Randomised study of screening for colorectal cancer with faecaloccult-blood
|
|
|
- Blaze Bridges
- 5 years ago
- Views:
Transcription
1 Articles Randomised study of screening for colorectal cancer with faecaloccult-blood test Ole Kronborg, Claus Fenger, Jørn Olsen, Ole Dan Jørgensen, Ole Søndergaard Summary Background Case-control studies and a voluntary-based follow-up study have suggested that repeated screening with faecal-occult-blood (FOB) tests can lead to a reduction in mortality from colorectal cancer (CRC). The aim of this randomised study was to compare mortality rates after FOB tests every 2 years during a 10-year period with those of unscreened similar controls. Methods people aged years lived in Funen, Denmark, in August, 1985, and were considered for inclusion in our study. Before randomisation we excluded individuals who had CRC or precursor adenomas and those who had taken part in a previous pilot study. Randomisation of people in blocks of 14 allocated three per 14 to the screening group (30 967), three per 14 to the control group (30 966), and eight not to be enrolled in the study (75 552). Controls were not told about the study and continued to use health-care facilities as normal. Hemoccult-II blood tests (with dietary restrictions but without rehydration) were sent to screening-group participants. Only those participants who completed the first screening round were invited for further screening five rounds of screening during a 10-year period. Participants with positive tests were asked to attend a full examination and were offered colonoscopy whenever possible. The primary endpoint was death from CRC. Findings Of the screening-group participants, (67%) completed the first screening round and were invited for further screening; more than 90% accepted repeated screenings. During the 10-year study, 481 people in the screening group had a diagnosis of CRC, compared with 483 unscreened controls. There were 205 deaths attributable to CRC in the screening group, compared with 249 deaths in controls. CRC mortality, including deaths attributable to complications from CRC treatment, was significantly lower in the screening group than in controls (mortality ratio 0 82 [95% CI ]) p=0 03). Interpretation Our findings indicate that biennial screening by FOB tests can reduce CRC mortality. This study is being continued to improve its statistical power and to assess Departments of Surgery A (Prof O Kronborg MD, O D Jørgensen MD), Pathology (C Fenger MD), and Statistics (O Søndergaard PhD), Odense University Hospital, DK 5000 Odense C, Denmark; and Danish Epidemiology Science Centre, Aarhus University, Denmark (Prof J Olsen MD) Correspondence to: Prof Ole Kronborg the effect of the removal of more precursor adenomas in the screening-group participants than in controls on CRC incidence. Lancet 1996; 348: See Commentary page 1463 Introduction Denmark has high incidence and mortality rates for colorectal cancer (CRC) the incidence of colonic cancer is currently increasing and mortality remains constant, whereas incidence and mortality of rectal cancer are declining. Early stages of CRC are commonly found in only 10 15% of patients with symptoms. However, there is evidence that earlier diagnosis and treatment of CRC in symptom-free patients may reduce mortality. Two casecontrol studies of screening with faecal-occult-blood (FOB) tests reported reductions in CRC mortality rates of 31% 1 and 57% 2 (the latter reduction was found only in women). Similarly, Winawer and colleagues non-randomised study 3 showed that annual rigid sigmoidoscopy and FOB tests, rather than sigmoidoscopy alone, led to a reduction in mortality. Mandel and colleagues voluntary-based randomised study in Minnesota 4 (ie, all participants were informed about randomisation), reported a 33% reduction in CRC mortality rates after 13 years in patients who were offered annual screening for FOB, but a non-significant reduction of 6% in those who were offered biennial screening. Four randomised population trials of screening with FOB tests are under way in Europe, 5 8 but no mortality figures have until now been reported. The main aim of this study was to compare deaths from CRC after biennial screening by FOB tests with deaths from CRC in a similar unscreened population (controls) during a 10-year period. Methods This study followed a pilot study of compliance in screening for CRC in which of 685 people, 460 (67%) accepted the Hemoccult-II test. 9 We intended to use three screening rounds with FOB tests during a 5-year period, followed by 5 years of follow-up based on passive case detection. However, after 5 years, the compliance was good and we decided to continue biennial screening for a further 5 years; thus, the study period was from August, 1985, to August, Based on the assumption of a CRC mortality rate of 0 9 per 1000 person-years and an annual withdrawal rate of at least 1% from death and other causes, 10 we estimated that about controls and people in the screening group were required to give a power of 0 70 and a significance level of 0 05 in detecting a 25% reduction in CRC mortality. Vol 348 November 30,
2 Age (years) Screening Control Men Women Men Women (n=14 864) (n=16 103) (n=14 850) (n=16 116) (17%) 2547 (16%) 2590 (17%) 2515 (16%) (18%) 2701 (17%) 2711 (18%) 2770 (17%) (18%) 2762 (17%) 2571 (17%) 2688 (17%) (17%) 2849 (18%) 2502 (17%) 2877 (18%) (15%) 2593 (16%) 2311 (16%) 2589 (16%) (13%) 2367 (15%) 1926 (13%) 2395 (15%) (2%) 284 (2%) 239 (2%) 282 (2%) Table 1: Age and sex of participants at initial screening In 1985, people aged years were living in Funen. Before randomisation we excluded individuals with known CRC, precursors of CRC (adenomas), and distant spread from all types of malignant disorders; these individuals were identified by linkage with hospital inpatient files, the county authorities, and the Civil registration System. People who had taken part in the pilot study were also excluded. We used a central randomisation procedure based on the population register of the county. The inhabitants of Funen were listed according to social security number, but married women were placed after their husbands. Balanced randomisation was done in groups of 14 (three to screening, three to the control group, and eight not enrolled). The computerised randomisation programme was adjusted for married couples, who were always allocated to the same group people were assigned biennial screening and were assigned no screening (controls). The primary end part was death attributable to CRC. Controls were not told about the study and continued to use health-care facilities as usual. This approach was judged to be ethical, and was necessary to obtain an accurate evaluation of general population screening; if the controls had been aware of the aims and interventions used in the study, their behaviour might not have been representative of the general population. Throughout the 10-year study, we obtained information on all newly diagnosed cases of CRC and precursor adenomas and death certificates for all participants (controls and screening) from the Funen patient database and the county public-health officer. Detailed information on all cases of CRC and adenomas is stored in a central database. In addition, we referred to the Danish National Registry of Patients three times during the study (the last time was in November, 1995). We also crosschecked with the Danish Cancer Society in late 1995 to confirm screening attended first screening and invited to repeat attended all five screening rounds August, 1995, 481 cases of CRC 205 died from CRC Figure 1: Study profile inhabitants aged years 2515 inhabitants excluded August, 1985, randomised not screened (controls) August, 1995, 483 cases of CRC 249 died from CRC not enrolled Screening round Number of people invited Number of people for screening screened (67%) (93%) (94%) (94%) (92%) Table 2: Compliance during repeated screening that no cases of CRC had been missed. Information from death certificates was stored in the database system. Death was certified as due to CRC in patients who had a previous diagnosis of CRC, or had CRC at the time of their death when one of the following criteria was met: histiologically or clinically confirmed distant spread; carcinomatosis or invasion of neighbouring organs; CRC judged to be unresectable; or CRC with perforation causing peritonitis. We were unaware of the participants screening status during the assessment of death certificates. When we were unable to decide whether CRC was the cause of death, we referred the case to an independent review committee (pathologist, surgeon, specialist in internal medicine, oncologist, general practitioner). 11 Death from complications attributable to CRC was included in the analysis of CRC mortality. Dukes staging of tumours and classification of adenomas were done by one investigator (CF) under masked conditions. 12 The Hemoccult-II test has been previously described. 13 The tests were carried out with dietary restrictions (no red meat, fresh fruit, iron preparations, vitamin C, aspirin, or other nonsteroidal antirheumatics during 3 days before samples were taken), but the completed slides were not rehydrated. Participants were asked to provide two faecal samples from each of three consecutive stools. Completed tests were sent to the Department of Clinical Chemistry, Odense University Hospital, Denmark, and were processed by three technicians. Individuals with positive tests (one or more blue slides) were invited for interview, physical examination, and full colonoscopy. A double-contrast barium enema was offered when full colonoscopy could not be obtained. We sent invitations to participants in the screening group; two reminder letters were sent during the initial screening round and a further reminder was sent during the following four screening rounds. Each screening round took 1 year to complete. Only individuals who agreed to take part in the first screening round were invited for further screening. The protocol automatically excluded from invitation people who died or had CRC or adenomas detected between randomisation and the first screening invitations. However, these individuals were included in the follow-up analyses. All analyses were intention to treat. Screening rounds Positive tests Number of individuals % of population tested Investigations undertaken after positive test Complete colonoscopy Incomplete colonoscopy and DCBE Incomplete colorectal examination No colorectal examination Colorectal carcinoma Number of cases Predictive value (%) of positive FOB test Adenoma 10 mm Number of cases Predictive value (%) of positive FOB test DCBE=double-contrast barium enema. Table 3: Screening-group individuals who underwent further investigations after a positive FOB test and predictive value of a positive test for neoplasia 1468 Vol 348 November 30, 1996
