Title: Reproducibility of the bronchoconstrictive response to eucapnic voluntary hyperpnoea
|
|
|
- Paulina Griffith
- 6 years ago
- Views:
Transcription
1 Title: Reproducibility of the bronchoconstrictive response to eucapnic voluntary hyperpnoea Authors: Williams NC, Johnson MA, Hunter KA, Sharpe GR Affiliation: Sport, Health and Performance Enhancement (SHAPE) Research Group, School of Science and Technology, Nottingham Trent University, Nottingham, NG11 8NS, UK Corresponding Author Dr Michael A Johnson School of Science and Technology Nottingham Trent University Nottingham NG11 8NS UK Telephone:+44 (0) Fax: +44 (0) Michael.johnson@ntu.ac.uk Abbreviations: EVH, eucapnic voluntary hyperpnoea; HIB, hyperpnoea-induced bronchoconstriction; EIB, exercise-induced bronchoconstriction; FVC, forced vital capacity; FEV 1, forced expiratory volume in 1 s; MVV, maximal voluntary ventilation;, minute ventilation; AUC, area under the curve; CV, coefficient of variation; SMC, smallest meaningful change. 1
2 Abstract Background: Eucapnic voluntary hyperpnoea (EVH) is considered an effective bronchoprovocation challenge for identifying exercise-induced bronchoconstriction (EIB). However, the reproducibility of the hyperpnoea-induced bronchoconstriction (HIB) response elicited by EVH remains unknown and was therefore the focus of this study. Methods: Two cohorts of 16 physically active males (each cohort comprised 8 controls and 8 with physician diagnosis of asthma) participated in two studies of the short- and long-term reproducibility of the bronchoconstrictive response to an EVH test with dry air. EVH was performed on days 0, 7, 14, and 21 (short-term study), and 0, 35, and 70 (long-term study). HIB was diagnosed by a 10% fall in forced expiratory volume in 1 s (F 1 ) after EVH. Results: On day 0 of the short-term study, FEV 1 fell by 2 1% (P < 0.05) and 27 18% (P < 0.01) from pre- to post-evh in control and HIB-positive groups respectively. The post-evh fall in FEV 1 did not differ across the short-term study test days. In the HIB-positive group, the day-to-day coefficient of variation, reproducibility, and smallest meaningful change for the fall in FEV 1 were 12%, 328 ml, and 164 ml, respectively. On day 0 of the long-term study, FEV 1 fell by 2 2% and 25 18% (P < 0.01) after EVH in control and HIB-positive groups respectively. The post-evh fall in FEV 1 did not differ across the long-term study test days. In the HIB-positive group, the day-to-day coefficient of variation, reproducibility, and smallest meaningful change for the fall in FEV 1 were 10%, 196 ml, and 98 ml respectively. Conclusion: The EVH test elicits a reproducible bronchoconstrictive response in physically active males with physician diagnosed asthma. These data thus support the clinical utility of the EVH test for EIB screening and monitoring. Key words: Exercise-induced bronchoconstriction; asthma; eucapnic voluntary hyperpnoea; reproducibility. 2
3 Introduction Asthma affects 5-10% of the population in developed countries 1 and is the most common chronic medical condition reported among Olympic athletes with a prevalence of around 8%. 2 At least 80% of individuals with clinically diagnosed asthma 3 and up to 50% of particular elite athlete populations 4 will also experience exercise-induced bronchoconstriction (EIB). EIB is characterised by transient airway narrowing during or after exercise and is ascribed to airway drying and subsequent changes in airway osmolality, which results in degranulation of inflammatory cells and release of inflammatory mediators. 5,6 Diagnosis of EIB should not be based exclusively on self-reported symptoms 7-9 as they lack sensitivity and specificity Instead, EIB diagnosis should be objective and based on a fall in forced expiratory volume in 1 s (FEV 1 ) after an exercise challenge, or a surrogate for exercise such as eucapnic voluntary hyperpnoea (EVH). 7,9 Exercise challenges are highly specific, but they lack sensitivity and thus the rate of false-negative diagnoses can be high. 13,15 Exercise challenges are also difficult to standardise due to changing environmental conditions and ventilatory responses, which determine the degree of EIB. 15,16 The EVH test comprises 6 min of voluntary hyperpnoea using a dry gas and high minute ventilation ( ). Hyperpnoeainduced bronchoconstriction (HIB) is diagnosed when FEV 1 falls by 10%. 17,18 The EVH test can be tightly controlled, has high specificity and sensitivity for diagnosing EIB, and results in fewer false-negative diagnoses compared with exercise challenges. 15,19-21 It is therefore considered a superior bronchoprovocation challenge for identifying EIB. 15,22 The clinical utility of the EVH test critically depends on the extent to which it elicits a reproducible day-to-day fall in FEV 1. Reproducibility is determined by the measurement error and within-individual fluctuation, which may increase with longer time intervals. 23 However, few studies have examined the reproducibility of HIB elicited by EVH across different time 3
4 intervals and using robust methods. Some studies failed to use appropriate statistical techniques to evaluate reproducibility, 17 whereas others examined elite swimmers 14 who may have a unique EIB pathophysiology. 24,25 Price et al. 26 reported poor reproducibility for the fall in FEV 1 (95% limits of agreement: -10.7% to 9.5%) after EVH in 32 individuals (6 with physician diagnosed asthma) with borderline HIB ( 10% fall in FEV 1 ). The reproducibility of HIB elicited by EVH in individuals with physician diagnosed asthma and more severe HIB is therefore unknown. Thus, the aim of the present study was to evaluate the short- (21 days) and long- (70 days) term test-retest reproducibility of HIB elicited by EVH in individuals with physician diagnosed asthma who were also positive for HIB during initial screening. Methods Following approval from the Nottingham Trent University Human Ethics Committee, two cohorts of 16 physically active (completing 4-6 hours of aerobic exercise per week) males provided written informed consent to participate in a short-term (4 EVH tests each separated by 7 days) or long-term (3 EVH tests each separated by 35 days) study of HIB reproducibility. All participants were non-smokers and had no history of smoking. Each cohort comprised 8 control participants and 8 HIB-positive participants. Inclusion criteria for HIB-positive participants included physician diagnosis of asthma, a baseline FEV 1 >65% of predicted, 17 and a 10% fall in FEV 1 following EVH. 9 On commencing the short-term study, HIB-positive participants were taking the following prescribed medication: N = 5, short acting β2 agonists; N = 1, combination of short acting β2 agonists and inhaled corticosteroids; N = 1, combination of short and long acting β2 agonists and inhaled corticosteroids; N = 1, combination of short acting β2 agonists, inhaled corticosteroids, and leukotriene modifiers. On commencing the long-term study, HIB-positive participants were taking the following 4
5 prescribed medication: N = 5, short acting β2 agonists; N = 1 short acting β2 agonists and inhaled corticosteroids; N = 2, short and long acting β2 agonists and inhaled corticosteroids. Inclusion criteria for the HIB-positive group did not consider changes of medication prior to starting the study, but exclusion criteria included a change in medication during the study. Throughout the study, participants adhered to their usual habitual exercise regime and avoided strenuous exercise during the 48 h prior to testing. 18 Pulmonary function and EVH test Baseline pulmonary function (forced vital capacity (FVC) and FEV 1 ) was assessed according to published guidelines 27 using a pneumotachograph (Pneumotrac, Vitalograph, Buckinghm, UK) as previously described. 28,29 For the 2 weeks prior to each EVH test, participants were free from any chest or upper respiratory tract infection. 19 On EVH test days participants abstained from caffeine and alcohol as they can influence asthma exacerbations, 30,31 and arrived at the laboratory at least 2 h post-prandial. For each participant, EVH tests were performed at the same time of day. Participants with asthma ceased their medication prior to each EVH test (inhaled corticosteroids and leukotriene modifiers: 4 days; inhaled long acting β2 agonists: 2 days; anti-histamines: 2 days; inhaled short acting β2 agonists: the day of the test). 18,19 The EVH test comprised 6 min of voluntary hyperpnoea at a target of 85% of the predicted maximal voluntary ventilation (MVV) (30 x baseline FEV 1 ). 17,18 Participants breathed through a flanged mouthpiece (Series 9060; Hans Rudolph, Missouri, USA) connected to a flow sensor (ZAN variable orifice pneumotach; Nspire Health, Oberthulba, Germany) that was calibrated using a 3 L syringe. Gas concentrations were measured using fast responding laser diode absorption spectroscopy sensors, which were calibrated using gases of known concentration (5% CO 2, 15% O 2, balance N 2 ; BOC, Guilford, UK), and 5
6 ventilatory and pulmonary gas exchange variables were measured breath-by-breath (ZAN 600USB; Nspire Health) as previously described. 28,29 A two-way non-rebreathing valve (2700 Series; Hans Rudolph) was connected distally to the flow sensor and the inspiratory port was connected via a 1.2 m length of corrugated tubing (internal diameter: 35 mm) to a 150 L capacity Douglas bag. Participants inspired from the Douglas bag which was continuously filled with gases of known concentration (21% O 2, 5% CO 2, balance N 2 ; BOC). 32 The inspired gas was at room temperature (19-21 C) and of low humidity (<3%). During EVH, participants faced a computer monitor and received real-time visual feedback of, and endtidal CO 2 was continuously monitored to ensure that isocapnia was maintained. After EVH, pulmonary function was assessed in duplicate at 3, 6 and 16 min, and the highest values recorded were used for subsequent analysis. After the EVH test, HIB-positive participants were supervised in the laboratory until their FEV 1 was within 10% of their baseline FEV 1. Statistical analysis The short- and long-term reproducibility studies were analysed separately using the Statistical Package for the Social Sciences (SPSS, Chicago, IL). Between-group comparisons (HIB-positive vs. control) for baseline FVC and FEV 1 were made using independent samples t-tests. One-way repeated measures ANOVA followed by Bonferroni adjusted pairwise comparisons was used to evaluate the within-group effects of day (short-term study: day 0, 7, 14, and 21; long-term study: day 0, 35, and 70) on baseline FVC and FEV 1. One-way repeated measures ANOVA followed by Bonferroni adjusted pairwise comparisons was used to evaluate the within-group effects of time after EVH (3, 6, and 16 min) on FVC and FEV 1. On all occasions there were no differences between these time points for FVC and FEV 1 and, therefore, the three values were averaged and used for further analyses, including reproducibility statistics. One-way repeated measures ANOVA followed by Bonferroni adjusted pairwise comparisons was used to evaluate the within-group effects of day on the 6
