Distribution and degranulation of airway mast cells in normal and asthmatic subjects
|
|
|
- Bennett Skinner
- 6 years ago
- Views:
Transcription
1 Eur Respir J 22; 19: DOI: / Printed in UK all rights reserved Copyright #ERS Journals Ltd 22 European Respiratory Journal ISSN Distribution and degranulation of airway mast cells in normal and asthmatic subjects N.G. Carroll, S. Mutavdzic #, A.L. James # Distribution and degranulation of airway mast cells in normal and asthmatic subjects. N.G. Carroll, S. Mutavdzic, A.L. James. #ERS Journals Ltd 22. ABSTRACT: It was hypothesized that the distribution and activation of mast cells across the airway wall may reflect their function in asthma. The density of mast cells (intact and degranulated) within airway compartments in cartilaginous and membranous airways, obtained from autopsies on patients with fatal asthma, nonfatal asthma, and nonasthmatic control cases have been examined. In cartilaginous airways, the mean SE density of mast cells in control cases was 27 9 cells?mm -2. It was similar in nonfatal asthma (24 2 cells?mm -2 ) but reduced (pv.5) in fatal asthma cases (16 2 cells?mm -2 ). In membranous airways, the density of mast cells in control cases was cells?mm -2 and was higher (pv.5) in cases of nonfatal (27 51 cells?mm -2 ) and fatal asthma ( cells?mm -2 ). Mast-cell density was greatest on the smooth muscle and mucous glands in cartilaginous airways and on the smooth muscle and outer airway wall in membranous airways. The percentage of degranulated mast cells was higher (pv.5) in cases of asthma, related to disease severity, and was higher in cartilaginous than membranous airways. Degranulation was greatest on the smooth muscle in fatal asthma cases. Mast-cell distribution and degranulation varies between cartilaginous and membranous airways and across the airway wall. Degranulation of mast cells is related to asthma severity. The increased degranulation in proximal airways may reflect stimulation via the inhaled route. Eur Respir J 22; 19: Faculty of Regional Professional Studies, Edith Cowen University, Bunbury and # Dept of Pulmonary Physiology, Sir Charles Gairdner Hospital, Nedlands, Western Australia. Correspondence: N. Carroll, Faculty of Regional Professional Studies, Edith Cowen University, Robertson Drive, Bunbury, WA 623, Australia. Fax: n.carroll@ecu.edu.au Keywords: Asthma,mastcells,pathology Received: August Accepted after revision November This study was supported by the Asthma Foundation of Western Australia, National Health and Medical Research Council, Australia. Asthma is a disease characterized by airway inflammation [1] and remodelling [2]. It has been suggested, but not proven, that inflammation results in remodelling. The extent to which inflammatory cells interact with airway wall structures (which are subject to remodelling) depends on the distribution of inflammatory cells across the airway wall. Two studies [3, 4] have shown an increase in the numbers of mast cells found on the smooth muscle layer in isolated sensitized human bronchi compared with nonsensitized airways. Mast cells are present in varying numbers in patients with asthma [5 1]. Their role in inflammatory reactions relates to their ability to store and release, or synthesize de novo, mediators of inflammation [11]. The multiple actions of mast-cell derived mediators suggest that mast cells might interact with airway structures. When mast cells are activated they become partly or completely degranulated [5]. However, the extent to which this occurs in asthma and its relationship to disease severity has not been quantified. A further rationale for studying the distribution of inflammatory cells across the airway wall in large and small airways is to determine the degree to which assessing inflammation by sampling the proximal bronchial tree is representative of airway inflammation in the distal bronchial tree. Therefore, the aim of this study was to examine the distribution of mast cells and their degree of degranulation within the airway wall of the large and small airways of subjects without respiratory disease and compare them with patients with asthma. Cases Methods The left or right lung was obtained at Coroner9s autopsy if the cause of death was asthma or if death occurred suddenly, without chest trauma or illness (other than asthma). Medical histories were obtained retrospectively from family members, usual medical practitioner and hospital files. As described previously [2], cases were categorized as follows. 1) Control: no history of asthma, wheeze, use of asthma medications or other lung disease; 2) nonfatal asthma: sudden nonrespiratory death but with a definite history of asthma; and 3) fatal asthma: death due only to asthma. Cases were excluded from the study if details of medical history could not be obtained. Ethical approval for the study was obtained from the Sir Charles Gairdner Hospital9s Ethics Committee. Histological preparation Lungs were fixed in formalin and transverse blocks of all large conducting airways down to the
2 88 N.G. CARROLL ET AL. subsegmental level were cut, resulting in large cartilaginous airways per case, from which five were randomly selected for this study. Six parenchymal sections (36261 cm) were taken at random from the midsaggital slice of the lung. Tissue sections were cut (5 mm) and stained using the immunoperoxidase technique with the antimast cell tryptase monoclonal antibody AA1 (Dako Patts, Copenhagen, Denmark). Airway dimensions Airway dimensions (inner and outer airway wall thickness and areas of smooth muscle, submucosal mucous glands and cartilage) were measured as previously described [2]. The basement membrane perimeter (Pbm) was directly traced using a camera lucida and a digitizing tablet. Cell counts Mast cells with a visible nucleus were counted and expressed as total number in each of the previously discussed compartments and cells?mm -2 of each compartment area (cell density). The percentage of total airway mast-cell count in each airway compartment was calculated. Mast-cell degranulation At high power (64), positively-stained nucleated mast cells were classified as intact if they were dense, compact, had unbroken cytoplasmic boundaries and did not have any surrounding positively stained granules (fig. 1). All other nucleated tryptase positive cells were classified as degranulated (fig. 2). Degranulated cells were expressed as a per cent of the total number of nucleated AA1-positive cells for the whole airway section and for each compartment. Intraobserver error was calculated for airway Fig. 2. A transverse section of a large cartilaginous airway showing mast cell tryptase positive cells (arrows) present in the airway wall showing damaged epithelium (EPI), airway smooth muscle (ASM) and submucosal mucous glands (SMG). In this section, most mast cells demonstrate a lack of dense homogeneous staining and an abundance of extracellular tryptase positivity (arrows) and were classified as degranulated mast cells. Scale bar=1 mm. dimensions, cell counts and degranulation index, as previously described [2]. All measurements were made by one observer (N.G. Carroll), blinded to case histories. Data analysis The mean of each case group, calculated from the means of each case, was used for analysis. Bartlett9s test for homogeneity of variances was performed. Where data was normally distributed, differences between groups were tested using parametric analysis (one way analysis of variance (ANOVA)) and where data was not normally distributed, nonparametric tests (Kruskal-Wallis nonparametric ANOVA) were used followed by Dunn9s multiple comparison test. A probability value of v5% was considered significant. Results Subject characteristics The cases of fatal asthma were generally severe, as defined by treatment requirements and symptoms, and had measurable airflow obstruction (table 1). The cases of nonfatal asthma were generally mild with infrequent symptoms. Total airway wall Fig. 1. A transverse section of a large cartilaginous airway showing mast cell tryptase positive cells (arrows) present in the airway wall including epithelium (EPI), airway smooth muscle (ASM) and submucosal mucous glands (SMG). Most mast cells demonstrate dense homogeneous staining with little extracellular tryptase positivity and were classified as intact mast cells. Scale bar=1 mm. There were no significant differences in the size (Pbm) of the cartilaginous or membranous airways examined in each of the three case groups (table 2). In cartilaginous airways, the absolute number and density of mast cells on transverse section were higher (pv.5) in cases of nonfatal asthma and control cases compared with cases of fatal asthma. In membranous airways they were higher (pv.5) in
