Volume 20 Number 5 are radiolucent and their eventual distribution is only inferred from the preprocedural imaging. Hepaticoenteric anastomoses are pr
|
|
|
- Bruce Morrison
- 6 years ago
- Views:
Transcription
1 Incorporating Cone-beam CT into the Treatment Planning for Yttrium-90 Radioembolization John D. Louie, MD, Nishita Kothary, MD, William T. Kuo, MD, Gloria L. Hwang, MD, Lawrence V. Hofmann, MD, Michael L. Goris, MD, Andrei H. Iagaru, MD, and Daniel Y. Sze, MD, PhD PURPOSE: To prepare for yttrium-90 (90Y) microsphere radioembolization therapy, digital subtraction angiography (DSA) and technetium- 99m labeled macroaggregated albumin (99mTc MAA) scintigraphy are used for treatment planning and detection of potential nontarget embolization. The present study was performed to determine if cone-beam computed tomography (CBCT) affects treatment planning as an adjunct to these conventional imaging modalities. MATERIALS AND METHODS: From March 2007 to August 2008, 42 consecutive patients (21 men, 21 women; mean age, 59 years; range, y) who underwent radioembolization were evaluated by CBCT in addition to DSA and 99m Tc MAA scintigraphy during treatment planning, and their records were retrospectively reviewed. The contrastenhanced territories shown by CBCT with selective intraarterial contrast agent administration were used to predict intrahepatic and possible extrahepatic distribution of microspheres. RESULTS: In 22 of 42 cases (52%), extrahepatic enhancement or incomplete tumor perfusion seen on CBCT affected the treatment plan. In 14 patients (33%), the findings were evident exclusively on CBCT and not detected by DSA. When comparing CBCT versus 99mTc MAA scintigraphy, CBCT showed eight cases of extrahepatic enhancement (19%) that were not evident on 99mTc MAA imaging. CBCT findings directed the additional embolization of vessels or repositioning of the catheter for better contrast agent and microsphere distribution. One case of gastric ulcer from nontarget embolization caused by reader error was observed. CONCLUSIONS: CBCT can provide additional information about tumor and tissue perfusion not currently detectable by DSA or 99mTc MAA imaging, which should optimize 90Y microsphere delivery and reduce nontarget embolization. J Vasc Interv Radiol 2009; 20: Abbreviations: CBCT cone-beam CT, DSA digital subtraction angiography, GDA gastroduodenal, gated albumin, RGA right gastric CONE-beam computed tomography (CBCT), which produces CT-like images in an angiography suite, is un- From the Division of Vascular and Interventional Radiology, Department of Radiology, Stanford University Medical Center, 300 Pasteur Drive, H-3630, Stanford, CA Received September 8, 2008; final revision received January 7, 2009; accepted January 9, Address correspondence to J.D.L.; jdlouie@stanford.edu N.K. and L.V.H. have received research grants from Siemens (Erlangen, Germany); D.Y.S. serves as a paid consultant to MediGene (San Diego, California), Pain Therapeutics (San Francisco, California), and Jennerex Biotherapeutics (San Francisco, California). None of the other authors have identified a conflict of interest. SIR, 2009 DOI: /j.jvir dergoing rapidly increasing use in the field of interventional radiology. Early case reports indicated the usefulness of CBCT in difficult neurovascular interventions, transjugular intrahepatic portosystemic shunt creation, endoleak repair, splenic embolization, and hepatic malignancy treatment (1 3). An interesting offshoot of modern flat-panel fluoroscopy technology, CBCT has been shown to provide anatomic information in addition to that detected by digital subtraction angiography (DSA) during hepatic arterial interventions, and this information can impact patient management in 19% of hepatic malignancy treatments (4). For transarterial chemoembolization, 99m Tc MAA technetium-99m-macroaggre- CBCT has improved catheter placement planning and diagnostic confidence in the selected catheter position for more selective chemotherapy infusion (5,6). These benefits of applying CBCT technology to chemoembolization may have even greater impact on patients undergoing radioembolization. Before radioembolization, meticulous planning with DSA and technetium- 99m labeled macroaggregated albumin (99mTc MAA) scintigraphy needs to be performed to avoid nontarget embolization and to ensure adequate delivery of microspheres to all the tumors. This attention to the vascular anatomy is important, because the microspheres themselves
2 Volume 20 Number 5 are radiolucent and their eventual distribution is only inferred from the preprocedural imaging. Hepaticoenteric anastomoses are preemptively coil-embolized to prevent nontarget embolization, which could otherwise produce severe gastrointestinal complications (7). In a recent review of the literature, the median rate of ulceration was 8%, with 6% requiring surgical intervention (8). The spatial resolution and three-dimensional dataset produced by CBCT could theoretically supplement the traditional tools of DSA and 99mTc MAA scintigraphy to prevent extrahepatic 90 Y microsphere deposition and to predict which tissues will be affected. This study examines whether CBCT changes the treatment planning for radioembolization, and whether its routine use is warranted. MATERIALS AND METHODS Between March 2007 and August 2008, 42 consecutive patients (21 men, 21 women; mean age, 59 years; age range, y) who underwent preprocedural CBCT evaluation for radioembolization of hepatic-dominant malignancies were included in this retrospective study. The underlying primary tumors, in descending order of frequency, included colon, neuroendocrine, melanoma, cholangiocarcinoma, lung, hepatocellular, ovarian, pancreatic, granulosa cell, sarcoma, bladder, ampullary, hemangiopericytoma, endometrial, breast, leiomyosarcoma, and adenocarcinoma of unknown primary lesion. Selection criteria were based on multidisciplinary consensus panel report from the radioembolization brachytherapy oncology consortium (9). Data were handled in accordance with Health Insurance Portability and Accountability Act regulations, and the study was granted an exemption from obtaining patient consent by our institutional review board. The radioembolization process was divided into two outpatient sessions, performed 1 2 weeks apart. During the first session, the patients underwent hepatic DSA imaging and coil embolizations to close natural hepaticoenteric anastomoses and accessory arteries, such as the gastroduodenal (GDA), right gastric (RGA), supraduodenal, falciform, Louie et al and accessory phrenic. During the initial vascular mapping, DSA images were obtained with a 5-F catheter placed at the common or proper hepatic, injecting contrast medium (Visipaque 320; GE Healthcare, Princeton, New Jersey) at 3 5 ml/sec for 2 4 seconds. Superselective DSA images were obtained with microcatheters and hand injections in vessels that potentially needed embolization. CBCT was used as an adjunct to DSA as a problemsolving tool when tissue perfusion or vascular anatomy was unclear. In addition, at the conclusion of each angiographic session, CBCT was performed to delineate the vascular territory served by the planned catheter placement, and therefore to predict distribution of the microspheres. The microcatheter was placed in the anticipated microsphere implantation vessel, which was the common or proper for whole-liver treatment. More selective lobar treatment required the microcatheter to be placed in the right or left. Anatomic variants, such as a replaced right, would also be evaluated with CBCT if it was the planned delivery vessel or if there was uncertainty of tumor perfusion. If there was a particular of uncertain tissue perfusion, CBCT images were obtained with superselective injection in the questionable. To ensure no contrast agent reflux, which would yield erroneous findings, the CBCT injection rates were approximately half the DSA injection rates. In addition, all the raw images from the CBCT acquisition were inspected for reflux. After CBCT, the patients underwent 99mTc MAA arterial administration and planar and single-photon emission CT scintigraphy to measure the proportion shunted into the lungs and to evaluate for any extrahepatic deposition. During the second session of the radioembolization process, the patients underwent confirmatory DSA and CBCT studies to evaluate for any interim changes in perfusion before administration of the 90Y resin microspheres (SIR-Spheres; Sirtex Medical, Sydney, Australia). If any extrahepatic perfusion was detected on the 99mTc MAA scintigraphy or on the current DSA or CBCT, additional coil embolization or catheter reposition was performed until CBCT showed no evidence of persistent extrahepatic enhancement. 