Pneumococcal vaccines for children and adults with bronchiectasis (Review)
|
|
|
- Carol Anthony
- 5 years ago
- Views:
Transcription
1 Pneumococcal vaccines for children and adults with bronchiectasis (Review) Chang CC, Singleton RJ, Morris PS, Chang AB This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in The Cochrane Library 2009, Issue 2
2 T A B L E O F C O N T E N T S HEADER ABSTRACT PLAIN LANGUAGE SUMMARY BACKGROUND OBJECTIVES METHODS RESULTS Figure Figure DISCUSSION AUTHORS CONCLUSIONS ACKNOWLEDGEMENTS REFERENCES CHARACTERISTICS OF STUDIES DATA AND ANALYSES WHAT S NEW HISTORY CONTRIBUTIONS OF AUTHORS DECLARATIONS OF INTEREST SOURCES OF SUPPORT INDEX TERMS i
3 [Intervention Review] Pneumococcal vaccines for children and adults with bronchiectasis Christina C Chang 1, Rosalyn J Singleton 2, Peter S Morris 3, Anne B Chang 3 1 Department of Infectious Diseases, The Alfred Hospital, Monash University, Prahran, Australia. 2 Arctic Investigations Program and Alaska Native Tribal Health Consortium, Centers for Disease Control and Prevention, National Center for Infectious Diseases Anchorage, Alaska, USA. 3 Child Health Division, Menzies School of Health Research, Charles Darwin University, Darwin, Australia Contact address: Christina C Chang, Department of Infectious Diseases, The Alfred Hospital, Monash University, Commercial Road, Prahran, Victoria, 3181, Australia. christina.chang@monash.edu. christina.chang@med.monash.edu.au ccchang339@hotmail.com. Editorial group: Cochrane Airways Group. Publication status and date: Edited (no change to conclusions), published in Issue 6, Review content assessed as up-to-date: 4 December Citation: Chang CC, Singleton RJ, Morris PS, Chang AB. Pneumococcal vaccines for children and adults with bronchiectasis. Cochrane Database of Systematic Reviews 2009, Issue 2. Art. No.: CD DOI: / CD pub3. Background A B S T R A C T Bronchiectasis is increasingly recognized as a major cause of respiratory morbidity especially in developing countries. Even in affluent countries, bronchiectasis is increasingly seen in some community subsections (e.g. Aboriginal communities) and occurs as a comorbidity and disease modifier in respiratory diseases such as chronic obstructive pulmonary disease (COPD). Respiratory exacerbations in people with bronchiectasis are associated with reduced quality of life, accelerated pulmonary decline, hospitalisation and even death. Conjugate pneumococcal vaccine is part of the routine infant immunisation schedule in many countries. Current recommendations for additional pneumococcal vaccination include children and adults with chronic suppurative disease. Objectives To evaluate the effectiveness of pneumococcal vaccine as routine management in children and adults with bronchiectasis in (a) reducing the severity and frequency of respiratory exacerbations and (b) pulmonary decline. Search methods The Cochrane Register of Controlled Trials (CENTRAL), the Cochrane Airways Group Specialised Register, MEDLINE and EMBASE databases were searched by the Cochrane Airways Group. Pharmaceutical manufacturers of pneumococcal vaccines were also contacted. The latest searches were performed in November Selection criteria All randomised controlled trials that utilised pneumococcal vaccine on children and adults with bronchiectasis. All types of pneumococcal vaccines were included. Data collection and analysis Results of searches were reviewed against pre-determined criteria for inclusion. No eligible trials were identified and thus no data was available for analysis. One small non-randomised controlled trial in children was reported. 1
4 Main results One randomised controlled open label study in 167 adults with chronic lung disease (bronchiectasis and other diseases associated with bronchiectasis) compared 23-valent pneumococcal (PV) and influenza vaccine with influenza vaccine alone (control group). The study found a significant reduction in acute infective respiratory exacerbations in the PV group compared to the control group, OR=0.48 (95%CI 0.26, 0.88); number needed to treat to benefit = 6 (95%CI 4, 32) over 2-years. There was however no difference in episodes of pneumonia between groups and no data on pulmonary decline was available. In another study, a benefit in elimination of Strep. pneumoniae in the sputum was found in a non-randomised trial in children but no clinical effect was described. Authors conclusions Current but limited evidence support the use of 23-valent pneumococcal vaccine as routine management in adults with bronchiectasis. Circumstantial evidence also support the use of routine 23-valent pneumococcal vaccination in children with bronchiectasis. Further randomised controlled trials examining the efficacy of this intervention using various vaccine types in different age groups are needed. There is no data on the efficacy of pneumococcal vaccine on pulmonary decline. With the lack of evidence in how often the vaccine should be given, it is recommended that health providers adhere to national guidelines. P L A I N L A N G U A G E S U M M A R Y Pneumonia (pneumococcal) vaccines for children and adults with bronchiectasis In many countries pneumonia vaccination (for the protection against infection of the bacteria pneumococcus), is part of the immunisation schedule for infants as well as for people with bronchiectasis. In this review, our search for randomised control trials that examined the effectiveness of pneumococcal vaccines for people with bronchiectasis revealed one randomised and one quasi-controlled trial. We conclude that, albeit the limitations of the review, adults and children (when age appropriate) with bronchiectasis should be vaccinated with the 23-valent polysaccharide pneumococcal vaccine as suggested in many national guidelines. Due to absence of data on how often the vaccine should be given, we recommend that national guidelines be followed until further evidence is available. B A C K G R O U N D Bronchiectasis, sometimes termed an orphan s disease (Callahan 2002) is increasingly recognized as a major cause of respiratory morbidity especially in developing countries (Karadag 2005) and in pockets of affluent countries (Chang 2003, Singleton 2000). Of diverse aetiology, bronchiectasis is often a result of repeated respiratory infections or may be due to rare immune deficiencies. Increasingly recognised as a common final pathway for a variety of diseases, it is seen to complicate both common and uncommon respiratory illnesses such as COPD, bronchiolitis obliterans, pan bronchiolitis (Poletti 2006), pneumoconiosis (Altin 2004), interstitial lung disease and sarcoidosis (Patel 2004, Chang 1998, Lewis 2002) and also secondary pulmonary illnesses such as autoimmune diseases and post tuberculosis (TB) (Buckles 1951). Its coexistence increases the morbidity and mortality of the underlying disease (Patel 2004, Lewis 2002, Keistinen 1997). For instance, bronchiectasis is reported to occur in 29-50% of COPD (Patel 2004, O Brien 2000) and when present, increases the severity and frequency of respiratory exacerbations (Patel 2004, Gursel 2006). Thus, management of the symptoms and prevention of progression of bronchiectasis is important. The dominant symptoms and signs of bronchiectasis are a productive or wet cough, dyspnoea on exertion and presence of other respiratory signs (clubbing, chest wall deformity, respiratory noises such as wheeze or crepitations on auscultation). In the long term, pulmonary decline may occur (Keistinen 1997, Twiss 2006). Children and adults with bronchiectasis suffer from recurrent acute exacerbations, some necessitating inpatient care. Effective management regimes for bronchiectasis should improve quality of life, reduce the frequency and severity of respiratory exacerbations and rate of pulmonary decline. Cole s vicious circle hypothesis suggests microbial colonization or infection as a key factor in its pathophysiology as this often leads to bronchial obstruction and a normal or exaggerated inflammatory response (Cole 1986). Treatment modalities that prevent or limit respiratory infections should thus, prevent or reduce respiratory decline. Respiratory infection alone increases morbidity and reduces the quality of life in those with 2
5 bronchiectasis (Martinez-Garcia 2005). Pneumococcal respiratory infections is a common respiratory pathogen in acute (Lucero 2004) and chronic respiratory diseases (Devitt 1977). Prevention of pneumococcal infections through the use of pneumococcal vaccine should in turn, be a useful routine management modality for children and adults with bronchiectasis. Indeed 5-yearly pneumococcal vaccination is recommended for patients with bronchiectasis (Chang 2002). Pneumococcal vaccines are available in two major types; the older pneumococcal polysaccharide vaccine and the more recent pneumococcal conjugate vaccine. The 23-valent polysaccharide vaccine (PPV23) contains polysaccharide antigen from 23 serotypes and vaccine efficacy against invasive disease is estimated at 38-53% (Conaty 2004). Although clinical trials in younger adults have generally shown efficacy against pneumococcal pneumonia and, or bacteraemia, the trial evidence in the elderly is less robust (Honkanen 1999). Effectiveness in case-control studies generally range from 56-81% except Forrester et al who demonstrated no effectiveness (Forrester 1987). The PPV23 vaccine is relatively ineffective in young children aged under 2 years (Lee 2003). The heptavalent pneumococcal conjugated vaccine (PCV7) is directed against seven serotypes and recommended for use in children less than 5 years of age (McEllistrem 2005). Universal childhood vaccination in the United States has resulted in 70% decrease in invasive pneumococcal disease (IPD) in children <2 years and indirectly, contributed to prevention of adult IPD (Lexau 2005). The possibility of replacement serotype disease mandates continued data surveillance (McEllistrem 2005). Vaccines also incur cost and can result in adverse reactions, mostly occurring as local pain and swelling (Walker 2005, Jackson 2006). A review on the efficacy of pneumococcal vaccines for bronchiectasis will help guide clinical practice. Efficacy of pneumococcal vaccines for other chronic respiratory diseases (Sheikh 2002, Granger 2006) and otitis media (Straetemans 2004) are covered in other Cochrane reviews. This systematic review will evaluate the evidence of efficacy of pneumococcal vaccination in children and adults with bronchiectasis. O B J E C T I V E S To evaluate the effectiveness of pneumococcal vaccine as routine management in