Hypertonic saline challenge in an adult epidemiological survey
|
|
|
- David Kennedy
- 6 years ago
- Views:
Transcription
1 Occup. Med. Vol. 46,. 3, pp ,996 Copyright 996 Rapid Science Publishers for SOM Printed in Great Britain. All rights reserved /96 ORIGINAL PAPERS Hypertonic saline challenge in an adult epidemiological survey S. J. Rabone,* W. O. Phoon, f S. D. Anderson,* K. C. Wan, s M. Seneviratne," L. Gutierrez" and J. Brannan* *5 Johnston Crescent Lane Cove, Australia 2066, a Worksafe Australia, GPO Box 58, Sydney NSW, Australia 200, ^Department of Occupational Health, University of Sydney, PO Box 88, Pymble NSWAustralia 2073, ^Department of Thoracic Medicine, Royal Prince Alfred Hospital, Camperdown NSW, Australia 2050, ^Department of Occupational Health, Safety and Welfare of Western Australia, PO Box 294 West Perth WA, Australia 6005 Bronchial provocation tests using pharmacological agents such as methacholine or histamine are used in epidemiological studies to identify asthma despite recognition of limitations in specificity, positive predictive value and availability of reagents. Hypertonic saline (4.5%) bronchial challenge (HSBC), although less sensitive than pharmacological challenges, is reportedly highly specific in diagnosing current asthma. Added advantages are that reagents are cheap, stable and recognized by participants. Thus, HSBC may offer benefits over pharmacological tests in epidemiological surveys. This paper reports on the second field survey using the test, a study of 99 adults from the timber industry in Western Australia. The test is described and critically appraised as a practical epidemiological tool for assessing asthma prevalence. At a cutoff point of 20% FEV, fall, HSBC was positive in 8% of subjects, appeared specific for asthma, was safe, well-accepted and easy to use in the field. Key words: Asthma; bronchial provocation tests; sputum; epidemiological methods. Occup. Med. Vol. 46,77-85,996 Received 4 August 995; accepted infinalform 3 March 996. INTRODUCTION A diagnosis of asthma in occupational settings has often been made on the basis of clinical examination by a medical practitioner, questionnaire surveys and spirometry. This approach does not give an index of the underlying physiological abnormalities of asthma, i.e. airway hyperresponsiveness, and for this reason is inaccurate. To overcome this problem The European Respiratory Society recommends the combination of airway hyperresponsiveness and recent wheezing (in the last year) as a definition of asthma for epidemiology. 2 The most commonly used tests in the field have been inhalation of aerosols of methacholine and histamine. These pharmacological agents act directly on smooth muscle to cause contraction, and consequently are known as direct challenges. They are excellent tests for identifying airway hyperresponsive- Correspondence and reprint requests to: S. J. Rabone, 5 Johnston Crescent Lane Cove, Australia ness but their role in identifying current asthma in the random population has been questioned. 3 The reason relates to the specificity of the challenge to identify current asthma and the subsequent high proportion of false positive results. For example, Enarson et a/. 3 found a sensitivity of 47%, specificity of 85% and positive predictive value of only 2% for methacholine challenge in identifying questionnaire-diagnosed asthma. They used a cutoff of PC20 (provocative concentration causing a 20% drop in FEVi) of < 8mg/ml to identify subjects who had ever had asthma amongst a group of workers employed mainly in timber and grain industries. Similarly, using the same PC20 cutoff value, Cockcroft et al. 4 recently reported a specificity of 93%, sensitivity of 00% and a positive predictive value of 29% for histamine in identifying current asthma in a random group of 500 college students. There are other bronchial provocation tests that are thought to be more specific for asthma than direct challenges. These include cold air, exercise, distilled water and hyperosmolar saline. These tests are known "as 'indirect challenges' and cause the airways to narrow by the endogenous release of mediators. 5 ' 6 ' 7 Thus, both
2 78 Occup. Med. Vol. 46, 996 cellular and neural pathways involved in the asthmatic response are tested with indirect challenges. It is for this reason they are considered to be more specific for asthma, while less sensitive for detecting bronchial hyperresponsiveness. Hypertonic saline bronchial challenge (HSBC) has an advantage over exercise testing in that it produces a dose-response curve while also identifying persons responsive to exercise and hyperventilation. Challenge with 4.5% NaCl is well established in hospital-based laboratories and recently the challenge has been used successfully in an epidemiological study of asthma in school children. 8 In the industrial setting, challenge with hyperosmolar saline appears to have some advantages over challenge with pharmacological agents. The equipment required for the test is easily obtained, sodium chloride BP is cheap, readily available for use in humans and the test is well tolerated. Salt is an easily recognized substance and not one perceived to be harmful, so higher rates of participation in the test might be expected. In laboratorybased populations the sensitivity of the challenge has been shown to be about 80% 9 and the specificity 00%, 0 using a cutoff point of > 20% FEVi fall for a positive test. In an epidemiological survey 8 of schoolchildren, using a cutoff point of > 5% FEVi fall, sensitivity and specificity of the test in identifying 'current wheeze' were 47% and 92% respectively, and the positive predictive value was 8%. serious adverse events have been reported using HSBC either in the laboratory or in the field. Cough is the only commonly reported side-effect. The maximum airway response occurs usually within -2 minutes following the last exposure to the aerosol" and late reactions are very uncommon. Because there are no reports of the use of HSBC in industrial surveys, and because of the potential advantages of the test, it was decided to investigate its use and acceptability in an industrial setting, on employees from work sites in the timber and particleboard industries of Western Australia. This paper addresses the practical aspects of using HSBC to detect airway hyperresponsiveness and assesses its use in epidemiological surveys. MATERIALS AND METHODS The study was a cross-sectional survey of 99 employees in six worksites of two timber industry companies in Western Australia. It included completion of a questionnaire, height measurement, baseline spirometry and the 4.5% saline bronchial challenge. Materials The materials necessary for performing the 4.5% saline bronchial challenge test, complying with the protocol of Smith and Anderson 2 and the European Respiratory Society, 2 are presented in Table. Questionnaire Self-administered questionnaire. The questionnaire included questions on age, gender, medical conditions requiring intervention over a recent time period, 3 respiratory symptoms, 4 and smoking habits. Seven questions were taken from the International Union Against Tuberculosis and Lung Disease Questionnaire (IUAT Bronchial Symptoms Questionnaire, 986), M and most of these questions (except those on cough) have been shown to be associated with bronchial hyperresponsiveness to histamine. 4 A series of questions designed to determine disease prevalence by asking the reasons for seeking interventions for recent health complaints were taken from the National Table. Equipment used for HSBC Equipment required Ultrasonic nebulisers Large bore, non-rebreathing expiratory valves 35mm mouthpieces for the Hans Rudolph Valve Spirometers and mouthpieces Spirometer calibrating syringe Electronic balance, to 0. g, max capacity > kg 4.5% Sodium chloride solution Bronchodilator Resuscitation equipment, including bronchodilators, corticosteroids, oxygen supply with attachments for artificial respiration Miscellaneous: electronic stopwatch, noseclips, hand calculator, towels and tissues* Equipment used" DeVilbiss 900 and De Vilbiss (De Vilbiss Health Care Inc, Somerset, PA, USA) Hans Rudolph 2700B with saliva trap (Kansas City Mo. USA) Vacumed (Ventura, CA, USA) part number 00 Vitalograph Alpha electronic, Vitalograph model S bellows. (Vitalograph Ltd, Buckingham, UK) Vitallograph litre syringe (Cat ) Sartorius PT200 (Sartorius GmbH Goettingen Germany) Sodium chloride BP, distilled water, beakers for weighing, litre containers for storage Salbutamol respirator solution 5mg/2.5ml, inhalers 00ug/dose Oxy-viva (CIGWELD, Melbourne, Australia) dexamethasone 8mg/ml injection, adrenaline mg/ml injection, 25 gauge hypodermic needles, 2 and 5ml syringes * Two sets of equipment were used in the survey. Towels and tissues are important because the test provokes salivation
3 S. J. Rabone ef a/.: Hypertonic saline challenge 79 Health Survey conducted by the Australian Bureau of Statistics. 3 Administered questionnaire. In order to determine subject acceptance of the 4.5% saline bronchial challenge, participants were asked to record their reactions following the test in one of four categories. The categories were: () very uncomfortable (never again); (2) uncomfortable (not again unless I have to); (3) mildly uncomfortable (minor inconvenience to have it again) and (4) no problems. METHODS Selection and characteristics of participants Eligibility for entry to the study was confined to employees from six worksites of two timber companies in Western Australia. Recruitment involved announcement of a 'health survey' by both management and employee-representative groups, a video demonstration of study procedures and distribution of a one-page information leaflet. On the back of this leaflet, recipients were asked whether they wished to participate in the study, and if they did, whether by completing a questionnaire only, or by full participation. From the list of volunteers, a sample from each worksite was chosen to participate in the study. The number of subjects in each sample depended on the rate of volunteering in the four small worksites (where all volunteers were included) or on the time constraints of the investigative team at the larger worksites (where random sampling of volunteers due at work occurred). The sample of 99 consisted of eight subjects from a chemical factory making formaldehyde-urea and melamine-urea for particleboard production, from a pine sawmill, 35 from the main particleboard producing plant, from a hardwood timber mill/processing centre, seven (no females) from a hardwood mill and 26 from a hardwood processing centre. There were six females. Mean age was 38 years (range 9-6). Ninety were employed as labourers, drivers of machinery or as plant operators. Nine were employed as tradesmen, para professionals and managers. Twenty-seven smoked, 32 were ex-smokers and 39 had never smoked. Hyperosmolar 4.5% saline bronchial challenge Current use and timing of medications were ascertained, with particular attention to asthma medications. Height was measured. The HSBC was performed using the techniques of Smith and Anderson 9 ' 2 which have been adopted by the European Respiratory Society. 2 Exposures were for 0.5,, 2, 4 and 8 minutes. After each exposure the participant performed FEVi on two occasions and the best was recorded. The procedure was stopped if FEVi fell below 80% of baseline, if the subject requested cessation or after a total of 5.5 minutes exposure. Participants were observed for 20 minutes following the test. Those who recorded falls in FEVi greater than 5% were administered inhaled bronchodilator (salbutamol 5mg) via nebuliser or 200ug via inhaler and observed until FEVi improved to within 0% of baseline value. In the case of non-response to bronchodilator, further measures were taken at the discretion of the medical practitioner (see below). The test was deemed positive if the final FEVi (following the 8 minute exposure or following cessation of the test) was 5% below baseline. This protocol differed from that of the European Respiratory Society in the following respects: medications were not requested to be withheld before the test, the test was not stopped after 5ml had been nebulised (although subjects who received < 5ml and who did not have a fall in FEVi > 5% were excluded from analysis), FEVi measurements were performed seconds following each exposure and bronchodilator was not given routinely at the completion of the test. Data analysis Statistical Analysis Software ( SAS Institute Inc, Cary, NC, USA) was used. Falls in FEV, > 5% and 20% of baseline recordings were determined and allocated to dichotomous variables, l asthl5' and 'asth20'. Cohen's kappa statistic 5 was chosen as a measure of agreement between dichotomous responses to respiratory symptom questions and these variables. The statistic is the observed proportion of responses in agreement adjusted for expected chance agreement, and ranges from - to +. 6 Dose-response graphs were constructed for all subjects who were 'asthl5' positive, and PDis FEVi values (the provoking dose of 4.5% saline required to cause a 5% FEVi reduction) calculated by linear interpolation from these graphs. In addition to analyzing PD5, all data was analyzed using log dose-response ratios, calculated as logio (per cent fall in FEVi divided by total dose of 4.5% saline delivered in ml). In order to investigate relationships between a positive HSBC test and respiratory questionnaire responses, multiple logistic regression analysis (Proc Logistic SAS) was performed using 'asthls' as the dependent variable and dichotomous responses to IUAT questions, 3, 7 and (see Table 2) and the chronic bronchitis question 'have you brought up phlegm from your chest on most mornings for at least 3 months each year for the last 2 years?' A stepwise backward elimination procedure was used which eliminated the least significant variable and stopped when the residual % 2 became significant at the 5% level. Gender and age were independent variables in a separate analysis with 'asthl5' as the dependent variable. Multiple linear regression (Proc GLM-SAS) was used to analyze the same relationships for 'FEVifall', the per cent fall in FEVi from baseline value following the HSBC.
