Original Paper. Urol Int 2017;98:40 48 DOI: /
|
|
|
- Lisa York
- 5 years ago
- Views:
Transcription
1 Urologia Internationalis Original Paper Urol Int 17;98: 48 DOI: / Received: March 29, 16 Accepted after revision: June 6, 16 Published online: August 4, 16 Differences in Patient Characteristics among Men Choosing Open or Robot-Assisted Radical Prostatectomy in Contemporary Practice Analysis of Surveillance, Epidemiology, and End Results Database Jonas Schiffmann a, d Alessandro Larcher a, e, f Maxine Sun a Zhe Tian a Jérémie Berdugo a, b Ion Leva a, b Hugues Widmer c Jean-Baptiste Lattouf c Kevin Zorn c Alexander Haese d Shahrokh F. Shariat g Fred Saad c Francesco Montorsi e, f Markus Graefen d Pierre I. Karakiewicz a, c a Cancer Prognostics and Health Outcomes Unit, b Department of Pathology, and c Department of Urology, University of Montreal Health Center, Montreal, Canada; d Martini-Clinic, Prostate Cancer Center Hamburg- Eppendorf, Hamburg, Germany; e Urological Research Institute, IRCCS Ospedale San Raffaele, and f Department of Urology, Vita-Salute San Raffaele University, Milan, Italy; g Department of Urology, Medical University of Vienna, Vienna, Austria Key Words Characteristics Open radical prostatectomy Pelvic lymph node dissection Prostate cancer Robot-assisted radical prostatectomy Abstract Objective: To examine characteristics of robot-assisted () and open radical prostatectomy () patients. Patients and Methods: We relied on the Surveillance, Epidemiology, and End Results-Medicare-linked database and focused on prostate cancer patients between 8 and 9. In multivariable logistic regression analyses, we predicted. Results: Of 5,915 patients, 3,476 (58.8) underwent and 2,439 (41.2). Patients within intermediate (OR 1.4, p =.1) or highest (OR 1.5, p =.2) education stra- ta and those treated by surgeons with a high volume (OR 2.2, p <.1) were more likely to undergo. Conversely, those residing in rural areas (OR.7, p =.5) and those with clinical stage T2 or higher (OR.7, p =.6) were less likely to undergo. Additionally, patients from the Southwest were less likely to undergo (OR.4, p <.1), but those from the Northern Plains were more likely to undergo (OR 1.4, p =.2) than their counterparts from the East. Finally, patients were neither younger nor healthier than patients. Conclusions: Several patient characteristics such as education, region of residence and population density affect the likelihood of vs. treatment. Similarly, clinical stage and surgeon characteristics also affect the assignment to one or other treatment modality. 16 S. Karger AG, Basel karger@karger.com 16 S. Karger AG, Basel Jonas Schiffmann, MD Martini-Clinic Prostate Cancer Center University Medical Center Hamburg-Eppendorf Martinistrasse 52, DE 246 Hamburg (Germany) klinikum-braunschweig.de
2 Introduction Radical prostatectomy (RP) represents the standard of care for localized prostate cancer (PCa) [1, 2]. Over the past decade, robot-assisted RP () has gradually replaced the traditional open RP () [3]. Despite the massive preference for, there are no randomized data supporting the benefit of relative to. Available population data demonstrate short-term advantages of relative to, such as fewer blood transfusions, fewer complications and shorter length of hospital stay [4]. Additionally, is at least equivalent [5] if not superior [6] to in terms of margin rates [7]. Moreover, the advantage of pelvic lymph node dissection (PLND) extent and/or yield at vs. is also being debated [8, 9]. For example, population-based studies observed an underuse of PLND at [1, 11]. Conversely, institutional data support the comparable feasibility of PLND at [12 14]. However, long-term data from the United States demonstrate urinary and erectile dysfunction benefits favoring [15]. These observations question the strong preference toward instead of. Since treatment decisions might be made on a subjective basis, it may be difficult to determine the characteristics of patients who opt for, instead of [16]. Based on these considerations, we decided to examine patient, clinical, pathological and surgical characteristics of individuals who either opt for or, within the most recent Surveillance, Epidemiology, and End Results (SEER)-Medicare linked database. Materials and Methods Population Sources This study relied on the most recent version of the SEER-Medicare linked database. The SEER registries cover approximately 28 of the United States population with Medicare administrative data. Medicare covers approximately 97 of Americans aged 65 years. Linkage to the SEER database is complete for approximately 93 of cases. [17]. Study Population Overall, 6,31 patients with histologically confirmed PCa (international classification of disease for oncology site code 61.9, histologic code 81) aged 65 years or older treated with RP from October 1, 8 to December 31, 9 were identified from the SEER-Medicare database. This time frame was selected as a specific modifier code for robotic-assisted approach was introduced on October 1, 8 (ICD-9 clinical modification procedure code: 17.42). The latter allows for accurate identification of. Patients who underwent were also abstracted. Exclusion criteria consisted of patients aged > years (n = 97), metastatic disease (n = 26), unknown tumor stage (n = 13), unknown tumor grade (n = 123), and unknown PLND status (n = 19). This resulted in 5,915 assessable patients. Covariates For each patient, age at diagnosis, race, population density (urban vs. rural), marital status (married vs. unmarried), census tract percent with 4-year college education (very low: 14.3, low: , high: and very high: 42.3), census tract annual median income, region of residence, pathological Gleason score, preoperative prostate-specific antigen (PSA), clinical and pathological tumor stage, PLND status, nodal stage, and surgical volume (low: 2, intermediate: 3 6 and high: 7 cases/ year) were assigned using the SEER data. The Charlson comorbidity index (CCI) was derived from the Medicare claims 1 year prior to PCa diagnosis, and categorized as, 1, 2, and 3, using a previously validated algorithm [18]. Statistical Analyses Means, medians and interquartile ranges were reported for continuous variables. Frequencies and proportions were reported for categorical variables. The independent t test and chi-square tests were used to compare the statistical significance of differences in means and proportions, respectively. Additionally, logistic regression analyses predicting were performed. Adjustment was made for surgical volume, region of residence, education, population density, clinical tumor stage, age, PSA, CCI, race, marital status and income. All statistical tests were performed using R. All tests were 2-sided with a significance level set at p <.5. Results Baseline Descriptives We identified 5,915 PCa patients treated with RP. Of these total number of patients, 2,439 (41.2) were treated with and 3,476 (58.8) with. Several important patient characteristics that distinguish between and were identified. patients had a lower median age (68 vs. 69 years, p =.4), without significant differences according to age categories (p =.2) compared to those who opted for. patients were more from the 2 highest income and education categories. Specifically, patients treated with were more frequently from the annual income category ranging from (US$) 5,955 69,389: 26. vs and that above 69,389: 29. vs (p <.1). Similarly, patients treated with were more frequently from the second highest (: 26.3 vs. : 23.4) and highest education strata (: 28.5 vs. :.5) than their counterparts treated with (p <.1). Additionally, patients treated with more frequently resided in urban centers (9.6 vs. 84.2, p < Patient Characteristics vs. Urol Int 17;98: 48 DOI: /
3 .1). Statistically significant differences emerged with respect to region of residence. For example, patients treated with were less likely to reside in the Southwest of the United States compared to patients treated with (3.4 vs. 11.5, p <.1). Of note is the absence of statistically significant or clinically meaningful differences with respect to age (65 66, 67 68, or 72 years) and CCI (, 1, 2 or 3). Regarding the clinical characteristics of patients treated with, we also identified several important observations. First, the serum PSA values of patient were more frequently 1 ng/ml (: 75. vs. 69.3, p <.1). Second, the clinical tumor stage distribution revealed that more patients harbored stages ct2a or lower at diagnosis (: 88.8 vs. : 84.9, p <.1). Finally, patients more frequently harbored a Gleason score 7 (85.8 vs. 83.4, p <.1). Last but not least, we also identified important pathological and surgical differences between and patients. For example, patients were more frequently diagnosed with pt3 stage than their counterparts (24.4 vs. 21.8, p =.6). The proportion of patients with missing pathological stage was lower at (6.4 vs. 8.2). Similarly, the proportion of PLND at was also statistically and significantly lower than at (49.4 vs. 71.8, p <.1). As a consequence, the rate of pathologically proven lymph node invasion (pn1) at RP was significantly lower at than at (1.4 vs. 3.4, p <.1). Finally, patients were more frequently treated by urologists within the highest surgeon volume tertile than patients (42.5 vs. 21.8, p <.1; table 1 ; fig. 1 ). Logistic Regression Analyses Predicting In the second part of the analyses, we relied on multivariable logistic regression models to predict the odds of undergoing instead of. According to these analyses, 5 predictors achieved independent predictor status: education level, region of residence, urban vs. rural population density, clinical T stage and surgical volume. Of patient characteristics (education, region of residence and population density), those within the highest and second highest education groups were respectively 1.5- and 1.4-fold more likely to undergo than patients from the very low education group (all p.2). Region of residence, specifically patients from the Southwest of the United States had a lower probability of undergoing relative to patients residing in the East (OR.4, 95 CI.3.6, p <.1). Finally, patients residing in rural areas were 3 less likely to undergo an compared to their counterparts from urban centers (OR.7, 95 CI.5.9, p =.5). Of clinical variables, clinical tumor stage achieved independent predictor status. Specifically, patients with ct2c or higher were less likely to undergo an then their counterparts with stage ct2a or lower (OR.7, 95 CI.5.9, p =.6). Additionally, individuals operated by surgeons within the highest surgical volume tertile were more likely to undergo then their counterparts treated by surgeons in the lowest volume tertile (OR 2.2, 95 CI , p <.1). Finally, neither age (65 66 vs. 72 years: OR.8, 95 CI.6 1., p =.59) nor CCI (CCI vs. 3: OR.9, 95 CI.7 1.2, p =.6) achieved independent predictor status ( table 2 ). Discussion To date there are no clearly established criteria for selecting over. We investigated patient characteristics within the SEER-Medicare linked database to examine potential differences between and patients. Our analyses detected several important findings. First, important patient characteristics differed between and. Specifically, patients were younger, had higher income, higher education, and were more likely to reside in urban areas than those who opted for. Taken together, these observations indicate that important patient characteristics may favor access to. Our data cannot determine whether such patients more aggressively seek or whether they are more frequently selected for by their treating surgeons. Second, patients treated with also had more favorable clinical characteristics. Specifically, patients more frequently had PSA 1 ng/ml (75. vs. 69.3, p <.1) and clinical tumor stage ct2a (88.8 vs. 84.9, p <.1) than patients. This observation may indicate a selection bias toward more favorable clinical characteristics when is contemplated. Alternatively, it may suggest that patients with more aggressive PCa characteristics opt for or that surgeons recommend to such patients more frequently. Third, with respect to pathological and surgical characteristics, a statistically and significantly lower proportion of patients with lymph node invasion were treated with (1.4 vs. 3.4, p <.1). The substantially lower rate of PLND within the patients (49.4 vs. 71.8, p <.1) explains the latter observation. Although, by itself should not limit PLND rates 42 Urol Int 17;98: 48 DOI: / Schiffmann et al.
