Key words: Asthma, remodeling, MMP-9, TIMP-1, ISS. 1 The potential role of MMP-9 in matrix remodeling
|
|
|
- Leslie Hudson
- 6 years ago
- Views:
Transcription
1 Remodeling associated expression of matrix metalloproteinase 9 but not tissue inhibitor of metalloproteinase 1 in airway epithelium: Modulation by immunostimulatory DNA Jae Youn Cho, MD, PhD, a Marina Miller, MD, PhD, a Kirsti McElwain, BS, a Shauna McElwain, BS, a Jung Yeon Shim, MD, a,b Eyal Raz, MD, a and David H. Broide, MBChB a San Diego, Calif, and Seoul, Korea Background: Matrix metalloproteinase 9 (MMP-9) and its tissue inhibitor of metalloproteinase 1 (TIMP-1) are hypothesized to play a role in the pathogenesis of airway remodeling in asthma. Objective: We have used a mouse model of airway remodeling to determine the pattern of expression of MMP-9 and TIMP-1 in airway epithelium and peribronchial cells, and assess whether TIMP-1, an inhibitor of MMP-9, is expressed at the same sites in the airway. In addition, we have investigated whether immunostimulatory sequences (ISSs) of DNA modulate levels of expression of MMP-9, TIMP-1, and peribronchial fibrosis. Methods: Levels of lung MMP-9 and TIMP-1 were assessed by zymography, ELISA, and immunohistochemistry. Results: Repetitive ovalbumin challenge induced a significant increase in levels of MMP-9, TIMP-1, and peribronchial collagen deposition. The pattern of expression of MMP-9 and TIMP-1 in the remodeled airway was significantly different. MMP-9 but not TIMP-1 was expressed in airway epithelium, whereas both MMP-9 and TIMP-1 were expressed in peribronchial inflammatory cells. ISS significantly reduced expression of MMP-9 in airway epithelium (which immunostained positive for Toll receptor 9), as well as in peribronchial inflammatory cells. In vitro studies demonstrated that ISS inhibited bone marrow macrophage generation of MMP-9. Conclusion: Allergen-induced peribronchial fibrosis is associated with expression of MMP-9 and TIMP-1 at different anatomical sites in the remodeled airway. The ability of ISS to inhibit the expression of MMP-9 in airway epithelium (a site where its inhibitor TIMP-1 is not induced by allergen challenge) may be important in determining whether ISS contributes to reductions in airway remodeling by reducing levels of MMP-9. Clinical implications: Immunostimulatory sequences of DNA, which are being investigated as novel therapeutics in asthma, inhibit airway remodeling in mice as well as epithelial expression of MMP-9, an enzyme that degrades the extracellular matrix proteins surrounding the airway. (J Allergy Clin Immunol 2006;117: ) From a the Department of Medicine, University of California San Diego, and b the Sungkyunkwan University School of Medicine, Seoul. Dr Broide is supported by National Institutes of Health grant AI Received for publication April 4, 2005; revised December 1, 2005; accepted for publication December 5, Reprint requests: David Broide, MBChB, University of California San Diego, Basic Science Building, Room 5090, 9500 Gilman Drive, La Jolla, CA dbroide@ucsd.edu /$32.00 Ó 2006 American Academy of Allergy, Asthma and Immunology doi: /j.jaci Key words: Asthma, remodeling, MMP-9, TIMP-1, ISS Matrix metalloproteinases (MMPs) are a family of extracellular proteases that are responsible for the degradation of the extracellular matrix during tissue remodeling. 1 The potential role of MMP-9 in matrix remodeling in asthma is suggested from studies in human beings with asthma demonstrating elevated levels of MMP-9 in bronchoalveolar lavage (BAL) and sputum Studies in mouse models of asthma have also demonstrated an important role for MMP-9 in allergen-induced acute airway inflammatory responses but have not yet investigated the role of MMP-9 in airway remodeling. MMPs are synthesized as secreted or transmembrane proenzymes and are processed to an active form by the removal of an amino terminal propeptide which, when not cleaved, blocks access to the catalytic site. 1 Tissue inhibitor of metalloproteinases (TIMPs) are specific inhibitors of MMPs that bind noncovalently in a 1:1 molar ratio with activated MMPs. 1 TIMPs are produced by a wide variety of cells and are induced by several cytokines and growth factors. In contrast with previous studies that have examined the role of MMP-9 in mediating the acute inflammatory response to ovalbumin challenge in mouse models of asthma, in this study we have investigated the airway pattern of expression of MMP-9 and its inhibitor TIMP-1 during episodes of airway remodeling induced in a mouse model by repetitive allergen challenge. Because MMPs have the potential to play an important role in the degradation of the extracellular matrix during tissue remodeling, we considered it important to determine whether MMP-9, an MMP that is highly expressed in sputum and BAL in patients with asthma, 2-11 is expressed in the airway during periods of airway remodeling, and whether TIMP-1, an endogenous inhibitor of MMP-9, is expressed in the same anatomical distribution in the remodeled airway. The mouse model of airway remodeling we have used is associated with allergen-induced structural changes in the airway including peribronchial fibrosis with deposition of collagen III and collagen V, and increased thickness of the peribronchial smooth muscle layer The T H 2 cytokine dependence of the allergen induced airway remodeling is suggested from studies in IL-5 deficient mice that have significantly reduced levels of airway remodeling. 17 Studies in human beings with asthma have also
2 J ALLERGY CLIN IMMUNOL VOLUME 117, NUMBER 3 Cho et al 619 Abbreviations used BAL: Bronchoalveolar lavage CpG: Cytosine phosphorothioate guanosine ISS: Immunostimulatory sequences of DNA MMP: Matrix metalloproteinase TIMP: Tissue inhibitor of metalloproteinase TLR-9: Toll receptor 9 demonstrated an important role for IL-5 in airway remodeling. 19 In addition to examining the expression of MMP-9 and TIMP-1 in the remodeled airways of mice challenged with allergen, we have also investigated whether immunostimulatory sequences (ISSs) of DNA containing a cytosine phosphorothioate guanosine (CpG) DNA motif modulate allergen induced expression of MMP-9 and TIMP-1 in the remodeled airway. Previous studies have demonstrated that ISS is effective in inhibiting acute allergen induced eosinophilic airway inflammation, T H 2 cytokine expression, mucus expression, and airway hyperreactivity In addition, when ISS is administered before allergen challenge in mice, it can prevent features of airway remodeling including the development of peribronchial fibrosis. 16 More recent studies have also demonstrated that ISS can reverse established airway remodeling in mice when ISS is first administered after the development of allergen induced airway remodeling. 18 Currently there is no information regarding the effect of ISS on allergen-induced expression of MMP-9, which has been implicated in tissue remodeling. We have therefore investigated whether ISS modulates expression of MMP-9 and its inhibitor TIMP-1 in the remodeled airways of allergenchallenged mice. METHODS Induction of allergen-induced airway remodeling The methods we have used to administer ovalbumin allergen to induce airway remodeling in mice have previously been described In brief, BALB/c mice (16 mice/group; Jackson Laboratory, Bar Harbor, Me) were used when they reached 8 to 10 weeks of age. Mice were immunized subcutaneously on days 0, 7, 14, and 21 with 25 mg ovalbumin (grade V; Sigma-Aldrich, St Louis, Mo) adsorbed to 1 mg alum (Sigma-Aldrich) in 200 ml normal saline. Intranasal ovalbumin challenges (20 ng/50 ml in PBS) were administered on days 27, 29, and 31 under isoflurane (Vedco, Inc, St Joseph, Mo) anesthesia. Intranasal ovalbumin challenges were then repeated twice a week for 1 to 3 months. Age-matched and sex-matched control mice were sensitized but not challenged with ovalbumin during the 3-month study. Mice were killed 24 hours after the final ovalbumin challenge, and BAL fluid and lungs were analyzed. All animal experimental protocols were approved by the University of California, San Diego, Animal Subjects Committee. Therapeutic intervention with ISS Different groups of mice (16 mice/group) were administered intraperitoneal endotoxin-free (<1 ng/mg DNA) phosphorothioate ISSoligodeoxynucleotide (ODN) (5 9 -TGACTGTGAACGTTCGAGAT GA-3 9 ; Trilink, San Diego, Calif; 100 mg in 100 ml sterile, endotoxin-free PBS), mutated ODN (M-ODN) (5 9 -TGACTGTGAAGG TTGGAGATGA-3 9 ), which lacks the CpG motif present in ISS, or diluent control starting 1 day before the first intranasal ovalbumin challenge on day 27, and then continuing every other week 1 day before intranasal challenges for 3 months. Measurement of MMP-9 Gelatin zymography. Gelatin zymogaphy 12 was performed to detect MMP-9 in BAL fluid in the different groups of mice. Samples of BAL fluid were added to loading buffer and separated in 10% SDSpolyacrylamide gels that contained 0.1% gelatin. SDS was removed by two 30-minute washes with 2.5% Triton-X 100 before incubation of gels for 24 hours at 37 C in developing buffer (BioRad, Hercules, Calif). Gelatin gels were stained with 0.25% Coomassie Blue and the optical density of the MMP-9 band determined by Unscan-it software (Silk Scientific, Orem, Utah). Results are expressed as MMP-9 zymography units (arbitrary units/ml) 13 on the basis of the computer analysis. A MMP-9 standard (Chemicon, Temecula, Calif) was used as a positive control. ELISA. The activity of MMP-9 in lung was assayed by ELISA (sensitivity 5 ng/ml) according to the manufacturer s instructions (Chemicon). Homogenized lung supernatants were prepared by using methods previously described in this laboratory for measurement of cytokines in lung. 16,18 Immunohistochemical detection of MMP-9 in lung sections. A primary mab directed against MMP-9 (Chemicon) was used for immunohistochemical detection of MMP-9 in the lung sections using the immunoperoxidase method as previously described in this laboratory Total peribronchial MMP-9 immunoreactivity was assessed and includes all immunoreactivity for MMP-9 extending from the lumenal aspect of the epithelium to the adventitia (ie, epithelium, submucosa, adventitia). The immunostained lung sections were also analyzed to determine the anatomical distribution of expression of MMP-9 in the airway (eg, epithelial versus peribronchial inflammatory cells). The total area of MMP-9 immunostaining (peribronchial MMP-9 immunoreactivity) as well as MMP-9 immunostaining in epithelium or in peribronchial inflammatory cells in each paraffin embedded lung was outlined and quantified by using a light microscope attached to an image analysis system (Image-Pro Plus; Media Cybernetics, Silver Springs, Md). The unit area of computer program images were calibrated and standardized with a slide micrometer. Results are expressed as the area of immunostaining per micrometer length of basement membrane of bronchioles 150 to 200 mm of internal diameter. Between 3 and 5 bronchioles were counted in each slide. For all experiments that require morphometric analysis of lung tissues, the slides are coded and analyzed by technicians blind to the study group. Each slide is also analyzed in the same predetermined sequence to minimize observer bias. All slides to be analyzed in a particular experiment are stained in the same batch under identical staining conditions and analyzed under the same light microscope conditions (magnification, gain, illumination). Immunohistochemical detection of Toll receptor 9 in airway epithelial cells in lung sections. A primary mab directed against Toll receptor 9 (TLR-9; Chemicon) was used for immunohistochemical detection of TLR-9 in the lung sections using the immunoperoxidase method as previously described in this laboratory Effect of ISS on macrophage MMP-9 expression in vitro. To determine whether ISS directly modulates levels of macrophage expression of MMP-9, bone marrow derived macrophages were incubated with LPS (10 mg/ml) in triplicate for 24 hours in the presence or absence of ISS or M-ODN (10 mg/ml) as previously described in this laboratory. 18 Supernatants were collected and assayed for MMP-9 by using the zymography assay as described.
