CLINICAL SCIENCES. Clinical Significance of Central Corneal Thickness in the Management of Glaucoma
|
|
|
- Ellen Pitts
- 5 years ago
- Views:
Transcription
1 CLINICAL SCIENCES Clinical Significance of Central Corneal Thickness in the Management of Glaucoma Carolyn Y. Shih, MD; Joshua S. Graff Zivin, PhD; Stephen L. Trokel, MD; James C. Tsai, MD Objective: To evaluate the effect of central corneal thickness determination on the clinical management of patients with glaucoma and glaucoma suspect. Methods: A cross-sectional retrospective study was performed on 188 consecutive patients. Mean ultrasound pachymetry measurements of central corneal thickness and corresponding Goldmann applanation tonometry measurements were obtained. Intraocular pressures (IOPs) were corrected using linear and mathematical (Orssengo- Pye) algorithms. Measurement-significant outcomes were defined as an IOP adjustment of 1.5 mm Hg or greater and outcomes-significant results as an IOP adjustment of 3.0 mm Hg or greater. Changes in therapy such as the use of eyedrops and addition or cancellation of laser therapy or surgery were then noted for those individuals with measurement- or outcomes-significant changes. Results: Using the linear correction scale, 105 (55.9%) of 188 patients had at least a measurement-significant adjustment in their IOP measurements: 67 (35.6%) had adjustments between 1.5 and 3.0 mm Hg, while 38 (20.2%) had an outcomes-significant IOP adjustment ( 3.0 mm Hg). Among the 188 patients, 16 (8.5%) had a change in eyedrop therapy, 4 (2.1%) had a change regarding laser therapy, and 6 (3.2%) had a change in the decision regarding glaucoma surgery. Using the exponential correction (Orssengo-Pye) scale, similar percentages were obtained. Conclusion: Pachymetry-measured central corneal thickness has a significant effect on the clinical management of patients with glaucoma and glaucoma suspect. Arch Ophthalmol. 2004;122: From the Edward S. Harkness Eye Institute, Department of Ophthalmology, College of Physicians and Surgeons (Drs Shih, Trokel, and Tsai), and Department of Health Policy and Management, Mailman School of Public Health (Dr Graff Zivin), Columbia University, New York, NY. The authors have no relevant financial interest in this article. OVER THE PAST 50 YEARS, central corneal thickness (CCT) measurement has been an important variable in the assessment of intraocular pressure (IOP) values in patients undergoing refractive and corneal transplant surgery, as well as in contact lens wearers. 1 Studies by Ehlers and Hansen 2 and Whitacre et al 3 stressed that IOP measurements should be adjusted for CCT. However, the incorporation of CCT-adjusted IOP measurements into daily clinical practice was limited until recently, when the Ocular Hypertension Treatment Study 4 reported that CCT was a strong predictor for the development of primary open-angle glaucoma in patients with ocular hypertension. In particular, this study demonstrated that subjects with decreased CCT measurements had an increased risk of developing primary open-angle glaucoma (for every 40-µm decrease in CCT, the relative risk was 1.71). Moreover, individuals with CCTs of 555 µm or less had a3times greater risk of developing glaucoma compared with patients with CCTs of greater than 588 µm. Moreover, with millions of individuals having undergone laser in situ keratomileusis surgery, 5,6 there is a growing concern that the process of removing corneal tissue during this surgery (with resulting thinner corneas) will lead to an increased difficulty in diagnosing glaucoma, because this surgery tends to alter IOP measurements and may in turn require greater emphasis on the assessment of the optic disc and visual fields for the diagnosis and treatment of glaucoma. 7,8 CME course available at As summarized in a meta-analysis by Doughty and Zaman 1 on the effect of CCT on IOP measurements, studies 9,10 have hypothesized that CCT and IOP are related to or interdependent on one another, except at gross extremes. Furthermore, variations in mean CCT have been observed in patients with different types of glaucoma Altogether, these studies suggest that IOP measurements are affected 1270
2 by CCT values. In fact, misdiagnosis often occurs when CCT is not considered, because generally patients with normal-tension glaucoma have thinner corneas and those with glaucoma suspect have thicker corneas. 11 According to manometric data from Ehlers and colleagues, 14 44% of patients with normal-tension glaucoma would be reclassified as having primary open-angle glaucoma, and 35% of patients with ocular hypertension would be reclassified as having normal IOPs. Furthermore, Herndon et al 15 found that as many as 65% of patients with ocular hypertension could be reclassified as having normal IOPs. Believing corneal pachymetry to be essential to the care of patients, Tanaka stated that... performing pachymetry may influence the management of all patients by allowing clinicians to (1) observe or pursue less aggressive treatment of patients with pseudo-ocular hypertension; (2) modify the target intraocular pressure in patients with glaucoma; and (3) detect an elevated intraocular pressure in otherwise normal patients with thin corneas and normal applanation readings. 16(p544) There is growing consensus that routine measurement of CCT may be critical for the proper management of patients with glaucoma and glaucoma suspect not only for cost reasons, but most important, for effective quality care. Therefore, we hypothesized that CCT has a significant effect on the clinical management of patients with the diagnoses of glaucoma and glaucoma suspect. To evaluate the effect of incorporating CCT measurements into daily clinical practice, we performed a cross-sectional retrospective study of consecutive patients seen for glaucoma care. METHODS A cross-sectional retrospective study was performed on 188 consecutive patients seen at an academic medical center glaucoma practice between June 20, 2002, and August 20, Patients with known corneal pathologic conditions (eg, with corneal edema or those who had undergone penetrating keratoplasty) were excluded from the study. However, patients who had undergone refractive surgery were not excluded from the study. Three consecutive ultrasound pachymetry (Sonomed, Inc, Lake Success, NY) measurements of CCT were obtained from each eye, and a mean value was then computed. Measurements were performed under topical anesthesia. The corresponding Goldmann applanation tonometry (GAT) measurements were obtained at each of these visits with the use of fluorescein solution (in most cases, only one measurement was taken). These GAT measurements were performed by one of us (J.C.T.). In most cases, the CCT measurements were performed before applanation tonometry. In all cases, the CCT measurements were done before gonioscopy. Given the small number of patients in the study, variables such as the number and type of glaucoma medications taken by each patient were not considered in subset analysis (eg, to determine whether differences were observed in CCT for patients taking topical carbonic anhydrase inhibitors). Analyses included the mean CCT and GAT values of the right eye of patients. If reliable CCT or GAT values were unobtainable from the right eye, then the corresponding measurements from the left eye were collected. Institutional review board approval was obtained for the retrospective data collection and analysis. The recorded IOP measurements were then adjusted for CCT using 545 µm as the reference value ( in a review 1 of 80 studies using ultrasound pachymetry, the mean±sd CCT was 544±34 µm). The IOP data were corrected using a linear algorithm and a mathematical model. The linear correction scale (based on extensive literature review) added or subtracted 2.5 mm Hg for every 50-µm difference in CCT from the reference value of 545 µm (ie, a 1.0-mm Hg change for every 20-µm difference in CCT from the reference value of 545 µm). A correction factor (CF) of 2.5 mm Hg (for every 50-µm deviation from the reference CCT value) was used, because various CFs in the literature have ranged from approximately 1.00 to 3.57 mm Hg for every 50-µm deviation. In fact, in the study by Ehlers and Hansen, 2 the CF reported was 3.57 mm Hg per 50-µm deviation (ie, about 5 mm Hg for every 70 µm), and the metaanalysis of 134 studies by Doughty and Zaman 1 found that the slope of the regression line created by the data resulted in 3.33 mm Hg per 50-µm deviation. Furthermore, in a cannulation study of 125 patients undergoing phacoemulsification cataract surgery with corresponding manometric water column and Perkins tonometry measurements, Pillunat and colleagues 17 calculated an approximate 2.5-mm Hg change in IOP for every 50-µm difference in corneal thickness. Adjustments of IOP were made according to the following linear formula: Corrected IOP = Measured IOP (CCT 545)/ mm Hg. Sensitivity analyses of the linear model were performed, substituting 2.0 and 3.0 mm Hg as the CFs (for every 50-µm deviation from the reference CCT of 545 µm). To provide a comparison, a mathematical formula derived by Orssengo and Pye 18 was used, because the formula accounts for factors such as the anterior radius of curvature, thickness, and Poisson ratio of the cornea. The formula is as follows: True IOP = Goldmann applanation IOP K, where K is a complex CF dependent on applanted area, radius of curvature of the anterior cornea, center thickness of the cornea, and Poisson s ratio of the cornea. A standard radius of curvature of the anterior cornea (7.74 mm) was used for the purpose of this study as it was not calculated for individual patients. In regard to CCT-adjusted IOP values, measurementsignificant adjustments were defined as IOP corrections of 1.5 mm Hg or greater (in either direction). Although there may be differences in opinion regarding the value of key CFs, our analysis suggests that 1.5 and 3.0 mm Hg are appropriate cutoff values for determining potential outcome effects. Although results of the Early Manifest Glaucoma Trial 19 and the Ocular Hypertension Treatment Study 4 suggest a 10% difference in outcome for each millimeter of mercury, this figure was derived from extrapolated data. As a conservative measure, we opted to set our first cutoff slightly higher at 1.5 mm Hg. The 1.5-mm Hg figure was arrived at because a change as small as 1.0 mm Hg is noted to be measurement significant in clinical trials; the Early Manifest Glaucoma Trial reported that each higher (or lower) millimeter of mercury of IOP on follow-up was associated with an approximate 10% increased (or decreased) risk of progression in patients with early manifest glaucoma. 