3 Screening group Controls Positive test Before invitation* Non-responders Interval cancers Total Stage of CRC Dukes A (22%) 54 (11%) Dukes B (34%) 177 (37%) Dukes C (19%) 111 (23%) Distant spread (20%) 114 (24%) No classification (5%) 27 (5%) Total CRC Adenoma 10 mm *Had CRC diagnosed or died after randomisation but before first invitation. Invited to first round but did not respond. Had a negative FOB test at first screening round but had a diagnosis of CRC made between screenings (includes two patients who refused further examination after a positive test). Table 4: Stage of CRC and presence of large adenomas in screening and control groups between August, 1985, and August, 1995 Incidence and mortality rates were calculated as the number of cases of CRC divided by the total time of observation. Between August, 1985, and August, 1995, all participants were considered to be at risk of CRC; after this period, or in the event of death, the screening status of all participants who were followed up was assessed. No interim assessments were done. We used control-group data as the denominator to calculate relative incidence and mortality rates of CRC. 95% CI values were calculated by the multiplicative poisson model. Poisson models were compared by the likelihood ratio test. Cumulative survival was calculated by the life-table method and compared by the log-rank test. Proportions were compared by the 2 test. The study was approved by the regional ethics committee, and the population registers were approved by the registry board of Funen. Results The groups were well matched in terms of age and sex at the initial screening (table 1). The age and sex distributions of the groups did not change substantially during the study. The study profile shows overall patient numbers during the 10-year study (figure 1). 205 people died between randomisation and planned invitation for screening. Of the people who were alive at the end of the follow-up, 1145 had moved away from Funen and six had emigrated from Denmark. The number of individuals who completed the FOB test at each screening is shown in table participants completed five screening rounds. During the first round of screening, the proportion of positive tests ranged from 0 6% to 1 7% according to age and sex; the proportion was higher in men than in women and in the elderly than in the younger participants. During the second and third screening rounds, the proportion of positive tests decreased (0 5% 1 3% and 0 5% 1 5%). However, during the last screening round, after 10 years of followup, the proportion of positive tests increased substantially ( %); the proportion of positive tests was highest in individuals older than 79 years (2 8% in women, 4 6% in men). Cause of death Number of people in Number of people in screening group control group (n=6228) (n=6303) Cardiovascular disease 2497 (40 1%) 2443 (38 8%) Lung disease 614 (9 9%) 623 (9 9%) Other benign disease and trauma 824 (13 2%) 779 (12 4%) Malignant disorders other 1624 (26 1%) 1721 (27 3%) than CRC Unknown 464 (7 4%) 488 (7 7%) CRC 182 (2 9%) 230 (3 6%) Complications arising from 23 (0 4%) 19 (0 3%) treatment of CRC Table 5: Causes of death in screening and control groups between August, 1985, and August, 1995 More than 85% of those with positive tests underwent full colonoscopy (table 3). The predictive value of a positive FOB test for detection of CRC ranged from 17% in the first screening round (37 cases among 215 positive), to 9% at the final screening (25 cases among 261 positive tests). The predictive values of a positive test for detection of large adenomas ranged from 32% at the first round to 21% at the final round (table 3). The distribution of stages of CRC during the 10-year study is shown in table 4. None of the participants with adenomas of 10 mm or more had CRC, but some had additional smaller adenomas. The proportion of stage A CRC was significantly lower in the control group than in the screening group (11 vs 22%, p<0 01), whereas the proportion of more advanced CRC (stage C, distant spread, and no classification) was significantly higher in the control group than in the screening group (table 4). Local surgery, including polypectomy for CRC, was done in 49 (10%) of the 481 screening-group participants and in 24 (5%) of the 483 controls (p<0 01). Curative surgery was achieved in 331 patients in the screening group and in 287 controls (p<0 01). Of the individuals in the screening group, were alive on Aug 1, 1995, compared with of the controls. We obtained certificates for all participants who died in Denmark. The distribution of causes of death other than CRC was similar in both groups (table 5). There were 33 suicides in the screening group and 41 in the control group; none of these individuals had CRC. Screening group Control group Observation time in years CRC Number of patients Incidence rate (per 1000 person-years) Incidence ratio (95% CI) 1 00 ( ) Death from CRC Number of deaths Mortality rate Mortality ratio (95% CI) 0 79 ( ) Death from CRC and complications from treatment Number of deaths Mortality rate Mortality ratio (95% CI) 0 82 ( ) Death from all causes Number of deaths Mortality rate Mortality ratio (95% CI) 0 99 ( ) Controls are the reference group. Table 6: Incidence and mortality rates for CRC between August, 1985, and August, 1995 Vol 348 November 30,
4 Cumulative mortality (per 1000) Time (years) Figure 2: Biennial cumulative mortality rates for CRC including deaths attributable to complications from CRC Vertical bars=95% CI. After the first screening, the difference in CRC incidence rates between the groups grew smaller and at 10 years the cumulative incidence of CRC was similar (table 6). By contrast, the cumulative CRC mortality rate was significantly higher in controls than in screeninggroup participants, irrespective of whether complications arising from treatment for CRC were excluded. The ratio of CRC mortality rates in screening and control groups was significantly less than 1 0 (table 6, figure 2). Mortality rates for all causes of death did not differ significantly between the groups. The necropsy rate was 24% in both groups. The CRC mortality ratio, which included deaths attributable to complications from CRC treatment was: 0 80 (95% CI ) in men; 0 85 ( ) in women; 0 84 ( ) in individuals 60 years or older at start of follow-up; and 0 77 ( ) in those younger than 60 years. In the screening group, the mortality ratios for left-sided cancer (rectum and sigmoid) and cancer in the remaining colon were 0 87 ( ) and 0 72 ( ), respectively. The cumulative survival of patients with CRC is shown in figure 3. The survival rate was higher in patients with screen-detected CRC than in controls (log-rank test p<0 01). Non-responders had the lowest survival rate of all subgroups and controls (p=0 12). Interval cases of CRC had a higher survival rate than controls (p=0 05). The overall cumulative survival in patients with CRC was significantly higher in the screening group than in the Cumulative survival Screening (n = ) Control (n = ) Screen-detected (n = 120) Screening group (n = 481) Interval (n = 148) Control group (n = 483) Non-responder (n = 195) Time (years) Figure 3: Cumulative survival in screening (by subgroups) and control groups Subgroup of patients who died or had CRC diagnosed between randomisation and first invitation omitted. control group (p<0 01). Within stages of CRC, no significant difference was found in cumulative survival between the screening group and controls, but screening-group patients with Dukes stage A tumours tended to have a better survival than those in the control group (p=0 13). Discussion We found that after 10 years of follow-up, screening by FOB every 2 years (Hemoccult-II without rehydration) led to a reduction of 18% in CRC mortality, which was independent of sex and age, in individuals aged years. Of the participants who were screened at least once only 892 (4 3%) underwent colonoscopy. Our findings contrast with those of the Minnesota study, 4 in which 38% of people who were screened annually during a period of 13 years had colonoscopy (with an intermission of 3 years), and even after biennial screening 28% had at least one colonoscopy; but there was no significant reduction in mortality from CRC. Our study was truly representative of the general population. Our findings can, therefore, be extrapolated to general population screening. By contrast, the Minnesota study included only volunteers with a low CRC mortality. In this study, mortality from causes other than CRC was similar in the screening and control groups, which suggests that comparability was achieved by randomisation. The finding that mortality attributable to complications from CRC treatment was similar in the groups was unexpected, particularly because more patients had local surgery in the screening group than in the control group. However, the number of deaths was small 23 and 19, respectively and we believe that this finding may be due to chance. Although annual screening might reduce the present high rate of interval cancers, it would also increase costs and the proportion of false-positive FOB results. Nevertheless, even if we used annual screening and increased the rate of colonoscopies from 4 3% to 8 6%, this rate would be less than a quarter that of the Minnesota study, due to the lower rate of positive tests with the Hemoccult-II test without rehydration used at Funen. The 18% reduction in mortality from CRC reported here would prevent 360 of the 2000 deaths from CRC in Denmark per year. Colonoscopic expertise and economic resources for screening with rehydrated Hemoccult-II are not currently available in Denmark. Although annual screening with the unhydrated test is a possibility, such screening should be introduced only after further studies have been done and more data on side-effects and cost are available. False-negative tests can lead to a delay in presentation and in subsequent treatment, but in our study patients with interval cancers had a higher survival rate than controls. This finding may reflect earlier diagnosis of CRC rather than later death (lead-time bias). The rate of interval cancers might be reduced by the introduction of annual screening. The difference in rates of death from CRC increased between the groups over time. The slight difference in mortality at 10 years means that this study needs to be continued; screening rounds 6 and 7 will be carried out throughout 1996 and 1997 to assess compliance for repeated screenings and the effect of increasing age. Economic analyses of cost per life-year saved are also in progress Vol 348 November 30, 1996
