The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better?
|
|
|
- Alexander Doyle
- 5 years ago
- Views:
Transcription
1 Int Surg 2016;101:58 63 DOI: /INTSURG-D The Choice of Palliative Treatment for Biliary and Duodenal Obstruction in Patients With Unresectable Pancreatic Cancer: Is Surgery Bypass Better? Qinghui Fu 1, Ying Chen 2, Xiaohan Liu 3 1 Department of SICU, the Second Affiliated Hospital of Zhejiang University School of Medicine, Hangzhou China 2 Fourth Affiliated Hospital of China Medical University, Shenyang, China 3 Yanshan University, Qinhuangdao, China This study aimed to investigate the clinical significance of palliative operation for carcinoma of pancreas between bypass surgery and interventional therapy. Most patients with locally advanced pancreatic cancer cannot undergo resection and show obstructive jaundice at presentation. Methods of palliation in these patients comprise biliary stent or surgical bypass. We retrospectively analyzed the clinical data of 53 patients who underwent palliative treatment with incurable locally advanced pancreatic ductal adenocarcinoma. This retrospective study compared morbidity, mortality, hospital stay, readmission rate, and survival in these patients. A total of 31 patients underwent biliary bypass surgery, and 22 had interventional therapy. There was no significant difference in the patients basic condition before operation and in the 30-day mortality between surgical palliation and intervention. However, there were some differences in the early complications, survival time, successful biliary drainage, and recurrent jaundice. Through analysis of these clinical data and the published studies, we conclude that surgical bypass is a better effective palliative method for patients than biliary and duodenum stent with locally advanced pancreatic cancer. Patients need to be carefully selected in consideration of operative risk and perceived overall survival. Corresponding author: Qinghui Fu, Department of SICU, the Second Affiliated Hospital of Zhejiang University School of Medicine, Hangzhou , Zhejiang Province, China. Tel.: þ ; @qq.com 58 Int Surg 2016;101
2 THE COMPARISON BETWEEN SURGICAL BYPASS AND INTERVENTIONAL THERAPY FU Key words: Obstructive jaundice Pancreatic cancer Surgical bypass Biliary stent Interventional therapy Pancreatic cancer is the fourth leading cause of cancer-related mortality in the world. 1 About 80% of patients who have received a diagnosis of pancreatic cancer already have other organ metastasis, as well as local tumor in the late stage. 2 Therefore, appropriate palliation for the main symptoms, such as obstructive jaundice, duodenal obstruction, and pain, is most important. However, there is controversy on how to provide better palliative treatment for these patients. Several therapeutic methods can be options. Some surgeons hold the view favoring resection surgery in the palliative way, arguing that it could offer a survival advantage or better palliation and has equivalent morbidity and mortality rates to surgical bypass, 3 but some surgeons do not agree with this view. Comparing to palliative resection, biliary bypass (choledochojejunostomy and cholecystojejunostomy) and biliary stent are also the choices of palliative treatment. The advantage of biliary stents is that the procedure is mini-invasive, which is well tolerated by patients. However, this method is limited by the recurrence of jaundice secondary to stent migration or accretion. Tumor progression and duodenal invasion may cause therapy to fail. Some surgeons also thought that surgical bypass was the best palliative treatment for carcinoma of the pancreas 4 because stenting of the biliary system requires periodic changes of the endoprosthesis and causes associated hospitalization. 5 Therefore, there is controversy on how to provide effective palliative treatment for those patients who have locally advanced pancreatic cancer. The goal of therapy for these patients is to obtain the most complete and prolonged remission of symptoms possible, with the least intervention-related morbidity and mortality. 6 The aim of this research was to compare morbidity and mortality rates and the effectiveness of palliative methods between patients matched for tumor size and clinical stage who underwent surgical bypass or biliary and duodenal stent for locally advanced pancreatic cancer. Patients and Methods Patients and data collection We carried out a retrospective analysis of patients who underwent palliative treatment with primary cancer of the head of the pancreas, requiring palliation of their malignant obstructive jaundice in our hospital from January 2008 to December Excluded from this research were any patients who underwent palliative resection, had no obstructive jaundice at the time of diagnosis, or had other periampullary cancer (distal bile duct, ampulla of Vater, and duodenum). All patients with metastatic disease proven by radiologic or surgical assessment were excluded. Patients with histologic diagnoses other than adenocarcinoma were also excluded. The tumors of these patients were unresectable because of local vascular invasion to the superior mesenteric vein, portal vein, superior mesenteric artery, hepatic artery, or celiac artery. The tumor size was cm in the surgical bypass group, and in the stent group. The tumors of these patients were all in stage 3 according to the NCCN guideline of pancreatic adenocarcinoma. The definition of hospital stay was the time of being in the hospital after the patient s surgical or interventional procedure. Information and data on shortand long-term morbidity in terms of postoperative complications and hospital readmissions and mortality were collected. Long-term disease-specific survival data were collected by telephoning the number of patients from hospital records. All patients undergoing interventional therapy underwent biliary stenting following percutaneous transhepatic cholangial drainage (PTCD) and duodenal stent if clinical symptoms of gastric outlet obstruction were present. All patients undergoing palliative surgery underwent a double bypass comprising a hepatojejunostomy-en-y and gastrojejunostomy. This study complied with the standards of the Helsinki Declaration and current ethics guideline and was approved by the Institutional Ethics Board. Statistical analysis Survival time is defined as counting from the day of surgery until death. According to the medical records, survival or death information can be obtained by telephone contact with patients relatives. Description of continuous data were expressed as mean and standard deviation (SD). Statistical analysis of continuous data used the Student t-test or Mann-Whitney U test for parametric and nonparametric data, respectively. Statistical Int Surg 2016;101 59
