When an athlete can t catch his breath. For personal use only
|
|
|
- Denis Bates
- 5 years ago
- Views:
Transcription
1 For mass reproduction, content licensing and permissions contact Dowden Health Media. FAMILY PRACTICE THE JOURNAL OF Michael A. Krafczyk, MD, and F. Dale Bautista, MD St. Luke s Hospital, Bethlehem, Pa krafczm@slhn.org IN THIS ARTICLE Drugs banned from competition Page 456 EIB medications Page 457 When an athlete can t catch his breath A patient who s fine during practice but runs out of breath before the game s over may have exercise-induced bronchoconstriction. This practical guide can help. Practice recommendations Don t rely on self-reported symptoms to diagnose exercise-induced bronchoconstriction (EIB) (A). Copyright Dowden Health Media Indirect testing is the best way to diagnose EIB in patients who do not have underlying asthma (A). Short-acting β2-agonists should be first-line management in EIB (A). Strength of recommendation (SOR) For personal use only A Good-quality patient-oriented evidence B Inconsistent or limited-quality patient-oriented evidence C Consensus, usual practice, opinion, disease-oriented evidence, case series Luke, a 16-year-old basketball player, complains that he can t finish a game without running out of breath. He says things are at their worst when the game is close and when it s nearing the end. He doesn t have the problem during practice, or when he is playing other sports. The team physician suggested using an albuterol inhaler half an hour before game time and when he has symptoms, but he gets only minimal relief. Now he has come to you. His vital signs, lung exam, and cardiac exam are normal. Results of pulmo- nary function tests with pre- and postalbuterol challenge done a year ago were also normal. Does Luke have exerciseinduced bronchoconstriction (EIB)? How can you be sure? And what can you do to help? Symptoms like Luke s are common among athletes of all abilities. They may add up to EIB, a condition with an estimated prevalence of 6% to 12% in the general population or they may not. 1 One study showed that only a third of athletes with symptoms or prior diagnosis of EIB had positive objective testing for the condition, and current studies show that reported symptoms are not an accurate guide in athletes like Luke who do not have underlying asthma. 2,3 To treat him correctly, you will need to nail down the diagnosis with additional tests. 3,4 Shortness of breath that s worse than expected EIB can have many different presentations. The most common symptom is cough associated with exercise. 3 Other common signs and symptoms include wheezing, chest tightness, and more severe than expected or worsening shortness of breath. More unusual symptoms 454 VOL 58, NO 9 / SEPTEMBER 2009 THE JOURNAL OF FAMILY PRACTICE
2 include a decrease in performance or fatigue out of proportion to workload. Often patients with EIB have other associated medical conditions, such as allergic rhinitis. Bronchoconstriction usually occurs with maximal or near maximal exertion. Generally, it takes 5 to 8 minutes of exercising at 80% of maximal heart rate to trigger EIB. Classically, the symptoms peak 5 to 10 minutes after exercise begins. 5 Rule out cardiac problems. If EIB is the correct diagnosis, the physical exam is usually normal. The importance of the physical exam is to evaluate for other diagnoses with similar presentations. Conditions to rule out include cardiac problems, exercise-induced hyperventilation, upper and lower respiratory infections or abnormalities, exercise-induced laryngeal dysfunction, exercise-induced anaphylaxis, and gastroesophageal reflux disease (GERD). The differential diagnosis for EIB is summarized in TABLE 1. Test for asthma. Once you have gone through the differential diagnosis and are comfortable that the symptoms are respiratory, the next step should be pulmonary function tests (PFT), pre- and post-albuterol challenge. Findings of obstruction, such as reduced forced expiratory volume in 1 second (FEV1) or increased lung volume, are consistent with a diagnosis of asthma. In that case, no further workup is needed unless the patient is unresponsive to asthma treatment. In athletes like Luke who do not have asthma and have a normal nonprovocative spirometry, you can move on to either provocative spirometry or empiric treatment. Perform provocative spirometry Direct spirometry is commonly done with a methacholine challenge. This test is less sensitive than indirect testing for EIB patients who do not have underlying asthma. TABLE 1 ETIOLOGY Pulmonary Cardiac Laryngeal Gastroesophageal Allergic Other Is it EIB, or something else? POSSIBLE DIAGNOSES Exercise-induced hyperventilation (pseudo-asthma syndrome) Restrictive lung disease Cystic fibrosis Upper and lower respiratory infections Foreign body aspiration Coronary artery disease Congenital and acquired heart defects Cardiomyopathy Congestive heart failure Exercise-induced laryngeal dysfunction Vocal cord dysfunction Laryngeal prolapse Laryngomalacia Gastroesophageal reflux disease Exercise-induced anaphylaxis Athlete is out of shape EIB, exercise-induced bronchoconstriction. Source: Weiler JM, et al. J Allergy Clin Immunol The gold standard for indirect testing is eucapnic voluntary hyperventilation (EVH). Because EVH requires special equipment, however, it may not be an option in your office. The more reasonable choice is exercise challenge testing, which can be done either in your office or in the milieu the basketball court, for example where the athlete s symptoms usually occur. In an exercise challenge, you get a baseline spirometry measurement, have the athlete exercise to 80% to 90% of maximal heart rate, and then repeat spirometry at short intervals after exercise ends. If you do an exercise challenge in the office, you can reduce falsenegative results by maintaining an ambient temperature between 68 and 77 F (20-25 C) with a relative humidity of less than 50%. 6,7 Or try empiric treatment Empiric treatment is a reasonable strategy for athletes with EIB symptoms, worth trying both for athletes who have underlying asthma and for those who do not. CONTINUED FAST TRACK It typically takes 5 to 8 minutes of exercising at 80% of maximal heart rate to trigger exercise-induced bronchoconstriction. VOL 58, NO 9 / SEPTEMBER
3 FAMILY PRACTICE THE JOURNAL OF Is that drug banned from competition? Certain medications used in the treatment of asthma and exercise-induced bronchoconstriction (EIB) are considered performance-enhancing drugs and either banned or restricted in athletic competition. The regulatory bodies that make these designations in the United States are the National Collegiate Athletic Association (NCAA) and the International Olympic Committee World Anti-Doping Agency (IOC-WADA). These organizations update their list of banned substances yearly and make the current list available on the Web. You can find the NCAA list at BANNED%20SUBSTANCESb.doc and the IOC-WADA list at www. wada-ama.org/rtecontent/document/2009_prohibited_list_eng_ Final_20_Sept_08.pdf. The IOC-WADA allows competing athletes to use inhaled corticosteroids and β2 agonists, but requires athletes with asthma to provide documentation that the medication is for therapeutic use. Glucocorticosteroids and oral β2 agonists remain prohibited by the IOC-WADA, but only oral β2 agonists are banned by the NCAA. The NCAA warns that student athletes are responsible for knowing which substances are on the banned list and advises them to consult for more information. To avoid disqualifying a patient from sports participation, check medications you prescribe with the official lists and be sure your FAST EIB TRACK patient has the documentation he or she needs to qualify for a therapeutic use exemption. If the athlete with asthma responds to treatment, the problem is solved. For the athlete who does not have asthma, however, there are some exceptions to this approach specifically, the elite athlete. In the elite athlete, you will need to confirm the diagnosis because many of the substances used to treat EIB are restricted by governing bodies such as the International Olympic Committee (IOC) and require provocative testing to obtain a therapeutic use exemption. 8 There is some debate as to whether nonelite athletes also need bronchoprovocative testing. Some recommendations advise testing all elite and competitive athletes and restricting empiric treatment to recreational athletes. 1 For more information on banned or restricted medications, see Is that drug banned from competition? at left. If you take the empiric approach and the athlete does not respond to treatment, consider further testing to rule out other, more serious problems. In Luke s case, where empiric treatment with albuterol has failed, indirect testing would be the next step. Medicate before exercise: SABAs and LABAs Prophylaxis for EIB usually starts with an inhaled short-acting β2 agonist (SABA) such as albuterol or pirbuterol, taken 15 minutes before starting to exercise. 9,10 The effectiveness of both shortand long-acting β2 agonists decreases with frequent use, which may be Luke s problem. For that reason, patients with mild EIB may choose to use pretreatment medication only for more demanding exercise sessions. 11 Advise EIB patients who need daily pretreatment to try adjunctive therapy (discussed at greater length, below.) Longer-acting β2 agonists (LABAs) such as salmeterol or formoterol may be effective for prolonged or all-day exercise, but may lose their prophylactic effect with prolonged use. 12 Furthermore, the US Food and Drug Administration (FDA) has advised against using LABAs alone because of the possibility of severe asthma episodes or death. LABAs should be used only in conjunction with daily therapy with inhaled corticosteroids. The properties of these and other EIB medications are summarized in TABLE 2. Cromolyn, antileukotrienes are options, too Mast cell stabilizers (cromolyn) can be used with β2 agonists as prophylactic therapy. When these agents are used together, they have an additive effect. 13 The athlete may take them 10 minutes to an hour before exercise. Make sure your patient knows that mast cell stabilizers can- 456 VOL 58, NO 9 / SEPTEMBER 2009 THE JOURNAL OF FAMILY PRACTICE
