Review Article Neurotropic Melanoma: The Management of Localised Disease
|
|
|
- Kellie Lucinda Knight
- 5 years ago
- Views:
Transcription
1 Skin Cancer Volume 2012, Article ID , 6 pages doi: /2012/ Review Article Neurotropic Melanoma: The Management of Localised Disease Jeremy Croker, 1 Bryan Burmeister, 2 and Matthew Foote 2 1 Radiation Oncology Queensland, Liz Plummer Cancer Center, Lake and Grove Streets, Cairns, QLD 4870, Australia 2 Division of Cancer Services, Princess Alexandra Hospital, University of Queensland, 199 Ipswich Road Woolloongabba, QLD 4102, Australia Correspondence should be addressed to Matthew Foote, matthew foote@health.qld.gov.au Received 6 August 2012; Accepted 23 September 2012 Academic Editor: Giuseppe Argenziano Copyright 2012 Jeremy Croker et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Neurotropic melanoma is a rare subtype of cutaneous malignant melanoma. Compared with conventional melanoma, it is more locally aggressive with an increased tendency for local recurrence but less likely for nodal or distant metastases. These tumours can be a diagnostic dilemma with a variety of morphological, histopathological, and immunophenotypical expressions. The often amelanotic, benign appearance may lead to treatment issues such as late presentation, diagnostic delay, misdiagnosis, insufficient surgical margins, and recurrence with resulting poor outcome. The neurotropic nature of the disease and prevalence in the head and neck region can result in perineural and neural invasion along named large nerves into the brain with resulting neuropathies. Wide local excision with adjuvant radiotherapy where indicated remains the current practice for treatment with chemotherapy predominately being reserved as a salvage treatment for patients with disseminated disease. 1. Introduction Neurotropic melanoma (NM) is a rare variant of cutaneous melanoma with a high incidence of local recurrence and low rate of distant metastases [1, 2]. Appearance of these lesions is highly variable and can mimic benign lesions which create diagnosis and therapeutic difficulties [3 6]. Neurotropic melanoma often displays desmoplasia. Desmoplastic neurotropic melanoma (DNM) is a well-described neurotropic subtype of desmoplastic melanoma (DM) [7]. However, diagnostic criteria to differentiate DNM from DM are not well described [8]. Neurotropism describes direct invasion into neural structures (intraneural) or surrounding nerve (perineural) infiltration or cells exhibiting neural or nerve sheath differentiation [1, 3, 4, 7]. Neurotropism can be associated with worse prognosis in melanoma due to its propensity for deep invasion at the primary site and potential for positive margins at the excision site due to neural extension [9]. Neurotropic melanoma, DNM, and DM have higher local recurrence rates when treated with surgical excision alone [1, 4]. A systemic review of 14 studies involving DM demonstrated local recurrence rates ranging from 7 to 56% [3]. This is compared with a rate of 3% for other melanoma [9]. Regional, nodal, and distant metastatic disease rates are lower than with other forms of cutaneous melanoma [1 3, 6, 7, 10]. Long-term control of local disease is therefore paramount [1]. This paper reviews current literature regarding this rare melanoma variant, describing its defining characteristics, exploring the diagnostic challenges, current therapeutic approach, and future treatment and research directions. 2. Historical Perspective First described in 1971 by Conley et al. [11], DM is a primarily dermal subtype of invasive cutaneous melanoma comprising dermal spindle cells separated by collagen fibres or fibrous stroma [5, 12]. Reed and Leonard [13] in 1979 delineated DNM as a subset of DM expressing Schwannian differentiation and neurotropic characteristics which may extend beyond the desmoplastic component. Over a 10-year study period at the Sydney Melanoma Unit, DNM represented 90 (1.3%) of the total 6791 new patients examined [12]. Desmoplastic neurotropic melanoma represents at least 30% of DM [1, 4, 5] andhasbeenreportedinupto82%of cases in certain DM series [14].
2 2 Skin Cancer There have been several hundred cases of NM described in series and discussion surrounds the differentiation of NM, DNM,and DM [2, 14]. Kayet al. [14] proposed the description desmoplastic melanoma with neurotropism for DNM as both DM and DNM were likely different phenotypes of the same tumour. Another hypothesis is that these tumours exist within a neuroectodermal tumour continuum, similar to nerve sheath tumours, as reflected in their propensity for neurotropism and their immunohistochemical profile [5, 6, 15]. Less common is NM without desmoplasia, whereby melanomas are solid spindle or epithelioid cell origin and have a nondesmoplastic growth phase but perineural or endoneurial involvement [5, 9, 16]. 3. Clinical Considerations 3.1. Presentation. Due to rarity of the disease, there is limited epidemiological data or descriptions of the natural history of NM [6]. Neurotropic melanoma provides a diagnostic challenge as it presents differently to other melanomas, often as slow-growing, painless, innocuous-appearing amelanotic lesions [5 7, 12, 17], leading to misdiagnosis and/or late diagnosis with associated poorer prognosis [4, 5]. Lesions may be discrete discoid papule, nondescript plaque, and thickening or nodular and ulcerative in nature [3, 4, 7]. The benign appearance may lead to insufficient initial excision margins [7]. Lesions most often are associated with lentigo maligna (melanoma in situ) [6] but they may occur with other melanoma types [12, 18]. Macroscopically they may resemble squamous cell or basal cell carcinomas, dermatofibromas, sarcomas, cysts, or scar tissue [3, 5, 17]. Size of lesions varies from 4 to 60 mm [19]. Margins of the lesions are often ill defined and satellite lesions present [6]. The less common are de novo tumours in which there is no intraepidermal melanocytic component. In rare circumstances, a conventional melanoma may reoccur as a DNM [19]. Cases of NM reported in the literature have been exclusively Caucasian. Approximately two-thirds of cases are male, which is a larger percentage than with conventional melanoma [3, 4, 14]. The ratio of male to female is even higher in those who undergo radiotherapy, suggesting males have more advanced disease at presentation [4]. Presentation is most common in the seventh decade of life [4, 12, 14]. This is older for other forms of cutaneous melanoma (median age of 46 years) [4]. Over half of DNM and NM lesions are located on the head and neck [1, 3 6, 12, 14, 19, 20]. This is compared with 19%forothermelanomas[4]. The location of lesions on the head or neck has been associated with poorer outcomes. Lesions on the extremities (upper more than lower limbs) are more common than on the trunk [3, 4, 17]. However, any anatomical site may be involved including oral, conjunctival, and genital sites [6]. As with other forms of cutaneous melanoma, sun exposure is a risk factor for NM and DNM, [1, 3, 4, 12, 14, 21, 22] as is fair skin [12, 20]. Nodal metastases at initial presentation or recurrence are not as common as other cutaneous melanomas, with an incidence range of 6 to 11% [4, 6, 12, 17]. There are reports of low yield from lymph node biopsy (SLNB) [7, 17]. Chen et al. [4] hypothesise that the lower occurrence of nodal metastases with DM (including DNM) may be due to their possible differing biology and natural history compared to other melanoma [4]. Distant NM metastatic disease is uncommon compared with other forms of melanoma. Site of initial metastatic spread is more commonly the central nervous system (CNS) for NM than for melanomas that do not demonstrate neurotropism [9]. The reported rate of CNS metastases was 13% for DNM, 9% for DM, and 5% for a comparison melanoma group as may be expected with a neural invasive tumours. Another study of DNM reported 17.9% of 128 cases reviewed had distant metastases, with the lung being the most common site [4]. Other metastatic sites include brain, liver, skin, and bone [21, 23]. Neural extension or invasion can occur along large or small nerves, [6, 24] including cranial nerves, [2, 6, 7, 13, 18, 24, 25] most commonly the facial and trigeminal nerves [12, 18, 26]. Extended latent periods can exist between initial diagnosis and neural involvement that usually presents as a symptomatic neuropathy [7, 18, 25, 26]. Perineural spread of disease can occur beyond the skull base into Meckel s cave, the cavernous sinus and brain, and also expand in an antegrade fashion to include other cranial nerves [18]. An average latent period of 4.9 years (range years) between initial diagnosis and recurrence into cranial nerves was reported in an eight-case respective study in 2004 [12, 18]. Presentation may include cranial nerve palsies, pain, numbness, difficulty with mastication, associated atrophy of jaw muscles, and the absence of corneal reflexes [7, 18, 25, 26]. One case of large nerve invasion outside of the head and neck involving the dorsal cutaneous branch of a spinal nerve has been reported [12]. Care must therefore be taken with patients who present with neuropathies where a previous suspicious lesion has been excised. Patients may present with multiple local recurrences in the scar line of previously excised lesions likely due to inadequate excision [7, 17, 23]. Metastases may resemble their primaries or other forms of cutaneous melanoma [6]. Recurrence may occur as skip lesions, in areas particularly with perineural invasion where previous margins were clear [2]. Extensive neural spread can make cure difficult [19]. Initial presentation of NM, DNM, and DM tends to be at a more advanced stage compared with other melanoma subtypes [1, 2, 6, 7, 17]. Quinn et al. [12] reported that only 28% of patients presented with American Joint Committee on Cancer Stage I disease compared with the overall melanoma rate of 80%. Presence of neurotropism within a melanoma is an independent risk factor for local recurrence [1, 9, 12, 27, 28]. Local recurrence rate of 20% for DNM has been reported [12] occurring sooner than melanoma [21, 23]. However, overall DNM survival rates are better than for other melanoma [9, 12] Investigation and Diagnosis. Diagnosis of NM, as with DM, can be difficult [5, 8, 14, 29, 30]. The list of differential diagnoses is extensive including both benign and