3 FU THE COMPARISON BETWEEN SURGICAL BYPASS AND INTERVENTIONAL THERAPY Table 1 Basic condition of patients before surgical bypass or interventional palliation Surgical double bypass Interventional therapy P value No. of patients Male, n 19 8 Female, n Mean age, y Total bilirubin, mmol/l Direct bilirubin, mmol/l Alanine aminotransferase, mmol/l ALP, mmol/l Albumin, g/l Tumor size, cm ALP, alkaline phosphatase. analysis of proportions used a v 2 test or Fisher exact test. Kaplan-Meier survival curve was used to calculate the incidence of cumulative event, and was tested by the use of log rank. In all analyses, a P value,0.05 was considered statistically significant. The clinical results were analyzed using a statistical analysis program package (SPSS 19.0, SPSS Inc, Chicago, Illinois). Results In this research, a total of 53 patients were included. Of these, 31 underwent palliative surgery and 22 underwent interventional therapy. Basic demographic and hematologic data are displayed in Table 1. The tumor size and stage are displayed in Table 1. No other values differed statistically between the groups. There were no significant differences in mortality rates between the patients who underwent palliative surgery and those who underwent palliative biliary and duodenal stent (Table 2). In the surgical group, no one was dead within 30 days. In the stent group, causes of death were cholangitis. Treatment of surgical palliation was successful in 29 of the 31 patients. Treatment of palliative stenting was successful in 21 of the 22 patients. The success was determined by normalization of the serum bilirubin levels and symptom improvement (Table 2). In the surgical group, the mean maximal preoperative bilirubin level was mmol/l, and the mean minimal postoperative level was mmol/l. In the stent group, the mean maximal preoperative bilirubin level was mmol/l, and the mean minimal postoperative level was mmol/l. There were 7 patients who had experienced complications within 30 days in surgical palliation group. Of these 7 patients, 4 had wound infections, 1 patient had upper gastrointestinal bleeding, and 2 had postoperative prolonged ileus. There was 1 patient who had experienced complications within 30 days in the palliative stenting group, and the main problem for this patient was stent blockage. In the first admission period, the postoperative stay of the palliative Table 2 Basic condition of patients after surgical bypass or interventional palliation Surgical double bypass Interventional therapy P value Total bilirubin, mmol/l ,0.001 Direct bilirubin, mmol/l ,0.001 Alanine aminotransferase, mmol/l ALP, mmol/l Mean postoperative hospital stay during the first admission period, days ,0.05 Mean survival, mo ,0.001 Early complications in 30 days, No. 7 1 NS 30-day mortality, n 0 1 NS Readmission reason, n Cholangitis 2 3 NS Gastrointestinal obstruction 0 5 NS Recurrent jaundice 2 6 NS ALP, alkaline phosphatase; NS, not significant. 60 Int Surg 2016;101
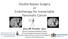
4 THE COMPARISON BETWEEN SURGICAL BYPASS AND INTERVENTIONAL THERAPY FU Fig. 1 Actuarial Kaplan-Meier survival analysis of patients who underwent surgical double bypass compared with patients who received interventional therapy. surgery group was longer than that of the palliative stenting group. Although the patients who underwent a surgical bypass had a longer postoperative hospital stay during the first hospitalization, they had a longer overall survival than patients who underwent interventional treatment (Fig. 1). The main reasons for readmission were gastrointestinal obstruction and recurrent jaundice in both groups. There were 14 patients in the palliative stenting group who had complications for readmission because of acute cholangitis, recurrent jaundice, and gastric outlet obstruction. Of these 14 palliative stenting patients, 5 developed intractable vomiting, which had radiologic evidence of gastric outlet obstruction. Recurrent jaundice occurred in 6 patients in the palliative stenting group. In the palliative surgery group there were 4 patients who had complications for readmissions because of acute cholangitis or recurrent jaundice. In the palliative surgery group, 2 patients had acute cholangitis and 2 patients had recurrent jaundice. Discussion In this single-center retrospective trial of comparison between bypass surgery and interventional therapy, we found that surgical bypass can be performed with mortality rates equivalent to those of biliary stenting in selected patients. Our findings agree with those of two previous retrospective studies of incurable, locally advanced pancreatic ductal adenocarcinoma that compared morbidity, mortality, hospital stay, readmission rate, and survival. In a study of 56 patients, Scott et al 7 reported that surgical bypass can be performed with morbidity and mortality rates equivalent to those of biliary stenting in selected patients, but with a significantly lower risk of readmission. In a similar study involving 69 patients, Kim et al 8 reported that the patients who underwent surgical palliation had a longer hospital-free survival rate, although they had a longer postoperative hospital stay during the first admission period. From our study and these 2 studies, we can find that surgical bypass can be performed with mortality and morbidity rates similar to those for interventional therapy, but with a longer hospital stay during the first admission period. Rates of late complications and readmissions were higher for patients who underwent palliative biliary stenting than for those who underwent surgical bypass. Obstructive jaundice is present in approximately 90% of patients with pancreatic cancer at the time of diagnosis. 9 Relief of obstructive jaundice should always be a major therapeutic goal, because jaundice is harmful for the liver and other organs. Therefore, the best palliative treatment for obstructive jaundice should be simple, have less trauma, have a low mortality and recurrence rate, produce a better quality of life for patients, and offer a shorter time in the perioperative period of overall survival time. Percutaneous or endoscopic palliation of obstructive jaundice can resolve biliary compression with lower early morbidity compared with open biliary bypass surgery. A study implied that for surgical bypass, the mortality rate is 1% to 5%, and the operative morbidity rate is 20% to 30%. 10 Stent occlusion and the growth of tumor may be the main reason for recurrent jaundice. Patients have to be in the hospital for treatment again and again in their limited survival time. Past study by Castaño et al 11 shows that interventional therapy may be associated with fewer early complications and surgical bypass with fewer late complications. Past study by Kim et al 8 shows that, compared with biliary stent, surgical biliary bypass has higher success rates in relieving obstructive jaundice, and patients have lower rates of recurrent jaundice as well as longer survival time and longer median hospital-free survival. Above all, because of its morbidity and mortality rates similar to those of biliary stent, and its lower rates of late complications and readmissions, surgical bypass can be a better choice for obstructive jaundice. Int Surg 2016;101 61
5 FU THE COMPARISON BETWEEN SURGICAL BYPASS AND INTERVENTIONAL THERAPY At the time of diagnosis, only about 19% of pancreatic cancer patients present with symptoms of gastric and duodenal obstruction, such as nausea and vomiting. About 30% to 50% of all patients will eventually develop malignant gastric outlet obstruction during the course of their disease. 12 Gastrojejunostomy and duodenal stenting are the only choices for these patients. At present, the success rate for placement of duodenal stents is 92% to 100%. The recovery of digestive system is rapid, usually within24 hours in 75% to 93% of cases. 13 Some new studies have shown similar success rate for these two techniques, but with fewer complications, more rapid resumption of alimentation, and shorter hospitalization for endoscopic treatment. 14 However, there are some problems for endoscopic treatment, such as a greater risk of stent migration, and a duodenal stent may impair function of the biliary stent in approximately 20% of cases. 15 Therefore, the patients who undergo endoscopic palliation of a biliary obstruction with gastric outlet obstruction cannot benefit. In our hospital, it is our policy to perform a gastrojejunostomy at the time of biliary bypass. The use of a routine gastrojejunostomy in some studies showed that gastrojejunostomies can be performed with no increase in morbidity and mortality. 16 They also hold the view that a gastrojejunostomy and biliary bypass be undertaken as a single procedure. In the present study, 5 patients in the endoscopic stent group developed gastric outlet obstruction. This also supports the use of prophylactic gastrojejunostomy in patients who underwent operative intervention. Gastrointestinal obstruction also could be treated by large-diameter metal stents by interventional therapy. 