Cell transplantation therapy for spinal cord injury
|
|
|
- Brittney Lyons
- 6 years ago
- Views:
Transcription
1 r e v i e w Cell transplantation therapy for spinal cord injury Peggy Assinck 1,2,6, Greg J Duncan 1,3,6, Brett J Hilton 1,3,6, Jason R Plemel 4,6 & Wolfram Tetzlaff 1,3,5 Spinal cord injury can lead to severe motor, sensory and autonomic dysfunction. Currently, there is no effective treatment for the injured spinal cord. The transplantation of Schwann cells, neural stem cells or progenitor cells, olfactory ensheathing cells, oligodendrocyte precursor cells and mesenchymal stem cells has been investigated as potential therapies for spinal cord injury. However, little is known about the mechanisms through which these individual cell types promote repair and functional improvements. The five most commonly proposed mechanisms include neuroprotection, immunomodulation, axon regeneration, neuronal relay formation and myelin regeneration. A better understanding of the mechanisms whereby these cells promote functional improvements, as well as an appreciation of the obstacles in implementing these therapies and effectively modeling spinal cord injury, will be important to make cell transplantation a viable clinical option and may lead to the development of more targeted therapies. An estimated three million people live with traumatic spinal cord injury (SCI) worldwide, with ~180,000 new cases reported each year 1. Spontaneous recovery is limited, and there is still no treatment for the injured spinal cord itself. Cell transplantation has emerged as a potential strategy to promote repair following SCI. Several early phase clinical trials have been completed showing that cell transplantation is generally feasible 2,3 but the efficacy and long-term safety remain unproven. Although cell transplantation remains intensely studied, surprisingly little is known about the mechanisms through which transplanted cells promote repair and mediate functional improvements. Here we define a mechanism broadly as an interaction, either direct or indirect, between transplanted cells and host cells that affects histological or functional outcomes following SCI. These interactions can be defined at the systems, cellular and/or molecular level. Unlike drugs or implanted biomaterials, transplanted cells are capable of responding to cues provided by the injured microenvironment and altering their environmental interactions. This makes defining specific therapeutic interactions between transplanted cells and host tissue a challenge. However, mechanistic information is also often lacking because of limitations in experimental design and a lack of critical interpretation. In this review, we discuss the five most commonly proposed mechanisms through which cell transplantation is thought to promote functional benefits following SCI: neuroprotection, immunomodulation, axon sprouting and/or regeneration, neuronal relay formation, 1 International Collaboration on Repair Discoveries, University of British Columbia, Vancouver, Canada. 2 Graduate Program in Neuroscience, University of British Columbia, Vancouver, Canada. 3 Department of Zoology, University of British Columbia, Vancouver, Canada. 4 Department of Clinical Neurosciences and the Hotchkiss Brain Institute, University of Calgary, Calgary, Canada. 5 Department of Surgery, University of British Columbia, Vancouver, Canada. 6 These authors contributed equally to this work. Correspondence should be addressed to W.T. (tetzlaff@icord.org). Received 23 June 2016; accepted 22 February 2017; published online 25 April 2017; doi: /nn.4541 and myelin regeneration. We address their definitions, discuss how researchers might provide more definitive evidence that they mediate functional improvements and highlight the obstacles to making cell transplantation a viable treatment option. Historical perspective The history of cell transplantation for CNS repair has multiple origins. Jorge Francisco Tello, in the laboratory of Santiago Ramon y Cajal, transplanted pre-degenerated peripheral nerve segments onto the proximal stumps of severed optic nerves and observed retinal axons growing into these nerves 4. This was almost forgotten until experiments by Richardson, David and Aguayo demonstrated that adult spinal axons can grow long distances into peripheral nerve grafts 5. In 1975, Richard Bunge envisioned treating SCI with Schwann cells, and the pioneering work by Bunge, Bunge and Wood on in vitro cultures of Schwann cells for spinal cord repair has led to recent clinical trials 6. Transplanting neural and non-neural tissues from both embryonic and adult sources into the mammalian CNS has an equally rich history 7. The notion that fetal tissue can promote CNS repair was established by Anders Björklund and colleagues, who replaced lost cell types in models of Parkinson s and Huntington s disease 8. Transplantation of fetal spinal cord tissue into injured spinal cord resulted in successful graft survival, differentiation of transplanted cells, connectivity and host graft integration 9. Intraspinal grafting of human fetal spinal cord tissue is both feasible and safe in humans 10. Current approaches owe a great deal to these researchers, who established the capacity of transplanted cells to differentiate, promote axon growth and myelinate within the injured spinal cord. Candidate cell types Numerous cell types have been assessed for their capacity to treat SCI with transplantation. The most widely studied are Schwann cells, neural stem and progenitor cells (NSPCs), oligodendrocyte precursor cells (OPCs), olfactory ensheathing cells (OECs) and mesenchymal stem cells (MSCs) 11. Schwann cells are the myelinating glia of the nature neuroscience VOLUME 20 NUMBER 5 MAY
2 R e v i e w Table 1 Cell sources and proposed mechanisms of cited transplantation work Schwann cells: peripheral myelinating glia required for the regeneration of axons following nerve injury. Source \ Species \ Age \ Cotransplant agent Sciatic nerve \ rat \ adult \ none 101,104,132,embedded in Matrigel 61,65,67,73, intraspinal camp 25, embedded in Matrigel with OEC cotransplant and systematic chondroitinase ABC 65 Proposed mechanism Neuroprotection 61,101, axon regeneration and sprouting 25,65,67,73,101,104,132, myelination 25,65,67,101 Back skin \ rat 102 or mouse 26 \ neonatal \ none 26,102 Neuroprotection 26,102, axon regenerationand sprouting 26,102, myelination 26,102 Olfactory ensheathing cells (OEC)s: glia that support the axonal growth of olfactory receptor neurons into the olfactory bulb. Source\ Species \ Age \ Cotransplant agent Olfactory bulb \ rat 27,42,62,65,101,132 or mouse 43 \ adult \ none 27,42,43,62,101,132 embedded in Matrigel with Schwann cell cotransplant and systematic chondroitinase ABC 65 Proposed mechanism Neuroprotection 27,42,62,101, axon regeneration and sprouting 27,43,62,65,101,132 Lamina propria \ mice \ neonatal \ none 43,44 axon regeneration and sprouting 43,44 MSCs and multipotent adult progenitor cells (MAPC)s: multipotent progenitors found in tissues such as adult bone marrow isolated by virtue of their adherence during tissue culturing and/or distinct cell surface markers. Source \ Species \ Age \ Cotransplant agent Proposed mechanism Tibia or femur bone marrow \ rat \ adult \ none 30,33,56, cells overexpressing BDNF 35, camp injected into DRG to precondition neurons with intraspinal NT-3 64, or intraspinal BDNF along with BDNF overexpression in transplanted cells 71 Neuroprotection 33,35,56, immunomodulation 30,56, axon regeneration and sprouting 64,71 Iliac crest (pelvic) bone marrow 55 or MAPCs 57 \ human \ adult \ none 55,57 Neuroprotection 55,57,, immunomodulation 55,57 NSPCs: multipotent progenitors isolated from the CNS and often grown as neurospheres with the capacity to differentiate into neurons and glia. Source \ Species \ Age \ Cotransplant agent Proposed mechanism Spinal cord \ rat \ adult 30,110,115 or embryonic 39 41,63,86,87,89,113 \ none 30, cells infected with neurogenin-2 overexpressing retrovirus 115, transplanted as a graft 39 41,86,87, cells infected with D15A retrovirus which secretes a bioactive growth factor with BDNF and NT3 activities 113 or overexpressing CNTF 110, dissociated cells suspended in fibrin gel with growth factor cocktail 63,89 Brain \ mouse \ embryonic 112,117 or adult 54,111,116,139 \ none 54, cells from a shiverer mouse 116,117, exogenous FGF and/or PDGF 112, exogenous PDGF, FGF, EGF for 1 week 111 and 1 week of chondroitinase ABC 139 Neuroprotection 113, immunomodulation 30, axon regeneration and sprouting 63,87,89,115, relay formation 63 myelinogenesis 110,113 Neuroprotection 54,116,117, myelinogenesis 111,112,139, axon regeneration and sprouting 116,117 Brain \ human \ fetal 14,90 \ none 14,90, retroviral overexpression of Olig2 114 Neuroprotection 114, myelinogenesis 114 Spinal cord \ human \ fetal \ transplanted in fibrin matrix with trophic factor cocktail 63 Axon regenerating and sprouting 63, relay formation 63 Embryonic stem cell derived or inducible pluripotent stem cell (ipsc)-derived neural precursor cells: cells derived from immortalized cell lines or from adult tissues and induced into pluripotent stem cells. Cells are then differentiated into desirable cell type prior to transplantation. Source \ Species \ Age \ Cotransplant agent Proposed mechanism Stem cells \ human \ embryonic \ predifferentiated into OPCs 32,108, sorted for NSPCs and transplanted in fibrin matrix with growth factor cocktail 63 Fibroblasts \ human \ adult \ ipscs differentiated into NSPCs 121,128, with fibrin matrix and growth factor cocktail 12,68 Neuroprotection 32, immunomodulation 32 axon regeneration and sprouting 63, relay formation 63, myelinogenesis 108 Neuroprotection 128, axon regeneration and sprouting 12,68,121,128, relay formation 12,68 Peripheral blood monocytes, fetal lung fibroblasts or BMSCs predifferentiated into OPCs \ Neuroprotection 109, myelinogenesis 109 mouse \ adult or fetal \ none 109 An overview of the cell types discussed in this review with a description of tissue sources and mechanisms the original authors of the studies cited proposed as mediating either anatomical or functional improvements. Only primary articles with cell transplantations following SCI are included here. Cells were grouped first by their generic cell type and then by the anatomical source of the cells. The proposed mechanisms are limited to the major mechanisms discussed in the review: neuroprotection, immunomodulation, axonal sprouting and regeneration, relay formation, and myelination. Cotransplant agents include biomaterials transplanted with the cells, exogenous factors and genetic modifications to the cells; immunosuppressants, growth factors used during cell culturing or antigens used in cell sorting were not included. Commas between cotransplant agents indicate different experiments. Species refers to the host species the cells were harvested from. peripheral nervous system; they guide regenerating axons following peripheral nerve injury. NSPCs are multipotent progenitors, typically grown as neurospheres that can differentiate into neurons, astrocytes, oligodendrocytes and oligodendrocyte precursor cells in vitro. OECs are glia that support olfactory receptor axon growth into the olfactory bulb. MSCs are multipotent progenitors found in many tissues, including bone marrow. Cells for transplantation can be generated from adult and embryonic sources, induced pluripotent stem cells 12 and, potentially, via direct conversion technology 13. Transplanted cells often vary with respect to the species, age and source from which they are derived, as well as culture conditions and co-treatments (Table 1). Comparisons between studies, even those that focus on a particular cell type, are challenging, as the cell name (for example, NSPC or MSC) can be an umbrella term for an assortment of cells that differ due to these variables. The timing after injury and location of cell transplantation can also influence transplanted cell fate. NSPCs transplanted into host parenchyma predominantly differentiate into oligodendrocytes, while lesion-site transplantation leads to more astrocyte differentiation 14. Following transplantation, cells are hypothesized to mediate functional improvements following SCI through a variety of mechanisms, including neuroprotection, immunomodulation, axon sprouting and/or regeneration, and myelin regeneration. Mechanisms of action of transplanted cells Neuroprotection. Primary trauma to the spinal cord triggers a complex cascade of secondary damage (Fig. 1). One proposed mechanism underlying functional improvements following cell transplantation is neuroprotection: the mitigation of this secondary 638 VOLUME 20 NUMBER 5 MAY 2017 nature neuroscience
