State of the Art. Remodeling in Asthma SUBEPITHELIAL FIBROSIS EPITHELIAL ALTERATION. Céline Bergeron 1, Wisam Al-Ramli 2, and Qutayba Hamid 2
|
|
|
- Edith McBride
- 6 years ago
- Views:
Transcription
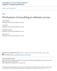
1 State of the Art Remodeling in Asthma Céline Bergeron 1, Wisam Al-Ramli 2, and Qutayba Hamid 2 1 Hotel-Dieu Hospital, Centre Hospitalier de l Université de Montréal, University of Montreal, Montréal, Quebec, Canada; and 2 Meakins-Christie Laboratories, McGilll University, Health Centre Research Institute, Montréal, Canada Airway remodeling refers to the structural changes that occur in both the large and the small airways of miscellaneous diseases, including asthma. In asthma, airway structural changes include subepithelial fibrosis, increased smooth muscle mass, enlargement of glands, neovascularization, and epithelial alterations. Although controversial, airway remodeling is commonly attributed to the underlying chronic inflammatory process. These remodeling changes contribute to thickening of airway walls and consequently lead to airway narrowing, bronchial hyperresponsiveness, airway edema, and mucous hypersecretion. Airway remodeling is associated with poorer clinical outcome among patients with asthma. Early diagnosis and prevention of airway remodeling has the potential to decrease disease severity, to improve control, and to prevent disease expression. In this article, we briefly provide an update on the characteristic features of airway remodeling observed in asthma and their clinical consequences. Keywords: remodeling; asthma; inflammation Airway remodeling in asthma was first described in 1922 by Hubert and Koessler in cases of fatal asthma (reviewed in Reference 1). Airway remodeling has been documented in all degrees of asthma severities and in both large and small airways (2). Airway remodeling refers to structural changes in airways of subjects with asthma which are not seen in healthy subjects. Figure 1 summarizes airway remodeling features. Structural changes include loss of epithelial integrity (3), thickening of basement membrane (4), subepithelial fibrosis (5), goblet cell and submucosal gland enlargement (6, 7), increased smooth muscle mass (6), decreased cartilage integrity (8), and increased airway vascularity (9, 10). Figure 2 shows remodeling features in asthma. It is believed that these changes largely stem from an ongoing chronic inflammatory process that involves activation of inflammatory cells including CD4 1 T cells, eosinophils, neutrophils, and mast cells (11 15). Duration of asthma has been associated with reduced lung function, increased hyperresponsiveness and asthma symptoms, as well as greater use of medication (5, 16, 17), and the remodeling process has been proposed to explain these features. EPITHELIAL ALTERATION Epithelial alterations in asthma include epithelial shedding, loss of ciliated cells, goblet cell hyperplasia, up-regulation of growthfactor release, and the overexpression of receptors, such as epidermal growth factor receptors (EGFR) (3, 6, 18 20). The (Received in original form August 19, 2008; accepted in final form February 27, 2009) Correspondence and requests for reprints should be addressed to Qutayba Hamid, M.D., Ph.D., Meakins-Christie Laboratories, McGill University, 3626 St Urbain Street, Montréal, PQ, H2X 2P2 Canada. qutayba.hamid@mcgill.ca Proc Am Thorac Soc Vol 6. pp , 2009 DOI: /pats RM Internet address: process of epithelial shedding is currently controversial and still a matter of debate, as some propose the detachment to be simply an artifact of physical tissue sampling of the asthmatic airways (20, 21). Studies suggest that either the asthmatic epithelium has a weakened attachment to the basement membrane or that asthmatic epithelial cells have a higher turnover compared with epithelial cells from healthy control subjects. Clinically, the extent of epithelial injury is correlated to airway hyperresponsiveness (17, 22), clearly suggesting that the degree of epithelial loss and/or turnover is related to asthma development and severity. The intact airway epithelium normally provides a physical protective barrier against inhaled small particles such as allergens. The loss of epithelium surface and the resultant denudation of the basement membrane may decrease this protective effect and increase the propensity for allergic insult on the airway. SUBEPITHELIAL FIBROSIS A second important feature of airway remodeling is the subepithelial fibrosis. Since it was first observed in 1922 (reviewed in Reference 1) in cases of fatal asthma, subepithelial fibrosis has been reported in all severities of asthma (5, 17) as well as in subjects with atopic rhinitis (23, 24), and even in children with difficult-to-treat asthma (25, 26). The subepithelial fibrosis occurs in the lamina reticularis layer just below the basement membrane, which leads to thickening of the basement membrane just underneath the epithelium. Fibrosis is a result of increased deposition of extracellular matrix (ECM) proteins, including collagens I, III, and V; fibronectin; tenascin; lumican; and biglycan (4, 27 30) by fibroblasts. Some variable correlations have been found between the severity of asthma, airway hyperresponsiveness or attack score, and subepithelial collagen types I and III deposition in the airways (31 34). Subepithelial fibrosis has been associated with the severity of asthma, and in severe asthma, increased airway wall thickness is observed (35). Proteoglycan deposition in the ECM and bronchial fibroblast production of proteoglycans also correlate with airway responsiveness in subjects with asthma (27, 36). An imbalance between ECM proteins production and degradation has also been found in asthmatic airways. The level of proteases and antiproteases may favor a profibrotic balance. Interstitial cells, macrophages, and neutrophils are the major sources of proteases and antiproteases. Matrix metalloproteinases (MMPs) are a family of proteases implicated in collagen degradation. MMP-2, MMP-3, MMP-8, and MMP-9 are the MMPs related to asthma (37 40). Among these, MMP-9 levels are reported to be significantly higher in the sputum of patients with asthma compared with control subjects (39). MMPs are implicated in airway inflammation through their influence on eosinophil trafficking (41) and in airway remodeling, not only by matrix reorganization but also by its effects on angiogenesis (42) and smooth muscle hyperplasia (43, 44). Elevated sputum
2 302 PROCEEDINGS OF THE AMERICAN THORACIC SOCIETY VOL Figure 1. Main characteristics of airway remodeling. Airway remodeling refers to structural changes in airways of individuals with asthma; these changes include (1) epithelial alteration, (2) subepithelial fibrosis, (3) increased smooth muscle mass, (4) goblet and mucous gland hyperplasia, (5) angiogenesis, (6) loss of cartilage integrity, and (7) inflammation. MMP-9 levels are associated with a fall in FEV 1 after allergen challenge and are linked to asthma severity (41, 45). Bronchoalveolar lavage level of MMP-8 inversely correlates with FEV 1 in patients with asthma (38). It has also been proposed that the remodeling process might be beneficial in airway diseases. Lambert and colleagues (46) have suggested that airway wall thickening may protect against bronchoconstriction. Collagen deposition in subepithelial matrix may inhibit narrowing by making the airway wall stiffer, representing an additional load on airway smooth muscle (24). Hyaluronan and versican deposition in and around the smooth muscle also counteracts airway narrowing and smooth muscle shortening. Experiments conducted on rat models of allergeninduced asthma suggested that airway responsiveness may increase after airway inflammation, but may decrease with airway deposition of fibronectin and collagen (47). INCREASED SMOOTH MUSCLE MASS Respiratory airway smooth muscle is the critical effector cell modulating airway tone. In asthmatic airways the smooth muscle mass is increased due to