Treatment of obstructive epiphora in adults by balloon dacryocystoplasty
|
|
|
- Aubrey Harvey
- 5 years ago
- Views:
Transcription
1 692 Uludag University, Department of Radiology, Bursa, Turkey Z Yazici M Parlak G Savci Uludag University, Department of Ophthalmology, Bursa, Turkey B Yazici H Erturk Correspondence to: Zeynep Yazici, MD, Department of Radiology, Uludag University, School of Medicine, Gorukle Campus, 16059, Gorukle, Bursa, Turkey. Accepted for publication 10 December 1998 Treatment of obstructive epiphora in adults by balloon dacryocystoplasty Zeynep Yazici, Bulent Yazici, Mufit Parlak, Haluk Erturk, Gursel Savci Abstract Aims To determine the eycacy of dacryocystoplasty with balloon dilatation in the treatment of complete and partial obstruction of the lacrimal drainage system. Methods The procedure was performed on 26 patients with epiphora due to complete (n=16) or partial (n=10) obstruction of the lacrimal drainage system. A flexible tipped guide wire was introduced through the superior canaliculus into the inferior meatus and manipulated out of the nasal cavity. A 3 mm balloon was then introduced in a retrograde direction over the guide wire and dilated at the obstruction site. Results The procedure was technically successful in all patients with partial obstruction, but unsuccessful in four of 16 cases with complete obstruction. Reobstruction occurred in eight of 12 patients with complete obstruction, and in five of 10 patients with partial obstruction. The overall success rate was 25% for complete and 50% for partial obstructions. The mean follow up was 14 months (8 37 months). Conclusion Although the balloon dacryocystoplasty is a simple and minimally invasive technique, the outcome from our study indicates that it is not advisable for treatment of complete obstruction of the lacrimal drainage system. Balloon dilatation may prove suitable for the treatment of patients with partial obstruction below the level of the lacrimal sac, especially in those who are poor candidates for surgery, or who do not wish to undertake dacryocystorhinostomy. Even in the partial obstruction group the success rate was only 50%, so that further modification to the technique and controlled studies are likely to be required before it could be recommended for general use. (Br J Ophthalmol 1999;83: ) In adults, epiphora is usually secondary to the obstruction of the nasolacrimal duct. The aetiology of the obstruction is mostly an idiopathic inflammation of the lacrimal drainage system (LDS). 1 Surgical treatment of obstructive epiphora is usually carried out either by recanalising the occluded lacrimal system such as by probing or silicone intubation, or by creating an anastomosis between the lacrimal sac and the nasal cavity to bypass the obstruction such as dacryocystorhinostomy (DCR). Dacryocystorhinostomy has a high success rate Br J Ophthalmol 1999;83: but it is an incisional surgical procedure. 2 It may require general anaesthesia for the comfort of both the patient and the physician. Probing and silicone intubation are usually the treatment choice for the obstructive epiphora in children. The evectiveness of these methods, however, is quite limited in adults, probably because of the diverences in the underlying cause of the obstruction. 3 4 The obstruction is usually caused by fibrosis as a result of idiopathic inflammation in adults, and imperforated Hasner s valve in children. Balloon dacryocystoplasty (BD) is a new method based on the recanalisation of the occluded lacrimal system. 5 In this study, we investigated the eycacy of BD in 26 adult patients with obstructive epiphora. Materials and methods Between January 1995 and May 1997, BD was performed in 16 patients with complete obstruction and 10 patients with partial obstruction of the LDS (20 women and six men; age range years; mean age 41 years). The average interval between the onset of symptomatic epiphora and the balloon dilatation was 34 months, with a range of 4 months to 15 years. Obstruction was idiopathic in all cases. All patients complained of moderate to severe epiphora. Each patient had an ophthalmic evaluation before the procedure to rule out an acute inflammatory process, and underwent digital subtraction dacryocystography (DCG) to determine the site and type of the obstruction. Patients with active dacryocystitis and canalicular obstruction were excluded from the study. Local infiltration anaesthesia of the medial canthus with 2% lignocaine, topical conjunctival anaesthesia with 0.4% benoxinate hydrochloride, and nasal anaesthesia with 2% lignocaine and 0.5% phenylephrine spray were employed in the first eight patients. The remainder did not receive infiltration anaesthesia of the medial canthus. Following anaesthesia, in six patients a lacrimal probe of a lacrimal intubation set (Lacrimal intubation set 5010, Visitec, Sarasota, FL, USA) was introduced via the superior punctum and advanced through the obstruction site under fluoroscopic control. Then, a floppy tipped guide wire was advanced from the superior punctum into the inferior meatus, where a bayonet-shaped nasal forceps was used to catch the tip of the guide wire and was extended out of the nose. In the next 20 patients, neither lacrimal probe nor nasal forceps was used. Following the insertion of soft tip of the or inch guide wire (either straight or angled tipped: Ultra-select
2 Treatment of obstructive epiphora in adults by balloon dacryocystoplasty 693 Figure 1 False passage creation. (A) Correct position of the guide wire. (B) The line of the guide wire is rather medial than usual trace. (C) Dacryocystogram obtained after balloon dacryocystoplasty shows that contrast medium is passing to the nasal cavity through the false passage. nitinol guide wire, Microvena Corp, Minnesota, USA or Flexfinder, Flexmedics Corp, Minnesota, USA) via the superior punctum proximal to the obstructed segment, a 24 or 22 gauge plastic arterial sheath was introduced over the guide wire. Then, both the guide wire and the sheath were gently manipulated while trying to pass the guide wire through the obstruction site. This procedure was performed under fluoroscopy in lateral projection to see the trace of the guide wire through the LDS. After the tip of the guide wire was manipulated out of the nose, the sheath was removed superiorly from the canaliculus. A catheter with a 3 mm in diameter and 2 cm long balloon (Sure pass PTCA catheter, NuMed Canada Inc, Ontario, Canada or Dacryocystic duct dilation set, William Cook Europe A/S, Bjaevershov, Denmark) was introduced retrogradely over the guide wire and placed at the level of the obstruction under fluoroscopic control. In order to prevent damage to the canaliculi, special attention was paid not to place it higher than the sac. The balloon was inflated three to four times for 1 minute using a balloon inflation device. A radiograph was taken during balloon inflation to ensure the correct positioning of the balloon. By leaving the wire in place, the balloon catheter was removed inferiorly. DCG was performed by injecting the contrast medium via the inferior punctum to verify passage. The dilatation procedure was repeated when DCG revealed that the dilatation of the stenotic segment was not suycient. Following the final dilatation, DCG was repeated to verify the success of the procedure. After completion of the intervention, the balloon was removed inferiorly and the wire superiorly. The LDS was irrigated with sterile saline. Topical antibiotic and steroid eye drops were administered postoperatively for 1 week in addition to oral antibiotic and antiinflammatory therapy for 5 days. On the following day, canalicular irrigation was performed to dislodge a possible clot. Within the first month after the procedure, canalicular irrigation was repeated weekly to determine the patency of the LDS. The patients were contacted every 2 months to obtain follow up information; patients having post-treatment epiphora underwent DCG. Results The follow up period ranged from 8 to 37 months (mean 14 months). Obstruction was at the lacrimal sac in five patients, the junction between the lacrimal sac and nasolacrimal duct in 14, in the nasolacrimal duct in five, and the divuse stricture in two. Sixteen patients had complete obstruction and 10 had partial obstruction. In four patients who had complete obstruction (one junctional and three in the lacrimal sac), BD could not be technically achieved. The failure in three patients was due to the inability to pass the guide wire through the obstruction site, and in one patient it was due to the creation of a false passage by the lacrimal probe (Fig 1). The technique was successful in 22 obstructed lacrimal ducts, consisting of 12 complete and 10 partial obstructions with a technical success rate of 85%.The patients who did not receive medial canthal anaesthesia tolerated the operation well. No major complication was seen. The average time to perform the procedure was 47 minutes; the range was between 35 and 68 minutes. Reobstruction occurred in 13 patients (eight complete obstruction and five partial obstruction). In seven of these 13 patients, reobstruction was observed within 2 months following the operation. Reobstruction occurred in five of six patients in whom a lacrimal probe was used to pass the obstruction site. No patency could be achieved in any complete obstruction located at the lacrimal sac. In one patient with severe partial obstruction, the type of the obstruction became complete after BD. During the follow up period, LDS remained patent after BD in 50% of the patients with partial obstruction and in 25% of those with complete obstruction (Figs 2 and 3). The overall success rate was 35% (Table 1).
