Optimising inhaled mannitol for cystic fibrosis in an adult population
|
|
|
- Alban Stanley
- 5 years ago
- Views:
Transcription
1 Patrick A. Flume Moira L. Aitken Diana Bilton Penny Agent Brett Charlton Emma Forster Howard G. Fox Helge Hebestreit John Kolbe Jonathan B Zuckerman Brenda M. Button Diana Bilton, Department of Respiratory Medicine, Royal Brompton Hospital, Sydney Street, London, UK d.bilton@rbht.nhs.uk Optimising inhaled mannitol for cystic fibrosis in an adult population Abstract There has been remarkable progress in the treatment of cystic fibrosis (CF) patients over the past 20 years. However, limitations of standard therapies have highlighted the need for a convenient alternative treatment to effectively target the pathophysiologic basis of CF-related disease by improving mucociliary clearance of airway secretions and consequently improve lung function and reduce respiratory exacerbations. Mannitol is an osmotic agent available as a dry powder, dispensed in a convenient disposable inhaler device for the treatment of adult patients with CF. Inhalation of mannitol as a dry powder is thought to change the viscoelastic properties of airway secretions, increase the hydration of the airway surface liquid and contribute to increased mucociliary and cough clearance of retained secretions. In two large phase 3 studies [1, 2], long-term use of inhaled mannitol resulted in a significant and clinically meaningful improvement in lung function relative to control in adult CF subjects and had an acceptable safety profile. Clinical experience with inhaled mannitol confirms that it is safe and effective. A minority of patients are unable to tolerate the medication. However, through training in proper inhaler technique and setting clear expectations regarding therapeutic effects, both the tolerance and adherence necessary for long term efficacy can be positively influenced. Educational aims To discuss the importance of airway clearance treatments in the management of cystic fibrosis. To describe the clinical data that supports the use of mannitol in adult patients with cystic fibrosis. To highlight the role of mannitol tolerance testing in screening for hyperresponsiveness. To provide practical considerations for patient education in use of mannitol inhaler. Conflict of interest Pharmaxis Limited sponsored the study. The study sponsor participated in the study design, data collection, data analysis, data interpretation and writing of the reports. Following completion of the trials, the data were held and analysed by the sponsor. The corresponding author had full access to all of the data, and had final responsibility for publication. ERS 2015 HERMES syllabus link: module B.15.1, E.1.1 As a result of an erratum, the online version of this article has been revised DOI: /
2 Optimising inhaled mannitol for cystic fibrosis Key points Inhaled mannitol is a safe and effective option in adult patients with cystic fibrosis. Mannitol tolerance testing effectively screens for hyperresponsiveness prior to initiation of therapy. Physiotherapists and respiratory therapists play an integral role in the introduction and maintenance of dry powder inhalation therapy. Patient training and follow-up is important for optimising longer term adherence. Introduction Chronic airways infection and inflammation is associated with considerable morbidity and early mortality in patients with cystic fibrosis (CF) [3]. In CF, the lung airway surface liquid is depleted, resulting in a defective mucociliary clearance. This contributes to retained airways phlegm, which promotes infection and inflammation within the airway lumen and wall, leading to airway remodelling. Initial reversible injury eventually results in refractory bronchiectasis and progressive loss of lung function [4]. Mechanical clearance of secretions from the airways is a primary therapy for CF patients, with a number of airway clearance therapies (ACTs) recommended in current guidelines [5]. There are recommended medications given by inhalation, including hypertonic saline and recombinant human deoxyribonuclease (rh DNase), that are used as an adjunct to ACTs. These agents alter the rheological properties of airway phlegm, thereby easing its clearance from the airways [5]. Inhaled rh DNase improves lung function by digesting high molecular weight DNA that is typically released in the CF airways by dead neutrophils and which contributes to the secretion viscosity [6, 7]. Inhaled hypertonic saline has been investigated as both an alternative and parallel treatment to rhdnase [8]. It has been demonstrated to increase airway surface liquid volume in vitro and modestly improve lung function in patients with CF [9 12]. Although recommended in guidelines, hypertonic saline is not a regulatory approved treatment and there are widely recognised tolerability issues in some patients [13, 14]. In addition, the administration of nebulised saline is time consuming and is associated with poor adherence [8]. This highlights the need for a convenient alternative treatment to effectively improve clearance of airway secretions and lung function. The naturally occurring sugar alcohol, mannitol, is an osmotic agent that has been studied as a dry powder formulated as 3-micron spheres for optimised inhaled use through a convenient disposable inhaler device for the treatment of patients with CF [15]. Inhalation of mannitol as a dry powder is thought to change the viscoelastic properties of airway phlegm, increase the hydration of the airway surface liquid and contribute to increased clearance of the retained secretions through mucociliary activity and productive cough (see video showing mannitol's mode of action, presented in the supplementary material alongside the online version of this article at breathe.ersjournals.com) [16]. As it does not require refrigeration, nebulisation, routine equipment cleaning or sterilisation, mannitol may provide a convenient treatment for CF patients, or an alternative option for adults who already have a high treatment burden (see fig. 1) [17]. Two recent, near identical, randomised, multicentre, double-blind, controlled, parallel-group phase 3 studies (CF301 and CF302) investigated the safety and efficacy of inhaled mannitol in subjects with CF over a period of 6 months [1, 2, 18]. These studies demonstrated clinically relevant benefits of inhaled mannitol even in study populations that were heavily treated with standard therapies. Inhaled mannitol was recently approved for use in adults in Europe. It is therefore relevant to present data specific to adult patients, distinct from the paediatric subjects who were included in previous publications. The pooled data from adult subjects (aged 18 years) in CF301 and CF302 are presented here and are derived using the statistical methodologies applied to the overall populations [18]. Methods Upon passing a mannitol tolerance test given to subjects at screening (sequential administrations of incremental doses of mannitol up to a maximum dose of 400 mg to assess hyperresponsiveness), subjects were randomised 3:2 to receive either mannitol 400 mg or control medication (mannitol 50 mg), respectively, twice daily for 26 weeks. A 50 mg subtherapeutic dose of mannitol was selected as control for the phase 3 studies using capsules indistinguishable from the active ones. The use of a placebo, such as inhalation-grade lactose was not feasible because safety data were not available for the quantities required for these clinical trials and blinding would be further complicated by the different taste of lactose. Similarly, nonrespirable mannitol was also considered unsuitable for use as a control due to concern that the large particle size might act as an irritant and any resultant lung function deterioration would make assessment problematic. Both studies had an open-label phase, in which participating subjects received mannitol for an additional 26 weeks or longer. Detailed methodologies of the studies have 40
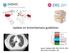
3 Optimising inhaled mannitol for cystic fibrosis in an adult population Spinning chamber Piercing buttons Mouthpiece Filter Piercing chamber Figure 1 Mannitol inhaler. been published previously [1, 2, 18]. Enrolled subjects had a diagnosis of CF with a defined range of baseline forced expiration volume in 1 s (FEV1) between 30 and 90% of predicted (study CF301), and between 40 and 90% of predicted (study CF302). Continuation of all approved CF therapies aside from hypertonic saline was permitted. The primary efficacy outcome for both studies was FEV1 [18]. Additional efficacy outcomes assessed included the post-dose sputum weight and frequency of pulmonary exacerbations. Subgroups were analysed based on rhdnase use and safety was assessed based on adverse events and monitoring of laboratory parameters. Results A total of 390 adult subjects were screened for inclusion, of whom 341 were randomised to receive either mannitol (n=207) or control (n=134). Overall, 141 subjects from the mannitol group and 102 subjects from the control group completed the 26-week double-blind phase. As shown in figure 2, a total of 130 and 94 adult subjects from the mannitol and control groups, respectively, consented to enter the optional open-label phase and received 400 mg mannitol twice daily. Baseline characteristics of the adult subjects were generally comparable between treatment groups (table 1). However, there were more male subjects in the mannitol group (61.4 versus 53.0% in the control group), and more subjects receiving rhdnase treatment in the control group (63.4 versus 58.9% in the mannitol group). Effects of mannitol on lung function Study CF301 and study CF302 both demonstrated a statistically significant improvement in lung function (FEV1 and forced vital capacity (FVC)) in the subgroup of adult patients compared with control (difference in FEV1 for CF301 and CF302 respectively was ml (95% CI ; p<0.001) and ml (95% CI ; p=0.038)). For the pooled analysis, 317 adult subjects (188 mannitol and 129 control) had FEV1 data at baseline and one post-baseline visit. Over 26 weeks, mannitol improved lung function as demonstrated by a mean absolute change in FEV1 from baseline compared with control of ml (95% CI ; p=0.001) and a relative change in % predicted for normal compared with control of +4.72% (95% CI ; p=0.001). Statistically significant improvements in FEV1 were sustained over the duration of the double-blind phase (fig. 3). Improvements in lung function were maintained for an additional 26 weeks in mannitol-treated subjects who consented to enter the open-label phase, indicating that the beneficial effects of mannitol on lung function can be sustained with prolonged treatment (fig. 4). The individual subject response at week 6 was highly predictive of longer-term FEV1 changes as shown in figure 5. Furthermore, 41
