Modified endoscopic dacryocystorhinostomy with posterior lacrimal sac flap for nasolacrimal duct obstruction!"#$%&'()*+,-*&'!./0(&
|
|
|
- Jasper Burns
- 6 years ago
- Views:
Transcription
1 Key words: Dacryocystorhinostomy; Endoscopy; Lacrimal apparatus diseases!!"#$%!"! KSC Yuen LYM Lam MWY Tse DDN Chan BWC Wong WM Chan Hong Kong Med J 00;:9-00 Department of Ophthalmology and Visual Sciences, The Chinese University of Hong Kong, Prince of Wales Hospital, Shatin, Hong Kong KSC Yuen, MRCS LYM Lam, FRCS (Edin) MWY Tse, FRCS (Edin) DDN Chan, FRCS (Edin) BWC Wong, MRCS WM Chan, MRCP, FRCS (Edin) Correspondence to: Prof WM Chan ( cwm67@netvigator.com) ORIGINAL ARTICLE Modified endoscopic dacryocystorhinostomy with posterior lacrimal sac flap for nasolacrimal duct obstruction!"#$%&'()*+,-*&'!./0(& Objectives. To evaluate a new technique of modified endoscopic dacryocystorhinostomy involving the creation of a large posterior flap at the lacrimal sac and to compare its success rate with that of the conventional endoscopic method of excising the entire medial lacrimal sac wall as a surgical treatment for epiphora caused by nasolacrimal duct obstruction. Design. Retrospective, interventional, and comparative case series. Setting. University teaching hospital, Hong Kong. Patients and methods. Only adults with primary nasolacrimal duct obstruction were included. Consecutive endoscopic dacryocystorhinostomy was performed using two different techniques from July 99 to June 001. The new technique involved the creation of a large posterior flap at the medial lacrimal sac wall, reflecting it posteriorly, followed by removal of the remaining small anterior flap (the LSF group). Other patients had the entire medial lacrimal sac wall excised (the ELS group). Main outcome measures. Surgical success was defined by free fluorescein drainage from the conjunctival sac into the rhinostomy site at least months after silicone stent removal. Results. Ninety-nine procedures were performed in 99 patients. The success rate was 89.1% (1/6) in the LSF group and 71.7% (8/) in the ELS group. The difference between the two groups was statistically significant (Chi squared test, P=0.01). Conclusions. Our new and modified technique of endonasal dacryocystorhinostomy has a greater success rate than conventional endonasal dacryocystorhinostomy. A large-scale prospective randomised controlled trial to further evaluate the efficacy and safety of this surgical technique is under way.!"#$%&'()* +,-./01)6789):;!"# $%&'()*+,-./01+67'8&9:;!"#$%&'()*+,-./01 #6789:;<=>!"#$!"#$%&#'()*+,-./0!"#$%&!"#!"#$%&'()*+,-./0"NVVV T OMMN S!"#$%&'()*+,-./0(6789'(:;<=!"#$%&'()*+,-+./0+67,=E F!"#$%&'()*+,=E!"F!"#$!"#$%&'()*+,-./0678$9!"#$%&'()"*+,-./0 VV!"#$VV!"# $%&'()UVKNB=EQNLQSF!"TNKTB=EPULRPF!"#$%&'(!)*+,=E!"mZMKMPNF!"#$%&#'()*+,-."$/0%&#'()*"1*!"#$%&'()*+$,-./067%6&89:;<=!"#$%& 9 Hong Kong Med J Vol 6 December 00
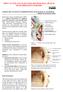
2 Modified endoscopic dacryocystorhinostomy Introduction Although endonasal dacryocystorhinostomy was described by Caldwell 1 as early as 9, it did not gain popularity until the development of effective endonasal illumination systems and endoscopic instrumentations in the past decade. Today, endoscopic dacryocystorhinostomy (EnDCR) can be performed using laser assistance,, radio-surgical electrodes, or other mechanical means including powered burr and rongeurs. Endoscopic dacryocystorhinostomy has two significant advantages over the external approach: external cutaneous scarring can be avoided, and the medial canthal ligament is not disrupted, thus preserving the normal pumping function of the nasolacrimal sac. The reported success rates of EnDCR vary from % to 96%, 6,7 and in general are lower than that of the external approach performed by many ophthalmologists. 8 The differences in the rate may be related to the lack of sutured apposition of the nasal and lacrimal sac mucosa, and the smaller bony ostium as compared with external dacryocystorhinostomy. 9 The benefits of mitomycin C and stenting of the rhinostomy site in EnDCR remain unclear., Some authors have claimed that stenting may actually increase the chance of surgical failure by inducing the formation of granulation tissue at the rhinostomy site. 1 Recently, there has been increasing interest in modifying the way of handling lacrimal sac wall and nasal mucosa in order to improve the surgical success of EnDCR. Traditionally, the medial lacrimal sac wall is either incised alone, or is excised completely after removal of the nasal mucosa and the bone of lacrimal fossa. Tsirbas and Wormald 1,1 described a technique that might increase the chance of apposition of the nasal and lacrimal sac mucosa. The technique involved creating a C-shaped nasal mucosal flap and a large anterior lacrimal sac flap, and they reported an anatomical success rate of 9% (Fig 1). The aims of this study are to develop a new modified EnDCR technique of handling the lacrimal sac flap, and to compare its success rate with that of the conventional method of excising the entire medial lacrimal sac wall. Methods Patients who received EnDCR between July 99 and June 001 were retrospectively identified and had their records reviewed. All surgeries were performed by two surgeons at the Department of Ophthalmology and Visual Sciences, Prince of Wales Hospital, Hong Kong. The inclusion criteria were adults with primary nasolacrimal duct obstruction and no other lacrimal disease. Patients were excluded if there was inaccessibility to their hospital files, a history of or presented with acute dacryocystitis, previous lacrimal surgery, or a follow-up period of less than months after silicone stent removal. Hospital files were reviewed for demographic information, mode of presentation, history of any lacrimal disease or surgery, details related to the EnDCR, and followup duration. The diagnosis of nasolacrimal duct obstruction was based on preoperative lacrimal probing, syringing results, and intra-operative findings. Postoperative findings including patency of rhinostomy site, presence or absence of free fluorescein flow into rhinostomy site from the conjunctival sac, and any surgery-related complications were gathered and analysed. (a) (b) CC ASF ASF NMF NMF IT IT Fig 1. Creation and reflection of the C-shaped nasal mucosal flap and large anterior lacrimal sac flap (a) Creation of C-shaped nasal mucosal flap (NMF) and large anterior lacrimal sac flap (ASF). : middle turbinate; IT: inferior turbinate; CC: internal opening of common canaliculus (b) Reflection of the NMF anteriorly onto the lateral nasal wall Hong Kong Med J Vol 6 December 00 9
3 Yuen et al (a) (b) Fig. Surgical technique of creating posterior lacrimal sac flap (a) Removal of lacrimal fossa bone showing underlying medial lacrimal sac wall. A: frontal process of right maxillary bone; B: medial lacrimal sac wall; C: middle turbinate. Solid line indicates the line of incision of the medial lacrimal sac wall (b) Creation of a large posterior lacrimal sac flap. A: frontal process of right maxillary bone; B: bicanalicular silicone intubation; C: posterior lacrimal sac flap Surgical technique of creating posterior lacrimal sac flap The nasal mucosa was decongested with ribbon gauze soaked with % cocaine and 1: 000 adrenaline (1:1 dilution). The lateral nasal mucosa anterior to the middle turbinate was injected with local anaesthetic (% xylocaine with 1: adrenaline). For surgery under local anaesthesia, a regional anterior ethmoidal nerve block ( ml of % xylocaine with 1: adrenaline) was added. 0 Ο and 0 Ο Storz endoscopes (Storz, California, US) equipped with three-chip cameras were used during the surgery. The location of the lacrimal sac was identified by inserting a -gauze fibre-optic light probe used in vitreoretinal surgery (Bausch and Lomb, New York, US) through one of the canaliculi into the lacrimal sac, and then observing the transmitted light with the nasoendoscope. A vertical incision of nasal mucosa was made just anterior to the maxillary line by a crescent knife used for cataract surgery (Alcon, Texas, US). The incision began at the level of the head of the middle turbinate to the level of the inferior end of the middle turbinate. A nasal mucosal flap was lifted with a Freer elevator and then excised completely with straight Blakesley forceps. The underlying bone of the lacrimal fossa, including the lacrimal bone and the frontal process of the maxilla, was removed with a -mm Kerrison rongeur. The bony ostium was created as large as possible with or without uncinectomy in order to fully expose the medial lacrimal sac wall (Fig a). The medial lacrimal sac wall was tented with a Bowman s probe before it was vertically incised with a crescent knife at the junction between the anterior one third and posterior two thirds of the lacrimal sac wall. Small horizontal cuts were made superiorly and inferiorly with the same crescent knife to facilitate the reflection of the large posterior lacrimal flap backwards. Adequate horizontal cuts were made to ensure that the posterior lacrimal sac flap would sit flatter on the lateral nasal mucosal wall. The small remaining anterior lacrimal sac was excised with a -mm Kerrison rongeur. Adequate exposure was achieved to allow bicanalicular silicone intubation (BD Vistec, Warks, United Kingdom) without difficulty at the end of surgery (Fig b). Dental sponges soaked with 0.0% mitomycin C were applied to the rhinostomy site for minutes, followed by 0-mL normal saline irrigation. All patients received postoperative oral antibiotics (cefuroxime 00 mg twice a day) for to 7 days and eye drops containing antibiotics and steroid (gutt maxitrol times a day). Nasal douching was carried out times a day at home as instructed until the wound was completely healed. Patients were routinely followed up at out-patient clinics at weeks 1 and ; months 1,, and ; and then every months postoperatively. Regular nasoendoscopic examinations were performed to remove blood clots or debris obstructing the rhinostomy site. This examination was also able to assess the patency of the rhinostomy site and determine healing before the stent was removed. Surgical success of the two groups was compared using the Chi squared test. Results A total of EnDCR from patients were identified from the records. Of those, three patients were excluded 96 Hong Kong Med J Vol 6 December 00