3 DISTRIBUTION OF MAST CELLS IN ASTHMA 881 Table 1. Subject characteristics Control Nonfatal Fatal Subjects n Male/female 5/3 4/4 4/4 Age yrs mean SD Treatment n Bronchodilator 8 8 Inhaled corticosteroid 2 8 Oral corticosteroid 6 Asthma symptoms Nil Weekly 3 of 8 Daily 7 of 8 Occasional 5 of 8 Occasional 1 of 8 Time off work or hospitalization due to asthma n 1 7 Duration of asthma yrs mean (range) Nil 14 (2 36) 18 (2 4) Lung function FEV1 % pred mean (range) NA NA 68 (35 9) FEV1: forced expiratory volume in one second; NA: not available. Table 2. Mast cell counts across the total airway wall in cartilaginous and membranous airways from cases of nonfatal and fatal asthma and controls Control Nonfatal asthma Fatal asthma Cartilaginous Membranous Cartilaginous Membranous Cartilaginous Membranous n Pbm mm mean SD Total mast cell count # # Mast cell density cells?mm # # Degranulated cells % } ,} 86 3 # 75 4 #,} Data are presented as mean SEM unless otherwise stated. Pbm: basement membrane perimeter. : pv.5 compared with control and nonfatal asthma cases; # :pv.5 compared with control cases; } :pv.5 compared with cartilaginous airways. cases of fatal and nonfatal asthma compared with control cases (table 2). Mast-cell density in airway wall compartments Cartilaginous airways. Figure 3a shows mast-cell density in different airway wall compartments in cartilaginous airways. In control cases, the density of mast cells variedw5-fold across the airway wall, being highest on the smooth muscle (74 17 cells?mm -2 ), intermediate in the inner airway wall (35 3 cells?mm -2 ), submucosal glands (39 9 cells?mm -2 ) and outer airway wall (7 1 cells?mm -2 ) and was lowest in the epithelium (1.5.4 cells?mm -2 ) and lumen (.2.1 cells?mm -2 ). In submucosal mucous glands, all mast cells were seen within the supporting stromal tissue surrounding glands and no cells were noted within individual serous or mucinous acini. Similar patterns were observed in the nonfatal and fatal cases of asthma. Compared with control cases, however, the density was significantly lower (pv.5) in the smooth muscle, the inner airway wall and the epithelium of nonfatal and fatal cases. The density of mast cells in the lumen was higher (pv.5) in the fatal cases compared with nonfatal cases of asthma, and both were higher than control cases (pv.5). The density of mast cells on submucosal glands was significantly higher (pv.5) in nonfatal compared with fatal cases of asthma and controls. In the outer airway wall there were no significant differences between the case groups. Membranous airways. Figure 3b shows mast-cell density in different airway wall compartments in membranous airways. In control cases, the highest density of mast cells was on the smooth muscle (21 27 cells?mm -2 ) and in the outer airway wall area ( cells?mm -2 ). The density in the inner wall area (78 12 cells?mm -2 ), lumen (1.5 cells?mm -2 ) and epithelium (.8.6 cells?mm -2 ) were significantly lower. In the nonfatal cases, the density of mast cells was significantly higher (pv.5) on the smooth muscle and in both the inner and the outer airway wall areas compared with control cases. In the fatal cases, the density of mast cells was higher in the outer wall area, lumen and epithelium, compared with control cases. The overall density of mast cells in membranous airways was an order of magnitude higher than in the cartilaginous airways (table 2 and fig. 3a and b). Per cent of total mast cells in different airway wall compartments Cartilaginous airways. Figure 4a shows the per cent of total mast cells in different airway wall compartments in cartilaginous airways. Within the airway wall, the distribution of mast cells into the different compartments was similar in the three case groups except the submucosal mucous glands where the per cent of total mast cells was higher in the asthma cases. The highest percentages of mast cells were seen in both the inner and outer airway wall reflecting the greater area
4 882 N.G. CARROLL ET AL. a) b) Mast cell density cells mm # Lumen EPI WAi ASM WAo Gland a) b) Total mast cells % Lumen EPI WAi ASM WAo Gland Mast cell density cells mm Lumen EPI WAi ASM WAo Fig. 3. Mast-cell density in a) cartilaginous and b) membranous airways. EPI: epithelium; WAi: inner airway wall; ASM: airway smooth muscle; WAo: outer airway wall; Gland: submucosal mucous glands. h: control; u: nonfatal asthma cases; q: fatal asthma cases. : pv.5 compared with control cases; # :pv.5 compared with control and nonfatal cases; } : pv.5 compared with control and fatal cases. Total mast cells % Lumen EPI WAi ASM WAo Fig. 4. Per cent of total mast cells in a) cartilaginous and b) membranous airways. EPI: epithelium; WAi: inner airway wall; ASM: airway smooth muscle; WAo: outer airway wall; Gland: submucosal mucous glands. h: control; u: nonfatal asthma cases; q: fatal asthma cases. : pv.5 compared with control cases; # : pv.5 compared with control and nonfatal cases. of these compartments on transverse section. In the epithelium, the per cent of mast cells was higher (pv.5) in the control cases compared with the fatal and nonfatal asthma cases, whereas in the airway lumen, the per cent of mast cells was higher (pv.5) in fatal than nonfatal asthma cases and control cases. Membranous airways. Figure 4b shows the per cent of total mast cells in different airway wall compartments in membranous airways. The greatest percentage of mast cells was observed in the outer airway wall, the largest compartment in membranous airways. In the cases of fatal asthma, the per cent of mast cells was higher (pv.5) in the outer airway wall and airway lumen but was lower (pv.5) in the inner airway wall and on the airway smooth muscle compared with control and nonfatal asthma cases. Fatal asthma and control cases had a higher per cent (pv.5) of total mast cells in the epithelium than the cases of nonfatal asthma. Degranulation The average percentage of degranulated mast cells was higher (pv.5) in cartilaginous airways than in membranous airways in all case groups. Compared with control cases, the percentage of degranulated mast cells was higher (pv.5) in cases of nonfatal asthma and higher again in cases of fatal asthma (table 2). The differences in degranulation between the control and asthma case groups were similar in the different airway wall compartments, in both cartilaginous (fig. 5a) and membranous (fig. 5b) airways for the three case groups. However, degranulation was significantly higher on the airway smooth muscle mast cells in cases of fatal asthma compared with both control and nonfatal asthma cases. The coefficient of variation for intraobserver error was 3% for airway dimensions, 11% for cell counts and 1% for the degranulation index. Discussion Insights can be gained from examining the distribution of mast cells across the airway wall. Firstly, the extent to which small samples from bronchial biopsies of large cartilaginous airways are representative of inflammatory processes deeper in the airway wall or in more distal sites in the bronchial tree can be assessed. The present study has shown that mast-cell density in the inner wall differs from that in the outer airway wall, smooth muscle and mucous glands. Moreover, the density in proximal airways was much lower than that in distal airways. Secondly, the relatively higher density of cells in smooth muscle