3 Skin Cancer 3 Figure 2: Low power ( 20) view of skin with epidermis on the left and subcutis on the right. At this magnification we can identify nodules within the subcutis: at the centre, at the bottom, centre top, and on the right in the middle. Figure 1: T1 Axial Fat Saturated, Gadolinium enhanced MRI scan of the head. This image displays the case of a 48-year-old man with a previous excision of a neurotropic melanoma of the face. Approximately one year from wide local excision he presented with facial pain and biopsy proven recurrence of neurotropic melanoma involving the mandibular division of the trigeminal nerve, filling the cavernous sinus and prepontine cistern with obvious brainstem compression. malignant pathology. Delay in diagnosis can arise from a benign histopathological appearance [19]. Consideration of the diagnosis is key to early diagnosis and improved outcome [25]. A high index of suspicion and careful examination of skin, particularly in the head and neck region including the scalp and mucous membranes, is required for patients with potential melanocytic abnormalities. Particular attention needs to be taken in those with a previous history of melanoma to check for recurrence. Imaging is a key investigation for NM with suspected neural invasion. MRI can illustrate enhancement and thickening of neural structures or adjacent tissue planes, intracranial changes such as expansion or erosion of the skull base, mass in Meckel s cave, and bulging of the cavernous sinus which suggests perineural invasion as outlined in Figure 1 [7, 12, 18]. However, perineural enhancement on MRI offers multiple differential diagnoses including varying neoplastic, infectious, and inflammatory pathologies. The use of FDG-PET scanning for diagnosis and staging NM has been little reported but the potential use exists, with the ability to demonstrate tumoural hypermetabolic activity associated with either the primary tumour, recurrence, or perineural spread [26]. For histopathological diagnosis, biopsy is required. This may be either excision of the entire lesion, open biopsy, core biopsy, or fine needle aspiration (FNA) biopsy of suspect lesions. As FNA biopsy of desmoplastic lesions has a low yield impairing diagnosis in NM [18] and has been associated with discrepant diagnostic opinions, [30] it is typically not recommended Histopathology. Diagnosis of DNM and NM can be a challenge for pathologists [2, 8, 14, 15, 30]. The histogeneses of NM, DNM, and DM are uncertain displaying both melanocytic and neuroectodermal properties and a variety of histogenic and immunophenotypic profiles [5, 6, 14]. Lesions may be associated with intraepidermal melanocytic proliferation (often lentigo maligna or superficial spreading melanoma) lesions but epithelioid and spindle cell components may also be involved [6, 14]. Microscopically NM is often poorly circumscribed, varying in size with extension into neural tissue, subcutaneous tissue, deep reticular layers, and fascia (Figure 2) [3]. The histopathological appearance is characteristically slender, hyperchromatic spindle cells and nuclei with mild to moderate amounts of cytological atypia, with or without neuroid differentiation [3, 5]. The majority of lesions are paucicellular. Vascular invasion is rare [5, 6]. Melanosomes may be difficult to locate and Schwannian differentiation may be present [19]. Neurotropic extension of spindle cells circumferentially around dermal nerves or thickened nerve tissue with abnormal cells in deeper tissue layers is distinct (Figure 3) [5]. Foci of neurotropism may be located beyond the margins of the main tumour. Melanomas with neurotropism usually have a high Breslow thickness and advanced Clark s level (IV or V) at the time of presentation compared to other melanomas [3, 5, 9, 12, 17, 22]. Quinn et al. [12] reported that all DNMs were >1.5 mm thick in one of the largest DNM series published. Thickness within DNM lesion is a significant poor prognostic factor for overall survival. Difficulty in diagnosis may contribute to the reason for high Breslow and Clark s levels at presentation. The mitotic rate is variable but more commonly low or intermediate in NM (0 4/mm 2 )[5, 9, 12]. However, high
4 4 Skin Cancer Figure 3: High power ( 400) view of a nodule shows a nerve (bottom half) surrounded by melanoma (darker spindle cells on the left and top). The tumour cells at the top of the picture are arranged in a fasciculated (bundled) growth pattern, similar to the nerve next to it. mitotic rate (i.e., >4/mm 2 ) has been found to be a significant prognostic factor for time to recurrence and overall survival. Immunophenotypically, NM and DNM also present a diagnostic dilemma, [30] lacking uniformity in expression of diagnostic antigens. Neurotropic Melanoma is almost uniformly positive for vimentin and S-100 [6, 15, 17] and less commonly positive for other melanocytic markers such as HMB-45, Melan-A, NKIC3, and Leu-7 [2, 8, 15, 19, 25]. However, S-100 is not specific for melanocytes and if the lesion is negative for S-100 it can make differentiation from other spindle cell lesions difficult. In addition, S- 100 is common in neural tissue including neural tumours, chondrocytes, lipocytes, and dendritic cells which also can impede diagnosis [2, 5]. However, benefit may be conveyed in staining margins of resected lesions with S-100 to assess for adequate resection to assess the extent of invasion [5, 25]. Nerve growth factor receptor p75 has potential as an ancillary diagnostic stain to enable more reliable diagnosis [5, 15, 31]. There are currently no specific genetic assays for NM, DNM, or DM. However, frequent allelic loss at the neurofibromatosis type 1 (NF1) gene locus and high prevalence of basic fibroblast growth factor (bfgf) in cell nuclei offers potential of genetic assays and possible targeted gene therapy in the future [5] Prognosis. Prognostic factors for cutaneous melanoma such as stage, tumour thickness, depth of invasion, and dermal mitotic rate apply to NM [5, 14, 17]. There are conflicting data as to the significance of neurotropism in melanoma as a poor prognostic factor for survival [9, 10, 17]. Baer et al. [9] reported 8-year survival for patients with DM as 90%, which decreased to 60% with the presence of neurotropism. The largest series thus far for DNM by Quinn et al. [12] reported significant increase in local recurrence when neurotropism was present but this had no significant impact on survival. In this series, DM and DNM 5-year survival was 72 and 58% at 10 years. Poor prognosis in DNM and NM is associated with age, male gender, and head and neck locations of primary lesions, high Breslow thickness, close (<1cm) or positive surgical margins. These are also the predictors of local recurrence [1, 4, 5, 12, 14, 28, 32]. While locally aggressive, DNM prognosis is better compared with similar staged conventional melanoma, emphasising the importance for local control [4]. Chen et al. [4] reported recurrence in 6.3% of DNM with a median time to local recurrence of 10 months. Local recurrence confers increased risk of further local recurrence and systemic metastases [3] which in turn is a poor prognostic marker [23]. Given the propensity for local recurrence, close, regular followup is recommended [21]. Perineural invasion into large nerves confers a poor prognosis, often altering the goal of treatment from cure to palliation [12, 18]. Untreated patients with intracranial metastases with neurological symptoms have a median survival of one month. Intracranial disease treated with radiotherapy can greatly extend median survival of patients by more than 8 months [7]. 4. Management 4.1. Surgical. Depending on the size, site, and level of suspicion of a lesion, it may be initially biopsied or completely excised. However, once a diagnosis of DNM or NM is made, prompt wide local excision (WLE) with clear margins is the definitive management [3, 4, 12, 18, 23]. A minimum margin of 2 cm is recommended for NM to decrease the risk of local recurrence [1, 3, 5, 7, 12, 17]. Deep margins should include the fascia due to the invasive nature of the disease [23]. The need for extensive margins has meant that patients often require reresection [4, 6]. The location of the lesions particularly on the head and neck coupled with the invasive propensity can present problems to achieve reasonable margins whilst preserving function and cosmesis [2, 12, 21]. These factors and the benign appearance of some of these lesions may contribute to insufficient margins at time of initial resection. In areas such as the nose, there may be the need for local or free flaps to ensure sufficient margins are accomplished [21]. The increased morbidity and impact on quality of life of ongoing re-resection for local recurrence are important considerations in treatment [17]. For NM, there is a correlation between positive <1cmor unknown margin status and local recurrence of DM [4, 17, 21, 23]. Given that neurotropism is associated with increased recurrence rates, nerves identified at surgery should be marked for specific histopathological analysis to examine presence of invasion [9]. The low incidence of nodal metastatic spread has meant that regional lymph node sampling and dissection are not routine when lesions are excised. Resections are undertaken when clinical palpable nodes are present and at the discretion of the surgeon [21]. Some argue that SLNB with lymphoscintigraphy is the most appropriate evaluation of nodal and micrometastatic spread to inform treatment