19(p48) Furthermore, Parrish et al 20 defined a 1.5- mm Hg difference as significant in their randomized clinical trial comparing the IOP-lowering effects of topical prostaglandin analogues. Other authors have defined similar differences in IOP (eg, 1.75 mm Hg) as being significant between study groups. 21 Any CCT-associated IOP adjustments of 3.0 mm Hg or greater (in either direction) were designated as outcomes significant. A 3.0-mm Hg decrease in the initial IOP corresponded to an almost 50% reduction in the risk of glaucoma observed in the population-based Baltimore Eye Survey. 22 Moreover, per findings in the Early Manifest Glaucoma Trial 19 (in which each 1.0-mm Hg reduction in IOP corresponded to a 10% decreased risk of progression of glaucoma), a 3.0-mm Hg reduction in IOP would result in an approximate 30% decreased risk of glaucoma progression. 1271
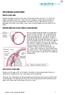
3 Patients, No. Table 1. Demographics of Study Population No. (%) Demographic (N = 188) Age, mean ± SD, y 71.4 ± 13.8 Men 69 (36.7) Women 119 (63.3) Race African American 26 (13.8) White 151 (80.3) Asian 11 (5.9) Right eye 185 (98.4) Left eye 3 (1.6) No. of glaucoma medications used by patient, mean ± SD 1.8 ± 1.4 Central corneal thickness, mean ± SD, µm ± 53.8 Intraocular pressure, mean ± SD, mm Hg 15.8 ± 4.8 Diagnosis Narrow-angle glaucoma 1 (0.5) Traumatic glaucoma 2 (1.1) Pigmentary glaucoma 2 (1.1) Primary angle-closure glaucoma 6 (3.2) Inflammatory glaucoma 4 (2.1) Pseudoexfoliation glaucoma 10 (5.3) Ocular hypertension 11 (5.9) Glaucoma suspect 18 (9.6) Normal-tension glaucoma 21 (11.2) Chronic angle-closure glaucoma 26 (13.8) Primary open-angle glaucoma 87 (46.3) Central Corneal Thickness, µm Distribution of ultrasound pachymetry central corneal thickness among 188 patients in the study population (mean [SD], [53.8]). The medical charts were reviewed, and notations that indicated the effect of CCT evaluation on the treatment plan were evaluated. Alterations in the glaucoma treatment plan were then noted for patients with measurement- and outcomessignificant IOP adjustments (ie, 1.5 and 3.0 mm Hg, respectively). These changes in therapy included (1) addition or discontinuation of antiglaucoma medications, (2) recommendation or deferment of glaucoma laser procedures, or (3) recommendation or deferment of glaucoma incisional surgery. Linear regression calculations were performed to ascertain the effect of variables such as age, race, and sex on adjustments in IOP following CCT measurements. Table 2. Measurement and Clinically Significant Changes Made After Central Corneal Thickness Measurements* Characteristic Measurement-significant changes 1.5 mm Hg Measurement-significant changes 3.0 mm Hg Outcomes-significant changes 3.0 mm Hg Change in glaucoma medical therapy Change in recommendation for glaucoma laser surgery Change in recommendation for glaucoma incisional surgery RESULTS Orssengo-Pye Model Linear Model 119 (63.3) 105 (55.9) 39 (20.7) 67 (35.6) 80 (42.6) 38 (20.2) 19 (10.1) 16 (8.5) 4 (2.1) 4 (2.1) 5 (2.7) 6 (3.2) *Data are expressed as number (percentage) among 188 subjects. ±2.5 mm Hg per 50-µm deviation from 545 µm. One hundred eighty-eight subjects were included in the study. The CCT and GAT were analyzed from the right eye; when neither of these readings was reliable, the CCT and GAT from the left eye were used (3/188 [1.6%]). Table 1 gives the demographic characteristics of the study population. Sixty-nine men (36.7%) and 119 women (63.3%) were enrolled. The mean±sd age of the subjects was 71.4±13.8 years. One hundred fifty-one (80.3%) of the patients were white, 26 (13.8%) were African American, and 11 (5.9%) were Asian. The mean±sd CCT was 553.0±53.6 µm for women and 557.0±54.0 µm for men (P.50). The mean±sd CCT for African Americans was 539.3±53.0 µm, and it was 562.2±53.5 µm and 572.4±56.5 µm for whites and Asians, respectively (P.15). The mean±sd CCT measurement for the entire sample was 554.5±53.8 µm (Figure). The mean±sd IOP recorded was 15.8±4.6 mm Hg. The most common initial diagnosis was primary open-angle glaucoma, in 87 patients (46.3%). The next most prevalent diagnoses were chronic angle-closure glaucoma in 26 patients (13.8%), normal-tension glaucoma in 21 patients (11.2%), glaucoma suspect in 18 patients (9.6%), and ocular hypertension in 11 patients (5.9%). Using the Orssengo-Pye model, 119 patients (63.3%) had at least a measurement-significant adjustment in their IOP after CCT assessment (Table 2). Thirty-nine patients (20.7%) had adjustments between 1.5 and 3.0 mm Hg, while 22 (11.7%) had outcomes-significant IOP changes ( 3.0-mm Hg adjustment made to IOP). Of those patients who had at least a measurement-significant change to their IOP, 28 patients (14.9%) had a change in their treatment plan as a result of adjustments made to their IOP following CCT correction. Of these patients, 19 (10.1%) had a change in their medication regimen, 4 (2.1%) had a change in whether they had laser surgery, and 5 (2.7%) had a change in whether they had glaucoma surgery. Similar percentages were obtained using the linear model (Table 2). One hundred five patients (55.9%) had 1272
4 Table 3. Sensitivity Analysis of Measurement and Clinically Significant Changes Using Linear Model* Characteristic 2.0 mm Hg 2.5 mm Hg 3.0 mm Hg Measurementsignificant changes 1.5 mm Hg Measurementsignificant changes 3.0 mm Hg Outcomes-significant changes 3.0 mm Hg Change in glaucoma medical therapy Change in recommendation for glaucoma laser surgery Change in recommendation for glaucoma incisional surgery Abbreviations: CCT, central corneal thickness; IOP, intraocular pressure. *Data are expressed as percentage among 188 subjects. Corrected IOP = Measured IOP (CCT 545)/ mm Hg. Corrected IOP = Measured IOP (CCT 545)/ mm Hg. Corrected IOP = Measured IOP (CCT 545)/ mm Hg. at least a measurement-significant adjustment to their IOP, with 67 (35.6%) having less than a 3.0-mm Hg correction and 38 (20.2%) having an outcomes-significant correction ( 3.0 mm Hg in either direction). Among the 188 patients, 26 (13.8%) had a change in their treatment plan as a result of CCT-associated IOP correction. Sixteen patients (8.5%) had a change in medication therapy, 4 patients (2.1%) had a deferment or addition of laser surgery, and 6 patients (3.2%) had a change in whether they would receive glaucoma surgery. Sensitivity analyses were performed following substitution of the linear CF (with 2.0-, 2.5-, and 3.0- mm Hg CFs; Table 3). With the more conservative CF of 2.0 mm Hg per 50-µm deviation in CCT, 43.6% of patients experienced at least a measurement-significant adjustment in their IOP measurements. With the less conservative adjustment of 3.0 mm Hg per 50-µm deviation, the percentage of patients with measurement-significant changes in IOP was 63.3%. Although the percentage of patients with measurement-significant changes less than 3.0 mm Hg remained relatively similar (33.5%-35.6%), the percentage of patients with outcomes-significant changes varied greatly depending on the adjustment used; 10.1% of the patients experienced outcomes-significant changes with the 2.0- mm Hg CF, compared with 29.4% of patients when using the 3.0-mm Hg CF. The percentage of patients who experienced changes in medical or surgical therapy varied slightly based on the CF used (Table 3). The percentage of patients who had a change in medication therapy ranged between 8.0% and 9.1% (with the 2.0- and 3.0-mm Hg CFs, respectively), while the percentage of patients with a change in the recommendation of laser surgery ranged from 1.6% (with the 2.0- and 3.0-mm Hg CFs) to 2.1% (with the 2.5-mm Hg CF). The percentage of patients with a change in recommendation of glaucoma incisional surgery ranged between 2.7% (with the 2.0-mm Hg CF) and 3.2% (with the 2.5- and 3.0-mm Hg CFs) (Table 3). Based on the Orssengo-Pye mathematical model, we compared the effects of IOP adjustment in regard to clinical management between different racial groups (Table 4). Measurement-significant IOP corrections were found in 69.3% of African Americans, 62.9% of whites, and 