Fiberoptic Videolaryngoscopy During Bicycle Ergometry: A Diagnostic Tool for Exercise- Induced Vocal Cord Dysfunction
|
|
|
- Veronica Black
- 6 years ago
- Views:
Transcription
1 The Laryngoscope VC 2009 The American Laryngological, Rhinological and Otological Society, Inc. Fiberoptic Videolaryngoscopy During Bicycle Ergometry: A Diagnostic Tool for Exercise- Induced Vocal Cord Dysfunction Hanna Tervonen, MD; Minna M. Niskanen, MD, PhD; Anssi R. Sovijärvi, MD, PhD; Auli S. Hakulinen, MD; Erkki A. Vilkman, MD, PhD; Leena-Maija Aaltonen, MD, PhD Additional Supporting Information may be found in the online version of this article. From the Department of Otorhinolaryngology Head and Neck Surgery (H.T., E.A.V., L.-M.A.), the Department of Surgery (M.M.N.), the Department of Clinical Physiology and Nuclear Medicine (A.R.S.), and Department of Dermatology and Allergy (A.S.H.), Helsinki University Central Hospital, Helsinki, Finland. Editor s Note: This Manuscript was accepted for publication January 28, Send correspondence to Hanna Tervonen, MD, Department of Otorhinolaryngology Head and Neck Surgery, Helsinki University Central Hospital, POB 220, FIN HUS, Helsinki, Finland. hanna. tervonen@hotmail.com DOI: /lary Objectives/Hypothesis: Exercise-induced vocal cord dysfunction is difficult to diagnose because the paradoxical vocal cord adduction should be observed during exercise. Our goal was to develop and validate a new diagnostic method for exercise-induced vocal cord dysfunction by combining continuous fiberoptic laryngoscopy with a bicycle ergometry test. Methods: Thirty consecutive patients referred to a laryngologist because of suspicion of exercise-induced vocal cord dysfunction and 15 healthy controls underwent the exercise test until dyspnea or exhaustion rated as 18 19/20 on the Borg scale. Laryngeal findings, electrocardiography, blood pressure, heart rate, and respiratory rate were monitored, and forced expiratory flow in the first second was measured before and after the exercise. The medical history was assessed by use of a structured questionnaire. Results: Among the 30 patients, 27 (90%) performed the test successfully, as did all controls. Diagnostic signs of inspiratory stridor, supraglottic collapse, and vocal cord adduction appeared in five (19%) patients but in none of the controls. Of the 30 patients referred, the laryngologist considered 25 to be suspect. Of them, 9 (36%) showed signs diagnostic or highly suspect for exercise-induced vocal cord dysfunction. Of the 15 patients whose dyspnea could be induced during the test, nine (60%) were suspected of having exercise-induced vocal cord dysfunction. Conclusions: Fiberoptic videolaryngoscopy during bicycle ergometry was a well-tolerated and relatively easily established diagnostic tool that could induce dyspnea in more than one half the patients examined. If the symptom of dyspnea appeared, the most frequent diagnosis was exercise- induced vocal cord dysfunction. Key Words: Diagnosis, exercise, paradoxical vocal cord movement, vocal cord dysfunction. Laryngoscope, 119: , 2009 INTRODUCTION Vocal cord dysfunction (VCD) is a condition with paradoxical closure of the vocal cords typically during inspiration. Such closure limits airflow, causing dyspnea and stridor, a condition often misdiagnosed and mistreated as asthma. 1 Other typical symptoms of VCD are dysphonia, dysphagia, and cough. 2 In some patients, VCD symptoms are related only to exercise, in others only to rest, and some get symptoms both in exercise and rest. 1,3,4 The pathophysiology of VCD is still poorly understood, and its etiology may be multifactorial. Suggested etiological factors, alone or combined, are infections, 5 physical exercise, 6,7 laryngeal sensitivity to various stimuli, 8 and psychosomatic and psychological stress. 7 Visualization of a paradoxical movement of the vocal cords during the dyspnea attack is the gold standard for VCD diagnosis. 3,4,6,7,9 Incidence of VCD in the general population is not widely established, but exercise-induced VCD (EIVCD) in patients with exertional dyspnea in one study showed an incidence of 15%. 3 Shortness of breath and wheezing during exercise in generally healthy adolescents is often caused by exerciseinduced asthma (EIA). 10 However, EIVCD alone or a combination with EIA and EIVCD can also cause these symptoms. 1 EIVCD, a subgroup of VCD, typically appears suddenly during very hard exercise and the symptoms are also resolved within a few seconds or minutes after stopping or just slowing down, and athletes have learned to limit their activity to avoid such attacks. 11 Because EIVCD is an episodic symptom not always appearing in the same exercise surroundings, a negative result in any provocation test does not preclude the diagnosis. 4
2 Characteristics* TABLE I. Characteristics/Patient History. No. of Patients, n ¼ 30 (%) Females Asthma Regular use of inhaled corticosteroids Regular use of antireflux medicine 3 10 Chronic cough 5 17 Chronic need for throat clearing Nonsmokers Chest pain at rest 2 7 Chest pain during exercise 4 13 History of Symptoms Other Than Dyspnea During EIVCD Attack Dysphonia Dysphagia 7 23 Numbness of hands 5 17 Anxiety 6 20 Patient and Test Preparation None of the patients tested or controls had any ongoing respiratory infection and all patients continued their medications before testing. Calibration of the equipment (ECG device, spirometer) was performed before each test as advised by the manufacturers. Ear, nose, and throat (ENT) examination was performed on all. Forced expiratory volume in the first second (FEV1), baseline 12-lead ECG, blood pressure, heart rate, and respiratory rate were measured before the start of the exercise. The test followed a schedule similar to that of an ordinary work-conducted cardiovascular exercise test (Fig. 1). Test Set-Up, Protocol, and Result Interpretation A stationary bicycle (E 80 Tunturi, Tunturi Oy, Turku, Finland) was used for the test, as were transnasal fiberoptic scope (Olympus D ENF type P3, Olympus-Optical, Tokyo, Japan) connected to computer-based videolaryngostroboscopy equipment (Rehder Partners, Hamburg, Germany) and continuous 12-lead- ECG monitoring (Nihon Kohden Cardiofax V, Nihon Kohden *Median age of the patients 27.8 years (range, years). EIVCD ¼ excercise induced vocal cord dysfunction. Heimdal et al. have published promising results of a new diagnostic method for EIVCD based on continuous laryngoscopy during treadmill exercise. However, as all subjects tested were young (ages, years) and mostly healthy volunteers, the utility of the procedure in patients in all age groups is unknown. 6 An earlier study of 10 young (16 32 years) healthy volunteers using a stationary bicycle combined with continuous laryngoscopy determined the incidence of exercise-induced laryngomalacia. Its test setting lacked a patient group, and electrocardiogram (ECG), blood pressure, heart rate, and respiratory rate monitoring. 12 The goal of our study was to develop and evaluate a new tool for the challenging diagnostics of EIVCD, appropriate for a laryngeal outpatient department and suitable for patients of various ages and physical conditions by combining fiberoptic videolaryngoscopy with a bicycle exercise test. MATERIALS AND METHODS We examined 30 consecutive patients referred to our clinic by pulmonary, allergy, and sports medicine specialists because of a suspicion of EIVCD; 25 of them had symptoms only during hard exercise. Patients median age was 27.8 years (range, ); 24 (80%) were female. There were 13 patients with coexisting asthma (Table I). The asthma diagnosis was based on the criteria of Global Initiative for Asthma (GINA). 13 As controls we examined 15 healthy volunteers. The median control group age was 33.4 years (range, ); 10 (67%) were female. All patients and controls underwent the same research protocol. Data from medical history (other possible illnesses and actual medication, subjective symptoms and smoking habits) were collected with a questionnaire. Informed consent was obtained from all individuals, and the human experimentation guidelines of the Helsinki University Central Hospital were followed. The study was approved by the Ethics Review Board of the Helsinki and Uusimaa Hospital District. Fig. 1. A photo and a schematic presentation of the laryngeal team performing exercise test. 1 ¼ patient; 2 ¼ ear, nose, and throat specialist; 3 ¼ anesthesiologist; 4 ¼ nurse; 5 ¼ computerbased videolaryngostroboscopy equipment; 6 ¼ 12-lead electrocardiogram monitor. [Color figure can be viewed in the online issue, which is available at