4 Table 1. Descriptive statistics of 5,915 patients treated with RP for localized prostate cancer performed between October 1, 8 and December 31, 9, within the SEER-Medicare linked database stratified according to the surgical approach Parameter Overall (n = 5,915) (n = 2,439; 41.2) (n = 3,476; 58.8) p value Patient age, years.4 Mean (median) 69.1 (68.) 69.2 (69.) 69. (68.) IQR Range Patient age categories, n () ,498 (25.3) 4 (24.8) 894 (25.7) ,531 (25.9) 615 (25.2) 916 (26.4) ,55 (26.2) 637 (26.1) 913 (26.3) 72 1,336 (22.6) 583 (23.9) 753 (21.7) Race, n ().3 White 4,869 (82.3) 1,996 (81.8) 2,873 (82.7) Black 53 (9.) 235 (9.6) 295 (8.5) Other 516 (8.7) 8 (8.5) 38 (8.9) Marital status, n ().2 Married 4,6 (77.9) 1,8 (77.1) 2,726 (78.4) Unmarried 1,39 (22.1) 559 (22.9) 75 (21.6) Income in US$/year, n () <.1 38,12 1,4 (24.7) 73 (29.9) 73 (21.) 38,13 5,954 1,481 (25.) 648 (26.6) 833 (24.) 5,955 69,389 1,486 (25.1) 581 (23.8) 95 (26.) 69,39 1,488 (25.2) 4 (19.7) 1,8 (29.) Education, n () <.1 Very low 1,468 (24.8) 711 (29.2) 757 (21.8) Low 1,474 (24.9) 658 (27.) 816 (23.5) High 1,483 (25.1) 57 (23.4) 913 (26.3) Very high 1,49 (25.2) 5 (.5) 99 (28.5) Population density, n () <.1 Urban 5,2 (87.9) 2,53 (84.2) 3,149 (9.6) Rural 713 (12.1) 386 (15.8) 327 (9.4) Region of residence, n () <.1 East 2,48 (34.6) 4 (33.) 1,244 (35.8) Northern plains 5 (1.2) 221 (9.1) 384 (11.) Pacific coast 2,865 (48.4) 1,134 (46.5) 1,731 (49.8) Southwest 397 (6.7) 2 (11.5) 117 (3.4) CCI, n ().1 4, (69.) 1,648 (67.6) 2,432 (7.) 1 2 (1.2) 248 (1.2) 354 (1.2) (11.) 292 (12.) 361 (1.4) 3 5 (9.8) 251 (1.3) 329 (9.5) PSA, ng/ml, n () <.1 1 4,298 (72.7) 1,691 (69.3) 2,7 (75.) (11.6) 38 (12.6) 376 (1.8) > 286 (4.8) 146 (6.) 1 (4.) Unknown 647 (1.9) 294 (12.1) 353 (1.2) Clinical tumor stage, n () <.1 ct2a 5,155 (87.2) 2,7 (84.9) 3,85 (88.8) ct2b 156 (2.6) 74 (3.) 82 (2.4) ct2c 4 (1.2) 295 (12.1) 39 (8.9) Pelvic lymph node dissection, n () <.1 Performed 3,468 (58.6) 1,751 (71.8) 1,717 (49.4) Not performed 2,447 (41.4) 688 (28.2) 1,759 (5.6) Gleason score, n () <.1 6 1,783 (3.1) 779 (31.9) 1,4 (28.9) 7 3,235 (54.7) 1,257 (51.5) 1,978 (56.9) (15.2) 3 (16.5) 494 (14.2) Patient Characteristics vs. Urol Int 17;98: 48 DOI: /
5 Table 1. (continued) Parameter Overall (n = 5,915) (n = 2,439; 41.2) (n = 3,476; 58.8) p value Pathological tumor stage, n ().6 pt2 4,54 (68.5) 1,678 (68.8) 2,376 (68.4) pt3 1,3 (23.3) 532 (21.8) 848 (24.4) pt4 56 (.9) 28 (1.1) 28 (.8) Missing 425 (7.2) 1 (8.2) 224 (6.4) Nodal stage, n () <.1 pn/nx 5,786 (97.8) 2,357 (96.6) 3,429 (98.6) pn1 129 (2.2) 82 (3.4) 47 (1.4) Organ-confined tumor ( pt2, N/NX), n () 4,25 (68.) 1,658 (68.) 2,367 (68.1).9 Surgical volume, n () <.1 Low 875 (34.1) 423 (37.1) 452 (31.7) Intermediate 836 (32.6) 468 (41.1) 368 (25.8) High 854 (33.3) 248 (21.8) 6 (42.5) IQR = Interquartile range. [12 14], several authors reported lower PLND rates at than [1, 11, 19]. These differences may be due to a learning curve effect and may eventually disappear with increasing surgeon experience [14, ]. For now, if PLND is clearly indicated, might represent a safer choice. patients were also more likely to harbor more favorable Gleason score ( 7) (85.8 vs. 83.4, p <.1). Nonetheless, a surprisingly higher proportion of patients were classified as pathological tumor stage pt3 (24.4 vs. 21.8, p =.6). This finding appears counterintuitive, unless the pathological assessment of the specimens is more meticulous than that of specimens. It was not surprising to observe that a substantially and highly statistically and significantly higher proportion of patients were treated by high-volume surgeons (42.5 vs. 21.8, p <.1). This observation may suggest that is more frequently offered by highly skilled surgeons, who perform a higher number of s on an individual basis. To the best of our knowledge, this is the first study that relied on the SEER-Medicare database that focused on explicit differences between and patients. However, several other authors relied on the SEER-Medicare database to examine other endpoints, such as PLND and surgical volume [1, 11, 19]. For example, Hu et al. [19] relied on SEER-Medicare data of 5,448 PCa patients treated between 4 and 6 with either (72.5) or minimally invasive RP (MIRP) (27.5) without being able to truly identify due to the absence of specific codes. Overall, PLND was more frequently performed in patients treated with compared to those treated with MIRP ( vs. 43.3). Additionally, it was also recorded that MIRP was more often performed by surgeons from the highest surgical volume strata compared to those treated with (55. vs. 31.5, p <.1). Our analysis updates these findings with special focus on that is validated by the -specific code. Similarly, higher PLND rates at vs. were also recorded in single-institutional series [21 23]. Additionally, our data validate previous observations from institutional studies. For example, Sooriakumaran et al. [6] relied on 22,393 PCa patients treated between and 11 at 14 different centers of excellence. Of those, 7,697 (34.4) men were treated with, 4,918 (22.) with LARP and 9,778 (43.6) with, respectively. Patients who opted for were less likely to harbor high-risk PCa vs. those who opt for LARP respectively (7. vs vs. 13.3, p <.1). Unlike in our study, patients treated with were less likely to harbor pt3 disease (5. vs. 6.9 vs. 11.1, p <.1). Finally, like in our study, those patients who opted for were less likely to harbor Gleason score 8 (7.7 vs. 6.2 vs. 1., p <.1). Regarding age, Smith et al. [24] compared 1,747 PCa patients treated at a single institution between 2 and 6 with either (n = 1,238) or (n = 59). Unlike in our study, no differences according to age were recorded between and patients (p =.3). Sev- 44 Urol Int 17;98: 48 DOI: / Schiffmann et al.
