Pulmonary distribution, regulation, and functional role of Trk receptors in a murine model of asthma
|
|
|
- Corey Osborne
- 5 years ago
- Views:
Transcription
1 Pulmonary distribution, regulation, and functional role of Trk receptors in a murine model of asthma Christina Nassenstein, MD, PhD, a * David Dawbarn, PhD, b * Kenneth Pollock, PhD, c Shelley Jane Allen, PhD, b Veit Johannes Erpenbeck, MD, PhD, a Emma Spies, a Norbert Krug, MD, a and Armin Braun, PhD a Hannover, Germany, and Bristol and Surrey, United Kingdom Background: Neurotrophins have been implicated in the pathogenesis of asthma because of their ability to promote hyperreactivity of sensory neurons and to induce airway inflammation. Hyperreactivity of sensory nerves is one key mechanism of airway hyperreactivity that is defined as an abnormal reactivity of the airways to unspecific stimuli, such as cold air and cigarette smoke. Neurotrophins use a dualreceptor system consisting of Trk receptor tyrosine kinases and the structurally unrelated p75 neurotrophin receptor. Objective: The aim of this study was to characterize the distribution, allergen-dependent regulation, and functional relevance of the Trk receptors in allergic asthma. Methods: BALB/c mice were sensitized to ovalbumin. After provocation with ovalbumin or vehicle aerosol, respectively, Trk receptor expression was analyzed in lung tissue by means of fluorescence microscopy and quantitative RT-PCR. To assess the functional relevance of Trk receptors in asthma, we tested the effects of the intranasally administered pan-trk receptor decoy REN1826. Allergic airway inflammation was quantified and lung function was measured by using head-out body plethysmography. Results: Trk receptors were expressed in neurons, airway smooth muscle cells, and cells of the inflammatory infiltrate surrounding the bronchi and upregulated after allergen challenge. Local application of REN1826 reduced IL-4 and IL-5 cytokine levels but had no effect on IL-13 levels or the cellular composition of bronchoalveolar lavage fluid cells. Furthermore, REN1826 decreased broncho-obstruction in response to sensory stimuli, indicating a diminished hyperreactivity of From a the Fraunhofer Institute of Toxicology and Experimental Medicine, Hannover; b the Henry Wellcome Laboratories, University of Bristol; and c ReNeuron Ltd, Guildford, Surrey. *These authors contributed equally to this study. Supported by a grant from the Deutsche Forschungsgemeinschaft (SFB 587, B4) and by direct financial support from ReNeuron Ltd and the Fraunhofer Society. Disclosure of potential conflict of interest: C. Nassenstein has received grant support from the German Research Foundation. D. Dawbarn has received grant support from Wellcome Trust and ReNeuron PLC. S. J. Allen has received grant support from Wellcome Trust and ReNeuron PLC. K. Pollock is employed by ReNeuron Ltd. The rest of the authors have declared that they have no conflict of interest. Received for publication January 25, 2006; revised March 22, 2006; accepted for publication April 24, Available online July 5, Reprint requests: Armin Braun, PhD, Immunology and Allergology, Fraunhofer Institute of Toxicology and Experimental Medicine, Nikolai-Fuchs-Str. 1, Hannover, Germany. braun@item.fraunhofer.de /$32.00 Ó 2006 American Academy of Allergy, Asthma and Immunology doi: /j.jaci sensory nerves, but did not influence airway smooth muscle hyperreactivity in response to methacholine. Conclusion: These results emphasize the important role of Trk receptor signaling in the development of asthma. Clinical implications: Our data indicate that blocking of Trk receptor signaling might reduce asthma symptoms. (J Allergy Clin Immunol 2006;118: ) Key words: Sensory nerves, airway hyperreactivity, airway inflammation, reflex bronchospasm, capsaicin Asthma is a chronic inflammatory disorder of the airways in which many cells and cellular elements play a role. In susceptible individuals this inflammation causes recurrent episodes of wheezing, breathlessness, chest tightness, and coughing. The inflammation also causes an associated increase in the existing bronchial hyperreactivity to a variety of stimuli. 1 On the basis of this definition, research activities of recent years were focused on discovering the immunologic events leading to allergic airway inflammation. However, it becomes clear that mediators of induce dysfunction in sensory nerves characterized by a long-lasting change of activity that becomes independent from inflammation during chronification. Growing evidence suggests that neurotrophins (NTs), such as nerve growth factor (NGF), brain-derived neurotrophic factor (BDNF), NT-3, and NT-4, might be important mediators for plasticity of sensory nerves in several disorders associated with inflammation, including allergic asthma. 2,3 Thus local application of NGF and BDNF induces airway hyperreactivity by contributing to an altered neuronal control of airway smooth muscle cells. 3,4 Antagonism of NGF inhibited allergeninduced allergic early-phase reactions and suppressed allergic inflammation in a murine model of asthma, whereas local treatment with NGF increased the influx of eosinophils into the lung. 5 NTs influence either directly by promoting survival and activation 6 and augmenting cytokine synthesis 2 or indirectly through amplification of proinflammatory neuropeptide synthesis in sensory neurons. 7 NTs exert individual cellular effects by means of interaction with 2 structurally unrelated receptors, the p75 NT receptor (p75ntr), which belongs to the TNF receptor superfamily, and the Trk receptor tyrosine kinases. Although p75ntr is capable of binding to all 597
2 598 Nassenstein et al J ALLERGY CLIN IMMUNOL SEPTEMBER 2006 Abbreviations used BALF: Bronchoalveolar lavage fluid BDNF: Brain-derived neurotrophic factor EF 50 : Tidal midexpiratory flow HBP: Head-out body plethysmography MCh: Methacholine NGF: Nerve growth factor NT: Neurotrophin OVA: Ovalbumin P75NTR: p75 neurotrophin receptor PC: Provocative concentration PD: Provocative dose REN1826: Pan-Trk receptor decoy (soluble TrkAd5 of a TrkA splice variant) Tb: Time of braking TBS: Tris-buffered saline TRPV1: Transient receptor potential vanilloid 1 mature NTs with equivalent affinity but unique kinetics, the Trk receptors exhibit ligand selectivity. Thus TrkA has been identified as the preferred receptor for NGF, TrkB for both BDNF and NT-4, and TrkC for NT-3. p75ntr and Trk receptors can form heteromeric complexes when both receptors are coexpressed, 8 resulting in an altered affinity and specificity of the Trk-NT interaction through conformational changes in Trk receptor proteins. 9 This is functionally associated with a prolonged survival after binding of NTs to neurons, 10 as well as to immune cells. 11 Under conditions in which concomitant Trk signaling is impaired, p75ntr can promote cell death in a variety of cell types, 12 whereas survival predominantly reflects Trk activation. 13 Because mechanisms involved in the regulation of sensory nerve and immune cell function play a central role in the pathogenesis of allergic airway diseases, we hypothesized that Trk receptors might play an important role in asthma. To address this question, we analyzed Trk receptor expression and its allergen-dependent regulation in murine lungs, constructed a novel soluble Trk receptor fragment (pan-trk receptor decoy [REN1826]) capable of binding all NTs with a high affinity, and investigated its effects after local application in a well-established mouse model of allergic asthma. REN1826 vector construction, protein expression, and purification To investigate the functional role of all Trk receptors, we generated REN1826. Details are provided in the Online Repository at Treatment protocol All animals were OVA sensitized, as previously described. 5 Aerosol challenges with either PBS (negative controls) or 1% OVA-PBS (positive controls and treatment groups) were performed on days 26, 27, and 35. Intranasal treatment with vehicle (negative and positive control groups) or 50, 200, or 800 ng of REN1826 per animal (treatment groups), respectively, was performed before each allergen challenge and consecutively every 2 days until day Lung function was assessed by using head-out body plethysmography (HBP) in response to capsaicin at days 28 and 36 and in response to methacholine (MCh) at day 29. Bronchoalveolar lavage was performed at day 36, as previously described (see Fig E1 in the Online Repository at 2 Quantification and localization of Trk receptor expression Trk receptor mrna expression was assessed by using real-time RT-PCR in murine lung tissue after exsanguination. To localize Trk receptor expression in the murine lung, we performed immunohistochemistry. Detailed protocols including primer sequences (Table E1) are provided in the Online Repository at Assessment of lung function Airway hyperreactivity was measured in response to inhaled capsaicin and MCh by using HBP in conscious and spontaneously breathing animals, as previously described. 14 Baseline measurements were followed by aerosol provocation with vehicle (10% EtOH in PBS for capsaicin and PBS for MCh, respectively) and increasing doses of capsaicin or MCh generated by a Pari Master aerosol generator (Pari-Werke, Starnberg, Germany). Changes of the time of braking (Tb) in response to capsaicin were used as a surrogate marker to assess a hyperreactivity of afferent sensory nerves of the airways. 3,14 The tidal midexpiratory airflow (EF 50 ; in milliliters per second) was analyzed to assess broncho-obstruction after capsaicin or MCh challenge, respectively, to evaluate the role of Trk receptors for reflex bronchospasm or smooth muscle constriction, respectively. The provocative concentration (PC; capsaicin [in micrograms per milliliter]) or the provocative dose (PD; MCh [in micrograms]) causing a decrease in EF 50 to 25% (capsaicin) or 50% (MCh) of the vehicle value was calculated after extrapolation of the dose-response curves and is expressed as PC 25 EF 50 (capsaicin) or PD 50 EF 50 (MCh). Details are provided in the Online Repository at www. jacionline.org. METHODS Animals Six- to 8-week-old female BALB/c mice were obtained from Charles River, Sulzfeld, Germany. They were fed with ovalbumin (OVA) free laboratory food and tap water ad libitum and held in a regular 12-hour dark-light cycle at a temperature of 22 C. All animal care practices and experimental procedures were performed in concordance with the German animal protection law under a protocol approved by the appropriate governmental authority (Bezirksregierung Hannover). Differential cell count Cytospin preparations from bronchoalveolar lavage fluid (BALF) cells were stained according to the Pappenheim standard protocol. Details are provided in the Online Repository at Assessment of cytokine levels in BALF The measurement of cytokines in BALF was performed in duplicate according to the manufacturer s recommendation (DuoSet ELISA Development Kit; R&D Systems, Wiesbaden, Germany). The detection limit was 12.5 pg/ml for all cytokines.