coordinated increase in size (hypertrophy) and number (hyperplasia) of airway smooth muscle cells. Importantly, the asthmatic smooth muscle cells take on not only the secretory and proliferative phenotype, but can also migrate to the subepithelial area of the asthmatic airways (6, 48, 49). Smooth muscle cells are known to actively participate in the inflammatory and remodeling processes though their release of proinflammatory cytokines, chemokines, and ECM proteins (50 52), and may therefore contribute to the pathogenesis of asthma. Migration of smooth muscle cells is a recently described feature of airway remodeling. We have shown that chemokines have the ability to induce human airway smooth muscle cell migration and to increase their contractility Figure 2. (A) Endobronchial biopsy stained with hematoxylin and eosin of a subject with asthma showing goblet (G) cell hyperplasia. (B) Endobronchial biopsy stained with hematoxylin and eosin of a subject with asthma showing extensive total subepithelial fibrosis (F) and increased smooth muscle (SMC) mass. (C) Lung biopsy showing a small airway from a subject with asthma showing increased smooth muscle mass and submucosal fibrosis. Reprinted by permission from Reference 65. in vitro, implementing another avenue which may significantly contribute to the overall airflow obstruction in these patients (49). The importance of smooth muscle mass has been correlated to asthma severity (53). GOBLET AND MUCOUS GLAND HYPERPLASIA Goblet cells hyperplasia and submucosal gland hyperplasia are seen in asthmatic airways of both adults and children; it is a feature particularly evident in fatal asthma (6, 7, 26). Functional consequences of these abnormalities mostly refer to increased
3 Bergeron, Al-Ramli, and Hamid: Remodeling in Asthma 303 sputum production, airway narrowing from sputum secretion, and increased airway wall thickness (6). ANGIOGENESIS Vascular alterations include increased size of airway wall vessels and angiogenesis (9). Changes in the airway wall microvasculature can contribute to airway wall edema and result from angiogenesis. Increased airway vascularity is seen in asthma (9, 10) in association with a greater expression of the vascular endothelial growth factor (VEGF) (54). Clinical consequences of airway wall angiogenesis are reduced airway caliber via airway wall edema, and increased inflammatory and remodeling mediators delivery into the airway wall having subsequent influence on structural and inflammatory cells. LOSS OF CARTILAGE INTEGRITY Cartilage is an important determinant of airway wall stiffness and integrity. Decreased cartilage volume and increased cartilage proteoglycan degradation are seen in asthmatic airways (8). Reduced cartilage integrity may result in a more powerful bronchoconstriction from airway smooth muscle bundles load reduction. Cartilage degradation can contribute to chronic airway obstruction, and allow more powerful bronchoconstriction for a given degree of airway smooth muscle contraction (55). INFLAMMATION Inflammation is another component of airway remodeling. There is good evidence that asthma is a heterogeneous disease. Airways of individuals with mild and moderate asthma are characterized by a Th2 profile inflammation, in which there is an overabundance of eosinophils, mast cells, and Th2 lymphocytes. These inflammatory cells release mediators which then trigger bronchoconstriction, mucus secretion, and, possibly, remodeling. The number of infiltrating leukocytes such as mast cells, eosinophils, and CD8 1 and CD45 1 T cells correlates with airway hyperresponsiveness in patients treated with inhaled corticosteroids (ICS) (56). The inflammatory mediators that drive this process include Th2 cytokines (IL-4, IL-5, IL-9, and IL-13), transforming growth factor (TGF)-b, granulocyte/macrophagecolony stimulating factor (GM-CSF), lipid mediators, and histamine. Some of these mediators have potent remodeling properties, such as TGF-b, IL-11, and IL-17 (31, 57, 58). Recently, a new subtype of T cells has been implicated in the pathogenesis of asthma, particularly in severe asthma, where the importance of noneosinophilic or neutrophilic inflammation is well described. This subtype of T cells are called Th-17, which secrete IL-17 A and F and might be involved in airway remodeling. TOOLS USED TO MEASURE AIRWAY REMODELING Airway remodeling is clinically defined as persistent airflow obstruction despite aggressive antiinflammatory therapies. The standard assessment of remodeling is obtained by surgical lung specimen or airway tissues sampled through flexible bronchoscopy. Flexible bronchoscopy is a minimally invasive technique, but requires specialist expertise; tools have been developed to bypass the biopsy sampling. Among these tools, indirect analysis of blood, urine, or sputum remodeling markers have been developed. However, we can only gain an insight into the ongoing fibrotic process, and we do not know if the fluid variations in remodeling markers have significant consequences in the diseased airway walls. Other alternative tools, including high-resolution computed tomography, endobronchial ultrasounds, and lung function measurement can also be used as screening tools, but modulation of airway remodeling will need to be confirmed on airway wall specimen. Clinicians should consider airway remodeling in all subjects with asthma and rhinitis. Fixed airflow obstruction is regarded as a late and irreversible manifestation of airway remodeling. For this reason, even without good and easily available tools to confirm the presence of remodeling, clinicians should use controlling medications to prevent development or worsening of airway and tissue remodeling. REMODELING IN ALLERGIC DISEASES IS NOT RESTRICTED TO THE AIRWAYS Allergen exposure triggers in sensitized subjects an inflammatory response that will be expressed in the targeted organ, such as the nasal mucosa, the skin, and the airway mucosa. Allergic rhinitis, atopic dermatitis, and asthma share many pathologic features. In fact, the same profile of inflammation, mediators, and adhesion molecules are observed in upper and lower allergic airway diseases as well as skin allergic disease. There is a common cellular inflammation pattern characterized by eosinophil, mast cell, and CD4 1 T cell influx (59, 60). Mediators, including histamine, cysteinyl-leukotrienes, interleukin (IL)-4, IL-5, IL-13, RANTES, and eotaxin are expressed in both upper and lower airways (61, 62). Although initial inflammation induced by allergens is similar in upper and lower airways, long-term structural consequences differ. In allergic rhinitis, minimal epithelial shedding is observed with less subsequent degree of basement membrane thickening (reviewed in Reference 63). Atopic dermatitis is also characterized by remodeling with increased expression of profibrotic cytokines (including TGF-b, IL-11, and IL-17) and increased subepithelial deposition of collagen (64). Remodeling is observed in all atopic diseases, which reinforces the hypothesis that remodeling is an inflammatory driven process. CONCLUSIONS The features of airway remodeling include subepithelial fibrosis, elevated numbers and volume of mucous cells in the epithelium, increased amounts of airway smooth muscle, and increased vascularization of the airway wall. It is important to understand the etiology of airway remodeling in asthma to develop therapies that inhibit or reverse it. The concern that asthma is associated with airway remodeling and loss of pulmonary function prompts clinicians to consider early recognition and early intervention. Currently, antiinflammatory drugs, including steroids, form the basis of asthma therapy. However, their effects on remodeling and chronic structural changes in the airways remains to be elucidated. It is for this reason that new treatments should be directed not only against inflammation itself but also against these chronic changes in the asthmatic lungs. Conflict of Interest Statement: None of the authors has a financial relationship with a commercial entity that has an interest in the subject of this manusript. References 1. Redington AE, Howarth PH. Airway wall remodelling in asthma. Thorax 1997;52: James AL, Maxwell PS, Pearce-Pinto G, Elliot JG, Carroll NG. The relationship of reticular basement membrane thickness to airway wall remodeling in asthma. Am J Respir Crit Care Med 2002;166: Naylor B. The shedding of the mucosa of the bronchial tree in asthma. Thorax 1962;17: Roche WR, Beasley R, Williams JH, Holgate ST. Subepithelial fibrosis in the bronchi of asthmatics. Lancet 1989;1:
4 304 PROCEEDINGS OF THE AMERICAN THORACIC SOCIETY VOL Elias JA, Zhu Z, Chupp G, Homer RJ. Airway remodeling in asthma. J Clin Invest 1999;104: Carroll N, Elliot J, Morton A, James A. The structure of large and small airways in nonfatal and fatal asthma. Am Rev Respir Dis 1993;147: Aikawa T, Shimura S, Sasaki H, Ebina M, Takishima T. Marked goblet cell hyperplasia with mucus accumulation in the airways of patients who died of severe acute asthma attack. Chest 1992;101: Haraguchi M, Shimura S, Shirato K. Morphometric analysis of bronchial cartilage in chronic obstructive pulmonary disease and bronchial asthma. Am J Respir Crit Care Med 1999;159: Li X, Wilson JW. Increased vascularity of the bronchial mucosa in mild asthma. Am J Respir Crit Care Med 1997;156: Tanaka H, Yamada G, Saikai T, Hashimoto M, Tanaka S, Suzuki K, Fujii M, Takahashi H, Abe S. Increased airway vascularity in newly diagnosed asthma using a high-magnification bronchovideoscope. Am J Respir Crit Care Med 2003;168: Metcalfe DD, Baram D, Mekori YA. Mast cells. Physiol Rev 1997;77: Kroegel C, Virchow JC Jr, Luttmann W, Walker C, Warner JA. Pulmonary immune cells in health and disease: the eosinophil leucocyte (Part I). Eur Respir J 1994;7: Mosmann TR, Cherwinski H, Bond MW, Giedlin MA, Coffman RL. Two types of murine helper T cell clone: I. Definition according to profiles of lymphokine activities and secreted proteins. J Immunol 1986;136: Le Gros G, Ben-Sasson SZ, Seder R, Finkelman FD, Paul WE. Generation of interleukin 4 (IL-4)-producing cells in vivo and in vitro: IL-2 and IL-4 are required for in vitro generation of IL-4- producing cells. J Exp Med 1990;172: Swain SL, Weinberg AD, English M, Huston G. IL-4 directs the development of Th2-like helper effectors. J Immunol 1990;145: Zeiger RS, Dawson C, Weiss S. Relationships between duration of asthma and asthma severity among children in the Childhood Asthma Management Program (CAMP). J Allergy Clin Immunol 1999;103: Boulet LP, Laviolette M, Turcotte H, Cartier A, Dugas M, Malo JL, Boutet M. Bronchial subepithelial fibrosis correlates with airway responsiveness to methacholine. Chest 1997;112: Laitinen LA, Heino M, Laitinen A, Kava T, Haahtela T. Damage of the airway epithelium and bronchial reactivity in patients with asthma. Am Rev Respir Dis 1985;131: Montefort S, Roberts JA, Beasley R, Holgate ST, Roche WR. The site of disruption of the bronchial epithelium in asthmatic and nonasthmatic subjects. Thorax 1992;47: Ordonez C, Ferrando R, Hyde DM, Wong HH, Fahy JV. Epithelial desquamation in asthma: artifact or pathology? Am J Respir Crit Care Med 2000;162: Boulet LP, Turcotte H, Carrier G, Boutet M, Laviolette M. Increased maximal airway response to methacholine during seasonal allergic rhinitis in nonasthmatic subjects: relationships with airway wall thickness and inflammation. Eur Respir J 1995;8: Jeffery PK, Wardlaw AJ, Nelson FC, Collins JV, Kay AB. Bronchial biopsies in asthma. An ultrastructural, quantitative study and correlation with hyperreactivity. Am Rev Respir Dis 1989;140: Chakir J, Laviolette M, Boutet M, Laliberte R, Dube J, Boulet LP. Lower airways remodeling in nonasthmatic subjects with allergic rhinitis. Lab Invest 1996;75: Milanese M, Crimi E, Scordamaglia A, Riccio A, Pellegrino R, Canonica GW, Brusasco V. On the functional consequences of bronchial basement membrane thickening. J Appl Physiol 2001;91: Payne DN, Rogers AV, Adelroth E, Bandi V, Guntupalli KK, Bush A, Jeffery PK. Early thickening of the reticular basement membrane in children with difficult asthma. Am J Respir Crit Care Med 2003;167: Jenkins HA, Cool C, Szefler SJ, Covar R, Brugman S, Gelfand EW, Spahn JD. Histopathology of severe childhood asthma: a case series. Chest 2003;124: Huang J, Olivenstein R, Taha R, Hamid Q, Ludwig M. Enhanced proteoglycan deposition in the airway wall of atopic asthmatics. Am J Respir Crit Care Med 1999;160: Laitinen A, Altraja A, Kampe M, Linden M, Virtanen I, Laitinen LA. Tenascin is increased in airway basement membrane of asthmatics and decreased by an inhaled steroid. Am J Respir Crit Care Med 1997; 156: Wilson JW, Li X. The measurement of reticular basement membrane and submucosal collagen in the asthmatic airway. Clin Exp Allergy 1997;27: Karjalainen EM, Lindqvist A, Laitinen LA, Kava T, Altraja A, Halme M, Laitinen A. Airway inflammation and basement membrane tenascin in newly diagnosed atopic and nonatopic asthma. Respir Med 2003;97: Minshall E, Chakir J, Laviolette M, Molet S, Zhu Z, Olivenstein R, Elias JA, Hamid Q. IL-11 expression is increased in severe asthma: association with epithelial cells and eosinophils. J Allergy Clin Immunol 2000;105: Hoshino M, Nakamura Y, Sim JJ. Expression of growth factors and remodelling of the airway wall in bronchial asthma. Thorax 1998;53: Chetta A, Foresi A, Del Donno M, Bertorelli G, Pesci A, Olivieri D. Airways remodeling is a distinctive feature of asthma and is related to severity of disease. Chest 1997;111: Chu HW, Halliday JL, Martin RJ, Leung DY, Szefler SJ, Wenzel SE. Collagen deposition in large airways may not differentiate severe asthma from milder forms of the disease. Am J Respir Crit Care Med 1998;158: Little SA, Sproule MW, Cowan MD, Macleod KJ, Robertson M, Love JG, Chalmers GW, McSharry CP, Thomson NC. High resolution computed tomographic assessment of airway wall thickness in chronic asthma: reproducibility and relationship with lung function and severity. Thorax 2002;57: Westergren-Thorsson G, Chakir J, Lafreniere-Allard MJ, Boulet LP, Tremblay GM. Correlation between airway responsiveness and proteoglycan production by bronchial fibroblasts from normal and asthmatic subjects. Int J Biochem Cell Biol 2002;34: Lemjabbar H, Gosset P, Lamblin C, Tillie I, Hartmann D, Wallaert B, Tonnel AB, Lafuma C. Contribution of 92 kda gelatinase/type IV collagenase in bronchial inflammation during status asthmaticus. Am J Respir Crit Care Med 1999;159: Prikk K, Maisi P, Pirila E, Reintam MA, Salo T, Sorsa T, Sepper R. Airway obstruction correlates with collagenase-2 (MMP-8) expression and activation in bronchial asthma. Lab Invest 2002;82: Vignola AM, Riccobono L, Mirabella A, Profita M, Chanez P, Bellia V, Mautino G, D accardi P, Bousquet J, Bonsignore G. Sputum metalloproteinase-9/tissue inhibitor of metalloproteinase-1 ratio correlates with airflow obstruction in asthma and chronic bronchitis. Am J Respir Crit Care Med 1998;158: Suzuki R, Kato T, Miyazaki Y, Iwata M, Noda Y, Takagi K, Nakashima N, Torii K. Matrix metalloproteinases and tissue inhibitors of matrix metalloproteinases in sputum from patients with bronchial asthma. J Asthma 2001;38: Wenzel SE, Balzar S, Cundall M, Chu HW. Subepithelial basement membrane immunoreactivity for matrix metalloproteinase 9: association with asthma severity, neutrophilic inflammation, and wound repair. J Allergy Clin Immunol 2003;111: Johnson C, Sung HJ, Lessner SM, Fini ME, Galis ZS. Matrix metalloproteinase-9 is required for adequate angiogenic revascularization of ischemic tissues: potential role in capillary branching. Circ Res 2003;94: Johnson C, Galis ZS. Matrix metalloproteinase-2 and -9 differentially regulate smooth muscle cell migration and cell-mediated collagen organization. Arterioscler Thromb Vasc Biol 2003;24: Johnson S, Knox A. Autocrine production of matrix metalloproteinase-2 is required for human airway smooth muscle proliferation. Am J Physiol 1999;277:L1109 L Cataldo DD, Bettiol J, Noel A, Bartsch P, Foidart JM, Louis R. Matrix metalloproteinase-9, but not tissue inhibitor of matrix metalloproteinase-1, increases in the sputum from allergic asthmatic patients after allergen challenge. Chest 2002;122: Lambert RK, Codd SL, Alley MR, Pack RJ. Physical determinants of bronchial mucosal folding. J Appl Physiol 1994;77: Palmans E, Kips JC, Pauwels RA. Prolonged allergen exposure induces structural airway changes in sensitized rats. Am J Respir Crit Care Med 2000;161: Johnson PR, Burgess JK. Airway smooth muscle and fibroblasts in the pathogenesis of asthma. Curr Allergy Asthma Rep 2004;4: Joubert P, Lajoie-Kadoch S, Labonte I, Gounni AS, Maghni K, Wellemans V, Chakir J, Laviolette M, Hamid Q, Lamkhioued B. CCR3 expression and function in asthmatic airway smooth muscle cells. J Immunol 2005;175:
5 Bergeron, Al-Ramli, and Hamid: Remodeling in Asthma Panettieri RA Jr. Airway smooth muscle: an immunomodulatory cell. J Allergy Clin Immunol 2002;110:S269 S Hakonarson H, Maskeri N, Carter C, Grunstein MM. Regulation of TH1- and TH2-type cytokine expression and action in atopic asthmatic sensitized airway smooth muscle. J Clin Invest 1999;103: Johnson PR. Role of human airway smooth muscle in altered extracellular matrix production in asthma. Clin Exp Pharmacol Physiol 2001; 28: Benayoun L, Druilhe A, Dombret MC, Aubier M, Pretolani M. Airway structural alterations selectively associated with severe asthma. Am J Respir Crit Care Med 2003;167: Hoshino M, Takahashi M, Aoike N. Expression of vascular endothelial growth factor, basic fibroblast growth factor, and angiogenin immunoreactivity in asthmatic airways and its relationship to angiogenesis. J Allergy Clin Immunol 2001;107: Noble PB, Turner DJ, Mitchell HW. Relationship of airway narrowing, compliance, and cartilage in isolated bronchial segments. J Appl Physiol 2002;92: Sont JK, Han J, van Krieken JM, Evertse CE, Hooijer R, Willems LN, Sterk PJ. Relationship between the inflammatory infiltrate in bronchial biopsy specimens and clinical severity of asthma in patients treated with inhaled steroids. Thorax 1996;51: Molet S, Hamid Q, Davoine F, Nutku E, Taha R, Pagé N, Olivenstein R, Elias J, Chakir J. IL-17 is increased in asthmatic airways and induces human bronchial fibroblasts to produce cytokines. J Allergy Clin Immunol 2001;108: Chakir J, Shannon J, Molet S, Fukakusa M, Elias J, Laviolette M, Boulet LP, Hamid Q. Airway remodeling-associated mediators in moderate to severe asthma: effect of steroids on TGF-beta, IL-11, IL-17, and type I and type III collagen expression. J Allergy Clin Immunol 2003; 111: Bradley BL, Azzawi M, Jacobson M, Assoufi B, Collins JV, Irani AM, Schwartz LB, Durham SR, Jeffery PK, Kay AB. Eosinophils, T- lymphocytes, mast cells, neutrophils, and macrophages in bronchial biopsy specimens from atopic subjects with asthma: comparison with biopsy specimens from atopic subjects without asthma and normal control subjects and relationship to bronchial hyperresponsiveness. J Allergy Clin Immunol 1991;88: Varga EM, Jacobson MR, Till SJ, Masuyama K, O Brien F, Rak S, Lund V, Scadding GK, Hamid QA, Durham SR. Cellular infiltration and cytokine mrna expression in perennial allergic rhinitis. Allergy 1999; 54: KleinJan A, Dijkstra MD, Boks SS, Severijnen LA, Mulder PG, Fokkens WJ. Increase in IL-8, IL-10, IL-13, and RANTES mrna levels (in situ hybridization) in the nasal mucosa after nasal allergen provocation. J Allergy Clin Immunol 1999;103: Nag S, Lamkhioued B, Renzi PM. Interleukin-2-induced increased airway responsiveness and lung Th2 cytokine expression occur after antigen challenge through the leukotriene pathway. Am J Respir Crit Care Med 2002;165: Bousquet J, Jacquot W, Vignola AM, Bachert C, Van Cauwenberge P. Allergic rhinitis: a disease remodeling the upper airways? J Allergy Clin Immunol 2004;113: Toda M, Leung DY, Molet S, Boguniewicz M, Taha R, Christodoulopoulos P, Fukuda T, Elias JA, Hamid QA. Polarized in vivo expression of IL-11 and IL-17 between acute and chronic skin lesions. J Allergy Clin Immunol 2003;111: Joubert P, Hamid Q. Role of airway smooth muscle in airway remodeling. J Allergy Clin Immunol 2005;116:
Bronchial hyperresponsiveness is generally assessed by
 Provocation With Adenosine 5 -Monophosphate Increases Sputum Eosinophils* Maarten van den Berge, MD; H.A.M. Kerstjens, PhD; D.M. de Reus; H.F. Kauffman, PhD; G.H. Koëter, PhD; and D.S. Postma, PhD (CHEST
Provocation With Adenosine 5 -Monophosphate Increases Sputum Eosinophils* Maarten van den Berge, MD; H.A.M. Kerstjens, PhD; D.M. de Reus; H.F. Kauffman, PhD; G.H. Koëter, PhD; and D.S. Postma, PhD (CHEST
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Airway Inflammation in Asthma Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan.
 REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
Differences in proteoglycan deposition in the airways of moderate and severe asthmatics
 Eur Respir J 2007; 29: 71 77 DOI: 10.1183/09031936.00047905 CopyrightßERS Journals Ltd 2007 Differences in proteoglycan deposition in the airways of moderate and severe asthmatics L. Pini*, Q. Hamid*,
Eur Respir J 2007; 29: 71 77 DOI: 10.1183/09031936.00047905 CopyrightßERS Journals Ltd 2007 Differences in proteoglycan deposition in the airways of moderate and severe asthmatics L. Pini*, Q. Hamid*,
Airway pathology in asthma
 Eur Respir J 2001; 18: Suppl. 34: 18s 23s DOI: 10.1183/09031936.01.00229501 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0904-1850 ISBN 1-904097-20-0
Eur Respir J 2001; 18: Suppl. 34: 18s 23s DOI: 10.1183/09031936.01.00229501 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0904-1850 ISBN 1-904097-20-0
Impact of Asthma in the U.S. per Year. Asthma Epidemiology and Pathophysiology. Risk Factors for Asthma. Childhood Asthma Costs of Asthma
 American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
Kun Jiang 1, He-Bin Chen 1, Ying Wang 1, Jia-Hui Lin 2, Yan Hu 1, Yu-Rong Fang 1
 Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Monitoring sputum eosinophils in mucosal inflammation and remodelling: a pilot study
 Eur Respir J 2010; 35: 48 53 DOI: 10.1183/09031936.00130008 CopyrightßERS Journals Ltd 2010 Monitoring sputum eosinophils in mucosal inflammation and remodelling: a pilot study J. Chakir*, L. Loubaki*,
Eur Respir J 2010; 35: 48 53 DOI: 10.1183/09031936.00130008 CopyrightßERS Journals Ltd 2010 Monitoring sputum eosinophils in mucosal inflammation and remodelling: a pilot study J. Chakir*, L. Loubaki*,
Sputum matrix metalloproteases: comparison between chronic obstructive pulmonary disease and asthma
 Respiratory Medicine (25) 99, 73 71 Sputum matrix metalloproteases: comparison between chronic obstructive pulmonary disease and asthma S.V. Culpitt, D.F. Rogers, S.L. Traves, P.J. Barnes, L.E. Donnelly
Respiratory Medicine (25) 99, 73 71 Sputum matrix metalloproteases: comparison between chronic obstructive pulmonary disease and asthma S.V. Culpitt, D.F. Rogers, S.L. Traves, P.J. Barnes, L.E. Donnelly
RESPIRATORY BLOCK. Bronchial Asthma. Dr. Maha Arafah Department of Pathology KSU
 RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Repeated allergen exposure changes collagen composition in airways of sensitised Brown Norway rats
 Eur Respir J 22; 2: 28 28 DOI: 1.1183/931936.2.242 Printed in UK all rights reserved Copyright #ERS Journals Ltd 22 European Respiratory Journal ISSN 93-1936 Repeated allergen exposure changes collagen
Eur Respir J 22; 2: 28 28 DOI: 1.1183/931936.2.242 Printed in UK all rights reserved Copyright #ERS Journals Ltd 22 European Respiratory Journal ISSN 93-1936 Repeated allergen exposure changes collagen
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Mechanisms of remodeling in asthmatic airways
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2012 Mechanisms of remodeling in asthmatic airways Adrian Shifren Washington University School of Medicine in St.
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2012 Mechanisms of remodeling in asthmatic airways Adrian Shifren Washington University School of Medicine in St.
