Br a i n s t e m hemangioblastomas account for approximately
|
|
|
- Nigel Holmes
- 5 years ago
- Views:
Transcription
1 J Neurosurg 114: , 2011 Long-term outcome after resection of brainstem hemangioblastomas in von Hippel-Lindau disease Clinical article Jo s h u a J. Wi n d, M.D., 1,2 Ka m r a n D. Ba k h t i a n, M.S., 1 Je n n i f e r A. Sw e e t, M.D., 1,2 Ga u t a m U. Me h ta, M.D., 1 Jay e s h P. Th a w a n i, M.D., 1 As h o k R. As t h a g i r i, M.D., 1 Ed w a r d H. Ol d f i e l d, M.D., 1,3 a n d Ru s s e l l R. Lo n s e r, M.D. 1 1 Surgical Neurology Branch, National Institute of Neurological Disorders and Stroke, National Institutes of Health, Bethesda, Maryland; 2 Department of Neurological Surgery, George Washington University Medical Center, Washington, DC; and 3 Department of Neurological Surgery, University of Virginia Health System, Charlottesville, Virginia Object. Brainstem hemangioblastomas are frequently encountered in patients with von Hippel-Lindau (VHL) disease. These tumors can cause significant morbidity, and their optimal management has not been defined. To better define the outcome and management of these tumors, the authors analyzed the long-term results in patients who underwent resection of brainstem hemangioblastomas. Methods. Consecutive patients with VHL disease who underwent resection of brainstem hemangioblastomas with a follow-up of 12 months or more were included in this study. Serial functional assessments, radiographic examinations, and operative records were analyzed. Results. Forty-four patients (17 male and 27 female) underwent 51 operations for resection of 71 brainstem hemangioblastomas. The most common presenting symptoms were headache, swallowing difficulties, singultus, gait difficulties, and sensory abnormalities. The mean follow-up was 5.9 ± 5.0 years (range years). Immediately after 34 operations (66.7%), the patients remained at their preoperative functional status; they improved after 8 operations (15.7%) and worsened after 9 operations (17.6%) as measured by the McCormick scale. Eight (88.9%) of the 9 patients who were worse immediately after resection returned to their preoperative status within 6 months. Two patients experienced functional decline during long-term follow-up (beginning at 2.5 and 5 years postoperatively) caused by extensive VHL disease associated CNS disease. Conclusions. Generally, resection of symptomatic brainstem hemangioblastomas is a safe and effective management strategy in patients with VHL disease. Most patients maintain their preoperative functional status, although long-term decline in functional status may occur due to VHL disease associated progression. (DOI: / JNS10839) Ke y Wo r d s brainstem hemangioblastoma outcome surgical treatment von Hippel-Lindau disease Br a i n s t e m hemangioblastomas account for approximately 10% 15% of CNS hemangioblastomas in VHL disease. 4,19 They are highly vascular, benign tumors that are derived from embryologically arrested hemangioblasts. 20 Brainstem hemangioblastomas are frequently located in the medullary region, 29 but rarely they can be present in other brainstem locations. Patients with brainstem hemangioblastomas most often present with coughing, singultus, swallowing difficulties, headache, nausea, vomiting, sensory abnormalities, and ataxia. 29 Despite the potential morbidity associated with brainstem hemangioblastomas in VHL disease, information describing the long-term follow-up of patients with VHL Abbreviations used in this paper: KPS = Karnofsky Performance Scale; NIH = National Institutes of Health; VHL = von Hippel- Lindau. disease with surgically treated brainstem hemangioblastomas is limited. Subsequently, the treatment and outcome of patients with these tumors has not been defined. We describe and analyze the surgical results of patients with VHL disease and brainstem hemangioblastomas treated at the NIH. Methods Patient Population Patients with VHL disease who underwent surgical treatment of brainstem hemangioblastomas at the NIH between 1988 and 2009 with 12 or more months of follow-up were included in this study. All patients met the clinical criteria for diagnosis of VHL disease. 10,13 To provide long-term follow-up data, this analysis also in J Neurosurg / Volume 114 / May 2011
2 Brainstem hemangioblastomas cluded updated clinical data from patients with brainstem hemangioblastomas that have been previously reported. 29 Patient Evaluation Clinical Evaluation. Clinical information was obtained using hospital charts, clinic notes, and operative reports. Clinical assessments were performed preoperatively, immediately postoperatively, and at 6- to 12-month intervals after surgery. Neurological function was assessed, and a functional grade was assigned based on the classification scheme described by McCormick and colleagues 16 (Table 1), and KPS scores were determined for each patient based on clinical evaluations. 9 Imaging Evaluation. Magnetic resonance imaging was performed in each patient preoperatively and postoperatively at 6- to 12-month intervals associated with clinic visits. Tumor volumes were calculated for each imaging study using contrast-enhanced T1-weighted MR imaging by determining the product of the largest tumor diameters in the anteroposterior, mediolateral, and dorsoventral planes and then dividing by two. 15 Syringobulbia (if present) volumes were calculated on T2-weighted MR images using the same equation. Tumors were classified by MR imaging as completely intramedullary, primarily extramedullary ( 50% of the tumor mass was extramedullary), or combined intra- and extramedullary (< 50% of the tumor mass was extramedullary). Surgical Technique The technique used for brainstem hemangioblastoma resection has been previously described. 29 Because most brainstem hemangioblastomas are located in the obex, we use a posterior midline approach to remove most brainstem hemangioblastomas. Briefly, the patient is placed in cranial fixation and positioned prone with neck flexion. A midline suboccipital incision is made, and a midline suboccipital craniectomy is performed with or without the addition of a C-1 laminectomy depending on tumor size. The dura is opened in a Y-shaped fashion. Under the operative microscope, the cerebellar tonsils are separated and retracted laterally. If the tumor has a pial presentation, it is circumferentially dissected along the tumor margins using bipolar cauterization and microscissors, individually interrupting the feeding and draining vessels, and dissecting precisely at the interface of the surface of the tumor and the normal tissue until the tumor is removed en bloc. A midline myelotomy is performed with a diamond knife to provide access to portions of tumors without a surface presentation. J Neurosurg / Volume 114 / May 2011 TABLE 1: McCormick clinical grading scale for neurological funcion 16 Grade I II III IV Definition neurologically normal; mild focal deficit not significantly affecting function of involved limb; mild spasticity or reflex abnormality; normal gait presence of sensorimotor deficit affecting function of involved limb; mild to moderate gait difficulty; severe pain or dysesthetic syndrome impairing patient s quality of life; still functions & ambulates independently more severe neurological deficit; requires cane/brace for ambulation or significant bilateral upper-extremity impairment; may or may not function independently severe deficit; requires wheelchair or cane/brace w/ bilat upper-extremity impairment; usually not independent * Reprinted from McCormick et al: J Neurosurg 72: , Statistical Analysis Ordinal logistic regression models were used to assess the relationship between patient, operative, and tumor variables, and changes in McCormick grade and KPS score. The proportion of patients who remained at or below their preoperative McCormick scale grade was determined by Kaplan-Meier analysis of long-term outcomes. Time-to-event data were calculated as the time between the first operation at NIH for brainstem hemangioblastoma and later functional decline. Statistical analyses were performed using the software R (R version 2.8.2, The R Foundation for Statistical Computing). Statistical significance was determined using a 2-sided p value < Mean values are reported as mean ± SDs throughout. Results Patient Characteristics Forty-four patients who underwent surgical treatment of brainstem hemangioblastomas at NIH with 12 or more months of follow-up were identified. The 44 patients underwent 51 operations for resection of 71 brainstem hemangioblastomas. The mean patient age at time of surgery was 35.7 ± 10.8 years (range years). There were 19 operations in male patients (37.3%) and 32 in female patients (62.7%). The mean follow-up was 5.9 ± 5.0 years (range years). Ten operations (19.6%) had follow-up for months, 15 operations (29.4%) for months, and 24 operations (47.1%) for longer than 48 months. Patients underwent 1.2 ± 0.5 operations (range 1 3 operations) for brainstem hemangioblastomas. The most frequent presenting signs and symptoms were headache, swallowing difficulties, and singultus (Table 2). The median preoperative McCormick grade was I (range I IV). The median preoperative KPS score was 80 (range ). Tumor Characteristics The mean resected tumor volume was 0.9 ± 1.3 cm 3 (range cm 3 ). Twelve operations (23.5%) included multiple brainstem hemangioblastomas that were resected contemporaneously (range 2 4). The mean combined tumor volume in these patients was 1.2 ± 1.6 cm 3 (range cm 3 ). Two operations (3.9%) were for tumors with associated intratumoral cysts, whereas 31 operations (60.8%) were for tumors with associated syringobulbia (peritumoral cyst). The mean total syringobulbia volume in these cases was 2.3 ± 2.2 cm 3 (range cm 3 ). The combined mean tumor and syringobulbia volume 1313
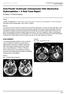
