An estimated 3 million people are
|
|
|
- Easter Brown
- 6 years ago
- Views:
Transcription
1 clinical focus An exploration of self-efficacy and self-management in COPD patients Edwina Simpson and Martyn Jones Abstract Aim: This study examined if self-efficacy in managing chronic obstructive pulmonary disease is associated with better mood, less breathlessness and fewer exacerbations; what helps or hinders patients in managing their chronic obstructive pulmonary disease (COPD); and patients suggestions to improve the selfmanagement support they receive. Background: COPD is the fifth leading cause of death in the UK, and it has been suggested that supporting self-efficacy and self-management could improve patient outcomes and reduce demands for NHS resources. Methods: An exploratory, descriptive survey involving the collection of both quantitative and semistructured qualitative data was chosen. Participants were randomly selected from four GP practices across the north east of Scotland. Results: Higher levels of self-efficacy were associated with lower levels of breathlessness, lower levels of anxiety and lower levels of depression in COPD patients. There was no association between high self-efficacy and exacerbation rates. Conclusion: Increasing self-efficacy and reducing anxiety and depression in patients living with COPD are important focus points for self-management support. Key words: Chronic obstructive pulmonary disease COPD Self-efficacy Self-management An estimated 3 million people are affected by chronic obstructive pulmonary disease (COPD) in the UK. About have been diagnosed with the condition and an estimated 2 million people are undiagnosed (National Institute for Health and Care Excellence (NICE), 2010). NICE states: Chronic obstructive pulmonary disease (COPD) is characterised by airflow obstruction. The airflow obstruction is usually progressive, not fully reversible and does not change markedly over several months. The disease is predominantly caused by smoking. There is no single diagnostic test for COPD. Making a diagnosis relies on clinical judgement based on a combination of history, physical examination and confirmation of the presence of airflow obstruction using spirometry (NICE, 2010). Edwina Simpson is COPD Specialist Nurse, Primary Care, NHS Tayside, Dundee and Martyn C Jones is Personal Chair of Healthcare, Research School of Nursing and Midwifery, University of Dundee Accepted for publication: October 2013 Most GP practices have access to a spirometer. This equipment measures the volume and flow rate of breathing. In healthy people, more than 70% of forced vital capacity (FVC) is exhaled in the first second; obstruction or airflow limitation is defined as FEV1/FVC<70% (Kelly, 2009). In COPD, severity is graded according to FEV1% predicted the volume of air exhaled in the first second of the FVC. The main symptoms associated with COPD are a chronic productive cough, breathlessness and wheeze. Anxiety, depression and acute exacerbations feature predominantly in the natural history of COPD (Kelly, 2009). Exacerbations are defined by NICE (2010) as a sustained worsening of the patient s symptoms from their usual, stable state, which is greater than the day-to-day variations and is acute on onset (NICE, 2010). Exacerbations carry a high mortality; within 90 days of admission for an exacerbation, 33% of patients with COPD are readmitted and almost 14% have died (Scullion, 2009). The average cost of treating a COPD patient in Scotland is estimated to be per patient per year (Long Term Conditions Collaborative, 2009). With an increasingly ageing population and predicted reductions in the NHS workforce, governments and healthcare providers are engaged in initiatives to develop new ways of supporting patients living with long-term conditions such as COPD to manage their own health (Rijken et al, 2008). Research suggests that improving self-efficacy (SE) and promoting self-management could reduce some of the burden on the NHS. Many theorists including Monninkhof (Harris et al, 2008) believe that patients SE their sense of confidence in their competence to manage their condition has been established as the route to better outcomes such as a reduction in exacerbations. According to this approach, increasing patients SE is likely to support them in changing their behaviour and lead to more effective self-management. Empowering patients to manage their longterm conditions is likely to involve a major change to the working practices of some health professionals (Health Foundation, 2012). The idea of self-management support implies there will be a change in the role of the health professional from an authoritarian position in delivering education and information to supporting patients to help them build confidence and make choices that lead to better self-management and outcomes (Coleman and Newton, 2005). This study also set out to discover what patients thought would help them to manage their COPD. Identifying where COPD patients commonly have low self-efficacy is likely to assist COPD nurses in identifying strategies to support patients to increase their SE and consequently improve their self-management. Improved patient self-management has the potential to reduce rates of exacerbation and hospital admission (Scullion, 2009). Rationale for study The evidence from studies including Cochrane reviews (Monninkhoff, 2003; Effing et al, 2009) suggests that further research is needed before firm conclusions can be drawn on what constitutes successful self-management support in COPD. Research in this area has not focused on SE and does not seem to have sought patients views on how they self-manage their condition. British Journal of Nursing, 2013, Vol 22, No
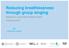
2 This study attempted to identify the barriers faced by patients when self-managing their COPD and what patients thought health professionals could do to assist them to selfmanage COPD. The use of SE, mood and symptom questionnaires and scales can help identify situations where COPD patients commonly experience low SE. The study focused on measuring patients levels of selfefficacy in relation to: Anxiety/depression Exacerbation rates Breathlessness. This study gained patients views on selfmanagement using a cross-sectional patient self-report survey. We are not aware of any other studies using the same combination of assessment methods; these involved measuring breathlessness with the Medical Research Council (MRC) dyspnoea scale (Bestall et al, 1999; Ozalevli and Ucan, 2006), mood using the hospital anxiety and depression (HAD) scale (Zigmond and Snaith, 1983), and exacerbation rates using the COPD selfefficacy scale (Wigal, 1991). Full ethical approval was granted by both the local research and ethics committee and the Caldicott guardian. Data search Four databases were chosen and searched for evidence in the literature of effective self-management/se in the care of COPD patients: MEDLINE, CINAHL Plus, OVID Online and the Cochrane Library (Figure 1). Two separate searches were undertaken. The search terms entered were: Self-management in COPD Self-efficacy in COPD. Thirty-four studies meeting the criteria were found; some of these are cited in this paper. Excluded studies included those that mentioned SE or self-management in their text but were rejected as their abstracts and conclusions showed they mentioned the topics only briefly. Studies that focused completely on pulmonary rehabilitation were rejected as their focus was more on the benefits of exercise. The study focused on Cochrane reviews and randomised controlled trials (RCTs) as they are regarded as producing the most robust evidence (Education for Health, 2008). Literature review Monninkhof s (2003) Cochrane review aimed to clarify the effectiveness of selfmanagement programmes in COPD. This systematic review of eight RCTs and one Self-efficacy and selfmanagement searched; Ovid Online, Cinahl Plus, Medline and the Cochrane Library Number of articles found and screened: 115 Number of articles with full text discussing either self-efficacy or self-management meeting the criteria: 34 Figure 1. Results of data search Number of articles excluded: 81 Excluded articles: pulmonary: 10; foreign language: 8; >10 yrs old: 15; triplicates: 20; not suitable: 28 controlled clinical trial assessed the efficacy of self-management education in patients with COPD. The self-management programmes reviewed used various methods of education including group and individualised sessions and providing written material. The education components targeted smoking cessation, managing exacerbations and improving exercise or nutrition. The review showed that self-management education had no effect on hospital admissions, emergency unit visits, days lost from work and lung function but led to an increased use of courses of antibiotics and oral steroids. Study limitations included participants having different diagnostic criteria and the educational components being of varying duration. In addition, a wide variation in outcome measures meant that insufficient data were obtained to make recommendations. The outcomes measured also varied in appropriateness. Days lost from work may not be relevant as many COPD patients are over retirement age. COPD patients are also prone to anxiety/depression and may not retain educational information. As COPD is a