Artificial External Glottic Device for Passive Lung Insufflation
|
|
|
- Cory Stevenson
- 6 years ago
- Views:
Transcription
1 Original Article pissn: , eissn: Yonsei Med J 52(6): , 2011 Artificial External Glottic Device for Passive Lung Insufflation Dong Hyun Kim, 1 Seong-Woong Kang, 2 Yoon Ghil Park, 2 Won Ah Choi, 2 and Hye Ree Lee 3 1 Department of Rehabilitation Medicine, College of Medicine, Kyung Hee University, Seoul; 2 Department of Rehabilitation Medicine and Rehabilitation Institute of Muscular Disease, Yonsei University College of Medicine, Seoul; 3 Department of Family Medicine, Yonsei University College of Medicine, Seoul, Korea. Received: March 18, 2011 Revised: August 22, 2011 Accepted: August 23, 2011 Corresponding author: Dr. Won Ah Choi, Department of Rehabilitation Medicine and Rehabilitation Institute of Muscular Disease, Yonsei University College of Medicine 211 Eonju-ro, Gangnam-gu, Seoul , Korea. Tel: , Fax: skyler02@wku.ac.kr The authors have no financial conflicts of interest. Purpose: For patients with neuromuscular disease, air stacking, which inflates the lungs to deep volumes, is important for many reasons. However, neuromuscular patients with severe glottic dysfunction or indwelling tracheostomy tubes cannot air stack effectively. For these patients, we developed a device that permits deep lung insufflations substituting for glottic function. Materials and Methods: Thirty-seven patients with bulbar-innervated muscle weakness and/or tracheostomies were recruited. Twenty-three had amyotrophic lateral sclerosis, and 14 were tetraplegic patients due to cervical spinal cord injury. An artificial external glottic device (AEGD) was used to permit passive deep lung insufflation. In order to confirm the utility of AEGD, vital capacity, maximum insufflation capacity (MIC), and lung insufflation capacity (LIC) with AEGD (LICA) were measured. Results: For 30 patients, MICs were initially zero. However, with the use of the AEGD, LICA was measurable for all patients. The mean LICA was 1,622.7±526.8 ml. Although MIC was measurable for the remaining 7 patients without utilizing the AEGD, it was significantly less than LICA, which was 1,084.3±259.9 ml and 1,862.9±248 ml, respectively (p<0.05). Conclusion: The AEGD permits lung insufflation by providing deeper lung volumes than possible by air stacking. Key Words: Air stacking, lung insufflation, maximal insufflation capacity INTRODUCTION Copyright: Yonsei University College of Medicine 2011 This is an Open Access article distributed under the terms of the Creative Commons Attribution Non- Commercial License ( licenses/by-nc/3.0) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Neuromuscular disease (NMD) is characterized by progressive weakening of skeletal, respiratory, and or bulbar-innervated muscles. 1 NMD patients have decrements in vital capacity (VC), lung and chest wall compliance, and coughing capacity. These patients cannot fully expand their chests, which leads to stiffening of the joints and tissues of the rib cage. 1,2 This in turn results in a reduction in chest wall compliance. 2 Reduction in lung and chest wall compliance may also be related to alterations in the elastic properties of lung tissues by chronically limited range of activity. 3 Normal breathing consists of varying tidal volumes with intermittent deep breaths or sighs. 1,4 Even in people with normal lungs, periodic hyperinflation is required to prevent closure of lung units. 1 For NMD patients, who cannot expand the lungs fully due to respiratory muscle weakness, periodic deep 972
2 AEGD for Passive Lung Insufflation insufflation by air-stacking is essential. 1 Air stacking involves the use of a manual resuscitator or a volume-cycled ventilator to deliver volumes of air that are consecutively held by glottic closure until no more air can be retained. 5 The maximum lung volume that can be held by air stacking is the maximum insufflation capacity (MIC). 6 In 2000, Kang and Bach 1 demonstrated that the MIC could significantly exceed VC for patients with NMD. However, patients presenting weak or no glottic closure due to bulbar muscle dysfunction or indwelling tracheostomy cannot air stack. Lung insufflation can only be given by bypassing glottis dysfunction in these patients, and the maximum passive lung insufflation volume achieved in this manner is defined as the lung insufflation capacity (LIC). 7 In this study, we designed a device that provides external control of an artificial glottic opening and closure for patients with bulbar innervated muscle weakness or who have indwelling tracheostomy tubes. We attempted to investigate the effectiveness of air stacking by replacing dysfunctional glottises with the newly designed device. Fig. 1. A fully assembled apparatus for measuring LIC with the artificial external glottic device (LICA): a resuscitation bag is connected to the AEGD. Connection part (A); Control part (B). LIC, lung insufflation capacity; AEGD, artificial external glottic device; LICA, LIC with AGED. One-way valve Insufflation port MATERIALS AND METHODS Patients The study consisted of 37 subjects with bulbar innervated muscle weakness or indwelling tracheostomy tubes. Bulbar-innervated muscle weakness was defined by clinically apparent dysarthria and/or dysphagia and impaired glottic function. Exclusion criteria were: inability to cooperate due to severe cognitive impairment; medical instability; and severe overriding lung and airway disease. A Patient connection port Exsufflation port Methods Artificial external glottic device (AEGD) An AEGD has a connection and a control part (Fig. 1). The connection part is a T-shaped plastic adaptor. The control part is designed to artificially modulate glottic opening and closure. The connection part As shown in Fig. 2, the connection part consists of a patient connection port, the insufflation port, and the exhalation port. The patient connection port is connected directly to the patient s airway through a tracheostomy tube or an oronasal mask (Fig. 2A). A manual resuscitator delivers air via B Fig. 2. Connection part of the artificial external glottic device (AEGD). (A) Disconnected view of the connection part. (B) Photograph of the connection part. 973
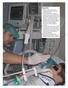
3 Dong Hyun Kim, et al. Thirty-seven patients (24 males, 13 females; mean age, 48; range, years) met the criteria, and were included in this study. Mean±standard deviation values of all the pathe insufflation port, which is located in the middle of the connection part and at a right angle. It has a one-way valve (Fig. 2A). The exsufflation port is connected to the control part. The control part The control part of the AEGD artificially modulates glottic a A a B b b Fig. 3. Diagram of the control part of the artificial external glottic device (AEGD). (A) Demounted view of the control part: control part is connected to the connection part through (a), and measurement apparatus such as a spirometer through (b), the external glottic function is controlled by an externally exposed part (c) of the pushing bar a', air flows from (a) to (b) like an opening of a normal glottis. (B) Photograph of the control part of AEGD: ports connecting to the connection part (a); to the measurement apparatus such as a spirometer (b); and to the external control of the glottis (c). c c a' opening and closure by pushing a button. The tip of the button protrudes from the outer wall of the control part. Pushing the button permits the air to flow from the patient to the spirometer connected to the control part. When the button is pressed, the concave portion of the bar is exposed to the connecting tube, and the patient can exhale. A spring is inserted in the connecting axis of the bar, and this axis is designed to pass through the center of the hole in a disc (Fig. 3). When the button is not pressed, airflow from the connecting tube is completely interrupted by the bar, which is fixed due to the recoil of the spring and support action of the disc hole. Therefore, patients are permitted to exhale after passive lung insufflations by pressing the AEGD button to open. Clinical evaluation This study was approved by the institutional review board, and informed consent was obtained from all of the study candidates. All lung volumes were measured by Micro Spirometer (Micro Medical Ltd., Rochester, Kent, UK) in a sitting position, and recorded as the greatest observed value in at least three attempts. Outcome measurements were as follows: 1) For the measurement of VC, all subjects were asked to take a deep breath, and then exhale the maximally held volume of air into the spirometer. 2) MIC was then measured as described. 1 The maximum value that was observed in at least three attempts was recorded. 3) LIC with AEGD (LICA) was measured by using the same manual resuscitator with MIC after connecting an AEGD to the measurement apparatus (Fig. 4). The largest value in three or more attempts was recorded as the LICA. Data analysis A paired t-test was used to determine the statistical significance between VC and LICA, and MIC and LICA. The Kruskal-Wallis method was used to determine the statistical significance among VC, MIC, and LICA. Data was analyzed using SPSS 12.0 b, and a p-value <0.05 was considered statistically significant. RESULTS Fig. 4. Actual application of the apparatus for the measurement of LICA. LICA, LIC with AEGD. 974
