The Role of Tumor Vascularity in Predicting Survival after Yttrium-90 Radioembolization for Liver Metastases
|
|
|
- Clarence O’Neal’
- 5 years ago
- Views:
Transcription
1 The Role of Tumor Vascularity in Predicting Survival after Yttrium-90 Radioembolization for Liver Metastases Kent T. Sato, MD, Reed A. Omary, MD, Christopher Takehana, MD, Saad Ibrahim, MD, Robert J. Lewandowski, MD, Robert K. Ryu, MD, and Riad Salem, MD, MBA PURPOSE: It is unclear what role pretreatment tumor vascularity plays in determining outcomes after yttrium-90 radioembolization. A hypothesis was tested that radiographic vascularity of a tumor does not affect patient survival. MATERIALS AND METHODS: In this two-institution retrospective study, 137 patients with metastatic liver disease underwent 90 Y radioembolization. Primary sites were categorized as colon, neuroendocrine, and other. All patients underwent triphasic contrast-enhanced computed tomography (CT) or magnetic resonance imaging, as well as detailed hepatic angiography. Two board-certified interventional radiologists interpreted all images and evaluated them for the presence of enhancement. Median survival times, as well as 1- and 2-year survival rates, were compared between patients with hypervascular and hypovascular tumors on (i) cross-sectional imaging and (ii) angiography with use of the log-rank statistic ( 0.05). RESULTS: On angiography, 108 patients had hypervascular tumors and 29 had hypovascular tumors. Median survival times for the two subgroups were 300 days and 261 days, respectively (P.95). On CT, 24 patients had hypervascular tumors and 113 had hypovascular tumors. Median survival times for these subgroups were 306 days and 284 days, respectively (P.67). Eighty-four patients tumors that were hypovascular on CT were hypervascular on angiography. There were no statistical differences in survival between patients with hypervascular and hypovascular tumors, regardless if vascularity was defined based on CT or angiography. CONCLUSIONS: Radiographic vascular appearance of liver tumors, regardless of imaging modality, does not affect survival after radioembolization. Therefore, hypovascular tumors should not be considered contraindicated for radioembolization. J Vasc Interv Radiol 2009; 20: From the Department of Radiology, Northwestern University, 251 East Huron, Room 4-710R Feinberg, Chicago, IL Received November 10, 2008; final revision received August 21, 2009; accepted August 24, Address correspondence to K.T.S.; k-sato@northwestern.edu From the 2008 SIR Annual Meeting. R.S. serves as a paid consultant for MDS Nordion. None of the other authors have identified a conflict of interest. SIR, 2009 DOI: /j.jvir METASTATIC liver disease is the most common form of hepatic malignancy, as the liver is a common site of metastasis for many tumors. Surgical resection is the only curative treatment for metastatic liver disease, but fewer than 20% of patients are candidates for surgery (1). For patients with unresectable disease, systemic chemotherapy is available; however, when these therapies fail, there is no consensus on how to treat these patients. Liver-directed therapies such as transarterial chemoembolization, bland embolization, and radioembolization with yttrium-90 microspheres have been used for patients in whom first- and second-line therapies fail. Radioembolization has been shown to be beneficial and well tolerated for metastatic disease (2,3), and its use for the treatment of liver metastasis is steadily increasing. Radioembolization relies on two fundamental principles: (i) liver tumors receive the majority of their blood supply from the hepatic artery (4) and (ii) tumor neovascularity is more dense than native hepatic vasculature and therefore allows the radioembolic particles to be concentrated within the tumor relative to normal liver tissue. Therefore, radioembolization theoretically depends on the hypervascularity of the tumors, with the goals to maximize concentration of microspheres within the tumor and minimize radiation exposure to surrounding normal hepatic parenchyma. With the use of digital subtraction angiography or cross-sectional imaging, contrast agent enhancement of liver metastases can vary. Depending on 1564
2 Volume 20 Number 12 Sato et al 1565 the primary tumor, liver metastases can be hypervascular or hypovascular. The rich blood supply of hypervascular tumors suggests that they would concentrate the 90 Y microspheres more and should therefore show a better response than hypovascular tumors. However, radioembolization has been shown to be effective in the treatment of a variety of metastases (5 7) regardless of vascularity. This suggests that there may be more to vascularity than enhancement alone. It is unclear what role pretreatment tumor vascularity plays in determining outcomes after 90 Y radioembolization. In this study, we tested the hypothesis that hypovascular liver metastases, as defined by angiography or cross-sectional imaging (ie, computed tomography [CT] or magnetic resonance [MR] imaging), are not associated with reduced survival after 90 Y radioembolization compared with hypervascular tumors. MATERIALS AND METHODS Clinical Setting and Patient Sample Between 2003 and 2006, 137 patients with chemotherapy-refractory disease presenting with liver-dominant hepatic metastases from various primary malignancies were treated at two institutions. Institution A was a large communitybased hospital with a large oncology practice. Institution B was a large academic practice, also with a large volume of oncology procedures. Pretreatment imaging consisted of a CT examination whenever possible, but when patients could not undergo contrast-enhanced CT or presented to us with an MR imaging study on initial consultation, CT was not performed. Survival and follow-up data from both institutions were obtained and included in this analysis. The Institutional Review Boards from both institutions approved the study protocol, and all patients signed an informed consent allowing use of their data. All data were stored in a fashion compliant with the Health Insurance Portability and Accountability Act. The sites of the primary malignancy were categorized as colon, neuroendocrine, and noncolorectal/nonneuroendocrine (ie, other ). This group included patients with the following primary malignancies: breast, pancreas, lung, cholangiocarcinoma, melanoma, renal, esophageal, ovarian, adenocarcinoma of unknown origin, lymphoma, gastric, duodenal, bladder, angiosarcoma, squamous cell, thyroid, adrenal, and parotid. CT Technique All CT scans were performed on a Lightspeed scanner (GE Healthcare, Princeton, New Jersey) or a Somatom 16-slice scanner (Siemens Medical Solutions, Erlangen, Germany). A triphasic contrast-enhanced liver protocol was employed that used a standard power injector (Medrad, Indianola, Pennsylvania) connected to an intravenous catheter to inject 125 ml of Omnipaque 350 (GE Healthcare) at a rate of 4 5 ml/sec. Arterial-phase scans were obtained 40 seconds after the start of the intravenous injection and venous-phase imaging was performed 90 seconds after the start of injection. Angiography Technique Angiography was performed with Angiostar, Multistar, or Axiom Artis equipment (Siemens Medical Solutions). Hepatic arterial angiography was performed selectively in the right or left hepatic artery. Selective arterial catheterization was performed with a Renegade Hi-Flo microcatheter (Boston Scientific, Natick, Massachusetts). Injection rates varied depending on the caliber of the hepatic artery as well as the level of flow within it but were 1 3 ml/sec as injected through a power injector (Medrad, Indianola, Pennsylvania). The contrast agent used was Omnipaque 350 (GE Healthcare, Milwaukee, Wisconsin), and a typical volume of 6 12 ml was used per injection, depending on the size of the liver being examined. Radioembolization Technique Radioembolization was performed with TheraSphere (MDS Nordion, Ottawa, Ontario, Canada). TheraSphere has received a Humanitarian Device Exemption from the United States Food and Drug Administration for use in hepatocellular carcinoma. For this study, all patients received permission for off-label use per the published Food and Drug Administration guidelines for Humanitarian Device Exemptions in disease conditions other than the approved indication. Depending on the extent of disease within the liver at the time of presentation, patients received bilobar (ie, right and left lobe) or unilobar treatment. For bilobar treatment, the first lobe treatment was followed by the second lobe treatment approximately 30 days later. No whole-liver infusions were performed. Lobar treatment was targeted to deliver an absorbed dose of 120 Gy according to previously published dosimetry techniques (8). Infusion of TheraSphere was performed by one of four interventional radiologists (K.T.S., R.J.L., R.K.R., R.S.) with 5, 2, 8, and 8 years of experience, respectively. For those patients who received bilobar treatment, imaging was repeated just before the second lobar treatment (30 45 days) and again at the third month. Patients undergoing unilobar treatment were scheduled for 30-day imaging, which was repeated every 3 months until the patient s death. Laboratory and clinical parameters (including lymphocyte counts) were assessed at each clinic visit and classified according the National Cancer Institute Common Toxicity Criteria, version 3.0. Procedural complications were classified according to the standards established by the Society of Interventional Radiology (9). All patients were prescribed a 2-week course of proton pump inhibitors. Nondiabetic patients received a 5-day methylprednisolone dose pack to counteract fatigue. Data Analysis Two board-certified attending interventional radiologists retrospectively reviewed and interpreted the pretreatment CT and angiographic images simultaneously and evaluated them for the presence of enhancement by consensus. Sixteen patients did not have a pretreatment contrast-enhanced CT study because of allergies or renal dysfunction and underwent MR imaging. For the sake of data analysis, these patients were grouped with the CT group and evaluated based on the same criteria. Tumors were classified as hypervascular if they enhanced greater than the surrounding hepatic parenchyma on imaging. Tumors were deemed hypervascular if they showed a distinct tumor blush relative to the normal hepatic parenchyma on angiography. The primary endpoint of the study was survival specific to the groups defined as having hypervascular and hypovascular tumors on both imaging modalities. Me-