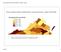
6 38,12 US$/year years years years 72 years White Black Other 38,13 5,954 US$/year 5,955 69,389 US$/year 69,39 US$/year a p =.2 b p =.3 c p <.1 d Very low Low High Very high p <.1 e Urban centers Rural areas p <.1 f Low Intermediate High p <.1 g PSA <1 ng/ml PSA > ng/ml PSA 1 ng/ml Unknown p <.1 h >ct2b ct2b <ct2b p <.1 i Gleason score 6 Gleason score 7 Gleason score 8 1 p <.1 j Unknown pt2 pt3 pt4 p =.6 k pno/x pn1 p <.1 l PLND No PLND p <.1 Fig. 1. Descriptive differences between 5,915 PCa patients treated with RP performed between October 1, 8 and December 31, 9, within the SEER-Medicare linked database stratified according to vs., according to age ( a ), race ( b ), annual income ( c ), education ( d ), population density ( e ), surgical volume ( f ), PSA level ( g ), clinical tumor stage ( h ), Gleason score ( i ), pathological tumor stage ( j ), nodal stage ( k ) and PLND ( l ), respectively. eral others also found no significant differences in age between and patients [21, 24]. Conversely, with respect to age and comorbidities, Briganti et al. [22] found patients were younger and healthier. The authors relied on 2,511 PCa patients treated between 6 and 1 with either (25.4) or (74.6) at a single institution. patients were younger (median 62.6 vs years, p <.1), healthier (CCI 2: 6.9 vs. 1.9, p <.1), had lower median body mass index (25 vs. 26, p <.1) and were Patient Characteristics vs. Urol Int 17;98: 48 DOI: /
7 Table 2. Univariable and multivariable logistic regression analyses evaluating the predictors of in 5,915 patients treated with RP for localized prostate cancer between October 1, 8 and December 31, 9, within the SEER-Medicare-linked database Univariable analyses Multivariable analyses OR (95 CI) p value OR (95 CI) p value Surgical volume Low 1 (ref.) 1 (ref.) Intermediate.7 (.6.9).2.7 (.6.9).1 High 2.9 ( ) < ( ) <.1 Region of residence East 1 (ref.) 1 (ref.) Norther plain 1.1 (.9 1.4) ( ).2 Pacific coast 1. (.9 1.1).8.9 (.7 1.1).3 Southwest.3 (.2.3).3.4 (.3.6) <.1 Education Very low 1 (ref.) 1 (ref.) Low 1.2 (1. 1.3) (.8 1.3).7 High 1.5 ( ) < ( ).1 Very high 1.9 ( ) < ( ).2 Population density Urban 1 (ref.) 1 (ref.) Rural.6 (.5.7) <.1.7 (.5.9).5 Clinical tumor stage ct2a 1 (ref.) 1 (ref.) ct2b.7 (.5 1.).7.6 (.4 1.).53 ct2c.7 (.6.8) <.1.7 (.5.9).6 Patient age, years (ref.) 1 (ref.) (.9 1.2).9.9 (.7 1.1) (.8 1.1).7.8 (.7 1.1) (.8 1.).7.8 (.6 1.).59 PSA, ng/ml <1 1 (ref.) 1 (ref.) 1.8 (.7.9).5.98 (.8 1.3).9 >.6 (.5.8) <.1.8 (.6 1.2).3 Unknown.8 (.7.9).3.8 (.6 1.).7 CCI 1 (ref.) 1 (ref.) 1 1. (.8 1.2).7.9 (.7 1.2) (.7 1.).4.8 (.6 1.) (.8 1.1).2.9 (.7 1.2).6 Race White 1 (ref.) 1 (ref.) Black.9 (.7 1.1).1.9 (.7 1.2).5 Other 1. (.9 1.2) (.9 1.6).3 Marital status Married 1 (ref.) 1 (ref.) Unmarried.9 (.8 1.1).2.96 (.8 1.2).7 Income in US$/year 38,12 1 (ref.) 1 (ref.) 38,13 5, ( ).1.99 (.8 1.3).97 5,955 69, ( ) < ( ).1 69, ( ) < (.9 1.8).2 46 Urol Int 17;98: 48 DOI: / Schiffmann et al.
8 less likely to harbor high-risk PCa (5.8 vs. 24.1, p <.1) compared to those treated with. The clinical implications of our findings are manifold. First, our findings show that higher education provides better access to. This finding warrants attention at the level of access to. Less well-educated individuals should be given higher consideration or should be encouraged to opt for, if indicated. Second, more favorable clinical characteristics of patients indicate a selection bias toward better surgical candidates. This dissemination may indicate that surgeons prefer to treat patients with more favorable characteristics. Alternatively, this may indicate that surgeons avoid operating patients with more complex or challenging pathology. Third, lower rates of PLND indicate the potentially increased technical difficulty of vs.. The highly significant difference in PLND rates cannot be expected by more favorable clinical stage prior to, alone. Despite its strengths, our study has limitations. First, our cohort exclusively originates from the Medicare, with an age distribution of over 65 years. The results might not be generalizable to younger patients. However, PCa rates are highest in people aged years with a median age at diagnosis of 66 years [25]. Second, additional limitations, known to affect SEER-Medicare derived analyses are also operational, such as for example use of claims data or lack of detailed parameters that are included in prospective trials. For example, the individual access to treatment or distance to next from the region of residence was not available within our data. Additionally, we cannot report if patients had to pay an additional fee to be treated with. Third, since availability of may differ substantially in other countries, our results might not be generalizable to other populations. Finally, other limitations are also operational. Conclusion may be preferred by highly educated, urban residents from the East or Northern Plains of the United States. Those individuals may have better access to. Additionally, is more frequently performed in patients with more favorable PCa characteristics and patients are more frequently treated by surgeons with a high volume of patients. Conversely, patients less frequently benefit from PLND. These observations warrant further attention to decrease the effect of potential barriers to and/or optimize use. Disclosure Statement and Ethical Standards The authors declare that there are no financial disclosures or conflict of interest regarding this manuscript. The study was performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. References 1 Mohler J, Bahnson RR, Boston B, et al: NCCN clinical practice guidelines in oncology: prostate cancer. J Natl Compr Canc Netw 1; 8: Heidenreich A, Bastian PJ, Bellmunt J, et al: EAU guidelines on prostate cancer. Part 1: screening, diagnosis, and local treatment with curative intent-update 13. Eur Urol 14; 65: Lowrance WT, Eastham JA, Savage C, et al: Contemporary open and robotic radical prostatectomy practice patterns among urologists in the United States. J Urol 12; 187: Trinh QD, Sammon J, Sun M, et al: Perioperative outcomes of robot-assisted radical prostatectomy compared with open radical prostatectomy: results from the nationwide inpatient sample. Eur Urol 12; 61: Tewari A, Sooriakumaran P, Bloch DA, et al: Positive surgical margin and perioperative complication rates of primary surgical treatments for prostate cancer: a systematic review and meta-analysis comparing retropubic, laparoscopic, and robotic prostatectomy. Eur Urol 12; 62: Sooriakumaran P, Srivastava A, Shariat SF, et al: A multinational, multi-institutional study comparing positive surgical margin rates among open, laparoscopic, and robotassisted radical prostatectomy patients. Eur Urol 14; 66: Bütow Z, Schunk S, Janssen M, et al: Quality of preoperative biopsy is a risk factor for positive surgical margins in organ-confined prostate cancer treated with nerve-sparing robot-assisted radical prostatectomy. Urol Int 15; 95: Schiffmann J, Haese A, Leyh-Bannurah SR, et al: Adherence of the indication to European Association of Urology guideline recommended pelvic lymph node dissection at a high-volume center: differences between open and robot-assisted radical prostatectomy. Eur J Surg Oncol 15; 41: Schiffmann J, Haese A, Lenz J, et al: Differences in patient characteristics among men choosing open or robot-assisted radical prostatectomy in contemporary practice at a European high-volume center. Urol Int 16; 97: Gandaglia G, Trinh QD, Hu JC, et al: The impact of robot-assisted radical prostatectomy on the use and extent of pelvic lymph node dissection in the post-dissemination period. Eur J Surg Oncol 14; : Feifer AH, Elkin EB, Lowrance WT, et al: Temporal trends and predictors of pelvic lymph node dissection in open or minimally invasive radical prostatectomy. Cancer 11; 117: Yee DS, Katz DJ, Godoy G, et al: Extended pelvic lymph node dissection in robotic-assisted radical prostatectomy: surgical technique and initial experience. Urology 1; 75: Patient Characteristics vs. Urol Int 17;98: 48 DOI: /
9 13 Feicke A, Baumgartner M, Talimi S, et al: Robotic-assisted laparoscopic extended pelvic lymph node dissection for prostate cancer: surgical technique and experience with the first 99 cases. Eur Urol 9; 55: Ploussard G, Briganti A, de la Taille A, et al: Pelvic lymph node dissection during robotassisted radical prostatectomy: efficacy, limitations, and complications-a systematic review of the literature. Eur Urol 14; 65: Hu JC, Gu X, Lipsitz SR, et al: Comparative effectiveness of minimally invasive vs open radical prostatectomy. JAMA 9; 32: Fowler FJ Jr, Gerstein BS, Barry MJ: How patient centered are medical decisions?: results of a national survey. JAMA Intern Med 13; 173: Warren JL, Klabunde CN, Schrag D, et al: Overview of the SEER-Medicare data: content, research applications, and generalizability to the United States elderly population. Med Care 2; (8 suppl):iv-3 IV Klabunde CN, Potosky AL, Legler JM, et al: Development of a comorbidity index using physician claims data. J Clin Epidemiol ; 53: Hu JC, Prasad SM, Gu X, et al: Determinants of performing radical prostatectomy pelvic lymph node dissection and the number of lymph nodes removed in elderly men. Urology 11; 77: 2 6. Merseburger AS, Herrmann TR, Shariat SF, et al: EAU guidelines on robotic and single-site surgery in urology. Eur Urol 13; 64: Williams SB, Chen MH, D Amico AV, et al: Radical retropubic prostatectomy and robotic-assisted laparoscopic prostatectomy: likelihood of positive surgical margin(s). Urology 1; 76: Briganti A, Bianchi M, Sun M, et al: Impact of the introduction of a robotic training programme on prostate cancer stage migration at a single tertiary referral centre. BJU Int 13; 111: Cooperberg MR, Kane CJ, Cowan JE, et al: Adequacy of lymphadenectomy among men undergoing robot-assisted laparoscopic radical prostatectomy. BJU Int 1; 15: Smith JA Jr, Chan RC, Chang SS, et al: A comparison of the incidence and location of positive surgical margins in robotic assisted laparoscopic radical prostatectomy and open retropubic radical prostatectomy. J Urol 7; 178: ; discussion Howlader NNA, Krapcho M, Garshell J, Neyman N, Altekruse SF, Kosary CL, Yu M, Ruhl J, Tatalovich Z, Cho H, Mariotto A, Lewis DR, Chen HS, Feuer EJ, Cronin KA (eds): SEER Cancer Statistics Review, National Cancer Institute. csr/1975_1/, based on November 12 SEER data submission, posted to the SEER web site, Urol Int 17;98: 48 DOI: / Schiffmann et al.