5 The finding that screening led to a smaller reduction in mortality from rectal and sigmoid cancer than from cancers of the upper colon supports the recommendations for screening trials that include flexible sigmoidoscopy. The removal of precursor adenomas in 413 screeninggroup participants compared with 174 controls did not affect CRC incidence in the screening group. The adenoma-carcinoma sequence may have a duration of several years and any reduction in CRC incidence because of polyp removal during colonoscopy will be investigated in the forthcoming years of our study. In conclusion, biennial screening with Hemoccult-II in individuals aged years reduced CRC mortality after 10 years of follow-up and five screening rounds. CRC is common among elderly people, and the reduction in mortality achieved by FOB screening cannot currently be achieved by any other known preventive measure. Better screening methods may become available in the future, but until then, screening by FOB tests is a feasible option. We thank: the Danish Cancer Society, Helsefonden, the county of Funen, the Danish Research Council, the University of Odense, the Albani Foundation, and several smaller foundations for their support; Darley Peterson and Kirsten Grinsted for secretarial assistance; and the staff of the Department of Clinical Biochemistry, Odense University for technical assistance. References 1 Selby JV, Friedman GD, Quesenbury CP, Weiss NS. Effect of fecal occult blood testing on mortality from colorectal cancer: a casecontrol study. Ann Int Med 1993; 118: Wahrendorf J, Robra B, Wiebelt H, Oberhausen R, Weiland M, Dhom G. Effectiveness of colorectal cancer screening: results from a population-based case-control evaluation in Saarland, Germany. Eur J Cancer Prev 1993; 2: Winawer SJ, Flehinger BJ, Schottenfeld D, Miller DG. Screening for colorectal cancer with fecal occult blood testing and sigmoidoscopy. J Natl Cancer Inst 1993; 85: Mandel JS, Bond JH, Church TR, et al. Reducing mortality from colorectal cancer by screening for fecal occult blood. N Engl J Med 1993; 328: Hardcastle JD,Thomas WM, Chamberlain J, et al. Randomised controlled trial of faecal occult blood screening for colorectal cancer: results for first subjects. Lancet 1989; ii: Kewenter J, Björck S, Haglind E, et al. Screening and re-screening for colorectal cancer: a controlled trial of fecal occult blood testing in subjects. Cancer 1988; 62: Faivre J, Arveux P, Milan C, Durand G, Lamour J, Bedenne L. Participation in mass screening for colorectal cancer: results of screening and rescreening from the Burgundy study. Eur J Cancer Prev 1991; 1: Kronborg O, Fenger C, Olsen J, Bech K, Søndergaard O. Repeated screening for colorectal cancer with fecal occult blood test: a prospective randomized study at Funen, Denmark. Scand J Gastroenterol 1989; 24: Adamsen S, Kronborg O. Acceptability and compliance in screening for colorectal cancer with fecal occult blood test. Scand J Gastroenterol 1984; 19: Taylor WF, Fantana RS. Biometric design of the Mayo lung project for early detection and localization of bronchogenic carcinoma. Cancer 1972; 30: Kronborg O, Fenger C, Worm J, et al. Causes of death during the first 5 years of a randomized trial of mass screening for colorectal cancer with fecal occult blood test. Scand J Gastroenterol 1992; 27: Bech K, Kronborg O, Fenger C. Adenoma and hyperplastic polyps in screening studies. World J Surg 1991; 15: Klaaborg K, Madsen MS, Søndergaard O, Kronborg O. Participation in mass screening for colorectal cancer with fecal occult blood test. Scand J Gastroenterol 1986; 21: Vol 348 November 30,
C olorectal cancer (CRC) is the second most common
 CANCER Effect of faecal occult blood screening on mortality from colorectal cancer: results from a randomised controlled trial J H Scholefield, S Moss, F Sufi, C M Mangham, J D Hardcastle... See end of
CANCER Effect of faecal occult blood screening on mortality from colorectal cancer: results from a randomised controlled trial J H Scholefield, S Moss, F Sufi, C M Mangham, J D Hardcastle... See end of
Colorectal Cancer Screening What are my options?
 069-Colorectal cancer (Rosen) 1/23/04 12:59 PM Page 69 What are my options? Wayne Rosen, MD, FRCSC As presented at the 37th Annual Mackid Symposium: Cancer Care in the Community (May 22, 2003) There are
069-Colorectal cancer (Rosen) 1/23/04 12:59 PM Page 69 What are my options? Wayne Rosen, MD, FRCSC As presented at the 37th Annual Mackid Symposium: Cancer Care in the Community (May 22, 2003) There are
THE EFFECT OF FECAL OCCULT-BLOOD SCREENING ON THE INCIDENCE OF COLORECTAL CANCER
 THE EFFECT OF FECAL OCCULT-BLOOD SCREENING ON THE INCIDENCE OF COLORECTAL CANCER JACK S. MANDEL, PH.D., M.P.H., TIMOTHY R. CHURCH, PH.D., JOHN H. BOND, M.D., FRED EDERER, M.A., MINDY S. GEISSER, M.S.,
THE EFFECT OF FECAL OCCULT-BLOOD SCREENING ON THE INCIDENCE OF COLORECTAL CANCER JACK S. MANDEL, PH.D., M.P.H., TIMOTHY R. CHURCH, PH.D., JOHN H. BOND, M.D., FRED EDERER, M.A., MINDY S. GEISSER, M.S.,
The Canadian Cancer Society estimates that in
 How Do I Screen For Colorectal Cancer? By Ted M. Ross, MD, FRCS(C); and Naomi Ross, RD, BSc To be presented at the University of Toronto s Primary Care Today sessions (October 3, 2003) The Canadian Cancer
How Do I Screen For Colorectal Cancer? By Ted M. Ross, MD, FRCS(C); and Naomi Ross, RD, BSc To be presented at the University of Toronto s Primary Care Today sessions (October 3, 2003) The Canadian Cancer
SCREENING FOR COLON AND RECTAL CANCER
 Review Article SCREENING FOR COLON AND RECTAL CANCER Jack S. Mandel, PhD, MPH School of Public Health, University of Minnesota Introduction Approximately 138,200 new cases and 55,300 deaths occured in
Review Article SCREENING FOR COLON AND RECTAL CANCER Jack S. Mandel, PhD, MPH School of Public Health, University of Minnesota Introduction Approximately 138,200 new cases and 55,300 deaths occured in
Estimation of screening test (Hemoccult ) sensitivity in colorectal cancer mass screening
 doi: 1.154/ bjoc.21.1752, available online at http://www.idealibrary.com on http://www.bjcancer.com Estimation of screening test (Hemoccult ) sensitivity in colorectal cancer mass screening JL Jouve 1,
doi: 1.154/ bjoc.21.1752, available online at http://www.idealibrary.com on http://www.bjcancer.com Estimation of screening test (Hemoccult ) sensitivity in colorectal cancer mass screening JL Jouve 1,
C olorectal adenomas are reputed to be precancerous
 568 COLORECTAL CANCER Incidence and recurrence rates of colorectal adenomas estimated by annually repeated colonoscopies on asymptomatic Japanese Y Yamaji, T Mitsushima, H Ikuma, H Watabe, M Okamoto, T
568 COLORECTAL CANCER Incidence and recurrence rates of colorectal adenomas estimated by annually repeated colonoscopies on asymptomatic Japanese Y Yamaji, T Mitsushima, H Ikuma, H Watabe, M Okamoto, T
Fecal occult blood tests: a cost-effectiveness analysis Gyrd-Hansen D
 Fecal occult blood tests: a cost-effectiveness analysis Gyrd-Hansen D Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS EED. Each abstract
Fecal occult blood tests: a cost-effectiveness analysis Gyrd-Hansen D Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion on NHS EED. Each abstract
Citation for published version (APA): Wijkerslooth de Weerdesteyn, T. R. (2013). Population screening for colorectal cancer by colonoscopy
 UvA-DARE (Digital Academic Repository) Population screening for colorectal cancer by colonoscopy de Wijkerslooth, T.R. Link to publication Citation for published version (APA): Wijkerslooth de Weerdesteyn,
UvA-DARE (Digital Academic Repository) Population screening for colorectal cancer by colonoscopy de Wijkerslooth, T.R. Link to publication Citation for published version (APA): Wijkerslooth de Weerdesteyn,
The effectiveness of telephone reminders and SMS messages on compliance with colorectal cancer screening: an open-label, randomized controlled trial
 Page1 of 5 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 The effectiveness of telephone reminders and SMS messages on compliance with colorectal cancer screening: an
Page1 of 5 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 The effectiveness of telephone reminders and SMS messages on compliance with colorectal cancer screening: an
Updates in Colorectal Cancer Screening & Prevention
 Updates in Colorectal Cancer Screening & Prevention Swati G. Patel, MD MS Assistant Professor of Medicine Division of Gastroenterology & Hepatology Gastrointestinal Cancer Risk and Prevention Clinic University
Updates in Colorectal Cancer Screening & Prevention Swati G. Patel, MD MS Assistant Professor of Medicine Division of Gastroenterology & Hepatology Gastrointestinal Cancer Risk and Prevention Clinic University
Papers. A systematic review of the effects of screening for colorectal cancer using the faecal occult blood test, Hemoccult. Abstract.