4 AEGD for Passive Lung Insufflation tients totaled were 794±391 ml for VC, 1,084±260 ml for MIC, and 1,668±493 ml for LICA measurements. When candidates were divided by diagnosis (Table 1), only 6 from the ALS group and 1 from the cervical spinal cord injury group could somewhat air stack. The remaining 30 patients failed to air stack due to glottic dysfunction, thus MICs were checked as zero. AEGD either maximized the ability to air stack or enabled passive lung insufflation even for those who initially failed. Consequently, LICA significantly exceeded the MIC for all of the candidates (p<0.05). In accordance with underlying pulmonary function, 37 patients were subdivided into groups 1, 2 or 3 (Table 2). Group 1 included three patients who presented severe inspiratory and expiratory muscle weakness with tracheostomies. Since their respiratory muscles were too weak to even take a deep breath in and out, VCs and MICs were essentially 0 ml. Group 2 included 27 patients whose MICs were initially 0 ml. After applying the AEGD, LICAs were successfully measured in both groups. The other 7 patients who had the minimal residual glottic function to hold and stack a little volume of air were named as Group 3. Although MIC-VC difference was greater than 0 ml, when using AEGD, the LICA was greater than MIC or VC in this group (p<0.05). DISCUSSION Just as limb range of motion helps avert limb contractures, assisted lung insufflations help to maintain compliance for patients with diminished VCs. 1 However, NMDs with glottic dysfunction and/or tracheostomized patients can not benefit from air stacking, because they cannot prevent leakage of inhaled air from the lungs. 8,9 Besides the inability to maintain pulmonary compliance, these patients also present difficulty with coughing due to respiratory muscle weakness and/or glottic dysfunction. Thus effective cough mechanisms can be hindered, which in turn results in the failure of eliminating airway secretions. 10,11 Bach had already defined a simple technique to provide deep lung insufflations, and called the deep passive lung insufflations attained this way as LIC. 7 He used a manual resuscitator connected to a spirometer, and simply occluded the expiratory port of the spirometer with fingers while providing an additional volume of air with the manual resuscitator bag. Through this method, he was not only able to give deep lung insufflations, but also quantified the volumes. In this study, on the other hand, we developed a clean, mechanical device to substitute for dysfunctional glottises. Despite the methodological difference, our handheld device is conceptually identical to Bach s simple method in providing deep lung insufflations and quantifying them. Although Bach s method is convenient in that does not require any device, AEGD is a clean technique that might provide more precise control and measurement of the glottic function by preventing possible air leaks. In addition, quantification of coughing ability was also possible with AEGD by changing the measurement apparatus to a peak flow meter. Table 1. Comparison of Pulmonary Function Parameters Under Diagnostic Classification Diagnosis No. Tracheostomy Age (yrs) VC (ml) LICA (ml) ALS ± ± ,543.9±438.7 SCI ± ± ,872.1±524.2 VC, vital capacity; LICA, lung insufflation capacity with artificial external glottic device; SD, standard deviation; ALS, amyotrophic lateral sclerosis; SCI, spinal cord injury. Mean values±sd (ml). Table 2. Comparison of Pulmonary Function Test Parameters Under Different Conditions VC (ml) MIC (ml) LICA (ml) Group 1 (n=3) UC UC 1,453.3±585.3 Group 2 (n=27) 780.4±424.7 UC 1,641.5±528.7* Group 3 (n=7) 850± ± ,862.9±248, VC, vital capacity; MIC, maximum insufflation capacity; LICA, lung insufflation capacity with the artificial external glottic device; SD, standard deviation; UC, uncheckable. Mean values±sd (ml). *p<0.05, comparison between VC and LICA in group 2. p<0.05, comparison between MIC and LICA in group 3. p<0.05, comparison among VC, MIC and LICA in group
5 Dong Hyun Kim, et al. Recruited candidates are another distinguishing factor. Although the previous study 7 presented a larger number of patients, the majority of the patients had relatively intact bulbar muscle function whose ability to air stack was spared. However, in this study, air stacking was essentially impossible in more than two thirds of the patients. About 70% of the candidates had tracheostomy tubes, and the remaining patients were bulbar-dominant ALS who showed severe glottic dysfunction. Limitations of this study include the fact that in the process of connecting the AEGD with measuring instruments, the value could be underestimated, because the exhaled air passes the connection system at a right-angled. Consequently, the fully assembled apparatus for measurement had a relatively long pathway for expiratory flow. Speed of the flow can also be a problem. Thus, measured MICA values may actually be greater than those reported in this study. In conclusion, NMD patients need to practice regular deep lung insufflations. The artificial external glottic device enables passive lung insufflations even for patients with severe bulbar-innervated muscle impairment or tracheostomy tubes, whose ability to air stack is poor. ACKNOWLEDGEMENTS This study was supported by a research grant of Jaewon Foundation for 2007 ( ). REFERENCES 1. Kang SW, Bach JR. Maximum insufflation capacity. Chest 2000; 118: Estenne M, Heilporn A, Delhez L, Yernault JC, De Troyer A. Chest wall stiffness in patients with chronic respiratory muscle weakness. Am Rev Respir Dis 1983;128: Estenne M, Gevenois PA, Kinnear W, Soudon P, Heilporn A, De Troyer A. Lung volume restriction in patients with chronic respiratory muscle weakness: the role of microatelectasis. Thorax 1993;48: Hoffman LA. Ineffective airway clearance related to neuromuscular dysfunction. Nurs Clin North Am 1987;22: Kang SW, Bach JR. Maximum insufflation capacity: vital capacity and cough flows in neuromuscular disease. Am J Phys Med Rehabil 2000;79: Bach JR, Bianchi C, Vidigal-Lopes M, Turi S, Felisari G. Lung inflation by glossopharyngeal breathing and air stacking in Duchenne muscular dystrophy. Am J Phys Med Rehabil 2007;86: Bach JR, Mahajan K, Lipa B, Saporito L, Goncalves M, Komaroff E. Lung insufflation capacity in neuromuscular disease. Am J Phys Med Rehabil 2008;87: Leith DE. Cough. In: Brain JD, Proctor D, Reid L, editors. Lung biology in health and disease. New York: Marcel Dekker; p Similowski T, Attali V, Bensimon G, Salachas F, Mehiri S, Arnulf I, et al. Diaphragmatic dysfunction and dyspnoea in amyotrophic lateral sclerosis. Eur Respir J 2000;15: Hanayama K, Ishikawa Y, Bach JR. Amyotrophic lateral sclerosis. Successful treatment of mucous plugging by mechanical insufflation-exsufflation. Am J Phys Med Rehabil 1997;76: Bach JR. Mechanical insufflation-exsufflation. Comparison of peak expiratory flows with manually assisted and unassisted coughing techniques. Chest 1993;104:
Neuromuscular diseases are characterized by progressive
 Maximum Insufflation Capacity* Seong-Woong Kang, MD, PhD; and John R. Bach, MD, FCCP Objective: To investigate the effect of deep lung insufflations on maximum insufflation capacities (MICs) and peak cough
Maximum Insufflation Capacity* Seong-Woong Kang, MD, PhD; and John R. Bach, MD, FCCP Objective: To investigate the effect of deep lung insufflations on maximum insufflation capacities (MICs) and peak cough
A Comparison of Cough Assistance Techniques in Patients with Respiratory Muscle Weakness
 Original Article Yonsei Med J 2016 Nov;57(6):1488-1493 pissn: 0513-5796 eissn: 1976-2437 A Comparison of Cough Assistance Techniques in Patients with Respiratory Muscle Weakness Sun Mi Kim 1,2, Won Ah