4 Modified endoscopic dacryocystorhinostomy Table 1. Endoscopic dacryocystorhinostomy with lacrimal sac flap (the LSF group) Case Sex/Age (years) F/6 F/9 F/7 F/ F/8 F/ F/77 F/68 F/0 M/7 F/60 F/60 F/6 F/8 F/ F/ M/7 F/6 F/79 M/9 F/1 F/67 F/ F/ F/0 M/7 M/0 F/7 F/71 F/ M/6 F/ F/6 F/71 F/0 F/8 Laterality Anaesthesia* Surgeon Mucocele Intubation period Follow-up period Surgical success * denotes local anaesthesia, general anaesthesia denotes LYM Lam, MWY Tse As defined by free fluorescein drainage from the conjunctival sac into the rhinostomy site at least months after silicone stent removal denotes granulation tissue formation at rhinostomy site Complications two due to incomplete hospital files, and one due to a loss of follow-up before stent removal. Of the remaining 99 patients, 6 patients received EnDCR with lacrimal sac flap (the LSF group) (Table 1) and the other patients had EnDCR with the entire medial lacrimal wall excised (the ELS group) (Table ). In the LSF group, 87.0% (0/6) patients were female with a mean age of 7. (range, ; standard deviation [SD], 1.) years. In the ELS group, 9.% (0/) patients were female with a mean age of 6.1 (range, ; SD, 1.) years. Mucocele were present in 6.1% (1/6) of the LSF group and 8.% (/) of the ELS group. Approximately.% (/6) of the LFS group and 9.% (/) of ELS group had the operation under general anaesthesia. The average silicone stent removal time was.7 (range,.0-.0; SD, 0.9) months in the LSF group and.0 (range,.0-6.0; SD, 0.9) months in the ELS group. Cheese-wiring of lacrimal punctum did not occur in patients of the LSF group but in 1.9% (1/) of the patients in the ELS group, from whom the stent was removed months postoperatively. The rhinostomy site was complicated by granulation tissue formation in 6.% (/6) of the LSF group and in.0% (9/) of the ELS group. other surgical complications were reported in either group. Hong Kong Med J Vol 6 December 00 97
5 Yuen et al Table. Endoscopic dacryocystorhinostomy with entire medial lacrimal sac wall excision (the ELS group) Case Sex/Age (years) F/67 F/7 F/8 F/71 F/ F/9 F/7 M/7 F/7 F/88 F/6 M/67 F/1 F/76 F/6 F/6 M/ F/6 F/ F/ F/6 F/ F/8 F/68 F/ F/90 F/7 F/7 F/ F/1 F/ F/ F/6 F/7 F/7 F/77 F/7 F/77 F/7 F/80 F/8 F/ F/7 F/66 F/6 F/7 Laterality Anaesthesia* Surgeon Mucocele Intubation Period Follow-up Period Surgical Success * denotes local anaesthesia, general anaesthesia denotes LYM Lam, MWY Tse As defined by free fluorescein drainage from the conjunctival sac into the rhinostomy site at least months after silicone stent removal CW denotes cheese-wiring of lacrimal punctum, granulation tissue formation at rhinostomy site Complications CW The success rate was 89.1% (1/6) in the LSF group and 71.7% (8/) in the ELS group with a statistically significant difference (Chi squared test, P=0.01). In all failure cases, the rhinostomy sites were completely closed by scar tissue. Discussion Despite the many advantages offered by EnDCR, many surgeons are still concerned that its success rate is lower than that of the external approach, which is commonly higher than 90%., When compared with external dacryocystorhinostomy, the reasons may be related to the lack of sutured apposition of the nasal and lacrimal sac mucosa and the smaller bony ostium. Surgical failure occurs when the lacrimal sac does not marsupialise on the lateral nasal mucosal wall. There are very few large-scale prospective randomised controlled trials in the literature to support the benefits of 98 Hong Kong Med J Vol 6 December 00
6 Modified endoscopic dacryocystorhinostomy the various adjunctive measures in EnDCR. Mitomycin C, an alkylating agent with inhibitory effects on fibroblasts, has been shown to cause a decrease in both the density and cellularity of nasal mucosal specimens taken from EnDCR. However, its role in preventing closure of the rhinostomy site following EnDCR remains uncertain. A study by Camara et al reported a statistically significant difference in the success rates comparing laser-assisted EnDCR with and without mitomycin C. However, Zilelioglu et al found no such benefit of mitomycin C in their study of EnDCR. Bicanalicular intubation, most often by silicone stenting, is one approach to prevent closure of the rhinostomy site. However, some surgeons are concerned that intubation might increase the chance of rhinostomy site closure by granulation tissue formation. 1, The combination of 0.0% mitomycin C and bicanalicular silicone intubation in this study represents a novel approach to increasing the success rate of EnDCR. Conventionally in EnDCR, the lateral nasal mucosal wall is removed completely to expose the underlying lacrimal fossa, then the medial lacrimal sac is either incised alone or excised completely to create a rhinostomy site. Patency of the rhinostomy site depends on anastomosis of the cut edges of the nasal and lacrimal sac mucosa. However, without sutured apposition, one cannot predict the pattern of anastomosis between the cut edges of the nasal and lacrimal sac mucosa. If lacrimal-to-lacrimal or nasalto-nasal mucosa anastomosis occurs, the rhinostomy site will be closed. To overcome this problem, Tsirbas and Wormald 1,1 reported a technique of creating a C-shaped lateral nasal mucosal flap and a large anterior lacrimal sac flap to promote close apposition between the two mucosal surfaces. In this study, we report another technique to encourage apposition of the nasal and lacrimal sac mucosa. Reflecting a large lacrimal sac flap posteriorly increases the distance between the edges of the lacrimal sac mucosa, thus reducing the chance of re-closure. The posterior flap also promotes marsupialisation of the lacrimal sac due to the close apposition of the lacrimal sac and the nasal mucosa. The surgical success rate of this new technique (89.1%) is comparable to those reported using other methods of EnDCR. When compared with the more conventional method of excising the entire medial lacrimal sac wall performed by the same surgeons, the surgical success of this new technique is statistically significantly higher (Chi squared test, P=0.01). Our technique does not require the acquisition of new surgical skills by surgeons. The horizontal cuts of the lacrimal sac wall can be performed immediately after the vertical incision when the crescent knife is still inside the lacrimal sac. Once reflected backwards with enough relaxing horizontal cuts, the posterior flap would tend to sit naturally on the lateral nasal mucosa without flipping forward again. We excised the anterior sac flap with the sharp cutting edges of a Kerrison rongeur instead of using Blakesley forceps to avoid tearing of the lacrimal sac mucosa. It is also important not to create too small an anterior lacrimal sac flap, which is difficult to excise and incomplete excision might increase the chance of surgical failure. Apart from cheese-wiring of the lacrimal punctum and the formation of granulation tissue at the rhinostomy site, no other significant surgical complication was reported. Orbital fat prolapse and frontal sinusitis could occur if dissection is taken too posteriorly into the uncinate. All failure cases in the study had closed rhinostomy sites observed by nasoendoscopic examination. However, the timing of rhinostomy site closure after stent removal was not clear due to the retrospective nature of the study. synaechia between the lateral nasal mucosa and the middle turbinate was noted in these failure cases. There are a few shortcomings of the study. Firstly, the retrospective study design did not allow patient randomisation to different surgical methods. Even though the two groups of patients were comparable in terms of their mean age, sex distribution, and proportion of mucocele, it is not certain why one surgical method was chosen instead of the other by the attending surgeon. A small and scarred nasolacrimal sac might be difficult for flap creation, thus leading the surgeon to excise the medial sac wall completely. A prospective randomised study is warranted to eliminate this potential bias. Secondly, the average size of the bony ostium in both groups, which may be a determining factor for the outcome, was not recorded due to the retrospective nature of the study. It was, however, a routine practice to create an as large bony ostium as possible by the surgeons to fully expose the lacrimal sac. Thirdly, there was no standardised protocol for the duration of postoperative stenting. The average silicone stent removal time was.7 (range,.0-.0; SD, 0.9) months in the LSF group and.0 (range,.0-6.0; SD, 0.9) months in the ELS group. It is uncertain why the stent was kept in some patients for as long as to 6 months postoperatively in the study. However, in this study surgical failure did not appear to be related to prolonged stenting. Of the 0 patients with surgical failure, only two had intubation time of more than months. Granulation tissue complicating the rhinostomy site was more common in the ELS group than in the LSF group (.0% [9/] and 6.% [/6], respectively). It has been postulated that a long intubation period may lead to granulation tissue formation at the rhinostomy site and subsequent surgical failure. 1,0 In our study, the patients with granulation tissue were found to have a lower success rate due to closure of the rhinostomy site (66.6% in both LSF and ESF groups). Their mean intubation period, however, was only.7 (range,.0-.0; SD, 0.7) months, which was similar to the mean intubation period of other patients in the study. Finally, the relatively small sample size should be taken into consideration while interpreting the study result. Hong Kong Med J Vol 6 December 00 99
