Goblet cell carcinoid of the appendix diagnostic challenges and treatment updates: a case report and review of the literature
|
|
|
- Sharon Gibbs
- 5 years ago
- Views:
Transcription
1 Gilmore et al. Journal of Medical Case Reports (2018) 12:275 CASE REPORT Open Access Goblet cell carcinoid of the appendix diagnostic challenges and treatment updates: a case report and of the literature Gregory Gilmore 1, Kristin Jensen 2, Shreyas Saligram 1, Thomas P. Sachdev 1 and Subramanyeswara R. Arekapudi 1* Abstract Background: Goblet cell carcinoid is a rare but distinct entity of appendiceal tumors which is a hybrid or mixed tumor consisting of both epithelial (glandular) and neuroendocrine elements containing goblet cells. This entity is important to recognize and appropriately grade as it tends to be more aggressive than typical carcinoid tumors, often presenting with metastatic disease. As a result, the 5-year overall survival is 14 22% in stage III IV disease. GCC therefore warrants more aggressive surgical and medical (chemotherapy) interventions than typical carcinoid tumors. Through this case report we give a brief update on GCC pathological features, staging, surgical management, and the literature as a guide to indications for chemotherapy and choice of agents. Case presentation: We present the case of a 77-year-old Caucasian man with a history of stage I adenocarcinoma of transverse colon status post transverse colectomy who was incidentally found on surveillance colonoscopy to have an abnormal appendiceal orifice lesion. A biopsy revealed an appendiceal goblet cell carcinoid and he underwent a right hemicolectomy which revealed a pathologic stage III GCC for which he received eight cycles of adjuvant chemotherapy with capecitabine. Conclusions: It is essential that patients who have tumors > 2 cm, are pt3 or pt4, have higher grade histology with signet ring (Tang grade B or grade C), locally advanced, or with positive surgical margins on appendectomy undergo a right hemicolectomy. Although there is no category 1 evidence, consensus recommendations are that patients with stage II (particularly Tang B and C) and stage III GCC be offered adjuvant chemotherapy with a regimen based on 5-fluorouracil, as these patients are known to have high rates of relapse. Keywords: Goblet cell carcinoid, Appendix, Chemotherapy Background Primary cancers of the appendix are quite rare representing less than 1% of all gastrointestinal malignancies with an annual incidence of approximately 1.2 cases per 100,000 people in the USA [1]. Although a small organ, tumors of the appendix can develop into cancers with significant morphologic diversity and thus are further classified into adenocarcinoma, carcinoid (neuroendocrine tumors; NETs), mucinous tumors, signet ring cell * Correspondence: drarekapudi@gmail.com; sarekapudi@fresno.ucsf.edu 1 Department of Medicine, Veterans Affairs Central California Health Care System, University of California San Francisco, 2615 E Clinton Ave, Fresno, CA 93703, USA Full list of author information is available at the end of the article tumors, and goblet cell carcinoids (GCCs). GCC is exceedingly rare accounting for approximately 14 19% of primary appendix cancers [1, 2]. It is a distinct entity as a hybrid or mixed tumor consisting of both epithelial (glandular) and neuroendocrine elements containing goblet cells. GCC is more common in Caucasians with a mean age at diagnosis of 58, and there is no known difference in incidence between males and females [1, 3 5]. At this time there are no known or established risk factors that increase a person s probability of developing GCC [6]. As with most tumors of the appendix, GCC frequently presents with acute abdominal pain and clinical findings of appendicitis in 50 60% of cases [7 9]. It The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
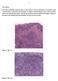
2 Gilmore et al. Journal of Medical Case Reports (2018) 12:275 Page 2 of 7 is often diagnosed incidentally during appendectomy or ileocecal resection and confirmed on surgical pathology [10]. Prognosis is very good if diagnosed at stage I or II, but significantly worsens in stage III or IV disease (5-year overall survival 22% and 14% respectively) [11]. Disease-specific 5-year survival for all patients presenting with GCC is 58 81% [2, 12, 13]. Due to the rarity of GCC there are no randomized trials or clinical guidelines for treatment but adjuvant 5-fluorouracil (5-FU)-based regimen is recommended for stage III or stage IV disease [8, 9, 13]. This rare entity is important to recognize and appropriately diagnose as the biology of this disease is more aggressive than typical carcinoid tumor and treatment needs to be tailored accordingly. Unfortunately, there are limited data to guide adjuvant treatment and most appropriate chemotherapy regimen. In this case report we the presently available literature to help guide treatment decisions for those patients diagnosed as having GCC. Case presentation We present a case of a 77-year-old Caucasian man with past medical history of stage I adenocarcinoma of transverse colon status post laparoscopically assisted segmented transverse colectomy in April Other medical history included type 2 diabetes, hypertension, hypothyroidism, and benign prostatic hypertrophy. Medications at the time of diagnosis included aspirin, metformin, lisinopril, and levothyroxine. His family history included lung cancer in his father who was a tobacco smoker. Our patient was a former tobacco smoker but denied history of alcohol or drug abuse and had no history of occupational or chemical exposure. He presented for follow-up screening colonoscopy approximately 2 years later in July 2016 at which time he was asymptomatic. His Eastern Cooperative Oncology Group (ECOG) performance status was grade 1. On clinical examination he was afebrile, mildly hypertensive with blood pressure 146/81, heart rate 78, respiratory rate of 16 with oxygen saturation of 96% on room air. He had normal cardiac rate and rhythm, and no abnormal breath sounds on respiratory examination. His abdomen had normal bowel sounds on auscultation, was soft and non-tender without distension. A neurologic examination demonstrated normal neurologic function without sensory deficits and normal muscle strength. On colonoscopy, he was found to have an abnormalappearing appendiceal orifice which was biopsied; pathology was suggestive of mucinous adenocarcinoma with signet ring cell features versus a goblet cell-type carcinoid tumor of the appendix (Fig. 1). The appendiceal orifice appeared normal on previous colonoscopies in March and December of Pre-colonoscopy complete blood count (CBC) revealed white blood cell (WBC) count of Fig. 1 Image from colonoscopy showing the abnormal-appearing appendiceal orifice (indicated by arrow) from which biopsies were taken /ul (reference range 4 11), hemoglobin 13.9 g/dl (reference range 14 17) with mean corpuscular volume (MCV) of 82.3 fl (reference range 80 94), and platelet count of 171 K/mm 3 (reference range ). Pre-colonoscopy basic chemistry including sodium, potassium, chloride, bicarbonate, and creatinine were all within normal limits. On histological examination the tumor was present as infiltrative small nests and clusters of cells with small nuclei compressed by abundant cytoplasmic mucin vacuoles, giving a signet ring appearance (Figs. 2 and 3). Given the location of the lesion at the appendiceal orifice, the diagnosis of goblet cell carcinoid was strongly suspected, but definitive diagnosis was deferred to complete resection. Further laboratory workup with tumor markers and neuroendocrine markers revealed carcinoembryonic antigen (CEA) of 3.1 ng/ml (reference Fig. 2 At low magnification, the tumor is seen infiltrating normal colonic glands, as nests and small rounded clusters of cells, many of which are distended by mucin. (Hematoxylin and eosin)
3 Gilmore et al. Journal of Medical Case Reports (2018) 12:275 Page 3 of 7 Fig. 3 Higher magnification of the tumor highlights the mucin as well as the cytologically bland nuclei compressed to the edges of the cells. (Hematoxylin and eosin) range ) and chromogranin A, and 24-hour urine 5-hydroxyindoleacetic acid (5-HIAA) within normal limits. A computed tomography (CT) scan of his chest, abdomen, and pelvis showed a thickened appendix (12 mm) without evidence of fat stranding (Fig. 4). There was no significant lymphadenopathy, no colonic masses seen, and no evidence of distant metastatic disease. After surgical evaluation, he underwent a right hemicolectomy in August Both specimens from colonoscopy and right hemicolectomy were sent for expert consultation. On pathologic, the bulk of the tumor involved the appendix, essentially obliterating the lumen, with diffuse spread into the mesoappendix and serosal adipose tissue. Both perineural and lymphovascular invasion were noted. Six of 14 lymph nodes harbored metastatic carcinoma. In areas of the appendiceal wall, the nests of signet ring cells coalesced into pools of mucin containing floating cells, indicating frank mucinous carcinoma, so-called adenocarcinoma ex-goblet cell carcinoid (Fig. 5), Tang group B. Immunohistochemistry for synaptophysin highlighted scattered occasional peripheral endocrine cells, as is characteristic of goblet cell carcinoid (Fig. 6). The final pathologic staging of the patient's tumor was pt3 N1 M0, stage III as per American joint committee on cancer staging manual, 7th edition [14]. Postoperatively, we discussed treatment options including adjuvant chemotherapy; our patient was initially against adjuvant chemotherapy due to prior experiences with family members, but he agreed to it after the rationale was explained. He was given adjuvant capecitabine with a goal of eight cycles. Given his age, the first four cycles of capecitabine were given at a 25% dose reduction of 1500 mg twice daily for days 1 14 every 21 days. As he tolerated therapy well, the dose was increased to 2000 mg twice daily for days 1 14 every 21 days for cycles five to eight. He completed eight cycles of capecitabine and tolerated treatment well other than mild hand and foot syndrome which developed during the last two cycles. A follow-up CT scan at 6 and 12 months after completion of adjuvant chemotherapy showed no evidence of recurrent disease. A repeat colonoscopy at 1 year from original diagnosis was also negative for any malignant-appearing lesions. We are continuing surveillance with history and physical with CEA every 3 months, and CT of his chest, abdomen, and pelvis every 6 months for the first 2 years and then annually for up to 5 years. At the current time he remains disease free at 2 years from time of diagnosis. Fig. 4 Computed tomography scan of the chest, abdomen, and pelvis showing a thickened appendix at 12 mm in diameter as indicated by arrow Fig. 5 The lower half of the field indicates what was once the appendiceal lumen, but which now shows small nests of cells distended by mucin. In the upper half and right side of the field, the nests have coalesced to form large infiltrating pools of mucin, some of which contain cells floating within the mucin. (Hematoxylin and eosin)
4 Gilmore et al. Journal of Medical Case Reports (2018) 12:275 Page 4 of 7 Fig. 6 An immunohistochemical stain for synaptophysin highlights scattered peripheral endocrine cells within the tumor nests. (Synaptophysin) Discussion We presented the case of a 77-year-old Caucasian man who had a history of early stage I colon cancer and was later diagnosed as having a second primary stage III GCC, Tang group B. He underwent a right hemicolectomy followed by adjuvant chemotherapy with the orally administered fluoropyrimidine capecitabine for eight cycles. Most patients with Tang group B or Tang group C GCC have metastatic disease at time of diagnosis [13]. Fortunately, this patient had stage III GCC at diagnosis due to the fact it was found incidentally on surveillance colonoscopy. Due to limited literature in regard to adjuvant treatment options for a Tang group B or C patient without metastatic disease, it was challenging to develop an evidence-based treatment plan. Goblet cell carcinoid is typically diagnosed postoperatively after an appendectomy or ileocecal resection and is confirmed by a pathologist in the post-surgical specimen. It is important to correctly identify tumors as GCC and categorize appropriately by Tang s classification as particularly higher grade GCCs exhibit more aggressive behavior and this should influence postoperative management decisions [13, 15]. The overall prognosis for GCC falls between that of appendiceal adenocarcinoma, which has a poorer prognosis, and NETs, which has a better prognosis [1, 3]. The differential diagnosis for GCC includes adenocarcinoma of appendix, signet ring cell tumors, carcinoid tumors, and mucinous-benign tumors of the appendix. GCC is an unusual entity, histologically distinct from typical carcinoid. Conventional carcinoids are typically cellular, and are composed of relatively small uniform cells arranged in moderately sized solid nests, cords, or ribbons. While mucinous differentiation may be seen in conventional carcinoids, it is typically a focal finding. Immunohistochemical staining for synaptophysin or chromogranin in a conventional carcinoid will highlight sheets of cells, nearly every cell in the tumor, in contrast with the rare scattered peripheral endocrine cells seen in goblet cell carcinoid. Once a goblet cell carcinoid has become frankly malignant, most authors advocate using the term carcinoma (or adenocarcinoma) ex-goblet cell carcinoid to avoid any potential confusion with conventional carcinoid tumor. The plethora of proposed and historic names for goblet cell carcinoid (mucinous carcinoid, adenocarcinoid, and crypt cell carcinoma) has contributed to the confusion surrounding this entity. There are several different classification/staging systems used for GCC including the 2010 World Health Organization (WHO) classification for appendix tumors, the 2010 AJCC (TNM classifications) staging, and recently proposed Tang et al. classification specific for GCC of the appendix [8]. The AJCC stages tumors as stage I (T1, N0, M0), stage II (T2/T3, N0, M0), stage III (any T, N1, M0), and stage IV (any T, any N, M1) [14]. The Tang classification uses histologic features of the tumor at the primary site to classify GCC tumors into three groups. The following groups are designated using the histologic features which include the arrangements of goblet cells, degree of atypia, and degree of desmoplasia: Typical GCC (group A), adenocarcinoma ex-gcc, signet ring cell (group B), and adenocarcinoma ex-gcc, poorly differentiated (group C). As demonstrated by Tang et al., tumors classified moving from group A to C represent progressively more aggressive phenotypes and worse prognosis with all patients in group C presenting with metastatic disease [13]. Our patient was staged by AJCC (TNM) staging as T3, N1, M0, stage IIIB. The tumor obliterated the lumen of his appendix with nests/clusters of signet ring cells coalesced into pools of mucin, indicating frank mucinous carcinoma. It was thus classified by Tang classification as group B, adenocarcinoma ex-gcc, signet ring cell. Due to the rarity of GCC, there are no Category 1-based guidelines from large randomized control trials on which to base treatment decisions. The mainstay of treatment for non-metastatic disease is surgical resection. However, the extent of surgical resection with appendectomy versus right hemicolectomy is debated. Since many GCCs are found incidentally after appendectomy, the need for further complete oncologic resection (that is, right hemicolectomy) is an important question. Both the North American and European Neuroendocrine Tumor Societies recommend right hemicolectomy as standard first-line treatment for GCC even after appendectomy due to high risk of metastases and improvement in prognosis [4, 8, 16]. However, in several published analyses, there is evidence to suggest limited or no benefit of right hemicolectomy, primarily in patients with low grade and/or limited disease burden. A meta-analysis of 13 studies including 100 total patients
5 Gilmore et al. Journal of Medical Case Reports (2018) 12:275 Page 5 of 7 Table 1 Goblet cell carcinoid outcomes by different chemotherapy regimens Study Type of N Stage Histology Treatment CR PFS Overall survival study 3 years Garin et al. [23] 2002 Case report 1 IV Adenocarcinoid 5-FU + LV (LV5FU2) 1 cycle followed by FOLFOX 4 9 months Yes (at 8 months) Pham et al. [11] 2006 Retrospective 57 I 8 II 20 III 6 IV 23 Goblet cell carcinoid 5-FU + LV-based chemotherapy (N = 27, Stage II IV) Cx versus No Cx Stage II III Mean (months): 47 versus 32 months (p = 0.383) 5 year (%): 43 versus 56 Stage IV Mean (months): 39 versus 29 (p = 0.281) 5 year (%): 26 versus 0 Toumpanakis et al. [24] 2007 Retrospective 15 I IV Goblet cell appendiceal carcinoid RH in all patients without metastasis. Stage IV (3) 2- VP-16 + cisplatin 1 5-FU + cisplatin +streptozotocin. 11/15 no disease (median follow-up 30 months) Median 30 months follow up: 11 alive with no disease 1 alive with metastatic disease 3 died of metastatic disease (9 14 months) Tang et al. [13] 2008 Retrospective 63 I 2 II 18 III 3 IV 40 Tang group A 30 B 26 C 7 Goblet cell carcinoid FOLFOX FOLFIRI (33/63) Stage III (2/3) Group B (14/26) Group A 86% Group B 15% Group C 0% DSS % (Tang groups) 3 years Group A 100% Group B 85% Group C 17% 5 years Group A 100% Group B 36% Group C 0% Bilen et al. [25] 2013 Case series 1 Metastatic Poorly differentiated adenocarcinoma arising from goblet cell carcinoid FOLFOX followed by CRS and HIPEC (mitomycin-c) pcr Disease free at 7 months Clift et al. [22] 2018 Retrospective 21 I 1 II 10 III 5 IV 5 Tang group A 8 B 10 C 3 Goblet cell carcinoid Appendectomy: 12 (completion RH: 8) RH: 6 Other resections: 3 6 received adjuvant cx with CAPOX 5 dead of disease, 1 alive with no disease DFS: 1-year: 94.7% 3-year: 74.2% 5-year: 74.2% Mean OS (1-, 3-, and 5-year OS) 80.3 months (79.4%, 60%, and 60%) Group A: 73.1 months (85.7%, 85.7%, 51.4%) Group B: 83.7 months (all 66.7%) Group C: 28.5 months (66.7%, 66.7%, not reached) 5-FU 5-fluorouracil, CAPOX capecitabine/oxaliplatin, CR complete response, CRS cytoreductive surgery, Cx chemotherapy, DFS disease-free survival, DSS disease specific survival, FOLFIRI 5-FU/LV/irinotecan, FOLFOX 5-Fu/LV/oxaliplatin, HIPEC hyperthermic intraperitoneal chemotherapy, LV leucovorin, OS overall survival, pcr pathologic complete response, PFS progression-free survival, RH right hemicolectomy, VP-16 etoposide