 A systematic review of the effects of screening for colorectal cancer using the faecal occult blood test, Hemoccult Bernie Towler, Les Irwig, Paul Glasziou, Jan Kewenter, David Weller, Chris Silagy Abstract
A systematic review of the effects of screening for colorectal cancer using the faecal occult blood test, Hemoccult Bernie Towler, Les Irwig, Paul Glasziou, Jan Kewenter, David Weller, Chris Silagy Abstract
Screening for colorectal cancer
 Postgrad Med J (1994) 70, 469-474 A) The Fellowship of Postgraduate Medicine, 1994 Review Article Screening for colorectal cancer D.H. Bennett and J.D. Hardcastle Department ofsurgery, E Floor, West Block,
Postgrad Med J (1994) 70, 469-474 A) The Fellowship of Postgraduate Medicine, 1994 Review Article Screening for colorectal cancer D.H. Bennett and J.D. Hardcastle Department ofsurgery, E Floor, West Block,
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE
 SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
SCREENING FOR BOWEL CANCER USING FLEXIBLE SIGMOIDOSCOPY REVIEW APPRAISAL CRITERIA FOR THE UK NATIONAL SCREENING COMMITTEE The Condition 1. The condition should be an important health problem Colorectal
THE NEW ZEALAND MEDICAL JOURNAL
 THE NEW ZEALAND MEDICAL JOURNAL Vol 120 No 1258 ISSN 1175 8716 A survey of colonoscopy capacity in New Zealand s public hospitals Andrew Yeoman, Susan Parry Abstract Aims Population screening for colorectal
THE NEW ZEALAND MEDICAL JOURNAL Vol 120 No 1258 ISSN 1175 8716 A survey of colonoscopy capacity in New Zealand s public hospitals Andrew Yeoman, Susan Parry Abstract Aims Population screening for colorectal
C olorectal cancer (CRC) is one of the leading causes of
 1329 COLON Testing for faecal calprotectin (PhiCal) in the Norwegian Colorectal Cancer Prevention trial on flexible sigmoidoscopy screening: comparison with an immunochemical test for occult blood (FlexSure
1329 COLON Testing for faecal calprotectin (PhiCal) in the Norwegian Colorectal Cancer Prevention trial on flexible sigmoidoscopy screening: comparison with an immunochemical test for occult blood (FlexSure
COLORECTAL SCREENING PROGRAMME: IMPACT ON THE HOSPITAL S PATHOLOGY SERVICES SINCE ITS INTRODUCTION.
 The West London Medical Journal 2009 Vol No 1 pp 23-31 COLORECTAL SCREENING PROGRAMME: IMPACT ON THE HOSPITAL S PATHOLOGY SERVICES SINCE ITS INTRODUCTION. Competing interests: None declared ABSTRACT Sarah
The West London Medical Journal 2009 Vol No 1 pp 23-31 COLORECTAL SCREENING PROGRAMME: IMPACT ON THE HOSPITAL S PATHOLOGY SERVICES SINCE ITS INTRODUCTION. Competing interests: None declared ABSTRACT Sarah
F rectal cancer have been almost constant over the
 Screening and Rescreening for Colorectal Cancer A Controlled Trial of Fecal Occult Blood Testing in 27,700 Subjects J. KEWENTER, MD, PHD; s. BJORK, MD, PHD,* EVA HAGLIND, MD, PHD," L. SMITH, MD, PHD,'
Screening and Rescreening for Colorectal Cancer A Controlled Trial of Fecal Occult Blood Testing in 27,700 Subjects J. KEWENTER, MD, PHD; s. BJORK, MD, PHD,* EVA HAGLIND, MD, PHD," L. SMITH, MD, PHD,'
Frequency of Diagnosis of Colorectal Cancer with Double Contrast Barium Enema
 Bahrain Medical Bulletin, Vol.24, No.3, September 2002 Frequency of Diagnosis of Colorectal Cancer with Double Contrast Barium Enema Najeeb S Jamsheer, MD, FRCR* Neelam. Malik, MD, MNAMS** Objective: To
Bahrain Medical Bulletin, Vol.24, No.3, September 2002 Frequency of Diagnosis of Colorectal Cancer with Double Contrast Barium Enema Najeeb S Jamsheer, MD, FRCR* Neelam. Malik, MD, MNAMS** Objective: To
Michael V. Maciosek, PhD, Leif I. Solberg, MD, Ashley B. Coffield, MPA, Nichol M. Edwards, MS, Michael J. Goodman, PhD
 Colorectal Cancer Screening Health Impact and Cost Effectiveness Michael V. Maciosek, PhD, Leif I. Solberg, MD, Ashley B. Coffield, MPA, Nichol M. Edwards, MS, Michael J. Goodman, PhD Background: Colorectal
Colorectal Cancer Screening Health Impact and Cost Effectiveness Michael V. Maciosek, PhD, Leif I. Solberg, MD, Ashley B. Coffield, MPA, Nichol M. Edwards, MS, Michael J. Goodman, PhD Background: Colorectal
Colonoscopy screening for colorectal cancer: the outcomes of two recruitment methods
 Colonoscopy screening for colorectal cancer: the outcomes of two recruitment methods Mike Corbett, Sharon L Chambers, Bruce Shadbolt, Lybus C Hillman and Doug Taupin One in 20 Australians will develop
Colonoscopy screening for colorectal cancer: the outcomes of two recruitment methods Mike Corbett, Sharon L Chambers, Bruce Shadbolt, Lybus C Hillman and Doug Taupin One in 20 Australians will develop
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Zauber AG, Winawer SJ, O Brien MJ, et al. Colonoscopic polypectomy
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Zauber AG, Winawer SJ, O Brien MJ, et al. Colonoscopic polypectomy
Colorectal Cancer Screening. Dr Kishor Muniyappa 2626 Care Drive, Suite 101 Tallahassee, FL Ph:
 Colorectal Cancer Screening Dr Kishor Muniyappa 2626 Care Drive, Suite 101 Tallahassee, FL 32308 Ph: 850-297-0351 What we ll be talking about How common is colorectal cancer? What is colorectal cancer?
Colorectal Cancer Screening Dr Kishor Muniyappa 2626 Care Drive, Suite 101 Tallahassee, FL 32308 Ph: 850-297-0351 What we ll be talking about How common is colorectal cancer? What is colorectal cancer?