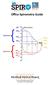
4 80 Occup. Med. Vol. 46, 996 Table 2. Agreement between luat questions and 4.5% hyperosmolar bronchial challenge at 5% FEVi fall cutoff. Numbers in parentheses are results at 20% cutoff. Question luat number' Positive HSBC T Kappa* Have you ever had wheezing or whistling in your chest at any time in the last 2 months? Have you at any time in the last 2 months had attacks of shortness of breath that come on during the day when you are not doing anything strenuous? Have you, at any time in the last 2 months, been woken at night by an attack of coughing? Do you usually cough first thing in the morning? Do you usually bring up phlegm from your chest first thing in the morning? Have you ever had an attack of asthma? Have you had an attack of asthma at any time in the last 2 months? Have you brought up phlegm from your chest on most mornings for at least 3 months each year for the last 2 years? National Health Survey asthma estimate Do you feel you have problems with your breathing? Have you at any time in the last 2 months felt chest tightness when you were not doing anything strenuous? * The luat number refers to the position of the question in the luat Bronchial Symptoms Questionnaire (5) 8(2) 3(3) 2(4) 7(2) 8(5) 4() (6) 3() 2(6) 4(4) (3) 4(4) (3) 3 () 2(6) 5(5) 0 (2) 4(3) (4) 4(3) (4) 8 (20) 56 (62) () 63 (7) 2 (26) 53 (56) 3 (6) 6 (66) 20 (22) 54 (60) 3(3) 7 (79) 2(2) 72 (80) 2 (4) 62 (68) 5(5) 69 (77) 3(4) 6 (68) 5 (6) 59 (66) 0.8 (0.22) 0.05 (0.20) 0.5 (-0.0) 0.09 (-0.03) (-0.06) 0.3 (0.53) 0.32 (0.58) 0.05 (-0.02) 0.3 (0.55) 0.09 (0.6) 0.06 (0.3) Positive 4.5% hypeitonic Saline Challenge test is defined as > 5% reduction (or, in parentheses, > 20% reduction) in baseline FEVi during or following the test. Cohen's Kappa Statistic (range - to +) is a measure of agreement between question responses and saline challenge responses. RESULTS Rate of volunteering Records are complete for only one of the two companies in the study. At this company, 07 employees were approached by receiving an information leaflet. Seventy agreed to full participation in the study, 2 wanted to answer the questionnaire only and 25 did not want to be involved. 4.5% hyperosmolar saline bronchial challenge Ten subjects who underwent testing were excluded from analysis. Of these, six were excluded because nebuliser output was < ml/minute, and they had not developed a fall in FEVi at this lower output of saline and subsequent smaller saline dose. Two were excluded because of incomplete data on nebuliser output. One subject with previous asthma had inhaled salbutamol 5 minutes before the test and another could not use the spirometer in a reproducible way. The results of per cent FEVi changes from baseline readings are plotted against the total dose of 4.5% saline delivered during the test for the 89 subjects in Figure. Fifteen subjects had a positive test when defined as FEVi fall greater than 5% of baseline, and Figure. Final FEVi changes by the total dose of 4.5% saline for 89 subjects. A positive test is defined as > 5% fall in FEVi by the end of the test. A borderline test is a negative test with a dose-response ratio (DRR) in the same range as several subjects who had a positive test. One subject is not included on the graph (volume = ml, FEVi increase = 23%). Percent FEV, Change t afcliiw Ktp«K I g B 00 0=EXCLUDED (low nebuliser output) = POSITIVE TEST 2 BORDERLINE TEST (negative test, low Dose- RespoDSe RJOO) 3= NEGATIVE TEST 3 J J 2 I J 3 J 3 J J 3 3 I J as la is ]o as la is»e «s Volume of 4.5% saline delivered (ml) -
5 S. J. Rabone et a/.: Hypertonic saline challenge 8 Figure 2. Individual log cumulative dose response curves for 5 subjects with positive HSBC with 5% as the cutoff point. Nine curves show a 'classical' response seen in asthmatic subjects (nos. 2, 5, 6, 7, 8,, 3, 4, 5). Curve no. 0 shows dilatation followed by constriction which has been reported by Rodwell ef a/. 22 Cumulative dose (ml) seven at a fall of greater than 20%. The individual log dose-response curves for the 5 subjects are presented in Figure 2. The prevalence of positive tests was 6.9% (95% CI ). Ten of the fifteen had baseline FEVi values > 80% predicted 7 (mean 02.%, SD 4.7%). The remaining five had mean FEVi 7.2% (SD 6.6%) of predicted value. The median PD5FEV value (dose of saline administered which caused a 5% fall in FEVi) was 5.64ml with a range of Nine of the fifteen had PD5 values > 6. lml and would be considered mildly responsive. The other six had moderately severe responses. 8 The per cent fall of FEVi from baseline at the end of the 4.5% saline appeared mildly positively skewed with a mean fall of 6.8% (SD = 9.6) and median of 4.3% (range ). 'Borderline' responses (see Figure ) were defined as those who did not have a 5% fall in FEVi but who had a dose response ratio (DRR = % FEVi fall/total saline dose) in the same range as those with the 5% fall. Higher DRR values indicate greater bronchial hyperresponsiveness. Eight subjects with a fall in FEVi ranging from 9.5%-3.95% had log DRR values in the range , and eight subjects with a fall in FEVi >5% also fell in that range. The distribution of log dose response ratios is presented in Figure 3. The present study did not inquire about former wheeze, but found that the 95th percentile for per cent fall in FEVi subjects who answered no to IUAT question about 'current wheeze' ('Have you ever had wheezing or whistling in your chest at any time in the last 2 months?') was 6.9% and the 90th percentile 6.%. Figure 4 shows the effect on sensitivity, specificity and positive predictive value of the test in diagnosing Figure 3. Distribution of log dose-response ratios for 89 subjects. This shows that eight subjects with FEN^ falls of <5% had dose response ratios in the range -0.3 to -0.0, as did eight people with FEVi falls > 5% (positive tests). Thus, the results for these eight subjects with negative challenge tests are considered borderline. DFEV fall > 5% FEV fall <5% -2B-U -U-L6 4JU-U 4.JD-4J mui MBL59 unu9 Log Dose Response Ratio
6 82 Occup. Med. Vol. 46, 996 'current wheeze' when the definition of a positive test is changed from an FEVi fall of 5% to other values. If 5% fall is the cutoff point, specificity was 0.88 (95% CI ) sensitivity 0.28 (95% CI ) and positive predictive value 47%. With 20% as the cutoff, prevalence was 7/89 (7.9%), specificity was 0.97 (95% CI ), sensitivity 20% (95% CI ) and positive predictive value 7%. Figure 5 stratifies subjects into classes indicating how much their FEVi fell and shows the proportion of respondents who reported 'current wheeze' in each class. Comparison between self-administered question responses and hyperosmolar bronchial challenge responses These comparisons, presented in Table 2, show that the question most in agreement with a positive hyperosmolar bronchial challenge is the question 'have you had an attack of asthma at any time in the last 2 months?' which is question 2 in the IUAT Bronchial Symptoms Questionnaire (986). 'Have you ever had an attack of asthma?' and the National Health Survey questions asking about recent requirements for medical advice, treatment or medications 3 were close behind. Other questions agreed poorly with the test. The logistic regression analyses showed that only one of the four questions analyzed significantly predicted a positive HSBC at the 5% level. That question was 'have you ever had an attack of asthma?' (X 2 = 7.5, ldf, p = ). The same question was the only significant predictor of percentage FEVi fall following HSBC (f= 0.73,, 8S df, p = 0.005). Subjects who responded positively to the question had a mean percentage fall in FEVi of 7.6%, and those who did not had a mean percentage FEVi fall of 5.8%. Neither age nor gender were related to HSBC outcomes at less than p = 0.5. Test safety and adverse reactions Only one subject who recorded a fall in FEVi > 5% did not respond promptly (within 20 minutes) and adequately (to within 0% of baseline) to inhaled bronchodilator. He was Caucasian, lean, aged 47 and had smoked 20 unfiltered cigarettes per day since his late teens. He gave negative responses to questions from the questionnaire related to cough, shortness of breath, chest whistling and wheezing, chest tightness, asthma and the taking of medications. His baseline FEV, and FVC were 2.7 litres (predicted = 3.50) 7 and 4.27 litres respectively. Following administration of 4.5% saline, his FEVi changed as follows: 0.5 min, 2.7; min, 2.94; 2 min, 2.77; 4 min, 2.54 and 8 min,.87 litres. He noticed chest tightness and mild dyspnoea. Bronchodilator (5mg salbutamol) was given by nebuliser and his mild distress eased over 0 minutes. FEVi was recorded at.74 litres 20 minutes later. He was observed and his FEVi spontaneously improved to 3.42 litres three hours after the test. This value, being higher than his baseline reading, suggests that he had bronchoconstriction at the time of the test. Bronchial hyperresponsiveness and smoking relationship between smoking status and a positive test was found. Five of 22 smokers, four of 29 exsmokers and six of 37 never-smokers had positive responses to the challenge. Subject acceptability of HSBC Responses to the administered questionnaire showed that 65 reported 