6 Gilmore et al. Journal of Medical Case Reports (2018) 12:275 Page 6 of 7 demonstrated a failure rate of 7% with appendectomy alone versus 10% in extended resection (p = 0.29); the authors concluded no benefit of right hemicolectomy in patients with localized disease with low grade histology [17]. Several other small studies evaluating extent of surgical resection in GCCs have suggested there is no benefit to right hemicolectomy in those with small (< 1 cm), localized, low grade tumors without high risk features such as positive resection margins [18, 19]. In a retrospective analysis of Surveillance, Epidemiology, and End Results (SEER) data evaluating 3137 patients with appendiceal NETs (typical NETs, typical GCC, and signet ring cell adenocarcinoma), after adjusting for age, stage, and histology, there was no significant survival benefit for right hemicolectomy versus appendectomy for typical NETs (p = 0.21) or typical GCC (p = 0.94). However, in those with signet ring cell adenocarcinoma histology, they found a statistically significant benefit in survival for right hemicolectomy versus appendectomy alone (p =0.01) [20]. In addition, analysis by Tang et al. demonstrated that histology rather than size of tumor should be used as a determining factor to decide the extent of oncologic resection (appendectomy versus right hemicolectomy) with higher grades (groups B and C) benefiting from more extensive resection. Therefore, based on these data, it is reasonable to consider appendectomy alone in those patients with tumor < 2 cm and localized to appendix with negative surgical margins, those with typical GCC group A histology, and those with pt1 or pt2 tumors. For all other patients which include those with tumors > 2 cm, locally advanced stage, positive margins, histology with signet ring group B or group C, or pt3 or pt4 tumors it is recommended to perform a right hemicolectomy [8, 11, 13, 21]. Owing to the rarity of GCC, we do not have randomized control trials or evidenced-based guidelines for choice of systemic chemotherapy. The available data are primarily anecdotal for clinician experience or published small case series. Since metastatic GCC most resembles that of colon adenocarcinoma, the selection of adjuvant chemotherapy has been extrapolated from colorectal adenocarcinoma with recommendations for regimens based on 5-FU. The most commonly used regimens historically are FOLFOX (5-FU, leucovorin, oxaliplatin) or FOLFIRI (5-FU, folic acid, irinotecan). In general, chemotherapy is recommended for select stage II and all stage III and IV disease, as well as in the setting of recurrence [8]. A retrospective of the Mayo Clinic database from 1984 to 2004 had a prospective follow-up of 57 patients with GCC. Of these, 27 patients received chemotherapy with primarily regimens based on 5-FU which showed a trend toward mean survival benefit but it was not statistically significant. The mean survival for combined stage II to III patients who received chemotherapy was 47 months with chemotherapy versus 32 months with no chemotherapy (p = 0.383). For stage IV patients, mean survival was 39 and 29 months, respectively (p =0.281)[11]. In another UK, single center study of patients with confirmed GCC, 18 patients received chemotherapy, 16 with curative intent. The most commonly received systemic chemotherapy regimens were either FOLFOX or single agent capecitabine. The results of this study showed no improvement in disease-free survival (DFS) (p = 0.870), and, in fact, patients who received adjuvant chemotherapy had a shorter DFS (21.3 versus 75.9 months). This finding is probably due to selection bias with patients with more advanced disease receiving adjuvant chemotherapy [7]. Most recently, in an article based on their institutional experience and of available literature, Clift et al. proposed that chemotherapy be offered to all patients with stage II GCC or a primary tumor classified as Tang B/C, and any stage III/IV patients treated with curative intent [22]. Additional case series and retrospective s reporting different choices of chemotherapy regimens and their outcomes are detailed in Table 1. Based on a of the literature, our patient was offered adjuvant chemotherapy given he was stage IIIB and classified as Tang group B. The choice of capecitabine single agent versus a multi-agent regimen was decided based on his age and, primarily, his preference for oral treatment and minimal toxicities. The overall survival for patients with GCC varies based on different series and classifications or staging systems used. Overall prognosis is good for patients with early stage disease but much poorer for those who present with late stage disease. Based on Tang s classification for groups A, B, and C, the mean overall survival was 199 months, 43 months, and 31 months, respectively. The 5-year overall survival statistics were 100%, 36%, and 0% respectively. It was also noted that a large percentage (63%) of patients with GCC presented with stage IV disease. The 5-year overall data based on AJCC (TNM) staging system is 100% for stage I, 76% for stage II, 22% for stage III, and 14% for stage IV [13]. Conclusions GCC is a rare but distinct entity of appendiceal tumors. It is essential to accurately diagnose GCC as it is more aggressive in nature than typical carcinoid tumor, and often presents with metastatic disease. Right hemicolectomy is recommended for tumors > 2 cm, pt3 or T4, higher grade histology with signet rings, or with positive surgical margins on appendectomy. Lastly, despite lack of category 1 evidence, consensus recommendations are patients with stage II (particularly Tang B and C) and stage III GCC should be offered adjuvant chemotherapy with a regimen based on 5-FU.
7 Gilmore et al. Journal of Medical Case Reports (2018) 12:275 Page 7 of 7 Funding No specific funding was allocated for this case report presentation. Our institution s Research department is willing to contribute to the publication costs if necessary. Authors contributions GG wrote the first draft of manuscript. KJ provided the pathology pictures with legends and participated in final editing. SS and TS provided critical of paper and participated in final. SA conceptualized the manuscript, guided GG through first draft and provided critical along with final draft preparation and submission. All authors read and approved the final manuscript. Ethics approval and consent to participate Not applicable. This submission represents case report only. We have not included any data that compromise patient identification. The only images submitted are hematoxylin and eosin (H&E) stain pictures from pathology. Our local Institutional policy does not require Institutional Review Board (IRB)/Ethics committee approval for submission of case reports with de-identified patient pictures/images. We have obtained consent from the patient to publish the case description and pathology slide pictures and if necessary imaging pictures. Consent for publication A written full informed consent was obtained from the patient for publication of this case report and corresponding images. A copy of the written consent is available for by Editor-in-Chief of this journal. Competing interests The authors declare that they have no competing interests. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Department of Medicine, Veterans Affairs Central California Health Care System, University of California San Francisco, 2615 E Clinton Ave, Fresno, CA 93703, USA. 2 Department of Pathology, Veterans Affairs Palo Alto Health Care System, Stanford Hospital and Clinics, Palo Alto, CA 94304, USA. Received: 2 February 2018 Accepted: 1 August 2018 References 1. McCusker ME, Coté TR, Clegg LX, Sobin LH. Primary malignant neoplasms of the appendix: a population-based study from the surveillance, epidemiology and end-results program, Cancer. 2002;94(12): Turaga KK, Pappas SG, Gamblin TC. Importance of histologic subtype in the staging of appendiceal tumors. Ann Surg Oncol. 2012;19(5): McGory ML, Maggard MA, Kang H, O Connell JB, Ko CY. Malignancies of the appendix: beyond case series reports. Dis Colon Rectum. 2005;48(12): Pape U, Perren A, Niederle B, Gross D, Gress T, Costa F, Arnold R, Denecke T, Plöckinger U, Salazar R, Grossman A. ENETS Consensus Guidelines for the management of patients with neuroendocrine neoplasms from the jejunoileum and the appendix including goblet cell carcinoid. Neuroendocrinology. 2012;95(2): Pahlavan PS, Kanthan R. Goblet cell carcinoid of the appendix. World J Surg Oncol. 2005;3: Jiang Y, Long H, Wang W, Liu H, Tang Y, Zhang X. Clinicopathological features and immunoexpression profiles of goblet cell carcinoid and typical carcinoid of the appendix. Pathol Oncol Res. 2011;17(1): Park K, Blessing K, Kerr K, Chetty U, Gilmour H. Goblet cell carcinoid of the appendix. Gut. 1990;31(3): Shenoy S. Goblet cell carcinoids of the appendix: Tumor biology, mutations and management strategies. World J Gastrointest Surg. 2016;8(10): Kelly KJ. Management of Appendix Cancer. Clin Colon Rectal Surg. 2015; 28(4): Lamarca A, Nonaka D, Lopez Escola C, Hubner RA, O Dwyer S, Chakrabarty B, Fulford P, Valle JW. Appendiceal Goblet Cell Carcinoids: Management Considerations from a Reference Peritoneal Tumor Service Centre and ENETS Centre of Excellence. Neuroendocrinology. 