Original Article Yonsei Med J 2016 Nov;57(6):1488-1493 pissn: 0513-5796 eissn: 1976-2437 A Comparison of Cough Assistance Techniques in Patients with Respiratory Muscle Weakness Sun Mi Kim 1,2, Won Ah
How Respiratory Muscle Strength Correlates with Cough Capacity in Patients with Respiratory Muscle Weakness
 Original Article DOI 10.3349/ymj.2010.51.3.392 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(3): 392-397, 2010 How Respiratory Muscle Strength Correlates with Cough Capacity in Patients with Respiratory
Original Article DOI 10.3349/ymj.2010.51.3.392 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(3): 392-397, 2010 How Respiratory Muscle Strength Correlates with Cough Capacity in Patients with Respiratory
Respiratory Muscle Strength and Cough Capacity in Patients with Duchenne Muscular Dystrophy
 Yonsei Medical Journal Vol. 47, No. 2, pp. 184-190, 2006 Respiratory Muscle Strength and Cough Capacity in Patients with Duchenne Muscular Dystrophy Seong-Woong Kang, Yeoun-Seung Kang, Hong-Seok Sohn,
Yonsei Medical Journal Vol. 47, No. 2, pp. 184-190, 2006 Respiratory Muscle Strength and Cough Capacity in Patients with Duchenne Muscular Dystrophy Seong-Woong Kang, Yeoun-Seung Kang, Hong-Seok Sohn,
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the
 Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
MND Study Day. Martin Latham CNS Leeds Sleep Service
 MND Study Day Martin Latham CNS Leeds Sleep Service Objectives: Identifying individuals at risk. Understand issues related to NIV. Understand issues related to secretion management Improve outcomes. Identifying
MND Study Day Martin Latham CNS Leeds Sleep Service Objectives: Identifying individuals at risk. Understand issues related to NIV. Understand issues related to secretion management Improve outcomes. Identifying
Motor Neurone Disease NICE to manage Management of ineffective cough. Alex Long Specialist NIV/Respiratory physiotherapist June 2016
 Motor Neurone Disease NICE to manage Management of ineffective cough Alex Long Specialist NIV/Respiratory physiotherapist June 2016 Content NICE guideline recommendations Respiratory involvement in MND
Motor Neurone Disease NICE to manage Management of ineffective cough Alex Long Specialist NIV/Respiratory physiotherapist June 2016 Content NICE guideline recommendations Respiratory involvement in MND
Respiratory Management- Your Questions Answered! Michelle Chatwin, PhD Consultant Physiotherapist
 Respiratory Management- Your Questions Answered! Michelle Chatwin, PhD Consultant Physiotherapist Why Are People Affected Differently Neuromuscular Disease; A Spectrum Its severity varies widely within
Respiratory Management- Your Questions Answered! Michelle Chatwin, PhD Consultant Physiotherapist Why Are People Affected Differently Neuromuscular Disease; A Spectrum Its severity varies widely within
Airway clearance in neuromuscular weakness
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY REVIEW Airway clearance in neuromuscular weakness LEANNE MAREE GAULD MBBS FRACP MD Royal Children's Hospital, Herston, Australia. Correspondence to Dr Leanne Maree
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY REVIEW Airway clearance in neuromuscular weakness LEANNE MAREE GAULD MBBS FRACP MD Royal Children's Hospital, Herston, Australia. Correspondence to Dr Leanne Maree
Noninvasive Respiratory Management for Patients with Spinal Cord Injury and Neuromuscular Disease
 Review Article 2012 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran ISSN: 1735-0344 Tanaffos 2012; 11 (1): 7-11 TANAFFOS Noninvasive Respiratory Management for Patients with
Review Article 2012 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran ISSN: 1735-0344 Tanaffos 2012; 11 (1): 7-11 TANAFFOS Noninvasive Respiratory Management for Patients with
The objectives of this presentation are to
 1 The objectives of this presentation are to 1. Review the mechanics of airway clearance 2. Understand the difference between secretion mobilization and secretion clearance 3. Identify conditions that
1 The objectives of this presentation are to 1. Review the mechanics of airway clearance 2. Understand the difference between secretion mobilization and secretion clearance 3. Identify conditions that
[N] = No product variation, policy applies as stated [Y] = Standard product coverage varies from application of this policy, see below
![[N] = No product variation, policy applies as stated [Y] = Standard product coverage varies from application of this policy, see below [N] = No product variation, policy applies as stated [Y] = Standard product coverage varies from application of this policy, see below](/thumbs/94/119510114.jpg) Original Issue Date (Created): May 3, 2004 Most Recent Review Date (Revised): September 24, 2013 Effective Date: November 1, 2013 I. POLICY Mechanical insufflation-exsufflation (MI-E) may be considered
Original Issue Date (Created): May 3, 2004 Most Recent Review Date (Revised): September 24, 2013 Effective Date: November 1, 2013 I. POLICY Mechanical insufflation-exsufflation (MI-E) may be considered
Home Mechanical Ventilation in South Korea
 Original Article http://dx.doi.org/10.3349/ymj.2014.55.6.1729 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 55(6):1729-1735, 2014 Home Mechanical Ventilation in South Korea Dong Hyun Kim, 1 Seong-Woong
Original Article http://dx.doi.org/10.3349/ymj.2014.55.6.1729 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 55(6):1729-1735, 2014 Home Mechanical Ventilation in South Korea Dong Hyun Kim, 1 Seong-Woong
PULMONARY FUNCTION. VOLUMES AND CAPACITIES
 PULMONARY FUNCTION. VOLUMES AND CAPACITIES The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer (spiro = breath, meter = to measure). A bell spirometer
PULMONARY FUNCTION. VOLUMES AND CAPACITIES The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer (spiro = breath, meter = to measure). A bell spirometer
CoughAssist E70. More than just a comfortable cough. Flexible therapy that brings more comfort to your patients airway clearance
 CoughAssist E70 More than just a comfortable cough Flexible therapy that brings more comfort to your patients airway clearance Flexible, customisable loosening and clearing therapy An effective cough is
CoughAssist E70 More than just a comfortable cough Flexible therapy that brings more comfort to your patients airway clearance Flexible, customisable loosening and clearing therapy An effective cough is
Cough Augmentation in Subjects With Duchenne Muscular Dystrophy: Comparison of Air Stacking via a Resuscitator Bag Versus Mechanical Ventilation
 Cough Augmentation in Subjects With Duchenne Muscular Dystrophy: Comparison of Air Stacking via a Resuscitator Bag Versus Mechanical Ventilation Michel Toussaint PhD, Kurt Pernet MPhysio, Marc Steens MPhysio,
Cough Augmentation in Subjects With Duchenne Muscular Dystrophy: Comparison of Air Stacking via a Resuscitator Bag Versus Mechanical Ventilation Michel Toussaint PhD, Kurt Pernet MPhysio, Marc Steens MPhysio,
Preventing Respiratory Complications of Muscular Dystrophy
 Preventing Respiratory Complications of Muscular Dystrophy Jonathan D. Finder, MD Professor of Pediatrics University of Pittsburgh School of Medicine Children s Hospital of Pittsburgh Introduction Respiratory
Preventing Respiratory Complications of Muscular Dystrophy Jonathan D. Finder, MD Professor of Pediatrics University of Pittsburgh School of Medicine Children s Hospital of Pittsburgh Introduction Respiratory
The great majority of neuromuscular disease morbidity. Prevention of Pulmonary Morbidity for Patients With Neuromuscular Disease*
 Prevention of Pulmonary Morbidity for Patients With Neuromuscular Disease* Alice C. Tzeng, MD; and John R. Bach, MD, FCCP Study objective: To evaluate the effects of a respiratory muscle aid protocol on
Prevention of Pulmonary Morbidity for Patients With Neuromuscular Disease* Alice C. Tzeng, MD; and John R. Bach, MD, FCCP Study objective: To evaluate the effects of a respiratory muscle aid protocol on
Pulmonary Rehabilitation in Acute Spinal Cord Injury. Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university
 Pulmonary Rehabilitation in Acute Spinal Cord Injury Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university Causes of spinal cord injury Traumatic injury Motor vehicle
Pulmonary Rehabilitation in Acute Spinal Cord Injury Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university Causes of spinal cord injury Traumatic injury Motor vehicle
Is mechanical insufflation exsufflation (M-IE) useful in children with neuromuscular disease?
