D uodenal polyps in familial adenomatous polyposis
|
|
|
- Kelly Simpson
- 5 years ago
- Views:
Transcription
1 381 COLON CANCER Duodenal adenomatosis in familial adenomatous polyposis SBülow, J Björk, I J Christensen, O Fausa, H Järvinen, F Moesgaard, H F A Vasen, the DAF Study Group... See end of article for authors affiliations... Correspondence to: Dr S Bülow, The Danish Polyposis Register, Hvidovre University Hospital, DK 2650 Hvidovre, Denmark; sbulow@dadlnet.dk Accepted 30 September Gut 2004;53: doi: /gut Background: The prevalence of duodenal carcinoma is much higher in familial adenomatous polyposis (FAP) than in the background population, and duodenal adenomatosis is found in most polyposis patients. Aims: To describe the long term natural history of duodenal adenomatosis in FAP and evaluate if cancer prophylactic surveillance of the duodenum is indicated. Methods: A prospective five nation study was carried out in the Nordic countries and the Netherlands. Patients: A total of 368 patients were examined by gastroduodenoscopy at two year intervals during the period Results: At the first endoscopy, 238 (65%) patients had duodenal adenomas at a median age of 38 years. Median follow up was 7.6 years. The cumulative incidence of adenomatosis at age 70 years was 90% (95% confidence interval (CI) %), and of Spigelman stage IV 52% (95% CI 28 76%). The probability of an advanced Spigelman score increased during the study period (p,0.0001) due to an increasing number and size of adenomas. Two patients had asymptomatic duodenal carcinoma at their first endoscopy while four developed carcinoma during the study at a median age of 52 years (range 26 58). The cumulative incidence rate of cancer was 4.5% at age 57 years (95% CI %) and the risk was higher in patients with Spigelman stage IV at their first endoscopy than in those with stages 0 III (p,0.01). Conclusions: The natural course of duodenal adenomatosis has now been described in detail. The high incidence and increasing severity of duodenal adenomatosis with age justifies prophylactic examination, and a programme is presented for upper gastrointestinal endoscopic surveillance. D uodenal polyps in familial adenomatous polyposis (FAP) were first described almost a century ago; 1 duodenal carcinoma was reported in and the first series of upper gastrointestinal endoscopic screening was published in The increasing use of prophylactic examination and early colectomy has caused a substantial reduction in the incidence of colorectal cancer which has led to improvement in prognosis. 4 Over the last decades, the pattern of causes of death has changed, and today duodenal cancer is one of the major causes of death. 5 Duodenal adenomatosis is found in the majority of polyposis patients and may lead to carcinoma development. In 1989, Spigelman et al published an endoscopic and histological classification system for evaluation of the severity of duodenal adenomatosis, 6 and the Spigelman classification has become the gold standard in several studies of duodenal adenomatosis Regular upper gastrointestinal endoscopic surveillance of polyposis patients has been recommended 17 but detailed knowledge of the course and development of duodenal adenomatosis is a necessary condition to justify such a recommendation. The aims of the present Nordic-Dutch prospective multicentre study were to describe the long term natural history of duodenal adenomatosis, to evaluate if cancer prophylactic endoscopic surveillance of the duodenum is indicated, and possibly to identify subgroups at high risk of carcinoma development. PATIENTS AND METHODS In 1990, patients with histologically verified FAP, aged 20 years or more, in Denmark, Finland, Norway, Sweden, and the Netherlands were invited to undergo regular upper gastrointestinal endoscopy according to a set protocol. Exclusion criteria were previous duodenal or periampullary carcinoma. The study was coordinated from the five national polyposis registries, and patients were examined as outpatients in regional hospitals at intervals of two years during the study period Sedation included diazepam or midazolam, and butylscopolamine was added for duodenal examination. A standard forward viewing endoscope was used. Gastric polyps were biopsied and removed with the exception of typical fundic gland polyposis. The size of the duodenal polyps was measured by an open biopsy forceps, and the Spigelman classification 6 was adopted for evaluation of endoscopic and histological staging. In patients without visible polyps, at least six random biopsies were taken from the mucosal folds of the second and upper third part of the duodenum, including the papilla region. One pathologist from each country evaluated the biopsies. The study was organised by a project leader, a study group, and regional contact persons in the examining departments (see appendix). The data were entered into a central database in the Danish Polyposis Register, and the five national ethics committees approved the study. 10 The Kaplan-Meier method was used to calculate cumulative rates of the endpoints of adenomatosis and adenomatosis Spigelman stage IV as a function of time from entry into the study. The Cox proportional hazards model was used to test for associations between the two endpoints and other covariates. Evaluation of the development of duodenal adenomatosis with time was performed using a generalised linear model assuming a multinomial distribution with cumulative logits as the link function and taking repeated measures into account. Estimates were obtained by generalised estimating equations. 18 For these calculations, endoscopies were classified as entry, 2, 4, 6, or 8 years, allocating each... Abbreviations: FAP, familial adenomatous polyposis; HR, hazard ratio
2 382 Bülow, Björk, Christensen, et al endoscopy to the nearest time point. Statistical calculations were done using SAS (v 8.2; SAS Institute, Cary, North Carolina, USA). A p value of less than 5% was considered significant. RESULTS First endoscopy A total of 368 patients (182 males and 186 females) entered the study in Denmark (n = 108), Finland (n = 65), Holland (n = 35), Norway (n = 59), and Sweden (n = 101). Median ages at diagnosis of FAP, at colectomy, and at the first upper gastrointestinal endoscopy in the study were 25 years (range 6 67), 26 years (range 9 67), and 37 years (range 20 81), respectively. Seven patients had various types of local excision of duodenal polyps before entering the study. Fundic gland polyps were seen in 198 (54%), gastric adenomas in 37 (10%), and gastric hyperplastic polyps in nine (2%) patients. Duodenal polyps were seen in 228 patients, in whom histological examination showed adenomas in 209 and normal mucosa in 19. Random biopsies showed adenomatous tissue in 28 patients without visible polyps at endoscopy. In total, 238 patients (65%) had duodenal adenomas, of whom 12% were invisible. Median age at diagnosis of duodenal adenomas was 38 years (range 20 81). The Spigelman classification in 366 classifiable patients was stage 0, 123 (34%); stage I, 55 (15%); stage II, 97 (27%); stage III, 64 (17%); and stage IV, 27 (7%) (fig 1). Two patients (0.5%) had a duodenal carcinoma. Development of adenomatosis The median number of endoscopies was 4 (range 1 5; 131 with five endoscopies, 57 with four, 52 with three, 45 with two, and 83 with one), and the median follow up period was 7.6 years (range ). The distribution according to Spigelman stage at the follow up endoscopies is shown in fig 1. During the observation period, 12 patients had open duodenotomy with polyp excision. The incidence of adenomas at entry was 65% (238 patients) and among the remaining 90 patients with follow up, 65% (95% confidence interval (CI) 53 77%) had demonstrated adenoma development within eight years from entry. Median age of patients entering the study with adenomas was 38 years (range 18 No of patients (%) Spigelman stage 4 6 Time after entry (years) Figure 1 Spigelman classification in classifiable patients in relation to time after entry into the study ) whereas median age was 35 years (range 20 75) for those without adenomas and with follow up. The cumulative incidence of adenomatosis development in 128 patients without adenomas at study entry was 50% after six years (95% confidence interval (CI) 5 8) and 68% after eight years (95% CI 56 80%) (fig 2). Including age, sex, and time from diagnosis to entry (dichotomised at 15 years) in a Cox proportional hazards model, no significant effect of the covariates was demonstrated (p = 0.51, p = 0.98, and p = 0.53, respectively). The cumulative incidence by age in this group was 73% at age 70 years (95% CI 57 89). Combining the latter with the age distribution in 238 patients with adenomas at entry, resulted in a 90% incidence of adenomatosis (95% CI %) at age 70 years. The incidence of Spigelman stage IV adenomatosis at entry was 7% (27/366, two missing). Among 339 patients with Spigelman stage,iv at entry, the cumulative incidence of stage IV was 15% (95% CI 10 20%) (fig 3) at eight years after entry. Including sex, age, time from diagnosis to entry, and Spigelman stage at entry (scored by its value: 0, 1, 2, 3) in a Cox proportional hazards model, age (p = 0.01; hazard ratio (HR) = 1.04; 95% CI ), time from diagnosis to entry (p = 0.04; HR = 2.1; 95% CI ), and Spigelman stage (p = ; HR = 2.0; 95% CI ) were significant. The cumulative incidence of stage IV among 257 patients with Spigelman stage,iv at entry and with follow up was 52% at age 70 years (95% CI 28 76%). Evaluation of changes in the components of the Spigelman classification was based on 283/285 patients with at least two endoscopies; two patients without adenomas at the first endoscopy were excluded. The repeated measures model included endoscopy number, adenoma at entry, time from diagnosis to entry, age, and sex, and demonstrated a significant increase in Spigelman stage over time (p,0.0001). Significant covariates were adenoma at entry (p,0.0001) and time from diagnosis (p,0.0001) but not age (p = 0.60) or sex (p = 0.29). The estimated cumulative probabilities are shown in table 1. A similar analysis of histological type suggested no significant changes over time (p = 0.7). Dysplasia was also not significant (p = 0.07). Size showed a significant increase over time (p,0.0001) adjusted for time from diagnosis (p = 0.001) and adenoma at entry (p,0.0001). Similarly, the number of polyps indicated a significant increase (p,0.0001), with both time from diagnosis as well as adenoma at entry being significant (p,0.0001). Duodenal carcinoma During the follow up period, four patients (1.1%) developed a duodenal carcinoma, and the total incidence of carcinoma was 6/368 (1.6%; 95% CI %). Median age at diagnosis Figure 2 Cumulative incidence Time to adenoma (months) At risk Cumulative incidence of adenomatosis development.