2016;103(5): Pham TH, Wolff B, Abraham SC, Drelichman E. Surgical and chemotherapy treatment outcomes of goblet cell carcinoid: a tertiary cancer center experience. Ann Surg Oncol. 2006;13(3): Hsu C, Rashid A, Xing Y, Chiang Y, Chagpar RB, Fournier KF, Chang GJ, You YN, Feig BW, Cormier JN. Varying malignant potential of appendiceal neuroendocrine tumors: importance of histologic subtype. J Surg Oncol. 2013;107(2): Tang LH, Shia J, Soslow RA, Dhall D, Wong WD, O Reilly E, Qin J, Paty P, Weiser MR, Guillem J, Temple L, Sobin LH, Klimstra DS. Pathologic classification and clinical behavior of the spectrum of goblet cell carcinoid tumors of the appendix. Am J Surg Pathol. 2008;32(10): Edge SB, Byrd DR, Compton CC, Fritz AG, Greene FL, Trotti A, editors. AJCC cancer staging manual (7th ed). New York, NY: Springer; McConnell YJ, Mack LA, Gui X, Carr NJ, Sideris L, Temple WJ, Dubé P, Chandrakumaran K, Moran BJ, Cecil TD. Cytoreductive surgery with hyperthermic intraperitoneal chemotherapy: an emerging treatment option for advanced goblet cell tumors of the appendix. Ann Surg Oncol. 2014;21(6): Boudreaux JP, Klimstra DS, Hassan MM, Woltering EA, Jensen RT, Goldsmith SJ, Nutting C, Bushnell DL, Caplin ME, Yao JC. The NANETS consensus guideline for the diagnosis and management of neuroendocrine tumors: well-differentiated neuroendocrine tumors of the Jejunum, Ileum, Appendix, and Cecum. Pancreas. 2010;39(6): Varisco B, McAlvin B, Dias J, Franga D. Adenocarcinoid of the appendix: is right hemicolectomy necessary? A meta-analysis of retrospective chart s. Am Surg. 2004;70(7): Bucher P, Gervaz P, Ris F, Oulhaci W, Egger J, Morel P. Surgical treatment of appendiceal adenocarcinoid (goblet cell carcinoid). World J Surg. 2005; 29(11): Byrn JC, Wang J, Divino CM, Nguyen SQ, Warner RRP. Management of goblet cell carcinoid. J Surg Oncol. 2006;94(5): Shaib W, Krishna K, Kim S, Goodman M, Rock J, Chen Z, Brutcher E, Staley CI, Maithel SK, Abdel-Missih S, El-Rayes BF, Bekaii-Saab T. Appendiceal Neuroendocrine, Goblet and Signet-Ring Cell Tumors: A Spectrum of Diseases with Different Patterns of Presentation and Outcome. Cancer Res Treat. 2016;48(2): Taggart MW, Abraham SC, Overman MJ, Mansfield PF, Rashid A. Goblet cell carcinoid tumor, mixed goblet cell carcinoid-adenocarcinoma, and adenocarcinoma of the appendix: comparison of clinicopathologic features and prognosis. Arch Pathol Lab Med. 2015;139(6): Clift AK, Kornasiewicz O, Drymousis P, Faiz O, Wasan HS, Kinross JM, Cecil T, Frilling A. Goblet cell carcinoid of the appendix: rare but aggressive neoplasms with challenging management. Endocrine connections. 2018;7(2): Garin L, Corbinais S, Boucher E, Blanchot J, Le Guilcher P, Raoul J. Case Report: Adenocarcinoid of the Appendix Vermiformis: Complete and Persistent Remission After Chemotherapy (Folfox) of a Metastatic Case. Dig Dis Sci. 2002;47(12): Toumpanakis C, Standish RA, Baishnab E, Winslet MC, Caplin ME. Goblet cell carcinoid tumors (adenocarcinoid) of the appendix. Dis Colon Rectum. 2007; 50(3): Bilen MA, Taggart MW, Fournier K, Ellis LM, Mansfield PF, Eng C, Royal RE, Overman MJ. Pathologic complete response in poorly differentiated adenocarcinomas of the appendix: A case series. Acta Oncol. 2013;52(5):
GOBLET CELL CARCINOID. Hanlin L. Wang, MD, PhD University of California Los Angeles
 GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
GOBLET CELL CARCINOID
 GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
GOBLET CELL CARCINOID. Hanlin L. Wang, MD, PhD University of California Los Angeles
 GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles hanlinwang@mednet.ucla.edu Goblet cell carcinoid (GCC) is a unique type of mixed endocrine-exocrine neoplasm, almost exclusively
GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles hanlinwang@mednet.ucla.edu Goblet cell carcinoid (GCC) is a unique type of mixed endocrine-exocrine neoplasm, almost exclusively
1: Department of Surgery and Cancer, Imperial College London, London, UK. 2: Department of Surgery, Warsaw Medical University, Warsaw, Poland
 Page 1 of 25 Endocrine Connections Publish Ahead of Print, published on January 15, 2018 as doi:10.1530/ec-17-0311 Goblet cell carcinomas of the appendix: rare but aggressive neoplasms with challenging
Page 1 of 25 Endocrine Connections Publish Ahead of Print, published on January 15, 2018 as doi:10.1530/ec-17-0311 Goblet cell carcinomas of the appendix: rare but aggressive neoplasms with challenging
Management of an Appendiceal Mass - Approach to acute presentation of appendiceal neoplasms
 Management of an Appendiceal Mass - Approach to acute presentation of appendiceal neoplasms Dr. Claudia LY WONG, Department of Surgery, Kwong Wah Hospital Joint Hospital Surgical Grand Round Presentation,
Management of an Appendiceal Mass - Approach to acute presentation of appendiceal neoplasms Dr. Claudia LY WONG, Department of Surgery, Kwong Wah Hospital Joint Hospital Surgical Grand Round Presentation,
Appendiceal Neuroendocrine, Goblet and Signet-Ring Cell Tumors: A Spectrum of Diseases with Different Patterns of Presentation and Outcome
 Appendiceal Neuroendocrine, Goblet and Signet-Ring Cell Tumors: A Spectrum of Diseases with Different Patterns of Presentation and Outcome Walid Shaib, Emory University Kavya Krishna, Ohio State University
Appendiceal Neuroendocrine, Goblet and Signet-Ring Cell Tumors: A Spectrum of Diseases with Different Patterns of Presentation and Outcome Walid Shaib, Emory University Kavya Krishna, Ohio State University
Chibueze Onyemkpa 1, Alan Davis 1, Michael McLeod 1, Tolutope Oyasiji 1,2. Original Article
 Original Article Typical carcinoids, goblet cell carcinoids, mixed adenoneuroendocrine carcinomas, neuroendocrine carcinomas and adenocarcinomas of the appendix: a comparative analysis of survival profile
Original Article Typical carcinoids, goblet cell carcinoids, mixed adenoneuroendocrine carcinomas, neuroendocrine carcinomas and adenocarcinomas of the appendix: a comparative analysis of survival profile
Pre-operative assessment of patients for cytoreduction and HIPEC
 Pre-operative assessment of patients for cytoreduction and HIPEC Washington Hospital Center Washington, DC, USA Ovarian Cancer Surgery New Strategies Bergamo, Italy May 5, 2011 Background Cytoreductive
Pre-operative assessment of patients for cytoreduction and HIPEC Washington Hospital Center Washington, DC, USA Ovarian Cancer Surgery New Strategies Bergamo, Italy May 5, 2011 Background Cytoreductive
Lymph node ratio as a prognostic factor in stage III colon cancer
 Lymph node ratio as a prognostic factor in stage III colon cancer Emad Sadaka, Alaa Maria and Mohamed El-Shebiney. Clinical Oncology department, Faculty of Medicine, Tanta University, Egypt alaamaria1@hotmail.com
Lymph node ratio as a prognostic factor in stage III colon cancer Emad Sadaka, Alaa Maria and Mohamed El-Shebiney. Clinical Oncology department, Faculty of Medicine, Tanta University, Egypt alaamaria1@hotmail.com
Surgical Management of Neuroendocrine Tumors of the Gut. Richard Hodin MD Professor of Surgery Massachusetts General Hospital Harvard Medical School
 Surgical Management of Neuroendocrine Tumors of the Gut Richard Hodin MD Professor of Surgery Massachusetts General Hospital Harvard Medical School Sites of GI Carcinoid Tumors Small intestine 44% Rectum
Surgical Management of Neuroendocrine Tumors of the Gut Richard Hodin MD Professor of Surgery Massachusetts General Hospital Harvard Medical School Sites of GI Carcinoid Tumors Small intestine 44% Rectum
Goblet Cell Carcinoids of the Appendix
 40 Ulster Med J 2006; 75 (1) 40-45 The Ulster Medical Journal Review Goblet Cell Carcinoids of the Appendix R Arnold, K McCallion, C McGailie Accepted 14 October 2005 INTRODUCTION Carcinoid tumours are
40 Ulster Med J 2006; 75 (1) 40-45 The Ulster Medical Journal Review Goblet Cell Carcinoids of the Appendix R Arnold, K McCallion, C McGailie Accepted 14 October 2005 INTRODUCTION Carcinoid tumours are
Appendix adenocarcinomas are rare and heterogeneous
 ORIGINAL CONTRIBUTION Predicting Survival After Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy for Appendix Adenocarcinoma Omer Aziz, Ph.D., F.R.C.S. 1,2 Ihab Jaradat, F.R.C.S. 1 Bipasha
ORIGINAL CONTRIBUTION Predicting Survival After Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy for Appendix Adenocarcinoma Omer Aziz, Ph.D., F.R.C.S. 1,2 Ihab Jaradat, F.R.C.S. 1 Bipasha
Signet-Ring Cell Carcinoma of the Colon: A Case Report and Review of the Literature
 Published online: November 4, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1662 6575/15/0083 0466$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0 International
Published online: November 4, 2015 2015 The Author(s) Published by S. Karger AG, Basel 1662 6575/15/0083 0466$39.50/0 This article is licensed under the Creative Commons Attribution-NonCommercial 4.0 International
11/21/13 CEA: 1.7 WNL
 Case Scenario 1 A 70 year-old white male presented to his primary care physician with a recent history of rectal bleeding. He was referred for imaging and a colonoscopy and was found to have adenocarcinoma.
Case Scenario 1 A 70 year-old white male presented to his primary care physician with a recent history of rectal bleeding. He was referred for imaging and a colonoscopy and was found to have adenocarcinoma.