children and adults with bronchiectasis in (a) reducing the severity and frequency of respiratory exacerbations and (b) pulmonary decline. Types of studies All randomised controlled trials using pneumococcal vaccine in patients with bronchiectasis. Types of participants Adults or children with bronchiectasis (defined clinically or radiologically). Exclusion criteria: Participants with other diseases where bronchiectasis is not present. Types of interventions All randomised controlled trials that utilised pneumococcal vaccine on children and adults with bronchiectasis. All types of pneumococcal vaccines were included. Types of outcome measures Attempts were made to obtain data on at least one of the following outcome measures: (A) for short term effectiveness (12 months or less) a) proportions of participants who had respiratory exacerbations b) proportions of participants who were hospitalised, c) total numbers of days with respiratory symptoms d) total number of hospitalised days e) mean difference in bronchiectasis severity control (QOL, cough diary, Likert scale, visual analogue scale, level of interference of cough, cough diary, etc), f) proportions experiencing adverse effects of the intervention, (e.g. local reaction, exacerbation immediately post vaccination, systemic effects (myalgia, fever, fatigue), etc) Outcomes (a) to (e) will be examined globally as well as also specifically to proven pneumococcal infections (from airway specimens or rising titres) (B) for medium to long term outcomes (more than 1 year) g) radiology scores (high resolution computed tomography scans or chest radiograph) h) lung function I) bronchiectasis severity control (QOL, cough diary, Likert scale, visual analogue scale, level of interference of cough, cough diary, etc), j) relevant airway markers of inflammation. k) other non-respiratory outcomes (otitis media, bacteraemia, meningitis, etc) caused by pneumococcus. M E T H O D S Criteria for considering studies for this review Search methods for identification of studies The following topic search strategy was used to identify relevant randomised controlled trials from electronic databases: 3
6 ( bronchiectasis OR suppurative lung disease ) AND ((vaccin* OR immunis*) AND (pneum*)) (all as textword or index terms). For the full strategies see Appendix 1. Trials were identified from the following sources: 1. The Cochrane Airways Group Specialised Trials Register 2. The Cochrane Central Register of Controlled Trials (CEN- TRAL) 3. MEDLINE (1966 to Nov 2008). Topic search strategy combined with the RCT search filter as outlined in the Airways Group module. 4. OLDMEDLINE (1950 to 1965). Topic search strategy combined with the RCT search filter as outlined in the Airways Group module. 5. EMBASE (1980 to Nov 2008).Topic search strategy combined with the RCT search filter as outlined in the Airways Group module. 6. The list of references in relevant publications. 7. Written communication with the authors of trials would have been included in the review if necessary. 7. Pharmaceutical companies that manufacture pneumococcal vaccines. Data collection and analysis Retrieval of studies: From the title, abstract, or descriptors, two reviewers (CC, AC) independently reviewed literature searches to identify potentially relevant trials for full review. Searches of bibliographies and texts were conducted to identify additional studies. From the full text using specific criteria, the same two reviewers independently selected trials for inclusion. Agreement would have been measured using kappa statistics. Disagreement would have been resolved by adjudication (RS and PM). It was planned that trials that satisfied the inclusion criteria would have been reviewed and the following information recorded: study setting, year of study, source of funding, patient recruitment details (including number of eligible subjects), inclusion and exclusion criteria, other symptoms, randomisation and allocation concealment method, numbers of participants randomised, blinding (masking) of participants, care providers and outcome assessors, dose and type of intervention, duration of therapy, co-interventions, numbers of patients not followed up, reasons for withdrawals from study protocol (clinical, side-effects, refusal and other), details on side-effects of therapy, and whether intention-to-treat analyses were possible. Data would have been extracted on the outcomes described previously. Further information would have been requested from the authors when required. The Revman 5 risk of bias tool as outlined in the Cochrane handbook (Higgins 2008) was utilised. STATISTICS Results from studies that met the inclusion criteria and reported any of the outcomes of interest were included in the meta-analyses when possible. For continuous variables, the summary weighted odds ratio and 95% confidence interval (fixed effects model) would have been calculated (Cochrane statistical package, RevMan version 5). Studies using cross-over designs would be of limited value and it was planned that only the first arm of the cross-study (if any) would be utilised. Numbers needed to treat for benefit (NNTB) was calculated from the pooled OR and its 95% CI applied to a specified baseline risk using an online calculator (Cates 2003). If studies reported outcomes using different measurement scales, the standardised mean difference would have been estimated. Any heterogeneity between the study results would have been described and tested to see if it reached statistical significance using a chisquared test. The 95% confidence interval estimated using a random effects model would have been included whenever there are concerns about statistical heterogeneity. SUB-GROUP ANALYSIS: The following a priori sub-group analyses was planned: 1. children (aged 18 years or less) and adults (>18 years) 2. types of pneumococcal vaccine 3. type of control group 4. participant type (bronchiectasis as primary disease vs bronchiectasis as co-existent disease) 5. severity of bronchiectasis (based on lung function) Sensitivity analyses were also planned to assess the impact of the potentially important factors on the overall outcomes: a) study quality; b) variation in the inclusion criteria; c) differences in the medications used in the intervention and comparison groups; d) differences in outcome measures; e) analysis using random effects model; f) analysis by treatment received ; and g) analysis by intention-to-treat. R E S U L T S Description of studies In the original search (2006) the Airways Group specialised register/search identified 44 potentially relevant titles. After assessing the abstracts, 3 publications were considered for inclusion into review including one non-english article (Russian). Of the 3 potentially relevant publication but none fulfilled the study eligibility criteria (see Table of excluded studies). No additional studies were found in the review articles. No additional data were available from the two pharmaceutical companies contacted (Merck Sharp & Dohme and Wyeth in Australia). The 2007 search revealed 5 abstracts of which none fulfilled the inclusion criteria. The 2008 search revealed 8 papers and one study (Furumoto 2008) was included. 4
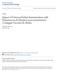
7 The included study has been described in the Characteristics of included studies table. Some subjects had very severe lung disease (59 on home oxygen, 11 on home ventilation). The study was included as some subjects were clearly described as having bronchiectasis. The respiratory condition the other subjects had, has a large overlap with bronchiectasis especially when the disease is severe. Subjects were followed up for 2 years. There were no randomised controlled studies in children that assessed clinical outcomes. There was one quasi controlled study (Ryzhov 2005) that utilised a comparative group published in Russian (Ryzhov 2005). In this study (Ryzhov 2005) in children with chronic lung disease (including bronchiectasis), 25 were vaccinated with PPV23, 13 with Haemophilus influenzae vaccine and 40 children were not vaccinated. As there was otherwise little data, this study could not be included in the meta-analysis. Risk of bias in included studies Please see risk of bias table in included studies section. The sole randomised study (Furumoto 2008) included in this review has high risk of performance and detection bias. Effects of interventions Adults Effect on exacerbations (Analysis 1.1): For number of people having had any respiratory exacerbations, the PV23 group was significantly better (less subjects with exacerbations) then the control group, OR 0.53 (95%CI 0.29, 0.99) Figure 1, NNTB over 2-years was 7 (95%CI 4, 424). With further evaluation, the difference between groups was mainly related to infective exacerbations (i.e. respiratory symptoms with increase in blood white cell count or serum C-reactive protein, as described in Characteristics of included studies). Comparing the PV23 group to controls, the OR for infective exacerbations was OR=0.48 (95%CI 0.26, 0.88); number needed to treat to benefit= 6 (95%CI 4, 32) over 2-years, see Figure 2. That for non-infective exacerbations was non significant, OR 1.42 (0.48, 4.19). Figure 1. Forest plot of comparison: 1 Adults, outcome: 1.2 Number of people with acute respiratory exacerbation. 5
8 Figure 2. Cates plot for NNT (B) over 2-years in reduction of infective exacerbation comparing PV23 vaccination to control in adults with chronic lung disease Effect on pneumonia (Analysis 1.2): There was no difference between groups for the outcome of pneumonia Other outcomes: Furumoto 2008 did not report on any pulmonary function. Seven subjects in each group (8.4% of the cohort studied) died during the follow up period of the study. Children There was only one study in children with bronchiectasis and this study utilised a comparative group, (i.e. a non-randomised study) published in Russian (Ryzhov 2005). In this study (Ryzhov 2005) in children with chronic lung disease (including bronchiectasis), 25 were vaccinated with PPV23, 13 with Haemophilus influenzae vaccine and 40 children were not vaccinated. The authors described that, a year after vaccination with PPV23, S. pneumoniae were isolated in monoculture in 3 out of 25 cases (88% elimination) (Ryzhov 2005). It was not possible to perform any relevant sub-analysis. D I S C U S S I O N In this review that evaluated the efficacy of pneumococcal vaccine in people with bronchiectasis for pulmonary outcomes, we found only one randomised controlled trial that was subject to bias as it was an open-labelled trial. Nevertheless the study in 167 adults with chronic lung disease found that PV23 vaccination significantly reduced the number of people with respiratory exacerbation with NNTB of 7 (95%CI 4, 424) over 2-years. The majority of this effect related to infective exacerbations, NNTB 6 (95%CI 4, 32) over 2-years. There was no difference between groups on number with pneumonia and no data for pulmonary decline was found. One controlled study that was not randomised (Ryzhov 2005) described efficacy with respect to microbiology of the sputum (88% elimination of S pneumoniae) but clinical evaluation was not examined in children. Large trials and meta-analysis have demonstrated that pneumococcal vaccination protects children and adults from invasive pneumococcal disease (de Roux 2005), thus many recommendations exist for regular pneumococcal vaccination for those at risk (including patients with suppurative lung disease). This Cochrane 6
