Bench Comparative Assessment of Mechanically Assisted Cough Devices
|
|
|
- Rosamond Higgins
- 5 years ago
- Views:
Transcription
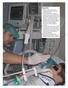
1 Bench Comparative Assessment of Mechanically Assisted Cough Devices Pamela Frigerio PT, Federico Longhini MD, Maurizio Sommariva PT, Enrica G Stagni PT, Francesco Curto MD, Tiziana Redaelli MD, Marco Ciboldi DEng, Anita K Simonds MD, and Paolo Navalesi MD BACKGROUND: Mechanically assisted cough devices are used in patients with impaired cough to avoid secretion accumulation. We compared 5 mechanically assisted cough devices by bench testing using a breathing simulator and assessed their user-friendliness. METHODS: We measured inspiratory and expiratory airway pressures and peak expiratory flow, the strongest indicator of cough efficacy. We performed 2 bench tests: 1) to ascertain the differences between preset and actual settings in 3 different machines of each mechanically assisted cough device and 2) to assess the effects of varying respiratory impedance and air leaks on performance of the devices. We also evaluated the user-friendliness of the devices by measuring the time required and errors in accomplishing 4 tasks by 10 physicians unfamiliar with mechanically assisted cough devices compared with product specialists from the distributing companies. Physicians also scored the ease of use. RESULTS: Four mechanically assisted cough devices during insufflation and all 5 during exsufflation showed differences between preset and actual airway pressures. All but one device showed uneven actual pressure values between models of the same type. Peak expiratory flow was significantly influenced by the mechanical properties in 2 devices and by air leaks in 4 devices. The median time to accomplish all tasks by the product specialist (10 [interquartile range of 2 29] s) was overall significantly shorter compared with all physicians (from 19 [14 65] to 36 [19 116] s). The number of procedural errors, but not the perceived ease of use, differed significantly between the devices. CONCLUSIONS: The performance of different mechanically assisted cough devices was erratic and included variance between models from the same manufacturer; it was affected by respiratory system impedance and air leaks. Time and rate of errors for performing procedures were elevated. These findings indicate that the devices are not interchangeable and that the settings should be targeted for each patient with the specific machine being used. Improvements in reliability, performance, and user-friendliness are advisable. Key words: cough; physical therapy modalities; respiratory therapy; pulmonary medicine; mechanical ventilators; critical care. [Respir Care 2015;60(7): Daedalus Enterprises] Introduction Impaired cough with retention of tracheobronchial secretions is a common complication of neuromuscular disorders. Ineffective cough can lead to tracheotomy for the sole purpose of airway suctioning in patients with severe respiratory failure. 1 Accordingly, intensive chest physical Ms Frigerio, Ms Stagni, and Dr Redaelli are affiliated with the Spinal Cord Unit; Mr Sommariva and Dr Curto are affiliated with the Neurocritical Care Unit, Department of Neuroscience; and Dr Ciboldi is affiliated with Department of Clinical Engineering, Niguarda Cà Granda Hospital, Milan, Italy. Drs Longhini and Navalesi are affiliated with the Department of Translational Medicine, Eastern Piedmont University A. Avogadro, Novara, Italy, and the Division of Anaesthesia and Intensive Care, Sant Andrea Hospita (ASL VC), Vercelli, Italy. Dr Simonds is affiliated with the National Heart & Lung Institute Respiratory Biomedical Research Unit, Royal Brompton & Harefield NHS Foundation Trust, London, United Kingdom. Dr Navalesi is also affiliated with CRRF Mons Luigi Novarese, Moncrivello, Italy. Supplementary material related to this paper is available at RESPIRATORY CARE JULY 2015 VOL 60 NO 7 975
2 therapy, including cough assistance, is often prescribed to enhance secretion clearance. 2,3 Cough assistance is traditionally based on inspiratory volume increase and manual abdominal thrust and/or chest compression. Mechanically assisted cough devices can also be used for this purpose, with either an endotracheal artificial airway 4 or a mask. 5 These devices sequentially apply positive and negative (subatmospheric) pressure to the airway, creating a pressure gradient to promote a peak expiratory flow (PEF) sufficient to remove secretions from the large airways. SEE THE RELATED EDITORIAL ON PAGE 1081 Several studies have demonstrated the effectiveness of mechanically assisted cough devices and, in some cases, superiority to manual techniques 6-8 in achieving secretion clearance in both acute 9,10 and chronic 11,12 subjects with ineffective cough with shorter periods of treatment. 13 As a result, these devices are being increasingly used, and their commercial availability in Europe has risen concomitantly. The use of mechanically assisted cough devices has been proposed for ICU patients as a means to facilitate successful extubation. 9 Despite the increased availability of mechanically assisted cough devices, to our knowledge, no study has evaluated and compared different devices to ascertain whether their performances are equivalent. As the performances of other devices such as home ventilators have been shown in bench studies to vary significantly, 14 we designed this bench study to evaluate and compare 5 mechanically assisted cough devices that are commercially available in Europe with respect to reliability, intra-device reproducibility, and response to varying respiratory mechanics and presence of air leaks. Moreover, considering the lack of homogeneity among mechanically assisted cough devices with respect to control screens and buttons, we also evaluated the userfriendliness of these 5 devices for ICU physicians. Methods The study was performed on 2 consecutive days in November 2012 in the laboratory of the Department of Clinical Engineering at the Niguarda Cà Granda Hospital in QUICK LOOK Current knowledge Impaired cough with retention of secretions is a common complication of neuromuscular disease. Ineffective cough can lead to tracheostomy to facilitate airway suctioning in patients with respiratory failure. Intensive chest physical therapy, including cough assistance, is indicated to enhance secretion clearance. Mechanically assisted cough devices sequentially apply positive and negative pressure to the airway, creating a pressure gradient and enhancing peak expiratory flow to remove airway secretions. What this paper contributes to our knowledge The performance of different mechanically assisted cough devices in a model system varied widely. Devices from the same manufacturers performed differently. Changes in respiratory system impedance and air leaks significantly impacted device performance. Ease of use and time to set up the devices also differed greatly. Improved reliability of mechanically assisted cough devices is needed. Milan, Italy. The 5 mechanically assisted cough devices tested are listed in Table 1. The devices were connected to a breathing simulator (ASL 5000, IngMar Medical, Pittsburgh, Pennsylvania). Two different bench tests were conducted. Both tests were performed in automatic mode, with the inspiratory and expiratory airway pressures (P aw ) set at 40 and 40 cm H 2 O, respectively, and the inspiratory (T I ) and expiratory (T E ) times both set 3 s, without pause in between. Immediately after the first cycle of insufflation-exsufflation, 5 consecutive respiratory cycles were recorded and averaged. Both bench tests were performed once by the same bioengineer in the Laboratory of Clinical Engineering, without familiarity with the devices under evaluation. In addition, we performed a test to evaluate the user-friendliness of the 5 devices. Table 1. Mechanically Assisted Cough Devices Tested in This Study Dr Navalesi has disclosed relationships with Intersurgical, Maquet, Dräger, Breas, Covidien, GlaxoSmithKline, Hill-Rom, and Linde AG. Dr Simonds has disclosed a relationship with ResMed. The other authors have disclosed no conflicts of interest. Correspondence: Paolo Navalesi MD, Department of Translational Medicine, Eastern Piedmont University A. Avogadro, Via Solaroli 17, Novara, Italy. paolo.navalesi@med.unipmn.it. DOI: /respcare Ventilator Nippy cough assistor CoughAssist New Negavent DA-3 PLUS Pegaso New Negavent DA-3 PLUS Mini Pegaso Pulsar Manufacturer B&D Electromedical (Warwickshire, UK) Philips Healthcare (Best, The Netherlands) Dima Italia (Bologna, Italy) Dima Italia Siare Engineering International Group (Bologna, Italy) 976 RESPIRATORY CARE JULY 2015 VOL 60 NO 7
