tissue at follow-up, endoscopic removal was performed in the outpatient clinic. Minor inflammation near the canaliculi was easily managed using antibiotic eye drops and oral antibiotics (Table 5). Table 4. Site of obstruction diagnosed after surgery Double-tube intubation group (n = 79) Single wide-diameter tube intubation group (n = 68) Monocanaliculus 36 (45.6) 21 (30.9) Superior 4 (5.1) 5 (7.4) Inferior 21 (26.6) 11 (16.2) Both 11 (13.9) 5 (7.4) Common canaliculus 43 (54.4) 47 (69.1) Values are presented as number (%). Table 5. Comparison of the postoperative complications of the two groups Double-tube intubation group (n = 79) Single wide-diameter tube intubation group (n = 68) p-value Granuloma 38 (48.1) 18 (26.5) * Reobstruction 7 (8.9) 8 (11.8) * Reoperation 1 (1.3) 2 (2.9) Inflammation 4 (5.1) 1 (1.5) Punctal slit 1 (1.3) 0 (0.0) None 34 (43.0) 42 (61.8) * Values are presented as number (%). * By Pearson s chi-square test; By Fisher s exact test. 5
6 Korean J Ophthalmol Vol.31, No.1, 2017 Discussion Successful treatment of canalicular obstruction continues to present a therapeutic challenge. Although CDCR is the standard treatment in patients with extensive canalicular obstruction, many studies have reported relatively high rates of complications and poor patient satisfaction [12]. Owing to the development of surgical techniques and instruments, endonasal DCR, a less invasive method, is now widely used to treat canalicular obstruction. Following DCR, silicone tubes are inserted into each canaliculus in order to prevent adherence of the mucosal lining of the ducts during healing and to maintain long-term patency. Various instruments and methods have been described for achieving increased anatomical and functional success rates in lacrimal intubation [2,4,9,10,13]. The aim of this study was to compare the clinical efficacies of two different intubation methods double silicone intubation and single wide-diameter tube intubation. The efficacy of double silicone intubation has been reported by many studies. Demirci and Elner [6] assessed the results of double silicone intubation and reported that 79% of the patients included in their study experienced symptom resolution. Additionally, Hwang et al. [7] reported anatomical and functional success rates of 96.5% and 88.3%, respectively, while Paik et al. [14] reported rates of 91.4% and 82.8%. They suggested that double silicone intubation might be a more successful procedure for the treatment of canalicular obstruction than balloon catheter dilatation, at a considerably lesser cost [6]. The reasons for the higher success rates of double silicone intubation in comparison to the other techniques are the greater dilation of the lacrimal system achieved by this method and prevention of restenosis after stent removal. In double-tube bicanalicular intubation, complications such as punctal or canalicular slitting can be expected while inserting the second tube into the punctum already occupied by the first tube. However, none of the previous studies have reported any serious complications during this procedure. Moreover, enlargement of the lacrimal punctum with an incision facilitates the entrance of the second silicone tube. Additionally, these complications can be avoided by advancing the tubes gently according to the contours of the canaliculus. During double silicone intubation, patients might experience local discomfort because of the greater dilation of the canaliculus; however, most patients tolerate this discomfort well. In the present study, the surgical results of double-tube intubation after endonasal DCR showed success rates similar to those reported in the previous studies. Yildiz et al. [10] and Hurwitz [2] introduced another intubation method employing a single wide-diameter tube. Hurwitz [2] suggested that wide-diameter stents would dilate the lacrimal system more easily and successfully. Yildiz et al. [10] reported no failures or difficulties related to the larger tube size, and Hurwitz [2] reported relief of epiphora in six of seven patients and no complications other than one case of punctal granuloma. The anatomical and functional success rates of single wide-diameter tube intubation in the present study were 88.2% and 89.7%, respectively, which are consistent with those reported in previous studies on the outcomes of wide-stent intubation. In the present study, although the mean follow-up period in the double-tube intubation group was slightly longer than that in the single wide-diameter tube intubation group, the difference between the two groups was not statistically significant (p = 0.828). We removed the silicone tubes in a routine procedure around 3 months after DCR by cutting their interpunctal portions and retracting the ends from the nose. Based on the theory that retention of a stent within the nasolacrimal system might widen the canalicular space and prevent adhesion of the mucosal lining, intubation for longer duration might help increase the success rates of this procedure. Demirci and Elner [6] reported that scarring responses reach their final configuration in approximately 1 year. However, Paik et al. [14] stated that tube stenting for a longer duration is not required to achieve effective treatment. In our study, the overall success rates of both groups after 3 months of intubation (82.3% and 80.9% in the double-tube and single wide-diameter tube intubation groups, respectively) were similar to those reported in previous studies. In this study, we examined follow-up visits that occurred more than 3 months after surgery. Six months after surgery, the success rates in both groups were similar to those observed 3 months after surgery. However, 12 months after surgery, the anatomical and functional success rates had declined in the double-tube intubation group. Further research is needed to verify these results because many patients were lost to follow up. However, the higher success rate in the single wide-diameter tube group at 12 months indicates that it may be advantageous to use single wide-diameter tube in 6
7 SC Choi, et al. The Efficacy of 0.94 mm Silicone Tube in Canalicular Obstruction treating canalicular stenosis and/or obstruction. We compared the efficacies of double silicone tube intubation and single 0.94-mm silicone tube intubation in the treatment of distal or common canalicular obstruction. Both methods showed high overall success rates (82.3% and 80.9% in the double-tube and single wide-diameter tube intubation groups, respectively) consistent with those reported previously. There were no significant differences in any of the clinical characteristics between the two groups. Patients who underwent double silicone intubation were diagnosed with common canalicular obstruction in 54.4% of the cases and monocanalicular obstruction in 45.6% of the cases. In the single wide-diameter intubation group, 69.1% of the eyes showed common canalicular obstruction, and 30.9% showed monocanalicular obstruction. The proportions of each of the diagnoses were different between the two groups; however, the differences were not statistically significant (p = 0.068). Single wide-diameter silicone intubation is advantageous since the procedure does not require additional procedures for the management of the puncta, such as dilatation or punctoplasty, and has a lower risk of inflammation compared to double silicone intubation. The presence of two tubes in a canaliculus might induce greater friction between the tubes and, consequently, greater irritation of the eye. Single wide-diameter silicone intubation exhibits as high a success rate as double silicone intubation, with fewer complications such as inflammation and ocular irritation. We, therefore, suggest that single wide-diameter silicone intubation could be a better primary choice for the treatment of monocanalicular or common canalicular stenosis/obstruction compared to double silicone intubation. There are several limitations to the present study. First, our study was retrospective, and the two different types of surgeries were not performed simultaneously. Additionally, the mean follow-up period in our study was shorter than that in similar previous studies. After removal of the tubes, the patients included in our study did not often present