Portage Health Cardiopulmonary Policy. Cardiopulmonary. To provide guidelines for process and procedure with pulmonary function tests.
|
|
|
- Grant Byrd
- 5 years ago
- Views:
Transcription
1 Subject: Pulmonary Function Testing Scope: Cardiopulmonary Effective Date: 6/90 Revised: 3/99, 5/02, 6/09, 6/12 Approved by: Deb Young Approval Date: Portage Health Cardiopulmonary Policy Cardiopulmonary I. Statement of Purpose To provide guidelines for process and procedure with pulmonary function tests. II. Definitions Pulmonary Function Test -A general term that refers to a wide assortment of studies which assess various aspects of lung functions. Methacholine Challenge A drug given (methacholine) during a PFT to help differentiate a diagnosis of asthma and in certain circumstance to assist in the managing of asthma III. Statement of Policy 3.1. Pulmonary Function Test (PFT) administration is the responsibility of the Cardiopulmonary Department which, upon a physician's order, will test both in-patients and out-patients as promptly as the staffing schedule will allow If testing is to include bronchodilator therapy, the practitioner should also have an aerosol nebulizer or a metered dose inhaler, supply of tubing, a gas supply (room air or oxygen) capable of providing a flow rate of at least 5-6 lpm, and the PFT specific bronchodilator If a particular bronchodilator is not specified, 2.5 mg Albuterol nebulizer treatment for before and after pulmonary function test and should be used; for a Methacholine Challenge. Combivent MDI or Duoneb should be used Contraindication for the Methacholine Challenge is pregnancy and nursing Patient compliance is necessary to perform accurate and viable test results. Patient education must be complete and consent obtained prior to the test Scope of Service: Patient must be able to follow directions and possess the ability to consistently reproduce deep breaths; must weigh less than 500 pounds for all tests except for the Body Box Test (Plethysmography) where the weight limit is less than 350 pounds. IV. Procedure 4.1. Patient preparation prior to the test
2 4.1.1 All tests require, absence of smoking and alcohol for 24 hours prior, no eating for 2 hours prior, no coffee, tea, cola or chocolate for 6 hours prior to the test and no strenuous exercise for 30 minutes before the test The following inhalers must be held for 12 hours: Albuterol Atrovent Combivent Cromolyn Sodium DuoNeb Maxair Proventil Ventolin Intal Nasocort Nasonex The following long acting medications need to be held for up to 48 hours: Advair Brovana Dulera Flovent Pulmicort Severent Singulair Spiriva Symbicort Theophylline The following antihistamines must be held for 48 hours: Allegra Benadryl Claritin Zyrtec Validate that the above criteria is met and that the patient education is complete Turn on computer, monitor, and printer by activating master power switch Attach clean spirometry tubing to pneumotach and insert a clean, disposable mouthpiece and filter Enter system set-up information at prompt on monitor Calibration - Perform calibrations at the start of each new day of PFT testing. (See Flow and Body Box Addendum 1 and 2.) 4.6. Enter New Patient Information Enter patient data in new patient screen 4.7. Pulmonary Function Screen Test See attached Flow Volume Loops Procedure. (Addendum 3) 4.8. Before and After Pulmonary Function Test See attached Flow Volume Loops Procedure. (Addendum 3) Perform 3 viable FVC Maneuvers.
3 Administer Repeat Be Administer bronchodilator Prepare a nebulizer setup for administration of the bronchodilator, explaining the treatment technique to the patient Unless otherwise specified by the patient's physician, a 2.5 mg Albuterol sulfate in 3.0 cc NS will be administered bronchodilator as outlined in nebulizer or MDI procedure The patient must wait for 15 minutes after test before resuming study Post Bronchodilator of PFT the FVC test procedures sure to select "Post-BD" from "Pre/Post" menu for each procedure Report 4.9. Methacholine Select PHS Auto Report, if pediatric patient under the age of 18select PHS-Auto report MGH and sent to MGH for interpretation See Methacholine Challenge (Addendum 4) 4.9. PFT Complete Perform Flow Volume Loop, (Addendum 3) Perform DLCO Single Breathe Diffusion (Addendum 5) Perform Plethysmography (Addendum 6) Repeat Flow Volume Loop with Bronchodialator Post Flow Volume Loop
4 Addendum 1 Performing the Calibration Flow Calibration Vmax Spectra 1. Connect the syringe to the Mass Flow Sensor. 2. Select [F1} to begin Calibration. 3. Stroke the syringe two times and [Space Continue]. The system automatically Zero the sensor. 4. When the calibration screen is displayed, stroke the syringe 5 times, completely displayed strokes fall within the yellow target zones. When 50% or more of the stroke is in the yellow target zone the column on the right will turn green indicating the zones that have been completed. The zones must be met within 3 minutes or 15 strokes but may be completed in as few as four. When all the zone criteria have been met, the yellow target graph will automatically advance to the verification screen. 5. Stroke the syringe 5 more times, completely filling and emptying the syringe with each stroke. The first stroke will be discarded. The strokes should vary in flow rates. One stroke on or just above the lower red lines (.5 LPS). Two strokes in-between the two red, dotted lines (3LBS). One stroke above the upper red dotted lines (6 8 LPS). Again, be careful not to bang the syringe at the end of each stroke. 6. The calibration sequence will end automatically. 7. [F3] to store. ATS Standards Calibrate the Mass Flow Sensor daily. If continuous testing is being performed, calibrate the sensor every 4 hours. If a filter is used for patient testing, a filter should be in-line when calibrating. Reproducibility Standards Each of the eight strokes must be within +/- 3% of 3 liters. The strikes are averaged and compared to the predicted. The % Target values should be between 97 and 103. Important Information Vmax will automatically measure temperature and pressure. If desired, these values may be entered in the [Setup] menu. A calibration must be performed if either one of these parameters is modified.
5 Addendum 2 Performing the Calibration Body Box Calibration 1. From the [Flow Sensor Calibration] screen, select [F4]. 2. Be sure the oxygen tank is turned on, the large bore tubing (white) is connected and the body box door is closed. 3. [F1] to begin the calibration. The test will run automatically. ATS Standards Calibrate the box daily Reproducibility Standards The %Target must be between 97% and 103%. Important Information Do not touch the body box while the test is being performed.
6 Addendum 3 Flow Volume Loops Performing the Maneuver 1. Press [F1] to begin data collection. 2. Obtain 2 4 stable tidal breaths. 3. Instruct patient to inhale maximally and perform a forceful exhalation. 4. Instruct the patient to do a rapid, maximal expiration. 5. Select [End] to end test. ATS Standards The Volume of Extrapolation must be less than 5% of the Best VC, or 150 cc s. At the end of expiration, no volume change for 1 second. The expiration phase must be at least 6 seconds long. Reproducibility Standards The Best FVC and at least one other must be within 200 cc s. The Best FEV1 and at least one other must be within 200 cc s. The Best Peak Flow and at least one other must be within 10%. Best Test Criteria Largest FVC from acceptable trials. Largest FEV1 from acceptable trials. Highest PEF from acceptable trials. All other parameters come from the trial with the largest SUM of FVC + FEV1. Testing Information Maximum inspiration must be at least 1 ½ times the tidal volume. If the patient has trouble getting 1 ½ times tidal volume on inspiration, such as pediatrics or geriatrics, press [F1] anytime during the collection of the loop and the Vmax will record it as the maneuver. To obtain tidal volume loop perform at least 3 tidal breaths before the maneuver.
