Extubation of Patients With Neuromuscular Weakness
|
|
|
- Alexis Hopkins
- 6 years ago
- Views:
Transcription
1 CHEST Original Research CRITICAL CARE MEDICINE Extubation of Patients With Neuromuscular Weakness A New Management Paradigm John Robert Bach, MD ; Miguel R. Gonçalves, PT ; Irram Hamdani, MD ; and Joao Carlos Winck, MD, PhD Background: Successful extubation conventionally necessitates the passing of spontaneous breathing trials (SBTs) and ventilator weaning parameters. We report successful extubation of patients with neuromuscular disease (NMD) and weakness who could not pass them. Methods: NMD-specific extubation criteria and a new extubation protocol were developed. Data were collected on 157 consecutive unweanable patients, including 83 transferred from other hospitals who refused tracheostomies. They could not pass the SBTs before or after extubation. Once the pulse oxyhemoglobin saturation (Sp o 2 ) was maintained at 95% in ambient air, patients were extubated to full noninvasive mechanical ventilation (NIV) support and aggressive mechanically assisted coughing (MAC). Rather than oxygen, NIV and MAC were used to maintain or return the Sp o 2 to 95%. Extubation success was defined as not requiring reintubation during the hospitalization and was considered as a function of diagnosis, preintubation NIV experience, and vital capacity and assisted cough peak flows (CPF) at extubation. Results: Before hospitalization 96 (61%) patients had no experience with NIV, 41 (26%) used it, 24 h per day, and 20 (13%) were continuously NIV dependent. The first-attempt protocol extubation success rate was 95% (149 patients). All 98 extubation attempts on patients with assisted CPF 160 L/m were successful. The dependence on continuous NIV and the duration of dependence prior to intubation correlated with extubation success ( P,.005). Six of eight patients who initially failed extubation succeeded on subsequent attempts, so only two with no measurable assisted CPF underwent tracheotomy. Conclusions: Continuous volume-cycled NIV via oral interfaces and masks and MAC with oximetry feedback in ambient air can permit safe extubation of unweanable patients with NMD. CHEST 2010; 137(5): Abbreviations: ALS 5 amyotrophic lateral sclerosis; CCM 5 critical care myopathy; CPF 5 cough peak flows; IPPV 5 intermittent positive pressure ventilation; MAC 5 mechanically assisted coughing; NIV 5 noninvasive mechanical ventilation; NMD 5 neuromuscular disease; PAP 5 positive airway pressure; SBT 5 spontaneous breathing trial; SMA 1 5 spinal muscular atrophy type 1; Spo 2 5 pulse oxyhemoglobin saturation; VC 5 vital capacity Conventional extubation attempts follow successful spontaneous breathing trials (SBTs) and the passing of ventilator weaning parameters, 1 otherwise patients undergo tracheotomy. Patients are often extubated to supplemental oxygen and bilevel positive airway pressure (PAP), but settings are infrequently reported,2 and extubation studies report very few if any patients with neuromuscular disease (NMD) (eg, 18 of 162, 3 17 of ) and completely exclude unweanable patients. 5-7 Patients with preexisting NMD make up only 4% to 12.5% of cases in critical care, 8-10 but about 25% in weaning centers. 11 While acquired critical care myopathy (CCM) is common, it is an often unrecognized 12,13 cause of extubation failure by conventional approaches There are no guidelines for extubating unweanable patients with NMD and CCM. Many are dependent on noninvasive mechanical ventilation (NIV) with no autonomous breathing ability for years before being intubated, and they refuse tracheotomy Further, these patients can have ineffective cough peak flows (CPFs), which can result in extubation failure due to airway secretion accumulation, but very few studies CHEST / 137 / 5 / MAY,
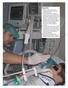
2 have reported CPF 2,21 and none systematically used mechanically assisted coughing (mechanical insufflationexsufflation with exsufflation-timed abdominal thrust) (MAC). 4,24 There are no ventilator weaning parameters that address the ability to expel secretions. With success in decannulating unweanable patients with traumatic tetraplegia and others to continuous MAC and NIV, which includes noninvasive intermittent positive pressure ventilation (IPPV) and high-span bilevel PAP, 20,25-27 we used similar criteria to extubate unweanable patients with NMD and CCM and report the success rates. Materials and Methods The data were gathered in two centers, with 113 patients in New Jersey and 44 in Portugal, using the inclusion criteria described in Table 1. The study was approved by the institutions review boards. All intubated patients were treated conventionally except for the use of MAC via the tube. Although virtually unknown in critical care, MAC has been instrumental in avoiding pneumonia, respiratory failure, and hospitalizations for NIVdependent patients with NMD Vital capacities (VCs) (Wright Mark 3 spirometer; Ferraris Ltd; London, England) and unassisted and assisted CPFs (Access Peak Flowmeter; Health Scan Products Inc.; Cedar Grove, NJ) were measured within 12 months before intubation for the local patients (group 1). The other 83 intubated patients were transferred intubated from other hospitals after one to four failed extubation attempts (group 2) or after failing multiple SBTs (group 3). VC was measured via the tube with the cuff inflated following clearing of the airways by MAC just prior to extubation. Patients were ready for extubation and inclusion in this study only when all Table 1 criteria were satisfied and SBTs failed, as described Patients had to experience immediate distress, precipitous oxyhemoglobin desaturation, and hypercapnia without stabilization before return to full ventilatory support both before and immediately postextubation. Local patients were considered to be group 1 because their greater experience with NIV and MAC could have affected outcomes. All transferred patients had been told that extubation and survival were not possible without tracheotomy. We reported that the risk for extubation failure is high when assisted CPF cannot attain 160 L/m. 22 Considering that patients with advanced averbal bulbar amyotrophic lateral sclerosis (ALS) can rarely attain a CPF of 160 L/m 34,35 we generally did not accept such patients for transfer (exclusion criteria). Local patients with Manuscript received September 11, 2009; revision accepted November 29, Affiliations: From the Department of Physical Medicine and Rehabilitation (Dr Bach ) and the Department of Medicine (Dr Hamdani), University of Medicine and Dentistry of New Jersey the New Jersey Medical School, Newark, NJ; and the Lung Function and Ventilation Unit, Pulmonary Medicine Department, Intensive Care and Emergency Department (Mr Gonçalves ), and the Pulmonary Medicine Department (Dr Winck), Faculty of Medicine University, Hospital of S. João, Porto, Portugal. Correspondence to: John R. Bach, MD, Department of Physical Medicine and Rehabilitation, University Hospital B-403, 150 Bergen St, Newark, NJ 07103; bachjr@umdnj.edu. Reproduction of this article is prohibited without written permission from the American College of Chest Physicians ( site/misc/reprints.xhtml ). DOI: /chest a CPF, 160 L/m were offered extubation if acknowledging that three extubation failures would necessitate tracheotomy. Other, at least temporary, exclusion criteria were medical instability, inadequate cooperation, and imminent surgery. 20,35 Protocol Table 1 Extubation Criteria for Unweanable Ventilator-Dependent Patients Afebrile and normal WBC count Aged 4 y and older No ventilator-free breathing tolerance with 7-cm pressure support in ambient air on the basis of NMD or CCM VC, 20% of normal Pa co 2 40 mm Hg at peak inspiratory pressures, 35 cm H 2 O on full-setting assist/control mode at a rate of 10-13/min Sp o 2 95% for 12 h or more in ambient air All oxyhemoglobin desaturations, 95% reversed by MAC and suctioning via translaryngeal tube Fully alert and cooperative, receiving no sedative medications Chest radiograph abnormalities cleared or clearing Air leakage via upper airway sufficient for vocalization upon cuff deflation CCM 5 critical care myopathy; MAC 5 mechanically assisted coughing; NMD 5 neuromuscular disease; Spo 2 5 pulse oxyhemoglobin saturation; VC 5 vital capacity. While intubated, sufficient ventilatory support was used to maintain normocapnia and normal respiratory rates. MAC (CoughAssist; Respironics, Inc.; Murrysville, PA) was used at 40 to 2 40 cm H 2 O or greater to rapidly achieve clinically full chest expansion to clinically complete emptying of the lungs, with exsufflation-timed abdominal thrusts. The MAC sessions were up to every 20 min to maintain or return the pulse oxyhemoglobin saturation ( S p o 2 ) to 95% in ambient air. Tracheotomy would have been recommended if the Table 1 criteria could not be met within 2 weeks of transfer. Once the Table 1 criteria were met, the orogastric or nasogastric tube was removed to facilitate postextubation nasal NIV. The patient was then extubated directly to NIV on assist/control of 800 to 1,500 ml, at a rate of 10 to 14 min in ambient air. Pressure control of at least 18 cm H 2 O was used if abdominal distension developed. The NIV was provided via a combination of nasal, oronasal, and mouthpiece interfaces. 36 Assisted CPF and CPF obtained by abdominal thrust following air stacking were measured within 3 h as the patient received full volume-cycled NIV support. Patients kept 15-mm angled mouthpieces accessible ( Fig 1 ), and weaned themselves, when possible, by taking fewer and fewer IPPVs as tolerated. Diurnal nasal IPPV was used for those who could not secure the mouthpiece. Patients took as much of the delivered volumes as desired. They used nasal or oronasal interfaces ( Figs 2, 3 ) for nighttime ventilation. For episodes of Sp o 2, 95%, ventilator positive inspiratory pressure, interface or tubing air leakage, CO 2 retention, ventilator settings, and MAC were considered. Patients were taught to maximally expand their lungs by air stacking (retaining consecutive) ventilator delivered volumes to the largest volume the glottis could hold. 37 Once the lunges were air stacked, an abdominal thrust was provided to manually assist the cough, 29,37 and these assisted CPFs were measured. For patients using pressure-cycling, air stacking volumes were provided by manual resuscitator. The therapists, nurses, and in particular, the family and personal care attendants provided MAC via oronasal interfaces up to every 20 min until the Sp o 2 no longer dipped below 95% and the patients felt clear of secretions. In seven cases, the postextubation oral intake was considered unsafe, so open 1034 Original Research