607 Yttrium-90 resin microspheres were then administered as described in detail elsewhere, including a multidisciplinary consensus report (7,9). The prescribed activity calculation was based on the consensus recommendation of the body surface area method, which has a favorable toxicity profile and similar response and survival outcomes as the empiric method. In the dose calculations for 90Y resin microspheres, exact volume measurements are not required, unlike for glass microspheres. However, the percentage of perfused liver in relation to the whole liver as seen on CBCT was used in the calculation of the delivery dose, especially in cases of partial liver radioembolization. No dose adjustment was made for catheter repositions, although there was a risk of reflux, especially for resin microspheres. If nearstasis of forward blood flow was observed during implantation, the entire dose was not delivered to prevent reflux. After delivery of the microspheres, patients were discharged the same day with a 10-day oral methylprednisolone taper regimen, 30-day course of proton pump inhibitor, and analgesic and antiemetic agents as needed. Patients were seen in clinic 1 month after radioembolization and followed for at least 3 months to monitor for possible complications. DSA and CBCT images were obtained with use of a ceiling mounted angiographic C-arm system with 30cm 40-cm flat-panel detector (Axiom Artis dta; Siemens, Erlangen, Germany). Patients were positioned with arms abducted, and extraneous metallic objects such as oxygen saturation and cardiac monitoring leads and cables were kept out of the field. The CBCT images (ie, DynaCT) were obtained by rotating the C-arm 200 around the patient in 8 seconds. The detector acquired images every 0.5 for a total of 419 images. Contrast medium (Visipaque 320; GE Healthcare) was diluted 1:1 with normal saline solution and injected at approximately half the rate of a DSA run, from 0.1 to 4 ml/sec depending on the size of the, rate of flow, and type of microcatheter. For all CBCT studies, a 4-second imaging delay was prescribed to allow injected contrast medium to enhance parenchymal tissue before data acquisition, and contrast medium was injected throughout the data acquisition period to keep the arterial tree enhanced. The 4-second imaging
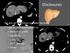
3 608 Cone-beam CT in Treatment Planning for 90 Y Radioembolization May 2009 JVIR delay, combined with the 8-second acquisition period, made the total injection time 12 seconds. The volumetric data set was transferred to a separate postprocessing workstation (Syngo-X; Siemens) for three-dimensional reconstruction. Image correction algorithms were applied for scatter, beam hardening, ring artifact, and truncation. The CT-type dataset was viewed as three-dimensional and multiplanar reconstructed images. The DSA, 99mTc MAA scintigraphy, and CBCT studies were retrospectively evaluated to determine whether CBCT changed the treatment plan for radioembolization. Specifically, additional embolization of hepaticoenteric anastomoses, embolization of accessory hepatic arteries, embolization of parasitized nonhepatic arteries, and changes in planned positioning of the microcatheter at the time of 90Y resin microsphere administration were tallied. RESULTS A total of 132 CBCT acquisitions were obtained in 42 patients, for an average of 3.1 studies per patient (range, 1 7 studies), during 91 outpatient sessions. In this group, 30 patients (71%) received single-session whole-liver treatment, 10 (24%) received partial liver treatment, and two (5%) did not receive treatment as a result of worsening liver function. In 22 of 42 patients (52%), findings of extrahepatic enhancement (n 18; 43%), incomplete perfusion of the tumor (n 8; 19%), or both (n 4; 10%) affected the treatment plan. Extrahepatic enhancement most often involved stomach, duodenum, or pancreas (Figs 1,2). Incomplete perfusion of the tumors was most often a result of previously unrecognized accessory hepatic arteries or parasitized extrahepatic arteries (Fig 3). Embolization of these unrecognized vessels redirects the blood flow away from the accessory and extrahepatic vessels to the in which the microspheres are injected, as evidenced by altered contrast enhancement, leading to presumed deposition of microspheres into areas of tumor. Of the 22 cases in which CBCT affected the treatment plan, 14 patients (33%) had unexpected CBCT findings that actually resulted in real change of the treatment plan. Additional embolization was performed in eight patients, catheter position was moved in four patients, and Figure 1. Images from a 59-year-old man with bilobar hepatocellular carcinoma, previously treated with hepatic resection and multiple chemoembolizations, who presented for radioembolization. (a) angiogram shows stasis of flow to the coil-embolized GDA. Embolization coils were placed in the accessory left and a branch of the left gastric, and the arteries to segments 2 and 3 were now filled through collateral circulation from segment 4. No remaining hepaticoenteric anastomoses were identified by DSA. (b) Arterial contrast-enhanced CBCT from the same catheter location showed enhancement in the posterior gastric antrum (arrow) that was not detected by DSA. Extensive beam-hardening artifacts were also seen from the radiopaque coils and catheters, partially obscuring the gastric parenchyma. (c) The origin of the RGA could not be identified by DSA despite angiography in multiple obliquities. As a result, the left gastric was selected and coils were deposited at the origin of the RGA (arrow) via the left-to-right gastric anastomosis. (d) Follow-up contrast-enhanced CBCT showed no residual enhancement in the gastric wall (arrow) after the coil placement. Note linear beam-hardening streak artifacts extending through the anterior and posterior gastric walls. both were performed in two patients (Table 1). These unexpected findings of potential nontarget embolization or incomplete inclusion of the treatment area were not demonstrated by DSA or 99mTc MAA imaging, even in retrospect. In the other eight cases (19%), the CBCT findings were also detected on DSA, but identification of the end organ perfused was equivocal (Table 2). CBCT allowed the operator to confirm hepatic or nonhepatic tissue enhancement, and therefore embolize vessels or reposition catheters with greater confidence (Fig 4). When comparing CBCT versus 99mTc MAA single-photon emission CT studies during the same treatment period, CBCT showed nine cases of extrahepatic enhancement, of which only one was detected by 99mTc MAA scintigraphy. Scintigraphy failed to identify the other eight as a result of limitations in spatial resolution. During the 3-month follow-up of the patients, one case of nontarget radioembolization induced gastric ulcer was seen with endoscopic biopsy confirmation. On retrospective review of the CBCT images, enhancement of the gastric wall was identified, probably
4 Volume 20 Number 5 Louie et al 609 Figure 2. Images from a 57-year-old woman with chemotherapy-refractory lung metastases to both lobes of the liver who presented for radioembolization. (a) hepatic arteriogram shows no flow into the GDA and RGA after coil embolization and no extrahepatic enhancement. (b) Contrast-enhanced CBCT shows enhancement in the duodenum and pancreatic head (arrow) that was not seen on DSA. This was treated by repositioning the microcatheter more distally into the liver and sequentially delivering the microspheres into the right and left hepatic arteries. CBCT in each hepatic vessel confirmed absence of the duodenal and pancreatic enhancement before radioembolization. supplied by a collateral vessel feeding the coil-embolized RGA. This enhancement, partly obscured by beamhardening artifact, was missed by the authors at the time of the CBCT study. However, in retrospect, CBCT accurately portrayed the nontarget perfusion of the stomach in this single case of a complication. DISCUSSION CBCT provides three-dimensional data and higher sensitivity to x-ray attenuation compared with DSA, and has superior spatial resolution to 99mTc MAA scintigraphy. DSA shows intraluminal enhancement of arteries with superior spatial and temporal resolution, but territorial parenchymal perfusion is limited by the projectional nature of the technology. In contrast, CBCT is able to delineate territorial tissue perfusion in three dimensions, with an attenuation resolution of approximately 10 HU. The clinical impact of these capabilities is only just being explored. We found that these theoretical advantages translate into real changes in patient care in a high proportion of patients undergoing radioembolization. In 33% of the cases, CBCT showed the po- tential for hazardous nontarget embolization and/or incomplete tumor perfusion that conventional DSA was unable to portray. Delivery of the 90Y microspheres without recognizing these vascular patterns could have led to ulcers or pancreatitis, or to incomplete tumor treatment (10). The CBCT information prompted additional