State-of-the-art: vision on the future. Urology
 State-of-the-art: vision on the future Urology Francesco Montorsi MD FRCS Professor and Chairman Department of Urology San Raffaele Hospital Vita-Salute San Raffaele University Milan, Italy Disclosures
State-of-the-art: vision on the future Urology Francesco Montorsi MD FRCS Professor and Chairman Department of Urology San Raffaele Hospital Vita-Salute San Raffaele University Milan, Italy Disclosures
NIH Public Access Author Manuscript World J Urol. Author manuscript; available in PMC 2012 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
EUROPEAN UROLOGY 61 (2012)
 EUROPEAN UROLOGY 61 (2012) 480 487 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by A. Heidenreich on pp. 488 490 of this issue
EUROPEAN UROLOGY 61 (2012) 480 487 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by A. Heidenreich on pp. 488 490 of this issue
Best Papers. F. Fusco
 Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
Best Papers UROLOGY F. Fusco Best papers - 2015 RP/RT Oncological outcomes RP/RT IN ct3 Utilization trends RP/RT Complications Evolving role of elnd /Salvage LND This cohort reflects the current clinical
The Impact of Insurance Status on Tumor Characteristics and Treatment Selection in Contemporary Patients With Prostate Cancer
 Original Research 1351 The Impact of Insurance Status on Tumor Characteristics and Treatment Selection in Contemporary Patients With Prostate Cancer Nicola Fossati, MD a,b ; Daniel P. Nguyen, MD c ; Quoc-Dien
Original Research 1351 The Impact of Insurance Status on Tumor Characteristics and Treatment Selection in Contemporary Patients With Prostate Cancer Nicola Fossati, MD a,b ; Daniel P. Nguyen, MD c ; Quoc-Dien
Predictors of Palliative Therapy Receipt in Stage IV Colorectal Cancer
 Predictors of Palliative Therapy Receipt in Stage IV Colorectal Cancer Osayande Osagiede, MBBS, MPH 1,2, Aaron C. Spaulding, PhD 2, Ryan D. Frank, MS 3, Amit Merchea, MD 1, Dorin Colibaseanu, MD 1 ACS
Predictors of Palliative Therapy Receipt in Stage IV Colorectal Cancer Osayande Osagiede, MBBS, MPH 1,2, Aaron C. Spaulding, PhD 2, Ryan D. Frank, MS 3, Amit Merchea, MD 1, Dorin Colibaseanu, MD 1 ACS
Comparison of open and robotic-assisted prostatectomy: The University of British Columbia experience
 Original research Comparison of open and robotic-assisted prostatectomy: The University of British Columbia experience Louis-Olivier Gagnon, MD; S. Larry Goldenberg, MD, FRCSC; Kenny Lynch, MD; Antonio
Original research Comparison of open and robotic-assisted prostatectomy: The University of British Columbia experience Louis-Olivier Gagnon, MD; S. Larry Goldenberg, MD, FRCSC; Kenny Lynch, MD; Antonio
Correspondence should be addressed to Taha Numan Yıkılmaz;
 Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
A Non Cancer-Related Survival Benefit Is Associated With Partial Nephrectomy
 EUROPEAN UROLOGY 61 (2012) 725 731 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Kidney Cancer Editorial by Alexander Kutikov, Marc C. Smaldone, Brian L.
EUROPEAN UROLOGY 61 (2012) 725 731 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Kidney Cancer Editorial by Alexander Kutikov, Marc C. Smaldone, Brian L.
Conclusions. Keywords
 The impact of androgen-deprivation therapy (ADT) on the risk of cardiovascular (CV) events in patients with non-metastatic prostate cancer: a population-based study Giorgio Gandaglia*, Maxine Sun*, Ioana
The impact of androgen-deprivation therapy (ADT) on the risk of cardiovascular (CV) events in patients with non-metastatic prostate cancer: a population-based study Giorgio Gandaglia*, Maxine Sun*, Ioana
How to select the right patient for the right treatment: What role does sexuality play in Pca treatment?
 How to select the right patient for the right treatment: What role does sexuality play in Pca treatment? Andrea Salonia, MD, PhD, FECSM Università Vita-Salute San Raffaele Director, URI-Urological Research
How to select the right patient for the right treatment: What role does sexuality play in Pca treatment? Andrea Salonia, MD, PhD, FECSM Università Vita-Salute San Raffaele Director, URI-Urological Research
External validation of the Briganti nomogram to estimate the probability of specimen-confined disease in patients with high-risk prostate cancer
 External validation of the Briganti nomogram to estimate the probability of specimen-confined disease in patients with high-risk prostate cancer Mathieu Roumiguié, Jean-Baptiste Beauval, Thomas Filleron*,
External validation of the Briganti nomogram to estimate the probability of specimen-confined disease in patients with high-risk prostate cancer Mathieu Roumiguié, Jean-Baptiste Beauval, Thomas Filleron*,
Patterns and Correlates of Prostate Cancer Treatment in Older Men
 CLINICAL RESEARCH STUDY Patterns and Correlates of Prostate Cancer Treatment in Older Men Calpurnyia B. Roberts, PhD, a,b Peter C. Albertsen, MD, c Yu-Hsuan Shao, PhD, d Dirk F. Moore, PhD, d,g Amit R.
CLINICAL RESEARCH STUDY Patterns and Correlates of Prostate Cancer Treatment in Older Men Calpurnyia B. Roberts, PhD, a,b Peter C. Albertsen, MD, c Yu-Hsuan Shao, PhD, d Dirk F. Moore, PhD, d,g Amit R.
Original Paper. Urol Int 2015;95: DOI: /
 Urologia Internationalis Original Paper Published online: July 3, 2015 First Nomogram Predicting the Probability of Lymph Node Involvement in Prostate Cancer Patients Undergoing Radioisotope Guided Sentinel
Urologia Internationalis Original Paper Published online: July 3, 2015 First Nomogram Predicting the Probability of Lymph Node Involvement in Prostate Cancer Patients Undergoing Radioisotope Guided Sentinel
Lung and Bronchus Cancer Statistics in Virginia - Maps. July
 July 2011 4 July 2011 5 July 2011 6 July 2011 7 Lung and Bronchus Cancer Statistics in Virginia - Notes Sources: Incidence and percent local staging (VA Cancer Registry); mortality (VDH Division of Health
July 2011 4 July 2011 5 July 2011 6 July 2011 7 Lung and Bronchus Cancer Statistics in Virginia - Notes Sources: Incidence and percent local staging (VA Cancer Registry); mortality (VDH Division of Health
ABSTRACT ORIGINAL RESEARCH. Margit Pohle. Ahmed Magheli. Tom Fischer. Carsten Kempkensteffen. Jonas Busch. Hannes Cash. Kurt Miller.
 Adv Ther (2017) 34:576 585 DOI 10.1007/s12325-016-0469-4 ORIGINAL RESEARCH The Effect of Evolving Strategies in the Surgical Management of Organ-Confined Prostate Cancer: Comparison of Data from 2005 to
Adv Ther (2017) 34:576 585 DOI 10.1007/s12325-016-0469-4 ORIGINAL RESEARCH The Effect of Evolving Strategies in the Surgical Management of Organ-Confined Prostate Cancer: Comparison of Data from 2005 to
da Vinci Surgery in Urology Clinical Literature, Health Economics and HTA update 2011 to 2013
 da Vinci Surgery in Urology Clinical Literature, Health Economics and HTA update 2011 to 2013 Robotic surgery s primary contribution has centered on its ability to enable complex surgeries to be performed
da Vinci Surgery in Urology Clinical Literature, Health Economics and HTA update 2011 to 2013 Robotic surgery s primary contribution has centered on its ability to enable complex surgeries to be performed
J Clin Oncol 25: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 25 NUMBER 24 AUGUST 20 2007 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T A Nomogram Predicting 10-Year Life Expectancy in Candidates for Radical Prostatectomy or Radiotherapy for Prostate
VOLUME 25 NUMBER 24 AUGUST 20 2007 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T A Nomogram Predicting 10-Year Life Expectancy in Candidates for Radical Prostatectomy or Radiotherapy for Prostate
Robotic assisted pelvic lymph node dissection for prostate cancer: frequency of nodal metastases and oncological outcomes
 UROLCHI World J Urol DOI 10.1007/s00345-015-1515-6 ORIGINAL ARTICLE Robotic assisted pelvic lymph node dissection for prostate cancer: frequency of nodal metastases and oncological outcomes Rodrigo A.
UROLCHI World J Urol DOI 10.1007/s00345-015-1515-6 ORIGINAL ARTICLE Robotic assisted pelvic lymph node dissection for prostate cancer: frequency of nodal metastases and oncological outcomes Rodrigo A.
National Trends in the Management of Low and Intermediate Risk Prostate Cancer in the United States
 National Trends in the Management of Low and Intermediate Risk Prostate Cancer in the United States Adam B. Weiner, Sanjay G. Patel, Ruth Etzioni and Scott E. Eggener* From the Pritzker School of Medicine
National Trends in the Management of Low and Intermediate Risk Prostate Cancer in the United States Adam B. Weiner, Sanjay G. Patel, Ruth Etzioni and Scott E. Eggener* From the Pritzker School of Medicine
Factors Associated with Initial Treatment for Clinically Localized Prostate Cancer
 Factors Associated with Initial Treatment for Clinically Localized Prostate Cancer Preliminary Results from the National Program of Cancer Registries Patterns of Care Study (PoC1) NAACCR Annual Meeting
Factors Associated with Initial Treatment for Clinically Localized Prostate Cancer Preliminary Results from the National Program of Cancer Registries Patterns of Care Study (PoC1) NAACCR Annual Meeting
A Nomogram Predicting Long-term Biochemical Recurrence After Radical Prostatectomy
 1254 A Nomogram Predicting Long-term Biochemical Recurrence After Radical Prostatectomy Nazareno Suardi, MD 1,2 Christopher R. Porter, MD 3 Alwyn M. Reuther, MD 4 Jochen Walz, MD 1,5 Koichi Kodama, MD
1254 A Nomogram Predicting Long-term Biochemical Recurrence After Radical Prostatectomy Nazareno Suardi, MD 1,2 Christopher R. Porter, MD 3 Alwyn M. Reuther, MD 4 Jochen Walz, MD 1,5 Koichi Kodama, MD
Objective. Patients and Methods. Conclusion. Results. Keywords. Introduction
 Functional and oncological outcomes of patients aged
Functional and oncological outcomes of patients aged
Overview of All SEER-Medicare Publications
 Overview of All SEER-Medicare Publications Outcomes Insights, Inc. Mark D. Danese, MHS, PhD Claire Cangialose February 22, 2017 Overview Information was extracted from the National Cancer Institute (NCI)
Overview of All SEER-Medicare Publications Outcomes Insights, Inc. Mark D. Danese, MHS, PhD Claire Cangialose February 22, 2017 Overview Information was extracted from the National Cancer Institute (NCI)
Predictors of time to biochemical recurrence in a radical prostatectomy cohort within the PSA-era
 ORIGINAL RESEARCH Predictors of time to biochemical recurrence in a radical prostatectomy cohort within the PSA-era Ahva Shahabi, MPH, PhD; 1* Raj Satkunasivam, MD; 2* Inderbir S. Gill, MD; 2 Gary Lieskovsky,
ORIGINAL RESEARCH Predictors of time to biochemical recurrence in a radical prostatectomy cohort within the PSA-era Ahva Shahabi, MPH, PhD; 1* Raj Satkunasivam, MD; 2* Inderbir S. Gill, MD; 2 Gary Lieskovsky,
concordance indices were calculated for the entire model and subsequently for each risk group.