7 Addendum 4 Methacholine Challenge test Procedure The purpose of a Methacholine Challenge test is to determine the reactivity of a patient s airways. Pre- procedure; Check order Make sure Methacholine challenge test is ordered. Ordering physician should fax over a physician signed consent form for the Methacholine challenge. Gather necessary equipment. o Filter, nose clips, mouthpiece, and spacer. o Methacholine solutions. o Syringes. o Dosimeter. Explain Procedure. Test Procedure. Enter patient information Choose new study on Main Menu. Enter patient information Click on F3 to save entered information and move to the next screen. PFT menu (#5) Choose Provocholine Cum Dose from menu at the top of the screen on the right side labeled TEST PROTOCOL. Click on flow volume loop and perform at least 3 FVC maneuvers to establish a baseline. The baseline FEV1 must be 80% of predicted to proceed with testing. Failure by the patient to product three consistent FVC s will result in technician discontinuing the Methacholine Challenge test. Pre and post bronchodilator will be performed instead. Administer 5 breaths via dosimeter of the Koch s solution to patient. Wait two minutes. Change the blue "Pre indicator in the lower right hand corner of the screen to baseline and do an FVC maneuver. Repeat FVC if the FEV1 result is not close to the baseline FEV1 result. You will continue administering Methacholine and doing FVC maneuvers until the FEV1 results show a drop of 20% or more. So, if the FEV1 result is close to the baseline go on. Administer level of.025mg. Change the blue Baseline indicator in the lower right hand corner of the screen to pink Level 1 and do an FVC maneuver. Repeat if necessary. Continue with the same steps until you have given all the doses of Methacholine or the FEV1 drops by 20% or more. Administer four (4) puffs of Combivent via spacer or Duoneb.
8 Wait fifteen (15) minutes. Change the pink level indicator to the red Post. After 15 minutes repeat the FVC to establish the return of the patient s FEV1 to baseline or within 10% of baseline. Possible Hazards and side effects Severs bronchospasms. Flushing of the face and neck. Generalized sweating. Salivation. Transient and slight fall in blood pressure. Increased pulse rate. Irritation of the throat. Cough. Headache. Post Test Add comments to test and print results. Send one copy with face sheet to Pulmonologists at MGH for interpretation. A 2 nd copy of the preliminary report, the face sheet, permission to treat, and original order if the patient brought it in to Medical Records.
9 Addendum 5 Single Breath Diffusion [DLCO] Performing the maneuver From main menu chose pulmonary function then choose single breath DLCO Press [F1] to begin test. This will start the automatic calibration it takes about 45 seconds. The screen will automatically go to the DLCO testing screen. Instruct the patient to breathe normally, them exhale maximally. During expiration, select [F12]. A [Continue to expire] message will appear. After the screen changes, instruct the patient to perform a fast maximal inspiration and then to hold their breath. Have the patient relax against the shutter, but remind them to keep their lips tight. After approximately 10 seconds the balloons will deflate, then instruct the patient to exhale completely at a moderate rate of speed. The test will end automatically. ATS Standards The patient IVC must be at least 90% of the best VC value. The Breath Hold Time should be 10 seconds and must be within 9 to 11 seconds. During Breath Hold have the patient relax against the shutter, or have a slightly negative pressure against the shutter. The [Patient Dead Space Volume] in the [Setup] screen, should be recorded at 1cc per pound of the patient s ideal weight. The Mead Jones breath hold time calculation method should be used. Reproducibility Standards The DLCO values must be within 10% of each other. Best Time Criteria DLCO Average of all trials VA Average of all IVC trials. IVC Average of all trials Testing Information This test is reported in STPD. Wait 5 minutes between trials. If DLCO is performed after a Nitrogen Washout, the same rule applies (5 minutes). Any oxygen in the lung above 21% will cause a decrease in the DLCO value. The patient should be sitting quietly for 5 minutes before starting this test.
10 If there is a hemoglobin (Hb) or carboxy-hemoglobin (COHb) value on this patient, it may be entered in the Patient Demographics [Other] or in DLCO under the pull down menu [Test]. The [Extra Dead Space Volume] should be entered for each item connected to the Mass Flow Sensor. If using a Microguard Filter only, enter.050 in this box. To add a Sensormedics rubber mouthpiece in addition to the Microguard add.030 more making the total extra deadspace volume.080. Use the [F2] delete key on trials with questionable values since the DLCO, VA, and IVC are the average of all the trials. The computer will place the collection box at a Discard value of 750 ccs and a Collection value of 1,000 ccs. If the patients VC is less the 2 liters, the Discard value can be dropped to 500ccs. The placement of the collection box should be placed anywhere on the vertical portion of the graph, representing the anatomical deadspace of the patient. The patient s IVC should not reach TLC in less than 1 second, but before 2 ½ seconds into the maneuver. The first green dotted vertical line on the graph is the 2 ½ second mark. For patients with chronic lung disease, this may be increased to 4 seconds.
11 Plethysmography Addendum 6 Performing the maneuver Before performing the tests below, make sure the patient has been inside the box with the door shut for at least one minute. This ensures that the box is thermally equilibrated. The 22 mm clear gas hose should be disconnected from the balloon valve assembly, while the large white hose should remain attached from the box to the right side of the balloon valve assembly. Panting Raw/FRC with Vtg 1. From the main menu, select pulmonary function then select plethysmography 2. Press [F1] to begin data collection. 3. Observe four stable tidal breaths. After the red dotted ERV line appears, instruct the patient to do a maximum inspiration, maximum expiration, then return to normal tidal breathing. 4. Press [F1] to begin the Raw/vtg maneuver. 5. Instruct the patient to begin panting. Panting is one to three times per second, around 50 cc s of volume. 6. The patient will pant for 8 seconds through an open circuit. Then, the circuit will become occluded and the patient will pant for eight more seconds. The circuit will open automatically after the second set of pants. Warn the patient that during the maneuver the circuit will become occluded for a few seconds. 7. Press [End]. Resting Raw with Vtg (Patient is unable to pant) 1. Press [F1] to begin data collection. 2. Observe four stable tidal breaths. After the red dotted ERV line appears, instruct the patient to do a maximum inspiration, maximum expiration, then return to normal tidal breathing. 3. Press [F1] to begin the Raw/vtg maneuver. FRC PL (Vtg) Resting 1. In the RAW and VTG protocol set the collection method to none for Raw and resting for Vtg. [F3} store. 2. Press [F1] to begin data collection. 3. Observe four stable tidal breaths After the red dotted ERV line appears, instruct the patient to do a maximum inspiration, maximum expiration, then return to normal tidal breathing. 4. Press [F1] to begin the Vtg maneuver. 5. The circuit will occlude. Instruct the patient to take one inspiratory breath and then breathe normally. 6. Press [End}. ATS Standards There are no standards for this maneuver. Reproducibility Standards The Raw s must be within 10% of each other. The FRC PL s must be within 10% of each other. The largest VC and at least one other must be within 200 cc s of each other. Best Test Criteria VC Largest from FVC, VC, or FIVC from any trial FRC PL Average from all trials of FRC ERV Average of all trials of ERV
12 IC An average of all trials Vt Average of all trials of Vt RAW Average of all trials of Raw Vtg Average of all trials of Vtg. Testing Information The Vtg loops must be evaluated after each trial by selecting the [F7] key. The Raw loops must be evaluated after each trial by selecting the [F7] key. The slope for each of the Vtg and Raw loops must be placed in the proper position. The correct position is parallel to both sides of the loop, down the center of the loop between the dotted lines. Any loops that are not acceptable must be deleted using the [F2] key so that they are not included in the averaging. For patients that are showing a rise in their ERV baseline, the [F9] key can be used to adjust the end-tidal point. Note that this is not a system artifact but a physiologic state. Another solution to this situation is to do the test by separating the VC and the FRC maneuvers. Remember to select [FRC (Vtg) Only] in the plethysmography [Test Setup] screen, if this is being done. In the [Test Setup] screen, the [Filter Raw] should be set to [0.050] for the resistance of the filter. In the [Test Setup] screen, the [Total Deadspace] should be entered in cc s. If you are using the Microguard filter 50 cc s should be entered. If there is also a rubber mouthpiece add 30 more cc s. The most important procedure to perform correctly is the panting maneuver. The maneuver should be done at a rate of 1 to 3 times per second, with a volume of not more than 50 cc s. The most common problem is patients panting too deeply. Instruct the patient to pant baby puffs of air. If patients are have a difficult time Panting correctly, switch to the Resting modes. The software can handle patient of up to 500 pounds. The body box can handle a patient of up to 350 pounds as long as their shoulders are not touching the sides of the box. If any part of the body is touching the box, the data will be invalid. The Plexiglas windows CANNOT be cleaned with ammonia or alcohol, as it will damage the finish.