Colon Screening in 2014 Offering Patients a Choice. Clark A Harrison MD The Nevada Colon Cancer Partnership
 Colon Screening in 2014 Offering Patients a Choice Clark A Harrison MD The Nevada Colon Cancer Partnership Objectives 1. Understand the incidence and mortality rates for CRC in the US. 2. Understand risk
Colon Screening in 2014 Offering Patients a Choice Clark A Harrison MD The Nevada Colon Cancer Partnership Objectives 1. Understand the incidence and mortality rates for CRC in the US. 2. Understand risk
Colorectal Cancer Screening: Technical Report Prepared for the National Commission on Prevention Priorities
 Colorectal Cancer Screening: Technical Report Prepared for the National Commission on Prevention Priorities Version 06.1; last updated May 11, 2006 Prepared by Michael V. Maciosek, PhD* Leif I. Solberg,
Colorectal Cancer Screening: Technical Report Prepared for the National Commission on Prevention Priorities Version 06.1; last updated May 11, 2006 Prepared by Michael V. Maciosek, PhD* Leif I. Solberg,
GUAIAC tests for fecal occult blood detect the pseudoperoxidase
 Vol. 334 No. 3 COMPARISON OF FECAL OCCULT-BLOOD TESTS FOR COLORECTAL-CANCER SCREENING 155 A COMPARISON OF FECAL OCCULT-BLOOD TESTS FOR COLORECTAL-CANCER SCREENING JAMES E. ALLISON, M.D., IRENE S. TEKAWA,
Vol. 334 No. 3 COMPARISON OF FECAL OCCULT-BLOOD TESTS FOR COLORECTAL-CANCER SCREENING 155 A COMPARISON OF FECAL OCCULT-BLOOD TESTS FOR COLORECTAL-CANCER SCREENING JAMES E. ALLISON, M.D., IRENE S. TEKAWA,
Cite this article as: BMJ, doi: /bmj c (published 5 July 2004)
 Cite this article as: BMJ, doi:10.1136/bmj.38153.491887.7c (published 5 July 2004) Results of the first round of a demonstration pilot of screening for colorectal cancer in the United Kingdom UK Colorectal
Cite this article as: BMJ, doi:10.1136/bmj.38153.491887.7c (published 5 July 2004) Results of the first round of a demonstration pilot of screening for colorectal cancer in the United Kingdom UK Colorectal
Colorectal cancer screening
 26 Colorectal cancer screening BETHAN GRAF AND JOHN MARTIN Colorectal cancer is theoretically a preventable disease and is ideally suited to a population screening programme, as there is a long premalignant
26 Colorectal cancer screening BETHAN GRAF AND JOHN MARTIN Colorectal cancer is theoretically a preventable disease and is ideally suited to a population screening programme, as there is a long premalignant
T. Rubeca 1, S. Rapi 2, M. Confortini 1, M. Brogioni 2, G. Grazzini 1, M. Zappa 1, D. Puliti 1, G. Castiglione 1, S. Ciatto 1
 The International Journal of Biological Markers, Vol. 21 no. 3, pp. 157-161 2006 Wichtig Editore Evaluation of diagnostic accuracy of screening by fecal occult blood testing (FOBT). Comparison of FOB Gold
The International Journal of Biological Markers, Vol. 21 no. 3, pp. 157-161 2006 Wichtig Editore Evaluation of diagnostic accuracy of screening by fecal occult blood testing (FOBT). Comparison of FOB Gold
CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING
 CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING This guideline is designed to assist practitioners by providing the framework for colorectal cancer (CRC) screening, and is not intended to replace
CLINICAL PRACTICE GUIDELINE FOR COLORECTAL CANCER SCREENING This guideline is designed to assist practitioners by providing the framework for colorectal cancer (CRC) screening, and is not intended to replace
Cost-effectiveness Model for Colon Cancer Screening
 GASTROENTEROLOGY 1995;109:1781-1790 Cost-effectiveness Model for Colon Cancer Screening DAVID A. LIEBERMAN Division of Gastroenterology, Department of Medicine, Oregon Health Sciences University, and Portland
GASTROENTEROLOGY 1995;109:1781-1790 Cost-effectiveness Model for Colon Cancer Screening DAVID A. LIEBERMAN Division of Gastroenterology, Department of Medicine, Oregon Health Sciences University, and Portland
Measuring performance and quality indicators of CRC screening
 Measuring performance and quality indicators of CRC screening Ondřej MÁJEK Institute of Biostatistics and Analyses, Masaryk University Institute of Biostatistics and Analyses, Masaryk University, Brno
Measuring performance and quality indicators of CRC screening Ondřej MÁJEK Institute of Biostatistics and Analyses, Masaryk University Institute of Biostatistics and Analyses, Masaryk University, Brno
Screening for GI Cancer Past Present and Future. Prof. Bob Steele University of Dundee
 Screening for GI Cancer Past Present and Future Prof. Bob Steele University of Dundee Worldwide Cancer Incidence Rates UK Cancer Incidence Rates Screening The detection of disease in asymptomatic subjects
Screening for GI Cancer Past Present and Future Prof. Bob Steele University of Dundee Worldwide Cancer Incidence Rates UK Cancer Incidence Rates Screening The detection of disease in asymptomatic subjects
Northern Ireland Bowel Cancer Screening Programme. Pathways. Version 4 1 st October 2013
 Northern Ireland Bowel Cancer Screening Programme Pathways These changes will be version controlled, led by the Quality Assurance Director for the Programme. Any updated versions will be circulated and
Northern Ireland Bowel Cancer Screening Programme Pathways These changes will be version controlled, led by the Quality Assurance Director for the Programme. Any updated versions will be circulated and
R. J. L. F. Loffeld, 1 P. E. P. Dekkers, 2 and M. Flens Introduction
 ISRN Gastroenterology Volume 213, Article ID 87138, 5 pages http://dx.doi.org/1.1155/213/87138 Research Article The Incidence of Colorectal Cancer Is Decreasing in the Older Age Cohorts in the Zaanstreek
ISRN Gastroenterology Volume 213, Article ID 87138, 5 pages http://dx.doi.org/1.1155/213/87138 Research Article The Incidence of Colorectal Cancer Is Decreasing in the Older Age Cohorts in the Zaanstreek
Screening & Surveillance Guidelines
 Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Chapter 2 Screening & Surveillance Guidelines I. Eligibility Coloradans ages 50 and older (average risk) or under 50 at elevated risk for colon cancer (personal or family history) that meet the following
Global colorectal cancer screening appropriate or practical? Graeme P Young, Flinders University WCC, Melbourne
 Global colorectal cancer screening appropriate or practical? Graeme P Young, Flinders University. 2014 WCC, Melbourne Outline WHO criteria to justify screening Appropriateness: Global variation in incidence
Global colorectal cancer screening appropriate or practical? Graeme P Young, Flinders University. 2014 WCC, Melbourne Outline WHO criteria to justify screening Appropriateness: Global variation in incidence
Improving Outcomes in Colorectal Cancer: The Science of Screening. Colorectal Cancer (CRC)
 Improving Outcomes in Colorectal Cancer: The Science of Screening Tennessee Primary Care Association October 23, 2014 Durado Brooks, MD, MPH Director, Prostate and Colorectal Cancers Colorectal Cancer
Improving Outcomes in Colorectal Cancer: The Science of Screening Tennessee Primary Care Association October 23, 2014 Durado Brooks, MD, MPH Director, Prostate and Colorectal Cancers Colorectal Cancer
NHS KINGSTON. Contents
 NHS KINGSTON Contents 1. Background... 2 2. Targets and quality standards... 2 3. Service provision and performance... 3 Uptake... 3 Investigations... 6 Cancer detection... 7 Age extension... 7 4. Quality
NHS KINGSTON Contents 1. Background... 2 2. Targets and quality standards... 2 3. Service provision and performance... 3 Uptake... 3 Investigations... 6 Cancer detection... 7 Age extension... 7 4. Quality
Cancer Screening Programmes BOWEL CANCER SCREENING. The Facts
 Cancer Screening Programmes BOWEL CANCER SCREENING The Facts What is the aim of this leaflet? This leaflet gives you information about bowel cancer, and the benefits and risks of bowel cancer screening.
Cancer Screening Programmes BOWEL CANCER SCREENING The Facts What is the aim of this leaflet? This leaflet gives you information about bowel cancer, and the benefits and risks of bowel cancer screening.