3 J ALLERGY CLIN IMMUNOL VOLUME 118, NUMBER 3 Nassenstein et al 599 FIG 1. Trk receptor mrna expression in murine lung tissue 24 hours after allergen challenge. A, End-point analysis revealed the expected product lengths. B, Quantification of Trk mrna expression is shown (n 5 8 per group). PBGD, Porphobilinogen deaminase (housekeeping gene); RNA, RNA control; POS, positive control group; NEG, negative control group. **P <.01. Statistical analysis Statistical analysis was performed with GraphPad Prism Version 4.0 (GraphPad Software, San Diego, Calif). Details are provided in the Online Repository at RESULTS Allergen-dependent regulation of Trk mrna expression in the murine lung To investigate Trk receptor expression in lung tissue and to test its potential allergen-dependent regulation in the lung, we performed quantitative RT-PCR in lung tissue obtained from the positive control group (OVA-sensitized and OVA-challenged animals, intranasal treatment with vehicle) or negative control group (OVAsensitized and PBS-challenged animals, intranasal treatment with vehicle), respectively. No difference in TrkA mrna expression levels was observed, whereas TrkB and TrkC mrna expression levels in the lung tissue were upregulated in the positive control group (Fig 1). Localization of Trk receptor expression in the murine lung Cellular distribution of Trk receptors in the murine lung was investigated by means of immunohistochemistry. Immunoreactivity for all Trk receptors was detected in large bundles of nerve fibers, as well as on terminal subepithelial varicosities, most likely reflecting sensory nerves adjacent to the airways. Furthermore, TrkA and TrkC expression was observed in airway smooth muscle cells. The Trk expression pattern in neuronal cells and airway smooth muscle cells did not differ between the animals of the positive and negative control groups (data not shown). In addition, expression of all Trks was detected in inflammatory infiltrates surrounding the bronchi and blood vessels. Trk expression in immune cells was detected exclusively in the lungs of the positive control group (Fig 2). Further analysis revealed that TrkA 1, TrkB 1, and TrkC 1 cells of the inflammatory infiltrate belonged to different immune cell subtypes, including T cells, B cells, and antigen-presenting cells. In contrast, none of these receptors was expressed by eosinophils (Table I and Fig E2 in the Online Repository at REN1826 protein expression To study the functional relevance of Trk receptors, we generated REN1826. The molecular weight of purified recombinant REN1826 was tested by means of matrixassisted laser desorption/ionization time-of-flight and showed the correct predicted molecular weight, including the initiating methionine (data not shown). Endotoxin testing revealed that the preparation was endotoxin free. Hyperreactivity of afferent sensory nerves in response to capsaicin Tb was determined by means of HBP on days 28 and 36 in response to capsaicin to analyze the functional consequences of Trk receptors on afferent sensory nerves. Tb baseline values did not differ among the different groups and days of assessment. As described before, 14 the aerosol
4 600 Nassenstein et al J ALLERGY CLIN IMMUNOL SEPTEMBER 2006 FIG 2. Immunohistochemical localization of Trk receptors in the murine lungs. Left row, Trk receptor expression in the trachea. Right row, Trk receptor expression in cells of the inflammatory infiltrate surrounding the bronchi. Inserts, Corresponding isotype controls. White bars represent 50 mm. The figure shows representative results from one of 4 independent experiments. N, Nerves; SM, smooth muscle; E, epithelium; L, airway lumen. TABLE I. Expression and distribution of Trk receptors in murine lung tissue TrkA TrkB TrkC Epithelium Nerves Airway smooth muscle CD45 1 immune cells 1* 1* 1* CD3 1 T lymphocytes 1* 2 1* CD19 1 B lymphocytes 1* 1* 1* MHC II 1 antigen-presenting 1* 1* 1* cells MBP 1 eosinophils MBP, Major basic protein. *Expression can be observed only after allergen provocation. of the vehicle control caused a slight prolongation of Tb in all investigated groups, which was further enhanced by increasing doses of capsaicin aerosol. Hyperreactivity in sensory nerves, as indicated by a markedly prolonged Tb in response to capsaicin aerosol, was observed in the positive control groups when compared with the negative control groups. Intranasal treatment with REN1826 in OVA-sensitized and OVA-challenged animals reduced hyperreactivity of sensory nerves in a dose-dependent manner. Contrary to day 28, hyperreactivity was also absent in those animals that received 50 ng of REN1826 when measurements were repeated on day 36 to evaluate a sustained effect of repeatedly administered REN1826 after iterated allergen challenge (Fig 3). Hyperreactivity of sensory nerves in response to capsaicin was measured
5 J ALLERGY CLIN IMMUNOL VOLUME 118, NUMBER 3 Nassenstein et al 601 FIG 3. Hyperreactivity of sensory nerves to capsaicin. A, Original monitor picture during capsaicin aerosol challenge. B, Dose-response curves at days 28 and 36. C, Exemplary statistical analysis for Tb during aerosol challenge with 100 mg/ml capsaicin (n 5 16 per group). *P <.05; **P <.01. neg, Negative control group; pos, positive control group. in an independent experiment after intratracheal treatment with vehicle (positive and negative control groups) or 200 ng of REN1826 to confirm that these results are related to pulmonary deposition of intranasally applied REN1826. Changes in Tb were similar to those obtained after intranasal treatment with REN1826 (data not shown). Broncho-obstruction in response to capsaicin The EF 50 was measured and the PC 25 EF 50 (in micrograms per milliliter) values were calculated to assess broncho-obstruction in response to selective activation of afferent sensory nerve fibers; low values correspond to an increased broncho-obstruction. No difference in EF 50 baseline values and EF 50 values after inhalation of the vehicle control was seen between the investigated groups. The PC 25 EF 50 values were significant lower in the positive control group compared with those in the negative control group. Intranasal treatment with REN1826 increased the PC 25 EF 50 in a dose-dependent manner both on day 28 and on day 36 (Fig 4). Similar results were observed after intratracheal application of REN1826 (data not shown). Broncho-obstruction in response to MCh MCh aerosol provocation was performed on day 29 by using HBP to investigate the contribution of Trk receptors to the development of airway smooth muscle cell hyperreactivity. No difference in EF 50 baseline values and EF 50 values after inhalation of vehicle control was seen among the investigated groups (data not shown). Hyperreactivity of airway smooth muscle cells to MCh was observed in the positive control group, indicated by a significantly lower PD 50 EF 50 compared with that of the negative control group. This response was not altered by intranasal treatment with REN1826 (Fig 5) or after intratracheal application (data not shown).
6 602 Nassenstein et al J ALLERGY CLIN IMMUNOL SEPTEMBER 2006 FIG 4. Broncho-obstruction to inhaled capsaicin. The PC (in micrograms per milliliter) of capsaicin causing a 25% decrease in EF 50 of the appropriate vehicle control was calculated (PC 25 EF 50 [in micrograms per milliliter]; n 5 16 per group). *P <.05; **P <.01. neg, Negative control group; pos, positive control group. DISCUSSION FIG 5. Broncho-obstruction to inhaled MCh. The PD (in micrograms) of MCh causing a 50% decrease in EF 50 of the appropriate vehicle control was calculated (PD 50 EF 50 [in micrograms]; n 5 16 per group). *P <.05. neg, Negative control group; pos, positive control group. Airway inflammation To investigate the effect of Trk receptors on airway inflammation, we assessed cytokine levels, as well as differential cell counts, in the BALF. As expected, marked increases in T H 2 cytokine levels (IL-4, IL-5, and IL-13) and the numbers of eosinophils, lymphocytes, and neutrophils were observed in the positive control animals when compared with the negative control animals. IFN-g levels of all groups were under the detection limit of the appropriate ELISA (data not shown). IL-4 and IL-5 levels were dose-dependently reduced by intranasal treatment with REN1826, whereas IL-13 levels and the numbers of infiltrating inflammatory cells, including eosinophils and lymphocytes, remained unaffected (Fig 6 and Table II). There were no differences in BALF recovery between the different groups. In this study the expression, distribution, and function of Trk receptors in the murine airways were analyzed. Trk receptors were expressed in airway smooth muscle cells and nerve fibers of healthy control mice and additionally in cells of the inflammatory infiltrate surrounding the bronchi and blood vessels of allergen-challenged animals. These results were associated with a marked increase in mrna levels of TrkB and TrkC in the inflamed lung tissue. Our data are therefore consistent with the results that were observed in the human lung sections showing Trk receptor expression in various cells types in healthy individuals 15 and in infiltrating cells after allergen provocation in patients with asthma. 6 The functional relevance of Trk receptor expression in asthma development was demonstrated by inhibition of Trk receptor binding with REN1826 before repetitive allergen challenges in a mouse model of allergic asthma. Our results clearly indicate that Trk receptors are involved in hyperreactivity of afferent sensory nerve fibers, reflex broncho-obstruction to capsaicin, and airway inflammation. Responsiveness of bronchial and pulmonary sensory nerve fibers was measured on the basis of prolongation of Tb as a central reflex mechanism after stimulation with capsaicin. Capsaicin is an exogenous agonist of the transient receptor potential vanilloid 1 (TRPV1) that is expressed almost selectively in C and Ad nociceptive fibers (reviewed in Szallasi and Blumberg 16 ). Although capsaicin was used as a surrogate to assess functional changes in sensory nerve fibers, it is likely that responses to stimulation with capsaicin reflect the responses to endogenous TRPV1 ligands. Endogenous ligands of this receptor, which might also play a role in allergic asthma, are acids and lipid mediators, such as anandamide and lipoxygenase products. In addition, stimulation of G-coupled receptors, such as the bradykinin B2 receptor, exert their effects, probably through activation of TRPV1 (reviewed in Suh and Oh 17 ).
