The CBCL predicts DSM bipolar disorder in children: a receiver operating characteristic curve analysis
|
|
|
- Gillian Conley
- 6 years ago
- Views:
Transcription
1 Bipolar Disorders 2005: 7: Copyright ª Blackwell Munksgaard 2005 BIPOLAR DISORDERS Original Article The CBCL predicts DSM bipolar disorder in children: a receiver operating characteristic curve analysis Faraone SV, Althoff RR, Hudziak JJ, Monuteaux M, Biederman J. The CBCL predicts DSM bipolar disorder in children: a receiver operating characteristic curve analysis. Bipolar Disord 2005: 7: ª Blackwell Munksgaard, 2005 Background: No clear consensus has been reached yet on how best to characterize children who suffer from pediatric bipolar disorder (PBD). The CBCL-PBD profile on the Child Behavior Checklist (CBCL) has been consistently reported showing deviant findings on the Attention Problems, Aggressive Behavior, and Anxious-Depressed subscales. Aim: To examine the sensitivity and specificity of the proposed CBCL- PBD profile for determining DSM diagnosis of PBD. Methods: We applied receiver operating characteristic (ROC) curve analysis to data from 471 probands from two family studies of attentiondeficit hyperactivity disorder and their 410 siblings. Results: The CBCL-PBD score demonstrated an area under the curve (AUC) of 0.97 for probands and 0.82 for siblings for current diagnosis of PBD, suggesting that the CBCL-PBD provided a highly efficient way of identifying subjects with a current diagnosis of PBD in this sample. Conclusions: These findings suggest that the CBCL-PBD may provide a highly efficient way of screening for childhood bipolar disorder. Stephen V Faraone a, Robert R Althoff b,c, James J Hudziak d, Michael Monuteaux b,c and Joseph Biederman b,c a Medical Genetics Research Program and Department of Psychiatry and Behavioral Sciences, SUNY Upstate Medical University, Syracuse, NY, b Department of Psychiatry, Massachusetts General Hospital, c Department of Psychiatry, Harvard Medical School, Boston, MA, d Department of Psychiatry, University of Vermont, Burlington, VT, USA Key words: aggression ADHD attention-deficit hyperactivity disorder bipolar affective disorder CBCL Child Behavior Checklist pediatric bipolar Received 25 May 2005, revised and accepted for publication 26 September 2005 Corresponding author: Stephen V Faraone PhD, Department of Psychiatry and Behavioral Sciences, SUNY Upstate Medical University, 750 East Adams St, Syracuse, NY 13210, USA. Fax: (315) ; faraones@upstate.edu There is a growing body of literature describing children who show symptoms of affective lability, agitation, aggression, and behavioral dyscontrol. How to best characterize these children and whether to identify them as pediatric bipolar disorder (PBD) has been the focus of considerable study (1 11). The cluster of symptoms that occur in PBD share many, but not all, of the characteristics of late-onset bipolar affective disorder (12), and some modifications of Diagnostic and Statistical Manual (DSM) criteria for pediatric populations (2, 13) have been proposed (14). Despite these diagnostic difficulties, a growing body of literature The authors of this paper do not have any commercial associations that might pose a conflict of interest in connection with this manuscript. 518 suggests that the diagnosis of bipolar disorder in youth is valid (12, 15) and the diagnosis has gained sufficient acceptance for the American Academy of Child and Adolescent Psychiatry to have issued treatment guidelines (2, 3, 7, 9, 10, 13, 14, 16 18). One of the diagnostic uncertainties in the diagnosis of PBD has been its relationship with attention-deficit hyperactivity disorder (ADHD) given the high comorbidity between the two disorders (5, 10, 18, 19) To address this issue, Biederman et al. (20) described a profile on the Child Behavior Checklist (CBCL; 21) which occurs in children with PBD that is discrete from the CBCL profiles in children without either ADHD or PBD, and more importantly, is different from children with ADHD alone. This profile was subsequently replicated by other groups and confirmed by meta-analysis (22 27). This profile on the
2 ROC of the CBCL-PBD CBCL is characterized by deviance on the Attention Problems, Aggressive Behavior, and Anxious/ Depressed syndrome scales. In contrast, ADHD children without bipolar disorder show deviance largely limited to the Attention Problems scale alone. In a recent set of studies we used a general population sample of over 21,000 twins to assess the validity of the CBCL-PBD profile (28). We hypothesized that, given the well established high heritability of bipolar disorder (17), the CBCL- PBD profile should be equally heritable. These data showed that the CBCL-PBD profile was highly heritable (54 68%) and had a population prevalence consistent with epidemiologic studies of bipolar disorder (1% of boys and girls at ages 7, 10, and 12). Subsequently this phenotype was tested using latent class analysis (LCA) and shown to emerge a priori from the data using LCA. The CBCL-PBD latent class was highly heritable and associated with marked increases in suicidal ideation when compared with children who did not fall into this severe class with up to 22% of the children with PBD positive for one of the two suicidal items (ÔDeliberately harms self or attempts suicideõ and ÔTalks about killing selfõ) on the maternal report of the CBCL (29). Kahana et al. (30) extended analysis of the CBCL-PBD profile further by using a multiinformant approach of investigating the relationship between the CBCL, the Teacher Report Form and the Youth Self Report forms of the Achenbach scales. They used logistic regression and receiver operating characteristic (ROC) analysis to evaluate the diagnostic efficiency of the CBCL as a predictor of PBD. They found that the sample of PBD children was significantly different (after adjusting for multiple comparisons) from their ÔAnyÕ category of controls on the CBCL on all subscales and differed from children with other disruptive behavior disorders on all scales except Social Problems and Attention Problems. The highest T-scores in PBD children were on the Aggressive, Attention, Anxious/ Depressed, and Delinquent subscales. Although their ROC analyses suggested the CBCL had a high level of predictive validity for PBD ( ), they concluded that the sensitivity and specificity of prediction was too low for clinical use. Unfortunately, they did not evaluate the diagnostic efficiency of the CBCL profile that had been validated by the research review above, which implicated the Attention Problems, Aggression, and Anxious/Depressed subscales. Additionally, to the best of our determination, Kahana et al. did not distinguish between current and lifetime diagnoses of the disorders, a distinction that is critical in the clinical assessment of children. To address these issues, the present work evaluated the diagnostic efficiency of the CBCL as a predictor of PBD using data from two family studies of ADHD (31, 32). We hypothesized that the attention problems, aggression and anxiety/ depression subscales of the CBCL would allow for accurate determination of PBD status in predicting lifetime and current diagnoses of PBD. Furthermore, because of the known genetic contributions to this disorder (4, 5, 10, 18, 28, 29, 33, 34) we hypothesized that a similar pattern would be seen in siblings of the PBD children. Methods Subjects We studied two groups of boys: 133 ADHD probands and 118 non-adhd comparisons. Their ages were 10.5 ± 2.9 and 11.6 ± 3.6, respectively. These groups had 126 and 96 siblings, respectively, who provided data. Their ages were 10.7 ± 3.0 and 11.1 ± 2.8, respectively. We also studied two groups of girls: 109 ADHD probands and 111 non- ADHD comparisons (ages 11.1 ± 3.3 and 12.2 ± 3.1, respectively). These groups had 90 and 98 siblings, respectively, who provided data. Their ages were 11.5 ± 3.7 and 11.9 ± 3.4, respectively. All ADHD subjects met full DSM-III-R diagnostic criteria for ADHD at the time of the clinical referral; at the time of recruitment they all had active symptoms of the disorder. Following the guidelines of the Institutional Review Board of the parent institution and in accord with the Helsinki Declaration of 1975, parents gave written informed consent for participation of children and the children participated only if they assented to the study procedures. The ascertainment procedures were identical for boy and girl probands. We identified psychiatrically referred ADHD probands from lists of consecutive patients from the pediatric psychiatry clinic at the Massachusetts General Hospital. Seventy-seven pediatrically referred ADHD probands were identified from lists of children having evidence of ADHD in the computerized medical record of a Health Maintenance Organization. Within each setting, we selected normal controls from lists of outpatients at pediatric medical clinics. We selected potential ADHD families if evidence in the medical record and the results of an initial interview suggested a child might have ADHD. 519
3 Faraone et al. We selected potential control families if evidence in the medical record and the results of an initial interview suggested a child did not have ADHD. Assessment procedures We used DSM-III-R-based structured interviews. Psychiatric assessments of youth used the Schedule for Affective Disorders and Schizophrenia for School-Age Children: Epidemiologic Version (Kiddie SADS-E; 35). Diagnoses were based on independent interviews with the mothers and direct interviews with the child. Children younger than 12 years of age (n ¼ 245) were not interviewed directly. To assess childhood diagnoses in the parents, we administered modules from the Kiddie SADS-E. We assessed dimensional measures of psychopathology with the CBCL (21). Interviewers were blind to the proband s diagnosis and ascertainment site. The direct interviews of mothers and the direct interviews of children were conducted by different raters. When interviewing mothers, the mother s interview about their children was sequenced after the direct interview with the mother about herself in about 90% of families. Raters were trained and supervised by board-certified psychiatrists. Final diagnostic assignment was made after blind review of all available information by a Diagnostic Committee chaired by Dr Biederman and composed of three board-certified child and adolescent psychiatrists and licensed clinical psychologists. The interviewers were instructed to take extensive notes about the symptoms for each disorder. These notes and the structured interview data were reviewed by the diagnostic committee so that the Committee can make a Best Estimate diagnosis as described by Leckman et al. (36). Definite diagnoses were assigned to subjects who met all diagnostic criteria. Diagnoses presented for review were considered definite only if a consensus is achieved that criteria are met to a degree that would be considered clinically meaningful. By Ôclinically meaningfulõ we mean that the data collected from the structured interview indicated that the diagnosis should be a clinical concern due to the nature of the symptoms, the associated impairment, and the coherence of the clinical picture. To combine discrepant parent and offspring reports, we used the most severe diagnosis from either source as the consensus diagnosis, unless the diagnosticians suspected that the source was not supplying reliable information. Interviewers of subjects were blind to their original ascertainment group (case or control), to all prior data 520 collected from that subject and to his or her family members. To be given the lifetime diagnosis of BPD, the child had to meet full DSM-III-R criteria for a manic episode with associated impairment. Thus, a child must have met criterion A for a period of extreme and persistently elevated, expansive or irritable mood, plus criterion B, manifested by three (four if the mood is irritable only) of seven symptoms during the period of mood disturbance, plus criterion C, associated impairment. To be given a current diagnosis of BPD, the child had to meet these criteria within the month prior to the interview. Statistical analyses Following the method of Hudziak et al. (28), we defined the CBCL-PBD score as the sum of the three CBCL scales that had been implicated in PBD by the studies reviewed in the Introduction: Attention Problems, Aggressive Behavior, and Anxious/Depressed. We used logistic regression to evaluate the statistical significance of the CBCL- PBD score as a predictor of the BPD diagnosis and used ROC analysis to evaluate the diagnostic efficiency of significant findings. Receiver operating characteristic analysis assesses the diagnostic efficiency of tests and to adjust cutpoints for clinical or research purposes (37) and has been widely applied to assessing the accuracy of diagnostic tests (38 40). On the ROC graph, the sensitivity (true positive rate) of different cutpoints on the test are graphed on the y-axis along with 1 minus the specificity (the false-positive rate) of the cutpoints on the x-axis to determine the ability of the test to optimize both measures for each point on the test. The higher the graph extends towards the upper left corner of the graph, the higher the discriminatory power of the test. Receiver operating characteristic analysis summarizes diagnostic efficiency with the area under the curve (AUC) statistic. The AUC ranges from 0.5 (when the test does not predict the disorder in any way) to 1.0 (when the test predicts the disorder perfectly). The AUC has two useful properties. First, it is equivalent to the Mann Whitney U-statistic computed from a comparison of the CBCL-PBD score between the bipolar disorder and non-bipolar disorder groups (41). Second, it equals the probability that a randomly selected member of the bipolar disorder group will have a more extreme CBCL-PBD score than a randomly selected member of the non-bipolar disorder group (41, 42).