 Is mechanical insufflation exsufflation (M-IE) useful in children with neuromuscular disease? Cross Canada Rounds ProCon debate January 2017 Dr K Keown Respiratory Fellow BC Children s Hospital Structure
Is mechanical insufflation exsufflation (M-IE) useful in children with neuromuscular disease? Cross Canada Rounds ProCon debate January 2017 Dr K Keown Respiratory Fellow BC Children s Hospital Structure
Benefit of Forced Expiratory Technique for Weak Cough in a Patient with Bulbar Onset Amyotrophic Lateral Sclerosis
 Original Article Benefit of Forced Expiratory Technique for Weak Cough in a Patient with Bulbar Onset Amyotrophic Lateral Sclerosis J. Phys. Ther. Sci. 16: 137 141, 2004 MITSUAKI ISHII, RPT 1) 1) Department
Original Article Benefit of Forced Expiratory Technique for Weak Cough in a Patient with Bulbar Onset Amyotrophic Lateral Sclerosis J. Phys. Ther. Sci. 16: 137 141, 2004 MITSUAKI ISHII, RPT 1) 1) Department
LUNG VOLUME RECRUITMENT IN NEUROMUSCULAR DISEASE
 LUNG VOLUME RECRUITMENT IN NEUROMUSCULAR DISEASE Sherri Katz, MDCM, MSc, FRCPC Pediatric Respirologist Children s Hospital of Eastern Ontario University of Ottawa Disclosures Research funding from CIHR,
LUNG VOLUME RECRUITMENT IN NEUROMUSCULAR DISEASE Sherri Katz, MDCM, MSc, FRCPC Pediatric Respirologist Children s Hospital of Eastern Ontario University of Ottawa Disclosures Research funding from CIHR,
Understanding Breathing Muscle Weakness
 Understanding Breathing Muscle Weakness A N D R E A L. K L E I N P R E S I D E N T / F O U N D E R B R E A T H E W I T H M D w w w.facebook.com/ b r e a t h e w i t h m d h t t p : / / w w w. b r e a t
Understanding Breathing Muscle Weakness A N D R E A L. K L E I N P R E S I D E N T / F O U N D E R B R E A T H E W I T H M D w w w.facebook.com/ b r e a t h e w i t h m d h t t p : / / w w w. b r e a t
Pulmonary Functions and Effect of Incentive Spirometry During Acute and Post Acute Period in Tetraplegia
 IJPMR 13, April 2002; 28-34 Pulmonary Functions and Effect of Incentive Spirometry During Acute and Post Acute Period in Tetraplegia Dr M Joshi, M.D., Research Associate Dr N Mathur, M.S., DNB, Associate
IJPMR 13, April 2002; 28-34 Pulmonary Functions and Effect of Incentive Spirometry During Acute and Post Acute Period in Tetraplegia Dr M Joshi, M.D., Research Associate Dr N Mathur, M.S., DNB, Associate
The difference is clear. CoughAssist clears airways with the force of a natural cough
 The difference is clear CoughAssist clears airways with the force of a natural cough When only a real cough will do CoughAssist is a noninvasive therapy that safely and consistently removes secretions
The difference is clear CoughAssist clears airways with the force of a natural cough When only a real cough will do CoughAssist is a noninvasive therapy that safely and consistently removes secretions
Bench Assessment of a New Insufflation-Exsufflation Device
 Bench Assessment of a New Insufflation-Exsufflation Device Véronique Porot MD and Claude Guérin MD PhD BACKGROUND: The Nippy Clearway is a new mechanical insufflation-exsufflation device used to assist
Bench Assessment of a New Insufflation-Exsufflation Device Véronique Porot MD and Claude Guérin MD PhD BACKGROUND: The Nippy Clearway is a new mechanical insufflation-exsufflation device used to assist
Mechanical Ventilation of the Patient with Neuromuscular Disease
 Mechanical Ventilation of the Patient with Neuromuscular Disease Dean Hess PhD RRT Associate Professor of Anesthesia, Harvard Medical School Assistant Director of Respiratory Care, Massachusetts General
Mechanical Ventilation of the Patient with Neuromuscular Disease Dean Hess PhD RRT Associate Professor of Anesthesia, Harvard Medical School Assistant Director of Respiratory Care, Massachusetts General
Terapias no farmacológicas de aclaramiento de la vía aérea y soporte respiratorio muscular en
 Terapias no farmacológicas de aclaramiento de la vía aérea y soporte respiratorio muscular en el paciente ventilado: Estado del arte João Carlos Winck, MD, PhD Coordinator of the Respiratory Medicine Unit
Terapias no farmacológicas de aclaramiento de la vía aérea y soporte respiratorio muscular en el paciente ventilado: Estado del arte João Carlos Winck, MD, PhD Coordinator of the Respiratory Medicine Unit
Management of Ventilatory Insufficiency in Neuromuscular Patients Using Mechanical Ventilator Supported by the Korean Government
 ORIGINAL ARTICLE Rehabilitation & Sports Medicine http://dx.doi.org/0.3346/jkms.06.3.6.976 J Korean Med Sci 06; 3: 976-98 Management of Ventilatory Insufficiency in Neuromuscular Patients Using Mechanical
ORIGINAL ARTICLE Rehabilitation & Sports Medicine http://dx.doi.org/0.3346/jkms.06.3.6.976 J Korean Med Sci 06; 3: 976-98 Management of Ventilatory Insufficiency in Neuromuscular Patients Using Mechanical
MedStar Health considers Cough Assist Devices medically necessary for the following indications:
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.047.MH Cough Assist Devices This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.047.MH Cough Assist Devices This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
6- Lung Volumes and Pulmonary Function Tests
 6- Lung Volumes and Pulmonary Function Tests s (PFTs) are noninvasive diagnostic tests that provide measurable feedback about the function of the lungs. By assessing lung volumes, capacities, rates of
6- Lung Volumes and Pulmonary Function Tests s (PFTs) are noninvasive diagnostic tests that provide measurable feedback about the function of the lungs. By assessing lung volumes, capacities, rates of
Respiratory Muscle Aids to Avert Respiratory Failure and Tracheostomy
 Respiratory Muscle Aids to Avert Respiratory Failure and Tracheostomy John R. Bach, M.D. DoctorBach.com Abstract The purpose of this article is to describe the use of noninvasive inspiratory and expiratory
Respiratory Muscle Aids to Avert Respiratory Failure and Tracheostomy John R. Bach, M.D. DoctorBach.com Abstract The purpose of this article is to describe the use of noninvasive inspiratory and expiratory
Limits of Effective Cough-Augmentation Techniques in Patients With Neuromuscular Disease
 Limits of Effective Cough-Augmentation Techniques in Patients With Neuromuscular Disease Michel Toussaint PT PhD, Louis J Boitano MSc RRT, Vincent Gathot MSc PT, Marc Steens MSc PT, and Philippe Soudon
Limits of Effective Cough-Augmentation Techniques in Patients With Neuromuscular Disease Michel Toussaint PT PhD, Louis J Boitano MSc RRT, Vincent Gathot MSc PT, Marc Steens MSc PT, and Philippe Soudon
Lung volume recruitment acutely increases respiratory system compliance in individuals with severe respiratory muscle weakness
 ORIGINAL ARTICLE RESPIRATORY MUSCLE WEAKNESS Lung volume recruitment acutely increases respiratory system compliance in individuals with severe respiratory muscle weakness Yannick Molgat-Seon 1, Liam M.