7 average FVC and FEV 1 measured after EVH. In HIB-positive participants the area under the curve for % F 1 during the 16 min period after EVH (AUC 0-16 % F 1 ) was calculated using the trapezoidal rule. Day-to-day variation in baseline FVC and FEV 1, and the fall in FEV 1 after EVH, was calculated as the within-participant coefficient of variation (CV). Measurement error and reproducibility were calculated for FVC and FEV 1 measured before and after EVH. The same statistics were also calculated for the absolute change in FVC and FEV 1 from baseline to post- EVH. The smallest meaningful change was subsequently determined. 33,34 Statistical significance was set at P < Results are presented as mean SD, unless otherwise indicated. Results No participants were excluded during the course of the study. Participant characteristics and baseline (mean across study days) pulmonary function before EVH are shown in Table 1. In both short- and long-term studies FVC before EVH did not differ between HIB-positive and control groups. In the short-term study there was a trend for baseline FEV 1 to be lower in the HIB-positive group compared with the control group (P = 0.056). In the long-term study baseline FEV 1 was lower in the HIB-positive group compared with the control group (P < 0.05). The mean target during EVH was therefore lower in the HIB-positive group compared with the control group in both short-term ( vs L min -1, P = 0.056) and long-term ( vs L min -1, P < 0.05) studies. In both studies and in both groups FVC and FEV 1 measured before EVH, and therefore the target during EVH, were not different between test days. The achieved during EVH was not different between test days in both short-term (HIB-positive: L min -1, range 7
8 L min -1, 86 11% MVV; control: L min -1, range L min -1, 84 2% MVV) and long-term (HIB-positive: L min -1, range L min -1, 88 9% MVV; control: L min -1, range L min -1, 82 4% MVV) studies. End-tidal CO 2 during EVH ( mmhg) was not different from rest ( mmhg) with a mean difference of mmhg (range: mmhg) (data pooled from both groups and both studies). Short term study Control group On day 0 of the short-term study, FVC was unchanged after EVH in the control group. Conversely, FEV 1 fell 3 2% 3 min after EVH (P < 0.05) and remained below baseline throughout the post-evh period (P < 0.05). The fall in FEV 1 after EVH was not different between the 4 short-term study days (Table 2). HIB-positive group On day 0 of the short-term study, FVC fell 11 14% 3 min after EVH in the HIBpositive group (P < 0.05) and remained below baseline throughout the post-evh period (P < 0.05). The fall in FVC after EVH was not different between the 4 short-term study days (Table 2). On day 0 of the short-term study, FEV 1 fell 27 18% 3 min after EVH (P < 0.01) and remained below baseline throughout the post-evh period (6 min: P < 0.01; 16 min: P < 0.05). The fall in FEV 1 after EVH was not different between the 4 short-term study days (Table 2). All HIB-positive participants experienced a >10% fall in FEV 1 after every EVH test and the consistency of the fall between days is shown in Figure 1. The AUC 0-16 % F 1 on day 0 of the short-term study was The AUC 0-16 % F 1 was not different between the 4 short-term study days. Between-day reproducibility in pulmonary function for 8
9 the short-term study is shown in Table 3. In the HIB-positive group, the smallest meaningful change for the fall in FEV 1 after EVH represented 17% of the absolute fall. Long term study Control group On day 0 of the long-term study, FVC was unchanged after EVH in the control group, whereas FEV 1 fell 3 1% 6 min after EVH (P < 0.01). FEV 1 at 3 and 16 min after EVH was not different from baseline. The fall in FEV 1 was not different between the 3 long-term study days (Table 4). HIB-positive group On day 0 of the long-term study, FVC fell 20 15% 6 min after EVH in the HIBpositive group (P < 0.05). There was also a trend for FVC to be lower than baseline 3 (P = 0.07) and 16 min (P = 0.09) after EVH. The fall in FVC after EVH was not different between the 3 long-term study days (Table 4). On day 0 of the long-term study, FEV 1 fell 27 19% 3 min after EVH (P < 0.05) and remained below baseline throughout the post-evh period (6 min: P < 0.01; 16 min: P < 0.05). The fall in FEV 1 was not different between the 3 long-term study days (Table 4). All HIB-positive participants experienced a >10% fall in FEV 1 after every EVH test and the consistency of the fall between days is shown in Figure 2. The AUC 0-16% F 1 on day 0 of the long-term study was The AUC 0-16 % F 1 was not different between the 3 long-term study days. Between-day reproducibility in pulmonary function for the long-term study is shown in Table 5. In the HIB-positive group, the smallest meaningful change for the fall in FEV 1 after EVH represented 11% of the absolute fall. 9
10 Discussion The present study is the first to report the reproducibility of the bronchoconstrictive response elicited by the 6 min EVH test in recreationally active males with physician diagnosed asthma. The main finding was that the EVH test elicits a reproducible fall in FEV 1 when evaluated over short- (21 days) and long-term (70 days) periods. These data therefore support the clinical utility of the EVH test for EIB screening and monitoring. The EVH test is an indirect bronchoprovocation test that is considered a suitable objective surrogate for identifying EIB. 9,35 The test can be tightly controlled and standardised, results in fewer false-negative EIB diagnoses compared with exercise challenges, and can diagnose EIB in previously undiagnosed and asymptomatic individuals. 15,19-21 The clinical utility of the EVH test is, in part, dependent on the extent to which it elicits a reproducible fall in FEV 1. Two previous studies reported good reproducibility for the fall in FEV 1 after two EVH tests performed on separate occasions; however, one failed to use appropriate statistical techniques to evaluate reproducibility, 17 and the other studied competitive swimmers 14 who may have a unique EIB pathophysiology. 24,25 The degree of HIB can be classified as mild ( % fall in FEV 1 ), moderate ( % fall in FEV 1 ), or severe ( 30% fall in F 1 ), 18 and Price et al. 26 have raised concerns regarding the reproducibility of HIB in individuals demonstrating a mild or borderline ( 10%) post-evh fall in FEV 1, which may result in misdiagnosis of EIB. Conversely, in the present study the post-evh fall in FEV 1 was highly reproducible for all HIB-positive participants, including those with mild HIB (Figures 1 and 2). Although the reasons for this inter-study discrepancy remain unclear, only 6 of 32 participants studied by Price et al. 26 had physician diagnosed asthma and the post-evh fall in FEV 1 (10 8%) was much smaller than in the present study ( 27%). Our data show that in 10
11 recreationally active males with physician diagnosed asthma the degree of HIB elicited by EVH is reproducible for up to 70 days irrespective of HIB severity. Based on patient perception of change, the minimal important difference for improvement or worsening in FEV 1 is 10% from baseline. 36 The post-evh fall in FEV 1 in the control groups is thus unlikely to have clinical significance. In the HIB-positive groups the mean FEV 1 at baseline was 4.03 and 3.75 L in the short- and long-term studies respectively, and thus an improvement or worsening in FEV 1 of 403 and 375 ml respectively would be perceptible. The smallest meaningful change for the post-evh fall in FEV 1 in the short- (164 ml) and long-term (98 ml) studies therefore demonstrates that the EVH test is sufficiently sensitive to detect clinically relevant changes in HIB that might occur with, for example, a therapeutic intervention. It is essential that isocapnia is maintained during EVH because hyperpnoea-induced hypocapnia can cause bronchoconstriction in individuals with asthma, whereas hypercapnia can cause bronchodilation in individuals with and without asthma. 37 The gold standard EVH gas mixture (4.5-5% CO 2 ) is based on the work of Phillips et al. 32 who showed that isocapnia is maintained over a range of from L min -1. Although in the present study the achieved during EVH exceeded this range, end-tidal CO 2 scarcely deviated from rest and, therefore, the observed HIB was not influenced by hypocapnia or hypercapnia. The present study therefore extends the findings of Phillips et al. 32 by showing that an EVH gas mixture containing 5% CO 2 can maintain isocapnia over a range of from L min -1. Limitations Caution is warranted when generalising the present findings to women. Changes in sex hormones during the menstrual cycle have been linked with cyclic changes in lung function in women with and without asthma, 38 and around half of women with asthma 11
12 experience an aggravation of asthma symptoms and increased medication use during the premenstrual or menstrual phase. 39,40 Women are also 2.38 times less likely than males to achieve a of 60% MVV during EVH (a criterion for an adequate test), although they may also experience bronchoconstriction at a lower than men. 41 These confounders may influence the ability of the EVH test to elicit a reproducible fall in FEV 1 in women with asthma. Further studies are therefore needed to establish the utility of the EVH test in women with asthma, including whether a reproducible bronchoconstrictive response is elicited across different time intervals and phases of the menstrual cycle. The EVH test is very provocative and may not represent the ventilatory and environmental challenges associated with most forms of exercise. 19 However, exercise challenges are difficult to standardise and they lack sensitivity, which can result in falsenegative diagnoses. Thus, a positive HIB diagnosis from the EVH test identifies that an individual is at risk of EIB and should therefore explore appropriate pharmacological treatment. Conclusions In conclusion, the degree of HIB elicited by the EVH test is reproducible over short- (21 days) and long-term (70 days) periods in recreationally active males with physician diagnosed asthma. These data support the clinical utility of the EVH test for EIB screening and monitoring, and for evaluating the effectiveness of therapeutic interventions for reducing EIB. Acknowledgements None 12
