Populations Interventions Comparators Outcomes Individuals: With non-neoplastic intracranial conditions (e.g., arteriovenous malformations) Surgery
|
|
|
- Marion Robbins
- 5 years ago
- Views:
Transcription
1 Protocol Stereotactic Radiosurgery and Stereotactic Body Radiotherapy (60110) Medical Benefit Effective Date: 07/01/17 Next Review Date: 03/19 Preauthorization No Review Dates: 11/07, 07/08, 01/09, 01/10, 03/11, 01/12, 09/12, 09/13, 03/14, 03/15, 03/16, 03/17, 03/18 Preauthorization is not required. The following protocol contains medical necessity criteria that apply for this service. The criteria are also applicable to services provided in the local Medicare Advantage operating area for those members, unless separate Medicare Advantage criteria are indicated. If the criteria are not met, reimbursement will be denied and the patient cannot be billed. Please note that payment for covered services is subject to eligibility and the limitations noted in the patient s contract at the time the services are rendered. Populations Interventions Comparators Outcomes Individuals: With non-neoplastic intracranial conditions (e.g., arteriovenous malformations) Individuals: With non-neoplastic intracranial conditions (e.g., trigeminal neuralgia) Interventions of interest are: Stereotactic radiosurgery Interventions of interest are: Stereotactic radiosurgery Comparators of interest are: Other forms of radiotherapy Surgery Combinations of other forms of radiotherapy, surgery, or chemotherapy Medical therapy Comparators of interest are: Other forms of radiotherapy Surgery Combinations of other forms of radiotherapy, surgery, or chemotherapy Medical therapy Relevant outcomes include: Overall survival Symptoms Treatment-related morbidity Relevant outcomes include: Overall survival Symptoms Treatment-related morbidity Individuals: With non-neoplastic neurologic disorders (e.g., epilepsy, tremor and movement disorders, chronic pain) Interventions of interest are: Stereotactic radiosurgery Comparators of interest are: Other forms of radiotherapy Surgery Combinations of other forms of radiotherapy, surgery, or chemotherapy Medical therapy Comparators of interest are: Other forms of radiotherapy Surgery Combinations of other forms of radiotherapy, surgery, or chemotherapy Relevant outcomes include: Overall survival Symptoms Treatment-related morbidity Individuals: With benign neoplastic intracranial lesion(s) (e.g., acoustic neuromas, pituitary adenoma, meningiomas) Interventions of interest are: Stereotactic radiosurgery Relevant outcomes include: Overall survival Symptoms Treatment-related morbidity Page 1 of 19
2 Populations Interventions Comparators Outcomes Individuals: With benign neoplastic intracranial lesion(s) (craniopharyngioma, glomus jugulare tumors) Individuals: With malignant neoplastic intracranial lesion(s) (e.g., gliomas, astrocytomas) Individuals: With malignant neoplastic intracranial lesion(s) (e.g., brain metastases) Individuals: With uveal melanoma Individuals: With benign or malignant extracranial lesion(s) (e.g., extracranial primary and metastatic tumors) a Interventions of interest are: Stereotactic radiosurgery Interventions of interest are: Stereotactic radiosurgery Interventions of interest are: Stereotactic radiosurgery Interventions of interest are: Stereotactic radiosurgery Interventions of interest are: Stereotactic body radiotherapy Comparators of interest are: Other forms of radiotherapy Surgery Combinations of other forms of radiotherapy, surgery, or chemotherapy Comparators of interest are: Other forms of radiotherapy Surgery Combinations of other forms of radiotherapy, surgery, or chemotherapy Comparators of interest are: Other forms of radiotherapy Surgery Combinations of other forms of radiotherapy, surgery, or chemotherapy Comparators of interest are: Other forms of radiotherapy Surgery Combinations of other forms of radiotherapy, surgery, or chemotherapy Comparators of interest are: Other forms of radiotherapy Surgery Combinations of radiotherapy, surgery, or chemotherapy Relevant outcomes include: Overall survival Symptoms Treatment-related morbidity Relevant outcomes include: Overall survival Symptoms Treatment-related morbidity Relevant outcomes include: Overall survival Symptoms Treatment-related morbidity Relevant outcomes include: Overall survival Symptoms Treatment-related morbidity Relevant outcomes include: Overall survival Symptoms Treatment-related morbidity a Extracranial lesions include: primary spinal or vertebral body tumors, primary and metastatic tumors of the liver; primary pancreatic cancer; primary and metastatic renal cell carcinoma; metastatic adrenal cancer, and oligometastases. Description Stereotactic radiosurgery (SRS) and stereotactic body radiotherapy (SBRT) are 3-dimensional conformal radiotherapy methods that deliver highly focused, convergent radiotherapy beams on a target that is defined with 3- dimensional imaging techniques with the ability to spare adjacent radiosensitive structures. Stereotactic radiosurgery primarily refers to such radiotherapy applied to intracranial lesions. Stereotactic body radiotherapy refers to therapy generally applied other areas of the body. Both techniques differ from conventional externalbeam radiotherapy, which involves exposing large areas of tissue to relatively broad fields of radiation over multiple sessions. Summary of Evidence Stereotactic Radiosurgery For individuals who have non-neoplastic intracranial conditions (e.g., arteriovenous malformations, trigeminal neuralgia), non-neoplastic neurologic conditions (e.g., epilepsy, tremor and movement disorders, chronic pain), Page 2 of 19
3 benign neoplastic intracranial lesion(s) (e.g., acoustic neuromas, pituitary adenoma, meningiomas, craniopharyngioma, glomus jugulare tumors), and malignant neoplastic intracranial lesion(s) (e.g., gliomas, astrocytomas), or uveal melanoma who receive SRS, the evidence includes randomized controlled trials, non-randomized retrospective cohort studies, and observational studies or case series. Relevant outcomes are over-all survival, symptoms, and treatment-related morbidity. General limitations of the body of evidence include a lack of trials that directly compare SRS and comparators, patient heterogeneity within and between studies, and failure to use standardized methods to collect and report outcomes (benefits and harms). There are several contextual factors to consider, such as SRS offers a noninvasive, highly precise radiotherapy alternative to surgery (particularly important for patients unable to undergo resection due to the presence of underlying comorbidities), intracranial lesions often are difficult to access surgically (and may be associated with a high risk for devastating adverse sequelae), intracranial lesions typically are located adjacent to vital organs and structures that are highly susceptible to radiation toxicities, and the accuracy and precision of SRS in this context make this technique a viable alternative to standard, nonconformal external-beam radiotherapy. Finally, given the rarity of many of the conditions under review, direct comparative trials are unlikely. The evidence is sufficient to determine that the technology results in a meaningful improvement in the net health outcome for patients with: arteriovenous malformations; acoustic neuromas; pituitary adenomas, nonresectable; residual, or recurrent meningiomas; primary malignancies of the central nervous system; and trigeminal neuralgia refractory to medical management. The evidence is insufficient to determine the effects of the technology on health outcomes in patients with: craniopharyngiomas; glomus jugulare tumors; epilepsy; functional disorders other than trigeminal neuralgia; tremors; chronic pain; and uveal melanoma. For individuals with craniopharyngiomas or glomus jugulare tumors, there was strong clinical support for SRS. Contextual factors considered included the rarity of these tumors, low likelihood of high-quality trials, and the potential for reduced harm compared with surgery. Stereotactic Body Radiotherapy For individuals who have benign or malignant extracranial lesion(s) (e.g., extracranial primary and metastatic tumors) who receive SBRT, the evidence includes a few randomized controlled trials, nonrandomized cohort studies, and case series. Relevant outcomes are overall survival, symptoms, and treatment-related morbidity. Limitations of the evidence include a lack of comparative trials, heterogeneity between patients and treatment schedules and planning techniques, and failure to use standardized methods to collect and report outcomes. SBRT has been shown to improve outcomes (reduce pain) in patients with spinal (vertebral) tumors. Page 3 of 19
4 The evidence is insufficient to determine the effects of the technology on health outcomes for patients with: spinal or vertebral body tumors (primary) in patients who have received prior radiotherapy; solid tumors, primary or metastatic, of the liver, pancreas, kidney, adrenal glands; oligometastases, except metastases to the spine. There was strong clinical support for the use of SBRT in patients with the condition listed below. Contextual factors were considered (e.g., the lack of alternatives in inoperable patients, and the potential for reduced harm compared with surgery). spinal or vertebral body tumors (primary) in patients who have received prior radiotherapy. Policy Stereotactic radiosurgery using a gamma ray or linear accelerator unit may be considered medically necessary for the following indications: arteriovenous malformations; acoustic neuromas; pituitary adenomas; non-resectable, residual, or recurrent meningiomas; craniopharyngiomas; glomus jugulare tumors; primary malignancies of the central nervous system, including but not limited to high-grade gliomas (initial treatment or treatment of recurrence); trigeminal neuralgia refractory to medical management. Stereotactic body radiotherapy may be considered medically necessary for the following indication: spinal or vertebral body tumors (primary) in patients who have received prior radiotherapy. When stereotactic radiosurgery or stereotactic body radiotherapy are performed using fractionation (defined in the Policy Guidelines) for the medically necessary indications described above, it may be considered medically necessary. Investigational applications of stereotactic radiosurgery include, but are not limited to, the treatment of seizures and functional disorders (other than trigeminal neuralgia), including chronic pain, tremor, and uveal melanoma. Stereotactic body radiotherapy is investigational for primary and metastatic tumors of the liver, pancreas, kidney, and adrenal glands except as outlined in the policy statements above. Policy Guidelines Radiation Source This protocol addresses the use of SRS and SRBT delivered by gamma ray or high-energy photons generated by a linear accelerator (LINAC) unit. The use of charged particle (proton or helium ion) radiotherapies is addressed in the Charged-Particle (Proton or Helium Ion) Radiotherapy Protocol. Page 4 of 19