SPIROMETRY. Marijke Currie (CRFS) Care Medical Ltd Phone: Copyright CARE Medical ltd
 SPIROMETRY Marijke Currie (CRFS) Care Medical Ltd Phone: 0800 333 808 Email: sales@caremed.co.nz What is spirometry Spirometry is a physiological test that measures the volume of air an individual can
SPIROMETRY Marijke Currie (CRFS) Care Medical Ltd Phone: 0800 333 808 Email: sales@caremed.co.nz What is spirometry Spirometry is a physiological test that measures the volume of air an individual can
What do pulmonary function tests tell you?
 Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Performing a Methacholine Challenge Test
 powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
powder for solution, for inhalation Performing a Methacholine Challenge Test Provocholine is a registered trademark of Methapharm Inc. Copyright Methapharm Inc. 2016. All rights reserved. Healthcare professionals
BETTER SPIROMETRY. Marijke Currie (CRFS) Care Medical Ltd Phone: Copyright CARE Medical ltd
 BETTER SPIROMETRY Marijke Currie (CRFS) Care Medical Ltd Phone: 0800 333 808 Email: sales@caremed.co.nz What is spirometry Spirometry is a physiological test that measures the volume of air an individual
BETTER SPIROMETRY Marijke Currie (CRFS) Care Medical Ltd Phone: 0800 333 808 Email: sales@caremed.co.nz What is spirometry Spirometry is a physiological test that measures the volume of air an individual
#7 - Respiratory System
 #7 - Respiratory System Objectives: Study the parts of the respiratory system Observe slides of the lung and trachea Perform spirometry to measure lung volumes Define and understand the lung volumes and
#7 - Respiratory System Objectives: Study the parts of the respiratory system Observe slides of the lung and trachea Perform spirometry to measure lung volumes Define and understand the lung volumes and
6- Lung Volumes and Pulmonary Function Tests
 6- Lung Volumes and Pulmonary Function Tests s (PFTs) are noninvasive diagnostic tests that provide measurable feedback about the function of the lungs. By assessing lung volumes, capacities, rates of
6- Lung Volumes and Pulmonary Function Tests s (PFTs) are noninvasive diagnostic tests that provide measurable feedback about the function of the lungs. By assessing lung volumes, capacities, rates of
MSRC AIR Course Karla Stoermer Grossman, MSA, BSN, RN, AE-C
 MSRC AIR Course Karla Stoermer Grossman, MSA, BSN, RN, AE-C Explain the importance of objective measures in the management of asthma Explain the different types of objective measures used in the management
MSRC AIR Course Karla Stoermer Grossman, MSA, BSN, RN, AE-C Explain the importance of objective measures in the management of asthma Explain the different types of objective measures used in the management
PULMONARY FUNCTION TESTS
 Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
It is recommended that a mask and protective eyewear be worn when providing care to a patient with a cough
 UNIVERSITY HEALTH NETWORK POLICY #: PAGE 1 OF 7 POLICY AND PROCEDURE MANUAL: RESPIRATORY THERAPY DEPT PATIENT CARE SECTION ORIGINAL DATE: 04/03 ISSUED BY: SITE LEADER APPROVED BY: Infection Prevention
UNIVERSITY HEALTH NETWORK POLICY #: PAGE 1 OF 7 POLICY AND PROCEDURE MANUAL: RESPIRATORY THERAPY DEPT PATIENT CARE SECTION ORIGINAL DATE: 04/03 ISSUED BY: SITE LEADER APPROVED BY: Infection Prevention
UNIT TWO: OVERVIEW OF SPIROMETRY. A. Definition of Spirometry
 UNIT TWO: OVERVIEW OF SPIROMETRY A. Definition of Spirometry Spirometry is a medical screening test that measures various aspects of breathing and lung function. It is performed by using a spirometer,
UNIT TWO: OVERVIEW OF SPIROMETRY A. Definition of Spirometry Spirometry is a medical screening test that measures various aspects of breathing and lung function. It is performed by using a spirometer,
PULMONARY FUNCTION TESTING. Purposes of Pulmonary Tests. General Categories of Lung Diseases. Types of PF Tests
 PULMONARY FUNCTION TESTING Wyka Chapter 13 Various AARC Clinical Practice Guidelines Purposes of Pulmonary Tests Is lung disease present? If so, is it reversible? If so, what type of lung disease is present?
PULMONARY FUNCTION TESTING Wyka Chapter 13 Various AARC Clinical Practice Guidelines Purposes of Pulmonary Tests Is lung disease present? If so, is it reversible? If so, what type of lung disease is present?
Breathing and pulmonary function
 EXPERIMENTAL PHYSIOLOGY EXPERIMENT 5 Breathing and pulmonary function Ying-ying Chen, PhD Dept. of Physiology, Zhejiang University School of Medicine bchenyy@zju.edu.cn Breathing Exercise 1: Tests of pulmonary
EXPERIMENTAL PHYSIOLOGY EXPERIMENT 5 Breathing and pulmonary function Ying-ying Chen, PhD Dept. of Physiology, Zhejiang University School of Medicine bchenyy@zju.edu.cn Breathing Exercise 1: Tests of pulmonary
2.0 Scope: This document is to be used by the DCS staff when collecting participants spirometry measurements using the TruFlow Easy-On Spirometer.
 Title: Spirometry Version Date: 2017-MAR-21 Document Effective Date: 2017-MAY-15 Number: Data Collection Site (DCS) Version: 2.3 Number of Pages: SOP_DCS_0012 6 1.0 Purpose: The purpose of this document
Title: Spirometry Version Date: 2017-MAR-21 Document Effective Date: 2017-MAY-15 Number: Data Collection Site (DCS) Version: 2.3 Number of Pages: SOP_DCS_0012 6 1.0 Purpose: The purpose of this document
Spirometry and Flow Volume Measurements
 Spirometry and Flow Volume Measurements Standards & Guidelines December 1998 To serve the public and guide the medical profession Revision Dates: December 1998 Approval Date: June 1998 Originating Committee:
Spirometry and Flow Volume Measurements Standards & Guidelines December 1998 To serve the public and guide the medical profession Revision Dates: December 1998 Approval Date: June 1998 Originating Committee:
Quality Assurance Mapping Your QC Program Equipment and Test Quality. Susan Blonshine RRT, RPFT, FAARC, AE-C
 Quality Assurance Mapping Your QC Program Equipment and Test Quality Susan Blonshine RRT, RPFT, FAARC, AE-C How to Begin Gather resources Define PF scope of service Procedures performed Equipment Describe
Quality Assurance Mapping Your QC Program Equipment and Test Quality Susan Blonshine RRT, RPFT, FAARC, AE-C How to Begin Gather resources Define PF scope of service Procedures performed Equipment Describe
I. Subject: Medication Delivery by Metered Dose Inhaler (MDI)
 I. Subject: Medication Delivery by Metered Dose Inhaler (MDI) II. Policy: Aerosol medication administration by metered dose inhaler will be performed upon a physician's order by Respiratory Therapy personnel.