5 DISTRIBUTION OF MAST CELLS IN ASTHMA 883 a) b) % of total mast cells % of total mast cells WAi ASM WAo Gland WAi ASM WAo and mucous glands suggests that they may be important in regulating the function of these tissues. Thirdly, the relation of mast-cell degranulation to asthma severity suggests an active role as effector cells in airway wall inflammation. Fourthly, the higher number of degranulated mast cells in cartilaginous compared with membranous bronchioles is consistent with an inhaled stimulus activating these cells. Mast-cell numbers in this study were expressed both as total numbers per transverse section and as density (the number of cells?mm -2 of area measured). This method of cell number estimation is a profile count of cells within a 3-dimensional (3D) structure and may be subject to bias if certain conditions are not met [12]. Firstly, sampling of tissues and fields of interest for measurements need to be performed in a systematic random fashion. Secondly, all cells of interest must have an equal probability of being counted. This depends largely on cell size and orientation. Thirdly, the reference area for measurements (i.e. a 2-dimensional (2D) profile area) should be related to the 3D volume that the profile represents if absolute cell number in the airway volume are to be determined. In the present study, the sampling processes, from lung collection to individual airway # # Fig. 5. Per cent of degranulated mast cells in a) cartilaginous and b) membranous airways. WAi: inner airway wall; ASM: airway smooth muscle; WAo: outer airway wall; Gland: submucosal mucous glands. h: control; u: nonfatal asthma cases; q: fatal asthma cases. : pv.5 compared with control cases; # :pv.5 compared with control and nonfatal cases. blocks and sections, were systematic and random. Cells were identified using immunohistochemical staining but only counted if nucleated. The size of the mast-cell nucleus does not vary significantly [13] and is small compared with the reference section in which it was measured in this study. Because the authors were unable to define an initial reference volume for the whole lung, and did not use a "lookup" section, the 2D profile counts in this study could not be converted into a 3D volume estimate of absolute cell numbers. However, since nucleus size and orientation were not likely to have systematically changed between groups, the authors felt that these limitations would not affect comparisons between groups. Since measurement variability is predominantly due to subject and tissue-block variability [14], a large number of randomly-selected airways from different sites in the lung were examined and the mean data from each case was used to compare cell numbers between groups. Therefore, comparisons of relative cell densities between the groups in this study are valid and make the data directly comparable with the many other published studies that have reported cell numbers in this way. Previous studies of mast-cell numbers in the airways have shown that compared with control cases, those with asthma have higher [5, 6], decreased [8], or similar [9, 1, 15, 16] numbers of mast cells. The variation between studies may be due to variations in asthma severity, use of different methodologies, effects of treatment and variations in the degree of degranulation [17 2]. To the authors9 knowledge, no previous studies have systematically quantified mast-cell degranulation. The higher concentrations of mast-cell derived mediators, such as histamine, prostaglandin D 2 (PGD 2 ), leukotriene C4 (LTC4) and tryptase seen in bronchoalveolar lavage (BAL) fluid in the early- and late-phase asthmatic reaction following local-allergen challenge [21], suggest mastcell degranulation. The amount of degranulation was greatest in fatal asthma cases, suggesting increased mast-cell activation in these cases. In addition, increased degranulation may have caused underestimation of the number of mast cells in these cases (i.e. by not counting cells where there were no granules left). The amount of mast-cell degranulation was found to be greatest in the submucosal mucous glands and on the airway smooth muscle layer in fatal asthma cases. PESCI et al. [22] showed an increase in the number of degranulated mast cells in the mucous glands of patients with chronic bronchitis, a disease characterized by excessive mucus production, and BRADDING [11] observed that interleukin-6 positive mast cells are concentrated in close proximity to submucosal mucous glands [7]. It is well documented that mast-cell derived proteases are capable of acting as potent secretagogues and that histamine, which is stored in and secreted from activated mast cells, stimulates smooth muscle shortening and vasodilatation [23]. The authors have shown previously that increased secretion of mucus into the airway lumen combined with moderate amounts of smooth-muscle shortening in vivo, may give rise to exaggerated airway narrowing [24], which may contribute to sudden fatal
6 884 N.G. CARROLL ET AL. asthma attacks [25]. These findings suggest the mast cell to be an important effector cell during an acute attack of asthma. The finding that the density of mast cells was highest on the smooth-muscle layer compared with other airway wall compartments is similar to the findings of AMMIT et al. [3] and BERGER et al. [4]. The present study is the first quantitative evidence that mast cells are the predominant cell within the airway smooth-muscle layer in both nonasthmatics and asthmatics, and that those present on the smooth muscle layer in cases of fatal asthma are mostly degranulated. CONNELL [8] noted accumulation of mast cells near the smooth-muscle layer in cartilaginous bronchi from cases of fatal asthma. During an acute episode of asthma, activation of mast cells might cause abnormal release of chemical mediators, resulting in excessive stimulation of smooth muscle and mucous glands. This hypothesis is supported by the findings of elevated amounts of mast-cell derived mediators in BAL fluid from cases of asthma following allergen challenge [26] and lower numbers of mast cells in biopsies obtained from patients during an episode of asthma than during symptom-free periods [27]. One potential mechanism that may cause mast cell numbers in the airway wall to be reduced during asthma exacerbations is the movement of cells from the airway wall into the airway lumen. This is supported by the observation in this study of a higher percentage of mast cells in the lumen of fatal asthma cases compared with nonfatal asthma and nonasthmatic control cases. In addition, higher numbers of mast cells are observed in the sputum of atopic asthmatics after allergen-inhalation challenge [2]. Another potential mechanism for reduced mast-cell numbers is increased apoptosis of cells. While the degree of mast-cell apoptosis was not assessed in this study and therefore cannot be excluded as a mechanism for reducing cell numbers, persistent inflammatory conditions are usually characterized by delayed or impaired apoptosis. The degree of mast-cell degranulation in the present study was higher in the cartilaginous (proximal) airways compared with the membranous (distal) airways. It is tempting to speculate that a major reason for this is that the predominant stimulus for mast-cell degranulation occurs close to the mucosal surface of the airway and, to a greater extent, in the proximal bronchial tree, due to an inhaled stimulus. In the present study, the level of mast-cell degranulation in the mucous glands in all cases of asthma was significantly higher than that observed in the outer airway wall, suggesting selective stimulation of mast cells. A mechanism that may explain this, is the fact that neuropeptides are capable of inducing mastcell degranulation [28] and there is an abundance of cholinergic nerves present in the airway epithelium that have local axonal pathways to submucosal mucous glands [29]. Thus, stimulation of these nerves at the mucosal surface and subsequent release of neuropeptides may lead to increased mast-cell degranulation of mucous glands. The density of mast cells was lower in the cartilaginous airways than the membranous airways in asthma cases compared with control cases. Similarly, the study of CONNELL [8] also reported decreased numbers of mast cells in the airway wall in cartilaginous airways from fatal asthma cases compared with control cases. Studies examining the numbers of mast cells in bronchial biopsies from the proximal bronchial tree in cases of mild asthma show variation, in that some studies show an increase in mast cells within the airway wall [5, 3], some in the epithelium only [6], and others showed no difference at all [9, 1, 15, 16]. This variation may be due to degranulation, apoptosis or the effects of anti-inflammatory treatment. Nonetheless, the present study clearly demonstrates that bronchial biopsy obtained from the proximal bronchial tree may not always represent the pattern of inflammation across the airway wall or along the entire length of the bronchial tree. In conclusion, in addition to their clearly defined role in immunoglobulin-e-dependent responses to antigenic stimulation in atopic disorders such as asthma, it is possible that mast cells may markedly amplify many features of the host response to nonspecific acute inflammatory stimuli, such as that seen in asthmatics in response to exercise, cold air and hypertonic saline inhalation. The separate activity of mast cells in the airways should be considered in both short-term and long-term treatment strategies. References 1. Djukanovic WR, Roche WR, Wilson JW, et al. Mucosal inflammation