Goblet Cell Carcinoid Tumor, Mixed Goblet Cell Carcinoid-Adenocarcinoma, and Adenocarcinoma of the Appendix
 Goblet Cell Carcinoid Tumor, Mixed Goblet Cell Carcinoid-Adenocarcinoma, and Adenocarcinoma of the Appendix Comparison of Clinicopathologic Features and Prognosis Melissa W. Taggart, MD; Susan C. Abraham,
Goblet Cell Carcinoid Tumor, Mixed Goblet Cell Carcinoid-Adenocarcinoma, and Adenocarcinoma of the Appendix Comparison of Clinicopathologic Features and Prognosis Melissa W. Taggart, MD; Susan C. Abraham,
Appendix cancer mimicking ovarian cancer
 Int J Gynecol Cancer 2002, 12, 768 772 CORRESPONDENCE AND BRIEF REPORTS Appendix cancer mimicking ovarian cancer P. A. GEHRIG *, J. F. BOGGESS*, D. W. OLLILA, P. A. GROBEN & L. VAN LE* *Division of Gynecologic
Int J Gynecol Cancer 2002, 12, 768 772 CORRESPONDENCE AND BRIEF REPORTS Appendix cancer mimicking ovarian cancer P. A. GEHRIG *, J. F. BOGGESS*, D. W. OLLILA, P. A. GROBEN & L. VAN LE* *Division of Gynecologic
RECTAL CANCER CLINICAL CASE PRESENTATION
 RECTAL CANCER CLINICAL CASE PRESENTATION Francesco Sclafani Medical Oncologist, Clinical Research Fellow The Royal Marsden NHS Foundation Trust, London, UK esmo.org Disclosure I have nothing to declare
RECTAL CANCER CLINICAL CASE PRESENTATION Francesco Sclafani Medical Oncologist, Clinical Research Fellow The Royal Marsden NHS Foundation Trust, London, UK esmo.org Disclosure I have nothing to declare
Disclosure of Relevant Financial Relationships
 Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
Patient Presentation. 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201
 Patient Presentation 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201 CT shows: Thickening of the right hemidiaphragm CT shows: Fluid in the right paracolic sulcus CT shows: Large
Patient Presentation 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201 CT shows: Thickening of the right hemidiaphragm CT shows: Fluid in the right paracolic sulcus CT shows: Large
High risk stage II colon cancer
 High risk stage II colon cancer Joel Gingerich, MD, FRCPC Assistant Professor Medical Oncologist University of Manitoba CancerCare Manitoba Disclaimer No conflict of interests 16 October 2010 Overview
High risk stage II colon cancer Joel Gingerich, MD, FRCPC Assistant Professor Medical Oncologist University of Manitoba CancerCare Manitoba Disclaimer No conflict of interests 16 October 2010 Overview
The Impact of Adjuvant Chemotherapy in Pulmonary Large Cell Neuroendocrine Carcinoma (LCNC)
 The Impact of Adjuvant Chemotherapy in Pulmonary Large Cell Neuroendocrine Carcinoma (LCNC) Disclosure None Background Torino, Italy LCNC Rare tumor (2% to 3% all resected primary lung cancers) Preoperative
The Impact of Adjuvant Chemotherapy in Pulmonary Large Cell Neuroendocrine Carcinoma (LCNC) Disclosure None Background Torino, Italy LCNC Rare tumor (2% to 3% all resected primary lung cancers) Preoperative
Gastrointestinal Neuroendocrine Tumors: A Closer Look at the Characteristics of These Diverse Tumors
 Gastrointestinal Neuroendocrine Tumors: A Closer Look at the Characteristics of These Diverse Tumors Jaume Capdevila, MD, PhD Vall d'hebron University Hospital Vall d'hebron Institute of Oncology (VHIO)
Gastrointestinal Neuroendocrine Tumors: A Closer Look at the Characteristics of These Diverse Tumors Jaume Capdevila, MD, PhD Vall d'hebron University Hospital Vall d'hebron Institute of Oncology (VHIO)
A916: rectum: adenocarcinoma
 General facts of colorectal cancer The colon has cecum, ascending, transverse, descending and sigmoid colon sections. Cancer can start in any of the r sections or in the rectum. The wall of each of these
General facts of colorectal cancer The colon has cecum, ascending, transverse, descending and sigmoid colon sections. Cancer can start in any of the r sections or in the rectum. The wall of each of these
Metachronous metastasis to inguinal lymph nodes from sigmoid colon adenocarcinoma with abdominal wall metastasis: a case report
 Tanabe et al. BMC Cancer (2019) 19:180 https://doi.org/10.1186/s12885-019-5386-x CASE REPORT Metachronous metastasis to inguinal lymph nodes from sigmoid colon adenocarcinoma with abdominal wall metastasis:
Tanabe et al. BMC Cancer (2019) 19:180 https://doi.org/10.1186/s12885-019-5386-x CASE REPORT Metachronous metastasis to inguinal lymph nodes from sigmoid colon adenocarcinoma with abdominal wall metastasis:
Appendiceal Adenocarcinoma with Suppurative Appendicitis: Case Report and Literature Review
 Appendiceal adenocarcinoma presenting with acute appendicitis 155 Appendiceal Adenocarcinoma with Suppurative Appendicitis: Case Report and Literature Review Va-Kei Kok 1, Teh-Kuang Wang 2, Hsi-Che Shen
Appendiceal adenocarcinoma presenting with acute appendicitis 155 Appendiceal Adenocarcinoma with Suppurative Appendicitis: Case Report and Literature Review Va-Kei Kok 1, Teh-Kuang Wang 2, Hsi-Che Shen
Disclosures. Outline. What IS tumor budding?? Tumor Budding in Colorectal Carcinoma: What, Why, and How. I have nothing to disclose
 Tumor Budding in Colorectal Carcinoma: What, Why, and How Disclosures I have nothing to disclose Soo-Jin Cho, MD, PhD Assistant Professor UCSF Dept of Pathology Current Issues in Anatomic Pathology 2017
Tumor Budding in Colorectal Carcinoma: What, Why, and How Disclosures I have nothing to disclose Soo-Jin Cho, MD, PhD Assistant Professor UCSF Dept of Pathology Current Issues in Anatomic Pathology 2017
CASE STUDIES IN COLORECTAL CANCER: A ROUNDTABLE DISCUSSION
 CASE STUDIES IN COLORECTAL CANCER: A ROUNDTABLE DISCUSSION PROVIDED AS AN EDUCATIONAL SERVICE BY THE INSTITUTE FOR CONTINUING HEALTHCARE EDUCATION SUPPORTED BY AN EDUCATIONAL GRANT FROM GENENTECH LEARNING
CASE STUDIES IN COLORECTAL CANCER: A ROUNDTABLE DISCUSSION PROVIDED AS AN EDUCATIONAL SERVICE BY THE INSTITUTE FOR CONTINUING HEALTHCARE EDUCATION SUPPORTED BY AN EDUCATIONAL GRANT FROM GENENTECH LEARNING
Joseph Misdraji, M.D. GI pathology Unit Massachusetts General Hospital
 Joseph Misdraji, M.D. GI pathology Unit Massachusetts General Hospital jmisdraji@partners.org Low-grade appendiceal mucinous neoplasm (LAMN) High-grade appendiceal mucinous neoplasm (HAMN) Adenocarcinoma
Joseph Misdraji, M.D. GI pathology Unit Massachusetts General Hospital jmisdraji@partners.org Low-grade appendiceal mucinous neoplasm (LAMN) High-grade appendiceal mucinous neoplasm (HAMN) Adenocarcinoma
Regional lymph node involvement and outcomes in appendiceal neuroendocrine tumors: a SEER database analysis
 /, 2017, Vol. 8, (No. 59), pp: 99541-99551 Regional lymph node involvement and outcomes in appendiceal neuroendocrine tumors: a SEER database analysis Amir Mehrvarz Sarshekeh 1, Shailesh Advani 1, Daniel
/, 2017, Vol. 8, (No. 59), pp: 99541-99551 Regional lymph node involvement and outcomes in appendiceal neuroendocrine tumors: a SEER database analysis Amir Mehrvarz Sarshekeh 1, Shailesh Advani 1, Daniel
Locally Advanced Colon Cancer. Feiran Lou MD. MS. Richmond University Medical Center Department of Surgery
 Locally Advanced Colon Cancer Feiran Lou MD. MS. Richmond University Medical Center Department of Surgery Case 34 yo man presented with severe RLQ abdominal pain X 24 hrs. No nausea/vomiting/fever. + flatus.
Locally Advanced Colon Cancer Feiran Lou MD. MS. Richmond University Medical Center Department of Surgery Case 34 yo man presented with severe RLQ abdominal pain X 24 hrs. No nausea/vomiting/fever. + flatus.
Surveillance of Small Rectal Carcinoid Tumors in the Absence of Metastatic Disease
 Ann Surg Oncol (2012) 19:3486 3490 DOI 10.1245/s10434-012-2442-z ORIGINAL ARTICLE ENDOCRINE TUMORS Surveillance of Small Rectal Carcinoid Tumors in the Absence of Metastatic Disease Sara E. Murray, MD
Ann Surg Oncol (2012) 19:3486 3490 DOI 10.1245/s10434-012-2442-z ORIGINAL ARTICLE ENDOCRINE TUMORS Surveillance of Small Rectal Carcinoid Tumors in the Absence of Metastatic Disease Sara E. Murray, MD
NET und NEC. Endoscopic and oncologic therapy
 NET und NEC Endoscopic and oncologic therapy Classification well-differentiated NET - G1 and G2 - carcinoid poorly-differentiated NEC - G3 - like SCLC well differentiated NET G3 -> elevated proliferation
NET und NEC Endoscopic and oncologic therapy Classification well-differentiated NET - G1 and G2 - carcinoid poorly-differentiated NEC - G3 - like SCLC well differentiated NET G3 -> elevated proliferation
COLORECTAL CANCER CASES
 COLORECTAL CANCER CASES Case #1 Case #2 Colorectal Cancer Case 1 A 52 year-old female attends her family physician for her yearly complete physical examination. Her past medical history is significant
COLORECTAL CANCER CASES Case #1 Case #2 Colorectal Cancer Case 1 A 52 year-old female attends her family physician for her yearly complete physical examination. Her past medical history is significant
HIPEC Controversies in the Indications and Application of Regional Chemotherapy for Peritoneal Surface Malignancies
 HIPEC Controversies in the Indications and Application of Regional Chemotherapy for Peritoneal Surface Malignancies Crescent City Cancer Update: GI and HPB Saturday September 24, 2016 George M. Fuhrman,
HIPEC Controversies in the Indications and Application of Regional Chemotherapy for Peritoneal Surface Malignancies Crescent City Cancer Update: GI and HPB Saturday September 24, 2016 George M. Fuhrman,
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
BC CRC Update Unusual Colorectal Tumors
 BC CRC Update Unusual Colorectal Tumors Anthony MacLean, MD, FRCSC, FACS, FASCRS Colorectal Surgeon Foothills Medical Centre Clinical Associate Professor of Surgery and Oncology University of Calgary I
BC CRC Update Unusual Colorectal Tumors Anthony MacLean, MD, FRCSC, FACS, FASCRS Colorectal Surgeon Foothills Medical Centre Clinical Associate Professor of Surgery and Oncology University of Calgary I
6 Department of Pathology, University of California at San Francisco Medical Center, San
 The Impact of Stage, Grade, and Mucinous Histology on the Efficacy of Systemic Chemotherapy in Adenocarcinomas of the Appendix: Analysis of the National Cancer Data Base Elliot A. Asare, MD 1,2 ; Carolyn
The Impact of Stage, Grade, and Mucinous Histology on the Efficacy of Systemic Chemotherapy in Adenocarcinomas of the Appendix: Analysis of the National Cancer Data Base Elliot A. Asare, MD 1,2 ; Carolyn
COLON CANCER PERITONEAL CARCINOMATOSIS TREATMENT Prof. Annibale Donini
 UNIVERSITY OF PERUGIA Department of General and Emergency Surgery Chief: Prof. Annibale Donini COLON CANCER PERITONEAL CARCINOMATOSIS TREATMENT Prof. Annibale Donini COLON CANCER IS A HIGHLY FREQUENT NEOPLASIA
UNIVERSITY OF PERUGIA Department of General and Emergency Surgery Chief: Prof. Annibale Donini COLON CANCER PERITONEAL CARCINOMATOSIS TREATMENT Prof. Annibale Donini COLON CANCER IS A HIGHLY FREQUENT NEOPLASIA
Syllabus. Appendiceal GCC and LAMN Navigating the Alphabet Soup in the Appendix. Appendiceal tumors. Summary provided Complete presentation
 2016 Current Issues in Surgical Pathology Appendiceal GCC and LAMN Navigating the Alphabet Soup in the Appendix Syllabus Summary provided Complete presentation sanjay.kakar@ucsf.edu Sanjay Kakar, MD University
2016 Current Issues in Surgical Pathology Appendiceal GCC and LAMN Navigating the Alphabet Soup in the Appendix Syllabus Summary provided Complete presentation sanjay.kakar@ucsf.edu Sanjay Kakar, MD University
AJCC 7 th Edition Staging Disease Site Webinar Colorectum
 AJCC 7 th Edition Staging Disease Site Webinar Colorectum Donna M. Gress, RHIT, CTR Validating science. Improving patient care. This presentation was supported by the Cooperative Agreement Number DP13-1310
AJCC 7 th Edition Staging Disease Site Webinar Colorectum Donna M. Gress, RHIT, CTR Validating science. Improving patient care. This presentation was supported by the Cooperative Agreement Number DP13-1310
7 th Edition Staging. AJCC 7 th Edition Staging. Disease Site Webinar. Colorectum. Overview. This webinar is sponsored by
 AJCC 7 th Edition Staging Colorectum Donna M. Gress, RHIT, CTR Validating science. Improving patient care. This presentation was supported by the Cooperative Agreement Number DP13-1310 from The Centers
AJCC 7 th Edition Staging Colorectum Donna M. Gress, RHIT, CTR Validating science. Improving patient care. This presentation was supported by the Cooperative Agreement Number DP13-1310 from The Centers
Surgical Management of Advanced Stage Colon Cancer. Nathan Huber, MD 6/11/14
 Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Kathleen A. Cummins 1, Gregory B. Russell 2, Konstantinos I. Votanopoulos 1, Perry Shen 1, John H. Stewart 1, Edward A. Levine 1.