4 Exercise-induced bronchoconstriction TABLE 2 EIB medications MEDICATION INDICATION DOSE CAUTIONS COMMENT Short-acting β2 agonists (SABAs) Albuterol, pirbuterol Pre-exercise 2 puffs pre-exercise May cause tachycardia, First-line treatment prophylaxis, acute treatment or 2 puffs every 4-6 h as needed hypokalemia. Tachyphylaxis can develop with frequent use. Mast cell stabilizers Cromolyn Inhaled corticosteroids Flunisolide, fluticasone, budesonide, triamcinolone, beclomethasone, mometasone Leukotriene inhibitors Zafirlukast Montelukast Zileuton Combinations Inhaled fluticasone and salmeterol Inhaled budesonide and formoterol Pre-exercise treatment, pre-exercise prophylaxis EIB, exercise-induced bronchoconstriction. 2 puffs min before exercise Variable None Can cause oral candidiasis, hoarseness. Best combined with SABA. Tell patients not to use for rescue. Tell patients this is not a rescue inhaler. 20 mg PO, bid None Variable response. Works well with inhaled corticosteroids. Low side-effect profile. 10 mg PO daily or up to 2 h pre-exercise None 1200 mg PO, bid Risk of elevated liver function tests. Variable doses (100/50, 250/50, 500/50 mcg/spray); 1 puff bid Variable doses (80/4.5, 160/4.5 mcg/spray); 1 puff bid Can cause oral candidiasis, hoarseness, tachycardia, hypokalemia. Tachyphylaxis can develop with frequent use. Can cause oral candidiasis, hoarseness, tachycardia, hypokalemia. Tachyphylaxis can develop with frequent use. Variable response. Works well with inhaled corticosteroids. Low side-effect profile. Variable response. Low side-effect profile. Tell FAST patients TRACK this is not a rescue inhaler. Evaluate all the gravidas a factors atta deliomite das effects before the internal dypsom Tell patients this is not a rescue inhaler. Adapted from the National Asthma Education and Prevention Program. Expert Panel Report 3: Guidelines for the diagnosis and management of asthma. 9 not be used as a rescue inhaler or bronchodilator. Inhaled corticosteroids (flunisolide, fluticasone, others) may be needed for athletes with poorly controlled chronic asthma; they can also be used as adjunct preventive treatment for athletes who have EIB with no underlying chronic asthma Often, inhaled corticosteroids are used as combination therapy with a LABA or an antileukotriene agent (montelukast, zafirlukast; see below). Recent research shows that montelukast in combination with inhaled corticosteroids is more efficacious than LABA with inhaled corticosteroids. 14,17 Antileukotriene agents can be especially helpful for EIB in patients with mild, stable asthma. 18 Patients who do respond to antileukotriene agents usually respond very favorably. Antileukotrienes offer a reasonable alternative to inhaled corti- VOL 58, NO 9 / SEPTEMBER
5 FAMILY PRACTICE THE JOURNAL OF FAST TRACK LABAs should be used only in conjunction with daily therapy with inhaled corticosteroids. costeroids and LABAs. They have a low side-effect profile and should be considered as daily prophylaxis. 19,20 The effects of montelukast are evident as early as 2 hours after administration, and bronchoprotective effects can last as long as 24 hours. 21,22 For that reason, montelukast is especially useful in children whose exercise patterns are not always predictable. Be prepared for acute exacerbations. Prophylactic medication does not always prevent acute exacerbations. When that happens, your EIB patient will need to use a β2 agonist as rescue therapy. Make sure your patient knows that none of the other medications are effective bronchodilators in acute exacerbations. Remember, too, that EIB cannot be effectively treated if the athlete has poorly controlled chronic asthma. Underlying causes of asthma exacerbations like allergies or respiratory infections must be addressed and stabilized first, following guidelines of the National Asthma Education and Prevention Program (NAEPP). 9 You can access the guidelines at asthgdln.htm. These tips can help the athlete Encourage athletes with EIB to keep up their exercise routines, because cardiovascular fitness has a beneficial effect on this condition. Fit individuals breathe more slowly, which reduces the likelihood of exacerbations. Of note, though: Certain sports are easier on patients with EIB. Patients may want to keep this in mind when deciding which team they want to go out for. Specifically, indoor sports, where air temperature, humidity, and exposure to allergens are controlled, and sports like baseball, sprinting, or football, which require less prolonged aerobic endurance, are good options. Tell athletes whose sports require cold, dry conditions ice skating, or skiing, for instance to try breathing through a scarf or mask to keep inspired air warm and less irritating. And tell all athletes with EIB to warm up properly before they start to compete. 23 That means a 15-minute warm-up at moderate exertion, followed by a 15- to 30-minute rest period. The rest period is the time to take their medication. When therapy fails When an EIB patient fails to respond despite multiple drug therapy, it s time to reconsider other diagnoses, such as vocal cord dysfunction and severe GERD, which may mimic symptoms of EIB. On the horizon. Other therapies for possible treatment of EIB are being studied. These include omega-3 fatty acid dietary supplementation and inhaled enoxaparin. 24,25 Data are currently insufficient to recommend use of these agents in clinical practice. As for Luke, indirect testing via exercise challenge was positive for EIB. Adjunctive therapy with montelukast was added to his albuterol inhaler, and the combination has worked well for him. He s still playing basketball, and enjoying it. Correspondence Michael A. Krafczyk, MD, FAAFP, St. Luke s Sports Medicine, 153 Brodhead Rd, Bethlehem, PA 18017; krafczm@slhn.org Acknowledgements The authors thank Ken Rundell, PhD, for reviewing this article. Dr. Rundell is director of the Human Physiology Laboratory at the Keith J. O Neill Center of Marywood University, Scranton, Pa. Disclosure The authors reported no potential conflict of interest relevant to this article. References 1. Holzer K, Brukner P. Screening of athletes for exercise-induced bronchoconstriction. Clin J Sport Med. 2004;14: Hallstrand TS, Curtis JR, Koepsell TD, et al. Effectiveness of screening examinations to detect unrecognized exercise-induced bronchoconstriction. J Pediatr. 2002;141: Rundell KW, Mayers LB, Wilber RL, et al. Self-reported symptoms of exercise-induced asthma in the elite athlete. Med Sci Sports Exerc. 2001;33: Weiler JM, Bonini S, Coifman R, et al. Ad Hoc Committee of Sports Medicine Committee, American Academy of Allergy, Asthma, and Immunology Work Group Report: exercise-induced asthma. J Allergy Clin Immunol. 2007;119: Parsons JP, Mastronarde JG. Exercise-induced 458 VOL 58, NO 9 / SEPTEMBER 2009 THE JOURNAL OF FAMILY PRACTICE