7 J ALLERGY CLIN IMMUNOL VOLUME 118, NUMBER 3 Nassenstein et al 603 NTs contribute to the onset of an enhanced sensitivity of afferent sensory nerve fibers to capsaicin, 3,5 for example by potentiating the response to TRPV1 agonists. 18 The results of our study indicate that Trk receptor signaling is important in the development of hyperreactive sensory nerves in allergic asthma. Therefore it might be likely that the pathways responsible for transducing the Trk-dependent sensitization of TRPV1 in asthma are comparable with those in thermal hyperalgesia. NGF-induced rapid sensitization of nociceptive sensory neurons to painful thermal stimuli depends on activation of second messengers of the Trk cascade, including phosphatidylinositol-39-kinase, protein kinase C, and calcium-calmodulin dependent protein kinase II. 19 However, because p75ntr is also involved in the increased excitability of sensory neurons, as has been demonstrated both in vitro 20 and in vivo in a mouse model of allergic asthma, 14 our data support the hypothesis that NTs probably bind to heteromeric complexes consisting of Trk and p75ntr 8,9 on sensory nerves innervating the airways. This assumption has to be confirmed experimentally. Subsequent activation of sensitized neurons (eg, by TRPV1 agonists, 21 ozone, exercise, and a variety of inflammatory mediators [reviewed in Joos et al 22 ]) could increase broncho-obstruction by both central reflex pathways facilitating efferent parasympathetic nerve activity and by local or axon reflexes characterized by release of neuropeptides from sensory nerve endings We have shown in our study that capsaicin-induced broncho-obstruction is also inhibited by local application of a pan-trk receptor decoy, indicating that NT signaling through Trk receptors is involved in reflex bronchospasm. NTs might influence reflex bronchospasm through upregulation of neuropeptide synthesis in ganglion neurons 26 and increase of the number of neuropeptide-immunoreactive nodose ganglion neurons projecting to the airways during. 27,28 After antidromic transport, neuropeptides are then stored in peripheral endings. Stimulation of sensory nerve endings in the respiratory tract results in a local axon reflex and finally in neuropeptide release, 29 which can then act on a number of effector cells, including airway smooth muscle cells. 30 The functional role of neuropeptides in NT-induced airway hyperreactivity has been emphasized by inhibiting broncho-obstruction after application of a neurokinin 1 receptor antagonist. 31 These mechanisms leading to broncho-obstruction can be facilitated by a heightened parasympathetic vagal reflex activity on stimulation of afferent endings of sensory nerves. 32,33 Although this assumption is compatible with our observation that blocking of Trk receptor signaling reduces hyperreactivity of sensory neurons in the airways and in the following broncho-obstruction, it could not be ruled out that Trk receptors might also directly influence cholinergic neurons and airway smooth muscle cells, in which we could observe TrkA and TrkC receptor immunoreactivity. Lung function was assessed in response to MCh to investigate the role of Trk receptors on airway smooth muscle cells. We saw an enhanced responsiveness FIG 6. Cytokine levels in BALF. Cytokine levels were measured in BALF 24 hours after last aerosol challenge. Levels of IL-4 (A), IL-5 (B), and IL-13 (C) were significantly increased in the positive control group (pos) compared with those in the negative control group (neg). Treatment with REN1826 partly reduced IL-4 and IL-5 levels (n 5 16 per group). *P <.05; **P <.01. of OVA-sensitized and OVA aerosol challenged animals to MCh, but this effect was not altered by treatment with REN1826, indicating that Trk receptor signaling in airway smooth muscle cells does not contribute to reflex bronchoobstruction after stimulation of afferent sensory nerves.
8 604 Nassenstein et al J ALLERGY CLIN IMMUNOL SEPTEMBER 2006 TABLE II. Distribution of leukocyte subpopulations in BALF Recovery (ml) Macrophages (cells ) Lymphocytes (cells ) Eosinophils (cells ) Neutrophils (cells ) Negative control ** ** ** Positive control ng of REN ng of REN ng of REN Cell numbers are given in absolute numbers (means 6 SEM; n 5 16 per group). **P <.01 compared with positive control. Because of the fact that disruption of p75ntr signaling also had no effect on broncho-obstruction in response to MCh, 14 we propose that NTs and Trk receptors in vivo are not involved in the development of hyperreactivity of airway smooth muscle cells, as could be suggested by in vitro studies. 34 The influence of Trk receptors on cholinergic nerves remains to be investigated. Although it has been suggested that NTs exert proinflammatory properties contributing to allergic airway inflammation (reviewed in Nassenstein et al 35 ), the role of Trk receptors has not yet been investigated. In this study we could demonstrate Trk receptor immunoreactivity in immune cells of the airways exclusively after allergen challenge. This observation was accompanied by increased mrna levels for TrkB and TrkC in the inflamed lung, indicating that Trk receptors might be involved in mediating proinflammatory properties of NTs. NTs are known to promote lymphocyte development and to increase neuropeptide production. In addition, they modulate cytokine synthesis and might play a critical role in regulating the T H 1/T H 2 balance (reviewed in Nassenstein et al 35 ). The relevance of the latter hypothesis has been shown in a mouse model of allergic asthma. Mononuclear cells of OVA-sensitized animals responded to exogenously added NGF with a dose-dependent increase in T H 2 cytokine production, whereas synthesis of IFN-g remained unaffected. 2 Our data indicate that Trk receptors, in particular TrkA and TrkC, are involved in regulation of cytokine synthesis in vivo, as indicated by decreased IL-4 and IL-5 levels but sustained IFN-g levels after local application of REN1826 in our mouse model of asthma. Because previous studies revealed that airway inflammation in asthma is also p75ntr dependent, 14 we suggest that NTs might bind to heteromeric complexes consisting of Trk and p75ntr in immune cells. 8,9 Although it has been demonstrated that NTs contribute to airway eosinophilia in a mouse model of allergic asthma, 2 probably through direct interaction with those cells, 6 antagonization of Trk-mediated signals had no influence on cell infiltration in our study. Therefore we suggest that eosinophilia in our mouse model is to a large extent dependent on p75ntr, but not on Trk, expression. 14 Nevertheless, there is an ongoing discussion about functional differences of eosinophils in mice and human subjects. 36 Therefore the functional role of Trk receptors in human eosinophils remains to be investigated. Because Trk receptors are expressed in immune cells and several in vitro studies indicate that NTs can directly affect immune cell function, can be complimentarily modulated by Trk-dependent activation of sensory nerves. Direct evidence for this so-called neurogenic inflammation in the airways characterized by enhanced neuropeptide release of sensory neurons came from Quarcoo et al. 37 In this study application of a dual neurokinin 1 neurokinin 2 antagonist in NGF-transgenic mice partly inhibited airway inflammation. However, the involvement of neurogenic inflammation in human subjects is still uncertain because initial clinical studies with strategies to block neurogenic inflammation have not been encouraging. 38 The observations of our study indicate that Trk receptors might play an important role in the development of hyperreactivity of sensory nerves, leading to reflex bronchospasm in patients with asthma. The latter is probably due to an increased local release of neuropeptides and facilitation of cholinergic neurotransmission. In contrast, Trk receptor signaling has no direct role on the hyperreactivity of airway smooth muscle cells but might play an important role in allergic airway inflammation. On the basis of these results, it becomes more and more evident that NT antagonism (eg, with a Trk receptor antagonist, such as REN1826) might be effective in inhibiting hyperreactivity of sensory nerves that could be responsible for many symptoms of asthma, including broncho-obstruction after inhalation of smoke or cold air and exercise. We thank Drs Nancy A. Lee and James J. Lee (Mayo Clinic Scottsdale) for providing the rat anti-mouse major basic protein antibody. We also gratefully acknowledge the statistical advice of Professor Hartmut Hecker, Institute Biometry, University Medical School, Hannover, Germany, and the excellent technical assistance of Sabine Schild and Olaf Macke. REFERENCES 1. National Institutes of Health. Global initiative for asthma. Natl Heart Lung Blood Inst Publ 1995; Publication no Braun A, Appel E, Baruch R, Herz U, Botchkarev V, Paus R, et al. Role of nerve growth factor in a mouse model of allergic airway inflammation and asthma. Eur J Immunol 1998;28: Braun A, Lommatzsch M, Neuhaus-Steinmetz U, Quarcoo D, Glaab T, McGregor GP, et al. Brain-derived neurotrophic factor (BDNF)