5 Fractionation Fractionated SRS refers to SRS or SBRT performed more than once on a specific site. SRS is most often single-fraction treatment; however, multiple fractions may be necessary when lesions are near critical structures. SBRT is commonly delivered over three to five fractions. Medicare Advantage Medically necessary indications for SRS/SBRT (for Cranial and Spinal Lesions only): 1. Primary central nervous system malignancies, generally used as a boost or salvage therapy for lesions < 5 cm. 2. Primary involving the brain or spine parenchyma, meninges/dura, or immediately adjacent bony structures. 3. Benign brain tumors and spinal tumors such as meningiomas, acoustic neuromas, other schwannomas, pituitary adenomas, pineocytomas, craniopharyngiomas, glomus tumors, hemangioblastomas. 4. Cranial arteriovenous malformations, cavernous malformations, and hemangiomas. 5. Other cranial non-neoplastic conditions such as trigeminal neuralgia and select cases of medically refractory epilepsy. 6. As a boost treatment for larger cranial or spinal lesions that have been treated initially with external beam radiation therapy or surgery (e.g., sarcomas, chondrosarcomas, chordomas, and nasopharyngeal or paranasal sinus malignancies). 7. Relapse in a previously irradiated cranial or spinal field where the additional stereotactic precision is required to avoid unacceptable vital tissue radiation. Limitations for SRS/SBRT (for Cranial and Spinal Lesions). SRS is considered not medically necessary under the following circumstances: 1. Treatment for anything other than a severe symptom or serious threat to life or critical functions. 2. Treatment unlikely to result in functional improvement or clinically meaningful disease stabilization, not otherwise achievable. 3. Patients with wide-spread extra-cranial metastases with limited life expectancy unlikely to gain clinical benefit within their remaining life. 4. Patients with poor performance status (Karnofsky Performance Status less than 40 or an ECOG Performance greater than three) (see Medicare Advantage Policy Guidelines) 5. Cobalt-60 pallidotomy. Medically necessary indications for Stereotactic Body Radiation Therapy (SBRT): 1. SBRT is indicated for primary tumors and tumors metastatic to the liver, kidney, adrenal gland, or pancreas. 2. SBRT is indicated for treatment of pelvic and head and neck tumors that have recurred after primary irradiation. Page 5 of 19
6 3. SBRT treatment, of any body site or internal organ, is indicated for treatment of recurrence in or near previously irradiated regions when a high level of precision and accuracy or a high dose per fraction is indicated to minimize the risk of injury to surrounding normal tissues and treatment with conventional methods is not appropriate or safe for the particular patient (medical records must describe the specific circumstances). Limitations for Stereotactic Body Radiation Therapy (SBRT); 1. Primary treatment of lesions of bone (primary), uterus, ovary, and other internal organs not listed in the policy statements above is considered not medically necessary. 2. SBRT is considered not medically necessary under the following circumstances for any condition: a. Treatment is unlikely to result in clinical cancer control and/or functional improvement. b. The tumor burden cannot be completely targeted with acceptable risk to critical normal structures. c. The patient has a poor performance status (Karnofsky Performance Status less than 40 or Eastern Cooperative Oncology Group (ECOG) Status of three or worse). d. Recurrent (other than pelvic and head and neck tumors) or metastatic disease could be treated by conventional methods (record must describe why other radiation therapy measures are not appropriate or safe for the particular patient). Medicare Advantage Policy Guidelines Since the goal of SBRT is to maximize the potency of the radiotherapy by completing an entire course of treatment within an extremely accelerated time frame, any course of radiation treatment extending beyond five fractions is not considered SBRT. SBRT is meant to represent a complete course of treatment and not to be used as a boost following a conventionally fractionated course of treatment. Karnofsky Performance Status Scale 100 Normal; no complaints, no evidence of disease 90 Able to carry on normal activity; minor signs or symptoms of disease 80 Normal activity with effort; some signs or symptoms of disease 70 Cares for self; unable to carry on normal activity or to do active work 60 Requires occasional assistance but is able to care for most needs 50 Requires considerable assistance and frequent medical care 40 Disabled; requires special care and assistance 30 Severely disabled; hospitalization is indicated although death not imminent 20 Very sick; hospitalization necessary; active supportive treatment is necessary 10 Moribund, fatal processes progressing rapidly 0 Dead ECOG Performance Status Scale Grade 0: Fully active, able to carry on all pre-disease performance without restriction. Grade 1: Restricted in physically strenuous activity but ambulatory and able to carry out work of a light or sedentary nature, e.g., light house work, office work. Page 6 of 19
7 Grade 2: Ambulatory and capable of all self-care but unable to carry out and work activities. Up and about more than 50% of waking hours. Grade 3: Capable of only limited self-care, confined to bed or chair more than 50% of waking hours. Grade 4: Completely disabled. Cannot carry on any self-care. Totally confined to bed or chair. Grade 5: Dead Background Conformal Radiotherapy SRS and SBRT are techniques that use highly focused, conformal radiation beams to treat both neoplastic and non-neoplastic conditions. Although SRS and SBRT may be completed with one session (single-fraction), SRS typically refers to a single-session procedure to ablate the target lesion. However, either technique may require additional sessions (typically not more than five) over a course of days, referred to as fractionated radiotherapy. Platforms available for SRS and SBRT are distinguished by their source of radiation; they include gamma radiation from cobalt 60 sources; high-energy photons from LINAC systems; and particle beams (e.g., protons). Particle beam therapy is not covered in this protocol. SRS and SBRT have been used for a range of malignant and nonmalignant conditions. A comprehensive review that encompasses all potential uses is beyond the scope of this protocol. Thus, a brief introduction follows of common applications of SRS and SBRT for which published evidence has been identified in database searches. Stereotactic Radiosurgery Non-Neoplastic Intracranial Conditions Treated With SRS ARTERIOVENOUS MALFORMATIONS An arteriovenous malformation (AVM) comprises a tangled network of vessels in which blood passes from arteries to veins without intervening capillaries. AVMs range in size from small, barely detectable lesions to large lesions that can occupy an entire hemisphere. SRS incites an inflammatory response in the vessels, which results in ongoing fibrosis with eventual complete obliteration of the lesion over the course of months to years. This latency period is variable, depending on the size of the AVM and the dose distribution of the radiosurgery. During this latency period, an ongoing but declining risk of hemorrhage is present. In contrast, surgical excision provides an immediate effect on the risk of hemorrhage. Total surgical extirpation of the lesion, if possible, is the desired form of therapy to avoid future hemorrhage. However, a small subset of AVMs because of their size or location cannot be excised without serious neurologic sequelae. SRS is an alternative in selected patients. TRIGEMINAL NEURALGIA Trigeminal neuralgia is a disorder of the fifth cranial (i.e., trigeminal) nerve that causes episodes of intense, stabbing pain in the face. The International Classification of Headache Disorders has defined classical trigeminal neuralgia as both idiopathic and related to vascular compression. Painful trigeminal neuropathy is caused by other conditions; post herpetic, posttraumatic, secondary to multiple sclerosis plaque or a space occupying lesion. 1 Although trigeminal neuralgia is initially treated medically, in a substantial number of cases, drug treatment is either ineffective or the adverse effects become intolerable. Neurosurgical options include microvascular decompression which involves craniotomy, peripheral neurectomy or rhizotomy. Rhizotomy is a technique to percutaneously isolate the nerve and apply ablation techniques such as balloon compression, radiofrequency ablation or chemical injection. SRS of the proximal trigeminal nerve root has been investigated as an alternative Page 7 of 19
8 to these neurosurgical treatments. There is a latency period of approximately one month for the effect to be observed. OTHER NEUROLOGIC DISORDERS Seizure disorders are initially treated medically. Surgical treatment is only considered in those instances when the seizures have proven refractory to all attempts at aggressive medical management, when the frequency and severity of the seizures are so frequent and severe as to significantly diminish quality of life, and when the seizure focus can be localized to a focal lesion in a region of the brain that is accessible to resection. SRS has been investigated as an alternative to neurosurgical resection. For chronic pain that is refractory to a variety of medical and psychological treatments, there are a variety of surgical alternatives. Neurodestructive procedures include cordotomy, myelotomy, dorsal root entry zone lesions, and stereotactic radiofrequency thalamotomy. SRS targeting the thalamus has been considered an investigative alternative to these neurodestructive procedures. SRS for the destruction of the thalamic nuclei (thalamotomy) has been proposed for a treatment of essential tremor and other forms of tremor (i.e., secondary to Parkinson disease, multiple sclerosis, or other neurologic conditions), as an alternative to medical therapy or surgical therapy in extreme cases. Neoplastic Conditions Treated With SRS PRIMARY INTRACRANIAL TUMORS Acoustic neuromas, also called vestibular schwannomas, are benign tumors originating on the eighth cranial nerve, sometimes associated with neurofibromatosis, which can be linked to significant morbidity and even death if their growth compresses vital structures. The tumors arise from the Schwann cell sheath surrounding either the vestibular or cochlear branches of the eighth cranial nerve. Treatment options include complete surgical excision using microsurgical techniques; radiosurgery has also been used extensively, either as a primary treatment or as a treatment of recurrence after incomplete surgical resection. Pituitary adenomas are benign tumors with symptoms related to hormone production (i.e., functioning adenomas) or neurologic symptoms due to their impingement on surrounding neural structures. Surgical treatment options for pituitary adenomas include excision, conventional radiotherapy, or SRS. Surgical excision is typically offered to patients with functioning adenomas; this is because complete removal of the adenoma leads to more rapid control of autonomous hormone production. The effects of SRS on hormone production are delayed or incomplete. In patients with nonfunctioning adenomas, the treatment goal is to control growth; complete removal of the adenoma is not necessary. Conventional radiotherapy has been used in this setting with an approximate 90% success rate with few complications. Craniopharyngiomas are benign tumors that arise from pituitary embryonic tissue at the base of the gland. However, because of proximity to the optic pathways, pituitary gland, and hypothalamus, these tumors may cause severe and permanent damage to these critical structures and can even be life-threatening. Total surgical resection is often difficult. A glomus jugulare tumor is a rare, benign tumor arising in the skull temporal bone that involves middle and inner ear structure. No consensus exists on optimal management to control tumor burden while minimizing treatment-related morbidity. SRS has been used for the treatment of other primary brain tumors, including gliomas, meningiomas, and primitive neuroectodermal tumors (i.e., medulloblastoma, pineoblastoma). Treatment of primary brain tumors such as gliomas is more challenging, due to their generally larger size and infiltrative borders. UVEAL MELANOMA Page 8 of 19