17 They are more expensive than conventional stents; metallic stents are purported to have longer patency, but this treatment also has its limitations. Metallic and large-diameter stents may still become occluded by tumor ingrowth or overgrowth. The survival of patients who underwent bypass was longer than that of those who underwent stenting. This may also be influenced by our policy of selecting the patients, and the fact that patients with distant pancreatic metastases were excluded from the study. It is accepted that through avoiding recurrent admissions for jaundice and concurrent cholangitis, surgical bypass may contribute to the increased survival in this group, in spite of these considerations. A potential limitation of this study is that it is a retrospective, single-center study. Therefore, a large-scale prospective validation study is needed to confirm the results. In conclusion, we hold the view that the surgical double bypass is an effective method of palliating patients with locally advanced pancreatic adenocarcinoma. Although stent therapy offers a shorter hospital stay and a lower rate of early complications, it involves a higher rate of late complications and a higher rate of readmission than surgical bypass. Meanwhile, we have shown that surgical bypass can be performed with mortality rates and therapy success equivalent to those of endoscopic stenting, and that it results in a lower rate of late complications. Surgical bypass in this study was associated with prolonged survival compared with palliative stenting. Although the precise reasons for this remain unclear, it should be an important consideration when considering palliation for patients with pancreatic cancer. References 1. Parkin DM, Bray F, Ferlay J, Pisani P. Global cancer statistics, CA Cancer J Clin 2005;55(2): Ouaïssi M, Giger U, Louis G, Sielezneff I, Farges O, Sastre B. Ductal adenocarcinoma of the pancreatic head: a focus on current diagnostic and surgical concepts. World J Gastroenterol 2012;18(24): Kymionis GD, Konstadoulakis MM, Leandros E, Manouras A, Apostolou A, Alexiou D et al. Effect of curative versus palliative surgical treatment for stage III pancreatic cancer patients. J R Coll Surg Edinb 1999;165(6): Taylor MC, McLeod RS, Langer B. Biliary stenting versus bypass surgery for the palliation of malignant distal bile duct obstruction: a meta-analysis. Liver Transpl 2000, 6(3): Assfalg V, Hüser N, Michalski C, Gillen S, Kleeff J, Friess H. Palliative interventional and surgical therapy for unresectable pancreatic cancer. Cancers (Basel) 2011;3(1): Maire F, Sauvanet A. Palliation of biliary and duodenal obstruction inpatients with unresectable pancreatic cancer: endoscopy or surgery? J Visc Surg 2013;150(3 Suppl):S27 S31 7. Scott EN, Garcea G, Doucas H, Steward WP, Dennison AR, Berry DP. Surgical bypass vs. endoscopic stenting for pancreatic ductal adenocarcinoma. HPB (Oxford) 2009;11(2): Kim HO, Hwang SI, Kim H, Shin JH. Quality of survival in patients treated for malignant biliary obstruction caused by unresectable pancreatic head cancer: surgical versus nonsurgical palliation. Hepatobiliary Pancreat Dis Int 2008;7(6): Karapanos K, Nomikos IN. Current surgical aspects of palliative treatment for unresectable pancreatic cancer. Cancers (Basel) 2011;3(1): Int Surg 2016;101
6 THE COMPARISON BETWEEN SURGICAL BYPASS AND INTERVENTIONAL THERAPY FU 10. Lesurtel M, Dehni N, Tiret E, Parc R, Paye F. Palliative surgery for unresectable pancreatic and periampullary cancer: a reappraisal. J Gastrointest Surg 2006;10(2): Castaño R, Lopes TL, Alvarez O, Calvo V, Luz LP, Artifon EL. Nitinol biliary stent versus surgery for palliation of distal malignant biliary obstruction. Surg Endosc 2010;24(9): Lillemoe KD. Palliative therapy for pancreatic cancer. Surg Oncol Clin N Am 1998;7(1): Gaidos JK, Draganov PV. Treatment of malignant gastric outlet obstruction with endoscopically placed self-expandable metal stents. World J Gastroenterol 2009;15(35): Kneuertz PJ, Cunningham SC, Cameron JL. Palliative surgical management of patients with unresectable pancreatic adenocarcinoma: trends and lessons learned from a large, single institution experience. J Gastrointest Surg 2011;15(11): Kim KO, Kim TN, Lee HC. Effectiveness of combined biliary and duodenal stenting in patients with malignant biliary and duodenal obstruction. Scand J Gastroenterol 2012;47(8 9): Lillemoe KD, Cameron JL, Hardacre JM. Is prophylactic gastrojejunostomy indicated for unresectable periampullary cancer? Ann Surg 1999;230(3): ; discussion Maetani I, Ogawa S, Hoshi H. Self-expanding metal stents for palliative treatment of malignant biliary and duodenal stenoses. Endoscopy 1994;26(8): Int Surg 2016;101 63
Peripancreatic carcinoma in most patients may
 Original Article / Pancreas Quality of survival in patients treated for malignant biliary obstruction caused by unresectable pancreatic head cancer: surgical versus non-surgical palliation Hyung Ook Kim,
Original Article / Pancreas Quality of survival in patients treated for malignant biliary obstruction caused by unresectable pancreatic head cancer: surgical versus non-surgical palliation Hyung Ook Kim,
Endoscopic Management of Biliary Strictures. Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center
 Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Endoscopic Management of Biliary Strictures Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Malignant Biliary Strictures Etiologies: Pancreatic
Стенты «Ella-cs» Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts»
 Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Уважаемые коллеги! Высылаем очередной выпуск «Issue of ELLA Abstracts» A. Esophageal Stenting and related topics 1 AMJG 2009; 104:1329 1330 Letters to Editor Early Tracheal Stenosis Post Esophageal Stent
Prophylactic Biliary and Gastrointestinal Bypass for Unresectable Pancreatic Head Cancer: A Retrospective Case Series
 ORIGINAL ARTICLE Prophylactic Biliary and Gastrointestinal Bypass for Unresectable Pancreatic Head Cancer: A Retrospective Case Series Yoshihiro Miyasaka, Yasuhisa Mori, Kohei Nakata, Takao Ohtsuka, Masafumi
ORIGINAL ARTICLE Prophylactic Biliary and Gastrointestinal Bypass for Unresectable Pancreatic Head Cancer: A Retrospective Case Series Yoshihiro Miyasaka, Yasuhisa Mori, Kohei Nakata, Takao Ohtsuka, Masafumi
Double Bypass Surgery vs Endotherapy for Irresectable Pancreatic Cancer
 Double Bypass Surgery vs Endotherapy for Irresectable Pancreatic Cancer Jones AO Omoshoro-Jones General & Hepatopancreatobiliary Surgery Chris Hani-Baragwanath Academic Hospital Faculty of Health Sciences,
Double Bypass Surgery vs Endotherapy for Irresectable Pancreatic Cancer Jones AO Omoshoro-Jones General & Hepatopancreatobiliary Surgery Chris Hani-Baragwanath Academic Hospital Faculty of Health Sciences,
3/28/2012. Periampullary Tumors. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Eric K. Nakakura Ko Olina, HI
 Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
5/17/2013. Pancreatic Cancer. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Case presentation. Differential diagnosis
 Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter?
 Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter? Q. Lina Hu, MD; Jason B. Liu, MD, MS; Ryan J. Ellis, MD, MS; Jessica Y. Liu, MD, MS; Anthony
Preoperative Biliary Drainage Among Patients With Resectable Hepatobiliary Malignancy: Does Technique Matter? Q. Lina Hu, MD; Jason B. Liu, MD, MS; Ryan J. Ellis, MD, MS; Jessica Y. Liu, MD, MS; Anthony
FAST TRACK MANAGEMENT OF PANCREATIC CANCER
 FAST TRACK MANAGEMENT OF PANCREATIC CANCER Jawad Ahmad Consultant Hepatobiliary Surgeon University Hospital Coventry and Warwickshire NHS Trust Part 1. Fast Track Surgery for Pancreatic Cancer Part 2.