 Original Article Peritoneal dissemination from high-grade appendiceal cancer treated with cytoreductive surgery (CRS) and hyperthermic intraperitoneal chemotherapy (HIPEC) Kathleen A. Cummins 1, Gregory
Original Article Peritoneal dissemination from high-grade appendiceal cancer treated with cytoreductive surgery (CRS) and hyperthermic intraperitoneal chemotherapy (HIPEC) Kathleen A. Cummins 1, Gregory
SCOPE TODAYS SESSION. Case 1: Case 2. Basic Theory Stuff: Heavy Stuff. Basic Questions. Basic Questions
 MONDAY TEACHING SCOPE TODAYS SESSION Case 1: Basic Questions Case 2 Basic Questions Basic Theory Stuff: AJCC TNM + Stage Group for Carcinoid of the Appendix Management of Carcinoid of the Appendix (NCCN)
MONDAY TEACHING SCOPE TODAYS SESSION Case 1: Basic Questions Case 2 Basic Questions Basic Theory Stuff: AJCC TNM + Stage Group for Carcinoid of the Appendix Management of Carcinoid of the Appendix (NCCN)
Clinical Study Small Bowel Tumors: Clinical Presentation, Prognosis, and Outcomein33PatientsinaTertiaryCareCenter
 Hindawi Publishing Corporation Journal of Oncology Volume 2008, Article ID 212067, 5 pages doi:10.1155/2008/212067 Clinical Study Small Bowel Tumors: Clinical Presentation, Prognosis, and Outcomein33PatientsinaTertiaryCareCenter
Hindawi Publishing Corporation Journal of Oncology Volume 2008, Article ID 212067, 5 pages doi:10.1155/2008/212067 Clinical Study Small Bowel Tumors: Clinical Presentation, Prognosis, and Outcomein33PatientsinaTertiaryCareCenter
Colon, Rectum, and Appendix. Presentation Outline. Overview Tumor Characteristics
 Colon, Rectum, and Appendix 2011 Reporting Requirements and CSv02.03.02 NCCN/ASCO Treatment Guidelines by Stage FCDS 2011 Educational Webcast Series September 15, 2011 Steven Peace, CTR Presentation Outline
Colon, Rectum, and Appendix 2011 Reporting Requirements and CSv02.03.02 NCCN/ASCO Treatment Guidelines by Stage FCDS 2011 Educational Webcast Series September 15, 2011 Steven Peace, CTR Presentation Outline
Colon, Rectum, and Appendix
 Colon, Rectum, and Appendix 2011 Reporting Requirements and CSv02.03.02 NCCN/ASCO Treatment Guidelines by Stage FCDS 2011 Educational Webcast Series September 15, 2011 Steven Peace, CTR Presentation Outline
Colon, Rectum, and Appendix 2011 Reporting Requirements and CSv02.03.02 NCCN/ASCO Treatment Guidelines by Stage FCDS 2011 Educational Webcast Series September 15, 2011 Steven Peace, CTR Presentation Outline
Basic Data. Birthday: Gender:Female Admission date:
 Basic Data Birthday:1951-07-02 Gender:Female Admission date:2004-06-28 Chief Complaint A protruding mass over RLQ abdomen for many years. Present Illness & Past History Pseudomyxoma peritonei s/p laparotomy
Basic Data Birthday:1951-07-02 Gender:Female Admission date:2004-06-28 Chief Complaint A protruding mass over RLQ abdomen for many years. Present Illness & Past History Pseudomyxoma peritonei s/p laparotomy
Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach
 Case Reports in Surgery Volume 2013, Article ID 560712, 4 pages http://dx.doi.org/10.1155/2013/560712 Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach Shigeo
Case Reports in Surgery Volume 2013, Article ID 560712, 4 pages http://dx.doi.org/10.1155/2013/560712 Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach Shigeo
Staging Challenges in Lower GI Cancers. Disclosure of Relevant Financial Relationships. AJCC 8 th edition and CAP protocol updates
 Staging Challenges in Lower GI Cancers Sanjay Kakar, MD University of California, San Francisco March 05, 2017 Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education
Staging Challenges in Lower GI Cancers Sanjay Kakar, MD University of California, San Francisco March 05, 2017 Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education
WHAT SHOULD WE DO WITH TUMOUR BUDDING IN EARLY COLORECTAL CANCER?
 CANCER STAGING TNM and prognosis in CRC WHAT SHOULD WE DO WITH TUMOUR BUDDING IN EARLY COLORECTAL CANCER? Alessandro Lugli, MD Institute of Pathology University of Bern Switzerland Maastricht, June 19
CANCER STAGING TNM and prognosis in CRC WHAT SHOULD WE DO WITH TUMOUR BUDDING IN EARLY COLORECTAL CANCER? Alessandro Lugli, MD Institute of Pathology University of Bern Switzerland Maastricht, June 19
Peritoneal Involvement in Stage II Colon Cancer
 Anatomic Pathology / PERITONEAL INVOLVEMENT IN STAGE II COLON CANCER Peritoneal Involvement in Stage II Colon Cancer A.M. Lennon, MB, MRCPI, H.E. Mulcahy, MD, MRCPI, J.M.P. Hyland, MCh, FRCS, FRCSI, C.
Anatomic Pathology / PERITONEAL INVOLVEMENT IN STAGE II COLON CANCER Peritoneal Involvement in Stage II Colon Cancer A.M. Lennon, MB, MRCPI, H.E. Mulcahy, MD, MRCPI, J.M.P. Hyland, MCh, FRCS, FRCSI, C.