9 Melanoma of the uvea (choroid, ciliary body, and iris) is the most common, primary, malignant, intraocular tumor in adults. Established treatment modalities include enucleation, local resection, brachytherapy, and proton beam radiotherapy. The main objectives of treating the tumor are twofold: (1) to reduce the risk of metastatic spread; and (2) to salvage the eye with useful vision (if feasible). Treatment selection depends on tumor size and location, associated ocular findings, the status of the other eye, as well as other individual factors, including age, life expectancy, quality of life issues, concurrent systemic diseases, and patient expectations. Stereotactic Body Radiotherapy Extracranial Primary Tumors Treated With SBRT Surgical resection is the preferred treatment of hepatocellular carcinoma although at the time of diagnosis, less than 20% of patients are amenable to definitive surgical management due to advanced local disease or comorbidities. These patients may be candidates for local ablative therapies, including radiofrequency ablation and chemoembolization. Radiation may be considered as an alternative to local ablative/embolization therapies or if these therapies fail. Radiation may be part of the treatment plan for pancreatic cancer, resectable or unresectable disease, and may be used in the adjuvant or neoadjuvant setting. Localized renal cell carcinoma is conventionally treated surgically; local ablative methods may also be an option. Preoperative and adjuvant external radiation have not improved survival. However, because renal cell cancer brain metastases although radioresistant to conventional external radiation have been responsive to radiosurgery, interest remains in the possibility of treating primary kidney cancer with SBRT. Extracranial Metastatic Tumors Treated With SBRT Oligometastases are defined as isolated sites of metastasis, with the entire burden of disease being recognized as a finite number of discrete lesions that can be potentially cured with local therapies. 2 In general, the indications for SBRT for oligometastases are the same as for metastasectomy. Recently proposed specific criteria for the use of SBRT in patients with oligometastases include the following: a controlled primary, favorable histology, limited metastatic disease, metachronous appearance of metastases, young age, and good performance status. 2 Management of metastatic solid tumors has historically focused on systemic treatment with palliative intent. However, surgical treatment of oligometastatic disease is now common practice in some clinical settings. 3 Although a cure may be possible in some patients with oligometastatic disease, the aim of SBRT in this setting is mainly to achieve local control and delay progression, which may also postpone the need for further treatment. Metastases from NSCLC to the adrenal gland are common, and systemic treatment is the most frequent therapeutic option. Nevertheless, in patients suffering from an isolated adrenal metastasis, a survival benefit could be achieved after surgical resection. Spinal Primary Tumors Treated With SBRT SBRT to the spine has been most widely studied in patients requiring reirradiation, but interest has also developed in the use of SBRT for the initial treatment of spinal tumors. Regulatory Status Several devices that use cobalt 60 radiation (gamma ray devices) for SRS have been cleared for marketing by the U.S. Food and Drug Administration (FDA) through the 510(k) process. The most commonly used gamma ray device, approved in May 1999, is the Gamma Knife (Elekta, Stockholm; product code IWB), which is a fixed Page 9 of 19
10 device used only for intracranial lesions. Gamma ray emitting devices that use cobalt 60 degradation are also regulated through the U.S. Nuclear Regulatory Commission. A number of LINAC movable platforms that generate high-energy photons have been cleared for marketing by FDA through the 510(k) process. Examples include the Novalis Tx (Novalis, Westchester, IL); the TrueBeam STx (Varian Medical Systems, Palo Alto, CA; approved December 2012; FDA product code IYE); and the CyberKnife Robotic Radiosurgery System (Accuray, Sunnyvale, CA; approved December 1998; FDA product code MUJ). LINAC-based devices may be used for intracranial and extracranial lesions. Related Protocols Charged-Particle (Proton or Helium Ion) Radiotherapy for Neoplastic Conditions Intensity-Modulated Radiotherapy: Abdomen and Pelvis Intensity-Modulated Radiotherapy: Central Nervous System Tumors Intracavitary Balloon Catheter Brain Brachytherapy for Malignant Gliomas Services that are the subject of a clinical trial do not meet our Technology Assessment Protocol criteria and are considered investigational. For explanation of experimental and investigational, please refer to the Technology Assessment Protocol. It is expected that only appropriate and medically necessary services will be rendered. We reserve the right to conduct prepayment and postpayment reviews to assess the medical appropriateness of the above-referenced procedures. Some of this protocol may not pertain to the patients you provide care to, as it may relate to products that are not available in your geographic area. References We are not responsible for the continuing viability of web site addresses that may be listed in any references below. 1. Headache Classification Committee of the International Headache Society. The International Classification of Headache Disorders, 3rd edition (beta version). Cephalalgia. Jul 2013; 33(9): PMID Alongi F, Arcangeli S, Filippi AR, et al. Review and uses of stereotactic body radiation therapy for oligometastases. Oncologist. 2012; 17(8): PMID Tree AC, Khoo VS, Eeles RA, et al. Stereotactic body radiotherapy for oligometastases. Lancet Oncol. Jan 2013; 14(1):e PMID Mohr JP, Parides MK, Stapf C, et al. Medical management with or without interventional therapy for unruptured brain arteriovenous malformations (ARUBA): a multicentre, non-blinded, randomised trial. Lancet. Feb ; 383(9917): PMID Magro E, Gentric JC, Darsaut TE, et al. Responses to ARUBA: a systematic review and critical analysis for the design of future arteriovenous malformation trials. J Neurosurg. Feb 2017; 126(2): PMID Mau CY, Sabourin VM, Gandhi CD, et al. SLAM: Stereotactic Radiosurgery of Large Arteriovenous Malformations: meta-analysis of hemorrhage in high-grade Pollock-Flickinger arteriovenous malformations. World Neurosurg. Jan 2016; 85: PMID Bowden G, Kano H, Tonetti D, et al. Stereotactic radiosurgery for arteriovenous malformations of the cerebellum. J Neurosurg. Mar 2014; 120(3): PMID Page 10 of 19
11 8. Fokas E, Henzel M, Wittig A, et al. Stereotactic radiosurgery of cerebral arteriovenous malformations: longterm follow-up in 164 patients of a single institution. J Neurol. Aug 2013; 260(8): PMID Kano H, Kondziolka D, Flickinger JC, et al. Stereotactic radiosurgery for arteriovenous malformations, Part 6: multistaged volumetric management of large arteriovenous malformations. J Neurosurg. Jan 2012; 116(1): PMID Matsuo T, Kamada K, Izumo T, et al. Linear accelerator-based radiosurgery alone for arteriovenous malformation: more than 12 years of observation. Int J Radiat Oncol Biol Phys. Jul ; 89(3): PMID Paul L, Casasco A, Kusak ME, et al. Results for a series of 697 AVMs reated by Gamma Knife: Influence of angiographic features on the obliteration rate. Neurosurgery. Jul ; 75(5): ; dicussion ; quiz 583. PMID Potts MB, Sheth SA, Louie J, et al. Stereotactic radiosurgery at a low marginal dose for the treatment of pediatric arteriovenous malformations: obliteration, complications, and functional outcomes. J Neurosurg Pediatr. Jul 2014; 14(1):1-11. PMID Cohen-Inbar O, Lee CC, Xu Z, et al. A quantitative analysis of adverse radiation effects following Gamma Knife radiosurgery for arteriovenous malformations. J Neurosurg. Oct 2015; 123(4): PMID Ding D, Starke RM, Kano H, et al. Stereotactic radiosurgery for Spetzler-Martin Grade III arteriovenous malformations: an international multicenter study. J Neurosurg. Apr :1-13. PMID Ding D, Starke RM, Kano H, et al. Radiosurgery for cerebral arteriovenous malformations in A Randomized Trial of Unruptured Brain Arteriovenous Malformations (ARUBA)-eligible patients: a multicenter study. Stroke. Feb 2016; 47(2): PMID Ding D, Xu Z, Yen CP, et al. Radiosurgery for cerebral arteriovenous malformations in elderly patients: effect of advanced age on outcomes after intervention. World Neurosurg. Sep 2015; 84(3): PMID Hanakita S, Shin M, Koga T, et al. Risk reduction of cerebral stroke after stereotactic radiosurgery for small unruptured brain arteriovenous malformations. Stroke. May 2016; 47(5): PMID Starke RM, Kano H, Ding D, et al. Stereotactic radiosurgery for cerebral arteriovenous malformations: evaluation of long-term outcomes in a multicenter cohort. J Neurosurg. Mar :1-9. PMID El-Ghanem M, Kass-Hout T, Kass-Hout O, et al. Arteriovenous Malformations in the Pediatric Population: Review of the Existing Literature. Interv Neurol. Sep 2016; 5(3-4): PMID Tonetti D, Kano H, Bowden G, et al. Hemorrhage during pregnancy in the latency interval after stereotactic radiosurgery for arteriovenous malformations. J Neurosurg. Dec 2014; 121 Suppl: PMID Yen CP, Schlesinger D, Sheehan JP. Gamma Knife(R) radiosurgery for trigeminal neuralgia. Expert Rev Med Devices. Nov 2011; 8(6): PMID Dhople AA, Adams JR, Maggio WW, et al. Long-term outcomes of Gamma Knife radiosurgery for classic trigeminal neuralgia: implications of treatment and critical review of the literature. Clinical article. J Neurosurg. Aug 2009; 111(2): PMID Zakrzewska JM, Akram H. Neurosurgical interventions for the treatment of classical trigeminal neuralgia. Cochrane Database Syst Rev. Sep (9):Cd PMID Blue Cross and Blue Shield Association. Special report: stereotactic radiosurgery for intracranial lesions by gamma beam, linear accelerator, and proton beam methods. Jan 1999: PMID Feng ES, Sui CB, Wang TX, et al. Stereotactic radiosurgery for the treatment of mesial temporal lobe epilepsy. Acta Neurol Scand. Dec 2016; 134(6): PMID Regis J, Bartolomei F, Rey M, et al. Gamma knife surgery for mesial temporal lobe epilepsy. J Neurosurg. Dec 2000; 93 Suppl 3: PMID Schrottner O, Eder HG, Unger F, et al. Radiosurgery in lesional epilepsy: brain tumors. Stereotact Funct Neurosurg. Oct 1998; 70 Suppl 1: PMID Page 11 of 19