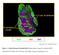
3 620 Cho et al J ALLERGY CLIN IMMUNOL MARCH 2006 FIG 1. Peribronchial distribution of expression of MMP-9 and TIMP-1: modulation by ISS. Minimal levels of either MMP-9 (A) or TIMP-1 (D) immunostaining are noted in nonovalbumin-challenged mice. Repetitive ovalbumin (OVA) challenge induced significantly increased levels of expression of MMP-9 (B) and TIMP-1 (E) that were significantly inhibited by ISS (C and F). Repetitive OVA challenge induced MMP-9 (B), but not TIMP-1 (E), expression in epithelial cells. Measurement of TIMP-1 TIMP-1 ELISA. The concentrations of TIMP-1 in homogenized lung supernatants was assayed by ELISA (sensitivity 37 pg/ml) according to the manufacturer s instructions (R&D Systems Inc, Minneapolis, Minn). Immunohistochemical detection of TIMP-1 in lung sections. Immunohistochemical detection of TIMP-1 in lung sections used a primary mab directed against TIMP-1 (Chemicon), and similar immunohistochemistry and image analysis methods as described for quantitation of epithelial versus peribronchial inflammatory cell expression of MMP-9. Quantitation of peribronchial fibrosis Peribronchial trichrome staining. The area of peribronchial trichrome staining in paraffin embedded lung was outlined and quantified by using a light microscope attached to an image analysis system as previously described Results are expressed as the area of trichrome staining per micrometer length of basement membrane of bronchioles 150 to 200 mm of internal diameter. At least 10 bronchioles were counted in each slide. Lung collagen assay. The amount of lung collagen was measured as previously described in this laboratory with a collagen assay kit that uses a dye reagent that selectively binds to the [Gly-X-Y]n tripeptide sequence of mammalian collagens (Biocolor, Newtownabbey, United Kingdom). In all experiments, a collagen standard was used to calibrate the assay. BAL eosinophil levels Bronchoalveolar lavage eosinophil counts were performed as previously described Statistical analysis Results in the different groups of mice were compared by ANOVA using the nonparametric Kruskal-Wallis test followed by posttesting using the Dunn multiple comparison of means. All results are presented as means 6 SEMs. A statistical software package (Graph Pad Prism, San Diego, Calif) was used for the analysis. P values of <.05 were considered statistically significant. RESULTS Immunohistochemical detection of epithelial cell vs peribronchial cells expressing MMP-9 and TIMP-1 in the remodeled airway: Effect of ISS Minimal peribronchial expression of either MMP-9 (Fig 1, A)orTIMP-1(Fig 1, D) was noted in nonovalbuminchallenged mice by immunohistochemistry. In contrast, both MMP-9 (Fig 1, B) and TIMP-1 (Fig 1, E) were significantly expressed after repetitive ovalbumin challenge for 3 months in the remodeled airway. However, the peribronchial distribution of MMP-9 expression differed from that of TIMP-1 expression in the remodeled airway in that MMP-9 was expressed in airway epithelium (Fig 1, B) whereas TIMP-1 was not expressed in airway epithelium (Fig 1, E). Both MMP-9 (Fig 1, B) and TIMP-1 (Fig 1, E) were expressed in peribronchial inflammatory cells and the peribronchial extracellular matrix. Quantitative analysis of MMP-9 expression by immunohistochemistry and image analysis demonstrated that ovalbumin challenge for 1 or 3 months induced significant increased numbers of MMP-9 1 peribronchial inflammatory cells (ovalbumin vs no ovalbumin; P 5.001; Fig 2, A) as well as significant increased levels of MMP-9 immunostaining in airway epithelial cells (ovalbumin vs no ovalbumin; P 5.001; Fig 2, B). ISS significantly reduced the numbers of MMP-9 1 peribronchial inflammatory cells
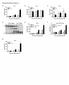
4 J ALLERGY CLIN IMMUNOL VOLUME 117, NUMBER 3 Cho et al 621 FIG 2. Expression of MMP-9: modulation by ISS. Levels of MMP-9 were assessed by counting the number of MMP-9 1 peribronchial cells (A), epithelial MMP-9 immunostaining (B), MMP-9 as assessed by ELISA (C), zymography (D and E), and peribronchial MMP-9 immunostaining (F). D, Lane 1 is MMP-9 standard, lane 2 is no ovalbumin (OVA), lane 3 is OVA, and lane 4 is OVA 1 ISS. (ovalbumin vs ovalbumin 1 ISS; P 5.001; Fig 1, B and C; Fig 2, A), as well as levels of MMP-9 immunostaining in airway epithelial cells (ovalbumin vs ovalbumin 1 ISS; P 5.001; Fig 1, B and C; Fig 2, B) when administered for 1 or 3 months. Quantitative analysis of TIMP-1 expression by immunohistochemistry and image analysis demonstrated that ovalbumin challenge for 1 or 3 months increased the numbers of TIMP-1 1 peribronchial inflammatory cells (ovalbumin vs no ovalbumin; P 5.001; Fig 1, D and E; Fig 3, A) but did not induce significant TIMP-1 compared with MMP-9 immunostaining in airway epithelial cells (Fig 1, B and E; Fig 2, B; Fig 3, B). ISS significantly reduced the number of TIMP-1 1 peribronchial inflammatory cells (ovalbumin vs ovalbumin 1 ISS; P 5.001; Fig 1, E and F; Fig 3, A). Quantitation of MMP-9 in lung by ELISA, zymography, and peribronchial immunostaining: Effect of ISS Significantly increased lung levels of MMP-9 were detected after ovalbumin challenge for 1 or 3 months using 3 different methods to quantitate MMP-9, including MMP-9 ELISA ( vs ng MMP-9/mg lung protein; ovalbumin 3 months vs no ovalbumin 3 months; P 5.001; Fig 2, C), MMP-9 zymography ( vs MMP-9 zymography units; ovalbumin 3 months vs no ovalbumin 3 months; P 5.001; Fig 2, D and E), and peribronchial MMP-9 immunostaining and image analysis quantitation ( vs mm 2 /mm circumference of bronchiole; ovalbumin 3 months vs no ovalbumin 3 months; P 5.001; Fig 2, F). Level of inhibition of MMP-9 in remodeled airway induced by ISS Levels of inhibition of MMP-9 induced by ISS were in general greater after 3 months of ISS administration compared with 1 month of ISS administration (Fig 2). Five different quantitative measurements of MMP-9 (MMP-9 1 immunostaining of epithelium; MMP-9 1 peribronchial cells; peribronchial MMP-9 immunostaining which includes extracellular matrix deposition of MMP- 9; ELISA; zymography) were used to assess the effect of ISS on levels of MMP-9 in the remodeled airway. Administration of ISS for 3 months significantly reduced the number of peribronchial MMP-9 1 cells (P 5.001; Fig 2, A), epithelial MMP-9 immunostaining (P 5.001; Fig 2, B), and levels of peribronchial MMP-9 immunostaining (P 5.001; Fig 2, F), and also had a statistically significant effect on reducing levels of MMP-9 as assessed by ELISA (P 5.05; Fig 2, C) and by MMP-9 zymography (Fig 2, E; P 5.01; ISS 1 ovalbumin vs ovalbumin). Administration of ISS for 1 month significantly reduced the number of peribronchial MMP-9 1 cells (P 5.001; Fig 2, A) and epithelial MMP-9 immunostaining (P 5.001; Fig 2, B) as well as levels of lung MMP-9 as assessed by ELISA (P 5.003; Fig 2, C; ISS 1 ovalbumin vs ovalbumin), and modestly reduced levels of BAL MMP-9 (P 5.05; Fig 2, E), but did not significantly reduce peribronchial MMP-9 immunostaining (Fig 2, F).