3 Bench Test 1 Three different machines of each mechanically assisted cough device were tested in a single experimental condition (simulated compliance of 40 ml/cm H 2 O, simulated resistance of 10 cm H 2 O/L/s, no air leaks). Bench Test 2 We used the best performing of the 3 machines evaluated in bench test 1 for each mechanically assisted cough device. The response to varying simulated respiratory mechanical properties, with and without air leaks, was evaluated mimicking 4 conditions: (1) compliance of 40 ml/cm H 2 O and resistance of 10 cm H 2 O/L/s without air leaks, (2) compliance of 40 ml/cm H 2 O and resistance of 10 cm H 2 O/L/s with air leaks, (3) compliance of 60 ml/cm H 2 O and resistance of 20 cm H 2 O/L/s without air leaks, and (4) compliance of 60 ml/cm H 2 O and resistance of 20 cm H 2 O/L/s with air leaks. User-Friendliness Test One product specialist for each mechanically assisted cough device, indicated by the company distributors, and 10 physicians, randomly drawn by lot from the neuro-icu medical staff and without previous experience with any of the 5 devices under evaluation, were selected to test userfriendliness. One week before the test, the physicians received information on the functions of all 5 devices. 15 Physicians were asked to perform a 4-task test for each mechanically assisted cough device. The order of evaluation of the devices was randomized for each physician. The test consisted of 4 separate phases: (1) start-up (starting the assembled device), (2) recognizing parameters (inspiratory and expiratory P aw,t I,T E, and the pause in between, requested according to a randomized sequence), (3) varying settings (inspiratory P aw of 40 cm H 2 O, expiratory P aw of 40 cm H 2 O, T I of 4 s, T E of 3 s, pause of 1 s), and (4) stop (ie, turning off the machine and activating the standby mode, if available). Data Analysis Data of the 2 bench tests were recorded from the ASL 5000 data output array and analyzed offline. T I,T E, PEF, and inspiratory tidal volume (V T ) were obtained from the flow tracing, whereas inspiratory and expiratory P aw and time to reach 90% of preset inspiratory and expiratory P aw (T 90I and T 90E, respectively) were obtained from the P aw tracing. In bench test 1, inspiratory and expiratory P aw were analyzed to evaluate whether the difference between preset and actual values was in accordance with the 4% tolerance limit indicated by the European Commission requirements ( CEI EN ). 16 To assess variability of each model, the test was performed on 3 machines obtained from the commercial distributors. In bench test 2, we evaluated the performance of the mechanically assisted cough devices under different simulated conditions. Inspiratory and expiratory Paw, PEF, V T,T 90I, and T 90E were determined for each device and compared. In the user-friendliness test, the time required to perform tasks was measured with a precision stopwatch by a second bioengineer in the laboratory of the Department of Clinical Engineering with extensive knowledge of all 5 mechanically assisted cough devices and awareness of the tasks to be accomplished. For all tasks, the time measurement was interrupted upon achievement of the specific objective or at a maximum limit of 5 min. In addition, the physicians graded the ease of use of each device, both overall and separately for each single task, using a visual analog scale on a 10-cm line marked with 0 on the left for very difficult and 10 on the right for very easy. Finally, the errors made by the physicians during test execution were counted and expressed both as absolute values and percent of the overall actions required during the test. Statistical Analysis Data are expressed as median (interquartile range) unless specified otherwise and were compared by analysis of variance on ranks (Kruskal-Wallis test). The Dunn post hoc test was used to ascertain differences between either selected pairs of conditions (bench test 2) or all mechanically assisted cough devices (user-friendliness test), as appropriate. We considered P.05 to be significant. Bench Test 1 Results As shown in Figure 1A, the discrepancy between preset and actual inspiratory and expiratory P aw was within the 4% tolerance limits for 2 mechanically assisted cough devices (Nippy and Pulsar) only. Furthermore, all devices but one (Nippy) showed uneven inspiratory and expiratory P aw with the 3 machines tested. As shown in Figure 1B, discrepancies were observed between preset and actual T I and T E. All devices but one (Pulsar) for T I and all but 2 devices (Nippy and Pulsar) for T E showed erratic values with the 3 machines tested. Bench Test 2 Figure 2A shows inspiratory P aw,v T, and T 90I, and Figure 2B shows expiratory P aw, PEF, and T 90E. Inspira- RESPIRATORY CARE JULY 2015 VOL 60 NO 7 977
4 Fig. 1. Discrepancy between preset and actual airway pressures. A: inspiratory and expiratory airway pressure (P aw ) medians of 5 respiratory cycles obtained with each individual mechanically assisted cough device (white symbols). The median values of the overall 15 measurements (black symbols) are also displayed for each type of device. Dashed lines indicate the 4% tolerance limits according to the European Commission regulation for mechanical ventilators. B: inspiratory (T I ) and expiratory (T E ) time medians are shown for each device. tory P aw was significantly affected by mechanical properties with one device only (Pegaso) and to varying extents by the presence of air leaks with the other 4 devices. V T was affected by the simulated mechanical properties with the Nippy device and to varying extents by air leaks with the other 4 devices. T 90I was unaffected by mechanical properties or air leaks with the CoughAssist; by mechanical properties with the Pegaso, Mini Pegaso, and Pulsar; and by air leaks with the Nippy. Expiratory P aw was affected by mechanical properties with the Pegaso and to varying extents by air leaks with the other 4 devices. PEF was influenced by mechanical properties with the Mini Pegaso and Pulsar and by air leaks with the Nippy, CoughAssist, Pegaso and Mini Pegaso. T 90E was affected by mechanical properties with the Mini Pegaso and by air leaks with the other 4 devices. User-Friendliness Test All 10 physicians completed all 4 tasks. Table 2 shows (1) the median (interquartile range) of the time spent by the 10 physicians to accomplish the 4 tasks individually and overall, (2) the scores on the ease of accomplishment of the tasks by the physicians, and (3) the errors made by the physicians during task execution. Overall, the Pegaso and Pulsar showed the shortest and longest times of execution, respectively. In addition, there were wide and significant differences between the mechanically assisted cough devices with respect to the individual tasks. The scores on the ease of use were no different overall and showed significant differences only for the start-up and recognizing-parameters tasks. The CoughAssist resulted in significantly more errors overall, as opposed to the Pegaso (P.04), Mini Pegaso (P.04), and Pulsar (P.03). This was due primarily to the recognizing-parameters task. The Nippy showed no significant difference with respect to all tasks compared with the other devices. As shown in Figure 3, the overall median time spent to accomplish the 4 tasks by the product specialists using each of the 5 devices (gray bar) was significantly shorter compared with that achieved by the 10 physicians (white bars) (P.02). Discussion In this study, we found that only 2 of the 5 mechanically assisted cough devices complied with the 4% tolerance limit for the discrepancy between preset and actual inspiratory and expiratory P aw. Moreover, for all devices but one, the actual inspiratory and expiratory P aw of the 3 machines tested were discrepant. In addition, the performance of the 5 devices was affected differently by the simulated mechanical properties, the air leaks, or both. Finally, the time spent to accomplish 4 tasks (separately and overall) assigned to 10 ICU physicians was largely and significantly different between devices. The ease of accomplishment of the tasks was not significantly different between the devices overall, whereas there were relatively small significant differences between devices with respect to 2 individual tasks (ie, start-up and recognizing parameters). Our bench study is the first to evaluate and compare several mechanically assisted cough devices. In a previously published bench study comparing the Nippy and CoughAssist operating with varying mechanical properties (but without considering air leaks), PEF was found to be greater with the Nippy. 17 It is of note that in a previous bench evaluation performed to assess the impact of various artificial airways on the performance of the CoughAssist, the same authors reported quite different PEF values with an identical setup. 18 In keeping with these contradictory findings, 17,18 we found uneven inspiratory and expiratory P aw (see Fig. 1A) and T I and T E (see Fig. 1B) between the 3 machines tested for each device. Furthermore, though all 978 RESPIRATORY CARE JULY 2015 VOL 60 NO 7
5 Fig. 2. Mechanically assisted cough device performance with varying mechanical properties and air leaks. A: Inspiratory airway pressure (P aw ), tidal volume (V T ), and time to reach 90% of preset inspiratory P aw (T 90I ) in different simulated conditions. B: Expiratory P aw, peak expiratory flow (PEF), and time to reach 90% of preset expiratory P aw (T 90E ) in different simulated conditions. Dashed lines indicate preset inspiratory (A) and expiratory (B) P aw.*p.05, compliance of 40 ml/cm H 2 O and resistance of 10 cm H 2 O/L/s with air leaks (C40R10L) vs compliance of 40 ml/cm H 2 O and resistance of 10 cm H 2 O/L/s without air leaks (C40R10). P.05, compliance of 60 ml/cm H 2 O and resistance of 20 cm H 2 O/L/s with air leaks (C60R20L) vs compliance of 60 ml/cm H 2 O and resistance of 20 cm H 2 O/L/s without air leaks (C60R20). P.05, C60R20 vs C40R10; P.05, C60R20L vs C40R10L. (For exact P values, see the supplementary materials at 5 devices had the European Conformity mark, only 2 devices conformed overall to the European Community 4% tolerance limit for mechanical ventilators with respect to the difference between preset and actual P aw. In addition, although the 4% tolerance limit corresponds in our study to a difference between preset and actual inspiratory and expiratory P aw of only 1.6 cm H 2 O (a relatively small value of limited clinical importance), some machines markedly exceeded the 4% limit (see Fig. 1A). These discrepancies may be more relevant in particular scenarios, such as when the mechanically assisted cough device is applied with a tracheotomy or endotracheal tube rather than de- RESPIRATORY CARE JULY 2015 VOL 60 NO 7 979
