Risk-adapted Therapy of Pediatric Hodgkin Lymphoma in Upper Egypt Ghazaly MH 1, Ali AM 2, Hamza HA 3, Mohamed AM 2
|
|
|
- Juniper Malone
- 5 years ago
- Views:
Transcription
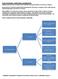
1 Ghazaly et al. SECI Oncology 2014 Risk-adapted Therapy of Pediatric Hodgkin Lymphoma in Upper Egypt Ghazaly MH 1, Ali AM 2, Hamza HA 3, Mohamed AM 2 1 Department of Pediatrics, Faculty of Medicine, Assiut University 2 Pediatric Oncology Department, South Egypt Cancer Institute, Assiut University 3 Radiotheray Department, South Egypt Cancer Institute, Assiut University Correspondence should be addressed to Amira M Mohamed at Pediatric Oncology Department, South Egypt Cancer Institute, El-Methak St., Assiut, Egypt, amirasherit@yahoo.com Accepted 2 December 2014 Abstract Background: Hodgkin's lymphoma (HL) is a highly curable malignant disease. Risk-adapted therapy for children with HL is directed toward high survival, minimal toxicity and optimal quality of life. Objectives: To assess the outcome of the HL patients treated with risk-adapted therapy approach at pediatric oncology department in South Egypt Cancer Institute and to assess the prognostic factors of survival in pediatric HL patients. Methods: This prospective study was carried out from January 2009 to January 2014, with median follow up of 36.5 months (range 8-58 months). Thirty four patients were eligible for this study stratified into three risk groups: low risk (LR), intermediate risk (IMR) and high risk (HR). Patients treated with two, four and six cycles respectively of alternating ABVD/COEP chemotherapy followed by involved-field radiation therapy (IFRT): 15 Gy for patients achieved complete response, and 25.5 Gy for those achieved partial response. Results: Six patients were LR, 18 patients were IMR and 10 patients were HR. Six patients had events, progressive disease in 3 patients, relapse in 2 patients, and death in one patient due to fever neutropenia. The 3-years overall survival (OS) and event free survival (EFS) rates (± SE) were 91.2% ± 5.3% and 82.3% ± 7.3% respectively. Multivariate analysis revealed "B" symptoms and anemia were the significant independent factors for inferior EFS, however, hypoalbuminemia and anemia were the significant independent factor for lower OS. Conclusion: Risk-adapted combined-modality therapy with ABVD/COEP and involved-field radiation therapy has high efficacy and minimal toxicity in the treatment of pediatric HL. Introduction Hodgkin's lymphoma (HL) is a highly curable malignant disease. Contemporary treatment for children and adolescents with Hodgkin s disease often uses a combined-modality approach with multi-agent chemotherapy and involved-field radiotherapy. This approach has yielded excellent results, with long-term disease-free survival ranged from 85% to % in patients with early-stage disease and of more than 60% in those with more advanced disease [1]. Because cure is likely for the majority of children presenting with HL, attention to long-term treatment complications has become increasingly important. Risk-adapted therapy for children with HL is directed toward high survival, minimal toxicity and optimal quality of life. This approach assigns intensity of therapy according to the risk criteria at presentation, with the parameters most frequently used to assign risk are the presence of "B" symptoms, bulk of presenting mass, mediastinal lymphadenopathy, extra nodal extension, number of involved nodal regions and Ann Arbor stage [2]. The objectives of this study are to assess the outcome of the HL patients treated with risk-adapted therapy approach at pediatric oncology department in South Egypt Cancer Institute (SECI) and to assess the prognostic factors of survival in pediatric HL patients. Patients and Methods This prospective study was carried out at the Pediatric Oncology Department and Radiotherapy Department, SECI, Assiut University during the period from January 2009 to January Informed consent was obtained from patient's family, and the study was approved by our institutional review board. Eligible patients had histologically confirmed HL, previously untreated and aged 16 years. For each patient, pretreatment evaluation included history and physical examination, laboratory investigations {complete blood picture (CBC), liver enzymes, albumin, bilirubin, serum
2 Ghazaly et al. SECI Oncology 2014 Page 2 of 8 urea and creatinine, erythrocytic sedimentation rate (ESR), lactic dehydrogenase (LDH), thyroid function test (TFT), sex hormones and bone marrow biopsy was done for patients with systemic (B) symptoms or stages (II-IV)}, chest X-ray and cervical, thoracic, abdominal and pelvic computed tomography (CT) scan with contrast. Pulmonary function test and echocardiography were done as baseline for follow up. Excisional biopsy was obtained from presenting lymphadenopathy and specimens were subjected to morphological studies and immunohistochemical tests by using CD15, CD30 and CD20, histopathological classification was done according to Revised European American Lymphoma classification/ World Health Organization (REAL/WHO) classification system [3]. Patients were staged by Cotswolds' modification of Ann Arbor staging system [4]. Risk assessment: patients were categorized into three risk groups: low risk (LR): included patients with stage IA, IIA without unfavorable features ("B" symptoms, bulky disease 10 cm, hilar lymphadenopathy, involvement of more than 4 lymph node regions and extra nodal extension to contiguous structures), intermediate risk (IMR): localized disease (stage I, II) with one or more of unfavorable features and patients with stage IIIA, high risk (HR): stage IIIB and IV [5]. Treatment: All patients received combination chemotherapy followed by involved field radiotherapy. Combination Chemotherapy was in the form of ABVD cycle (Adriamycin, bleomycin, vincristine and doxorubicin) alternating with COEP cycle (cyclophosphamide, oncovin (vincristine), etoposide and prednisone), table (1) [6], patients received different number of cycles according to risk stratification. Two alternating cycles for low risk group, four alternating cycles for intermediate risk group and six alternating cycles for high risk group. Radiotherapy was delivered to all initially involved sites. Patients who achieved early complete remission (CR) after two cycles of chemotherapy received 15 Gy and patients who achieved partial response (PR) received 25.5 Gy with modification based on patient s age, the presence of bulky disease, normal tissue concerns and potential acute and long-term effects. Radiation therapy was given using antero-posterior/postero-anterior fields, and started within 4 weeks of last chemotherapy cycle. Gross target volume was enlarged lymph node, clinical target volume was the anatomical compartment of enlarged lymph node and planning target volume was 1 cm margin to clinical target volume. An anterior laryngeal block was used if it did not shield involved nodes in case of radiation therapy to cervical region. If the axillae were to be treated, humeral head blocks were used. Evaluation of remission: Patient's response was evaluated by physical examination, laboratory investigations according to initial positive findings and radiological examination CT scan according to the initial positive findings. Monitoring of response was done every 2 cycles of chemotherapy with early response after first 2 cycles. Complete response (CR): was defined as resolution of all tumor- related constitutional symptoms and disappearance of all measurable nodal disease (Patients with residual disease in the mediastinum will be considered as showing a CR if there is a >70% reduction of mediastinal tumor volume or abdominal tumor). Partial response (PR): was defined as at least 50% reduction in the sum of the products of 2 perpendicular diameters of all measurable lesions with disappearance of all constitutional symptoms if initially present. Stable disease (SD): was defined as neither sufficient shrinkage (< 50%) to qualify for partial response, nor sufficient increase (> 25%) nor appearance of new lesions to qualify for progressive disease. Progressive disease (PD): was defined as an increase in the product of two perpendicular diameters of any measurable lesion by >25% over the size at presentation or appearance of new lesions [7]. Table (1): Combination Chemotherapy [6] Drug Dose/Route Day(s) ABVD Protocol includes: Doxorubicin Bleomycin Vinblastin Decarbazine (repeat every 28 days) COEP Protocol includes: Cyclophosphamide Vincristine (Oncovin) Etoposide* Prednisone (repeat every 28 days) ICE protocol Ifosfamide with Mesna Carboplatin Etoposide (repeated every 21 days) 25 mg/ m2 IV 10 mg/ m2 IV 6 mg/ m2 IV 375 mg/ m2 IV 800 mg/ m2 IV 1.5 mg/ m2 IV 60 mg/ m2 IV 40 mg/ m2/ day PO 1800 mg/m2iv 450 mg/m2iv mg/m2iv d1, 15. d1, 15. d1, 15. d1, 15. d1,15 d1,15 d1,15 d1,15 then gradual withdrawal. D1 3 D1 D1 3 *Procarbazine is substituted by etoposide in COEP regimen. After-therapy monitoring: After completion of chemotherapy, patients was followed monthly in the first year, every 3 months in the 2 nd and 3 rd years.. Follow-up examinations was done by physical examination, chest X-ray, routine laboratory investigations (CBC and ESR) and CT scans according to initial presentation. Specific evaluation of late effects including hormonal assessment (TFT and sex hormones), pulmonary function test, echocardiography and examination of bone and soft tissues was done. Statistical analysis: Overall survival (OS) was calculated from the first day of chemotherapy to the date of the last follow up or death due to any cause. Event free survival (EFS) was calculated from the first day of chemotherapy to an event (death due to any cause, progression after PR, relapse or a second malignancy) or to the date of the last follow up contact for patients who did not experience any event. OS and EFS were estimated with Kaplan-Meier method and differences were assessed by the log-rank test. Coxregression was used in multivariate analysis.