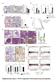
5 622 Cho et al J ALLERGY CLIN IMMUNOL MARCH 2006 FIG 3. Expression of TIMP-1 and collagen: modulation by ISS. The number of TIMP-1 1 peribronchial cells (A), epithelial TIMP-1 immunostaining (B), lung TIMP-1 measured by ELISA (C), peribronchial TIMP-1 stained area (D), levels of lung collagen (E), and peribronchial trichrome staining (F) were assessed at 1 and 3 months in mice challenged with ovalbumin (OVA) and treated with ISS. Repetitive ovalbumin challenge induces expression of TIMP-1 Increased numbers of TIMP-1 1 peribronchial cells (P 5.001; Fig 3, A) and TIMP-1 in the peribronchial extracellular matrix (Fig 1, E) were detected by immunohistochemistry after ovalbumin challenge. In contrast, ovalbumin challenge induced minimal TIMP-1 immunostaining in airway epithelial cells (Fig 1, E;Fig 3, B). Levels of lung TIMP-1 as measured by ELISA were also significantly increased in mice exposed to repetitive ovalbumin challenge ( vs ng TIMP-1/mg lung protein; ovalbumin 3 months vs no ovalbumin 3 months; P 5.001; Fig 3, C). The area of peribronchial TIMP-1 immunostaining in mice repetitively challenged with ovalbumin was also significantly greater than in control nonovalbumin-challenged mice ( vs mm 2 /mm circumference of bronchiole; P 5.001; Fig 3, D). Effect of ISS on TIMP-1 expression in vivo Immunostimulatory sequences of DNA administered for either 1 or 3 months significantly reduced levels of lung TIMP-1 as assessed by significant reductions in the number of peribronchial TIMP-1 1 cells (P 5.001; Fig 3, A) and level of peribronchial TIMP-1 immunostaining (P 5.001; Fig 3, D) in mice exposed to repetitive ovalbumin challenge. ISS administered for 3 months, but not for 1 month, reduced levels of lung TIMP-1 as assessed by ELISA (P 5.01; Fig 3, C). Effect of ISS on peribronchial collagen deposition Levels of total lung collagen (P 5.001; Fig 3, E) and the area of peribronchial trichrome staining (P 5.001; Fig 3, F) were significantly greater in mice that were repetitively challenged with ovalbumin for 1 or 3 months compared with control nonovalbumin-challenged mice. Administration of ISS to mice repetitively challenged with ovalbumin significantly reduced levels of lung collagen (P 5.05; Fig 3, E) at both 1 and 3 months. ISS reduced the area of peribronchial trichrome (P 5.001) staining at 3 months, but not at 1 month (Fig 3, F). Comparison of MMP-9, TIMP-1, and collagen expression after 1 month or 3 months of allergen challenge Overall, these studies show that MMP-9 (Fig 2), TIMP- 1(Fig 3), and lung collagen (Fig 3, E and F) are significantly induced after ovalbumin challenge for 1 month at approximately similar levels as noted after 3 months of ovalbumin challenge. The effect of ISS on reducing levels of MMP-9, TIMP-1, and collagen is not significantly different at 1 versus 3 months, although there appears to be a trend for greater ISS inhibitory effects on reducing levels of MMP-9 (Fig 2, E and F), TIMP-1 (Fig 3, C), and trichrome staining (Fig 3, F) at 3 months compared with 1 month. In contrast with the inhibitory effect of ISS on MMP-9, TIMP-1, and fibrosis, administration of an M-ODN to mice for as long as 3 months had no significant
6 J ALLERGY CLIN IMMUNOL VOLUME 117, NUMBER 3 Cho et al 623 FIG 4. Expression of TLR-9 by airway epithelial cells. Lung sections of nonovalbumin-challenged mice were stained with a control species and isotype matched antibody (A), and an anti TLR-9 Ab (B). After ovalbumin (OVA) challenge, epithelial cells in lung sections stained with an anti TLR-9 Ab continued to express TLR-9, as did peribronchial mononuclear cells (C). effect on reducing any of the parameters of ovalbumin induced MMP-9, TIMP-1, collagen, or trichrome staining (data not shown). Expression of TLR-9 the receptor for ISS by airway epithelial cells Lung sections of nonovalbumin-challenged mice stained with an anti TLR-9 Ab demonstrated significant staining of airway epithelial cells (Fig 4, B). A control species and isotype matched antibody did not stain airway epithelial cells in nonovalbumin-challenged lung sections (Fig 4, A). After ovalbumin challenge epithelial cells continued to express TLR-9, as did peribronchial mononuclear cells (Fig 4, C). Effect of ISS on macrophage MMP-9 expression in vitro Bone marrow derived macrophages incubated with LPS expressed significantly higher levels of MMP-9 in the supernatant compared with cells cultured in media alone ( vs MMP-9 zymography units; LPS vs no LPS; P 5.01). Incubation of bone marrow derived macrophages with ISS significantly reduced levels of MMP-9 expression in the supernatant ( vs MMP-9 zymography units; ISS 1 LPS vs LPS; P 5.05). Effect of ISS on BAL eosinophilia The absolute number of BAL eosinophils in mice sensitized to ovalbumin and repetitively challenged with ovalbumin was significantly greater than in control nonovalbumin-challenged mice ( vs BAL eosinophils; ovalbumin 3 months vs no ovalbumin 3 months; P ). Administration of ISS before initiation of repetitive ovalbumin challenges significantly reduced the absolute number of BAL eosinophils ( vs BAL eosinophils; ISS 1 ovalbumin 3 months vs ovalbumin 3 months; P 5.001). DISCUSSION In this study, we have demonstrated that allergen induced airway remodeling is associated with significantly increased levels of expression of MMP-9 and its inhibitor TIMP-1. Interestingly, immunostaining of lungs derived from mice with remodeled airways demonstrated a distinctly different pattern of MMP-9 expression compared with TIMP-1 expression in the remodeled airway, with MMP-9, but not TIMP-1, expressed in airway epithelium. Thus, the localized absence of expression of TIMP-1, an endogenous MMP-9 inhibitor, in the airway epithelium of mice with remodeled airways could contribute to the continued function of MMP-9 in the airway epithelium. In addition, we have demonstrated that ISS can inhibit expression of MMP-9 in airway epithelium in vivo, a tissue site where TIMP-1 is not significantly expressed in the remodeled airway. We have also demonstrated that airway epithelial cells in mouse lung express TLR-9, the receptor for ISS, raising the possibility that ISS could inhibit MMP-9 by acting directly on airway epithelial cells and/or acting indirectly on epithelial cells through effects on innate immune cells expressing TLR-9. To determine whether ISS could be acting on either innate immune cells (ie, TLR-9 expressing macrophages) or airway epithelial cells to inhibit MMP-9 expression, we performed in vitro studies with macrophages and epithelial cells to determine whether ISS inhibited MMP-9 expression. These studies demonstrated that ISS inhibited macrophage expression of MMP-9, suggesting that ISS effects on macrophages could contribute to reduced MMP-9 expression in the remodeled airway. Although we demonstrated that TLR-9 was expressed by a mouse airway epithelial cell line MLE-12 (data not shown), we were unable to induce MMP-9 expression in this cell line, making assessment of the ability of ISS to modulate airway epithelial MMP- 9 expression in this cell line not feasible (data not shown). Interestingly, the human airway epithelial transformed cell line BEAS 2B and primary human bronchial epithelial cells express TLR-9 as assessed by RT-PCR. 23 However,