9 review has significant limitations with the lack of studies.. Whilst we cannot always wait for perfect data, others have cautioned against availability creep with respect to the gap between policy and evidence (Jefferson 2006). Until additional RCTs are undertaken to examine the question, we cannot be absolutely confident with the findings of this review that routine pneumococcal vaccination in children and adults with bronchiectasis is beneficial. The feasibility of performing RCTs in this target group is in question. For now, as children and adults with bronchiectasis are at increased risk for pneumonia and pneumococcal disease and there is some evidence that pneumococcal vaccine can reduce pneumonia and invasive pneumococcal disease (Lucero 2004), it would be prudent that providers follow guidelines from the national bodies such as Advisory Committee on Immunization Practices (in USA) (ACIP) and NIPS (Australia) (NIPS) regarding recommendations for pneumococcal vaccination of persons with bronchiectasis. It is debatable whether the study (Furumoto 2008) we have included in this review fulfilled all the inclusion criteria, specifically that related to the diagnosis. We decided to include the study because a subgroup definitely had bronchiectasis and all the lung conditions in the subjects have a large overlap with bronchiectasis especially when the disease is severe. Although the study did not describe the severity of the chronic lung disease in all the subjects, it is likely that they were in the severe spectrum (35.3% of cohort was on ambulatory oxygen and 6.6% was on home ventilation). Unless a HRCT scan is performed on each subject, it is very difficult to ascertain whether radiological bronchiectasis is present. The study was also limited with a risk of performance and detection bias. Nevertheless, in infective exacerbations where the greatest significance between groups was found, objective blood tests were utilised. There was no data on how frequent pneumococcal vaccine should be given after the initial vaccination. Some advocate repeating PV23 after 5 years. In the absence of data on frequency of vaccination, we advocate that national guidelines be adhered to. A U T H O R S C O N C L U S I O N S Implications for practice Limited evidence support the routine use of polysaccharide 23-valent pneumococcal vaccine in adults with chronic lung disease including those with bronchiectasis. Other circumstantial data also suggests that pneumococcal vaccination is beneficial in children. There is no data on the efficacy of pneumococcal vaccine on pulmonary decline. There is also no data on how often the vaccination should be repeated. With the lack of evidence on this, it is recommended that health providers adhere to national guidelines. Individual risk factors for adverse events should be taken into account. Implications for research Randomised controlled trials to establish the efficacy of pneumococcal vaccination in reducing severity and frequency of respiratory exacerbations and pulmonary decline in people with bronchiectasis are needed. As vaccine response alters with age, age-based cohorts should include young children (less than 2 years), children, adults and older adults. Various vaccine types and microbiological surveillance for possible serotype replacement should also be examined in these RCTs. However the difficulty in performing a RCT in the target group is acknowledged. A C K N O W L E D G E M E N T S We thank Toby Lasserson and Chris Cates from the Airways Group for their advice, supportive role and comments to the protocol and review. We are also grateful to Susan Hansen and Elizabeth Arnold for performing the relevant searches and obtaining the articles. We also thank Dr. Vasiliy Vlassov for translation of the Russian article. R E F E R E N C E S References to studies included in this review Furumoto 2008 {published data only} Furumoto A, Ohkusa Y, Chen M, Kawakami K, Masaki H, Sueyasu Y, et al.additive effect of pneumococcal vaccine and influenza vaccine on acute exacerbation in patients with chronic lung disease. Vaccine 2008;26(33): References to studies excluded from this review Ryzhov 2005 {published data only} Ryzhov AA, Katosova LK, Kostinov MP, Volkov IK, Magarshak OO. Evaluation of the influence of the bacterial vaccines Pneumo-23 and Act-HIB on the course of the chronic inflammatory process of the respiratory organs in children. Zhurnal Mikrobiologii, Epidemiologii i Immunobiologii 2005;30(3):84 7. van Kessel 2005 {published data only} van Kessel DA, van Velzen-Blad H, van den Bosch JM, Rijkers GT. Impaired pneumococcal antibody response in bronchiectasis of unknown aetiology. European Respiratory Journal 2005;25(3): Vendrell 2005 {published data only} Vendrell M, De Gracia J, Rodrigo MJ, Cruz MJ, Alvarez A, Garcia M, et al.antibody production deficiency with normal IgG levels in bronchiectasis of unknown etiology. Chest 2005;127(1):
10 Additional references ACIP ACIP. Advisory Committee on Immunization Practices. (accessed Dec 2006). Altin 2004 Altin R, Savranlar A, Kart L, Mahmutyazicioglu K, Ozdemir H, Akdag B, et al.presence and HRCT quantification of bronchiectasis in coal workers. European Journal of Radiology 2004;52(2): Buckles 1951 Buckles MG, Potts WL, Davidson HB, Neptune WB. Bronchography in pulmonary tuberculosis, with histopathologic correlation in 82 resections. American Review of Tuberculosis 1951;64(4): Callahan 2002 Callahan CW, Redding GJ. Bronchiectasis in children: orphan disease or persistent problem?. Pediatric pulmonology 2002;33(6): Cates 2003 Cates CJ, Jefferson TO, Bara AI, Rowe BH. Vaccines for preventing influenza in people with asthma (Cochrane Review). Cochrane Database of Systematic Reviews 2003, Issue 4. [Art. No.: CD DOI: / CD pub2.] Chang 1998 Chang AB, Masel JP, Masters B. Post-infectious bronchiolitis obliterans: clinical, radiological and pulmonary function sequelae. Pediatric Radiology 1998;28(1): Chang 2002 Chang AB, Grimwood K, Mulholland EK, Torzillo PJ. Bronchiectasis in Indigenous children in remote Australian communities. Medical Journal of Australia 2002;177(4): Chang 2003 Chang AB, Masel JP, Boyce NC, Wheaton G, Torzillo PJ. Non-CF bronchiectasis-clinical and HRCT evaluation. Pediatric Pulmonology 2003;35: Cole 1986 Cole PJ. Inflammation: a two edged sword. The model of bronchiectasis. European Journal Respiratory Disease 1986; 147(Suppl):6 15. Conaty 2004 Conaty S, Watson L, Dinnes J, Waugh N. The effectiveness of pneumococcal polysaccharide vaccines in adults: a systematic review of observational studies and comparison with results from randomised controlled trials. Vaccine 2004;22(23-24): de Roux 2005 de Roux A, Lode H. Pneumococcal vaccination. European Respiratory Journal 2005;26(6): Devitt 1977 Devitt L, Riley I, Hansman D. Human infection caused by penicillin-insensitive pneumococci. Medical Journal of Australia 1977;1(16): Forrester 1987 Forrester HL, Jahnigen DW, LaForce FM. Inefficacy of pneumococcal vaccine in a high-risk population. American Journal of Medicine 1987;83(3): Granger 2006 Granger R, Walters J, Poole PJ, Lasserson TJ, Mangtani P, Cates CJ, et al.injectable vaccines for preventing pneumococcal infection in patients with chronic obstructive pulmonary disease (Cochrane Review). Cochrane Database of Systematic Reviews 2006, Issue 4. [Art. No.: CD DOI: / CD pub2.] Gursel 2006 Gursel G. Does coexistence with bronchiectasis influence intensive care unit outcome in patients with chronic obstructive pulmonary disease?. Heart Lung 2006;35(1): Higgins 2008 Higgins JPT, Green S (editors). Cochrane Handbook for Systematic Reviews of Interventions Version [updated September 2008]. The Cochrane Collaboration. Available from handbook.org, Honkanen 1999 Honkanen PO, Keistinen T, Miettinen L, Herva E, Sankilampi U, Laara E, et al.incremental effectiveness of pneumococcal vaccine on simultaneously administered influenza vaccine in preventing pneumonia and pneumococcal pneumonia among persons aged 65 years or older. Vaccine 1999;17(20-21): Jackson 2006 Jackson LA, Nelson JC, Whitney CG, Neuzil KM, Benson P, Malais D, et al.assessment of the safety of a third dose of pneumococcal polysaccharide vaccine in the Vaccine Safety Datalink population. Vaccine 2006;24(2): Jefferson 2006 Jefferson T. Influenza vaccination: policy versus evidence. BMJ 2006;333(7574): Karadag 2005 Karadag B, Karakoc F, Ersu R, Kut A, Bakac S, Dagli E. Non-cystic-fibrosis bronchiectasis in children: a persisting problem in developing countries. Respiration 2005;72(3): Keistinen 1997 Keistinen T, Saynajakangas O, Tuuponen T, Kivela SL. Bronchiectasis: an orphan disease with a poorly-understood prognosis. European Respiratory Journal 1997;10(12): Lee 2003 Lee CJ, Lee LH, Frasch CE. Protective immunity of pneumococcal glycoconjugates. Critical Reviews in Microbiology 2003;29(4):