3 Ghazaly et al. SECI Oncology 2014 Page 3 of 8 Results From January 2009 to January patients with previously untreated HL were enrolled into this study. Patients' characteristics: are shown in table (2). The median age was 8 years (range 4-16 years). Twenty patients (60%) were males and 14 patients (40%) were females with male to female ratio 1.4:1. Four patients (11.8%) were stage I, 16 patients (47.1%) were stage II, 12 patients (35.3%) were stage III and 2 patients (5.8%) were stage IV. Risk stratification revealed 6 patients (17.6%) in LR group, 18 patients (52.9%) in IMR group and 10 patients (29.4%) in HR group. Twenty one patients (61.8%) had systemic "B" symptoms. Bulky disease was reported in 9 patients (26.5%) with 6 patients (17.6%) had bulky mediastinal mass and 3 patients (8.8%) had bulky peripheral nodal mass. Cervical lymph node enlargement was the most predominant site 85.3% followed by axillary in 50%, abdomen in 47% and mediastinum in 28.6%. Extra nodal involvement was recorded in 9 patients (26.5%), splenomegaly in 17.6%, hepatomegaly in 14.7%. Nineteen patients (58.8%) had 4 nodal regions. Twenty six patients (76.5%) had mixed cellularity, 14 patients had nodular sclerosis and 3 patients had lymphocytic predominant. Four patients (11.8%) had leukocytosis, 19 patients (55.9%) had anemia, ESR was elevated in 14 patients (41.2%). Response to treatment: After 2 cycles of chemotherapy, 12 patients (35.3%) achieved CR (five patients (83.3%) in LR, 6 patients (33.3%) in IMR and one patient (10%) in HR), 22 patients (64.7%) had PR. At the end of chemotherapy, Thirty-three out of 34 patients (97.1%) evaluated, 30/33 patients (90.9%) had CR ( 6 patients (%) in LR, 17 patients (94.4%) in IMR and 7 patients (70%) in HR) and 3/33 patients (9.1%) had PD (one patient in IMR and 2 patients in HR). Treatment failure: There were 5 treatment failures, 3/33 patients (9.1%) had progressive disease (one patient of IMR group and two of HR group) and 2/30 patients (6.7%) had relapse (two of HR group). One patient relapsed outside the irradiated field, the other relapsed within and outside the irradiated field. They occurred at 7, 22 months after completion of radiotherapy. Both were salvaged by second line chemotherapy ICE (ifosfamide, carboplatin and etoposide) table (1) followed by radiotherapy with complete remission in one patient and partial remission in the other patient who died from hepatocellular failure. Toxicity: Morbidity was mostly observed in HR group. As regard to the early complications, bone marrow suppression was the most frequent complication (8.8%) followed by chest infection. Acute gonadal failure occurred in one patient (post pubertal) after receiving pelvic radiotherapy in spite of oophrepexy and she is now on hormonal therapy. Late effects of treatment were detected in patients on follow up in the form of hypothyroidism in 2 patients (8.8%) and restrictive pulmonary function in one patient (2.9%) while no cardiac complications occurred. Table (2): Patient Characteristics Patient Characteristics Age Range Mean ± SD Median Gender Male Female Ratio Systemic symptoms Absent Present Clinical presentation* Cervical lymphadenopathy Axillary lymphadenopathy Abdominal lymphadenopathy Mediastinal lymphadenopathy hepatomegaly Splenomegaly Bulky Disease No Yes Mediastinal Peripheral node No. of Nodal Regions <4 4 Stage I II III IV Risk Groups LR IMR HR White Blood Cells (10 3 /mm 3 ) 13.5 >13.5 Hemoglobin Level (g/dl) 11gm <11gm Serum Albumin (g/dl) 4gm <4gm Histological subtype Mixed cellularity Nodular sclerosis Lymphocytic rich All Patients (n=34) 4-16 y. 8.5 y. ± 3 8Y. 20(60%) 14(40%) 1.43:1 13(38.2%) 21(61.8%) 29(85.3%) 17(50%) 16(47.1%) 10(28.6%) 5(14.7%) 6(17.6%) 25(73.5%) 9(26.5%) 6(66.7%) 3(33.3%) 15(44.1%) 19(55.9%) 4(11.8%) 16(47.1%) 12(35.3%) 2(5.8%) 6(17.6%) 18(53%) 10(29.4%) 30(88.2%) 4 (11.8%) 16(47.1%) 18(52.9%) 15(44.1%) 19(55.9%) 26(76.5%) 5 (14.7%) 3 (8.8%) Survival analysis: The 3-years OS and EFS rates (± SE) were 91.2% ± 5.3% and 82.3% ± 7.3% respectively (Fig 1, 2). Factors affecting OS and EFS are shown in table (3). For patients with low, intermediate and high
4 Ghazaly et al. SECI Oncology 2014 Page 4 of 8 risk groups, 3-year OS were %, 94.4% ± 5.4% versus 80% ± 13.4% respectively (p=0.07) and 3-year EFS were %, 94.4% ± 5.4% versus 50% ± 17.4% respectively (p=0.005) (Fig 3, 4). For patients with B symptoms, 3-year EFS and OS were 71.4% ± 10.5%, 85.7% ± 7.9% respectively compared with patients without B symptoms % (p=0.048), % (p=0.21). 3-year EFS and OS for patients without bulky disease were 92% ± 5.8%, 96% ± 3.9% respectively which differ than those with bulky disease 55.6%± 17.3% (p=0.025), 77.8%± 15.3% (p=0.054). For patients without extra nodal extension, 3-year EFS and OS were 96%± 3.9%, % respectively that significantly differ than with extra nodal extension 44.4%± 16.6% (p=<0.001), 77.8%± 14.8% (p=0.02). The 3-year EFS for patients with stage I, II, III and IV was %, 93.8%± 6.1%, 75%± 12.5% and 0% respectively with significant difference in between (p= 0.007). Patients without leukocytosis had 3-year EFS and OS of 90% ± 11.6% and 93.3%± 5.2% compared with patients with leukocytosis 25%± 21.7% (p=0.006) and 75%±21.7% (p=0.391), 3-year EFS and OS for patients without lymphopenia 87.1%± 7.1%, 96.7%±3.2% respectively, compared with those with lymphopenia 33.3%± 21.2% (p=0.019) and 0.333± 21.2% (p=0.004). Three-year EFS for patients without anemia % is significantly better than those with anemia (66.7%±12.8%) (p= 0.018), 3-year EFS for patients with normal ESR is significantly better than with high ESR (p= 0.031) (95%± 4.9% versus 64.3%± 14.8%) and 3-year EFS for patients without hypoalbuminemia is significantly better than with hypoalbuminemia (p=0.018) (% versus 66.7%±12.8%). Multivariate analysis revealed that the significant independent factors for inferior EFS were "B" symptoms (p=0.047, HR: 2.1, 95% CI: ) and anemia (p=0.025, HR: 3.8, 95% CI: ). However, the significant independent factors for lower OS were hypoalbuminemia (p=0.013, HR: 5.4, 95% CI: ) and anemia (p= 0.048, HR: 2.6, 95% CI: ). Fig (2): Event Free Survival (EFS) in 34 HL patients Fig (3): Overall survival distributions by risk groups Fig (1): Overall Survival (OS) in 34 HL patients Fig (4): Event-free survival distributions by risk groups
5 Ghazaly et al. SECI Oncology 2014 Page 5 of 8 Table (3): Factors Affecting the Overall Survival (OS) and Event Free Survival (EFS) Variable 3-Year OS 3-Year EFS % SE (%) P value % SE (%) P value Risk Group Low Intermediate High Stage I II III IV Extra nodal Involvement Absent Present Systemic Symptoms Absent Present Bulky Disease Absent Present Leukocytosis (10 3 /mm 3 ) 13.5 >13.5 Lymphopenia (10 3 /mm 3 ) 600 >600 Hemoglobin Level (g/dl) 11 <11 ESR (mm/h) <50 50 Serum Albumin (g/dl) 4 gm <4gm Discussion Hodgkin lymphoma is a neoplasm in which survival and cure has improved dramatically over the 50 years with survival rate reaching 94%. Because cure is likely for the majority of children and adolescents presenting with HL, attention to long-term treatment complications has become increasingly important. Risk-adapted combined modality treatment protocols, which assign intensity of therapy according to risk features at diagnosis have become a standard treatment approach for pediatric malignancies that are highly curable with contemporary therapy while reducing therapy-related complications [8]. In the current study, the median age was 8 years which is less than that reported by El Badawy et al [8] and Ebeid et al [9] and similar to median age reported by Gao et al which was 7.7 years [10] this may be explained by the different number of patients reported in these studies: 121 patients in El Badawy et al, 27 patients in Ebeid et al. The majority of patient's age was found below 10 years (64.7%) which was in agreement with Gao et al [10] which was 71.4%, but less than that reported by Kelly et al [11] with most of patient's age above 10 years (89.8%). This can be explained by effect of low socio economic status, large family size and high incidence of EBV infection in our developing countries. There is slight predominance of males in our study (1.4:1) similar to that reported by Hudson et al [2] and Ali et al [12] but lower than the ratio reported by El Badawy et al [8]. In our study, the clinical presentation of nodal disease is comparable to what was reported in the literature as cervical lymphadenopathy was the most predominant site reported in (85.3%) followed by axillary, abdominal and mediastinal involvement which is also in agreement with other studies reported by El Badawy et al [8] and Kelly et al [11]. Extra nodal involvement occurred in 9 patients (26.5%) which in agreement to what was reported by Hudson et al [2]. 61.8% of patients had systemic "B" symptoms which is comparable to Schwatez et al [7] and El Badawy et al [8]. Bulky disease was seen in 9 patients (26.7%) (mediastinum in 6 patients and peripheral lymph nodes in 3 patients) which is similar to Ali et al [12]. Regarding the stage, 73.2% of our patients had an advanced stage disease, this is in agreement with what