embolizations and catheter repositions that would not have occurred with DSA alone. CBCT helps optimize catheter placement to maximize the number of treated tumors while minimizing the risk for nontarget embolization. Although routine selective radioembolization would reduce nontarget embolization, most patients have multifocal disease in most segments of the liver, which requires a more central injection to treat all tumors. Whole-liver treatment, which was performed in 71% of the patients in the present series, is more likely to benefit from CBCT because of the more proximal point of delivery. The utility of increased sensitivity to tissue perfusion was first documented with the use of CBCT for transarterial chemoembolization. Small hepatocellular carcinomas were not well visualized with DSA, but could be identified with CBCT (11). CBCT s ability to recognize subtle tissue perfusion offers potential incremental improvement in the field of radioembolization. Compared with chemoembolization, radioembolization has the common potential of ischemic injury to bowel, but poses the added risk of persistent radiation damage from a fixed radiation source. As a result, there is an inherent higher risk of morbidity from nontarget embolization with 90Y resin microspheres, which can be mitigated with CBCT. In addition, contrastenhanced CBCT with contrast medium injected at the site of planned microsphere delivery can also reveal territories where radioembolization will be ineffective because unenhanced regions are unlikely to receive microsphere deposition, a finding in 19% of our patients. These unenhanced regions with tumor were often supplied by small accessory hepatic arteries, which were coil-embolized before microsphere administration. The use of two-dimensional projectional DSA to map arterial anatomy may be confusing because of superimpositions. However, as is true of other cross-sectional modalities, CBCT allows for multiplanar reconstructions that enable manipulation of the images to differentiate adjacent or overlapping or-
5 610 Cone-beam CT in Treatment Planning for 90 Y Radioembolization Figure 3. Images from a 44-year-old woman with bilobar colorectal metastases who presented for radioembolization. (a) hepatic arteriogram shows no flow into the GDA, RGA, and falciform after coil embolization, and enhancement of what appeared to be the entire liver. (b) Contrast-enhanced CBCT shows region in segment 6 devoid of enhancement (arrow). (c) A small pancreaticoduodenal branch of the superior mesenteric supplied collateral flow to an accessory right (arrow), which arose from the previously coil-embolized GDA. This collateral branch was not noticed on the original flush aortogram, but with the aid of CBCT the was coil-embolized. (d) Contrast-enhanced CBCT with injection of contrast medium in the common after coil embolization of the collateral vessel showed rerouting of contrast agent to segment 6 (arrow). gans and arteries. For example, parasitized blood supply from the phrenic or intercostal arteries could be clearly shown to supply intrahepatic tumors on CBCT. In addition, parenchymal blushes of gastric, esophageal, pancreatic, or duodenal DSA images in patients with cachexia who have empty gastrointestinal tracts were sometimes difficult to differentiate from enhancement of adjacent liver, particularly if the hepatic enhancement pattern was distorted by tumor involvement. In 19% of our patients, DSA interpretation was equivocal about the identity of the end organs perfused, and CBCT clarified the perfusion question and increased confidence in the treatment plan. Differentiation between adjacent or- gans is an even greater challenge for Tc MAA scintigraphy, even with three-dimensional single-photon emission CT. Although scintigraphy is excellent for lung shunt evaluation, identification of extrahepatic enhancement is extremely limited by poor spatial resolution. In this series, there were nine cases of extrahepatic enhancement, all of which were detected by CBCT. In contrast, the 99mTc MAA scintigraphy studies missed eight of the nine cases that were detected by CBCT. Despite the increased sensitivity to extrahepatic perfusion afforded by CBCT, one patient (2.4%) did have a gastric ulcer from nontarget radioembolization, which was confirmed by endoscopic biopsy. The patient recovered after conservative management with a 99m May 2009 JVIR high-dose pantoprazole and sucralfate. Retrospective review of the DSA and CBCT images showed subtle perfusion of the gastric antrum via a newly appeared collateral vessel from the left, feeding the already coilembolized RGA. This accessory RGA was not recognized prospectively, representing a human error rather than a deficiency of the technology. Because our sample size is small, a larger number of patients will need to be studied to confirm that a significant reduction in the complication rate can be achieved by routine use of CBCT. Although CBCT has the advantage of multiplanar reconstruction and increased sensitivity to attenuation differences, it is subject to serious artifacts. For instance, it is more prone to beamhardening streak artifacts than is conventional CT. These artifacts can be caused by the routine placement of coils adjacent to organs of interest, by the presence of gas within hollow viscera, and by the presence of radiopaque catheters and surgical clips. These artifacts can mimic enhancement of visceral walls. One can usually distinguish between artifact and true enhancement by looking for nonlinear enhancement that does not extend beyond anatomic boundaries. Other potential disadvantages of incorporating routine use of CBCT into the radioembolization protocol include additional contrast medium administered, additional radiation exposure to the patient, additional time expended, and discomfort in patients with limited shoulder range of motion. However, because of the higher sensitivity of CBCT to attenuation differences, the amount of contrast medium used for one CBCT acquisition is actually identical to that used in one DSA acquisition. One CBCT acquisition also results in patient radiation exposure equivalent to only one or two DSA acquisitions. Our institution s equipment is adjusted to acquire DSA images at 3.60 Gy per image and CBCT images at 0.36 Gy per image. For an 8-second rotational scan in which 419 images are acquired, the dosage is equivalent to that of 42 DSA images, or a 10.5-second DSA run at four frames per second. The radiation is distributed over a larger surface area and volume because of the 200 rotation, whereas DSA delivers the radiation more focally. Although the abdomen dosage has not been studied, calculations for CBCT of
6 Volume 20 Number 5 Louie et al Table 1 Unexpected CBCT Findings Not Seen in DSA or Planning before Radioembolization Pt. No. Vessel Injected Replaced proper Replaced right m Extrahepatic Enhancement and duodenum Pancreas and duodenum Omentum, anterior abdominal wall, stomach Pancreas and duodenum Incomplete Hepatic Perfusion Additional Embolizations segment 6 Falciform and accessory right branch of SMA medial aspect of tumor when replaced right injected segments 2 and 3 Duodenum Extrahepatic draining vein Duodenum and esophagus Distally in segment 4a/4b Distally in proper More distally Accessory left RGA part of segment 6 Missing peripheral enhancement in multiple segments Missing peripheral enhancement in multiple segments portions of segments 5 and 6 Reposition of Catheter Middle arising from the celiac axis Hilar lymph nodes and greater omentum 611 Tc MAA Scintigraphy and Corresponding Changes in Treatment More distally Dorsal pancreatic, right T9, T10, T12 intercostal arteries Right inferior phrenic Right inferior phrenic Accessory right branch of SMA More distally to avoid stomach Repositioned for better evaluation Supraduodenal and pancreaticoduodenal arteries Accessory left gastric/esophageal Note.SMA superior mesenteric. Table 2 Equivocal End-organ Perfusion Clarified by CBCT that Led to Corresponding Adjustment of Treatment Plan* Pt. No. Vessel Injected Extrahepatic Enhancement Incomplete Hepatic Perfusion Pancreatic Left Cystic Distal left hepatic RGA hepatic Pancreatic Segmental splenic Pancreas Gallbladder and hilar lymph nodes Left hemidiaphragm Dorsal pancreatic Accessory left gastric Cystic Accessory left phrenic RGA RGA Pancreas Missing perfusion of portions of segments 2 and 3 * No repositioning of the catheter was necessary in any of the cases listed. Additional Embolizations Dorsal pancreatic Parasitized superior branches of splenic supplying left lobe of liver