for follow-up; this might largely have been due to the relief of symptoms. Finally, our study did not assess the efficacy of the 0.64-mm single-tube intubation. However, many previous studies have reported the success rates of single, double, and wide-diameter intubations. The results of our study indicate that double silicone tube stenting and single wide-diameter tube stenting in endoscopic DCR are effective treatments for patients with distal or common canalicular obstruction. Conflict of Interest No potential conflict of interest relevant to this article was reported. References 1. Bartley GB, Gustafson RO. Complications of malpositioned Jones tubes. Am J Ophthalmol 1990;109: Hurwitz JJ. A new, wider-diameter Crawford tube for stenting in the lacrimal drainage system. Ophthal Plast Reconstr Surg 2004;20: Crawford JS. Intubation of obstructions in the lacrimal system. Can J Ophthalmol 1977;12: Inatani M, Yamauchi T, Fukuchi M, et al. Direct silicone intubation using Nunchaku-style tube (NST-DSI) to treat lacrimal passage obstruction. Acta Ophthalmol Scand 2000;78: Lauring L. Silicone intubation of the lacrimal system: pitfalls, problems and complications. Ann Ophthalmol 1976;8: Demirci H, Elner VM. Double silicone tube intubation for the management of partial lacrimal system obstruction. Ophthalmology 2008;115: Hwang SW, Khwarg SI, Kim JH, et al. Bicanalicular double silicone intubation in external dacryocystorhinostomy and canaliculoplasty for distal canalicular obstruction. Acta Ophthalmol 2009;87: Kashkouli MB, Pakdel F, Kiavash V. Assessment and management of proximal and incomplete symptomatic obstruction of the lacrimal drainage system. Middle East Afr J Ophthalmol 2012;19: Kim SJ, Kim SD. The surgical results of endonasal DCR with two silicone tubes in common canalicular obstruction. J Korean Ophthalmol Soc 2007;48: Yildiz M, Yazici B, Akova B, Karatas A. A new and simple silicone intubation method for dacryocystorhinostomy. Eur J Gen Med 2011;8: Munk PL, Lin DT, Morris DC. Epiphora: treatment by means of dacryocystoplasty with balloon dilation of the nasolacrimal drainage apparatus. Radiology 1990;177: Liarakos VS, Boboridis KG, Mavrikakis E, Mavrikakis I. 7
8 Korean J Ophthalmol Vol.31, No.1, 2017 Management of canalicular obstructions. Curr Opin Ophthalmol 2009;20: Kurihashi K. Bicanalicular silicone intubation using threepiece silicone tubing: direct silicone intubation. Ophthalmologica 1993;206: Paik JS, Cho WK, Yang SW. Bicanalicular double silicone stenting in endoscopic dacryocystorhinostomy with lacrimal trephination in distal or common canalicular obstruction. Eur Arch Otorhinolaryngol 2012;269:
Study of success rates in endoscopic dacryocystorhinostomy with and without stenting. dacryocystorhinostomy with and
 Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
NASOLACRIMAL DUCT OBSTRUCTION (BLOCKED TEAR DUCT) AND TEARY EYE - PATIENT INFORMATION
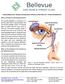 NASOLACRIMAL DUCT OBSTRUCTION (BLOCKED TEAR DUCT) AND TEARY EYE - PATIENT INFORMATION What is lacrimal sac and nasolacrimal duct? The lacrimal apparatus is composed of a lacrimal gland (tear producing
NASOLACRIMAL DUCT OBSTRUCTION (BLOCKED TEAR DUCT) AND TEARY EYE - PATIENT INFORMATION What is lacrimal sac and nasolacrimal duct? The lacrimal apparatus is composed of a lacrimal gland (tear producing
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 80/ Oct. 05, 2015 Page 14022
 STUDY ON MANAGEMENT OF EPIPHORA IN PATIENTS WITH OBSTRUCTION AT VARIOUS LEVELS OF NASOLACRIMAL APPARATUS S. Shivranjani 1, Jaishree Dwivedi 2, Neha Mithal 3, Sandeep Mithal 4 HOW TO CITE THIS ARTICLE:
STUDY ON MANAGEMENT OF EPIPHORA IN PATIENTS WITH OBSTRUCTION AT VARIOUS LEVELS OF NASOLACRIMAL APPARATUS S. Shivranjani 1, Jaishree Dwivedi 2, Neha Mithal 3, Sandeep Mithal 4 HOW TO CITE THIS ARTICLE:
Evaluation of Tear Film Lipid Layer Thickness Measurements Obtained Using an Ocular Surface Interferometer in Nasolacrimal Duct Obstruction Patients
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(6):445-450 https://doi.org/10.3341/kjo.2018.0012 Original Article Evaluation of Tear Film Lipid Layer Thickness Measurements Obtained Using
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(6):445-450 https://doi.org/10.3341/kjo.2018.0012 Original Article Evaluation of Tear Film Lipid Layer Thickness Measurements Obtained Using
Original Article Bicanalicular intubation procedure for acquired punctual stenosis
 Int J Clin Exp Med 2018;11(10):10815-10819 www.ijcem.com /ISSN:1940-5901/IJCEM0074867 Original Article Bicanalicular intubation procedure for acquired punctual stenosis Ying Chen 1, Xia Zhang 1, Liguo
Int J Clin Exp Med 2018;11(10):10815-10819 www.ijcem.com /ISSN:1940-5901/IJCEM0074867 Original Article Bicanalicular intubation procedure for acquired punctual stenosis Ying Chen 1, Xia Zhang 1, Liguo
Minimally Invasive Technique of Dacryocystorhinostomy
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Protocol Mohammad Idrees* Consultant Ophthalmology, REDO Eye Hospital, Rawalpindi, Pakistan *Corresponding Author: Mohammad Idrees, Consultant Ophthalmology,
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Protocol Mohammad Idrees* Consultant Ophthalmology, REDO Eye Hospital, Rawalpindi, Pakistan *Corresponding Author: Mohammad Idrees, Consultant Ophthalmology,
Yunhai Tu, 1 Zhenbin Qian, 2 Jiao Zhang, 1 Wencan Wu, 1 and Tianlin Xiao Introduction. 2. Patients and Methods
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 201, Article ID 67909, 7 pages http://dx.doi.org/10.11/201/67909 Clinical Study Endoscopic Endonasal Dacryocystorhinostomy Combined with Canaliculus
Hindawi Publishing Corporation Journal of Ophthalmology Volume 201, Article ID 67909, 7 pages http://dx.doi.org/10.11/201/67909 Clinical Study Endoscopic Endonasal Dacryocystorhinostomy Combined with Canaliculus
Philippine Journal of OPHTHALMOLOGY ABSTRACT
 Original Article Philippine Journal of OPHTHALMOLOGY Surgical Technique and Preliminary Results of Transcanalicular Endoscopic Lacrimal Duct Recanalization and Balloon Dacryoplasty with Silicone Intubation
Original Article Philippine Journal of OPHTHALMOLOGY Surgical Technique and Preliminary Results of Transcanalicular Endoscopic Lacrimal Duct Recanalization and Balloon Dacryoplasty with Silicone Intubation
THE EXTERNAL DACRYOCYSTORHINOSTOMY (DCR)
 Outcome of External Dacryocystorhinostomy Combined With Membranectomy of a Distal Canalicular Obstruction KOSTAS G. BOBORIDIS, MD, CATEY BUNCE, DSC, AND GEOFFREY E. ROSE, FRCS, FRCOPHTH PURPOSE: To investigate
Outcome of External Dacryocystorhinostomy Combined With Membranectomy of a Distal Canalicular Obstruction KOSTAS G. BOBORIDIS, MD, CATEY BUNCE, DSC, AND GEOFFREY E. ROSE, FRCS, FRCOPHTH PURPOSE: To investigate
Preoperative Computed Tomography Findings for Patients with Nasolacrimal Duct Obstruction or Stenosis
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):243-250 http://dx.doi.org/10.3341/kjo.2016.30.4.243 Original Article Preoperative Computed Tomography Findings for Patients with Nasolacrimal
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):243-250 http://dx.doi.org/10.3341/kjo.2016.30.4.243 Original Article Preoperative Computed Tomography Findings for Patients with Nasolacrimal
Effects of Nasopore Packing on Dacryocystorhinostomy
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(2):73-80 http://dx.doi.org/10.3341/kjo.2013.27.2.73 Effects of Nasopore Packing on Dacryocystorhinostomy Original Article Sun Young Jang 1,
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(2):73-80 http://dx.doi.org/10.3341/kjo.2013.27.2.73 Effects of Nasopore Packing on Dacryocystorhinostomy Original Article Sun Young Jang 1,
Pediatric Epiphora. Lacrimal drainage system begins to develop at the. Pediatric Ophthalmology. Saurbhi Khurana MD, FICO
 Pediatric Ophthalmology Pediatric Epiphora Saurbhi Khurana MD, FICO Saurbhi Khurana MD, FICO, A.K Grover MD, MNAMS, FRCS (Glasgow) FIMSA, FICO Vision Eye Centre, Siri Fort Road, New Delhi Lacrimal drainage
Pediatric Ophthalmology Pediatric Epiphora Saurbhi Khurana MD, FICO Saurbhi Khurana MD, FICO, A.K Grover MD, MNAMS, FRCS (Glasgow) FIMSA, FICO Vision Eye Centre, Siri Fort Road, New Delhi Lacrimal drainage
Repeat DCR with Silicone Tube intubation : A Prospective Study.