in asthma. Am Rev Respir Dis 199; 142: Carroll NG, Elliot J, Morton AR, James AL. The structure of large and small airways in nonfatal and fatal asthma. Am Rev Respir Dis 1993; 147: Ammit AJ, Bekir SS, Johnson PRA, Hughes JM, Armour CL, Black JL. Mast cell numbers are increased in the smooth muscle of human sensitized isolated bronchi. Am J Respir Crit Care Med 1997; 155: Berger P, Walls AF, Marthan R, Tunon-de-Lara JM. Immunoglobulin E-induced passive sensitization of human airways: An immunohistochemical study. Am J Respir Crit Care Med 1998; 157: Pesci A, Foresi A, Bertorelli AC, Oliveri D. Histochemical characteristics and degranulation of mast cells in epithelium and lamina propria of bronchial biopsies from asthmatic and normal subjects. Am Rev Respir Dis 1993; 147: Laitinen LA, Laitinen A, Haahtela T. Airway mucosal inflammation even in patients with newly diagnosed asthma. Am Rev Respir Dis 1993; 147: Wardlaw AJ, Dunnett S, Gleich GJ, Collins JV, Kay AB. Eosinophils and mast cells in bronchoalveolar lavage in mild asthma: relationship to bronchial hyperreactivity. Am Rev Respir Dis 1988; 137: Connell JT. Asthmatic deaths: role of the mast cell. JAMA 1971; 215: Bradley BL, Azzawi M, Jacobson M, et al. Eosinophils, T-lymphocytes, mast cells, neutrophils, and macrophages in bronchial biopsy specimens from atopic subjects with asthma: comparison with biopsy
7 DISTRIBUTION OF MAST CELLS IN ASTHMA 885 specimens from atopic subjects without asthma and normal control subjects and relationship to bronchial hyperresponsiveness. J Allergy Clin Immunol 1991; 88: Djukanovic R, Wilson JW, Britten KM, et al. Quantitation of mast cells and eosinophils in the bronchial mucosa of symptomatic atopic asthmatics and healthy control subjects using immunohistochemistry. Am Rev Respir Dis 199; 142: Bradding P. Interleukins (IL)-4, -5, -6 and TNFa in normal and asthmatic airways: evidence for the human mast cell as an important source of these cytokines. Am J Respir Cell Mol Biol 1994; 1: Weibel ER, Gomez DM. A principle for counting tissue structures on random sections. J Appl Physiol 1962; 17: Jeffery PK, Heard BE, Kay AB. Do mast cells degranulate in the bronchial mucosa of mildly symptomatic atopic asthmatic subjects? Am Rev Respir Dis 1992; 145: A Gundersen H, Osterby R. Optimizing sampling efficiency of stereological studies in biology. J Microscopy 1981; 121: Beasley R, Roche W, Roberts JA, Holgate ST. Cellular events in the bronchi in mild asthma and after bronchial provocation. Am Rev Respir Dis 1989; 139: Vignola AM, Chanez P, Campbell AM, et al. Airway inflammation in mild intermittent and in persistent asthma. Am J Respir Crit Care Med 1998; 157: Trigg CJ, Manolitsas ND, Wang J, et al. Placebocontrolled immunopathologic study of four months of inhaled corticosteroids in asthma. Am J Respir Crit Care Med 1994; 15: Djukanovic R, Wilson JW, Britten K, et al. Effect of an inhaled corticosteroid on airway inflammation and symptoms in asthma. Am Rev Respir Dis 1992; 145: Bentley AM, Hamid Q, Robinson DS, et al. Prednisolone treatment in asthma: Reduction in the numbers of eosinophils, T cells, tryptase-only positive mast cells, and modulation of IL-4, IL-5, and interferongamma cytokine gene expression within the bronchial mucosa. Am J Respir Crit Care Med 1996; 153: Gauvreau GM, Lee JM, Watson RM, Irani AM, Schwartz LB, O9Byrne PM. Increased numbers of both airway basophils and mast cells in sputum after allergen inhalation challenge of atopic asthmatics. Am J Respir Crit Care Med 2; 161: Metzger WJ, Zavala D, Richerson HB, et al. Local allergen challenge and bronchoalveolar lavage of allergic asthmatic lungs. Description of the model and local airway inflammation. Am Rev Respir Dis 1987; 135: Pesci A, Rossi GA, Bertorelli G, Aufiero A, Zanon P, Olivieri D. Mast cells in the airway lumen and bronchial mucosa of patients with chronic bronchitis. Am J Respir Crit Care Med 1994; 149: Nadel JA. Biologic effects of mast cell enzymes. Am Rev Respir Dis 1992; 145: s37 s James AL, Carroll NG. The theoretical effects of mucous gland discharge on airway resistance in asthma. Chest 1995; 17: 11s. 25. Carroll NG, Carello S, Cooke C, James A. Airway structure and inflammatory cells in fatal attacks of asthma. Eur Respir J 1996; 9: Liu MC, Bleecker ER, Lichtenstein LW, et al. Evidence for elevated levels of histamine, prostaglandin D 2, and other bronchoconstricting prostaglandins in the airways of subjects with mild asthma. Am Rev Respir Dis 199; 142: Bhat KN, Arroyave CM, Marney SR, Stevenson DD, Tan EM. Plasma histamine changes during provoked bronchospasm in asthmatic patients. J Allergy Clin Immunol 1976; 58: Forsythe P, McGarvey LP, Heaney LG, MacMahon J, Ennis M. Sensory neuropeptides induce histamine release from bronchoalveolar lavage cells in both nonasthmatic coughers and cough variant asthmatics. Clin Exp Allergy 2; 3: Jeffery PK. Structural, immunological and neural elements of the normal human airway wall. In: Busse WW, Holgate ST, eds. Asthma and Rhinitis 2nd Edn. Oxford, Blackwell Scientific, 2; pp Lozewicz S, Gomez E, Ferguson H, Davies RJ. Inflammatory cells in the airways in asthma. BMJ 1988; 297:
RESPIRATORY BLOCK. Bronchial Asthma. Dr. Maha Arafah Department of Pathology KSU
 RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
Impact of Asthma in the U.S. per Year. Asthma Epidemiology and Pathophysiology. Risk Factors for Asthma. Childhood Asthma Costs of Asthma
 American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
The distribution of eosinophils and lymphocytes in the large and small airways of asthmatics.
 Eur Respir J 997; : 292 3 DOI:.83/93936.97.2292 Printed in UK - all rights reserved Copyright ERS Journals Ltd 997 European Respiratory Journal ISSN 93-936 The distribution of eosinophils and lymphocytes
Eur Respir J 997; : 292 3 DOI:.83/93936.97.2292 Printed in UK - all rights reserved Copyright ERS Journals Ltd 997 European Respiratory Journal ISSN 93-936 The distribution of eosinophils and lymphocytes
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline
 Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air
 Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Mechanisms of action of bronchial provocation testing
 Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network
 Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network Robert.kruklitis@lvh.com Correlation of a Asthma pathophyisology with basic science Asthma (Physiology) Bronchodilators
Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network Robert.kruklitis@lvh.com Correlation of a Asthma pathophyisology with basic science Asthma (Physiology) Bronchodilators
Chronic Cough Due to Nonasthmatic Eosinophilic Bronchitis. ACCP Evidence-Based Clinical Practice Guidelines
 Chronic Cough Due to Nonasthmatic Eosinophilic Bronchitis ACCP Evidence-Based Clinical Practice Guidelines Christopher E. Brightling, MBBS, PhD, FCCP Objectives: Nonasthmatic eosinophilic bronchitis is
Chronic Cough Due to Nonasthmatic Eosinophilic Bronchitis ACCP Evidence-Based Clinical Practice Guidelines Christopher E. Brightling, MBBS, PhD, FCCP Objectives: Nonasthmatic eosinophilic bronchitis is
Life-long asthma and its relationship to COPD. Stephen T Holgate School of Medicine University of Southampton
 Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Air Flow Limitation. In most serious respiratory disease, a key feature causing morbidity and functional disruption is air flow imitation.
 Asthma Air Flow Limitation In most serious respiratory disease, a key feature causing morbidity and functional disruption is air flow imitation. True whether reversible, asthma and exercise-induced bronchospasm,
Asthma Air Flow Limitation In most serious respiratory disease, a key feature causing morbidity and functional disruption is air flow imitation. True whether reversible, asthma and exercise-induced bronchospasm,
Implications on therapy. Prof. of Medicine and Allergy Faculty of Medicine, Cairo University
 Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
MAST CELLS IN AIRWAY SMOOTH MUSCLE IN ASTHMA MAST-CELL INFILTRATION OF AIRWAY SMOOTH MUSCLE IN ASTHMA. Study Subjects
 MAST-CELL INFILTRATION OF AIRWAY SMOOTH MUSCLE IN ASTHMA CHRISTOPHER E. BRIGHTLING, M.B., B.S., PETER BRADDING, D.M., FIONA A. SYMON, PH.D., STEPHEN T. HOLGATE, M.D., D.SC., ANDREW J. WARDLAW, PH.D., AND
MAST-CELL INFILTRATION OF AIRWAY SMOOTH MUSCLE IN ASTHMA CHRISTOPHER E. BRIGHTLING, M.B., B.S., PETER BRADDING, D.M., FIONA A. SYMON, PH.D., STEPHEN T. HOLGATE, M.D., D.SC., ANDREW J. WARDLAW, PH.D., AND
asthma. A role of histamine in atopic asthma.