 ; 2010 Urological Oncology ACCURACY OF KATTAN NOMOGRAM KORETS ET AL. BJUI Accuracy of the Kattan nomogram across prostate cancer risk-groups Ruslan Korets, Piruz Motamedinia, Olga Yeshchina, Manisha Desai
; 2010 Urological Oncology ACCURACY OF KATTAN NOMOGRAM KORETS ET AL. BJUI Accuracy of the Kattan nomogram across prostate cancer risk-groups Ruslan Korets, Piruz Motamedinia, Olga Yeshchina, Manisha Desai
EUROPEAN UROLOGY 60 (2011)
 EUROPEAN UROLOGY 60 (2011) 920 930 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by Monique J. Roobol and Eveline A.M. Heijnsdijk
EUROPEAN UROLOGY 60 (2011) 920 930 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by Monique J. Roobol and Eveline A.M. Heijnsdijk
Comparative Analysis Research of Robotic Assisted Laparoscopic Prostatectomy
 Comparative Analysis Research of Robotic Assisted Laparoscopic Prostatectomy By: Jonathan Barlaan; Huy Nguyen Mentor: Julio Powsang, MD Reader: Richard Wilder, MD May 2, 211 Abstract Introduction: The
Comparative Analysis Research of Robotic Assisted Laparoscopic Prostatectomy By: Jonathan Barlaan; Huy Nguyen Mentor: Julio Powsang, MD Reader: Richard Wilder, MD May 2, 211 Abstract Introduction: The
Colorectal Cancer Statistics in Virginia - Maps. July
 July 2011 5 July 2011 6 July 2011 7 July 2011 8 Colorectal Cancer Statistics in Virginia - Notes Sources: Incidence and percent local staging (VA Cancer Registry); mortality (VDH Division of Health Statistics);
July 2011 5 July 2011 6 July 2011 7 July 2011 8 Colorectal Cancer Statistics in Virginia - Notes Sources: Incidence and percent local staging (VA Cancer Registry); mortality (VDH Division of Health Statistics);
The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters.
 An Exploration of Risk Stratification for Active Surveillance and Androgen Deprivation Therapy Side Effects for Prostate Cancer Utilizing Data From the Surveillance, Epidemiology, and End Results Database
An Exploration of Risk Stratification for Active Surveillance and Androgen Deprivation Therapy Side Effects for Prostate Cancer Utilizing Data From the Surveillance, Epidemiology, and End Results Database
CONTEMPORARY UPDATE OF PROSTATE CANCER STAGING NOMOGRAMS (PARTIN TABLES) FOR THE NEW MILLENNIUM
 RAPID COMMUNICATION CME ARTICLE CONTEMPORARY UPDATE OF PROSTATE CANCER STAGING NOMOGRAMS (PARTIN TABLES) FOR THE NEW MILLENNIUM ALAN W. PARTIN, LESLIE A. MANGOLD, DANA M. LAMM, PATRICK C. WALSH, JONATHAN
RAPID COMMUNICATION CME ARTICLE CONTEMPORARY UPDATE OF PROSTATE CANCER STAGING NOMOGRAMS (PARTIN TABLES) FOR THE NEW MILLENNIUM ALAN W. PARTIN, LESLIE A. MANGOLD, DANA M. LAMM, PATRICK C. WALSH, JONATHAN
Early radical cystectomy in NMIBC Marko Babjuk
 Early radical cystectomy in NMIBC Marko Babjuk Dept. of Urology, 2nd Faculty of Medicine, Hospital Motol, Praha, Czech Republic We Are The European Association of Urology We Are Urologists, residents,
Early radical cystectomy in NMIBC Marko Babjuk Dept. of Urology, 2nd Faculty of Medicine, Hospital Motol, Praha, Czech Republic We Are The European Association of Urology We Are Urologists, residents,
Clinical Study Oncologic Outcomes of Surgery in T3 Prostate Cancer: Experience of a Single Tertiary Center
 Advances in Urology Volume 22, Article ID 64263, 8 pages doi:.55/22/64263 Clinical Study Oncologic Outcomes of Surgery in T3 Prostate Cancer: Experience of a Single Tertiary Center D. Milonas, G. Smailyte,
Advances in Urology Volume 22, Article ID 64263, 8 pages doi:.55/22/64263 Clinical Study Oncologic Outcomes of Surgery in T3 Prostate Cancer: Experience of a Single Tertiary Center D. Milonas, G. Smailyte,
da Vinci Prostatectomy My Greek personal experience
 da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
da Vinci Prostatectomy My Greek personal experience Vassilis Poulakis MD, PhD, FEBU Ass. Prof. of Urology Director of Urologic Clinic Doctors Hospital Athens Laparoscopy - golden standard in Urology -
Introduction. Original Article
 bs_bs_banner International Journal of Urology (2015) 22, 363 367 doi: 10.1111/iju.12704 Original Article Prostate-specific antigen level, stage or Gleason score: Which is best for predicting outcomes after
bs_bs_banner International Journal of Urology (2015) 22, 363 367 doi: 10.1111/iju.12704 Original Article Prostate-specific antigen level, stage or Gleason score: Which is best for predicting outcomes after
Role and extension of lymph node dissection in kidney, bladder and prostate cancer. Omar Ghanem (PGY3 ) Moderator: Dr A. Noujem 30 th March 2017
 Role and extension of lymph node dissection in kidney, bladder and prostate cancer Omar Ghanem (PGY3 ) Moderator: Dr A. Noujem 30 th March 2017 Bladder Cancer LN dissection in Bladder cancer 25% of patients
Role and extension of lymph node dissection in kidney, bladder and prostate cancer Omar Ghanem (PGY3 ) Moderator: Dr A. Noujem 30 th March 2017 Bladder Cancer LN dissection in Bladder cancer 25% of patients
Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery
 Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Prostate Cancer Your prostate is a walnut-sized gland that is part of the male reproductive system. The prostate
Facing Prostate Cancer Surgery? Learn about minimally invasive da Vinci Surgery The Condition: Prostate Cancer Your prostate is a walnut-sized gland that is part of the male reproductive system. The prostate
Preoperative Gleason score, percent of positive prostate biopsies and PSA in predicting biochemical recurrence after radical prostatectomy
 JBUON 2013; 18(4): 954-960 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Gleason score, percent of positive prostate and PSA in predicting biochemical
JBUON 2013; 18(4): 954-960 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Gleason score, percent of positive prostate and PSA in predicting biochemical
Biochemical recurrence-free survival and pathological outcomes after radical prostatectomy for high-risk prostate cancer
 Beauval et al. BMC Urology (2016) 16:26 DOI 10.1186/s12894-016-0146-6 RESEARCH ARTICLE Open Access Biochemical recurrence-free survival and pathological outcomes after radical prostatectomy for high-risk
Beauval et al. BMC Urology (2016) 16:26 DOI 10.1186/s12894-016-0146-6 RESEARCH ARTICLE Open Access Biochemical recurrence-free survival and pathological outcomes after radical prostatectomy for high-risk
DAYS IN PANCREATIC CANCER
 HOSPITAL AND MEDICAL CARE DAYS IN PANCREATIC CANCER Annals of Surgical Oncology, March 27, 2012 Casey B. Duncan, Kristin M. Sheffield, Daniel W. Branch, Yimei Han, Yong-Fang g Kuo, James S. Goodwin, Taylor
HOSPITAL AND MEDICAL CARE DAYS IN PANCREATIC CANCER Annals of Surgical Oncology, March 27, 2012 Casey B. Duncan, Kristin M. Sheffield, Daniel W. Branch, Yimei Han, Yong-Fang g Kuo, James S. Goodwin, Taylor
Hospitalization Costs for Radical Prostatectomy Attributable to Robotic Surgery
 EUROPEAN UROLOGY 64 (2013) 11 16 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by Yair Lotan on pp. 17 18 of this issue Hospitalization
EUROPEAN UROLOGY 64 (2013) 11 16 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by Yair Lotan on pp. 17 18 of this issue Hospitalization
Oncologic Outcome of Robot-Assisted Laparoscopic Prostatectomy in the High-Risk Setting
 END-2010-0305-ver9-Engel_1P.3d 09/17/10 2:42pm Page 1 END-2010-0305-ver9-Engel_1P Type: research-article JOURNAL OF ENDOUROLOGY Volume 24, Number 00, XXXX 2010 ª Mary Ann Liebert, Inc. Pp. &&& &&& DOI:
END-2010-0305-ver9-Engel_1P.3d 09/17/10 2:42pm Page 1 END-2010-0305-ver9-Engel_1P Type: research-article JOURNAL OF ENDOUROLOGY Volume 24, Number 00, XXXX 2010 ª Mary Ann Liebert, Inc. Pp. &&& &&& DOI:
Information Content of Five Nomograms for Outcomes in Prostate Cancer
 Anatomic Pathology / NOMOGRAMS IN PROSTATE CANCER Information Content of Five Nomograms for Outcomes in Prostate Cancer Tarek A. Bismar, MD, 1 Peter Humphrey, MD, 2 and Robin T. Vollmer, MD 3 Key Words:
Anatomic Pathology / NOMOGRAMS IN PROSTATE CANCER Information Content of Five Nomograms for Outcomes in Prostate Cancer Tarek A. Bismar, MD, 1 Peter Humphrey, MD, 2 and Robin T. Vollmer, MD 3 Key Words:
A comparison of preliminary oncologic outcome and postoperative complications between patients undergoing either open or robotic radical cystectomy
 ORIGINAL ARTICLE Vol. 42 (4): 663-670, July - August, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0393 A comparison of preliminary oncologic outcome and postoperative complications between patients undergoing
ORIGINAL ARTICLE Vol. 42 (4): 663-670, July - August, 2016 doi: 10.1590/S1677-5538.IBJU.2015.0393 A comparison of preliminary oncologic outcome and postoperative complications between patients undergoing
Predictive factors of late biochemical recurrence after radical prostatectomy