13 References 1. Wenzel SE. Asthma phenotypes: the evolution from clinical to molecular approaches. Nat Med 2012; 18: Fitch KD. An overview of asthma and airway hyper-responsiveness in Olympic athletes. Br J Sports Med 2012; 46: Anderson SD. Exercise-induced bronchoconstriction in the 21st century. J Am Osteopath Assoc 2011; 111:S Ali Z, Norsk P, Ulrik CS. Mechanisms and management of exercise-induced asthma in elite athletes. J Asthma 2012; 49: Hallstrand TS, Altemeier WA, Aitken ML, Henderson WR,Jr. Role of cells and mediators in exercise-induced bronchoconstriction. Immunol Allergy Clin North Am 2013; 33:313,28, vii. 6. Hallstrand TS. New insights into pathogenesis of exercise-induced bronchoconstriction. Curr Opin Allergy Clin Immunol 2012; 12: Anderson SD, Kippelen P. Assessment and prevention of exercise-induced bronchoconstriction. Br J Sports Med 2012; 46: Boulet LP, O'Byrne PM. Asthma and exercise-induced bronchoconstriction in athletes. N Engl J Med 2015; 372: Parsons JP, Hallstrand TS, Mastronarde JG, Kaminsky DA, Rundell KW, Hull JH, et al. An official American Thoracic Society clinical practice guideline: exercise-induced bronchoconstriction. Am J Respir Crit Care Med 2013; 187: Ansley L, Kippelen P, Dickinson J, Hull JH. Misdiagnosis of exercise-induced bronchoconstriction in professional soccer players. Allergy 2012; 67: Parsons JP, Kaeding C, Phillips G, Jarjoura D, Wadley G, Mastronarde JG. Prevalence of exercise-induced bronchospasm in a cohort of varsity college athletes. Med Sci Sports Exerc 2007; 39: Rundell KW, Im J, Mayers LB, Wilber RL, Szmedra L, Schmitz HR. Self-reported symptoms and exercise-induced asthma in the elite athlete. Med Sci Sports Exerc 2001; 33: Rundell KW, Wilber RL, Szmedra L, Jenkinson DM, Mayers LB, Im J. Exercise-induced asthma screening of elite athletes: field versus laboratory exercise challenge. Med Sci Sports Exerc 2000; 32: Stadelmann K, Stensrud T, Carlsen KH. Respiratory symptoms and bronchial responsiveness in competitive swimmers. Med Sci Sports Exerc 2011; 43:
14 15. Dickinson JW, Whyte GP, McConnell AK, Harries MG. Screening elite winter athletes for exercise induced asthma: a comparison of three challenge methods. Br J Sports Med 2006; 40:179,82; discussion Rundell KW, Slee JB. Exercise and other indirect challenges to demonstrate asthma or exercise-induced bronchoconstriction in athletes. J Allergy Clin Immunol 2008; 122:238,46; quiz Argyros GJ, Roach JM, Hurwitz KM, Eliasson AH, Phillips YY. Eucapnic voluntary hyperventilation as a bronchoprovocation technique: development of a standarized dosing schedule in asthmatics. Chest 1996; 109: Anderson SD, Argyros GJ, Magnussen H, Holzer K. Provocation by eucapnic voluntary hyperpnoea to identify exercise induced bronchoconstriction. Br J Sports Med 2001; 35: Dickinson J, McConnell A, Whyte G. Diagnosis of exercise-induced bronchoconstriction: eucapnic voluntary hyperpnoea challenges identify previously undiagnosed elite athletes with exercise-induced bronchoconstriction. Br J Sports Med 2011; 45: Molphy J, Dickinson J, Hu J, Chester N, Whyte G. Prevalence of bronchoconstriction induced by eucapnic voluntary hyperpnoea in recreationally active individuals. J Asthma 2014; 51: Rundell KW, Anderson SD, Spiering BA, Judelson DA. Field exercise vs laboratory eucapnic voluntary hyperventilation to identify airway hyperresponsiveness in elite cold weather athletes. Chest 2004; 125: Anderson SD. Indirect challenge tests: Airway hyperresponsiveness in asthma: its measurement and clinical significance. Chest 2010; 138:25S-30S. 23. Chinn S, Schouten JP. Reproducibility of non-specific bronchial challenge in adults: implications for design, analysis and interpretation of clinical and epidemiological studies. Thorax 2005; 60: Bougault V, Boulet LP. Airway dysfunction in swimmers. Br J Sports Med 2012; 46: Bougault V, Turmel J, St-Laurent J, Bertrand M, Boulet LP. Asthma, airway inflammation and epithelial damage in swimmers and cold-air athletes. Eur Respir J 2009; 33: Price OJ, Ansley L, Hull JH. Diagnosing exercise-induced bronchoconstriction with eucapnic voluntary hyperpnea: is one test enough? J Allergy Clin Immunol Pract 2015; 3: Miller MR, Hankinson J, Brusasco V, Burgos F, Casaburi R, Coates A, et al. Standardisation of spirometry. Eur Respir J 2005; 26:
15 28. Johnson MA, Mills DE, Brown DM, Bayfield KJ, Gonzalez JT, Sharpe GR. Inspiratory loading intensity does not influence lactate clearance during recovery. Med Sci Sports Exerc 2012; 44: Mills DE, Johnson MA, McPhilimey MJ, Williams NC, Gonzalez JT, Barnett YA, et al. The effects of inspiratory muscle training on plasma interleukin-6 concentration during cycling exercise and a volitional mimic of the exercise hyperpnea. J Appl Physiol (1985) 2013; 115: Duffy P, Phillips YY. Caffeine consumption decreases the response to bronchoprovocation challenge with dry gas hyperventilation. Chest 1991; 99: Vally H, Thompson PJ. Alcoholic drinks and asthma. Clin Exp Allergy 2002; 32: Phillips YY, Jaeger JJ, Laube BL, Rosenthal RR. Eucapnic voluntary hyperventilation of compressed gas mixture. A simple system for bronchial challenge by respiratory heat loss. Am Rev Respir Dis 1985; 131: Bland JM, Altman DG. Measurement error. BMJ 1996; 313: Hopkins WG. Measures of reliability in sports medicine and science. Sports Med 2000; 30: Anderson SD, Kippelen P. Assessment and prevention of exercise-induced bronchoconstriction. Br J Sports Med 2012; 46: Santanello NC, Zhang J, Seidenberg B, Reiss TF, Barber BL. What are minimal important changes for asthma measures in a clinical trial? Eur Respir J 1999; 14: van den Elshout FJ, van Herwaarden CL, Folgering HT. Effects of hypercapnia and hypocapnia on respiratory resistance in normal and asthmatic subjects. Thorax 1991; 46: Farha S, Asosingh K, Laskowski D, Hammel J, Dweik RA, Wiedemann HP, et al. Effects of the menstrual cycle on lung function variables in women with asthma. Am J Respir Crit Care Med 2009; 180: Murphy VE, Gibson PG. Premenstrual asthma: prevalence, cycle-to-cycle variability and relationship to oral contraceptive use and menstrual symptoms. J Asthma 2008; 45: Pereira Vega A, Sanchez Ramos JL, Maldonado Perez JA, Alvarez Gutierrez FJ, Ignacio Garcia JM, Vazquez Oliva R, et al. Variability in the prevalence of premenstrual asthma. Eur Respir J 2010; 35: Brummel NE, Mastronarde JG, Rittinger D, Philips G, Parsons JP. The clinical utility of eucapnic voluntary hyperventilation testing for the diagnosis of exercise-induced bronchospasm. J Asthma 2009; 46:
16 Table 1. Participant characteristics and baseline pulmonary function (pooled data across all test days) for short- and long-term studies. Values are mean SD. *Significant difference between groups in the long-term study (P < 0.05). Short-term study Long-term study HIB-positive Control HIB-positive Control Age (yr) Height (cm) Body mass (kg) FVC (L) % predicted FEV 1 (L) * % predicted HIB, hyperpnoea-induced bronchoconstriction; FVC, forced vital capacity; FEV 1, forced expiratory volume in 1 s. 16
17 Table 2 Relative and absolute changes in pulmonary function after eucapnic voluntary hyperpnoea (EVH) performed on 4 separate days in the short-term study. Values represent the mean ± SD of the three post-evh measurements. Day Change % ml % ml % ml % ml EIB-positive Control ΔFVC ΔFEV ΔFVC ΔFEV FVC, forced vital capacity; FEV 1, forced expiratory volume in 1 s. 17
18 Table 3 Between-day reproducibility in baseline pulmonary function and the fall in pulmonary function after eucapnic voluntary hyperpnoea performed on 4 separate days (day 0, 7, 14, and 21) in the short-term study. HIB-positive Day-to-day CV (%) Measurement error Reproducibility SMC Baseline FVC (ml) Baseline FEV 1 (ml) Fall in FEV 1 (ml) Control Baseline FVC (ml) Baseline FEV 1 (ml) CV, coefficient of variation; SMC, smallest meaningful change; HIB, hyperpnoea-induced bronchoconstriction; FVC, forced vital capacity; FEV 1, forced expiratory volume in 1 s. 18
19 Table 4 Relative and absolute changes in pulmonary function after eucapnic voluntary hyperpnoea (EVH) in the long-term study. Values represent the mean ± SD of the three post- EVH measurements. Day Change % ml % ml % ml EIB-positive Control ΔFVC ΔFEV ΔFVC ΔFEV FVC, forced vital capacity; FEV 1, forced expiratory volume in 1. 19
20 Table 5 Between-day reproducibility in baseline pulmonary function and the fall in pulmonary function after eucapnic voluntary hyperpnoea performed on 3 separate days (day 0, 35, and 70) in the long-term study. HIB-positive Day-to-day CV (%) Measurement error Reproducibility SMC Baseline FVC (ml) Baseline FEV 1 (ml) Fall in FEV 1 (ml) Control Baseline FVC (ml) Baseline FEV 1 (ml) CV, coefficient of variation; SMC, smallest meaningful change; FVC, forced vital capacity; FEV 1, forced expiratory volume in 1 s. 20
21 Figure 1. Individual falls in forced expiratory volume in 1 s (FEV 1 ) after eucapnic voluntary hyperpnoea (EVH) in the short-term study. Data are for HIB-positive participants only, with identical symbols representing the same HIB-positive participant. 21
22 Figure 2. Individual falls in forced expiratory volume in 1 s (FEV 1 ) after eucapnic voluntary hyperpnoea (EVH) in the long-term study. Data are for HIB-positive participants only, with identical symbols representing the same HIB-positive participant. 22
THE ROLE OF IMPULSE OSCILLOMETRY IN DETECTING AIRWAY DYSFUNCTION IN ATHLETES
 THE ROLE OF IMPULSE OSCILLOMETRY IN DETECTING AIRWAY DYSFUNCTION IN ATHLETES Word count: 3097 Abstract word count: 250 Running title: Detecting airway dysfunction in athletes. Key words: Asthma, Diagnosis,
THE ROLE OF IMPULSE OSCILLOMETRY IN DETECTING AIRWAY DYSFUNCTION IN ATHLETES Word count: 3097 Abstract word count: 250 Running title: Detecting airway dysfunction in athletes. Key words: Asthma, Diagnosis,
Prevalence of Exercise-Induced Bronchoconstriction Measured by Standardized Testing in Healthy College Athletes
 Prevalence of Exercise-Induced Bronchoconstriction Measured by Standardized Testing in Healthy College Athletes David Burnett PhD RRT AE-C, Steve Burns PhD, Samantha Merritt MSc, Jo Wick PhD, and Matthew
Prevalence of Exercise-Induced Bronchoconstriction Measured by Standardized Testing in Healthy College Athletes David Burnett PhD RRT AE-C, Steve Burns PhD, Samantha Merritt MSc, Jo Wick PhD, and Matthew
Prevalence of Exercise-Induced Bronchoconstriction Measured by Standardized Testing in Healthy College Athletes
 Prevalence of Exercise-Induced Bronchoconstriction Measured by Standardized Testing in Healthy College Athletes David M Burnett PhD RRT AE-C, Steve Burns PhD, Samantha Merritt MSc, Jo Wick PhD, and Matthew
Prevalence of Exercise-Induced Bronchoconstriction Measured by Standardized Testing in Healthy College Athletes David M Burnett PhD RRT AE-C, Steve Burns PhD, Samantha Merritt MSc, Jo Wick PhD, and Matthew
Beta 2 adrenoceptor agonists and the Olympic Games in Athens
 Beta 2 adrenoceptor agonists and the Olympic Games in Athens 1 Appendix A of the Olympic Movement Anti-Doping Code, the List of Prohibited Substances and Prohibited Methods dated 1 st January 2003 states
Beta 2 adrenoceptor agonists and the Olympic Games in Athens 1 Appendix A of the Olympic Movement Anti-Doping Code, the List of Prohibited Substances and Prohibited Methods dated 1 st January 2003 states
Eucapnic Voluntary Hyperpnea: Gold Standard for Diagnosing Exercise-Induced Bronchoconstriction in Athletes?