 Repeat DCR with Silicone Tube intubation : A Prospective Study. Dr Imtiyaz A Lone Assistant Professor Department of Ophthalmology SKIMS Medical College Bemina, Srinagar, India Dr Bashir A Malik Sr. Resident
Repeat DCR with Silicone Tube intubation : A Prospective Study. Dr Imtiyaz A Lone Assistant Professor Department of Ophthalmology SKIMS Medical College Bemina, Srinagar, India Dr Bashir A Malik Sr. Resident
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
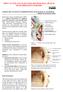 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY ENDOSCOPIC DACRYOCYSTORHINOSTOMY (DCR) SURGICAL TECHNIQUE Hisham Wasl, Darlene Lubbe Endoscopic dacryocystorhinostomy (DCR) is a surgical
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY ENDOSCOPIC DACRYOCYSTORHINOSTOMY (DCR) SURGICAL TECHNIQUE Hisham Wasl, Darlene Lubbe Endoscopic dacryocystorhinostomy (DCR) is a surgical
Non-endoscopic Mechanical Endonasal Dacryocystorhinostomy
 Surgical Technique Non-endoscopic Mechanical Endonasal Dacryocystorhinostomy Mohammad Etezad Razavi 1, MD; Morteza Noorollahian 2, MD; Alireza Eslampoor 1, MD 1 Khatam-al-Anbia Eye Research Center, Mashhad
Surgical Technique Non-endoscopic Mechanical Endonasal Dacryocystorhinostomy Mohammad Etezad Razavi 1, MD; Morteza Noorollahian 2, MD; Alireza Eslampoor 1, MD 1 Khatam-al-Anbia Eye Research Center, Mashhad
The clinical value of dacryoscintigraphy in the selection of surgical approach for patients with functional lacrimal duct obstruction
 ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 19, No. 6, 479 483, 2005 The clinical value of dacryoscintigraphy in the selection of surgical approach for patients with functional lacrimal duct obstruction
ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 19, No. 6, 479 483, 2005 The clinical value of dacryoscintigraphy in the selection of surgical approach for patients with functional lacrimal duct obstruction
Nasal Endoscopic Dacryocystorhinostomy The Nizamabad experience
 Original Research Article Nasal Endoscopic Dacryocystorhinostomy The Nizamabad experience Anand Acharya 1*, Modini P. 2, G. Lakpati 3 1 Associate Professor, ENT Department, GMC, Nizamabad, India 2 Associate
Original Research Article Nasal Endoscopic Dacryocystorhinostomy The Nizamabad experience Anand Acharya 1*, Modini P. 2, G. Lakpati 3 1 Associate Professor, ENT Department, GMC, Nizamabad, India 2 Associate
Self-Securing Monocanalicular Stent for Treatment of Nasolacrimal Duct Obstruction
 J Med Sci 2004;24(4):199-204 http://jms.ndmctsgh.edu.tw/2404199.pdf Copyright 2004 JMS Shang-Yi Chiang, et al. Self-Securing Monocanalicular Stent for Treatment of Nasolacrimal Duct Obstruction Shang-Yi
J Med Sci 2004;24(4):199-204 http://jms.ndmctsgh.edu.tw/2404199.pdf Copyright 2004 JMS Shang-Yi Chiang, et al. Self-Securing Monocanalicular Stent for Treatment of Nasolacrimal Duct Obstruction Shang-Yi
Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy
 SV Manjunatha Rao, MM Rajshekar Original Article 10.5005/jp-journals-10013-1284 Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy 1 SV Manjunatha Rao, 2 MM Rajshekar ABSTRACT
SV Manjunatha Rao, MM Rajshekar Original Article 10.5005/jp-journals-10013-1284 Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy 1 SV Manjunatha Rao, 2 MM Rajshekar ABSTRACT
Acute Dacryocystitis with Abscess: Endonasal Dacryocystorhinostomy, the Primary Treatment of Choice
 10.5005/jp-journals-10013-1129 ORIGINAL ARTICLE Acute Dacryocystitis with Abscess: Endonasal Dacryocystorhinostomy, the Primary Treatment of Choice Sudhir M Naik, Sarika S Naik ABSTRACT Background/objectives:
10.5005/jp-journals-10013-1129 ORIGINAL ARTICLE Acute Dacryocystitis with Abscess: Endonasal Dacryocystorhinostomy, the Primary Treatment of Choice Sudhir M Naik, Sarika S Naik ABSTRACT Background/objectives:
DACRYOCYSTORHINOSTOMY; A COMPARATIVE STUDY OF THE RESULTS WITH AND WITHOUT SILICON INTUBATION IN PAKISTANI PATIENTS OF CHRONIC DACRYOCYSTITIS
 DACRYOCYSTORHINOSTOMY 81 ORIGINAL PROF-1230 DACRYOCYSTORHINOSTOMY; A COMPARATIVE STUDY OF THE RESULTS WITH AND WITHOUT SILICON INTUBATION IN PAKISTANI PATIENTS OF CHRONIC DACRYOCYSTITIS DR. MUHAMMAD NAWAZ,
DACRYOCYSTORHINOSTOMY 81 ORIGINAL PROF-1230 DACRYOCYSTORHINOSTOMY; A COMPARATIVE STUDY OF THE RESULTS WITH AND WITHOUT SILICON INTUBATION IN PAKISTANI PATIENTS OF CHRONIC DACRYOCYSTITIS DR. MUHAMMAD NAWAZ,
Shreya M. Shah, Mehul A. Shah & Chintan Patel
 Cannula dacryocystorhinostomy: a simple, innovative and cost-effective method of lacrimal surgery Shreya M. Shah, Mehul A. Shah & Chintan Patel International Ophthalmology The International Journal of
Cannula dacryocystorhinostomy: a simple, innovative and cost-effective method of lacrimal surgery Shreya M. Shah, Mehul A. Shah & Chintan Patel International Ophthalmology The International Journal of
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD
 St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-EYES Fax: 314-997-3911 Toll Free: 866-869-3937 NASOLACRIMAL DUCT SURGERY (Post-Op
St. Louis Eye Care Specialists, LLC Andrew N. Blatt, MD 675 Old Ballas Rd. Suite 220 St. Louis, MO 63141 Phone: 314-997-EYES Fax: 314-997-3911 Toll Free: 866-869-3937 NASOLACRIMAL DUCT SURGERY (Post-Op
Outcomes of external dacryocystorhinostomy and endoscopic endonasal dacryocystorhinostomy in the management of nasolacrimal duct obstruction
 Original article Outcomes of external dacryocystorhinostomy and endoscopic endonasal dacryocystorhinostomy in the management of nasolacrimal duct obstruction Duwal S, Saiju R Tilganga Institute of Ophthalmology,
Original article Outcomes of external dacryocystorhinostomy and endoscopic endonasal dacryocystorhinostomy in the management of nasolacrimal duct obstruction Duwal S, Saiju R Tilganga Institute of Ophthalmology,
Clinical Results of Endoscopic Dacryocystorhinostomy using a Microdebrider
 Clinical Results of Endoscopic Dacryocystorhinostomy using a Microdebrider Sung Wook Yoon, MD, Young Sun Yoon, MD, Su Hyung Lee, MD Department of Ophthalmology, Dongkang General Hospital, Ulsan, Korea
Clinical Results of Endoscopic Dacryocystorhinostomy using a Microdebrider Sung Wook Yoon, MD, Young Sun Yoon, MD, Su Hyung Lee, MD Department of Ophthalmology, Dongkang General Hospital, Ulsan, Korea
Treatment of obstructive epiphora in adults by balloon dacryocystoplasty
 692 Uludag University, Department of Radiology, Bursa, Turkey Z Yazici M Parlak G Savci Uludag University, Department of Ophthalmology, Bursa, Turkey B Yazici H Erturk Correspondence to: Zeynep Yazici,