7 624 Cho et al J ALLERGY CLIN IMMUNOL MARCH 2006 incubation of these epithelial cells with CpG did not induce GM-CSF or macrophage inflammatory protein 3-a release. 23 Thus, both mouse and human airway epithelial cells express TLR-9, but its function in epithelial cells in terms of modulating allergen induced MMP-9 or other mediator generation is currently unknown. To determine whether MMP-9 plays a role in the pathogenesis of airway remodeling, we have recently performed studies of airway remodeling in MMP-9 deficient mice (Lim et al, unpublished data, January 2006). In these studies, we demonstrated that ovalbumin-challenged MMP-9 deficient mice have reduced levels of peribronchial fibrosis compared with ovalbumin-challenged wildtype mice, suggesting that MMP-9 does play a role in promoting airway remodeling. However, because airway remodeling is reduced but not ablated in MMP-9 deficient mice, MMPs other than MMP-9 and/or alternate mediators that regulate collagen synthesis and breakdown are also likely to contribute to airway remodeling. We have also demonstrated that repetitive ovalbumin challenge not only induces expression of MMP-9 but also induces expression of an inhibitor of MMP-9, TIMP-1. At the transcriptional level, MMP-9 and TIMP-1 may be coregulated, such that activators of MMP-9 and TIMP-1 transcription (eg, LPS) will affect both genes in the same direction. 24 The effect of ISS on MMP-9 and TIMP-1 transcription is similar to that of corticosteroids, which are also able to inhibit both MMP-9 and TIMP-1 expression by macrophages. 25 The net effect of induction of MMP-9 as well as its inhibitor TIMP-1 on MMP-9 function will be dependent on the ratios of MMP-9 and TIMP-1 expressed, the localization of MMP-9 and TIMP-1 in the airway, and MMP-9 regulatory pathways other than TIMPs that play key roles in localizing the pericellular proteolytic activity of MMPs. 25 One of the assays that we have used to measure MMP-9 in BAL fluid is a functional assay assessing cleavage of the MMP-9 substrate gelatin. This functional MMP-9 zymography assay demonstrated significantly increased levels of MMP-9 bioactivity in BAL fluid after ovalbumin challenge, suggesting that although TIMP-1 had also been induced by repetitive ovalbumin challenge, it did not prevent repetitive ovalbumin challenge from inducing significant MMP-9 bioactivity in BAL. In summary, in this study we have demonstrated that allergen induced airway remodeling is associated with expression of MMP-9 in the remodeled airway in airway epithelium, as well as in peribronchial cells and the extracellular matrix. Administration of ISS to mice exposed to repetitive ovalbumin challenge significantly reduces levels of MMP-9 expression and peribronchial fibrosis. In vitro studies demonstrate that ISS can directly inhibit macrophage expression of MMP-9, and further studies are needed to determine whether ISS directly inhibits MMP-9 expression by airway epithelial cells that we have identified to express TLR-9 in lung sections. In vivo studies demonstrate that repetitive allergen challenge induces MMP-9 but not TIMP-1 expression in epithelium, providing a potential for increased MMP-9 bioactivity in the epithelium in the localized absence of its inhibitor. The ability of ISS to inhibit MMP-9 expression in epithelium may thus be particularly important to inhibiting MMP-9 function at this epithelial site where no expression of the MMP-9 inhibitor TIMP-1 is present. REFERENCES 1. Parks WC, Shapiro SD. Matrix metalloproteinases in lung biology. Respir Res 2001;2: Lemjabbar H, Gosset P, Lamblin C, Tillie I, Hartmann D, Wallaert B, et al. Contribution of 92 kda gelatinase/type IV collagenase in bronchial inflammation during status asthmaticus. Am J Respir Crit Care Med 1999;159: Vignola AM, Riccobono L, Mirabella A, Profita M, Chanez P, Bellia V, et al. Sputum metalloproteinase-9/tissue inhibitor of metalloproteinase-1 ratio correlates with airflow obstruction in asthma and chronic bronchitis. Am J Respir Crit Care Med 1998;158: Mautino G, Oliver N, Chanez P, Bousquet J, Capony F. Increased release of matrix metalloproteinase-9 in bronchoalveolar lavage fluid and by alveolar macrophages of asthmatics. Am J Respir Cell Mol Biol 1997; 17: Hoshino M, Nakamura Y, Sim J, Shimojo J, Isogai S. Bronchial subepithelial fibrosis and expression of matrix metalloproteinase-9 in asthmatic airway inflammation. J Allergy Clin Immunol 1998;102: Lee YC, Lee HB, Rhee YK, Song CH. The involvement of matrix metalloproteinase-9 in airway inflammation of patients with acute asthma. Clin Exp Allergy 2001;31: Tanaka H, Miyazaki N, Oashi K, Tanaka S, Ohmichi M, Abe S. Sputum matrix metalloproteinase-9: tissue inhibitor of metalloproteinase-1 ratio in acute asthma. J Allergy Clin Immunol 2000;105: Hoshino M, Takahashi M, Takai Y, Sim J. Inhaled corticosteroids decrease subepithelial collagen deposition by modulation of the balance between matrix metalloproteinase-9 and tissue inhibitor of metalloproteinase-1 expression in asthma. J Allergy Clin Immunol 1999;104: Bosse M, Chakir J, Rouabhia M, Boulet LP, Audette M, Laviolette M. Serum matrix metalloproteinase-9: tissue inhibitor of metalloproteinase-1 ratio correlates with steroid responsiveness in moderate to severe asthma. Am J Respir Crit Care Med 1999;159: Kelly EA, Busse WW, Jarjour NN. Increased matrix metalloproteinase-9 in the airway after allergen challenge. Am J Respir Crit Care Med 2000; 162: Dahlen B, Shute J, Howarth P. Immunohistochemical localisation of the matrix metalloproteinases MMP-3 and MMP-9 within the airways in asthma. Thorax 1999;54: Kumagai K, Ohno I, Okada S, Ohkawara Y, Suzuki K, Shinya T, et al. Inhibition of matrix metalloproteinases prevents allergen-induced airway inflammation in a murine model of asthma. J Immunol 1999;162: Cataldo DD, Tournoy KG, Vermaelen K, Munaut C, Foidart JM, Louis R, et al. Matrix metalloproteinase-9 deficiency impairs cellular infiltration and bronchial hyperresponsiveness during allergen-induced airway inflammation. Am J Pathol 2002;161: Vermaelen KY, Cataldo D, Tournoy K, Maes T, Dhulst A, Louis R, et al. Matrix metalloproteinase-9-mediated dendritic cell recruitment into the airways is a critical step in a mouse model of asthma. J Immunol 2003;171: Corry DB, Kiss A, Song LZ, Song L, Xu J, Lee SH, et al. Overlapping and independent contributions of MMP2 and MMP9 to lung allergic inflammatory cell egression through decreased CC chemokines. FASEB J 2004;18: Cho JY, Miller M, Baek KJ, Han JW, Nayar J, Rodriguez M, et al. Immunostimulatory DNA inhibits transforming growth factor-beta expression and airway remodeling. Am J Respir Cell Mol Biol 2004;30: Cho JY, Miller M, Baek KJ, Han JW, Nayar J, Lee SY, et al. Inhibition of airway remodeling in IL-5-deficient mice. J Clin Invest 2004;113: Cho JY, Miller M, Baek KJ, Han JW, Nayar J, Lee SY, et al. Immunostimulatory DNA reverses established allergen-induced airway remodeling. J Immunol 2004;173: Flood-Page P, Menzies-Gow A, Phipps S, Ying S, Wangoo A, Ludwig MS, et al. Anti-IL-5 treatment reduces deposition of ECM proteins in the bronchial subepithelial basement membrane of mild atopic asthmatics. J Clin Invest 2003;112:
8 J ALLERGY CLIN IMMUNOL VOLUME 117, NUMBER 3 Cho et al Broide D, Schwarze J, Tighe H, Gifford T, Nguyen MD, Malek S, et al. Immunostimulatory DNA sequences inhibit IL-5, eosinophilic inflammation, and airway hyperresponsiveness in mice. J Immunol 1998;161: Kline JN, Waldschmidt TJ, Businga TR, Lemish JE, Weinstock JV, Thorne PS, et al. Modulation of airway inflammation by CpG oligodeoxynucleotides in a murine model of asthma. J Immunol 1998;160: Sur S, Wild JS, Choudhury BK, Sur N, Alam R, Klinman DM. Long term prevention of allergic lung inflammation in a mouse model of asthma by CpG oligodeoxynucleotides. J Immunol 1999;162: Sha Q, Truong-Tran AQ, Pitt JR, Beck LA, Schleimer RP. Activation of airway epithelial cells by toll-like receptor agonists. Am J Respir Cell Mol Biol 2004;31: Shapiro SD, Campbell EJ, Kobayashi DK, Welgus HG. Dexamethasone selectively modulates basal and lipopolysaccharide-induced metalloproteinase and tissue inhibitor of metalloproteinase production by human alveolar macrophages. J Immunol 1991;146: Kheradmand F, Rishi K. The role of proteases in airway remodeling. In: Eissa NT, Huston D, editors. Therapeutic targets in airway inflammation: lung biology in health and disease, Vol 177. New York: Marcel Dekker; p
Inhibition of airway remodeling in IL-5 deficient mice
 Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Sputum matrix metalloproteases: comparison between chronic obstructive pulmonary disease and asthma
 Respiratory Medicine (25) 99, 73 71 Sputum matrix metalloproteases: comparison between chronic obstructive pulmonary disease and asthma S.V. Culpitt, D.F. Rogers, S.L. Traves, P.J. Barnes, L.E. Donnelly
Respiratory Medicine (25) 99, 73 71 Sputum matrix metalloproteases: comparison between chronic obstructive pulmonary disease and asthma S.V. Culpitt, D.F. Rogers, S.L. Traves, P.J. Barnes, L.E. Donnelly
COPD lungs show an attached stratified mucus layer that separate. bacteria from the epithelial cells resembling the protective colonic
 COPD lungs show an attached stratified mucus layer that separate bacteria from the epithelial cells resembling the protective colonic mucus SUPPLEMENTARY TABLES AND FIGURES Tables S1 S8, page 1 and separate
COPD lungs show an attached stratified mucus layer that separate bacteria from the epithelial cells resembling the protective colonic mucus SUPPLEMENTARY TABLES AND FIGURES Tables S1 S8, page 1 and separate
Circulating MMP-9 and TIMP-1 in acute exacerbations and after remission induced by oral corticosteroids in asthmatic children.