3 J. J. Wind et al. TABLE 2: Preoperative clinical characteristics Symptomatic Presentation No. of Cases (%) headache 30 (58.8) swallowing difficulties 17 (33.3) singultus 16 (31.4) gait difficulties 16 (31.4) ataxia 15 (29.4) visual disturbances 13 (25.5) limb paresthesias 13 (25.5) decreased sensation in upper extremities 13 (25.5) decreased sensation in lower extremities 12 (23.5) nausea or vomiting 12 (23.5) speech difficulties 10 (19.6) lower-extremity weakness 9 (17.6) vertigo 8 (15.7) upper-extremity weakness 7 (13.7) fatigue or changes in sleep/wake cycle 6 (11.8) coughing 8 (15.7) anorexia 2 (3.9) was 3.0 ± 2.4 cm 3 (range cm 3 ). Eleven tumors (33.3%) with associated syringobulbia also demonstrated peritumoral edema, but 22 tumors (66.7%) with associated syringobulbia did not have associated peritumoral edema. All tumors without associated syringobulbia demonstrated peritumoral edema. Thirty-eight (74.5%) of the 51 operations were for tumors in the obex (Fig. 1), 12 (23.5%) were for tumors at the cervicomedullary junction, and 1 (2.0%) was for a tumor in the anterolateral pontomedullary junction. Fig. 1. Axial (A) and sagittal (C) postcontrast T1-weighted and axial (B) and sagittal (D) T2-weighted MR images obtained in a patient with VHL disease and a brainstem hemangioblastoma in the region of the obex. Immediate Postoperative Outcome. The median immediate postoperative McCormick grade remained at I (range I IV). Thirty-four operations (66.7%) produced no change in immediate postoperative McCormick grades (compared with preoperative grade). After the operations, patients in 8 cases (15.7%) had improvement in their immediate postoperative McCormick grades. Patients in 9 cases (17.6%) had worsening of their immediate postoperative McCormick grades. Seven (77.8%) of these were Surgical Characteristics The mean number of tumors resected at each operation was 1.4 ± 0.9 (range 1 4). A myelotomy was required to gain access to the tumor in 21 operations (41.2%). While a tumor-associated cyst was entered during the course of tumor resection in 18 (54.5%) of the 33 tumors with associated syringobulbia, it was not entered in the remaining 15 tumors (45.5%) associated with syringobulbia. Radiographic Outcomes All tumors (100%) demonstrated gross-total resection on postoperative contrast-enhanced MR imaging. There was no evidence of tumor recurrence in any case at the last follow-up. Edema surrounding tumors (56.9% of tumors) resolved in all cases (100%). All (100%) of the 33 tumors with associated syringobulbia demonstrated collapse of syringobulbia at the last radiographic examination (Fig. 2). The radiographic collapse of syringobulbia occurred regardless of whether the cyst or syrinx was entered during tumor resection. Clinical Outcomes Fig. 2. Preoperative sagittal postcontrast T1-weighted (A) and T2- weighted (C) and postoperative sagittal postcontrast T1-weighted (B) and T2-weighted (D) MR images demonstrating the resolution of tumorrelated syringobulbia following resection of a brainstem hemangioblastoma J Neurosurg / Volume 114 / May 2011
4 Brainstem hemangioblastomas a deterioration of 1 grade, and 2 (22.2%) were a deterioration of 2 grades. The median immediate postoperative KPS score remained at 80 (range ). After 6 operations (11.8%), the patients required placement of a tracheostomy or gastrostomy for exacerbation of lower cranial nerve dysfunction. Patients in 5 (83.3%) of these cases immediately worsened as a result of surgery (by 1 McCormick grade in 3 patients and by 2 McCormick grades in 2 patients) and 1 patient (16.7%) had significant preoperative functional deficits that remained at the same grade postoperatively (McCormick Grade II). All but 1 deterioration in McCormick grade was transient and resolved by 6 months (mean time to recovery 3.2 ± 1.5 months, range months). Short-Term Outcome (6 Months). The median 6-month postoperative McCormick grade was I (range I IV). The median 6-month postoperative KPS score was 90 (range ). Patients in 39 cases (76.5%) had stable 6-month postoperative functional status compared with preoperative status, as measured by McCormick grade. Patients in 11 cases (21.6%) had improved, and 1 (2.0%) had worsened compared with preoperative status. Eight (88.9%) of the 9 cases in which the patient experienced immediate postoperative worsening of their functional status returned to their preoperative grade within 6 months (mean time to recovery of the 9 patients was 3.2 ± 1.5 months; range months). Four (66.7%) of the 6 patients who had placement of tracheostomy or gastrostomy after surgery had them removed during short-term follow-up; 2 (50%) of these 4 patients underwent removal by 3 months (mean time to removal 2.0 months, range months). Two patients (3.9%) required tracheostomy and gastrostomy (1 patient) or gastrostomy (1 patient) through long-term follow-up. Long-Term Outcome (Longer Than 12 Months). The median McCormick grade at final follow-up was I (range I IV). The median KPS score at final follow-up was 90 (range ). Patients in 38 cases (74.5%) had stable long-term postoperative functional status compared with preoperative status. Patients in 10 cases (19.6%) had improved, and those in 3 cases (5.9%) had worsened compared with the preoperative status. Kaplan-Meier analysis was performed to demonstrate the number of patients who remained at or below their preoperative McCormick grade throughout long-term follow-up, including the last known McCormick grades before death (Fig. 3). After stable immediate postoperative McCormick grades, 2 patients experienced 1 grade worsening of their McCormick grade over the course of long-term follow-up due to progression of extensive CNS disease. Six patients died during long-term follow-up (mean age at death 45.5 ± 5.5 years, range years) of CNS progression of VHL disease or complications related to renal cell carcinoma. Analysis of Preoperative Variables and Outcomes. Univariate ordinal logistic regression analysis was performed to determine if preoperative patient characteristics were associated with functional decline in McCormick grade or KPS score immediately after surgery, at 6 months after resection, or at long-term follow-up. Variables analyzed J Neurosurg / Volume 114 / May 2011 Fig. 3. Kaplan-Meier analysis of last recorded McCormick grades demonstrating that most patients with VHL disease and brainstem hemangioblastomas remain stable over the long term. The proportion of patients who remained functionally stable according to their McCormick grade at 2, 5, 10, and 15 years follow-up was 98%, 94%, 94%, and 94%. The dashed lines indicate 95% CIs. Tick marks represent censored data at the point of last follow-up. included patient sex, age, number of tumors, need for myelotomy, intramedullary tumor location with or without a surface presentation, tumor size, presence of syringobulbia, and combined volume of tumor and syringobulbia (Table 3). Only the presence of syringobulbia had a trend toward being associated with better immediate postoperative McCormick grades (p = 0.07). Postoperative Complications Postoperative complications included pneumonia (in 5 patients), gastrointestinal ulceration (in 3 patients), development of new hydrocephalus requiring placement of a ventriculoperitoneal shunt (in 1 patient), deep vein thrombosis (in 1 patient), and CSF leak (in 1 patient). Pneumonias occurred in patients with exacerbated lower cranial nerve dysfunction and aspiration. These patients were treated with intravenous antibiotic administration and tube feeding until resolution of lower cranial nerve dysfunction. Gastrointestinal ulceration was treated with proton pump inhibitor therapy in 2 cases but required surgical repair in the third case. Deep vein thrombosis was treated with anticoagulation for 6 weeks. The CSF leak was successfully treated with lumbar drainage for 4 days. Histological Results All resected tumors were histopathologically diagnostic for hemangioblastomas. The tumors were composed of polygonal, lipid-laden cells with a rich vascular network and they exhibited positive reaction to neuronspecific enolase on immunohistochemical analysis. No tumor had evidence of metastatic deposit. 1315
5 J. J. Wind et al. TABLE 3: Analysis of factors influencing immediate postoperative, 6-month, and final follow-up McCormick grade* Factor Von Hippel-Lindau Disease Immediate Postop Discussion p Value 6-Mo Follow-Up Final Follow-Up sex age no. of tumors need for myelotomy intramedullary tumor location w/o surface presentation largest tumor vol presence of syringobulbia cyst/syrinx entered at time of op tumor & syringobulbia vol * The analysis was performed using ordinal regression. Von Hippel-Lindau disease is a multisystem tumor syndrome that occurs in roughly 1 in every 39,000 live births. 13 It is inherited in an autosomal dominant pattern, with a penetrance of greater than 90% by 60 years of age. 1 Von Hippel-Lindau disease has been linked to mutations in the VHL gene, a tumor suppressor gene located on the short arm of chromosome 3. 11,13 Patients with VHL disease are prone to develop tumors in visceral organs and the nervous system. Visceral tumors and cysts can occur in the kidneys, adrenal glands, pancreas, epididymis, and broad ligament. Tumors also develop within the CNS. Sixty percent to 80% of patients with VHL disease develop CNS tumors, including hemangioblastomas of the cerebellum, brainstem, spine, and retina, as well as endolymphatic sac tumors. 13 The most frequent locations of CNS hemangioblastomas in patients with VHL disease are the cerebellum and spinal cord, followed by the brainstem. 18,26 Previous Studies The literature regarding long-term management of brainstem hemangioblastomas in VHL disease is limited. Most studies examining brainstem hemangioblastoma treatment often analyze a combination of VHL disease and sporadic tumors. 21,23,27,29,30 The management of hemangioblastomas in patients with VHL disease presents complexity not present in patients with sporadic hemangioblastomas, as those with VHL disease often harbor multiple hemangioblastomas in multiple locations throughout the craniospinal axis, and patients with VHL disease experience growth of existing hemangioblastomas as well as development of new hemangioblastomas over their lifetimes. Furthermore, visceral VHL disease associated lesions add complexity to the treatment of these patients. Clinical Implications Surgery for VHL Disease Associated Hemangioblastomas. Similar to other neurosurgical disorders, the indications for resection of brainstem hemangioblastomas in VHL disease are based on their natural history. Several important aspects of the behavior of VHL disease associated hemangioblastomas must be taken into consideration when deciding to resect these tumors. Patients with VHL disease will frequently develop multiple new tumors during their lifetime. Previously, in long-term analysis, it was found that 45% of symptomatic hemangioblastomas requiring resection were not apparent on initial radiographic studies. 