692 Uludag University, Department of Radiology, Bursa, Turkey Z Yazici M Parlak G Savci Uludag University, Department of Ophthalmology, Bursa, Turkey B Yazici H Erturk Correspondence to: Zeynep Yazici,
Study of outcomes of endonasal dacryocystorhinostomy in relation with sex distribution in Indian population
 Original article: Study of outcomes of endonasal dacryocystorhinostomy in relation with sex distribution in Indian population 1Dr. Mayur Ingale, 2 Dr. Vinod Shinde, 3 Dr.Paresh Chavan, 4 Dr.SudeepChoudhary
Original article: Study of outcomes of endonasal dacryocystorhinostomy in relation with sex distribution in Indian population 1Dr. Mayur Ingale, 2 Dr. Vinod Shinde, 3 Dr.Paresh Chavan, 4 Dr.SudeepChoudhary
Repair of Eyelid Trauma
 Repair of Eyelid Trauma Yunia Irawati, MD Plastic Reconstruction Division, Department of Ophthalmology FKUI / RSCM Introduction Eyelid trauma defined as a trauma to external surface of the lids with or
Repair of Eyelid Trauma Yunia Irawati, MD Plastic Reconstruction Division, Department of Ophthalmology FKUI / RSCM Introduction Eyelid trauma defined as a trauma to external surface of the lids with or
Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy
 Graefes Arch Clin Exp Ophthalmol (2012) 250:1509 1513 DOI 10.1007/s00417-012-1992-x OCULOPLASTICS AND ORBIT Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy Jae Wook
Graefes Arch Clin Exp Ophthalmol (2012) 250:1509 1513 DOI 10.1007/s00417-012-1992-x OCULOPLASTICS AND ORBIT Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy Jae Wook
External lacrimal punctum grading: Reliability and interobserver variation
 European Journal of Ophthalmology / Vol. 18 no. 4, 2008 / pp. 507-511 External lacrimal punctum grading: Reliability and interobserver variation M.B. KASHKOULI 1, N. NILFORUSHAN 1, M. NOJOMI 2, R. REZAEE
European Journal of Ophthalmology / Vol. 18 no. 4, 2008 / pp. 507-511 External lacrimal punctum grading: Reliability and interobserver variation M.B. KASHKOULI 1, N. NILFORUSHAN 1, M. NOJOMI 2, R. REZAEE
Stent technique for endoscopic dacryocystorhinostomy Our expertise
 Romanian Journal of Rhinology, Vol. 6, No. 21, January - March 2016 ORIGINAL STUDY Stent technique for endoscopic dacryocystorhinostomy Our expertise Vlad Budu 1, Tatiana Decuseara 1, Bogdan Mocanu 2,
Romanian Journal of Rhinology, Vol. 6, No. 21, January - March 2016 ORIGINAL STUDY Stent technique for endoscopic dacryocystorhinostomy Our expertise Vlad Budu 1, Tatiana Decuseara 1, Bogdan Mocanu 2,
Modified endoscopic dacryocystorhinostomy with posterior lacrimal sac flap for nasolacrimal duct obstruction!"#$%&'()*+,-*&'!./0(&
 Key words: Dacryocystorhinostomy; Endoscopy; Lacrimal apparatus diseases!!"#$%!"! KSC Yuen LYM Lam MWY Tse DDN Chan BWC Wong WM Chan Hong Kong Med J 00;:9-00 Department of Ophthalmology and Visual Sciences,
Key words: Dacryocystorhinostomy; Endoscopy; Lacrimal apparatus diseases!!"#$%!"! KSC Yuen LYM Lam MWY Tse DDN Chan BWC Wong WM Chan Hong Kong Med J 00;:9-00 Department of Ophthalmology and Visual Sciences,
A Comparative Study of Endoscopic Endonasal Dacryocystorhinostomy with and without Intraoperative Mitomycin-C Application
 10.5005/jp-journals-10013-1140 ORIGINAL ARTICLE A Comparative Study of Endoscopic Endonasal Dacryocystorhinostomy with and without Intraoperative Mitomycin-C Application Raman Wadhera, Sat Paul Gulati,
10.5005/jp-journals-10013-1140 ORIGINAL ARTICLE A Comparative Study of Endoscopic Endonasal Dacryocystorhinostomy with and without Intraoperative Mitomycin-C Application Raman Wadhera, Sat Paul Gulati,
Management of epiphora and lacrimal obstruction in adults
 Management of epiphora and lacrimal obstruction in adults Louis Savar, MD 1,2, Stuart R. Seiff, MD, FACS 1,2, Angela Maria Dolmetsch, MD 3 1. Department of Ophthalmology, University of California, San
Management of epiphora and lacrimal obstruction in adults Louis Savar, MD 1,2, Stuart R. Seiff, MD, FACS 1,2, Angela Maria Dolmetsch, MD 3 1. Department of Ophthalmology, University of California, San
Original Article Effect of revision dacryocystorhinostomy under nasal endoscopy on recrudescent dacryocystitis
 Int J Clin Exp Pathol 2017;10(12):11717-11722 www.ijcep.com /ISSN:1936-2625/IJCEP0052246 Original Article Effect of revision dacryocystorhinostomy under nasal endoscopy on recrudescent dacryocystitis Jintao
Int J Clin Exp Pathol 2017;10(12):11717-11722 www.ijcep.com /ISSN:1936-2625/IJCEP0052246 Original Article Effect of revision dacryocystorhinostomy under nasal endoscopy on recrudescent dacryocystitis Jintao
Frequency of Nasal Septal Perforation at the Suture Fixation Site of a Silastic Sheet Inserted during Nasal Surgery
 Soonchunhyang Medical Science 17(2):53-57, December 2011 pissn: 2233-4289 I eissn: 2233-4297 ORIGINAL ARTICLE Frequency of Nasal Septal Perforation at the Suture Fixation Site of a Silastic Sheet Inserted
Soonchunhyang Medical Science 17(2):53-57, December 2011 pissn: 2233-4289 I eissn: 2233-4297 ORIGINAL ARTICLE Frequency of Nasal Septal Perforation at the Suture Fixation Site of a Silastic Sheet Inserted
Clinical Study Comparison of Transcanalicular Multidiode Laser Dacryocystorhinostomy with and without Silicon Tube Intubation
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 2016, Article ID 6719529, 5 pages http://dx.doi.org/10.1155/2016/6719529 Clinical Study Comparison of Transcanalicular Multidiode Laser Dacryocystorhinostomy
Hindawi Publishing Corporation Journal of Ophthalmology Volume 2016, Article ID 6719529, 5 pages http://dx.doi.org/10.1155/2016/6719529 Clinical Study Comparison of Transcanalicular Multidiode Laser Dacryocystorhinostomy
Evaluation of the Canalicular Entrance Into the Lacrimal Sac: An Anatomical Study
 ANATOMY &PHYSIOLOGY Evaluation of the Canalicular Entrance Into the Lacrimal Sac: An Anatomical Study Christopher I. Zoumalan, M.D.*, Jeffrey M. Joseph, M.D.*, Gary J. Lelli, Jr., M.D., Kira L. Segal,
ANATOMY &PHYSIOLOGY Evaluation of the Canalicular Entrance Into the Lacrimal Sac: An Anatomical Study Christopher I. Zoumalan, M.D.*, Jeffrey M. Joseph, M.D.*, Gary J. Lelli, Jr., M.D., Kira L. Segal,
Intranasal location of lacrimal sac in Thai cadavers
 Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Balloon Dacryoplasty: Indications, Techniques and Outcomes
 INTERNATIONAL JOURNAL OF HEALTH RESEARCH IN MODERN INTEGRATED MEDICAL SCIENCES (IJHRMIMS), ISSN XXXX (P), ISSN XXXX (O), Oct-Dec 2014 15 Review Article Balloon Dacryoplasty: Indications, Techniques and
INTERNATIONAL JOURNAL OF HEALTH RESEARCH IN MODERN INTEGRATED MEDICAL SCIENCES (IJHRMIMS), ISSN XXXX (P), ISSN XXXX (O), Oct-Dec 2014 15 Review Article Balloon Dacryoplasty: Indications, Techniques and