 Egypt J Pediatr Allergy Immunol 2006; 4(1):23-29. Original article Circulating MMP-9 and TIMP-1 in acute exacerbations and after remission induced by oral corticosteroids in asthmatic children. Background
Egypt J Pediatr Allergy Immunol 2006; 4(1):23-29. Original article Circulating MMP-9 and TIMP-1 in acute exacerbations and after remission induced by oral corticosteroids in asthmatic children. Background
Role of Tyk-2 in Th9 and Th17 cells in allergic asthma
 Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Neutrophil-derived matrix metalloproteinase-9 is increased in severe asthma and poorly inhibited by glucocorticoids
 Neutrophil-derived matrix metalloproteinase-9 is increased in severe asthma and poorly inhibited by glucocorticoids Meghan Cundall, MS, a Yongchang Sun, MD, b Christina Miranda, MS, PA, a John B. Trudeau,
Neutrophil-derived matrix metalloproteinase-9 is increased in severe asthma and poorly inhibited by glucocorticoids Meghan Cundall, MS, a Yongchang Sun, MD, b Christina Miranda, MS, PA, a John B. Trudeau,
Time Sequence of Airway Remodeling in a Mouse Model of Chronic Asthma: the Relation with Airway Hyperresponsiveness
 J Korean Med Sci 7; : 183-91 ISSN 111-893 Copyright The Korean Academy of Medical Sciences Time Sequence of Airway Remodeling in a Mouse Model of Chronic Asthma: the Relation with Airway Hyperresponsiveness
J Korean Med Sci 7; : 183-91 ISSN 111-893 Copyright The Korean Academy of Medical Sciences Time Sequence of Airway Remodeling in a Mouse Model of Chronic Asthma: the Relation with Airway Hyperresponsiveness
The recruitment of bone marrow-derived eosinophils from
 Anti-Siglec-F Antibody Reduces Allergen-Induced Eosinophilic Inflammation and Airway Remodeling 1 Dae Jin Song,* Jae Youn Cho,* Sang Yeub Lee,* Marina Miller,* Peter Rosenthal,* Pejman Soroosh, Michael
Anti-Siglec-F Antibody Reduces Allergen-Induced Eosinophilic Inflammation and Airway Remodeling 1 Dae Jin Song,* Jae Youn Cho,* Sang Yeub Lee,* Marina Miller,* Peter Rosenthal,* Pejman Soroosh, Michael
Soluble ADAM33 initiates airway remodeling to promote susceptibility for. Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David I Wilson,
 Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Identifying Biologic Targets to Attenuate or Eliminate Asthma Exacerbations
 Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Research Article Matrix Metalloproteinases-9 (MMPs-9) and -12 Are Upregulated in the Airways of Mice with Chronic Airway Inflammation and Remodeling
 International Scholarly Research Network ISRN Pulmonology Volume 2012, Article ID 840489, 7 pages doi:10.5402/2012/840489 Research Article Matrix Metalloproteinases-9 (MMPs-9) and -12 Are Upregulated in
International Scholarly Research Network ISRN Pulmonology Volume 2012, Article ID 840489, 7 pages doi:10.5402/2012/840489 Research Article Matrix Metalloproteinases-9 (MMPs-9) and -12 Are Upregulated in
Distinct structural changes occur in the airways of. Matrix Metalloproteinase-9 Expression in Asthma*
 Matrix Metalloproteinase-9 Expression in Asthma* Effect of Asthma Severity, Allergen Challenge, and Inhaled Corticosteroids Waldo Mattos, MD; Sam Lim, MBBS; Richard Russell, MB; Anon Jatakanon, MD; K.
Matrix Metalloproteinase-9 Expression in Asthma* Effect of Asthma Severity, Allergen Challenge, and Inhaled Corticosteroids Waldo Mattos, MD; Sam Lim, MBBS; Richard Russell, MB; Anon Jatakanon, MD; K.
Interplay between matrix metalloproteinase-9 and tissue inhibitor of matrix metalloproteinase-1 in acute asthma exacerbation and airway remodeling
 Egyptian Journal of Chest Diseases and Tuberculosis (2012) 61, 35 39 The Egyptian Society of Chest Diseases and Tuberculosis Egyptian Journal of Chest Diseases and Tuberculosis www.elsevier.com/locate/ejcdt
Egyptian Journal of Chest Diseases and Tuberculosis (2012) 61, 35 39 The Egyptian Society of Chest Diseases and Tuberculosis Egyptian Journal of Chest Diseases and Tuberculosis www.elsevier.com/locate/ejcdt
Original Article CXCR4 inhibitor attenuates allergen-induced lung inflammation by down-regulating MMP-9 and ERK1/2
 Int J Clin Exp Pathol 2015;8(6):6700-6707 www.ijcep.com /ISSN:1936-2625/IJCEP0007873 Original Article CXCR4 inhibitor attenuates allergen-induced lung inflammation by down-regulating MMP-9 and ERK1/2 Huilong
Int J Clin Exp Pathol 2015;8(6):6700-6707 www.ijcep.com /ISSN:1936-2625/IJCEP0007873 Original Article CXCR4 inhibitor attenuates allergen-induced lung inflammation by down-regulating MMP-9 and ERK1/2 Huilong
Immunostimulatory oligonucleotides block allergic airway inflammation by inhibiting Th2 cell activation and IgE-mediated cytokine induction
 Immunostimulatory oligonucleotides block allergic airway inflammation by inhibiting Th2 cell activation and IgE-mediated cytokine induction Edith M. Hessel, 1 Mabel Chu, 1 Jennifer O. Lizcano, 1 Bonnie
Immunostimulatory oligonucleotides block allergic airway inflammation by inhibiting Th2 cell activation and IgE-mediated cytokine induction Edith M. Hessel, 1 Mabel Chu, 1 Jennifer O. Lizcano, 1 Bonnie
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Bronchial Hyperresponsiveness. Defining Asthma: Clinical Criteria. Impaired Ventilation in Asthma. Dynamic Imaging of Asthma
 Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Supplementary Information
 Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Airway Inflammation and Allergen Specific IgE Production May Persist Longer Than Airway Hyperresponsiveness in Mice
 J Korean Med Sci 24; 19: 69-73 ISSN 111-8934 Copyright The Korean Academy of Medical Sciences Airway Inflammation and Allergen Specific IgE Production May Persist Longer Than Airway Hyperrespoiveness in
J Korean Med Sci 24; 19: 69-73 ISSN 111-8934 Copyright The Korean Academy of Medical Sciences Airway Inflammation and Allergen Specific IgE Production May Persist Longer Than Airway Hyperrespoiveness in
Kun Jiang 1, He-Bin Chen 1, Ying Wang 1, Jia-Hui Lin 2, Yan Hu 1, Yu-Rong Fang 1
 Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Original Article Changes in interleukin-17 and transforming growth factor beta 1 levels in serum and bronchoalveolar lavage fluid and their clinical significance among children with asthma Kun Jiang 1,
Eosinophilic esophagitis (EoE) is a clinicopathologic disorder
 ORIGINAL ARTICLE: GASTROENTEROLOGY Siglec-F Inhibition Reduces Esophageal Eosinophilia and Angiogenesis in a Mouse Model of Eosinophilic Esophagitis Eitan Rubinstein, y Jae Youn Cho, y Peter Rosenthal,
ORIGINAL ARTICLE: GASTROENTEROLOGY Siglec-F Inhibition Reduces Esophageal Eosinophilia and Angiogenesis in a Mouse Model of Eosinophilic Esophagitis Eitan Rubinstein, y Jae Youn Cho, y Peter Rosenthal,
Abstract. IgE. IgE Th2. x x IL-4 IL-5 IgE CD4 +
 D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
Supplemental Table 1. Primer sequences for transcript analysis
 Supplemental Table 1. Primer sequences for transcript analysis Primer Sequence (5 3 ) Primer Sequence (5 3 ) Mmp2 Forward CCCGTGTGGCCCTC Mmp15 Forward CGGGGCTGGCT Reverse GCTCTCCCGGTTTC Reverse CCTGGTGTGCCTGCTC
Supplemental Table 1. Primer sequences for transcript analysis Primer Sequence (5 3 ) Primer Sequence (5 3 ) Mmp2 Forward CCCGTGTGGCCCTC Mmp15 Forward CGGGGCTGGCT Reverse GCTCTCCCGGTTTC Reverse CCTGGTGTGCCTGCTC
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Matrix metalloproteinases and TIMP-1 production by peripheral blood granulocytes from COPD patients and asthmatics
 Matrix metalloproteinases and TIMP-1 production by peripheral blood granulocytes from COPD patients and asthmatics D. Cataldo 1,2, C. Munaut 2, A. Noël 2, F. Frankenne 2, P. Bartsch 1, J. M. Foidart 2,
Matrix metalloproteinases and TIMP-1 production by peripheral blood granulocytes from COPD patients and asthmatics D. Cataldo 1,2, C. Munaut 2, A. Noël 2, F. Frankenne 2, P. Bartsch 1, J. M. Foidart 2,
Impact of Asthma in the U.S. per Year. Asthma Epidemiology and Pathophysiology. Risk Factors for Asthma. Childhood Asthma Costs of Asthma
 American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
Allergen-induced peribronchial fibrosis and mucus production mediated by I B kinase -dependent genes in airway epithelium
 Allergen-induced peribronchial fibrosis and mucus production mediated by I B kinase -dependent genes in airway epithelium David H. Broide*, Toby Lawrence, Taylor Doherty*, Jae Youn Cho*, Marina Miller*,
Allergen-induced peribronchial fibrosis and mucus production mediated by I B kinase -dependent genes in airway epithelium David H. Broide*, Toby Lawrence, Taylor Doherty*, Jae Youn Cho*, Marina Miller*,
Interleukin-4 and interleukin-13 induce fibronectin production by human lung fibroblasts