6 Ghazaly et al. SECI Oncology 2014 Page 6 of 8 was reported by Schwartz et al [7] and Ebeid et al [9]. The majority of patients (58.8%) had 4 regions which is similar to Kulyova et al [13], and unlike what's reported by Morais et al [14]. The distribution of risk groups of our study was 17.6% in LR, 53% in IMR and 29.4% in HR group which was similar to Gao et al [10] and differ from the results reported by Ali et al [12]. Although nodular sclerosis histological subtype was reported to be the predominant histological subtype by Hudson et al [2] and Kelly et al [11]. In the current study, the mixed cellularity subtype form the predominant type (76.5%) followed by nodular sclerosis subtype and lymphocytic predominant subtype which is similar to El Badawy [8], Gao et al [10] and Ali et al [12]. Bazzeh et al [15] reported that mixed cellularity subtype was more prevalent in children less than 10 years old, but less likely in older children/adolescents which is in agreement with our study with the majority of patient's age was found below 10 years. The explanation of high prevalence of mixed cellularity subtype may be explained by increased risk factors in developing countries rather than developed countries which also can explain the high frequency of advanced stages and "B" symptoms which is associated with mixed cellularity subtype other than nodular sclerosis subtype. Leukocytosis recorded in 4 patients (11.8%) which is slightly less than that was reported by Hudson et al [2] and Smith et al [16]. Elevated ESR was found in 41.2% which is in agreement with Hudson et al [2] but Morais et al [14] found that the majority of patients had elevated ESR level 69.5%. Anemia occurred in 19 patients (55.9%) which is much higher than reported by Hudson et al [2], Morais et al [14] and Smith et al [16]. This may be due to associated malnutrition and low socioeconomic level in our country. Early response was reported in 12 patients (35.3%) 83.3% in LR, 35.3% in IMR and 10% in HR group which is higher than that reported by Hudson et al [2] and lower than that reported by Ali et al [12]. There were 5 treatment failures, either initial disease progression (9.1%) or relapse (6.7%) which is less than reported by El Badawy et al [8] and Krasin et al [17] and much lower than reported by Hudson et al [2] and Ali et al [12]. The difference may be related to number of patients in those studies. Combination chemotherapy is used alone or followed by low-dose involved field radiotherapy (IFRT) [16]. It had been evaluated by European and American investigators, in the most recent GPOH-HD 2002 study, the German investigators confirmed the efficacy of the OPPA/OEPA chemotherapy regimens and aimed to further decrease treatment intensity by omitting radiation therapy in patients with favorable risk only who achieved complete remission after chemotherapy [18]. In the United States, CCG-5942 results indicated a higher number of relapses in the group of patients who were not irradiated, patients with complete response who were randomized to receive radiation had superior disease control compared to patients randomized to no irradiation (3 year EFS 92% versus 87%) [19]. Also in COG- AHOD0431 with response-based therapy revealed lower EFS in patients of favorable risk with CR who didn't receive RT than patients with PR who received RT (2- year EFS 80% versus 88%) and they suggest that response to Chemotherapy alone not adequate to identify patients can be treated without RT after abbreviated chemotherapy [20]. Three years OS and EFS (± SE) were 91.2% ± 5.3% and 82.3%± 7.3% respectively. There is no significant difference in 3-year OS for patients with LR, IMR and HR groups (p=0.07), but 3-year EFS for patients with LR and IMR groups is significantly better than HR group (p=0.005) (%, 94.4%± 5.4% versus 50%± 17.4%). The 3-year OS and EFS of LR group in our result was (% and % respectively) which is comparable with Ali et al [12], Nachman et al [19] and Donaldson et al [21]. In our study, the 3-year OS and EFS of IMR group was 94.4%± 5.4% and 94.4%± 5.4% respectively which is in agreement to the result of El Badawy et al [8], Ali et al [ 12] and Ruhl et al [22]. Three-year OS and EFS 80%± 13.4% and 5%± 17.4% for HR group in the current study which is higher than what was reported by Gao et al [10] and Ali et al [12] and less than which was reported by Mauz- Korholz et al [18]. Univariate analysis of prognostic factors of OS and EFS revealed that there was significant influence of advanced stage, extra nodal involvement, "B" symptoms, bulky disease, leukocytosis, lymphopenia, anemia, hypoalbuminemia and elevated ESR on inferior EFS while this was not translated into significant affection of the OS except for extra nodal involvement and lymphopenia. In Egypt, Ali et al [12] reported that many factors greatly affect EFS and OS which were histology, "B" symptoms, disease bulk and response to therapy but Smith et al [16] reported that there were many factors affecting OS and DFS as stage, histology, "B" symptoms, bulky disease, number of nodal regions, leukocytosis, anemia and elevated ESR. There are multiple prognostic factors identified in selected multi-institutional studies, In the Stanford/St. Jude/Dana Farber Cancer Institute consortium, male gender; stage IIB, IIIB, or IV disease; white blood cell count of 11,500/mm 3 or higher; and hemoglobin lower than 11.0 g/dl were significant prognostic factors for inferior disease-free survival and overall survival (OS) [16], in the Society for Paediatric Oncology and Haematology (GPOH-95) study, "B" symptoms, histology, and male gender were adverse prognostic factors for EFS on multivariate analysis [23]. In the Children Cancer Group (CCG-5942) study, the combination of "B" symptoms and bulky disease was associated with an inferior outcome [19], and in St. Jude study, Hudson et al found that only leukocytosis and
7 Ghazaly et al. SECI Oncology 2014 Page 7 of 8 anemia were both associated with worse outcome (p=.046 and p=.003 respectively) [2]. In our study, multivariate analysis revealed that B symptoms (p=0.047, HR: 2.1, 95% CI: ) and hemoglobin <11gm (p=0.025, HR: 3.8, 95% CI: ) are the significant independent factors for inferior EFS. In Egypt, Ali et al [12] found that lymphocytic depletion pathological subtype was the only significant predictor of lower EFS and El- Badway et al [8] reported that only statistically significant prognostic indicator for OS and DFS was the relation between the DFS and the initial response to chemotherapy. OPPA OS PD PR REAL/WHO SD SE SECI TFT Oncovin, procarbazine, prednisone, and adriamycin. Overall survival. Progressive disease. Partial response. Revised European American Lymphoma classification/ World Health Organization. Stable disease. Standard error. South Egypt Cancer Institute. Thyroid function test. Conclusion Treatment results of HL in pediatric oncology department, SECI, Assiut University using risk-adapted combined-modality therapy with ABVD/COEP and IFRT has high efficacy with minimal toxicity. "B" symptoms and anaemia were the significant independent factors for lower EFS but hypoalbuminemia and anemia were significant factors for inferior OS. Conflict of Interests The authors declare that they have no conflict of interests. Authors Contribution All the work was done by the corresponding author under supervision and guidance by the remaining authors. Abbreviations ABVD Adriamycin, bleomycin, vinblastine, and decarbazine.. CBC Complete blood count. CCG Children cancer group. CI Confidence interval. COEP Cyclophosphamide, vincristine, etoposide, prednisone. COG Children s Oncology Group. CR Complete response. CT Computed tomography. EFS Event-free survival. ESR Erythrocytic sedimentation rate. GPOH German paediatric oncology and haematology. Gy Gray HL Hodgkin lymphoma. HR High risk. ICE Ifosfamide, carboplatin and etoposide. IFRH Involved field radiotherapy. IMR Intermediate risk LDH Lactic dehydrogenase. LR Low risk. OEPA Oncovin, etoposide, prednisone, and adriamycin. References [1] Pacquement H, Landman-Parker J, Leblanc T, Habrand JL, Terrier-Lacombe MJ, Bertrand Y, Perel Y,Robert A, Coze C, Thuret I, Donadieu J, Schaison G, Leverger G, Lemerle J and Oberlin O.: Localized childhood Hodgkin s disease: Response-adapted chemotherapy with etoposide, bleomycin, vinblastine, and prednisone before low-dose radiation therapy Results of the French Society of Pediatric Oncology Study MDH90. J Clin Oncol, : p [2] Hundson MM, Krasin M, and Link MP, Donaldson SS, Billups C, Merchant TE, Kun L, Billet AL, Kaste S, Tarbell NJ, Howard S, Friedmann AM, Hurwitz CA, Young JA, Marcus KC, Rai S, Cowan T and Weinstein HJ: Risk-adapted, combined- Modality therapy with VAMP/ COP and response- based, Involved- field radiation for Unfavorable Pediatric Hodgkin's Disease. Journal of Clinical Oncology, (22): p [3] Eberle FC, Mani H and Jaffe ES: Histopathology of Hodgkin s Lymphoma. Cancer J, (2009). 15: [4] Lister TA, Crowther D, Sutcliffe SB, Glatstein E, Canellos GP, Young RC, Rosenberg SA, Coltman CA and Tubiana M: Report of a committee convened to discuss the evaluation and staging of patients with Hodgkin s disease: Cotswolds meeting. J Clin Oncol, (11): [5] Tsuji SY, Chan LW, Dophne A and Kogan H: Pediatric (non-cns) Trs. In: Handbook of Evidence-Based Radiation Oncology. 2 nd Ed, 2010: [6] Lanzkowsky P: Hodgkin lymphoma. In: Manual of Pediatric Hematology and Oncology, 5 th ed. 2011, [7] Schwartz CL, Constine LS, Villaluna D, London WB, Hutchison RE, Sposto R, Lipshultz SE, Turner CS, Alarcon PA and Chauvenet A: A risk-adapted, response-based approach using ABVE-PC for children and adolescents with intermediate- and high-risk Hodgkin lymphoma: the results of P9425. Blood, : [8] El Badawy S, Aboulnaga S, Abou Gamal A, Mokhless A, Zamzam M, Sidhom I, Ebeid E and