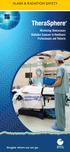
3 1566 Tumor Vascularity to Predict Survival after Liver Radioembolization December 2009 JVIR Figure 1. Images from a 45-year-old woman with metastatic neuroendocrine tumors who is being evaluated for treatment with 90 Y. (a) CT scan of the liver obtained during the arterial phase shows a hypervascular mass (arrow) within the left lobe of the liver. (b) Selective left hepatic arteriography shows multiple hypervascular enhancing masses (arrowheads) corresponding with the masses seen on CT. Figure 2. Images from a 67-year-old man with metastatic rectal carcinoma. (a) CT scan shows a large hypodense mass (arrow) in the right lobe of the liver, which does not enhance relative to the liver parenchyma during the arterial phase. (b) Selective common hepatic arteriography does not demonstrate any appreciable enhancement in the large mass. dian days of survival, as well as 1- and 2-year survival percentages, were compared between the hypervascular and hypovascular imaging groups as well as the hypervascular and hypovascular angiography groups using the log-rank statistic, with an value of Additionally, a subgroup analysis was performed for median days of survival in patients with hypervascular or hypovascular tumors on angiography and imaging scans with use of 2 analyses, with an value of RESULTS Patient Demographics One hundred thirty-seven patients underwent a total of 225 administrations of 90 Y TheraSphere via transcatheter intraarterial infusion. The median age of the patients was 61 years, and there were 66 men and 71 women in the patient cohort. Primary malignancies included colon (n 51), breast (n 21), neuroendocrine (n 19), cholangiocarcinoma (n 7), pancreas (n 6), lung (n 5), melanoma (n 5), renal (n 4), esophageal (n 3),
4 Volume 20 Number 12 Sato et al 1567 Figure 3. Images from a 59-year-old man with metastatic sigmoid colon carcinoma. (a) Arterial-phase CT does not clearly demonstrate a lesion, which is in the region of the arrowheads. (b) Equilibrium-phase image, which was windowed for more contrast, shows an area of hypodensity relative to the normal liver (arrowheads). (c) Selective right hepatic angiography shows a hypervascular enhancing mass in the right lobe of the liver (arrowheads). adenocarcinoma with unknown primary tumor (n 3), ovary (n 2), and adrenal, angiosarcoma, bladder, cervical, duodenal, gallbladder, gastric, lymphoma, parotid, squamous cell carcinoma, and thyroid (n 1 each). Cross-sectional Imaging Classification A total of 137 patients were studied. Of those, 121 had contrast-enhanced CT and 16 had contrast-enhanced MR imaging. On cross-sectional imaging, 24 of 137 patients (18%) were found to have hypervascular tumors (Fig 1) and 113 (82%) had hypovascular tumors (Fig 2). Eighty-four of the 113 patients (74%) whose tumors were deemed hypovascular on cross-sectional imaging were found to have hypervascular tumors on angiography (Fig 3). Digital Subtraction Angiographic Classification Of the 137 patients, 108 (79%) had lesions that appeared hypervascular on angiography, whereas only 29 (21%) had tumors that appeared hypovascular. Further evaluation of the data revealed that 29 of 137 patients (21%) had tumors that were hypovascular on both angiography and crosssectional imaging, whereas 24 patients (18%) had tumors that were found to be hypervascular on both imaging modalities. Survival After radioembolization, the angiographically hypervascular tumor group exhibited a 1-year survival rate of 48.5% and a 2-year survival rate of 25.9%. The median survival time for the hypervascular tumor group was 300 days. For the angiographically hypovascular tumor group, the 1-year survival rate was similar at 47.9% and the 2-year survival rate was 32.8%. The median survival time for this group was 261 days. There were no statistical differences in survival between patients with hypervascular tumors and those with hypovascular tumors, regardless of the modality used (P.05).
5 1568 Tumor Vascularity to Predict Survival after Liver Radioembolization December 2009 JVIR Table 1 Survival Outcomes among Patients with Hypervascular and Hypovascular Tumors Vascularity On cross-sectional imaging, only 18% of the patients exhibited hypervascular tumors, whereas 82% of tumors were considered hypovascular. After radioembolization, results were very similar to the angiography group. Patients with hypervascular tumors on cross-sectional imaging had a 1-year survival rate of 47.6% and a 2-year survival rate of 30.5%. The median survival rate for the hypervascular tumor group was 306 days. Patients with hypovascular tumors exhibited a 48.3% 1-year survival rate and a 31.1% 2-year survival rate. The median survival time for this group was 284 days (Table 1). In addition, the subgroup analysis of combined tumor vascularity as defined by angiography and cross-sectional imaging also demonstrated no statistical difference in survival between hypervascular and hypovascular tumors. Of the 137 patients, 24 exhibited tumor hypervascularity on cross-sectional imaging and angiography, and had a median survival of 305 days. Twenty-nine patients had hypovascular tumors on cross-sectional imaging and angiography, and had a median survival of 224 days (P.57; Table 2). DISCUSSION No. of Pts. Mean Survival (d) Median Survival (d) Overall Survival (%) On angiography Hypervascular Hypovascular On CT/MR imaging Hypervascular Hypovascular y 2y P Value Table 2 Median Survival after 90 Y Radioembolization as a Function of CT/MR Imaging Tumor Vascularity Vascularity No. of Pts. Median Survival (d)* Hypervascular Hypovascular * P value between groups:.3227 ( 2 test) In an attempt to refine selection criteria for patients undergoing radioembolization, identification of pretreatment variables that may predict the response of a tumor to radioembolization becomes crucial. In the present study of 137 patients, we found that the enhancement patterns of tumors did not appear to affect survival of these patients after radioembolization. Specifically, patients with hypervascular tumors did not have a significant survival advantage versus those with hypovascular tumors. The mechanism of action for radioembolization is flow-directed deposition of the radioactive microspheres into the vascular bed of liver tumors. Because of this, one would expect that patients with hypervascular tumors should have the radioactive microspheres concentrate to a greater degree in the tumors compared with those with hypovascular tumors, and therefore have a better response. However, because it has been shown that both hypovascular and hypervascular tumors respond well to radioembolization (8), our goal was to study the role of vascularity in the success of radioembolization. As there is no accepted objective measure of enhancement, the determination of tumor vascularity on crosssectional imaging and catheter angiography was subjectively determined by two interventional radiologists. Our results show that the response of tumors to radioembolization is independent of enhancement patterns. In addition, enhancement on one imaging modality does not correlate with enhancement on another modality. These confounding data further demonstrate the difficulty in using enhancement as a measure of tumor perfusion. Our results may in fact be secondary to an inadequate means to measure true tumor perfusion, indicating a discrepancy between actual tumor perfusion and radiographic enhancement. These findings were echoed in a study by Taniai et al (10), who examined the response of liver metastases to chemoembolization. Similarly to our study, they characterized metastatic colorectal tumors as hypervascular and hypovascular by angiography and contrastenhanced CT. They found that, although patients with tumors with early angiographic hypervascularity showed a slight trend toward improved survival, there was no significant difference in survival between patients hypervascular and hypovascular tumors. These findings raise the question of how much tumor enhancement really correlates with tumor vascularity. Tumor enhancement depends not only on tumor blood flow, blood volume, and contrast agent concentration, but also on vessel permeability. In some tumors, newly developed tumor vessels demonstrated increased fenestrations in the basement membrane that results in increased permeability (11). This increase in permeability is one reason these tumors exhibit intense enhancement on cross-sectional imaging. However, not all neovascularity demonstrates this high permeability, so some tumors may possess a network of new vasculature, but the tumors may not enhance as much as others. Recently, methods of measuring tissue perfusion other than tissue enhancement have been evaluated. Tissue perfusion is a reflection of overall blood flow to a volume of tissue over time. Contrast enhancement is a phenomenon that relies on two main factors. First, there must be perfusion of the tissue in question to carry the contrast material to the target tissue. Second, there is diffusion of the contrast material across the cell membranes, which allows it to be detected. Even with dynamic contrast scans, images are obtained from one point in time; not in a