5 Skin Cancer 5 decisionmaking [17, 23]. However, given a lack of research regarding SLNB in either NM or DM and the low yield of reported SLNB, the benefit of the procedure is still being debated [4, 5]. A tumour that has already demonstrated perineural spread, either on imaging or symptomatic neuropathy, may be unsuitable for definitive surgery and may require palliative radiotherapy or chemotherapy [12, 18] Radiotherapy. Adjuvant radiotherapy after surgery is often considered particularly in high-risk regions like the head and neck where wide surgical margins are difficult to achieve. Currently, radiotherapy is considered in the postoperative setting for recurrent lesions or where margins are positive or deemed inadequate [4, 7, 20]. Radiotherapy as definitive treatment for inoperable disease has been shown to provide local control of disease [20]. In this case the radiotherapy volume should encompass all of the gross disease (including the primary site), the named nerve extending to the skull base, and neural foramina and any evidence of intracranial disease [2, 4]. Inmany cases, however, those with inoperable disease are incurable and radiotherapy is effective in the palliation of these patients. Limited data are available for the use of only radiotherapy for treatment of NM. Chen et al. [4] reported on 128 cases of DNM, of which 21% underwent adjuvant radiotherapy. The authors found that those patients who underwent radiotherapyhadmoreadvancedtumoursandlessadequate surgical margins. Foote et al. [1] reported on 24 patients that received radiotherapy for DM including DNM. The median dose was48gyin20fractionsover4weeks(doserange48 60 Gy, fraction range 20 30). The 3-year in-field relapse-free survival was 91%, 3-year relapse-free survival was 86%, and 3-year overall survival was 83% [1]. Noprospectiverandomisedtrialstodatehaveevaluated radiotherapy preventing local recurrence following surgical excision. A randomised trial of postoperative radiation treatment following wide excision of neurotropic melanoma of the head and neck is currently underway with the Trans Tasman Radiation Oncology Group (TROG 08.09)/Australia and New Zealand Melanoma Trials Group (ANZMTG 01.09) Chemotherapy. Chemotherapy is not routinely offered for treatment of localised NM. It has been utilised for patients with hematogenously disseminated disease. For disseminated disease palliative chemotherapy regimens have included use of chemotherapy and immunotherapy agents such as dacarbazine (DTIC), ipilimumab (IPI), interferonα, aldesleukin, and BRAF inhibitors such as vemurafenib (in patients with BRAF-mutated melanoma). There have been no dedicated studies regarding efficacy of chemotherapy treatments in disseminated NM or DNM disease [2, 7]. 5. Conclusion Neurotropic melanoma is a rare but locally aggressive variant of melanoma. It is varied and often benign appearance makes diagnosis challenging and may contribute to advanced stage at presentation and propensity of local recurrence. Low rates of nodal and distant metastatic disease highlight the importance of local control. This is achieved through excision of lesion with wide margins of at least 2 cm and adjuvant radiotherapy where indicated. Potential exists for clarification in diagnostic criteria for NM and evaluation of adjuvant radiotherapy. Abbreviations CNS: Central nervous system DM: Desmoplastic melanoma DNM: Desmoplastic neurotropic melanoma IPI: Ipilimumab NM: Neurotropic melanoma MRI: Magnetic Resonance Imaging SLNB: Sentinel lymph node biopsy TROG: Trans Tasman radiation oncology group. Conflict of Interests The authors have no conflict of interest to declare. Acknowledgment The authors would like to thank Dr. Samuel Boros of the Department of Pathology at the Princess Alexandra Hospital for his assistance with the images for this paper. References [1] M.C.Foote,B.Burmeister,E.Burmeister,G.Bayley,andB.M. Smithers, Desmoplastic melanoma: the role of radiotherapy in improving local control, ANZ Surgery, vol. 78, no. 4, pp , [2] T. D. Anderson, R. S. Weber, D. Guerry et al., Desmoplastic neurotropic melanoma of the head and neck: the role of radiation therapy, Head and Neck, vol. 24, no. 12, pp , [3] M. B. Lens, J. A. Newton-Bishop, and A. P. Boon, Desmoplastic malignant melanoma: a systematic review, British Journal of Dermatology, vol. 152, no. 4, pp , [4] J. Y. Chen, G. Hruby, R. A. Scolyer et al., Desmoplastic neurotropic melanoma: a clinicopathologic analysis of 128 cases, Cancer, vol. 113, no. 10, pp , [5] S. W. McCarthy, R. A. Scolyer, and A. A. Palmer, Desmoplasticmelanoma:adiagnostictrapfortheunwary, Pathology, vol. 36, no. 5, pp , [6] J. A. Carlson, G. R. Dickersin, A. J. Sober, and R. L. Barnhill, Desmoplastic neurotropic melanoma. A clinicopathologic analysis of 28 cases, Cancer, vol. 75, pp , [7] D. Lin, M. Kashani-Sabet, T. McCalmont, and M. I. Singer, Neurotropic melanoma invading the inferior alveolar nerve, the American Academy of Dermatology, vol. 53, no. 2, pp. S120 S122, [8] R. Murali, H. M. Shaw, K. Lai et al., Prognostic factors in cutaneous desmoplastic melanoma: a study of 252 patients, Cancer, vol. 116, no. 17, pp , [9] S. C. Baer, D. Schultz, M. Synnestvedt, and D. E. Elder, Desmoplasia and neurotropism. Prognostic variables in
6 6 Skin Cancer patients with stage I melanoma, Cancer, vol. 76, pp , [10] D. P. Livestro, A. Muzikansky, E. M. Kaine et al., Biology of desmoplastic melanoma: a case-control comparison with other melanomas, Clinical Oncology, vol. 23, no. 27, pp , [11]J.Conley,R.Lattes,andW.Orr, Desmoplasticmalignant melanoma (a rare variant of spindle cell melanoma), Cancer, vol. 28, no. 4, pp , [12] M. J. Quinn, K. A. Crotty, J. F. Thompson, A. S. Coates, C. J. O Brien, and W. H. McCarthy, Desmoplastic and desmoplastic neurotropic melanoma: experience with 280 patients, Cancer, vol. 83, no. 6, pp , [13] R. J. Reed and D. D. Leonard, Neurotropic melanoma. A variant of desmoplastic melanoma, American Surgical Pathology, vol. 3, no. 4, pp , [14] P. A. Kay, A. D. Pinheiro, C. M. Lohse et al., Desmoplastic melanoma of the head and neck: histopathologic and immunohistochemical study of 28 cases, International Journal of Surgical Pathology, vol. 12, no. 1, pp , [15] V. Winnepenninckx, R. de Vos, M. Stas, and J. J. van den Oord, New phenotypical and ultrastructural findings in spindle cell (desmoplastic/neurotropic) melanoma, Applied Immunohistochemistry and Molecular Morphology, vol. 11, no. 4, pp , [16] R. L. Barnhill and J. L. Bolognia, Neurotropic melanoma with prominent melanization, Cutaneous Pathology, vol. 22, no. 5, pp , [17] K. E. Posther, M. A. Selim, P. J. Mosca et al., Histopathologic characteristics, recurrence patterns, and survival of 129 patients with desmoplastic melanoma, Annals of Surgical Oncology, vol. 13, no. 5, pp , [18] P. C. Chang, N. J. Fischbein, T. H. McCalmont et al., Perineural spread of malignant melanoma of the head and neck: clinical and imaging features, American Neuroradiology, vol. 25, no. 1, pp. 5 11, [19] S. S. Banerjee and M. Harris, Morphological and immunophenotypic variations in malignant melanoma, Histopathology, vol. 36, no. 5, pp , [20] H. E. Newlin, C. G. Morris, R. J. Amdur, and W. M. Mendenhall, Neurotropic melanoma of the head and neck with clinical perineural invasion, American Clinical Oncology, vol. 28, no. 4, pp , [21] T. Papadopoulos, K. Rasiah, J. F. Thompson, M. J. Quinn, andk.a.crotty, Melanomaofthenose, British Surgery, vol. 84, no. 7, pp , [22] V. de Giorgi, S. Sestini, D. Massi, and T. Lotti, Melanocytic aggregation in the skin: diagnostic clues from lentigines to melanoma, Dermatologic Clinics, vol. 25, no. 3, pp , [23] D. E. Jaroszewski, B. A. Pockaj, D. J. DiCaudo, and U. Bite, The clinical behavior of desmoplastic melanoma, American Surgery, vol. 182, no. 6, pp , [24] E. E. Mack and E. C. Gomez, Neurotropic melanoma. A case report and review of the literature, Neuro-Oncology, vol. 13, no. 2, pp , [25] H. Walters, E. Lewis, R. Wolper, A. T. Yachnis, J. Green, and S. Lewis, Neurotropic melanoma of the trigeminal nerve: a case of atypical facial pain, Oral and Maxillofacial Surgery, vol. 66, no. 3, pp , [26] G. Moulin-Romsee, M. Benamor, and S. Neuenschwander, Desmoplastic neurotropic melanoma in a patient with trigeminal neuralgia: FDG PET/CT and MRI, Clinical Nuclear Medicine, vol. 33, no. 5, pp , [27] B. Egbert, R. Kempson, and R. Sagebiel, Desmoplastic malignant melanoma. A clinicohistopathologic study of 25 cases, Cancer, vol. 62, no. 9, pp , [28]S.JainandP.W.Allen, Desmoplasticmalignantmelanoma and its variants. A study of 45 cases, American Surgical Pathology, vol. 13, no. 5, pp , [29] T. Murakami, T. Kiyosawa, S. Murata, K. Usui, M. Ohtsuki, and H. Nakagawa, Malignant schwannoma with melanocytic differentiation arising in a patient with neurofibromatosis, British Dermatology, vol. 143, no. 5, pp , [30] Z. K. Arbiser, A. L. Folpe, and S. W. Weiss, Consultative (expert) second opinions in soft tissue pathology: analysis of problem-prone diagnostic situations, American Clinical Pathology, vol. 116, no. 4, pp , [31]R.Lazova,I.Tantcheva-Poor,andA.C.Sigal, P75nerve growth factor receptor staining is superior to S100 in identifying spindle cell and desmoplastic melanoma, the American Academy of Dermatology, vol. 63, no. 5, pp , [32] B. M. Smithers, G. R. McLeod, and J. H. Little, Desmoplastic melanoma: patterns of recurrence, World Surgery, vol. 16, no. 2, pp , 1992.