6 Table 2. Time, Ease of Use, and Errors for Accomplishment of Tasks Nippy CoughAssist Pegaso Mini Pegaso Pulsar Time, s Start-up 13 (12 22) 3 (2 4) 26 (22 34) a 37 (32 58) b 76 (57 111) c,d Recognizing parameters 20 (18 22) 68 (44 84) e 17 (14 19) f 19 (16 38) g 23 (17 30) h Varying settings 103 (91 139) 83 (52 113) 67 (62 92) 83 (63 112) 153 ( ) d,i,j Stop 67 (22 91) 7 (5 17) e 5 (3 72) k 8 (7 14) l 23 (17 62) i Overall 217 ( ) 151 ( ) 127 ( ) m 181 ( ) 309 ( ) h,i Visual analog scale ease of use, cm Start-up 9.4 ( ) 9.6 ( ) 7.2 ( ) a 7.2 ( ) n 5.4 ( ) c,d Recognizing parameters 9.5 ( ) 7.2 ( ) o 9.4 ( ) a 9.4 ( ) n 8.3 ( ) Varying settings 9.2 ( ) 7.0 ( ) 8.9 ( ) 8.1 ( ) 7.3 ( ) Stop 8.9 ( ) 9.3 ( ) 9.4 ( ) 8.8 ( ) 6.4 ( ) Overall 8.8 ( ) 7.7 ( ) 8.8 ( ) 8.9 ( ) 6.9 ( ) Errors, % (n) Start-up 0 (0), (0) 0 (0), (0) 0 (0), (0) 0 (0), (0) 0 (0), (0) Recognizing parameters 0 (0 20), (4) 40 (15 45), (18) 0 (0), (1) p 0 (0), (2) n 0 (0), (0) h Varying settings 0 (0 30), (7) 0 (0 40), (10) 0 (0), (0) 0 (0), (0) 0 (0), (1) Stop 0 (0), (0) 0 (0), (0) 0 (0), (0) 0 (0), (0) 0 (0), (0) Overall 0 (0 21), (11) 21 (12 31), (28) 0 (0), (1) p 0 (0), (2) n 0 (0), (1) h Data are expressed as median (interquartile range). a P.02 Pegaso vs CoughAssist b P.001 Mini Pegaso vs CoughAssist c P.001 Pulsar vs Nippy d P.001 Pulsar vs CoughAssist e P.01 CoughAssist vs Nippy f P.001 Pegaso vs CoughAssist g P.01 Mini Pegaso vs CoughAssist h P.03 Pulsar vs CoughAssist i P.001 Pulsar vs Pegaso j P.02 Pulsar vs Mini Pegaso k P.001 Pegaso vs Nippy l P.02 Mini Pegaso vs Nippy m P.02 Pegaso vs Nippy n P.04 Mini Pegaso vs CoughAssist o P.004 CoughAssist vs Nippy p P.04 Pegaso vs CoughAssist Fig. 3. Time for performing all the tests on all mechanically assisted cough devices by ICU physicians The graph shows the overall median time spent to accomplish all tasks by the product specialists (grey bar) compared with 10 ICU physicians (white bars). * P.02, product specialists vs physicians. livered via a face mask or mouthpiece. Furthermore, we do not know whether the variance between actual and preset values is greater or less marked at insufflation-exsufflation pressure settings other than 40 to 40 cm H 2 O. In a bench test of one mechanically assisted cough device (CoughAssist) at 3 different preset inspiratory and expiratory P aw with 4 simulated mechanical properties, Guérin et al 18 showed that varying the size of the artificial airway (ie, the additional airway resistance imposed by the tube) affects PEF, which is the strongest indicator of cough efficacy. Our study expands this observation, demonstrating that the performance of these devices is affected by the mechanical properties of the respiratory system and by the presence of air leaks. In fact, we found not only PEF, but also V T, the actual inspiratory and expiratory P aw,t 90I, and T 90E to fluctuate with all mechanically assisted cough devices, although to remarkably varying extents. As shown in Figure 4, V T, actual inspiratory and expiratory P aw,t 90I, and T 90E are all determinants of PEF. Gonzalez-Bermejo et al 19 reported the limited userfriendliness of home ventilators and stressed the importance of this considering the increasing number of medical and nonmedical health-care professionals required to manage the technical aspects of these machines when caring for patients receiving home ventilation. The authors found that for most ventilators, the ICU physicians were slower than the specialist technician in completing the required tasks. Furthermore, the physicians scored the overall ease of use as no different between ventilators. With a similar study design, the present study extends those observations to mechanically assisted cough devices. The time taken by each task differed between devices, and overall, ICU physicians were slower than the product specialist. Also, consistent with the former study, physicians scored ease of 980 RESPIRATORY CARE JULY 2015 VOL 60 NO 7
7 Fig. 4. Determinants of peak expiratory flow (PEF), which is the strongest indicator of cough efficacy. The magnitude of PEF is directly influenced by the pressure applied to the airway opening (P aw ) during the expiratory phase, the time to reach 90% of preset expiratory P aw (T 90E ), and the volume insufflated during the inspiratory phase (tidal volume [V T ]), corresponding to the pre-tussive volume and resulting from the extent of the inspiratory P aw and the speed of achievement of the time to reach 90% of preset inspiratory P aw (T 90I ). use overall as no different between devices. Importantly, however, the only device with an analog interface (CoughAssist) produced the highest incidence of errors in the recognizing-parameters task and received the lowest score. Our study has limitations. First, it has the intrinsic limitation of any bench evaluation that attempts in a strictly controlled environment to simulate situations that are definitely more complex and dynamically variable in the clinical setting. Although no recommendation or specific requirement exists for bench evaluations, 20 in particular for these devices, we attempted to mimic the most common clinical settings and scenarios. It is clear that the huge discrepancies we found between preset and actual values and the inhomogeneous behavior of machines of the same model indicate that some mechanically assisted cough devices might not produce PEF high enough to achieve adequate airway clearance. 1,9,21 Second, we extended the 4% tolerance limit (originally intended for mechanical ventilators) to mechanically assisted cough devices, which may be considered arbitrary and potentially unfair. Lacking specific criteria, we chose the evaluation regulations in force for the instruments more closely resembling these devices. Third, a blinded assessment of mechanically assisted cough devices is not feasible; nonetheless, neither the bioengineer who performed the bench testing nor the physicians involved in the user-friendliness test had previous experience with any of the devices under evaluation. Fourth, we differ from North America but are similar to many other European countries in that we do not have respiratory therapists in our hospitals and thus performed our userfriendliness evaluation by interviewing ICU physicians. Therefore, the results of our evaluation might not be applicable to other health-care professionals or nonprofessional caregivers. Considering ICU physicians familiarity with similar but more complex devices such as mechanical ventilators, the user-friendliness of mechanically assisted cough devices might be even worse for other categories of users. Finally, we tested all of the devices available in our country at the time the study was performed. It is notable that only one device is presently available for clinical use in North America. We are aware that some new mechanically assisted cough devices have since been introduced in the market, and the manufacturers have updated some of those evaluated here. Although we share this limitation with any study evaluating medical devices, we believe that the message of this study remains valid for both clinicians and manufacturers. Conclusions The performance of different mechanically assisted cough devices was extremely variable, even between machines of the same model, and is affected by respiratory system impedance and air leaks. The time taken to set up and operate the devices and the number of procedural errors made by the ICU physicians were high. These findings indicate that the devices are not interchangeable and that the settings should be targeted for each patient with the specific machine utilized. A substantial improvement in reliability, reproducibility of performance, and userfriendliness is advised. REFERENCES 1. Bach JR, Saporito LR. Criteria for extubation and tracheostomy tube removal for patients with ventilatory failure. A different approach to weaning. Chest 1996;110(6): Bach JR, Gonçalves MR, Hon A, Ishikawa Y, De Vito EL, Prado F, Dominguez ME. Changing trends in the management of end-stage neuromuscular respiratory muscle failure: recommendations of an international consensus. Am J Phys Med Rehabil 2013;92(3): Tzeng AC, Bach JR. Prevention of pulmonary morbidity for patients with neuromuscular disease. Chest 2000;118(5): Toussaint M. The use of mechanical insufflation-exsufflation via artificial airways. Respir Care 2011;56(8): Sancho J, Servera E, Díaz J, Marín J. Efficacy of mechanical insufflation-exsufflation in medically stable patients with amyotrophic lateral sclerosis. Chest 2004;125(4): Bach JR. Mechanical insufflation-exsufflation. Comparison of peak expiratory flows with manually assisted and unassisted coughing techniques. Chest 1993;104(5): Chatwin M, Ross E, Hart N, Nickol AH, Polkey MI, Simonds AK. Cough augmentation with mechanical insufflation/exsufflation in patients with neuromuscular weakness. Eur Respir J 2003;21(3): Mustfa N, Aiello M, Lyall RA, Nikoletou D, Olivieri D, Leigh PN, et al. Cough augmentation in amyotrophic lateral sclerosis. Neurology 2003;61(9): Bach JR, Gonçalves MR, Hamdani I, Winck JC. Extubation of patients with neuromuscular weakness: a new management paradigm. Chest 2010;137(5): Gonçalves MR, Honrado T, Winck JC, Paiva JA. Effects of mechanical insufflation-exsufflation in preventing respiratory failure after extubation: a randomized controlled trial. Crit Care 2012;16(2):R Bach JR, Rajaraman R, Ballanger F, Tzeng AC, Ishikawa Y, Kulessa R, Bansal T. Neuromuscular ventilatory insufficiency: effect of home RESPIRATORY CARE JULY 2015 VOL 60 NO 7 981
8 mechanical ventilator use v oxygen therapy on pneumonia and hospitalization rates. Am J Phys Med Rehabil 1998;77(1): Vitacca M, Paneroni M, Trainini D, Bianchi L, Assoni G, Saleri M, et al. At home and on demand mechanical cough assistance program for patients with amyotrophic lateral sclerosis. Am J Phys Med Rehabil 2010;89(5): Chatwin M, Simonds AK. The addition of mechanical insufflation/ exsufflation shortens airway-clearance sessions in neuromuscular patients with chest infection. Respir Care 2009;54(11): Blakeman TC, Rodriquez D Jr, Hanseman D, Branson RD. Bench evaluation of 7 home-care ventilators. Respir Care 2011;56(11): Navalesi P, Frigerio P. Cough assistance in mechanically ventilated neuromuscular patients. In: Vincent JL. Update in intensive care. Berlin: Springer-Verlag; 2004; Council of the European Communities. Council Directive 93/42/EEC of 14 June 1993 concerning medical devices. eu/lexuriserv/lexuriserv.do?uri CONSLEG:1993L0042: :en:PDF. Accessed March 17, Porot V, Guérin C. Bench assessment of a new insufflation-exsufflation device. Respir Care 2013;58(9): Guérin C, Bourdin G, Leray V, Delannoy B, Bayle F, Germain M, Richard JC. Performance of the CoughAssist insufflation-exsufflation device in the presence of an endotracheal tube or tracheostomy tube: a bench study. Respir Care 2011;56(8): Gonzalez-Bermejo J, Laplanche V, Husseini FE, Duguet A, Derenne JP, Similowski T. Evaluation of the user-friendliness of 11 home mechanical ventilators. Eur Respir J 2006;27(6): Olivieri C, Costa R, Conti G, Navalesi P. Bench studies evaluating devices for non-invasive ventilation: critical analysis and future perspectives. Intensive Care Med 2012;38(1): Smina M, Salam A, Khamiees M, Gada P, Amoateng-Adjepong Y, Manthous CA. Cough peak flows and extubation outcomes. Chest 2003;124(1): This article is approved for Continuing Respiratory Care Education credit. For information and to obtain your CRCE (free to AARC members) visit RESPIRATORY CARE JULY 2015 VOL 60 NO 7