12 28. Whang CJ, Kwon Y. Long-term follow-up of stereotactic Gamma Knife radiosurgery in epilepsy. Stereotact Funct Neurosurg. Jan 1996; 66(Suppl 1): PMID Niranjan A, Raju SS, Kooshkabadi A, et al. Stereotactic radiosurgery for essential tremor: Retrospective analysis of a 19-year experience. Mov Disord. May 2017; 32(5): PMID Witjas T, Carron R, Krack P, et al. A prospective single-blind study of Gamma Knife thalamotomy for tremor. Neurology. Nov ; 85(18): PMID Kondziolka D, Ong JG, Lee JY, et al. Gamma Knife thalamotomy for essential tremor. J Neurosurg. Jan 2008; 108(1): PMID Kooshkabadi A, Lunsford LD, Tonetti D, et al. Gamma Knife thalamotomy for tremor in the magnetic resonance imaging era. J Neurosurg. Apr 2013; 118(4): PMID Lim SY, Hodaie M, Fallis M, et al. Gamma knife thalamotomy for disabling tremor: a blinded evaluation. Arch Neurol. May 2010; 67(5): PMID Ohye C, Higuchi Y, Shibazaki T, et al. Gamma knife thalamotomy for Parkinson disease and essential tremor: a prospective multicenter study. Neurosurgery. Mar 2012; 70(3): ; discussion PMID Young RF, Jacques S, Mark R, et al. Gamma knife thalamotomy for treatment of tremor: long-term results. J Neurosurg. Dec 2000; 93 Suppl 3: PMID Roberts DG, Pouratian N. Stereotactic radiosurgery for the treatment of chronic intractable pain: a systematic review. Oper Neurosurg (Hagerstown). Oct ; 13(5): PMID Persson O, Bartek J, Jr., Shalom NB, et al. Stereotactic radiosurgery vs. fractionated radiotherapy for tumor control in vestibular schwannoma patients: a systematic review. Acta Neurochir (Wien). Jun 2017; 159(6): PMID Muzevic D, Legcevic J, Splavski B, et al. Stereotactic radiotherapy for vestibular schwannoma. Cochrane Database Syst Rev. Dec (12):Cd PMID Badakhshi H, Muellner S, Wiener E, et al. Image-guided stereotactic radiotherapy for patients with vestibular schwannoma. A clinical study. Strahlenther Onkol. Jun 2014; 190(6): PMID Williams BJ, Xu Z, Salvetti DJ, et al. Gamma Knife surgery for large vestibular schwannomas: a single-center retrospective case-matched comparison assessing the effect of lesion size. J Neurosurg. Aug 2013; 119(2): PMID Woolf DK, Williams M, Goh CL, et al. Fractionated stereotactic radiotherapy for acoustic neuromas: longterm outcomes. Clin Oncol (R Coll Radiol). Dec 2013; 25(12): PMID Pollock BE, Driscoll CL, Foote RL, et al. Patient outcomes after vestibular schwannoma management: a prospective comparison of microsurgical resection and stereotactic radiosurgery. Neurosurgery. Jul 2006; 59(1):77-85; discussion PMID Meijer OW, Vandertop WP, Baayen JC, et al. Single-fraction vs. fractionated linac-based stereotactic radiosurgery for vestibular schwannoma: a single-institution study. Int J Radiat Oncol Biol Phys. Aug ; 56(5): PMID Chung HT, Ma R, Toyota B, et al. Audiologic and treatment outcomes after linear accelerator-based stereotactic irradiation for acoustic neuroma. Int J Radiat Oncol Biol Phys. Jul ; 59(4): PMID Chang SD, Gibbs IC, Sakamoto GT, et al. Staged stereotactic irradiation for acoustic neuroma. Neurosurgery. Jun 2005; 56(6): ; discussion PMID Chen Y, Li ZF, Zhang FX, et al. Gamma knife surgery for patients with volumetric classification of nonfunctioning pituitary adenomas: a systematic review and meta-analysis. Eur J Endocrinol. Oct 2013; 169(4): PMID Lee CC, Kano H, Yang HC, et al. Initial Gamma Knife radiosurgery for nonfunctioning pituitary adenomas. J Neurosurg. Mar 2014; 120(3): PMID Sheehan JP, Starke RM, Mathieu D, et al. Gamma Knife radiosurgery for the management of nonfunctioning pituitary adenomas: a multicenter study. J Neurosurg. Aug 2013; 119(2): PMID Page 12 of 19
13 49. Hashizume C, Mori Y, Kobayashi T, et al. Stereotactic radiotherapy using Novalis for craniopharyngioma adjacent to optic pathways. J Neurooncol. Jun 2010; 98(2): PMID Hasegawa T, Kobayashi T, Kida Y. Tolerance of the optic apparatus in single-fraction irradiation using stereotactic radiosurgery: evaluation in 100 patients with craniopharyngioma. Neurosurgery. Apr 2010; 66(4): ; discussion PMID Combs SE, Thilmann C, Huber PE, et al. Achievement of long-term local control in patients with craniopharyngiomas using high precision stereotactic radiotherapy. Cancer. Jun ; 109(11): PMID Lee CC, Yang HC, Chen CJ, et al. Gamma Knife surgery for craniopharyngioma: report on a 20-year experience. J Neurosurg. Dec 2014; 121 Suppl: PMID Ivan ME, Sughrue ME, Clark AJ, et al. A meta-analysis of tumor control rates and treatment-related morbidity for patients with glomus jugulare tumors. J Neurosurg. May 2011; 114(5): PMID Wakefield DV, Venable GT, VanderWalde NA, et al. Comparative neurologic outcomes of salvage and definitive Gamma Knife radiosurgery for glomus jugulare: a 20-year experience. J Neurol Surg B Skull Base. Jun 2017; 78(3): PMID Ibrahim R, Ammori MB, Yianni J, et al. Gamma Knife radiosurgery for glomus jugulare tumors: a singlecenter series of 75 cases. J Neurosurg. May 2017; 126(5): PMID El-Shehaby AM, Reda WA, Abdel Karim KM, et al. Gamma Knife radiosurgery for low-grade tectal gliomas. Acta Neurochir (Wien). Feb 2015; 157(2): PMID Clark GM, McDonald AM, Nabors LB, et al. Hypofractionated stereotactic radiosurgery with concurrent bevacizumab for recurrent malignant gliomas: the University of Alabama at Birmingham experience. Neurooncol Pract. Dec 2014; 1(4): PMID Cabrera AR, Cuneo KC, Desjardins A, et al. Concurrent stereotactic radiosurgery and bevacizumab in recurrent malignant gliomas: a prospective trial. Int J Radiat Oncol Biol Phys. Aug ; 86(5): PMID Cuneo KC, Vredenburgh JJ, Sampson JH, et al. Safety and efficacy of stereotactic radiosurgery and adjuvant bevacizumab in patients with recurrent malignant gliomas. Int J Radiat Oncol Biol Phys. Apr ; 82(5): PMID Dodoo E, Huffmann B, Peredo I, et al. Increased survival using delayed gamma knife radiosurgery for recurrent high-grade glioma: a feasibility study. World Neurosurg. Nov 2014; 82(5):e PMID Furdova A, Sramka M, Chorvath M, et al. Stereotactic radiosurgery in intraocular malignant melanoma-- retrospective study. Neuro Endocrinol Lett. Mar 2014; 35(1): PMID Sarici AM, Pazarli H. Gamma-knife-based stereotactic radiosurgery for medium- and large-sized posterior uveal melanoma. Graefes Arch Clin Exp Ophthalmol. Jan 2013; 251(1): PMID Muller K, Naus N, Nowak PJ, et al. Fractionated stereotactic radiotherapy for uveal melanoma, late clinical results. Radiother Oncol. Feb 2012; 102(2): PMID Furdova A, Slezak P, Chorvath M, et al. No differences in outcome between radical surgical treatment (enucleation) and stereotactic radiosurgery in patients with posterior uveal melanoma. Neoplasma. 2010; 57(4): PMID Roos D. What is the randomised evidence for surgery and stereotactic radiosurgery for patients with solitary (or few) brain metastases? Int J Evid Based Healthc. Mar 2011; 9(1): PMID Park HS, Chiang VL, Knisely JP, et al. Stereotactic radiosurgery with or without whole-brain radiotherapy for brain metastases: an update. Expert Rev Anticancer Ther. Nov 2011; 11(11): PMID Patil CG, Pricola K, Garg SK, et al. Whole brain radiation therapy (WBRT) alone versus WBRT and radiosurgery for the treatment of brain metastases. Cochrane Database Syst Rev. Jun (6):CD PMID Patil CG, Pricola K, Sarmiento JM, et al. Whole brain radiation therapy (WBRT) alone versus WBRT and radiosurgery for the treatment of brain metastases. Cochrane Database Syst Rev. Sep (9):Cd PMID Page 13 of 19
14 69. Chang DT, Schellenberg D, Shen J, et al. Stereotactic radiotherapy for unresectable adenocarcinoma of the pancreas. Cancer. Feb ; 115(3): PMID Kondziolka D, Patel A, Lunsford LD, et al. Stereotactic radiosurgery plus whole brain radiotherapy versus radiotherapy alone for patients with multiple brain metastases. Int J Radiat Oncol Biol Phys. Sep ; 45(2): PMID Weltman E, Salvajoli JV, Brandt RA, et al. Radiosurgery for brain metastases: a score index for predicting prognosis. Int J Radiat Oncol Biol Phys. Mar ; 46(5): PMID Yu C, Chen JC, Apuzzo ML, et al. Metastatic melanoma to the brain: prognostic factors after gamma knife radiosurgery. Int J Radiat Oncol Biol Phys. Apr ; 52(5): PMID Aoyama H, Shirato H, Tago M, et al. Stereotactic radiosurgery plus whole-brain radiation therapy vs. stereotactic radiosurgery alone for treatment of brain metastases: a randomized controlled trial. JAMA. Jun ; 295(21): PMID Raizer J. Radiosurgery and whole-brain radiation therapy for brain metastases: either or both as the optimal treatment. JAMA. Jun ; 295(21): PMID Tian LJ, Zhuang HQ, Yuan ZY. A comparison between cyberknife and neurosurgery in solitary brain metastases from non-small cell lung cancer. Clin Neurol Neurosurg. Oct 2013; 115(10): PMID Yamamoto M, Serizawa T, Shuto T, et al. Stereotactic radiosurgery for patients with multiple brain metastases (JLGK0901): a multi-institutional prospective observational study. Lancet Oncol. Apr 2014; 15(4): PMID Rava P, Leonard K, Sioshansi S, et al. Survival among patients with 10 or more brain metastases treated with stereotactic radiosurgery. J Neurosurg. Aug 2013; 119(2): PMID Raldow AC, Chiang VL, Knisely JP, et al. Survival and intracranial control of patients with 5 or more brain metastases treated with gamma knife stereotactic radiosurgery. Am J Clin Oncol. Oct 2013; 36(5): PMID Yomo S, Hayashi M. Upfront stereotactic radiosurgery in patients with brain metastases from small cell lung cancer: retrospective analysis of 41 patients. Radiat Oncol. Jul ; 9(1):152. PMID Zehetmayer M. Stereotactic photon beam irradiation of uveal melanoma. Dev Ophthalmol. 2012; 49: PMID Eibl-Lindner K, Furweger C, Nentwich M, et al. Robotic radiosurgery for the treatment of medium and large uveal melanoma. Melanoma Res. Feb 2016; 26(1): PMID Reynolds MM, Arnett AL, Parney IF, et al. Gamma knife radiosurgery for the treatment of uveal melanoma and uveal metastases. Int J Retina Vitreous. Jun 2017; 3:17. PMID Dunavoelgyi R, Dieckmann K, Gleiss A, et al. Local tumor control, visual acuity, and survival after hypofractionated stereotactic photon radiotherapy of choroidal melanoma in 212 patients treated between 1997 and Int J Radiat Oncol Biol Phys. Sep ; 81(1): PMID Wackernagel W, Holl E, Tarmann L, et al. Local tumour control and eye preservation after gamma-knife radiosurgery of choroidal melanomas. Br J Ophthalmol. Feb 2014; 98(2): PMID Gerszten PC, Ozhasoglu C, Burton SA, et al. CyberKnife frameless stereotactic radiosurgery for spinal lesions: clinical experience in 125 cases. Neurosurgery. Jul 2004; 55(1):89-98; discussion PMID Degen JW, Gagnon GJ, Voyadzis JM, et al. CyberKnife stereotactic radiosurgical treatment of spinal tumors for pain control and quality of life. J Neurosurg Spine. May 2005; 2(5): PMID Gerszten PC, Burton SA, Ozhasoglu C, et al. Radiosurgery for spinal metastases: clinical experience in 500 cases from a single institution. Spine (Phila Pa 1976). Jan ; 32(2): PMID Chang EL, Shiu AS, Mendel E, et al. Phase I/II study of stereotactic body radiotherapy for spinal metastasis and its pattern of failure. J Neurosurg Spine. Aug 2007; 7(2): PMID Page 14 of 19