Tissue repair. (3&4 of 4)
 Tissue repair (3&4 of 4) What will we discuss today: Regeneration in tissue repair Scar formation Cutaneous wound healing Pathologic aspects of repair Regeneration in tissue repair Labile tissues rapid
Tissue repair (3&4 of 4) What will we discuss today: Regeneration in tissue repair Scar formation Cutaneous wound healing Pathologic aspects of repair Regeneration in tissue repair Labile tissues rapid
Distribution and degranulation of airway mast cells in normal and asthmatic subjects
 Eur Respir J 22; 19: 879 885 DOI: 1.1183/931936.2.27582 Printed in UK all rights reserved Copyright #ERS Journals Ltd 22 European Respiratory Journal ISSN 93-1936 Distribution and degranulation of airway
Eur Respir J 22; 19: 879 885 DOI: 1.1183/931936.2.27582 Printed in UK all rights reserved Copyright #ERS Journals Ltd 22 European Respiratory Journal ISSN 93-1936 Distribution and degranulation of airway
C urrent understanding of asthma defines it
 163 OCCASIONAL REVIEW Pharmacotherapy and airway remodelling in asthma? P A Beckett, P H Howarth... Over the last few decades attention has largely focused on airway inflammation in asthma, but more recently
163 OCCASIONAL REVIEW Pharmacotherapy and airway remodelling in asthma? P A Beckett, P H Howarth... Over the last few decades attention has largely focused on airway inflammation in asthma, but more recently
Life-long asthma and its relationship to COPD. Stephen T Holgate School of Medicine University of Southampton
 Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline
 Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Property of Presenter
 Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Induced sputum to assess airway inflammation: a study of reproducibility
 Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Bronchial asthma is a chronic inflammatory disorder
 Increased Expression of the Chemoattractant Cytokines Eotaxin, Monocyte Chemotactic Protein-4, and Interleukin-16 in Induced Sputum in Asthmatic Patients* Rame A. Taha, MD; Sophie Laberge, MD; Qutayba
Increased Expression of the Chemoattractant Cytokines Eotaxin, Monocyte Chemotactic Protein-4, and Interleukin-16 in Induced Sputum in Asthmatic Patients* Rame A. Taha, MD; Sophie Laberge, MD; Qutayba
Specificity of basement membrane thickening in severe asthma
 Specificity of basement membrane thickening in severe asthma Arnaud Bourdin, MD, a Dorine Neveu, PhD, b Isabelle Vachier, PhD, a Fabrice Paganin, MD, PhD, a Philippe Godard, MD, a and Pascal Chanez, MD,
Specificity of basement membrane thickening in severe asthma Arnaud Bourdin, MD, a Dorine Neveu, PhD, b Isabelle Vachier, PhD, a Fabrice Paganin, MD, PhD, a Philippe Godard, MD, a and Pascal Chanez, MD,
Pathogenesis of asthma
 Med Clin N Am 86 (2002) 925 936 Pathogenesis of asthma Nizar N. Jarjour, MD*, Elizabeth A.B. Kelly, PhD Section of Pulmonary and Critical Care Medicine, 600 Highland Avenue, CSC K4/930, University of Wisconsin
Med Clin N Am 86 (2002) 925 936 Pathogenesis of asthma Nizar N. Jarjour, MD*, Elizabeth A.B. Kelly, PhD Section of Pulmonary and Critical Care Medicine, 600 Highland Avenue, CSC K4/930, University of Wisconsin
University of Groningen
 University of Groningen Reticular basement membrane in asthma and COPD Liesker, Jeroen J W; ten Hacken, Nick H.T.; Zeinstra - Smith, Mieke; Rutgers, Steven R; Postma, Dirkje S; Timens, Willem Published
University of Groningen Reticular basement membrane in asthma and COPD Liesker, Jeroen J W; ten Hacken, Nick H.T.; Zeinstra - Smith, Mieke; Rutgers, Steven R; Postma, Dirkje S; Timens, Willem Published
ORIGINAL ARTICLE. Epithelial Shedding of the Inferior Turbinate in Perennial Allergic and Nonallergic Rhinitis
 ORIGINAL ARTICLE Epithelial Shedding of the Inferior Turbinate in Perennial Allergic and Nonallergic Rhinitis A Riddle to Solve Gilead Berger, MD; Joelle Bernheim, MD; Dov Ophir, MD Objective: To examine
ORIGINAL ARTICLE Epithelial Shedding of the Inferior Turbinate in Perennial Allergic and Nonallergic Rhinitis A Riddle to Solve Gilead Berger, MD; Joelle Bernheim, MD; Dov Ophir, MD Objective: To examine
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Epithelial Desquamation in Asthma Artifact or Pathology?
 Epithelial Desquamation in Asthma Artifact or Pathology? CLAUDIA ORDOÑEZ, RON FERRANDO, DALLAS M. HYDE, HOFER H. WONG, and JOHN V. FAHY Departments of Pediatrics and Medicine and the Cardiovascular Research
Epithelial Desquamation in Asthma Artifact or Pathology? CLAUDIA ORDOÑEZ, RON FERRANDO, DALLAS M. HYDE, HOFER H. WONG, and JOHN V. FAHY Departments of Pediatrics and Medicine and the Cardiovascular Research
IgE-mediated allergy in elderly patients with asthma
 Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Bronchial Hyperresponsiveness. Defining Asthma: Clinical Criteria. Impaired Ventilation in Asthma. Dynamic Imaging of Asthma
 Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
COPYRIGHTED MATERIAL. Definition and Pathology CHAPTER 1. John Rees
 CHAPTER 1 Definition and Pathology John Rees Sherman Education Centre, Guy s Hospital, London, UK OVERVIEW Asthma is an overall descriptive term but there are a number of more or less distinct phenotypes
CHAPTER 1 Definition and Pathology John Rees Sherman Education Centre, Guy s Hospital, London, UK OVERVIEW Asthma is an overall descriptive term but there are a number of more or less distinct phenotypes
Anti-IL-5 treatment reduces deposition of ECM proteins in the bronchial subepithelial basement membrane of mild atopic asthmatics
 Anti-IL-5 treatment reduces deposition of ECM proteins in the bronchial subepithelial basement membrane of mild atopic asthmatics Patrick Flood-Page, 1 Andrew Menzies-Gow, 1 Simon Phipps, 1 Sun Ying, 2
Anti-IL-5 treatment reduces deposition of ECM proteins in the bronchial subepithelial basement membrane of mild atopic asthmatics Patrick Flood-Page, 1 Andrew Menzies-Gow, 1 Simon Phipps, 1 Sun Ying, 2
Interleukin-4 and interleukin-13 induce fibronectin production by human lung fibroblasts
 Allergology International (2001) 50: 197 202 Original Article Interleukin-4 and interleukin-13 induce fibronectin production by human lung fibroblasts Tatsuya Machino, Shu Hashimoto, Yasuhiro Gon, Kosei
Allergology International (2001) 50: 197 202 Original Article Interleukin-4 and interleukin-13 induce fibronectin production by human lung fibroblasts Tatsuya Machino, Shu Hashimoto, Yasuhiro Gon, Kosei
Implications on therapy. Prof. of Medicine and Allergy Faculty of Medicine, Cairo University
 Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
Comparative Study of Nasal Smear and Biopsy in Patients of Allergic Rhinitis
 Indian J Allergy Asthma Immunol 2002; 16(1) : 27-31 Comparative Study of Nasal Smear and Biopsy in Patients of Allergic Rhinitis Rakesh Chanda, Ajay Kumar Aggarwal, G.S. Kohli, T.S. Jaswal*, and K.B. Gupta**
Indian J Allergy Asthma Immunol 2002; 16(1) : 27-31 Comparative Study of Nasal Smear and Biopsy in Patients of Allergic Rhinitis Rakesh Chanda, Ajay Kumar Aggarwal, G.S. Kohli, T.S. Jaswal*, and K.B. Gupta**
Airway Remodeling in Asthma and its Influence on Clinical Pathophysiology
 Tohoku J. Exp. Med., 2006, Airway 209, Remodeling 75-87 in Asthma and Clinical Pathophysiology 75 Invited Review Airway Remodeling in Asthma and its Influence on Clinical Pathophysiology KOHEI YAMAUCHI
Tohoku J. Exp. Med., 2006, Airway 209, Remodeling 75-87 in Asthma and Clinical Pathophysiology 75 Invited Review Airway Remodeling in Asthma and its Influence on Clinical Pathophysiology KOHEI YAMAUCHI
What effect does asthma treatment have on airway remodeling? Current perspectives
 Clinical reviews in allergy and immunology Series editors: Donald Y. M. Leung, MD, PhD, and Dennis K. Ledford, MD What effect does asthma treatment have on airway remodeling? Current perspectives Sheharyar
Clinical reviews in allergy and immunology Series editors: Donald Y. M. Leung, MD, PhD, and Dennis K. Ledford, MD What effect does asthma treatment have on airway remodeling? Current perspectives Sheharyar
Circulating MMP-9 and TIMP-1 in acute exacerbations and after remission induced by oral corticosteroids in asthmatic children.