4 Optimising inhaled mannitol for cystic fibrosis 390 Adult subjects screened 27 (6.9%) failed the mannitol tolerance test 22 (5.6%) not randomised for other reasons 341 Subjects randomised (ITT) 207 Mannitol subjects 134 Control subjects 66 (31.9%) Withdrawals 33 (15.9%) Due to AEs 22 (10.6%) Withdrew consent 6 (2.9%) Physician decision 5 (2.4%) Other 32 (23.9%) Withdrawals 12 (9.0%) Due to AEs 18 (13.4%) Withdrew consent 1 (0.7%) Physician decision 1 (0.7%) Other 141 (68.1%) Completed 26 week DBP 102 (76.1%) Completed 26 week DBP 224 subjects entered the OLP (92.2%) of those completing the DBP entered the OLP 177 subjects completed the OLP (79.0%) of those entering the OLP completed this phase of the study Figure 2 Disposition of adult subjects in studies CF-301 and CF-302. AE: adverse event; OLP: open-label phase; DBP: double-blind phase; ITT: intention-to-treat. subjects in whom FEV1 improved over 26 weeks suffered fewer exacerbations (see fig. 6). In subjects who had received control medication (mannitol 50 mg twice daily) in the double-blind phase, the mean FEV1 increased upon switching treatment to mannitol 400 mg twice daily in the open-label phase. At week 52, the mean FEV1 had increased by 74.7 ml in these subjects. Lung function in other subgroups of adult subjects To assess the efficacy of inhaled mannitol when used in conjunction with best standard care, lung function scores were compared in various treatment groups. Improvements were seen irrespective of rhdnase, tobramycin or colistin use, as shown in figure 7. Effects of mannitol on the frequency of pulmonary exacerbations Overall, adult subjects treated with inhaled mannitol had a meaningful trend in reduction in risk for pulmonary exacerbations during the 26-week double-blind phase, with a relative risk versus control of 0.76 (95% CI ). This appeared to be driven by mannitol-treated subjects who had improved FEV1 between baseline and week 26. These subjects had a significantly reduced frequency of pulmonary exacerbations relative to those whose lung function did not respond (relative risk 0.4; p=0.03). Withdrawals, education and compliance There are challenges associated with the introduction of an inhaled dry powder, particularly 42
5 Optimising inhaled mannitol for cystic fibrosis in an adult population Table 1 Baseline characteristics of adult subjects enrolled in CF-301 and CF-302 Characteristic Age years Mannitol 400 mg twice daily (n=207) Control 50 mg twice daily (n=134) Mean±sd 28.3± ±8.46 Range Sex n (%) Male 127 (61.4) 71 (53.0) FEV1 % predicted Mean±sd 59.8± ±15.8 Median (range) 60.4 ( ) 54.2 ( ) FEV1 L Mean±sd 2.34 (0.80) 2.16 (0.70) Median (range) 2.20 ( ) 2.02 ( ) BMI kg m 2 Mean±sd 22.6± ±3.25 Range rhdnase treatment n (%) 122 (58.9) 85 (63.4) Inhaled antibiotics n (%) Tobramycin 72 (34.8) 47 (35.1) Colistin 62 (30.0) 39 (29.1) Systemic antibodies n (%) Azithromcyin 121 (58.5) 75 (56.0) Drugs for obstructive airway disease n (%) Short-acting bronchodilator # 201 (97.1) 126 (94.0) Inhaled corticosteroids 135 (65.2) 93 (69.4) BMI: body mass index; FEV1: forced expiration volume in 1 s. # : salbutamol (albuterol) or terbutaline; : includes subjects on combination of an inhaled corticosteroid and a β agonist. at large doses. In study CF301, there was a dropout rate of 35.3%, which led to additional instruction of study coordinators to teach subjects proper inhaler technique with reinforcement and additional training provided during study CF302. The withdrawal rate in study CF302 was 20.5%, a 41.9% reduction compared with CF301. Overall, median treatment compliance as measured by capsule returns in adult subjects who stayed on medication for the duration of the study was over 88% and 91% in the mannitol and control groups, respectively. Overall, mannitol was well tolerated by adult subjects with CF, although there was a higher drop-out rate overall in the mannitol group compared with the control group Safety Adverse events in adults were experienced by similar proportions of adult subjects in both 43
6 Optimising inhaled mannitol for cystic fibrosis Mean FEV1 change from baseline ml Week 0 Difference 89.8 ml p<0.001 Difference 84.2 ml p=0.006 Overall effect in adults 99.5 ml (95% CI ) p<0.001 versus control Week 6 Mannitol Week 14 Control Difference ml p<0.001 Figure 3 Change in FEV1 from baseline sustained during double-blind phase of studies (intention-to-treat). Mean FEV1 change from baseline ml Week 0 Week 6 Week 14 Week 26 Week 38 Week 26 Week 52 Mannitol Control Mannitol Mannitol open-label ex-control Figure 4 Sustained improvements in lung function from baseline in patients who completed the double-blind phase and entered the open-label extension phase. Mean relative change in % pred FEV1 across 26 weeks treatment 60 Slope = 0.726; p< Week Relative change in % pred FEV1 at week 6 Figure 5 Scatter plot showing correlation between FEV1 response at week 6 and over 26 weeks. Week 26 treatment groups (see table 2). Adverse events were generally mild or moderate, and consistent with CF and its standard therapies. There was a greater incidence of adverse events leading to discontinuation in mannitol-treated subjects compared with those on control Mean exacerbation rate per 26 weeks Difference: 0.4; p= # 0 >0 Mean change in FEV1 (% predicted) from baseline to week 26 Figure 6 Exacerbation rate by change from baseline in FEV1 during study period. (15.5% and 9.0% respectively). The most frequently reported adverse event in both treatment groups was condition aggravated (pulmonary exacerbation). Serious adverse events that were considered related to treatment were infrequent (3.4% for mannitol, 1.5% for control). Respiratory adverse events are of special interest with inhaled therapies. The most commonly reported respiratory adverse events occurring more frequently in mannitol-treated subjects were cough, haemoptysis and pharyngeal pain. As haemoptysis is frequently a component of pulmonary exacerbations, haemop tysis occurring as a component of a pulmonary exacerbation was noted if it occurred, regardless of whether it was reported separately as a haemoptysis adverse event. The incidence of exacerbation-related haemoptysis episodes in mannitol treated subjects was lower than the incidence in the control group (mannitol 4.8% versus control 9.7%). The total incidence of haemoptysis, including all events reported as a haemoptysis adverse event or those occurring as part of an exacerbation was marginally lower in the mannitol arm (15.5% and 17.9%, for mannitol and control, respectively). There was no change in growth of CF organisms with mannitol and no difference in growth between mannitol and control over 26 weeks. Clinical experience with inhaled mannitol Clinical experience with inhaled mannitol in 20 patients was recently presented [19]. Positive and negative factors that may influence adherence were reported. Positive factors identified included the brevity and simplicity of 44
7 Optimising inhaled mannitol for cystic fibrosis in an adult population administration with inhalation of 10 capsules taking about 5 min. The inhaler is breath actuated, portable and disposable. It requires no special care and does not require sterilisation. All of these features are intended to improve acceptability of the preparation. Negative factors that were identified included excessive coughing on inhalation in some patients and no perceived short-term benefit. These responses highlight the importance of education, particularly on correct inhalation technique, to the acceptance and effectiveness of this therapy as part of daily care. A trial of approximately 6 weeks is therefore encouraged before efficacy is reviewed meaning that an early review of response can be used to inform a decision whether to continue and so help manage adherence/treatment burden. For the management of hacking, dry and irritated cough, patients were advised to slow down the speed of inhalation, take sips of water between capsules and take time to settle the cough. Productive cough was managed by patients taking a moment between capsules to get control of their coughing and by practicing controlled huffing and coughing to clear secretions between inhalations. Patients tend to accommodate cough well, provided expectations are set, and the positive implication of a productive cough is understood. In this clinical experience, ACT was generally more effective following inhaled mannitol administration. Cough that was productive of phlegm was often increased and some patients reported a reduction in non-productive paroxysmal coughing. The change in cough character was described as less intrusive and disruptive to daily life. Discussion Inhaled mannitol has been demonstrated to be a safe, effective treatment for adult patients with CF, and it can be used in addition to best standard care. This form of therapy addresses many of the complaints patients have with other aerosol