By: Tania Cortas, MD Arizona Oncology 03/10/2015
 By: Tania Cortas, MD Arizona Oncology 03/10/2015 Epidemiology In the United States, CRC incidence rates have declined about 2 to 3 percent per year over the last 15 years Death rates from CRC have declined
By: Tania Cortas, MD Arizona Oncology 03/10/2015 Epidemiology In the United States, CRC incidence rates have declined about 2 to 3 percent per year over the last 15 years Death rates from CRC have declined
OFCCR CLINICAL DIAGNOSIS AND TREATMENT FORM
 OFCCR CLINICAL DIAGNOSIS AND TREATMENT FORM Name: _, OFCCR # _ OCGN # _ OCR Group # _ HIN# Sex: MALE FEMALE UNKNOWN Date of Birth: DD MMM YYYY BASELINE DIAGNOSIS & TREATMENT 1. Place of Diagnosis: Name
OFCCR CLINICAL DIAGNOSIS AND TREATMENT FORM Name: _, OFCCR # _ OCGN # _ OCR Group # _ HIN# Sex: MALE FEMALE UNKNOWN Date of Birth: DD MMM YYYY BASELINE DIAGNOSIS & TREATMENT 1. Place of Diagnosis: Name
Well-differentiated Papillary Mesothelioma of the Pleura Diagnosed by Video-Assisted Thoracic Surgical Pleural Biopsy : A Case Report
 Showa Univ J Med Sci 25 1, 67 72, March 2013 Case Report Well-differentiated Papillary Mesothelioma of the Pleura Diagnosed by Video-Assisted Thoracic Surgical Pleural Biopsy : A Case Report Yuri TOMITA
Showa Univ J Med Sci 25 1, 67 72, March 2013 Case Report Well-differentiated Papillary Mesothelioma of the Pleura Diagnosed by Video-Assisted Thoracic Surgical Pleural Biopsy : A Case Report Yuri TOMITA
Metastatic mechanism of spermatic cord tumor from stomach cancer
 Int Canc Conf J (2013) 2:191 195 DOI 10.1007/s13691-013-0-9 CANCER BOARD CONFERENCE Metastatic mechanism of spermatic cord tumor from stomach cancer Masahiro Seike Yoshikazu Kanazawa Ryuji Ohashi Tadashi
Int Canc Conf J (2013) 2:191 195 DOI 10.1007/s13691-013-0-9 CANCER BOARD CONFERENCE Metastatic mechanism of spermatic cord tumor from stomach cancer Masahiro Seike Yoshikazu Kanazawa Ryuji Ohashi Tadashi
Serotonin- and Somatostatin-Positive Goblet Cell Carcinoid of the Duodenum
 2012 66 4 351 356 Serotonin- and Somatostatin-Positive Goblet Cell Carcinoid of the Duodenum a b* c c c a a b d a c b d 352 Ohara et al. received remedies at another hospital. Hematemesis then recurred
2012 66 4 351 356 Serotonin- and Somatostatin-Positive Goblet Cell Carcinoid of the Duodenum a b* c c c a a b d a c b d 352 Ohara et al. received remedies at another hospital. Hematemesis then recurred
Kentaro Tominaga, Kenya Kamimura, Junji Yokoyama and Shuji Terai
 doi: 10.2169/internalmedicine.1700-18 http://internmed.jp CASE REPORT Usefulness of Capsule Endoscopy and Double-balloon Enteroscopy for the Diagnosis of Multiple Carcinoid Tumors in the Small Intestine:
doi: 10.2169/internalmedicine.1700-18 http://internmed.jp CASE REPORT Usefulness of Capsule Endoscopy and Double-balloon Enteroscopy for the Diagnosis of Multiple Carcinoid Tumors in the Small Intestine:
BOWEL CANCER. Causes of bowel cancer
 A cancer is an abnormality in an organ that grows without control. The growth is often quite slow, but will continue unabated until it is detected. It can cause symptoms by its presence in the organ or
A cancer is an abnormality in an organ that grows without control. The growth is often quite slow, but will continue unabated until it is detected. It can cause symptoms by its presence in the organ or
Management of a Solitary Bone Metastasis to the Tibia from Colorectal Cancer
 354 Management of a Solitary Bone Metastasis to the Tibia from Colorectal Cancer Anastasia S. Chalkidou a Panagiotis Padelis a Anastasios L. Boutis b a Clinical Oncology Department, Theagenion Cancer Hospital
354 Management of a Solitary Bone Metastasis to the Tibia from Colorectal Cancer Anastasia S. Chalkidou a Panagiotis Padelis a Anastasios L. Boutis b a Clinical Oncology Department, Theagenion Cancer Hospital
Specialised Services Policy: CP02 Hyperthermic Intraperitoneal Chemotherapy (HIPEC) and Cytoreductive Surgery for treatment of Pseudomyxoma Peritonei
 Specialised Services Policy: CP02 Hyperthermic Intraperitoneal Chemotherapy (HIPEC) of Pseudomyxoma Peritonei Document Author: Assistant Medical Director Executive Lead: Medical Director Approved by: Management
Specialised Services Policy: CP02 Hyperthermic Intraperitoneal Chemotherapy (HIPEC) of Pseudomyxoma Peritonei Document Author: Assistant Medical Director Executive Lead: Medical Director Approved by: Management
Lower lymph node yield following neoadjuvant therapy for rectal cancer has no clinical significance
 Original Article Lower lymph node yield following neoadjuvant therapy for rectal cancer has no clinical significance Dedrick Kok Hong Chan 1,2, Ker-Kan Tan 1,2 1 Division of Colorectal Surgery, University
Original Article Lower lymph node yield following neoadjuvant therapy for rectal cancer has no clinical significance Dedrick Kok Hong Chan 1,2, Ker-Kan Tan 1,2 1 Division of Colorectal Surgery, University
Update on 2015 WHO Classification of Lung Adenocarcinoma 1/3/ Mayo Foundation for Medical Education and Research. All rights reserved.
 1 Our speaker for this program is Dr. Anja Roden, an associate professor of Laboratory Medicine and Pathology at Mayo Clinic as well as consultant in the Anatomic Pathology Laboratory and co-director of
1 Our speaker for this program is Dr. Anja Roden, an associate professor of Laboratory Medicine and Pathology at Mayo Clinic as well as consultant in the Anatomic Pathology Laboratory and co-director of
COLON CANCER CARE GUIDELINES NON-METASTATIC DISEASE
 COLON CANCER CARE GUIDELINES NON-METASTATIC DISEASE Guideline Authors: Todd S. Crocenzi, M.D.; Mark Whiteford, M.D.; Matthew Solhjem, M.D.; Carlo Bifulco, M.D.; Melissa Li, M.D.; Christopher Cai, M.D.;
COLON CANCER CARE GUIDELINES NON-METASTATIC DISEASE Guideline Authors: Todd S. Crocenzi, M.D.; Mark Whiteford, M.D.; Matthew Solhjem, M.D.; Carlo Bifulco, M.D.; Melissa Li, M.D.; Christopher Cai, M.D.;
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
3/27/2017. Pulmonary Pathology Specialty Conference. Disclosure of Relevant Financial Relationships. Clinical History:
 Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Advanced duodenal carcinoma: Chemotherapy efficacy and analysis of prognostic factors
 Oncology and Translational Medicine DOI 10.1007/s10330-015-0094-8 February 2016, Vol. 2, No. 1, P16 P20 ORIGINAL ARTICLE Advanced duodenal carcinoma: Chemotherapy efficacy and analysis of prognostic factors
Oncology and Translational Medicine DOI 10.1007/s10330-015-0094-8 February 2016, Vol. 2, No. 1, P16 P20 ORIGINAL ARTICLE Advanced duodenal carcinoma: Chemotherapy efficacy and analysis of prognostic factors
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Prof. Dr. Aydın ÖZSARAN
 Prof. Dr. Aydın ÖZSARAN Adenocarcinomas of the endometrium Most common gynecologic malignancy in developed countries Second most common in developing countries. Adenocarcinomas, grade 1 and 2 endometrioid
Prof. Dr. Aydın ÖZSARAN Adenocarcinomas of the endometrium Most common gynecologic malignancy in developed countries Second most common in developing countries. Adenocarcinomas, grade 1 and 2 endometrioid
S1.04 Principal clinician. G1.01 Comments. G2.01 *Specimen dimensions (prostate) S2.02 *Seminal vesicles
 Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Sex Male
Prostate Cancer Histopathology Reporting Proforma (Radical Prostatectomy) Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth Sex Male
Rare Case of Metastatic Colorectal Cancer to Uretral Meatus with Rapid Progression and Fatal Outcomes
 Rare Case of Metastatic Colorectal Cancer to Uretral Meatus with Rapid Progression and Fatal Outcomes Marwane Andaloussi Benatiya Department of Urology, Hassan 2 Hospital, Agadir, Morocco Zakaria El Asri
Rare Case of Metastatic Colorectal Cancer to Uretral Meatus with Rapid Progression and Fatal Outcomes Marwane Andaloussi Benatiya Department of Urology, Hassan 2 Hospital, Agadir, Morocco Zakaria El Asri
Color Codes Pathology and Genetics Medicine and Clinical Pathology Surgery Imaging
 Saturday, November 5, 2005 8:30-10:30 a. m. Poorly Differentiated Endocrine Carcinomas Chairman: E. Van Cutsem, Leuven, Belgium 9:00-9:30 a. m. Working Group Sessions Pathology and Genetics Group leaders:
Saturday, November 5, 2005 8:30-10:30 a. m. Poorly Differentiated Endocrine Carcinomas Chairman: E. Van Cutsem, Leuven, Belgium 9:00-9:30 a. m. Working Group Sessions Pathology and Genetics Group leaders:
Colon, or Colorectal, Cancer Information
 Colon, or Colorectal, Cancer Information Definition Colon, or colorectal, cancer is cancer that starts in the large intestine (colon) or the rectum (end of the colon). Other types of cancer can affect
Colon, or Colorectal, Cancer Information Definition Colon, or colorectal, cancer is cancer that starts in the large intestine (colon) or the rectum (end of the colon). Other types of cancer can affect
Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms
 Hindawi Publishing Corporation Volume 2015, Article ID 153932, 5 pages http://dx.doi.org/10.1155/2015/153932 Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms Shiuan-Li
Hindawi Publishing Corporation Volume 2015, Article ID 153932, 5 pages http://dx.doi.org/10.1155/2015/153932 Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms Shiuan-Li
Carcinoembryonic Antigen
 Other Names/Abbreviations CEA 190.26 - Carcinoembryonic Antigen Carcinoembryonic antigen (CEA) is a protein polysaccharide found in some carcinomas. It is effective as a biochemical marker for monitoring
Other Names/Abbreviations CEA 190.26 - Carcinoembryonic Antigen Carcinoembryonic antigen (CEA) is a protein polysaccharide found in some carcinomas. It is effective as a biochemical marker for monitoring
Case history: Figure 1. H&E, 5x. Figure 2. H&E, 20x.