3 694 Yazici, Yazici, Parlak, et al Figure 2 (A) Dacryocystogram shows partial passage of contrast medium through the partially obstructed nasolacrimal duct. (B) Dacryocystogram obtained after balloon dacryocystoplasty demonstrates resolution of the obstructed segment. Figure 3 (A) Dacryocystogram shows the complete obstruction at the junction between lacrimal sac and nasolacrimal duct. (B) Dacryocystogram following balloon dacryocystoplasty reveals complete resolution of the obstruction site. Table 1 Obstruction site Success versus obstruction site Complete obstruction Partial obstruction Total Lacrimal sac 0/5 0/5 (0%) Junction* 3/9 2/5 5/14 (36%) Nasolacrimal duct 1/2 2/3 3/5 (60%) DiVuse stricture 1/2 1/2 (50%) Total (n=26) 4/16 (25%) 5/10 (50%) 9/26 (35%) *Junction refers to the junction between the nasolacrimal sac and duct. Discussion Although the success rate of external DCR is high, it is an invasive treatment of obstructive epiphora. In the past decade, endonasal endoscopic DCR, BD, and non-surgical treatment with stents have been proposed as an alternative to DCR. 5 7 The major technical diyculty of BD is to pass the soft tipped guide wire against an anatomical obstruction While it is diycult to pass the obstruction with a soft tipped guide wire, a hard tipped guide wire tends to create a false passage and is more traumatic. 12 Therefore the soft tipped guide wire has been widely used Robinson et al 10 and Ilgit et al 9 passed the obstruction site with a 21 gauge curved lacrimal cannula and a 20 gauge soft plastic arterial sheath supported intraluminally with a guiding lacrimal probe, respectively. We used the lacrimal probe to pass the obstruction site in our first six patients. However, a false passage was created in one of these patients. When the films obtained for this case were compared with others, we realised that the line of the guide wire was rather more medial than the usual trace. McCullough reported a similar event. 11 We think that the inappropriate passage of the wire was probably due to the perforation of the thin lacrimal bone by the probe and the advancement of the guide wire through this opening. The thickness of the lacrimal bone at the lacrimal sac fossa is mostly less than 100 µm, so that it can be easily penetrated with most surgical instruments. 15 In the literature, the creation of a false passage has been reported to be through the submucosa or periosteum The lacrimal probe was not used in the remaining patients in order to reduce the traumatic evects of the procedure. With the flexible guide wire, no false passage was created. The introduction of the guide wire through a plastic arterial sheath seems to facilitate the manipulation. McCullough modified the guide wire by reducing the length of the floppy tip for the same purpose. 11 The diyculty in bringing forward the guide wire through the external nare can be overcome by using a haemostat under nasal endoscopic guidance or a hook. In our experience, to direct the guide wire anteriorly with an angled tip was easy under fluoroscopic monitoring in the lateral projection. While it was easier to advance the guide wire through the obstruction site with the straight tip, the angled tip facilitated the advancement of the guide wire through the nare. Therefore, in some patients we first used a straight tipped guide wire to pass the obstruction, and after creating a track we replaced it with an angled tipped guide wire. Munk et al were the first to perform retrograde balloon dilatation in adults with obstructive epiphora. 5 There are several reports on BD with a significant diverence in the success rates, varying from 23% to 89% Janssen et al stated that the diverences in results could be explained by diverences in patient selection and diverent dacryocystoplasty techniques. 14 However, on reviewing the literature, we think that it is hard to find a satisfactory explanation for the wide range in the success rates. Munk et al and McCullough included 18 patients (89% partial) and 22 patients (100% partial), respectively, with postsaccal obstructions in their studies Munk et al and McCullough used the same sized balloon. Although the patient selection and the size of the balloon were similar in both studies, the durations of balloon inflation were
4 Treatment of obstructive epiphora in adults by balloon dacryocystoplasty 695 diverent. Munk et al and McCullough inflated the balloon two or three times for seconds each time and twice for 5 minutes each, respectively. Their overall success rates were 72% (Munk et al) and 68% (McCullough). These results show that the diverence in the duration of balloon inflation may not avect the success rates significantly. Lee et al included 20 patients with partial obstruction at the junction and nasolacrimal duct. 13 Ilgit et al had 14 patients with partial obstruction at the nasolacrimal duct. 9 They both inflated the 4 mm diameter balloon for at least 5 minutes. The overall success rates for partial obstruction in these two reports were 25% and 100%, respectively. Although there was not a significant diverence in the techniques and the type and the site of the obstruction, there was a remarkable diverence between the results. Ilgit et al concluded that their higher overall success rate compared with that reported by Lee et al might be attributed to the diverent average intervals between the epiphora and the BD. 9 However, Janssen et al did not find any statistically significant diverence in the success rate between patients with epiphora for 1 year or less and those with epiphora for more than 1 year. 14 According to the results of the previous studies, it seems that the treatment of epiphora by BD is more successful for partial obstructions than for complete obstructions, and in nasolacrimal duct obstructions than in obstructions of the lacrimal sac or the canaliculi Our results tend to confirm these observations. In our study, the results of BD in partial obstruction were better than those in complete obstruction (50% versus 25%). We obtained the highest patency rate (60%) in the patients with nasolacrimal duct obstruction. But the relatively small number of patients in this group as opposed to the other groups does not allow us to make further conclusions in terms of the site of the obstruction. The success rate was significantly lower in patients in whom a lacrimal probe was used to pass the obstruction site. It is obvious that the traumatic evect of the procedure to the LDS is an essential factor in the failure of BD. In their widely quoted clinicopathological study, Linberg and McCormick reported that the reason of primary acquired nasolacrimal duct obstruction in the early phase is active chronic inflammation along the entire length of the narrowed nasolacrimal duct, where fibrous obliteration eventuates in the late phase. 1 Although BD resolves the obstruction, it does not remedy the primary inflammatory process, which is likely to avect the recurrence of the obstruction. As the balloon is inflated with pressure against the stenotic area, the mucosa of the nasolacrimal duct gets crushed which probably causes development of inflammatory reaction and haemorrhage, eventually increasing the likelihood of the development of the reobstruction. For this reason, the use of topical or systemic anti-inflammatory agents to reduce the early inflammatory reaction and saline irrigation following the operation to dislodge the clot formation have been suggested to prevent the development of reobstruction However, this treatment regimen may not be successful in all cases, as demonstrated by our study. A potential criticism of the present study may be that the radiation dose to the eye during BD was not measured. Indeed, interventional radiological procedures take much more time than do routine diagnostic x ray examinations; therefore, there is increased risk of radiation exposure to the patients and the personnel involved. The clinical threshold for the development of radiation induced cataract in acute exposure is 5 Gy (2 10 Gy). 17 The radiation dose to the head during the interventional neuroradiological procedures is much smaller than the threshold level for the eye. Since BD generally takes less time than neuroangiointerventional procedures, we can assume that the radiation dose to the eye did not reach the critical level in the present study. The success rates reported in the literature for simple probing in adults are almost identical to the success rate found in our study. 19 It would be unlikely to produce a persistent patency with probing or BD in a long standing obstruction when a dense fibrous tissue has already developed. Balloon dacryocystoplasty with subsequent silicone intubation or stent placement seems to ensure the patency of the system Our overall success rate with BD is low compared with DCR; however, BD is less traumatic, easier to perform, and could be more promising in some cases. Further investigations may improve the eycacy of this method. 1 Linberg JV, McCormick SA. Primary acquired nasolacrimal duct obstruction: a clinicopathologic report and biopsy technique. Ophthalmology 1986;93: Tarbet KJ, Custer PL. External dacryocystorhinostomy: surgical success, patient satisfaction, economic cost. Ophthalmology 1995;102: Bell TAG. An investigation into the eycacy of probing the nasolacrimal duct as a treatment for epiphora in adults. Trans Ophthalmol Soc UK 1986;105: Becker BB, Berry FD, Koller H. Balloon catheter dilatation for treatment of congenital nasolacrimal duct obstruction. Am J Ophthalmol 1996;121: Munk PL, Lin DTC, Morris DC. Epiphora: treatment by means of dacryocystoplasty with balloon dilation of the nasolacrimal drainage apparatus. Radiology 1990;177: Shun-shin GA, Thurairajan G. External dacryocystorhinostomy an end of an era? Br J Ophthalmol 1997;81: Song HY, Ahn HS, Park CK,et al. Complete obstruction of the nasolacrimal system. Part II. Treatment with lacrimal metallic stents. Radiology 1993;186: Song HY, Ahn HS, Park CK,et al. Complete obstruction of the nasolacrimal system. Part I. Treatment with balloon dilation. Radiology 1993;186: Ilgit ET, Yuksel D, Unal M, et al. Transluminal balloon dilatation of the lacrimal drainage system for the treatment of epiphora. Am J Roentgen 1995;165: Robinson R, Turner N, Brettle P, et al. The treatment of epiphora with balloon dacryocystoplasty. Eye 1993;7: McCullough KM. Naso-lacrimal duct balloon dilatation. Clin Radiol 1994;49: Berkefeld J, Kirchner J, Muller HM, et al. Balloon dacryocystoplasty: indications and contraindications. Radiology 1997;205: Lee JM, Song HY, Han YM, et al. Balloon dacryocystoplasty: results in the treatment of complete and partial obstructions of the nasolacrimal system. Radiology 1994;192: Janssen AG, Mansour K, Bos JJ. Obstructed nasolacrimal duct system in epiphora: long-term results of dacryocystoplasty by means of balloon dilation. Radiology 1997;205: Hartikainen J, Aho HJ, Seppa H,et al. Lacrimal bone thickness at the lacrimal sac fossa. Ophthalmic Surg Lasers 1996; 27:
5 696 Yazici, Yazici, Parlak, et al 16 Kumar E. Technical note: non-surgical treatment of epiphora by balloon dacryocystoplasty-the technique. Br J Radiol 1995;68: Kuwayama N, Takaku A, Endo S, et al. Radiation exposure in endovascular surgery of the head and neck. Am J Neuroradiol 1994;15: Bergeron P, Carrier R, Roy D, et al. Radiation doses to patients in neurointerventional procedures. Am J Neuroradiol 1994;15: Bell TAG. An investigation into the eycacy of probing the nasolacrimal duct as a treatment for epiphora in adults. Trans Ophthalmol Soc UK 1986;105: Steinkogler FJ, Huber E, Kuchar A, et al. Retrograde dilation of postsaccal lacrimal stenosis. Ann Otol Rhinol Laryngol 1994;103: Song HY, Jin YH, Kim JH, et al. Nonsurgical placement of a nasolacrimal polyurethane stent: long term evectiveness. Radiology 1996;200: Br J Ophthalmol: first published as /bjo on 1 June Downloaded from on 17 April 2019 by guest. Protected by copyright.