8 Ghazaly et al. SECI Oncology 2014 Page 8 of 8 Hussein H: Risk Adapted Combined Modality Treatment in Children with Hodgkin's Disease: NCI, Cairo. Journal of the Egyptian Nat. Cancer Inst, : June: [9] Ebeid EN, Zaghloul M and Khairy M: Clinical outcome of pediatric Hodgkin's disease in upper Egypt. Journal of Clinical Oncology, 2006 ASCO Annual Meeting Proceeding (post-meeting Edition). 24: [10] Gao Y J, Tang J Y, pan C, Lu FJ, Xue HL and Chen J: Risk-adapted chemotherapy without procarbazine in treatment of children with Hodgkin lymphoma. World J Pediatr (1); [11] Kelly KM, Sposto R, Hutchinson R, Massey V, McCarten K, Perkins S, Lones M, Villaluna D and Weiner M: BEACOPP chemotherapy is highly effective regimen in children and adolescents with high-risk Hodgkin lymphoma: a report from the Children's Oncology Group. Blood Journal (9): [12] Ali A, Sayed H, Farrag A and El-Sayed M: Riskbased combined-modality therapy of pediatric Hodgkin's lymphoma: A retrospective study. Leukemia Research ; [13] Kulyova S A and Kolygin B A: Hodgkin s Lymphoma in Children and Adolescents: A Saint Petersburg Hodgkin s Lymphoma Group Study. Journal of Oncology 2011, 2011; 1-6. [14] Morais A, Barros M H M, Hassan R, Morais VLL and Muniz MTC: Number of involved anatomic areas as a risk predictor in pediatric Hodgkin s lymphoma: a retrospective study. J Pediatr (Rio J) 2009; 85(3): [15] Bazzeh F, Rihani R, Howards S and Sultan I: Comparing adult and pediatric Hodgkin lymphoma in the Surveillance, Epidemiology and End Results Program, : an analysis of cases. Leukemia Lymphoma Dec; 51 (12): [16] Smith RS, Chen Q, Hudson MM, Link MP, Kun L, Weinstein H, Billett A, Marcus KJ, Tarbell NJ and Donaldson SS: Prognostic Factors for Children With Hodgkin s Disease Treated With Combined-Modality Therapy. J Clin Oncol 2003, 21: [17] Krasin MJ, Rai SN, Kun LE, Merchant TE, Metzger ML, Kaste SC, Howard SC and Hudson MM: Patterns of Treatment Failure in Pediatric and Young Adult Patients With Hodgkin s Disease: Local Disease Control With Combined- Modality Therapy. J Clin Oncol 2005, 23: [18] Mauz-Korholz C, Hasenclever D, Do rffel W, Ruschke K, Pelz T, Voigt A, Stiefel M, Winkler M, Vilser C, Dieckmann K, Karlen J, Bergstrasser E, Fossa A, Mann G, Hummel M, Klapper W, Stein H, Vordermark D, Kluge R and Ko rholz D: Procarbazine-Free OEPA-COPDAC Chemotherapy in Boys and Standard OPPA- COPP in Girls Have Comparable Effectiveness in Pediatric Hodgkin s Lymphoma: The GPOH- HD-2002 Study. Journal of Clinical Oncology (23): p [19] Nachman JB, Sposto R, Herzog P, Gilchrist GS, Wolden SL, Thomson J, Kadin ME, Pattengale P, Davis C, Hutchinson RJ and White K: Randomized comparison of low-dose involved-field radiotherapy and no radiotherapy for children with Hodgkin s disease who achieve a complete response to chemotherapy. J Clin Oncol 2002, 20: [20] Keller FG, Nachman J, Constine LS, Thomson J, McCarten KM, Chen L and Schwartz C: A Phase III Study for the Treatment of Children and Adolescents with Newly Diagnosed Low Risk Hodgkin Lymphoma (HL): American Society of Hematology, [21] Donaldson SS, Hudson MM, Lamborn KR, Link MP, Kun L, Billett AL, Marcus KC, Hurwitz CA, Young JA, Tarbell NJ and Weinstein HJ: VAMP and low-dose, involved-field radiation for children and adolescents with favorable, earlystage Hodgkin s disease: results of a prospective clinical trial. J Clin Oncol 2002, 20: [22] Ruhl U, Albrecht MR, Lueders H, Merciniak H and Doerffel W: The German multinational GPOH-HD 95 trial: treatment results and analysis of failures in pediatric Hodgkins disease using combination chemotherapy with and without radiation. Int J Radiat Oncol Biol Phys 2004, 60: S131. [23] Ruhl U, Albrecht M, Dieckmann K, Lüders H, Marciniak H, Schellenberg D, Wickmann L and Dörffel W. : Response-adapted radiotherapy in the treatment of pediatric Hodgkin s disease: an interim report at 5 years of the German GPOH- HD 95 trial. Int J Radiat Oncol Biol Phys 2001, 51:
Radiation and Hodgkin s Disease: A Changing Field. Sravana Chennupati Radiation Oncology PGY-2
 Radiation and Hodgkin s Disease: A Changing Field Sravana Chennupati Radiation Oncology PGY-2 History of Present Illness 19 yo previously healthy male college student began having pain in his R shoulder
Radiation and Hodgkin s Disease: A Changing Field Sravana Chennupati Radiation Oncology PGY-2 History of Present Illness 19 yo previously healthy male college student began having pain in his R shoulder
Childhood Hodgkin International Prognostic Score (CHIPS) Predicts event-free survival in Hodgkin Lymphoma: A Report from the Children's Oncology Group
 Childhood Hodgkin International Prognostic Score (CHIPS) Predicts event-free survival in Hodgkin Lymphoma: A Report from the Children's Oncology Group Cindy L. Schwartz, UT MD Anderson Cancer Center Lu
Childhood Hodgkin International Prognostic Score (CHIPS) Predicts event-free survival in Hodgkin Lymphoma: A Report from the Children's Oncology Group Cindy L. Schwartz, UT MD Anderson Cancer Center Lu
Printed by Martina Huckova on 10/3/2011 3:04:43 PM. For personal use only. Not approved for distribution. Copyright 2011 National Comprehensive
 NCCN Categories of Evidence and Consensus Category 1: The recommendation is based on high-level evidence (e.g. randomized controlled trials) and there is uniform NCCN consensus. Category 2A: The recommendation
NCCN Categories of Evidence and Consensus Category 1: The recommendation is based on high-level evidence (e.g. randomized controlled trials) and there is uniform NCCN consensus. Category 2A: The recommendation
PET-adapted therapies in the management of younger patients (age 60) with classical Hodgkin lymphoma
 PET-adapted therapies in the management of younger patients (age 60) with classical Hodgkin lymphoma Ryan Lynch MD Assistant Professor, University of Washington Assistant Member, Fred Hutchinson Cancer
PET-adapted therapies in the management of younger patients (age 60) with classical Hodgkin lymphoma Ryan Lynch MD Assistant Professor, University of Washington Assistant Member, Fred Hutchinson Cancer
Serum levels of soluble CD30 improve International Prognostic Score in predicting the outcome of advanced Hodgkin s lymphoma
 Original article Annals of Oncology 13: 1908 1914, 2002 DOI: 10.1093/annonc/mdf333 Serum levels of soluble CD30 improve International Prognostic Score in predicting the outcome of advanced Hodgkin s lymphoma
Original article Annals of Oncology 13: 1908 1914, 2002 DOI: 10.1093/annonc/mdf333 Serum levels of soluble CD30 improve International Prognostic Score in predicting the outcome of advanced Hodgkin s lymphoma
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Hodgkin s Lymphoma in Children Aged 6 Years Or Below- Long Term Follow Up Results Giri G V
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Hodgkin s Lymphoma in Children Aged 6 Years Or Below- Long Term Follow Up Results Giri G V
Pediatric Hodgkin Lymphoma Treated at Cancer Institute, Chennai, India: Long-Term Outcome
 original report Pediatric Hodgkin Lymphoma Treated at Cancer Institute, Chennai, India: Long-Term Outcome Venkatraman Radhakrishnan Manikandan Dhanushkodi Trivadi S. Ganesan Prasanth Ganesan Shirley Sundersingh
original report Pediatric Hodgkin Lymphoma Treated at Cancer Institute, Chennai, India: Long-Term Outcome Venkatraman Radhakrishnan Manikandan Dhanushkodi Trivadi S. Ganesan Prasanth Ganesan Shirley Sundersingh
German Hodgkin Study Group
 German Hodgkin Study Group Deutsche Hodgkin Studiengruppe Avoiding Relapse of Hodgkin Lymphoma: Have We Moved The Needle? Andreas Engert, MD Chairman, German Hodgkin Study Group University Hospital of
German Hodgkin Study Group Deutsche Hodgkin Studiengruppe Avoiding Relapse of Hodgkin Lymphoma: Have We Moved The Needle? Andreas Engert, MD Chairman, German Hodgkin Study Group University Hospital of
THE EORTC-GELA TREATMENT STRATEGY IN CLINICAL STAGES I-II HL Results of the H9-F and H9-U trials (#20982)
 EORTC Lymphoma Group THE EORTC-GELA TREATMENT STRATEGY IN CLINICAL STAGES I-II HL Results of the H9-F and H9-U trials (#20982) J. Thomas, C. Fermé, E.M. Noordijk, H. Eghbali and M. Henry-Amar 7th International
EORTC Lymphoma Group THE EORTC-GELA TREATMENT STRATEGY IN CLINICAL STAGES I-II HL Results of the H9-F and H9-U trials (#20982) J. Thomas, C. Fermé, E.M. Noordijk, H. Eghbali and M. Henry-Amar 7th International
Comparison of Three Radiation Dose Levels after EBVP Regimen in Favorable Supradiaphragmatic Clinical Stages I-II Hodgkin s Lymphoma (HL):
 Comparison of Three Radiation Dose Levels after EBVP Regimen in Favorable Supradiaphragmatic Clinical Stages I-II Hodgkin s Lymphoma (HL): Preliminary Results of the EORTC-GELA H9-F Trial H. Eghbali, P.
Comparison of Three Radiation Dose Levels after EBVP Regimen in Favorable Supradiaphragmatic Clinical Stages I-II Hodgkin s Lymphoma (HL): Preliminary Results of the EORTC-GELA H9-F Trial H. Eghbali, P.