 Allergology International (2001) 50: 197 202 Original Article Interleukin-4 and interleukin-13 induce fibronectin production by human lung fibroblasts Tatsuya Machino, Shu Hashimoto, Yasuhiro Gon, Kosei
Allergology International (2001) 50: 197 202 Original Article Interleukin-4 and interleukin-13 induce fibronectin production by human lung fibroblasts Tatsuya Machino, Shu Hashimoto, Yasuhiro Gon, Kosei
Bronchial hyperresponsiveness is generally assessed by
 Provocation With Adenosine 5 -Monophosphate Increases Sputum Eosinophils* Maarten van den Berge, MD; H.A.M. Kerstjens, PhD; D.M. de Reus; H.F. Kauffman, PhD; G.H. Koëter, PhD; and D.S. Postma, PhD (CHEST
Provocation With Adenosine 5 -Monophosphate Increases Sputum Eosinophils* Maarten van den Berge, MD; H.A.M. Kerstjens, PhD; D.M. de Reus; H.F. Kauffman, PhD; G.H. Koëter, PhD; and D.S. Postma, PhD (CHEST
The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma
 Ph.D Thesis The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma By Attila Kiss M.D. Semmelweis University Doctoral School Semmelweis University Faculty of Pulmonology
Ph.D Thesis The role of exogen proteases in Th 2 cell differentiation and in the pathogenesis of asthma By Attila Kiss M.D. Semmelweis University Doctoral School Semmelweis University Faculty of Pulmonology
Diagnosis and Management of Fungal Allergy Monday, 9-139
 Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Diagnosis and Management of Fungal Allergy Monday, 9-139 13-2010 Alan P. Knutsen,, MD Director, Pediatric Allergy & Immunology Director, Jeffrey Modell Diagnostic Center for Primary Immunodeficiencies
Effects of CpG oligodeoxynucleotide on transcription factors GATA-3 and T-bet mrna expression in asthmatic mice
 Acta Pharmacologica Sinica 2005 Sep; 26 (9): 1117 1122 Full-length article Effects of CpG oligodeoxynucleotide on transcription factors GATA-3 and T-bet mrna expression in asthmatic mice Zu-qun WU 1,2,
Acta Pharmacologica Sinica 2005 Sep; 26 (9): 1117 1122 Full-length article Effects of CpG oligodeoxynucleotide on transcription factors GATA-3 and T-bet mrna expression in asthmatic mice Zu-qun WU 1,2,
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung
 IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
IKKα Causes Chromatin Modification on Pro-Inflammatory Genes by Cigarette Smoke in Mouse Lung Se-Ran Yang, Samantha Valvo, Hongwei Yao, Aruna Kode, Saravanan Rajendrasozhan, Indika Edirisinghe, Samuel
IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells
 IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells Jennifer A. Mitchel, Silvio Antoniak, Joo-Hyeon Lee, Sae-Hoon Kim, Maureen McGill, David I. Kasahara,
IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells Jennifer A. Mitchel, Silvio Antoniak, Joo-Hyeon Lee, Sae-Hoon Kim, Maureen McGill, David I. Kasahara,
Airway Inflammation in Asthma Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan.
 REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
Phenotypes of asthma; implications for treatment. Medical Grand Rounds Feb 2018 Jim Martin MD DSc
 Phenotypes of asthma; implications for treatment Medical Grand Rounds Feb 2018 Jim Martin MD DSc No conflicts to declare Objectives To understand the varied clinical forms of asthma To understand the pathobiologic
Phenotypes of asthma; implications for treatment Medical Grand Rounds Feb 2018 Jim Martin MD DSc No conflicts to declare Objectives To understand the varied clinical forms of asthma To understand the pathobiologic
Interleukin-13 Dependent Expression of Matrix Metalloproteinase-12 Is Required for the Development of Airway Eosinophilia in Mice
 Interleukin-13 Dependent Expression of Matrix Metalloproteinase-12 Is Required for the Development of Airway Eosinophilia in Mice Mahmoud A. Pouladi, Clinton S. Robbins, Filip K. Swirski, Meghan Cundall,
Interleukin-13 Dependent Expression of Matrix Metalloproteinase-12 Is Required for the Development of Airway Eosinophilia in Mice Mahmoud A. Pouladi, Clinton S. Robbins, Filip K. Swirski, Meghan Cundall,
Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma
 Research article Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma Mang Yu, 1 Michael R. Eckart, 2 Alexander A. Morgan, 3 Kaori Mukai, 1 Atul J. Butte, 3 Mindy Tsai, 1 and Stephen
Research article Identification of an IFN-γ/mast cell axis in a mouse model of chronic asthma Mang Yu, 1 Michael R. Eckart, 2 Alexander A. Morgan, 3 Kaori Mukai, 1 Atul J. Butte, 3 Mindy Tsai, 1 and Stephen
B220 CD4 CD8. Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN
 B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
Epithelial interleukin-25 is a key mediator in Th2-high, corticosteroid-responsive
 Online Data Supplement: Epithelial interleukin-25 is a key mediator in Th2-high, corticosteroid-responsive asthma Dan Cheng, Zheng Xue, Lingling Yi, Huimin Shi, Kan Zhang, Xiaorong Huo, Luke R. Bonser,
Online Data Supplement: Epithelial interleukin-25 is a key mediator in Th2-high, corticosteroid-responsive asthma Dan Cheng, Zheng Xue, Lingling Yi, Huimin Shi, Kan Zhang, Xiaorong Huo, Luke R. Bonser,
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
JOURNAL OF PHYSIOLOGY AND PHARMACOLOGY 2008, 59, Suppl 6,
 JOURNAL OF PHYSIOLOGY AND PHARMACOLOGY 2008, 59, Suppl 6, 145 152 www.jpp.krakow.pl B. BRAJER 1, H. BATURA-GABRYEL 1, A. NOWICKA 1, B. KUZNAR-KAMINSKA 1, A. SZCZEPANIK 2 CONCENTRATION OF MATRIX METALLOPROTEINASE-9
JOURNAL OF PHYSIOLOGY AND PHARMACOLOGY 2008, 59, Suppl 6, 145 152 www.jpp.krakow.pl B. BRAJER 1, H. BATURA-GABRYEL 1, A. NOWICKA 1, B. KUZNAR-KAMINSKA 1, A. SZCZEPANIK 2 CONCENTRATION OF MATRIX METALLOPROTEINASE-9
Increase in macrophage elastase (MMP-12) in lungs from patients with chronic obstructive pulmonary disease
 Inflamm. res. 54 (2005) 31 36 1023-3830/05/010031-06 DOI 10.1007/s00011-004-1319-4 Birkhäuser Verlag, Basel, 2005 Inflammation Research Increase in macrophage elastase (MMP-12) in lungs from patients with
Inflamm. res. 54 (2005) 31 36 1023-3830/05/010031-06 DOI 10.1007/s00011-004-1319-4 Birkhäuser Verlag, Basel, 2005 Inflammation Research Increase in macrophage elastase (MMP-12) in lungs from patients with
Property of Presenter
 Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Have We Missed A Role For Neutrophils In Asthma? In Steroid-Refractory Asthma? Erwin W. Gelfand, MD Chairman, Department of Pediatrics National Jewish Health Professor of Pediatrics and Immunology University
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation
 Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
Abhd2 regulates alveolar type Ⅱ apoptosis and airway smooth muscle remodeling: a key target of COPD research
 Abhd2 regulates alveolar type Ⅱ apoptosis and airway smooth muscle remodeling: a key target of COPD research Shoude Jin Harbin Medical University, China Background COPD ------ a silent killer Insidious,
Abhd2 regulates alveolar type Ⅱ apoptosis and airway smooth muscle remodeling: a key target of COPD research Shoude Jin Harbin Medical University, China Background COPD ------ a silent killer Insidious,
Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice
 Disease Models & Mechanisms, 75-8 (9) doi:1.14/dmm.1859 RESEARCH ARTICLE Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice Franco A. DiGiovanni
Disease Models & Mechanisms, 75-8 (9) doi:1.14/dmm.1859 RESEARCH ARTICLE Concurrent dual allergen exposure and its effects on airway hyperresponsiveness, inflammation and remodeling in mice Franco A. DiGiovanni
CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma
 Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Raemdonck et al. Respiratory Research (2016)17:45 DOI 10.1186/s12931-016-0359-y RESEARCH CD4 + and CD8 + T cells play a central role in a HDM driven model of allergic asthma Open Access Kristof Raemdonck
Supplementary Figure 1 Protease allergens induce IgE and IgG1 production. (a-c)
 1 Supplementary Figure 1 Protease allergens induce IgE and IgG1 production. (a-c) Serum IgG1 (a), IgM (b) and IgG2 (c) concentrations in response to papain immediately before primary immunization (day
1 Supplementary Figure 1 Protease allergens induce IgE and IgG1 production. (a-c) Serum IgG1 (a), IgM (b) and IgG2 (c) concentrations in response to papain immediately before primary immunization (day
Pathogenesis of asthma
 Med Clin N Am 86 (2002) 925 936 Pathogenesis of asthma Nizar N. Jarjour, MD*, Elizabeth A.B. Kelly, PhD Section of Pulmonary and Critical Care Medicine, 600 Highland Avenue, CSC K4/930, University of Wisconsin
Med Clin N Am 86 (2002) 925 936 Pathogenesis of asthma Nizar N. Jarjour, MD*, Elizabeth A.B. Kelly, PhD Section of Pulmonary and Critical Care Medicine, 600 Highland Avenue, CSC K4/930, University of Wisconsin
Topical nanocrystalline silver cream inhibits expression of matrix metalloproteinase-9 in animal models of allergic contact dermatitis.