Minimally Invasive Technique of Dacryocystorhinostomy
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Protocol Mohammad Idrees* Consultant Ophthalmology, REDO Eye Hospital, Rawalpindi, Pakistan *Corresponding Author: Mohammad Idrees, Consultant Ophthalmology,
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Protocol Mohammad Idrees* Consultant Ophthalmology, REDO Eye Hospital, Rawalpindi, Pakistan *Corresponding Author: Mohammad Idrees, Consultant Ophthalmology,
Repeat DCR with Silicone Tube intubation : A Prospective Study.
 Repeat DCR with Silicone Tube intubation : A Prospective Study. Dr Imtiyaz A Lone Assistant Professor Department of Ophthalmology SKIMS Medical College Bemina, Srinagar, India Dr Bashir A Malik Sr. Resident
Repeat DCR with Silicone Tube intubation : A Prospective Study. Dr Imtiyaz A Lone Assistant Professor Department of Ophthalmology SKIMS Medical College Bemina, Srinagar, India Dr Bashir A Malik Sr. Resident
Study of success rates in endoscopic dacryocystorhinostomy with and without stenting. dacryocystorhinostomy with and
 Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
The role of interventional radiology in the treatment of epiphora
 Review Article on Interventional Radiology in Glands The role of interventional radiology in the treatment of epiphora Francesca Patella 1, Silvia Panella 1, Stefania Zannoni 1, Maria Laura Jannone 1,
Review Article on Interventional Radiology in Glands The role of interventional radiology in the treatment of epiphora Francesca Patella 1, Silvia Panella 1, Stefania Zannoni 1, Maria Laura Jannone 1,
DACRYOCYSTORHINOSTOMY; A COMPARATIVE STUDY OF THE RESULTS WITH AND WITHOUT SILICON INTUBATION IN PAKISTANI PATIENTS OF CHRONIC DACRYOCYSTITIS
 DACRYOCYSTORHINOSTOMY 81 ORIGINAL PROF-1230 DACRYOCYSTORHINOSTOMY; A COMPARATIVE STUDY OF THE RESULTS WITH AND WITHOUT SILICON INTUBATION IN PAKISTANI PATIENTS OF CHRONIC DACRYOCYSTITIS DR. MUHAMMAD NAWAZ,
DACRYOCYSTORHINOSTOMY 81 ORIGINAL PROF-1230 DACRYOCYSTORHINOSTOMY; A COMPARATIVE STUDY OF THE RESULTS WITH AND WITHOUT SILICON INTUBATION IN PAKISTANI PATIENTS OF CHRONIC DACRYOCYSTITIS DR. MUHAMMAD NAWAZ,
NASOLACRIMAL DUCT OBSTRUCTION (BLOCKED TEAR DUCT) AND TEARY EYE - PATIENT INFORMATION
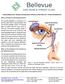 NASOLACRIMAL DUCT OBSTRUCTION (BLOCKED TEAR DUCT) AND TEARY EYE - PATIENT INFORMATION What is lacrimal sac and nasolacrimal duct? The lacrimal apparatus is composed of a lacrimal gland (tear producing
NASOLACRIMAL DUCT OBSTRUCTION (BLOCKED TEAR DUCT) AND TEARY EYE - PATIENT INFORMATION What is lacrimal sac and nasolacrimal duct? The lacrimal apparatus is composed of a lacrimal gland (tear producing
Balloon Dacryoplasty: Indications, Techniques and Outcomes
 INTERNATIONAL JOURNAL OF HEALTH RESEARCH IN MODERN INTEGRATED MEDICAL SCIENCES (IJHRMIMS), ISSN XXXX (P), ISSN XXXX (O), Oct-Dec 2014 15 Review Article Balloon Dacryoplasty: Indications, Techniques and
INTERNATIONAL JOURNAL OF HEALTH RESEARCH IN MODERN INTEGRATED MEDICAL SCIENCES (IJHRMIMS), ISSN XXXX (P), ISSN XXXX (O), Oct-Dec 2014 15 Review Article Balloon Dacryoplasty: Indications, Techniques and
Comparison of the Efficacies of 0.94 mm and Double Silicone Tubes for Treatment of Canalicular Obstruction
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(1):1-8 ht tps://doi.org/10.3341/k jo.2017.31.1.1 Original Article Comparison of the Efficacies of 0.94 mm and Double Silicone Tubes for Treatment
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(1):1-8 ht tps://doi.org/10.3341/k jo.2017.31.1.1 Original Article Comparison of the Efficacies of 0.94 mm and Double Silicone Tubes for Treatment
Pediatric Epiphora. Lacrimal drainage system begins to develop at the. Pediatric Ophthalmology. Saurbhi Khurana MD, FICO
 Pediatric Ophthalmology Pediatric Epiphora Saurbhi Khurana MD, FICO Saurbhi Khurana MD, FICO, A.K Grover MD, MNAMS, FRCS (Glasgow) FIMSA, FICO Vision Eye Centre, Siri Fort Road, New Delhi Lacrimal drainage
Pediatric Ophthalmology Pediatric Epiphora Saurbhi Khurana MD, FICO Saurbhi Khurana MD, FICO, A.K Grover MD, MNAMS, FRCS (Glasgow) FIMSA, FICO Vision Eye Centre, Siri Fort Road, New Delhi Lacrimal drainage
Self-Securing Monocanalicular Stent for Treatment of Nasolacrimal Duct Obstruction
 J Med Sci 2004;24(4):199-204 http://jms.ndmctsgh.edu.tw/2404199.pdf Copyright 2004 JMS Shang-Yi Chiang, et al. Self-Securing Monocanalicular Stent for Treatment of Nasolacrimal Duct Obstruction Shang-Yi
J Med Sci 2004;24(4):199-204 http://jms.ndmctsgh.edu.tw/2404199.pdf Copyright 2004 JMS Shang-Yi Chiang, et al. Self-Securing Monocanalicular Stent for Treatment of Nasolacrimal Duct Obstruction Shang-Yi
Philippine Journal of OPHTHALMOLOGY ABSTRACT
 Original Article Philippine Journal of OPHTHALMOLOGY Surgical Technique and Preliminary Results of Transcanalicular Endoscopic Lacrimal Duct Recanalization and Balloon Dacryoplasty with Silicone Intubation
Original Article Philippine Journal of OPHTHALMOLOGY Surgical Technique and Preliminary Results of Transcanalicular Endoscopic Lacrimal Duct Recanalization and Balloon Dacryoplasty with Silicone Intubation
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/24545
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/24545
Obstruction of the LDS, resulting in inadequate drainage of
 ORIGINAL RESEARCH B. Coskun E. Ilgit B. Onal O. Konuk G. Erbas MR Dacryocystography in the Evaluation of Patients with Obstructive Epiphora Treated by Means of Interventional Radiologic Procedures BACKGROUND
ORIGINAL RESEARCH B. Coskun E. Ilgit B. Onal O. Konuk G. Erbas MR Dacryocystography in the Evaluation of Patients with Obstructive Epiphora Treated by Means of Interventional Radiologic Procedures BACKGROUND
Shreya M. Shah, Mehul A. Shah & Chintan Patel
 Cannula dacryocystorhinostomy: a simple, innovative and cost-effective method of lacrimal surgery Shreya M. Shah, Mehul A. Shah & Chintan Patel International Ophthalmology The International Journal of
Cannula dacryocystorhinostomy: a simple, innovative and cost-effective method of lacrimal surgery Shreya M. Shah, Mehul A. Shah & Chintan Patel International Ophthalmology The International Journal of
THE EXTERNAL DACRYOCYSTORHINOSTOMY (DCR)
 Outcome of External Dacryocystorhinostomy Combined With Membranectomy of a Distal Canalicular Obstruction KOSTAS G. BOBORIDIS, MD, CATEY BUNCE, DSC, AND GEOFFREY E. ROSE, FRCS, FRCOPHTH PURPOSE: To investigate
