Pulmonary Pathway & Assessment/Plan of Care: Acute. Pulmonary Risk Factors & Pulmonary History
|
|
|
- Madeleine Jennings
- 6 years ago
- Views:
Transcription
1 Pulmonary Risk Factors & Pulmonary History Pulmonary History: Asthma Bronchitis COPD Emphysema Cystic Fibrosis Pneumonia (last 30d) Other: Smoking: Never Current Cigs/Day Previous Year Quit Alcohol Use Stress Source/Management Normal Activity Level Did the patient receive the Influenza Vaccine? Yes No Date/Notes: Did the patient receive Pneumonia Vaccines PCV13? Yes No Date/Notes: Did the patient receive Pneumonia Vaccines PPSV23? Yes No Date/Notes: Did the patient use oxygen in the home prior to admit: Yes No If Yes, how many liters, via what and how often did they wear it? Did the patient have nebulizer treatments in the home prior to admit: Yes No If Yes, what medicine and how often? If the resident had respiratory equipment in the home prior to admit, which company did they use? Thyroid Disease Yes No Liver Disease Yes No GI Disease Yes No Renal Disease Yes No Hemoptysis Yes No Loss of Appetite Yes No Tremors Yes No Acute Past Medical History Review of Current Respiratory Medications Cancer Yes No Bleeding Disorder Yes No Insomnia Yes No Hay fever Yes No Eczema Yes No Weight loss Yes No Antihistamines Yes No Inhaled Corticosteroids Yes No Decongestants Yes No Antimuscarinic (Ipratropium, Tiotroium)_ Yes No Expectorants Yes No Short Acting Bronchodilator (Albuterol, Xopenex) Yes No Antitussives Yes No Long Acting Bronchodilator (Advair, Symbicort) Yes No Oral Corticosteroids Yes No Anti-cholinergic Yes No Did the resident have temporary medications in place for an acute condition like antibiotics/steroids/breathing treatments? No Yes If yes is the temporary treatment in place complete? No Yes Is there a stop date? No Yes Current Respiratory Is the resident currently using an incentive spirometer? No Yes How frequent are the using it? Oxygen Use: No Yes (Liters/via/ how long) CPAP or BiPAP: No Yes (Settings) Labs done in the last 72 Hours (Make sure they are in the active medical record) CXR Yes No CBC Yes No BMP Yes No If No is checked Proceed To establish a baseline obtain CBC and BMP if it has not been done in the last 72 hours. Signature: Date: Other New orders: Signature: Date: Temperature: Apical Pulse: Baseline Vital Signs Oxygen Sat: Base Line Respiration:
2 Assessment Color: Pink Pale Jaundiced Ashen Cyanotic Other Temperature: Warm Cool Cold Other Heart Rhythm: Regular Irregular Pacemaker Other Nail Beds: Normal Cyanotic Clubbing Capillary Refill: < 3 seconds >3 seconds Cough: Strong Moderate Weak Absent Sputum: N/A Scant Moderate Copious Color Respirations: Labored Intercostal Use Deep Shallow Chest shape: Normal Pectus Carinatum Pectus Excavatum Barrel Chest Lung Sounds: C = Clear W= Wheeze (Rhonchi) R = Rales (Crackles) D = Diminished PR = Plural Rub (Indicate C, W, R, D or PR next to each line) RUL LUL LUL RUL RLL RML LLL LLL RML RLL Signature: Date:
3 Pulmonary Pathway & Assessment/Plan of Care: Acute Plan of Care Precautions: Physical Activity in conjunction with Therapy: Therapy Evaluation Nursing/Dietary Patient has an acute Pulmonary disease. Throughout the next 7 days patient will maintain effective airway clearance as evidenced by: No decline in energy or increased fatigue No c/o chest pain No c/o of SOA Maintain O2 Sat of: Monitor Vital Signs daily to monitor for changes Monitor respiratory status - Notify physician if change is noted Administer respiratory treatments as ordered Encourage use of the Incentive Spirometer 10 times every 1-2 hours Frequent rest periods to avoid fatigue and decrease the O2 demand Other: Mobility/Therapy During the next 7 days therapy staff will assess the patient s current level of function and develop an activity plan. Patient and direct care staff will be educated to improve the success of exercise, mobility and activity. Resident will participate in therapy and activity limits/precautions will be established. Education Needs Assess cognition and communication to maximize patient s potential and compliance. Complete tug test if applicable Assess level and recommend nursing /restorative additional waking program. Complete standardized modified Borg Scale and 6 minute walk test if applicable By day 7 patient and/or caretaker will be able to verbally voice understanding of the following: Identify 3 symptoms of pulmonary disease Understand energy conservation Resident will use IS 10 x every 1-2hr Provide verbal and written education Educate patient on energy conservation Educate patient on incentive spirometer use Social Services Identify patient s level of commitment. Identify psychosocial factors that may affect overall health. By day 7 psychosocial risk factors will be identified to promote multidimensional health Complete Quality of Life Index on admit and again at day 7 if applicable Complete interview to identify any mood symptom indicators Staff/Title/Date: Staff/Title/Date: Staff/Title/Date: Staff/Title/Date:
4 Chronic Nursing Patient has chronic pulmonary disease. Throughout the next 60 days patient will maintain effective breathing patterns and remain free from hospitalization Maintain respiratory rate of Monitor Vital Signs daily to monitor for changes Apical Rate: Frequent rest periods to avoid fatigue and decrease the O2 demand Maintain O2 Sat of: Weekly respiratory focused assessment Therapy Patient will be independent and mobile with all care needs in their projected transition location. Patient will: Able to function independently with all adl s for at least 48 hours before discharge Activity tolerance will be improved per Borg Scale Continue PT/OT/SLP per individual plan of care Perform the modified Borg assessment weekly if applicable Education All Disciplines Patient will be taught how to monitor their respiratory status with emphasis on early detection of these symptoms to prevent Properly identify when respiratory symptoms are worse and when to call the physician. Properly identify health eating habits Properly identify exercise and rest balance Social Worker hospitalization. Patient will learn to: Review Living with chronic respiratory disease Information booklet Teach patient how to utilize home respiratory therapy treatments like inhalers and or nebulizers Instruct patient during therapy to recognize symptoms of fatigue and need to rest Prior to discharge risk factors for psychosocial deficits will be minimized to promote multidimensional health. Patient will remain motivated with a high level of commitment. Patient will have interventions in place to reduce psychosocial factors that may affect overall health Community resources will be engaged if needed Complete Quality of Life Index within 1-3 days before discharge. Teach patient coping mechanisms r/t chronic disease to reduce stress Refer to community resources as needed Staff/Title/Date: Staff/Title/Date: Staff/Title/Date: Staff/Title/Date: Staff/Title/Date: Staff/Title/Date:
5 Weekly Assessment Pulmonary History Pulmonary History: Asthma Bronchitis COPD Emphysema Cystic Fibrosis Pneumonia (last 30d) Other: Antihistamines Yes No Decongestants Yes No Expectorants Yes No Antitussives Yes No Oral Corticosteroids Yes No Anti-cholinergic Yes No Review of Current Respiratory Medications Inhaled Corticosteroids Yes No Antimuscarinic (Ipratropium, Tiotroium)_ Yes No Short Acting Bronchodilator (Albuterol, Xopenex) Yes No Long Acting Bronchodilator (Advair, Symbicort) Yes No Did the resident have temporary medications in place for an acute condition like antibiotics/steroids/breathing treatments? No Yes If yes is the temporary treatment in place complete? No Yes Is there a stop date? No Yes Current Respiratory Is the resident currently using an incentive spirometer? No Yes How frequent are the using it? Oxygen Use: No Yes (Liters/via/ how long) CPAP or BiPAP: No Yes (Settings) Temperature: Apical Pulse: Vital Signs Oxygen Sat range for the last week: Respiration range for the last week: Assessment Color: Pink Pale Jaundiced Ashen Cyanotic Other Temperature: Warm Cool Cold Other Heart Rhythm: Regular Irregular Pacemaker Other Nail Beds: Normal Cyanotic Clubbing Capillary Refill: < 3 seconds >3 seconds Cough: Strong Moderate Weak Absent Sputum: N/A Scant Moderate Copious Color Respirations: Labored Intercostal Use Deep Shallow Chest shape: Normal Pectus Carinatum Pectus Excavatum Barrel Chest
6 Lung Sounds: C = Clear W= Wheeze (Rhonchi) R = Rales (Crackles) D = Diminished PR = Plural Rub (Indicate C, W, R, D or PR next to each line) Has there been a change since last respiratory assessment? No Yes If yes explain in detail: Evaluation Does the resident Continue to show S/S of acute distress? No Yes If No is checked and resident has a hx of pulmonary disease Proceed If Yes is checked If the resident has a history of pulmonary disease proceed to chronic phase of clinical pathway Signature: Date: If the resident if free of acute distress notify physician to modify plan of care to home routine so teaching can begin. If resident does not have a chronic lung condition discontinue weekly assessments. Signature: Date: If yes is checked continue current plan of care. If resident s symptoms are worse notify physician. Signature: Date: Signature: Date:
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Presented by UIC College of Nursing
 Presented by UIC College of Nursing Describe COPD. Identify red flags for a COPD exacerbation. Identify COPD triggers or risk factors. Differentiate between long-acting inhalers and emergency use inhalers.
Presented by UIC College of Nursing Describe COPD. Identify red flags for a COPD exacerbation. Identify COPD triggers or risk factors. Differentiate between long-acting inhalers and emergency use inhalers.
Chronic Obstructive Pulmonary Disease 1/18/2018
 Presented by UIC College of Nursing Describe COPD. Identify red flags for a COPD exacerbation. Identify COPD triggers or risk factors. Differentiate between long acting inhalers and emergency use inhalers.
Presented by UIC College of Nursing Describe COPD. Identify red flags for a COPD exacerbation. Identify COPD triggers or risk factors. Differentiate between long acting inhalers and emergency use inhalers.
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory System Anatomy Respiratory system: all the structures that contribute to
 1 2 3 4 5 6 7 8 Chapter 15 Respiratory Emergencies Respiratory Distress Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine.
1 2 3 4 5 6 7 8 Chapter 15 Respiratory Emergencies Respiratory Distress Patients often complain about dyspnea. Shortness of breath Symptom of many different conditions Cause can be difficult to determine.