therapies which often lead to reduced adherence. That is, the disposable capsule-based dry-powder inhaler is portable and easy to use, greatly reducing the time of treatment. The portable inhaler is also convenient for adults, enabling them to maintain an active lifestyle. It appears from published studies that inhaled mannitol was not well tolerated by some subjects. This may have contributed to a significant withdrawal rate related to difficulties Adults Adult rhdnase users Adult rhdnase non-users Adult tobramycin users Adult tobramycin non-users Adult colistin users Adult colistin non-users ( ), 227 (135, 92) Favours control Favours mannitol Difference FEV1 ml: mannitol versus control with inhaling the dry powder. The differences in the withdrawal rates between studies CF301 and CF302 however, seem to highlight the importance of education and training in achieving good treatment adherence. These data suggest that demonstration and reinforcement of proper inhaler technique and setting clear expectations with respect to treatment effects may increase the proportion of patients who could benefit from this novel medication. The physiotherapist or respiratory therapist will play a key role in the introduction and maintenance of inhaled mannitol therapy for patients with CF. Patients who are prescribed mannitol will first undergo a mannitol tolerance test to be certain that clinically significant bronchospasm will not occur, and the mannitol tolerance test has been shown to be an effective screening procedure to identify those patients at risk for bronchospasm. The mannitol tolerance test also provides a valuable opportunity to educate patients about the proper use of the inhaler, including loading capsules, inhaler technique and the appropriate inspiratory flow rate. Patients should be informed about the possible side effects of inhaled mannitol including cough, which is considered part of its therapeutic effect. As this is the first opportunity for patients to experience taking inhaled mannitol, it would be ideally conducted by a CF healthcare professional (such as a physiotherapist or respiratory therapist) who has experience with the product. Patients may be encouraged by findings from the phase 3 studies, in which not only was the response at week 6 highly predictive of long-term FEV1 improvement, but also subjects Difference (95% CI), n (M, C) ( ), 317 (188, 129) ( ), 191 (111, 80) ( ), 112 (67, 45) ( ), 126 (77, 49) ( ), 205 (121, 84) ( ), 90 (53, 37) Figure 7 FEV1 (ml) changes in mannitol treated patients by concomitant therapy. 45
8 Optimising inhaled mannitol for cystic fibrosis Table 2 Summary of adverse events in pooled adult analysis Mannitol 400 mg twice daily (n=207) Control 50 mg twice daily (n=134) Patients with 1 AE Patients with 1 AE leading to discontinuation from the study AEs by MedDRA preferred term (occurring in 10% patients overall) # Condition aggravated Headache Cough Lower respiratory tract infection Bacteria sputum identified Nasopharyngitis Haemoptysis Patients with 1 SAE SAEs by MedDRA preferred term (occurring in 1% patients overall) # Condition aggravated Haemoptysis Lower respiratory tract infection Constipation Pneumonia Intestinal obstruction Catheterisation venous AE: adverse event; SAE: serious adverse event; MedDRA: Medical Dictionary for Regulatory Activities. # : patients are counted once for each unique preferred term identified from the CRF verbatim text; : refers to haemoptysis reported as an AE, but does not include all haemoptysis events that were recorded as part of an exacerbation. Overall incidence of haemoptysis including events reported exclusively as part of an exacerbation was 15.5% in mannitol arm and 17.9% in control. in whom the FEV1 improved over 26 weeks suffered fewer exacerbations. Therefore, all patients should be informed of this milestone and they should be evaluated with spirometry after approximately 6 weeks of treatment. As chronic therapy is necessary for long-term treatment benefit, follow-up of patients is important and should be used to monitor treatment adherence, and to encourage correct dosing (400 mg twice daily) and inhaler technique. Tips for optimal use of inhaled mannitol When preparing for a dose, patients should breathe out away from the inhaler, to prevent caking of the mannitol powder in the device and optimal dispersal of the dry powder. The capsule should be pierced a single time and the inhaler tilted downward to allow the capsule to fall into the spinning chamber. The patient should inhale with the head tilted slightly upward, breathing in deeply at an even, steady rate sufficient to make the capsule spin (see table 3). The rotating capsule will make an audible rattle indicating satisfactory inspiratory flow. Rapid inhalation may result in cough, in which case the patient should slow down their inhalation rate. The capsule should be checked after inspiration and if powder is still present, the patient should inhale a second time. After taking in the dose from each capsule, the patient should hold their breath for 5 s. There should not be a long delay between inhalations. The 10 capsules used during a dosing session should be inhaled closely together over about 5 min and, with practice, a full dose can be taken in 3 5 min (see supplementary video for overview of inhalation technique). 46
9 Optimising inhaled mannitol for cystic fibrosis in an adult population Table 3 Tips for use of inhaled mannitol Only remove capsules immediately before use. Pierce capsules once only. Tilt inhaler so mouth-piece faces slightly downward which allows capsule to drop forward into spinning chamber. Keep inhaler tilted in this way and breathe out completely away from the inhaler. With the head tilted upwards, the patient should inhale deeply at an even, steady rate that is fast enough to make the capsule spin - the capsule will make a rattling sound in the inhaler when inspiratory flow is sufficient. The inhalation rate may be slowed down if coughing occurs controlled coughing should be encouraged where possible. After the dose from each capsule is inhaled, the patient must breath hold for 5 s exhale and cough AWAY from the inhaler to prevent humidity build-up within the device. The 10 capsules should be taken closely together over a 3 5 min. A sip of water may be taken throughout the challenge to relieve cough and/or dry throat. See the supplementary material for video showing mannitol inhalation technique. Conclusion Inhaled mannitol is now available for adult patients with CF as an adjunctive therapy to augment airway clearance. Designated CF care team members will play vital roles in the evaluation and education of the patient who is prescribed inhaled mannitol. There are clear lessons that have been learned about this new dry powder therapy which should prove useful to the therapists in their discussions with patients about inhaled mannitol. Follow-up of patients is important to help ensure long-term benefit, and should be used to monitor adherence to treatment and encourage correct dosing. Acknowledgements We thank staff at Insight Medical Writing (Oxford, UK) for their assistance in preparing a first draft of this manuscript and Joanne Leadbetter (Pharmaxis Ltd) for her assistance with statistical analysis. All authors helped to interpret data, write the manuscript and have seen and approved the final version. Diana Bilton and Moira L. Aitken were the Global Principal Investigators for CF301/CF302, respectively, and had full access to all the data in the study and had final responsibility to submit for publication. John Kolbe was New Zealand Lead Regional Investigator for CF301. Moira L Aitken, Patrick A Flume and Jonathan Zuckerman were on the CF302 Steering Committee. Helge Hebestreit was Lead Regional Investigator for Germany for CF302. Brett Charlton designed the CF301 and CF302 studies, approved the statistical plans, and was the Sponsor s Responsible Medical Officer. Howard Fox approved the statistical plans and assisted in the design of CF302. Author affiliations: Patrick A. Flume: Pulmonary and Critical Care Medicine, Medical University of South Carolina, Charleston, SC, USA. Moira L. Aitken: Pulmonary and Critical Care Medicine, University of Washington Medical Center, Seattle, WA, USA. Diana Bilton: Department of Respiratory Medicine, Royal Brompton Hospital, London, UK. Penny Agent: Rehabilitation & Therapies, Royal Brompton & Harefield NHS Foundation Trust, Royal Brompton Hospital, London, UK. Brett Charlton: Pharmaxis Ltd, Frenchs Forest, NSW, Australia. Emma Forster: Bristol Royal Infirmary, University Hospitals Bristol NHS Foundation Trust, Bristol, UK. Howard G. Fox: Pharmaxis Ltd, Frenchs Forest, NSW, Australia. Helge Hebestreit: Department of Pediatric Pulmonology, Allergology and Cystic Fibrosis, Universitats Kinderklinik, Wurzburg, Germany. John Kolbe: Department of Medicine, University of Auckland, Auckland, New Zealand. Jonathan B Zuckerman: Tufts University School of Medicine, Maine Medical Centre, Portland, ME, USA. Brenda M. Button: Faculty of Medicine, Nursing and Health Sciences, Monash University, Melbourne, VIC, Australia. Conflict of interest: Diana Bilton has received fees for chairing an advisory board for Pharmaxis. Diana Bilton, John Kolbe, Moira Aitken, Patrick Flume, Jonathan Zucherman and Helge Hebestreit were all investigators during the studies and their institutions received standard clinical trial support from Pharmaxis. Investigators received travel support for the investigator meetings. No Investigator received any personal funding to participate in the study. Brett Charlton is the Medical Director of and holds stock options in Pharmaxis Ltd. Howard Fox is Chief Medical Officer of and holds stock options in Pharmaxis Ltd. References 1. Bilton D, Robinson P, Cooper P, et al. Inhaled dry powder mannitol in cystic fibrosis: an efficacy and safety study. Eur Respir J 2011; 38: Aitken ML, Bellon G, De Boeck K, et al. Long-term inhaled dry powder mannitol in cystic fibrosis: an international randomized study. Am J Respir Crit Care Med 2012; 185: Flume PA. Pulmonary complications of cystic fibrosis. Respir Care 2009; 54:
10 Optimising inhaled mannitol for cystic fibrosis 4. Boucher RC. Evidence for airway surface dehydration as the initiating event in CF airway disease. J Int Med 2007; 261: Flume PA, Robinson KA, O Sullivan BP, et al. Cystic fibrosis pulmonary guidelines: airway clearance therapies. Respir Care 2009; 54: Flume PA, O Sullivan BP, Robinson KA, et al. Cystic fibrosis pulmonary guidelines: chronic medications for maintenance of lung health. Am J Respir Crit Care Med 2007; 176: Shak S, Capon DJ, Hellmiss R, et al. Recombinant human DNase I reduces the viscosity of cystic fibrosis sputum. Proc Natl Acad Sci USA 1990; 87: Ratjen F. Restoring airway surface liquid in cystic fibrosis. N Engl J Med 2006; 354: Donaldson SH, Bennett WD, Zeman KL, et al. Mucus clearance and lung function in cystic fibrosis with hypertonic saline. N Engl J Med 2006; 354: Robinson M, Hemming AL, Regnis JA, et al. Effect of increasing doses of hypertonic saline on mucociliary clearance in patients with cystic fibrosis. Thorax 1997; 52: Elkins MR, Bye PT. Inhaled hypertonic saline as a therapy for cystic fibrosis. Curr Opin Pulm Med 2006; 12: Wark P, McDonald VM. Nebulised hypertonic saline for cystic fibrosis. Cochrane Database Syst Rev 2009; CD Suri R, Metcalfe C, Lees B, et al. Comparison of hypertonic saline and alternate-day or daily recombinant human deoxyribonuclease in children with cystic fibrosis: a randomised trial. Lancet 2001; 358: Robinson M, Daviskas E, Eberl S, et al. The effect of inhaled mannitol on bronchial mucus clearance in cystic fibrosis patients: a pilot study. Eur Respir J 1999; 14: Hurt K, Bilton D. Inhaled mannitol for the treatment of cystic fibrosis. Expert Rev Respir Med 2012; 6: Daviskas E, Rubin BK. Effect of inhaled dry powder mannitol on mucus and its clearance. Expert Rev Respir Med 2013; 7: Pettit RS, Johnson CE. Airway-rehydrating agents for the treatment of cystic fibrosis: past, present, and future. Ann Pharmacother 2011; 45: Bilton D, Bellon G, Charlton B, et al. Pooled analysis of two large randomised phase III inhaled mannitol studies in cystic fibrosis. J Cyst Fibros 2013; 12: Button BM, Finlayson F, Borg B, et al. Clinical impact of inhaled mannitol in an adult cystic fibrosis population. J Cyst Fibros 2013; 1: S98. 48
National Horizon Scanning Centre. Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis. April 2008
 Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis April 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not
Mannitol dry powder for inhalation (Bronchitol) for cystic fibrosis April 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not
CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions
 CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions Issue 1: Hypertonic Saline Summary: Preserving lung function is a crucial element in the care of the individual with
CYSTIC FIBROSIS FOUNDATION INFO-POD Information You Need to Make Benefits Decisions Issue 1: Hypertonic Saline Summary: Preserving lung function is a crucial element in the care of the individual with
TITLE: Hypertonic Saline Nebules for Patients with Cystic Fibrosis and Bronchioectasis: A Review of the Clinical and Cost-Effectiveness
 TITLE: Hypertonic Saline Nebules for Patients with Cystic Fibrosis and Bronchioectasis: A Review of the Clinical and Cost-Effectiveness DATE: 16 March 2009 CONTEXT AND POLICY ISSUES: Hypertonic saline
TITLE: Hypertonic Saline Nebules for Patients with Cystic Fibrosis and Bronchioectasis: A Review of the Clinical and Cost-Effectiveness DATE: 16 March 2009 CONTEXT AND POLICY ISSUES: Hypertonic saline
Cystic fibrosis (CF) is characterised by a. Inhaled dry powder mannitol in cystic fibrosis: an efficacy and safety study
 Eur Respir J 2011; 38: 1071 1080 DOI: 10.1183/09031936.00187510 CopyrightßERS 2011 Inhaled dry powder mannitol in cystic fibrosis: an efficacy and safety study D. Bilton*, P. Robinson #, P. Cooper ", C.G.
Eur Respir J 2011; 38: 1071 1080 DOI: 10.1183/09031936.00187510 CopyrightßERS 2011 Inhaled dry powder mannitol in cystic fibrosis: an efficacy and safety study D. Bilton*, P. Robinson #, P. Cooper ", C.G.
About the National Centre for Pharmacoeconomics
 Cost-effectiveness of mannitol dry powder for inhalation (Bronchitol ) for the treatment of adult patients with cystic fibrosis as an add-on therapy to best standard of care. The NCPE has issued a recommendation
Cost-effectiveness of mannitol dry powder for inhalation (Bronchitol ) for the treatment of adult patients with cystic fibrosis as an add-on therapy to best standard of care. The NCPE has issued a recommendation
Correspondence: Dr Sushil K. Kabra, Professor, Department of Pediatrics, AIIMS, New Delhi , India.
 JOURNAL OF TROPICAL PEDIATRICS, VOL. 58, NO. 5, 2012 Comparison of Effects of 3 and 7% Hypertonic Saline Nebulization on Lung Function in Children with Cystic Fibrosis: A Double-Blind Randomized, Controlled
JOURNAL OF TROPICAL PEDIATRICS, VOL. 58, NO. 5, 2012 Comparison of Effects of 3 and 7% Hypertonic Saline Nebulization on Lung Function in Children with Cystic Fibrosis: A Double-Blind Randomized, Controlled
Nebulised hypertonic saline for cystic fibrosis.
 Revista: Cochrane Database Syst Rev. 2003;(1):CD001506. Nebulised hypertonic saline for cystic fibrosis. Autor: Wark PA, McDonald V. Source: Department of Respiratory Medicine, John Hunter Hospital, Locked
Revista: Cochrane Database Syst Rev. 2003;(1):CD001506. Nebulised hypertonic saline for cystic fibrosis. Autor: Wark PA, McDonald V. Source: Department of Respiratory Medicine, John Hunter Hospital, Locked
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data. The synopsis
abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data. The synopsis
Appendix D Clinical specialist statement template
 Appendix D Colistimethate sodium powder and tobramycin powder for inhalation for the treatment of pseudomonas lung infection in cystic fibrosis Thank you for agreeing to give us a statement on your organisation
Appendix D Colistimethate sodium powder and tobramycin powder for inhalation for the treatment of pseudomonas lung infection in cystic fibrosis Thank you for agreeing to give us a statement on your organisation
Hypertonic Saline (7%) Administration Guideline (adults)
 Hypertonic Saline (7%) Administration Guideline (adults) Full Title of Guideline: Author (include email and role): Hypertonic Saline (7%) Administration Guideline for Practice (Adults) Clair Martin, Senior
Hypertonic Saline (7%) Administration Guideline (adults) Full Title of Guideline: Author (include email and role): Hypertonic Saline (7%) Administration Guideline for Practice (Adults) Clair Martin, Senior
Comparison of inhaled mannitol, daily rhdnase and a combination of both in children with cystic fibrosis: a randomised trial
 1 Royal Brompton Hospital & Imperial College, London, UK; 2 Great Ormond Street Hospital, London, UK; 3 University of Bristol, Bristol, UK Correspondence to: Dr C Minasian, Department of Paediatric Respiratory
1 Royal Brompton Hospital & Imperial College, London, UK; 2 Great Ormond Street Hospital, London, UK; 3 University of Bristol, Bristol, UK Correspondence to: Dr C Minasian, Department of Paediatric Respiratory
Comparison of inhaled mannitol, daily rhdnase, and a combination. of both in children with cystic fibrosis: a randomised trial
 Thorax Online First, published on December 8, 2009 as 10.1136/thx.2009.116970 Comparison of inhaled mannitol, daily rhdnase, and a combination of both in children with cystic fibrosis: a randomised trial
Thorax Online First, published on December 8, 2009 as 10.1136/thx.2009.116970 Comparison of inhaled mannitol, daily rhdnase, and a combination of both in children with cystic fibrosis: a randomised trial
Small Volume Nebulizer Treatment (Hand-Held)
 Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Donaldson SH, Bennett WD, Zeman KL, et al. Mucus clearance
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Donaldson SH, Bennett WD, Zeman KL, et al. Mucus clearance
Clinical Commissioning Policy: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (all ages)
 Clinical Commissioning Policy: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (all ages) NHS England Reference: 1732P NHS England INFORMATION READER BOX Directorate
Clinical Commissioning Policy: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (all ages) NHS England Reference: 1732P NHS England INFORMATION READER BOX Directorate
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment: Objectives: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Innovative products for r espiratory rrespiratory d iseases diseases April 2012
 Innovative products for respiratory diseases April 2012 Pharmaxis - company overview Objectives Employees Development of products for respiratory diseases 153 involved in research and development, clinical
Innovative products for respiratory diseases April 2012 Pharmaxis - company overview Objectives Employees Development of products for respiratory diseases 153 involved in research and development, clinical
GETTING STARTED WITH MANNITOL CHALLENGE TESTING. Rick Ballard, RRT, RPFT Applications/Education Specialist MGC Diagnostics
 GETTING STARTED WITH MANNITOL CHALLENGE TESTING Rick Ballard, RRT, RPFT Applications/Education Specialist MGC Diagnostics OBJECTIVES Indications for provocation testing Identify candidates for testing
GETTING STARTED WITH MANNITOL CHALLENGE TESTING Rick Ballard, RRT, RPFT Applications/Education Specialist MGC Diagnostics OBJECTIVES Indications for provocation testing Identify candidates for testing
SYNOPSIS. Study center(s) This study was conducted in the United States (128 centers).