7 Yuen et al Conclusions We have described an improved approach to EnDCR. The method involves a new and easy technique of fashioning the large posterior lacrimal sac flap and excising the remaining small anterior sac flap. This method also promotes close apposition between the lacrimal sac and nasal mucosa. This retrospective non-randomised review showed that the success rate of this technique is statistically better than the conventional method involving excision of the entire medial lacrimal sac wall. A large-scale prospective randomised controlled trial to study the efficacy of this surgical method is under way. References 1. Caldwell GM. Two new operations for obstruction of the nasal duct, with preservation of the canaliculi, with an incidental description of a new lacrymal probe. N Y Med J 9;7:81.. Woog JJ, Metson R, Puliafito CA. Holmium: YAG endonasal laser dacryocystorhinostomy. Am J Ophthalmol 9;1:1-.. Boush, Lemke BN, Dortzbach RK. Results of endonasal laser-assisted dacryocystorhinostomy. Ophthalmology 9;1: Javate RM, Campomanes BS Jr, Co ND, et al. The endoscope and the radiofrequency unit in DCR surgery. Ophthal Plast Reconstr Surg 9;:-8.. Yung MW, Hardman-Lea S. Endoscopic inferior dacryocystorhinostomy. Clin Otolaryngol 98;: Sprekelsen MB, Barberan. Endoscopic dacryocystorhinostomy: surgical technique and results. Laryngoscope 96;6: Yung MW, Hardman-Lea S. Analysis of the results of surgical endoscopic dacryocystorhinostomy: effect of the level of obstruction. Br J Ophthalmol 00;86: Malhotra R, Wright M, Olver JM. A consideration of the time taken to do dacryo-cystorhinostomy (DCR) surgery. Eye 00;: Shun-Shin, Thurairajan G. External dacryocystorhinsotomy an end of an era? Br J Ophthalmol 97;81:7-7.. Zilelioglu G, Ugurbas SH, Anadolu Y, Akiner M, Akturk T. Adjunctive use of mitomycin C on endoscopic lacrimal surgery. Br J Ophthalmol 98;8:6-6.. Selig YK, Biesman BS, Rebeiz EE. Topical application of mitomycin C in endoscopic dacryocystorhinostomy. Am J Rhinol 000;1: Unlu HH, Toprak B, Aslan A, Guler C. Comparison of surgical outcomes in primary endoscopic dacryocystorhinostomy with and without silicone intubation. Ann Otol Rhinol Laryngol 00;1: Tsirbas A, Wormald PJ. Mechanical endonasal dacryocystorhinostomy with mucosal flaps. Br J Ophthalmol 00;87: Tsirbas A, Wormald PJ. Endonasal dacryocystorhinostomy with mucosal flaps. Am J Ophthalmol 00;: Hartikainen J, Grenman R, Puukka P, Seppa H. Prospective randomized comparison of external dacryocystorhinostomy and endonasal laser dacryocystorhinostomy. Ophthalmology 98;: Rosen N, Sharir M, Moverman DC, Rosner M. Dacryocystorhinostomy with silicone tubes: evaluation of cases. Ophthalmic Surg 89; 0:1-9.. Ugurbas SH, Zilelioglu G, Sargon MF, Anadolu Y, Akiner M, Akturk T. Histopathologic effects of mitomycin-c on endoscopic transnasal dacryocystorhinostomy. Ophthalmic Surg Lasers 97;8:00-.. Camara JG, Bengzon AU, Henson RD. The safety and efficacy of mitomycin C in endonasal endoscopic laser-assisted dacryocystorhinostomy. Ophthal Plast Reconstr Surg 000;:-8.. Allen K, Berlin AJ. Dacryocystorhinostomy failure: association with nasolacrimal silicone intubation. Ophthalmic Surg 89;0: Onerci M, Orhan M, Ogretmenoglu O, Irkec M. Long-term results and reasons for failure of intranasal endoscopic dacryocystorhinostomy. Acta Otolaryngol 000;:-. 00 Hong Kong Med J Vol 6 December 00
Non-endoscopic Mechanical Endonasal Dacryocystorhinostomy
 Surgical Technique Non-endoscopic Mechanical Endonasal Dacryocystorhinostomy Mohammad Etezad Razavi 1, MD; Morteza Noorollahian 2, MD; Alireza Eslampoor 1, MD 1 Khatam-al-Anbia Eye Research Center, Mashhad
Surgical Technique Non-endoscopic Mechanical Endonasal Dacryocystorhinostomy Mohammad Etezad Razavi 1, MD; Morteza Noorollahian 2, MD; Alireza Eslampoor 1, MD 1 Khatam-al-Anbia Eye Research Center, Mashhad
Study of success rates in endoscopic dacryocystorhinostomy with and without stenting. dacryocystorhinostomy with and
 Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
A Comparative Study of Endoscopic Endonasal Dacryocystorhinostomy with and without Intraoperative Mitomycin-C Application
 10.5005/jp-journals-10013-1140 ORIGINAL ARTICLE A Comparative Study of Endoscopic Endonasal Dacryocystorhinostomy with and without Intraoperative Mitomycin-C Application Raman Wadhera, Sat Paul Gulati,
10.5005/jp-journals-10013-1140 ORIGINAL ARTICLE A Comparative Study of Endoscopic Endonasal Dacryocystorhinostomy with and without Intraoperative Mitomycin-C Application Raman Wadhera, Sat Paul Gulati,
Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy
 Graefes Arch Clin Exp Ophthalmol (2012) 250:1509 1513 DOI 10.1007/s00417-012-1992-x OCULOPLASTICS AND ORBIT Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy Jae Wook
Graefes Arch Clin Exp Ophthalmol (2012) 250:1509 1513 DOI 10.1007/s00417-012-1992-x OCULOPLASTICS AND ORBIT Success rate and complications of endonasal dacryocystorhinostomy with unciformectomy Jae Wook
INTERVENTIONAL PROCEDURES PROGRAMME
 Prepared by ASERNIP-S Introduction NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of Endoscopic Dacryocystorhinostomy This overview has
Prepared by ASERNIP-S Introduction NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of Endoscopic Dacryocystorhinostomy This overview has
To analyse the success rate of external Dacryocystorhinostomy related with anatomical osteotomy size made during surgery
 2018; 4(1): 354-358 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(1): 354-358 www.allresearchjournal.com Received: 23-11-2017 Accepted: 24-12-2017 Pandit VK Associate Professor,
2018; 4(1): 354-358 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(1): 354-358 www.allresearchjournal.com Received: 23-11-2017 Accepted: 24-12-2017 Pandit VK Associate Professor,
A randomized placebo controlled trial of Mitomycin - C in surgical outcome of primary endoscopic dacryocystorhinostomy
 Al Am een J Med Sci 2013; 6(3):231-236 US National Library of Medicine enlisted journal ISSN 0974-1143 ORIGI NAL ARTICLE C O D E N : A A J MB G A randomized placebo controlled trial of Mitomycin - C in
Al Am een J Med Sci 2013; 6(3):231-236 US National Library of Medicine enlisted journal ISSN 0974-1143 ORIGI NAL ARTICLE C O D E N : A A J MB G A randomized placebo controlled trial of Mitomycin - C in
Anatomical and Functional Evaluation of Conventional vs Inferior Endoscopic Dacryocystorhinostomy in Study Cases of Idiopathic Chronic Dacryocystitis
 Kuldeep Thakur et al ORIGINAL ARTICLE 10.5005/jp-journals-10013-1314 Anatomical and Functional Evaluation of Conventional vs Inferior Endoscopic Dacryocystorhinostomy in Study Cases of Idiopathic Chronic
Kuldeep Thakur et al ORIGINAL ARTICLE 10.5005/jp-journals-10013-1314 Anatomical and Functional Evaluation of Conventional vs Inferior Endoscopic Dacryocystorhinostomy in Study Cases of Idiopathic Chronic
Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy
 SV Manjunatha Rao, MM Rajshekar Original Article 10.5005/jp-journals-10013-1284 Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy 1 SV Manjunatha Rao, 2 MM Rajshekar ABSTRACT
SV Manjunatha Rao, MM Rajshekar Original Article 10.5005/jp-journals-10013-1284 Dacryocystorhinostomy Stent Insertion in Initial Endoscopic Dacryocystorhinostomy 1 SV Manjunatha Rao, 2 MM Rajshekar ABSTRACT
Endonasal Dacryocystorhinostomy done with and without Silicon Tube Stents: A Comparative Case Series Analysis Study
 10.5005/jp-journals-10001-1116 RESEARCH ARTICLE Endonasal Dacryocystorhinostomy done with and without Silicon Tube Stents: A Comparative Case Series Analysis Study Sudhir M Naik, Annapurna S Mushannavar,
10.5005/jp-journals-10001-1116 RESEARCH ARTICLE Endonasal Dacryocystorhinostomy done with and without Silicon Tube Stents: A Comparative Case Series Analysis Study Sudhir M Naik, Annapurna S Mushannavar,
ORIGINAL ARTICLE. Intranasal Localization of the Lacrimal Sac
 ORIGINAL ARTICLE Intranasal Localization of the Lacrimal Sac Mustafa Orhan, MD; Canan Y. Saylam, MD; Raşit Midilli, MD Objective: To optimize the approach to the lacrimal sac during intranasal dacryocystorhinostomy.