less variable disease than asthma, it can be more difficult to show positive results. A Cochrane review by Effing et al (2009) built on the results of Monninkhof s (2003) Cochrane review by assessing the settings, methods and efficacy of COPD selfmanagement education programmes on health outcomes and use of healthcare services. The method was a systematic review of 15 group comparisons drawn from 14 RCTs. A total of patients were recruited for the trials, of whom participated. The various RCTs followed up patients from periods of 8 weeks to 12 months. The studies reviewed examined a broad spectrum of self-management interventions, including individualised education on COPD, breathing and coughing techniques, relaxation exercises, energy conservation and adapting a healthy lifestyle as well as action plans to identify and treat exacerbations. The self-management education included smoking cessation, selftreatment of exacerbations and improving exercise and nutrition. A significant reduction was seen in the probability of at least one hospital admission for about 36% for patients receiving selfmanagement education compared with those receiving usual care, combined with an improvement in their health-related quality of life. However, because of the heterogeneity in interventions, study populations, follow-up time and outcome measures, the data were insufficient to be used to formulate clear recommendations regarding specific facets of self-management education programmes in COPD. Effing et al (2009) recognised the limitations of their study and recommended further research with larger RCTs and a longerterm follow-up before conclusions could be drawn. They added that it may be useful to choose only studies that measure the same variables, thereby reducing the heterogeneity. Similar conclusions were drawn by Bourbeau and van der Palen (2009), who suggested that further research was needed to increase our understanding of the effectiveness of the specific components of self-management programmes and how best to support COPD patients in self-management. This Cochrane review discussed the increase in the use of antibiotics and steroids, and suggested that self-management education with the addition of action plans resulted in patients recognising their exacerbations and treating them promptly, which resulted in less severe exacerbations. However, in the first author s experience, this is not suitable for all patients as some will take them inappropriately, despite having written guidance. Wood-Baker et al (2006) examined the efficacy of the components of action plans in the self-management of COPD. This longitudinal RCT prospective parallel group study compared written action plans to usual practice. All patients received an information booklet on COPD and an individual educational session with a respiratory nurse. Topics included smoking cessation, exercise, sputum clearance, nutrition, stress management, 1106 British Journal of Nursing, 2013, Vol 22, No 19
3 clinical focus inhaler use and support services. Intervention group members also received a written selfmanagement plan and were encouraged to contact their GP during the early stages of an exacerbation. Patients were followed up every three months for a year. Intervention group members were more likely to have had treatment with antibiotics; there were no differences between the groups in numbers of GP visits and hospital admissions. These findings are similar to those of Monninkhof et al s (2003) review. Wood-Baker et al s (2006) study had several limitations including a lack of blinding; the use of self-reporting, which is open to error as some participants cannot recall events accurately; and insufficient power to determine differences between interventions. In addition, many patients only received one educational session, which may limit the amount of information they retained. The majority of patients had stopped smoking at the time they enrolled onto this study. The results may have differed had more smokers been included. Research questions This study was designed to answer the following questions: Is self-efficacy in managing COPD associated with improved mood, reduced breathlessness and reduced exacerbations in patients? What helps or hinders patients in managing their COPD? What suggestions do patients with COPD have to improve the self-management support that they receive? Study inclusion criteria All patients included in this study: Had a definite diagnosis of COPD Were aged years Had an FEV1/FVC <70% Had an Fev1% predicted value of 20 79%. So that participants would be representative of patients seen at COPD clinics, both smokers and non-smokers were included. Methodology A descriptive survey involving the collection of quantitative and qualitative data was chosen to best answer the research questions. This survey comprised a questionnaire with validated scales and semistructured questions. Study participants received an information sheet, a consent form and a COPD questionnaire. The questionnaire had 10 questions; these included open questions to allow patients to express themselves and closed questions to maintain their interest. The COPD questionnaire included: Visual analogue scales measuring confidence in both recognising and treating an exacerbation. The scales for each had a range, with 0= Not at all confident and 100= Very confident. The patients marked an X on the line to determine how confident they were. The Wigal COPD self-efficacy scale. This measures how confident patients are in managing their breathlessness in certain situations. It lists 47 specific situations. This scale has proven acceptability, reliability and validity (Wigal et al, 1991). The MRC dyspnoea scale. This is on a scale of 1 5, with 1 representing no breathlessness except on strenuous exercise and 5 representing being too breathless to leave the house or being breathless when dressing or undressing. A higher score suggests more advanced disease. This breathlessness scale is commonly used in COPD as it has been proven to be acceptable, reliable and valid (Bestall et al, 1999: Ozalevli and Ucan, 2006). HAD scale. This is a 14-item self-report instrument for the detection of anxiety and depression in patients. It has two domains, each with seven statements on emotions or emotional situations. Patients express their agreement with the statements on a scale of 0 3, which leads to a maximal score of 21 points for each domain. Scores of 8 11 per domain suggest the presence of the mood disorder; scores >11 indicate a probable presence (Trappenburg et al, 2009). The HAD has proven acceptability, reliability and validity (Zigmond and Snaith, 1983). The first researcher measured self-efficacy using the COPD self-efficacy scale and the two visual analogue scales in confidence in recognising and confidence in treating an exacerbation separately. Data analysis Pearson s r correlation and independent sample t-test was chosen as the most appropriate statistical test for the numerical data meeting assumptions of normality. Spearman s rho non-parametric test was used for the nominal/ ordinal data. Qualitative data were analysed by content analysis, which is a process of analysing qualitative material for recurring themes and patterns (Polit et al, 2001). Correlation, according to Education for Health (2008), shows the relationship between the data of two continuous study variables. The data were analysed using the SPSS 18 statistical analysis package. Results Study population Two hundred and fifty patients were contacted, with 48 completing the study, giving a 19.2% response rate. Table 1 shows the characteristics of the study population. Participants were aged years, and the mean age was 69 years. The majority of patients were still smoking. There were equal numbers of men and women. The majority of patients had moderate COPD with FEV1=50 79% predicted. The most common score on the MRC dyspnoea scale was 3; people with this score walk more slowly than their contemporaries on level ground because of breathlessness, or have to stop to take a breath when walking at their own pace. Exacerbation rates were also recorded (Table 4). Table 1. Study population characteristics Frequency Percentage Disease severity Moderate COPD FEV % Disease severity Severe COPD FEV % Sex Male Female Smoking Non-smoker Smoker MRC dyspnoea scale score MRC 1 MRC 2 MRC 3 MRC 4 MRC British Journal of Nursing, 2013, Vol 22, No