3 Before the Test During the Test TABLE II. Schematic Test Protocol. Immediately After the Test 10 Min After the Test Calculated Parameters Heart rate Heart rate FEV1 ECG Heart rate % of maximum Respiratory rate Respiratory rate* ECG Changes in respiratory rate RR* RR Changes in RR FEV1 SaO 2 Changes in FEV1 SaO 2 ECG Changes in SaO 2 ECG Total duration of test Topical anesthesia of the nose *No longer measured in routine clinical use. FEV1 ¼ forced expiratory volume in the first second; ECG ¼ electrocardiogram; RR ¼ blood pressure; SaO 2 ¼ oxygen saturation. Corp., Tokyo, Japan). Before patients were studied, this set-up was tested on a volunteer staff member from our clinic. After baseline measurements (FEV1, oxygen saturation, ECG, blood pressure, heart rate, and respiratory rate) topical anesthesia with 2% lidocaine on a cotton stick was applied inside the patient s nostril for 7 minutes to prevent the irritation by the fiberoptic. The lower parts of the nasopharynx and larynx were not anesthetized, to avoid possible masquerading of the symptoms, so no local anesthetic spray was used. Thereafter, the patient mounted a bicycle adjusted to proper height. The transnasal fiberoptic scope connected to computer-based videolaryngoscopy equipment was then inserted to the optimal position for visualization of the larynx, and the patient started pedalling. The fiberoptic scope was held in place by the otorhinolaryngologist to ensure the optimal position of the scope during the whole exercise. The work load started at 40 watts (W) for women and 50 W for men, and the load was added every 4 minutes in 40 W or 50 W increments supervised by an anesthesiologist. Pedalling speed was 60 rpm. Blood pressure, heart rate, and respiratory rate were measured during the 3rd minute at every exercise step (Table II). The patient estimated the rate of perceived exertion at the end of each load step by using the Borg scale. The Borg scale measures perceived exertion in sports, and particularly in exercise testing, and is used to document the patient s subjective exertion during a test. The original scale, introduced by Gunnar Borg, rated exertion on a scale of 6 to All subjects continued pedalling until the typical symptoms of dyspnea appeared or until exhaustion (Borg scale 18 19/20). After completing four exercise steps (160 W for women, 200 W for men), a few highly athletic patients reported tiredness of muscles without respiratory symptoms. They were asked to pedal with no speed limit a load of 120 W/150 W until exhaustion. The test result was considered diagnostic for EIVCD if inspiratory stridor, supraglottic collapse of arytenoids, and aryepiglottic folds toward the aditus of the larynx and vocal cord adduction were noticed. If all of these signs appeared without vocal cord adduction in the end, the result was considered to be highly suspect for EIVCD. The test was performed and scored every time by the same two physicians who simultaneously made the decision after a short unanimous discussion. Statistical Analysis Descriptive parameters were calculated to describe distributions of variables. Two-sided Fisher exact test was used to determine any associations between two categorical variables. By using the Mann-Whitney or Student t test, we analyzed differences in mean values for continuous variables. The Kolmogorov-Smirnov test was performed to determine whether two distributions differed. Analyses were performed with SAS software version 8.02 (SAS Institute Inc., Cary, NC). RESULTS Test Results: Tolerability, Symptoms and Laryngeal Findings For all age groups, the test was relatively easy to perform and well tolerated. We had three patients in the age group 60 years and eight patients 16 years, and the youngest one was a 10-year-old female. The test was successfully performed for 27 (90%) patients and all controls. Three of the 30 patients interrupted the test: one patient s laryngeal spasm was triggered by FEV1 measurement, another experienced a panic attack during the preparation phase, and the third patient s test was interrupted by vasovagal collapse during local anesthesia of the nose. Laryngeal anatomy and function before exercise test was normal in all patients. During the test, the typical dyspnea in their history could be induced in 15 (56%) of the patients. Of these, nine (60%) had EIVCD (n ¼ 5) or a high suspicion of EIVCD (n ¼ 4), showing collapse of arytenoids and aryepiglottic folds toward the aditus of the larynx; in five EIVCD patients this supraglottic collapse was followed by adduction of the vocal cords. All EIVCD patients showed a glottic narrowing of at least 90%, leaving only a minimal posterior chink open (video is included in the online version of this article). Inspiratory stridor was audible during subjective symptom of dyspnea in all of the nine patients. Laryngeal function was normal in all controls during the test, and no subjective symptoms of dyspnea appeared. Soon after the test was started, physiological slight and fast adduction of vocal cords during expiration was seen for a short period in 13 (87%) of the 15 controls. This was seen very briefly and only during expiration, caused no subjective symptoms, and did not considerably narrow the glottic level. 1778
4 Test Results: Other Findings The median exercise test duration for patients was 18.6 minutes (range, ), and for controls 15.7 minutes (range, ). All patients and controls were able to reach the heart rate (HR) minimum of 85% of the predicted maximal HR, (220 age in years)/ minutes, by the end of the test. An asthma-like attack with expiratory stridor and dyspnea, but without reduction in FEV1, occurred in one patient, and another patient showed decreased ST level without chest pain in ECG during the test; in subsequent cardiological examinations, coronary artery disease showed in the latter. No others had severe ECG changes. Blood pressure and breathing rate responses to exercise were normal in all patients and controls. Oxygen saturation momentarily decreased to under 90% in four (15%) of the patients and in one (7%) of the controls. Neither the patients nor the control reported any symptoms during these short periods of decreased oxygen saturation. No control used regular medication or reported any history of dyspnea, continuous cough, or need to clear the throat. One of the controls was a smoker. No statistically significant differences appeared between patients and controls by age (P ¼.0815, Kolmogorov-Smirnov Test), or by gender (P ¼.4639, Fisher exact test, 2-sided). DISCUSSION Of those patients referred to our clinic because of suspicion of EIVCD, our test identified one third. Continuous transnasal fiberoptic videolaryngoscopy during bicycle ergometry proved a well-tolerated and relatively easily performed diagnostic method. It could be performed on patients from 10 to 69 years of age, and the instrumentation needed for testing was easily available. In addition to the physicians, two nurses and a resident were involved in our pilot study, but for the test setting a nurse and two physicians (anesthesiologist and ENT specialist) are required. Our protocol with slowly increasing work load was suitable for elderly patients and for those with impaired physical condition. Younger and more athletic patients needed the fast unlimited pedalling step at the end of the test to create the circumstances at which the symptom typically occurs. It is possible to establish a test setting in an ordinary laryngeal outpatient department at the relatively low extra cost of a stationary bicycle, ECG monitor, and FEV1 measuring equipment. However, because the test set-up is based on two physicians and a nurse, and the number of suspected VCD patients is limited, this diagnostic tool is especially suitable for tertiary care units and offices of the academic laryngologists. Our test s benefit in comparison with the test from Heimdal is that it can be performed on the patients in different age groups and physical conditions. In addition, our test set-up is technically less demanding, and space requirements favor an ergometer as compared to a treadmill in the often crowded facilities. Our patients stated that the exercise-induced dyspnea does not appear every time identically, even if the level, mode, and the surroundings of the exercise are the same, in accordance to previous studies. 