ORIGINAL ARTICLE Intranasal Localization of the Lacrimal Sac Mustafa Orhan, MD; Canan Y. Saylam, MD; Raşit Midilli, MD Objective: To optimize the approach to the lacrimal sac during intranasal dacryocystorhinostomy.
Repeat DCR with Silicone Tube intubation : A Prospective Study.
 Repeat DCR with Silicone Tube intubation : A Prospective Study. Dr Imtiyaz A Lone Assistant Professor Department of Ophthalmology SKIMS Medical College Bemina, Srinagar, India Dr Bashir A Malik Sr. Resident
Repeat DCR with Silicone Tube intubation : A Prospective Study. Dr Imtiyaz A Lone Assistant Professor Department of Ophthalmology SKIMS Medical College Bemina, Srinagar, India Dr Bashir A Malik Sr. Resident
Intranasal location of lacrimal sac in Thai cadavers
 Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY ENDOSCOPIC DACRYOCYSTORHINOSTOMY (DCR) SURGICAL TECHNIQUE Hisham Wasl, Darlene Lubbe Endoscopic dacryocystorhinostomy (DCR) is a surgical
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY ENDOSCOPIC DACRYOCYSTORHINOSTOMY (DCR) SURGICAL TECHNIQUE Hisham Wasl, Darlene Lubbe Endoscopic dacryocystorhinostomy (DCR) is a surgical
Clinical Results of Endoscopic Dacryocystorhinostomy using a Microdebrider
 Clinical Results of Endoscopic Dacryocystorhinostomy using a Microdebrider Sung Wook Yoon, MD, Young Sun Yoon, MD, Su Hyung Lee, MD Department of Ophthalmology, Dongkang General Hospital, Ulsan, Korea
Clinical Results of Endoscopic Dacryocystorhinostomy using a Microdebrider Sung Wook Yoon, MD, Young Sun Yoon, MD, Su Hyung Lee, MD Department of Ophthalmology, Dongkang General Hospital, Ulsan, Korea
THE EXTERNAL DACRYOCYSTORHINOSTOMY (DCR)
 Outcome of External Dacryocystorhinostomy Combined With Membranectomy of a Distal Canalicular Obstruction KOSTAS G. BOBORIDIS, MD, CATEY BUNCE, DSC, AND GEOFFREY E. ROSE, FRCS, FRCOPHTH PURPOSE: To investigate
Outcome of External Dacryocystorhinostomy Combined With Membranectomy of a Distal Canalicular Obstruction KOSTAS G. BOBORIDIS, MD, CATEY BUNCE, DSC, AND GEOFFREY E. ROSE, FRCS, FRCOPHTH PURPOSE: To investigate
Comparison of outcome of external DCR and endonasal DCR surgery among the rural population
 Original article: Comparison of outcome of external DCR and endonasal DCR surgery among the rural population 1 Dr Aniket Lathi*, 2 Dr C Anand Kumar, 3 Dr Nitin Kulkarni, 4 Dr Ashish Gupta, 5 Dr Shruti
Original article: Comparison of outcome of external DCR and endonasal DCR surgery among the rural population 1 Dr Aniket Lathi*, 2 Dr C Anand Kumar, 3 Dr Nitin Kulkarni, 4 Dr Ashish Gupta, 5 Dr Shruti
Minimally Invasive Technique of Dacryocystorhinostomy
 Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Protocol Mohammad Idrees* Consultant Ophthalmology, REDO Eye Hospital, Rawalpindi, Pakistan *Corresponding Author: Mohammad Idrees, Consultant Ophthalmology,
Cronicon OPEN ACCESS EC OPHTHALMOLOGY Research Protocol Mohammad Idrees* Consultant Ophthalmology, REDO Eye Hospital, Rawalpindi, Pakistan *Corresponding Author: Mohammad Idrees, Consultant Ophthalmology,
Outcomes of external dacryocystorhinostomy and endoscopic endonasal dacryocystorhinostomy in the management of nasolacrimal duct obstruction
 Original article Outcomes of external dacryocystorhinostomy and endoscopic endonasal dacryocystorhinostomy in the management of nasolacrimal duct obstruction Duwal S, Saiju R Tilganga Institute of Ophthalmology,
Original article Outcomes of external dacryocystorhinostomy and endoscopic endonasal dacryocystorhinostomy in the management of nasolacrimal duct obstruction Duwal S, Saiju R Tilganga Institute of Ophthalmology,
International Journal of Pharma and Bio Sciences
 Research Article Otorhinolaryngology International Journal of Pharma and Bio Sciences ISSN 0975-6299 COMPARATIVE RESULTS OF ENDOSCOPIC VERSUS EXTERNAL DACRYOCYSTORHINOSTOMY FOR ACQUIRED NASO-LACRIMAL DUCT
Research Article Otorhinolaryngology International Journal of Pharma and Bio Sciences ISSN 0975-6299 COMPARATIVE RESULTS OF ENDOSCOPIC VERSUS EXTERNAL DACRYOCYSTORHINOSTOMY FOR ACQUIRED NASO-LACRIMAL DUCT
DACRYOCYSTORHINOSTOMY; A COMPARATIVE STUDY OF THE RESULTS WITH AND WITHOUT SILICON INTUBATION IN PAKISTANI PATIENTS OF CHRONIC DACRYOCYSTITIS
 DACRYOCYSTORHINOSTOMY 81 ORIGINAL PROF-1230 DACRYOCYSTORHINOSTOMY; A COMPARATIVE STUDY OF THE RESULTS WITH AND WITHOUT SILICON INTUBATION IN PAKISTANI PATIENTS OF CHRONIC DACRYOCYSTITIS DR. MUHAMMAD NAWAZ,
DACRYOCYSTORHINOSTOMY 81 ORIGINAL PROF-1230 DACRYOCYSTORHINOSTOMY; A COMPARATIVE STUDY OF THE RESULTS WITH AND WITHOUT SILICON INTUBATION IN PAKISTANI PATIENTS OF CHRONIC DACRYOCYSTITIS DR. MUHAMMAD NAWAZ,
Nasal Endoscopic Dacryocystorhinostomy The Nizamabad experience
 Original Research Article Nasal Endoscopic Dacryocystorhinostomy The Nizamabad experience Anand Acharya 1*, Modini P. 2, G. Lakpati 3 1 Associate Professor, ENT Department, GMC, Nizamabad, India 2 Associate
Original Research Article Nasal Endoscopic Dacryocystorhinostomy The Nizamabad experience Anand Acharya 1*, Modini P. 2, G. Lakpati 3 1 Associate Professor, ENT Department, GMC, Nizamabad, India 2 Associate
Endonasal dacryocystorhinostomy was first. Reliable technique of Endoscopic Dacryocystorhinostomy A Pilot Study. Main Article
 Main Article Reliable technique of Endoscopic Dacryocystorhinostomy A Pilot Study Sudip Kumar Das, 1 Chiranjib Das, 1 Amit Bikram Maiti, 2 Ruma Guha, 3 Subhendu Chowdhury 1 ABSTRACT Introduction Over last
Main Article Reliable technique of Endoscopic Dacryocystorhinostomy A Pilot Study Sudip Kumar Das, 1 Chiranjib Das, 1 Amit Bikram Maiti, 2 Ruma Guha, 3 Subhendu Chowdhury 1 ABSTRACT Introduction Over last
Acute Dacryocystitis with Abscess: Endonasal Dacryocystorhinostomy, the Primary Treatment of Choice
 10.5005/jp-journals-10013-1129 ORIGINAL ARTICLE Acute Dacryocystitis with Abscess: Endonasal Dacryocystorhinostomy, the Primary Treatment of Choice Sudhir M Naik, Sarika S Naik ABSTRACT Background/objectives:
10.5005/jp-journals-10013-1129 ORIGINAL ARTICLE Acute Dacryocystitis with Abscess: Endonasal Dacryocystorhinostomy, the Primary Treatment of Choice Sudhir M Naik, Sarika S Naik ABSTRACT Background/objectives:
Stent technique for endoscopic dacryocystorhinostomy Our expertise
 Romanian Journal of Rhinology, Vol. 6, No. 21, January - March 2016 ORIGINAL STUDY Stent technique for endoscopic dacryocystorhinostomy Our expertise Vlad Budu 1, Tatiana Decuseara 1, Bogdan Mocanu 2,
