Comparison of handheld rebound tonometry with Goldmann applanation tonometry in children with glaucoma: a cohort study For peer review only
|
|
|
- Patricia Fisher
- 5 years ago
- Views:
Transcription
1 BMJ Open Comparison of handheld rebound tonometry with Goldmann applanation tonometry in children with glaucoma: a cohort study Journal: BMJ Open Manuscript ID: bmjopen--00 Article Type: Research Date Submitted by the Author: -Jul- Complete List of Authors: Dahlmann-Noor, Annegret; NIHR Biomedical Research Centre at Moorfields Eye Hospital NHS Foundation Trust and UCL Institute of Ophthalmology, Paediatric Ophthalmology Bunce, Catey; Moorfields Eye Hospital NHS Foundation Trust, Research and Development Puertas, Renata; Moorfields Eye Hospital, Glaucoma Tabasa-Lim, Shenille; Moorfields Eye Hospital, Paediatric Ophthalmology El-Karmouty, Ahmed; Moorfields Eye Hospital, Glaucoma Kadhim, Mustafa; Moorfields Eye Hospital, Glaucoma Wride, Nicholas; Moorfields Eye Hospital, Glaucoma Lewis, Amanda; Moorfields Eye Hospital, Glaucoma Grosvenor, Dawn; Moorfields Eye Hospital, Glaucoma Rai, Poornima; Moorfields Eye Hospital, Glaucoma Papadopoulos, Maria; Moorfields Eye Hospital, Glaucoma brookes, john; Moorfields Eye Hospital, Glaucoma Khaw, Peng; NIHR Biomedical Research Centre at Moorfields Eye Hospital NHS Foundation Trust and UCL Institute of Ophthalmology, Glaucoma <b>primary Subject Heading</b>: Ophthalmology Secondary Subject Heading: Paediatrics, Evidence based practice Keywords: Paediatric ophthalmology < OPHTHALMOLOGY, Community child health < PAEDIATRICS, Glaucoma < OPHTHALMOLOGY BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
2 Page of BMJ Open 0 Handheld rebound tonometry in children with glaucoma Authors Annegret Hella Dahlmann-Noor Renata Puertas Shenille Tabasa-Lim Ahmed El-Karmouty Mustafa Kadhim Nicholas Wride Amanda Lewis Dawn Grosvenor Poornima Rai Maria Papadopoulos John Brookes Catey Bunce Peng Tee Khaw Corresponding author: Annegret Dahlmann-Noor, Moorfields Eye Hospital, City Road, London ECV PD; annegret.dahlmann-noor@moorfields.nhs.uk Funding statement: This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. Acknowledgements: The authors are grateful for the support from Fight for Sight and the Helen Hamlyn Trust. The research took place at the National Institute for Health Research (NIHR) Biomedical Research Centre at Moorfields Eye Hospital NHS Foundation Trust and UCL Institute of Ophthalmology. The views expressed are those of the author(s) and not necessarily those of the NHS, the NIHR or the Department of Health. Competing Interests Statement: None of the authors have competing interests to declare. Contributorship Statement: AHDN and CB designed the trial and prepared the manuscript. AHDN, RP, STL, AE, PR, MK, NW, AL, DG, MP, JB and PTK facilitated recruitment, obtained informed consent, acquired data and completed case report forms. AHDN entered data onto the electronic database. CB analysed the data. All authors reviewed the manuscript. BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
3 BMJ Open Page of 0 Abstract Objective: To test agreement of two methods to measure intraocular pressure (IOP): rebound tonometry (RBT) and gold standard Goldmann applanation (GAT) tonometry in children with glaucoma Design: observational prospective cohort study Setting: tertiary paediatric glaucoma clinic at a single centre Participants: 0 children with glaucoma, mean (SD) age. (.), of whom were male Primary and secondary outcome measures: intraocular pressure, central corneal thickness, child preference for measurement method Results: Limits of agreement for intra- and interobserver were respectively (-.,.) mmhg and (-.,.) mmhg. RBT frequently gave higher readings than GAT and the magnitude of disagreement depended on the level of IOP being assessed. Differences of 0mmHg were not uncommon. RBT was the preferred method for 0% of children. Conclusions: There is poor agreement between RBT and GAT in children with glaucoma. RBT frequently and significantly overestimates IOP. However, normal RBT readings are likely to be accurate and may spare children an EUA. High RBT readings should prompt the practitioner to use another standard method of IOP measurement if possible, or consider the RBT measurement in the context of clinical findings before referring the child to a specialist clinic or considering EUA. BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
4 Page of BMJ Open 0 Background/Introduction Glaucoma is a potentially blinding condition. Raised intraocular pressure (IOP) is an important risk factor for the development and progression of optic nerve damage in glaucoma, and is the target of both medical and surgical treatment. There are no published figures on how many children have an IOP test per year, but both community optometrists and hospital clinics regularly perform IOP measurement as part of a comprehensive eye examination. For all practitioners IOP measurements in young children are challenging. The current gold standard measurement technique is Goldmann applanation tonometry (GAT) on a slit lamp, or handheld Perkins applanation tonometry (PAT) during an examination under anaesthesia (EUA). GAT requires the instillation of topical anaesthetics and a high degree of co-operation from the child. Frequently children are unable to suppress the natural reflex of moving backward or closing their eyes. This leads to repeated attempts being made at obtaining a reading, prolonged examination times and distress to children and families. In 0 a new device to measure intraocular pressure became available, the icare rebound tonometer (RBT). Its main advantage over other instruments is that no topical anaesthesia is required. In addition, it is a hand-held device, which children may perceive as less intimidating and allows examiners to move with the child when required. The RBT acquires six readings in quick succession by propelling a fine sensor tip less than mm in diameter against the central cornea from the instrument base held at a distance of -mm from the surface of the eye. [] [] After contact, the probe bounces back; the higher the IOP the faster the rebound. Measurements are taken within 0. seconds. The force impacting on the cornea is minimal and does usually not even trigger the highly sensitive blink reflex. The instrument display then shows the average of the six readings and whether the standard deviation (SD) is low, medium or high. Since its introduction, RBT has become very popular and is now being used in many children s eye services and by many community-based optometrists. Two surveys of tonometry practice in children (Table and reference []) indicate that for most paediatric ophthalmologists in the UK, RBT has become the preferred method to measure IOP in children. Whilst the device is considered easy to use, many users report that RBT measurements tend to be higher than GAT measurements (Table ). Data comparing RBT performance with GAT in children with glaucoma are scarce and limited to one study only. [] Studies which have compared RBT with non-contact tonometry and tonopen in healthy children indicate good intra- and interobserver reliability and good agreement. [] [] [] In children with glaucoma good agreement has been reported with both PAT [] and GAT, [] although RBT measurements are consistently higher than PAT or GAT readings. In adults with healthy eyes, glaucoma or ocular hypertension, papers have reported good agreement between the RBT and GAT, albeit with systematically higher measurements on RBT. [] [0] [] [] [] [] [] BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
5 BMJ Open Page of 0 Accuracy of RBT may be affected by levels of IOP [] [] and central corneal thickness (CCT), [] [] [] it might not be CCT alone but rather other corneal properties (hysteresis and resistance) that affect IOP measurement. [] These parameters are not routinely assessed in clinics and impossible to assess in young children. We carried out the present study to evaluate the accuracy and reliability of RBT in children with glaucoma as compared to GAT. Secondary objectives were to investigate the influence of IOP and CCT, and to determine children s preference for RBT or GAT. Methods Patients We recruited children and teenagers between the age of and years with an established diagnosis of primary or secondary glaucoma, attending our tertiary paediatric glaucoma service at Moorfields Eye Hospital. The study was approved by the local research ethics committee. All parents/guardians gave written informed consent and children were invited to give assent. The sample size was determined by recommendations for Bland-Altman analysis. [] Protocol Three observers took the measurements required for this study. Observer measured the IOP in one eye by RBT. In children with glaucoma in both eyes, readings were taken from the right eye. In children with glaucoma only in the left eye, readings were taken from the left eye. Observer recorded two consecutive averagerbt readings from six measurements and the SD indicated by the device. One repeat average RBT measurement was obtained by a second observer and recorded separately. Following instillation of a drop of proxymethacaine, observer recorded CCT on ultrasound pachymetry. The third observer recorded IOP on GAT and asked the child which instrument they preferred. All data were recorded on a Case Report Form which also recorded the child s diagnosis and ethnic background. At the end of the study, data were entered into a computerised database. Data analysis Summary statistics were produced for demographic factors and for IOP readings made by each observer and method (Tables and ). Repeat readings made by observer using RBT were used to estimate intraobserver agreement using the Bland-Altmann limits of agreement method. [] The same method was used to determine interobserver agreement, analysing RBT reading from observer and the RBT reading obtained by observer. Agreement between RBT and GAT was analysed based on reading from observer and GAT recorded by observer. A histogram for CCT was plotted in two age bands (under and over 0 years of age). Child preference for either device was summarised by descriptive statistical methods. Results Demographics BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
6 Page of BMJ Open 0 We carried out the study between //0 and //0. We enrolled n=0 children with a confirmed diagnosis of glaucoma. Age ranged from. to years (mean., SD. years). boys and girls took part (Table ). In children the right eye was the study eye, and in n= children the left eye. Analysis of first RBT reading by observer One hundred and two datasets were analysed. Data were missing for subjects. In participants the variability reading on the RBT was high. Nineteen sets of data were therefore excluded from analysis. Analysis of second RBT reading by observer There were nine missing values, and children with high SD scores. Cross-tabulation of the first and second reading by observer showed that readings were missing on both occasions for three children, and missing only on the second occasion for six children. Six children had high SD scores on both measurements. Analysis of RBT reading by observer Data was missing on children. This was due to the trial being run within a busy tertiary centre clinic, with observers not always able to complete this part of the examination. Excluding RBT data with high variability readings, we were left with measurements by observer (reading ), measurements by observer (reading ), and measurements by observer. Analysis of GAT data GAT readings were missing in datasets. Most of these children had complex ocular pathology (corneal graft n=, microphthalmos/sunken socket n=, nystagmus n=, microcornea n=, congenital glaucoma and multiple surgery n=, Sturge Weber syndrome n=). One child was very anxious and difficult to examine. Two children were glaucoma suspects, and in three cases no comment was available explaining missing GAT. Analysis of IOP readings by RBT and GAT The mean RBT reading (SD) by observer was.mmhg (.), RBT reading by observer was. mmhg (.), observer RBT was. mmhg (.), and GAT was mmhg (.). Reproducibility of RBT readings: intra- and inter-observer variability Data were available for children who had two readings by observer. The mean difference between the readings was 0. (SD.). A t-test revealed no evidence of systematic bias between reading and reading (( df)=0., p=0.). The distribution of the differences appeared symmetric. The Bland Altman plot showed no systematic relationship between the average measure and the difference, and limits of agreement were computed as (-.,.) mmhg (Fig. A). First RBT reading by observer and RBT reading by observer were available for cases. The mean difference between readings was 0. mmhg (.). A t-test revealed no evidence of systematic bias between observers (t()=0., p=0.). Again, the data appeared symmetric. The Bland-Altman plot showed no systematic relationship, limits of agreement were (-.,.) mmhg (Fig. B). Agreement between GAT and RBT BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