4 This leads us to the conclusion that most probably no single optimal way to test EIVCD exists, and variations in testing method in different surroundings might be required for this complicated diagnosis. Therefore, in this series, the negative test result did not rule EIVCD out, but the positive result ruled it in. Reproducibility of our test was not tested. Our test set-up is intended for both clinical and research applications. ECG monitoring throughout the test was very informative and important also in the aspect of safety, whereas in blood pressure and breathing rate responses no significant differences between patients and controls occurred. Findings from the study allowed us to simplify the procedure; we no longer measure blood pressure and respiratory rate during the test. The nonsymptomatic short periods of blood oxygen level decreases were most likely due to equipment bias; oxygen level was measured from the fingertip, and the equipment did not always remain optimally in place, especially after sweating. In line with previous studies, EIVCD findings resolved within a few seconds when the exercise slowed or stopped. 7 This confirms the value of direct visualization of the vocal cords during the symptoms in the diagnosis of laryngeal dyspnea. 3,4,6,7,9 On the other hand, the patient s subjective feeling of dyspnea at laryngeal level was not always accurate; six (40%) of the patients who reported subjective laryngeal dyspnea had a wide open larynx visualized simultaneously in fiberoptic videolaryngoscopy. In our series the fiberoptic videolaryngoscope was held manually to maintain optimal positioning. The head piece holding the laryngo-fiberscope used by Heimdal et al. 6 would allow the test to be done with only one physician, but visualization of the vocal cords might sometimes be lost, and the in-place fixed headpiece itself can lead to a panic reaction, especially for patients who can hardly bear the fiberoptic scope alone. Moreover, because our test was performed with a stationary bicycle, patient movement was limited so that the scope could be manually held. It is possible to instruct a nurse on holding the fiberoptic instead of the ENT specialist, who is able to check the test result later from the digital video. A quantitative measurement of glottic narrowing is needed, and we are working further to solve this problem in our future studies. In all five EIVCD patients, the laryngeal signs began with the collapse of the posterior supraglottic structures and aryepiglottic folds, followed by an adduction of the vocal cords. Four other patients, considered highly suspicious of EIVCD, showed similar supraglottic adduction without progression to vocal cord adduction. Staging and the relevance of other laryngeal findings, such as slight adduction of arytenoid cartilages without subjective symptom of dyspnea during the exercise test, still remain challenging; are they presymptoms for EIVCD, prognostic for the later progress to EIVCD, or just normal physiological variants? In line with previous studies, we had a dominance of female patients, and coexisting asthma was diagnosed in almost one half of the patients. 9 Infection can also 1779
5 trigger VCD. 5 Interestingly, we had one male patient with a serologically confirmed pertussis found in one of his family members about 3 months before at the time his own cough and dyspnea symptoms began. Unfortunately, the patient himself was not tested at that time, although his symptoms were evidence for the disease. His laryngeal spasm was induced after forced expiration to the spirometer. Of patients with established EIVCD in our study, 19% (5/27) was a low prevalence. However, the typical symptom of dyspnea appeared only to 15 patients during the test. This result may reflect the limited sensitivity of our test, but perhaps also the difficulties in the diagnosis of dyspnea. It is possible that some of those 12 patients without symptoms during the test could have been diagnosed with a treadmill test or by retesting them with a more individually modified version of our test set-up. Individual modifying means shorter exercise steps (3 minutes) and/or the possibility to pedal with no speed limit and with a lesser load than 120 W/150 W until exhaustion. One should also remember that some of these 12 patients are most likely true negative cases whose symptoms are not induced by exercise, although the feeling of dyspnea is present during physical exercise. Although examined by many physicians specialized in airway problems, those with exercise-induced dyspnea, not being asthma or EIA, often remain without an accurate diagnosis. On the other hand, after we had interviewed all patients referred to us for the exercise test, five (17%) of the 30 had a history of dyspnea that did not quite meet the criteria of EIVCD. However, the exercise test was still administered all the patients referred. These five patients were included in the group of 12 patients whose symptoms were not induced during the test; it seems evident that the test detected no false positive cases. The classification of laryngeal disorders is difficult. Laryngospasm is defined as a spasmodic closure of the glottic aperture or a sudden forceful and abnormal closing of the vocal cords causing sudden brief episodes of dyspnea and stridor. VCD is characterized by involuntary, paradoxical adduction of the vocal cords and false cords typically during inspiration, with closure of the vocal cords maintained sometimes during an entire respiratory cycle. 15 The relationship between VCD and laryngeal spasm is not clear; are they separate conditions or different manifestations of specific laryngeal pathology? However, in EIVCD the trigger of the symptom is physical stress and the patients are otherwise free of symptoms. There has not been a clinically relevant test method for EIVCD before the one introduced by Heimdal et al. 6 Using that method or our test set-up will definitely improve diagnostic accuracy of EIVCD because methods used earlier for diagnostic purposes in EIVCD, such as laryngoscopy after the exercise or spirometry, are far from optimal. Diagnosis of EIVCD requires visualization of the paradoxical movement of the vocal cords during exercise. To verify this, some effort and costs are needed. On the other hand, a better differential diagnostics of dyspnea often saves money and other resources. Moreover, the potentially severe side effects of high-dose corticosteroids and other asthma drugs are avoided Therefore a consultation with an ear, nose, and throat specialist in diagnosing unclear exercise-induced dyspnea is recommended. CONCLUSION Fiberoptic videolaryngoscopy during bicycle ergometry was a well-tolerated and relatively easily established diagnostic tool that induced dyspnea in more than one half the patients examined. If the symptom of dyspnea appeared, the most frequent finding was exerciseinduced vocal cord dysfunction. The test was suitable for a laryngeal outpatient department and applicable to patients of various ages and physical conditions. Acknowledgments The authors thank the staff of the Phoniatric and Laryngological Outpatient Department and ENT Clinic Research Laboratory, especially Tuula Säämänen, Eija Nenye, Leena Juvonen, and Kirsi Käppi for excellent technical assistance and coordination of the study, and acknowledge Sonja Lumme for statistical analysis. BIBLIOGRAPHY 1. Newman K, Mason U, Schmaling K. Clinical features of vocal cord dysfunction. Am J Respir Crit Care Med 1995; 152: Vertigan A, Theodoros D, Gibson P, Winkworth A. The relationship between chronic cough and paradoxical vocal fold movement: a review of the literature. J Voice 2006; 20: Morris M, Deal L, Bean D, Grbach V, Morgan J. Vocal cord dysfunction in patients with exertional dyspnea. Chest 1999;116: Wood R, Milgrom H. Vocal cord dysfunction. J Allergy Clin Immunol 1996;98: Taramarcaz P, Grissel T, Borgas T, Gibson P. Transient postviral vocal cord dysfunction. J Allergy Clin Immunol 2004;114: Heimdal J-H, Roksund O, Halvorsen T, Skadberg B, Olofsson J. Continuous laryngoscopy exercise test: a method for visualizing laryngeal dysfunction during exercise. Laryngoscope 2006;116: Rundell K, Spiering B. Inspiratory stridor in elite athletes. Chest 2003;123: Ayres J, Gabbot P. Vocal cord dysfunction and laryngeal hyperresponsiveness: a function of altered autonomic balance? Thorax 2002;57: Altman K, Mirza N, Ruiz C, Sataloff R. Paradoxical vocal fold motion: presentation and treatment options. J Voice 2000;14: Mutasim A-H, Tannous B, Weinberger M. Exercise-induced dyspnea in children and adolescents: if not asthma then what? Ann Allergy Asthma Immunol 2005;94: Mathers-Schmidt B, Brilla L. Inspiratory muscle training in exercise-induced paradoxical vocal fold motion. J Voice 2005;19: Bent J, Kim J, Wilson J, Miller D, Bauman N, Smith R. Pediatric exercise-induced laryngomalacia. Ann Otol Rhinol Laryngol 1996;105: Global Strategy for Asthma Management and Prevention. Global Initiative for Asthma (GINA); Borg G. Physical Performance and Perceived Exertion. Lund, Sweden: Gleerup; 1962: Andrianopoulos M, Gallivan G, Gallivan H. PVCM, PVCD, EPL, and irritable larynx syndrome. What are we talking about and how do we treat it? J Voice 2000;14:
Why Can t I breathe? Asthma vs. Vocal Cord Dysfunction (VCD) Lindsey Frohn, M.S., CCC-SLP Madonna Rehabilitation Hospital (Lincoln, NE)
 Why Can t I breathe? Asthma vs. Vocal Cord Dysfunction (VCD) Lindsey Frohn, M.S., CCC-SLP Madonna Rehabilitation Hospital (Lincoln, NE) Objectives Examine Vocal Cord Dysfunction Examine Exercise Induced
Why Can t I breathe? Asthma vs. Vocal Cord Dysfunction (VCD) Lindsey Frohn, M.S., CCC-SLP Madonna Rehabilitation Hospital (Lincoln, NE) Objectives Examine Vocal Cord Dysfunction Examine Exercise Induced
Not all who wheeze have asthma
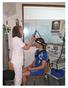 Not all who wheeze have asthma Educational aims Exercise-induced asthma is frequently found among children, adolescents and young adults. The diagnosis of asthma should be documented by variable lung function,
Not all who wheeze have asthma Educational aims Exercise-induced asthma is frequently found among children, adolescents and young adults. The diagnosis of asthma should be documented by variable lung function,
Laryngeal and respiratory patterns in patients with paradoxical vocal fold motion
 Respiratory Medicine (2011) 105, 1891e1895 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Laryngeal and respiratory patterns in patients with paradoxical vocal fold motion
Respiratory Medicine (2011) 105, 1891e1895 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Laryngeal and respiratory patterns in patients with paradoxical vocal fold motion
Exertional dyspnea and inspiratory stridor of 2 years duration: A tale of 2 wheezes
 Maintenance of Certification clinical management series Series editor: James T. Li, MD, PhD Exertional dyspnea and inspiratory stridor of 2 years duration: A tale of 2 wheezes Kaiser Lim, MD, a,b and James
Maintenance of Certification clinical management series Series editor: James T. Li, MD, PhD Exertional dyspnea and inspiratory stridor of 2 years duration: A tale of 2 wheezes Kaiser Lim, MD, a,b and James
Exercise induced laryngeal obstruction: a review of diagnosis and management
 Eur Arch Otorhinolaryngol (2017) 274:1781 1789 DOI 10.1007/s00405-016-4338-1 REVIEW ARTICLE Exercise induced laryngeal obstruction: a review of diagnosis and management Savinda Liyanagedara 1 Robert McLeod
Eur Arch Otorhinolaryngol (2017) 274:1781 1789 DOI 10.1007/s00405-016-4338-1 REVIEW ARTICLE Exercise induced laryngeal obstruction: a review of diagnosis and management Savinda Liyanagedara 1 Robert McLeod
Laryngospasm and Asthma
 Variable Presentations of Laryngospasm Thomas Murry, PhD Lucian Sulica, MD Lowell Gurey, MD Weill Cornell Medical College New York, New York Variable Presentations of Laryngospasm Laryngospasm: Sudden-onset,
Variable Presentations of Laryngospasm Thomas Murry, PhD Lucian Sulica, MD Lowell Gurey, MD Weill Cornell Medical College New York, New York Variable Presentations of Laryngospasm Laryngospasm: Sudden-onset,
VCD and Asthma: SLP Perspective. Jeff Searl, Ph.D., CCC-SLP Department of Communicative Sciences & Disorders Michigan State University
 VCD and Asthma: SLP Perspective Jeff Searl, Ph.D., CCC-SLP Department of Communicative Sciences & Disorders Michigan State University The Name Issue 1983 Vocal Cord Dysfunction (VCD) coined by Christopher
VCD and Asthma: SLP Perspective Jeff Searl, Ph.D., CCC-SLP Department of Communicative Sciences & Disorders Michigan State University The Name Issue 1983 Vocal Cord Dysfunction (VCD) coined by Christopher
Patient Information Series
 A M E R I C A N T H O R A C I C S O C I E T Y Patient Information Series What Is Vocal Cord Dysfunction (VCD)? Vocal Cord Dysfunction means that your vocal cords do not act normally. With VCD, instead
A M E R I C A N T H O R A C I C S O C I E T Y Patient Information Series What Is Vocal Cord Dysfunction (VCD)? Vocal Cord Dysfunction means that your vocal cords do not act normally. With VCD, instead
Symptoms & Treatment of Vocal Cord Dysfunction / Paradoxical Vocal Fold Motion
 Symptoms & Treatment of Vocal Cord Dysfunction / Paradoxical Vocal Fold Motion Florence B. Blager, Ph.D., CCC-SLP Professor Emeritus Department of Otolaryngology University of Colorado Denver and Department
Symptoms & Treatment of Vocal Cord Dysfunction / Paradoxical Vocal Fold Motion Florence B. Blager, Ph.D., CCC-SLP Professor Emeritus Department of Otolaryngology University of Colorado Denver and Department
Does Treatment of Paradoxical Vocal Fold Movement Disorder Decrease Asthma Medication Use?
 The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Does Treatment of Paradoxical Vocal Fold Movement Disorder Decrease Asthma Medication Use? Scott Kramer,
The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Does Treatment of Paradoxical Vocal Fold Movement Disorder Decrease Asthma Medication Use? Scott Kramer,
Anatomy and Physiology
 Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Letters to the Editor
 Letters to the Editor Masqueraders of exercise-induced vocal cord dysfunction To the Editor: Vocal cord dysfunction (VCD) is well known to asthma specialists as a masquerader of asthma that should be considered
Letters to the Editor Masqueraders of exercise-induced vocal cord dysfunction To the Editor: Vocal cord dysfunction (VCD) is well known to asthma specialists as a masquerader of asthma that should be considered
Anita Gheller-Rigoni, DO, FACAAI Allergist-Immunologist. Exercise-Induced Vocal Cord Dysfunction
 Anita Gheller-Rigoni, DO, FACAAI Allergist-Immunologist Exercise-Induced Vocal Cord Dysfunction Objectives 1. Understand the concept of vocal cord dysfunction 2. Recognize the difference between exercised
Anita Gheller-Rigoni, DO, FACAAI Allergist-Immunologist Exercise-Induced Vocal Cord Dysfunction Objectives 1. Understand the concept of vocal cord dysfunction 2. Recognize the difference between exercised
L.J. Hoeve and R.H.M. van Poppelen * (Received 12 July 1989) (Accepted 10 August 1989)
 International Journal of Pediatric Otorhinolaryngolo~. 18 (1990) 241-245 Elsevier 241 PEDOT 00617 Fiberoptic laryngoscopy under in neonates general anesthesia L.J. Hoeve and R.H.M. van Poppelen * Lkpar?ments
International Journal of Pediatric Otorhinolaryngolo~. 18 (1990) 241-245 Elsevier 241 PEDOT 00617 Fiberoptic laryngoscopy under in neonates general anesthesia L.J. Hoeve and R.H.M. van Poppelen * Lkpar?ments
Paradoxical Vocal Fold Motion Disorder in the Elite Athlete: Experience at a Large Division I University
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Paradoxical Vocal Fold Motion Disorder in the Elite Athlete: Experience at a Large Division I University
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Paradoxical Vocal Fold Motion Disorder in the Elite Athlete: Experience at a Large Division I University
Association of breathing sound spectra with glottal dimensions in exercise-induced vocal cord dysfunction
 https://helda.helsinki.fi Association of breathing sound spectra with glottal dimensions in exercise-induced vocal cord dysfunction Geneid, Ahmed 2017-11 Geneid, A, Aaltonen, L -M, Porra, L, Peltonen,
https://helda.helsinki.fi Association of breathing sound spectra with glottal dimensions in exercise-induced vocal cord dysfunction Geneid, Ahmed 2017-11 Geneid, A, Aaltonen, L -M, Porra, L, Peltonen,
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing
 Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Afferent nerves, interactions of, in cough, 20 21 Airway, eosinophilic inflammation of, 124 narrowing of, in asthma, 126 protection of, terms
Note: Page numbers of article titles are in boldface type. A Afferent nerves, interactions of, in cough, 20 21 Airway, eosinophilic inflammation of, 124 narrowing of, in asthma, 126 protection of, terms
Vocal cord dysfunction: Beyond severe asthma
 Respiratory Medicine (2010) 104, 504e509 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Vocal cord dysfunction: Beyond severe asthma Jonathan P. Parsons a, *, Cathy Benninger
Respiratory Medicine (2010) 104, 504e509 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Vocal cord dysfunction: Beyond severe asthma Jonathan P. Parsons a, *, Cathy Benninger
S P I R O M E T R Y. Objectives. Objectives 2/5/2019
 S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
Evaluating dyspnea: A practical approach -- When to consider cardiopulmonary exercise testing.