Romanian Journal of Rhinology, Vol. 6, No. 21, January - March 2016 ORIGINAL STUDY Stent technique for endoscopic dacryocystorhinostomy Our expertise Vlad Budu 1, Tatiana Decuseara 1, Bogdan Mocanu 2,
Yunhai Tu, 1 Zhenbin Qian, 2 Jiao Zhang, 1 Wencan Wu, 1 and Tianlin Xiao Introduction. 2. Patients and Methods
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 201, Article ID 67909, 7 pages http://dx.doi.org/10.11/201/67909 Clinical Study Endoscopic Endonasal Dacryocystorhinostomy Combined with Canaliculus
Hindawi Publishing Corporation Journal of Ophthalmology Volume 201, Article ID 67909, 7 pages http://dx.doi.org/10.11/201/67909 Clinical Study Endoscopic Endonasal Dacryocystorhinostomy Combined with Canaliculus
Study of outcomes of endonasal dacryocystorhinostomy in relation with sex distribution in Indian population
 Original article: Study of outcomes of endonasal dacryocystorhinostomy in relation with sex distribution in Indian population 1Dr. Mayur Ingale, 2 Dr. Vinod Shinde, 3 Dr.Paresh Chavan, 4 Dr.SudeepChoudhary
Original article: Study of outcomes of endonasal dacryocystorhinostomy in relation with sex distribution in Indian population 1Dr. Mayur Ingale, 2 Dr. Vinod Shinde, 3 Dr.Paresh Chavan, 4 Dr.SudeepChoudhary
Original Article Effect of revision dacryocystorhinostomy under nasal endoscopy on recrudescent dacryocystitis
 Int J Clin Exp Pathol 2017;10(12):11717-11722 www.ijcep.com /ISSN:1936-2625/IJCEP0052246 Original Article Effect of revision dacryocystorhinostomy under nasal endoscopy on recrudescent dacryocystitis Jintao
Int J Clin Exp Pathol 2017;10(12):11717-11722 www.ijcep.com /ISSN:1936-2625/IJCEP0052246 Original Article Effect of revision dacryocystorhinostomy under nasal endoscopy on recrudescent dacryocystitis Jintao
Problems / Complications, Success Rate Endoscopic Dacryocystorhinostomy
 Original Article Problems / Complications, Success Rate Endoscopic Dacryocystorhinostomy Khawaja Khalid Shoaib, Salahuddin Ahmad, Muhammad Manzoor, Sabihuddin Ahmed, Iftikhar Aslam Syed Nadeem ul Haq Pak
Original Article Problems / Complications, Success Rate Endoscopic Dacryocystorhinostomy Khawaja Khalid Shoaib, Salahuddin Ahmad, Muhammad Manzoor, Sabihuddin Ahmed, Iftikhar Aslam Syed Nadeem ul Haq Pak
Application of biodegradable collagen matrix (Ologen ) implants in Dacryocystorhinostomy surgeries, a randomized clinical study
 Marey et al. BMC Ophthalmology (2018) 18:254 https://doi.org/10.1186/s12886-018-0901-4 RESEARCH ARTICLE Open Access Application of biodegradable collagen matrix (Ologen ) implants in Dacryocystorhinostomy
Marey et al. BMC Ophthalmology (2018) 18:254 https://doi.org/10.1186/s12886-018-0901-4 RESEARCH ARTICLE Open Access Application of biodegradable collagen matrix (Ologen ) implants in Dacryocystorhinostomy
Shreya M. Shah, Mehul A. Shah & Chintan Patel
 Cannula dacryocystorhinostomy: a simple, innovative and cost-effective method of lacrimal surgery Shreya M. Shah, Mehul A. Shah & Chintan Patel International Ophthalmology The International Journal of
Cannula dacryocystorhinostomy: a simple, innovative and cost-effective method of lacrimal surgery Shreya M. Shah, Mehul A. Shah & Chintan Patel International Ophthalmology The International Journal of
ENDONASAL CARBON-DIOXIDE LASER ASSISTED DACRYOCYS- TORHINOSTOMY VERSES EXTERNAL DACRYOCYSTORHINOSTOMY
 9 Main Article ENDONASAL CARBON-DIOXIDE LASER ASSISTED DACRYOCYS- TORHINOSTOMY VERSES EXTERNAL DACRYOCYSTORHINOSTOMY Ashok Verma, Mazin Al Khabori, Rajiv Zutshi* ABSTRACT: This is a prospective, non- randomized
9 Main Article ENDONASAL CARBON-DIOXIDE LASER ASSISTED DACRYOCYS- TORHINOSTOMY VERSES EXTERNAL DACRYOCYSTORHINOSTOMY Ashok Verma, Mazin Al Khabori, Rajiv Zutshi* ABSTRACT: This is a prospective, non- randomized
Philippine Journal of OPHTHALMOLOGY ABSTRACT
 Original Article Philippine Journal of OPHTHALMOLOGY Surgical Technique and Preliminary Results of Transcanalicular Endoscopic Lacrimal Duct Recanalization and Balloon Dacryoplasty with Silicone Intubation
Original Article Philippine Journal of OPHTHALMOLOGY Surgical Technique and Preliminary Results of Transcanalicular Endoscopic Lacrimal Duct Recanalization and Balloon Dacryoplasty with Silicone Intubation
Morphological and morphometrical study of the nasal opening of nasolacrimal duct in man
 O R I G I N A L A R T I C L E Folia Morphol. Vol. 73, No. 3, pp. 321 330 DOI: 10.5603/FM.2014.0049 Copyright 2014 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Morphological and morphometrical study of
O R I G I N A L A R T I C L E Folia Morphol. Vol. 73, No. 3, pp. 321 330 DOI: 10.5603/FM.2014.0049 Copyright 2014 Via Medica ISSN 0015 5659 www.fm.viamedica.pl Morphological and morphometrical study of
Endonasal endoscopic scalpel-forceps dacryocystorhinostomy vs endocanalicular diode laser dacryocystorhinostomy
 Eur J Ophthalmol 2012; 00 ( 00) : 000-000 DOI: 10.5301/ejo.5000157 ORIGINAL ARTICLE Endonasal endoscopic scalpel-forceps dacryocystorhinostomy vs endocanalicular diode laser dacryocystorhinostomy Juan
Eur J Ophthalmol 2012; 00 ( 00) : 000-000 DOI: 10.5301/ejo.5000157 ORIGINAL ARTICLE Endonasal endoscopic scalpel-forceps dacryocystorhinostomy vs endocanalicular diode laser dacryocystorhinostomy Juan
Balloon Dacryoplasty: Indications, Techniques and Outcomes
 INTERNATIONAL JOURNAL OF HEALTH RESEARCH IN MODERN INTEGRATED MEDICAL SCIENCES (IJHRMIMS), ISSN XXXX (P), ISSN XXXX (O), Oct-Dec 2014 15 Review Article Balloon Dacryoplasty: Indications, Techniques and
INTERNATIONAL JOURNAL OF HEALTH RESEARCH IN MODERN INTEGRATED MEDICAL SCIENCES (IJHRMIMS), ISSN XXXX (P), ISSN XXXX (O), Oct-Dec 2014 15 Review Article Balloon Dacryoplasty: Indications, Techniques and
Dacryocystorh i nostomy in South West England
 Dacryocystorh i nostomy in South West England BlJAN BEIGI, WILLIAM WESTLAKE, BERNARD CHANG, CATHERINE MARSH, JOHN JACOB, JUDITH CHATFIELD B. Beigi W. Westlake B. Chang C. Marsh J. Jacob Department of Ophthalmology
Dacryocystorh i nostomy in South West England BlJAN BEIGI, WILLIAM WESTLAKE, BERNARD CHANG, CATHERINE MARSH, JOHN JACOB, JUDITH CHATFIELD B. Beigi W. Westlake B. Chang C. Marsh J. Jacob Department of Ophthalmology
Comparison of the Efficacies of 0.94 mm and Double Silicone Tubes for Treatment of Canalicular Obstruction
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(1):1-8 ht tps://doi.org/10.3341/k jo.2017.31.1.1 Original Article Comparison of the Efficacies of 0.94 mm and Double Silicone Tubes for Treatment