Overview of COPD INTRODUCTION
 Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview. Baseline Vital Signs. Chapter 5. Baseline Vital Signs and SAMPLE History. Baseline Vital Signs. SAMPLE History
 Chapter 5 Baseline Vital Signs and SAMPLE History Slide 1 Baseline Vital Signs Breathing Skin Pupils Blood Pressure Overview Vital Sign Reassessment SAMPLE History Slide 2 Baseline Vital Signs Slide 3
Chapter 5 Baseline Vital Signs and SAMPLE History Slide 1 Baseline Vital Signs Breathing Skin Pupils Blood Pressure Overview Vital Sign Reassessment SAMPLE History Slide 2 Baseline Vital Signs Slide 3
COPD. Helen Suen & Lexi Smith
 COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
Function of the Respiratory System. Exchange CO2 (on expiration) for O2 (on inspiration)
 Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Anatomy Review. Anatomy Review. Respiratory Emergencies CHAPTER 16
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
Respiratory Emergencies
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
Chapter 16. Objectives. Objectives. Respiratory Emergencies
 Chapter 16 Respiratory Emergencies Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key
Chapter 16 Respiratory Emergencies Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights reserved. Objectives 1. Define key
Chronic Obstructive Pulmonary Disease (COPD) Clinical Guideline
 Chronic Obstructive Pulmonary Disease (COPD) Clinical These clinical guidelines are designed to assist clinicians by providing an analytical framework for the evaluation and treatment of patients. They
Chronic Obstructive Pulmonary Disease (COPD) Clinical These clinical guidelines are designed to assist clinicians by providing an analytical framework for the evaluation and treatment of patients. They
Objectives. Case Presentation. Respiratory Emergencies
 Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Chapter 19 - Respiratory_Emergencies
 Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
Firefighter Pre-Hospital Care Program Recruit Presentation. Respiratory Emergencies
 Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
PATHOLOGY & PATHOPHYSIOLOGY
 PATHOLOGY & PATHOPHYSIOLOGY DISORDERS OF THE RESPIRATORY SYSTEM DISORDERS OF THE RESPIRATORY SYSTEM Disorders of the Respiratory System Infections Degenerative Tumours Immune Trauma Congenital Upper respiratory
PATHOLOGY & PATHOPHYSIOLOGY DISORDERS OF THE RESPIRATORY SYSTEM DISORDERS OF THE RESPIRATORY SYSTEM Disorders of the Respiratory System Infections Degenerative Tumours Immune Trauma Congenital Upper respiratory
Baseline Vital Signs and SAMPLE History. Chapter 5
 Baseline Vital Signs and SAMPLE History Chapter 5 Baseline Vital Signs and SAMPLE History Assessment is the most complex skill EMT-Bs learn. During assessment you will: Gather key information. Evaluate
Baseline Vital Signs and SAMPLE History Chapter 5 Baseline Vital Signs and SAMPLE History Assessment is the most complex skill EMT-Bs learn. During assessment you will: Gather key information. Evaluate
COPD/Asthma. Prudence Twigg, AGNP
 COPD/Asthma Prudence Twigg, AGNP COPD/Asthma Qualifying Diagnosis Known diagnosis of COPD/asthma or CXR showing COPD with hyperinflated lungs and no infiltrates + two or more: Wheezing, SOB, increased
COPD/Asthma Prudence Twigg, AGNP COPD/Asthma Qualifying Diagnosis Known diagnosis of COPD/asthma or CXR showing COPD with hyperinflated lungs and no infiltrates + two or more: Wheezing, SOB, increased
COPD Treatable. Preventable.
 My COPD Action Plan Patient s Copy (Patient s Name) Date Canadian Respiratory COPD Treatable. Preventable. This is to tell me how I will take care of myself when I have a COPD flare-up. My goals are My
My COPD Action Plan Patient s Copy (Patient s Name) Date Canadian Respiratory COPD Treatable. Preventable. This is to tell me how I will take care of myself when I have a COPD flare-up. My goals are My
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
What do pulmonary function tests tell you?
 Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013 DEFINITIONS General Impression - EMT develops a plan of action from the
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013 DEFINITIONS General Impression - EMT develops a plan of action from the
1 I *********IF YOU ARE NOT ON ALLERGY SHOTS PLEASE SKIP THIS SECTION AND MOVE TO PAGE 2********* NAME: AGE: ---- ID (For Office Use Only):
 NAME: AGE: ---- Date of Appointment:. ID (For Office Use Only): RETURN VISIT Date of Visit: Main Reason for visit: Reevaluation Family Doctor: Symptoms worse _ New problem _ Yearly follow up _ Follow up/office
NAME: AGE: ---- Date of Appointment:. ID (For Office Use Only): RETURN VISIT Date of Visit: Main Reason for visit: Reevaluation Family Doctor: Symptoms worse _ New problem _ Yearly follow up _ Follow up/office
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Bronchoconstriction is also treated with medications that inhibit bronchiolar constriction such as: Ipratropium (Atrovent)
 Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Vital Signs and SAMPLE History
 CHAPTER 9 Vital Signs and SAMPLE History Overall Assessment Scheme Scene Size-Up Initial Assessment Trauma Physical Exam Vital Signs & SAMPLE History Medical SAMPLE History Physical Exam & Vital Signs
CHAPTER 9 Vital Signs and SAMPLE History Overall Assessment Scheme Scene Size-Up Initial Assessment Trauma Physical Exam Vital Signs & SAMPLE History Medical SAMPLE History Physical Exam & Vital Signs
3. Identify the importance in the prehospital setting for the administration of nebulized bronchodilator.
 TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
EXACERBATION ASSESSMENT FORM
 EXACERBATION ASSESSMENT FORM ID NUMBER: 0a) Form Completion Date... 0b) Staff Code... Administrative Information 1) Date of clinic visit: 2) What type of Event is this?... Participant/HCU-triggered...