 Evaluating dyspnea: A practical approach -- When to consider cardiopulmonary exercise testing. ABSTRACT: Shortness of breath is a common complaint associated with a number of conditions. Although the results
Evaluating dyspnea: A practical approach -- When to consider cardiopulmonary exercise testing. ABSTRACT: Shortness of breath is a common complaint associated with a number of conditions. Although the results
DIFFICULT ASTHMA. Dr. Prathyusha Dr. S.Balasubramanian KKCTH
 DIFFICULT ASTHMA Dr. Prathyusha Dr. S.Balasubramanian KKCTH CASE SUMMARY 11 yr old girl, Neyveli Treated as moderate persistent asthma x 5 years On Seroflo [ LABA + steroid ] 250 2 puffs BD and intermittent
DIFFICULT ASTHMA Dr. Prathyusha Dr. S.Balasubramanian KKCTH CASE SUMMARY 11 yr old girl, Neyveli Treated as moderate persistent asthma x 5 years On Seroflo [ LABA + steroid ] 250 2 puffs BD and intermittent
Exercise-induced laryngeal obstruction: natural history and evect of surgical treatment
 Eur Arch Otorhinolaryngol (2011) 268:1485 1492 DOI 10.1007/s00405-011-1656-1 LARYNGOLOGY Exercise-induced laryngeal obstruction: natural history and evect of surgical treatment Robert Christiaan Maat Magnus
Eur Arch Otorhinolaryngol (2011) 268:1485 1492 DOI 10.1007/s00405-011-1656-1 LARYNGOLOGY Exercise-induced laryngeal obstruction: natural history and evect of surgical treatment Robert Christiaan Maat Magnus
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
Respiratory Compromise and Swallowing
 Speech Pathology and Respiratory Care April 11, 2013 By Angela Parcaro-Tucker, MA, CCC-SLP, LSVT How can Speech Therapy help? 1 Respiratory Compromise and Swallowing Swallowing is a complex sequence of
Speech Pathology and Respiratory Care April 11, 2013 By Angela Parcaro-Tucker, MA, CCC-SLP, LSVT How can Speech Therapy help? 1 Respiratory Compromise and Swallowing Swallowing is a complex sequence of
Vocal cord dysfunction
 Key points VCD is an increasingly recognised co-existing feature in asthmatics. VCD may arise from an alteration in the autonomic balance between the glottis and central control areas, with potential aggravation
Key points VCD is an increasingly recognised co-existing feature in asthmatics. VCD may arise from an alteration in the autonomic balance between the glottis and central control areas, with potential aggravation
What do pulmonary function tests tell you?
 Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Asthma and Vocal Cord Dysfunction
 Asthma and Vocal Cord Dysfunction Amy L. Marks DO, FACOP Pediatric Allergy and Immunology Assistant Professor of Pediatrics Oakland University William Beaumont School of Medicine Objectives: Understanding
Asthma and Vocal Cord Dysfunction Amy L. Marks DO, FACOP Pediatric Allergy and Immunology Assistant Professor of Pediatrics Oakland University William Beaumont School of Medicine Objectives: Understanding
Dynamic CT evaluation and follow up of adult patients with suspected vocal cord dysfunction
 Dynamic CT evaluation and follow up of adult patients with suspected vocal cord dysfunction Poster No.: C-0935 Congress: ECR 2010 Type: Scientific Exhibit Topic: Chest Authors: K. K. Lau; Melbourne, Victoria/AU
Dynamic CT evaluation and follow up of adult patients with suspected vocal cord dysfunction Poster No.: C-0935 Congress: ECR 2010 Type: Scientific Exhibit Topic: Chest Authors: K. K. Lau; Melbourne, Victoria/AU
Procedures/Risks: pulmonology, sleep, critical care
 Procedures/Risks: pulmonology, sleep, critical care Bronchoscopy (and bronchoaveolar lavage) Purpose: The purpose of the bronchoscopy is to collect cells and fluid from the lung, so that information can
Procedures/Risks: pulmonology, sleep, critical care Bronchoscopy (and bronchoaveolar lavage) Purpose: The purpose of the bronchoscopy is to collect cells and fluid from the lung, so that information can
ABCs of VCD DEFINITION. Incidence of VCD. Outline VCD TERMINOLOGY. VCD: Early Reports
 Outline ABCs of VCD Rohit Katial, MD, FAAAAI, FACP Professor of Medicine Program Director, Allergy & Immunology Director, Weinberg Clinical Research Unit Director, A/I Clinical Services Definition Demographics
Outline ABCs of VCD Rohit Katial, MD, FAAAAI, FACP Professor of Medicine Program Director, Allergy & Immunology Director, Weinberg Clinical Research Unit Director, A/I Clinical Services Definition Demographics
Spirometry: FEVER DISEASE DIABETES HOW RELIABLE IS THIS? 9/2/2010 BUT WHAT WE PRACTICE: Spirometers are objective tools
 SPIROMETRY PRINCIPLES, PROCEDURE AND QA Spirometry: Dr. Rahul Kodgule CHEST RESEARCH FOUNDATION, PUNE FEVER ISCHAEMIC HEART DISEASE DIABETES BUT WHAT WE PRACTICE: Spirometers are objective tools to diagnose
SPIROMETRY PRINCIPLES, PROCEDURE AND QA Spirometry: Dr. Rahul Kodgule CHEST RESEARCH FOUNDATION, PUNE FEVER ISCHAEMIC HEART DISEASE DIABETES BUT WHAT WE PRACTICE: Spirometers are objective tools to diagnose
Vocal cord dysfunction (VCD),
 One Hundred Case Series of in a Military Treatment Facility Clifford Nolt, MD; Michael Ott, MD; Ryann Ennis, MA, CCC-SLP; and Jose Roman, MD The authors evaluation of vocal cord dysfunction cases reveals
One Hundred Case Series of in a Military Treatment Facility Clifford Nolt, MD; Michael Ott, MD; Ryann Ennis, MA, CCC-SLP; and Jose Roman, MD The authors evaluation of vocal cord dysfunction cases reveals
Discordant Symptoms Simplified. Kristy T. Duggan, MD November 2, 2017 ACP Oregon Chapter Meeting Salem, OR
 Discordant Symptoms Simplified Kristy T. Duggan, MD November 2, 2017 ACP Oregon Chapter Meeting Salem, OR Once upon a time I can t breathe! Over the last week Difficulty breathing Happens randomly (rest/exertion)
Discordant Symptoms Simplified Kristy T. Duggan, MD November 2, 2017 ACP Oregon Chapter Meeting Salem, OR Once upon a time I can t breathe! Over the last week Difficulty breathing Happens randomly (rest/exertion)
The Validity and Reliability of the Reflux Finding Score (RFS)
 The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. The Validity and Reliability of the Reflux Finding Score (RFS)
The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. The Validity and Reliability of the Reflux Finding Score (RFS)
LUNG FUNCTION TESTING: SPIROMETRY AND MORE
 LUNG FUNCTION TESTING: SPIROMETRY AND MORE OBJECTIVES 1. To describe other lung function testing for toddlers and those who cannot perform spirometry 2. To describe a lung function test on infants 3. To
LUNG FUNCTION TESTING: SPIROMETRY AND MORE OBJECTIVES 1. To describe other lung function testing for toddlers and those who cannot perform spirometry 2. To describe a lung function test on infants 3. To
S P I R O M E T R Y. Objectives. Objectives 3/12/2018
 S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
Dear Professor Schmid-Grendelmeier (EAACI Vice President Education & Specialty),
 28 May 2017 Subject: EAACI Allergopharma Award, Final Report Dear Professor Schmid-Grendelmeier (EAACI Vice President Education & Specialty), I am very honoured and grateful to have received the EAACI-Allergopharma
28 May 2017 Subject: EAACI Allergopharma Award, Final Report Dear Professor Schmid-Grendelmeier (EAACI Vice President Education & Specialty), I am very honoured and grateful to have received the EAACI-Allergopharma
A NEW WAY TO DIAGNOSE BREATHING PROBLEMS