3 review a the control group. An increase in spared tissue is generally correlated with improvements in sensorimotor function in preclinical models of injury19 21 and in humans with SCI22 (Box 1). Quantification of lesion volume is also sometimes performed to assess neuroprotection but is confounded by decreasing lesion volume over time due to the ongoing shrinkage of the spinal cord, without necessarily increasing spared tissue23. Uninjured b Subacute (1 2 weeks after injury) c Chronic (6 8 weeks after injury) Axon with end bulb Growing axon Myelinating oligodendrocyte Astrocyte Oligodendrocyte myelin Reactive astrocyte + OPC or NG2 cell Schwann cell myelin Myelin debris Neuron Microglia Activated microglia or macrophages Fibroblast or stromal cell Figure 1 The pathophysiology of spinal cord injury in the absence of cell transplantation. The uninjured rat spinal cord and the contused rat spinal cord at specific stages post-sci. After SCI, cells are typically transplanted at the subacute (defined here as 1 2 weeks after injury) or chronic (defined here as beginning 6 8 weeks after injury) stages. (a) Uninjured spinal cord contains axons wrapped in myelin. OPCs, microglia and astrocytes are found throughout white and gray matter. Neuronal somata can be seen in gray matter. (b) Spinal cord contusion in rat induces a secondary injury cascade. At the subacute stage, there is considerable loss of neurons, axons, oligodendrocytes and myelin. Axons die back from the lesion site and myelin debris accumulates. Activated microglia, hematogenous macrophages and other inflammatory cells are recruited to the lesion site. Astrocytes become reactive by extending processes and proliferating and along with fibrotic cells forming a scar. OPCs and other cells also staining for the neural/glial antigen-2 (NG2+ cells) also proliferate and are recruited to the scar. (c) At the chronic stage (6 8 weeks after injury) astrocytes and other cells further thicken the scar, and in rats, a fluid-filled cavity is frequently formed at the lesion center. Activated microglia and macrophages persist within the lesion, though at reduced numbers compared to the subacute period. Some OPCs differentiate into new oligodendrocytes that produce myelin, and Schwann cells are often found myelinating axons near or in the lesion epicenter. damage to protect the tissue. Many cell types are thought to promote neuroprotection, including Schwann cells, NSPCs, MSCs, OECs and OPCs11,18 (Table 1). Neuroprotection is believed to be the underlying mechanism when there is more spared (normal-appearing) tissue adjacent to the injury site in a cell-transplanted group compared to in nature neuroscience VOLUME 20 NUMBER 5 MAY 2017 Do transplanted cells promote neuroprotection? Transplantation is likely to promote neuroprotection through different mechanisms than those classically attributed to protection, such as therapies that prevent excitotoxicity. Yet there are several caveats to studies that propose neuroprotection as a mechanism of action. First, classical neuroprotective agents that are known to reduce secondary damage are only effective within the first hours (rarely a day) after injury24, yet cell transplantation is often performed 1 2 weeks after the injury to improve graft survival11. Even at these later time points of transplantation when known mediators of secondary damage have already been released transplantation has been associated with increased tissue sparing, as evidenced by increased thickness of spared white matter surrounding the contusion epicenter In the weeks after injury, there is ongoing cellular injury and apoptosis of oligodendrocytes28; transplanted cells may rescue oligodendrocytes or prevent ongoing degeneration by unknown mechanisms. Second, many cell transplantation candidates might contribute to the appearance of increased spared white matter by producing myelin in the adjacent parenchyma on spared axons. Schwann cell myelination is particularly relevant in this regard, as it requires more space than oligodendrocyte myelin and might enlarge the cross-sectional area of white matter tracts29. Third, cell transplantation could enhance axon regeneration and sprouting, followed by myelination in the parenchyma surrounding the injury site. If there are more myelinated axons or regenerated fibers, this could in itself increase the cross-sectional area adjacent to the injury site. Thus, an increase in spared tissue adjacent to the injury site might reflect bona fide protection, a regenerative response that increases the amount of white matter adjacent to the injury site or a combination of both. Molecules secreted by transplanted cells. One widely proposed mechanism underlying neuroprotection mediated by transplanted cells is the secretion of bioactive molecules such as trophic factors and cytokines. Many cell types, including MSCs, NSPCs and Schwann cells, have the capacity to secrete trophic factors and cytokines in vitro or to increase the presence of these factors after transplantation These factors may potentially enhance host cell survival, regulate gliosis, modulate inflammation and/or improve the regeneration of blood vessels. However, the increase in these factors and their neuroprotective properties is, for the most part, correlative. There are few studies which systemically employ cell-type specific deletion to investigate which cell-derived factor(s) is (are) necessary for neuroprotection. These studies require the transplantation of cells that are modified and diminished in their capacity to express/secrete specific factors35. For example, the neuroprotective effects of transplanted MSCs from bone marrow (BMSCs) after SCI are reduced when secretion of brainderived neurotrophic factor (BDNF) is impaired35. However, BDNF knockdown also reduces BMSC survival, leaving it unclear whether the reduction of spared tissue is a result of diminished BDNF secretion directly or whether it is secondary to some other BMSC-mediated neuroprotective effect that hinges on cell survival. Moving forward, it will be important to understand the secretome of transplanted cells and to use factor specific loss-of-function experiments while 639
4 R e v i e w Box 1 What is functional recovery in spinal cord injury? Recovery is defined in the Oxford English Dictionary as a return to a normal state of health, mind, or strength. In most animal models of SCI there are significant spontaneous improvements. For example, after the commonly used moderate thoracic contusion, there is initially flaccid paralysis of the hindlimbs, but within weeks animals regain weight-supported stepping. However, recovery to a normal state, comparable to an uninjured animal, is not seen. As a field, SCI researchers use the term functional recovery to refer to a statistically significant functional improvement in a treatment group versus control, although true recovery as such is rarely observed. Hence, we should avoid using this general term and refer to specific improvements. Importantly, since no effective treatment for SCI has been translated, it is unclear what degree of functional improvement in preclinical animal models is clinically relevant. Although we focus on motor improvements, treatment can also promote sensory or autonomic functional improvement, which can be more highly prioritized by those with injury 133. promoting survival of the cells by other means to determine whether these factors are beneficial after transplantation. Preventing blood vessel loss or improving angiogenesis. There is widespread blood vessel loss after SCI, which induces local hypoxia within and adjacent to the injury site 36,37. The proliferation of endothelial cells, or angiogenesis, occurs as early as 3 d and stops by 10 d after SCI, but only after 14 d does vessel perfusion recover to baseline levels 38. Restoration of oxygen and nutrients within spared tissue is rarely discussed but might be a general mechanism by which transplanted cells influence outcome. Transplant-derived secreted molecules might promote blood vessel protection and regeneration. Fetal tissue grafts re-establish oxygen levels within the graft and adjacent to the injury site 39, which is correlated with elevated blood vessel density in and around the transplant site 40. Fetal tissue grafts also elevate glucose utilization, suggesting an overall increase in metabolism compared to SCI injured controls 41. Transplanted OECs increase vasculature within the graft and align vasculature along the length of the spinal cord 42 44, but whether they, or any other transplanted cell type, accelerate tissue reoxygenation and nutrient access after injury is unknown. The use of in vivo live imaging techniques with vital dyes or genetically encoded fluorescence resonance energy transfer (FRET) sensors to measure dynamic changes in tissue oxygen 45, glucose 46 and/or other tissue metabolites 37, coupled with injury and transplantation, will improve our understanding of the dynamic metabolic changes after SCI and how transplantation might regulate these processes. In these investigations of tissue oxidation and metabolites, large animal models such as pigs may be of use, since they permit the placement of dialysis probes or pressure sensors into the spinal cord 37. Immunomodulation. Many repair mechanisms rely on beneficial aspects of inflammation 47 49, yet certain aspects of inflammation cause damage to spared tissue. The complex nature of inflammation is best exemplified by the phenotypic separation of macrophages and potentially microglia into neurotoxic, proinflammatory M1 and immunoregulatory M2 subsets, the latter of which secretes factors that promote axon growth 50,51 and enhance remyelination 52. While the M1 or M2 designation reflects an oversimplification and there are other macrophage activation states 53, they are yet to be described in vivo after SCI 50. Cell transplantation can provide benefits through immunomodulation, by attenuating detrimental inflammation or stimulating beneficial inflammation. Whether transplanted cells directly alter inflammation is confounded by putative neuroprotective mechanisms; transplanted cells might alter inflammation indirectly by dampening tissue damage. Still, few studies dissect the direct interactions between transplanted cells and immune cells; instead, they measure global changes in cytokine release or the abundance of immune cells after SCI 11. These findings are, thus, correlative. For example, NSPC transplantation improves ankle movement and hindlimb placement in association with a slight increase in the abundance of T cells, a decrease in B cells and reduced M1-like macrophages following SCI 54. NSPCs express and secrete many factors that could regulate inflammation, yet demonstrating a causal role would require transplanting cells with specific genetic modifications of candidate genes of interest. MSCs can also modify the immune response after injury by elevating levels of anti-inflammatory and reducing levels of proinflammatory cytokines when transplanted 3 or 7 d after SCI 55,56. Intraspinal transplantation of MSCs 1 week after SCI is associated with a polarization of macrophages toward an M2 phenotype and away from an M1 phenotype, which is correlated with increased spared white matter 55. Despite a lack of cell entry into the spinal cord, intravenous delivery of MSCs 1 d after contusive SCI is associated with increased forelimb hindlimb coordination and improved micturition, which correlates with increased spared tissue and an elevation in M2 markers 57. There is also decreased proinflammatory cytokine production in the spleen and blood, indicating a systemic change in the inflammatory state. Importantly, there is no need for neural integration of MSCs: conditioned medium from MSCs can improve motor function after SCI, suggesting that cell transplantation may not be required to achieve functional benefits 31. Axon regeneration and/or sprouting. The primary cause of sustained dysfunction following SCI is the disruption of functional connections in the CNS. As such, a major goal is to promote axon regeneration and plasticity. Major impediments to axon growth following SCI include the formation of a scar around the injury site 58, CNS myelin 59 and the diminished growth capacity of adult mammalian central neurons, particularly after axotomy 60. In humans, in addition to the formation of a scar around the injury site, SCI sites can contain cavities filled with extracellular fluid that lack a substrate for axon growth, but most such sites also harbor tissue septae that can serve as a bridge and might be important as a site of attachment for transplanted cell integration and axon growth 16. Bridge formation. The most well-established mechanism through which cell transplantation can promote axon growth is through the formation of bridges across the lesion site (Fig. 2a). We define a bridge as a multicellular structure comprised of transplanted cells that crosses the lesion site (rostrally to caudally) and provides a substrate onto which axons can grow. Transplanted-cell-secreted molecules, such as laminin, also provide a substrate for axon growth. Evidence that cellular bridging leads to axon regeneration is typically an association of host axons with transplanted cells within the bridge following a complete transection SCI that cuts all descending and ascending axons at the level of injury. Schwann cells 61, OECs 62, NSPCs 63 and MSCs 64 can form bridges following SCI leading to axon regeneration, which can generally be accentuated by combining cells with biomaterials 63,65,66 or trophic factors 6,63. However, stimulating large numbers of axons to exit these bridges at the distal interface remains a challenge VOLUME 20 NUMBER 5 MAY 2017 nature neuroscience