6 Volume 20 Number 12 Sato et al 1569 dynamic fashion over a period of time. Transcatheter intraarterial perfusion MR imaging is a new technique that has been used to measure such objective tumor perfusion changes during transarterial chemoembolization (12 15). High perfusion values may represent not only a higher microvessel density, but also intrinsically greater angiogenic activity of the tumor as a secondary response to tissue hypoxia. This is significant in the setting of radioembolization, as tissue hypoxia has also been shown to offer resistance to radiation therapy (16). Hypoxia is known to upregulate vascular endothelial growth factor and hypoxia-inducible factor 1 (17 19). If a hypoxic tumor were to upregulate vascular endothelial growth factor expression, this may result in higher membrane permeability and the tumor may appear hypervascular on imaging because of the increased enhancement seen. Because not all tumors produce vascular endothelial growth factor, this is likely not the only factor affecting enhancement, but it does suggest that neovascularity by itself does not necessarily correspond with contrast enhancement. Further study into innovative methods of evaluating tissue perfusion may help us understand our findings better. There were several limitations to this study. First, the method of defining hypervascular and hypovascular tumors based on different imaging techniques was subjective. A more rigorous objective method such as transcatheter intraarterial perfusion MR imaging (15) would be preferable, but this technique is still not widely available. Second, our cohort of patients included patients with many different primary tumors. Regardless of vascularity, the underlying malignancy may have more of an effect on survival than vascularity. In the future, further subgroup analysis could be performed within each of the major tumor groups comparing vascularity and survival. Finally, although the determination of vascularity was based on consensus opinion by two boardcertified attending interventional radiologists, no intra- or interobserver variability was tested. In conclusion, radiographic vascular appearance of liver tumors, regardless of imaging modality, does not appear to significantly affect survival after treatment with radioembolization. Therefore, tumor hypovascularity should not be considered a contraindication for 90 Y radioembolization. References 1. Sasson AR, Sigurdson ER. Surgical treatment of liver metastases. Semin Oncol 2002; 29: Mulcahy MF, Lewandowski RJ, Ibrahim SM, et al. Radioembolization of colorectal hepatic metastases using yttrium-90 microspheres. Cancer 2009; 115: Lewandowski RJ, Thurston KG, Goin JE, et al. 90Y Microsphere (Thera- Sphere) treatment for unresectable colorectal cancer metastases of the liver: response to treatment at targeted doses of Gy as measured by [18F]fluorodeoxyglucose positron emission tomography and computed tomographic imaging. J Vasc Interv Radiol 2005; 16: Breedis C, Young G. The blood supply of neoplasms in the liver. Am J Pathol 1954; 30: Herba MJ, Thirlwell MP. Radioembolization for hepatic metastases. Semin Oncol 2002; 29: Wong CY, Salem R, Raman S, et al. Evaluating 90Y-glass microsphere treatment response of unresectable colorectal liver metastases by [18F]FDG PET: a comparison with CT or MRI. Eur J Nucl Med Mol Imaging 2002; 29: Stubbs RS, Cannan RJ, Mitchell AW. Selective internal radiation therapy (SIRT) with 90yttrium microspheres for extensive colorectal liver metastases. Hepatogastroenterology 2001; 48: Salem R, Thurston KG. Radioembolization with yttrium-90 microspheres: a state-of-the-art brachytherapy treatment for primary and secondary liver malignancies. Part 3: comprehensive literature review and future direction. J Vasc Interv Radiol 2006; 17: Omary RA, Bettmann MA, Cardella JF, et al. Quality improvement guidelines for the reporting and archiving of interventional radiology procedures. J Vasc Interv Radiol 2003; 14(suppl):S293 S Taniai N, Onda M, Tajiri T, et al. Good embolization response for colorectal liver metastases with hypervascularity. Hepatogastroenterology 2002; 49: Dvorak HF, Brown LF, Detmar M, Dvorak AM. Vascular permeability factor/vascular endothelial growth factor, microvascular hyperpermeability, and angiogenesis. Am J Pathol 1995; 146: Wang D, Bangash AK, Rhee TK, et al. Liver tumors: monitoring embolization in rabbits with VX2 tumors transcatheter intraarterial first-pass perfusion MR imaging. Radiology 2007; 245: Virmani S, Wang D, Harris KR, et al. Comparison of transcatheter intraarterial perfusion MR imaging and fluorescent microsphere perfusion measurements during transcatheter arterial embolization of rabbit liver tumors. J Vasc Interv Radiol 2007; 18: Lewandowski RJ, Wang D, Gehl J, et al. A comparison of chemoembolization endpoints using angiographic versus transcatheter intraarterial perfusion/mr imaging monitoring. J Vasc Interv Radiol 2007; 18: Larson AC, Wang D, Atassi B, et al. Transcatheter intraarterial perfusion: MR monitoring of chemoembolization for hepatocellular carcinoma feasibility of initial clinical translation. Radiology 2008; 246: Harada H, Kizaka-Kondoh S, Li G, et al. Significance of HIF-1-active cells in angiogenesis and radioresistance. Oncogene 2007; 26: Byrne AM, Bouchier-Hayes DJ, Harmey JH. Angiogenic and cell survival functions of vascular endothelial growth factor (VEGF). J Cell Mol Med 2005; 9: Hicklin DJ, Ellis LM. Role of the vascular endothelial growth factor pathway in tumor growth and angiogenesis. J Clin Oncol 2005; 23: Rhee TK, Young JY, Larson AC, et al. Effect of transcatheter arterial embolization on levels of hypoxia-inducible factor-1alpha in rabbit VX2 liver tumors. J Vasc Interv Radiol 2007; 18:
Embolotherapy for Cholangiocarcinoma: 2016 Update
 Embolotherapy for Cholangiocarcinoma: 2016 Update Igor Lobko,MD Chief, Division Vascular and Interventional Radiology Long Island Jewish Medical Center GEST 2016 Igor Lobko, M.D. No relevant financial
Embolotherapy for Cholangiocarcinoma: 2016 Update Igor Lobko,MD Chief, Division Vascular and Interventional Radiology Long Island Jewish Medical Center GEST 2016 Igor Lobko, M.D. No relevant financial
Yttrium-90 Radioembolization of Malignant Tumors of the Liver: Gallbladder Effects
 Vascular and Interventional Radiology Original Research Sag et al. Radioembolization of Liver Tumors Vascular and Interventional Radiology Original Research Alan A. Sag 1 Michael A. Savin 2 Nirish R. Lal
Vascular and Interventional Radiology Original Research Sag et al. Radioembolization of Liver Tumors Vascular and Interventional Radiology Original Research Alan A. Sag 1 Michael A. Savin 2 Nirish R. Lal
Clinical trials evaluating the use of Yttrium-90. Copyright HMP Communications
 Optimizing Reimbursement for Radioembolization: The Importance of Adequate Documentation Rishi Chopra, MS 1 ; Jason C. Hoffmann, MD 1 ; Amanjit S. Baadh, MD 2 From 1 Winthrop University Hospital, Department
Optimizing Reimbursement for Radioembolization: The Importance of Adequate Documentation Rishi Chopra, MS 1 ; Jason C. Hoffmann, MD 1 ; Amanjit S. Baadh, MD 2 From 1 Winthrop University Hospital, Department
Radioembolization of Colorectal Hepatic Metastases Using Yttrium-90 Microspheres
 Radioembolization of Colorectal Hepatic Metastases Using Yttrium-90 Microspheres Mary F. Mulcahy, MD 1, Robert J. Lewandowski, MD 2, Saad M. Ibrahim, MD 2, Kent T. Sato, MD 2, Robert K. Ryu, MD 2, Bassel
Radioembolization of Colorectal Hepatic Metastases Using Yttrium-90 Microspheres Mary F. Mulcahy, MD 1, Robert J. Lewandowski, MD 2, Saad M. Ibrahim, MD 2, Kent T. Sato, MD 2, Robert K. Ryu, MD 2, Bassel
Trans-arterial radioembolisation (TARE) of unresectable HCC using Y-90 microspheres: is it dangerous in case of portal vein thrombosis?
 Trans-arterial radioembolisation (TARE) of unresectable HCC using Y-90 microspheres: is it dangerous in case of portal vein thrombosis? Poster No.: C-1634 Congress: ECR 2014 Type: Authors: Keywords: DOI:
Trans-arterial radioembolisation (TARE) of unresectable HCC using Y-90 microspheres: is it dangerous in case of portal vein thrombosis? Poster No.: C-1634 Congress: ECR 2014 Type: Authors: Keywords: DOI:
Minimizing Unnecessary Radiation Exposure to Healthcare Professionals and Patients Imagine where we can go.