Bench Assessment of a New Insufflation-Exsufflation Device
 Bench Assessment of a New Insufflation-Exsufflation Device Véronique Porot MD and Claude Guérin MD PhD BACKGROUND: The Nippy Clearway is a new mechanical insufflation-exsufflation device used to assist
Bench Assessment of a New Insufflation-Exsufflation Device Véronique Porot MD and Claude Guérin MD PhD BACKGROUND: The Nippy Clearway is a new mechanical insufflation-exsufflation device used to assist
CoughAssist E70. More than just a comfortable cough. Flexible therapy that brings more comfort to your patients airway clearance
 CoughAssist E70 More than just a comfortable cough Flexible therapy that brings more comfort to your patients airway clearance Flexible, customisable loosening and clearing therapy An effective cough is
CoughAssist E70 More than just a comfortable cough Flexible therapy that brings more comfort to your patients airway clearance Flexible, customisable loosening and clearing therapy An effective cough is
The difference is clear. CoughAssist clears airways with the force of a natural cough
 The difference is clear CoughAssist clears airways with the force of a natural cough When only a real cough will do CoughAssist is a noninvasive therapy that safely and consistently removes secretions
The difference is clear CoughAssist clears airways with the force of a natural cough When only a real cough will do CoughAssist is a noninvasive therapy that safely and consistently removes secretions
Performance of the CoughAssist Insufflation-Exsufflation Device in the Presence of an Endotracheal Tube or Tracheostomy Tube: A Bench Study
 Performance of the CoughAssist Insufflation-Exsufflation Device in the Presence of an or : A Bench Study Claude Guérin MD PhD, Gaël Bourdin MD, Véronique Leray MD, Bertrand Delannoy MD, Frédérique Bayle
Performance of the CoughAssist Insufflation-Exsufflation Device in the Presence of an or : A Bench Study Claude Guérin MD PhD, Gaël Bourdin MD, Véronique Leray MD, Bertrand Delannoy MD, Frédérique Bayle
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the
 Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Respiratory Management- Your Questions Answered! Michelle Chatwin, PhD Consultant Physiotherapist
 Respiratory Management- Your Questions Answered! Michelle Chatwin, PhD Consultant Physiotherapist Why Are People Affected Differently Neuromuscular Disease; A Spectrum Its severity varies widely within
Respiratory Management- Your Questions Answered! Michelle Chatwin, PhD Consultant Physiotherapist Why Are People Affected Differently Neuromuscular Disease; A Spectrum Its severity varies widely within
Terapias no farmacológicas de aclaramiento de la vía aérea y soporte respiratorio muscular en
 Terapias no farmacológicas de aclaramiento de la vía aérea y soporte respiratorio muscular en el paciente ventilado: Estado del arte João Carlos Winck, MD, PhD Coordinator of the Respiratory Medicine Unit
Terapias no farmacológicas de aclaramiento de la vía aérea y soporte respiratorio muscular en el paciente ventilado: Estado del arte João Carlos Winck, MD, PhD Coordinator of the Respiratory Medicine Unit
Commissioning Policy for Cough Assist Requests
 Commissioning Policy for Cough Assist Requests 1 DOCUMENT CONTROL Reference Number (lead in specific policy area to provide once policy ratified) Version Draft Version 0.3 071015 Status Sponsor(s)/Author(s)
Commissioning Policy for Cough Assist Requests 1 DOCUMENT CONTROL Reference Number (lead in specific policy area to provide once policy ratified) Version Draft Version 0.3 071015 Status Sponsor(s)/Author(s)
Alternative title: Confessions of a Mucus Enthusiast. Mechanical Insufflation Exsufflation for airway secretion clearance and lung expansion therapy
 Mechanical Insufflation Exsufflation for airway secretion clearance and lung expansion therapy Alternative title: Confessions of a Mucus Enthusiast Marty Davig, RRT RCP Philips Respironics Inc. Objectives
Mechanical Insufflation Exsufflation for airway secretion clearance and lung expansion therapy Alternative title: Confessions of a Mucus Enthusiast Marty Davig, RRT RCP Philips Respironics Inc. Objectives
A Comparison of Cough Assistance Techniques in Patients with Respiratory Muscle Weakness
 Original Article Yonsei Med J 2016 Nov;57(6):1488-1493 pissn: 0513-5796 eissn: 1976-2437 A Comparison of Cough Assistance Techniques in Patients with Respiratory Muscle Weakness Sun Mi Kim 1,2, Won Ah
Original Article Yonsei Med J 2016 Nov;57(6):1488-1493 pissn: 0513-5796 eissn: 1976-2437 A Comparison of Cough Assistance Techniques in Patients with Respiratory Muscle Weakness Sun Mi Kim 1,2, Won Ah
Key points. k Ineffective cough is a major cause of
 Breathe review cough.qxd 21/05/2008 16:06 Page 2 Key points k Ineffective cough is a major cause of k k k mortality and morbidity in patients with neuromuscular disease. A normal cough requires the inspiratory
Breathe review cough.qxd 21/05/2008 16:06 Page 2 Key points k Ineffective cough is a major cause of k k k mortality and morbidity in patients with neuromuscular disease. A normal cough requires the inspiratory
Operation Manual for clinical use of SIARE Pulsar
 Operation Manual for clinical use of SIARE Pulsar This manual is for clinical use only 1-12 INDEX 1) Indications /Contraindications and cautions 2) Questions to ask before using a MI-E machine 3) Guideline
Operation Manual for clinical use of SIARE Pulsar This manual is for clinical use only 1-12 INDEX 1) Indications /Contraindications and cautions 2) Questions to ask before using a MI-E machine 3) Guideline
The objectives of this presentation are to
 1 The objectives of this presentation are to 1. Review the mechanics of airway clearance 2. Understand the difference between secretion mobilization and secretion clearance 3. Identify conditions that
1 The objectives of this presentation are to 1. Review the mechanics of airway clearance 2. Understand the difference between secretion mobilization and secretion clearance 3. Identify conditions that
Preventing Respiratory Complications of Muscular Dystrophy
 Preventing Respiratory Complications of Muscular Dystrophy Jonathan D. Finder, MD Professor of Pediatrics University of Pittsburgh School of Medicine Children s Hospital of Pittsburgh Introduction Respiratory
Preventing Respiratory Complications of Muscular Dystrophy Jonathan D. Finder, MD Professor of Pediatrics University of Pittsburgh School of Medicine Children s Hospital of Pittsburgh Introduction Respiratory
Simulation of Late Inspiratory Rise in Airway Pressure During Pressure Support Ventilation
 Simulation of Late Inspiratory Rise in Airway Pressure During Pressure Support Ventilation Chun-Hsiang Yu MD, Po-Lan Su MD, Wei-Chieh Lin MD PhD, Sheng-Hsiang Lin PhD, and Chang-Wen Chen MD MSc BACKGROUND:
Simulation of Late Inspiratory Rise in Airway Pressure During Pressure Support Ventilation Chun-Hsiang Yu MD, Po-Lan Su MD, Wei-Chieh Lin MD PhD, Sheng-Hsiang Lin PhD, and Chang-Wen Chen MD MSc BACKGROUND:
My CoughAssist. A patient guide to CoughAssist E70
 My CoughAssist A patient guide to CoughAssist E70 A natural part of life Coughing. We often think of a cough as a symptom of a cold or a means to clear our throat. Truth is, the ability to cough is essential
My CoughAssist A patient guide to CoughAssist E70 A natural part of life Coughing. We often think of a cough as a symptom of a cold or a means to clear our throat. Truth is, the ability to cough is essential
Mechanical Insufflation-Exsufflation Versus Conventional Chest Physiotherapy in Children With Cerebral Palsy
 Mechanical Insufflation-Exsufflation Versus Conventional Chest Physiotherapy in Children With Cerebral Palsy Rasintra Siriwat MD, Jitladda Deerojanawong MD, Suchada Sritippayawan MD, Sumalee Hantragool
Mechanical Insufflation-Exsufflation Versus Conventional Chest Physiotherapy in Children With Cerebral Palsy Rasintra Siriwat MD, Jitladda Deerojanawong MD, Suchada Sritippayawan MD, Sumalee Hantragool
Motor Neurone Disease NICE to manage Management of ineffective cough. Alex Long Specialist NIV/Respiratory physiotherapist June 2016
 Motor Neurone Disease NICE to manage Management of ineffective cough Alex Long Specialist NIV/Respiratory physiotherapist June 2016 Content NICE guideline recommendations Respiratory involvement in MND
Motor Neurone Disease NICE to manage Management of ineffective cough Alex Long Specialist NIV/Respiratory physiotherapist June 2016 Content NICE guideline recommendations Respiratory involvement in MND
Artificial External Glottic Device for Passive Lung Insufflation
 Original Article http://dx.doi.org/10.3349/ymj.2011.52.6.972 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 52(6):972-976, 2011 Artificial External Glottic Device for Passive Lung Insufflation Dong Hyun
Original Article http://dx.doi.org/10.3349/ymj.2011.52.6.972 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 52(6):972-976, 2011 Artificial External Glottic Device for Passive Lung Insufflation Dong Hyun
A Comparison of Leak Compensation in Acute Care Ventilators During Noninvasive and Invasive Ventilation: A Lung Model Study
 A Comparison of Leak Compensation in Acute Care Ventilators During Noninvasive and Invasive Ventilation: A Lung Model Study Jun Oto MD PhD, Christopher T Chenelle, Andrew D Marchese, and Robert M Kacmarek
A Comparison of Leak Compensation in Acute Care Ventilators During Noninvasive and Invasive Ventilation: A Lung Model Study Jun Oto MD PhD, Christopher T Chenelle, Andrew D Marchese, and Robert M Kacmarek