3 Duodenal adenomatosis in FAP 383 Figure 3 Cumulative incidence Time to Spigelman stage IV (months) At risk Cumulative incidence of Spigelman stage IV. of duodenal cancer in the six patients was 52 years (range 26 58) and the cumulative incidence rate was 4.5% at age 57 years (95% CI %). Spigelman stages at the previous endoscopies in the four patients who developed duodenal cancer were II II, IV III IV III, III III II IV, and IV IV IV IV, respectively. Among 27 patients with Spigelman stage IV at the first endoscopy, two (7%) later developed a carcinoma compared with 2/339 (0.7%) with Spigelman stages 0 III (p,0.01). The cumulative crude five year survival after duodenal cancer was 44% (95% CL 22 67). DISCUSSION The present study is the largest series of FAP patients followed prospectively with regular upper endoscopy. The advantages of the study were that it was based on five national polyposis registers with a high completeness of registration, it included a 10 year study period, and random biopsies were taken in patients without visible duodenal polyps. The disadvantages were the use of forward viewing endoscopy and decreasing patient compliance throughout the study period. The former may have led to underestimation of the stage of adenomatosis whereas decreasing patient compliance may have had the opposite effect as it cannot be ruled out that more patients with advanced duodenal adenomatosis continued to participate in the study. Findings at the first endoscopy demonstrated that the prevalence of duodenal adenomatosis was 65%. This is similar to values of 58 74% in major series in the literature, which are comparable concerning age at diagnosis of FAP and at the first endoscopy (table 2). It is interesting that 12% of adenomas were diagnosed only histologically and this underlines the importance of multiple random biopsies in patients without visible polyps. It has been stated that side viewing endoscopy is the ideal procedure for evaluation of duodenal adenomatosis 9 but as this procedure is only used routinely by endoscopists performing ERCP, we considered the standard use of side viewing endoscopy to be unrealistic in this multicentre study. In our opinion, future studies of the natural course or treatment of duodenal adenomatosis should include a combination of forward and side viewing endoscopy as well as random biopsies. We found the same proportion of adenomatosis Spigelman stage IV as in the Swedish study, 14 in contrast with the Finnish result of only 2%. 12 Median age of patients in the latter study was four years younger, and an updated analysis showed 3.6% Spigelman stage IV, thus indicating that the difference is probably not real (H Järvinen, personal communication). The follow up examinations confirmed the results of the Nordic studies and showed that the lifetime risk of duodenal adenomatosis is approaching 100% We found a lifetime risk of Spigelman stage IV of 52%, with a broad confidence Table 1 Estimated cumulative probabilities (probability that the stage is less than or equal to 0, 1, 2, or 3) for Spigelman stages for patients entering with and without adenomas, and with time from diagnosis to entry dichotomised at 15 years (familial adenomatous polyposis (FAP) time) No of endoscopies Spigelman stage +Adenoma FAP time,15 y +Adenoma FAP time.15 y Table 2 Proposed programme for surveillance and treatment of duodenal adenomatosis Spigelman stage 0 Spigelman stage I Spigelman stage II Spigelman stage III Spigelman stage IV 2Adenoma FAP time,15 y Endoscopy* at intervals of 5 y EndoscopyÀ at intervals of 5 y EndoscopyÀ at intervals of 3 y EndoscopyÀ at intervals of 1 2 y Endoscopic ultrasonography Consider pancreas sparing or pylorus sparing duodenectomy *Including multiple random biopsies from mucosal folds in patients without visible polyps. ÀIncluding multiple biopsies from polyps. 2Adenoma FAP time.15 y
4 384 Bülow, Björk, Christensen, et al Table 3 Patient series, including results of upper gastrointestinal endoscopy follow up Cumul. incidence (%) of duodenal cancer at 75 y Duodenal cancer (%) Cumul. incidence (%) of Spigelman stage IV at y Findings at first endoscopy Cumul. incidence (%) of duodenal adenomas at y Spigelman stage IV (%) Duodenal adenomas (%) Age at endoscopy Age at diagnosis of FAP Mean No of endoscopies Endoscopy type* No of patients Author (ref No) Year Church SV+FV Nugent SV Debinski Heiskanen SV/FV À 30À 4À Björk FV Kadmon FV Groves SV Present study 368 FV ` *FV, forward viewing endoscope; SV, side viewing endoscope. ÀAt age 80 years. `At age 57 years. interval, compared with 30% in the Finnish study 12 and 20% in the Swedish study. 14 The explanation for these discrepancies could be statistical uncertainty (at age 60 years the cumulated incidence was 22%), different biopsy policies, and different observation periods. In the Swedish study, only the papilla region was included, and the Spigelman classification was calculated without considering the remaining duodenum. In the Finnish study, the observation period was three years shorter than in our present study. Detailed analysis of changes in Spigelman classification during the study period demonstrated an increasing number of polyps and size of polyps but no statistically significant change in histological type or degree of dysplasia. This resulted in an overall worsening of the Spigelman score and stage with time. The results in the literature concerning a possible change in Spigelman stage with time are confusing, as some studies report little or no change while others have shown 50 75% progression Our present results are based on a high number of patients followed regularly for 10 years, with an improved statistical method of evaluation. Twelve patients had duodenal polyp excision, and periodic sulindac treatment may have been used in a small number of patients for rectal adenomatosis or desmoid tumours. The influence of this on the development or progression of duodenal adenomatosis is however considered minimal. 14 Therefore, we believe that our results are valid and indicate that the Spigelman stage will progress with time and patient age, as recently indicated. 15 The unchanged distribution of histological type with time was expected but the lack of change in degree of dysplasia is surprising and conflicts with the increasing proportion of patients with Spigelman stage IV with time. It is possible that severe degree of dysplasia should add more points to the total Spigelman score and therefore we propose that validation of the Spigelman classification should be undertaken. This could be done in the setting of a multicentre study under the auspices of the Leeds Castle Polyposis Group. The overall incidence of 1.6% for duodenal carcinoma in this five nation study is similar to most other series but lower than in a recent 10 year follow up study from St Mark s Hospital. 17 During follow up, carcinoma developed in 2/26 patients with Spigelman stage IV at their first endoscopy compared with 3/11 in the Swedish study 14 and 4/11 in the St Mark s study. 17 These values are small and probably not different, thus indicating a higher risk of carcinoma development in patients with Spigelman stage IV than in those with stages 0 III. This is another indication of the existence of a duodenal adenoma-carcinoma sequence similar to the well documented sequence in the colon and rectum. The ideal treatment of duodenal adenomatosis includes complete and lasting destruction of adenomas with a minimum risk of complications and no functional problems. Such a treatment is not yet available but several options have been tried. Endoscopic treatment with Nd-YAG laser or electrocautery implies a risk of perforation and pancreatitis, and requires repeated endoscopies. 19 Photodynamic therapy seems promising but has not yet been validated. 20 Duodenotomy with polypectomy is feasible but inevitably leads to recurrence. 21 Radical surgical treatment has included total pancreatico-duodenectomy (Whipple s operation), which is presently used only in patients with carcinomas. A less comprehensive procedure is recommended as a cancer prophylactic operation in patients with severe adenomatosis: pylorus sparing or pancreas sparing duodenectomy result in few complications and good quality of life. 22 Pharmacological trials have included sulindac, calcium, calciferol, and celecoxib. In small series, sulindac had little or no effect, and calcium and calciferol had no effect. 25 A randomised controlled trial showed that celecoxib 800 mg daily resulted
5 Duodenal adenomatosis in FAP 385 in a reduction in duodenal adenomatosis 26 but there are as yet no long term results concerning adenomatosis development or a cancer protective effect. Several studies have tried to identify a genotype-phenotype relation between specific mutation sites of the APC gene and the severity of duodenal adenomatosis but the results have been inconsistent. Five studies indicated correlations with mutations in codon , 27 codon , 28 exon 15, 29 after codon 1400, 30 and exon 10 15, 31 respectively, whereas two studies found no correlation between mutation sites and the severity of adenomatosis or carcinoma development. 17 During the last decades, endoscopic surveillance of the duodenum has been recommended. An evaluation of the effect of such a policy showed a lifetime risk of 3 5% of duodenal cancer, and decision analysis demonstrated that regular surveillance resulted in an increase in life expectancy of seven months. 33 Endoscopic ultrasonography has been recommended in patients with Spigelman stages III IV to ensure that invasive growth has not occurred. 9 A recent study presented a detailed surveillance programme, including endoscopy at intervals of 1 5 years depending on the Spigelman stage. Patients with stages II and III are considered for chemoprevention and endoscopic treatment, and those with stage IV should be offered a pancreas preserving duodenectomy. 