 Topical nanocrystalline silver cream inhibits expression of matrix metalloproteinase-9 in animal models of allergic contact dermatitis. K C Bhol, P J Schechter NUCRYST Pharmaceuticals Inc, Wakefield, MA
Topical nanocrystalline silver cream inhibits expression of matrix metalloproteinase-9 in animal models of allergic contact dermatitis. K C Bhol, P J Schechter NUCRYST Pharmaceuticals Inc, Wakefield, MA
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis
 Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Chronic Cough Due to Nonasthmatic Eosinophilic Bronchitis. ACCP Evidence-Based Clinical Practice Guidelines
 Chronic Cough Due to Nonasthmatic Eosinophilic Bronchitis ACCP Evidence-Based Clinical Practice Guidelines Christopher E. Brightling, MBBS, PhD, FCCP Objectives: Nonasthmatic eosinophilic bronchitis is
Chronic Cough Due to Nonasthmatic Eosinophilic Bronchitis ACCP Evidence-Based Clinical Practice Guidelines Christopher E. Brightling, MBBS, PhD, FCCP Objectives: Nonasthmatic eosinophilic bronchitis is
Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline
 Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
RESPIRATORY BLOCK. Bronchial Asthma. Dr. Maha Arafah Department of Pathology KSU
 RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
Monitoring sputum eosinophils in mucosal inflammation and remodelling: a pilot study
 Eur Respir J 2010; 35: 48 53 DOI: 10.1183/09031936.00130008 CopyrightßERS Journals Ltd 2010 Monitoring sputum eosinophils in mucosal inflammation and remodelling: a pilot study J. Chakir*, L. Loubaki*,
Eur Respir J 2010; 35: 48 53 DOI: 10.1183/09031936.00130008 CopyrightßERS Journals Ltd 2010 Monitoring sputum eosinophils in mucosal inflammation and remodelling: a pilot study J. Chakir*, L. Loubaki*,
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
MMP-9 protein level does not reflect overall MMP activity in the airways of patients with COPD
 Respiratory Medicine (2008) 102, 845 851 MMP-9 protein level does not reflect overall MMP activity in the airways of patients with Gillian E. Lowrey a,b, Neil Henderson b, John D. Blakey b, Jonathan M.
Respiratory Medicine (2008) 102, 845 851 MMP-9 protein level does not reflect overall MMP activity in the airways of patients with Gillian E. Lowrey a,b, Neil Henderson b, John D. Blakey b, Jonathan M.
December 7, 2010 Future Use of Biologics in Allergy and Asthma
 December 7, 2010 Future Use of Biologics in Allergy and Asthma Lanny J. Rosenwasser, M.D. Dee Lyons/Missouri Endowed Chair in Immunology Research Professor of Pediatrics Allergy-Immunology Division Childrens
December 7, 2010 Future Use of Biologics in Allergy and Asthma Lanny J. Rosenwasser, M.D. Dee Lyons/Missouri Endowed Chair in Immunology Research Professor of Pediatrics Allergy-Immunology Division Childrens
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과
 감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic
 Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Chemical Chaperones Mitigate Experimental Asthma By Attenuating Endoplasmic Reticulum Stress Lokesh Makhija, BE, Veda Krishnan, MSc, Rakhshinda Rehman, MTech, Samarpana Chakraborty, MSc, Shuvadeep Maity,
Interleukin-17 cytokine signalling in patients with asthma
 BACK TO BASICS CYTOKINE SIGNALLING IN ASTHMA Interleukin-17 cytokine signalling in patients with asthma Anders Lindén 1,2 and Barbro Dahlén 2 Affiliations: 1 Unit for Lung and Airway Research, Institute
BACK TO BASICS CYTOKINE SIGNALLING IN ASTHMA Interleukin-17 cytokine signalling in patients with asthma Anders Lindén 1,2 and Barbro Dahlén 2 Affiliations: 1 Unit for Lung and Airway Research, Institute
Alveolar macrophages modulate allergic inflammation in a murine model of asthma
 EXPERIMENTAL and MOLECULAR MEDICINE, Vol. 43, No. 5, 275-280, May 2011 Alveolar macrophages modulate allergic inflammation in a murine model of asthma Bo-Ram Bang 1,2, Eunyoung Chun 1,2, Eun-Jin Shim 1,2,
EXPERIMENTAL and MOLECULAR MEDICINE, Vol. 43, No. 5, 275-280, May 2011 Alveolar macrophages modulate allergic inflammation in a murine model of asthma Bo-Ram Bang 1,2, Eunyoung Chun 1,2, Eun-Jin Shim 1,2,
Fibrosis and Remodeling in EoE
 Fibrosis and Remodeling in EoE Seema S. Aceves, M.D., Ph.D. Division of Allergy, Immunology University of California, San Diego Rady Children s Hospital, San Diego Faculty Disclosure Co-inventor of OVB
Fibrosis and Remodeling in EoE Seema S. Aceves, M.D., Ph.D. Division of Allergy, Immunology University of California, San Diego Rady Children s Hospital, San Diego Faculty Disclosure Co-inventor of OVB
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Functional Effects of TGF-beta1 on Mesenchymal Stem Cell Mobilization in Cockroach Allergen Induced Asthma
 Functional Effects of TGF-beta1 on Mesenchymal Stem Cell Mobilization in Cockroach Allergen Induced Asthma Pei-Song Gao, MD, PhD Division of Allergy & Clinical Immunology Johns Hopkins University School
Functional Effects of TGF-beta1 on Mesenchymal Stem Cell Mobilization in Cockroach Allergen Induced Asthma Pei-Song Gao, MD, PhD Division of Allergy & Clinical Immunology Johns Hopkins University School
CONTRACTING ORGANIZATION: West Virginia University Research Corporation Morgantown, WV
 AD Award Number: DAMD17-2-1-23 TITLE: Bone Marrow Function in Development of Childhood Asthma PRINCIPAL INVESTIGATOR: Mary Beth Hogan, M.D. CONTRACTING ORGANIZATION: West Virginia University Research Corporation
AD Award Number: DAMD17-2-1-23 TITLE: Bone Marrow Function in Development of Childhood Asthma PRINCIPAL INVESTIGATOR: Mary Beth Hogan, M.D. CONTRACTING ORGANIZATION: West Virginia University Research Corporation
DNA vaccine, peripheral T-cell tolerance modulation 185
 Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
10.00 PBS OVA OVA+isotype antibody 8.00 OVA+anti-HMGB1. PBS Methatroline (mg/ml)
 RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
RESEARCH ARTICLE Penh (100% of PBS) 1 PBS 8.00 +anti-hmgb1 6.00 4.00 p=0.054 Cellular & Molecular Immunology advance online publication, PBS 3.12 6.25 Methatroline (mg/ml) Neutrophil isolation and culture
Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response
 Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Combining an epithelial repair factor and antifibrotic with a corticosteroid offers optimal treatment for allergic airways disease
 BJP British Journal of Pharmacology RESEARCH PAPER British Journal of Pharmacology (2016) 173 2016 2029 2016 Combining an epithelial repair factor and antifibrotic with a corticosteroid offers optimal
BJP British Journal of Pharmacology RESEARCH PAPER British Journal of Pharmacology (2016) 173 2016 2029 2016 Combining an epithelial repair factor and antifibrotic with a corticosteroid offers optimal
Current Asthma Therapy: Little Need to Phenotype. Phenotypes of Severe Asthma. Cellular Phenotypes 12/7/2012
 Subbasement Membrane Thickness(µm) 12/7/212 Current Asthma Therapy: Little Need to Phenotype Phenotypes of Severe Asthma Most mild and to some degree moderate asthmatics respond well to currently available
Subbasement Membrane Thickness(µm) 12/7/212 Current Asthma Therapy: Little Need to Phenotype Phenotypes of Severe Asthma Most mild and to some degree moderate asthmatics respond well to currently available
The activin A antagonist follistatin inhibits asthmatic airway remodelling
 Additional supplementary files are published online only. To view these files please visit the journal online (http://dx. doi.org/10.1136/thoraxjnl- 2011-201128). 1 Department of Immunology, Monash University,
Additional supplementary files are published online only. To view these files please visit the journal online (http://dx. doi.org/10.1136/thoraxjnl- 2011-201128). 1 Department of Immunology, Monash University,
The activin A antagonist follistatin inhibits asthmatic airway remodelling
 Thorax Online First, published on October 10, 2012 as 10.1136/thoraxjnl-2011-201128 Asthma Additional supplementary files are published online only. To view these files please visit the journal online
Thorax Online First, published on October 10, 2012 as 10.1136/thoraxjnl-2011-201128 Asthma Additional supplementary files are published online only. To view these files please visit the journal online
Special Issue on CleanWAS 2015
 Open Life Sci. 2016; 11: 498 505 Special Issue on CleanWAS 2015 Open Access Yujuan Chen, Yanlu Gao, Muhammad Aqeel Ashraf, Wei Gao* Effects of the Traditional Chinese Medicine on Airway Remodeling in Rats
Open Life Sci. 2016; 11: 498 505 Special Issue on CleanWAS 2015 Open Access Yujuan Chen, Yanlu Gao, Muhammad Aqeel Ashraf, Wei Gao* Effects of the Traditional Chinese Medicine on Airway Remodeling in Rats
Induced sputum to assess airway inflammation: a study of reproducibility
 Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Supplementary Figure 1: STAT3 suppresses Kras-induced lung tumorigenesis
 Supplementary Figure 1: STAT3 suppresses Kras-induced lung tumorigenesis (a) Immunohistochemical (IHC) analysis of tyrosine 705 phosphorylation status of STAT3 (P- STAT3) in tumors and stroma (all-time
Supplementary Figure 1: STAT3 suppresses Kras-induced lung tumorigenesis (a) Immunohistochemical (IHC) analysis of tyrosine 705 phosphorylation status of STAT3 (P- STAT3) in tumors and stroma (all-time
TITLE: Genes Associated with Food Allergy and Eosinophilic Esophagitis
 AD Award Number: W81XWH-1-1-75 TITLE: Genes Associated with Food Allergy and Eosinophilic Esophagitis PRINCIPAL INVESTIGATOR: Dr. David Broide CONTRACTING ORGANIZATION: University of California, San Diego
AD Award Number: W81XWH-1-1-75 TITLE: Genes Associated with Food Allergy and Eosinophilic Esophagitis PRINCIPAL INVESTIGATOR: Dr. David Broide CONTRACTING ORGANIZATION: University of California, San Diego
GSI Canine IL-5 ELISA Kit-2 Plates DataSheet
 Interleukin5 (IL5) is a secreted glycoprotein that belongs to the α-helical group of cytokines (1, 2, 3). Unlike other family members, it is present as a covalently linked antiparallel dimer (4, 5). IL-5
Interleukin5 (IL5) is a secreted glycoprotein that belongs to the α-helical group of cytokines (1, 2, 3). Unlike other family members, it is present as a covalently linked antiparallel dimer (4, 5). IL-5
CHAPTER I INTRODUCTION. Nowadays chronic kidney disease (CKD) becomes one. of the most common diseases found in the population.