7 BMJ Open Page of 0 We used data from first RBT reading by observer. These and GAT data were available for children. The mean difference was -. mmhg (.). A t-test showed evidence of systematic bias (t()=-., p<0.00). The Bland Altman plot also showed evidence of a relationship between the magnitude of the difference between methods and the magnitude of the measurement, with smaller differences being seen with lower measurements. This would imply that limits of agreement cannot be simply produced. Stratifying data at mmhg allows production of LOA. These are -.+/-.*. for readings less than mmhg, and -.+/-.*. for readings greater than mmhg. Based on these analyses, agreement between the two methods appears poor and not clinically acceptable. As demonstrated by the graph (Fig C), RBT frequently gave higher readings than GAT. Differences of 0mmHg were not uncommon. Pachymetry data Pachymetry measurements were obtained in n= children, of whom had IOP measurements taken by both RBT and GAT. As expected for the study population we found a high prevalence of increased pachymetry values (Fig D). Defining the normal range as -um, two readings were below the normal range (, um), and readings were above the normal range; of these, seven participants had both RBT and GAT measurements. Pachymetry and RBT readings Disagreement between GAT and RBT readings was greater with higher pachymetry readings, p=0.00. Patient preference Eleven children preferred GAT, 0 preferred RBT, and gave no preference. BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
8 Page of BMJ Open 0 Discussion The main finding of the present study is that the agreement of RBT and GAT appears poor in children with glaucoma. Since previous studies have largely concluded that there is good agreement between RBT and applanation tonometry, this observation was a surprise. We believe that this discrepancy may in part be due to the fact that many studies have considered correlation rather than agreement. It is quite possible for methods to correlate well, but to disagree by amounts that are of real clinical relevance. Our data provide strong evidence of a linear association between measures made by GAT and RBT - but linear association is not the same as agreement, which is why Bland and Altman advocated the Limits of Agreement method. [] The present study is the second to compare RBT and GAT in children with glaucoma. The only other study into RBT in this population also included children with suspected glaucoma, excluded readings from children who were nervous or squeezing during the RBT measurement, and repeated RBT readings until a measurement with minimal variability was obtained, or three readings had been taken. [] Whilst this guaranteed the vast majority of readings had either minimal or low variability, this approach means that the operator manually reduced device errors an approach often not possible in a busy clinic setting. The results of this study are comparable to those presented in our work: the authors report that RBT were higher than GAT readings in %, and within +/- mmhg of GAT in %. [] Our view is that disagreements of greater than mm Hg are of concern if they can impact on the management of the child. The only other study exploring the use of RBT in children with glaucoma compared it with Perkins applanation tonometry (PAT). [] The authors performed RBT and PAT in random order, which means that RBT measurements were performed after administration of topical anaesthesia. According to the manufacturer s manual topical anaesthesia may reduce the RBT reading. [] [] Again, the authors repeated RBT measurements when the variability indicator was high or IOP > mmhg with medium standard variation, excluding readings with erroneous device performance. The authors found greater disagreement with higher IOP measurements, yet did not provide limits of agreement stratified by IOP, or present regression-based limits of agreement. Interestingly, the graphs show that RBT measurements were consistently higher up to mmhg, which is consistent with our findings. Both PAT and RBT readings were higher in cases of increased corneal thickness, another finding that agrees with our report. Other paediatric studies of RBT are limited to healthy children, and none used GAT as comparator. [] [] [] Difference in study population is likely to be a contributory factor explaining why agreement between RBT and GAT was significantly poorer in our study than in others. Comparisons with GAT have been conducted in adults with glaucoma, but excluding significant other pathologies such as astigmatism, microphthalmos, buphthalmos, dry eyes, nystagmus. [] [] [] [] Results in studies with mixed populations (adults with glaucoma/ocular hypertension and healthy adults) also reported good GAT/RBT agreement. [] [] [] However, all studies except two used topical anaesthesia before RBT. Interestingly, the two studies who did not use topical anaesthesia found significant differences between GAT and RBT, with RBT overestimating IOP by to mmhg. [] [] Three studies performed on healthy adults without topical anaesthesia reported good agreement between RBT and GAT, [] [] [0] whilst three others reported significant differences in some cases. [] [] [] The main limitation of these studies might be the inclusion of normal eyes with normal IOP only. Findings from this population cannot be generalised to subjects with raised IOP. BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
9 BMJ Open Page of 0 Sequence of tests may also explain differences in findings. Applanation tonometry, especially repeated measurements, can progressively lower IOP by a mechanism know as aqueous massage. [] [] [] Our study design avoided this effect by obtaining RBT before GAT measurements. Studies that obtained GAT before RBT or conducted tests in random order [] [] [] [] [] may have induced IOP lowering, thereby erroneously obtaining lower RBT readings. Similar to other groups [] [] [] [] we found increased disagreement between RBT and GAT with higher CCT values. However, we found that even in children with pachymetry readings of um, disagreements could be greater than 0 mmhg. Our study confirms reports [][][] that the hand-held RBT has high acceptability in children. Since we started this work in 0, it has become widely available and popular in many community optometric practices and hospital eye units in the UK (Table ). [] Seventy percent of the children enrolled in this study had a clear preference for the new device which does not require instillation of anaesthetic eye drops and no prolonged sitting in an uncomfortable position. On the basis of previously published reports and our own work, we would recommend the use of the RBT in children, but advise practitioners to be cautious in the interpretation of findings, particularly in children with thicker corneas. It is reassuring that measurement discrepancies tend to reflect a systematic over-reading by the RBT: normal values obtained by this method are likely correct, and the IOP is unlikely to be high. This in turn can re-assure examiners and spare children the need for other IOP measurement methods and even examinations under anaesthesia. High RBT readings, on the other side, should not automatically trigger a trip to the operating theatre, but should prompt the examiner to seek confirmation of IOP level by another established technique. BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
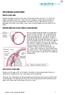
10 Page of BMJ Open 0 Legends Table. Survey of current paediatric tonometry practice in the UK. Using an electronic mailing list, we contacted of paediatric ophthalmologists in the UK. The survey ran for 0 days, from February to,, and collected replies. Table. Demographic details of study participants. Table : Agreement (inter observer, Intra observer and with GAT) for RBT Fig.. Tonometry and pachymetry results. A: Intraobserver agreement of RBT measurements. B: Interobserver agreement of RBT measurements. C: Agreement between RBT and GAT measurements. D: Distribution of corneal thickness as determined by pachymetry. BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
11 BMJ Open Page 0 of 0 Tables and Figures In which setting do you work and measure IOP in children? Do you run a specialist paediatric glaucoma service? In how many children do you measure the IOP per month? Teaching hospital District general hospital Community clinic What is your preferred method to measure IOP in children? If you are using a RBT, how easy do you find it to use? In your experience, are RBT readings accurate as compared to Goldmann applanation tonometry readings? Yes No Less than Between and More than RBT Goldmann/Perkins applanation Tonopen Air puff Very easy Moderately easy Not at all easy Not applicable As accurate as Goldmann RBT tend to be higher than GAT readings RBT tend to be lower than GAT readings.%.%.%.% 0.% %.%.%.%.%.%.% %.%.%.%.%.%.% Table. Survey of current paediatric tonometry practice in the UK. Using an electronic mailing list, we contacted of paediatric ophthalmologists in the UK. The survey ran for 0 days, from February to,, and collected replies. BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
12 Page of BMJ Open 0 Sex Male:female (n : Age (Years) Mean (SD). (.) Laterality Right:left : Ethnicity Caucasian Mixed Asian or Asian British Carribbean/African/Any other Black background Other ethnic groups (incl. Chinese) Not stated or not recorded Pachymetry Median (IQR)* (, ) * IQR : interquartile range, children had no pachymetry readings Table : Demographic factors of the children under investigation BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
13 BMJ Open Page of 0 Mean difference SD difference LOA Intra observer (n = ) 0.. (-.,.) Inter-observer (n = ) 0.. (-.,.) ICare-GAT (n = ) -.. < mmhg :(-.,.0) >= mmhg :(-.0, 0.0) Table : Agreement (inter observer, Intra observer and with GAT) for RBT BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
14 Page of BMJ Open 0 References. Kontiola AI, Goldblum D, Mittag T, et al. The induction/impact tonometer: a new instrument to measure intraocular pressure in the rat. Experimental eye research 0;():-. Kontiola A, Puska P. Measuring intraocular pressure with the Pulsair 00 and Rebound tonometers in elderly patients without an anesthetic. Graefe's archive for clinical and experimental ophthalmology = Albrecht von Graefes Archiv fur klinische und experimentelle Ophthalmologie 0;():-. Chan WH, Lloyd IC, Ashworth JL, et al. Measurement of intraocular pressure in children in the UK. Eye (London, England) ;():-. Flemmons MS, Hsiao YC, Dzau J, et al. Icare rebound tonometry in children with known and suspected glaucoma. J Aapos ;():-. Kageyama M, Hirooka K, Baba T, et al. Comparison of ICare rebound tonometer with noncontact tonometer in healthy children. Journal of glaucoma ;():-. Sahin A, Basmak H, Niyaz L, et al. Reproducibility and tolerability of the ICare rebound tonometer in school children. Journal of glaucoma 0;():-. Sahin A, Basmak H, Yildirim N. The influence of central corneal thickness and corneal curvature on intraocular pressure measured by tono-pen and rebound tonometer in children. Journal of glaucoma 0;():-. Martinez-de-la-Casa JM, Garcia-Feijoo J, Saenz-Frances F, et al. Comparison of rebound tonometer and Goldmann handheld applanation tonometer in congenital glaucoma. Journal of glaucoma 0;():-. Fernandes P, Diaz-Rey JA, Queiros A, et al. Comparison of the ICare rebound tonometer with the Goldmann tonometer in a normal population. Ophthalmic Physiol Opt 0;():- 0. Davies LN, Bartlett H, Mallen EA, et al. Clinical evaluation of rebound tonometer. Acta ophthalmologica Scandinavica 0;():-. Brusini P, Salvetat ML, Zeppieri M, et al. Comparison of ICare tonometer with Goldmann applanation tonometer in glaucoma patients. Journal of glaucoma 0;():-. Nakamura M, Darhad U, Tatsumi Y, et al. Agreement of rebound tonometer in measuring intraocular pressure with three types of applanation tonometers. American journal of ophthalmology 0;():-. Sahin A, Niyaz L, Yildirim N. Comparison of the rebound tonometer with the Goldmann applanation tonometer in glaucoma patients. Clinical & experimental ophthalmology 0;():-. Pakrou N, Gray T, Mills R, et al. Clinical comparison of the Icare tonometer and Goldmann applanation tonometry. Journal of glaucoma 0;():-. Rehnman JB, Martin L. Comparison of rebound and applanation tonometry in the management of patients treated for glaucoma or ocular hypertension. Ophthalmic Physiol Opt 0;():-. Munkwitz S, Elkarmouty A, Hoffmann EM, et al. Comparison of the icare rebound tonometer and the Goldmann applanation tonometer over a wide IOP range. Graefe's archive for clinical and experimental ophthalmology = Albrecht von Graefes Archiv fur klinische und experimentelle Ophthalmologie 0;():-. Chui WS, Lam A, Chen D, et al. The influence of corneal properties on rebound tonometry. Ophthalmology 0;():0-. Bland JM, Altman DG. Applying the right statistics: analyses of measurement studies. Ultrasound Obstet Gynecol 0;():-. Tiolat. icare Tonometer: User's and Maintenance Manual. Helsinki.. Baudouin C, Gastaud P. Influence of topical anesthesia on tonometric values of intraocular pressure. Ophthalmologica. Journal international d'ophtalmologie. International journal of ophthalmology ;():- BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