7 612 Cone-beam CT in Treatment Planning for 90 Y Radioembolization May 2009 JVIR microspheres would travel through collateral vessels to regions previously supplied by the embolized accessory and parasitized arteries. These smaller vessels that supply tumor would otherwise be untreated becasue of the increased risk of reflux. In conclusion, we found CBCT to be a sensitive and useful problem-solving tool when questions of perfusion were raised in patients undergoing radioembolization. Treatment plans were altered in one third of our patients based on findings suggesting potential nontarget embolization or incomplete tumor treatment. Change in catheter placement or additional embolizations were performed in response to the findings, which were generally beneath the threshold of detectability by DSA and by nuclear scintigraphy. Figure 4. (a) Right inferior phrenic arteriogram in a 74-year-old woman with cholangiocarcinoma shows enhancement of the diaphragm, but is equivocal in identifying hepatic enhancement. (b) Contrast-enhanced CBCT in the same patient shows enhancement of a hepatic tumor (arrow) fed by the right phrenic that was difficult to resolve on DSA. (c) Selective distal left hepatic arteriogram in a 44-year-old woman with bilobar colorectal metastases shows a tortuous vessel of uncertain destination (arrow). Coils were already placed in the GDA in this patient, and contrast-enhanced CBCT (d) demonstrated anterior abdominal wall (arrow) and omental enhancement with communication with superior epigastric branches that were not seen on DSA, confirming that this tortuous vessel represented a falciform. the head and neck indicate a reduction in total radiation dose of as much as 90% compared with DSA. The reduction reflects primarily the lower milliamperage and thus the dose per frame (12). The amount of time required to acquire and process CBCT images is also equivalent to that of approximately two to three DSA acquisitions, but the CBCT data acquired may actually supplant the data conventionally obtained from an even greater number of DSA acquisitions, resulting in a net decrease in time and radiation dose. Our study is limited by the noncontrolled retrospective design and its small sample size. We assumed that embolization of parasitized and accessory arteries would consolidate blood flow to all tumors via the main. CBCT showed successful consolidation by complete parenchymal and tumor enhancement during one central contrast agent injection. However, the mean 30- m diameter and specific gravity of 1.6 mg/ml of the 90Y resin microspheres may make them behave differently from the smaller contrast agent molecules as they flow through intrahepatic collateral vessels of unknown size. Therefore, distribution of microspheres may or may not be the same as distribution of contrast medium. Contrast enhancement predicted the pattern of microsphere deposition, but this was not confirmed by explant pathologic examination. Further studies need to be performed to evaluate the assumption that References 1. Heran NS, Song JK, Namba K, Smith W, Niimi Y, Berenstein A. The utility of DynaCT in neuroendovascular procedures. AJNR Am J Neuroradiol 2006; 27: Sze DY, Strobel N, Fahrig R, Moore T, Busque S, Frisoli JK. Transjugular intrahepatic portosystemic shunt creation in a polycystic liver facilitated by hybrid crosssectional/angiographic imaging. J Vasc Interv Radiol 2006; 17: Hirota S, Nakao N, Yamamoto S, et al. Cone-beam CT with flat-detector digital angiography system: early experience in abdominal interventional procedures. Cardiovasc Intervent Radiol 2006; 29: Wallace MJ, Murthy R, Kamat PP, et al. Impact of C-arm CT on hepatic arterial interventions for hepatic malignancies. J Vasc Interv Radiol 2007; 18: Virmani S, Ryu RK, Sato KT, et al. Effect of C-arm angiographic CT on transcatheter arterial chemoembolization of liver tumors. J Vasc Interv Radiol 2007; 18: Liapi E, Hong K, Georgiades CS, Geschwind JFH. Three-dimensional rotational angiography: introduction of an adjunctive tool for successful transarterial chemoembolization. J Vasc Interv Radiol 2005; 16: Murthy R, Nunez R, Szklaruk F, et al. Yttrium-90 microsphere therapy for hepatic malignancy: devices, indications, technical considerations, and potential complications. Radiographics 2005; 25(suppl):S41 S Murthy R, Brown DB, Salem R, et al. Gastrointestinal complications associated with hepatic arterial yttrium-90
8 Volume 20 Number 5 microsphere therapy. J Vasc Interv Radiol 2007; 18: Kennedy A, Nag S, Salem R, et al. Recommendations for radioembolization of hepatic malignancies using yttrium-90 microsphere brachytherapy: a consensus panel report from the radioembolization brachytherapy oncology Louie et al consortium. Int J Radiat Oncol Biol Phys 2007; 68: Liu D, Salem R, Bui JT, et al. Angiographic considerations in patients undergoing liver directed therapy. J Vasc Interv Radiol 2005; 16: Kakeda S, Korogi Y, Ohnari N, et al. Usefulness of cone-beam volume CT 613 with flat panel detectors in conjunction with catheter angiography for transcatheter arterial embolization. J Vasc Interv Radiol 2007; 18: Bridcut RR, Murphy E, Workman A, Flynn P, Winder RJ. Patient dose from 3D rotational neurovascular studies. Br J Radiol 2007; 80:
SELECTIVE INTERNAL RADIATION THERAPY FOR TREATMENT OF LIVER CANCER
 SELECTIVE INTERNAL RADIATION THERAPY FOR TREATMENT OF LIVER CANCER SIR-Spheres*: A New Treatment Option for Non-Resectable Liver Tumors Treatment Overview SIRT: Selective Internal Radiation Therapy Concept
SELECTIVE INTERNAL RADIATION THERAPY FOR TREATMENT OF LIVER CANCER SIR-Spheres*: A New Treatment Option for Non-Resectable Liver Tumors Treatment Overview SIRT: Selective Internal Radiation Therapy Concept
SORAMIC: NM Procedures
 : NM Procedures J. Ruf Klinik für Radiologie und Nuklearmedizin : NM Procedures Evaluation - 99m Tc MAA Scintigraphy Lung shunt assessment Treatment activity determination Therapy - 90 Y-SIR-Spheres Procedure
: NM Procedures J. Ruf Klinik für Radiologie und Nuklearmedizin : NM Procedures Evaluation - 99m Tc MAA Scintigraphy Lung shunt assessment Treatment activity determination Therapy - 90 Y-SIR-Spheres Procedure
The use of minimally invasive procedures to
 Yttrium-90 Radioembolization Mapping and Therapy What to do and what to avoid. BY PAVAN K. KAVALI, MD; RIPAL T. GANDHI, MD; AND SUVRANU GANGULI, MD The use of minimally invasive procedures to manage primary
Yttrium-90 Radioembolization Mapping and Therapy What to do and what to avoid. BY PAVAN K. KAVALI, MD; RIPAL T. GANDHI, MD; AND SUVRANU GANGULI, MD The use of minimally invasive procedures to manage primary
Selective Internal Radiation Therapy. Jefferson R. Pagsisihan, MD, DPSNM The Medical City St. Luke s Medical Center
 Selective Internal Radiation Therapy Jefferson R. Pagsisihan, MD, DPSNM The Medical City St. Luke s Medical Center S Selective Internal Radiation Therapy catheter-based liver directed modality for patients
Selective Internal Radiation Therapy Jefferson R. Pagsisihan, MD, DPSNM The Medical City St. Luke s Medical Center S Selective Internal Radiation Therapy catheter-based liver directed modality for patients
Minimizing Unnecessary Radiation Exposure to Healthcare Professionals and Patients Imagine where we can go.
 ALARA & RADIATION SAFETY Minimizing Unnecessary Radiation Exposure to Healthcare Professionals and Patients Imagine where we can go. What is ALARA? As Low As Reasonably Achievable The use of radiation
ALARA & RADIATION SAFETY Minimizing Unnecessary Radiation Exposure to Healthcare Professionals and Patients Imagine where we can go. What is ALARA? As Low As Reasonably Achievable The use of radiation
The Role of Tumor Vascularity in Predicting Survival after Yttrium-90 Radioembolization for Liver Metastases
 The Role of Tumor Vascularity in Predicting Survival after Yttrium-90 Radioembolization for Liver Metastases Kent T. Sato, MD, Reed A. Omary, MD, Christopher Takehana, MD, Saad Ibrahim, MD, Robert J. Lewandowski,
The Role of Tumor Vascularity in Predicting Survival after Yttrium-90 Radioembolization for Liver Metastases Kent T. Sato, MD, Reed A. Omary, MD, Christopher Takehana, MD, Saad Ibrahim, MD, Robert J. Lewandowski,
Radioembolization of the Liver. Michael Meuse, M.D. Vascular and Interventional Radiology
 Radioembolization of the Liver Michael Meuse, M.D. Vascular and Interventional Radiology Brachytherapy Principle Radiation is accepted as a standard treatment option for liver cancer Radiation will break
Radioembolization of the Liver Michael Meuse, M.D. Vascular and Interventional Radiology Brachytherapy Principle Radiation is accepted as a standard treatment option for liver cancer Radiation will break
HOW I DO IT: SIRT for Hepatocellular Carcinoma
 HOW I DO IT: SIRT for Hepatocellular Carcinoma Philip Chong-hei KWOK Department of Radiology and Imaging Queen Elizabeth Hospital HONG KONG SAR, CHINA Declaration I have no financial interest to declare
HOW I DO IT: SIRT for Hepatocellular Carcinoma Philip Chong-hei KWOK Department of Radiology and Imaging Queen Elizabeth Hospital HONG KONG SAR, CHINA Declaration I have no financial interest to declare
Minimizing Unnecessary Radiation Exposure to Healthcare Professionals and Patients Imagine where we can go.