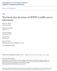
4 ROC of the CBCL-PBD Results The prevalence of a lifetime history of bipolar disorder was 4.7% (n ¼ 22) for probands and 3.4% (n ¼ 14) for siblings. For current bipolar disorder the prevalence figures were 2.8% (n ¼ 13) and 2.0% (n ¼ 8), respectively. The clinical and familial features of bipolar disorder in these children have been described in prior publications (3). For probands, the mean CBCL-PBD score was 170 ± 26. For siblings it was 158 ± 18. The logistic regression model predicting lifetime PBD diagnoses from CBCL-PBD scores was significant for both probands (z ¼ 6.5, p < 0.001) and siblings (z ¼ 5.9, p < 0.001). These results are shown graphically in the ROC curves in Fig. 1A,B for probands and siblings, respectively. The AUC was 0.89 for probands and 0.85 for siblings suggesting that the CBCL-PBD provided a highly efficient way of identifying subjects with a lifetime history of PBD in this sample. Sensitivity and specificity values at various cutpoints are given in Table 1. A Table 1. Sensitivity, specificity, positive predictive power, and negative predictive power at various cutpoints of the Child Behavior Checklistpediatric bipolar disorder Score threshold Sensitivity Specificity Positive predictive power Diagnostic accuracy statistics Proband lifetime Sibling lifetime Proband current Sibling current Negative predictive power B Area under ROC curve = The logistic regression model predicting lifetime PBD diagnoses from CBCL-PBD scores was significant for both probands (z ¼ 5.0, p < 0.001) and siblings (z ¼ 5.3, p < 0.001). The corresponding ROC curves are given in Fig. 2A,B, respectively. The AUC was 0.97 for probands and 0.82 for siblings suggesting that the CBCL-PBD score was highly efficient for identifying current PBD in both samples. Area under ROC curve = Fig. 1. Receiver operating characteristic (ROC) curve for Child Behavior Checklist-pediatric bipolar disorder (CBCL- PBD) in probands (A) with a lifetime diagnosis of PBD (B) and siblings. Discussion The diagnosis of PBD is a complicated and nontrivial enterprise. It involves careful examination of the child and parental reporting of the child s history. No screening test can substitute for the judgment of well-trained clinicians in making the diagnosis. The results here provide evidence for the utility of a CBCL score based on the attention, aggression, and anxiety/depression subscales to predict structured interview diagnoses of bipolar disorder in children. This value of this score and its potential for generalizability is underscored by the 521
5 Faraone et al. A B Area under ROC curve = Area under ROC curve = Fig. 2. Receiver operating characteristic (ROC) curve for Child Behavior Checklist-pediatric bipolar disorder (CBCL- PBD) in probands (A) with current diagnosis of PBD (B) and siblings. fact that the CBCL profile from which it was derived has been replicated across multiple age groups (20, 23 27), multiple treatment settings (inpatient, outpatient), and multiple cultures (American, Dutch, Brazilian, Australian). Notably, as measured by the AUC statistic, the diagnostic efficiency of CBCL predictions of current diagnoses of BPD (0.97) equals the diagnostic efficiency of Troponin-T as a predictor of acute myocardial infarction in an emergency room setting (AUC ¼ 0.94; 43). There continues to be much debate in the field about the diagnostic definition of PBD (7, 15), which is influenced by clinical traditions, interview methods, and differing interpretations of the nature of a mood episode. In contrast to these diagnostic issues, the CBCL is not affected by clinical tradition, interviewer training, or clinical interpretations. It relies solely on parental answers to questionnaire items. Thus, if it could be shown to be a valid predictor of PBD diagnoses, it would provide clinicians with a useful screening tool and 522 researchers with an easy method of measuring PBD psychopathology. One can choose cutpoints on the CBCL-PBD to fit the purpose of the clinician or the investigator. For example, if the clinician specifically wants to screen his or her clinical population for PBD and is willing to accept lower specificity, then a higher cutpoint can be used, which would result in higher number of false positives and more children tested. If instead, a researcher would like to investigate whether there is a high percentage of children with PBD in an epidemiological sample and wants to be assured that the children screened will have PBD, a cutpoint can be used, which will result in fewer false positives, but more false negatives. We conducted our analyses for the ADHD probands and their siblings to correspond to the ascertainment scheme of the original project. These two samples address different issues about the diagnostic accuracy of CBCL-PBD scores for PBD. The proband sample was a mix of ADHD subjects who had been referred to either psychiatric or pediatric clinics. Controls were selected from the same sites. The sibling sample consisted of the siblings of these probands. Thus, we might have expected the diagnostic accuracy of the CBCL- PBD to be greater for the probands because discriminating clinically referred cases is usually easier than cases in the population. Our results showed that this was true for current diagnoses but not for lifetime diagnoses. We did not find dramatic differences in the AUCs between lifetime and current diagnoses. For siblings, the AUCs for lifetime and current diagnoses were nearly identical (0.85 and 0.82, respectively). For probands, the AUC was somewhat less for lifetime (0.89) compared with current (0.97) diagnoses. Given that the CBCL inquires about behaviors that have occurred in the past 6 months, we would have expected CBCL-PBD scores to be more accurate for current, rather than lifetime, diagnoses. The unexpected accuracy of the CBCL for lifetime diagnoses may be due to the fact that, because PBD is such a severe disorder, children are rarely symptom free for a 6-month period. Our findings should be evaluated in light of methodological limitations. Although raters administering the structured diagnostic interviews were highly selected, trained, and supervised, they were not clinicians. Although our assessment methods may not elicit the same quality of information as of clinician interviews, in prior work we have shown 90% agreement between expert clinician-derived diagnoses of pediatric BPD and the structured interview diagnoses of non-clinical raters (44). Because our sample had originally been
6 ROC of the CBCL-PBD collected for a family study of ADHD, our findings may not generalize to other populations. Because our sample was collected through ADHD subjects, it provides an illustration of the ability of the CBCL-PBD score to discriminate bipolar diagnoses but cannot be used to define cutpoints for clinical use. As an illustration of the potential of the method, consider Fig. 2A, which presents results for current diagnoses in probands. Reading from the lower left-hand corner of the plot, each successive point corresponds to an increase of one point of the CBCL-PBD scale. For low scores, sensitivity is very low, which means that few PBD cases would be identified. But because low scores have a low false-positive rate (1 specificity), few false positives are identified. As we climb up the curve from the lower left to upper right corner, sensitivity increases dramatically without a large increase in the false-positive rate. For example, the score with a sensitivity of 75% has a false-positive rate of 10%. Although this false-positive rate is too high for substituting the CBCL-PBD for the PBD diagnosis, it does suggest that the CBCL score could be useful for screening in clinical contexts and as a quantitative trait for research studies. Despite these limitations, our work suggests that the CBCL-PBD has the potential to be a useful screening instrument for bipolar disorder in children. Specifically, the elevations on the Attention Problems, Aggressive Behavior, and Anxious/ Depressed subscales can be used to create a subscale that is highly heritable and predictive of PBD diagnoses. Our results suggest the efficiency of the measure to predict PBD is somewhat increased if the symptoms of PBD are current rather than lifetime and if the subject had been referred for a psychiatric disorder. Acknowledgements This work was supported, in part, by NIH grants RO1HD37999 and RO1MH66877 to S. Faraone and a grant from Johnson & Johnson to J. Biederman. References 1. Biederman J, Faraone SV, Keenan K, Tsuang MT. Evidence of familial association between attention deficit disorder and major affective disorders. Arch Gen Psychiatry 1991; 48: Geller B, Luby J. Child and adolescent bipolar disorder: a review of the