3 in means were compared using the Wilcoxon rank test. A P value.05 was considered significant. Univariate comparisons of potential predictive factors for failure or success were run with the Fisher exact test for categorical variables and the Wilcoxon rank-sums test for continuous variables. Results Figure 1. A 10-year-old girl with neurofibromatosis status postspinal cord tumor resection, extubated with a vital capacity (VC) of 180 ml and no ventilator-free breathing ability, using a 15-mm angled mouthpiece (Malincrodt-Puritan-Bennett; Pleasanton, CA) for ventilatory support. Current VC 380 ml and minimal ventilatorfree breathing ability. The patient provided written consent for the use of this photograph. modified Stamm gastrostomies were performed under local anesthesia using NIV, as in Figure 2, without complication. 38 Extubation was considered successful if the patient was discharged without reintubation. When reintubation was necessary, the patient was again extubated after achieving the Table 1 criteria. Multiple failures necessitated tracheotomy. Extubation success was considered as a function of diagnosis, patient group, VC, CPF, and preintubation NIV experience. VC was measured 3 to 6 months after extubation. The total days intubated were compared pretransfer and posttransfer. Statistical Analysis Results are expressed as mean 6 SD. Statistical analyses were carried out using SPSS 12.0 (SPSS, Inc.; Chicago, IL). Differences Figure 2. A 20-year-old man with Duchenne muscular dystrophy transferred for extubation after failing three extubations over a 26-day period. He used a 15-mm angled mouthpiece, as in Figure 1, for daytime ventilatory support and a lip-seal phalange with nasal prongs for nocturnal ventilatory support. His VC was 260 ml at extubation in October 2007 and 720 ml in July See Figure 1 legend for expansion of the abbreviation. The patient provided written consent for the use of this photograph. The 157 patients, mean age years, included 139 (89%) with NMD who were intubated for acute respiratory failure and compromise due to pneumonia and/or surgery and 18 patients with CCM (11%). The 74 local patients (group 1) were intubated at our institutions, and 83 others were intubated elsewhere. Demographic data are in Table 2. VC and CPF data are in Table 3. Twenty (13%) of the 157 patients had been continuously NIV dependent for 12.2 years (range ) before being intubated. Forty-one (26%) used NIV part-time (, 24 h/d), and 96 (61%) used no NIV before intubation. All patients satisfied the Table 1 criteria in, 2 weeks. Univariate comparisons of potential predictive factors for extubation success yielded significant differences for continuous NIV use ( P,.0001) and for the duration of continuous NIV use and MAC use prior to intubation ( P ), indicating that experience with NIV and MAC was significant in predicting success. Given only 15 failures in eight patients, it was not possible to run multivariable logistic regression models considering diagnosis, patient group, VC, and CPF. Of 172 extubations on 157 patients, all 98 on patients with assisted CPF 160 L/m were successful. Fifty-nine of 74 attempts (80%) on patients with CPF, 160 L/m were successful, including 52 of 60 (87%) at first extubation. Six patients who initially failed, succeeded on second (four patients) and third (three patients) attempts. One with advanced bulbar ALS and one with facioscapulohumeral muscular dystrophy, both with no measurable assisted CPF, failed a total of five extubations and underwent tracheotomy. Only one of the eight who failed any extubation attempt had preintubation experience with NIV and MAC, but she and several others had suboptimal postextubation care provider support for aggressive MAC. She and eight patients with bulbar ALS with little residual bulbar-innervated muscle function required oro-nasal interfaces for a closed system of postextubation NIV (Hybrid NE; Teleflex Medical; Research Triangle Park, NC) ( Fig 2 ). All nine had gastrostomy tubes for total enteral nutrition. One lip-seal nocturnal NIV user for 28 years prior to intubation was extubated back to lip-seal NIV ( Fig 3 ). 36 Data on VC, CPF, and duration of NIV use as a function of postextubation weaning capacity are included in Table 4. Weaning from full-time to part-time CHEST / 137 / 5 / MAY,
4 Figure 3. A 59-year-old woman with spinal cord injury at birth and 31 years of dependence on a daytime mouthpiece and nocturnal lip-seal (seen here) ventilation. She was extubated back to noninvasive mechanical ventilation despite a VC of 130 ml and no autonomous breathing ability and continued to use simple 15-mm angled-mouthpiece ventilation for daytime ventilatory support and lip-seal ventilation overnight with the nose clipped to prevent air leakage. Current VC is 340 ml. She is employed full-time as a psychologist. See Figure 1 legend for expansion of the abbreviation. The patient provided written consent for the use of this photograph. NIV took 3 to 21 days and was usually accomplished at home. As supine VC increased to approach 1,000 ml, we encouraged patients to sleep without NIV but with Sp o 2 and end-tidal CO 2 monitoring, and when these remained stable for 2 weeks to discontinue NIV. The mean extubation VCs and assisted CPFs for the 29 patients 18 years of age who were successfully extubated at first attempt despite assisted CPF, 160 L/m were ml (range ) and L/m (range 0-150), respectively. No clinically or radiographically apparent barotrauma was noted for any patients. The 83 patients in groups 2 and 3 had been intubated for days (range ) before transfer and days (range ) on our units before extubation ( P,.005). Upon admission, on 21% fraction of inspired O 2, 71 (85%) of the patients Sp o 2 levels settled below 95%. Increased NIV support to normalize CO 2 and especially MAC normalized Sp o 2 generally within 24 to 48 h to satisfy a criterion for extubation. The intensivists and respiratory therapists estimated that noninvasive treatment necessitated more time than invasive respiratory treatment. The extubation itself required about 1.5 h for a specifically trained respiratory therapist to train the patients and care providers in NIV and MAC. In part because only one local nursing/rehabilitation facility would accept NIV users, all except one patient who had a tracheostomy were discharged home. One hundred thirty-one patients are alive using NIV ( Table 4 ). Nine patients (6%) died of cardiac failure, six (4%) from lung disease/respiratory failure, two (2%) with bulbar ALS died after tracheotomy from sepsis and decubiti, and nine (6%) died of unknown causes. Although offered, no patients accepted tracheotomy following successful extubation. Discussion There are no extubation studies on continuously NIVdependent patients with NMD. 6 A recent controlled Table 2 Demographic Data Characteristics Group 1a Group 2b Group 3c Total Subjects, No. (%) 74 (47) 45 (29) 38 (24) 157 (100) Sex, No. (%) 52 male (70) 28 male (62) 17 male (45) 97 male (62) 22 female (30) 17 female (38) 21 female (55) 60 female (38) Diagnoses, No. (%) ICUMy, 15 (20) SMA, 10 (22) SMA, 10 (26) SMA, 25 (16) SCI, 13 (18) MD, 9 (20) DMD, 9 (24) MD, 22 (14) ALS, 11 (15) DMD, 8 (18) MD, 5 (13) DMD, 20 (13) MG, 9 (12) MG, 6 (13) PPS, 5 (13) SCI, 17 (11) MD, 8 (11) PPS, 4 (9) onmd, 4 (11) ALS, 16(10) onmd, 8 (11) onmd, 4 (9) SCI, 3 (8) onmd, 16 (10) SMA, 5 (7) ALS, 3 (7) ALS, 2 (5) ICUMy, 15 (10) DMD, 3 (4) SCI, 1 (2)... MG, 15 (10) PPS, 2 (3) PPS. 11 (7) Use of NIV preintubation, No. (%) No NIV, 51 (69) No NIV, 24 (53) No NIV, 21 (55) No NIV, 96 (61) Cont, 10 (14) Cont, 7 (16) Cont, 3 (8) Cont, 20 (13) Noct, 13 (17) Noct, 14 (31) Noct, 14 (37) Noct, 41 (26) ALS 5 amyotrophic lateral sclerosis; Cont 5 continuous noninvasive ventilation; DMD 5 Duchenne muscular dystrophy; ICUMy 5 ICU-acquired neuromuscular disease; MD 5 muscular dystrophy; MG 5 myasthenia gravis; NIV 5 noninvasive ventilation; Noct 5 nocturnal noninvasive ventilation; onmd 5 other neuromuscular disease; PPS 5 postpolio syndrome; SCI 5 spinal cord injury; SMA 5 spinal muscular atrophy, including types 1, 2, and 3, and other neuromuscular disease. alocal patients. b Patients transferred after failing extubations in other institutions. c Patients transferred after failing multiple spontaneous breathing trials in other institutions Original Research
5 Table 3 Pulmonary Function Characteristics Group 1 a Group 2 b Group 3 c Total Subjects, n (%) 74 (47%) 45 (29) 37 (24%) 157 Assisted CPF at extubation, L/min VC at extubation, ml VC 3-6 mo postextubation, ml 1, Intergroup differences were not statistically significantly different except for postextubation VC, with that of group 1 being greater than for groups 2 and 3 ( P,.05). CPF 5 cough peak flows. See Table 1 for expansion of the other abbreviation. alocal patients. b Patients transferred after failing extubations in other institutions. c Patients transferred after failing multiple spontaneous breathing trials in other institutions. postextubation respiratory failure study of 106 patients included only two with restrictive syndromes, but none with NMD, and all had passed SBTs. They were extubated to supplemental O 2 alone or in conjunction with bilevel PAP at spans up to 14 cm H 2 O, pressures inadequate for normal alveolar ventilation for our patients. 39 A metaanalysis of 12 extubation studies to bilevel PAP demonstrated decreased mortality, ventilator-associated pneumonia, length of stay, and resort to tracheotomy, but unweanable patients with NMD were uniformly excluded. 6 Eligibility for extubation was based on readiness for weaning and failure of SBTs after 30 min or more. 6 While this justifies extubation to NIV for patients who primarily have lung/airways disease with some autonomous breathing ability and for whom Sp o 2. 90% may be acceptable with or without supplemental O 2, our patients had no ability to sustain breathing before or after extubation with VCs as low as 0 ml. Thus, no control group extubation to O 2 or less than full NIV would be possible, ethical, or permissible by any review board. While there are always limitations of uncontrolled studies when comparing two approaches, this was a study of only one approach to extubate patients not previously considered extubatable. For our long-term NIV users, aspiration causing persistent Sp o 2, 95% despite continuous NIV and MAC in ambient air is the indication for tracheotomy. 35 Besides hypoventilation, ineffective CPF have been associated with extubation failure. 21,22 MAC is essentially noninvasive suctioning via noninvasive or invasive interfaces. It can clear the left airways that are often not cleared by invasive suctioning and can acutely increase VC and Sp o 2. 30,40,41 Our success stemmed not only from providing continuous fullsetting NIV via a variety of interfaces but also from frequent and aggressive MAC to expel secretions and maintain or return Sp o 2. 95%. In our earlier study of extubation/decannulation to NIV, considering the extent of need for NIV, age, VC, and maximum assisted CPF, only assisted CPF 160 L/m predicted success in 62 extubation/decannulation attempts on 49 consecutive patients, including 34 with no ventilator-free breathing ability. 22 None of the 15 attempts on those with maximum CPF, 160 L/m succeeded, as opposed to an 87% first-attempt extubation success rate in this study. The most likely reasons for the difference between then and now are: baseline Sp o 2 criterion for extubation of 92% vs 95%, and thus the earlier patients had more residual airway secretions or lung disease at extubation; 5% vs 39% of patients with pre-extubation experience with NIV and MAC; less hospital staff experience with NIV and MAC; 50 of 62 patients were decanulated, not extubated; the patients were in various hospital locations; and MAC was used less often and without family involvement. 22 The 87% first-attempt extubation success rate on patients with maximum CPF, 160 L/m in this study is greater than the 82.4% (61 of 74) success rate reported for extubating NIV-dependent infants with spinal muscular atrophy type 1 (SMA 1), according to an almost identical protocol. 42 The difference may be the result of the ability of these patients, as opposed to babies, to cooperate with NIV and MAC. The SMA 1 infants may have also had more severe bulbar-innervated muscle dysfunction. Thus, while higher than those Table 4 Postextubation Long-Term Noninvasive Ventilation Use for 155 Patients Characteristics Weaned in 1 wk Weaned to Part-Time NIV Unweanable Subjects, n VC at extubation, ml CPF at extubation, L/min VC 6 mo postextubation, ml Duration ventilator use, mo (range) (1-204) (1-228) See Tables 1 and 3 for expansion of abbreviations. CHEST / 137 / 5 / MAY,