 Sports Med (2016) 46:1083 1093 DOI 10.1007/s40279-016-0491-3 REVIEW ARTICLE Eucapnic Voluntary Hyperpnea: Gold Standard for Diagnosing Exercise-Induced Bronchoconstriction in Athletes? James H. Hull 1,2
Sports Med (2016) 46:1083 1093 DOI 10.1007/s40279-016-0491-3 REVIEW ARTICLE Eucapnic Voluntary Hyperpnea: Gold Standard for Diagnosing Exercise-Induced Bronchoconstriction in Athletes? James H. Hull 1,2
Exercise-Induced Bronchoconstriction EIB
 Exercise-Induced Bronchoconstriction EIB Case 1 14 yo boy, freshman in high school Complains of shortness of breath 2 minutes into a mile-run in his first gym class Same complains in his 2 nd gym class
Exercise-Induced Bronchoconstriction EIB Case 1 14 yo boy, freshman in high school Complains of shortness of breath 2 minutes into a mile-run in his first gym class Same complains in his 2 nd gym class
NON-SPECIFIC BRONCHIAL HYPERESPONSIVENESS. J. Sastre. Allergy Service
 NON-SPECIFIC BRONCHIAL HYPERESPONSIVENESS J. Sastre. Allergy Service Asthma: definition Asthma is a syndrome defined on basis of three main aspects: 1- Symptoms due to variable and reversible airway obstruction
NON-SPECIFIC BRONCHIAL HYPERESPONSIVENESS J. Sastre. Allergy Service Asthma: definition Asthma is a syndrome defined on basis of three main aspects: 1- Symptoms due to variable and reversible airway obstruction
Role of bronchoprovocation tests in identifying exercise-induced bronchoconstriction in a non-athletic population: a pilot study
 Original Article Role of bronchoprovocation tests in identifying exercise-induced bronchoconstriction in a non-athletic population: a pilot study Jessica H. Y. Tan 1 *, Wui Mei Chew 1 *, Therese S. Lapperre
Original Article Role of bronchoprovocation tests in identifying exercise-induced bronchoconstriction in a non-athletic population: a pilot study Jessica H. Y. Tan 1 *, Wui Mei Chew 1 *, Therese S. Lapperre
Bronchial challenge tests: usefulness, availability and limitations
 This article is based on a postgraduate course from the Barcelona 2010 ERS Annual Congress S.D. Anderson Bronchial challenge tests: usefulness, availability and limitations Introduction Indirect challenges
This article is based on a postgraduate course from the Barcelona 2010 ERS Annual Congress S.D. Anderson Bronchial challenge tests: usefulness, availability and limitations Introduction Indirect challenges
+ Asthma and Athletics
 + Asthma and Athletics Shaylon Rettig, MD, MBA Champion Sports Medicine + Financial Disclosure Dr. Shaylon Rettig has no relevant financial relationships with commercial interests to disclose. + Asthma
+ Asthma and Athletics Shaylon Rettig, MD, MBA Champion Sports Medicine + Financial Disclosure Dr. Shaylon Rettig has no relevant financial relationships with commercial interests to disclose. + Asthma
Asthma Management for the Athlete
 Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
(EVH), 60%) 1, 5, 10, 15 5 (2) 5% CO2, 21% O2,
 A Comparison of Two Challenge Tests for Identifying Exercise-Induced Bronchospasm in Figure Skaters* Edward T. Mannix, PhD; Felice Manfredi, MD; and Mark O. Farber, MD Objectives: Studies documenting the
A Comparison of Two Challenge Tests for Identifying Exercise-Induced Bronchospasm in Figure Skaters* Edward T. Mannix, PhD; Felice Manfredi, MD; and Mark O. Farber, MD Objectives: Studies documenting the
Downloaded on T22:37:55Z. Title. A study to assess the prevalence of exercise-induced bronchoconstriction in inter-county hurling.
 Title Author(s) A study to assess the prevalence of exercise-induced bronchoconstriction in inter-county hurling Hunt, Eithne B.; Murphy, B.; Murphy, C.; Crowley, T.; Cronin, Owen; Hay, S.; Stack, M.;
Title Author(s) A study to assess the prevalence of exercise-induced bronchoconstriction in inter-county hurling Hunt, Eithne B.; Murphy, B.; Murphy, C.; Crowley, T.; Cronin, Owen; Hay, S.; Stack, M.;
This version was downloaded from Northumbria Research Link:
 Citation: Vakali, Sofia, Vogiatzis, Ioannis, Florou, A., Giavi, S., Zakynthinos, S., Papadopoulos, N.G. and Gratziou, Ch. (2017) Exercise-induced bronchoconstriction among athletes: Assessment of bronchial
Citation: Vakali, Sofia, Vogiatzis, Ioannis, Florou, A., Giavi, S., Zakynthinos, S., Papadopoulos, N.G. and Gratziou, Ch. (2017) Exercise-induced bronchoconstriction among athletes: Assessment of bronchial
Mechanisms of action of bronchial provocation testing
 Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
ADVANCES IN THE DIAGNOSIS OF EXERCISE-INDUCED BRONCHOCONSTRICTION
 ADVANCES IN THE DIAGNOSIS OF EXERCISE-INDUCED BRONCHOCONSTRICTION Oliver J. Price 1, James H. Hull 1, 2, Les Ansley 1 1 Faculty of Health and Life Sciences, Northumbria University, Newcastle, United Kingdom
ADVANCES IN THE DIAGNOSIS OF EXERCISE-INDUCED BRONCHOCONSTRICTION Oliver J. Price 1, James H. Hull 1, 2, Les Ansley 1 1 Faculty of Health and Life Sciences, Northumbria University, Newcastle, United Kingdom
Diagnostic Exercise Challenge Testing
 Curr Allergy Asthma Rep (2011) 11:482 490 DOI 10.1007/s11882-011-0225-4 PEDIATRIC ALLERGY AND IMMUNOLOGY (JAY M. PORTNOY AND CHRISTINA E. CIACCIO, SECTION EDITORS) Diagnostic Exercise Challenge Testing
Curr Allergy Asthma Rep (2011) 11:482 490 DOI 10.1007/s11882-011-0225-4 PEDIATRIC ALLERGY AND IMMUNOLOGY (JAY M. PORTNOY AND CHRISTINA E. CIACCIO, SECTION EDITORS) Diagnostic Exercise Challenge Testing
Eucapnic Voluntary Hyperventilation as a Bronchoprovocation Technique*
 Eucapnic Voluntary Hyperventilation as a Bronchoprovocation Technique* Development of a Standardized Dosing Schedule in Asthmatics Gregory]. Argyros, MD, FCCP; James M. Roach, MD, FCCP; Kenneth M. Hurwitz,
Eucapnic Voluntary Hyperventilation as a Bronchoprovocation Technique* Development of a Standardized Dosing Schedule in Asthmatics Gregory]. Argyros, MD, FCCP; James M. Roach, MD, FCCP; Kenneth M. Hurwitz,
Bronchial Challenges and Respiratory Symptoms in Elite Swimmers and Winter Sport Athletes
 CHEST Supplement AIRWAY HYPERRESPONSIVENESS IN ASTHMA: ITS MEASUREMENT AND CLINICAL SIGNIFICANCE Bronchial Challenges and Respiratory Symptoms in Elite Swimmers and Winter Sport Athletes Airway Hyperresponsiveness
CHEST Supplement AIRWAY HYPERRESPONSIVENESS IN ASTHMA: ITS MEASUREMENT AND CLINICAL SIGNIFICANCE Bronchial Challenges and Respiratory Symptoms in Elite Swimmers and Winter Sport Athletes Airway Hyperresponsiveness
Alternatives to exercise challenge for the objective assessment of exerciseinduced
 Alternatives to exercise challenge for the objective assessment of exerciseinduced bronchospasm: eucapnic voluntary hyperpnoea and the osmotic challenge tests Educational aims To describe alternative tests
Alternatives to exercise challenge for the objective assessment of exerciseinduced bronchospasm: eucapnic voluntary hyperpnoea and the osmotic challenge tests Educational aims To describe alternative tests
Sergio Bonini. Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy.