past 10 years. J Am Acad Child Adolesc Psychiatry 1997; 36: Biederman J, Faraone S, Mick E et al. Attention-deficit hyperactivity disorder and juvenile mania: an overlooked comorbidity? J Am Acad Child Adolesc Psychiatry 1996; 35: Faraone SV, Biederman J, Mennin D, Russell R. Bipolar and antisocial disorders among relatives of ADHD children: parsing familial subtypes of illness. Am J Med Genet 1998; 81: Faraone SV, Biederman J, Mennin D, Wozniak J, Spencer T. Attention-deficit hyperactivity disorder with bipolar disorder: a familial subtype? J Am Acad Child Adolesc Psychiatry 1997; 36: ; discussion Weller EB, Weller RA, Fristad MA. Bipolar disorder in children: misdiagnosis, underdiagnosis, and future directions. J Am Acad Child Adolesc Psychiatry 1995; 34: Biederman J, Klein RG, Pine DS, Klein DF. Resolved: mania is mistaken for ADHD in prepubertal children. J Am Acad Child Adolesc Psychiatry 1998; 37: Faedda GL, Baldessarini RJ, Suppes T, Tondo L, Becker I, Lipschitz DS. Pediatric-onset bipolar disorder: a neglected clinical and public health problem. Harv Rev Psychiatry 1995; 3: Biederman J, Mick E, Faraone SV, Spencer T, Wilens TE, Wozniak J. Pediatric mania: a developmental subtype of bipolar disorder? Biol Psychiatry 2000; 48: Faraone SV, Biederman J, Wozniak J, Mundy E, Mennin D, O Donnell D. Is comorbidity with ADHD a marker for juvenile-onset mania? J Am Acad Child Adolesc Psychiatry 1997; 36: Biederman J, Munir K, Knee D et al. High rate of affective disorders in probands with attention deficit disorder and in their relatives: a controlled family study. Am J Psychiatry 1987; 144: Coyle JT, Pine DS, Charney DS et al. Depression and bipolar support alliance consensus statement on the unmet needs in diagnosis and treatment of mood disorders in children and adolescents. J Am Acad Child Adolesc Psychiatry 2003; 42: Wozniak J, Biederman J, Kiely K et al. Mania-like symptoms suggestive of childhood-onset bipolar disorder in clinically referred children. J Am Acad Child Adolesc Psychiatry 1995; 34: Faedda GL, Baldessarini RJ, Glovinsky IP, Austin NB. Pediatric bipolar disorder: phenomenology and course of illness. Bipolar Disord 2004; 6: Kowatch RA, Youngstrom EA, Danielyan A, Findling RL. Review and meta-analysis of the phenomenology and clinical characteristics of mania in children and adolescents. Bipolar Disord 2005; 7: Kowatch RA, Fristad M, Birmaher B, Wagner KD, Findling RL, Hellander M. Treatment guidelines for children and adolescents with bipolar disorder. J Am Acad Child Adolesc Psychiatry 2005; 44: Faraone SV, Glatt SJ, Tsuang MT. The genetics of pediatric-onset bipolar disorder. Biol Psychiatry 2003; 53: Faraone SV, Biederman J, Monuteaux MC. Attention deficit hyperactivity disorder with bipolar disorder in girls: further evidence for a familial subtype? J Affect Disord 2001; 64: Wozniak J, Spencer T, Biederman J et al. The clinical characteristics of unipolar versus bipolar major depression in ADHD youth. J Affect Disord 2004; 82 (Suppl. 1): S59 S Biederman J, Wozniak J, Kiely K et al. CBCL clinical scales discriminate prepubertal children with structured interviewderived diagnosis of mania from those with ADHD. J Am Acad Child Adolesc Psychiatry 1995; 34:
7 Faraone et al. 21. Achenbach TM. Manual for the Child Behavior Checklist/ 4-18 and 1991 Profile. Burlington, VT: University of Vermont, Mick E, Biederman J, Pandina G, Faraone SV. A preliminary meta-analysis of the child behavior checklist in pediatric bipolar disorder. Biol Psychiatry 2003; 53: Wals M, Hillegers MH, Reichart CG, Ormel J, Nolen WA, Verhulst FC. Prevalence of psychopathology in children of a bipolar parent. J Am Acad Child Adolesc Psychiatry 2001; 40: Carlson GA, Kelly KL. Manic symptoms in psychiatrically hospitalized children what do they mean? J Affect Disord 1998; 51: Geller B, Warner K, Williams M, Zimerman B. Prepubertal and young adolescent bipolarity versus ADHD: assessment and validity using the WASH-U-KSADS, CBCL and TRF. J Affect Disord 1998; 51: Hazell PL, Lewin TJ, Carr VJ. Confirmation that Child Behavior Checklist clinical scales discriminate juvenile mania from attention deficit hyperactivity disorder. J Paediatr Child Health 1999; 35: Dienes KA, Chang KD, Blasey CM, Adleman NE, Steiner H. Characterization of children of bipolar parents by parent report CBCL. J Psychiatr Res 2002; 36: Hudziak JJ, Althoff RR, Rettew DC, Derks EM, Faraone SV, Boomsma DI. The prevalence and genetic architecture of CBCL-juvenile bipolar disorder. Biol Psychiatry in press. 29. Althoff RR, Faraone SV, Rettew DC, Morley CP, Hudziak JJ. Family, twin, adoption, and molecular genetic studies of juvenile bipolar disorder. Bipolar Disord in press. 30. Kahana SY, Youngstrom EA, Findling RL, Calabrese JR. Employing parent, teacher, and youth self-report checklists in identifying pediatric bipolar spectrum disorders: an examination of diagnostic accuracy and clinical utility. J Child Adolesc Psychopharmacol 2003; 13: Biederman J, Faraone SV, Keenan K et al. Further evidence for family-genetic risk factors in attention deficit hyperactivity disorder: patterns of comorbidity in probands and relatives in psychiatrically and pediatrically referred samples. Arch Gen Psychiatry 1992; 49: Biederman J, Faraone SV, Mick E et al. Clinical correlates of ADHD in females: findings from a large group of girls ascertained from pediatric and psychiatric referral sources. J Am Acad Child Adolesc Psychiatry 1999; 38: Smoller JW, Finn CT. Family, twin, and adoption studies of bipolar disorder. Am J Med Genet 2003; 123C: Faraone SV, Glatt SJ, Su J, Tsuang MT. Three potential susceptibility loci shown by a genome-wide scan for regions influencing the age at onset of mania. Am J Psychiatry 2004; 161: Orvaschel H, Puig-Antich J. Schedule for Affective Disorders and Schizophrenia for School-Age Children: Epidemiologic Version. Fort Lauderdale, FL: Nova University, Leckman JF, Sholomskas D, Thompson WD, Belanger A, Weissman MM. Best estimate of lifetime psychiatric diagnosis: a methodological study. Arch Gen Psychiatry 1982; 39: McNeil BJ, Hanley JA. Statistical approaches to the analysis of receiver operating characteristic (ROC) curves. Med Decis Making 1984; 4: Swets JA. Sensitivities and specificities of diagnostic tests. JAMA 1982; 248: Siegel B, Vukicevic J, Elliott GR, Kraemer HC. The use of signal detection theory to assess DSM-III-R criteria for autistic disorder. J Am Acad Child Adolesc Psychiatry 1989; 28: Siegel B, Vukicevic J, Spitzer RL. Using signal detection methodology to revise DSM-III-R: re-analysis of the DSM-III-R national field trials for autistic disorder. J Psychiatr Res 1990; 24: Hanley JA, McNeil BJ. The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology 1982; 143: Colditz GA, Miller JN, Mosteller F. Measuring gain in the evaluation of medical technology. The probability of a better outcome. Int J Technol Assess Health Care 1988; 4: Collinson PO, Stubbs PJ, Kessler AC. Multicentre evaluation of the diagnostic value of cardiac troponin T, CK- MB mass, and myoglobin for assessing patients with suspected acute coronary syndromes in routine clinical practice. Heart 2003; 89: Wozniak J, Monuteaux M, Richards JE, Lai K, Faraone SV, Biederman J. Convergence between structured diagnostic interviews and clinical assessment on the diagnosis of pediatric-onset mania. Biol Psychiatry 2003; 53:
More boys than girls with attention deficit hyperactivity
 Why More Boys Than Girls With ADHD Receive Treatment: A Study of Dutch Twins Eske M. Derks, 1 James J. Hudziak, 2,3 and Dorret I. Boomsma 1 1 Department of Biological Psychology,Vrije Universiteit,Amsterdam,
Why More Boys Than Girls With ADHD Receive Treatment: A Study of Dutch Twins Eske M. Derks, 1 James J. Hudziak, 2,3 and Dorret I. Boomsma 1 1 Department of Biological Psychology,Vrije Universiteit,Amsterdam,
J. Indian Assoc. Child Adolesc. Ment. Health 2012; 8(1):1-5. Editorial
 1 J. Indian Assoc. Child Adolesc. Ment. Health 2012; 8(1):1-5 Editorial Controversies in Paediatric Bipolar Disorder Vivek Agarwal 1, Sivakumar T 2 1.Editor JIACAM & Associate Professor, Department of
1 J. Indian Assoc. Child Adolesc. Ment. Health 2012; 8(1):1-5 Editorial Controversies in Paediatric Bipolar Disorder Vivek Agarwal 1, Sivakumar T 2 1.Editor JIACAM & Associate Professor, Department of
The existence, prevalence, and taxonomy of juvenile bipolar
 Longitudinal Stability of the CBCL-Juvenile Bipolar Disorder Phenotype: A Study in Dutch Twins Dorret I. Boomsma, Irene Rebollo, Eske M. Derks, Toos C.E.M. van Beijsterveldt, Robert R. Althoff, David C.
Longitudinal Stability of the CBCL-Juvenile Bipolar Disorder Phenotype: A Study in Dutch Twins Dorret I. Boomsma, Irene Rebollo, Eske M. Derks, Toos C.E.M. van Beijsterveldt, Robert R. Althoff, David C.