5 r e v i e w Heterogeneity of axon growth. There is significant heterogeneity in the capacity of different axon populations to grow onto bridges. While there are many documented cases of brainstem, propriospinal and sensory ascending axons on bridges of various sources, there are limited examples of robust corticospinal regeneration onto a transplanted cell bridge 68. To date, the most robust corticospinal axon regeneration observed is onto NSPCs suspended in fibrin with growth factors 63,68. Understanding this heterogeneity is essential given the importance of corticospinal function in humans 69. It appears that this capacity relates to two factors primarily. First, the ability of axons to grow onto bridges correlates with their intrinsic growth capacity (with sensory neurons having arguably the highest and corticospinal neurons the lowest) 70 and can be accentuated by the application of treatments that heighten growth potential 25,63,64,71. Second, the homotypic nature of the graft that is, its similarity to the axons original substrate may be an important factor. Robust corticospinal regeneration onto NSPCs only occurs when the cells are derived from or driven toward a caudal neural fate, similar to what is observed in the spinal cord, where corticospinal axons normally project. When derived from telencephalon, NSPCs are incapable of supporting corticospinal regeneration 68. Deciphering molecular differences underlying this may detail the factor(s) necessary to induce corticospinal regeneration, opening up the possibility of enhancing corticospinal regeneration onto cell types of other origin or without the need for transplantation. Modification of the glial scar. An additional mechanism through which cell transplantation is thought to promote axon growth is by modifying the astrocyte response to injury. Glial fibrillary acidic protein (GFAP)-positive reactive astrocytes in proximity to SCI lesion sites can be an unfavorable substrate for axon growth and can secrete growth-inhibitory molecules 58. The age-dependent decline in axon regeneration in the adult mammalian CNS is accompanied by increased GFAP immunoreactivity in the vicinity of lesions 72. There is evidence that cell transplantation can modify astrogliosis in a way that promotes axon regeneration. Following Schwann cell transplantation along with Matrigel, regenerating axons can be found in direct association with GFAP-positive astrocyte processes that elongate in association with transplanted Schwann cell processes 73. Regenerating axons grow within a basal lamina tunnel alongside transplanted cells and GFAP-positive astrocyte processes, and the extent of axon regeneration correlates with the number of astrocyte processes found within the bridge 73. Therefore, it is likely that these astrocytes are in part mediating the regeneration observed. In some cases of transplantation following SCI, a modification of astrogliosis following cell transplantation is observed based on a change in GFAP immunoreactivity 26,68, yet it is unclear if this promotes axon growth. Reactive astrocytes help restrict secondary damage by forming a compact scar protecting outside tissue from a non-neural lesion core comprised of inflammatory cells and fibroblasts 58,74,75. Preventing astrocyte scar formation does not promote axon regeneration following SCI 74. Instead, it results in fewer axons present in the vicinity of the lesion site 76. A diverse mix of factors modifies reactive gliosis following CNS injury 74. While some of these molecules may be expressed by transplanted cells 77, no transplanted cell has been specifically demonstrated to secrete factors that regulate astrogliosis in loss-of-function experiments. Given that a common transplantation site is the non-neural lesion core, there are likely many interactions between transplanted cells and lesion cells that will be important to identify to establish the mechanisms through which cell transplantation promotes axon growth and to consider transplantation a rational option to safely modify astrogliosis. a b Bridge formation Relay formation Axon Axon with endbulb Regenerating axon Regenerated and synapsed axon Host neuron Transplant-derived bridging cell Transplant-derived neuron Regenerated and synapsed transplant-derived axon Figure 2 Repair of neuronal connectivity following SCI after cell transplantation. Cell transplantation may promote the repair of neuronal connectivity through the formation of a bridge or relay. (a) Transplanted cells, such as Schwann cells, can support axon growth by providing a bridge across the injury site. Axons, which frequently have a tortuous appearance in the bridge, are often unable to re-enter host tissue. (b) Transplanted cells may improve the connectivity through the formation of a relay. Such relays occur when host axons synapse onto transplant-derived neurons, which harbor a capacity to extend axons long distances from the injury and synapse with host neurons. Caveats to axon growth assessments. Although enhancing axon growth is considered one primary objective of cell transplantation strategies following SCI, there are significant challenges to interpreting these data. Some compensatory axonal plasticity occurs after SCI in the absence of treatment 78. If cell transplantation protects against axonal degeneration, it might be associated with a higher axon density without actually promoting de novo axon growth. In the context of bridge formation in incomplete models of SCI such as contusions, a direct physical interaction between host axons and transplanted cells might arise without representing axon growth. The term axon regeneration has historically been ambiguous, but a growing consensus has defined the term to mean regrowth of a transected axon 70. In contusion SCI models, wherein transplantation studies often occur, there is typically considerable tissue sparing, leaving ambiguity as to what extent axons have been severed. The development of injury models that completely cut a projecting system of axons 70,79 and clearing technologies that permit 3-dimensional reconstruction of tissue 80 will aid interpretation in this regard. Axon growth: not always functionally beneficial. It is important to realize that axon growth is not always associated with improved function. Overexpression of Sox11 in corticospinal neurons promotes nature neuroscience VOLUME 20 NUMBER 5 MAY
6 R e v i e w axon regeneration but impairs forelimb function on pellet reaching and horizontal ladder tasks 81. OEC transplantation into complete transection SCI sites promotes axon regeneration and reconnection of descending pathways across the lesion site as evidenced electrophysiologically 62. The combination of this transplantation with step training to facilitate the reorganization of regenerating axons into functional circuits and with quipazine, a 5-HT 2A (serotonin) agonist that activates lumbosacral locomotor networks, results in increased frequency of plantar stepping in some rats. However, in other rats, retransection of the spinal cord to interrupt regenerating axons is associated with rats making significantly more plantar steps, providing evidence that regeneration actually suppressed this function 62. This highlights the complexity of directing functional improvement, which may require activity-based approaches to consolidate axons into mature networks 82. Indeed, little is known about how regenerating axons can be directed toward forming functional synapses with target neurons, given that robust axon regeneration remains a formidable challenge. It will be important to assess causal roles for specific populations of axons in recovery. Traditionally, it has not been possible to distinguish such causality and merely correlative evidence has been presented. However, with the development of reversible neuronal silencing technologies, it is now possible for researchers to assess the extent to which specific neuronal populations are incorporated into functional circuits underlying functional changes 83,84. Neuronal relays. An alternative approach to reconnecting segments following SCI is through the formation of neuronal relays. When transplanted cells are capable of neuronal differentiation, survival, axon outgrowth and synapse formation with host neurons, a relay circuit can form between descending axons and newly differentiated transplanted neurons (Fig. 2b). Early studies demonstrated that axons could project into and arise from embryonic day 14 rat spinal cord tissue grafts following their transplantation into spinal cord cavities Human neuroblasts implanted into lesioned adult striatum can extend axons along myelinated fiber tracts for distances up to 20 mm 88. NSPCs can differentiate into neurons with a capacity for relay formation 63. In the latter study 63 cells were embedded within a fibrin matrix to aid in their retention within a complete transection site and included a cocktail of (initially) 10 trophic factors (four were used in later studies) plus a protease inhibitor to support cell survival and vascular ingrowth. When grafting was implemented 2 weeks after complete transection, host axons synapsed onto newly differentiated neurons, which extended large numbers of axons long distances rostral or caudal to injury. This approach resulted in significant hindlimb functional improvement: grafted rats had movement about each joint of the hindlimb, in contrast to minimalto-no movement in controls, and this was abolished following retransection at the rostral graft host interface. Translational concerns. One concern with transplantation of NSPCs is the migration of cells to other areas of the CNS, where they can form ectopic colonies that might trigger abnormal activity and/or compress tissue 89. Following thoracic SCI, human NSPCs transplanted into the spared parenchyma proliferate and migrate several millimeters toward and away from the injury epicenter 90. To limit migration, cells can be embedded in a fibrin matrix that stabilizes them within the lesion. One possibility is that ectopic colony formation relies on inconsistent gelation of this matrix, although this remains to be tested. It will be important to establish the efficacy of this fibrin-matrix approach in more clinically relevant models of injury, given that complete transections rarely occur in humans. An additional translational concern is OPC/NG2 + Transplant-derived OPC/NG2 + Oligodendrocyte myelin Schwann cell myelin Myelinating cell transplantation Myelinating host oligodendrocyte Myelinating transplantderived oligodendrocyte Transplant-derived oligodendrocyte myelin Figure 3 Regeneration of oligodendrocyte-derived myelin with cell transplantation. Transplanting precursors of myelinating glia can result in the formation of new myelin sheaths. Transplanted OPCs or NSPCs compete with endogenous OPCs to remyelinate axons. the administration of trophic factors that, while necessary for graft survival, can instigate sensory dysfunction 91. Still, while these possible complications need to be addressed, the principle of using NSPCs as relays may provide a new means to promote repair and opens up an exciting avenue to study mechanisms underlying axon growth in the injured CNS environment. Myelin regeneration. Loss of myelin is observed early after SCI in both rodents 92,93 and humans 16,22. Concurrent with myelin loss, oligodendrocyte apoptosis occurs for weeks after contusive SCI in rodents, nonhuman primates and humans 28,94. Demyelination impairs conduction and severs an important metabolic shuttle between oligodendrocytes and axons 95,96. Replacing lost oligodendrocytes and myelin improves conduction 97,98 and may protect axons from degeneration. Myelin regeneration, the process by which transplanted cells produce myelin around axons that have lost their myelin sheaths, has been targeted as a mechanism to enhance recovery following SCI (Fig. 3). Myelin regeneration following cell transplantation. Transplantation of Schwann cells, OPCs or NSPCs capable of producing oligodendrocytes can be used to enhance myelin regeneration after SCI 11,99,100. Transplanting Schwann cells in the acute or subacute setting after rodent thoracic SCI increases the number of axons with peripheral myelin and is often correlated with modest improvements in forelimb hindlimb coordination during open field testing 26,101. Transplanted Schwann cells can myelinate axons 25,26,65,67,102 and enhance endogenous Schwann cell myelination 102,103. However, attributing any improvement in function to myelination by Schwann cells is confounded by their propensity to enhance axon growth 25,26,65,67,73,101,102,104 (Table 1). There is also uncertainty about whether peripheral myelin found within the spinal cord following transplantation forms around demyelinated spared axons or if this represents myelination of newly grown axons. Therefore, it is not known to what extent spared axons are remyelinated by transplanted Schwann cells, nor is the contribution of this myelin to functional improvements proven. Ascending or descending axons should be traced in combination with Schwann cell transplantation to examine their contribution to remyelination of spared axons. Transplantation of Schwann cells incapable of producing 642 VOLUME 20 NUMBER 5 MAY 2017 nature neuroscience