6 for a comparable infant population, the success rate was significantly less (87% vs 100%) ( P,.05) than for patients with assisted CPF 160 L/m. Unmeasurable assisted CPFs indicate an inability to close the glottis and are associated with stridor, saliva aspiration, and less effective NIV and MAC. An NIV/MAC protocol has been used to avoid over 100 hospitalizations for continuously ventilatordependent (NIV) patients with NMD. 20,35 Here we considered unweanable patients with NMD for whom intubation could not be avoided. Upon extubation, most patients with a VC of 200 ml or more eventually were weaned from continuous to part-time NIV by taking fewer and fewer mouthpiece IPPVs. Thus, the paradigm of weaning then extubation can be changed to extubation to permit self-weaning for patients with NMD. The notion that early tracheotomy after intubation somehow facilitates ventilator weaning 43 should be reassessed for patients with NMD. NIV is also associated with over 75% fewer ventilator-associated pneumonias. 6,44 Use of mouthpieces rather than masks interfaced in acute-care facilitated speech, oral intake, comfort, and glossopharyngeal breathing 45 ; eliminated the risk of skin pressure sores; and permitted air stacking to maintain pulmonary compliance, 37,45 diminish atelectasis, and facilitate manually assisted coughing. The purpose here was not to facilitate ventilator weaning or to consider long-term outcomes, but to extubate unweanable patients. Benefits included no mortality, fewer days intubated, no tracheostomies, and return home. Decannulation, too, can facilitate ventilator weaning. 46 Avoidance of tracheostomy for continuous ventilator (NIV) users can also better maintain quality of life, significantly diminish long-term pneumonia and respiratory hospitalization rates, 50 maximize ventilator-free breathing, 46 and facilitate return home. 49 In conclusion, unweanable intubated patients with NMD who satisfy specific criteria can be successfully extubated to full NIV and MAC. Patients with measurable assisted cough flows should no longer be advised to refuse intubation for fear of extubation failure and tracheotomy. We no longer consider tracheotomy for any ventilator-dependent patients with NMD who satisfy Table 1 criteria, and now offer extubation to most with CPF, 160 L/m. Acknowledgments Author contributions: Dr Bach: wrote all drafts of the paper and, with Dr Hamdani, extubated all the patients in New Jersey. Mr Gonçalves: performed the extubations on all of the patients in Portugal, gathered data on the Portuguese patients, and added material to the text of the manuscript. Dr Hamdani: performed the extubations on some of the patients in New Jersey, gathered data on the New Jersey patients, and added material to the text of the manuscript. Dr Winck: oversaw the extubations on all of the Portuguese patients and added material to the introductory and Discussion sections of the manuscript. Financial /nonfinancial disclosures: The authors have reported to CHEST the following conflicts of interest: Respironics, Inc, is the manufacturer of the CoughAssist, a device mentioned in this article. Dr Winck has been reimbursed by Respironics, Inc, for attending a sleep conference, received 4,500 for organizing two postgraduate courses on noninvasive ventilation for Respironics, Inc, and received 500 for lectures in a conference sponsored by Respironics, Inc. Mr Gonçalves received lecture honoraria of 4,000 from Respironics, Inc, for two postgraduate courses on noninvasive ventilation. Drs Bach and Hamdani have reported no conflicts of interest exist with any companies/organizations whose products or services may be discussed in this article. Other contributions: We wish to thank Teresa Honrado, MD; Teresa Oliveira, MD; and Celeste Dias, MD, as well as the ICU medical, respiratory therapy, and nursing staffs of both institutions for their assistance and support in treating the patients. References 1. Boles JM, Bion J, Connors A, et al. Weaning from mechanical ventilation. Eur Respir J ;29(5): Caples SM, Gay PC. Noninvasive positive pressure ventilation in the intensive care unit: a concise review. Crit Care Med ;33(11): Ferrer M, Valencia M, Nicolas JM, Bernadich O, Badia JR, Torres A. Early noninvasive ventilation averts extubation failure in patients at risk: a randomized trial. Am J Respir Crit Care Med ;173(2): Frutos-Vivar F, Ferguson ND, Esteban A, et al. Risk factors for extubation failure in patients following a successful spontaneous breathing trial. Chest ;130(6): Templeton M, Palazzo MG. Chest physiotherapy prolongs duration of ventilation in the critically ill ventilated for more than 48 hours. Intensive Care Med ;33(11): Burns KE, Adhikari NKJ, Keenan SP, Meade M. Use of non-invasive ventilation to wean critically ill adults off invasive ventilation: meta-analysis and systematic review. BMJ ;338: Nava S, Ambrosino N, Clini E, et al. Noninvasive mechanical ventilation in the weaning of patients with respiratory failure due to chronic obstructive pulmonary disease. A randomized, controlled trial. Intern Med ;128(9): Esteban A, Anzueto A, Frutos F, et al ; Mechanical Ventilation International Study Group. Characteristics and outcomes in adult patients receiving mechanical ventilation: a 28-day international study. JAMA ;287(3): Antonelli M, Conti G, Moro ML, et al. Predictors of failure of noninvasive positive pressure ventilation in patients with acute hypoxemic respiratory failure: a multi-center study. Intensive Care Med ;27(11): Ceriana P, Delmastro M, Rampulla C, Nava S. Demographics and clinical outcomes of patients admitted to a respiratory intensive care unit located in a rehabilitation center. Respir Care ;48(7): Pilcher DV, Bailey MJ, Treacher DF, Hamid S, Williams AJ, Davidson AC. Outcomes, cost and long term survival of patients referred to a regional weaning centre. Thorax ; 60 ( 3 ): De Jonghe B, Sharshar T, Lefaucheur JP, et al ; Groupe de Réflexion et d Etude des Neuromyopathies en Réanimation. Paresis acquired in the intensive care unit: a prospective multicenter study. JAMA ;288(22): Deem S, Lee CM, Curtis JR. Acquired neuromuscular disorders in the intensive care unit. Am J Respir Crit Care Med ;168(7): Original Research
7 14. Simonds AK. Streamlining weaning: protocols and weaning units. Thorax ;60 (3 ): Winck JC, Gonçalves M. Muscles and lungs: fatal attraction, but time for intervention. Monaldi Arch Chest Dis ;63 (3 ): Epstein SK. Weaning the unweanable : liberating patients from prolonged mechanical ventilation. Crit Care Med ;35 (11 ): Benditt JO, Boitano L. Respiratory treatment of amyotrophic lateral sclerosis. Phys Med Rehabil Clin N Am ; 19 ( 3 ): Benditt JO. Full-time noninvasive ventilation: possible and desirable. Respir Care ;52 (9 ): Soudon P, Steens M, Toussaint M. A comparison of invasive versus noninvasive full-time mechanical ventilation in Duchenne muscular dystrophy. Chron Respir Dis ;5 (2 ): Gomez-Merino E, Bach JR. Duchenne muscular dystrophy: prolongation of life by noninvasive ventilation and mechanically assisted coughing. Am J Phys Med Rehabil ; 81 ( 6 ): Smina M, Salam A, Khamiees M, Gada P, Amoateng-Adjepong Y, Manthous CA. Cough peak flows and extubation outcomes. Chest ;124 (1 ): Bach JR, Saporito LR. Criteria for extubation and tracheostomy tube removal for patients with ventilatory failure. A different approach to weaning. Chest ;110 (6 ): Salam A, Tilluckdharry L, Amoateng-Adjepong Y, Manthous CA. Neurologic status, cough, secretions and extubation outcomes. Intensive Care Med ;30 (7 ): Ferrer M, Esquinas A, Arancibia F, et al. Noninvasive ventilation during persistent weaning failure: a randomized controlled trial. Am J Respir Crit Care Med ;168 (1 ): Bach JR, Alba AS. Noninvasive options for ventilatory support of the traumatic high level quadriplegic patient. Chest ;98 (3 ): Bach JR. New approaches in the rehabilitation of the traumatic high level quadriplegic. Am J Phys Med Rehabil ; 70 ( 1 ): Bach JR. Amyotrophic lateral sclerosis: prolongation of life by noninvasive respiratory AIDS. Chest ;122 (1 ): Tzeng AC, Bach JR. Prevention of pulmonary morbidity for patients with neuromuscular disease. Chest ;118 (5 ): Bach JR. Mechanical insufflation-exsufflation. Comparison of peak expiratory flows with manually assisted and unassisted coughing techniques. Chest ;104 (5 ): Winck JC, Gonçalves MR, Lourenço C, Viana P, Almeida J, Bach JR. Effects of mechanical insufflation-exsufflation on respiratory parameters for patients with chronic airway secretion encumbrance. Chest ;126 (3 ): Ely EW, Baker AM, Dunagan DP, et al. Effect on the duration of mechanical ventilation of identifying patients capable of breathing spontaneously. N Engl J Med ; 335 ( 25 ): Meade M, Guyatt G, Sinuff T, et al. Trials comparing alternative weaning modes and discontinuation assessments. Chest ;120 (6 Suppl ):425S-437S. 33. MacIntyre NR, Cook DJ, Ely EW Jr, et al ; American College of Chest Physicians ; American Association for Respiratory Care ; American College of Critical Care Medicine. Evidencebased guidelines for weaning and discontinuing ventilatory support: a collective task force facilitated by the American College of Chest Physicians; the American Association for Respiratory Care; and the American College of Critical Care Medicine. Chest ;120 (6 Suppl ):375S-395S. 34. Sancho J, Servera E, Díaz J, Marín J. Predictors of ineffective cough during a chest infection in patients with stable amyotrophic lateral sclerosis. Am J Respir Crit Care Med ;175 (12 ): Bach JR, Bianchi C, Aufiero E. Oximetry and indications for tracheotomy for amyotrophic lateral sclerosis. Chest ;126 (5 ): Bach JR, Alba AS, Saporito LR. Intermittent positive pressure ventilation via the mouth as an alternative to tracheostomy for 257 ventilator users. Chest ;103 (1 ): Bach JR, Kang SW. Disorders of ventilation: weakness, stiffness, and mobilization. Chest ;117 (2 ): Bach JR, Gonzalez M, Sharma A, Swan K, Patel A. Open gastrostomy for noninvasive ventilation users with neuromuscular disease. Am J Phys Med Rehabil ;87 (1 ): Ferrer M, Sellares J, Valencia M, et al. Non-invasive ventilation after extubation in hypercapnic patients with chronic respiratory disorders: randomised controlled trial. Lancet ; 374 (9695): Bach JR, Ishikawa Y, Kim H. Prevention of pulmonary morbidity for patients with Duchenne muscular dystrophy. Chest ;112 (4 ): Servera E, Sancho J, Zafra MJ, Catalá A, Vergara P, Marín J. Alternatives to endotracheal intubation for patients with neuromuscular diseases. Am J Phys Med Rehabil ; 84 ( 11 ): Bach JR, Niranjan V, Weaver B. Spinal muscular atrophy type 1: a noninvasive respiratory management approach. Chest ;117 (4 ): Blot F, Melot C ; Commission d Epidémiologie et de Recherche Clinique. Indications, timing, and techniques of tracheostomy in 152 French ICUs. Chest ;127 (4 ): Kollef MH. Avoidance of tracheal intubation as a strategy to prevent ventilator-associated pneumonia. Intensive Care Med ;25 (6 ): Bach JR, Bianchi C, Vidigal-Lopes M, Turi S, Felisari G. Lung inflation by glossopharyngeal breathing and air stacking in Duchenne muscular dystrophy. Am J Phys Med Rehabil ;86 (4 ): Bach JR, Goncalves M. Ventilator weaning by lung expansion and decannulation. Am J Phys Med Rehabil ;83 (7 ): Bourke SC, Bullock RE, Williams TL, Shaw PJ, Gibson GJ. Noninvasive ventilation in ALS: indications and effect on quality of life. Neurology ;61 (2 ): Viroslav J, Rosenblatt R, Tomazevic SM. Respiratory management, survival, and quality of life for high-level traumatic tetraplegics. Respir Care Clin N Am ;2 (2 ): Bach JR, Intintola P, Alba AS, Holland IE. The ventilatorassisted individual. Cost analysis of institutionalization vs rehabilitation and in-home management. Chest ;101 (1 ): Bach JR, Rajaraman R, Ballanger F, et al. Neuromuscular ventilatory insufficiency: effect of home mechanical ventilator use v oxygen therapy on pneumonia and hospitalization rates. Am J Phys Med Rehabil ;77 (1 ): CHEST / 137 / 5 / MAY,