 CHAPTER I INTRODUCTION I.1 Background Nowadays chronic kidney disease (CKD) becomes one of the most common diseases found in the population. Based on community survey that is held by PERNEFRI (Perhimpunan
CHAPTER I INTRODUCTION I.1 Background Nowadays chronic kidney disease (CKD) becomes one of the most common diseases found in the population. Based on community survey that is held by PERNEFRI (Perhimpunan
The role of mucosal innate immunity in allergic rhinitis Ji-Hwan Ryu
 The role of mucosal innate immunity in allergic rhinitis Ji-Hwan Ryu Research Center for Human Natural Defense system College of Medicine Yonsei University Mucosal epithelium in innate immunity Mucosal
The role of mucosal innate immunity in allergic rhinitis Ji-Hwan Ryu Research Center for Human Natural Defense system College of Medicine Yonsei University Mucosal epithelium in innate immunity Mucosal
COPYRIGHTED MATERIAL. Definition and Pathology CHAPTER 1. John Rees
 CHAPTER 1 Definition and Pathology John Rees Sherman Education Centre, Guy s Hospital, London, UK OVERVIEW Asthma is an overall descriptive term but there are a number of more or less distinct phenotypes
CHAPTER 1 Definition and Pathology John Rees Sherman Education Centre, Guy s Hospital, London, UK OVERVIEW Asthma is an overall descriptive term but there are a number of more or less distinct phenotypes
The Effect of BTP on the Development of Allergic Asthma in Mice
 93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
C urrent understanding of asthma defines it
 163 OCCASIONAL REVIEW Pharmacotherapy and airway remodelling in asthma? P A Beckett, P H Howarth... Over the last few decades attention has largely focused on airway inflammation in asthma, but more recently
163 OCCASIONAL REVIEW Pharmacotherapy and airway remodelling in asthma? P A Beckett, P H Howarth... Over the last few decades attention has largely focused on airway inflammation in asthma, but more recently
Small Airways Disease. Respiratory Function In Small Airways And Asthma. Pathophysiologic Changes in the Small Airways of Asthma Patients
 Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained
 1 2 3 4 5 6 7 8 9 10 11 Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained jejunum sections ( 200 magnification;
1 2 3 4 5 6 7 8 9 10 11 Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained jejunum sections ( 200 magnification;
colorimetric sandwich ELISA kit datasheet
 colorimetric sandwich ELISA kit datasheet For the quantitative detection of human IL5 in serum, plasma, cell culture supernatants and urine. general information Catalogue Number Product Name Species cross-reactivity
colorimetric sandwich ELISA kit datasheet For the quantitative detection of human IL5 in serum, plasma, cell culture supernatants and urine. general information Catalogue Number Product Name Species cross-reactivity
COPD: From Phenotypes to Endotypes. MeiLan K Han, M.D., M.S. Associate Professor of Medicine University of Michigan, Ann Arbor, MI
 COPD: From Phenotypes to Endotypes MeiLan K Han, M.D., M.S. Associate Professor of Medicine University of Michigan, Ann Arbor, MI Presenter Disclosures MeiLan K. Han Consulting Research support Novartis
COPD: From Phenotypes to Endotypes MeiLan K Han, M.D., M.S. Associate Professor of Medicine University of Michigan, Ann Arbor, MI Presenter Disclosures MeiLan K. Han Consulting Research support Novartis
Supplementary information
 Supplementary information Supplementary Figure S1: Ex[Ca 2+ ]-induced IL-1ß production of monocytes primed with different TLR ligands IL-1ß release of CD14+ monocytes in response to stimulation for 16
Supplementary information Supplementary Figure S1: Ex[Ca 2+ ]-induced IL-1ß production of monocytes primed with different TLR ligands IL-1ß release of CD14+ monocytes in response to stimulation for 16
Immunostimulatory DNA inhibits IL-4 dependent IgE synthesis by human B cells
 Immunostimulatory DNA inhibits IL-4 dependent IgE synthesis by human B cells Anthony A. Horner, MD, a,c George F. Widhopf, PhD, a,c Jan A. Burger, MD, a,c Kenji Takabayashi, PhD, a,c Nadya Cinman, BA,
Immunostimulatory DNA inhibits IL-4 dependent IgE synthesis by human B cells Anthony A. Horner, MD, a,c George F. Widhopf, PhD, a,c Jan A. Burger, MD, a,c Kenji Takabayashi, PhD, a,c Nadya Cinman, BA,
Chronic cough is defined as a cough persisting for. Airway Inflammation as an Assessment of Chronic Nonproductive Cough*
 Airway Inflammation as an Assessment of Chronic Nonproductive Cough* Sang Yeub Lee, MD ; Jae Youn Cho, MD; Jae Jeong Shim, MD; Han Kyeom Kim, MD; Kyung Ho Kang, MD, FCCP; Se Hwa Yoo, MD; and Kwang Ho In,
Airway Inflammation as an Assessment of Chronic Nonproductive Cough* Sang Yeub Lee, MD ; Jae Youn Cho, MD; Jae Jeong Shim, MD; Han Kyeom Kim, MD; Kyung Ho Kang, MD, FCCP; Se Hwa Yoo, MD; and Kwang Ho In,
Introduction. Acute sodium overload produces renal tubulointerstitial inflammation in normal rats
 Acute sodium overload produces renal tubulointerstitial inflammation in normal rats MI Roson, et al. Kidney International (2006) Introduction Present by Kanya Bunnan and Wiraporn paebua Tubular sodium
Acute sodium overload produces renal tubulointerstitial inflammation in normal rats MI Roson, et al. Kidney International (2006) Introduction Present by Kanya Bunnan and Wiraporn paebua Tubular sodium
To compare the relative amount of of selected gene expression between sham and
 Supplementary Materials and Methods Gene Expression Analysis To compare the relative amount of of selected gene expression between sham and mice given renal ischemia-reperfusion injury (IRI), ncounter
Supplementary Materials and Methods Gene Expression Analysis To compare the relative amount of of selected gene expression between sham and mice given renal ischemia-reperfusion injury (IRI), ncounter
Distinction and Overlap. Allergy Dpt, 2 nd Pediatric Clinic, University of Athens
 Asthma Phenotypes: Distinction and Overlap Nikos Papadopoulos Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Asthma as a syndrome From the Iliad to ADAM 33 and back again Bronchoconstriction,
Asthma Phenotypes: Distinction and Overlap Nikos Papadopoulos Allergy Dpt, 2 nd Pediatric Clinic, University of Athens Asthma as a syndrome From the Iliad to ADAM 33 and back again Bronchoconstriction,
(a) Significant biological processes (upper panel) and disease biomarkers (lower panel)
 Supplementary Figure 1. Functional enrichment analyses of secretomic proteins. (a) Significant biological processes (upper panel) and disease biomarkers (lower panel) 2 involved by hrab37-mediated secretory
Supplementary Figure 1. Functional enrichment analyses of secretomic proteins. (a) Significant biological processes (upper panel) and disease biomarkers (lower panel) 2 involved by hrab37-mediated secretory