11 Lewis 2002 Lewis MM, Mortelliti MP, Yeager H, Jr, Tsou E. Clinical bronchiectasis complicating pulmonary sarcoidosis: case series of seven patients. Sarcoidosis, vasculitis, and diffuse lung diseases 2002;19(2): Lexau 2005 Lexau CA, Lynfield R, Danila R, Pilishvili T, Facklam R, Farley MM, et al.changing epidemiology of invasive pneumococcal disease among older adults in the era of pediatric pneumococcal conjugate vaccine. JAMA 2005; 294(16): Lucero 2004 Lucero MG, Dulalia VE, Parreno RN, Lim-Quianzon DM, Nohynek H, Makela H, et al.pneumococcal conjugate vaccines for preventing vaccine-type invasive pneumococcal disease and pneumonia with consolidation on x-ray in children under two years of age (Cochrane Review). Cochrane Database of Systematic Reviews 2004, Issue 4. [Art. No.: CD DOI: / CD ] Martinez-Garcia 2005 Martinez-Garcia MA, Perpina-Tordera M, Roman-Sanchez P, Soler-Cataluna JJ. Quality-of-life determinants in patients with clinically stable bronchiectasis. Chest 2005;128(2): McEllistrem 2005 McEllistrem MC, Adams JM, Patel K, Mendelsohn AB, Kaplan SL, Bradley JS, et al.acute otitis media due to penicillin-nonsusceptible Streptococcus pneumoniae before and after the introduction of the pneumococcal conjugate vaccine. Clinical Infectious Diseases 2005;40(12): NIPS National Immunisation Program. publishing.nsf/content/nips accessed Dec O Brien 2000 O Brien C, Guest PJ, Hill SL, Stockley RA. Physiological and radiological characterisation of patients diagnosed with chronic obstructive pulmonary disease in primary care. Thorax 2000;55(8): Patel 2004 Patel IS, Vlahos I, Wilkinson TM, Lloyd-Owen SJ, Donaldson GC, Wilks M, et al.bronchiectasis, exacerbation indices, and inflammation in chronic obstructive pulmonary disease. American Journal of Respiratory & Critical Care Medicine 2004;170(4): Poletti 2006 Poletti V, Casoni G, Chilosi M, Zompatori M. Diffuse panbronchiolitis. European Respiratory Journal 2006;28(4): Sheikh 2002 Sheikh A, Alves B, Dhami S. Pneumococcal vaccine for asthma (Cochrane Review). Cochrane Database of Systematic Reviews 2002, Issue 1. [DOI: / CD002165] Singleton 2000 Singleton RJ, Morris A, Redding G, Poll J, Holck P, Martinez P, et al.bronchiectasis in Alaska Native children: causes and clinical courses. Pediatric Pulmonology 2000;29 (3): Straetemans 2004 Straetemans M, Sanders EAM, Veenhoven RH, Schilder AGM, Damoiseaux RAMJ, Zielhuis GA. Pneumococcal vaccines for preventing otitis media (Cochrane Review). Cochrane Database of Systematic Reviews 2004, Issue 1. [DOI: / CD pub2] Twiss 2006 Twiss J, Stewart AW, Byrnes CA. Longitudinal pulmonary function of childhood bronchiectasis and comparison with cystic fibrosis. Thorax 2006;61(5): Walker 2005 Walker FJ, Singleton RJ, Bulkow LR, Strikas RA, Butler JC. Reactions after 3 or more doses of pneumococcal polysaccharide vaccine in adults in Alaska. Clinical Infectious Diseases 2005;40(12): Indicates the major publication for the study 9
12 C H A R A C T E R I S T I C S O F S T U D I E S Characteristics of included studies [ordered by study ID] Furumoto 2008 Methods Participants Interventions Outcomes Notes Multicentre parallel RCT involving 13 hospitals in the district of Kyushu and Okinawa (Japan) between November 2001 and April Subjects were seen monthly and with exacerbations, they visited a study physician 191 enrolled but 167 completed. All had chronic lung disease (COPD (n=55), bronchiectasis (20), sequelae of pulmonary tuberculosis (50), sarcoidosis (1), interstitial lung disease (9), diffuse pan bronchiolitis (5), pneumoconiosis (14), bronchial asthma (13)) Inclusion criteria were patients with chronic lung disease who previously experienced acute exacerbations, were able to comply with a schedule of monthly clinical visits and were between 40 and 80 years of age. Exclusion criteria: Patients who were pregnant or had immunocompromised conditions (e.g. active malignant diseases, renal insufficiency in dialysis or HIV infection, hypogammaglobulinaemia, anatomical or functional asplenia and who had previously received 23-valent PV Mean age: pneumococcal vaccine (PV) with influenza vaccine (IV) group=67.8, SD 9. 5 years; IV alone group=70.1 SD 7.4 years Gender: PV group=60 (69%), IV group=46 (57.5%) Home O2 use: PV group=27 (31%), IV group=32 (40%) Home non-invasive pressure ventilation: PV group=6 (6.9%), IV group=5 (6.3%) 23-valent pneumococcal vaccine (PV) and influenza vaccine (IV) compared to influenza vaccine alone. PV + IV group were separately immunized with 0.5 ml of PV and 0.5 ml of IV on separate occasions in 1month intervals, the participants in the IV group were immunized with 0.5 ml of IV alone Pneumonia defined as either clinical symptoms (cough, sputum or fever) plus increased white blood cell counts or serum C-reactive protein, and the appearance of a new infiltration on a chest radiograph Acute respiratory exacerbation defined by presence of criteria: (1) increased dyspnoea, (2) increased sputum volume and (3) increased sputum purulence, and (4) absence of newly appeared infiltration on a chest radiograph. Acute exacerbation was diagnosed when two of the three respiratory symptoms existed or when one of these and one of additional symptoms, such as a fever without any other causes or increased cough was present Acute infective respiratory exacerbation: above plus when the laboratory examinations revealed an increase in white blood cell counts (WCC) or serum C-reactive protein (CRP), in addition to the clinical symptoms of acute exacerbation Acute non-infective respiratory exacerbation: clinical symptoms of acute exacerbation without increase in WCC or serum CRP Follow-up period was 2-years. As all diseases in the inclusion list develop bronchiectasis, paper included Risk of bias Bias Authors judgement Support for judgement 10
13 Furumoto 2008 (Continued) Random sequence generation (selection bias) Unclear risk Not described Allocation concealment (selection bias) Low risk Use of envelopes Blinding (performance bias and detection bias) Pneumonia Blinding (performance bias and detection bias) Acute infective respiratory exacerbation High risk High risk Open label trial Open label trial Blinding (performance bias and detection bias) Acute non-infective respiratory exacerbation Incomplete outcome data (attrition bias) Pneumonia Incomplete outcome data (attrition bias) Acute infective respiratory exacerbation Incomplete outcome data (attrition bias) Acute non-infective respiratory exacerbation Low risk Low risk Unclear risk Unclear risk Defined by objective blood results; thus presumed blinded outcome Proportion of possible missing outcomes highly unlikely to have clinical relevant impact on intervention effect estimate (low numbers of drop outs and outcomes in both groups episodes per person year) Numbers lost and withdrawn in both groups given (7 in active arm, 17 in control arm) Numbers lost and withdrawn in both groups given (7 in active arm, 17 in control arm) Characteristics of excluded studies [ordered by study ID] Study Ryzhov 2005 van Kessel 2005 Reason for exclusion Non RCT. This study in Russian was a comparative study in 40 controls (unvaccinated ) and 25 children with chronic lung disease (including bronchiectasis) using Pneumovax 23. Hib vaccination was examined in another group Non RCT. Study examined antibody response to polysaccharide pneumococcal vaccine in 26 patients with bronchiectasis of unknown aetiology 11
14 (Continued) Vendrell 2005 Non RCT. Study examined antibody response to a pneumococcal unconjugate vaccine and an Haemophilus influenzae type b conjugate vaccine in all consecutive adult patients with bronchiectasis of unknown etiology 12
15 D A T A A N D A N A L Y S E S Comparison 1. Adults Outcome or subgroup title No. of studies No. of participants Statistical method Effect size 1 Number of people with one 1 Odds Ratio (M-H, Fixed, 95% CI) Subtotals only or more acute respiratory exacerbation 1.1 Any exacerbation Odds Ratio (M-H, Fixed, 95% CI) 0.53 [0.29, 0.99] 1.2 Infective exacerbations Odds Ratio (M-H, Fixed, 95% CI) 0.48 [0.26, 0.88] 1.3 Non-infective Odds Ratio (M-H, Fixed, 95% CI) 1.42 [0.48, 4.19] exacerbations 2 Number of subjects with pneumonia Odds Ratio (M-H, Fixed, 95% CI) 1.00 [0.43, 2.33] W H A T S N E W Last assessed as up-to-date: 4 December Date Event Description 5 June 2014 Amended PLS title amended H I S T O R Y Protocol first published: Issue 1, 2007 Review first published: Issue 2, 2007 Date Event Description 12 March 2009 Amended Contact details changed 4 December 2008 New citation required and conclusions have changed Study on 167 people added to review 12 November 2008 New search has been performed Literature search re-run 16 April 2008 Amended Converted to new review format. 13
16 (Continued) 10 December 2006 New citation required and conclusions have changed Substantive amendment C O N T R I B U T I O N S O F A U T H O R S For the protocol: Protocol was written by both CC and AC. RS reviewed the protocol. For the review: CC and AC selected articles from search, extracted data and wrote the review. RS and PM contributed to writing the review and would have been adjudicators if disagreements had occurred. D E C L A R A T I O N S O F None declared. I N T E R E S T S O U R C E S O F S U P P O R T Internal sources Royal Children s Hospital Foundation, Brisbane, Australia. External sources National Health and Medical Research Council, Australia. I N D E X T E R M S Medical Subject Headings (MeSH) Bronchiectasis [ complications]; Pneumococcal Infections [ prevention & control]; Pneumococcal Vaccines [ therapeutic use]; Respiration Disorders [ prevention & control] MeSH check words Adult; Child; Humans 14
Inhaled steroids for bronchiectasis (Review)
 Kapur N, Bell S, Kolbe J, Chang AB This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in The Cochrane Library 2009, Issue 1 http://www.thecochranelibrary.com
Kapur N, Bell S, Kolbe J, Chang AB This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in The Cochrane Library 2009, Issue 1 http://www.thecochranelibrary.com
Surgery versus non-surgical treatment for bronchiectasis (Review)
 Surgery versus non-surgical treatment for bronchiectasis (Review) Warburton CJ, Corless JA This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in
Surgery versus non-surgical treatment for bronchiectasis (Review) Warburton CJ, Corless JA This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in
pneumonia 2015;6:48 56
 pneumonia 2015 Aug 21;6:48 56 pneumonia Brief Report Anne B Chang a,b, Heidi Smith-Vaughan a,c, Theo P Sloots f, Patricia C Valery a, David Whiley f, Jemima Beissbarth a, Paul J Torzillo d,e a Menzies
pneumonia 2015 Aug 21;6:48 56 pneumonia Brief Report Anne B Chang a,b, Heidi Smith-Vaughan a,c, Theo P Sloots f, Patricia C Valery a, David Whiley f, Jemima Beissbarth a, Paul J Torzillo d,e a Menzies
Pneumococcal vaccines. Safety & Efficacy. Prof. Rajesh Kumar, MD PGIMER School of Public Health Chandigarh
 Pneumococcal vaccines Safety & Efficacy Prof. Rajesh Kumar, MD PGIMER School of Public Health Chandigarh Disclosure Slide X X I DO NOT have any significant or other financial relationships with industry
Pneumococcal vaccines Safety & Efficacy Prof. Rajesh Kumar, MD PGIMER School of Public Health Chandigarh Disclosure Slide X X I DO NOT have any significant or other financial relationships with industry
COPD Bronchiectasis Overlap Syndrome.