54.6% of Asians (P=.62). Of those patients with measurement-significant IOP adjustments, 30.6% of African Americans had a change in their therapy, compared with 13.3% of whites and 0% of Asians (P.05). Furthermore, 15.3% of African Americans had a change in medication therapy, compared with 9.9% of whites; 11.5% of African-Americans had a change in whether they had laser therapy, compared with 0.7% of whites; and 3.8% of the African Americans had a change in whether they had glaucoma surgery, compared with 2.7% of whites (P.05 for all). The only statistically significant difference observed was that African Americans and whites were more likely to experience outcomes-significant IOP changes ( 3.0 mm Hg) than Asians (P.05). There were significant sex differences seen when using the Orssengo-Pye model (Table 5). As such, 73.9% of the men had a measurement-significant change in their IOP, compared with 57.1% of the women (P=.03). Furthermore, 14.5% of the men had a change in their medication therapy, compared with 7.6% of the women (P=.14). Among men, 4.3% had a change in whether they would have glaucoma surgery, compared with 1.8% of the women. The only category in which women had a greater change in therapy was laser surgery, in which 2.8% of the women had this change vs 1.4% of the men. COMMENT Although some authors 11,23 have reported that patients may be misdiagnosed because of the absence of CCT determination or the subsequent adjustment of IOP, we are not aware of any studies that have assessed the effect of CCT-associated IOP adjustments on glaucoma clinical management. In our study, approximately half of the 188 eyes examined required an adjustment in IOP measurement of 1.5 mm Hg or greater. We chose 1.5 mm Hg as a key correction end point, because this value is often cited as a significant difference in clinical studies assessing IOP efficacy between medications. Furthermore, it is not known whether these calculated adjustments in IOP are relevant to clinical management. Based on our analysis, there appears to be clinical usefulness in these IOP corrections, as approximately 8% to 10% of the patients had a change in their medication therapy, about 2% had a change in the recommendation (or deferment) of laser procedures, and about 3% had a change in the recommendation (or deferment) of glaucoma incisional surgery. However, because our study was cross-sectional and there are no long-term data to support the clinical implications of these changes, it is impossible to extrapolate the true effect of these IOP adjustments and the resultant changes in clinical decisions on patient outcomes. 1273
5 Table 4. Results According to Race (Using Orssengo-Pye Model)* Individual or Racial Population Characteristic White (n = 151) African American (n = 26) Asian (n = 11) Individual Central corneal thickness, mean ± SD, µm ± ± ± 56.5 Measurement-significant changes 1.5 mm Hg Measurement-significant changes 3.0 mm Hg Outcomes-significant changes 3.0 mm Hg Racial population Change in glaucoma medical therapy Change in recommendation for glaucoma laser therapy Change in recommendation for glaucoma incisional surgery *Data are expressed as percentages unless otherwise indicated. P.05. Table 5. Results According to Sex (Using Orssengo-Pye Model)* Individual or Sex Population Characteristic Male (n = 69) Female (n = 119) Individual Central corneal thickness, mean ± SD, µm ± ± 53.6 Measurement-significant changes 1.5 mm Hg Measurement-significant changes 3.0 mm Hg Outcomes-significant changes 3.0 mm Hg Sex population Change in glaucoma medical therapy Change in recommendation for glaucoma laser therapy Change in recommendation for glaucoma incisional surgery *Data are expressed as percentages unless otherwise indicated. P =.03, t test. Because there is controversy regarding the IOP correction algorithm, we performed the CCT-associated adjustments based on the most prominent formulas used, a linear model derived based on a literature search and a mathematical model developed by Orssengo and Pye. 18 A comparison of the 2 correction formulas yielded similar results. A sensitivity analysis yielded results that were nonmonotonic in 2 instances (ie, the percentage of patients with measurement-significant changes 3.0 mm Hg and the percentage of patients with changes in laser surgery recommendation). Because the category-significant changes less than 3.0 mm Hg were an intermediate category between no change and changes greater than 3.0 mm Hg, as one moved from more to less conservative CFs (ie, mm Hg per 50-µm change), there was an initial increase followed by a slight decrease as more patients were shifted into the 3.0-mm Hg range or greater (eg, the large increase to 29.4% with the 3.0-mm Hg CF). With regard to the recommendation for laser surgery, the move to less conservative CFs (ie, 3.0 mm Hg per 50-µm change) may have caused a shift in the need for glaucoma filtration surgery (rather than laser surgery) in the one patient affected. Regardless of the models and correction algorithms studied, adjustments for IOP based on CCT are critical for clinical management. The only statistically significant difference between races was that Asians were less likely to experience outcomes-significant changes compared with whites and African Americans (when the Orssengo-Pye model was used). The lack of greater statistical significance between groups may be due to several factors, including that our patient sample (from a tertiary care practice) may not be representative of the general population. The patients analyzed were already diagnosed as having glaucoma or glaucoma suspect. Furthermore, sample sizes of the different races were not large enough to generate statistical power, with only 26 African Americans and 11 Asians included in the study. For example, the populationbased Barbados eye studies of a predominantly black community (1142 participants) reported that black participants tended to have thinner corneas than white participants. 24 Limitations of this study include its retrospective analysis and its short duration. Patients were seen in an academic medical center glaucoma practice, with most having well-controlled glaucoma (mean IOP, approximately 16.0 mm Hg). Moreover, there was no way to confirm the true IOP of patients, because they were not taken to the operating room to have their anterior chambers cannulated for IOP assessment. 25 Finally, we do not know whether our definitions of measurement-significant ( 1.5 mm Hg) and outcomes-significant ( 3.0 mm Hg) results are useful for accurately assessing the extent of the IOP adjustments. Another limitation of this study is that it addresses CCTs obtained using ultrasound pachymetry, which is only one method of measuring CCT. Studies 26,27 have shown that, depending on the method used, statistically 1274
6 different CCTs may be obtained. Ventura et al 13 noted that optical low coherence reflectometry represents the most precise pachymetric method available, with its measurements reproducible to 1 µm. In the future, appropriate refinement of the correction formula may need to be undertaken, depending on the corneal pachymetric method adopted. This study presents preliminary data regarding the effects of CCT-adjusted IOP on clinical management of patients with glaucoma and glaucoma suspect. Because this was a cross-sectional study, further randomized controlled studies are needed to elucidate the effects of CCT on clinical management and consequent long-term patient outcomes. Given these future studies, it may be easier to delineate clear and effective treatment guidelines. Additional studies are needed to better test the consistency of these results across different racial and ethnic groups. Submitted for publication July 16, 2003; final revision received January 2, 2004; accepted March 4, This study was supported by the Columbia University Homer McK. Rees Scholar Award (Dr Tsai) and Eye Surgery Fund (Dr Tsai) and by an unrestricted departmental grant from Research to Prevent Blindness, New York. Correspondence: James C. Tsai, MD, Edward S. Harkness Eye Institute, Department of Ophthalmology, College of Physicians and Surgeons, Columbia University, 635 W 165th St, New York, NY (jct2002@columbia.edu). REFERENCES 1. Doughty M, Zaman M. Human corneal thickness and its impact on intraocular pressure measures: a review and meta-analysis approach. Surv Ophthalmol. 2000; 44: Ehlers N, Hansen FK. Central corneal thickness in low-tension glaucoma. Acta Ophthalmol (Copenh). 1974;52: Whitacre M, Stein R, Hassanein K. The effect of corneal thickness on applanation tonometry. Am J Ophthalmol. 1993;115: Gordon M, Beiser J, Brandt J, et al. The Ocular Hypertension Treatment Study: baseline factors that predict the onset of primary open-angle glaucoma. Arch Ophthalmol. 2002;120: Priglinger S, Neubauer A, May C, et al. Optical coherence tomography for the detection of laser in situ keratomileusis in donor corneas. Cornea. 2003;22: Seiler T. Does refractive surgery really make eyeglasses superfluous? Schweiz Rundsch Med Prax. 2001;90: Emara B, Probst L, Tingey D, et al. Correlation of intraocular pressure and central corneal thickness in normal myopic eyes after laser in situ keratomileusis. J Cataract Refract Surg. 1998;24: El Danasoury M, El Maghraby A, Coorpender S. Change in intraocular pressure in myopic eyes measured with contact and non-contact tonometers after laser in situ keratomileusis. J Refract Surg. 2001;17: Emara B, Probst LE, Tingey DP, Kennedy DW, Willms LJ, Machat J. Correlation of intraocular pressure and central corneal thickness in normal myopic eyes and after laser in situe keratomileusis. J Cataract Refract Surg. 1998;24: Lowe RF. Central corneal thickness: ocular correlations in normal eyes and those with primary angle-closure glaucoma. Br J Ophthalmol. 