1 Alternatively, not all VHL disease associated CNS hemangioblastomas evident on MR imaging will become symptomatic and require resection. Furthermore, CNS hemangioblastomas have a saltatory growth pattern, with periods of growth and quiescence (often lasting years). Subsequently, radiographic progression does not necessarily correlate with symptom development, and defined radiographic features to predict symptom formation are yet to be established. Surgical intervention is reserved for patients with early symptoms to maintain long-term function but prevent additional unnecessary operations. Therefore, we have avoided operating on patients with asymptomatic VHL disease who harbor brainstem hemangioblastomas. Clinical Presentation. Presenting signs and symptoms are listed in Table 2. Many symptoms (swallowing difficulties, singultus, nausea, vomiting, coughing, and speech difficulties) were attributable to local pathology affecting lower cranial nerve nuclei or tracts. Tumors at the obex may manifest with clinical symptoms due to their proximity to the area postrema, hypoglossal nucleus, dorsal motor nucleus, nucleus ambiguus of the vagus nerve, and nucleus tractus solitarius. The nuclei gracilis and cuneatus are located just lateral to the obex and may also account for symptomatic presentation that includes paresthesias, hypesthesias, or proprioceptive difficulties. Disruption of brainstem satiety pathways by tumors such as hemangioblastomas could lead to interference with normal physiological satiety. 24 Larger tumors can obstruct CSF outflow from the fourth ventricle, resulting in obstructive hydrocephalus and more generalized symptoms of headache, nausea and vomiting. Patient Outcome. Overall, most patients remained at their preoperative baseline after surgery. We analyzed McCormick grade and KPS scores preoperatively, immediately postoperatively, at the 6-month follow-up, and at the last follow-up. Patients in 9 cases (17.6%) experienced worsening of their immediate postoperative McCormick grade. All but 1 McCormick grade deterioration was transient, resolving by 6 months (mean time to recovery 3.2 ± 1.5 months, range months). Due to CNS progression of VHL disease, patients in 2 cases (3.9%) experienced late clinical worsening over the course of long-term follow-up after stable immediate postoperative neurological function. Thus, most patients maintain their preoperative functional status, and surgery offers a lasting treatment that prevents progressive functional decline 1316 J Neurosurg / Volume 114 / May 2011
6 Brainstem hemangioblastomas attributable to the treated brainstem hemangioblastoma. Patients with VHL disease will experience new CNS and non-cns lesions that may ultimately contribute to functional decline. 1,26 Tumor Control. Previous studies have described rates of subtotal resection of brainstem hemangioblastomas as high as 15%. 21,27,30 Incomplete resection of hemangioblastomas frequently leads to the need for resection of recurrent tumors at a later time. In this series, imaging confirmed complete resection in all tumors, and there was no evidence of tumor recurrence over long-term followup. These findings underscore the importance of careful circumferential dissection at the margin of the tumor, allowing complete resection in all brainstem hemangioblastomas in this series. Complete resection can translate to lasting patient benefit and cure. Effect on Syringobulbia. Syringobulbia was present in most cases (66.7%) preoperatively. All patients demonstrated resolution of their syringobulbia postoperatively as a consequence of tumor resection, whether or not the syrinx or cyst was entered at the time of resection. Previous analysis demonstrated that tumor vascular permeability leads to increased interstitial pressure and peritumoral edema. 6,14 Once the volume of fluid extravasated through the highly permeable tumor vasculature exceeds the capacity of the surrounding tissue to reabsorb edema, a cyst may develop. Because the tumor is the sole source of syringobulbia, no attempt was made to surgically address the peritumoral cyst in terms of resection, fenestration, or cyst fluid shunting, as resolution of syringobulbia occurs following tumor resection. Complications. Mortality associated with the resection of brainstem hemangioblastomas varies widely within the literature, with contemporary series documenting rates as high as 24%. 5,21,27,29,30 Published data on surgical morbidity includes rates of gastrointestinal hemorrhage in patients with solid brainstem hemangioblastomas as high as 30% and cranial neuropathies as high as 21.2%. 30 As in those studies, complications in this series were related to the unique anatomy of the region where these tumors were located. For example, dysfunction of the descending hypothalamic autonomic fibers to the dorsal motor nucleus of the vagus nerve may alter parasympathetic innervation to the gastrointestinal tract and account for gastroduodenal ulceration (5.9%) immediately after surgery in our patients. 3,12 Use of perioperative gastrointestinal prophylaxis with H2-blockers or proton pump inhibitors may reduce the incidence of this complication. Factors Affecting Outcome. While previous reports have suggested that larger brainstem tumors are associated with increasing surgical morbidity and mortality, 27,30 detailed analysis in our series of patients did not confirm this hypothesis. To determine preoperative patient factors that may predict outcomes in patients undergoing surgery for brainstem hemangioblastomas, we performed regression analysis of these factors with respect to immediate postoperative, 6-month, and last McCormick grade. There was a trend toward the presence of syringobulbia being associated with improved immediate postoperative J Neurosurg / Volume 114 / May 2011 McCormick grade. This may be explained by the fact that syringobulbia may facilitate resection of the hemangioblastoma by minimizing the need for surgical tissue manipulation. Alternatively, this association may be due to the fact that syringobulbia is associated with preoperative symptoms that improve with surgical treatment and subsequent syringobulbia resolution. This trend disappeared by the 6-month follow-up examinations and is likely due to the fact that the majority of patients were at their baseline preoperative McCormick grade by 6-month followup. Radiation Therapy Stereotactic radiosurgery has been proposed as an alternative treatment strategy for CNS hemangioblastomas. These reports have presented excellent control rates within short-term follow-up, with some reports of control rates exceeding 90% at 2 and 5 years. 7,8,17,22,25,28 Recent long-term prospective evaluation of radiosurgery for the treatment of cerebellar and brainstem hemangioblastomas in VHL disease revealed favorable control rates at 2 and 5 years but declining efficacy in tumor control over time, reaching 61% and 51% at 10 and 15 years, respectively. 2 Furthermore, exacerbation of neurological deficits as a result of increased peritumoral edema after radiosurgery may limit the use of this modality in symptomatic patients. Investigation of the natural history of hemangioblastomas in VHL disease has demonstrated a saltatory growth pattern of these tumors, and periods of tumor quiescence coinciding with treatment may inaccurately suggest tumor control after radiosurgical treatment. 1 Subsequently, whether stereotactic radiosurgery results in significant control of these tumors over the long term compared with the natural history of the tumor remains to be determined. Conclusions Patient outcomes over long-term follow-up demonstrate that most patients with VHL disease and brainstem hemangioblastomas experience stable or improved neurological function after resection. Despite the successful treatment of brainstem hemangioblastomas in patients with VHL disease, some patients develop late deterioration of their functional status due to progression of their disease elsewhere in the craniospinal axis or systemically. Disclosure This research was supported by the Intramural Research Program of the National Institute of Neurological Disorders and Stroke at the National Institutes of Health. Author contributions to the study and manuscript preparation include the following. Conception and design: Lonser, Wind, Bakhtian, Oldfield. Acquisition of data: Lonser, Wind, Bakhtian, Sweet, Thawani, Asthagiri, Oldfield. Analysis and interpretation of data: all authors. Drafting the article: Lonser, Wind, Oldfield. Critically revising the article: Lonser, Wind, Bakhtian, Sweet, Mehta, Asthagiri, Oldfield. Reviewed final version of the manuscript and approved it for submission: all authors. Statistical analysis: Lonser, Bakhtian, Mehta. Administrative/technical/material support: Lonser. Study supervision: Lonser, Oldfield. 1317