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE
 COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
COLORECTAL CANCER FAISALGHANISIDDIQUI MBBS; FCPS; PGDIP-BIOETHICS; MCPS-HPE PROFESSOR OF SURGERY & DIRECTOR, PROFESSIONAL DEVELOPMENT CENTRE J I N N A H S I N D H M E D I C A L U N I V E R S I T Y faisal.siddiqui@jsmu.edu.pk
Guidelines for Breast, Cervical and Colorectal Cancer Screening
 Guidelines for Breast, Cervical and Colorectal Cancer Screening Your recommendation counts. Talk to your patients about screening for cancer. CancerCare Manitoba provides organized, population-based screening
Guidelines for Breast, Cervical and Colorectal Cancer Screening Your recommendation counts. Talk to your patients about screening for cancer. CancerCare Manitoba provides organized, population-based screening
treated successfully. The predictive value of a positive test varied
 Detecting Colorectal Cancer with a Large Scale Fecal Occult Blood Testing Program DAVID 1. GREGORIO, PhD, MS PERI LOLACHI, MPH HOLGER HANSEN, MD, DrPH The authors are with the University of Connecticut,
Detecting Colorectal Cancer with a Large Scale Fecal Occult Blood Testing Program DAVID 1. GREGORIO, PhD, MS PERI LOLACHI, MPH HOLGER HANSEN, MD, DrPH The authors are with the University of Connecticut,
The relative economics of screening for colorectal cancer, breast cancer and cervical cancer
 Critical Reviews in Oncology/Hematology 32 (1999) 133 144 www.elsevier.com/locate/critrevonc The relative economics of screening for colorectal cancer, breast cancer and cervical cancer Dorte Gyrd-Hansen*
Critical Reviews in Oncology/Hematology 32 (1999) 133 144 www.elsevier.com/locate/critrevonc The relative economics of screening for colorectal cancer, breast cancer and cervical cancer Dorte Gyrd-Hansen*
Colorectal Cancer Screening. Paul Berg MD
 Colorectal Cancer Screening Paul Berg MD What is clinical integration? AMA Definition The means to facilitate the coordination of patient care across conditions, providers, settings, and time in order
Colorectal Cancer Screening Paul Berg MD What is clinical integration? AMA Definition The means to facilitate the coordination of patient care across conditions, providers, settings, and time in order
The New England Journal of Medicine
 The New England Journal of Medicine Copyright 2001 by the Massachusetts Medical Society VOLUME 345 A UGUST 23, 2001 NUMBER 8 ONE-TIME SCREENING FOR COLORECTAL CANCER WITH COMBINED FECAL OCCULT-BLOOD TESTING
The New England Journal of Medicine Copyright 2001 by the Massachusetts Medical Society VOLUME 345 A UGUST 23, 2001 NUMBER 8 ONE-TIME SCREENING FOR COLORECTAL CANCER WITH COMBINED FECAL OCCULT-BLOOD TESTING
Supplementary Online Content
 Supplementary Online Content Meester R.G.S, Doubeni CA, Lansdorp-Vogelaar, et al. Variation in adenoma detection rate and the lifetime benefits and cost of colorectal cancer screening: a microsimulation
Supplementary Online Content Meester R.G.S, Doubeni CA, Lansdorp-Vogelaar, et al. Variation in adenoma detection rate and the lifetime benefits and cost of colorectal cancer screening: a microsimulation
Colorectal Cancer Screening and Surveillance
 1 Colorectal Cancer Screening and Surveillance Jeffrey Lee MD, MAS Assistant Clinical Professor of Medicine University of California, San Francisco jeff.lee@ucsf.edu Objectives Review the various colorectal
1 Colorectal Cancer Screening and Surveillance Jeffrey Lee MD, MAS Assistant Clinical Professor of Medicine University of California, San Francisco jeff.lee@ucsf.edu Objectives Review the various colorectal
CENTERS FOR DISEASE CONTROL AND PREVENTION CENTERS FOR DISEASE CONTROL AND PREVENTION. Incidence Male. Incidence Female.
 A Call to Action: Prevention and Early Detection of Colorectal Cancer (CRC) 5 Key Messages Screening reduces mortality from CRC All persons aged 50 years and older should begin regular screening High-risk
A Call to Action: Prevention and Early Detection of Colorectal Cancer (CRC) 5 Key Messages Screening reduces mortality from CRC All persons aged 50 years and older should begin regular screening High-risk
COLON CANCER SCREENING: AN UPDATE
 Overview COLON CANCER SCREENING: AN UPDATE Siddharth Verma, DO, JD Rutgers New Jersey Medical School Background Screening Updates in Specific Populations African Americans CRC in the younger age USPSTF
Overview COLON CANCER SCREENING: AN UPDATE Siddharth Verma, DO, JD Rutgers New Jersey Medical School Background Screening Updates in Specific Populations African Americans CRC in the younger age USPSTF
Performance Characteristics and Comparison of Two Fecal Occult Blood Tests in Patients Undergoing Colonoscopy
 Dig Dis Sci (2007) 52:1009 1013 DOI 10.1007/s10620-006-9383-y ORIGINAL ARTICLE Performance Characteristics and Comparison of Two Fecal Occult Blood Tests in Patients Undergoing Colonoscopy Marcia Cruz-Correa
Dig Dis Sci (2007) 52:1009 1013 DOI 10.1007/s10620-006-9383-y ORIGINAL ARTICLE Performance Characteristics and Comparison of Two Fecal Occult Blood Tests in Patients Undergoing Colonoscopy Marcia Cruz-Correa
removal of adenomatous polyps detects important effectively as follow-up colonoscopy after both constitute a low-risk Patients with 1 or 2
 Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
COLORECTAL CANCER. Colorectal Cancer (CRC) 3 rd most common cancer in U.S. 3 rd deadliest cancer in U.S. 12/4/2014
 The heart and science of medicine. UVMHealth.org/CancerCenter COLORECTAL CANCER Claire Verschraegen, MD Co-Director University of Vermont Cancer Center 1 Colorectal Cancer (CRC) 3 rd most common cancer
The heart and science of medicine. UVMHealth.org/CancerCenter COLORECTAL CANCER Claire Verschraegen, MD Co-Director University of Vermont Cancer Center 1 Colorectal Cancer (CRC) 3 rd most common cancer
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines
 Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
UK Bowel Cancer screening Dr Voi Shim Wong BsC MD FRCP. Consultant Gastroenterologist Accredited BCSP colonoscopist Whittington + UCL Hospitals
 UK Bowel Cancer screening 2017 Dr Voi Shim Wong BsC MD FRCP Consultant Gastroenterologist Accredited BCSP colonoscopist Whittington + UCL Hospitals Bowel Cancer Contents UK Bowel Cancer Screening Programme
UK Bowel Cancer screening 2017 Dr Voi Shim Wong BsC MD FRCP Consultant Gastroenterologist Accredited BCSP colonoscopist Whittington + UCL Hospitals Bowel Cancer Contents UK Bowel Cancer Screening Programme
Setting The setting was secondary care. The economic study was carried out in Australia.
 Cost-effectiveness of colorectal cancer screening: comparison of community-based flexible sigmoidoscopy with fecal occult blood testing and colonoscopy O'Leary B A, Olynyk J K, Neville A M, Platell C F
Cost-effectiveness of colorectal cancer screening: comparison of community-based flexible sigmoidoscopy with fecal occult blood testing and colonoscopy O'Leary B A, Olynyk J K, Neville A M, Platell C F
HOW TO EVALUATE ACTIVITIES INTENDED TO INCREASE AWARENESS AND USE OF COLORECTAL CANCER SCREENING. Using your toolkit to conduct an evaluation
 EVALUATION TOOLKIT HOW TO EVALUATE ACTIVITIES INTENDED TO INCREASE AWARENESS AND USE OF COLORECTAL CANCER SCREENING Using your toolkit to conduct an evaluation Welcome Mary Doroshenk, MA Director National
EVALUATION TOOLKIT HOW TO EVALUATE ACTIVITIES INTENDED TO INCREASE AWARENESS AND USE OF COLORECTAL CANCER SCREENING Using your toolkit to conduct an evaluation Welcome Mary Doroshenk, MA Director National
Colorectal cancer screening in asymptomatic populations
 590 Colorectal cancer screening in asymptomatic populations Gut 1995; 36: 590-598 Gastroenterology Research Unit, Leicester General Hospital, Leicester A R Hart A C B Wicks J F Mayberry Correspondence
590 Colorectal cancer screening in asymptomatic populations Gut 1995; 36: 590-598 Gastroenterology Research Unit, Leicester General Hospital, Leicester A R Hart A C B Wicks J F Mayberry Correspondence
Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care
 Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
Quality ID #343: Screening Colonoscopy Adenoma Detection Rate National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Outcome DESCRIPTION:
The Prevalence Rate and Anatomic Location of Colorectal Adenoma and Cancer Detected by Colonoscopy in Average-Risk Individuals Aged Years
 American Journal of Gastroenterology ISSN 0002-9270 C 2006 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2006.00430.x Published by Blackwell Publishing The Prevalence Rate and Anatomic Location
American Journal of Gastroenterology ISSN 0002-9270 C 2006 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2006.00430.x Published by Blackwell Publishing The Prevalence Rate and Anatomic Location
Colorectal Cancer Screening: Cost-Effectiveness and Adverse events October, 2005
 Colorectal Cancer Screening: Cost-Effectiveness and Adverse events October, 2005 David Lieberman MD Chief, Division of Gastroenterology Oregon Health and Science University Portland VAMC Portland, Oregon