 ALARA & RADIATION SAFETY Minimizing Unnecessary Radiation Exposure to Healthcare Professionals and Patients Imagine where we can go. What is ALARA? As Low As Reasonably Achievable The use of radiation
ALARA & RADIATION SAFETY Minimizing Unnecessary Radiation Exposure to Healthcare Professionals and Patients Imagine where we can go. What is ALARA? As Low As Reasonably Achievable The use of radiation
Intra-arterial Therapy in Management of HCC: ctace, DEB-TACE, and Y90 Radioembolization
 Intra-arterial Therapy in Management of HCC: ctace, DEB-TACE, and Y90 Radioembolization Department of Radiology, National Cancer Center In Joon Lee Contents Conventional TACE Role of TACE in management
Intra-arterial Therapy in Management of HCC: ctace, DEB-TACE, and Y90 Radioembolization Department of Radiology, National Cancer Center In Joon Lee Contents Conventional TACE Role of TACE in management
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Lung Perfusion Analysis New Pathways in Lung Imaging. Case Study Brochure PLA 309 Hospital
 Lung Perfusion Analysis New Pathways in Lung Imaging Case Study Brochure PLA 309 Hospital http://www.toshibamedicalsystems.com Toshiba Medical Systems Corporation 2012 all rights reserved. Design and specifications
Lung Perfusion Analysis New Pathways in Lung Imaging Case Study Brochure PLA 309 Hospital http://www.toshibamedicalsystems.com Toshiba Medical Systems Corporation 2012 all rights reserved. Design and specifications
TRANSEARTERIAL CHEMO- EMBOLIZATION FOR HEPATIC METASTASES FROM NEURO-ENDOCINE NEOPLASIA AND HEPATOMA DR SAMIA AHMAD
 UNIVERSITY OF PRETORIA STEVE BIKO ACADEMIC HOSPITAL SOUTH AFRICA TRANSEARTERIAL CHEMO- EMBOLIZATION FOR HEPATIC METASTASES FROM NEURO-ENDOCINE NEOPLASIA AND HEPATOMA DR SAMIA AHMAD 1 INTRODUCTION Hepatic
UNIVERSITY OF PRETORIA STEVE BIKO ACADEMIC HOSPITAL SOUTH AFRICA TRANSEARTERIAL CHEMO- EMBOLIZATION FOR HEPATIC METASTASES FROM NEURO-ENDOCINE NEOPLASIA AND HEPATOMA DR SAMIA AHMAD 1 INTRODUCTION Hepatic
COMPARING Y90 DEVICES
 COMPARING Y90 DEVICES William S Rilling MD, FSIR Professor of Radiology and Surgery Director, Vascular and Interventional Radiology Medical College of Wisconsin DISCLOSURES Research support : Siemens,
COMPARING Y90 DEVICES William S Rilling MD, FSIR Professor of Radiology and Surgery Director, Vascular and Interventional Radiology Medical College of Wisconsin DISCLOSURES Research support : Siemens,
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System
 Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Y90 SIRT Therapy Dosimetric Aspects
 Y90 SIRT Therapy Dosimetric Aspects David Chee-Eng Ng MBBS, BSc, MSc, MRCP, FAMS, FRCP (Edin) Head and Senior Consultant, Department of Nuclear Medicine and PET Singapore General Hospital Adjunct Assistant
Y90 SIRT Therapy Dosimetric Aspects David Chee-Eng Ng MBBS, BSc, MSc, MRCP, FAMS, FRCP (Edin) Head and Senior Consultant, Department of Nuclear Medicine and PET Singapore General Hospital Adjunct Assistant
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
SIR 2008 Annual Meeting Film Panel Case: Radiation-induced Angiosarcoma
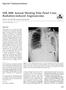 Special Communications SIR 2008 Annual Meeting Film Panel Case: Radiation-induced Angiosarcoma Daniel Y. Sze, MD, PhD, and Judy H. Huang, MD J Vasc Interv Radiol 2008; 19:1133 1137 HISTORY From the Division
Special Communications SIR 2008 Annual Meeting Film Panel Case: Radiation-induced Angiosarcoma Daniel Y. Sze, MD, PhD, and Judy H. Huang, MD J Vasc Interv Radiol 2008; 19:1133 1137 HISTORY From the Division
Superselective vs. lobar transarterial ethiodized oil-chemoembolization - occurrence and clinical significance of non-target embolization
 Superselective vs. lobar transarterial ethiodized oil-chemoembolization - occurrence, p. 13-22 Interventional HR J Original Article Superselective vs. lobar transarterial ethiodized oil-chemoembolization
Superselective vs. lobar transarterial ethiodized oil-chemoembolization - occurrence, p. 13-22 Interventional HR J Original Article Superselective vs. lobar transarterial ethiodized oil-chemoembolization
Tips and tricks. Camillo Aliberti, Massimo Tilli
 Tips and tricks Camillo Aliberti, Massimo Tilli Unit of Oncological Diagnostic and Interventional Radiology, Delta Hospital AUSL Ferrara, Ferrara Italy camy.ali@libero.it mtilli72@libero.it Intra-arterial
Tips and tricks Camillo Aliberti, Massimo Tilli Unit of Oncological Diagnostic and Interventional Radiology, Delta Hospital AUSL Ferrara, Ferrara Italy camy.ali@libero.it mtilli72@libero.it Intra-arterial
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Clinical trials evaluating the use of Yttrium-90. Copyright HMP Communications
 Optimizing Reimbursement for Radioembolization: The Importance of Adequate Documentation Rishi Chopra, MS 1 ; Jason C. Hoffmann, MD 1 ; Amanjit S. Baadh, MD 2 From 1 Winthrop University Hospital, Department
Optimizing Reimbursement for Radioembolization: The Importance of Adequate Documentation Rishi Chopra, MS 1 ; Jason C. Hoffmann, MD 1 ; Amanjit S. Baadh, MD 2 From 1 Winthrop University Hospital, Department
Yttrium-90 Radioembolization of Malignant Tumors of the Liver: Gallbladder Effects
 Vascular and Interventional Radiology Original Research Sag et al. Radioembolization of Liver Tumors Vascular and Interventional Radiology Original Research Alan A. Sag 1 Michael A. Savin 2 Nirish R. Lal
Vascular and Interventional Radiology Original Research Sag et al. Radioembolization of Liver Tumors Vascular and Interventional Radiology Original Research Alan A. Sag 1 Michael A. Savin 2 Nirish R. Lal
Liver imaging takes a step forward with Ingenia
 Publication for the Philips MRI Community ISSUE 49 2013 / 2 Liver imaging takes a step forward with Ingenia Lyon South Hospital strives to move from several studies first CT, then MR or PET to using just
Publication for the Philips MRI Community ISSUE 49 2013 / 2 Liver imaging takes a step forward with Ingenia Lyon South Hospital strives to move from several studies first CT, then MR or PET to using just
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
ALARA and Radiation Safety
 ALARA and Radiation Safety Experience the power of TheraSphere and deliver hope where it s needed most. Imagine where we can go. btg-im.com What is TheraSphere? TheraSphere is indicated for radiation treatment
ALARA and Radiation Safety Experience the power of TheraSphere and deliver hope where it s needed most. Imagine where we can go. btg-im.com What is TheraSphere? TheraSphere is indicated for radiation treatment
Postpancreatectomy Hemorrhage: Imaging and Interventional Radiological Treatment
 Postpancreatectomy Hemorrhage: Imaging and Interventional Radiological Treatment Poster No.: C-1422 Congress: ECR 2014 Type: Educational Exhibit Authors: T. Matsuura, K. Takase, T. Hasegawa, H. Ota, K.
Postpancreatectomy Hemorrhage: Imaging and Interventional Radiological Treatment Poster No.: C-1422 Congress: ECR 2014 Type: Educational Exhibit Authors: T. Matsuura, K. Takase, T. Hasegawa, H. Ota, K.
CT angiography techniques. Boot camp
 CT angiography techniques Boot camp Overview Basic concepts Contrast administration arterial opacification Time scan acquisition during the arterial phase Protocol examples Helical non-gated CTA Pulmonary
CT angiography techniques Boot camp Overview Basic concepts Contrast administration arterial opacification Time scan acquisition during the arterial phase Protocol examples Helical non-gated CTA Pulmonary
Nasogastric tube. Stomach. Pylorus. Duodenum 1. Duodenum 2. Duodenum 3. Duodenum 4
 Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Esophagus Barium Swallow Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach and Duodenum 4 year old Upper GI Nasogastric tube Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum 4
Role of Three-Dimensional Rotational Angiography in the Treatment of Spinal Dural Arteriovenous Fistulas
 Open Access Case Report DOI: 10.7759/cureus.1932 Role of Three-Dimensional Rotational Angiography in the Treatment of Spinal Dural Arteriovenous Fistulas Yigit Ozpeynirci 1, Bernd Schmitz 2, Melanie Schick
Open Access Case Report DOI: 10.7759/cureus.1932 Role of Three-Dimensional Rotational Angiography in the Treatment of Spinal Dural Arteriovenous Fistulas Yigit Ozpeynirci 1, Bernd Schmitz 2, Melanie Schick
Embolotherapy for Cholangiocarcinoma: 2016 Update
 Embolotherapy for Cholangiocarcinoma: 2016 Update Igor Lobko,MD Chief, Division Vascular and Interventional Radiology Long Island Jewish Medical Center GEST 2016 Igor Lobko, M.D. No relevant financial
Embolotherapy for Cholangiocarcinoma: 2016 Update Igor Lobko,MD Chief, Division Vascular and Interventional Radiology Long Island Jewish Medical Center GEST 2016 Igor Lobko, M.D. No relevant financial
Vascular. Experiences Using an Angiography System with a Inch FPD - CT-Like Imaging of the Neck and Abdomen - 1.