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2017;31(1):1-8 ht tps://doi.org/10.3341/k jo.2017.31.1.1 Original Article Comparison of the Efficacies of 0.94 mm and Double Silicone Tubes for Treatment
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Treatment of obstructive epiphora in adults by balloon dacryocystoplasty
 692 Uludag University, Department of Radiology, Bursa, Turkey Z Yazici M Parlak G Savci Uludag University, Department of Ophthalmology, Bursa, Turkey B Yazici H Erturk Correspondence to: Zeynep Yazici,
692 Uludag University, Department of Radiology, Bursa, Turkey Z Yazici M Parlak G Savci Uludag University, Department of Ophthalmology, Bursa, Turkey B Yazici H Erturk Correspondence to: Zeynep Yazici,
Effects of Nasopore Packing on Dacryocystorhinostomy
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(2):73-80 http://dx.doi.org/10.3341/kjo.2013.27.2.73 Effects of Nasopore Packing on Dacryocystorhinostomy Original Article Sun Young Jang 1,
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2013;27(2):73-80 http://dx.doi.org/10.3341/kjo.2013.27.2.73 Effects of Nasopore Packing on Dacryocystorhinostomy Original Article Sun Young Jang 1,
NASOLACRIMAL DUCT OBSTRUCTION (BLOCKED TEAR DUCT) AND TEARY EYE - PATIENT INFORMATION
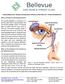 NASOLACRIMAL DUCT OBSTRUCTION (BLOCKED TEAR DUCT) AND TEARY EYE - PATIENT INFORMATION What is lacrimal sac and nasolacrimal duct? The lacrimal apparatus is composed of a lacrimal gland (tear producing
NASOLACRIMAL DUCT OBSTRUCTION (BLOCKED TEAR DUCT) AND TEARY EYE - PATIENT INFORMATION What is lacrimal sac and nasolacrimal duct? The lacrimal apparatus is composed of a lacrimal gland (tear producing
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 80/ Oct. 05, 2015 Page 14022
 STUDY ON MANAGEMENT OF EPIPHORA IN PATIENTS WITH OBSTRUCTION AT VARIOUS LEVELS OF NASOLACRIMAL APPARATUS S. Shivranjani 1, Jaishree Dwivedi 2, Neha Mithal 3, Sandeep Mithal 4 HOW TO CITE THIS ARTICLE:
STUDY ON MANAGEMENT OF EPIPHORA IN PATIENTS WITH OBSTRUCTION AT VARIOUS LEVELS OF NASOLACRIMAL APPARATUS S. Shivranjani 1, Jaishree Dwivedi 2, Neha Mithal 3, Sandeep Mithal 4 HOW TO CITE THIS ARTICLE:
Analysis of Functional and Anatomic Success Following Endonasal Dacryocystorhinostomy
 Annais af Otology, Riiinology & Laryngology 0(4):3-38. 0 Annals Publishing Company. All rights reserved. Analysis of Functional and Anatomic Success Following Endonasal Dacryocystorhinostomy Barbara Zuercher,
Annais af Otology, Riiinology & Laryngology 0(4):3-38. 0 Annals Publishing Company. All rights reserved. Analysis of Functional and Anatomic Success Following Endonasal Dacryocystorhinostomy Barbara Zuercher,
The modified endoscopic pre-lacrimal approach: how I do it
 Specialty Techniques Page 1 of 6 The modified endoscopic pre-lacrimal approach: how I do it Leslie T. Koh 1, Rataphol C. Dhepnorrarat 2 1 Department of Otolaryngology-Head & Neck Surgery, Changi General
Specialty Techniques Page 1 of 6 The modified endoscopic pre-lacrimal approach: how I do it Leslie T. Koh 1, Rataphol C. Dhepnorrarat 2 1 Department of Otolaryngology-Head & Neck Surgery, Changi General
Congenital lacrimal fistula
 Ugurbas 6-03-2000 14:59 Pagina 22 European Journal of Ophthalmology / Vol. 10 no. 1, 2000 / pp. 22-26 S.H. UǦURBAŞ, G. ZILELIOǦLU Department of Ophthalmology, Ankara University Faculty of Medicine, Ankara
Ugurbas 6-03-2000 14:59 Pagina 22 European Journal of Ophthalmology / Vol. 10 no. 1, 2000 / pp. 22-26 S.H. UǦURBAŞ, G. ZILELIOǦLU Department of Ophthalmology, Ankara University Faculty of Medicine, Ankara
Original Article Bicanalicular intubation procedure for acquired punctual stenosis
 Int J Clin Exp Med 2018;11(10):10815-10819 www.ijcem.com /ISSN:1940-5901/IJCEM0074867 Original Article Bicanalicular intubation procedure for acquired punctual stenosis Ying Chen 1, Xia Zhang 1, Liguo
Int J Clin Exp Med 2018;11(10):10815-10819 www.ijcem.com /ISSN:1940-5901/IJCEM0074867 Original Article Bicanalicular intubation procedure for acquired punctual stenosis Ying Chen 1, Xia Zhang 1, Liguo
Repair of Eyelid Trauma
 Repair of Eyelid Trauma Yunia Irawati, MD Plastic Reconstruction Division, Department of Ophthalmology FKUI / RSCM Introduction Eyelid trauma defined as a trauma to external surface of the lids with or
Repair of Eyelid Trauma Yunia Irawati, MD Plastic Reconstruction Division, Department of Ophthalmology FKUI / RSCM Introduction Eyelid trauma defined as a trauma to external surface of the lids with or
Pediatric Epiphora. Lacrimal drainage system begins to develop at the. Pediatric Ophthalmology. Saurbhi Khurana MD, FICO
 Pediatric Ophthalmology Pediatric Epiphora Saurbhi Khurana MD, FICO Saurbhi Khurana MD, FICO, A.K Grover MD, MNAMS, FRCS (Glasgow) FIMSA, FICO Vision Eye Centre, Siri Fort Road, New Delhi Lacrimal drainage
Pediatric Ophthalmology Pediatric Epiphora Saurbhi Khurana MD, FICO Saurbhi Khurana MD, FICO, A.K Grover MD, MNAMS, FRCS (Glasgow) FIMSA, FICO Vision Eye Centre, Siri Fort Road, New Delhi Lacrimal drainage
Lacrimal drainage surgery in patients with rare nasal diseases
 (2007) 21, 1361 1366 & 2007 Nature Publishing Group All rights reserved 0950-222X/07 $30.00 www.nature.com/eye Lacrimal drainage surgery in patients with rare nasal diseases CLINICAL STUDY Abstract Aim
(2007) 21, 1361 1366 & 2007 Nature Publishing Group All rights reserved 0950-222X/07 $30.00 www.nature.com/eye Lacrimal drainage surgery in patients with rare nasal diseases CLINICAL STUDY Abstract Aim
Evaluation of the Canalicular Entrance Into the Lacrimal Sac: An Anatomical Study
 ANATOMY &PHYSIOLOGY Evaluation of the Canalicular Entrance Into the Lacrimal Sac: An Anatomical Study Christopher I. Zoumalan, M.D.*, Jeffrey M. Joseph, M.D.*, Gary J. Lelli, Jr., M.D., Kira L. Segal,
ANATOMY &PHYSIOLOGY Evaluation of the Canalicular Entrance Into the Lacrimal Sac: An Anatomical Study Christopher I. Zoumalan, M.D.*, Jeffrey M. Joseph, M.D.*, Gary J. Lelli, Jr., M.D., Kira L. Segal,
Preoperative Computed Tomography Findings for Patients with Nasolacrimal Duct Obstruction or Stenosis
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):243-250 http://dx.doi.org/10.3341/kjo.2016.30.4.243 Original Article Preoperative Computed Tomography Findings for Patients with Nasolacrimal
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):243-250 http://dx.doi.org/10.3341/kjo.2016.30.4.243 Original Article Preoperative Computed Tomography Findings for Patients with Nasolacrimal
Chapter Six. 1 of 6 11/3/2008 2:21 PM.