15 89. Sahgal A, Atenafu EG, Chao S, et al. Vertebral compression fracture after spine stereotactic body radiotherapy: a multi-institutional analysis with a focus on radiation dose and the spinal instability neoplastic score. J Clin Oncol. Sep ; 31(27): PMID Solda F, Lodge M, Ashley S, et al. Stereotactic radiotherapy (SABR) for the treatment of primary non-small cell lung cancer; systematic review and comparison with a surgical cohort. Radiother Oncol. Oct 2013; 109(1):1-7. PMID Jeppesen SS, Schytte T, Jensen HR, et al. Stereotactic body radiation therapy versus conventional radiation therapy in patients with early stage non-small cell lung cancer: an updated retrospective study on local failure and survival rates. Acta Oncol. Oct 2013; 52(7): PMID Hof H, Muenter M, Oetzel D, et al. Stereotactic single-dose radiotherapy (radiosurgery) of early stage nonsmall-cell lung cancer (NSCLC). Cancer. Jul ; 110(1): PMID Allibhai Z, Taremi M, Bezjak A, et al. The impact of tumor size on outcomes after stereotactic body radiation therapy for medically inoperable early-stage non-small cell lung cancer. Int J Radiat Oncol Biol Phys. Dec ; 87(5): PMID Harkenrider MM, Bertke MH, Dunlap NE. Stereotactic body radiation therapy for unbiopsied early-stage lung cancer: a multi-institutional analysis. Am J Clin Oncol. Aug 2014; 37(4): PMID Timmerman R, Paulus R, Galvin J, et al. Stereotactic body radiation therapy for inoperable early stage lung cancer. Jama. Mar ; 303(11): PMID Stanic S, Paulus R, Timmerman RD, et al. No clinically significant changes in pulmonary function following stereotactic body radiation therapy for early-stage peripheral non-small cell lung cancer: an analysis of RTOG Int J Radiat Oncol Biol Phys. Apr ; 88(5): PMID Chang JY, Senan S, Paul MA, et al. Stereotactic ablative radiotherapy versus lobectomy for operable stage I non-small-cell lung cancer: a pooled analysis of two randomised trials. Lancet Oncol. Jun 2015; 16(6): PMID Fernando HC, Timmerman R. American College of Surgeons Oncology Group Z4099/Radiation Therapy Oncology Group 1021: a randomized study of sublobar resection compared with stereotactic body radiotherapy for high-risk stage I non-small cell lung cancer. J Thorac Cardiovasc Surg. Sep 2012; 144(3):S PMID Zheng X, Schipper M, Kidwell K, et al. Survival outcome after stereotactic body radiation therapy and surgery for stage i non-small cell lung cancer: a meta-analysis. Int J Radiat Oncol Biol Phys. Jul ; 90(3): PMID Nguyen NP, Garland L, Welsh J, et al. Can stereotactic fractionated radiation therapy become the standard of care for early stage non-small cell lung carcinoma. Cancer Treat Rev. Dec 2008; 34(8): PMID Koto M, Takai Y, Ogawa Y, et al. A phase II study on stereotactic body radiotherapy for stage I non-small cell lung cancer. Radiother Oncol. Dec 2007; 85(3): PMID Kupelian PA, Komaki R, Allen P. Prognostic factors in the treatment of node-negative nonsmall cell lung carcinoma with radiotherapy alone. Int J Radiat Oncol Biol Phys. Oct ; 36(3): PMID Yu JB, Soulos PR, Cramer LD, et al. Comparative effectiveness of surgery and radiosurgery for stage I nonsmall cell lung cancer. Cancer. Jul ; 121(14): PMID Ezer N, Veluswamy RR, Mhango G, et al. Outcomes after Stereotactic Body Radiotherapy versus Limited Resection in Older Patients with Early-Stage Lung Cancer. J Thorac Oncol. Aug 2015; 10(8): PMID Crabtree TD, Puri V, Robinson C, et al. Analysis of first recurrence and survival in patients with stage I nonsmall cell lung cancer treated with surgical resection or stereotactic radiation therapy. J Thorac Cardiovasc Surg. Apr 2014; 147(4): ; discussion PMID Port JL, Parashar B, Osakwe N, et al. A propensity-matched analysis of wedge resection and stereotactic body radiotherapy for early stage lung cancer. Ann Thorac Surg. Jul ; 98(4): PMID Page 15 of 19
Original Date: April 2016 Page 1 of 7 FOR CMS (MEDICARE) MEMBERS ONLY
 National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIATION THERAPY: STEREO RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: Please refer to pages 5-6 LCD
National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIATION THERAPY: STEREO RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: Please refer to pages 5-6 LCD
This LCD recognizes these two distinct treatment approaches and is specific to treatment delivery:
 National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: 77371, 77372, 77373 LCD ID Number: L33410 J-N FL Responsible
National Imaging Associates, Inc. Clinical guidelines STEREOTACTIC RADIOSURGERY (SRS) AND STEREOTACTIC BODY RADIATION THERAPY (SBRT) CPT4 Codes: 77371, 77372, 77373 LCD ID Number: L33410 J-N FL Responsible
Medical Benefit Effective Date: 01/01/13 Next Review Date: 09/13 Preauthorization* No Review Dates: 11/07, 07/08, 01/09, 01/10, 03/11, 01/12, 09/12
 Protocol Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy (60110) Medical Benefit Effective Date: 01/01/13 Next Review Date: 09/13 Preauthorization* No Review Dates: 11/07, 07/08, 01/09,
Protocol Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy (60110) Medical Benefit Effective Date: 01/01/13 Next Review Date: 09/13 Preauthorization* No Review Dates: 11/07, 07/08, 01/09,
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2017
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2017
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/20/2015
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 11/20/2015
Stereotactic Radiosurgery and Stereotactic Body Radiotherapy
 Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Policy Number: 6.01.10 Last Review: 11/2018 Origination: 1/1989 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Policy Number: 6.01.10 Last Review: 11/2018 Origination: 1/1989 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2015
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 04/01/2015
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Page 1 of 74 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Stereotactic Radiosurgery and Stereotactic
Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Page 1 of 74 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Stereotactic Radiosurgery and Stereotactic
Medical Policy. MP Stereotactic Radiosurgery and Stereotactic Body Radiotherapy
 Medical Policy MP 6.01.10 BCBSA Ref. Policy: 6.01.10 Last Review: 10/18/2018 Effective Date: 10/18/2018 Section: Radiation Related Policies 8.01.10 Charged-Particle (Proton or Helium Ion) Radiotherapy
Medical Policy MP 6.01.10 BCBSA Ref. Policy: 6.01.10 Last Review: 10/18/2018 Effective Date: 10/18/2018 Section: Radiation Related Policies 8.01.10 Charged-Particle (Proton or Helium Ion) Radiotherapy
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 03/01/2013 Section:
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 03/01/2013 Section:
Medical Policy Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Medical Policy Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Table of Contents Policy: Commercial Coding Information Information Pertaining to All Policies Policy: Medicare Description
Medical Policy Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Table of Contents Policy: Commercial Coding Information Information Pertaining to All Policies Policy: Medicare Description
Populations Interventions Comparators Outcomes Individuals: With nonmalignant or malignant intracranial lesion(s) a
 Protocol Stereotactic Radiosurgery and Stereotactic Body Radiotherapy (60110) Medical Benefit Effective Date: 07/01/17 Next Review Date: 03/18 Preauthorization No Review Dates: 11/07, 07/08, 01/09, 01/10,
Protocol Stereotactic Radiosurgery and Stereotactic Body Radiotherapy (60110) Medical Benefit Effective Date: 07/01/17 Next Review Date: 03/18 Preauthorization No Review Dates: 11/07, 07/08, 01/09, 01/10,
Description. Section: Therapy Effective Date: January 15, 2015 Subsection: Therapy Original Policy Date: September 13, 2012 Subject:
 Last Review Status/Date: December 2014 Page: 1 of 51 Description Stereotactic radiosurgery (SRS) and stereotactic body radiotherapy (SBRT) are radiotherapy methods that entail delivering highly focused,
Last Review Status/Date: December 2014 Page: 1 of 51 Description Stereotactic radiosurgery (SRS) and stereotactic body radiotherapy (SBRT) are radiotherapy methods that entail delivering highly focused,
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 04/01/2014 Section:
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: Original Effective Date: MM.05.008 05/12/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 04/01/2014 Section:
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: 6.01.10 Last Review: 11/2013 Origination: 1/1989 Next Review: 11/2014 Policy Blue Cross and Blue Shield of Kansas City (Blue
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Policy Number: 6.01.10 Last Review: 11/2013 Origination: 1/1989 Next Review: 11/2014 Policy Blue Cross and Blue Shield of Kansas City (Blue
Subject: Stereotactic Radiosurgery and Stereotactic Body Radiotherapy. Revision Date(s):
 Subject: Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Guidance Number: MCG-224 Revision Date(s): Original Effective Date: 12/18/14 DESCRIPTION OF PROCEDURE/SERVICE/PHARMACEUTICAL Stereotactic
Subject: Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Guidance Number: MCG-224 Revision Date(s): Original Effective Date: 12/18/14 DESCRIPTION OF PROCEDURE/SERVICE/PHARMACEUTICAL Stereotactic
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: charged_particle_radiotherapy 3/12/96 5/2017 5/2018 5/2017 Description of Procedure or Service Charged-particle
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: charged_particle_radiotherapy 3/12/96 5/2017 5/2018 5/2017 Description of Procedure or Service Charged-particle
MEDICAL POLICY SUBJECT: STEREOTACTIC RADIOSURGERY AND STEREOTACTIC BODY RADIATION THERAPY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: STEREOTACTIC RADIOSURGERY PAGE: 1 OF: 9 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: STEREOTACTIC RADIOSURGERY PAGE: 1 OF: 9 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Chapter 5 Section 3.1
 Radiology Chapter 5 Section 3.1 Issue Date: March 27, 1991 Authority: 32 CFR 199.4(b)(2), (b)(2)(x), (c)(2)(viii), and (g)(15) 1.0 CPT 1 PROCEDURE CODES 37243, 61793, 61795, 77261-77421, 77427-77799, 0073T
Radiology Chapter 5 Section 3.1 Issue Date: March 27, 1991 Authority: 32 CFR 199.4(b)(2), (b)(2)(x), (c)(2)(viii), and (g)(15) 1.0 CPT 1 PROCEDURE CODES 37243, 61793, 61795, 77261-77421, 77427-77799, 0073T
Stereotactic Radiosurgery and Proton Beam Therapy
 Last Review Date: January 12, 2018 Number: MG.MM.RA.13i Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: January 12, 2018 Number: MG.MM.RA.13i Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Medical Policy Manual Surgery, Policy No. 16 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Next Review: June 2018 Last Review: August 2017 Effective: October 1, 2017 IMPORTANT REMINDER
Medical Policy Manual Surgery, Policy No. 16 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Next Review: June 2018 Last Review: August 2017 Effective: October 1, 2017 IMPORTANT REMINDER
Stereotactic Radiosurgery. Extracranial Stereotactic Radiosurgery. Linear accelerators. Basic technique. Indications of SRS
 Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
Stereotactic Radiosurgery Extracranial Stereotactic Radiosurgery Annette Quinn, MSN, RN Program Manager, University of Pittsburgh Medical Center Using stereotactic techniques, give a lethal dose of ionizing
20. Background. Oligometastases. Oligometastases: bone (including spine) and lymph nodes
 125 20. Oligometastases Background The oligometastatic state can be defined as 1 3 isolated metastatic sites, typically occurring more than six months after successful treatment of primary disease. 1 In
125 20. Oligometastases Background The oligometastatic state can be defined as 1 3 isolated metastatic sites, typically occurring more than six months after successful treatment of primary disease. 1 In
Dosimetry, see MAGIC; Polymer gel dosimetry. Fiducial tracking, see CyberKnife radiosurgery
 Subject Index Acoustic neuroma, neurofibromatosis type 2 complications 103, 105 hearing outcomes 103, 105 outcome measures 101 patient selection 105 study design 101 tumor control 101 105 treatment options
Subject Index Acoustic neuroma, neurofibromatosis type 2 complications 103, 105 hearing outcomes 103, 105 outcome measures 101 patient selection 105 study design 101 tumor control 101 105 treatment options
Subject: Stereotactic Radiosurgery and Stereotactic Body Radiotherapy
 Subject: Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Policy Number: MCP-224 Revision Date(s): 12/13/2017 Original Effective Date: 12/18/2014 Review Date: 12/16/2015, 9/15/2016, 9/13/2017,
Subject: Stereotactic Radiosurgery and Stereotactic Body Radiotherapy Policy Number: MCP-224 Revision Date(s): 12/13/2017 Original Effective Date: 12/18/2014 Review Date: 12/16/2015, 9/15/2016, 9/13/2017,
Background Principles and Technical Development
 Contents Part I Background Principles and Technical Development 1 Introduction and the Nature of Radiosurgery... 3 Definitions of Radiosurgery... 5 Consequences of Changing Definitions of Radiosurgery...
Contents Part I Background Principles and Technical Development 1 Introduction and the Nature of Radiosurgery... 3 Definitions of Radiosurgery... 5 Consequences of Changing Definitions of Radiosurgery...