 Vascular Experiences Using an Angiography System with a 17 17 Inch FPD - CT-Like Imaging of the Neck and Abdomen - Department of Radiology, University Hospital, Kyoto Prefectural University of Medicine
Vascular Experiences Using an Angiography System with a 17 17 Inch FPD - CT-Like Imaging of the Neck and Abdomen - Department of Radiology, University Hospital, Kyoto Prefectural University of Medicine
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 6/23/2012 Radiology Quiz of the Week # 78 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Combined Anatomical and Functional Imaging with Revolution * CT
 GE Healthcare Case studies Combined Anatomical and Functional Imaging with Revolution * CT Jean-Louis Sablayrolles, M.D. Centre Cardiologique du Nord, Saint-Denis, France Case 1 Whole Brain Perfusion and
GE Healthcare Case studies Combined Anatomical and Functional Imaging with Revolution * CT Jean-Louis Sablayrolles, M.D. Centre Cardiologique du Nord, Saint-Denis, France Case 1 Whole Brain Perfusion and
3 Circulatory Pathways
 40 Chapter 3 Circulatory Pathways Systemic Arteries -Arteries carry blood away from the heart to the various organs of the body. -The aorta is the longest artery in the body; it branches to give rise to
40 Chapter 3 Circulatory Pathways Systemic Arteries -Arteries carry blood away from the heart to the various organs of the body. -The aorta is the longest artery in the body; it branches to give rise to
Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER
 1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
1 Block 3: DISSECTION 2 CELIAC TRUNK, JEJUNUM/ILEUM, LARGE INTESTINE, DUODENUM, PANCREAS, PORTAL VEIN; MOBILIZATION OF THE LIVER Attempt to complete as much as you can of the dissection explained in the
Corporate Medical Policy
 Corporate Medical Policy Intensity Modulated Radiation Therapy (IMRT) of Abdomen and File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_abdomen_and_pelvis
Corporate Medical Policy Intensity Modulated Radiation Therapy (IMRT) of Abdomen and File Name: Origination: Last CAP Review: Next CAP Review: Last Review: intensity_modulated_radiation_therapy_imrt_of_abdomen_and_pelvis
Lin Yang, Xiao Ming Zhang, Yong Jun Ren, Nan Dong Miao, Xiao Hua Huang, and Guo Li Dong
 Radiology Research and Practice Volume 2013, Article ID 535272, 6 pages http://dx.doi.org/10.1155/2013/535272 Clinical Study The Features of Extrahepatic Collateral Arteries Related to Hepatic Artery Occlusion
Radiology Research and Practice Volume 2013, Article ID 535272, 6 pages http://dx.doi.org/10.1155/2013/535272 Clinical Study The Features of Extrahepatic Collateral Arteries Related to Hepatic Artery Occlusion
Trans-arterial radioembolisation (TARE) of unresectable HCC using Y-90 microspheres: is it dangerous in case of portal vein thrombosis?
 Trans-arterial radioembolisation (TARE) of unresectable HCC using Y-90 microspheres: is it dangerous in case of portal vein thrombosis? Poster No.: C-1634 Congress: ECR 2014 Type: Authors: Keywords: DOI:
Trans-arterial radioembolisation (TARE) of unresectable HCC using Y-90 microspheres: is it dangerous in case of portal vein thrombosis? Poster No.: C-1634 Congress: ECR 2014 Type: Authors: Keywords: DOI:
Cone-beam CT findings during prostate artery embolization for benign prostatic hyperplasia-induced lower urinary tract symptoms: a case report
 Chen et al. BMC Urology (2017) 17:120 DOI 10.1186/s12894-017-0311-6 CASE REPORT Cone-beam CT findings during prostate artery embolization for benign prostatic hyperplasia-induced lower urinary tract symptoms:
Chen et al. BMC Urology (2017) 17:120 DOI 10.1186/s12894-017-0311-6 CASE REPORT Cone-beam CT findings during prostate artery embolization for benign prostatic hyperplasia-induced lower urinary tract symptoms:
SIRT Dosimetry: Sometimes Less Is More
 SIRT Dosimetry: Sometimes Less Is More Navesh K. Sharma, DO, PhD Assistant Professor, Departments of Radiation Oncology, Diagnostic Radiology and Nuclear Medicine Medical Director, Radiation Oncology,
SIRT Dosimetry: Sometimes Less Is More Navesh K. Sharma, DO, PhD Assistant Professor, Departments of Radiation Oncology, Diagnostic Radiology and Nuclear Medicine Medical Director, Radiation Oncology,
Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition
 22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
22 Limited en bloc Resection of the Gastroesophageal Junction with Isoperistaltic Jejunal Interposition J.R. Izbicki, W.T. Knoefel, D. C. Broering ] Indications Severe dysplasia in the distal esophagus
Hilar cholangiocarcinoma. Frank Wessels, Maarten van Leeuwen, UMCU utrecht
 Hilar cholangiocarcinoma Frank Wessels, Maarten van Leeuwen, UMCU utrecht Content Anatomy Biliary strictures (Hilar) Cholangiocarcinoom Staging Biliary tract 1 st order Ductus hepatica dextra Ductus hepaticus
Hilar cholangiocarcinoma Frank Wessels, Maarten van Leeuwen, UMCU utrecht Content Anatomy Biliary strictures (Hilar) Cholangiocarcinoom Staging Biliary tract 1 st order Ductus hepatica dextra Ductus hepaticus
The gastroduodenal artery: Radiological anatomy, imaging and endovascular intervention
 The gastroduodenal artery: Radiological anatomy, imaging and endovascular intervention Poster No.: C-2049 Congress: ECR 2010 Type: Educational Exhibit Topic: Interventional Radiology Authors: R. D. White,
The gastroduodenal artery: Radiological anatomy, imaging and endovascular intervention Poster No.: C-2049 Congress: ECR 2010 Type: Educational Exhibit Topic: Interventional Radiology Authors: R. D. White,
Liver Perfusion Analysis New Frontiers in Dynamic Volume Imaging. Case Study Brochure Chang Gung Memorial Hospital.
 New Frontiers in Dynamic Volume Imaging dynamic volume CT Case Study Brochure Chang Gung Memorial Hospital http://www.toshibamedicalsystems.com Toshiba Medical Systems Corporation 2010-2011. All rights
New Frontiers in Dynamic Volume Imaging dynamic volume CT Case Study Brochure Chang Gung Memorial Hospital http://www.toshibamedicalsystems.com Toshiba Medical Systems Corporation 2010-2011. All rights
Post-Y90 Radioembolisation imaging with bremsstrahlung SPECT-CT and PET-CT
 Post-Y90 Radioembolisation imaging with bremsstrahlung SPECT-CT and PET-CT Poster No.: C-2264 Congress: ECR 2012 Type: Scientific Exhibit Authors: S.-C. M. Wang, S. Evans, B. Camden, D. Farlow; Westmead,
Post-Y90 Radioembolisation imaging with bremsstrahlung SPECT-CT and PET-CT Poster No.: C-2264 Congress: ECR 2012 Type: Scientific Exhibit Authors: S.-C. M. Wang, S. Evans, B. Camden, D. Farlow; Westmead,
Spontaneous portosystemic venous shunts in liver cirrhosis: Anatomy, pathophysiology, hemodynamic changes and imaging findings
 Spontaneous portosystemic venous shunts in liver cirrhosis: Anatomy, pathophysiology, hemodynamic changes and imaging findings Poster No.: C-3193 Congress: ECR 2010 Type: Educational Exhibit Topic: Vascular
Spontaneous portosystemic venous shunts in liver cirrhosis: Anatomy, pathophysiology, hemodynamic changes and imaging findings Poster No.: C-3193 Congress: ECR 2010 Type: Educational Exhibit Topic: Vascular
INCIDENTAL FINDING DURING CARDIOMYOPATHY WORKUP
 Originally Posted: February 01, 2015 INCIDENTAL FINDING DURING CARDIOMYOPATHY WORKUP Resident(s): Mariya Gusman, M.D. Attending(s): Raul Palacios, M.D. Program/Dept(s): Brooke Army Medical Center DISCLAIMER
Originally Posted: February 01, 2015 INCIDENTAL FINDING DURING CARDIOMYOPATHY WORKUP Resident(s): Mariya Gusman, M.D. Attending(s): Raul Palacios, M.D. Program/Dept(s): Brooke Army Medical Center DISCLAIMER
The Clinical Utility of Yttrium-90 PET after SIRT
 The Clinical Utility of Yttrium-90 PET after SIRT Dr Yung Hsiang Kao Department of Nuclear Medicine Austin Health Melbourne, Australia 2 nd Asia Pacific Symposium on Liver-Directed Y-90 Microspheres Therapy
The Clinical Utility of Yttrium-90 PET after SIRT Dr Yung Hsiang Kao Department of Nuclear Medicine Austin Health Melbourne, Australia 2 nd Asia Pacific Symposium on Liver-Directed Y-90 Microspheres Therapy
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Variations In Branching Pattern Of Coeliac Trunk
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. IV (Nov. 2015), PP 54-58 www.iosrjournals.org Variations In Branching Pattern Of Coeliac
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 11 Ver. IV (Nov. 2015), PP 54-58 www.iosrjournals.org Variations In Branching Pattern Of Coeliac
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Radioembolization: technical aspects
 Radioembolization: technical aspects Rita Golfieri Unità Operativa Radiologia Malpighi Azienda Ospedaliero-Universitaria di Bologna Policlinico S. Orsola - Malpighi La sottoscritta dichiara di non aver
Radioembolization: technical aspects Rita Golfieri Unità Operativa Radiologia Malpighi Azienda Ospedaliero-Universitaria di Bologna Policlinico S. Orsola - Malpighi La sottoscritta dichiara di non aver
Renal vascular evaluation with 64 Multislice Computerized Tomography Daniela Stoisa, Fabrizzio E. Galiano, Andrés Quaranta, Roberto L.
 Renal vascular evaluation with 64 Multislice Computerized Tomography Daniela Stoisa, Fabrizzio E. Galiano, Andrés Quaranta, Roberto L. Villavicencio Footnote Diagnóstico Médico Oroño. Bv. Oroño 1515. 2000.