4 Table 2. Correlation between self-efficacy scales and anxiety and depression Pearson s r bivariate was used to examine relationships between variables that were normally distributed COPD self-efficacy scale Missing scores replaced Mean SD n COPD self-efficacy scale score Depression Anxiety VAS confidence in ability to recognise an exacerbation Depression ** 1 Anxiety ** 0.805** 1 VAS confidence in ability to ** 0.486** 0.501** 1 recognise an exacerbation Vas confidence in ability to treat an exacerbation ** 0.615** 0.599** 0.804** 1 P*<0.05, **<0.01, ***<0.001; VAS: visual analogue scale VAS confidence in ability to treat an exacerbation Table 3. Correlation between self-efficacy scales and the MRC dyspnoea scale Spearman s rho non-parametric test was used as the variable was ordinal Mean SD n COPD self-efficacy scale score VAS confidence in ability to recognise an exacerbation VAS confidence in ability to treat an exacerbation MRC dyspnoea scale score 1 5 COPD self-efficacy scale VAS confidence in ability to ** 1 recognise an exacerbation VAS confidence in ability to ** 0.829** 1 treat an exacerbation MRC dyspnoea scale ** 0.500** ** 1 P*<0.05, **<0.01,***<0.001; VAS: visual analogue scale Table 4. Means of the exacerbation rate and anxiety/depression for patients who have visited GP in last 6 months with an exacerbation Have you had an appointment in the last 6 months for an exacerbation? n Mean SD Standard error mean Anxiety total No Yes Depression total No Yes confidence in recognising and confidence in treating an exacerbation, the dyspnoea scale and the COPD self-efficacy scale are all positively correlated. This suggests that people who have higher self-efficacy have less breathlessness they scored less on the MRC dyspnoea scale. There were no significant differences in anxiety (t-test result) and depression (t-test result) for patients who had had an appointment for an exacerbation in the last 6 months. Research question: correlation The study s first question was: is self-efficacy in managing COPD associated with improved mood, reduced breathlessness and reduced exacerbation? In testing the normality of the variables, all variables were normally distributed using the Kolmogorov-Smirnov test. Table 2 shows there were positive correlations between high visual analogue scale scores in confidence in recognising and treating an exacerbation, high confidence in the COPD self-efficacy scale and lower levels of anxiety and depression. The p value is <0.05 in all of the variables, which suggests that COPD patients who are more confident in recognising and treating an exacerbation and more confident at controlling their breathlessness have less anxiety and depression. The COPD selfefficacy scale measures the control of managing breathlessness in certain situations and the two visual analogue scales measure confidence in recognising and confidence in treating an exacerbation. To establish if higher levels of self-efficacy reduced breathlessness, it was also necessary to see if there was a positive correlation between the two visual analogue scales, the COPD self-efficacy scale and the MRC dyspnoea scale; a non-parametric test was used for the MRC scale as the variable level is ordinal (Table 3). The P values are all <0.05, which suggests that the visual analogue scales scores of Qualitative data The qualitative data were collected from the COPD questionnaire. The study s second question was: what helps or hinders patients in managing their COPD? The data suggested that patients were aware that smoking and weight gain increased breathlessness. They also commented that taking their medication as prescribed and pacing themselves helped control their breathlessness. The study s third question was: what suggestions do patients with COPD have to improve the self-management support that they receive? The data suggested that keeping patients up to date with new medications, being there when they needed advice, offering 1108 British Journal of Nursing, 2013, Vol 22, No 19
5 clinical focus Key points Anxiety, depression and acute exacerbations feature predominantly in the natural history of chronic obstructive pulmonary disease (COPD) Governments and healthcare providers are engaged in initiatives to develop new ways of supporting patients living with long-term conditions such as COPD to manage their own health increasing self-efficacy is likely to lead to behaviour change and more effective selfmanagement People with long-term conditions may need self-management support to cope more effectively with the psychological effects of their illness a written progress chart annually and believing them when they said they were having an exacerbation would all be helpful. Discussion and conclusion Although the response rate was poor, the patient sample was randomly selected and robust processes were in place to reduce selection bias. The first researcher was blind to the random selection and the participants identifiable information. The study population was a true sample of COPD patients across four GP practices in north east Scotland including men and women, smokers, non-smokers and those with moderate or severe COPD. This study looked to see if there was an association between self-efficacy, mood, breathlessness and exacerbations. The results show there is an association between higher levels of self-efficacy, reduced breathlessness (Table 3) and lower levels of anxiety and depression (Table 2). Patients who had high scores on the COPD self-efficacy scale which concerns their ability to control their breathlessness in certain situations had lower anxiety and depression levels. Those who said they were more confident at recognising an exacerbation and treating one had less anxiety/ depression and breathlessness. However, exacerbation rates were the same for people with high and low self-efficacy levels. We should therefore focus on increasing self-efficacy and reducing anxiety and depression in patients living with COPD (Effing et al, 2009).The COPD team of nurses in this NHS setting have received training in health behaviour change. These skills, used in combination with this study s findings, will enable us to assist patients with problem solving, achieving their goals and enhancing behaviour change. Future research Further research is needed, using a larger sample, preferably over a prolonged period of time. The outcome measures should focus on behaviour change, the attainment of goals and/or self-efficacy scores, as opposed to exacerbation rates or GP visits (Bourbeau and van der Palen, 2009). Past studies have focused mainly on exacerbations; acute exacerbations feature predominantly in the natural history of COPD (Kelly, 2009) so it may not always be possible to prevent them. BJN Conflict of interest: none. Bestall JC, Paul EA, Garrod R, Garnham R, Jones PW, Wedzicha JA (1999) Usefulness of the Medical Research Council (MRC) dyspnoea scale as a measure of disability in patients with chronic obstructive pulmonary disease. Thorax 54(7): Bourbeau J, van der Palen J (2009) Promoting effective selfmanagement programmes to improve COPD. Eur Respir J 33(3): Coleman MT, Newton KS (2005) Supporting self-management in patients with chronic illness. Am Fam Physician 72(8): Education for Health (2008) Simply Evidence-Based Healthcare: a Practical Pocket Book. 2nd edn. Education for Health, Warwick Effing T, Monninkhof EM, van der Valk PD et al (2007) Selfmanagement education for patients with chronic obstructive pulmonary disease. Cochrane Database Syst Rev 4: CD Harris M, Smith BJ, Veale A (2008) Patient education programmes can they provide outcomes in COPD? Int J Chron Obstruct Pulmon Dis 3(1): Health Foundation (2012) About Self Management Support. The Health Foundation, London. health.org.uk/about-self-management-support/ (accessed 13 October 2013) Kelly C (2009) Management of stable COPD. Indep Nurse. Special section 4 7 Long Term Conditions Collaborative (2009) Improving Self Management Support. Scottish Government, Edinburgh. www. scotland.gov.uk/resource/doc/274194/ pdf Monninkhof EM, van der Valk PD, van der Palen J et al (2003) Self-management education for chronic obstructive pulmonary disease. Cochrane Database Syst Rev 1: CD National Clinical Guideline Centre (2010) Chronic obstructive pulmonary disease: management of chronic obstructive pulmonary disease in adults in primary and secondary care. London: National Clinical Guideline Centre. nice.org.uk National Institute for Health and Clinical Excellence (2010) Chronic Obstructive Pulmonary Disease: Management of Chronic Obstructive Pulmonary Disease in Adults in Primary and Secondary Care (Partial Update) (CG101). NICE, London. org.uk/cg101 Ozalevli S, Ucan ES (2006) The comparison of different dyspnoea scales in patients with COPD. J Eval Clin Pract 12(5): Polit DF, Beck CT, Hungler BP (2001) Methods of data collection. In: Polit DF, Beck CT, Hungler BP (2001) Essentials of Nursing Research: Methods, Appraisal and Utilization (5th edn). Philadelphia: Lippincott. Rijken M, Jones M, Heijmans, Dixon A (2008) Supporting selfmanagement. In: Nolte E (author) and Mckee M (author/ ed). Caring for People With Chronic Conditions: a Health System Perspective. McGraw Hill, Maidenhead: Scullion J (2008) Patient-focused outcomes in chronic obstructive pulmonary disease. Nurs Stand 22(21), 50 6 Scullion J (2009) Managing COPD exacerbations. Indep Nurse Professional Development for Nurse Prescribers: COPD supplement, October, 6 7 Trappenburg JC, Koevoets L, de Weert-van Oene GH et al (2009) Action plan to enhance self-management and early detection of exacerbations in COPD patients; a multicenter RCT. BMC Pulm Med 9: 52 Wigal JK, Creer TL, Kotses H (1991) The COPD self-efficacy scale. Chest 99(5): Wood-Baker R, McGlone S, Venn A, Walters EH (2006) Written action plans in chronic obstructive pulmonary disease increase appropriate treatment for acute exacerbations. Respirology 11(5): Zigmond AS, Snaith RP (1983) The hospital anxiety and depression scale. Acta Psychiatr Scand 67(6): British Journal of Nursing, 2013, Vol 22, No
6 Copyright of British Journal of Nursing is the property of Mark Allen Publishing Ltd and its content may not be copied or ed to multiple sites or posted to a listserv without the copyright holder's express written permission. However, users may print, download, or articles for individual use.