7 J. J. Wind et al. References 1. Ammerman JM, Lonser RR, Dambrosia J, Butman JA, Oldfield EH: Long-term natural history of hemangioblastomas in patients with von Hippel-Lindau disease: implications for treatment. J Neurosurg 105: , Asthagiri AR, Mehta GU, Zach L, Li X, Butman JA, Camphausen KA, et al: Prospective evaluation of radiosurgery for hemangioblastomas in von Hippel-Lindau disease. Neuro Oncol 12:80 86, Baumgartner JE, Wilson CB: Removal of posterior fossa and spinal hemangioblastomas, in Wilson CB (ed): Neurosurgical Procedures: Personal Approaches to Classic Operations. Baltimore: Williams & Wilkins, 1992, pp Filling-Katz MR, Choyke PL, Oldfield E, Charnas L, Patronas NJ, Glenn GM, et al: Central nervous system involvement in Von Hippel-Lindau disease. Neurology 41:41 46, Fukushima T, Sakamoto S, Iwaasa M, Hayashi S, Yamamoto M, Utsunomiya H, et al: Intramedullary hemangioblastoma of the medulla oblongata two case reports and review of the literature. Neurol Med Chir (Tokyo) 38: , Gläsker S, Vortmeyer AO, Lonser RR, Lubensky IA, Okamoto H, Xia JB, et al: Proteomic analysis of hemangioblastoma cyst fluid. Cancer Biol Ther 5: , Jawahar A, Kondziolka D, Garces YI, Flickinger JC, Pollock BE, Lunsford LD: Stereotactic radiosurgery for hemangioblastomas of the brain. Acta Neurochir (Wien) 142: , Kano H, Niranjan A, Mongia S, Kondziolka D, Flickinger JC, Lunsford LD: The role of stereotactic radiosurgery for intracranial hemangioblastomas. Neurosurgery 63: , Karnofsky DA, Burchenal JH: The clinical evaluation of chemotherapeutic agents in cancer, in MacLeod CM (ed): Evaluation of Chemotherapeutic Agents. New York: Columbia University Press, 1949, pp Lamiell JM, Salazar FG, Hsia YE: von Hippel-Lindau disease affecting 43 members of a single kindred. Medicine (Baltimore) 68:1 29, Latif F, Tory K, Gnarra J, Yao M, Duh FM, Orcutt ML, et al: Identification of the von Hippel-Lindau disease tumor suppressor gene. Science 260: , Lewis EA: Gastroduodenal ulceration and haemorrhage of neurogenic origin. Br J Surg 60: , Lonser RR, Glenn GM, Walther M, Chew EY, Libutti SK, Linehan WM, et al: von Hippel-Lindau disease. Lancet 361: , Lonser RR, Vortmeyer AO, Butman JA, Glasker S, Finn MA, Ammerman JM, et al: Edema is a precursor to central nervous system peritumoral cyst formation. Ann Neurol 58: , Lundin P, Pedersen F: Volume of pituitary macroadenomas: assessment by MRI. J Comput Assist Tomogr 16: , McCormick PC, Torres R, Post KD, Stein BM: Intramedullary ependymoma of the spinal cord. J Neurosurg 72: , Moss JM, Choi CY, Adler JR Jr, Soltys SG, Gibbs IC, Chang SD: Stereotactic radiosurgical treatment of cranial and spinal hemangioblastomas. Neurosurgery 65:79 85, Neumann HP, Eggert HR, Scheremet R, Schumacher M, Mohadjer M, Wakhloo AK, et al: Central nervous system lesions in von Hippel-Lindau syndrome. J Neurol Neurosurg Psychiatry 55: , Neumann HP, Eggert HR, Weigel K, Friedburg H, Wiestler OD, Schollmeyer P: Hemangioblastomas of the central nervous system. A 10-year study with special reference to von Hippel-Lindau syndrome. J Neurosurg 70:24 30, Park DM, Zhuang Z, Chen L, Szerlip N, Maric I, Li J, et al: von Hippel-Lindau disease-associated hemangioblastomas are derived from embryologic multipotent cells. PLoS Med 4:e60, Parker F, Aghakhani N, Ducati LG, Yacubian-Fernandes A, Silva MV, David P, et al: Results of microsurgical treatment of medulla oblongata and spinal cord hemangioblastomas: a comparison of two distinct clinical patient groups. J Neurooncol 93: , Patrice SJ, Sneed PK, Flickinger JC, Shrieve DC, Pollock BE, Alexander E III, et al: Radiosurgery for hemangioblastoma: results of a multiinstitutional experience. Int J Radiat Oncol Biol Phys 35: , Rachinger J, Buslei R, Prell J, Strauss C: Solid haemangioblastomas of the CNS: a review of 17 consecutive cases. Neurosurg Rev 32:37 48, Song DK, Lonser RR: Pathological satiety caused by brainstem hemangioblastoma. Case report. J Neurosurg Pediatr 2: , Tago M, Terahara A, Shin M, Maruyama K, Kurita H, Nakagawa K, et al: Gamma knife surgery for hemangioblastomas. J Neurosurg 102 Suppl: , Wanebo JE, Lonser RR, Glenn GM, Oldfield EH: The natural history of hemangioblastomas of the central nervous system in patients with von Hippel-Lindau disease. J Neurosurg 98: 82 94, Wang C, Zhang J, Liu A, Sun B: Surgical management of medullary hemangioblastoma. Report of 47 cases. Surg Neurol 56: , Wang EM, Pan L, Wang BJ, Zhang N, Zhou LF, Dong YF, et al: The long-term results of gamma knife radiosurgery for hemangioblastomas of the brain. J Neurosurg 102 Suppl: , Weil RJ, Lonser RR, DeVroom HL, Wanebo JE, Oldfield EH: Surgical management of brainstem hemangioblastomas in patients with von Hippel-Lindau disease. J Neurosurg 98:95 105, Zhou LF, Du G, Mao Y, Zhang R: Diagnosis and surgical treatment of brainstem hemangioblastomas. Surg Neurol 63: , 2005 Manuscript submitted June 4, Accepted September 13, Please include this information when citing this paper: published online October 8, 2010; DOI: / JNS Address correspondence to: Russell R. Lonser, M.D., Surgical Neurology Branch, National Institute of Neurological Disorders and Stroke, National Institutes of Health, Building 10, Room 3D20, Bethesda, Maryland lonserr@ninds.nih.gov J Neurosurg / Volume 114 / May 2011
Disclosures. Neurological Manifestations of Von Hippel Lindau Syndrome. Objectives. Overview. None No conflicts of interest
 Neurological Manifestations of Von Hippel Lindau Syndrome ARNOLD B. ETAME MD, PhD NEURO-ONCOLOGY/NEUROSURGERY Moffitt Cancer Center Disclosures None No conflicts of interest VHL Alliance Annual Family
Neurological Manifestations of Von Hippel Lindau Syndrome ARNOLD B. ETAME MD, PhD NEURO-ONCOLOGY/NEUROSURGERY Moffitt Cancer Center Disclosures None No conflicts of interest VHL Alliance Annual Family
Integra Foundation Award: Long-term Natural History of Hemangioblastomas in von Hippel-Lindau Disease: Implications for Treatment
 CHAPTER 38 Integra Foundation Award: Long-term Natural History of Hemangioblastomas in von Hippel-Lindau Disease: Implications for Treatment Joshua M. Ammerman, M.D., Russell R. Lonser, M.D., James Dambrosia,
CHAPTER 38 Integra Foundation Award: Long-term Natural History of Hemangioblastomas in von Hippel-Lindau Disease: Implications for Treatment Joshua M. Ammerman, M.D., Russell R. Lonser, M.D., James Dambrosia,
Spinal Cord Hemangioblastomas in von Hippel-Lindau Disease: Management of Asymptomatic and Symptomatic Tumors
 Original Article http://dx.doi.org/10.3349/ymj.2012.53.6.1073 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 53(6):1073-1080, 2012 Spinal Cord Hemangioblastomas in von Hippel-Lindau Disease: Management
Original Article http://dx.doi.org/10.3349/ymj.2012.53.6.1073 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 53(6):1073-1080, 2012 Spinal Cord Hemangioblastomas in von Hippel-Lindau Disease: Management
FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR HAEMANGIOBLASTOMA
 1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR HAEMANGIOBLASTOMA QUESTIONS TO BE ADDRESSED: 1. What is the evidence for the clinical effectiveness
1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR HAEMANGIOBLASTOMA QUESTIONS TO BE ADDRESSED: 1. What is the evidence for the clinical effectiveness
Haemangioblastomas of the central nervous system in von Hippel Lindau Syndrome involving cerebellum and spinal cord
 Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article Haemangioblastomas of the central nervous system in von Hippel Lindau Syndrome involving cerebellum and spinal cord V.A. Kiran Kumar,
Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article Haemangioblastomas of the central nervous system in von Hippel Lindau Syndrome involving cerebellum and spinal cord V.A. Kiran Kumar,
G. Aksu, C. Ulutin, M. Fayda, M. Saynak Gulhane Military Faculty of Medicine, Department of Radiation Oncology, Ankara, Turkey CLINICAL CASE.
 Journal of BUON 10: 405-409, 2005 2005 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Cerebellar and multiple spinal hemangioblastomas and intraventricular meningioma managed with subtotal
Journal of BUON 10: 405-409, 2005 2005 Zerbinis Medical Publications. Printed in Greece CLINICAL CASE Cerebellar and multiple spinal hemangioblastomas and intraventricular meningioma managed with subtotal
Clinical Factors Predicting Outcomes After Surgical Resection for Sporadic Cerebellar Hemangioblastomas
 Clinical Factors Predicting Outcomes After Surgical Resection for Sporadic Cerebellar Hemangioblastomas Masafumi Fukuda, Tetsuro Takao, Tetsuya Hiraishi, Junichi Yoshimura, Naoki Yajima, Akihiko Saito,
Clinical Factors Predicting Outcomes After Surgical Resection for Sporadic Cerebellar Hemangioblastomas Masafumi Fukuda, Tetsuro Takao, Tetsuya Hiraishi, Junichi Yoshimura, Naoki Yajima, Akihiko Saito,
The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease
 AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
AJNR Am J Neuroradiol 24:1570 1574, September 2003 The Natural History of Cerebellar Hemangioblastomas in von Hippel-Lindau Disease Andrew Slater, Niall R. Moore, and Susan M. Huson BACKGROUND AND PURPOSE:
Disseminated Hemangioblastoma of the Central Nervous System without Von Hippel-Lindau Disease
 CASE REPORT Brain Tumor Res Treat 2014;2(2):96-101 / pissn 2288-2405 / eissn 2288-2413 http://dx.doi.org/10.14791/btrt.2014.2.2.96 Disseminated Hemangioblastoma of the Central Nervous System without Von
CASE REPORT Brain Tumor Res Treat 2014;2(2):96-101 / pissn 2288-2405 / eissn 2288-2413 http://dx.doi.org/10.14791/btrt.2014.2.2.96 Disseminated Hemangioblastoma of the Central Nervous System without Von
DIRECT SURGERY FOR INTRA-AXIAL
 Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
Kitakanto Med. J. (S1) : 23 `28, 1998 23 DIRECT SURGERY FOR INTRA-AXIAL BRAINSTEM LESIONS Kazuhiko Kyoshima, Susumu Oikawa, Shigeaki Kobayashi Department of Neurosurgery, Shinshu University School of Medicine,
We have previously reported good clinical results
 J Neurosurg 113:48 52, 2010 Gamma Knife surgery as sole treatment for multiple brain metastases: 2-center retrospective review of 1508 cases meeting the inclusion criteria of the JLGK0901 multi-institutional
J Neurosurg 113:48 52, 2010 Gamma Knife surgery as sole treatment for multiple brain metastases: 2-center retrospective review of 1508 cases meeting the inclusion criteria of the JLGK0901 multi-institutional
10/11/2018. Disclosures TOC. von Hippel-Lindau disease. CNS correlations
 Disclosures CLINICAL DEBATE: Optimal Treatment of Hemangioblastomas Ashok R. Asthagiri, MD Ian McCutcheon, MD TOC Background ELST Asymptomatic growth Peritumoral edema Pregnancy Radiosurgery Difficult
Disclosures CLINICAL DEBATE: Optimal Treatment of Hemangioblastomas Ashok R. Asthagiri, MD Ian McCutcheon, MD TOC Background ELST Asymptomatic growth Peritumoral edema Pregnancy Radiosurgery Difficult
Stereotactic radiosurgery for intracranial hemangioblastomas: a retrospective international outcome study
 clinical article J Neurosurg 122:1469 1478, 2015 Stereotactic radiosurgery for intracranial hemangioblastomas: a retrospective international outcome study Hideyuki Kano, MD, PhD, 1 Takashi Shuto, MD, 2
clinical article J Neurosurg 122:1469 1478, 2015 Stereotactic radiosurgery for intracranial hemangioblastomas: a retrospective international outcome study Hideyuki Kano, MD, PhD, 1 Takashi Shuto, MD, 2
Surgical management of brainstem hemangioblastomas in patients with von Hippel Lindau disease
 J Neurosurg 98:95 105, 2003 Surgical management of brainstem hemangioblastomas in patients with von Hippel Lindau disease ROBERT J. WEIL, M.D., RUSSELL R. LONSER, M.D., HETTY L. DEVROOM, R.N., JOHN E.