17 The present results indicate that regular endoscopic surveillance of the duodenum should be offered to all FAP patients, and our proposed surveillance programme is shown in table 3. The first endoscopy should be carried out at the age of 30 years and include multiple random biopsies taken from the duodenal mucosa in patients without visible polyps. We find the present evidence of endoscopic therapy too weak to justify a general recommendation outside specialised centres. Endoscopic ultrasonography is recommended for evaluation of patients with Spigelman stage IV, severe dysplasia, or large adenomas in order to ensure that invasive growth can be ruled out. In order to delay progression to Spigelman stage IV, it seems justified to treat patients with stage III with celecoxib 800 mg daily. Patients with Spigelman stage IV should be informed about cancer prophylactic surgery. Endoscopic surveillance (including endoscopic ultrasonography) and chemoprevention are recommended at intervals of three months in patients who are not suitable or refuse surgery. In conclusion, the long term natural history of duodenal adenomatosis in FAP is now known in detail and it has been documented that the incidence and severity of adenomatosis increase with age. There is thus convincing evidence to justify recommendation of regular endoscopic surveillance in all FAP patients. Furthermore, a high risk group for carcinoma development (Spigelman stage IV) has been identified. Chemoprevention with celecoxib may prove to delay worsening of duodenal adenomatosis. Patients with Spigelman stage IV should be offered prophylactic surgery, with pancreas preserving or pylorus sparing duodenectomy being the procedures of choice. We propose that the surveillance programme should be evaluated prospectively in an international multicentre study. ACKNOWLEDGEMENTS The study was supported by Ingeborg Roikjers Fond and The Nordic Cooperative Board for Medical Research.... Authors affiliations SBülow, F Moesgaard, The Danish Polyposis Register, Hvidovre University Hospital, Copenhagen, Denmark J Björk, The Swedish Polyposis Register, Karolinska Sjukhuset, Stockholm, Sweden I J Christensen, The Finsen Laboratory, Copenhagen, Denmark O Fausa, The Norwegian Polyposis Register, Rikshospitalet, Oslo, Norway HJärvinen, The Finnish Polyposis Register, Helsinki University Central Hospital, Helsinki, Finland H F A Vasen, The Dutch Polyposis Register, The Netherlands Foundation for the Detection of Hereditary Tumours, Leiden, the Netherlands APPENDIX The DAF Study Group included: H Järvinen, A Kahri, and J-P Mecklin (Finland); T Alm, J Björk, R Hultcrantz, and C Rubio (Sweden); S Norheim Andersen, A Bakka, and O Fausa (Norway); G Griffioen, F Nagengast, GJA Offerhaus, and H Vasen (the Netherlands); S Bülow, IJ Christensen, H Højen, F Moesgaard, AM Mogensen, and LB Svendsen (Denmark). The regional contact persons included: OB Andersen, J La Cour Andersen, C Kirk Axelsson, I Balslev, T Bremholm Sørensen, F Burchharth, HE Bøgh, P Crone, A Fischer, HJ Frederiksen, O Hart Hansen, H Harling, KE Juul Jensen, A Skov Jensen, V Jensen, J Jepsen, P Jess, A Kruse, E Larsen, S Laurberg, A Lauridsen, A Marckmann, O Lawaetz, G Madsen, T Nilsson, V Møller Pedersen, H Raskov, PC Rasmussen, O Roikjær, N Qvist, K Sørensen, T Bonnesen, P Wamberg, C Werner, and M Øster (Denmark); J-P Mecklin, A-L Karvonen, M Pääkkönen, and I Kellokumpu (Finland) EMH Matthus-Vliegen, P de Ruyter, and B Taal (Holland) and L-K Enander, K Furugård, D-A Hallbäck, and H-O Håkansson (Sweden). REFERENCES 1 Funkenstein O. Über Polyposis intestinalis. Z Klin Med Berlin 1904;55: Cabot RC. Case records of the Massachusetts General Hospital. Case N Engl J Med 1935;212: Yao T, Iida M, Ohsato K, et al. Duodenal lesions in familial polyposis of the colon. Gastroenterology 1977;73: Bülow S, Bülow C, Nielsen TF, et al. Centralized registration, prophylactic examination, and treatment results in improved prognosis in familial adenomatous polyposis. Results from the Danish Polyposis Register. Scand J Gastroenterol 1995;30: Arvanitis ML, Jagelman DG, Fazio VW, et al. Mortality in patients with familial adenomatous polyposis. Dis Colon Rectum 1990;33: Spigelman AD, Williams CB, Talbot IC, et al. Upper gastrointestinal cancer in patients with familial adenomatous polyposis. Lancet 1989;2: Church JM, McGannon E, Hull-Boiner S, et al. Gastroduodenal polyps in patients with familial adenomatous polyposis. Dis Colon Rectum 1992;35: Nugent KP, Spigelman AD, Williams CB, et al. Surveillance of duodenal polyps in familial adenomatous polyposis: progress report. J R Soc Med 1994;87: Debinski HS, Spigelman AD, Hatfield A, et al. Upper intestinal surveillance in familial adenomatous polyposis. Eur J Cancer 1995;31A: Bülow S, Alm T, Fausa O, et al. Duodenal adenomatosis in familial adenomatous polyposis. DAF Project Group. Int J Colorectal Dis 1995;10: Burke CA, Beck GJ, Church JM, et al. The natural history of untreated duodenal and ampullary adenomas in patients with familial adenomatous polyposis followed in an endoscopic surveillance program. Gastrointest Endosc 1999;49: Heiskanen I, Kellokumpu I, Järvinen H. Management of duodenal adenomas in 98 patients with familial adenomatous polyposis. Endoscopy 1999;31: Saurin JC, Ligneau B, Lepretre J, et al. Prospective evaluation of duodenal polyposis progression in familial adenomatous polyposis (FAP) patients, and genotype-phenotype correlation. Digestive Disease Week, San Diego, California, USA, 2000: abstract Björk J, Åkerbrant H, Iselius L, et al. Periampullary adenomas and adenocarcinomas in familial adenomatous polyposis: cumulative risks and APC gene mutations. Gastroenterology 2001;121: Mozaar KL, Madlensky L, Berk T, et al. Slow progression of periampullary neoplasia in familial adenomatous polyposis. J Gastrointest Surg 2002;6: Kadmon M, Tandara A, Herfarth C. Duodenal adenomatosis in familial adenomatous polyposis coli. A review of the literature and results from the Heidelberg Polyposis Register. Int J Colorectal Dis 2001;16: Groves CJ, Saunders BP, Spigelman AD, et al. Duodenal cancer in patients with familial adenomatous polyposis (FAP): results of a 10 year prospective study. Gut 2002;50: Liang K-Y, Zeger SL. Longitudinal data analysis using generalized linear models. Biometrika 1986;73: Norton ID, Geller A, Petersen BT, et al. Endoscopic surveillance and ablative therapy for periampullary adenomas. Am J Gastroenterol 2001;96:101 6.
6 386 Bülow, Björk,Christensen,etal 20 Mlkvy P, Messmann H, Debinski H, et al. Photodynamic therapy for polyps in familial adenomatous polyposis a pilot study. Eur J Cancer 1995;31A: Penna C, Phillips RK, Tiret E, et al. Surgical polypectomy of duodenal adenomas in familial adenomatous polyposis: experience of two European centres. Br J Surg 1993;80: Sarmiento JM, Thompson GB, Nagorney DM, et al. Pancreas-sparing duodenectomy for duodenal polyposis. Arch Surg 2002;137: Nugent KP, Farmer KC, Spigelman AD, et al. Randomized controlled trial of the effect of sulindac on duodenal and rectal polyposis and cell proliferation in patients with familial adenomatous polyposis. Br J Surg 1993;80: Richard CS, Berk T, Bapat BV, et al. Sulindac for periampullary polyps in FAP patients. Int J Colorectal Dis 1997;12: Seow-Choen F, Vijayan V, Keng V. Prospective randomized study of sulindac versus calcium and calciferol for upper gastrointestinal polyps in familial adenomatous polyposis. Br J Surg 1996;83: Phillips RK, Wallace MH, Lynch PM, et al. A randomised, double blind, placebo controlled study of celecoxib, a selective cyclooxygenase 2 inhibitor, on duodenal polyposis in familial adenomatous polyposis. Gut 2002;50: Enomoto M, Konishi M, Iwama T, et al. The relationship between frequencies of extracolonic manifestations and the position of APC germline mutation in patients with familial adenomatous polyposis. Jpn J Clin Oncol 2000;30: Saurin JC, Ligneau B, Ponchon T, et al. The influence of mutation site and age on the severity of duodenal polyposis in patients with familial adenomatous polyposis. Gastrointest Endosc 2002;55: Norheim Andersen S, Løvig T, Fausa O, et al. Germline and somatic mutations in exon 15 of the APC gene and K-ras mutations in duodenal adenomas in patients with familial adenomatous polyposis. Scand J Gastroenterol 1999;34: Groves C, Lamlum H, Crabtree M, et al. Mutation cluster region, association between germline and somatic mutations and genotype-phenotype correlation in upper gastrointestinal familial adenomatous polypsis. Am J Path 2002;160: Matsumoto T, Iida M, Kobori Y, et al. Genetic predisposition to clinical manifestations in familial adenomatous polyposis with special reference to duodenal lesions. Am J Gastroenterol 2002;97: Sanabria JR, Croxford R, Berk TC, et al. Familial segregation in the occurrence and severity of periampullary neoplasms in familial adenomatous polyposis. Am J Surg 1996;171: Vasen HF, Bülow S, Myrhøj T, et al. Decision analysis in the management of duodenal adenomatosis in familial adenomatous polyposis. Gut 1997;40: GI SNAPSHOT... Large bowel obstruction due to a benign uterine leiomyoma Question A 44 year old woman was admitted with a two week history of colicky abdominal pain, vomiting, and constipation. Past medical history included Ehlers Danlos syndrome type IV with a history of spontaneous retroperitoneal haemorrhage treated conservatively. She was also known to have large uterine leiomyomas for which she was on hormonal therapy and was awaiting a hysterectomy. On examination she had abdominal distension with generalised vague tenderness and some suprapubic fullness. Digital rectal examination revealed an empty rectum with a large pelvic mass bimanually palpable anteriorly. Chest x ray was normal but supine abdominal x ray revealed faeces filled distended loops of large bowel with minimal air in the rectum. Routine blood tests were within normal limits. She was initially treated conservatively with laxatives and enemas which did not improve her symptoms. On the fourth day of admission she developed severe colicky abdominal pain, persistent vomiting, gross abdominal distension, and obstipation. See page 430 for answer R P C Chaparala A S Fawole N S Ambrose Department of Academic Surgical Gastroenterology, St James s University Hospital,, Leeds, UK A H Chapman Department of Radiology, St James s University Hospital, Leeds, UK Correspondence to: Mr A S Fawole Department of Academic Surgical Gastroenterology, St James s University Hospital, Beckett St, Leeds LS9 7TF, UK; pamshina@aol.com Figure 1 The investigation that was performed is shown. What investigation is demonstrated and what does it show?