LUNG VOLUME RECRUITMENT IN NEUROMUSCULAR DISEASE
 LUNG VOLUME RECRUITMENT IN NEUROMUSCULAR DISEASE Sherri Katz, MDCM, MSc, FRCPC Pediatric Respirologist Children s Hospital of Eastern Ontario University of Ottawa Disclosures Research funding from CIHR,
LUNG VOLUME RECRUITMENT IN NEUROMUSCULAR DISEASE Sherri Katz, MDCM, MSc, FRCPC Pediatric Respirologist Children s Hospital of Eastern Ontario University of Ottawa Disclosures Research funding from CIHR,
Understanding Breathing Muscle Weakness
 Understanding Breathing Muscle Weakness A N D R E A L. K L E I N P R E S I D E N T / F O U N D E R B R E A T H E W I T H M D w w w.facebook.com/ b r e a t h e w i t h m d h t t p : / / w w w. b r e a t
Understanding Breathing Muscle Weakness A N D R E A L. K L E I N P R E S I D E N T / F O U N D E R B R E A T H E W I T H M D w w w.facebook.com/ b r e a t h e w i t h m d h t t p : / / w w w. b r e a t
The Addition of Mechanical Insufflation/Exsufflation Shortens Airway-Clearance Sessions in Neuromuscular Patients With Chest Infection
 The Addition of Mechanical Insufflation/Exsufflation Shortens Airway-Clearance Sessions in Neuromuscular Patients With Chest Infection Michelle Chatwin PhD and Anita K Simonds MD BACKGROUND: Mechanical
The Addition of Mechanical Insufflation/Exsufflation Shortens Airway-Clearance Sessions in Neuromuscular Patients With Chest Infection Michelle Chatwin PhD and Anita K Simonds MD BACKGROUND: Mechanical
Bringing Advanced Technology to Airway Clearance
 Bringing Advanced Technology to Airway Clearance NIPPY Clearway Sales Training - Objectives Overview of MRD specification Introduction to the device Understanding the modes Key Messaging Questions Overview
Bringing Advanced Technology to Airway Clearance NIPPY Clearway Sales Training - Objectives Overview of MRD specification Introduction to the device Understanding the modes Key Messaging Questions Overview
Efficacy of Mechanical Insufflation-Exsufflation in Extubating Unweanable Subjects With Restrictive Pulmonary Disorders
 Efficacy of Mechanical Insufflation-Exsufflation in Extubating Unweanable Subjects With Restrictive Pulmonary Disorders John R Bach MD, Diane M Sinquee MD, Louis R Saporito RRT, Amanda L Botticello PhD
Efficacy of Mechanical Insufflation-Exsufflation in Extubating Unweanable Subjects With Restrictive Pulmonary Disorders John R Bach MD, Diane M Sinquee MD, Louis R Saporito RRT, Amanda L Botticello PhD
[N] = No product variation, policy applies as stated [Y] = Standard product coverage varies from application of this policy, see below
![[N] = No product variation, policy applies as stated [Y] = Standard product coverage varies from application of this policy, see below [N] = No product variation, policy applies as stated [Y] = Standard product coverage varies from application of this policy, see below](/thumbs/94/119510114.jpg) Original Issue Date (Created): May 3, 2004 Most Recent Review Date (Revised): September 24, 2013 Effective Date: November 1, 2013 I. POLICY Mechanical insufflation-exsufflation (MI-E) may be considered
Original Issue Date (Created): May 3, 2004 Most Recent Review Date (Revised): September 24, 2013 Effective Date: November 1, 2013 I. POLICY Mechanical insufflation-exsufflation (MI-E) may be considered
Extubation of Patients With Neuromuscular Weakness
 CHEST Original Research CRITICAL CARE MEDICINE Extubation of Patients With Neuromuscular Weakness A New Management Paradigm John Robert Bach, MD ; Miguel R. Gonçalves, PT ; Irram Hamdani, MD ; and Joao
CHEST Original Research CRITICAL CARE MEDICINE Extubation of Patients With Neuromuscular Weakness A New Management Paradigm John Robert Bach, MD ; Miguel R. Gonçalves, PT ; Irram Hamdani, MD ; and Joao
Noninvasive Respiratory Management for Patients with Spinal Cord Injury and Neuromuscular Disease
 Review Article 2012 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran ISSN: 1735-0344 Tanaffos 2012; 11 (1): 7-11 TANAFFOS Noninvasive Respiratory Management for Patients with
Review Article 2012 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran ISSN: 1735-0344 Tanaffos 2012; 11 (1): 7-11 TANAFFOS Noninvasive Respiratory Management for Patients with
Jesús Sancho MD, Enric Bures MD, Saray de La Asunción RN, and Emilio Servera MD RESPIRATORY CARE AUGUST 2016 VOL 61 NO
 Effect of High-Frequency Oscillations on Cough Peak Flows Generated by Mechanical In-Exsufflation in Medically Stable Subjects With Amyotrophic Lateral Sclerosis Jesús Sancho MD, Enric Bures MD, Saray
Effect of High-Frequency Oscillations on Cough Peak Flows Generated by Mechanical In-Exsufflation in Medically Stable Subjects With Amyotrophic Lateral Sclerosis Jesús Sancho MD, Enric Bures MD, Saray
MedStar Health considers Cough Assist Devices medically necessary for the following indications:
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.047.MH Cough Assist Devices This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.047.MH Cough Assist Devices This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
MND Study Day. Martin Latham CNS Leeds Sleep Service
 MND Study Day Martin Latham CNS Leeds Sleep Service Objectives: Identifying individuals at risk. Understand issues related to NIV. Understand issues related to secretion management Improve outcomes. Identifying
MND Study Day Martin Latham CNS Leeds Sleep Service Objectives: Identifying individuals at risk. Understand issues related to NIV. Understand issues related to secretion management Improve outcomes. Identifying
Mechanical Ventilation of the Patient with Neuromuscular Disease
 Mechanical Ventilation of the Patient with Neuromuscular Disease Dean Hess PhD RRT Associate Professor of Anesthesia, Harvard Medical School Assistant Director of Respiratory Care, Massachusetts General
Mechanical Ventilation of the Patient with Neuromuscular Disease Dean Hess PhD RRT Associate Professor of Anesthesia, Harvard Medical School Assistant Director of Respiratory Care, Massachusetts General
The great majority of neuromuscular disease morbidity. Prevention of Pulmonary Morbidity for Patients With Neuromuscular Disease*
 Prevention of Pulmonary Morbidity for Patients With Neuromuscular Disease* Alice C. Tzeng, MD; and John R. Bach, MD, FCCP Study objective: To evaluate the effects of a respiratory muscle aid protocol on
Prevention of Pulmonary Morbidity for Patients With Neuromuscular Disease* Alice C. Tzeng, MD; and John R. Bach, MD, FCCP Study objective: To evaluate the effects of a respiratory muscle aid protocol on
The addition of non-invasive ventilation during exercise training in COPD patients. Enrico Clini and Michelle Chatwin
 Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
Comparison of patient spirometry and ventilator spirometry
 GE Healthcare Comparison of patient spirometry and ventilator spirometry Test results are based on the Master s thesis, Comparison between patient spirometry and ventilator spirometry by Saana Jenu, 2011
GE Healthcare Comparison of patient spirometry and ventilator spirometry Test results are based on the Master s thesis, Comparison between patient spirometry and ventilator spirometry by Saana Jenu, 2011
The Influence of Altered Pulmonarv
 The Influence of Altered Pulmonarv J Mechanics on the Adequacy of Controlled Ventilation Peter Hutchin, M.D., and Richard M. Peters, M.D. W ' hereas during spontaneous respiration the individual determines
The Influence of Altered Pulmonarv J Mechanics on the Adequacy of Controlled Ventilation Peter Hutchin, M.D., and Richard M. Peters, M.D. W ' hereas during spontaneous respiration the individual determines
The Effects of Breathing Exercise with Intermittent Positive Pressure Ventilator on Pulmonary Function in Patients with Cervical Spinal Cord Injury
 NEUROTHERAPY 6 Sang-Su Hwang, Sang-Mi 대한신경치료학회지 Chung, Kyoung-Bo 제권제Lee 호 The Effects of Breathing Exercise with Intermittent Positive Pressure Ventilator on Pulmonary Function in Patients with Cervical
NEUROTHERAPY 6 Sang-Su Hwang, Sang-Mi 대한신경치료학회지 Chung, Kyoung-Bo 제권제Lee 호 The Effects of Breathing Exercise with Intermittent Positive Pressure Ventilator on Pulmonary Function in Patients with Cervical
King s Research Portal
 King s Research Portal DOI: 10.1002/14651858.CD011833.pub2 Document Version Publisher's PDF, also known as Version of record Link to publication record in King's Research Portal Citation for published
King s Research Portal DOI: 10.1002/14651858.CD011833.pub2 Document Version Publisher's PDF, also known as Version of record Link to publication record in King's Research Portal Citation for published
GE Healthcare. Non Invasive Ventilation (NIV) For the Engström Ventilator. Relief, Relax, Recovery
 GE Healthcare Non Invasive Ventilation (NIV) For the Engström Ventilator Relief, Relax, Recovery COPD is currently the fourth leading cause of death in the world, and further increases in the prevalence
GE Healthcare Non Invasive Ventilation (NIV) For the Engström Ventilator Relief, Relax, Recovery COPD is currently the fourth leading cause of death in the world, and further increases in the prevalence
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
KENNEDY DISEASE PULMONARY CONSIDERATIONS: SCIENCE & MANAGEMENT STRATEGIES
 KENNEDY DISEASE PULMONARY CONSIDERATIONS: SCIENCE & MANAGEMENT STRATEGIES When you can t breathe nothing else matters American Lung Association Noah Lechtzin, MD; MHS Associate Professor of Medicine Johns
KENNEDY DISEASE PULMONARY CONSIDERATIONS: SCIENCE & MANAGEMENT STRATEGIES When you can t breathe nothing else matters American Lung Association Noah Lechtzin, MD; MHS Associate Professor of Medicine Johns
Mechanical Ventilation Principles and Practices
 Mechanical Ventilation Principles and Practices Dr LAU Chun Wing Arthur Department of Intensive Care Pamela Youde Nethersole Eastern Hospital 6 October 2009 In this lecture, you will learn Major concepts
Mechanical Ventilation Principles and Practices Dr LAU Chun Wing Arthur Department of Intensive Care Pamela Youde Nethersole Eastern Hospital 6 October 2009 In this lecture, you will learn Major concepts
What s New About Proning?