15 BMJ Open Page of 0. Lundvall A, Svedberg H, Chen E. Application of the ICare rebound tonometer in healthy infants. Journal of glaucoma ;():-. Martinez-de-la-Casa JM, Garcia-Feijoo J, Vico E, et al. Effect of corneal thickness on dynamic contour, rebound, and goldmann tonometry. Ophthalmology 0;():-. van der Jagt LH, Jansonius NM. Three portable tonometers, the TGDc-0, the ICARE and the Tonopen XL, compared with each other and with Goldmann applanation tonometry*. Ophthalmic Physiol Opt 0;():-. Jorge J, Fernandes P, Queiros A, et al. Comparison of the IOPen and icare rebound tonometers with the Goldmann tonometer in a normal population. Ophthalmic Physiol Opt;():0-. Poostchi A, Mitchell R, Nicholas S, et al. The icare rebound tonometer: comparisons with Goldmann tonometry, and influence of central corneal thickness. Clinical & experimental ophthalmology 0;():-. Krakau CE, Wilke K. On repeated tonometry. Acta Ophthalmol (Copenh) ;():- BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
16 Page of BMJ Open 0 xmm (0 x 0 DPI) BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
17 BMJ Open Comparison of handheld rebound tonometry with Goldmann applanation tonometry in children with glaucoma: a cohort study Journal: BMJ Open Manuscript ID: bmjopen--00.r Article Type: Research Date Submitted by the Author: -Nov- Complete List of Authors: Dahlmann-Noor, Annegret; NIHR Biomedical Research Centre at Moorfields Eye Hospital NHS Foundation Trust and UCL Institute of Ophthalmology, Paediatric Ophthalmology Bunce, Catey; Moorfields Eye Hospital NHS Foundation Trust, Research and Development Puertas, Renata; Moorfields Eye Hospital, Glaucoma Tabasa-Lim, Shenille; Moorfields Eye Hospital, Paediatric Ophthalmology El-Karmouty, Ahmed; Moorfields Eye Hospital, Glaucoma Kadhim, Mustafa; Moorfields Eye Hospital, Glaucoma Wride, Nicholas; Moorfields Eye Hospital, Glaucoma Lewis, Amanda; Moorfields Eye Hospital, Glaucoma Grosvenor, Dawn; Moorfields Eye Hospital, Glaucoma Rai, Poornima; Moorfields Eye Hospital, Glaucoma Papadopoulos, Maria; Moorfields Eye Hospital, Glaucoma brookes, john; Moorfields Eye Hospital, Glaucoma Khaw, Peng; NIHR Biomedical Research Centre at Moorfields Eye Hospital NHS Foundation Trust and UCL Institute of Ophthalmology, Glaucoma <b>primary Subject Heading</b>: Ophthalmology Secondary Subject Heading: Paediatrics, Evidence based practice Keywords: Paediatric ophthalmology < OPHTHALMOLOGY, Community child health < PAEDIATRICS, Glaucoma < OPHTHALMOLOGY BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
18 Page of BMJ Open 0 Handheld rebound tonometry in children with glaucoma Authors Annegret Hella Dahlmann-Noor Renata Puertas Shenille Tabasa-Lim Ahmed El-Karmouty Mustafa Kadhim Nicholas Wride Amanda Lewis Dawn Grosvenor Poornima Rai Maria Papadopoulos John Brookes Catey Bunce Peng Tee Khaw Corresponding author: Annegret Dahlmann-Noor, Moorfields Eye Hospital, City Road, London ECV PD; annegret.dahlmann-noor@moorfields.nhs.uk Funding statement: This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. Acknowledgements: The authors are grateful for the support from Fight for Sight and the Helen Hamlyn Trust. The research took place at the National Institute for Health Research (NIHR) Biomedical Research Centre at Moorfields Eye Hospital NHS Foundation Trust and UCL Institute of Ophthalmology. The views expressed are those of the author(s) and not necessarily those of the NHS, the NIHR or the Department of Health. Competing Interests Statement: None of the authors have competing interests to declare. Contributorship Statement: AHDN and CB designed the trial and prepared the manuscript. AHDN, RP, STL, AE, PR, MK, NW, AL, DG, MP, JB and PTK facilitated recruitment, obtained informed consent, acquired data and completed case report forms. AHDN entered data onto the electronic database. CB analysed the data. All authors reviewed the manuscript. BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
19 BMJ Open Page of 0 Abstract Objective: To test agreement of two methods to measure intraocular pressure (IOP): rebound tonometry (RBT) and gold standard Goldmann applanation (GAT) tonometry in children with glaucoma Design: observational prospective cohort study Setting: tertiary paediatric glaucoma clinic at a single centre Participants: 0 individuals attending a paediatric glaucoma clinic, mean (SD) age. (.), of whom were male Interventions: n/a Primary and secondary outcome measures: intraocular pressure, central corneal thickness, child preference for measurement method Results: Limits of agreement for intra- and interobserver were respectively (-.,.) mmhg and (-.,.) mmhg. RBT frequently gave higher readings than GAT and the magnitude of disagreement depended on the level of IOP being assessed. Differences of 0mmHg were not uncommon. RBT was the preferred method for 0% of children. Conclusions: There is poor agreement between RBT and GAT in children with glaucoma. RBT frequently and significantly overestimates IOP. However, normal RBT readings are likely to be accurate and may spare children an examination under anaesthesia (EUA). High RBT readings should prompt the practitioner to use another standard method of IOP measurement if possible, or consider the RBT measurement in the context of clinical findings before referring the child to a specialist clinic or considering EUA. Trial registration: n/a Article Summary Article focus BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
20 Page of BMJ Open 0 Measuring intraocular pressure (IOP) is critical in diagnosis and monitoring of glaucoma, and is often difficult in children. Rebound tonometry (RBT) may be more child-friendly than other tonometry methods. Agreement between RBT and reference standard Goldmann applanation tonometry (GAT) in children and young people attending glaucoma clinics has not been sufficiently evaluated. Key messages Agreement between RBT and GAT is poor in children and young people with glaucoma; RBT frequently and significantly overestimates IOP. Normal RBT readings are likely to be accurate and may spare children an examination under anaesthesia. High RBT readings should prompt the practitioner to use another standard method of IOP measurement, if possible. Strengths and limitations of this study This study focuses on a cohort of children and young people attending a paediatric glaucoma clinic, a population in whom accurate tonometry is required for correct diagnosis and management. Statistical analysis is based on the limits of agreement method rather than correlation. BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
21 BMJ Open Page of 0 Background/Introduction Glaucoma is a potentially blinding condition. Raised intraocular pressure (IOP) is an important risk factor for the development and progression of optic nerve damage in glaucoma, and is the target of both medical and surgical treatment. There are no published figures on how many children have an IOP test per year, but both community optometrists and hospital clinics regularly perform IOP measurement as part of a comprehensive eye examination. For all practitioners IOP measurements in young children are challenging. The current reference standard for tonometry is the Goldmann applanation tonometer (GAT, ISO ) mounted on a slit lamp. The Perkins tonometer (PAT), as the hand-held version of GAT, is a suitable reference standard for IOP measurements for patients in the supine position, and hence for children during an examination under anaesthesia (EUA). Another commonly used handheld tonometer is the Reichert Tono-Pen R, but for comparison of diagnostic test accuracy, we opted for the reference standard devices. GAT requires the instillation of topical anaesthetics and a high degree of co-operation from the child. Frequently children are unable to suppress the natural reflex of moving backward or closing their eyes. This leads to repeated attempts being made at obtaining a reading, prolonged examination times and distress to children and families. In 0 a new device to measure intraocular pressure became available, the icare rebound tonometer (RBT). Its main advantage over other instruments is that no topical anaesthesia is required. In addition, it is a hand-held device, which children may perceive as less intimidating and allows examiners to move with the child when required. The RBT acquires six readings in quick succession by propelling a fine sensor tip less than mm in diameter against the central cornea from the instrument base held at a distance of -mm from the surface of the eye. [] [] After contact, the probe bounces back; the higher the IOP the faster the rebound. Measurements are taken within 0. seconds. The force impacting on the cornea is minimal and does usually not even trigger the highly sensitive blink reflex. The instrument display then shows the average of the six readings and whether the standard deviation (SD) is low, medium or high. Since its introduction, RBT has become very popular and is now being used in many children s eye services and by many community-based optometrists. Two surveys of tonometry practice in children (Table and reference []) indicate that for most paediatric ophthalmologists in the UK, RBT has become the preferred method to measure IOP in children. Whilst the device is considered easy to use, many users report that RBT measurements tend to be higher than GAT measurements (Table ). Data comparing RBT performance with GAT in children with glaucoma are scarce and limited to one study only. [] Studies which have compared RBT with non-contact tonometry and tonopen in healthy children indicate good intra- and interobserver reliability and good agreement. [] [] [] In children with glaucoma good agreement has been reported with both PAT [] and GAT, [] although RBT measurements are consistently higher than PAT or GAT readings. In adults with healthy eyes, glaucoma or ocular hypertension, papers have reported good agreement between the RBT and GAT, albeit with systematically higher measurements on RBT. [] [0] [] [] [] [] [] BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
22 Page of BMJ Open 0 Accuracy of RBT may be affected by levels of IOP, [] [] central corneal thickness (CCT) [] [] [] and other corneal properties such as hysteresis and resistance. [] The latter parameters are not routinely assessed in clinics and impossible to assess in young children. We carried out the present study to evaluate the accuracy and reliability of RBT in children with glaucoma as compared to GAT. Secondary objectives were to investigate the influence of CCT on IOP measurements by RBT, and to determine children s preference for RBT or GAT. Methods Patients We recruited consecutive subjects attending our tertiary paediatric glaucoma service at Moorfields Eye Hospital. The study was approved by the local research ethics committee. All parents/guardians gave written informed consent and children were invited to give assent. The sample size was determined by recommendations for Bland-Altman analysis. [] Protocol Three observers took the measurements required for this study. Observer measured the IOP in one eye by RBT. In children with glaucoma in both eyes, readings were taken from the right eye. In children with glaucoma only in the left eye, readings were taken from the left eye. Observer recorded two consecutive averagerbt readings from six measurements and the SD indicated by the device. One repeat average RBT measurement was obtained by a second observer and recorded separately. Following instillation of a drop of proxymethacaine, observer recorded CCT on ultrasound pachymetry. The third observer recorded IOP on GAT and asked the child which instrument they preferred. All data were recorded on a Case Report Form which also recorded the child s diagnosis and ethnic background. At the end of the study, data were entered into a computerised database. Data analysis Summary statistics were produced for demographic factors and for IOP readings made by each observer and method (Tables and ). Repeat readings made by observer using RBT were used to estimate intraobserver agreement using the Bland-Altmann limits of agreement method. [] The same method was used to determine interobserver agreement, analysing RBT reading from observer and the RBT reading obtained by observer. Agreement between RBT and GAT was analysed based on reading from observer and GAT recorded by observer. A histogram for CCT was plotted in two age bands (under and over 0 years of age). Child preference for either device was summarised by descriptive statistical methods. Results Demographics We carried out the study between //0 and //0. We enrolled n=0 children with a confirmed diagnosis of glaucoma. Age ranged from. to years (mean., SD. years). BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