 1 of 6 11/3/2008 2:21 PM Email : myousefmian@hotmail.com Chapter Six FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
1 of 6 11/3/2008 2:21 PM Email : myousefmian@hotmail.com Chapter Six FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
Syringing And Probing Under Local Anesthesia In Infants
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 3 Number 2 V Sharma, S Vaidya, S Shrivastava Citation V Sharma, S Vaidya, S Shrivastava.. The Internet Journal of Ophthalmology
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 3 Number 2 V Sharma, S Vaidya, S Shrivastava Citation V Sharma, S Vaidya, S Shrivastava.. The Internet Journal of Ophthalmology
Management of epiphora and lacrimal obstruction in adults
 Management of epiphora and lacrimal obstruction in adults Louis Savar, MD 1,2, Stuart R. Seiff, MD, FACS 1,2, Angela Maria Dolmetsch, MD 3 1. Department of Ophthalmology, University of California, San
Management of epiphora and lacrimal obstruction in adults Louis Savar, MD 1,2, Stuart R. Seiff, MD, FACS 1,2, Angela Maria Dolmetsch, MD 3 1. Department of Ophthalmology, University of California, San
Endoscopic transnasal orbital decompression for thyrotoxic orbitopathy
 Key words: Endoscopes; Exophthalmos; Keratitis; Orbital diseases; Thyrotoxicosis "# " APW Yuen KYW Kwan E Chan AWC Kung KSL Lam Hong Kong Med J 2002;8:406-10 Queen Mary Hospital, 102 Pokfulam Road, Hong
Key words: Endoscopes; Exophthalmos; Keratitis; Orbital diseases; Thyrotoxicosis "# " APW Yuen KYW Kwan E Chan AWC Kung KSL Lam Hong Kong Med J 2002;8:406-10 Queen Mary Hospital, 102 Pokfulam Road, Hong
Effectiveness of sedation in dacryocystorhinostomy surgery
 Original article Effectiveness of sedation in dacryocystorhinostomy surgery Tuladhar S 1, Adhikari S 1, Bhattarai B K 2 Departments of 1 Ophthalmology and 2 Anesthesiology and Critical Care B P Koirala
Original article Effectiveness of sedation in dacryocystorhinostomy surgery Tuladhar S 1, Adhikari S 1, Bhattarai B K 2 Departments of 1 Ophthalmology and 2 Anesthesiology and Critical Care B P Koirala
Comparative Study Of Probing Done with and without Endoscopic Assistance
 Comparative Study Of Probing Done with and without Endoscopic Assistance Ishan Acharya 1, Jitendra Jethani 2, Monika Jethani 3 Department of Ophthalmic Plastic Surgery, Orbit, Ocular Oncology and Ocular
Comparative Study Of Probing Done with and without Endoscopic Assistance Ishan Acharya 1, Jitendra Jethani 2, Monika Jethani 3 Department of Ophthalmic Plastic Surgery, Orbit, Ocular Oncology and Ocular
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
Self-Securing Monocanalicular Stent for Treatment of Nasolacrimal Duct Obstruction
 J Med Sci 2004;24(4):199-204 http://jms.ndmctsgh.edu.tw/2404199.pdf Copyright 2004 JMS Shang-Yi Chiang, et al. Self-Securing Monocanalicular Stent for Treatment of Nasolacrimal Duct Obstruction Shang-Yi
J Med Sci 2004;24(4):199-204 http://jms.ndmctsgh.edu.tw/2404199.pdf Copyright 2004 JMS Shang-Yi Chiang, et al. Self-Securing Monocanalicular Stent for Treatment of Nasolacrimal Duct Obstruction Shang-Yi
External vs. endonasal dacryocystorhinostomy: has the current view changed?
 ACTA otorhinolaryngologica italica 2014;34:29-35 Rhinology External vs. endonasal dacryocystorhinostomy: has the current view changed? Dacriocistorinostomia esterna ed endonasale a confronto: si è modificata
ACTA otorhinolaryngologica italica 2014;34:29-35 Rhinology External vs. endonasal dacryocystorhinostomy: has the current view changed? Dacriocistorinostomia esterna ed endonasale a confronto: si è modificata
Clinical Study Comparison of Transcanalicular Multidiode Laser Dacryocystorhinostomy with and without Silicon Tube Intubation
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 2016, Article ID 6719529, 5 pages http://dx.doi.org/10.1155/2016/6719529 Clinical Study Comparison of Transcanalicular Multidiode Laser Dacryocystorhinostomy
Hindawi Publishing Corporation Journal of Ophthalmology Volume 2016, Article ID 6719529, 5 pages http://dx.doi.org/10.1155/2016/6719529 Clinical Study Comparison of Transcanalicular Multidiode Laser Dacryocystorhinostomy
Technique Guide. Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures.
 Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
ISSN: Volume 4 Issue Role of Modified Endoscopic Medial Maxillectomy in persistent chronic maxillary. sinusitis
 ISSN: 2250-0359 Volume 4 Issue 3 2014 Role of Modified Endoscopic Medial Maxillectomy in persistent chronic maxillary sinusitis Thulasidas P ¹ Venkatraman V ² ¹ Sinus and Nose Hospital, Chennai, India,
ISSN: 2250-0359 Volume 4 Issue 3 2014 Role of Modified Endoscopic Medial Maxillectomy in persistent chronic maxillary sinusitis Thulasidas P ¹ Venkatraman V ² ¹ Sinus and Nose Hospital, Chennai, India,
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis
 Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
ORIGINAL ARTICLE. Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the Anterior Ethmoid
 Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures.
 Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Procedures. Technique Guide This publication is not intended for distribution in the USA. Instruments and implants approved
Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q
 The British Association of Plastic Surgeons (2004) 57, 37 44 Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q M. Kakibuchi*,
The British Association of Plastic Surgeons (2004) 57, 37 44 Combination of transconjunctival and endonasal-transantral approach in the repair of blowout fractures involving the orbital floor q M. Kakibuchi*,
Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
Reasons for Failure and Surgical Revisions. Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology
 Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Comparison of nonlaser nonendoscopic endonasal dacryocystorhinostomy with external dacryocystorhinostomy
 Comparison of nonlaser nonendoscopic endonasal dacryocystorhinostomy with external dacryocystorhinostomy Randy A. Walker,* MD; Ahmed Al-Ghoul, { MD, FRCS(C); M. Ronan Conlon,* MD, FRCS(C) ABSTRACT N RÉSUMÉ
Comparison of nonlaser nonendoscopic endonasal dacryocystorhinostomy with external dacryocystorhinostomy Randy A. Walker,* MD; Ahmed Al-Ghoul, { MD, FRCS(C); M. Ronan Conlon,* MD, FRCS(C) ABSTRACT N RÉSUMÉ
Lower Eyelid Malposition
 Oculoplastic Surgeon s DDX for the Red Eye Geeta Belsare Been,MD The Center for Facial Plastic Surgery Barrington, IL Lower Eyelid Malposition Ectropion Involutional Cicatricial Paralytic Entropion Involutional
Oculoplastic Surgeon s DDX for the Red Eye Geeta Belsare Been,MD The Center for Facial Plastic Surgery Barrington, IL Lower Eyelid Malposition Ectropion Involutional Cicatricial Paralytic Entropion Involutional
Mucocele of paranasal sinuses
 From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
The sebaceous glands (glands of Zeis) open directly into the eyelash follicles, ciliary glands (glands of Moll) are modified sweat glands that open
 The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
Role of Modified Endoscopic Medial Maxillectomy in Persistent Chronic Maxillary Sinusitis
 THIEME Original Research 159 Role of Modified Endoscopic Medial Maxillectomy in Persistent Chronic Maxillary Sinusitis Ponnaiah Thulasidas 1 Venkatraman Vaidyanathan 2 1 Department of Otolaryngology Head
THIEME Original Research 159 Role of Modified Endoscopic Medial Maxillectomy in Persistent Chronic Maxillary Sinusitis Ponnaiah Thulasidas 1 Venkatraman Vaidyanathan 2 1 Department of Otolaryngology Head
Inverted papilloma of the maxillary sinus and endoscopic endonasal medial maxillectomy
 Romanian Journal of Rhinology, Vol. 3, No. 9, January - March 2013 ORIGINAL STUDY Inverted papilloma of the maxillary sinus and endoscopic endonasal medial maxillectomy Philippe Eloy ENT&HNS Department,
Romanian Journal of Rhinology, Vol. 3, No. 9, January - March 2013 ORIGINAL STUDY Inverted papilloma of the maxillary sinus and endoscopic endonasal medial maxillectomy Philippe Eloy ENT&HNS Department,
Anatomical Analysis of the Frontal Recess Cells in Endoscopic Sinus Surgery An Indian Perspective
 ORIGINAL ARTICLE Anatomical Analysis of the Frontal Recess Cells in Endoscopic Sinus Surgery An Indian Perspective 1 Dhingra Shruti, 2 Agarwal AK, 3 Passey JC, 4 Kaul JM 1 Resident, Department of Otolaryngology
ORIGINAL ARTICLE Anatomical Analysis of the Frontal Recess Cells in Endoscopic Sinus Surgery An Indian Perspective 1 Dhingra Shruti, 2 Agarwal AK, 3 Passey JC, 4 Kaul JM 1 Resident, Department of Otolaryngology