2007 ANNUAL SITE STUDY HODGKIN S LYMPHOMA
 2007 ANNUAL SITE STUDY HODGKIN S LYMPHOMA SUSQUEHANNA HEALTH David B. Nagel, M.D. April 11, 2008 Hodgkin s lymphoma was first described by Thomas Hodgkin in 1832. It remained an incurable malignancy until
2007 ANNUAL SITE STUDY HODGKIN S LYMPHOMA SUSQUEHANNA HEALTH David B. Nagel, M.D. April 11, 2008 Hodgkin s lymphoma was first described by Thomas Hodgkin in 1832. It remained an incurable malignancy until
HODGKIN LYMPHOMA Updated February 2016 by Dr. Manna (PGY 5 Hematology Resident, University of Calgary)
 HODGKIN LYMPHOMA Updated February 2016 by Dr. Manna (PGY 5 Hematology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr. Matt Cheung (Staff
HODGKIN LYMPHOMA Updated February 2016 by Dr. Manna (PGY 5 Hematology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr. Matt Cheung (Staff
Guidelines for management of Pediatric Hodgkin Lymphoma
 Guidelines for management of Pediatric Hodgkin Lymphoma Section of Leukemia/Lymphoma Department of Pediatric Hematology/Oncology King Faisal Specialist Hospital and Research Center Riyadh TABLE OF CONTENTS
Guidelines for management of Pediatric Hodgkin Lymphoma Section of Leukemia/Lymphoma Department of Pediatric Hematology/Oncology King Faisal Specialist Hospital and Research Center Riyadh TABLE OF CONTENTS
CURRENTLY MORE THAN 90% OF
 ORIGINAL CONTRIBUTION Association Between Radiotherapy vs Radiotherapy Based on Early Response to VAMP Chemotherapy and Survival Among Children With Favorable-Risk Hodgkin Lymphoma Monika L. Metzger, MD,
ORIGINAL CONTRIBUTION Association Between Radiotherapy vs Radiotherapy Based on Early Response to VAMP Chemotherapy and Survival Among Children With Favorable-Risk Hodgkin Lymphoma Monika L. Metzger, MD,
Limited-Stage Disease: Optimal Use of Chemotherapy and Radiation Treatment
 HODGKIN LYMPHOMA: CLINICAL CHALLENGES Limited-Stage Disease: Optimal Use of Chemotherapy and Radiation Treatment John Radford 1 1 Professor of Medical Oncology, Christie Hospital and The University of
HODGKIN LYMPHOMA: CLINICAL CHALLENGES Limited-Stage Disease: Optimal Use of Chemotherapy and Radiation Treatment John Radford 1 1 Professor of Medical Oncology, Christie Hospital and The University of
Professor Maurice Tubiana
 Professor Maurice Tubiana The French way of life Dr. Odile Schweisguth Pediatric Radiation Oncology Daniele Sarrazin Pediatric Radiation Oncology Stanford Visitors from France A Massiot 1958 Courbevoie
Professor Maurice Tubiana The French way of life Dr. Odile Schweisguth Pediatric Radiation Oncology Daniele Sarrazin Pediatric Radiation Oncology Stanford Visitors from France A Massiot 1958 Courbevoie
Update in Pediatric Hodgkin Lymphoma
 Update in Pediatric Hodgkin Lymphoma Jeff Deyo, MD, PhD Medical Director, Baton Rouge Affiliate St Jude Children s Research Hospital Our Lady of the Lake Children s Hospital Acadiana Potpourri, August
Update in Pediatric Hodgkin Lymphoma Jeff Deyo, MD, PhD Medical Director, Baton Rouge Affiliate St Jude Children s Research Hospital Our Lady of the Lake Children s Hospital Acadiana Potpourri, August
Treatment of Forty Adult Patients with Hodgkin Disease; Baghdad Teaching Hospital Experience
 Original Article Treatment of Forty Adult Patients with Hodgkin Disease; Baghdad Teaching * Alaadin S. Naji* Ahmed A. AL - Saffar* Mazin A. Shubbar* Bassam F. Matti* Adil Siwan* Ammar F. Majeed* Ali M.Jawad*
Original Article Treatment of Forty Adult Patients with Hodgkin Disease; Baghdad Teaching * Alaadin S. Naji* Ahmed A. AL - Saffar* Mazin A. Shubbar* Bassam F. Matti* Adil Siwan* Ammar F. Majeed* Ali M.Jawad*
Effective local and systemic therapy is necessary for the cure of Ewing tumor Most chemotherapy regimens are a combination of cyclophosphamide,
 Ewing Tumor Perez Ewing tumor is the second most common primary tumor of bone in childhood, and also occurs in soft tissues Ewing tumor is uncommon before 8 years of age and after 25 years of age In the
Ewing Tumor Perez Ewing tumor is the second most common primary tumor of bone in childhood, and also occurs in soft tissues Ewing tumor is uncommon before 8 years of age and after 25 years of age In the
ARRO Case: Pediatric High Risk Classical Hodgkin Lymphoma
 ARRO Case: Pediatric High Risk Classical Hodgkin Lymphoma Steven Seyedin, MD (PGY-3) Faculty Advisor: Dr. John Buatti, MD, FASTRO Department of Radiation Oncology University of Iowa Hospital and Clinics
ARRO Case: Pediatric High Risk Classical Hodgkin Lymphoma Steven Seyedin, MD (PGY-3) Faculty Advisor: Dr. John Buatti, MD, FASTRO Department of Radiation Oncology University of Iowa Hospital and Clinics
First Line Management of Classical Hodgkin Lymphoma
 First Line Management of Classical Hodgkin Lymphoma George Follows Cambridge University Hospitals NHS Foundation Trust george.follows@addenbrookes.nhs.uk The controversial areas Early stage non-bulky /
First Line Management of Classical Hodgkin Lymphoma George Follows Cambridge University Hospitals NHS Foundation Trust george.follows@addenbrookes.nhs.uk The controversial areas Early stage non-bulky /
Advanced stage HL The old and new match: BEACOPP
 27.03.2015 1 Advanced stage HL The old and new match: BEACOPP Peter Borchmann German Hodgkin Study Group University of Cologne, Germany Which answer is wrong? For patients with advanced stage HL, treatment
27.03.2015 1 Advanced stage HL The old and new match: BEACOPP Peter Borchmann German Hodgkin Study Group University of Cologne, Germany Which answer is wrong? For patients with advanced stage HL, treatment
children and young people:
 Hodgkin lymphoma in children and young people: State of the art Professor W. Hamish Wallace RHSC 2016 Childhood Cancer 1971-2010 One-, Five- and Ten-Year Actuarial Survival (%), Children (Aged 0-14),
Hodgkin lymphoma in children and young people: State of the art Professor W. Hamish Wallace RHSC 2016 Childhood Cancer 1971-2010 One-, Five- and Ten-Year Actuarial Survival (%), Children (Aged 0-14),
Lymphomas and multiple myeloma 12/23/2018 1
 60 Lymphomas and multiple myeloma 12/23/2018 1 Lymphomas Lymphoma is cancer of the lymphatic system. Lymphomas are subdivided into two main categories: Hodgkin's lymphoma (HL) and non- Hodgkin's lymphoma
60 Lymphomas and multiple myeloma 12/23/2018 1 Lymphomas Lymphoma is cancer of the lymphatic system. Lymphomas are subdivided into two main categories: Hodgkin's lymphoma (HL) and non- Hodgkin's lymphoma
LEUKAEMIA and LYMPHOMA. Dr Mubarak Abdelrahman Assistant Professor Jazan University
 LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary)
 NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
Lung hilar Ga-67 uptake in patients with lymphoma following chemotherapy
 ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 18, No. 5, 391 397, 2004 Lung hilar Ga-67 uptake in patients with lymphoma following chemotherapy Emel Ceylan GUNAY,* Bilge Volkan SALANCI,* Ibrahim BARISTA**
ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 18, No. 5, 391 397, 2004 Lung hilar Ga-67 uptake in patients with lymphoma following chemotherapy Emel Ceylan GUNAY,* Bilge Volkan SALANCI,* Ibrahim BARISTA**
PET-imaging: when can it be used to direct lymphoma treatment?
 PET-imaging: when can it be used to direct lymphoma treatment? Luca Ceriani Nuclear Medicine and PET-CT centre Oncology Institute of Southern Switzerland Bellinzona Disclosure slide I declare no conflict
PET-imaging: when can it be used to direct lymphoma treatment? Luca Ceriani Nuclear Medicine and PET-CT centre Oncology Institute of Southern Switzerland Bellinzona Disclosure slide I declare no conflict
Treatment of Early Stage Hodgkin Lymphoma. Massimo Federico University of Modena and Reggio Emilia Città di Lecce Hospital - GVM Care & Research
 Treatment of Early Stage Hodgkin Lymphoma Massimo Federico University of Modena and Reggio Emilia Città di Lecce Hospital - GVM Care & Research Conflict of Interest Disclosure I hereby declare the following
Treatment of Early Stage Hodgkin Lymphoma Massimo Federico University of Modena and Reggio Emilia Città di Lecce Hospital - GVM Care & Research Conflict of Interest Disclosure I hereby declare the following
Relapsed/Refractory Hodgkin Lymphoma
 Relapsed/Refractory Hodgkin Lymphoma Anas Younes, MD Chief, Lymphoma Service Memorial Sloan-Kettering Cancer Center New York, New York, United States Case Study 32-year-old woman was diagnosed with stage
Relapsed/Refractory Hodgkin Lymphoma Anas Younes, MD Chief, Lymphoma Service Memorial Sloan-Kettering Cancer Center New York, New York, United States Case Study 32-year-old woman was diagnosed with stage
Lugano classification: Role of PET-CT in lymphoma follow-up
 CAR Educational Exhibit: ID 084 Lugano classification: Role of PET-CT in lymphoma follow-up Charles Nhan 4 Kevin Lian MD Charlotte J. Yong-Hing MD FRCPC Pete Tonseth 3 MD FRCPC Department of Diagnostic
CAR Educational Exhibit: ID 084 Lugano classification: Role of PET-CT in lymphoma follow-up Charles Nhan 4 Kevin Lian MD Charlotte J. Yong-Hing MD FRCPC Pete Tonseth 3 MD FRCPC Department of Diagnostic
Dr. Noelle O Rourke Beatson Oncology Centre, Glasgow RADIOTHERAPY FOR LYMPHOMA???
 Dr. Noelle O Rourke Beatson Oncology Centre, Glasgow RADIOTHERAPY FOR LYMPHOMA??? History of Radiotherapy 1895 Rontgen describes X-rays 1896 Becquerel radioactivity 1905 Radiation is used to treat tumours
Dr. Noelle O Rourke Beatson Oncology Centre, Glasgow RADIOTHERAPY FOR LYMPHOMA??? History of Radiotherapy 1895 Rontgen describes X-rays 1896 Becquerel radioactivity 1905 Radiation is used to treat tumours
Large cell immunoblastic Diffuse histiocytic (DHL) Lymphoblastic lymphoma Diffuse lymphoblastic Small non cleaved cell Burkitt s Non- Burkitt s
 Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
CHOP CHEMOTHERAPY OF INTERMEDIATE AND HIGH-GRADE NON-HODGKIN S LYMPHOMA
 Aria Oncologicu Vol., No. 8, pp. 95-99, 1994 CHOP CHEMOTHERAPY OF INTERMEDIATE AND HIGH-GRADE NON-HODGKIN S LYMPHOMA MARTA LLANOS, JOSEP TABERNERO, JOAN BRUNET, MARGARITAMENEDO, CINTA PALLARES, LUIS DE
Aria Oncologicu Vol., No. 8, pp. 95-99, 1994 CHOP CHEMOTHERAPY OF INTERMEDIATE AND HIGH-GRADE NON-HODGKIN S LYMPHOMA MARTA LLANOS, JOSEP TABERNERO, JOAN BRUNET, MARGARITAMENEDO, CINTA PALLARES, LUIS DE
End-of-treatment but not interim PET scan predicts outcome in nonbulky limited-stage Hodgkin s lymphoma
 original article Annals of Oncology 22: 910 915, 2011 doi:10.1093/annonc/mdq549 Published online 15 October 2010 original article End-of-treatment but not interim PET scan predicts outcome in nonbulky
original article Annals of Oncology 22: 910 915, 2011 doi:10.1093/annonc/mdq549 Published online 15 October 2010 original article End-of-treatment but not interim PET scan predicts outcome in nonbulky
All India Institute of Medical Sciences, New Delhi, INDIA. Department of Pediatric Surgery, Medical Oncology, and Radiology
 All India Institute of Medical Sciences, New Delhi, INDIA Department of Pediatric Surgery, Medical Oncology, and Radiology Clear cell sarcoma of the kidney- rare renal neoplasm second most common renal
All India Institute of Medical Sciences, New Delhi, INDIA Department of Pediatric Surgery, Medical Oncology, and Radiology Clear cell sarcoma of the kidney- rare renal neoplasm second most common renal
Elderly Patients with Hodgkin s Lymphoma: FIL experience. Massimo Federico University of Modena and Reggio Emilia
 Elderly Patients with Hodgkin s Lymphoma: FIL experience Massimo Federico University of Modena and Reggio Emilia RESULTS OF VbMp CHEMOTHERAPY REGIMEN IN ELDERLY PATIENTS WITH HODGKIN DISEASE: THE GISL
Elderly Patients with Hodgkin s Lymphoma: FIL experience Massimo Federico University of Modena and Reggio Emilia RESULTS OF VbMp CHEMOTHERAPY REGIMEN IN ELDERLY PATIENTS WITH HODGKIN DISEASE: THE GISL
Lymphocyte Predominant Hodgkin s Lymphoma. Case Presentation. How would you treat the patient?