7 r e v i e w Box 2 Is remyelination an optimal target for cell transplantation after SCI? The capacity of transplanted cells to myelinate is the rationale for several human trials. However, considerable debate remains regarding the capacity of endogenous OPCs to effectively myelinate denuded axons following SCI and whether demyelinated axons persist long after injury 92,93,100,107,134. In animal models, there are reports of demyelinated axons persisting for months after injury 93,135,136. However, these studies examined cross sections where it is difficult to differentiate between severed axons that persist near the lesion without myelin and axons that were spared but have become demyelinated. Tracing spared axons through the lesion found no evidence that a population of intact, chronically demyelinated axons remains following SCI, suggesting that endogenous myelin regeneration is highly efficient in rodents 92,107. The persistence of chronically demyelinated axons after human SCI has only been examined in a handful of studies, in which it is generally noted that few demyelinated axons persist 16,22,137 except in cases of persistent cord compression, which may result in ongoing demyelination 137,138. This raises questions regarding whether myelin regeneration is even a plausible therapeutic strategy at later timepoints after injury. No study which observes improved motor function 132,139 following transplantation of chronically myelinating cells has demonstrated an enhanced total number of remyelinated fibers in the spinal cord. Functional benefits in these studies could be the result of enhanced axon growth and/or sparing, which are also observed 132,139. Thus, transplantation of cells to myelinate seems premature as it is unclear whether myelin regeneration is a proven target 100. myelin, such as cells derived from trembler (Pmp22 Tr ) mutant mice 105, may be useful in establishing a causal relationship between myelin regeneration and functional improvements. Extensive endogenous remyelination occurs following contusive injuries in rodents 106,107, and thus remyelination as a therapeutic approach after SCI is contentious (Box 2). Transplanted OPCs or NSPCs are likely to compete with endogenous remyelinating cells for denuded axons. Several studies have found an increase in the number of myelinated axons at endpoint, which is suggestive of enhanced remyelination and is correlated with improved forelimb hindlimb coordination or enhanced frequency of plantar stepping 111. However, the differentiation of transplanted cells into oligodendrocytes does not always result in improved motor recovery, particularly if the level of remyelination is not sufficient to promote an overall increase in the number of myelinated fibers 112. Transplanted cells engineered to overexpress trophic factors 110,113 or transcription factors 114,115 enhance oligodendrogenesis 110, and functional improvements compared to naive cells. Improving the differentiation of transplanted cells to oligodendrocytes with exogenous factors or genetic modification may be necessary to increase remyelination over the level attained by host precursors. Given the efficacy of endogenous remyelination, it is possible that enhancing this process may promote functional improvements without the need for cell transplantation (Box 3). Is remyelination by transplanted cells causally related to functional improvements? Recent studies have tested whether myelination by transplanted cells is required for functional improvement. NSPCs derived from shiverer (Mbp shi ) mice were transplanted after SCI 116,117. Shiverer mice are capable of producing oligodendrocytes but are incapable of compact myelin formation 118. In contrast to wildtype cells, transplanted shiverer-derived NSPCs fail to promote functional improvements after SCI 116,117, implying that transplanted cells must generate compact myelin to promote functional improvements. However, shiverer oligodendrocytes are capable of ensheathing axons , and it is possible that these cells displaced endogenous cells which would otherwise have remyelinated demyelinated axons. The total number of remyelinated axons was not quantified after shiverer NSPC transplantation, and it remains unclear whether endogenous remyelination was affected in these studies. Thus, caution is warranted when interpreting these results and concluding that improved myelin regeneration is required for transplanted cells to promote recovery. Conditionally depleting specific cell types, such as myelinating oligodendrocytes, within the transplanted cell population 119 or removing a critical factor essential for myelinogenesis and axon ensheathment from transplanted cells will complement the shiverer studies above and help elucidate the role of remyelination specifically in recovery associated with cell transplantation. Future perspectives In addition to enhancing our mechanistic understanding of repair by transplanted cells, there should be additional efforts to: 1. Improve risk assessments. Each transplantation candidate carries specific risks during translation that are often poorly understood 115. Options for risk assessment include transplantation into large animals that live longer than rodents and allowing long-term assessments of the tumorigenic potential of human cells that may not thrive in a rodent microenvironment 120. Tumor formation is a major risk, particularly in cases where cells are derived from a pluripotent stage 121. Another risk of transplantation is increasing the likelihood of infections. With injuries at T3 or above, there is a large systemic decrease of immune function, termed CNS injuryinduced immune deficiency syndrome (CIDS) 122,123. The use of immunosuppressants might further weaken immune function and should be tested thoroughly to ensure that an increased risk of infection is not observed 124. There might be an upside of CIDS, as such patients may be less likely to reject allogeneic transplants. Box 3 Can we stimulate the endogenous cellular response after SCI in lieu of transplantation? Stimulating the endogenous cellular response to injury could be a strategy to improve outcomes without the use of exogenous cells. Neural/glial antigen 2 (NG2) expressing OPCs are the major proliferating cell type after SCI and are the primary producer of new oligodendrocytes 106, Growth factor and ferritin treatments increase OPC proliferation and stimulate oligodendrogenesis 144,145. The scar is also produced by highly proliferative astrocytes 143, type A pericytes 146, ependymal cells 143,147,148 and perivascular collagen1α1 cells 149. Some inflammatory cells facilitate endogenous repair processes, including axon regeneration, sprouting and myelin regeneration 49,51,52. There is also evidence that cell transplantation can affect endogenous responses. Schwann cell transplantation into the injured spinal cord can increase the number of endogenous Schwann cells 26,104, although the value of this is yet to be determined. Understanding how exogenous cells modify the host endogenous cell response might enable us to target the endogenous cell response to injury in a way that avoids the need for cell transplantation, with its associated risks of invasiveness, immunosuppression and the possibility of tumor formation. nature neuroscience VOLUME 20 NUMBER 5 MAY
8 R e v i e w 2. Align preclinical models more closely with the clinical situation. The majority of preclinical data is based on mild to moderately severe thoracic contusion injury models, and these are not severe enough to justify clinical translation with cell transplantation 125. Functionally incomplete thoracic injuries occur infrequently in humans (approximately 5% of cases in Canada) 126. Over 60% of human SCIs occur in cervical spinal segments, and many lead to complete or severe incomplete loss of sensorimotor function 126. Patients with cervical injuries are expected to benefit the most from cell therapies, as regaining two segments of function could mean regaining independence and greatly improved quality of life 127. In addition, many studies have been undertaken in immunodeficient animals that have vastly different immune responses to SCI 128. Such alterations of the immune system can overcome rejection of transplanted cells and may better reveal the tumorigenic potential of a human cell in a rodent. However, these immunodeficient models may not accurately model the human situation. 3. Assess efficacy in the chronic stage of injury. Most preclinical transplantation studies have been performed ~1 2 weeks after injury 129. While this has guided several clinical trials, a later transplantation time point will help reduce the number of subjects required for a clinical trial since their outcome trajectory is more predictable 130. However, the SCI microenvironment changes drastically from the acute to the chronic setting, and this can affect cell survival and differentiation 131. Unfortunately, few preclinical studies have been performed with treatment initiation at 2 months after injury, and those that have been conducted at the time this paper was written demonstrate marginal or no functional benefits 14,108,111,132. Despite this, trials in humans with chronic injuries have been approved and initiated ( Conclusion Despite efforts to match preclinical models to human SCI, no amount of preclinical animal investigation can guarantee the safety and success of a cell treatment in human trials. The validity of preclinical SCI animal models remains unproven until a treatment is successfully translated, and only a human trial (albeit experimental in nature) will provide necessary data on the efficacy and safety of cells. Still, researchers should do what is possible to improve therapeutic effect sizes, and thus the likelihood of success, and to minimize the risks before taking a cell-transplantation approach to trial. With several clinical trials ongoing, cell transplantation for spinal cord repair remains an important avenue for further research. To date, causal relationships between functional improvements and particular mechanisms have rarely been established. Usually, only correlative evidence is provided, and the effect sizes are modest. Unfortunately, this is enough to fuel stem-cell tourism with unproven cell treatments in clinics worldwide. Still, while few studies have demonstrated which interactions between transplanted cells and host tissue mediate functional benefits, thanks to technological advances, there has never been a better time to investigate this. By more accurately modeling human SCI and through rigorous interpretation, the field can further advance cell transplantation strategies for spinal cord repair. Acknowledgments P.A. received a Canadian Institute for Health Research (CIHR) Frederick Banting and Charles Best Canadian Graduate Scholarship Doctoral Award and the CIHR Transplantation Training Program Award. G.J.D. was supported by a Multiple Sclerosis Society of Canada Doctoral Scholarship and the CIHR Transplantation Training Program Award. B.J.H. holds a CIHR Frederick Banting and Charles Best Canadian Graduate Scholarship Doctoral Award, a Zoology Graduate Fellowship and a CIHR Transplantation Training Program Award. J.R.P. is supported by the Donna Joan Oxford Postdoctoral Fellowship Award from the Multiple Sclerosis Society of Canada and by postdoctoral fellowship awards from CIHR, Alberta Innovates Health Solutions and T. Chen Fong. W.T. receives support from the John and Penny Ryan British Columbia Leadership Chair in Spinal Cord Research and from CIHR FRN COMPETING FINANCIAL INTERESTS The authors declare no competing financial interests. Reprints and permissions information is available online at reprints/index.html. 1. Lee, B.B., Cripps, R.A., Fitzharris, M. & Wing, P.C. The global map for traumatic spinal cord injury epidemiology: update 2011, global incidence rate. Spinal Cord 52, (2014). 