 Egypt J Pediatr Allergy Immunol 2006; 4(1):23-29. Original article Circulating MMP-9 and TIMP-1 in acute exacerbations and after remission induced by oral corticosteroids in asthmatic children. Background
Egypt J Pediatr Allergy Immunol 2006; 4(1):23-29. Original article Circulating MMP-9 and TIMP-1 in acute exacerbations and after remission induced by oral corticosteroids in asthmatic children. Background
Increased Leukotriene E 4 in the Exhaled Breath Condensate of Children With Mild Asthma*
 CHEST Original Research Increased Leukotriene E 4 in the Exhaled Breath Condensate of Children With Mild Asthma* Atsushi Shibata, MD; Toshio Katsunuma, MD, PhD; Morimitsu Tomikawa, MD; Aiko Tan, MD; Keisuke
CHEST Original Research Increased Leukotriene E 4 in the Exhaled Breath Condensate of Children With Mild Asthma* Atsushi Shibata, MD; Toshio Katsunuma, MD, PhD; Morimitsu Tomikawa, MD; Aiko Tan, MD; Keisuke
Respiratory pathophysiologic responses Inflammation of small airways in asthma
 Respiratory pathophysiologic responses Inflammation of small airways in asthma Qutayba Hamid, MD, PhD, a Yunling Song, MD, a Thomas C. Kotsimbos, MD, a Eleanor Minshall, PhD," Tony R. Bai, MD, b Richard
Respiratory pathophysiologic responses Inflammation of small airways in asthma Qutayba Hamid, MD, PhD, a Yunling Song, MD, a Thomas C. Kotsimbos, MD, a Eleanor Minshall, PhD," Tony R. Bai, MD, b Richard
Current reviews of allergy and clinical immunology (Supported by a grant from Astra Pharmaceuticals, Westborough, Mass)
 Current reviews of allergy and clinical immunology (Supported by a grant from Astra Pharmaceuticals, Westborough, Mass) Series editor: Harold S. Nelson, MD Airway remodeling and persistent airway obstruction
Current reviews of allergy and clinical immunology (Supported by a grant from Astra Pharmaceuticals, Westborough, Mass) Series editor: Harold S. Nelson, MD Airway remodeling and persistent airway obstruction
Hans-Peter Hauber, MD, Celine Bergeron, MD, Masao Toda, MD, Mario Kontolemos, BSc, Kenneth J. Holroyd, Roy C. Levitt, MD, and Qutayba Hamid, MD, PhD
 ORIGINAL ARTICLE Up-Regulation of Interleukin-9 and the Interleukin-9- Associated Calcium-Activated Chloride Channel hclca1 in Nasal Mucosa Following In Vivo Allergen Challenge Hans-Peter Hauber, MD, Celine
ORIGINAL ARTICLE Up-Regulation of Interleukin-9 and the Interleukin-9- Associated Calcium-Activated Chloride Channel hclca1 in Nasal Mucosa Following In Vivo Allergen Challenge Hans-Peter Hauber, MD, Celine
R emodelling of the airway wall in patients with asthma
 242 ORIGINAL ARTICLE Correlation between the bronchial subepithelial layer and whole airway wall thickness in patients with asthma K Kasahara, K Shiba, T Ozawa, K Okuda, M Adachi... See end of article
242 ORIGINAL ARTICLE Correlation between the bronchial subepithelial layer and whole airway wall thickness in patients with asthma K Kasahara, K Shiba, T Ozawa, K Okuda, M Adachi... See end of article
The distribution of eosinophils and lymphocytes in the large and small airways of asthmatics.
 Eur Respir J 997; : 292 3 DOI:.83/93936.97.2292 Printed in UK - all rights reserved Copyright ERS Journals Ltd 997 European Respiratory Journal ISSN 93-936 The distribution of eosinophils and lymphocytes
Eur Respir J 997; : 292 3 DOI:.83/93936.97.2292 Printed in UK - all rights reserved Copyright ERS Journals Ltd 997 European Respiratory Journal ISSN 93-936 The distribution of eosinophils and lymphocytes
Diagnosis and Management of Fungal Allergy Monday, 9-139
 Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
COPD: From Phenotypes to Endotypes. MeiLan K Han, M.D., M.S. Associate Professor of Medicine University of Michigan, Ann Arbor, MI
 COPD: From Phenotypes to Endotypes MeiLan K Han, M.D., M.S. Associate Professor of Medicine University of Michigan, Ann Arbor, MI Presenter Disclosures MeiLan K. Han Consulting Research support Novartis
COPD: From Phenotypes to Endotypes MeiLan K Han, M.D., M.S. Associate Professor of Medicine University of Michigan, Ann Arbor, MI Presenter Disclosures MeiLan K. Han Consulting Research support Novartis
Phenotypes of asthma; implications for treatment. Medical Grand Rounds Feb 2018 Jim Martin MD DSc
 Phenotypes of asthma; implications for treatment Medical Grand Rounds Feb 2018 Jim Martin MD DSc No conflicts to declare Objectives To understand the varied clinical forms of asthma To understand the pathobiologic
Phenotypes of asthma; implications for treatment Medical Grand Rounds Feb 2018 Jim Martin MD DSc No conflicts to declare Objectives To understand the varied clinical forms of asthma To understand the pathobiologic
Steroid Response in Refractory Asthmatics
 review korean j intern med 2012;27:143-148 pissn 1226-3303 eissn 2005-6648 Steroid Response in Refractory Asthmatics An-Soo Jang Department of Internal Medicine, Soonchunhyang University Bucheon Hospital,
review korean j intern med 2012;27:143-148 pissn 1226-3303 eissn 2005-6648 Steroid Response in Refractory Asthmatics An-Soo Jang Department of Internal Medicine, Soonchunhyang University Bucheon Hospital,
Chronic Cough Due to Nonasthmatic Eosinophilic Bronchitis. ACCP Evidence-Based Clinical Practice Guidelines
 Chronic Cough Due to Nonasthmatic Eosinophilic Bronchitis ACCP Evidence-Based Clinical Practice Guidelines Christopher E. Brightling, MBBS, PhD, FCCP Objectives: Nonasthmatic eosinophilic bronchitis is
Chronic Cough Due to Nonasthmatic Eosinophilic Bronchitis ACCP Evidence-Based Clinical Practice Guidelines Christopher E. Brightling, MBBS, PhD, FCCP Objectives: Nonasthmatic eosinophilic bronchitis is
Immunological Lung Diseases
 Emphysema and Fibrosis Universitätsklinik für Pneumologie Prof. Thomas Geiser Head Div. of Pulmonary Medicine and Laboratory of Lung Research, MU50 thomas.geiser@insel.ch The healthy lung: The pathway
Emphysema and Fibrosis Universitätsklinik für Pneumologie Prof. Thomas Geiser Head Div. of Pulmonary Medicine and Laboratory of Lung Research, MU50 thomas.geiser@insel.ch The healthy lung: The pathway
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) asthma Relationship to patient age and the proportions of bronchoalveolar cells
 28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
Distinction and Overlap. Allergy Dpt, 2 nd Pediatric Clinic, University of Athens
 Asthma Phenotypes: Distinction and Overlap Nikos Papadopoulos Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Asthma as a syndrome From the Iliad to ADAM 33 and back again Bronchoconstriction,
Asthma Phenotypes: Distinction and Overlap Nikos Papadopoulos Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Asthma as a syndrome From the Iliad to ADAM 33 and back again Bronchoconstriction,
Respiratory Pharmacology PCTH 400 Asthma and β-agonists
 Respiratory Pharmacology PCTH 400 Asthma and β-agonists Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Director, Centre of
Respiratory Pharmacology PCTH 400 Asthma and β-agonists Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Director, Centre of
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air
 Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Variation in the measurements of basement membrane thickness and inflammatory cell number in bronchial biopsies
 Eur Respir J 1998; 12: 811 815 DOI: 10.1183/09031936.98.12040811 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 0903-1936 Variation in the measurements
Eur Respir J 1998; 12: 811 815 DOI: 10.1183/09031936.98.12040811 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 0903-1936 Variation in the measurements
MAST CELLS IN AIRWAY SMOOTH MUSCLE IN ASTHMA MAST-CELL INFILTRATION OF AIRWAY SMOOTH MUSCLE IN ASTHMA. Study Subjects
 MAST-CELL INFILTRATION OF AIRWAY SMOOTH MUSCLE IN ASTHMA CHRISTOPHER E. BRIGHTLING, M.B., B.S., PETER BRADDING, D.M., FIONA A. SYMON, PH.D., STEPHEN T. HOLGATE, M.D., D.SC., ANDREW J. WARDLAW, PH.D., AND
MAST-CELL INFILTRATION OF AIRWAY SMOOTH MUSCLE IN ASTHMA CHRISTOPHER E. BRIGHTLING, M.B., B.S., PETER BRADDING, D.M., FIONA A. SYMON, PH.D., STEPHEN T. HOLGATE, M.D., D.SC., ANDREW J. WARDLAW, PH.D., AND
Asthma comprises different phenotypes. Relationship between past airway pathology and current lung function in preschool wheezers
 Eur Respir J ; 8: 6 DOI:.8/996.69 CopyrightßERS Relationship between past airway pathology and current lung function in preschool wheezers S. Sonnappa*,#, C.M. Bastardo*, S. Saglani ", A. Bush " and P.
Eur Respir J ; 8: 6 DOI:.8/996.69 CopyrightßERS Relationship between past airway pathology and current lung function in preschool wheezers S. Sonnappa*,#, C.M. Bastardo*, S. Saglani ", A. Bush " and P.