 1 What s New About Proning? J. Brady Scott, MSc, RRT-ACCS, AE-C, FAARC Director of Clinical Education and Assistant Professor Department of Cardiopulmonary Sciences Division of Respiratory Care Rush University
1 What s New About Proning? J. Brady Scott, MSc, RRT-ACCS, AE-C, FAARC Director of Clinical Education and Assistant Professor Department of Cardiopulmonary Sciences Division of Respiratory Care Rush University
Adapting to the Worsening of the LTMV Patient
 14 èmes Journées Internationales de Ventilation à Domicile LYON, 26-28 mars 2015 Adapting to the Worsening of the LTMV Patient Andrea Vianello Fisiopatologia e Terapia Intensiva Respiratoria Ospedale-Università
14 èmes Journées Internationales de Ventilation à Domicile LYON, 26-28 mars 2015 Adapting to the Worsening of the LTMV Patient Andrea Vianello Fisiopatologia e Terapia Intensiva Respiratoria Ospedale-Università
Delay Between Actuation and Shaking of a Hydrofluoroalkane Fluticasone Pressurized Metered-Dose Inhaler
 Delay Between Actuation and Shaking of a Hydrofluoroalkane Fluticasone Pressurized Metered-Dose Inhaler Ariel Berlinski MD, Dirk von Hollen, John N Pritchard PhD, and Ross HM Hatley PhD BACKGROUND: Inhaled
Delay Between Actuation and Shaking of a Hydrofluoroalkane Fluticasone Pressurized Metered-Dose Inhaler Ariel Berlinski MD, Dirk von Hollen, John N Pritchard PhD, and Ross HM Hatley PhD BACKGROUND: Inhaled
Airway clearance in neuromuscular weakness
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY REVIEW Airway clearance in neuromuscular weakness LEANNE MAREE GAULD MBBS FRACP MD Royal Children's Hospital, Herston, Australia. Correspondence to Dr Leanne Maree
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY REVIEW Airway clearance in neuromuscular weakness LEANNE MAREE GAULD MBBS FRACP MD Royal Children's Hospital, Herston, Australia. Correspondence to Dr Leanne Maree
Hyperinflation Therapy and the Tools to Accomplish It!! Bill Barnes, RN, RRT Good Shepherd Rehabilitation Network
 Hyperinflation Therapy and the Tools to Accomplish It!! Bill Barnes, RN, RRT Good Shepherd Rehabilitation Network HYPERINFLATION THERAPY Challenges in Post Acute Care Deconditioning Malnutrition Hydration
Hyperinflation Therapy and the Tools to Accomplish It!! Bill Barnes, RN, RRT Good Shepherd Rehabilitation Network HYPERINFLATION THERAPY Challenges in Post Acute Care Deconditioning Malnutrition Hydration
WHAT DO YOU WANT FROM A HOME VENTILATION SYSTEM? 8322_RS_HomeNIV_brochure_v14.ind1 1 4/7/06 12:57:35
 WHAT DO YOU WANT FROM A HOME VENTILATION SYSTEM? 8322_RS_HomeNIV_brochure_v14.ind1 1 4/7/06 12:57:35 D I L E M M A DIFFERENT VENTILATORS DIFFERENT ALGORITHMS TO KNOW YOU VE CHANGED PATIENT LIVES?PATIENT??
WHAT DO YOU WANT FROM A HOME VENTILATION SYSTEM? 8322_RS_HomeNIV_brochure_v14.ind1 1 4/7/06 12:57:35 D I L E M M A DIFFERENT VENTILATORS DIFFERENT ALGORITHMS TO KNOW YOU VE CHANGED PATIENT LIVES?PATIENT??
Ventilator Waveforms: Interpretation
 Ventilator Waveforms: Interpretation Albert L. Rafanan, MD, FPCCP Pulmonary, Critical Care and Sleep Medicine Chong Hua Hospital, Cebu City Types of Waveforms Scalars are waveform representations of pressure,
Ventilator Waveforms: Interpretation Albert L. Rafanan, MD, FPCCP Pulmonary, Critical Care and Sleep Medicine Chong Hua Hospital, Cebu City Types of Waveforms Scalars are waveform representations of pressure,
Alma Mater University of Bologna. Respiratory and Critical Care Sant Orsola Hospital, Bologna, Italy
 Alma Mater University of Bologna Respiratory and Critical Care Sant Orsola Hospital, Bologna, Italy Conflict of Interest I have affiliations with, special interests, or have conducted business with the
Alma Mater University of Bologna Respiratory and Critical Care Sant Orsola Hospital, Bologna, Italy Conflict of Interest I have affiliations with, special interests, or have conducted business with the
Cough Augmentation in Subjects With Duchenne Muscular Dystrophy: Comparison of Air Stacking via a Resuscitator Bag Versus Mechanical Ventilation
 Cough Augmentation in Subjects With Duchenne Muscular Dystrophy: Comparison of Air Stacking via a Resuscitator Bag Versus Mechanical Ventilation Michel Toussaint PhD, Kurt Pernet MPhysio, Marc Steens MPhysio,
Cough Augmentation in Subjects With Duchenne Muscular Dystrophy: Comparison of Air Stacking via a Resuscitator Bag Versus Mechanical Ventilation Michel Toussaint PhD, Kurt Pernet MPhysio, Marc Steens MPhysio,
Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo
 Instant dowload and all chapters Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo https://testbanklab.com/download/test-bank-pilbeams-mechanical-ventilation-physiologicalclinical-applications-6th-edition-cairo/
Instant dowload and all chapters Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo https://testbanklab.com/download/test-bank-pilbeams-mechanical-ventilation-physiologicalclinical-applications-6th-edition-cairo/
Cough assist T70 for the Tracheostomy Child
 Patient and Family Education Cough assist 70 for the racheostomy Child with or without a ventilator What is a Cough assist device? he Cough assist 70 device removes mucus (secretions) from your child s
Patient and Family Education Cough assist 70 for the racheostomy Child with or without a ventilator What is a Cough assist device? he Cough assist 70 device removes mucus (secretions) from your child s
Problem-solving Respiratory Issues in Children With Neuromuscular Disease. December 13, 2018 Eliezer Be eri, M.D.
 Problem-solving Respiratory Issues in Children With Neuromuscular Disease December 13, 2018 Eliezer Be eri, M.D. About Our Presenter Eliezer Be eri, M.D. Alyn Rehabilitation Hospital Jerusalem, Israel
Problem-solving Respiratory Issues in Children With Neuromuscular Disease December 13, 2018 Eliezer Be eri, M.D. About Our Presenter Eliezer Be eri, M.D. Alyn Rehabilitation Hospital Jerusalem, Israel
Evaluation of Endotracheal Tube Scraping on Airway Resistance
 Evaluation of Endotracheal Tube Scraping on Airway Resistance J Brady Scott MSc RRT-ACCS AE-C FAARC, Meagan N Dubosky MSc RRT-ACCS RRT-NPS AE-C, David L Vines, MHS RRT FAARC, Adewunmi S Sulaiman MSc RRT,
Evaluation of Endotracheal Tube Scraping on Airway Resistance J Brady Scott MSc RRT-ACCS AE-C FAARC, Meagan N Dubosky MSc RRT-ACCS RRT-NPS AE-C, David L Vines, MHS RRT FAARC, Adewunmi S Sulaiman MSc RRT,
Limits of Effective Cough-Augmentation Techniques in Patients With Neuromuscular Disease
 Limits of Effective Cough-Augmentation Techniques in Patients With Neuromuscular Disease Michel Toussaint PT PhD, Louis J Boitano MSc RRT, Vincent Gathot MSc PT, Marc Steens MSc PT, and Philippe Soudon
Limits of Effective Cough-Augmentation Techniques in Patients With Neuromuscular Disease Michel Toussaint PT PhD, Louis J Boitano MSc RRT, Vincent Gathot MSc PT, Marc Steens MSc PT, and Philippe Soudon
Use of Mechanical Insufflation-Exsufflation Devices for Airway Clearance in Subjects With Neuromuscular Disease
 Use of Mechanical Insufflation-Exsufflation Devices for Airway Clearance in Subjects With Neuromuscular Disease Catherine Auger MSc, Vanessa Hernando PharmD PhD, and Hubert Galmiche PharmD Introduction
Use of Mechanical Insufflation-Exsufflation Devices for Airway Clearance in Subjects With Neuromuscular Disease Catherine Auger MSc, Vanessa Hernando PharmD PhD, and Hubert Galmiche PharmD Introduction
Evaluation of a Nasal Cannula in Noninvasive Ventilation Using a Lung Simulator
 Evaluation of a Nasal in Noninvasive Ventilation Using a Lung Simulator Narayan P Iyer MD and Robert Chatburn MHHS RRT-NPS FAARC BACKGROUND: Nasal noninvasive ventilation (NIV) is a common form of noninvasive
Evaluation of a Nasal in Noninvasive Ventilation Using a Lung Simulator Narayan P Iyer MD and Robert Chatburn MHHS RRT-NPS FAARC BACKGROUND: Nasal noninvasive ventilation (NIV) is a common form of noninvasive
AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL
 AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL A. Definition of Therapy: 1. Cough machine: 4 sets of 5 breaths with a goal of I:E pressures approximately the same of 30-40. Inhale time = 1 second, exhale
AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL A. Definition of Therapy: 1. Cough machine: 4 sets of 5 breaths with a goal of I:E pressures approximately the same of 30-40. Inhale time = 1 second, exhale
Cough Assist. Information for patients, families and carers Therapy Services
 Cough Assist Information for patients, families and carers Therapy Services PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 16 Table of contents Why do I need a Cough
Cough Assist Information for patients, families and carers Therapy Services PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 16 Table of contents Why do I need a Cough
Is mechanical insufflation exsufflation (M-IE) useful in children with neuromuscular disease?