9 J ALLERGY CLIN IMMUNOL VOLUME 118, NUMBER 3 Nassenstein et al 605 contributes to neuronal dysfunction in a model of allergic airway inflammation. Br J Pharmacol 2004;141: Braun A, Quarcoo D, Schulte-Herbruggen O, Lommatzsch M, Hoyle G, Renz H. Nerve growth factor induces airway hyperresponsiveness in mice. Int Arch Allergy Immunol 2001;124: Path G, Braun A, Meents N, Kerzel S, Quarcoo D, Raap U, et al. Augmentation of allergic early-phase reaction by nerve growth factor. Am J Respir Crit Care Med 2002;166: Nassenstein C, Braun A, Erpenbeck VJ, Lommatzsch M, Schmidt S, Krug N, et al. The neurotrophins nerve growth factor, brain-derived neurotrophic factor, neurotrophin-3, and neurotrophin-4 are survival and activation factors for eosinophils in patients with allergic bronchial asthma. J Exp Med 2003;198: Goedert M, Stoeckel K, Otten U. Biological importance of the retrograde axonal transport of nerve growth factor in sensory neurons. Proc Natl Acad Sci U S A 1981;78: Bibel M, Hoppe E, Barde YA. Biochemical and functional interactions between the neurotrophin receptors trk and p75ntr. EMBO J 1999; 18: Esposito D, Patel P, Stephens RM, Perez P, Chao MV, Kaplan DR, et al. The cytoplasmic and transmembrane domains of the p75 and Trk A receptors regulate high affinity binding to nerve growth factor. J Biol Chem 2001;276: Lee KF, Davies AM, Jaenisch R. p75-deficient embryonic dorsal root sensory and neonatal sympathetic neurons display a decreased sensitivity to NGF. Development 1994;120: Caroleo MC, Costa N, Bracci-Laudiero L, Aloe L. Human monocyte/ macrophages activate by exposure to LPS overexpress NGF and NGF receptors. J Neuroimmunol 2001;113: Dechant G. Molecular interactions between neurotrophin receptors. Cell Tissue Res 2001;305: Huang EJ, Reichardt LF. Neurotrophins: roles in neuronal development and function. Annu Rev Neurosci 2001;24: Kerzel S, Path G, Nockher WA, Quarcoo D, Raap U, Groneberg DA, et al. Pan-neurotrophin receptor p75 contributes to neuronal hyperreactivity and airway inflammation in a murine model of experimental asthma. Am J Respir Cell Mol Biol 2003;28: Ricci A, Felici L, Mariotta S, Mannino F, Schmid G, Terzano C, et al. Neurotrophin and neurotrophin receptor protein expression in the human lung. Am J Respir Cell Mol Biol 2004;30: Szallasi A, Blumberg PM. Vanilloid (capsaicin) receptors and mechanisms. Pharmacol Rev 1999;51: Suh YG, Oh U. Activation and activators of TRPV1 and their pharmaceutical implication. Curr Pharm Des 2005;11: Shu X, Mendell LM. Nerve growth factor acutely sensitizes the response of adult rat sensory neurons to capsaicin. Neurosci Lett 1999;274: Bonnington JK, McNaughton PA. Signalling pathways involved in the sensitisation of mouse nociceptive neurones by nerve growth factor. J Physiol 2003;551(suppl):S Zhang YH, Nicol GD. NGF-mediated sensitization of the excitability of rat sensory neurons is prevented by a blocking antibody to the p75 neurotrophin receptor. Neurosci Lett 2004;366: Saria A, Theodorsson-Norheim E, Gamse R, Lundberg JM. Release of substance P- and substance K-like immunoreactivities from the isolated perfused guinea-pig lung. Eur J Pharmacol 1984;106: Joos GF, Germonpre PR, Pauwels RA. Role of tachykinins in asthma. Allergy 2000;55: Szolcsanyi J, Bartho L. Capsaicin-sensitive non-cholinergic excitatory innervation of the guinea-pig tracheobronchial smooth muscle. Neurosci Lett 1982;34: Mazzone SB, Canning BJ. Synergistic interactions between airway afferent nerve subtypes mediating reflex bronchospasm in guinea pigs. Am J Physiol Regul Integr Comp Physiol 2002;283:R Fuller RW, Dixon CM, Barnes PJ. Bronchoconstrictor response to inhaled capsaicin in humans. J Appl Physiol 1985;58: Lindsay RM, Harmar AJ. Nerve growth factor regulates expression of neuropeptide genes in adult sensory neurons. Nature 1989;337: Hunter DD, Myers AC, Undem BJ. Nerve growth factor-induced phenotypic switch in guinea pig airway sensory neurons. Am J Respir Crit Care Med 2000;161: Fischer A, McGregor GP, Saria A, Philippin B, Kummer W. Induction of tachykinin gene and peptide expression in guinea pig nodose primary afferent neurons by allergic airway inflammation. J Clin Invest 1996;98: Barnes PJ. Asthma as an axon reflex. Lancet 1986;1: Lundberg JM, Martling CR, Saria A. Substance P and capsaicininduced contraction of human bronchi. Acta Physiol Scand 1983; 119: de Vries A, Dessing MC, Engels F, Henricks PA, Nijkamp FP. Nerve growth factor induces a neurokinin-1 receptor-mediated airway hyperresponsiveness in guinea pigs. Am J Respir Crit Care Med 1999;159: Barnes PJ. Neural mechanisms in asthma. Br Med Bull 1992;48: Hahn HL. Role of the parasympathetic nervous system and of cholinergic mechanisms in bronchial hyperreactivity. Bull Eur Physiopathol Respir 1986;22(suppl 7): Bachar O, Adner M, Uddman R, Cardell LO. Nerve growth factor enhances cholinergic innervation and contractile response to electric field stimulation in a murine in vitro model of chronic asthma. Clin Exp Allergy 2004;34: Nassenstein C, Kerzel S, Braun A. Neurotrophins and neurotrophin receptors in allergic asthma. Prog Brain Res 2004;146: Malm-Erjefalt M, Persson CG, Erjefalt JS. Degranulation status of airway tissue eosinophils in mouse models of allergic airway inflammation. Am J Respir Cell Mol Biol 2001;24: Quarcoo D, Schulte-Herbruggen O, Lommatzsch M, Schierhorn K, Hoyle GW, Renz H, et al. Nerve growth factor induces increased airway inflammation via a neuropeptide-dependent mechanism in a transgenic animal model of allergic airway inflammation. Clin Exp Allergy 2004; 34: Barnes PJ. Neurogenic inflammation in the airways. Respir Physiol 2001; 125:
Mechanisms of asthma and allergic inflammation Perspectives in asthma. Neurotrophins and asthma: Novel insight into neuroimmune interaction
 Perspectives in asthma Guest editor: William W. Busse, MD Neurotrophins and asthma: Novel insight into neuroimmune interaction Wolfgang Andreas Nockher, MD, MSc, and Harald Renz, MD Marburg, Germany There
Perspectives in asthma Guest editor: William W. Busse, MD Neurotrophins and asthma: Novel insight into neuroimmune interaction Wolfgang Andreas Nockher, MD, MSc, and Harald Renz, MD Marburg, Germany There
Inflammation-Induced Airway Hypersensitivity: From Ion Channels to Patients
 Inflammation-Induced Airway Hypersensitivity: From Ion Channels to Patients Lu-Yuan Lee, Ph.D. Airway Sensory Neurobiology Laboratory Department of Physiology University of Kentucky Medical Center BACKGROUND
Inflammation-Induced Airway Hypersensitivity: From Ion Channels to Patients Lu-Yuan Lee, Ph.D. Airway Sensory Neurobiology Laboratory Department of Physiology University of Kentucky Medical Center BACKGROUND
Role of the Brain-Lung Axis in Fatigue
 Role of the Brain-Lung Axis in Fatigue Y.S. Prakash, M.D., Ph.D. Professor of Anesthesiology and Physiology Chair, Department of Physiology & BME Mayo Clinic Rochester, Minnesota, USA Fatigue in Chronic
Role of the Brain-Lung Axis in Fatigue Y.S. Prakash, M.D., Ph.D. Professor of Anesthesiology and Physiology Chair, Department of Physiology & BME Mayo Clinic Rochester, Minnesota, USA Fatigue in Chronic
Brain-derived neurotrophic factor (BDNF) contributes to neuronal dysfunction in a model of allergic airway inflammation
 British Journal of Pharmacology (2004) 141, 431 440 & 2004 Nature Publishing Group All rights reserved 0007 1188/04 $25.00 www.nature.com/bjp Brain-derived neurotrophic factor (BDNF) contributes to neuronal
British Journal of Pharmacology (2004) 141, 431 440 & 2004 Nature Publishing Group All rights reserved 0007 1188/04 $25.00 www.nature.com/bjp Brain-derived neurotrophic factor (BDNF) contributes to neuronal
The contribution of neurotrophins to the pathogenesis of allergic asthma
 594 Biochemical Society Transactions (2006) Volume 34, part 4 The contribution of neurotrophins to the pathogenesis of allergic asthma S. Rochlitzer, C. Nassenstein and A. Braun 1 Immunology and Allergology,