 Assessment of EIA in the community and in athletes: the role of standardized questionnaires Sergio Bonini Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy se.bonini@gmail.com
Assessment of EIA in the community and in athletes: the role of standardized questionnaires Sergio Bonini Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy se.bonini@gmail.com
Tina M. Evans, PhD, ATC; Kenneth W. Rundell, PhD; Kenneth C. Beck, PhD; Alan M. Levine, PhD; and Jennifer M. Baumann, MS, RD, LDN
 Airway Narrowing Measured by Spirometry and Impulse Oscillometry Following Room Temperature and Cold Temperature Exercise* Tina M. Evans, PhD, ATC; Kenneth W. Rundell, PhD; Kenneth C. Beck, PhD; Alan M.
Airway Narrowing Measured by Spirometry and Impulse Oscillometry Following Room Temperature and Cold Temperature Exercise* Tina M. Evans, PhD, ATC; Kenneth W. Rundell, PhD; Kenneth C. Beck, PhD; Alan M.
Joint Session ACOFP and AOASM: Exercise Induced Asthma. Bruce Dubin, DO, JD, FCLM, FACOI
 Joint Session ACOFP and AOASM: Exercise Induced Asthma Bruce Dubin, DO, JD, FCLM, FACOI ACOFP FULL DISCLOSURE FOR CME ACTIVITIES Please check where applicable and sign below. Provide additional pages as
Joint Session ACOFP and AOASM: Exercise Induced Asthma Bruce Dubin, DO, JD, FCLM, FACOI ACOFP FULL DISCLOSURE FOR CME ACTIVITIES Please check where applicable and sign below. Provide additional pages as
Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma
 Original Article Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma Feng-Jia Chen, Huai Liao, Xin-Yan Huang, Can-Mao Xie Department of Respiratory
Original Article Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma Feng-Jia Chen, Huai Liao, Xin-Yan Huang, Can-Mao Xie Department of Respiratory
Exercise and Asthma: What patients and doctors can do to improve outcomes
 Exercise and Asthma: What patients and doctors can do to improve outcomes Timothy Craig, DO Professor of Medicine and Pediatrics Distinguished Educator Program Director Penn State University Hershey, PA,
Exercise and Asthma: What patients and doctors can do to improve outcomes Timothy Craig, DO Professor of Medicine and Pediatrics Distinguished Educator Program Director Penn State University Hershey, PA,
Perception of Exercise-Induced Bronchoconstriction in College Athletes
 Perception of Exercise-Induced Bronchoconstriction in College Athletes David M Burnett PhD RRT AE-C, John P Vardiman PhD ATC, Jake A Deckert MSc, Jaimie L Ward and Matthew R Sharpe MD BACKGROUND: Exercise-induced
Perception of Exercise-Induced Bronchoconstriction in College Athletes David M Burnett PhD RRT AE-C, John P Vardiman PhD ATC, Jake A Deckert MSc, Jaimie L Ward and Matthew R Sharpe MD BACKGROUND: Exercise-induced
Exercise-Induced Bronchospasm. Michael A Lucia, MD, FCCP Asst Clinical Professor, UNR School of Medicine Sierra Pulmonary & Sleep Institute
 Exercise-Induced Bronchospasm Michael A Lucia, MD, FCCP Asst Clinical Professor, UNR School of Medicine Sierra Pulmonary & Sleep Institute EIB Episodic bronchoconstriction with exercise May be an exacerbation
Exercise-Induced Bronchospasm Michael A Lucia, MD, FCCP Asst Clinical Professor, UNR School of Medicine Sierra Pulmonary & Sleep Institute EIB Episodic bronchoconstriction with exercise May be an exacerbation
Comparing the effect of physical activity on pulmonary function of Kerman s professional endurance runners and non-athletes
 International Research Journal of Applied and Basic Sciences 2013 Available online at www.irjabs.com ISSN 2251-838X / Vol, 5 (12): 1552-1556 Science Explorer Publications Comparing the effect of physical
International Research Journal of Applied and Basic Sciences 2013 Available online at www.irjabs.com ISSN 2251-838X / Vol, 5 (12): 1552-1556 Science Explorer Publications Comparing the effect of physical
Efficacy of a Heat Exchanger Mask in Cold Exercise-Induced Asthma* David A. Beuther, MD; and Richard J. Martin, MD, FCCP
 Original Research ASTHMA Efficacy of a Heat Exchanger Mask in Cold Exercise-Induced Asthma* David A. Beuther, MD; and Richard J. Martin, MD, FCCP Study objectives: To determine the efficacy of a novel
Original Research ASTHMA Efficacy of a Heat Exchanger Mask in Cold Exercise-Induced Asthma* David A. Beuther, MD; and Richard J. Martin, MD, FCCP Study objectives: To determine the efficacy of a novel
Asthma, rhinitis, other respiratory diseases
 Responses to bronchial challenge submitted for approval to use inhaled β 2 -agonists before an event at the 2002 Winter Olympics Sandra D. Anderson, PhD, DSc, a Kenneth Fitch, MD, FACSM, b Clare P. Perry,
Responses to bronchial challenge submitted for approval to use inhaled β 2 -agonists before an event at the 2002 Winter Olympics Sandra D. Anderson, PhD, DSc, a Kenneth Fitch, MD, FACSM, b Clare P. Perry,
Ass. Prof. Pulmonary and Crit.Care Medical School,University of Athens
 Diagnosis i of Exercise Induced Asthma Ch. Gratziou Ass. Prof. Pulmonary and Crit.Care Medical School,University of Athens Other Diagnostic Challenges for Exercise Induced Asthma Do we need other tests
Diagnosis i of Exercise Induced Asthma Ch. Gratziou Ass. Prof. Pulmonary and Crit.Care Medical School,University of Athens Other Diagnostic Challenges for Exercise Induced Asthma Do we need other tests
TUE PHYSICIAN GUIDELINES Medical Information to Support the Decisions of TUE Committees Asthma ASTHMA
 1. Medical Condition ASTHMA is a syndrome of the respiratory airways manifested by recurrent episodic symptoms. It is associated with variable airway obstruction that is reversible either spontaneously
1. Medical Condition ASTHMA is a syndrome of the respiratory airways manifested by recurrent episodic symptoms. It is associated with variable airway obstruction that is reversible either spontaneously
Ventilatory functions response to breathing training versus aerobic training in asthmatic children
 Egypt J Pediatr Allergy Immunol 2012;10(1):33-37. Original article Ventilatory functions response to breathing training versus aerobic training in asthmatic children Background: There is worldwide public
Egypt J Pediatr Allergy Immunol 2012;10(1):33-37. Original article Ventilatory functions response to breathing training versus aerobic training in asthmatic children Background: There is worldwide public
B.A. Wilson*, O. Bar-Or**, P.M. O'Byrne +
 Eur Respir J, 1994, 7, 2174 2178 DOI: 10.1183/09031936.94.07122174 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 The effects of indomethacin
Eur Respir J, 1994, 7, 2174 2178 DOI: 10.1183/09031936.94.07122174 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 The effects of indomethacin
Sensitivity and Specificity of Self Reported Symptoms for Exercise Induced Bronchospasm Diagnosis in Children
 Original Article Iran J Pediatr Mar 2009; Vol 19 (No 1), Pp:47-51 Sensitivity and Specificity of Self Reported Symptoms for Exercise Induced Bronchospasm Diagnosis in Children Behroz Bavarian 1,2, MD;
Original Article Iran J Pediatr Mar 2009; Vol 19 (No 1), Pp:47-51 Sensitivity and Specificity of Self Reported Symptoms for Exercise Induced Bronchospasm Diagnosis in Children Behroz Bavarian 1,2, MD;
TUEC Guidelines Medical Information to Support the Decisions of TUE Committees Asthma ASTHMA
 1. Medical Condition ASTHMA is a syndrome of the respiratory airways manifested by recurrent episodic symptoms. It is associated with variable airway obstruction that is reversible either spontaneously
1. Medical Condition ASTHMA is a syndrome of the respiratory airways manifested by recurrent episodic symptoms. It is associated with variable airway obstruction that is reversible either spontaneously
Conflicts of Interest
 Exercise and Asthma: What patients and doctors can do to improve outcomes Timothy Craig, DO Professor of Medicine and Pediatrics Distinguished Educator Program Director Penn State University Hershey, PA,
Exercise and Asthma: What patients and doctors can do to improve outcomes Timothy Craig, DO Professor of Medicine and Pediatrics Distinguished Educator Program Director Penn State University Hershey, PA,
Research Article Exercise-Induced Asthma Symptoms and Nighttime Asthma: Are They Similar to AHR?