Viral infections in airway remodeling
 Viral infections in airway remodeling Nikos Papadopoulos As. Proffesor,Head, Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Overview Acute events may have long term consequences Remodeling appears
Viral infections in airway remodeling Nikos Papadopoulos As. Proffesor,Head, Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Overview Acute events may have long term consequences Remodeling appears
2010 Health Press Ltd.
 Fast Facts Fast Facts: Asthma Third edition Stephen T Holgate MD DSc FRCP FMedSci MRC Clinical Professor of Immunopharmacology School of Medicine Southampton General Hospital Southampton, UK Jo Douglass
Fast Facts Fast Facts: Asthma Third edition Stephen T Holgate MD DSc FRCP FMedSci MRC Clinical Professor of Immunopharmacology School of Medicine Southampton General Hospital Southampton, UK Jo Douglass
Chronic cough is defined as a cough persisting for. Airway Inflammation as an Assessment of Chronic Nonproductive Cough*
 Airway Inflammation as an Assessment of Chronic Nonproductive Cough* Sang Yeub Lee, MD ; Jae Youn Cho, MD; Jae Jeong Shim, MD; Han Kyeom Kim, MD; Kyung Ho Kang, MD, FCCP; Se Hwa Yoo, MD; and Kwang Ho In,
Airway Inflammation as an Assessment of Chronic Nonproductive Cough* Sang Yeub Lee, MD ; Jae Youn Cho, MD; Jae Jeong Shim, MD; Han Kyeom Kim, MD; Kyung Ho Kang, MD, FCCP; Se Hwa Yoo, MD; and Kwang Ho In,
Relationships between thickening of reticular basement membrane and the clinical features in children with asthma
 Relationships between thickening of reticular basement membrane and the clinical features in children with asthma Eun Soo Kim Department of Medicine The Graduate School, Yonsei University Relationships
Relationships between thickening of reticular basement membrane and the clinical features in children with asthma Eun Soo Kim Department of Medicine The Graduate School, Yonsei University Relationships
CURRENT DEVELOPMENTS IN THE PHYSIOLOGY AND MANAGEMENT OF ASTHMA. V. I. IYAWE and M. I. EBOMOYI
 19 Nigerian Journal Of Physiological Sciences 20 (1-2): 19-29@ Physiological Society Of Nigeria, 2005 Available online/abstracted at http://www.biolineinternational.org.br/njps; www.ajol.info/journals.njp;
19 Nigerian Journal Of Physiological Sciences 20 (1-2): 19-29@ Physiological Society Of Nigeria, 2005 Available online/abstracted at http://www.biolineinternational.org.br/njps; www.ajol.info/journals.njp;
Air Flow Limitation. In most serious respiratory disease, a key feature causing morbidity and functional disruption is air flow imitation.
 Asthma Air Flow Limitation In most serious respiratory disease, a key feature causing morbidity and functional disruption is air flow imitation. True whether reversible, asthma and exercise-induced bronchospasm,
Asthma Air Flow Limitation In most serious respiratory disease, a key feature causing morbidity and functional disruption is air flow imitation. True whether reversible, asthma and exercise-induced bronchospasm,
Key words: Asthma, remodeling, MMP-9, TIMP-1, ISS. 1 The potential role of MMP-9 in matrix remodeling
 Remodeling associated expression of matrix metalloproteinase 9 but not tissue inhibitor of metalloproteinase 1 in airway epithelium: Modulation by immunostimulatory DNA Jae Youn Cho, MD, PhD, a Marina
Remodeling associated expression of matrix metalloproteinase 9 but not tissue inhibitor of metalloproteinase 1 in airway epithelium: Modulation by immunostimulatory DNA Jae Youn Cho, MD, PhD, a Marina
Disclosures. Learning Objective. Biological therapies. Biologics with action against 11/30/2011. Biologic Asthma Therapies and Individualized Medicine
 Biologic Asthma Therapies and Individualized Medicine Mark S. Dykewicz, MD Director, Allergy & Immunology Fellowship Program Director Wake Forest University School of Medicine Winston-Salem, North Carolina
Biologic Asthma Therapies and Individualized Medicine Mark S. Dykewicz, MD Director, Allergy & Immunology Fellowship Program Director Wake Forest University School of Medicine Winston-Salem, North Carolina
Investigation and assessment of airway and lung inflammation: we now have the tools, what are the questions?
 Eur Respir J 1998; 11: 524 528 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 0903-1936 EDITORIAL Investigation and assessment of airway and lung
Eur Respir J 1998; 11: 524 528 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1998 European Respiratory Journal ISSN 0903-1936 EDITORIAL Investigation and assessment of airway and lung
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis
 Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Mechanisms of asthma and allergic inflammation. asthma, despite treatment with corticosteroids. (J Allergy Clin Immunol 2005;115:280-6.
 Oral corticosteroids decrease eosinophil and CC chemokine expression but increase neutrophil, IL-8, and IFN-g inducible protein 10 expression in asthmatic airway mucosa Motonori Fukakusa, MD, PhD, a Celine
Oral corticosteroids decrease eosinophil and CC chemokine expression but increase neutrophil, IL-8, and IFN-g inducible protein 10 expression in asthmatic airway mucosa Motonori Fukakusa, MD, PhD, a Celine
Bronchial Subepithelial Fibrosis Correlates With Airway Responsiveness to Methacholine*
 Bronchial Subepithelial Fibrosis Correlates With Airway Responsiveness to Methacholine* LouisPhilippe Boulet, MD, FCCP; Michel Laviolette, MD, CSPQ; Helene Turcotte, MSc; Andre Cartier, MD; Mario Dugas,
Bronchial Subepithelial Fibrosis Correlates With Airway Responsiveness to Methacholine* LouisPhilippe Boulet, MD, FCCP; Michel Laviolette, MD, CSPQ; Helene Turcotte, MSc; Andre Cartier, MD; Mario Dugas,
COPD and Asthma: Similarities and differences Prof. Peter Barnes
 and Asthma: Similarities and Differences and Asthma: 1 Imperial College Peter Barnes FRS, FMedSci, National Heart & Lung Institute Imperial College, London, UK p.j.barnes@imperial.ac.uk Royal Brompton
and Asthma: Similarities and Differences and Asthma: 1 Imperial College Peter Barnes FRS, FMedSci, National Heart & Lung Institute Imperial College, London, UK p.j.barnes@imperial.ac.uk Royal Brompton
A sthma is now accepted as a disease characterised by airway
 309 ORIGINAL ARTICLE Airway inflammation, basement membrane thickening and bronchial hyperresponsiveness in asthma C Ward, M Pais, R Bish, D Reid, B Feltis, D Johns, E H Walters... See end of article for
309 ORIGINAL ARTICLE Airway inflammation, basement membrane thickening and bronchial hyperresponsiveness in asthma C Ward, M Pais, R Bish, D Reid, B Feltis, D Johns, E H Walters... See end of article for
Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network
 Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network Robert.kruklitis@lvh.com Correlation of a Asthma pathophyisology with basic science Asthma (Physiology) Bronchodilators
Robert Kruklitis, MD, PhD Chief, Pulmonary Medicine Lehigh Valley Health Network Robert.kruklitis@lvh.com Correlation of a Asthma pathophyisology with basic science Asthma (Physiology) Bronchodilators
Pulmonary Perspective
 Pulmonary Perspective Severe Asthma in Adults Sally Wenzel National Jewish Medical and Research Center, Denver, Colorado Severe asthma remains poorly understood and frustrating to care for, partly because
Pulmonary Perspective Severe Asthma in Adults Sally Wenzel National Jewish Medical and Research Center, Denver, Colorado Severe asthma remains poorly understood and frustrating to care for, partly because
Harkness, Louise M; Kanabar, Varsha; Sharma, Hari S; Westergren-Thorsson, Gunilla; Larsson Callerfelt, Anna-Karin
 Pulmonary vascular changes in asthma and COPD. Harkness, Louise M; Kanabar, Varsha; Sharma, Hari S; Westergren-Thorsson, Gunilla; Larsson Callerfelt, Anna-Karin Published in: Pulmonary Pharmacology & Therapeutics
Pulmonary vascular changes in asthma and COPD. Harkness, Louise M; Kanabar, Varsha; Sharma, Hari S; Westergren-Thorsson, Gunilla; Larsson Callerfelt, Anna-Karin Published in: Pulmonary Pharmacology & Therapeutics
Subclinical phenotypes of asthma
 1 Subclinical phenotypes of asthma P Bradding DM FRCP*, RH Green MD FRCP* * Institute for Lung Health and Department of Respiratory Medicine, Glenfield Hospital, Leicester, UK Department of Infection,
1 Subclinical phenotypes of asthma P Bradding DM FRCP*, RH Green MD FRCP* * Institute for Lung Health and Department of Respiratory Medicine, Glenfield Hospital, Leicester, UK Department of Infection,
Rising Incidence of Asthma
 Controlling Severe Asthma through Advanced Diagnosis and Treatment Strategies James F. Donohue, MD Professor of Medicine Division of Pulmonary and Critical Care Medicine University of North Carolina at
Controlling Severe Asthma through Advanced Diagnosis and Treatment Strategies James F. Donohue, MD Professor of Medicine Division of Pulmonary and Critical Care Medicine University of North Carolina at
Distinct structural changes occur in the airways of. Matrix Metalloproteinase-9 Expression in Asthma*
 Matrix Metalloproteinase-9 Expression in Asthma* Effect of Asthma Severity, Allergen Challenge, and Inhaled Corticosteroids Waldo Mattos, MD; Sam Lim, MBBS; Richard Russell, MB; Anon Jatakanon, MD; K.