 Lymphocyte Predominant Hodgkin s Lymphoma Wei Ai, MD, PhD Assistant Clinical Professor University of California, San Francisco January 2010 Case Presentation 32 yo male, diagnosed with stage IIIA lymphocyte
Lymphocyte Predominant Hodgkin s Lymphoma Wei Ai, MD, PhD Assistant Clinical Professor University of California, San Francisco January 2010 Case Presentation 32 yo male, diagnosed with stage IIIA lymphocyte
Lymphoma Case Scenario 1
 Lymphoma Case Scenario 1 HISTORY: A 23-year-old healthy female presented with a month-long history of persistent headache of increasing severity. She noted episodic nausea and vomiting in association with
Lymphoma Case Scenario 1 HISTORY: A 23-year-old healthy female presented with a month-long history of persistent headache of increasing severity. She noted episodic nausea and vomiting in association with
Pediatric Oncology. Vlad Radulescu, MD
 Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
RESEARCH ARTICLE. Effects of Radiotherapy on the Risk of Developing Secondary Malignant Neoplasms in Hodgkin s Lymphoma Survivors
 DOI:http://dx.doi.org/10.7314/APJCP.2016.17.2.749 Effects of Radiotherapy on Risk of Developing Secondary Malignant Neoplasms in Hodgkin s Lymphoma Survivors RESEARCH ARTICLE Effects of Radiotherapy on
DOI:http://dx.doi.org/10.7314/APJCP.2016.17.2.749 Effects of Radiotherapy on Risk of Developing Secondary Malignant Neoplasms in Hodgkin s Lymphoma Survivors RESEARCH ARTICLE Effects of Radiotherapy on
Lancashire and South Cumbria Haematology NSSG Guidelines for Follicular Lymphoma:
 1 Lancashire and South Cumbria Haematology NSSG Guidelines for Follicular Lymphoma: 2018-19 1.1 Pretreatment evaluation The following tests should be performed: FBC, U&Es, creat, LFTs, calcium, LDH, Igs/serum
1 Lancashire and South Cumbria Haematology NSSG Guidelines for Follicular Lymphoma: 2018-19 1.1 Pretreatment evaluation The following tests should be performed: FBC, U&Es, creat, LFTs, calcium, LDH, Igs/serum
Radiotherapy Alone Versus Combined-Modality Therapy for Initial Treatment of Early Stage Hodgkin's Lymphoma
 Radiotherapy Alone Versus Combined-Modality Therapy for Initial Treatment of Early Stage Hodgkin's Lymphoma Hanan Shawky Gamal El-Deen * and Amr Abd- El Aziz Ghannam Clinical Oncology Department, Tanta
Radiotherapy Alone Versus Combined-Modality Therapy for Initial Treatment of Early Stage Hodgkin's Lymphoma Hanan Shawky Gamal El-Deen * and Amr Abd- El Aziz Ghannam Clinical Oncology Department, Tanta
Treatment Outcome of Pediatric Patients with Mature B Cell Lymphoma Receiving Fab LMB96 Protocol at the National Cancer Institute, Cairo University
 Journal of the Egyptian Nat. Cancer Inst., Vol. 22,. 4, December: 21-28, 21 Treatment Outcome of Pediatric Patients with Mature B Cell Lymphoma Receiving Fab LMB96 Protocol at the National Cancer Institute,
Journal of the Egyptian Nat. Cancer Inst., Vol. 22,. 4, December: 21-28, 21 Treatment Outcome of Pediatric Patients with Mature B Cell Lymphoma Receiving Fab LMB96 Protocol at the National Cancer Institute,
Update: Non-Hodgkin s Lymphoma
 2008 Update: Non-Hodgkin s Lymphoma ICML 2008: Update on non-hodgkin s lymphoma Diffuse Large B-cell Lymphoma Improved outcome of elderly patients with poor-prognosis diffuse large B-cell lymphoma (DLBCL)
2008 Update: Non-Hodgkin s Lymphoma ICML 2008: Update on non-hodgkin s lymphoma Diffuse Large B-cell Lymphoma Improved outcome of elderly patients with poor-prognosis diffuse large B-cell lymphoma (DLBCL)
Hodgkin's Lymphoma. Symptoms. Types
 Hodgkin's lymphoma (Hodgkin's disease) usually develops in the lymphatic system, a part of the body's immune system. This system carries disease-fighting white blood cells throughout the body. Lymph tissue
Hodgkin's lymphoma (Hodgkin's disease) usually develops in the lymphatic system, a part of the body's immune system. This system carries disease-fighting white blood cells throughout the body. Lymph tissue
Long-term risk of second malignancy after treatment of Hodgkin s disease: the influence of treatment, age and follow-up time
 Original article Annals of Oncology 13: 1786 1791, 2002 DOI: 10.1093/annonc/mdf289 Long-term risk of second malignancy after treatment of Hodgkin s disease: the influence of treatment, age and follow-up
Original article Annals of Oncology 13: 1786 1791, 2002 DOI: 10.1093/annonc/mdf289 Long-term risk of second malignancy after treatment of Hodgkin s disease: the influence of treatment, age and follow-up
Radiation therapy has a dramatic effect on lymphomas, and has played an important role in treating Hodgkin
 COUNTERPOINTS Current Controversies in Hematology and Oncology Can Radiotherapy Be Omitted in Patients With Localized Hodgkin Lymphoma? Radiation therapy has a dramatic effect on lymphomas, and has played
COUNTERPOINTS Current Controversies in Hematology and Oncology Can Radiotherapy Be Omitted in Patients With Localized Hodgkin Lymphoma? Radiation therapy has a dramatic effect on lymphomas, and has played
Original Articles. Etoposide, vinblastine, adriamycin and prednisolone (EVAP) combination chemotherapy as first-line treatment for Hodgkin s disease
 RUPALI et al. : AETIOLOGY OF PROLONGED FEVER IN HIV-INFECTED ADULTS Original Articles 189 Etoposide, vinblastine, adriamycin and prednisolone (EVAP) combination chemotherapy as first-line treatment for
RUPALI et al. : AETIOLOGY OF PROLONGED FEVER IN HIV-INFECTED ADULTS Original Articles 189 Etoposide, vinblastine, adriamycin and prednisolone (EVAP) combination chemotherapy as first-line treatment for
Lymphocyte-Depleted Classical Hodgkin s Lymphoma: A Comprehensive Analysis From the German Hodgkin Study Group
 Published Ahead of Print on September 12, 211 as 1.12/JCO.211.36.473 The latest version is at http://jco.ascopubs.org/cgi/doi/1.12/jco.211.36.473 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R
Published Ahead of Print on September 12, 211 as 1.12/JCO.211.36.473 The latest version is at http://jco.ascopubs.org/cgi/doi/1.12/jco.211.36.473 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R
Pediatric Lymphoma Update from the Children s Oncology Group
 Pediatric Lymphoma Update from the Children s Oncology Group Stephan D. Voss, MD, PhD Department of Radiology Boston Children s Hospital Harvard Medical School Staging Assessment Disclosures None Acknowledgements:
Pediatric Lymphoma Update from the Children s Oncology Group Stephan D. Voss, MD, PhD Department of Radiology Boston Children s Hospital Harvard Medical School Staging Assessment Disclosures None Acknowledgements:
Practical Application of PET adapted Therapy in Hodgkin Lymphoma
 Practical Application of PET adapted Therapy in Hodgkin Lymphoma Matthew Matasar, MD Lymphoma and Adult BMT Services Director, Lymphoma Survivorship Clinic Memorial Sloan Kettering Cancer Center New York,
Practical Application of PET adapted Therapy in Hodgkin Lymphoma Matthew Matasar, MD Lymphoma and Adult BMT Services Director, Lymphoma Survivorship Clinic Memorial Sloan Kettering Cancer Center New York,
Hodgkin Lymphoma: Umberto Ricardi
 Hodgkin Lymphoma: Radiation Volumes Umberto Ricardi Università di Torino The changing role of RT in the cure of HL From Maximal use as a single agent To Combination of chemotherapy and full dose-full volume
Hodgkin Lymphoma: Radiation Volumes Umberto Ricardi Università di Torino The changing role of RT in the cure of HL From Maximal use as a single agent To Combination of chemotherapy and full dose-full volume
Lymphoma co existing with Tuberculosis granulomatous
 Available online at www.worldscientificnews.com WSN 90 (2017) 265-270 EISSN 2392-2192 SHORT COMMUNICATION Lymphoma co existing with Tuberculosis granulomatous Madeeha Subhan 1, *, Waleed Sadiq 2 1 Ayub
Available online at www.worldscientificnews.com WSN 90 (2017) 265-270 EISSN 2392-2192 SHORT COMMUNICATION Lymphoma co existing with Tuberculosis granulomatous Madeeha Subhan 1, *, Waleed Sadiq 2 1 Ayub
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Schaapveld M, Aleman BMP, van Eggermond AM, et al. Second cancer
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Schaapveld M, Aleman BMP, van Eggermond AM, et al. Second cancer
LYSA PET adapted programs. O. Casasnovas Hematology department Hopital Le Bocage, CHU Dijon, France
 LYSA PET adapted programs O. Casasnovas Hematology department Hopital Le Bocage, CHU Dijon, France 3 phase III trials DLBCL LNH 09-1B: aaipi = 0, 18 80y : ongoing GAINED: aaipi = 1-3, 18 60y : ongoing
LYSA PET adapted programs O. Casasnovas Hematology department Hopital Le Bocage, CHU Dijon, France 3 phase III trials DLBCL LNH 09-1B: aaipi = 0, 18 80y : ongoing GAINED: aaipi = 1-3, 18 60y : ongoing
Hodgkin Lymphoma PROVIDING THE LATEST INFORMATION FOR PATIENTS & CAREGIVERS. Revised 2018
 PROVIDING THE LATEST INFORMATION FOR PATIENTS & CAREGIVERS Hodgkin Lymphoma Revised 2018 Supported by an independent educational grant from Merck & Co., Inc. and Seattle Genetics, Inc. A six-word narrative