 Drug product: Drug substance(s): Document No.: Edition No.: Study code: Date: SYMBICORT pmdi 160/4.5 µg Budesonide/formoterol SD-039-0725 17 February 2005 SYNOPSIS A Twelve-Week, Randomized, Double-blind,
Drug product: Drug substance(s): Document No.: Edition No.: Study code: Date: SYMBICORT pmdi 160/4.5 µg Budesonide/formoterol SD-039-0725 17 February 2005 SYNOPSIS A Twelve-Week, Randomized, Double-blind,
PULMONARY-ALLERGY DRUGS ADVISORY COMMITTEE MEETING January 30, 2013
 PULMONARY-ALLERGY DRUGS ADVISORY COMMITTEE MEETING January 30, 2013 NDA# 202049: mannitol inhalation powder (proposed trade name Bronchitol) for oral inhalation sponsored by Pharmaxis, for the management
PULMONARY-ALLERGY DRUGS ADVISORY COMMITTEE MEETING January 30, 2013 NDA# 202049: mannitol inhalation powder (proposed trade name Bronchitol) for oral inhalation sponsored by Pharmaxis, for the management
TORCH: Salmeterol and Fluticasone Propionate and Survival in COPD
 TORCH: and Propionate and Survival in COPD April 19, 2007 Justin Lee Pharmacy Resident University Health Network Outline Overview of COPD Pathophysiology Pharmacological Treatment Overview of the TORCH
TORCH: and Propionate and Survival in COPD April 19, 2007 Justin Lee Pharmacy Resident University Health Network Outline Overview of COPD Pathophysiology Pharmacological Treatment Overview of the TORCH
Clinical Commissioning Policy: Dornase alfa inhaled therapy for primary ciliary dyskinesia (all ages)
 Clinical Commissioning Policy: Dornase alfa inhaled therapy for primary ciliary dyskinesia (all ages) Reference: NHS England: 16029/P NHS England INFORMATION READER BOX Directorate Medical Operations and
Clinical Commissioning Policy: Dornase alfa inhaled therapy for primary ciliary dyskinesia (all ages) Reference: NHS England: 16029/P NHS England INFORMATION READER BOX Directorate Medical Operations and
Experience the Powder of Non-nebulized Pa Treatment
 For people 6 years and older with cystic fibrosis (CF), Pseudomonas aeruginosa (Pa), and FEV 1 25% to 80% predicted and who do not have Burkholderia cepacia. Experience the Powder of Non-nebulized Pa Treatment
For people 6 years and older with cystic fibrosis (CF), Pseudomonas aeruginosa (Pa), and FEV 1 25% to 80% predicted and who do not have Burkholderia cepacia. Experience the Powder of Non-nebulized Pa Treatment
4.6 Small airways disease
 4.6 Small airways disease Author: Jean-Marc Fellrath 1. INTRODUCTION Small airways are defined as any non alveolated and noncartilaginous airway that has an internal diameter of 2 mm. Several observations
4.6 Small airways disease Author: Jean-Marc Fellrath 1. INTRODUCTION Small airways are defined as any non alveolated and noncartilaginous airway that has an internal diameter of 2 mm. Several observations
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data. The synopsis
abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data. The synopsis
Adults with cystic fibrosis prefer hypertonic saline before or during airway clearance techniques: a randomised crossover trial
 Dentice et al: Timing of hypertonic saline and airway clearance in cystic fibrosis Adults with cystic fibrosis prefer hypertonic saline before or during airway clearance techniques: a randomised crossover
Dentice et al: Timing of hypertonic saline and airway clearance in cystic fibrosis Adults with cystic fibrosis prefer hypertonic saline before or during airway clearance techniques: a randomised crossover
Journal Club The ELITE Trial. Sandra Katalinic, Pharmacy Resident University Hospital of Northern British Columbia April 28, 2010
 Journal Club The ELITE Trial Sandra Katalinic, Pharmacy Resident University Hospital of Northern British Columbia April 28, 2010 Overview Journal article Title, journal, authors, funding Abstract Introduction
Journal Club The ELITE Trial Sandra Katalinic, Pharmacy Resident University Hospital of Northern British Columbia April 28, 2010 Overview Journal article Title, journal, authors, funding Abstract Introduction
Aerosol Therapy. Aerosol Therapy. RSPT 1410 Humidity & Aerosol Therapy Part 4
 1 RSPT 1410 Humidity & Part 4 Wilkins Chapter 36; p. 801-806 2 Stability: the tendency for aerosol particles to remain in Size: the the particle, the greater the tendency toward stability the the particle,
1 RSPT 1410 Humidity & Part 4 Wilkins Chapter 36; p. 801-806 2 Stability: the tendency for aerosol particles to remain in Size: the the particle, the greater the tendency toward stability the the particle,
CYSTIC FIBROSIS INPATIENT PROTOCOL PURPOSE POLICY STATEMENTS SITE APPLICABILITY PRACTICE LEVEL/COMPETENCIES DEFINITIONS EQUIPMENT
 PURPOSE Physiotherapy role for inpatients with cystic fibrosis. POLICY STATEMENTS On admission to hospital all patients will be assessed by the physiotherapist within 24 hours. Physiotherapists have standing
PURPOSE Physiotherapy role for inpatients with cystic fibrosis. POLICY STATEMENTS On admission to hospital all patients will be assessed by the physiotherapist within 24 hours. Physiotherapists have standing
Clinical Commissioning Policy Proposition: Dornase alfa inhaled therapy for primary ciliary dyskinesia (all ages)
 Clinical Commissioning Policy Proposition: Dornase alfa inhaled therapy for primary ciliary dyskinesia (all ages) Reference: NHS England E03X05/01 Information Reader Box (IRB) to be inserted on inside
Clinical Commissioning Policy Proposition: Dornase alfa inhaled therapy for primary ciliary dyskinesia (all ages) Reference: NHS England E03X05/01 Information Reader Box (IRB) to be inserted on inside
Innovative products for r espiratory rrespiratory d iseases diseases September 2012
 Innovative products for respiratory diseases September 2012 Pharmaxis - company overview Summary A pharmaceutical company which develops therapeutic products for human chronic respiratory diseases. Headquartered
Innovative products for respiratory diseases September 2012 Pharmaxis - company overview Summary A pharmaceutical company which develops therapeutic products for human chronic respiratory diseases. Headquartered
Turning Science into Real Life Roflumilast in Clinical Practice. Roland Buhl Pulmonary Department Mainz University Hospital
 Turning Science into Real Life Roflumilast in Clinical Practice Roland Buhl Pulmonary Department Mainz University Hospital Therapy at each stage of COPD I: Mild II: Moderate III: Severe IV: Very severe
Turning Science into Real Life Roflumilast in Clinical Practice Roland Buhl Pulmonary Department Mainz University Hospital Therapy at each stage of COPD I: Mild II: Moderate III: Severe IV: Very severe
NG80. Asthma: diagnosis, monitoring and chronic asthma management (NG80)
 Asthma: diagnosis, monitoring and chronic asthma management (NG80) NG80 NICE has checked the use of its content in this product and the sponsor has had no influence on the content of this booklet. NICE
Asthma: diagnosis, monitoring and chronic asthma management (NG80) NG80 NICE has checked the use of its content in this product and the sponsor has had no influence on the content of this booklet. NICE
COPD. Breathing Made Easier
 COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
Inhaled Hypertonic Saline In Adults Hospitalized For Exacerbation Of Cystic Fibrosis Lung Disease: A Retrospective Study For peer review only
 BMJ Open Inhaled Hypertonic Saline In Adults Hospitalized For Exacerbation Of Cystic Fibrosis Lung Disease: A Retrospective Study Journal: BMJ Open Manuscript ID: bmjopen--0000 Article Type: Research Date
BMJ Open Inhaled Hypertonic Saline In Adults Hospitalized For Exacerbation Of Cystic Fibrosis Lung Disease: A Retrospective Study Journal: BMJ Open Manuscript ID: bmjopen--0000 Article Type: Research Date
Forward Looking Statements
 Therapeutic products for respiratory diseases January 2010 Forward Looking Statements This presentation may contain forward-looking statements that are based on management s current expectations ti and
Therapeutic products for respiratory diseases January 2010 Forward Looking Statements This presentation may contain forward-looking statements that are based on management s current expectations ti and
Clinical Commissioning Policy Proposition: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (Adults)
 Clinical Commissioning Policy Proposition: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (Adults) Reference: NHS England 1621 First published: Month Year Prepared
Clinical Commissioning Policy Proposition: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (Adults) Reference: NHS England 1621 First published: Month Year Prepared
Sodium Chloride Inhalation for the Treatment of Cystic Fibrosis: A Review of the Clinical Evidence, Cost-Effectiveness and Guidelines
 TITLE: Sodium Chloride Inhalation for the Treatment of Cystic Fibrosis: A Review of the Clinical Evidence, Cost-Effectiveness and Guidelines DATE: 2 August 2012 CONTEXT AND POLICY ISSUES Cystic fibrosis
TITLE: Sodium Chloride Inhalation for the Treatment of Cystic Fibrosis: A Review of the Clinical Evidence, Cost-Effectiveness and Guidelines DATE: 2 August 2012 CONTEXT AND POLICY ISSUES Cystic fibrosis
Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis
 Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis Vallières, E., Tumelty, K., Tunney, M. M., Hannah, R., Hewitt, O., Elborn, J. S., & Downey, D. G. (2017). Efficacy of Pseudomonas
Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis Vallières, E., Tumelty, K., Tunney, M. M., Hannah, R., Hewitt, O., Elborn, J. S., & Downey, D. G. (2017). Efficacy of Pseudomonas
Effect of mannitol and repetitive coughing on the sputum properties in bronchiectasis
 Respiratory Medicine (2010) 104, 371e377 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Effect of mannitol and repetitive coughing on the sputum properties in bronchiectasis
Respiratory Medicine (2010) 104, 371e377 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Effect of mannitol and repetitive coughing on the sputum properties in bronchiectasis
aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A.
 aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A. 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and
aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A. 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and
Pocket Guide to Inhaler Technique A Step-By-Step Guide for Healthcare Professionals
 Pocket Guide to Inhaler Technique A Step-By-Step Guide for Healthcare Professionals Endorsed by NHSGGC Respiratory Managed Clinical Network; June 2016 Designed by Medical Illustration Services Contents
Pocket Guide to Inhaler Technique A Step-By-Step Guide for Healthcare Professionals Endorsed by NHSGGC Respiratory Managed Clinical Network; June 2016 Designed by Medical Illustration Services Contents
SYNOPSIS. Date 15 June 2004
 Drug product Drug substance(s) Document No. Edition No. Study code SYMBICORT pmdi 160/4.5 mg per actuation Budesonide/formoterol SD-039-0719 Date 15 June 2004 SYNOPSIS A Six-Month, Randomized, Open-Label
Drug product Drug substance(s) Document No. Edition No. Study code SYMBICORT pmdi 160/4.5 mg per actuation Budesonide/formoterol SD-039-0719 Date 15 June 2004 SYNOPSIS A Six-Month, Randomized, Open-Label
Performing a Methacholine Challenge Test
 powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
What is Cystic Fibrosis? CYSTIC FIBROSIS. Genetics of CF
 What is Cystic Fibrosis? CYSTIC FIBROSIS Lynne M. Quittell, M.D. Director, CF Center Columbia University Chronic, progressive and life limiting autosomal recessive genetic disease characterized by chronic
What is Cystic Fibrosis? CYSTIC FIBROSIS Lynne M. Quittell, M.D. Director, CF Center Columbia University Chronic, progressive and life limiting autosomal recessive genetic disease characterized by chronic
Roflumilast (Daxas) for chronic obstructive pulmonary disease
 Roflumilast (Daxas) for chronic obstructive pulmonary disease August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
Roflumilast (Daxas) for chronic obstructive pulmonary disease August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
Update on bronchiectasis guidelines. James Chalmers MD, PhD, FRCPE, FERS University of Dundee, UK
 Update on bronchiectasis guidelines James Chalmers MD, PhD, FRCPE, FERS University of Dundee, UK University of Dundee Bronchiectasis guidelines 2017 2010 2006 2008 2015 2015 Currently valid guidelines
Update on bronchiectasis guidelines James Chalmers MD, PhD, FRCPE, FERS University of Dundee, UK University of Dundee Bronchiectasis guidelines 2017 2010 2006 2008 2015 2015 Currently valid guidelines
Asthma. UVM. University of Vermont. Alicia Jacobs MD Fletcher Allen Health Care and the University of Vermont
 University of Vermont ScholarWorks @ UVM Family Medicine Scholarly Works 6-14-2013 Asthma Alicia Jacobs MD Fletcher Allen Health Care and the University of Vermont Follow this and additional works at:
University of Vermont ScholarWorks @ UVM Family Medicine Scholarly Works 6-14-2013 Asthma Alicia Jacobs MD Fletcher Allen Health Care and the University of Vermont Follow this and additional works at:
Shared Care Guideline
 Shared Care Guideline Gentamicin for Nebulisation For the long term prophylaxis of chronic lung infections in non CF bronchiectasis Executive Summary Indication Nebulised gentamicin is indicated in patients
Shared Care Guideline Gentamicin for Nebulisation For the long term prophylaxis of chronic lung infections in non CF bronchiectasis Executive Summary Indication Nebulised gentamicin is indicated in patients
Summary A pharmaceutical company which develops therapeutic products for
 Innovative products for respiratory diseases Annual General Meeting October 2012 Pharmaxis - company overview Summary A pharmaceutical company which develops therapeutic products for human chronic respiratory
Innovative products for respiratory diseases Annual General Meeting October 2012 Pharmaxis - company overview Summary A pharmaceutical company which develops therapeutic products for human chronic respiratory
Nebulised anti-pseudomonal antibiotics for cystic fibrosis (Review)
 Nebulised anti-pseudomonal antibiotics for cystic fibrosis (Review) Ryan G, Mukhopadhyay S, Singh M This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published
Nebulised anti-pseudomonal antibiotics for cystic fibrosis (Review) Ryan G, Mukhopadhyay S, Singh M This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: exhaled_nitric_oxide_measurement 2/2009 3/2018 3/2019 3/2018 Description of Procedure or Service Asthma is
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: exhaled_nitric_oxide_measurement 2/2009 3/2018 3/2019 3/2018 Description of Procedure or Service Asthma is
Bronchiectasis. Grant Waterer. Professor of Medicine, University of Western Australia Adjunct Professor of Medicine, Northwestern University, Chicago
 Bronchiectasis Grant Waterer MBBS PhD MBA FRACP FCCP Professor of Medicine, University of Western Australia Adjunct Professor of Medicine, Northwestern University, Chicago Conflicts of Interest I have
Bronchiectasis Grant Waterer MBBS PhD MBA FRACP FCCP Professor of Medicine, University of Western Australia Adjunct Professor of Medicine, Northwestern University, Chicago Conflicts of Interest I have
Lead team presentation: Roflumilast for treating chronic obstructive pulmonary disease [ID984]
![Lead team presentation: Roflumilast for treating chronic obstructive pulmonary disease [ID984] Lead team presentation: Roflumilast for treating chronic obstructive pulmonary disease [ID984]](/thumbs/85/91889043.jpg) Lead team presentation: Roflumilast for treating chronic obstructive pulmonary disease [ID984] 1 st Appraisal Committee meeting Background & Clinical Effectiveness John McMurray 11 th January 2016 For
Lead team presentation: Roflumilast for treating chronic obstructive pulmonary disease [ID984] 1 st Appraisal Committee meeting Background & Clinical Effectiveness John McMurray 11 th January 2016 For
roflumilast 500 microgram tablets (Daxas ) SMC No. (635/10) Nycomed Ltd
 roflumilast 500 microgram tablets (Daxas ) SMC No. (635/10) Nycomed Ltd 06 August 2010 (Issued 10 September 2010) The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
roflumilast 500 microgram tablets (Daxas ) SMC No. (635/10) Nycomed Ltd 06 August 2010 (Issued 10 September 2010) The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
ARIDOL (mannitol inhalation powder) Full Prescribing Information and Test Kit Instructions. Bronchial Challenge Test Kit
 NDC 44178-0552-1 ARIDOL (mannitol inhalation powder) Bronchial Challenge Test Kit Full Prescribing Information and Test Kit Instructions Please see accompanying Full Prescribing Information, Boxed Warning,
NDC 44178-0552-1 ARIDOL (mannitol inhalation powder) Bronchial Challenge Test Kit Full Prescribing Information and Test Kit Instructions Please see accompanying Full Prescribing Information, Boxed Warning,
CCLI. Bronchiectasis Treatment Antibiotics. Charles Haworth. Physician / Patient Conference, Georgetown University, May 2017
 Physician / Patient Conference, Georgetown University, May 2017 Bronchiectasis Treatment Antibiotics Charles Haworth CCLI Cambridge Centre for Lung Infection Disclosures Educational talks and / or consultancy
Physician / Patient Conference, Georgetown University, May 2017 Bronchiectasis Treatment Antibiotics Charles Haworth CCLI Cambridge Centre for Lung Infection Disclosures Educational talks and / or consultancy
The long term effect of inhaled hypertonic saline 6% in non-cystic fibrosis bronchiectasis
 Respiratory Medicine (2012) 106, 661e667 Available online at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed The long term effect of inhaled hypertonic saline 6% in non-cystic fibrosis
Respiratory Medicine (2012) 106, 661e667 Available online at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed The long term effect of inhaled hypertonic saline 6% in non-cystic fibrosis
ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS. Version 3.0 1
 ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS Version 3.0 1 1. NAME OF THE MEDICINAL PRODUCT Bronchitol 40 mg inhalation powder, hard capsules 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each hard capsule
ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS Version 3.0 1 1. NAME OF THE MEDICINAL PRODUCT Bronchitol 40 mg inhalation powder, hard capsules 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each hard capsule
I. Subject: Medication Delivery by Metered Dose Inhaler (MDI)
 I. Subject: Medication Delivery by Metered Dose Inhaler (MDI) II. Policy: Aerosol medication administration by metered dose inhaler will be performed upon a physician's order by Respiratory Therapy personnel.