Noninvasive Respiratory Management for Patients with Spinal Cord Injury and Neuromuscular Disease
 Review Article 2012 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran ISSN: 1735-0344 Tanaffos 2012; 11 (1): 7-11 TANAFFOS Noninvasive Respiratory Management for Patients with
Review Article 2012 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran ISSN: 1735-0344 Tanaffos 2012; 11 (1): 7-11 TANAFFOS Noninvasive Respiratory Management for Patients with
The great majority of neuromuscular disease morbidity. Prevention of Pulmonary Morbidity for Patients With Neuromuscular Disease*
 Prevention of Pulmonary Morbidity for Patients With Neuromuscular Disease* Alice C. Tzeng, MD; and John R. Bach, MD, FCCP Study objective: To evaluate the effects of a respiratory muscle aid protocol on
Prevention of Pulmonary Morbidity for Patients With Neuromuscular Disease* Alice C. Tzeng, MD; and John R. Bach, MD, FCCP Study objective: To evaluate the effects of a respiratory muscle aid protocol on
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the
 Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Preventing Respiratory Complications of Muscular Dystrophy
 Preventing Respiratory Complications of Muscular Dystrophy Jonathan D. Finder, MD Professor of Pediatrics University of Pittsburgh School of Medicine Children s Hospital of Pittsburgh Introduction Respiratory
Preventing Respiratory Complications of Muscular Dystrophy Jonathan D. Finder, MD Professor of Pediatrics University of Pittsburgh School of Medicine Children s Hospital of Pittsburgh Introduction Respiratory
Respiratory Muscle Aids to Avert Respiratory Failure and Tracheostomy
 Respiratory Muscle Aids to Avert Respiratory Failure and Tracheostomy John R. Bach, M.D. DoctorBach.com Abstract The purpose of this article is to describe the use of noninvasive inspiratory and expiratory
Respiratory Muscle Aids to Avert Respiratory Failure and Tracheostomy John R. Bach, M.D. DoctorBach.com Abstract The purpose of this article is to describe the use of noninvasive inspiratory and expiratory
Duchenne Muscular Dystrophy
 Authors: Elia Gomez-Merino, MD John R. Bach, MD Affiliations: From the Department of Pulmonary Medicine, Hospital Clinico Universitario de San Juan, San Juan de Alicante, Spain (EGM), and the Department
Authors: Elia Gomez-Merino, MD John R. Bach, MD Affiliations: From the Department of Pulmonary Medicine, Hospital Clinico Universitario de San Juan, San Juan de Alicante, Spain (EGM), and the Department
The difference is clear. CoughAssist clears airways with the force of a natural cough
 The difference is clear CoughAssist clears airways with the force of a natural cough When only a real cough will do CoughAssist is a noninvasive therapy that safely and consistently removes secretions
The difference is clear CoughAssist clears airways with the force of a natural cough When only a real cough will do CoughAssist is a noninvasive therapy that safely and consistently removes secretions
Mechanical Ventilation of the Patient with Neuromuscular Disease
 Mechanical Ventilation of the Patient with Neuromuscular Disease Dean Hess PhD RRT Associate Professor of Anesthesia, Harvard Medical School Assistant Director of Respiratory Care, Massachusetts General
Mechanical Ventilation of the Patient with Neuromuscular Disease Dean Hess PhD RRT Associate Professor of Anesthesia, Harvard Medical School Assistant Director of Respiratory Care, Massachusetts General
MND Study Day. Martin Latham CNS Leeds Sleep Service
 MND Study Day Martin Latham CNS Leeds Sleep Service Objectives: Identifying individuals at risk. Understand issues related to NIV. Understand issues related to secretion management Improve outcomes. Identifying
MND Study Day Martin Latham CNS Leeds Sleep Service Objectives: Identifying individuals at risk. Understand issues related to NIV. Understand issues related to secretion management Improve outcomes. Identifying
Efficacy of Mechanical Insufflation-Exsufflation in Extubating Unweanable Subjects With Restrictive Pulmonary Disorders
 Efficacy of Mechanical Insufflation-Exsufflation in Extubating Unweanable Subjects With Restrictive Pulmonary Disorders John R Bach MD, Diane M Sinquee MD, Louis R Saporito RRT, Amanda L Botticello PhD
Efficacy of Mechanical Insufflation-Exsufflation in Extubating Unweanable Subjects With Restrictive Pulmonary Disorders John R Bach MD, Diane M Sinquee MD, Louis R Saporito RRT, Amanda L Botticello PhD
Motor Neurone Disease NICE to manage Management of ineffective cough. Alex Long Specialist NIV/Respiratory physiotherapist June 2016
 Motor Neurone Disease NICE to manage Management of ineffective cough Alex Long Specialist NIV/Respiratory physiotherapist June 2016 Content NICE guideline recommendations Respiratory involvement in MND
Motor Neurone Disease NICE to manage Management of ineffective cough Alex Long Specialist NIV/Respiratory physiotherapist June 2016 Content NICE guideline recommendations Respiratory involvement in MND
Understanding Breathing Muscle Weakness
 Understanding Breathing Muscle Weakness A N D R E A L. K L E I N P R E S I D E N T / F O U N D E R B R E A T H E W I T H M D w w w.facebook.com/ b r e a t h e w i t h m d h t t p : / / w w w. b r e a t
Understanding Breathing Muscle Weakness A N D R E A L. K L E I N P R E S I D E N T / F O U N D E R B R E A T H E W I T H M D w w w.facebook.com/ b r e a t h e w i t h m d h t t p : / / w w w. b r e a t
Mouthpiece ventilation and complementary techniques in patients with neuromuscular disease: A brief clinical review and update
 Review Article Mouthpiece ventilation and complementary techniques in patients with neuromuscular disease: A brief clinical review and update Chronic Respiratory Disease 2016, Vol. 14(2) 1 7 ª The Author(s)
Review Article Mouthpiece ventilation and complementary techniques in patients with neuromuscular disease: A brief clinical review and update Chronic Respiratory Disease 2016, Vol. 14(2) 1 7 ª The Author(s)
Artificial External Glottic Device for Passive Lung Insufflation
 Original Article http://dx.doi.org/10.3349/ymj.2011.52.6.972 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 52(6):972-976, 2011 Artificial External Glottic Device for Passive Lung Insufflation Dong Hyun
Original Article http://dx.doi.org/10.3349/ymj.2011.52.6.972 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 52(6):972-976, 2011 Artificial External Glottic Device for Passive Lung Insufflation Dong Hyun
Pediatric Patients. Neuromuscular Disease. Teera Kijmassuwan, MD Phetcharat Netmuy, B.N.S., MA Oranee Sanmaneechai, MD : Preceptor
 Patient Management Pediatric Patients with Neuromuscular Disease Teera Kijmassuwan, MD Phetcharat Netmuy, B.N.S., MA Oranee Sanmaneechai, MD : Preceptor Case Thai boy 1 year old Present with Respiratory
Patient Management Pediatric Patients with Neuromuscular Disease Teera Kijmassuwan, MD Phetcharat Netmuy, B.N.S., MA Oranee Sanmaneechai, MD : Preceptor Case Thai boy 1 year old Present with Respiratory
CoughAssist E70. More than just a comfortable cough. Flexible therapy that brings more comfort to your patients airway clearance
 CoughAssist E70 More than just a comfortable cough Flexible therapy that brings more comfort to your patients airway clearance Flexible, customisable loosening and clearing therapy An effective cough is
CoughAssist E70 More than just a comfortable cough Flexible therapy that brings more comfort to your patients airway clearance Flexible, customisable loosening and clearing therapy An effective cough is
Neuromuscular diseases are characterized by progressive
 Maximum Insufflation Capacity* Seong-Woong Kang, MD, PhD; and John R. Bach, MD, FCCP Objective: To investigate the effect of deep lung insufflations on maximum insufflation capacities (MICs) and peak cough
Maximum Insufflation Capacity* Seong-Woong Kang, MD, PhD; and John R. Bach, MD, FCCP Objective: To investigate the effect of deep lung insufflations on maximum insufflation capacities (MICs) and peak cough
Alternative title: Confessions of a Mucus Enthusiast. Mechanical Insufflation Exsufflation for airway secretion clearance and lung expansion therapy
 Mechanical Insufflation Exsufflation for airway secretion clearance and lung expansion therapy Alternative title: Confessions of a Mucus Enthusiast Marty Davig, RRT RCP Philips Respironics Inc. Objectives
Mechanical Insufflation Exsufflation for airway secretion clearance and lung expansion therapy Alternative title: Confessions of a Mucus Enthusiast Marty Davig, RRT RCP Philips Respironics Inc. Objectives
Terapias no farmacológicas de aclaramiento de la vía aérea y soporte respiratorio muscular en
 Terapias no farmacológicas de aclaramiento de la vía aérea y soporte respiratorio muscular en el paciente ventilado: Estado del arte João Carlos Winck, MD, PhD Coordinator of the Respiratory Medicine Unit
Terapias no farmacológicas de aclaramiento de la vía aérea y soporte respiratorio muscular en el paciente ventilado: Estado del arte João Carlos Winck, MD, PhD Coordinator of the Respiratory Medicine Unit
Amyotrophic Lateral Sclerosis: Predictors for Prolongation of Life by Noninvasive Respiratory Aids
 828 Amyotrophic Lateral Sclerosis: Predictors for Prolongation of Life by Noninvasive Respiratory Aids John Robert Bach, AID ABSTRACT. Bach JR. Amyotrophic lateral sclerosis: predictors for prolongation
828 Amyotrophic Lateral Sclerosis: Predictors for Prolongation of Life by Noninvasive Respiratory Aids John Robert Bach, AID ABSTRACT. Bach JR. Amyotrophic lateral sclerosis: predictors for prolongation
Problem-solving Respiratory Issues in Children With Neuromuscular Disease. December 13, 2018 Eliezer Be eri, M.D.