 A NEW WAY TO DIAGNOSE BREATHING PROBLEMS Breathing problems are the second most common cause of poor performance in racehorses. The nasal passages and throat (pharynx and larynx) in their simplest form
A NEW WAY TO DIAGNOSE BREATHING PROBLEMS Breathing problems are the second most common cause of poor performance in racehorses. The nasal passages and throat (pharynx and larynx) in their simplest form
Exercise-induced laryngeal obstruction
 Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Medicine 1300 Exercise-induced laryngeal obstruction Prevalence, laryngeal findings and evaluation of treatment KATARINA NORLANDER
Digital Comprehensive Summaries of Uppsala Dissertations from the Faculty of Medicine 1300 Exercise-induced laryngeal obstruction Prevalence, laryngeal findings and evaluation of treatment KATARINA NORLANDER
Laryngoscopy Examinations
 Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Asthma Management for the Athlete
 Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Objectives. Phil Slocum, D.O. FCCP, FACOI, FCCM, FACP Professor of Medicine. All that wheezes (or has intermittent dyspnea) is not asthma
 * Phil Slocum, D.O. FCCP, FACOI, FCCM, FACP Professor of Medicine Objectives All that wheezes (or has intermittent dyspnea) is not asthma Ockham's Razor does not work in evaluating patients with shortness
* Phil Slocum, D.O. FCCP, FACOI, FCCM, FACP Professor of Medicine Objectives All that wheezes (or has intermittent dyspnea) is not asthma Ockham's Razor does not work in evaluating patients with shortness
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Appendix (i) The ABCDE approach to the sick patient
 Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
The Paediatric Voice Clinic
 The Paediatric Voice Clinic Smillie I 1, McManus K 1, Cohen W 2, Wynne D1. Department of Paediatric Otolaryngology, Royal Hospital for Sick Children, Glasgow. 2 School of Psychological Sciences and Health,
The Paediatric Voice Clinic Smillie I 1, McManus K 1, Cohen W 2, Wynne D1. Department of Paediatric Otolaryngology, Royal Hospital for Sick Children, Glasgow. 2 School of Psychological Sciences and Health,
Office Based Spirometry
 Osteopathic Family Physician (2014)1, 14-18 Scott Klosterman, DO; Woodson Crenshaw, OMS4 Spartanburg Regional Family Medicine Residency Program; Edward Via College of Osteopathic Medicine - Virginia Campus
Osteopathic Family Physician (2014)1, 14-18 Scott Klosterman, DO; Woodson Crenshaw, OMS4 Spartanburg Regional Family Medicine Residency Program; Edward Via College of Osteopathic Medicine - Virginia Campus
Vocal Cord Dysfunction The Great Masquerader
 Vocal Cord Dysfunction The Great Masquerader Dr. Mary Noseworthy MD FRCPC Pediatric Respirologist Alberta health Service Clinical Assistant Professor University of Calgary Asthma and Home Oxygen Clinical
Vocal Cord Dysfunction The Great Masquerader Dr. Mary Noseworthy MD FRCPC Pediatric Respirologist Alberta health Service Clinical Assistant Professor University of Calgary Asthma and Home Oxygen Clinical
PARADOXICAL T V C D. ANTONIO (T) YSUNZA M.D. Ph.D. BEAUMONT ROYAL OAK
 PARADOXICAL T V C D ANTONIO (T) YSUNZA M.D. Ph.D. BEAUMONT ROYAL OAK GOALS P T V C D: WHAT IS IT? DIAGNOSIS DIFFERENTIAL DIAGNOSIS PATHOPHYSIOLOGY TREATMENT ACUTE TREATMENT LONG TERM MUNCHAUSEN STRIDOR
PARADOXICAL T V C D ANTONIO (T) YSUNZA M.D. Ph.D. BEAUMONT ROYAL OAK GOALS P T V C D: WHAT IS IT? DIAGNOSIS DIFFERENTIAL DIAGNOSIS PATHOPHYSIOLOGY TREATMENT ACUTE TREATMENT LONG TERM MUNCHAUSEN STRIDOR
Breathing and pulmonary function
 EXPERIMENTAL PHYSIOLOGY EXPERIMENT 5 Breathing and pulmonary function Ying-ying Chen, PhD Dept. of Physiology, Zhejiang University School of Medicine bchenyy@zju.edu.cn Breathing Exercise 1: Tests of pulmonary
EXPERIMENTAL PHYSIOLOGY EXPERIMENT 5 Breathing and pulmonary function Ying-ying Chen, PhD Dept. of Physiology, Zhejiang University School of Medicine bchenyy@zju.edu.cn Breathing Exercise 1: Tests of pulmonary
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery. By: Lillian Han
 Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Paradoxical Vocal Fold Motion (Vocal Cord Dysfunction)
 Paradoxical Vocal Fold Motion (Vocal Cord Dysfunction) Evaluation and Treatment Christina Kang, MM, MS, CCC-SLP Association of Asthma Educators July 21, 2018 2016 MFMER slide-1 Disclosure Relevant financial
Paradoxical Vocal Fold Motion (Vocal Cord Dysfunction) Evaluation and Treatment Christina Kang, MM, MS, CCC-SLP Association of Asthma Educators July 21, 2018 2016 MFMER slide-1 Disclosure Relevant financial
Wheeze. Dr Jo Harrison
 Wheeze Dr Jo Harrison 9.9.14 Wheeze - Physiology a continuous musical sound that lasts longer than 250 msec. can be high-pitched or low-pitched, consist of single or multiple notes, and occur during inspiration
Wheeze Dr Jo Harrison 9.9.14 Wheeze - Physiology a continuous musical sound that lasts longer than 250 msec. can be high-pitched or low-pitched, consist of single or multiple notes, and occur during inspiration
Supplementary Online Content
 Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Validity and reliability of grade scoring in the diagnosis of exercise-induced laryngeal obstruction
 ORIGINAL ARTICLE EILO Validity and reliability of grade scoring in the diagnosis of exercise-induced laryngeal obstruction Emil Schwarz Walsted 1,2, James H. Hull 2, Jeppe Hvedstrup 1, Robert Christiaan
ORIGINAL ARTICLE EILO Validity and reliability of grade scoring in the diagnosis of exercise-induced laryngeal obstruction Emil Schwarz Walsted 1,2, James H. Hull 2, Jeppe Hvedstrup 1, Robert Christiaan
Vocal cord dysfunction: a functional cause of respiratory distress
 Miles Weinberger 1,2, Devang Doshi 3 miles-weinberger@uiowa.edu 1 University of Iowa, Iowa City, IA, USA. 2 Rady Children s Hospital, University of California, San Diego, CA, USA. 3 Oakland University,
Miles Weinberger 1,2, Devang Doshi 3 miles-weinberger@uiowa.edu 1 University of Iowa, Iowa City, IA, USA. 2 Rady Children s Hospital, University of California, San Diego, CA, USA. 3 Oakland University,
Anatomy & Physiology 2 Canale. Respiratory System: Exchange of Gases
 Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Anyone who smokes and/or has shortness of breath and sputum production could have COPD
 COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM
 CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
Chronic Cough. Dr Peter George Consultant Respiratory Physician Royal Brompton and Harefield Hospitals
 Chronic Cough Dr Peter George Consultant Respiratory Physician Royal Brompton and Harefield Hospitals Overview Common causes of chronic cough Important diagnoses not to miss How to investigate a cough
Chronic Cough Dr Peter George Consultant Respiratory Physician Royal Brompton and Harefield Hospitals Overview Common causes of chronic cough Important diagnoses not to miss How to investigate a cough
Play acting Asthma attack
 1 ASTHMA Date: 16/10/06 By: ismile Health Info Inforeach Communications Sdn Bhd. Tel: 03-42946368 You cough, wheeze and feel tightness in your chest. Suddenly, your airways narrow and you gasp for breath.
1 ASTHMA Date: 16/10/06 By: ismile Health Info Inforeach Communications Sdn Bhd. Tel: 03-42946368 You cough, wheeze and feel tightness in your chest. Suddenly, your airways narrow and you gasp for breath.