Colorectal Cancer Screening: Cost-Effectiveness and Adverse events October, 2005 David Lieberman MD Chief, Division of Gastroenterology Oregon Health and Science University Portland VAMC Portland, Oregon
Summary. Cezary ŁozińskiABDF, Witold KyclerABCDEF. Rep Pract Oncol Radiother, 2007; 12(4):
 Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Rep Pract Oncol Radiother, 2007; 12(4): 201-206 Original Paper Received: 2006.12.19 Accepted: 2007.04.02 Published: 2007.08.31 Authors Contribution: A Study Design B Data Collection C Statistical Analysis
Structured Follow-Up after Colorectal Cancer Resection: Overrated. R. Taylor Ripley University of Colorado Grand Rounds April 23, 2007
 Structured Follow-Up after Colorectal Cancer Resection: Overrated R. Taylor Ripley University of Colorado Grand Rounds April 23, 2007 Guidelines for Colonoscopy Production: Surveillance US Multi-Society
Structured Follow-Up after Colorectal Cancer Resection: Overrated R. Taylor Ripley University of Colorado Grand Rounds April 23, 2007 Guidelines for Colonoscopy Production: Surveillance US Multi-Society
Bowel Cancer Screening
 Bowel Cancer Screening Dr John Hancock FRCP Consultant Gastroenterologist University Hospital of North Tees Outline Background Current bowel cancer screening programme Tees Screening Centre Future Flexi
Bowel Cancer Screening Dr John Hancock FRCP Consultant Gastroenterologist University Hospital of North Tees Outline Background Current bowel cancer screening programme Tees Screening Centre Future Flexi
The most common methods currently used to investigate the colon (alone or in combination) include:
 CCO No.9 Oct 2002 Before CCO decides to undertake a health technology assessment, a pre-assessment of the literature is performed. Pre-assessments are based on a limited literature search; they are not
CCO No.9 Oct 2002 Before CCO decides to undertake a health technology assessment, a pre-assessment of the literature is performed. Pre-assessments are based on a limited literature search; they are not
John Croese, Stephen Fairley, John Masson. Gastroenterology, Townsville Hospital, Queensland. School of Population Health, University of Queensland
 Guaiac versus immunochemical tests: faecal occult blood test screening for colorectal cancer in a rural community Abstract Objective: To describe patient participation and clinical performance in a colorectal
Guaiac versus immunochemical tests: faecal occult blood test screening for colorectal cancer in a rural community Abstract Objective: To describe patient participation and clinical performance in a colorectal
Diagnostics for the early detection and prevention of colon cancer. Publication of DeeP-C Study Data in New England Journal of Medicine March 2014
 Diagnostics for the early detection and prevention of colon cancer Publication of DeeP-C Study Data in New England Journal of Medicine March 2014 Safe Harbor Statement Certain statements made in this presentation
Diagnostics for the early detection and prevention of colon cancer Publication of DeeP-C Study Data in New England Journal of Medicine March 2014 Safe Harbor Statement Certain statements made in this presentation
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci. Colon polyps. Colorectal cancer
 Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Colon polyps Colorectal cancer Harrison s Principles of Internal Medicine 18 Ed. 2012 Colorectal cancer 70% Colorectal cancer CRC and colon
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Colon polyps Colorectal cancer Harrison s Principles of Internal Medicine 18 Ed. 2012 Colorectal cancer 70% Colorectal cancer CRC and colon
Increasing the number of older persons in the United
 Current Capacity for Endoscopic Colorectal Cancer Screening in the United States: Data from the National Cancer Institute Survey of Colorectal Cancer Screening Practices Martin L. Brown, PhD, Carrie N.
Current Capacity for Endoscopic Colorectal Cancer Screening in the United States: Data from the National Cancer Institute Survey of Colorectal Cancer Screening Practices Martin L. Brown, PhD, Carrie N.
DR.RUPNATHJI( DR.RUPAK NATH )
 8. Screening for Colorectal Cancer Burden of Suffering RECOMMENDATION Screening for colorectal cancer is recommended for all persons aged 50 and older with annual fecal occult blood testing (FOBT), or
8. Screening for Colorectal Cancer Burden of Suffering RECOMMENDATION Screening for colorectal cancer is recommended for all persons aged 50 and older with annual fecal occult blood testing (FOBT), or
Colorectal cancer screening guidelines clearly recommend. Comparing Risks and Benefits of Colorectal Cancer Screening in Elderly Patients
 GASTROENTEROLOGY 2005;129:1163 1170 Comparing Risks and Benefits of Colorectal Cancer Screening in Elderly Patients CYNTHIA W. KO* and AMNON SONNENBERG *Department of Medicine, University of Washington,
GASTROENTEROLOGY 2005;129:1163 1170 Comparing Risks and Benefits of Colorectal Cancer Screening in Elderly Patients CYNTHIA W. KO* and AMNON SONNENBERG *Department of Medicine, University of Washington,
We couldn t have made it any easier.
 We couldn t have made it any easier. To save lives For over thirty years Hemoccult has been the gold standard for fecal occult blood tests (FOBTs). In fact, our name has become synonymous with FOBTs. Now
We couldn t have made it any easier. To save lives For over thirty years Hemoccult has been the gold standard for fecal occult blood tests (FOBTs). In fact, our name has become synonymous with FOBTs. Now
Cost-effectiveness of colonoscopy in screening for colorectal cancer Sonnenberg A, Delco F, Inadomi J M
 Cost-effectiveness of colonoscopy in screening for colorectal cancer Sonnenberg A, Delco F, Inadomi J M Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion
Cost-effectiveness of colonoscopy in screening for colorectal cancer Sonnenberg A, Delco F, Inadomi J M Record Status This is a critical abstract of an economic evaluation that meets the criteria for inclusion
A microsimulation study of the benefits and costs of screening for colorectal cancer Christopher Eric Stevenson
 A microsimulation study of the benefits and costs of screening for colorectal cancer Christopher Eric Stevenson A thesis submitted for the degree of Doctor of Philosophy of The Australian National University
A microsimulation study of the benefits and costs of screening for colorectal cancer Christopher Eric Stevenson A thesis submitted for the degree of Doctor of Philosophy of The Australian National University
patients over the age of 40
 Postgraduate Medical Journal (1988) 64, 364-368 Frank rectal bleeding: a prospective study of causes in patients over the age of 40 P.S.Y. Cheung, S.K.C. Wong, J. Boey and C.K. Lai Department of Surgery,
Postgraduate Medical Journal (1988) 64, 364-368 Frank rectal bleeding: a prospective study of causes in patients over the age of 40 P.S.Y. Cheung, S.K.C. Wong, J. Boey and C.K. Lai Department of Surgery,
Screening for colorectal cancer in a factory-based population
 Br. J. Cancer (1983), 48, 843-847 Screening for colorectal cancer in a factory-based population with Fecatest F.I. Lee Department of Gastroenterology, Victoria Hospital, Blackpool. Summary This report
Br. J. Cancer (1983), 48, 843-847 Screening for colorectal cancer in a factory-based population with Fecatest F.I. Lee Department of Gastroenterology, Victoria Hospital, Blackpool. Summary This report
Debate: General surveillance/screening for colon cancer in a resource constrained environment is imperative
 Debate: General surveillance/screening for colon cancer in a resource constrained environment is imperative Dr. Meryl Oyomno Department of surgery, University of Pretoria INTRODUCTION Screening is the
Debate: General surveillance/screening for colon cancer in a resource constrained environment is imperative Dr. Meryl Oyomno Department of surgery, University of Pretoria INTRODUCTION Screening is the
The New Grade A: USPSTF Updated Colorectal Cancer Screening Guidelines, What does it all mean?
 The New Grade A: USPSTF Updated Colorectal Cancer Screening Guidelines, What does it all mean? Robert A. Smith, PhD Cancer Control, Department of Prevention and Early Detection American Cancer Society
The New Grade A: USPSTF Updated Colorectal Cancer Screening Guidelines, What does it all mean? Robert A. Smith, PhD Cancer Control, Department of Prevention and Early Detection American Cancer Society
Interventions to Improve Follow-up of Positive Results on Fecal Blood Tests
 Interventions to Improve Follow-up of Positive Results on Fecal Blood Tests Results of a systematic review, Kaiser experience, and implications for the Canton of Vaud Kevin Selby, M.D. Kevin.Selby@hospvd.ch
Interventions to Improve Follow-up of Positive Results on Fecal Blood Tests Results of a systematic review, Kaiser experience, and implications for the Canton of Vaud Kevin Selby, M.D. Kevin.Selby@hospvd.ch
Rx Only. Detecting Cancer In Blood.