 COPD Bronchiectasis Overlap Syndrome. John R Hurst 1, J Stuart Elborn 2, and Anthony De Soyza 3 on Behalf of the BRONCH-UK Consortium (D Bilton, J Bradley, JS Brown, J Duckers, F Copeland, A Floto, J Foweraker,
COPD Bronchiectasis Overlap Syndrome. John R Hurst 1, J Stuart Elborn 2, and Anthony De Soyza 3 on Behalf of the BRONCH-UK Consortium (D Bilton, J Bradley, JS Brown, J Duckers, F Copeland, A Floto, J Foweraker,
Breathing exercises for chronic obstructive pulmonary disease (Protocol)
 Breathing exercises for chronic obstructive pulmonary disease (Protocol) Holland AE, Hill C, McDonald CF This is a reprint of a Cochrane protocol, prepared and maintained by The Cochrane Collaboration
Breathing exercises for chronic obstructive pulmonary disease (Protocol) Holland AE, Hill C, McDonald CF This is a reprint of a Cochrane protocol, prepared and maintained by The Cochrane Collaboration
Pneumococcal polysaccharide vaccines: Systematic review and meta-analysis of randomised controlled efficacy trials
 Pneumococcal polysaccharide vaccines: Systematic review and meta-analysis of randomised controlled efficacy trials Pippa Scott, Anke Huss, Matthias Egger Institute of Social & Preventive Medicine (ISPM)
Pneumococcal polysaccharide vaccines: Systematic review and meta-analysis of randomised controlled efficacy trials Pippa Scott, Anke Huss, Matthias Egger Institute of Social & Preventive Medicine (ISPM)
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Goyal V, Grimwood K, Byrnes CA, et al. Amoxicillin
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Goyal V, Grimwood K, Byrnes CA, et al. Amoxicillin
The Bacteriology of Bronchiectasis in Australian Indigenous children
 The Bacteriology of Bronchiectasis in Australian Indigenous children Kim Hare, Amanda Leach, Peter Morris, Heidi Smith-Vaughan, Anne Chang Presentation outline What is bronchiectasis? Our research at Menzies
The Bacteriology of Bronchiectasis in Australian Indigenous children Kim Hare, Amanda Leach, Peter Morris, Heidi Smith-Vaughan, Anne Chang Presentation outline What is bronchiectasis? Our research at Menzies
Summary of Indigenous health: respiratory disease
 Summary of Indigenous health: respiratory disease Ellie Kirov and Neil Thomson Australian Indigenous HealthInfoNet www.healthinfonet.ecu.edu.au This summary of respiratory disease in the Australian Indigenous
Summary of Indigenous health: respiratory disease Ellie Kirov and Neil Thomson Australian Indigenous HealthInfoNet www.healthinfonet.ecu.edu.au This summary of respiratory disease in the Australian Indigenous
Haemophilus influenzae
 Haemophilus influenzae type b Severe bacterial infection, particularly among infants During late 19th century believed to cause influenza Immunology and microbiology clarified in 1930s Haemophilus influenzae
Haemophilus influenzae type b Severe bacterial infection, particularly among infants During late 19th century believed to cause influenza Immunology and microbiology clarified in 1930s Haemophilus influenzae
Vaccines for preventing pneumococcal infection in adults (Review)
 Vaccines for preventing pneumococcal infection in adults (Review) Moberley S, Holden J, Tatham DP, Andrews RM This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Vaccines for preventing pneumococcal infection in adults (Review) Moberley S, Holden J, Tatham DP, Andrews RM This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
BCG vaccine and tuberculosis
 PART 2: Vaccination for special risk groups 2.1 Vaccination for Aboriginal and Torres Strait Islander people Aboriginal and Torres Strait Islander people historically had a very high burden of infectious
PART 2: Vaccination for special risk groups 2.1 Vaccination for Aboriginal and Torres Strait Islander people Aboriginal and Torres Strait Islander people historically had a very high burden of infectious
EPIREVIEW INVASIVE PNEUMOCOCCAL DISEASE, NSW, 2002
 EPIREVIEW INVASIVE PNEUMOCOCCAL DISEASE, NSW, 2002 Robyn Gilmour Communicable Diseases Branch NSW Department of Health BACKGROUND Infection with the bacterium Streptococcus pneumoniae is a major cause
EPIREVIEW INVASIVE PNEUMOCOCCAL DISEASE, NSW, 2002 Robyn Gilmour Communicable Diseases Branch NSW Department of Health BACKGROUND Infection with the bacterium Streptococcus pneumoniae is a major cause
Adult Pneumococcal Disease
 Adult Pneumococcal Disease S. pneumoniae and pneumococcal disease The bacterium Streptococcus pneumoniae causes pneumococcal disease S. pneumoniae is commonly found in human nasopharynx (nose and throat)
Adult Pneumococcal Disease S. pneumoniae and pneumococcal disease The bacterium Streptococcus pneumoniae causes pneumococcal disease S. pneumoniae is commonly found in human nasopharynx (nose and throat)
Adult Pneumococcal Disease
 Adult Pneumococcal Disease S. pneumoniae and pneumococcal disease The bacterium Streptococcus pneumoniae causes pneumococcal disease S. pneumoniae is commonly found in human nasopharynx (nose and throat)
Adult Pneumococcal Disease S. pneumoniae and pneumococcal disease The bacterium Streptococcus pneumoniae causes pneumococcal disease S. pneumoniae is commonly found in human nasopharynx (nose and throat)
PEER REVIEW HISTORY ARTICLE DETAILS TITLE (PROVISIONAL)
 PEER REVIEW HISTORY BMJ Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form (http://bmjopen.bmj.com/site/about/resources/checklist.pdf)
PEER REVIEW HISTORY BMJ Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form (http://bmjopen.bmj.com/site/about/resources/checklist.pdf)
Systematic reviews and meta-analyses of observational studies (MOOSE): Checklist.
 Systematic reviews and meta-analyses of observational studies (MOOSE): Checklist. MOOSE Checklist Infliximab reduces hospitalizations and surgery interventions in patients with inflammatory bowel disease:
Systematic reviews and meta-analyses of observational studies (MOOSE): Checklist. MOOSE Checklist Infliximab reduces hospitalizations and surgery interventions in patients with inflammatory bowel disease:
Pneumococcal Disease and Pneumococcal Vaccines
 Pneumococcal Disease and Epidemiology and Prevention of - Preventable Diseases Note to presenters: Images of vaccine-preventable diseases are available from the Immunization Action Coalition website at
Pneumococcal Disease and Epidemiology and Prevention of - Preventable Diseases Note to presenters: Images of vaccine-preventable diseases are available from the Immunization Action Coalition website at
Pneumococcal: Disease & Vaccine
 Pneumococcal: Disease & Vaccine Wednesday 15 June 2016 Wednesday 28 June 2016 Start time in your state: 7:30pm = QLD, NSW, VIC, TAS, ACT 7:00pm = SA, NT 5:30pm = WA Your presenter tonight Angela Newbound,
Pneumococcal: Disease & Vaccine Wednesday 15 June 2016 Wednesday 28 June 2016 Start time in your state: 7:30pm = QLD, NSW, VIC, TAS, ACT 7:00pm = SA, NT 5:30pm = WA Your presenter tonight Angela Newbound,
Chronic Lung Disease in vertically HIV infected children. Dr B O Hare Senior Lecturer in Paediatrics and Child Health, COM, Blantyre
 Chronic Lung Disease in vertically HIV infected children Dr B O Hare Senior Lecturer in Paediatrics and Child Health, COM, Blantyre Natural history of HIV in vertically infected children without and with
Chronic Lung Disease in vertically HIV infected children Dr B O Hare Senior Lecturer in Paediatrics and Child Health, COM, Blantyre Natural history of HIV in vertically infected children without and with
vaccination. Children enrolled in these clusters between 6 weeks and 6 months of age received a 2-dose primary vaccination schedule.
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Incidence per 100,000
 Streptococcus pneumoniae Surveillance Report 2005 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services Updated: March 2007 Background
Streptococcus pneumoniae Surveillance Report 2005 Oregon Active Bacterial Core Surveillance (ABCs) Office of Disease Prevention & Epidemiology Oregon Department of Human Services Updated: March 2007 Background
Cochrane Pregnancy and Childbirth Group Methodological Guidelines
 Cochrane Pregnancy and Childbirth Group Methodological Guidelines [Prepared by Simon Gates: July 2009, updated July 2012] These guidelines are intended to aid quality and consistency across the reviews
Cochrane Pregnancy and Childbirth Group Methodological Guidelines [Prepared by Simon Gates: July 2009, updated July 2012] These guidelines are intended to aid quality and consistency across the reviews
Systematic Review of RCTs of Haemophilus influenzae Type b Conjugate Vaccines: Efficacy and immunogenicity
 Supplementary text 1 Systematic Review of RCTs of Haemophilus influenzae Type b Conjugate Vaccines: Efficacy and immunogenicity Review protocol Pippa Scott, Shelagh Redmond, Nicola Low and Matthias Egger
Supplementary text 1 Systematic Review of RCTs of Haemophilus influenzae Type b Conjugate Vaccines: Efficacy and immunogenicity Review protocol Pippa Scott, Shelagh Redmond, Nicola Low and Matthias Egger
Impact of pneumococcal conjugate vaccine: US experience Stephanie Schrag Centers for Disease Control and Prevention Atlanta, GA
 Impact of pneumococcal conjugate vaccine: US experience Stephanie Schrag Centers for Disease Control and Prevention Atlanta, GA San Jose, Costa Rica, August 2007 Pneumococcal Conjugate Vaccine Introduction
Impact of pneumococcal conjugate vaccine: US experience Stephanie Schrag Centers for Disease Control and Prevention Atlanta, GA San Jose, Costa Rica, August 2007 Pneumococcal Conjugate Vaccine Introduction
Dr Conroy Wong. Professor Richard Beasley. Dr Sarah Mooney. Professor Innes Asher
 Professor Richard Beasley University of Otago Director Medical Research Institute of New Zealand Wellington Dr Sarah Mooney Physiotherapy Advanced Clinician Counties Manukau Health NZ Respiratory and Sleep
Professor Richard Beasley University of Otago Director Medical Research Institute of New Zealand Wellington Dr Sarah Mooney Physiotherapy Advanced Clinician Counties Manukau Health NZ Respiratory and Sleep
Bronchiectasis Domiciliary treatment. Prof. Adam Hill Royal Infirmary and University of Edinburgh
 Bronchiectasis Domiciliary treatment Prof. Adam Hill Royal Infirmary and University of Edinburgh Plan of talk Background of bronchiectasis Who requires IV antibiotics Domiciliary treatment Results to date.
Bronchiectasis Domiciliary treatment Prof. Adam Hill Royal Infirmary and University of Edinburgh Plan of talk Background of bronchiectasis Who requires IV antibiotics Domiciliary treatment Results to date.
Conference Bronchiectasis A Growing Problem
 Conference 2015 Bronchiectasis A Growing Problem Bronchiectasis (in Children) What is it? Why such a concern in NZ? What to look out for? Management Positives? Just a note that the bar for diagnosis, referral
Conference 2015 Bronchiectasis A Growing Problem Bronchiectasis (in Children) What is it? Why such a concern in NZ? What to look out for? Management Positives? Just a note that the bar for diagnosis, referral
Author's response to reviews
 Author's response to reviews Title: Pneumococcal vaccination and otitis media in Australian Aboriginal infants: comparison of two birth cohorts before and after introduction of vaccination Authors: Grant
Author's response to reviews Title: Pneumococcal vaccination and otitis media in Australian Aboriginal infants: comparison of two birth cohorts before and after introduction of vaccination Authors: Grant
Chapter 16 Pneumococcal Infection. Pneumococcal Infection. August 2015
 Chapter 16 16 PPV introduced for at risk 1996 PCV7 introduced for at risk 2002 and as routine 2008 PCV13 replaced PCV7 in 2010 NOTIFIABLE In some circumstances, advice in these guidelines may differ from
Chapter 16 16 PPV introduced for at risk 1996 PCV7 introduced for at risk 2002 and as routine 2008 PCV13 replaced PCV7 in 2010 NOTIFIABLE In some circumstances, advice in these guidelines may differ from
Pneumococcal pneumonia
 Pneumococcal pneumonia Wei Shen Lim Consultant Respiratory Physician & Honorary Professor of Medicine Nottingham University Hospitals NHS Trust University of Nottingham Declarations of interest Unrestricted
Pneumococcal pneumonia Wei Shen Lim Consultant Respiratory Physician & Honorary Professor of Medicine Nottingham University Hospitals NHS Trust University of Nottingham Declarations of interest Unrestricted
Patient characteristics Intervention Comparison Length of followup
 ORAL MUCOLYTICS Ref ID: 2511 Bachh AA, Shah NN, Bhargava R et al. Effect oral N- in COPD - A randomised controlled trial. JK Practitioner. 2007; 14(1):12-16. Ref ID: 2511 RCT Single blind; unclear allocation
ORAL MUCOLYTICS Ref ID: 2511 Bachh AA, Shah NN, Bhargava R et al. Effect oral N- in COPD - A randomised controlled trial. JK Practitioner. 2007; 14(1):12-16. Ref ID: 2511 RCT Single blind; unclear allocation
Cochrane Breast Cancer Group
 Cochrane Breast Cancer Group Version and date: V3.2, September 2013 Intervention Cochrane Protocol checklist for authors This checklist is designed to help you (the authors) complete your Cochrane Protocol.