1969;53: Shah S, Chatterjee A, Mathai M, et al. Relationship between corneal thickness and measured intraocular pressure in a general ophthalmology clinic. Ophthalmology. 1999;106: Tomlinson A, Leighton DA. Ocular dimensions in low tension glaucoma compared with open-angle glaucoma and the normal. Br J Ophthalmol. 1972;56: Ventura AC, Bohnke M, Mojon DS. Central corneal thickness measurements in patients with normal tension glaucoma, primary open angle glaucoma, pseudoexfoliation glaucoma, or ocular hypertension. Br J Ophthalmol. 2001;85: Ehlers N, Bramsen T, Sperling S. Applanation tonometry and central corneal thickness. Acta Ophthalmol (Copenh). 1975;53: Herndon LW, Choudhri SA, Cox T, et al. Central corneal thickness in normal, glaucomatous, and ocular hypertensive eyes. Arch Ophthalmol. 1997;115: Tanaka GH. Corneal pachymetry: a prerequisite for applanation tonometry? Arch Ophthalmol. 1998;116: Pillunat LE, Kohlhaas M, Boehm AG, et al. Effect of corneal thickness, curvature, and axial length on Goldmann applanation tonometry [ARVO abstract]. Paper presented at: 2003 Annual Meeting of Association for Research in Vision and Ophthalmology (ARVO); May 4-8, 2003; Fort Lauderdale, Fla. Abstract Orssengo GJ, Pye DC. Determination of the true intraocular pressure and modulus of elasticity of the human cornea in vivo. Bull Math Biol. 1999;61: Leske MC, Heijl A, Hussein M, et al. Factors for glaucoma progression and the effect of treatment. Arch Ophthalmol. 2003;121: Parrish RK, Palmberg P, Sheu WP, XLT Study Group. A comparison of latanoprost, bimatoprost, and travoprost in patients with elevated intraocular pressure: a 12-week, randomized, masked-evaluator multicenter study. Am J Ophthalmol. 2003;135: Noecker R, Dirks M, Choplin N, et al. A six-month randomized clinical trial comparing the intraocular pressure lowering efficacy of bimatoprost and latanoprost in patients with ocular hypertension or glaucoma. Am J Ophthalmol. 2003; 135: Palmberg P. Answers from the Ocular Hypertension Treatment Study [editorial]. Arch Ophthalmol. 2002;120: Copt RP, Thomas R, Mermoud A. Corneal thickness in ocular hypertension, primary open-angle glaucoma, and normal tension glaucoma. Arch Ophthalmol. 1999; 117: Nemesure B, Wu SY, Hennis A, Leske MC, Barbados Eye Study Group. Corneal thickness and intraocular pressure in the Barbados eye studies. Arch Ophthalmol. 2003;121: Green K. Techniques of intraocular pressure determination. Lens Eye Toxic Res. 1990;7: Giraldez Fernandez M, Diaz Rey A, Cervino A, et al. A comparison of two pachymetric systems: slit scanning and ultrasonic. CLAO J. 2002;28: Gonzalez-Meijome J, Cervino A, Yebra-Pimentel E, et al. Central and peripheral corneal thickness measurement with Orbscan II and topographical ultrasound pachymetry. J Cataract Refract Surg. 2003;29:
CLINICAL SCIENCES. Effect of Central Corneal Thickness, Corneal Curvature, and Axial Length on Applanation Tonometry
 CLINICAL SCIENCES Effect of Central Corneal Thickness, Corneal Curvature, and Axial Length on Applanation Tonometry Markus Kohlhaas, MD; Andreas G. Boehm, MD; Eberhard Spoerl, PhD; Antje Pürsten, Dipl-Ing
CLINICAL SCIENCES Effect of Central Corneal Thickness, Corneal Curvature, and Axial Length on Applanation Tonometry Markus Kohlhaas, MD; Andreas G. Boehm, MD; Eberhard Spoerl, PhD; Antje Pürsten, Dipl-Ing
Correlating central corneal thickness and intraocular pressure in ocular hypertension and glaucoma
 VOL. 3 NO. 1 PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE JUNE 07 Jonathan G. Soriano, MD 1 Ma. Margarita L. Lat-Luna, MD 1, 3 Patricia M. Khu, MD 1, 1 Department of Ophthalmology and Visual
VOL. 3 NO. 1 PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE JUNE 07 Jonathan G. Soriano, MD 1 Ma. Margarita L. Lat-Luna, MD 1, 3 Patricia M. Khu, MD 1, 1 Department of Ophthalmology and Visual
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Pachymetry Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Pachymetry Professional Institutional Original Effective Date: March 11, 2004 Original Effective
Pachymetry Page 1 of 8 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Pachymetry Professional Institutional Original Effective Date: March 11, 2004 Original Effective
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND PACHYMETRY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
INTRODUCTION S. HERDENER, D. HAFIZOVIC, M. PACHE, S. LAUTEBACH, J. FUNK. University Eye Hospital, Freiburg - Germany
 European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 39-43 Is the PASCAL -Tonometer suitable for measuring intraocular pressure in clinical routine? Long- and short-term reproducibility of dynamic
European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 39-43 Is the PASCAL -Tonometer suitable for measuring intraocular pressure in clinical routine? Long- and short-term reproducibility of dynamic
Central corneal thickness among glaucoma patients attending Menelik II Hospital, Addis Ababa, Ethiopia
 Original article Central corneal thickness among glaucoma patients attending Menelik II Hospital, Addis Ababa, Ethiopia Zelalem Gizachew 1, Abiy Mulugeta 1* Abstract Background: Glaucoma is one of the
Original article Central corneal thickness among glaucoma patients attending Menelik II Hospital, Addis Ababa, Ethiopia Zelalem Gizachew 1, Abiy Mulugeta 1* Abstract Background: Glaucoma is one of the
Role of central corneal thickness measurement in management of open angle glaucoma and glaucoma suspects in Calabar, Nigeria
 Original Research Article Role of central corneal thickness measurement in management of open angle glaucoma and glaucoma suspects in Calabar, Nigeria Nkanga DG 1,2, Ibanga AA 1,2, Nkanga ED 2, Etim BA
Original Research Article Role of central corneal thickness measurement in management of open angle glaucoma and glaucoma suspects in Calabar, Nigeria Nkanga DG 1,2, Ibanga AA 1,2, Nkanga ED 2, Etim BA
Central corneal thickness determined with optical coherence tomography in various types of glaucoma
 Br J Ophthalmol 2000;84:1233 1237 1233 Department of Ophthalmology, Ludwig-Maximilians- University, Munich, Germany M Bechmann M J Thiel B Roesen S Ullrich M W Ulbig K Ludwig Correspondence to: Martin
Br J Ophthalmol 2000;84:1233 1237 1233 Department of Ophthalmology, Ludwig-Maximilians- University, Munich, Germany M Bechmann M J Thiel B Roesen S Ullrich M W Ulbig K Ludwig Correspondence to: Martin
Central corneal thickness and vascular risk factors in normal tension glaucoma
 Central corneal thickness and vascular risk factors in normal tension glaucoma Aoife Doyle, Ahmed Bensaid and Yves Lachkar L Institut du Glaucome, Fondation Hoˆpital St. Joseph, Paris, France ABSTRACT.
Central corneal thickness and vascular risk factors in normal tension glaucoma Aoife Doyle, Ahmed Bensaid and Yves Lachkar L Institut du Glaucome, Fondation Hoˆpital St. Joseph, Paris, France ABSTRACT.
Effect of corneal parameters on measurements using the pulsatile ocular blood flow tonograph and Goldmann applanation tonometer
 518 EXTENDED REPORT Effect of corneal parameters on measurements using the pulsatile ocular blood flow tonograph and Goldmann applanation tonometer P Gunvant, M Baskaran, L Vijaya, I S Joseph, R J Watkins,
518 EXTENDED REPORT Effect of corneal parameters on measurements using the pulsatile ocular blood flow tonograph and Goldmann applanation tonometer P Gunvant, M Baskaran, L Vijaya, I S Joseph, R J Watkins,
Central Corneal Thickness (CCT) among Glaucoma and Non Glaucoma Patients in a Hospital Based Population
 ISSN 2278 0211 (Online) Central Corneal Thickness (CCT) among Glaucoma and Non Glaucoma Patients in a Hospital Based Population Dr. Sheldon James Goudinho Professor, Department of Ophthalmology, Dr. Somervell
ISSN 2278 0211 (Online) Central Corneal Thickness (CCT) among Glaucoma and Non Glaucoma Patients in a Hospital Based Population Dr. Sheldon James Goudinho Professor, Department of Ophthalmology, Dr. Somervell
Jose M. Martinez-de-la-Casa, Julian Garcia-Feijoo, Ana Fernandez-Vidal, Carmen Mendez-Hernandez, and Julian Garcia-Sanchez METHODS
 Ocular Response Analyzer versus Goldmann Applanation Tonometry for Intraocular Pressure Measurements Jose M. Martinez-de-la-Casa, Julian Garcia-Feijoo, Ana Fernandez-Vidal, Carmen Mendez-Hernandez, and
Ocular Response Analyzer versus Goldmann Applanation Tonometry for Intraocular Pressure Measurements Jose M. Martinez-de-la-Casa, Julian Garcia-Feijoo, Ana Fernandez-Vidal, Carmen Mendez-Hernandez, and
Dina H. Erickson, O.D., a Denise Goodwin, O.D., a Michael Rollins, O.D., b Amber Belaustegui, O.D., c and Chad Anderson a
 Optometry (2009) 80, 169-174 Comparison of dynamic contour tonometry and Goldmann applanation tonometry and their relationship to corneal properties, refractive error, and ocular pulse amplitude Dina H.
Optometry (2009) 80, 169-174 Comparison of dynamic contour tonometry and Goldmann applanation tonometry and their relationship to corneal properties, refractive error, and ocular pulse amplitude Dina H.