ORIGINAL ARTICLE RESPIRATORY MUSCLE WEAKNESS Lung volume recruitment acutely increases respiratory system compliance in individuals with severe respiratory muscle weakness Yannick Molgat-Seon 1, Liam M.
Effect of air stacking training on pulmonary function, respiratory strength and peak cough flow in persons with cervical spinal cord injury
 Original Article https://doi.org/10.14474/ptrs.2018.7.4.147 pissn 2287-7576 eissn 2287-7584 Phys Ther Rehabil Sci 2018, 7 (4), 147-153 www.jptrs.org Effect of air stacking training on pulmonary function,
Original Article https://doi.org/10.14474/ptrs.2018.7.4.147 pissn 2287-7576 eissn 2287-7584 Phys Ther Rehabil Sci 2018, 7 (4), 147-153 www.jptrs.org Effect of air stacking training on pulmonary function,
RESPIRATORY COMPLICATIONS are the primary cause
 ORIGINAL ARTICLE Lung Volume Recruitment Slows Pulmonary Function Decline in Duchenne Muscular Dystrophy Douglas A. McKim, MD, Sherri L. Katz, MDCM, Nicholas Barrowman, PhD, Andy Ni, MSc, Carole LeBlanc,
ORIGINAL ARTICLE Lung Volume Recruitment Slows Pulmonary Function Decline in Duchenne Muscular Dystrophy Douglas A. McKim, MD, Sherri L. Katz, MDCM, Nicholas Barrowman, PhD, Andy Ni, MSc, Carole LeBlanc,
The Effects of Breathing Exercise with Intermittent Positive Pressure Ventilator on Pulmonary Function in Patients with Cervical Spinal Cord Injury
 NEUROTHERAPY 6 Sang-Su Hwang, Sang-Mi 대한신경치료학회지 Chung, Kyoung-Bo 제권제Lee 호 The Effects of Breathing Exercise with Intermittent Positive Pressure Ventilator on Pulmonary Function in Patients with Cervical
NEUROTHERAPY 6 Sang-Su Hwang, Sang-Mi 대한신경치료학회지 Chung, Kyoung-Bo 제권제Lee 호 The Effects of Breathing Exercise with Intermittent Positive Pressure Ventilator on Pulmonary Function in Patients with Cervical
Amyotrophic Lateral Sclerosis: Predictors for Prolongation of Life by Noninvasive Respiratory Aids
 828 Amyotrophic Lateral Sclerosis: Predictors for Prolongation of Life by Noninvasive Respiratory Aids John Robert Bach, AID ABSTRACT. Bach JR. Amyotrophic lateral sclerosis: predictors for prolongation
828 Amyotrophic Lateral Sclerosis: Predictors for Prolongation of Life by Noninvasive Respiratory Aids John Robert Bach, AID ABSTRACT. Bach JR. Amyotrophic lateral sclerosis: predictors for prolongation
Alternative title: Confessions of a Mucus Enthusiast. Mechanical Insufflation Exsufflation for airway secretion clearance and lung expansion therapy
 Mechanical Insufflation Exsufflation for airway secretion clearance and lung expansion therapy Alternative title: Confessions of a Mucus Enthusiast Marty Davig, RRT RCP Philips Respironics Inc. Objectives
Mechanical Insufflation Exsufflation for airway secretion clearance and lung expansion therapy Alternative title: Confessions of a Mucus Enthusiast Marty Davig, RRT RCP Philips Respironics Inc. Objectives
Operation Manual for clinical use of SIARE Pulsar
 Operation Manual for clinical use of SIARE Pulsar This manual is for clinical use only 1-12 INDEX 1) Indications /Contraindications and cautions 2) Questions to ask before using a MI-E machine 3) Guideline
Operation Manual for clinical use of SIARE Pulsar This manual is for clinical use only 1-12 INDEX 1) Indications /Contraindications and cautions 2) Questions to ask before using a MI-E machine 3) Guideline
Commissioning Policy for Cough Assist Requests
 Commissioning Policy for Cough Assist Requests 1 DOCUMENT CONTROL Reference Number (lead in specific policy area to provide once policy ratified) Version Draft Version 0.3 071015 Status Sponsor(s)/Author(s)
Commissioning Policy for Cough Assist Requests 1 DOCUMENT CONTROL Reference Number (lead in specific policy area to provide once policy ratified) Version Draft Version 0.3 071015 Status Sponsor(s)/Author(s)
Respiratory Physiology In-Lab Guide
 Respiratory Physiology In-Lab Guide Read Me Study Guide Check Your Knowledge, before the Practical: 1. Understand the relationship between volume and pressure. Understand the three respiratory pressures
Respiratory Physiology In-Lab Guide Read Me Study Guide Check Your Knowledge, before the Practical: 1. Understand the relationship between volume and pressure. Understand the three respiratory pressures
Airway Clearance Applications in the Elderly and in Patients With Neurologic or Neuromuscular Compromise
 Airway Clearance Applications in the Elderly and in Patients With Neurologic or Neuromuscular Compromise Carl F Haas MLS RRT FAARC, Paul S Loik RRT, and Steven E Gay MD MSc Introduction The Normal Clearance
Airway Clearance Applications in the Elderly and in Patients With Neurologic or Neuromuscular Compromise Carl F Haas MLS RRT FAARC, Paul S Loik RRT, and Steven E Gay MD MSc Introduction The Normal Clearance
Department of Rehabilitation Medicine, Gangnam Severance Hospital, Seoul; 2
 Original Article Ann Rehabil Med 2017;41(2):306-312 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2017.41.2.306 Annals of Rehabilitation Medicine Correlation of Serum Creatine Kinase Level
Original Article Ann Rehabil Med 2017;41(2):306-312 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2017.41.2.306 Annals of Rehabilitation Medicine Correlation of Serum Creatine Kinase Level
Ventilator Waveforms: Interpretation
 Ventilator Waveforms: Interpretation Albert L. Rafanan, MD, FPCCP Pulmonary, Critical Care and Sleep Medicine Chong Hua Hospital, Cebu City Types of Waveforms Scalars are waveform representations of pressure,
Ventilator Waveforms: Interpretation Albert L. Rafanan, MD, FPCCP Pulmonary, Critical Care and Sleep Medicine Chong Hua Hospital, Cebu City Types of Waveforms Scalars are waveform representations of pressure,
My CoughAssist. A patient guide to CoughAssist E70
 My CoughAssist A patient guide to CoughAssist E70 A natural part of life Coughing. We often think of a cough as a symptom of a cold or a means to clear our throat. Truth is, the ability to cough is essential
My CoughAssist A patient guide to CoughAssist E70 A natural part of life Coughing. We often think of a cough as a symptom of a cold or a means to clear our throat. Truth is, the ability to cough is essential
Respiratory System Mechanics
 M56_MARI0000_00_SE_EX07.qxd 8/22/11 3:02 PM Page 389 7 E X E R C I S E Respiratory System Mechanics Advance Preparation/Comments 1. Demonstrate the mechanics of the lungs during respiration if a bell jar
M56_MARI0000_00_SE_EX07.qxd 8/22/11 3:02 PM Page 389 7 E X E R C I S E Respiratory System Mechanics Advance Preparation/Comments 1. Demonstrate the mechanics of the lungs during respiration if a bell jar
Problem-solving Respiratory Issues in Children With Neuromuscular Disease. December 13, 2018 Eliezer Be eri, M.D.