Cochrane Breast Cancer Group Version and date: V3.2, September 2013 Intervention Cochrane Protocol checklist for authors This checklist is designed to help you (the authors) complete your Cochrane Protocol.
Anticholinergics for prolonged non-specific cough in children (Review)
 Anticholinergics for prolonged non-specific cough in children (Review) Chang AB, McKean MC, Morris PS This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published
Anticholinergics for prolonged non-specific cough in children (Review) Chang AB, McKean MC, Morris PS This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published
MCH-Immunization Conference. September 2012
 MCH-Immunization Conference September 2012 Rosalyn Singleton MD Arctic Investigations Program-CDC Alaska Native Tribal Health Consortium, Anchorage, AK DISCLAIMER: The results and conclusions presented
MCH-Immunization Conference September 2012 Rosalyn Singleton MD Arctic Investigations Program-CDC Alaska Native Tribal Health Consortium, Anchorage, AK DISCLAIMER: The results and conclusions presented
Community Acquired Pneumonia
 April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
9/12/2018. Pneumococcal Disease and Pneumococcal Vaccines. Streptococcus pneumoniae. Pneumococcal Disease. Adult Track. Gram-positive bacteria
 Centers for Disease Control and Prevention National Center for Immunization and Respiratory Diseases Pneumococcal Disease and Pneumococcal Vaccines Adult Track Chapter 17 Photographs and images included
Centers for Disease Control and Prevention National Center for Immunization and Respiratory Diseases Pneumococcal Disease and Pneumococcal Vaccines Adult Track Chapter 17 Photographs and images included
Communicable Disease. Introduction
 Communicable Disease HIGHLIGHTS Seniors have the highest incidence rates of tuberculosis compared to other age groups. The incidence rates for TB have been higher among Peel seniors compared to Ontario
Communicable Disease HIGHLIGHTS Seniors have the highest incidence rates of tuberculosis compared to other age groups. The incidence rates for TB have been higher among Peel seniors compared to Ontario
Exhaled nitric oxide levels to guide treatment for adults with asthma (Review) Petsky, Helen L.; Kew, Kayleigh M.; Turner, Catherine; Chang, Anne
 Charles Darwin University Petsky, Helen L.; Kew, Kayleigh M.; Turner, Catherine; Chang, Anne Published in: Cochrane Database of Systematic Reviews DOI: 10.1002/14651858.CD011440.pub2 Published: 01/09/2016
Charles Darwin University Petsky, Helen L.; Kew, Kayleigh M.; Turner, Catherine; Chang, Anne Published in: Cochrane Database of Systematic Reviews DOI: 10.1002/14651858.CD011440.pub2 Published: 01/09/2016
Rationale and design of CAPITA: a RCT of 13-valent conjugated pneumococcal vaccine efficacy among older adults
 ORIGINAL ARTICLE Rationale and design of CAPITA: a RCT of 13-valent conjugated pneumococcal vaccine efficacy among older adults E. Hak 1,2*, D.E. Grobbee 1, E.A.M. Sanders 2, T.J.M. Verheij 1, M. Bolkenbaas
ORIGINAL ARTICLE Rationale and design of CAPITA: a RCT of 13-valent conjugated pneumococcal vaccine efficacy among older adults E. Hak 1,2*, D.E. Grobbee 1, E.A.M. Sanders 2, T.J.M. Verheij 1, M. Bolkenbaas
Exhaled nitric oxide levels to guide treatment for children with asthma (Review)
 Charles Darwin University Petsky, Helen L.; Kew, Kayleigh M.; Chang, Anne Published in: Cochrane Database of Systematic Reviews DOI: 10.1002/14651858.CD011439.pub2 Published: 08/11/2016 Document Version
Charles Darwin University Petsky, Helen L.; Kew, Kayleigh M.; Chang, Anne Published in: Cochrane Database of Systematic Reviews DOI: 10.1002/14651858.CD011439.pub2 Published: 08/11/2016 Document Version
To view past issues, go to: The New 13-Valent Pneumococcal Conjugate Vaccine (PCV13)
 From the Texas Department of State Health Services Immunization Branch The goal of the Vaccine Advisory is to disseminate, in a timely manner, practical information related to vaccines, vaccine-preventable
From the Texas Department of State Health Services Immunization Branch The goal of the Vaccine Advisory is to disseminate, in a timely manner, practical information related to vaccines, vaccine-preventable
Gastro-oesophageal reflux treatment for prolonged nonspecific cough in children and adults (Review)
 Gastro-oesophageal reflux treatment for prolonged nonspecific cough in children and adults (Review) Chang AB, Lasserson TJ, Gaffney J, Connor FL, Garske LA This is a reprint of a Cochrane review, prepared
Gastro-oesophageal reflux treatment for prolonged nonspecific cough in children and adults (Review) Chang AB, Lasserson TJ, Gaffney J, Connor FL, Garske LA This is a reprint of a Cochrane review, prepared
Pulmonary rehabilitation following exacerbations of chronic obstructive pulmonary disease(review)
 Cochrane Database of Systematic Reviews Pulmonary rehabilitation following exacerbations of chronic obstructive pulmonary disease(review) Puhan MA, Gimeno-Santos E, Cates CJ, Troosters T Puhan MA, Gimeno-Santos
Cochrane Database of Systematic Reviews Pulmonary rehabilitation following exacerbations of chronic obstructive pulmonary disease(review) Puhan MA, Gimeno-Santos E, Cates CJ, Troosters T Puhan MA, Gimeno-Santos
Differential diagnosis
 Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Database of Abstracts of Reviews of Effects (DARE) Produced by the Centre for Reviews and Dissemination Copyright 2017 University of York.
 A comparison of the cost-effectiveness of five strategies for the prevention of non-steroidal anti-inflammatory drug-induced gastrointestinal toxicity: a systematic review with economic modelling Brown
A comparison of the cost-effectiveness of five strategies for the prevention of non-steroidal anti-inflammatory drug-induced gastrointestinal toxicity: a systematic review with economic modelling Brown
Surveillance report Published: 6 April 2016 nice.org.uk. NICE All rights reserved.
 Surveillance report 2016 Chronic obstructive pulmonary disease in over 16s: diagnosis and management (2010) NICE guideline CG101 Surveillance report Published: 6 April 2016 nice.org.uk NICE 2016. All rights
Surveillance report 2016 Chronic obstructive pulmonary disease in over 16s: diagnosis and management (2010) NICE guideline CG101 Surveillance report Published: 6 April 2016 nice.org.uk NICE 2016. All rights
Nebulised hypertonic saline for cystic fibrosis.
 Revista: Cochrane Database Syst Rev. 2003;(1):CD001506. Nebulised hypertonic saline for cystic fibrosis. Autor: Wark PA, McDonald V. Source: Department of Respiratory Medicine, John Hunter Hospital, Locked
Revista: Cochrane Database Syst Rev. 2003;(1):CD001506. Nebulised hypertonic saline for cystic fibrosis. Autor: Wark PA, McDonald V. Source: Department of Respiratory Medicine, John Hunter Hospital, Locked
Vaccine Efficacy IPD and Pneumonia
 Vaccine Efficacy IPD and Pneumonia Hanna Nohynek, MD PhD National Public Health Institute Helsinki, Finland for 3rd Regional Pneumococcal Symposium Istanbul, Turkey February 13-14, 2008 Vaccine efficacy
Vaccine Efficacy IPD and Pneumonia Hanna Nohynek, MD PhD National Public Health Institute Helsinki, Finland for 3rd Regional Pneumococcal Symposium Istanbul, Turkey February 13-14, 2008 Vaccine efficacy
Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H
 Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H Authors' objectives To systematically review the incidence of deep vein
Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H Authors' objectives To systematically review the incidence of deep vein
Non-cystic fibrosis bronchiectasis in childhood: longitudinal growth and lung function
 1 Portex Anaesthesia, Intensive Therapy and Respiratory Unit, UCL, Institute of Child Health, London, UK; 2 Department of Respiratory Medicine, Great Ormond Street Hospital for Children NHS Trust, London,
1 Portex Anaesthesia, Intensive Therapy and Respiratory Unit, UCL, Institute of Child Health, London, UK; 2 Department of Respiratory Medicine, Great Ormond Street Hospital for Children NHS Trust, London,
Streptococcus pneumoniae CDC
 Streptococcus pneumoniae CDC Pneumococcal Disease Infection caused by the bacteria, Streptococcus pneumoniae» otitis media 20 million office visits (28-55% Strep)» pneumonia 175,000 cases annually» meningitis
Streptococcus pneumoniae CDC Pneumococcal Disease Infection caused by the bacteria, Streptococcus pneumoniae» otitis media 20 million office visits (28-55% Strep)» pneumonia 175,000 cases annually» meningitis
ACIP Recommendations for Pneumococcal 13-valent Conjugate and 23-valent Polysaccharide Vaccine Use among Adults
 ACIP Recommendations for Pneumococcal 13-valent Conjugate and 23-valent Polysaccharide Vaccine Use among Adults National Center for Immunization & Respiratory Diseases Respiratory Diseases Branch ACIP
ACIP Recommendations for Pneumococcal 13-valent Conjugate and 23-valent Polysaccharide Vaccine Use among Adults National Center for Immunization & Respiratory Diseases Respiratory Diseases Branch ACIP
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE
 Last Updated: Version 4.4 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Set: Immunization Set Measure ID#: Measure Information Form Collected For: CMS Voluntary Only The Joint Commission
Last Updated: Version 4.4 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARDS FOR HOSPITAL CARE Measure Set: Immunization Set Measure ID#: Measure Information Form Collected For: CMS Voluntary Only The Joint Commission
Impact of Universal Infant Immunization with Pneumococcal (Streptococcus pneumonia) Conjugate Vaccines in Alaska
 Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects 8-2008 Impact of Universal Infant Immunization with Pneumococcal (Streptococcus pneumonia)
Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects 8-2008 Impact of Universal Infant Immunization with Pneumococcal (Streptococcus pneumonia)
Systematic review of observational data on effectiveness of Haemophilus influenzae
 Systematic review of observational data on effectiveness of Haemophilus influenzae type b (Hib) vaccines to allow optimization of vaccination schedules Charlotte Jackson, Andrea Mann, Punam Mangtani, Paul
Systematic review of observational data on effectiveness of Haemophilus influenzae type b (Hib) vaccines to allow optimization of vaccination schedules Charlotte Jackson, Andrea Mann, Punam Mangtani, Paul
Impact of vaccination on epidemiology in adults
 Impact of vaccination on epidemiology in adults Jan Verhaegen 1. Data on prospective study on IPD in Belgium (2009-2011) 2. Evolution of capsular types of invasive isolates from adults after introduction
Impact of vaccination on epidemiology in adults Jan Verhaegen 1. Data on prospective study on IPD in Belgium (2009-2011) 2. Evolution of capsular types of invasive isolates from adults after introduction
Influenza vaccine for patients with chronic obstructive pulmonary disease (Review)
 Influenza vaccine for patients with chronic obstructive pulmonary disease (Review) Poole P, Chacko EE, Wood-Baker R, Cates CJ This is a reprint of a Cochrane review, prepared and maintained by The Cochrane
Influenza vaccine for patients with chronic obstructive pulmonary disease (Review) Poole P, Chacko EE, Wood-Baker R, Cates CJ This is a reprint of a Cochrane review, prepared and maintained by The Cochrane