I. Subject: Medication Delivery by Metered Dose Inhaler (MDI) II. Policy: Aerosol medication administration by metered dose inhaler will be performed upon a physician's order by Respiratory Therapy personnel.
Content Indica c tion Lung v olumes e & Lung Indica c tions i n c paci c ties
 Spirometry Content Indication Indications in occupational medicine Contraindications Confounding factors Complications Type of spirometer Lung volumes & Lung capacities Spirometric values Hygiene &
Spirometry Content Indication Indications in occupational medicine Contraindications Confounding factors Complications Type of spirometer Lung volumes & Lung capacities Spirometric values Hygiene &
Your Inhaler Devices & You
 1 Your Inhaler Devices & You COUNSEL ON THE APPROPRIATE USE OF A: METERED DOSE INHALER (MDI) DRY POWDER INHALER (DPI) DISCUSS THE APPROPRIATE USAGE OF A PEAK FLOW METER AND SPACER/HOLDING CHAMBER DEVICE
1 Your Inhaler Devices & You COUNSEL ON THE APPROPRIATE USE OF A: METERED DOSE INHALER (MDI) DRY POWDER INHALER (DPI) DISCUSS THE APPROPRIATE USAGE OF A PEAK FLOW METER AND SPACER/HOLDING CHAMBER DEVICE
2.0 Scope: This document is to be used by the DCS staff when collecting participants spirometry measurements using the TruFlow Easy-On Spirometer.
 Title: Spirometry Version Date: 2014-AUG-20 Effective Date: 2014-OCT-15 Data Collection Site (DCS) Version: 2.2 Document Number: Number of Pages: SOP_DCS_0012 7 1.0 Purpose: The purpose of this document
Title: Spirometry Version Date: 2014-AUG-20 Effective Date: 2014-OCT-15 Data Collection Site (DCS) Version: 2.2 Document Number: Number of Pages: SOP_DCS_0012 7 1.0 Purpose: The purpose of this document
Spirometry: Introduction
 Spirometry: Introduction Dr. Badri Paudel 1 2 GMC Spirometry Spirometry is a method of assessing lung function by measuring the volume of air the patient can expel from the lungs after a maximal expiration.
Spirometry: Introduction Dr. Badri Paudel 1 2 GMC Spirometry Spirometry is a method of assessing lung function by measuring the volume of air the patient can expel from the lungs after a maximal expiration.
Credential Maintenance Program
 First Quarter of the Calendar 5 I. INSTRUMENTATION / EQUIPMENT 1 4 5 A. Set Up, Maintain, Calibrate 1 2 3 1. Blood gas analyzers 2. CO-oximeters / hemoximeters 3. Spirometers (for example, diagnostic,
First Quarter of the Calendar 5 I. INSTRUMENTATION / EQUIPMENT 1 4 5 A. Set Up, Maintain, Calibrate 1 2 3 1. Blood gas analyzers 2. CO-oximeters / hemoximeters 3. Spirometers (for example, diagnostic,
MANAGING ASTHMA. Nancy Davis, RRT, AE-C
 MANAGING ASTHMA Nancy Davis, RRT, AE-C What is asthma? Asthma is a chronic respiratory disease characterized by episodes or attacks of inflammation and narrowing of small airways in response to asthma
MANAGING ASTHMA Nancy Davis, RRT, AE-C What is asthma? Asthma is a chronic respiratory disease characterized by episodes or attacks of inflammation and narrowing of small airways in response to asthma
Respiratory Physiology In-Lab Guide
 Respiratory Physiology In-Lab Guide Read Me Study Guide Check Your Knowledge, before the Practical: 1. Understand the relationship between volume and pressure. Understand the three respiratory pressures
Respiratory Physiology In-Lab Guide Read Me Study Guide Check Your Knowledge, before the Practical: 1. Understand the relationship between volume and pressure. Understand the three respiratory pressures
MEDIUM-FLOW PNEUMOTACH TRANSDUCER
 MEDIUM-FLOW PNEUMOTACH TRANSDUCER SS11LA for MP3x and MP45 System TSD117 & TSD117-MRI for MP150/MP100 System RX117 Replacement Airflow Head See also: AFT series of accessories for airflow and gas analysis
MEDIUM-FLOW PNEUMOTACH TRANSDUCER SS11LA for MP3x and MP45 System TSD117 & TSD117-MRI for MP150/MP100 System RX117 Replacement Airflow Head See also: AFT series of accessories for airflow and gas analysis
Getting Spirometry Right It Matters! Performance, Quality Assessment, and Interpretation. Susan Blonshine RRT, RPFT, AE-C, FAARC
 Getting Spirometry Right It Matters! Performance, Quality Assessment, and Interpretation Susan Blonshine RRT, RPFT, AE-C, FAARC Objectives Sample Title Recognize acceptable spirometry that meets the start
Getting Spirometry Right It Matters! Performance, Quality Assessment, and Interpretation Susan Blonshine RRT, RPFT, AE-C, FAARC Objectives Sample Title Recognize acceptable spirometry that meets the start
Spirometry Technique Maximizing Effort, Comprehension & Coordination
 Spirometry Technique Maximizing Effort, Comprehension & Coordination Carl Mottram, RRT RPFT FAARC Director - Pulmonary Function Labs & Rehabilitation Associate Professor of Medicine - Mayo Clinic College
Spirometry Technique Maximizing Effort, Comprehension & Coordination Carl Mottram, RRT RPFT FAARC Director - Pulmonary Function Labs & Rehabilitation Associate Professor of Medicine - Mayo Clinic College
Pulmonary Function Testing
 Pulmonary Function Testing Let s catch our breath Eddie Needham, MD, FAAFP Program Director Emory Family Medicine Residency Program Learning Objectives The Astute Learner will: Become familiar with indications
Pulmonary Function Testing Let s catch our breath Eddie Needham, MD, FAAFP Program Director Emory Family Medicine Residency Program Learning Objectives The Astute Learner will: Become familiar with indications
Nancy Davis, RRT, AE-C
 Nancy Davis, RRT, AE-C Asthma Statistics 25.6 million Americans diagnosed with asthma 6.8 million are children 10.5 million missed school days per year 14.2 lost work days for adults Approximately 10%
Nancy Davis, RRT, AE-C Asthma Statistics 25.6 million Americans diagnosed with asthma 6.8 million are children 10.5 million missed school days per year 14.2 lost work days for adults Approximately 10%
PFT Interpretation and Reference Values
 PFT Interpretation and Reference Values September 21, 2018 Eric Wong Objectives Understand the components of PFT Interpretation of PFT Clinical Patterns How to choose Reference Values 3 Components Spirometry
PFT Interpretation and Reference Values September 21, 2018 Eric Wong Objectives Understand the components of PFT Interpretation of PFT Clinical Patterns How to choose Reference Values 3 Components Spirometry
PULMONARY FUNCTION TEST(PFT)
 PULMONARY FUNCTION TEST(PFT) Objectives: By the end of the present lab, students should be able to: 1. Record lung volumes and capacities and compare them with those of a typical person of the same gender,
PULMONARY FUNCTION TEST(PFT) Objectives: By the end of the present lab, students should be able to: 1. Record lung volumes and capacities and compare them with those of a typical person of the same gender,
S P I R O M E T R Y. Objectives. Objectives 2/5/2019
 S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
Physiology lab (RS) First : Spirometry. ** Objectives :-