7 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Diabetes Research International Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Obesity Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
Neurotropic cutaneous malignant melanoma with contiguous spread to spinal cord, an extremely rare presentation
 Case Report Neurotropic cutaneous malignant melanoma with contiguous spread to spinal cord, an extremely rare presentation Sheikh Asad, Idrees Sher, Jens Peters-Willke, Peter Jessup Departments of Neurosurgery
Case Report Neurotropic cutaneous malignant melanoma with contiguous spread to spinal cord, an extremely rare presentation Sheikh Asad, Idrees Sher, Jens Peters-Willke, Peter Jessup Departments of Neurosurgery
Desmoplastic Melanoma R/O BCC. Clinical Information. 74 y.o. man with lesion on left side of neck r/o BCC
 R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Interesting Case Series. Desmoplastic Melanoma
 Interesting Case Series Desmoplastic Melanoma Anthony Maurice Kordahi, MD, Joshua B. Elston, MD, Ellen M. Robertson, MD, and C. Wayne Cruse, MD Division of Plastic Surgery, Department of Surgery, University
Interesting Case Series Desmoplastic Melanoma Anthony Maurice Kordahi, MD, Joshua B. Elston, MD, Ellen M. Robertson, MD, and C. Wayne Cruse, MD Division of Plastic Surgery, Department of Surgery, University
Summary and Introduction
 www.medscape.com Summary and Introduction Summary Background: Desmoplastic melanoma (DM) is an uncommonly encountered type of malignant melanoma. The clinical appearance of DM can be highly variable and
www.medscape.com Summary and Introduction Summary Background: Desmoplastic melanoma (DM) is an uncommonly encountered type of malignant melanoma. The clinical appearance of DM can be highly variable and
Desmoplastic Melanoma: Clinical Behavior and Management Implications
 Desmoplastic Melanoma: Clinical Behavior and Management Implications Collier S. Pace, MD, a Jyoti P. Kapil, MD, b Luke G. Wolfe, MS, c Brian J. Kaplan, MD, c and James P. Neifeld, MD c a Division of Plastic
Desmoplastic Melanoma: Clinical Behavior and Management Implications Collier S. Pace, MD, a Jyoti P. Kapil, MD, b Luke G. Wolfe, MS, c Brian J. Kaplan, MD, c and James P. Neifeld, MD c a Division of Plastic
Clinical Study Mucosal Melanoma in the Head and Neck Region: Different Clinical Features and Same Outcome to Cutaneous Melanoma
 ISRN Dermatology Volume 2013, Article ID 586915, 5 pages http://dx.doi.org/10.1155/2013/586915 Clinical Study Mucosal Melanoma in the Head and Neck Region: Different Clinical Features and Same Outcome
ISRN Dermatology Volume 2013, Article ID 586915, 5 pages http://dx.doi.org/10.1155/2013/586915 Clinical Study Mucosal Melanoma in the Head and Neck Region: Different Clinical Features and Same Outcome
Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor
 Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy
 Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy Dale Han, MD Assistant Professor Department of Surgery Section of Surgical Oncology No disclosures Background Desmoplastic melanoma (DM)
Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy Dale Han, MD Assistant Professor Department of Surgery Section of Surgical Oncology No disclosures Background Desmoplastic melanoma (DM)
Case Report Metastatic Malignant Melanoma of Parotid Gland with a Regressed Primary Tumor
 Case Reports in Otolaryngology Volume 2016, Article ID 5393404, 4 pages http://dx.doi.org/10.1155/2016/5393404 Case Report Metastatic Malignant Melanoma of Parotid Gland with a Regressed Primary Tumor
Case Reports in Otolaryngology Volume 2016, Article ID 5393404, 4 pages http://dx.doi.org/10.1155/2016/5393404 Case Report Metastatic Malignant Melanoma of Parotid Gland with a Regressed Primary Tumor
1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter.
 Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Case Scenario 1 Worksheet. Primary Site C44.4 Morphology 8743/3 Laterality 0 Stage/ Prognostic Factors
 CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
Malignant Peripheral Nerve Sheath Tumor
 C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
Cutaneous Melanoma: Epidemiology (USA) The Sentinel Node in Head and Neck Melanoma. Cutaneous Melanoma: Epidemiology (USA)
 The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
Journal of International Academy of Forensic Science & Pathology (JIAFP)
 Journal of International Academy of Forensic Science & Pathology (JIAFP) ISSN 2395-0722 MICROCYSTIC ADNEXAL CARCINOMA-A CASE REPORT WITH REVIEW OF LITERATURE Case Report Sulakshana M S 1,Natarajan M 2
Journal of International Academy of Forensic Science & Pathology (JIAFP) ISSN 2395-0722 MICROCYSTIC ADNEXAL CARCINOMA-A CASE REPORT WITH REVIEW OF LITERATURE Case Report Sulakshana M S 1,Natarajan M 2
Dermatopathology. Dr. Rafael Botella Estrada. Hospital La Fe de Valencia
 Dermatopathology Dr. Rafael Botella Estrada. Hospital La Fe de Valencia Melanoma and mimics Dr. Martin Mihm Malignant lesions result from the accumulation of mutations Class I lesions (benign) Class II
Dermatopathology Dr. Rafael Botella Estrada. Hospital La Fe de Valencia Melanoma and mimics Dr. Martin Mihm Malignant lesions result from the accumulation of mutations Class I lesions (benign) Class II
Clinical Pathological Conference. Malignant Melanoma of the Vulva
 Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
أملس عضلي غرن = Leiomyosarcoma. Leiomyosarcoma 1 / 5
 Leiomyosarcoma 1 / 5 EPIDEMIOLOGY Exact incidence is unknown, but older studies suggest that leiomyosarcomas comprise approximately 3 percent of soft-tissue sarcomas. Superficial leiomyosarcoma occurs
Leiomyosarcoma 1 / 5 EPIDEMIOLOGY Exact incidence is unknown, but older studies suggest that leiomyosarcomas comprise approximately 3 percent of soft-tissue sarcomas. Superficial leiomyosarcoma occurs
Histopathology of Melanoma
 THE YALE JOURNAL OF BIOLOGY AND MEDICINE 48, 409-416 (1975) Histopathology of Melanoma G. J. WALKER SMITH Department ofpathology, Yale University School ofmedicine, 333 Cedar Street, New Haven, Connecticut
THE YALE JOURNAL OF BIOLOGY AND MEDICINE 48, 409-416 (1975) Histopathology of Melanoma G. J. WALKER SMITH Department ofpathology, Yale University School ofmedicine, 333 Cedar Street, New Haven, Connecticut
WHAT DOES THE PATHOLOGY REPORT MEAN?