2. Mackay-Sim, A. & St John, J.A. Olfactory ensheathing cells from the nose: clinical application in human spinal cord injuries. Exp. Neurol. 229, (2011). 3. Saberi, H. et al. Safety of intramedullary Schwann cell transplantation for postrehabilitation spinal cord injuries: 2-year follow-up of 33 cases. J. Neurosurg. Spine 15, (2011). 4. Ramón y Cajal, S., DeFelipe, J. & Jones, E.G. Cajal s Degeneration and Regeneration of the Nervous System (Oxford Univ. Press, 1991). 5. David, S. & Aguayo, A.J. Axonal elongation into peripheral nervous system bridges after central nervous system injury in adult rats. Science 214, (1981). 6. Bunge, M.B. Efficacy of Schwann Cell (SC) transplantation for spinal cord repair is improved with combinatorial strategies. J. Physiol. (Lond.) 594, (2016). 7. Das, G.D. Neural transplantation: an historical perspective. Neurosci. Biobehav. Rev. 14, (1990). 8. Björklund, A. & Lindvall, O. Cell replacement therapies for central nervous system disorders. Nat. Neurosci. 3, (2000). 9. Bregman, B.S. et al. Recovery of function after spinal cord injury: mechanisms underlying transplant-mediated recovery of function differ after spinal cord injury in newborn and adult rats. Exp. Neurol. 123, 3 16 (1993). 10. Wirth, E.D. III et al. Feasibility and safety of neural tissue transplantation in patients with syringomyelia. J. Neurotrauma 18, (2001). 11. Tetzlaff, W. et al. A systematic review of cellular transplantation therapies for spinal cord injury. J. Neurotrauma 28, (2011). 12. Lu, P. et al. Long-distance axonal growth from human induced pluripotent stem cells after spinal cord injury. Neuron 83, (2014). 13. Yang, N. et al. Generation of oligodendroglial cells by direct lineage conversion. Nat. Biotechnol. 31, (2013). 14. Piltti, K.M., Salazar, D.L., Uchida, N., Cummings, B.J. & Anderson, A.J. Safety of epicenter versus intact parenchyma as a transplantation site for human neural stem cells for spinal cord injury therapy. Stem Cells Transl. Med. 2, (2013). 15. Kwon, B.K., Tetzlaff, W., Grauer, J.N., Beiner, J. & Vaccaro, A.R. Pathophysiology and pharmacologic treatment of acute spinal cord injury. Spine J. 4, (2004). 16. Norenberg, M.D., Smith, J. & Marcillo, A. The pathology of human spinal cord injury: defining the problems. J. Neurotrauma 21, (2004). 17. Oyinbo, C.A. Secondary injury mechanisms in traumatic spinal cord injury: a nugget of this multiply cascade. Acta Neurobiol. Exp. (Warsz.) 71, (2011). 18. Raisman, G. Olfactory ensheathing cells - another miracle cure for spinal cord injury? Nat. Rev. Neurosci. 2, (2001). 19. Plemel, J.R. et al. A graded forceps crush spinal cord injury model in mice. J. Neurotrauma 25, (2008). 20. Basso, D.M., Beattie, M.S. & Bresnahan, J.C. Graded histological and locomotor outcomes after spinal cord contusion using the NYU weight-drop device versus transection. Exp. Neurol. 139, (1996). 21. Schucht, P., Raineteau, O., Schwab, M.E. & Fouad, K. Anatomical correlates of locomotor recovery following dorsal and ventral lesions of the rat spinal cord. Exp. Neurol. 176, (2002). 22. Kakulas, B.A. Neuropathology: the foundation for new treatments in spinal cord injury. Spinal Cord 42, (2004). 23. Rabchevsky, A.G., Fugaccia, I., Sullivan, P.G., Blades, D.A. & Scheff, S.W. Efficacy of methylprednisolone therapy for the injured rat spinal cord. J. Neurosci. Res. 68, 7 18 (2002). 24. Kwon, B.K. et al. A systematic review of non-invasive pharmacologic neuroprotective treatments for acute spinal cord injury. J. Neurotrauma 28, (2011). 25. Pearse, D.D. et al. camp and Schwann cells promote axonal growth and functional recovery after spinal cord injury. Nat. Med. 10, (2004). 26. Biernaskie, J. et al. Skin-derived precursors generate myelinating Schwann cells that promote remyelination and functional recovery after contusion spinal cord injury. J. Neurosci. 27, (2007). 27. Barbour, H.R., Plant, C.D., Harvey, A.R. & Plant, G.W. Tissue sparing, behavioral recovery, supraspinal axonal sparing/regeneration following sub-acute glial transplantation in a model of spinal cord contusion. BMC Neurosci. 14, 106 (2013). 644 VOLUME 20 NUMBER 5 MAY 2017 nature neuroscience
regenerative medicine in the brain and the spinal cord spinal cord injuries
 regenerative medicine in the brain and the spinal cord spinal cord injuries primary and secondary events during SCI traumatic spinal cord injury (SCI) traumatic spinal cord injury (SCI) main goal is to
regenerative medicine in the brain and the spinal cord spinal cord injuries primary and secondary events during SCI traumatic spinal cord injury (SCI) traumatic spinal cord injury (SCI) main goal is to
Olfactory ensheathing glia
 Olfactory ensheathing glia From Wikipedia, the free encyclopedia Neuroglia of the brain shown by Golgi's method. Olfactory ensheathing glia (OEG), also known as olfactory ensheathing cells (OECs) or olfactory
Olfactory ensheathing glia From Wikipedia, the free encyclopedia Neuroglia of the brain shown by Golgi's method. Olfactory ensheathing glia (OEG), also known as olfactory ensheathing cells (OECs) or olfactory
Symptoms of spinal cord injury:
 Symptoms of spinal cord injury: involuntary muscle spasms loss of voluntary movement sensation, balance control of breathing autonomic functions (blood pressure) bladder, sexual, bowel control All due
Symptoms of spinal cord injury: involuntary muscle spasms loss of voluntary movement sensation, balance control of breathing autonomic functions (blood pressure) bladder, sexual, bowel control All due
Adult Nervous System
 Adult Nervous System What is the capacity of the PNS and CNS for repair? WHY? Why discuss this now? Potential for repair depends on cellular properties of nerve and glial cells. http://neuroscience.uth.tmc.edu/s1/chapter09.html
Adult Nervous System What is the capacity of the PNS and CNS for repair? WHY? Why discuss this now? Potential for repair depends on cellular properties of nerve and glial cells. http://neuroscience.uth.tmc.edu/s1/chapter09.html
New Approaches to Repair of Spinal Cord Injury
 New Approaches to Repair of Spinal Cord Injury 1 WHY IS THE SPINAL CORD SO VULNERABLE? Peripheral Nerve Spinal Cord Schwann Cell Myelin DRG Neuron Oligodendrocyte Myelin Collagen Axon 2 3 WHY IS THE SPINAL
New Approaches to Repair of Spinal Cord Injury 1 WHY IS THE SPINAL CORD SO VULNERABLE? Peripheral Nerve Spinal Cord Schwann Cell Myelin DRG Neuron Oligodendrocyte Myelin Collagen Axon 2 3 WHY IS THE SPINAL
Brain Development III
 Brain Development III Neural Development In the developing nervous system there must be: 1. The formation of different regions of the brain. 2. The ability of a neuron to differentiate. 3. The ability
Brain Development III Neural Development In the developing nervous system there must be: 1. The formation of different regions of the brain. 2. The ability of a neuron to differentiate. 3. The ability
Cells of the nervous system
 Neurobiology Cells of the nervous system Anthony Heape 2011 1 Cells of the nervous system Neuroglia : part 2 The non excitable cells of the nervous system that provide support to neuronal survival and
Neurobiology Cells of the nervous system Anthony Heape 2011 1 Cells of the nervous system Neuroglia : part 2 The non excitable cells of the nervous system that provide support to neuronal survival and
Is Spinal Cord Repair a Reality? Schwann Cell Transplantation for Subacute Spinal Cord Injury
 Is Spinal Cord Repair a Reality? Schwann Cell Transplantation for Subacute Spinal Cord Injury James Guest MD, PhD, FACS Clinical Professor of Neurological Surgery, Neurosurgery and the Miami Project to
Is Spinal Cord Repair a Reality? Schwann Cell Transplantation for Subacute Spinal Cord Injury James Guest MD, PhD, FACS Clinical Professor of Neurological Surgery, Neurosurgery and the Miami Project to
BioMed Central. Jeannette E Davies*, Christoph Pröschel, Ningzhe Zhang, Mark Noble, Margot Mayer-Pröschel and Stephen JA Davies* Research article
 BioMed Central Open Access Research article Transplanted astrocytes derived from BMP- or CNTF-treated glialrestricted precursors have opposite effects on recovery and allodynia after spinal cord injury
BioMed Central Open Access Research article Transplanted astrocytes derived from BMP- or CNTF-treated glialrestricted precursors have opposite effects on recovery and allodynia after spinal cord injury
Helen R Barbour 2, Christine D Plant 1, Alan R Harvey 3 and Giles W Plant 1,2*
 Barbour et al. BMC Neuroscience 2013, 14:106 RESEARCH ARTICLE Open Access Tissue sparing, behavioral recovery, supraspinal axonal sparing/regeneration following sub-acute glial transplantation in a model
Barbour et al. BMC Neuroscience 2013, 14:106 RESEARCH ARTICLE Open Access Tissue sparing, behavioral recovery, supraspinal axonal sparing/regeneration following sub-acute glial transplantation in a model
Nerve tissue & the Nervous System
 Nerve tissue & the Nervous System The human nervous system, by far the most complex system in the body, is formed by a network of many billion nerve cells (neurons), all assisted by many more supporting
Nerve tissue & the Nervous System The human nervous system, by far the most complex system in the body, is formed by a network of many billion nerve cells (neurons), all assisted by many more supporting
Axon Guidance. Matthew Blewitt
 Axon Guidance Matthew Blewitt Overview Axonal development PNS regeneration CNS regeneration Future directions Brain Repair Axonal Development Neurite growth cone www.anatomy.unimelb.edu.au http://kalil.anatomy.wisc.edu/articles/kalil_dent_curropneurobiol_2005.pdf
Axon Guidance Matthew Blewitt Overview Axonal development PNS regeneration CNS regeneration Future directions Brain Repair Axonal Development Neurite growth cone www.anatomy.unimelb.edu.au http://kalil.anatomy.wisc.edu/articles/kalil_dent_curropneurobiol_2005.pdf
Progress Report for NJCSCR (Yu-Wen Chang)
 Progress Report for NJCSCR (Yu-Wen Chang) Overall Plan Summary: Traumatic injury to the spinal cord initiates a cascade of degenerative processes, known as secondary injury, which include various inflammatory
Progress Report for NJCSCR (Yu-Wen Chang) Overall Plan Summary: Traumatic injury to the spinal cord initiates a cascade of degenerative processes, known as secondary injury, which include various inflammatory
SUPPLEMENTARY FIG. S2. Representative counting fields used in quantification of the in vitro neural differentiation of pattern of dnscs.
 Supplementary Data SUPPLEMENTARY FIG. S1. Representative counting fields used in quantification of the in vitro neural differentiation of pattern of anpcs. A panel of lineage-specific markers were used
Supplementary Data SUPPLEMENTARY FIG. S1. Representative counting fields used in quantification of the in vitro neural differentiation of pattern of anpcs. A panel of lineage-specific markers were used
Neurodevelopment II Structure Formation. Reading: BCP Chapter 23
 Neurodevelopment II Structure Formation Reading: BCP Chapter 23 Phases of Development Ovum + Sperm = Zygote Cell division (multiplication) Neurogenesis Induction of the neural plate Neural proliferation
Neurodevelopment II Structure Formation Reading: BCP Chapter 23 Phases of Development Ovum + Sperm = Zygote Cell division (multiplication) Neurogenesis Induction of the neural plate Neural proliferation
Tissue renewal and Repair. Nisamanee Charoenchon, PhD Department of Pathobiology, Faculty of Science
 Tissue renewal and Repair Nisamanee Charoenchon, PhD Email: nisamanee.cha@mahidol.ac.th Department of Pathobiology, Faculty of Science Topic Objectives 1. Describe processes of tissue repair, regeneration
Tissue renewal and Repair Nisamanee Charoenchon, PhD Email: nisamanee.cha@mahidol.ac.th Department of Pathobiology, Faculty of Science Topic Objectives 1. Describe processes of tissue repair, regeneration
Spinal cord injury (SCI) throughout history
 Overview of Cellular Therapies in Spinal Cord Injuries Jesse OWENS Biomedical Program, University of Alaska, Anchorage, Alaska Spinal cord injury (SCI) throughout history has been considered untreatable.
Overview of Cellular Therapies in Spinal Cord Injuries Jesse OWENS Biomedical Program, University of Alaska, Anchorage, Alaska Spinal cord injury (SCI) throughout history has been considered untreatable.
Human Anatomy and Physiology - Problem Drill 11: Neural Tissue & The Nervous System
 Human Anatomy and Physiology - Problem Drill 11: Neural Tissue & The Nervous System Question No. 1 of 10 The human body contains different types of tissue. The tissue is formed into organs and organ systems.
Human Anatomy and Physiology - Problem Drill 11: Neural Tissue & The Nervous System Question No. 1 of 10 The human body contains different types of tissue. The tissue is formed into organs and organ systems.