6 Exercise-induced bronchoconstriction bronchoconstriction in athletes. Chest. 2005; 128: Rundell KW, Slee JB. Exercise and other indirect challenges to demonstrate asthma or exerciseinduced bronchoconstriction in athletes. J Allergy Clin Immunol. 2008;122: Rundell KW, Wilber RL, Szmedra L, et al. Exerciseinduced asthma screening of elite athletes: field versus laboratory exercise challenges. Med Sci Sports Exerc. 2000;32: Fitch KD, Sue-Chu M, Anderson SD, et al. Asthma and the elite athlete: summary of the International Olympic Committee s Consensus Conference, Lausanne Switzerland. January 22-24, J Allergy Clin Immunol. 2008;122: National Asthma Education and Prevention Program. Expert Panel Report 3: Guidelines for the diagnosis and management of asthma. Bethesda, MD: National Heart, Lung, and Blood Institute; NIH publication no Available at: asthgdln.htm. Accessed September 1, Anderson S, Seale JP, Ferris L, et al. An evaluation of pharmacotherapy for exercise-induced asthma. J Allergy Clin Immunol. 1979;64: Hancox RJ, Subbarao P, Kamada D, et al. β2- Agonist tolerance and exercise-induced bronchospasm. Am Respir Crit Care Med. 2002;165: Inman M, O Byrne PM. The effect of regular inhaled albuterol on exercise-induced bronchoconstriction. Am J Respir Crit Care Med. 1996;153: Latimer KM, O Byrne PM, Morris MM, et al. Bronchoconstriction stimulated by airway cooling: better protection with combined inhalation of terbutaline sulphate and cromolyn sodium than with either alone. Am Rev Respir Dis. 1983;128: Stelmach I, Grzelewski T, Majak P, et al. Effect of different antiasthmatic treatments on exerciseinduced bronchoconstriction in children with asthma. J Allergy Clin Immunol. 2008;121: Koh MS, Tee A, Lasserson TJ, et al. Inhaled corticosteroids compared to placebo for prevention of exercise induced bronchoconstriction. Cochrane Database Syst Rev. 2007;(3):CD Jonasson G, Carlsen KH, Hultquist C. Low-dose budesonide improves exercise-induced bronchospasm in schoolchildren. Pediatr Allergy Immunol. 2000;11: Storms W, Chervinsky P, Ghannam AF, et al. Challenge-Rescue Study Group. Respir Med. 2004; 98: Leff JA, Busse WW, Pearlman D, et al. Montelukast, a leukotriene-receptor antagonist for the treatment of mild asthma and exercise-induced bronchoconstriction. N Engl J Med. 1998;339: Steinshamn S, Sandsund M, Sue-Chu M, et al. Effects of montelukast and salmeterol on physical performance and exercise economy in adult asthmatics with exercise-induced bronchoconstriction. Chest. 2004;126: Storms W. Update on montelukast and its role in the treatment of asthma, allergic rhinitis, and exercise-induced bronchoconstriction. Expert Opin Pharmacother. 2007;8: Pearlman DS, van Adelsberg J, Philip G, et al. Onset and duration of protection against exercise-induced bronchoconstriction by a single oral dose of montelukast. Ann Allergy Asthma Immunol. 2006;97: Philip G, Villaran C, Pearlman DS, et al. Protection against exercise-induced bronchoconstriction two hours after a single oral dose of montelukast. J Asthma. 2007;44: Storms WW. Review of exercise-induced asthma. Med Sci Sports Exerc. 2003;35: Mickleborough TD, Lindley MR, Ionescu AA, et al. Protective effect of fish oil supplementation on exercise-induced bronchoconstriction in asthma. Chest. 2006;129: Ahmed T, Gonzalez BJ, Danta I. Prevention of exercise-induced bronchoconstriction by inhaled lowmolecular-weight heparin. Am J Respir Crit Care Med. 1999;160: An emerging strategy for the prevention of HPV infection and disease in males 0.5 CME/CE CREDIT CLICK ON JFP SUPPLEMENTS AT This supplement was sponsored by SciMed and supported by an educational grant from Merck & Co., Inc.
+ Asthma and Athletics
 + Asthma and Athletics Shaylon Rettig, MD, MBA Champion Sports Medicine + Financial Disclosure Dr. Shaylon Rettig has no relevant financial relationships with commercial interests to disclose. + Asthma
+ Asthma and Athletics Shaylon Rettig, MD, MBA Champion Sports Medicine + Financial Disclosure Dr. Shaylon Rettig has no relevant financial relationships with commercial interests to disclose. + Asthma
Asthma Management for the Athlete
 Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Exercise-Induced Bronchospasm. Michael A Lucia, MD, FCCP Asst Clinical Professor, UNR School of Medicine Sierra Pulmonary & Sleep Institute
 Exercise-Induced Bronchospasm Michael A Lucia, MD, FCCP Asst Clinical Professor, UNR School of Medicine Sierra Pulmonary & Sleep Institute EIB Episodic bronchoconstriction with exercise May be an exacerbation
Exercise-Induced Bronchospasm Michael A Lucia, MD, FCCP Asst Clinical Professor, UNR School of Medicine Sierra Pulmonary & Sleep Institute EIB Episodic bronchoconstriction with exercise May be an exacerbation
Exercise-Induced Bronchoconstriction EIB
 Exercise-Induced Bronchoconstriction EIB Case 1 14 yo boy, freshman in high school Complains of shortness of breath 2 minutes into a mile-run in his first gym class Same complains in his 2 nd gym class
Exercise-Induced Bronchoconstriction EIB Case 1 14 yo boy, freshman in high school Complains of shortness of breath 2 minutes into a mile-run in his first gym class Same complains in his 2 nd gym class
Exercise and Asthma: What patients and doctors can do to improve outcomes
 Exercise and Asthma: What patients and doctors can do to improve outcomes Timothy Craig, DO Professor of Medicine and Pediatrics Distinguished Educator Program Director Penn State University Hershey, PA,
Exercise and Asthma: What patients and doctors can do to improve outcomes Timothy Craig, DO Professor of Medicine and Pediatrics Distinguished Educator Program Director Penn State University Hershey, PA,
Sergio Bonini. Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy.
 Assessment of EIA in the community and in athletes: the role of standardized questionnaires Sergio Bonini Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy se.bonini@gmail.com
Assessment of EIA in the community and in athletes: the role of standardized questionnaires Sergio Bonini Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy se.bonini@gmail.com
Diagnosis, Assessment, Monitoring and Pharmacological Treatment of Asthma
 Diagnosis, Assessment, Monitoring and Pharmacological Treatment of Asthma Magnitude of Asthma - India Delhi Childhood asthma: 10.9% Adults: 8% Other Cities 3 to 18% Chhabra SK et al Ann Allergy Asthma
Diagnosis, Assessment, Monitoring and Pharmacological Treatment of Asthma Magnitude of Asthma - India Delhi Childhood asthma: 10.9% Adults: 8% Other Cities 3 to 18% Chhabra SK et al Ann Allergy Asthma
**This form MUST accompany a TUE Application for a Beta-2 Agonist if submitted to USADA**
 **This form MUST accompany a TUE Application for a Beta-2 Agonist if submitted to USADA** PHYSICIAN- You must select one of the Objective Tests in the Table below and report the result. Please take note
**This form MUST accompany a TUE Application for a Beta-2 Agonist if submitted to USADA** PHYSICIAN- You must select one of the Objective Tests in the Table below and report the result. Please take note
ARE CURRENT SPORT REGULATIONS FAIR TO ALLERGIC ATHLETES?
 ARE CURRENT SPORT REGULATIONS FAIR TO ALLERGIC ATHLETES? Sergio Bonini Second University of Naples & Institute of Neurobiology and Molecular Medicine, Italian National Research Council (INMM-CNR), Rome,
ARE CURRENT SPORT REGULATIONS FAIR TO ALLERGIC ATHLETES? Sergio Bonini Second University of Naples & Institute of Neurobiology and Molecular Medicine, Italian National Research Council (INMM-CNR), Rome,
Asthma in Pediatric Patients. DanThuy Dao, D.O., FAAP. Disclosures. None
 Asthma in Pediatric Patients DanThuy Dao, D.O., FAAP Disclosures None Objectives 1. Discuss the evaluation and management of asthma in a pediatric patient 2. Accurately assess asthma severity and level
Asthma in Pediatric Patients DanThuy Dao, D.O., FAAP Disclosures None Objectives 1. Discuss the evaluation and management of asthma in a pediatric patient 2. Accurately assess asthma severity and level
Role of Leukotriene Receptor Antagonists in the Treatment of Exercise-Induced Bronchoconstriction: A Review
 Review Article Role of Leukotriene Receptor Antagonists in the Treatment of Exercise-Induced Bronchoconstriction: A Review George S. Philteos, MD, FRCP(C); Beth E. Davis, BSc; Donald W. Cockcroft, MD,
Review Article Role of Leukotriene Receptor Antagonists in the Treatment of Exercise-Induced Bronchoconstriction: A Review George S. Philteos, MD, FRCP(C); Beth E. Davis, BSc; Donald W. Cockcroft, MD,
Beta 2 adrenoceptor agonists and the Olympic Games in Athens
 Beta 2 adrenoceptor agonists and the Olympic Games in Athens 1 Appendix A of the Olympic Movement Anti-Doping Code, the List of Prohibited Substances and Prohibited Methods dated 1 st January 2003 states
Beta 2 adrenoceptor agonists and the Olympic Games in Athens 1 Appendix A of the Olympic Movement Anti-Doping Code, the List of Prohibited Substances and Prohibited Methods dated 1 st January 2003 states
JANUARY Guide to the WADA Prohibited List and Therapeutic Use Exemptions
 JANUARY 2018 Guide to the WADA Prohibited List and Therapeutic Use Exemptions Contents The WADA Prohibited List 3 Therapeutic Use Exemptions (TUEs) 5 Requirements for asthma TUEs 9 2 The WADA Prohibited
JANUARY 2018 Guide to the WADA Prohibited List and Therapeutic Use Exemptions Contents The WADA Prohibited List 3 Therapeutic Use Exemptions (TUEs) 5 Requirements for asthma TUEs 9 2 The WADA Prohibited
Asthma in the Athlete
 Asthma in the Athlete Jorge E. Gomez, MD Associate Professor Texas Children s Hospital Baylor College of Medicine Assist Team Physician UH Understand how we diagnose asthma Objectives Be familiar with
Asthma in the Athlete Jorge E. Gomez, MD Associate Professor Texas Children s Hospital Baylor College of Medicine Assist Team Physician UH Understand how we diagnose asthma Objectives Be familiar with
Asthma in Pregnancy. Asthma. Chronic Airway Inflammation. Objective Measures of Airflow. Peak exp. flow rate (PEFR)
 Chronic Airway Inflammation Asthma in Pregnancy Robin Field, MD Maternal Fetal Medicine Kaiser Permanente San Francisco Asthma Chronic airway inflammation increased airway responsiveness to a variety of
Chronic Airway Inflammation Asthma in Pregnancy Robin Field, MD Maternal Fetal Medicine Kaiser Permanente San Francisco Asthma Chronic airway inflammation increased airway responsiveness to a variety of
I have no perceived conflicts of interest or commercial relationships to disclose.