The Association of Central corneal thickness with Intra-ocular Pressure and Refractive Error in a Nigerian Population
 Peer Reviewed, Open Access, Free Published Quarterly Mangalore, South India ISSN 0972-5997 Volume 6, Issue 3; Jul-Sep 2007 Original Article The Association of Central corneal thickness with Intra-ocular
Peer Reviewed, Open Access, Free Published Quarterly Mangalore, South India ISSN 0972-5997 Volume 6, Issue 3; Jul-Sep 2007 Original Article The Association of Central corneal thickness with Intra-ocular
Interest in central corneal thickness (CCT) and glaucoma was. Central Corneal Thickness and Glaucoma in East Asian People.
 Glaucoma Central Corneal Thickness and Glaucoma in East Asian People Alexander C. Day, 1,2 David Machin, 3 Tin Aung, 4 Gus Gazzard, 2 Rahat Husain, 4 Paul T. K. Chew, 5 Peng T. Khaw, 1,2,6 Steve K. L.
Glaucoma Central Corneal Thickness and Glaucoma in East Asian People Alexander C. Day, 1,2 David Machin, 3 Tin Aung, 4 Gus Gazzard, 2 Rahat Husain, 4 Paul T. K. Chew, 5 Peng T. Khaw, 1,2,6 Steve K. L.
Central Corneal Thickness and its Association with Ocular Parameters
 Central Corneal Thickness and its Association with Ocular Parameters Authors: An-Fei Li 1,2 Mei-Ju Chen 1,2 Affiliations: 1 Department of Ophthalmology, Taipei Veterans General Hospital 2 National Yang-Ming
Central Corneal Thickness and its Association with Ocular Parameters Authors: An-Fei Li 1,2 Mei-Ju Chen 1,2 Affiliations: 1 Department of Ophthalmology, Taipei Veterans General Hospital 2 National Yang-Ming
Central Corneal Thickness in Primary Angle Closure and Open Angle Glaucoma
 Original Article Central Corneal Thickness in Primary Angle Closure and Open Angle Glaucoma Sasan Moghimi 1,2, MD; Hamidreza Torabi 1, MD; Hesam Hashemian 1, MD; Heydar Amini 1, MD; Shan Lin 2, MD 1 Department
Original Article Central Corneal Thickness in Primary Angle Closure and Open Angle Glaucoma Sasan Moghimi 1,2, MD; Hamidreza Torabi 1, MD; Hesam Hashemian 1, MD; Heydar Amini 1, MD; Shan Lin 2, MD 1 Department
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma
 Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
True IOP No Doubt Facts and Figures Figures. Ziemer Ophthalmic Systems AG a Ziemer Group Company Allmendstrasse 11 CH-2562 Port, Switzerland
 True IOP No Doubt Facts and Figures Figures and Facts Ziemer Ophthalmic Systems AG a Ziemer Group Company Allmendstrasse 11 CH-2562 Port, Switzerland There is increasing evidence that DCT measures IOP
True IOP No Doubt Facts and Figures Figures and Facts Ziemer Ophthalmic Systems AG a Ziemer Group Company Allmendstrasse 11 CH-2562 Port, Switzerland There is increasing evidence that DCT measures IOP
Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India
 Original article: Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India 1Dr. Apala Bhattacharya, 2 Dr Gautam Bhaduri,
Original article: Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India 1Dr. Apala Bhattacharya, 2 Dr Gautam Bhaduri,
Central corneal thickness and normal tension glaucoma: A cross-sectional study
 Optometry (2006) 77, 134-140 Central corneal thickness and normal tension glaucoma: A cross-sectional study Michael Sullivan-Mee, O.D., a Kathy D. Halverson, O.D., a Mollie C. Saxon, O.D., a Glenn B. Saxon,
Optometry (2006) 77, 134-140 Central corneal thickness and normal tension glaucoma: A cross-sectional study Michael Sullivan-Mee, O.D., a Kathy D. Halverson, O.D., a Mollie C. Saxon, O.D., a Glenn B. Saxon,
Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
Trabeculectomy is an effective method for lowering
 ORIGINAL STUDY Refractive Outcome of Cataract Surgery in Eyes With Prior Trabeculectomy: Risk Factors for Postoperative Myopia Oliver L. Yeh, MD, Karine D. Bojikian, MD, Mark A. Slabaugh, MD, and Philip
ORIGINAL STUDY Refractive Outcome of Cataract Surgery in Eyes With Prior Trabeculectomy: Risk Factors for Postoperative Myopia Oliver L. Yeh, MD, Karine D. Bojikian, MD, Mark A. Slabaugh, MD, and Philip
Accuracy and Repeatability of a New Portable Ultrasound Pachymeter
 Accuracy and Repeatability of a New Portable Ultrasound Pachymeter Queirós A 1, González-Méijome JM 1, Fernandes P 1, Jorge J 1, Almeida J B 1, Parafita MA 2 1 Department of Physics (Optometry), School
Accuracy and Repeatability of a New Portable Ultrasound Pachymeter Queirós A 1, González-Méijome JM 1, Fernandes P 1, Jorge J 1, Almeida J B 1, Parafita MA 2 1 Department of Physics (Optometry), School
Collaboration in the care of glaucoma patients and glaucoma suspects. Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012
 Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Ever since the recognition that certain forms of blindness. Central corneal thickness, tonometry, and glaucoma risk a guide for the perplexed
 CJO LECTURE 2007 Central corneal thickness, tonometry, and glaucoma risk a guide for the perplexed James D. Brandt, MD ABSTRACT RÉSUMÉ The results of the Ocular Hypertension Treatment Study (OHTS) brought
CJO LECTURE 2007 Central corneal thickness, tonometry, and glaucoma risk a guide for the perplexed James D. Brandt, MD ABSTRACT RÉSUMÉ The results of the Ocular Hypertension Treatment Study (OHTS) brought
Laser in situ keratomileusis (LASIK) has
 Changes in Intraocular Pressure After Laser in situ Keratomileusis Khaled M. Rashad, MD; Ahmed A. Bahnassy, MSc, PhD ABSTRACT PURPOSE: To evaluate changes in intraocular pressure (IOP) measurements by
Changes in Intraocular Pressure After Laser in situ Keratomileusis Khaled M. Rashad, MD; Ahmed A. Bahnassy, MSc, PhD ABSTRACT PURPOSE: To evaluate changes in intraocular pressure (IOP) measurements by
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Based on the studies by Goldmann and Schmidt 1 and Ehlers. Central Corneal Thickness Correlated with Glaucoma Damage and Rate of Progression
 Central Corneal Thickness Correlated with Glaucoma Damage and Rate of Progression Jost B. Jonas, 1,2 Andrea Stroux, 3,4 Isabel Velten, 1 Anselm Juenemann, 1 Peter Martus, 3 and Wido M. Budde 1,2 PURPOSE.
Central Corneal Thickness Correlated with Glaucoma Damage and Rate of Progression Jost B. Jonas, 1,2 Andrea Stroux, 3,4 Isabel Velten, 1 Anselm Juenemann, 1 Peter Martus, 3 and Wido M. Budde 1,2 PURPOSE.
Circadian variations in central corneal thickness and intraocular pressure in patients with glaucoma
 SCIENTIFIC REPORT Circadian variations in central corneal thickness and intraocular pressure in patients with glaucoma P Fogagnolo, L Rossetti, F Mazzolani, N Orzalesi... Br J Ophthalmol ;9:. doi: 1.113/bjo.5.795
SCIENTIFIC REPORT Circadian variations in central corneal thickness and intraocular pressure in patients with glaucoma P Fogagnolo, L Rossetti, F Mazzolani, N Orzalesi... Br J Ophthalmol ;9:. doi: 1.113/bjo.5.795
Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015
 Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015 Jimmy Lai Clinical Professor Department of Ophthalmology The University of Hong Kong 1 Primary Angle Closure Glaucoma PACG
Management of Angle Closure Glaucoma Hospital Authority Convention 18 May 2015 Jimmy Lai Clinical Professor Department of Ophthalmology The University of Hong Kong 1 Primary Angle Closure Glaucoma PACG
9/25/2017 CASE. 67 years old On 2 topical meds since 3 years. Rx: +3.0 RE LE
 CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
Glaucoma Clinical Update. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial
 Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial Boel Bengtsson, PhD, 1 M. Cristina Leske, MD, MPH, 2 Leslie Hyman, PhD, 2 Anders Heijl, MD, PhD, 1 Early
Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial Boel Bengtsson, PhD, 1 M. Cristina Leske, MD, MPH, 2 Leslie Hyman, PhD, 2 Anders Heijl, MD, PhD, 1 Early
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T.
 STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
STUDY OF EFFECTIVENESS OF LENS EXTRACTION AND PCIOL IMPLANTATION IN PRIMARY ANGLE CLOSURE GLAUCOMA Sudhakar Rao P 1, K. Revathy 2, T. Sreevathsala 3 HOW TO CITE THIS ARTICLE: Sudhakar Rao P, K. Revathy,
Glaucoma: Diagnostic Modalities
 Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Glaucoma: Diagnostic Modalities - Dr. Barun Kumar Nayak, Dr. Sarika Ramugade Glaucoma is a leading cause of blindness in the world, especially in older people. Early detection and treatment by ophthalmologist
Recent evidence has stressed the clinical role of the assessment
 Underestimate of Tonometric Readings after Photorefractive Keratectomy Increases at Higher Intraocular Pressure Levels Ciro Tamburrelli, Andrea Giudiceandrea, Agostino Salvatore Vaiano, Carmela Grazia
Underestimate of Tonometric Readings after Photorefractive Keratectomy Increases at Higher Intraocular Pressure Levels Ciro Tamburrelli, Andrea Giudiceandrea, Agostino Salvatore Vaiano, Carmela Grazia
Present relevant clinical findings of four landmark glaucoma trials OHTS, EMGT, CNTGS and CIGTS.