 JJCO Japanese Journal of Clinical Oncology Japanese Journal of Clinical Oncology, 2017, 47(3) 233 238 doi: 10.1093/jjco/hyw181 Advance Access Publication Date: 9 December 2016 Original Article Original
JJCO Japanese Journal of Clinical Oncology Japanese Journal of Clinical Oncology, 2017, 47(3) 233 238 doi: 10.1093/jjco/hyw181 Advance Access Publication Date: 9 December 2016 Original Article Original
Prostate Cancer and Prostatic Disease (2014), Macmillan Publishers Limited All rights reserved /14
 Prostate Cancer and Prostatic Disease (2014), 1 7 2014 Macmillan Publishers Limited All rights reserved 1365-7852/14 www.nature.com/pcan ORIGINAL ARTICLE Predicting prostate cancer-specific outcome after
Prostate Cancer and Prostatic Disease (2014), 1 7 2014 Macmillan Publishers Limited All rights reserved 1365-7852/14 www.nature.com/pcan ORIGINAL ARTICLE Predicting prostate cancer-specific outcome after
Controversies in Prostate Cancer Screening
 Controversies in Prostate Cancer Screening William J Catalona, MD Northwestern University Chicago Disclosure: Beckman Coulter, a manufacturer of PSA assays, provides research support PSA Screening Recommendations
Controversies in Prostate Cancer Screening William J Catalona, MD Northwestern University Chicago Disclosure: Beckman Coulter, a manufacturer of PSA assays, provides research support PSA Screening Recommendations
Prostate Cancer Treatment for Economically Disadvantaged Men
 Prostate Cancer Treatment for Economically Disadvantaged Men A Comparison of County Hospitals and Private Providers J. Kellogg Parsons, MD, MHS 1,2 ; Lorna Kwan, MPH 3 ; Sarah E. Connor, MPH 4 ; David
Prostate Cancer Treatment for Economically Disadvantaged Men A Comparison of County Hospitals and Private Providers J. Kellogg Parsons, MD, MHS 1,2 ; Lorna Kwan, MPH 3 ; Sarah E. Connor, MPH 4 ; David
Risk Factors for Clinical Metastasis in Men Undergoing Radical Prostatectomy and Immediate Adjuvant Androgen Deprivation Therapy
 RESEARCH ARTICLE Risk Factors for Clinical Metastasis in Men Undergoing Radical Prostatectomy and Immediate Adjuvant Androgen Deprivation Therapy Satoru Taguchi, Hiroshi Fukuhara*, Shigenori Kakutani,
RESEARCH ARTICLE Risk Factors for Clinical Metastasis in Men Undergoing Radical Prostatectomy and Immediate Adjuvant Androgen Deprivation Therapy Satoru Taguchi, Hiroshi Fukuhara*, Shigenori Kakutani,
Providing Treatment Information for Prostate Cancer Patients
 Providing Treatment Information for Prostate Cancer Patients For all patients with localized disease on biopsy For all patients with adverse pathology after prostatectomy See what better looks like Contact
Providing Treatment Information for Prostate Cancer Patients For all patients with localized disease on biopsy For all patients with adverse pathology after prostatectomy See what better looks like Contact
RAPN. in T1b Renal Masses? A. Mottrie. G. Denaeyer, P. Schatteman, G. Novara
 RAPN in T1b Renal Masses? A. Mottrie G. Denaeyer, P. Schatteman, G. Novara Department of Urology O.L.V. Clinic Aalst OLV Vattikuti Robotic Surgery Institute Aalst Belgium Guidelines on Renal Cell Carcinoma
RAPN in T1b Renal Masses? A. Mottrie G. Denaeyer, P. Schatteman, G. Novara Department of Urology O.L.V. Clinic Aalst OLV Vattikuti Robotic Surgery Institute Aalst Belgium Guidelines on Renal Cell Carcinoma
Radical Prostatectomy in High-Risk Prostate Cancer Patients: Results of a Single- Institution Study
 Original Article Songklanagarind Medical Journal Radical Prostatectomy in High-Risk Prostate Cancer Patients: Results of a Single- Institution Study Virote Chalieopanyarwong, M.D., Worapat Attawettayanon,
Original Article Songklanagarind Medical Journal Radical Prostatectomy in High-Risk Prostate Cancer Patients: Results of a Single- Institution Study Virote Chalieopanyarwong, M.D., Worapat Attawettayanon,
Post Radical Prostatectomy Radiation in Intermediate and High Risk Group Prostate Cancer Patients - A Historical Series
 Post Radical Prostatectomy Radiation in Intermediate and High Risk Group Prostate Cancer Patients - A Historical Series E. Z. Neulander 1, Z. Wajsman 2 1 Department of Urology, Soroka UMC, Ben Gurion University,
Post Radical Prostatectomy Radiation in Intermediate and High Risk Group Prostate Cancer Patients - A Historical Series E. Z. Neulander 1, Z. Wajsman 2 1 Department of Urology, Soroka UMC, Ben Gurion University,
Cancer of the Breast (Female) - Cancer Stat Facts
 Page 1 of 9 Home Statistical Summaries Cancer Stat Facts Cancer of the Breast (Female) Cancer Stat Facts: Female Breast Cancer Statistics at a Glance At a Glance Estimated New Cases in 2016 % of All New
Page 1 of 9 Home Statistical Summaries Cancer Stat Facts Cancer of the Breast (Female) Cancer Stat Facts: Female Breast Cancer Statistics at a Glance At a Glance Estimated New Cases in 2016 % of All New
Who are Candidates for Laparoscopic or Open Radical Nephrectomy. Arieh Shalhav
 Who are Candidates for Laparoscopic or Open Radical Nephrectomy Arieh Shalhav Fritz Duda Chair of Urologic Surgery Professor of Surgery and the Comprehensive Cancer Research Center Who are Candidates for
Who are Candidates for Laparoscopic or Open Radical Nephrectomy Arieh Shalhav Fritz Duda Chair of Urologic Surgery Professor of Surgery and the Comprehensive Cancer Research Center Who are Candidates for
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #104 (NQF 0390): Prostate Cancer: Combination Androgen Deprivation Therapy for High Risk or Very High Risk Prostate Cancer National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS
Quality ID #104 (NQF 0390): Prostate Cancer: Combination Androgen Deprivation Therapy for High Risk or Very High Risk Prostate Cancer National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS
Prostate Cancer Incidence
 Prostate Cancer: Prevention, Screening and Treatment Philip Kantoff MD Dana-Farber Cancer Institute Professor of fmedicine i Harvard Medical School Prostate Cancer Incidence # of patients 350,000 New Cases
Prostate Cancer: Prevention, Screening and Treatment Philip Kantoff MD Dana-Farber Cancer Institute Professor of fmedicine i Harvard Medical School Prostate Cancer Incidence # of patients 350,000 New Cases
Jaspreet S. Sandhu,*,, Geoffrey T. Gotto,*, Luis A. Herran, Peter T. Scardino, James A. Eastham and Farhang Rabbani
 Age, Obesity, Medical Comorbidities and Surgical Technique are Predictive of Symptomatic Anastomotic Strictures After Contemporary Radical Prostatectomy Jaspreet S. Sandhu,*,, Geoffrey T. Gotto,*, Luis
Age, Obesity, Medical Comorbidities and Surgical Technique are Predictive of Symptomatic Anastomotic Strictures After Contemporary Radical Prostatectomy Jaspreet S. Sandhu,*,, Geoffrey T. Gotto,*, Luis
Percent Surviving 5 Years 89.4%
 Page 1 of 8 Surveillance, Epidemiology, and End Results Program Turning Cancer Data Into Discovery Home Statistical Summaries Cancer Stat Fact Sheets Cancer of the Breast SEER Stat Fact Sheets: Breast
Page 1 of 8 Surveillance, Epidemiology, and End Results Program Turning Cancer Data Into Discovery Home Statistical Summaries Cancer Stat Fact Sheets Cancer of the Breast SEER Stat Fact Sheets: Breast
Robot-Assisted Radical Prostatectomy
 John W. Davis Editor Robot-Assisted Radical Prostatectomy Beyond the Learning Curve 123 Apex: The Crossroads of Functional Recovery and Oncologic Control 10 Fatih Atug I nt rod u c ti on Prostate cancer
John W. Davis Editor Robot-Assisted Radical Prostatectomy Beyond the Learning Curve 123 Apex: The Crossroads of Functional Recovery and Oncologic Control 10 Fatih Atug I nt rod u c ti on Prostate cancer
1 Oregon Health & Science University, Portland, OR 2 Stritch School of Medicine, Loyola University Chicago, Chicago, IL
 Current treatment practices for limited-stage small cell lung cancer: A survey of US radiation oncologists on the timing of thoracic radiotherapy with chemotherapy Matthew J. Farrell 1, Jehan Yahya 1,
Current treatment practices for limited-stage small cell lung cancer: A survey of US radiation oncologists on the timing of thoracic radiotherapy with chemotherapy Matthew J. Farrell 1, Jehan Yahya 1,
Local treatment for metastatic prostate cancer: A systematic review
 International Journal of Urology (2018) 25, 390--403 doi: 10.1111/iju.13535 Review Article Local treatment for metastatic prostate cancer: A systematic review Derya Tilki, 1,2 Raisa S Pompe, 1,3 Marco
International Journal of Urology (2018) 25, 390--403 doi: 10.1111/iju.13535 Review Article Local treatment for metastatic prostate cancer: A systematic review Derya Tilki, 1,2 Raisa S Pompe, 1,3 Marco
Since the beginning of the prostate-specific antigen (PSA) era in the. Characteristics of Insignificant Clinical T1c Prostate Tumors
 2001 Characteristics of Insignificant Clinical T1c Prostate Tumors A Contemporary Analysis Patrick J. Bastian, M.D. 1 Leslie A. Mangold, B.A., M.S. 1 Jonathan I. Epstein, M.D. 2 Alan W. Partin, M.D., Ph.D.