594 Biochemical Society Transactions (2006) Volume 34, part 4 The contribution of neurotrophins to the pathogenesis of allergic asthma S. Rochlitzer, C. Nassenstein and A. Braun 1 Immunology and Allergology,
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Learning Outcomes. Systems Pharmacology PHAR3320. Nerves of the Respiratory Tract. Dr Fernandes
 Systems Pharmacology PHAR3320 Nerves of the Respiratory Tract Dr Fernandes Learning Outcomes By the end of this lecture, students should be able to describe nerve pathways that innervate the airways discuss
Systems Pharmacology PHAR3320 Nerves of the Respiratory Tract Dr Fernandes Learning Outcomes By the end of this lecture, students should be able to describe nerve pathways that innervate the airways discuss
Nerve growth factor enhances cough and airway obstruction via TrkA receptor- and TRPV1-dependent mechanisms
 c Additional methods are published online only at http:// thorax.bmj.com/content/vol64/ issue9 Department of Applied Therapeutics, Faculty of Pharmacy, Kuwait University, Kuwait Correspondence to: Dr A
c Additional methods are published online only at http:// thorax.bmj.com/content/vol64/ issue9 Department of Applied Therapeutics, Faculty of Pharmacy, Kuwait University, Kuwait Correspondence to: Dr A
Airway epithelial cells produce neurotrophins and promote the survival of eosinophils during allergic airway inflammation
 Airway epithelial cells produce neurotrophins and promote the survival of eosinophils during allergic airway inflammation Christian Hahn, PhD, Ariyan Pirayesh Islamian, Harald Renz, MD, and Wolfgang Andreas
Airway epithelial cells produce neurotrophins and promote the survival of eosinophils during allergic airway inflammation Christian Hahn, PhD, Ariyan Pirayesh Islamian, Harald Renz, MD, and Wolfgang Andreas
Role of Tyk-2 in Th9 and Th17 cells in allergic asthma
 Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Soluble ADAM33 initiates airway remodeling to promote susceptibility for. Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David I Wilson,
 Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Revised Suppl. Data: Soluble ADAM33 1 Soluble ADAM33 initiates airway remodeling to promote susceptibility for allergic asthma in early life Elizabeth R. Davies, Joanne F.C. Kelly, Peter H. Howarth, David
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al.
 Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al. Chapter 75: Approach to Infants and Children with Asthma
Allergy and Immunology Review Corner: Chapter 75 of Middleton s Allergy Principles and Practice, 7 th Edition, edited by N. Franklin Adkinson, et al. Chapter 75: Approach to Infants and Children with Asthma
Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline
 Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Pathology of Asthma Dr Rodney Itaki Lecturer Division of Pathology Anatomical Pathology Discipline Bronchial Asthma Definition: chronic, relapsing inflammatory lung disorder characterised by reversible
Supplementary Information
 Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Supplementary Information TABLE S1. SUBJECT CHARACTERISTICS* Normal Control Subjects Subjects with Asthma p Value Number 23 48 Age (years) 35±10 35±10 0.75 Sex, M:F (% F) 9:12 (57) 17:26 (60) 0.76 FEV1
Systems Pharmacology Respiratory Pharmacology. Lecture series : General outline
 Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Systems Pharmacology 3320 2017 Respiratory Pharmacology Associate Professor Peter Henry (Rm 1.34) Peter.Henry@uwa.edu.au Division of Pharmacology, School of Biomedical Sciences Lecture series : General
Allergen-induced substance P synthesis in large-diameter sensory neurons innervating the lungs
 Allergen-induced substance P synthesis in large-diameter sensory neurons innervating the lungs Benjamas Chuaychoo, MD, Dawn D. Hunter, PhD, Allen C. Myers, PhD, Marian Kollarik, MD, PhD, and Bradley J.
Allergen-induced substance P synthesis in large-diameter sensory neurons innervating the lungs Benjamas Chuaychoo, MD, Dawn D. Hunter, PhD, Allen C. Myers, PhD, Marian Kollarik, MD, PhD, and Bradley J.
Respiratory Research. Open Access. Abstract. BioMed Central
 Respiratory Research BioMed Central Research Invasive versus noninvasive measurement of allergic and cholinergic airway responsiveness in mice Thomas Glaab 1,2, Michaela Ziegert 1, Ralf Baelder 1, Regina
Respiratory Research BioMed Central Research Invasive versus noninvasive measurement of allergic and cholinergic airway responsiveness in mice Thomas Glaab 1,2, Michaela Ziegert 1, Ralf Baelder 1, Regina
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling
 E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
E-1 Role of IgE and IgE receptors in allergic airway inflammation and remodeling Ruby Pawankar, MD, Ph.D. FRCP, FAAAAI Prof. Div of Allergy, Dept of Pediatrics Nippon Medical School Tokyo, Japan pawankar.ruby@gmail.com
Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma
 6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
6 Modulation of hyperresponsiveness by glutathione in a murine in vivo model of allergic asthma J. Kloek, I. Van Ark, G. Folkerts, F. De Clerck,, N. Bloksma,, F.P. Nijkamp. Department of Pharmacology and
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis
 Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Potent and Selective CRTh2 Antagonists are Efficacious in Models of Asthma, Allergic Rhinitis and Atopic Dermatitis Laura L. Carter, Yoshi Shiraishi, Yooseob Shin, Laurence Burgess, Christine Eberhardt,
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Induced sputum to assess airway inflammation: a study of reproducibility
 Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Clinical and Experimental Allergy. 1997. Volume 27. pages 1138-1144 Induced sputum to assess airway inflammation: a study of reproducibility A. SPANEVELLO, G. B. MIGLIORI. A. SHARARA*, L. BALLARDlNIt,
Chapter 2 Electrophysiologically Identified Airway Receptors: Main Characteristics
 Chapter 2 Electrophysiologically Identified Airway Receptors: Main Characteristics The most generally accepted classification discriminates mechanosensory slowly adapting (stretch) receptors (SARs), rapidly
Chapter 2 Electrophysiologically Identified Airway Receptors: Main Characteristics The most generally accepted classification discriminates mechanosensory slowly adapting (stretch) receptors (SARs), rapidly
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과
 감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
감초 (Glycyrrhiza uralensis Fisch, GLU) 가천식모델생쥐의 BALF 내면역세포및 Cytokine 에미치는효과 Effects of Glycyrrhiza uralensis Fisch on Immunocyte and Cytokine Production in Asthma Model Mouse Young-Joo Han, Yang-Chun Park
Advanced Receptor Psychopharmacology
 Advanced Receptor Psychopharmacology Otsuka Pharmaceutical Development & Commercialization, Inc. 2017 Otsuka Pharmaceutical Development & Commercialization, Inc., Rockville, MD February 2017 Lundbeck,
Advanced Receptor Psychopharmacology Otsuka Pharmaceutical Development & Commercialization, Inc. 2017 Otsuka Pharmaceutical Development & Commercialization, Inc., Rockville, MD February 2017 Lundbeck,
Neurotrophins in allergic diseases: From neuronal growth factors to intercellular signaling molecules
 Neurotrophins in allergic diseases: From neuronal growth factors to intercellular signaling molecules Wolfgang Andreas Nockher, MD, MSc, and Harald Renz, MD Marburg, Germany Understanding the complex pathophysiology
Neurotrophins in allergic diseases: From neuronal growth factors to intercellular signaling molecules Wolfgang Andreas Nockher, MD, MSc, and Harald Renz, MD Marburg, Germany Understanding the complex pathophysiology
EXPERIMENTAL AND THERAPEUTIC MEDICINE 8: , 2014
 1402 Lung dendritic cells undergo maturation and polarization towards a T helper type 2 stimulating phenotype in a mouse model of asthma: Role of nerve growth factor QINGWU QIN 1*, ZHAN WANG 1*, PINHUA
1402 Lung dendritic cells undergo maturation and polarization towards a T helper type 2 stimulating phenotype in a mouse model of asthma: Role of nerve growth factor QINGWU QIN 1*, ZHAN WANG 1*, PINHUA
Inhibition of nerve growth factor/tyrosine kinase
 European Review for Medical and Pharmacological Sciences Inhibition of nerve growth factor/tyrosine kinase receptor A signaling ameliorates airway remodeling in chronic allergic airway inflammation L.-W.
European Review for Medical and Pharmacological Sciences Inhibition of nerve growth factor/tyrosine kinase receptor A signaling ameliorates airway remodeling in chronic allergic airway inflammation L.-W.