 ALARA & RADIATION SAFETY Minimizing Unnecessary Radiation Exposure to Healthcare Professionals and Patients Imagine where we can go. What is ALARA? As Low As Reasonably Achievable The use of radiation
ALARA & RADIATION SAFETY Minimizing Unnecessary Radiation Exposure to Healthcare Professionals and Patients Imagine where we can go. What is ALARA? As Low As Reasonably Achievable The use of radiation
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Tips and tricks. Camillo Aliberti, Massimo Tilli
 Tips and tricks Camillo Aliberti, Massimo Tilli Unit of Oncological Diagnostic and Interventional Radiology, Delta Hospital AUSL Ferrara, Ferrara Italy camy.ali@libero.it mtilli72@libero.it Intra-arterial
Tips and tricks Camillo Aliberti, Massimo Tilli Unit of Oncological Diagnostic and Interventional Radiology, Delta Hospital AUSL Ferrara, Ferrara Italy camy.ali@libero.it mtilli72@libero.it Intra-arterial
The Egyptian Journal of Hospital Medicine (October 2017) Vol.69(1), Page
 The Egyptian Journal of Hospital Medicine (October 2017) Vol.69(1), Page 1674-1679 Radioembolization in Treatment of Hepatocellular Carcinoma with Portal Vein Invasion Elsahhar Ahmed Hetta, Osama Mohamed
The Egyptian Journal of Hospital Medicine (October 2017) Vol.69(1), Page 1674-1679 Radioembolization in Treatment of Hepatocellular Carcinoma with Portal Vein Invasion Elsahhar Ahmed Hetta, Osama Mohamed
Radioembolization of the Liver. Michael Meuse, M.D. Vascular and Interventional Radiology
 Radioembolization of the Liver Michael Meuse, M.D. Vascular and Interventional Radiology Brachytherapy Principle Radiation is accepted as a standard treatment option for liver cancer Radiation will break
Radioembolization of the Liver Michael Meuse, M.D. Vascular and Interventional Radiology Brachytherapy Principle Radiation is accepted as a standard treatment option for liver cancer Radiation will break
RADIATION SEGMENTECTOMY. Robert J Lewandowski, MD
 RADIATION SEGMENTECTOMY Robert J Lewandowski, MD Robert Lewandowski, M.D. Consultant/Advisory Board: Cook Medical, LLC, Arsenal, BTG International, Boston Scientific Corp., ABK Reference Unlabeled/Unapproved
RADIATION SEGMENTECTOMY Robert J Lewandowski, MD Robert Lewandowski, M.D. Consultant/Advisory Board: Cook Medical, LLC, Arsenal, BTG International, Boston Scientific Corp., ABK Reference Unlabeled/Unapproved
TRANSEARTERIAL CHEMO- EMBOLIZATION FOR HEPATIC METASTASES FROM NEURO-ENDOCINE NEOPLASIA AND HEPATOMA DR SAMIA AHMAD
 UNIVERSITY OF PRETORIA STEVE BIKO ACADEMIC HOSPITAL SOUTH AFRICA TRANSEARTERIAL CHEMO- EMBOLIZATION FOR HEPATIC METASTASES FROM NEURO-ENDOCINE NEOPLASIA AND HEPATOMA DR SAMIA AHMAD 1 INTRODUCTION Hepatic
UNIVERSITY OF PRETORIA STEVE BIKO ACADEMIC HOSPITAL SOUTH AFRICA TRANSEARTERIAL CHEMO- EMBOLIZATION FOR HEPATIC METASTASES FROM NEURO-ENDOCINE NEOPLASIA AND HEPATOMA DR SAMIA AHMAD 1 INTRODUCTION Hepatic
SELECTIVE INTERNAL RADIATION THERAPY FOR TREATMENT OF LIVER CANCER
 SELECTIVE INTERNAL RADIATION THERAPY FOR TREATMENT OF LIVER CANCER SIR-Spheres*: A New Treatment Option for Non-Resectable Liver Tumors Treatment Overview SIRT: Selective Internal Radiation Therapy Concept
SELECTIVE INTERNAL RADIATION THERAPY FOR TREATMENT OF LIVER CANCER SIR-Spheres*: A New Treatment Option for Non-Resectable Liver Tumors Treatment Overview SIRT: Selective Internal Radiation Therapy Concept
Diffusion-weighted MR Imaging for Determination of Hepatocellular Carcinoma Response to Yttrium-90 Radioembolization
 Diffusion-weighted MR Imaging for Determination of Hepatocellular Carcinoma Response to Yttrium-90 Radioembolization Jie Deng, MS, Frank H. Miller, MD, Thomas K. Rhee, MD, Kent T. Sato, MD, Mary F. Mulcahy,
Diffusion-weighted MR Imaging for Determination of Hepatocellular Carcinoma Response to Yttrium-90 Radioembolization Jie Deng, MS, Frank H. Miller, MD, Thomas K. Rhee, MD, Kent T. Sato, MD, Mary F. Mulcahy,
INCIDENTAL FINDING DURING CARDIOMYOPATHY WORKUP
 Originally Posted: February 01, 2015 INCIDENTAL FINDING DURING CARDIOMYOPATHY WORKUP Resident(s): Mariya Gusman, M.D. Attending(s): Raul Palacios, M.D. Program/Dept(s): Brooke Army Medical Center DISCLAIMER
Originally Posted: February 01, 2015 INCIDENTAL FINDING DURING CARDIOMYOPATHY WORKUP Resident(s): Mariya Gusman, M.D. Attending(s): Raul Palacios, M.D. Program/Dept(s): Brooke Army Medical Center DISCLAIMER
Radioembolization as Salvage Therapy for Hepatic Metastasis of Uveal Melanoma: A Single- Institution Experience
 Vascular and Interventional Radiology Original Research Gonsalves et al. Radioembolization of Hepatic Metastasis of Uveal Melanoma Vascular and Interventional Radiology Original Research Carin F. Gonsalves
Vascular and Interventional Radiology Original Research Gonsalves et al. Radioembolization of Hepatic Metastasis of Uveal Melanoma Vascular and Interventional Radiology Original Research Carin F. Gonsalves
SORAMIC: NM Procedures
 : NM Procedures J. Ruf Klinik für Radiologie und Nuklearmedizin : NM Procedures Evaluation - 99m Tc MAA Scintigraphy Lung shunt assessment Treatment activity determination Therapy - 90 Y-SIR-Spheres Procedure
: NM Procedures J. Ruf Klinik für Radiologie und Nuklearmedizin : NM Procedures Evaluation - 99m Tc MAA Scintigraphy Lung shunt assessment Treatment activity determination Therapy - 90 Y-SIR-Spheres Procedure
COMPARING Y90 DEVICES
 COMPARING Y90 DEVICES William S Rilling MD, FSIR Professor of Radiology and Surgery Director, Vascular and Interventional Radiology Medical College of Wisconsin DISCLOSURES Research support : Siemens,
COMPARING Y90 DEVICES William S Rilling MD, FSIR Professor of Radiology and Surgery Director, Vascular and Interventional Radiology Medical College of Wisconsin DISCLOSURES Research support : Siemens,
Minimizing Unnecessary Radiation Exposure to Healthcare Professionals and Patients Imagine where we can go.
 ALARA & RADIATION SAFETY Minimizing Unnecessary Radiation Exposure to Healthcare Professionals and Patients Imagine where we can go. What is ALARA? As Low As Reasonably Achievable The use of radiation
ALARA & RADIATION SAFETY Minimizing Unnecessary Radiation Exposure to Healthcare Professionals and Patients Imagine where we can go. What is ALARA? As Low As Reasonably Achievable The use of radiation
Description. Section: Therapy Effective Date: July 15, 2014 Subsection: Therapy Original Policy Date: June 7, 2012 Subject: Page: 1 of 23
 Last Review Status/Date: June 2014 Page: 1 of 23 Description Radioembolization (RE), referred to as selective internal radiation therapy or SIRT in older literature, is the intra-arterial delivery of small
Last Review Status/Date: June 2014 Page: 1 of 23 Description Radioembolization (RE), referred to as selective internal radiation therapy or SIRT in older literature, is the intra-arterial delivery of small
Disclosures. I am on the Onyx speaker bureau I am a paid consultant to. Boston Scientific CeloNova Cook MDS Nordion Sirtex
 Disclosures I am on the Onyx speaker bureau I am a paid consultant to Boston Scientific CeloNova Cook MDS Nordion Sirtex Comparing Y90 Devices Matthew S. Johnson MD, FSIR Indiana University School of Medicine
Disclosures I am on the Onyx speaker bureau I am a paid consultant to Boston Scientific CeloNova Cook MDS Nordion Sirtex Comparing Y90 Devices Matthew S. Johnson MD, FSIR Indiana University School of Medicine
PET IMAGING (POSITRON EMISSION TOMOGRAPY) FACT SHEET
 Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Targeted Transarterial Therapy of Vx-2 Rabbit Liver Tumor with Yttrium-90 Labeled Ferromagnetic Particles Using an External Magnetic Field
 Targeted Transarterial Therapy of Vx-2 Rabbit Liver Tumor with Yttrium-90 Labeled Ferromagnetic Particles Using an External Magnetic Field HICHAM KOBEITER 1, CHRISTOS S. GEORGIADES 2, TINA LEAKAKOS 3,
Targeted Transarterial Therapy of Vx-2 Rabbit Liver Tumor with Yttrium-90 Labeled Ferromagnetic Particles Using an External Magnetic Field HICHAM KOBEITER 1, CHRISTOS S. GEORGIADES 2, TINA LEAKAKOS 3,
ABDOMINAL DIFFUSION WEIGHTED MR
 ABDOMINAL DIFFUSION WEIGHTED MR Frank Miller, M.D. FACR Professor of Radiology Chief, Body Imaging Section Medical Director, MR Imaging Northwestern University Feinberg School of Medicine fmiller@northwestern.edu
ABDOMINAL DIFFUSION WEIGHTED MR Frank Miller, M.D. FACR Professor of Radiology Chief, Body Imaging Section Medical Director, MR Imaging Northwestern University Feinberg School of Medicine fmiller@northwestern.edu
Re: Request to Retire Article (A54072) Restricting Medicare Coverage of Treatment with Yttrium-90 Microspheres
 February 7, 2017 Arthur Lurvey, MD 900 42nd Street S, PO Box 6781 Fargo, ND 58108-6781 Charles E. Haley, MD 900 42nd Street S, P.O. Box 6740 Fargo, ND 58108-6740 Gary Oakes, MD 900 42nd Street S, P.O.
February 7, 2017 Arthur Lurvey, MD 900 42nd Street S, PO Box 6781 Fargo, ND 58108-6781 Charles E. Haley, MD 900 42nd Street S, P.O. Box 6740 Fargo, ND 58108-6740 Gary Oakes, MD 900 42nd Street S, P.O.
PRIOR AUTHORIZATION Prior authorization is required for BlueCHiP for Medicare members and recommended for Commercial products.