 Is mechanical insufflation exsufflation (M-IE) useful in children with neuromuscular disease? Cross Canada Rounds ProCon debate January 2017 Dr K Keown Respiratory Fellow BC Children s Hospital Structure
Is mechanical insufflation exsufflation (M-IE) useful in children with neuromuscular disease? Cross Canada Rounds ProCon debate January 2017 Dr K Keown Respiratory Fellow BC Children s Hospital Structure
Use of Cough Peak Flow Measured by a Ventilator to Predict Re-Intubation When a Spirometer Is Unavailable
 Use of Cough Peak Flow Measured by a Ventilator to Predict Re-Intubation When a Spirometer Is Unavailable Linfu Bai MD and Jun Duan MD BACKGROUND: A ventilator includes the function to measure flow velocity.
Use of Cough Peak Flow Measured by a Ventilator to Predict Re-Intubation When a Spirometer Is Unavailable Linfu Bai MD and Jun Duan MD BACKGROUND: A ventilator includes the function to measure flow velocity.
Mouthpiece ventilation and complementary techniques in patients with neuromuscular disease: A brief clinical review and update
 Review Article Mouthpiece ventilation and complementary techniques in patients with neuromuscular disease: A brief clinical review and update Chronic Respiratory Disease 2016, Vol. 14(2) 1 7 ª The Author(s)
Review Article Mouthpiece ventilation and complementary techniques in patients with neuromuscular disease: A brief clinical review and update Chronic Respiratory Disease 2016, Vol. 14(2) 1 7 ª The Author(s)
The intelligent solution. System One Sleep Therapy System uses advanced intelligence to deliver excellent care while making patient management easy
 The intelligent solution System One Sleep Therapy System uses advanced intelligence to deliver excellent care while making patient management easy Proven efficacy The System One REMstar Auto algorithm
The intelligent solution System One Sleep Therapy System uses advanced intelligence to deliver excellent care while making patient management easy Proven efficacy The System One REMstar Auto algorithm
Difficult weaning from mechanical ventilation
 Difficult weaning from mechanical ventilation Paolo Biban, MD Director, Neonatal and Paediatric Intensive Care Unit Division of Paediatrics, Major City Hospital Azienda Ospedaliera Universitaria Integrata
Difficult weaning from mechanical ventilation Paolo Biban, MD Director, Neonatal and Paediatric Intensive Care Unit Division of Paediatrics, Major City Hospital Azienda Ospedaliera Universitaria Integrata
7 Initial Ventilator Settings, ~05
 Abbreviations (inside front cover and back cover) PART 1 Basic Concepts and Core Knowledge in Mechanical -- -- -- -- 1 Oxygenation and Acid-Base Evaluation, 1 Review 01Arterial Blood Gases, 2 Evaluating
Abbreviations (inside front cover and back cover) PART 1 Basic Concepts and Core Knowledge in Mechanical -- -- -- -- 1 Oxygenation and Acid-Base Evaluation, 1 Review 01Arterial Blood Gases, 2 Evaluating
Journal Club American Journal of Respiratory and Critical Care Medicine. Zhang Junyi
 Journal Club 2018 American Journal of Respiratory and Critical Care Medicine Zhang Junyi 2018.11.23 Background Mechanical Ventilation A life-saving technique used worldwide 15 million patients annually
Journal Club 2018 American Journal of Respiratory and Critical Care Medicine Zhang Junyi 2018.11.23 Background Mechanical Ventilation A life-saving technique used worldwide 15 million patients annually
Benefit of Forced Expiratory Technique for Weak Cough in a Patient with Bulbar Onset Amyotrophic Lateral Sclerosis
 Original Article Benefit of Forced Expiratory Technique for Weak Cough in a Patient with Bulbar Onset Amyotrophic Lateral Sclerosis J. Phys. Ther. Sci. 16: 137 141, 2004 MITSUAKI ISHII, RPT 1) 1) Department
Original Article Benefit of Forced Expiratory Technique for Weak Cough in a Patient with Bulbar Onset Amyotrophic Lateral Sclerosis J. Phys. Ther. Sci. 16: 137 141, 2004 MITSUAKI ISHII, RPT 1) 1) Department
Duchenne Muscular Dystrophy
 Authors: Elia Gomez-Merino, MD John R. Bach, MD Affiliations: From the Department of Pulmonary Medicine, Hospital Clinico Universitario de San Juan, San Juan de Alicante, Spain (EGM), and the Department
Authors: Elia Gomez-Merino, MD John R. Bach, MD Affiliations: From the Department of Pulmonary Medicine, Hospital Clinico Universitario de San Juan, San Juan de Alicante, Spain (EGM), and the Department
Ron Hosp, MS-HSA, RRT Regional Respiratory Specialist. This program has been approved for 1 hour of continuing education credit.
 Ron Hosp, MS-HSA, RRT Regional Respiratory Specialist This program has been approved for 1 hour of continuing education credit. Course Objectives Identify at least four goals of home NIV Identify candidates
Ron Hosp, MS-HSA, RRT Regional Respiratory Specialist This program has been approved for 1 hour of continuing education credit. Course Objectives Identify at least four goals of home NIV Identify candidates
Oxygen Therapy. 7. Partial Initiation of therapy
 Oxygen Therapy 1. Nasal Initiation of therapy Cannula 2. Alteration of therapy 3. Change of equipment 4. Simple Mask Initiation of therapy 5. Alteration of therapy 6. Change of equipment 7. Partial Initiation
Oxygen Therapy 1. Nasal Initiation of therapy Cannula 2. Alteration of therapy 3. Change of equipment 4. Simple Mask Initiation of therapy 5. Alteration of therapy 6. Change of equipment 7. Partial Initiation
Invest to Save: Jackie Baillie MSP (Chair, Cross Party Group on Muscular Dystrophy) Eileen McCallum
 Invest to Save: Invest to Save: I am pleased to welcome this briefing, which puts forward the case for investing in preventative services for people with neuromuscular conditions in Scotland. I pay tribute
Invest to Save: Invest to Save: I am pleased to welcome this briefing, which puts forward the case for investing in preventative services for people with neuromuscular conditions in Scotland. I pay tribute
Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor
 Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
An ideal ventilator for neuromuscular patients. F. Lofaso, Raymond Poincaré Hospital Inserm U 1179
 An ideal ventilator for neuromuscular patients F. Lofaso, Raymond Poincaré Hospital Inserm U 1179 Neuromuscular diseasescausing progressive respiratoryfailure Cerebral diseases: strokes, tumors. Brainstem:primaryhypoventilation,
An ideal ventilator for neuromuscular patients F. Lofaso, Raymond Poincaré Hospital Inserm U 1179 Neuromuscular diseasescausing progressive respiratoryfailure Cerebral diseases: strokes, tumors. Brainstem:primaryhypoventilation,
Airway pressure release ventilation (APRV) in PICU: Current evidence. Chor Yek Kee Sarawak General Hospital
 Airway pressure release ventilation (APRV) in PICU: Current evidence Chor Yek Kee Sarawak General Hospital Outline Brief introduction of APRV History of APRV Common confusion in APRV Features of APRV and
Airway pressure release ventilation (APRV) in PICU: Current evidence Chor Yek Kee Sarawak General Hospital Outline Brief introduction of APRV History of APRV Common confusion in APRV Features of APRV and
Evaluation of a systematic approach to weaning of tracheotomized neurological patients: an early interrupted randomized controlled trial
 DOI 10.1186/s13613-015-0098-0 RESEARCH Open Access Evaluation of a systematic approach to weaning of tracheotomized neurological patients: an early interrupted randomized controlled trial Rosanna Vaschetto
DOI 10.1186/s13613-015-0098-0 RESEARCH Open Access Evaluation of a systematic approach to weaning of tracheotomized neurological patients: an early interrupted randomized controlled trial Rosanna Vaschetto
Proportional Assist Ventilation (PAV) (NAVA) Younes ARRD 1992;145:114. Ventilator output :Triggering, Cycling Control of flow, rise time and pressure
 Conflict of Interest Disclosure Robert M Kacmarek Unconventional Techniques Using Your ICU Ventilator!" 5-5-17 FOCUS Bob Kacmarek PhD, RRT Massachusetts General Hospital, Harvard Medical School, Boston,
Conflict of Interest Disclosure Robert M Kacmarek Unconventional Techniques Using Your ICU Ventilator!" 5-5-17 FOCUS Bob Kacmarek PhD, RRT Massachusetts General Hospital, Harvard Medical School, Boston,
Cough Augmentation Techniques in the Critically Ill: A Canadian National Survey
 Cough Augmentation Techniques in the Critically Ill: A Canadian National Survey Louise Rose RN PhD, Neill K Adhikari MDCM MSc, Joseph Poon, David Leasa MD FRCPC, and Douglas A McKim MD FRCPC DABSM; on