 Problem-solving Respiratory Issues in Children With Neuromuscular Disease December 13, 2018 Eliezer Be eri, M.D. About Our Presenter Eliezer Be eri, M.D. Alyn Rehabilitation Hospital Jerusalem, Israel
Problem-solving Respiratory Issues in Children With Neuromuscular Disease December 13, 2018 Eliezer Be eri, M.D. About Our Presenter Eliezer Be eri, M.D. Alyn Rehabilitation Hospital Jerusalem, Israel
Performance of the CoughAssist Insufflation-Exsufflation Device in the Presence of an Endotracheal Tube or Tracheostomy Tube: A Bench Study
 Performance of the CoughAssist Insufflation-Exsufflation Device in the Presence of an or : A Bench Study Claude Guérin MD PhD, Gaël Bourdin MD, Véronique Leray MD, Bertrand Delannoy MD, Frédérique Bayle
Performance of the CoughAssist Insufflation-Exsufflation Device in the Presence of an or : A Bench Study Claude Guérin MD PhD, Gaël Bourdin MD, Véronique Leray MD, Bertrand Delannoy MD, Frédérique Bayle
The objectives of this presentation are to
 1 The objectives of this presentation are to 1. Review the mechanics of airway clearance 2. Understand the difference between secretion mobilization and secretion clearance 3. Identify conditions that
1 The objectives of this presentation are to 1. Review the mechanics of airway clearance 2. Understand the difference between secretion mobilization and secretion clearance 3. Identify conditions that
Ron Hosp, MS-HSA, RRT Regional Respiratory Specialist. This program has been approved for 1 hour of continuing education credit.
 Ron Hosp, MS-HSA, RRT Regional Respiratory Specialist This program has been approved for 1 hour of continuing education credit. Course Objectives Identify at least four goals of home NIV Identify candidates
Ron Hosp, MS-HSA, RRT Regional Respiratory Specialist This program has been approved for 1 hour of continuing education credit. Course Objectives Identify at least four goals of home NIV Identify candidates
[N] = No product variation, policy applies as stated [Y] = Standard product coverage varies from application of this policy, see below
![[N] = No product variation, policy applies as stated [Y] = Standard product coverage varies from application of this policy, see below [N] = No product variation, policy applies as stated [Y] = Standard product coverage varies from application of this policy, see below](/thumbs/94/119510114.jpg) Original Issue Date (Created): May 3, 2004 Most Recent Review Date (Revised): September 24, 2013 Effective Date: November 1, 2013 I. POLICY Mechanical insufflation-exsufflation (MI-E) may be considered
Original Issue Date (Created): May 3, 2004 Most Recent Review Date (Revised): September 24, 2013 Effective Date: November 1, 2013 I. POLICY Mechanical insufflation-exsufflation (MI-E) may be considered
Adapting to the Worsening of the LTMV Patient
 14 èmes Journées Internationales de Ventilation à Domicile LYON, 26-28 mars 2015 Adapting to the Worsening of the LTMV Patient Andrea Vianello Fisiopatologia e Terapia Intensiva Respiratoria Ospedale-Università
14 èmes Journées Internationales de Ventilation à Domicile LYON, 26-28 mars 2015 Adapting to the Worsening of the LTMV Patient Andrea Vianello Fisiopatologia e Terapia Intensiva Respiratoria Ospedale-Università
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
A Comparison of Cough Assistance Techniques in Patients with Respiratory Muscle Weakness
 Original Article Yonsei Med J 2016 Nov;57(6):1488-1493 pissn: 0513-5796 eissn: 1976-2437 A Comparison of Cough Assistance Techniques in Patients with Respiratory Muscle Weakness Sun Mi Kim 1,2, Won Ah
Original Article Yonsei Med J 2016 Nov;57(6):1488-1493 pissn: 0513-5796 eissn: 1976-2437 A Comparison of Cough Assistance Techniques in Patients with Respiratory Muscle Weakness Sun Mi Kim 1,2, Won Ah
Bench Assessment of a New Insufflation-Exsufflation Device
 Bench Assessment of a New Insufflation-Exsufflation Device Véronique Porot MD and Claude Guérin MD PhD BACKGROUND: The Nippy Clearway is a new mechanical insufflation-exsufflation device used to assist
Bench Assessment of a New Insufflation-Exsufflation Device Véronique Porot MD and Claude Guérin MD PhD BACKGROUND: The Nippy Clearway is a new mechanical insufflation-exsufflation device used to assist
LUNG VOLUME RECRUITMENT IN NEUROMUSCULAR DISEASE
 LUNG VOLUME RECRUITMENT IN NEUROMUSCULAR DISEASE Sherri Katz, MDCM, MSc, FRCPC Pediatric Respirologist Children s Hospital of Eastern Ontario University of Ottawa Disclosures Research funding from CIHR,
LUNG VOLUME RECRUITMENT IN NEUROMUSCULAR DISEASE Sherri Katz, MDCM, MSc, FRCPC Pediatric Respirologist Children s Hospital of Eastern Ontario University of Ottawa Disclosures Research funding from CIHR,
Patients with acute neurologic disease and respiratory failure are typically. Noninvasive Mechanical Ventilation in Acute Neurologic Disorders
 TREATMENT UPDATE Noninvasive Mechanical Ventilation in Acute Neurologic Disorders Eelco F.M. Wijdicks, MD Department of Neurology, Division of Critical Care Neurology, Mayo Clinic College of Medicine,
TREATMENT UPDATE Noninvasive Mechanical Ventilation in Acute Neurologic Disorders Eelco F.M. Wijdicks, MD Department of Neurology, Division of Critical Care Neurology, Mayo Clinic College of Medicine,
Respiratory Management- Your Questions Answered! Michelle Chatwin, PhD Consultant Physiotherapist
 Respiratory Management- Your Questions Answered! Michelle Chatwin, PhD Consultant Physiotherapist Why Are People Affected Differently Neuromuscular Disease; A Spectrum Its severity varies widely within
Respiratory Management- Your Questions Answered! Michelle Chatwin, PhD Consultant Physiotherapist Why Are People Affected Differently Neuromuscular Disease; A Spectrum Its severity varies widely within
KENNEDY DISEASE PULMONARY CONSIDERATIONS: SCIENCE & MANAGEMENT STRATEGIES
 KENNEDY DISEASE PULMONARY CONSIDERATIONS: SCIENCE & MANAGEMENT STRATEGIES When you can t breathe nothing else matters American Lung Association Noah Lechtzin, MD; MHS Associate Professor of Medicine Johns
KENNEDY DISEASE PULMONARY CONSIDERATIONS: SCIENCE & MANAGEMENT STRATEGIES When you can t breathe nothing else matters American Lung Association Noah Lechtzin, MD; MHS Associate Professor of Medicine Johns
Commissioning Policy for Cough Assist Requests
 Commissioning Policy for Cough Assist Requests 1 DOCUMENT CONTROL Reference Number (lead in specific policy area to provide once policy ratified) Version Draft Version 0.3 071015 Status Sponsor(s)/Author(s)
Commissioning Policy for Cough Assist Requests 1 DOCUMENT CONTROL Reference Number (lead in specific policy area to provide once policy ratified) Version Draft Version 0.3 071015 Status Sponsor(s)/Author(s)
Home Mechanical Ventilation in South Korea
 Original Article http://dx.doi.org/10.3349/ymj.2014.55.6.1729 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 55(6):1729-1735, 2014 Home Mechanical Ventilation in South Korea Dong Hyun Kim, 1 Seong-Woong
Original Article http://dx.doi.org/10.3349/ymj.2014.55.6.1729 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 55(6):1729-1735, 2014 Home Mechanical Ventilation in South Korea Dong Hyun Kim, 1 Seong-Woong
WEANING READINESS & SPONTANEOUS BREATHING TRIAL MONITORING
 CLINICAL EVIDENCE GUIDE WEANING READINESS & SPONTANEOUS BREATHING TRIAL MONITORING Weaning readiness and spontaneous breathing trial monitoring protocols can help you make the right weaning decisions at
CLINICAL EVIDENCE GUIDE WEANING READINESS & SPONTANEOUS BREATHING TRIAL MONITORING Weaning readiness and spontaneous breathing trial monitoring protocols can help you make the right weaning decisions at
Extubation Failure & Delay in Brain-Injured Patients
 Extubation Failure & Delay in Brain-Injured Patients Niall D. Ferguson, MD, FRCPC, MSc Director, Critical Care Medicine University Health Network & Mount Sinai Hospital Associate Professor of Medicine
Extubation Failure & Delay in Brain-Injured Patients Niall D. Ferguson, MD, FRCPC, MSc Director, Critical Care Medicine University Health Network & Mount Sinai Hospital Associate Professor of Medicine
Key points. k Ineffective cough is a major cause of
 Breathe review cough.qxd 21/05/2008 16:06 Page 2 Key points k Ineffective cough is a major cause of k k k mortality and morbidity in patients with neuromuscular disease. A normal cough requires the inspiratory
Breathe review cough.qxd 21/05/2008 16:06 Page 2 Key points k Ineffective cough is a major cause of k k k mortality and morbidity in patients with neuromuscular disease. A normal cough requires the inspiratory
DIAPHRAGM PACING AND NONINVASIVE RESPIRATORY MANAGEMENT OF AMYOTROPHIC LATERAL SCLEROSIS/MOTOR NEURON DISEASE
 DIAPHRAGM PACING AND NONINVASIVE RESPIRATORY MANAGEMENT OF AMYOTROPHIC LATERAL SCLEROSIS/MOTOR NEURON DISEASE KEDAR R. MAHAJAN, MD, PhD, JOHN ROBERT BACH, MD, LOU SAPORITO, BS, and NICK PEREZ, MD Department