EXACERBATION ASSESSMENT FORM ID NUMBER: 0a) Form Completion Date... 0b) Staff Code... Administrative Information 1) Date of clinic visit: 2) What type of Event is this?... Participant/HCU-triggered...
RESPIRATORY EMERGENCIES. Michael Waters MD April 2004
 RESPIRATORY EMERGENCIES Michael Waters MD April 2004 ASTHMA Asthma is a chronic inflammatory disease of the airways with variable or reversible airway obstruction Characterized by increased sensitivity
RESPIRATORY EMERGENCIES Michael Waters MD April 2004 ASTHMA Asthma is a chronic inflammatory disease of the airways with variable or reversible airway obstruction Characterized by increased sensitivity
EXACERBATION ASSESSMENT FORM
 EXACERBATION ASSESSMENT FORM ID NUMBER: VERSION: 1.0 05/27/14 0a) Form Completion Date... 0b) Staff Code... Instructions: This form should be completed when a participant comes to the clinical center for
EXACERBATION ASSESSMENT FORM ID NUMBER: VERSION: 1.0 05/27/14 0a) Form Completion Date... 0b) Staff Code... Instructions: This form should be completed when a participant comes to the clinical center for
Running head: BEST-PRACTICE NURSING CARE FOR PATIENTS WITH 1 CHRONIC OBSTRUCTIVE PULMONARY DISEASE
 Running head: BEST-PRACTICE NURSING CARE FOR PATIENTS WITH 1 CHRONIC OBSTRUCTIVE PULMONARY DISEASE Best-Practice Nursing Care for Patients with Chronic Obstructive Pulmonary Disease Jessica N. Anderson,
Running head: BEST-PRACTICE NURSING CARE FOR PATIENTS WITH 1 CHRONIC OBSTRUCTIVE PULMONARY DISEASE Best-Practice Nursing Care for Patients with Chronic Obstructive Pulmonary Disease Jessica N. Anderson,
Respiratory Emergencies. Lesson Goal. Lesson Objectives 9/10/2012
 Respiratory Emergencies Lesson Goal Assess and provide timely treatment & transport to patients experiencing respiratory emergencies Lesson Objectives List parts of respiratory system and how they work
Respiratory Emergencies Lesson Goal Assess and provide timely treatment & transport to patients experiencing respiratory emergencies Lesson Objectives List parts of respiratory system and how they work
RESPIRATORY ASSESSMENT JENNY CASEY RESPIRATORY SERVICES LEAD ACE
 RESPIRATORY ASSESSMENT JENNY CASEY RESPIRATORY SERVICES LEAD ACE What does respiratory assessment involve? Subjective Assessment Objective Assessment Inspection, palpation, percussion and auscultation
RESPIRATORY ASSESSMENT JENNY CASEY RESPIRATORY SERVICES LEAD ACE What does respiratory assessment involve? Subjective Assessment Objective Assessment Inspection, palpation, percussion and auscultation
Provider Respiratory Inservice
 Provider Respiratory Inservice 2 Welcome Opening Remarks We will cover: Definition of Asthma & COPD Evidence based guidelines for diagnosis, evaluation, and management of asthma Evidence based guidelines
Provider Respiratory Inservice 2 Welcome Opening Remarks We will cover: Definition of Asthma & COPD Evidence based guidelines for diagnosis, evaluation, and management of asthma Evidence based guidelines
Cardiovascular and Respiratory Disorders
 Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Cardiovascular and Respiratory Disorders Blood Pressure Normal blood pressure is 120/80 mmhg (millimeters of mercury) Hypertension is when the resting blood pressure is too high Systolic BP is 140 mmhg
Chronic Obstructive Pulmonary Disease (COPD)
 James Paget University Hospitals NHS Foundation Trust Great Yarmouth and Waveney Clinical Commissioning Group HealthEast Chronic Obstructive Pulmonary Disease (COPD) Information and Advice for Patients
James Paget University Hospitals NHS Foundation Trust Great Yarmouth and Waveney Clinical Commissioning Group HealthEast Chronic Obstructive Pulmonary Disease (COPD) Information and Advice for Patients
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
OBSERVATION UNIT ASTHMA PATHWAY OUTLINE Westmoreland Hospital PAGE 1 OF 5
 PAGE 1 OF 5 Exclusion Criteria: (Reason to admit to hospital) A. New EKG changes except sinus tachycardia B. Respiratory Rate > 40 C. Signs/symptoms of Heart Failure D. Impending respiratory failure or
PAGE 1 OF 5 Exclusion Criteria: (Reason to admit to hospital) A. New EKG changes except sinus tachycardia B. Respiratory Rate > 40 C. Signs/symptoms of Heart Failure D. Impending respiratory failure or
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
NORTHERN VIRGINIA PULMONARY AND CRITICAL CARE ASSOCIATES, P.C.