 Problem-solving Respiratory Issues in Children With Neuromuscular Disease December 13, 2018 Eliezer Be eri, M.D. About Our Presenter Eliezer Be eri, M.D. Alyn Rehabilitation Hospital Jerusalem, Israel
Problem-solving Respiratory Issues in Children With Neuromuscular Disease December 13, 2018 Eliezer Be eri, M.D. About Our Presenter Eliezer Be eri, M.D. Alyn Rehabilitation Hospital Jerusalem, Israel
The Influence of Altered Pulmonarv
 The Influence of Altered Pulmonarv J Mechanics on the Adequacy of Controlled Ventilation Peter Hutchin, M.D., and Richard M. Peters, M.D. W ' hereas during spontaneous respiration the individual determines
The Influence of Altered Pulmonarv J Mechanics on the Adequacy of Controlled Ventilation Peter Hutchin, M.D., and Richard M. Peters, M.D. W ' hereas during spontaneous respiration the individual determines
KENNEDY DISEASE PULMONARY CONSIDERATIONS: SCIENCE & MANAGEMENT STRATEGIES
 KENNEDY DISEASE PULMONARY CONSIDERATIONS: SCIENCE & MANAGEMENT STRATEGIES When you can t breathe nothing else matters American Lung Association Noah Lechtzin, MD; MHS Associate Professor of Medicine Johns
KENNEDY DISEASE PULMONARY CONSIDERATIONS: SCIENCE & MANAGEMENT STRATEGIES When you can t breathe nothing else matters American Lung Association Noah Lechtzin, MD; MHS Associate Professor of Medicine Johns
Respiratory Training. Standard Operations Manuel For Outcome Measures Version 2.0 April Page 1 of 11
 Respiratory Training Page 1 of 11 Index Background... 2 SVC and FVC TESTING... 3 Clarification of used terms:... 3 Step 1) Preparation... 3 Step 2) Calibration... 3 Step 3) Adjusting the set-up menu...
Respiratory Training Page 1 of 11 Index Background... 2 SVC and FVC TESTING... 3 Clarification of used terms:... 3 Step 1) Preparation... 3 Step 2) Calibration... 3 Step 3) Adjusting the set-up menu...
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Respiratory therapy. Anja Raab. Doktorandin Clinical Trial Unit. Anja Raab, MSc. Physiotherapist and Phd-student SPZ Nottwil. June 17th of
 Respiratory therapy Anja Raab Anja Raab, MSc Doktorandin Clinical Trial Unit Physiotherapist and Phd-student SPZ Nottwil 1 Content Basis for an effective respiratory therapy Posture Interaction of 3 essential
Respiratory therapy Anja Raab Anja Raab, MSc Doktorandin Clinical Trial Unit Physiotherapist and Phd-student SPZ Nottwil 1 Content Basis for an effective respiratory therapy Posture Interaction of 3 essential
I. Subject: Medication Delivery by Metered Dose Inhaler (MDI)
 I. Subject: Medication Delivery by Metered Dose Inhaler (MDI) II. Policy: Aerosol medication administration by metered dose inhaler will be performed upon a physician's order by Respiratory Therapy personnel.
I. Subject: Medication Delivery by Metered Dose Inhaler (MDI) II. Policy: Aerosol medication administration by metered dose inhaler will be performed upon a physician's order by Respiratory Therapy personnel.
ORIGINAL RESEARCH. Optimum Insufflation Capacity and Peak Cough Flow in Neuromuscular Disorders. Abstract. Uwe Mellies 1 and Christof Goebel 2
 Optimum Insufflation Capacity and Peak Cough Flow in Neuromuscular Disorders Uwe Mellies 1 and Christof Goebel 2 1 Department of Pediatric Pulmonology, University of Essen, Childrens Hospital, Essen, Germany;
Optimum Insufflation Capacity and Peak Cough Flow in Neuromuscular Disorders Uwe Mellies 1 and Christof Goebel 2 1 Department of Pediatric Pulmonology, University of Essen, Childrens Hospital, Essen, Germany;
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
F: Respiratory Care. College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59
 F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
F: Respiratory Care College of Licensed Practical Nurses of Alberta, Competency Profile for LPNs, 3rd Ed. 59 Competency: F-1 Airway Management F-1-1 F-1-2 F-1-3 F-1-4 F-1-5 Demonstrate knowledge and ability
Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology
 Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
I Need to Cough Ways to Keep Your Airways Clear
 I Need to Cough Ways to Keep Your Airways Clear 2018 Annual Cure SMA Conference Richard Kravitz, MD Duke University School of Medicine Duke University Medical Center Durham, North Carolina Presenters Jane
I Need to Cough Ways to Keep Your Airways Clear 2018 Annual Cure SMA Conference Richard Kravitz, MD Duke University School of Medicine Duke University Medical Center Durham, North Carolina Presenters Jane
H: Respiratory Care. Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79
 H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
H: Respiratory Care Saskatchewan Association of Licensed Practical Nurses, Competency Profile for LPNs, 3rd Ed. 79 Competency: H-1 Airway Management H-1-1 H-1-2 H-1-3 H-1-4 H-1-5 Demonstrate knowledge
Supporting information leaflet (6): Chest Physiotherapy: Lung Volume Recruitment Techniques and Cough Augmentation (Assisted Cough Techniques)
 Acute Services Division Supporting information leaflet (6): Chest Physiotherapy: Lung Volume Recruitment Techniques and Cough Augmentation (Assisted Cough Techniques) Introduction For many people with
Acute Services Division Supporting information leaflet (6): Chest Physiotherapy: Lung Volume Recruitment Techniques and Cough Augmentation (Assisted Cough Techniques) Introduction For many people with
Ron Hosp, MS-HSA, RRT Regional Respiratory Specialist. This program has been approved for 1 hour of continuing education credit.