'no problems', 9 found it 'mildly uncomfortable', nobody found it 'uncomfortable' and only one person found the HSBC 'very uncomfortable'. This indicates a high level of acceptance. However, acceptance was less amongst those with a positive HSBC, since out of 2 recorded responses seven had 'no problems', four found it 'mildly uncomfortable' and one responded that the test was 'very uncomfortable'. He was a 50 year old ex-smoker with no previous history of asthma or breathing problems. DISCUSSION It has been demonstrated in this study that the 4.5% saline bronchial challenge test can be successfully used for measurements of bronchial responsiveness in industrial field settings. Sixty-five per cent of people approached using an information leaflet underwent the test. This percentage is less than the 8% participation Cockcroft et al. 4 obtained for histamine challenge after telephoning students, although many other factors apart from the nature of the challenging agent would be expected to influence participation rates. The data obtained in this study are consistent with results from previous published studies. Data of Anderson et al. is on 80 healthy subjects referred for SCUBA diving examinations revealed that the distribution of per cent fall of FEVi from baseline at the end of the 4.5% saline challenge was mildly positively skewed with a mean of 7.2% (SD = 8.2) and median of 4.5% (range ). The study of Riedler et al} recorded a median PD5FEV value of.75ml with range 0.24^0.4. Riedler et al. found that the 95th percentile for per cent fall in FEVi amongst children who did not report 'current wheeze' (a positive response to IUAT question, see Table 2) or 'former wheeze' ('have you ever had wheezing or whistling in the chest at any time in the past') was 5%, and the 90th percentile 3.4%. Riedler et al. also determined that the sensitivity and specificity of the 4.5% salt challenge for detecting current wheeze diagnosed by questionnaire (IUAT question ) were 47% (95% CI ) and 92% (95% CI ). Results from the present study amongst timber industry employees can be best compared to the study
7 S. J. Rabone ef a/.: Hypertonic saline challenge 83 Table 3. Comparison of methacholine and hypertonic saline challenge results in detecting positive responses to the question 'have you ever had an attack of asthma?' 4.5% saline challenge at 5% fall cutoff 4.5% saline challenge at (b) 20% FEV\ fall cutoff Methacholine challenge at PC20 s Bmg/ml cutoff n =,392' 47 (34-59) 85 (83-87) 2 ( 8-6) 97 (92-98) Sensitivity Specificity Positive predictive value Negative predictive value 57 (20-94) T 86 (79-94) 27 ( 4-49) 96 (9-00) 57 (20-94) 96 (92-00) 57 (20-94) 96 (92-00) * number of subjects in the study 95% confidence interval Figure 4. Sensitivity, specificity and positive predictive value of the 4.5% hyperosmolar challenge for diagnosing 'current wheeze' at different FEV fall cutoff points. Ninety five per cent confidence limits of the sensitivity and specificity estimates are shown. Figure 5. Per cent positive responses to IUAT questions and 2 for respondents grouped by %FEVi fall during 4.5% hypertonic saline challenge. The graph shows no increase in the proportion of positive responses below 9.9% FEV fall. P r o P o r t i o n 'Sereitivity / Positive Predictive Value %FBflfall cutoff point far+test of Enarson et al? of,392 workers (mainly timber and grain industries) using methacholine challenge, because a common questionnaire definition of asthma exists. The sensitivity, specificity, positive and negative predictive values of both the HSBC and the methacholine challenge in detecting positive responses to the questionnaire question 'have you ever had an attack of asthma?' are shown in Table 3. In this comparison, the HSBC at 20% FEVi fall cutoff has superior positive prediction and specificity whilst matching methacholine's sensitivity. Departures from the protocol of Smith and Anderson deserve mention. A bronchodilator drug was not given routinely following the tests. The reasons for this were: that medical practitioners were present; that to give a pharmacologically active agent prophylactically seemed unnecessary in the absence of any fall in FEVi over the time of observation; and that FEVi is not expected to fall further minute after test completion.' l However these reasons do not consider subjects with current unsuspected bronchospasm undergoing the test. Bronchial hyperresponsiveness in these subjects may not be detected until administration of bronchodilator following the test reveals that their baseline FEVi has I350 Q, CurrentWheeze D 02, Asthma in last 2 months Rse, Oto 5 to 0to 5 to rc2 4.9, 9.9, 49, 09, n=36 n=3 n=4 rt=8 Percent FEVI fall >m9, been underestimated. It is therefore recommended that brochodilator be given following the challenge and the response measured. Further FEVi fall following completion of the HSBC was demonstrated by one subject in the study. This is possibly of concern because previous information 9 did not suggest that such a fall would occur. This man had undetected bronchospasm when commencing the test (because his baseline FEVI of 2.7 litres increased to 3.42 litres 3 hours after the test following administered bronchodilator) and had a positive test. The protocol of giving bronchodilator after the test, followed by checking FEVi, left us alerted and prepared. He recovered; nevertheless, more research is required on larger numbers of people to document patterns of recovery. The large variation in nebuliser output between tests performed over the standard 5.5 minutes is possibly of concern (see Figure ), although it has been shown that few negative responses will change to positive by merely administering more saline, 8 the rate of change of osmolarity in the airways being more important. Nebuliser output is recognized to vary with tidal volume and respiratory rate in children, 20 and these
8 84 Occup. Med. Vol. 46, 996 possibly accounted for part of the variation. Nevertheless, to minimize measurement error, weighing of the saline canister and tubing must be performed meticulously without loss of saline. The definition of a positive test at a cutoff point of > 5% FEVi fall is arbitrary. The decision as to what cutoff point is appropriate will depend on the circumstances of the investigator, and the desirability for a sensitive or specific test. Whereas the necessity for an exact definition is acknowledged to enable practical usage of the test in epidemiological settings, the possible limitations of a cutoff point of 5% for population studies deserve consideration. Given that the data from this study come from a small group of subjects exposed to (possibly asthmagenic) wood dusts and may not generalize to other populations, they suggest that a cutoff point for a positive test which provides high specificity (see Figure 3 and Table 3) and which separates individuals who appear to react to inhaled saline differently (see Figures and 4) lies above 5%. Figure shows that responses of nine individuals (those with FEVi falls > 9%) appear separate from the rest. Separation of those with FEVi falls from 5-9% appears less clear. In epidemiological surveys there is usually responsibility to provide subjects with results and interpretation of procedures, and high specificity aids interpretation. The doseresponse ratio, by considering the rate of saline administration, may offer some future advantages in defining cutoff points for the test. A cutoff of 20% FEVi fall in this study produced an asthma prevalence estimate of 7.9%, consistent with the estimate of participants (see Table 2). For the above reasons, a 20% cutoff point appears more appropriate for epidemiological surveys. Responses to inhaled histamine have been quantified and classified by Cockcroft et a/. 2 to provide predictions of current symptomatic asthma; for example, Cockcroft et al. state that a histamine challenge PC 2 o below 2mg/ml is diagnostic of current symptomatic asthma and that a PC 2 o greater than 8mg/ml virtually excludes current asthma. This type of information is of obvious use in interpreting results, and after appropriate research should become available for the HSBC. At that stage the best cutoff points for different applications will be apparent. The equipment and expertise required to perform the HSBC are similar to those required for methacholine or histamine challenge; both procedures can be performed by one person in a non-laboratory setting. This study, in support of the study of Riedler et a/., 8 shows that the HSBC is safe, well-tolerated and produces results comparable to those obtained in laboratories. Potential advantages of the indirect mechanism of action of HSBC in causing broncoconstriction have not been demonstrated at this stage by a direct comparison between pharmacological challenge and HSBC. The differing methods of defining questionnairediagnosed asthma, of recruiting subjects into studies and of defining cutoff points have prevented accurate direct comparison between measures of bronchial responsiveness in the general population. The use of HSBC as an epidemiological tool for estimating asthma prevalence is uncertain, but given the difficulties normally involved in estimating asthma prevalence and the desirability to