Extracolonic Manifestations in Familial Adenomatous Polyposis
 Govaresh 2003; 8: 178-83 Extracolonic Manifestations in Familial Adenomatous Polyposis Narimantas Evaldas Samalavicius Department of Surgery, Vilnius Center University Hospital, Vilnius, Lithuania ABSTRACT
Govaresh 2003; 8: 178-83 Extracolonic Manifestations in Familial Adenomatous Polyposis Narimantas Evaldas Samalavicius Department of Surgery, Vilnius Center University Hospital, Vilnius, Lithuania ABSTRACT
colorectal cancer Colorectal cancer hereditary sporadic Familial 1/12/2018
 colorectal cancer Adenocarcinoma of the colon and rectum is the third most common site of new cancer cases and deaths in men (following prostate and lung or bronchus cancer) and women (following breast
colorectal cancer Adenocarcinoma of the colon and rectum is the third most common site of new cancer cases and deaths in men (following prostate and lung or bronchus cancer) and women (following breast
Endoscopic techniques for surveillance and treatment of FAP
 Endoscopic techniques for surveillance and treatment of FAP Evelien Dekker MD PhD Department of Gastroenterology & Hepatology Academic Medical Center Amsterdam The Netherlands FAP: endoscopic surveillance
Endoscopic techniques for surveillance and treatment of FAP Evelien Dekker MD PhD Department of Gastroenterology & Hepatology Academic Medical Center Amsterdam The Netherlands FAP: endoscopic surveillance
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions. South Island Cancer Nurses Network September 2013
 For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
For identification, support and follow up related to Familial Gastrointestinal Cancer conditions South Island Cancer Nurses Network September 2013 Who are we? Specialist multidisciplinary team: Nurse coordinators,
Latest Endoscopic Guidelines for FAP, HNPCC, IBD, and the General Population
 Latest Endoscopic Guidelines for FAP, HNPCC, IBD, and the General Population David T. Rubin, M.D. Assistant Professor of Medicine Inflammatory Bowel Disease Center MacLean Center for Clinical Medical Ethics
Latest Endoscopic Guidelines for FAP, HNPCC, IBD, and the General Population David T. Rubin, M.D. Assistant Professor of Medicine Inflammatory Bowel Disease Center MacLean Center for Clinical Medical Ethics
GI Polyp syndromes in children. Screening and surveillance, surgery.
 Dr Warren Hyer Consultant Paediatric Gastroenterologist St Mark s Hospital, UK GI Polyp syndromes in children Screening and surveillance, surgery. No conflict of interests to declare Objectives Understand
Dr Warren Hyer Consultant Paediatric Gastroenterologist St Mark s Hospital, UK GI Polyp syndromes in children Screening and surveillance, surgery. No conflict of interests to declare Objectives Understand
PENETRANCE ACTIONABILITY SIGNIFICANCE/BURDEN OF DISEASE NEXT STEPS. YES ( 1 of above) YES (Proceed to Stage II)
 Stage I: Binning Dashboard GENE/GENE PANEL: APC ACTIONABILITY 1. Is there a qualifying resource, such as a practice guideline or systematic review, for the genetic condition? 2. Does the practice guideline
Stage I: Binning Dashboard GENE/GENE PANEL: APC ACTIONABILITY 1. Is there a qualifying resource, such as a practice guideline or systematic review, for the genetic condition? 2. Does the practice guideline
Familial Adenomatous Polyposis
 Familial Adenomatous Polyposis 1 in 10,000 incidence 100 s to 1000 s of colonic adenomas by teens Cancer risk: colon, gastric, duodenum (periampulla), small bowel, pancreas, papillary thyroid, childhood
Familial Adenomatous Polyposis 1 in 10,000 incidence 100 s to 1000 s of colonic adenomas by teens Cancer risk: colon, gastric, duodenum (periampulla), small bowel, pancreas, papillary thyroid, childhood
Variables affecting penetrance of gastric and duodenal phenotype in familial adenomatous polyposis patients
 Sample et al. BMC Gastroenterology (2018) 18:115 https://doi.org/10.1186/s12876-018-0841-8 RESEARCH ARTICLE Variables affecting penetrance of gastric and duodenal phenotype in familial adenomatous polyposis
Sample et al. BMC Gastroenterology (2018) 18:115 https://doi.org/10.1186/s12876-018-0841-8 RESEARCH ARTICLE Variables affecting penetrance of gastric and duodenal phenotype in familial adenomatous polyposis
Duodenal adenomas Management. Dr Stratis Alexandridis Consultant Gastroenterologist BRI
 Duodenal adenomas Management Dr Stratis Alexandridis Consultant Gastroenterologist BRI Introduction Ampullary and non ampullary polyps of the duodenum are diagnosed within and outside genetic syndromes.
Duodenal adenomas Management Dr Stratis Alexandridis Consultant Gastroenterologist BRI Introduction Ampullary and non ampullary polyps of the duodenum are diagnosed within and outside genetic syndromes.
Risk factors for advanced duodenal and ampullary adenomatosis in familial adenomatous polyposis: a prospective, single-center study
 Risk factors for advanced duodenal and ampullary adenomatosis in familial adenomatous polyposis: a prospective, single-center study Authors M. Sulbaran 1,F.G.Campos 2, U. Ribeiro Jr. 2,H.S.Kishi 3,P.Sakai
Risk factors for advanced duodenal and ampullary adenomatosis in familial adenomatous polyposis: a prospective, single-center study Authors M. Sulbaran 1,F.G.Campos 2, U. Ribeiro Jr. 2,H.S.Kishi 3,P.Sakai
Familial and Hereditary Colon Cancer
 Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Prognosis after Treatment of Villous Adenomas
 Prognosis after Treatment of Villous Adenomas of the Colon and Rectum JOHN CHRISTIANSEN, M.D., PREBEN KIRKEGAARD, M.D., JYTTE IBSEN, M.D. With the existing evidence of neoplastic polyps of the colon and
Prognosis after Treatment of Villous Adenomas of the Colon and Rectum JOHN CHRISTIANSEN, M.D., PREBEN KIRKEGAARD, M.D., JYTTE IBSEN, M.D. With the existing evidence of neoplastic polyps of the colon and
C olorectal adenomas are reputed to be precancerous
 568 COLORECTAL CANCER Incidence and recurrence rates of colorectal adenomas estimated by annually repeated colonoscopies on asymptomatic Japanese Y Yamaji, T Mitsushima, H Ikuma, H Watabe, M Okamoto, T
568 COLORECTAL CANCER Incidence and recurrence rates of colorectal adenomas estimated by annually repeated colonoscopies on asymptomatic Japanese Y Yamaji, T Mitsushima, H Ikuma, H Watabe, M Okamoto, T
ORIGINAL ARTICLE. Extracolonic Manifestations of Familial Adenomatous Polyposis After Proctocolectomy
 ORIGINAL ARTICLE Extracolonic Manifestations of Familial Adenomatous Polyposis After Proctocolectomy Hagit Tulchinsky, MD; Andrei Keidar, MD; Hana Strul, MD; Gideon Goldman, MD; Joseph M. Klausner, MD;
ORIGINAL ARTICLE Extracolonic Manifestations of Familial Adenomatous Polyposis After Proctocolectomy Hagit Tulchinsky, MD; Andrei Keidar, MD; Hana Strul, MD; Gideon Goldman, MD; Joseph M. Klausner, MD;
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS. Family Health Clinical Genetics. Clinical Genetics department
 GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
GENETIC MANAGEMENT OF A FAMILY HISTORY OF FAP or MUTYH ASSOCIATED POLYPOSIS Full Title of Guideline: Author (include email and role): Division & Speciality: GUIDELINES FOR THE GENETIC MANAGEMENT OF A FAMILY
Familial and Hereditary Colon Cancer
 Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Familial and Hereditary Colon Cancer Aasma Shaukat, MD, MPH, FACG, FASGE, FACP GI Section Chief, Minneapolis VAMC Associate Professor, Division of Gastroenterology, Department of Medicine, University of
Pathology reports, related operative reports and consult letters must be provided with a request for assessment.