Self-management plan for COPD
 Sheffield Clinical Commissioning Group Sheffield Teaching Hospitals NHS Foundation Trust Self-management plan for COPD This is your personal management plan The aim of the plan is to help you have better
Sheffield Clinical Commissioning Group Sheffield Teaching Hospitals NHS Foundation Trust Self-management plan for COPD This is your personal management plan The aim of the plan is to help you have better
Care Bundle. Adult patients with COPD
 Care Bundle Adult patients with COPD Version 2 July 2014 What is a care bundle? A care bundle is a set of interventions that, when used together, significantly improve patient outcomes. The measures chosen
Care Bundle Adult patients with COPD Version 2 July 2014 What is a care bundle? A care bundle is a set of interventions that, when used together, significantly improve patient outcomes. The measures chosen
Chronic Obstructive Pulmonary Disease (COPD) Measures Document
 Chronic Obstructive Pulmonary Disease (COPD) Measures Document COPD Version: 3 - covering patients discharged between 01/10/2017 and present. Programme Lead: Jo Higgins Clinical Lead: Dr Paul Albert Number
Chronic Obstructive Pulmonary Disease (COPD) Measures Document COPD Version: 3 - covering patients discharged between 01/10/2017 and present. Programme Lead: Jo Higgins Clinical Lead: Dr Paul Albert Number
Chronic obstructive pulmonary disease
 0 Chronic obstructive pulmonary disease Implementing NICE guidance June 2010 NICE clinical guideline 101 What this presentation covers Background Scope Key priorities for implementation Discussion Find
0 Chronic obstructive pulmonary disease Implementing NICE guidance June 2010 NICE clinical guideline 101 What this presentation covers Background Scope Key priorities for implementation Discussion Find
INITIATING A COPD CLINIC: PROTOCOL & ASSESSMENT
 COPD Resource Pack Section 2A INITIATING A COPD CLINIC: PROTOCOL & ASSESSMENT In this section: 1. Initiating a COPD Clinic 2. Equipment for a COPD Clinic 3. Primary Care Chronic Obstructive Pulmonary Disease
COPD Resource Pack Section 2A INITIATING A COPD CLINIC: PROTOCOL & ASSESSMENT In this section: 1. Initiating a COPD Clinic 2. Equipment for a COPD Clinic 3. Primary Care Chronic Obstructive Pulmonary Disease
Self-Management Plan for COPD
 Self-Management Plan for COPD This is your personal management plan. The aim of this plan is to help you have better control of your chronic obstructive pulmonary disease (COPD). It will enable you to
Self-Management Plan for COPD This is your personal management plan. The aim of this plan is to help you have better control of your chronic obstructive pulmonary disease (COPD). It will enable you to
JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES
 JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES Authors Dr Ian Benton Respiratory Consultant COCH Penny Rideal Respiratory Nurse COCH Kirti Burgul Respiratory Pharmacist COCH Pam
JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES Authors Dr Ian Benton Respiratory Consultant COCH Penny Rideal Respiratory Nurse COCH Kirti Burgul Respiratory Pharmacist COCH Pam
Self-Management Plan for COPD
 Self-Management Plan for COPD This is your personal management plan. The aim of this plan is to help you have better control of your chronic obstructive pulmonary disease (COPD). It will enable you to
Self-Management Plan for COPD This is your personal management plan. The aim of this plan is to help you have better control of your chronic obstructive pulmonary disease (COPD). It will enable you to
Commissioning for Better Outcomes in COPD
 Commissioning for Better Outcomes in COPD Dr Matt Kearney Primary Care & Public Health Advisor Respiratory Programme, Department of Health General Practitioner, Runcorn November 2011 What are the Commissioning
Commissioning for Better Outcomes in COPD Dr Matt Kearney Primary Care & Public Health Advisor Respiratory Programme, Department of Health General Practitioner, Runcorn November 2011 What are the Commissioning
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Chronic obstructive pulmonary disease: the management of adults with chronic obstructive pulmonary disease in primary and secondary
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Chronic obstructive pulmonary disease: the management of adults with chronic obstructive pulmonary disease in primary and secondary
Self-Management Plan for COPD
 Self-Management Plan for COPD This is your personal management plan. Bring it with you every time you see a nurse or doctor about your COPD The aim of this plan is to help you have better control of your
Self-Management Plan for COPD This is your personal management plan. Bring it with you every time you see a nurse or doctor about your COPD The aim of this plan is to help you have better control of your
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 DRAFT NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Chronic obstructive pulmonary disease: the management of adults with chronic obstructive pulmonary disease in primary
DRAFT NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Chronic obstructive pulmonary disease: the management of adults with chronic obstructive pulmonary disease in primary
Changing Healthcare Forever mycopd
 Changing Healthcare Forever mycopd Introducing mycopd, from my mhealth. mycopd is the most comprehensive, user friendly and intuitive COPD App available on any device. Built by COPD experts, and externally
Changing Healthcare Forever mycopd Introducing mycopd, from my mhealth. mycopd is the most comprehensive, user friendly and intuitive COPD App available on any device. Built by COPD experts, and externally
UNDERSTANDING COPD MEDIA BACKGROUNDER
 UNDERSTANDING COPD MEDIA BACKGROUNDER What is COPD? Chronic Obstructive Pulmonary Disease (COPD) also called emphysema and/or chronic obstructive bronchitis* is a preventable lung disease caused by the
UNDERSTANDING COPD MEDIA BACKGROUNDER What is COPD? Chronic Obstructive Pulmonary Disease (COPD) also called emphysema and/or chronic obstructive bronchitis* is a preventable lung disease caused by the
Chronic Obstructive Pulmonary Disease (COPD).
 Chronic Obstructive Pulmonary Disease (COPD). Linde: Living healthcare 02 03 Chronic Obstructive Pulmonary Disease (COPD). A pocket guide for healthcare professionals. COPD the facts Moderate to severe
Chronic Obstructive Pulmonary Disease (COPD). Linde: Living healthcare 02 03 Chronic Obstructive Pulmonary Disease (COPD). A pocket guide for healthcare professionals. COPD the facts Moderate to severe
VA/DoD Clinical Practice Guideline Management of COPD Pocket Guide
 VA/DoD Clinical Practice Guideline Management of COPD Pocket Guide MODULE A: MAAGEMET OF COPD 1 2 Patient with suspected or confirmed COPD presents to primary care [ A ] See sidebar A Perform brief clinical
VA/DoD Clinical Practice Guideline Management of COPD Pocket Guide MODULE A: MAAGEMET OF COPD 1 2 Patient with suspected or confirmed COPD presents to primary care [ A ] See sidebar A Perform brief clinical
Self-management education for patients with chronic obstructive pulmonary disease (Review)
 Self-management education for patients with chronic obstructive pulmonary disease (Review) Effing T, Monninkhof EEM, van der Valk PP, Zielhuis GGA, Walters EH, van der Palen JJ, Zwerink M This is a reprint
Self-management education for patients with chronic obstructive pulmonary disease (Review) Effing T, Monninkhof EEM, van der Valk PP, Zielhuis GGA, Walters EH, van der Palen JJ, Zwerink M This is a reprint
Asthma Tutorial. Trainer MRW. Consider the two scenarios, make an attempt at the questions, what guidance have you used?
 Registrar: LG PR RS Topic Asthma and COPD Asthma Tutorial Trainer MRW Date of Tutorial 18 th Jan 2007 Objectives of the tutorial How to diagnose What investigations and when Treatment guidelines QoF Criteria
Registrar: LG PR RS Topic Asthma and COPD Asthma Tutorial Trainer MRW Date of Tutorial 18 th Jan 2007 Objectives of the tutorial How to diagnose What investigations and when Treatment guidelines QoF Criteria
aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A.
 aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A. 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and
aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A. 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and
Shared Decision Making chronic obstructive pulmonary disease (COPD)
 Shared Decision Making chronic obstructive disease (COPD) Next clinical review date March 2018 Deciding what to do about COPD This short decision aid is to help you decide what treatment, or combination
Shared Decision Making chronic obstructive disease (COPD) Next clinical review date March 2018 Deciding what to do about COPD This short decision aid is to help you decide what treatment, or combination
Development of a self-reported Chronic Respiratory Questionnaire (CRQ-SR)
 954 Department of Respiratory Medicine, University Hospitals of Leicester, Glenfield Hospital, Leicester LE3 9QP, UK J E A Williams S J Singh L Sewell M D L Morgan Department of Clinical Epidemiology and
954 Department of Respiratory Medicine, University Hospitals of Leicester, Glenfield Hospital, Leicester LE3 9QP, UK J E A Williams S J Singh L Sewell M D L Morgan Department of Clinical Epidemiology and
The distribution of COPD in UK general practice using the new GOLD classification
 ORIGINAL ARTICLE COPD The distribution of COPD in UK general practice using the new GOLD classification John Haughney 1, Kevin Gruffydd-Jones 2, June Roberts 3, Amanda J. Lee 4, Alison Hardwell 5 and Lorcan
ORIGINAL ARTICLE COPD The distribution of COPD in UK general practice using the new GOLD classification John Haughney 1, Kevin Gruffydd-Jones 2, June Roberts 3, Amanda J. Lee 4, Alison Hardwell 5 and Lorcan
Chronic Obstructive Pulmonary Disease, shortened to COPD, is an umbrella term for a group of conditions which cause long-term damage to the airways.