The comparison of behavioral and emotional problems in children with a bipolar parent and children with healthy parents in Zahedan, Iran, 2011
 The comparison of behavioral and emotional problems in children with a bipolar parent and children with healthy parents in Zahedan, Iran, 2011 Mahboubeh Firoozkouhi Moghaddam, Nour Mohammad Bakhshani,
The comparison of behavioral and emotional problems in children with a bipolar parent and children with healthy parents in Zahedan, Iran, 2011 Mahboubeh Firoozkouhi Moghaddam, Nour Mohammad Bakhshani,
NIH Public Access Author Manuscript Psychol Assess. Author manuscript; available in PMC 2011 September 1.
 NIH Public Access Author Manuscript Published in final edited form as: Psychol Assess. 2010 September ; 22(3): 609 617. doi:10.1037/a0019699. Assessment of Dysregulated Children Using the Child Behavior
NIH Public Access Author Manuscript Published in final edited form as: Psychol Assess. 2010 September ; 22(3): 609 617. doi:10.1037/a0019699. Assessment of Dysregulated Children Using the Child Behavior
APPENDIX 11: CASE IDENTIFICATION STUDY CHARACTERISTICS AND RISK OF BIAS TABLES
 APPENDIX 11: CASE IDENTIFICATION STUDY CHARACTERISTICS AND RISK OF BIAS TABLES 1 Study characteristics table... 3 2 Methodology checklist: the QUADAS-2 tool for studies of diagnostic test accuracy... 4
APPENDIX 11: CASE IDENTIFICATION STUDY CHARACTERISTICS AND RISK OF BIAS TABLES 1 Study characteristics table... 3 2 Methodology checklist: the QUADAS-2 tool for studies of diagnostic test accuracy... 4
Differentiating MDD vs. Bipolar Depression In Youth
 Differentiating MDD vs. Bipolar Depression In Youth Mai Uchida, M.D. Staff Physician Clinical and Research Programs in Pediatric Psychopharmacology Massachusetts General Hospital Disclosures Neither I
Differentiating MDD vs. Bipolar Depression In Youth Mai Uchida, M.D. Staff Physician Clinical and Research Programs in Pediatric Psychopharmacology Massachusetts General Hospital Disclosures Neither I
University of Groningen. Children of bipolar parents Wals, Marjolein
 University of Groningen Children of bipolar parents Wals, Marjolein IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Children of bipolar parents Wals, Marjolein IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna
 University of Groningen Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna IMPORTANT NOTE: You are advised to consult the publisher's
University of Groningen Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna IMPORTANT NOTE: You are advised to consult the publisher's
SUMMARY AND DISCUSSION
 Risk factors for the development and outcome of childhood psychopathology SUMMARY AND DISCUSSION Chapter 147 In this chapter I present a summary of the results of the studies described in this thesis followed
Risk factors for the development and outcome of childhood psychopathology SUMMARY AND DISCUSSION Chapter 147 In this chapter I present a summary of the results of the studies described in this thesis followed
Bipolar disorder in children and young people on the autism spectrum
 Exclusively sponsored by: Bipolar disorder in children and young people on the autism spectrum We are members of a multidisciplinary tertiary second opinion referral service for youth (under age 18 years)
Exclusively sponsored by: Bipolar disorder in children and young people on the autism spectrum We are members of a multidisciplinary tertiary second opinion referral service for youth (under age 18 years)
CONTROVERSIES AND NEW DIRECTIONS
 BIPOLAR Introduction DISORDER IN CHILDHOOD AND EARLY ADOLESCENCE Introduction MELISSA P. D ELBELLO, DAVID AXELSON, and BARBARA GELLER CONTROVERSIES AND NEW DIRECTIONS Although the existence and diagnostic
BIPOLAR Introduction DISORDER IN CHILDHOOD AND EARLY ADOLESCENCE Introduction MELISSA P. D ELBELLO, DAVID AXELSON, and BARBARA GELLER CONTROVERSIES AND NEW DIRECTIONS Although the existence and diagnostic
BEHAVIOR PROBLEMS AND SUBTYPES OF ATTENTION-DEFICIT HYPERACTIVITY DISORDER WITH COMORBIDITIES
 BEHAVIOR PROBLEMS AND SUBTYPES OF ATTENTION-DEFICIT HYPERACTIVITY DISORDER WITH COMORBIDITIES Ruu-Fen Tzang 1,2 and Yue-Cune Chang 3 1 Department of Psychiatry, Mackay Memorial Hospital, 2 Mackay Medicine,
BEHAVIOR PROBLEMS AND SUBTYPES OF ATTENTION-DEFICIT HYPERACTIVITY DISORDER WITH COMORBIDITIES Ruu-Fen Tzang 1,2 and Yue-Cune Chang 3 1 Department of Psychiatry, Mackay Memorial Hospital, 2 Mackay Medicine,
University of Groningen. Children of bipolar parents Wals, Marjolein
 University of Groningen Children of bipolar parents Wals, Marjolein IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Children of bipolar parents Wals, Marjolein IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Differentiating Unipolar vs Bipolar Depression in Children
 Differentiating Unipolar vs Bipolar Depression in Children Mai Uchida, M.D. Director, Center for Early Identification and Prevention of Pediatric Depression Massachusetts General Hospital Assistant Professor
Differentiating Unipolar vs Bipolar Depression in Children Mai Uchida, M.D. Director, Center for Early Identification and Prevention of Pediatric Depression Massachusetts General Hospital Assistant Professor
Aggregation of psychopathology in a clinical sample of children and their parents
 Aggregation of psychopathology in a clinical sample of children and their parents PA R E N T S O F C H I LD R E N W I T H PSYC H O PAT H O LO G Y : PSYC H I AT R I C P R O B LEMS A N D T H E A S SO C I
Aggregation of psychopathology in a clinical sample of children and their parents PA R E N T S O F C H I LD R E N W I T H PSYC H O PAT H O LO G Y : PSYC H I AT R I C P R O B LEMS A N D T H E A S SO C I
Deficits in Emotional Regulation in ADHD
 Deficits in Emotional Regulation in ADHD Joseph Biederman, MD Professor of Psychiatry Harvard Medical School Chief, Clinical and Research Programs in Pediatric Psychopharmacology and Adult ADHD Massachusetts
Deficits in Emotional Regulation in ADHD Joseph Biederman, MD Professor of Psychiatry Harvard Medical School Chief, Clinical and Research Programs in Pediatric Psychopharmacology and Adult ADHD Massachusetts
RANZCP 2010 AUCKLAND, NEW ZEALAND
 RANZCP 2010 AUCKLAND, NEW ZEALAND Dr Veronica Stanganelli et al. RANZCP 2010 1 INTRODUCTION Bipolar disorder within young people has been debated for years. It is still controversial in DSM V (1), whether
RANZCP 2010 AUCKLAND, NEW ZEALAND Dr Veronica Stanganelli et al. RANZCP 2010 1 INTRODUCTION Bipolar disorder within young people has been debated for years. It is still controversial in DSM V (1), whether
Discriminative Validity of the General Behavior Inventory Using Youth Report
 Journal of Abnormal Child Psychology, Vol. 31, No. 1, February 2003, pp. 29 39 ( C 2003) Discriminative Validity of the General Behavior Inventory Using Youth Report Carla Kmett Danielson, 1 Eric A. Youngstrom,
Journal of Abnormal Child Psychology, Vol. 31, No. 1, February 2003, pp. 29 39 ( C 2003) Discriminative Validity of the General Behavior Inventory Using Youth Report Carla Kmett Danielson, 1 Eric A. Youngstrom,
Paediatric Bipolar Disorder & Transitions to adult services. Adi Sharma on behalf of ABS
 Paediatric Bipolar Disorder & Transitions to adult services Adi Sharma on behalf of ABS Talk Paediatric Bipolar Disorder [PBD]: Why bother DMDD Comorbidity and/or Differential Diagnoses: EUPD, ADHD & ASD
Paediatric Bipolar Disorder & Transitions to adult services Adi Sharma on behalf of ABS Talk Paediatric Bipolar Disorder [PBD]: Why bother DMDD Comorbidity and/or Differential Diagnoses: EUPD, ADHD & ASD
Current concepts in the validity, diagnosis and treatment of paediatric bipolar disorder
 International Journal of Neuropsychopharmacology (2003), 6, 293 300. Copyright f 2003 CINP DOI: 10.1017/S1461145703003547 Current concepts in the validity, diagnosis and treatment of paediatric bipolar
International Journal of Neuropsychopharmacology (2003), 6, 293 300. Copyright f 2003 CINP DOI: 10.1017/S1461145703003547 Current concepts in the validity, diagnosis and treatment of paediatric bipolar
The shift in nosology from the Diagnostic PROCEEDINGS FROM CHILDHOOD TO ADOLESCENCE: DIAGNOSIS AND COMORBIDITY ISSUES * Thomas J. Spencer, MD ABSTRACT
 FROM CHILDHOOD TO ADOLESCENCE: DIAGNOSIS AND COMORBIDITY ISSUES * Thomas J. Spencer, MD ABSTRACT Attention-deficit/hyperactivity disorder (ADHD) tends to manifest differently in adolescents than in children,
FROM CHILDHOOD TO ADOLESCENCE: DIAGNOSIS AND COMORBIDITY ISSUES * Thomas J. Spencer, MD ABSTRACT Attention-deficit/hyperactivity disorder (ADHD) tends to manifest differently in adolescents than in children,
Pediatric Mania: A Developmental Subtype of Bipolar Disorder?
 Pediatric Mania: A Developmental Subtype of Bipolar Disorder? Joseph Biederman, Eric Mick, Stephen V. Faraone, Thomas Spencer, Timothy E. Wilens, and Janet Wozniak Despite ongoing controversy, the view
Pediatric Mania: A Developmental Subtype of Bipolar Disorder? Joseph Biederman, Eric Mick, Stephen V. Faraone, Thomas Spencer, Timothy E. Wilens, and Janet Wozniak Despite ongoing controversy, the view
Attention Deficit Disorder. Evaluation Scale-Home Version 16. The Attention Deficit Disorders. Evaluation Scale-School Version 17
 The Development of an Educational and Screening Instrument for Attention Deficit Hyperactivity Disorder in a Pediatric Residency Program Stephen P. Amos, Ph.D., Robert Wittler, M.D., Corrie Nevil, M.D.,
The Development of an Educational and Screening Instrument for Attention Deficit Hyperactivity Disorder in a Pediatric Residency Program Stephen P. Amos, Ph.D., Robert Wittler, M.D., Corrie Nevil, M.D.,
NIH Public Access Author Manuscript J Am Acad Child Adolesc Psychiatry. Author manuscript; available in PMC 2011 November 1.