J Neurosurg 98:95 105, 2003 Surgical management of brainstem hemangioblastomas in patients with von Hippel Lindau disease ROBERT J. WEIL, M.D., RUSSELL R. LONSER, M.D., HETTY L. DEVROOM, R.N., JOHN E.
Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report
 Neurosurg Focus 5 (3):Article 9, 1998 Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report Dean Chou, M.D., Prakash Sampath, M.D., and Henry Brem, M.D. Departments of Neurological
Neurosurg Focus 5 (3):Article 9, 1998 Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report Dean Chou, M.D., Prakash Sampath, M.D., and Henry Brem, M.D. Departments of Neurological
Von Hippel Lindau Disease, Involvement of Multiple Members of the Same Families
 ORIGINAL ARTICLE Von Hippel Lindau Disease, Involvement of Multiple Members of the Same Families AMIR AZIZ, YASER-UD-DIN HOTI, KHURRAM ISHAQ Tariq Salah-ud-Din Department of Neurosurgery Unit II, Lahore
ORIGINAL ARTICLE Von Hippel Lindau Disease, Involvement of Multiple Members of the Same Families AMIR AZIZ, YASER-UD-DIN HOTI, KHURRAM ISHAQ Tariq Salah-ud-Din Department of Neurosurgery Unit II, Lahore
What Every Spine Surgeon Should Know About Neurosurgical Issues
 What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
What Every Spine Surgeon Should Know About Neurosurgical Issues Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA Objectives Main intraspinal lesions Chiari malformation
Multifocal central nervous system hemangioblastoma: a case report and review of the literature
 Multifocal central nervous system hemangioblastoma: a case report and review of the literature L.Z. Chu 1,3, Z.Z. Guan 1,2, J. Liu 3, H. Yang 3, X.L. Qi 2, M.G. Dong 3, Y.M. Chen 3, Y.N. Xiang 1 and Y.
Multifocal central nervous system hemangioblastoma: a case report and review of the literature L.Z. Chu 1,3, Z.Z. Guan 1,2, J. Liu 3, H. Yang 3, X.L. Qi 2, M.G. Dong 3, Y.M. Chen 3, Y.N. Xiang 1 and Y.
Lecturer. Prof. Dr. Ali K. Al-Shalchy MBChB/ FIBMS/ MRCS/ FRCS 2014
 Lecturer Prof. Dr. Ali K. Al-Shalchy MBChB/ FIBMS/ MRCS/ FRCS 2014 Dorsal root: The dorsal root carries both myelinated and unmyelinated afferent fibers to the spinal cord. Posterior gray column: Long
Lecturer Prof. Dr. Ali K. Al-Shalchy MBChB/ FIBMS/ MRCS/ FRCS 2014 Dorsal root: The dorsal root carries both myelinated and unmyelinated afferent fibers to the spinal cord. Posterior gray column: Long
TUMOURS IN THE REGION OF FORAMEN MAGNUM
 TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
TUMOURS IN THE REGION OF FORAMEN MAGNUM Abstract Pages with reference to book, From 119 To 122 Naim-ur-Rahman ( Department of Neurosurgery, Rawalpindi Medical College, Rawalpindi. ) A very unusual case
ASJ. Microsurgical Treatment of Sporadic and von Hippel-Lindau Disease Associated Spinal Hemangioblastomas: A Single-Institution Experience
 Asian Spine Journal 548 Joe M. Das Clinical et al. Study Asian Spine J 217;11(4):548-555 https://doi.org/1.4184/asj.217.11.4.548 Asian Spine J 217;11(4):548-555 Microsurgical Treatment of Sporadic and
Asian Spine Journal 548 Joe M. Das Clinical et al. Study Asian Spine J 217;11(4):548-555 https://doi.org/1.4184/asj.217.11.4.548 Asian Spine J 217;11(4):548-555 Microsurgical Treatment of Sporadic and
Tumors of the Endolymphatic Sac in von Hippel Lindau Disease
 The new england journal of medicine brief report Tumors of the Endolymphatic Sac in von Hippel Lindau Disease Russell R. Lonser, M.D., H. Jeffrey Kim, M.D., John A. Butman, M.D., Ph.D., Alexander O. Vortmeyer,
The new england journal of medicine brief report Tumors of the Endolymphatic Sac in von Hippel Lindau Disease Russell R. Lonser, M.D., H. Jeffrey Kim, M.D., John A. Butman, M.D., Ph.D., Alexander O. Vortmeyer,
Update on Pediatric Brain Tumors
 Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Von Hippel-Lindau (VHL) Syndrome: A Critical Insight
 114 Review Article Von Hippel-Lindau (VHL) Syndrome: A Critical Insight Tapan Behl*, Ishneet Kaur, Puneet Sudan, Monika Sharma, Heena Goel Department of Pharmacology, Doaba Group of Colleges, Kharar, Mohali,
114 Review Article Von Hippel-Lindau (VHL) Syndrome: A Critical Insight Tapan Behl*, Ishneet Kaur, Puneet Sudan, Monika Sharma, Heena Goel Department of Pharmacology, Doaba Group of Colleges, Kharar, Mohali,
Adult intramedullary astrocytomas of the spinal cord
 J Neurosurg 77:355-359, 1992 Adult intramedullary astrocytomas of the spinal cord FRED J. EPSTEIN, M.D., JEAN-PIERRE FARMER, M.D., F.R.C.S., AND DIANA FREED Division of Pediatric Neurosurgery, Department
J Neurosurg 77:355-359, 1992 Adult intramedullary astrocytomas of the spinal cord FRED J. EPSTEIN, M.D., JEAN-PIERRE FARMER, M.D., F.R.C.S., AND DIANA FREED Division of Pediatric Neurosurgery, Department
Stereotactic radiosurgery for hemangiomas and ependymomas of the spinal cord
 Neurosurg Focus 15 (5):Article 10, 2003, Click here to return to Table of Contents Stereotactic radiosurgery for hemangiomas and ependymomas of the spinal cord STEPHEN I. RYU, M.D., DANIEL H. KIM, M.D.,
Neurosurg Focus 15 (5):Article 10, 2003, Click here to return to Table of Contents Stereotactic radiosurgery for hemangiomas and ependymomas of the spinal cord STEPHEN I. RYU, M.D., DANIEL H. KIM, M.D.,
WHOLE SPECTRUM OF NATURAL PROGRESSION OF HAEMANGIOBLASTOMA SEEN WITHIN A SINGLE PATIENT: A VERY RARE CASE REPORT AND LITERATURE REVIEW
 WHOLE SPECTRUM OF NATURAL PROGRESSION OF HAEMANGIOBLASTOMA SEEN WITHIN A SINGLE PATIENT: A VERY RARE CASE REPORT AND LITERATURE REVIEW *Sunil Munakomi, Binod Bhattarai Department of Neurosurgery, College
WHOLE SPECTRUM OF NATURAL PROGRESSION OF HAEMANGIOBLASTOMA SEEN WITHIN A SINGLE PATIENT: A VERY RARE CASE REPORT AND LITERATURE REVIEW *Sunil Munakomi, Binod Bhattarai Department of Neurosurgery, College
BRAIN & SPINAL LESIONS: NOT JUST A SCIENCE. Rimas V. Lukas, MD Associate Professor Director of Medical Neuro-Oncology University of Chicago
 BRAIN & SPINAL LESIONS: NOT JUST A SCIENCE Rimas V. Lukas, MD Associate Professor Director of Medical Neuro-Oncology University of Chicago OVERVIEW Background Clinical Presentation Clinical Management
BRAIN & SPINAL LESIONS: NOT JUST A SCIENCE Rimas V. Lukas, MD Associate Professor Director of Medical Neuro-Oncology University of Chicago OVERVIEW Background Clinical Presentation Clinical Management
The NIHSS score is 4 (considering 2 pts for the ataxia involving upper and lower limbs.