23 BMJ Open Page of 0 boys and girls took part (Table ). In children the right eye was the study eye, and in n= children the left eye. Analysis of first RBT reading by observer One hundred and two datasets were analysed. Data were missing for subjects. The RBT automatically indicates a higher than normal standard deviation of the acquired measurements by displaying a flashing P or a line in the Up position following the measurement. These are indicators of poor reliability, and the manufacturer recommends repeating the measurement. We excluded participants in whom measurements displayed these poor reliability parameters. Nineteen sets of data were therefore excluded from analysis. Analysis of second RBT reading by observer There were nine missing values, and children with poor reliability scores. Cross-tabulation of the first and second reading by observer showed that readings were missing on both occasions for three children, and missing only on the second occasion for six children. Six children had poor reliability indicators on both measurements. Analysis of RBT reading by observer Data was missing on children. This was due to the trial being run within a busy tertiary centre clinic, with observers not always able to complete this part of the examination. Excluding RBT data with poor reliability indicators, we were left with measurements by observer (reading ), measurements by observer (reading ), and measurements by observer. Analysis of GAT data GAT readings were missing in datasets. Most of these children had complex ocular pathology (corneal graft n=, microphthalmos/sunken socket n=, nystagmus n=, microcornea n=, congenital glaucoma and multiple surgery n=, Sturge Weber syndrome n=). One child was very anxious and difficult to examine. Two children were glaucoma suspects, and in three cases no comment was available explaining missing GAT. Analysis of IOP readings by RBT and GAT The mean RBT reading (SD) by observer was.mmhg (.), RBT reading by observer was. mmhg (.), observer RBT was. mmhg (.), and GAT was mmhg (.). Reproducibility of RBT readings: intra- and inter-observer variability Data were available for children who had two readings by observer. The mean difference between the readings was 0. (SD.). A t-test revealed no evidence of systematic bias between reading and reading (( df)=0., p=0.). The distribution of the differences appeared symmetric. The Bland Altman plot showed no systematic relationship between the average measure and the difference, and limits of agreement were computed as (-.,.) mmhg (Fig. A). First RBT reading by observer and RBT reading by observer were available for cases. The mean difference between readings was 0. mmhg (.). A t-test revealed no evidence of systematic bias between observers (t()=0., p=0.). Again, the data appeared symmetric. The Bland-Altman plot showed no systematic relationship, limits of agreement were (-.,.) mmhg (Fig. B). BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
24 Page of BMJ Open 0 Agreement between GAT and RBT We used data from first RBT reading by observer. These and GAT data were available for children. The mean difference was -. mmhg (.). A t-test showed evidence of systematic bias (t()=-., p<0.00). The Bland Altman plot also showed evidence of a relationship between the magnitude of the difference between methods and the magnitude of the measurement, with smaller differences being seen with lower measurements. This would imply that limits of agreement cannot be simply produced. Stratifying data at mmhg removed evidence of bias and limits of agreement were then computed as (-.,.) mmhg for for readings less than mmhg, and (-.0, 0.0) mmhg for readings greater than mmhg. Based on these analyses, agreement between the two methods appears poor and not clinically acceptable. As demonstrated by the graph (Fig C), RBT frequently gave higher readings than GAT. Differences of 0mmHg were not uncommon. Pachymetry data Pachymetry measurements were obtained in n= children, of whom had IOP measurements taken by both RBT and GAT (Fig D). Defining the normal range as -um, two readings were below the normal range (, um), and readings were above the normal range; of these, seven participants had both RBT and GAT measurements. Of the children with CCT greater than um, one had corneal clouding/oedema and enlarged cornea, and in two children multiple previous glaucoma interventions were recorded. None of these children had nystagmus, aphakic glaucoma, aniridia or anterior segment dysgenesis syndromes, or other confounding corneal abnormalities. Pachymetry and RBT readings Disagreement between GAT and RBT readings was greater with higher pachymetry readings, p=0.00. Patient preference Eleven children preferred GAT, 0 preferred RBT, and gave no preference. BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
25 BMJ Open Page of 0 Discussion The main finding of the present study is that the agreement of RBT and GAT appears poor in children with glaucoma. Since previous studies have largely concluded that there is good agreement between RBT and applanation tonometry, this observation was a surprise. We believe that this discrepancy may in part be due to the fact that many studies have considered correlation rather than agreement. It is quite possible for methods to correlate well, but to disagree by amounts that are of real clinical relevance. Our data provide strong evidence of a linear association between measures made by GAT and RBT - but linear association is not the same as agreement, which is why Bland and Altman advocated the Limits of Agreement method. [] The present study is the second to compare RBT and GAT in children with glaucoma. The only other study into RBT in this population also included children with suspected glaucoma, excluded readings from children who were nervous or squeezing during the RBT measurement, and repeated RBT readings until a measurement with minimal variability was obtained, or three readings had been taken. [] Whilst this guaranteed the vast majority of readings had either minimal or low variability, this approach means that the operator manually reduced device errors. The results of this study are comparable to those presented in our work: the authors report that RBT were higher than GAT readings in %, and within +/- mmhg of GAT in %. [] Our view is that disagreements of greater than mm Hg are of concern if they can impact on the management of the child. The only other study exploring the use of RBT in children with glaucoma compared it with Perkins applanation tonometry (PAT). [] The authors performed RBT and PAT in random order, which means that RBT measurements were performed after administration of topical anaesthesia. According to the manufacturer s manual topical anaesthesia may reduce the RBT reading. [] [] Again, the authors repeated RBT measurements when the variability indicator was high or IOP > mmhg with medium standard variation, excluding readings with erroneous device performance. The authors found greater disagreement with higher IOP measurements, yet did not provide limits of agreement stratified by IOP, or present regression-based limits of agreement. Interestingly, the graphs show that RBT measurements were consistently higher up to mmhg, which is consistent with our findings. Both PAT and RBT readings were higher in cases of increased corneal thickness, another finding that agrees with our report. Other paediatric studies of RBT are limited to healthy children, and none used GAT as comparator. [] [] [] Difference in study population is likely to be a contributory factor explaining why agreement between RBT and GAT was significantly poorer in our study than in others. Comparisons with GAT have been conducted in adults with glaucoma, but excluding significant other pathologies such as astigmatism, microphthalmos, buphthalmos, dry eyes, nystagmus. [] [] [] [] Results in studies with mixed populations (adults with glaucoma/ocular hypertension and healthy adults) also reported good GAT/RBT agreement. [] [] [] However, all studies except two used topical anaesthesia before RBT. Interestingly, the two studies who did not use topical anaesthesia found significant differences between GAT and RBT, with RBT overestimating IOP by to mmhg. [] [] Three studies performed on healthy adults without topical anaesthesia reported good agreement between RBT and GAT, [] [] [0] whilst three others reported significant differences in some cases. [] [] [] The main limitation of these studies might be the inclusion of normal eyes with normal IOP only. Findings from this population cannot be generalised to subjects with raised IOP. Sequence of tests may also explain differences in findings. Applanation tonometry, especially BMJ Open: first published as 0./bmjopen--00 on April. Downloaded from on July by guest. Protected by copyright.
Comparison of handheld rebound tonometry with Goldmann applanation tonometry in children with glaucoma: a cohort study
 Open Access Research Comparison of handheld rebound tonometry with Goldmann applanation tonometry in children with glaucoma: a cohort study Annegret Hella Dahlmann-Noor, 1 Renata Puertas, 2 Shenille Tabasa-Lim,
Open Access Research Comparison of handheld rebound tonometry with Goldmann applanation tonometry in children with glaucoma: a cohort study Annegret Hella Dahlmann-Noor, 1 Renata Puertas, 2 Shenille Tabasa-Lim,
Comparison of icare Tonometer with Pulsair and Tonopen in Domiciliary Work
 Optometry in Practice Vol 6 (2005) 33 39 Comparison of icare Tonometer with Pulsair and Tonopen in Domiciliary Work Dawn E C Roberts BSc(Hons) MSc MCOptom Healthcall Optical Services, Luton, Bedfordshire,
Optometry in Practice Vol 6 (2005) 33 39 Comparison of icare Tonometer with Pulsair and Tonopen in Domiciliary Work Dawn E C Roberts BSc(Hons) MSc MCOptom Healthcall Optical Services, Luton, Bedfordshire,
Kobe University Repository : Kernel
 Kobe University Repository : Kernel タイトル Title 著者 Author(s) 掲載誌 巻号 ページ Citation 刊行日 Issue date 資源タイプ Resource Type 版区分 Resource Version 権利 Rights DOI JaLCDOI URL Agreement of Rebound Tonometer in Measuring
Kobe University Repository : Kernel タイトル Title 著者 Author(s) 掲載誌 巻号 ページ Citation 刊行日 Issue date 資源タイプ Resource Type 版区分 Resource Version 権利 Rights DOI JaLCDOI URL Agreement of Rebound Tonometer in Measuring
Agreement between methods of measurement
 Agreement between methods of measurement Gabriela Czanner PhD CStat Department of Biostatistics Department of Eye and Vision Science University of Liverpool and Clinical Eye Research Center Royal Liverpool
Agreement between methods of measurement Gabriela Czanner PhD CStat Department of Biostatistics Department of Eye and Vision Science University of Liverpool and Clinical Eye Research Center Royal Liverpool
Effect of corneal parameters on measurements using the pulsatile ocular blood flow tonograph and Goldmann applanation tonometer
 518 EXTENDED REPORT Effect of corneal parameters on measurements using the pulsatile ocular blood flow tonograph and Goldmann applanation tonometer P Gunvant, M Baskaran, L Vijaya, I S Joseph, R J Watkins,
518 EXTENDED REPORT Effect of corneal parameters on measurements using the pulsatile ocular blood flow tonograph and Goldmann applanation tonometer P Gunvant, M Baskaran, L Vijaya, I S Joseph, R J Watkins,
pat hways Medtech innovation briefing Published: 15 March 2016 nice.org.uk/guidance/mib57
 pat hways Icare rebound tonometer to measure intraocular pressure Medtech innovation briefing Published: 15 March 2016 nice.org.uk/guidance/mib57 Summary Icare products are the only devices that currently
pat hways Icare rebound tonometer to measure intraocular pressure Medtech innovation briefing Published: 15 March 2016 nice.org.uk/guidance/mib57 Summary Icare products are the only devices that currently
The innovative aspects are that ORA G3 is currently the only device capable of measuring corneal hysteresis.