 Physiology lab (RS) ** Objectives :- 1. Spirometry in general. 2. Spirogram (volumes and capacities). 3. The importance of vital capacity in diagnosis. 4. Flow volume loop. 5. Miss Arwa s part (the practical
Physiology lab (RS) ** Objectives :- 1. Spirometry in general. 2. Spirogram (volumes and capacities). 3. The importance of vital capacity in diagnosis. 4. Flow volume loop. 5. Miss Arwa s part (the practical
Using an Inhaler and Nebulizer
 Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
What You Need to Know about Metered-Dose Inhalers and the HFA Propellant
 What You Need to Know about Metered- Inhalers and the HFA Propellant There are a number ways to deliver inhaled medication. They include: Metered-dose inhaler () Metered-dose inhaler with spacer/holding
What You Need to Know about Metered- Inhalers and the HFA Propellant There are a number ways to deliver inhaled medication. They include: Metered-dose inhaler () Metered-dose inhaler with spacer/holding
Small Volume Nebulizer Treatment (Hand-Held)
 Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Office Spirometry Guide
 Office Spirometry Guide MD Spiro 803 Webster Street, Lewiston ME 04240 Telephone 207-786-7808 1-800-588-3381 Fax 207-786-7280 www.mdspiro.com e-mail: sales@mdspiro.com Why should you perform spirometry
Office Spirometry Guide MD Spiro 803 Webster Street, Lewiston ME 04240 Telephone 207-786-7808 1-800-588-3381 Fax 207-786-7280 www.mdspiro.com e-mail: sales@mdspiro.com Why should you perform spirometry
PATIENT INFORMATION FORM
 PATIENT INFORMATION FORM "I am going to ask you a number of questions about your asthma. The set of questions is somewhat long, but I will try to move through it fairly quickly so that we can complete
PATIENT INFORMATION FORM "I am going to ask you a number of questions about your asthma. The set of questions is somewhat long, but I will try to move through it fairly quickly so that we can complete
S P I R O M E T R Y. Objectives. Objectives 3/12/2018
 S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
S P I R O M E T R Y Dewey Hahlbohm, PA-C, AE-C Objectives To understand the uses and importance of spirometry testing To perform spirometry testing including reversibility testing To identify normal and
Inhalation devices, proper technique and cleaning
 Preventing Your Symptoms and Taking Your Medications Inhalation devices, proper technique and cleaning Knowing how to use your medications properly is important because inhaled drugs are meant to get directly
Preventing Your Symptoms and Taking Your Medications Inhalation devices, proper technique and cleaning Knowing how to use your medications properly is important because inhaled drugs are meant to get directly
Independent Health Facilities
 Independent Health Facilities Assessment Protocol for Pulmonary Function Studies INSTRUCTIONS: Please complete ( ) the attached protocol during the assessment. Ensure that all the questions have been answered,
Independent Health Facilities Assessment Protocol for Pulmonary Function Studies INSTRUCTIONS: Please complete ( ) the attached protocol during the assessment. Ensure that all the questions have been answered,
Pulmonary Function Tests. Mohammad Babai M.D Occupational Medicine Specialist
 Pulmonary Function Tests Mohammad Babai M.D Occupational Medicine Specialist www.drbabai.com Pulmonary Function Tests Pulmonary Function Tests: Spirometry Peak-Flow metry Bronchoprovocation Tests Body
Pulmonary Function Tests Mohammad Babai M.D Occupational Medicine Specialist www.drbabai.com Pulmonary Function Tests Pulmonary Function Tests: Spirometry Peak-Flow metry Bronchoprovocation Tests Body
Spirometry: FEVER DISEASE DIABETES HOW RELIABLE IS THIS? 9/2/2010 BUT WHAT WE PRACTICE: Spirometers are objective tools
 SPIROMETRY PRINCIPLES, PROCEDURE AND QA Spirometry: Dr. Rahul Kodgule CHEST RESEARCH FOUNDATION, PUNE FEVER ISCHAEMIC HEART DISEASE DIABETES BUT WHAT WE PRACTICE: Spirometers are objective tools to diagnose
SPIROMETRY PRINCIPLES, PROCEDURE AND QA Spirometry: Dr. Rahul Kodgule CHEST RESEARCH FOUNDATION, PUNE FEVER ISCHAEMIC HEART DISEASE DIABETES BUT WHAT WE PRACTICE: Spirometers are objective tools to diagnose
You Take My Breath Away. Student Information Page 5C Part 1
 You Take My Breath Away Student Information Page 5C Part 1 Students with asthma or other respiratory problems should not participate in this activity because it involves repeated maximal inhalations and
You Take My Breath Away Student Information Page 5C Part 1 Students with asthma or other respiratory problems should not participate in this activity because it involves repeated maximal inhalations and
Appendix M: Device Technique
 Nursing Care of Dyspnea: The 6th Vital Sign in Individuals with Chronic Obstructive Pulmonary Disease (COPD) Appendix M: Device Technique Medications: Inhalation Devices Medications come in many forms.
Nursing Care of Dyspnea: The 6th Vital Sign in Individuals with Chronic Obstructive Pulmonary Disease (COPD) Appendix M: Device Technique Medications: Inhalation Devices Medications come in many forms.
Pulmonary Function Laboratory ATS Accreditation Are you prepared? Susan Blonshine RRT, RPFT, FAARC, AE-C
 Pulmonary Function Laboratory ATS Accreditation Are you prepared? Susan Blonshine RRT, RPFT, FAARC, AE-C Why Quality Consistent, accurate, reliable results Cost-effective Diagnosis Misclassification Reduce
Pulmonary Function Laboratory ATS Accreditation Are you prepared? Susan Blonshine RRT, RPFT, FAARC, AE-C Why Quality Consistent, accurate, reliable results Cost-effective Diagnosis Misclassification Reduce
PULMONARY FUNCTION. VOLUMES AND CAPACITIES
 PULMONARY FUNCTION. VOLUMES AND CAPACITIES The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer (spiro = breath, meter = to measure). A bell spirometer
PULMONARY FUNCTION. VOLUMES AND CAPACITIES The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer (spiro = breath, meter = to measure). A bell spirometer
How to Use Inhaled Medications for Asthma and COPD
 How to Use Inhaled Medications for Asthma and COPD This information is not intended to diagnose health problems or to take the place of medical advice or care you receive from your physician or other health
How to Use Inhaled Medications for Asthma and COPD This information is not intended to diagnose health problems or to take the place of medical advice or care you receive from your physician or other health
ADASUVE (LOXAPINE) INHALATION POWDER. EDUCATION PROGRAM for HEALTHCARE PROFESSIONALS
 ADASUVE (LOXAPINE) INHALATION POWDER EDUCATION PROGRAM for HEALTHCARE PROFESSIONALS August2017 December 2012 PMR-JUN-2017-0017 ADASUVE Risk Evaluation and Mitigation Strategy (REMS) Education Program Content
ADASUVE (LOXAPINE) INHALATION POWDER EDUCATION PROGRAM for HEALTHCARE PROFESSIONALS August2017 December 2012 PMR-JUN-2017-0017 ADASUVE Risk Evaluation and Mitigation Strategy (REMS) Education Program Content