 NORTHERN VIRGINIA PULMONARY AND CRITICAL CARE ASSOCIATES, P.C. Past Medical History AIDS/HIV disease Anemia Asthma Bronchitis Cancer Date of last Chest X-ray Diabetes Mellitus, Type I Diabetes Mellitus,
NORTHERN VIRGINIA PULMONARY AND CRITICAL CARE ASSOCIATES, P.C. Past Medical History AIDS/HIV disease Anemia Asthma Bronchitis Cancer Date of last Chest X-ray Diabetes Mellitus, Type I Diabetes Mellitus,
Chronic Obstructive Pulmonary Disease (COPD)
 Chronic Obstructive Pulmonary Disease (COPD) Health Promotion and Education Program Rev. 2014 2014, MMM Healthcare, Inc. - PMC Medicare Choice, Inc. Reproduction of this material is prohibited. MP-HEP-PPT-200-01-021914-E
Chronic Obstructive Pulmonary Disease (COPD) Health Promotion and Education Program Rev. 2014 2014, MMM Healthcare, Inc. - PMC Medicare Choice, Inc. Reproduction of this material is prohibited. MP-HEP-PPT-200-01-021914-E
Chapter 15 - Respiratory Emergencies
 1 2 3 4 5 6 7 National EMS Education Standard Competencies (1 of 5) Medicine Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
1 2 3 4 5 6 7 National EMS Education Standard Competencies (1 of 5) Medicine Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
Topic: Baseline Vitals and Sample History Company Drill
 Baseline Vitals and Sample History Company Drill Instructor Guide Session Reference: 1 Topic: Baseline Vitals and Sample History Company Drill Level of Instruction: 2 Time Required: Three Hours Materials
Baseline Vitals and Sample History Company Drill Instructor Guide Session Reference: 1 Topic: Baseline Vitals and Sample History Company Drill Level of Instruction: 2 Time Required: Three Hours Materials
Reference Guide for Group Education
 A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 5 Plan of Action: Part I Overview of the Plan of Action and Management of Respiratory Infections Plan of Action: Objectives
A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 5 Plan of Action: Part I Overview of the Plan of Action and Management of Respiratory Infections Plan of Action: Objectives
Arizona Grand Medical Center 3777 Crossings Drive Prescott, AZ 86305
 Patient Information Arizona Grand Medical Center 3777 Crossings Drive Prescott, AZ 86305 Home Phone: Cell Phone: Last Name: First Name: MI Mailing Address: APT City/State/Zip Sex: Male Female Birthdate:
Patient Information Arizona Grand Medical Center 3777 Crossings Drive Prescott, AZ 86305 Home Phone: Cell Phone: Last Name: First Name: MI Mailing Address: APT City/State/Zip Sex: Male Female Birthdate:
The Goal of the Respiratory Assessment. Two Parts of the Respiratory Assessment
 The Respiratory System Respiratory Assessment of the Adult Patient Mary Douglas, MSN, RN Nurse Educator Minneapolis VA Health Care System Respiratory system: moves oxygen into the body and carbon dioxide
The Respiratory System Respiratory Assessment of the Adult Patient Mary Douglas, MSN, RN Nurse Educator Minneapolis VA Health Care System Respiratory system: moves oxygen into the body and carbon dioxide
Exam 1 Review. Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies
 Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
Exam 1 Review Cardiopulmonary Symptoms Physical Examination Clinical Laboratory Studies WBC Count Differential A patient had been admitted to the hospital for acute shortness of breath. A CXR examination
Chronic Obstructive Pulmonary Disease. Information about medication and an Action Plan to use if your condition gets worse due to an infection
 Chronic Obstructive Pulmonary Disease Information about medication and an Action Plan to use if your condition gets worse due to an infection Information about your medication Your usual treatment Inhalers
Chronic Obstructive Pulmonary Disease Information about medication and an Action Plan to use if your condition gets worse due to an infection Information about your medication Your usual treatment Inhalers
CPAP. Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device. Charlottesville Albemarle Rescue Squad - CPAP
 CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
Pulmonary Predicaments in Primary Care Peter F. Bidey, DO
 Pulmonary Predicaments in Primary Care Peter F. Bidey, DO Pulmonary Predicaments in Primary Care Peter F. Bidey, D.O. Clinical Instructor -Family Medicine Philadelphia College of Osteopathic Medicine
Pulmonary Predicaments in Primary Care Peter F. Bidey, DO Pulmonary Predicaments in Primary Care Peter F. Bidey, D.O. Clinical Instructor -Family Medicine Philadelphia College of Osteopathic Medicine
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Chapter 9 Vital Signs and SAMPLE History DOT Directory
 Chapter 9 Vital Signs and SAMPLE History U.S. Objectives U.S. Objectives are covered and/or supported by the PowerPoint Slide Program and Notes for Emergency Care, 11th Ed. Please see the Chapter 9 correlation
Chapter 9 Vital Signs and SAMPLE History U.S. Objectives U.S. Objectives are covered and/or supported by the PowerPoint Slide Program and Notes for Emergency Care, 11th Ed. Please see the Chapter 9 correlation
Anyone who smokes and/or has shortness of breath and sputum production could have COPD
 COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
5/3/2012 PRESENTATION GOALS RESPIRATORY THERAPISTS ROLE IN END OF LIFE CARE FOR THE PULMONARY PATIENT