Matrix Metalloproteinase-9 Expression in Asthma* Effect of Asthma Severity, Allergen Challenge, and Inhaled Corticosteroids Waldo Mattos, MD; Sam Lim, MBBS; Richard Russell, MB; Anon Jatakanon, MD; K.
The natural history of asthma and early intervention
 The natural history of asthma and early intervention Stanley J. Szefler, MD Denver, Colo The understanding of the natural history of asthma has changed significantly during the last 4 decades, with the
The natural history of asthma and early intervention Stanley J. Szefler, MD Denver, Colo The understanding of the natural history of asthma has changed significantly during the last 4 decades, with the
asthma. A role of histamine in atopic asthma.
 14 Histamine and LTC4 in atopic asthma Release of histamine and leukotriene C 4 from bronchoalveolar cells III patients with bronchial asthma. A role of histamine in atopic asthma. Fumihiro Mitsunobu,
14 Histamine and LTC4 in atopic asthma Release of histamine and leukotriene C 4 from bronchoalveolar cells III patients with bronchial asthma. A role of histamine in atopic asthma. Fumihiro Mitsunobu,
ASTHMA ASTHMA DISEASE SUMMARY. Risk Factors
 ASTHMA Risk Factors Family history of asthma or other atopic diseases (eczema, hayfever) Having eczema or hayfever currently or as a child Living in an industrialised area more exposure to airborne pollutants,
ASTHMA Risk Factors Family history of asthma or other atopic diseases (eczema, hayfever) Having eczema or hayfever currently or as a child Living in an industrialised area more exposure to airborne pollutants,
How immunology informs the design of immunotherapeutics.
 How immunology informs the design of immunotherapeutics. Stephen R Durham Allergy and Clinical Immunology, Royal Brompton Hospital and Imperial College London WAO Cancun Mon Dec 5 th 2011 How immunology
How immunology informs the design of immunotherapeutics. Stephen R Durham Allergy and Clinical Immunology, Royal Brompton Hospital and Imperial College London WAO Cancun Mon Dec 5 th 2011 How immunology
Do current treatment protocols adequately prevent airway remodeling in children with mild intermittent asthma?
 Respiratory Medicine (2006) 100, 458 462 Do current treatment protocols adequately prevent airway remodeling in children with mild intermittent asthma? Haim S. Bibi a,, David Feigenbaum a, Mariana Hessen
Respiratory Medicine (2006) 100, 458 462 Do current treatment protocols adequately prevent airway remodeling in children with mild intermittent asthma? Haim S. Bibi a,, David Feigenbaum a, Mariana Hessen
Interplay between matrix metalloproteinase-9 and tissue inhibitor of matrix metalloproteinase-1 in acute asthma exacerbation and airway remodeling
 Egyptian Journal of Chest Diseases and Tuberculosis (2012) 61, 35 39 The Egyptian Society of Chest Diseases and Tuberculosis Egyptian Journal of Chest Diseases and Tuberculosis www.elsevier.com/locate/ejcdt
Egyptian Journal of Chest Diseases and Tuberculosis (2012) 61, 35 39 The Egyptian Society of Chest Diseases and Tuberculosis Egyptian Journal of Chest Diseases and Tuberculosis www.elsevier.com/locate/ejcdt
Mechanisms of action of bronchial provocation testing
 Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers?
 Disclosures: Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers? Stanley Fineman, MD Past-President, American College of Allergy, Asthma & Immunology Adjunct Associate
Disclosures: Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers? Stanley Fineman, MD Past-President, American College of Allergy, Asthma & Immunology Adjunct Associate
Bronchial gland duct ectasia in fatal bronchial asthma: association with interstitial emphysema
 J Clin Pathol 1989;42:1026-1031 Bronchial gland duct ectasia in fatal bronchial asthma: association with interstitial emphysema A CLUROE, L HOLLOWAY, K THOMSON, G PURDIE,I R BEASLEY* From the Departments
J Clin Pathol 1989;42:1026-1031 Bronchial gland duct ectasia in fatal bronchial asthma: association with interstitial emphysema A CLUROE, L HOLLOWAY, K THOMSON, G PURDIE,I R BEASLEY* From the Departments
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma
 Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Current Asthma Therapy: Little Need to Phenotype. Phenotypes of Severe Asthma. Cellular Phenotypes 12/7/2012
 Subbasement Membrane Thickness(µm) 12/7/212 Current Asthma Therapy: Little Need to Phenotype Phenotypes of Severe Asthma Most mild and to some degree moderate asthmatics respond well to currently available
Subbasement Membrane Thickness(µm) 12/7/212 Current Asthma Therapy: Little Need to Phenotype Phenotypes of Severe Asthma Most mild and to some degree moderate asthmatics respond well to currently available
Inhibition of airway remodeling in IL-5 deficient mice
 Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Clinical significance of airway inflammation in bronchcial asthma. Comparison with chronic obstructive bronchiolitis.
 24 Airway inflammation in asthma Clinical significance of airway inflammation in bronchcial asthma. Comparison with chronic obstructive bronchiolitis. Yoshiro Tanizaki, Hikaru Kitani, Takashi Mifune, Fumihiro
24 Airway inflammation in asthma Clinical significance of airway inflammation in bronchcial asthma. Comparison with chronic obstructive bronchiolitis. Yoshiro Tanizaki, Hikaru Kitani, Takashi Mifune, Fumihiro
Review Article Airway Epithelium in Atopic and Nonatopic Asthma: Similarities and Differences
 International Scholarly Research Network ISRN Allergy Volume 2011, Article ID 195846, 7 pages doi:10.5402/2011/195846 Review Article Airway Epithelium in Atopic and Nonatopic Asthma: Similarities and Differences
International Scholarly Research Network ISRN Allergy Volume 2011, Article ID 195846, 7 pages doi:10.5402/2011/195846 Review Article Airway Epithelium in Atopic and Nonatopic Asthma: Similarities and Differences
Viral-Induced Asthma:
 Viral-Induced : Sorting through the Studies Malcolm R. Sears, MB, FRACP, FRCPC Presented at the Respirology Update Continuing Education Program, January 2005 Viral-associated wheezing is common and not
Viral-Induced : Sorting through the Studies Malcolm R. Sears, MB, FRACP, FRCPC Presented at the Respirology Update Continuing Education Program, January 2005 Viral-associated wheezing is common and not
Airwayin ammationinasthmawithincomplete reversibility of air ow obstruction $
 Vol. 97 (2003) 739^744 Airwayin ammationinasthmawithincomplete reversibility of air ow obstruction $ L-P. BOULET*, H.TURCOTTE,O.TURCOT AND J.CHAKIR Ho pitallaval,2725,cheminsainte-foy,sainte-foy,queł bec
Vol. 97 (2003) 739^744 Airwayin ammationinasthmawithincomplete reversibility of air ow obstruction $ L-P. BOULET*, H.TURCOTTE,O.TURCOT AND J.CHAKIR Ho pitallaval,2725,cheminsainte-foy,sainte-foy,queł bec
Safety, PK and PD of ARRY-502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies
 Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
Safety, PK and PD of ARRY502, a CRTh2 Antagonist, in Healthy Subjects with a History of Seasonal Allergies L. Burgess*, L. Anderson, C. Nugent, N. Klopfenstein, C. Eberhardt, L. Carter, C. Kass, S. RojasCaro,
THE PROMISE OF NEW AND NOVEL DRUGS. Pyng Lee Respiratory & Critical Care Medicine National University Hospital
 THE PROMISE OF NEW AND NOVEL DRUGS Pyng Lee Respiratory & Critical Care Medicine National University Hospital Pyng_lee@nuhs.edu.sg Asthma Prevalence, Morbidity, Mortality 235 million suffer from asthma
THE PROMISE OF NEW AND NOVEL DRUGS Pyng Lee Respiratory & Critical Care Medicine National University Hospital Pyng_lee@nuhs.edu.sg Asthma Prevalence, Morbidity, Mortality 235 million suffer from asthma
Airway inflammation assessed by invasive and noninvasive means in severe asthma: Eosinophilic and noneosinophilic phenotypes
 Airway inflammation assessed by invasive and noninvasive means in severe asthma: Eosinophilic and noneosinophilic phenotypes Catherine Lemière, MD, MSc, a Pierre Ernst, MD, b Ron Olivenstein, MD, b Yasuhiro
Airway inflammation assessed by invasive and noninvasive means in severe asthma: Eosinophilic and noneosinophilic phenotypes Catherine Lemière, MD, MSc, a Pierre Ernst, MD, b Ron Olivenstein, MD, b Yasuhiro