 Epi procolon is an FDA-approved blood test for colorectal cancer screening for patients who are unwilling or unable to be screened by recommended methods. Rx Only Intended Use, Contraindications, Warnings,
Epi procolon is an FDA-approved blood test for colorectal cancer screening for patients who are unwilling or unable to be screened by recommended methods. Rx Only Intended Use, Contraindications, Warnings,
Cancer Screenings and Early Diagnostics
 Cancer Screenings and Early Diagnostics Ankur R. Parikh, D.O. Medical Director, Center for Advanced Individual Medicine Hematologist/Medical Oncologist Atlantic Regional Osteopathic Convention April 6
Cancer Screenings and Early Diagnostics Ankur R. Parikh, D.O. Medical Director, Center for Advanced Individual Medicine Hematologist/Medical Oncologist Atlantic Regional Osteopathic Convention April 6
Colorectal Cancer. Mark Chapman. MA MS FRCS EBSQ(coloproct) 21 st March 2018 Consultant Coloproctologist
 Colorectal Cancer Mark Chapman MA MS FRCS EBSQ(coloproct) 21 st March 2018 Consultant Coloproctologist Overview Epidemiology of colorectal cancer Adenoma carcinoma sequence Tumour diagnosis & staging Treatment
Colorectal Cancer Mark Chapman MA MS FRCS EBSQ(coloproct) 21 st March 2018 Consultant Coloproctologist Overview Epidemiology of colorectal cancer Adenoma carcinoma sequence Tumour diagnosis & staging Treatment
Health Professional Information
 Bowel Screening Wales Health Professional Information 2011 www.bowelscreeningwales.org.uk Version 2.0 Acknowledgements Bowel Screening Wales would like to express their sincere thanks to the English and
Bowel Screening Wales Health Professional Information 2011 www.bowelscreeningwales.org.uk Version 2.0 Acknowledgements Bowel Screening Wales would like to express their sincere thanks to the English and
Provider Contribution to Overuse and Underuse of Colorectal Cancer Screening (mostly colonoscopy)
 Provider Contribution to Overuse and Underuse of Colorectal Cancer Screening (mostly colonoscopy) James S. Goodwin, MD George and Cynthia Mitchell Distinguished Chair in Geriatric Medicine Director, Sealy
Provider Contribution to Overuse and Underuse of Colorectal Cancer Screening (mostly colonoscopy) James S. Goodwin, MD George and Cynthia Mitchell Distinguished Chair in Geriatric Medicine Director, Sealy
BOWEL CANCER. Cancer information.
 BOWEL CANCER Cancer information www.cancervic.org.au What is bowel cancer? Bowel cancer is the second most common cancer in both men and women in Australia1 and is more common in people over the age of
BOWEL CANCER Cancer information www.cancervic.org.au What is bowel cancer? Bowel cancer is the second most common cancer in both men and women in Australia1 and is more common in people over the age of
Prognosis after Treatment of Villous Adenomas
 Prognosis after Treatment of Villous Adenomas of the Colon and Rectum JOHN CHRISTIANSEN, M.D., PREBEN KIRKEGAARD, M.D., JYTTE IBSEN, M.D. With the existing evidence of neoplastic polyps of the colon and
Prognosis after Treatment of Villous Adenomas of the Colon and Rectum JOHN CHRISTIANSEN, M.D., PREBEN KIRKEGAARD, M.D., JYTTE IBSEN, M.D. With the existing evidence of neoplastic polyps of the colon and
Colorectal Neoplasia. Dr. Smita Devani MBChB, MRCP. Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi
 Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Colorectal Neoplasia Dr. Smita Devani MBChB, MRCP Consultant Physician and Gastroenterologist Aga Khan University Hospital, Nairobi Case History BT, 69yr male Caucasian History of rectal bleeding No change
Page 1. Cancer Screening for Women I have no conflicts of interest. Overview. Breast, Colon, and Lung Cancer. Jeffrey A.
 Cancer Screening for Women 2017 Breast, Colon, and Lung Cancer Jeffrey A. Tice, MD Professor of Medicine Division of General Internal Medicine University of California, San Francisco I have no conflicts
Cancer Screening for Women 2017 Breast, Colon, and Lung Cancer Jeffrey A. Tice, MD Professor of Medicine Division of General Internal Medicine University of California, San Francisco I have no conflicts
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Colorectal cancer: colonoscopic surveillance for prevention of colorectal cancer in patients with ulcerative colitis, Crohn
DECISION MODEL AND COST-EFFECTIVENESS ANALYSIS OF COLORECTAL CANCER
 DECISION MODEL AND COST-EFFECTIVENESS ANALYSIS OF COLORECTAL CANCER SCREENING AND SURVEILLANCE GUIDELINES FOR AVERAGE-RISK ADULTS Rezaul K. Khandker, Jane D. Dulski, Jeffrey B. Kilpatrick, Randall P. Ellis,
DECISION MODEL AND COST-EFFECTIVENESS ANALYSIS OF COLORECTAL CANCER SCREENING AND SURVEILLANCE GUIDELINES FOR AVERAGE-RISK ADULTS Rezaul K. Khandker, Jane D. Dulski, Jeffrey B. Kilpatrick, Randall P. Ellis,
Appendix 1 This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors.
 Appendix 1 This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Appendix to: Cenin DR, St John DJB, Ledger MJN, et al. Optimising the
Appendix 1 This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Appendix to: Cenin DR, St John DJB, Ledger MJN, et al. Optimising the
Section I Early Colorectal Cancer
 Section I Early Colorectal Cancer CHAPTER 1 SETTING THE SCENE 1.1 Colorectal Cancer in Australia Colorectal Cancer is unequivocally a major health problem in Australia. It is the most common cancer reported
Section I Early Colorectal Cancer CHAPTER 1 SETTING THE SCENE 1.1 Colorectal Cancer in Australia Colorectal Cancer is unequivocally a major health problem in Australia. It is the most common cancer reported
Bowel Cancer Information Leaflet THE DIGESTIVE SYSTEM
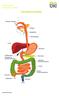 THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
University of Dundee. Published in: Journal of Medical Screening DOI: / Publication date: 2016
 University of Dundee Interval cancers using a quantitative faecal immunochemical test (FIT) for haemoglobin when colonoscopy capacity is limited Digby, Jayne; Fraser, Callum G.; Carey, Francis A.; Lang,
University of Dundee Interval cancers using a quantitative faecal immunochemical test (FIT) for haemoglobin when colonoscopy capacity is limited Digby, Jayne; Fraser, Callum G.; Carey, Francis A.; Lang,
Deakin Research Online
 Deakin Research Online This is the authors final peer reviewed (post print) version of the item published as: Tran, Ben, Keating, Catherine L., Ananda, Sumitra S., Kosmider, Suzanne, Jones, Ian, Croxford,
Deakin Research Online This is the authors final peer reviewed (post print) version of the item published as: Tran, Ben, Keating, Catherine L., Ananda, Sumitra S., Kosmider, Suzanne, Jones, Ian, Croxford,
Transforming Cancer Services for London
 Programme Director Paul Roche Status Draft Owner Laura Boyd Version 0.4 Author Jennifer Layburn Date 15/05/13 Transforming Cancer Services for London Best Practice Commissioning Pathway for the early detection
Programme Director Paul Roche Status Draft Owner Laura Boyd Version 0.4 Author Jennifer Layburn Date 15/05/13 Transforming Cancer Services for London Best Practice Commissioning Pathway for the early detection
Screening for Colorectal Cancer in Chinese: Comparison of Fecal Occult Blood Test, Flexible Sigmoidoscopy, and Colonoscopy
 GASTROENTEROLOGY 2003;124:608 614 Screening for Colorectal Cancer in Chinese: Comparison of Fecal Occult Blood Test, Flexible Sigmoidoscopy, and Colonoscopy JOSEPH J. Y. SUNG,* FRANCIS K. L. CHAN,* WAI
GASTROENTEROLOGY 2003;124:608 614 Screening for Colorectal Cancer in Chinese: Comparison of Fecal Occult Blood Test, Flexible Sigmoidoscopy, and Colonoscopy JOSEPH J. Y. SUNG,* FRANCIS K. L. CHAN,* WAI
Colorectal cancer screening A puzzle of tests and strategies
 Colorectal cancer screening A puzzle of tests and strategies A. Van Gossum, MD, PhD Head of the Clinic of Intestinal Diseases and Nutritional Support Department of Gastroenterology Hôpital Erasme ULB -
Colorectal cancer screening A puzzle of tests and strategies A. Van Gossum, MD, PhD Head of the Clinic of Intestinal Diseases and Nutritional Support Department of Gastroenterology Hôpital Erasme ULB -