FAST TRACK MANAGEMENT OF PANCREATIC CANCER Jawad Ahmad Consultant Hepatobiliary Surgeon University Hospital Coventry and Warwickshire NHS Trust Part 1. Fast Track Surgery for Pancreatic Cancer Part 2.
Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas
 CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic
 Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic cancer Section AA Cancer Centre Referrals In the absence of metastatic
Intended for use by Clinicians and Health Care Providers involved in the Management or Referral of adult patients with pancreatic cancer Section AA Cancer Centre Referrals In the absence of metastatic
Interventional Endoscopy in PB Malignancy
 Interventional Endoscopy in PB Malignancy 7 th Annual Symposium on GI Cancers St Louis, Missouri Sept 20 th, 2008 David L Carr-Locke MA, MB BChir, DRCOG, FRCP, FACG, FASGE Director, Endoscopy Institute,
Interventional Endoscopy in PB Malignancy 7 th Annual Symposium on GI Cancers St Louis, Missouri Sept 20 th, 2008 David L Carr-Locke MA, MB BChir, DRCOG, FRCP, FACG, FASGE Director, Endoscopy Institute,
Expandable stents in digestive pathology present use in an emergency hospital
 ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
ORIGINAL ARTICLES Article received on November30, 2015 and accepted for publishing on December15, 2015. Expandable stents in digestive pathology present use in an emergency hospital Mădălina Ilie 1, Vasile
Surgical bypass vs. endoscopic stenting for pancreatic ductal adenocarcinoma
 DOI:10.1111/j.1477-2574.2008.00015.x HPB ORIGINAL ARTICLE Surgical bypass vs. endoscopic stenting for pancreatic ductal adenocarcinoma Edwina N. Scott, Giuseppe Garcea, Helena Doucas, Will P. Steward,
DOI:10.1111/j.1477-2574.2008.00015.x HPB ORIGINAL ARTICLE Surgical bypass vs. endoscopic stenting for pancreatic ductal adenocarcinoma Edwina N. Scott, Giuseppe Garcea, Helena Doucas, Will P. Steward,
Surgical Management of Pancreatic Cancer
 I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
Colonic stenting anno 2014
 Jeanin E. van Hooft, MD, PhD Gastroenterologist Academic Medical Centre Dept. of Gastroenterology and Hepatology Amsterdam, Netherlands Annual meeting of Colonic Stent Safe Procedure Research Group May
Jeanin E. van Hooft, MD, PhD Gastroenterologist Academic Medical Centre Dept. of Gastroenterology and Hepatology Amsterdam, Netherlands Annual meeting of Colonic Stent Safe Procedure Research Group May
Enteral stenting for gastric outlet obstruction and afferent limb syndrome following pancreaticoduodenectomy
 CASE SERIES Annals of Gastroenterology (2014) 27, 1-5 Enteral stenting for gastric outlet obstruction and afferent limb syndrome following pancreaticoduodenectomy Wilson T. Kwong a, Syed M. Fehmi a, Andrew
CASE SERIES Annals of Gastroenterology (2014) 27, 1-5 Enteral stenting for gastric outlet obstruction and afferent limb syndrome following pancreaticoduodenectomy Wilson T. Kwong a, Syed M. Fehmi a, Andrew
Surgical. Gastroenterology. Evaluating the efficacy of tumor markers CA 19-9 and CEA to predict operability and survival in pancreatic malignancies
 Tropical Gastroenterology 2010;31(3):190 194 Surgical Gastroenterology Evaluating the efficacy of tumor markers and CEA to predict operability and survival in pancreatic malignancies Jay Mehta, Ramkrishna
Tropical Gastroenterology 2010;31(3):190 194 Surgical Gastroenterology Evaluating the efficacy of tumor markers and CEA to predict operability and survival in pancreatic malignancies Jay Mehta, Ramkrishna
Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser
 16 Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser I. Zuber-Jerger F. Kullmann Department of Internal Medicine I, University of Regensburg, Regensburg, Germany Key Words Broken
16 Trimming of a Broken Migrated Biliary Metal Stent with the Nd:YAG Laser I. Zuber-Jerger F. Kullmann Department of Internal Medicine I, University of Regensburg, Regensburg, Germany Key Words Broken
Pylorus Preserving Pancreaticoduodenectomy
 REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
Obstructive Jaundice; A Clinical Study of Malignant Causes.
 DOI: 10.21276/aimdr.2018.4.1.SG6 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Obstructive Jaundice; A Clinical Study of Malignant Causes. Bhuban Mohan Das 1, Sushil Kumar Patnaik 1, Chitta Ranjan
DOI: 10.21276/aimdr.2018.4.1.SG6 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Obstructive Jaundice; A Clinical Study of Malignant Causes. Bhuban Mohan Das 1, Sushil Kumar Patnaik 1, Chitta Ranjan
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
STRICTURES OF THE BILE DUCTS Session No.: 5. Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy
 STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
STRICTURES OF THE BILE DUCTS Session No.: 5 Andrea Tringali Digestive Endoscopy Unit Catholic University Rome - Italy Drainage of biliary strictures. The history before 1980 Surgical bypass Percutaneous
Palliative Laparoscopic Hepatico- and Gastrojejunostomy for Advanced Pancreatic Cancer
 SCIENTIFIC PAPER Palliative Laparoscopic Hepatico- and Gastrojejunostomy for Advanced Pancreatic Cancer Paolo Gentileschi, MD, Subhash Kini, MD, Michel Gagner, MD, FACS, FRCSC ABSTRACT Only 10% to 20%
SCIENTIFIC PAPER Palliative Laparoscopic Hepatico- and Gastrojejunostomy for Advanced Pancreatic Cancer Paolo Gentileschi, MD, Subhash Kini, MD, Michel Gagner, MD, FACS, FRCSC ABSTRACT Only 10% to 20%
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Prevention Of Pancreaticojejunal Fistula After Whipple Procedure
 ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
Topics: Staging and treatment for pancreatic cancer. Staging systems for pancreatic cancer: Differences between the Japanese and UICC systems
 M. J Hep Kobari Bil Pancr and S. Surg Matsuno: (1998) Staging 5:121 127 system for pancreatic cancer 121 Topics: Staging and treatment for pancreatic cancer Staging systems for pancreatic cancer: Differences
M. J Hep Kobari Bil Pancr and S. Surg Matsuno: (1998) Staging 5:121 127 system for pancreatic cancer 121 Topics: Staging and treatment for pancreatic cancer Staging systems for pancreatic cancer: Differences
Outcomes of pancreaticoduodenectomy in patients with metastatic cancer
 Korean J Hepatobiliary Pancreat Surg 2014;18:147-151 http://dx.doi.org/.14701/kjhbps.2014.18.4.147 Original Article Outcomes of pancreaticoduodenectomy in patients with metastatic cancer Joo Hwa Kwak,
Korean J Hepatobiliary Pancreat Surg 2014;18:147-151 http://dx.doi.org/.14701/kjhbps.2014.18.4.147 Original Article Outcomes of pancreaticoduodenectomy in patients with metastatic cancer Joo Hwa Kwak,
Malignant Obstructive Jaundice has dismal
 Proceeding S.Z.P.G.M.L vol: 22(2}: pp. 79-83, 2008. Anatomic Level of Biliary Obstruction and Outcome of Pre-Operative Biliary Stenting in Malignant Obstructive Jaundice -A Shaikh Zayed Hospital Experience
Proceeding S.Z.P.G.M.L vol: 22(2}: pp. 79-83, 2008. Anatomic Level of Biliary Obstruction and Outcome of Pre-Operative Biliary Stenting in Malignant Obstructive Jaundice -A Shaikh Zayed Hospital Experience
Maximize Control. Minimize Migration.