 NIH Public Access Author Manuscript Published in final edited form as: J Am Acad Child Adolesc Psychiatry. 2010 November ; 49(11): 1105 1116.e1. doi:10.1016/j.jaac. 2010.08.006. Adult Outcomes of Childhood
NIH Public Access Author Manuscript Published in final edited form as: J Am Acad Child Adolesc Psychiatry. 2010 November ; 49(11): 1105 1116.e1. doi:10.1016/j.jaac. 2010.08.006. Adult Outcomes of Childhood
Practice Parameter for the Assessment and Treatment of Children and Adolescents with Bipolar Disorder,
 Practice Parameter for the Assessment and Treatment of Children and Adolescents with Bipolar Disorder, Journal of the Academy of Child and Adolescent Psychiatry, 1997 Primary Authors: Jon McClellan MD
Practice Parameter for the Assessment and Treatment of Children and Adolescents with Bipolar Disorder, Journal of the Academy of Child and Adolescent Psychiatry, 1997 Primary Authors: Jon McClellan MD
Quality of Life in Children With Psychiatric Disorders: Self-, Parent, and Clinician Report
 Quality of Life in Children With Psychiatric Disorders: Self-, Parent, and Clinician Report DENNIS BASTIAANSEN, M.D., HANS M. KOOT, PH.D., ROBERT F. FERDINAND, M.D., PH.D., AND FRANK C. VERHULST, M.D.,
Quality of Life in Children With Psychiatric Disorders: Self-, Parent, and Clinician Report DENNIS BASTIAANSEN, M.D., HANS M. KOOT, PH.D., ROBERT F. FERDINAND, M.D., PH.D., AND FRANK C. VERHULST, M.D.,
Comprehensive Quick Reference Handout on Pediatric Bipolar Disorder By Jessica Tomasula
 Comprehensive Quick Reference Handout on Pediatric Bipolar Disorder By Jessica Tomasula Official Name Bipolar Disorder; also referred to as Manic Depression Definitions (DSM-IV-TR, 2000) Bipolar I Disorder
Comprehensive Quick Reference Handout on Pediatric Bipolar Disorder By Jessica Tomasula Official Name Bipolar Disorder; also referred to as Manic Depression Definitions (DSM-IV-TR, 2000) Bipolar I Disorder
Research has shown that adverse childhood experiences
 Article Differential Effect of Environmental Adversity by Gender: Rutter s Index of Adversity in a Group of Boys and Girls With and Without ADHD Joseph Biederman, M.D. Stephen V. Faraone, Ph.D. Michael
Article Differential Effect of Environmental Adversity by Gender: Rutter s Index of Adversity in a Group of Boys and Girls With and Without ADHD Joseph Biederman, M.D. Stephen V. Faraone, Ph.D. Michael
S P O U S A L R ES E M B L A N C E I N PSYCHOPATHOLOGY: A C O M PA R I SO N O F PA R E N T S O F C H I LD R E N W I T H A N D WITHOUT PSYCHOPATHOLOGY
 Aggregation of psychopathology in a clinical sample of children and their parents S P O U S A L R ES E M B L A N C E I N PSYCHOPATHOLOGY: A C O M PA R I SO N O F PA R E N T S O F C H I LD R E N W I T H
Aggregation of psychopathology in a clinical sample of children and their parents S P O U S A L R ES E M B L A N C E I N PSYCHOPATHOLOGY: A C O M PA R I SO N O F PA R E N T S O F C H I LD R E N W I T H
A dimensional approach to developmental psychopathology
 International Journal of Methods in Psychiatric Research Published online in Wiley InterScience (www.interscience.wiley.com).217 A dimensional approach to developmental psychopathology JAMES J. HUDZIAK,
International Journal of Methods in Psychiatric Research Published online in Wiley InterScience (www.interscience.wiley.com).217 A dimensional approach to developmental psychopathology JAMES J. HUDZIAK,
A randomized controlled clinical trial of Citalopram versus Fluoxetine in children and adolescents with obsessive-compulsive disorder (OCD)
 Eur Child Adolesc Psychiatry (2009) 18:131 135 DOI 10.1007/s00787-007-0634-z ORIGINAL CONTRIBUTION Javad Alaghband-Rad Mitra Hakimshooshtary A randomized controlled clinical trial of Citalopram versus
Eur Child Adolesc Psychiatry (2009) 18:131 135 DOI 10.1007/s00787-007-0634-z ORIGINAL CONTRIBUTION Javad Alaghband-Rad Mitra Hakimshooshtary A randomized controlled clinical trial of Citalopram versus
University of Groningen. Children of bipolar parents Wals, Marjolein
 University of Groningen Children of bipolar parents Wals, Marjolein IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Children of bipolar parents Wals, Marjolein IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 BadgerCare Plus Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice
BadgerCare Plus Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice
Psychosocial problems in attention-deficit hyperactivity disorder with oppositional defiant disorder
 Psychiatry and Clinical Neurosciences (2002), 56, 365 369 Regular Article Psychosocial problems in attention-deficit hyperactivity disorder with oppositional defiant disorder YUZURU HARADA, md, phd, 1
Psychiatry and Clinical Neurosciences (2002), 56, 365 369 Regular Article Psychosocial problems in attention-deficit hyperactivity disorder with oppositional defiant disorder YUZURU HARADA, md, phd, 1
BroadcastMed Bipolar, Borderline, Both? Diagnostic/Formulation Issues in Mood and Personality Disorders
 BroadcastMed Bipolar, Borderline, Both? Diagnostic/Formulation Issues in Mood and Personality Disorders BRIAN PALMER: Hi. My name is Brian Palmer. I'm a psychiatrist here at Mayo Clinic. Today, we'd like
BroadcastMed Bipolar, Borderline, Both? Diagnostic/Formulation Issues in Mood and Personality Disorders BRIAN PALMER: Hi. My name is Brian Palmer. I'm a psychiatrist here at Mayo Clinic. Today, we'd like
History of Maltreatment and Psychiatric Impairment in Children in Outpatient Psychiatric Treatment
 University of Connecticut DigitalCommons@UConn Honors Scholar Theses Honors Scholar Program Spring 5-10-2009 History of Maltreatment and Psychiatric Impairment in Children in Outpatient Psychiatric Treatment
University of Connecticut DigitalCommons@UConn Honors Scholar Theses Honors Scholar Program Spring 5-10-2009 History of Maltreatment and Psychiatric Impairment in Children in Outpatient Psychiatric Treatment
Anxiety disorders in mothers and their children: prospective longitudinal community study
 Anxiety disorders in mothers and their children: prospective longitudinal community study Andrea Schreier, Hans-Ulrich Wittchen, Michael Höfler and Roselind Lieb Summary The relationship between DSM IV
Anxiety disorders in mothers and their children: prospective longitudinal community study Andrea Schreier, Hans-Ulrich Wittchen, Michael Höfler and Roselind Lieb Summary The relationship between DSM IV
Birth Order and Sibling Gender Ratio of a Clinical Sample of Children and Adolescents Diagnosed with Attention Deficit Hyperactivity Disorder
 Birth Order and Sibling Gender Ratio of a Clinical Sample Original Article Birth Order and Sibling Gender Ratio of a Clinical Sample of Children and Adolescents Diagnosed with Attention Deficit Hyperactivity
Birth Order and Sibling Gender Ratio of a Clinical Sample Original Article Birth Order and Sibling Gender Ratio of a Clinical Sample of Children and Adolescents Diagnosed with Attention Deficit Hyperactivity
The criterion validity of the Borderline Personality Features Scale for Children
 Journal of Personality Disorders, 25(4), 492 503, 2011 2011 The Guilford Press The criterion validity of the Borderline Personality Features Scale for Children in an adolescent inpatient setting Bonny
Journal of Personality Disorders, 25(4), 492 503, 2011 2011 The Guilford Press The criterion validity of the Borderline Personality Features Scale for Children in an adolescent inpatient setting Bonny
Bipolar Disorder in Youth
 Bipolar Disorder in Youth Janet Wozniak, M.D. Associate Professor of Psychiatry Director, Pediatric Bipolar Disorder Research Program Harvard Medical School Massachusetts General Hospital Pediatric-Onset
Bipolar Disorder in Youth Janet Wozniak, M.D. Associate Professor of Psychiatry Director, Pediatric Bipolar Disorder Research Program Harvard Medical School Massachusetts General Hospital Pediatric-Onset
Pediatric Bipolar Disorder and ADHD
 Pediatric Bipolar Disorder and ADHD Janet Wozniak, M.D. Director, Pediatric Bipolar Disorder Research Program Associate Professor Psychiatry Massachusetts General Hospital Harvard Medical School Disclosures
Pediatric Bipolar Disorder and ADHD Janet Wozniak, M.D. Director, Pediatric Bipolar Disorder Research Program Associate Professor Psychiatry Massachusetts General Hospital Harvard Medical School Disclosures
Childhood ADHD is a risk factor for some Psychiatric Disorders and co-morbidities
 Childhood ADHD is a risk factor for some Psychiatric Disorders and co-morbidities By: Dr. Ehsane M. Gad M.B.B.Ch CABMSPsych. D.P.P Post-Fellow Aus. Consultant Child Psychiatry Childhood ADHD and emergence
Childhood ADHD is a risk factor for some Psychiatric Disorders and co-morbidities By: Dr. Ehsane M. Gad M.B.B.Ch CABMSPsych. D.P.P Post-Fellow Aus. Consultant Child Psychiatry Childhood ADHD and emergence
Clinical evaluation of children testing positive in screening tests for attention-deficit/hyperactivity disorder: A preliminary report
 Eur. J. Psychiat. Vol. 23, N. 2, (115-120) 2009 Keywords: Attention deficit hyperactivity disorder; Diagnosis; Psychiatric assessment; Screening tests. Clinical evaluation of children testing positive
Eur. J. Psychiat. Vol. 23, N. 2, (115-120) 2009 Keywords: Attention deficit hyperactivity disorder; Diagnosis; Psychiatric assessment; Screening tests. Clinical evaluation of children testing positive
Youthdale Treatment Centres
 Youthdale Treatment Centres 227 Victoria Street, Toronto, ON M5B 1T8 PEG 205 Final Report August 1, 2007 Stephens R and Guerra R."Longitudinal functional and behavioural outcomes of youth with neuropsychiatric
Youthdale Treatment Centres 227 Victoria Street, Toronto, ON M5B 1T8 PEG 205 Final Report August 1, 2007 Stephens R and Guerra R."Longitudinal functional and behavioural outcomes of youth with neuropsychiatric
5 COMMON QUESTIONS WHEN TREATING DEPRESSION
 5 COMMON QUESTIONS WHEN TREATING DEPRESSION Do Antidepressants Increase the Possibility of Suicide? Will I Accidentally Induce Mania if I Prescribe an SSRI? Are Depression Medications Safe and Effective
5 COMMON QUESTIONS WHEN TREATING DEPRESSION Do Antidepressants Increase the Possibility of Suicide? Will I Accidentally Induce Mania if I Prescribe an SSRI? Are Depression Medications Safe and Effective
Depressive Disorder in Children and Adolescents: Dysthymic Disorder and the Use of Self-Rating Scales in Assessment
 Depressive Disorder in Children and Adolescents: Dysthymic Disorder and the Use of Self-Rating Scales in Assessment Stuart Fine, MB, FRCP (C), Marlene Moretti, MA, Glenn Haley, MA, Simon Fraser University.