 Page 1 of 6 Polyposis Syndromes Inherited risk for colorectal cancer is associated with a number of polyposis syndromes (genes), some of which are well-defined and others are less common. Identification
Page 1 of 6 Polyposis Syndromes Inherited risk for colorectal cancer is associated with a number of polyposis syndromes (genes), some of which are well-defined and others are less common. Identification
Summary. Cezary ŁozińskiABDF, Witold KyclerABCDEF. Rep Pract Oncol Radiother, 2007; 12(4):
 Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
YES NO UNKNOWN. Stage I: Rule-Out Dashboard ACTIONABILITY PENETRANCE SIGNIFICANCE/BURDEN OF DISEASE NEXT STEPS. YES ( 1 of above)
 Stage I: Rule-Out Dashboard GENE/GENE PANEL: SMAD4, BMPR1A DISORDER: Juvenile Polyposis Syndrome HGNC ID: 6670, 1076 OMIM ID: 174900, 175050 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource,
Stage I: Rule-Out Dashboard GENE/GENE PANEL: SMAD4, BMPR1A DISORDER: Juvenile Polyposis Syndrome HGNC ID: 6670, 1076 OMIM ID: 174900, 175050 ACTIONABILITY PENETRANCE 1. Is there a qualifying resource,
Precision Cancer Prevention: Hereditary Polyposis Syndromes
 Precision Cancer Prevention: Hereditary Polyposis Syndromes N. Jewel Samadder, MD, MSC, FRCPC HUNTSMAN CANCER INSTITUTE UNIVERSITY OF UTAH Familial Adenomatous Polyposis Familial Adenomatous Polyposis
Precision Cancer Prevention: Hereditary Polyposis Syndromes N. Jewel Samadder, MD, MSC, FRCPC HUNTSMAN CANCER INSTITUTE UNIVERSITY OF UTAH Familial Adenomatous Polyposis Familial Adenomatous Polyposis
Upper gastrointestinal tract polyps in familial
 Upper gastrointestinal tract polyps in familial adenomatosis coli H JARVINEN, M NYBERG, AND P PELTOKALLIO Gut, 1983, 24, 333-339 From the Second Department of Surgery, Helsinki University Central Hospital,
Upper gastrointestinal tract polyps in familial adenomatosis coli H JARVINEN, M NYBERG, AND P PELTOKALLIO Gut, 1983, 24, 333-339 From the Second Department of Surgery, Helsinki University Central Hospital,
Hereditary Gastric Cancer
 Hereditary Gastric Cancer Dr Bastiaan de Boer Consultant Pathologist Department of Anatomical Pathology PathWest Laboratory Medicine, QE II Medical Centre Clinical Associate Professor School of Pathology
Hereditary Gastric Cancer Dr Bastiaan de Boer Consultant Pathologist Department of Anatomical Pathology PathWest Laboratory Medicine, QE II Medical Centre Clinical Associate Professor School of Pathology
Familial adenomatous polyposis (FAP) is an autosomal
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:1237 1242 Risk of Developing Adenomas and Carcinomas in the Ileal Pouch in Patients With Familial Adenomatous Polyposis PIETER FRIEDERICH,* ANDREA E. DE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:1237 1242 Risk of Developing Adenomas and Carcinomas in the Ileal Pouch in Patients With Familial Adenomatous Polyposis PIETER FRIEDERICH,* ANDREA E. DE
Quality of and compliance with colonoscopy in Lynch Syndrome surveillance: are we getting it right?
 Quality of and compliance with colonoscopy in Lynch Syndrome surveillance: are we getting it right? Hartery K 1, Sukha A 1, Thomas-Gibson S 1, Thomas H 1,2, Latchford A 1,2. 1 Wolfson Endoscopy Unit, St.
Quality of and compliance with colonoscopy in Lynch Syndrome surveillance: are we getting it right? Hartery K 1, Sukha A 1, Thomas-Gibson S 1, Thomas H 1,2, Latchford A 1,2. 1 Wolfson Endoscopy Unit, St.
LIST OF ABBREVIATIONS
 Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Gastroenter oenterology 2005 Royal College of Physicians of Edinburgh Screening and surveillance for upper and lower gastrointestinal cancer JN Plevris Consultant Gastroenterologist and Honorary Senior
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines
 Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Fundic Gland Polyposis in Patients Without Familial Adenomatosis Coli: Its Incidence and Clinical Features
 GASTROENTEROLOGY 1984;86;1437-42 ALIMENTARY TRACT Fundic Gland Polyposis in Patients Without Familial Adenomatosis Coli: Its Incidence and Clinical Features MITSUO IIDA, TSUNEYOSHI YAO, HIDENOBU WATANABE,
GASTROENTEROLOGY 1984;86;1437-42 ALIMENTARY TRACT Fundic Gland Polyposis in Patients Without Familial Adenomatosis Coli: Its Incidence and Clinical Features MITSUO IIDA, TSUNEYOSHI YAO, HIDENOBU WATANABE,
27
 26 27 28 29 30 31 32 33 34 35 Diagnosis:? Diagnosis: Juvenile Polyposis with BMPR1A Mutation 36 Juvenile Polyposis Syndrome Rare Autosomal Dominant Disorder with Multiple Juvenile Polyps in GI Tract Juvenile
26 27 28 29 30 31 32 33 34 35 Diagnosis:? Diagnosis: Juvenile Polyposis with BMPR1A Mutation 36 Juvenile Polyposis Syndrome Rare Autosomal Dominant Disorder with Multiple Juvenile Polyps in GI Tract Juvenile
Risk of Colorectal Cancer (CRC) Hereditary Syndromes in GI Cancer GENETIC MALPRACTICE
 Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Identifying the Patient at Risk for an Inherited Syndrome Sapna Syngal, MD, MPH, FACG Director, Gastroenterology Director, Familial GI Program Dana-Farber/Brigham and Women s Cancer Center Associate Professor
Hereditary Colorectal Cancer Syndromes Miguel A. Rodriguez-Bigas, MD
 Hereditary Colorectal Cancer Syndromes Miguel A. Rodriguez-Bigas, MD Living Beyond Cancer A-Z January 12,2019 Hereditary CRC Syndromes Objectives are to discuss the : Most common Hereditary CRC syndromes
Hereditary Colorectal Cancer Syndromes Miguel A. Rodriguez-Bigas, MD Living Beyond Cancer A-Z January 12,2019 Hereditary CRC Syndromes Objectives are to discuss the : Most common Hereditary CRC syndromes
Prevention of Bowel Cancer: which patients do I send for colonoscopy?
 Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Long-term Treatment With Sulindac in Familial Adenomatous Polyposis: A Prospective Cohort Study
 GASTROENTEROLOGY 2002;122:641 645 Long-term Treatment With Sulindac in Familial Adenomatous Polyposis: A Prospective Cohort Study MARCIA CRUZ CORREA, LINDA M. HYLIND, KATHARINE E. ROMANS, SUSAN V. BOOKER,
GASTROENTEROLOGY 2002;122:641 645 Long-term Treatment With Sulindac in Familial Adenomatous Polyposis: A Prospective Cohort Study MARCIA CRUZ CORREA, LINDA M. HYLIND, KATHARINE E. ROMANS, SUSAN V. BOOKER,
Frequency of Diagnosis of Colorectal Cancer with Double Contrast Barium Enema
 Bahrain Medical Bulletin, Vol.24, No.3, September 2002 Frequency of Diagnosis of Colorectal Cancer with Double Contrast Barium Enema Najeeb S Jamsheer, MD, FRCR* Neelam. Malik, MD, MNAMS** Objective: To
Bahrain Medical Bulletin, Vol.24, No.3, September 2002 Frequency of Diagnosis of Colorectal Cancer with Double Contrast Barium Enema Najeeb S Jamsheer, MD, FRCR* Neelam. Malik, MD, MNAMS** Objective: To
Classification of polyposis syndromes two major groups. Adenomatous polyposis syndromes. Hamartomatous polyposis syndromes
 Hereditary polyposis syndromes Classification of polyposis syndromes two major groups adenomatous and non-adenomatous polyposis syndromes Adenomatous polyposis syndromes Familial adenomatous polyposis(fap)
Hereditary polyposis syndromes Classification of polyposis syndromes two major groups adenomatous and non-adenomatous polyposis syndromes Adenomatous polyposis syndromes Familial adenomatous polyposis(fap)
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal surgery prior as factor in laparoscopic colorectal surgery, 554 555 Abscess(es) CRC presenting as, 539 540 Adenocarcinoma of
Index Note: Page numbers of article titles are in boldface type. A Abdominal surgery prior as factor in laparoscopic colorectal surgery, 554 555 Abscess(es) CRC presenting as, 539 540 Adenocarcinoma of
Mr Chris Wakeman. General Surgeon University of Otago, Christchurch. 12:15-12:40 Management of Colorectal Cancer
 Mr Chris Wakeman General Surgeon University of Otago, Christchurch 12:15-12:40 Management of Colorectal Cancer Bowel cancer Chris Wakeman Colorectal Surgeon Christchurch Sam Simon (Simpsons) Elizabeth
Mr Chris Wakeman General Surgeon University of Otago, Christchurch 12:15-12:40 Management of Colorectal Cancer Bowel cancer Chris Wakeman Colorectal Surgeon Christchurch Sam Simon (Simpsons) Elizabeth
This is the portion of the intestine which lies between the small intestine and the outlet (Anus).
 THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
PMS2 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table
 PMS2 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
PMS2 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) PMS2 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
Large Colorectal Adenomas An Approach to Pathologic Evaluation
 Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
University of Groningen
 University of Groningen Incidence of small bowel neoplasia in Lynch syndrome assessed by video capsule endoscopy Haanstra, Jasmijn; Al-Toma, Abdul; Dekker, Evelien; Vanhoutvin, Steven A L W; Nagengast,
University of Groningen Incidence of small bowel neoplasia in Lynch syndrome assessed by video capsule endoscopy Haanstra, Jasmijn; Al-Toma, Abdul; Dekker, Evelien; Vanhoutvin, Steven A L W; Nagengast,
removal of adenomatous polyps detects important effectively as follow-up colonoscopy after both constitute a low-risk Patients with 1 or 2
 Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Review article: the incidence and prevalence of colorectal cancer in inflammatory bowel disease
 Aliment Pharmacol Ther 23; 18 (Suppl. 2): 1 5. Review article: the incidence and prevalence of colorectal cancer in inflammatory bowel disease P. MUNKHOLM Department of Medical Gastroenterology, Hvidovre
Aliment Pharmacol Ther 23; 18 (Suppl. 2): 1 5. Review article: the incidence and prevalence of colorectal cancer in inflammatory bowel disease P. MUNKHOLM Department of Medical Gastroenterology, Hvidovre
Digestive Health Southwest Endoscopy 2016 Quality Report
 Digestive Health 2016 Quality Report Our 2016 our quality and value management program focused on one primary area of interest: Performing high quality colonoscopy High quality Colonoscopy We selected
Digestive Health 2016 Quality Report Our 2016 our quality and value management program focused on one primary area of interest: Performing high quality colonoscopy High quality Colonoscopy We selected
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY
 OPEN ACCESS TEXTBOOK OF GENERAL SURGERY COLORECTAL POLYPS P Goldberg POLYP A polyp is a localised elevated lesion arising from a epithelial surface. If it has a stalk it is called a pedunculated polyp
OPEN ACCESS TEXTBOOK OF GENERAL SURGERY COLORECTAL POLYPS P Goldberg POLYP A polyp is a localised elevated lesion arising from a epithelial surface. If it has a stalk it is called a pedunculated polyp
Content. Diagnostic approach and clinical management of Lynch Syndrome: guidelines. Terminology. Identification of Lynch Syndrome
 of Lynch Syndrome: guidelines 17/03/2009 Content Terminology Lynch Syndrome Presumed Lynch Syndrome Familial Colorectal Cancer Identification of Lynch Syndrome Amsterdam II criteria Revised Bethesda Guidelines
of Lynch Syndrome: guidelines 17/03/2009 Content Terminology Lynch Syndrome Presumed Lynch Syndrome Familial Colorectal Cancer Identification of Lynch Syndrome Amsterdam II criteria Revised Bethesda Guidelines
Colonic Polyp. Najmeh Aletaha. MD
 Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Citation for published version (APA): Wijkerslooth de Weerdesteyn, T. R. (2013). Population screening for colorectal cancer by colonoscopy
 UvA-DARE (Digital Academic Repository) Population screening for colorectal cancer by colonoscopy de Wijkerslooth, T.R. Link to publication Citation for published version (APA): Wijkerslooth de Weerdesteyn,
UvA-DARE (Digital Academic Repository) Population screening for colorectal cancer by colonoscopy de Wijkerslooth, T.R. Link to publication Citation for published version (APA): Wijkerslooth de Weerdesteyn,
Structured Follow-Up after Colorectal Cancer Resection: Overrated. R. Taylor Ripley University of Colorado Grand Rounds April 23, 2007
 Structured Follow-Up after Colorectal Cancer Resection: Overrated R. Taylor Ripley University of Colorado Grand Rounds April 23, 2007 Guidelines for Colonoscopy Production: Surveillance US Multi-Society
Structured Follow-Up after Colorectal Cancer Resection: Overrated R. Taylor Ripley University of Colorado Grand Rounds April 23, 2007 Guidelines for Colonoscopy Production: Surveillance US Multi-Society
Endoscopic Corner CASE 1. Sirimontaporn N Klaikaew N Imraporn B Rerknimitr R
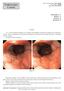 Endoscopic Corner Sirimontaporn N, et al. THAI J GASTROENTEROL 2010 Vol. 11 No. 3 Sept. - Dec. 2010 171 Sirimontaporn N Klaikaew N Imraporn B Rerknimitr R CASE 1 A 47- year-old female presented to the
Endoscopic Corner Sirimontaporn N, et al. THAI J GASTROENTEROL 2010 Vol. 11 No. 3 Sept. - Dec. 2010 171 Sirimontaporn N Klaikaew N Imraporn B Rerknimitr R CASE 1 A 47- year-old female presented to the
B Base excision repair, in MUTYH-associated polyposis and colorectal cancer, BRAF testing, for hereditary colorectal cancer, 696
 Index Note: Page numbers of article titles are in boldface type. A Adenomatous polyposis, familial. See Familial adenomatous polyposis. Anal anastomosis, ileal-pouch, proctocolectomy with, in FAP, 591
Index Note: Page numbers of article titles are in boldface type. A Adenomatous polyposis, familial. See Familial adenomatous polyposis. Anal anastomosis, ileal-pouch, proctocolectomy with, in FAP, 591
Page 1. Is the Risk This High? Dysplasia in the IBD Patient. Dysplasia in the Non IBD Patient. Increased Risk of CRC in Ulcerative Colitis
 Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Objectives. Definitions. Colorectal Cancer Screening 5/8/2018. Payam Afshar, MS, MD Kaiser Permanente, San Diego. Colorectal cancer background
 Colorectal Cancer Screening Payam Afshar, MS, MD Kaiser Permanente, San Diego Objectives Colorectal cancer background Colorectal cancer screening populations Colorectal cancer screening modalities Colonoscopy
Colorectal Cancer Screening Payam Afshar, MS, MD Kaiser Permanente, San Diego Objectives Colorectal cancer background Colorectal cancer screening populations Colorectal cancer screening modalities Colonoscopy
Colon Cancer Screening & Surveillance. Amit Patel, MD PGY-4 GI Fellow
 Colon Cancer Screening & Surveillance Amit Patel, MD PGY-4 GI Fellow Epidemiology CRC incidence and mortality rates vary markedly around the world. Globally, CRC is the third most commonly diagnosed cancer
Colon Cancer Screening & Surveillance Amit Patel, MD PGY-4 GI Fellow Epidemiology CRC incidence and mortality rates vary markedly around the world. Globally, CRC is the third most commonly diagnosed cancer
Personalized Aspirin Therapy
 Personalized Aspirin Therapy Nadir Arber, MD, MSc, MHA Head - Integrated Cancer Prevention Center Tel Aviv Medical Centre and Tel Aviv University Heidelberg 2014 CRC is Preventable Early detection Chemoprevention
Personalized Aspirin Therapy Nadir Arber, MD, MSc, MHA Head - Integrated Cancer Prevention Center Tel Aviv Medical Centre and Tel Aviv University Heidelberg 2014 CRC is Preventable Early detection Chemoprevention
Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER
 Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER Epidemiology of CRC Colorectal cancer (CRC) is a common and lethal disease Environmental
Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER Epidemiology of CRC Colorectal cancer (CRC) is a common and lethal disease Environmental
ACG Clinical Guideline: Genetic Testing and Management of Hereditary Gastrointestinal Cancer Syndromes
 ACG Clinical Guideline: Genetic Testing and Management of Hereditary Gastrointestinal Cancer Syndromes Sapna Syngal, MD, MPH, FACG, 1,2,3 Randall E. Brand, MD, FACG, 4 James M. Church, MD, FACG, 5,6,7
ACG Clinical Guideline: Genetic Testing and Management of Hereditary Gastrointestinal Cancer Syndromes Sapna Syngal, MD, MPH, FACG, 1,2,3 Randall E. Brand, MD, FACG, 4 James M. Church, MD, FACG, 5,6,7
MSH6 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table
 MSH6 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
MSH6 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MSH6 Summary Cancer Risk Table CANCER Colorectal GENETIC CANCER RISK High Risk Endometrial High Risk
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kaminski MF, Regula J, Kraszewska E, et al. Quality indicators
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kaminski MF, Regula J, Kraszewska E, et al. Quality indicators
Gastrointestinal polyposis syndromes for the general gastroenterologist
 TRAINING MATTERS CURRICULUM BASED CLINICAL REVIEWS Gastrointestinal polyposis syndromes for the general gastroenterologist Joanna J Hurley, 1,2 Iain Ewing, 3 Julian R Sampson, 2 Sunil Dolwani 1 1 Department
TRAINING MATTERS CURRICULUM BASED CLINICAL REVIEWS Gastrointestinal polyposis syndromes for the general gastroenterologist Joanna J Hurley, 1,2 Iain Ewing, 3 Julian R Sampson, 2 Sunil Dolwani 1 1 Department