MSRC AIR Course Karla Stoermer Grossman, MSA, BSN, RN, AE-C
 MSRC AIR Course Karla Stoermer Grossman, MSA, BSN, RN, AE-C Explain the importance of objective measures in the management of asthma Explain the different types of objective measures used in the management
MSRC AIR Course Karla Stoermer Grossman, MSA, BSN, RN, AE-C Explain the importance of objective measures in the management of asthma Explain the different types of objective measures used in the management
CLINICAL SIGNIFICANCE OF PULMONARY FUNCTION TESTS
 CLINICAL SIGNIFICANCE OF PULMONARY FUNCTION TESTS Upper Airway Obstruction* John C. Acres, M.D., and Meir H. Kryger, M.D.t chronic upper airway obstruction is frequently unrecognized or misdiagnosed as
CLINICAL SIGNIFICANCE OF PULMONARY FUNCTION TESTS Upper Airway Obstruction* John C. Acres, M.D., and Meir H. Kryger, M.D.t chronic upper airway obstruction is frequently unrecognized or misdiagnosed as
Meenu Singh, Joseph L. Mathew, Prabhjot Malhi, B.R. Srinivas and Lata Kumar
 Comparison of Improvement in Quality of Life Score with Objective Parameters of Pulmonary Function in Indian Asthmatic Children Receiving Inhaled Corticosteroid Therapy Meenu Singh, Joseph L. Mathew, Prabhjot
Comparison of Improvement in Quality of Life Score with Objective Parameters of Pulmonary Function in Indian Asthmatic Children Receiving Inhaled Corticosteroid Therapy Meenu Singh, Joseph L. Mathew, Prabhjot
Lung Disease and Your Throat
 Lung Disease and Your Throat Presented by Beth Causa Speech Pathologist Wollongong Speech Pathology With sincere thanks to Kate Baumwol Speech Pathologist, Western Health (Perth) For sharing the contents
Lung Disease and Your Throat Presented by Beth Causa Speech Pathologist Wollongong Speech Pathology With sincere thanks to Kate Baumwol Speech Pathologist, Western Health (Perth) For sharing the contents
+ Asthma and Athletics
 + Asthma and Athletics Shaylon Rettig, MD, MBA Champion Sports Medicine + Financial Disclosure Dr. Shaylon Rettig has no relevant financial relationships with commercial interests to disclose. + Asthma
+ Asthma and Athletics Shaylon Rettig, MD, MBA Champion Sports Medicine + Financial Disclosure Dr. Shaylon Rettig has no relevant financial relationships with commercial interests to disclose. + Asthma
Continuous laryngoscopy quantitates laryngeal behaviour in exercise and recovery
 ERJ Express. Published on July, 6 as doi:.8/99.6-6 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Continuous laryngoscopy quantitates laryngeal behaviour in exercise and recovery J. Tod Olin, Matthew S. Clary,
ERJ Express. Published on July, 6 as doi:.8/99.6-6 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Continuous laryngoscopy quantitates laryngeal behaviour in exercise and recovery J. Tod Olin, Matthew S. Clary,
Physiology lab (RS) First : Spirometry. ** Objectives :-
 Physiology lab (RS) ** Objectives :- 1. Spirometry in general. 2. Spirogram (volumes and capacities). 3. The importance of vital capacity in diagnosis. 4. Flow volume loop. 5. Miss Arwa s part (the practical
Physiology lab (RS) ** Objectives :- 1. Spirometry in general. 2. Spirogram (volumes and capacities). 3. The importance of vital capacity in diagnosis. 4. Flow volume loop. 5. Miss Arwa s part (the practical
Chapter 11 The Respiratory System
 Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
B Unit III Notes 6, 7 and 8
 The Respiratory System Why do we breathe? B. 2201 Unit III Notes 6, 7 and 8 Respiratory System We know that our cells respire to produce ATP (energy). All organisms need energy to live, so that s why we
The Respiratory System Why do we breathe? B. 2201 Unit III Notes 6, 7 and 8 Respiratory System We know that our cells respire to produce ATP (energy). All organisms need energy to live, so that s why we
Inducible laryngeal obstruction: an official joint European Respiratory Society and European Laryngological Society statement
 TASK FORCE REPORT ERS/ELS STATEMENT Inducible laryngeal obstruction: an official joint European Respiratory Society and European Laryngological Society statement Thomas Halvorsen 1, Emil Schwarz Walsted
TASK FORCE REPORT ERS/ELS STATEMENT Inducible laryngeal obstruction: an official joint European Respiratory Society and European Laryngological Society statement Thomas Halvorsen 1, Emil Schwarz Walsted
Patient Resources: Syncope
 Patient Resources: Syncope Overview Syncope is the medical term for fainting or loss of consciousness. Fainting can occur for a few different reasons. The autonomic (involuntary) nervous system helps to
Patient Resources: Syncope Overview Syncope is the medical term for fainting or loss of consciousness. Fainting can occur for a few different reasons. The autonomic (involuntary) nervous system helps to
Pediatric Endoscopic Airway Management With Posterior Cricoid Rib Grafting
 The Laryngoscope VC 2011 The American Laryngological, Rhinological and Otological Society, Inc. Pediatric Endoscopic Airway Management With Posterior Cricoid Rib Grafting Matthew J. Provenzano, MD; Stephanie
The Laryngoscope VC 2011 The American Laryngological, Rhinological and Otological Society, Inc. Pediatric Endoscopic Airway Management With Posterior Cricoid Rib Grafting Matthew J. Provenzano, MD; Stephanie
Unilateral Supraglottoplasty for Severe Laryngomalacia in Children. Nasser A Fageeh, MD, FRCSC, FACS*
 Bahrain Medical Bulletin, Vol. 37, No. 1, March 2015 Unilateral Supraglottoplasty for Severe Laryngomalacia in Children Nasser A Fageeh, MD, FRCSC, FACS* Objective: To study the efficacy of Unilateral
Bahrain Medical Bulletin, Vol. 37, No. 1, March 2015 Unilateral Supraglottoplasty for Severe Laryngomalacia in Children Nasser A Fageeh, MD, FRCSC, FACS* Objective: To study the efficacy of Unilateral
Financial Disclosure. Exercise Induced Bronchospasm BHR. Exercise Induced Asthma
 Financial Disclosure Exercise Induced Bronchospasm Elizabeth Bailey MSN, CRNP Allergy & Asthma Specialists BREATHE II March, 23, 2012 I have no commercial conflicts of interest and no financial relationships
Financial Disclosure Exercise Induced Bronchospasm Elizabeth Bailey MSN, CRNP Allergy & Asthma Specialists BREATHE II March, 23, 2012 I have no commercial conflicts of interest and no financial relationships
The VCDQ a Questionnaire for Symptom Monitoring in Vocal Cord Dysfunction
 Article The VCDQ a Questionnaire for Symptom Monitoring in Vocal Cord Dysfunction Fowler, Stephen J., Thurston, Andrew, Chesworth, Brigit, Cheng, Vinton, Constantinou, Panayiotis, Vyas, Aashish, Lillie,
Article The VCDQ a Questionnaire for Symptom Monitoring in Vocal Cord Dysfunction Fowler, Stephen J., Thurston, Andrew, Chesworth, Brigit, Cheng, Vinton, Constantinou, Panayiotis, Vyas, Aashish, Lillie,
Reference Guide for Group Education
 A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 1 Introduction to Living Well with COPD Education Program Participants Expectations Towards the Program Health in COPD
A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 1 Introduction to Living Well with COPD Education Program Participants Expectations Towards the Program Health in COPD
Spirometry and Flow Volume Measurements
 Spirometry and Flow Volume Measurements Standards & Guidelines December 1998 To serve the public and guide the medical profession Revision Dates: December 1998 Approval Date: June 1998 Originating Committee:
Spirometry and Flow Volume Measurements Standards & Guidelines December 1998 To serve the public and guide the medical profession Revision Dates: December 1998 Approval Date: June 1998 Originating Committee:
I Can t Breathe! Physiology and Evaluation of the Dyspneic Patient. Christopher Parker, MD Pulmonology, Norman Regional Health Systems
 I Can t Breathe! Physiology and Evaluation of the Dyspneic Patient Christopher Parker, MD Pulmonology, Norman Regional Health Systems Photo by James Heilman, MD / CC BY-SA 3.0 Disclosures No Financial
I Can t Breathe! Physiology and Evaluation of the Dyspneic Patient Christopher Parker, MD Pulmonology, Norman Regional Health Systems Photo by James Heilman, MD / CC BY-SA 3.0 Disclosures No Financial
Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant. Tara Brennan, MD 2,3
 Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant Tara Brennan, MD 2,3 Jeffrey C. Rastatter, MD, FAAP 1,2 1 Department of Otolaryngology, Northwestern
Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant Tara Brennan, MD 2,3 Jeffrey C. Rastatter, MD, FAAP 1,2 1 Department of Otolaryngology, Northwestern
Sleep Apnea. What is sleep apnea? How does it occur? What are the symptoms?