Renal vascular evaluation with 64 Multislice Computerized Tomography Daniela Stoisa, Fabrizzio E. Galiano, Andrés Quaranta, Roberto L. Villavicencio Footnote Diagnóstico Médico Oroño. Bv. Oroño 1515. 2000.
ACR SIR PRACTICE PARAMETER FOR RADIOEMBOLIZATION WITH MICROSPHERE BRACHYTHERAPY DEVICE (RMBD) FOR TREATMENT OF LIVER MALIGNANCIES
 The American College of Radiology, with more than 30,000 members, is the principal organization of radiologists, radiation oncologists, and clinical medical physicists in the United States. The College
The American College of Radiology, with more than 30,000 members, is the principal organization of radiologists, radiation oncologists, and clinical medical physicists in the United States. The College
Improvement of Image Quality with ß-Blocker Premedication on ECG-Gated 16-MDCT Coronary Angiography
 16-MDCT Coronary Angiography Shim et al. 16-MDCT Coronary Angiography Sung Shine Shim 1 Yookyung Kim Soo Mee Lim Received December 1, 2003; accepted after revision June 1, 2004. 1 All authors: Department
16-MDCT Coronary Angiography Shim et al. 16-MDCT Coronary Angiography Sung Shine Shim 1 Yookyung Kim Soo Mee Lim Received December 1, 2003; accepted after revision June 1, 2004. 1 All authors: Department
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management. Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC
 An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
An Overview of Post-EVAR Endoleaks: Imaging Findings and Management Ravi Shergill BSc Sean A. Kennedy MD Mark O. Baerlocher MD FRCPC Disclosure Slide Mark O. Baerlocher: Current: Consultant for Boston
PET IMAGING (POSITRON EMISSION TOMOGRAPY) FACT SHEET
 Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
General Nuclear Medicine
 General Nuclear Medicine What is General Nuclear Medicine? What are some common uses of the procedure? How should I prepare? What does the equipment look like? How does the procedure work? How is the procedure
General Nuclear Medicine What is General Nuclear Medicine? What are some common uses of the procedure? How should I prepare? What does the equipment look like? How does the procedure work? How is the procedure
Y-90 Microsphere Therapy: Nuclear Medicine Perspective
 Y-90 Microsphere Therapy: Nuclear Medicine Perspective Carl Hoh, M.D. Dept. Radiology UCSD Medical Center ckhoh@ucsd.edu Learning Objectives Role of Nuclear Medicine in patient selection Technical Issues
Y-90 Microsphere Therapy: Nuclear Medicine Perspective Carl Hoh, M.D. Dept. Radiology UCSD Medical Center ckhoh@ucsd.edu Learning Objectives Role of Nuclear Medicine in patient selection Technical Issues
Ultrasound. Computed tomography. Case studies. Utility of IQon Spectral CT in. cardiac imaging
 Ultrasound Computed tomography Case studies Utility of IQon Spectral CT in cardiac imaging Cardiac imaging is a challenging procedure where it is necessary to image a motion-free heart. This requires a
Ultrasound Computed tomography Case studies Utility of IQon Spectral CT in cardiac imaging Cardiac imaging is a challenging procedure where it is necessary to image a motion-free heart. This requires a
Abdomen Sonography Examination Content Outline
 Abdomen Sonography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 Anatomy, Perfusion, and Function Pathology, Vascular Abnormalities, Trauma, and Postoperative Anatomy
Abdomen Sonography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 Anatomy, Perfusion, and Function Pathology, Vascular Abnormalities, Trauma, and Postoperative Anatomy
Gastroduodenal injury after radioembolization of hepatic tumors
 Gastroduodenal injury after radioembolization of hepatic tumors Cristina Carretero, M.D., 1 Miguel Munoz-Navas, M.D., Ph.D., 1 Maite Betes, M.D., Ph.D., 1 Ramon Angos, M.D., Ph.D., 1 Jose C. Subtil, M.D.,
Gastroduodenal injury after radioembolization of hepatic tumors Cristina Carretero, M.D., 1 Miguel Munoz-Navas, M.D., Ph.D., 1 Maite Betes, M.D., Ph.D., 1 Ramon Angos, M.D., Ph.D., 1 Jose C. Subtil, M.D.,
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Anatomy of the SMALL INTESTINE. Dr. Noman Ullah Wazir PMC
 Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Anatomy of the SMALL INTESTINE Dr. Noman Ullah Wazir PMC SMALL INTESTINE The small intestine, consists of the duodenum, jejunum, and illium. It extends from the pylorus to the ileocecal junction were the
Case Scenarios. 12/28/12 MRI Liver: multiple focal arterially enhancing liver lesions, indeterminate. Repeat MRI in 4 months.
 Case Scenarios Case Scenario 1 A 63 year old black female presented with a history of liver lesions present for the past three years being monitored by serial scans. The patient has a history of esophageal
Case Scenarios Case Scenario 1 A 63 year old black female presented with a history of liver lesions present for the past three years being monitored by serial scans. The patient has a history of esophageal
Gastro-Intestinal Bleeding- Interventional Radiology turning off the tap. Simon McPherson, Vascular Interventional Radiologist, Leeds
 Gastro-Intestinal Bleeding- Interventional Radiology turning off the tap Simon McPherson, Vascular Interventional Radiologist, Leeds Scale UK 100,000 /year Commonest Vascular IR on-call 75% UGIB 65% NVUGIB
Gastro-Intestinal Bleeding- Interventional Radiology turning off the tap Simon McPherson, Vascular Interventional Radiologist, Leeds Scale UK 100,000 /year Commonest Vascular IR on-call 75% UGIB 65% NVUGIB
100% pure beta emitter Decays to zirconium-90 Physical half-life of 64.1 hours (2.67 days) 94% of radiation delivered within 11 days
 100% pure beta emitter Decays to zirconium-90 Physical half-life of 64.1 hours (2.67 days) 94% of radiation delivered within 11 days TheraSphere [US package insert]. Surrey, UK: Biocompatibles UK Ltd,
100% pure beta emitter Decays to zirconium-90 Physical half-life of 64.1 hours (2.67 days) 94% of radiation delivered within 11 days TheraSphere [US package insert]. Surrey, UK: Biocompatibles UK Ltd,
Gastrointestinal tract
 Gastrointestinal tract Colloidal liver-spleen imaging Presented by: Jehad Felemban Introduction: To obtain better anatomic display of liver and spleen architecture, we use (CT Ultrasound). (Radionuclide
Gastrointestinal tract Colloidal liver-spleen imaging Presented by: Jehad Felemban Introduction: To obtain better anatomic display of liver and spleen architecture, we use (CT Ultrasound). (Radionuclide
The Egyptian Journal of Hospital Medicine (October 2017) Vol.69(1), Page
 The Egyptian Journal of Hospital Medicine (October 2017) Vol.69(1), Page 1674-1679 Radioembolization in Treatment of Hepatocellular Carcinoma with Portal Vein Invasion Elsahhar Ahmed Hetta, Osama Mohamed
The Egyptian Journal of Hospital Medicine (October 2017) Vol.69(1), Page 1674-1679 Radioembolization in Treatment of Hepatocellular Carcinoma with Portal Vein Invasion Elsahhar Ahmed Hetta, Osama Mohamed
Hepatic metastases of neuroendocrine tumors: treatment options and outcomes of local patients treated with radioembolization
 Hepatic metastases of neuroendocrine tumors: treatment options and outcomes of local patients treated with radioembolization JP King PGY2 May 22, 2015 Neuroendocrine Tumor (NET) WHO Classification Location
Hepatic metastases of neuroendocrine tumors: treatment options and outcomes of local patients treated with radioembolization JP King PGY2 May 22, 2015 Neuroendocrine Tumor (NET) WHO Classification Location
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Radioembolization (Y90)
 Scan for mobile link. Radioembolization (Y90) Radioembolization is a minimally invasive procedure that combines embolization and radiation therapy to treat liver cancer. Tiny glass or resin beads filled
Scan for mobile link. Radioembolization (Y90) Radioembolization is a minimally invasive procedure that combines embolization and radiation therapy to treat liver cancer. Tiny glass or resin beads filled
Anatomical and Functional MRI of the Pancreas
 Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Anatomical and Functional MRI of the Pancreas MA Bali, MD, T Metens, PhD Erasme Hospital Free University of Brussels Belgium mbali@ulb.ac.be Introduction The use of MRI to investigate the pancreas has
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Locoregional Treatments for HCC Applications in Transplant Candidates. Locoregional Treatments for HCC Applications in Transplant Candidates