Pulmonary Function Technologists (PFT) Detailed Content Outline
 I. INSTRUMENTATION / EQUIPMENT 7 15 8 30 A. Set Up, Maintain, Calibrate 3 5 2 10 1. Blood gas analyzers 2. CO-oximeters / hemoximeters 3. Spirometers (for example, diagnostic, screening, portable) 4. Peak
I. INSTRUMENTATION / EQUIPMENT 7 15 8 30 A. Set Up, Maintain, Calibrate 3 5 2 10 1. Blood gas analyzers 2. CO-oximeters / hemoximeters 3. Spirometers (for example, diagnostic, screening, portable) 4. Peak
SS11LA Pneumotach Transducer
 BIOPAC Systems, Inc. 42 Aero Camino Goleta, CA 93117 Ph (805) 685-0066 Fax (805) 685-0067 www.biopac.com info@biopac.com SS11LA Pneumotach Transducer The SS11LA can be used to measure respiratory flow
BIOPAC Systems, Inc. 42 Aero Camino Goleta, CA 93117 Ph (805) 685-0066 Fax (805) 685-0067 www.biopac.com info@biopac.com SS11LA Pneumotach Transducer The SS11LA can be used to measure respiratory flow
19 LUNG FUNCTION USING NDD EASY ON-PC
 UK Data Archive Study Number 7251 - Understanding Society: Nurse Health Assessment 19 LUNG FUNCTION USING NDD EASY ON-PC 19.1 Introduction Lung function tests objectively assess respiratory function and
UK Data Archive Study Number 7251 - Understanding Society: Nurse Health Assessment 19 LUNG FUNCTION USING NDD EASY ON-PC 19.1 Introduction Lung function tests objectively assess respiratory function and
Chapter 3. Pulmonary Function Study Assessments. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 3 Pulmonary Function Study Assessments 1 Introduction Pulmonary function studies are used to: Evaluate pulmonary causes of dyspnea Differentiate between obstructive and restrictive pulmonary disorders
Chapter 3 Pulmonary Function Study Assessments 1 Introduction Pulmonary function studies are used to: Evaluate pulmonary causes of dyspnea Differentiate between obstructive and restrictive pulmonary disorders
Coexistence of confirmed obstruction in spirometry and restriction in body plethysmography, e.g.: COPD + pulmonary fibrosis
 Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Appendix E: Device Technique
 Adult Asthma Care Guidelines for Nurses: Promoting Control of Asthma Appendix E: Device Technique Medications: Inhalation Devices Adapted with permission from The Lung Association: www.lung.ca/asthma/manage/devices.html
Adult Asthma Care Guidelines for Nurses: Promoting Control of Asthma Appendix E: Device Technique Medications: Inhalation Devices Adapted with permission from The Lung Association: www.lung.ca/asthma/manage/devices.html
behaviour are out of scope of the present review.
 explained about the test, a trial may be done before recording the results. The maneuver consists initially of normal tidal breathing. The subject then inhales to maximally fill the lungs. This is followed
explained about the test, a trial may be done before recording the results. The maneuver consists initially of normal tidal breathing. The subject then inhales to maximally fill the lungs. This is followed
NEBULIZERS, METERED DOSE INHALERS, AND DRY POWDER INHALERS
 NEBULIZERS, METERED DOSE INHALERS, AND DRY POWDER INHALERS Douglas S. Gardenhire, Ed.D, RRT-NPS MODULE 1 Manipulate Small Volume Nebulizers by Order or Protocol 1 Objectives for Module 1 At the end of
NEBULIZERS, METERED DOSE INHALERS, AND DRY POWDER INHALERS Douglas S. Gardenhire, Ed.D, RRT-NPS MODULE 1 Manipulate Small Volume Nebulizers by Order or Protocol 1 Objectives for Module 1 At the end of
Spirometry. Obstruction. By Helen Grim M.S. RRT. loop will have concave appearance. Flows decreased consistent with degree of obstruction.
 1 2 Spirometry By Helen Grim M.S. RRT 3 4 Obstruction loop will have concave appearance. Flows decreased consistent with degree of obstruction. Volumes may be normal, but can decrease with severity of
1 2 Spirometry By Helen Grim M.S. RRT 3 4 Obstruction loop will have concave appearance. Flows decreased consistent with degree of obstruction. Volumes may be normal, but can decrease with severity of
10/18/2012. Penn State University Children s Hospital JODIE STABINSKI CRNP MSN AE-C
 Penn State University Children s Hospital JODIE STABINSKI CRNP MSN AE-C Daily: Long-Term Control Corticosteroids (inhaled and systemic) Long-acting beta 2 -agonists (Serevent, Foradil) Methylxanthines
Penn State University Children s Hospital JODIE STABINSKI CRNP MSN AE-C Daily: Long-Term Control Corticosteroids (inhaled and systemic) Long-acting beta 2 -agonists (Serevent, Foradil) Methylxanthines
RELEASED. first steps. Icon Icon name What it means
 Icon Icon name What it means Connection The connection icon appears green when the Sensor feature is on and your transmitter is successfully communicating with your pump. The connection icon appears gray
Icon Icon name What it means Connection The connection icon appears green when the Sensor feature is on and your transmitter is successfully communicating with your pump. The connection icon appears gray
Spirometric protocol
 Spirometric protocol Spirometry is the most common of the Pulmonary Function Test, that measures lung function, specifically the amount (volume) and/or speed (flow) of air that can be inhaled and exhaled.
Spirometric protocol Spirometry is the most common of the Pulmonary Function Test, that measures lung function, specifically the amount (volume) and/or speed (flow) of air that can be inhaled and exhaled.
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Asthma Education. The Keys to Asthma Prevention and Control. what to do when one s asthma is flared! Lucile Packard Children s Hospital.
 Asthma Education Lucile Packa r d Children s H o spit al Created by Rachel Lawler RN, MSN, cpnp, AE-C, NPAT Pulmonary Pediatric Nurse Practitioner Lucile Packard Children s Hospital The Keys to Asthma
Asthma Education Lucile Packa r d Children s H o spit al Created by Rachel Lawler RN, MSN, cpnp, AE-C, NPAT Pulmonary Pediatric Nurse Practitioner Lucile Packard Children s Hospital The Keys to Asthma
How to Perform Spirometry
 Purpose How to Perform Spirometry This guideline provides recommendations regarding best practice to support high quality spirometry practice for KINNECT Pre-Employment Medicals. Scope This guideline provides
Purpose How to Perform Spirometry This guideline provides recommendations regarding best practice to support high quality spirometry practice for KINNECT Pre-Employment Medicals. Scope This guideline provides
Respiratory Training. Standard Operations Manuel For Outcome Measures Version 2.0 April Page 1 of 11
 Respiratory Training Page 1 of 11 Index Background... 2 SVC and FVC TESTING... 3 Clarification of used terms:... 3 Step 1) Preparation... 3 Step 2) Calibration... 3 Step 3) Adjusting the set-up menu...
Respiratory Training Page 1 of 11 Index Background... 2 SVC and FVC TESTING... 3 Clarification of used terms:... 3 Step 1) Preparation... 3 Step 2) Calibration... 3 Step 3) Adjusting the set-up menu...