 1 Case history: A 49 year-old female presented with a 5 year history of chronic anal fissure. The patient s past medical history is otherwise unremarkable. On digital rectal examination there was a very
1 Case history: A 49 year-old female presented with a 5 year history of chronic anal fissure. The patient s past medical history is otherwise unremarkable. On digital rectal examination there was a very
A215- Urinary bladder cancer tissues
 A215- Urinary bladder cancer tissues (formalin fixed) For research use only Specifications: No. of cases: 45 Tissue type: Urinary bladder cancer tissues No. of spots: 2 spots from each cancer case (90
A215- Urinary bladder cancer tissues (formalin fixed) For research use only Specifications: No. of cases: 45 Tissue type: Urinary bladder cancer tissues No. of spots: 2 spots from each cancer case (90
Presentation material is for education purposes only. All rights reserved URMC Radiology Page 1 of 98
 Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Carcinoid Tumors: The Beginning and End. Surgical Oncology Update 2011 Chris Baliski MD, FRCS BC Cancer Agency, CSI October 21, 2011
 Carcinoid Tumors: The Beginning and End Surgical Oncology Update 2011 Chris Baliski MD, FRCS BC Cancer Agency, CSI October 21, 2011 1 st described by Oberndofer(1907) Karzinoide = cancer like Arise from
Carcinoid Tumors: The Beginning and End Surgical Oncology Update 2011 Chris Baliski MD, FRCS BC Cancer Agency, CSI October 21, 2011 1 st described by Oberndofer(1907) Karzinoide = cancer like Arise from
Kaoru Takeshima, Kazuo Yamafuji, Atsunori Asami, Hideo Baba, Nobuhiko Okamoto, Hidena Takahashi, Chisato Takagi, and Kiyoshi Kubochi
 Case Reports in Surgery Volume 2016, Article ID 4548798, 5 pages http://dx.doi.org/10.1155/2016/4548798 Case Report Successful Resection of Isolated Para-Aortic Lymph Node Recurrence from Advanced Sigmoid
Case Reports in Surgery Volume 2016, Article ID 4548798, 5 pages http://dx.doi.org/10.1155/2016/4548798 Case Report Successful Resection of Isolated Para-Aortic Lymph Node Recurrence from Advanced Sigmoid
Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms
 Case Reports in Pathology Volume 2015, Article ID 153932, 5 pages http://dx.doi.org/10.1155/2015/153932 Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms Shiuan-Li
Case Reports in Pathology Volume 2015, Article ID 153932, 5 pages http://dx.doi.org/10.1155/2015/153932 Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms Shiuan-Li
Analysis of the outcome of young age tongue squamous cell carcinoma
 Jeon et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:41 DOI 10.1186/s40902-017-0139-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Analysis of the outcome of
Jeon et al. Maxillofacial Plastic and Reconstructive Surgery (2017) 39:41 DOI 10.1186/s40902-017-0139-8 Maxillofacial Plastic and Reconstructive Surgery RESEARCH Open Access Analysis of the outcome of
Planned relaparotomy following curative resection of a locally advanced gastrointestinal cancer
 Planned relaparotomy following curative resection of a locally advanced gastrointestinal cancer PD Dr. med. Michel Adamina, MSc Department of Surgery Agenda Prerequisite for successful CRS HIPEC Planned
Planned relaparotomy following curative resection of a locally advanced gastrointestinal cancer PD Dr. med. Michel Adamina, MSc Department of Surgery Agenda Prerequisite for successful CRS HIPEC Planned
ADJUVANT CHEMOTHERAPY...
 Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
PNET 3/7/2015. GI and Pancreatic NETs. The Postgraduate Course in Breast and Endocrine Surgery. Decision Tree. GI and Pancreatic NETs.
 GI and Pancreatic NETs The Postgraduate Course in Breast and Endocrine Surgery Disclosures Ipsen NET Advisory Board Marines Memorial Club and Hotel San Francisco, CA Eric K Nakakura San Francisco, CA March
GI and Pancreatic NETs The Postgraduate Course in Breast and Endocrine Surgery Disclosures Ipsen NET Advisory Board Marines Memorial Club and Hotel San Francisco, CA Eric K Nakakura San Francisco, CA March
Terumitsu; Nagayasu, Takeshi
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation A rare case of segmental ulcerative Tominaga, Tetsuro; Nonaka, Takashi; Shuichi; Kunizaki, Masaki; Sumida, Terumitsu; Nagayasu, Takeshi Acta medica
NAOSITE: Nagasaki University's Ac Title Author(s) Citation A rare case of segmental ulcerative Tominaga, Tetsuro; Nonaka, Takashi; Shuichi; Kunizaki, Masaki; Sumida, Terumitsu; Nagayasu, Takeshi Acta medica
Primary Small Cell Carcinoma Of The Bladder: A Case Report And Review Of The Literature
 ISPUB.COM The Internet Journal of Urology Volume 7 Number 1 Primary Small Cell Carcinoma Of The Bladder: A Case Report And Review Of The Literature T Hsieh, J Aragon-Ching, J Saia, T Sotelo Citation T
ISPUB.COM The Internet Journal of Urology Volume 7 Number 1 Primary Small Cell Carcinoma Of The Bladder: A Case Report And Review Of The Literature T Hsieh, J Aragon-Ching, J Saia, T Sotelo Citation T
Surgical Management of Metastatic Colon Cancer: analysis of the Surveillance, Epidemiology and End Results (SEER) database
 Surgical Management of Metastatic Colon Cancer: analysis of the Surveillance, Epidemiology and End Results (SEER) database Hadi Khan, MD 1, Adam J. Olszewski, MD 2 and Ponnandai S. Somasundar, MD 1 1 Department
Surgical Management of Metastatic Colon Cancer: analysis of the Surveillance, Epidemiology and End Results (SEER) database Hadi Khan, MD 1, Adam J. Olszewski, MD 2 and Ponnandai S. Somasundar, MD 1 1 Department
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Case Scenario 1. The patient agreed to a CT guided biopsy of the left upper lobe mass. This was performed and confirmed non-small cell carcinoma.
 Case Scenario 1 An 89 year old male patient presented with a progressive cough for approximately six weeks for which he received approximately three rounds of antibiotic therapy without response. A chest
Case Scenario 1 An 89 year old male patient presented with a progressive cough for approximately six weeks for which he received approximately three rounds of antibiotic therapy without response. A chest
Despite advances in our understanding of appendiceal. An Update on the Diagnosis, Grading, and Staging of Appendiceal Mucinous Neoplasms
 REVIEW ARTICLE An Update on the Diagnosis, Grading, and Staging of Appendiceal Mucinous Neoplasms Mark A. Valasek, MD, PhD* and Reetesh K. Pai, MD Abstract: Despite advances in our understanding of appendiceal
REVIEW ARTICLE An Update on the Diagnosis, Grading, and Staging of Appendiceal Mucinous Neoplasms Mark A. Valasek, MD, PhD* and Reetesh K. Pai, MD Abstract: Despite advances in our understanding of appendiceal
TREATMENT OF PERITONEAL COLORECTAL CARCINOMATOSIS
 TREATMENT OF PERITONEAL COLORECTAL CARCINOMATOSIS Anna Lepistö, MD, PhD Department of Colorectal Surgery, Abdominal Center, Helsinki University Hospital Incidence, prevalence and risk factors for peritoneal
TREATMENT OF PERITONEAL COLORECTAL CARCINOMATOSIS Anna Lepistö, MD, PhD Department of Colorectal Surgery, Abdominal Center, Helsinki University Hospital Incidence, prevalence and risk factors for peritoneal
Regional Therapy for Management of Peritoneal Carcinomatosis from Gastrointestinal Malignancies
 Regional Therapy for Management of Peritoneal Carcinomatosis from Gastrointestinal Malignancies Byrne Lee, MD FACS Chief, Mixed Tumor Surgery Service City of Hope Division of Surgical Oncology September
Regional Therapy for Management of Peritoneal Carcinomatosis from Gastrointestinal Malignancies Byrne Lee, MD FACS Chief, Mixed Tumor Surgery Service City of Hope Division of Surgical Oncology September
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL RECTAL CANCER GI Site Group Rectal Cancer Authors: Dr. Jennifer Knox, Dr. Mairead McNamara 1. INTRODUCTION 3 2. SCREENING AND
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL RECTAL CANCER GI Site Group Rectal Cancer Authors: Dr. Jennifer Knox, Dr. Mairead McNamara 1. INTRODUCTION 3 2. SCREENING AND
How much colon should be resected?
 Colon Cancer Surgical Standard of Care and Operative Techniques Madhulika G. Varma MD Professor and Chief Section of Colorectal Surgery University of California, San Francisco How much colon should be
Colon Cancer Surgical Standard of Care and Operative Techniques Madhulika G. Varma MD Professor and Chief Section of Colorectal Surgery University of California, San Francisco How much colon should be
Fig. 59 Malignant phaeochromocytoma, hepatic metastasis.
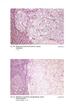 Fig. 59 Malignant phaeochromocytoma, hepatic metastasis. X 120 Hyperte nsion Fig. 60 Malignant sympathetic paraganglioma, lymph node metastasis Primary in bladder. x 1 20 Hypertension Fig. 61 Malignant
Fig. 59 Malignant phaeochromocytoma, hepatic metastasis. X 120 Hyperte nsion Fig. 60 Malignant sympathetic paraganglioma, lymph node metastasis Primary in bladder. x 1 20 Hypertension Fig. 61 Malignant
Case Conference. Craig Morgenthal Department of Surgery Long Island College Hospital
 Case Conference Craig Morgenthal Department of Surgery Long Island College Hospital Neoadjuvant versus Adjuvant Radiation Therapy in Rectal Carcinoma Epidemiology American Cancer Society statistics for
Case Conference Craig Morgenthal Department of Surgery Long Island College Hospital Neoadjuvant versus Adjuvant Radiation Therapy in Rectal Carcinoma Epidemiology American Cancer Society statistics for
Are goblet cell carcinoids a group of heterogeneous tumors?
 Are goblet cell carcinoids a group of heterogeneous tumors? Jirka Macak a,c, Kristina Nemejcova b, Jana Dvorackova a,c Background. Goblet cell carcinoids belong to neuroendocrine tumors, according to the
Are goblet cell carcinoids a group of heterogeneous tumors? Jirka Macak a,c, Kristina Nemejcova b, Jana Dvorackova a,c Background. Goblet cell carcinoids belong to neuroendocrine tumors, according to the