 ASTHMA BASICS Michelle Dickens RN FNP-C AE-C Nurse Practitioner/Certified Asthma Educator Ferrell Duncan Allergy/Asthma/Immunology Coordinator, CoxHealth Asthma Center DISCLOSURES I have no perceived conflicts
ASTHMA BASICS Michelle Dickens RN FNP-C AE-C Nurse Practitioner/Certified Asthma Educator Ferrell Duncan Allergy/Asthma/Immunology Coordinator, CoxHealth Asthma Center DISCLOSURES I have no perceived conflicts
Dual-Controller Asthma Therapy: Rationale and Clinical Benefits
 B/1 Dual-Controller Asthma Therapy: Rationale and Clinical Benefits MODULE B The 1997 National Heart, Lung, and Blood Institute (NHLBI) Expert Panel guidelines on asthma management recommend a 4-step approach
B/1 Dual-Controller Asthma Therapy: Rationale and Clinical Benefits MODULE B The 1997 National Heart, Lung, and Blood Institute (NHLBI) Expert Panel guidelines on asthma management recommend a 4-step approach
Asthma By Mayo Clinic staff
 MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution, use the reprints
MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution, use the reprints
Asthma Description. Asthma is a disease that affects the lungs defined as a chronic inflammatory disorder of the airways.
 Asthma Asthma Description Asthma is a disease that affects the lungs defined as a chronic inflammatory disorder of the airways. Symptoms of asthma In susceptible individuals, this inflammation causes recurrent
Asthma Asthma Description Asthma is a disease that affects the lungs defined as a chronic inflammatory disorder of the airways. Symptoms of asthma In susceptible individuals, this inflammation causes recurrent
II: Moderate Worsening airflow limitations Dyspnea on exertion, cough, and sputum production; patient usually seeks medical
 Table 3.1. Classification of COPD Severity Stage Pulmonary Function Test Findings Symptoms I: Mild Mild airflow limitations +/ Chronic cough and sputum production; patient unaware of abnormal FEV 1 80%
Table 3.1. Classification of COPD Severity Stage Pulmonary Function Test Findings Symptoms I: Mild Mild airflow limitations +/ Chronic cough and sputum production; patient unaware of abnormal FEV 1 80%
Conflicts of Interest
 Exercise and Asthma: What patients and doctors can do to improve outcomes Timothy Craig, DO Professor of Medicine and Pediatrics Distinguished Educator Program Director Penn State University Hershey, PA,
Exercise and Asthma: What patients and doctors can do to improve outcomes Timothy Craig, DO Professor of Medicine and Pediatrics Distinguished Educator Program Director Penn State University Hershey, PA,
Financial Disclosure. Exercise Induced Bronchospasm BHR. Exercise Induced Asthma
 Financial Disclosure Exercise Induced Bronchospasm Elizabeth Bailey MSN, CRNP Allergy & Asthma Specialists BREATHE II March, 23, 2012 I have no commercial conflicts of interest and no financial relationships
Financial Disclosure Exercise Induced Bronchospasm Elizabeth Bailey MSN, CRNP Allergy & Asthma Specialists BREATHE II March, 23, 2012 I have no commercial conflicts of interest and no financial relationships
ASTHMA IN THE PEDIATRIC POPULATION
 ASTHMA IN THE PEDIATRIC POPULATION SEARCH Rotation 2 August 23, 2010 Objectives Define asthma as a chronic disease Discuss the morbidity of asthma in pediatrics Discuss a few things that a health center
ASTHMA IN THE PEDIATRIC POPULATION SEARCH Rotation 2 August 23, 2010 Objectives Define asthma as a chronic disease Discuss the morbidity of asthma in pediatrics Discuss a few things that a health center
Current Asthma Management: Opportunities for a Nutrition-Based Intervention
 Current Asthma Management: Opportunities for a Nutrition-Based Intervention Stanley J. Szefler, MD Approximately 22 million Americans, including 6 million children, have asthma. It is one of the most prevalent
Current Asthma Management: Opportunities for a Nutrition-Based Intervention Stanley J. Szefler, MD Approximately 22 million Americans, including 6 million children, have asthma. It is one of the most prevalent
TUE PHYSICIAN GUIDELINES Medical Information to Support the Decisions of TUE Committees Asthma ASTHMA
 1. Medical Condition ASTHMA is a syndrome of the respiratory airways manifested by recurrent episodic symptoms. It is associated with variable airway obstruction that is reversible either spontaneously
1. Medical Condition ASTHMA is a syndrome of the respiratory airways manifested by recurrent episodic symptoms. It is associated with variable airway obstruction that is reversible either spontaneously
Xolair (Omalizumab) Drug Prior Authorization Protocol (Medical Benefit & Part B Benefit)
 Line of Business: All Lines of Business Effective Date: August 16, 2017 Xolair (Omalizumab) Drug Prior Authorization Protocol (Medical Benefit & Part B Benefit) This policy has been developed through review
Line of Business: All Lines of Business Effective Date: August 16, 2017 Xolair (Omalizumab) Drug Prior Authorization Protocol (Medical Benefit & Part B Benefit) This policy has been developed through review
In 2002, it was reported that 72 of 1000
 REPORTS Aligning Patient Care and Asthma Treatment Guidelines Eric Cannon, PharmD Abstract This article describes how the National Asthma Education and Prevention Program Guidelines for the Diagnosis and
REPORTS Aligning Patient Care and Asthma Treatment Guidelines Eric Cannon, PharmD Abstract This article describes how the National Asthma Education and Prevention Program Guidelines for the Diagnosis and
Case-Compare Impact Report
 Case-Compare Impact Report October 8, 20 For CME Activity: Developed through an independent educational grant from Genentech: Moderate to Severe Persistent Asthma: A Case-Based Panel Discussion (March
Case-Compare Impact Report October 8, 20 For CME Activity: Developed through an independent educational grant from Genentech: Moderate to Severe Persistent Asthma: A Case-Based Panel Discussion (March
Asthma and Vocal Cord Dysfunction
 Asthma and Vocal Cord Dysfunction Amy L. Marks DO, FACOP Pediatric Allergy and Immunology Assistant Professor of Pediatrics Oakland University William Beaumont School of Medicine Objectives: Understanding
Asthma and Vocal Cord Dysfunction Amy L. Marks DO, FACOP Pediatric Allergy and Immunology Assistant Professor of Pediatrics Oakland University William Beaumont School of Medicine Objectives: Understanding
Asthma medications: Know your options - MayoClinic.com. Asthma medications: Know your options
 MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution, use the reprints
MayoClinic.com reprints This single copy is for your personal, noncommercial use only. For permission to reprint multiple copies or to order presentation-ready copies for distribution, use the reprints
Exercise testing, exerciseinduced asthma and sports
 Basics in Asthma Exercise testing, exerciseinduced asthma and sports Educational aims To inform about the occurrence of EIA, particularly in top athletes. To describe how EIA can be diagnosed. To describe
Basics in Asthma Exercise testing, exerciseinduced asthma and sports Educational aims To inform about the occurrence of EIA, particularly in top athletes. To describe how EIA can be diagnosed. To describe
12/18/2017. Disclosures. Asthma Management Updates: A Focus on Long-acting Muscarinic Antagonists and Intermittent Inhaled Corticosteroid Dosing
 Asthma Management Updates: A Focus on Long-acting Muscarinic Antagonists and Intermittent Inhaled Corticosteroid Dosing Diana M. Sobieraj, PharmD, BCPS Assistant Professor University of Connecticut School
Asthma Management Updates: A Focus on Long-acting Muscarinic Antagonists and Intermittent Inhaled Corticosteroid Dosing Diana M. Sobieraj, PharmD, BCPS Assistant Professor University of Connecticut School
Asthma Management Updates: A Focus on Long-acting Muscarinic Antagonists and Intermittent Inhaled Corticosteroid Dosing
 Asthma Management Updates: A Focus on Long-acting Muscarinic Antagonists and Intermittent Inhaled Corticosteroid Dosing Diana M. Sobieraj, PharmD, BCPS Assistant Professor University of Connecticut School
Asthma Management Updates: A Focus on Long-acting Muscarinic Antagonists and Intermittent Inhaled Corticosteroid Dosing Diana M. Sobieraj, PharmD, BCPS Assistant Professor University of Connecticut School
Clinical Practice Guideline: Asthma
 Clinical Practice Guideline: Asthma INTRODUCTION A critical aspect of the diagnosis and management of asthma is the precise and periodic measurement of lung function both before and after bronchodilator
Clinical Practice Guideline: Asthma INTRODUCTION A critical aspect of the diagnosis and management of asthma is the precise and periodic measurement of lung function both before and after bronchodilator
Is it Under Diagnosed?