 14 Histamine and LTC4 in atopic asthma Release of histamine and leukotriene C 4 from bronchoalveolar cells III patients with bronchial asthma. A role of histamine in atopic asthma. Fumihiro Mitsunobu,
14 Histamine and LTC4 in atopic asthma Release of histamine and leukotriene C 4 from bronchoalveolar cells III patients with bronchial asthma. A role of histamine in atopic asthma. Fumihiro Mitsunobu,
2010 Health Press Ltd.
 Fast Facts Fast Facts: Asthma Third edition Stephen T Holgate MD DSc FRCP FMedSci MRC Clinical Professor of Immunopharmacology School of Medicine Southampton General Hospital Southampton, UK Jo Douglass
Fast Facts Fast Facts: Asthma Third edition Stephen T Holgate MD DSc FRCP FMedSci MRC Clinical Professor of Immunopharmacology School of Medicine Southampton General Hospital Southampton, UK Jo Douglass
Clinical significance of airway inflammation in bronchcial asthma. Comparison with chronic obstructive bronchiolitis.
 24 Airway inflammation in asthma Clinical significance of airway inflammation in bronchcial asthma. Comparison with chronic obstructive bronchiolitis. Yoshiro Tanizaki, Hikaru Kitani, Takashi Mifune, Fumihiro
24 Airway inflammation in asthma Clinical significance of airway inflammation in bronchcial asthma. Comparison with chronic obstructive bronchiolitis. Yoshiro Tanizaki, Hikaru Kitani, Takashi Mifune, Fumihiro
Airway pathology in asthma
 Eur Respir J 2001; 18: Suppl. 34: 18s 23s DOI: 10.1183/09031936.01.00229501 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0904-1850 ISBN 1-904097-20-0
Eur Respir J 2001; 18: Suppl. 34: 18s 23s DOI: 10.1183/09031936.01.00229501 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0904-1850 ISBN 1-904097-20-0
Airway Inflammation in Asthma Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan.
 REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
COPYRIGHTED MATERIAL. Definition and Pathology CHAPTER 1. John Rees
 CHAPTER 1 Definition and Pathology John Rees Sherman Education Centre, Guy s Hospital, London, UK OVERVIEW Asthma is an overall descriptive term but there are a number of more or less distinct phenotypes
CHAPTER 1 Definition and Pathology John Rees Sherman Education Centre, Guy s Hospital, London, UK OVERVIEW Asthma is an overall descriptive term but there are a number of more or less distinct phenotypes
Variation in the measurements of basement membrane thickness and inflammatory cell number in bronchial biopsies
 Eur Respir J 1998; 12: 811 815 DOI: 10.1183/09031936.98.12040811 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 0903-1936 Variation in the measurements
Eur Respir J 1998; 12: 811 815 DOI: 10.1183/09031936.98.12040811 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 0903-1936 Variation in the measurements
Small Airways Disease. Respiratory Function In Small Airways And Asthma. Pathophysiologic Changes in the Small Airways of Asthma Patients
 Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Bronchial Hyperresponsiveness. Defining Asthma: Clinical Criteria. Impaired Ventilation in Asthma. Dynamic Imaging of Asthma
 Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al.
 Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al. Chapter 75: Approach to Infants and Children with Asthma
Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al. Chapter 75: Approach to Infants and Children with Asthma
Respiratory pathophysiologic responses Inflammation of small airways in asthma
 Respiratory pathophysiologic responses Inflammation of small airways in asthma Qutayba Hamid, MD, PhD, a Yunling Song, MD, a Thomas C. Kotsimbos, MD, a Eleanor Minshall, PhD," Tony R. Bai, MD, b Richard
Respiratory pathophysiologic responses Inflammation of small airways in asthma Qutayba Hamid, MD, PhD, a Yunling Song, MD, a Thomas C. Kotsimbos, MD, a Eleanor Minshall, PhD," Tony R. Bai, MD, b Richard
Bronchoscopy with bronchial biopsies. Quantitative morphology using bronchial biopsies. P.G. Woodruff and A.L. Innes
 Eur Respir Rev 2006; 15: 101, 157 161 DOI: 10.1183/09059180.00010106 CopyrightßERSJ Ltd 2006 Quantitative morphology using bronchial biopsies P.G. Woodruff and A.L. Innes ABSTRACT: Bronchoscopy with bronchial
Eur Respir Rev 2006; 15: 101, 157 161 DOI: 10.1183/09059180.00010106 CopyrightßERSJ Ltd 2006 Quantitative morphology using bronchial biopsies P.G. Woodruff and A.L. Innes ABSTRACT: Bronchoscopy with bronchial
IgE-mediated allergy in elderly patients with asthma
 Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Comparative Study of Nasal Smear and Biopsy in Patients of Allergic Rhinitis
 Indian J Allergy Asthma Immunol 2002; 16(1) : 27-31 Comparative Study of Nasal Smear and Biopsy in Patients of Allergic Rhinitis Rakesh Chanda, Ajay Kumar Aggarwal, G.S. Kohli, T.S. Jaswal*, and K.B. Gupta**
Indian J Allergy Asthma Immunol 2002; 16(1) : 27-31 Comparative Study of Nasal Smear and Biopsy in Patients of Allergic Rhinitis Rakesh Chanda, Ajay Kumar Aggarwal, G.S. Kohli, T.S. Jaswal*, and K.B. Gupta**
Induced sputum to assess airway inflammation: a study of reproducibility
 Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Property of Presenter
 Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
On completion of this chapter you should be able to: discuss the stepwise approach to the pharmacological management of asthma in children
 7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
7 Asthma Asthma is a common disease in children and its incidence has been increasing in recent years. Between 10-15% of children have been diagnosed with asthma. It is therefore a condition that pharmacists
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007 Hosted by: Australian Small Animal Veterinary Association (ASAVA) Australian Small Animal Veterinary Association (ASAVA)