Mechanisms of action of bronchial provocation testing
 Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Mechanisms of action of bronchial provocation testing TSANZ / ANZSRS Masterclass: April 3rd, 2016 13:00 13:30 John D. Brannan PhD Scientific Director - Dept. Respiratory & Sleep Medicine John Hunter Hospital,
Small Airways Disease. Respiratory Function In Small Airways And Asthma. Pathophysiologic Changes in the Small Airways of Asthma Patients
 Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Impact of Asthma in the U.S. per Year. Asthma Epidemiology and Pathophysiology. Risk Factors for Asthma. Childhood Asthma Costs of Asthma
 American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
American Association for Respiratory Care Asthma Educator Certification Prep Course Asthma Epidemiology and Pathophysiology Robert C. Cohn, MD, FAARC MetroHealth Medical Center Cleveland, OH Impact of
Abstract. IgE. IgE Th2. x x IL-4 IL-5 IgE CD4 +
 D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
D. o ƒf 6,''!" # + % %$ '& ' '' & " k n k x k k k k k x k IgE k x IgE Ò1Ó k Ò2Ó v k x IgE Th2 x } x x IL-4 IL-5 IgE IgE j IFN-γ IgG j j CD4 + { k d «d j B7 w k k x IgE k 1 k Abstract Parental immunization
IgE-mediated allergy in elderly patients with asthma
 Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Allergology international (1997) 46: 237-241 Original Article IgE-mediated allergy in elderly patients with asthma Fumihiro Mitsunobu, Takashi Mifune, Yasuhiro Hosaki, Kouzou Ashida, Hirofumi Tsugeno,
Prolonged exposure to NT-3 attenuates cholinergic nerve-mediated contractions in cultured murine airways.
 Prolonged exposure to NT-3 attenuates cholinergic nerve-mediated contractions in cultured murine airways. Bachar, Ofir; Adner, Mikael; Uddman, Rolf; Cardell, Lars-Olaf Published in: Respiratory Physiology
Prolonged exposure to NT-3 attenuates cholinergic nerve-mediated contractions in cultured murine airways. Bachar, Ofir; Adner, Mikael; Uddman, Rolf; Cardell, Lars-Olaf Published in: Respiratory Physiology
Brain-derived neurotrophic factor in asthmatic children.
 Egypt J Pediatr Allergy Immunol 2003; 1(2): 102-9. Original article Brain-derived neurotrophic factor in asthmatic children. Background: Brain-derived neurotrophic factor (BDNF) regulates the crosstalk
Egypt J Pediatr Allergy Immunol 2003; 1(2): 102-9. Original article Brain-derived neurotrophic factor in asthmatic children. Background: Brain-derived neurotrophic factor (BDNF) regulates the crosstalk
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Bronchial Hyperresponsiveness. Defining Asthma: Clinical Criteria. Impaired Ventilation in Asthma. Dynamic Imaging of Asthma
 Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Defining Asthma: Clinical Criteria Defining Asthma: Bronchial Hyperresponsiveness Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine,
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Defining Asthma: Clinical Criteria. Defining Asthma: Bronchial Hyperresponsiveness
 Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Defining Asthma: Clinical Criteria Atopy 34% Recent wheeze 20% Asthma 11% AHR 19% n = 807 From: Woolcock, AJ. Asthma in Textbook of Respiratory Medicine, 2nd ed. Murray, Nadel, eds.(saunders:philadelphia)
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Life-long asthma and its relationship to COPD. Stephen T Holgate School of Medicine University of Southampton
 Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
COPYRIGHTED MATERIAL. Definition and Pathology CHAPTER 1. John Rees
 CHAPTER 1 Definition and Pathology John Rees Sherman Education Centre, Guy s Hospital, London, UK OVERVIEW Asthma is an overall descriptive term but there are a number of more or less distinct phenotypes
CHAPTER 1 Definition and Pathology John Rees Sherman Education Centre, Guy s Hospital, London, UK OVERVIEW Asthma is an overall descriptive term but there are a number of more or less distinct phenotypes
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
COPD, Asthma, Or Something In Between? Sharon R. Rosenberg Assistant Professor of Medicine Northwestern University December 4, 2013
 COPD, Asthma, Or Something In Between? Sharon R. Rosenberg Assistant Professor of Medicine Northwestern University December 4, 2013 None Disclosures Definitions Asthma Asthma is a chronic inflammatory
COPD, Asthma, Or Something In Between? Sharon R. Rosenberg Assistant Professor of Medicine Northwestern University December 4, 2013 None Disclosures Definitions Asthma Asthma is a chronic inflammatory
Novel biomarkers of chemical-induced asthma: a murine model. Jeroen Vanoirbeek
 Novel biomarkers of chemical-induced asthma: a murine model Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide 2. Reversible airflow limitation, airway
Novel biomarkers of chemical-induced asthma: a murine model Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide 2. Reversible airflow limitation, airway
RESPIRATORY BLOCK. Bronchial Asthma. Dr. Maha Arafah Department of Pathology KSU
 RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
Chapter 7. Anticholinergic (Parasympatholytic) Bronchodilators. Mosby items and derived items 2008, 2002 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 7 Anticholinergic (Parasympatholytic) Bronchodilators Clinical Indications for Use Indication for anticholinergic bronchodilator COPD maintenance Indication for combined anticholinergic and β-agonist
Chapter 7 Anticholinergic (Parasympatholytic) Bronchodilators Clinical Indications for Use Indication for anticholinergic bronchodilator COPD maintenance Indication for combined anticholinergic and β-agonist
Adenosine 5 0 -monophosphate increases levels of leukotrienes in breath condensate in asthma
 Respiratory Medicine (2004) 98, 651 655 Adenosine 5 0 -monophosphate increases levels of leukotrienes in breath condensate in asthma E. Bucchioni, Z. Csoma, L. Allegra, K.F. Chung, P.J. Barnes, S.A. Kharitonov*
Respiratory Medicine (2004) 98, 651 655 Adenosine 5 0 -monophosphate increases levels of leukotrienes in breath condensate in asthma E. Bucchioni, Z. Csoma, L. Allegra, K.F. Chung, P.J. Barnes, S.A. Kharitonov*
Airway Inflammation in Asthma Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan.
 REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
REVIEW ARTICLE Chih-Yung Chiu 1,2, Kin-Sun Wong 2 1 Department of Pediatrics, Chang Gung Memorial Hospital, Keelung, Taiwan. 2 Division of Pediatric Pulmonology, Department of Pediatrics, Chang Gung Memorial
IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells
 IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells Jennifer A. Mitchel, Silvio Antoniak, Joo-Hyeon Lee, Sae-Hoon Kim, Maureen McGill, David I. Kasahara,
IL-13 Augments Compressive Stress-induced Tissue Factor Expression in Human Airway Epithelial Cells Jennifer A. Mitchel, Silvio Antoniak, Joo-Hyeon Lee, Sae-Hoon Kim, Maureen McGill, David I. Kasahara,
Understanding How Allergic Responses End: The Allergy Resolvome. Lipid mediators
 Understanding How Allergic Responses End: The Allergy Resolvome Lipid mediators Koichiro Asano Tokai University School of Medicine, Kanagawa, JAPAN ko-asano@tokai-u.jp Resolution of granulocytic inflammation
Understanding How Allergic Responses End: The Allergy Resolvome Lipid mediators Koichiro Asano Tokai University School of Medicine, Kanagawa, JAPAN ko-asano@tokai-u.jp Resolution of granulocytic inflammation
Neural integration and allergic disease
 Neural integration and allergic disease Bradley J. Undem, PhD, Radhika Kajekar, PhD, Dawn D. Hunter, PhD, and Allen C. Myers, PhD Baltimore, Md Changes in neural activity play a key role in many symptoms
Neural integration and allergic disease Bradley J. Undem, PhD, Radhika Kajekar, PhD, Dawn D. Hunter, PhD, and Allen C. Myers, PhD Baltimore, Md Changes in neural activity play a key role in many symptoms
SERIES 'OCCUPATIONAL ASTHMA' Edited by C. Mapp
 Eur Respir J, 1994, 7, 555 568 DOI: 10.1183/09031936.94.07030555 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 SERIES 'OCCUPATIONAL ASTHMA'
Eur Respir J, 1994, 7, 555 568 DOI: 10.1183/09031936.94.07030555 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1994 European Respiratory Journal ISSN 0903-1936 SERIES 'OCCUPATIONAL ASTHMA'
Pharmacology of Pain Transmission and Modulation
 Pharmacology of Pain Transmission and Modulation 2 Jürg Schliessbach and Konrad Maurer Nociceptive Nerve Fibers Pain is transmitted to the central nervous system via thinly myelinated Aδ and unmyelinated
Pharmacology of Pain Transmission and Modulation 2 Jürg Schliessbach and Konrad Maurer Nociceptive Nerve Fibers Pain is transmitted to the central nervous system via thinly myelinated Aδ and unmyelinated
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
ASTHMA TREATMENT EFFICACY ASSESSMENT BY FeNO MEASUREMENT
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 ASTHMA TREATMENT EFFICACY ASSESSMENT BY FeNO MEASUREMENT Dana ALEXANDRESCU 1 Abstract: The author of
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 ASTHMA TREATMENT EFFICACY ASSESSMENT BY FeNO MEASUREMENT Dana ALEXANDRESCU 1 Abstract: The author of
EFFECT OF CHRONIC AIRWAY INFLAMMATION INDUCED BY ALLERGEN SENSITIZATION ON VAGAL BRONCHOPULMONARY SENSORY NERVES IN RATS
 University of Kentucky UKnowledge University of Kentucky Doctoral Dissertations Graduate School 2008 EFFECT OF CHRONIC AIRWAY INFLAMMATION INDUCED BY ALLERGEN SENSITIZATION ON VAGAL BRONCHOPULMONARY SENSORY
University of Kentucky UKnowledge University of Kentucky Doctoral Dissertations Graduate School 2008 EFFECT OF CHRONIC AIRWAY INFLAMMATION INDUCED BY ALLERGEN SENSITIZATION ON VAGAL BRONCHOPULMONARY SENSORY
RESPIRATORY PHARMACOLOGY - ASTHMA. Primary Exam Teaching - Westmead ED
 RESPIRATORY PHARMACOLOGY - ASTHMA Primary Exam Teaching - Westmead ED Sympathomimetic agents MOA: relax airway smooth muscle and inhibit broncho constricting mediators from mast cells May also inhibit
RESPIRATORY PHARMACOLOGY - ASTHMA Primary Exam Teaching - Westmead ED Sympathomimetic agents MOA: relax airway smooth muscle and inhibit broncho constricting mediators from mast cells May also inhibit
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Afferent nerves, interactions of, in cough, 20 21 Airway, eosinophilic inflammation of, 124 narrowing of, in asthma, 126 protection of, terms
Note: Page numbers of article titles are in boldface type. A Afferent nerves, interactions of, in cough, 20 21 Airway, eosinophilic inflammation of, 124 narrowing of, in asthma, 126 protection of, terms
Inhibition of airway remodeling in IL-5 deficient mice
 Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Inhibition of airway remodeling in IL-5 deficient mice See the related Commentary beginning on page 507. Jae Youn Cho, Marina Miller, Kwang Je Baek, Ji Won Han, Jyothi Nayar, Sook Young Lee, Kirsti McElwain,
Coordination of trophic interactions by separate developmental programs in sensory neurons and their target fields
 Coordination of trophic interactions by separate developmental programs in sensory neurons and their target fields ALUN M. DAVIES, YVES LÄRMET, EDWINA WRIGHT and KRISTINE S. VOGEL Department o f Anatomy,
Coordination of trophic interactions by separate developmental programs in sensory neurons and their target fields ALUN M. DAVIES, YVES LÄRMET, EDWINA WRIGHT and KRISTINE S. VOGEL Department o f Anatomy,
Mouse Total IgA Antibody Detection Kit
 Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Mouse Total IgA Antibody Detection Kit Catalog # 3019 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION The total IgA levels in specimens are often determined in mouse disease models involving
Sergio Bonini. Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy.