 Asthma in Icehockey Is it Under Diagnosed? Dr. med. B. Villiger CEO, Schweizer Paraplegiker Zentrum Nottwil Asthma bronchiale Mechanism Inflammation Remodelling Bronchial Hyperreactivity Airway - obstruction
Asthma in Icehockey Is it Under Diagnosed? Dr. med. B. Villiger CEO, Schweizer Paraplegiker Zentrum Nottwil Asthma bronchiale Mechanism Inflammation Remodelling Bronchial Hyperreactivity Airway - obstruction
TUEC Guidelines Medical Information to Support the Decisions of TUE Committees Asthma ASTHMA
 1. Medical Condition ASTHMA is a syndrome of the respiratory airways manifested by recurrent episodic symptoms. It is associated with variable airway obstruction that is reversible either spontaneously
1. Medical Condition ASTHMA is a syndrome of the respiratory airways manifested by recurrent episodic symptoms. It is associated with variable airway obstruction that is reversible either spontaneously
31 - Respiratory System
 31 - Respiratory System Asthma 1. Asthma has two components. Name the two components. 2. What are the common triggers of asthma? (LP p319) (e.g., pets) Upper respiratory infections ( ) 3. Describe a normal
31 - Respiratory System Asthma 1. Asthma has two components. Name the two components. 2. What are the common triggers of asthma? (LP p319) (e.g., pets) Upper respiratory infections ( ) 3. Describe a normal
Ass. Prof. Pulmonary and Crit.Care Medical School,University of Athens
 Diagnosis i of Exercise Induced Asthma Ch. Gratziou Ass. Prof. Pulmonary and Crit.Care Medical School,University of Athens Other Diagnostic Challenges for Exercise Induced Asthma Do we need other tests
Diagnosis i of Exercise Induced Asthma Ch. Gratziou Ass. Prof. Pulmonary and Crit.Care Medical School,University of Athens Other Diagnostic Challenges for Exercise Induced Asthma Do we need other tests
Alberta Childhood Asthma Pathway for Primary Care
 Asthma Diagnosis Box 1 Diagnosis: Based on symptom pattern, careful and thorough history of symptoms (wheeze, cough, night waking and activity limitations), and assessment of family history of asthma and
Asthma Diagnosis Box 1 Diagnosis: Based on symptom pattern, careful and thorough history of symptoms (wheeze, cough, night waking and activity limitations), and assessment of family history of asthma and
The Acute & Maintenance Treatment of Asthma via Aerosolized Medications
 The Acute & Maintenance Treatment of Asthma via Aerosolized Medications Douglas S. Gardenhire, EdD, RRT-NPS, FAARC Associate Professor and Chairman Department of Respiratory Therapy Objectives Define Asthma.
The Acute & Maintenance Treatment of Asthma via Aerosolized Medications Douglas S. Gardenhire, EdD, RRT-NPS, FAARC Associate Professor and Chairman Department of Respiratory Therapy Objectives Define Asthma.
Key points Intermittent doses of inhaled 2
 Key points Intermittent doses of inhaled 2 -agonists are the treatment of choice to block exercise-induced asthma/exercise-induced bronchoconstriction (EIA/EIB) if taken immediately before exercising.
Key points Intermittent doses of inhaled 2 -agonists are the treatment of choice to block exercise-induced asthma/exercise-induced bronchoconstriction (EIA/EIB) if taken immediately before exercising.
Significance. Asthma Definition. Focus on Asthma
 Focus on Asthma (Relates to Chapter 29, Nursing Management: Obstructive Pulmonary Diseases, in the textbook) Asthma Definition Chronic inflammatory disorder of airways Causes airway hyperresponsiveness
Focus on Asthma (Relates to Chapter 29, Nursing Management: Obstructive Pulmonary Diseases, in the textbook) Asthma Definition Chronic inflammatory disorder of airways Causes airway hyperresponsiveness
Asthma Management in Pregnancy HEATHER HOWE, MD UNIVERSITY OF UTAH PULMONARY DIVISION
 Asthma Management in Pregnancy HEATHER HOWE, MD UNIVERSITY OF UTAH PULMONARY DIVISION Asthma Management in Pregnancy Effects of asthma on pregnancy outcomes Effects of pregnancy on asthma control Management
Asthma Management in Pregnancy HEATHER HOWE, MD UNIVERSITY OF UTAH PULMONARY DIVISION Asthma Management in Pregnancy Effects of asthma on pregnancy outcomes Effects of pregnancy on asthma control Management
Adult Asthma Clinical Practice Guideline Summary
 Adult Asthma Clinical Practice Guideline Summary The following evidence-based guideline was developed to assist Primary Care physicians and other clinicians in the management of asthma in adults. It was
Adult Asthma Clinical Practice Guideline Summary The following evidence-based guideline was developed to assist Primary Care physicians and other clinicians in the management of asthma in adults. It was
Asthma. Rachel Miller, MD, FAAAAI Director Allergy and Immunology New York Presbyterian Hospital. Figure 1 Asthma Prevalence,
 Asthma Rachel Miller, MD, FAAAAI Director Allergy and Immunology New York Presbyterian Hospital Figure 1 Asthma Prevalence, 1980-2000 * Gap between 1995-1996 and 1997 indicates a break in trend due to
Asthma Rachel Miller, MD, FAAAAI Director Allergy and Immunology New York Presbyterian Hospital Figure 1 Asthma Prevalence, 1980-2000 * Gap between 1995-1996 and 1997 indicates a break in trend due to
Asthma Update A/Prof. John Abisheganaden. Senior Consultant, Dept Of Respiratory & Crit Care Medicine Tan Tock Seng Hospital
 Asthma Update - 2013 A/Prof. John Abisheganaden Senior Consultant, Dept Of Respiratory & Crit Care Medicine Tan Tock Seng Hospital Asthma A complex syndrome Multifaceted disease Heterogeneous Genetic and
Asthma Update - 2013 A/Prof. John Abisheganaden Senior Consultant, Dept Of Respiratory & Crit Care Medicine Tan Tock Seng Hospital Asthma A complex syndrome Multifaceted disease Heterogeneous Genetic and
ASTHMA. Epidemiology. Pathophysiology. Diagnosis. IAP UG Teaching slides
 BRONCHIAL ASTHMA ASTHMA Epidemiology Pathophysiology Diagnosis 2 CHILDHOOD ASTHMA Childhood bronchial asthma is characterized by Airway obstruction which is reversible Airway inflammation Airway hyper
BRONCHIAL ASTHMA ASTHMA Epidemiology Pathophysiology Diagnosis 2 CHILDHOOD ASTHMA Childhood bronchial asthma is characterized by Airway obstruction which is reversible Airway inflammation Airway hyper
Function of the Respiratory System. Exchange CO2 (on expiration) for O2 (on inspiration)
 Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Improving the Management of Asthma to Improve Patient Adherence and Outcomes
 Improving the Management of Asthma to Improve Patient Adherence and Outcomes Robert Sussman, MD Atlantic Health System Overlook Medical Center Asthma Remains a Serious Health Risk in the US Every day in
Improving the Management of Asthma to Improve Patient Adherence and Outcomes Robert Sussman, MD Atlantic Health System Overlook Medical Center Asthma Remains a Serious Health Risk in the US Every day in
Asthma. doh.sd.gov/statistics/2009brfss/asthma.pdf