PROVIDING THE LATEST INFORMATION FOR PATIENTS & CAREGIVERS Hodgkin Lymphoma Revised 2018 Supported by an independent educational grant from Merck & Co., Inc. and Seattle Genetics, Inc. A six-word narrative
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center
 LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
XVIII. Management of nodular lymphocyte predominant Hodgkin lymphoma
 Hematological Oncology Hematol Oncol 2015; 33: 90 95 Published online in Wiley Online Library (wileyonlinelibrary.com).2226 Supplement Article XVIII. Management of nodular lymphocyte predominant Hodgkin
Hematological Oncology Hematol Oncol 2015; 33: 90 95 Published online in Wiley Online Library (wileyonlinelibrary.com).2226 Supplement Article XVIII. Management of nodular lymphocyte predominant Hodgkin
Addition of rituximab is not associated with survival benefit compared with CHOP alone for patients with stage I diffuse large B-cell lymphoma
 Original Article Addition of rituximab is not associated with survival benefit compared with CHOP alone for patients with stage I diffuse large B-cell lymphoma Bo Jia 1, Yuankai Shi 1, Suyi Kang 1, Sheng
Original Article Addition of rituximab is not associated with survival benefit compared with CHOP alone for patients with stage I diffuse large B-cell lymphoma Bo Jia 1, Yuankai Shi 1, Suyi Kang 1, Sheng
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL RESPONSE ASSESSMENT LYMPHOMA CHAPTER 11B REVISED: SEPTEMBER 2016
 LYMPHOMA Definitions of Response According to Non Hodgkin s Lymphoma (NHL) Criteria Listed below is the new NCI Lymphoma criteria for evaluation and endpoint definitions for Non Hodgkin s Lymphoma response
LYMPHOMA Definitions of Response According to Non Hodgkin s Lymphoma (NHL) Criteria Listed below is the new NCI Lymphoma criteria for evaluation and endpoint definitions for Non Hodgkin s Lymphoma response
Supplementary Appendix to manuscript submitted by Trappe, R.U. et al:
 Supplementary Appendix to manuscript submitted by Trappe, R.U. et al: Response to rituximab induction is a predictive marker in B-cell post-transplant lymphoproliferative disorder and allows successful
Supplementary Appendix to manuscript submitted by Trappe, R.U. et al: Response to rituximab induction is a predictive marker in B-cell post-transplant lymphoproliferative disorder and allows successful
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Hodgkin. The PET World. Sally Barrington
 Hodgkin The PET World Sally Barrington PET-CT Staging in HL PET-CT changes stage 15-30% RATHL - Advanced HL 1171 pts Stage by PET-CT compared with cect and BMB 20% stage change; upstaging 14% Most upstaging
Hodgkin The PET World Sally Barrington PET-CT Staging in HL PET-CT changes stage 15-30% RATHL - Advanced HL 1171 pts Stage by PET-CT compared with cect and BMB 20% stage change; upstaging 14% Most upstaging
Review Article. Current Strategies in the Treatment of Childhood Hodgkin s Disease
 Review Article Current Strategies in the Treatment of Childhood Hodgkin s Disease Laxman S. Arya Veronique Dinand Dramatic changes in the treatment of childhood Hodgkin s disease have taken place during
Review Article Current Strategies in the Treatment of Childhood Hodgkin s Disease Laxman S. Arya Veronique Dinand Dramatic changes in the treatment of childhood Hodgkin s disease have taken place during
THORACIC MALIGNANCIES
 THORACIC MALIGNANCIES Summary for Malignant Malignancies. Lung Ca 1 Lung Cancer Non-Small Cell Lung Cancer Diagnostic Evaluation for Non-Small Lung Cancer 1. History and Physical examination. 2. CBCDE,
THORACIC MALIGNANCIES Summary for Malignant Malignancies. Lung Ca 1 Lung Cancer Non-Small Cell Lung Cancer Diagnostic Evaluation for Non-Small Lung Cancer 1. History and Physical examination. 2. CBCDE,
One, the UK RAPID trial, including patients with early stage disease stage 1 and 2A nonbulky.
 Martin Hutchings, MD, PhD Department of Hematology The Finsen Centre, National Hospital Copenhagen University Hospital Copenhagen, Denmark Welcome to Managing Hodgkin Lymphoma. My name is Martin Hutchings.
Martin Hutchings, MD, PhD Department of Hematology The Finsen Centre, National Hospital Copenhagen University Hospital Copenhagen, Denmark Welcome to Managing Hodgkin Lymphoma. My name is Martin Hutchings.
Aggressive Lymphomas - Current. Dr Kevin Imrie Physician-in-Chief, Sunnybrook Health Sciences Centre
 Aggressive Lymphomas - Current Dr Kevin Imrie Physician-in-Chief, Sunnybrook Health Sciences Centre Conflicts of interest I have no conflicts of interest to declare Outline What does aggressive lymphoma
Aggressive Lymphomas - Current Dr Kevin Imrie Physician-in-Chief, Sunnybrook Health Sciences Centre Conflicts of interest I have no conflicts of interest to declare Outline What does aggressive lymphoma
Rituximab and Combination Chemotherapy in Treating Patients With Non- Hodgkin's Lymphoma
 Page 1 of 5 Home Search Study Topics Glossary Search Full Text View Tabular View No Study Results Posted Related Studies Rituximab and Combination Chemotherapy in Treating Patients With Non- Hodgkin's
Page 1 of 5 Home Search Study Topics Glossary Search Full Text View Tabular View No Study Results Posted Related Studies Rituximab and Combination Chemotherapy in Treating Patients With Non- Hodgkin's
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Cell Transplantation for Hodgkin Lymphoma File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_cell_transplantation_for_hodgkin_lymphoma
Corporate Medical Policy Hematopoietic Cell Transplantation for Hodgkin Lymphoma File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_cell_transplantation_for_hodgkin_lymphoma
Hodgkin s Lymphoma (Hodgkin s Disease, HD) PI HD-1 Protocol
 1 Hodgkin s Lymphoma (Hodgkin s Disease, HD) PI HD-1 Protocol NCCN Pacific Island Working Group Clinical Members Scott Macfarlane Peter Bradbeer Jane Skeen Rob Corbett Radhika Sandilya PI HD-1 Updated
1 Hodgkin s Lymphoma (Hodgkin s Disease, HD) PI HD-1 Protocol NCCN Pacific Island Working Group Clinical Members Scott Macfarlane Peter Bradbeer Jane Skeen Rob Corbett Radhika Sandilya PI HD-1 Updated
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113)
 Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Doppler ultrasound of the abdomen and pelvis, and color Doppler
 - - - - - - - - - - - - - Testicular tumors are rare in children. They account for only 1% of all pediatric solid tumors and 3% of all testicular tumors [1,2]. The annual incidence of testicular tumors
- - - - - - - - - - - - - Testicular tumors are rare in children. They account for only 1% of all pediatric solid tumors and 3% of all testicular tumors [1,2]. The annual incidence of testicular tumors
NON HODGKINS LYMPHOMA: AGGRESSIVE Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary)
 NON HODGKINS LYMPHOMA: AGGRESSIVE Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and
NON HODGKINS LYMPHOMA: AGGRESSIVE Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and
Strategies for the Treatment of Elderly DLBCL Patients, New Combination Therapy in NHL, and Maintenance Rituximab Therapy in FL
 New Evidence reports on presentations given at ASH 2009 Strategies for the Treatment of Elderly DLBCL Patients, New Combination Therapy in NHL, and Maintenance Rituximab Therapy in FL From ASH 2009: Non-Hodgkin
New Evidence reports on presentations given at ASH 2009 Strategies for the Treatment of Elderly DLBCL Patients, New Combination Therapy in NHL, and Maintenance Rituximab Therapy in FL From ASH 2009: Non-Hodgkin
Head and Neck: DLBCL
 Head and Neck: DLBCL Nikhil G. Thaker Chelsea C. Pinnix Valerie K. Reed Bouthaina S. Dabaja Department of Radiation Oncology MD Anderson Cancer Center Case 60 yo male Presented with right cervical LAD
Head and Neck: DLBCL Nikhil G. Thaker Chelsea C. Pinnix Valerie K. Reed Bouthaina S. Dabaja Department of Radiation Oncology MD Anderson Cancer Center Case 60 yo male Presented with right cervical LAD
Hodgkin Lymphoma. Erica, Hodgkin lymphoma survivor
 Hodgkin Lymphoma Erica, Hodgkin lymphoma survivor Revised 2016 Publication Update Hodgkin Lymphoma The Leukemia & Lymphoma Society wants you to have the most up-to-date information about blood cancer treatment.
Hodgkin Lymphoma Erica, Hodgkin lymphoma survivor Revised 2016 Publication Update Hodgkin Lymphoma The Leukemia & Lymphoma Society wants you to have the most up-to-date information about blood cancer treatment.
State of the Art Radiotherapy for Pediatric Tumors. Suzanne L. Wolden, MD Memorial Sloan-Kettering Cancer Center
 State of the Art Radiotherapy for Pediatric Tumors Suzanne L. Wolden, MD Memorial Sloan-Kettering Cancer Center Introduction Progress and success in pediatric oncology Examples of low-tech and high-tech
State of the Art Radiotherapy for Pediatric Tumors Suzanne L. Wolden, MD Memorial Sloan-Kettering Cancer Center Introduction Progress and success in pediatric oncology Examples of low-tech and high-tech
Staging Laparotomy in the Management of Hodgkin s Disease: Is it Still Necessary?