 RESPIRATORY THERAPISTS ROLE IN END OF LIFE CARE FOR THE PULMONARY PATIENT Presented by Carrie Black Bourassa, LRT, RRT PRESENTATION GOALS Define palliative care Define hospice care Discuss pulmonary hospice
RESPIRATORY THERAPISTS ROLE IN END OF LIFE CARE FOR THE PULMONARY PATIENT Presented by Carrie Black Bourassa, LRT, RRT PRESENTATION GOALS Define palliative care Define hospice care Discuss pulmonary hospice
Self-management plan for COPD
 Sheffield Clinical Commissioning Group Sheffield Teaching Hospitals NHS Foundation Trust Self-management plan for COPD This is your personal management plan The aim of the plan is to help you have better
Sheffield Clinical Commissioning Group Sheffield Teaching Hospitals NHS Foundation Trust Self-management plan for COPD This is your personal management plan The aim of the plan is to help you have better
Care of the Patient with a Respiratory Disorder
 Care of the Patient with a Respiratory Disorder 1 Slide 1 Overview of Anatomy and Physiology External respiration Exchange of oxygen and carbon dioxide between the lung and the environment Internal respiration
Care of the Patient with a Respiratory Disorder 1 Slide 1 Overview of Anatomy and Physiology External respiration Exchange of oxygen and carbon dioxide between the lung and the environment Internal respiration
PEDIATRIC ACUTE ASTHMA SCORE (P.A.A.S.) GUIDELINES. >97% 94% to 96% 91%-93% <90% Moderate to severe expiratory wheeze
 Inclusion: Children experiencing acute asthma exacerbation 24 months to 18 years of age with a diagnosis of asthma Patients with a previous history of asthma (Consider differential diagnosis for infants
Inclusion: Children experiencing acute asthma exacerbation 24 months to 18 years of age with a diagnosis of asthma Patients with a previous history of asthma (Consider differential diagnosis for infants
PATIENT INFORMATION Chronic Obstructive Pulmonary Disease (COPD) Fact Sheet
 PATIENT INFORMATION Chronic Obstructive Pulmonary Disease (COPD) Fact Sheet What is COPD? COPD is a general term, which includes the conditions chronic asthma, chronic bronchitis and emphysema. It is due
PATIENT INFORMATION Chronic Obstructive Pulmonary Disease (COPD) Fact Sheet What is COPD? COPD is a general term, which includes the conditions chronic asthma, chronic bronchitis and emphysema. It is due
New Patient Sleep Intake
 New Patient Sleep Intake Name: Date of Birth: Primary Care Physician: Date of Visit: Referring Physician and/or Other Physicians: Retail Pharmacy: Mail Order Pharmacy: Address: Mail Order Phone #: Phone
New Patient Sleep Intake Name: Date of Birth: Primary Care Physician: Date of Visit: Referring Physician and/or Other Physicians: Retail Pharmacy: Mail Order Pharmacy: Address: Mail Order Phone #: Phone
COPD. The goals of COPD. about. you quit. If you. efforts to quit. Heart
 How Is COPD Treated? COPD has no cure yet. However, lifestyle changes and treatments can help you feel better, stay more active, and slow the progress of the disease. The goals of COPD treatment include:
How Is COPD Treated? COPD has no cure yet. However, lifestyle changes and treatments can help you feel better, stay more active, and slow the progress of the disease. The goals of COPD treatment include:
St. Dominic Jackson Memorial Hospital. Pulmonary Services. Therapist Driven Protocol. Assess and Treat Aerosol Therapy
 St. Dominic Jackson Memorial Hospital Pulmonary Services Therapist Driven Protocol Assess and Treat Aerosol Therapy Purpose The purpose of the Therapist Driven Protocol (TDP) aerosol therapy is to create
St. Dominic Jackson Memorial Hospital Pulmonary Services Therapist Driven Protocol Assess and Treat Aerosol Therapy Purpose The purpose of the Therapist Driven Protocol (TDP) aerosol therapy is to create
Examination of the Respiratory System
 Examination of the Respiratory System Wash your hands & Introduce the exam to your patient Positioning & Draping while seated or standing, the patient should be exposed to the waist? patients can be uncovered
Examination of the Respiratory System Wash your hands & Introduce the exam to your patient Positioning & Draping while seated or standing, the patient should be exposed to the waist? patients can be uncovered
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Room # Critical Care & Pulmonary Consultants, P.C.
 Room # Critical Care & Pulmonary Consultants, P.C. Health History You have been scheduled for an appointment with Critical Care and Pulmonary Consultants, P.C. This health history will help us facilitate
Room # Critical Care & Pulmonary Consultants, P.C. Health History You have been scheduled for an appointment with Critical Care and Pulmonary Consultants, P.C. This health history will help us facilitate
Chronic Obstructive Pulmonary Disease, shortened to COPD, is an umbrella term for a group of conditions which cause long-term damage to the airways.
 10 Common QuESTIonS AbouT CoPD Chronic Obstructive Pulmonary Disease, shortened to COPD, is an umbrella term for a group of conditions which cause long-term damage to the airways. COPD includes: chronic
10 Common QuESTIonS AbouT CoPD Chronic Obstructive Pulmonary Disease, shortened to COPD, is an umbrella term for a group of conditions which cause long-term damage to the airways. COPD includes: chronic
Chronic Obstructive Pulmonary Disease
 Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
PALS Pulseless Arrest Algorithm.