2013 Health Press Ltd.
 Fast Facts Fast Facts: Asthma Fourth edition Stephen T Holgate MD DSc FRCP FMedSci MRC Clinical Professor of Immunopharmacology School of Medicine Southampton General Hospital Southampton, UK Jo A Douglass
Fast Facts Fast Facts: Asthma Fourth edition Stephen T Holgate MD DSc FRCP FMedSci MRC Clinical Professor of Immunopharmacology School of Medicine Southampton General Hospital Southampton, UK Jo A Douglass
COPD and Asthma: Similarities and differences Prof. Peter Barnes
 and Asthma: Similarities and Differences and Asthma: 1 Imperial College Peter Barnes FRS, FMedSci, National Heart & Lung Institute Imperial College, London, UK p.j.barnes@imperial.ac.uk Royal Brompton
and Asthma: Similarities and Differences and Asthma: 1 Imperial College Peter Barnes FRS, FMedSci, National Heart & Lung Institute Imperial College, London, UK p.j.barnes@imperial.ac.uk Royal Brompton
THE PROMISE OF NEW AND NOVEL DRUGS. Pyng Lee Respiratory & Critical Care Medicine National University Hospital
 THE PROMISE OF NEW AND NOVEL DRUGS Pyng Lee Respiratory & Critical Care Medicine National University Hospital Pyng_lee@nuhs.edu.sg Asthma Prevalence, Morbidity, Mortality 235 million suffer from asthma
THE PROMISE OF NEW AND NOVEL DRUGS Pyng Lee Respiratory & Critical Care Medicine National University Hospital Pyng_lee@nuhs.edu.sg Asthma Prevalence, Morbidity, Mortality 235 million suffer from asthma
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis
 Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
The role of lung function testing in the assessment of and treatment of: AIRWAYS DISEASE
 The role of lung function testing in the assessment of and treatment of: AIRWAYS DISEASE RHYS JEFFERIES ARTP education Learning Objectives Examine the clinical features of airways disease to distinguish
The role of lung function testing in the assessment of and treatment of: AIRWAYS DISEASE RHYS JEFFERIES ARTP education Learning Objectives Examine the clinical features of airways disease to distinguish
Asthma for Primary Care: Assessment, Control, and Long-Term Management
 Asthma for Primary Care: Assessment, Control, and Long-Term Management Learning Objectives After participating in this educational activity, participants should be better able to: 1. Choose the optimal
Asthma for Primary Care: Assessment, Control, and Long-Term Management Learning Objectives After participating in this educational activity, participants should be better able to: 1. Choose the optimal
Chronic cough is defined as a cough persisting for. Airway Inflammation as an Assessment of Chronic Nonproductive Cough*
 Airway Inflammation as an Assessment of Chronic Nonproductive Cough* Sang Yeub Lee, MD ; Jae Youn Cho, MD; Jae Jeong Shim, MD; Han Kyeom Kim, MD; Kyung Ho Kang, MD, FCCP; Se Hwa Yoo, MD; and Kwang Ho In,
Airway Inflammation as an Assessment of Chronic Nonproductive Cough* Sang Yeub Lee, MD ; Jae Youn Cho, MD; Jae Jeong Shim, MD; Han Kyeom Kim, MD; Kyung Ho Kang, MD, FCCP; Se Hwa Yoo, MD; and Kwang Ho In,
Respiratory Pharmacology
 Allergy Targets of allergies Type I Histamine Leukotrienes Prostaglandins Bradykinin Hypersensitivity reactions Asthma Characterised by Triggered by Intrinsic Extrinsic (allergic) Mediators Result Early
Allergy Targets of allergies Type I Histamine Leukotrienes Prostaglandins Bradykinin Hypersensitivity reactions Asthma Characterised by Triggered by Intrinsic Extrinsic (allergic) Mediators Result Early
Outline FEF Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications?
 Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Difference in the onset mechansisms of attacks between atopic and nonatopic asthma. A role of leukotriene C 4
 Difference in onset mechanism between atopic and nonatopic asthma 21 Difference in the onset mechansisms of attacks between atopic and nonatopic asthma. A role of leukotriene C 4 Kouzou Ashida, Takashi
Difference in onset mechanism between atopic and nonatopic asthma 21 Difference in the onset mechansisms of attacks between atopic and nonatopic asthma. A role of leukotriene C 4 Kouzou Ashida, Takashi
ASTHMA ASTHMA DISEASE SUMMARY. Risk Factors
 ASTHMA Risk Factors Family history of asthma or other atopic diseases (eczema, hayfever) Having eczema or hayfever currently or as a child Living in an industrialised area more exposure to airborne pollutants,
ASTHMA Risk Factors Family history of asthma or other atopic diseases (eczema, hayfever) Having eczema or hayfever currently or as a child Living in an industrialised area more exposure to airborne pollutants,
Mast cell numbers in airway smooth muscle and PC 20 AMP in asthma and COPD
 Respiratory Medicine (2007) 101, 882 887 Mast cell numbers in airway smooth muscle and PC 20 AMP in asthma and COPD J.J.W. Liesker a, N.H.T. ten Hacken a,, S.R. Rutgers a, M. Zeinstra-Smith b, D.S. Postma
Respiratory Medicine (2007) 101, 882 887 Mast cell numbers in airway smooth muscle and PC 20 AMP in asthma and COPD J.J.W. Liesker a, N.H.T. ten Hacken a,, S.R. Rutgers a, M. Zeinstra-Smith b, D.S. Postma
Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) asthma Relationship to patient age and the proportions of bronchoalveolar cells
 28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
Pathophysiology of the cysteinyl leukotrienes and effects of leukotriene receptor antagonists in asthma
 Allergy 2001: 56: Suppl. 66: 7 11 Printed in UK. All rights reserved Copyright # Munksgaard 2001 ALLERGY ISSN 0108-1675 Pathophysiology of the cysteinyl leukotrienes and effects of leukotriene receptor
Allergy 2001: 56: Suppl. 66: 7 11 Printed in UK. All rights reserved Copyright # Munksgaard 2001 ALLERGY ISSN 0108-1675 Pathophysiology of the cysteinyl leukotrienes and effects of leukotriene receptor
Kun Jiang 1, He-Bin Chen 1, Ying Wang 1, Jia-Hui Lin 2, Yan Hu 1, Yu-Rong Fang 1
 Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Asthma. Rachel Miller, MD, FAAAAI Director Allergy and Immunology New York Presbyterian Hospital. Figure 1 Asthma Prevalence,
 Asthma Rachel Miller, MD, FAAAAI Director Allergy and Immunology New York Presbyterian Hospital Figure 1 Asthma Prevalence, 1980-2000 * Gap between 1995-1996 and 1997 indicates a break in trend due to
Asthma Rachel Miller, MD, FAAAAI Director Allergy and Immunology New York Presbyterian Hospital Figure 1 Asthma Prevalence, 1980-2000 * Gap between 1995-1996 and 1997 indicates a break in trend due to
Diagnosis and Management of Fungal Allergy Monday, 9-139
 Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Increased peak expiratory flow variation in asthma: severe persistent increase but not nocturnal worsening of airway inflammation
 Eur Respir J 998; : 5655 DOI:.83/93936.98.356 Printed in UK - all rights reserved Copyright ERS Journals Ltd 998 European Respiratory Journal ISSN 93-936 Increased peak expiratory flow variation in asthma:
Eur Respir J 998; : 5655 DOI:.83/93936.98.356 Printed in UK - all rights reserved Copyright ERS Journals Ltd 998 European Respiratory Journal ISSN 93-936 Increased peak expiratory flow variation in asthma:
Identifying Biologic Targets to Attenuate or Eliminate Asthma Exacerbations
 Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Dual-Controller Asthma Therapy: Rationale and Clinical Benefits
 B/1 Dual-Controller Asthma Therapy: Rationale and Clinical Benefits MODULE B The 1997 National Heart, Lung, and Blood Institute (NHLBI) Expert Panel guidelines on asthma management recommend a 4-step approach
B/1 Dual-Controller Asthma Therapy: Rationale and Clinical Benefits MODULE B The 1997 National Heart, Lung, and Blood Institute (NHLBI) Expert Panel guidelines on asthma management recommend a 4-step approach
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Immunomodulators: Anti-IgE mab. Thomas B. Casale, MD Professor of Medicine Chief, Allergy/Immunology Creighton University Omaha, NE
 Immunomodulators: Anti-IgE mab Thomas B. Casale, MD Professor of Medicine Chief, Allergy/Immunology Creighton University Omaha, NE Objectives To explain the rationale behind IgE blockade To discuss which
Immunomodulators: Anti-IgE mab Thomas B. Casale, MD Professor of Medicine Chief, Allergy/Immunology Creighton University Omaha, NE Objectives To explain the rationale behind IgE blockade To discuss which
Mucosal inflammation in severe glucocorticoiddependent
 Eur Respir J 1999; 13: 1245±1252 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 93-1936 Mucosal inflammation in severe glucocorticoiddependent asthma
Eur Respir J 1999; 13: 1245±1252 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 93-1936 Mucosal inflammation in severe glucocorticoiddependent asthma
The Link Between Viruses and Asthma
 The Link Between Viruses and Asthma CATHERINE KIER, MD Professor of Clinical Pediatrics Division Chief, Pediatric Pulmonary, and Cystic Fibrosis Center Director, Pediatric Sleep Disorders Center SUNY Stony
The Link Between Viruses and Asthma CATHERINE KIER, MD Professor of Clinical Pediatrics Division Chief, Pediatric Pulmonary, and Cystic Fibrosis Center Director, Pediatric Sleep Disorders Center SUNY Stony
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma
 Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Is reslizumab effective in improving quality of life and asthma control in adolescent and adult patients with poorly controlled eosinophilic asthma?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is reslizumab effective in improving
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2018 Is reslizumab effective in improving
Age-related changes of IgE-mediated allergic reaction in patients with late onset asthma.