 Maximize Control. Minimize Migration. New SHORT WIRE Delivery System SHORT W IRE BILIARY ENDOPROSTHESIS Improved treatment of biliary strictures The self-expanding, fully covered metal stent is intended
Maximize Control. Minimize Migration. New SHORT WIRE Delivery System SHORT W IRE BILIARY ENDOPROSTHESIS Improved treatment of biliary strictures The self-expanding, fully covered metal stent is intended
Together, putting patients first
 The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
The Role of a Gastroenterologist in the Diagnosis and Management of Pancreatic Cancer Sarah Jowett, Consultant Gastroenterologist Bradford Teaching Hospitals Trust Leeds Regional Study Day, 12 September
Placement of self-expanding metal stents is a safe and effective palliative
 Diagn Interv Radiol 2012; 18:360 364 Turkish Society of Radiology 2012 ABDOMINAL IMAGING ORIGINAL ARTICLE Placement of duodenal stents across the duodenal papilla may predispose to acute pancreatitis:
Diagn Interv Radiol 2012; 18:360 364 Turkish Society of Radiology 2012 ABDOMINAL IMAGING ORIGINAL ARTICLE Placement of duodenal stents across the duodenal papilla may predispose to acute pancreatitis:
Endoscopic Management of the Iatrogenic CBD Injury
 The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy
 Korean J Hepatobiliary Pancreat Surg 2011;15:152-156 Original Article Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy Suzy Kim 1,#, Kyubo
Korean J Hepatobiliary Pancreat Surg 2011;15:152-156 Original Article Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy Suzy Kim 1,#, Kyubo
Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*)
 Hiroshima Journal of Medical Sciences Vol. 33, No. 2, 179,...183, June, 1984 HJM 33-24 179 Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*) Tsuneo TAN AKA, Motomu KODAMA, Rokuro
Hiroshima Journal of Medical Sciences Vol. 33, No. 2, 179,...183, June, 1984 HJM 33-24 179 Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*) Tsuneo TAN AKA, Motomu KODAMA, Rokuro
RESEARCH ARTICLE. Clinical Efficacy of Endoscopic Pancreatic Drainage for Pain Relief with Malignant Pancreatic Duct Obstruction
 DOI:http://dx.doi.org/10.7314/APJCP.2014.15.16.6823 RESEARCH ARTICLE Clinical Efficacy of Endoscopic Pancreatic Drainage for Pain Relief with Malignant Pancreatic Duct Obstruction Fei Gao 1 *, Shuren Ma
DOI:http://dx.doi.org/10.7314/APJCP.2014.15.16.6823 RESEARCH ARTICLE Clinical Efficacy of Endoscopic Pancreatic Drainage for Pain Relief with Malignant Pancreatic Duct Obstruction Fei Gao 1 *, Shuren Ma
ESPEN Congress Brussels Stenting of the esophagus and small bowel. Jean-Marc Dumonceau
 ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
ESPEN Congress Brussels 2005 Stenting of the esophagus and small bowel Jean-Marc Dumonceau Stenting of the esophagus and small bowel Jean-Marc Dumonceau, Div. of Gastroenterology Geneva, Switzerland Indication:
A Guide for Patients Living with a Biliary Metal Stent
 A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
A Guide for Patients Living with a Biliary Metal Stent What is a biliary metal stent? A biliary metal stent (also known as a bile duct stent ) is a flexible metallic tube specially designed to hold your
Factors affecting morbidity and mortality after surgery for obstructive jaundice: a review of 373 patients
 Progress report Gut, 1983, 24, 845-852 Factors affecting morbidity and mortality after surgery for obstructive jaundice: a review of 373 patients A retrospective study of 373 patients undergoing surgery
Progress report Gut, 1983, 24, 845-852 Factors affecting morbidity and mortality after surgery for obstructive jaundice: a review of 373 patients A retrospective study of 373 patients undergoing surgery
Surgical Bypass versus Endoscopic Stenting for Unresectable Head Pancreatic Cancer, Which Palliative Treatment Is Better in Developing
 Open Journal of Gastroenterology, 2017, 7, 154-164 http://www.scirp.org/journal/ojgas ISSN Online: 2163-9469 ISSN Print: 2163-9450 Surgical Bypass versus Endoscopic Stenting for Unresectable Head Pancreatic
Open Journal of Gastroenterology, 2017, 7, 154-164 http://www.scirp.org/journal/ojgas ISSN Online: 2163-9469 ISSN Print: 2163-9450 Surgical Bypass versus Endoscopic Stenting for Unresectable Head Pancreatic
To evaluate 792 patients with malignant biliary obstruction after inner-stents drainage procedure
 To evaluate 792 patients with malignant biliary obstruction after inner-stents drainage procedure Zhu wei, Zhang xiquan, Pan xiaolin, Dong ge, Guo feng. The Cardio-Interventional Center, The 148th PLA
To evaluate 792 patients with malignant biliary obstruction after inner-stents drainage procedure Zhu wei, Zhang xiquan, Pan xiaolin, Dong ge, Guo feng. The Cardio-Interventional Center, The 148th PLA
ORIGINAL ARTICLE. A Preoperative Biliary Stent Is Associated With Increased Complications After Pancreatoduodenectomy
 ORIGINAL ARTICLE A Preoperative Biliary Stent Is Associated With Increased Complications After Pancreatoduodenectomy Martin J. Heslin, MD; Ari D. Brooks, MD; Steven N. Hochwald, MD; Lawrence E. Harrison,
ORIGINAL ARTICLE A Preoperative Biliary Stent Is Associated With Increased Complications After Pancreatoduodenectomy Martin J. Heslin, MD; Ari D. Brooks, MD; Steven N. Hochwald, MD; Lawrence E. Harrison,
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction
 A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
PANCREATIC CANCER GUIDELINES
 PANCREATIC CANCER GUIDELINES North-East London Cancer Network & Barts and the London HPB Centre PROTOCOL FOR MANAGEMENT OF PANCREATIC CANCER (SEPTEMBER 2010) I. PRE-REFERRAL GUIDELINES Screening 1. Offer
PANCREATIC CANCER GUIDELINES North-East London Cancer Network & Barts and the London HPB Centre PROTOCOL FOR MANAGEMENT OF PANCREATIC CANCER (SEPTEMBER 2010) I. PRE-REFERRAL GUIDELINES Screening 1. Offer
Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study
 Original article Annals of Gastroenterology (2013) 26, 346-352 Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study Subhankar Chakraborty
Original article Annals of Gastroenterology (2013) 26, 346-352 Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study Subhankar Chakraborty
Inflammation-based Prognostic Score Predicts Biliary Stent Patency in Patients with Unresectable Malignant Biliary Obstruction
 Inflammation-based Prognostic Score Predicts Biliary Stent Patency in Patients with Unresectable Malignant Biliary Obstruction YOSHIMI IWASAKI, MITSURU ISHIZUKA, MASATO KATO, JUNJI KITA, MITSUGI SHIMODA
Inflammation-based Prognostic Score Predicts Biliary Stent Patency in Patients with Unresectable Malignant Biliary Obstruction YOSHIMI IWASAKI, MITSURU ISHIZUKA, MASATO KATO, JUNJI KITA, MITSUGI SHIMODA
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
Hepatobiliary Malignancies Retrospective Study at Truman Medical Center
 Hepatobiliary Malignancies 206-207 Retrospective Study at Truman Medical Center Brandon Weckbaugh MD, Prarthana Patel & Sheshadri Madhusudhana MD Introduction: Hepatobiliary malignancies are cancers which
Hepatobiliary Malignancies 206-207 Retrospective Study at Truman Medical Center Brandon Weckbaugh MD, Prarthana Patel & Sheshadri Madhusudhana MD Introduction: Hepatobiliary malignancies are cancers which
Management of Cholangiocarcinoma. Roseanna Lee, MD PGY-5 Kings County Hospital
 Management of Cholangiocarcinoma Roseanna Lee, MD PGY-5 Kings County Hospital Case Presentation 37 year old male from Yemen presented with 2 week history of epigastric pain, anorexia, jaundice and puritis.