I. Subject: Medication Delivery by Metered Dose Inhaler (MDI) II. Policy: Aerosol medication administration by metered dose inhaler will be performed upon a physician's order by Respiratory Therapy personnel.
PRODUCT INFORMATION. BRONCHITOL Mannitol powder for inhalation
 PRODUCT INFORMATION BRONCHITOL Mannitol powder for inhalation Name of the Medicine Mannitol. Also known as D-mannitol. The empirical formula is C 6 H 14 O 6. Molecular weight is 182.2 CAS number: 69-65-8.
PRODUCT INFORMATION BRONCHITOL Mannitol powder for inhalation Name of the Medicine Mannitol. Also known as D-mannitol. The empirical formula is C 6 H 14 O 6. Molecular weight is 182.2 CAS number: 69-65-8.
Appendix M: Device Technique
 Nursing Care of Dyspnea: The 6th Vital Sign in Individuals with Chronic Obstructive Pulmonary Disease (COPD) Appendix M: Device Technique Medications: Inhalation Devices Medications come in many forms.
Nursing Care of Dyspnea: The 6th Vital Sign in Individuals with Chronic Obstructive Pulmonary Disease (COPD) Appendix M: Device Technique Medications: Inhalation Devices Medications come in many forms.
SYNOPSIS 2/198 CSR_BDY-EFC5825-EN-E02. Name of company: TABULAR FORMAT (For National Authority Use only)
 SYNOPSIS Title of the study: A randomized, double-blind, placebo-controlled, parallel-group, fixed-dose (rimonabant 20 mg) multicenter study of long-term glycemic control with rimonabant in treatment-naïve
SYNOPSIS Title of the study: A randomized, double-blind, placebo-controlled, parallel-group, fixed-dose (rimonabant 20 mg) multicenter study of long-term glycemic control with rimonabant in treatment-naïve
Bronchial reactions to the inhalation of high-dose tobramycin in cystic fibrosis
 Eur Respir J 2002; 20: 122 126 DOI: 10.1183/09031936.02.00264002 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 Bronchial reactions to the
Eur Respir J 2002; 20: 122 126 DOI: 10.1183/09031936.02.00264002 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 Bronchial reactions to the
A NEBULISERS AND NEBULISED MEDICATION. Generic Guide for the use of nebulisers and nebulised medication
 A NEBULISERS AND NEBULISED MEDICATION Generic Guide for the use of nebulisers and nebulised medication Aim The aim of this guide is to provide a template for those who wish to develop their own nebuliser
A NEBULISERS AND NEBULISED MEDICATION Generic Guide for the use of nebulisers and nebulised medication Aim The aim of this guide is to provide a template for those who wish to develop their own nebuliser
Jennifer R Bishop, Odette J Erskine and Peter G Middleton
 Timing of dornase alpha inhalation does not affect the efficacy of an airway clearance regimen in adults with cystic fibrosis: a randomised crossover trial Jennifer R Bishop, Odette J Erskine and Peter
Timing of dornase alpha inhalation does not affect the efficacy of an airway clearance regimen in adults with cystic fibrosis: a randomised crossover trial Jennifer R Bishop, Odette J Erskine and Peter
Northumbria Healthcare NHS Foundation Trust. Bronchiectasis. Issued by Respiratory Medicine
 Northumbria Healthcare NHS Foundation Trust Bronchiectasis Issued by Respiratory Medicine The aim of this booklet is to help you manage your bronchiectasis. It contains information which you should find
Northumbria Healthcare NHS Foundation Trust Bronchiectasis Issued by Respiratory Medicine The aim of this booklet is to help you manage your bronchiectasis. It contains information which you should find
The Use of Active Cycle of Breathing Technique (ACBT) In Pulmonary Physiotherapy: A Critical Review of the Literature Lauro G. Villegas Jr.
 The Use of Active Cycle of Breathing Technique (ACBT) In Pulmonary Physiotherapy: A Critical Review of the Literature Lauro G. Villegas Jr., PTRP Keywords: Active Cycle of Breathing Technique (ACBT), Pulmonary
The Use of Active Cycle of Breathing Technique (ACBT) In Pulmonary Physiotherapy: A Critical Review of the Literature Lauro G. Villegas Jr., PTRP Keywords: Active Cycle of Breathing Technique (ACBT), Pulmonary
Therapeutic products for respiratory and autoimmune diseases. Annual General Meeting
 Therapeutic products for respiratory and autoimmune diseases Annual General Meeting November 2007 Summary Objective Lead products Discovery Listings Location Facility Employees Cash (30/6/07) Shares outstanding
Therapeutic products for respiratory and autoimmune diseases Annual General Meeting November 2007 Summary Objective Lead products Discovery Listings Location Facility Employees Cash (30/6/07) Shares outstanding
Prescribing guidelines: Management of COPD in Primary Care
 Prescribing guidelines: Management of COPD in Primary Care Establish diagnosis of COPD in patients 35 years with appropriate symptoms with history, examination and spirometry (FEV1/FVC ratio < 70%) Establish
Prescribing guidelines: Management of COPD in Primary Care Establish diagnosis of COPD in patients 35 years with appropriate symptoms with history, examination and spirometry (FEV1/FVC ratio < 70%) Establish
Chronic Obstructive Pulmonary Disease (COPD) Self-management plan
 Chronic Obstructive Pulmonary Disease (COPD) Self-management plan Respiratory Respiratory Nurses Royal Lancaster Infirmary & Westmorland General Hospital 01524 583608 Furness General Hospital 01229 403584
Chronic Obstructive Pulmonary Disease (COPD) Self-management plan Respiratory Respiratory Nurses Royal Lancaster Infirmary & Westmorland General Hospital 01524 583608 Furness General Hospital 01229 403584
CPT (Current Procedural Terminology) and Drug Coding Guidance
 CPT (Current Procedural Terminology) and Drug Coding Guidance Aridol (mannitol inhalation powder) Bronchial Challenge Test Kit NDC 44178-0552-1 The CPT codes provided are consistent with AMA guidance for
CPT (Current Procedural Terminology) and Drug Coding Guidance Aridol (mannitol inhalation powder) Bronchial Challenge Test Kit NDC 44178-0552-1 The CPT codes provided are consistent with AMA guidance for
ADASUVE (LOXAPINE) INHALATION POWDER. EDUCATION PROGRAM for HEALTHCARE PROFESSIONALS
 ADASUVE (LOXAPINE) INHALATION POWDER EDUCATION PROGRAM for HEALTHCARE PROFESSIONALS August2017 December 2012 PMR-JUN-2017-0017 ADASUVE Risk Evaluation and Mitigation Strategy (REMS) Education Program Content
ADASUVE (LOXAPINE) INHALATION POWDER EDUCATION PROGRAM for HEALTHCARE PROFESSIONALS August2017 December 2012 PMR-JUN-2017-0017 ADASUVE Risk Evaluation and Mitigation Strategy (REMS) Education Program Content
Respiratory Physiology In-Lab Guide
 Respiratory Physiology In-Lab Guide Read Me Study Guide Check Your Knowledge, before the Practical: 1. Understand the relationship between volume and pressure. Understand the three respiratory pressures
Respiratory Physiology In-Lab Guide Read Me Study Guide Check Your Knowledge, before the Practical: 1. Understand the relationship between volume and pressure. Understand the three respiratory pressures
Non pharmacological approaches to asthma: Physiotherapy. Claire Hepworth Specialist Respiratory Physiotherapist
 Non pharmacological approaches to asthma: Physiotherapy Claire Hepworth Specialist Respiratory Physiotherapist Good breathing control Buteyko therapy & research How to clear the nose effectively Managing
Non pharmacological approaches to asthma: Physiotherapy Claire Hepworth Specialist Respiratory Physiotherapist Good breathing control Buteyko therapy & research How to clear the nose effectively Managing
Study No.: Title: Rationale: Phase: Study Period Study Design: Centres: Indication: Treatment: Objectives : Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
C.S. HAWORTH 1, A. WANNER 2, J. FROEHLICH 3, T. O'NEAL 3, A. DAVIS 4, I. GONDA 3, A. O'DONNELL 5
 Inhaled Liposomal Ciprofloxacin in Patients With Non-Cystic Fibrosis Bronchiectasis and Chronic Pseudomonas aeruginosa: Results From Two Parallel Phase III Trials (ORBIT-3 and -4) C.S. HAWORTH 1, A. WANNER
Inhaled Liposomal Ciprofloxacin in Patients With Non-Cystic Fibrosis Bronchiectasis and Chronic Pseudomonas aeruginosa: Results From Two Parallel Phase III Trials (ORBIT-3 and -4) C.S. HAWORTH 1, A. WANNER
How can I benefit most from my COPD medications?