 50 Changes in IgE-mediated allergic reaction with aglllg Age-related changes of IgE-mediated allergic reaction in patients with late onset asthma. Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou
50 Changes in IgE-mediated allergic reaction with aglllg Age-related changes of IgE-mediated allergic reaction in patients with late onset asthma. Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou
Monitoring sputum eosinophils in mucosal inflammation and remodelling: a pilot study
 Eur Respir J 2010; 35: 48 53 DOI: 10.1183/09031936.00130008 CopyrightßERS Journals Ltd 2010 Monitoring sputum eosinophils in mucosal inflammation and remodelling: a pilot study J. Chakir*, L. Loubaki*,
Eur Respir J 2010; 35: 48 53 DOI: 10.1183/09031936.00130008 CopyrightßERS Journals Ltd 2010 Monitoring sputum eosinophils in mucosal inflammation and remodelling: a pilot study J. Chakir*, L. Loubaki*,
Persistence of sputum eosinophilia in children with controlled asthma when compared with healthy children
 Eur Respir J 1998; 11: 848 853 DOI: 10.1183/09031936.98.11040848 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 0903-1936 Persistence of sputum eosinophilia
Eur Respir J 1998; 11: 848 853 DOI: 10.1183/09031936.98.11040848 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 0903-1936 Persistence of sputum eosinophilia
(b) Stomach s function 1. Dilution of food materials 2. Acidification of food (absorption of dietary Fe in small intestine) 3. Partial chemical digest
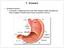 (1) General features a) Stomach is widened portion of gut-tube: between tubular and spherical; Note arranged of smooth muscle tissue in muscularis externa. 1 (b) Stomach s function 1. Dilution of food
(1) General features a) Stomach is widened portion of gut-tube: between tubular and spherical; Note arranged of smooth muscle tissue in muscularis externa. 1 (b) Stomach s function 1. Dilution of food
As-needed (intermittent) inhaled corticosteroid for mild asthma
 1 3.2.2008 CIPP VIII 8 th International Congress on Pediatric Pulmonology, Nice 2008 As-needed (intermittent) inhaled corticosteroid for mild asthma Tari Haahtela, Professor Skin and Allergy Hospital,
1 3.2.2008 CIPP VIII 8 th International Congress on Pediatric Pulmonology, Nice 2008 As-needed (intermittent) inhaled corticosteroid for mild asthma Tari Haahtela, Professor Skin and Allergy Hospital,
IL-5 production by bronchoalveolar lavage and peripheral blood mononuclear cells in asthma and atopy
 Eur Respir J, 1997; 1: 624 632 DOI: 1.1183/931936.97.13624 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 93-1936 IL-5 production by bronchoalveolar
Eur Respir J, 1997; 1: 624 632 DOI: 1.1183/931936.97.13624 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1997 European Respiratory Journal ISSN 93-1936 IL-5 production by bronchoalveolar
Obstructive Lung Diseases. By: Shefaa Qa qa
 Obstructive Lung Diseases By: Shefaa Qa qa Obstructive lung diseases (or airway diseases) are characterized by an increase in resistance to airflow due to partial or complete obstruction at any level from
Obstructive Lung Diseases By: Shefaa Qa qa Obstructive lung diseases (or airway diseases) are characterized by an increase in resistance to airflow due to partial or complete obstruction at any level from
Asthma Management for the Athlete
 Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
Asthma Management for the Athlete Khanh Lai, MD Assistant Professor Division of Pediatric Pulmonary and Sleep Medicine University of Utah School of Medicine 2 nd Annual Sports Medicine Symposium: The Pediatric
ASTHMA. Epidemiology. Pathophysiology. Diagnosis. IAP UG Teaching slides
 BRONCHIAL ASTHMA ASTHMA Epidemiology Pathophysiology Diagnosis 2 CHILDHOOD ASTHMA Childhood bronchial asthma is characterized by Airway obstruction which is reversible Airway inflammation Airway hyper
BRONCHIAL ASTHMA ASTHMA Epidemiology Pathophysiology Diagnosis 2 CHILDHOOD ASTHMA Childhood bronchial asthma is characterized by Airway obstruction which is reversible Airway inflammation Airway hyper
Asthma mortality in Danish children and young adults, 1973± 1994: epidemiology and validity of death certificates
 Eur Respir J 2000; 15: 844±848 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 Asthma mortality in Danish children and young adults, 1973±
Eur Respir J 2000; 15: 844±848 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 Asthma mortality in Danish children and young adults, 1973±
Increased Leukotriene E 4 in the Exhaled Breath Condensate of Children With Mild Asthma*
 CHEST Original Research Increased Leukotriene E 4 in the Exhaled Breath Condensate of Children With Mild Asthma* Atsushi Shibata, MD; Toshio Katsunuma, MD, PhD; Morimitsu Tomikawa, MD; Aiko Tan, MD; Keisuke
CHEST Original Research Increased Leukotriene E 4 in the Exhaled Breath Condensate of Children With Mild Asthma* Atsushi Shibata, MD; Toshio Katsunuma, MD, PhD; Morimitsu Tomikawa, MD; Aiko Tan, MD; Keisuke
Emily DiMango, MD Asthma II
 Emily DiMango, MD Asthma II Director John Edsall/John Wood Asthma Center Columbia University Medical Center HP 2000 Goal: 2.25/1,000 Comparison of Asthma Hospitalization Rates in Children Aged 0-14 in
Emily DiMango, MD Asthma II Director John Edsall/John Wood Asthma Center Columbia University Medical Center HP 2000 Goal: 2.25/1,000 Comparison of Asthma Hospitalization Rates in Children Aged 0-14 in
Airway smooth muscle in health and disease; methods of measurement and relation to function
 Eur Respir J 2000; 15: 782±789 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 SERIES "THE AIRWAY SMOOTH MUSCLE CELL" Edited by F. Chung
Eur Respir J 2000; 15: 782±789 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 SERIES "THE AIRWAY SMOOTH MUSCLE CELL" Edited by F. Chung
Prelab #4 BLOOD; BONE MARROW; RESPIRATORY; INTEGUEMENT Page 1
 Prelab #4 BLOOD; BONE MARROW; RESPIRATORY; INTEGUEMENT Page 1 Blood Slide 101 This a classic slide of blood cells using a Wright stain. Inspect red blood cells and their appearance. Note the approximate
Prelab #4 BLOOD; BONE MARROW; RESPIRATORY; INTEGUEMENT Page 1 Blood Slide 101 This a classic slide of blood cells using a Wright stain. Inspect red blood cells and their appearance. Note the approximate
Distinction and Overlap. Allergy Dpt, 2 nd Pediatric Clinic, University of Athens
 Asthma Phenotypes: Distinction and Overlap Nikos Papadopoulos Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Asthma as a syndrome From the Iliad to ADAM 33 and back again Bronchoconstriction,
Asthma Phenotypes: Distinction and Overlap Nikos Papadopoulos Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Asthma as a syndrome From the Iliad to ADAM 33 and back again Bronchoconstriction,
Asthma- THE most common Pediatric Disease JENNIFER MCDANIEL, RRT- NPS
 Asthma- THE most common Pediatric Disease JENNIFER MCDANIEL, RRT- NPS Asthma Usually acquire before the age of 10 These patients exhibit hyper-reactive airways Spasm Constriction Swelling Secretions are
Asthma- THE most common Pediatric Disease JENNIFER MCDANIEL, RRT- NPS Asthma Usually acquire before the age of 10 These patients exhibit hyper-reactive airways Spasm Constriction Swelling Secretions are
APSR RESPIRATORY UPDATES
 APSR RESPIRATORY UPDATES Volume 4, Issue 7 Newsletter Date: July 2012 APSR EDUCATION PUBLICATION Inside this issue: Quantitative imaging of airways Small-Airway Obstruction and Emphysema in Chronic Obstructive