 Neuroscience case 5 1. Speech comprehension, ability to speak, and word use were normal in Mr. Washburn, indicating that aphasia (cortical language problem) was not involved. However, he did have a problem
Neuroscience case 5 1. Speech comprehension, ability to speak, and word use were normal in Mr. Washburn, indicating that aphasia (cortical language problem) was not involved. However, he did have a problem
Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report
 ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report A Babbu, R Katheerayson Citation A Babbu, R Katheerayson..
ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report A Babbu, R Katheerayson Citation A Babbu, R Katheerayson..
Chiari Malformations. Google. Objectives Seventh Annual NKY TBI Conference 3/22/13. Kerry R. Crone, M.D.
 Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
The Genetics of VHL. Proper tissue growth - controlled traffic. How human cells and tissue grow and die?
 How human cells and tissue grow and die? The Genetics of VHL Xia Wang MD PhD Oct, 2017 Proper tissue growth - controlled traffic Normal tissue growth is regulated by many genetic factors Safe traffic is
How human cells and tissue grow and die? The Genetics of VHL Xia Wang MD PhD Oct, 2017 Proper tissue growth - controlled traffic Normal tissue growth is regulated by many genetic factors Safe traffic is
MINERVA MEDICA COPYRIGHT
 ORIGINAL ARTICLES J NEUROSURG SCI 2008;52:29-36 Neurosurgical treatment of von Hippel-Lindau-associated hemangioblastomas: benefits, risks and outcome G. PAVESI 1, A. FELETTI 2, S. BERLUCCHI 1, G. OPOCHER
ORIGINAL ARTICLES J NEUROSURG SCI 2008;52:29-36 Neurosurgical treatment of von Hippel-Lindau-associated hemangioblastomas: benefits, risks and outcome G. PAVESI 1, A. FELETTI 2, S. BERLUCCHI 1, G. OPOCHER
Estimating the Risks of Adverse Radiation Effects After Gamma Knife Radiosurgery for Arteriovenous Malformations
 Estimating the Risks of Adverse Radiation Effects After Gamma Knife Radiosurgery for Arteriovenous Malformations Hideyuki Kano, MD, PhD; John C. Flickinger, MD; Daniel Tonetti, MD; Alan Hsu, MD; Huai-che
Estimating the Risks of Adverse Radiation Effects After Gamma Knife Radiosurgery for Arteriovenous Malformations Hideyuki Kano, MD, PhD; John C. Flickinger, MD; Daniel Tonetti, MD; Alan Hsu, MD; Huai-che
Sporadic hemangioblastoma of the filum terminale: Case report and review of literature
 DOI: 10.2478/romneu-2018-0064 Article Sporadic hemangioblastoma of the filum terminale: Case report and review of literature Prashant S. Gade, Vernon Velho, Harish Naik, Laxmikant Bhople INDIA Romanian
DOI: 10.2478/romneu-2018-0064 Article Sporadic hemangioblastoma of the filum terminale: Case report and review of literature Prashant S. Gade, Vernon Velho, Harish Naik, Laxmikant Bhople INDIA Romanian
Leptomeningeal Carcinomatosis: Risks, Detection, and Treatment. Goldie Kurtz, MD, FRCPC Department of Radiation Oncology University of Pennsylvania
 Leptomeningeal Carcinomatosis: Risks, Detection, and Treatment Goldie Kurtz, MD, FRCPC Department of Radiation Oncology University of Pennsylvania May 13, 2016 Disclosures None to declare 2 Outline Epidemiology
Leptomeningeal Carcinomatosis: Risks, Detection, and Treatment Goldie Kurtz, MD, FRCPC Department of Radiation Oncology University of Pennsylvania May 13, 2016 Disclosures None to declare 2 Outline Epidemiology
Chiari malformations. A fact sheet for patients and carers
 A fact sheet for patients and carers Chiari malformations This fact sheet provides information on Chiari malformations. It focuses on Chiari malformations in adults. Our fact sheets are designed as general
A fact sheet for patients and carers Chiari malformations This fact sheet provides information on Chiari malformations. It focuses on Chiari malformations in adults. Our fact sheets are designed as general
FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA
 1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA QUESTIONS TO BE ADDRESSED: SUMMARY 1. What is the evidence for the clinical
1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA QUESTIONS TO BE ADDRESSED: SUMMARY 1. What is the evidence for the clinical
Neurosurgery. Neurosurgery
 Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Neurological Change after Gamma Knife Radiosurgery for Brain Metastases Involving the Motor Cortex
 ORIGINAL ARTICLE Brain Tumor Res Treat 2016;4(2):111-115 / pissn 2288-2405 / eissn 2288-2413 http://dx.doi.org/10.14791/btrt.2016.4.2.111 Neurological Change after Gamma Knife Radiosurgery for Brain Metastases
ORIGINAL ARTICLE Brain Tumor Res Treat 2016;4(2):111-115 / pissn 2288-2405 / eissn 2288-2413 http://dx.doi.org/10.14791/btrt.2016.4.2.111 Neurological Change after Gamma Knife Radiosurgery for Brain Metastases
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Nature and Science 2017;15(7) Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus
 Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus Mohamed Mahmoud Abohashima; Ahmed Mohamed Hasan Salem; Magdy Asaad El-Hawary Neurosurgery department, Faculty of Medicine, Al-azhar
Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus Mohamed Mahmoud Abohashima; Ahmed Mohamed Hasan Salem; Magdy Asaad El-Hawary Neurosurgery department, Faculty of Medicine, Al-azhar
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION. Mustafa Rashid Issa
 THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
Pediatric Brain Tumors: Updates in Treatment and Care
 Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
Survival and Intracranial Control of Patients With 5 or More Brain Metastases Treated With Gamma Knife Stereotactic Radiosurgery
 ORIGINAL ARTICLE Survival and Intracranial Control of Patients With 5 or More Brain Metastases Treated With Gamma Knife Stereotactic Radiosurgery Ann C. Raldow, BS,* Veronica L. Chiang, MD,w Jonathan P.
ORIGINAL ARTICLE Survival and Intracranial Control of Patients With 5 or More Brain Metastases Treated With Gamma Knife Stereotactic Radiosurgery Ann C. Raldow, BS,* Veronica L. Chiang, MD,w Jonathan P.
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Selecting the Optimal Treatment for Brain Metastases
 Selecting the Optimal Treatment for Brain Metastases Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Understand the benefits, limitations,
Selecting the Optimal Treatment for Brain Metastases Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Understand the benefits, limitations,
Surgical Treatment of Hemangioblastoma in the Pituitary Stalk: An Extremely Rare Case
 Technical Report Yonsei Med J 2016 Mar;57(2):518-522 pissn: 0513-5796 eissn: 1976-2437 Surgical Treatment of Hemangioblastoma in the Pituitary Stalk: An Extremely Rare Case Jaejoon Lim, Sunghyun Noh, and
Technical Report Yonsei Med J 2016 Mar;57(2):518-522 pissn: 0513-5796 eissn: 1976-2437 Surgical Treatment of Hemangioblastoma in the Pituitary Stalk: An Extremely Rare Case Jaejoon Lim, Sunghyun Noh, and
Brain metastases: changing visions
 Brain metastases: changing visions Roberto Spiegelmann, MD Baiona, 2014 Head, Stereotactic Radiosurgery Unit Dept of Neurosurgery, Chaim Sheba Medical Center Tel Hashomer, Israel The best current estimate
Brain metastases: changing visions Roberto Spiegelmann, MD Baiona, 2014 Head, Stereotactic Radiosurgery Unit Dept of Neurosurgery, Chaim Sheba Medical Center Tel Hashomer, Israel The best current estimate
An information leaflet for patients and families. Von Hippel- Lindau Disease
 An information leaflet for patients and families Von Hippel- Lindau Disease What is Von Hippel-Lindau disease? Von Hippel-Lindau (VHL) disease is a rare inherited disorder caused by a genetic alteration
An information leaflet for patients and families Von Hippel- Lindau Disease What is Von Hippel-Lindau disease? Von Hippel-Lindau (VHL) disease is a rare inherited disorder caused by a genetic alteration
Leptomeningeal metastasis: management and guidelines. Emilie Le Rhun Lille, FR Zurich, CH
 Leptomeningeal metastasis: management and guidelines Emilie Le Rhun Lille, FR Zurich, CH Definition of LM LM is defined as the spread of tumor cells within the leptomeninges and the subarachnoid space
Leptomeningeal metastasis: management and guidelines Emilie Le Rhun Lille, FR Zurich, CH Definition of LM LM is defined as the spread of tumor cells within the leptomeninges and the subarachnoid space
NON MALIGNANT BRAIN TUMOURS Facilitator. Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol
 NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
Organization of The Nervous System PROF. SAEED ABUEL MAKAREM
 Organization of The Nervous System PROF. SAEED ABUEL MAKAREM Objectives By the end of the lecture, you should be able to: List the parts of the nervous system. List the function of the nervous system.
Organization of The Nervous System PROF. SAEED ABUEL MAKAREM Objectives By the end of the lecture, you should be able to: List the parts of the nervous system. List the function of the nervous system.