 Course title: The Glaucoma Compass Course length: 1 hour +/- 31 slides Corse Description: Even with the technology and available information, glaucoma decision making can still be confusing. How should
Course title: The Glaucoma Compass Course length: 1 hour +/- 31 slides Corse Description: Even with the technology and available information, glaucoma decision making can still be confusing. How should
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study
 Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
FUTURE DRAFT Local Coverage Determination (LCD) for Corneal Pachymetry (DL32410)
 FUTURE DRAFT Local Coverage Determination (LCD) for Corneal Pachymetry (DL32410) Please note: This is a Draft policy. Draft LCDs are works in progress that are available on the Medicare Coverage Database
FUTURE DRAFT Local Coverage Determination (LCD) for Corneal Pachymetry (DL32410) Please note: This is a Draft policy. Draft LCDs are works in progress that are available on the Medicare Coverage Database
Glaucoma. Glaucoma. Optic Disc Cupping
 Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
PRACTICAL APPROACH TO MEDICAL MANAGEMENT OF GLAUCOMA
 PRACTICAL APPROACH TO MEDICAL MANAGEMENT OF GLAUCOMA DR. RAVI THOMAS, DR. RAJUL PARIKH, DR. SHEFALI PARIKH IJO MAY 2008 PRESENTER AT JDOS : DR. RAHUL SHUKLA T.N. SHUKLA EYE HOSPITAL TERMINOLOGY POAG: PRIMARY
PRACTICAL APPROACH TO MEDICAL MANAGEMENT OF GLAUCOMA DR. RAVI THOMAS, DR. RAJUL PARIKH, DR. SHEFALI PARIKH IJO MAY 2008 PRESENTER AT JDOS : DR. RAHUL SHUKLA T.N. SHUKLA EYE HOSPITAL TERMINOLOGY POAG: PRIMARY
Clinical decision making based on data from GDx: One year observations
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2002 Clinical decision making based on data from GDx: One year observations James C. Bobrow Washington University
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2002 Clinical decision making based on data from GDx: One year observations James C. Bobrow Washington University
Glaucoma. How is Glaucoma Diagnosed? Glaucoma Testing
 Glaucoma How is Glaucoma Diagnosed? Glaucoma Testing There is no single test for glaucoma. The diagnosis is made by evaluating the patient from a number of perspectives, using specialized instruments.
Glaucoma How is Glaucoma Diagnosed? Glaucoma Testing There is no single test for glaucoma. The diagnosis is made by evaluating the patient from a number of perspectives, using specialized instruments.
Changes in Central Corneal Thickness over Time
 Changes in Central Corneal Thickness over Time The Ocular Hypertension Treatment Study James D. Brandt, MD, 1 Mae O. Gordon, PhD, 2 Julia A. Beiser, MS, 2 Shan C. Lin, MD, 3 Monica Y. Alexander, MD, 4
Changes in Central Corneal Thickness over Time The Ocular Hypertension Treatment Study James D. Brandt, MD, 1 Mae O. Gordon, PhD, 2 Julia A. Beiser, MS, 2 Shan C. Lin, MD, 3 Monica Y. Alexander, MD, 4
CENTRAL CORNEAL THICKNESS STUDY CCTS
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 CENTRAL CORNEAL THICKNESS STUDY CCTS A Prospective Study of Central Corneal Thickness in Children Less than 18 Years Old PROTOCOL Version 1.0 April 4,
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 CENTRAL CORNEAL THICKNESS STUDY CCTS A Prospective Study of Central Corneal Thickness in Children Less than 18 Years Old PROTOCOL Version 1.0 April 4,
1/31/2018. Course Objectives. Diagnostic Testing. Optic Nerve Damage ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY TECHNICIAN: -SDP
 ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY KNOW THE DISEASE PROCESS TECHNICIAN: EXPLAIN PROCESS OF EXAMINATION Presenters: Dana McMahan, COA Nicole Smith, COA Engage with patient s, help alleviate
ANATOMY AND PHYSIOLOGY OF A GLAUCOMA WORK-UP/TONOMETRY KNOW THE DISEASE PROCESS TECHNICIAN: EXPLAIN PROCESS OF EXAMINATION Presenters: Dana McMahan, COA Nicole Smith, COA Engage with patient s, help alleviate
LARGE DISCS WITH LARGE CUPS A DIAGNOSTIC CHALLENGE IN AFRICAN PATIENTS. Darshana Soma
 LARGE DISCS WITH LARGE CUPS A DIAGNOSTIC CHALLENGE IN AFRICAN PATIENTS Darshana Soma A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, in partial
LARGE DISCS WITH LARGE CUPS A DIAGNOSTIC CHALLENGE IN AFRICAN PATIENTS Darshana Soma A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, in partial
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors
 CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
4/06/2013. Medication Observation POAG. Proportion. Native American 0.1% 0.4%
 Clinical Research in Glaucoma: Putting Science into Practice J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS)
Clinical Research in Glaucoma: Putting Science into Practice J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS)
Peretyagin O.A., Cand. Med. Sc., Ass. Prof.; Dmitriev S.K., Dr. Med. Sc., Prof.; Lazar Yu.M., Cand. Med. Sc.; Tatarina Yu.A., Junior Research Fellow
 Changes in corneoscleral rigidity and corneal thickness at various target intraocular pressures in patients with stabilized primary open-angle glaucoma Peretyagin O.A., Cand. Med. Sc., Ass. Prof.; Dmitriev
Changes in corneoscleral rigidity and corneal thickness at various target intraocular pressures in patients with stabilized primary open-angle glaucoma Peretyagin O.A., Cand. Med. Sc., Ass. Prof.; Dmitriev
Regional Institute of Ophthalmology, Indira Gandhi Institute of Medical Sciences, Patna, India 2
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(5):399-407 http://dx.doi.org/10.3341/kjo.2014.28.5.399 Original Article Comparing the Efficacy of (0.005%), Bimatoprost (0.03%), Travoprost
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(5):399-407 http://dx.doi.org/10.3341/kjo.2014.28.5.399 Original Article Comparing the Efficacy of (0.005%), Bimatoprost (0.03%), Travoprost
Morphological Study of Corneal Endothelium and Corneal Thickness in Pseudoexfoliation Syndrome
 LABORATORY INVESTIGATIONS Morphological Study of Corneal Endothelium and Corneal Thickness in Pseudoexfoliation Syndrome Kenji Inoue*,, Kazuko Okugawa*,, Tetsuro Oshika and Shiro Amano *Department of Ophthalmology,
LABORATORY INVESTIGATIONS Morphological Study of Corneal Endothelium and Corneal Thickness in Pseudoexfoliation Syndrome Kenji Inoue*,, Kazuko Okugawa*,, Tetsuro Oshika and Shiro Amano *Department of Ophthalmology,
CHARTING THE NEW COURSE FOR MIGS
 CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure Glaucoma
 Original Article DOI 10.3349/ymj.2009.50.2.206 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(2):206-210, 2009 Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure
Original Article DOI 10.3349/ymj.2009.50.2.206 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(2):206-210, 2009 Inaccuracy of Intraocular Lens Power Prediction for Cataract Surgery in Angle-Closure
The Relative Frequency and Risk Factors of Primary Open Angle Glaucoma and Angle Closure Glaucoma
 Original Article The Relative Frequency and Risk Factors of Primary Open Angle Glaucoma and Angle Closure Glaucoma Naila Ali, Syed Ali Wajid, Nasir Saeed, Muhammad Daud Khan Pak J Ophthalmol 07, Vol. 23
Original Article The Relative Frequency and Risk Factors of Primary Open Angle Glaucoma and Angle Closure Glaucoma Naila Ali, Syed Ali Wajid, Nasir Saeed, Muhammad Daud Khan Pak J Ophthalmol 07, Vol. 23
THE CHRONIC GLAUCOMAS
 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA? People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
Refractive corneal surgery (RCS) using a laser, such as. Glaucoma Progression in Eyes with a History of Refractive Corneal Surgery.
 Glaucoma Glaucoma Progression in Eyes with a History of Refractive Corneal Surgery Yoon Jeon Kim, 1 Sung-Cheol Yun, 2 Jung Hwa Na, 3 Hung Won Tchah, 1 Jong Jin Jung, 3 and Kyung Rim Sung 1 PURPOSE. To
Glaucoma Glaucoma Progression in Eyes with a History of Refractive Corneal Surgery Yoon Jeon Kim, 1 Sung-Cheol Yun, 2 Jung Hwa Na, 3 Hung Won Tchah, 1 Jong Jin Jung, 3 and Kyung Rim Sung 1 PURPOSE. To
THE CHRONIC GLAUCOMAS
 THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
THE CHRONIC GLAUCOMAS WHAT IS GLAUCOMA People with glaucoma have lost some of their field of all round vision. It is often the edge or periphery that is lost. That is why the condition can be missed until
Clinical Profile of Primary Open Angle Glaucoma Suspects.