Management of Cholangiocarcinoma Roseanna Lee, MD PGY-5 Kings County Hospital Case Presentation 37 year old male from Yemen presented with 2 week history of epigastric pain, anorexia, jaundice and puritis.
EGIS BILIARY STENT. 1. Features & Benefits 2. Ordering information 3. References
 EGIS BILIARY STENT 1. Features & Benefits 2. Ordering information 3. References 1. Features & Benefits (1) Features Superior flexibility & conformability 4 Types Single bare, Single cover, Double bare,
EGIS BILIARY STENT 1. Features & Benefits 2. Ordering information 3. References 1. Features & Benefits (1) Features Superior flexibility & conformability 4 Types Single bare, Single cover, Double bare,
Y A L E S C H O O L O F M E D I C I N E. This is a CME accredited activity. The presenters and there are no conflicts of interest.
 This is a CME accredited activity. The presenters and there are no conflicts of interest. Pain in Pancreatic Cancer More than 50% of patients with pancreatic cancer suffer from abdominal and back pain
This is a CME accredited activity. The presenters and there are no conflicts of interest. Pain in Pancreatic Cancer More than 50% of patients with pancreatic cancer suffer from abdominal and back pain
Surgical Treatment for Carcinoma of the Ampulla of Vater and Residual Pancreatic Function before and after Pancreaticoduodenectomy*)
 Hiroshima Journal of Medical Sciences Vol. 32, No. 4, 455,-...,460, December, 1983 HIJM 32-68 455 Surgical Treatment for Carcinoma of the Ampulla of Vater and Residual Pancreatic Function before and after
Hiroshima Journal of Medical Sciences Vol. 32, No. 4, 455,-...,460, December, 1983 HIJM 32-68 455 Surgical Treatment for Carcinoma of the Ampulla of Vater and Residual Pancreatic Function before and after
Jennifer Hsieh 1, Amar Thosani 1, Matthew Grunwald 2, Satish Nagula 1, Juan Carlos Bucobo 1, Jonathan M. Buscaglia 1. Introduction
 How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
How We Do It Serial insertion of bilateral uncovered metal stents for malignant hilar obstruction using an 8 Fr biliary system: a case series of 17 consecutive patients Jennifer Hsieh 1, Amar Thosani 1,
Afferent Loop Syndrome: Treatment by Means of the Placement of Dual Stents
 Vascular and Interventional Radiology Original Research Han et al. Use of Dual Stents for Treatment of Afferent Loop Syndrome Vascular and Interventional Radiology Original Research Kichang Han 1 Ho-Young
Vascular and Interventional Radiology Original Research Han et al. Use of Dual Stents for Treatment of Afferent Loop Syndrome Vascular and Interventional Radiology Original Research Kichang Han 1 Ho-Young
Guidelines for the management of patients with pancreatic cancer periampullary and ampullary carcinomas
 v1 GUIDELINES Guidelines for the management of patients with pancreatic cancer periampullary and ampullary carcinomas Pancreatic Section of the British Society of Gastroenterology, Pancreatic Society of
v1 GUIDELINES Guidelines for the management of patients with pancreatic cancer periampullary and ampullary carcinomas Pancreatic Section of the British Society of Gastroenterology, Pancreatic Society of
Neoadjuvant radiotherapy for pancreatic cancer: rationale and outcomes
 Review Article Neoadjuvant radiotherapy for pancreatic cancer: rationale and outcomes Rohan Deraniyagala, Emily D. Tanzler The University of Florida College of Medicine Department of Radiation Oncology,
Review Article Neoadjuvant radiotherapy for pancreatic cancer: rationale and outcomes Rohan Deraniyagala, Emily D. Tanzler The University of Florida College of Medicine Department of Radiation Oncology,
Clinical Study Small Bowel Tumors: Clinical Presentation, Prognosis, and Outcomein33PatientsinaTertiaryCareCenter
 Hindawi Publishing Corporation Journal of Oncology Volume 2008, Article ID 212067, 5 pages doi:10.1155/2008/212067 Clinical Study Small Bowel Tumors: Clinical Presentation, Prognosis, and Outcomein33PatientsinaTertiaryCareCenter
Hindawi Publishing Corporation Journal of Oncology Volume 2008, Article ID 212067, 5 pages doi:10.1155/2008/212067 Clinical Study Small Bowel Tumors: Clinical Presentation, Prognosis, and Outcomein33PatientsinaTertiaryCareCenter
Early Infectious Complications of Percutaneous Metallic Stent Insertion for Malignant Biliary Obstruction
 Vascular and Interventional Radiology Original Research Sol et al. Stent Insertion in Biliary Obstruction Vascular and Interventional Radiology Original Research Yu Li Sol 1 Chang Won Kim 1 Ung Bae Jeon
Vascular and Interventional Radiology Original Research Sol et al. Stent Insertion in Biliary Obstruction Vascular and Interventional Radiology Original Research Yu Li Sol 1 Chang Won Kim 1 Ung Bae Jeon
Cholangiocarcinoma. GI Practice Guideline. Michael Sanatani, MD, FRCPC (Medical Oncologist) Barbara Fisher, MD, FRCPC (Radiation Oncologist)
 Cholangiocarcinoma GI Practice Guideline Michael Sanatani, MD, FRCPC (Medical Oncologist) Barbara Fisher, MD, FRCPC (Radiation Oncologist) Approval Date: October 2006 This guideline is a statement of consensus
Cholangiocarcinoma GI Practice Guideline Michael Sanatani, MD, FRCPC (Medical Oncologist) Barbara Fisher, MD, FRCPC (Radiation Oncologist) Approval Date: October 2006 This guideline is a statement of consensus
Chronic Pancreatitis
 Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
Gastro Foundation Fellows Weekend 2017 Chronic Pancreatitis Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Aetiology in SA Alcohol (up to 80%) Idiopathic Tropical Obstruction Autoimmune
WallFlex Stents Technique Spotlights
 WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
Surgery for hilar cholangiocirconoma
 Department of Surgery University Hospital RWTH Aachen Surgery for hilar cholangiocirconoma Ulf Peter Neumann Agenda Operating on the most complex tumor in HBP Surgery Preoperative management Does the patient
Department of Surgery University Hospital RWTH Aachen Surgery for hilar cholangiocirconoma Ulf Peter Neumann Agenda Operating on the most complex tumor in HBP Surgery Preoperative management Does the patient
Outcomes associated with robotic approach to pancreatic resections
 Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic Duct Obstruction: Is Endoscopic Sphincterotomy Needed?
 Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Gastroenterology Research and Practice Volume 2013, Article ID 375613, 6 pages http://dx.doi.org/10.1155/2013/375613 Clinical Study Covered Metal Stenting for Malignant Lower Biliary Stricture with Pancreatic
Tumor Overgrowth After Expandable Metallic Stent Placement: Experience in 583 Patients With Malignant Gastroduodenal Obstruction
 Vascular and Interventional Radiology Original Research Jang et al. Stent Placement for Malignant Gastroduodenal Obstruction Vascular and Interventional Radiology Original Research Jong Keon Jang 1 Ho-Young
Vascular and Interventional Radiology Original Research Jang et al. Stent Placement for Malignant Gastroduodenal Obstruction Vascular and Interventional Radiology Original Research Jong Keon Jang 1 Ho-Young
Palliative Treatment of Obstructive Jaundice in Patients with Carcinoma of the Pancreatic Head or Distal Biliary Tree. Endoscopic Stent Placement vs
 ORIGINAL ARTICLE Palliative Treatment of Obstructive Jaundice in Patients with Carcinoma of the Pancreatic Head or Distal Biliary Tree. Endoscopic Placement vs. Hepaticojejunostomy Marius Distler 1, Stephan
ORIGINAL ARTICLE Palliative Treatment of Obstructive Jaundice in Patients with Carcinoma of the Pancreatic Head or Distal Biliary Tree. Endoscopic Placement vs. Hepaticojejunostomy Marius Distler 1, Stephan
Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated with stent failure
 Kato et al. BMC Surgery (2017) 17:11 DOI 10.1186/s12893-017-0209-y RESEARCH ARTICLE Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated
Kato et al. BMC Surgery (2017) 17:11 DOI 10.1186/s12893-017-0209-y RESEARCH ARTICLE Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated
Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment
 Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment Andrew W. Bowman, MD PhD Assistant Professor of Radiology Mayo Clinic Florida SCBT-MR Annual Meeting Nashville,
Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment Andrew W. Bowman, MD PhD Assistant Professor of Radiology Mayo Clinic Florida SCBT-MR Annual Meeting Nashville,
Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W.
 UvA-DARE (Digital Academic Repository) Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W. Link to publication Citation for published version (APA): van den Berg, M. W.
UvA-DARE (Digital Academic Repository) Endoscopic stent placement throughout the gastrointestinal tract van den Berg, M.W. Link to publication Citation for published version (APA): van den Berg, M. W.
What to expect with major vascular reconstruction during Whipple procedures: a single institution experience and literature review
 Original Article What to expect with major vascular reconstruction during Whipple procedures: a single institution experience and literature review Matthew S. Jorgensen 1, Tariq Almerey 2, Houssam Farres
Original Article What to expect with major vascular reconstruction during Whipple procedures: a single institution experience and literature review Matthew S. Jorgensen 1, Tariq Almerey 2, Houssam Farres
WallFlex Biliary RX Fully Covered Stent System Prescriptive Information
 Caution/Rx Only: Federal Law (USA) restricts this device to sale by or on the order of a physician. Warning Contents supplied STERILE using an ethylene oxide (EO) process. Do not use if sterile barrier
Caution/Rx Only: Federal Law (USA) restricts this device to sale by or on the order of a physician. Warning Contents supplied STERILE using an ethylene oxide (EO) process. Do not use if sterile barrier
Prognostic factors for survival of patients with ampullary carcinoma after local resection. Abstract
 UPPER GI ANZJSurg.com Prognostic factors for survival of patients with ampullary carcinoma after local resection Xiangqian Zhao, Jiahong Dong, Xiaoqiang Huang, Wenzhi Zhang and Kai Jiang Hospital and Institute
UPPER GI ANZJSurg.com Prognostic factors for survival of patients with ampullary carcinoma after local resection Xiangqian Zhao, Jiahong Dong, Xiaoqiang Huang, Wenzhi Zhang and Kai Jiang Hospital and Institute
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Douglas G. Adler MD. ACG Regional Postgraduate Course - Nashville, TN Copyright 2013 American College of Gastroenterology
 Enteral Stents 2013: State of the Art Douglas G. Adler MD Associate Professor of Medicine Director of Therapeutic Endoscopy University of Utah School of Medicine Huntsman Cancer Center Esophageal Stents
Enteral Stents 2013: State of the Art Douglas G. Adler MD Associate Professor of Medicine Director of Therapeutic Endoscopy University of Utah School of Medicine Huntsman Cancer Center Esophageal Stents
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Metal versus plastic stents for malignant biliary obstruction: An update meta-analysis
 Clinics and Research in Hepatology and Gastroenterology (2013) xxx, xxx xxx Available online at www.sciencedirect.com ORIGINAL ARTICLE Metal versus plastic stents for malignant biliary obstruction: An
Clinics and Research in Hepatology and Gastroenterology (2013) xxx, xxx xxx Available online at www.sciencedirect.com ORIGINAL ARTICLE Metal versus plastic stents for malignant biliary obstruction: An
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Minimally Invasive Esophagectomy- Valuable. Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006
 Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Percutaneous biliary drainage catheter insertion in patients with extensive hepatic metastatic tumor burden
 Original Article Percutaneous biliary drainage catheter insertion in patients with extensive hepatic metastatic tumor burden Eun L. Langman 1, Paul V. Suhocki 1, Herbert I. Hurwitz 2, Michael A. Morse
Original Article Percutaneous biliary drainage catheter insertion in patients with extensive hepatic metastatic tumor burden Eun L. Langman 1, Paul V. Suhocki 1, Herbert I. Hurwitz 2, Michael A. Morse
Evaluation of a 12-mm diameter covered self-expandable end bare metal stent for malignant biliary obstruction
 Evaluation of a 12-mm diameter covered self-expandable end bare metal stent for malignant biliary obstruction Authors Kazunori Nakaoka, Senju Hashimoto, Naoto Kawabe, Takuji Nakano, Toshiki Kan, Masashi
Evaluation of a 12-mm diameter covered self-expandable end bare metal stent for malignant biliary obstruction Authors Kazunori Nakaoka, Senju Hashimoto, Naoto Kawabe, Takuji Nakano, Toshiki Kan, Masashi
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Is a Metallic Stent Useful for Non Resectable Esophageal Cancer?