Dr Stephen Child. General Physician Auckland. 14:20-14:40 Secondary Care Perspective
 Dr Stephen Child General Physician Auckland 14:20-14:40 Secondary Care Perspective Wheeze Witchery Stephen Child MD, FRACP, FRCPC General Physician Respiratory Interest Director of Clinical Training Auckland
Dr Stephen Child General Physician Auckland 14:20-14:40 Secondary Care Perspective Wheeze Witchery Stephen Child MD, FRACP, FRCPC General Physician Respiratory Interest Director of Clinical Training Auckland
Pneumococcal Vaccines The Impact Of Conjugate Vaccine
 Pneumococcal Vaccines The Impact Of Conjugate Vaccine 1 / 5 2 / 5 3 / 5 Pneumococcal Vaccines The Impact Of Pneumococcal vaccine. The pneumococcal vaccine protects against serious and potentially fatal
Pneumococcal Vaccines The Impact Of Conjugate Vaccine 1 / 5 2 / 5 3 / 5 Pneumococcal Vaccines The Impact Of Pneumococcal vaccine. The pneumococcal vaccine protects against serious and potentially fatal
Prevention of pneumococcal disease in Canadian adults Old and New. Allison McGeer, MSc, MD, FRCPC Mount Sinai Hospital University of Toronto
 Prevention of pneumococcal disease in Canadian adults Old and New Allison McGeer, MSc, MD, FRCPC Mount Sinai Hospital University of Toronto Objectives Review epidemiology of pneumococcal disease in adults
Prevention of pneumococcal disease in Canadian adults Old and New Allison McGeer, MSc, MD, FRCPC Mount Sinai Hospital University of Toronto Objectives Review epidemiology of pneumococcal disease in adults
Economic Evaluation of a Universal Childhood Pneumococcal Conjugate Vaccination Strategy in Ireland
 Volume 11 Number 5 2008 VALUE IN HEALTH Economic Evaluation of a Universal Childhood Pneumococcal Conjugate Vaccination Strategy in Ireland Lesley Tilson, BSc (Pharm), PhD, 1 Cara Usher, BSc, PhD, 1 Karina
Volume 11 Number 5 2008 VALUE IN HEALTH Economic Evaluation of a Universal Childhood Pneumococcal Conjugate Vaccination Strategy in Ireland Lesley Tilson, BSc (Pharm), PhD, 1 Cara Usher, BSc, PhD, 1 Karina
Adult Pneumococcal Disease
 Adult Pneumococcal Disease Reviewed and updated July 2018 S. pneumoniae and pneumococcal disease The bacterium Streptococcus pneumoniae causes pneumococcal disease S. pneumoniae is commonly found in human
Adult Pneumococcal Disease Reviewed and updated July 2018 S. pneumoniae and pneumococcal disease The bacterium Streptococcus pneumoniae causes pneumococcal disease S. pneumoniae is commonly found in human
Pneumococcal vaccination in UK: an update. Dr Richard Pebody Immunisation Department Health Protection Agency Centre for Infections
 Pneumococcal vaccination in UK: an update Dr Richard Pebody Immunisation Department Health Protection Agency Centre for Infections Leading infectious causes of mortality, 2000 WHO estimates 3.5 Deaths
Pneumococcal vaccination in UK: an update Dr Richard Pebody Immunisation Department Health Protection Agency Centre for Infections Leading infectious causes of mortality, 2000 WHO estimates 3.5 Deaths
Table 1 23 Pneumococcal Capsular Types Included in PNEUMOVAX 23
 PRODUCT INFORMATION NAME OF THE MEDICINE: PNEUMOVAX 23 (pneumococcal vaccine, polyvalent, MSD) DESCRIPTION: PNEUMOVAX 23 (Pneumococcal Vaccine, Polyvalent, MSD), is a sterile, liquid vaccine for intramuscular
PRODUCT INFORMATION NAME OF THE MEDICINE: PNEUMOVAX 23 (pneumococcal vaccine, polyvalent, MSD) DESCRIPTION: PNEUMOVAX 23 (Pneumococcal Vaccine, Polyvalent, MSD), is a sterile, liquid vaccine for intramuscular
Benefits of the pneumococcal immunisation programme in children in the United Kingdom
 Benefits of the pneumococcal immunisation programme in children in the United Kingdom 2006-2014 Professor Mary P E Slack mpeslack@gmail.com March 2015 Disclosure of interest The presenter has received
Benefits of the pneumococcal immunisation programme in children in the United Kingdom 2006-2014 Professor Mary P E Slack mpeslack@gmail.com March 2015 Disclosure of interest The presenter has received
HIV AND LUNG HEALTH. Stephen Aston Infectious Diseases SpR Royal Liverpool University Hospital
 HIV AND LUNG HEALTH Stephen Aston Infectious Diseases SpR Royal Liverpool University Hospital Introduction HIV infection exerts multiple effects on pulmonary immune responses: Generalised state of immune
HIV AND LUNG HEALTH Stephen Aston Infectious Diseases SpR Royal Liverpool University Hospital Introduction HIV infection exerts multiple effects on pulmonary immune responses: Generalised state of immune
Impacto de la vacuna conjugada en EUA
 Impacto de la vacuna conjugada en EUA Richard Facklam, PhD, Distinguished Consultant, Retired, Centers for Disease Control and Prevention Atlanta, GA Bogotá, Colombia, February 2008 Pneumococcal Conjugate
Impacto de la vacuna conjugada en EUA Richard Facklam, PhD, Distinguished Consultant, Retired, Centers for Disease Control and Prevention Atlanta, GA Bogotá, Colombia, February 2008 Pneumococcal Conjugate
Experience with maternal pertussis and PCV13 immunisation in England
 Experience with maternal pertussis and PCV13 immunisation in England Immunisation, Hepatitis & Blood Safety department Public Health England 5th RIVM Vaccine Preventable Diseases Research day 18 th November
Experience with maternal pertussis and PCV13 immunisation in England Immunisation, Hepatitis & Blood Safety department Public Health England 5th RIVM Vaccine Preventable Diseases Research day 18 th November
Systematic review of observational data on effectiveness of Haemophilus influenzae
 Systematic review of observational data on effectiveness of Haemophilus influenzae type b (Hib) vaccines to allow optimization of vaccination schedules Charlotte Jackson, Andrea Mann, Punam Mangtani, Paul
Systematic review of observational data on effectiveness of Haemophilus influenzae type b (Hib) vaccines to allow optimization of vaccination schedules Charlotte Jackson, Andrea Mann, Punam Mangtani, Paul
Application for inclusion, change or deletion of a medicine in the WHO Model List of Essential Medicines
 Application for inclusion, change or deletion of a medicine in the WHO Model List of Essential Medicines We are a group of authors within an external affiliated non-government organisation, the Cochrane
Application for inclusion, change or deletion of a medicine in the WHO Model List of Essential Medicines We are a group of authors within an external affiliated non-government organisation, the Cochrane
Controlled Trials. Spyros Kitsiou, PhD
 Assessing Risk of Bias in Randomized Controlled Trials Spyros Kitsiou, PhD Assistant Professor Department of Biomedical and Health Information Sciences College of Applied Health Sciences University of
Assessing Risk of Bias in Randomized Controlled Trials Spyros Kitsiou, PhD Assistant Professor Department of Biomedical and Health Information Sciences College of Applied Health Sciences University of
Chest radiographs for acute lower respiratory tract infections
 Bond University epublications@bond Faculty of Health Sciences & Medicine Publications Faculty of Health Sciences & Medicine 1-2-2014 Chest radiographs for acute lower respiratory tract infections Amy Cao
Bond University epublications@bond Faculty of Health Sciences & Medicine Publications Faculty of Health Sciences & Medicine 1-2-2014 Chest radiographs for acute lower respiratory tract infections Amy Cao
PROSPERO International prospective register of systematic reviews
 PROSPERO International prospective register of systematic reviews The effect of probiotics on functional constipation: a systematic review of randomised controlled trials EIRINI DIMIDI, STEPHANOS CHRISTODOULIDES,
PROSPERO International prospective register of systematic reviews The effect of probiotics on functional constipation: a systematic review of randomised controlled trials EIRINI DIMIDI, STEPHANOS CHRISTODOULIDES,
Prophylactic antibiotic therapy for chronic obstructive pulmonary disease(copd)(review)
 Cochrane Database of Systematic Reviews Prophylactic antibiotic therapy for chronic obstructive pulmonary disease(copd)(review) HerathSC,PooleP Herath SC, Poole P. Prophylactic antibiotic therapy for chronic
Cochrane Database of Systematic Reviews Prophylactic antibiotic therapy for chronic obstructive pulmonary disease(copd)(review) HerathSC,PooleP Herath SC, Poole P. Prophylactic antibiotic therapy for chronic
T A B L E O F C O N T E N T S
 Short-term psychodynamic psychotherapies for anxiety, depression and somatoform disorders (Unknown) Abbass AA, Hancock JT, Henderson J, Kisely S This is a reprint of a Cochrane unknown, prepared and maintained
Short-term psychodynamic psychotherapies for anxiety, depression and somatoform disorders (Unknown) Abbass AA, Hancock JT, Henderson J, Kisely S This is a reprint of a Cochrane unknown, prepared and maintained
Pneumococcal Vaccine Effectiveness. Steven Black, MD Center for Global Health Cincinnati Children s s Hospital Cincinnati, Ohio USA
 Pneumococcal Vaccine Effectiveness Steven Black, MD Center for Global Health Cincinnati Children s s Hospital Cincinnati, Ohio USA Overview Possible effectiveness outcomes for pneumococcal vaccines Pre-licensure
Pneumococcal Vaccine Effectiveness Steven Black, MD Center for Global Health Cincinnati Children s s Hospital Cincinnati, Ohio USA Overview Possible effectiveness outcomes for pneumococcal vaccines Pre-licensure
Gastro-oesophageal reflux treatment for prolonged nonspecific cough in children and adults (Review)
 Gastro-oesophageal reflux treatment for prolonged nonspecific cough in children and adults (Review) Chang AB, Lasserson TJ, Gaffney J, Connor FL, Garske LA This is a reprint of a Cochrane review, prepared
Gastro-oesophageal reflux treatment for prolonged nonspecific cough in children and adults (Review) Chang AB, Lasserson TJ, Gaffney J, Connor FL, Garske LA This is a reprint of a Cochrane review, prepared
PROSPERO International prospective register of systematic reviews
 PROSPERO International prospective register of systematic reviews High-dose chemotherapy followed by autologous haematopoietic cell transplantation for children, adolescents and young adults with first
PROSPERO International prospective register of systematic reviews High-dose chemotherapy followed by autologous haematopoietic cell transplantation for children, adolescents and young adults with first
PLACEMENT OPERATIONS - FREQUENTLY ASKED QUESTIONS
 PLACEMENT OPERATIONS - FREQUENTLY ASKED QUESTIONS IMMUNISATION AND HEALTH RECORDS Q: When should I commence my immunisations? A: All immunisation requirements must be completed prior to placement. It is
PLACEMENT OPERATIONS - FREQUENTLY ASKED QUESTIONS IMMUNISATION AND HEALTH RECORDS Q: When should I commence my immunisations? A: All immunisation requirements must be completed prior to placement. It is
THE EPIDEMIOLOGY OF RESPIRATORY SYNCYTIAL VIRUS INFECTIONS IN NSW CHILDREN,
 THE EPIDEMIOLOGY OF RESPIRATORY SYNCYTIAL VIRUS INFECTIONS IN NSW CHILDREN, 1992 1997 Susan Lister * and Peter McIntyre National Centre for Immunisation Research and Surveillance of Vaccine Preventable
THE EPIDEMIOLOGY OF RESPIRATORY SYNCYTIAL VIRUS INFECTIONS IN NSW CHILDREN, 1992 1997 Susan Lister * and Peter McIntyre National Centre for Immunisation Research and Surveillance of Vaccine Preventable
Influenza vaccines in 2016: why, who, what?