 10 Common QuESTIonS AbouT CoPD Chronic Obstructive Pulmonary Disease, shortened to COPD, is an umbrella term for a group of conditions which cause long-term damage to the airways. COPD includes: chronic
10 Common QuESTIonS AbouT CoPD Chronic Obstructive Pulmonary Disease, shortened to COPD, is an umbrella term for a group of conditions which cause long-term damage to the airways. COPD includes: chronic
Community pulmonary rehabilitation: a multidisciplinary approach
 Community pulmonary rehabilitation: a multidisciplinary approach Lindsay Welch Pulmonary rehabilitation is a well-evidenced programme of therapy for patients with chronic obstructive pulmonary disease
Community pulmonary rehabilitation: a multidisciplinary approach Lindsay Welch Pulmonary rehabilitation is a well-evidenced programme of therapy for patients with chronic obstructive pulmonary disease
Reference Guide for Group Education
 A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 1 Introduction to Living Well with COPD Education Program Participants Expectations Towards the Program Health in COPD
A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 1 Introduction to Living Well with COPD Education Program Participants Expectations Towards the Program Health in COPD
MULTICARE Health System Care of the Adult Chronic Obstructive Pulmonary Disease (COPD) Patient
 Clinical Guideline Ver. 2.0 MULTICARE Health System Care of the Adult Chronic Obstructive Pulmonary Disease (COPD) Patient Target Audience: The target audience for this clinical guideline is all MHS providers
Clinical Guideline Ver. 2.0 MULTICARE Health System Care of the Adult Chronic Obstructive Pulmonary Disease (COPD) Patient Target Audience: The target audience for this clinical guideline is all MHS providers
CARE OF THE ADULT COPD PATIENT
 CARE OF THE ADULT COPD PATIENT Target Audience: The target audience for this clinical guideline is all MultiCare providers and staff including those associated with our Clinically Integrated Network. The
CARE OF THE ADULT COPD PATIENT Target Audience: The target audience for this clinical guideline is all MultiCare providers and staff including those associated with our Clinically Integrated Network. The
Reference Guide for Group Education
 A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 5 Plan of Action: Part I Overview of the Plan of Action and Management of Respiratory Infections Plan of Action: Objectives
A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 5 Plan of Action: Part I Overview of the Plan of Action and Management of Respiratory Infections Plan of Action: Objectives
Chronic Obstructive Pulmonary Disease (COPD) Treatment Guidelines
 Chronic Obstructive Pulmonary Disease (COPD) Treatment Guidelines Where appropriate the following should be offered before commencing inhaled treatment: Offer treatment and support to stop smoking. Smoking
Chronic Obstructive Pulmonary Disease (COPD) Treatment Guidelines Where appropriate the following should be offered before commencing inhaled treatment: Offer treatment and support to stop smoking. Smoking
roflumilast 500 microgram tablets (Daxas ) SMC No. (635/10) Nycomed Ltd
 roflumilast 500 microgram tablets (Daxas ) SMC No. (635/10) Nycomed Ltd 06 August 2010 (Issued 10 September 2010) The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
roflumilast 500 microgram tablets (Daxas ) SMC No. (635/10) Nycomed Ltd 06 August 2010 (Issued 10 September 2010) The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
COPD in primary care: reminder and update
 COPD in primary care: reminder and update Managing COPD continues to be a major feature of primary care, particularly in practices with a high proportion of M ori and Pacific peoples. COPDX clinical practice
COPD in primary care: reminder and update Managing COPD continues to be a major feature of primary care, particularly in practices with a high proportion of M ori and Pacific peoples. COPDX clinical practice
Coordination of palliative care in community settings. Summary report
 Coordination of palliative care in community settings Summary report This resource may also be made available on request in the following formats: 0131 314 5300 nhs.healthscotland-alternativeformats@nhs.net
Coordination of palliative care in community settings Summary report This resource may also be made available on request in the following formats: 0131 314 5300 nhs.healthscotland-alternativeformats@nhs.net
Screening for chronic obstructive pulmonary disease (COPD) in the general adult population
 Screening for chronic obstructive pulmonary disease (COPD) in the general adult population External review against programme appraisal criteria for the UK National Screening Committee Version: FINAL Author:
Screening for chronic obstructive pulmonary disease (COPD) in the general adult population External review against programme appraisal criteria for the UK National Screening Committee Version: FINAL Author:
Reducing breathlessness through group singing
 Reducing breathlessness through group singing Singing for Lung Health Impact Report February 2018 mt milestone tweed The singing helps you to expand your lungs and your life, it helps you to not limit
Reducing breathlessness through group singing Singing for Lung Health Impact Report February 2018 mt milestone tweed The singing helps you to expand your lungs and your life, it helps you to not limit
Guideline for the Diagnosis and Management of COPD
 Guideline for the Diagnosis and Management of COPD Introduction Chronic obstructive pulmonary disease (COPD) is a respiratory disorder largely caused by smoking. It is characterized by progressive, partially
Guideline for the Diagnosis and Management of COPD Introduction Chronic obstructive pulmonary disease (COPD) is a respiratory disorder largely caused by smoking. It is characterized by progressive, partially
Wales Primary Care COPD Audit
 Wales Primary Care COPD Audit 2014-15 Next steps for improvement National Chronic Obstructive Pulmonary Disease (COPD) Audit Programme 2016 The audit programme partnership Working in strategic partnership:
Wales Primary Care COPD Audit 2014-15 Next steps for improvement National Chronic Obstructive Pulmonary Disease (COPD) Audit Programme 2016 The audit programme partnership Working in strategic partnership:
COPD: early detection, screening and case-finding: what is the evidence? Prof. Jan-Willem Lammers, Md PhD Department of Respiratory Diseases
 COPD: early detection, screening and case-finding: what is the evidence? Prof. Jan-Willem Lammers, Md PhD Department of Respiratory Diseases «If you test one smoker with cough every day You will diagnose
COPD: early detection, screening and case-finding: what is the evidence? Prof. Jan-Willem Lammers, Md PhD Department of Respiratory Diseases «If you test one smoker with cough every day You will diagnose
Chronic Obstructive Pulmonary Disease. Information about medication and an Action Plan to use if your condition gets worse due to an infection
 Chronic Obstructive Pulmonary Disease Information about medication and an Action Plan to use if your condition gets worse due to an infection Information about your medication Your usual treatment Inhalers
Chronic Obstructive Pulmonary Disease Information about medication and an Action Plan to use if your condition gets worse due to an infection Information about your medication Your usual treatment Inhalers
An Outcomes Strategy for COPD and Asthma: NHS Companion Document IMPACT REPORT
 An Outcomes Strategy for COPD and Asthma: NHS Companion Document IMPACT REPORT 1 DH INFORMATION READER BOX Policy Clinical Estates HR / Workforce Commissioner Development IM & T Management Provider Development
An Outcomes Strategy for COPD and Asthma: NHS Companion Document IMPACT REPORT 1 DH INFORMATION READER BOX Policy Clinical Estates HR / Workforce Commissioner Development IM & T Management Provider Development
Changing Landscapes in COPD New Zealand Respiratory Conference
 Changing Landscapes in COPD New Zealand Respiratory Conference Dr Robert Young BMedSc MBChB DPhil (Oxon) FRACP FRCP Associate Professor Consultant Physician Changing Landscapes in COPD: Summary 1. Overview
Changing Landscapes in COPD New Zealand Respiratory Conference Dr Robert Young BMedSc MBChB DPhil (Oxon) FRACP FRCP Associate Professor Consultant Physician Changing Landscapes in COPD: Summary 1. Overview
Copyright General Practice Airways Group. Reproduction Prohibited
 Primary Care Respiratory Journal (2004) 13, 84 88 REVIEW The NICE COPD Guidelines 2004 what are the messages for primary care? David Bellamy*,1 James Fisher Medical Centre, 4 Tolpuddle Gardens, Muscliffe,
Primary Care Respiratory Journal (2004) 13, 84 88 REVIEW The NICE COPD Guidelines 2004 what are the messages for primary care? David Bellamy*,1 James Fisher Medical Centre, 4 Tolpuddle Gardens, Muscliffe,
Algorithm for the use of inhaled therapies in COPD
 Berkshire West Integrated Care System Representing Berkshire West Clinical Commisioning Group Royal Berkshire NHS Foundation Trust Berkshire Healthcare NHS Foundation Trust Berkshire West Primary Care
Berkshire West Integrated Care System Representing Berkshire West Clinical Commisioning Group Royal Berkshire NHS Foundation Trust Berkshire Healthcare NHS Foundation Trust Berkshire West Primary Care
COPD in Korea. Division of Pulmonary, Allergy and Critical Care Medicine of Hallym University Medical Center Park Yong Bum
 COPD in Korea Division of Pulmonary, Allergy and Critical Care Medicine of Hallym University Medical Center Park Yong Bum Mortality Rate 1970-2002, USA JAMA,2005 Global Burden of Disease: COPD WHO & World
COPD in Korea Division of Pulmonary, Allergy and Critical Care Medicine of Hallym University Medical Center Park Yong Bum Mortality Rate 1970-2002, USA JAMA,2005 Global Burden of Disease: COPD WHO & World
Comparisons of health status scores with MRC grades in COPD: implications for the GOLD 2011 classification
 ORIGINAL ARTICLE COPD Comparisons of health status scores with MRC grades in COPD: implications for the GOLD 2011 classification Paul W. Jones 1, Lukasz Adamek 2, Gilbert Nadeau 2 and Norbert Banik 3 Affiliations:
ORIGINAL ARTICLE COPD Comparisons of health status scores with MRC grades in COPD: implications for the GOLD 2011 classification Paul W. Jones 1, Lukasz Adamek 2, Gilbert Nadeau 2 and Norbert Banik 3 Affiliations:
Pulmonary Rehabilitation in COPD-An Important Non-pharmacological Treatment
 122 Review Article Pulmonary Rehabilitation in COPD-An Important Non-pharmacological Treatment Department of Adult Nursing, Maharajgunj Nursing Campus, Institute of Medicine, Tribhuvan University, Kathmandu,
122 Review Article Pulmonary Rehabilitation in COPD-An Important Non-pharmacological Treatment Department of Adult Nursing, Maharajgunj Nursing Campus, Institute of Medicine, Tribhuvan University, Kathmandu,
Defining COPD. Georgina Grantham Community Respiratory Team Leader/ Respiratory Nurse Specialist
 Defining COPD Georgina Grantham Community Respiratory Team Leader/ Respiratory Nurse Specialist Defining COPD Chronic Obstructive Pulmonary Disease (COPD) is a common, preventable and treatable disease
Defining COPD Georgina Grantham Community Respiratory Team Leader/ Respiratory Nurse Specialist Defining COPD Chronic Obstructive Pulmonary Disease (COPD) is a common, preventable and treatable disease
Algorithm for the use of inhaled therapies in COPD Version 2 May 2017
 Algorithm for the use of inhaled therapies in COPD This document has been revised by the Berkshire West Respiratory Network to support clinicians in selecting the most appropriate, cost effective treatments
Algorithm for the use of inhaled therapies in COPD This document has been revised by the Berkshire West Respiratory Network to support clinicians in selecting the most appropriate, cost effective treatments
Surveillance report Published: 6 April 2016 nice.org.uk. NICE All rights reserved.