Depressive Disorder in Children and Adolescents: Dysthymic Disorder and the Use of Self-Rating Scales in Assessment Stuart Fine, MB, FRCP (C), Marlene Moretti, MA, Glenn Haley, MA, Simon Fraser University.
NIH Public Access Author Manuscript J Am Acad Child Adolesc Psychiatry. Author manuscript; available in PMC 2015 April 01.
 NIH Public Access Author Manuscript Published in final edited form as: J Am Acad Child Adolesc Psychiatry. 2014 April ; 53(4): 408 416. doi:10.1016/j.jaac.2013.12.026. Disruptive Mood Dysregulation Disorder
NIH Public Access Author Manuscript Published in final edited form as: J Am Acad Child Adolesc Psychiatry. 2014 April ; 53(4): 408 416. doi:10.1016/j.jaac.2013.12.026. Disruptive Mood Dysregulation Disorder
Current. A bad boy s behavior problems CASES THAT TEST YOUR SKILLS
 Two weeks after changing medications, a hyperactive 11-year-old becomes manic and attempts suicide. Is the new regimen or an undiagnosed mental disorder to blame? A. Kenneth Fuller, MD Chief of psychiatry
Two weeks after changing medications, a hyperactive 11-year-old becomes manic and attempts suicide. Is the new regimen or an undiagnosed mental disorder to blame? A. Kenneth Fuller, MD Chief of psychiatry
Disruptive Mood Dysregulation Disorder
 Walden University ScholarWorks School of Counseling Publications College of Social and Behavioral Sciences 2015 Disruptive Mood Dysregulation Disorder Brandy L. Gilea Walden University Rachel M. O Neill
Walden University ScholarWorks School of Counseling Publications College of Social and Behavioral Sciences 2015 Disruptive Mood Dysregulation Disorder Brandy L. Gilea Walden University Rachel M. O Neill
Early risk factors for adult bipolar disorder in adolescents with mood disorders: a 15-year follow-up of a community sample
 Päären et al. BMC Psychiatry (2014) 14:363 DOI 10.1186/s12888-014-0363-z RESEARCH ARTICLE Open Access Early risk factors for adult bipolar disorder in adolescents with mood disorders: a 15-year follow-up
Päären et al. BMC Psychiatry (2014) 14:363 DOI 10.1186/s12888-014-0363-z RESEARCH ARTICLE Open Access Early risk factors for adult bipolar disorder in adolescents with mood disorders: a 15-year follow-up
Severe Mood Dysregulation in Children and Adolescents Research Findings Support Diagnostic Validity of Pediatric Bipolar Disorder
 Severe Mood Dysregulation in Children and Adolescents Research Findings Support Diagnostic Validity of Pediatric Bipolar Disorder Janet Wozniak, M.D. Associate Professor of Psychiatry Director, Pediatric
Severe Mood Dysregulation in Children and Adolescents Research Findings Support Diagnostic Validity of Pediatric Bipolar Disorder Janet Wozniak, M.D. Associate Professor of Psychiatry Director, Pediatric
Disentangling chronological age from age of onset in children and adolescents with obsessive compulsive disorder
 International Journal of Neuropsychopharmacology (2001), 4, 169 178. Copyright 2001 CINP Disentangling chronological age from age of onset in children and adolescents with obsessive compulsive disorder
International Journal of Neuropsychopharmacology (2001), 4, 169 178. Copyright 2001 CINP Disentangling chronological age from age of onset in children and adolescents with obsessive compulsive disorder
Title: ADHD: Symptom Reduction in Follow up Period CMS ID: PP3 NQF #: N/A
 Source(s) Office of the National Coordinator for Health Information Technology/Centers for Medicare & Medicaid Services Measure Domain Effective Clinical Care: Outcome Brief Abstract Description Percentage
Source(s) Office of the National Coordinator for Health Information Technology/Centers for Medicare & Medicaid Services Measure Domain Effective Clinical Care: Outcome Brief Abstract Description Percentage
New Research in Depression and Anxiety
 New Research in Depression and Anxiety Robert Glassman Introduction Depression and anxiety are some of the most common disorders of childhood and adolescence. New research in these areas explores important
New Research in Depression and Anxiety Robert Glassman Introduction Depression and anxiety are some of the most common disorders of childhood and adolescence. New research in these areas explores important
PSYCHOPATHOLOGY AND DEVELOPMENT: TRAJECTORIES OF PSYCHOPATHOLOGY FROM EARLY ADOLESCENCE THROUGH YOUNG ADULTHOOD
 Psychopathology and Develoment, 1 PSYCHOPATHOLOGY AND DEVELOPMENT: TRAJECTORIES OF PSYCHOPATHOLOGY FROM EARLY ADOLESCENCE THROUGH YOUNG ADULTHOOD Marc S. Schulz*, Stuart T. Hauser**, Joseph P. Allen***,
Psychopathology and Develoment, 1 PSYCHOPATHOLOGY AND DEVELOPMENT: TRAJECTORIES OF PSYCHOPATHOLOGY FROM EARLY ADOLESCENCE THROUGH YOUNG ADULTHOOD Marc S. Schulz*, Stuart T. Hauser**, Joseph P. Allen***,
Managing ADHD in the Primary Care Setting
 Managing ADHD in the Primary Care Setting Andrea E. Spencer, MD Assistant Professor of Psychiatry Boston University School of Medicine Boston Medical Center March 17, 2017 Disclosures Neither I nor my
Managing ADHD in the Primary Care Setting Andrea E. Spencer, MD Assistant Professor of Psychiatry Boston University School of Medicine Boston Medical Center March 17, 2017 Disclosures Neither I nor my
Adolescent depression
 Diagnostic skills can differentiate 40 VOL. 1, NO. 7 / JULY 2002 teen angst from psychopathology Ann Wagner, PhD Chief, Autism and Pervasive Developmental Disorders Intervention Research Program Benedetto
Diagnostic skills can differentiate 40 VOL. 1, NO. 7 / JULY 2002 teen angst from psychopathology Ann Wagner, PhD Chief, Autism and Pervasive Developmental Disorders Intervention Research Program Benedetto
Change in resolved plans and suicidal ideation factors of suicidality after participation in an intensive outpatient treatment program
 Journal of Affective Disorders 103 (2007) 63 68 www.elsevier.com/locate/jad Research report Change in resolved plans and suicidal ideation factors of suicidality after participation in an intensive outpatient
Journal of Affective Disorders 103 (2007) 63 68 www.elsevier.com/locate/jad Research report Change in resolved plans and suicidal ideation factors of suicidality after participation in an intensive outpatient
With additional support from Florida International University and The Children s Trust.
 The Society for Clinical Child and Adolescent Psychology (SCCAP): Initiative for Dissemination of Evidence-based Treatments for Childhood and Adolescent Mental Health Problems With additional support from
The Society for Clinical Child and Adolescent Psychology (SCCAP): Initiative for Dissemination of Evidence-based Treatments for Childhood and Adolescent Mental Health Problems With additional support from
Impact of Comorbidities on Self-Esteem of Children with Attention Deficit Hyperactivity Disorder
 The International Journal of Indian Psychology ISSN 2348-5396 (e) ISSN: 2349-3429 (p) Volume 3, Issue 3, No.1, DIP: 18.01.011/20160303 ISBN: 978-1-365-03416-9 http://www.ijip.in April - June, 2016 Impact
The International Journal of Indian Psychology ISSN 2348-5396 (e) ISSN: 2349-3429 (p) Volume 3, Issue 3, No.1, DIP: 18.01.011/20160303 ISBN: 978-1-365-03416-9 http://www.ijip.in April - June, 2016 Impact
The latent class structure of ADHD is stable across informants
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2006 The latent class structure of ADHD is stable across informants Robert R. Althoff University of Vermont William
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2006 The latent class structure of ADHD is stable across informants Robert R. Althoff University of Vermont William
Mood lability among offspring of parents with bipolar disorder and community controls
 Bipolar Disorders 2013: 15: 253 263 Original Article 2013 John Wiley and Sons A/S Published by Blackwell Publishing Ltd. BIPOLAR DISORDERS Mood lability among offspring of parents with bipolar disorder
Bipolar Disorders 2013: 15: 253 263 Original Article 2013 John Wiley and Sons A/S Published by Blackwell Publishing Ltd. BIPOLAR DISORDERS Mood lability among offspring of parents with bipolar disorder
Bipolar Disorder Sarah Brown
 Bipolar Disorder Sarah Brown Introduction Bipolar disorder, also referred to as Manic Depressive Illness, is an affective disorder characterized by alternating periods of mania and depression. A person
Bipolar Disorder Sarah Brown Introduction Bipolar disorder, also referred to as Manic Depressive Illness, is an affective disorder characterized by alternating periods of mania and depression. A person
To justify their expense, specialty
 mcd1.qxd 12/13/01 12:34 PM Page 57 Severity of Children s Psychopathology and Impairment and Its Relationship to Treatment Setting Brett M. McDermott, M.B.B.S., F.R.A.N.Z.C.P. Robert McKelvey, M.D., F.R.A.N.Z.C.P.
mcd1.qxd 12/13/01 12:34 PM Page 57 Severity of Children s Psychopathology and Impairment and Its Relationship to Treatment Setting Brett M. McDermott, M.B.B.S., F.R.A.N.Z.C.P. Robert McKelvey, M.D., F.R.A.N.Z.C.P.