base such estimations on objective data, it is a measurement of bronchial hyperresponsiveness (amongst several) that warrants full investigation. Ideally, part of that investigation will involve a direct comparison between pharmacological challenge and the HSBC on the same subjects. ACKNOWLEDGMENTS The authors thank Mrs Kathleen Howell of the Department of Occupational Health and Safety of Western Australia for her assistance in data collection. Mr Gerard Turner and Mr Gregory Van Hazendonk organized the study in their respective companies. The authors also thank the managements and employees of the companies for supporting the study. REFERENCES. Stenton S, Beach J, Avery A, Hendrick D. The value of questionnaires and spirometry in asthma surveillance programmes in the workplace. Occup Med 993; 43: Sterk P, Fabbri L, Quanjer P et al. Airway responsiveness, standardised challenge testing with pharmacological, physical and sensitising stimuli in adults. EurRespirJ 993; 6(Suppll6): Enarson D, Vedal S, Schulzer M, DyBuncio A, Chan-Yeung M. Asthma, asthma-like symptoms, chronic bronchitis and the degree of bronchial hyperresponsiveness in epidemiologic surveys. Am Rev Respir Dis. 987; 36: Cockcroft D, Murdock K, Berscheid B and Gore B. Sensitivity and specificity of histamine PC20 determination in a random selection of young college students. J Allergy Clin Immunol 992; 89: Eggleston P, Kagey-Sobotka A, Schleimer R, Iichtenstein L. Interaction between hyperosmolar and IgE-mediated histamine release from mast cells. Am Rev Resp Dis 984; 30: Silber G, Proud D, Warner J, Nacliero R, Kagey-Sobotka A, Lichtenstein L et al. In vivo release of inflammatory mediators by hyperosmolar solutions. Am Rev Resp Dis 988; 27; Belcher N, Murdock R, Dalton N, House F, Clark TJH, Rees P, Lee T. A comparison of mediator and catecholamine release between exercise- and hypertonic saline-induced asthma. Am Rev Respir Dis 988; 37: Riedler J, Reade T, Dalton M, Hoist D, Robertson C. Hypertonic saline challenge in an epidemiologic survey of asthma in children. Am J Respir Crit Care Med 994; 50: Smith C, Anderson S. Inhalational challenge using hypertonic saline in asthmatic subjects: a comparison with responses to hyperpnoea, methacholine and water. Eur Respir J 990; 3: Araki H, Sly PD. Inhalation of hypertonic saline as a bronchial challenge in children with mild asthma and normal children. J Allergy Clin Immunol 989; 84(): Smith C, Anderson S. A comparison between the airway response to isocapnic hyperventilation and hypertonic saline in subjects with asthma. EurRespirJ 989; 2:
9 S. J. Rabone et a/.: Hypertonic saline challenge Smith C, Anderson S. Inhalation provocation tests using nonisotonic aerosols. J Allergy Clin Immunol 989; 84: Australian Bureau of Statistics National Health Survey Users' Guide. Commonwealth Government Printer, Canberra, Burney PGJ, Chin S. Britton J, Tattersfield A, Papacosta A. What Symptoms predict the bronchial response to histamine? Evaluation in a community survey of the bronchial symptoms questionnaire 984 of the International Union Against Tuberculosis and Lung Disease. EurJResp Disease 989; 8: Armitage P, Berry G. Statistical Methods in Medical Research. 3rd ed. Blackwell Scientific Publications, 994: Chinn S, Burney P. On measuring repeatability of data from Self-Administered Questionnaires. International Journal of Epidemiology 987; 6: Goldman A, Becklake M. Respiratory function tests: rmal values at medium altitude and the prediction of normal results. Am Rev Respir Dis 959; 79: 457^ Anderson S, Smith C, Rodwell L, du Toit J, Reidler J, Robertson C. The use of nonisotonic aerosols for evaluating bronchial hyperresponsiveness. In: Spector SL, ed. Provocation Testing in ClinicalProcrtce. New York: Marcel Dekker Inc, 994: Rodwell L. The role of hyperosmolar challenge in the assessment and treatment of asthma. Unpublished PhD thesis, Faculty of Medicine, University of Sydney, 994: Riedler M, Robertson C. Effect of tidal volume on the output and particle size distribution of hypertonic saline from an ultrasonic nebuliser. Eur Resp Journal 994; 7: Cockcroft D, Berscheid B, Murdock K. Sensitivity and specificity of histamine PC20 measurements in a random population. J Allergy Clin Immunol 985; 75: 42 A. 22. Rodwell L, Anderson S, du Toit J, Seale J. The effect of inhaled frusemide on airway sensitivity to inhaled 4.5% sodium chloride aerosol in asthmatic subjects. Thorax 993; 48:
J. Riedler, C.F. Robertson
 Eur Respir J, 1994, 7, 998 1002 DOI: 10.1183/09031936.94.07050998 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 TECHNICAL NOTE Effect of
Eur Respir J, 1994, 7, 998 1002 DOI: 10.1183/09031936.94.07050998 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 TECHNICAL NOTE Effect of
Mechanisms of action of bronchial provocation testing
 Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Prevalence of bronchial hyperresponsiveness and
 Thorax 1987;42:361-368 Prevalence of bronchial hyperresponsiveness and asthma in a rural adult population A J WOOLCOCK, J K PEAT, C M SALOME, K YAN, S D ANDERSON, R E SCHOEFFEL, G McCOWAGE, T KILLALEA
Thorax 1987;42:361-368 Prevalence of bronchial hyperresponsiveness and asthma in a rural adult population A J WOOLCOCK, J K PEAT, C M SALOME, K YAN, S D ANDERSON, R E SCHOEFFEL, G McCOWAGE, T KILLALEA
Role of bronchoprovocation tests in identifying exercise-induced bronchoconstriction in a non-athletic population: a pilot study
 Original Article Role of bronchoprovocation tests in identifying exercise-induced bronchoconstriction in a non-athletic population: a pilot study Jessica H. Y. Tan 1 *, Wui Mei Chew 1 *, Therese S. Lapperre
Original Article Role of bronchoprovocation tests in identifying exercise-induced bronchoconstriction in a non-athletic population: a pilot study Jessica H. Y. Tan 1 *, Wui Mei Chew 1 *, Therese S. Lapperre
responsiveness in asthmatic patients and smokers
 63 Department of Pulmonology B Auffarth D S Postma G H Koeter Th W van der Mark Department of Allergology J G R de Monchy University Hospital, 973 EZ Groningen, The Netherlands Reprint requests to: Professor
63 Department of Pulmonology B Auffarth D S Postma G H Koeter Th W van der Mark Department of Allergology J G R de Monchy University Hospital, 973 EZ Groningen, The Netherlands Reprint requests to: Professor
C. Wojnarowski*, K. Storm Van's Gravesande*, J. Riedler**, I. Eichler*, C. Gartner*, T. Frischer*
 Eur Respir J, 1996, 9, 1896 191 DOI: 1.1183/931936.96.991896 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 93-1936 Comparison of bronchial challenge
Eur Respir J, 1996, 9, 1896 191 DOI: 1.1183/931936.96.991896 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 93-1936 Comparison of bronchial challenge
Variation in nebulizer aerosol output and weight output from the Mefar dosimeter: implications for multicentre studies
 Eur Respir J 1997; 10: 452 456 DOI: 10.1183/09031936.97.10020452 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 0903-1936 Variation in nebulizer aerosol
Eur Respir J 1997; 10: 452 456 DOI: 10.1183/09031936.97.10020452 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 0903-1936 Variation in nebulizer aerosol
Performing a Methacholine Challenge Test
 powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
Perception of respiratory symptoms after methacholine-induced bronchoconstriction in a general population
 Eur Respir J 1998; 12: 189 193 DOI: 1.1183/931936.98.125189 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 93-1936 Perception of respiratory symptoms
Eur Respir J 1998; 12: 189 193 DOI: 1.1183/931936.98.125189 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 93-1936 Perception of respiratory symptoms
Respiratory symptoms questionnaire for asthma epidemiology: validity and reproducibility
 214 Department of Occupational and Environmental Medicine, National Heart and Lung nstitute, Emmanuel Kaye Building, Manresa Road, London SW3 6LR K M Venables N Farrer L Sharp B J Graneek A J Newman Taylor
214 Department of Occupational and Environmental Medicine, National Heart and Lung nstitute, Emmanuel Kaye Building, Manresa Road, London SW3 6LR K M Venables N Farrer L Sharp B J Graneek A J Newman Taylor
Predictors of obstructive lung disease among seafood processing workers along the West Coast of the Western Cape Province
 Predictors of obstructive lung disease among seafood processing workers along the West Coast of the Western Cape Province Adams S 1, Jeebhay MF 1, Lopata AL 2, Bateman ED 3, Smuts M 4, Baatjies R 1, Robins
Predictors of obstructive lung disease among seafood processing workers along the West Coast of the Western Cape Province Adams S 1, Jeebhay MF 1, Lopata AL 2, Bateman ED 3, Smuts M 4, Baatjies R 1, Robins
Beta 2 adrenoceptor agonists and the Olympic Games in Athens
 Beta 2 adrenoceptor agonists and the Olympic Games in Athens 1 Appendix A of the Olympic Movement Anti-Doping Code, the List of Prohibited Substances and Prohibited Methods dated 1 st January 2003 states
Beta 2 adrenoceptor agonists and the Olympic Games in Athens 1 Appendix A of the Olympic Movement Anti-Doping Code, the List of Prohibited Substances and Prohibited Methods dated 1 st January 2003 states
Outline FEF Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications?
 Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
O ccupational asthma (OA) is the most commonly
 58 ORIGINAL ARTICLE Changes in rates and severity of compensation claims for asthma due to diisocyanates: a possible effect of medical surveillance measures S M Tarlo, G M Liss, K S Yeung... See end of
58 ORIGINAL ARTICLE Changes in rates and severity of compensation claims for asthma due to diisocyanates: a possible effect of medical surveillance measures S M Tarlo, G M Liss, K S Yeung... See end of
Predictive value of respiratory symptoms and bronchial hyperresponsiveness to diagnose asthma in New Zealand
 Respiratory Medicine (2006) 100, 2107 2111 Predictive value of respiratory symptoms and bronchial hyperresponsiveness to diagnose asthma in New Zealand D. Sistek a,, K. Wickens b, R. Amstrong c, W. D Souza
Respiratory Medicine (2006) 100, 2107 2111 Predictive value of respiratory symptoms and bronchial hyperresponsiveness to diagnose asthma in New Zealand D. Sistek a,, K. Wickens b, R. Amstrong c, W. D Souza
Life-long asthma and its relationship to COPD. Stephen T Holgate School of Medicine University of Southampton
 Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Josef Riedler* Agnes Gamper* Waltraud Eder* Gerd Oberfeld**
 September 1997 Prevalence of bronchial hyperresponsiveness to 4.5% saline and its relation to asthma and allergy symptoms in Austrian children Correspondence: Josef Riedler* Agnes Gamper* Waltraud Eder*
September 1997 Prevalence of bronchial hyperresponsiveness to 4.5% saline and its relation to asthma and allergy symptoms in Austrian children Correspondence: Josef Riedler* Agnes Gamper* Waltraud Eder*
Clinical Variables Are Poor Selection Criteria for the Use of Methacholine Bronchoprovocation in Symptomatic Subjects
 Clinical Variables Are Poor Selection Criteria for the Use of Methacholine Bronchoprovocation in Symptomatic Subjects Annie Lin Parker MD and Muhanned Abu-Hijleh MD OBJECTIVE: Airway hyperresponsiveness
Clinical Variables Are Poor Selection Criteria for the Use of Methacholine Bronchoprovocation in Symptomatic Subjects Annie Lin Parker MD and Muhanned Abu-Hijleh MD OBJECTIVE: Airway hyperresponsiveness
C.S. Ulrik *, V. Backer **
 Eur Respir J, 1996, 9, 1696 1700 DOI: 10.1183/09031936.96.09081696 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Increased bronchial responsiveness
Eur Respir J, 1996, 9, 1696 1700 DOI: 10.1183/09031936.96.09081696 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Increased bronchial responsiveness
Validation of Questionnaire and Bronchial Hyperresponsiveness against Respiratory Physician Assessment in the Diagnosis of Asthma
 International Journal of Epidemiology O International EpkJemlologlcal Association 1996 Vol. 25,. 3 Printed in Great Britain Validation of Questionnaire and Bronchial Hyperresponsiveness against Respiratory
International Journal of Epidemiology O International EpkJemlologlcal Association 1996 Vol. 25,. 3 Printed in Great Britain Validation of Questionnaire and Bronchial Hyperresponsiveness against Respiratory
Busselton is a coastal city in southwestern Western
 Obstructive airway disease in 46e65-year-old people in Busselton, Western Australia, 1966e2015 Arthur (Bill) Musk 1, Michael Hunter 2,3, Jennie Hui 2,4, Matthew W Knuiman 2, Mark Divitini 2, John P Beilby
Obstructive airway disease in 46e65-year-old people in Busselton, Western Australia, 1966e2015 Arthur (Bill) Musk 1, Michael Hunter 2,3, Jennie Hui 2,4, Matthew W Knuiman 2, Mark Divitini 2, John P Beilby
Adenosine 5 0 -monophosphate increases levels of leukotrienes in breath condensate in asthma
 Respiratory Medicine (2004) 98, 651 655 Adenosine 5 0 -monophosphate increases levels of leukotrienes in breath condensate in asthma E. Bucchioni, Z. Csoma, L. Allegra, K.F. Chung, P.J. Barnes, S.A. Kharitonov*
Respiratory Medicine (2004) 98, 651 655 Adenosine 5 0 -monophosphate increases levels of leukotrienes in breath condensate in asthma E. Bucchioni, Z. Csoma, L. Allegra, K.F. Chung, P.J. Barnes, S.A. Kharitonov*
For the last 15 years, 4.5% hypertonic saline
 VOLUME 45 May - June 2005 NUMBER 5-6 Original Article The use of 4.5% hypertonic saline challenge test in diagnosing asthma in children with chronic recurrent cough Bambang Supriyatno, MD; Dina Medina,
VOLUME 45 May - June 2005 NUMBER 5-6 Original Article The use of 4.5% hypertonic saline challenge test in diagnosing asthma in children with chronic recurrent cough Bambang Supriyatno, MD; Dina Medina,
Asthma Management for the Athlete
 Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Airway calibre as a confounder in interpreting
 702 Medical Department TTA 7511, State University Hospital, Copenhagen, Denmark A Dirksen F Madsen T Engel L Frolund J H Heing H Mosbech Reprint requests to: Dr A Dirksen, Department of Pulmonary Medicine
702 Medical Department TTA 7511, State University Hospital, Copenhagen, Denmark A Dirksen F Madsen T Engel L Frolund J H Heing H Mosbech Reprint requests to: Dr A Dirksen, Department of Pulmonary Medicine
Respiratory symptoms and ventilatory function
 Thorax (1972), 27, 454. Respiratory symptoms and ventilatory function changes in relation to length of exposure to cotton dust E. ZUgKIN and F. VALIC Andrija Stampar School of Public Health, Zagreb University,
Thorax (1972), 27, 454. Respiratory symptoms and ventilatory function changes in relation to length of exposure to cotton dust E. ZUgKIN and F. VALIC Andrija Stampar School of Public Health, Zagreb University,
Revised Protocol: Criteria for Designating Substances as. Occupational Asthmagens on the AOEC List of. Exposure Codes
 Revised Protocol: Criteria for Designating Substances as Occupational Asthmagens on the AOEC List of Exposure Codes Revised September 2008 1 I. Introduction This is a project to evaluate the current AOEC
Revised Protocol: Criteria for Designating Substances as Occupational Asthmagens on the AOEC List of Exposure Codes Revised September 2008 1 I. Introduction This is a project to evaluate the current AOEC
UNIT TWO: OVERVIEW OF SPIROMETRY. A. Definition of Spirometry
 UNIT TWO: OVERVIEW OF SPIROMETRY A. Definition of Spirometry Spirometry is a medical screening test that measures various aspects of breathing and lung function. It is performed by using a spirometer,
UNIT TWO: OVERVIEW OF SPIROMETRY A. Definition of Spirometry Spirometry is a medical screening test that measures various aspects of breathing and lung function. It is performed by using a spirometer,
E pidemiologic studies of adults rely on selfadministered. Questionnaire Items That Predict Asthma and Other Respiratory Conditions in Adults*
 Questionnaire Items That Predict Asthma and Other Respiratory Conditions in Adults* fun Bai, MPH; Jennifer K. Peat, PhD; Geoffrey Berry, PhD; Guy B. Marks, PhD; and Ann]. Woolcock, MD, FCCP The International
Questionnaire Items That Predict Asthma and Other Respiratory Conditions in Adults* fun Bai, MPH; Jennifer K. Peat, PhD; Geoffrey Berry, PhD; Guy B. Marks, PhD; and Ann]. Woolcock, MD, FCCP The International
GETTING STARTED WITH MANNITOL CHALLENGE TESTING. Rick Ballard, RRT, RPFT Applications/Education Specialist MGC Diagnostics
 GETTING STARTED WITH MANNITOL CHALLENGE TESTING Rick Ballard, RRT, RPFT Applications/Education Specialist MGC Diagnostics OBJECTIVES Indications for provocation testing Identify candidates for testing
GETTING STARTED WITH MANNITOL CHALLENGE TESTING Rick Ballard, RRT, RPFT Applications/Education Specialist MGC Diagnostics OBJECTIVES Indications for provocation testing Identify candidates for testing
polyvinylchloride dust
 Thorax 1983;38:834-839 Clinical studies of workers exposed to polyvinylchloride dust CA SOUTAR, S GAULD From the Institute of Occupational Medicine, Edinburgh ABsTRAcr A previous study showed that exposure
Thorax 1983;38:834-839 Clinical studies of workers exposed to polyvinylchloride dust CA SOUTAR, S GAULD From the Institute of Occupational Medicine, Edinburgh ABsTRAcr A previous study showed that exposure
Value of measuring diurnal peak flow variability in the recognition of asthma: a study in general practice
 Eur Respir J ; : DOI:./.. Printed in UK - all rights reserved Copyright ERS Journals Ltd European Respiratory Journal ISSN - Value of measuring diurnal peak flow variability in the recognition of asthma:
Eur Respir J ; : DOI:./.. Printed in UK - all rights reserved Copyright ERS Journals Ltd European Respiratory Journal ISSN - Value of measuring diurnal peak flow variability in the recognition of asthma:
pulmonary function and peak flow variability in adults
 Thorax 1995;50:121-126 Department of Epidemiology and Statistics, University of Groningen, 971AV Groningen, The Netherlands H M Boezen J P Schouten B Rijcken Department of Pulnonology, University Hospital
Thorax 1995;50:121-126 Department of Epidemiology and Statistics, University of Groningen, 971AV Groningen, The Netherlands H M Boezen J P Schouten B Rijcken Department of Pulnonology, University Hospital
Exercise-induced bronchial hyperresponsiveness and parental ISAAC questionnaire responses
 Eur Respir J, 1996, 9, 1356 1362 DOI: 1.1183/931936.96.971356 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 93-1936 Exercise-induced bronchial hyperresponsiveness
Eur Respir J, 1996, 9, 1356 1362 DOI: 1.1183/931936.96.971356 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 93-1936 Exercise-induced bronchial hyperresponsiveness
Cut-off points defining normal and asthmatic bronchial reactivity to exercise and inhalation challenges in children and young adults
 Eur Respir J 1999; 14: 659±668 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 0903-1936 Cut-off points defining normal and asthmatic bronchial reactivity
Eur Respir J 1999; 14: 659±668 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 0903-1936 Cut-off points defining normal and asthmatic bronchial reactivity
Cross-sectional assessment of workers with repeated exposure to chlorine over a three year period
 Eur Respir J, 1995, 8, 2046 2054 DOI: 10.1183/09031936.95.08122046 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1995 European Respiratory Journal ISSN 0903-1936 Cross-sectional assessment
Eur Respir J, 1995, 8, 2046 2054 DOI: 10.1183/09031936.95.08122046 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1995 European Respiratory Journal ISSN 0903-1936 Cross-sectional assessment
Airway Hyperresponsiveness to Hypertonic Saline as a Predictive Index of Exercise-Induced Bronchoconstriction
 The Korean Journal of Internal Medicine: 20:284-289, 2005 Airway Hyperresponsiveness to Hypertonic Saline as a Predictive Index of Exercise-Induced Bronchoconstriction Inseon S. Choi, M.D., Se-Woong Chung,
The Korean Journal of Internal Medicine: 20:284-289, 2005 Airway Hyperresponsiveness to Hypertonic Saline as a Predictive Index of Exercise-Induced Bronchoconstriction Inseon S. Choi, M.D., Se-Woong Chung,
Spirometry: Introduction
 Spirometry: Introduction Dr. Badri Paudel 1 2 GMC Spirometry Spirometry is a method of assessing lung function by measuring the volume of air the patient can expel from the lungs after a maximal expiration.