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT
 SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
SUCCESSFUL TREATMENT OF METASTATIC BRAIN TUMOR BY CYBERKNIFE: A CASE REPORT Cheng-Ta Hsieh, 1 Cheng-Fu Chang, 1 Ming-Ying Liu, 1 Li-Ping Chang, 2 Dueng-Yuan Hueng, 3 Steven D. Chang, 4 and Da-Tong Ju 1
4.x Oligometastases: evidence for dose-fractionation
 4.x Oligometastases: evidence for dose-fractionation Background 4.x.1. The oligometastatic state can be defined as 1-3 isolated metastatic sites, typically occurring more than six months after successful
4.x Oligometastases: evidence for dose-fractionation Background 4.x.1. The oligometastatic state can be defined as 1-3 isolated metastatic sites, typically occurring more than six months after successful
Public Statement: Medical Policy Statement:
 Medical Policy Title: Stereotactic ARBenefits Approval: 07/25/2012 Radiosurgery Effective Date: 01/01/2012 Document: ARB0321 Revision Date: Code(s): 77371 Radiation treatment delivery, Stereotactic radiosurgery
Medical Policy Title: Stereotactic ARBenefits Approval: 07/25/2012 Radiosurgery Effective Date: 01/01/2012 Document: ARB0321 Revision Date: Code(s): 77371 Radiation treatment delivery, Stereotactic radiosurgery
Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy
 Medical Policy Manual Surgery, Policy No. 16 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Next Review: June 2019 Last Review: February 2019 Effective: February 15, 2019 IMPORTANT REMINDER
Medical Policy Manual Surgery, Policy No. 16 Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Next Review: June 2019 Last Review: February 2019 Effective: February 15, 2019 IMPORTANT REMINDER
IMAGE-GUIDED RADIOSURGERY USING THE GAMMA KNIFE
 IMAGE-GUIDED RADIOSURGERY USING THE GAMMA KNIFE L. D. LUNSFORD INTRODUCTION Image guided brain surgery became a reality in the mid-1970s after the introduction of the first methods to obtain axial imaging
IMAGE-GUIDED RADIOSURGERY USING THE GAMMA KNIFE L. D. LUNSFORD INTRODUCTION Image guided brain surgery became a reality in the mid-1970s after the introduction of the first methods to obtain axial imaging
Otolaryngologist s Perspective of Stereotactic Radiosurgery
 Otolaryngologist s Perspective of Stereotactic Radiosurgery Douglas E. Mattox, M.D. 25 th Alexandria International Combined ORL Conference April 18-20, 2007 Acoustic Neuroma Benign tumor of the schwann
Otolaryngologist s Perspective of Stereotactic Radiosurgery Douglas E. Mattox, M.D. 25 th Alexandria International Combined ORL Conference April 18-20, 2007 Acoustic Neuroma Benign tumor of the schwann
Clinical Appropriateness Guidelines: Radiation Oncology
 Clinical Appropriateness Guidelines: Radiation Oncology Proton Beam Treatment Guidelines Effective Date: September 5, 2017 Proprietary Date of Origin: 05/14/2014 Last revised: 01/08/2015 Last reviewed:
Clinical Appropriateness Guidelines: Radiation Oncology Proton Beam Treatment Guidelines Effective Date: September 5, 2017 Proprietary Date of Origin: 05/14/2014 Last revised: 01/08/2015 Last reviewed:
Medical Policy Manual. Topic: Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy. Date of Origin: January 1996
 Medical Policy Manual Topic: Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Date of Origin: January 1996 Section: Surgery Last Reviewed Date: June 2014 Policy No: 16 Effective Date:
Medical Policy Manual Topic: Stereotactic Radiosurgery and Stereotactic Body Radiation Therapy Date of Origin: January 1996 Section: Surgery Last Reviewed Date: June 2014 Policy No: 16 Effective Date:
STEREOTACTIC RADIATION THERAPY. Monique Blanchard ANUM Radiation Oncology Epworth HealthCare
 STEREOTACTIC RADIATION THERAPY Monique Blanchard ANUM Radiation Oncology Epworth HealthCare Overview Stereotactic radiation therapy at Epworth Healthcare What is stereotactic radiation therapy? Delivery
STEREOTACTIC RADIATION THERAPY Monique Blanchard ANUM Radiation Oncology Epworth HealthCare Overview Stereotactic radiation therapy at Epworth Healthcare What is stereotactic radiation therapy? Delivery
Patients Treated with Leksell Gamma Knife
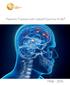 Patients Treated with Leksell Gamma Knife 1968-2016 TREATMENTS REPORTED 2016 BY REGION AND INDICATION INDICATION Asia excl. Europe Latin Middle East & Africa North Grand Total Benign Tumors 12283 9778
Patients Treated with Leksell Gamma Knife 1968-2016 TREATMENTS REPORTED 2016 BY REGION AND INDICATION INDICATION Asia excl. Europe Latin Middle East & Africa North Grand Total Benign Tumors 12283 9778
STEREOTACTIC RADIOSURGERY & STEREOTACTIC BODY RADIATION THERAPY
 STEREOTACTIC RADIOSURGERY & STEREOTACTIC BODY RADIATION THERAPY Protocol: NEU017 Effective Date: November 1, 2017 Table of Contents Page COMMERCIAL & MEDICAID COVERAGE RATIONALE... 1 MEDICARE COVERAGE
STEREOTACTIC RADIOSURGERY & STEREOTACTIC BODY RADIATION THERAPY Protocol: NEU017 Effective Date: November 1, 2017 Table of Contents Page COMMERCIAL & MEDICAID COVERAGE RATIONALE... 1 MEDICARE COVERAGE
Gamma Knife Radiosurgery
 Gamma Knife Radiosurgery A Team Approach to Treating Patients George Bovis, MD Patrick Sweeney, MD Jagan Venkatesan, MS Matt White, MS Illinois Gamma Knife Center Elk Grove Village, IL Disclosures Shareholders
Gamma Knife Radiosurgery A Team Approach to Treating Patients George Bovis, MD Patrick Sweeney, MD Jagan Venkatesan, MS Matt White, MS Illinois Gamma Knife Center Elk Grove Village, IL Disclosures Shareholders
Chapter 28 Emerging Indications in Stereotactic Radiosurgery: The First Application of Cellular Surgery
 Chapter 28 Emerging Indications in Stereotactic Radiosurgery: The First Application of Cellular Surgery Douglas Kondziolka, M.D., M.Sc., F.R.C.S.C., L. Dade Lunsford, M.D., John C. Flickinger, M.D., and
Chapter 28 Emerging Indications in Stereotactic Radiosurgery: The First Application of Cellular Surgery Douglas Kondziolka, M.D., M.Sc., F.R.C.S.C., L. Dade Lunsford, M.D., John C. Flickinger, M.D., and
Specialised Services Policy: CP22. Stereotactic Radiosurgery
 Specialised Services Policy: CP22 Document Author: Assistant Director of Planning Executive Lead: Director of Planning ad Performance Approved by: Management Group Issue Date: 01 July 2015 Review Date:
Specialised Services Policy: CP22 Document Author: Assistant Director of Planning Executive Lead: Director of Planning ad Performance Approved by: Management Group Issue Date: 01 July 2015 Review Date:
Oncology Clinical Service Line System-wide Consensus Guidelines: Treatment of Stage I Lung Cancer
 Oncology Clinical Service Line System-wide Consensus Guidelines: Treatment of Stage I Lung Cancer These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes
Oncology Clinical Service Line System-wide Consensus Guidelines: Treatment of Stage I Lung Cancer These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes
Reference: NHS England B01X26
 Clinical Commissioning Policy Proposition: The use of Stereotactic Ablative Radiotherapy (SABR) as a treatment option for patients with Hepatocellular carcinoma or Cholangiocarcinoma Reference: NHS England
Clinical Commissioning Policy Proposition: The use of Stereotactic Ablative Radiotherapy (SABR) as a treatment option for patients with Hepatocellular carcinoma or Cholangiocarcinoma Reference: NHS England
Optimal Management of Isolated HER2+ve Brain Metastases
 Optimal Management of Isolated HER2+ve Brain Metastases Eliot Sims November 2013 Background Her2+ve patients 15% of all breast cancer Even with adjuvant trastuzumab 10-15% relapse Trastuzumab does not
Optimal Management of Isolated HER2+ve Brain Metastases Eliot Sims November 2013 Background Her2+ve patients 15% of all breast cancer Even with adjuvant trastuzumab 10-15% relapse Trastuzumab does not
Extracranial doses in stereotactic and conventional radiotherapy for pituitary adenomas
 JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 7, NUMBER 2, SPRING 2006 Extracranial doses in stereotactic and conventional radiotherapy for pituitary adenomas Thomas Samuel Ram, a Paul B. Ravindran,
JOURNAL OF APPLIED CLINICAL MEDICAL PHYSICS, VOLUME 7, NUMBER 2, SPRING 2006 Extracranial doses in stereotactic and conventional radiotherapy for pituitary adenomas Thomas Samuel Ram, a Paul B. Ravindran,
Selecting the Optimal Treatment for Brain Metastases
 Selecting the Optimal Treatment for Brain Metastases Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Understand the benefits, limitations,
Selecting the Optimal Treatment for Brain Metastases Clinical Practice Today CME Co-provided by Learning Objectives Upon completion, participants should be able to: Understand the benefits, limitations,
DRAFT Local Coverage Determination (LCD) for Radiology: Stereotactic Radiosurgery (SRS) and Stereotactic Body Radiation Therapy (SBRT) (DL32973)
 DRAFT Local Coverage Determination (LCD) for Radiology: Stereotactic Radiosurgery (SRS) and Stereotactic Body Radiation Therapy (SBRT) (DL32973) Please note: This is a Draft policy. Draft LCDs are works
DRAFT Local Coverage Determination (LCD) for Radiology: Stereotactic Radiosurgery (SRS) and Stereotactic Body Radiation Therapy (SBRT) (DL32973) Please note: This is a Draft policy. Draft LCDs are works
Gamma Knife Radiosurgery A tool for treating intracranial conditions. CNSA Annual Congress 2016 Radiation Oncology Pre-congress Workshop
 Gamma Knife Radiosurgery A tool for treating intracranial conditions CNSA Annual Congress 2016 Radiation Oncology Pre-congress Workshop ANGELA McBEAN Gamma Knife CNC State-wide Care Coordinator Gamma Knife
Gamma Knife Radiosurgery A tool for treating intracranial conditions CNSA Annual Congress 2016 Radiation Oncology Pre-congress Workshop ANGELA McBEAN Gamma Knife CNC State-wide Care Coordinator Gamma Knife
Stereotactic ablative body radiotherapy for renal cancer
 1 EVIDENCE SUMMARY REPORT Stereotactic ablative body radiotherapy for renal cancer Questions to be addressed 1. What is the clinical effectiveness of stereotactic ablative body radiotherapy for inoperable
1 EVIDENCE SUMMARY REPORT Stereotactic ablative body radiotherapy for renal cancer Questions to be addressed 1. What is the clinical effectiveness of stereotactic ablative body radiotherapy for inoperable
NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) BONE (Version , 03/28/18)
 BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
Reference: NHS England: 16022/P
 Clinical Commissioning Policy: The use of Stereotactic Ablative Radiotherapy (SABR) as a treatment option for patients with Hepatocellular carcinoma or Cholangiocarcinoma Reference: NHS England: 16022/P
Clinical Commissioning Policy: The use of Stereotactic Ablative Radiotherapy (SABR) as a treatment option for patients with Hepatocellular carcinoma or Cholangiocarcinoma Reference: NHS England: 16022/P
8/2/2018. Acknowlegements: TCP SPINE. Disclosures
 A Presentation for the AAPM Annual meeting, Aug 2, 2018 Nashville, TN Stereotactic Radiosurgery for Spinal Metastases: Tumor Control Probability Analyses and Recommended Reporting Standards for Future
A Presentation for the AAPM Annual meeting, Aug 2, 2018 Nashville, TN Stereotactic Radiosurgery for Spinal Metastases: Tumor Control Probability Analyses and Recommended Reporting Standards for Future
Clinical Policy: Stereotactic Body Radiation Therapy Reference Number: CP.MP.22 Last Review Date: 01/18
 Clinical Policy: Reference Number: CP.MP.22 Last Review Date: 01/18 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description
Clinical Policy: Reference Number: CP.MP.22 Last Review Date: 01/18 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description
Survival and Intracranial Control of Patients With 5 or More Brain Metastases Treated With Gamma Knife Stereotactic Radiosurgery
 ORIGINAL ARTICLE Survival and Intracranial Control of Patients With 5 or More Brain Metastases Treated With Gamma Knife Stereotactic Radiosurgery Ann C. Raldow, BS,* Veronica L. Chiang, MD,w Jonathan P.
ORIGINAL ARTICLE Survival and Intracranial Control of Patients With 5 or More Brain Metastases Treated With Gamma Knife Stereotactic Radiosurgery Ann C. Raldow, BS,* Veronica L. Chiang, MD,w Jonathan P.