Pediatric Bipolar Disorder: Advances in Diagnosis and Research
 Pediatric Bipolar Disorder: Advances in Diagnosis and Research Janet Wozniak, M.D. Associate Professor of Psychiatry Director, Pediatric Bipolar Disorder Research Program Harvard Medical School Massachusetts
Pediatric Bipolar Disorder: Advances in Diagnosis and Research Janet Wozniak, M.D. Associate Professor of Psychiatry Director, Pediatric Bipolar Disorder Research Program Harvard Medical School Massachusetts
Written by Dr. Taylor Saturday, 20 February :10 - Last Updated Tuesday, 26 August :06
 ADHD and Generalized Anziety Disorder by Susan Hill, Ph.D. While discriminating between disorders within a category of the Diagnostic and Statistical Manual - fourth edition (DSM-IV) can be challenging,
ADHD and Generalized Anziety Disorder by Susan Hill, Ph.D. While discriminating between disorders within a category of the Diagnostic and Statistical Manual - fourth edition (DSM-IV) can be challenging,
University of Utrecht Master psychology, Child- and Youth Psychology THESIS
 University of Utrecht Master psychology, Child- and Youth Psychology THESIS Parents of Children with ADHD, ODD or Comorbid ADHD and ODD: Do their Parenting Practices Differ? Desiree Kluijtmans, 3270173
University of Utrecht Master psychology, Child- and Youth Psychology THESIS Parents of Children with ADHD, ODD or Comorbid ADHD and ODD: Do their Parenting Practices Differ? Desiree Kluijtmans, 3270173
University of Groningen. Children of bipolar parents Wals, Marjolein
 University of Groningen Children of bipolar parents Wals, Marjolein IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Children of bipolar parents Wals, Marjolein IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Sinhala translation of child behaviour checklist: validity and reliability
 Sinhala translation of child behaviour checklist: validity and reliability B C V Senaratna 1, H Perera 2 and P Fonseka 3 Abstract Objective To translate the child behaviour checklist (CBCL) into Sinhala
Sinhala translation of child behaviour checklist: validity and reliability B C V Senaratna 1, H Perera 2 and P Fonseka 3 Abstract Objective To translate the child behaviour checklist (CBCL) into Sinhala
Downloaded by Guangxi University for Nationalities from online.liebertpub.com at 02/19/18. For personal use only. ABSTRACT
 JOURNAL OF CHILD AND ADOLESCENT PSYCHOPHARMACOLOGY Volume 12, Number 1, 2002 Mary Ann Liebert, Inc. Pp. 3 9 Phenomenology of Prepubertal and Early Adolescent Bipolar Disorder: Examples of Elated Mood,
JOURNAL OF CHILD AND ADOLESCENT PSYCHOPHARMACOLOGY Volume 12, Number 1, 2002 Mary Ann Liebert, Inc. Pp. 3 9 Phenomenology of Prepubertal and Early Adolescent Bipolar Disorder: Examples of Elated Mood,
Correspondence of Pediatric Inpatient Behavior Scale (PIBS) Scores with DSM Diagnosis and Problem Severity Ratings in a Referred Pediatric Sample
 1 1999 Florida Conference on Child Health Psychology Gainesville, FL Correspondence of Pediatric Inpatient Behavior Scale (PIBS) Scores with DSM Diagnosis and Problem Severity Ratings in a Referred Pediatric
1 1999 Florida Conference on Child Health Psychology Gainesville, FL Correspondence of Pediatric Inpatient Behavior Scale (PIBS) Scores with DSM Diagnosis and Problem Severity Ratings in a Referred Pediatric
Citation for published version (APA): Noordhof, A. (2010). In the absence of a gold standard Groningen: s.n.
 University of Groningen In the absence of a gold standard Noordhof, Arjen IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen In the absence of a gold standard Noordhof, Arjen IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
Assessment and Diagnosis
 Amaze Position Statement Assessment and Diagnosis Key points Autism assessment and diagnostic services should be available to all people who require them, irrespective of age, gender, locality, financial
Amaze Position Statement Assessment and Diagnosis Key points Autism assessment and diagnostic services should be available to all people who require them, irrespective of age, gender, locality, financial
MOOD AND ANXIETY SYMPTOMS: POTENTIAL RISK INDICATORS FOR MAJOR MOOD DISORDERS AMONG HIGH-RISK OFFSPRING OF BIPOLAR PARENTS. Courtney Grace Heisler
 MOOD AND ANXIETY SYMPTOMS: POTENTIAL RISK INDICATORS FOR MAJOR MOOD DISORDERS AMONG HIGH-RISK OFFSPRING OF BIPOLAR PARENTS by Courtney Grace Heisler Submitted in partial fulfilment of the requirements
MOOD AND ANXIETY SYMPTOMS: POTENTIAL RISK INDICATORS FOR MAJOR MOOD DISORDERS AMONG HIGH-RISK OFFSPRING OF BIPOLAR PARENTS by Courtney Grace Heisler Submitted in partial fulfilment of the requirements
Suicide is the third leading cause of death among
 DA 00464 134 Ghaziuddin et al. DEPRESSION AND ANXIETY 11:134 138 (2000) ANXIETY CONTRIBUTES TO SUICIDALITY IN DEPRESSED ADOLESCENTS Neera Ghaziuddin, M.D., 1 * Cheryl A. King, Ph.D., 2 Michael W. Naylor,
DA 00464 134 Ghaziuddin et al. DEPRESSION AND ANXIETY 11:134 138 (2000) ANXIETY CONTRIBUTES TO SUICIDALITY IN DEPRESSED ADOLESCENTS Neera Ghaziuddin, M.D., 1 * Cheryl A. King, Ph.D., 2 Michael W. Naylor,
Genetic Influences on Childhood Competencies: A Twin Study
 Genetic Influences on Childhood Competencies: A Twin Study JAMES J. HUDZIAK, M.D., WILLIAM COPELAND, B.A., LAWRENCE P. RUDIGER, PH.D., THOMAS M. ACHENBACH, PH.D., ANDREW C. HEATH, D.PHIL., AND RICHARD
Genetic Influences on Childhood Competencies: A Twin Study JAMES J. HUDZIAK, M.D., WILLIAM COPELAND, B.A., LAWRENCE P. RUDIGER, PH.D., THOMAS M. ACHENBACH, PH.D., ANDREW C. HEATH, D.PHIL., AND RICHARD
FAMILY AND ADOLESCENT MENTAL HEALTH: THE PEDIATRICIAN S ROLE
 FAMILY AND ADOLESCENT MENTAL HEALTH: THE PEDIATRICIAN S ROLE Mark Cavitt, M.D. Medical Director, Pediatric Psychiatry All Children s Hospital/Johns Hopkins Medicine OBJECTIVES Review the prevalence of
FAMILY AND ADOLESCENT MENTAL HEALTH: THE PEDIATRICIAN S ROLE Mark Cavitt, M.D. Medical Director, Pediatric Psychiatry All Children s Hospital/Johns Hopkins Medicine OBJECTIVES Review the prevalence of
Disruptive mood dysregulation disorder in offspring of parents with depression and bipolar disorder
 The British Journal of Psychiatry (2017) 210, 408 412. doi: 10.1192/bjp.bp.117.198754 Disruptive mood dysregulation disorder in offspring of parents with depression and bipolar disorder Lukas Propper,
The British Journal of Psychiatry (2017) 210, 408 412. doi: 10.1192/bjp.bp.117.198754 Disruptive mood dysregulation disorder in offspring of parents with depression and bipolar disorder Lukas Propper,
Is ADHD Always a Childhood Onset Disorder? Towards Understanding Adult Onset ADHD
 Is ADHD Always a Childhood Onset Disorder? Towards Understanding Adult Onset ADHD Joseph Biederman, MD Professor of Psychiatry Harvard Medical School Chief, Clinical and Research Programs in Pediatric
Is ADHD Always a Childhood Onset Disorder? Towards Understanding Adult Onset ADHD Joseph Biederman, MD Professor of Psychiatry Harvard Medical School Chief, Clinical and Research Programs in Pediatric
NIH Public Access Author Manuscript Bipolar Disord. Author manuscript; available in PMC 2014 May 01.