The Comparison of the Result of Epiduroscopic Laser Neural Decompression between FBSS or Not
 Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
A new classification system of nasal contractures
 Original Article J Cosmet Med 2017;1(2):106-111 https://doi.org/10.25056/jcm.2017.1.2.106 pissn 2508-8831, eissn 2586-0585 A new classification system of nasal contractures Geunuck Chang 1, Donghak Jung
Original Article J Cosmet Med 2017;1(2):106-111 https://doi.org/10.25056/jcm.2017.1.2.106 pissn 2508-8831, eissn 2586-0585 A new classification system of nasal contractures Geunuck Chang 1, Donghak Jung
A new method for identifying the cut ends in canalicular laceration
 www.nature.com/scientificreports OPEN ecei e : 23 une 201 ccepte : 25 anuar 2017 u is e : 24 e ruar 2017 A new method for identifying the cut ends in canalicular laceration Wenyan Peng 1, Yandong Wang
www.nature.com/scientificreports OPEN ecei e : 23 une 201 ccepte : 25 anuar 2017 u is e : 24 e ruar 2017 A new method for identifying the cut ends in canalicular laceration Wenyan Peng 1, Yandong Wang
Tear Meniscus Volume Changes in Dacryocystorhinostomy Evaluated With Quantitative Measurement Using Anterior Segment Optical Coherence Tomography
 Clinical and Epidemiologic Research Tear Meniscus Volume Changes in Dacryocystorhinostomy Evaluated With Quantitative Measurement Using Anterior Segment Optical Coherence Tomography Kazuyoshi Ohtomo, Takashi
Clinical and Epidemiologic Research Tear Meniscus Volume Changes in Dacryocystorhinostomy Evaluated With Quantitative Measurement Using Anterior Segment Optical Coherence Tomography Kazuyoshi Ohtomo, Takashi
INTERVENTIONAL PROCEDURES PROGRAMME
 Prepared by ASERNIP-S Introduction NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of Endoscopic Dacryocystorhinostomy This overview has
Prepared by ASERNIP-S Introduction NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of Endoscopic Dacryocystorhinostomy This overview has
Congenital lacrimal fistula
 Ugurbas 6-03-2000 14:59 Pagina 22 European Journal of Ophthalmology / Vol. 10 no. 1, 2000 / pp. 22-26 S.H. UǦURBAŞ, G. ZILELIOǦLU Department of Ophthalmology, Ankara University Faculty of Medicine, Ankara
Ugurbas 6-03-2000 14:59 Pagina 22 European Journal of Ophthalmology / Vol. 10 no. 1, 2000 / pp. 22-26 S.H. UǦURBAŞ, G. ZILELIOǦLU Department of Ophthalmology, Ankara University Faculty of Medicine, Ankara
Reconstructions of Traumatic Lacrimal Canalicular Lacerations: A 5 Years Experience
 The Open Access Journal of Science and Technology Vol. 3 (2015), Article ID 101121, 6 pages doi:10.11131/2015/101121 Publishing House http://www.agialpress.com/ Clinical Study Reconstructions of Traumatic
The Open Access Journal of Science and Technology Vol. 3 (2015), Article ID 101121, 6 pages doi:10.11131/2015/101121 Publishing House http://www.agialpress.com/ Clinical Study Reconstructions of Traumatic
To analyse the success rate of external Dacryocystorhinostomy related with anatomical osteotomy size made during surgery
 2018; 4(1): 354-358 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(1): 354-358 www.allresearchjournal.com Received: 23-11-2017 Accepted: 24-12-2017 Pandit VK Associate Professor,
2018; 4(1): 354-358 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(1): 354-358 www.allresearchjournal.com Received: 23-11-2017 Accepted: 24-12-2017 Pandit VK Associate Professor,
International Journal of Pharma and Bio Sciences
 Research Article Otorhinolaryngology International Journal of Pharma and Bio Sciences ISSN 0975-6299 COMPARATIVE RESULTS OF ENDOSCOPIC VERSUS EXTERNAL DACRYOCYSTORHINOSTOMY FOR ACQUIRED NASO-LACRIMAL DUCT
Research Article Otorhinolaryngology International Journal of Pharma and Bio Sciences ISSN 0975-6299 COMPARATIVE RESULTS OF ENDOSCOPIC VERSUS EXTERNAL DACRYOCYSTORHINOSTOMY FOR ACQUIRED NASO-LACRIMAL DUCT
Value of nasal endoscopy and probing in the diagnosis and management of children with congenital epiphora
 314 Department of Ophthalmology, Ninewells Hospital, Dundee DD1 9SY, UK C J MacEwen JDHYoung C W Barras Department of Otolaryngology B Ram P S White Correspondence to: Dr MacEwen c.j.macewen@dundee.ac.uk
314 Department of Ophthalmology, Ninewells Hospital, Dundee DD1 9SY, UK C J MacEwen JDHYoung C W Barras Department of Otolaryngology B Ram P S White Correspondence to: Dr MacEwen c.j.macewen@dundee.ac.uk
Management of Congenital Nasolacrimal Duct Obstruction: Comparison of Probing Vs Conservative Medical Approach
 Bahrain Medical Bulletin, Vol. 22, No. 1, March 2000 Management of Congenital Nasolacrimal Duct Obstruction: Comparison of Probing Vs Conservative Medical Approach Basel T Baarah, MD* Wael Abu-Laban, MD**
Bahrain Medical Bulletin, Vol. 22, No. 1, March 2000 Management of Congenital Nasolacrimal Duct Obstruction: Comparison of Probing Vs Conservative Medical Approach Basel T Baarah, MD* Wael Abu-Laban, MD**
POLYTHENE TUBES IN CANALICULUS SURGERY*
 Brit. J. Ophthal. (1963) 47, 203. POLYTHENE TUBES IN CANALICULUS SURGERY* BY T. P. GRIFFITHt From the Corneo-Plastic Unit and Regional Eye Bank, Queen Victoria Hospital, East Grinstead, Sussex CANALICULUS
Brit. J. Ophthal. (1963) 47, 203. POLYTHENE TUBES IN CANALICULUS SURGERY* BY T. P. GRIFFITHt From the Corneo-Plastic Unit and Regional Eye Bank, Queen Victoria Hospital, East Grinstead, Sussex CANALICULUS
Dacryocystorh i nostomy in South West England
 Dacryocystorh i nostomy in South West England BlJAN BEIGI, WILLIAM WESTLAKE, BERNARD CHANG, CATHERINE MARSH, JOHN JACOB, JUDITH CHATFIELD B. Beigi W. Westlake B. Chang C. Marsh J. Jacob Department of Ophthalmology
Dacryocystorh i nostomy in South West England BlJAN BEIGI, WILLIAM WESTLAKE, BERNARD CHANG, CATHERINE MARSH, JOHN JACOB, JUDITH CHATFIELD B. Beigi W. Westlake B. Chang C. Marsh J. Jacob Department of Ophthalmology
Factors Influencing the Prevalence of Amblyopia in Children with Anisometropia
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(4):225-229 DOI: 10.3341/kjo.2010.24.4.225 Factors Influencing the Prevalence of Amblyopia in Children with Anisometropia Original Article Chong
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(4):225-229 DOI: 10.3341/kjo.2010.24.4.225 Factors Influencing the Prevalence of Amblyopia in Children with Anisometropia Original Article Chong
Puncto-Canalicular Microsurgery
 Puncto-Canalicular Microsurgery By Ossama T Nada Lecturer of Ophthalmology Ain Shams University MD, PhD, FRCSG Egyptian Ophthalmological Society Meeting 2018 Figure 10-9 (A) A hard stop with canalicular