Update on early management of acute spinal cord injuries. Mr Jonathon L Richards Orthopaedic & Spinal surgeon
 Update on early management of acute spinal cord injuries Mr Jonathon L Richards Orthopaedic & Spinal surgeon Overview: Aetiology/Cost Pathophysiology Early surgical intervention Emerging therapies Steroids
Update on early management of acute spinal cord injuries Mr Jonathon L Richards Orthopaedic & Spinal surgeon Overview: Aetiology/Cost Pathophysiology Early surgical intervention Emerging therapies Steroids
In vivo reprogramming reactive glia into ipscs to produce new neurons in the
 In vivo reprogramming reactive glia into ipscs to produce new neurons in the cortex following traumatic brain injury Xiang Gao 1, Xiaoting Wang 1, Wenhui Xiong 1, Jinhui Chen 1, * 1 Spinal Cord and Brain
In vivo reprogramming reactive glia into ipscs to produce new neurons in the cortex following traumatic brain injury Xiang Gao 1, Xiaoting Wang 1, Wenhui Xiong 1, Jinhui Chen 1, * 1 Spinal Cord and Brain
Reaction to Injury & Regeneration. Steven McLoon Department of Neuroscience University of Minnesota
 Reaction to Injury & Regeneration Steven McLoon Department of Neuroscience University of Minnesota 1 Course News Dec 4 (Mon) Dec 6 (Wed) adult neurogenesis injury & regeneration Dec 8 (Fri) research paper
Reaction to Injury & Regeneration Steven McLoon Department of Neuroscience University of Minnesota 1 Course News Dec 4 (Mon) Dec 6 (Wed) adult neurogenesis injury & regeneration Dec 8 (Fri) research paper
TITLE: Harnessing GPR17 Biology for Treating Demyelinating Disease
 AD Award Number: W81XWH-10-1-0723 TITLE: Harnessing GPR17 Biology for Treating Demyelinating Disease PRINCIPAL INVESTIGATOR: Qing Lu, Ph.D. CONTRACTING ORGANIZATION: University of Texas Southwestern Medical
AD Award Number: W81XWH-10-1-0723 TITLE: Harnessing GPR17 Biology for Treating Demyelinating Disease PRINCIPAL INVESTIGATOR: Qing Lu, Ph.D. CONTRACTING ORGANIZATION: University of Texas Southwestern Medical
Strategies for Neuronal Regeneration after Spinal Cord Injury
 Magnetic Shield Corporation. (1997). Electromagnetic Shielding. Riley, K. (1995). Tracing EMFs in Building wiring and grounding. Tucson, AZ: Magnetic Sciences International. Posted in Uncategorized Tags:
Magnetic Shield Corporation. (1997). Electromagnetic Shielding. Riley, K. (1995). Tracing EMFs in Building wiring and grounding. Tucson, AZ: Magnetic Sciences International. Posted in Uncategorized Tags:
Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline
 Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline Module 11.1 Overview of the Nervous System (Figures 11.1-11.3) A. The nervous system controls our perception and experience
Chapter 11 Introduction to the Nervous System and Nervous Tissue Chapter Outline Module 11.1 Overview of the Nervous System (Figures 11.1-11.3) A. The nervous system controls our perception and experience
THE NEUROBIOLOGY OF THE NEURON AND THE NEUROGLIA
 THE NEUROBIOLOGY OF THE NEURON AND THE NEUROGLIA DEFINITION OF A NEURON Neuron is the name given to the nerve cell and all its processes. Neurons are excitable cells that are specialized for the reception
THE NEUROBIOLOGY OF THE NEURON AND THE NEUROGLIA DEFINITION OF A NEURON Neuron is the name given to the nerve cell and all its processes. Neurons are excitable cells that are specialized for the reception
Nervous System. Master controlling and communicating system of the body. Secrete chemicals called neurotransmitters
 Nervous System Master controlling and communicating system of the body Interacts with the endocrine system to control and coordinate the body s responses to changes in its environment, as well as growth,
Nervous System Master controlling and communicating system of the body Interacts with the endocrine system to control and coordinate the body s responses to changes in its environment, as well as growth,
April 29, Neurophysiology. Chul-Kyu Park, Ph.D. Assistant Professor Department of Physiology, Graduate School of Medicine, Gachon University,
 April 29, 2016 Neurophysiology Chul-Kyu Park, Ph.D. Assistant Professor Department of Physiology, Graduate School of Medicine, Gachon University, Cells in the brain Neurons glia 1. Astrocytes 2. Microglia
April 29, 2016 Neurophysiology Chul-Kyu Park, Ph.D. Assistant Professor Department of Physiology, Graduate School of Medicine, Gachon University, Cells in the brain Neurons glia 1. Astrocytes 2. Microglia
Brain Plasticity. Brain Plasticity. Recovery from Deprivation 1/2/11. Dogma. Modern neuroscience. Deprivation can lower IQ. Deprivation reversed
 Brain Plasticity Brain Plasticity Dogma Adult brain is stable, unchanging Lose neurons Do not grow/repair neurons Modern neuroscience Brain changes throughout life plasticity Extra capacity Face life s
Brain Plasticity Brain Plasticity Dogma Adult brain is stable, unchanging Lose neurons Do not grow/repair neurons Modern neuroscience Brain changes throughout life plasticity Extra capacity Face life s
Development of the Nervous System 1 st month
 Development of the Nervous System 1 st month day 1 - fertilization of egg day 6 - uterine implantation day 18 - trilaminar (3-layered) disc (blastoderm, embryo) ectoderm (dorsal) - nervous system and skin
Development of the Nervous System 1 st month day 1 - fertilization of egg day 6 - uterine implantation day 18 - trilaminar (3-layered) disc (blastoderm, embryo) ectoderm (dorsal) - nervous system and skin
FGF22 signaling regulates synapse formation during postinjury remodeling of the spinal cord
 Manuscript EMBO-2014-90578 FGF22 signaling regulates synapse formation during postinjury remodeling of the spinal cord Anne Jacobi, Kristina Loy, Anja M Schmalz, Mikael Hellsten, Hisashi Umemori, Martin
Manuscript EMBO-2014-90578 FGF22 signaling regulates synapse formation during postinjury remodeling of the spinal cord Anne Jacobi, Kristina Loy, Anja M Schmalz, Mikael Hellsten, Hisashi Umemori, Martin
Nerve Cells and Behavior
 Nerve Cells and Behavior 27 th September, 2016 Touqeer Ahmed Ph.D. Atta-ur-Rahman School of Applied Biosciences National University of Sciences and Technology Nervous System and Behavior Nervous system
Nerve Cells and Behavior 27 th September, 2016 Touqeer Ahmed Ph.D. Atta-ur-Rahman School of Applied Biosciences National University of Sciences and Technology Nervous System and Behavior Nervous system
Human Anatomy and Physiology- Problem Drill 04: Tissues of the Body
 Human Anatomy and Physiology- Problem Drill 04: Tissues of the Body Question No. 1 of 10 A biopsy sample is obtained from a lesion on the right cheek of a male patient. A technician in the histology lab
Human Anatomy and Physiology- Problem Drill 04: Tissues of the Body Question No. 1 of 10 A biopsy sample is obtained from a lesion on the right cheek of a male patient. A technician in the histology lab
B-cell. Astrocyte SCI SCI. T-cell
 RF #2015 P-01 PI: Azizul Haque, PhD Grant Title: Targeting Enolase in Spinal Cord Injury 12-month Technical Progress Report Progress Report (First Six Months): Enolase is one of the most abundantly expressed
RF #2015 P-01 PI: Azizul Haque, PhD Grant Title: Targeting Enolase in Spinal Cord Injury 12-month Technical Progress Report Progress Report (First Six Months): Enolase is one of the most abundantly expressed
Lecture 3 (Oct 5 th ): NEURONS AND NERVE IMPULSES Lecture Outline
 Lecture 3 (Oct 5 th ): NEURONS AND NERVE IMPULSES Lecture Outline 1) CNS vs. PNS 2) Structure of Neurons parts of a neuron: soma, dendrites, axons 3) Glial Cells 4) Mitosis and Regeneration in Neurons
Lecture 3 (Oct 5 th ): NEURONS AND NERVE IMPULSES Lecture Outline 1) CNS vs. PNS 2) Structure of Neurons parts of a neuron: soma, dendrites, axons 3) Glial Cells 4) Mitosis and Regeneration in Neurons
Neurons vs. glia. Traditionally, glia have been viewed as passive cells that help to maintain the function of neurons.
 GLIA Neurons vs. glia The defining characteristic of a neuron is its ability to transmit rapid electrical signals in the form of action potentials. All other neural cells that lack this property are broadly
GLIA Neurons vs. glia The defining characteristic of a neuron is its ability to transmit rapid electrical signals in the form of action potentials. All other neural cells that lack this property are broadly
New Therapies for Spinal Cord Injury Ann M. Parr, MD, PhD, FAANS, FRCSC Director of Spinal Neurosurgery Assistant Professor University of Minnesota
 New Therapies for Spinal Cord Injury Ann M. Parr, MD, PhD, FAANS, FRCSC Director of Spinal Neurosurgery Assistant Professor University of Minnesota Neurological Conditions for Stem Cell Therapy Application
New Therapies for Spinal Cord Injury Ann M. Parr, MD, PhD, FAANS, FRCSC Director of Spinal Neurosurgery Assistant Professor University of Minnesota Neurological Conditions for Stem Cell Therapy Application
First in human:irv Weissman, Stanford University
 First in human:irv Weissman, Stanford University The case for making human mouse chimeras to understand the function of human tissue stem cells from normal or genetically diseased donors Blood-Forming
First in human:irv Weissman, Stanford University The case for making human mouse chimeras to understand the function of human tissue stem cells from normal or genetically diseased donors Blood-Forming
CNS third year med students Summary of midterm material H Awad
 CNS third year med students 2018 Summary of midterm material H Awad Dear All This presentation summaries the main important topics covered in the midterm material ( lectures 1-6) There will be two questions
CNS third year med students 2018 Summary of midterm material H Awad Dear All This presentation summaries the main important topics covered in the midterm material ( lectures 1-6) There will be two questions
Nervous System. Electrical Signals.III Signal Transmission at Synapses Neurotransmitters.V Neural Circuits.VI
 Nervous System Overview.I Histology.II Electrical Signals.III Signal Transmission at Synapses Neurotransmitters.V Neural Circuits.VI Repairs.VII Pathology.VIII.IV 1 Controls and integrates all body activities
Nervous System Overview.I Histology.II Electrical Signals.III Signal Transmission at Synapses Neurotransmitters.V Neural Circuits.VI Repairs.VII Pathology.VIII.IV 1 Controls and integrates all body activities
Neurogenesis in Adult Central Nervous System: Death of a Dogma
 Aristotle University of Thessaloniki, Greece, Nov. 2007 Neurogenesis in Adult Central Nervous System: Death of a Dogma Anton B. Tonchev Division of Cell Biology, Varna University of Medicine, Bulgaria
Aristotle University of Thessaloniki, Greece, Nov. 2007 Neurogenesis in Adult Central Nervous System: Death of a Dogma Anton B. Tonchev Division of Cell Biology, Varna University of Medicine, Bulgaria
SCIRF Award #2016 I-03 PI: Azizul Haque, PhD Grant Title: Neuron-specific Enolase and SCI
 SCIRF Award #2016 I-03 PI: Azizul Haque, PhD Grant Title: Neuron-specific Enolase and SCI 10-month Technical Progress Report Enolase is a multifunctional glycolytic enzyme involved in growth control, hypoxia,
SCIRF Award #2016 I-03 PI: Azizul Haque, PhD Grant Title: Neuron-specific Enolase and SCI 10-month Technical Progress Report Enolase is a multifunctional glycolytic enzyme involved in growth control, hypoxia,
Nerve Cell Flashcards
 1. What does the word innervates mean? Refers to a nerve supplying a muscle or organ. For example, The phrenic nerve innervates the diaphragm muscle. 2. 3 parts of the Nervous System 1. Central Nervous
1. What does the word innervates mean? Refers to a nerve supplying a muscle or organ. For example, The phrenic nerve innervates the diaphragm muscle. 2. 3 parts of the Nervous System 1. Central Nervous
The Nervous System: Neural Tissue Pearson Education, Inc.
 13 The Nervous System: Neural Tissue Introduction Nervous System Characteristics Controls and adjust the activity of the body Provides swift but brief responses The nervous system includes: Central Nervous
13 The Nervous System: Neural Tissue Introduction Nervous System Characteristics Controls and adjust the activity of the body Provides swift but brief responses The nervous system includes: Central Nervous
Cells of the Nervous System
 Cells of the Nervous System Layout of the Nervous System Central Nervous System (CNS) Brain (in the skull) Spinal Cord (in the spine) Interprets sensory input, initiates movement, and mediates complex
Cells of the Nervous System Layout of the Nervous System Central Nervous System (CNS) Brain (in the skull) Spinal Cord (in the spine) Interprets sensory input, initiates movement, and mediates complex
Biology 218 Human Anatomy
 Chapter 17 Adapted form Tortora 10 th ed. LECTURE OUTLINE A. Overview of the Nervous System (p. 537) 1. The nervous system and the endocrine system are the body s major control and integrating centers.
Chapter 17 Adapted form Tortora 10 th ed. LECTURE OUTLINE A. Overview of the Nervous System (p. 537) 1. The nervous system and the endocrine system are the body s major control and integrating centers.
Man and his environment
 Man and his environment Dr. Elriah M. Makie 0122858517 Nervous Tissue BSc.M.Sc.MBBS Introduction The nervous system is divided into two main parts: The central nervous system (CNS) comprising the brain
Man and his environment Dr. Elriah M. Makie 0122858517 Nervous Tissue BSc.M.Sc.MBBS Introduction The nervous system is divided into two main parts: The central nervous system (CNS) comprising the brain
Internship Research Paper. Locomotion and Motor Neuron Plasticity after Incomplete Spinal Cord Injury. Completed at St.
 Internship Research Paper Locomotion and Motor Neuron Plasticity after Incomplete Spinal Cord Injury Completed at St. Joseph s Hospital Barrow Neurological Institute Dr. Thomas Hamm By Anivarya Kumar Introduction
Internship Research Paper Locomotion and Motor Neuron Plasticity after Incomplete Spinal Cord Injury Completed at St. Joseph s Hospital Barrow Neurological Institute Dr. Thomas Hamm By Anivarya Kumar Introduction
BIOL241 - Lecture 12a
 Cranial Nerves, source: training.seer.cancer.gov Nervous System Overview BIOL241 - Lecture 12a 1 Topics Divisions of the NS: CNS and PNS Structure and types of neurons Synapses Structure and function of
Cranial Nerves, source: training.seer.cancer.gov Nervous System Overview BIOL241 - Lecture 12a 1 Topics Divisions of the NS: CNS and PNS Structure and types of neurons Synapses Structure and function of
συν together απτειν to clasp 2h Neuroscience with Pharmacology Functions and Mechanisms of Reflexes Cogito, ergo sum ( I think therefore I am ) Down
 2h Neuroscience with Pharmacology Functions and Mechanisms of Reflexes Neuroscience is studied at many different levels: from brain, to system, network, neurone, synapse, and molecule... Top Up Down René
2h Neuroscience with Pharmacology Functions and Mechanisms of Reflexes Neuroscience is studied at many different levels: from brain, to system, network, neurone, synapse, and molecule... Top Up Down René
NURSE-UP INTRODUCTION TO THE NERVOUS SYSTEM
 NURSE-UP INTRODUCTION TO THE NERVOUS SYSTEM FUNCTIONS OF THE NERVOUS SYSTEM Body s primary communication and control system. Integrates and regulates body function Collects information specialized nervous
NURSE-UP INTRODUCTION TO THE NERVOUS SYSTEM FUNCTIONS OF THE NERVOUS SYSTEM Body s primary communication and control system. Integrates and regulates body function Collects information specialized nervous
Myelin suppresses axon regeneration by PIR-B/SHPmediated inhibition of Trk activity
 Manuscript EMBO-2010-76298 Myelin suppresses axon regeneration by PIR-B/SHPmediated inhibition of Trk activity Yuki Fujita, Shota Endo, Toshiyuki Takai and Toshihide Yamashita Corresponding author: Toshihide
Manuscript EMBO-2010-76298 Myelin suppresses axon regeneration by PIR-B/SHPmediated inhibition of Trk activity Yuki Fujita, Shota Endo, Toshiyuki Takai and Toshihide Yamashita Corresponding author: Toshihide
Introduction and aims of the study
 Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Introduction and aims of the study 1 Chapter 1 Motor neuron diseases include the most incapacitating and life-threatening illnesses but also rather benign disorders with only mild symptoms and slow progression.