 Medical Coverage Policy Radioembolization for Primary and Metastatic Tumors of the Liver EFFECTIVE DATE: 10 06 2009 POLICY LAST UPDATED: 08 02 2016 OVERVIEW Radioembolization (RE), referred to as selective
Medical Coverage Policy Radioembolization for Primary and Metastatic Tumors of the Liver EFFECTIVE DATE: 10 06 2009 POLICY LAST UPDATED: 08 02 2016 OVERVIEW Radioembolization (RE), referred to as selective
Selective internal radiation therapy with 90y microspheres for liver metastases: single-centre experience
 Selective internal radiation therapy with 90y microspheres for liver metastases: single-centre experience Poster No.: C-0718 Congress: ECR 2011 Type: Scientific Exhibit Authors: A. Presidente, G. Lombardi,
Selective internal radiation therapy with 90y microspheres for liver metastases: single-centre experience Poster No.: C-0718 Congress: ECR 2011 Type: Scientific Exhibit Authors: A. Presidente, G. Lombardi,
Radioembolization for Primary and Metastatic Tumors of the Liver
 Radioembolization for Primary and Metastatic Tumors of the Liver Policy Number: 8.01.43 Last Review: 8/2017 Origination: 8/2006 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue
Radioembolization for Primary and Metastatic Tumors of the Liver Policy Number: 8.01.43 Last Review: 8/2017 Origination: 8/2006 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue
Chemosaturation: Indication, Technique and Outcome
 Chemosaturation: Indication, Technique and Outcome Thomas J Vogl, S Koch, B Gebauer, W Willinek, C Engelke, R Bruening, F Wacker, A Enk I D I R: Institute of Diagnostic and Interventional Radiology Goethe
Chemosaturation: Indication, Technique and Outcome Thomas J Vogl, S Koch, B Gebauer, W Willinek, C Engelke, R Bruening, F Wacker, A Enk I D I R: Institute of Diagnostic and Interventional Radiology Goethe
Radioembolization for Primary and Metastatic Tumors of the Liver
 Radioembolization for Primary and Metastatic Tumors of the Liver Policy Number: 8.01.43 Last Review: 8/2018 Origination: 8/2006 Next Review: 8/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Radioembolization for Primary and Metastatic Tumors of the Liver Policy Number: 8.01.43 Last Review: 8/2018 Origination: 8/2006 Next Review: 8/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
SIRT in the Management of Metastatic Neuroendocrine Tumors
 SIRT in the Management of Metastatic Neuroendocrine Tumors Navesh K. Sharma, DO, PhD Assistant Professor, Departments of Radiation Oncology, Diagnostic Radiology and Nuclear Medicine Medical Director,
SIRT in the Management of Metastatic Neuroendocrine Tumors Navesh K. Sharma, DO, PhD Assistant Professor, Departments of Radiation Oncology, Diagnostic Radiology and Nuclear Medicine Medical Director,
Internal Pair Production of 90 Y Permits Hepatic Localization of Microspheres Using Routine PET: Proof of Concept
 Internal Pair Production of Y Permits Hepatic Localization of Microspheres Using Routine PET: Proof of Concept Vanessa L. Gates 1, Abdulredha A.H. Esmail 2, Karen Marshall 3, Stewart Spies 1, and Riad
Internal Pair Production of Y Permits Hepatic Localization of Microspheres Using Routine PET: Proof of Concept Vanessa L. Gates 1, Abdulredha A.H. Esmail 2, Karen Marshall 3, Stewart Spies 1, and Riad
Clinical Study Yttrium-90 Radioembolization for Colorectal Cancer Liver Metastases: A Single Institution Experience
 International Journal of Surgical Oncology Volume 20, Article ID 5726, 9 pages doi:0.55/20/5726 Clinical Study Yttrium-90 Radioembolization for Colorectal Cancer Liver Metastases: A Single Institution
International Journal of Surgical Oncology Volume 20, Article ID 5726, 9 pages doi:0.55/20/5726 Clinical Study Yttrium-90 Radioembolization for Colorectal Cancer Liver Metastases: A Single Institution
International Journal of Current Medical Sciences- Vol. 6, Issue,, pp , June, 2016 A B S T R A C T
 ISSN: 2320-8147 International Journal of Current Medical Sciences- Vol. 6, Issue,, pp. 122-126, June, 2016 COMPUTED TOMOGRAPHY IN HEPATIC METASTASES Ananthakumar P and Adaikkappan M., Available online
ISSN: 2320-8147 International Journal of Current Medical Sciences- Vol. 6, Issue,, pp. 122-126, June, 2016 COMPUTED TOMOGRAPHY IN HEPATIC METASTASES Ananthakumar P and Adaikkappan M., Available online
The Frequency and Significance of Small (15 mm) Hepatic Lesions Detected by CT
 535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
535 Elizabeth C. Jones1 Judith L. Chezmar Rendon C. Nelson Michael E. Bernardino Received July 22, 1991 ; accepted after revision October 16, 1991. Presented atthe annual meeting ofthe American Aoentgen
YTTRIUM-90 MICROSPHERES FOR THE TREATMENT OF HEPATOCELLULAR CARCINOMA: A REVIEW
 doi:10.1016/j.ijrobp.2006.02.061 Int. J. Radiation Oncology Biol. Phys., Vol. 66, No. 2, Supplement, pp. S83 S88, 2006 Copyright 2006 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/06/$
doi:10.1016/j.ijrobp.2006.02.061 Int. J. Radiation Oncology Biol. Phys., Vol. 66, No. 2, Supplement, pp. S83 S88, 2006 Copyright 2006 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/06/$
ALARA and Radiation Safety
 ALARA and Radiation Safety Experience the power of TheraSphere and deliver hope where it s needed most. Imagine where we can go. btg-im.com What is TheraSphere? TheraSphere is indicated for radiation treatment
ALARA and Radiation Safety Experience the power of TheraSphere and deliver hope where it s needed most. Imagine where we can go. btg-im.com What is TheraSphere? TheraSphere is indicated for radiation treatment
Intra-arterial Therapy in Management of HCC: ctace, DEB-TACE, and Y90 Radioembolization
 Intra-arterial Therapy in Management of HCC: ctace, DEB-TACE, and Y90 Radioembolization Department of Radiology, National Cancer Center In Joon Lee Contents Conventional TACE Role of TACE in management
Intra-arterial Therapy in Management of HCC: ctace, DEB-TACE, and Y90 Radioembolization Department of Radiology, National Cancer Center In Joon Lee Contents Conventional TACE Role of TACE in management
Ruolo della interventistica per le secondarietà epatiche e di altre sedi
 Ruolo della interventistica per le secondarietà epatiche e di altre sedi Giancarlo Bizzarri Dipartimento di Diagnostica per Immagini e Radiologia Interventistica Ospedale Regina Apostolorum, Albano Laziale
Ruolo della interventistica per le secondarietà epatiche e di altre sedi Giancarlo Bizzarri Dipartimento di Diagnostica per Immagini e Radiologia Interventistica Ospedale Regina Apostolorum, Albano Laziale
The use of minimally invasive procedures to
 Yttrium-90 Radioembolization Mapping and Therapy What to do and what to avoid. BY PAVAN K. KAVALI, MD; RIPAL T. GANDHI, MD; AND SUVRANU GANGULI, MD The use of minimally invasive procedures to manage primary
Yttrium-90 Radioembolization Mapping and Therapy What to do and what to avoid. BY PAVAN K. KAVALI, MD; RIPAL T. GANDHI, MD; AND SUVRANU GANGULI, MD The use of minimally invasive procedures to manage primary
Transarterial Therapies for the Treatment of Intrahepatic Cholangiocarcinoma
 21 Transarterial Therapies for the Treatment of Intrahepatic Cholangiocarcinoma Joseph J. Zechlinski, MD 1 William S. Rilling, MD, FSIR 1 1 Division of Interventional Radiology, Medical College of Wisconsin,
21 Transarterial Therapies for the Treatment of Intrahepatic Cholangiocarcinoma Joseph J. Zechlinski, MD 1 William S. Rilling, MD, FSIR 1 1 Division of Interventional Radiology, Medical College of Wisconsin,
SIRT in Neuroendocrine Tumors
 SIRT in Neuroendocrine Tumors Marnix G.E.H. Lam, MD PhD Professor of Nuclear Medicine AVL Amsterdam UMC Utrecht ENETS Center of Excellence, The Netherlands Disclosure of speaker s interests Consultant
SIRT in Neuroendocrine Tumors Marnix G.E.H. Lam, MD PhD Professor of Nuclear Medicine AVL Amsterdam UMC Utrecht ENETS Center of Excellence, The Netherlands Disclosure of speaker s interests Consultant
Index. C Cancer, Carcinoid syndrome, 413. D DCIS. See Ductal carcinoma in situ (DCIS) DEB-TACE. See Drug eluting beads-tace (DEB-TACE)
 Index A Ablation, 179 199, 843 853 devices, 179, 199 liver tumors, 527 techniques, 516 Ablative radiation therapy, 456 Accelerated partial breast, 894, 896 898 Adaptive radiation therapy, 586, 598, 602
Index A Ablation, 179 199, 843 853 devices, 179, 199 liver tumors, 527 techniques, 516 Ablative radiation therapy, 456 Accelerated partial breast, 894, 896 898 Adaptive radiation therapy, 586, 598, 602
HEPATIC METASTASES. We can state 3 types of metastases depending on their treatment options:
 HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
HEPATIC METASTASES 1. Definition Metastasis means the spread of cancer. Cancerous cells can separate from the primary tumor and enter the bloodstream or the lymphatic system (the one that produces, stores,
Regional Therapy for Metastatic Neuroendocrine Tumors. Janette Durham, MD Professor of Radiology University of Colorado School of Medicine
 Regional Therapy for Metastatic Neuroendocrine Tumors Janette Durham, MD Professor of Radiology University of Colorado School of Medicine Introduce regional therapy for mnet Arterial therapies Injection
Regional Therapy for Metastatic Neuroendocrine Tumors Janette Durham, MD Professor of Radiology University of Colorado School of Medicine Introduce regional therapy for mnet Arterial therapies Injection
Radioembolization with Lipiodol for the Treatment of Hepatocellular Carcinoma and Liver Metastases
 Radioembolization with Lipiodol for the Treatment of Hepatocellular Carcinoma and Liver Metastases Pr Francesco Giammarile CHLS Lyon Faculté de Lyon Sud «Aut tace aut loquere meliora silentio» Malignant
Radioembolization with Lipiodol for the Treatment of Hepatocellular Carcinoma and Liver Metastases Pr Francesco Giammarile CHLS Lyon Faculté de Lyon Sud «Aut tace aut loquere meliora silentio» Malignant
Selective Internal Radiation Therapy. Jefferson R. Pagsisihan, MD, DPSNM The Medical City St. Luke s Medical Center
 Selective Internal Radiation Therapy Jefferson R. Pagsisihan, MD, DPSNM The Medical City St. Luke s Medical Center S Selective Internal Radiation Therapy catheter-based liver directed modality for patients
Selective Internal Radiation Therapy Jefferson R. Pagsisihan, MD, DPSNM The Medical City St. Luke s Medical Center S Selective Internal Radiation Therapy catheter-based liver directed modality for patients
Guidelines for SIRT in HCC An Evolution
 Guidelines for SIRT in HCC An Evolution 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore The challenge of HCC Surgery is potentially curative in early
Guidelines for SIRT in HCC An Evolution 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore The challenge of HCC Surgery is potentially curative in early
100% pure beta emitter Decays to zirconium-90 Physical half-life of 64.1 hours (2.67 days) 94% of radiation delivered within 11 days
 100% pure beta emitter Decays to zirconium-90 Physical half-life of 64.1 hours (2.67 days) 94% of radiation delivered within 11 days TheraSphere [US package insert]. Surrey, UK: Biocompatibles UK Ltd,
100% pure beta emitter Decays to zirconium-90 Physical half-life of 64.1 hours (2.67 days) 94% of radiation delivered within 11 days TheraSphere [US package insert]. Surrey, UK: Biocompatibles UK Ltd,
Selective Internal Radiation Therapy with SIR-Spheres in Patients with Nonresectable Liver Tumors
 CANCER BIOTHERAPY & RADIOPHARMACEUTICALS Volume 20, Number 2, 2005 Mary Ann Liebert, Inc. Selective Internal Radiation Therapy with SIR-Spheres in Patients with Nonresectable Liver Tumors Gabriele Pöpperl,
CANCER BIOTHERAPY & RADIOPHARMACEUTICALS Volume 20, Number 2, 2005 Mary Ann Liebert, Inc. Selective Internal Radiation Therapy with SIR-Spheres in Patients with Nonresectable Liver Tumors Gabriele Pöpperl,
8/1/2017. Disclosures. Outline. SAM Imaging Education Course 90Y-Microsphere Therapy: Emerging Trends and Future Directions
 SAM Imaging Education Course Y-Microsphere Therapy: Emerging Trends and Future Directions Matt Vanderhoek, PhD Henry Ford Health System, Detroit, MI Vanessa Gates, MS Northwestern University, Chicago,
SAM Imaging Education Course Y-Microsphere Therapy: Emerging Trends and Future Directions Matt Vanderhoek, PhD Henry Ford Health System, Detroit, MI Vanessa Gates, MS Northwestern University, Chicago,
SIRT Dosimetry: Sometimes Less Is More
 SIRT Dosimetry: Sometimes Less Is More Navesh K. Sharma, DO, PhD Assistant Professor, Departments of Radiation Oncology, Diagnostic Radiology and Nuclear Medicine Medical Director, Radiation Oncology,
SIRT Dosimetry: Sometimes Less Is More Navesh K. Sharma, DO, PhD Assistant Professor, Departments of Radiation Oncology, Diagnostic Radiology and Nuclear Medicine Medical Director, Radiation Oncology,
Selection Criteria and Insertion of SIRT into HCC Treatment Guidelines
 Selection Criteria and Insertion of SIRT into HCC Treatment Guidelines 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore Pierce Chow FRCSE PhD SIRT in
Selection Criteria and Insertion of SIRT into HCC Treatment Guidelines 2 nd Asia Pacific Symposium on Liver- Directed Y-90 Microspheres Therapy 1st November 2014, Singapore Pierce Chow FRCSE PhD SIRT in
Volume 20 Number 5 Siddiqi and Devlin 665 Figure 1. Axial CT image in portal venous phase before treatment with 90 Y spheres. Low-density areas, some
 Radiation Lobectomy A Minimally Invasive Treatment Model for Liver Cancer: Case Report Nasir H. Siddiqi, MD, Phillip M. Devlin, MD Chemotherapy-resistant colon carcinoma metastases to a patient s right
Radiation Lobectomy A Minimally Invasive Treatment Model for Liver Cancer: Case Report Nasir H. Siddiqi, MD, Phillip M. Devlin, MD Chemotherapy-resistant colon carcinoma metastases to a patient s right
Staging & Current treatment of HCC
 Staging & Current treatment of HCC Dr.: Adel El Badrawy Badrawy; ; M.D. Staging & Current ttt of HCC Early stage HCC is typically silent. HCC is often advanced at first manifestation. The selective ttt
Staging & Current treatment of HCC Dr.: Adel El Badrawy Badrawy; ; M.D. Staging & Current ttt of HCC Early stage HCC is typically silent. HCC is often advanced at first manifestation. The selective ttt
NIH Public Access Author Manuscript Int J Radiat Oncol Biol Phys. Author manuscript; available in PMC 2013 July 01.
 NIH Public Access Author Manuscript Published in final edited form as: Int J Radiat Oncol Biol Phys. 2012 July 1; 83(3): 887 894. doi:10.1016/j.ijrobp.2011.07.041. Radioembolization for Neuroendocrine
NIH Public Access Author Manuscript Published in final edited form as: Int J Radiat Oncol Biol Phys. 2012 July 1; 83(3): 887 894. doi:10.1016/j.ijrobp.2011.07.041. Radioembolization for Neuroendocrine
Radiofrequency Ablation versus Microwave Ablation in HCC and Liver Metastases
 Radiofrequency Ablation versus Microwave Ablation in HCC and Liver Metastases Thomas J. Vogl, B. Panahi, N. Nour-Eldin I D I R: Institute of Diagnostic and Interventional Radiology Goethe University Frankfurt,
Radiofrequency Ablation versus Microwave Ablation in HCC and Liver Metastases Thomas J. Vogl, B. Panahi, N. Nour-Eldin I D I R: Institute of Diagnostic and Interventional Radiology Goethe University Frankfurt,
Y90 SIRT Therapy Dosimetric Aspects
 Y90 SIRT Therapy Dosimetric Aspects David Chee-Eng Ng MBBS, BSc, MSc, MRCP, FAMS, FRCP (Edin) Head and Senior Consultant, Department of Nuclear Medicine and PET Singapore General Hospital Adjunct Assistant
Y90 SIRT Therapy Dosimetric Aspects David Chee-Eng Ng MBBS, BSc, MSc, MRCP, FAMS, FRCP (Edin) Head and Senior Consultant, Department of Nuclear Medicine and PET Singapore General Hospital Adjunct Assistant
Radioembolization for Primary and Metastatic Tumors of the Liver
 Page: 1 of 28 Last Review Status/Date: September 2015 Description Radioembolization (RE), also referred to as selective internal radiotherapy (SIRT), is the intra-arterial delivery of small beads (microspheres)
Page: 1 of 28 Last Review Status/Date: September 2015 Description Radioembolization (RE), also referred to as selective internal radiotherapy (SIRT), is the intra-arterial delivery of small beads (microspheres)
POSITRON EMISSION TOMOGRAPHY (PET)
 Status Active Medical and Behavioral Health Policy Section: Radiology Policy Number: V-27 Effective Date: 08/27/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Radiology Policy Number: V-27 Effective Date: 08/27/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Radioembolization with Yttrium-90 microspheres for patients with unresectable hepatocellular carcinoma
 Original Article Radioembolization with Yttrium-90 microspheres for patients with unresectable hepatocellular carcinoma Munveer Singh Bhangoo 1, Diraj R. Karnani 1, Paul N. Hein 2, Huan Giap 3, Harry Knowles
Original Article Radioembolization with Yttrium-90 microspheres for patients with unresectable hepatocellular carcinoma Munveer Singh Bhangoo 1, Diraj R. Karnani 1, Paul N. Hein 2, Huan Giap 3, Harry Knowles
Title: What is the role of pre-operative PET/PET-CT in the management of patients with