 Influenza vaccines in 2016: why, who, what? Heath Kelly Founding Head, Epidemiology Unit, Victorian Infectious Diseases Reference Laboratory Adjunct Professor, National Centre for Epidemiology and Population
Influenza vaccines in 2016: why, who, what? Heath Kelly Founding Head, Epidemiology Unit, Victorian Infectious Diseases Reference Laboratory Adjunct Professor, National Centre for Epidemiology and Population
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
OREGON PUBLIC HEALTH, DHS IMMUNIZATION PROTOCOL FOR PHARMACISTS. PNEUMOCOCCAL POLYSACCHARIDE VACCINE 23-Valent Vaccine
 OREGON PUBLIC HEALTH, DHS IMMUNIZATION PROTOCOL FOR PHARMACISTS PNEUMOCOCCAL POLYSACCHARIDE VACCINE 23-Valent Vaccine Revisions as of 2/24/10 Pneumovax 23 should not be given concurrently with Zostavax
OREGON PUBLIC HEALTH, DHS IMMUNIZATION PROTOCOL FOR PHARMACISTS PNEUMOCOCCAL POLYSACCHARIDE VACCINE 23-Valent Vaccine Revisions as of 2/24/10 Pneumovax 23 should not be given concurrently with Zostavax
Annual Epidemiological Report
 August 2018 Annual Epidemiological Report Key Facts Streptococcus 1Pneumoniae (invasive) in Ireland, 2017 In 2017, 415 confirmed cases of invasive pneumococcal diseases (IPD) were reported in Ireland,
August 2018 Annual Epidemiological Report Key Facts Streptococcus 1Pneumoniae (invasive) in Ireland, 2017 In 2017, 415 confirmed cases of invasive pneumococcal diseases (IPD) were reported in Ireland,
Journal Club 3/4/2011
 Journal Club 3/4/2011 Maternal HIV Infection and Antibody Responses Against Vaccine-Preventable Diseases in Uninfected Infants JAMA. 2011 Feb 9;305(6):576-84. Jones et al Dept of Pediatrics, Imperial College,
Journal Club 3/4/2011 Maternal HIV Infection and Antibody Responses Against Vaccine-Preventable Diseases in Uninfected Infants JAMA. 2011 Feb 9;305(6):576-84. Jones et al Dept of Pediatrics, Imperial College,
Surveillance of invasive pneumococcal infection in Belgium
 Surveillance of invasive pneumococcal infection in Belgium National Reference Laboratory Start in 198 Laboratory Microbiology UH Leuven (prof. J. Vandepitte) Capsular type determination Antibiotic susceptibility
Surveillance of invasive pneumococcal infection in Belgium National Reference Laboratory Start in 198 Laboratory Microbiology UH Leuven (prof. J. Vandepitte) Capsular type determination Antibiotic susceptibility
This is the publisher s version. This version is defined in the NISO recommended practice RP
 Journal Article Version This is the publisher s version. This version is defined in the NISO recommended practice RP-8-2008 http://www.niso.org/publications/rp/ Suggested Reference Chong, J., Karner, C.,
Journal Article Version This is the publisher s version. This version is defined in the NISO recommended practice RP-8-2008 http://www.niso.org/publications/rp/ Suggested Reference Chong, J., Karner, C.,
Bronchiectasis (non-cystic fibrosis), acute exacerbation: antimicrobial prescribing
 National Institute for Health and Care Excellence Bronchiectasis (non-cystic fibrosis), acute exacerbation: antimicrobial prescribing Evidence review NICE guideline NG117 December 2018 Disclaimer The
National Institute for Health and Care Excellence Bronchiectasis (non-cystic fibrosis), acute exacerbation: antimicrobial prescribing Evidence review NICE guideline NG117 December 2018 Disclaimer The
Antimicrobial Stewardship in Community Acquired Pneumonia
 Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
Antimicrobial Stewardship in Community Acquired Pneumonia Medicine Review Course 2018 Dr Lee Tau Hong Consultant Department of Infectious Diseases National Centre for Infectious Diseases Scope 1. Diagnosis
The McMaster at night Pediatric Curriculum
 The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
The McMaster at night Pediatric Curriculum Community Acquired Pneumonia Based on CPS Practice Point Pneumonia in healthy Canadian children and youth and the British Thoracic Society Guidelines on CAP Objectives
Streptococcus Pneumoniae
 Streptococcus Pneumoniae (Invasive Pneumococcal Disease) DISEASE REPORTABLE WITHIN 24 HOURS OF DIAGNOSIS Per N.J.A.C. 8:57, healthcare providers and administrators shall report by mail or by electronic
Streptococcus Pneumoniae (Invasive Pneumococcal Disease) DISEASE REPORTABLE WITHIN 24 HOURS OF DIAGNOSIS Per N.J.A.C. 8:57, healthcare providers and administrators shall report by mail or by electronic
Quick Literature Searches
 Quick Literature Searches National Pediatric Nighttime Curriculum Written by Leticia Shanley, MD, FAAP Institution: University of Texas Southwestern Medical Center Case 1 It s 1:00am and you have just
Quick Literature Searches National Pediatric Nighttime Curriculum Written by Leticia Shanley, MD, FAAP Institution: University of Texas Southwestern Medical Center Case 1 It s 1:00am and you have just
WHO INFLUENZA VACCINE RECOMMENDATION
 WHO INFLUENZA VACCINE RECOMMENDATION Strategic Advisory Group of Experts (SAGE) on Immunization SAGE Working Group on Influenza Vaccine and Immunization 1 Evidence Evaluation: Conceptual Matrix Target
WHO INFLUENZA VACCINE RECOMMENDATION Strategic Advisory Group of Experts (SAGE) on Immunization SAGE Working Group on Influenza Vaccine and Immunization 1 Evidence Evaluation: Conceptual Matrix Target
PNEUMONIA : PROMISE FULFILLED? Regina Berba MD FPSMID
 PNEUMONIA : PROMISE FULFILLED? Regina Berba MD FPSMID Objectives of Lecture Know the quality of current evidence based guidelines on immunization Appreciate the performance of pneumonia vaccines in terns
PNEUMONIA : PROMISE FULFILLED? Regina Berba MD FPSMID Objectives of Lecture Know the quality of current evidence based guidelines on immunization Appreciate the performance of pneumonia vaccines in terns
Immunology and the middle ear Andrew Riordan
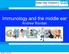 Immunology and the middle ear Andrew Riordan The Immune system is NOT there; To baffle medical students To keep Immunologists in a job To encourage experiments on mice The Immune system IS there as a defence
Immunology and the middle ear Andrew Riordan The Immune system is NOT there; To baffle medical students To keep Immunologists in a job To encourage experiments on mice The Immune system IS there as a defence
WF RESPIRATORY SYSTEM. RESPIRATORY MEDICINE
 WF RESPIRATORY SYSTEM. RESPIRATORY MEDICINE 1 Societies 11 History 13 Dictionaries. Encyclopaedias. Bibliographies Use for general works only. Classify with specific aspect where possible 15 Classification.
WF RESPIRATORY SYSTEM. RESPIRATORY MEDICINE 1 Societies 11 History 13 Dictionaries. Encyclopaedias. Bibliographies Use for general works only. Classify with specific aspect where possible 15 Classification.
Evelyn A. Kluka, MD FAAP November 30, 2011
 Evelyn A. Kluka, MD FAAP November 30, 2011 > 80% of children will suffer from at least one episode of AOM by 3 years of age 40% will have > 6 recurrences by age 7 years Most common diagnosis for which
Evelyn A. Kluka, MD FAAP November 30, 2011 > 80% of children will suffer from at least one episode of AOM by 3 years of age 40% will have > 6 recurrences by age 7 years Most common diagnosis for which
Data extraction. Specific interventions included in the review Dressings and topical agents in relation to wound healing.
 Systematic reviews of wound care management: (2) dressings and topical agents used in the healing of chronic wounds Bradley M, Cullum N, Nelson E A, Petticrew M, Sheldon T, Torgerson D Authors' objectives
Systematic reviews of wound care management: (2) dressings and topical agents used in the healing of chronic wounds Bradley M, Cullum N, Nelson E A, Petticrew M, Sheldon T, Torgerson D Authors' objectives