 DOI: 10.21276/aimdr.2018.4.2.OT3 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Clinical Profile of Primary Open Angle Glaucoma Suspects. Pradnya Abhinav Mohan 1 1 Fellow Phaco-surgery, Department
DOI: 10.21276/aimdr.2018.4.2.OT3 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Clinical Profile of Primary Open Angle Glaucoma Suspects. Pradnya Abhinav Mohan 1 1 Fellow Phaco-surgery, Department
Immersion Vs Contact Biometery for Axial Length Measurement before Phacoemulsification
 Original Article Immersion Vs Contact Biometery for Axial Length Measurement before Phacoemulsification with Foldable IOL Irum Abbas, Atif Mansoor Ahmad, Tahir Mahmood Pak J Ophthalmol 2009, Vol. 25 No.
Original Article Immersion Vs Contact Biometery for Axial Length Measurement before Phacoemulsification with Foldable IOL Irum Abbas, Atif Mansoor Ahmad, Tahir Mahmood Pak J Ophthalmol 2009, Vol. 25 No.
NIIOS. Cornea Specialist, Melles Cornea Clinic, NIIOS, Rotterdam, the Netherlands Naval Hospital, Athens, Greece VASILIS S.
 Cornea Specialist, Melles Cornea Clinic, NIIOS, Rotterdam, the Netherlands Naval Hospital, Athens, Greece Goldman applanation tonometry is still the gold standard for measuring IOP, but its accuracy is
Cornea Specialist, Melles Cornea Clinic, NIIOS, Rotterdam, the Netherlands Naval Hospital, Athens, Greece Goldman applanation tonometry is still the gold standard for measuring IOP, but its accuracy is
Central corneal thickness (CCT) measurement is a critical
 ARTICLE Topographic Paracentral Corneal Thickness With Pentacam and Orbscan: Effect of Acoustic Factor Javier González-Pérez, O.D., M.Sc., Ph.D., Jose M. González-Méijome, O.D., Ph.D., María T. Rodríguez
ARTICLE Topographic Paracentral Corneal Thickness With Pentacam and Orbscan: Effect of Acoustic Factor Javier González-Pérez, O.D., M.Sc., Ph.D., Jose M. González-Méijome, O.D., Ph.D., María T. Rodríguez
Article Central Corneal Thickness In Individuals With And Without Pseudo Exfoliation Syndrome A Prospective Study
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 7 (May. 2018), PP 19-26 www.iosrjournals.org Article Central Corneal Thickness In Individuals
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 7 (May. 2018), PP 19-26 www.iosrjournals.org Article Central Corneal Thickness In Individuals
The Role of the RNFL in the Diagnosis of Glaucoma
 Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1
 Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
WARNING LETTER DEPARTMENT OF HEALTH & HUMAN SERVICES TRANSMITTED BY FACSIMILE
 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Rockville, MD 20857 TRANSMITTED BY FACSIMILE David E.I. Pyott President and Chief Executive Officer PO Box 19534
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Rockville, MD 20857 TRANSMITTED BY FACSIMILE David E.I. Pyott President and Chief Executive Officer PO Box 19534
Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
 Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Central Cornea Thickness in Glaucoma and Non- Glaucoma African Population
 Ophthalmology Research: An International Journal 6(4): 1-8, 2016; Article no.or.31121 ISSN: 2321-7227 SCIENCEDOMAIN international www.sciencedomain.org Central Cornea Thickness in Glaucoma and Non- Glaucoma
Ophthalmology Research: An International Journal 6(4): 1-8, 2016; Article no.or.31121 ISSN: 2321-7227 SCIENCEDOMAIN international www.sciencedomain.org Central Cornea Thickness in Glaucoma and Non- Glaucoma
Glaucoma is the most frequent
 Refined glaucoma referral practice offers prospect of improved capacity and expanded role for primary eye care professionals BY ROD MCNEIL Glaucoma is the most frequent cause of irreversible blindness
Refined glaucoma referral practice offers prospect of improved capacity and expanded role for primary eye care professionals BY ROD MCNEIL Glaucoma is the most frequent cause of irreversible blindness
The second most common causes of blindness worldwide. ( after cataract) The commonest cause of irreversible blindness in the world Estimated that 3%
 The second most common causes of blindness worldwide. ( after cataract) The commonest cause of irreversible blindness in the world Estimated that 3% of our population age > 40 have glaucoma In the past:
The second most common causes of blindness worldwide. ( after cataract) The commonest cause of irreversible blindness in the world Estimated that 3% of our population age > 40 have glaucoma In the past:
Efficacy of latanoprost in management of chronic angle closure glaucoma. Kumar S 1, Malik A 2 Singh M 3, Sood S 4. Abstract
 Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Effect of Selective Laser Trabeculoplasty in Glaucoma Patients with High or Low Central Corneal Thickness
 Research Article imedpub Journals http://www.imedpub.com Effect of Selective Laser Trabeculoplasty in Glaucoma Patients with High or Low Central Corneal Thickness Abstract Purpose: Comparison of the effect
Research Article imedpub Journals http://www.imedpub.com Effect of Selective Laser Trabeculoplasty in Glaucoma Patients with High or Low Central Corneal Thickness Abstract Purpose: Comparison of the effect
Training Checking Vision Tonometry
 Training 101-2 Checking Vision Tonometry Checking Vision The classic example of an eye chart is the Snellen eye chart, in general they show 11 rows of capital letters. The top row contains one letter (usually
Training 101-2 Checking Vision Tonometry Checking Vision The classic example of an eye chart is the Snellen eye chart, in general they show 11 rows of capital letters. The top row contains one letter (usually
Original Article Effects of topical travoprost 0.004% on intraocular pressure and corneal biomechanical properties in an animal model
 Original Article Effects of topical travoprost 0.004% on intraocular pressure and corneal biomechanical properties in an animal model Gabriel Lazcano-Gomez, MD, a David Ancona-Lezama, MD, b Felix Gil-Carrasco,
Original Article Effects of topical travoprost 0.004% on intraocular pressure and corneal biomechanical properties in an animal model Gabriel Lazcano-Gomez, MD, a David Ancona-Lezama, MD, b Felix Gil-Carrasco,
Glaucoma is the leading cause of irreversible blindness in
 CLINICAL SCIENCE Determinants of Postoperative Corneal Edema and Impact on Goldmann Intraocular Pressure Yuqiang Huang, MBBS,* Mingzhi Zhang, MD,* Chukai Huang, MBBS,* Bin Chen, PhD,* Dennis S. C. Lam,
CLINICAL SCIENCE Determinants of Postoperative Corneal Edema and Impact on Goldmann Intraocular Pressure Yuqiang Huang, MBBS,* Mingzhi Zhang, MD,* Chukai Huang, MBBS,* Bin Chen, PhD,* Dennis S. C. Lam,
Comparison of Goldmann applanation tonometry and dynamic contour tonometry in healthy and glaucomatous eyes
 (2009) 23, 262 269 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye CLINICAL STUDY Comparison of Goldmann applanation tonometry and dynamic contour tonometry
(2009) 23, 262 269 & 2009 Macmillan Publishers Limited All rights reserved 0950-222X/09 $32.00 www.nature.com/eye CLINICAL STUDY Comparison of Goldmann applanation tonometry and dynamic contour tonometry
The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters.
 A Study of the Safety and Efficacy of Travoprost 0.004%/Timolol 0.5% Ophthalmic Solution Compared to Latanoprost 0.005% and Timolol 0.5% Dosed Concomitantly in Patients with Open-Angle Glaucoma or Ocular
A Study of the Safety and Efficacy of Travoprost 0.004%/Timolol 0.5% Ophthalmic Solution Compared to Latanoprost 0.005% and Timolol 0.5% Dosed Concomitantly in Patients with Open-Angle Glaucoma or Ocular
Relationship between central corneal thickness and parameters of optic nerve head topography in healthy subjects
 European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 32-38 Relationship between central corneal thickness and parameters of optic nerve head topography in healthy subjects A.B. CANKAYA, U. ELGIN,
European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 32-38 Relationship between central corneal thickness and parameters of optic nerve head topography in healthy subjects A.B. CANKAYA, U. ELGIN,
INTRODUCTION MIKLOS SCHNEIDER 1, GABOR BORGULYA 2, ANDRAS SERES 1, ZOLTAN Z. NAGY 1, JANOS NEMETH 1
 European Journal of Ophthalmology / Vol. 19 no. 2, 2009 / pp. 180-187 Central corneal thickness measurements with optical coherence tomography and ultrasound pachymetry in healthy subjects and in patients
European Journal of Ophthalmology / Vol. 19 no. 2, 2009 / pp. 180-187 Central corneal thickness measurements with optical coherence tomography and ultrasound pachymetry in healthy subjects and in patients
Elements for a public summary. Overview of disease epidemiology
 VI.2 VI.2.1 Elements for a public summary Overview of disease epidemiology Glaucoma is an eye disease that can result in damage to the optic nerve and loss of vision (blindness). It is the major cause
VI.2 VI.2.1 Elements for a public summary Overview of disease epidemiology Glaucoma is an eye disease that can result in damage to the optic nerve and loss of vision (blindness). It is the major cause
Goals. Glaucoma PARA PEARL TO DO. Vision Loss with Glaucoma
 Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Correspondence should be addressed to Fusako Fujimura;
 BioMed Research International Volume 2013, Article ID 370592, 5 pages http://dx.doi.org/10.1155/2013/370592 Research Article Repeatability and Reproducibility of Measurements Using a NT-530P Noncontact
BioMed Research International Volume 2013, Article ID 370592, 5 pages http://dx.doi.org/10.1155/2013/370592 Research Article Repeatability and Reproducibility of Measurements Using a NT-530P Noncontact
Glaucoma Disease Progression Role of Intra Ocular Pressure. Is Good Enough, Low Enough?