 Melanoma WHAT IS MELANOMA? Melanoma is a type of cancer that affects cells called melanocytes. These cells are found mainly in skin but also in the lining of other areas such as nose and rectum, and also
Melanoma WHAT IS MELANOMA? Melanoma is a type of cancer that affects cells called melanocytes. These cells are found mainly in skin but also in the lining of other areas such as nose and rectum, and also
Research Article A Clinicopathological Analysis of Soft Tissue Sarcoma with Telangiectatic Changes
 Sarcoma Volume 2015, Article ID 740571, 5 pages http://dx.doi.org/10.1155/2015/740571 Research Article A Clinicopathological Analysis of Soft Tissue Sarcoma with Telangiectatic Changes Hiroshi Kobayashi,
Sarcoma Volume 2015, Article ID 740571, 5 pages http://dx.doi.org/10.1155/2015/740571 Research Article A Clinicopathological Analysis of Soft Tissue Sarcoma with Telangiectatic Changes Hiroshi Kobayashi,
Melanoma Underwriting Presented at 2018 AHOU Conference. Hank George FALU
 Melanoma Underwriting Presented at 2018 AHOU Conference Hank George FALU MELANOMA EPIDEMIOLOGY 70-80,000 American cases annually Majority are in situ or thin > 20% are diagnosed age 45 8-9,000 melanoma
Melanoma Underwriting Presented at 2018 AHOU Conference Hank George FALU MELANOMA EPIDEMIOLOGY 70-80,000 American cases annually Majority are in situ or thin > 20% are diagnosed age 45 8-9,000 melanoma
World Articles of Ear, Nose and Throat Page 1
 World Articles of Ear, Nose and Throat ---------------------Page 1 Primary Malignant Melanoma of the Tongue: A Case Report Authors: Nanayakkara PR*, Arudchelvam JD** Ariyaratne JC*, Mendis K*, Jayasekera
World Articles of Ear, Nose and Throat ---------------------Page 1 Primary Malignant Melanoma of the Tongue: A Case Report Authors: Nanayakkara PR*, Arudchelvam JD** Ariyaratne JC*, Mendis K*, Jayasekera
Case Report Multiple Giant Cell Tumors of Tendon Sheath Found within a Single Digit of a 9-Year-Old
 Case Reports in Orthopedics Volume 2016, Article ID 1834740, 4 pages http://dx.doi.org/10.1155/2016/1834740 Case Report Multiple Giant Cell Tumors of Tendon Sheath Found within a Single Digit of a 9-Year-Old
Case Reports in Orthopedics Volume 2016, Article ID 1834740, 4 pages http://dx.doi.org/10.1155/2016/1834740 Case Report Multiple Giant Cell Tumors of Tendon Sheath Found within a Single Digit of a 9-Year-Old
Primary Cutaneous Melanoma Pathology Reporting Proforma DD MM YYYY. *Tumour site. *Specimen laterality. *Specimen type
 Primary Cutaneous Melanoma Pathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth DD MM YYYY Sex Male Female
Primary Cutaneous Melanoma Pathology Reporting Proforma Includes the International Collaboration on Cancer reporting dataset denoted by * Family name Given name(s) Date of birth DD MM YYYY Sex Male Female
Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach
 Case Reports in Surgery Volume 2013, Article ID 560712, 4 pages http://dx.doi.org/10.1155/2013/560712 Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach Shigeo
Case Reports in Surgery Volume 2013, Article ID 560712, 4 pages http://dx.doi.org/10.1155/2013/560712 Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach Shigeo
Case Report A Case of Primary Submandibular Gland Oncocytic Carcinoma
 Case Reports in Otolaryngology Volume 2013, Article ID 384238, 4 pages http://dx.doi.org/10.1155/2013/384238 Case Report A Case of Primary Submandibular Gland Oncocytic Carcinoma Kunihiko Tokashiki, Kiyoaki
Case Reports in Otolaryngology Volume 2013, Article ID 384238, 4 pages http://dx.doi.org/10.1155/2013/384238 Case Report A Case of Primary Submandibular Gland Oncocytic Carcinoma Kunihiko Tokashiki, Kiyoaki
1/10/2018. Soft Tissue Tumors Showing Melanocytic Differentiation. Overview. Desmoplastic/ Spindle Cell Melanoma
 2016 MFMER slide-1 2016 MFMER slide-2 2016 MFMER slide-3 Soft Tissue Tumors Showing Melanocytic Differentiation Andrew L. Folpe, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic, Rochester,
2016 MFMER slide-1 2016 MFMER slide-2 2016 MFMER slide-3 Soft Tissue Tumors Showing Melanocytic Differentiation Andrew L. Folpe, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic, Rochester,
Kentaro Tanaka, 1 Hiroki Mori, 1 Mutsumi Okazaki, 1 Aya Nishizawa, 2 and Hiroo Yokozeki Introduction. 2. Case Presentation
 Case Reports in Oncological Medicine Volume 2013, Article ID 259326, 4 pages http://dx.doi.org/10.1155/2013/259326 Case Report Long-Term Treatment Outcome after Only Popliteal Lymph Node Dissection for
Case Reports in Oncological Medicine Volume 2013, Article ID 259326, 4 pages http://dx.doi.org/10.1155/2013/259326 Case Report Long-Term Treatment Outcome after Only Popliteal Lymph Node Dissection for
R. F. Falkenstern-Ge, 1 S. Bode-Erdmann, 2 G. Ott, 2 M. Wohlleber, 1 and M. Kohlhäufl Introduction. 2. Histology
 Case Reports in Oncological Medicine Volume 2013, Article ID 167585, 4 pages http://dx.doi.org/10.1155/2013/167585 Case Report Late Lung Metastasis of a Primary Eccrine Sweat Gland Carcinoma 10 Years after
Case Reports in Oncological Medicine Volume 2013, Article ID 167585, 4 pages http://dx.doi.org/10.1155/2013/167585 Case Report Late Lung Metastasis of a Primary Eccrine Sweat Gland Carcinoma 10 Years after
Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc
 1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
1 Benign versus Cancerous Lesions How to tell the difference FMF 2014 Christie Freeman MD, CCFP, DipPDerm, MSc Benign lesions Seborrheic Keratoses: Warty, stuck-on Genetics and birthdays Can start in late
Metastatic Melanoma. Cynthia Kwong February 16, 2017 SUNY Downstate Medical Center Department of Surgery Grand Rounds
 Metastatic Melanoma Cynthia Kwong February 16, 2017 SUNY Downstate Medical Center Department of Surgery Grand Rounds Case Presentation 77 year old male with previous history of scalp melanoma and thyroid
Metastatic Melanoma Cynthia Kwong February 16, 2017 SUNY Downstate Medical Center Department of Surgery Grand Rounds Case Presentation 77 year old male with previous history of scalp melanoma and thyroid
Malignant tumors of melanocytes: Part 1. Deba P Sarma, MD., Omaha
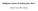 Malignant tumors of melanocytes: Part 1 Deba P Sarma, MD., Omaha The melanocytic tumor is one of the most difficult and confusing areas in Dematopathology. It is true that most (95%) of such lesions are
Malignant tumors of melanocytes: Part 1 Deba P Sarma, MD., Omaha The melanocytic tumor is one of the most difficult and confusing areas in Dematopathology. It is true that most (95%) of such lesions are
An Overview of Melanoma. Harriet Kluger, M.D. Associate Professor Section of Medical Oncology Yale Cancer Center
 An Overview of Melanoma Harriet Kluger, M.D. Associate Professor Section of Medical Oncology Yale Cancer Center Melanoma Statistics Median age at presentation 45-55 55 years Incidence: 2003 54,200 cases
An Overview of Melanoma Harriet Kluger, M.D. Associate Professor Section of Medical Oncology Yale Cancer Center Melanoma Statistics Median age at presentation 45-55 55 years Incidence: 2003 54,200 cases
Epithelial Cancer- NMSC & Melanoma
 Epithelial Cancer- NMSC & Melanoma David Chin MB, BCh, BAO, LRCP, LRCS (Ireland) MCh(MD), PhD (UQ), FRCS, FRACS (Plast) Plastic & Reconstructive Surgeon Visiting Scientist Melanoma Genomic Group & Drug
Epithelial Cancer- NMSC & Melanoma David Chin MB, BCh, BAO, LRCP, LRCS (Ireland) MCh(MD), PhD (UQ), FRCS, FRACS (Plast) Plastic & Reconstructive Surgeon Visiting Scientist Melanoma Genomic Group & Drug
Dr Rosalie Stephens. Mr Richard Martin. Medical Oncologist Auckland City Hospital Auckland
 Dr Rosalie Stephens Medical Oncologist Auckland City Hospital Auckland Mr Richard Martin General Surgeon Melanoma Unit Team Waitemata District Health Board Auckland 8:30-9:25 WS #99: Interactive Case Studies
Dr Rosalie Stephens Medical Oncologist Auckland City Hospital Auckland Mr Richard Martin General Surgeon Melanoma Unit Team Waitemata District Health Board Auckland 8:30-9:25 WS #99: Interactive Case Studies
Cutaneous Malignancies: A Primer COPYRIGHT. Marissa Heller, M.D.