DIAPHRAGM PACING AND NONINVASIVE RESPIRATORY MANAGEMENT OF AMYOTROPHIC LATERAL SCLEROSIS/MOTOR NEURON DISEASE KEDAR R. MAHAJAN, MD, PhD, JOHN ROBERT BACH, MD, LOU SAPORITO, BS, and NICK PEREZ, MD Department
An ideal ventilator for neuromuscular patients. F. Lofaso, Raymond Poincaré Hospital Inserm U 1179
 An ideal ventilator for neuromuscular patients F. Lofaso, Raymond Poincaré Hospital Inserm U 1179 Neuromuscular diseasescausing progressive respiratoryfailure Cerebral diseases: strokes, tumors. Brainstem:primaryhypoventilation,
An ideal ventilator for neuromuscular patients F. Lofaso, Raymond Poincaré Hospital Inserm U 1179 Neuromuscular diseasescausing progressive respiratoryfailure Cerebral diseases: strokes, tumors. Brainstem:primaryhypoventilation,
Weaning from Mechanical Ventilation. Dr Azmin Huda Abdul Rahim
 Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
Noninvasive ventilation for avoidance of reintubation in patients with various cough strength
 Duan et al. Critical Care (2016) 20:316 DOI 10.1186/s13054-016-1493-0 RESEARCH Open Access Noninvasive ventilation for avoidance of reintubation in patients with various cough strength Jun Duan *, Xiaoli
Duan et al. Critical Care (2016) 20:316 DOI 10.1186/s13054-016-1493-0 RESEARCH Open Access Noninvasive ventilation for avoidance of reintubation in patients with various cough strength Jun Duan *, Xiaoli
GE Healthcare. Non Invasive Ventilation (NIV) For the Engström Ventilator. Relief, Relax, Recovery
 GE Healthcare Non Invasive Ventilation (NIV) For the Engström Ventilator Relief, Relax, Recovery COPD is currently the fourth leading cause of death in the world, and further increases in the prevalence
GE Healthcare Non Invasive Ventilation (NIV) For the Engström Ventilator Relief, Relax, Recovery COPD is currently the fourth leading cause of death in the world, and further increases in the prevalence
MedStar Health considers Cough Assist Devices medically necessary for the following indications:
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.047.MH Cough Assist Devices This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.047.MH Cough Assist Devices This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
The Role of Noninvasive Ventilation in the Ventilator Discontinuation Process
 The Role of Noninvasive Ventilation in the Ventilator Discontinuation Process Dean R Hess PhD RRT FAARC Introduction NIV to Shorten the Length of Invasive Ventilation NIV to Prevent Extubation Failure
The Role of Noninvasive Ventilation in the Ventilator Discontinuation Process Dean R Hess PhD RRT FAARC Introduction NIV to Shorten the Length of Invasive Ventilation NIV to Prevent Extubation Failure
Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor
 Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Bi-Level Therapy: Boosting Comfort & Compliance in Apnea Patients
 Bi-Level Therapy: Boosting Comfort & Compliance in Apnea Patients Objectives Describe nocturnal ventilation characteristics that may indicate underlying conditions and benefits of bilevel therapy for specific
Bi-Level Therapy: Boosting Comfort & Compliance in Apnea Patients Objectives Describe nocturnal ventilation characteristics that may indicate underlying conditions and benefits of bilevel therapy for specific
Liberation from Mechanical Ventilation in Critically Ill Adults
 Liberation from Mechanical Ventilation in Critically Ill Adults 2017 ACCP/ATS Clinical Practice Guidelines Timothy D. Girard, MD, MSCI Clinical Research, Investigation, and Systems Modeling of Acute Illness
Liberation from Mechanical Ventilation in Critically Ill Adults 2017 ACCP/ATS Clinical Practice Guidelines Timothy D. Girard, MD, MSCI Clinical Research, Investigation, and Systems Modeling of Acute Illness
PAPER DE LA VNI EN LA RETIRADA DE LA VENTILACIÓ INVASIVA I FRACÀS D EXTUBACIÓ
 PAPER DE LA VNI EN LA RETIRADA DE LA VENTILACIÓ INVASIVA I FRACÀS D EXTUBACIÓ Dr. Miquel Ferrer UVIIR, Servei de Pneumologia, Hospital Clínic, IDIBAPS, CibeRes, Barcelona. E- mail: miferrer@clinic.ub.es
PAPER DE LA VNI EN LA RETIRADA DE LA VENTILACIÓ INVASIVA I FRACÀS D EXTUBACIÓ Dr. Miquel Ferrer UVIIR, Servei de Pneumologia, Hospital Clínic, IDIBAPS, CibeRes, Barcelona. E- mail: miferrer@clinic.ub.es
Cough Augmentation in Subjects With Duchenne Muscular Dystrophy: Comparison of Air Stacking via a Resuscitator Bag Versus Mechanical Ventilation
 Cough Augmentation in Subjects With Duchenne Muscular Dystrophy: Comparison of Air Stacking via a Resuscitator Bag Versus Mechanical Ventilation Michel Toussaint PhD, Kurt Pernet MPhysio, Marc Steens MPhysio,
Cough Augmentation in Subjects With Duchenne Muscular Dystrophy: Comparison of Air Stacking via a Resuscitator Bag Versus Mechanical Ventilation Michel Toussaint PhD, Kurt Pernet MPhysio, Marc Steens MPhysio,
AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL
 AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL A. Definition of Therapy: 1. Cough machine: 4 sets of 5 breaths with a goal of I:E pressures approximately the same of 30-40. Inhale time = 1 second, exhale
AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL A. Definition of Therapy: 1. Cough machine: 4 sets of 5 breaths with a goal of I:E pressures approximately the same of 30-40. Inhale time = 1 second, exhale
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Respiratory Management of Facioscapulohumeral Muscular Dystrophy. Nicholas S. Hill, MD Tufts Medical Center Boston, MA
 Respiratory Management of Facioscapulohumeral Muscular Dystrophy Nicholas S. Hill, MD Tufts Medical Center Boston, MA Respiratory Involvement in FSHD Very variable time of onset rate of progression Muscles
Respiratory Management of Facioscapulohumeral Muscular Dystrophy Nicholas S. Hill, MD Tufts Medical Center Boston, MA Respiratory Involvement in FSHD Very variable time of onset rate of progression Muscles
MINERVA MEDICA COPYRIGHT
 EUR J PHYS REHABIL MED 2010;46:581-97 Physical medicine respiratory muscle aids to avert respiratory complications of pediatric chest wall and vertebral deformity and muscle dysfunction The purpose of
EUR J PHYS REHABIL MED 2010;46:581-97 Physical medicine respiratory muscle aids to avert respiratory complications of pediatric chest wall and vertebral deformity and muscle dysfunction The purpose of
UCH WEANING FROM MECHANICAL VENTILATION PATHWAY
 UCH WEANING FROM MECHANICAL VENTILATION PATHWAY WAKE WARM AND WEAN. POST OPERATIVE PATIENTS WHO HAVE BEEN VENTILATED < 24 HOURS DAILY EXTUBATION SCREEN A DAILY SCREEN TO BE CARRIED OUT ON ALL PATIENTS
UCH WEANING FROM MECHANICAL VENTILATION PATHWAY WAKE WARM AND WEAN. POST OPERATIVE PATIENTS WHO HAVE BEEN VENTILATED < 24 HOURS DAILY EXTUBATION SCREEN A DAILY SCREEN TO BE CARRIED OUT ON ALL PATIENTS
Noninvasive Mechanical Ventilation in Children ศ.พญ.อร ณวรรณ พฤทธ พ นธ หน วยโรคระบบหายใจเด ก ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร โรงพยาบาลรามาธ บด
 Noninvasive Mechanical Ventilation in Children ศ.พญ.อร ณวรรณ พฤทธ พ นธ หน วยโรคระบบหายใจเด ก ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร โรงพยาบาลรามาธ บด Noninvasive Mechanical Ventilation Provide support without
Noninvasive Mechanical Ventilation in Children ศ.พญ.อร ณวรรณ พฤทธ พ นธ หน วยโรคระบบหายใจเด ก ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร โรงพยาบาลรามาธ บด Noninvasive Mechanical Ventilation Provide support without
Operation Manual for clinical use of SIARE Pulsar
 Operation Manual for clinical use of SIARE Pulsar This manual is for clinical use only 1-12 INDEX 1) Indications /Contraindications and cautions 2) Questions to ask before using a MI-E machine 3) Guideline
Operation Manual for clinical use of SIARE Pulsar This manual is for clinical use only 1-12 INDEX 1) Indications /Contraindications and cautions 2) Questions to ask before using a MI-E machine 3) Guideline
POLICY. Number: Title: APPLICATION OF NON INVASIVE VENTILATION FOR ACUTE RESPIRATORY FAILURE. Authorization
 POLICY Number: 7311-60-024 Title: APPLICATION OF NON INVASIVE VENTILATION FOR ACUTE RESPIRATORY FAILURE Authorization [ ] President and CEO [ x ] Vice President, Finance and Corporate Services Source:
POLICY Number: 7311-60-024 Title: APPLICATION OF NON INVASIVE VENTILATION FOR ACUTE RESPIRATORY FAILURE Authorization [ ] President and CEO [ x ] Vice President, Finance and Corporate Services Source:
Do Not Cite. For Public Comment Period DRAFT MEASURE #3: Evaluation of Pulmonary Status Ordered MUSCULAR DYSTROPHY
 MEASURE #3: Evaluation of Pulmonary Status Ordered MUSCULAR DYSTROPHY Measure Description All patients diagnosed with a muscular dystrophy who had a pulmonary status evaluation* ordered. Measure Components
MEASURE #3: Evaluation of Pulmonary Status Ordered MUSCULAR DYSTROPHY Measure Description All patients diagnosed with a muscular dystrophy who had a pulmonary status evaluation* ordered. Measure Components
Keeping Patients Off the Vent: Bilevel, HFNC, Neither?
 Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
Keeping Patients Off the Vent: Bilevel, HFNC, Neither? Robert Kempainen, MD Pulmonary and Critical Care Medicine Hennepin County Medical Center University of Minnesota School of Medicine Objectives Summarize
Abbreviations: DMD=Duchenne muscular dystrophy; IPPV=intermittent positive pressure ventilation; Sa0 2
 Prevention of Pulmonary Morbidity for Patients With Duchenne Muscular Dystrophy* John R. Bach, MD, FCCP; Yuka Ishikawa, MD; and Heakyung Kim, MD Study objective: To evaluate the effects of a new respiratory
Prevention of Pulmonary Morbidity for Patients With Duchenne Muscular Dystrophy* John R. Bach, MD, FCCP; Yuka Ishikawa, MD; and Heakyung Kim, MD Study objective: To evaluate the effects of a new respiratory
Predictors of Successful Noninvasive Ventilation Treatment for Patients Suffering Acute Respiratory Failure
 ORIGINAL ARTICLE Predictors of Successful Noninvasive Ventilation Treatment for Patients Suffering Acute Respiratory Failure Ming-Shian Lin 1, How-Ran Guo 2,3, Ming-Hua Huang 4, Cheng-Ren Chen 1, Chen-Long
ORIGINAL ARTICLE Predictors of Successful Noninvasive Ventilation Treatment for Patients Suffering Acute Respiratory Failure Ming-Shian Lin 1, How-Ran Guo 2,3, Ming-Hua Huang 4, Cheng-Ren Chen 1, Chen-Long
Interdisciplinary Care of the Patient with Amyotrophic Lateral Sclerosis Respiratory Therapy Care
 Peggy Cox, RRT, RN Frazier Rehab Institute Pulmonary Rehab Interdisciplinary Care of the Patient with Amyotrophic Lateral Sclerosis Respiratory Therapy Care Disclosure I have the following relevant financial
Peggy Cox, RRT, RN Frazier Rehab Institute Pulmonary Rehab Interdisciplinary Care of the Patient with Amyotrophic Lateral Sclerosis Respiratory Therapy Care Disclosure I have the following relevant financial
Hypoventilation? Obstructive Sleep Apnea? Different Tests, Different Treatment
 Hypoventilation? Obstructive Sleep Apnea? Different Tests, Different Treatment Judith R. Fischer, MSLS, Editor, Ventilator-Assisted Living (fischer.judith@sbcglobal.net) Thanks to Josh Benditt, MD, University
Hypoventilation? Obstructive Sleep Apnea? Different Tests, Different Treatment Judith R. Fischer, MSLS, Editor, Ventilator-Assisted Living (fischer.judith@sbcglobal.net) Thanks to Josh Benditt, MD, University
Limits of Effective Cough-Augmentation Techniques in Patients With Neuromuscular Disease
 Limits of Effective Cough-Augmentation Techniques in Patients With Neuromuscular Disease Michel Toussaint PT PhD, Louis J Boitano MSc RRT, Vincent Gathot MSc PT, Marc Steens MSc PT, and Philippe Soudon
Limits of Effective Cough-Augmentation Techniques in Patients With Neuromuscular Disease Michel Toussaint PT PhD, Louis J Boitano MSc RRT, Vincent Gathot MSc PT, Marc Steens MSc PT, and Philippe Soudon
Mechanical Insufflation-Exsufflation Versus Conventional Chest Physiotherapy in Children With Cerebral Palsy
 Mechanical Insufflation-Exsufflation Versus Conventional Chest Physiotherapy in Children With Cerebral Palsy Rasintra Siriwat MD, Jitladda Deerojanawong MD, Suchada Sritippayawan MD, Sumalee Hantragool
Mechanical Insufflation-Exsufflation Versus Conventional Chest Physiotherapy in Children With Cerebral Palsy Rasintra Siriwat MD, Jitladda Deerojanawong MD, Suchada Sritippayawan MD, Sumalee Hantragool
Measure #6: ALS Noninvasive Ventilation Treatment for Respiratory Insufficiency Discussed Amyotrophic Lateral Sclerosis
 Measure #6: ALS Noninvasive Ventilation Treatment for Respiratory Insufficiency Discussed Amyotrophic Lateral Sclerosis Measure Description Percentage of patients diagnosed with ALS and respiratory insufficiency
Measure #6: ALS Noninvasive Ventilation Treatment for Respiratory Insufficiency Discussed Amyotrophic Lateral Sclerosis Measure Description Percentage of patients diagnosed with ALS and respiratory insufficiency
High Flow Oxygen Therapy in Acute Respiratory Failure. Laurent Brochard Toronto
 High Flow Oxygen Therapy in Acute Respiratory Failure Laurent Brochard Toronto Conflicts of interest Our clinical research laboratory has received research grants for clinical research projects from the
High Flow Oxygen Therapy in Acute Respiratory Failure Laurent Brochard Toronto Conflicts of interest Our clinical research laboratory has received research grants for clinical research projects from the
Mechanical Ventilation Principles and Practices
 Mechanical Ventilation Principles and Practices Dr LAU Chun Wing Arthur Department of Intensive Care Pamela Youde Nethersole Eastern Hospital 6 October 2009 In this lecture, you will learn Major concepts
Mechanical Ventilation Principles and Practices Dr LAU Chun Wing Arthur Department of Intensive Care Pamela Youde Nethersole Eastern Hospital 6 October 2009 In this lecture, you will learn Major concepts
Management of Ventilatory Insufficiency in Neuromuscular Patients Using Mechanical Ventilator Supported by the Korean Government
 ORIGINAL ARTICLE Rehabilitation & Sports Medicine http://dx.doi.org/0.3346/jkms.06.3.6.976 J Korean Med Sci 06; 3: 976-98 Management of Ventilatory Insufficiency in Neuromuscular Patients Using Mechanical
ORIGINAL ARTICLE Rehabilitation & Sports Medicine http://dx.doi.org/0.3346/jkms.06.3.6.976 J Korean Med Sci 06; 3: 976-98 Management of Ventilatory Insufficiency in Neuromuscular Patients Using Mechanical
NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity
 NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Use of NIV 1998-2010 50 45 40 35 30 25 20 15 10 5 0 1998
NIV in Acute Respiratory Failure: Where we fail? Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Use of NIV 1998-2010 50 45 40 35 30 25 20 15 10 5 0 1998
Noninvasive ventilation: Selection of patient, interfaces, initiation and weaning
 CME article Johnson S, et al: Noninvasive ventilation Noninvasive ventilation: Selection of patient, interfaces, initiation and weaning Saumy Johnson, Ramesh Unnikrishnan * Email: ramesh.unnikrishnan@manipal.edu
CME article Johnson S, et al: Noninvasive ventilation Noninvasive ventilation: Selection of patient, interfaces, initiation and weaning Saumy Johnson, Ramesh Unnikrishnan * Email: ramesh.unnikrishnan@manipal.edu
Home Mechanical Ventilation. Anthony Bateman
 Home Mechanical Ventilation Anthony Bateman What is Long Term Ventilation? LTV is the provision of respiratory support to individuals with non-acute respiratory failure Progression of expected disease
Home Mechanical Ventilation Anthony Bateman What is Long Term Ventilation? LTV is the provision of respiratory support to individuals with non-acute respiratory failure Progression of expected disease
Dr. CK NG Department of Medicine Queen Elizabeth Hospital Kowloon Central Cluster
 Ng CK, O WH, Lit MPK, Lee KH, Chan HF, Chan YC, Cheung YF, Hui YT, Chu S, Chong HM, Yu David, Chan JHM and Chan JWM Dr. CK NG Department of Medicine Queen Elizabeth Hospital Kowloon Central Cluster Neuromuscular
Ng CK, O WH, Lit MPK, Lee KH, Chan HF, Chan YC, Cheung YF, Hui YT, Chu S, Chong HM, Yu David, Chan JHM and Chan JWM Dr. CK NG Department of Medicine Queen Elizabeth Hospital Kowloon Central Cluster Neuromuscular
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Motor neurone disease: the use of non-invasive ventilation in the management of motor neurone disease 1.1 Short title Motor
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Motor neurone disease: the use of non-invasive ventilation in the management of motor neurone disease 1.1 Short title Motor
Index. sleep.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acquired central hypoventilation syndrome, NPPV in children with, 475 Acute cardiogenic pulmonary edema, PAP therapy in, 394 395 Adaptive
Index Note: Page numbers of article titles are in boldface type. A Acquired central hypoventilation syndrome, NPPV in children with, 475 Acute cardiogenic pulmonary edema, PAP therapy in, 394 395 Adaptive
(Non)-invasive ventilation: transition from PICU to home. Christian Dohna-Schwake
 (Non)-invasive ventilation: transition from PICU to home Christian Dohna-Schwake Increased use of NIV in PICUs over last 15 years First choice of respiratory support in many diseases Common temporary indications:
(Non)-invasive ventilation: transition from PICU to home Christian Dohna-Schwake Increased use of NIV in PICUs over last 15 years First choice of respiratory support in many diseases Common temporary indications:
Is mechanical insufflation exsufflation (M-IE) useful in children with neuromuscular disease?