 Allergy Volume 2009, Article ID 378245, 6 pages doi:10.1155/2009/378245 Research Article Exercise-Induced Asthma Symptoms and Nighttime Asthma: Are They Similar to AHR? V. Backer and L. M. Rasmussen Department
Allergy Volume 2009, Article ID 378245, 6 pages doi:10.1155/2009/378245 Research Article Exercise-Induced Asthma Symptoms and Nighttime Asthma: Are They Similar to AHR? V. Backer and L. M. Rasmussen Department
**This form MUST accompany a TUE Application for a Beta-2 Agonist if submitted to USADA**
 **This form MUST accompany a TUE Application for a Beta-2 Agonist if submitted to USADA** PHYSICIAN- You must select one of the Objective Tests in the Table below and report the result. Please take note
**This form MUST accompany a TUE Application for a Beta-2 Agonist if submitted to USADA** PHYSICIAN- You must select one of the Objective Tests in the Table below and report the result. Please take note
Exercise-Induced Bronchoconstriction and Vocal Cord Dysfunction
 Exercise-Induced Bronchoconstriction and Vocal Cord Dysfunction 2 Christopher Kempe and Jonathan P. Parsons Exercise-induced bronchoconstriction (EIB) describes acute, transient airway narrowing that occurs
Exercise-Induced Bronchoconstriction and Vocal Cord Dysfunction 2 Christopher Kempe and Jonathan P. Parsons Exercise-induced bronchoconstriction (EIB) describes acute, transient airway narrowing that occurs
When an athlete can t catch his breath. For personal use only
 For mass reproduction, content licensing and permissions contact Dowden Health Media. FAMILY PRACTICE THE JOURNAL OF Michael A. Krafczyk, MD, and F. Dale Bautista, MD St. Luke s Hospital, Bethlehem, Pa
For mass reproduction, content licensing and permissions contact Dowden Health Media. FAMILY PRACTICE THE JOURNAL OF Michael A. Krafczyk, MD, and F. Dale Bautista, MD St. Luke s Hospital, Bethlehem, Pa
Assessment of accuracy and applicability of a new electronic peak flow meter and asthma monitor
 Eur Respir J 18; 12: 45 42 DOI: 18/1.8.5 Printed in UK - all rights reserved Copyright ERS Journals Ltd 18 European Respiratory Journal ISSN - 1 Assessment of accuracy and applicability of a new electronic
Eur Respir J 18; 12: 45 42 DOI: 18/1.8.5 Printed in UK - all rights reserved Copyright ERS Journals Ltd 18 European Respiratory Journal ISSN - 1 Assessment of accuracy and applicability of a new electronic
Asthma. In Europe ~30 million children and adults under 45 have asthma. On average 3 people a day die from asthma in the UK
 Dr Neil Williams Nottingham Trent University College of Science and Technology Department of Sport Science Email: neil.williams@ntu.ac.uk @NeilW_ExPhys 1 Asthma In Europe ~30 million children and adults
Dr Neil Williams Nottingham Trent University College of Science and Technology Department of Sport Science Email: neil.williams@ntu.ac.uk @NeilW_ExPhys 1 Asthma In Europe ~30 million children and adults
BJSM Online First, published on May 29, 2010 as /bjsm Original article
 BJSM Online First, published on May 29, 2010 as 10.1136/bjsm.2009.071043 Original article 1 Department of Lung Medicine, St Olavs Hospital, University Hospital of Trondheim, Trondheim, Norway 2 Department
BJSM Online First, published on May 29, 2010 as 10.1136/bjsm.2009.071043 Original article 1 Department of Lung Medicine, St Olavs Hospital, University Hospital of Trondheim, Trondheim, Norway 2 Department
Airways hyperresponsiveness to different inhaled combination therapies in adolescent asthmatics
 Airways hyperresponsiveness to different inhaled combination therapies in adolescent asthmatics Daniel Machado 1, MD Celso Pereira 1,2, MD, PhD Beatriz Tavares 1, MD Graça Loureiro 1, MD António Segorbe-Luís
Airways hyperresponsiveness to different inhaled combination therapies in adolescent asthmatics Daniel Machado 1, MD Celso Pereira 1,2, MD, PhD Beatriz Tavares 1, MD Graça Loureiro 1, MD António Segorbe-Luís
Financial Disclosure. Exercise Induced Bronchospasm BHR. Exercise Induced Asthma
 Financial Disclosure Exercise Induced Bronchospasm Elizabeth Bailey MSN, CRNP Allergy & Asthma Specialists BREATHE II March, 23, 2012 I have no commercial conflicts of interest and no financial relationships
Financial Disclosure Exercise Induced Bronchospasm Elizabeth Bailey MSN, CRNP Allergy & Asthma Specialists BREATHE II March, 23, 2012 I have no commercial conflicts of interest and no financial relationships
M alcolm Sue - Chu, 1,2 John D B r ann an, 3 S andr a D A nder son, 3 Nor a Che w, 4 L ei f Bjer m er 5
 A ir w ay hy per r e sponsi ve ne s s to me t hacholine, adenosine 5-monophosphate, mannitol, eucapnic voluntary hyperpnoea and fi eld exercise challenge in elite cross-country skiers M alcolm Sue - Chu,
A ir w ay hy per r e sponsi ve ne s s to me t hacholine, adenosine 5-monophosphate, mannitol, eucapnic voluntary hyperpnoea and fi eld exercise challenge in elite cross-country skiers M alcolm Sue - Chu,
PREDICTION EQUATIONS FOR LUNG FUNCTION IN HEALTHY, LIFE TIME NEVER-SMOKING MALAYSIAN POPULATION
 Prediction Equations for Lung Function in Healthy, Non-smoking Malaysian Population PREDICTION EQUATIONS FOR LUNG FUNCTION IN HEALTHY, LIFE TIME NEVER-SMOKING MALAYSIAN POPULATION Justin Gnanou, Brinnell
Prediction Equations for Lung Function in Healthy, Non-smoking Malaysian Population PREDICTION EQUATIONS FOR LUNG FUNCTION IN HEALTHY, LIFE TIME NEVER-SMOKING MALAYSIAN POPULATION Justin Gnanou, Brinnell
Running, walking, and hyperventilation causing
 Thorax, 1979, 34, 582-586 Running, walking, and hyperventilation causing asthma in children H KILHAM, M TOOLEY, AND M SILVERMAN From the Department of Paediatrics, Hammersmith Hospital, London W12 OHS,
Thorax, 1979, 34, 582-586 Running, walking, and hyperventilation causing asthma in children H KILHAM, M TOOLEY, AND M SILVERMAN From the Department of Paediatrics, Hammersmith Hospital, London W12 OHS,
Prevalence of respiratory symptoms in an athlete population
 Respiratory Medicine (2003) 97, 955 963 Prevalence of respiratory symptoms in an athlete population H!el"ene Turcotte, Jean-Bruno Langdeau, Guy Thibault, Louis-Philippe Boulet* Centre de Recherche de l
Respiratory Medicine (2003) 97, 955 963 Prevalence of respiratory symptoms in an athlete population H!el"ene Turcotte, Jean-Bruno Langdeau, Guy Thibault, Louis-Philippe Boulet* Centre de Recherche de l
Medical Emergencies at Moderate and High Altitude
 Medical Emergencies at Moderate and High Altitude Annalisa Cogo Clinica Pneumologica e Centro Studi Biomedici Applicati allo Sport Università di Ferrara Payer Hutte, Ortler Mountain Environment Barometric
Medical Emergencies at Moderate and High Altitude Annalisa Cogo Clinica Pneumologica e Centro Studi Biomedici Applicati allo Sport Università di Ferrara Payer Hutte, Ortler Mountain Environment Barometric
asthma to appear, and it is typically the last symptom to disappear with treatment. 15 Even after treatment with
 Exercise-Induced Bronchoconstriction in the 21st Century Sandra D. Anderson, PhD, DSc Exercise-induced bronchoconstriction (EIB) is the term used to describe the transient narrowing of the lower airways
Exercise-Induced Bronchoconstriction in the 21st Century Sandra D. Anderson, PhD, DSc Exercise-induced bronchoconstriction (EIB) is the term used to describe the transient narrowing of the lower airways
Relationship Between FEV1& PEF in Patients with Obstructive Airway Diseases
 OBSTRUCTIVE THE IRAQI POSTGRADUATE AIRWAY MEDICAL DISEASES JOURNAL Relationship Between FEV1& PEF in Patients with Obstructive Airway Diseases Muhammed.W.AL.Obaidy *, Kassim Mhamed Sultan*,Basil Fawzi
OBSTRUCTIVE THE IRAQI POSTGRADUATE AIRWAY MEDICAL DISEASES JOURNAL Relationship Between FEV1& PEF in Patients with Obstructive Airway Diseases Muhammed.W.AL.Obaidy *, Kassim Mhamed Sultan*,Basil Fawzi
This is a cross-sectional analysis of the National Health and Nutrition Examination
 SUPPLEMENTAL METHODS Study Design and Setting This is a cross-sectional analysis of the National Health and Nutrition Examination Survey (NHANES) data 2007-2008, 2009-2010, and 2011-2012. The NHANES is
SUPPLEMENTAL METHODS Study Design and Setting This is a cross-sectional analysis of the National Health and Nutrition Examination Survey (NHANES) data 2007-2008, 2009-2010, and 2011-2012. The NHANES is
Pulmonary Function Testing
 In the Clinic Pulmonary Function Testing Hawa Edriss MD, Gilbert Berdine MD The term PFT encompasses three different measures of lung function: spirometry, lung volumes, and diffusion capacity. In this
In the Clinic Pulmonary Function Testing Hawa Edriss MD, Gilbert Berdine MD The term PFT encompasses three different measures of lung function: spirometry, lung volumes, and diffusion capacity. In this
EVect of breathing circuit resistance on the measurement of ventilatory function
 9 Department of Respiratory Medicine, The Alfred Hospital and Monash University Medical School, Melbourne, Victoria, Australia 311 D P Johns C M Ingram S Khov P D Rochford E H Walters Correspondence to:
9 Department of Respiratory Medicine, The Alfred Hospital and Monash University Medical School, Melbourne, Victoria, Australia 311 D P Johns C M Ingram S Khov P D Rochford E H Walters Correspondence to:
It is advisable to refer to the publisher s version if you intend to cite from the work.