Outcome of External Dacryocystorhinostomy Combined With Membranectomy of a Distal Canalicular Obstruction KOSTAS G. BOBORIDIS, MD, CATEY BUNCE, DSC, AND GEOFFREY E. ROSE, FRCS, FRCOPHTH PURPOSE: To investigate
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 80/ Oct. 05, 2015 Page 14022
 STUDY ON MANAGEMENT OF EPIPHORA IN PATIENTS WITH OBSTRUCTION AT VARIOUS LEVELS OF NASOLACRIMAL APPARATUS S. Shivranjani 1, Jaishree Dwivedi 2, Neha Mithal 3, Sandeep Mithal 4 HOW TO CITE THIS ARTICLE:
STUDY ON MANAGEMENT OF EPIPHORA IN PATIENTS WITH OBSTRUCTION AT VARIOUS LEVELS OF NASOLACRIMAL APPARATUS S. Shivranjani 1, Jaishree Dwivedi 2, Neha Mithal 3, Sandeep Mithal 4 HOW TO CITE THIS ARTICLE:
Value of nasal endoscopy and probing in the diagnosis and management of children with congenital epiphora
 314 Department of Ophthalmology, Ninewells Hospital, Dundee DD1 9SY, UK C J MacEwen JDHYoung C W Barras Department of Otolaryngology B Ram P S White Correspondence to: Dr MacEwen c.j.macewen@dundee.ac.uk
314 Department of Ophthalmology, Ninewells Hospital, Dundee DD1 9SY, UK C J MacEwen JDHYoung C W Barras Department of Otolaryngology B Ram P S White Correspondence to: Dr MacEwen c.j.macewen@dundee.ac.uk
To analyse the success rate of external Dacryocystorhinostomy related with anatomical osteotomy size made during surgery
 2018; 4(1): 354-358 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(1): 354-358 www.allresearchjournal.com Received: 23-11-2017 Accepted: 24-12-2017 Pandit VK Associate Professor,
2018; 4(1): 354-358 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(1): 354-358 www.allresearchjournal.com Received: 23-11-2017 Accepted: 24-12-2017 Pandit VK Associate Professor,
MR Dacryocystography: Comparison with Dacryocystography and CT Dacryocystography
 AJNR Am J Neuroradiol 21:1145 1150, June/July 2000 MR Dacryocystography: Comparison with Dacryocystography and CT Dacryocystography Luigi Manfrè, Marcello de Maria, Enzo Todaro, Adriana Mangiameli, Francesco
AJNR Am J Neuroradiol 21:1145 1150, June/July 2000 MR Dacryocystography: Comparison with Dacryocystography and CT Dacryocystography Luigi Manfrè, Marcello de Maria, Enzo Todaro, Adriana Mangiameli, Francesco
Study of outcomes of endonasal dacryocystorhinostomy in relation with sex distribution in Indian population
 Original article: Study of outcomes of endonasal dacryocystorhinostomy in relation with sex distribution in Indian population 1Dr. Mayur Ingale, 2 Dr. Vinod Shinde, 3 Dr.Paresh Chavan, 4 Dr.SudeepChoudhary
Original article: Study of outcomes of endonasal dacryocystorhinostomy in relation with sex distribution in Indian population 1Dr. Mayur Ingale, 2 Dr. Vinod Shinde, 3 Dr.Paresh Chavan, 4 Dr.SudeepChoudhary
Syringing And Probing Under Local Anesthesia In Infants
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 3 Number 2 V Sharma, S Vaidya, S Shrivastava Citation V Sharma, S Vaidya, S Shrivastava.. The Internet Journal of Ophthalmology
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 3 Number 2 V Sharma, S Vaidya, S Shrivastava Citation V Sharma, S Vaidya, S Shrivastava.. The Internet Journal of Ophthalmology
Non-endoscopic Mechanical Endonasal Dacryocystorhinostomy
 Surgical Technique Non-endoscopic Mechanical Endonasal Dacryocystorhinostomy Mohammad Etezad Razavi 1, MD; Morteza Noorollahian 2, MD; Alireza Eslampoor 1, MD 1 Khatam-al-Anbia Eye Research Center, Mashhad
Surgical Technique Non-endoscopic Mechanical Endonasal Dacryocystorhinostomy Mohammad Etezad Razavi 1, MD; Morteza Noorollahian 2, MD; Alireza Eslampoor 1, MD 1 Khatam-al-Anbia Eye Research Center, Mashhad
Stent technique for endoscopic dacryocystorhinostomy Our expertise
 Romanian Journal of Rhinology, Vol. 6, No. 21, January - March 2016 ORIGINAL STUDY Stent technique for endoscopic dacryocystorhinostomy Our expertise Vlad Budu 1, Tatiana Decuseara 1, Bogdan Mocanu 2,
Romanian Journal of Rhinology, Vol. 6, No. 21, January - March 2016 ORIGINAL STUDY Stent technique for endoscopic dacryocystorhinostomy Our expertise Vlad Budu 1, Tatiana Decuseara 1, Bogdan Mocanu 2,
Original Article Bicanalicular intubation procedure for acquired punctual stenosis
 Int J Clin Exp Med 2018;11(10):10815-10819 www.ijcem.com /ISSN:1940-5901/IJCEM0074867 Original Article Bicanalicular intubation procedure for acquired punctual stenosis Ying Chen 1, Xia Zhang 1, Liguo
Int J Clin Exp Med 2018;11(10):10815-10819 www.ijcem.com /ISSN:1940-5901/IJCEM0074867 Original Article Bicanalicular intubation procedure for acquired punctual stenosis Ying Chen 1, Xia Zhang 1, Liguo
Modified endoscopic dacryocystorhinostomy with posterior lacrimal sac flap for nasolacrimal duct obstruction!"#$%&'()*+,-*&'!./0(&
 Key words: Dacryocystorhinostomy; Endoscopy; Lacrimal apparatus diseases!!"#$%!"! KSC Yuen LYM Lam MWY Tse DDN Chan BWC Wong WM Chan Hong Kong Med J 00;:9-00 Department of Ophthalmology and Visual Sciences,
Key words: Dacryocystorhinostomy; Endoscopy; Lacrimal apparatus diseases!!"#$%!"! KSC Yuen LYM Lam MWY Tse DDN Chan BWC Wong WM Chan Hong Kong Med J 00;:9-00 Department of Ophthalmology and Visual Sciences,
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
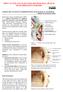 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY ENDOSCOPIC DACRYOCYSTORHINOSTOMY (DCR) SURGICAL TECHNIQUE Hisham Wasl, Darlene Lubbe Endoscopic dacryocystorhinostomy (DCR) is a surgical
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY ENDOSCOPIC DACRYOCYSTORHINOSTOMY (DCR) SURGICAL TECHNIQUE Hisham Wasl, Darlene Lubbe Endoscopic dacryocystorhinostomy (DCR) is a surgical
Evaluation of Tear Film Lipid Layer Thickness Measurements Obtained Using an Ocular Surface Interferometer in Nasolacrimal Duct Obstruction Patients
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(6):445-450 https://doi.org/10.3341/kjo.2018.0012 Original Article Evaluation of Tear Film Lipid Layer Thickness Measurements Obtained Using
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2018;32(6):445-450 https://doi.org/10.3341/kjo.2018.0012 Original Article Evaluation of Tear Film Lipid Layer Thickness Measurements Obtained Using
Computed tomographic dacryocystography as compared with X-ray dacryocystography in patients with dacryostenosis
 Computed tomographic dacryocystography as compared with X-ray dacryocystography in patients with dacryostenosis Poster No.: C-1887 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M.