 pat hways ORA G3 to measure corneal hysteresis Medtech innovation briefing Published: 18 June 2018 nice.org.uk/guidance/mib150 Summary The technology described in this briefing is Ocular Response Analyzer
pat hways ORA G3 to measure corneal hysteresis Medtech innovation briefing Published: 18 June 2018 nice.org.uk/guidance/mib150 Summary The technology described in this briefing is Ocular Response Analyzer
NIIOS. Cornea Specialist, Melles Cornea Clinic, NIIOS, Rotterdam, the Netherlands Naval Hospital, Athens, Greece VASILIS S.
 Cornea Specialist, Melles Cornea Clinic, NIIOS, Rotterdam, the Netherlands Naval Hospital, Athens, Greece Goldman applanation tonometry is still the gold standard for measuring IOP, but its accuracy is
Cornea Specialist, Melles Cornea Clinic, NIIOS, Rotterdam, the Netherlands Naval Hospital, Athens, Greece Goldman applanation tonometry is still the gold standard for measuring IOP, but its accuracy is
Clinical Study Evaluation of the New Digital Goldmann Applanation Tonometer for Measuring Intraocular Pressure
 Ophthalmology, Article ID 461681, 5 pages http://dx.doi.org/1.1155/214/461681 Clinical Study Evaluation of the New Digital Goldmann Applanation Tonometer for Measuring Intraocular Pressure Yuta Sakaue,
Ophthalmology, Article ID 461681, 5 pages http://dx.doi.org/1.1155/214/461681 Clinical Study Evaluation of the New Digital Goldmann Applanation Tonometer for Measuring Intraocular Pressure Yuta Sakaue,
INTRODUCTION S. HERDENER, D. HAFIZOVIC, M. PACHE, S. LAUTEBACH, J. FUNK. University Eye Hospital, Freiburg - Germany
 European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 39-43 Is the PASCAL -Tonometer suitable for measuring intraocular pressure in clinical routine? Long- and short-term reproducibility of dynamic
European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 39-43 Is the PASCAL -Tonometer suitable for measuring intraocular pressure in clinical routine? Long- and short-term reproducibility of dynamic
Clinical Study Short-Term Effect of Standard Automated Perimetry Testing on Intraocular Pressure in Patients with Open-Angle Glaucoma
 ISRN Ophthalmology Volume 2013, Article ID 956504, 5 pages http://dx.doi.org/10.1155/2013/956504 Clinical Study Short-Term Effect of Standard Automated Perimetry Testing on Intraocular Pressure in Patients
ISRN Ophthalmology Volume 2013, Article ID 956504, 5 pages http://dx.doi.org/10.1155/2013/956504 Clinical Study Short-Term Effect of Standard Automated Perimetry Testing on Intraocular Pressure in Patients
LOCSU Community Services. Glaucoma Repeat Readings & OHT Monitoring Community Service Pathway. Issued by Local Optical Committee Support Unit May 2009
 LOCSU Community Services Glaucoma Repeat Readings & OHT Monitoring Community Service Pathway Issued by Local Optical Committee Support Unit May 2009 [Revised November 2013] Contents Page Executive Summary...
LOCSU Community Services Glaucoma Repeat Readings & OHT Monitoring Community Service Pathway Issued by Local Optical Committee Support Unit May 2009 [Revised November 2013] Contents Page Executive Summary...
GLAUCOMA REPEAT READINGS PATHWAY
 GLAUCOMA REPEAT READINGS PATHWAY Level 1a: Goldmann style applanation tonometry repeat readings A first level community service for IOP refinement where other signs of glaucoma are not present will reduce
GLAUCOMA REPEAT READINGS PATHWAY Level 1a: Goldmann style applanation tonometry repeat readings A first level community service for IOP refinement where other signs of glaucoma are not present will reduce
Clinical Study Comprasion of ICare Rebound Tonometer and Goldmann Applanation Tonometer in High Myopia
 Hindawi Publishing Corporation e Scientific World Journal Volume 2014, Article ID 869460, 5 pages http://dx.doi.org/10.1155/2014/869460 Clinical Study Comprasion of ICare Rebound Tonometer and Goldmann
Hindawi Publishing Corporation e Scientific World Journal Volume 2014, Article ID 869460, 5 pages http://dx.doi.org/10.1155/2014/869460 Clinical Study Comprasion of ICare Rebound Tonometer and Goldmann
City, University of London Institutional Repository
 City Research Online City, University of London Institutional Repository Citation: Dabasia, P. L., Lawrenson, J. & Murdoch, I. E. (2015). Evaluation of a new rebound tonometer for self-measurement of intraocular
City Research Online City, University of London Institutional Repository Citation: Dabasia, P. L., Lawrenson, J. & Murdoch, I. E. (2015). Evaluation of a new rebound tonometer for self-measurement of intraocular
Clinical Evaluation of Glaucoma in Children
 Curr Ophthalmol Rep (2013) 1:106 112 DOI 10.1007/s40135-013-0012-6 DIAGNOSIS AND MONITORING OF GLAUCOMA (S SMITH, SECTION EDITOR) Clinical Evaluation of Glaucoma in Children Nicholas G. Strouthidis Maria
Curr Ophthalmol Rep (2013) 1:106 112 DOI 10.1007/s40135-013-0012-6 DIAGNOSIS AND MONITORING OF GLAUCOMA (S SMITH, SECTION EDITOR) Clinical Evaluation of Glaucoma in Children Nicholas G. Strouthidis Maria
LOCSU Community Services. Glaucoma Repeat Readings & OHT Monitoring Community Service Pathway. Issued by Local Optical Committee Support Unit May 2009
 LOCSU Community Services Glaucoma Repeat Readings & OHT Monitoring Community Service Pathway Issued by Local Optical Committee Support Unit May 2009 [Revised May 2016, Version 3.3] Contents Page Executive
LOCSU Community Services Glaucoma Repeat Readings & OHT Monitoring Community Service Pathway Issued by Local Optical Committee Support Unit May 2009 [Revised May 2016, Version 3.3] Contents Page Executive
Retrospective analysis of risk factors for late presentation of chronic glaucoma
 24 Glaxo Department of Ophthalmic Epidemiology, Moorfields Eye Hospital, City Road, London EC1V 2PD S Fraser C Bunce R Wormald Correspondence to: Mr S G Fraser. Accepted for publication 31 July 1998 Retrospective
24 Glaxo Department of Ophthalmic Epidemiology, Moorfields Eye Hospital, City Road, London EC1V 2PD S Fraser C Bunce R Wormald Correspondence to: Mr S G Fraser. Accepted for publication 31 July 1998 Retrospective
Kathryn L. Wotman, DVM, DACVIM Jeffrey E. Bowersox, DVM, DACVO. Veterinary Specialty Center of Delaware
 Kathryn L. Wotman, DVM, DACVIM Jeffrey E. Bowersox, DVM, DACVO Veterinary Specialty Center of Delaware Contact Lensesuse in Veterinary Ophthalmology -Corneal erosions Spontaneous Chronic Corneal Epithelial
Kathryn L. Wotman, DVM, DACVIM Jeffrey E. Bowersox, DVM, DACVO Veterinary Specialty Center of Delaware Contact Lensesuse in Veterinary Ophthalmology -Corneal erosions Spontaneous Chronic Corneal Epithelial
The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (8), Page
 The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (8), Page 1371-1376 Relationship Between Corneal Astigmatism and Intraocular Pressure Abdulrahman E. Algarni 1, Mohammad Abahussin 2, Nuha
The Egyptian Journal of Hospital Medicine (January 2018) Vol. 70 (8), Page 1371-1376 Relationship Between Corneal Astigmatism and Intraocular Pressure Abdulrahman E. Algarni 1, Mohammad Abahussin 2, Nuha
Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
Comparison of Intraocular Pressure Measurements by the Ocular Response Analyzer and Goldmann Applanation Tonometer after Penetrating Keratoplasty
 Comparison of Intraocular Pressure Measurements by the Ocular Response Analyzer and Goldmann Applanation Tonometer after Penetrating Keratoplasty in Keratoconic Patients Sepehr Feizi, MD 1 Mohammad Pakravan,
Comparison of Intraocular Pressure Measurements by the Ocular Response Analyzer and Goldmann Applanation Tonometer after Penetrating Keratoplasty in Keratoconic Patients Sepehr Feizi, MD 1 Mohammad Pakravan,
Comparison of a New Non-Contact Tonometer with Goldmann Applanation
 Eye (1989) 3, 332-337 Comparison of a New Non-Contact Tonometer with Goldmann Applanation M. J. MOSELEY, N. M. EVANS and A. R. FIELDER Leicester Summary A comparison of a new non-contact tonometer (Keeler
Eye (1989) 3, 332-337 Comparison of a New Non-Contact Tonometer with Goldmann Applanation M. J. MOSELEY, N. M. EVANS and A. R. FIELDER Leicester Summary A comparison of a new non-contact tonometer (Keeler
1 Birmingham and Midland Eye Centre, City Hospital, Birmingham, 2 Ophthalmic Research Group, Life and Health Sciences, Aston
 Accuracy of Goldmann, Ocular Response Analyser, Pascal and TonoPen XL Tonometry in Keratoconic and Normal Eyes Susan P Mollan MB CHB MRCOphth 1, James S Wolffsohn BSc PhD PgDip MCOptom 2, Maged Nessim
Accuracy of Goldmann, Ocular Response Analyser, Pascal and TonoPen XL Tonometry in Keratoconic and Normal Eyes Susan P Mollan MB CHB MRCOphth 1, James S Wolffsohn BSc PhD PgDip MCOptom 2, Maged Nessim
1/31/2018. Course Objectives. Diagnostic Testing. Optic Nerve Damage ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY TECHNICIAN: -SDP
 ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY KNOW THE DISEASE PROCESS TECHNICIAN: EXPLAIN PROCESS OF EXAMINATION Presenters: Dana McMahan, COA Nicole Smith, COA Engage with patient s, help alleviate
ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY KNOW THE DISEASE PROCESS TECHNICIAN: EXPLAIN PROCESS OF EXAMINATION Presenters: Dana McMahan, COA Nicole Smith, COA Engage with patient s, help alleviate
Evaluation of the Effect of Diabetes Mellitus on Corneal Biomechanics
 The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (4), Page 782-788 Abd Elmagid Mohamed Tag Eldin, Abdulmoez Haddad Ahmed, Amr Khalil Abdelmonem* Ophthalmology department, Faculty of Medicine,
The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (4), Page 782-788 Abd Elmagid Mohamed Tag Eldin, Abdulmoez Haddad Ahmed, Amr Khalil Abdelmonem* Ophthalmology department, Faculty of Medicine,
Closed Angle Glaucoma Or Narrow Angle Glaucoma. What s is a closed angle type of glaucoma,
 Closed Angle Glaucoma Or Narrow Angle Glaucoma What s is a closed angle type of glaucoma, This is where the iris is found to be blocking the drainage of the eye through the trabecular meshwork. The eye
Closed Angle Glaucoma Or Narrow Angle Glaucoma What s is a closed angle type of glaucoma, This is where the iris is found to be blocking the drainage of the eye through the trabecular meshwork. The eye
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Approach to Childhood Glaucoma. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Approach to Childhood Glaucoma. These podcasts are designed to give medical students an overview of key topics in pediatrics.