 Glaucoma Disease Progression Role of Intra Ocular Pressure Is Good Enough, Low Enough? Glaucoma Diseases Progression Key Considerations Good number of patients may be diagnosed only after some damage the
Glaucoma Disease Progression Role of Intra Ocular Pressure Is Good Enough, Low Enough? Glaucoma Diseases Progression Key Considerations Good number of patients may be diagnosed only after some damage the
ORIGINAL ARTICLE RISK FACTORS FOR DEVELOPMENT OF ANGLE CLOSURE GLAUCOMA IN EYES WITH SHALLOW ANTERIOR CHAMBER
 RISK FACTORS FOR DEVELOPMENT OF ANGLE CLOSURE GLAUCOMA IN EYES WITH SHALLOW ANTERIOR CHAMBER Sundeep 1, Niveditha H 2, Pooja Patil 3, N V V Himamshu 4, Vinutha B V 5, Liji P 6, M S Smitha Gowda 7, Nivedhitha
RISK FACTORS FOR DEVELOPMENT OF ANGLE CLOSURE GLAUCOMA IN EYES WITH SHALLOW ANTERIOR CHAMBER Sundeep 1, Niveditha H 2, Pooja Patil 3, N V V Himamshu 4, Vinutha B V 5, Liji P 6, M S Smitha Gowda 7, Nivedhitha
INTRODUCTION J. DAWCZYNSKI, E. KOENIGSDOERFFER, R. AUGSTEN, J. STROBEL. Department of Ophthalmology, University Hospital Jena, Jena - Germany
 European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
European Journal of Ophthalmology / Vol. 17 no. 3, 2007 / pp. 363-367 Anterior segment optical coherence tomography for evaluation of changes in anterior chamber angle and depth after intraocular lens
CLINICAL SCIENCES. tonometry (GAT) has become the gold standard against which other tonometers
 CLINICAL SCIENCES Dynamic Contour Tonometry A Comparative Study on Human Cadaver Eyes Christoph Kniestedt, MD; Michelle Nee, MD; Robert L. Stamper, MD Objective: To compare intraocular pressure measurements
CLINICAL SCIENCES Dynamic Contour Tonometry A Comparative Study on Human Cadaver Eyes Christoph Kniestedt, MD; Michelle Nee, MD; Robert L. Stamper, MD Objective: To compare intraocular pressure measurements
Prevalence Of Primary Open Angle Glaucoma in Diabetic Patients
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. III (June. 2017), PP 147-151 www.iosrjournals.org Prevalence Of Primary Open Angle Glaucoma
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. III (June. 2017), PP 147-151 www.iosrjournals.org Prevalence Of Primary Open Angle Glaucoma
Ocular Rigidity Evaluation After Photorefractive Keratectomy: An Experimental Study
 BIOMECHANICS Ocular Rigidity Evaluation After Photorefractive Keratectomy: An Experimental Study George D. Kymionis, MD, PhD; Vasilios F. Diakonis, MD; George Kounis, BSc; Spyridon Charisis, MD; Dimitrios
BIOMECHANICS Ocular Rigidity Evaluation After Photorefractive Keratectomy: An Experimental Study George D. Kymionis, MD, PhD; Vasilios F. Diakonis, MD; George Kounis, BSc; Spyridon Charisis, MD; Dimitrios
Diabetes, Hyperglycemia, and Central Corneal Thickness
 Diabetes, Hyperglycemia, and Central Corneal Thickness The Singapore Malay Eye Study Daniel H. W. Su, MMed(Ophth), FRCS(Ed), 1 Tien Y. Wong, PhD, FRCS(Ed), 1,2,3 Wan-Ling Wong, BSc, 1 Seang-Mei Saw, PhD,
Diabetes, Hyperglycemia, and Central Corneal Thickness The Singapore Malay Eye Study Daniel H. W. Su, MMed(Ophth), FRCS(Ed), 1 Tien Y. Wong, PhD, FRCS(Ed), 1,2,3 Wan-Ling Wong, BSc, 1 Seang-Mei Saw, PhD,
[TRAVOPROST] 40 MICROGRAMS/ML, EYE DROPS, SOLUTION RISK MANAGEMENT PLAN. TRAVOPR-v
![[TRAVOPROST] 40 MICROGRAMS/ML, EYE DROPS, SOLUTION RISK MANAGEMENT PLAN. TRAVOPR-v [TRAVOPROST] 40 MICROGRAMS/ML, EYE DROPS, SOLUTION RISK MANAGEMENT PLAN. TRAVOPR-v](/thumbs/94/119684929.jpg) [TRAVOPROST] 40 MICROGRAMS/ML, EYE DROPS, SOLUTION RISK MANAGEMENT PLAN TRAVOPR-v2-270214 VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Studies estimated that 3-6 million people
[TRAVOPROST] 40 MICROGRAMS/ML, EYE DROPS, SOLUTION RISK MANAGEMENT PLAN TRAVOPR-v2-270214 VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Studies estimated that 3-6 million people
Ocular hypertension is present in approximately 8%
 ORIGINAL STUDY The Probability of Glaucoma From Ocular Hypertension Determined by Ophthalmologists in Comparison to a Risk Calculator Steven L. Mansberger, MD, MPH and George A. Cioffi, MD Objective: To
ORIGINAL STUDY The Probability of Glaucoma From Ocular Hypertension Determined by Ophthalmologists in Comparison to a Risk Calculator Steven L. Mansberger, MD, MPH and George A. Cioffi, MD Objective: To
Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography
 Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
GLAUCOMA REPEAT READINGS PATHWAY
 GLAUCOMA REPEAT READINGS PATHWAY Level 1a: Goldmann style applanation tonometry repeat readings A first level community service for IOP refinement where other signs of glaucoma are not present will reduce
GLAUCOMA REPEAT READINGS PATHWAY Level 1a: Goldmann style applanation tonometry repeat readings A first level community service for IOP refinement where other signs of glaucoma are not present will reduce
Investigation of the relationship between central corneal thickness and retinal nerve fiber layer thickness in ocular hypertension
 Acta Medica Anatolia Volume 2 Issue 1 2014 Investigation of the relationship between central corneal thickness and retinal nerve fiber layer thickness in ocular hypertension Remzi Mısır 1, Sinan Sarıcaoğlu
Acta Medica Anatolia Volume 2 Issue 1 2014 Investigation of the relationship between central corneal thickness and retinal nerve fiber layer thickness in ocular hypertension Remzi Mısır 1, Sinan Sarıcaoğlu
NON-INVASIVE OCULAR RIGIDITY MEASUREMENT: A DIFFERENTIAL TONOMETRY APPROACH
 ORIGINAL ARTICLE NON-INVASIVE OCULAR RIGIDITY MEASUREMENT: A DIFFERENTIAL TONOMETRY APPROACH Efstathios T. Detorakis 1,2, Emmanuela Tsaglioti 1, George Kymionis 1,2 Institute of Vision & Optics, University
ORIGINAL ARTICLE NON-INVASIVE OCULAR RIGIDITY MEASUREMENT: A DIFFERENTIAL TONOMETRY APPROACH Efstathios T. Detorakis 1,2, Emmanuela Tsaglioti 1, George Kymionis 1,2 Institute of Vision & Optics, University
Comparison of IOP measurement by ocular response analyzer, dynamic contour, Goldmann applanation, and noncontact tonometry
 European Journal of Ophthalmology / Vol. 19 no. 6, 2009 / pp. 936-941 Comparison of IOP measurement by ocular response analyzer, dynamic contour, Goldmann applanation, and noncontact tonometry BANU ONCEL,
European Journal of Ophthalmology / Vol. 19 no. 6, 2009 / pp. 936-941 Comparison of IOP measurement by ocular response analyzer, dynamic contour, Goldmann applanation, and noncontact tonometry BANU ONCEL,
Closed Angle Glaucoma Or Narrow Angle Glaucoma. What s is a closed angle type of glaucoma,
 Closed Angle Glaucoma Or Narrow Angle Glaucoma What s is a closed angle type of glaucoma, This is where the iris is found to be blocking the drainage of the eye through the trabecular meshwork. The eye
Closed Angle Glaucoma Or Narrow Angle Glaucoma What s is a closed angle type of glaucoma, This is where the iris is found to be blocking the drainage of the eye through the trabecular meshwork. The eye