Computed tomographic dacryocystography as compared with X-ray dacryocystography in patients with dacryostenosis Poster No.: C-1887 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M.
Nasolacrimal duct obstruction: the relationship with nasal allergy
 Romanian Journal of Rhinology, Vol. 7, No. 27, July - September 2017 DOI: 10.1515/rjr-2017-0018 Original study Nasolacrimal duct obstruction: the relationship with nasal allergy Desiderio Passali 1, Leandro
Romanian Journal of Rhinology, Vol. 7, No. 27, July - September 2017 DOI: 10.1515/rjr-2017-0018 Original study Nasolacrimal duct obstruction: the relationship with nasal allergy Desiderio Passali 1, Leandro
The clinical value of dacryoscintigraphy in the selection of surgical approach for patients with functional lacrimal duct obstruction
 ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 19, No. 6, 479 483, 2005 The clinical value of dacryoscintigraphy in the selection of surgical approach for patients with functional lacrimal duct obstruction
ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 19, No. 6, 479 483, 2005 The clinical value of dacryoscintigraphy in the selection of surgical approach for patients with functional lacrimal duct obstruction
RECOMMENDED INSTRUCTIONS FOR USE
 Rapid Exchange PTCA Dilatation Catheter RECOMMENDED INSTRUCTIONS FOR USE Available in diameters 1.25mm to 4.5mm and in lengths 09mm to 40mm Caution: This device should be used only by physicians trained
Rapid Exchange PTCA Dilatation Catheter RECOMMENDED INSTRUCTIONS FOR USE Available in diameters 1.25mm to 4.5mm and in lengths 09mm to 40mm Caution: This device should be used only by physicians trained
Outcomes of external dacryocystorhinostomy and endoscopic endonasal dacryocystorhinostomy in the management of nasolacrimal duct obstruction
 Original article Outcomes of external dacryocystorhinostomy and endoscopic endonasal dacryocystorhinostomy in the management of nasolacrimal duct obstruction Duwal S, Saiju R Tilganga Institute of Ophthalmology,
Original article Outcomes of external dacryocystorhinostomy and endoscopic endonasal dacryocystorhinostomy in the management of nasolacrimal duct obstruction Duwal S, Saiju R Tilganga Institute of Ophthalmology,
Nasal Endoscopic Dacryocystorhinostomy The Nizamabad experience
 Original Research Article Nasal Endoscopic Dacryocystorhinostomy The Nizamabad experience Anand Acharya 1*, Modini P. 2, G. Lakpati 3 1 Associate Professor, ENT Department, GMC, Nizamabad, India 2 Associate
Original Research Article Nasal Endoscopic Dacryocystorhinostomy The Nizamabad experience Anand Acharya 1*, Modini P. 2, G. Lakpati 3 1 Associate Professor, ENT Department, GMC, Nizamabad, India 2 Associate
Acute Dacryocystitis with Abscess: Endonasal Dacryocystorhinostomy, the Primary Treatment of Choice
 10.5005/jp-journals-10013-1129 ORIGINAL ARTICLE Acute Dacryocystitis with Abscess: Endonasal Dacryocystorhinostomy, the Primary Treatment of Choice Sudhir M Naik, Sarika S Naik ABSTRACT Background/objectives:
10.5005/jp-journals-10013-1129 ORIGINAL ARTICLE Acute Dacryocystitis with Abscess: Endonasal Dacryocystorhinostomy, the Primary Treatment of Choice Sudhir M Naik, Sarika S Naik ABSTRACT Background/objectives:
INTERVENTIONAL PROCEDURES PROGRAMME
 Prepared by ASERNIP-S Introduction NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of Endoscopic Dacryocystorhinostomy This overview has
Prepared by ASERNIP-S Introduction NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of Endoscopic Dacryocystorhinostomy This overview has
Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile)
 Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Congenital lacrimal fistula
 Ugurbas 6-03-2000 14:59 Pagina 22 European Journal of Ophthalmology / Vol. 10 no. 1, 2000 / pp. 22-26 S.H. UǦURBAŞ, G. ZILELIOǦLU Department of Ophthalmology, Ankara University Faculty of Medicine, Ankara
Ugurbas 6-03-2000 14:59 Pagina 22 European Journal of Ophthalmology / Vol. 10 no. 1, 2000 / pp. 22-26 S.H. UǦURBAŞ, G. ZILELIOǦLU Department of Ophthalmology, Ankara University Faculty of Medicine, Ankara
Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases
 Chin J Radiol 2003; 28: 137-142 137 Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases SHE-MENG CHENG SUK-PING NG FEI-SHIH YANG SHIN-LIN SHIH Department
Chin J Radiol 2003; 28: 137-142 137 Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases SHE-MENG CHENG SUK-PING NG FEI-SHIH YANG SHIN-LIN SHIH Department
Management of Congenital Nasolacrimal Duct Obstruction: Comparison of Probing Vs Conservative Medical Approach
 Bahrain Medical Bulletin, Vol. 22, No. 1, March 2000 Management of Congenital Nasolacrimal Duct Obstruction: Comparison of Probing Vs Conservative Medical Approach Basel T Baarah, MD* Wael Abu-Laban, MD**
Bahrain Medical Bulletin, Vol. 22, No. 1, March 2000 Management of Congenital Nasolacrimal Duct Obstruction: Comparison of Probing Vs Conservative Medical Approach Basel T Baarah, MD* Wael Abu-Laban, MD**
A simple and evolutional approach proven to recanalise the nasolacrimal duct obstruction
 See Editorial, p 1416 1 Department of ENT, First Affiliated Hospital, Sun Yat-sen University, Guangzhou, PR China; 2 State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University,
See Editorial, p 1416 1 Department of ENT, First Affiliated Hospital, Sun Yat-sen University, Guangzhou, PR China; 2 State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University,
Evaluation of the Canalicular Entrance Into the Lacrimal Sac: An Anatomical Study
 ANATOMY &PHYSIOLOGY Evaluation of the Canalicular Entrance Into the Lacrimal Sac: An Anatomical Study Christopher I. Zoumalan, M.D.*, Jeffrey M. Joseph, M.D.*, Gary J. Lelli, Jr., M.D., Kira L. Segal,
ANATOMY &PHYSIOLOGY Evaluation of the Canalicular Entrance Into the Lacrimal Sac: An Anatomical Study Christopher I. Zoumalan, M.D.*, Jeffrey M. Joseph, M.D.*, Gary J. Lelli, Jr., M.D., Kira L. Segal,
Intranasal location of lacrimal sac in Thai cadavers
 Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Yunhai Tu, 1 Zhenbin Qian, 2 Jiao Zhang, 1 Wencan Wu, 1 and Tianlin Xiao Introduction. 2. Patients and Methods
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 201, Article ID 67909, 7 pages http://dx.doi.org/10.11/201/67909 Clinical Study Endoscopic Endonasal Dacryocystorhinostomy Combined with Canaliculus
Hindawi Publishing Corporation Journal of Ophthalmology Volume 201, Article ID 67909, 7 pages http://dx.doi.org/10.11/201/67909 Clinical Study Endoscopic Endonasal Dacryocystorhinostomy Combined with Canaliculus
Technique Guide. Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures.
 Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Treatment of Maxillary Sinusitis Using the SinuSys Vent-Os Sinus Dilation System
 WHITE PAPER Treatment of Maxillary Sinusitis Using the SinuSys Vent-Os Sinus Dilation System Jerome Hester, MD Chief Medical Officer SinuSys Corporation Palo Alto, California USA Introduction Establishment
WHITE PAPER Treatment of Maxillary Sinusitis Using the SinuSys Vent-Os Sinus Dilation System Jerome Hester, MD Chief Medical Officer SinuSys Corporation Palo Alto, California USA Introduction Establishment
POLYTHENE TUBES IN CANALICULUS SURGERY*
 Brit. J. Ophthal. (1963) 47, 203. POLYTHENE TUBES IN CANALICULUS SURGERY* BY T. P. GRIFFITHt From the Corneo-Plastic Unit and Regional Eye Bank, Queen Victoria Hospital, East Grinstead, Sussex CANALICULUS
Brit. J. Ophthal. (1963) 47, 203. POLYTHENE TUBES IN CANALICULUS SURGERY* BY T. P. GRIFFITHt From the Corneo-Plastic Unit and Regional Eye Bank, Queen Victoria Hospital, East Grinstead, Sussex CANALICULUS
Repair of Eyelid Trauma
 Repair of Eyelid Trauma Yunia Irawati, MD Plastic Reconstruction Division, Department of Ophthalmology FKUI / RSCM Introduction Eyelid trauma defined as a trauma to external surface of the lids with or
Repair of Eyelid Trauma Yunia Irawati, MD Plastic Reconstruction Division, Department of Ophthalmology FKUI / RSCM Introduction Eyelid trauma defined as a trauma to external surface of the lids with or
Comparison of outcome of external DCR and endonasal DCR surgery among the rural population
 Original article: Comparison of outcome of external DCR and endonasal DCR surgery among the rural population 1 Dr Aniket Lathi*, 2 Dr C Anand Kumar, 3 Dr Nitin Kulkarni, 4 Dr Ashish Gupta, 5 Dr Shruti
Original article: Comparison of outcome of external DCR and endonasal DCR surgery among the rural population 1 Dr Aniket Lathi*, 2 Dr C Anand Kumar, 3 Dr Nitin Kulkarni, 4 Dr Ashish Gupta, 5 Dr Shruti
Application of biodegradable collagen matrix (Ologen ) implants in Dacryocystorhinostomy surgeries, a randomized clinical study
 Marey et al. BMC Ophthalmology (2018) 18:254 https://doi.org/10.1186/s12886-018-0901-4 RESEARCH ARTICLE Open Access Application of biodegradable collagen matrix (Ologen ) implants in Dacryocystorhinostomy
Marey et al. BMC Ophthalmology (2018) 18:254 https://doi.org/10.1186/s12886-018-0901-4 RESEARCH ARTICLE Open Access Application of biodegradable collagen matrix (Ologen ) implants in Dacryocystorhinostomy
Management of epiphora and lacrimal obstruction in adults
 Management of epiphora and lacrimal obstruction in adults Louis Savar, MD 1,2, Stuart R. Seiff, MD, FACS 1,2, Angela Maria Dolmetsch, MD 3 1. Department of Ophthalmology, University of California, San
Management of epiphora and lacrimal obstruction in adults Louis Savar, MD 1,2, Stuart R. Seiff, MD, FACS 1,2, Angela Maria Dolmetsch, MD 3 1. Department of Ophthalmology, University of California, San
Clinical Results of Endoscopic Dacryocystorhinostomy using a Microdebrider
 Clinical Results of Endoscopic Dacryocystorhinostomy using a Microdebrider Sung Wook Yoon, MD, Young Sun Yoon, MD, Su Hyung Lee, MD Department of Ophthalmology, Dongkang General Hospital, Ulsan, Korea
Clinical Results of Endoscopic Dacryocystorhinostomy using a Microdebrider Sung Wook Yoon, MD, Young Sun Yoon, MD, Su Hyung Lee, MD Department of Ophthalmology, Dongkang General Hospital, Ulsan, Korea
Morphological and morphometrical study of the nasal opening of nasolacrimal duct in man
 O R I G I N A L A R T I C L E Folia Morphol. Vol. 73, No. 3, pp. 321 330 DOI: 10.5603/FM.2014.0049 Copyright 2014 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Morphological and morphometrical study of
O R I G I N A L A R T I C L E Folia Morphol. Vol. 73, No. 3, pp. 321 330 DOI: 10.5603/FM.2014.0049 Copyright 2014 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Morphological and morphometrical study of
Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy
 SV Manjunatha Rao, MM Rajshekar Original Article 10.5005/jp-journals-10013-1284 Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy 1 SV Manjunatha Rao, 2 MM Rajshekar ABSTRACT
SV Manjunatha Rao, MM Rajshekar Original Article 10.5005/jp-journals-10013-1284 Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy 1 SV Manjunatha Rao, 2 MM Rajshekar ABSTRACT
ORIGINAL ARTICLE. Intranasal Localization of the Lacrimal Sac
 ORIGINAL ARTICLE Intranasal Localization of the Lacrimal Sac Mustafa Orhan, MD; Canan Y. Saylam, MD; Raşit Midilli, MD Objective: To optimize the approach to the lacrimal sac during intranasal dacryocystorhinostomy.
ORIGINAL ARTICLE Intranasal Localization of the Lacrimal Sac Mustafa Orhan, MD; Canan Y. Saylam, MD; Raşit Midilli, MD Objective: To optimize the approach to the lacrimal sac during intranasal dacryocystorhinostomy.
Translaryngeal tracheostomy
 Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Biliary Metal Stents MAKING A DIFFERENCE TO HEALTH
 Biliary Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Biliary Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Evaluation of lacrimal apparatus
 From the SelectedWorks of Balasubramanian Thiagarajan September 18, 2012 Evaluation of lacrimal apparatus Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/9/ Evaluation of lacrimal
From the SelectedWorks of Balasubramanian Thiagarajan September 18, 2012 Evaluation of lacrimal apparatus Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/9/ Evaluation of lacrimal
Evaluation of lacrimal apparatus
 Evaluation of lacrimal apparatus Balasubramanian Thiagarajan Introduction: Dacryocystorhinostomy as a treatment modality for epiphora is commonly being performed endonasally using a nasal endoscope by
Evaluation of lacrimal apparatus Balasubramanian Thiagarajan Introduction: Dacryocystorhinostomy as a treatment modality for epiphora is commonly being performed endonasally using a nasal endoscope by
Recanalisation of urethral strictures with new-generation temporary covered biocompatible metal endoprostheses
 Acta Chirurgica Iugoslavica (ACI) Vol: LIV, (3) 2007, pages 123-127 SCIENTIFIC PAPER UDC: 616.65-007.271-089.819.5 Recanalisation of urethral strictures with new-generation temporary covered biocompatible
Acta Chirurgica Iugoslavica (ACI) Vol: LIV, (3) 2007, pages 123-127 SCIENTIFIC PAPER UDC: 616.65-007.271-089.819.5 Recanalisation of urethral strictures with new-generation temporary covered biocompatible
Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy
 Graefes Arch Clin Exp Ophthalmol (2012) 250:1509 1513 DOI 10.1007/s00417-012-1992-x OCULOPLASTICS AND ORBIT Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy Jae Wook
Graefes Arch Clin Exp Ophthalmol (2012) 250:1509 1513 DOI 10.1007/s00417-012-1992-x OCULOPLASTICS AND ORBIT Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy Jae Wook
Preoperative Computed Tomography Findings for Patients with Nasolacrimal Duct Obstruction or Stenosis
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):243-250 http://dx.doi.org/10.3341/kjo.2016.30.4.243 Original Article Preoperative Computed Tomography Findings for Patients with Nasolacrimal
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):243-250 http://dx.doi.org/10.3341/kjo.2016.30.4.243 Original Article Preoperative Computed Tomography Findings for Patients with Nasolacrimal
Dr. Najah طب بغداد. Lecture: 14
 2015 2016 The lacrimal apparatus The lacrimal system consists of: Lecture: 14 Dr. Najah طب بغداد 1- Secretory portion: Comprises the following: a- The lacrimal gland: Which is divided into palpebral (Aqueoussecretion)
2015 2016 The lacrimal apparatus The lacrimal system consists of: Lecture: 14 Dr. Najah طب بغداد 1- Secretory portion: Comprises the following: a- The lacrimal gland: Which is divided into palpebral (Aqueoussecretion)
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures.
 Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Titanium Wire With Barb and Needle
 For Canthal Tendon Procedures Titanium Wire With Barb and Needle Surgical Technique Table of Contents Introduction Titanium Wire With Barb and Needle 2 Indications 2 Surgical Technique Preoperative Planning
For Canthal Tendon Procedures Titanium Wire With Barb and Needle Surgical Technique Table of Contents Introduction Titanium Wire With Barb and Needle 2 Indications 2 Surgical Technique Preoperative Planning
A Comparative Study of Endoscopic Endonasal Dacryocystorhinostomy with and without Intraoperative Mitomycin-C Application
 10.5005/jp-journals-10013-1140 ORIGINAL ARTICLE A Comparative Study of Endoscopic Endonasal Dacryocystorhinostomy with and without Intraoperative Mitomycin-C Application Raman Wadhera, Sat Paul Gulati,
10.5005/jp-journals-10013-1140 ORIGINAL ARTICLE A Comparative Study of Endoscopic Endonasal Dacryocystorhinostomy with and without Intraoperative Mitomycin-C Application Raman Wadhera, Sat Paul Gulati,
Dacryocystorh i nostomy in South West England
 Dacryocystorh i nostomy in South West England BlJAN BEIGI, WILLIAM WESTLAKE, BERNARD CHANG, CATHERINE MARSH, JOHN JACOB, JUDITH CHATFIELD B. Beigi W. Westlake B. Chang C. Marsh J. Jacob Department of Ophthalmology
Dacryocystorh i nostomy in South West England BlJAN BEIGI, WILLIAM WESTLAKE, BERNARD CHANG, CATHERINE MARSH, JOHN JACOB, JUDITH CHATFIELD B. Beigi W. Westlake B. Chang C. Marsh J. Jacob Department of Ophthalmology
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013
 FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
Effectiveness of sedation in dacryocystorhinostomy surgery
 Original article Effectiveness of sedation in dacryocystorhinostomy surgery Tuladhar S 1, Adhikari S 1, Bhattarai B K 2 Departments of 1 Ophthalmology and 2 Anesthesiology and Critical Care B P Koirala
Original article Effectiveness of sedation in dacryocystorhinostomy surgery Tuladhar S 1, Adhikari S 1, Bhattarai B K 2 Departments of 1 Ophthalmology and 2 Anesthesiology and Critical Care B P Koirala
Anatomical and Functional Evaluation of Conventional vs Inferior Endoscopic Dacryocystorhinostomy in Study Cases of Idiopathic Chronic Dacryocystitis
 Kuldeep Thakur et al ORIGINAL ARTICLE 10.5005/jp-journals-10013-1314 Anatomical and Functional Evaluation of Conventional vs Inferior Endoscopic Dacryocystorhinostomy in Study Cases of Idiopathic Chronic
Kuldeep Thakur et al ORIGINAL ARTICLE 10.5005/jp-journals-10013-1314 Anatomical and Functional Evaluation of Conventional vs Inferior Endoscopic Dacryocystorhinostomy in Study Cases of Idiopathic Chronic
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
Comparative Study Of Probing Done with and without Endoscopic Assistance
 Comparative Study Of Probing Done with and without Endoscopic Assistance Ishan Acharya 1, Jitendra Jethani 2, Monika Jethani 3 Department of Ophthalmic Plastic Surgery, Orbit, Ocular Oncology and Ocular
Comparative Study Of Probing Done with and without Endoscopic Assistance Ishan Acharya 1, Jitendra Jethani 2, Monika Jethani 3 Department of Ophthalmic Plastic Surgery, Orbit, Ocular Oncology and Ocular
Lessons for Successful Subintimal Angioplasty in SFA CTO
 Lessons for Successful Subintimal Angioplasty in SFA CTO John R. Laird Professor of Medicine Medical Director of the Vascular Center UC Davis Medical Center CTOs in the Periphery Presence of Total Occlusion
Lessons for Successful Subintimal Angioplasty in SFA CTO John R. Laird Professor of Medicine Medical Director of the Vascular Center UC Davis Medical Center CTOs in the Periphery Presence of Total Occlusion
Therapeutic Bronchoscopy Etiology - Benign Stenosis Post - intubation Trauma Post - operative Inflammatory Idiopathic
 Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Original Article Effect of revision dacryocystorhinostomy under nasal endoscopy on recrudescent dacryocystitis
 Int J Clin Exp Pathol 2017;10(12):11717-11722 www.ijcep.com /ISSN:1936-2625/IJCEP0052246 Original Article Effect of revision dacryocystorhinostomy under nasal endoscopy on recrudescent dacryocystitis Jintao
Int J Clin Exp Pathol 2017;10(12):11717-11722 www.ijcep.com /ISSN:1936-2625/IJCEP0052246 Original Article Effect of revision dacryocystorhinostomy under nasal endoscopy on recrudescent dacryocystitis Jintao
Sialendoscopy for Obstructive Salivary Gland Disorders
 Disclosures Sialendoscopy for Obstructive Salivary Gland Disorders None Otolaryngology Head Jolie Chang, MD Assistant Professor Otolaryngology, Head University of California, San Francisco November 8,
Disclosures Sialendoscopy for Obstructive Salivary Gland Disorders None Otolaryngology Head Jolie Chang, MD Assistant Professor Otolaryngology, Head University of California, San Francisco November 8,
Chronic Total Occlusion (CTO) Technologies
 to receive our latest news and key activities. Chronic Total Occlusion (CTO) Technologies Re-open vital channels LinkedIn page Follow us on CORDIS EMEA OUTBACK LTD Re-Entry Catheter True Lumen Re-Entry
to receive our latest news and key activities. Chronic Total Occlusion (CTO) Technologies Re-open vital channels LinkedIn page Follow us on CORDIS EMEA OUTBACK LTD Re-Entry Catheter True Lumen Re-Entry
Rhinology Products. Rhinology Products. Superior solutions for superior patient care.
 Rhinology Products Superior solutions for superior patient care. The Doyle Open-Lumen Splint addresses the problem of potential closure of the airway lumen by a hypertrophied turbinate. We also offer the
Rhinology Products Superior solutions for superior patient care. The Doyle Open-Lumen Splint addresses the problem of potential closure of the airway lumen by a hypertrophied turbinate. We also offer the
Congenital Nasolacrimal Duct Obstruction (CNLDO)
 June 2007 Ramesh Murthy - Congenital Nasolacrimal Duct Obstruction 191 OPHTHALMIC SURGERY Congenital Nasolacrimal Duct Obstruction (CNLDO) Dr. Ramesh Murthy MD FRCS Introduction CNLDO is a common problem
June 2007 Ramesh Murthy - Congenital Nasolacrimal Duct Obstruction 191 OPHTHALMIC SURGERY Congenital Nasolacrimal Duct Obstruction (CNLDO) Dr. Ramesh Murthy MD FRCS Introduction CNLDO is a common problem
Introduction 3. What is Peripheral Vascular Disease? 5. What Are Some of the Symptoms of Peripheral Vascular Disease? 6
 Patient Information Table of Contents Introduction 3 What is Peripheral Vascular Disease? 5 What Are Some of the Symptoms of Peripheral Vascular Disease? 6 What Causes Peripheral Vascular Disease? 7 How
Patient Information Table of Contents Introduction 3 What is Peripheral Vascular Disease? 5 What Are Some of the Symptoms of Peripheral Vascular Disease? 6 What Causes Peripheral Vascular Disease? 7 How
Colonic Metal Stents MAKING A DIFFERENCE TO HEALTH
 Colonic Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Colonic Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium range.
Allium Round Posterior Urethral Stent System (RPS) Instructions For Use
 Allium Round Posterior Urethral Stent System (RPS) Instructions For Use Manufactured by Allium Ltd. 2 Ha-Eshel St. Caesarea Industrial Park 38900 Israel Device Name: Allium Round Posterior Urethral Stent
Allium Round Posterior Urethral Stent System (RPS) Instructions For Use Manufactured by Allium Ltd. 2 Ha-Eshel St. Caesarea Industrial Park 38900 Israel Device Name: Allium Round Posterior Urethral Stent
BIOPSY GUN. Delivered in sterile peel-open package. Device is made of Stainless Steel and PP material.