Spirometry: Introduction Dr. Badri Paudel 1 2 GMC Spirometry Spirometry is a method of assessing lung function by measuring the volume of air the patient can expel from the lungs after a maximal expiration.
Online Data Supplement. Prevalence of Chronic Obstructive Pulmonary Disease in Korea: Results of a Population-based Spirometry Survey
 Online Data Supplement Prevalence of Chronic Obstructive Pulmonary Disease in Korea: Results of a Population-based Spirometry Survey Dong Soon Kim, MD, Young Sam Kim MD, Kee Suk Chung MD, Jung Hyun Chang
Online Data Supplement Prevalence of Chronic Obstructive Pulmonary Disease in Korea: Results of a Population-based Spirometry Survey Dong Soon Kim, MD, Young Sam Kim MD, Kee Suk Chung MD, Jung Hyun Chang
Western Red Cedar Asthma SS-433
 SS-433 November 2014 Table of Contents Background information... 3 Introduction... 3 Occupational exposure limits... 4 Resources... 5 SS-433 November 2014 Page 2 Background information Western Red Cedar
SS-433 November 2014 Table of Contents Background information... 3 Introduction... 3 Occupational exposure limits... 4 Resources... 5 SS-433 November 2014 Page 2 Background information Western Red Cedar
Effect of particle size of bronchodilator aerosols on lung distribution and pulmonary function in patients
 Thorax 1987;42:457-461 Effect of particle size of bronchodilator aerosols on lung distribution and pulmonary function in patients with chronic asthma D M MITCHELL, M A SOLOMON, S E J TOLFREE, M SHORT,
Thorax 1987;42:457-461 Effect of particle size of bronchodilator aerosols on lung distribution and pulmonary function in patients with chronic asthma D M MITCHELL, M A SOLOMON, S E J TOLFREE, M SHORT,
Fish consumption and respiratory symptoms among young adults in a Norwegian community.
 Eur Respir J 1; 1: 6 1 DOI: 10./0016..1006 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1 European Respiratory Journal ISSN 00-16 Fish consumption and respiratory symptoms among young
Eur Respir J 1; 1: 6 1 DOI: 10./0016..1006 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1 European Respiratory Journal ISSN 00-16 Fish consumption and respiratory symptoms among young
normal and asthmatic males
 Lung volume and its subdivisions in normal and asthmatic males MARGARET I. BLACKHALL and R. S. JONES1 Thorax (1973), 28, 89. Institute of Child Health, University of Liverpool, Alder Hey Children's Hospital,
Lung volume and its subdivisions in normal and asthmatic males MARGARET I. BLACKHALL and R. S. JONES1 Thorax (1973), 28, 89. Institute of Child Health, University of Liverpool, Alder Hey Children's Hospital,
THE NEW ZEALAND MEDICAL JOURNAL
 THE NEW ZEALAND MEDICAL JOURNAL Vol 120 No 1267 ISSN 1175 8716 Is Salamol less effective than Ventolin? A randomised, blinded, crossover study in New Zealand Catherina L Chang, Manisha Cooray, Graham Mills,
THE NEW ZEALAND MEDICAL JOURNAL Vol 120 No 1267 ISSN 1175 8716 Is Salamol less effective than Ventolin? A randomised, blinded, crossover study in New Zealand Catherina L Chang, Manisha Cooray, Graham Mills,
Methacholine versus Mannitol Challenge in the Evaluation of Asthma
 Methacholine versus Mannitol Challenge in the Evaluation of Asthma 1645-1800 AAAAI San Antonio Texas February 25 th 2013 Sandra D Anderson PhD, DSc Clinical Professor Royal Prince Alfred Hospital, Camperdown
Methacholine versus Mannitol Challenge in the Evaluation of Asthma 1645-1800 AAAAI San Antonio Texas February 25 th 2013 Sandra D Anderson PhD, DSc Clinical Professor Royal Prince Alfred Hospital, Camperdown
CIRCULAR INSTRUCTION REGARDING ESTABLISHMENT OF IMPAIRMENT DUE TO OCCUPATIONAL LUNG DISEASE FOR THE PURPOSES OF AWARDING PERMANENT DISABLEMENT
 Circular Instruction 195 CIRCULAR INSTRUCTION REGARDING ESTABLISHMENT OF IMPAIRMENT DUE TO OCCUPATIONAL LUNG DISEASE FOR THE PURPOSES OF AWARDING PERMANENT DISABLEMENT COMPENSATION FOR OCCUPATIONAL INJURIES
Circular Instruction 195 CIRCULAR INSTRUCTION REGARDING ESTABLISHMENT OF IMPAIRMENT DUE TO OCCUPATIONAL LUNG DISEASE FOR THE PURPOSES OF AWARDING PERMANENT DISABLEMENT COMPENSATION FOR OCCUPATIONAL INJURIES
Content Indica c tion Lung v olumes e & Lung Indica c tions i n c paci c ties
 Spirometry Content Indication Indications in occupational medicine Contraindications Confounding factors Complications Type of spirometer Lung volumes & Lung capacities Spirometric values Hygiene &
Spirometry Content Indication Indications in occupational medicine Contraindications Confounding factors Complications Type of spirometer Lung volumes & Lung capacities Spirometric values Hygiene &
NON-SPECIFIC BRONCHIAL HYPERESPONSIVENESS. J. Sastre. Allergy Service
 NON-SPECIFIC BRONCHIAL HYPERESPONSIVENESS J. Sastre. Allergy Service Asthma: definition Asthma is a syndrome defined on basis of three main aspects: 1- Symptoms due to variable and reversible airway obstruction
NON-SPECIFIC BRONCHIAL HYPERESPONSIVENESS J. Sastre. Allergy Service Asthma: definition Asthma is a syndrome defined on basis of three main aspects: 1- Symptoms due to variable and reversible airway obstruction
Occupational asthma is a disease characterised. Workplace-specific challenges as a contribution to the diagnosis of occupational asthma
 Eur Respir J 2008; 32: 997 1003 DOI: 10.1183/09031936.00100207 CopyrightßERS Journals Ltd 2008 Workplace-specific challenges as a contribution to the diagnosis of occupational asthma J-P. Rioux, J-L. Malo,
Eur Respir J 2008; 32: 997 1003 DOI: 10.1183/09031936.00100207 CopyrightßERS Journals Ltd 2008 Workplace-specific challenges as a contribution to the diagnosis of occupational asthma J-P. Rioux, J-L. Malo,
Chronic rhinitis in workers at risk of reactive airways dysfunction syndrome due to exposure to chlorine
 334 Department of Chest Medicine, Hôpital du Sacré-Coeur, Montreal, Canada C Leroyer J-L Malo D Gautrin 3365 Place de Rouen, Trois-Rivières, Canada D Girard Occupamed, Trois-Rivières, Canada J-G Dufour
334 Department of Chest Medicine, Hôpital du Sacré-Coeur, Montreal, Canada C Leroyer J-L Malo D Gautrin 3365 Place de Rouen, Trois-Rivières, Canada D Girard Occupamed, Trois-Rivières, Canada J-G Dufour
workers exposed to asbestos and synthetic mineral fibres
 British Journal of Industrial Medicine 1987;44:90-95 Determinants of respiratory symptoms in insulation workers exposed to asbestos and synthetic mineral fibres P ERNST, S SHAPIRO, R E DALES, MARGARET
British Journal of Industrial Medicine 1987;44:90-95 Determinants of respiratory symptoms in insulation workers exposed to asbestos and synthetic mineral fibres P ERNST, S SHAPIRO, R E DALES, MARGARET
Peak flow rate in relation to forced expiratory volume in hemp workers
 Brit. J. industr. Med., 1971, 28, 159-163 Peak flow rate in relation to forced expiratory volume in hemp workers v v I E. ZUSKIN and F. VALIC Department of Occupational Health, Andrija Stampar School of
Brit. J. industr. Med., 1971, 28, 159-163 Peak flow rate in relation to forced expiratory volume in hemp workers v v I E. ZUSKIN and F. VALIC Department of Occupational Health, Andrija Stampar School of
On completion of this chapter you should be able to: discuss the stepwise approach to the pharmacological management of asthma in children
 7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
Asthma Assessment & Review
 ASTHMA RESOURCE PACK Section 5B Asthma Assessment & Review In this section: 1. Primary Care initial assessment and review Asthma Resource Pack Section 5B: Asthma Assessment & Review Version 3.0 Last Updated:
ASTHMA RESOURCE PACK Section 5B Asthma Assessment & Review In this section: 1. Primary Care initial assessment and review Asthma Resource Pack Section 5B: Asthma Assessment & Review Version 3.0 Last Updated:
Supplementary Online Content
 Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
(Asthma) Diagnosis, monitoring and chronic asthma management
 Dubai Standards of Care 2018 (Asthma) Diagnosis, monitoring and chronic asthma management Preface Asthma is one of the most common problem dealt with in daily practice. In Dubai, the management of chronic
Dubai Standards of Care 2018 (Asthma) Diagnosis, monitoring and chronic asthma management Preface Asthma is one of the most common problem dealt with in daily practice. In Dubai, the management of chronic
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Office Based Spirometry
 Osteopathic Family Physician (2014)1, 14-18 Scott Klosterman, DO; Woodson Crenshaw, OMS4 Spartanburg Regional Family Medicine Residency Program; Edward Via College of Osteopathic Medicine - Virginia Campus
Osteopathic Family Physician (2014)1, 14-18 Scott Klosterman, DO; Woodson Crenshaw, OMS4 Spartanburg Regional Family Medicine Residency Program; Edward Via College of Osteopathic Medicine - Virginia Campus
Atopy, non-allergic bronchial reactivity, and past history as determinants of work related symptoms in seasonal grain handlers
 British Journal of Industrial Medicine 1986;43:396-400 Atopy, non-allergic bronchial reactivity, and past history as determinants of work related symptoms in seasonal grain handlers W 0 C M COOKSON, G
British Journal of Industrial Medicine 1986;43:396-400 Atopy, non-allergic bronchial reactivity, and past history as determinants of work related symptoms in seasonal grain handlers W 0 C M COOKSON, G
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Young Yoo, MD; Jinho Yu, MD; Do Kyun Kim, MD; and Young Yull Koh, MD
 Original Research ASTHMA Percentage Fall in FVC at the Provocative Concentration of Methacholine Causing a 20% Fall in FEV 1 in Symptomatic Asthma and Clinical Remission During Adolescence* Young Yoo,
Original Research ASTHMA Percentage Fall in FVC at the Provocative Concentration of Methacholine Causing a 20% Fall in FEV 1 in Symptomatic Asthma and Clinical Remission During Adolescence* Young Yoo,
C.J. Gore*, A.J. Crockett**, D.G. Pederson +, M.L. Booth ++, A. Bauman #, N. Owen ##
 Eur Respir J, 1995, 8: 773 782 DOI: 10.1183/09031936.95.08050773 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1995 European Respiratory Journal ISSN 0903-1936 Spirometric standards for
Eur Respir J, 1995, 8: 773 782 DOI: 10.1183/09031936.95.08050773 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1995 European Respiratory Journal ISSN 0903-1936 Spirometric standards for
Spirometry: an essential clinical measurement
 Shortness of breath THEME Spirometry: an essential clinical measurement BACKGROUND Respiratory disease is common and amenable to early detection and management in the primary care setting. Spirometric
Shortness of breath THEME Spirometry: an essential clinical measurement BACKGROUND Respiratory disease is common and amenable to early detection and management in the primary care setting. Spirometric
Sergio Bonini. Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy.