 Is mechanical insufflation exsufflation (M-IE) useful in children with neuromuscular disease? Cross Canada Rounds ProCon debate January 2017 Dr K Keown Respiratory Fellow BC Children s Hospital Structure
Is mechanical insufflation exsufflation (M-IE) useful in children with neuromuscular disease? Cross Canada Rounds ProCon debate January 2017 Dr K Keown Respiratory Fellow BC Children s Hospital Structure
Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo
 Instant dowload and all chapters Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo https://testbanklab.com/download/test-bank-pilbeams-mechanical-ventilation-physiologicalclinical-applications-6th-edition-cairo/
Instant dowload and all chapters Test Bank Pilbeam's Mechanical Ventilation Physiological and Clinical Applications 6th Edition Cairo https://testbanklab.com/download/test-bank-pilbeams-mechanical-ventilation-physiologicalclinical-applications-6th-edition-cairo/
ORIGINAL CONTRIBUTION. Noninvasive Ventilation in Myasthenic Crisis. is defined by the appearance
 ORIGINAL CONTRIBUTION Noninvasive Ventilation in Myasthenic Crisis Janaka Seneviratne, MBBS; Jay Mandrekar, PhD; Eelco F. M. Wijdicks, MD; Alejandro A. Rabinstein, MD Background: Myasthenic crisis (MC)
ORIGINAL CONTRIBUTION Noninvasive Ventilation in Myasthenic Crisis Janaka Seneviratne, MBBS; Jay Mandrekar, PhD; Eelco F. M. Wijdicks, MD; Alejandro A. Rabinstein, MD Background: Myasthenic crisis (MC)
NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP)
 Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Introduction NIV - BI-LEVEL POSITIVE AIRWAY PRESSURE (BIPAP) Noninvasive ventilation (NIV) is a method of delivering oxygen by positive pressure mask that allows for the prevention or postponement of invasive
Benefit of Forced Expiratory Technique for Weak Cough in a Patient with Bulbar Onset Amyotrophic Lateral Sclerosis
 Original Article Benefit of Forced Expiratory Technique for Weak Cough in a Patient with Bulbar Onset Amyotrophic Lateral Sclerosis J. Phys. Ther. Sci. 16: 137 141, 2004 MITSUAKI ISHII, RPT 1) 1) Department
Original Article Benefit of Forced Expiratory Technique for Weak Cough in a Patient with Bulbar Onset Amyotrophic Lateral Sclerosis J. Phys. Ther. Sci. 16: 137 141, 2004 MITSUAKI ISHII, RPT 1) 1) Department
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION
 CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
CONTINUOUS POSITIVE AIRWAY PRESSURE (CPAP) DEFINITION Method of maintaining low pressure distension of lungs during inspiration and expiration when infant breathing spontaneously Benefits Improves oxygenation
Hyperinflation Therapy and the Tools to Accomplish It!! Bill Barnes, RN, RRT Good Shepherd Rehabilitation Network
 Hyperinflation Therapy and the Tools to Accomplish It!! Bill Barnes, RN, RRT Good Shepherd Rehabilitation Network HYPERINFLATION THERAPY Challenges in Post Acute Care Deconditioning Malnutrition Hydration
Hyperinflation Therapy and the Tools to Accomplish It!! Bill Barnes, RN, RRT Good Shepherd Rehabilitation Network HYPERINFLATION THERAPY Challenges in Post Acute Care Deconditioning Malnutrition Hydration
Airway clearance in neuromuscular weakness
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY REVIEW Airway clearance in neuromuscular weakness LEANNE MAREE GAULD MBBS FRACP MD Royal Children's Hospital, Herston, Australia. Correspondence to Dr Leanne Maree
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY REVIEW Airway clearance in neuromuscular weakness LEANNE MAREE GAULD MBBS FRACP MD Royal Children's Hospital, Herston, Australia. Correspondence to Dr Leanne Maree
The Effect of a Mechanical Ventilation Discontinuation Protocol in Patients with Simple and Difficult Weaning: Impact on Clinical Outcomes
 The Effect of a Mechanical Ventilation Discontinuation Protocol in Patients with Simple and Difficult Weaning: Impact on Clinical Outcomes Pooja Gupta MD, Katherine Giehler RRT, Ryan W Walters MSc, Katherine
The Effect of a Mechanical Ventilation Discontinuation Protocol in Patients with Simple and Difficult Weaning: Impact on Clinical Outcomes Pooja Gupta MD, Katherine Giehler RRT, Ryan W Walters MSc, Katherine
Respiratory Muscle Strength and Cough Capacity in Patients with Duchenne Muscular Dystrophy
 Yonsei Medical Journal Vol. 47, No. 2, pp. 184-190, 2006 Respiratory Muscle Strength and Cough Capacity in Patients with Duchenne Muscular Dystrophy Seong-Woong Kang, Yeoun-Seung Kang, Hong-Seok Sohn,
Yonsei Medical Journal Vol. 47, No. 2, pp. 184-190, 2006 Respiratory Muscle Strength and Cough Capacity in Patients with Duchenne Muscular Dystrophy Seong-Woong Kang, Yeoun-Seung Kang, Hong-Seok Sohn,
Airway Clearance Applications in the Elderly and in Patients With Neurologic or Neuromuscular Compromise
 Airway Clearance Applications in the Elderly and in Patients With Neurologic or Neuromuscular Compromise Carl F Haas MLS RRT FAARC, Paul S Loik RRT, and Steven E Gay MD MSc Introduction The Normal Clearance
Airway Clearance Applications in the Elderly and in Patients With Neurologic or Neuromuscular Compromise Carl F Haas MLS RRT FAARC, Paul S Loik RRT, and Steven E Gay MD MSc Introduction The Normal Clearance
Weaning guidelines for Spinal Cord Injured patients in Critical Care Units
 RISCI Respiratory Information for Spinal Cord Injury UK Weaning guidelines for Spinal Cord Injured patients in Critical Care Units Introduction It is an unfortunate fact that Spinal Cord Injury Centres
RISCI Respiratory Information for Spinal Cord Injury UK Weaning guidelines for Spinal Cord Injured patients in Critical Care Units Introduction It is an unfortunate fact that Spinal Cord Injury Centres
Home Mechanical Ventilation:
 Home Mechanical Ventilation: A Global A Global View View Nicholas Hill MD Tufts Medical Center Boston MA Nicholas S Hill MD Tufts Medical Center Boston, MA Disclosures Research Grants MAB Breathe Technologies
Home Mechanical Ventilation: A Global A Global View View Nicholas Hill MD Tufts Medical Center Boston MA Nicholas S Hill MD Tufts Medical Center Boston, MA Disclosures Research Grants MAB Breathe Technologies
When a patient is not able to fully sustain the muscular work of breathing. A Ventilator Requirement Index ORIGINAL RESEARCH ARTICLE.
 Authors: John R. Bach, MD Miguel Goncalves, RT Michal Eisenberg, MD Yuka Ishikawa, MD Eric Altschuler, MD João Carlos Winck, MD, PhD Eugene Komaroff, PhD Affiliations: From the Department of Physical Medicine
Authors: John R. Bach, MD Miguel Goncalves, RT Michal Eisenberg, MD Yuka Ishikawa, MD Eric Altschuler, MD João Carlos Winck, MD, PhD Eugene Komaroff, PhD Affiliations: From the Department of Physical Medicine
King s Research Portal
 King s Research Portal DOI: 10.1002/14651858.CD011833.pub2 Document Version Publisher's PDF, also known as Version of record Link to publication record in King's Research Portal Citation for published
King s Research Portal DOI: 10.1002/14651858.CD011833.pub2 Document Version Publisher's PDF, also known as Version of record Link to publication record in King's Research Portal Citation for published
Evaluation of cough peak expiratory flow as a predictor of successful mechanical ventilation discontinuation: a narrative review of the literature
 Jiang et al. Journal of Intensive Care (2017) 5:33 DOI 10.1186/s40560-017-0229-9 REVIEW Evaluation of cough peak expiratory flow as a predictor of successful mechanical ventilation discontinuation: a narrative
Jiang et al. Journal of Intensive Care (2017) 5:33 DOI 10.1186/s40560-017-0229-9 REVIEW Evaluation of cough peak expiratory flow as a predictor of successful mechanical ventilation discontinuation: a narrative
Spontaneous Breathing Trial and Mechanical Ventilation Weaning Process
 Page 1 of 5 ASSESSMENT INTERVENTION Patient receiving mechanical ventilation Baseline ventilatory mode/ settings RT and RN to assess criteria 1 for SBT Does patient meet criteria? RT to initiate SBT Does
Page 1 of 5 ASSESSMENT INTERVENTION Patient receiving mechanical ventilation Baseline ventilatory mode/ settings RT and RN to assess criteria 1 for SBT Does patient meet criteria? RT to initiate SBT Does
Prolonged Invasive Ventilation Following Acute Ventilatory Failure in COPD* Weaning Results, Survival, and the Role of Noninvasive Ventilation
 CHEST Prolonged Invasive Ventilation Following Acute Ventilatory Failure in COPD* Weaning Results, Survival, and the Role of Noninvasive Ventilation Timothy G. Quinnell, MRCP; Samantha Pilsworth, BSc;
CHEST Prolonged Invasive Ventilation Following Acute Ventilatory Failure in COPD* Weaning Results, Survival, and the Role of Noninvasive Ventilation Timothy G. Quinnell, MRCP; Samantha Pilsworth, BSc;
I Need to Cough Ways to Keep Your Airways Clear
 I Need to Cough Ways to Keep Your Airways Clear 2018 Annual Cure SMA Conference Richard Kravitz, MD Duke University School of Medicine Duke University Medical Center Durham, North Carolina Presenters Jane
I Need to Cough Ways to Keep Your Airways Clear 2018 Annual Cure SMA Conference Richard Kravitz, MD Duke University School of Medicine Duke University Medical Center Durham, North Carolina Presenters Jane
Noninvasive Ventilation: Non-COPD Applications
 Noninvasive Ventilation: Non-COPD Applications NONINVASIVE MECHANICAL VENTILATION Why Noninvasive Ventilation? Avoids upper A respiratory airway trauma system lacerations, protective hemorrhage strategy
Noninvasive Ventilation: Non-COPD Applications NONINVASIVE MECHANICAL VENTILATION Why Noninvasive Ventilation? Avoids upper A respiratory airway trauma system lacerations, protective hemorrhage strategy
7 Initial Ventilator Settings, ~05
 Abbreviations (inside front cover and back cover) PART 1 Basic Concepts and Core Knowledge in Mechanical -- -- -- -- 1 Oxygenation and Acid-Base Evaluation, 1 Review 01Arterial Blood Gases, 2 Evaluating
Abbreviations (inside front cover and back cover) PART 1 Basic Concepts and Core Knowledge in Mechanical -- -- -- -- 1 Oxygenation and Acid-Base Evaluation, 1 Review 01Arterial Blood Gases, 2 Evaluating
Policy Specific Section: October 1, 2010 January 21, 2013
 Medical Policy Bi-level Positive Airway Pressure (BPAP/NPPV) Type: Medical Necessity/Not Medical Necessity Policy Specific Section: Durable Medical Equipment Original Policy Date: Effective Date: October
Medical Policy Bi-level Positive Airway Pressure (BPAP/NPPV) Type: Medical Necessity/Not Medical Necessity Policy Specific Section: Durable Medical Equipment Original Policy Date: Effective Date: October
Hospital outcomes and long-term survival after referral to a specialized weaning unit
 British Journal of Anaesthesia, 118 (4): 563 9 (2017) doi: 10.1093/bja/aex031 Critical Care CRITICAL CARE Hospital outcomes and long-term survival after referral to a specialized weaning unit M. G. Davies*,
British Journal of Anaesthesia, 118 (4): 563 9 (2017) doi: 10.1093/bja/aex031 Critical Care CRITICAL CARE Hospital outcomes and long-term survival after referral to a specialized weaning unit M. G. Davies*,