Lecture 4 The BRAINSTEM Medulla Oblongata
 Lecture 4 The BRAINSTEM Medulla Oblongata Introduction to brainstem 1- Medulla oblongata 2- Pons 3- Midbrain - - - occupies the posterior cranial fossa of the skull. connects the narrow spinal cord
Lecture 4 The BRAINSTEM Medulla Oblongata Introduction to brainstem 1- Medulla oblongata 2- Pons 3- Midbrain - - - occupies the posterior cranial fossa of the skull. connects the narrow spinal cord
Medical Neuroscience Tutorial Notes
 Medical Neuroscience Tutorial Notes Blood Supply to the Brain MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. LEARNING OBJECTIVES After study of the assigned learning
Medical Neuroscience Tutorial Notes Blood Supply to the Brain MAP TO NEUROSCIENCE CORE CONCEPTS 1 NCC1. The brain is the body's most complex organ. LEARNING OBJECTIVES After study of the assigned learning
Year 2003 Paper two: Questions supplied by Tricia
 question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Organization of The Nervous System PROF. MOUSAED ALFAYEZ & DR. SANAA ALSHAARAWY
 Organization of The Nervous System PROF. MOUSAED ALFAYEZ & DR. SANAA ALSHAARAWY Objectives At the end of the lecture, the students should be able to: List the parts of the nervous system. List the function
Organization of The Nervous System PROF. MOUSAED ALFAYEZ & DR. SANAA ALSHAARAWY Objectives At the end of the lecture, the students should be able to: List the parts of the nervous system. List the function
Stereotactic Radiosurgery of World Health Organization Grade II and III Intracranial Meningiomas
 Stereotactic Radiosurgery of World Health Organization Grade II and III Intracranial Meningiomas Treatment Results on the Basis of a 22-Year Experience Bruce E. Pollock, MD 1,2 ; Scott L. Stafford, MD
Stereotactic Radiosurgery of World Health Organization Grade II and III Intracranial Meningiomas Treatment Results on the Basis of a 22-Year Experience Bruce E. Pollock, MD 1,2 ; Scott L. Stafford, MD
NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE
 THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
Hemangioblastoma located in the posterior incisural space mimicking a tentorial meningioma: a case report
 Rabadán et al. Journal of Medical Case Reports (2016) 10:183 DOI 10.1186/s13256-016-0962-z CASE REPORT Open Access Hemangioblastoma located in the posterior incisural space mimicking a tentorial meningioma:
Rabadán et al. Journal of Medical Case Reports (2016) 10:183 DOI 10.1186/s13256-016-0962-z CASE REPORT Open Access Hemangioblastoma located in the posterior incisural space mimicking a tentorial meningioma:
Chapter 13. The Spinal Cord & Spinal Nerves. Spinal Cord. Spinal Cord Protection. Meninges. Together with brain forms the CNS Functions
 Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
Spinal Cord Chapter 13 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward
Otolaryngologist s Perspective of Stereotactic Radiosurgery
 Otolaryngologist s Perspective of Stereotactic Radiosurgery Douglas E. Mattox, M.D. 25 th Alexandria International Combined ORL Conference April 18-20, 2007 Acoustic Neuroma Benign tumor of the schwann
Otolaryngologist s Perspective of Stereotactic Radiosurgery Douglas E. Mattox, M.D. 25 th Alexandria International Combined ORL Conference April 18-20, 2007 Acoustic Neuroma Benign tumor of the schwann
S YRINGOMYELIA and syringobulbia are
 Syringomyelia: A Look at Surgical Therapy J. GRAFTON LOVE, M.D. AND RICHARD A. OLAFSON, M.D. Mayo Clinic and Mayo Foundation, Section of Neurologic Surgery, and Mayo Graduate School of Medicine, University
Syringomyelia: A Look at Surgical Therapy J. GRAFTON LOVE, M.D. AND RICHARD A. OLAFSON, M.D. Mayo Clinic and Mayo Foundation, Section of Neurologic Surgery, and Mayo Graduate School of Medicine, University
Brain and Spine Tumors
 Brain and Spine Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases
Brain and Spine Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Long-term results of gamma knife surgery for growth hormone producing pituitary adenoma: is the disease difficult to cure?
 J Neurosurg (Suppl) 102:119 123, 2005 Long-term results of gamma knife surgery for growth hormone producing pituitary adenoma: is the disease difficult to cure? TATSUYA KOBAYASHI, M.D., PH.D., YOSHIMASA
J Neurosurg (Suppl) 102:119 123, 2005 Long-term results of gamma knife surgery for growth hormone producing pituitary adenoma: is the disease difficult to cure? TATSUYA KOBAYASHI, M.D., PH.D., YOSHIMASA
RECURRENT ADRENAL DISEASE. Megan Applewhite Endorama 2/19/2015 SR , SC
 RECURRENT ADRENAL DISEASE Megan Applewhite Endorama 2/19/2015 SR 2412318, SC 3421561 Category: Adrenal Attendings: Angelos & Grogan PATIENT #1 36yo woman with a hx of Cushing s Syndrome and right adrenalectomy
RECURRENT ADRENAL DISEASE Megan Applewhite Endorama 2/19/2015 SR 2412318, SC 3421561 Category: Adrenal Attendings: Angelos & Grogan PATIENT #1 36yo woman with a hx of Cushing s Syndrome and right adrenalectomy
Brainstem. By Dr. Bhushan R. Kavimandan
 Brainstem By Dr. Bhushan R. Kavimandan Development Ventricles in brainstem Mesencephalon cerebral aqueduct Metencephalon 4 th ventricle Mylencephalon 4 th ventricle Corpus callosum Posterior commissure
Brainstem By Dr. Bhushan R. Kavimandan Development Ventricles in brainstem Mesencephalon cerebral aqueduct Metencephalon 4 th ventricle Mylencephalon 4 th ventricle Corpus callosum Posterior commissure
Nervous System The Brain and Spinal Cord Unit 7b
 Nervous System The Brain and Spinal Cord Unit 7b Chetek High School Mrs. Michaelsen 9.12 Meninges A. Meninges 1. The organs of the CNS are covered by membranes a. The meninges are divided into 3 layers:
Nervous System The Brain and Spinal Cord Unit 7b Chetek High School Mrs. Michaelsen 9.12 Meninges A. Meninges 1. The organs of the CNS are covered by membranes a. The meninges are divided into 3 layers:
Case Report Optic Nerve Hemangioblastoma: A Case Report
 Case Reports in Pathology Volume 2012, Article ID 915408, 4 pages doi:10.1155/2012/915408 Case Report Optic Nerve Hemangioblastoma: A Case Report Holly Zywicke, 1 Cheryl Ann Palmer, 2 Michael S. Vaphiades,
Case Reports in Pathology Volume 2012, Article ID 915408, 4 pages doi:10.1155/2012/915408 Case Report Optic Nerve Hemangioblastoma: A Case Report Holly Zywicke, 1 Cheryl Ann Palmer, 2 Michael S. Vaphiades,
MRI. 3p25-p26.
 3p25-p26 e-mail:hamidshafi@yahoo.com (epididymis cyst) (cerebellar (Retinal hemangioblastoma) angioma) Violaris Violaris Jartell Chew J Babol Univ Med Sci; 11(4); Oct-Nov 2009 Von Hippel-Lindau Syndrome;
3p25-p26 e-mail:hamidshafi@yahoo.com (epididymis cyst) (cerebellar (Retinal hemangioblastoma) angioma) Violaris Violaris Jartell Chew J Babol Univ Med Sci; 11(4); Oct-Nov 2009 Von Hippel-Lindau Syndrome;
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Serial Follow-up MR Imaging after Gamma Knife Radiosurgery for Vestibular Schwannoma
 AJNR Am J Neuroradiol 21:1540 1546, September 2000 Serial Follow-up MR Imaging after Gamma Knife Radiosurgery for Vestibular Schwannoma Hiroyuki Nakamura, Hidefumi Jokura, Kou Takahashi, Nagatoshi Boku,
AJNR Am J Neuroradiol 21:1540 1546, September 2000 Serial Follow-up MR Imaging after Gamma Knife Radiosurgery for Vestibular Schwannoma Hiroyuki Nakamura, Hidefumi Jokura, Kou Takahashi, Nagatoshi Boku,
Alleinige Radiochirurgie und alleinige Systemtherapie zwei «extreme» Entwicklungen in der Behandlung von Hirnmetastasen?
 Department of Radiation Oncology Chairman: Prof. Dr. Matthias Guckenberger Alleinige Radiochirurgie und alleinige Systemtherapie zwei «extreme» Entwicklungen in der Behandlung von Hirnmetastasen? Matthias
Department of Radiation Oncology Chairman: Prof. Dr. Matthias Guckenberger Alleinige Radiochirurgie und alleinige Systemtherapie zwei «extreme» Entwicklungen in der Behandlung von Hirnmetastasen? Matthias
Management of pediatric brain tumors, strategies and long term outcome
 Management of pediatric brain tumors, strategies and long term outcome SAN The Sudanese association of neurosurgeons By Dr. Abubakr Darrag Salim Ahmed Dr. Mohammed Awad Elzain Khartoum Sudan Pediatric
Management of pediatric brain tumors, strategies and long term outcome SAN The Sudanese association of neurosurgeons By Dr. Abubakr Darrag Salim Ahmed Dr. Mohammed Awad Elzain Khartoum Sudan Pediatric
Results of Surgery of Cerebellopontine angle Tumors
 Original Article Iranian Journal of Otorhinolaryngology, Vol. 27(1), Serial No.78, Jan 2015 Abstract Results of Surgery of Cerebellopontine angle Tumors Faramarz Memari 1, * Fatemeh Hassannia 1, Seyed
Original Article Iranian Journal of Otorhinolaryngology, Vol. 27(1), Serial No.78, Jan 2015 Abstract Results of Surgery of Cerebellopontine angle Tumors Faramarz Memari 1, * Fatemeh Hassannia 1, Seyed
Long term neuroimaging and clinical outcome of brain Arteriovenous Malformations (bavm) treated with stereotactic radiosurgery (SRS).