2001 Characteristics of Insignificant Clinical T1c Prostate Tumors A Contemporary Analysis Patrick J. Bastian, M.D. 1 Leslie A. Mangold, B.A., M.S. 1 Jonathan I. Epstein, M.D. 2 Alan W. Partin, M.D., Ph.D.
J Clin Oncol 28: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 28 NUMBER 1 JANUARY 1 2010 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Clinical Results of Long-Term Follow-Up of a Large, Active Surveillance Cohort With Localized Prostate Cancer
VOLUME 28 NUMBER 1 JANUARY 1 2010 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Clinical Results of Long-Term Follow-Up of a Large, Active Surveillance Cohort With Localized Prostate Cancer
Zonal Origin of Localized Prostate Cancer Does not Affect the Rate of Biochemical Recurrence after Radical Prostatectomy
 european urology 51 (2007) 949 955 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Zonal Origin of Localized Prostate Cancer Does not Affect the Rate of Biochemical
european urology 51 (2007) 949 955 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prostate Cancer Zonal Origin of Localized Prostate Cancer Does not Affect the Rate of Biochemical
pissn , eissn Open Access Original Article
 pissn 1598-2998, eissn 2005-9256 Original Article https://doi.org/10.4143/crt.2016.494 Open Access Re-stratification of Patients with High-Risk Prostate Cancer According to the NCCN Guidelines among Patients
pissn 1598-2998, eissn 2005-9256 Original Article https://doi.org/10.4143/crt.2016.494 Open Access Re-stratification of Patients with High-Risk Prostate Cancer According to the NCCN Guidelines among Patients
Accepted for publication 3 January 2005
 Original Article RACIAL DIFFERENCES IN PSA DOUBLING TIME AND RECURRENCE TEWARI et al. In a multi-institutional study authors from the USA and Austria attempt to determine if there are differences in several
Original Article RACIAL DIFFERENCES IN PSA DOUBLING TIME AND RECURRENCE TEWARI et al. In a multi-institutional study authors from the USA and Austria attempt to determine if there are differences in several
Use of the cell cycle progression (CCP) score for predicting systemic disease and response to radiation of biochemical recurrence
 Cancer Biomarkers 17 (2016) 83 88 83 DOI 10.3233/CBM-160620 IOS Press Use of the cell cycle progression (CCP) score for predicting systemic disease and response to radiation of biochemical recurrence Michael
Cancer Biomarkers 17 (2016) 83 88 83 DOI 10.3233/CBM-160620 IOS Press Use of the cell cycle progression (CCP) score for predicting systemic disease and response to radiation of biochemical recurrence Michael
Salvage Radical Prostatectomy for Radiation-recurrent Prostate Cancer: A Multi-institutional Collaboration
 EUROPEAN UROLOGY 60 (2011) 205 210 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by Markus Graefen on pp. 211 213 of this issue
EUROPEAN UROLOGY 60 (2011) 205 210 available at www.sciencedirect.com journal homepage: www.europeanurology.com Platinum Priority Prostate Cancer Editorial by Markus Graefen on pp. 211 213 of this issue
The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters
 A Contemporary, Population-Based Analysis of the Incidence, Cost, Outcomes, and Preoperative Risk Prediction of Postoperative Delirium Following Major Urologic Cancer Surgeries The Harvard community has
A Contemporary, Population-Based Analysis of the Incidence, Cost, Outcomes, and Preoperative Risk Prediction of Postoperative Delirium Following Major Urologic Cancer Surgeries The Harvard community has
Diet, Physical Activity, Weight & Cancer Survivorship: Perspectives from the NCI
 Diet, Physical Activity, Weight & Cancer Survivorship: Perspectives from the NCI American Institute for Cancer Research Meeting October 21, 2010 Catherine M. Alfano, Ph.D. Program Director & Behavioral
Diet, Physical Activity, Weight & Cancer Survivorship: Perspectives from the NCI American Institute for Cancer Research Meeting October 21, 2010 Catherine M. Alfano, Ph.D. Program Director & Behavioral
ROBOTIC VS OPEN RADICAL CYSTECTOMY
 ROBOTIC VS OPEN RADICAL CYSTECTOMY A REVIEW Colin Lundeen December 14, 2016 Objectives Review the history of radical cystectomy Critically analyze recent RCTs comparing open radical cystectomy (ORC) to
ROBOTIC VS OPEN RADICAL CYSTECTOMY A REVIEW Colin Lundeen December 14, 2016 Objectives Review the history of radical cystectomy Critically analyze recent RCTs comparing open radical cystectomy (ORC) to
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #104 (NQF 0390): Prostate Cancer: Adjuvant Hormonal Therapy for High Risk or Very High Risk Prostate Cancer National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL
Measure #104 (NQF 0390): Prostate Cancer: Adjuvant Hormonal Therapy for High Risk or Very High Risk Prostate Cancer National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL
Relationship between surgical volume and patient outcomes
 7 Relationship between surgical volume and patient outcomes MASSIMILIANO SPALIVIERO AND JAMES A. EASTHAM The authors discuss the inverse relationship between hospital volume of surgical procedures and
7 Relationship between surgical volume and patient outcomes MASSIMILIANO SPALIVIERO AND JAMES A. EASTHAM The authors discuss the inverse relationship between hospital volume of surgical procedures and
Laparoscopic Surgery. The Da Vinci Robot. Limits of Laparoscopy. What Robotics Offers. Robotic Urologic Surgery: A New Era in Patient Care
 Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Laparoscopic Surgery Robotic Urologic Surgery: A New Era in Patient Care Laparoscopic technique was introduced in urologic surgery in the 1990s Benefits: Improved recovery time, decreased morbidity Matthew
Reducing overtreatment of prostate cancer by radical prostatectomy in Eastern Ontario: a population-based cohort study
 Reducing overtreatment of prostate cancer by radical prostatectomy in Eastern Ontario: a population-based cohort study Luke Witherspoon MD MSc, Johnathan L. Lau BSc, Rodney H. Breau MD MSc, Christopher
Reducing overtreatment of prostate cancer by radical prostatectomy in Eastern Ontario: a population-based cohort study Luke Witherspoon MD MSc, Johnathan L. Lau BSc, Rodney H. Breau MD MSc, Christopher
Radical Prostatectomy and Pelvic Lymph Node Dissection in Kaiser Permanente Southern California: 15-Year Experience
 Radical Prostatectomy and Pelvic Lymph Node Dissection in Kaiser Permanente Southern California: 15-Year Experience Pooya Banapour, MD 1 ; Andrew Schumacher, MD 2 ; Jane C Lin 3 ; David S Finley, MD 1
Radical Prostatectomy and Pelvic Lymph Node Dissection in Kaiser Permanente Southern California: 15-Year Experience Pooya Banapour, MD 1 ; Andrew Schumacher, MD 2 ; Jane C Lin 3 ; David S Finley, MD 1
A comparative study of radical prostatectomy and permanent seed brachytherapy for low- and intermediate-risk prostate cancer
 ORIGINAL RESEARCH A comparative study of radical prostatectomy and permanent seed brachytherapy for low- and intermediate-risk prostate cancer Daniel Taussky, MD; 1 Véronique Ouellet, MD; 2 Guila Delouya,
ORIGINAL RESEARCH A comparative study of radical prostatectomy and permanent seed brachytherapy for low- and intermediate-risk prostate cancer Daniel Taussky, MD; 1 Véronique Ouellet, MD; 2 Guila Delouya,
Adverse Effects of Robotic-Assisted Laparoscopic Versus Open Retropubic Radical Prostatectomy Among a Nationwide Random Sample of Medicare-Age Men
 Published Ahead of Print on January 3, 2012 as 10.1200/JCO.2011.36.8621 The latest version is at http://jco.ascopubs.org/cgi/doi/10.1200/jco.2011.36.8621 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R
Published Ahead of Print on January 3, 2012 as 10.1200/JCO.2011.36.8621 The latest version is at http://jco.ascopubs.org/cgi/doi/10.1200/jco.2011.36.8621 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R
GUIDELINES ON PROSTATE CANCER
 10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
10 G. Aus (chairman), C. Abbou, M. Bolla, A. Heidenreich, H-P. Schmid, H. van Poppel, J. Wolff, F. Zattoni Eur Urol 2001;40:97-101 Introduction Cancer of the prostate is now recognized as one of the principal
Surgical Management of Metastatic and Locally Recurrent Kidney Cancer: Does it Make Sense?