 Staging Laparotomy in the Management of Hodgkin s Disease: Is it Still Necessary? PRATIK S. MULTANI, MICHAEL L. GROSSBARD Department of Medicine and Hematology/Oncology Unit, Massachusetts General Hospital,
Staging Laparotomy in the Management of Hodgkin s Disease: Is it Still Necessary? PRATIK S. MULTANI, MICHAEL L. GROSSBARD Department of Medicine and Hematology/Oncology Unit, Massachusetts General Hospital,
Update in Lymphoma Imaging
 Update in Lymphoma Imaging Victorine V. Muse, MD Lymphoma Update in Lymphoma Imaging Victorine V Muse, MD Heterogeneous group of lymphoid neoplasms divided into two broad histological categories Hodgkin
Update in Lymphoma Imaging Victorine V. Muse, MD Lymphoma Update in Lymphoma Imaging Victorine V Muse, MD Heterogeneous group of lymphoid neoplasms divided into two broad histological categories Hodgkin
Hodgkin Lymphoma-Unfavorable Clinical Stage I and II EVIDENCE TABLE
 . Kaplan HS. Evidence for a tumoricidal dose level in the radiotherapy of Hodgkin's disease. Cancer Res. 966;6(6):-4.. Rosenberg SA, Kaplan HS. Evidence for an orderly progression in the spread of Hodgkin's
. Kaplan HS. Evidence for a tumoricidal dose level in the radiotherapy of Hodgkin's disease. Cancer Res. 966;6(6):-4.. Rosenberg SA, Kaplan HS. Evidence for an orderly progression in the spread of Hodgkin's
NK/T cell lymphoma Recent advances. Y.L Kwong University Department of Medicine Queen Mary Hospital
 NK/T cell lymphoma Recent advances Y.L Kwong University Department of Medicine Queen Mary Hospital Natural killer cell lymphomas NK cell lymphomas are mainly extranodal lymphomas Clinical classification
NK/T cell lymphoma Recent advances Y.L Kwong University Department of Medicine Queen Mary Hospital Natural killer cell lymphomas NK cell lymphomas are mainly extranodal lymphomas Clinical classification
NIH Public Access Author Manuscript Expert Opin Pharmacother. Author manuscript; available in PMC 2011 December 1.
 NIH Public Access Author Manuscript Published in final edited form as: Expert Opin Pharmacother. 2010 December ; 11(17): 2891 2906. doi:10.1517/14656566.2010.515979. Hodgkin s Lymphoma Therapy: Past, Present,
NIH Public Access Author Manuscript Published in final edited form as: Expert Opin Pharmacother. 2010 December ; 11(17): 2891 2906. doi:10.1517/14656566.2010.515979. Hodgkin s Lymphoma Therapy: Past, Present,
Evolving Approaches to Primary Treatment of Hodgkin Lymphoma
 Evolving Approaches to Primary Treatment of Hodgkin Lymphoma Joseph M. Connors Two challenges confront the clinician treating Hodgkin lymphoma today: achieving a high level of effectiveness while minimizing
Evolving Approaches to Primary Treatment of Hodgkin Lymphoma Joseph M. Connors Two challenges confront the clinician treating Hodgkin lymphoma today: achieving a high level of effectiveness while minimizing
Outcome of acute leukemia patients with central nervous system (CNS) involvement treated with total body or CNS irradiation before transplantation
 Original Article Page 1 of 9 Outcome of acute leukemia patients with central nervous system (CNS) involvement treated with total body or CNS irradiation before transplantation Wen-Han Kuo 1, Yu-Hsuan Chen
Original Article Page 1 of 9 Outcome of acute leukemia patients with central nervous system (CNS) involvement treated with total body or CNS irradiation before transplantation Wen-Han Kuo 1, Yu-Hsuan Chen
Gemcitabine and Carboplatin in Patients with Refractory or Progressive Metastatic Breast Cancer after Treatment
 DOI: 10.18056/seci2014.6 Gemcitabine and Carboplatin in Patients with Refractory or Progressive Metastatic Breast Cancer after Treatment Zedan A 1, Soliman M 2, Sedik MF 1 1 Medical Oncology Department,
DOI: 10.18056/seci2014.6 Gemcitabine and Carboplatin in Patients with Refractory or Progressive Metastatic Breast Cancer after Treatment Zedan A 1, Soliman M 2, Sedik MF 1 1 Medical Oncology Department,
Nodular lymphocyte-predominant Hodgkin lymphoma: a unique disease deserving unique management
 HODGKIN LYMPHOMA: NEW INSIGHTS AND NEW APPROACHES Nodular lymphocyte-predominant Hodgkin lymphoma: a unique disease deserving unique management Dennis A. Eichenauer 1,2 and Andreas Engert 1,2 1 First Department
HODGKIN LYMPHOMA: NEW INSIGHTS AND NEW APPROACHES Nodular lymphocyte-predominant Hodgkin lymphoma: a unique disease deserving unique management Dennis A. Eichenauer 1,2 and Andreas Engert 1,2 1 First Department
Hodgkin s Lymphoma: Biology and Treatment Strategies for Primary, Refractory, and Relapsed Disease
 Hodgkin s Lymphoma: Biology and Treatment Strategies for Primary, Refractory, and Relapsed Disease Volker Diehl, Harald Stein, Michael Hummel, Raphael Zollinger, and Joseph M. Connors Hodgkin s lymphomas
Hodgkin s Lymphoma: Biology and Treatment Strategies for Primary, Refractory, and Relapsed Disease Volker Diehl, Harald Stein, Michael Hummel, Raphael Zollinger, and Joseph M. Connors Hodgkin s lymphomas
On behalf of the Israel Cooperative Lymphoma Group. A. Avigdor, S. Bulvik, I. Levi, E. Dann, A. Nagler, I. Ben-Bassat and A.
 Two cycles of escalated BEACOPP followed by four cycles of ABVD utilizing early-interim PET/CT scan for patients with advanced highrisk Hodgkin s lymphoma A. Avigdor, S. Bulvik, I. Levi, E. Dann, A. Nagler,
Two cycles of escalated BEACOPP followed by four cycles of ABVD utilizing early-interim PET/CT scan for patients with advanced highrisk Hodgkin s lymphoma A. Avigdor, S. Bulvik, I. Levi, E. Dann, A. Nagler,
Hodgkin Lymphoma Status of the art of treatment
 11.05.2016 1 Hodgkin Lymphoma Status of the art of treatment Peter Borchmann German Hodgkin Study Group University of Cologne, Germany Question No 1: Which statement regarding 1 st line treatment of early
11.05.2016 1 Hodgkin Lymphoma Status of the art of treatment Peter Borchmann German Hodgkin Study Group University of Cologne, Germany Question No 1: Which statement regarding 1 st line treatment of early
FAST FACTS Eligibility Reviewed and Verified By MD/DO/RN/LPN/CRA Date MD/DO/RN/LPN/CRA Date Consent Version Dated
 Page 1 of 5 COG-AEWS1221: Randomized Phase 3 Trial Evaluating the Addition of the IGF-1R Monoclonal Antibody Ganitumab (AMG 479, NSC# 750008, IND# 120449) to Multiagent Chemotherapy for Patients with Newly
Page 1 of 5 COG-AEWS1221: Randomized Phase 3 Trial Evaluating the Addition of the IGF-1R Monoclonal Antibody Ganitumab (AMG 479, NSC# 750008, IND# 120449) to Multiagent Chemotherapy for Patients with Newly
NK/T cell lymphoma Hong Kong Experience with L-Asparaginase containing regimens. Y.L. Kwong University Department of Medicine Queen Mary Hospital
 NK/T cell lymphoma Hong Kong Experience with L-Asparaginase containing regimens Y.L. Kwong University Department of Medicine Queen Mary Hospital Management of NK cell malignancies Principles 1. Accurate
NK/T cell lymphoma Hong Kong Experience with L-Asparaginase containing regimens Y.L. Kwong University Department of Medicine Queen Mary Hospital Management of NK cell malignancies Principles 1. Accurate
Results of LSA2-L, Therapy in Children with High-Risk Acute Lyrnphoblastic Leukemia and Non-Hodgkin's Lymphoma *
 Haematology and Blood Transfusion Vol. 28 Modem Trends in Human Leukemia V Edited by Neth, Gallo, Greaves, Moore, Winkler @ Springer-Verlag Berlin Heidelberg 1983 Results of LSA2-L, Therapy in Children
Haematology and Blood Transfusion Vol. 28 Modem Trends in Human Leukemia V Edited by Neth, Gallo, Greaves, Moore, Winkler @ Springer-Verlag Berlin Heidelberg 1983 Results of LSA2-L, Therapy in Children
Dr Sneha Shah Tata Memorial Hospital, Mumbai.
 Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Radiotherapy in DLCL is often worthwhile. Dr. Joachim Yahalom Memorial Sloan-Kettering, New York
 Radiotherapy in DLCL is often worthwhile Dr. Joachim Yahalom Memorial Sloan-Kettering, New York The case for radiotherapy Past: Pre-Rituximab randomized trials Present: R-CHOP as backbone, retrospective
Radiotherapy in DLCL is often worthwhile Dr. Joachim Yahalom Memorial Sloan-Kettering, New York The case for radiotherapy Past: Pre-Rituximab randomized trials Present: R-CHOP as backbone, retrospective
Poor-prognostic advanced Germ Cell Tumors
 14-10-16 Poor-prognostic advanced Germ Cell Tumors Karim Fizazi, MD, PhD Institut Gustave Roussy, France Metastatic GCT: Prognosis (IGCCC) Good prognosis Intermediate prognosis Poor prognosis J Clin Oncol
14-10-16 Poor-prognostic advanced Germ Cell Tumors Karim Fizazi, MD, PhD Institut Gustave Roussy, France Metastatic GCT: Prognosis (IGCCC) Good prognosis Intermediate prognosis Poor prognosis J Clin Oncol
Prognostic Value of Early Introduction of Second Line in Patients with Diffuse Large B Cell Lymphoma
 Med. J. Cairo Univ., Vol. 84, No., December: 443-447, 6 www.medicaljournalofcairouniversity.net Prognostic Value of Early Introduction of Second Line in Patients with Diffuse Large B Cell Lymphoma HAMDY
Med. J. Cairo Univ., Vol. 84, No., December: 443-447, 6 www.medicaljournalofcairouniversity.net Prognostic Value of Early Introduction of Second Line in Patients with Diffuse Large B Cell Lymphoma HAMDY
Hodgkin Lymphoma in Older Patients
 Hodgkin Lymphoma in Older Patients Andrew M. Evens, DO, MSc March 26 th, 2015 Professor of Medicine Chief, Division of Hematology/Oncology Director, Tufts Cancer Center Tufts Medical Center Elderly Hodgkin
Hodgkin Lymphoma in Older Patients Andrew M. Evens, DO, MSc March 26 th, 2015 Professor of Medicine Chief, Division of Hematology/Oncology Director, Tufts Cancer Center Tufts Medical Center Elderly Hodgkin
Lung Cancer Non-small Cell Local, Regional, Small Cell, Other Thoracic Cancers: The Question Isn t Can We, but Should We
 Lung Cancer Non-small Cell Local, Regional, Small Cell, Other Thoracic Cancers: The Question Isn t Can We, but Should We Edward Garon, MD, MS Associate Professor Director- Thoracic Oncology Program David
Lung Cancer Non-small Cell Local, Regional, Small Cell, Other Thoracic Cancers: The Question Isn t Can We, but Should We Edward Garon, MD, MS Associate Professor Director- Thoracic Oncology Program David