 Ron Hosp, MS-HSA, RRT Regional Respiratory Specialist This program has been approved for 1 hour of continuing education credit. Course Objectives Identify at least four goals of home NIV Identify candidates
Ron Hosp, MS-HSA, RRT Regional Respiratory Specialist This program has been approved for 1 hour of continuing education credit. Course Objectives Identify at least four goals of home NIV Identify candidates
Min Hur, Eun-Hee Kim, In-Kyung Song, Ji-Hyun Lee, Hee-Soo Kim, and Jin Tae Kim INTRODUCTION. Clinical Research
 Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Duchenne Muscular Dystrophy
 Authors: Elia Gomez-Merino, MD John R. Bach, MD Affiliations: From the Department of Pulmonary Medicine, Hospital Clinico Universitario de San Juan, San Juan de Alicante, Spain (EGM), and the Department
Authors: Elia Gomez-Merino, MD John R. Bach, MD Affiliations: From the Department of Pulmonary Medicine, Hospital Clinico Universitario de San Juan, San Juan de Alicante, Spain (EGM), and the Department
Effects of Core Stability Training on Postural Control Ability and Respiratory Function in Chronic Stroke Patients
 , pp.181-186 http://dx.doi.org/10.14257/astl.2015.88.38 Effects of Core Stability Training on Postural Control Ability and Respiratory Function in Chronic Stroke Patients Kyung Yoon Kim 1, Sung Pil Chun
, pp.181-186 http://dx.doi.org/10.14257/astl.2015.88.38 Effects of Core Stability Training on Postural Control Ability and Respiratory Function in Chronic Stroke Patients Kyung Yoon Kim 1, Sung Pil Chun
RESPIRATORY COMPLICATIONS AFTER SCI
 SHEPHERD.ORG RESPIRATORY COMPLICATIONS AFTER SCI NORMA I RIVERA, RRT, RCP RESPIRATORY EDUCATOR SHEPHERD CENTER 2020 Peachtree Road, NW, Atlanta, GA 30309-1465 404-352-2020 DISCLOSURE STATEMENT I have no
SHEPHERD.ORG RESPIRATORY COMPLICATIONS AFTER SCI NORMA I RIVERA, RRT, RCP RESPIRATORY EDUCATOR SHEPHERD CENTER 2020 Peachtree Road, NW, Atlanta, GA 30309-1465 404-352-2020 DISCLOSURE STATEMENT I have no
Key points. k Ineffective cough is a major cause of
 Breathe review cough.qxd 21/05/2008 16:06 Page 2 Key points k Ineffective cough is a major cause of k k k mortality and morbidity in patients with neuromuscular disease. A normal cough requires the inspiratory
Breathe review cough.qxd 21/05/2008 16:06 Page 2 Key points k Ineffective cough is a major cause of k k k mortality and morbidity in patients with neuromuscular disease. A normal cough requires the inspiratory
The Role of Facemask Spirometry in Motor Neurone Disease (MND) Respiratory Sleep and Support Centre, Papworth Hospital NHS Trust, Papworth
 The Role of Facemask Spirometry in Motor Neurone Disease (MND) Banerjee SK 1, Davies MG 1, Sharples LD 2, Smith IE 1 1 Respiratory Sleep and Support Centre, Papworth Hospital NHS Trust, Papworth Everard,
The Role of Facemask Spirometry in Motor Neurone Disease (MND) Banerjee SK 1, Davies MG 1, Sharples LD 2, Smith IE 1 1 Respiratory Sleep and Support Centre, Papworth Hospital NHS Trust, Papworth Everard,
Relation between the Peripherofacial Psoriasis and Scalp Psoriasis
 pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 4, 2016 http://dx.doi.org/10.5021/ad.2016.28.4.422 ORIGINAL ARTICLE Relation between the Peripherofacial Psoriasis and Scalp Psoriasis Kyung Ho
pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 4, 2016 http://dx.doi.org/10.5021/ad.2016.28.4.422 ORIGINAL ARTICLE Relation between the Peripherofacial Psoriasis and Scalp Psoriasis Kyung Ho
Pulmonary Function Testing. Ramez Sunna MD, FCCP
 Pulmonary Function Testing Ramez Sunna MD, FCCP Lecture Overview General Introduction Indications and Uses Technical aspects Interpretation Patterns of Abnormalities When to perform a PFT 1. Evaluation
Pulmonary Function Testing Ramez Sunna MD, FCCP Lecture Overview General Introduction Indications and Uses Technical aspects Interpretation Patterns of Abnormalities When to perform a PFT 1. Evaluation
acapella vibratory PEP Therapy System Maximizing Therapy Effectiveness, Empowering Patient Compliance
 acapella vibratory PEP Therapy System Maximizing Therapy Effectiveness, Empowering Patient Compliance Investigating Questions Each acapella vibratory PEP therapy system uniquely provides PEP therapy by
acapella vibratory PEP Therapy System Maximizing Therapy Effectiveness, Empowering Patient Compliance Investigating Questions Each acapella vibratory PEP therapy system uniquely provides PEP therapy by
Weaning guidelines for Spinal Cord Injured patients in Critical Care Units
 RISCI Respiratory Information for Spinal Cord Injury UK Weaning guidelines for Spinal Cord Injured patients in Critical Care Units Introduction It is an unfortunate fact that Spinal Cord Injury Centres
RISCI Respiratory Information for Spinal Cord Injury UK Weaning guidelines for Spinal Cord Injured patients in Critical Care Units Introduction It is an unfortunate fact that Spinal Cord Injury Centres
Mouthpiece ventilation and complementary techniques in patients with neuromuscular disease: A brief clinical review and update
 Review Article Mouthpiece ventilation and complementary techniques in patients with neuromuscular disease: A brief clinical review and update Chronic Respiratory Disease 2016, Vol. 14(2) 1 7 ª The Author(s)
Review Article Mouthpiece ventilation and complementary techniques in patients with neuromuscular disease: A brief clinical review and update Chronic Respiratory Disease 2016, Vol. 14(2) 1 7 ª The Author(s)
North Wales Critical Care Network
 North Wales Critical Care Network Weaning Guidelines for SPINAL CORD INJURED patients in North Wales Critical Care Units NWCCN Spinal Cord Injury Weaning Guidelines_APPROVED February 2014 Page 1 Weaning
North Wales Critical Care Network Weaning Guidelines for SPINAL CORD INJURED patients in North Wales Critical Care Units NWCCN Spinal Cord Injury Weaning Guidelines_APPROVED February 2014 Page 1 Weaning
DIAPHRAGM PACING AND NONINVASIVE RESPIRATORY MANAGEMENT OF AMYOTROPHIC LATERAL SCLEROSIS/MOTOR NEURON DISEASE
 DIAPHRAGM PACING AND NONINVASIVE RESPIRATORY MANAGEMENT OF AMYOTROPHIC LATERAL SCLEROSIS/MOTOR NEURON DISEASE KEDAR R. MAHAJAN, MD, PhD, JOHN ROBERT BACH, MD, LOU SAPORITO, BS, and NICK PEREZ, MD Department
DIAPHRAGM PACING AND NONINVASIVE RESPIRATORY MANAGEMENT OF AMYOTROPHIC LATERAL SCLEROSIS/MOTOR NEURON DISEASE KEDAR R. MAHAJAN, MD, PhD, JOHN ROBERT BACH, MD, LOU SAPORITO, BS, and NICK PEREZ, MD Department
Chapter 10. The Respiratory System Exchange of Gases. Copyright 2009 Pearson Education, Inc.
 Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Small Volume Nebulizer Treatment (Hand-Held)
 Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Chapter 11 The Respiratory System
 Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Original Article. Annals of Rehabilitation Medicine
 Original Article Ann Rehabil Med 2017;41(6):1055-1064 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2017.41.6.1055 Annals of Rehabilitation Medicine Long-Term Outcome of Amyotrophic Lateral
Original Article Ann Rehabil Med 2017;41(6):1055-1064 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2017.41.6.1055 Annals of Rehabilitation Medicine Long-Term Outcome of Amyotrophic Lateral
Performance of the CoughAssist Insufflation-Exsufflation Device in the Presence of an Endotracheal Tube or Tracheostomy Tube: A Bench Study
 Performance of the CoughAssist Insufflation-Exsufflation Device in the Presence of an or : A Bench Study Claude Guérin MD PhD, Gaël Bourdin MD, Véronique Leray MD, Bertrand Delannoy MD, Frédérique Bayle
Performance of the CoughAssist Insufflation-Exsufflation Device in the Presence of an or : A Bench Study Claude Guérin MD PhD, Gaël Bourdin MD, Véronique Leray MD, Bertrand Delannoy MD, Frédérique Bayle
Estimation of Stellate Ganglion Block Injection Point Using the Cricoid Cartilage as Landmark Through X-ray Review
 Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL
 AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL A. Definition of Therapy: 1. Cough machine: 4 sets of 5 breaths with a goal of I:E pressures approximately the same of 30-40. Inhale time = 1 second, exhale
AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL A. Definition of Therapy: 1. Cough machine: 4 sets of 5 breaths with a goal of I:E pressures approximately the same of 30-40. Inhale time = 1 second, exhale
P Sivasothy, L Brown, I E Smith, J M Shneerson
 438 Respiratory Support and Sleep Centre, Papworth Hospital, Papworth Everard, Cambridge CB3 8RE, UK P Sivasothy L Brown I E Smith J M Shneerson Correspondence to: Dr P Sivasothy ps247@cus.cam.ac.uk Received
438 Respiratory Support and Sleep Centre, Papworth Hospital, Papworth Everard, Cambridge CB3 8RE, UK P Sivasothy L Brown I E Smith J M Shneerson Correspondence to: Dr P Sivasothy ps247@cus.cam.ac.uk Received
Jesús Sancho MD, Enric Bures MD, Saray de La Asunción RN, and Emilio Servera MD RESPIRATORY CARE AUGUST 2016 VOL 61 NO
 Effect of High-Frequency Oscillations on Cough Peak Flows Generated by Mechanical In-Exsufflation in Medically Stable Subjects With Amyotrophic Lateral Sclerosis Jesús Sancho MD, Enric Bures MD, Saray
Effect of High-Frequency Oscillations on Cough Peak Flows Generated by Mechanical In-Exsufflation in Medically Stable Subjects With Amyotrophic Lateral Sclerosis Jesús Sancho MD, Enric Bures MD, Saray
The respiratory system
 The respiratory system Practical 1 Objectives Respiration, ventilation Intrapleural and intrapulmonary pressure Mechanism of inspiration and expiration Composition of the atmosphere and the expired air
The respiratory system Practical 1 Objectives Respiration, ventilation Intrapleural and intrapulmonary pressure Mechanism of inspiration and expiration Composition of the atmosphere and the expired air
Oxygenation. Chapter 45. Re'eda Almashagba 1
 Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
Oxygenation Chapter 45 Re'eda Almashagba 1 Respiratory Physiology Structure and function Breathing: inspiration, expiration Lung volumes and capacities Pulmonary circulation Respiratory gas exchange: oxygen,
The estimation of pulmonary functions in various body postures in normal subjects
 International Journal of Advances in Medicine Ganapathi LV et al. Int J Adv Med. 2015 Aug;2(3):250-254 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20150554
International Journal of Advances in Medicine Ganapathi LV et al. Int J Adv Med. 2015 Aug;2(3):250-254 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20150554
Anatomy & Physiology 2 Canale. Respiratory System: Exchange of Gases
 Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
RSPT Tracheal Aspiration. Tracheal Aspiration. RSPT 1410 Tracheal Aspiration
 1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
S P I R O M E T R Y. Objectives. Objectives 2/5/2019
 S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
Ch 16 A and P Lecture Notes.notebook May 03, 2017
 Table of Contents # Date Title Page # 1. 01/30/17 Ch 8: Muscular System 1 2. 3. 4. 5. 6. 7. 02/14/17 Ch 9: Nervous System 12 03/13/17 Ch 10: Somatic and Special Senses 53 03/27/17 Ch 11: Endocrine System
Table of Contents # Date Title Page # 1. 01/30/17 Ch 8: Muscular System 1 2. 3. 4. 5. 6. 7. 02/14/17 Ch 9: Nervous System 12 03/13/17 Ch 10: Somatic and Special Senses 53 03/27/17 Ch 11: Endocrine System
Conference Proceedings
 Conference Proceedings Mechanical Insufflation-Exsufflation for Airway Mucus Clearance Douglas N Homnick MD MPH Introduction Cough and Airway Clearance Mechanical Insufflation-Exsufflation The CoughAssist
Conference Proceedings Mechanical Insufflation-Exsufflation for Airway Mucus Clearance Douglas N Homnick MD MPH Introduction Cough and Airway Clearance Mechanical Insufflation-Exsufflation The CoughAssist
COMPREHENSIVE RESPIROMETRY
 INTRODUCTION Respiratory System Structure Complex pathway for respiration 1. Specialized tissues for: a. Conduction b. Gas exchange 2. Position in respiratory pathway determines cell type Two parts Upper
INTRODUCTION Respiratory System Structure Complex pathway for respiration 1. Specialized tissues for: a. Conduction b. Gas exchange 2. Position in respiratory pathway determines cell type Two parts Upper
Pediatric Patients. Neuromuscular Disease. Teera Kijmassuwan, MD Phetcharat Netmuy, B.N.S., MA Oranee Sanmaneechai, MD : Preceptor
 Patient Management Pediatric Patients with Neuromuscular Disease Teera Kijmassuwan, MD Phetcharat Netmuy, B.N.S., MA Oranee Sanmaneechai, MD : Preceptor Case Thai boy 1 year old Present with Respiratory
Patient Management Pediatric Patients with Neuromuscular Disease Teera Kijmassuwan, MD Phetcharat Netmuy, B.N.S., MA Oranee Sanmaneechai, MD : Preceptor Case Thai boy 1 year old Present with Respiratory
Cough assist T70 for the Tracheostomy Child
 Patient and Family Education Cough assist 70 for the racheostomy Child with or without a ventilator What is a Cough assist device? he Cough assist 70 device removes mucus (secretions) from your child s
Patient and Family Education Cough assist 70 for the racheostomy Child with or without a ventilator What is a Cough assist device? he Cough assist 70 device removes mucus (secretions) from your child s
Respiratory care and ventilation
 Respiratory care and ventilation There are many different neuromuscular conditions in which weakness of the breathing muscles requires monitoring and treatment and may eventually need some form of mechanical
Respiratory care and ventilation There are many different neuromuscular conditions in which weakness of the breathing muscles requires monitoring and treatment and may eventually need some form of mechanical
Adapting to the Worsening of the LTMV Patient
 14 èmes Journées Internationales de Ventilation à Domicile LYON, 26-28 mars 2015 Adapting to the Worsening of the LTMV Patient Andrea Vianello Fisiopatologia e Terapia Intensiva Respiratoria Ospedale-Università
14 èmes Journées Internationales de Ventilation à Domicile LYON, 26-28 mars 2015 Adapting to the Worsening of the LTMV Patient Andrea Vianello Fisiopatologia e Terapia Intensiva Respiratoria Ospedale-Università
Relationship between supramaximal flow during cough and mortality in motor neurone disease
 Eur Respir J 22; 19: 434 438 DOI: 1.1183/931936.2.8272 Printed in UK all rights reserved Copyright ERS Journals Ltd 22 European Respiratory Journal ISSN 93-1936 Relationship between supramaximal flow during
Eur Respir J 22; 19: 434 438 DOI: 1.1183/931936.2.8272 Printed in UK all rights reserved Copyright ERS Journals Ltd 22 European Respiratory Journal ISSN 93-1936 Relationship between supramaximal flow during
#7 - Respiratory System
 #7 - Respiratory System Objectives: Study the parts of the respiratory system Observe slides of the lung and trachea Perform spirometry to measure lung volumes Define and understand the lung volumes and
#7 - Respiratory System Objectives: Study the parts of the respiratory system Observe slides of the lung and trachea Perform spirometry to measure lung volumes Define and understand the lung volumes and
Lab 4: Respiratory Physiology and Pathophysiology
 Lab 4: Respiratory Physiology and Pathophysiology This exercise is completed as an in class activity and including the time for the PhysioEx 9.0 demonstration this activity requires ~ 1 hour to complete
Lab 4: Respiratory Physiology and Pathophysiology This exercise is completed as an in class activity and including the time for the PhysioEx 9.0 demonstration this activity requires ~ 1 hour to complete