 Title: What is the role of pre-operative PET/PET-CT in the management of patients with potentially resectable colorectal cancer liver metastasis? Pablo E. Serrano, Julian F. Daza, Natalie M. Solis June
Title: What is the role of pre-operative PET/PET-CT in the management of patients with potentially resectable colorectal cancer liver metastasis? Pablo E. Serrano, Julian F. Daza, Natalie M. Solis June
Y-90 Microsphere Therapy: Nuclear Medicine Perspective
 Y-90 Microsphere Therapy: Nuclear Medicine Perspective Carl Hoh, M.D. Dept. Radiology UCSD Medical Center ckhoh@ucsd.edu Learning Objectives Role of Nuclear Medicine in patient selection Technical Issues
Y-90 Microsphere Therapy: Nuclear Medicine Perspective Carl Hoh, M.D. Dept. Radiology UCSD Medical Center ckhoh@ucsd.edu Learning Objectives Role of Nuclear Medicine in patient selection Technical Issues
Clinical indications for positron emission tomography
 Clinical indications for positron emission tomography Oncology applications Brain and spinal cord Parotid Suspected tumour recurrence when anatomical imaging is difficult or equivocal and management will
Clinical indications for positron emission tomography Oncology applications Brain and spinal cord Parotid Suspected tumour recurrence when anatomical imaging is difficult or equivocal and management will
Newcastle HPB MDM updated radiology imaging protocol recommendations. Author Dr John Scott. Consultant Radiologist Freeman Hospital
 Newcastle HPB MDM updated radiology imaging protocol recommendations Author Dr John Scott. Consultant Radiologist Freeman Hospital This document is intended as a guide to aid radiologists and clinicians
Newcastle HPB MDM updated radiology imaging protocol recommendations Author Dr John Scott. Consultant Radiologist Freeman Hospital This document is intended as a guide to aid radiologists and clinicians
Hepatic metastases of neuroendocrine tumors: treatment options and outcomes of local patients treated with radioembolization
 Hepatic metastases of neuroendocrine tumors: treatment options and outcomes of local patients treated with radioembolization JP King PGY2 May 22, 2015 Neuroendocrine Tumor (NET) WHO Classification Location
Hepatic metastases of neuroendocrine tumors: treatment options and outcomes of local patients treated with radioembolization JP King PGY2 May 22, 2015 Neuroendocrine Tumor (NET) WHO Classification Location
Radioembolization: technical aspects
 Radioembolization: technical aspects Rita Golfieri Unità Operativa Radiologia Malpighi Azienda Ospedaliero-Universitaria di Bologna Policlinico S. Orsola - Malpighi La sottoscritta dichiara di non aver
Radioembolization: technical aspects Rita Golfieri Unità Operativa Radiologia Malpighi Azienda Ospedaliero-Universitaria di Bologna Policlinico S. Orsola - Malpighi La sottoscritta dichiara di non aver
Superselective vs. lobar transarterial ethiodized oil-chemoembolization - occurrence and clinical significance of non-target embolization
 Superselective vs. lobar transarterial ethiodized oil-chemoembolization - occurrence, p. 13-22 Interventional HR J Original Article Superselective vs. lobar transarterial ethiodized oil-chemoembolization
Superselective vs. lobar transarterial ethiodized oil-chemoembolization - occurrence, p. 13-22 Interventional HR J Original Article Superselective vs. lobar transarterial ethiodized oil-chemoembolization
Current Treatment of Colorectal Metastases. Dr. Thavanathan Surgical Grand Rounds February 1, 2005
 Current Treatment of Colorectal Metastases Dr. Thavanathan Surgical Grand Rounds February 1, 2005 25% will have metastases at initial presentation 25-50% 50% will develop metastases later 40% of potentially
Current Treatment of Colorectal Metastases Dr. Thavanathan Surgical Grand Rounds February 1, 2005 25% will have metastases at initial presentation 25-50% 50% will develop metastases later 40% of potentially
Locoregional Treatments for HCC Applications in Transplant Candidates. Locoregional Treatments for HCC Applications in Transplant Candidates
 Locoregional Treatments for HCC Applications in Transplant Candidates Matthew Casey, MD March 31, 2016 Locoregional Treatments for HCC Applications in Transplant Candidates *No disclosures *Off-label uses
Locoregional Treatments for HCC Applications in Transplant Candidates Matthew Casey, MD March 31, 2016 Locoregional Treatments for HCC Applications in Transplant Candidates *No disclosures *Off-label uses
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
CT Contrast Protocols for Different Organ Imaging
 CT Contrast Protocols for Different Organ Imaging g Paul Shreve, M.D. Advanced Radiology Services, P.C. & Spectrum Health Grand Rapids, MI, USA Correlative Imaging Council Society of Nuclear Medicine 56
CT Contrast Protocols for Different Organ Imaging g Paul Shreve, M.D. Advanced Radiology Services, P.C. & Spectrum Health Grand Rapids, MI, USA Correlative Imaging Council Society of Nuclear Medicine 56
Management of Rare Liver Tumours
 Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
Conformal external beam radiation or selective internal radiation therapy a comparison of treatment outcomes for hepatocellular carcinoma
 Original Article Conformal external beam radiation or selective internal radiation therapy a comparison of treatment outcomes for hepatocellular carcinoma Oluwadamilola T. Oladeru 1, Joseph A. Miccio 1,
Original Article Conformal external beam radiation or selective internal radiation therapy a comparison of treatment outcomes for hepatocellular carcinoma Oluwadamilola T. Oladeru 1, Joseph A. Miccio 1,
Hepatobiliary Malignancies Retrospective Study at Truman Medical Center
 Hepatobiliary Malignancies 206-207 Retrospective Study at Truman Medical Center Brandon Weckbaugh MD, Prarthana Patel & Sheshadri Madhusudhana MD Introduction: Hepatobiliary malignancies are cancers which
Hepatobiliary Malignancies 206-207 Retrospective Study at Truman Medical Center Brandon Weckbaugh MD, Prarthana Patel & Sheshadri Madhusudhana MD Introduction: Hepatobiliary malignancies are cancers which
IMPLANTABLE BETA-EMITTING MICROSPHERES FOR TREATMENT OF MALIGNANT TUMORS
 UnitedHealthcare Oxford Clinical Policy IMPLANTABLE BETA-EMITTING MICROSPHERES FOR TREATMENT OF MALIGNANT TUMORS Policy Number: CANCER 036.9 T2 Effective Date: January 1, 2017 Table of Contents Page INSTRUCTIONS
UnitedHealthcare Oxford Clinical Policy IMPLANTABLE BETA-EMITTING MICROSPHERES FOR TREATMENT OF MALIGNANT TUMORS Policy Number: CANCER 036.9 T2 Effective Date: January 1, 2017 Table of Contents Page INSTRUCTIONS
INTRAARTERIAL TREATMENT OF COLORECTAL LIVER METASTASES. Dr. Joan Falcó Interventional Radiology UDIAT. Hospital Universitari Parc Taulí
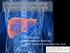 INTRAARTERIAL TREATMENT OF COLORECTAL LIVER METASTASES Dr. Joan Falcó Interventional Radiology UDIAT. Hospital Universitari Parc Taulí STRATEGIES FOR CRLM LIVER METASTASES Extended indications Resectable
INTRAARTERIAL TREATMENT OF COLORECTAL LIVER METASTASES Dr. Joan Falcó Interventional Radiology UDIAT. Hospital Universitari Parc Taulí STRATEGIES FOR CRLM LIVER METASTASES Extended indications Resectable
RADIOEMBOLIZZAZIONE NEI TUMORI EPATICI: STATO DELL ARTE. clic per modificare lo stile del sottotitolo dello schem
 XII Congresso Nazionale AIMN 2015 16-19 Aprile 2015 Rimini RADIOEMBOLIZZAZIONE NEI TUMORI EPATICI: STATO DELL ARTE clic per modificare lo stile del sottotitolo dello schem Marco Maccauro Nuclear Medicine
XII Congresso Nazionale AIMN 2015 16-19 Aprile 2015 Rimini RADIOEMBOLIZZAZIONE NEI TUMORI EPATICI: STATO DELL ARTE clic per modificare lo stile del sottotitolo dello schem Marco Maccauro Nuclear Medicine
Hepatocellular carcinoma (HCC) is a malignant liver neoplasm
 Diagn Interv Radiol 2011; 17:328 333 Turkish Society of Radiology 2011 ABDOMINAL IMAGING ORIGINAL ARTICLE Correlation of dynamic multidetector CT findings with pathological grades of hepatocellular carcinoma
Diagn Interv Radiol 2011; 17:328 333 Turkish Society of Radiology 2011 ABDOMINAL IMAGING ORIGINAL ARTICLE Correlation of dynamic multidetector CT findings with pathological grades of hepatocellular carcinoma
Nuclear Medicine and PET. D. J. McMahon rev cewood
 Nuclear Medicine and PET D. J. McMahon 150504 rev cewood 2018-02-15 Key Points Nuclear Medicine and PET: Imaging: Understand how Nuc Med & PET differ from Radiography & CT by the source of radiation. Be
Nuclear Medicine and PET D. J. McMahon 150504 rev cewood 2018-02-15 Key Points Nuclear Medicine and PET: Imaging: Understand how Nuc Med & PET differ from Radiography & CT by the source of radiation. Be