 Surveillance report 2016 Chronic obstructive pulmonary disease in over 16s: diagnosis and management (2010) NICE guideline CG101 Surveillance report Published: 6 April 2016 nice.org.uk NICE 2016. All rights
Surveillance report 2016 Chronic obstructive pulmonary disease in over 16s: diagnosis and management (2010) NICE guideline CG101 Surveillance report Published: 6 April 2016 nice.org.uk NICE 2016. All rights
RESPIRATORY CARE IN GENERAL PRACTICE
 RESPIRATORY CARE IN GENERAL PRACTICE Definitions of Asthma and COPD Asthma is due to inflammation of the air passages in the lungs and affects the sensitivity of the nerve endings in the airways so they
RESPIRATORY CARE IN GENERAL PRACTICE Definitions of Asthma and COPD Asthma is due to inflammation of the air passages in the lungs and affects the sensitivity of the nerve endings in the airways so they
Rosemary Plum Prescriptive Solutions Ltd SIMPLE Respiratory 2015
 + A SERVICE FOR COMMUNITY PHARMACY Rosemary Plum Prescriptive Solutions Ltd + n Why Pharmacy? High patient footfall 450 diagnosed asthma patients Walk-in service Medicines skills and expertise Structured
+ A SERVICE FOR COMMUNITY PHARMACY Rosemary Plum Prescriptive Solutions Ltd + n Why Pharmacy? High patient footfall 450 diagnosed asthma patients Walk-in service Medicines skills and expertise Structured
QOF indicator area: Chronic Obstructive Pulmonary disease (COPD)
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Cost impact statement: Chronic Obstructive Pulmonary Disease QOF indicator area:
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE QUALITY AND OUTCOMES FRAMEWORK (QOF) INDICATOR DEVELOPMENT PROGRAMME Cost impact statement: Chronic Obstructive Pulmonary Disease QOF indicator area:
This is the publisher s version. This version is defined in the NISO recommended practice RP
 Journal Article Version This is the publisher s version. This version is defined in the NISO recommended practice RP-8-2008 http://www.niso.org/publications/rp/ Suggested Reference Chong, J., Karner, C.,
Journal Article Version This is the publisher s version. This version is defined in the NISO recommended practice RP-8-2008 http://www.niso.org/publications/rp/ Suggested Reference Chong, J., Karner, C.,
National COPD Audit Programme
 National COPD Audit Programme Planning for every breath National Chronic Obstructive Pulmonary Disease (COPD) Audit Programme: Primary care audit () 2015 17 Data analysis and methodology Section 4: Providing
National COPD Audit Programme Planning for every breath National Chronic Obstructive Pulmonary Disease (COPD) Audit Programme: Primary care audit () 2015 17 Data analysis and methodology Section 4: Providing
A Validation Study for the Korean Version of Chronic Obstructive Pulmonary Disease Assessment Test (CAT)
 http://dx.doi.org/10.4046/trd.2013.74.6.256 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2013;74:256-263 CopyrightC2013. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
http://dx.doi.org/10.4046/trd.2013.74.6.256 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2013;74:256-263 CopyrightC2013. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
National COPD Audit Programme
 National COPD Audit Programme Planning for every breath Primary Care Audit (Wales) 2015-17 Findings and quality improvement The audit programme partnership Working in strategic partnership: Supported by:
National COPD Audit Programme Planning for every breath Primary Care Audit (Wales) 2015-17 Findings and quality improvement The audit programme partnership Working in strategic partnership: Supported by:
Manuscript type: Research letter
 TITLE PAGE Chronic breathlessness associated with poorer physical and mental health-related quality of life (SF-12) across all adult age groups. Authors Currow DC, 1,2,3 Dal Grande E, 4 Ferreira D, 1 Johnson
TITLE PAGE Chronic breathlessness associated with poorer physical and mental health-related quality of life (SF-12) across all adult age groups. Authors Currow DC, 1,2,3 Dal Grande E, 4 Ferreira D, 1 Johnson
Dear Reader, What was the study about? Why was the research needed? BI NCT
 Dear Reader, Sponsors of clinical studies create study reports. A study report describes how the study was done and what the results of the study were. This is a summary of such a report. It is meant for
Dear Reader, Sponsors of clinical studies create study reports. A study report describes how the study was done and what the results of the study were. This is a summary of such a report. It is meant for
The product website contains useful information and videos that cover both the patient and the clinician interfaces for mycopd
 mycopd universal guidance The product website contains useful information and videos that cover both the patient and the clinician interfaces for mycopd https://mymhealth.com/mymhealth/mycopd The clinician
mycopd universal guidance The product website contains useful information and videos that cover both the patient and the clinician interfaces for mycopd https://mymhealth.com/mymhealth/mycopd The clinician
THE CHALLENGES OF COPD MANAGEMENT IN PRIMARY CARE An Expert Roundtable
 THE CHALLENGES OF COPD MANAGEMENT IN PRIMARY CARE An Expert Roundtable This activity is supported by an educational grant from Sunovion Pharmaceuticals Inc. COPD in the United States Third leading cause
THE CHALLENGES OF COPD MANAGEMENT IN PRIMARY CARE An Expert Roundtable This activity is supported by an educational grant from Sunovion Pharmaceuticals Inc. COPD in the United States Third leading cause
Confidence and understanding among general practitioners and practice nurses in the UK about diagnosis and management of COPD
 Respiratory Medicine (2007) 101, 2378 2385 Confidence and understanding among general practitioners and practice nurses in the UK about diagnosis and management of COPD D.M.G. Halpin a,, J.F. O Reilly
Respiratory Medicine (2007) 101, 2378 2385 Confidence and understanding among general practitioners and practice nurses in the UK about diagnosis and management of COPD D.M.G. Halpin a,, J.F. O Reilly
Attending a healthcare setting can be a daunting
 Visual symbols in healthcare settings for children with learning disabilities and autism spectrum disorder Irene Vaz Abstract Children with learning disabilities (LD) and autism spectrum disorder (ASD)
Visual symbols in healthcare settings for children with learning disabilities and autism spectrum disorder Irene Vaz Abstract Children with learning disabilities (LD) and autism spectrum disorder (ASD)
CHRONIC OBSTRUCTIVE PULMONARY DISEASE
 A F O C A l p O I N T l E A r N I N g p r O g r A m m E CHRONIC OBSTRUCTIVE PULMONARY DISEASE S E C O N D E D I T I O N BOOK 1 September 2013 FP120/1 CENTRE FOR PHARMACY POSTGRADUATE EDUCATION About CPPE
A F O C A l p O I N T l E A r N I N g p r O g r A m m E CHRONIC OBSTRUCTIVE PULMONARY DISEASE S E C O N D E D I T I O N BOOK 1 September 2013 FP120/1 CENTRE FOR PHARMACY POSTGRADUATE EDUCATION About CPPE
Better community respiratory care. Dr Roland Meyer Respiratory Physician Southern DHB August 2010
 Better community respiratory care Dr Roland Meyer Respiratory Physician Southern DHB August 2010 Integration : What is needed? Raise profile of disease Strong management in primary care Good communication
Better community respiratory care Dr Roland Meyer Respiratory Physician Southern DHB August 2010 Integration : What is needed? Raise profile of disease Strong management in primary care Good communication
Chronic Obstructive Pulmonary Disease (COPD) is a systematic disease with
 Chronic Obstructive Pulmonary Disease (COPD) is a systematic disease with considerable impact on several dimensions of daily life. Those that suffer from COPD can be submitted to rehabilitation programmes.