Puncto-Canalicular Microsurgery By Ossama T Nada Lecturer of Ophthalmology Ain Shams University MD, PhD, FRCSG Egyptian Ophthalmological Society Meeting 2018 Figure 10-9 (A) A hard stop with canalicular
Classification of Lacrimal Punctal Stenosis and Its Related Histopathological Feature in Patients with Epiphora
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(5):375-382 https://doi.org/10.3341/kjo.2016.0129 Classification of Lacrimal Punctal Stenosis and Its Related Histopathological Feature in Patients
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(5):375-382 https://doi.org/10.3341/kjo.2016.0129 Classification of Lacrimal Punctal Stenosis and Its Related Histopathological Feature in Patients
Application of biodegradable collagen matrix (Ologen ) implants in Dacryocystorhinostomy surgeries, a randomized clinical study
 Marey et al. BMC Ophthalmology (2018) 18:254 https://doi.org/10.1186/s12886-018-0901-4 RESEARCH ARTICLE Open Access Application of biodegradable collagen matrix (Ologen ) implants in Dacryocystorhinostomy
Marey et al. BMC Ophthalmology (2018) 18:254 https://doi.org/10.1186/s12886-018-0901-4 RESEARCH ARTICLE Open Access Application of biodegradable collagen matrix (Ologen ) implants in Dacryocystorhinostomy
Bicanalicular Intubation for Traumatic Unicanalicular Laceration
 Medical Science, Volume 9, Number 32, June 4, 2014 EISSN 2321 7367 RESEARCH OPHTHALMOLOGY Medical Science ISSN 2321 7359 The International Weekly Journal for Medicine Bicanalicular Intubation for Traumatic
Medical Science, Volume 9, Number 32, June 4, 2014 EISSN 2321 7367 RESEARCH OPHTHALMOLOGY Medical Science ISSN 2321 7359 The International Weekly Journal for Medicine Bicanalicular Intubation for Traumatic
Endonasal Dacryocystorhinostomy done with and without Silicon Tube Stents: A Comparative Case Series Analysis Study
 10.5005/jp-journals-10001-1116 RESEARCH ARTICLE Endonasal Dacryocystorhinostomy done with and without Silicon Tube Stents: A Comparative Case Series Analysis Study Sudhir M Naik, Annapurna S Mushannavar,
10.5005/jp-journals-10001-1116 RESEARCH ARTICLE Endonasal Dacryocystorhinostomy done with and without Silicon Tube Stents: A Comparative Case Series Analysis Study Sudhir M Naik, Annapurna S Mushannavar,
Problems / Complications, Success Rate Endoscopic Dacryocystorhinostomy
 Original Article Problems / Complications, Success Rate Endoscopic Dacryocystorhinostomy Khawaja Khalid Shoaib, Salahuddin Ahmad, Muhammad Manzoor, Sabihuddin Ahmed, Iftikhar Aslam Syed Nadeem ul Haq Pak
Original Article Problems / Complications, Success Rate Endoscopic Dacryocystorhinostomy Khawaja Khalid Shoaib, Salahuddin Ahmad, Muhammad Manzoor, Sabihuddin Ahmed, Iftikhar Aslam Syed Nadeem ul Haq Pak
Lacrimal drainage surgery in patients with rare nasal diseases
 (2007) 21, 1361 1366 & 2007 Nature Publishing Group All rights reserved 0950-222X/07 $30.00 www.nature.com/eye Lacrimal drainage surgery in patients with rare nasal diseases CLINICAL STUDY Abstract Aim
(2007) 21, 1361 1366 & 2007 Nature Publishing Group All rights reserved 0950-222X/07 $30.00 www.nature.com/eye Lacrimal drainage surgery in patients with rare nasal diseases CLINICAL STUDY Abstract Aim
Size Solution for Dry Eye
 The Size Solution for Dry Eye Plug1 is the culmination of almost 40 years experience in the punctal occlusion market. A unique dual-lobed design allows Plug1 to fit a wide range of punctum sizes* using
The Size Solution for Dry Eye Plug1 is the culmination of almost 40 years experience in the punctal occlusion market. A unique dual-lobed design allows Plug1 to fit a wide range of punctum sizes* using
Endonasal endoscopic scalpel-forceps dacryocystorhinostomy vs endocanalicular diode laser dacryocystorhinostomy
 Eur J Ophthalmol 2012; 00 ( 00) : 000-000 DOI: 10.5301/ejo.5000157 ORIGINAL ARTICLE Endonasal endoscopic scalpel-forceps dacryocystorhinostomy vs endocanalicular diode laser dacryocystorhinostomy Juan
Eur J Ophthalmol 2012; 00 ( 00) : 000-000 DOI: 10.5301/ejo.5000157 ORIGINAL ARTICLE Endonasal endoscopic scalpel-forceps dacryocystorhinostomy vs endocanalicular diode laser dacryocystorhinostomy Juan
Comparative Study Of Probing Done with and without Endoscopic Assistance
 Comparative Study Of Probing Done with and without Endoscopic Assistance Ishan Acharya 1, Jitendra Jethani 2, Monika Jethani 3 Department of Ophthalmic Plastic Surgery, Orbit, Ocular Oncology and Ocular
Comparative Study Of Probing Done with and without Endoscopic Assistance Ishan Acharya 1, Jitendra Jethani 2, Monika Jethani 3 Department of Ophthalmic Plastic Surgery, Orbit, Ocular Oncology and Ocular
Comparison of outcome of external DCR and endonasal DCR surgery among the rural population
 Original article: Comparison of outcome of external DCR and endonasal DCR surgery among the rural population 1 Dr Aniket Lathi*, 2 Dr C Anand Kumar, 3 Dr Nitin Kulkarni, 4 Dr Ashish Gupta, 5 Dr Shruti
Original article: Comparison of outcome of external DCR and endonasal DCR surgery among the rural population 1 Dr Aniket Lathi*, 2 Dr C Anand Kumar, 3 Dr Nitin Kulkarni, 4 Dr Ashish Gupta, 5 Dr Shruti
Relation between the Peripherofacial Psoriasis and Scalp Psoriasis
 pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 4, 2016 http://dx.doi.org/10.5021/ad.2016.28.4.422 ORIGINAL ARTICLE Relation between the Peripherofacial Psoriasis and Scalp Psoriasis Kyung Ho
pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 4, 2016 http://dx.doi.org/10.5021/ad.2016.28.4.422 ORIGINAL ARTICLE Relation between the Peripherofacial Psoriasis and Scalp Psoriasis Kyung Ho
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Dr. Najah طب بغداد. Lecture: 14
 2015 2016 The lacrimal apparatus The lacrimal system consists of: Lecture: 14 Dr. Najah طب بغداد 1- Secretory portion: Comprises the following: a- The lacrimal gland: Which is divided into palpebral (Aqueoussecretion)
2015 2016 The lacrimal apparatus The lacrimal system consists of: Lecture: 14 Dr. Najah طب بغداد 1- Secretory portion: Comprises the following: a- The lacrimal gland: Which is divided into palpebral (Aqueoussecretion)
Syringing And Probing Under Local Anesthesia In Infants
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 3 Number 2 V Sharma, S Vaidya, S Shrivastava Citation V Sharma, S Vaidya, S Shrivastava.. The Internet Journal of Ophthalmology
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 3 Number 2 V Sharma, S Vaidya, S Shrivastava Citation V Sharma, S Vaidya, S Shrivastava.. The Internet Journal of Ophthalmology
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Epiphora Decoded. VG: How do you go about evaluating patients of epiphora? Any special investigations?