Analysis of Lung Function
 Computer 21 Spirometry is a valuable tool for analyzing the flow rate of air passing into and out of the lungs. Flow rates vary over the course of a respiratory cycle (a single inspiration followed by
Computer 21 Spirometry is a valuable tool for analyzing the flow rate of air passing into and out of the lungs. Flow rates vary over the course of a respiratory cycle (a single inspiration followed by
Spirometry in primary care
 Spirometry in primary care Wednesday 13 th July 2016 Dr Rukhsana Hussain What is spirometry? A method of assessing lung function Measures volume of air a patient can expel after a full inspiration Recorded
Spirometry in primary care Wednesday 13 th July 2016 Dr Rukhsana Hussain What is spirometry? A method of assessing lung function Measures volume of air a patient can expel after a full inspiration Recorded
Office Based Spirometry
 Osteopathic Family Physician (2014)1, 14-18 Scott Klosterman, DO; Woodson Crenshaw, OMS4 Spartanburg Regional Family Medicine Residency Program; Edward Via College of Osteopathic Medicine - Virginia Campus
Osteopathic Family Physician (2014)1, 14-18 Scott Klosterman, DO; Woodson Crenshaw, OMS4 Spartanburg Regional Family Medicine Residency Program; Edward Via College of Osteopathic Medicine - Virginia Campus
Accurately Measuring Airway Resistance in the PFT Lab
 Accurately Measuring Airway Resistance in the PFT Lab Angela Lorenzo, MS, RRT, RPFT Adjunct Faculty, Long Island University Respiratory Care Division Disclaimer The views in this lecture are those of the
Accurately Measuring Airway Resistance in the PFT Lab Angela Lorenzo, MS, RRT, RPFT Adjunct Faculty, Long Island University Respiratory Care Division Disclaimer The views in this lecture are those of the
In order to diagnose lung diseases doctors
 You Take My Breath Away Activity 5C NOTE: This activity is designed to follow You Really Are Full of Hot Air! Activity Objectives: After completing You Really Are Full of Hot Air! Activity 5B, students
You Take My Breath Away Activity 5C NOTE: This activity is designed to follow You Really Are Full of Hot Air! Activity Objectives: After completing You Really Are Full of Hot Air! Activity 5B, students
Anyone who smokes and/or has shortness of breath and sputum production could have COPD
 COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
Procedures/Risks: pulmonology, sleep, critical care
 Procedures/Risks: pulmonology, sleep, critical care Bronchoscopy (and bronchoaveolar lavage) Purpose: The purpose of the bronchoscopy is to collect cells and fluid from the lung, so that information can
Procedures/Risks: pulmonology, sleep, critical care Bronchoscopy (and bronchoaveolar lavage) Purpose: The purpose of the bronchoscopy is to collect cells and fluid from the lung, so that information can
Patient assessment - spirometry
 Patient assessment - spirometry STEP 1 Learning objectives This module will provide you with an understanding of spirometry and the role it plays in aiding the diagnosis of lung diseases, particularly
Patient assessment - spirometry STEP 1 Learning objectives This module will provide you with an understanding of spirometry and the role it plays in aiding the diagnosis of lung diseases, particularly
Inhaled bronchodilators relax constricted airways and treat the noisy part of asthma: coughing, wheezing, choking and shortness of breath.
 Inhaled bronchodilators relax constricted airways and treat the noisy part of asthma: coughing, wheezing, choking and shortness of breath. AccuNeb inhalation 0.021% solution: 0.63mg/3mL 3-4 times solution
Inhaled bronchodilators relax constricted airways and treat the noisy part of asthma: coughing, wheezing, choking and shortness of breath. AccuNeb inhalation 0.021% solution: 0.63mg/3mL 3-4 times solution
Effective Date: August 31, 2006 SUBJECT: CARE AND USE OF NEBULIZER AND INTERMITTENT POSITIVE PRESSURE BREATHING DEVICE
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 421 Effective Date: August 31, 2006 SUBJECT: CARE AND USE OF NEBULIZER AND INTERMITTENT POSITIVE PRESSURE
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION - Treatments POLICY NUMBER: 421 Effective Date: August 31, 2006 SUBJECT: CARE AND USE OF NEBULIZER AND INTERMITTENT POSITIVE PRESSURE
SPIROMETRY METHOD. COR-MAN IN / EN Issue A, Rev INNOVISION ApS Skovvænget 2 DK-5620 Glamsbjerg Denmark
 SPIROMETRY METHOD COR-MAN-0000-006-IN / EN Issue A, Rev. 2 2013-07 INNOVISION ApS Skovvænget 2 DK-5620 Glamsbjerg Denmark Tel.: +45 65 95 91 00 Fax: +45 65 95 78 00 info@innovision.dk www.innovision.dk
SPIROMETRY METHOD COR-MAN-0000-006-IN / EN Issue A, Rev. 2 2013-07 INNOVISION ApS Skovvænget 2 DK-5620 Glamsbjerg Denmark Tel.: +45 65 95 91 00 Fax: +45 65 95 78 00 info@innovision.dk www.innovision.dk
Asthma. UVM. University of Vermont. Alicia Jacobs MD Fletcher Allen Health Care and the University of Vermont
 University of Vermont ScholarWorks @ UVM Family Medicine Scholarly Works 6-14-2013 Asthma Alicia Jacobs MD Fletcher Allen Health Care and the University of Vermont Follow this and additional works at:
University of Vermont ScholarWorks @ UVM Family Medicine Scholarly Works 6-14-2013 Asthma Alicia Jacobs MD Fletcher Allen Health Care and the University of Vermont Follow this and additional works at:
Basic approach to PFT interpretation. Dr. Giulio Dominelli BSc, MD, FRCPC Kelowna Respiratory and Allergy Clinic
 Basic approach to PFT interpretation Dr. Giulio Dominelli BSc, MD, FRCPC Kelowna Respiratory and Allergy Clinic Disclosures Received honorarium from Astra Zeneca for education presentations Tasked Asked
Basic approach to PFT interpretation Dr. Giulio Dominelli BSc, MD, FRCPC Kelowna Respiratory and Allergy Clinic Disclosures Received honorarium from Astra Zeneca for education presentations Tasked Asked
Methacholine Challenge Test
 PATIENT & CAREGIVER EDUCATION Methacholine Challenge Test This information will help you prepare for your methacholine challeng e test at Memorial Sloan Kettering (MSK). A methacholine (meth-a-kole-leen)
PATIENT & CAREGIVER EDUCATION Methacholine Challenge Test This information will help you prepare for your methacholine challeng e test at Memorial Sloan Kettering (MSK). A methacholine (meth-a-kole-leen)
DIAGNOSTIC ACCREDITATION PROGRAM. Spirometry Quality Control Plan
 DIAGNOSTIC ACCREDITATION PROGRAM Spirometry Quality Control Plan Table of Contents Introduction...1 Spirometry Definitions and Requirements...2 Spirometry Requirements... 2...4 Daily Quality Control (see
DIAGNOSTIC ACCREDITATION PROGRAM Spirometry Quality Control Plan Table of Contents Introduction...1 Spirometry Definitions and Requirements...2 Spirometry Requirements... 2...4 Daily Quality Control (see
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing
 In the Clinic Pulmonary Function Testing Hawa Edriss MD, Gilbert Berdine MD The term PFT encompasses three different measures of lung function: spirometry, lung volumes, and diffusion capacity. In this
In the Clinic Pulmonary Function Testing Hawa Edriss MD, Gilbert Berdine MD The term PFT encompasses three different measures of lung function: spirometry, lung volumes, and diffusion capacity. In this
PULMONARY FUNCTION TESTING. By: Gh. Pouryaghoub. MD Center for Research on Occupational Diseases (CROD) Tehran University of Medical Sciences (TUMS)
 PULMONARY FUNCTION TESTING By: Gh. Pouryaghoub. MD Center for Research on Occupational Diseases (CROD) Tehran University of Medical Sciences (TUMS) PULMONARY FUNCTION TESTS CATEGORIES Spirometry Lung volumes
PULMONARY FUNCTION TESTING By: Gh. Pouryaghoub. MD Center for Research on Occupational Diseases (CROD) Tehran University of Medical Sciences (TUMS) PULMONARY FUNCTION TESTS CATEGORIES Spirometry Lung volumes
Asthma. If an Ambulance is required - call immediately - do not delay. H & A Training PL RTO No:90871
 Asthma is a reversible breathing problem caused from sudden or progressive narrowing and spasming of the smaller airways and includes mucus production, which interferes with oxygen exchange. People who
Asthma is a reversible breathing problem caused from sudden or progressive narrowing and spasming of the smaller airways and includes mucus production, which interferes with oxygen exchange. People who
ASTHMA POLICY KYABRAM P-12 COLLEGE
 Asthma Policy ASTHMA POLICY KYABRAM P-12 COLLEGE THE VICTORIAN SCHOOLS ASTHMA POLICY 1. ASTHMA AWARENESS As asthma can affect up to one in five children and one in ten adults, it is important for teachers
Asthma Policy ASTHMA POLICY KYABRAM P-12 COLLEGE THE VICTORIAN SCHOOLS ASTHMA POLICY 1. ASTHMA AWARENESS As asthma can affect up to one in five children and one in ten adults, it is important for teachers
A NEBULISERS AND NEBULISED MEDICATION. Generic Guide for the use of nebulisers and nebulised medication
 A NEBULISERS AND NEBULISED MEDICATION Generic Guide for the use of nebulisers and nebulised medication Aim The aim of this guide is to provide a template for those who wish to develop their own nebuliser
A NEBULISERS AND NEBULISED MEDICATION Generic Guide for the use of nebulisers and nebulised medication Aim The aim of this guide is to provide a template for those who wish to develop their own nebuliser
Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology
 Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
. Type of solution/medication. Amount/dose to be delivered. Frequency/duration. Mode of administration.