 Locoregional Treatments for HCC Applications in Transplant Candidates Matthew Casey, MD March 31, 2016 Locoregional Treatments for HCC Applications in Transplant Candidates *No disclosures *Off-label uses
Locoregional Treatments for HCC Applications in Transplant Candidates Matthew Casey, MD March 31, 2016 Locoregional Treatments for HCC Applications in Transplant Candidates *No disclosures *Off-label uses
Abdominal ultrasound:
 Abdominal ultrasound: Non-traumatic acute abdomen Wittanee Na-ChiangMai, MD Department of Radiology ChiangMai University 26/04/2017 Contents Technique of examination Normal anatomy Emergency conditions
Abdominal ultrasound: Non-traumatic acute abdomen Wittanee Na-ChiangMai, MD Department of Radiology ChiangMai University 26/04/2017 Contents Technique of examination Normal anatomy Emergency conditions
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Interventional Radiology Original Research
 Interventional Radiology Original Research Seki et al. Side-Hole Catheter Placement for HAI Chemotherapy Interventional Radiology Original Research Hiroshi Seki 1 Toshirou Ozaki Makoto Shiina Seki H, Ozaki
Interventional Radiology Original Research Seki et al. Side-Hole Catheter Placement for HAI Chemotherapy Interventional Radiology Original Research Hiroshi Seki 1 Toshirou Ozaki Makoto Shiina Seki H, Ozaki
The role for contrast-enhanced ultrasonography outside of focal liver lesions
 The role for contrast-enhanced ultrasonography outside of focal liver lesions Paul S. Sidhu King s College Hospital, London, UK Introduction Contrast-enhanced ultrasonography (US) of focal liver lesions
The role for contrast-enhanced ultrasonography outside of focal liver lesions Paul S. Sidhu King s College Hospital, London, UK Introduction Contrast-enhanced ultrasonography (US) of focal liver lesions
Future Needs for Standards in 90 Y Microsphere Therapy. CIRMS 2012 Reed Selwyn, PhD, DABR 24 October 2012
 Future Needs for Standards in 90 Y Microsphere Therapy CIRMS 2012 Reed Selwyn, PhD, DABR 24 October 2012 Objectives I. General Description Microsphere Distribution Product Comparison II. Dosimetry Models
Future Needs for Standards in 90 Y Microsphere Therapy CIRMS 2012 Reed Selwyn, PhD, DABR 24 October 2012 Objectives I. General Description Microsphere Distribution Product Comparison II. Dosimetry Models
Radioembolization with Use of Yttrium-90 Resin Microspheres in Patients with Hepatocellular Carcinoma and Portal Vein Thrombosis
 Radioembolization with Use of Yttrium-90 Resin Microspheres in Patients with Hepatocellular Carcinoma and Portal Vein Thrombosis Mercedes Iñarrairaegui, MD, PhD, Kenneth G. Thurston, MA, Jose I. Bilbao,
Radioembolization with Use of Yttrium-90 Resin Microspheres in Patients with Hepatocellular Carcinoma and Portal Vein Thrombosis Mercedes Iñarrairaegui, MD, PhD, Kenneth G. Thurston, MA, Jose I. Bilbao,
Surgical anatomy of the biliary tract
 HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
Coils and plugs have emerged as the most commonly
 The MVP Micro Vascular Plug: A New Paradigm in Peripheral Embolization BY RIPAL T. GANDHI, MD, FSVM; BRIAN E. SCHIRF, MD; AND JONATHAN IGLESIAS, MD Coils and plugs have emerged as the most commonly employed
The MVP Micro Vascular Plug: A New Paradigm in Peripheral Embolization BY RIPAL T. GANDHI, MD, FSVM; BRIAN E. SCHIRF, MD; AND JONATHAN IGLESIAS, MD Coils and plugs have emerged as the most commonly employed
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Varian Acuity BrachyTherapy Suite One Room Integrated Image-Guided Brachytherapy
 Varian Acuity BrachyTherapy Suite One Room Integrated Image-Guided Brachytherapy The Acuity BrachyTherapy Suite Integrating Imaging, Planning, and Treatment in a Single Room Each component draws on the
Varian Acuity BrachyTherapy Suite One Room Integrated Image-Guided Brachytherapy The Acuity BrachyTherapy Suite Integrating Imaging, Planning, and Treatment in a Single Room Each component draws on the
General summary GENERAL SUMMARY
 General summary GENERAL SUMMARY In Chapter 2.1 the long-term results and prognostic factors of radiofrequency ablation (RFA) for unresectable colorectal liver metastases (CRLM) in a single center with
General summary GENERAL SUMMARY In Chapter 2.1 the long-term results and prognostic factors of radiofrequency ablation (RFA) for unresectable colorectal liver metastases (CRLM) in a single center with
Selection Criteria and Insertion of SIRT into HCC Treatment Guidelines
 Selection Criteria and Insertion of SIRT into HCC Treatment Guidelines 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore Pierce Chow FRCSE PhD SIRT in
Selection Criteria and Insertion of SIRT into HCC Treatment Guidelines 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore Pierce Chow FRCSE PhD SIRT in
8/1/2017. Clinical Indications and Applications of Realtime MRI-Guided Radiotherapy
 Clinical Indications and Applications of Realtime MRI-Guided Radiotherapy Michael F Bassetti MD PhD Assistant Professor, Department of Human Oncology University of Wisconsin, Madison. Carbone Cancer Center
Clinical Indications and Applications of Realtime MRI-Guided Radiotherapy Michael F Bassetti MD PhD Assistant Professor, Department of Human Oncology University of Wisconsin, Madison. Carbone Cancer Center
Ruolo della interventistica per le secondarietà epatiche e di altre sedi
 Ruolo della interventistica per le secondarietà epatiche e di altre sedi Giancarlo Bizzarri Dipartimento di Diagnostica per Immagini e Radiologia Interventistica Ospedale Regina Apostolorum, Albano Laziale
Ruolo della interventistica per le secondarietà epatiche e di altre sedi Giancarlo Bizzarri Dipartimento di Diagnostica per Immagini e Radiologia Interventistica Ospedale Regina Apostolorum, Albano Laziale
To describe the liver. To list main structures in porta hepatis.
 GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
GI anatomy Lecture: 6 د. عصام طارق Objectives: To describe the liver. To list main structures in porta hepatis. To define portal system & portosystemic anastomosis. To list parts of biliary system. To
Dual-Energy CT: The Technological Approaches
 Dual-Energy CT: The Technological Approaches Dushyant Sahani, M.D Director of CT Associate Professor of Radiology Massachusetts General Hospital Harvard Medical School Email-dsahani@partners.org Disclosure
Dual-Energy CT: The Technological Approaches Dushyant Sahani, M.D Director of CT Associate Professor of Radiology Massachusetts General Hospital Harvard Medical School Email-dsahani@partners.org Disclosure
BY DR NOMAN ULLAH WAZIR
 BY DR NOMAN ULLAH WAZIR The stomach (from ancient Greek word stomachos, stoma means mouth) is a muscular, hollow and the most dilated part of the GIT. It starts from the point where esophagus ends. It
BY DR NOMAN ULLAH WAZIR The stomach (from ancient Greek word stomachos, stoma means mouth) is a muscular, hollow and the most dilated part of the GIT. It starts from the point where esophagus ends. It
Disclosures. I am on the Onyx speaker bureau I am a paid consultant to. Boston Scientific CeloNova Cook MDS Nordion Sirtex
 Disclosures I am on the Onyx speaker bureau I am a paid consultant to Boston Scientific CeloNova Cook MDS Nordion Sirtex Comparing Y90 Devices Matthew S. Johnson MD, FSIR Indiana University School of Medicine
Disclosures I am on the Onyx speaker bureau I am a paid consultant to Boston Scientific CeloNova Cook MDS Nordion Sirtex Comparing Y90 Devices Matthew S. Johnson MD, FSIR Indiana University School of Medicine
Visceral Artery Aneurysms Endovascular vs. Open?
 Disclosures Visceral Artery Aneurysms Endovascular vs. Open? John S. Lane III, MD Professor and Acting Chief of Vascular Surgery UC San Diego, Department of Surgery None relevant UCSF Vascular Symposium,
Disclosures Visceral Artery Aneurysms Endovascular vs. Open? John S. Lane III, MD Professor and Acting Chief of Vascular Surgery UC San Diego, Department of Surgery None relevant UCSF Vascular Symposium,
Radioembolization with Lipiodol for the Treatment of Hepatocellular Carcinoma and Liver Metastases
 Radioembolization with Lipiodol for the Treatment of Hepatocellular Carcinoma and Liver Metastases Pr Francesco Giammarile CHLS Lyon Faculté de Lyon Sud «Aut tace aut loquere meliora silentio» Malignant
Radioembolization with Lipiodol for the Treatment of Hepatocellular Carcinoma and Liver Metastases Pr Francesco Giammarile CHLS Lyon Faculté de Lyon Sud «Aut tace aut loquere meliora silentio» Malignant
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