 NIH Public Access Author Manuscript Published in final edited form as: Bipolar Disord. 2013 May ; 15(3): 253 263. doi:10.1111/bdi.12060. Mood lability among offspring of parents with bipolar disorder and
NIH Public Access Author Manuscript Published in final edited form as: Bipolar Disord. 2013 May ; 15(3): 253 263. doi:10.1111/bdi.12060. Mood lability among offspring of parents with bipolar disorder and
Comorbidity With Substance Abuse P a g e 1
 Comorbidity With Substance Abuse P a g e 1 Comorbidity With Substance Abuse Introduction This interesting session provided an overview of recent findings in the diagnosis and treatment of several psychiatric
Comorbidity With Substance Abuse P a g e 1 Comorbidity With Substance Abuse Introduction This interesting session provided an overview of recent findings in the diagnosis and treatment of several psychiatric
Supplementary Online Content
 Supplementary Online Content Sourander A, McGrath PJ, Ristkari T, et al. Internet-assisted parent training intervention for disruptive behavior in 4-year-old children: a randomized clinical trial. JAMA
Supplementary Online Content Sourander A, McGrath PJ, Ristkari T, et al. Internet-assisted parent training intervention for disruptive behavior in 4-year-old children: a randomized clinical trial. JAMA
Preschool Bipolar Disorder
 Preschool Bipolar Disorder Joan L. Luby, MD*, MiniTandon, DO, Andy Belden, PhD KEYWORDS Preschool Bipolar Mania Despite significant progress over the last decade in the characterization and validation
Preschool Bipolar Disorder Joan L. Luby, MD*, MiniTandon, DO, Andy Belden, PhD KEYWORDS Preschool Bipolar Mania Despite significant progress over the last decade in the characterization and validation
A META-ANALYTICAL STUDY OF PEDIATRIC BIPOLAR DISORDER: SYMPTOMATOLOGY AND COMORBIDITY. A Dissertation. Presented to the Faculty of
 A META-ANALYTICAL STUDY OF PEDIATRIC BIPOLAR DISORDER: SYMPTOMATOLOGY AND COMORBIDITY A Dissertation Presented to the Faculty of Antioch University Seattle Seattle, WA. In Partial Fulfillment of the Requirements
A META-ANALYTICAL STUDY OF PEDIATRIC BIPOLAR DISORDER: SYMPTOMATOLOGY AND COMORBIDITY A Dissertation Presented to the Faculty of Antioch University Seattle Seattle, WA. In Partial Fulfillment of the Requirements
F. J. Cameron*, D. Smidts, K. Hesketh, M. Wake and E. A. Northam. Summary. Introduction. CHQ, BASC, maladjustment, children, screening
 Early detection of emotional and behavioural problems Oxford, DME Diabetic 0742-3071 Blackwell 20 Original Emotional UK Article article Medicine Publishing Science well-being: Ltd, Ltd. screening 2003
Early detection of emotional and behavioural problems Oxford, DME Diabetic 0742-3071 Blackwell 20 Original Emotional UK Article article Medicine Publishing Science well-being: Ltd, Ltd. screening 2003
PRESCRIBING PHYSICIANS PLEASE READ
 PRESCRIBING PHYSICIANS PLEASE READ USADA s mission is to protect the rights of clean athletes. Some athletes need to use stimulants to manage ADD/ADHD and the anti-doping community acknowledges and respects
PRESCRIBING PHYSICIANS PLEASE READ USADA s mission is to protect the rights of clean athletes. Some athletes need to use stimulants to manage ADD/ADHD and the anti-doping community acknowledges and respects
SCREENING FOR SOCIAL ANXIETY DISORDER WITH THE SELF-REPORT VERSION OF THE LIEBOWITZ SOCIAL ANXIETY SCALE
 DEPRESSION AND ANXIETY 26:34 38 (2009) Research Article SCREENING FOR SOCIAL ANXIETY DISORDER WITH THE SELF-REPORT VERSION OF THE LIEBOWITZ SOCIAL ANXIETY SCALE Nina K. Rytwinski, M.A., 1 David M. Fresco,
DEPRESSION AND ANXIETY 26:34 38 (2009) Research Article SCREENING FOR SOCIAL ANXIETY DISORDER WITH THE SELF-REPORT VERSION OF THE LIEBOWITZ SOCIAL ANXIETY SCALE Nina K. Rytwinski, M.A., 1 David M. Fresco,
Discriminative Validity of Parent Report of Hypomanic and Depressive Symptoms on the General Behavior Inventory
 Psychological Assessment 2001, Vol. 13, No. 2, 267-276 Copyright 2001 by the American Psychological Association, Inc. 1040-3590/01/55.00 DOI: 10.1037//1040-3590,13.2.267 Discriminative Validity of Parent
Psychological Assessment 2001, Vol. 13, No. 2, 267-276 Copyright 2001 by the American Psychological Association, Inc. 1040-3590/01/55.00 DOI: 10.1037//1040-3590,13.2.267 Discriminative Validity of Parent
A Comparison of Diagnostic Interviews for Children. A Senior Honors Thesis
 Running Head: Diagnostic Interviews for Children A Comparison of Diagnostic Interviews for Children A Senior Honors Thesis Presented in Partial Fulfillment of the Requirements for Graduation with Research
Running Head: Diagnostic Interviews for Children A Comparison of Diagnostic Interviews for Children A Senior Honors Thesis Presented in Partial Fulfillment of the Requirements for Graduation with Research
BIPOLAR DISORDER IN CHILDREN: A REVIEW OF THE LITERATURE KRISTY BAYNTON. A Final Project Submitted to the
 BIPOLAR DISORDER IN CHILDREN: A REVIEW OF THE LITERATURE BY KRISTY BAYNTON A Final Project Submitted to the Campus Alberta Applied Psychology: Counselling Initiative In partial fulfillment of the requirements
BIPOLAR DISORDER IN CHILDREN: A REVIEW OF THE LITERATURE BY KRISTY BAYNTON A Final Project Submitted to the Campus Alberta Applied Psychology: Counselling Initiative In partial fulfillment of the requirements
FAMILY THERAPY OR FAMILY BASED INTERVENTION FOR CHILDREN AND ADOLESCENTS WHO SUFFER FROM PSYCHIATRIC DISORDERS
 Client HMSA: PQSR 2009 Measure Title FAMILY THERAPY OR FAMILY BASED INTERVENTION FOR CHILDREN AND ADOLESCENTS WHO SUFFER FROM PSYCHIATRIC DISORDERS Disease State Psychiatry Indicator Classification Disease
Client HMSA: PQSR 2009 Measure Title FAMILY THERAPY OR FAMILY BASED INTERVENTION FOR CHILDREN AND ADOLESCENTS WHO SUFFER FROM PSYCHIATRIC DISORDERS Disease State Psychiatry Indicator Classification Disease
Chronic irritability in youth that may be misdiagnosed as bipolar disorder. Ellen Leibenluft, M.D.
 Chronic irritability in youth that may be misdiagnosed as bipolar disorder Ellen Leibenluft, M.D. Chief, Section on Bipolar Spectrum Disorders Emotion and Development Branch National Institute of Mental
Chronic irritability in youth that may be misdiagnosed as bipolar disorder Ellen Leibenluft, M.D. Chief, Section on Bipolar Spectrum Disorders Emotion and Development Branch National Institute of Mental
Depression in Children with Autism/Pervasive Developmental Disorders: A Case-Control Family History Study
 Journal of Autism and Developmental Disorders, Vol 28, No. 2, 1998 Depression in Children with Autism/Pervasive Developmental Disorders: A Case-Control Family History Study Mohammad Ghaziuddin1,2 and John
Journal of Autism and Developmental Disorders, Vol 28, No. 2, 1998 Depression in Children with Autism/Pervasive Developmental Disorders: A Case-Control Family History Study Mohammad Ghaziuddin1,2 and John
CASE 5 - Toy & Klamen CASE FILES: Psychiatry
 CASE 5 - Toy & Klamen CASE FILES: Psychiatry A 14-year-old boy is brought to the emergency department after being found in the basement of his home by his parents during the middle of a school day. The
CASE 5 - Toy & Klamen CASE FILES: Psychiatry A 14-year-old boy is brought to the emergency department after being found in the basement of his home by his parents during the middle of a school day. The
Page 1 of 7. Supplemental Analysis
 Data Supplement for Birmaher et al., Longitudinal Trajectories and Associated Baseline Predictors in Youths With Bipolar Spectrum Disorders. Am J Psychiatry (doi: 10.1176/appi.ajp.2014.13121577) Supplemental
Data Supplement for Birmaher et al., Longitudinal Trajectories and Associated Baseline Predictors in Youths With Bipolar Spectrum Disorders. Am J Psychiatry (doi: 10.1176/appi.ajp.2014.13121577) Supplemental
ADHD is a neurodevelopmental disorder most frequently
 10.1177/1087054705283650 ARTICLE Journal Magnússon of Attention et al. / Validity Disorders of Adult Rating Scales Validity of Self-Report and Informant Rating Scales of Adult ADHD Symptoms in Comparison
10.1177/1087054705283650 ARTICLE Journal Magnússon of Attention et al. / Validity Disorders of Adult Rating Scales Validity of Self-Report and Informant Rating Scales of Adult ADHD Symptoms in Comparison
Classification of mood disorders
 Classification of mood disorders Congress of Neuropsychiatry and Neuropsychology 2014 Poznań 27 November 2014 Jules Angst Department of Psychiatry, Psychotherapy and Psychosomatics Psychiatric Hospital,
Classification of mood disorders Congress of Neuropsychiatry and Neuropsychology 2014 Poznań 27 November 2014 Jules Angst Department of Psychiatry, Psychotherapy and Psychosomatics Psychiatric Hospital,
ORIGINAL ARTICLE INTRODUCTION METHODOLOGY. Ehsan Ullah Syed 1, Sajida Abdul Hussein 1, Syed Iqbal Azam 2 and Abdul Ghani Khan 3
 ORIGINAL ARTICLE Comparison of Urdu Version of Strengths and Difficulties Questionnaire (SDQ) and the Child Behaviour Check List (CBCL) Amongst Primary School Children in Karachi Ehsan Ullah Syed 1, Sajida
ORIGINAL ARTICLE Comparison of Urdu Version of Strengths and Difficulties Questionnaire (SDQ) and the Child Behaviour Check List (CBCL) Amongst Primary School Children in Karachi Ehsan Ullah Syed 1, Sajida