Supporting people at higher risk of bowel cancer
 #never2young Never too young: Supporting people at higher risk of bowel cancer Campaign briefing Supporting people at higher risk of bowel cancer Bowel cancer is the second most common cause of cancer
#never2young Never too young: Supporting people at higher risk of bowel cancer Campaign briefing Supporting people at higher risk of bowel cancer Bowel cancer is the second most common cause of cancer
GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY
 Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Timing of surgery in FAP
 Timing of surgery in FAP Sue Clark Consultant Colorectal Surgeon, The Polyposis Registry, St Mark s Hospital, London, UK. 0-5 5-10 10-15 15-20 20-25 25-30 30-35 35-40 40-45 45-50 50-55 55-60 60-65 65-70
Timing of surgery in FAP Sue Clark Consultant Colorectal Surgeon, The Polyposis Registry, St Mark s Hospital, London, UK. 0-5 5-10 10-15 15-20 20-25 25-30 30-35 35-40 40-45 45-50 50-55 55-60 60-65 65-70
EARLY DETECTION OF COLORECTAL CANCER. Epidemiology of CRC
 Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER Epidemiology of CRC Colorectal cancer (CRC) is a common and lethal disease Environmental
Razvan I. Arsenescu, MD Assistant Professor of Medicine Division of Digestive Diseases EARLY DETECTION OF COLORECTAL CANCER Epidemiology of CRC Colorectal cancer (CRC) is a common and lethal disease Environmental
Title Description Type / Priority
 Merit-based Incentive Payment system (MIPS) 2019 Qualified Clinical Data Registry (QCDR) Measure Specifications Summary Listing of QCDR measures supported by the NHCR Measure # NHCR4 NHCR5 GIQIC12 GIQIC15
Merit-based Incentive Payment system (MIPS) 2019 Qualified Clinical Data Registry (QCDR) Measure Specifications Summary Listing of QCDR measures supported by the NHCR Measure # NHCR4 NHCR5 GIQIC12 GIQIC15
Endoscopic Submucosal Dissection ESD
 Endoscopic Submucosal Dissection ESD Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated
Endoscopic Submucosal Dissection ESD Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated
Diagnostic values of dual focus narrow band imaging and probe-based confocal laser endomicroscopy in FAP-related duodenal adenoma
 E450 THIEME Diagnostic values of dual focus narrow band imaging and probe-based confocal laser endomicroscopy in FAP-related duodenal adenoma Authors Rapat Pittayanon 1, Rungsun Rerknimitr 1, Boonlert
E450 THIEME Diagnostic values of dual focus narrow band imaging and probe-based confocal laser endomicroscopy in FAP-related duodenal adenoma Authors Rapat Pittayanon 1, Rungsun Rerknimitr 1, Boonlert
Colorectal Neoplasia. Dr. Smita Devani MBChB, MRCP. Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi
 Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Hereditary nonpolyposis colorectal cancer (HNPCC)
 GASTROENTEROLOGY 2000;118:829 834 Controlled 15-Year Trial on Screening for Colorectal Cancer in Families With Hereditary Nonpolyposis Colorectal Cancer HEIKKI J. JÄRVINEN,* MARKKU AARNIO,* HARRI MUSTONEN,*
GASTROENTEROLOGY 2000;118:829 834 Controlled 15-Year Trial on Screening for Colorectal Cancer in Families With Hereditary Nonpolyposis Colorectal Cancer HEIKKI J. JÄRVINEN,* MARKKU AARNIO,* HARRI MUSTONEN,*
Can We Predict the Natural History of Ulcerative Colitis? Edward V Loftus, Jr, MD Professor of Medicine Mayo Clinic Rochester, Minnesota, USA
 Can We Predict the Natural History of Ulcerative Colitis? Edward V Loftus, Jr, MD Professor of Medicine Mayo Clinic Rochester, Minnesota, USA Endpoints Overview Hospitalization Surgery Colorectal cancer
Can We Predict the Natural History of Ulcerative Colitis? Edward V Loftus, Jr, MD Professor of Medicine Mayo Clinic Rochester, Minnesota, USA Endpoints Overview Hospitalization Surgery Colorectal cancer
Luminal Histological Outline and Colonic Adenoma Phenotypes
 Luminal Histological Outline and Colonic Adenoma Phenotypes CARLOS A. RUBIO Gastrointestinal and Liver Pathology Research Laboratory, Department of Pathology, Karolinska Institute and University Hospital,
Luminal Histological Outline and Colonic Adenoma Phenotypes CARLOS A. RUBIO Gastrointestinal and Liver Pathology Research Laboratory, Department of Pathology, Karolinska Institute and University Hospital,
Colorectal Cancer Prevention Quantity and Quality Count
 Colorectal Cancer Prevention Quantity and Quality Count Ernesto Drelichman, MD Gastrointestinal Surgery & Endoscopy Providence Hospital Key Messages Colorectal cancer can be prevented Screening reduces
Colorectal Cancer Prevention Quantity and Quality Count Ernesto Drelichman, MD Gastrointestinal Surgery & Endoscopy Providence Hospital Key Messages Colorectal cancer can be prevented Screening reduces
Phenotypic diverences in familial adenomatous polyposis based on APC gene mutation status
 Gut 1998;43:675 679 675 Research Group Human Genetics, University Hospital and Department of Human Genetics, University Children s Hospital, Basel, K Heinimann W Weber M Attenhofer Hj Müller Z Dobbie Department
Gut 1998;43:675 679 675 Research Group Human Genetics, University Hospital and Department of Human Genetics, University Children s Hospital, Basel, K Heinimann W Weber M Attenhofer Hj Müller Z Dobbie Department
Guidelines for Breast, Cervical and Colorectal Cancer Screening
 Guidelines for Breast, Cervical and Colorectal Cancer Screening Your recommendation counts. Talk to your patients about screening for cancer. CancerCare Manitoba provides organized, population-based screening
Guidelines for Breast, Cervical and Colorectal Cancer Screening Your recommendation counts. Talk to your patients about screening for cancer. CancerCare Manitoba provides organized, population-based screening
SMALL BOWEL ADENOCARCINOMA. Dr. C. Jeske
 SMALL BOWEL ADENOCARCINOMA Dr. C. Jeske Case presentation 54 year old female. Presents with OJ and weight loss. Abdominal examination only reveals a palpable gallbladder. ERCP reveals a circumferential
SMALL BOWEL ADENOCARCINOMA Dr. C. Jeske Case presentation 54 year old female. Presents with OJ and weight loss. Abdominal examination only reveals a palpable gallbladder. ERCP reveals a circumferential
HHS Public Access Author manuscript Gastrointest Endosc. Author manuscript; available in PMC 2015 April 29.
 Endoscopic papillectomy: risk factors for incomplete resection and recurrence during long-term follow-up Wiriyaporn Ridtitid, MD 1,2, Damien Tan, MD 1, Suzette E. Schmidt, BSN 1, Evan L. Fogel, MD 1, Lee
Endoscopic papillectomy: risk factors for incomplete resection and recurrence during long-term follow-up Wiriyaporn Ridtitid, MD 1,2, Damien Tan, MD 1, Suzette E. Schmidt, BSN 1, Evan L. Fogel, MD 1, Lee
Increased Prevalence of Colorectal Neoplasia in Korean Patients with Sporadic Duodenal Adenomas: A Case-Control Study
 Gut and Liver, Vol. 5, No. 4, December 2011, pp. 432-436 ORiginal Article Increased Prevalence of Colorectal Neoplasia in Korean Patients with Sporadic Duodenal Adenomas: A Case-Control Study Woo Chul
Gut and Liver, Vol. 5, No. 4, December 2011, pp. 432-436 ORiginal Article Increased Prevalence of Colorectal Neoplasia in Korean Patients with Sporadic Duodenal Adenomas: A Case-Control Study Woo Chul
Citation for published version (APA): Bartels, S. A. L. (2013). Laparoscopic colorectal surgery: beyond the short-term effects
 UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
MLH1 gene. Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Colorectal Cancer (HNPCC) MLH1 Summary Cancer Risk Table
 MLH1 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Cancer (HNPCC) MLH1 Summary Cancer Risk Table CANCER GENETIC CANCER RISK Endometrial Other MLH1 gene Overview Lynch syndrome 1,
MLH1 gene Associated Syndrome Name: Lynch syndrome/hereditary NonPolyposis Cancer (HNPCC) MLH1 Summary Cancer Risk Table CANCER GENETIC CANCER RISK Endometrial Other MLH1 gene Overview Lynch syndrome 1,
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE
 SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
F AP (familial adenomatous polyposis) is an autosomal
 97 CASE REPORT Intraductal papillary mucinous neoplasm of the pancreas in a patient with attenuated familial adenomatous polyposis R Chetty, S Salahshor, B Bapat, T Berk, M Croitoru, S Gallinger... A 67
97 CASE REPORT Intraductal papillary mucinous neoplasm of the pancreas in a patient with attenuated familial adenomatous polyposis R Chetty, S Salahshor, B Bapat, T Berk, M Croitoru, S Gallinger... A 67
White Rose Research Online URL for this paper: Version: Accepted Version
 This is a repository copy of Patients with Endoscopically Visible Polypoid Adenomatous Lesions Within the Extent of Ulcerative Colitis Have an Increased Risk of Colorectal Cancer Despite Endoscopic Resection.