 Comparable reductions in hyperpnoeainduced bronchoconstriction and markers of airway inflammation after supplementation with 6.2 and 3.1 g/d of long chain omega 3 polyunsaturated fatty acids in adults
Comparable reductions in hyperpnoeainduced bronchoconstriction and markers of airway inflammation after supplementation with 6.2 and 3.1 g/d of long chain omega 3 polyunsaturated fatty acids in adults
Performing a Methacholine Challenge Test
 powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers?
 Disclosures: Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers? Stanley Fineman, MD Past-President, American College of Allergy, Asthma & Immunology Adjunct Associate
Disclosures: Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers? Stanley Fineman, MD Past-President, American College of Allergy, Asthma & Immunology Adjunct Associate
Meenu Singh, Joseph L. Mathew, Prabhjot Malhi, B.R. Srinivas and Lata Kumar
 Comparison of Improvement in Quality of Life Score with Objective Parameters of Pulmonary Function in Indian Asthmatic Children Receiving Inhaled Corticosteroid Therapy Meenu Singh, Joseph L. Mathew, Prabhjot
Comparison of Improvement in Quality of Life Score with Objective Parameters of Pulmonary Function in Indian Asthmatic Children Receiving Inhaled Corticosteroid Therapy Meenu Singh, Joseph L. Mathew, Prabhjot
allergy Asia Pacific Original Article H. Haluk Akar *, Fulya Tahan, and Hatice Eke Gungor
 pissn 2233-8276 eissn 2233-8268 Original Article http://dx.doi.org/1.5415/ap.15.5.2.98 Asia Pac Allergy 15;5:98-12 The association of forced expiratory volume in one second and forced expiratory flow at
pissn 2233-8276 eissn 2233-8268 Original Article http://dx.doi.org/1.5415/ap.15.5.2.98 Asia Pac Allergy 15;5:98-12 The association of forced expiratory volume in one second and forced expiratory flow at
JANUARY Guide to the WADA Prohibited List and Therapeutic Use Exemptions
 JANUARY 2018 Guide to the WADA Prohibited List and Therapeutic Use Exemptions Contents The WADA Prohibited List 3 Therapeutic Use Exemptions (TUEs) 5 Requirements for asthma TUEs 9 2 The WADA Prohibited
JANUARY 2018 Guide to the WADA Prohibited List and Therapeutic Use Exemptions Contents The WADA Prohibited List 3 Therapeutic Use Exemptions (TUEs) 5 Requirements for asthma TUEs 9 2 The WADA Prohibited
Life-long asthma and its relationship to COPD. Stephen T Holgate School of Medicine University of Southampton
 Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
COPD. Breathing Made Easier
 COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
Difference Between The Slow Vital Capacity And Forced Vital Capacity: Predictor Of Hyperinflation In Patients With Airflow Obstruction
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 4 Number 2 Difference Between The Slow Vital Capacity And Forced Vital Capacity: Predictor Of Hyperinflation In Patients With Airflow Obstruction
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 4 Number 2 Difference Between The Slow Vital Capacity And Forced Vital Capacity: Predictor Of Hyperinflation In Patients With Airflow Obstruction
Correlation between spirometry values and pulmonary artery pressure in young. healthy subjects
 Correlation between spirometry values and pulmonary artery pressure in young healthy subjects Alon Grossman MD MHA 1, 2, Michal Benderly Ph. D 3, Alex Prokupetz MHA 1, Barak Gordon MD MHA 1, Ofra Kalter-Leibovici
Correlation between spirometry values and pulmonary artery pressure in young healthy subjects Alon Grossman MD MHA 1, 2, Michal Benderly Ph. D 3, Alex Prokupetz MHA 1, Barak Gordon MD MHA 1, Ofra Kalter-Leibovici
It is well established that a cold and dry ambient environment. Incidence of exercise-induced bronchospasm in Olympic winter sport athletes
 Incidence of exercise-induced bronchospasm in Olympic winter sport athletes RANDALL L. WILBER, KENNETH W. RUNDELL, LEON SZMEDRA, DAVID M. JENKINSON, JOOHEE IM, and SEAN D. DRAKE United States Olympic Committee,
Incidence of exercise-induced bronchospasm in Olympic winter sport athletes RANDALL L. WILBER, KENNETH W. RUNDELL, LEON SZMEDRA, DAVID M. JENKINSON, JOOHEE IM, and SEAN D. DRAKE United States Olympic Committee,
Adenosine 5 0 -monophosphate increases levels of leukotrienes in breath condensate in asthma
 Respiratory Medicine (2004) 98, 651 655 Adenosine 5 0 -monophosphate increases levels of leukotrienes in breath condensate in asthma E. Bucchioni, Z. Csoma, L. Allegra, K.F. Chung, P.J. Barnes, S.A. Kharitonov*
Respiratory Medicine (2004) 98, 651 655 Adenosine 5 0 -monophosphate increases levels of leukotrienes in breath condensate in asthma E. Bucchioni, Z. Csoma, L. Allegra, K.F. Chung, P.J. Barnes, S.A. Kharitonov*
What Makes a Difference in Exercise-Induced Bronchoconstriction: An 8 Year Retrospective Analysis
 What Makes a Difference in Exercise-Induced Bronchoconstriction: An 8 Year Retrospective Analysis Han-Ki Park 1,2, Jae-Woo Jung 2,3, Sang-Heon Cho 1,2, Kyung-Up Min 1,2, Hye-Ryun Kang 1,2 * 1 Department
What Makes a Difference in Exercise-Induced Bronchoconstriction: An 8 Year Retrospective Analysis Han-Ki Park 1,2, Jae-Woo Jung 2,3, Sang-Heon Cho 1,2, Kyung-Up Min 1,2, Hye-Ryun Kang 1,2 * 1 Department
TRENDS in Sport Sciences 2015; 1(22): ISSN
 REVIEW ARTICLE TRENDS in Sport Sciences 2015; 1(22): 17-21. ISSN 2299-9590 Asthma in athletes and the use of asthma treatment TOMASZ BALCEREK, PRZEMYSŁAW LUTOMSKI, MIKOŁAJ GRZESIAK Asthma is a common disease
REVIEW ARTICLE TRENDS in Sport Sciences 2015; 1(22): 17-21. ISSN 2299-9590 Asthma in athletes and the use of asthma treatment TOMASZ BALCEREK, PRZEMYSŁAW LUTOMSKI, MIKOŁAJ GRZESIAK Asthma is a common disease
COMMON RESPIRATORY DISORDERS IN ELITE SWIMMERS
 SPORTS SCIENCE COMMON RESPIRATORY DISORDERS IN ELITE SWIMMERS DIAGNOSIS AND MANAGEMENT Written by Jon Greenwell, United Kingdom Swimming is widely promoted as a suitable exercise to maintain cardiovascular
SPORTS SCIENCE COMMON RESPIRATORY DISORDERS IN ELITE SWIMMERS DIAGNOSIS AND MANAGEMENT Written by Jon Greenwell, United Kingdom Swimming is widely promoted as a suitable exercise to maintain cardiovascular
Bronchial hyperresponsiveness testing in athletes of the Swiss Paralympic team
 Osthoff et al. BMC Sports Science, Medicine, and Rehabilitation 2013, 5:7 RESEARCH Open Access Bronchial hyperresponsiveness testing in athletes of the Swiss Paralympic team Mirjam Osthoff 1, Franz Michel
Osthoff et al. BMC Sports Science, Medicine, and Rehabilitation 2013, 5:7 RESEARCH Open Access Bronchial hyperresponsiveness testing in athletes of the Swiss Paralympic team Mirjam Osthoff 1, Franz Michel
Not all who wheeze have asthma
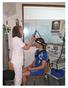 Not all who wheeze have asthma Educational aims Exercise-induced asthma is frequently found among children, adolescents and young adults. The diagnosis of asthma should be documented by variable lung function,
Not all who wheeze have asthma Educational aims Exercise-induced asthma is frequently found among children, adolescents and young adults. The diagnosis of asthma should be documented by variable lung function,
Outline FEF Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications?
 Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Budesonide treatment of moderate and severe asthma in children: A doseresponse
 Budesonide treatment of moderate and severe asthma in children: A doseresponse study Soren Pedersen, MD, PhD, and Ove Ramsgaard Hansen, MD Kolding, Denmark Objective: The purpose of the study was to evaluate
Budesonide treatment of moderate and severe asthma in children: A doseresponse study Soren Pedersen, MD, PhD, and Ove Ramsgaard Hansen, MD Kolding, Denmark Objective: The purpose of the study was to evaluate
Comparison of exhaled nitric oxide measurements between NIOX MINO â electrochemical and Ecomedics chemiluminescence analyzer
 Respiratory Medicine (2008) 102, 1667e1671 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed SHORT COMMUNICATION Comparison of exhaled nitric oxide measurements between
Respiratory Medicine (2008) 102, 1667e1671 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed SHORT COMMUNICATION Comparison of exhaled nitric oxide measurements between
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air
 Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Technical Assessment of Spirometers Connected in Series
 Technical Assessment of Spirometers Connected in Series Quentin Lefebvre, Thomas Vandergoten, Eric Derom MD PhD, Emilie Marchandise PhD, and Giuseppe Liistro MD PhD BACKGROUND: Office spirometers are now
Technical Assessment of Spirometers Connected in Series Quentin Lefebvre, Thomas Vandergoten, Eric Derom MD PhD, Emilie Marchandise PhD, and Giuseppe Liistro MD PhD BACKGROUND: Office spirometers are now
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Do current treatment protocols adequately prevent airway remodeling in children with mild intermittent asthma?