Chronic Obstructive Pulmonary Disease (COPD) is a systematic disease with considerable impact on several dimensions of daily life. Those that suffer from COPD can be submitted to rehabilitation programmes.
COPD GOLD Guidelines & Barnet inhaler choices. Dr Dean Creer, Respiratory Consultant, Royal Free London NHS Foundation Trust
 COPD GOLD Guidelines & Barnet inhaler choices Dr Dean Creer, Respiratory Consultant, Royal Free London NHS Foundation Trust GOLD 2017 Report: Chapters 1. Definition and Overview 2. Diagnosis and Initial
COPD GOLD Guidelines & Barnet inhaler choices Dr Dean Creer, Respiratory Consultant, Royal Free London NHS Foundation Trust GOLD 2017 Report: Chapters 1. Definition and Overview 2. Diagnosis and Initial
Anyone who smokes and/or has shortness of breath and sputum production could have COPD
 COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
Disclosure and Conflict of Interest 8/15/2017. Pharmacist Objectives. At the conclusion of this program, the pharmacist will be able to:
 Digging for GOLD Rebecca Young, PharmD, BCACP, Roosevelt University College of Pharmacy Assistant Professor of Clinical Sciences Practice Site Advocate Medical Group-Nesset Pavilion Disclosure and Conflict
Digging for GOLD Rebecca Young, PharmD, BCACP, Roosevelt University College of Pharmacy Assistant Professor of Clinical Sciences Practice Site Advocate Medical Group-Nesset Pavilion Disclosure and Conflict
Patient reported outcomes in respiratory diseases; How to assess clinical success in COPD
 Patient reported outcomes in respiratory diseases; How to assess clinical success in COPD Thys van der Molen, University of Groningen, Department of General Practice, The Netherlands Mr Valette Smoking
Patient reported outcomes in respiratory diseases; How to assess clinical success in COPD Thys van der Molen, University of Groningen, Department of General Practice, The Netherlands Mr Valette Smoking
Roflumilast (Daxas) for chronic obstructive pulmonary disease
 Roflumilast (Daxas) for chronic obstructive pulmonary disease August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
Roflumilast (Daxas) for chronic obstructive pulmonary disease August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
Asthma: Evaluate and Improve Your Practice
 Potential Barriers and Suggested Ideas for Change Key Activity: Initial assessment and management Rationale: The history and physical examination obtained from the patient and family interviews form the
Potential Barriers and Suggested Ideas for Change Key Activity: Initial assessment and management Rationale: The history and physical examination obtained from the patient and family interviews form the
Usefulness of the Medical Research Council (MRC) dyspnoea scale as a measure of disability in patients with chronic obstructive pulmonary disease
 Thorax 1999;54:581 586 581 Academic Department of Respiratory Medicine, St Bartholomew s and Royal London School of Medicine and Dentistry, London Chest Hospital, London, UK EAPaul R Garrod R Garnham J
Thorax 1999;54:581 586 581 Academic Department of Respiratory Medicine, St Bartholomew s and Royal London School of Medicine and Dentistry, London Chest Hospital, London, UK EAPaul R Garrod R Garnham J
ACE Programme SOMERSET INTEGRATED LUNG CANCER PATHWAY. Phases One and Two Final Report
 ACE Programme SOMERSET INTEGRATED LUNG CANCER PATHWAY Phases One and Two Final Report July 2017 Introduction This paper presents the learning and actions that have been generated from phase One and Two
ACE Programme SOMERSET INTEGRATED LUNG CANCER PATHWAY Phases One and Two Final Report July 2017 Introduction This paper presents the learning and actions that have been generated from phase One and Two
Respiratory disease is the poor relation of the big three.
 WHO ARE WE and WHAT DO WE DO? Live well with COPD was formed in July 2016 to provide support, advice and guidance for Chronic Obstructive Pulmonary Disease (COPD) to those in the Gosport, Fareham and surrounding
WHO ARE WE and WHAT DO WE DO? Live well with COPD was formed in July 2016 to provide support, advice and guidance for Chronic Obstructive Pulmonary Disease (COPD) to those in the Gosport, Fareham and surrounding
Asthma and COPD in older people lumping or splitting? Christine Jenkins Concord Hospital Woolcock Institute of Medical Research
 Asthma and COPD in older people lumping or splitting? Christine Jenkins Concord Hospital Woolcock Institute of Medical Research Concord Hospital Woolcock Institute of Medical Research Joe has asthma What
Asthma and COPD in older people lumping or splitting? Christine Jenkins Concord Hospital Woolcock Institute of Medical Research Concord Hospital Woolcock Institute of Medical Research Joe has asthma What
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Patient Reported Outcomes
 Patient Reported Outcomes INTRODUCTION TO CLINICAL RESEARCH A TWO-WEEK INTENSIVE COURSE, 2010 Milo Puhan, MD, PhD, Associate Professor Key messages Patient-reported outcomes (PRO) is a broad group of outcomes
Patient Reported Outcomes INTRODUCTION TO CLINICAL RESEARCH A TWO-WEEK INTENSIVE COURSE, 2010 Milo Puhan, MD, PhD, Associate Professor Key messages Patient-reported outcomes (PRO) is a broad group of outcomes
glycopyrronium 44 micrograms hard capsules of inhalation powder (Seebri Breezhaler ) SMC No. (829/12) Novartis Pharmaceuticals Ltd.