 What is sleep apnea? Sleep Apnea Sleep apnea is a serious sleep problem. If you have it, you stop breathing for more than 10 seconds at a time many times while you sleep. Another term for this problem
What is sleep apnea? Sleep Apnea Sleep apnea is a serious sleep problem. If you have it, you stop breathing for more than 10 seconds at a time many times while you sleep. Another term for this problem
The Respiratory System
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 14 The Respiratory System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 14 The Respiratory System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
ASTHMA CARE FOR CHILDREN BASKET OF CARE SUBCOMMITTEE Report to: Minnesota Department of Health. June 22, 2009
 This document is made available electronically by the Minnesota Legislative Reference Library as part of an ongoing digital archiving project. http://www.leg.state.mn.us/lrl/lrl.asp ASTHMA CARE FOR CHILDREN
This document is made available electronically by the Minnesota Legislative Reference Library as part of an ongoing digital archiving project. http://www.leg.state.mn.us/lrl/lrl.asp ASTHMA CARE FOR CHILDREN
behaviour are out of scope of the present review.
 explained about the test, a trial may be done before recording the results. The maneuver consists initially of normal tidal breathing. The subject then inhales to maximally fill the lungs. This is followed
explained about the test, a trial may be done before recording the results. The maneuver consists initially of normal tidal breathing. The subject then inhales to maximally fill the lungs. This is followed
Contents. Part A Clinical Evaluation of Laryngeal Disorders. 3 Videostroboscopy and Dynamic Voice Evaluation with Flexible Laryngoscopy...
 Contents Part A Clinical Evaluation of Laryngeal Disorders 1 Anatomy and Physiology of the Larynx....... 3 1.1 Anatomy.................................. 3 1.1.1 Laryngeal Cartilages........................
Contents Part A Clinical Evaluation of Laryngeal Disorders 1 Anatomy and Physiology of the Larynx....... 3 1.1 Anatomy.................................. 3 1.1.1 Laryngeal Cartilages........................
Some Facts About Asthma
 Some Facts About Asthma Contents What is asthma? Diagnosing asthma Asthma symptoms Asthma triggers Thanks What is asthma?? Asthma is a chronic lung-disease that inflames and narrows the airways (tubes
Some Facts About Asthma Contents What is asthma? Diagnosing asthma Asthma symptoms Asthma triggers Thanks What is asthma?? Asthma is a chronic lung-disease that inflames and narrows the airways (tubes
NOTE: The first appearance of terms in bold in the body of this document (except titles) are defined terms please refer to the Definitions section.
 TITLE SCOPE Provincial APPROVAL AUTHORITY Clinical Operations Executive Committee SPONSOR Pharmacy Services PARENT DOCUMENT TITLE, TYPE AND NUMBER Not applicable DOCUMENT # INITIAL EFFECTIVE DATE REVISION
TITLE SCOPE Provincial APPROVAL AUTHORITY Clinical Operations Executive Committee SPONSOR Pharmacy Services PARENT DOCUMENT TITLE, TYPE AND NUMBER Not applicable DOCUMENT # INITIAL EFFECTIVE DATE REVISION
Respiratory System. Chapter 9
 Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
IAEM Clinical Guideline 9 Laryngomalacia. Version 1 September, Author: Dr Farah Mustafa
 IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
IAEM Clinical Guideline 9 Laryngomalacia Version 1 September, 2016 Author: Dr Farah Mustafa Guideline lead: Dr Áine Mitchell, in collaboration with IAEM Clinical Guideline committee and Our Lady s Children
The Respiratory System Structures of the Respiratory System Structures of the Respiratory System Structures of the Respiratory System Nose Sinuses
 CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
Diagnosis. you have asthma? Get the answers. Your Asthma Basics series: Asthma Basics #1. Diagnosis Triggers Medications Kids
 Diagnosis Asthma Basics #1 Your Asthma Basics series: 1 2 3 Diagnosis Triggers Medications Kids Supported by unrestricted educational grants from: For more information from the Asthma Society of Canada:
Diagnosis Asthma Basics #1 Your Asthma Basics series: 1 2 3 Diagnosis Triggers Medications Kids Supported by unrestricted educational grants from: For more information from the Asthma Society of Canada:
In case of an urgent concern or emergency, call 911 or go to the nearest emergency department right away.
 Asthma Basics Patient and Family Education This teaching sheet contains general information only. Talk with your child s doctor or a member of your child s healthcare team about specific care of your child.
Asthma Basics Patient and Family Education This teaching sheet contains general information only. Talk with your child s doctor or a member of your child s healthcare team about specific care of your child.
Aeroallergens/Irritants and Vocal Cord Disorder Saturday, 08 October :48 - Last Updated Saturday, 08 October :44
 Aeroallergens/irritants effects on the respiratory system - Vocal Cord Dysfunction (VCD) Loss of voice with shortness of breath By Dr Sharyn Martin PhD The previous article dealt with the effects of aeroallergens/irritants
Aeroallergens/irritants effects on the respiratory system - Vocal Cord Dysfunction (VCD) Loss of voice with shortness of breath By Dr Sharyn Martin PhD The previous article dealt with the effects of aeroallergens/irritants
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
People with asthma who smoke. The combination of asthma, a chronic airway disease, and smoking increases the risk of COPD even more.
 COPD Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
COPD Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
Chronic Obstructive Pulmonary Disease (COPD) is a systematic disease with
 Chronic Obstructive Pulmonary Disease (COPD) is a systematic disease with considerable impact on several dimensions of daily life. Those that suffer from COPD can be submitted to rehabilitation programmes.
Chronic Obstructive Pulmonary Disease (COPD) is a systematic disease with considerable impact on several dimensions of daily life. Those that suffer from COPD can be submitted to rehabilitation programmes.
Performing a Methacholine Challenge Test
 powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
Date of Assessment: Assessed By: Questionnaire: Assessing Student Readiness to Self- Carry
 Student Name: Score: Date of Assessment: Assessed By: naire: Assessing Student Readiness to Self- Carry Having immediate access to quick- relief medicine is critical for people with asthma. The purpose
Student Name: Score: Date of Assessment: Assessed By: naire: Assessing Student Readiness to Self- Carry Having immediate access to quick- relief medicine is critical for people with asthma. The purpose
NON-SPECIFIC BRONCHIAL HYPERESPONSIVENESS. J. Sastre. Allergy Service
 NON-SPECIFIC BRONCHIAL HYPERESPONSIVENESS J. Sastre. Allergy Service Asthma: definition Asthma is a syndrome defined on basis of three main aspects: 1- Symptoms due to variable and reversible airway obstruction
NON-SPECIFIC BRONCHIAL HYPERESPONSIVENESS J. Sastre. Allergy Service Asthma: definition Asthma is a syndrome defined on basis of three main aspects: 1- Symptoms due to variable and reversible airway obstruction
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems The Respiratory System Functions of the Respiratory System Warms, moistens, and filters incoming air Nasal cavity Resonating chambers for speech and
The RESPIRATORY System Unit 3 Transportation Systems The Respiratory System Functions of the Respiratory System Warms, moistens, and filters incoming air Nasal cavity Resonating chambers for speech and