APSR RESPIRATORY UPDATES Volume 4, Issue 7 Newsletter Date: July 2012 APSR EDUCATION PUBLICATION Inside this issue: Quantitative imaging of airways Small-Airway Obstruction and Emphysema in Chronic Obstructive
ALLERGIC RHINITIS AND ASTHMA :
 ALLERGIC RHINITIS AND ASTHMA : from the Link to Emerging Therapies Allergic rhinitis and asthma are both chronic heterogeneous disorders, with an overlapping epidemiology of prevalence, health care costs
ALLERGIC RHINITIS AND ASTHMA : from the Link to Emerging Therapies Allergic rhinitis and asthma are both chronic heterogeneous disorders, with an overlapping epidemiology of prevalence, health care costs
Diagnosis and Management of Asthma in Children based on the British Thoracic Society and Scottish Intercollegiate Guidelines Network September 2016
 Diagnosis and Management of Asthma in Children based on the British Thoracic Society and Scottish Intercollegiate Guidelines Network September 2016 Diagnosis: There is no lower limit to the age at which
Diagnosis and Management of Asthma in Children based on the British Thoracic Society and Scottish Intercollegiate Guidelines Network September 2016 Diagnosis: There is no lower limit to the age at which
Current Asthma Therapy: Little Need to Phenotype. Phenotypes of Severe Asthma. Cellular Phenotypes 12/7/2012
 Subbasement Membrane Thickness(µm) 12/7/212 Current Asthma Therapy: Little Need to Phenotype Phenotypes of Severe Asthma Most mild and to some degree moderate asthmatics respond well to currently available
Subbasement Membrane Thickness(µm) 12/7/212 Current Asthma Therapy: Little Need to Phenotype Phenotypes of Severe Asthma Most mild and to some degree moderate asthmatics respond well to currently available
The Asthma Guidelines: Diagnosis and Assessment of Asthma
 The Asthma Guidelines: Diagnosis and Assessment of Asthma Christopher H. Fanta, M.D. Partners Asthma Center Brigham and Women s Hospital Harvard Medical School Objectives Know how the diagnosis of asthma
The Asthma Guidelines: Diagnosis and Assessment of Asthma Christopher H. Fanta, M.D. Partners Asthma Center Brigham and Women s Hospital Harvard Medical School Objectives Know how the diagnosis of asthma
Theophylline induces a reduction in circulating interleukin-4 and interleukin-5 in atopic asthmatics
 Eur Respir J 1999; 13: 53±58 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 0903-1936 Theophylline induces a reduction in circulating interleukin-4
Eur Respir J 1999; 13: 53±58 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 0903-1936 Theophylline induces a reduction in circulating interleukin-4
Basic mechanisms disturbing lung function and gas exchange
 Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Bronchial Asthma OBJECTIVES: Editing File
 Bronchial Asthma OBJECTIVES: Define bronchial asthma (BA). Know the two types of asthma 1. Extrinsic or atopic allergic. 2. Intrinsic asthma. Understand the pathogenesis of BA. Understand the morphological
Bronchial Asthma OBJECTIVES: Define bronchial asthma (BA). Know the two types of asthma 1. Extrinsic or atopic allergic. 2. Intrinsic asthma. Understand the pathogenesis of BA. Understand the morphological
Hypersensitivity is the term used when an immune response results in exaggerated or inappropriate reactions harmful to the host.
 Hypersensitivity is the term used when an immune response results in exaggerated or inappropriate reactions harmful to the host. Hypersensitivity vs. allergy Hypersensitivity reactions require a pre-sensitized
Hypersensitivity is the term used when an immune response results in exaggerated or inappropriate reactions harmful to the host. Hypersensitivity vs. allergy Hypersensitivity reactions require a pre-sensitized
How immunology informs the design of immunotherapeutics.
 How immunology informs the design of immunotherapeutics. Stephen R Durham Allergy and Clinical Immunology, Royal Brompton Hospital and Imperial College London WAO Cancun Mon Dec 5 th 2011 How immunology
How immunology informs the design of immunotherapeutics. Stephen R Durham Allergy and Clinical Immunology, Royal Brompton Hospital and Imperial College London WAO Cancun Mon Dec 5 th 2011 How immunology
Baseline airway hyperresponsiveness and its reversible component: role of airway inflammation and airway calibre
 Eur Respir J 2; 5: 248±253 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2 European Respiratory Journal ISSN 93-936 Baseline airway hyperresponsiveness and its reversible component: role
Eur Respir J 2; 5: 248±253 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2 European Respiratory Journal ISSN 93-936 Baseline airway hyperresponsiveness and its reversible component: role
Amanda Hess, MMS, PA-C President-Elect, AAPA-AAI Arizona Asthma and Allergy Institute Scottsdale, AZ
 Amanda Hess, MMS, PA-C President-Elect, AAPA-AAI Arizona Asthma and Allergy Institute Scottsdale, AZ Financial Disclosures Advanced Practiced Advisory Board for Circassia Learning Objectives 1. Briefly
Amanda Hess, MMS, PA-C President-Elect, AAPA-AAI Arizona Asthma and Allergy Institute Scottsdale, AZ Financial Disclosures Advanced Practiced Advisory Board for Circassia Learning Objectives 1. Briefly
Supplementary Information
 Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
7/7/2015. Somboon Chansakulporn, MD. History of variable respiratory symptoms. 1. Documented excessive variability in PFT ( 1 test)
 Definition of Asthma GINA 2010: Chronic inflammatory disorder of the airways Airway hyper-responsiveness Recurrent wheezing, breathlessness, chest tightness, coughing Variable, reversible airflow obstruction
Definition of Asthma GINA 2010: Chronic inflammatory disorder of the airways Airway hyper-responsiveness Recurrent wheezing, breathlessness, chest tightness, coughing Variable, reversible airflow obstruction
Abstract. IgE. IgE Th2. x x IL-4 IL-5 IgE CD4 +
 D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
Management of Bronchial Asthma in Adults..emerging role of anti-leukotriene
 Management of Bronchial Asthma in Adults..emerging role of anti-leukotriene Han-Pin Kuo MD, PhD Department of Thoracic Medicine Chang Gung University Chang Gung Memorial Hospital Taipei, Taiwan Bronchial
Management of Bronchial Asthma in Adults..emerging role of anti-leukotriene Han-Pin Kuo MD, PhD Department of Thoracic Medicine Chang Gung University Chang Gung Memorial Hospital Taipei, Taiwan Bronchial
Function of the Respiratory System. Exchange CO2 (on expiration) for O2 (on inspiration)
 Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Allergy overview. Mike Levin Division of Asthma and Allergy Department of Paediatrics University of Cape Town Red Cross Hospital
 Allergy overview Mike Levin Division of Asthma and Allergy Department of Paediatrics University of Cape Town Red Cross Hospital Adaptive Immune Responses Adaptive immune responses allow responses against
Allergy overview Mike Levin Division of Asthma and Allergy Department of Paediatrics University of Cape Town Red Cross Hospital Adaptive Immune Responses Adaptive immune responses allow responses against
Research Review. Salmeterol/fluticasone propionate (Seretide ) in COPD. Extended listing for salmeterol/fluticasone propionate in COPD
 Research Review Salmeterol/fluticasone propionate (Seretide ) in COPD Extended listing for salmeterol/fluticasone propionate in COPD In New Zealand, salmeterol/fluticasone propionate (SFC) (Seretide )
Research Review Salmeterol/fluticasone propionate (Seretide ) in COPD Extended listing for salmeterol/fluticasone propionate in COPD In New Zealand, salmeterol/fluticasone propionate (SFC) (Seretide )