 Surgical Management of Metastatic and Locally Recurrent Kidney Cancer: Does it Make Sense? Philippe E. Spiess, MD, FACS Associate Member Department of GU Oncology Department of Tumor Biology Moffitt Cancer
Surgical Management of Metastatic and Locally Recurrent Kidney Cancer: Does it Make Sense? Philippe E. Spiess, MD, FACS Associate Member Department of GU Oncology Department of Tumor Biology Moffitt Cancer
Aram Kim 4, Myong Kim 1, Se Un Jeong 2, Cheryn Song 1, Yong Mee Cho 2, Jae Yoon Ro 3 and Hanjong Ahn 1*
 Kim et al. BMC Urology (2018) 18:7 DOI 10.1186/s12894-018-0321-z RESEARCH ARTICLE Open Access Level of invasion into fibromuscular band is an independent factor for positive surgical margin and biochemical
Kim et al. BMC Urology (2018) 18:7 DOI 10.1186/s12894-018-0321-z RESEARCH ARTICLE Open Access Level of invasion into fibromuscular band is an independent factor for positive surgical margin and biochemical
Introduction. Key Words: high-grade prostatic intraepithelial neoplasia, HGPIN, radical prostatectomy, prostate biopsy, insignificant prostate cancer
 Prostate cancer after initial high-grade prostatic intraepithelial neoplasia and benign prostate biopsy Premal Patel, MD, 1 Jasmir G. Nayak, MD, 1,2 Zlatica Biljetina, MD, 4 Bryan Donnelly, MD 3, Kiril
Prostate cancer after initial high-grade prostatic intraepithelial neoplasia and benign prostate biopsy Premal Patel, MD, 1 Jasmir G. Nayak, MD, 1,2 Zlatica Biljetina, MD, 4 Bryan Donnelly, MD 3, Kiril
Evaluation of prognostic factors after radical prostatectomy in pt3b prostate cancer patients in Japanese population
 Japanese Journal of Clinical Oncology, 2015, 45(8) 780 784 doi: 10.1093/jjco/hyv077 Advance Access Publication Date: 15 May 2015 Original Article Original Article Evaluation of prognostic factors after
Japanese Journal of Clinical Oncology, 2015, 45(8) 780 784 doi: 10.1093/jjco/hyv077 Advance Access Publication Date: 15 May 2015 Original Article Original Article Evaluation of prognostic factors after
Incidence and Determinants of 1-Month Mortality after Cancer-Directed Surgery
 Annals of Oncology Advance Access published November 27, 2014 1 Incidence and Determinants of 1-Month Mortality after Cancer-Directed Surgery B.A. Mahal 1,*, G. Inverso 2,*, A.A. Aizer 3, D.R. Ziehr 1,
Annals of Oncology Advance Access published November 27, 2014 1 Incidence and Determinants of 1-Month Mortality after Cancer-Directed Surgery B.A. Mahal 1,*, G. Inverso 2,*, A.A. Aizer 3, D.R. Ziehr 1,
Presentation with lymphadenopathy
 Presentation with lymphadenopathy Theo M. de Reijke MD PhD FEBU Department of Urology Academic Medical Center Amsterdam Rationale for RRP in N+ disease Prevention local problems Better survival in limited
Presentation with lymphadenopathy Theo M. de Reijke MD PhD FEBU Department of Urology Academic Medical Center Amsterdam Rationale for RRP in N+ disease Prevention local problems Better survival in limited
Key words: prostatic neoplasms, risk groups, biochemical recurrence, clinical progression, prostate cancer specific mortality
 JJCO Japanese Journal of Clinical Oncology Japanese Journal of Clinical Oncology, 2016, 46(8) 762 767 doi: 10.1093/jjco/hyw061 Advance Access Publication Date: 20 May 2016 Original Article Original Article
JJCO Japanese Journal of Clinical Oncology Japanese Journal of Clinical Oncology, 2016, 46(8) 762 767 doi: 10.1093/jjco/hyw061 Advance Access Publication Date: 20 May 2016 Original Article Original Article
Prostate Cancer Local or distant recurrence?
 Prostate Cancer Local or distant recurrence? Diagnostic flowchart Vanessa Vilas Boas Urologist VFX Hospital FEBU PSA - only recurrence PSA recurrence: 27-53% of all patients undergoing treatment with curative
Prostate Cancer Local or distant recurrence? Diagnostic flowchart Vanessa Vilas Boas Urologist VFX Hospital FEBU PSA - only recurrence PSA recurrence: 27-53% of all patients undergoing treatment with curative
Adam Raben M.D. Helen F Graham Cancer Center
 Adam Raben M.D. Helen F Graham Cancer Center Is the biopsy sample representative of the extent of the disease in your patient with clinically low-risk prostate cancer? BIOPSY RP registry (n=8095) 3+3=6
Adam Raben M.D. Helen F Graham Cancer Center Is the biopsy sample representative of the extent of the disease in your patient with clinically low-risk prostate cancer? BIOPSY RP registry (n=8095) 3+3=6
estimating risk of BCR and risk of aggressive recurrence after RP was assessed using the concordance index, c.
 . JOURNAL COMPILATION 2008 BJU INTERNATIONAL Urological Oncology PREDICTION OF AGGRESSIVE RECURRENCE AFTER RP SCHROECK et al. BJUI BJU INTERNATIONAL Do nomograms predict aggressive recurrence after radical
. JOURNAL COMPILATION 2008 BJU INTERNATIONAL Urological Oncology PREDICTION OF AGGRESSIVE RECURRENCE AFTER RP SCHROECK et al. BJUI BJU INTERNATIONAL Do nomograms predict aggressive recurrence after radical
10/2/2018 OBJECTIVES PROSTATE HEALTH BACKGROUND THE PROSTATE HEALTH INDEX PHI*: BETTER PROSTATE CANCER DETECTION
 THE PROSTATE HEALTH INDEX PHI*: BETTER PROSTATE CANCER DETECTION Lenette Walters, MS, MT(ASCP) Medical Affairs Manager Beckman Coulter, Inc. *phi is a calculation using the values from PSA, fpsa and p2psa
THE PROSTATE HEALTH INDEX PHI*: BETTER PROSTATE CANCER DETECTION Lenette Walters, MS, MT(ASCP) Medical Affairs Manager Beckman Coulter, Inc. *phi is a calculation using the values from PSA, fpsa and p2psa
ROBOTIC ASSISTED RADICAL PROSTATECTOMY VERSUS OPEN RETROPUBIC RADICAL PROSTATECTOMY: WHERE DO WE STAND IN 2015?
 ROBOTIC ASSISTED RADICAL PROSTATECTOMY VERSUS OPEN RETROPUBIC RADICAL PROSTATECTOMY: WHERE DO WE STAND IN 2015? Mark Frydenberg 1, Declan G Murphy, 2,3,5 Daniel A Moon, 3,5 Nathan Lawrentschuk 2,3,4 1.
ROBOTIC ASSISTED RADICAL PROSTATECTOMY VERSUS OPEN RETROPUBIC RADICAL PROSTATECTOMY: WHERE DO WE STAND IN 2015? Mark Frydenberg 1, Declan G Murphy, 2,3,5 Daniel A Moon, 3,5 Nathan Lawrentschuk 2,3,4 1.
Understanding the risk of recurrence after primary treatment for prostate cancer. Aditya Bagrodia, MD
 Understanding the risk of recurrence after primary treatment for prostate cancer Aditya Bagrodia, MD Aditya.bagrodia@utsouthwestern.edu 423-967-5848 Outline and objectives Prostate cancer demographics
Understanding the risk of recurrence after primary treatment for prostate cancer Aditya Bagrodia, MD Aditya.bagrodia@utsouthwestern.edu 423-967-5848 Outline and objectives Prostate cancer demographics
When to perform preoperative chest computed tomography for renal cancer staging
 When to perform preoperative chest computed tomography for renal cancer staging Alessandro Larcher*, Paolo Dell Oglio*, Nicola Fossati*, Alessandro Nini*, Fabio Muttin*, Nazareno Suardi*, Francesco De
When to perform preoperative chest computed tomography for renal cancer staging Alessandro Larcher*, Paolo Dell Oglio*, Nicola Fossati*, Alessandro Nini*, Fabio Muttin*, Nazareno Suardi*, Francesco De
Patterns in the Treatment of Intermediate and High Risk Localized Prostate Cancer
 Patterns in the Treatment of Intermediate and High Risk Localized Prostate Cancer Jonathan E. Heinlen, M.D. Stephenson Oklahoma Cancer Center University of Oklahoma Health Sciences Center Disclosures I
Patterns in the Treatment of Intermediate and High Risk Localized Prostate Cancer Jonathan E. Heinlen, M.D. Stephenson Oklahoma Cancer Center University of Oklahoma Health Sciences Center Disclosures I
Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer
 Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Robot-assisted vs. Laparoscopic Partial Nephrectomy: utilization rates and perioperative outcomes
 ORIGINAL Article Vol. 39 (3): 377-386, May - June, 2013 doi: 10.1590/S1677-5538.IBJU.2013.03.11 Robot-assisted vs. Laparoscopic Partial Nephrectomy: utilization rates and perioperative outcomes Jesse D.
ORIGINAL Article Vol. 39 (3): 377-386, May - June, 2013 doi: 10.1590/S1677-5538.IBJU.2013.03.11 Robot-assisted vs. Laparoscopic Partial Nephrectomy: utilization rates and perioperative outcomes Jesse D.
UC San Francisco UC San Francisco Previously Published Works
 UC San Francisco UC San Francisco Previously Published Works Title The quantitative Gleason score improves prostate cancer risk assessment Permalink https://escholarship.org/uc/item/9wq7g6k5 Journal Cancer,
UC San Francisco UC San Francisco Previously Published Works Title The quantitative Gleason score improves prostate cancer risk assessment Permalink https://escholarship.org/uc/item/9wq7g6k5 Journal Cancer,
PSA Screening and Prostate Cancer. Rishi Modh, MD
 PSA Screening and Prostate Cancer Rishi Modh, MD ABOUT ME From Tampa Bay Went to Berkeley Prep University of Miami for Undergraduate - 4 years University of Miami for Medical School - 4 Years University
PSA Screening and Prostate Cancer Rishi Modh, MD ABOUT ME From Tampa Bay Went to Berkeley Prep University of Miami for Undergraduate - 4 years University of Miami for Medical School - 4 Years University
Untreated Gleason Grade Progression on Serial Biopsies during Prostate Cancer Active Surveillance: Clinical Course and Pathological Outcomes
 Untreated Gleason Grade Progression on Serial Biopsies during Prostate Cancer Active Surveillance: Clinical Course and Pathological Outcomes A. A. Hussein,* C. J. Welty,* N. Ameli,* J. E. Cowan, M. Leapman,*
Untreated Gleason Grade Progression on Serial Biopsies during Prostate Cancer Active Surveillance: Clinical Course and Pathological Outcomes A. A. Hussein,* C. J. Welty,* N. Ameli,* J. E. Cowan, M. Leapman,*