 Assessment of EIA in the community and in athletes: the role of standardized questionnaires Sergio Bonini Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy se.bonini@gmail.com
Assessment of EIA in the community and in athletes: the role of standardized questionnaires Sergio Bonini Professor of Internal Medicine, Second University of Naples INMM-CNR, Rome, Italy se.bonini@gmail.com
Effector T Cells and
 1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
Abhd2 regulates alveolar type Ⅱ apoptosis and airway smooth muscle remodeling: a key target of COPD research
 Abhd2 regulates alveolar type Ⅱ apoptosis and airway smooth muscle remodeling: a key target of COPD research Shoude Jin Harbin Medical University, China Background COPD ------ a silent killer Insidious,
Abhd2 regulates alveolar type Ⅱ apoptosis and airway smooth muscle remodeling: a key target of COPD research Shoude Jin Harbin Medical University, China Background COPD ------ a silent killer Insidious,
Asthma- THE most common Pediatric Disease JENNIFER MCDANIEL, RRT- NPS
 Asthma- THE most common Pediatric Disease JENNIFER MCDANIEL, RRT- NPS Asthma Usually acquire before the age of 10 These patients exhibit hyper-reactive airways Spasm Constriction Swelling Secretions are
Asthma- THE most common Pediatric Disease JENNIFER MCDANIEL, RRT- NPS Asthma Usually acquire before the age of 10 These patients exhibit hyper-reactive airways Spasm Constriction Swelling Secretions are
responsiveness in asthmatic patients and smokers
 63 Department of Pulmonology B Auffarth D S Postma G H Koeter Th W van der Mark Department of Allergology J G R de Monchy University Hospital, 973 EZ Groningen, The Netherlands Reprint requests to: Professor
63 Department of Pulmonology B Auffarth D S Postma G H Koeter Th W van der Mark Department of Allergology J G R de Monchy University Hospital, 973 EZ Groningen, The Netherlands Reprint requests to: Professor
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation
 Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
Signaling through Fc RIII is required for optimal T helper type (Th)2 responses and Th2-mediated airway inflammation Hozefa S. Bandukwala, 1 Bryan S. Clay, 1 Jiankun Tong, 2 Purvi D. Mody, 1 Judy L. Cannon,
Role of TRPV Receptors in Respiratory Diseases
 Role of TRPV Receptors in Respiratory Diseases Yanlin Jia, Lu-Yuan Lee To cite this version: Yanlin Jia, Lu-Yuan Lee. Role of TRPV Receptors in Respiratory Diseases. Biochimica et Biophysica Acta - Molecular
Role of TRPV Receptors in Respiratory Diseases Yanlin Jia, Lu-Yuan Lee To cite this version: Yanlin Jia, Lu-Yuan Lee. Role of TRPV Receptors in Respiratory Diseases. Biochimica et Biophysica Acta - Molecular
Bronchial asthma. MUDr. Mojmír Račanský Odd. Alergologie a klinické imunologie FNOL Ústav Imunologie LF UPOL
 Bronchial asthma MUDr. Mojmír Račanský Odd. Alergologie a klinické imunologie FNOL Ústav Imunologie LF UPOL DEFINITION ASTHMA BRONCHIALE = Asthma is a chronic inflammatory disorder of the airways in which
Bronchial asthma MUDr. Mojmír Račanský Odd. Alergologie a klinické imunologie FNOL Ústav Imunologie LF UPOL DEFINITION ASTHMA BRONCHIALE = Asthma is a chronic inflammatory disorder of the airways in which
Outline FEF Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications?
 Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Implications on therapy. Prof. of Medicine and Allergy Faculty of Medicine, Cairo University
 Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
Implications on therapy Dr. Hisham Tarraf MD,FRCP(Edinb.) Prof. of Medicine and Allergy Faculty of Medicine, Cairo University Need for better understanding Global health problem Impact on quality of life
The Pain Pathway. dorsal root ganglion. primary afferent nociceptor. TRP: Transient Receptor Potential
 Presented by Issel Anne L. Lim 1 st Year PhD Candidate Biomedical Engineering Johns Hopkins University 580.427/580.633 Ca Signals in Biological Systems Outline The Pain Pathway TRP: Transient Receptor
Presented by Issel Anne L. Lim 1 st Year PhD Candidate Biomedical Engineering Johns Hopkins University 580.427/580.633 Ca Signals in Biological Systems Outline The Pain Pathway TRP: Transient Receptor
special communication
 Am J Physiol Lung Cell Mol Physiol 280: L565 L573, 2001. special communication Tidal midexpiratory flow as a measure of airway hyperresponsiveness in allergic mice THOMAS GLAAB, 1 ANGELIKA DASER, 2 ARMIN
Am J Physiol Lung Cell Mol Physiol 280: L565 L573, 2001. special communication Tidal midexpiratory flow as a measure of airway hyperresponsiveness in allergic mice THOMAS GLAAB, 1 ANGELIKA DASER, 2 ARMIN
Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response
 Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
Research article Role of C5 in the development of airway inflammation, airway hyperresponsiveness, and ongoing airway response Tao Peng, 1 Liming Hao, 2 Joseph A. Madri, 2 Xiao Su, 1 Jack A. Elias, 3 Gregory
ASTHMA. Epidemiology. Pathophysiology. Diagnosis. IAP UG Teaching slides
 BRONCHIAL ASTHMA ASTHMA Epidemiology Pathophysiology Diagnosis 2 CHILDHOOD ASTHMA Childhood bronchial asthma is characterized by Airway obstruction which is reversible Airway inflammation Airway hyper
BRONCHIAL ASTHMA ASTHMA Epidemiology Pathophysiology Diagnosis 2 CHILDHOOD ASTHMA Childhood bronchial asthma is characterized by Airway obstruction which is reversible Airway inflammation Airway hyper
Nerve growth factor exacerbates allergic lung inflammation and airway remodeling in a rat model of chronic asthma
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 6: 1251-1258, 2013 Nerve growth factor exacerbates allergic lung inflammation and airway remodeling in a rat model of chronic asthma YUN-GANG YANG, WEI-MIN TIAN, HAN
EXPERIMENTAL AND THERAPEUTIC MEDICINE 6: 1251-1258, 2013 Nerve growth factor exacerbates allergic lung inflammation and airway remodeling in a rat model of chronic asthma YUN-GANG YANG, WEI-MIN TIAN, HAN
Mouse Anti-OVA IgM Antibody Assay Kit
 Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
Mouse Anti-OVA IgM Antibody Assay Kit Catalog # 3017 For Research Use Only - Not Human or Therapeutic Use INTRODUCTION Ovalbumin (OVA) is a widely used antigen for inducing allergic reactions in experimental
COUGH REFLEX SENSITIVITY TESTING IN ASTHMATIC PATIENTS AND HEALTHY VOLUNTEERS. Comenius University, Slovak Republic. A bstract
 ACTA MEDICA MAR TINIANA 2013 Suppl. 1 DOI: 10.2478/acm-2013-0003 21 COUGH REFLEX SENSITIVITY TESTING IN ASTHMATIC PATIENTS AND HEALTHY VOLUNTEERS Neuschlova M. 1, Pecova R. 2 1 Department of Microbiology
ACTA MEDICA MAR TINIANA 2013 Suppl. 1 DOI: 10.2478/acm-2013-0003 21 COUGH REFLEX SENSITIVITY TESTING IN ASTHMATIC PATIENTS AND HEALTHY VOLUNTEERS Neuschlova M. 1, Pecova R. 2 1 Department of Microbiology
Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) asthma Relationship to patient age and the proportions of bronchoalveolar cells
 28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
28 Bronchial hyperresponsiveness in type I Bronchial hyperresponsiveness in type Ia (simple bronchoconstriction) Relationship to patient age and the proportions of bronchoalveolar cells Kouzou Ashida,
Absence of Tachykinin Involvement in Leukotriene D 4 and Antigen-Induced Contraction of Guinea Pig Isolated Bronchus 1
 0022-3565/97/2833-1102$03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 283, No. 3 Copyright 1997 by The American Society for Pharmacology and Experimental Therapeutics Printed in