Cough Augmentation Techniques in the Critically Ill: A Canadian National Survey Louise Rose RN PhD, Neill K Adhikari MDCM MSc, Joseph Poon, David Leasa MD FRCPC, and Douglas A McKim MD FRCPC DABSM; on
Pulmonary Rehabilitation in Acute Spinal Cord Injury. Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university
 Pulmonary Rehabilitation in Acute Spinal Cord Injury Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university Causes of spinal cord injury Traumatic injury Motor vehicle
Pulmonary Rehabilitation in Acute Spinal Cord Injury Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university Causes of spinal cord injury Traumatic injury Motor vehicle
Titration protocol reference guide
 PN 1079754_Cover:22037_Cov_Canada 11/22/10 Philips Healthcare is part of Royal Philips Electronics How to reach us www.philips.com/healthcare healthcare@philips.com Asia +49 7031 463 2254 Europe, Middle
PN 1079754_Cover:22037_Cov_Canada 11/22/10 Philips Healthcare is part of Royal Philips Electronics How to reach us www.philips.com/healthcare healthcare@philips.com Asia +49 7031 463 2254 Europe, Middle
High-Frequency Chest Wall Compression Therapy in Neurologically Impaired Children
 High-Frequency Chest Wall Compression Therapy in Neurologically Impaired Children Kathryn Fitzgerald MSN CPNP, Jessica Dugre MSN, Sobhan Pagala, Peter Homel PhD, Michael Marcus MD, and Mikhail Kazachkov
High-Frequency Chest Wall Compression Therapy in Neurologically Impaired Children Kathryn Fitzgerald MSN CPNP, Jessica Dugre MSN, Sobhan Pagala, Peter Homel PhD, Michael Marcus MD, and Mikhail Kazachkov
Landmark articles on ventilation
 Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Landmark articles on ventilation Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity ARDS AECC DEFINITION-1994 ALI Acute onset Bilateral chest infiltrates PCWP
Airway Clearance Devices
 Print Page 1 of 11 Wisconsin.gov home state agencies subject directory department of health services Search Welcome» August 2, 2018 5:18 PM Program Name: BadgerCare Plus and Medicaid Handbook Area: Durable
Print Page 1 of 11 Wisconsin.gov home state agencies subject directory department of health services Search Welcome» August 2, 2018 5:18 PM Program Name: BadgerCare Plus and Medicaid Handbook Area: Durable
Evaluation of Functional Characteristics of 4 Oscillatory Positive Pressure Devices in a Simulated Cystic Fibrosis Model
 Evaluation of Functional Characteristics of 4 Oscillatory Positive Pressure Devices in a Simulated Cystic Fibrosis Model Hillary Van Fleet MSc RRT, Diane K Dunn RRT-NPS, Neil L McNinch MSc RN, and Teresa
Evaluation of Functional Characteristics of 4 Oscillatory Positive Pressure Devices in a Simulated Cystic Fibrosis Model Hillary Van Fleet MSc RRT, Diane K Dunn RRT-NPS, Neil L McNinch MSc RN, and Teresa
FAILURE OF NONINVASIVE VENTILATION FOR DE NOVO ACUTE HYPOXEMIC RESPIRATORY FAILURE: ROLE OF TIDAL VOLUME
 FAILURE OF NONINVASIVE VENTILATION FOR DE NOVO ACUTE HYPOXEMIC RESPIRATORY FAILURE: ROLE OF TIDAL VOLUME Guillaume CARTEAUX, Teresa MILLÁN-GUILARTE, Nicolas DE PROST, Keyvan RAZAZI, Shariq ABID, Arnaud
FAILURE OF NONINVASIVE VENTILATION FOR DE NOVO ACUTE HYPOXEMIC RESPIRATORY FAILURE: ROLE OF TIDAL VOLUME Guillaume CARTEAUX, Teresa MILLÁN-GUILARTE, Nicolas DE PROST, Keyvan RAZAZI, Shariq ABID, Arnaud
Predicting Extubation Outcome by Cough Peak Flow Measured Using a Built-in Ventilator Flow Meter
 Predicting Extubation Outcome by Cough Peak Flow Measured Using a Built-in Ventilator Flow Meter Florent Gobert MD, Hodane Yonis MD, Romain Tapponnier MD, Raul Fernandez, Marie-Aude Labaune, Jean-François
Predicting Extubation Outcome by Cough Peak Flow Measured Using a Built-in Ventilator Flow Meter Florent Gobert MD, Hodane Yonis MD, Romain Tapponnier MD, Raul Fernandez, Marie-Aude Labaune, Jean-François
Small Volume Nebulizer Treatment (Hand-Held)
 Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Neuromuscular diseases are characterized by progressive
 Maximum Insufflation Capacity* Seong-Woong Kang, MD, PhD; and John R. Bach, MD, FCCP Objective: To investigate the effect of deep lung insufflations on maximum insufflation capacities (MICs) and peak cough
Maximum Insufflation Capacity* Seong-Woong Kang, MD, PhD; and John R. Bach, MD, FCCP Objective: To investigate the effect of deep lung insufflations on maximum insufflation capacities (MICs) and peak cough
The more you know, the more you can do
 The more you know, the more you can do How Duchenne muscular dystrophy affects lung function As life expectancy of patients with Duchenne muscular dystrophy (DMD) has increased over the past few decades,
The more you know, the more you can do How Duchenne muscular dystrophy affects lung function As life expectancy of patients with Duchenne muscular dystrophy (DMD) has increased over the past few decades,
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Motor neurone disease: the use of non-invasive ventilation in the management of motor neurone disease 1.1 Short title Motor
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Motor neurone disease: the use of non-invasive ventilation in the management of motor neurone disease 1.1 Short title Motor
Comparison of automated and static pulse respiratory mechanics during supported ventilation
 Comparison of automated and static pulse respiratory mechanics during supported ventilation Alpesh R Patel, Susan Taylor and Andrew D Bersten Respiratory system compliance ( ) and inspiratory resistance
Comparison of automated and static pulse respiratory mechanics during supported ventilation Alpesh R Patel, Susan Taylor and Andrew D Bersten Respiratory system compliance ( ) and inspiratory resistance
Cardiorespiratory Physiotherapy Tutoring Services 2017
 VENTILATOR HYPERINFLATION ***This document is intended to be used as an information resource only it is not intended to be used as a policy document/practice guideline. Before incorporating the use of
VENTILATOR HYPERINFLATION ***This document is intended to be used as an information resource only it is not intended to be used as a policy document/practice guideline. Before incorporating the use of
Disclaimer. Objectives. I can t cough it up! Airway Clearance Therapy. Heather Murgatroyd, RRT, RPSGT Field Clinical Specialist
 I can t cough it up! Airway Clearance Therapy Heather Murgatroyd, RRT, RPSGT Field Clinical Specialist 1 Disclaimer Name of presenter: Heather Murgatroyd, BA, RRT, RPSGT Name of employer: RespirTech I
I can t cough it up! Airway Clearance Therapy Heather Murgatroyd, RRT, RPSGT Field Clinical Specialist 1 Disclaimer Name of presenter: Heather Murgatroyd, BA, RRT, RPSGT Name of employer: RespirTech I
Hot Topics in Noninvasive Ventilation: Report of a Working Group at the International Symposium on Sleep-Disordered Breathing in Leuven, Belgium
 Hot Topics in Noninvasive Ventilation: Report of a Working Group at the International Symposium on Sleep-Disordered Breathing in Leuven, Belgium Bart Vrijsen PT MSc, Michelle Chatwin PT PhD, Oliver Contal
Hot Topics in Noninvasive Ventilation: Report of a Working Group at the International Symposium on Sleep-Disordered Breathing in Leuven, Belgium Bart Vrijsen PT MSc, Michelle Chatwin PT PhD, Oliver Contal
Interfacility Protocol Protocol Title:
 Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
Supplementary Online Content 2
 Supplementary Online Content 2 van Meenen DMP, van der Hoeven SM, Binnekade JM, et al. Effect of on demand vs routine nebulization of acetylcysteine with salbutamol on ventilator-free days in intensive
Supplementary Online Content 2 van Meenen DMP, van der Hoeven SM, Binnekade JM, et al. Effect of on demand vs routine nebulization of acetylcysteine with salbutamol on ventilator-free days in intensive
Airway Clearance Applications in the Elderly and in Patients With Neurologic or Neuromuscular Compromise
 Airway Clearance Applications in the Elderly and in Patients With Neurologic or Neuromuscular Compromise Carl F Haas MLS RRT FAARC, Paul S Loik RRT, and Steven E Gay MD MSc Introduction The Normal Clearance
Airway Clearance Applications in the Elderly and in Patients With Neurologic or Neuromuscular Compromise Carl F Haas MLS RRT FAARC, Paul S Loik RRT, and Steven E Gay MD MSc Introduction The Normal Clearance
Weaning from Mechanical Ventilation. Dr Azmin Huda Abdul Rahim
 Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