 Assessment of EIA in the community and in athletes: the role of standardized questionnaires Sergio Bonini Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy se.bonini@gmail.com
Assessment of EIA in the community and in athletes: the role of standardized questionnaires Sergio Bonini Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy se.bonini@gmail.com
Relationship between Methacholine Challenge Testing and exhaled Nitric Oxide in adult patients with suspected bronchial asthma
 O R I G I N A L A R T I C L E S Eur Ann Allergy Clin Immunol Vol 46, N 3, 109-113, 2014 M. Giovannini, M. Valli, V. Ribuffo, R. Melara, G. Cappiello, E. Businarolo, A. Andreani Relationship between Methacholine
O R I G I N A L A R T I C L E S Eur Ann Allergy Clin Immunol Vol 46, N 3, 109-113, 2014 M. Giovannini, M. Valli, V. Ribuffo, R. Melara, G. Cappiello, E. Businarolo, A. Andreani Relationship between Methacholine
Asthma Description. Asthma is a disease that affects the lungs defined as a chronic inflammatory disorder of the airways.
 Asthma Asthma Description Asthma is a disease that affects the lungs defined as a chronic inflammatory disorder of the airways. Symptoms of asthma In susceptible individuals, this inflammation causes recurrent
Asthma Asthma Description Asthma is a disease that affects the lungs defined as a chronic inflammatory disorder of the airways. Symptoms of asthma In susceptible individuals, this inflammation causes recurrent
Alternatives to exercise challenge for the objective assessment of exerciseinduced
 Alternatives to exercise challenge for the objective assessment of exerciseinduced bronchospasm: eucapnic voluntary hyperpnoea and the osmotic challenge tests Educational aims To describe alternative tests
Alternatives to exercise challenge for the objective assessment of exerciseinduced bronchospasm: eucapnic voluntary hyperpnoea and the osmotic challenge tests Educational aims To describe alternative tests
How to treat COPD? What is the mechanism of dyspnea? Smoking cessation
 : The Increasing Role of the FP Alan Kaplan, MD, CCFP(EM) Presented at the Primary Care Today: Education Conference and Medical Exposition, Toronto, Ontario, May 2006. Chronic obstructive pulmonary disease
: The Increasing Role of the FP Alan Kaplan, MD, CCFP(EM) Presented at the Primary Care Today: Education Conference and Medical Exposition, Toronto, Ontario, May 2006. Chronic obstructive pulmonary disease
FEV1 predicts length of stay and in-hospital mortality in patients undergoing cardiac surgery
 EUROPEAN SOCIETY OF CARDIOLOGY CONGRESS 2010 FEV1 predicts length of stay and in-hospital mortality in patients undergoing cardiac surgery Nicholas L Mills, David A McAllister, Sarah Wild, John D MacLay,
EUROPEAN SOCIETY OF CARDIOLOGY CONGRESS 2010 FEV1 predicts length of stay and in-hospital mortality in patients undergoing cardiac surgery Nicholas L Mills, David A McAllister, Sarah Wild, John D MacLay,
Office Spirometry Guide
 Office Spirometry Guide MD Spiro 803 Webster Street, Lewiston ME 04240 Telephone 207-786-7808 1-800-588-3381 Fax 207-786-7280 www.mdspiro.com e-mail: sales@mdspiro.com Why should you perform spirometry
Office Spirometry Guide MD Spiro 803 Webster Street, Lewiston ME 04240 Telephone 207-786-7808 1-800-588-3381 Fax 207-786-7280 www.mdspiro.com e-mail: sales@mdspiro.com Why should you perform spirometry
Efficacy of a Heat Exchanger Mask in Cold Exercise-Induced Asthma* David A. Beuther, MD; and Richard J. Martin, MD, FCCP
 Original Research ASTHMA Efficacy of a Heat Exchanger Mask in Cold Exercise-Induced Asthma* David A. Beuther, MD; and Richard J. Martin, MD, FCCP Study objectives: To determine the efficacy of a novel
Original Research ASTHMA Efficacy of a Heat Exchanger Mask in Cold Exercise-Induced Asthma* David A. Beuther, MD; and Richard J. Martin, MD, FCCP Study objectives: To determine the efficacy of a novel
Aerosol recovery from large-volume reservoir delivery systems is highly dependent on the static properties of the reservoir
 Eur Respir J 1999; 13: 668±672 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 0903-1936 Aerosol recovery from large-volume reservoir delivery systems
Eur Respir J 1999; 13: 668±672 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 0903-1936 Aerosol recovery from large-volume reservoir delivery systems
Joint Session ACOFP and AOASM: Exercise Induced Asthma. Bruce Dubin, DO, JD, FCLM, FACOI
 Joint Session ACOFP and AOASM: Exercise Induced Asthma Bruce Dubin, DO, JD, FCLM, FACOI ACOFP FULL DISCLOSURE FOR CME ACTIVITIES Please check where applicable and sign below. Provide additional pages as
Joint Session ACOFP and AOASM: Exercise Induced Asthma Bruce Dubin, DO, JD, FCLM, FACOI ACOFP FULL DISCLOSURE FOR CME ACTIVITIES Please check where applicable and sign below. Provide additional pages as
Bronchial Provocation Results: What Does It Mean?
 Bronchial Provocation Results: What Does It Mean? Greg King 1 Department of Respiratory Medicine, Royal North Shore Hospital, St Leonards 2065 2 Woolcock Institute of Medical Research and Sydney Medical
Bronchial Provocation Results: What Does It Mean? Greg King 1 Department of Respiratory Medicine, Royal North Shore Hospital, St Leonards 2065 2 Woolcock Institute of Medical Research and Sydney Medical
COPD in primary care: reminder and update
 COPD in primary care: reminder and update Managing COPD continues to be a major feature of primary care, particularly in practices with a high proportion of M ori and Pacific peoples. COPDX clinical practice
COPD in primary care: reminder and update Managing COPD continues to be a major feature of primary care, particularly in practices with a high proportion of M ori and Pacific peoples. COPDX clinical practice
Meenu Singh, Joseph L. Mathew, Prabhjot Malhi, B.R. Srinivas and Lata Kumar
 Comparison of Improvement in Quality of Life Score with Objective Parameters of Pulmonary Function in Indian Asthmatic Children Receiving Inhaled Corticosteroid Therapy Meenu Singh, Joseph L. Mathew, Prabhjot
Comparison of Improvement in Quality of Life Score with Objective Parameters of Pulmonary Function in Indian Asthmatic Children Receiving Inhaled Corticosteroid Therapy Meenu Singh, Joseph L. Mathew, Prabhjot
CHRONIC COUGH AS THE PRESENTING MANIFESTATION OF BRONCHIAL ASTHMA
 CHRONIC COUGH AS THE PRESENTING MANIFESTATION OF BRONCHIAL ASTHMA T C Goh Dept of Medicine Toa Payoh Hospital Singapore 1129 T C Goh, MBBS, MRCP (UK), AM Registrar SYNOPSIS Bronchial asthma may present
CHRONIC COUGH AS THE PRESENTING MANIFESTATION OF BRONCHIAL ASTHMA T C Goh Dept of Medicine Toa Payoh Hospital Singapore 1129 T C Goh, MBBS, MRCP (UK), AM Registrar SYNOPSIS Bronchial asthma may present
M.M. Haby*, J.K. Peat*, C.M. Mellis**, S.D. Anderson +, A.J. Woolcock*
 Eur Respir J, 1995, 8, 729 736 DOI: 10.1183/09031936.95.08050729 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1995 European Respiratory Journal ISSN 0903-1936 An exercise challenge for
Eur Respir J, 1995, 8, 729 736 DOI: 10.1183/09031936.95.08050729 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1995 European Respiratory Journal ISSN 0903-1936 An exercise challenge for
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/21235
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/21235
Frequency of nocturnal symptoms in asthmatic children attending a hospital out-patient clinic
 Eur Respir J, 1995, 8, 2076 2080 DOI: 10.1183/09031936.95.08122076 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1995 European Respiratory Journal ISSN 0903-1936 Frequency of nocturnal
Eur Respir J, 1995, 8, 2076 2080 DOI: 10.1183/09031936.95.08122076 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1995 European Respiratory Journal ISSN 0903-1936 Frequency of nocturnal
Ass. Prof. Pulmonary and Crit.Care Medical School,University of Athens
 Diagnosis i of Exercise Induced Asthma Ch. Gratziou Ass. Prof. Pulmonary and Crit.Care Medical School,University of Athens Other Diagnostic Challenges for Exercise Induced Asthma Do we need other tests
Diagnosis i of Exercise Induced Asthma Ch. Gratziou Ass. Prof. Pulmonary and Crit.Care Medical School,University of Athens Other Diagnostic Challenges for Exercise Induced Asthma Do we need other tests
Airway responsiveness and job selection: a study in coal miners and non-mining controls
 Occupational and Environmental Medicine 1995;52:745-749 National Institute for Occupational Safety and Health, Division of Respiratory Disease Studies, Morgantown, West Virginia, USA E L Petsonk D M Mannino
Occupational and Environmental Medicine 1995;52:745-749 National Institute for Occupational Safety and Health, Division of Respiratory Disease Studies, Morgantown, West Virginia, USA E L Petsonk D M Mannino
FEVI before (5% predicted) 62 (49-77) 59 (44-77) FEV, after (% predicted) 92 (84-108) 89 (69-107) to the entire group received aerosol isoprenaline.