 Page 1 of 9 (Large, Medium Volume, and Aerogen Continuous Nebulizer) Purpose Scope Physician's Order To standardize the use of continuous aerosol therapy as a modality used for the rescue of patients with
Page 1 of 9 (Large, Medium Volume, and Aerogen Continuous Nebulizer) Purpose Scope Physician's Order To standardize the use of continuous aerosol therapy as a modality used for the rescue of patients with
Variation in lung with normal, quiet breathing. Minimal lung volume (residual volume) at maximum deflation. Total lung capacity at maximum inflation
 r Total lung capacity at maximum inflation Variation in lung with normal, quiet breathing Volume of lungs at end of normal inspiration (average 2,200 ml) Minimal lung volume (residual volume) at maximum
r Total lung capacity at maximum inflation Variation in lung with normal, quiet breathing Volume of lungs at end of normal inspiration (average 2,200 ml) Minimal lung volume (residual volume) at maximum
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
GENERAL INFORMATION. Page 1 z 11
 GENERAL INFORMATION MySpiroo is a personal, connected and ultraportable spirometer with a dedicated mobile application for your smartphone. The device encompasses all of the most important and widely used
GENERAL INFORMATION MySpiroo is a personal, connected and ultraportable spirometer with a dedicated mobile application for your smartphone. The device encompasses all of the most important and widely used
2008 IPAC-RS Conference Doing the Right Thing Science, Quality and Patient Focus
 2008 IPAC-RS Conference Doing the Right Thing Science, Quality and Patient Focus Patient Perspective Alpha-1 1 Foundation John W. Walsh Patient Focus Personal perspective Challenges and lessons Importance
2008 IPAC-RS Conference Doing the Right Thing Science, Quality and Patient Focus Patient Perspective Alpha-1 1 Foundation John W. Walsh Patient Focus Personal perspective Challenges and lessons Importance
Lung Pathophysiology & PFTs
 Interpretation of Pulmonary Function Tests (PFTs) Course # 1612 2:00 5:00pm Friday February 22, 2013 Lung Pathophysiology & PFTs Mark F. Sands MD, FCCP, FAAAAI Division of Allergy, Immunology & Rheumatology
Interpretation of Pulmonary Function Tests (PFTs) Course # 1612 2:00 5:00pm Friday February 22, 2013 Lung Pathophysiology & PFTs Mark F. Sands MD, FCCP, FAAAAI Division of Allergy, Immunology & Rheumatology
Breezhaler. Open to see clear capsule. How do I use my Breezhaler? Care of my Breezhaler
 Breezhaler 3 Pull cap off Press buttons once and release Breathe in rapidly and steadily. Hold. Open. Place capsule in chamber. Close (click). Breathe out 4 Open to see clear capsule. If not all clear
Breezhaler 3 Pull cap off Press buttons once and release Breathe in rapidly and steadily. Hold. Open. Place capsule in chamber. Close (click). Breathe out 4 Open to see clear capsule. If not all clear
DLCO Webinar Q&A Dr. Christine Oropez answers post-presentation FAQs
 DLCO Webinar Q&A Dr. Christine Oropez answers post-presentation FAQs If you re setting up bio controls, should they be measured at a specific window because of diurnal changes in DLCO? I would not necessarily
DLCO Webinar Q&A Dr. Christine Oropez answers post-presentation FAQs If you re setting up bio controls, should they be measured at a specific window because of diurnal changes in DLCO? I would not necessarily
How can I benefit most from my COPD medications?
 Fact Sheet: COPD Medications and Delivery Devices How can I benefit most from my COPD medications? COPD medications can improve your symptoms. By taking the right medication at the right time, you can
Fact Sheet: COPD Medications and Delivery Devices How can I benefit most from my COPD medications? COPD medications can improve your symptoms. By taking the right medication at the right time, you can
Facility Information for Initial Assessment
 DIAGNOSTIC ACCREDITATION PROGRAM 300 669 Howe Street Telephone: 604-733-7758 Vancouver BC V6C 0B4 Toll Free: 1-800-461-3008 (in BC) www.cpsbc.ca Fax: 604-733-3503 Facility Information for Initial Assessment
DIAGNOSTIC ACCREDITATION PROGRAM 300 669 Howe Street Telephone: 604-733-7758 Vancouver BC V6C 0B4 Toll Free: 1-800-461-3008 (in BC) www.cpsbc.ca Fax: 604-733-3503 Facility Information for Initial Assessment
I. Subject: Continuous Aerosolization of Bronchodilators
 I. Subject: Continuous Aerosolization of Bronchodilators II. Indications: A. Acute airflow obstruction in which treatment with an aerosolized bronchodilator is desired for an extended period of time, i.e.
I. Subject: Continuous Aerosolization of Bronchodilators II. Indications: A. Acute airflow obstruction in which treatment with an aerosolized bronchodilator is desired for an extended period of time, i.e.
Essen%als of Spirometry and Assessment
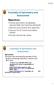 Essen%als of Spirometry and Assessment Objectives: 1. Review spirometric acceptability, reproducibility and reporting standards 2. Discuss lung volumes and capacities 3. Discuss Pre & Post bronchodilator
Essen%als of Spirometry and Assessment Objectives: 1. Review spirometric acceptability, reproducibility and reporting standards 2. Discuss lung volumes and capacities 3. Discuss Pre & Post bronchodilator
Vitalograph Alpha Spirometer
 Product Catalogue Vitalograph Alpha Spirometer Dedicated all-in-one desktop unit Simple to use Rapid and low cost testing Clear and bright color screen Accurate Fleisch pneumotachograph Measures VC, FVC,
Product Catalogue Vitalograph Alpha Spirometer Dedicated all-in-one desktop unit Simple to use Rapid and low cost testing Clear and bright color screen Accurate Fleisch pneumotachograph Measures VC, FVC,
Kickin Asthma. Workbook for Children with Asthma. Name:
 Kickin Asthma Workbook for Children with Asthma Name: Why Have You Been Invited to Kickin Asthma? You have been invited to Kickin Asthma because you have asthma. Asthma is a disease of your air tubes that
Kickin Asthma Workbook for Children with Asthma Name: Why Have You Been Invited to Kickin Asthma? You have been invited to Kickin Asthma because you have asthma. Asthma is a disease of your air tubes that