Non-contact Tonometry Synchronized with Cardiac Rhythm
 Non-contact Tonometry Synchronized with Cardiac Rhythm and its Relationship with Blood Pressure Queirós A 1, González-Méijome JM 1, Fernandes P 1, Jorge J 1, Almeida J B 1, Parafita MA 2 1 Department of
Non-contact Tonometry Synchronized with Cardiac Rhythm and its Relationship with Blood Pressure Queirós A 1, González-Méijome JM 1, Fernandes P 1, Jorge J 1, Almeida J B 1, Parafita MA 2 1 Department of
CENTRAL CORNEAL THICKNESS STUDY CCTS
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 CENTRAL CORNEAL THICKNESS STUDY CCTS A Prospective Study of Central Corneal Thickness in Children Less than 18 Years Old PROTOCOL Version 1.0 April 4,
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 CENTRAL CORNEAL THICKNESS STUDY CCTS A Prospective Study of Central Corneal Thickness in Children Less than 18 Years Old PROTOCOL Version 1.0 April 4,
PRESCRIBING IN GLAUCOMA: GUIDELINES FOR NZ OPTOMETRISTS
 PRESCRIBING IN GLAUCOMA: GUIDELINES FOR NZ OPTOMETRISTS Introduction Independent prescribing relates to the capacity to use clinical judgement in respect of diagnosis and treatment. It does not mean working
PRESCRIBING IN GLAUCOMA: GUIDELINES FOR NZ OPTOMETRISTS Introduction Independent prescribing relates to the capacity to use clinical judgement in respect of diagnosis and treatment. It does not mean working
Jose M. Martinez-de-la-Casa, Julian Garcia-Feijoo, Ana Fernandez-Vidal, Carmen Mendez-Hernandez, and Julian Garcia-Sanchez METHODS
 Ocular Response Analyzer versus Goldmann Applanation Tonometry for Intraocular Pressure Measurements Jose M. Martinez-de-la-Casa, Julian Garcia-Feijoo, Ana Fernandez-Vidal, Carmen Mendez-Hernandez, and
Ocular Response Analyzer versus Goldmann Applanation Tonometry for Intraocular Pressure Measurements Jose M. Martinez-de-la-Casa, Julian Garcia-Feijoo, Ana Fernandez-Vidal, Carmen Mendez-Hernandez, and
Accuracy and Repeatability of a New Portable Ultrasound Pachymeter
 Accuracy and Repeatability of a New Portable Ultrasound Pachymeter Queirós A 1, González-Méijome JM 1, Fernandes P 1, Jorge J 1, Almeida J B 1, Parafita MA 2 1 Department of Physics (Optometry), School
Accuracy and Repeatability of a New Portable Ultrasound Pachymeter Queirós A 1, González-Méijome JM 1, Fernandes P 1, Jorge J 1, Almeida J B 1, Parafita MA 2 1 Department of Physics (Optometry), School
CLINICAL SCIENCES. Effect of Central Corneal Thickness, Corneal Curvature, and Axial Length on Applanation Tonometry
 CLINICAL SCIENCES Effect of Central Corneal Thickness, Corneal Curvature, and Axial Length on Applanation Tonometry Markus Kohlhaas, MD; Andreas G. Boehm, MD; Eberhard Spoerl, PhD; Antje Pürsten, Dipl-Ing
CLINICAL SCIENCES Effect of Central Corneal Thickness, Corneal Curvature, and Axial Length on Applanation Tonometry Markus Kohlhaas, MD; Andreas G. Boehm, MD; Eberhard Spoerl, PhD; Antje Pürsten, Dipl-Ing
Glaucoma: Diagnostic Modalities
 Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
The Common Clinical Competency Framework for Non-medical Ophthalmic Healthcare Professionals in Secondary Care
 The Common Clinical Competency Framework for Non-medical Ophthalmic Healthcare Professionals in Secondary Care Glaucoma November 2016 Association of Health Professions in Ophthalmology General basic competences
The Common Clinical Competency Framework for Non-medical Ophthalmic Healthcare Professionals in Secondary Care Glaucoma November 2016 Association of Health Professions in Ophthalmology General basic competences
Correspondence should be addressed to Fusako Fujimura;
 BioMed Research International Volume 2013, Article ID 370592, 5 pages http://dx.doi.org/10.1155/2013/370592 Research Article Repeatability and Reproducibility of Measurements Using a NT-530P Noncontact
BioMed Research International Volume 2013, Article ID 370592, 5 pages http://dx.doi.org/10.1155/2013/370592 Research Article Repeatability and Reproducibility of Measurements Using a NT-530P Noncontact
Glaucoma. Glaucoma. Optic Disc Cupping
 Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
Glaucoma Intraocular Pressure What Will I Notice?
 Glaucoma Glaucoma is the name given to a group of eye conditions in which the optic nerve at the back of the eye is slowly damaged. The diagnosis of glaucoma is made when your optometrist or ophthalmologist
Glaucoma Glaucoma is the name given to a group of eye conditions in which the optic nerve at the back of the eye is slowly damaged. The diagnosis of glaucoma is made when your optometrist or ophthalmologist
True IOP No Doubt Facts and Figures Figures. Ziemer Ophthalmic Systems AG a Ziemer Group Company Allmendstrasse 11 CH-2562 Port, Switzerland
 True IOP No Doubt Facts and Figures Figures and Facts Ziemer Ophthalmic Systems AG a Ziemer Group Company Allmendstrasse 11 CH-2562 Port, Switzerland There is increasing evidence that DCT measures IOP
True IOP No Doubt Facts and Figures Figures and Facts Ziemer Ophthalmic Systems AG a Ziemer Group Company Allmendstrasse 11 CH-2562 Port, Switzerland There is increasing evidence that DCT measures IOP
Comparison of Central Corneal Thickness Measurements with Pentacam, Orbscan II, and Ultrasound Pachymeter
 Comparison of Central Corneal Thickness Measurements with Pentacam, Orbscan II, and Ultrasound Pachymeter Abbas-Ali Yekta, PhD 1 Hassan Hashemi, MD 2,3 Mehdi KhabazKhoob, MSc 3 Asghar Dostdar, MSc 4 Shiva
Comparison of Central Corneal Thickness Measurements with Pentacam, Orbscan II, and Ultrasound Pachymeter Abbas-Ali Yekta, PhD 1 Hassan Hashemi, MD 2,3 Mehdi KhabazKhoob, MSc 3 Asghar Dostdar, MSc 4 Shiva
Comparison of IOP measurement by ocular response analyzer, dynamic contour, Goldmann applanation, and noncontact tonometry
 European Journal of Ophthalmology / Vol. 19 no. 6, 2009 / pp. 936-941 Comparison of IOP measurement by ocular response analyzer, dynamic contour, Goldmann applanation, and noncontact tonometry BANU ONCEL,
European Journal of Ophthalmology / Vol. 19 no. 6, 2009 / pp. 936-941 Comparison of IOP measurement by ocular response analyzer, dynamic contour, Goldmann applanation, and noncontact tonometry BANU ONCEL,
Dina H. Erickson, O.D., a Denise Goodwin, O.D., a Michael Rollins, O.D., b Amber Belaustegui, O.D., c and Chad Anderson a
 Optometry (2009) 80, 169-174 Comparison of dynamic contour tonometry and Goldmann applanation tonometry and their relationship to corneal properties, refractive error, and ocular pulse amplitude Dina H.
Optometry (2009) 80, 169-174 Comparison of dynamic contour tonometry and Goldmann applanation tonometry and their relationship to corneal properties, refractive error, and ocular pulse amplitude Dina H.