 Tl.orax, 1980, 35, 298-302 Lung elastic recoil and reduced airflow in clinically stable asthma D S McCARTHY AND M SIGURDSON From the Department of Medicine, University ofmanitoba, Respiratory Division,
Tl.orax, 1980, 35, 298-302 Lung elastic recoil and reduced airflow in clinically stable asthma D S McCARTHY AND M SIGURDSON From the Department of Medicine, University ofmanitoba, Respiratory Division,
3.0 METHODS. 3.1 Participants
 3.0 METHODS 3.1 Participants There were initially twenty participants studied in this experiment. The age range was between 18-50 years of age. The nine workers came from a private landscape company with
3.0 METHODS 3.1 Participants There were initially twenty participants studied in this experiment. The age range was between 18-50 years of age. The nine workers came from a private landscape company with
Birth characteristics and asthma symptoms in young adults: results from a population-based cohort study in Norway
 Eur Respir J 998; 2: 6 7 DOI:./996.98.266 Printed in UK - all rights reserved Copyright ERS Journals Ltd 998 European Respiratory Journal ISSN 9-96 Birth characteristics and asthma symptoms in young adults:
Eur Respir J 998; 2: 6 7 DOI:./996.98.266 Printed in UK - all rights reserved Copyright ERS Journals Ltd 998 European Respiratory Journal ISSN 9-96 Birth characteristics and asthma symptoms in young adults:
Bronchoconstriction in potroom workers
 British Journal of Inidustrial Medicine, 1979, 36, 211-215 M. SARIC, E. ZUSKIN*, AND M. GOMZI From the Institute for Meclical Research and Occupational Health, Zagreb and the *Andrija Stampar School of
British Journal of Inidustrial Medicine, 1979, 36, 211-215 M. SARIC, E. ZUSKIN*, AND M. GOMZI From the Institute for Meclical Research and Occupational Health, Zagreb and the *Andrija Stampar School of
SGRQ Questionnaire assessing respiratory disease-specific quality of life. Questionnaire assessing general quality of life
 SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
Effect of peak expiratory flow data quantity on diagnostic sensitivity and specificity in occupational asthma
 Eur Respir J 2004; 23: 730 734 DOI: 10.1183/09031936.04.00027304 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2004 European Respiratory Journal ISSN 0903-1936 Effect of peak expiratory
Eur Respir J 2004; 23: 730 734 DOI: 10.1183/09031936.04.00027304 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2004 European Respiratory Journal ISSN 0903-1936 Effect of peak expiratory
A diagnosis of asthma is made on the basis of compatible
 383 ASTHMA Exhaled nitric oxide in the diagnosis of asthma: comparison with bronchial provocation tests N Berkman, A Avital, R Breuer, E Bardach, C Springer, S Godfrey... See end of article for authors
383 ASTHMA Exhaled nitric oxide in the diagnosis of asthma: comparison with bronchial provocation tests N Berkman, A Avital, R Breuer, E Bardach, C Springer, S Godfrey... See end of article for authors
Lisa M Bradshaw, David Fishwick, Tania Slater, Neil Pearce
 150 Wellington Asthma Research Group, Department of Medicine, Wellington School of Medicine, PO Box 7343, Mein Street, Wellington, New Zealand L M Bradshaw D Fishwick T Slater N Pearce Correspondence to:
150 Wellington Asthma Research Group, Department of Medicine, Wellington School of Medicine, PO Box 7343, Mein Street, Wellington, New Zealand L M Bradshaw D Fishwick T Slater N Pearce Correspondence to:
ADULT ASTHMA GUIDE SUMMARY. This summary provides busy health professionals with key guidance for assessing and treating adult asthma.
 ADULT ASTHMA GUIDE SUMMARY This summary provides busy health professionals with key guidance for assessing and treating adult asthma. Its source document Asthma and Respiratory Foundation NZ Adult Asthma
ADULT ASTHMA GUIDE SUMMARY This summary provides busy health professionals with key guidance for assessing and treating adult asthma. Its source document Asthma and Respiratory Foundation NZ Adult Asthma
Treatment of acute asthmatic exacerbations with an increased dose of inhaled steroid
 12 Paediatrics and Child Health, Dunedin School of Medicine, PO Box 913, University of Otago Medical School, Dunedin, New Zealand J Garrett Preventive and Social Medicine, Dunedin School of Medicine S
12 Paediatrics and Child Health, Dunedin School of Medicine, PO Box 913, University of Otago Medical School, Dunedin, New Zealand J Garrett Preventive and Social Medicine, Dunedin School of Medicine S
File: Spirometry-Vimeo 720p-MP3 for Audio Podcasting.mp3 Duration: 0:07:09 Date: 05/02/2014 START AUDIO
 BMJ LEARNING VIDEO TRANSCRIPT File: Spirometry-Vimeo 720p-MP3 for Audio Podcasting.mp3 Duration: 0:07:09 Date: 05/02/2014 START AUDIO Dr Kevin Gruffyd-Jones: Spirometry is important in several ways. Firstly,
BMJ LEARNING VIDEO TRANSCRIPT File: Spirometry-Vimeo 720p-MP3 for Audio Podcasting.mp3 Duration: 0:07:09 Date: 05/02/2014 START AUDIO Dr Kevin Gruffyd-Jones: Spirometry is important in several ways. Firstly,
PREDICTION EQUATIONS FOR LUNG FUNCTION IN HEALTHY, LIFE TIME NEVER-SMOKING MALAYSIAN POPULATION
 Prediction Equations for Lung Function in Healthy, Non-smoking Malaysian Population PREDICTION EQUATIONS FOR LUNG FUNCTION IN HEALTHY, LIFE TIME NEVER-SMOKING MALAYSIAN POPULATION Justin Gnanou, Brinnell
Prediction Equations for Lung Function in Healthy, Non-smoking Malaysian Population PREDICTION EQUATIONS FOR LUNG FUNCTION IN HEALTHY, LIFE TIME NEVER-SMOKING MALAYSIAN POPULATION Justin Gnanou, Brinnell
Asthma: diagnosis and monitoring
 Asthma: diagnosis and monitoring NICE guideline: short version Draft for second consultation, July 01 This guideline covers assessing, diagnosing and monitoring suspected or confirmed asthma in adults,
Asthma: diagnosis and monitoring NICE guideline: short version Draft for second consultation, July 01 This guideline covers assessing, diagnosing and monitoring suspected or confirmed asthma in adults,
Benzalkonium Chloride Induced Bronchoconstriction in Patients with Stable Bronchial Asthma
 The Korean Journal of Internal Medicine : 22:244-248, 2007 Benzalkonium Chloride Induced Bronchoconstriction in Patients with Stable Bronchial Asthma Byoung Hoon Lee, M.D. and Sang-Hoon Kim, M.D. Department
The Korean Journal of Internal Medicine : 22:244-248, 2007 Benzalkonium Chloride Induced Bronchoconstriction in Patients with Stable Bronchial Asthma Byoung Hoon Lee, M.D. and Sang-Hoon Kim, M.D. Department
Asthma Management. Photo from
 Asthma Management 1 Photo from www.nhlbi.nih.gov Course Overview 1. Recognition of the symptoms and signs Basic Knowledge of asthma Recognition of common symptoms Recognition of the signs of asthma including
Asthma Management 1 Photo from www.nhlbi.nih.gov Course Overview 1. Recognition of the symptoms and signs Basic Knowledge of asthma Recognition of common symptoms Recognition of the signs of asthma including
Abnormal Spirometry Medical Risk in Aviation Conference Royal Aeronautical Society, Dec 2017
 Abnormal Spirometry Medical Risk in Aviation Conference Royal Aeronautical Society, Dec 2017 Professor Howard Branley MBChB MSc MD FCCP FRCP FRAeS Consultant in Respiratory Medicine What I want to cover
Abnormal Spirometry Medical Risk in Aviation Conference Royal Aeronautical Society, Dec 2017 Professor Howard Branley MBChB MSc MD FCCP FRCP FRAeS Consultant in Respiratory Medicine What I want to cover