We have previously reported good clinical results
 J Neurosurg 113:48 52, 2010 Gamma Knife surgery as sole treatment for multiple brain metastases: 2-center retrospective review of 1508 cases meeting the inclusion criteria of the JLGK0901 multi-institutional
J Neurosurg 113:48 52, 2010 Gamma Knife surgery as sole treatment for multiple brain metastases: 2-center retrospective review of 1508 cases meeting the inclusion criteria of the JLGK0901 multi-institutional
Artificial Pancreas Device Systems. Populations Interventions Comparators Outcomes. pump. pump
 Protocol Artificial Pancreas Device Systems (10130) Medical Benefit Effective Date: 04/01/18 Next Review Date: 01/19 Preauthorization Yes Review Dates: 03/15, 03/16, 03/17, 01/18 Preauthorization is required.
Protocol Artificial Pancreas Device Systems (10130) Medical Benefit Effective Date: 04/01/18 Next Review Date: 01/19 Preauthorization Yes Review Dates: 03/15, 03/16, 03/17, 01/18 Preauthorization is required.
Palliative radiotherapy in lung cancer
 New concepts and insights regarding the role of radiation therapy in metastatic disease Umberto Ricardi University of Turin Department of Oncology Radiation Oncology Palliative radiotherapy in lung cancer
New concepts and insights regarding the role of radiation therapy in metastatic disease Umberto Ricardi University of Turin Department of Oncology Radiation Oncology Palliative radiotherapy in lung cancer
Protocol. Intensity-Modulated Radiation Therapy (IMRT): Central Nervous System Tumors
 Intensity-Modulated Radiation Therapy (IMRT): Central Nervous (80159) Medical Benefit Effective Date: 03/01/14 Next Review Date: 03/15 Preauthorization No Review Dates: 07/12, 07/13, 03/14 The following
Intensity-Modulated Radiation Therapy (IMRT): Central Nervous (80159) Medical Benefit Effective Date: 03/01/14 Next Review Date: 03/15 Preauthorization No Review Dates: 07/12, 07/13, 03/14 The following
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: January 15, 2019 Related Policies: 8.01.46 Intensity-Modulated Radiotherapy of the Lung 8.01.48 Intensity-Modulated Radiotherapy: Cancer of the Thyroid 8.01.49
FEP Medical Policy Manual Effective Date: January 15, 2019 Related Policies: 8.01.46 Intensity-Modulated Radiotherapy of the Lung 8.01.48 Intensity-Modulated Radiotherapy: Cancer of the Thyroid 8.01.49
Management of single brain metastasis: a practice guideline
 PRACTICE GUIDELINE SERIES Management of single brain metastasis: a practice guideline A. Mintz MD,* J. Perry MD, K. Spithoff BHSc, A. Chambers MA, and N. Laperriere MD on behalf of the Neuro-oncology Disease
PRACTICE GUIDELINE SERIES Management of single brain metastasis: a practice guideline A. Mintz MD,* J. Perry MD, K. Spithoff BHSc, A. Chambers MA, and N. Laperriere MD on behalf of the Neuro-oncology Disease
Therapy of Non-Operable early stage NSCLC
 SBRT Stage I NSCLC Therapy of Non-Operable early stage NSCLC Dr. Adnan Al-Hebshi MD, FRCR(UK), FRCP(C), ABR King Faisal Specialist Hospital & Research Centre This is our territory Early Stages NSCLC Surgical
SBRT Stage I NSCLC Therapy of Non-Operable early stage NSCLC Dr. Adnan Al-Hebshi MD, FRCR(UK), FRCP(C), ABR King Faisal Specialist Hospital & Research Centre This is our territory Early Stages NSCLC Surgical
PEDIATRIC ORBITAL TUMORS RADIOTHERAPY PLANNING
 PEDIATRIC ORBITAL TUMORS RADIOTHERAPY PLANNING ANATOMY ANATOMY CONT ANATOMY CONT. ANATOMY CONT. EYE OF A CHILD Normal tissue tolerance doses (in conventional #) TD 5/5 TD 50/5 Endpoint Gy Gy Optic nerve
PEDIATRIC ORBITAL TUMORS RADIOTHERAPY PLANNING ANATOMY ANATOMY CONT ANATOMY CONT. ANATOMY CONT. EYE OF A CHILD Normal tissue tolerance doses (in conventional #) TD 5/5 TD 50/5 Endpoint Gy Gy Optic nerve
Treatment of oligometastases: Lung
 Treatment of oligometastases: Lung Themadag Catharina ZH 30 March 2017 Max Dahele Radiation Oncologist Vumc, Amsterdam m.dahele@vumc.nl Do you all treat lung oligometastases? What is your definition of
Treatment of oligometastases: Lung Themadag Catharina ZH 30 March 2017 Max Dahele Radiation Oncologist Vumc, Amsterdam m.dahele@vumc.nl Do you all treat lung oligometastases? What is your definition of
Treatment of oligometastatic NSCLC
 Treatment of oligometastatic NSCLC Jarosław Kużdżał Department of Thoracic Surgery Jagiellonian University Collegium Medicum, John Paul II Hospital, Cracow New idea? 14 NSCLC patients with solitary extrathoracic
Treatment of oligometastatic NSCLC Jarosław Kużdżał Department of Thoracic Surgery Jagiellonian University Collegium Medicum, John Paul II Hospital, Cracow New idea? 14 NSCLC patients with solitary extrathoracic
IEHP UM Subcommittee Approved Authorization Guidelines Proton Beam Radiation Therapy for Prostate Cancer
 Policy: The use of Proton Beam Therapy (PBT) in Prostate cancer has not been established as more effective than other forms of External Beam Radiation Therapies (EBRT s), such as Intensity Modulated Radiation
Policy: The use of Proton Beam Therapy (PBT) in Prostate cancer has not been established as more effective than other forms of External Beam Radiation Therapies (EBRT s), such as Intensity Modulated Radiation
Bone Metastases Radiation Therapy Physician Worksheet Pages 2-5. Brain Metastases Radiation Therapy Physician Worksheet Pages 6-9
 evicore Healthcare needs to collect sufficient clinical history and treatment plan information relevant to a request for radiation therapy treatment to establish the medical necessity of the service. evicore
evicore Healthcare needs to collect sufficient clinical history and treatment plan information relevant to a request for radiation therapy treatment to establish the medical necessity of the service. evicore
MP Charged-Particle (Proton or Helium Ion) Radiotherapy for Neoplastic Conditions
 Medical Policy BCBSA Ref. Policy: 8.01.10 Last Review: 07/25/2018 Effective Date: 07/25/2018 Section: Therapy Related Policies 6.01.10 Stereotactic Radiosurgery and Stereotactic Body Radiotherapy 8.01.46
Medical Policy BCBSA Ref. Policy: 8.01.10 Last Review: 07/25/2018 Effective Date: 07/25/2018 Section: Therapy Related Policies 6.01.10 Stereotactic Radiosurgery and Stereotactic Body Radiotherapy 8.01.46
Protocol. Intensity-Modulated Radiotherapy: Central Nervous System Tumors
 Intensity-Modulated Radiotherapy: Central Nervous System (80159) Medical Benefit Effective Date: 07/01/17 Next Review Date: 03/18 Preauthorization No Review Dates: 07/12, 07/13, 03/14, 03/15, 03/16, 03/17,
Intensity-Modulated Radiotherapy: Central Nervous System (80159) Medical Benefit Effective Date: 07/01/17 Next Review Date: 03/18 Preauthorization No Review Dates: 07/12, 07/13, 03/14, 03/15, 03/16, 03/17,
Tania Kaprealian, M.D. Assistant Professor UCLA Department of Radiation Oncology August 22, 2015
 Tania Kaprealian, M.D. Assistant Professor UCLA Department of Radiation Oncology August 22, 2015 Most common brain tumor, affecting 8.5-15% of cancer patients. Treatment options: Whole brain radiation
Tania Kaprealian, M.D. Assistant Professor UCLA Department of Radiation Oncology August 22, 2015 Most common brain tumor, affecting 8.5-15% of cancer patients. Treatment options: Whole brain radiation
Clinical Treatment Planning
 Radiation Therapy Services Benefits to Change for the CSHCN Services Program Effective October 1, 2008, benefits for radiation therapy services will change for the Children with Special Health Care Needs
Radiation Therapy Services Benefits to Change for the CSHCN Services Program Effective October 1, 2008, benefits for radiation therapy services will change for the Children with Special Health Care Needs
Stereotactic body radiation therapy versus surgery for patients with stage I non-small cell lung cancer
 Review Article Page 1 of 9 Stereotactic body radiation therapy versus surgery for patients with stage I non-small cell lung cancer Tomoki Kimura Department of Radiation Oncology, Hiroshima University Hospital,
Review Article Page 1 of 9 Stereotactic body radiation therapy versus surgery for patients with stage I non-small cell lung cancer Tomoki Kimura Department of Radiation Oncology, Hiroshima University Hospital,
The Role of Radiation Therapy in the Treatment of Brain Metastases. Matthew Cavey, M.D.