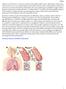 is an obstructive or restrictive condition which inhibits airflow due to inflammation of the airway. This obstruction occurs via increased edema in the small bronchioles walls as well as greater production
is an obstructive or restrictive condition which inhibits airflow due to inflammation of the airway. This obstruction occurs via increased edema in the small bronchioles walls as well as greater production
Effective Date: 4/27/2016 Version: 1.0 Approval By: CCC Clinical Delivery Steering Planned Review Date: 4/27/2017
 Protocol Title: Adult Asthma Protocol Effective Date: 4/27/2016 Version: 1.0 Approval By: CCC Clinical Delivery Steering Planned Review Date: 4/27/2017 1 Purpose & Objective This protocol provides evidence-based
Protocol Title: Adult Asthma Protocol Effective Date: 4/27/2016 Version: 1.0 Approval By: CCC Clinical Delivery Steering Planned Review Date: 4/27/2017 1 Purpose & Objective This protocol provides evidence-based
Asthma and the competitive swimmer
 Asthma and the competitive swimmer Introduction: One in seven children and one in 25 adults in Great Britain have asthma and the number is growing. Thus every swim squad or club will have a number of asthmatics
Asthma and the competitive swimmer Introduction: One in seven children and one in 25 adults in Great Britain have asthma and the number is growing. Thus every swim squad or club will have a number of asthmatics
Diagnosis. you have asthma? Get the answers. Your Asthma Basics series: Asthma Basics #1. Diagnosis Triggers Medications Kids
 Diagnosis Asthma Basics #1 Your Asthma Basics series: 1 2 3 Diagnosis Triggers Medications Kids Supported by unrestricted educational grants from: For more information from the Asthma Society of Canada:
Diagnosis Asthma Basics #1 Your Asthma Basics series: 1 2 3 Diagnosis Triggers Medications Kids Supported by unrestricted educational grants from: For more information from the Asthma Society of Canada:
Asthma training. Mike Levin Division of Asthma and Allergy Red Cross Hospital
 Asthma training Mike Levin Division of Asthma and Allergy Red Cross Hospital Introduction Physiology Diagnosis Severity Treatment Control Stage 3 of guidelines Acute asthma Drug delivery Conclusion Overview
Asthma training Mike Levin Division of Asthma and Allergy Red Cross Hospital Introduction Physiology Diagnosis Severity Treatment Control Stage 3 of guidelines Acute asthma Drug delivery Conclusion Overview
Lack of tolerance to the protective effect of montelukast in exercise-induced bronchoconstriction in children
 Eur Respir J 2006; 28: 291 295 DOI: 10.1183/09031936.06.00020606 CopyrightßERS Journals Ltd 2006 Lack of tolerance to the protective effect of montelukast in exercise-induced bronchoconstriction in children
Eur Respir J 2006; 28: 291 295 DOI: 10.1183/09031936.06.00020606 CopyrightßERS Journals Ltd 2006 Lack of tolerance to the protective effect of montelukast in exercise-induced bronchoconstriction in children
Role of bronchoprovocation tests in identifying exercise-induced bronchoconstriction in a non-athletic population: a pilot study
 Original Article Role of bronchoprovocation tests in identifying exercise-induced bronchoconstriction in a non-athletic population: a pilot study Jessica H. Y. Tan 1 *, Wui Mei Chew 1 *, Therese S. Lapperre
Original Article Role of bronchoprovocation tests in identifying exercise-induced bronchoconstriction in a non-athletic population: a pilot study Jessica H. Y. Tan 1 *, Wui Mei Chew 1 *, Therese S. Lapperre
Allergic Conditions in Sports. Seth Smith, MD, CAQ-SM, PharmD TPC Course February 7, 2016
 Allergic Conditions in Sports Seth Smith, MD, CAQ-SM, PharmD TPC Course February 7, 2016 Goals and Objectives Describe diagnosis and management of exercise-induced bronchospasm/bronchoconstriction (EIB)
Allergic Conditions in Sports Seth Smith, MD, CAQ-SM, PharmD TPC Course February 7, 2016 Goals and Objectives Describe diagnosis and management of exercise-induced bronchospasm/bronchoconstriction (EIB)
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
EIB in adults and children
 Onset and duration of protection against exercise-induced bronchoconstriction by a single oral dose of montelukast David S. Pearlman, MD*; Janet van Adelsberg, MD ; George Philip, MD ; Stephen A. Tilles,
Onset and duration of protection against exercise-induced bronchoconstriction by a single oral dose of montelukast David S. Pearlman, MD*; Janet van Adelsberg, MD ; George Philip, MD ; Stephen A. Tilles,
On completion of this chapter you should be able to: discuss the stepwise approach to the pharmacological management of asthma in children
 7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
Exercise-induced asthma is a common disease affecting
 Exercise-Induced Asthma Exercise-induced asthma is a common disease affecting at least 15 million people in the United States. The etiology of exercise-induced asthma is not completely understood, although
Exercise-Induced Asthma Exercise-induced asthma is a common disease affecting at least 15 million people in the United States. The etiology of exercise-induced asthma is not completely understood, although
THE ROLE OF IMPULSE OSCILLOMETRY IN DETECTING AIRWAY DYSFUNCTION IN ATHLETES
 THE ROLE OF IMPULSE OSCILLOMETRY IN DETECTING AIRWAY DYSFUNCTION IN ATHLETES Word count: 3097 Abstract word count: 250 Running title: Detecting airway dysfunction in athletes. Key words: Asthma, Diagnosis,
THE ROLE OF IMPULSE OSCILLOMETRY IN DETECTING AIRWAY DYSFUNCTION IN ATHLETES Word count: 3097 Abstract word count: 250 Running title: Detecting airway dysfunction in athletes. Key words: Asthma, Diagnosis,
Meeting the Challenges of Asthma
 Presenter Disclosure Information 11:05 11:45am Meeting the Challenge of Asthma SPEAKER Christopher Fanta, MD The following relationships exist related to this presentation: Christopher Fanta, MD: No financial
Presenter Disclosure Information 11:05 11:45am Meeting the Challenge of Asthma SPEAKER Christopher Fanta, MD The following relationships exist related to this presentation: Christopher Fanta, MD: No financial
Asthma. Definition. Symptoms
 Asthma Definition Asthma is a condition in which your airways narrow and swell and produce extra mucus. This can make breathing difficult and trigger coughing, wheezing and shortness of breath. For some
Asthma Definition Asthma is a condition in which your airways narrow and swell and produce extra mucus. This can make breathing difficult and trigger coughing, wheezing and shortness of breath. For some
Exercise-Induced Bronchoconstriction and Vocal Cord Dysfunction
 Exercise-Induced Bronchoconstriction and Vocal Cord Dysfunction 2 Christopher Kempe and Jonathan P. Parsons Exercise-induced bronchoconstriction (EIB) describes acute, transient airway narrowing that occurs