 glycopyrronium 44 micrograms hard capsules of inhalation powder (Seebri Breezhaler ) SMC No. (829/12) Novartis Pharmaceuticals Ltd. 07 December 2012 The Scottish Medicines Consortium (SMC) has completed
glycopyrronium 44 micrograms hard capsules of inhalation powder (Seebri Breezhaler ) SMC No. (829/12) Novartis Pharmaceuticals Ltd. 07 December 2012 The Scottish Medicines Consortium (SMC) has completed
damage, a result of chronic inflammation that differs from that seen in asthma and is usually caused by tobacco smoke. 1
 COPD Exacerbations Is Self-Management A Treatment Option? Hetal Dhruve, Specialist Respiratory & Allergy Pharmacist, Barts Health NHS Trust; Matthew Hodson, Nurse Consultant, Homerton University Hospital
COPD Exacerbations Is Self-Management A Treatment Option? Hetal Dhruve, Specialist Respiratory & Allergy Pharmacist, Barts Health NHS Trust; Matthew Hodson, Nurse Consultant, Homerton University Hospital
Northumbria Healthcare NHS Foundation Trust. Bronchiectasis. Issued by Respiratory Medicine
 Northumbria Healthcare NHS Foundation Trust Bronchiectasis Issued by Respiratory Medicine The aim of this booklet is to help you manage your bronchiectasis. It contains information which you should find
Northumbria Healthcare NHS Foundation Trust Bronchiectasis Issued by Respiratory Medicine The aim of this booklet is to help you manage your bronchiectasis. It contains information which you should find
How to treat COPD? What is the mechanism of dyspnea? Smoking cessation
 : The Increasing Role of the FP Alan Kaplan, MD, CCFP(EM) Presented at the Primary Care Today: Education Conference and Medical Exposition, Toronto, Ontario, May 2006. Chronic obstructive pulmonary disease
: The Increasing Role of the FP Alan Kaplan, MD, CCFP(EM) Presented at the Primary Care Today: Education Conference and Medical Exposition, Toronto, Ontario, May 2006. Chronic obstructive pulmonary disease
Patient information leaflet. A study of low dose theophylline in Chronic Obstructive Pulmonary Disease (COPD)
 Patient information leaflet A study of low dose theophylline in Chronic Obstructive Pulmonary Disease (COPD) Theophylline With Inhaled CorticoSteroids (TWICS) study. We would like to invite you to take
Patient information leaflet A study of low dose theophylline in Chronic Obstructive Pulmonary Disease (COPD) Theophylline With Inhaled CorticoSteroids (TWICS) study. We would like to invite you to take
Chronic Obstructive Pulmonary Disease (COPD)
 James Paget University Hospitals NHS Foundation Trust Great Yarmouth and Waveney Clinical Commissioning Group HealthEast Chronic Obstructive Pulmonary Disease (COPD) Information and Advice for Patients
James Paget University Hospitals NHS Foundation Trust Great Yarmouth and Waveney Clinical Commissioning Group HealthEast Chronic Obstructive Pulmonary Disease (COPD) Information and Advice for Patients
Chronic Obstructive Pulmonary Disease
 Page 1 of 5 Chronic Obstructive Pulmonary Disease Chronic Obstructive Pulmonary Disease (COPD) is an 'umbrella' term for people with chronic bronchitis, emphysema, or both. With COPD the airflow to the
Page 1 of 5 Chronic Obstructive Pulmonary Disease Chronic Obstructive Pulmonary Disease (COPD) is an 'umbrella' term for people with chronic bronchitis, emphysema, or both. With COPD the airflow to the
Commissioning Brief - Background Information. Sputum colour charts to guide antibiotic self-treatment of acute exacerbation of COPD
 Commissioning Brief - Background Information Sputum colour charts to guide antibiotic self-treatment of acute exacerbation of COPD HTA no 17/128 This background document provides further information to
Commissioning Brief - Background Information Sputum colour charts to guide antibiotic self-treatment of acute exacerbation of COPD HTA no 17/128 This background document provides further information to
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Bode index as a predictor of severity in patients with chronic obstructive pulmonary disease.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. VII (May. 2016), PP 93-100 www.iosrjournals.org Bode index as a predictor of severity
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. VII (May. 2016), PP 93-100 www.iosrjournals.org Bode index as a predictor of severity
Design - Multicentre prospective cohort study. Setting UK Community Pharmacies within one CCG area within the UK
 Enabling Patient Health Improvements through COPD (EPIC) Medicines Optimisation within Community Pharmacy: a prospective cohort study Abstract Objectives To improve patients ability to manage their own
Enabling Patient Health Improvements through COPD (EPIC) Medicines Optimisation within Community Pharmacy: a prospective cohort study Abstract Objectives To improve patients ability to manage their own
ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS
 R2 (REVISED MANUSCRIPT BLUE 200208-877OC) ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS Mario Castro, M.D., M.P.H. Nina A. Zimmermann R.N. Sue
R2 (REVISED MANUSCRIPT BLUE 200208-877OC) ONLINE DATA SUPPLEMENT - ASTHMA INTERVENTION PROGRAM PREVENTS READMISSIONS IN HIGH HEALTHCARE UTILIZERS Mario Castro, M.D., M.P.H. Nina A. Zimmermann R.N. Sue
Can Audit and Feedback Reduce Antibiotic Prescribing in Dentistry?
 February 2015: RAPiD Audit and Feedback Trial Summary Can Audit and Feedback Reduce Antibiotic Prescribing in Dentistry? Antimicrobial resistance is a serious threat to global public health and patient
February 2015: RAPiD Audit and Feedback Trial Summary Can Audit and Feedback Reduce Antibiotic Prescribing in Dentistry? Antimicrobial resistance is a serious threat to global public health and patient
Smoking cessation interventions and services
 National Institute for Health and Care Excellence Guideline version (Final) Smoking cessation interventions and services [E] Evidence reviews for advice NICE guideline NG92 Evidence reviews FINAL These
National Institute for Health and Care Excellence Guideline version (Final) Smoking cessation interventions and services [E] Evidence reviews for advice NICE guideline NG92 Evidence reviews FINAL These
Community COPD Service Protocol
 Community COPD Service Protocol Acknowledgements This protocol is based on the following documents: 1. Chronic obstructive pulmonary disease: Management of chronic obstructive pulmonary disease in adults
Community COPD Service Protocol Acknowledgements This protocol is based on the following documents: 1. Chronic obstructive pulmonary disease: Management of chronic obstructive pulmonary disease in adults
Managing Exacerbations of COPD (Version 3.0)
 Managing Exacerbations of COPD (Version 3.0) Guideline Readership This guideline is intended for use in patients with a confirmed diagnosis of a chronic obstructive pulmonary disease (COPD) exacerbation.
Managing Exacerbations of COPD (Version 3.0) Guideline Readership This guideline is intended for use in patients with a confirmed diagnosis of a chronic obstructive pulmonary disease (COPD) exacerbation.
Your COPD action plan
 Your COPD action plan Patient name: Better Breathing 0161 206 3159 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: MED24(17). Review date: July 2019 Your COPD Action Plan This
Your COPD action plan Patient name: Better Breathing 0161 206 3159 All Rights Reserved 2017. Document for issue as handout. Unique Identifier: MED24(17). Review date: July 2019 Your COPD Action Plan This
DATE: 09 December 2009 CONTEXT AND POLICY ISSUES:
 TITLE: Tiotropium Compared with Ipratropium for Patients with Moderate to Severe Chronic Obstructive Pulmonary Disease: A Review of the Clinical Effectiveness DATE: 09 December 2009 CONTEXT AND POLICY
TITLE: Tiotropium Compared with Ipratropium for Patients with Moderate to Severe Chronic Obstructive Pulmonary Disease: A Review of the Clinical Effectiveness DATE: 09 December 2009 CONTEXT AND POLICY
Promoting Drug Users Respiratory Health
 Promoting Drug Users Respiratory Health Lloyd Baron IAD Research Assistant, Centre for Public Health, Liverpool John Moores University L.R.Baron@ljmu.ac.uk Outline Background terminology and COPD explanation
Promoting Drug Users Respiratory Health Lloyd Baron IAD Research Assistant, Centre for Public Health, Liverpool John Moores University L.R.Baron@ljmu.ac.uk Outline Background terminology and COPD explanation
Patient Assessment Quality of Life
 Patient Assessment Quality of Life STEP 1 Learning objectives This module will provide you with an understanding of the importance of assessing Quality of Life (QoL) in patients and the role that quality
Patient Assessment Quality of Life STEP 1 Learning objectives This module will provide you with an understanding of the importance of assessing Quality of Life (QoL) in patients and the role that quality
2/4/2019. GOLD Objectives. GOLD 2019 Report: Chapters
 GOLD Objectives To provide a non biased review of the current evidence for the assessment, diagnosis and treatment of patients with COPD. To highlight short term and long term treatment objectives organized
GOLD Objectives To provide a non biased review of the current evidence for the assessment, diagnosis and treatment of patients with COPD. To highlight short term and long term treatment objectives organized
C hronic obstructive pulmonary disease (COPD) is a serious
 394 CHRONIC OBSTRUCTIVE PULMONARY DISEASE Self-management education for patients with chronic obstructive pulmonary disease: a systematic review E Monninkhof, P van der Valk, J van der Palen, C van Herwaarden,
394 CHRONIC OBSTRUCTIVE PULMONARY DISEASE Self-management education for patients with chronic obstructive pulmonary disease: a systematic review E Monninkhof, P van der Valk, J van der Palen, C van Herwaarden,
Policy position statement Chronic Obstructive Pulmonary Disease (COPD) May 2017 Introduction
 Policy position statement Chronic Obstructive Pulmonary Disease (COPD) May 2017 Introduction The British Lung Foundation recommends: Improvements to COPD diagnosis speed and accuracy through better symptom
Policy position statement Chronic Obstructive Pulmonary Disease (COPD) May 2017 Introduction The British Lung Foundation recommends: Improvements to COPD diagnosis speed and accuracy through better symptom