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Seung Pil Bang, Chong Eun Lee and Yu Cheol Kim *
 Bang et al. BMC Ophthalmology (2017) 17:199 DOI 10.1186/s12886-017-0593-1 RESEARCH ARTICLE Open Access Comparison of intraocular pressure as measured by three different non-contact tonometers and goldmann
Bang et al. BMC Ophthalmology (2017) 17:199 DOI 10.1186/s12886-017-0593-1 RESEARCH ARTICLE Open Access Comparison of intraocular pressure as measured by three different non-contact tonometers and goldmann
The effect of corneal thickness on intraocular pressure measurement in patients with corneal pathology
 1395 SCIENTIFIC REPORT The effect of corneal thickness on intraocular pressure measurement in patients with corneal pathology A C Browning, A Bhan, A P Rotchford, S Shah, H S Dua... Background/aim: To
1395 SCIENTIFIC REPORT The effect of corneal thickness on intraocular pressure measurement in patients with corneal pathology A C Browning, A Bhan, A P Rotchford, S Shah, H S Dua... Background/aim: To
Deep anterior lamellar keratoplasty (DALK) is considered
 Cornea Comparison of the Ocular Response Analyzer and the Goldmann Applanation Tonometer for Measuring Intraocular Pressure after Deep Anterior Lamellar Keratoplasty Sepehr Feizi, 1,2 Ali Hashemloo, 1,2
Cornea Comparison of the Ocular Response Analyzer and the Goldmann Applanation Tonometer for Measuring Intraocular Pressure after Deep Anterior Lamellar Keratoplasty Sepehr Feizi, 1,2 Ali Hashemloo, 1,2
Reproducibility and Clinical Relevance of the Ocular Response Analyzer in Nonoperated Eyes: Corneal Biomechanical and Tonometric Implications
 Reproducibility and Clinical Relevance of the Ocular Response Analyzer in Nonoperated Eyes: Corneal Biomechanical and Tonometric Implications Javier Moreno-Montañés, 1 Miguel J. Maldonado, 1 Noelia García,
Reproducibility and Clinical Relevance of the Ocular Response Analyzer in Nonoperated Eyes: Corneal Biomechanical and Tonometric Implications Javier Moreno-Montañés, 1 Miguel J. Maldonado, 1 Noelia García,
Self-monitoring of disease has long been of proven value. For
 Pressure Phosphene Self-Tonometry: A Comparison with Goldmann Tonometry in Glaucoma Patients Dennis S. C. Lam, 1 Dexter Y. L. Leung, 1 Thomas Y. H. Chiu, 1 Dorothy S. P. Fan, 1 Eva Y. Y. Cheung, 1 Tien-Yin
Pressure Phosphene Self-Tonometry: A Comparison with Goldmann Tonometry in Glaucoma Patients Dennis S. C. Lam, 1 Dexter Y. L. Leung, 1 Thomas Y. H. Chiu, 1 Dorothy S. P. Fan, 1 Eva Y. Y. Cheung, 1 Tien-Yin
Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective cohort study
 Nesaratnam et al. BMC Ophthalmology (2015) 15:17 DOI 10.1186/s12886-015-0007-1 RESEARCH ARTICLE Open Access Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective
Nesaratnam et al. BMC Ophthalmology (2015) 15:17 DOI 10.1186/s12886-015-0007-1 RESEARCH ARTICLE Open Access Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective
LOCSU/WOPEC Courses to support the development of local enhanced eye care services. Excellence in Education for Eye Care Professionals
 LOCSU/WOPEC Courses to support the development of local enhanced eye care services Excellence in Education for Eye Care Professionals LOCSU/WOPEC training courses are designed to support the delivery of
LOCSU/WOPEC Courses to support the development of local enhanced eye care services Excellence in Education for Eye Care Professionals LOCSU/WOPEC training courses are designed to support the delivery of
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
Make a more confident glaucoma risk assessment with Corneal Hysteresis, a superior predictor of glaucoma progression.
 Make a more confident glaucoma risk assessment with Corneal Hysteresis, a superior predictor of glaucoma progression. Advancing Eye Care. American Innovation. Reichert Ocular Response Analyzer G3. Make
Make a more confident glaucoma risk assessment with Corneal Hysteresis, a superior predictor of glaucoma progression. Advancing Eye Care. American Innovation. Reichert Ocular Response Analyzer G3. Make
Analysis of differences in intraocular pressure evaluation performed with contact and non-contact devices
 Lanza et al. BMC Ophthalmology (2018) 18:233 https://doi.org/10.1186/s12886-018-0900-5 RESEARCH ARTICLE Open Access Analysis of differences in intraocular pressure evaluation performed with contact and
Lanza et al. BMC Ophthalmology (2018) 18:233 https://doi.org/10.1186/s12886-018-0900-5 RESEARCH ARTICLE Open Access Analysis of differences in intraocular pressure evaluation performed with contact and
THE CHRONIC GLAUCOMAS
 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
Glaucoma Care Pathway
 PRIMARY CARE OPTOMETRY UPDATE Glaucoma Care Pathway March 2018 Colleagues, In June 2017 the Health and Social Care Board provided you with the second Glaucoma Care Pathway Primary Care Optometry Update,
PRIMARY CARE OPTOMETRY UPDATE Glaucoma Care Pathway March 2018 Colleagues, In June 2017 the Health and Social Care Board provided you with the second Glaucoma Care Pathway Primary Care Optometry Update,
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND PACHYMETRY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
For peer review only. BMJ Open. For peer review only - Journal: BMJ Open
 The effectiveness of schemes that refine referrals between primary and secondary care - the United Kingdom experience with glaucoma referrals: The Health Innovation & Education Cluster (HIEC) Glaucoma
The effectiveness of schemes that refine referrals between primary and secondary care - the United Kingdom experience with glaucoma referrals: The Health Innovation & Education Cluster (HIEC) Glaucoma
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier
 Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name OMIM number for disease 231300 Disease alternative names Please provide any alternative
Proposal form for the evaluation of a genetic test for NHS Service Gene Dossier Test Disease Population Triad Disease name OMIM number for disease 231300 Disease alternative names Please provide any alternative
Primary Angle Closure Glaucoma
 www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
www.eyesurgeonlondon.co.uk Primary Angle Closure Glaucoma What is Glaucoma? Glaucoma is a condition in which there is damage to the optic nerve. This nerve carries visual signals from the eye to the brain.
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma
 Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
England. Suspect OHT/Glaucoma. Repeat Readings Service Common Pathway
 England Suspect OHT/Glaucoma Repeat Readings Service Common Pathway Greater Manchester Local Eye Health Network April 2015 Contents Page Executive Summary... 3 Background... 5 NICE Guidance and Quality
England Suspect OHT/Glaucoma Repeat Readings Service Common Pathway Greater Manchester Local Eye Health Network April 2015 Contents Page Executive Summary... 3 Background... 5 NICE Guidance and Quality
Role of central corneal thickness measurement in management of open angle glaucoma and glaucoma suspects in Calabar, Nigeria
 Original Research Article Role of central corneal thickness measurement in management of open angle glaucoma and glaucoma suspects in Calabar, Nigeria Nkanga DG 1,2, Ibanga AA 1,2, Nkanga ED 2, Etim BA
Original Research Article Role of central corneal thickness measurement in management of open angle glaucoma and glaucoma suspects in Calabar, Nigeria Nkanga DG 1,2, Ibanga AA 1,2, Nkanga ED 2, Etim BA
Use of the Arden grating test for screening
 British Journal of Ophthalmology, 19, 64, 591-596 Use of the rden grating test for screening ROBERT G. WETHERHED From Moorfields Eye Hospital, City Road, London EC] V PD SUMMRY One hundred and forty patients
British Journal of Ophthalmology, 19, 64, 591-596 Use of the rden grating test for screening ROBERT G. WETHERHED From Moorfields Eye Hospital, City Road, London EC] V PD SUMMRY One hundred and forty patients
Immersion Vs Contact Biometery for Axial Length Measurement before Phacoemulsification
 Original Article Immersion Vs Contact Biometery for Axial Length Measurement before Phacoemulsification with Foldable IOL Irum Abbas, Atif Mansoor Ahmad, Tahir Mahmood Pak J Ophthalmol 2009, Vol. 25 No.
Original Article Immersion Vs Contact Biometery for Axial Length Measurement before Phacoemulsification with Foldable IOL Irum Abbas, Atif Mansoor Ahmad, Tahir Mahmood Pak J Ophthalmol 2009, Vol. 25 No.
glaucoma and ocular hypertension
 British Journal of Ophthalmology, 1980, 64, 852-857 Colour vision in patients with chronic simple glaucoma and ocular hypertension D. POINOOSAWMY, S. NAGASUBRAMANIAN, AND J. GLOSTER From the Glaucoma Unit,
British Journal of Ophthalmology, 1980, 64, 852-857 Colour vision in patients with chronic simple glaucoma and ocular hypertension D. POINOOSAWMY, S. NAGASUBRAMANIAN, AND J. GLOSTER From the Glaucoma Unit,
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Pachymetry Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Pachymetry Professional Institutional Original Effective Date: March 11, 2004 Original Effective
Pachymetry Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Pachymetry Professional Institutional Original Effective Date: March 11, 2004 Original Effective
EFFECTS OF PREDNISOLONE EYE DROPS*t
 Brit. J. Ophthal. (1967) 51, 398 EFFECTS OF PREDNISOLONE EYE DROPS*t A TRIAL OF THE EFFECTS OF PREDNISOLONE PHOSPHATE EYE DROPS ON THE INTRA-OCULAR PRESSURE OF NORMAL VOLUNTEERS BY T. G. RAMSELL, W. TRILLWOOD,
Brit. J. Ophthal. (1967) 51, 398 EFFECTS OF PREDNISOLONE EYE DROPS*t A TRIAL OF THE EFFECTS OF PREDNISOLONE PHOSPHATE EYE DROPS ON THE INTRA-OCULAR PRESSURE OF NORMAL VOLUNTEERS BY T. G. RAMSELL, W. TRILLWOOD,
Correlating central corneal thickness and intraocular pressure in ocular hypertension and glaucoma
 VOL. 3 NO. 1 PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE JUNE 07 Jonathan G. Soriano, MD 1 Ma. Margarita L. Lat-Luna, MD 1, 3 Patricia M. Khu, MD 1, 1 Department of Ophthalmology and Visual
VOL. 3 NO. 1 PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE JUNE 07 Jonathan G. Soriano, MD 1 Ma. Margarita L. Lat-Luna, MD 1, 3 Patricia M. Khu, MD 1, 1 Department of Ophthalmology and Visual
This is the author s version of a work that was submitted/accepted for publication in the following source:
 This is the author s version of a work that was submitted/accepted for publication in the following source: Zeri, Fabrizio, De Cusatis, Mario, lupelli, luigi, & Swann, Peter G. (2016) The measurement of
This is the author s version of a work that was submitted/accepted for publication in the following source: Zeri, Fabrizio, De Cusatis, Mario, lupelli, luigi, & Swann, Peter G. (2016) The measurement of
The role of education in the promotion of red reflex assessments
 RESEARCH The role of education in the promotion of red reflex assessments WJ Muen 1,2 M Hindocha 1 MA Reddy 1,2 1 Department of Ophthalmology, Barts and the London NHS Trust, Whitechapel Road, London E1
RESEARCH The role of education in the promotion of red reflex assessments WJ Muen 1,2 M Hindocha 1 MA Reddy 1,2 1 Department of Ophthalmology, Barts and the London NHS Trust, Whitechapel Road, London E1
Medical Management of Glaucoma
 Medical Management of Glaucoma Medical Management of Glaucoma Keith Barton Consultant Ophthalmologist Moorfields Eye Hospital Foundation Trust Honorary Reader Department of Epidemiology and Genetics Institute