This is a repository copy of Patients with Endoscopically Visible Polypoid Adenomatous Lesions Within the Extent of Ulcerative Colitis Have an Increased Risk of Colorectal Cancer Despite Endoscopic Resection.
The effectiveness of telephone reminders and SMS messages on compliance with colorectal cancer screening: an open-label, randomized controlled trial
 Page1 of 5 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 The effectiveness of telephone reminders and SMS messages on compliance with colorectal cancer screening: an
Page1 of 5 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 The effectiveness of telephone reminders and SMS messages on compliance with colorectal cancer screening: an
Screening for Colorectal Cancer in the Elderly. The Broad Perspective
 Screening for Colorectal Cancer in the Elderly Charles J. Kahi, MD, MSCR Indiana University School of Medicine Richard L. Roudebush VA Medical Center Indianapolis, Indiana ACG Regional Midwest Course Symposium
Screening for Colorectal Cancer in the Elderly Charles J. Kahi, MD, MSCR Indiana University School of Medicine Richard L. Roudebush VA Medical Center Indianapolis, Indiana ACG Regional Midwest Course Symposium
Colorectal Cancer Screening: Cost-Effectiveness and Adverse events October, 2005
 Colorectal Cancer Screening: Cost-Effectiveness and Adverse events October, 2005 David Lieberman MD Chief, Division of Gastroenterology Oregon Health and Science University Portland VAMC Portland, Oregon
Colorectal Cancer Screening: Cost-Effectiveness and Adverse events October, 2005 David Lieberman MD Chief, Division of Gastroenterology Oregon Health and Science University Portland VAMC Portland, Oregon
Pathology in Slovenian CRC screening programme:
 Pathology in Slovenian CRC screening programme: Findings, organisation and quality assurance Snježana Frković Grazio University Medical Center Ljubljana, Slovenia Slovenia s population: 2 million Incidence
Pathology in Slovenian CRC screening programme: Findings, organisation and quality assurance Snježana Frković Grazio University Medical Center Ljubljana, Slovenia Slovenia s population: 2 million Incidence
Colon and Rectum: 2018 Solid Tumor Rules
 2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING Colon and Rectum: 2018 Solid Tumor Rules 1 Colon and Rectum Solid Tumor Rules Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent
2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING Colon and Rectum: 2018 Solid Tumor Rules 1 Colon and Rectum Solid Tumor Rules Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent
Technical and Endoscopic Factors in. in CDH1 Mutation Carriers
 Technical and Endoscopic Factors in Gastric Cancer Surveillance in CDH Mutation Carriers Carol A. Burke,3,5, Michael Cruise 2,5, Lisa LaGuardia 3,5, Margaret O Malley 3,5, Matthew Kalady 3,5, James Church
Technical and Endoscopic Factors in Gastric Cancer Surveillance in CDH Mutation Carriers Carol A. Burke,3,5, Michael Cruise 2,5, Lisa LaGuardia 3,5, Margaret O Malley 3,5, Matthew Kalady 3,5, James Church
Extensive Surgery in LS factoring in gene and gender. Gabriela Möslein
 Extensive Surgery in LS factoring in gene and gender Gabriela Möslein Where we are coming from. Non polyposis colon cancer Recommend subtotal colectomy at the time of the first colon cancer Recommend prophylactic
Extensive Surgery in LS factoring in gene and gender Gabriela Möslein Where we are coming from. Non polyposis colon cancer Recommend subtotal colectomy at the time of the first colon cancer Recommend prophylactic
ACG Clinical Guideline: Colorectal Cancer Screening
 ACG Clinical Guideline: Colorectal Cancer Screening Douglas K. Rex, MD, FACG 1, David A. Johnson, MD, FACG 2, Joseph C. Anderson, MD 3, Phillip S. Schoenfeld, MD, MSEd, MSc (Epi), FACG 4, Carol A. Burke,
ACG Clinical Guideline: Colorectal Cancer Screening Douglas K. Rex, MD, FACG 1, David A. Johnson, MD, FACG 2, Joseph C. Anderson, MD 3, Phillip S. Schoenfeld, MD, MSEd, MSc (Epi), FACG 4, Carol A. Burke,
Detecting and managing hereditary colorectal cancer syndromes in your practice
 PERSONALIZING PATIENT CARE CME CREDIT EDUCATIONAL OBJECTIVE: Readers will assess their patients personal and family histories and suspect hereditary colorectal cancer syndromes if red flags are present
PERSONALIZING PATIENT CARE CME CREDIT EDUCATIONAL OBJECTIVE: Readers will assess their patients personal and family histories and suspect hereditary colorectal cancer syndromes if red flags are present
Principles of diagnosis, work-up and therapy The Gastroenterologist s role
 Principles of diagnosis, work-up and therapy The Gastroenterologist s role Dr. Christos G. Toumpanakis MD PhD FRCP Consultant in Gastroenterology/Neuroendocrine Tumours Hon. Senior Lecturer University
Principles of diagnosis, work-up and therapy The Gastroenterologist s role Dr. Christos G. Toumpanakis MD PhD FRCP Consultant in Gastroenterology/Neuroendocrine Tumours Hon. Senior Lecturer University
Twenty years of familial adenomatosis polyposis syndromes in the Singapore Polyposis Registry: an analysis of outcomes
 Original Article Singapore Med J 2011; 52(4) 246 Twenty years of familial adenomatosis polyposis syndromes in the Singapore Polyposis Registry: an analysis of outcomes Chew M H, Quah H Teh K L, Loi T T
Original Article Singapore Med J 2011; 52(4) 246 Twenty years of familial adenomatosis polyposis syndromes in the Singapore Polyposis Registry: an analysis of outcomes Chew M H, Quah H Teh K L, Loi T T
2018 National Academy of Medicine Annual Meeting
 2018 National Academy of Medicine Annual Meeting October 15, 2018 Targeting Cancer with Precision Prevention Ernest Hawk, M.D., M.P.H. What is Precision Prevention? The concept of precision medicine prevention
2018 National Academy of Medicine Annual Meeting October 15, 2018 Targeting Cancer with Precision Prevention Ernest Hawk, M.D., M.P.H. What is Precision Prevention? The concept of precision medicine prevention
Measuring the quality of colonoscopy: Where are we now and where are we going?
 Measuring the quality of colonoscopy: Where are we now and where are we going? Timothy D. Imler, MD Division of Gastroenterology and Hepatology, Indiana University School of Medicine, Indianapolis, Indiana
Measuring the quality of colonoscopy: Where are we now and where are we going? Timothy D. Imler, MD Division of Gastroenterology and Hepatology, Indiana University School of Medicine, Indianapolis, Indiana
Frameshift Mutations (Deletion at Codon 1309 and Codon 849) in the APC Gene in Iranian FAP Patients: a Case Series and Review of the Literature
 IJMCM Summer 2014, Vol 3, No 3 Case Series Frameshift Mutations (Deletion at Codon 1309 and Codon 849) in the APC Gene in Iranian FAP Patients: a Case Series and Review of the Literature Seyed Mohammad
IJMCM Summer 2014, Vol 3, No 3 Case Series Frameshift Mutations (Deletion at Codon 1309 and Codon 849) in the APC Gene in Iranian FAP Patients: a Case Series and Review of the Literature Seyed Mohammad
MULTIPLE CARCINOMAS OF THE LARGE INTESTINE- CASE REPORT AND A REVIEW OF THE LITERATURE
 MULTIPLE CARCINOMAS OF THE LARGE INTESTINE- CASE REPORT AND A REVIEW OF THE LITERATURE Abstract Pages with reference to book, From 147 To 149 Masood Hameed, Mushtaq Ahmed ( Surgical Unit I, Civil Hospital,
MULTIPLE CARCINOMAS OF THE LARGE INTESTINE- CASE REPORT AND A REVIEW OF THE LITERATURE Abstract Pages with reference to book, From 147 To 149 Masood Hameed, Mushtaq Ahmed ( Surgical Unit I, Civil Hospital,