 The Role of Radiation Therapy in the Treatment of Brain Metastases Matthew Cavey, M.D. Objectives Provide information about the prospective trials that are driving the treatment of patients with brain
The Role of Radiation Therapy in the Treatment of Brain Metastases Matthew Cavey, M.D. Objectives Provide information about the prospective trials that are driving the treatment of patients with brain
Stereotactic Radiosurgery/Fractionated Stereotactic Radiotherapy for Acoustic Neuroma (Vestibular Schwannomas)
 Strategic Commissioning Group West Midlands Commissioning Policy (WM/38) Stereotactic Radiosurgery/Fractionated Stereotactic Radiotherapy for Acoustic Neuroma (Vestibular Schwannomas) Version 1 July 2010
Strategic Commissioning Group West Midlands Commissioning Policy (WM/38) Stereotactic Radiosurgery/Fractionated Stereotactic Radiotherapy for Acoustic Neuroma (Vestibular Schwannomas) Version 1 July 2010
Disclosures. Overview 8/3/2016. SRS: Cranial and Spine
 SRS: Cranial and Spine Brian Winey, Ph.D. Department of Radiation Oncology Massachusetts General Hospital Harvard Medical School Disclosures Travel and research funds from Elekta Travel funds from IBA
SRS: Cranial and Spine Brian Winey, Ph.D. Department of Radiation Oncology Massachusetts General Hospital Harvard Medical School Disclosures Travel and research funds from Elekta Travel funds from IBA
Leksell Gamma Knife Icon. Treatment information
 Leksell Gamma Knife Icon Treatment information You may be feeling frightened or overwhelmed by your recent diagnosis. It can be confusing trying to process a diagnosis, understand a new and challenging
Leksell Gamma Knife Icon Treatment information You may be feeling frightened or overwhelmed by your recent diagnosis. It can be confusing trying to process a diagnosis, understand a new and challenging
ANALYSIS OF TREATMENT OUTCOMES WITH LINAC BASED STEREOTACTIC RADIOSURGERY IN INTRACRANIAL ARTERIOVENOUS MALFORMATIONS
 ANALYSIS OF TREATMENT OUTCOMES WITH LINAC BASED STEREOTACTIC RADIOSURGERY IN INTRACRANIAL ARTERIOVENOUS MALFORMATIONS Dr. Maitri P Gandhi 1, Dr. Chandni P Shah 2 1 Junior resident, Gujarat Cancer & Research
ANALYSIS OF TREATMENT OUTCOMES WITH LINAC BASED STEREOTACTIC RADIOSURGERY IN INTRACRANIAL ARTERIOVENOUS MALFORMATIONS Dr. Maitri P Gandhi 1, Dr. Chandni P Shah 2 1 Junior resident, Gujarat Cancer & Research
Oncology Clinical Service Line System-wide Consensus Guidelines: Treatment of Stage I Lung Cancer
 Oncology Clinical Service Line System-wide Consensus Guidelines: Treatment of Stage I Lung Cancer These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes
Oncology Clinical Service Line System-wide Consensus Guidelines: Treatment of Stage I Lung Cancer These guidelines apply to clinical interventions that have well-documented outcomes, but whose outcomes
Tecniche Radioterapiche U. Ricardi
 Tecniche Radioterapiche U. Ricardi UNIVERSITA DEGLI STUDI DI TORINO Should we always rely on stage? T4N0M0 Stage IIIB T2N3M0 Early stage NSCLC The treatment of choice for early-stage NSCLC is anatomic
Tecniche Radioterapiche U. Ricardi UNIVERSITA DEGLI STUDI DI TORINO Should we always rely on stage? T4N0M0 Stage IIIB T2N3M0 Early stage NSCLC The treatment of choice for early-stage NSCLC is anatomic
Charged-Particle (Proton or Helium Ion) Radiotherapy for Neoplastic Conditions
 Charged-Particle (Proton or Helium Ion) Radiotherapy for Neoplastic Conditions Policy Number: 8.01.10 Last Review: 11/2017 Origination: 11/2006 Next Review: 11/2018 Policy Blue Cross and Blue Shield of
Charged-Particle (Proton or Helium Ion) Radiotherapy for Neoplastic Conditions Policy Number: 8.01.10 Last Review: 11/2017 Origination: 11/2006 Next Review: 11/2018 Policy Blue Cross and Blue Shield of
Protocol. Charged-Particle (Proton or Helium Ion) Radiation Therapy
 Protocol Charged-Particle (Proton or Helium Ion) Radiation Therapy (80110) Medical Benefit Effective Date: 03/01/14 Next Review Date: 03/15 Preauthorization Yes Review Dates: 03/09, 03/10, 03/11, 03/12,
Protocol Charged-Particle (Proton or Helium Ion) Radiation Therapy (80110) Medical Benefit Effective Date: 03/01/14 Next Review Date: 03/15 Preauthorization Yes Review Dates: 03/09, 03/10, 03/11, 03/12,
Evidence Based Medicine for Gamma Knife Radiosurgery. Metastatic Disease GAMMA KNIFE SURGERY
 GAMMA KNIFE SURGERY Metastatic Disease Evidence Based Medicine for Gamma Knife Radiosurgery Photos courtesy of Jean Régis, Timone University Hospital, Marseille, France Brain Metastases The first report
GAMMA KNIFE SURGERY Metastatic Disease Evidence Based Medicine for Gamma Knife Radiosurgery Photos courtesy of Jean Régis, Timone University Hospital, Marseille, France Brain Metastases The first report
Current Status and Future Medical Perspectives at MedAustron. U. Mock EBG MedAustron GmbH
 Current Status and Future Medical Perspectives at MedAustron U. Mock EBG MedAustron GmbH Cancer treatment facility Ion beam therapy with protons and carbon ions Research facility Medical physics Radiobiology
Current Status and Future Medical Perspectives at MedAustron U. Mock EBG MedAustron GmbH Cancer treatment facility Ion beam therapy with protons and carbon ions Research facility Medical physics Radiobiology
and Strength of Recommendations
 ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
Clinical Commissioning Policy: Arteriovenous Malformations. December Reference : NHSCB/D5/4
 Clinical Commissioning Policy: Arteriovenous Malformations December 2012 Reference : NHSCB/D5/4 NHS Commissioning Board Clinical Commissioning Policy: Arteriovenous Malformations First published: December
Clinical Commissioning Policy: Arteriovenous Malformations December 2012 Reference : NHSCB/D5/4 NHS Commissioning Board Clinical Commissioning Policy: Arteriovenous Malformations First published: December
Artificial Pancreas Device Systems. Populations Interventions Comparators Outcomes Individuals: With type 1 diabetes
 Protocol Artificial Pancreas Device Systems Medical Benefit Effective Date: 07/01/18 Next Review Date: 01/20 Preauthorization Yes Review Dates: 03/15, 03/16, 03/17, 01/18, 05/18, 01/19 Preauthorization
Protocol Artificial Pancreas Device Systems Medical Benefit Effective Date: 07/01/18 Next Review Date: 01/20 Preauthorization Yes Review Dates: 03/15, 03/16, 03/17, 01/18, 05/18, 01/19 Preauthorization
FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA
 1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA QUESTIONS TO BE ADDRESSED: SUMMARY 1. What is the evidence for the clinical
1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR PILOCYTIC ASTROCYTOMA QUESTIONS TO BE ADDRESSED: SUMMARY 1. What is the evidence for the clinical
Current Concepts and Trends in Spinal Radiosurgery. Edward M. Marchan
 Current Concepts and Trends in Spinal Radiosurgery Edward M. Marchan Spinal Neoplasia The spine is the most common site of skeletal metastatic disease. (70%) 40% of bony metastases involve the vertebrae
Current Concepts and Trends in Spinal Radiosurgery Edward M. Marchan Spinal Neoplasia The spine is the most common site of skeletal metastatic disease. (70%) 40% of bony metastases involve the vertebrae
NON MALIGNANT BRAIN TUMOURS Facilitator. Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol
 NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
Clinically Proven Metabolically-Guided TomoTherapy SM Treatments Advancing Cancer Care
 Clinically Proven Metabolically-Guided TomoTherapy SM Treatments Advancing Cancer Care Institution: San Raffaele Hospital Milan, Italy By Nadia Di Muzio, M.D., Radiotherapy Department (collaborators: Berardi
Clinically Proven Metabolically-Guided TomoTherapy SM Treatments Advancing Cancer Care Institution: San Raffaele Hospital Milan, Italy By Nadia Di Muzio, M.D., Radiotherapy Department (collaborators: Berardi
Corporate Medical Policy
 Corporate Medical Policy Radiofrequency Ablation of Miscellaneous Solid Tumors Excluding File Name: Origination: Last CAP Review: Next CAP Review: Last Review: radiofrequency_ablation_of_miscellaneous_solid_tumors
Corporate Medical Policy Radiofrequency Ablation of Miscellaneous Solid Tumors Excluding File Name: Origination: Last CAP Review: Next CAP Review: Last Review: radiofrequency_ablation_of_miscellaneous_solid_tumors
Clinical Commissioning Policy: The use of Stereotactic Ablative Radiotherapy (SABR) in the treatment of oligometastatic disease
 Clinical Commissioning Policy: The use of Stereotactic Ablative Radiotherapy (SABR) in the treatment of oligometastatic disease Reference: NHS England: 16032/P 2 NHS England INFORMATION READER BOX Directorate
Clinical Commissioning Policy: The use of Stereotactic Ablative Radiotherapy (SABR) in the treatment of oligometastatic disease Reference: NHS England: 16032/P 2 NHS England INFORMATION READER BOX Directorate
cryosurgical_ablation_of_miscellaneous_solid_tumors 1/2007 5/2017 5/2018 5/2017
 Corporate Medical Policy Cryosurgical Ablation of Miscellaneous Solid Tumors Other File Name: Origination: Last CAP Review: Next CAP Review: Last Review: cryosurgical_ablation_of_miscellaneous_solid_tumors
Corporate Medical Policy Cryosurgical Ablation of Miscellaneous Solid Tumors Other File Name: Origination: Last CAP Review: Next CAP Review: Last Review: cryosurgical_ablation_of_miscellaneous_solid_tumors
Stereotactic Ablative Radiotherapy for Prostate Cancer
 Stereotactic Ablative Radiotherapy for Prostate Cancer Laurie Cuttino, MD Associate Professor of Radiation Oncology VCU Massey Cancer Center Director of Radiation Oncology Sarah Cannon Cancer Center at
Stereotactic Ablative Radiotherapy for Prostate Cancer Laurie Cuttino, MD Associate Professor of Radiation Oncology VCU Massey Cancer Center Director of Radiation Oncology Sarah Cannon Cancer Center at
FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR EPENDYMOMA
 1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR EPENDYMOMA QUESTIONS TO BE ADDRESSED: 1. What is the evidence for the clinical effectiveness
1 EVIDENCE SUMMARY REPORT FOR PUBLIC CONSULTATION ONLY STEREOTACTIC RADIOSURGERY/ STEROTACTIC RADIOTHERAPY FOR EPENDYMOMA QUESTIONS TO BE ADDRESSED: 1. What is the evidence for the clinical effectiveness
Brain Tumor Treatment
 Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
RADIATION THERAPY SERVICES CSHCN SERVICES PROGRAM PROVIDER MANUAL
 RADIATION THERAPY SERVICES CSHCN SERVICES PROGRAM PROVIDER MANUAL APRIL 2018 CSHCN PROVIDER PROCEDURES MANUAL APRIL 2018 RADIATION THERAPY SERVICES Table of Contents 34.1 Enrollment......................................................................
RADIATION THERAPY SERVICES CSHCN SERVICES PROGRAM PROVIDER MANUAL APRIL 2018 CSHCN PROVIDER PROCEDURES MANUAL APRIL 2018 RADIATION THERAPY SERVICES Table of Contents 34.1 Enrollment......................................................................
ARROCase Brain Metastases
 ARROCase Brain Metastases Colin Hill*, Daniel M. Trifiletti*, Timothy N. Showalter*, Jason P. Sheehan Radiation Oncology* and Neurosurgery University of Virginia Charlottesville, VA Case: HPI 64 year old
ARROCase Brain Metastases Colin Hill*, Daniel M. Trifiletti*, Timothy N. Showalter*, Jason P. Sheehan Radiation Oncology* and Neurosurgery University of Virginia Charlottesville, VA Case: HPI 64 year old
Stereotactic Radiosurgery for Brain Metastasis: Changing Treatment Paradigms. Overall Clinical Significance 8/3/13
 Stereotactic Radiosurgery for Brain Metastasis: Changing Treatment Paradigms Jason Sheehan, MD, PhD Departments of Neurosurgery and Radiation Oncology University of Virginia, Charlottesville, VA USA Overall
Stereotactic Radiosurgery for Brain Metastasis: Changing Treatment Paradigms Jason Sheehan, MD, PhD Departments of Neurosurgery and Radiation Oncology University of Virginia, Charlottesville, VA USA Overall
Radiation Therapy Services
 Radiation Therapy Services Chapter.1 Enrollment..................................................................... -2.2 Benefits, Limitations, and Authorization Requirements...........................
Radiation Therapy Services Chapter.1 Enrollment..................................................................... -2.2 Benefits, Limitations, and Authorization Requirements...........................
Stereotactic radiosurgery for the treatment of melanoma and renal cell carcinoma brain metastases
 ONCOLOGY REPORTS 29: 407-412, 2013 Stereotactic radiosurgery for the treatment of melanoma and renal cell carcinoma brain metastases SHELLY LWU 1, PABLO GOETZ 1, ERIC MONSALVES 1, MANDANA ARYAEE 1, JULIUS
ONCOLOGY REPORTS 29: 407-412, 2013 Stereotactic radiosurgery for the treatment of melanoma and renal cell carcinoma brain metastases SHELLY LWU 1, PABLO GOETZ 1, ERIC MONSALVES 1, MANDANA ARYAEE 1, JULIUS
Disclosures. Neurological Manifestations of Von Hippel Lindau Syndrome. Objectives. Overview. None No conflicts of interest
 Neurological Manifestations of Von Hippel Lindau Syndrome ARNOLD B. ETAME MD, PhD NEURO-ONCOLOGY/NEUROSURGERY Moffitt Cancer Center Disclosures None No conflicts of interest VHL Alliance Annual Family
Neurological Manifestations of Von Hippel Lindau Syndrome ARNOLD B. ETAME MD, PhD NEURO-ONCOLOGY/NEUROSURGERY Moffitt Cancer Center Disclosures None No conflicts of interest VHL Alliance Annual Family