 Respiratory Medicine (2006) 100, 458 462 Do current treatment protocols adequately prevent airway remodeling in children with mild intermittent asthma? Haim S. Bibi a,, David Feigenbaum a, Mariana Hessen
Respiratory Medicine (2006) 100, 458 462 Do current treatment protocols adequately prevent airway remodeling in children with mild intermittent asthma? Haim S. Bibi a,, David Feigenbaum a, Mariana Hessen
Lung Function Basics of Diagnosis of Obstructive, Restrictive and Mixed Defects
 Lung Function Basics of Diagnosis of Obstructive, Restrictive and Mixed Defects Use of GOLD and ATS Criteria Connie Paladenech, RRT, RCP, FAARC Benefits and Limitations of Pulmonary Function Testing Benefits
Lung Function Basics of Diagnosis of Obstructive, Restrictive and Mixed Defects Use of GOLD and ATS Criteria Connie Paladenech, RRT, RCP, FAARC Benefits and Limitations of Pulmonary Function Testing Benefits
Relationship between Methacholine Challenge Testing and exhaled Nitric Oxide in adult patients with suspected bronchial asthma
 O R I G I N A L A R T I C L E S Eur Ann Allergy Clin Immunol Vol 46, N 3, 109-113, 2014 M. Giovannini, M. Valli, V. Ribuffo, R. Melara, G. Cappiello, E. Businarolo, A. Andreani Relationship between Methacholine
O R I G I N A L A R T I C L E S Eur Ann Allergy Clin Immunol Vol 46, N 3, 109-113, 2014 M. Giovannini, M. Valli, V. Ribuffo, R. Melara, G. Cappiello, E. Businarolo, A. Andreani Relationship between Methacholine
Exercise induced airway obstruction in children: Patho-physiology and diagnostics Driessen, J.M.M.
 UvA-DARE (Digital Academic Repository) Exercise induced airway obstruction in children: Patho-physiology and diagnostics Driessen, J.M.M. Link to publication Citation for published version (APA): Driessen,
UvA-DARE (Digital Academic Repository) Exercise induced airway obstruction in children: Patho-physiology and diagnostics Driessen, J.M.M. Link to publication Citation for published version (APA): Driessen,
PULMONARY FUNCTION TESTING. Purposes of Pulmonary Tests. General Categories of Lung Diseases. Types of PF Tests
 PULMONARY FUNCTION TESTING Wyka Chapter 13 Various AARC Clinical Practice Guidelines Purposes of Pulmonary Tests Is lung disease present? If so, is it reversible? If so, what type of lung disease is present?
PULMONARY FUNCTION TESTING Wyka Chapter 13 Various AARC Clinical Practice Guidelines Purposes of Pulmonary Tests Is lung disease present? If so, is it reversible? If so, what type of lung disease is present?
Stability of the EasyOne ultrasonic spirometer for use in general practice
 Blackwell Publishing AsiaMelbourne, AustraliaRESRespirology1323-77992006 Blackwell Publishing Asia Pty Ltd2006113306310MiscellaneousCalibration of an ultrasonic spirometerjae Walters et al. Respirology
Blackwell Publishing AsiaMelbourne, AustraliaRESRespirology1323-77992006 Blackwell Publishing Asia Pty Ltd2006113306310MiscellaneousCalibration of an ultrasonic spirometerjae Walters et al. Respirology
Original Contributions
 Original Contributions Comparison of a New Desktop Spirometer (Spirospec) with a Laboratory Spirometer in a Respiratory Out-Patient Clinic François Swart, Macé M Schuurmans MD, Johannes C Heydenreich,
Original Contributions Comparison of a New Desktop Spirometer (Spirospec) with a Laboratory Spirometer in a Respiratory Out-Patient Clinic François Swart, Macé M Schuurmans MD, Johannes C Heydenreich,
LUNG FUNCTION TESTING: SPIROMETRY AND MORE
 LUNG FUNCTION TESTING: SPIROMETRY AND MORE OBJECTIVES 1. To describe other lung function testing for toddlers and those who cannot perform spirometry 2. To describe a lung function test on infants 3. To
LUNG FUNCTION TESTING: SPIROMETRY AND MORE OBJECTIVES 1. To describe other lung function testing for toddlers and those who cannot perform spirometry 2. To describe a lung function test on infants 3. To
GETTING STARTED WITH MANNITOL CHALLENGE TESTING. Rick Ballard, RRT, RPFT Applications/Education Specialist MGC Diagnostics
 GETTING STARTED WITH MANNITOL CHALLENGE TESTING Rick Ballard, RRT, RPFT Applications/Education Specialist MGC Diagnostics OBJECTIVES Indications for provocation testing Identify candidates for testing
GETTING STARTED WITH MANNITOL CHALLENGE TESTING Rick Ballard, RRT, RPFT Applications/Education Specialist MGC Diagnostics OBJECTIVES Indications for provocation testing Identify candidates for testing
Dyspneic athlete FIELD MANAGEMENT OF SPORTS INJURIES (J KINDERKNECHT, SECTION EDITOR) David Krey & Thomas Best. Introduction
 Curr Rev Musculoskelet Med (2014) 7:373 380 DOI 10.1007/s12178-014-9236-9 FIELD MANAGEMENT OF SPORTS INJURIES (J KINDERKNECHT, SECTION EDITOR) Dyspneic athlete David Krey & Thomas Best Published online:
Curr Rev Musculoskelet Med (2014) 7:373 380 DOI 10.1007/s12178-014-9236-9 FIELD MANAGEMENT OF SPORTS INJURIES (J KINDERKNECHT, SECTION EDITOR) Dyspneic athlete David Krey & Thomas Best Published online:
RESPIRATORY MUSCLE TRAINING
 RESPIRATORY MUSCLE TRAINING RESPIRATORY MUSCLE FATIGUE RESPIRATORY MUSCLE TRAINING During heavy exercise, breathing frequency rises to 40 to 50 breaths per minute. Tidal volume is 3 to 4 litres. This gives
RESPIRATORY MUSCLE TRAINING RESPIRATORY MUSCLE FATIGUE RESPIRATORY MUSCLE TRAINING During heavy exercise, breathing frequency rises to 40 to 50 breaths per minute. Tidal volume is 3 to 4 litres. This gives
SPIROMETRY METHOD. COR-MAN IN / EN Issue A, Rev INNOVISION ApS Skovvænget 2 DK-5620 Glamsbjerg Denmark
 SPIROMETRY METHOD COR-MAN-0000-006-IN / EN Issue A, Rev. 2 2013-07 INNOVISION ApS Skovvænget 2 DK-5620 Glamsbjerg Denmark Tel.: +45 65 95 91 00 Fax: +45 65 95 78 00 info@innovision.dk www.innovision.dk
SPIROMETRY METHOD COR-MAN-0000-006-IN / EN Issue A, Rev. 2 2013-07 INNOVISION ApS Skovvænget 2 DK-5620 Glamsbjerg Denmark Tel.: +45 65 95 91 00 Fax: +45 65 95 78 00 info@innovision.dk www.innovision.dk
Office Based Spirometry
 Osteopathic Family Physician (2014)1, 14-18 Scott Klosterman, DO; Woodson Crenshaw, OMS4 Spartanburg Regional Family Medicine Residency Program; Edward Via College of Osteopathic Medicine - Virginia Campus
Osteopathic Family Physician (2014)1, 14-18 Scott Klosterman, DO; Woodson Crenshaw, OMS4 Spartanburg Regional Family Medicine Residency Program; Edward Via College of Osteopathic Medicine - Virginia Campus
Peak Expiratory Flow Is Not a Quality Indicator for Spirometry*
 Original Research PULMONARY FUNCTION TESTING Peak Expiratory Flow Is Not a Quality Indicator for Spirometry* Peak Expiratory Flow Variability and FEV 1 Are Poorly Correlated in an Elderly Population Matthew
Original Research PULMONARY FUNCTION TESTING Peak Expiratory Flow Is Not a Quality Indicator for Spirometry* Peak Expiratory Flow Variability and FEV 1 Are Poorly Correlated in an Elderly Population Matthew
Outcome, classification and management of wheezing in preschool children Paul L.P. Brand
 Outcome, classification and management of wheezing in preschool children Paul L.P. Brand Princess Amalia Children s Clinic Isala klinieken, Zwolle the Netherlands p.l.p.brand@isala.nl Valle de la Luna,
Outcome, classification and management of wheezing in preschool children Paul L.P. Brand Princess Amalia Children s Clinic Isala klinieken, Zwolle the Netherlands p.l.p.brand@isala.nl Valle de la Luna,
THE NEW ZEALAND MEDICAL JOURNAL
 THE NEW ZEALAND MEDICAL JOURNAL Vol 120 No 1267 ISSN 1175 8716 Is Salamol less effective than Ventolin? A randomised, blinded, crossover study in New Zealand Catherina L Chang, Manisha Cooray, Graham Mills,
THE NEW ZEALAND MEDICAL JOURNAL Vol 120 No 1267 ISSN 1175 8716 Is Salamol less effective than Ventolin? A randomised, blinded, crossover study in New Zealand Catherina L Chang, Manisha Cooray, Graham Mills,
NG80. Asthma: diagnosis, monitoring and chronic asthma management (NG80)
 Asthma: diagnosis, monitoring and chronic asthma management (NG80) NG80 NICE has checked the use of its content in this product and the sponsor has had no influence on the content of this booklet. NICE
Asthma: diagnosis, monitoring and chronic asthma management (NG80) NG80 NICE has checked the use of its content in this product and the sponsor has had no influence on the content of this booklet. NICE
Bronchoconstriction in Response to Deep Inhalation During Spirometry Testing
 Bronchoconstriction in Response to Deep Inhalation During Spirometry Testing Jeffrey M Haynes RRT RPFT Introduction In healthy individuals, airway resistance has an inverse relationship with lung volume.
Bronchoconstriction in Response to Deep Inhalation During Spirometry Testing Jeffrey M Haynes RRT RPFT Introduction In healthy individuals, airway resistance has an inverse relationship with lung volume.
Aerobic Conditioning in Mild Asthma Decreases the Hyperpnea of Exercise and Improves Exercise and Ventilatory Capacity*
 preliminary report Aerobic Conditioning in Mild Asthma Decreases the Hyperpnea of Exercise and Improves Exercise and Ventilatory Capacity* Teal S. Hallstrand, MD; Peter W. Bates, MD, FCCP; and Robert B.
preliminary report Aerobic Conditioning in Mild Asthma Decreases the Hyperpnea of Exercise and Improves Exercise and Ventilatory Capacity* Teal S. Hallstrand, MD; Peter W. Bates, MD, FCCP; and Robert B.