Medical Management of Glaucoma Medical Management of Glaucoma Keith Barton Consultant Ophthalmologist Moorfields Eye Hospital Foundation Trust Honorary Reader Department of Epidemiology and Genetics Institute
Policy #: 354 Latest Review Date: July 2011
 Name of Policy: Corneal Hysteresis Policy #: 354 Latest Review Date: July 2011 Category: Medicine Policy Grade: Active Policy but no longer scheduled for regular literature reviews and updates. Background/Definitions:
Name of Policy: Corneal Hysteresis Policy #: 354 Latest Review Date: July 2011 Category: Medicine Policy Grade: Active Policy but no longer scheduled for regular literature reviews and updates. Background/Definitions:
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE. Glaucoma: diagnosis and management of chronic open angle glaucoma and ocular hypertension
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Glaucoma: diagnosis and management of chronic open angle glaucoma and ocular hypertension 1.1 Short title Glaucoma 2 Background
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Glaucoma: diagnosis and management of chronic open angle glaucoma and ocular hypertension 1.1 Short title Glaucoma 2 Background
INTRODUCTION J. DAWCZYNSKI, E. KOENIGSDOERFFER, R. AUGSTEN, J. STROBEL. Department of Ophthalmology, University Hospital Jena, Jena - Germany
 European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
Enhanced Scheme Evaluation Project (ESEP) Robert Harper On behalf of the ESEP team
 Enhanced Scheme Evaluation Project (ESEP) Robert Harper On behalf of the ESEP team ESEP Team Project Leads: Robert Harper and John Lawrenson Co-applicants: David Edgar, Cecilia Fenerty, David Henson, Ian
Enhanced Scheme Evaluation Project (ESEP) Robert Harper On behalf of the ESEP team ESEP Team Project Leads: Robert Harper and John Lawrenson Co-applicants: David Edgar, Cecilia Fenerty, David Henson, Ian
The Causes of Distress in Paediatric Outpatients Receiving Dilating Drops *
 Open Journal of Ophthalmology, 2012, 2, 21-25 http://dx.doi.org/10.4236/ojoph.2012.22005 Published Online May 2012 (http://www.scirp.org/journal/ojoph) 21 The Causes of Distress in Paediatric Outpatients
Open Journal of Ophthalmology, 2012, 2, 21-25 http://dx.doi.org/10.4236/ojoph.2012.22005 Published Online May 2012 (http://www.scirp.org/journal/ojoph) 21 The Causes of Distress in Paediatric Outpatients
CLASS-y Laser Treats Glaucoma
 Article # 404 Comments About the Author Released: Author: Category: March 12th, 2014 Issue #0314 Ehud Assia Feature S S S S S CLASS-y Laser Treats Glaucoma Transforming complex, invasive and risky glaucoma
Article # 404 Comments About the Author Released: Author: Category: March 12th, 2014 Issue #0314 Ehud Assia Feature S S S S S CLASS-y Laser Treats Glaucoma Transforming complex, invasive and risky glaucoma
Commissioning Guide: Glaucoma (Long Version)
 Draft for Consultation Commissioning Guide: Glaucoma (Long Version) March 2015 Contents Section page 1. ABBREVIATIONS 4 2. Introduction: Glaucoma 5 3. Commissioning Guidance for Glaucoma 7 4. HIGH VALUE
Draft for Consultation Commissioning Guide: Glaucoma (Long Version) March 2015 Contents Section page 1. ABBREVIATIONS 4 2. Introduction: Glaucoma 5 3. Commissioning Guidance for Glaucoma 7 4. HIGH VALUE
BMJ Open. For peer review only -
 Initial Experience Using A Femtosecond Laser Cataract Surgery System At A UK National Health Service Cataract Surgery Day Care Centre. Journal: BMJ Open Manuscript ID bmjopen--0 Article Type: Research
Initial Experience Using A Femtosecond Laser Cataract Surgery System At A UK National Health Service Cataract Surgery Day Care Centre. Journal: BMJ Open Manuscript ID bmjopen--0 Article Type: Research
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study
 Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
INTRODUCTION MIKLOS SCHNEIDER 1, GABOR BORGULYA 2, ANDRAS SERES 1, ZOLTAN Z. NAGY 1, JANOS NEMETH 1
 European Journal of Ophthalmology / Vol. 19 no. 2, 2009 / pp. 180-187 Central corneal thickness measurements with optical coherence tomography and ultrasound pachymetry in healthy subjects and in patients
European Journal of Ophthalmology / Vol. 19 no. 2, 2009 / pp. 180-187 Central corneal thickness measurements with optical coherence tomography and ultrasound pachymetry in healthy subjects and in patients
Retinal Nerve Fiber Analysis: the Role It Plays in Assessing Glaucoma Grace Martin, CPOT
 Retinal Nerve Fiber Analysis: the Role It Plays in Assessing Glaucoma Grace Martin, CPOT Every day, patients experiencing visual difficulties are seen in the optometric practice. This can range from a
Retinal Nerve Fiber Analysis: the Role It Plays in Assessing Glaucoma Grace Martin, CPOT Every day, patients experiencing visual difficulties are seen in the optometric practice. This can range from a
THE CHRONIC GLAUCOMAS
 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
Community Eye Care Pathway Developments in South Staffs (or: How we Bridge the North/South Divide )
 Community Eye Care Pathway Developments in South Staffs (or: How we Bridge the North/South Divide ) Mark McCracken Joint Vice Chair (South) Staffordshire LOC Staffordshire Community Eye Care Pathways North
Community Eye Care Pathway Developments in South Staffs (or: How we Bridge the North/South Divide ) Mark McCracken Joint Vice Chair (South) Staffordshire LOC Staffordshire Community Eye Care Pathways North
CLINICAL SCIENCES. Clinical Significance of Central Corneal Thickness in the Management of Glaucoma
 CLINICAL SCIENCES Clinical Significance of Central Corneal Thickness in the Management of Glaucoma Carolyn Y. Shih, MD; Joshua S. Graff Zivin, PhD; Stephen L. Trokel, MD; James C. Tsai, MD Objective: To
CLINICAL SCIENCES Clinical Significance of Central Corneal Thickness in the Management of Glaucoma Carolyn Y. Shih, MD; Joshua S. Graff Zivin, PhD; Stephen L. Trokel, MD; James C. Tsai, MD Objective: To
Glaucoma: diagnosis and management (large print version)
 Glaucoma: diagnosis and management (large print version) 1 November 2017 Recommendations People have the right to be involved in discussions and make informed decisions about their care, as described in
Glaucoma: diagnosis and management (large print version) 1 November 2017 Recommendations People have the right to be involved in discussions and make informed decisions about their care, as described in
Comparison of intraocular pressure measurement with Schiotz tonometer and Tono-Pen Vet tonometer in healthy dogs
 J Vet Res 62, 243-247, 2018 DOI:10.2478/jvetres-2018-0018 Comparison of intraocular pressure measurement with Schiotz and Tono-Pen Vet in healthy dogs Karolina Wrześniewska, Jacek Madany, Dagmara Winiarczyk
J Vet Res 62, 243-247, 2018 DOI:10.2478/jvetres-2018-0018 Comparison of intraocular pressure measurement with Schiotz and Tono-Pen Vet in healthy dogs Karolina Wrześniewska, Jacek Madany, Dagmara Winiarczyk
Glaucoma is the most frequent
 Refined glaucoma referral practice offers prospect of improved capacity and expanded role for primary eye care professionals BY ROD MCNEIL Glaucoma is the most frequent cause of irreversible blindness
Refined glaucoma referral practice offers prospect of improved capacity and expanded role for primary eye care professionals BY ROD MCNEIL Glaucoma is the most frequent cause of irreversible blindness
Moorfields Research and Innovation. Participating in research at Moorfields Eye Hospital NHS Foundation Trust. hope trust care
 Moorfields Research and Innovation Participating in research at Moorfields Eye Hospital NHS Foundation Trust hope trust care take part At Moorfields, we conduct clinical studies (including trials) with
Moorfields Research and Innovation Participating in research at Moorfields Eye Hospital NHS Foundation Trust hope trust care take part At Moorfields, we conduct clinical studies (including trials) with
Intraocular pressure (IOP) is the main risk factor for the
 The Circadian Curve of Intraocular Pressure: Can We Estimate Its Characteristics during Office Hours? Paolo Fogagnolo, 1 Nicola Orzalesi, 2 Antonio Ferreras, 3,4 and Luca Rossetti 2 PURPOSE. To verify
The Circadian Curve of Intraocular Pressure: Can We Estimate Its Characteristics during Office Hours? Paolo Fogagnolo, 1 Nicola Orzalesi, 2 Antonio Ferreras, 3,4 and Luca Rossetti 2 PURPOSE. To verify
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Noel de Jesus Atienza, MD, MSc and Joseph Anthony Tumbocon, MD
 Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Sonographic measurement of the epiglottis in normal Chinese adults
 Hong Kong Journal of Emergency Medicine Sonographic measurement of the epiglottis in normal Chinese adults CW Chau, HH Chan, CP Wong, TW Wong, CC Lau Objectives: (1) To assess the normal range of thickness
Hong Kong Journal of Emergency Medicine Sonographic measurement of the epiglottis in normal Chinese adults CW Chau, HH Chan, CP Wong, TW Wong, CC Lau Objectives: (1) To assess the normal range of thickness
LOCSU Community Services
 LOCSU Community Services Pre- and Post-Operative Cataract Community Service Pathway Issued by Local Optical Committee Support Unit December 2008 [Revised 14 March 2016, Version 3.2] Contents Page Outline
LOCSU Community Services Pre- and Post-Operative Cataract Community Service Pathway Issued by Local Optical Committee Support Unit December 2008 [Revised 14 March 2016, Version 3.2] Contents Page Outline
Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India
 Original article: Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India 1Dr. Apala Bhattacharya, 2 Dr Gautam Bhaduri,
Original article: Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India 1Dr. Apala Bhattacharya, 2 Dr Gautam Bhaduri,
Comparative study of new imaging technologies for the diagnosis of glaucoma: Protocol Approved by the Ethics Committee
 Comparative study of new imaging technologies for the diagnosis of glaucoma: Protocol Approved by the Ethics Committee HTA 09/22/111. Applicants: Augusto Azuara-Blanco (CI), Jennifer Burr,, Rodolfo Hernández,
Comparative study of new imaging technologies for the diagnosis of glaucoma: Protocol Approved by the Ethics Committee HTA 09/22/111. Applicants: Augusto Azuara-Blanco (CI), Jennifer Burr,, Rodolfo Hernández,
Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors
 CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
Structural changes of the anterior chamber following cataract surgery during infancy
 Structural changes of the anterior chamber following cataract surgery during infancy Matthew Nguyen, Emory University Marla Shainberg, Emory University Allen Beck, Emory University Scott Lambert, Emory
Structural changes of the anterior chamber following cataract surgery during infancy Matthew Nguyen, Emory University Marla Shainberg, Emory University Allen Beck, Emory University Scott Lambert, Emory
Tonometer validation and intraocular pressure reference values in the normal chinchilla (Chinchilla lanigera)
 Veterinary Ophthalmology (2018) 21, 1, 4 9 DOI:10.1111/vop.12468 Tonometer validation and intraocular pressure reference values in the normal chinchilla (Chinchilla lanigera) Kevin C. Snyder,*, Andrew
Veterinary Ophthalmology (2018) 21, 1, 4 9 DOI:10.1111/vop.12468 Tonometer validation and intraocular pressure reference values in the normal chinchilla (Chinchilla lanigera) Kevin C. Snyder,*, Andrew