 Cutaneous Malignancies: A Primer Marissa Heller, M.D. Associate Director of Dermatologic Surgery Department of Dermatology Beth Israel Deaconess Medical Center December 10, 2016 Skin Cancer Non-melanoma
Cutaneous Malignancies: A Primer Marissa Heller, M.D. Associate Director of Dermatologic Surgery Department of Dermatology Beth Israel Deaconess Medical Center December 10, 2016 Skin Cancer Non-melanoma
Case Report: Chondroid Syringoma of the Cheek
 Cronicon OPEN ACCESS Dina Amin 1 *, Abdullah Al-Gorashi 2 and Rahaf Y Al-Habbab 2 1 Assistant Consultant Al-Noor Specialist Hospital, Saudi Arabia, Clinical fellow University of Alabama, USA 2 Department
Cronicon OPEN ACCESS Dina Amin 1 *, Abdullah Al-Gorashi 2 and Rahaf Y Al-Habbab 2 1 Assistant Consultant Al-Noor Specialist Hospital, Saudi Arabia, Clinical fellow University of Alabama, USA 2 Department
Malignant tumors of melanocytes : Part 3. Deba P Sarma, MD., Omaha
 Malignant tumors of melanocytes : Part 3 Deba P Sarma, MD., Omaha Let s go over one case of melanoma using the following worksheet. Of the various essential information that needs to be included in the
Malignant tumors of melanocytes : Part 3 Deba P Sarma, MD., Omaha Let s go over one case of melanoma using the following worksheet. Of the various essential information that needs to be included in the
Neuroradiology Case of the Day
 Neuroradiology Case of the Day 76 th CAR Annual Meeting, Montreal, Quebec April 27, 2013 Eugene Yu, MD Assistant Professor of Radiology and Otolaryngology-Head and Neck Surgery Head and Neck Imaging Princess
Neuroradiology Case of the Day 76 th CAR Annual Meeting, Montreal, Quebec April 27, 2013 Eugene Yu, MD Assistant Professor of Radiology and Otolaryngology-Head and Neck Surgery Head and Neck Imaging Princess
Protocol applies to melanoma of cutaneous surfaces only.
 Melanoma of the Skin Protocol applies to melanoma of cutaneous surfaces only. Procedures Biopsy (No Accompanying Checklist) Excision Re-excision Protocol revision date: January 2005 Based on AJCC/UICC
Melanoma of the Skin Protocol applies to melanoma of cutaneous surfaces only. Procedures Biopsy (No Accompanying Checklist) Excision Re-excision Protocol revision date: January 2005 Based on AJCC/UICC
Updates on Melanoma: Are You Following the Latest Guidelines of Care? Jerry Brewer, MD
 Updates on Melanoma: Are You Following the Latest Guidelines of Care? Jerry Brewer, MD Disclosure Statement Update on Melanoma Are You Following the Latest Guidelines of Care? I, Jerry D. Brewer, MD, do
Updates on Melanoma: Are You Following the Latest Guidelines of Care? Jerry Brewer, MD Disclosure Statement Update on Melanoma Are You Following the Latest Guidelines of Care? I, Jerry D. Brewer, MD, do
A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL
 A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL OBJECTIVES Discuss current trends and changing concepts in our understanding of
A PRACTICAL APPROACH TO ATYPICAL MELANOCYTIC LESIONS BIJAN HAGHIGHI M.D, DIRECTOR OF DERMATOPATHOLOGY, ST. JOSEPH HOSPITAL OBJECTIVES Discuss current trends and changing concepts in our understanding of
Update on 8 th Edition Cutaneous AJCC Staging of Primary Cutaneous Melanoma. Michael T. Tetzlaff MD, PhD
 Update on 8 th Edition Cutaneous AJCC Staging of Primary Cutaneous Melanoma Michael T. Tetzlaff MD, PhD Associate Professor Departments of Pathology (Dermatopathology) and Translational and Molecular Pathology
Update on 8 th Edition Cutaneous AJCC Staging of Primary Cutaneous Melanoma Michael T. Tetzlaff MD, PhD Associate Professor Departments of Pathology (Dermatopathology) and Translational and Molecular Pathology
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more
 Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
Benign and malignant epithelial lesions: Seborrheic keratosis: A common benign pigmented epidermal tumor occur in middle-aged or older persons more common on the trunk; but extremities, head and neck are
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
Da Costa was the first to coin the term. Marjolin s Ulcer: A Case Report and Literature Review. Case Report. Introduction
 E-Da Medical Journal 2016;3(2):24-28 Case Report Marjolin s Ulcer: A Case Report and Literature Review Yue-Chiu Su 1, Li-Ren Chang 2 Marjolin s ulcer is an aggressive cutaneous malignancy, which is common
E-Da Medical Journal 2016;3(2):24-28 Case Report Marjolin s Ulcer: A Case Report and Literature Review Yue-Chiu Su 1, Li-Ren Chang 2 Marjolin s ulcer is an aggressive cutaneous malignancy, which is common
Clinical Case Conference Melanoma
 Clinical Case Conference Melanoma Epidemiology ~60,000 cases and 8,000 deaths per year in US Caucasian:African American = 10:1 15% arise from existing nevi 91% are cutaneous 15% are LN+ at presentation
Clinical Case Conference Melanoma Epidemiology ~60,000 cases and 8,000 deaths per year in US Caucasian:African American = 10:1 15% arise from existing nevi 91% are cutaneous 15% are LN+ at presentation
Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms
 Case Reports in Pathology Volume 2015, Article ID 153932, 5 pages http://dx.doi.org/10.1155/2015/153932 Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms Shiuan-Li
Case Reports in Pathology Volume 2015, Article ID 153932, 5 pages http://dx.doi.org/10.1155/2015/153932 Case Report Tumor-to-Tumor Metastasis: Lung Carcinoma Metastasizing to Thyroid Neoplasms Shiuan-Li
STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD
 STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD WHAT DO YOU DO WHEN THIS SHOWS UP IN YOUR OFFICE? besides panicking KEY PRINCIPLE!!! Reactive zone is the edema, neovascularity and inflammation
STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD WHAT DO YOU DO WHEN THIS SHOWS UP IN YOUR OFFICE? besides panicking KEY PRINCIPLE!!! Reactive zone is the edema, neovascularity and inflammation
Contrast with Australian Guidelines A/Pr Pascale Guitera,
 Contrast with Australian Guidelines A/Pr Pascale Guitera, Dermatologist, Sydney University NO CONFLICT OF INTEREST Sydney Melanoma Diagnostic Centre, RPAH 2011 2008 225 pages 16 pages http://www.cancer.org.au/file/healthprofessionals/clinica
Contrast with Australian Guidelines A/Pr Pascale Guitera, Dermatologist, Sydney University NO CONFLICT OF INTEREST Sydney Melanoma Diagnostic Centre, RPAH 2011 2008 225 pages 16 pages http://www.cancer.org.au/file/healthprofessionals/clinica
David B. Troxel, MD. Common Medicolegal Situations: Misdiagnosis of Melanoma
 Common Medicolegal Situations: Misdiagnosis of Melanoma David B. Troxel, MD Medical Director, The Doctors Company, Napa, California Clinical Professor Emeritus, University of California at Berkeley Past
Common Medicolegal Situations: Misdiagnosis of Melanoma David B. Troxel, MD Medical Director, The Doctors Company, Napa, California Clinical Professor Emeritus, University of California at Berkeley Past
Springer Healthcare. Staging and Diagnosing Cutaneous Melanoma. Concise Reference. Dirk Schadendorf, Corinna Kochs, Elisabeth Livingstone
 Concise Reference Staging and Diagnosing Cutaneous Melanoma Dirk Schadendorf, Corinna Kochs, Elisabeth Livingstone Extracted from Handbook of Cutaneous Melanoma: A Guide to Diagnosis and Treatment Published
Concise Reference Staging and Diagnosing Cutaneous Melanoma Dirk Schadendorf, Corinna Kochs, Elisabeth Livingstone Extracted from Handbook of Cutaneous Melanoma: A Guide to Diagnosis and Treatment Published
Epidemiology. Objectives 8/28/2017
 Case based Discussion of Head and Neck Melanoma: Review of Epidemiology, Risk Factors, Identification, Treatments and Prevention Jacqueline M. Doucette MS FNP-C Objectives Define and identify melanoma
Case based Discussion of Head and Neck Melanoma: Review of Epidemiology, Risk Factors, Identification, Treatments and Prevention Jacqueline M. Doucette MS FNP-C Objectives Define and identify melanoma
Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology
 Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology Outline Germline testing CDKN2A BRCA2 BAP1 Somatic testing Gene expression profiling (GEP) BRAF Germline vs Somatic testing
Genetic Testing: When should it be ordered? Julie Schloemer, MD Dermatology Outline Germline testing CDKN2A BRCA2 BAP1 Somatic testing Gene expression profiling (GEP) BRAF Germline vs Somatic testing
Case Report Micromelanomas: A Review of Melanomas 2mmand a Case Report
 Case Reports in Oncological Medicine, Article ID 206260, 4 pages http://dx.doi.org/10.1155/2014/206260 Case Report Micromelanomas: A Review of Melanomas 2mmand a Case Report Sharad P. Paul 1,2,3 1 Skin
Case Reports in Oncological Medicine, Article ID 206260, 4 pages http://dx.doi.org/10.1155/2014/206260 Case Report Micromelanomas: A Review of Melanomas 2mmand a Case Report Sharad P. Paul 1,2,3 1 Skin
Perineural Tumor Spread. In Head & Neck Cancer
 Head and Neck Imaging Conference University of Perineural Tumor Spread In Head & Neck Cancer Philip Chapman MD University of Alabama, Birmingham OBJECTIVES: 1. Define (PNTS) 2. Distinguish from pathologic
Head and Neck Imaging Conference University of Perineural Tumor Spread In Head & Neck Cancer Philip Chapman MD University of Alabama, Birmingham OBJECTIVES: 1. Define (PNTS) 2. Distinguish from pathologic
Mandana Moosavi 1 and Stuart Kreisman Background