0022-3565/97/2833-1102$03.00/0 THE JOURNAL OF PHARMACOLOGY AND EXPERIMENTAL THERAPEUTICS Vol. 283, No. 3 Copyright 1997 by The American Society for Pharmacology and Experimental Therapeutics Printed in
Biomerker onderzoek voor isocyanaatgeïnduceerd
 CGC en NVAB meeting, 6 Juni 2013, s-hertogenbosch Biomerker onderzoek voor isocyanaatgeïnduceerd astma Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide
CGC en NVAB meeting, 6 Juni 2013, s-hertogenbosch Biomerker onderzoek voor isocyanaatgeïnduceerd astma Jeroen Vanoirbeek Asthma 1. Chronic airway disease: prevalence: 5-10%, 300.000 people affected world-wide
State of Science for Respiratory Sensitization
 State of Science for Respiratory Sensitization Dose-Response Models for the OEL-Derivation of Chemicals Jürgen Pauluhn Global Drug Discovery, Bayer HealthCare, Bayer Pharma AG, Wuppertal, Germany Hannover
State of Science for Respiratory Sensitization Dose-Response Models for the OEL-Derivation of Chemicals Jürgen Pauluhn Global Drug Discovery, Bayer HealthCare, Bayer Pharma AG, Wuppertal, Germany Hannover
Potential Rebalancing of the Immune System by Anti-CD52 Therapy
 Potential Rebalancing of the Immune System by Anti-CD52 Therapy Johanne Kaplan, PhD VP Neuroimmunology Research Genzyme March 26, 2013 RESTRICTED USE SEE TRAINING MEMO 2011 DO Genzyme NOT 1COPY Corporation
Potential Rebalancing of the Immune System by Anti-CD52 Therapy Johanne Kaplan, PhD VP Neuroimmunology Research Genzyme March 26, 2013 RESTRICTED USE SEE TRAINING MEMO 2011 DO Genzyme NOT 1COPY Corporation
Treatment of asthmatic bronchoconstriction by percutaneous low voltage vagal nerve stimulation: case report.
 ISPUB.COM The Internet Journal of Asthma, Allergy and Immunology Volume 7 Number 2 Treatment of asthmatic bronchoconstriction by percutaneous low voltage vagal nerve stimulation: case P Sepulveda, G Bohill,
ISPUB.COM The Internet Journal of Asthma, Allergy and Immunology Volume 7 Number 2 Treatment of asthmatic bronchoconstriction by percutaneous low voltage vagal nerve stimulation: case P Sepulveda, G Bohill,
12/10/2009. Department of Pathology, Case Western Reserve University. Mucosal Cytokine Network in IBD
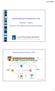 Cytokine-Mediated Inflammation in IBD Theresa T. Pizarro Department of Pathology, Case Western Reserve University Mucosal Cytokine Network in IBD Andoh, et al., 2008 1 Interleukin-1 (IL-1) Family Cytokine
Cytokine-Mediated Inflammation in IBD Theresa T. Pizarro Department of Pathology, Case Western Reserve University Mucosal Cytokine Network in IBD Andoh, et al., 2008 1 Interleukin-1 (IL-1) Family Cytokine
Identifying Biologic Targets to Attenuate or Eliminate Asthma Exacerbations
 Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Identifying Biologic Targets to Attenuate or Eliminate Exacerbations exacerbations are a major cause of disease morbidity and costs. For both children and adults, viral respiratory infections are the major
Bilateral Vagotomy as a Tool for Determining Autonomic Involvement in Airway Responses in Mouse Models of Asthma
 Chapter 17 Bilateral Vagotomy as a Tool for Determining Autonomic Involvement in Airway Responses in Mouse Models of Asthma Abstract This chapter describes the use of bilateral vagotomy as a tool for determining
Chapter 17 Bilateral Vagotomy as a Tool for Determining Autonomic Involvement in Airway Responses in Mouse Models of Asthma Abstract This chapter describes the use of bilateral vagotomy as a tool for determining
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing
 Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
Chronic inflammation of the airways Hyperactive bronchi Shortness of breath Tightness in chest Coughing Wheezing Components of the respiratory system Nasal cavity Pharynx Trachea Bronchi Bronchioles Lungs
B220 CD4 CD8. Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN
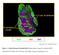 B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
Acute lung injury in children : from viral infection and mechanical ventilation to inflammation and apoptosis Bern, R.A.
 UvA-DARE (Digital Academic Repository) Acute lung injury in children : from viral infection and mechanical ventilation to inflammation and apoptosis Bern, R.A. Link to publication Citation for published
UvA-DARE (Digital Academic Repository) Acute lung injury in children : from viral infection and mechanical ventilation to inflammation and apoptosis Bern, R.A. Link to publication Citation for published
Pathophysiology of Pain
 Pathophysiology of Pain Wound Inflammatory response Chemical mediators Activity in Pain Path PAIN http://neuroscience.uth.tmc.edu/s2/chapter08.html Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University
Pathophysiology of Pain Wound Inflammatory response Chemical mediators Activity in Pain Path PAIN http://neuroscience.uth.tmc.edu/s2/chapter08.html Chris Cohan, Ph.D. Dept. of Pathology/Anat Sci University
Intracellular MHC class II molecules promote TLR-triggered innate. immune responses by maintaining Btk activation
 Intracellular MHC class II molecules promote TLR-triggered innate immune responses by maintaining Btk activation Xingguang Liu, Zhenzhen Zhan, Dong Li, Li Xu, Feng Ma, Peng Zhang, Hangping Yao and Xuetao
Intracellular MHC class II molecules promote TLR-triggered innate immune responses by maintaining Btk activation Xingguang Liu, Zhenzhen Zhan, Dong Li, Li Xu, Feng Ma, Peng Zhang, Hangping Yao and Xuetao
Full Paper. Hiroyasu Hirose, Jian Jiang, and Masaru Nishikibe*
 J Pharmacol Sci 92, 209 217 (2003) Journal of Pharmacological Sciences 2003 The Japanese Pharmacological Society Full Paper Effects of Muscarinic Receptor Antagonists With or Without M 2 Antagonist Activity
J Pharmacol Sci 92, 209 217 (2003) Journal of Pharmacological Sciences 2003 The Japanese Pharmacological Society Full Paper Effects of Muscarinic Receptor Antagonists With or Without M 2 Antagonist Activity
The Effect of BTP on the Development of Allergic Asthma in Mice
 93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
93 The Effect of BTP on the Development of Allergic Asthma in Mice Alana Curry, McNair Scholar, Virginia State University Faculty Advisor: Avery August, Ph.D Associate Professor of Immunology Department
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air
 Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Allergic diseases and treatment. Feng Qian ( 钱峰 )
 Allergic diseases and treatment Feng Qian ( 钱峰 ) fengqian@sjtu.edu.cn Hypersensitivity Antigen Host Adaptive responses protective to the host harmful to the host The deleterious consequences of the adaptive
Allergic diseases and treatment Feng Qian ( 钱峰 ) fengqian@sjtu.edu.cn Hypersensitivity Antigen Host Adaptive responses protective to the host harmful to the host The deleterious consequences of the adaptive
Systems Neuroscience November 21, 2017 The autonomic nervous system
 Systems Neuroscience November 21, 2017 The autonomic nervous system Daniel C. Kiper kiper@ini.phys.ethz.ch http: www.ini.unizh.ch/~kiper/system_neurosci.html How is the organization of the autonomic nervous
Systems Neuroscience November 21, 2017 The autonomic nervous system Daniel C. Kiper kiper@ini.phys.ethz.ch http: www.ini.unizh.ch/~kiper/system_neurosci.html How is the organization of the autonomic nervous