 Original Article Is a Metallic Stent Useful for Non Resectable Esophageal Cancer? Shinsuke Wada, MD, 1 Tsuyoshi Noguchi, MD, 1 Shinsuke Takeno, MD, 1 Hatsuo Moriyama, MD, 1 Tsuyoshi Hashimoto, MD, 1 Yuzo
Original Article Is a Metallic Stent Useful for Non Resectable Esophageal Cancer? Shinsuke Wada, MD, 1 Tsuyoshi Noguchi, MD, 1 Shinsuke Takeno, MD, 1 Hatsuo Moriyama, MD, 1 Tsuyoshi Hashimoto, MD, 1 Yuzo
Bilateral stenting methods for hilar biliary obstructions
 RAPID COMMUNICATION Bilateral stenting methods for hilar biliary obstructions Wandong Hong, I Shanxi Chen, II Qihuai Zhu, I Huichun Chen, III Jingye Pan, IV Qingke Huang I* I First Affiliated Hospital
RAPID COMMUNICATION Bilateral stenting methods for hilar biliary obstructions Wandong Hong, I Shanxi Chen, II Qihuai Zhu, I Huichun Chen, III Jingye Pan, IV Qingke Huang I* I First Affiliated Hospital
Endoscopic biliary self-expandable metallic stent in malignant biliary obstruction with or without sphincterotomy: systematic review and meta-analysis
 Review Endoscopic biliary self-expandable metallic in malignant biliary obstruction with or without sphincterotomy: systematic review and meta-analysis Authors Benedetto Mangiavillano 1, 2, Amedeo Montale
Review Endoscopic biliary self-expandable metallic in malignant biliary obstruction with or without sphincterotomy: systematic review and meta-analysis Authors Benedetto Mangiavillano 1, 2, Amedeo Montale
Intra-arterial chemotherapy for patients with
 Annals of the Royal College of Surgeons of England (980) vol 62 ASPECTS OF TREATMENT* ntra-arterial chemotherapy for patients with inoperable carcinoma of the pancreas Lord Smith of Marlow KBE MS PPRCS
Annals of the Royal College of Surgeons of England (980) vol 62 ASPECTS OF TREATMENT* ntra-arterial chemotherapy for patients with inoperable carcinoma of the pancreas Lord Smith of Marlow KBE MS PPRCS
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical analysis of 29 cases of nasal mucosal malignant melanoma
 1166 Clinical analysis of 29 cases of nasal mucosal malignant melanoma HUANXIN YU and GANG LIU Department of Otorhinolaryngology Head and Neck Surgery, Tianjin Huanhu Hospital, Tianjin 300060, P.R. China
1166 Clinical analysis of 29 cases of nasal mucosal malignant melanoma HUANXIN YU and GANG LIU Department of Otorhinolaryngology Head and Neck Surgery, Tianjin Huanhu Hospital, Tianjin 300060, P.R. China
Review Article Fully Covered Self-Expandable Metal Stents for Treatment of Both Benign and Malignant Biliary Disorders
 Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
Hindawi Publishing Corporation Diagnostic and Therapeutic Endoscopy Volume 2012, Article ID 498617, 5 pages doi:10.1155/2012/498617 Review Article Fully Covered Self-Expandable Metal Stents for Treatment
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Published: Address correspondence to Vidal-Jove Joan:
 Oncothermia Journal 7:111-114 (2013) Complete responses after hyperthermic ablation by ultrasound guided high intensity focused ultrasound (USgHIFU) plus cystemic chemotherapy (SC) for locally advanced
Oncothermia Journal 7:111-114 (2013) Complete responses after hyperthermic ablation by ultrasound guided high intensity focused ultrasound (USgHIFU) plus cystemic chemotherapy (SC) for locally advanced
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction
 Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
Navigating the Biliary Tract with CT & MR: An Imaging Approach to Bile Duct Obstruction Ann S. Fulcher, MD Medical College of Virginia Virginia Commonwealth University Richmond, Virginia Objectives To
Long term survival study of de-novo metastatic breast cancers with or without primary tumor resection
 Long term survival study of de-novo metastatic breast cancers with or without primary tumor resection Dr. Michael Co Division of Breast Surgery Queen Mary Hospital The University of Hong Kong Conflicts
Long term survival study of de-novo metastatic breast cancers with or without primary tumor resection Dr. Michael Co Division of Breast Surgery Queen Mary Hospital The University of Hong Kong Conflicts
Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study
 Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Study title Subtotal cholecystectomy for complicated acute cholecystitis: a multicenter prospective observational study Primary Investigator: Kazuhide Matsushima, MD Co-Primary investigator: Zachary Warriner,
Clinical Study Pancreatic Resections for Advanced M1-Pancreatic Carcinoma: The Value of Synchronous Metastasectomy
 HPB Surgery Volume 2010, Article ID 579672, 6 pages doi:10.1155/2010/579672 Clinical Study Pancreatic Resections for Advanced M1-Pancreatic Carcinoma: The Value of Synchronous Metastasectomy S. K. Seelig,
HPB Surgery Volume 2010, Article ID 579672, 6 pages doi:10.1155/2010/579672 Clinical Study Pancreatic Resections for Advanced M1-Pancreatic Carcinoma: The Value of Synchronous Metastasectomy S. K. Seelig,
Author s response to reviews
 Author s response to reviews Title: Neoadjuvant chemotherapy versus surgery first for resectable pancreatic cancer (Norwegian Pancreatic Cancer Trial - 1 (NorPACT)) - Study protocol for a national, multicentre
Author s response to reviews Title: Neoadjuvant chemotherapy versus surgery first for resectable pancreatic cancer (Norwegian Pancreatic Cancer Trial - 1 (NorPACT)) - Study protocol for a national, multicentre
Pancreaticoduodenectomy the anatomy and the surgical approaches
 Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreatic cancer remains one of the most formidable
 ORIGINAL ARTICLES Long-term Results of Intraoperative Electron Beam Irradiation () for Patients With Unresectable Pancreatic Cancer Christopher G. Willett, MD,* Carlos Fernandez Del Castillo, MD, Helen
ORIGINAL ARTICLES Long-term Results of Intraoperative Electron Beam Irradiation () for Patients With Unresectable Pancreatic Cancer Christopher G. Willett, MD,* Carlos Fernandez Del Castillo, MD, Helen
Neoadjuvant therapy prior to surgical resection for previously explored pancreatic cancer patients is associated with improved survival
 Original Article Neoadjuvant therapy prior to surgical resection for previously explored pancreatic cancer patients is associated with improved survival Fengchun Lu 1,2, Kevin C. Soares 1, Jin He 1, Ammar
Original Article Neoadjuvant therapy prior to surgical resection for previously explored pancreatic cancer patients is associated with improved survival Fengchun Lu 1,2, Kevin C. Soares 1, Jin He 1, Ammar
Afternoon Session Cases
 Afternoon Session Cases Case 1 19 year old woman Presented with abdominal pain to community hospital Mild incr WBC a14, 000, Hg normal, lipase 100 (normal to 75) US 5.2 x 3.7 x 4 cm mass in porta hepatis
Afternoon Session Cases Case 1 19 year old woman Presented with abdominal pain to community hospital Mild incr WBC a14, 000, Hg normal, lipase 100 (normal to 75) US 5.2 x 3.7 x 4 cm mass in porta hepatis