Development of the Nervous System. Leah Militello, class of 2018
 Development of the Nervous System Leah Militello, class of 2018 Learning Objectives 1. Describe the formation and fate of the neural tube and neural crest including timing and germ layer involved. 2. Describe
Development of the Nervous System Leah Militello, class of 2018 Learning Objectives 1. Describe the formation and fate of the neural tube and neural crest including timing and germ layer involved. 2. Describe
Human Histology The Nervous System. Dr. Rawaa Salim Hameed
 Human Histology The Nervous System Dr. Rawaa Salim Hameed The organization of the nervous system Anatomically, the nervous system is divided into:- Neurohistology Structurally, nerve tissue consists of
Human Histology The Nervous System Dr. Rawaa Salim Hameed The organization of the nervous system Anatomically, the nervous system is divided into:- Neurohistology Structurally, nerve tissue consists of
Fundamentals of the Nervous System and Nervous Tissue. Nervous System. Basic Divisions of the Nervous System C H A P T E R 12.
 C H A P T E R 12 Fundamentals of the Nervous System and Nervous Tissue Nervous System Sensory input Integration Motor output Figure 12.1 Basic Divisions of the Nervous System Brain CNS Spinal cord Nerves
C H A P T E R 12 Fundamentals of the Nervous System and Nervous Tissue Nervous System Sensory input Integration Motor output Figure 12.1 Basic Divisions of the Nervous System Brain CNS Spinal cord Nerves
2401 : Anatomy/Physiology
 Dr. Chris Doumen Week 5 2401 : Anatomy/Physiology Introduction Neural Tissue TextBook Readings Pages 388 through 397. Make use of the figures in your textbook ; a picture is worth a thousand words! Work
Dr. Chris Doumen Week 5 2401 : Anatomy/Physiology Introduction Neural Tissue TextBook Readings Pages 388 through 397. Make use of the figures in your textbook ; a picture is worth a thousand words! Work
Supplementary Information
 Supplementary Information Title Degeneration and impaired regeneration of gray matter oligodendrocytes in amyotrophic lateral sclerosis Authors Shin H. Kang, Ying Li, Masahiro Fukaya, Ileana Lorenzini,
Supplementary Information Title Degeneration and impaired regeneration of gray matter oligodendrocytes in amyotrophic lateral sclerosis Authors Shin H. Kang, Ying Li, Masahiro Fukaya, Ileana Lorenzini,
10.1: Introduction. Cell types in neural tissue: Neurons Neuroglial cells (also known as neuroglia, glia, and glial cells) Dendrites.
 10.1: Introduction Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cell types in neural tissue: Neurons Neuroglial cells (also known as neuroglia, glia, and glial
10.1: Introduction Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cell types in neural tissue: Neurons Neuroglial cells (also known as neuroglia, glia, and glial
Cellular Transplantation Strategies for Spinal Cord Injury and Translational Neurobiology
 NeuroRx : The Journal of the American Society for Experimental NeuroTherapeutics Cellular Transplantation Strategies for Spinal Cord Injury and Translational Neurobiology Paul J. Reier College of Medicine
NeuroRx : The Journal of the American Society for Experimental NeuroTherapeutics Cellular Transplantation Strategies for Spinal Cord Injury and Translational Neurobiology Paul J. Reier College of Medicine
! BIOL 2401! Week 5. Nervous System. Nervous System
 Collin County Community College! BIOL 2401! Week 5 Nervous System 1 Nervous System The process of homeostasis makes sure that the activities that occur in the body are maintained within normal physiological
Collin County Community College! BIOL 2401! Week 5 Nervous System 1 Nervous System The process of homeostasis makes sure that the activities that occur in the body are maintained within normal physiological
Cell Birth and Death. Chapter Three
 Cell Birth and Death Chapter Three Neurogenesis All neurons and glial cells begin in the neural tube Differentiated into neurons rather than ectoderm based on factors we have already discussed If these
Cell Birth and Death Chapter Three Neurogenesis All neurons and glial cells begin in the neural tube Differentiated into neurons rather than ectoderm based on factors we have already discussed If these
BIOH111. o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system
 BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
BIOH111 o Cell Module o Tissue Module o Integumentary system o Skeletal system o Muscle system o Nervous system o Endocrine system Endeavour College of Natural Health endeavour.edu.au 1 TEXTBOOK AND REQUIRED/RECOMMENDED
Major Structures of the Nervous System. Brain, cranial nerves, spinal cord, spinal nerves, ganglia, enteric plexuses and sensory receptors
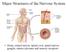 Major Structures of the Nervous System Brain, cranial nerves, spinal cord, spinal nerves, ganglia, enteric plexuses and sensory receptors Nervous System Divisions Central Nervous System (CNS) consists
Major Structures of the Nervous System Brain, cranial nerves, spinal cord, spinal nerves, ganglia, enteric plexuses and sensory receptors Nervous System Divisions Central Nervous System (CNS) consists
12 Anatomy and Physiology of Peripheral Nerves
 12 Anatomy and Physiology of Peripheral Nerves Introduction Anatomy Classification of Peripheral Nerves Sensory Nerves Motor Nerves Pathologies of Nerves Focal Injuries Regeneration of Injured Nerves Signs
12 Anatomy and Physiology of Peripheral Nerves Introduction Anatomy Classification of Peripheral Nerves Sensory Nerves Motor Nerves Pathologies of Nerves Focal Injuries Regeneration of Injured Nerves Signs
Cell transplantation to the rescue: Repairing the injured spinal cord. Mary Bartlett Bunge, PhD
 Cell transplantation to the rescue: Repairing the injured spinal cord Mary Bartlett Bunge, PhD Christine E. Lynn Distinguished Professor of Neuroscience Professor of Cell Biology, Neurological Surgery,
Cell transplantation to the rescue: Repairing the injured spinal cord Mary Bartlett Bunge, PhD Christine E. Lynn Distinguished Professor of Neuroscience Professor of Cell Biology, Neurological Surgery,
Chapter 7. The Nervous System
 Chapter 7 The Nervous System General overview of the nervous system functions Sensory input (info travels in along afferent pathways) Integration (information is processed) Sensory neurons Spinal cord
Chapter 7 The Nervous System General overview of the nervous system functions Sensory input (info travels in along afferent pathways) Integration (information is processed) Sensory neurons Spinal cord
Microglia-derived extracellular vesicles regulate the proliferation and differentiation of oligodendrocyte precursor cells
 University of Turin CNR Institute of Neuroscience Microglia-derived extracellular vesicles regulate the proliferation and differentiation of oligodendrocyte precursor cells Roberta Parolisi Turin, December
University of Turin CNR Institute of Neuroscience Microglia-derived extracellular vesicles regulate the proliferation and differentiation of oligodendrocyte precursor cells Roberta Parolisi Turin, December
Biology Dr. Khalida Ibrahim Nervous system The nervous system is responsible for communication between different regions of the body, it is divided
 Biology Dr. Khalida Ibrahim Nervous system The nervous system is responsible for communication between different regions of the body, it is divided into: CNS (central nervous system) = brain + spinal cord
Biology Dr. Khalida Ibrahim Nervous system The nervous system is responsible for communication between different regions of the body, it is divided into: CNS (central nervous system) = brain + spinal cord
Chapter 12 The Nervous System INTRODUCTION TO THE NERVOUS SYSTEM. Central Nervous System (CNS): STRUCTURE BRAIN SPINAL CORD NERVES
 Chapter 12 The Nervous System PowerPoint by John McGill Supplemental Notes by Beth Wyatt INTRODUCTION TO THE NERVOUS SYSTEM STRUCTURE BRAIN SPINAL CORD NERVES Central Nervous System (CNS): Brain Spinal
Chapter 12 The Nervous System PowerPoint by John McGill Supplemental Notes by Beth Wyatt INTRODUCTION TO THE NERVOUS SYSTEM STRUCTURE BRAIN SPINAL CORD NERVES Central Nervous System (CNS): Brain Spinal
Chapter 2 Microenvironment Within the Injured Spinal Cord Focusing on IL-6
 Chapter 2 Microenvironment Within the Injured Spinal Cord Focusing on IL-6 Masaya Nakamura Abstract In recent years, a variety of studies have been conducted towards the goal of achieving regeneration
Chapter 2 Microenvironment Within the Injured Spinal Cord Focusing on IL-6 Masaya Nakamura Abstract In recent years, a variety of studies have been conducted towards the goal of achieving regeneration
Nervous tissue, charachteristics, neurons, glial cells
 Nervous tissue, charachteristics, neurons, glial cells Functional Organization of Nervous Tissue The Nervous System Components Brain, spinal cord, nerves, sensory receptors Responsible for Sensory perceptions,
Nervous tissue, charachteristics, neurons, glial cells Functional Organization of Nervous Tissue The Nervous System Components Brain, spinal cord, nerves, sensory receptors Responsible for Sensory perceptions,
Functional Organization of Nervous Tissue. Nervous tissue, charachteristics, neurons, glial cells. The Nervous System. The Nervous System 21/12/2010
 Nervous tissue, charachteristics, neurons, glial cells Functional Organization of Nervous Tissue The Nervous System Components Brain, spinal cord, nerves, sensory receptors Responsible for Sensory perceptions,
Nervous tissue, charachteristics, neurons, glial cells Functional Organization of Nervous Tissue The Nervous System Components Brain, spinal cord, nerves, sensory receptors Responsible for Sensory perceptions,
Nervous Tissue and Histology of CNS
 Nervous Tissue and Histology of CNS Functions of Nervous System Like the CPU of a computer, the nervous system is the master controlling system of the body. It is designed to constantly and rapidly adjust
Nervous Tissue and Histology of CNS Functions of Nervous System Like the CPU of a computer, the nervous system is the master controlling system of the body. It is designed to constantly and rapidly adjust
Table of Contents: Chapter 1 The organization of the spinal cord Charles Watson and Gulgun Kayalioglu
 Table of Contents: Chapter 1 The organization of the spinal cord Charles Watson and Gulgun Kayalioglu The gross anatomy of the spinal cord Spinal cord segments Spinal nerves Spinal cord gray and white
Table of Contents: Chapter 1 The organization of the spinal cord Charles Watson and Gulgun Kayalioglu The gross anatomy of the spinal cord Spinal cord segments Spinal nerves Spinal cord gray and white
What Cell Make Up the Brain and Spinal Cord
 What Cell Make Up the Brain and Spinal Cord Jennifer LaVail, Ph.D. (http://anatomy.ucsf.edu/pages/lavaillab/index.html) What kinds of cells are these?" Neuron?" Epithelial cell?" Glial cell?" What makes
What Cell Make Up the Brain and Spinal Cord Jennifer LaVail, Ph.D. (http://anatomy.ucsf.edu/pages/lavaillab/index.html) What kinds of cells are these?" Neuron?" Epithelial cell?" Glial cell?" What makes
Growth Factors. BIT 230 Walsh Chapter 7
 Growth Factors BIT 230 Walsh Chapter 7 3 Definitions Autocrine: a mode of hormone action in which a hormone affects the function of the cell type that produced it. Paracrine: Relating to the release of
Growth Factors BIT 230 Walsh Chapter 7 3 Definitions Autocrine: a mode of hormone action in which a hormone affects the function of the cell type that produced it. Paracrine: Relating to the release of
Improvement of Peripheral Regeneration with G-CSF in a Rat Model of Sciatic Nerve Repair
 Improvement of Peripheral Regeneration with G-CSF in a Rat Model of Sciatic Nerve Repair YENFU CHEN, MD 1, YAO-LUNG KUO, MD 2,3,4, I-Ming Jou, Prof, 3. 1 Department of Orthopaedics, National Cheng Kung
Improvement of Peripheral Regeneration with G-CSF in a Rat Model of Sciatic Nerve Repair YENFU CHEN, MD 1, YAO-LUNG KUO, MD 2,3,4, I-Ming Jou, Prof, 3. 1 Department of Orthopaedics, National Cheng Kung
A. Subdivisions of the Nervous System: 1. The two major subdivisions of the nervous system:
 BIO 211: ANATOMY & PHYSIOLOGY I 1 Ch 10 A Ch 10 B CHAPTER 10 NERVOUS SYSTEM 1 BASIC STRUCTURE and FUNCTION Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill.