 Experts Corner Epiphora Decoded The development over the years in understanding pathophysiology of Lacrimal System disorder has undergone a sea-size change. The improvement in stenting material, laser-advances
Experts Corner Epiphora Decoded The development over the years in understanding pathophysiology of Lacrimal System disorder has undergone a sea-size change. The improvement in stenting material, laser-advances
A randomized placebo controlled trial of Mitomycin - C in surgical outcome of primary endoscopic dacryocystorhinostomy
 Al Am een J Med Sci 2013; 6(3):231-236 US National Library of Medicine enlisted journal ISSN 0974-1143 ORIGI NAL ARTICLE C O D E N : A A J MB G A randomized placebo controlled trial of Mitomycin - C in
Al Am een J Med Sci 2013; 6(3):231-236 US National Library of Medicine enlisted journal ISSN 0974-1143 ORIGI NAL ARTICLE C O D E N : A A J MB G A randomized placebo controlled trial of Mitomycin - C in
Research Article How Important Is the Etiology in the Treatment of Epiphora?
 Ophthalmology Volume 2016, Article ID 1438376, 6 pages http://dx.doi.org/10.1155/2016/1438376 Research Article How Important Is the Etiology in the Treatment of Epiphora? Mahmut OLuz Ulusoy, 1 Sertaç Argun
Ophthalmology Volume 2016, Article ID 1438376, 6 pages http://dx.doi.org/10.1155/2016/1438376 Research Article How Important Is the Etiology in the Treatment of Epiphora? Mahmut OLuz Ulusoy, 1 Sertaç Argun
A simple and evolutional approach proven to recanalise the nasolacrimal duct obstruction
 See Editorial, p 1416 1 Department of ENT, First Affiliated Hospital, Sun Yat-sen University, Guangzhou, PR China; 2 State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University,
See Editorial, p 1416 1 Department of ENT, First Affiliated Hospital, Sun Yat-sen University, Guangzhou, PR China; 2 State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University,
The Clinical Effects of Carthami-Flos Pharmacopuncture on Posterior Neck pain of Menopausal Women
 ISSN 2093-6966 Journal of Pharmacopuncture 71 http://dx.doi.org/10.3831/kpi.2011.14.4.071 Received : Nov 10, 2011 Revised : Nov 25, 2011 Accepted : Nov 30, 2011 KEY WORDS: Carthami-Flos; Neck pain, Pharmacopuncture;
ISSN 2093-6966 Journal of Pharmacopuncture 71 http://dx.doi.org/10.3831/kpi.2011.14.4.071 Received : Nov 10, 2011 Revised : Nov 25, 2011 Accepted : Nov 30, 2011 KEY WORDS: Carthami-Flos; Neck pain, Pharmacopuncture;
Superior Rectus Muscle Recession for Residual Head Tilt after Inferior Oblique Muscle Weakening in Superior Oblique Palsy
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(4):285-289 http://dx.doi.org/10.3341/kjo.2012.26.4.285 Original Article Superior Rectus Muscle Recession for Residual Head Tilt after Inferior
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2012;26(4):285-289 http://dx.doi.org/10.3341/kjo.2012.26.4.285 Original Article Superior Rectus Muscle Recession for Residual Head Tilt after Inferior
Initial placement 24FR Pull PEG kit REORDER NO:
 Initial placement 24FR Pull PEG kit REORDER NO: 00710805 INSTRUCTIONS FOR USE 1 of 5 These products have been manufactured not to include latex. Intended Use: The Initial placement 24FR Pull PEG kit is
Initial placement 24FR Pull PEG kit REORDER NO: 00710805 INSTRUCTIONS FOR USE 1 of 5 These products have been manufactured not to include latex. Intended Use: The Initial placement 24FR Pull PEG kit is
Endonasal dacryocystorhinostomy was first. Reliable technique of Endoscopic Dacryocystorhinostomy A Pilot Study. Main Article
 Main Article Reliable technique of Endoscopic Dacryocystorhinostomy A Pilot Study Sudip Kumar Das, 1 Chiranjib Das, 1 Amit Bikram Maiti, 2 Ruma Guha, 3 Subhendu Chowdhury 1 ABSTRACT Introduction Over last
Main Article Reliable technique of Endoscopic Dacryocystorhinostomy A Pilot Study Sudip Kumar Das, 1 Chiranjib Das, 1 Amit Bikram Maiti, 2 Ruma Guha, 3 Subhendu Chowdhury 1 ABSTRACT Introduction Over last
Estimation of Stellate Ganglion Block Injection Point Using the Cricoid Cartilage as Landmark Through X-ray Review
 Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Endoscopic Examination in Postmortem Examination
 Korean J Leg Med 2017;41:94-99 Original Article Endoscopic Examination in Postmortem Examination Joo-Young Na 1, Ji Hye Park 2 1 Biomedical Research Institute, Chonnam National University Hospital, Gwangju,
Korean J Leg Med 2017;41:94-99 Original Article Endoscopic Examination in Postmortem Examination Joo-Young Na 1, Ji Hye Park 2 1 Biomedical Research Institute, Chonnam National University Hospital, Gwangju,
Functional Endoscopic Sinus Surgery
 WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
Microscopic Characteristics of Lower Eyelid Retractors in Koreans
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(5):344-348 http://dx.doi.org/10.3341/kjo.2011.25.5.344 Original Article Microscopic Characteristics of Lower Eyelid Retractors in Koreans Won-Kyung
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2011;25(5):344-348 http://dx.doi.org/10.3341/kjo.2011.25.5.344 Original Article Microscopic Characteristics of Lower Eyelid Retractors in Koreans Won-Kyung
ORIGINAL ARTICLE. Intranasal Localization of the Lacrimal Sac
 ORIGINAL ARTICLE Intranasal Localization of the Lacrimal Sac Mustafa Orhan, MD; Canan Y. Saylam, MD; Raşit Midilli, MD Objective: To optimize the approach to the lacrimal sac during intranasal dacryocystorhinostomy.
ORIGINAL ARTICLE Intranasal Localization of the Lacrimal Sac Mustafa Orhan, MD; Canan Y. Saylam, MD; Raşit Midilli, MD Objective: To optimize the approach to the lacrimal sac during intranasal dacryocystorhinostomy.