Exercise-Induced Bronchoconstriction and Vocal Cord Dysfunction 2 Christopher Kempe and Jonathan P. Parsons Exercise-induced bronchoconstriction (EIB) describes acute, transient airway narrowing that occurs
Get Healthy Stay Healthy
 Asthma Management WHAT IS ASTHMA? Asthma causes swelling and inflammation in the breathing passages that lead to your lungs. When asthma flares up, the airways tighten and become narrower. This keeps the
Asthma Management WHAT IS ASTHMA? Asthma causes swelling and inflammation in the breathing passages that lead to your lungs. When asthma flares up, the airways tighten and become narrower. This keeps the
GINA. At-A-Glance Asthma Management Reference. for adults, adolescents and children 6 11 years. Updated 2017
 GINA At-A-Glance Asthma Management Reference for adults, adolescents and children 6 11 years Updated 2017 This resource should be used in conjunction with the Global Strategy for Asthma Management and
GINA At-A-Glance Asthma Management Reference for adults, adolescents and children 6 11 years Updated 2017 This resource should be used in conjunction with the Global Strategy for Asthma Management and
Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network
 Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network Robert.kruklitis@lvh.com Correlation of a Asthma pathophyisology with basic science Asthma (Physiology) Bronchodilators
Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network Robert.kruklitis@lvh.com Correlation of a Asthma pathophyisology with basic science Asthma (Physiology) Bronchodilators
Emily DiMango, MD Asthma II
 Emily DiMango, MD Asthma II Director John Edsall/John Wood Asthma Center Columbia University Medical Center HP 2000 Goal: 2.25/1,000 Comparison of Asthma Hospitalization Rates in Children Aged 0-14 in
Emily DiMango, MD Asthma II Director John Edsall/John Wood Asthma Center Columbia University Medical Center HP 2000 Goal: 2.25/1,000 Comparison of Asthma Hospitalization Rates in Children Aged 0-14 in
ASTHMA AND SPORT. 88 Current Allergy & Clinical Immunology, June 2008 Vol 21, No. 2. Table I. Variables that affect the reporting of exerciseinduced
 ASTHMA AND SPORT Samuel Malamulele Risenga, BSc, MB ChB, DCH (SA), MMed (Paed), Dip Allergology (SA) Division of Paediatric Pulmonology, Department of Paediatrics and Child Health, University of Pretoria,
ASTHMA AND SPORT Samuel Malamulele Risenga, BSc, MB ChB, DCH (SA), MMed (Paed), Dip Allergology (SA) Division of Paediatric Pulmonology, Department of Paediatrics and Child Health, University of Pretoria,
Sensitivity and Specificity of Self Reported Symptoms for Exercise Induced Bronchospasm Diagnosis in Children
 Original Article Iran J Pediatr Mar 2009; Vol 19 (No 1), Pp:47-51 Sensitivity and Specificity of Self Reported Symptoms for Exercise Induced Bronchospasm Diagnosis in Children Behroz Bavarian 1,2, MD;
Original Article Iran J Pediatr Mar 2009; Vol 19 (No 1), Pp:47-51 Sensitivity and Specificity of Self Reported Symptoms for Exercise Induced Bronchospasm Diagnosis in Children Behroz Bavarian 1,2, MD;
Prevalence of Exercise-Induced Bronchoconstriction Measured by Standardized Testing in Healthy College Athletes
 Prevalence of Exercise-Induced Bronchoconstriction Measured by Standardized Testing in Healthy College Athletes David Burnett PhD RRT AE-C, Steve Burns PhD, Samantha Merritt MSc, Jo Wick PhD, and Matthew
Prevalence of Exercise-Induced Bronchoconstriction Measured by Standardized Testing in Healthy College Athletes David Burnett PhD RRT AE-C, Steve Burns PhD, Samantha Merritt MSc, Jo Wick PhD, and Matthew
Guideline for the Diagnosis and Management of Chronic Childhood Asthma
 Guideline for the Diagnosis and Management of Chronic Childhood Asthma Guideline developed by Larry A. Simmons, MD, FAAP, Associate Professor of Pediatrics, Department of Pediatrics, UAMS at Arkansas Children
Guideline for the Diagnosis and Management of Chronic Childhood Asthma Guideline developed by Larry A. Simmons, MD, FAAP, Associate Professor of Pediatrics, Department of Pediatrics, UAMS at Arkansas Children
Amanda Hess, MMS, PA-C President-Elect, AAPA-AAI Arizona Asthma and Allergy Institute Scottsdale, AZ
 Amanda Hess, MMS, PA-C President-Elect, AAPA-AAI Arizona Asthma and Allergy Institute Scottsdale, AZ Financial Disclosures Advanced Practiced Advisory Board for Circassia Learning Objectives 1. Briefly
Amanda Hess, MMS, PA-C President-Elect, AAPA-AAI Arizona Asthma and Allergy Institute Scottsdale, AZ Financial Disclosures Advanced Practiced Advisory Board for Circassia Learning Objectives 1. Briefly
VA/DoD Clinical Practice Guideline Management of COPD Pocket Guide
 VA/DoD Clinical Practice Guideline Management of COPD Pocket Guide MODULE A: MAAGEMET OF COPD 1 2 Patient with suspected or confirmed COPD presents to primary care [ A ] See sidebar A Perform brief clinical
VA/DoD Clinical Practice Guideline Management of COPD Pocket Guide MODULE A: MAAGEMET OF COPD 1 2 Patient with suspected or confirmed COPD presents to primary care [ A ] See sidebar A Perform brief clinical
Prevalence of Exercise-Induced Bronchoconstriction Measured by Standardized Testing in Healthy College Athletes
 Prevalence of Exercise-Induced Bronchoconstriction Measured by Standardized Testing in Healthy College Athletes David M Burnett PhD RRT AE-C, Steve Burns PhD, Samantha Merritt MSc, Jo Wick PhD, and Matthew
Prevalence of Exercise-Induced Bronchoconstriction Measured by Standardized Testing in Healthy College Athletes David M Burnett PhD RRT AE-C, Steve Burns PhD, Samantha Merritt MSc, Jo Wick PhD, and Matthew
Why Can t I breathe? Asthma vs. Vocal Cord Dysfunction (VCD) Lindsey Frohn, M.S., CCC-SLP Madonna Rehabilitation Hospital (Lincoln, NE)
 Why Can t I breathe? Asthma vs. Vocal Cord Dysfunction (VCD) Lindsey Frohn, M.S., CCC-SLP Madonna Rehabilitation Hospital (Lincoln, NE) Objectives Examine Vocal Cord Dysfunction Examine Exercise Induced
Why Can t I breathe? Asthma vs. Vocal Cord Dysfunction (VCD) Lindsey Frohn, M.S., CCC-SLP Madonna Rehabilitation Hospital (Lincoln, NE) Objectives Examine Vocal Cord Dysfunction Examine Exercise Induced
CLINICAL PRACTICE. Clinical Practice. N Engl J Med, Vol. 345, No. 17 October 25,
 CLINICAL PRACTICE Clinical Practice This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies is then presented, followed by a review
CLINICAL PRACTICE Clinical Practice This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies is then presented, followed by a review
Diagnosis, Treatment and Management of Asthma
 Diagnosis, Treatment and Management of Asthma Asthma is a complex disorder characterized by variable and recurring symptoms, airflow obstruction, bronchial hyperresponsiveness, and an underlying inflammation.
Diagnosis, Treatment and Management of Asthma Asthma is a complex disorder characterized by variable and recurring symptoms, airflow obstruction, bronchial hyperresponsiveness, and an underlying inflammation.