 Case Reports in Endocrinology Volume 2016, Article ID 6471081, 4 pages http://dx.doi.org/10.1155/2016/6471081 Case Report A Case Report of Dramatically Increased Thyroglobulin after Lymph Node Biopsy in
Case Reports in Endocrinology Volume 2016, Article ID 6471081, 4 pages http://dx.doi.org/10.1155/2016/6471081 Case Report A Case Report of Dramatically Increased Thyroglobulin after Lymph Node Biopsy in
Skin Cancer. 5 Warning Signs. American Osteopathic College of Occupational and Preventive Medicine OMED 2012, San Diego, Monday, October 8, 2012 C-1
 Skin Cancer AMERICAN OSTEOPATHIC COLLEGE OF OCCUPATIONAL & PREVENTIVE MEDICINE OMED 2012 October 8, 2012 E. Robert Wanat II, D.O., M.P.H. Learning Objectives: Identify the 3 Basic Types of Skin Cancer
Skin Cancer AMERICAN OSTEOPATHIC COLLEGE OF OCCUPATIONAL & PREVENTIVE MEDICINE OMED 2012 October 8, 2012 E. Robert Wanat II, D.O., M.P.H. Learning Objectives: Identify the 3 Basic Types of Skin Cancer
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Malignant melanoma: assessment and management of malignant melanoma 1.1 Short title Malignant Melanoma 2 The remit The Department
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Malignant melanoma: assessment and management of malignant melanoma 1.1 Short title Malignant Melanoma 2 The remit The Department
ANNEX 1 OBJECTIVES. At the completion of the training period, the fellow should be able to:
 1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
Financial disclosures
 Mesenchymal Neoplasms with Melanocytic Differentiation By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchcock Medical Center Geisel
Mesenchymal Neoplasms with Melanocytic Differentiation By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchcock Medical Center Geisel
Selected Pseudomalignant Soft Tissue Tumors of the Skin and Subcutis
 Selected Pseudomalignant Soft Tissue Tumors of the Skin and Subcutis Andrew L. Folpe, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic, Rochester, MN folpe.andrew@mayo.edu 2016 MFMER slide-1
Selected Pseudomalignant Soft Tissue Tumors of the Skin and Subcutis Andrew L. Folpe, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic, Rochester, MN folpe.andrew@mayo.edu 2016 MFMER slide-1
Invasive Papillary Breast Carcinoma
 410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
Melanoma Quality Reporting
 Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Primary Mucosal Desmoplastic Melanoma of Gingiva
 The Korean Journal of Pathology 2006; 40: 456-60 Primary Mucosal Desmoplastic Melanoma of Gingiva - A Case Report - Gawon Choi Jeong Won Kim Soon Yuhl Nam 1 Kyung-Ja Cho Departments of Pathology and 1
The Korean Journal of Pathology 2006; 40: 456-60 Primary Mucosal Desmoplastic Melanoma of Gingiva - A Case Report - Gawon Choi Jeong Won Kim Soon Yuhl Nam 1 Kyung-Ja Cho Departments of Pathology and 1
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Catholic University of Louvain, St - Luc University Hospital Head and Neck Oncology Programme. Anatomopathology. Pathology 1 Sept.
 Anatomopathology Pathology 1 Anatomopathology Biopsies Frozen section Surgical specimen Peculiarities for various tumor site References Pathology 2 Biopsies Minimum data, which should be given by the pathologist
Anatomopathology Pathology 1 Anatomopathology Biopsies Frozen section Surgical specimen Peculiarities for various tumor site References Pathology 2 Biopsies Minimum data, which should be given by the pathologist
Case Scenario 1 History and Physical 3/15/13 Imaging Pathology
 Case Scenario 1 History and Physical 3/15/13 The patient is an 84 year old white female who presented with an abnormal mammogram. The patient has a five year history of refractory anemia with ringed sideroblasts
Case Scenario 1 History and Physical 3/15/13 The patient is an 84 year old white female who presented with an abnormal mammogram. The patient has a five year history of refractory anemia with ringed sideroblasts
Multidisciplinary management of retroperitoneal sarcomas
 Multidisciplinary management of retroperitoneal sarcomas Eric K. Nakakura, MD UCSF Department of Surgery UCSF Comprehensive Cancer Center San Francisco, CA 7 th Annual Clinical Cancer Update North Lake
Multidisciplinary management of retroperitoneal sarcomas Eric K. Nakakura, MD UCSF Department of Surgery UCSF Comprehensive Cancer Center San Francisco, CA 7 th Annual Clinical Cancer Update North Lake
Update on Sarcomas of the Head and Neck. Kevin Harrington
 Update on Sarcomas of the Head and Neck Kevin Harrington Overview Classification and incidence of sarcomas Clinical presentation Challenges to treatment Management approaches Prognostic factors Radiation-induced
Update on Sarcomas of the Head and Neck Kevin Harrington Overview Classification and incidence of sarcomas Clinical presentation Challenges to treatment Management approaches Prognostic factors Radiation-induced
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Modalities of Radiation
 Modalities of Radiation Superficial radiotherapy Orthovoltage Megavoltage Photons Electrons Brachytherapy Interstitial Moulds When to refer? The vast majority of skin cancers will be managed without any
Modalities of Radiation Superficial radiotherapy Orthovoltage Megavoltage Photons Electrons Brachytherapy Interstitial Moulds When to refer? The vast majority of skin cancers will be managed without any
Management of the patient with Lymph Node Involvement. Michael A Henderson Peter MacCallum Cancer Center Univ of Melbourne
 Management of the patient with Lymph Node Involvement Michael A Henderson Peter MacCallum Cancer Center Univ of Melbourne Lymph Node Field Recurrence Most important prognostic factor for early stage melanoma
Management of the patient with Lymph Node Involvement Michael A Henderson Peter MacCallum Cancer Center Univ of Melbourne Lymph Node Field Recurrence Most important prognostic factor for early stage melanoma
Case Report A Case of Cystic Basal Cell Carcinoma Which Shows a Homogenous Blue/Black Area under Dermatoscopy
 Volume 20, Article ID 450472, 4 pages doi:0.55/20/450472 Case Report A Case of Cystic Basal Cell Carcinoma Which Shows a Homogenous Blue/Black Area under Dermatoscopy Akihiro Yoneta, Kohei Horimoto, Keiko
Volume 20, Article ID 450472, 4 pages doi:0.55/20/450472 Case Report A Case of Cystic Basal Cell Carcinoma Which Shows a Homogenous Blue/Black Area under Dermatoscopy Akihiro Yoneta, Kohei Horimoto, Keiko
Case Report Two Cases of Small Cell Cancer of the Maxillary Sinus Treated with Cisplatin plus Irinotecan and Radiotherapy
 Case Reports in Otolaryngology Volume 2013, Article ID 893638, 4 pages http://dx.doi.org/10.1155/2013/893638 Case Report Two Cases of Small Cell Cancer of the Maxillary Sinus Treated with Cisplatin plus
Case Reports in Otolaryngology Volume 2013, Article ID 893638, 4 pages http://dx.doi.org/10.1155/2013/893638 Case Report Two Cases of Small Cell Cancer of the Maxillary Sinus Treated with Cisplatin plus
The Relevance of Cytologic Atypia in Cutaneous Neural Tumors
 The Relevance of Cytologic Atypia in Cutaneous Neural Tumors Recent Findings - New Developments New Problems Zsolt B. Argenyi, M.D. Professor of Pathology & Dermatology Director of Dermatopathology Department
The Relevance of Cytologic Atypia in Cutaneous Neural Tumors Recent Findings - New Developments New Problems Zsolt B. Argenyi, M.D. Professor of Pathology & Dermatology Director of Dermatopathology Department
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Identifying Skin Cancer. Mary S. Stone MD Professor of Dermatology and Pathology University of Iowa Carver College of Medicine March, 2018
 Identifying Skin Cancer Mary S. Stone MD Professor of Dermatology and Pathology University of Iowa Carver College of Medicine March, 2018 American Cancer Society web site Skin Cancer Melanoma Non-Melanoma
Identifying Skin Cancer Mary S. Stone MD Professor of Dermatology and Pathology University of Iowa Carver College of Medicine March, 2018 American Cancer Society web site Skin Cancer Melanoma Non-Melanoma
ORAL MELANOMA Definition Epidemiology Clinical Presentation
 ORAL MELANOMA Definition Melanoma is a highly malignant neoplasia, arising from melanocytes, the cells that produce the brownish pigment melanin. Melanin is the determinant in skin colour and protects
ORAL MELANOMA Definition Melanoma is a highly malignant neoplasia, arising from melanocytes, the cells that produce the brownish pigment melanin. Melanin is the determinant in skin colour and protects
Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma of Thyroid
 Case Reports in Urology Volume 2013, Article ID 651081, 4 pages http://dx.doi.org/10.1155/2013/651081 Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma
Case Reports in Urology Volume 2013, Article ID 651081, 4 pages http://dx.doi.org/10.1155/2013/651081 Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma
Melanoma Update: 8th Edition of AJCC Staging System
 Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Melanoma Update: 8th Edition of AJCC Staging System Rosalie Elenitsas, M.D. Professor of Dermatology Director, Dermatopathology University of Pennsylvania DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY None
Dermatopathology: The tumor is composed of keratinocytes which show atypia, increase mitoses and abnormal mitoses.
 Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Squamous cell carcinoma (SCC): A common malignant tumor of keratinocytes arising in the epidermis, usually from a precancerous condition: 1- UV induced actinic keratosis, usually of low grade malignancy.
Disclosures. SLNB for Melanoma 25/02/2014 SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION
 8 th Canadian Melanoma Conference February 22, 2014 Rimrock Resort Hotel, Banff, Alberta SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION Christopher Bichakjian,
8 th Canadian Melanoma Conference February 22, 2014 Rimrock Resort Hotel, Banff, Alberta SENTINEL LYMPH NODE BIOPSY FOR MELANOMA: CURRENT GUIDELINES AND THEIR CLINICAL APPLICATION Christopher Bichakjian,
Michael T. Tetzlaff MD, PhD
 Update on American Joint Cancer Committee (AJCC) staging system for primary cutaneous melanoma Emphasis on concise and accurate reporting of primary and metastatic melanoma for effective risk stratification
Update on American Joint Cancer Committee (AJCC) staging system for primary cutaneous melanoma Emphasis on concise and accurate reporting of primary and metastatic melanoma for effective risk stratification
Index. Note: Page numbers of article titles are in boldface type. A Age as factor in melanoma, Anorectal melanoma RT for, 1035
 Index Note: Page numbers of article titles are in boldface type. A Age as factor in melanoma, 947 948 Anorectal melanoma RT for, 1035 B Bacille Calmette-Guerin (BCG) in melanoma, 1008 BCG. See Bacille
Index Note: Page numbers of article titles are in boldface type. A Age as factor in melanoma, 947 948 Anorectal melanoma RT for, 1035 B Bacille Calmette-Guerin (BCG) in melanoma, 1008 BCG. See Bacille
Directly Coded Summary Stage Melanoma
 Directly Coded Summary Stage Melanoma National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention and Control, National Program of Cancer Registries Directly Coded
Directly Coded Summary Stage Melanoma National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention and Control, National Program of Cancer Registries Directly Coded
Pathology of the skin. 2nd Department of Pathology, Semmelweis University
 Pathology of the skin 2nd Department of Pathology, Semmelweis University Histology of the skin Epidermis: Stratum corneum Stratum granulosum Stratum spinosum Stratum basale Dermis: papillary and reticular
Pathology of the skin 2nd Department of Pathology, Semmelweis University Histology of the skin Epidermis: Stratum corneum Stratum granulosum Stratum spinosum Stratum basale Dermis: papillary and reticular
Original Articles Primary orbital melanoma in association with cellular blue nevus
 Original Articles Primary orbital melanoma in association with cellular blue nevus Tarek El-Sawy, MD, PhD, a Mathieu F. Bakhoum, PhD, a Michael Tetzlaff, MD, PhD, b Qasiem J. Nasser, MD, a Victor G. Prieto,
Original Articles Primary orbital melanoma in association with cellular blue nevus Tarek El-Sawy, MD, PhD, a Mathieu F. Bakhoum, PhD, a Michael Tetzlaff, MD, PhD, b Qasiem J. Nasser, MD, a Victor G. Prieto,
Evening Specialty Conference Bone and Soft Tissue Pathology. Diagnostic pitfalls in bone and soft tissue pathology
 Evening Specialty Conference Bone and Soft Tissue Pathology. Case 1 Elizabeth G Demicco, MD, PhD Mount Sinai Hospital, New York Disclosure of Relevant Financial Relationships USCAP requires that all planners
Evening Specialty Conference Bone and Soft Tissue Pathology. Case 1 Elizabeth G Demicco, MD, PhD Mount Sinai Hospital, New York Disclosure of Relevant Financial Relationships USCAP requires that all planners
Case Report Long Term Survival and Continued Complete Response of Vemurafenib in a Metastatic Melanoma Patient with BRAF V600K Mutation
 Case Reports in Oncological Medicine Volume 2016, Article ID 2672671, 4 pages http://dx.doi.org/10.1155/2016/2672671 Case Report Long Term Survival and Continued Complete Response of Vemurafenib in a Metastatic
Case Reports in Oncological Medicine Volume 2016, Article ID 2672671, 4 pages http://dx.doi.org/10.1155/2016/2672671 Case Report Long Term Survival and Continued Complete Response of Vemurafenib in a Metastatic
Amelanotic melanoma of the skin detailed review of the problem
 of the skin detailed review of the problem Strahil Strashilov 1, Veselin Kirov 2, Angel Yordanov 3, Yoana Simeonova 4 and Miroslava Mihailova 5 1. Department of Plastic Restorative, Reconstructive and
of the skin detailed review of the problem Strahil Strashilov 1, Veselin Kirov 2, Angel Yordanov 3, Yoana Simeonova 4 and Miroslava Mihailova 5 1. Department of Plastic Restorative, Reconstructive and
Living Beyond Cancer Skin Cancer Detection and Prevention
 Living Beyond Cancer Skin Cancer Detection and Prevention Cutaneous Skin Cancers Identification Diagnosis Treatment options Prevention What is the most common cancer in people? What is the most common
Living Beyond Cancer Skin Cancer Detection and Prevention Cutaneous Skin Cancers Identification Diagnosis Treatment options Prevention What is the most common cancer in people? What is the most common
Skin Malignancies Non - Melanoma & Melanoma Marilyn Ng, MD Dept. of Surgery M&M Conference Downstate Medical Center July 19, 2012
 Skin Malignancies Non - Melanoma & Melanoma Marilyn Ng, MD Dept. of Surgery M&M Conference Downstate Medical Center July 19, 2012 Case Presentation 57 yo man with 3 month hx of a nonhealing < 1 cm right
Skin Malignancies Non - Melanoma & Melanoma Marilyn Ng, MD Dept. of Surgery M&M Conference Downstate Medical Center July 19, 2012 Case Presentation 57 yo man with 3 month hx of a nonhealing < 1 cm right
NAACCR Webinar Series 1
 Collecting Cancer Data: Melanoma 2013 2014 NAACCR Webinar Series April 3, 2014 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
Collecting Cancer Data: Melanoma 2013 2014 NAACCR Webinar Series April 3, 2014 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
Basement membrane in lobule.
 Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Management of Neck Metastasis from Unknown Primary
 Management of Neck Metastasis from Unknown Primary.. Definition Histologic evidence of malignancy in the cervical lymph node (s) with no apparent primary site of original tumour Diagnosis after a thorough
Management of Neck Metastasis from Unknown Primary.. Definition Histologic evidence of malignancy in the cervical lymph node (s) with no apparent primary site of original tumour Diagnosis after a thorough
Update on Cutaneous Mesenchymal Tumors. Thomas Brenn
 Update on Cutaneous Mesenchymal Tumors Thomas Brenn Cutaneous Mesenchymal Tumours Wide morphological and biological spectrum Myofibroblastic, smooth muscle, neural, vascular, apidocytic, undifferentiated;
Update on Cutaneous Mesenchymal Tumors Thomas Brenn Cutaneous Mesenchymal Tumours Wide morphological and biological spectrum Myofibroblastic, smooth muscle, neural, vascular, apidocytic, undifferentiated;