Unilateral lateral rectus muscle advancement surgery based on one-fourth of the angle of consecutive esotropia
 Kim and Lee BMC Ophthalmology (2017) 17:266 DOI 10.1186/s12886-017-0658-1 RESEARCH ARTICLE Open Access Unilateral lateral rectus muscle advancement surgery based on one-fourth of the angle of consecutive
Kim and Lee BMC Ophthalmology (2017) 17:266 DOI 10.1186/s12886-017-0658-1 RESEARCH ARTICLE Open Access Unilateral lateral rectus muscle advancement surgery based on one-fourth of the angle of consecutive
Double Y-stenting for tracheobronchial stenosis
 ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
The Results of Evisceration with Primary Porous Implant Placement in Patients with Endophthalmitis
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(5):279-283 DOI: 10.3341/kjo.2010.24.5.279 Original Article The Results of Evisceration with Primary Porous Implant Placement in Patients with
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2010;24(5):279-283 DOI: 10.3341/kjo.2010.24.5.279 Original Article The Results of Evisceration with Primary Porous Implant Placement in Patients with
Morphological and morphometrical study of the nasal opening of nasolacrimal duct in man
 O R I G I N A L A R T I C L E Folia Morphol. Vol. 73, No. 3, pp. 321 330 DOI: 10.5603/FM.2014.0049 Copyright 2014 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Morphological and morphometrical study of
O R I G I N A L A R T I C L E Folia Morphol. Vol. 73, No. 3, pp. 321 330 DOI: 10.5603/FM.2014.0049 Copyright 2014 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Morphological and morphometrical study of
Congenital Nasolacrimal Duct Obstruction (CNLDO)
 June 2007 Ramesh Murthy - Congenital Nasolacrimal Duct Obstruction 191 OPHTHALMIC SURGERY Congenital Nasolacrimal Duct Obstruction (CNLDO) Dr. Ramesh Murthy MD FRCS Introduction CNLDO is a common problem
June 2007 Ramesh Murthy - Congenital Nasolacrimal Duct Obstruction 191 OPHTHALMIC SURGERY Congenital Nasolacrimal Duct Obstruction (CNLDO) Dr. Ramesh Murthy MD FRCS Introduction CNLDO is a common problem
Nasolacrimal Duct Blockage
 The eyelids play a key role in protecting the eyes. They help spread moisture (tears) over the surface of the eyes when they close (for example, while blinking); thus, they help prevent the eyes from becoming
The eyelids play a key role in protecting the eyes. They help spread moisture (tears) over the surface of the eyes when they close (for example, while blinking); thus, they help prevent the eyes from becoming
Time Series Changes in Cataract Surgery in Korea
 pissn: 111-8942 eissn: 292-9382 Korean J Ophthalmol 218;32(3):182-189 https://doi.org/1.3341/kjo.217.72 Time Series Changes in Cataract Surgery in Korea Original Article Ju Hwan Song 1*, Jung Youb Kang
pissn: 111-8942 eissn: 292-9382 Korean J Ophthalmol 218;32(3):182-189 https://doi.org/1.3341/kjo.217.72 Time Series Changes in Cataract Surgery in Korea Original Article Ju Hwan Song 1*, Jung Youb Kang
Lower Eyelid Malposition
 Oculoplastic Surgeon s DDX for the Red Eye Geeta Belsare Been,MD The Center for Facial Plastic Surgery Barrington, IL Lower Eyelid Malposition Ectropion Involutional Cicatricial Paralytic Entropion Involutional
Oculoplastic Surgeon s DDX for the Red Eye Geeta Belsare Been,MD The Center for Facial Plastic Surgery Barrington, IL Lower Eyelid Malposition Ectropion Involutional Cicatricial Paralytic Entropion Involutional
The role of interventional radiology in the treatment of epiphora
 Review Article on Interventional Radiology in Glands The role of interventional radiology in the treatment of epiphora Francesca Patella 1, Silvia Panella 1, Stefania Zannoni 1, Maria Laura Jannone 1,
Review Article on Interventional Radiology in Glands The role of interventional radiology in the treatment of epiphora Francesca Patella 1, Silvia Panella 1, Stefania Zannoni 1, Maria Laura Jannone 1,
INFORMATION REGARDING YOUR NASAL SURGERY
 INFORMATION REGARDING YOUR NASAL SURGERY This document contains information about the following aspects of nasal surgery: Pre-op information: How to prepare for surgery. Procedure: Wat is done during surgery.
INFORMATION REGARDING YOUR NASAL SURGERY This document contains information about the following aspects of nasal surgery: Pre-op information: How to prepare for surgery. Procedure: Wat is done during surgery.
Obstruction of the LDS, resulting in inadequate drainage of
 ORIGINAL RESEARCH B. Coskun E. Ilgit B. Onal O. Konuk G. Erbas MR Dacryocystography in the Evaluation of Patients with Obstructive Epiphora Treated by Means of Interventional Radiologic Procedures BACKGROUND
ORIGINAL RESEARCH B. Coskun E. Ilgit B. Onal O. Konuk G. Erbas MR Dacryocystography in the Evaluation of Patients with Obstructive Epiphora Treated by Means of Interventional Radiologic Procedures BACKGROUND
Watery Eye. Watering of the eye (epiphora) Causes of overproduction of tears
 Watery Eye Watery Eye Tears are formed by the lacrimal gland, which lies beneath the outer part of the upper lid, and by cells in the conjunctival surface of the eye. Watering of the eye (epiphora) This
Watery Eye Watery Eye Tears are formed by the lacrimal gland, which lies beneath the outer part of the upper lid, and by cells in the conjunctival surface of the eye. Watering of the eye (epiphora) This
SINUS SURGERY. Dr Zenia Chow MBBS(hons), FRACS
 SINUS SURGERY Dr Zenia Chow MBBS(hons), FRACS Facial Plastic & Reconstructive Surgeon Otolaryngology, Head and Neck Surgeon ENDOSCOPIC SINUS SURGERY/FESS What are sinuses The sinuses are a connected system
SINUS SURGERY Dr Zenia Chow MBBS(hons), FRACS Facial Plastic & Reconstructive Surgeon Otolaryngology, Head and Neck Surgeon ENDOSCOPIC SINUS SURGERY/FESS What are sinuses The sinuses are a connected system
Computed tomographic dacryocystography as compared with X-ray dacryocystography in patients with dacryostenosis
 Computed tomographic dacryocystography as compared with X-ray dacryocystography in patients with dacryostenosis Poster No.: C-1887 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M.
Computed tomographic dacryocystography as compared with X-ray dacryocystography in patients with dacryostenosis Poster No.: C-1887 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M.
MEDIAL CANTHAL LIGAment
 CLINICAL SCIENCES Transcaruncular Medial Canthal Ligament Plication for Repair of Lower Eyelid Malposition Victor M. Elner, MD, PhD; Hakan Demirci, MD; Asa D. Morton, MD; Susan G. Elner, MD; Adam S. Hassan,
CLINICAL SCIENCES Transcaruncular Medial Canthal Ligament Plication for Repair of Lower Eyelid Malposition Victor M. Elner, MD, PhD; Hakan Demirci, MD; Asa D. Morton, MD; Susan G. Elner, MD; Adam S. Hassan,
Evaluation of lacrimal apparatus
 From the SelectedWorks of Balasubramanian Thiagarajan September 18, 2012 Evaluation of lacrimal apparatus Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/9/ Evaluation of lacrimal
From the SelectedWorks of Balasubramanian Thiagarajan September 18, 2012 Evaluation of lacrimal apparatus Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/9/ Evaluation of lacrimal
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/24545
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/24545