BIO 211: ANATOMY & PHYSIOLOGY I 1 Ch 10 A Ch 10 B CHAPTER 10 NERVOUS SYSTEM 1 BASIC STRUCTURE and FUNCTION Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill.
Chapter 7 Nerve tissue 1 Liu Jiamei
 Chapter 7 Nerve tissue 1 Liu Jiamei General description: nerve tissue nerve cells (neurons): show numerous long processes receive the stimulation make contact with each other, conduct the nerve impulse
Chapter 7 Nerve tissue 1 Liu Jiamei General description: nerve tissue nerve cells (neurons): show numerous long processes receive the stimulation make contact with each other, conduct the nerve impulse
Control of an injured spinal cord: Perspectives after regeneration
 Control of an injured spinal cord: Perspectives after regeneration Avis H. Cohen Department of Biology Institute for Systems Research Neurosciences and Cognitive Sciences University of Maryland College
Control of an injured spinal cord: Perspectives after regeneration Avis H. Cohen Department of Biology Institute for Systems Research Neurosciences and Cognitive Sciences University of Maryland College
Cephalization. Nervous Systems Chapter 49 11/10/2013. Nervous systems consist of circuits of neurons and supporting cells
 Nervous Systems Chapter 49 Cephalization Nervous systems consist of circuits of neurons and supporting cells Nervous system organization usually correlates with lifestyle Organization of the vertebrate
Nervous Systems Chapter 49 Cephalization Nervous systems consist of circuits of neurons and supporting cells Nervous system organization usually correlates with lifestyle Organization of the vertebrate
Contribution of microglia to tissue injury and repair in MS
 Contribution of microglia to tissue injury and repair in MS MS disease course histologic features Courtesy of Samuel Ludwin I ACUTE CHRONIC s ACTIVE CHRONIC Clinical Course Intra CNS Extra CNS Imaging
Contribution of microglia to tissue injury and repair in MS MS disease course histologic features Courtesy of Samuel Ludwin I ACUTE CHRONIC s ACTIVE CHRONIC Clinical Course Intra CNS Extra CNS Imaging
Examining the properties and therapeutic potential of glial restricted precursors in spinal cord injury
 NEURAL REGENERATION RESEARCH April 2016,Volume 11,Issue 4 www.nrronline.org INVITED REVIEW Examining the properties and therapeutic potential of glial restricted precursors in spinal cord injury Kazuo
NEURAL REGENERATION RESEARCH April 2016,Volume 11,Issue 4 www.nrronline.org INVITED REVIEW Examining the properties and therapeutic potential of glial restricted precursors in spinal cord injury Kazuo
Index Note: Page numbers of article titles are in boldface type.
 Neurosurg Clin N Am 18 (2007) 191 198 Index Note: Page numbers of article titles are in boldface type. A AC133 antigen, in brain tumor cancer cells, 32 35 Activity-based restoration therapy, for spinal
Neurosurg Clin N Am 18 (2007) 191 198 Index Note: Page numbers of article titles are in boldface type. A AC133 antigen, in brain tumor cancer cells, 32 35 Activity-based restoration therapy, for spinal
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 12 Nervous Tissue Introduction The purpose of the chapter is to: 1. Understand how the nervous system helps to keep controlled conditions within
Principles of Anatomy and Physiology 14 th Edition CHAPTER 12 Nervous Tissue Introduction The purpose of the chapter is to: 1. Understand how the nervous system helps to keep controlled conditions within
MYELINATION, DEVELOPMENT AND MULTIPLE SCLEROSIS 1
 MYELINATION, DEVELOPMENT AND MULTIPLE SCLEROSIS 1 Myelination, development and Multiple Sclerosis Randy Christensen Salt Lake Community College MYELINATION, DEVELOPMENT AND MULTIPLE SCLEROSIS 2 Myelination,
MYELINATION, DEVELOPMENT AND MULTIPLE SCLEROSIS 1 Myelination, development and Multiple Sclerosis Randy Christensen Salt Lake Community College MYELINATION, DEVELOPMENT AND MULTIPLE SCLEROSIS 2 Myelination,
sensory input receptors integration Human Anatomy motor output Ch. 7 effectors Structural classification
 Human Anatomy Ch. 7 I. The Nervous System A. General characteristics 1. body s control & communication center a. 3 overlapping functions 1) sensory input: receptors monitor stimuli 2) integration: processes,
Human Anatomy Ch. 7 I. The Nervous System A. General characteristics 1. body s control & communication center a. 3 overlapping functions 1) sensory input: receptors monitor stimuli 2) integration: processes,
Nervous Tissue Nervous tissue is the term for groups of organized cells in the nervous system, which is the organ system that controls the body s
 Nervous Tissue Nervous tissue is the term for groups of organized cells in the nervous system, which is the organ system that controls the body s movements, sends and carries signals to and from the different
Nervous Tissue Nervous tissue is the term for groups of organized cells in the nervous system, which is the organ system that controls the body s movements, sends and carries signals to and from the different
Review Article Endogenous Proliferation after Spinal Cord Injury in Animal Models
 Stem Cells International Volume 2012, Article ID 387513, 16 pages doi:10.1155/2012/387513 Review Article Endogenous Proliferation after Spinal Cord Injury in Animal Models Ashley McDonough 1, 2, 3 and
Stem Cells International Volume 2012, Article ID 387513, 16 pages doi:10.1155/2012/387513 Review Article Endogenous Proliferation after Spinal Cord Injury in Animal Models Ashley McDonough 1, 2, 3 and
CONTRACTING ORGANIZATION: University of Florida Gainsville, FL
 AD Award Number: W81XWH-11-1-0145 TITLE: Nerve Degeneration and Regeneration Associated with NF1 Tumors PRINCIPAL INVESTIGATOR: David F. Muir CONTRACTING ORGANIZATION: University of Florida Gainsville,
AD Award Number: W81XWH-11-1-0145 TITLE: Nerve Degeneration and Regeneration Associated with NF1 Tumors PRINCIPAL INVESTIGATOR: David F. Muir CONTRACTING ORGANIZATION: University of Florida Gainsville,
ORTHOPEDICS BONE Recalcitrant nonunions In total hip replacement total knee surgery increased callus volume
 ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
ORTHOPEDICS Orthopedics has to do with a variety of tissue: bone, cartilage, tendon, ligament, muscle. In this regard orthopedic and sports medicine share the same tissue targets. Orthopedics is mostly
MOLECULAR AND CELLULAR NEUROSCIENCE
 MOLECULAR AND CELLULAR NEUROSCIENCE BMP-218 November 4, 2014 DIVISIONS OF THE NERVOUS SYSTEM The nervous system is composed of two primary divisions: 1. CNS - Central Nervous System (Brain + Spinal Cord)
MOLECULAR AND CELLULAR NEUROSCIENCE BMP-218 November 4, 2014 DIVISIONS OF THE NERVOUS SYSTEM The nervous system is composed of two primary divisions: 1. CNS - Central Nervous System (Brain + Spinal Cord)
Meyers' A&P February 15, Unit 7. The Nervous System. I. Functions of the Nervous System. Monitors body's internal and external enviornments
 Unit 7 The Nervous System I. Functions of the Nervous System Monitors body's internal and external enviornments Integrates sensory information Coordinates voluntary & involuntary responses of many other
Unit 7 The Nervous System I. Functions of the Nervous System Monitors body's internal and external enviornments Integrates sensory information Coordinates voluntary & involuntary responses of many other
Microglia preconditioning (priming) in central nervous system pathologies
 Microglia preconditioning (priming) in central nervous system pathologies Florence Perrin florence.perrin@umontpellier.fr Montpellier, October 2018 1 Spanish anatomists Glia = glue in Greek Santiago Ramon
Microglia preconditioning (priming) in central nervous system pathologies Florence Perrin florence.perrin@umontpellier.fr Montpellier, October 2018 1 Spanish anatomists Glia = glue in Greek Santiago Ramon
Outline. Neuron Structure. Week 4 - Nervous System. The Nervous System: Neurons and Synapses
 Outline Week 4 - The Nervous System: Neurons and Synapses Neurons Neuron structures Types of neurons Electrical activity of neurons Depolarization, repolarization, hyperpolarization Synapses Release of
Outline Week 4 - The Nervous System: Neurons and Synapses Neurons Neuron structures Types of neurons Electrical activity of neurons Depolarization, repolarization, hyperpolarization Synapses Release of
Chapter 2: Cellular Mechanisms and Cognition
 Chapter 2: Cellular Mechanisms and Cognition MULTIPLE CHOICE 1. Two principles about neurons were defined by Ramón y Cajal. The principle of connectional specificity states that, whereas the principle
Chapter 2: Cellular Mechanisms and Cognition MULTIPLE CHOICE 1. Two principles about neurons were defined by Ramón y Cajal. The principle of connectional specificity states that, whereas the principle
Shift 1, 8 July 2018, 09:30-13:00
 Shift 1, 8 July 2018, 09:30-13:00 CNS patterning A001-A014 Stem cells: basic biology and postnatal neurogenesis - part I Development of neural systems: Molecular and genetic characterisationa Epigenetic
Shift 1, 8 July 2018, 09:30-13:00 CNS patterning A001-A014 Stem cells: basic biology and postnatal neurogenesis - part I Development of neural systems: Molecular and genetic characterisationa Epigenetic
The pathogenesis of nervous distemper
 Veterinary Sciences Tomorrow - 2004 The pathogenesis of nervous distemper Marc Vandevelde Canine distemper is a highly contagious viral disease of dogs and of all animals in the Canidae, Mustellidae and
Veterinary Sciences Tomorrow - 2004 The pathogenesis of nervous distemper Marc Vandevelde Canine distemper is a highly contagious viral disease of dogs and of all animals in the Canidae, Mustellidae and
Glial Cells: The Other Cells of the Nervous System
 Glial Cells: The Other Cells of the Nervous System 2. Astrocytes - Star Performers in the Neural Tissue Medha S Rajadhyaksha and Daya Manghani Medha S Rajadhyaksha is a reader in life sciences at Sophia
Glial Cells: The Other Cells of the Nervous System 2. Astrocytes - Star Performers in the Neural Tissue Medha S Rajadhyaksha and Daya Manghani Medha S Rajadhyaksha is a reader in life sciences at Sophia
Peripheral Nerve Grafts Support Regeneration after Spinal Cord Injury
 Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics REVIEW Peripheral Nerve Grafts Support Regeneration after Spinal Cord Injury Marie-Pascale Côté, Arthi A. Amin,
Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics REVIEW Peripheral Nerve Grafts Support Regeneration after Spinal Cord Injury Marie-Pascale Côté, Arthi A. Amin,