A comprehensive study on complications of endoscopic sinus surgery
 International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
Frequency of Nasal Septal Perforation at the Suture Fixation Site of a Silastic Sheet Inserted during Nasal Surgery
 Soonchunhyang Medical Science 17(2):53-57, December 2011 pissn: 2233-4289 I eissn: 2233-4297 ORIGINAL ARTICLE Frequency of Nasal Septal Perforation at the Suture Fixation Site of a Silastic Sheet Inserted
Soonchunhyang Medical Science 17(2):53-57, December 2011 pissn: 2233-4289 I eissn: 2233-4297 ORIGINAL ARTICLE Frequency of Nasal Septal Perforation at the Suture Fixation Site of a Silastic Sheet Inserted
Endoscopic transnasal dacryocystorhinostomy without stenting: results in 64 consecutive procedures
 ACTA otorhinolaryngologica italica 2010;30:294-298 Rhinology Endoscopic transnasal dacryocystorhinostomy without stenting: results in 64 consecutive procedures Dacriocistorinostomia endoscopica transnasale
ACTA otorhinolaryngologica italica 2010;30:294-298 Rhinology Endoscopic transnasal dacryocystorhinostomy without stenting: results in 64 consecutive procedures Dacriocistorinostomia endoscopica transnasale
The clinical value of dacryoscintigraphy in the selection of surgical approach for patients with functional lacrimal duct obstruction
 ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 19, No. 6, 479 483, 2005 The clinical value of dacryoscintigraphy in the selection of surgical approach for patients with functional lacrimal duct obstruction
ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 19, No. 6, 479 483, 2005 The clinical value of dacryoscintigraphy in the selection of surgical approach for patients with functional lacrimal duct obstruction
Endoscopic medial maxillectomy
 Operative Techniques in Otolaryngology (2010) 21, 111-116 Endoscopic medial maxillectomy Kelly Cunningham, MD, Kevin C. Welch, MD From the Department of Otolaryngology - Head and Neck Surgery, Loyola University
Operative Techniques in Otolaryngology (2010) 21, 111-116 Endoscopic medial maxillectomy Kelly Cunningham, MD, Kevin C. Welch, MD From the Department of Otolaryngology - Head and Neck Surgery, Loyola University
A simple and evolutional approach proven to recanalise the nasolacrimal duct obstruction
 See Editorial, p 1416 1 Department of ENT, First Affiliated Hospital, Sun Yat-sen University, Guangzhou, PR China; 2 State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University,
See Editorial, p 1416 1 Department of ENT, First Affiliated Hospital, Sun Yat-sen University, Guangzhou, PR China; 2 State Key Laboratory of Ophthalmology, Zhongshan Ophthalmic Center, Sun Yat-sen University,
Frontal sinus disease continues to be one of the great
 Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
REVISION ENDOSCOPIC FRONTAL SINUSOTOMY WITH MUCOPERIOSTEAL FLAP ADVANCEMENT
 CURRENT CONCEPTS IN THE SURGICAL MANAGEMENT OF FRONTAL SINUS DISEASE 00304665/01 $15.00 +.OO REVISION ENDOSCOPIC FRONTAL SINUSOTOMY WITH MUCOPERIOSTEAL FLAP ADVANCEMENT The Frontal Sinus Rescue Procedure
CURRENT CONCEPTS IN THE SURGICAL MANAGEMENT OF FRONTAL SINUS DISEASE 00304665/01 $15.00 +.OO REVISION ENDOSCOPIC FRONTAL SINUSOTOMY WITH MUCOPERIOSTEAL FLAP ADVANCEMENT The Frontal Sinus Rescue Procedure
Transnasal Endoscopic Sinonasal Surgery
 Reda kamel, Cadaveric dissection 1 Transnasal Endoscopic Sinonasal Surgery Cadaver Dissection Guide For Endoscopic Sinus Surgery Cairo University Egypt Reda Kamel Professor of Rhinology Cairo University
Reda kamel, Cadaveric dissection 1 Transnasal Endoscopic Sinonasal Surgery Cadaver Dissection Guide For Endoscopic Sinus Surgery Cairo University Egypt Reda Kamel Professor of Rhinology Cairo University
Bicanalicular Intubation for Traumatic Unicanalicular Laceration
 Medical Science, Volume 9, Number 32, June 4, 2014 EISSN 2321 7367 RESEARCH OPHTHALMOLOGY Medical Science ISSN 2321 7359 The International Weekly Journal for Medicine Bicanalicular Intubation for Traumatic
Medical Science, Volume 9, Number 32, June 4, 2014 EISSN 2321 7367 RESEARCH OPHTHALMOLOGY Medical Science ISSN 2321 7359 The International Weekly Journal for Medicine Bicanalicular Intubation for Traumatic
Chapter Five. 1 of 8 11/3/2008 2:52 PM.
 1 of 8 11/3/2008 2:52 PM Email : myousefmian@hotmail.com Chapter Five FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
1 of 8 11/3/2008 2:52 PM Email : myousefmian@hotmail.com Chapter Five FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
Bony orbit Roof The orbital plate of the frontal bone Lateral wall: the zygomatic bone and the greater wing of the sphenoid
 Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Tear Meniscus Volume Changes in Dacryocystorhinostomy Evaluated With Quantitative Measurement Using Anterior Segment Optical Coherence Tomography
 Clinical and Epidemiologic Research Tear Meniscus Volume Changes in Dacryocystorhinostomy Evaluated With Quantitative Measurement Using Anterior Segment Optical Coherence Tomography Kazuyoshi Ohtomo, Takashi
Clinical and Epidemiologic Research Tear Meniscus Volume Changes in Dacryocystorhinostomy Evaluated With Quantitative Measurement Using Anterior Segment Optical Coherence Tomography Kazuyoshi Ohtomo, Takashi
PROBLEM RECOMMENDATION
 PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
Septoplasty and Turbinoplasty Indications - Technique - Follow up - Pitfalls
 Septoplasty and Turbinoplasty Indications - Technique - Follow up - Pitfalls H.R. Briner ORL-Zentrum Klinik Hirslanden Zürich Septoplasty and Turbinoplasty Septoplasty Indications Technique Follow up Complications,
Septoplasty and Turbinoplasty Indications - Technique - Follow up - Pitfalls H.R. Briner ORL-Zentrum Klinik Hirslanden Zürich Septoplasty and Turbinoplasty Septoplasty Indications Technique Follow up Complications,
Proboscis lateralis: report of two cases
 The British Association of Plastic Surgeons (2003) 56, 704 708 CASE REPORT Proboscis lateralis: report of two cases Lütfi Eroğlu a, *, Osman Ata Uysal b a Faculty of Medicine, Department of Plastic and
The British Association of Plastic Surgeons (2003) 56, 704 708 CASE REPORT Proboscis lateralis: report of two cases Lütfi Eroğlu a, *, Osman Ata Uysal b a Faculty of Medicine, Department of Plastic and
JMSCR Vol 05 Issue 09 Page September 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
The cribriform plate. ethmoid bone. Ethmoid bone consists from: 1) A horizontal cribriform plate. 2) A perpendicular plate. 3) Two lateral labyrinths.
 ethmoid bone Ethmoid bone consists from: 1) A horizontal cribriform plate. 2) A perpendicular plate. 3) Two lateral labyrinths. The cribriform plate 1) Connect the two labyrinths to the perpendicular plate.
ethmoid bone Ethmoid bone consists from: 1) A horizontal cribriform plate. 2) A perpendicular plate. 3) Two lateral labyrinths. The cribriform plate 1) Connect the two labyrinths to the perpendicular plate.
Epiphora Decoded. VG: How do you go about evaluating patients of epiphora? Any special investigations?
 Experts Corner Epiphora Decoded The development over the years in understanding pathophysiology of Lacrimal System disorder has undergone a sea-size change. The improvement in stenting material, laser-advances
Experts Corner Epiphora Decoded The development over the years in understanding pathophysiology of Lacrimal System disorder has undergone a sea-size change. The improvement in stenting material, laser-advances
Exposure techniques in endoscopic skull base surgery: Posterior septectomy, medial maxillectomy, transmaxillary and transpterygoid approach
 European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 284 288 Available online at www.sciencedirect.com TECHNICAL NOTE Exposure techniques in endoscopic skull base surgery: Posterior
European Annals of Otorhinolaryngology, Head and Neck diseases (2012) 129, 284 288 Available online at www.sciencedirect.com TECHNICAL NOTE Exposure techniques in endoscopic skull base surgery: Posterior
Endoscopic Sinus Surgery in the Pediatric Age Group
 Endoscopic Sinus Surgery in the Pediatric Age Group Scott C. Manning Endoscopic Sinus Surgical Preparation and Technique Surgical Risks Every decision for therapy involves a risk-benefit analysis and a
Endoscopic Sinus Surgery in the Pediatric Age Group Scott C. Manning Endoscopic Sinus Surgical Preparation and Technique Surgical Risks Every decision for therapy involves a risk-benefit analysis and a