Staging Colorectal Cancer
 Staging Colorectal Cancer CT is recommended as the initial staging scan for colorectal cancer to assess local extent of the disease and to look for metastases to the liver and/or lung Further imaging for
Staging Colorectal Cancer CT is recommended as the initial staging scan for colorectal cancer to assess local extent of the disease and to look for metastases to the liver and/or lung Further imaging for
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of selective internal radiation therapy for non-resectable colorectal metastases
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of selective internal radiation therapy for non-resectable colorectal metastases
IMPLANTABLE BETA-EMITTING MICROSPHERES FOR TREATMENT OF MALIGNANT TUMORS
 UnitedHealthcare Commercial Medical Policy IMPLANTABLE BETA-EMITTING MICROSPHERES FOR TREATMENT OF MALIGNANT TUMORS Policy Number: 2017T0445N Effective Date: January 1, 2017 Table of Contents Page INSTRUCTIONS
UnitedHealthcare Commercial Medical Policy IMPLANTABLE BETA-EMITTING MICROSPHERES FOR TREATMENT OF MALIGNANT TUMORS Policy Number: 2017T0445N Effective Date: January 1, 2017 Table of Contents Page INSTRUCTIONS
Transarterial Chemoembolisation (TACE) with Drug-Eluting Beads
 Transarterial Chemoembolisation (TACE) with Drug-Eluting Beads A minimally invasive treatment for liver cancer Provided as an educational service by Biocompatibles UK Ltd, a BTG International group company
Transarterial Chemoembolisation (TACE) with Drug-Eluting Beads A minimally invasive treatment for liver cancer Provided as an educational service by Biocompatibles UK Ltd, a BTG International group company
Imaging of Hepatocellular Carcinoma After Treatment with Yttrium-90 Microspheres
 Keppke et al. Imaging of 90 Y-Treated Hepatocellular Carcinoma Hepatobiliary Imaging Original Research na L. Keppke 1 Riad Salem 1 Denise Reddy 1 Jie Huang 2 Jianhua Jin 2 ndrew C. Larson 1 Frank H. Miller
Keppke et al. Imaging of 90 Y-Treated Hepatocellular Carcinoma Hepatobiliary Imaging Original Research na L. Keppke 1 Riad Salem 1 Denise Reddy 1 Jie Huang 2 Jianhua Jin 2 ndrew C. Larson 1 Frank H. Miller
Section: Medicine Last Reviewed Date: July Policy No: 140 Effective Date: October 1, 2014
 Medical Policy Manual Topic: Radioembolization for Primary and Metastatic Tumors of the Liver Date of Origin: December 2, 2010 Section: Medicine Last Reviewed Date: July 2014 Policy No: 140 Effective Date:
Medical Policy Manual Topic: Radioembolization for Primary and Metastatic Tumors of the Liver Date of Origin: December 2, 2010 Section: Medicine Last Reviewed Date: July 2014 Policy No: 140 Effective Date:
Radioembolization for the treatment of hepatocellular carcinoma
 pissn 2287-2728 eissn 2287-285X Review https://doi.org/10.3350/cmh.2017.0004 Clinical and Molecular Hepatology 2017;23:109-114 Radioembolization for the treatment of hepatocellular carcinoma Hyo-Cheol
pissn 2287-2728 eissn 2287-285X Review https://doi.org/10.3350/cmh.2017.0004 Clinical and Molecular Hepatology 2017;23:109-114 Radioembolization for the treatment of hepatocellular carcinoma Hyo-Cheol
Evaluation of prognostic scoring systems for bone metastases using single center data
 MOLECULAR AND CLINICAL ONCOLOGY 3: 1361-1370, 2015 Evaluation of prognostic scoring systems for bone metastases using single center data HIROFUMI SHIMADA 1, TAKAO SETOGUCHI 2, SHUNSUKE NAKAMURA 1, MASAHIRO
MOLECULAR AND CLINICAL ONCOLOGY 3: 1361-1370, 2015 Evaluation of prognostic scoring systems for bone metastases using single center data HIROFUMI SHIMADA 1, TAKAO SETOGUCHI 2, SHUNSUKE NAKAMURA 1, MASAHIRO
Selective Internal Radiation Therapy (SIRT) in the multimodal approach to Hepatocellular Carcinoma
 Selective Internal Radiation Therapy (SIRT) in the multimodal approach to Hepatocellular Carcinoma International Course on THERANOSTICS and MOLECULAR RADIOTHERAPY Brussels, 4 october 2017 Vincent Donckier
Selective Internal Radiation Therapy (SIRT) in the multimodal approach to Hepatocellular Carcinoma International Course on THERANOSTICS and MOLECULAR RADIOTHERAPY Brussels, 4 october 2017 Vincent Donckier
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
IMPLANTABLE BETA-EMITTING MICROSPHERES FOR TREATMENT OF MALIGNANT TUMORS
 UnitedHealthcare Commercial Medical Policy IMPLANTABLE BETA-EMITTING MICROSPHERES FOR TREATMENT OF MALIGNANT TUMORS Policy Number: 2018T0445O Effective Date: February 1, 2018 Table of Contents Page INSTRUCTIONS
UnitedHealthcare Commercial Medical Policy IMPLANTABLE BETA-EMITTING MICROSPHERES FOR TREATMENT OF MALIGNANT TUMORS Policy Number: 2018T0445O Effective Date: February 1, 2018 Table of Contents Page INSTRUCTIONS
National Horizon Scanning Centre. Bevacizumab (Avastin) for glioblastoma multiforme - relapsed. August 2008
 Bevacizumab (Avastin) for glioblastoma multiforme - relapsed August 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
Bevacizumab (Avastin) for glioblastoma multiforme - relapsed August 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
SELECTIVE INTERNAL RADIATION THERAPY OR FROM COLORECTAL CANCER
 TITLE: SELECTIVE INTERNAL RADIATION THERAPY OR RADIOEMBOLIZATION FOR INOPERABLE LIVER METASTASES FROM COLORECTAL CANCER AUTHOR: Jeffrey A. Tice, MD Assistant Professor of Medicine Division of General Internal
TITLE: SELECTIVE INTERNAL RADIATION THERAPY OR RADIOEMBOLIZATION FOR INOPERABLE LIVER METASTASES FROM COLORECTAL CANCER AUTHOR: Jeffrey A. Tice, MD Assistant Professor of Medicine Division of General Internal
Radioembolization with Use of Yttrium-90 Resin Microspheres in Patients with Hepatocellular Carcinoma and Portal Vein Thrombosis
 Radioembolization with Use of Yttrium-90 Resin Microspheres in Patients with Hepatocellular Carcinoma and Portal Vein Thrombosis Mercedes Iñarrairaegui, MD, PhD, Kenneth G. Thurston, MA, Jose I. Bilbao,
Radioembolization with Use of Yttrium-90 Resin Microspheres in Patients with Hepatocellular Carcinoma and Portal Vein Thrombosis Mercedes Iñarrairaegui, MD, PhD, Kenneth G. Thurston, MA, Jose I. Bilbao,
MULTI-DISCIPLINARY MANAGEMENT OF INTERMEDIATE STAGE HCC
 Dr Apoorva Gogna MBBS FRCR FAMS Consultant Interventional Radiology Center Department of Diagnostic Radiology SingaporeGeneral Hospital MULTI-DISCIPLINARY MANAGEMENT OF INTERMEDIATE STAGE HCC CASE HISTORY
Dr Apoorva Gogna MBBS FRCR FAMS Consultant Interventional Radiology Center Department of Diagnostic Radiology SingaporeGeneral Hospital MULTI-DISCIPLINARY MANAGEMENT OF INTERMEDIATE STAGE HCC CASE HISTORY
MEDICAL POLICY SUBJECT: SELECTIVE INTERNAL RADIATION THERAPY (SIRT) FOR HEPATIC TUMORS. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: SELECTIVE INTERNAL PAGE: 1 OF: 8 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an
MEDICAL POLICY SUBJECT: SELECTIVE INTERNAL PAGE: 1 OF: 8 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product (including an
PET-CT versus MRI in the identification of hepatic metastases from colorectal carcinoma: An evidence based review of the current literature.
 PET-CT versus MRI in the identification of hepatic metastases from colorectal carcinoma: An evidence based review of the current literature. Poster No.: C-1275 Congress: ECR 2017 Type: Scientific Exhibit
PET-CT versus MRI in the identification of hepatic metastases from colorectal carcinoma: An evidence based review of the current literature. Poster No.: C-1275 Congress: ECR 2017 Type: Scientific Exhibit
Hepatobiliary and Pancreatic Malignancies
 Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Austin Radiological Association Nuclear Medicine Procedure PET SODIUM FLUORIDE BONE SCAN (F-18 NaF)
 Austin Radiological Association Nuclear Medicine Procedure PET SODIUM FLUORIDE BONE SCAN (F-18 NaF) Overview Indication Sodium Fluoride F18 injection is a radioactive diagnostic agent for positron emission
Austin Radiological Association Nuclear Medicine Procedure PET SODIUM FLUORIDE BONE SCAN (F-18 NaF) Overview Indication Sodium Fluoride F18 injection is a radioactive diagnostic agent for positron emission
SELECTIVE INTERNAL RADIOTHERAPY Y90 RADIOEMBOLIZATION
 THE NEXT OIS FRONTIER? SELECTIVE INTERNAL RADIOTHERAPY Y90 RADIOEMBOLIZATION David Sperling, MD, FSIR Vice Chair, Strategy and Development Department of Radiology Columbia University Medical Center David
THE NEXT OIS FRONTIER? SELECTIVE INTERNAL RADIOTHERAPY Y90 RADIOEMBOLIZATION David Sperling, MD, FSIR Vice Chair, Strategy and Development Department of Radiology Columbia University Medical Center David