 Fact Sheet: COPD Medications and Delivery Devices How can I benefit most from my COPD medications? COPD medications can improve your symptoms. By taking the right medication at the right time, you can
Fact Sheet: COPD Medications and Delivery Devices How can I benefit most from my COPD medications? COPD medications can improve your symptoms. By taking the right medication at the right time, you can
SYNOPSIS THIS IS A PRINTED COPY OF AN ELECTRONIC DOCUMENT. PLEASE CHECK ITS VALIDITY BEFORE USE.
 Drug product: Drug substance(s): Document No.: Edition No.: 1 Study code: Accolate Zafirlukast (ZD9188) 9188IL/0138 Date: 02 May 2007 SYNOPSIS A Multicenter, Randomized, Double-blind, -controlled, Parallel
Drug product: Drug substance(s): Document No.: Edition No.: 1 Study code: Accolate Zafirlukast (ZD9188) 9188IL/0138 Date: 02 May 2007 SYNOPSIS A Multicenter, Randomized, Double-blind, -controlled, Parallel
Aclidinium bromide/formoterol Endpoint category. RR Endpoint. [95% CI 2 ] Study. with event
![Aclidinium bromide/formoterol Endpoint category. RR Endpoint. [95% CI 2 ] Study. with event Aclidinium bromide/formoterol Endpoint category. RR Endpoint. [95% CI 2 ] Study. with event](/thumbs/90/102875145.jpg) Resolution by the Federal Joint Committee on an amendment to the Pharmaceutical Directive (AM-RL): Appendix XII Resolutions on the benefit assessment of pharmaceuticals with new active ingredients, in
Resolution by the Federal Joint Committee on an amendment to the Pharmaceutical Directive (AM-RL): Appendix XII Resolutions on the benefit assessment of pharmaceuticals with new active ingredients, in
Individual Study Table Referring to Part of the Dossier. Volume:
 Final Report M/100977/21Final Version () 2. SYNOPSIS A Title of Study: A PHASE IIa, RANDOMISED, DOUBLE-BLIND, MULTIPLE DOSE, PLACEBO CONTROLLED, 3 PERIOD CROSS-OVER, ASCENDING DOSE CLINICAL TRIAL TO ASSESS
Final Report M/100977/21Final Version () 2. SYNOPSIS A Title of Study: A PHASE IIa, RANDOMISED, DOUBLE-BLIND, MULTIPLE DOSE, PLACEBO CONTROLLED, 3 PERIOD CROSS-OVER, ASCENDING DOSE CLINICAL TRIAL TO ASSESS
Key points. Credit: Sheffield Teaching Hospitals NHS Foundation Trust
 Key points There have been significant advances in both inhalation medicines and delivery devices with intelligent nebulisers and dry-powder inhalers becoming commonplace in CF care. Inhaled medicines
Key points There have been significant advances in both inhalation medicines and delivery devices with intelligent nebulisers and dry-powder inhalers becoming commonplace in CF care. Inhaled medicines
Active Cycle of Breathing Technique
 Active Cycle of Breathing Technique Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when
Active Cycle of Breathing Technique Full Title of Guideline: Author (include email and role): Division & Speciality: Version: 3 Ratified by: Scope (Target audience, state if Trust wide): Review date (when
Pseudomonas aeruginosa eradication guideline
 SCOTTISH PAEDIATRIC CYSTIC FIBROSIS MCN Pseudomonas aeruginosa eradication guideline Date Created: 27 th June 2013 Date Approved by Steering Group: 30 th May 2014 Date of Review: 31 st May 2016 Lead Author:
SCOTTISH PAEDIATRIC CYSTIC FIBROSIS MCN Pseudomonas aeruginosa eradication guideline Date Created: 27 th June 2013 Date Approved by Steering Group: 30 th May 2014 Date of Review: 31 st May 2016 Lead Author:
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Committed to the research, development and commercialisation of human therapeutic products for chronic respiratory and autoimmune diseases
 ABN 75 082 811 630 Committed to the research, development and commercialisation of human therapeutic products for chronic respiratory and autoimmune diseases November 2003 Overview Our Objective to build
ABN 75 082 811 630 Committed to the research, development and commercialisation of human therapeutic products for chronic respiratory and autoimmune diseases November 2003 Overview Our Objective to build
umeclidinium, 55 micrograms, powder for inhalation (Incruse ) SMC No. (1004/14) GlaxoSmithKline
 umeclidinium, 55 micrograms, powder for inhalation (Incruse ) SMC No. (1004/14) GlaxoSmithKline 07 November 2014 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
umeclidinium, 55 micrograms, powder for inhalation (Incruse ) SMC No. (1004/14) GlaxoSmithKline 07 November 2014 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
Signs and Symptoms of Chest Infections
 Signs and Symptoms of Chest Infections Chest infection If you have been diagnosed with a lung condition you can be at greater risk of contracting a chest infection. Chest infections can be caused by a
Signs and Symptoms of Chest Infections Chest infection If you have been diagnosed with a lung condition you can be at greater risk of contracting a chest infection. Chest infections can be caused by a
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Moss RB, Flume PA, Elborn JS, et al, on behalf
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Moss RB, Flume PA, Elborn JS, et al, on behalf
Forward Looking Statements
 Therapeutic products for respiratory diseases September 2008 Forward Looking Statements This presentation may contain forward-looking statements that are based on management s current expectations and
Therapeutic products for respiratory diseases September 2008 Forward Looking Statements This presentation may contain forward-looking statements that are based on management s current expectations and
A Place For Airway Clearance Therapy In Today s Healthcare Environment
 A Place For Airway Clearance Therapy In Today s Healthcare Environment Michigan Society for Respiratory Care 2015 Fall Conference K. James Ehlen, MD October 6, 2015 Objectives Describe patients who will
A Place For Airway Clearance Therapy In Today s Healthcare Environment Michigan Society for Respiratory Care 2015 Fall Conference K. James Ehlen, MD October 6, 2015 Objectives Describe patients who will
Supplementary Medications during asthma attack. Prof. Dr Finn Rasmussen PhD. DrMedSc. Near East University Hospital North Cyprus
 Supplementary Medications during asthma attack Prof. Dr Finn Rasmussen PhD. DrMedSc. Near East University Hospital North Cyprus Conflicts of Interest None Definition of Asthma Airway narrowing that is
Supplementary Medications during asthma attack Prof. Dr Finn Rasmussen PhD. DrMedSc. Near East University Hospital North Cyprus Conflicts of Interest None Definition of Asthma Airway narrowing that is
Forward Looking Statements
 Therapeutic products for respiratory diseases October 2011 Forward Looking Statements This presentation may contain forward-looking statements that are based on management s current expectations and beliefs
Therapeutic products for respiratory diseases October 2011 Forward Looking Statements This presentation may contain forward-looking statements that are based on management s current expectations and beliefs
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data. The synopsis
abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data. The synopsis
Cystic Fibrosis the future
 Cystic Fibrosis the future Pathophysiologic cascade Abnormal Gene Abnormal CFTR Therapy Gene replacement Protein replacement Gene read through therapy Abnormal sodium chloride & water movement through
Cystic Fibrosis the future Pathophysiologic cascade Abnormal Gene Abnormal CFTR Therapy Gene replacement Protein replacement Gene read through therapy Abnormal sodium chloride & water movement through
PAEDIATRIC RESPIRATORY FAILURE. Tang Swee Fong Department of Paediatrics University Kebangsaan Malaysia Medical Centre
 PAEDIATRIC RESPIRATORY FAILURE Tang Swee Fong Department of Paediatrics University Kebangsaan Malaysia Medical Centre Outline of lecture Bronchiolitis Bronchopulmonary dysplasia Asthma ARDS Bronchiolitis
PAEDIATRIC RESPIRATORY FAILURE Tang Swee Fong Department of Paediatrics University Kebangsaan Malaysia Medical Centre Outline of lecture Bronchiolitis Bronchopulmonary dysplasia Asthma ARDS Bronchiolitis
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
TR Protocol Number: TR02-107
 TR02-107 A PLACEBO CONTROLLED, RANDOMIZED, PARALLEL COHORT, SAFETY AND TOLERABILITY STUDY OF TWO DOSE LEVELS OF LIPOSOMAL AMIKACIN FOR INHALATION (ARIKACE ) IN PATIENTS WITH BRONCHIECTASIS COMPLICATED
TR02-107 A PLACEBO CONTROLLED, RANDOMIZED, PARALLEL COHORT, SAFETY AND TOLERABILITY STUDY OF TWO DOSE LEVELS OF LIPOSOMAL AMIKACIN FOR INHALATION (ARIKACE ) IN PATIENTS WITH BRONCHIECTASIS COMPLICATED
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the
abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the