 Long term neuroimaging and clinical outcome of brain Arteriovenous Malformations (bavm) treated with stereotactic radiosurgery (SRS). Poster No.: C-2489 Congress: ECR 2012 Type: Scientific Exhibit Authors:
Long term neuroimaging and clinical outcome of brain Arteriovenous Malformations (bavm) treated with stereotactic radiosurgery (SRS). Poster No.: C-2489 Congress: ECR 2012 Type: Scientific Exhibit Authors:
Von Hippel-Lindau disease (VHL) Information for patients
 Von Hippel-Lindau disease (VHL) Information for patients This booklet has been written to answer some of the questions people may have about von Hippel-Lindau (VHL) disease. VHL is a rare disorder caused
Von Hippel-Lindau disease (VHL) Information for patients This booklet has been written to answer some of the questions people may have about von Hippel-Lindau (VHL) disease. VHL is a rare disorder caused
Hydrocephalus 1/16/2015. Hydrocephalus. Functions of Cerebrospinal fluid (CSF) Flow of CSF
 Hydrocephalus Hydrocephalus Ruth Arms, MSN, CNS-BC, SCRN Hydrocephalus is the buildup of fluid in the cavities (ventricles) deep within the brain. The excess fluid increases the size of the ventricles
Hydrocephalus Hydrocephalus Ruth Arms, MSN, CNS-BC, SCRN Hydrocephalus is the buildup of fluid in the cavities (ventricles) deep within the brain. The excess fluid increases the size of the ventricles
Kidney Cancer Causes, Risk Factors, and Prevention
 Kidney Cancer Causes, Risk Factors, and Prevention Risk Factors A risk factor is anything that affects your chance of getting a disease such as cancer. Learn more about the risk factors for kidney cancer.
Kidney Cancer Causes, Risk Factors, and Prevention Risk Factors A risk factor is anything that affects your chance of getting a disease such as cancer. Learn more about the risk factors for kidney cancer.
Department of Neurosurgery, Christliches Krankenhaus, Quakenbrück, Germany
 J Neurosurg Spine 19:12 26, 2013 AA, 2013 Treatment of intramedullary tumors: analysis of surgical morbidity and long-term results Clinical article Jörg Klekamp, M.D. Department of Neurosurgery, Christliches
J Neurosurg Spine 19:12 26, 2013 AA, 2013 Treatment of intramedullary tumors: analysis of surgical morbidity and long-term results Clinical article Jörg Klekamp, M.D. Department of Neurosurgery, Christliches
Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
Vertebral Artery Pseudoaneurysm
 Vertebral Artery Pseudoaneurysm T. W. Khanzada,K. R. Makhdoomi ( Department of Vascular Surgery, Liaquat National Postgraduate Medical Centre, Karachi. ) Vertebral artery (VA) pseudoaneurysms are exceedingly
Vertebral Artery Pseudoaneurysm T. W. Khanzada,K. R. Makhdoomi ( Department of Vascular Surgery, Liaquat National Postgraduate Medical Centre, Karachi. ) Vertebral artery (VA) pseudoaneurysms are exceedingly
Urgent and Emergent Pituitary Conditions
 Urgent and Emergent Pituitary Conditions PANKAJ A. GORE, MD DIRECTOR, BRAIN AND SKULL BASE T UMOR SURGERY PROVIDENCE B R AIN AND S PINE I NSTITUTE Urgent and Emergent Pituitary Conditions Neurosurgical
Urgent and Emergent Pituitary Conditions PANKAJ A. GORE, MD DIRECTOR, BRAIN AND SKULL BASE T UMOR SURGERY PROVIDENCE B R AIN AND S PINE I NSTITUTE Urgent and Emergent Pituitary Conditions Neurosurgical
LONG-TERM FOLLOW-UP OF ACOUSTIC SCHWANNOMA RADIOSURGERY WITH MARGINAL TUMOR DOSES OF 12 TO 13 Gy
 doi:10.1016/j.ijrobp.2007.01.001 Int. J. Radiation Oncology Biol. Phys., Vol. 68, No. 3, pp. 845 851, 2007 Copyright 2007 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/07/$ see front
doi:10.1016/j.ijrobp.2007.01.001 Int. J. Radiation Oncology Biol. Phys., Vol. 68, No. 3, pp. 845 851, 2007 Copyright 2007 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/07/$ see front
Surgical treatment of cerebellar hemangioblastomas
 SNI: Neurovascular OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Kazuhiro Hongo, M.D., Shinsui University, Matsomoto, Japan Original Article Surgical treatment
SNI: Neurovascular OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Kazuhiro Hongo, M.D., Shinsui University, Matsomoto, Japan Original Article Surgical treatment
RESEARCH HUMAN CLINICAL STUDIES
 TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Radiosurgery to the Surgical Cavity as Adjuvant Therapy for Resected Brain Metastasis Jared R. Robbins, MD* Samuel Ryu, MD* Steven
TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Radiosurgery to the Surgical Cavity as Adjuvant Therapy for Resected Brain Metastasis Jared R. Robbins, MD* Samuel Ryu, MD* Steven
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Capt. Nazim ATA Aerospace Medicine Specialist Turkish Air Force AAMIMO 2013
 F-15 Pilot with ACOUSTIC NEUROMA Capt. Nazim ATA Aerospace Medicine Specialist Turkish Air Force AAMIMO 2013 Disclosure Information 84 th Annual AsMA Scientific Meeting Nazim ATA I have no financial relationships
F-15 Pilot with ACOUSTIC NEUROMA Capt. Nazim ATA Aerospace Medicine Specialist Turkish Air Force AAMIMO 2013 Disclosure Information 84 th Annual AsMA Scientific Meeting Nazim ATA I have no financial relationships
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
Surgical Management of Solitary Nerve Sheath Tumors of the Cervical Spine: A Retrospective Case Analysis Based on Tumor Location and Extension
 ORIGINAL ARTICLE Neurol Med Chir (Tokyo) 54, 924 929, 2014 doi: 10.2176/nmc.oa.2014-0158 Online October 31, 2014 Surgical Management of Solitary Nerve Sheath Tumors of the Cervical Spine: A Retrospective
ORIGINAL ARTICLE Neurol Med Chir (Tokyo) 54, 924 929, 2014 doi: 10.2176/nmc.oa.2014-0158 Online October 31, 2014 Surgical Management of Solitary Nerve Sheath Tumors of the Cervical Spine: A Retrospective
Guide to Draw It to Know It Neuroanatomy (relative to Medical Neuro, UI-COM Urbana)
 Guide to Draw It to Know It Neuroanatomy (relative to Medical Neuro, UI-COM Urbana) Note: Sometimes DITKI goes into far more detail than is necessary for the course, and in other cases not enough. As helpful
Guide to Draw It to Know It Neuroanatomy (relative to Medical Neuro, UI-COM Urbana) Note: Sometimes DITKI goes into far more detail than is necessary for the course, and in other cases not enough. As helpful
Decompression of the spinal subarachnoid space as a solution for syringomyelia without Chiari malformation
 (2002) 40, 501 ± 506 ã 2002 International Society All rights reserved 1362 ± 4393/02 $25.00 www.nature.com/sc Original Article Decompression of the spinal subarachnoid space as a solution for syringomyelia
(2002) 40, 501 ± 506 ã 2002 International Society All rights reserved 1362 ± 4393/02 $25.00 www.nature.com/sc Original Article Decompression of the spinal subarachnoid space as a solution for syringomyelia
CS Tumor Size CS Extension CS Tumor Size/Ext Eval CS Lymph Nodes CS Lymph Nodes Eval Reg LN Pos Reg LN Exam CS Mets at DX CS Mets Eval
 C70.0, C71.0-C71.9 C70.0 Cerebral meninges C71.0 Cerebrum C71.1 Frontal lobe C71.2 Temporal lobe C71.3 Parietal lobe C71.4 Occipital lobe C71.5 Ventricle, NOS C71.6 Cerebellum, NOS C71.7 Brain stem C71.8
C70.0, C71.0-C71.9 C70.0 Cerebral meninges C71.0 Cerebrum C71.1 Frontal lobe C71.2 Temporal lobe C71.3 Parietal lobe C71.4 Occipital lobe C71.5 Ventricle, NOS C71.6 Cerebellum, NOS C71.7 Brain stem C71.8
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT
 SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
Update on IGKRF Activities
 Stereotactic radiosurgery research, education and publishing for the purpose of improving public health Fall 2016 In this issue: Update on IGKRF Activities The IGKRF Recently Published Articles Topics
Stereotactic radiosurgery research, education and publishing for the purpose of improving public health Fall 2016 In this issue: Update on IGKRF Activities The IGKRF Recently Published Articles Topics
Nervous System. Unit 6.6 (6 th Edition) Chapter 7.6 (7 th Edition)
 Nervous System Unit 6.6 (6 th Edition) Chapter 7.6 (7 th Edition) 1 Learning Objectives Identify the main parts (anatomy) of a neuron. Identify the 2 divisions of nervous system. Classify the major types
Nervous System Unit 6.6 (6 th Edition) Chapter 7.6 (7 th Edition) 1 Learning Objectives Identify the main parts (anatomy) of a neuron. Identify the 2 divisions of nervous system. Classify the major types