 PALS Pulseless Arrest Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Bradycardia Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Tachycardia Algorithm. Kleinman M
PALS Pulseless Arrest Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Bradycardia Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Tachycardia Algorithm. Kleinman M
AIRWAY & HEART ANOTOMY
 Objectives I CAN T BREATH Respiratory Emergencies Review of anatomical structures related to heart & lungs Differentiate differences between adult and pediatric airways Identify the need for airway assistance
Objectives I CAN T BREATH Respiratory Emergencies Review of anatomical structures related to heart & lungs Differentiate differences between adult and pediatric airways Identify the need for airway assistance
Protocol Update 2019
 Protocol Update 2019 There have been several questions revolving around protocol updates and how they are to be conducted. As many of you are aware there is a protocol submission process in the appendix
Protocol Update 2019 There have been several questions revolving around protocol updates and how they are to be conducted. As many of you are aware there is a protocol submission process in the appendix
Laser Vein Center Thomas Wright MD Page 1 of 4
 Demographics Laser Vein Center Thomas Wright MD Page 1 of 4 Patient Name: Address: City, St, Zip Primary Phone: Alternate: DOB: Social Security #: Insurance Information Primary Insurance ID# Group# Subscriber
Demographics Laser Vein Center Thomas Wright MD Page 1 of 4 Patient Name: Address: City, St, Zip Primary Phone: Alternate: DOB: Social Security #: Insurance Information Primary Insurance ID# Group# Subscriber
Cardiac & Pulmonary Rehab Individual Treatment Plan
 Initial Assessment Date: Re-Assessment Date: Re-Assessment Date: Follow-Up Discharge Date: Risk Assessment Risk Assessment Risk Assessment Risk Assessment BP SpO2 BP SpO2 BP SpO2 BP SpO2 HR Edema HR Edema
Initial Assessment Date: Re-Assessment Date: Re-Assessment Date: Follow-Up Discharge Date: Risk Assessment Risk Assessment Risk Assessment Risk Assessment BP SpO2 BP SpO2 BP SpO2 BP SpO2 HR Edema HR Edema
COPD. Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS
 IN THE NAME OF GOD COPD Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS Definition of COPD* COPD is a preventable and treatable chronic lung disease characterized by airflow limitation that is not fully
IN THE NAME OF GOD COPD Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS Definition of COPD* COPD is a preventable and treatable chronic lung disease characterized by airflow limitation that is not fully
NEW PATIENT QUESTIONNAIRE
 NEW PATIENT QUESTIONNAIRE Last Name: First Name: Date Form Completed: Referring Physician: Address: City: Sex: Marital Status: Race: Age: Married Caucasian Single Male Divorced African American Hispanic
NEW PATIENT QUESTIONNAIRE Last Name: First Name: Date Form Completed: Referring Physician: Address: City: Sex: Marital Status: Race: Age: Married Caucasian Single Male Divorced African American Hispanic
Name: (Last), (First), (Middle) Date of Birth: SS: Left or Right Handed: Complete Address: Phone: Home: Cell: Work:
 An Outpatient Department of PLEASE FILL OUT ALL INFORMATION COMPLETELY Date Completed Name: (Last), (First), (Middle) Date of Birth: SS: Left or Right Handed: Complete Address: Phone: Home: Cell: Work:
An Outpatient Department of PLEASE FILL OUT ALL INFORMATION COMPLETELY Date Completed Name: (Last), (First), (Middle) Date of Birth: SS: Left or Right Handed: Complete Address: Phone: Home: Cell: Work:
THE RESPIRATORY SYSTEM. Pages and
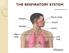 THE RESPIRATORY SYSTEM Pages 103-105 and 146-150 1 When the respiratory system is mentioned, people generally think of breathing, but breathing is only one of the activities of the respiratory system.
THE RESPIRATORY SYSTEM Pages 103-105 and 146-150 1 When the respiratory system is mentioned, people generally think of breathing, but breathing is only one of the activities of the respiratory system.
Epinephrine Intramuscular (IM) Injection Administration EMT Optional Scope Highlights
 Epinephrine Intramuscular (IM) Injection Administration EMT Optional Scope Highlights Nor-Cal EMS February 2018 version 1 Special Thank You To Seattle / King County EMS NY State Department of Health, Check
Epinephrine Intramuscular (IM) Injection Administration EMT Optional Scope Highlights Nor-Cal EMS February 2018 version 1 Special Thank You To Seattle / King County EMS NY State Department of Health, Check
COPD COPD. C - Chronic O - Obstructive P - Pulmonary D - Disease OBJECTIVES
 COPD C - Chronic O - Obstructive P - Pulmonary D - Disease 1 OBJECTIVES Following this presentation the participant should be able to demonstrate understanding of chronic lung disease by successful completion
COPD C - Chronic O - Obstructive P - Pulmonary D - Disease 1 OBJECTIVES Following this presentation the participant should be able to demonstrate understanding of chronic lung disease by successful completion
Exacerbations of COPD. Dr J Cullen
 Exacerbations of COPD Dr J Cullen Definition An AECOPD is a sustained worsening of the patient s clinical condition from their stable state that is beyond their usual day-to-day variation is acute in onset
Exacerbations of COPD Dr J Cullen Definition An AECOPD is a sustained worsening of the patient s clinical condition from their stable state that is beyond their usual day-to-day variation is acute in onset
2/12/2015. ASTHMA & COPD The Yin &Yang. Asthma General Information. Asthma General Information
 ASTHMA & COPD The Yin &Yang Arizona State Association of Physician Assistants March 6, 2015 Sedona, Arizona Randy D. Danielsen, PhD, PA-C, DFAAPA Dean & Professor A.T. Still University Asthma General Information
ASTHMA & COPD The Yin &Yang Arizona State Association of Physician Assistants March 6, 2015 Sedona, Arizona Randy D. Danielsen, PhD, PA-C, DFAAPA Dean & Professor A.T. Still University Asthma General Information
Worker Respirator Use Page 1 of 6
 Page 1 of 6 Medical Evaluation Report: TODAY S DATE EMPLOYER S NAME / COMPANY ADDRESS PHONE # FAX # Did the worker provide a completed respirator questionnaire for medical review? Yes Date respirator questionnaire
Page 1 of 6 Medical Evaluation Report: TODAY S DATE EMPLOYER S NAME / COMPANY ADDRESS PHONE # FAX # Did the worker provide a completed respirator questionnaire for medical review? Yes Date respirator questionnaire
JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES
 JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES Authors Dr Ian Benton Respiratory Consultant COCH Penny Rideal Respiratory Nurse COCH Kirti Burgul Respiratory Pharmacist COCH Pam
JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES Authors Dr Ian Benton Respiratory Consultant COCH Penny Rideal Respiratory Nurse COCH Kirti Burgul Respiratory Pharmacist COCH Pam
Anatomy & Physiology 2 Canale. Respiratory System: Exchange of Gases
 Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
PIDS AND RESPIRATORY DISORDERS
 PRIMARY IMMUNODEFICIENCIES PIDS AND RESPIRATORY DISORDERS PIDS AND RESPIRATORY DISORDERS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS COPD CT MRI IG PID Chronic obstructive pulmonary disease Computed tomography
PRIMARY IMMUNODEFICIENCIES PIDS AND RESPIRATORY DISORDERS PIDS AND RESPIRATORY DISORDERS 1 PRIMARY IMMUNODEFICIENCIES ABBREVIATIONS COPD CT MRI IG PID Chronic obstructive pulmonary disease Computed tomography
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
WF RESPIRATORY SYSTEM. RESPIRATORY MEDICINE
 WF RESPIRATORY SYSTEM. RESPIRATORY MEDICINE 1 Societies 11 History 13 Dictionaries. Encyclopaedias. Bibliographies Use for general works only. Classify with specific aspect where possible 15 Classification.