Q: Should patients with mild asthma
 1-MINUTE CONSULT CME CREDIT EDUCATIONAL OBJECTIVE: Readers will consider prescribing inhaled corticosteroids to their patients who have mild persistent asthma brief answers to specific clinical questions
1-MINUTE CONSULT CME CREDIT EDUCATIONAL OBJECTIVE: Readers will consider prescribing inhaled corticosteroids to their patients who have mild persistent asthma brief answers to specific clinical questions
Pulmonary Function Testing
 Pulmonary Function Testing Let s catch our breath Eddie Needham, MD, FAAFP Program Director Emory Family Medicine Residency Program Learning Objectives The Astute Learner will: Become familiar with indications
Pulmonary Function Testing Let s catch our breath Eddie Needham, MD, FAAFP Program Director Emory Family Medicine Residency Program Learning Objectives The Astute Learner will: Become familiar with indications
Asthma in the college health setting: diagnosis, treatment, pitfalls
 Asthma in the college health setting: diagnosis, treatment, pitfalls A 20-year-old college student with a history of asthma and allergic rhinitis, which were diagnosed in childhood, presents with cough
Asthma in the college health setting: diagnosis, treatment, pitfalls A 20-year-old college student with a history of asthma and allergic rhinitis, which were diagnosed in childhood, presents with cough
Perception of Exercise-Induced Bronchoconstriction in College Athletes
 Perception of Exercise-Induced Bronchoconstriction in College Athletes David M Burnett PhD RRT AE-C, John P Vardiman PhD ATC, Jake A Deckert MSc, Jaimie L Ward and Matthew R Sharpe MD BACKGROUND: Exercise-induced
Perception of Exercise-Induced Bronchoconstriction in College Athletes David M Burnett PhD RRT AE-C, John P Vardiman PhD ATC, Jake A Deckert MSc, Jaimie L Ward and Matthew R Sharpe MD BACKGROUND: Exercise-induced
Presented by the California Academy of Family Physicians 2013/California Academy of Family Physicians
 Family Medicine and Patient-Centered Asthma Care Presented by the California Academy of Family Physicians Faculty: Hobart Lee, MD Disclosures: Jeffrey Luther, MD, Program Director, Memorial Family Medicine
Family Medicine and Patient-Centered Asthma Care Presented by the California Academy of Family Physicians Faculty: Hobart Lee, MD Disclosures: Jeffrey Luther, MD, Program Director, Memorial Family Medicine
A comparison of the effects of oral montelukast and inhaled salmeterol on response to rescue bronchodilation after challenge
 Respiratory Medicine (2004) 98, 1051 1062 A comparison of the effects of oral montelukast and inhaled salmeterol on response to rescue bronchodilation after challenge William Storms a, Paul Chervinsky
Respiratory Medicine (2004) 98, 1051 1062 A comparison of the effects of oral montelukast and inhaled salmeterol on response to rescue bronchodilation after challenge William Storms a, Paul Chervinsky
James P. Kemp, MD; Margaret C. Minkwitz, PhD; Catherine M. Bonuccelli, MD; and Marshelle S. Warren, MD
 Therapeutic Effect of Zafirlukast as Monotherapy in Steroid-Naive Patients With Severe Persistent Asthma* James P. Kemp, MD; Margaret C. Minkwitz, PhD; Catherine M. Bonuccelli, MD; and Marshelle S. Warren,
Therapeutic Effect of Zafirlukast as Monotherapy in Steroid-Naive Patients With Severe Persistent Asthma* James P. Kemp, MD; Margaret C. Minkwitz, PhD; Catherine M. Bonuccelli, MD; and Marshelle S. Warren,
Asthma: Chronic Management. Yung-Yang Liu, MD Attending physician, Chest Department Taipei Veterans General Hospital April 26, 2015
 Asthma: Chronic Management Yung-Yang Liu, MD Attending physician, Chest Department Taipei Veterans General Hospital April 26, 2015 Global Strategy for Asthma Management and Prevention Evidence-based Implementation
Asthma: Chronic Management Yung-Yang Liu, MD Attending physician, Chest Department Taipei Veterans General Hospital April 26, 2015 Global Strategy for Asthma Management and Prevention Evidence-based Implementation
Joint Session ACOFP and AOASM: Exercise Induced Asthma. Bruce Dubin, DO, JD, FCLM, FACOI
 Joint Session ACOFP and AOASM: Exercise Induced Asthma Bruce Dubin, DO, JD, FCLM, FACOI ACOFP FULL DISCLOSURE FOR CME ACTIVITIES Please check where applicable and sign below. Provide additional pages as
Joint Session ACOFP and AOASM: Exercise Induced Asthma Bruce Dubin, DO, JD, FCLM, FACOI ACOFP FULL DISCLOSURE FOR CME ACTIVITIES Please check where applicable and sign below. Provide additional pages as
Combination Beta2-Agonist/Corticosteroid Inhalers Policy Number: Last Review: Origination: Next Review: Policy When Policy Topic is covered:
 Combina ation Beta2-Agonist/Corticosteroid Inhalers Policy Number: 5.01.572 Origination: 06/2014 Last Review: 07/2014 Next Review: 07/2015 Policy BCBSKC will provide coverage for the combination beta2-agonist/corticosteroid
Combina ation Beta2-Agonist/Corticosteroid Inhalers Policy Number: 5.01.572 Origination: 06/2014 Last Review: 07/2014 Next Review: 07/2015 Policy BCBSKC will provide coverage for the combination beta2-agonist/corticosteroid
Pulmonary Pearls. Medical Pearls. Case 1: Case 1 (cont.): Case 1: What is the Most Likely Diagnosis? Case 1 (cont.):
 Pulmonary Pearls Christopher H. Fanta, MD Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Medical Pearls Definition: Medical fact that is
Pulmonary Pearls Christopher H. Fanta, MD Pulmonary and Critical Care Division Brigham and Women s Hospital Partners Asthma Center Harvard Medical School Medical Pearls Definition: Medical fact that is
Bronchial asthma. MUDr. Mojmír Račanský Odd. Alergologie a klinické imunologie FNOL Ústav Imunologie LF UPOL
 Bronchial asthma MUDr. Mojmír Račanský Odd. Alergologie a klinické imunologie FNOL Ústav Imunologie LF UPOL DEFINITION ASTHMA BRONCHIALE = Asthma is a chronic inflammatory disorder of the airways in which
Bronchial asthma MUDr. Mojmír Račanský Odd. Alergologie a klinické imunologie FNOL Ústav Imunologie LF UPOL DEFINITION ASTHMA BRONCHIALE = Asthma is a chronic inflammatory disorder of the airways in which
Speaker Disclosure. Identification and Diagnosis of Asthma. Definition of Asthma. Objectives 11/9/2017
 Speaker Disclosure Identification and Diagnosis of Asthma Isabel L. Virella Lowell, MD, Associate Professor, Pulmonology and Sleep Medicine, University of Alabama at Birmingham Isabel Virella-Lowell, MD
Speaker Disclosure Identification and Diagnosis of Asthma Isabel L. Virella Lowell, MD, Associate Professor, Pulmonology and Sleep Medicine, University of Alabama at Birmingham Isabel Virella-Lowell, MD
(EVH), 60%) 1, 5, 10, 15 5 (2) 5% CO2, 21% O2,
 A Comparison of Two Challenge Tests for Identifying Exercise-Induced Bronchospasm in Figure Skaters* Edward T. Mannix, PhD; Felice Manfredi, MD; and Mark O. Farber, MD Objectives: Studies documenting the
A Comparison of Two Challenge Tests for Identifying Exercise-Induced Bronchospasm in Figure Skaters* Edward T. Mannix, PhD; Felice Manfredi, MD; and Mark O. Farber, MD Objectives: Studies documenting the
Efficacy of a Heat Exchanger Mask in Cold Exercise-Induced Asthma* David A. Beuther, MD; and Richard J. Martin, MD, FCCP
 Original Research ASTHMA Efficacy of a Heat Exchanger Mask in Cold Exercise-Induced Asthma* David A. Beuther, MD; and Richard J. Martin, MD, FCCP Study objectives: To determine the efficacy of a novel
Original Research ASTHMA Efficacy of a Heat Exchanger Mask in Cold Exercise-Induced Asthma* David A. Beuther, MD; and Richard J. Martin, MD, FCCP Study objectives: To determine the efficacy of a novel
Adult asthma management: focus on control
 Adult asthma management: focus on control Jennifer W. McCallister, MD Associate Professor Pulmonary, Allergy, Critical Care & Sleep Medicine The Ohio State University Wexner Medical Center Objectives Apply
Adult asthma management: focus on control Jennifer W. McCallister, MD Associate Professor Pulmonary, Allergy, Critical Care & Sleep Medicine The Ohio State University Wexner Medical Center Objectives Apply
Key features and changes to these four components of asthma care include:
 Guidelines for the Diagnosis and Management of Asthma in Adults Clinical Practice Guideline MedStar Health These guidelines are provided to assist physicians and other clinicians in making decisions regarding
Guidelines for the Diagnosis and Management of Asthma in Adults Clinical Practice Guideline MedStar Health These guidelines are provided to assist physicians and other clinicians in making decisions regarding
Objectives. Asthma in Primary Care. Definition. Epidemiology. Pathophysiology
 Objectives Asthma in Primary Care Jed Grant, PA-C Program Director, SJVC PA Program Staff PA, AMCH Emergency Department Apply the NAEPP guideline measures of severity and control including current impairment
Objectives Asthma in Primary Care Jed Grant, PA-C Program Director, SJVC PA Program Staff PA, AMCH Emergency Department Apply the NAEPP guideline measures of severity and control including current impairment
LivingWith Asthma. A Guide to Understanding Asthma...
 A Guide to Understanding... LivingWith Understanding Diagnosing Treating Frequently Asked Questions [2] A Guide to Understanding... Understanding What Is? (AZ-muh) is a chronic disease that affects your
A Guide to Understanding... LivingWith Understanding Diagnosing Treating Frequently Asked Questions [2] A Guide to Understanding... Understanding What Is? (AZ-muh) is a chronic disease that affects your
COMMON RESPIRATORY DISORDERS IN ELITE SWIMMERS
 SPORTS SCIENCE COMMON RESPIRATORY DISORDERS IN ELITE SWIMMERS DIAGNOSIS AND MANAGEMENT Written by Jon Greenwell, United Kingdom Swimming is widely promoted as a suitable exercise to maintain cardiovascular
SPORTS SCIENCE COMMON RESPIRATORY DISORDERS IN ELITE SWIMMERS DIAGNOSIS AND MANAGEMENT Written by Jon Greenwell, United Kingdom Swimming is widely promoted as a suitable exercise to maintain cardiovascular
Not all who wheeze have asthma
 Not all who wheeze have asthma Educational aims Exercise-induced asthma is frequently found among children, adolescents and young adults. The diagnosis of asthma should be documented by variable lung function,
Not all who wheeze have asthma Educational aims Exercise-induced asthma is frequently found among children, adolescents and young adults. The diagnosis of asthma should be documented by variable lung function,