 BIOPSY GUN Biopsy Gun is a reusable system for histological core biopsies. It has a throw (advancement) of 25mm and is used in conjunction with a single use needle. This device is used to obtain tissue
BIOPSY GUN Biopsy Gun is a reusable system for histological core biopsies. It has a throw (advancement) of 25mm and is used in conjunction with a single use needle. This device is used to obtain tissue
PRODUCTS FOR THE DIFFICULT AIRWAY. Courtesy of Cook Critical Care
 PRODUCTS FOR THE DIFFICULT AIRWAY Courtesy of Cook Critical Care EMERGENCY CRICOTHYROTOMY Thyroid Cartilage Access Site Cricoid Cartilage Identify the cricothyroid membrane between the cricoid and thyroid
PRODUCTS FOR THE DIFFICULT AIRWAY Courtesy of Cook Critical Care EMERGENCY CRICOTHYROTOMY Thyroid Cartilage Access Site Cricoid Cartilage Identify the cricothyroid membrane between the cricoid and thyroid
Gastric / EUS Metal Stents
 Gastric / EUS Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium
Gastric / EUS Metal Stents In a fast paced and maturing market, Diagmed Healthcare s Hanarostent has managed to continue to innovate and add unique and clinically superior features to its already premium
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Zenith Renu AAA Converter Graft. Device Description Planning and Sizing Deployment Sequence Patient Follow-Up
 Zenith Renu AAA Converter Graft Device Description Planning and Sizing Deployment Sequence Patient Follow-Up Device description: Device indications The Zenith Renu AAA Converter Graft with Z-Trak Introduction
Zenith Renu AAA Converter Graft Device Description Planning and Sizing Deployment Sequence Patient Follow-Up Device description: Device indications The Zenith Renu AAA Converter Graft with Z-Trak Introduction
Percutaneous Removal of Biliary Stone from Anomalous Right Hepatic Duct
 Percutaneous Removal of Biliary Stone from Anomalous Right Hepatic Duct Pages with reference to book, From 94 To 96 Tanveer ul Haq, Mohammed Younus Sheikh, Changes Khan Jadun, M.N. Ahmad, Yousuf H. Husen
Percutaneous Removal of Biliary Stone from Anomalous Right Hepatic Duct Pages with reference to book, From 94 To 96 Tanveer ul Haq, Mohammed Younus Sheikh, Changes Khan Jadun, M.N. Ahmad, Yousuf H. Husen
The Efficiency of Double Probing in Congenital Nasolacrimal Duct Obstruction
 Merit Research Journal of Medicine and Medical Sciences (ISSN: 2354-3238) Vol. 2(8) pp. 152-157, August, 2014 Available online http://www.meritresearchjournals.org/mms/index.htm Copyright 2014 Merit Research
Merit Research Journal of Medicine and Medical Sciences (ISSN: 2354-3238) Vol. 2(8) pp. 152-157, August, 2014 Available online http://www.meritresearchjournals.org/mms/index.htm Copyright 2014 Merit Research
Proboscis lateralis: report of two cases
 The British Association of Plastic Surgeons (2003) 56, 704 708 CASE REPORT Proboscis lateralis: report of two cases Lütfi Eroğlu a, *, Osman Ata Uysal b a Faculty of Medicine, Department of Plastic and
The British Association of Plastic Surgeons (2003) 56, 704 708 CASE REPORT Proboscis lateralis: report of two cases Lütfi Eroğlu a, *, Osman Ata Uysal b a Faculty of Medicine, Department of Plastic and
Endonasal Dacryocystorhinostomy done with and without Silicon Tube Stents: A Comparative Case Series Analysis Study
 10.5005/jp-journals-10001-1116 RESEARCH ARTICLE Endonasal Dacryocystorhinostomy done with and without Silicon Tube Stents: A Comparative Case Series Analysis Study Sudhir M Naik, Annapurna S Mushannavar,
10.5005/jp-journals-10001-1116 RESEARCH ARTICLE Endonasal Dacryocystorhinostomy done with and without Silicon Tube Stents: A Comparative Case Series Analysis Study Sudhir M Naik, Annapurna S Mushannavar,
Nasotracheal Intubation for Head and Neck Surgery
 Nasotracheal Intubation for Head and Neck Surgery Dr A J Cartwright Introduction History Anatomy Indications for Technique of Complications Contraindications Conclusions History First described in 1902
Nasotracheal Intubation for Head and Neck Surgery Dr A J Cartwright Introduction History Anatomy Indications for Technique of Complications Contraindications Conclusions History First described in 1902
Tear Meniscus Volume Changes in Dacryocystorhinostomy Evaluated With Quantitative Measurement Using Anterior Segment Optical Coherence Tomography
 Clinical and Epidemiologic Research Tear Meniscus Volume Changes in Dacryocystorhinostomy Evaluated With Quantitative Measurement Using Anterior Segment Optical Coherence Tomography Kazuyoshi Ohtomo, Takashi
Clinical and Epidemiologic Research Tear Meniscus Volume Changes in Dacryocystorhinostomy Evaluated With Quantitative Measurement Using Anterior Segment Optical Coherence Tomography Kazuyoshi Ohtomo, Takashi
Lacrimal drainage surgery in patients with rare nasal diseases
 (2007) 21, 1361 1366 & 2007 Nature Publishing Group All rights reserved 0950-222X/07 $30.00 www.nature.com/eye Lacrimal drainage surgery in patients with rare nasal diseases CLINICAL STUDY Abstract Aim
(2007) 21, 1361 1366 & 2007 Nature Publishing Group All rights reserved 0950-222X/07 $30.00 www.nature.com/eye Lacrimal drainage surgery in patients with rare nasal diseases CLINICAL STUDY Abstract Aim
Clinical Study Comparison of Transcanalicular Multidiode Laser Dacryocystorhinostomy with and without Silicon Tube Intubation
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 2016, Article ID 6719529, 5 pages http://dx.doi.org/10.1155/2016/6719529 Clinical Study Comparison of Transcanalicular Multidiode Laser Dacryocystorhinostomy
Hindawi Publishing Corporation Journal of Ophthalmology Volume 2016, Article ID 6719529, 5 pages http://dx.doi.org/10.1155/2016/6719529 Clinical Study Comparison of Transcanalicular Multidiode Laser Dacryocystorhinostomy
International Journal of Pharma and Bio Sciences
 Research Article Otorhinolaryngology International Journal of Pharma and Bio Sciences ISSN 0975-6299 COMPARATIVE RESULTS OF ENDOSCOPIC VERSUS EXTERNAL DACRYOCYSTORHINOSTOMY FOR ACQUIRED NASO-LACRIMAL DUCT
Research Article Otorhinolaryngology International Journal of Pharma and Bio Sciences ISSN 0975-6299 COMPARATIVE RESULTS OF ENDOSCOPIC VERSUS EXTERNAL DACRYOCYSTORHINOSTOMY FOR ACQUIRED NASO-LACRIMAL DUCT
Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully
 Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Physician Training Bifurcated system Proximal suprarenal stent Modular (aortic main body and two iliac legs) Full thickness woven polyester graft material Fully supported by self-expanding z-stents H&L-B
Document No. BMB/IFU/40 Rev No. & Date 00 & 15/11/2017 Issue No & Date 01 & 15/11/2017
 Central Venous Catheter Device Description Multi-lumen catheters incorporate separate, non-communicating vascular access lumens within a single catheter body. Minipunctur Access Sets And Trays: Used for
Central Venous Catheter Device Description Multi-lumen catheters incorporate separate, non-communicating vascular access lumens within a single catheter body. Minipunctur Access Sets And Trays: Used for
MICS & FEMORAL CANNULAE
 MICS & FEMORAL CANNULAE Cannulae that can High performance cannulae for direct and femoral cannulation, either in conventional or minimally invasive cardiac surgery 1. Pfeiffer et al. Interactive Cardiovascular
MICS & FEMORAL CANNULAE Cannulae that can High performance cannulae for direct and femoral cannulation, either in conventional or minimally invasive cardiac surgery 1. Pfeiffer et al. Interactive Cardiovascular
Introduction What Causes Peripheral Vascular Disease? How Do Doctors Treat Peripheral Vascular Disease?... 9
 Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Ureteral Stenting and Nephrostomy
 Scan for mobile link. Ureteral Stenting and Nephrostomy Ureteral stenting and nephrostomy help restore urine flow through blocked ureters and return the kidney to normal function. Ureters are long, narrow
Scan for mobile link. Ureteral Stenting and Nephrostomy Ureteral stenting and nephrostomy help restore urine flow through blocked ureters and return the kidney to normal function. Ureters are long, narrow