WF RESPIRATORY SYSTEM. RESPIRATORY MEDICINE 1 Societies 11 History 13 Dictionaries. Encyclopaedias. Bibliographies Use for general works only. Classify with specific aspect where possible 15 Classification.
Asthma in the Athlete
 Asthma in the Athlete Jorge E. Gomez, MD Associate Professor Texas Children s Hospital Baylor College of Medicine Assist Team Physician UH Understand how we diagnose asthma Objectives Be familiar with
Asthma in the Athlete Jorge E. Gomez, MD Associate Professor Texas Children s Hospital Baylor College of Medicine Assist Team Physician UH Understand how we diagnose asthma Objectives Be familiar with
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing
 Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
National Asthma Educator Certification Board Detailed Content Outline
 I. THE ASTHMA CONDITION 9 20 1 30 A. Pathophysiology 4 6 0 10 1. Teach an individual with asthma and their family using simple language by illustrating the following with appropriate educational aids a.
I. THE ASTHMA CONDITION 9 20 1 30 A. Pathophysiology 4 6 0 10 1. Teach an individual with asthma and their family using simple language by illustrating the following with appropriate educational aids a.
Chronic Obstructive Pulmonary Disease (COPD) Copyright 2014 by Mosby, an imprint of Elsevier Inc.
 Chronic Obstructive Pulmonary Disease () 8.18.18 Copyright 2014 by Mosby, an imprint of Elsevier Inc. Description Airflow limitation not fully reversible progressive Abnormal inflammatory response of lungs
Chronic Obstructive Pulmonary Disease () 8.18.18 Copyright 2014 by Mosby, an imprint of Elsevier Inc. Description Airflow limitation not fully reversible progressive Abnormal inflammatory response of lungs
COPD. Breathing Made Easier
 COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
CARE OF THE ADULT COPD PATIENT
 CARE OF THE ADULT COPD PATIENT Target Audience: The target audience for this clinical guideline is all MultiCare providers and staff including those associated with our Clinically Integrated Network. The
CARE OF THE ADULT COPD PATIENT Target Audience: The target audience for this clinical guideline is all MultiCare providers and staff including those associated with our Clinically Integrated Network. The
Respiratory Assessment
 Module Four Physical examination of Respiratory Assessment 1 THORACIC CAGE: Anterior thoracic cage Posterior thoracic cage 2 Reference lines: Anterior vertical lines Lateral vertical line Posterior vertical
Module Four Physical examination of Respiratory Assessment 1 THORACIC CAGE: Anterior thoracic cage Posterior thoracic cage 2 Reference lines: Anterior vertical lines Lateral vertical line Posterior vertical
Chronic Obstructive Pulmonary Disease
 Chronic Obstructive Pulmonary Disease 07 Contributor Dr David Tan Hsien Yung Definition, Diagnosis and Risk Factors for (COPD) Differential Diagnoses Goals of Management Management of COPD THERAPY AT EACH
Chronic Obstructive Pulmonary Disease 07 Contributor Dr David Tan Hsien Yung Definition, Diagnosis and Risk Factors for (COPD) Differential Diagnoses Goals of Management Management of COPD THERAPY AT EACH
Chronic Obstructive Pulmonary Disease
 Page 1 of 5 Chronic Obstructive Pulmonary Disease Chronic Obstructive Pulmonary Disease (COPD) is an 'umbrella' term for people with chronic bronchitis, emphysema, or both. With COPD the airflow to the
Page 1 of 5 Chronic Obstructive Pulmonary Disease Chronic Obstructive Pulmonary Disease (COPD) is an 'umbrella' term for people with chronic bronchitis, emphysema, or both. With COPD the airflow to the
Community COPD Service Protocol
 Community COPD Service Protocol Acknowledgements This protocol is based on the following documents: 1. Chronic obstructive pulmonary disease: Management of chronic obstructive pulmonary disease in adults
Community COPD Service Protocol Acknowledgements This protocol is based on the following documents: 1. Chronic obstructive pulmonary disease: Management of chronic obstructive pulmonary disease in adults
